Repeat Open-Heart Surgery
|
|
|
- Jack Floyd
- 5 years ago
- Views:
Transcription
1 Repeat Open-Heart Surgery Albert B. Iben, M.D., Edward J. Hurley, M.D., William W. Angell, M.D., and Norman E. Shumway, M.D. S econd open-heart operations will be performed with increasing frequency as experience in cardiac surgery grows. Progression of valvular or vessel disease, failure and fatigue of prosthetic materials, incomplete closure of septal defects, and technical errors comprise the etiology of repeat open-heart surgery. As soon after the first operation as difficulty is perceived, the reoperation must be planned. Failure to proceed early with corrective surgery is the leading cause of mortality in patients of this type. In a series of 768 consecutive intracardiac operations at the Stanford Medical Center, 40 patients underwent open-heart surgery for at least the second time; most of these 40 had been operated upon initially in this same clinic. Two patients had had two prior open procedures. There were 6 hospital or operative deaths. Not included in this report are patients who had had previous closed-heart operations. CASE MA TERIAL Among the 40 cases the aortic valve area by itself and in combination with the mitral valve accounted for 25 of the repeat open-heart procedures. The mitral valve alone was involved in 8 cases, and the second operation was required following ventricular septal defect closure in another 7. The reoperations were performed between twelve hours and eight years after the initial repair; data summarizing the histories of all 40 appears in Table 1. The earliest return to the operating room came in 2 instances of mediocystic disease of the aorta (Group I, Table 1). In both, difficulty with hemostasis was a serious problem. In 1, uncontrollable bleeding led to resection and replacement of the ascending aorta on cardiopulmonary bypass in a repeat operation after the aortic valve had been replaced at the first operation. This patient died two weeks later without regaining From the Division of Cardiovascular Surgery, Department of Surgery, Stanford University School of Medicine, Palo Alto, Calif. Supported in part by U.S. Public Health Service Grant No. HE Presented at the Second Annual Meeting of The Society of Thoracic Surgeons, Denver, Colo., Jan , THE ANNALS OF THORACIC SURGERY
2 TABLE 1. SUMMARY OF CASE MATERIAL, 40 REPEAT OPEN-HEART OPERATIONS (listed in order of description in text) Group, Age, Sex Group I 1. 59, Mt 2. 30, M Group I , M 2. 51, M 3. 46, Mt 4. 64, M 5. 33, Mt 6. 51, M 7. 41, M 8. 42, M 9. 61, Mt , F , M , M , M , F , M - Original Surgery ; ascending aortoplasty Aortic & mitral valvuloplas- ties Aortic & mitral valvuloplasties Repeat Surgery Resection ascending aorta Aortic & mitral valve replace- ment Aortic & mitral valve replacement Aortic & mitral valve replacement Aortic & mitral valve replacement thospita1 or operative death. Interval Between Open-Heart Procedures 12 hr. 12 hr. 11 mo. 1 yr. 8 mo. 3 yr. 4 mo. 1 yr. 11 mo. 2 yr. 4 yr. 2 mo. 3 yr. 2 mo. 3 yr. 5 mo. 2 yr. 7 mo. 2 yr. 6 mo. 2 yr. 6 mo. 2 yr. 1 mo. 4 yr. 2 yr. 6 mo. 3 yr. 2 mo.
3 ~ TABLE 1 (Continued) Group, Age, Sex Original Surgery Group I1 (Continued) , M , F Group I , M 2. 57, Mt 3. 51, M 4. 51, M 5. 62, M 6. 24, M Group IV 1. 58, F 2. 60, F 3. 58, F 4. 64, F 5. 42, F Aortic & mitral valvuloplas- ties Aortic & mitral valvuloplasties (mediocystic disease) (bacterial endocarditis) Mitral commissurotomy Mitral commissurotomy Mitral commissurotomy Mitral commissurotomy Mitral commissurotomy Interval Between Open-Heart Repeat Surgery Procedures Aortic & tricuspid valve re- placement 1. Mitral valve replacement 2. Aortic & tricuspid valve replacement Closure of leak about prosthesis Closure of leak about prosthesis Closure of leak about prosthesis Closure of leak about prosthesis Closure of leak about prosthesis Removal & replacement of aortic prosthesis Mitral valve replacement Mitral valve replacement Mitral valve replacement Mitral valve replacement Aortic & mitral valve replacement 2 yr. 2 yr. 1 mo. 1 yr. 7 mo. 5 mo. 6 mo. 1 yr. 1 mo. 11 mo. 3 mo. 2% mo. 2 yr. 7 mo. 1 yr. 6 mo. 1 yr. 2 mo. 1 yr. 5 mo. 1 yr.
4 Group V 1. 42, M Mitral valve replacement 2. 60, F Mitral valve replacement Group VI 1. 45, F Repair of acyanotic tetralogy of Fallot 2. 11, F 3. 11, F Closure of ventricular septal defect Repair of tetralogy of Fallot 4. 7, M Repair of tetralogy of Fallot 5. 12, M 6. 5, M Closure of ventricular septal defect Repair of tetralogy of Fallot 7. 3% Mt Closure of ventricular septal defect Group VII 1. 62, M Mitral valve replacement?hospital or operative death. Closure of leak about pros- thesis Removal & replacement of mitral prosthesis 1. Closure of residual ventricular septal defect 2. Excision of subvalvular aortic stenosis & aortic valve replacement Tricuspid annuloplasty Closure of residual ventricular septal defect Closure of residual ventricular septal defect Closure of residual ventricular septal defect Repair of ventricular aneurysm Closure of residual ventricular septal defect 4 mo. 3 mo. 1 yr. 6 yr. 3 mo. 8 yr. 2 yr- 2 yr. 4 mo. 1 yr. 9 mo. 1 yr. 6 mo. 2 yr. 10 mo. 4 mo.
5 IBEN, HURLEY, ANGELL, AND SHUMWAY consciousness. The duration of cerebral anoxia was prolonged due to the sudden exsanguination, but the heart recovered despite numerous episodes of arrest. Acute aortic insufficiency after valvuloplasty for leaflet prolapse was responsible for reoperation in the other patient, and aortic valve substitution was performed in the repeat operation within the first twelve hours. The patient recovered fully and is now well and active. As both cases were reoperated upon a few hours after the first procedure, their repeat operations tested well the facilities for emergency cardiopulmonary bypass. Forty-four of the original 768 cardiac surgery patients had both debridement and commissurotomy performed on the aortic valve either separately or in conjunction with mitral repair. Seventeen returned for further surgery (Group 11, Table 1). Eleven of the 17 originally had had aortic repair and returned for aortic replacement; 2 others required mitral substitution as well. Two of the 4 who had had combined aortic and mitral repair returned for replacement in both areas. Another patient required substitution of the aortic and tricuspid valves, while the fourth had the mitral valve replaced at a second operation and the aortic and tricuspid valves at a third. In almost all instances of progression of aortic disease, the process was calcified aortic stenosis and the valve was bicuspid in nature, possibly congenital in origin. Three patients died following the second procedure. Six times in 166 aortic valve replacements insufficiency developed around the prosthesis (Group 111, Table 1). Symptoms and signs of insufficiency appeared early, and repeat surgery was carried out within 2% to 13 months. The average interval was 6% months. One patient with mediocystic disease of the aorta had corrective surgery within 3 months when it was found that one-third of the prosthetic ring of the largest Starr-Edwards aortic valve had pulled away from the annulus. The shortest interval between operations in this group was in a 24-yearold male who had an aortic valve replacement following endocarditis. The initial operation was done as soon as blood cultures had cleared. Much of the annulus was weak and fragmented, holding sutures poorly and predisposing to leakage about the valve upholstery. At the second procedure, a new prosthesis was inserted, and the course was uneventful. One patient in this group died postoperatively. Open mitral commissurotomy in 5 patients was followed by mitral replacement in 4 and aortic and mitral substitution in 1 (Group IV, Table 1). The average time between operations was 18 months. Following mitral valve substitution in 146 of the original 768 cases, insufficiency appeared in 2 (Group V, Table 1). In 1 patient there was true leakage about the ring. In the other, a 60-year-old female, a thick fibrin clot was densely adherent to all metallic portions of the cage and ring of the Starr-Edwards prosthesis, making it impossible for the ball 338 THE ANNALS OF THORACIC SURGERY
6 Repeat Open-Heart Surgery to seat properly during systole. The valve was replaced and satisfactory function ensued. Reoperation was performed within 4 and 3 months, respectively. Spencer recently described a similar patient [61. Ventricular septal defect repairs produced a group of repeat operations extending up to eight years following the initial surgery (Group VI, Table 1). One patient in this category required two procedures for acyanotic tetralogy of Fallot and a third for a procedure consisting of aortic replacement, resection of subaortic stenosis, and closure of a still residual ventricular septal defect. Another patient required tricuspid annuloplasty almost eight years after closure of the septal defect. In all but 1 of the remaining cases, a residual ventricular septal defect was closed on the second operation. Following repair of a tetralogy of Fallot, a right ventricular aneurysm developed in 1 case and was resected eighteen months later. The only death occurred as a result of aortic valve injury during closure of a ventricular septal defect in a small child with pulmonary hypertension. A single case comprises Group VII (see Table 1). Replacement of the aortic valve was done 4 months following mitral valve substitution. Minimal aortic insufficiency was noted at the first surgery, and its severity was magnified by a competent mitral valve. PROCEDURE FOR REPEAT OPERATION The median sternotomy was used in all cases. When a previous lateral approach has been employed, the intact anterior pericardium allows for easy performance of the sternal split. In most instances, however, sternotomy has been used on the initial entry, and no attempt was made to close the pericardium. This leaves the aorta and right ventricle in close proximity to the undersurface of the sternum, which makes the reoperation incision somewhat hazardous even when care is exercised. It is the policy now to prime the heart-lung machine before the incision is begun. Even if the right ventricle or aorta is entered, the patient can be connected to extracorporeal circulation before irreversible brain injury results from hypoxia. After the sternum is approached through the skin and subcutaneous tissues, the wires of the earlier sternal closure are bared and removed. The electric bone saw is used for cutting the outer table along the line of healed bone. After dividing the upper midline abdominal musculature, the inner table of bone is divided from below upward, using a blunt cutting instrument such as a slightly curved Mayo scissors. With the scissor points visualized, the bone and adhesions are divided anterior to the ventricle and aorta. In order to avoid traction injury to the right ventricle, the self-retaining retractor is not used until the anterior chest wall is freed from the heart.
