Thoracic Aortic Aneurysm: Reading the Enemy s Playbook
|
|
|
- Meghan Nash
- 5 years ago
- Views:
Transcription
1 HOSPITAL CHRONICLES 2008, SUPPLEMENT: ATHENS CARDIOLOGY UPDATE 2008 Thoracic Aortic Aneurysm: Reading the Enemy s Playbook John A. Elefteriades, MD Yale University School of Medicine; Department of Surgery, Section of Cardiothoracic Surgery, New Haven, CT, USA Imagine if a sports team were able to read the opposing team s playbook; this would be a boon of major proportions. Aortic diseases represent a virulent opponent for cardiac specialists and for our patients. Over the last 10 years, at the Yale Center for Thoracic Aortic Disease, we have made a concerted effort to learn more about the natural history of aortic diseases based on a data set including information on 3000 patients and 9000 years of patient follow-up and 9000 serial imaging studies. This analysis has given us glimpses into the playbook of thoracic aortic diseases; these glimpses have corrolaries in terms of the appropriate role and timing of surgical intervention. Aortic dissection is one of the most catastrophic acute natural events that can befall the human being. The pain of this disorder is often described by those affected as the most severe pain imaginable. Because acute aortic dissection often masquerades as a heart attack, its true incidence is often underestimated. If a middle-aged or elderly person presents to the emergency room with acute onset of chest pain, clutches his chest, and promptly dies, he is likely to be signed out as a myocardial infarction. In actual fact, many such presentations represent undiagnosed aortic dissections. It takes autopsy series to document the true incidence of acute aortic dissection. Such series have indicated that aortic dissection is actually the most common lethal condition affecting the human aorta, more common than the better appreciated ruptured abdominal aortic aneurysm. [1] Furthermore, with the increasing frequency of 3-D imaging of the human body including the so-called drive-in CT scanners aortic pathology is being diagnosed more thoroughly. For all these reasons, acute aortic dissection is a condition of great importance not only to the surgical specialist, but also to the generalist and to other specialists such as emergency medicine, radiology, and cardiology. This chapter will address the natural history of aortic dissection. Its surgical treatment will be covered elsewhere in this text. E t i o l o g y Address for correspondence: john.elefteriades@yale.edu Marfan s syndrome, based on any of a large number of mutations on the fibrillin gene, is a well-known cause of aortic dissection. A patient with Marfan s disease, if denied surgical intervention, runs a 50% risk of developing aortic dissection during his lifetime. Marfan s disease accounts for about 5% of all cases of aortic dissection. A small number of other collagen vascular diseases (including Ehler-Danlos syndrome) cause an even smaller percentage of aortic dissections. As is well-known, the condition of cystic medial necrosis provides the anatomic backdrop in which the dissecting
2 Thoracic Aortic Aneurysm: Reading the Enemy s Playbook process can occur. Figure 1 provides a classic example of this pathologic entity. One can easily picture how a tear in the endothelium can permit blood under pressure to enter one of the intramedial lacunae and how such pressurized entry can split the aortic wall and propagate distally. Cystic medial necrosis is a non-specific degenerative condition of the media which can occur from one of the collagen vascular syndromes like Marfan s disease, from the effects of chronic hypertension, or from the aging process itself. Although the medial degeneration may take decades to develop, the process of dissection itself is literally instantaneous: one moment the aorta is whole, and a split second later, it is dissected. We have visualized this process by direct aortic examination and by echo in our laboratories in an animal model of experimental aortic dissection. [2] By naked eye and by echo, one can see the dissection extend from the proximal descending aorta, where we induce an intimal tear along the entire length of the aorta. By producing an intimal tear and then inducing severe iatrogenic hypertension (BP 300 mmhg, utilizing epinephrine injection), we can reliably produce these aortic phenomena and evaluate various surgical treatments. We are recognizing that many patients with aortic dissection do not fit any acknowledged syndrome of collagen vascular disease. In fact, Marfan s disease and the similar disorders account for only the tip of the iceberg of aortic dissection. Our own studies have indicated a strong genetic component in patients with thoracic aortic aneurysm and dissection among those patients without Marfan s disease. In fact, our construction of nearly 250 family trees of patients with thoracic aortic aneurysm or dissection has indicated that 21% of our probands have at one family member with a known aneurysm somewhere in the arterial tree. [3] Figure 2 shows the positive family trees from among our first hundred family trees. Note that the predominant method of inheritance is autosomal dominant, but that other genetic patterns are also expressed. The true rate of inheritance is likely much higher, as many family members may harbor aneurysms without being aware of their presence. We have undertaken intensive efforts aimed toward identifying the specific genetic aberrations that underlie these family transmissions. The patients with positive family trees showed a higher rate of growth of their aortas and a presentation with clinical disease at an earlier age, strongly supporting an inherent genetic defect of the aortic wall. It is interesting that aortic dissection has been shown to occur in circadian and diurnal patterns, with a preponderance of instances in the winter months and in the early morning hours. The reasons behind these patterns are unknown. Acute aortic dissection can also occur in pregnancy. Also, bicuspid aortic valve, a very common congenital condition (1-2% of the general population) predisposes to aortic dissection. One in twenty bicuspid patients will develop aortic dissection in his lifetime. Of note, dissection usually occurs before the onset of symptomatic aortic stenosis in these patients. Aortic Figure 1. Classic cystic medial necrosis. Note the drop-out of medial cell bodies and the cystic spaces within the media. Figure 2. Family trees of the first 21 patients in Yale series with positive family histories, drawn from among 100 interviewed families. The predominant pattern of inheritance is autosomal dominant. coarctation predisposes strongly to aortic dissection. Dissection can occur in pregnancy, threatening both mother and fetus. In the present era, cocaine use is emerging as an increasingly frequent cause of aortic dissection. 161
3 HOSPITAL CHRONICLES, SUPPLEMENT 2008 S y m p t o m s The symptoms of aortic dissection are well-known. Ascending aortic dissection usually produces substernal pain, and descending dissection produces posterior back pain in the interscapular region. It is interesting that nature perceives the pain of dissection via a splitting or tearing quality very much a propos to the pathologic process itself. Other symptoms are reflective of ischemia of the specific vascular branches that may be impaired or occluded by the dissection process. These are depicted in Figure 3. Dissection may produce ischemia of the brain, resulting in stroke; ischemia of the spinal cord, resulting in paraplegia; ischemia of the intestines, resulting in bowel necrosis; ischemia of the kidneys, resulting in renal failure or reno-vascular hypertension; or iliac artery ischemia, resulting in pulseless lower extremities. Figure 3 also indicates the means by which aortic dissection can lead to mortality. These are four: (1) intrapericardial rupture, producing cardiac tamponade, (2) acute aortic insufficiency, resulting in acute cardiogenic shock, (3) free intrapleural rupture, usually on the left side, and (4) vascular compromise, from any of the indicated branch arteries of the aorta. S u r v i v a l i m p a c t We have followed hundreds of patients longitudinally in our Yale Center for Thoracic Aortic Disease. This serial follow-up has demonstrated that thoracic aortic aneurysm disease is inherently a lethal disease. [4] Five-year survival overall is 63%. In all calculations, regardless of category, patients with aneurysm do more poorly than those with aneurysm without dissection. This can be seen in Figure 4. The five-year survival for patients with dissection is only 42%. This poorer outcome is understandable in view of the fact that, after dissection has occurred, the bloodstream is restrained by only a partial thickness of an intrinsically weak aortic wall. In fact, our data has indicated clearly that the dissected aorta grows more quickly than the non-dissected aorta, 0.37 cm / year, compared to 0.09 cm/year. This poor prognosis after realized dissection indicates how critically important it is to intervene before aortic dissection occurs. Our detailed studies of the natural history of the enlarged aorta have defined criteria which predict when dissection and rupture are likely to occur in an enlarged thoracic aorta. See Figure 5. We have identified hinge points for dissection or rupture at 6 cm for the ascending and 7 cm for the descending aorta. [4] We have recommended intervention at sizes smaller than these danger points, namely 5.5 cm for the ascending aorta and 6.5 cm for the descending aorta. It is well-known that patients with Marfan s disease can dissect at quite small sizes, and for this reason, we have decreased the intervention for Marfan s patients to lower levels, namely 5.0 cm for the ascending aorta and 6.0 cm for the descending aorta. We consider patients without Marfan s disease but Figure 3. Schematic depiction of the manners in which acute aortic dissection can take a patient s life. These include (1) intrapericardial rupture with tamponade, (2) acute aortic insufficiency, resulting in acute cardiogenic shock, (3) free intrapleural rupture, usually on the left side, and (4) vascular compromise, from any of the indicated branch arteries of the aorta. Figure 4. Long-term survival of patients with thoracic aortic aneurysms and dissections. 162
