Biofeedback as a Treatment of Fecal Incontinence or Constipation
|
|
|
- Moris Wilcox
- 6 years ago
- Views:
Transcription
1 Biofeedback as a Treatment of Fecal Incontinence or Constipation Policy Number: Last Review: 7/2014 Origination: 7/2008 Next Review: 7/2015 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide coverage for biofeedback as a treatment of fecal incontinence or constipation. This is considered investigational. Biofeedback and biofeedback devices are specifically excluded under many benefit plans. In addition, biofeedback and biofeedback devices are considered behavioral training and education/training in nature, and such services are specifically excluded under many benefit plans. When Policy Topic is covered Biofeedback for constipation in adults may be considered medically necessary for patients with dyssynergia-type constipation as demonstrated by meeting all 3 of the following criteria: 1. Symptoms of functional constipation that meet ROME III criteria (see Policy Guidelines). 2. Objective physiologic evidence of pelvic floor dyssynergia (see Policy Guidelines) demonstrated by inappropriate contraction of the pelvic floor muscles or less than 20% relaxation of basal resting sphincter pressure by manometry, imaging or EMG; 3. Failed a 3-month trial of standard treatments for constipation including laxatives, dietary changes, and exercises (as many of the previous as are tolerated). When Policy Topic is not covered Biofeedback is considered investigational as a treatment of constipation in adults and children in all other situations. Biofeedback is considered investigational as a treatment of fecal incontinence in adults and children. Considerations Rome III Diagnostic Criteria for Functional Gastrointestinal Disorders ( : Rome III diagnostic criteria for functional constipation* Must include two or more of the following: 1. Straining during at least 25% of defecations a. Lumpy or hard stools in at least 25% of defecations b. Sensation of incomplete evacuation for at least 25% of defecations c. Sensation of anorectal obstruction/blockage for at least 25% of defecations d. Manual maneuvers to facilitate at least 25% of defecations (e.g., digital evacuation, support of the pelvic floor) e. Fewer than three defecations per week 2. Loose stools are rarely present without the use of laxatives 3. Insufficient criteria for irritable bowel syndrome * Criteria fulfilled for the last 3 months with symptom onset at least 6 months prior to diagnosis Rome III diagnostic criterion for dyssynergic defecation:
2 Inappropriate contraction of the pelvic floor or less than 20% relaxation of basal resting sphincter pressure with adequate propulsive forces during attempted defecation Guidance on biofeedback protocol The recommended treatment course for patients with constipation who meet criteria is up to 6 biofeedback sessions over 3 months. This is consistent with the protocol used in key randomized trials showing benefit of biofeedback for selected patients. Description of Procedure or Service Biofeedback is a technique to teach patients self-regulation of physiological processes not generally considered to be under voluntary control; a variety of approaches and devices are available. Among other possible indications, biofeedback is proposed as a treatment of fecal incontinence and constipation. Background Biofeedback, a technique intended to teach patients self-regulation of certain physiologic processes not normally considered to be under voluntary control, is used to treat a variety of conditions and is proposed as a treatment of fecal incontinence and constipation. Fecal incontinence in adults is the recurrent uncontrolled passage of fecal material. Pathophysiology of the disorder ranges from abnormalities in intestinal motility (diarrhea or constipation), to poor rectal compliance, impaired rectal sensation, or weak or damaged pelvic floor muscles. There is no increase in mortality attributable to fecal incontinence. Morbidity includes skin breakdown and urinary tract infections. Fecal incontinence affects quality of life through restricting work, recreation, and activities related to getting out of the house, impaired social role function, diminished sexual activity, and increase of social isolation due to embarrassment. Fecal incontinence brings about loss of independence and mobility. It is the second most common reason for elderly institutionalization. The most common causes of fecal incontinence in adults are obstetric trauma coupled with age-related degeneration, previous anorectal surgery, rectal prolapse, and perineal trauma. In many individuals, the condition is multifactorial, involving a combination of structural, physiological, and psychosocial factors. Conventional interventions to treat fecal incontinence include dietary recommendations (e.g., fiber), bowel and toilet scheduling, and medications (e.g., bulking or antidiarrheal agents). Constipation refers to infrequent bowel movements and difficulty during defecation. Primary constipation is generally categorized into three groups. The most common type is normal-transit constipation in which there is a normal rate of stool movement but patients feel constipated and may complain of abdominal pain and/or bloating. In the second type, slow-transit constipation, stool moves more slowly through the colon and individuals often experience a limited urge to defecate. The third type, dyssynergic defecation, refers to a loss of ability to coordinate contractions of the pelvic floor muscles and to relax the anal sphincter during defecation. Patients often report an inability to defecate despite the urge to do so. There are also secondary causes of constipation such as the use of certain medications, including opioids and psychoactive drugs; neurologic, endocrine, or metabolic disorders; structural abnormalities; and lifestyle factors. Conventional treatment includes dietary recommendations (i.e., adequate fiber and fluid intake), use of supplemental bulking substances, exercises and medications. In children, most cases of fecal incontinence and constipation are functional, in which structural, endocrine, or metabolic diseases have been ruled out. Factors contributing to functional incontinence and constipation are fear and/or pain associated with large, hard stools. This leads to retentive posturing in approximately half the children with chronic constipation (i.e., the avoidance of defecation by purposefully contracting the external anal sphincter, also termed anismus or paradoxical sphincter contraction). Customary or conventional medical intervention includes dietary recommendations, bowel and toilet scheduling, education and softening agents. Behavioral interventions aim at restoring normal bowel habits through toilet training, reward and incentive contingency management programs, desensitization of phobia and fear, or skill-building and goal-setting techniques with home practice.
3 Counseling and psychotherapy provide support to the child and address social and psychological problems. Biofeedback training for fecal incontinence focuses on improving the ability to voluntarily contract the external anal sphincter and puborectalis muscles in response to rectal filling and to decrease delay in response to a sensation of distension. For constipation, the aim of biofeedback is to teach patients how to tighten and relax their external anal sphincter in order to pass bowel movements. Biofeedback attempts to improve rectal sensory perception, strength, coordination, or some combination of these three components. Sensory training involves inducing intrarectal pressure using a balloon feedback device. A manometric balloon probe is inserted into the rectum, and the balloon is filled with air to produce a sensation of rectal filling. Strength training uses either anal canal pressure (manometric) or intra-anal EMG feedback of pelvic floor muscles (PFM). The purpose is to strengthen the force of the PFM contraction without including rectal distention. Some training increases endurance (duration of external anal sphincter contraction), as well as its peak strength. Coordination training uses pressure feedback of intra-rectal balloon distention using a water-perfused catheter or Schuster-type balloon probe and PFM contractions in a simultaneous feedback display. The purpose of coordination training is to synchronize the contraction of the external anal sphincter with relaxation of the internal anal sphincter. Biofeedback techniques convert the physiologic measures from an intra-anal EMG sensor, anal manometric probe (measuring intra-anal pressure), or perianal surface EMG electrodes to either visual or audio display for feedback. Ultrasound has also been used to show patients contraction of the anal sphincter on a screen. Biofeedback training is done alone, or in combination with other behavioral therapies designed to teach relaxation. Training sessions are performed in a quiet, non-arousing environment. Regulatory Status A variety of biofeedback devices are cleared for marketing though the U.S. Food and Drug Administration s (FDA) 510(k) marketing clearance process. These devices are designated by the FDA as class II with special controls, and are exempt from the premarket notification requirements. The FDA defines a biofeedback device as an instrument that provides a visual or auditory signal corresponding to the status of one or more of a patient's physiological parameters (e.g., brain alpha wave activity, muscle activity, skin temperature, etc.) so that the patient can control voluntarily these physiological parameters. Rationale This policy was originally created in 2003 and was updated regularly with searches of the MEDLINE database. The most recent literature search was performed for the period November 2012 through November 21, Following is a summary of the key literature to date. Several methodologic difficulties exist in assessing biofeedback. For example, most interventions that include biofeedback are multimodal and include relaxation and behavioral instruction, which may have effects separate from those that may occur due to biofeedback. While studies may report a beneficial effect of multimodality treatment, without appropriate control conditions, it is impossible to isolate the specific contribution of biofeedback to the overall treatment effect. For example, relaxation, attention, or suggestion may account for the successful results that have been attributed to biofeedback. These are nonspecific therapeutic factors, some of which can be considered placebo effects. Moreover, it is important that studies demonstrate that biofeedback improves disease-related health outcomes, as opposed to potentially affecting only physiologic, intermediate outcomes, and that they address the durability of effects beyond the initial, short-term biofeedback training period. The relevant clinical outcome for biofeedback as a treatment in incontinence should be an overall change in the patient s symptoms. Reduction in episodes of fecal incontinence and increase in voluntary bowel movements are the primary clinical outcomes, and these are typically reported as the
4 percentage of individuals cured or improved. Achieving normal defecation dynamics (eg, anal pressure, squeeze pressure, sensory threshold, rectal inhibitory reflex, or defecation dynamics) does not correspond with symptom relief (ie, clinical outcomes). Anorectal physiology measurements are a poor proxy for changes in clinical symptoms. Patient symptoms are usually assessed through diary, questionnaire, or interview (completed by the patient and, in the case of children, parents). Fecal incontinence Does the addition of biofeedback to standard care reduce fecal incontinence, compared with standard care alone? Adults Numerous randomized controlled trials (RCT) on biofeedback treatment for fecal incontinence in adults have been published. There are also several systematic reviews of RCTs. In 2009, Enck et al identified 11 RCTs evaluating the efficacy of biofeedback therapy for fecal incontinence in adult populations.(1) Two RCTs were excluded, one because of the small sample size, and the other because it did not include an appropriate control group. The remaining 9 studies consisted of 5 comparisons of different modalities of biofeedback and 6 comparisons of electromyographic (EMG) biofeedback versus other types of therapy, mainly pelvic floor exercises (2 studies had multiple treatment groups and were included in both categories). The total number of patients included in the 9 studies was 540; sample sizes of individual studies ranged from 18 to 171. A meta-analysis of 5 studies did not find a significant difference in the efficacy of different types of biofeedback (pooled odds ratio [OR], 1.23; 95% confidence interval [CI], 0.74 to 2.20, p=0.38). Similarly, a meta-analysis of studies comparing biofeedback to other therapies did not find a significant difference in efficacy (pooled OR=1.19; 95% CI, 0.69 to 2.05). The outcome measure used in the analysis was not specified and appears to vary from study to study. Other systematic reviews have addressed biofeedback alone and in combination with other interventions. A 2013 systematic review by Vonthein et al identified 13 RCTS on biofeedback, electrical stimulation or their combination for treatment of fecal incontinence.(2) Ten trials included comparisons of biofeedback and an alternative treatment; some of the biofeedback interventions also involved other components such as sensory training and pelvic floor exercises. A meta-analysis of studies comparing biofeedback to a control intervention significantly favored biofeedback (relative risk, 2.12; 95% CI, 1.42 to 3.16). This study did not attempt to isolate the effect of biofeedback in multicomponent interventions that included pelvic floor exercise or other treatments. A 2012 Cochrane review identified 21 RCTs evaluating biofeedback and/or sphincter exercises for treating fecal incontinence in adults.(3) Most studies used multifaceted interventions, eg, biofeedback, education and sphincter exercise. In addition, a wide variety of control interventions were used. Three trials compared biofeedback plus sphincter exercises to sphincter exercises alone and 1 trial compared biofeedback plus 1 type of exercise to biofeedback to another type of exercise. The authors did not pool study findings due to heterogeneity among trials. Representative RCTs are described below In 2009, Heymen et al randomly assigned 168 individuals with fecal incontinence to 3 months of biweekly pelvic floor exercise training alone (n=85) or exercise training with manometric biofeedback (n=83).(4) Twenty-two patients in the exercise-only group and 38 in the biofeedback group improved during a 4-week run-in period and did not participate further, leaving 63 in the exercise group and 45 in the biofeedback group. The primary efficacy outcome was decrease in scores on the Fecal Incontinence Severity Instrument (FISI), a validated 4-item scale, from the end of the run-in to 3 months. The analysis included all patients who completed at least 1 treatment (a total of 15 patients dropped out). The authors reported that there was a greater reduction in FISI scores in the biofeedback group compared to the exercise-only group (p=0.01, exact scores were not reported). Complete continence (no staining) was reported by 13 of 63 (21%) in the exercise-only group and 20 of 45 (44%)
