Gastrointestinal Tract and Abdomen Benign Rectal, Anal, and Perineal Problems: Introduction
|
|
|
- Marsha Willis
- 6 years ago
- Views:
Transcription
1 To Print: Click your browser's PRINT button. NOTE: To view the article with Web enhancements, go to: Gastrointestinal Tract and Abdomen Benign Rectal, Anal, and Perineal Problems: Introduction David E. Beck, M.D., F.A.C.S., F.A.S.C.R.S. ACS Surgery Online. 2002; 2002 WebMD Inc. Posted 03/10/2006 In this chapter, I briefly review the evaluation and management of common benign conditions affecting the rectum, the anus, and the perineum: hemorrhoidal disease, anal fissures, anorectal abscesses and fistulas, pilonidal disease, hidradenitis suppurativa, pruritus ani, and solitary rectal ulcer syndrome (SRUS). For proper diagnosis and treatment of these conditions, an understanding of the relevant anatomy is essential [see Figure 1 -- omitted]. 1 The dentate line divides the rectal mucosa, which is generally insensate and is lined with columnar mucosa, from the anoderm below it, which is highly sensitive (because of the somatic innervation provided by the inferior hemorrhoidal nerve) and is lined with modified squamous mucosa. The anal canal is surrounded by two muscles. The internal anal sphincter, innervated by the autonomic nervous system, maintains resting anal tone and is under involuntary control. The external sphincter, innervated by somatic nerve fibers, generates the voluntary anal squeeze and plays the key role in maintaining anal continence. The area surrounding the anorectum is divided into four spaces perianal, ischioanal, supralevator, and intersphincteric (intermuscular) familiarity with which is particularly important in the evaluation of perirectal abscesses and fistulas. Hemorrhoids Hemorrhoids are fibromuscular cushions that line the anal canal. They are classically found in three locations: right anterior, right posterior, and left lateral. 2,3 On occasion, smaller secondary cushions may be found lying between these main cushions. Contrary to popular belief, hemorrhoids are not related to the superior hemorrhoidal artery and vein, to the portal vein, or to portal hypertension. 4 In fact, hemorrhoids are part of the normal anal anatomy. Their engorgement during straining or performance of the Valsalva maneuver is a component of the normal mechanism of fecal continence: it most likely completes the occlusion of the anal canal and prevents stool loss associated with nondefecatory straining. In the medical literature, however, the term hemorrhoid is used almost exclusively to refer to pathologic hemorrhoids, and I follow this usage throughout the remainder of the chapter. Hemorrhoids are broadly classified as either internal or external. Internal hemorrhoids are found proximal to the dentate line, whereas external hemorrhoids occur distally [see Figure 2 -- omitted]. External hemorrhoids are redundant folds of perianal skin that generally derive from previous anal swelling; they remain asymptomatic unless they are thrombosed and are treated entirely differently from internal hemorrhoids. Internal. Internal hemorrhoidal disease is manifested by two main symptoms: painless bleeding and protrusion. 4 Pain is rare because internal hemorrhoids originate above the dentate line in the insensate rectal mucosa. The most popular etiologic theory states that hemorrhoids result from chronic straining at defecation (with upright posture and heavy lifting possibly playing contributing roles as well). This straining not only causes hemorrhoidal engorgement but also generates forces that reduce the attachment between the hemorrhoids and the anal muscular wall. Continued straining causes further engorgement and bleeding, as well as hemorrhoidal prolapse. Internal hemorrhoids are classified into four grades on the basis of clinical findings and symptoms. Grade 1 represents bleeding without prolapse; grade 2, prolapse that spontaneously reduces; grade 3, prolapse necessitating manual reduction; and grade 4, irreducible prolapse. Page 1 sur 9
2 Questioning often reveals a long history of constipation and straining at defecation. Many patients with internal hemorrhoids are extensive bathroom readers, spending many hours in the bathroom each week. Symptoms start with painless bleeding and may progress to anal protrusion. The physical examination begins with visual inspection and may reveal prolapsing hemorrhoidal tissue appearing as a rosette of three distinct pink-purple hemorrhoidal groups. Hemorrhoidal prolapse must be distinguished from true full-thickness rectal prolapse. When hemorrhoidal prolapse is not present, anoscopy typically reveals redundant anorectal mucosa just proximal to the dentate line in the classic locations. Surgical treatment of hemorrhoids in a patient whose main disease process is Crohn disease, a pelvic floor abnormality, or fissure disease invariably yields imperfect results. It is especially important to recognize the anal pain and spasm associated with anal fissure because in patients with this problem, excision of the hemorrhoids without concomitant management of the fissure leads to increased postoperative pain and poor wound healing. Not uncommonly, patients are treated for hemorrhoids when the true primary condition is fissure disease.. Treatment of symptomatic internal hemorrhoids ranges from simple reassurance to operative hemorrhoid excision, depending on hemorrhoid grade [see Table 1 -- omitted]. Therapies may be classified into three categories: (1) diet and lifestyle modifications, (2) nonoperative and office procedures, and (3) operative hemorrhoidectomies. Diet and lifestyle modifications. For all patients with grade 1 or 2 hemorrhoids and most patients with grade 3 hemorrhoids, treatment should begin with efforts to correct constipation. Recommendations should include a highfiber diet, liberal water intake (six to eight 8 oz glasses of water daily), and fiber supplements (e.g., psyllium, methylcellulose, calcium polycarbophyl, and gum). Sitz baths are recommended for their soothing effect and their ability to relax the anal sphincter muscles. Topical creams may reduce some of the associated symptoms, though they do not affect the hemorrhoids themselves. Suppositories are not helpful, because they deliver medication to the rectum, not the anus. Patients are instructed to avoid prolonged trips to the bathroom and to read in the bathroom only when sitting atop the toilet lid. Nonoperative and office procedures. If initial diet and lifestyle modifications are not effective, there are a number of nonoperative therapies that may be tried next. At present, the main recommended options are rubber band ligation, infrared photocoagulation, and sclerotherapy. Rubber band ligation. Ligation of hemorrhoids with elastic bands is the method most commonly used in the outpatient setting [see 5:37 Anal Procedures for Benign Disease -- omitted]. 5 It is successful in two thirds to three quarters of all patients with grade 1 or 2 hemorrhoids. 2 Repeated banding may be necessary to resolve all symptoms. On rare occasions, patients do not respond to banding at all or cannot tolerate it. Some of these patients will respond to infrared coagulation; others may require formal hemorrhoidectomy. Complications of rubber band ligation include bleeding, pain, thrombosis, and life-threatening perineal sepsis. 5,6 The cardinal signs of perineal sepsis are significant pain, fever, and difficult urination. Patients in whom any of these symptoms develop require urgent evaluation and treatment with broad-spectrum antibiotics, coupled with selective debridement of any necrotic anal tissue. Infrared coagulation. The infrared coagulator generates infrared radiation, which coagulates tissue protein and evaporates water from cells. 7 The extent of the tissue destruction depends on the intensity and duration of the application. An anoscopic examination is performed, and the infrared coagulator is applied to the apex of each hemorrhoid at the top of the anal canal [see Figure 3 -- omitted]. Each hemorrhoid bundle receives three to four applications, each lasting 1 to 1.5 seconds. The infrared coagulator was designed to decrease blood flow to the region. It is not particularly effective for treating large amounts of prolapsing tissue; it is most useful for treating grade 1 and small grade 2 hemorrhoids. Overall, it is slightly less painful than rubber banding. Infrared coagulation is especially beneficial for patients in whom rubber band ligation fails because of pain or who have symptomatic internal hemorrhoids that are too small to band. Sclerotherapy. Sclerotherapy was once commonly employed to treat internal hemorrhoids, but with the advent of rubber band ligation, it has become less popular. The technique involves injection of a sclerosant into the anorectal submucosa to decrease vascularity and increase fibrosis. The agents used include phenol in oil, sodium morrhuate, and quinine urea. 2 Hemorrhoids are identified via anoscopy, and the sclerosant is infiltrated at the apex of the hemorrhoid (at the proximal anal rectal ring). After injection, patients occasionally experience a dull ache lasting 24 to 48 hours, but substantial bleeding and other significant complications are uncommon. Misplacement of Page 2 sur 9