4 Thoracic Aortic Aneurysm: Reading the Enemy s Playbook Table 1. Size criteria for resection of asymptomatic thoracic aortic aneurysms. Figure 5. Depiction of hinge points for lifetime natural history complications at various sizes of the aorta. The y-axis lists the probability of complication; complication refers to rupture or dissection. The x-axis shows aneurysm size. Figure a is for the ascending aorta. Figure b is for the descending aorta. The Yale Center for Thoracic Aortic Disease Recommended Surgical Intervention Criteria for Thoracic Aortic Aneurysms 1. Rupture 2. Acute Aortic dissection a. Ascending requires urgent operation b. Descending requires a complication- specific approach 3. Symptomatic states a. Pain consistent with rupture and unexplained by other causes b. Compression of adjacent organs, especially trachea, esophagus, or left main stem bronchus c. Significant aortic insufficiency in conjunction with ascending aortic aneurysm 4. Documented enlargement a. growth >1 cm/yr or substantial growth and aneurysm is rapidly approaching absolute size criteria 5. Absolute size (cm) Marfan s Non-Marfan s Ascending 5.0 cm 5.5 cm Descending 6.0 cm 6.5 cm with a family pattern of aortic disease just as vulnerable as Marfan s patients. We use these lower criteria for patients with a positive family history. See Table 1 for criteria for preemptive surgical intervention for aortic enlargement. It is important to emphasize that these criteria are specifically and only for asymptomatic patients. Presence of symptoms requires surgical extirpation of the aorta, regardless of size. We have recently been able to determine the yearly risk of rupture, dissection, or death for patients with enlarged aortas of various sizes. [5] These are depicted in Figure 6. This analysis was just recently completed, as calculation of yearly rates requires extremely robust statistical data. We now have observed about 150 hard aortic endpoints, permitting such statistical analysis. One can see that an aorta that has reached 6 cm imparts a risk of dissection of 3.9 % per year. The corresponding risks of rupture and death are 3.7 % and 11.8%. The yearly risk of rupture, dissection, or death is 14.1% per year. This data provides further substantiation of the validity of criteria which permit intervention before the dangerous dimension of 6 cm is reached. Very recently, we have been able to refine our analysis to Figure 6. Yearly rates of rupture, dissection, or death according to aneurysm size. permit estimation of rupture and dissection risk based on the patient s body size as well as the diameter of the aneurysm. This information is relayed in Table 2. By inputting body surface area and aneurysm size, one can categorize any specific patient into low, moderate, and high risk categories. 163
5 HOSPITAL CHRONICLES, SUPPLEMENT 2008 Table 2. Nomogram for computing risk category based on body size and aneurysm size. Aortic Size (cm) BSA 3,5 4,0 4,5 5,0 5,5 6,0 6,5 7,0 7,5 8,0 1,30 2,69 3,08 3,46 3,85 4,23 4,62 5,00 5,38 5,77 6,15 1,40 2,50 2,86 3,21 3,57 3,93 4,29 4,64 5,00 5,36 5,71 1,50 2,33 2,67 3,00 3,33 3,67 4,00 4,33 4,67 5,00 5,33 1,60 2,19 2,50 2,80 3,13 3,44 3,75 4,06 4,38 4,69 5,00 1,70 2,05 2,35 2,65 2,94 3,24 3,53 3,82 4,12 4,41 4,71 1,80 1,94 2,22 2,50 2,78 3,06 3,33 3,61 3,89 4,17 4,44 1,90 1,84 2,11 2,37 2,63 2,89 3,16 3,42 3,68 3,95 4,22 2,00 1,75 2,00 2,25 2,50 2,75 3,00 3,25 3,50 3,75 4,00 2,10 1,67 1,90 2,14 2,38 2,62 2,86 3,10 3,33 3,57 3,80 2,20 1,59 1,82 2,05 2,27 2,50 2,72 2,95 3,18 3,41 3,64 2,30 1,52 1,74 1,96 2,17 2,39 2,61 2,83 3,04 3,26 3,48 2,40 1,46 1,67 1,88 2,08 2,29 2,50 2,71 2,92 3,13 3,33 2,50 1,40 1,60 1,80 2,00 2,20 2,40 2,60 2,80 3,00 3,20 = low risk (~4% per yr) = moderate risk (~8% per yr) = severe risk (~20% per yr) A c u t e A o r t i c D i s s e c t i o n We will consider acute aortic dissection by the categories of ascending and descending dissection, as the presentations, sequellae, and treatments vary according to this distinction. A c u t e a s c e n d i n g d i s s e c t i o n It is well-known that acute aortic dissection of the ascending aorta is a lethal condition. It has been estimated that up to 90% of patients with acute aortic dissection will die from this disease, if not surgically treated, and that patients die at a rate of 20% in the first 24 hours, 60% within 2 weeks, and 90% within 3 months. [6] Because this natural history is well appreciated, we no longer allow acute ascending aortic dissection to express its natural history. Urgent surgical intervention is performed, to prevent the lethal development of intrapericardial rupture, coronary artery dissection with myocardial infarction, and acute aortic insufficiency with shock. Occasionally, two or three days have already passed since the onset of symptoms before diagnosis is made or the patient is transferred to a tertiary treatment center. Our review of patients with late recognition or referral has indicated that this subgroup of patient need not be operated in the middle of the night, but can await the next daytime operative slot. [7] This may be helpful to know, as complex aortic surgery usually can be carried much better to a successful outcome during regular working hours, when ideal staff and facilities are available. Occasionally, a patient presents with acute aortic dissection who cannot be operated because of completed stroke or should not be operated because of overwhelming age, debility, or comorbidity. We have found that vigorous anti-impulse therapy can produce some survivors in this setting. A c u t e d e s c e n d i n g d i s s e c t i o n Although an extremely serious disorder, acute descending dissection is less virulent than ascending aortic dissection. Accordingly, urgent surgical intervention is not frequently required. The so-called anti-impulse therapy is applied, so as to decrease the mechanical stresses on the aortic wall by means of medical treatment. This therapy usually involves a beta-blocker or calcium channel blocker to decrease strength or cardiac contraction and an afterload reducing agent to lower blood pressure. We have recommended a complication-specific approach to acute descending dissection. [8] For most patients, without rupture or ischemic vascular complications, medical therapy suffices. For patients with acute vascular occlusion, we use the fenestration procedure, which is quick, safe, and effective. Traditional replacement of the proximal descending aorta for acute descending dissection carries a very serious risk, with a mortality of nearly 50% and a rate of paraplegia 164
6 Thoracic Aortic Aneurysm: Reading the Enemy s Playbook or paresis amounting to 32% [9]. Fenestration is much simpler and more effective. Variations of fenestration can now be performed percutaneously at many centers. For realized rupture, only traditional aortic resection and graft replacement is appropriate. We have recently examined a consecutive series of 100 patients presenting to our center with acute descending aortic dissection. See Figure 7. Nine percent of patients died during the initial hospital admission. As can be seen in the figure, two-thirds of patients did fine with just anti-impulse therapy. The remaining 31% of patients developed specific vascular complications and required early or late surgical intervention. This data indicates again that uncomplicated acute descending dissection is a medical, not a surgical, phenomenon. Whether there is any appropriate role for routine percutaneous stent treatment of all patients with acute descending aortic dissection remains to be determined from clinical trials. Some experts have recommended such therapy, reasoning that reapplying the two layers early in the process may lessen later complications. going obliquely across the aortic lumen, it is not a typical dissection. See Figure 8. In contradistinction to aortic dissection, with an intimal flap, intramural hematoma and penetrating ulcer have no flap. Intramural hematoma is a concentric collection of blood in the wall of the aorta. Penetrating ulcer is an extension of blood beyond the media of the aortic wall. This looks just like a duodenal ulcer, but it is located in the aorta. See Figure 9. We have found these variant lesions to be even more virulent that typical aortic dissection. The rate of rupture at initial presentation is even higher than for typical dissection. [10] See Figure 10. Also, intramural hematoma and penetrating ulcer have a 50% or more likelihood of worsening or progressing to typical dissection, in mid-term follow-up. Also, patients treated medically for these variant dissection processes continue to die of rupture on medical treatment. For these reasons, we recommend nearly routing surgical therapy during the initial hospital admission for patients with intramural hematoma or penetrating ulcer of the aorta. Some centers have found V a r i a n t f o r m s o f a o r t i c d i s s e c t i o n : i n t r a m u r a l h e m a t o m a a n d p e n e t r a t i n g u c l e r o f t h e a o r t a In the current era of 3-D aortic imaging by transesophageal echocardiography, CT scan, and MRI imaging, it has become clear that variants of aortic dissection exist, which have been called intramural hematoma of the aorta and penetrating ulcer of the aorta. In interpreting these imaging studies, we use the principle no flap, no dissection ; that is, if there is no flap Figure 8. Schematic representation of three types of acute aortic dissection pathologies. Figure 7. Flow diagram of natural behavior of 100 consecutive cases of acute descending aortic dissection. Figure 9. An example of a penetrating ulcer of the thoracic aorta. Note the resemblance to duodenal ulcer. 165