5 in the biofeedback group; this difference was statistically significant (p=0.008). A study limitation was that only 108 of 168 randomized patients (64%) received the intervention, and therefore there may have been baseline differences in the treated groups that affected study outcomes. A stronger design is to randomize patients after, not before, a run-in period. In 2011, Bartlett et al in Australia published an RCT with 72 participants comparing 2 exercise regimens used with biofeedback for fecal incontinence.(5) The study did not find significant differences in outcomes with the 2 types of exercises. It is not possible to make conclusions about the efficacy of biofeedback from this study s findings because all participants received biofeedback. Norton et al reported in 2003 on the results of a trial that randomly assigned 171 patients with fecal incontinence to 1 of 4 groups: standard care (advice), advice plus instruction on sphincter exercises, hospital-based computer-assisted sphincter pressure biofeedback, and hospital biofeedback plus the use of a home EMG biofeedback device.(6) Outcomes included diary reports of incontinence, quality of life, and anal manometry measurements. The authors reported that biofeedback yielded no greater benefit than standard care. In 2003, Solomon et al reported on the results of a trial that randomly assigned 120 patients with mild to moderate fecal incontinence to 1 of 3 groups: biofeedback with anal manometry, biofeedback with transanal ultrasound, or pelvic floor exercises with feedback from digital examination alone.(7) There were no significant differences in outcomes among the treatment groups; all reported modest improvements. Children A Cochrane review on behavioral and cognitive interventions for children with fecal incontinence was published in 2006 and updated in 2011.(8,9) Of the 21 studies, 9 compared conventional treatment alone (ie, laxatives, toilet training, dietary advice) to conventional treatment plus biofeedback. Eight trials included children with functional fecal incontinence, and the ninth included children with fecal incontinence due to myelomeningocele (n=12). In 4 trials, children were included who had fecal incontinence due to constipation, and in 3 other trials, children had fecal incontinence due to constipation and pelvic floor dyssynergia. When data from the 9 studies were combined, 133 of 260 (51.2%) in the conventional treatment plus biofeedback group were not cured or improved at follow-up compared to 121 of 250 (48.4%) patients in the conventional only group. In a meta-analysis (random effects), this difference was not statistically significant (pooled OR=1.08, 95% CI, 0.63 to 1.84). The analysis combined 6- and 12-month follow-up data; 12-month data were used when available. The authors concluded that findings from RCTs do not support the claim that biofeedback training provides additional benefit to conventional treatment in the management of fecal incontinence associated with constipation. They also stated that, due to a lack of sufficient trials, they were unable to evaluate the effects of biofeedback in children with organic fecal incontinence. Constipation Does the addition of biofeedback to standard care improve refractory constipation, compared with standard care alone? Adults The Enck et al systematic review, described above in the section on fecal incontinence, also reviewed the literature on biofeedback for constipation.(1) Eight RCTs conducted in adults were identified. Four of these compared 2 types of biofeedback; a meta-analysis of these 4 studies did not find a significant benefit of 1 technique over another (pooled OR=1.44; 95% CI, 0.69 to 3.09; p=0.32). The other 4 studies compared biofeedback to another treatment. Comparison treatments (1 study each) were botulinum toxin, laxatives, diazepam, and best supportive care (diet, exercise, and laxatives). Two studies also included a third arm, in which treatment was a sham or placebo intervention. Three of the 4
6 studies included patients with dyssynergia-type constipation and the fourth included patients with anismus. A meta-analysis of the 4 studies comparing 1 treatment with another (using the active intervention arm as the comparison in the 3-arm trials) found a significantly greater benefit of biofeedback in improving constipation symptoms (pooled OR=3.23; 95% CI, 1.88 to 5.58; p<0.001). The results of this systematic review are limited by the heterogeneity in patient populations, comparison treatments, and outcome measures. The 2 three-arm studies and newer RCTs published after the Enck review are described below. Heymen et al included adults who met Rome II diagnostic criteria for pelvic floor dyssynergia, had 2 or more symptoms of functional constipation for at least 12 weeks in the past year, and had manometry or electromyography findings consistent with chronic constipation (eg, evidence of inadequate propulsive forces and incomplete evacuation).(10) Patients participated in a 4-week run-in period consisting of education on diet and exercise and provision of fiber and stool softeners. Those who still met eligibility criteria at the end of the run-in period (84 of 117, 72%) were randomly assigned to EMG biofeedback (n=30), diazepam 5 mg (n=30), or placebo medication (n=24). All participants were trained to perform pelvic floor exercises, and all received 6 biweekly visits over 3 months, each lasting approximately 50 minutes. Patients and investigators were blinded to which patients received active versus placebo medication but not to whether or not they received biofeedback. In an intention-to-treat (ITT) analysis after the 3-month intervention, the proportion of patients reporting adequate relief of constipation symptoms was 70% in the biofeedback group, 23% in the diazepam group, and 38% in the placebo group; biofeedback had a significantly greater benefit when compared either with diazepam (p<0.001) or placebo (p<0.017). A strength of this study was that it attempted to control for nonspecific effects of biofeedback, eg, increased contact with a health care provider and lifestyle modification advice, by including a run-in period and similar follow-up visits for all groups. Moreover, randomization did not occur until after the run-in period, so treatment groups were more likely to be similar at the start of the treatment phase. Rao et al included patients who met Rome II diagnostic criteria for functional constipation, had dyssynergia-type constipation and, when expelling a simulated stool, had either prolonged difficulty (at least 1 minute) or prolonged delay (at least 20% marker retention in colonic transfer).(11) All participants had failed routine management of constipation. A total of 77 patients were randomly assigned to receive 3 months of standard therapy, ie, education, dietary advice (n=24), standard therapy and biofeedback therapy (n=28), or standard therapy and sham feedback (n=24). Patients receiving active biofeedback received up to 6 biweekly 1-hour sessions: training was performed using a rectal manometry probe and software for displaying the biofeedback data. In the sham treatment group, patients also used a rectal manometry probe but did not receive visual and verbal feedback. Patients were not blinded to treatment group, but the manometry reader was unaware of treatment assignment. In an ITT analysis, after the 3-month intervention, patients in the biofeedback group reported a significantly greater increase in complete spontaneous bowel movements than the sham feedback group (p<0.05) and the standard treatment group (p<0.062). In addition, a greater proportion of the patients in the biofeedback group reported improved global bowel satisfaction compared to the sham feedback group (p=0.04), but the comparison with the standard treatment group was not significantly different. (The authors did not report exact numbers for either of these preceding primary analyses). Of the primary physiologic parameters, the ITT analysis found that the dyssynergia pattern was corrected in 79% of those in the biofeedback group, 4% in the sham group, and 8% in the standard treatment group. This difference was statistically significant in favor of the biofeedback group compared to each of the other groups (p<0.001 for both analyses). Moreover, the balloon expulsion time during simulated defecation decreased significantly more in the biofeedback group compared with sham (p=0.003) or standard treatment (p=0.03) (exact times not reported for the ITT analysis). A 2010 publication reported on 1-year findings of the Rao study in 13 of 21 (62%) patients in the biofeedback group and 13 of 23 (57%) in the standard treatment group.(12) Patients in the sham group were not included in this follow-up study. The extension study included visits at 3-month intervals, with additional advice provided as needed. Seven of the 13 (54%) biofeedback patients and all 13 patients in the standard treatment group completed the 1-year follow-up. Mean change in complete
7 spontaneous bowel movements (the primary outcome) favored the biofeedback group (increase of 2.9) compared to the standard treatment group (decrease of 0.2). The follow-up study suggests longer-term effectiveness of biofeedback for this patient population. However, the small numbers of patients who completed the 1-year follow-up, along with the drop-out rate in the biofeedback group, limit the conclusions that can be reached. A 2012 RCT by Hart et al included 21 patients with constipation who failed to respond to dietary and medical therapies.(13) (The study was not limited to patients with dyssynergia-type constipation.) The experimental arm consisted of biofeedback with an EMG rectal probe. Patients were taught to isolate the anal sphincter and receive feedback on the muscle activity of the external anal sphincter. In the control intervention, investigators attempted to control for the nonspecific effects of biofeedback by using biofeedback but no rectal probe. The comparison intervention involved biofeedback with bilateral EMGs in conjunction with surface electrodes placed on the trapezius or temporalis muscle and muscle tension reduction instruction. Both groups were given 6 treatment sessions (every other week for 12 weeks). A total of 15 of 21 patients (71%) completed the study and were included in the follow-up evaluation. The 2 primary outcome measures were the Constipation Severity Instrument (CSI) and the Irritable Bowel Syndrome Quality of Life Scale (IBS-QOL); both of these are multi-item self-report instruments. For the CSI, a lower score represents less severe symptoms and for the IBS-QOL, a higher score represents a higher quality of life. The authors did not report the possible maximum scores for either measure. The change in scores from baseline to follow-up assessments did not differ significantly between groups for either outcome measure. Mean scores on the CSI decreased from 46.5 to 30.0 in the anorectal biofeedback group and 41.2 to 34.9 in the biofeedback control group. Mean scores on IBS-QOL increased from 80.8 to 96.1 in the anorectal biofeedback group and from 90.6 to 96.7 in the biofeedback control group. The study had a small sample size and was likely underpowered to statistically significant difference between groups. Children No systematic reviews or meta-analyses on biofeedback for constipation in children, not associated with fecal incontinence, were identified. The literature search did identify the 1 RCT published since Van Ginkel et al in the Netherlands included 212 children at least 5 years old with constipation who met at least 2 of the following 4 criteria: (1) stool frequency fewer than 3 times per week; (2) 2 or more soiling and/or encopresis episodes per week; (3) periodic passage of very large amounts of stool every 7 to 30 days; or (4) a palpable abdominal or rectal fecal mass.