7 IBEN, HURLEY, ANGELL, AND SHUMWAY All adhesions about the heart are divided for total control and to permit local cooling [4, 51 in cases where the aorta has to be occluded. Dissection is extended to the points of great vessel control. Another area of danger during dissection is in the angle of junction between the inferior vena cava and the right atrium, as dense adhesions and a friable myocardium in this region can result in inadvertent entry to the heart. If posterior adhesions cannot be divided easily, their dissection is postponed until partial cardiopulmonary bypass decreases the heart size and makes its displacement of less hernodynamic consequence. When the patient is on total cardiopulmonary bypass, the appropriate repair is carried out. The aortic valve is approached through the line of the previous anterior curvilinear aortotomy. The mitral valve, as before, is exposed through a left atriotomy done anterior to the confluence of right pulmonary veins. Right ventriculotomies are made in the scar of the previous procedure. OPERATIVE DEATHS The patient in Group I who required early resection of the ascending aorta died of the complications of prolonged hypotension some 14 days after operation. In Group 11, in which aortic valve repair was followed by reoperation for valve replacement, there were 3 deaths: 1 at surgery, another within 72 hours of surgery, and the third some two weeks after aortic replacement. Repeat surgery was delayed in the first patient until heart failure with electrolyte derangement led to cardiac arrest with resuscitation early in the morning of the day of surgery. The operation was performed after his condition had improved only slightly and with the patient in renal shutdown and in the process of peritoneal dialysis. The second hospital death in this group occurred in a patient whose recurrent aortic stenosis had produced massive left ventricular hypertrophy. Thirty-six hours following aortic valve replacement recurrent bouts of ventricular fibrillation developed which were uncontrolled. The third patient expired following two weeks of coma, the result of central nervous system anoxia that began when a dissecting aneurysm was entered during sternotomy. Bypass was initiated within 12 minutes and aortic replacement was effected, but the brain insult was irreversible. There was one death in Group 111, in which insufficiency presented around an aortic valve prosthesis. Again, failure to reoperate on this individual early and a degree of coronary artery disease caused the unfavorable outcome. The single remaining death was the result of aortic insufficiency developing as a complication of the closure of a ventricular septa1 defect in a 3%-year-old child with severe pulmonary hypertension. 340 THE ANNALS OF THORACIC SURGERY
8 Repeat Open-Heart Szirgcry To summarize, there were 6 hospital or operative deaths among the 40 cases of repeat operations (an overall mortality of 15%). Surgery had been delayed beyond the optimum time in 4 of the 6 patients who died. DISC USSIOlV Regardless of how carefully each open-heart procedure is planned, a residual group will appear requiring repeat surgery, especially when acquired valvular lesions are concerned. Often these repeat patients must be operated upon when they are more severely ill than they were before the initial procedures. A mortality rate of 15% results, in our experience. This rate is relatively high compared with 2 deaths among 60 patients having multiple valve replacement during the same period of time at the Stanford Medical Center; it reflects well the increased risk a second open-heart operation carries. The greatest morbidity and mortality resides in cases of mitral valve disease, especially mitral stenosis. It is here where left ventricular reserve is decreased by the small ventricular size and involvement of the myocardium by old rheumatic disease. It may be that a less than perfect aortic valve will increase the morbidity if not recognized and replaced. It is in such instances that we deviate from our usual sequence of combined valve replacement and replace the aortic valve after the mitral valve substitution [ 11. Symptomatic patients should be reoperated upon as soon as persistent disease is noted in order to avoid increased risk. The problem should be located and plans made to correct it before signs and symptoms become severe. Of 44 patients who had aortic valvuloplasties, 17 returned for replacement of at least the aortic valve. However, many patients who underwent aortic valvular debridement are continuing to do well up to five years postoperatively. This procedure is used now only in the most ideal situation where the valve is clearly tricuspid and each commissure can be opened to the annulus without significant insufficiency. Leakage about prosthetic devices points out the need of meticulous suture techniques and proper sizing of the valvular annulus. The one case of clotting of a mitral prosthesis suggests the need for careful maintenance of anticoagulation. Patients with aortic valve prostheses appear to carry less risk of embolic phenomena, but every patient with a mitral valve prosthesis must be protected against clotting by anticoagulants and restoration of normal sinus rhythm whenever possible. Starr-Edwards prostheses were used in all cases of replacement. Mackenzie et al. 121 and March et al. [3] described the difficulties following ventricular septal defect closures. Their experience agrees to some extent with our own. The liberal use of the Teflon patch for closure of ventricular septal defects has led in recent years to the disappearance of residual septal defects.
9 IBEN, HURLEY, ANGELL, AND SHUMWAY SUMMARY Among 40 patients having multiple open-heart procedures, 38 had two and 2 patients had three open-heart operations. Although this represents a high-risk group of patients, a combined hospital and operative mortality rate of 15% was attained. Nine patients were in the seventh decade of life. Decision to operate early is of great importance in seeking a lower mortality. Four of the 6 hospital deaths were related to procrastination. Previous open-heart procedures do not preclude successful accomplishment of a second operation, if the appropriate anatomical considerations are observed. REFERENCES 1. Iben, A. B., Hurley, E. J., and Shumway, N. E. Surgery for combined lesions of the aortic and mitral valves. Amer. J. Surg. 110:262, Mackenzie, J. W., Sloan, H., Morris, J. D., and Stern, A. The problem of second open cardiotomies. J. Thorac. Cardiov. Surg. 44: 544, March, H. W., Gerbode, F., and Hultgren, H. N. The reopened ventricular septal defect. Circulation 24:256, Shumway, N. E., and Lower, R. R. Tropical cardiac hypothermia for extended periods of anoxic arrest. Surg. Forum 10:563, Shumway, N. E., Lower, R. R., and Stofer, R. C. Selective hypothermia of the heart in anoxic cardiac arrest. Surg. Gynec. Obstet. 109:750, Spencer, F. C., Trinkle, J. K., and Reeves, J. T. Successful replacement of a thrombosed mitral ball-valve prosthesis. J.A.M.A. 1954: 191, DISCUSSION DR. JOHANN L. EHRENHAFT (Iowa City, Iowa): It is always an agonizing experience for a surgeon to decide upon reoperation in patients who had previous open-cardiac procedures. All these patients present surgical failures of one type or another which need to be and can be corrected in most instances. Reoperation may not be necessary in all patients, but this decision must depend upon complete reevaluation of each patient and the proper timing for the procedure. The number of patients Dr. Iben presented is the same as we have in our series. In 770 heart operations using extracorporeal circulation, reoperation was necessary in 9 instances. This is only one-fourth the number reported by Dr. Iben needing reoperation. The reason for this difference might be that 'in our series the number of patients with valvular disease needing valve replacement were fewer and there were more patients with various congenital lesions. The patients who needed reoperation in our series had the following lesions: tetralogy of Fallot, 2 patients; interventricular septal defect, 1 patient; subaortic stenosis, 3 patients; and congenital calcific aortic stenosis, 1 patient. One other patient, now a 12-year-old boy, had two reoperations for congenital aortic insufficiency; in the first, at age 8, a Muller-Littlefield valve was inserted. This valve stiffened, and the patient developed subacute bacterial endocarditis. The valve was replaced after one and one-half years with a Magovern aortic prosthesis. It functioned well for about one year. Due to dislodgment and recurrent aortic insufficiency, this prosthesis was replaced with a Starr-Edwards prosthesis with ultimate complete recovery of the patient. The only fatality in our reoperated patients was 1 with a previous tetralogy of Fallot. This patient developed aortic insufficiency several years after the initial 342 THE ANNALS OF THORACIC SURGERY
10 Repeat Open-Heart Surgery repair, necessitating an aortic valve replacement. Death was due to cardiac arrhythmias in the immediate postoperative period. I would like to emphasize that reoperation is necessary after procedures considered failures or ones that did not completely correct the existing lesions. The stakes are definitely higher and the operative and postoperative problems more complex in reoperation. Nevertheless, one should never deny a patient the chance of complete recovery because the problems to achieve this aim are more difficult. The attitude must be an aggressive one, and it often will bring satisfactory results. DR. JAMES W. MACKENZIE (Columbia, Mo.): I would like to thank Dr. Iben and his coauthors for their usual lucid presentation and to support their thesis that previous open-heart surgery does not preclude a successful second operation. In 1962 we reported a series of 22 second open-heart operations carried out at the University of Michigan with Dr. Sloan and Dr. Morris. In this group, which included only congenital lesions, there were 5 deaths. Since then we have continued to apply an aggressive surgical approach to reoperation in patients with acquired heart disease who have obvious hemodynamic difficulty. There are a few problems we have encountered that I suppose are rather pedestrian but might merit some discussion. In terms of local adhesions, it would seem to us that about one year following operation is probably the worst time to schedule reoperation. This is obviously just a clinical impression. We have, when option was available, tried to use a separate surgical field, particularly in valvular replacement. This is quite often possible and probably desirable, not so much because the dissection is difficult but because the postoperative pulmonary problems are often greater when the same field is reentered. I would emphasize, as the authors have here, and as Dr. McGoon has