7 HOSPITAL CHRONICLES, SUPPLEMENT 2008 lower virulence than we have seen for these lesions; this may be related to the fact that all of our patients presented with acutely symptomatic hematoma or ulcer none were incidental findings on scans done for other reasons. C h r o n i c a s c e n d i n g d i s s e c t i o n Occasionally, a patient will present for evaluation with a chronic ascending aortic dissection. This presentation implies that the patient was one of the small minority (<10%) who survive this event without the benefit of surgical therapy. In some cases, there was an acute event, possibly weeks, months, or even years ago, and the diagnosis was missed. In other cases, no acute symptomatic event can be recalled whatsoever. In any case, this disorder does not require urgent therapy. Associated aortic insufficiency may mandate surgical intervention. Severe aortic enlargement may warrant intervention. We apply the same size criteria as for chronic non-dissected aneurysm, namely attainment of a diameter of 5.5 cm. Most patients need intervention for one of these reasons. Also, pain requires surgery. For the few patients who have a chronic dissection but do not have aortic insufficiency, dangerous aortic enlargement, or pain, optimal treatment is controversial. The natural history may not be very poor. Nonetheless, most authorities operate on these patients, albeit electively. C h r o n i c d e s c e n d i n g a o r t i c d i s s e c t i o n In our experience, longitudinal extension and new branch vessel occlusion are quite rare in chronic descending aortic dissection. The real issue with these cases is rupture. Rupture can and does occur, usually preceded by dilatation of the involved segment of aorta. In most patients, this dilatation occurs gradually, at one to three millimeters per year. In some patients, especially those with Marfan s disease, dilatation may occur very rapidly. For chronic descending aortic dissection, we operate pre-emptively to prevent rupture when the aorta has reached the same criterion that we apply for chronic non-dissected aneurysm, namely 6.5 cm. As always, if the patient has pain, surgery is always indicated, to prevent catastrophic rupture. A recent review by Dr. Griepp s group has found that, in patients with chronic descending aortic dissection, older age, chronic obstructive pulmonary disease, and elevated mean blood pressure were strongly predictive of rupture. [11] They make a strong point for earlier intervention for chronic descending aortic dissection, especially when those identified risk factors are operative. L o c a l i z e d d i s s e c t i o n s On occasion, dissection may be limited in longitudinal extent to the abdominal aorta or be confined to the carotid artery or the coronary arteries. The natural history of these localized dissections is being elucidated. Only about 1% of dissections are limited to the abdominal aorta. Natural history appears similar to that of descending aortic dissection, and complication-specific management, similar to that of descending aortic dissection, appears most appropriate. [12] Isolated coronary artery dissection is seen once or twice yearly in a busy catheterization laboratory, often manifesting on the basis of myocardial ischemia in a patient without traditional risk factors for arteriosclerosis. Myocardial infarction may result from coronary artery dissection, so, in the current era, stent therapy is applied at the time of angiographic diagnosis. C o n c l u s i o n Regarding the natural history of aortic dissection, one can say that this beast is quite a fierce one. Once it occurs, the impact on both short and long-term survival is severe. Although advances in imaging techniques and surgical sciences have succeeded to some extent in taming this disorder, it continues to exert quite a fierce impact on the human race. Once the aorta has been rent into two dissected layers, despite the most talented surgical efforts, the outlook for that aorta and consequently, for the patient will be irrevocably impaired. The best hope for taming this disorder in the future resides in predicting and preventing aortic dissection before it actually occurs. From the point of view of aortic size, natural history investigations have clarified quite well appropriate criterion levels for pre-emptive intervention. If the genetic studies underway bear fruit, it may be possible to predict the diathesis for dissection from a simple blood test. Perhaps understanding the genetic underpinnings of dissection disease may, in the future, permit conventional therapies aimed at strengthening the abnormal structural proteins coded by those genes. Even specific genetic remedies can be envisioned for the future. R e f e r e n c e s 1. Anagnostopoulos CE. Acute Aortic Dissection. University Park Press Morales DLS, Quin JA, Braxton JH, et al. Experimental confirmation of effectiveness of fenestration in acute aortic dissection. Ann Thorac Surg 1998;66: Coady MA, Davies RB, Roberts M, et al. Familial patterns of 166
8 Thoracic Aortic Aneurysm: Reading the Enemy s Playbook thoracic aortic aneurysm. Arch Surg 1999;134: Coady MA, Rizzo JA, Hammond GL, et al. What is the appropriate size criterion for resection of thoracic aortic aneurysm? J Thorac Cardiovasc Surg 1997;113: Davies RR, Goldstein LJ, Coady MA, et al. Yearly rupture rates for thoracic aortic aneurysms: Simple prediction based on size. Ann Thorac Surg 2001;73: Cohen LS. Diseases of the Aorta. In, Bennet JC, Plum F, Cecil Textbook of Medicine (20 th Edition). W.B. Saunders. Philadelphia Scholl FG, Coady MA, Davies R, et al. Interval or permanent nonoperative management of acute type A aortic dissection. Arch Surg 1999;134: Elefteriades JA, Hartleroad J, Gusberg RJ, et al. Long-term experience with descending aortic dissection: The complicationspecific approach. Ann Thorac Surg 1992;53: Svensson LG, Crawford ES, Hess KR, Coselli JS, Safi HJ. Dissection of the aorta and dissecting aortic aneurysms. Improving early and long-term surgical results. Circulation (5 Suppl)IV Coady MA, Rizzo JA, Elefteriades JA. Pathologic variants of thoracic aortic dissections: Penetrating atherosclerotic ulcers and intramural hematomas. Cardiol Clin Nor Am 1999;17: Juvonen T,Ergin MA, Galla JD, et al. Risk factors for rupture of chronic type B dissections. J Thorac Cardiovasc Surg 1999;117: Wagner FA, Cosman DV, Cohen JL, et al. Isolated dissection of the abdominal aorta: clinical presentation and therapeutic options. J Vasc Surg 2002;36:
Disclosures: Acute Aortic Syndrome. A. Michael Borkon, M.D. Director of CV Surgery Mid America Heart Institute Saint Luke s Hospital Kansas City, MO
 Acute Aortic Syndrome Disclosures: A. Michael Borkon, M.D. Director of CV Surgery Mid America Heart Institute Saint Luke s Hospital Kansas City, MO No financial relationships to disclose 1 Acute Aortic
Acute Aortic Syndrome Disclosures: A. Michael Borkon, M.D. Director of CV Surgery Mid America Heart Institute Saint Luke s Hospital Kansas City, MO No financial relationships to disclose 1 Acute Aortic
An aneurysm is a localized abnormal dilation of a blood vessel or the heart Types: 1-"true" aneurysm it involves all three layers of the arterial
 An aneurysm is a localized abnormal dilation of a blood vessel or the heart Types: 1-"true" aneurysm it involves all three layers of the arterial wall (intima, media, and adventitia) or the attenuated
An aneurysm is a localized abnormal dilation of a blood vessel or the heart Types: 1-"true" aneurysm it involves all three layers of the arterial wall (intima, media, and adventitia) or the attenuated
Thoracic Aortic Aneurysm: Reading the Enemy s Playbook
 YALE JOURNAL OF BIOLOGY AND MEDICINE 81 (2008), pp.175-186. Copyright 2008. REVIEW Thoracic Aortic Aneurysm: Reading the Enemy s Playbook John A. Elefteriades, MD Section of Cardiothoracic Surgery, Yale
YALE JOURNAL OF BIOLOGY AND MEDICINE 81 (2008), pp.175-186. Copyright 2008. REVIEW Thoracic Aortic Aneurysm: Reading the Enemy s Playbook John A. Elefteriades, MD Section of Cardiothoracic Surgery, Yale
AORTIC DISSECTION. DISSECTING ANEURYSMS OF THE AORTA or CLASSIFICATION
 DISSECTING ANEURYSMS OF THE AORTA or AORTIC DISSECTION CLASSIFICATION DeBakey classified aortic dissections into types I, II, and III :- Type I dissection the tear site originates in the ascending aorta,
DISSECTING ANEURYSMS OF THE AORTA or AORTIC DISSECTION CLASSIFICATION DeBakey classified aortic dissections into types I, II, and III :- Type I dissection the tear site originates in the ascending aorta,
Surgical indications in ascending aorta aneurysms: What do we know? Jean-Luc MONIN, MD, PhD. Institut Mutualiste Montsouris, Paris, FRANCE
 Surgical indications in ascending aorta aneurysms: What do we know? Jean-Luc MONIN, MD, PhD. Institut Mutualiste Montsouris, Paris, FRANCE Disclosures related to this talk : NONE 2 Clinical case A 40 year-old
Surgical indications in ascending aorta aneurysms: What do we know? Jean-Luc MONIN, MD, PhD. Institut Mutualiste Montsouris, Paris, FRANCE Disclosures related to this talk : NONE 2 Clinical case A 40 year-old
Diseases of the Aorta
 Diseases of the Aorta ASE Review 2018 Susan E Wiegers, MD, FASE, FACC Professor of Medicine My great friend Dr. Roberto Lang Disclosure None related to this presentation 1 Objectives Aneurysm Dissection
Diseases of the Aorta ASE Review 2018 Susan E Wiegers, MD, FASE, FACC Professor of Medicine My great friend Dr. Roberto Lang Disclosure None related to this presentation 1 Objectives Aneurysm Dissection
AORTIC DISSECTIONS Current Management. TOMAS D. MARTIN, MD, LAT Professor, TCV Surgery Director UF Health Aortic Disease Center University of Florida
 AORTIC DISSECTIONS Current Management TOMAS D. MARTIN, MD, LAT Professor, TCV Surgery Director UF Health Aortic Disease Center University of Florida DISCLOSURES Terumo Medtronic Cook Edwards Cryolife AORTIC
AORTIC DISSECTIONS Current Management TOMAS D. MARTIN, MD, LAT Professor, TCV Surgery Director UF Health Aortic Disease Center University of Florida DISCLOSURES Terumo Medtronic Cook Edwards Cryolife AORTIC
Case 9799 Stanford type A aortic dissection: US and CT findings
 Case 9799 Stanford type A aortic dissection: US and CT findings Accogli S, Aringhieri G, Scalise P, Angelini G, Pancrazi F, Bemi P, Bartolozzi C Department of Diagnostic and Interventional Radiology, University
Case 9799 Stanford type A aortic dissection: US and CT findings Accogli S, Aringhieri G, Scalise P, Angelini G, Pancrazi F, Bemi P, Bartolozzi C Department of Diagnostic and Interventional Radiology, University
Long-term Follow-up of Aortic Intramural Hematomas and Penetrating Ulcers
 Long-term Follow-up of Aortic Intramural Hematomas and Penetrating Ulcers Alan S. Chou, BA, Bulat A. Ziganshin, MD, Paris Charilaou, MD, Maryann Tranquilli, RN, John A. Rizzo, PhD, John A. Elefteriades,
Long-term Follow-up of Aortic Intramural Hematomas and Penetrating Ulcers Alan S. Chou, BA, Bulat A. Ziganshin, MD, Paris Charilaou, MD, Maryann Tranquilli, RN, John A. Rizzo, PhD, John A. Elefteriades,
Aortic CT: Intramural Hematoma. Leslie E. Quint, M.D.