(14) Participants were randomly assigned to 6 weeks of standard treatment, ie, education, laxatives (n=111) or standard treatment plus 2 sessions of anorectal manometry (n=91). During the manometry sessions, the child was asked to squeeze the sphincter as tight as possible 5 times. Squeeze pressure data were converted to digital values and transmitted to a computer; the data could be viewed by the child and parent. The data were discussed after the sessions, and instructions were given on how to perform defection exercises at home. Ten of 212 (5%) randomly assigned patients did not receive treatment, and the remainder completed the intervention. Treatment success was defined as achievement of 3 or more bowel movements per week and fewer than 1 soiling and/or encopresis episodes per 2 weeks while not receiving laxatives. At 6 weeks, 4 of 111 (4%) in the standard treatment group and 6 of 91 (7%) in the biofeedback group were considered to have successful treatment; this difference was not significantly different. There was also no statistically significant difference between groups at any other follow-up point. At the final 104-week follow-up, 36 of 83 (43%) patients in the standard treatment group and 23 of 65 (35%) in the biofeedback group were considered treatment successes. Data on 30% of the randomized patients were missing at the final follow-up. This intervention did not control for the nonspecific effects of biofeedback. Ongoing Clinical Trials Comparison of PTNS and Biofeedback for Fecal Incontinence (NCT )(15): This open-label study is randomizing 50 adults with fecal incontinence to treatment with posterior tibial nerve stimulation
8 (PTNS) or EMG biofeedback. The primary outcome is change in weekly episodes of fecal incontinence. The expected date of completion is December Summary There is a relatively large body of literature (ie, randomized controlled trials [RCTs] and systematic reviews) evaluating the efficacy of biofeedback for treating fecal incontinence and constipation. For the treatment of fecal incontinence, systematic reviews have not found that biofeedback provides additional benefit when offered in conjunction with conventional therapy, compared with conventional therapy alone. While 1 recent RCT found that there was a significantly greater decrease in fecal incontinence symptoms with biofeedback plus exercise training than with exercise training alone, the majority of trials do not show a significant benefit. Overall, the evidence is insufficient to conclude that biofeedback improves the net health outcome for adults and children with fecal incontinence; therefore, this treatment is considered investigational. For the treatment of constipation, a systematic review of RCTs found a benefit of biofeedback as a treatment of constipation in adults. Conclusions of the systematic review were limited by variability in patient populations, comparison groups and outcomes measures. However, detailed examination of several well-conducted RCTs focusing on patients with dyssynergia-type constipation suggests benefits in a subgroup of patients who meet criteria similar to trial participants. Thus, biofeedback may be considered medically necessary in adult patients with dyssynergia-type constipation who meet selection criteria and investigational for other patients with constipation. Practice Guidelines and Position Statements In 2013, the American Gastroenterological Association updated their position statement on constipation. The following statement on biofeedback was included: Pelvic floor retraining by biofeedback therapy rather than laxatives is recommended for defecatory disorders (Strong Recommendation, High-Quality Evidence). (16) In May 2010, the National Institute for Clinical Excellence issued a guideline on constipation in children and young people. The guideline states that biofeedback should not be used for ongoing treatment.(17) In June 2007, they issued a guideline on fecal incontinence in adults which states the following regarding biofeedback: The evidence we found did not show biofeedback to be more effective than standard care, exercises alone, or other conservative therapies. The limited number of studies and the small number of participants in each group of the studies make it difficult to come to any definitive conclusion about its effectiveness. (18) In 2008, the National Institutes of Health issued a state-of-the science statement on fecal and urinary incontinence based on a consensus conference held in December 2007.(19) Included in the conclusions was the following statement, pelvic floor muscle training and biofeedback are effective in preventing and reversing fecal and urinary incontinence in women for the first year after giving birth In December 2007, an Evidence Report/Technology Assessment, Prevention of Urinary and Fecal Incontinence in Adults,(20) based on research conducted by the Minnesota Evidence-based Practice Center under contract to the Agency for Healthcare Research and Quality, was issued. One of the research objectives was to review the effectiveness of clinical interventions to reduce the risk of incontinence. The authors identified 1 RCT that found twice the rate of control of fecal incontinence in women who had obstetric and sphincter trauma after biofeedback training with pelvic floor muscle training compared to muscle training alone. The review concluded that limited evidence supports a reduction in fecal incontinence after complex behavioral interventions, which include exercises augmented with biofeedback. In October 2007, the American Society of Colon and Rectal Surgeons released Practice Parameters for thetreatment of Fecal Incontinence.(21) The report stated that biofeedback can be considered as a
9 treatment option for patients who have not responded to dietary modification or medication (Level of Evidence: III; Grade of Recommendation: B). It also states that biofeedback may be considered in the early post-partum period for women with symptomatic sphincter weakness. Also, in 2007, they published Practice Parameters for the Evaluation and Management of Constipation.(22) They recommend biofeedback therapy for patients with symptomatic pelvic floor dyssynergia (Level of Evidence: Class II; Grade of Recommendation: B). Medicare National Coverage National Coverage Determination (NCD) for Biofeedback (30.1) Biofeedback therapy is covered under Medicare only when it is reasonable and necessary for the individual patient for muscle re-education of specific muscle groups or for treating pathological muscle abnormalities of spasticity, incapacitating muscle spasm, or weakness, and more conventional treatments (heat, cold, massage, exercise, support) have not been successful. This therapy is not covered for treatment of ordinary muscle tension states or for psychosomatic conditions.(23) References 1. Enck P, Van der Voort IR, Klosterhalfen S. Biofeedback therapy in fecal incontinence and constipation. Neurogastroenterol Motil 2009; 21(11): Vonthein R, Heimerl T, Schwandner T et al. Electrical stimulation and biofeedback for the treatment of fecal incontinence: a systematic review. Int J Colorectal Dis 2013; 28(11): Norton C, Cody JD. Biofeedback and/or sphincter exercises for the treatment of faecal incontinence in adults. Cochrane Database Syst Rev 2012; 7:CD Heymen S, Scarlett Y, Jones K et al. Randomized controlled trial shows biofeedback to be superior to pelvic floor exercises for fecal incontinence. Dis Colon Rectum 2009; 52(10): Bartlett L, Sloots K, Nowak M et al. Biofeedback for fecal incontinence: a randomized study comparing exercise regimens. Dis Colon Rectum 2011; 54(7): Norton C, Chelvanayagam S, Wilson-Barnett J et al. Randomized controlled trial of biofeedback for fecal incontinence. Gastroenterology 2003; 125(5): Solomon MJ, Pager CK, Rex J et al. Randomized, controlled trial of biofeedback with anal manometry, transanal ultrasound, or pelvic floor retraining with digital guidance alone in the treatment of mild to moderate fecal incontinence. Dis Colon Rectum 2003; 46(6): Brazzelli M, Griffiths P. Behavioural and cognitive interventions with or without other treatments for the management of faecal incontinence in children. Cochrane Database Syst Rev 2006; (2):CD Brazzelli M, Griffiths PV, Cody JD et al. Behavioural and cognitive interventions with or without other treatments for the management of faecal incontinence in children. Cochrane Database Syst Rev 2011; (12):CD Heymen S, Scarlett Y, Jones K et al. Randomized, controlled trial shows biofeedback to be superior to alternative treatments for patients with pelvic floor dyssynergia-type constipation. Dis Colon Rectum 2007; 50(4): Rao SS, Seaton K, Miller M et al. Randomized controlled trial of biofeedback, sham feedback and standard therapy for dyssynergic defecation. Clin Gastroenterol Hepatol 2007; 5(3): Rao SS, Valestin J, Brown CK et al. Long-term efficacy of biofeedback therapy for dyssynergic defection: randomized controlled trial. Am J Gastroenterol 2010; 105(4): Hart SL, Lee JW, Berian J et al. A randomized controlled trial of anorectal biofeedback for constipation. Int J Colorectal Dis 2012; 27(4): van Ginkel R, Buller HA, Boeckxstaens GE et al. The effect of anorectal manometry on the outcome of treatment in severe childhood constipation: a randomized controlled trial. Pediatrics 2001; 108(1):E Sponsored by Seoul National University Hospital. Comparison of PTNS and Biofeedback for Fecal Incontinence (NCT ). Available online at: American Gastroenterological Association. American Gastroenterological Association medical position statement on constipation. Available online at:
10 17. National Institute for Health and Clinical Excellence (NICE). Guideline 99: Constipation in children and young people Available online at: National Institute for Health and Clinical Excellence (NICE). Guideline 49: Faecal incontinence: the management of faecal incontinence in adults Available online at: Landefeld CS, Bowers BJ, Feld AD et al. National Institutes of Health State-of-the-Science Conference Statement: Prevention of fecal and urinary incontinence in adults. Ann Intern Med 2008; 148(6): Shamliyan T, Wyman J, Bliss DZ et al. Prevention of urinary and fecal incontinence in adults. Evid Rep Technol Assess (Full Rep) 2007; 161(AHRQ Publication No. 08-E003): Tjandra JJ, Dykes SL, Kumar RR et al. Standards Practice Task Force of the American Society of Colon Rectal Surgeons. Practice parameters for the treatment of fecal incontinence. Dis Colon Rectum 2007; 50(10): Ternent CA, Bastawrous AL, Morin NASPTFotASoC et al. Practice parameters for the evaluation and management of constipation. Dis Colon Rectum 2007; 50(12): National Coverage Determination (NCD) for Biofeedback Therapy (30.1). Available online at: %3A1%3ABiofeedback+Therapy Billing Coding/Physician Documentation Information Individual psychophysiological therapy incorporating biofeedback training by any modality (face-to-face with the patient), with psychotherapy (eg, insight oriented, behavior modifying or supportive psychotherapy); 30 minutes Individual psychophysiological therapy incorporating biofeedback training by any modality (face-to-face with the patient), with psychotherapy (eg, insight oriented, behavior modifying or supportive psychotherapy); 45 minutes Biofeedback training by any modality Biofeedback training, perineal muscles, anorectal or urethral sphincter, including EMG and/or manometry E0746 Electromyography (EMG), biofeedback device Additional Policy Key Words N/A Policy Implementation/Update Information 7/1/08 New policy; considered investigational. 7/1/09 No policy statement changes. 7/1/10 No policy statement changes. 7/1/11 Scope expanded to include constipation and title changed to reflect this change. Policy statement on constipation added which states that it is investigational. 7/1/12 No policy statement changes. 3/1/13 Statement added that biofeedback for constipation in adults may be considered medically necessary for patients with dyssynergia-type constipation who meet criteria. Investigational statement on constipation modified to indicate that it applies to all patients who do not meet criteria in medically necessary statement. 7/1/13 No policy statement changes. 7/1/14 No policy statement changes. State and Federal mandates and health plan contract language, including specific provisions/exclusions, take precedence over Medical Policy and must be considered first in determining eligibility for coverage. The medical policies contained herein are for informational purposes. The medical policies do not constitute medical advice or medical care. Treating health care providers are independent contractors and are neither employees nor agents Blue KC and are solely responsible for
11 diagnosis, treatment and medical advice. No part of this publication may be reproduced, stored in a retrieval system or transmitted, in any form or by any means, electronic, photocopying, or otherwise, without permission from Blue KC.