previously, that complete freeing of the heart is probably necessary, both for control of air and also for the possible necessity of defibrillation. In terms of the dissection of the heart from the surrounding adhesions, known to most of you, I am sure, is the need for sharp dissection. The tendency to carry out blunt dissection frequently results, unfortunately, in dissection in the fat along the coronary vessels; sometimes severe injury to the major coronary vessels or heart occurs. Cannulation of the ascending aorta, as recommended by Dr. DeWall and others, avoids the occasional problem of perfusion through damaged femoral vessels. DR. PETER AILEN (Vancouver, B.C., Canada): I would like to augment Dr. Iben s remarks on reoperation in open-heart surgery, specifically by dwelling on those patients with recurrent aortic valve disease. With increasing frequency, cardiac surgeons are seeing a return of patients who have survived palliative surgery of the aortic valve. At the time of reoperation one finds dense, widespread calcification into the aortic root and along the gnarled, deformed aortic cusps. There is an almost irresistible urge to remove every bit of calcium, regardless of the consequences. Indeed, as a result of this singleness of purpose, many of us have found ourselves in the undesirable position of having button-holed the root of the aorta, or even worse, of partially separating the aorta from its attachment to the left ventricle. I would make the point that one must resist this temptation, and excise the calcium flush with the aorta only, thereby leaving the base of the aorta undamaged. Under these circumstances extremely accurate and deep placement of sutures into the friable aortic root will insure firm anchorage of the valve pros thesis. DR. IBEN: We wish to thank the discussants for their remarks. It was our hope in preparing this paper that we would have discussion such as this, and that in sharing some of these problems we could to some extent dispel the feeling of loneliness that we have developed as a result of the lack of such reports in the literature over the years. In answer to some points made by Dr. Mackenzie concerning the time of VOL. 2, NO. 3, MAY,
11 IBEN, HURLEY, ANGELL, AND SHUMWAY reoperation in relation to the number of adhesions encountered, this has not been a problem in our series. We have always proceeded at a time when we felt it was necessary to act on a particular situation. The adhesions at any given time vary in individual patients. In closing, I would like to say that we frequently find consolation in having a living patient upon whom to perform a second operation. We are, however, perplexed by the 15% mortality rate in this group, which runs higher than the mortality rate we have had in our primary series, in which we have been fortunate to have had a 12% rate in mitral operations, a 5% rate in aortic operations, and an overall mortality rate of 7.3%. NOTICE FROM THE SOCIETY OF THORACIC SURGEONS Abstracts for papers to be presented at the 1967 Annual Meeting of The Society of Thoracic Surgeons are now being accepted. The meeting is to be held in Kansas City, Missouri, on January The deadline for receipts of abstracts is September 15, An original and six copies should be submitted to Francis X. Byron, M.D., Secretary, The Society of Thoracic Surgeons, City of Hope Medical Center, Duarte, California. Abstracts must summarize an original contribution and must not exceed 200 words in length. Abstracts received after the deadline or exceeding 200 words will not be considered. The program committee reserves the right to select papers for either 15- or 10-minute forum-type presentations. Essayists are reminded that the complete manuscript must be submitted in duplicate either to the editor of The Annals of Thoracic Surgery before the meeting or to the secretary of the Society at the meeting, immediately prior to presentation. FRANCIS X. BYRON, M.D. Secretary 344 THE ANNALS OF THORACIC SURGERY
Mechanical Bleeding Complications During Heart Surgery
 Mechanical Bleeding Complications During Heart Surgery Arthur C. Beall, Jr., M.D., Kenneth L. Mattox, M.D., Mary Martin, R.N., C.C.P., Bonnie Cromack, C.C.P., and Gary Cornelius, C.C.P. * Potential for
Mechanical Bleeding Complications During Heart Surgery Arthur C. Beall, Jr., M.D., Kenneth L. Mattox, M.D., Mary Martin, R.N., C.C.P., Bonnie Cromack, C.C.P., and Gary Cornelius, C.C.P. * Potential for
14 Valvular Stenosis
 14 Valvular Stenosis 14-1. Valvular Stenosis unicuspid valve FIGUE 14-1. This photograph shows severe valvular stenosis as it occurs in a newborn. There is a unicuspid, horseshoe-shaped leaflet with a
14 Valvular Stenosis 14-1. Valvular Stenosis unicuspid valve FIGUE 14-1. This photograph shows severe valvular stenosis as it occurs in a newborn. There is a unicuspid, horseshoe-shaped leaflet with a
Saphenous Vein Autograft Replacement
 Saphenous Vein Autograft Replacement of Severe Segmental Coronary Artery Occlusion Operative Technique Rene G. Favaloro, M.D. D irect operation on the coronary artery has been performed in 180 patients
Saphenous Vein Autograft Replacement of Severe Segmental Coronary Artery Occlusion Operative Technique Rene G. Favaloro, M.D. D irect operation on the coronary artery has been performed in 180 patients
Outcomes of Mitral Valve Repair for Mitral Regurgitation Due to Degenerative Disease
 Outcomes of Mitral Valve Repair for Mitral Regurgitation Due to Degenerative Disease TIRONE E. DAVID, MD ; SEMIN THORAC CARDIOVASC SURG 19:116-120c 2007 ELSEVIER INC. PRESENTED BY INTERN 許士盟 Mitral valve
Outcomes of Mitral Valve Repair for Mitral Regurgitation Due to Degenerative Disease TIRONE E. DAVID, MD ; SEMIN THORAC CARDIOVASC SURG 19:116-120c 2007 ELSEVIER INC. PRESENTED BY INTERN 許士盟 Mitral valve
Surgical treatment of ventricular septal defect
 Thorax (1965), 20, 278. VIKING OLOV BJORK From the Department of Thoracic Surgery, University Hospital, Uppsala, Sweden Since the first report of direct vision closure of ventricular septal defects in
Thorax (1965), 20, 278. VIKING OLOV BJORK From the Department of Thoracic Surgery, University Hospital, Uppsala, Sweden Since the first report of direct vision closure of ventricular septal defects in
Adult Echocardiography Examination Content Outline
 Adult Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 4 5 Anatomy and Physiology Pathology Clinical Care and Safety Measurement Techniques, Maneuvers,
Adult Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 4 5 Anatomy and Physiology Pathology Clinical Care and Safety Measurement Techniques, Maneuvers,
An anterior aortoventriculoplasty, known as the Konno-
 The Konno-Rastan Procedure for Anterior Aortic Annular Enlargement Mark E. Roeser, MD An anterior aortoventriculoplasty, known as the Konno-Rastan procedure, is a useful tool for the cardiac surgeon. Originally,
The Konno-Rastan Procedure for Anterior Aortic Annular Enlargement Mark E. Roeser, MD An anterior aortoventriculoplasty, known as the Konno-Rastan procedure, is a useful tool for the cardiac surgeon. Originally,
Results of Mitral Valve Replacement, with Special Reference to the Functional Tricuspid Insufficiency
 Results of Mitral Valve Replacement, with Special Reference to the Functional Tricuspid Insufficiency Ken-ichi ASANO, M.D., Masahiko WASHIO, M.D., and Shoji EGUCHI, M.D. SUMMARY (1) Surgical results of
Results of Mitral Valve Replacement, with Special Reference to the Functional Tricuspid Insufficiency Ken-ichi ASANO, M.D., Masahiko WASHIO, M.D., and Shoji EGUCHI, M.D. SUMMARY (1) Surgical results of
Replacement of the mitral valve in the presence of
 Mitral Valve Replacement in Patients with Mitral Annulus Abscess Christopher M. Feindel Replacement of the mitral valve in the presence of an abscess of the mitral annulus presents a major challenge to
Mitral Valve Replacement in Patients with Mitral Annulus Abscess Christopher M. Feindel Replacement of the mitral valve in the presence of an abscess of the mitral annulus presents a major challenge to
The modified Konno procedure, or subaortic ventriculoplasty,
 Modified Konno Procedure for Left Ventricular Outflow Tract Obstruction David P. Bichell, MD The modified Konno procedure, or subaortic ventriculoplasty, first described by Cooley and Garrett in1986, 1
Modified Konno Procedure for Left Ventricular Outflow Tract Obstruction David P. Bichell, MD The modified Konno procedure, or subaortic ventriculoplasty, first described by Cooley and Garrett in1986, 1
The pericardial sac is composed of the outer fibrous pericardium
 Pericardiectomy for Constrictive or Recurrent Inflammatory Pericarditis Mauricio A. Villavicencio, MD, Joseph A. Dearani, MD, and Thoralf M. Sundt, III, MD Anatomy and Preoperative Considerations The pericardial
Pericardiectomy for Constrictive or Recurrent Inflammatory Pericarditis Mauricio A. Villavicencio, MD, Joseph A. Dearani, MD, and Thoralf M. Sundt, III, MD Anatomy and Preoperative Considerations The pericardial
Aortic root enlargement is an invaluable surgical technique
 Aortic Root Enlargement in the Adult Christopher M. Feindel, MD, CM, FRCS(C) Aortic root enlargement is an invaluable surgical technique with which every cardiac surgeon performing aortic valve replacement
Aortic Root Enlargement in the Adult Christopher M. Feindel, MD, CM, FRCS(C) Aortic root enlargement is an invaluable surgical technique with which every cardiac surgeon performing aortic valve replacement
Ostium primum defects with cleft mitral valve
 Thorax (1965), 20, 405. VIKING OLOV BJORK From the Department of Thoracic Surgery, University Hospital, Uppsala, Sweden Ostium primum defects are common; by 1955, 37 operated cases had been reported by
Thorax (1965), 20, 405. VIKING OLOV BJORK From the Department of Thoracic Surgery, University Hospital, Uppsala, Sweden Ostium primum defects are common; by 1955, 37 operated cases had been reported by
Heart Valve Replacement
 Heart Valve Replacement Introduction Sometimes people have serious problems with the valves in their hearts. A heart valve repair or replacement surgery restores or replaces a defective heart valve. If
Heart Valve Replacement Introduction Sometimes people have serious problems with the valves in their hearts. A heart valve repair or replacement surgery restores or replaces a defective heart valve. If
Adult Cardiac Surgery
 Adult Cardiac Surgery Mahmoud ABU-ABEELEH Associate Professor Department of Surgery Division of Cardiothoracic Surgery School of Medicine University Of Jordan Adult Cardiac Surgery: Ischemic Heart Disease
Adult Cardiac Surgery Mahmoud ABU-ABEELEH Associate Professor Department of Surgery Division of Cardiothoracic Surgery School of Medicine University Of Jordan Adult Cardiac Surgery: Ischemic Heart Disease
CASE REPORT. Mycotic Aneurysm of Ascending Aorta Due to Sarcina Lutea. G. A. Lopez, M.D., and A. R. C. Dobell, M.D.