 Aortic CT: Intramural Hematoma Leslie E. Quint, M.D. 43 M Mid back pain X several months What type of aortic disease? A. Aneurysm with intraluminal thrombus B. Chronic dissection with thrombosed false
Aortic CT: Intramural Hematoma Leslie E. Quint, M.D. 43 M Mid back pain X several months What type of aortic disease? A. Aneurysm with intraluminal thrombus B. Chronic dissection with thrombosed false
Yearly Rupture or Dissection Rates for Thoracic Aortic Aneurysms: Simple Prediction Based on Size
 ORIGINAL ARTICLES: CARDIOVASCULAR Yearly Rupture or Dissection Rates for Thoracic Aortic Aneurysms: Simple Prediction Based on Size Ryan R. Davies, BA, Lee J. Goldstein, MD, Michael A. Coady, MD, Shawn
ORIGINAL ARTICLES: CARDIOVASCULAR Yearly Rupture or Dissection Rates for Thoracic Aortic Aneurysms: Simple Prediction Based on Size Ryan R. Davies, BA, Lee J. Goldstein, MD, Michael A. Coady, MD, Shawn
CT of Acute Thoracic Aortic Syndromes Stuart S. Sagel, M.D.
 CT of Acute Thoracic Aortic Syndromes Stuart S. Sagel, M.D. Thoracic Aortic Aneurysms Atherosclerotic Dissection Penetrating ulcer Mycotic Inflammatory (vasculitis) Traumatic Aortic Imaging Options Catheter
CT of Acute Thoracic Aortic Syndromes Stuart S. Sagel, M.D. Thoracic Aortic Aneurysms Atherosclerotic Dissection Penetrating ulcer Mycotic Inflammatory (vasculitis) Traumatic Aortic Imaging Options Catheter
Ascending Thoracic Aorta: Postsurgical CT Evaluation
 Ascending Thoracic Aorta: Postsurgical CT Evaluation Santiago Martinez Jimenez, MD GOALS Ascending Thoracic Aorta: Postsurgical CT Evaluation Santiago Martínez MD smartinez-jimenez@saint-lukes.org Saint
Ascending Thoracic Aorta: Postsurgical CT Evaluation Santiago Martinez Jimenez, MD GOALS Ascending Thoracic Aorta: Postsurgical CT Evaluation Santiago Martínez MD smartinez-jimenez@saint-lukes.org Saint
Echocardiographic Evaluation of the Aorta
 Echocardiographic Evaluation of the Aorta William F. Armstrong M.D. Director Echocardiography Laboratory Professor of Medicine University of Michigan The Aorta: What to Evaluate Dimensions / shape Atherosclerotic
Echocardiographic Evaluation of the Aorta William F. Armstrong M.D. Director Echocardiography Laboratory Professor of Medicine University of Michigan The Aorta: What to Evaluate Dimensions / shape Atherosclerotic
Update on Acute Aortic Syndrome
 SUNDAY Update on Acute Aortic Syndrome Diana Litmanovich, MD Learning objectives To be familiar with the definition, natural history, and imaging findings of acute aortic syndrome, including: I. Aortic
SUNDAY Update on Acute Aortic Syndrome Diana Litmanovich, MD Learning objectives To be familiar with the definition, natural history, and imaging findings of acute aortic syndrome, including: I. Aortic
Acute Aortic Syndromes
 Acute Aortic Syndromes Michael H. Picard, M.D. Massachusetts General Hospital Harvard Medical School No disclosures For everything you need to know about the aorta see Circulation 2010;121:e266-e369 And.
Acute Aortic Syndromes Michael H. Picard, M.D. Massachusetts General Hospital Harvard Medical School No disclosures For everything you need to know about the aorta see Circulation 2010;121:e266-e369 And.
Animesh Rathore, MD 4/21/17. Penetrating atherosclerotic ulcers of aorta
 Animesh Rathore, MD 4/21/17 Penetrating atherosclerotic ulcers of aorta Disclosures No financial disclosures Thank You Dr. Panneton for giving this lecture for me. I am stuck at Norfolk with an emergency
Animesh Rathore, MD 4/21/17 Penetrating atherosclerotic ulcers of aorta Disclosures No financial disclosures Thank You Dr. Panneton for giving this lecture for me. I am stuck at Norfolk with an emergency
IMAGING the AORTA. Mirvat Alasnag FACP, FSCAI, FSCCT, FASE June 1 st, 2011
 IMAGING the AORTA Mirvat Alasnag FACP, FSCAI, FSCCT, FASE June 1 st, 2011 September 11, 2003 Family is asking $67 million in damages from two doctors Is it an aneurysm? Is it a dissection? What type of
IMAGING the AORTA Mirvat Alasnag FACP, FSCAI, FSCCT, FASE June 1 st, 2011 September 11, 2003 Family is asking $67 million in damages from two doctors Is it an aneurysm? Is it a dissection? What type of
Acute Aortic Syndromes
 Acute Aortic Syndromes Carole J. Dennie, MD Acute Thoracic Aortic Syndromes Background Non-Traumatic Acute Thoracic Aortic Syndromes Carole Dennie MD FRCPC Associate Professor of Radiology and Cardiology
Acute Aortic Syndromes Carole J. Dennie, MD Acute Thoracic Aortic Syndromes Background Non-Traumatic Acute Thoracic Aortic Syndromes Carole Dennie MD FRCPC Associate Professor of Radiology and Cardiology
Asymptomatic Radiology / Clinical data Report / Cohort bias Referral bias. UCSF Vascular Symposium April 7-9, Acute Aortic Dissection
 Aortic Dissection: Natural History What is the Natural History of Aortic Dissection? UCSF Vascular Symposium April 7-9, 2011 Asymptomatic Radiology / Clinical data Report / Cohort bias Referral bias Stephen
Aortic Dissection: Natural History What is the Natural History of Aortic Dissection? UCSF Vascular Symposium April 7-9, 2011 Asymptomatic Radiology / Clinical data Report / Cohort bias Referral bias Stephen
Follow-up of Aortic Dissection: How, How Often, Which Consequences Euro Echo 2011
 Follow-up of Aortic Dissection: How, How Often, Which Consequences Euro Echo 2011 Susan E. Wiegers, MD, FASE Director of Clinical Echocardiography Hospital of the University of Pennsylvania Disclosure
Follow-up of Aortic Dissection: How, How Often, Which Consequences Euro Echo 2011 Susan E. Wiegers, MD, FASE Director of Clinical Echocardiography Hospital of the University of Pennsylvania Disclosure
CT angiography in type I acute aortic dissection complicated with malperfusion - a visual review of obstruciton patterns
 CT angiography in type I acute aortic dissection complicated with malperfusion - a visual review of obstruciton patterns Eneva M. St. Ekaterna University Hospital Report objectives 1. Review malperfusion
CT angiography in type I acute aortic dissection complicated with malperfusion - a visual review of obstruciton patterns Eneva M. St. Ekaterna University Hospital Report objectives 1. Review malperfusion
CURRENT UNDERSTANDING: ANATOMY & PHYSIOLOGY TYPE B AORTIC DISSECTION ANATOMY ANATOMY. Medial degeneration characterized by
 DISCLOSURES CURRENT UNDERSTANDING: INDIVIDUAL None & PHYSIOLOGY TYPE B AORTIC DISSECTION INSTITUTIONAL Cook, Inc Not discussing off-label use of anything Medial degeneration characterized by Smooth muscle
DISCLOSURES CURRENT UNDERSTANDING: INDIVIDUAL None & PHYSIOLOGY TYPE B AORTIC DISSECTION INSTITUTIONAL Cook, Inc Not discussing off-label use of anything Medial degeneration characterized by Smooth muscle
Diseases of the aorta
 Diseases of the aorta Aneurysm, dissection and aortitis are the main pathologies (Fig. 18.79 ). data:text/html;charset=utf-8,%3ch2%20id%3d%22cc5a0836d6aa490ca26dd7c15632b559%22%20style%3d%22margin%3a%201.3em%200px%200.5em%3b%20padding%3a%200px%3b%20border%3a%200px%3b%20font-fa
Diseases of the aorta Aneurysm, dissection and aortitis are the main pathologies (Fig. 18.79 ). data:text/html;charset=utf-8,%3ch2%20id%3d%22cc5a0836d6aa490ca26dd7c15632b559%22%20style%3d%22margin%3a%201.3em%200px%200.5em%3b%20padding%3a%200px%3b%20border%3a%200px%3b%20font-fa
Aneurysms & a Brief Discussion on Embolism
 Aneurysms & a Brief Discussion on Embolism Aneurysms, overview = congenital or acquired dilations of blood vessels or the heart True aneurysms -involve all three layers of the artery (intima, media, and
Aneurysms & a Brief Discussion on Embolism Aneurysms, overview = congenital or acquired dilations of blood vessels or the heart True aneurysms -involve all three layers of the artery (intima, media, and
B myonephropathic metabolic syndrome MNMS 33 CT DeBakey IIIb MNMS
 13 603 607 2004 B B myonephropathic metabolic syndrome MNMS33 CT DeBakey IIIb MNMS 20 A MNMSMNMS 13 603 607 2004 MNMS B malperfusion myonephropathic metabolic syndrome MNMS MNMS Haimovici 1 3 MNMS B MNMS
13 603 607 2004 B B myonephropathic metabolic syndrome MNMS33 CT DeBakey IIIb MNMS 20 A MNMSMNMS 13 603 607 2004 MNMS B malperfusion myonephropathic metabolic syndrome MNMS MNMS Haimovici 1 3 MNMS B MNMS
Acute Type B dissection. Closure of the infra diaphragmatic tear: how and when?
