INTERMEDIATE-TERM FOLLOW-UP RESULTS OF TRANSCATHETER CLOSURE OF VENTRICULAR SEPTAL DEFECT USING AMPLATZER DEVICE VERSUS NIT-OCCLUD LÊ VSD COIL SYSTEM
|
|
|
- Lindsay Poole
- 5 years ago
- Views:
Transcription
1 INTERMEDIATE-TERM FOLLOW-UP RESULTS OF TRANSCATHETER CLOSURE OF VENTRICULAR SEPTAL DEFECT USING AMPLATZER DEVICE VERSUS NIT-OCCLUD LÊ VSD COIL SYSTEM Kritvikrom Durongpisitkul 1, Paweena Chungsomprasong 1, Pornthip Panjasamarnwong 2, Suphalak Darunaitorn 3, Prakul Chanthong 1, Chodchanok Vijarnsorn 1, and Jarupim Soongswang 1 1 Division of Cardiology, Department of Pediatrics, Faculty of Medicine Siriraj Hospital, Mahidol University, Bangkok; 2 Pediatric Clinic, Siriraj Piyamaharajkarun Hospital, Bangkok; 3 Division of Pediatric Nursing, Department of Nursing, Faculty of Medicine Siriraj Hospital, Mahidol University, Bangkok, Thailand Abstract. Transcatheter ventricular septal defect (VSD) is an alternative method of VSD closure, especially in perimembranous (PmVSD) type and doubly committed subarterial (DCSA) type VSD. The aim of this retrospective study was to review and report intermediate-term (up to 5-years) results of transcatheter closure of VSD in patients who received Amplatzer device (device) or Nit- Occlud Lê VSD Coil System (coil). Of 247 patients who underwent transcatheter closure during the 2003 to 2015 study period, there were 240 (97.1%) successful procedures (187 device, 53 coil). Of the 240 included patients, 115 were male and 125 were female, and the median (range) age and weight were 12 years (range: 1-67) and 40.3 kg (range: 10-97), respectively. Median VSD size in the device group was larger than that of the coil group. [7 mm (range: 3-18) vs 5 mm (range: ); p<0.001]. Complete closure was comparable between groups. Sixty-nine (26%) of all patients had DCSA VSD. Twenty-six patients (49.1%) had DCSA VSD in the coil group, while only 43 patients (23%) had DCSA VSD in the device group. Although pre-closure aortic regurgitation (AR) was comparable between groups (22.9% vs 32%; p=0.448), AR was significantly higher in the coil group than in device group (p<0.001). When comparing VSD types, post-procedure AR was higher in DCSA VSD than in PmVSD (p=0.001). At the end of the 5-year follow-up, 98.6% of DCSA VSD had less than mild AR. Closure rates were comparable between closure methods for both PmVSD and DCSA VSD. The progression of AR was higher in DCSA VSD patients, but a majority of those patients had less than mild AR at end of 5 years. Key words: Ventricular Septal Defect, VSD, Amplatzer Device, Nit-Occlud Lê VSD Spiral Coil System INTRODUCTION Correspondence: Kritvikrom Durongpisitkul, MD, Division of Cardiology, Department of Pediatrics, Faculty of Medicine Siriraj Hospital, Mahidol University, 2 Wanglang Road, Bangkok Noi, Bangkok 10700, Thailand. Tel: +66 (0) ; Fax +66 (0) kritvikrom.dur@mahidol.ac.th Ventricular septal defect (VSD) is one of the most common congenital heart defects that is treated by surgical closure in Thailand (Sakornpant and Kojaranjit, 2011; Ratanasit et al, 2015). Several long-term complications of isolated VSD, including endocarditis and aortic regurgitation (AR), are well-recognized (Jortveit et al, 2016; Vol. 48 (Supplement 2)
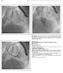
2 Southeast Asian J Trop Med Public Health Karonis et al, 2016). Transcatheter VSD closures have been performed at Siriraj Hospital since 2003 (Durongpisitkul et al, 2003). In 2011, we reported the initial success of transcatheter closure of VSD in 109 patients. Seventy-six patients were in the Amplatzer group (62 patients received the Amplatzer membranous device and 14 patients received the Amplatzer muscular device) and 33 patients were in the Nit-Occlud Lê VSD Coil group (Pfm coil), with a median follow-up duration of 8 months (6-76) (Chungsomprasong et al, 2011). However, longer-term follow-up evaluation of the extent of post-ar closure for both perimembranous VSD (PmVSD) and doubly committed subarterial (DCSA) VSD is an ongoing topic of interest among those who perform and study transcatheter closure of VSD (Tomita et al, 2004; Tomita et al, 2005; Chen et al, 2015b; Sanoussi et al, 2015; Amano et al, 2016). Accordingly, the aim of this retrospective study was to review and report intermediateterm (up to 5-years) results of transcatheter closure of VSD in patients who received Amplatzer device (device) or Nit-Occlud Lê VSD Coil System (coil). MATERIALS AND METHODS This retrospective study reviewed the medical charts of 240 patients that underwent transcatheter closure with either Amplatzer device or Nit-Occlud Lê VSD Coil System at Siriraj Hospital during the 2003 to 2015 study period. The protocol for this study was approved by the Siriraj Institutional Review Board (SIRB), Faculty of Medicine Siriraj Hospital, Mahidol University, Bangkok, Thailand (approval no. 584/2013). Indications for transcatheter closure of VSD included one or more of the following: (1) hemodynamic data indicative of left to right shunt Fig 1 Left ventriculography in steep left anterior oblique view (up to 90 degrees) shows delineation of VSD border of DCSA VSD. 50 Vol. 48 (Supplement 2) 2017
3 Transcatheter Closure of Ventricular Septal Defect by echocardiography or cardiac catheterization (Qp:Qs >1.5); (2) clinical signs and symptoms of heart failure; (3) evidence of left side chamber enlargement by echocardiography; (4) prolapsed coronary cusp with trivial to mild AR (Figs 1-2); (5) risk of prolapsed coronary cusp with right coronary cusp deformity index >0.3 or right coronary cusp imbalance index >1.3 (Tomita et al, 2004), or prolapse of non-coronary cusp (Tomita et al, 2005); and/or, (6) the size of the defect is not larger than the size of the available devices. Procedure A complete description of the procedure along with device selection was previously reported in detail (Durongpisitkul et al, 2003; Chungsomprasong et al, 2011). Briefly, all procedures were performed under general anesthesia with prophylactic antibiotics. All aortic valve prolapses and pre-closure AR were documented using transesophageal echocardiography (TEE). Complete right and left cardiac catheterization was performed. Left ventricular angiogram was performed to define the location and size of the defect. In cases of DCSA VSD, a steep LAO view (up to 90 degrees) was preferred due to delineation of the VSD border (Fig 1). Judkins Right catheter, LIMA, or Benston catheter were used for VSD engagement. In some cases the catheter curve was reshaped to facilitate passage into VSD tunnel. A complete arteriovenous loop of glide wire was performed. The delivery sheath (TorqueVue ; St. Jude Medical, St. Paul, MN) was inserted through the femoral vein and advanced along the wire to the Judkins Right catheter using the kissing technique into the right atrium, the right ventricle, and then through the VSD until the sheath reached the Fig 2 Left ventriculogram in steep left anterior oblique view shows Amplatzer Muscular VSD device (undersized by 1-2 mm) deployed with left ventricular disc open and at a position just below the prolapsed aortic cusp to avoid injury. Vol. 48 (Supplement 2)
4 Southeast Asian J Trop Med Public Health ascending aorta. The opposing Judkins Right catheter was advanced to push the tip of the sheath into the left ventricle apex. In some cases (particularly DCSA VSD cases), if access to the left ventricle apex could not be obtained, then the device or coil would be deployed via the ascending aorta. All Pfm coils were deployed via the ascending aorta. We selected the device size using measurements from both echocardiographic and angiographic methods. The original recommendation for selection of Amplatzer membranous VSD device size was to calculate the size from the square root of the longest diameter multiplied by the shortest diameter. However and given that the Amplatzer muscular VSD device is a symmetrical disc device, we generally choose a device size that is 1 mm less than or equal to the largest defect diameter. In DCSA VSD cases, we found that the superior border of the defect could not be well-delineated in some cases. In these cases, we intentionally started with an undersized Amplatzer muscular device to avoid injuring the aortic cusp, with the left ventricular disc positioned below the prolapsed aortic cusp (Fig 2). In 2006, the Nit-Occlud Lê VSD Spiral Coil System was introduced at our center. This system was used in patients that had PmVSD with aneurysm and an opening less than 6-8 mm. After 2008, the Nit-Occlud Lê VSD Coil was also adopted for use in patients with DSCA VSD (Fig 3). Patients were observed for catheter-related complications during the post-catheterization period. Infective endocarditis prophylaxis and antiplatelet dosage of aspirin were given for at least 6 months after successful procedure or until the defect was completely occluded. Statistical analysis Data analysis was performed using SPSS Sta- Fig 3 Steep left anterior oblique projection shows Nit-Occlud Lê VSD Coil System positioned in a doubly committed subaortic ventricular septal defect. Part of the left ventricular loop coil is open in the left ventricle, and the reversed loop coil is open in the right ventricle. 52 Vol. 48 (Supplement 2) 2017
5 Transcatheter Closure of Ventricular Septal Defect tistics version 20 (IBM, Armonk, NY). Chi-square test, independent t-test, or Mann-Whitney U test were used to compare the Amplatzer device group and the Pfm coil group. Nominal variables are reported as frequency or percentage, and continuous variables are presented as mean ± standard deviation if normally distributed and as median and range of non-normally distributed. Categorical data are reported as percentage (%). For all analyses, a p-value <0.05 was regarded as being statistically significant. RESULTS Transcatheter VSD closure was successfully performed in 240 of 247 patients (97.1%) dur- Table 1 Comparison of demographic, clinical, and hemodynamic characteristics between the Amplatzer device group and the Nit-Occlud Lê VSD Coil (Pfm coil) group. Amplatzer device (n=187) Pfm coil (n=53) p-value Age (yrs), median (range) 14 (1-67) 1 (1-29) <0.001 Weight (kg), median (range) 44 ( ) 26.6 ( ) <0.001 Height (cm), median (range) 151 (80-186) 129 (81-180) Gender (M:F) 88:99 27: VSD size (mm), median (range) 7 (3-18) 5 ( ) <0.001 VSD type, % Pm 57.8% 39.6% Pm with inlet extension/aneurysm 10.7% 11.3% DCSA 23.0% 49.1% Muscular 4.8% 0% Post-surgical repair 3.7% 0% Hemodynamic data, mean±sd Mean AO pressure (mmhg) 82±15 75± Mean PA pressure (mmhg) 22±7 20± Qp:Qs 1.75± ± Pulmonary arteriolar resistance (units m 2 ) 1.6± ± Flu time (min), mean±sd 22.4± ± Procedure time (min), mean±sd 81.8± ± LOS (days), mean±sd 1.7± ± A p-value<0.05 indicates statistical significance. VSD, ventricular septal defect; Pm, perimembranous; DCSA, doubly committed subarterial; AO, aortic pressure; PA, pulmonary arterial pressure; Qp:Qs, pulmonary blood flow : systemic blood flow; LOS, length of stay; SD, standard deviation. Vol. 48 (Supplement 2)