 CASE REPORT Mycotic Aneurysm of Ascending Aorta Due to Sarcina Lutea G. A. Lopez, M.D., and A. R. C. Dobell, M.D. ABSTRACT A patient developed a mycotic aneurysm of the aortic suture line after aortic
CASE REPORT Mycotic Aneurysm of Ascending Aorta Due to Sarcina Lutea G. A. Lopez, M.D., and A. R. C. Dobell, M.D. ABSTRACT A patient developed a mycotic aneurysm of the aortic suture line after aortic
Autologous Pulmonary Valve Replacement of the Diseased Aortic Valve
 Autologous Pulmonary Valve Replacement of the Diseased Aortic Valve By L. GONZALEZ-LAvIN, M.D., M. GEENS. M.D., J. SOMERVILLE, M.D., M.R.C.P., ANm D. N. Ross, M.B., CH.B., F.R.C.S. SUMMARY Living tissue
Autologous Pulmonary Valve Replacement of the Diseased Aortic Valve By L. GONZALEZ-LAvIN, M.D., M. GEENS. M.D., J. SOMERVILLE, M.D., M.R.C.P., ANm D. N. Ross, M.B., CH.B., F.R.C.S. SUMMARY Living tissue
Unusual Complications During Mitral Valve Replacement in the Presence of Calcification of the Annulus
 Unusual Complications During Mitral Valve Replacement in the Presence of Calcification of the Annulus Horace MacVaugh, 111, M.D., Claude R. Joyner, M.D., and Julian Johnson, M.D. ABSTRACT Replacement of
Unusual Complications During Mitral Valve Replacement in the Presence of Calcification of the Annulus Horace MacVaugh, 111, M.D., Claude R. Joyner, M.D., and Julian Johnson, M.D. ABSTRACT Replacement of
Basic principles of Rheumatic mitral valve Repair
 Basic principles of Rheumatic mitral valve Repair Prof. Gebrine El Khoury, MD DEPARTMENT OF CARDIOVASCULAR AND THORACIC SURGERY ST. LUC HOSPITAL - BRUSSELS, BELGIUM 1 Rheumatic MV disease MV repair confers
Basic principles of Rheumatic mitral valve Repair Prof. Gebrine El Khoury, MD DEPARTMENT OF CARDIOVASCULAR AND THORACIC SURGERY ST. LUC HOSPITAL - BRUSSELS, BELGIUM 1 Rheumatic MV disease MV repair confers
The stentless bioprosthesis has many salient features that
 Aortic Valve Replacement with the Medtronic Freestyle Xenograft Using the Subcoronary Implantation Technique D. Michael Deeb, MD The stentless bioprosthesis has many salient features that make it an attractive
Aortic Valve Replacement with the Medtronic Freestyle Xenograft Using the Subcoronary Implantation Technique D. Michael Deeb, MD The stentless bioprosthesis has many salient features that make it an attractive
University of Florida Department of Surgery. CardioThoracic Surgery VA Learning Objectives
 University of Florida Department of Surgery CardioThoracic Surgery VA Learning Objectives This service performs coronary revascularization, valve replacement and lung cancer resections. There are 2 faculty
University of Florida Department of Surgery CardioThoracic Surgery VA Learning Objectives This service performs coronary revascularization, valve replacement and lung cancer resections. There are 2 faculty
Minimal access aortic valve surgery has become one of
 Minimal Access Aortic Valve Surgery Through an Upper Hemisternotomy Approach Prem S. Shekar, MD Minimal access aortic valve surgery has become one of the accepted forms of surgical therapy for patients
Minimal Access Aortic Valve Surgery Through an Upper Hemisternotomy Approach Prem S. Shekar, MD Minimal access aortic valve surgery has become one of the accepted forms of surgical therapy for patients
Aortic valve repair is an accepted option for aortic valve
 Complex Aortic Valve Disease in Children Christopher W. Baird, MD,* and Pedro J. del Nido, MD Aortic valve repair is an accepted option for aortic valve pathologic conditions in children and young adults.
Complex Aortic Valve Disease in Children Christopher W. Baird, MD,* and Pedro J. del Nido, MD Aortic valve repair is an accepted option for aortic valve pathologic conditions in children and young adults.
In 1980, Bex and associates 1 first introduced the initial
 Technique of Aortic Translocation for the Management of Transposition of the Great Arteries with a Ventricular Septal Defect and Pulmonary Stenosis Victor O. Morell, MD, and Peter D. Wearden, MD, PhD In
Technique of Aortic Translocation for the Management of Transposition of the Great Arteries with a Ventricular Septal Defect and Pulmonary Stenosis Victor O. Morell, MD, and Peter D. Wearden, MD, PhD In
Long-term results of a strategy of aortic valve repair in the paediatric population: Should we avoid cusp extension?