 Acute Type B dissection. Closure of the infra diaphragmatic tear: how and when? Prof. Olgierd Rowiński II Department of Clinical Radiology Medical University of Warsaw Disclosure Speaker name: Olgierd
Acute Type B dissection. Closure of the infra diaphragmatic tear: how and when? Prof. Olgierd Rowiński II Department of Clinical Radiology Medical University of Warsaw Disclosure Speaker name: Olgierd
, David Stultz, MD. Aortic Dissection. David Stultz, MD October 7, 2003
 Aortic Dissection David Stultz, MD October 7, 2003 Background Incidence of 1 in 2000 in US Early mortality of 1%/hour for proximal dissection Two theories of formation Breach of intimal layer of aorta
Aortic Dissection David Stultz, MD October 7, 2003 Background Incidence of 1 in 2000 in US Early mortality of 1%/hour for proximal dissection Two theories of formation Breach of intimal layer of aorta
What Determines Aortic False Lumen Growth Post Dissection?
 Aortic Dissections What Determines Aortic False Lumen Growth Post Dissection? UCSF Vascular Symposium April 26, 2012 Most common aortic emergency Incidence of aortic dissections are 2/100,000 person-years
Aortic Dissections What Determines Aortic False Lumen Growth Post Dissection? UCSF Vascular Symposium April 26, 2012 Most common aortic emergency Incidence of aortic dissections are 2/100,000 person-years
Case Acute ascending thoracic aortic rupture due to penetrating atherosclerotic ulcer
 Case 12305 Acute ascending thoracic aortic rupture due to penetrating atherosclerotic ulcer Lopes Dias J, Costa NV, Leal C, Alves P, Bilhim T Section: Chest Imaging Published: 2014, Dec. 19 Patient: 68
Case 12305 Acute ascending thoracic aortic rupture due to penetrating atherosclerotic ulcer Lopes Dias J, Costa NV, Leal C, Alves P, Bilhim T Section: Chest Imaging Published: 2014, Dec. 19 Patient: 68
I-Hui Wu, M.D. Ph.D. Clinical Assistant Professor Cardiovascular Surgical Department National Taiwan University Hospital
 Comparisons of Aortic Remodeling and Outcomes after Endovascular Repair of Acute and Chronic Complicated Type B Aortic Dissections I-Hui Wu, M.D. Ph.D. Clinical Assistant Professor Cardiovascular Surgical
Comparisons of Aortic Remodeling and Outcomes after Endovascular Repair of Acute and Chronic Complicated Type B Aortic Dissections I-Hui Wu, M.D. Ph.D. Clinical Assistant Professor Cardiovascular Surgical
THORACIC AORTIC DISSECTION
 The Essence of Aortic Dissection THORACIC AORTIC DISSECTION Aortic dissection can be classified as acute if it s onset has been less than 14 days or chronic if its onset has been more than 14 days. Mortality
The Essence of Aortic Dissection THORACIC AORTIC DISSECTION Aortic dissection can be classified as acute if it s onset has been less than 14 days or chronic if its onset has been more than 14 days. Mortality
Optimal repair of acute aortic dissection
 Optimal repair of acute aortic dissection Dept. of Vascular Surgery, The 2nd Xiang-Yale Hospital, Central-South University, China Hunan Major Vessels Diseases Clinical Center Chang Shu Email:changshu01@yahoo.com
Optimal repair of acute aortic dissection Dept. of Vascular Surgery, The 2nd Xiang-Yale Hospital, Central-South University, China Hunan Major Vessels Diseases Clinical Center Chang Shu Email:changshu01@yahoo.com
Evolution of Thoracic Aortic Surgery A Rapidly Advancing Paradigm. October 15 th, 2014 Family Practice Evening Course University of Calgary
 Evolution of Thoracic Aortic Surgery A Rapidly Advancing Paradigm October 15 th, 2014 Family Practice Evening Course University of Calgary Jehangir Appoo Division of Cardiac Surgery Libin Cardiovascular
Evolution of Thoracic Aortic Surgery A Rapidly Advancing Paradigm October 15 th, 2014 Family Practice Evening Course University of Calgary Jehangir Appoo Division of Cardiac Surgery Libin Cardiovascular
Current Trends in. Torin P. Fitton, MD Division of Cardiothoracic Surgery Lahey Clinic NO DISCLOSURES. Aortic Syndromes
 Current Trends in Aortic Syndromes Torin P. Fitton, MD Division of Cardiothoracic Surgery Lahey Clinic NO DISCLOSURES Aortic Syndromes Aortic Aneurysm Aortic Dissection Intramural Hematoma (IMH) Penetrating
Current Trends in Aortic Syndromes Torin P. Fitton, MD Division of Cardiothoracic Surgery Lahey Clinic NO DISCLOSURES Aortic Syndromes Aortic Aneurysm Aortic Dissection Intramural Hematoma (IMH) Penetrating
AORTIC ANEURYSM. howmed.net
 AORTIC ANEURYSM howmed.net ANATOMY It is important to understand the anatomy of the aorta Need to know the extent of the aneurysm Need to know the vessels involved This helps with Medical or Surgical management
AORTIC ANEURYSM howmed.net ANATOMY It is important to understand the anatomy of the aorta Need to know the extent of the aneurysm Need to know the vessels involved This helps with Medical or Surgical management
Mohit Bhasin MD. Aortic Imaging and Follow-up
 Mohit Bhasin MD Aortic Imaging and Follow-up "There is no condition more conducive to clinical humility than aneurysm of the aorta. William Osler 55 yo F suddenly develops ventricular fibrillation Defibrillated
Mohit Bhasin MD Aortic Imaging and Follow-up "There is no condition more conducive to clinical humility than aneurysm of the aorta. William Osler 55 yo F suddenly develops ventricular fibrillation Defibrillated
Current treatment of Aortic Aneurysms and Dissections. Adam Keefer, MD, FACS Sean Hislop, MD, FACS
 Current treatment of Aortic Aneurysms and Dissections Adam Keefer, MD, FACS Sean Hislop, MD, FACS Patient 1 69 year old well-educated man with reoccurring pain in his upper abdomen and a pulsatile mass.
Current treatment of Aortic Aneurysms and Dissections Adam Keefer, MD, FACS Sean Hislop, MD, FACS Patient 1 69 year old well-educated man with reoccurring pain in his upper abdomen and a pulsatile mass.
Descending aorta replacement through median sternotomy
 Descending aorta replacement through median sternotomy Mitrev Z, Anguseva T, Belostotckij V, Hristov N. Special hospital for surgery Filip Vtori Skopje - Makedonija June, 2010 Cardiosurgery - Skopje 1
Descending aorta replacement through median sternotomy Mitrev Z, Anguseva T, Belostotckij V, Hristov N. Special hospital for surgery Filip Vtori Skopje - Makedonija June, 2010 Cardiosurgery - Skopje 1
Multimodality Imaging of the Thoracic Aorta
 Multimodality Imaging of the Thoracic Aorta Steven Goldstein MD, FACC Director Noninvasive Cardiology MedStar Heart and Vascular Institute Washington Hospital Center Saturday, October 8, 2016 DISCLOSURE
Multimodality Imaging of the Thoracic Aorta Steven Goldstein MD, FACC Director Noninvasive Cardiology MedStar Heart and Vascular Institute Washington Hospital Center Saturday, October 8, 2016 DISCLOSURE
Visceral aneurysm. Diagnosis and Interventions M.NEDEVSKA
 Visceral aneurysm Diagnosis and Interventions M.NEDEVSKA History 1953 De Bakeyand Cooley Visceral aneurysm VAAs rare, reported incidence of 0.01 to 0.2% on routine autopsies. Clinically important Potentially
Visceral aneurysm Diagnosis and Interventions M.NEDEVSKA History 1953 De Bakeyand Cooley Visceral aneurysm VAAs rare, reported incidence of 0.01 to 0.2% on routine autopsies. Clinically important Potentially
EVAR and TEVAR: Extending Their Use for Rupture and Traumatic Injury. Conflict of Interest. Hypotensive shock 5/5/2014. none
 EVAR and TEVAR: Extending Their Use for Rupture and Traumatic Injury Bruce H. Gray, DO MSVM FSCAI Professor of Surgery/Vascular Medicine USC SOM-Greenville Greenville, South Carolina none Conflict of Interest
EVAR and TEVAR: Extending Their Use for Rupture and Traumatic Injury Bruce H. Gray, DO MSVM FSCAI Professor of Surgery/Vascular Medicine USC SOM-Greenville Greenville, South Carolina none Conflict of Interest
Optimised management of type A aortic dissection with visceral malperfusion concept to reconsider
 Optimised management of type A aortic dissection with visceral malperfusion concept to reconsider Matthias Thielmann, MD, PhD, FAHA Thoracic and Cardiovascular Surgery, West-German Heart and Vascular Center
Optimised management of type A aortic dissection with visceral malperfusion concept to reconsider Matthias Thielmann, MD, PhD, FAHA Thoracic and Cardiovascular Surgery, West-German Heart and Vascular Center
Another pregnancy after a previous aortic dissection in pregnancy?