6 Southeast Asian J Trop Med Public Health ing the 2003 to 2015 study period. The procedure was unsuccessful in seven patients due to transient atrioventricular block during crossing of VSD in 2 patients, inability to engage VSD in 1 patient, and worsening of AR after deployment of device/coil in 4 patients. There were 215 isolated VSD patients. Twenty-five patients (10.4%) had comorbidity that required an additional procedure, such as device closure for atrial septal defect or PDA, or balloon valvuloplasty of pulmonary valve stenosis. Of 240 patients who had complete closure, there were 129 PmVSD, 25 Pm with extension to inlet or aneurysm, 69 DCSA (outlet) VSD, 9 muscular VSD, 1 inlet VSD, and 7 patch leakage VSD (5 from tetralogy of Fallot and 2 from complete atrioventricular septal defect). The average follow-up period was 49.5±42.9 months (median: 39.7). Residual shunt and AR were reported at intervals of 24 hours, one month, six months, one year, and five years. More than 70% of patients were followed-up for at least 5 years. Of 240 patients, 187 were in the Amplatzer device group (114 Amplatzer Muscular VSD device, 67 Amplatzer Membranous VSD device, 6 Amplatzer Duct Occluder, and 2 Amplatzer Duct Occluder II) (device group) and 53 were in the Nit-Occlud Lê VSD Coil group (coil group). Demographic, clinical, hemodynamic, and immediate procedural data are presented in Table 1. Patients in the device group were significantly older than patients in the coil group [median: 14 years (range: 1-67) vs 1 year (1-29); (p<0.001)]. Device group patients weighed more than coil group patients [median: 44 kg ( ) vs 26.6 kg ( ); p<0.001]. The median diameter of VSD was larger in the device group than in coil group [7 mm (3-18) vs 5 mm ( ); p<0.001]. There were no statistically significant differences in hemodynamic data during cardiac catheterization between groups, with the exception of high mean aortic blood pressure in the device group. Regarding VSD type, 57.8% of device group patients and 39.6% of coil group patients had PmVSD, whereas 23.0% of device group patients and 49.1% of coil group patients had DCSA VSD (p=004). Immediate procedure-related complications (Table 2) Of 240 patients who had successful procedure, VSD device or coil embolization were found in five patients in device group three patients in coil group. All devices were successfully retrieved and a larger sized device was deployed. Two of three cases in the coil group were replaced with an Amplatzer device, and the other was replaced with a larger Nit-Occlud Lê VSD Coil. Other immediate Table 2 Comparison of complications between the Amplatzer device group and the Nit-Occlud Lê VSD Coil (Pfm coil) group. Complications, n Amplatzer device (n=187) Pfm coil (n=53) p-value Embolization Hemolysis Blood transfusion Arterial occlusion Death A p-value<0.05 indicates statistical significance. 54 Vol. 48 (Supplement 2) 2017
7 Transcatheter Closure of Ventricular Septal Defect procedure-related complications are shown in Table 2. One patient who had Amplatzer perimembranous VSD device with residual shunt after closure developed hemolysis that required surgical removal of the device on day 5 postcatheterization. All other complications were resolved within a few days after the procedure. The one patient who died in this study had residual shunt from repair of tetralogy of Fallot and complete atrioventricular septal defect. The patient had severe pulmonary hypertension and residual VSD after surgical closure. The patient underwent transcatheter closure of the residual VSD and later developed severe pulmonary hypertension and hemorrhage within 48 hours, and died at 14 days after admission. Residual shunt Residual shunt was classified at trivial, small, or larger than moderate. At the 24-hour followup time point, patients in the device group had 19.8% trivial shunt, 0.5% small shunt, and 1.1% larger than moderate shunt, as compared to 20.8% trivial shunt, 0.0% small shunt, and Table 3 Comparison of residual shunt between the Amplatzer device group and the Nit-Occlud Lê VSD Coil (Pfm coil) group. Amplatzer device (n=187) Pfm coil (n=53) p-value Residual shunt at first day post-procedure, % Trivial Small Larger than moderate Residual shunt at 1-month post-procedure, % Trivial Small Larger than moderate Residual shunt at 6-months post-procedure, % Trivial Small Larger than moderate Residual shunt at 1-year post-procedure, % Trivial Small Larger than moderate Residual shunt at 5-years post-procedure, % Trivial Small Larger than moderate A p-value <0.05 indicates statistical significance. Vol. 48 (Supplement 2)
8 Southeast Asian J Trop Med Public Health 0.0% larger than moderate shunt in the coil group (p=0.832) (Table 3). Degree of residual shunt was not significantly different between groups at any follow-up time point. We found one patient in the device group (inlet with large multiple opening of VSD aneurysm) that improved from larger than moderate shunt to trivial shunt. One patient with DCSA VSD in the coil group had shunt progression that required a second procedure using an Amplatzer Muscular VSD device. Effect on bundle branch, atrioventricular block, and pacemaker implantation (Table 4) Pre- and post-procedure electrocardiogram (ECG) results were collected from both groups. We found that 12.2% of patients in the device group had right bundle branch block (RBBB), as compared to no patients in the coil group. Moreover, all RBBB appeared only in PmVSD patients. Post-procedure ECG showed new RBBB in 10 patients in the device group, as compared to 2 patients in the coil group (p=0.014). Five patients developed complete atrioventricular block (CAVB) within two weeks post-procedure (3 Amplatzer Membranous VSD device, 1 Amplatzer Muscular VSD device, and 1 Nit- Occlud Lê VSD Coil). One patient who received an Amplatzer Membranous VSD device (patient number 95; device year 2009) developed CAVB at one month. No CAVB was reported after the one-month time point. Three of five CAVB patients received hydrocortisone treatment, and CAVB was resolved in 2 of those 3 patients (one Amplatzer Membranous VSD device and one Nit-Occlud Lê VSD Coil). In total, four patients received permanent pace maker implantation (3 Amplatzer Membranous VSD device and 1 Amplatzer Muscular VSD device). Aortic regurgitation (AR) The severities of aortic regurgitation were classified as none, mild, moderate and severe according to European Association of Echocardiography (Lancellotti et al, 2010) as shown in Fig 4. Aortic valve prolapse (AVP) was found to be significantly lower in the device group than in the coil group (32.6% vs 50.9%; p=0.015), the Table 4 Comparison of ECG finding between the Amplatzer device group and the Nit-Occlud Lê VSD Coil (Pfm coil) group (N=214). Amplatzer device (n=164) Pfm coil (n=50) p-value RBBB, n (%) Pre-closure RBBB 20 (12.2) 0 (0) 0.01 Post-closure RBBB 30 (18.2) 1 (2) New-onset RBBB, n (%) 10 (6.1) 1 (2) Rhythm after closure, n (%) Normal sinus rhythm 170 (90.9) 52 (98.1) st degree AVB 10 (5.3) 0 (0) 2 nd degree AVB 2 (1.1) 0 (0) 3 rd degree AVB 5 (2.6) 1 (2) Permanent pacemaker, n (%) 4 (2.1) 0 (0) A p-value<0.05 indicates statistical significance. RBBB, right bundle branch block; AVB, atrioventricular block. 56 Vol. 48 (Supplement 2) 2017
9 Transcatheter Closure of Ventricular Septal Defect A B Fig 4 Post-Amplatzer VSD device closure, echocardiography demonstrate mild and moderate aortic regurgitation (Fig A and B, respectively). frequency of pre-procedure AR was comparable between the device group and the coil group for both trivial to mild (17% vs 24.5%) and moderate to severe (5.9% vs 7.5 %) (p=0.448). Regarding post-procedure degree of AR, progressive AR was significantly higher in the coil group than in the device group at every follow-up time point (Table 5). Worsening of AR, defined as change in degree of AR to the next level of severity, was found in 7 of 187 (3.7%) device group patients and in 11 of 53 (20.7%) coil group patients (p=0.191). Comparison between perimembranous VSD (PmVSD) and doubly committed subarterial VSD (DCSA VSD) groups (Tables 6, 7) Given the ongoing interest in the effectiveness of transcatheter closure between perimembranous VSD (PmVSD) and doubly committed subarterial (DCSA) VSD among those who perform and study transcatheter closure of VSD, we divided patients into the PmVSD group (including PmVSD with some extension into the muscle, and PmVSD with or without aneurysm or mus- Vol. 48 (Supplement 2)
10 Southeast Asian J Trop Med Public Health Table 5 Comparison of aortic regurgitation (AR) between the Amplatzer device group and the Nit-Occlud Lê VSD Coil (Pfm coil) group relative to pre-closure aortic valve prolapse, pre-closure AR, and postclosure. Amplatzer device (n=187) Pfm coil (n=53) p=value Pre-aortic valve prolapse, % Pre-closure AR, % None Trivial to mild Moderate to severe Post-procedure AR at 24 hours, % None Trivial to mild Moderate to severe Post-procedure AR at 1 month, % None Trivial to mild Moderate to severe Post-procedure AR at 6 months, % None Trivial to mild Moderate to severe Post-procedure AR at 1 year, % None Trivial to mild Moderate to severe Post-procedure AR at 5 years, % None Trivial to mild Moderate to severe Worsening AR, n (%) 7 (3.7) 11 (20.7) A p-value<0.05 indicates statistical significance. 58 Vol. 48 (Supplement 2) 2017
11 Transcatheter Closure of Ventricular Septal Defect cular defect) and DCSA VSD (outlet) type VSD group. After exclusion of 7 patch leakage VSD patients in our study, there were 233 patients, with 164 in the PmVSD group and 69 in the DCSA VSD group. The hemodynamic characteristics of both groups were comparable (Table 6). We found the mean defect size to be larger in the PmVSD group than in the DCSA VSD group (7.1±2.6 mm vs 5.6±1.8 mm; p=0.001). The devices used in each group were different (Table 6). Among patients with PmVSD, a larger number of Amplatzer devices was used than Nit-Occlud Lê VSD Coils (137 vs 27); however, more coils were used than devices in patients with DCSA VSD (43 vs 26; p=0.001). Degree of residual shunt was classified as trivial, small, or moderate. Residual shunt classification results at each time point between the PmVSD and Table 6 Comparison of demographic, clinical, and hemodynamic characteristics between perimembranous ventricular septal defect (PmVSD) group and doubly committed subaortic ventricular septal defect (DCSA VSD) group. Characteristics PmVSD (n=164) DCSA VSD (n=69) p-value Demographic Age (yrs), median (range) 12.5 (1-67) 12 (1-54) Weight (kg), median (range) 40.4 ( ) 37 ( ) Height (cm), median (range) (80-186) 147 (85-182) Gender (M:F) 88:99 27: VSD size (mm), median (range) 8 (2-20) 8 (4-16) <0.001 VSD device, n (%) Amplatzer device 137 (83.5) 43 (62.3) Pfm coil 27 (16.5) 26 (37.7) Hemodynamic data, mean±sd Mean AO (mmhg) 81±15 80± Mean PA (mmhg) 21±7 20± Qp:Qs 1.8± ± Pulmonary arteriolar resistance (units m 2 ) 1.6± ± Flu time (min), mean±sd 21.8± ± Procedure time (min), mean±sd 81.2± ± LOS (days), mean±sd 1.8± ± A p-value<0.05 indicates statistical significance. Pfm coil, Nit-Occlud Lê VSD Coil System; VSD, ventricular septal defect; Pm, perimembranous; DCSA, doubly committed subarterial; AO, aortic pressure; PA, pulmonary arterial pressure; Qp:Qs, pulmonary blood flow:systemic blood flow; LOS, length of stay; SD, standard deviation. Vol. 48 (Supplement 2)