 Long-term results of a strategy of aortic valve repair in the paediatric population: Should we avoid cusp extension? Y d Udekem, J Siddiqui, C Seaman, I Konstantinov, J Galati, M Cheung, C Brizard Royal
Long-term results of a strategy of aortic valve repair in the paediatric population: Should we avoid cusp extension? Y d Udekem, J Siddiqui, C Seaman, I Konstantinov, J Galati, M Cheung, C Brizard Royal
Hypoplasia of the aortic root1 The problem of aortic valve replacement
 Hypoplasia of the aortic root1 The problem of aortic valve replacement ROWAN NICKS, T. CARTMILL, and L. BERNSTEIN Department of Cardio-thoracic Surgery and the Hallstrom Institute of Cardiology, the Royal
Hypoplasia of the aortic root1 The problem of aortic valve replacement ROWAN NICKS, T. CARTMILL, and L. BERNSTEIN Department of Cardio-thoracic Surgery and the Hallstrom Institute of Cardiology, the Royal
LAB 12-1 HEART DISSECTION GROSS ANATOMY OF THE HEART
 LAB 12-1 HEART DISSECTION GROSS ANATOMY OF THE HEART Because mammals are warm-blooded and generally very active animals, they require high metabolic rates. One major requirement of a high metabolism is
LAB 12-1 HEART DISSECTION GROSS ANATOMY OF THE HEART Because mammals are warm-blooded and generally very active animals, they require high metabolic rates. One major requirement of a high metabolism is
The radial procedure was developed as an outgrowth
 The Radial Procedure for Atrial Fibrillation Takashi Nitta, MD The radial procedure was developed as an outgrowth of an alternative to the maze procedure. The atrial incisions are designed to radiate from
The Radial Procedure for Atrial Fibrillation Takashi Nitta, MD The radial procedure was developed as an outgrowth of an alternative to the maze procedure. The atrial incisions are designed to radiate from
Mitral valve infective endocarditis (IE) is the most
 Mitral Valve Replacement for Infective Endocarditis With Annular Abscess: Annular Reconstruction Gregory J. Bittle, MD, Murtaza Y. Dawood, MD, and James S. Gammie, MD Mitral valve infective endocarditis
Mitral Valve Replacement for Infective Endocarditis With Annular Abscess: Annular Reconstruction Gregory J. Bittle, MD, Murtaza Y. Dawood, MD, and James S. Gammie, MD Mitral valve infective endocarditis
Diversion of the inferior vena cava following repair of atrial septal defect causing hypoxemia
 Marshall University Marshall Digital Scholar Internal Medicine Faculty Research Spring 5-2004 Diversion of the inferior vena cava following repair of atrial septal defect causing hypoxemia Ellen A. Thompson
Marshall University Marshall Digital Scholar Internal Medicine Faculty Research Spring 5-2004 Diversion of the inferior vena cava following repair of atrial septal defect causing hypoxemia Ellen A. Thompson
PATCHING AND SECTION OF THE PULMONARY ORIFICE OF THE HEART.*
 Published Online: 1 July, 1914 Supp Info: http://doi.org/10.1084/jem.20.1.3 Downloaded from jem.rupress.org on December 24, 2018 PATCHING AND SECTION OF THE PULMONARY ORIFICE OF THE HEART.* BY THEODORE
Published Online: 1 July, 1914 Supp Info: http://doi.org/10.1084/jem.20.1.3 Downloaded from jem.rupress.org on December 24, 2018 PATCHING AND SECTION OF THE PULMONARY ORIFICE OF THE HEART.* BY THEODORE
Case 47 Clinical Presentation
 93 Case 47 C Clinical Presentation 45-year-old man presents with chest pain and new onset of a murmur. Echocardiography shows severe aortic insufficiency. 94 RadCases Cardiac Imaging Imaging Findings C
93 Case 47 C Clinical Presentation 45-year-old man presents with chest pain and new onset of a murmur. Echocardiography shows severe aortic insufficiency. 94 RadCases Cardiac Imaging Imaging Findings C
Appendix A.1: Tier 1 Surgical Procedure Terms and Definitions
 Appendix A.1: Tier 1 Surgical Procedure Terms and Definitions Tier 1 surgeries AV Canal Atrioventricular Septal Repair, Complete Repair of complete AV canal (AVSD) using one- or two-patch or other technique,
Appendix A.1: Tier 1 Surgical Procedure Terms and Definitions Tier 1 surgeries AV Canal Atrioventricular Septal Repair, Complete Repair of complete AV canal (AVSD) using one- or two-patch or other technique,
CJ Shuster A&P2 Lab Addenum Beef Heart Dissection 1. Heart Dissection. (taken from Johnson, Weipz and Savage Lab Book)
 CJ Shuster A&P2 Lab Addenum Beef Heart Dissection 1 Heart Dissection. (taken from Johnson, Weipz and Savage Lab Book) Introduction When you have finished examining the model, you are ready to begin your
CJ Shuster A&P2 Lab Addenum Beef Heart Dissection 1 Heart Dissection. (taken from Johnson, Weipz and Savage Lab Book) Introduction When you have finished examining the model, you are ready to begin your
Idiopathic Hypertrophic Subaortic Stenosis and Mitral Stenosis
 CASE REPORTS Idiopathic Hypertrophic Subaortic Stenosis and Mitral Stenosis Martin J. Nathan, M.D., Roman W. DeSanctis, M.D., Mortimer J. Buckley, M.D., Charles A. Sanders, M.D., and W. Gerald Austen,
CASE REPORTS Idiopathic Hypertrophic Subaortic Stenosis and Mitral Stenosis Martin J. Nathan, M.D., Roman W. DeSanctis, M.D., Mortimer J. Buckley, M.D., Charles A. Sanders, M.D., and W. Gerald Austen,
Ebstein s anomaly is defined by a downward displacement
 Repair of Ebstein s Anomaly Sylvain Chauvaud, MD Ebstein s anomaly is a tricuspid valve anomaly associated with poor right ventricular contractility in severe cases. Surgery is indicated in all symptomatic
Repair of Ebstein s Anomaly Sylvain Chauvaud, MD Ebstein s anomaly is a tricuspid valve anomaly associated with poor right ventricular contractility in severe cases. Surgery is indicated in all symptomatic
Heart Dissection. 5. Locate the tip of the heart or the apex. Only the left ventricle extends all the way to the apex.
 Heart Dissection Page 1 of 6 Background: The heart is a four-chambered, hollow organ composed primarily of cardiac muscle tissue. It is located in the center of the chest in between the lungs. It is the
Heart Dissection Page 1 of 6 Background: The heart is a four-chambered, hollow organ composed primarily of cardiac muscle tissue. It is located in the center of the chest in between the lungs. It is the
Multiple Valve Replacement
 Multiple Valve Replacement Review of Five Years' Experience By JOHN C. BIGELOW, M.D., RODNEY H. HERm, M.D., JAMES A. WOOD, M.D., AND ALBERT STARR, M.D. SUMMARY During the past 5i2 years 152 patients have
Multiple Valve Replacement Review of Five Years' Experience By JOHN C. BIGELOW, M.D., RODNEY H. HERm, M.D., JAMES A. WOOD, M.D., AND ALBERT STARR, M.D. SUMMARY During the past 5i2 years 152 patients have
The need for right ventricular outflow tract reconstruction
 Polytetrafluoroethylene Bicuspid Pulmonary Valve Implantation James A. Quintessenza, MD The need for right ventricular outflow tract reconstruction and pulmonary valve replacement is increasing for many
Polytetrafluoroethylene Bicuspid Pulmonary Valve Implantation James A. Quintessenza, MD The need for right ventricular outflow tract reconstruction and pulmonary valve replacement is increasing for many
Concomitant procedures using minimally access
 Surgical Technique on Cardiac Surgery Concomitant procedures using minimally access Nelson Santos Paulo Cardiothoracic Surgery, Centro Hospitalar de Vila Nova de Gaia, Oporto, Portugal Correspondence to:
Surgical Technique on Cardiac Surgery Concomitant procedures using minimally access Nelson Santos Paulo Cardiothoracic Surgery, Centro Hospitalar de Vila Nova de Gaia, Oporto, Portugal Correspondence to:
CorMatrix ECM Bioscaffold
 CorMatrix ECM Bioscaffold REMODEL. REGROW. RESTORE. CorMatrix ECM Bioscaffold provides a natural bioscaffold matrix that enables the body s own cells to repair and remodel damaged cardio-vascular tissue.
CorMatrix ECM Bioscaffold REMODEL. REGROW. RESTORE. CorMatrix ECM Bioscaffold provides a natural bioscaffold matrix that enables the body s own cells to repair and remodel damaged cardio-vascular tissue.
The Rastelli procedure has been traditionally used for repair
 En-bloc Rotation of the Truncus Arteriosus A Technique for Complete Anatomic Repair of Transposition of the Great Arteries/Ventricular Septal Defect/Left Ventricular Outflow Tract Obstruction or Double
En-bloc Rotation of the Truncus Arteriosus A Technique for Complete Anatomic Repair of Transposition of the Great Arteries/Ventricular Septal Defect/Left Ventricular Outflow Tract Obstruction or Double
Repair or Replacement
 Surgical intervention post MitraClip Device: Repair or Replacement Saudi Heart Association, February 21-24 Rüdiger Lange, MD, PhD Nicolo Piazza, MD, FRCPC, FESC German Heart Center, Munich, Germany Division
Surgical intervention post MitraClip Device: Repair or Replacement Saudi Heart Association, February 21-24 Rüdiger Lange, MD, PhD Nicolo Piazza, MD, FRCPC, FESC German Heart Center, Munich, Germany Division
Aortic valve replacement
 Aortic valve replacement VIKING OLOV BJORK From the Department of Thoracic Surgery, University Hospital, Uppsala, Sweden The removal of calcium from calcified aortic leaflets seldom results in perfect
Aortic valve replacement VIKING OLOV BJORK From the Department of Thoracic Surgery, University Hospital, Uppsala, Sweden The removal of calcium from calcified aortic leaflets seldom results in perfect
ABSTRACT One hundred thirty-eight children underwent
 Repeat Median Stemotomy in Pediatrics: Experience in 164 Consecutive Cases Serafin Y. DeLeon, M.D., Joseph LoCicero 111, M.D., Michel N. Ilbawi, M.D., and Farouk S. Idriss, M.D. ABSTRACT One hundred thirty-eight
Repeat Median Stemotomy in Pediatrics: Experience in 164 Consecutive Cases Serafin Y. DeLeon, M.D., Joseph LoCicero 111, M.D., Michel N. Ilbawi, M.D., and Farouk S. Idriss, M.D. ABSTRACT One hundred thirty-eight
AP2 Lab 3 Coronary Vessels, Valves, Sounds, and Dissection
 AP2 Lab 3 Coronary Vessels, Valves, Sounds, and Dissection Project 1 - BLOOD Supply to the Myocardium (Figs. 18.5 &18.10) The myocardium is not nourished by the blood while it is being pumped through the
AP2 Lab 3 Coronary Vessels, Valves, Sounds, and Dissection Project 1 - BLOOD Supply to the Myocardium (Figs. 18.5 &18.10) The myocardium is not nourished by the blood while it is being pumped through the
The Cardiovascular System Part I: Heart Outline of class lecture After studying part I of this chapter you should be able to:
 The Cardiovascular System Part I: Heart Outline of class lecture After studying part I of this chapter you should be able to: 1. Describe the functions of the heart 2. Describe the location of the heart,
The Cardiovascular System Part I: Heart Outline of class lecture After studying part I of this chapter you should be able to: 1. Describe the functions of the heart 2. Describe the location of the heart,
CAUTION- Investigational device. Limited by United States law to investigational use.