Biofeedback as a Treatment of Fecal Incontinence or Constipation
 2.01.64 Biofeedback as a Treatment of Fecal Incontinence or Constipation Section 2.0 Medicine Subsection Effective Date February 15, 2015 Original Policy Date December 15, 2014 Next Review Date December
2.01.64 Biofeedback as a Treatment of Fecal Incontinence or Constipation Section 2.0 Medicine Subsection Effective Date February 15, 2015 Original Policy Date December 15, 2014 Next Review Date December
Populations Interventions Comparators Outcomes Individuals: With fecal incontinence
 Protocol Biofeedback as a Treatment of Fecal Incontinence or Constipation (20164) Medical Benefit Effective Date: 07/01/13 Next Review Date: 03/19 Preauthorization No Review Dates: 09/07, 09/08, 09/09,
Protocol Biofeedback as a Treatment of Fecal Incontinence or Constipation (20164) Medical Benefit Effective Date: 07/01/13 Next Review Date: 03/19 Preauthorization No Review Dates: 09/07, 09/08, 09/09,
Biofeedback as a Treatment of Fecal Incontinence or Constipation
 Biofeedback as a Treatment of Fecal Incontinence or Constipation Policy Number: 2.01.64 Last Review: 7/2018 Origination: 7/2008 Next Review: 7/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue
Biofeedback as a Treatment of Fecal Incontinence or Constipation Policy Number: 2.01.64 Last Review: 7/2018 Origination: 7/2008 Next Review: 7/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue
Medical Policy. MP Biofeedback as a Treatment of Fecal Incontinence or Constipation
 Medical Policy MP 2.01.64 BCBSA Ref. Policy: 2.01.64 Last Review: 11/15/2018 Effective Date: 11/15/2018 Section: Medicine Related Policies 2.01.27 Biofeedback as a Treatment of Urinary Incontinence in
Medical Policy MP 2.01.64 BCBSA Ref. Policy: 2.01.64 Last Review: 11/15/2018 Effective Date: 11/15/2018 Section: Medicine Related Policies 2.01.27 Biofeedback as a Treatment of Urinary Incontinence in
MEDICAL POLICY SUBJECT: BIOFEEDBACK
 MEDICAL POLICY PAGE: 1 OF: 6 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases, medical policy criteria are not applied.
MEDICAL POLICY PAGE: 1 OF: 6 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases, medical policy criteria are not applied.
Biofeedback as a Treatment of Headache
 Biofeedback as a Treatment of Headache Policy Number: 2.01.29 Last Review: 7/2018 Origination: 7/2008 Next Review: 7/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) may provide coverage
Biofeedback as a Treatment of Headache Policy Number: 2.01.29 Last Review: 7/2018 Origination: 7/2008 Next Review: 7/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) may provide coverage
Biofeedback for Pelvic Floor Disorders and Incontinence
 The UNC Center for Functional GI & Motility Disorders www.med.unc.edu/ibs Biofeedback for Pelvic Floor Disorders and Incontinence Olafur S. Palsson, Psy.D. Associate Professor of Medicine UNC Center for
The UNC Center for Functional GI & Motility Disorders www.med.unc.edu/ibs Biofeedback for Pelvic Floor Disorders and Incontinence Olafur S. Palsson, Psy.D. Associate Professor of Medicine UNC Center for
Corporate Medical Policy
 Corporate Medical Policy Biofeedback File Name: Origination: Last CAP Review: Next CAP Review: Last Review: biofeedback 11/1994 2/2017 2/2018 9/2017 Description of Procedure or Service Biofeedback is a
Corporate Medical Policy Biofeedback File Name: Origination: Last CAP Review: Next CAP Review: Last Review: biofeedback 11/1994 2/2017 2/2018 9/2017 Description of Procedure or Service Biofeedback is a
Anorectal Diagnostic Overview
 Anorectal Diagnostic Overview 11-25-09 3.11.2010 2009 2010 Anorectal Manometry Overview Measurement of pressures and the annotation of rectal sensation throughout the rectum and anal canal to determine:
Anorectal Diagnostic Overview 11-25-09 3.11.2010 2009 2010 Anorectal Manometry Overview Measurement of pressures and the annotation of rectal sensation throughout the rectum and anal canal to determine:
Corporate Medical Policy
 Corporate Medical Policy Biofeedback as a Treatment of Pain File Name: Origination: Last CAP Review: Next CAP Review: Last Review: Biofeedback_as_a_treatment_of_pain 2/2017 5/2018 5/2019 5/2018 Description
Corporate Medical Policy Biofeedback as a Treatment of Pain File Name: Origination: Last CAP Review: Next CAP Review: Last Review: Biofeedback_as_a_treatment_of_pain 2/2017 5/2018 5/2019 5/2018 Description
Elderly Man With Chronic Constipation
 Elderly Man With Chronic Constipation Linda Nguyen, MD Director, Neurogastroenterology and Motility Clinical Assistant Professor Stanford University Overview Normal bowel function Defining Constipation:
Elderly Man With Chronic Constipation Linda Nguyen, MD Director, Neurogastroenterology and Motility Clinical Assistant Professor Stanford University Overview Normal bowel function Defining Constipation:
Vertebral Axial Decompression
 Vertebral Axial Decompression Policy Number: 8.03.09 Last Review: 11/2017 Origination: 11/2005 Next Review: 11/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide coverage
Vertebral Axial Decompression Policy Number: 8.03.09 Last Review: 11/2017 Origination: 11/2005 Next Review: 11/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide coverage
JNM Journal of Neurogastroenterology and Motility
 JNM Journal of Neurogastroenterology and Motility J Neurogastroenterol Motil, Vol. 19 No. 4 October, 2013 pissn: 2093-0879 eissn: 2093-0887 http://dx.doi.org/10.5056/jnm.2013.19.4.532 How to Interpret
JNM Journal of Neurogastroenterology and Motility J Neurogastroenterol Motil, Vol. 19 No. 4 October, 2013 pissn: 2093-0879 eissn: 2093-0887 http://dx.doi.org/10.5056/jnm.2013.19.4.532 How to Interpret
Corporate Medical Policy
 Corporate Medical Policy Biofeedback File Name: Origination: Last CAP Review: Next CAP Review: Last Review: biofeedback 11/1994 2/2018 2/2019 9/2018 Description of Procedure or Service Biofeedback is a
Corporate Medical Policy Biofeedback File Name: Origination: Last CAP Review: Next CAP Review: Last Review: biofeedback 11/1994 2/2018 2/2019 9/2018 Description of Procedure or Service Biofeedback is a
Fecal Incontinence. What is fecal incontinence?