12 Southeast Asian J Trop Med Public Health Table 7 Comparison of degree of aortic regurgitation (AR) between perimembranous ventricular septal defect (PmVSD) group and doubly committed subaortic ventricular septal defect (DCSA VSD) group. PmVSD (n=163) DCSA VSD (n=69) p-value Pre-aortic valve prolapse, % <0.001 Pre-closure AR, % None <0.001 Trivial to mild Moderate to severe Post-procedure AR at 24 hrs, % None <0.001 Trivial to mild Moderate to severe Post-procedure AR at 1 month, % None <0.001 Trivial to mild Moderate to severe Post-procedure AR at 6 months, % None <0.001 Trivial to mild Moderate to severe Post-procedure AR at 1 year, % None <0.001 Trivial to mild Moderate to severe Post-procedure AR at 5 years, % None <0.001 Trivial to mild Moderate to severe Worsening AR, n (%) 15/124 (9.1) 8/69 (11.6) <0.001 A p-value<0.05 indicates statistical significance. 60 Vol. 48 (Supplement 2) 2017
13 Transcatheter Closure of Ventricular Septal Defect DCSA groups were, as follows: 24 hours (19.0%, 0%, 0.6% vs 17.4%, 0%, 1.4%; p=0.792); 1 month (11.0%, 0%, 0% vs 15.9%, 0%, 1.4%; p=0.172); 6 months (11.0%, 0%, 0.6% vs 10.1%, 4.3%, 1.4%; p=0.198); 1 year (11.7%, 0%, 0% vs 11.6%, 0.9%, 2.9%; p=0.08); and, 5 years (12.9%, 0%, 0% vs 10.5%, 1.8%, 1.8%; p=0.235). Residual shunt findings were comparable between VSD types. Predictably, the degree of post-closure AR was significantly higher in the DCSA VSD group than in the PmVSD at any duration of follow-up (p<0.001). We observed a trend towards less progression of AR in the PmVSD group than in the DCSA VSD group at the 1-year follow-up time point (%AR trivial to mild 15.9% and 0.6% moderate to severe in the PmVSD group vs %AR 47.8% trivial to mild and 1.4% moderate to severe in the DCSA VSD group). Progression of AR was observed in 15 of 164 (9.1%) PmVSD patients and in 8 of 69 (11.6%) DCSA VSD patients (p<0.001) (Table 7). DISCUSSION We reported the intermediate-term follow-up results of transcatheter closure of VSD in 240 patients, with a success rate of 97.1%. Patients were divided into the Amplatzer device group (device group) and the Nit-Occlud Lê VSD Coil group (coil group). Mean VSD size in the device group was larger than in the coil group. One hundred thirty-seven devices and 27 coils were used to treat patients with PmVSD, and 43 devices and 26 coils were used to repair defects in patients with DCSA VSD (p=0.001). The one patient who died in this study had residual shunt from repair of tetralogy of Fallot with complete atrioventricular defect and died from complications of pulmonary hemorrhage two weeks after closure. Progressive post-procedure AR was higher in DCSA VSD than in PmVSD. In 2014, a systemic review entitled A systematic review on the efficacy and safety of transcatheter device closure of ventricular septal defects (VSD) reported that, from 37 publications and 4,406 patients, the pooled success rate of transcatheter closure in VSD was 96.6% (Yang et al, 2014), which was comparable to the 97.1% success rate found in our study. Regarding immediate residual shunt at 24 hours post-procedure, residual shunt rates were 19.8% trivial, 0.5% small, and 1.1% moderate for the device and 20.8% trivial, 0.0% small, and 0.0% moderate for the coil. Our rates were lower than the 25.5% (95% CI: ) pooled rate from the aforementioned meta-analysis group (Yang et al, 2014). At the 5-year follow-up time point, percentages of residual shunt were lower in both groups, as follows: 11.6% trivial, 0.8% small, and 0.8% moderate in the device group and 14.6% trivial, 0.0% small, and 0.0% moderate in the coil group. The percentage of residual shunt was comparable between the PmVSD and DCSA VSD groups. When transcatheter closure of VSD was first performed, CAVB could develop up to several years after the procedure was performed (Yip et al, 2005; Sullivan, 2007; Song et al, 2009). Pm- VSD defects were occluded using the Amplatzer Membranous VSD Occluder with good results during the early period (Hijazi et al, 2002; Durongpisitkul et al, 2003; Fu et al, 2006). However, we stopped using the Amplatzer Membranous VSD Occluder in 2008 after reports of CAVB started being published. One of the suspected causes of CAVB when using the Amplatzer Membranous VSD Occluder centered on its narrow 2 mm waist and an attempt to oversize the device in order to achieve a stable straddle position (Liu et al, 2004; Yip et al, 2005 Sullivan, 2007; Song et al, 2009; Kloecker et al, 2010; Erdem et al, 2012). We found the Amplatzer Muscular VSD device with a symmetrical disc and longer waist to be associated with less chance of oversizing and it allowed us to avoid force injuring the conducting system along the VSD anatomy. This allowed us to use undersize device by 1-2 mm when compare to largest defect diameter. Our initial results showed that only 4 Vol. 48 (Supplement 2)
14 Southeast Asian J Trop Med Public Health of 116 patients (3.4%) received a permanent pacemaker as a result of CAVB 3 from Amplatzer Membranous VSD device and 1 from oversizing of Amplatzer Muscular VSD device during the early years after the procedure was adopted. No patients have developed CAVB at our center since In the meta-analysis study by Yang, et al (2014), 85.3% of PmVSD type cases were closed, as compared to 53.4% in our study, and Amplatzer device or Nit-Occlud Lê VSD Coil were used in both studies. Forty-two percent of our patients (69 patients) were DCSA VSD, which was much higher than the proportion in most of the studies in the meta-analysis. Progressive AR in DCSA, even after surgical VSD closure, is a well-known long-term potential complication (Layangool et al, 2008; Menting et al, 2015; Sanoussi et al, 2015; Amano et al, 2016; Jortveit et al, 2016). Incidence of late AR progression among patients after repair of subpulmonic infundibular VSD was unexpectedly high at 7.7% (Amano et al, 2016; Rahmath et al, 2016). One study reported no difference in degree of AR after closure (Egbe et al, 2015). Our study found pre-closure AR to be comparable between the device and the coil (22.9% vs 32%; p=0.448). After closure, we found AR to be lower in the device than in the coil at 24 hours (24.1% vs 39.6%; p=0.025), 1 month (22.4% vs 40.4%; p=0.029), 6 months (23.1% vs 39.6%; p=0.048), 1 year (22.4% vs 41.5%; p=0.019), and at 5 years (23% vs 41.5%; p=0.024). In addition, there were 11 patients in the coil group and 7 patients in the device group (p=0.191) that had progressive AR after 5 years of follow-up. Patients with PmVSD had a lower proportion of pre-closure AR than patients with DCSA VSD (14.1% vs 50.7%; p<0.001). This trend was observed at each of the follow-up time points, as follows: 24 hours (14.7% vs 55.1%; p<0.01), 1 month (15.9% vs 47.8%; p<0.001, 6 months (16.5% vs 53.3%; p<0.001), 1 year (16.5% vs 47.8%; p=0.019), and 5 years (16.5% vs 49.2%; p<0.001). Our study found a higher proportion of AR than the pooled rate reported in the systemic review by Yang et al (2014). of 2.0% (95% CI: ). This difference between studies may have been due to a higher proportion of DCSA VSD or perhaps for double disc device design of VSD device. However, longer term follow-up may be needed to reveal the progression of aortic regurgitation. The Nit-Occlud Lê VSD coil was introduced in This system can be considered for closure in selected cases of DCSA VSD with less than mild AR. In this study, we encountered several instances in which the coil became trapped in the aortic valve while pulling from the aorta to the left ventricular outflow tract (LVOT) in patients with DCSA VSD. Over time and after developing a better understanding of patient anatomy in certain cases of DCSA VSD with only trivial AR and prolapsed AV with right coronary cusp deformity index close to 0.3 (Tomita et al, 2004) (protrudes less than 3 mm into the LVOT), we elected to use an Amplatzer Muscular VSD device that was slightly smaller (1-2 mm) than the defect in order to avoid injuring the AV. In contrast to the previous believe that a device may always cause injury to the aortic valve, we believed that a undersize device size (1-2 mm smaller than the defect size) of symmetrical disc Amplatzer Muscular VSD Occluder may safely deployed while avoiding injury to aortic valve similar to other devices that are used for DCSA VSD (Fu et al, 2006; Qin et al, 2008; Lertsapcharoen et al, 2013; Chen et al, 2015a; Chen et al, 2015b; Ghaderian et al, 2015; Tutar et al, 2015). Our study found that 98.6% of DCSA VSD patients had either no AR or trivial to mild AR at the 5-year follow-up. We found only 1 moderate AR DCSA VSD patient. That patient was in the Amplatzer device group and had progressed from mild to moderate AR. Based on these findings, we believe that both PmVSD and DCSA VSD with only trivial AR can be closed 62 Vol. 48 (Supplement 2) 2017
15 Transcatheter Closure of Ventricular Septal Defect using transcatheter method. In conclusion, transcatheter closure of VSD in both PmVSD and DCSA VSD can be achieved by using either the Amplatzer Device or the Nit-Occlud Lê VSD Spiral Coil System, with comparable closure rates between systems. The progression of AR was higher in DCSA VSD patients, but a majority of those patients had less than mild AR at end of 5 years. CONFLICTS OF INTEREST The authors hereby declare no personal or professional conflicts of interest regarding any aspect of this study. REFERENCES Amano M, Izumi C, Imamura S, et al. Progression of aortic regurgitation after subpulmonic infundibular ventricular septal defect repair. Heart 2016; 102: Chen F, Li P, Liu S, et al. Transcatheter closure of intracristal ventricular septal defect with mild aortic cusp prolapse using zero eccentricity ventricular septal defect occluder. Circ J 2015a; 79: Chen GL, Li HT, Li HR, Zhang ZW. Transcatheter closure of ventricular septal defect in patients with aortic valve prolapse and mild aortic regurgitation: feasibility and preliminary outcome. Asian Pac J Trop Med 2015b; 8: Chungsomprasong P, Durongpisitkul K, Vijarnsorn C, Soongswang J, Lê TP. The results of transcatheter closure of VSD using Amplatzer device and Nit Occlud Lê VSD coil. Catheter Cardiovasc Interv 2011; 78: Durongpisitkul K, Soongswang J, Laohaprasitiporn D, Nana A, Nutakul T. Transcatheter closure of perimembranous ventricular septal defect with immediate follow-up. J Med Assoc Thai 2003; 86: Egbe AC, Poterucha JT, Dearani JA, Warnes CA. Supracristal ventricular septal defect in adults: is it time for a paradigm shift? Int J Cardiol 2015; 198: Erdem S, Kizlltas A, Kucukosmanoglu O, Ozbarlas N. Temporary atrioventricular complete block that develops following the transcatheter closure of ventricular septal defect. Turk J Pediatr 2012; 54: Fu YC, Bass J, Amin Z, et al. Transcatheter closure of perimembranous ventricular septal defects using the new amplatzer membranous VSD occluder: results of the U.S. Phase i Trial. J Am Coll Cardiol 2006; 47: Ghaderian M, Merajie M, Mortezaeian H, Aarabi M, Mohammad Y, Shah Mohammadi A. Efficacy and safety of using amplatzer ductal occluder for transcatheter closure of perimembranous ventricular septal defect in pediatrics. Iran J Pediatr 2015; 25: e386. Hijazi ZM, Hakim F, Haweleh AA, et al. Catheter closure of perimembranous ventricular septal defects using the new Amplatzer membranous VSD occluder: initial clinical experience. Catheter Cardiovasc Interv 2002; 56: Jortveit J, Leirgul E, Eskedal L, et al. Mortality and complications in 3495 children with isolated ventricular septal defects. Arch Dis Child 2016; 101: Karonis T, Scognamiglio G, Babu-Narayan SV, et al. Clinical course and potential complications of small ventricular septal defects in adulthood: late development of left ventricular dysfunction justifies lifelong care. Int J Cardiol 2016; 208: Kloecker L, Emmel M, Sreeram N. Late complete left bundle branch block after transcatheter closure of a muscular ventricular septal defect. Cardiol Young 2010; 20: Lancellotti P, Tribouilloy C, Hagendorff A, et al. Vol. 48 (Supplement 2)