 CAUTION- Investigational device. Limited by United States law to investigational use. This booklet is provided to help you learn more about the Medtronic CoreValve U.S. Pivotal Trial. The purpose of the
CAUTION- Investigational device. Limited by United States law to investigational use. This booklet is provided to help you learn more about the Medtronic CoreValve U.S. Pivotal Trial. The purpose of the
The arterial switch operation has been the accepted procedure
 The Arterial Switch Procedure: Closed Coronary Artery Transfer Edward L. Bove, MD The arterial switch operation has been the accepted procedure for the repair of transposition of the great arteries (TGA)
The Arterial Switch Procedure: Closed Coronary Artery Transfer Edward L. Bove, MD The arterial switch operation has been the accepted procedure for the repair of transposition of the great arteries (TGA)
Surgical Management of TOF in Adults. Dr Flora Tsang Associate Consultant Department of Cardiothoracic Surgery Queen Mary Hospital
 Surgical Management of TOF in Adults Dr Flora Tsang Associate Consultant Department of Cardiothoracic Surgery Queen Mary Hospital Tetralogy of Fallot (TOF) in Adults Most common cyanotic congenital heart
Surgical Management of TOF in Adults Dr Flora Tsang Associate Consultant Department of Cardiothoracic Surgery Queen Mary Hospital Tetralogy of Fallot (TOF) in Adults Most common cyanotic congenital heart
THE SURGICAL TREATMENT OF SUPRAVALVULAR AORTIC STENOSIS BASED ON TWO CASES
 Thorax (1962), 17, 154. THE SURGICAL TREATMENT OF SUPRAVALVULAR AORTIC STENOSIS BASED ON TWO CASES BY SAM NORDSTROM AND TORSTEN SILANDER From the Clinic for Thoracic Surgery, Karolinska Sjukhuset, Stockholm,
Thorax (1962), 17, 154. THE SURGICAL TREATMENT OF SUPRAVALVULAR AORTIC STENOSIS BASED ON TWO CASES BY SAM NORDSTROM AND TORSTEN SILANDER From the Clinic for Thoracic Surgery, Karolinska Sjukhuset, Stockholm,
Tricuspid Valve Repair for Ebstein's Anomaly
 Tricuspid Valve Repair for Ebstein's Anomaly Joseph A. Dearani, MD, and Gordon K. Danielson, MD E bstein's anomaly is a malformation of the tricuspid valve and right ventricle that is characterized by
Tricuspid Valve Repair for Ebstein's Anomaly Joseph A. Dearani, MD, and Gordon K. Danielson, MD E bstein's anomaly is a malformation of the tricuspid valve and right ventricle that is characterized by
Disease of the aortic valve is frequently associated with
 Stentless Aortic Bioprosthesis for Disease of the Aortic Valve, Root and Ascending Aorta John R. Doty, MD, and Donald B. Doty, MD Disease of the aortic valve is frequently associated with morphologic abnormalities
Stentless Aortic Bioprosthesis for Disease of the Aortic Valve, Root and Ascending Aorta John R. Doty, MD, and Donald B. Doty, MD Disease of the aortic valve is frequently associated with morphologic abnormalities
Late Recovery of Conduction following Surgically Induced Atrioventricular Block
 Late Recovery of Conduction following Surgically Induced Atrioventricular Block Thomas W. Smith, M.D., James C. McFarland, M.D., Mortimer J. Buckley, M.D., and W. Gerald Austen, M.D. U se of long-term
Late Recovery of Conduction following Surgically Induced Atrioventricular Block Thomas W. Smith, M.D., James C. McFarland, M.D., Mortimer J. Buckley, M.D., and W. Gerald Austen, M.D. U se of long-term
Although most patients with Ebstein s anomaly live
 Management of Neonatal Ebstein s Anomaly Christopher J. Knott-Craig, MD, FACS Although most patients with Ebstein s anomaly live through infancy, those who present clinically as neonates are a distinct
Management of Neonatal Ebstein s Anomaly Christopher J. Knott-Craig, MD, FACS Although most patients with Ebstein s anomaly live through infancy, those who present clinically as neonates are a distinct
Congenital Heart Disease Cases
 Congenital Heart Disease Cases Sabrina Phillips, MD FACC FASE Mayo Clinic Congenital Heart Disease Center 2013 MFMER slide-1 No Disclosures 2013 MFMER slide-2 1 CASE 1 2013 MFMER slide-3 63 year old Woman
Congenital Heart Disease Cases Sabrina Phillips, MD FACC FASE Mayo Clinic Congenital Heart Disease Center 2013 MFMER slide-1 No Disclosures 2013 MFMER slide-2 1 CASE 1 2013 MFMER slide-3 63 year old Woman
PATIENT BOOKLET MEDTRONIC MITRAL AND TRICUSPID HEART VALVE REPAIR
 PATIENT BOOKLET MEDTRONIC MITRAL AND TRICUSPID HEART VALVE REPAIR ARE MEDTRONIC HEART VALVE REPAIR THERAPIES RIGHT FOR YOU? Prosthetic (artificial) heart valve repair products are used by physicians to
PATIENT BOOKLET MEDTRONIC MITRAL AND TRICUSPID HEART VALVE REPAIR ARE MEDTRONIC HEART VALVE REPAIR THERAPIES RIGHT FOR YOU? Prosthetic (artificial) heart valve repair products are used by physicians to
Anatomy determines the close vicinity of the sinuses of
 Aortic Valve Reimplantation According to the David Type I Technique Matthias Karck, MD, and Axel Haverich, MD Department of Thoracic and Cardiovascular Surgery, Hannover Medical School, Hannover, Germany.
Aortic Valve Reimplantation According to the David Type I Technique Matthias Karck, MD, and Axel Haverich, MD Department of Thoracic and Cardiovascular Surgery, Hannover Medical School, Hannover, Germany.
Surgical Repair of Congenital Aortic Stenosis
 Surgical Repair of Congenital Aortic Stenosis Maurice Adam, M.D., Ben F. Mitchel, M.D., Milton V. Davis, M.D., Alvis Johnson, M.D., Kathryn Willis, M.D., and Gladys J. Fashena, M.D. C ongenital aortic
Surgical Repair of Congenital Aortic Stenosis Maurice Adam, M.D., Ben F. Mitchel, M.D., Milton V. Davis, M.D., Alvis Johnson, M.D., Kathryn Willis, M.D., and Gladys J. Fashena, M.D. C ongenital aortic
Penetrating wounds of the heart and great vessels
 Thorax (1973), 28, 142. Penetrating wounds of the heart and great vessels A report of 30 patients C. E. ANAGNOSTOPOULOS and C. FREDERICK KITTLE Department of Surgery, Section of Thoracic and Cardiovascular
Thorax (1973), 28, 142. Penetrating wounds of the heart and great vessels A report of 30 patients C. E. ANAGNOSTOPOULOS and C. FREDERICK KITTLE Department of Surgery, Section of Thoracic and Cardiovascular
Right Ventricular Aneurysm Following Open Cardiotomy for Correction of Tetralogy of Fallot
 Right Ventricular Aneurysm Following Open Cardiotomy for Correction of Tetralogy of Fallot Juro Wada, M.D., Koji Ideda, M.D., Yutaka Kadowaki, M.D., and Shigeo Sugii, M.D. I n recent years, the development
Right Ventricular Aneurysm Following Open Cardiotomy for Correction of Tetralogy of Fallot Juro Wada, M.D., Koji Ideda, M.D., Yutaka Kadowaki, M.D., and Shigeo Sugii, M.D. I n recent years, the development
Repair of Complete Atrioventricular Septal Defects Single Patch Technique
 Repair of Complete Atrioventricular Septal Defects Single Patch Technique Fred A. Crawford, Jr., MD The first repair of a complete atrioventricular septal defect was performed in 1954 by Lillehei using
Repair of Complete Atrioventricular Septal Defects Single Patch Technique Fred A. Crawford, Jr., MD The first repair of a complete atrioventricular septal defect was performed in 1954 by Lillehei using
Late Results with Autogenous
 Late Results with Autogenous Tissue Heart Valves W. Sterling Edwards, M.D. ABSTRACT Five years of experience using unsupported and mounted fascia lata and pericardial heart valves in human beings is summarized.
Late Results with Autogenous Tissue Heart Valves W. Sterling Edwards, M.D. ABSTRACT Five years of experience using unsupported and mounted fascia lata and pericardial heart valves in human beings is summarized.