3 the sclerosant, resulting in significant perianal infection and fibrosis, has been reported, albeit rarely. Comparison of methods. A meta-analysis comparing a variety of modalities used to treat hemorrhoids found that rubber band ligation was superior to sclerotherapy for grade 1 through grade 3 hemorrhoids. 8 Patients who were treated with sclerotherapy or infrared coagulation were more likely to require further treatment than those treated with rubber band ligation. The authors concluded that hemorrhoidectomy should be reserved for patients in whom rubber band ligation or infrared coagulation fails or who have associated external hemorrhoidal disease. Hemorrhoidectomies. Various hemorrhoidectomies have been developed throughout the years. Although they differ with respect to detail, they incorporate similar basic principles namely, reduction of blood flow to the anorectal ring, removal of redundant hemorrhoidal tissue, and fixation of redundant mucosa and anoderm. 9 Open and closed hemorrhoidectomy. In the United Kingdom, open (Milligan and Morgan) hemorrhoidectomy, in which hemorrhoids are ligated and excised with the wound left open, is the most commonly performed operative excision procedure. In the United States, closed (Ferguson) hemorrhoidectomy is most commonly performed 10 ; this procedure is described more fully elsewhere [see 5:37 Anal Procedures for Benign Disease -- omitted]. With either type of hemorrhoidectomy, one, two, or three hemorrhoidal bundles may be excised. In performing a closed hemorrhoidectomy, it is essential to excise as little of the anoderm as possible: if large amounts are excised, closing the anal wounds or secondary healing can result in significant postoperative pain and perhaps even longterm anal stenosis. Stapled hemorrhoidectomy. Stapled hemorrhoidectomy or anoplasty (commonly known as the procedure for prolapsing hemorrhoids [PPH]) is increasingly being performed as an alternative to standard open or closed hemorrhoidectomy with the aim of reducing the pain associated with traditional surgical techniques. 9 PPH involves transanal circular stapling of redundant anorectal mucosa with a modified circular stapling instrument (PPH-01, Ethicon Endo-Surgery Inc., Cincinnati, Ohio). 11 Because no incisions are made in the somatically innervated, highly sensitive anoderm, there should, theoretically, be significantly less postoperative pain. Randomized, prospective trials comparing PPH with various operative hemorrhoidectomies and other therapies found it to be associated with significantly less pain then conventional treatments and to have similar complication rates. 9 PPH may, however, have a greater potential for disastrous complications (e.g., rectovaginal or rectourethral fistula from inclusion of too much tissue within the purse-string suture, perforation caused by placing the pursestring too high, and incontinence caused by placing the purse-string too low or too deep). Bleeding also remains a problem with PPH, and leaks have been reported. Finally, stapled hemorrhoidectomy has not yet been adequately compared with office procedures for grade 1 and 2 hemorrhoids and thus should not replace these techniques for treatment of minimally symptomatic hemorrhoidal disease. External. External hemorrhoids are asymptomatic except when secondary thrombosis occurs. Thrombosis may result from defecatory straining or extreme physical activity, or it may be a random event. 1 Patients present with constant anal pain of acute onset and often report feeling the sensation of sitting on a tender marble. Physical examination identifies the external thrombosis as a purple mass at the anal verge.. Treatment depends on the patient's symptoms [see Figure 4 -- omitted]. 4 In the first 24 to 72 hours after the onset of thrombosis, pain increases, and excision is warranted. After 72 hours, pain generally diminishes, and expectant treatment is all that is necessary. Patients should be advised that some drainage may occur. If operative treatment is chosen, the entire thrombosed hemorrhoid is excised with the patient under local anesthesia. Incision and drainage of the clot are avoided because they typically lead to rethrombosis and exacerbation of symptoms. Anal Fissure Anal fissures are tears or splits in the anoderm just distal to the dentate line. 12 They are characterized as acute or chronic. Generally, acute fissures are caused by the mechanical force generated by the passage of a large, hard bowel movement through an anal canal that is too small to accommodate it safely and easily (though they can also be caused by diarrhea). These mechanical forces usually cause a split to occur in the posterior midline: 90% of the fissures in females and 99% of those in males are located posteriorly. Either decreased local blood flow or increased mechanical stress may account for the propensity of these fissures to occur in this location. 13 Repeated injury (e.g., from hard or watery bowel movements) may result in the development of a chronic fissure. Page 3 sur 9
4 Symptoms associated with anal fissures include anal pain and bright-red rectal bleeding after bowel movements. The pain is usually described as a knifelike or tearing sensation, and the associated anal sphincter spasm may persist for several hours after each bowel movement. The bleeding is usually minor and is seen mainly on the toilet paper. Physical examination is difficult because the patient has an extremely tender anus and is fearful of further pain. Often, visual inspection with gentle eversion of the anoderm in the posterior midline is all that is required. Physical findings include a split in the anoderm approximately 1 cm long in the posterior midline just distal to the dentate line. In chronic fissures, the classic triad may be present: hypertrophy of the anal papilla, an anal fissure, and a sentinel skin tag [see Figure 5 -- omitted]. Once an anal fissure has been diagnosed, further examination is very painful, unrewarding, and unnecessary; more extensive investigations can be performed after the fissure has healed. Multiple fissures are unusual, as are fissures that occur away from the anterior or posterior midline; either should raise suspicions that other problems may be present [see Figure 6 -- omitted]. Acute fissures usually have been present for less than 4 to 6 weeks. As a rule, they are treated nonoperatively: fiber supplements, stool softeners, and generous intake of water, along with sitz baths and local anesthetic ointments, rapidly alleviate symptoms and usually bring about complete healing. Anal suppositories are avoided both because they are painful and because they rest in the rectum rather than the anal canal. Chronic fissures have been present for periods longer than 4 to 6 weeks. As noted (see above), they are typically characterized by an associated hypertrophied papilla, a skin tag, rolled skin edges, and exposed internal anal sphincter muscle at the base of the fissure. Chronic fissures respond less well to nonoperative measures than acute fissures do. The surgical procedure most frequently performed for anal fissure is lateral internal anal sphincterotomy [see 5:37 Anal Procedures for Benign Disease -- omitted], 14 which results in cure in 95% to 98% of patients. Complications of this procedure include incontinence to flatus (0% to 18% of cases), soiling (0% to 7%), fecal incontinence (0% to 0.17%), and various other problems (0% to 7%). 14 Several therapeutic alternatives for anal fissures have been proposed with the aim of avoiding the need for operation and the consequent risk of surgical complications. 15 On the basis of the theory that a fissure is actually an ischemic ulcer of the anoderm, topical nitroglycerin (NTG) ointment has been used to treat fissures, with success rates ranging from 48% to 78%. When metabolized, NTG releases nitric oxide, which is believed to be an inhibitory neurotransmitter for smooth muscle. The resulting neurogenic relaxation of the internal sphincter brings about a reduction in anal canal pressure, which diminishes pain and spasm. Typically, NTG is given in a concentration of 0.2% three to five times daily, but concentrations as high as 0.5% have been recommended. In practice, dosing is limited by NTG's side effects, which arise in as many as 88% of patients. Headaches are the predominant complaint, but dizziness, lightheadedness, and hypotension have also been reported. Caution must be exercised when NTG therapy is employed in patients receiving cardiac medications or those with sensitivities to nitrates. A meta-analysis comparing topical NTG therapy with sphincterotomy demonstrated that sphincterotomy results in better healing of chronic fissures. 16 Another nonsurgical option is the use of nifedipine gel or ointment, which also has met with varying degrees of success. Nifedipine acts as a calcium antagonist, preventing calcium from flowing into the sarcoplasm of smooth muscle and thereby reducing local demand for oxygen and mechanical contraction of the muscle. 12 Like NTG ointment, nifedipine ointment is usually applied topically in a 0.2% concentration, but it seems to have fewer side effects than NTG does. Nifedipine should be used with caution in cardiac patients and patients who have demonstrated previous sensitivities. One multicenter study reported a 95% complete healing rate after 21 days of treatment. 12 Topical 2% diltiazem has also been employed to treat chronic anal fissures, yielding a 67% healing rate. 12 Botulinum toxin has been reported to facilitate healing in 78% to 90% of anal fissure patients, with an 8% recurrence rate at 6 months. 15,17 The toxin, produced by the bacterium Clostridium botulinum, acts by inhibiting the release of acetylcholine at the presynaptic membrane. The resulting blockage of neurotransmission diminishes or eliminates spasms and contractions of the sphincter mechanism. Typically, 2.5 to 10 units are injected at two to Page 4 sur 9
5 four sites in the internal sphincter at the level of the dentate line. 18 Pain relief is generally noted within 24 hours, though it still takes days for the fissure to heal. Postinjection incontinence is rare. 12 The major drawback is the cost of the toxin, which may be as high as $400 per 100 unit vial. Anorectal Abscess Anorectal abscesses, like abscesses elsewhere in the body, are the result of local, walled-off infections. Most perirectal abscesses are of cryptogenic origin that is, they begin as infections in the anal glands that surround the anal canal and empty into the anal crypts at the dentate line. 18,19 It is thought that the ducts leading to and from these glands become obstructed by feces or traumatized tissue, and a secondary infection then develops that follows the path of least resistance, resulting in an anorectal abscess. Abscesses are categorized according to the space in which they occur: perianal, ischioanal, supralevator, or intersphincteric (intermuscular) [see Figure 7 -- omitted]. Perianal abscesses are the most common together with ischioanal abscesses, they account for more than 90% of perianal infections. Perianal abscesses occur in the perianal space immediately adjacent to the anal verge. Ischioanal abscesses are larger and often more complex than their perianal counterparts, and they usually manifest themselves as a tender buttock mass. Supralevator abscesses occur above the levator ani muscles and are characterized by poorly localized pain; they are exceedingly rare. Intersphincteric abscesses occur in the plane between the internal and external sphincter muscles, high within the anal canal; these are also rare. The location of an abscess is important in that it dictates subsequent therapy. 20 Regardless of location, all anorectal abscesses are associated with constant perianal pain. Accompanying symptoms may include fever, chills, and malaise. In rare cases, systemic toxicity may be evident. The history reveals rectal pain of gradual onset that progressively worsens until the time of presentation. Occasionally, spontaneous drainage decompresses the abscess, and the patient presents with a purulent discharge. As with fissures, visual inspection of the perineum often clinches the diagnosis. A fluctuant, erythematous, tender area identifies the abscess. In the rare event of a supralevator or intersphincteric abscess, there may be no external manifestations. When this is the case, the presence of a tender mass on digital examination above the anal canal, either adjacent to the rectal ampulla (supralevator abscess) or within the anal canal (intersphincteric abscess), provides the clue to the diagnosis. Treatment of anorectal abscesses consists of adequate drainage performed in the office, in the emergency department, or in the operating room. 18 Most abscesses can be drained in the office, but recurrent or complex abscesses, abscesses in immunosupressed hosts (including some diabetic patients), intersphincteric abscesses, and supralevator abscesses are more appropriately drained in the OR. Adequate drainage is essential and may be established in several ways. One method is to place a catheter (e.g., a 10 to 16 French Pezzar catheter) through a small stab incision [see 5:37 Anal Procedures for Benign Disease -- omitted]. 