16 Southeast Asian J Trop Med Public Health European Association of Echocardiography recommendations for the assessment of valvular regurgitation. Part 1: aortic and pulmonary regurgitation (native valve disease). Eur J Echocardiogr 2010; 11: Layangool T, Kirawittaya T, Sangtawesin C, et al. Natural aortic valve complications of ventricular septal defect: a prospective cohort study. J Med Assoc Thai 2008; 91 (Suppl 3): S53-9. Lertsapcharoen P, Srimahachota S, Charoonrut P. Transcatheter ventricular septal defect closure with a new nanoplatinum-coated nitinol device in a swine model. J Invasive Cardiol 2013; 25: Liu TL, Wang YL, Wang Y, et al. [Hemolysis and transient complete atrioventricular block after transcatheter closure of ventricular septal defect]. Zhonghua Er Ke Za Zhi 2004; 42: 871. Menting ME, Cuypers JA, Opic P, et al. The unnatural history of the ventricular septal defect: outcome up to 40 years after surgical closure. J Am Coll Cardiol 2015; 65: Qin Y, Chen J, Zhao X, et al. Transcatheter closure of perimembranous ventricular septal defect using a modified double-disk occluder. Am J Cardiol 2008; 101: Rahmath MR, Numan M, Dilawar M. Medium to long-term echo follow-up after ventricular septal defect device closure. Asian Cardiovasc Thorac Ann 2016; 24: Ratanasit N, Karaketklang K, Jakrapanichakul D, et al. Prevalence and echocardiographic characteristics of common congenital heart disease in adult patients at Siriraj Hospital: 10- year study. J Med Assoc Thai 2015; 98: Sakornpant P, Kojaranjit V. First National Adult Cardiac Surgical Database Report: Demonstrating practice of adult cardiac surgery in Thailand: measuring performance and outcome. Bangkok: The Society of Thoracie Surgeons of Thailand, Sanoussi A, Demanet H, Dessy H, et al. Managing ventricular septal defect with associated aortic regurgitation: two decades of experience. J Heart Valve Dis 2015; 24: Song ZY, Li YH, Chai H, et al. [Prognostic impact of heart block during transcatheter closure of ventricular septal defect]. Zhonghua Xin Xue Guan Bing Za Zhi 2009; 37: Sullivan ID. Transcatheter closure of perimembranous ventricular septal defect: Is the risk of heart block too high a price? Heart 2007; 93: Tomita H, Arakaki Y, Ono Y, Yamada O, Yagihara T, Echigo S. Severity indices of right coronary cusp prolapse and aortic regurgitation complicating ventricular septal defect in the outlet septum: which defect should be closed? Circ J 2004; 68: Tomita H, Arakaki Y, Ono Y, Yamada O, Yagihara T, Echigo S. Impact of noncoronary cusp prolapse in addition to right coronary cusp prolapse in patients with a perimembranous ventricular septal defect. Int J Cardiol 2005; 101: Tutar E, Ramoglu M, Ciftci O, Ucar T, Altin T. Transcatheter ventricular septal defect closure: should we feel comfortable after many years? Anatol J Cardiol 2015; 15: Yang L, Tai BC, Khin LW, Quek SC. A systematic review on the efficacy and safety of transcatheter device closure of ventricular septal defects (VSD). J Interv Cardiol 2014; 27: Yip WC, Zimmerman F, Hijazi ZM. Heart block and empirical therapy after transcatheter closure of perimembranous ventricular septal defect. Catheter Cardiovasc Interv 2005; 66: Vol. 48 (Supplement 2) 2017
Percutaneous VSD closure
 Percutaneous VSD closure Gianfranco Butera San Donato Milanese - Italy Patients selection Pts having hemodynamically significant VSD Left ventricular enlargement (left ventricular overload),defined as
Percutaneous VSD closure Gianfranco Butera San Donato Milanese - Italy Patients selection Pts having hemodynamically significant VSD Left ventricular enlargement (left ventricular overload),defined as
Type Size AP/PS RP/RS Qp/Qs. Ia Resistive <0.3 < Ib Resistive <0.3 < IIa Resistive <0.5 >2
 Transcatheter closure of VSD using Duct Occluder device Nguyen Lan Hieu, MD, PhD Hanoi Medical University Vietnam Heart Institute Anatomy of VSD 1. Perimembranous VSD: Aneurysm septal membranous(tv or
Transcatheter closure of VSD using Duct Occluder device Nguyen Lan Hieu, MD, PhD Hanoi Medical University Vietnam Heart Institute Anatomy of VSD 1. Perimembranous VSD: Aneurysm septal membranous(tv or
Perimembranous VSD: When Do We Ask For A Surgical Closure? LI Xin. Department of Cardiothoracic Surgery Queen Mary Hospital Hong Kong
 Perimembranous VSD: When Do We Ask For A Surgical Closure? LI Xin Department of Cardiothoracic Surgery Queen Mary Hospital Hong Kong Classification (by Kirklin) I. Subarterial (10%) Outlet, conal, supracristal,
Perimembranous VSD: When Do We Ask For A Surgical Closure? LI Xin Department of Cardiothoracic Surgery Queen Mary Hospital Hong Kong Classification (by Kirklin) I. Subarterial (10%) Outlet, conal, supracristal,
Giovanni Di Salvo MD, PhD, FESC Second University of Naples Monaldi Hospital
 Giovanni Di Salvo MD, PhD, FESC Second University of Naples Monaldi Hospital VSD is one of the most common congenital cardiac abnormalities in the newborn. It can occur as an isolated finding or in combination
Giovanni Di Salvo MD, PhD, FESC Second University of Naples Monaldi Hospital VSD is one of the most common congenital cardiac abnormalities in the newborn. It can occur as an isolated finding or in combination
Percutaneous VSD closure: Problems in the mid- and long-term
 Percutaneous VSD closure: Problems in the mid- and long-term Lee Benson MD Professor Pediatrics (Cardiology) Director, Cardiac Diagnostic & Interventional Unit The Hospital for Sick Children Toronto, Canada
Percutaneous VSD closure: Problems in the mid- and long-term Lee Benson MD Professor Pediatrics (Cardiology) Director, Cardiac Diagnostic & Interventional Unit The Hospital for Sick Children Toronto, Canada
Jian Fang 1, Shaobo Xie 2, Lunchao Ma 2, Chao Yang 2. Original Article
 Original Article Anatomic and surgical factors affecting the switch from minimally invasive transthoracic occlusion to open surgery during ventricular septal defect repair Jian Fang 1, Shaobo Xie 2, Lunchao
Original Article Anatomic and surgical factors affecting the switch from minimally invasive transthoracic occlusion to open surgery during ventricular septal defect repair Jian Fang 1, Shaobo Xie 2, Lunchao
Perimembranous ventricular septal defects (pmvsds) are
 Transcatheter Closure of Congenital Perimembranous Ventricular Septal Defect in Children Using Symmetric Occluders: An 8-Year Multiinstitutional Experience Lei Wang, MD, PhD,* Sancheng Cao, MD, Jun Li,
Transcatheter Closure of Congenital Perimembranous Ventricular Septal Defect in Children Using Symmetric Occluders: An 8-Year Multiinstitutional Experience Lei Wang, MD, PhD,* Sancheng Cao, MD, Jun Li,
Hybrid Muscular VSD Closure in Small Weight Children
 Hybrid Muscular VSD Closure in Small Weight Children Shakeel A Qureshi, on behalf of: John P. Cheatham, MD George H. Dunlap Endowed Chair in Interventional Cardiology Director Cardiac Catheterization &
Hybrid Muscular VSD Closure in Small Weight Children Shakeel A Qureshi, on behalf of: John P. Cheatham, MD George H. Dunlap Endowed Chair in Interventional Cardiology Director Cardiac Catheterization &
For Personal Use. Copyright HMP 2013
 Case Report J INVASIVE CARDIOL 2013;25(2):E42-E44 Percutaneous Closure of Iatrogenic Ventricular Septal Defect Following Surgical Aortic Valve Replacement Using Two Different Approaches Takashi Matsumoto,
Case Report J INVASIVE CARDIOL 2013;25(2):E42-E44 Percutaneous Closure of Iatrogenic Ventricular Septal Defect Following Surgical Aortic Valve Replacement Using Two Different Approaches Takashi Matsumoto,
CONGENITAL HEART DEFECTS IN ADULTS
 CONGENITAL HEART DEFECTS IN ADULTS THE ROLE OF CATHETER INTERVENTIONS Mario Carminati CONGENITAL HEART DEFECTS IN ADULTS CHD in natural history CHD with post-surgical sequelae PULMONARY VALVE STENOSIS
CONGENITAL HEART DEFECTS IN ADULTS THE ROLE OF CATHETER INTERVENTIONS Mario Carminati CONGENITAL HEART DEFECTS IN ADULTS CHD in natural history CHD with post-surgical sequelae PULMONARY VALVE STENOSIS
5.8 Congenital Heart Disease
 5.8 Congenital Heart Disease Congenital heart diseases (CHD) refer to structural or functional heart diseases, which are present at birth. Some of these lesions may be discovered later. prevalence of Chd
5.8 Congenital Heart Disease Congenital heart diseases (CHD) refer to structural or functional heart diseases, which are present at birth. Some of these lesions may be discovered later. prevalence of Chd
Efficacy and Safety of Using Amplatzer Ductal Occluder for Transcatheter Closure of Perimembranous Ventricular Septal Defect in Pediatrics
 Iran J Pediatr. 2015 April; 25(2):e386. Published online 2015 April 18. DOI: 10.5812/ijp.386 Research Article Efficacy and Safety of Using Amplatzer Ductal Occluder for Transcatheter Closure of Perimembranous
Iran J Pediatr. 2015 April; 25(2):e386. Published online 2015 April 18. DOI: 10.5812/ijp.386 Research Article Efficacy and Safety of Using Amplatzer Ductal Occluder for Transcatheter Closure of Perimembranous
Transcatheter closure of the patent ductus arteriosus using the new Amplatzer duct occluder: Initial clinical applications in children
 Transcatheter closure of the patent ductus arteriosus using the new Amplatzer duct occluder: Initial clinical applications in children Basil Thanopoulos, MD, PhD, a Nikolaos Eleftherakis, MD, a Konstantinos
Transcatheter closure of the patent ductus arteriosus using the new Amplatzer duct occluder: Initial clinical applications in children Basil Thanopoulos, MD, PhD, a Nikolaos Eleftherakis, MD, a Konstantinos
Risk Factors and Outcomes of Post-Procedure Heart Blocks After Transcatheter Device Closure of Perimembranous Ventricular Septal Defect
 JACC: CARDIOVASCULAR INTERVENTIONS VOL. 5, NO. 4, 2012 2012 BY THE AMERICAN COLLEGE OF CARDIOLOGY FOUNDATION ISSN 1936-8798/$36.00 PUBLISHED BY ELSEVIER INC. DOI: 10.1016/j.jcin.2012.01.015 Risk Factors
JACC: CARDIOVASCULAR INTERVENTIONS VOL. 5, NO. 4, 2012 2012 BY THE AMERICAN COLLEGE OF CARDIOLOGY FOUNDATION ISSN 1936-8798/$36.00 PUBLISHED BY ELSEVIER INC. DOI: 10.1016/j.jcin.2012.01.015 Risk Factors
Follow-up after VSD closure- what to look for?
 The 3rd Congress of Congenital heart disease Ventricular Septal Defect from A-Z January 9-11. 2013, Ho Chi Minh City, Vietnam Follow-up after VSD closure- what to look for? Nina Wunderlich University Hospital
The 3rd Congress of Congenital heart disease Ventricular Septal Defect from A-Z January 9-11. 2013, Ho Chi Minh City, Vietnam Follow-up after VSD closure- what to look for? Nina Wunderlich University Hospital
INTEGRATING ECHOCARDIOGRAPHY WITH CATHETER INTERVENTIONS FOR CONGENITAL HEART DISEASE. Krishna Kumar SevenHills Hospital, Mumbai, India
 INTEGRATING ECHOCARDIOGRAPHY WITH CATHETER INTERVENTIONS FOR CONGENITAL HEART DISEASE Krishna Kumar SevenHills Hospital, Mumbai, India Why talk about it? What is the big deal? Are we not stating the obvious?