 Scan for mobile link. Fecal Incontinence Fecal incontinence is the inability to control the passage of waste material from the body. It may be associated with constipation or diarrhea and typically occurs
Scan for mobile link. Fecal Incontinence Fecal incontinence is the inability to control the passage of waste material from the body. It may be associated with constipation or diarrhea and typically occurs
Vertebral Axial Decompression
 Vertebral Axial Decompression Policy Number: 8.03.09 Last Review: 11/2018 Origination: 11/2005 Next Review: 11/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide coverage
Vertebral Axial Decompression Policy Number: 8.03.09 Last Review: 11/2018 Origination: 11/2005 Next Review: 11/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide coverage
Posterior Tibial Nerve Stimulation for Voiding Dysfunction
 Posterior Tibial Nerve Stimulation for Voiding Dysfunction Corporate Medical Policy File name: Posterior Tibial Nerve Stimulation for Voiding Dysfunction File code: UM.NS.05 Origination: 8/2011 Last Review:
Posterior Tibial Nerve Stimulation for Voiding Dysfunction Corporate Medical Policy File name: Posterior Tibial Nerve Stimulation for Voiding Dysfunction File code: UM.NS.05 Origination: 8/2011 Last Review:
ACG Clinical Guideline: Management of Benign Anorectal Disorders
 ACG Clinical Guideline: Management of Benign Anorectal Disorders Arnold Wald, MD, MACG 1, Adil E. Bharucha, MBBS, MD 2, Bard C. Cosman, MD, MPH, FASCRS 3 and William E. Whitehead, PhD, MACG 4 1 Division
ACG Clinical Guideline: Management of Benign Anorectal Disorders Arnold Wald, MD, MACG 1, Adil E. Bharucha, MBBS, MD 2, Bard C. Cosman, MD, MPH, FASCRS 3 and William E. Whitehead, PhD, MACG 4 1 Division
A Nursing Assessment Tool for Adults With Fecal Incontinence
 Journal of Wound, Ostomy and Continence Nursing 2000, 279- A Nursing Assessment Tool for Adults With Fecal Incontinence Christine Norton, MA, RN, and Sonya Chelvanayagam, MSc, RN Abstract Fecal incontinence
Journal of Wound, Ostomy and Continence Nursing 2000, 279- A Nursing Assessment Tool for Adults With Fecal Incontinence Christine Norton, MA, RN, and Sonya Chelvanayagam, MSc, RN Abstract Fecal incontinence
Biofeedback has been reported to be an effective treatment
 ORIGINAL CONTRIBUTION Randomized Controlled Trial Shows Biofeedback to be Superior to Pelvic Floor Exercises for Fecal Incontinence Steve Heymen, Ph.D. Yolanda Scarlett, M.D. Kenneth Jones, Ph.D. Yehuda
ORIGINAL CONTRIBUTION Randomized Controlled Trial Shows Biofeedback to be Superior to Pelvic Floor Exercises for Fecal Incontinence Steve Heymen, Ph.D. Yolanda Scarlett, M.D. Kenneth Jones, Ph.D. Yehuda
GI Physiology - Investigating and treating patients with pelvic floor dysfunction. Lynne Smith Department of GI Physiology NGH Sheffield
 GI Physiology - Investigating and treating patients with pelvic floor dysfunction Lynne Smith Department of GI Physiology NGH Sheffield Aims o o o To give an overview of lower GI investigations To demonstrate
GI Physiology - Investigating and treating patients with pelvic floor dysfunction Lynne Smith Department of GI Physiology NGH Sheffield Aims o o o To give an overview of lower GI investigations To demonstrate
Human Anatomy rectum
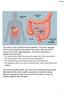 rectum The colon is also called the large intestine. The ileum (last part of the small intestine) connects to the cecum (first part of the colon) in the lower right abdomen. The rest of the colon is divided
rectum The colon is also called the large intestine. The ileum (last part of the small intestine) connects to the cecum (first part of the colon) in the lower right abdomen. The rest of the colon is divided
Posterior Tibial Nerve Stimulation
 Posterior Tibial Nerve Stimulation Policy Number: Original Effective Date: MM.02.025 01/01/2015 Lines of Business: Current Effective Date: HMO; PPO; QUEST Integration 02/01/2015 Section: Medicine Place(s)
Posterior Tibial Nerve Stimulation Policy Number: Original Effective Date: MM.02.025 01/01/2015 Lines of Business: Current Effective Date: HMO; PPO; QUEST Integration 02/01/2015 Section: Medicine Place(s)
Injectable Bulking Agents for the Treatment of Fecal Incontinence. Policy Specific Section: September 27, 2013 January 1, 2015
 Medical Policy Injectable Bulking Agents for the Treatment of Fecal Incontinence Type: Investigational / Experimental Policy Specific Section: Surgery Original Policy Date: Effective Date: September 27,
Medical Policy Injectable Bulking Agents for the Treatment of Fecal Incontinence Type: Investigational / Experimental Policy Specific Section: Surgery Original Policy Date: Effective Date: September 27,
NIH Public Access Author Manuscript Best Pract Res Clin Gastroenterol. Author manuscript; available in PMC 2012 February 1.
 NIH Public Access Author Manuscript Published in final edited form as: Best Pract Res Clin Gastroenterol. 2011 February ; 25(1): 159 166. doi:10.1016/j.bpg.2011.01.004. BIOFEEDBACK THERAPY FOR CONSTIPATION
NIH Public Access Author Manuscript Published in final edited form as: Best Pract Res Clin Gastroenterol. 2011 February ; 25(1): 159 166. doi:10.1016/j.bpg.2011.01.004. BIOFEEDBACK THERAPY FOR CONSTIPATION
Peripheral Subcutaneous Field Stimulation
 Peripheral Subcutaneous Field Stimulation Policy Number: 7.01.139 Last Review: 9/2014 Origination: 7/2013 Next Review: 1/2015 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide
Peripheral Subcutaneous Field Stimulation Policy Number: 7.01.139 Last Review: 9/2014 Origination: 7/2013 Next Review: 1/2015 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide
Paediatric constipation and functional non-retentive faecal soiling Voskuijl, W.P.
 UvA-DARE (Digital Academic Repository) Paediatric constipation and functional non-retentive faecal soiling Voskuijl, W.P. Link to publication Citation for published version (APA): Voskuijl, W. P. (2005).
UvA-DARE (Digital Academic Repository) Paediatric constipation and functional non-retentive faecal soiling Voskuijl, W.P. Link to publication Citation for published version (APA): Voskuijl, W. P. (2005).
CONSTIPATION. Atan Baas Sinuhaji
 CONSTIPATION Atan Baas Sinuhaji Sub Division of Pediatrics Gastroentero-Hepatolgy Department of ChildHealth,School of Medicine University of Sumatera Utara MEDAN DEFECATION REGULAR PATTERN CONSTIPATION
CONSTIPATION Atan Baas Sinuhaji Sub Division of Pediatrics Gastroentero-Hepatolgy Department of ChildHealth,School of Medicine University of Sumatera Utara MEDAN DEFECATION REGULAR PATTERN CONSTIPATION
Duc M. Vo, MD, FACS Northwest Surgical Specialists
 Duc M. Vo, MD, FACS Northwest Surgical Specialists Disclosures none Outline Definition Etiologies Exam findings Additional testing Medical management Surgical options What is fecal incontinence? Recurrent
Duc M. Vo, MD, FACS Northwest Surgical Specialists Disclosures none Outline Definition Etiologies Exam findings Additional testing Medical management Surgical options What is fecal incontinence? Recurrent
Management of Neurogenic Bowel Dysfunction. Fiona Paul, DNP, RN, CPNP Center for Motility and Functional Gastrointestinal Disorders
 Management of Neurogenic Bowel Dysfunction Fiona Paul, DNP, RN, CPNP Center for Motility and Functional Gastrointestinal Disorders DEFECATION Delivery of colon contents to the rectum Rectal compliance
Management of Neurogenic Bowel Dysfunction Fiona Paul, DNP, RN, CPNP Center for Motility and Functional Gastrointestinal Disorders DEFECATION Delivery of colon contents to the rectum Rectal compliance
New Advances in Biofeedback. Brigitte Fung Physiotherapist Kwong Wah Hospital
 New Advances in Biofeedback Brigitte Fung Physiotherapist Kwong Wah Hospital Content What is biofeedback Types of biofeedback Uses of biofeedback in UI Uses of Biofeedback in FI & Constipation What is
New Advances in Biofeedback Brigitte Fung Physiotherapist Kwong Wah Hospital Content What is biofeedback Types of biofeedback Uses of biofeedback in UI Uses of Biofeedback in FI & Constipation What is
Biofeedback Therapy A nurse led management service for functional bowel disorders
 Biofeedback Therapy A nurse led management service for functional bowel disorders Brigitte Collins Lead Nurse BSc, MSc GI Nursing, Dip/Hypnotherapy St Marks Hospital Is biofeedback necessary? Conservative
Biofeedback Therapy A nurse led management service for functional bowel disorders Brigitte Collins Lead Nurse BSc, MSc GI Nursing, Dip/Hypnotherapy St Marks Hospital Is biofeedback necessary? Conservative
Effect of biofeedback therapy on anorectal physiological parameters among patients with fecal evacuation disorder
 DOI 10.1007/s12664-017-0731-y ORIGINAL ARTICLE Effect of biofeedback therapy on anorectal physiological parameters among patients with fecal evacuation disorder Abhai Verma 1 & Asha Misra 1 & Uday C Ghoshal
DOI 10.1007/s12664-017-0731-y ORIGINAL ARTICLE Effect of biofeedback therapy on anorectal physiological parameters among patients with fecal evacuation disorder Abhai Verma 1 & Asha Misra 1 & Uday C Ghoshal
Common Gastrointestinal Problems in the Elderly
 Common Gastrointestinal Problems in the Elderly Brian Viviano, D.O. Objectives Understand the pathophysiology, clinical manifestations, diagnosis and management of GI diseases of the elderly. Differentiate
Common Gastrointestinal Problems in the Elderly Brian Viviano, D.O. Objectives Understand the pathophysiology, clinical manifestations, diagnosis and management of GI diseases of the elderly. Differentiate
Biofeedback provides long term benefit for patients with intractable, slow and normal transit constipation
 Gut 1998;42:517 521 517 St Mark s Hospital, London, UK E Chiotakakou-Faliakou M A Kamm AJRoy J B Storrie I C Turner Correspondence to: Dr M A Kamm, St Mark s Hospital, Northwick Park, Watford Road, Harrow,
Gut 1998;42:517 521 517 St Mark s Hospital, London, UK E Chiotakakou-Faliakou M A Kamm AJRoy J B Storrie I C Turner Correspondence to: Dr M A Kamm, St Mark s Hospital, Northwick Park, Watford Road, Harrow,
15. Prevention of UTI and lifestyle modifications
 15. Prevention of UTI and lifestyle modifications Key questions: Does improving poor voiding habits help prevent UTI recurrence? Does improving constipation help prevent UTI recurrence? Does increasing
15. Prevention of UTI and lifestyle modifications Key questions: Does improving poor voiding habits help prevent UTI recurrence? Does improving constipation help prevent UTI recurrence? Does increasing
SACRAL NERVE STIMULATION FOR EXPERIENCE IN CHILDREN
 SACRAL NERVE STIMULATION FOR COLORECTAL DISEASES: EXPERIENCE IN CHILDREN C. LOUIS-BORRIONE - JM. GUYS TIMONE-ENFANTS MARSEILLE SACRAL NEUROMODULATION IN CHILDREN 26 : Humphreys et al - 23 children with
SACRAL NERVE STIMULATION FOR COLORECTAL DISEASES: EXPERIENCE IN CHILDREN C. LOUIS-BORRIONE - JM. GUYS TIMONE-ENFANTS MARSEILLE SACRAL NEUROMODULATION IN CHILDREN 26 : Humphreys et al - 23 children with
Biofeedback pelvic floor exercise therapy for pelvic floor dyssynergia: an observational study
 International Surgery Journal Porwal A et al. Int Surg J. 2017 Oct;4(10):3461-3465 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20174516
International Surgery Journal Porwal A et al. Int Surg J. 2017 Oct;4(10):3461-3465 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20174516
Transtympanic Micropressure Applications as a Treatment of Meniere s Disease
 Transtympanic Micropressure Applications as a Treatment of Meniere s Disease Policy Number: 1.01.23 Last Review: 8/2014 Origination: 2/2006 Next Review: 8/2015 Policy Blue Cross and Blue Shield of Kansas
Transtympanic Micropressure Applications as a Treatment of Meniere s Disease Policy Number: 1.01.23 Last Review: 8/2014 Origination: 2/2006 Next Review: 8/2015 Policy Blue Cross and Blue Shield of Kansas
Constipation. What is constipation? What is the criteria for having constipation? What are the different types of constipation?