18 This measure allows the pus to drain through the catheter as the cavity closes down. A second option involves creating a larger elliptical incision. 20 Unroofing the abscess cavity allows it to heal without any need for packing. A small incision should be avoided because it would require painful packing to keep the skin open until the abscess cavity heals. The most difficult abscess to diagnose and manage is a deep postanal space abscess. Such abscesses are caused by fistulization from the posterior anal canal, usually in the bed of a chronic posterior fissure. The patient is highly uncomfortable and febrile, but there is no apparent sign of a problem perianally. A simple digital examination pushing posteriorly towards the coccyx and the deep postanal space will evoke severe pain, and this response should lead the examiner to suspect the diagnosis. The patient should be taken to the OR and anesthetized. On digital examination, the deep postanal space is often felt to be bulging. The diagnosis is confirmed by aspirating the space with an 18-gauge needle. Once the diagnosis is confirmed, an incision is made in the perianal skin posterior to the anal verge and deepened into the space, and the space is drained. In selected patients, a cutting seton is placed from the primary site in the posterior anal canal directly into the deep postanal space abscess. Horseshoe fistulas are dealt with as described elsewhere [see 5:37 Anal Procedures for Benign Disease -- omitted]. Page 5 sur 9
6 Fistula in Ano An anal fistula is a communication between the anal canal and the perianal skin. It usually begins in a crypt at the dentate line and follows a course either between the internal and external sphincters (the most common location), resulting in an ischioanal abscess, or above the sphincters, leading to a supralevator abscess. 18,20 After drainage of an abscess, one of three things typically occurs if a fistula is present: (1) the fistula heals spontaneously, and the patient experiences no further symptoms; (2) the abscess heals, only to recur in the future; or (3) the abscess heals, but a chronic draining fistula remains. Only the third scenario is addressed here. After drainage of one or more abscesses, a fistula is usually associated with chronic serosanguineous to seropurulent drainage. As long as the fistula remains open and draining, patients report little pain. If the fistula closes externally, however, an anorectal abscess may develop. Physical examination reveals a 2 to 3 mm opening in the perianal skin, with surrounding induration. Often, a fistula tract can be palpated as a firm cord running between the external opening and the anal canal. The relationship of the external opening to the internal opening is suggested by Goodsall's rule [see Figure 8 -- omitted]. Fistulas are classified into four main categories according to their relation to the anal sphincters [see Figure 9 -- omitted]: intersphincteric, transsphincteric, suprasphincteric, and extrasphincteric. 21 Essentially, all chronic fistulas call for surgical treatment, which consists of unroofing the entire fistula tract (fistulotomy) and leaving the wound open to heal secondarily. Fistulas that course through significant amounts of sphincter muscle, anterior fistulas in women, and fistulas associated with inflammatory bowel disease or weakened sphincter muscles, however, cannot be opened entirely, because incontinence will result. These fistulas may be partially opened, with the anal musculature left intact and encircled with a seton [see 5:37 Anal Procedures for Benign Disease -- omitted]. 20 Although some surgeons sequentially tighten the seton (making it a cutting seton), I prefer not to, because of the resultant patient discomfort. Another surgical option is to close the internal fistula opening with an advancement flap. 22 Advancement flap repairs result in high success rates with minimal effects on continence. Pilonidal Disease The term pilonidal disease is derived from the Latin words pilus ( hair ) and nidus ( nest ). 23 It denotes a chronic subcutaneous infection and foreign-body reaction to hairs embedded in the skin or to abnormalities of hair follicles in the natal cleft. 23 Pilonidal disease is most commonly seen in men between the onset of puberty and 40 years of age and in obese persons. 23 Pilonidal disease has three common presentations. First, nearly all patients experience an episode of acute abscess formation. Second, after the abscess resolves, either spontaneously or with medical assistance, a pilonidal sinus tract develops in many cases. Third, although most of these sinus tracts resolve, chronic disease or recurrent disease after treatment develops in a small minority of cases. Physical examination typically reveals one or more small (1 to 2 mm) dermal pits at the base of the intergluteal cleft [see Figure omitted]. Tracking from the pits (usually proceeding in a cranial and lateral direction) appears as areas of induration. If there is an associated abscess, the diseased area may be tender and erythematous, and draining pus may be evident. The more extensive the disease, the more prominent the findings. Treatment varies according to the stage of the disease. Abscesses must be drained. In one study, incision and drainage in an office setting with local anesthesia led to healing in 60% of patients. 24 As many as 40% of acute pilonidal abscesses treated with incision and drainage develop into chronic sinuses for which additional treatment is necessary. Several different approaches have been employed in the surgical treatment of pilonidal sinus tracts. A review of Page 6 sur 9
7 articles published over a period of 30 years on the treatment of pilonidal disease divided the procedures into the following four broad categories and reported the following findings Closed techniques (coring out follicles and brushing the tracts). These techniques necessitated shaving of the area but could be performed on an outpatient basis. Mean healing time was about 40 days, and recurrence rates were slightly higher than those seen with other forms of treatment. 2. Laying open (unroofing) the tracts with healing by granulation. This approach resulted in average healing times of 48 days and necessitated frequent outpatient dressing changes. The incidence of recurrent sinus formation was lower than 13%. 3. Wide and deep excision of the sinus alone. This procedure resulted in an average healing time of 72 days. The recurrence rate was similar to that of simple unroofing of the sinus tract with healing by granulation. 4. Excision and primary closure. This technique resulted in wound healing within 2 weeks in successful cases (19 days overall). However, primary wound healing failed in as many as 30% of patients, and the average recurrence rate was 15%. A nonoperative or conservative approach involving meticulous hair control (through natal cleft shaving), improved perineal hygiene, and limited lateral incision and drainage for treatment of abscess has been suggested as an alternative to conventional excision. 26 This approach has brought about a significant reduction in the number of excisional procedures and occupied-bed days. Even with proper treatment of pilonidal abscesses and sinuses, a small number of patients are left with persistent, nonhealing wounds. A number of more aggressive approaches have been advocated for treatment of complex or recurrent disease, including wide excision with split-thickness skin grafting, cleft closure, and excision with flap closure. 24,27 Flap techniques, as a group, have been found to lead to primary healing within 15 days in 90% of cases. 24 These aggressive approaches nevertheless have certain disadvantages. For nearly all of them, hospitalization and general anesthesia are mandatory. In addition, as many as 50% of procedures involving the use of skin flaps for wound coverage or closure in this setting result in some loss of skin sensation or some degree of flap-tip necrosis. My policy is to treat acute abscesses with drainage, followed by measures aimed at keeping the cleft free of hair. If a chronic sinus develops, it is managed with unroofing or, in selected patients, excision and closure. Flap procedures are reserved for cases of extensive, recurrent, and complex disease. 23 Hidradenitis Suppurativa Hidradenitis suppurativa is a chronic, recurrent inflammatory process involving the apocrine glands of the axilla, the groin, the perineum, and the perianal region. 28 The disease can result in chronically draining wounds and sinus tracts and can become quite painful and debilitating. 29 Occlusion of follicles and abnormalities of apocrine ducts are believed to be causative factors. Medical management may afford temporary relief of symptoms; however, most patients eventually require surgical therapy. 30 In select patients, incision and drainage or unroofing of sinuses may provide relief, but these measures should be reserved for cases of early and acute disease. Local excision provides adequate control of symptoms; however, recurrence rates higher than 50% may be anticipated. Wide excision with secondary granulation of perineal wounds constitutes the most definitive therapy and generally can be accomplished safely. 29 Perianal disease is associated with considerably lower recurrence rates than perineal disease is and thus can more often be managed with local excision alone. Pruritus Ani Pruritus ani is a dermatologic condition of the perianal skin characterized by uneasiness or itching in the area around the anus. 12,31 Multiple factors may predispose this area to irritation, including poor perianal hygiene (related to incontinence, diarrhea, or excessive hair), excessive moisture, irregularities of the perianal skin (from hemorrhoids, fistulas, or previous surgery), skin hypersensitivity, diet, decreased resistance to infection, and injury Page 7 sur 9