INTEGRATING ECHOCARDIOGRAPHY WITH CATHETER INTERVENTIONS FOR CONGENITAL HEART DISEASE Krishna Kumar SevenHills Hospital, Mumbai, India Why talk about it? What is the big deal? Are we not stating the obvious?
IMAGES. in PAEDIATRIC CARDIOLOGY. Abstract
 IMAGES in PAEDIATRIC CARDIOLOGY Images Paediatr Cardiol. 2008 Apr-Jun; 10(2): 11 17. PMCID: PMC3232589 Transcatheter closure of symptomatic aortopulmonary window in an infant F Pillekamp, 1 T Hannes, 1
IMAGES in PAEDIATRIC CARDIOLOGY Images Paediatr Cardiol. 2008 Apr-Jun; 10(2): 11 17. PMCID: PMC3232589 Transcatheter closure of symptomatic aortopulmonary window in an infant F Pillekamp, 1 T Hannes, 1
Percutaneous atrial septal defect closure with the Occlutech Figulla Flex ASD Occluder.
 Percutaneous atrial septal defect closure with the Occlutech Figulla Flex ASD Occluder. First case with a novel delivery system. Werner Budts, Md, PhD, FESC Congenital and Structural Cardiology University
Percutaneous atrial septal defect closure with the Occlutech Figulla Flex ASD Occluder. First case with a novel delivery system. Werner Budts, Md, PhD, FESC Congenital and Structural Cardiology University
TCTAP C-217 Bilateral Pulmonary Arterio Venus Fistula Managed by Vascular Plugs and Coil Manotosh Panja 1 1 BelleVue Clinic, India
 S450 JOURNAL OF THE AMERICAN COLLEGE OF CARDIOLOGY, VOL. 65, NO. 17, SUPPL S, 2015 Case Summary. Aneurysm at LVOT is a rare complication after Bentall operation and the aneurysm may increase in size. In
S450 JOURNAL OF THE AMERICAN COLLEGE OF CARDIOLOGY, VOL. 65, NO. 17, SUPPL S, 2015 Case Summary. Aneurysm at LVOT is a rare complication after Bentall operation and the aneurysm may increase in size. In
Case submission for CSI Asia-Pacific Case 2
 Case submission for CSI Asia-Pacific 2018- Case 2 Title Page Case category: Coarctation and ducts, valves Title: Simultaneous balloon aortic valvuloplasty with transcatheter closure of large hypertensive
Case submission for CSI Asia-Pacific 2018- Case 2 Title Page Case category: Coarctation and ducts, valves Title: Simultaneous balloon aortic valvuloplasty with transcatheter closure of large hypertensive
Imaging Evaluation of the Ventricular Septum
 Imaging Evaluation of the Ventricular Septum Craig E Fleishman, MD FACC FASE The Heart Center at Arnold Palmer Hospital for Children, Orlando SCAI Fall Fellows Course 2013 Las Vegas Disclosure Information
Imaging Evaluation of the Ventricular Septum Craig E Fleishman, MD FACC FASE The Heart Center at Arnold Palmer Hospital for Children, Orlando SCAI Fall Fellows Course 2013 Las Vegas Disclosure Information
Implantation of Cardioverter Defibrillator After Percutaneous Closure of Atrial Septal Defect
 The Ochsner Journal 10:27 31, 2010 f Academic Division of Ochsner Clinic Foundation Implantation of Cardioverter Defibrillator After Percutaneous Closure of Atrial Septal Defect Anas Bitar, MD, Maria Malaya
The Ochsner Journal 10:27 31, 2010 f Academic Division of Ochsner Clinic Foundation Implantation of Cardioverter Defibrillator After Percutaneous Closure of Atrial Septal Defect Anas Bitar, MD, Maria Malaya
Index. cardiology.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A ACHD. See Adult congenital heart disease (ACHD) Adult congenital heart disease (ACHD), 503 512 across life span prevalence of, 504 506
Index Note: Page numbers of article titles are in boldface type. A ACHD. See Adult congenital heart disease (ACHD) Adult congenital heart disease (ACHD), 503 512 across life span prevalence of, 504 506
ECHOCARDIOGRAPHIC APPROACH TO CONGENITAL HEART DISEASE: THE UNOPERATED ADULT
 ECHOCARDIOGRAPHIC APPROACH TO CONGENITAL HEART DISEASE: THE UNOPERATED ADULT Karen Stout, MD, FACC Divisions of Cardiology University of Washington Medical Center Seattle Children s Hospital NO DISCLOSURES
ECHOCARDIOGRAPHIC APPROACH TO CONGENITAL HEART DISEASE: THE UNOPERATED ADULT Karen Stout, MD, FACC Divisions of Cardiology University of Washington Medical Center Seattle Children s Hospital NO DISCLOSURES
Atrial Septal Defect Closure. Stephen Brecker Director, Cardiac Catheterisation Labs
 Stephen Brecker Director, Cardiac Catheterisation Labs ADVANCED ANGIOPLASTY Incorporating The Left Main 5 Plus Course Conflicts of Interest The following companies have supported educational courses held
Stephen Brecker Director, Cardiac Catheterisation Labs ADVANCED ANGIOPLASTY Incorporating The Left Main 5 Plus Course Conflicts of Interest The following companies have supported educational courses held
Patient guide: pfm Nit-Occlud PDA coil occlusion system. Catheter occlusion of. Patent Ductus Arteriosus. with the
 Patient guide: Catheter occlusion of Patent Ductus Arteriosus with the pfm Nit-Occlud PDA coil occlusion system pfm Produkte für die Medizin - AG Wankelstr. 60 D - 50996 Cologne Phone: +49 (0) 2236 96
Patient guide: Catheter occlusion of Patent Ductus Arteriosus with the pfm Nit-Occlud PDA coil occlusion system pfm Produkte für die Medizin - AG Wankelstr. 60 D - 50996 Cologne Phone: +49 (0) 2236 96
IMAGES. in PAEDIATRIC CARDIOLOGY
 IMAGES in PAEDIATRIC CARDIOLOGY Images Paediatr Cardiol. 2005 Jan-Mar; 7(1): 12 17. PMCID: PMC3232568 Stent implantation for coarctation facilitated by the anterograde trans-septal approach N Sreeram and
IMAGES in PAEDIATRIC CARDIOLOGY Images Paediatr Cardiol. 2005 Jan-Mar; 7(1): 12 17. PMCID: PMC3232568 Stent implantation for coarctation facilitated by the anterograde trans-septal approach N Sreeram and
Perventricular Closure of Muscular VSD s
 Perventricular Closure of Muscular VSD s Dr Damien Kenny, MB, MD Assistant Professor of Pediatrics Director of the Cardiac Catheterization Hybrid Suite Co-Director of the Rush Adult Congenital Heart Disease
Perventricular Closure of Muscular VSD s Dr Damien Kenny, MB, MD Assistant Professor of Pediatrics Director of the Cardiac Catheterization Hybrid Suite Co-Director of the Rush Adult Congenital Heart Disease
Case 47 Clinical Presentation
 93 Case 47 C Clinical Presentation 45-year-old man presents with chest pain and new onset of a murmur. Echocardiography shows severe aortic insufficiency. 94 RadCases Cardiac Imaging Imaging Findings C
93 Case 47 C Clinical Presentation 45-year-old man presents with chest pain and new onset of a murmur. Echocardiography shows severe aortic insufficiency. 94 RadCases Cardiac Imaging Imaging Findings C
CMR for Congenital Heart Disease
 CMR for Congenital Heart Disease * Second-line tool after TTE * Strengths of CMR : tissue characterisation, comprehensive access and coverage, relatively accurate measurements of biventricular function/
CMR for Congenital Heart Disease * Second-line tool after TTE * Strengths of CMR : tissue characterisation, comprehensive access and coverage, relatively accurate measurements of biventricular function/
Transcatheter Closure of Atrial Septal Defects with Superior-anterior Rim Deficiency Using Amplatzer Septal Occluder
 ORIGINAL ARTICLE Transcatheter Closure of Atrial Septal Defects with Superior-anterior Rim Deficiency Using Amplatzer Septal Occluder Chien-Fu Huang, 1 Chih-Yuan Fang, 2 Sheung-Fat Ko, 3 Shao-Ju Chien,
ORIGINAL ARTICLE Transcatheter Closure of Atrial Septal Defects with Superior-anterior Rim Deficiency Using Amplatzer Septal Occluder Chien-Fu Huang, 1 Chih-Yuan Fang, 2 Sheung-Fat Ko, 3 Shao-Ju Chien,
ΔΙΑΧΕΙΡΙΣΗ ΑΣΘΕΝΩΝ ΜΕ ΜΕΣΟΚΟΛΠΙΚΗ ΕΠΙΚΟΙΝΩΝΙΑ ΖΑΧΑΡΑΚΗ ΑΓΓΕΛΙΚΗ ΚΑΡΔΙΟΛΟΓΟΣ ΗΡΑΚΛΕΙΟ - ΚΡΗΤΗ
 ΔΙΑΧΕΙΡΙΣΗ ΑΣΘΕΝΩΝ ΜΕ ΜΕΣΟΚΟΛΠΙΚΗ ΕΠΙΚΟΙΝΩΝΙΑ ΖΑΧΑΡΑΚΗ ΑΓΓΕΛΙΚΗ ΚΑΡΔΙΟΛΟΓΟΣ ΗΡΑΚΛΕΙΟ - ΚΡΗΤΗ European Accreditation in TTE, TEE and CHD Echocardiography NOTHING TO DECLARE ATRIAL SEPTAL DEFECT TYPES SECUNDUM
ΔΙΑΧΕΙΡΙΣΗ ΑΣΘΕΝΩΝ ΜΕ ΜΕΣΟΚΟΛΠΙΚΗ ΕΠΙΚΟΙΝΩΝΙΑ ΖΑΧΑΡΑΚΗ ΑΓΓΕΛΙΚΗ ΚΑΡΔΙΟΛΟΓΟΣ ΗΡΑΚΛΕΙΟ - ΚΡΗΤΗ European Accreditation in TTE, TEE and CHD Echocardiography NOTHING TO DECLARE ATRIAL SEPTAL DEFECT TYPES SECUNDUM
ADULT CONGENITAL HEART DISEASE. Stuart Lilley
 ADULT CONGENITAL HEART DISEASE Stuart Lilley More adults than children have congenital heart disease Huge variety of congenital lesions from minor to major Heart failure, re-operation and arrhythmia are
ADULT CONGENITAL HEART DISEASE Stuart Lilley More adults than children have congenital heart disease Huge variety of congenital lesions from minor to major Heart failure, re-operation and arrhythmia are
Surgical Repair of Ventricular Septal Defect; Contemporary Results and Risk Factors for a Complicated Course
 Pediatr Cardiol (2017) 38:264 270 DOI 10.1007/s00246-016-1508-2 ORIGINAL ARTICLE Surgical Repair of Ventricular Septal Defect; Contemporary Results and Risk Factors for a Complicated Course Maartje Schipper
Pediatr Cardiol (2017) 38:264 270 DOI 10.1007/s00246-016-1508-2 ORIGINAL ARTICLE Surgical Repair of Ventricular Septal Defect; Contemporary Results and Risk Factors for a Complicated Course Maartje Schipper
The role of intraoperative TOE in congenital cardiac surgery
 The role of intraoperative TOE in congenital cardiac surgery Justiaan Swanevelder Dept of Anaesthesia Groote Schuur and Red Cross War Memorial Children s Hospitals University of Cape Town, South Africa
The role of intraoperative TOE in congenital cardiac surgery Justiaan Swanevelder Dept of Anaesthesia Groote Schuur and Red Cross War Memorial Children s Hospitals University of Cape Town, South Africa
For Personal Use. Copyright HMP 2013
 12-00415 Case Report J INVASIVE CARDIOL 2013;25(4):E69-E71 A Concert in the Heart. Bilateral Melody Valve Implantation in the Branch Pulmonary Arteries Nicola Maschietto, MD, PhD and Ornella Milanesi,
12-00415 Case Report J INVASIVE CARDIOL 2013;25(4):E69-E71 A Concert in the Heart. Bilateral Melody Valve Implantation in the Branch Pulmonary Arteries Nicola Maschietto, MD, PhD and Ornella Milanesi,
Echocardiographic assessment in Adult Patients with Congenital Heart Diseases
 Echocardiographic assessment in Adult Patients with Congenital Heart Diseases Athanasios Koutsakis Cardiologist, Cl. Research Fellow George Giannakoulas Ass. Professor in Cardiology 1st Cardiology Department,
Echocardiographic assessment in Adult Patients with Congenital Heart Diseases Athanasios Koutsakis Cardiologist, Cl. Research Fellow George Giannakoulas Ass. Professor in Cardiology 1st Cardiology Department,
Treatment of Inter-MitraClip Regurgitation Due to Posterior Leaflet Cleft by Use of The Amplatzer Vascular Plug II device
 Volume 1, Issue 3 Case Report ISSN: 2572-9292 Treatment of Inter-MitraClip Regurgitation Due to Posterior Leaflet Cleft by Use of The Amplatzer Vascular Plug II device Neha M. Mantri, Gagan D. Singh, Thomas
Volume 1, Issue 3 Case Report ISSN: 2572-9292 Treatment of Inter-MitraClip Regurgitation Due to Posterior Leaflet Cleft by Use of The Amplatzer Vascular Plug II device Neha M. Mantri, Gagan D. Singh, Thomas
HISTORY. Question: What category of heart disease is suggested by this history? CHIEF COMPLAINT: Heart murmur present since early infancy.