 What is constipation? is defined as having a bowel movement less than 3 times per week. It is usually associated with hard stools or difficulty passing stools. You may have pain while passing stools or
What is constipation? is defined as having a bowel movement less than 3 times per week. It is usually associated with hard stools or difficulty passing stools. You may have pain while passing stools or
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Constipation: management of idiopathic constipation in children in primary and secondary care 1.1 Short title Constipation
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Constipation: management of idiopathic constipation in children in primary and secondary care 1.1 Short title Constipation
Physical Therapy. Pelvic Floor Physical Therapy for Gastrointestinal Conditions. Objectives: Upon completion, participants will be able to:
 Pelvic Floor Physical Therapy for Gastrointestinal Conditions By Meghan Z. Markowski, PT, DPT, WCS, BCB-PMD Brigham and Women s s Hospital Department of Rehabilitation Services 850 Boylston Street, Suite
Pelvic Floor Physical Therapy for Gastrointestinal Conditions By Meghan Z. Markowski, PT, DPT, WCS, BCB-PMD Brigham and Women s s Hospital Department of Rehabilitation Services 850 Boylston Street, Suite
Biofeedback as a Treatment of Urinary Incontinence in Adults
 Biofeedback as a Treatment of Urinary Incontinence in Adults Policy Number: 2.01.27 Last Review: 10/2018 Origination: 7/2008 Next Review: 10/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue
Biofeedback as a Treatment of Urinary Incontinence in Adults Policy Number: 2.01.27 Last Review: 10/2018 Origination: 7/2008 Next Review: 10/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue
ANMS-ESNM position paper and consensus guidelines on biofeedback therapy for anorectal disorders
 Neurogastroenterology & Motility Neurogastroenterol Motil (2015) 27, 594 609 doi: 10.1111/nmo.12520 POSITION PAPER ANMS-ESNM position paper and consensus guidelines on therapy for anorectal disorders S.
Neurogastroenterology & Motility Neurogastroenterol Motil (2015) 27, 594 609 doi: 10.1111/nmo.12520 POSITION PAPER ANMS-ESNM position paper and consensus guidelines on therapy for anorectal disorders S.
Peripheral Subcutaneous Field Stimulation
 Peripheral Subcutaneous Field Stimulation Policy Number: 7.01.139 Last Review: 3/2018 Origination: 7/2013 Next Review: 9/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide
Peripheral Subcutaneous Field Stimulation Policy Number: 7.01.139 Last Review: 3/2018 Origination: 7/2013 Next Review: 9/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide
Pelvic Floor Stimulation as a Treatment of Urinary Incontinence
 Pelvic Floor Stimulation as a Treatment of Urinary Incontinence Policy Number: 1.01.17 Last Review: 2/2014 Origination: 2/2007 Next Review: 2/2015 Policy Blue Cross and Blue Shield of Kansas City (Blue
Pelvic Floor Stimulation as a Treatment of Urinary Incontinence Policy Number: 1.01.17 Last Review: 2/2014 Origination: 2/2007 Next Review: 2/2015 Policy Blue Cross and Blue Shield of Kansas City (Blue
Surgical Interruption of Pelvic Nerve Pathways for Primary and Secondary Dysmenorrhea
 Surgical Interruption of Pelvic Nerve Pathways for Primary and Secondary Dysmenorrhea Policy Number: 4.01.17 Last Review: 11/2013 Origination: 11/2007 Next Review: 11/2014 Policy Blue Cross and Blue Shield
Surgical Interruption of Pelvic Nerve Pathways for Primary and Secondary Dysmenorrhea Policy Number: 4.01.17 Last Review: 11/2013 Origination: 11/2007 Next Review: 11/2014 Policy Blue Cross and Blue Shield
Research Article Pelvic Muscle Rehabilitation: A Standardized Protocol for Pelvic Floor Dysfunction
 Advances in Urology, Article ID 487436, 7 pages http://dx.doi.org/1155/2014/487436 Research Article Pelvic Muscle Rehabilitation: A Standardized Protocol for Pelvic Floor Dysfunction Rodrigo Pedraza, 1,2
Advances in Urology, Article ID 487436, 7 pages http://dx.doi.org/1155/2014/487436 Research Article Pelvic Muscle Rehabilitation: A Standardized Protocol for Pelvic Floor Dysfunction Rodrigo Pedraza, 1,2
SUPPLEMENTARY INFORMATION Associated with
 Table1: Rome III and Rome IV diagnostic criteria for IBS, functional constipation and functional dyspepsia. Rome III diagnostic criteria 1,2 Rome IV diagnostic criteria 3,4 Diagnostic criteria for IBS
Table1: Rome III and Rome IV diagnostic criteria for IBS, functional constipation and functional dyspepsia. Rome III diagnostic criteria 1,2 Rome IV diagnostic criteria 3,4 Diagnostic criteria for IBS
Medical Policy. MP Ingestible ph and Pressure Capsule
 Medical Policy BCBSA Ref. Policy: 2.01.81 Last Review: 11/15/2018 Effective Date: 11/15/2018 Section: Medicine Related Policies 2.01.20 Esophageal ph Monitoring 6.01.33 Wireless Capsule Endoscopy as a
Medical Policy BCBSA Ref. Policy: 2.01.81 Last Review: 11/15/2018 Effective Date: 11/15/2018 Section: Medicine Related Policies 2.01.20 Esophageal ph Monitoring 6.01.33 Wireless Capsule Endoscopy as a
PREPARING FOR ANORECTOAL MANOMETRY. ManoScan Anorectal Manometry System
 PREPARING FOR ANORECTOAL MANOMETRY ManoScan Anorectal Manometry System WHAT IS ANORECTAL MANOMETRY? Anorectal manometry is a test used to evaluate the function and coordination of the sphincter and pelvic
PREPARING FOR ANORECTOAL MANOMETRY ManoScan Anorectal Manometry System WHAT IS ANORECTAL MANOMETRY? Anorectal manometry is a test used to evaluate the function and coordination of the sphincter and pelvic
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE The management of faecal incontinence in adults 1.1 Short title Faecal incontinence 2 Background (a) (b) (c) The National Institute
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE The management of faecal incontinence in adults 1.1 Short title Faecal incontinence 2 Background (a) (b) (c) The National Institute
PARTICULARS, SCHEDULE 2- THE SERVICES, A- SERVICE SPECIFICATIONS. A08/S/d Colorectal: Faecal Incontinence (Adult)
 A08/S/d 2013/14 NHS STANDARD CONTRACT FOR COLORECTAL: FAECAL INCONTINENCE (ADULT) PARTICULARS, SCHEDULE 2- THE SERVICES, A- SERVICE SPECIFICATIONS Service Specification No. Service Commissioner Lead Provider
A08/S/d 2013/14 NHS STANDARD CONTRACT FOR COLORECTAL: FAECAL INCONTINENCE (ADULT) PARTICULARS, SCHEDULE 2- THE SERVICES, A- SERVICE SPECIFICATIONS Service Specification No. Service Commissioner Lead Provider
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Constipation: the diagnosis and management of idiopathic childhood constipation in primary and secondary care 1.1 Short title
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Constipation: the diagnosis and management of idiopathic childhood constipation in primary and secondary care 1.1 Short title
Controlled randomised trial of visual biofeedback
 Gut 1995; 37: 95-99 Service de Medecine C, CHG de F6camp, 764 F6camp, France D Koutsomanis St Mark's Hospital, London EC1V 2PS J E Lennard-Jones A J Roy M A Kamm Correspondence to: Professor J E Lennard-Jones,
Gut 1995; 37: 95-99 Service de Medecine C, CHG de F6camp, 764 F6camp, France D Koutsomanis St Mark's Hospital, London EC1V 2PS J E Lennard-Jones A J Roy M A Kamm Correspondence to: Professor J E Lennard-Jones,
Facet Arthroplasty. Policy Number: Last Review: 9/2018 Origination: 9/2009 Next Review: 3/2019
 Facet Arthroplasty Policy Number: 7.01.120 Last Review: 9/2018 Origination: 9/2009 Next Review: 3/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide coverage for total facet
Facet Arthroplasty Policy Number: 7.01.120 Last Review: 9/2018 Origination: 9/2009 Next Review: 3/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide coverage for total facet
Chronic constipation in the elderly
 Chronic constipation in the elderly 1 Dec,2011 R 2 Natta Asanaleykha Epidemiology Definition Scope The impact of chronic constipation in the elderly Pathophysiology Evaluation the elderly patient with
Chronic constipation in the elderly 1 Dec,2011 R 2 Natta Asanaleykha Epidemiology Definition Scope The impact of chronic constipation in the elderly Pathophysiology Evaluation the elderly patient with
The efficacy of a multidisciplinary approach to the management of constipation: a case series
 Journal of the Association of Chartered Physiotherapists in Women s Health, Spring 2008, 102, 36 44 CLINICAL PAPER The efficacy of a multidisciplinary approach to the management of constipation: a case
Journal of the Association of Chartered Physiotherapists in Women s Health, Spring 2008, 102, 36 44 CLINICAL PAPER The efficacy of a multidisciplinary approach to the management of constipation: a case
3D Dynamic Ultrasound In Obstructed Defecation
 3D Dynamic Ultrasound In Obstructed Defecation By Ramy Salahudin Abdelkader Assist. Lecturer of General Surgery Cairo University Introduction Pelvic floor is complex system, with passive and active components
3D Dynamic Ultrasound In Obstructed Defecation By Ramy Salahudin Abdelkader Assist. Lecturer of General Surgery Cairo University Introduction Pelvic floor is complex system, with passive and active components
Research Article Efficacy of Adaptive Biofeedback Training in Treating Constipation-Related Symptoms
 Evidence-Based Complementary and Alternative Medicine Volume 2015, Article ID 959734, 5 pages http://dx.doi.org/10.1155/2015/959734 Research Article Efficacy of Adaptive Biofeedback Training in Treating
Evidence-Based Complementary and Alternative Medicine Volume 2015, Article ID 959734, 5 pages http://dx.doi.org/10.1155/2015/959734 Research Article Efficacy of Adaptive Biofeedback Training in Treating
Medical Policy Vertebral Axial Decompression Section 8.0 Therapy Subsection 8.03 Rehabilitation. Description. Related Policies.