8 to the perianal skin. 31 The variety of possible causes is what often makes pruritus ani difficult to treat. Some patients improve only after the offending agents or conditions are identified and specific therapy instituted. Fortunately, many patients' symptoms can be alleviated by the application of nonspecific treatments. A thorough history and physical examination are necessary to suggest possible causes of pruritus. Initial inspection of the perianal skin should be conducted with gentle retraction of the buttocks under bright lighting. A characteristic finding is erythematous or thickened perianal skin [see Figure omitted]. This thickening results in a pale, whitish appearance, with accentuation of the radial anal skin creases. In addition, the skin may be excoriated or ulcerated; this process, when combined with thickening, is referred to as lichenification. Occasionally, the skin is so excoriated that a large, coalescing, weeping ulcer forms. Digital rectal examination should be performed to assess the competence of the anal sphincter both at rest and during maximal squeeze. Anoscopy and proctosigmoidoscopy may be performed after the administration of an enema. The basic principles of therapy for pruritus ani are uncomplicated. If an inciting cause can be identified, it should of course be eliminated or corrected. Frequently, the inciting cause is elusive, but even so, most patients can still be effectively managed by applying several simple measures. Generally, patients should keep the perianal area dry and avoid further trauma to the area. The perianal area should be gently washed, never scrubbed. After showering, the area should be patted dry or dried with a hair dryer on a low heat setting. After bowel movements, the anus should be cleaned with moistened toilet paper. Excessive rubbing or wiping should be discouraged: scratching or rubbing the anal area damages the perianal skin, making it more susceptible to irritation. Patients should also be instructed to avoid irritating foods and drinks, such as tomatoes, peppers, citrus fruits and juices, coffee, colas, beer and other alcoholic beverages, milk, nuts, popcorn, and any other foodstuffs found to be associated with increased gas, indigestion, or diarrhea. After 2 weeks, food items eliminated from the diet can be reintroduced one at a time in an attempt to identify the offending agent more specifically. A regular bowel habit should be maintained with the help of fiber supplementation or a high-fiber diet. Patients should be instructed to eschew all proprietary creams, lotions, and emollients. If prescribed and supervised by a physician, however, a hydrocortisone cream may be applied sparingly to the affected area for a period of 1 week or less to attain control of symptoms. Occasionally, when pruritus ani is refractory to treatment, a candidal yeast infection is found to be present, in which case a trial of antifungal lotion, solution, or powder is worthwhile. The fundamental goal in the treatment of pruritus ani is to establish and maintain intact, healthy, clean, and dry perianal skin. When standard measures fail to elicit improvement, fungal and viral cultures and perhaps even biopsy may be necessary to exclude an infectious or neoplastic cause. Solitary Rectal Ulcer Syndrome SRUS is a clinical condition characterized by rectal bleeding, copious mucous discharge, anorectal pain, and difficult evacuation. 32 The name of the condition notwithstanding, SRUS patients can have a single rectal ulcer, multiple ulcers, or even no ulcers at all. When present, the ulcers usually occur on the anterior rectal wall, just above the anorectal ring; less commonly, they occur from just above the dentate line to 15 cm above it. The ulcers usually appear as shallow lesions with a punched-out gray-white base that is surrounded by hyperemia. 33 Colitis cystica profunda (CCF) is a benign condition that is related to SRUS and is characterized by mucin-filled cysts located deep to the muscularis mucosae. CCF is a pathologic diagnosis, of which the most important aspect is differentiation of CCF from colorectal adenocarcinoma. Precisely what causes SRUS and CCF remains unclear, but both conditions are known to be associated with chronic inflammation or trauma (e.g., internal intussception or prolapse of the rectum, direct digital trauma, or the forces associated with evacuating a hard stool). Endoscopic evaluation of the distal colon and rectum reveals the lesions described. For both CCF and SRUS, the differential diagnosis includes polyps, endometriosis, inflammatory granuloma, infection, drug-induced colitis, and mucus-producing adenocarcinoma. These entities can be confirmed or excluded by means of an adequate biopsy. Page 8 sur 9
9 Treatment is directed at alleviating symptoms or interfering with some of the proposed etiologic mechanisms. Conservative therapy (e.g., a high-fiber diet, lifestyle changes, and biofeedback) reduces symptoms in most patients and should be tried first. Patients without rectal intussusception are offered biofeedback for retraining their bowel function. Pharmacologic therapy (e.g., anti-inflammatory enemas and suppositories) has had only limited success but nonetheless may be worth trying before the decision is made to embark on surgery. If symptoms persist, localized resection may be considered in selected patients. Patients with prolapse are considered for perineal procedures (i.e., mucosal or perineal proctectomy) and abdominal procedures (i.e., fixation or resection and rectopexy). Patients without prolapse may be offered excision, for which the options range from a transanal excision to a major resection with coloanal pull-through. Understandably, surgeons have been hesitant to offer surgical therapy for this benign condition; the results are often unsatisfactory. 34 Click here to purchase the full chapter. Beck, David E, 5 Gastrointestinal Tract and Abdomen, 17 Benign Rectal, Anal, and Perineal Problems, ACS Surgery Online, Dale DC; Federman DD, Eds. WebMD Inc., New York, Disclaimer Figures, tables, videos, and sidebars are available in the subscription edition of ACS Surgery. David E. Beck, M.D., F.A.C.S., F.A.S.C.R.S., Chairman, Department of Colon and Rectal Surgery, Ochsner Clinic Foundation, New Orleans Page 9 sur 9
Hemorrhoids. Carlos R. Alvarez-Allende PGY-III Colorectal Surgery
 Hemorrhoids Carlos R. Alvarez-Allende PGY-III Colorectal Surgery Overview Anatomy Classification Etiology Incidence Symptoms Differential Diagnosis Medical Management Surgical Management Anatomy Anal canal
Hemorrhoids Carlos R. Alvarez-Allende PGY-III Colorectal Surgery Overview Anatomy Classification Etiology Incidence Symptoms Differential Diagnosis Medical Management Surgical Management Anatomy Anal canal
Common Office Anorectal Problems
 Common Office Anorectal Problems Sandra J. Beck, M.D., FACS, FASCRS Associate Professor of Colon and Rectal Surgery University of Kentucky Medical Center l None Disclosures Benign Anal Rectal Disease l
Common Office Anorectal Problems Sandra J. Beck, M.D., FACS, FASCRS Associate Professor of Colon and Rectal Surgery University of Kentucky Medical Center l None Disclosures Benign Anal Rectal Disease l
Office Management of Anorectal Disease. Waqar Qureshi, MD, FRCP, FACG, FASGE Professor Baylor College of Medicine Houston Texas
 Office Management of Anorectal Disease Waqar Qureshi, MD, FRCP, FACG, FASGE Professor Baylor College of Medicine Houston Texas Commonly seen Anorectal Disease Hemorrhoids Anal fissures Pruritus Abscesses
Office Management of Anorectal Disease Waqar Qureshi, MD, FRCP, FACG, FASGE Professor Baylor College of Medicine Houston Texas Commonly seen Anorectal Disease Hemorrhoids Anal fissures Pruritus Abscesses
Benign anorectal diseases
 Benign anorectal diseases Symptoms Bleeding Pruritus Discharge Fecal incontinence Diarrhea Constipation False need to defecate Examinations Clinical exam Anuscopy Rectosigmoidoscopy Endosonography MRI
Benign anorectal diseases Symptoms Bleeding Pruritus Discharge Fecal incontinence Diarrhea Constipation False need to defecate Examinations Clinical exam Anuscopy Rectosigmoidoscopy Endosonography MRI
Anterior anal fissure is much more common in women and may arise following vaginal delivery.
 ANAL FISSURE Definition An anal fissure (synonym: fissure-in-ano) is a longitudinal split in the anoderm of the distal anal canal which extends from the anal verge proximally towards, but not beyond, the
ANAL FISSURE Definition An anal fissure (synonym: fissure-in-ano) is a longitudinal split in the anoderm of the distal anal canal which extends from the anal verge proximally towards, but not beyond, the
, may spread caudally to present as a perianal abscess, laterally across the external sphincter to form an ischiorectal abscess or, rarely,
 ANORECTAL ABSCESSES , may spread caudally to present as a perianal abscess, laterally across the external sphincter to form an ischiorectal abscess or, rarely, superiorly above the anorectal junction
ANORECTAL ABSCESSES , may spread caudally to present as a perianal abscess, laterally across the external sphincter to form an ischiorectal abscess or, rarely, superiorly above the anorectal junction
ACG Clinical Guideline: Management of Benign Anorectal Disorders
 ACG Clinical Guideline: Management of Benign Anorectal Disorders Arnold Wald, MD, MACG 1, Adil E. Bharucha, MBBS, MD 2, Bard C. Cosman, MD, MPH, FASCRS 3 and William E. Whitehead, PhD, MACG 4 1 Division
ACG Clinical Guideline: Management of Benign Anorectal Disorders Arnold Wald, MD, MACG 1, Adil E. Bharucha, MBBS, MD 2, Bard C. Cosman, MD, MPH, FASCRS 3 and William E. Whitehead, PhD, MACG 4 1 Division
Anal Fissure: Finding the Root Cause
 Anal Fissure: Finding the Root Cause Michael A. Jobst, MD, FACS, FASCRS Surgical Associates, PC -- Lincoln, NE 27 th Annual Management of Colon and Rectal Diseases February 23, 2019 Objectives Differentiate
Anal Fissure: Finding the Root Cause Michael A. Jobst, MD, FACS, FASCRS Surgical Associates, PC -- Lincoln, NE 27 th Annual Management of Colon and Rectal Diseases February 23, 2019 Objectives Differentiate
2015 General Surgery Survival Guide
 2015 General Surgery Survival Guide Chapter 9: Hemorrhoids New codes in the block: 45350 & 45398 45350: Sigmoidoscopy, flexible; with band ligation(s) (eg, hemorrhoids) 45398: Colonoscopy, flexible; with
2015 General Surgery Survival Guide Chapter 9: Hemorrhoids New codes in the block: 45350 & 45398 45350: Sigmoidoscopy, flexible; with band ligation(s) (eg, hemorrhoids) 45398: Colonoscopy, flexible; with
Dr Stephanie Ulmer General Surgeon Middlemore Hospital Auckland
 Dr Stephanie Ulmer General Surgeon Middlemore Hospital Auckland 16:30-17:25 WS #168: Modern Treatment of Haemorrhoids 17:35-18:30 WS #180: Modern Treatment of Haemorrhoids (Repeated) BOTTOMS Science and
Dr Stephanie Ulmer General Surgeon Middlemore Hospital Auckland 16:30-17:25 WS #168: Modern Treatment of Haemorrhoids 17:35-18:30 WS #180: Modern Treatment of Haemorrhoids (Repeated) BOTTOMS Science and
Abscess. A abscess is a localized collection of pus in the skin and may occur on any skin surface and be formed in any part of body.