 HISTORY 18-year-old man. CHIEF COMPLAINT: Heart murmur present since early infancy. PRESENT ILLNESS: Although normal at birth, a heart murmur was heard at the six week check-up and has persisted since
HISTORY 18-year-old man. CHIEF COMPLAINT: Heart murmur present since early infancy. PRESENT ILLNESS: Although normal at birth, a heart murmur was heard at the six week check-up and has persisted since
Mitral Valve Disease, When to Intervene
 Mitral Valve Disease, When to Intervene Swedish Heart and Vascular Institute Ming Zhang MD PhD Interventional Cardiology Structure Heart Disease Conflict of Interest None Current ACC/AHA guideline Stages
Mitral Valve Disease, When to Intervene Swedish Heart and Vascular Institute Ming Zhang MD PhD Interventional Cardiology Structure Heart Disease Conflict of Interest None Current ACC/AHA guideline Stages
Transcatheter closure of ventricular septal defects with nitinol wire occluders of type patent ductus arteriosus
 Pediatric cardiology Transcatheter closure of ventricular septal defects with nitinol wire occluders of type patent ductus arteriosus Arkadiusz Wierzyk 1, Małgorzata Szkutnik 1, Roland Fiszer 1, Paweł
Pediatric cardiology Transcatheter closure of ventricular septal defects with nitinol wire occluders of type patent ductus arteriosus Arkadiusz Wierzyk 1, Małgorzata Szkutnik 1, Roland Fiszer 1, Paweł
Congenital heart disease: When to act and what to do?
 Leading Article Congenital heart disease: When to act and what to do? Duminda Samarasinghe 1 Sri Lanka Journal of Child Health, 2010; 39: 39-43 (Key words: Congenital heart disease) Congenital heart disease
Leading Article Congenital heart disease: When to act and what to do? Duminda Samarasinghe 1 Sri Lanka Journal of Child Health, 2010; 39: 39-43 (Key words: Congenital heart disease) Congenital heart disease
Transcatheter closure of right coronary artery fistula to the right ventricle
 Case Report Transcatheter closure of right coronary artery fistula to the right ventricle Abstract Coronary artery fistula (CAF) is an uncommon anomaly usually congenital but can be acquired. Although,
Case Report Transcatheter closure of right coronary artery fistula to the right ventricle Abstract Coronary artery fistula (CAF) is an uncommon anomaly usually congenital but can be acquired. Although,
Congenital heart disease. By Dr Saima Ali Professor of pediatrics
 Congenital heart disease By Dr Saima Ali Professor of pediatrics What is the most striking clinical finding in this child? Learning objectives By the end of this lecture, final year student should be able
Congenital heart disease By Dr Saima Ali Professor of pediatrics What is the most striking clinical finding in this child? Learning objectives By the end of this lecture, final year student should be able
Research Article A New Coated Nitinol Occluder for Transcatheter Closure of Ventricular Septal Defects in a Canine Model
 BioMed Research International Volume 2013, Article ID 507919, 7 pages http://dx.doi.org/10.1155/2013/507919 Research Article A New Coated Nitinol Occluder for Transcatheter Closure of Ventricular Septal
BioMed Research International Volume 2013, Article ID 507919, 7 pages http://dx.doi.org/10.1155/2013/507919 Research Article A New Coated Nitinol Occluder for Transcatheter Closure of Ventricular Septal
Absent Pulmonary Valve Syndrome
 Absent Pulmonary Valve Syndrome Fact sheet on Absent Pulmonary Valve Syndrome In this condition, which has some similarities to Fallot's Tetralogy, there is a VSD with narrowing at the pulmonary valve.
Absent Pulmonary Valve Syndrome Fact sheet on Absent Pulmonary Valve Syndrome In this condition, which has some similarities to Fallot's Tetralogy, there is a VSD with narrowing at the pulmonary valve.
Journal of the American College of Cardiology Vol. 33, No. 5, by the American College of Cardiology ISSN /99/$20.
 Journal of the American College of Cardiology Vol. 33, No. 5, 1999 1999 by the American College of Cardiology ISSN 0735-1097/99/$20.00 Published by Elsevier Science Inc. PII S0735-1097(99)00011-X Transcatheter
Journal of the American College of Cardiology Vol. 33, No. 5, 1999 1999 by the American College of Cardiology ISSN 0735-1097/99/$20.00 Published by Elsevier Science Inc. PII S0735-1097(99)00011-X Transcatheter
Adult Congenital Heart Disease: The New Reality. Disclosures
 Adult Congenital Heart Disease: The New Reality Kathryn Rouine-Rapp, MD Professor of Anesthesia Disclosures I have nothing to disclose 1 Outline Historic perspective Our reality Common lesions Guidelines
Adult Congenital Heart Disease: The New Reality Kathryn Rouine-Rapp, MD Professor of Anesthesia Disclosures I have nothing to disclose 1 Outline Historic perspective Our reality Common lesions Guidelines
DIAGNOSIS, MANAGEMENT AND OUTCOME OF HEART DISEASE IN SUDANESE PATIENTS
 434 E AST AFRICAN MEDICAL JOURNAL September 2007 East African Medical Journal Vol. 84 No. 9 September 2007 DIAGNOSIS, MANAGEMENT AND OUTCOME OF CONGENITAL HEART DISEASE IN SUDANESE PATIENTS K.M.A. Sulafa,
434 E AST AFRICAN MEDICAL JOURNAL September 2007 East African Medical Journal Vol. 84 No. 9 September 2007 DIAGNOSIS, MANAGEMENT AND OUTCOME OF CONGENITAL HEART DISEASE IN SUDANESE PATIENTS K.M.A. Sulafa,
TGA atrial vs arterial switch what do we need to look for and how to react
 TGA atrial vs arterial switch what do we need to look for and how to react Folkert Meijboom, MD, PhD, FES Dept ardiology University Medical entre Utrecht The Netherlands TGA + atrial switch: Follow-up
TGA atrial vs arterial switch what do we need to look for and how to react Folkert Meijboom, MD, PhD, FES Dept ardiology University Medical entre Utrecht The Netherlands TGA + atrial switch: Follow-up
Edwards Sapien. Medtronic CoreValve. Inoperable FDA approved High risk: in trials. FDA approved
 Transcatheter Aortic Valve Replacement Symptomatic Aortic Stenosis Asymptomatic Juan Crestanello, MD Interim Director, Division of Cardiac Surgery Associate Professor Division of Cardiac Surgery The Ohio
Transcatheter Aortic Valve Replacement Symptomatic Aortic Stenosis Asymptomatic Juan Crestanello, MD Interim Director, Division of Cardiac Surgery Associate Professor Division of Cardiac Surgery The Ohio
Cardiac MRI in ACHD What We. ACHD Patients
 Cardiac MRI in ACHD What We Have Learned to Apply to ACHD Patients Faris Al Mousily, MBChB, FAAC, FACC Consultant, Pediatric Cardiology, KFSH&RC/Jeddah Adjunct Faculty, Division of Pediatric Cardiology
Cardiac MRI in ACHD What We Have Learned to Apply to ACHD Patients Faris Al Mousily, MBChB, FAAC, FACC Consultant, Pediatric Cardiology, KFSH&RC/Jeddah Adjunct Faculty, Division of Pediatric Cardiology
Cardiac Catheterization Cases Primary Cardiac Diagnoses Facility 12 month period from to PRIMARY DIAGNOSES (one per patient)
 PRIMARY DIAGNOSES (one per patient) Septal Defects ASD (Atrial Septal Defect) PFO (Patent Foramen Ovale) ASD, Secundum ASD, Sinus venosus ASD, Coronary sinus ASD, Common atrium (single atrium) VSD (Ventricular
PRIMARY DIAGNOSES (one per patient) Septal Defects ASD (Atrial Septal Defect) PFO (Patent Foramen Ovale) ASD, Secundum ASD, Sinus venosus ASD, Coronary sinus ASD, Common atrium (single atrium) VSD (Ventricular
Transthoracic closure of atrial septal defect and ventricular septal defect without cardiopulmonary bypass
 Transthoracic closure of atrial septal defect and ventricular septal defect without cardiopulmonary bypass L. Wan, B.-T. Yu, Q.-C. Wu, L. Zeng, Q. Wang, J. Tang, Q.-R. Xu, H. Xu, W.-J. Wang, Y.-P. Cao
Transthoracic closure of atrial septal defect and ventricular septal defect without cardiopulmonary bypass L. Wan, B.-T. Yu, Q.-C. Wu, L. Zeng, Q. Wang, J. Tang, Q.-R. Xu, H. Xu, W.-J. Wang, Y.-P. Cao
Echocardiography in Adult Congenital Heart Disease
 Echocardiography in Adult Congenital Heart Disease Michael Vogel Kinderherz-Praxis München CHD missed in childhood Subsequent lesions after repaired CHD Follow-up of cyanotic heart disease CHD missed in
Echocardiography in Adult Congenital Heart Disease Michael Vogel Kinderherz-Praxis München CHD missed in childhood Subsequent lesions after repaired CHD Follow-up of cyanotic heart disease CHD missed in
Paediatrica Indonesiana
 Paediatrica Indonesiana VOLUME 53 July NUMBER 4 Original Article Transcatheter vs. surgical closure of patent ductus arteriosus: outcomes and cost analysis Mulyadi M Djer, Mochammading, Mardjanis Said
Paediatrica Indonesiana VOLUME 53 July NUMBER 4 Original Article Transcatheter vs. surgical closure of patent ductus arteriosus: outcomes and cost analysis Mulyadi M Djer, Mochammading, Mardjanis Said
Percutaneous Device Closure of Congenital VSDs Current techniques and results for treating ventricular septal defects.