 8.03.09 Vertebral Axial Decompression Section 8.0 Therapy Subsection 8.03 Rehabilitation Effective Date October 31, 2014 Original Policy Date June 28, 2007 Next Review Date October 2015 Description Vertebral
8.03.09 Vertebral Axial Decompression Section 8.0 Therapy Subsection 8.03 Rehabilitation Effective Date October 31, 2014 Original Policy Date June 28, 2007 Next Review Date October 2015 Description Vertebral
Bioimpedance Devices for Detection and Management of Lymphedema
 Bioimpedance Devices for Detection and Management of Lymphedema Policy Number: 2.01.82 Last Review: 5/2017 Origination: 1/2011 Next Review: 5/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue
Bioimpedance Devices for Detection and Management of Lymphedema Policy Number: 2.01.82 Last Review: 5/2017 Origination: 1/2011 Next Review: 5/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue
Chapter 31 Bowel Elimination
 Chapter 31 Bowel Elimination Defecation Defecation: the act of expelling feces from the body Peristalsis: rhythmic contractions of intestinal smooth muscle to facilitate defecation Gastrocolic reflex:
Chapter 31 Bowel Elimination Defecation Defecation: the act of expelling feces from the body Peristalsis: rhythmic contractions of intestinal smooth muscle to facilitate defecation Gastrocolic reflex:
Original Policy Date
 MP 7.01.39 Transurethral Microwave Thermotherapy Medical Policy Section Surgery Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature search/12:2013 Return to Medical
MP 7.01.39 Transurethral Microwave Thermotherapy Medical Policy Section Surgery Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature search/12:2013 Return to Medical
OPIOID-INDUCED CONSTIPATION DR ANDREW DAVIES
 OPIOID-INDUCED CONSTIPATION DR ANDREW DAVIES Introduction Introduction Mean faecal weight 128 g / cap / day Mean range 51-796 g Absolute range 15-1505 g Main factors affecting mass are caloric intake,
OPIOID-INDUCED CONSTIPATION DR ANDREW DAVIES Introduction Introduction Mean faecal weight 128 g / cap / day Mean range 51-796 g Absolute range 15-1505 g Main factors affecting mass are caloric intake,
Constipation in childhood is characterized by a low defecation frequency in combination with either involuntary loss of
 USE OF ROME II CRITERIA IN CHILDHOOD DEFECATION DISORDERS: APPLICABILITY IN CLINICAL AND RESEARCH PRACTICE WIEGER P. VOSKUIJL, MD, JAROM HEIJMANS, HUGO S. A. HEIJMANS, MD, PHD, JAN A. J. M. TAMINIAU,MD,PHD,
USE OF ROME II CRITERIA IN CHILDHOOD DEFECATION DISORDERS: APPLICABILITY IN CLINICAL AND RESEARCH PRACTICE WIEGER P. VOSKUIJL, MD, JAROM HEIJMANS, HUGO S. A. HEIJMANS, MD, PHD, JAN A. J. M. TAMINIAU,MD,PHD,
Pelvic Floor Therapy for the Oncology Patient
 Therapy for the Oncology Patient CARINA SIRACUSA, PT, DPT, WCS OHIOHEALTH PELVIC FLOOR PHYSICAL THERAPIST ONCOLOGY REHABILITATION PROGRAM COORDINATOR What does a pelvic floor therapist treat? Muscles Muscles
Therapy for the Oncology Patient CARINA SIRACUSA, PT, DPT, WCS OHIOHEALTH PELVIC FLOOR PHYSICAL THERAPIST ONCOLOGY REHABILITATION PROGRAM COORDINATOR What does a pelvic floor therapist treat? Muscles Muscles
Clinical Policy: Biofeedback Reference Number: CP.MP.168
 Clinical Policy: Reference Number: CP.MP.168 Effective Date: 07/17 Last Review Date: 07/17 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory and
Clinical Policy: Reference Number: CP.MP.168 Effective Date: 07/17 Last Review Date: 07/17 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory and
... SELECTED ABSTRACTS...
 ... SELECTED ABSTRACTS... The following abstracts, from medical journals containing literature on irritable bowel syndrome, were selected for their relevance to this supplement. A Technical Review for
... SELECTED ABSTRACTS... The following abstracts, from medical journals containing literature on irritable bowel syndrome, were selected for their relevance to this supplement. A Technical Review for
Efficacy and Safety of Lubiprostone. Laura Wozniak February 23, 2010 K30 Monthly Journal Club
 Efficacy and Safety of Lubiprostone Laura Wozniak February 23, 2010 K30 Monthly Journal Club Objectives Brief overview of constipation Review of article Discussion Constipation in Children 3-5% of all
Efficacy and Safety of Lubiprostone Laura Wozniak February 23, 2010 K30 Monthly Journal Club Objectives Brief overview of constipation Review of article Discussion Constipation in Children 3-5% of all
Diagnosis of Impaired Defecatory Function with Special Reference to Physiological Tests
 Defecatory Dysfunction Diagnosis of Impaired Defecatory Function with Special Reference to Physiological Tests JMAJ 46(9): 373 377, 2003 Masatoshi OYA, Masashi UENO, and Tetsuichiro MUTO Department of
Defecatory Dysfunction Diagnosis of Impaired Defecatory Function with Special Reference to Physiological Tests JMAJ 46(9): 373 377, 2003 Masatoshi OYA, Masashi UENO, and Tetsuichiro MUTO Department of
Lets talk about Faecal incontinence (FI) in Scleroderma
 Lets talk about Faecal incontinence (FI) in Scleroderma Dr. Shamaila Butt Gastroenterology Research Registrar GI Physiology unit University College Hospital London GI manifestations in Scleroderma Oesophagus
Lets talk about Faecal incontinence (FI) in Scleroderma Dr. Shamaila Butt Gastroenterology Research Registrar GI Physiology unit University College Hospital London GI manifestations in Scleroderma Oesophagus
Novel Options for the Management of Fecal Incontinence
 Novel Options for the Management of Fecal Incontinence Arnold Wald, MD, MACG University of Wisconsin School of Medicine and Public Health, Madison WI ANORECTAL CONTINENCE MECHANISMS Reservoir Elements
Novel Options for the Management of Fecal Incontinence Arnold Wald, MD, MACG University of Wisconsin School of Medicine and Public Health, Madison WI ANORECTAL CONTINENCE MECHANISMS Reservoir Elements
Populations Interventions Comparators Outcomes Individuals: With urinary incontinence (women)
 Protocol Biofeedback as a Treatment of Urinary Incontinence in Adults (20127) Medical Benefit Effective Date: 01/01/10 Next Review Date: 09/18 Preauthorization No Review Dates: 01/08, 11/08, 09/09, 09/10,
Protocol Biofeedback as a Treatment of Urinary Incontinence in Adults (20127) Medical Benefit Effective Date: 01/01/10 Next Review Date: 09/18 Preauthorization No Review Dates: 01/08, 11/08, 09/09, 09/10,
Intracellular Micronutrient Analysis
 Intracellular Micronutrient Analysis Policy Number: 2.04.73 Last Review: 1/2019 Origination: 1/2013 Next Review: 1/2020 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide coverage
Intracellular Micronutrient Analysis Policy Number: 2.04.73 Last Review: 1/2019 Origination: 1/2013 Next Review: 1/2020 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide coverage
2/5/2016. Evolving Surgical Treatment Approaches for Fecal Incontinence in Women: An Evidence and Cased-Based Approach
 Evolving Surgical Treatment Approaches for Fecal Incontinence in Women: An Evidence and Cased-Based Approach Holly E Richter, PhD, MD, FACOG, FACS J Marion Sims Professor Obstetrics and Gynecology Professor
Evolving Surgical Treatment Approaches for Fecal Incontinence in Women: An Evidence and Cased-Based Approach Holly E Richter, PhD, MD, FACOG, FACS J Marion Sims Professor Obstetrics and Gynecology Professor
Use of Functional Electrical Stimulation (FES) for chronic constipation & People with Multiple Sclerosis (PwMS)
 Use of Functional Electrical Stimulation (FES) for chronic constipation & People with Multiple Sclerosis (PwMS) Christine.singleton@bhamcommunity.nhs.uk Tel: 0121 446 3281 West Midlands Rehabilitation
Use of Functional Electrical Stimulation (FES) for chronic constipation & People with Multiple Sclerosis (PwMS) Christine.singleton@bhamcommunity.nhs.uk Tel: 0121 446 3281 West Midlands Rehabilitation
ACCIDENTAL BOWEL LEAKAGE: A PRACTICAL APPROACH TO EVALUATION. Tristi W. Muir, MD Chair, Department of OB/GYN Houston Methodist Hospital
 ACCIDENTAL BOWEL LEAKAGE: A PRACTICAL APPROACH TO EVALUATION Tristi W. Muir, MD Chair, Department of OB/GYN Houston Methodist Hospital Accidental Bowel Leakage What Gets the Woman into Your Office 67%
ACCIDENTAL BOWEL LEAKAGE: A PRACTICAL APPROACH TO EVALUATION Tristi W. Muir, MD Chair, Department of OB/GYN Houston Methodist Hospital Accidental Bowel Leakage What Gets the Woman into Your Office 67%
Hemorrhoids. Carlos R. Alvarez-Allende PGY-III Colorectal Surgery
 Hemorrhoids Carlos R. Alvarez-Allende PGY-III Colorectal Surgery Overview Anatomy Classification Etiology Incidence Symptoms Differential Diagnosis Medical Management Surgical Management Anatomy Anal canal
Hemorrhoids Carlos R. Alvarez-Allende PGY-III Colorectal Surgery Overview Anatomy Classification Etiology Incidence Symptoms Differential Diagnosis Medical Management Surgical Management Anatomy Anal canal
Pelvic Floor Stimulation as a Treatment of Urinary and Fecal Incontinence
 Pelvic Floor Stimulation as a Treatment of Urinary and Fecal Incontinence Policy Number: 1.01.17 Last Review: 2/2018 Origination: 2/2007 Next Review: 2/2019 Policy Blue Cross and Blue Shield of Kansas