Acute type A aortic dissection (Type I, proximal, ascending)
 Acute Type A Aortic Dissection R. Morton Bolman, III, MD Acute type A aortic dissection (Type I, proximal, ascending) is a true surgical emergency. It is estimated that patients suffering this calamity
Acute Type A Aortic Dissection R. Morton Bolman, III, MD Acute type A aortic dissection (Type I, proximal, ascending) is a true surgical emergency. It is estimated that patients suffering this calamity
Unit 6: Circulatory System. 6.2 Heart
 Unit 6: Circulatory System 6.2 Heart Functions of Circulatory System 1. The heart is the pump necessary to circulate blood to all parts of the body 2. Arteries, veins and capillaries are the structures
Unit 6: Circulatory System 6.2 Heart Functions of Circulatory System 1. The heart is the pump necessary to circulate blood to all parts of the body 2. Arteries, veins and capillaries are the structures
Open-Heart Surgery in Patients More than 65 Years Old
 Open-Heart Surgery in Patients More than 65 Years Old Donald A. Barnhorst, M.D., Emilio R. Giuliani, M.D., James R. Pluth, M.D., Gordon K. Danielson, M.D., Robert B. Wallace, M.D., and Dwight C. McGoon,
Open-Heart Surgery in Patients More than 65 Years Old Donald A. Barnhorst, M.D., Emilio R. Giuliani, M.D., James R. Pluth, M.D., Gordon K. Danielson, M.D., Robert B. Wallace, M.D., and Dwight C. McGoon,
Atrial fibrillation (AF) is associated with increased morbidity
 Ablation of Atrial Fibrillation with Concomitant Surgery Edward G. Soltesz, MD, MPH, and A. Marc Gillinov, MD Atrial fibrillation (AF) is associated with increased morbidity and mortality in coronary artery
Ablation of Atrial Fibrillation with Concomitant Surgery Edward G. Soltesz, MD, MPH, and A. Marc Gillinov, MD Atrial fibrillation (AF) is associated with increased morbidity and mortality in coronary artery
Mitral incompetence after repair of ostium
 Thorax (1965), 20, 40. Mitral incompetence after repair of ostium primum septal defects A. R. C. DOBELL, D. R. MURPHY, G. M. KARN, AND A. MARTINEZ-CARO From the Department of Cardiovascular Surgery, the
Thorax (1965), 20, 40. Mitral incompetence after repair of ostium primum septal defects A. R. C. DOBELL, D. R. MURPHY, G. M. KARN, AND A. MARTINEZ-CARO From the Department of Cardiovascular Surgery, the
Partial anomalous pulmonary venous connection to superior
 Cavo-Atrial Anastomosis Technique for Partial Anomalous Pulmonary Venous Connection to the Superior Vena Cava The Warden Procedure Robert A. Gustafson, MD Partial anomalous pulmonary venous connection
Cavo-Atrial Anastomosis Technique for Partial Anomalous Pulmonary Venous Connection to the Superior Vena Cava The Warden Procedure Robert A. Gustafson, MD Partial anomalous pulmonary venous connection
MATRIX VHD FORM. State the name of the patient ( Product Recipient ) for whom you are providing the information contained in this form.
 MATRIX VHD FORM A. Patient Information State the name of the patient ( Product Recipient ) for whom you are providing the information contained in this form. (First Name) (Middle Initial) (Last Name) (Date
MATRIX VHD FORM A. Patient Information State the name of the patient ( Product Recipient ) for whom you are providing the information contained in this form. (First Name) (Middle Initial) (Last Name) (Date
CMS Limitations Guide - Radiology Services
 CMS Limitations Guide - Radiology Services Starting October 1, 2015, CMS will update their existing medical necessity limitations on tests and procedures to correspond to ICD-10 codes. This limitations
CMS Limitations Guide - Radiology Services Starting October 1, 2015, CMS will update their existing medical necessity limitations on tests and procedures to correspond to ICD-10 codes. This limitations
Uptofate Study Summary
 CONGENITAL HEART DISEASE Uptofate Study Summary Acyanotic Atrial septal defect Ventricular septal defect Patent foramen ovale Patent ductus arteriosus Aortic coartation Pulmonary stenosis Cyanotic Tetralogy
CONGENITAL HEART DISEASE Uptofate Study Summary Acyanotic Atrial septal defect Ventricular septal defect Patent foramen ovale Patent ductus arteriosus Aortic coartation Pulmonary stenosis Cyanotic Tetralogy
Surgical AVR: Are there any contraindications? Pyowon Park Samsung Medical Center Seoul, Korea
 Surgical AVR: Are there any contraindications? Pyowon Park Samsung Medical Center Seoul, Korea Contents Decision making in surgical AVR in old age Clinical results of AVR with tissue valve Impact of 19mm
Surgical AVR: Are there any contraindications? Pyowon Park Samsung Medical Center Seoul, Korea Contents Decision making in surgical AVR in old age Clinical results of AVR with tissue valve Impact of 19mm
Surgical treatment of aneurysmal changes in the ascending aorta
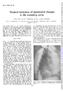 Thcrax (1966), 21, 240. Surgical treatment of aneurysmal changes in the ascending aorta VIKING OLOV BJORK AND LARS BJORK Fronit thle Depart-tneiet.s of Tlioracic Surgery and Diagnostic Radiology, University
Thcrax (1966), 21, 240. Surgical treatment of aneurysmal changes in the ascending aorta VIKING OLOV BJORK AND LARS BJORK Fronit thle Depart-tneiet.s of Tlioracic Surgery and Diagnostic Radiology, University
Ebstein s anomaly is a congenital malformation of the right
 Cone Reconstruction of the Tricuspid Valve for Ebstein s Anomaly: Anatomic Repair Joseph A. Dearani, MD, Emile Bacha, MD, and José Pedro da Silva, MD Division of Cardiovascular Surgery, Mayo Clinic, Rochester,
Cone Reconstruction of the Tricuspid Valve for Ebstein s Anomaly: Anatomic Repair Joseph A. Dearani, MD, Emile Bacha, MD, and José Pedro da Silva, MD Division of Cardiovascular Surgery, Mayo Clinic, Rochester,
The vast majority of patients, especially children, who
 Technique of Mechanical Pulmonary Valve Replacement John M. Stulak, MD, and Joseph A. Dearani, MD The vast majority of patients, especially children, who require pulmonary valve replacement (PVR), obtain
Technique of Mechanical Pulmonary Valve Replacement John M. Stulak, MD, and Joseph A. Dearani, MD The vast majority of patients, especially children, who require pulmonary valve replacement (PVR), obtain
Supplemental Table 1. ICD-9 Codes for Diagnoses and Procedures
 Supplemental Table 1. ICD-9 Codes for Diagnoses and Procedures ICD-9 Code Description Heart Failure 402.01 Malignant hypertensive heart disease with heart failure 402.11 Benign hypertensive heart disease
Supplemental Table 1. ICD-9 Codes for Diagnoses and Procedures ICD-9 Code Description Heart Failure 402.01 Malignant hypertensive heart disease with heart failure 402.11 Benign hypertensive heart disease
Following Mitral Valve Replacement
 Re air of a Subvalvular Le rt Ventricular Aneurysm Following Mitral Valve Replacement Darryl J. Sutorius, M.D., James A. Helmsworth, M.D., James A. Majeski, Ph.D., M.D., and Stephen F. Miller, M.D. ABSTRACT
Re air of a Subvalvular Le rt Ventricular Aneurysm Following Mitral Valve Replacement Darryl J. Sutorius, M.D., James A. Helmsworth, M.D., James A. Majeski, Ph.D., M.D., and Stephen F. Miller, M.D. ABSTRACT
Chapter 13 Worksheet Code It
 Class: Date: Chapter 13 Worksheet 3 2 1 Code It True/False Indicate whether the statement is true or false. 1. A cardiac catheterization diverts blood from the heart to the aorta. 2. Selective vascular
Class: Date: Chapter 13 Worksheet 3 2 1 Code It True/False Indicate whether the statement is true or false. 1. A cardiac catheterization diverts blood from the heart to the aorta. 2. Selective vascular
A new era in cardiac valve surgery has begun...