 Percutaneous Device Closure of Congenital VSDs Current techniques and results for treating ventricular septal defects. BY KARIM A. DIAB, MD; QI-LING CAO, MD; AND ZIYAD M. HIJAZI, MD, MPH During the past
Percutaneous Device Closure of Congenital VSDs Current techniques and results for treating ventricular septal defects. BY KARIM A. DIAB, MD; QI-LING CAO, MD; AND ZIYAD M. HIJAZI, MD, MPH During the past
Adult Echocardiography Examination Content Outline
 Adult Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 4 5 Anatomy and Physiology Pathology Clinical Care and Safety Measurement Techniques, Maneuvers,
Adult Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 4 5 Anatomy and Physiology Pathology Clinical Care and Safety Measurement Techniques, Maneuvers,
Anatomy of Atrioventricular Septal Defect (AVSD)
 Surgical challenges in atrio-ventricular septal defect in grown-up congenital heart disease Anatomy of Atrioventricular Septal Defect (AVSD) S. Yen Ho Professor of Cardiac Morphology Royal Brompton and
Surgical challenges in atrio-ventricular septal defect in grown-up congenital heart disease Anatomy of Atrioventricular Septal Defect (AVSD) S. Yen Ho Professor of Cardiac Morphology Royal Brompton and
Transcatheter Atrial Septal Defect Closure with Right Aortic Arch Is it really difficult? M Tokue, H Hara, K Sugi, M Nakamura
 5th Asia Pacific Congenital & Structural Heart Intervention Symposium 2014 10 12 October 2014, Hong Kong Convention and Exhibition Centre Organizer: Hong Kong Society of Congenital & Structural Heart Disease
5th Asia Pacific Congenital & Structural Heart Intervention Symposium 2014 10 12 October 2014, Hong Kong Convention and Exhibition Centre Organizer: Hong Kong Society of Congenital & Structural Heart Disease
Διαδερμική θεραπεία των παραβαλβιδικών διαφυγών Σ.Ράμμος
 ΔΜΙΝΑΡΙΟ ΔΠΙΣΗΜΟΝΙΚΩΝ ΔΝΩΔΩΝ ΔΛΛΗΝΙΚΟΤ ΚΟΛΛΔΓΙΟΤ ΚΑΡ ΙΟΛΟΓΙΑ 2-4.10.2015 Δπιζηημονική Ένωζη Δπεμβαηικής Καρδιολογίας Βαλβιδοπάθειες, Γιαδερμικές παρεμβάζεις Διαδερμική θεραπεία των παραβαλβιδικών διαφυγών
ΔΜΙΝΑΡΙΟ ΔΠΙΣΗΜΟΝΙΚΩΝ ΔΝΩΔΩΝ ΔΛΛΗΝΙΚΟΤ ΚΟΛΛΔΓΙΟΤ ΚΑΡ ΙΟΛΟΓΙΑ 2-4.10.2015 Δπιζηημονική Ένωζη Δπεμβαηικής Καρδιολογίας Βαλβιδοπάθειες, Γιαδερμικές παρεμβάζεις Διαδερμική θεραπεία των παραβαλβιδικών διαφυγών
Perioperative Management of DORV Case
 Perioperative Management of DORV Case James P. Spaeth, MD Department of Anesthesia Cincinnati Children s Hospital Medical Center University of Cincinnati Objectives: 1. Discuss considerations regarding
Perioperative Management of DORV Case James P. Spaeth, MD Department of Anesthesia Cincinnati Children s Hospital Medical Center University of Cincinnati Objectives: 1. Discuss considerations regarding
September 26, 2012 Philip Stockwell, MD Lifespan CVI Assistant Professor of Medicine (Clinical)
 September 26, 2012 Philip Stockwell, MD Lifespan CVI Assistant Professor of Medicine (Clinical) Advances in cardiac surgery have created a new population of adult patients with repaired congenital heart
September 26, 2012 Philip Stockwell, MD Lifespan CVI Assistant Professor of Medicine (Clinical) Advances in cardiac surgery have created a new population of adult patients with repaired congenital heart
Pediatric Echocardiography Examination Content Outline
 Pediatric Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 Anatomy and Physiology Normal Anatomy and Physiology 10% 2 Abnormal Pathology and Pathophysiology
Pediatric Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 Anatomy and Physiology Normal Anatomy and Physiology 10% 2 Abnormal Pathology and Pathophysiology
Transcatheter device occlusion of patent ductus arteriosus
 CONGENITAL HEART DISEASE The New Occlutech Duct Occluder: Immediate Results, Procedural Challenges, and Short-Term Follow-Up Vikram Kudumula, MRCPCH; Demetris Taliotis, MRCPCH; Christopher Duke, FRCP ABSTRACT:
CONGENITAL HEART DISEASE The New Occlutech Duct Occluder: Immediate Results, Procedural Challenges, and Short-Term Follow-Up Vikram Kudumula, MRCPCH; Demetris Taliotis, MRCPCH; Christopher Duke, FRCP ABSTRACT:
Perventricular Closure of Muscular VSD
 Perventricular Closure of Muscular VSD John P. Cheatham, MD, MSCAI George H. Dunlap Endowed Chair in Interventional Cardiology Co-Director, The Heart Center, Nationwide Children s Hospital Professor, Pediatrics
Perventricular Closure of Muscular VSD John P. Cheatham, MD, MSCAI George H. Dunlap Endowed Chair in Interventional Cardiology Co-Director, The Heart Center, Nationwide Children s Hospital Professor, Pediatrics
Uptofate Study Summary
 CONGENITAL HEART DISEASE Uptofate Study Summary Acyanotic Atrial septal defect Ventricular septal defect Patent foramen ovale Patent ductus arteriosus Aortic coartation Pulmonary stenosis Cyanotic Tetralogy
CONGENITAL HEART DISEASE Uptofate Study Summary Acyanotic Atrial septal defect Ventricular septal defect Patent foramen ovale Patent ductus arteriosus Aortic coartation Pulmonary stenosis Cyanotic Tetralogy
Glenmark Cardiac Centre Mumbai, India
 ASD device closure: Long term follow up Bharat Dalvi, MD Glenmark Cardiac Centre Mumbai, India Our experience 1998 to 2011 1566 patients 912 patients > 4 years FU Exclusive with ASO Clinical, electrocardiographic
ASD device closure: Long term follow up Bharat Dalvi, MD Glenmark Cardiac Centre Mumbai, India Our experience 1998 to 2011 1566 patients 912 patients > 4 years FU Exclusive with ASO Clinical, electrocardiographic
AMPLATZER Septal Occluder Structural Heart Therapy. Over 15 years of. Demonstrated. Clinical Experience. We ll show you our data. Ask to see theirs.
 AMPLATZER Septal Occluder Structural Heart Therapy Over 15 years of Demonstrated Clinical Experience We ll show you our data. Ask to see theirs. Leading the Standard of Care 1,2 The AMPLATZER Septal Occluder
AMPLATZER Septal Occluder Structural Heart Therapy Over 15 years of Demonstrated Clinical Experience We ll show you our data. Ask to see theirs. Leading the Standard of Care 1,2 The AMPLATZER Septal Occluder
Predictors of unfavorable outcome after atrial septal defect closure in adults
 after atrial septal defect closure in adults H. M. Gabriel 1, M. Humenberger 1, R. Rosenhek 1, GP. Diller 2, G. Kaleschke 2, TH. Binder 1, P. Probst 1, G. Maurer 1, H. Baumgartner 2 (1) Medical University
after atrial septal defect closure in adults H. M. Gabriel 1, M. Humenberger 1, R. Rosenhek 1, GP. Diller 2, G. Kaleschke 2, TH. Binder 1, P. Probst 1, G. Maurer 1, H. Baumgartner 2 (1) Medical University
AMPLATZER Septal Occluder
 AMPLATZER Septal Occluder A Patient s Guide to the Non-Surgical Closure of the Atrial Septal Defect Using the AMPLATZER Septal Occluder System leadership through innovation TM AGA Medical Corporation 5050
AMPLATZER Septal Occluder A Patient s Guide to the Non-Surgical Closure of the Atrial Septal Defect Using the AMPLATZER Septal Occluder System leadership through innovation TM AGA Medical Corporation 5050
CARDIAC CATHETERIZATION IN GROWN-UP PATIENTS WITH CONGENITAL HEART DISEASES INDICATIONS AND COMPLICATIONS
 Pak Heart J ORIGINAL ARTICLE CARDIAC CATHETERIZATION IN GROWN-UP PATIENTS WITH CONGENITAL HEART DISEASES INDICATIONS AND COMPLICATIONS 1 2 3 4 Mehboob Sultan, Asif Muhammad, Maad Ullah, Nadeem Sadiq, 5
Pak Heart J ORIGINAL ARTICLE CARDIAC CATHETERIZATION IN GROWN-UP PATIENTS WITH CONGENITAL HEART DISEASES INDICATIONS AND COMPLICATIONS 1 2 3 4 Mehboob Sultan, Asif Muhammad, Maad Ullah, Nadeem Sadiq, 5
Clinicians and Facilities: RESOURCES WHEN CARING FOR WOMEN WITH ADULT CONGENITAL HEART DISEASE OR OTHER FORMS OF CARDIOVASCULAR DISEASE!!
 Clinicians and Facilities: RESOURCES WHEN CARING FOR WOMEN WITH ADULT CONGENITAL HEART DISEASE OR OTHER FORMS OF CARDIOVASCULAR DISEASE!! Abha'Khandelwal,'MD,'MS' 'Stanford'University'School'of'Medicine'
Clinicians and Facilities: RESOURCES WHEN CARING FOR WOMEN WITH ADULT CONGENITAL HEART DISEASE OR OTHER FORMS OF CARDIOVASCULAR DISEASE!! Abha'Khandelwal,'MD,'MS' 'Stanford'University'School'of'Medicine'
Delayed Infective Endocarditis with Mycotic Aneurysm Rupture below the Mechanical Valved Conduit after the Bentall Procedure
 Case Report Acta Cardiol Sin 2014;30:341 345 Delayed Infective Endocarditis with Mycotic Aneurysm Rupture below the Mechanical Valved Conduit after the Bentall Procedure Mei-Ling Chen, 1,3 Michael Y. Chen,
Case Report Acta Cardiol Sin 2014;30:341 345 Delayed Infective Endocarditis with Mycotic Aneurysm Rupture below the Mechanical Valved Conduit after the Bentall Procedure Mei-Ling Chen, 1,3 Michael Y. Chen,
JOINT MEETING 2 Tricuspid club Chairpersons: G. Athanassopoulos, A. Avgeropoulou, M. Khoury, G. Stavridis
 JOINT MEETING 2 Tricuspid club Chairpersons: G. Athanassopoulos, A. Avgeropoulou, M. Khoury, G. Stavridis Similarities and differences in Tricuspid vs. Mitral Valve Anatomy and Imaging. Echo evaluation
JOINT MEETING 2 Tricuspid club Chairpersons: G. Athanassopoulos, A. Avgeropoulou, M. Khoury, G. Stavridis Similarities and differences in Tricuspid vs. Mitral Valve Anatomy and Imaging. Echo evaluation
First Transfemoral Aortic Valve Implantation In Bulgaria - Crossing The Valve With The Device Is Not Always
 ISPUB.COM The Internet Journal of Cardiology Volume 9 Number 2 First Transfemoral Aortic Valve Implantation In Bulgaria - Crossing The Valve With The Device Is Not T D, J P. Citation T D, J P.. First Transfemoral
ISPUB.COM The Internet Journal of Cardiology Volume 9 Number 2 First Transfemoral Aortic Valve Implantation In Bulgaria - Crossing The Valve With The Device Is Not T D, J P. Citation T D, J P.. First Transfemoral
LEFT VENTRICULAR OUTFLOW OBSTRUCTION WITH A VSD: OPTIONS FOR SURGICAL MANAGEMENT
 LEFT VENTRICULAR OUTFLOW OBSTRUCTION WITH A VSD: OPTIONS FOR SURGICAL MANAGEMENT 10-13 March 2017 Ritz Carlton, Riyadh, Saudi Arabia Zohair AlHalees, MD Consultant, Cardiac Surgery Heart Centre LEFT VENTRICULAR
LEFT VENTRICULAR OUTFLOW OBSTRUCTION WITH A VSD: OPTIONS FOR SURGICAL MANAGEMENT 10-13 March 2017 Ritz Carlton, Riyadh, Saudi Arabia Zohair AlHalees, MD Consultant, Cardiac Surgery Heart Centre LEFT VENTRICULAR
Management of HOCM: Non-Surgical Options
 Management of HOCM: Non-Surgical Options Howard C. Herrmann, MD, FACC, MSCAI John Bryfogle Professor of Cardiovascular Medicine and Surgery Health System Director for Interventional Cardiology Director,
Management of HOCM: Non-Surgical Options Howard C. Herrmann, MD, FACC, MSCAI John Bryfogle Professor of Cardiovascular Medicine and Surgery Health System Director for Interventional Cardiology Director,
Device closure of congenital ventricular septal defects with Amplatzer devices: first experiences in Turkey
 The Turkish Journal of Pediatrics 2008; 50: 106-113 Original Device closure of congenital ventricular septal defects with Amplatzer devices: first experiences in Turkey Alpay Çeliker, Süheyla Özkutlu,
The Turkish Journal of Pediatrics 2008; 50: 106-113 Original Device closure of congenital ventricular septal defects with Amplatzer devices: first experiences in Turkey Alpay Çeliker, Süheyla Özkutlu,
Fabien Praz, Andreas Wahl, Sophie Beney, Stephan Windecker, Heinrich P. Mattle*, Bernhard Meier
 Procedural Outcome after Percutaneous Closure of Patent Foramen Ovale using the Amplatzer PFO Occluder Without Intra-Procedural Echocardiography in 1,000 Patients Fabien Praz, Andreas Wahl, Sophie Beney,
Procedural Outcome after Percutaneous Closure of Patent Foramen Ovale using the Amplatzer PFO Occluder Without Intra-Procedural Echocardiography in 1,000 Patients Fabien Praz, Andreas Wahl, Sophie Beney,
CIPG Transcatheter Aortic Valve Replacement- When Is Less, More?