 Another pregnancy after a previous aortic dissection in pregnancy? Dr Leisa Freeman GUCH & Maternal Cardiology Unit Norfolk & Norwich University Hospital UK Arterial wall changes & haemodynamic effects
Another pregnancy after a previous aortic dissection in pregnancy? Dr Leisa Freeman GUCH & Maternal Cardiology Unit Norfolk & Norwich University Hospital UK Arterial wall changes & haemodynamic effects
Thoracic Aortic Aneurysm: Reading the Enemy s Playbook
 HOSPITAL CHRONICLES 2009, 4(1): 14 21 Review Thoracic Aortic Aneurysm: Reading the Enemy s Playbook John A. Elefteriades, MD A B S T R A C T Section of Cardiothoracic Surgery, Department of Surgery, Yale
HOSPITAL CHRONICLES 2009, 4(1): 14 21 Review Thoracic Aortic Aneurysm: Reading the Enemy s Playbook John A. Elefteriades, MD A B S T R A C T Section of Cardiothoracic Surgery, Department of Surgery, Yale
Open fenestration for complicated acute aortic B dissection
 Art of Operative Techniques Open fenestration for complicated acute aortic B dissection Santi Trimarchi 1, Sara Segreti 1, Viviana Grassi 1, Chiara Lomazzi 1, Marta Cova 1, Gabriele Piffaretti 2, Vincenzo
Art of Operative Techniques Open fenestration for complicated acute aortic B dissection Santi Trimarchi 1, Sara Segreti 1, Viviana Grassi 1, Chiara Lomazzi 1, Marta Cova 1, Gabriele Piffaretti 2, Vincenzo
2 nd International Meeting on Aortic Diseases Liege, Belgium September, 2010
 Bovine Aortic Arch Not a Benign Variant 2 nd International Meeting on Aortic Diseases Liege, Belgium September, 2010 John A. Elefteriades, MD William W.L. Glenn Professor and Chief, Section of Cardiac
Bovine Aortic Arch Not a Benign Variant 2 nd International Meeting on Aortic Diseases Liege, Belgium September, 2010 John A. Elefteriades, MD William W.L. Glenn Professor and Chief, Section of Cardiac
Neurological Complications of TEVAR. Frank J Criado, MD. Union Memorial-MedStar Health Baltimore, MD USA
 ISES Online Neurological Complications of Frank J Criado, MD TEVAR Union Memorial-MedStar Health Baltimore, MD USA frank.criado@medstar.net Paraplegia Incidence is 0-4% after surgical Rx of TAAs confined
ISES Online Neurological Complications of Frank J Criado, MD TEVAR Union Memorial-MedStar Health Baltimore, MD USA frank.criado@medstar.net Paraplegia Incidence is 0-4% after surgical Rx of TAAs confined
Abdominal Aortic Aneurysm - Part 1. Learning Objectives. Disclosure. University of Toronto Division of Vascular Surgery
 University of Toronto Division of Vascular Surgery Abdominal Aortic Aneurysm - Part 1 Dr Mark Wheatcroft & Dr Elisa Greco Vascular Surgeon, St Michael s Hospital, Toronto & University of Toronto Disclosure
University of Toronto Division of Vascular Surgery Abdominal Aortic Aneurysm - Part 1 Dr Mark Wheatcroft & Dr Elisa Greco Vascular Surgeon, St Michael s Hospital, Toronto & University of Toronto Disclosure
No Disclosure. Aortic Dissection in Japan. This. The Challenge of Acute and Chronic Type B Aortic Dissections with Endovascular Aortic Repair
 No Disclosure The Challenge of Acute and Chronic Type B Aortic Dissections with Endovascular Aortic Repair Toru Kuratani Department of Cardiovascular Surgery Osaka University Graduate School of Medicine,
No Disclosure The Challenge of Acute and Chronic Type B Aortic Dissections with Endovascular Aortic Repair Toru Kuratani Department of Cardiovascular Surgery Osaka University Graduate School of Medicine,
Percutaneous Approaches to Aortic Disease in 2018
 Percutaneous Approaches to Aortic Disease in 2018 Wendy Tsang, MD, SM Assistant Professor, University of Toronto Toronto General Hospital, University Health Network Case 78 year old F Lower CP and upper
Percutaneous Approaches to Aortic Disease in 2018 Wendy Tsang, MD, SM Assistant Professor, University of Toronto Toronto General Hospital, University Health Network Case 78 year old F Lower CP and upper
New ASE Guidelines: What you must know
 New ASE Guidelines: What you must know Federico M Asch MD, FASE, FACC Chair, ASE Guidelines and Standards Committee Medstar Washington Hospital Center Medstar Health Research Institute Georgetown University
New ASE Guidelines: What you must know Federico M Asch MD, FASE, FACC Chair, ASE Guidelines and Standards Committee Medstar Washington Hospital Center Medstar Health Research Institute Georgetown University
Familial Thoracic Aortic Aneurysms and Dissections Incidence, Modes of Inheritance, and Phenotypic Patterns
 Familial Thoracic Aortic Aneurysms and Dissections Incidence, Modes of Inheritance, and Phenotypic Patterns Gonzalo Albornoz, MD, Michael A. Coady, MD, Michele Roberts, MD, PhD, Ryan R. Davies, MD, Maryann
Familial Thoracic Aortic Aneurysms and Dissections Incidence, Modes of Inheritance, and Phenotypic Patterns Gonzalo Albornoz, MD, Michael A. Coady, MD, Michele Roberts, MD, PhD, Ryan R. Davies, MD, Maryann
Sports Participation in Patients with Inherited Diseases of the Aorta
 Sports Participation in Patients with Inherited Diseases of the Aorta Yonatan Buber, MD Adult Congenital Heart Service Leviev Heart Center Safra Childrens Hospital Disclosures None Patient Presentation
Sports Participation in Patients with Inherited Diseases of the Aorta Yonatan Buber, MD Adult Congenital Heart Service Leviev Heart Center Safra Childrens Hospital Disclosures None Patient Presentation
The Bicuspid Aortic Valve: New Frontiers in Genetics and Interventions
 The Bicuspid Aortic Valve: New Frontiers in Genetics and Interventions Westfälische Wilhelms-Universität Münster Helmut Baumgartner Adult Congenital and Valvular Heart Disease Center Dept. of Cardiology
The Bicuspid Aortic Valve: New Frontiers in Genetics and Interventions Westfälische Wilhelms-Universität Münster Helmut Baumgartner Adult Congenital and Valvular Heart Disease Center Dept. of Cardiology
The Petticoat Technique Managing Type B Dissection with both Early and Long Term Considerations
 The Petticoat Technique Managing Type B Dissection with both Early and Long Term Considerations Joseph V. Lombardi, MD Professor & Chief, Division of Vascular & Endovascular Surgery Department of Surgery,
The Petticoat Technique Managing Type B Dissection with both Early and Long Term Considerations Joseph V. Lombardi, MD Professor & Chief, Division of Vascular & Endovascular Surgery Department of Surgery,
Experience of endovascular procedures on abdominal and thoracic aorta in CA region
 Experience of endovascular procedures on abdominal and thoracic aorta in CA region May 14-15, 2015, Dubai Dr. Viktor Zemlyanskiy National Research Center of Emergency Care Astana, Kazakhstan Region Characteristics
Experience of endovascular procedures on abdominal and thoracic aorta in CA region May 14-15, 2015, Dubai Dr. Viktor Zemlyanskiy National Research Center of Emergency Care Astana, Kazakhstan Region Characteristics
Aortic Dissection in BAV Patients: The IRAD Experience and Beyond
 Aortic Dissection in BAV Patients: The IRAD Experience and Beyond Eduardo Bossone, MD, Ph.D, FESC, FACC Cardiology Division - Heart Dept. University of Salerno, Italy I have no financial relationships
Aortic Dissection in BAV Patients: The IRAD Experience and Beyond Eduardo Bossone, MD, Ph.D, FESC, FACC Cardiology Division - Heart Dept. University of Salerno, Italy I have no financial relationships
From Valve to Arch: How s Your Aorta? March 7, 2011
 From Valve to Arch: How s Your Aorta? March 7, 2011 Susan Housholder-Hughes, RN, MSN, ANP-BC, FAHA, AACC Nurse Practitioner, Multidisciplinary Aortic Program Cardiovascular Center Adjunct Clinical Instructor,
From Valve to Arch: How s Your Aorta? March 7, 2011 Susan Housholder-Hughes, RN, MSN, ANP-BC, FAHA, AACC Nurse Practitioner, Multidisciplinary Aortic Program Cardiovascular Center Adjunct Clinical Instructor,
Abdominal and thoracic aneurysm repair
 Abdominal and thoracic aneurysm repair William A. Gray MD Director, Endovascular Intervention Cardiovascular Research Foundation Columbia University Medical Center Abdominal Aortic Aneurysm Endografts
Abdominal and thoracic aneurysm repair William A. Gray MD Director, Endovascular Intervention Cardiovascular Research Foundation Columbia University Medical Center Abdominal Aortic Aneurysm Endografts
Endovascular Treatment of Malperfusion Syndrome
 Endovascular Treatment of Malperfusion Syndrome in Type B Aortic Dissection Department of Cardiology, Pusan National luniveristy i Hospital, Han Cheol Lee Endovascular Treatment Indication of Type B Aortic
Endovascular Treatment of Malperfusion Syndrome in Type B Aortic Dissection Department of Cardiology, Pusan National luniveristy i Hospital, Han Cheol Lee Endovascular Treatment Indication of Type B Aortic
Endovascular Management of Thoracic Aortic Pathology Stéphan Haulon, J Sobocinski, B Maurel, T Martin-Gonzalez, R Spear, A Hertault, R Azzaoui
 Endovascular Management of Thoracic Aortic Pathology Stéphan Haulon, J Sobocinski, B Maurel, T Martin-Gonzalez, R Spear, A Hertault, R Azzaoui Aortic Center, Lille University Hospital, France Disclosures
Endovascular Management of Thoracic Aortic Pathology Stéphan Haulon, J Sobocinski, B Maurel, T Martin-Gonzalez, R Spear, A Hertault, R Azzaoui Aortic Center, Lille University Hospital, France Disclosures
Animesh Rathore, MD 4/22/17. The Great Debate 45yo Man With Uncomplicated Acute TBAD: The Case For Medical Management
 Animesh Rathore, MD 4/22/17 The Great Debate 45yo Man With Uncomplicated Acute TBAD: The Case For Medical Management Disclosures Just a young vascular surgeon who would like to keep his job My opponent
Animesh Rathore, MD 4/22/17 The Great Debate 45yo Man With Uncomplicated Acute TBAD: The Case For Medical Management Disclosures Just a young vascular surgeon who would like to keep his job My opponent
UC SF An Algorithm to Choose Which Uncomplicated (Asymptomatic) Acute Type B Dissection Patients Should Undergo TEVAR. Disclosures.