 THE CENTER FOR VALVE SURGERY A new era in cardiac valve surgery has begun... Good Help to Those in Need Rawn Salenger, MD, FACS, Director, The Center for Valve Surgery Edward F. Lundy, MD, PhD, Chief of
THE CENTER FOR VALVE SURGERY A new era in cardiac valve surgery has begun... Good Help to Those in Need Rawn Salenger, MD, FACS, Director, The Center for Valve Surgery Edward F. Lundy, MD, PhD, Chief of
Right-Sided Bacterial Endocarditis
 New Concepts in the Treatment of the Uncontrollable Infection Agustin Arbulu, M.D., Ali Kafi, M.D., Norman W. Thorns, M.D., and Robert F. Wilson, M.D. ABSTRACT Our experience with 25 patients with right-sided
New Concepts in the Treatment of the Uncontrollable Infection Agustin Arbulu, M.D., Ali Kafi, M.D., Norman W. Thorns, M.D., and Robert F. Wilson, M.D. ABSTRACT Our experience with 25 patients with right-sided
Cardiac anaesthesia. Simon May
 Cardiac anaesthesia Simon May Contents Cardiac: Principles of peri-operative management for cardiac surgery Cardiopulmonary bypass, cardioplegia and off pump cardiac surgery Cardiac disease and its implications
Cardiac anaesthesia Simon May Contents Cardiac: Principles of peri-operative management for cardiac surgery Cardiopulmonary bypass, cardioplegia and off pump cardiac surgery Cardiac disease and its implications
S. Bert Litwin, MD. Preface
 Preface Because of the wide variety of anomalies encountered in congenital heart surgery, a broad understanding of the pathologic anatomy of defects is vitally important to the surgeon. More than in many
Preface Because of the wide variety of anomalies encountered in congenital heart surgery, a broad understanding of the pathologic anatomy of defects is vitally important to the surgeon. More than in many
Chapter 24: Diagnostic workup and evaluation: eligibility, risk assessment, FDA guidelines Ashwin Nathan, MD, Saif Anwaruddin, MD, FACC Penn Medicine
 Chapter 24: Diagnostic workup and evaluation: eligibility, risk assessment, FDA guidelines Ashwin Nathan, MD, Saif Anwaruddin, MD, FACC Penn Medicine Mitral regurgitation, regurgitant flow between the
Chapter 24: Diagnostic workup and evaluation: eligibility, risk assessment, FDA guidelines Ashwin Nathan, MD, Saif Anwaruddin, MD, FACC Penn Medicine Mitral regurgitation, regurgitant flow between the
Long-term results (22 years) of the Ross Operation a single institutional experience
 Long-term results (22 years) of the Ross Operation a single institutional experience Authors: Costa FDA, Schnorr GM, Veloso M,Calixto A, Colatusso D, Balbi EM, Torres R, Ferreira ADA, Colatusso C Department
Long-term results (22 years) of the Ross Operation a single institutional experience Authors: Costa FDA, Schnorr GM, Veloso M,Calixto A, Colatusso D, Balbi EM, Torres R, Ferreira ADA, Colatusso C Department
Expanding Relevance of Aortic Valve Repair Is Earlier Operation Indicated?
 Expanding Relevance of Aortic Valve Repair Is Earlier Operation Indicated? RM Suri, V Sharma, JA Dearani, HM Burkhart, RC Daly, LD Joyce, HV Schaff Division of Cardiovascular Surgery, Mayo Clinic, Rochester,
Expanding Relevance of Aortic Valve Repair Is Earlier Operation Indicated? RM Suri, V Sharma, JA Dearani, HM Burkhart, RC Daly, LD Joyce, HV Schaff Division of Cardiovascular Surgery, Mayo Clinic, Rochester,
Case # 1. Page: 8. DUKE: Adams
 Case # 1 Page: 8 1. The cardiac output in this patient is reduced because of: O a) tamponade physiology O b) restrictive physiology O c) coronary artery disease O d) left bundle branch block Page: 8 1.
Case # 1 Page: 8 1. The cardiac output in this patient is reduced because of: O a) tamponade physiology O b) restrictive physiology O c) coronary artery disease O d) left bundle branch block Page: 8 1.
NOTES. Left-Sided Cannulation of the Right. Atrium for Mitral Surgery. Ronald P. Grunwald, M.D., A. Attai-Lari, M.D., and George Robinson, M.D.
 NOTES Left-Sided Cannulation of the Right Atrium for Mitral Surgery Ronald P. Grunwald, M.D., A. Attai-Lari, M.D., and George Robinson, M.D. T here are several approaches to the mitral valve which yield
NOTES Left-Sided Cannulation of the Right Atrium for Mitral Surgery Ronald P. Grunwald, M.D., A. Attai-Lari, M.D., and George Robinson, M.D. T here are several approaches to the mitral valve which yield
Kinsing Ko, Thom de Kroon, Najim Kaoui, Bart van Putte, Nabil Saouti. St. Antonius Hospital, Nieuwegein, The Netherlands
 Minimal Invasive Mitral Valve Surgery After Previous Sternotomy Without Aortic Clamping: Short- and Long Term Results of a Single Surgeon Single Institution Kinsing Ko, Thom de Kroon, Najim Kaoui, Bart
Minimal Invasive Mitral Valve Surgery After Previous Sternotomy Without Aortic Clamping: Short- and Long Term Results of a Single Surgeon Single Institution Kinsing Ko, Thom de Kroon, Najim Kaoui, Bart
pulmonary valve on, 107 pulmonary valve vegetations on, 113
 INDEX Adriamycin-induced cardiomyopathy, 176 Amyloidosis, 160-161 echocardiographic abnormalities in, 160 intra-mural tumors similar to, 294 myocardial involvement in, 160-161 two-dimensional echocardiography
INDEX Adriamycin-induced cardiomyopathy, 176 Amyloidosis, 160-161 echocardiographic abnormalities in, 160 intra-mural tumors similar to, 294 myocardial involvement in, 160-161 two-dimensional echocardiography
The Edge-to-Edge Technique f For Barlow's Disease
 The Edge-to-Edge Technique f For Barlow's Disease Ottavio Alfieri, Michele De Bonis, Elisabetta Lapenna, Francesco Maisano, Lucia Torracca, Giovanni La Canna. Department of Cardiac Surgery, San Raffaele
The Edge-to-Edge Technique f For Barlow's Disease Ottavio Alfieri, Michele De Bonis, Elisabetta Lapenna, Francesco Maisano, Lucia Torracca, Giovanni La Canna. Department of Cardiac Surgery, San Raffaele
A brief history of valvular surgery
 Cardiac surgery Valvular heart disease University of Pecs, Medical Faculty Heart Institute A brief history of valvular surgery 1925. Souttar closed mitral commissurotomy 1960. McGoon plasty for mitral
Cardiac surgery Valvular heart disease University of Pecs, Medical Faculty Heart Institute A brief history of valvular surgery 1925. Souttar closed mitral commissurotomy 1960. McGoon plasty for mitral
Cardiology/Cardiothoracic
 Cardiology/Cardiothoracic ICD-9-CM to ICD-10-CM Code Mapper 800-334-5724 www.contexomedia.com 2013 ICD-9-CM 272.0 Pure hypercholesterolemia 272.2 Mixed hyperlipidemia 272.4 Other and hyperlipidemia 278.00
Cardiology/Cardiothoracic ICD-9-CM to ICD-10-CM Code Mapper 800-334-5724 www.contexomedia.com 2013 ICD-9-CM 272.0 Pure hypercholesterolemia 272.2 Mixed hyperlipidemia 272.4 Other and hyperlipidemia 278.00
Anatomy & Physiology
 1 Anatomy & Physiology Heart is divided into four chambers, two atrias & two ventricles. Atrioventricular valves (tricuspid & mitral) separate the atria from ventricles. they open & close to control flow
1 Anatomy & Physiology Heart is divided into four chambers, two atrias & two ventricles. Atrioventricular valves (tricuspid & mitral) separate the atria from ventricles. they open & close to control flow
Mitral Valve Disease, When to Intervene
 Mitral Valve Disease, When to Intervene Swedish Heart and Vascular Institute Ming Zhang MD PhD Interventional Cardiology Structure Heart Disease Conflict of Interest None Current ACC/AHA guideline Stages
Mitral Valve Disease, When to Intervene Swedish Heart and Vascular Institute Ming Zhang MD PhD Interventional Cardiology Structure Heart Disease Conflict of Interest None Current ACC/AHA guideline Stages
CONGENITAL HEART DISEASE (CHD)
 CONGENITAL HEART DISEASE (CHD) DEFINITION It is the result of a structural or functional abnormality of the cardiovascular system at birth GENERAL FEATURES OF CHD Structural defects due to specific disturbance
CONGENITAL HEART DISEASE (CHD) DEFINITION It is the result of a structural or functional abnormality of the cardiovascular system at birth GENERAL FEATURES OF CHD Structural defects due to specific disturbance
DISSECTION OF A SHEEP HEART
 DISSECTION OF A SHEEP HEART I. INTRODUCTION A. You will soon appreciate the point made previously the heart models just don t teach us what a real heart is like! Dissecting a sheep heart will give you
DISSECTION OF A SHEEP HEART I. INTRODUCTION A. You will soon appreciate the point made previously the heart models just don t teach us what a real heart is like! Dissecting a sheep heart will give you
Management of Difficult Aortic Root, Old and New solutions
 Management of Difficult Aortic Root, Old and New solutions Hani K. Najm MD, Msc, FRCSC,, FACC, FESC Chairman, Pediatric and Congenital Heart Surgery Cleveland Clinic Conflict of Interest None Difficult
Management of Difficult Aortic Root, Old and New solutions Hani K. Najm MD, Msc, FRCSC,, FACC, FESC Chairman, Pediatric and Congenital Heart Surgery Cleveland Clinic Conflict of Interest None Difficult
CMS Limitations Guide - Cardiovascular Services
 CMS Limitations Guide - Cardiovascular Services Starting October 1, 2015, CMS will update their existing medical necessity limitations on tests and procedures to correspond to ICD-10 codes. This limitations
CMS Limitations Guide - Cardiovascular Services Starting October 1, 2015, CMS will update their existing medical necessity limitations on tests and procedures to correspond to ICD-10 codes. This limitations