 CIPG 2013 Transcatheter Aortic Valve Replacement- When Is Less, More? James D. Rossen, M.D. Professor of Medicine and Neurosurgery Director, Cardiac Catheterization Laboratory and Interventional Cardiology
CIPG 2013 Transcatheter Aortic Valve Replacement- When Is Less, More? James D. Rossen, M.D. Professor of Medicine and Neurosurgery Director, Cardiac Catheterization Laboratory and Interventional Cardiology
Interventions in Adult Congenital Heart Disease: Role of CV Imaging. Associate Professor. ACHD mortality. Pillutla. Am Heart J 2009;158:874-9
 Interventions in Adult Congenital Heart Disease: Role of CV Imaging Sangeeta Shah MD, FACC, FASE Associate Professor ACHD mortality Pillutla. Am Heart J 2009;158:874-9 Adult Congenital Heart Disease Heterogenity
Interventions in Adult Congenital Heart Disease: Role of CV Imaging Sangeeta Shah MD, FACC, FASE Associate Professor ACHD mortality Pillutla. Am Heart J 2009;158:874-9 Adult Congenital Heart Disease Heterogenity
Transcatheter closure of patent foramen ovale using the internal jugular venous approach
 New methods in diagnosis and therapy Transcatheter closure of patent foramen ovale using the internal jugular venous approach Przemysław Węglarz 1,2, Ewa Konarska-Kuszewska 2, Tadeusz Zębik 2, Piotr Kuszewski
New methods in diagnosis and therapy Transcatheter closure of patent foramen ovale using the internal jugular venous approach Przemysław Węglarz 1,2, Ewa Konarska-Kuszewska 2, Tadeusz Zębik 2, Piotr Kuszewski
Muscular VSD Occluder
 Muscular VSD Occluder Instructions for Use Device Description The AMPLATZER Muscular VSD Occluder is a self-expanding, double-disc device made from a nitinol wire mesh. The 2 discs are linked together
Muscular VSD Occluder Instructions for Use Device Description The AMPLATZER Muscular VSD Occluder is a self-expanding, double-disc device made from a nitinol wire mesh. The 2 discs are linked together
Transcatheter Closure of Acute Myocardial Infarction VSD
 The 10 th Anniversary, Interventional Vascular Therapeutics ANGIOPLASTY SUMMIT 2005 TCT ASIA PACIFIC Transcatheter Closure of Acute Myocardial Infarction VSD Dr. Mullasari S Ajit Senior Consultant Cardiologist
The 10 th Anniversary, Interventional Vascular Therapeutics ANGIOPLASTY SUMMIT 2005 TCT ASIA PACIFIC Transcatheter Closure of Acute Myocardial Infarction VSD Dr. Mullasari S Ajit Senior Consultant Cardiologist
Index. interventional.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Alagille syndrome, pulmonary artery stenosis in, 143 145, 148 149 Amplatz devices for atrial septal defect closure, 42 46 for coronary
Index Note: Page numbers of article titles are in boldface type. A Alagille syndrome, pulmonary artery stenosis in, 143 145, 148 149 Amplatz devices for atrial septal defect closure, 42 46 for coronary
Anatomy & Physiology
 1 Anatomy & Physiology Heart is divided into four chambers, two atrias & two ventricles. Atrioventricular valves (tricuspid & mitral) separate the atria from ventricles. they open & close to control flow
1 Anatomy & Physiology Heart is divided into four chambers, two atrias & two ventricles. Atrioventricular valves (tricuspid & mitral) separate the atria from ventricles. they open & close to control flow
CASE REPORT: A THREE-MONTH-OLD BOY WITH INCOMPLETE KAWASAKI DISEASE AND EARLY SUPER-GIANT CORONARY ANEURYSM RESULTING IN DETRIMENTAL CARDIAC FUNCTION
 CASE REPORT: A THREE-MONTH-OLD BOY WITH INCOMPLETE KAWASAKI DISEASE AND EARLY SUPER-GIANT CORONARY ANEURYSM RESULTING IN DETRIMENTAL CARDIAC FUNCTION Prakul Chanthong, Pornrawee Plearntummakun, Chodchanok
CASE REPORT: A THREE-MONTH-OLD BOY WITH INCOMPLETE KAWASAKI DISEASE AND EARLY SUPER-GIANT CORONARY ANEURYSM RESULTING IN DETRIMENTAL CARDIAC FUNCTION Prakul Chanthong, Pornrawee Plearntummakun, Chodchanok
Incidence And Predictors Of Left Bundle Branch Block After Transcatheter Aortic Valve Implantation
 Incidence And Predictors Of Left Bundle Branch Block After Transcatheter Aortic Valve Implantation Ömer Aktug 1, MD; Guido Dohmen 2, MD; Kathrin Brehmer 1, MD; Verena Deserno 1 ; Ralf Herpertz 1 ; Rüdiger
Incidence And Predictors Of Left Bundle Branch Block After Transcatheter Aortic Valve Implantation Ömer Aktug 1, MD; Guido Dohmen 2, MD; Kathrin Brehmer 1, MD; Verena Deserno 1 ; Ralf Herpertz 1 ; Rüdiger
Anomalous muscle bundle of the right ventricle
 British Heart Journal, 1978, 40, 1040-1045 Anomalous muscle bundle of the right ventricle Its recognition and surgical treatment M. D. LI, J. C. COLES, AND A. C. McDONALD From the Department of Paediatrics,
British Heart Journal, 1978, 40, 1040-1045 Anomalous muscle bundle of the right ventricle Its recognition and surgical treatment M. D. LI, J. C. COLES, AND A. C. McDONALD From the Department of Paediatrics,
Adult Congenital Heart Disease: What All Echocardiographers Should Know Sharon L. Roble, MD, FACC Echo Hawaii 2016
 1 Adult Congenital Heart Disease: What All Echocardiographers Should Know Sharon L. Roble, MD, FACC Echo Hawaii 2016 DISCLOSURES I have no disclosures relevant to today s talk 2 Why should all echocardiographers
1 Adult Congenital Heart Disease: What All Echocardiographers Should Know Sharon L. Roble, MD, FACC Echo Hawaii 2016 DISCLOSURES I have no disclosures relevant to today s talk 2 Why should all echocardiographers
Since first successfully performed by Jatene et al, the
 Long-Term Predictors of Aortic Root Dilation and Aortic Regurgitation After Arterial Switch Operation Marcy L. Schwartz, MD; Kimberlee Gauvreau, ScD; Pedro del Nido, MD; John E. Mayer, MD; Steven D. Colan,
Long-Term Predictors of Aortic Root Dilation and Aortic Regurgitation After Arterial Switch Operation Marcy L. Schwartz, MD; Kimberlee Gauvreau, ScD; Pedro del Nido, MD; John E. Mayer, MD; Steven D. Colan,
Original Policy Date
 MP 7.01.46 Transcatheter Closure of Patent Ductus Arteriosus Medical Policy Section Surgery Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature search/12:2013 Return
MP 7.01.46 Transcatheter Closure of Patent Ductus Arteriosus Medical Policy Section Surgery Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature search/12:2013 Return
TGA Surgical techniques: tips & tricks (Arterial switch operation)
 TGA Surgical techniques: tips & tricks (Arterial switch operation) Seoul National University Children s Hospital Woong-Han Kim Surgical History 1951 Blalock and Hanlon, atrial septectomy 1954 Mustard et
TGA Surgical techniques: tips & tricks (Arterial switch operation) Seoul National University Children s Hospital Woong-Han Kim Surgical History 1951 Blalock and Hanlon, atrial septectomy 1954 Mustard et
Foetal Cardiology: How to predict perinatal problems. Prof. I.Witters Prof.M.Gewillig UZ Leuven
 Foetal Cardiology: How to predict perinatal problems Prof. I.Witters Prof.M.Gewillig UZ Leuven Cardiopathies Incidence : 8-12 / 1000 births ( 1% ) Most frequent - Ventricle Septum Defect 20% - Atrium Septum
Foetal Cardiology: How to predict perinatal problems Prof. I.Witters Prof.M.Gewillig UZ Leuven Cardiopathies Incidence : 8-12 / 1000 births ( 1% ) Most frequent - Ventricle Septum Defect 20% - Atrium Septum
Echocardiographic Guidance During Placement of the Buttoned Double-Disk Device for Atrial Septa1 Defect Closure
 Echocardiographic Guidance During Placement of the Buttoned Double-Disk Device for Atrial Septa1 Defect Closure L. LUANN MINICH, M.D., and A. REBECCA SNIDER, M.D. Department of Pediatrics, C.S. Mott Children
Echocardiographic Guidance During Placement of the Buttoned Double-Disk Device for Atrial Septa1 Defect Closure L. LUANN MINICH, M.D., and A. REBECCA SNIDER, M.D. Department of Pediatrics, C.S. Mott Children
Notes by Sandra Dankwa 2009 HF- Heart Failure DS- Down Syndrome IE- Infective Endocarditis ET- Exercise Tolerance. Small VSD Symptoms -asymptomatic
 Congenital Heart Disease: Notes. Condition Pathology PC Ix Rx Ventricular septal defect (VSD) L R shuntsdefect anywhere in the ventricle, usually perimembranous (next to the tricuspid valve) 30% 1)small
Congenital Heart Disease: Notes. Condition Pathology PC Ix Rx Ventricular septal defect (VSD) L R shuntsdefect anywhere in the ventricle, usually perimembranous (next to the tricuspid valve) 30% 1)small
Double outlet right ventricle: navigation of surgeon to chose best treatment strategy
 Double outlet right ventricle: navigation of surgeon to chose best treatment strategy Jan Marek Great Ormond Street Hospital & Institute of Cardiovascular Sciences, University College London Double outlet
Double outlet right ventricle: navigation of surgeon to chose best treatment strategy Jan Marek Great Ormond Street Hospital & Institute of Cardiovascular Sciences, University College London Double outlet
How to Assess and Treat Obstructive Lesions
 How to Assess and Treat Obstructive Lesions Erwin Oechslin, MD, FESC, FRCPC, Director, Congenital Cardiac Centre for Adults Peter Munk Cardiac Centre University Health Network/Toronto General Hospital
How to Assess and Treat Obstructive Lesions Erwin Oechslin, MD, FESC, FRCPC, Director, Congenital Cardiac Centre for Adults Peter Munk Cardiac Centre University Health Network/Toronto General Hospital