 Abscess A abscess is a localized collection of pus in the skin and may occur on any skin surface and be formed in any part of body. Ethyology Bacteria causing cutaneous abscesses are typically indigenous
Abscess A abscess is a localized collection of pus in the skin and may occur on any skin surface and be formed in any part of body. Ethyology Bacteria causing cutaneous abscesses are typically indigenous
DIAGNOSIS AND MANAGEMENT OF COMMON ANORECTAL DISORDERS. Lisa Coleman, DO, FASCRS, FACS Center for Colorectal Surgery TPMG Retreat 2017
 DIAGNOSIS AND MANAGEMENT OF COMMON ANORECTAL DISORDERS Lisa Coleman, DO, FASCRS, FACS Center for Colorectal Surgery TPMG Retreat 2017 The Heinous Anus Anal Abscess Anal Cancer Anal Fissure Anal Warts Cancer
DIAGNOSIS AND MANAGEMENT OF COMMON ANORECTAL DISORDERS Lisa Coleman, DO, FASCRS, FACS Center for Colorectal Surgery TPMG Retreat 2017 The Heinous Anus Anal Abscess Anal Cancer Anal Fissure Anal Warts Cancer
Department of General Surgery. Anus Benign. Lucy Yang PGY 2 Dr. Nawar Alkhamesi October 5, 2016
 Department of General Surgery Lucy Yang PGY 2 Dr. Nawar Alkhamesi October 5, 2016 Objectives Medical Expert: 1. Anal canal anatomy, histology, innervation and pelvic floor association 2. Etiology and management
Department of General Surgery Lucy Yang PGY 2 Dr. Nawar Alkhamesi October 5, 2016 Objectives Medical Expert: 1. Anal canal anatomy, histology, innervation and pelvic floor association 2. Etiology and management
A painful problem. Symptoms of haemorrhoids. Causes of haemorrhoids. Your evaluation
 A painful problem Haemorrhoids, cushions of swollen veins in the anal canal, are often a source of embarrassment. They shouldn t be they re a very common problem that affects all kinds of people, including
A painful problem Haemorrhoids, cushions of swollen veins in the anal canal, are often a source of embarrassment. They shouldn t be they re a very common problem that affects all kinds of people, including
Although disparate topics, these two different pathologic
 34 H E M O R R H O I D S A N D R E C T A L P R O L A P S E CHARLES N. HEADRICK MICHAEL J. STAMOS Although disparate topics, these two different pathologic entities are commonly misdiagnosed by both layperson
34 H E M O R R H O I D S A N D R E C T A L P R O L A P S E CHARLES N. HEADRICK MICHAEL J. STAMOS Although disparate topics, these two different pathologic entities are commonly misdiagnosed by both layperson
DISEASES OF THE COLON, RECTUM, & ANUS
 DISEASES OF THE COLON, RECTUM, & ANUS Rocco Ricciardi, MD, MPH Chief, Section of Colon & Rectal Surgery Massachusetts General Hospital Associate Professor of Surgery Harvard Medical School CASE 1 Hemorrhoid
DISEASES OF THE COLON, RECTUM, & ANUS Rocco Ricciardi, MD, MPH Chief, Section of Colon & Rectal Surgery Massachusetts General Hospital Associate Professor of Surgery Harvard Medical School CASE 1 Hemorrhoid
Bright-red bleeding: If you have piles, you might see bright-red bleeding on the toilet paper, in the toilet bowl or on the surface of the faeces.
 What are haemorrhoids/piles? In the inner lining of the anus there are three haemorrhoidal cushions of tissue, which help to seal the anus and contribute to the control of the bowels (continence). Often,
What are haemorrhoids/piles? In the inner lining of the anus there are three haemorrhoidal cushions of tissue, which help to seal the anus and contribute to the control of the bowels (continence). Often,
The Non-Operative Treatment of Hemorrhoids and Anal Fissures
 Hemorrhoids Current non-surgical treatments The Non-Operative Treatment of Hemorrhoids and Anal Fissures Presented by Mitchel Guttenplan, MD, FACS mitchguttenplan@yahoo.com 2007, Alan L. Goldman, M.D.,
Hemorrhoids Current non-surgical treatments The Non-Operative Treatment of Hemorrhoids and Anal Fissures Presented by Mitchel Guttenplan, MD, FACS mitchguttenplan@yahoo.com 2007, Alan L. Goldman, M.D.,
Anal Fissure. The basis of conservative treatment for an anal fissure is simple. If you have
 Anal Fissure An anal fissure is a cut in the anal canal resulting from trauma. Most people suffering from an anal fissure experience pain during or after defecation (the act of moving one s bowels, a number
Anal Fissure An anal fissure is a cut in the anal canal resulting from trauma. Most people suffering from an anal fissure experience pain during or after defecation (the act of moving one s bowels, a number
Perianal diseases. What causes pain in the bottom? What causes lumps around the bottom? What examination is likely?
 In association with: Primary Care Society for Gastroenterology INFORMATION ABOUT Perianal diseases www.corecharity.org.uk What are perianal diseases? What causes an itchy bottom? What causes pain in the
In association with: Primary Care Society for Gastroenterology INFORMATION ABOUT Perianal diseases www.corecharity.org.uk What are perianal diseases? What causes an itchy bottom? What causes pain in the
Fecal Incontinence. What is fecal incontinence?
 Scan for mobile link. Fecal Incontinence Fecal incontinence is the inability to control the passage of waste material from the body. It may be associated with constipation or diarrhea and typically occurs
Scan for mobile link. Fecal Incontinence Fecal incontinence is the inability to control the passage of waste material from the body. It may be associated with constipation or diarrhea and typically occurs
Treatment of haemorrhoids. Mr Rowan Collinson FRACS Colorectal and General Surgeon Auckland
 Treatment of haemorrhoids Mr Rowan Collinson FRACS Colorectal and General Surgeon Auckland Much overlap of haemorrhoidal symptoms with other conditions Is it just the haemorrhoids? what type of haemorrhoidal
Treatment of haemorrhoids Mr Rowan Collinson FRACS Colorectal and General Surgeon Auckland Much overlap of haemorrhoidal symptoms with other conditions Is it just the haemorrhoids? what type of haemorrhoidal
Suggestions for Perianal Care in patients with itching or irritation:
 Suggestions for Perianal Care in patients with itching or irritation: Itching (and sometimes pain, even intense pain) in the anal area is termed pruritis ani (proo-rii-tus a-ni) and is in essence adult
Suggestions for Perianal Care in patients with itching or irritation: Itching (and sometimes pain, even intense pain) in the anal area is termed pruritis ani (proo-rii-tus a-ni) and is in essence adult
PAUL E. SAVOCA, MD, FACS, FASCRS Consent Form for Hemorrhoidectomy
 PAUL E. SAVOCA, MD, FACS, FASCRS Consent Form for Hemorrhoidectomy The doctor has explained that I have the following condition: Hemorrhoids- abnormally enlarged anal veins. The following procedure will
PAUL E. SAVOCA, MD, FACS, FASCRS Consent Form for Hemorrhoidectomy The doctor has explained that I have the following condition: Hemorrhoids- abnormally enlarged anal veins. The following procedure will
To inject, to band or to excise? These were the alternatives for a colorectal surgeon
 CHAPTER 2 Hemorrhoids To inject, to band or to excise? These were the alternatives for a colorectal surgeon some 50 years ago, when sclerosant injection, rubber band ligation and hemorrhoidectomy were
CHAPTER 2 Hemorrhoids To inject, to band or to excise? These were the alternatives for a colorectal surgeon some 50 years ago, when sclerosant injection, rubber band ligation and hemorrhoidectomy were
Rectal Prolapse: A 10-Year Experience
 24 The Ochsner Journal Volume 7, Number 1, Spring 2007 25 Rectal Prolapse: A 10-Year Experience Figure 2. Physical examination. A. Concentric folds of prolapsed rectum. B. Radial folds of hemorrhoids (mucosal
24 The Ochsner Journal Volume 7, Number 1, Spring 2007 25 Rectal Prolapse: A 10-Year Experience Figure 2. Physical examination. A. Concentric folds of prolapsed rectum. B. Radial folds of hemorrhoids (mucosal
Clinical Role of Modified Seton Procedure and Coring Out for Treatment of Complex Anal Fistulas Associated With Hidradenitis Suppurativa
 Int Surg 2015;100:974 978 DOI: 10.9738/INTSURG-D-14-00237.1 Clinical Role of Modified Seton Procedure and Coring Out for Treatment of Complex Anal Fistulas Associated With Hidradenitis Suppurativa Yukihiko
Int Surg 2015;100:974 978 DOI: 10.9738/INTSURG-D-14-00237.1 Clinical Role of Modified Seton Procedure and Coring Out for Treatment of Complex Anal Fistulas Associated With Hidradenitis Suppurativa Yukihiko
POST-OPERATIVE INSTRUCTIONS FOLLOWING RECTAL OFFICE SURGERY
 POST-OPERATIVE INSTRUCTIONS FOLLOWING RECTAL OFFICE SURGERY 1. KEEP THE RECTAL AREA CLEAN AND DRY. After a bowel movement, clean your bottom with peri-anal cleansing pads (i.e. Tucks or baby-wipes), followed
POST-OPERATIVE INSTRUCTIONS FOLLOWING RECTAL OFFICE SURGERY 1. KEEP THE RECTAL AREA CLEAN AND DRY. After a bowel movement, clean your bottom with peri-anal cleansing pads (i.e. Tucks or baby-wipes), followed
World Journal of Pharmaceutical Research SJIF Impact Factor 5.990
 SJIF Impact Factor 5.990 Volume 4, Issue 9, 608-613. Review Article ISSN 2277 7105 AYURVEDIC MANAGEMENT OF HEMORRHOIDS *Dr Sunil Kumar Pandey Lecturer, Deptt. of Shalya Tantra, A & U Tibbia College & Hospital,
SJIF Impact Factor 5.990 Volume 4, Issue 9, 608-613. Review Article ISSN 2277 7105 AYURVEDIC MANAGEMENT OF HEMORRHOIDS *Dr Sunil Kumar Pandey Lecturer, Deptt. of Shalya Tantra, A & U Tibbia College & Hospital,
Colorectal procedure guide
 Colorectal procedure guide Illustrations by Lisa Clark Biodesign ADVANCED TISSUE REPAIR cookmedical.com 2 INDEX Anal fistula repair Using the Biodesign plug with no button.... 4 Anal fistula repair Using
Colorectal procedure guide Illustrations by Lisa Clark Biodesign ADVANCED TISSUE REPAIR cookmedical.com 2 INDEX Anal fistula repair Using the Biodesign plug with no button.... 4 Anal fistula repair Using
HREE Questions. Setting 3: Inpatient Facilities. Block
 Block HREE Questions Setting 3: Inpatient Facilities You have general admitting privileges to the hospital. You may see patients in the critical care unit, the pediatrics unit, the maternity unit, or recovery
Block HREE Questions Setting 3: Inpatient Facilities You have general admitting privileges to the hospital. You may see patients in the critical care unit, the pediatrics unit, the maternity unit, or recovery
Accidental Bowel Leakage (Fecal Incontinence)
 Accidental Bowel Leakage (Fecal Incontinence) What is Accidental Bowel Leakage (ABL)? Accidental bowel leakage is the inability to control solid or liquid stool. This is the inability to control gas and
Accidental Bowel Leakage (Fecal Incontinence) What is Accidental Bowel Leakage (ABL)? Accidental bowel leakage is the inability to control solid or liquid stool. This is the inability to control gas and
1/3/2008. Karen Burke Priscilla LeMone Elaine Mohn-Brown. Medical-Surgical Nursing Care, 2e Karen Burke, Priscilla LeMone, and Elaine Mohn-Brown
 Medical-Surgical Nursing Care Second Edition Karen Burke Priscilla LeMone Elaine Mohn-Brown Chapter 20 Caring for Clients with Bowel Disorders Diarrhea Pathophysiology Result from impaired water absorption
Medical-Surgical Nursing Care Second Edition Karen Burke Priscilla LeMone Elaine Mohn-Brown Chapter 20 Caring for Clients with Bowel Disorders Diarrhea Pathophysiology Result from impaired water absorption
PERIANAL PROBLEMS. ACS/ASE Medical Student Core Curriculum Perianal Problems INTRODUCTION
 INTRODUCTION PERIANAL PROBLEMS Understanding the perianal anatomy and histology can help a physician to understand how patients presenting with perianal symptoms can generate a list of differentiate diagnoses.