 An Algorithm to Choose Which Uncomplicated (Asymptomatic) Acute Type B Dissection Patients Should Undergo TEVAR Disclosures Royalties and research grant support from Cook Medical, Inc. Jade S. Hiramoto,
An Algorithm to Choose Which Uncomplicated (Asymptomatic) Acute Type B Dissection Patients Should Undergo TEVAR Disclosures Royalties and research grant support from Cook Medical, Inc. Jade S. Hiramoto,
Total Endovascular Repair Type A Dissection. Eric Herget Interventional Radiology
 Total Endovascular Repair Type A Dissection Eric Herget Interventional Radiology 65 year old male Acute Type A Dissection Severe Aortic Regurgitation No co-morbidities Management? Part II Evolving Global
Total Endovascular Repair Type A Dissection Eric Herget Interventional Radiology 65 year old male Acute Type A Dissection Severe Aortic Regurgitation No co-morbidities Management? Part II Evolving Global
Acute Aortic Dissection: Decision and Outcome
 Acute Aortic Dissection: Decision and Outcome Marc R. Moon, M.D. John M. Shoenberg Chair in CV Disease Chief, Cardiac Surgery Director, Center for Diseases of the Thoracic Aorta Washington University School
Acute Aortic Dissection: Decision and Outcome Marc R. Moon, M.D. John M. Shoenberg Chair in CV Disease Chief, Cardiac Surgery Director, Center for Diseases of the Thoracic Aorta Washington University School
Total endovascular techniques utilization in aortic dissection radical treatment
 Total endovascular techniques utilization in aortic dissection radical treatment Chang Shu, MD, PhD Vascular Surgery Center National Center for Cardiovascular Diseases. Fuwai Hospital, CAMS & PUMC Beijing,
Total endovascular techniques utilization in aortic dissection radical treatment Chang Shu, MD, PhD Vascular Surgery Center National Center for Cardiovascular Diseases. Fuwai Hospital, CAMS & PUMC Beijing,
The Journal of Thoracic and Cardiovascular Surgery
 Accepted Manuscript Chronic type A dissection: when to operate? Francois Dagenais, MD PII: S0022-5223(18)33131-3 DOI: https://doi.org/10.1016/j.jtcvs.2018.11.032 Reference: YMTC 13781 To appear in: The
Accepted Manuscript Chronic type A dissection: when to operate? Francois Dagenais, MD PII: S0022-5223(18)33131-3 DOI: https://doi.org/10.1016/j.jtcvs.2018.11.032 Reference: YMTC 13781 To appear in: The
Subject: Endovascular Stent Grafts for Disorders of the Thoracic Aorta
 02-33000-29 Original Effective Date: 04/15/03 Reviewed: 07/26/18 Revised: 08/15/18 Subject: Endovascular Stent Grafts for Disorders of the Thoracic Aorta THIS MEDICAL COVERAGE GUIDELINE IS NOT AN AUTHORIZATION,
02-33000-29 Original Effective Date: 04/15/03 Reviewed: 07/26/18 Revised: 08/15/18 Subject: Endovascular Stent Grafts for Disorders of the Thoracic Aorta THIS MEDICAL COVERAGE GUIDELINE IS NOT AN AUTHORIZATION,
Do the Data Support Endovascular Therapy for Descending Thoracic AD? Woong Chol Kang, M.D.
 Do the Data Support Endovascular Therapy for Descending Thoracic AD? Woong Chol Kang, M.D. Gil Hospital, Gachon University Incheon, Korea Classification of AD Acute vs. Chronic (2weeks) (IIIa, b) type
Do the Data Support Endovascular Therapy for Descending Thoracic AD? Woong Chol Kang, M.D. Gil Hospital, Gachon University Incheon, Korea Classification of AD Acute vs. Chronic (2weeks) (IIIa, b) type
Case Report Anomalous Left Main Coronary Artery: Case Series of Different Courses and Literature Review
 Case Reports in Vascular Medicine Volume 2013, Article ID 380952, 5 pages http://dx.doi.org/10.1155/2013/380952 Case Report Anomalous Left Main Coronary Artery: Case Series of Different Courses and Literature
Case Reports in Vascular Medicine Volume 2013, Article ID 380952, 5 pages http://dx.doi.org/10.1155/2013/380952 Case Report Anomalous Left Main Coronary Artery: Case Series of Different Courses and Literature
ACUTE AORTIC SYNDROMES
 ACUTE AORTIC SYNDROMES AGNETA FLINCK MD, PhD Dept. of Thoracic Radiology Sahlgrenska University Hospital ACUTE AORTIC SYNDROMES Aortic dissection Intramural hematoma (IMH) 5-20% Penetrating atherosclerotic
ACUTE AORTIC SYNDROMES AGNETA FLINCK MD, PhD Dept. of Thoracic Radiology Sahlgrenska University Hospital ACUTE AORTIC SYNDROMES Aortic dissection Intramural hematoma (IMH) 5-20% Penetrating atherosclerotic
Midterm follow-up of penetrating ulcer and intramural hematoma of the aorta
 Midterm follow-up of penetrating ulcer and intramural hematoma of the aorta Shawn L. Tittle, MD a Raymond J. Lynch, BS a Patricia E. Cole, MD b Harsimran S. Singh, BS a John A. Rizzo, PhD c Gary S. Kopf,
Midterm follow-up of penetrating ulcer and intramural hematoma of the aorta Shawn L. Tittle, MD a Raymond J. Lynch, BS a Patricia E. Cole, MD b Harsimran S. Singh, BS a John A. Rizzo, PhD c Gary S. Kopf,
SUPPLEMENTAL MATERIAL
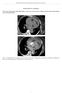 SUPPLEMENTL MTERIL Marie erna, Martin Kocher, Rohit Philip Thomas. cute aorta, overview of acute T findings and endovascular treatment options (doi: 10.5507/bp.2016.060) Fig. 1. : Non-enhanced T, hemopericardium
SUPPLEMENTL MTERIL Marie erna, Martin Kocher, Rohit Philip Thomas. cute aorta, overview of acute T findings and endovascular treatment options (doi: 10.5507/bp.2016.060) Fig. 1. : Non-enhanced T, hemopericardium
NON-ATHEROSCLEROTIC PATHOLOGY OF THE CAROTID ARTERIES
 NON-ATHEROSCLEROTIC PATHOLOGY OF THE CAROTID ARTERIES Leslie M. Scoutt, MD, FACR Professor of Diagnostic Radiology & Surgery Vice Chair, Dept of Radiology & Biomedical Imaging Chief, Ultrasound Section
NON-ATHEROSCLEROTIC PATHOLOGY OF THE CAROTID ARTERIES Leslie M. Scoutt, MD, FACR Professor of Diagnostic Radiology & Surgery Vice Chair, Dept of Radiology & Biomedical Imaging Chief, Ultrasound Section
La sindrome aortica acuta oggi
 University of Milan Thoracic Aortic Research Center La sindrome aortica acuta oggi Santi Trimarchi, MD, PhD Professore Associato di Chirurgia Vascolare, Università degli Studi di Milano Direttore, Divisione
University of Milan Thoracic Aortic Research Center La sindrome aortica acuta oggi Santi Trimarchi, MD, PhD Professore Associato di Chirurgia Vascolare, Università degli Studi di Milano Direttore, Divisione
The natural history of uncomplicated type B dissection, PAU and IMH: the IRAD knowledge. Santi Trimarchi, MD, PhD
 IRCCS Policlinico San Donato University of Milan Thoracic Aortic Research Center The natural history of uncomplicated type B dissection, PAU and IMH: the IRAD knowledge Santi Trimarchi, MD, PhD No COI
IRCCS Policlinico San Donato University of Milan Thoracic Aortic Research Center The natural history of uncomplicated type B dissection, PAU and IMH: the IRAD knowledge Santi Trimarchi, MD, PhD No COI
What Are the Current Guidelines for Treating Thoracic Aortic Disease?
 What Are the Current Guidelines for Treating Thoracic Aortic Disease? Eric M. Isselbacher, M.D. Director, MGH Healthcare Transformation Lab Co-Director, MGH Thoracic Aortic Center Associate Professor of
What Are the Current Guidelines for Treating Thoracic Aortic Disease? Eric M. Isselbacher, M.D. Director, MGH Healthcare Transformation Lab Co-Director, MGH Thoracic Aortic Center Associate Professor of
WHI Form Report of Cardiovascular Outcome Ver (For items 1-11, each question specifies mark one or mark all that apply.
 WHI Form - Report of Cardiovascular Outcome Ver. 6. COMMENTS To be completed by Physician Adjudicator Date Completed: - - (M/D/Y) Adjudicator Code: OMB# 095-044 Exp: 4/06 -Affix label here- Clinical Center/ID:
WHI Form - Report of Cardiovascular Outcome Ver. 6. COMMENTS To be completed by Physician Adjudicator Date Completed: - - (M/D/Y) Adjudicator Code: OMB# 095-044 Exp: 4/06 -Affix label here- Clinical Center/ID:
Aortic arch pathology. Cerebral ischemia following carotid artery stenosis.