Pelvic Floor Stimulation as a Treatment of Urinary and Fecal Incontinence Policy Number: 1.01.17 Last Review: 2/2018 Origination: 2/2007 Next Review: 2/2019 Policy Blue Cross and Blue Shield of Kansas
CONTINENCE MODULE 1 MIMIMUM STANDARDS FOR THE SPECIALIST ASSESSMENT & CONSERVATIVE MANAGEMENT OF FEMALE LOWER URINARY TRACT SYMPTOMS
 CONTINENCE MODULE 1 MIMIMUM STANDARDS FOR THE SPECIALIST ASSESSMENT & CONSERVATIVE MANAGEMENT OF FEMALE LOWER URINARY TRACT SYMPTOMS The minimum standards required to initiate specialised conservative
CONTINENCE MODULE 1 MIMIMUM STANDARDS FOR THE SPECIALIST ASSESSMENT & CONSERVATIVE MANAGEMENT OF FEMALE LOWER URINARY TRACT SYMPTOMS The minimum standards required to initiate specialised conservative
Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS
 Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS OhioHealth, Columbus Ohio Disclosures I have nothing to disclose Objectives Describe the role of a pelvic floor therapist in
Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS OhioHealth, Columbus Ohio Disclosures I have nothing to disclose Objectives Describe the role of a pelvic floor therapist in
Peripheral Subcutaneous Field Stimulation
 Peripheral Subcutaneous Field Stimulation Policy Number: 7.01.139 Last Review: 9/2018 Origination: 7/2013 Next Review: 3/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide
Peripheral Subcutaneous Field Stimulation Policy Number: 7.01.139 Last Review: 9/2018 Origination: 7/2013 Next Review: 3/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide
Peer reviewed article systematic review: The management of constipation using physical therapies including biofeedback
 Peer reviewed article systematic review: The management of constipation using physical therapies including biofeedback Abstract Constipation can be a symptom of many diseases and disorders. Functional
Peer reviewed article systematic review: The management of constipation using physical therapies including biofeedback Abstract Constipation can be a symptom of many diseases and disorders. Functional
Physiotherapy Management for Faecal Incontinence in Children. Amy Chung MSSc, Dip. (Acupuncture), P.D.PT 19 Sept 2009
 Physiotherapy Management for Faecal Incontinence in Children Amy Chung MSSc, Dip. (Acupuncture), P.D.PT 19 Sept 2009 Contents Introduction Overview of physiotherapy management Local experience - Continence
Physiotherapy Management for Faecal Incontinence in Children Amy Chung MSSc, Dip. (Acupuncture), P.D.PT 19 Sept 2009 Contents Introduction Overview of physiotherapy management Local experience - Continence
Bowel Function After Spinal Cord Injury
 Bowel Function After Spinal Cord Injury A resource for individuals with SCI and their supporters This presentation is based on SCI Model Systems research and was developed with support from the National
Bowel Function After Spinal Cord Injury A resource for individuals with SCI and their supporters This presentation is based on SCI Model Systems research and was developed with support from the National
PELVIC PHYSIOTHERAPY EDUCATION GUIDELINE
 PELVIC PHYSIOTHERAPY EDUCATION GUIDELINE Initiated at the International Continence Society (ICS) Annual Meeting in San Francisco 2009 Initially Adopted by the ICS Physiotherapy Committee September 2010
PELVIC PHYSIOTHERAPY EDUCATION GUIDELINE Initiated at the International Continence Society (ICS) Annual Meeting in San Francisco 2009 Initially Adopted by the ICS Physiotherapy Committee September 2010
Antigen Leukocyte Antibody Test
 Antigen Leukocyte Antibody Test Policy Number: 2.01.93 Last Review: 4/2014 Origination: 4/2014 Next Review: 4/2015 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide coverage for
Antigen Leukocyte Antibody Test Policy Number: 2.01.93 Last Review: 4/2014 Origination: 4/2014 Next Review: 4/2015 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide coverage for
Constipation in children
 Search date August 2003 Gregory Rubin QUESTIONS Effects of treatments...397 395 INTERVENTIONS CONSTIPATION Trade off between benefits and harms Cisapride with or without magnesium oxide*...397 Unknown
Search date August 2003 Gregory Rubin QUESTIONS Effects of treatments...397 395 INTERVENTIONS CONSTIPATION Trade off between benefits and harms Cisapride with or without magnesium oxide*...397 Unknown
Constipation. (Medical Aspects)
 Constipation (Medical Aspects) By Dr. Ehab Abdel Khalik MD. Anatomy of the anorectum The rectum is 12-15 15 cm. long. It connects with the sigmoid colon by the rectosigmoid junction which is believed to
Constipation (Medical Aspects) By Dr. Ehab Abdel Khalik MD. Anatomy of the anorectum The rectum is 12-15 15 cm. long. It connects with the sigmoid colon by the rectosigmoid junction which is believed to
Transtympanic Micropressure Applications as a Treatment of Meniere s Disease
 Transtympanic Micropressure Applications as a Treatment of Meniere s Disease Policy Number: 1.01.23 Last Review: 8/2017 Origination: 2/2006 Next Review: 8/2018 Policy Blue Cross and Blue Shield of Kansas
Transtympanic Micropressure Applications as a Treatment of Meniere s Disease Policy Number: 1.01.23 Last Review: 8/2017 Origination: 2/2006 Next Review: 8/2018 Policy Blue Cross and Blue Shield of Kansas
Clinical Policy Title: Injectable bulking agents for fecal incontinence
 Clinical Policy Title: Injectable bulking agents for fecal incontinence Clinical policy number: 08.02.04 Effective Date: October 1, 2015 Initial Review Date: May 20, 2015 Most Recent Review Date: June
Clinical Policy Title: Injectable bulking agents for fecal incontinence Clinical policy number: 08.02.04 Effective Date: October 1, 2015 Initial Review Date: May 20, 2015 Most Recent Review Date: June
Pelvic Floor Disorders. Amir Darakhshan MD FRCS (Gen Surg) Consultant Colorectal and General Surgeon
 Pelvic Floor Disorders Amir Darakhshan MD FRCS (Gen Surg) Consultant Colorectal and General Surgeon What is Pelvic Floor Disorder Surgical perspective symptoms of RED, FI or prolapse on the background
Pelvic Floor Disorders Amir Darakhshan MD FRCS (Gen Surg) Consultant Colorectal and General Surgeon What is Pelvic Floor Disorder Surgical perspective symptoms of RED, FI or prolapse on the background
Biofeedback as a Treatment of Headache
 2.01.29 Biofeedback as a Treatment of Headache Section 2.0 Medicine Subsection Effective Date September 30, 2014 Original Policy Date September 30, 2014 Next Review Date September 2015 Description Biofeedback
2.01.29 Biofeedback as a Treatment of Headache Section 2.0 Medicine Subsection Effective Date September 30, 2014 Original Policy Date September 30, 2014 Next Review Date September 2015 Description Biofeedback
Constipation. Information for adults. GI Motility Clinic (UMCCC University Medical Clinics of Campbelltown and Camden) Page 1
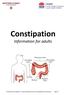 Constipation Information for adults GI Motility Clinic (UMCCC University Medical Clinics of Campbelltown and Camden) Page 1 Contents Role of the large intestine..3 Mass movements in the large intestine..4
Constipation Information for adults GI Motility Clinic (UMCCC University Medical Clinics of Campbelltown and Camden) Page 1 Contents Role of the large intestine..3 Mass movements in the large intestine..4
CONSERVATIVE MANAGEMENT OF URINARY INCONTINENCE IN WOMEN. Riette Vosloo Physiotherapist in Women s s Health
 CONSERVATIVE MANAGEMENT OF URINARY INCONTINENCE IN WOMEN Riette Vosloo Physiotherapist in Women s s Health CONSERVATIVE TREATMENT Any therapy that does not involve Pharmacologic intervention or Surgical
CONSERVATIVE MANAGEMENT OF URINARY INCONTINENCE IN WOMEN Riette Vosloo Physiotherapist in Women s s Health CONSERVATIVE TREATMENT Any therapy that does not involve Pharmacologic intervention or Surgical
A Case of Fecal Incontinence: Medical and Interventional Treatment Options
 A Case of Fecal Incontinence: Medical and Interventional Treatment Options HPI JP is a 69 year-old F with a 12-month history of FI. Her symptoms began after a colonoscopy She has been experiencing passive
A Case of Fecal Incontinence: Medical and Interventional Treatment Options HPI JP is a 69 year-old F with a 12-month history of FI. Her symptoms began after a colonoscopy She has been experiencing passive
Bioimpedance Devices for Detection and Management of Lymphedema
 Bioimpedance Devices for Detection and Management of Lymphedema Policy Number: 2.01.82 Last Review: 5/2018 Origination: 1/2011 Next Review: 5/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue
Bioimpedance Devices for Detection and Management of Lymphedema Policy Number: 2.01.82 Last Review: 5/2018 Origination: 1/2011 Next Review: 5/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue
from Bowel Control Problems twitter.com/voicesforpfd
 BREAK FREE from Bowel Control Problems POP Quiz THE NUMBER OF PEOPLE IN THE UNITED STATES WITH BOWEL CONTROL PROBLEMS: A. 6 million B. 12 million C. 18 million BOWEL CONTROL PROBLEMS Nearly 18 million
BREAK FREE from Bowel Control Problems POP Quiz THE NUMBER OF PEOPLE IN THE UNITED STATES WITH BOWEL CONTROL PROBLEMS: A. 6 million B. 12 million C. 18 million BOWEL CONTROL PROBLEMS Nearly 18 million