INTRODUCTION PERIANAL PROBLEMS Understanding the perianal anatomy and histology can help a physician to understand how patients presenting with perianal symptoms can generate a list of differentiate diagnoses.
Robotic Ventral Rectopexy
 Robotic Ventral Rectopexy What is a robotic ventral rectopexy? The term rectopexy refers to an operation in which the rectum (the part of the bowel nearest the anus) is put back into its normal position
Robotic Ventral Rectopexy What is a robotic ventral rectopexy? The term rectopexy refers to an operation in which the rectum (the part of the bowel nearest the anus) is put back into its normal position
Patient information leaflet. Royal Surrey County Hospital. NHS Foundation Trust. Haemorrhoids. Day Surgery Unit
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Haemorrhoids Day Surgery Unit What are haemorrhoids? The anal canal (back passage) contains cushions of tissue at the top of
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Haemorrhoids Day Surgery Unit What are haemorrhoids? The anal canal (back passage) contains cushions of tissue at the top of
Local Glyceryl Trinitrate Versus Lateral Internal Sphincterotomy In Management Of Anal Fissure
 ISPUB.COM The Internet Journal of Surgery Volume 22 Number 2 Local Glyceryl Trinitrate Versus Lateral Internal Sphincterotomy In Management Of Anal Fissure G El-Labban, G El-Gazzaz, E Hokamam Citation
ISPUB.COM The Internet Journal of Surgery Volume 22 Number 2 Local Glyceryl Trinitrate Versus Lateral Internal Sphincterotomy In Management Of Anal Fissure G El-Labban, G El-Gazzaz, E Hokamam Citation
THE PELVIC FLOOR, EPISIOTOMY AND PERINEAL REPAIR AND VAGINAL/RECTAL MEDICATIONS
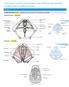 THE PELVIC FLOOR, EPISIOTOMY AND PERINEAL REPAIR AND VAGINAL/RECTAL MEDICATIONS MID2010 LEARNING OBJECTIVE 1 - REVIEW THE ANATOMY OF THE PELVIC FLOOR Superficial layers cavernosus Deep layer Coccygeus
THE PELVIC FLOOR, EPISIOTOMY AND PERINEAL REPAIR AND VAGINAL/RECTAL MEDICATIONS MID2010 LEARNING OBJECTIVE 1 - REVIEW THE ANATOMY OF THE PELVIC FLOOR Superficial layers cavernosus Deep layer Coccygeus
Perianal Fistula of Crohn s Disease
 Case 3 Perianal Fistula of Crohn s Disease A 16 year-old boy referred by surgeon due to perianal fistula since 6mo ago CC=perianal pain History of intermittent non-bloody diarrhea and mild abdominal pain
Case 3 Perianal Fistula of Crohn s Disease A 16 year-old boy referred by surgeon due to perianal fistula since 6mo ago CC=perianal pain History of intermittent non-bloody diarrhea and mild abdominal pain
Hemorrhoids. What are hemorrhoids? What is the cause? What are the symptoms?
 What are hemorrhoids? Hemorrhoids Hemorrhoids are swollen veins in the lower end of your intestine (rectum) or the anus. The anus is the opening where bowel movements pass out of your body. Hemorrhoids
What are hemorrhoids? Hemorrhoids Hemorrhoids are swollen veins in the lower end of your intestine (rectum) or the anus. The anus is the opening where bowel movements pass out of your body. Hemorrhoids
Constipation Information Leaflet THE DIGESTIVE SYSTEM. gutscharity.org.uk
 THE DIGESTIVE SYSTEM http://healthfavo.com/digestive-system-for-kids.html This factsheet is about Constipation Constipation is a symptom that can mean different things to different people but the usual
THE DIGESTIVE SYSTEM http://healthfavo.com/digestive-system-for-kids.html This factsheet is about Constipation Constipation is a symptom that can mean different things to different people but the usual
Gastrointestinal Hemorrhage, Lower
 Gastrointestinal Hemorrhage, Lower What is a lower gastrointestinal hemorrhage? A lower gastrointestinal (GI) hemorrhage, also called lower GI bleeding or rectal bleeding, is abnormal blood loss from the
Gastrointestinal Hemorrhage, Lower What is a lower gastrointestinal hemorrhage? A lower gastrointestinal (GI) hemorrhage, also called lower GI bleeding or rectal bleeding, is abnormal blood loss from the
Hemorrhoidal Disease: A Comprehensive Review
 COLLECTIVE REVIEWS Hemorrhoidal Disease: A Comprehensive Review Orit Kaidar-Person, MD, Benjamin Person, MD, Steven D Wexner, MD, FACS, FRCS, FRCS (Ed) Hemorrhoids are one of the most common conditions
COLLECTIVE REVIEWS Hemorrhoidal Disease: A Comprehensive Review Orit Kaidar-Person, MD, Benjamin Person, MD, Steven D Wexner, MD, FACS, FRCS, FRCS (Ed) Hemorrhoids are one of the most common conditions
Management Of Rectal Bleeding In The Community: How A Shared Care Approach Can Benefit Dr. Daniel Lee
 Management Of Rectal Bleeding In The Community: How A Shared Care Approach Can Benefit Dr. Daniel Lee MD, MMed (S'pore), FRCS (Edin) Associate Consultant Department of Surgery 9 January 2016 Incidence
Management Of Rectal Bleeding In The Community: How A Shared Care Approach Can Benefit Dr. Daniel Lee MD, MMed (S'pore), FRCS (Edin) Associate Consultant Department of Surgery 9 January 2016 Incidence
TURP - TransUrethral Resection of the Prostate
 TURP - TransUrethral Resection of the Prostate To learn about a TURP, you will need to know these words: The prostate is the sexual gland that makes a fluid which helps sperm move. It surrounds the urethra
TURP - TransUrethral Resection of the Prostate To learn about a TURP, you will need to know these words: The prostate is the sexual gland that makes a fluid which helps sperm move. It surrounds the urethra
Surgical Management for Defecation Dysfunction
 Defecatory Dysfunction Surgical Management for Defecation Dysfunction JMAJ 46(9): 378 383, 2003 Tatsuo TERAMOTO Professor, 1st Department of Surgery, School of Medicine, Toho University Abstract: Typical
Defecatory Dysfunction Surgical Management for Defecation Dysfunction JMAJ 46(9): 378 383, 2003 Tatsuo TERAMOTO Professor, 1st Department of Surgery, School of Medicine, Toho University Abstract: Typical
General Surgery. Haemorrhoids
 General Surgery Haemorrhoids Hemorrhoids_PRINT.indd 1 5/9/2016 5:50:45 PM A painful problem Haemorrhoids, cushions of swollen veins in the anal canal, are often a source of embarrassment. They shouldn
General Surgery Haemorrhoids Hemorrhoids_PRINT.indd 1 5/9/2016 5:50:45 PM A painful problem Haemorrhoids, cushions of swollen veins in the anal canal, are often a source of embarrassment. They shouldn
Principles of Surgery - Ano rectal region: Haemorrhoids
 Principles of Surgery - Ano rectal region: Haemorrhoids Maurice Brygel Director, Melbourne Hernia Clinic (www.hernia.net.au) Fellow, Royal Australian College of Surgeons (RACS) Correspondence Maurice Brygel
Principles of Surgery - Ano rectal region: Haemorrhoids Maurice Brygel Director, Melbourne Hernia Clinic (www.hernia.net.au) Fellow, Royal Australian College of Surgeons (RACS) Correspondence Maurice Brygel
The Management of Anorectal Abscess: An Inexpensive and Simple Alternative Technique to Incision and "Deroofing"
 The Management of Anorectal Abscess: An Inexpensive and Simple Alternative Technique to Incision and "Deroofing" William H. Isbister, MD; Stephen Kyle, MB From the Departments of Surgery, Wellington School
The Management of Anorectal Abscess: An Inexpensive and Simple Alternative Technique to Incision and "Deroofing" William H. Isbister, MD; Stephen Kyle, MB From the Departments of Surgery, Wellington School
Surgical Management of IBD in the Age of Biologics
 Surgical Management of IBD in the Age of Biologics Lisa S. Poritz, M.D Associate Professor of Surgery Division of Colon and Rectal Surgery Objectives Discuss surgical management of IBD When to operate
Surgical Management of IBD in the Age of Biologics Lisa S. Poritz, M.D Associate Professor of Surgery Division of Colon and Rectal Surgery Objectives Discuss surgical management of IBD When to operate
Patient Information Leaflet
 Patient Information Leaflet Haemorrhoid Operation What are haemorrhoids? Everyone has swellings in the anal canal (back passage) called anal cushions. These bulges in the lining of the anal canal act like
Patient Information Leaflet Haemorrhoid Operation What are haemorrhoids? Everyone has swellings in the anal canal (back passage) called anal cushions. These bulges in the lining of the anal canal act like
Case Presentation and Discussion on GI Bleeding Nolan Ortega Aludino, M.D.