 Important: -Subclavian Steal Syndrome -Cerebral ischemia Aortic arch pathology. Cerebral ischemia following carotid artery stenosis. Mina Aubeed & Alba Hernández Pinilla Aortic arch pathology Common arch
Important: -Subclavian Steal Syndrome -Cerebral ischemia Aortic arch pathology. Cerebral ischemia following carotid artery stenosis. Mina Aubeed & Alba Hernández Pinilla Aortic arch pathology Common arch
Acute dissections of the descending thoracic aorta (Debakey
 Endovascular Treatment of Acute Descending Thoracic Aortic Dissections Nimesh D. Desai, MD, PhD, and Joseph E. Bavaria, MD Acute dissections of the descending thoracic aorta (Debakey type III or Stanford
Endovascular Treatment of Acute Descending Thoracic Aortic Dissections Nimesh D. Desai, MD, PhD, and Joseph E. Bavaria, MD Acute dissections of the descending thoracic aorta (Debakey type III or Stanford
Multimodality Imaging in Aortic Diseases:
 Multimodality Imaging in Aortic Diseases: Federico M Asch MD, FASE, FACC Chair, ASE Guidelines and Standards Committee MedStar Washington Hospital Center MedStar Health Research Institute Georgetown University
Multimodality Imaging in Aortic Diseases: Federico M Asch MD, FASE, FACC Chair, ASE Guidelines and Standards Committee MedStar Washington Hospital Center MedStar Health Research Institute Georgetown University
Echocardiography as a diagnostic and management tool in medical emergencies
 Echocardiography as a diagnostic and management tool in medical emergencies Frank van der Heusen MD Department of Anesthesia and perioperative Care UCSF Medical Center Objective of this presentation Indications
Echocardiography as a diagnostic and management tool in medical emergencies Frank van der Heusen MD Department of Anesthesia and perioperative Care UCSF Medical Center Objective of this presentation Indications
Coronary artery Dissection. Dr TP Singh MD,DM
 Coronary artery Dissection Dr TP Singh MD,DM 52 M,Non HT, Non DM,Acute IWMI lysed within 4 hours D2 Coronary angiography RCA mid 90% discrete hazy stenosis LAD non significant ifi disease, LCx Normal Taken
Coronary artery Dissection Dr TP Singh MD,DM 52 M,Non HT, Non DM,Acute IWMI lysed within 4 hours D2 Coronary angiography RCA mid 90% discrete hazy stenosis LAD non significant ifi disease, LCx Normal Taken
Heart disease remains the leading cause of morbidity and mortality in industrialized nations. It accounts for nearly 40% of all deaths in the United
 Heart disease remains the leading cause of morbidity and mortality in industrialized nations. It accounts for nearly 40% of all deaths in the United States, totaling about 750,000 individuals annually
Heart disease remains the leading cause of morbidity and mortality in industrialized nations. It accounts for nearly 40% of all deaths in the United States, totaling about 750,000 individuals annually
Endovascular therapy for Ischemic versus Nonischemic complicated acute type B aortic dissection (catbad).
 Endovascular therapy for Ischemic versus Nonischemic complicated acute type B aortic dissection (catbad). AS. Eleshra, MD 1, T. Kölbel, MD, PhD 1, F. Rohlffs, MD 1, N. Tsilimparis, MD, PhD 1,2 Ahmed Eleshra
Endovascular therapy for Ischemic versus Nonischemic complicated acute type B aortic dissection (catbad). AS. Eleshra, MD 1, T. Kölbel, MD, PhD 1, F. Rohlffs, MD 1, N. Tsilimparis, MD, PhD 1,2 Ahmed Eleshra
A very short lecture.
 Medical Treatment of Type A Aortic Dissection: Tales of Turkeys, Tygon Tubing, and Evolving Paradigms The Houston Aortic Symposium April 4-6, 2008 John A. Elefteriades, MD William W.L. Glenn Professor
Medical Treatment of Type A Aortic Dissection: Tales of Turkeys, Tygon Tubing, and Evolving Paradigms The Houston Aortic Symposium April 4-6, 2008 John A. Elefteriades, MD William W.L. Glenn Professor
SURGICAL INTERVENTION IN AORTOPATHIES ZOHAIR ALHALEES, MD RIYADH, SAUDI ARABIA
 SURGICAL INTERVENTION IN AORTOPATHIES ZOHAIR ALHALEES, MD RIYADH, SAUDI ARABIA In patients born with CHD, dilatation of the aorta is a frequent feature at presentation and during follow up after surgical
SURGICAL INTERVENTION IN AORTOPATHIES ZOHAIR ALHALEES, MD RIYADH, SAUDI ARABIA In patients born with CHD, dilatation of the aorta is a frequent feature at presentation and during follow up after surgical
Complex Thoracic and Abdominal Aortic Repair Using Hybrid Techniques
 Complex Thoracic and Abdominal Aortic Repair Using Hybrid Techniques Tariq Almerey MD, January Moore BA, Houssam Farres MD, Richard Agnew MD, W. Andrew Oldenburg MD, Albert Hakaim MD Department of Vascular
Complex Thoracic and Abdominal Aortic Repair Using Hybrid Techniques Tariq Almerey MD, January Moore BA, Houssam Farres MD, Richard Agnew MD, W. Andrew Oldenburg MD, Albert Hakaim MD Department of Vascular
Early outcomes of acute retrograde dissection in the aortic arch and the ascending aorta data from IRAD
 Early outcomes of acute retrograde dissection in the aortic arch and the ascending aorta data from IRAD Foeke JH Nauta, MD, PhD Resident Cardiothoracic Surgery, Academic Medical Center, Amsterdam Disclosure
Early outcomes of acute retrograde dissection in the aortic arch and the ascending aorta data from IRAD Foeke JH Nauta, MD, PhD Resident Cardiothoracic Surgery, Academic Medical Center, Amsterdam Disclosure
Case 1. Aortic Disasters. Case 2. Case 3. Diagnosis, Imaging Techniques and Management
 Aortic Disasters Diagnosis, Imaging Techniques and Management Eric R. Snoey, MD Alameda County Medical Center Oakland, CA 1 Case 1 51 yo female presents with sharp anterior chest pain while at rest. She
Aortic Disasters Diagnosis, Imaging Techniques and Management Eric R. Snoey, MD Alameda County Medical Center Oakland, CA 1 Case 1 51 yo female presents with sharp anterior chest pain while at rest. She
TEVAR. (Thoracic Endovascular Aortic Repair) for Aneurysm and Dissection. Bruce Tjaden MD Vascular Surgery Fellow
 Department of Cardiothoracic & Vascular Surgery McGovern Medical School / The University of Texas Health Science Center at Houston TEVAR (Thoracic Endovascular Aortic Repair) for Aneurysm and Dissection
Department of Cardiothoracic & Vascular Surgery McGovern Medical School / The University of Texas Health Science Center at Houston TEVAR (Thoracic Endovascular Aortic Repair) for Aneurysm and Dissection
Natural History of a Dilated Ascending Aorta After Aortic Valve Replacement
 Circ J 2005; 69: 392 396 Natural History of a Dilated Ascending Aorta After Aortic Valve Replacement Katsuhiko Matsuyama, MD; Akihiko Usui, MD; Toshiaki Akita, MD; Masaharu Yoshikawa, MD; Masaomi Murayama,
Circ J 2005; 69: 392 396 Natural History of a Dilated Ascending Aorta After Aortic Valve Replacement Katsuhiko Matsuyama, MD; Akihiko Usui, MD; Toshiaki Akita, MD; Masaharu Yoshikawa, MD; Masaomi Murayama,
Advances in Treatment of Traumatic Aortic Transection
 Advances in Treatment of Traumatic Aortic Transection Himanshu J. Patel MD University of Michigan Medical Center Author Disclosures Consulting fees from WL Gore Inc. There is no disease more conducive
Advances in Treatment of Traumatic Aortic Transection Himanshu J. Patel MD University of Michigan Medical Center Author Disclosures Consulting fees from WL Gore Inc. There is no disease more conducive
THE BLOOD VESSELS. Manar hajeer, MD University of Jordan Faculty of medicine, pathology department.
 THE BLOOD VESSELS Manar hajeer, MD University of Jordan Faculty of medicine, pathology department. Vascular pathology: 1- Narrowing or complete obstruction of vessel lumina, either progressively (e.g.,
THE BLOOD VESSELS Manar hajeer, MD University of Jordan Faculty of medicine, pathology department. Vascular pathology: 1- Narrowing or complete obstruction of vessel lumina, either progressively (e.g.,
Acute Aortic Syndromes
 Acute Aortic Syndromes None Disclosures Smita Patel, M.B.B.S., M.R.C.P., F.R.C.R. Associate Professor, University of Michigan Ann Arbor, MI Objectives To review common CTA findings of acute aortic syndromes
Acute Aortic Syndromes None Disclosures Smita Patel, M.B.B.S., M.R.C.P., F.R.C.R. Associate Professor, University of Michigan Ann Arbor, MI Objectives To review common CTA findings of acute aortic syndromes
Treatment of acute type B aortic dissection: Current status
 MEET Cannes, 18. - 21.06.2009 Treatment of acute type B aortic dissection: Current status Christoph A. Nienaber, MD, FACC University of Rostock Department of Internal Medicine, Cardiology christoph.nienaber@med.uni-rostock.de
MEET Cannes, 18. - 21.06.2009 Treatment of acute type B aortic dissection: Current status Christoph A. Nienaber, MD, FACC University of Rostock Department of Internal Medicine, Cardiology christoph.nienaber@med.uni-rostock.de
Ischemic heart disease
 Ischemic heart disease Introduction In > 90% of cases: the cause is: reduced coronary blood flow secondary to: obstructive atherosclerotic vascular disease so most of the time it is called: coronary artery
Ischemic heart disease Introduction In > 90% of cases: the cause is: reduced coronary blood flow secondary to: obstructive atherosclerotic vascular disease so most of the time it is called: coronary artery
Malperfusion Syndromes Type B Aortic Dissection with Malperfusion
 Malperfusion Syndromes Type B Aortic Dissection with Malperfusion Jade S. Hiramoto, MD, MAS April 27, 2012 Associated with early mortality Occurs when there is end organ ischemia secondary to aortic branch
Malperfusion Syndromes Type B Aortic Dissection with Malperfusion Jade S. Hiramoto, MD, MAS April 27, 2012 Associated with early mortality Occurs when there is end organ ischemia secondary to aortic branch