 Case Presentation and Discussion on GI Bleeding Nolan Ortega Aludino, M.D. General Data R.L. R.L. 4343 years old MaleMale PacoPaco Manila Chief Complaint Anal Anal bleeding History of Present Illness 3
Case Presentation and Discussion on GI Bleeding Nolan Ortega Aludino, M.D. General Data R.L. R.L. 4343 years old MaleMale PacoPaco Manila Chief Complaint Anal Anal bleeding History of Present Illness 3
Rectal Cancer. About the Colon and Rectum. Symptoms. Colorectal Cancer Screening
 Patient information regarding care and surgery associated with RECTAL CANCER by Robert K. Cleary, M.D., John C. Eggenberger, M.D., Amalia J. Stefanou., M.D. location: Michigan Heart and Vascular Institute,
Patient information regarding care and surgery associated with RECTAL CANCER by Robert K. Cleary, M.D., John C. Eggenberger, M.D., Amalia J. Stefanou., M.D. location: Michigan Heart and Vascular Institute,
Patient Information Leaflet
 Patient Information Leaflet Your Haemorrhoid Operation What are haemorrhoids? Everyone has swellings in the anal canal (back passage) called anal cushions. These bulges in the lining of the anal canal
Patient Information Leaflet Your Haemorrhoid Operation What are haemorrhoids? Everyone has swellings in the anal canal (back passage) called anal cushions. These bulges in the lining of the anal canal
Chapter 34. Nursing Care of Patients with Lower Gastrointestinal Disorders
 Chapter 34 Nursing Care of Patients with Lower Gastrointestinal Disorders Lower Gastrointestinal System Small Intestines Large Intestines Rectum Anus Constipation Fecal Mass Held In Rectum Feces Become
Chapter 34 Nursing Care of Patients with Lower Gastrointestinal Disorders Lower Gastrointestinal System Small Intestines Large Intestines Rectum Anus Constipation Fecal Mass Held In Rectum Feces Become
Chapter 19 Hidradenitis Suppurativa
 1 Chapter 19 Hidradenitis Suppurativa Peter Nthumba Hidradenitis suppurativa is a chronic, recurrent, painful inflammatory skin disease, first described in 1833 by a French surgeon. Verneuil, another French
1 Chapter 19 Hidradenitis Suppurativa Peter Nthumba Hidradenitis suppurativa is a chronic, recurrent, painful inflammatory skin disease, first described in 1833 by a French surgeon. Verneuil, another French
Modern Management of Perianal Fistulas in Crohn s Disease (PFCD): Future Directions
 Modern Management of Perianal Fistulas in Crohn s Disease (PFCD): Future Directions Rami Ismail, Pharm.D., BCPS, BCCCP, CACP Lead Clinical staff Pharmacist, Cleveland Clinic Abu Dhabi Disclosure Information
Modern Management of Perianal Fistulas in Crohn s Disease (PFCD): Future Directions Rami Ismail, Pharm.D., BCPS, BCCCP, CACP Lead Clinical staff Pharmacist, Cleveland Clinic Abu Dhabi Disclosure Information
Piles / Sclerosing. Endoscopy Department. Patient information leaflet
 Piles / Sclerosing Endoscopy Department Patient information leaflet You will only be given this leaflet if you have been diagnosed with piles / sclerosing. The information below outlines the condition,
Piles / Sclerosing Endoscopy Department Patient information leaflet You will only be given this leaflet if you have been diagnosed with piles / sclerosing. The information below outlines the condition,
Discharge information for patients Fistula plug for anal fistula
 Discharge information for patients Fistula plug for anal fistula Clinical Sciences Building Colorectal Surgery 0161 206 1249 All Rights Reserved 2017. Document for issue as handout.. What is an anal fistula?
Discharge information for patients Fistula plug for anal fistula Clinical Sciences Building Colorectal Surgery 0161 206 1249 All Rights Reserved 2017. Document for issue as handout.. What is an anal fistula?
Pelvic Prolapse. A Patient Guide to Pelvic Floor Reconstruction
 Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
Surgical Treatment Of Hemorrhoids READ ONLINE
 Surgical Treatment Of Hemorrhoids READ ONLINE If you are searching for a book Surgical Treatment of Hemorrhoids in pdf format, then you've come to the right site. We present full variation of this book
Surgical Treatment Of Hemorrhoids READ ONLINE If you are searching for a book Surgical Treatment of Hemorrhoids in pdf format, then you've come to the right site. We present full variation of this book
Colorectal Surgery Benign Anal Conditions...
 Colorectal Surgery Benign Anal Conditions... Lee Dvorkin Consultant General, Colorectal & Laparoscopic Surgeon, NMUH Clinical Lead for General Surgery, NMH Senior Clinical Lecturer, UCLH Associate Professor
Colorectal Surgery Benign Anal Conditions... Lee Dvorkin Consultant General, Colorectal & Laparoscopic Surgeon, NMUH Clinical Lead for General Surgery, NMH Senior Clinical Lecturer, UCLH Associate Professor
Skin Integrity and Wound Care
 Skin Integrity and Wound Care By Dr. Amer Hasanien & Dr. Ali Saleh Skin Integrity and Wound Care Skin integrity: the presence of normal Skin & Uninterrupted skin layers by wounds. Factors affecting appearance
Skin Integrity and Wound Care By Dr. Amer Hasanien & Dr. Ali Saleh Skin Integrity and Wound Care Skin integrity: the presence of normal Skin & Uninterrupted skin layers by wounds. Factors affecting appearance
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION. 9 May 2007
 The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 9 May 2007 RECTOGESIC 4 mg/g, rectal ointment B/1 (CIP 376 537-0) Applicant : PROSTRAKAN PHARMA SAS Glyceryl trinitrate
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 9 May 2007 RECTOGESIC 4 mg/g, rectal ointment B/1 (CIP 376 537-0) Applicant : PROSTRAKAN PHARMA SAS Glyceryl trinitrate
Stapled transanal rectal resection for obstructed defaecation syndrome
 Stapled transanal rectal resection for obstructed Issued: June 2010 www.nice.org.uk/ipg351 NHS Evidence has accredited the process used by the NICE Interventional Procedures Programme to produce interventional
Stapled transanal rectal resection for obstructed Issued: June 2010 www.nice.org.uk/ipg351 NHS Evidence has accredited the process used by the NICE Interventional Procedures Programme to produce interventional
Crohn's disease CAUSES COURSE OF CROHN'S DISEASE TREATMENT. Sulfasalazine
 Crohn's disease Crohn's disease is an inflammatory condition of the digestive tract that affects children and adults. Common features of Crohn's disease include mouth sores, diarrhea, abdominal pain, weight
Crohn's disease Crohn's disease is an inflammatory condition of the digestive tract that affects children and adults. Common features of Crohn's disease include mouth sores, diarrhea, abdominal pain, weight
A Nursing Assessment Tool for Adults With Fecal Incontinence
 Journal of Wound, Ostomy and Continence Nursing 2000, 279- A Nursing Assessment Tool for Adults With Fecal Incontinence Christine Norton, MA, RN, and Sonya Chelvanayagam, MSc, RN Abstract Fecal incontinence
Journal of Wound, Ostomy and Continence Nursing 2000, 279- A Nursing Assessment Tool for Adults With Fecal Incontinence Christine Norton, MA, RN, and Sonya Chelvanayagam, MSc, RN Abstract Fecal incontinence
Small Bowel and Colon Surgery
 Small Bowel and Colon Surgery Why Do I Need a Small Bowel Resection? A variety of conditions can damage your small bowel. In severe cases, your doctor may recommend removing part of your small bowel. Conditions
Small Bowel and Colon Surgery Why Do I Need a Small Bowel Resection? A variety of conditions can damage your small bowel. In severe cases, your doctor may recommend removing part of your small bowel. Conditions
19th Annual International Colorectal Disease Symposium An International Exchange of Medical and Surgical Concepts
 Wednesday, February 13, 2008 7-9:00p Early Check-In / Registration (Grand Ballroom Foyer) Thursday, February 14, 2008 6:45 AM Breakfast (Caribbean Ballroom and Foyer) 7:00 AM Registration (Grand Ballroom
Wednesday, February 13, 2008 7-9:00p Early Check-In / Registration (Grand Ballroom Foyer) Thursday, February 14, 2008 6:45 AM Breakfast (Caribbean Ballroom and Foyer) 7:00 AM Registration (Grand Ballroom
Lee Jackson, M.D. Post-Operation Information and Instructions
 Post-Operation Information and Instructions While a robotic prostatectomy is performed routinely, it is still a relatively major surgery that will take some time and effort to recover from. The following
Post-Operation Information and Instructions While a robotic prostatectomy is performed routinely, it is still a relatively major surgery that will take some time and effort to recover from. The following
Anterior Sphincter Repair Operation
 Anterior Sphincter Repair Operation How will the operation help me? The investigations that you have had indicate that your anal sphincter is damaged or very weak, and this is why you are having trouble
Anterior Sphincter Repair Operation How will the operation help me? The investigations that you have had indicate that your anal sphincter is damaged or very weak, and this is why you are having trouble
Magnetic Resonance Imaging of Perianal Fistulas
 Magnetic Resonance Imaging of Perianal Fistulas Poster No.: C-0317 Congress: ECR 2014 Type: Authors: Keywords: DOI: Educational Exhibit A. P. Sathe, E. Soh, K. Y. Seto, B. Yeh, D. W. Y. chee, R. Quah,
Magnetic Resonance Imaging of Perianal Fistulas Poster No.: C-0317 Congress: ECR 2014 Type: Authors: Keywords: DOI: Educational Exhibit A. P. Sathe, E. Soh, K. Y. Seto, B. Yeh, D. W. Y. chee, R. Quah,
-15. -Alaa Albandi. -Dr. Mohammad Almohtasib. 0 P a g e
 -15 -Alaa Albandi - -Dr. Mohammad Almohtasib 0 P a g e In this last lecture, we will talk about the sigmoid colon, rectum, and anal canal. Sigmoid colon It has a mesentery called pelvic mesocolon or sigmoidal
-15 -Alaa Albandi - -Dr. Mohammad Almohtasib 0 P a g e In this last lecture, we will talk about the sigmoid colon, rectum, and anal canal. Sigmoid colon It has a mesentery called pelvic mesocolon or sigmoidal
At the outset, we want to clear up some terminology issues. IBS is COPYRIGHTED MATERIAL. What Is IBS?
 1 What Is IBS? At the outset, we want to clear up some terminology issues. IBS is the abbreviation that doctors use for irritable bowel syndrome, often when they are talking about people with IBS. We will
1 What Is IBS? At the outset, we want to clear up some terminology issues. IBS is the abbreviation that doctors use for irritable bowel syndrome, often when they are talking about people with IBS. We will
HIDRADENITIS SUPPURATIVA
 Print Close Window Note: Large images and tables on this page may necessitate printing in landscape mode. Copyright 2004-2005 The McGraw-Hill Companies. All rights reserved. Fitzpatrick Color Atlas, 5e
Print Close Window Note: Large images and tables on this page may necessitate printing in landscape mode. Copyright 2004-2005 The McGraw-Hill Companies. All rights reserved. Fitzpatrick Color Atlas, 5e
Hemorrhoids represent one of the most common
 THE JOURNAL OF FAMILY PRACTICE S U P P L E M E N T A new treatment option for grades III and IV hemorrhoids Glenn S. Parker, MD, FACS, FASCRS Chief, Division of Colon and Rectal Surgery, and Director,
THE JOURNAL OF FAMILY PRACTICE S U P P L E M E N T A new treatment option for grades III and IV hemorrhoids Glenn S. Parker, MD, FACS, FASCRS Chief, Division of Colon and Rectal Surgery, and Director,
Management of Common Paediatric Surgical G.I. Problems
 Management of Common Paediatric Surgical G.I. Problems Dr. Loh Ser Kheng Dale Lincoln Senior Consultant Department of Paediatric Surgery National University Hospital National University Health System Tongue
Management of Common Paediatric Surgical G.I. Problems Dr. Loh Ser Kheng Dale Lincoln Senior Consultant Department of Paediatric Surgery National University Hospital National University Health System Tongue
World Journal of Colorectal Surgery
 World Journal of Colorectal Surgery Volume 2, Issue 1 10 Article 12 LOCAL GLYCERYL TRINITRATE VERSUS LATERAL INTERNAL SPHINCTEROTOMY IN MANAGEMENT OF ANAL FISSURE gouda m. ellabban galal elkazaz emad hokam
World Journal of Colorectal Surgery Volume 2, Issue 1 10 Article 12 LOCAL GLYCERYL TRINITRATE VERSUS LATERAL INTERNAL SPHINCTEROTOMY IN MANAGEMENT OF ANAL FISSURE gouda m. ellabban galal elkazaz emad hokam
Abstract. Successful use of 0.2% Glyceryl Trinitrate ointment for anal fissures in Erbil city, Iraq. Abdulqadir M. Zangana (1) Kawa F.
 Successful use of 0.2% Glyceryl Trinitrate ointment for anal fissures in Erbil city, Iraq Abdulqadir M. Zangana (1) Kawa F. Dizaye (2) (1) Professor of Surgery, CABS-FICS-MD, Head of Department of surgery,
Successful use of 0.2% Glyceryl Trinitrate ointment for anal fissures in Erbil city, Iraq Abdulqadir M. Zangana (1) Kawa F. Dizaye (2) (1) Professor of Surgery, CABS-FICS-MD, Head of Department of surgery,
Saratoga Schenectady Endoscopy Center, LLC Burnt Hills, N.Y Hemorrhoids. National Digestive Diseases Information Clearinghouse
 Hemorrhoids National Digestive Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What are hemorrhoids? Hemorrhoids are swollen and inflamed veins
Hemorrhoids National Digestive Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What are hemorrhoids? Hemorrhoids are swollen and inflamed veins
Diagnosis of Impaired Defecatory Function with Special Reference to Physiological Tests
 Defecatory Dysfunction Diagnosis of Impaired Defecatory Function with Special Reference to Physiological Tests JMAJ 46(9): 373 377, 2003 Masatoshi OYA, Masashi UENO, and Tetsuichiro MUTO Department of
Defecatory Dysfunction Diagnosis of Impaired Defecatory Function with Special Reference to Physiological Tests JMAJ 46(9): 373 377, 2003 Masatoshi OYA, Masashi UENO, and Tetsuichiro MUTO Department of
ISSN: X Int. J. Curr. Res. Biol. Med. (2018). 3(2): 53-62
 INTERNATIONAL JOURNAL OF CURRENT RESEARCH IN BIOLOGY AND MEDICINE ISSN: 2455-944X www.darshanpublishers.com DOI:10.22192/ijcrbm Volume 3, Issue 2-2018 Original Research Article DOI: http://dx.doi.org/10.22192/ijcrbm.2018.03.02.009
INTERNATIONAL JOURNAL OF CURRENT RESEARCH IN BIOLOGY AND MEDICINE ISSN: 2455-944X www.darshanpublishers.com DOI:10.22192/ijcrbm Volume 3, Issue 2-2018 Original Research Article DOI: http://dx.doi.org/10.22192/ijcrbm.2018.03.02.009
General diagnostic considerations of the anorectal and perianal diseases III. Suppl. examinations Bloodwork, urinalysis (gen. state) Fine needle aspir
 Surgical anatomy (Anorectum) Surgery of the anorectum and the perianal region in small animals Dr. T. Németh, DVM, PhD, DipECVS Associate Professor and Head of Surgery Surgical anatomy (Anorectum) Surgical
Surgical anatomy (Anorectum) Surgery of the anorectum and the perianal region in small animals Dr. T. Németh, DVM, PhD, DipECVS Associate Professor and Head of Surgery Surgical anatomy (Anorectum) Surgical
INFORMED CONSENT FOR ANORECTAL PROCEDURES
 516-248-2422 www.crssny.com Locations in Nassau, Suffolk and Queens INFORMED CONSENT FOR ANORECTAL PROCEDURES You may undergo anoscopy or proctosigmoidoscopy as part of your rectal examination. These tests
516-248-2422 www.crssny.com Locations in Nassau, Suffolk and Queens INFORMED CONSENT FOR ANORECTAL PROCEDURES You may undergo anoscopy or proctosigmoidoscopy as part of your rectal examination. These tests
Chapter 19. Assisting With Bowel Elimination. Elsevier items and derived items 2014, 2010 by Mosby, an imprint of Elsevier Inc. All rights reserved.
 Chapter 19 Assisting With Bowel Elimination Normal Bowel Elimination Time and frequency of bowel movements (BMs) vary. To assist with bowel elimination, you need to know these terms: Defecation is the
Chapter 19 Assisting With Bowel Elimination Normal Bowel Elimination Time and frequency of bowel movements (BMs) vary. To assist with bowel elimination, you need to know these terms: Defecation is the
The Use of Glyceryl Tri-Nitrate Ointment in Treatment of Chronic Fissure in Ano
 Bahrain Medical Bulletin, Vol. 28, No. 4, December 2006 The Use of Glyceryl Tri-Nitrate Ointment in Treatment of Chronic Fissure in Ano Suhair Al-Saad, MBChB,FRCS I,CABS,* Hamdi Al- Shenawi, MBBS, FRCS
Bahrain Medical Bulletin, Vol. 28, No. 4, December 2006 The Use of Glyceryl Tri-Nitrate Ointment in Treatment of Chronic Fissure in Ano Suhair Al-Saad, MBChB,FRCS I,CABS,* Hamdi Al- Shenawi, MBBS, FRCS
Haemorrhoidal disorders -What is the optimal treatment?
 Haemorrhoidal disorders -What is the optimal treatment? Per-Olof Nyström, M.D., Ph.D. Professor of Surgery Karolinska Institutet and Karolinska University Hospital Huddinge Stockholm, Sweden The methods
Haemorrhoidal disorders -What is the optimal treatment? Per-Olof Nyström, M.D., Ph.D. Professor of Surgery Karolinska Institutet and Karolinska University Hospital Huddinge Stockholm, Sweden The methods
Cryotherapy for localised prostate cancer
 Cryotherapy for localised prostate cancer Introduction This leaflet is written for patients and their family. It provides information on prostate cryotherapy for prostate cancer which has not previously
Cryotherapy for localised prostate cancer Introduction This leaflet is written for patients and their family. It provides information on prostate cryotherapy for prostate cancer which has not previously
DIGESTIVE SYSTEM SURGICAL PROCEDURES December 22, 2015 (effective March 1, 2016) INTESTINES (EXCEPT RECTUM) Asst Surg Anae
 December 22, 2015 (effective March 1, 201) INTESTINES (EXCEPT RECTUM) Z513 Hydrostatic - Pneumatic dilatation of colon stricture(s) through colonoscope... 10.50 Z50 Fulguration of first polyp through colonoscope...
December 22, 2015 (effective March 1, 201) INTESTINES (EXCEPT RECTUM) Z513 Hydrostatic - Pneumatic dilatation of colon stricture(s) through colonoscope... 10.50 Z50 Fulguration of first polyp through colonoscope...
Procedure Specific Information Sheet Open Radical Prostatectomy
 Procedure Specific Information Sheet Open Radical Prostatectomy Dr Vasudevan has recommended that you have an open radical prostatectomy. This document gives you information on what to expect before, during
Procedure Specific Information Sheet Open Radical Prostatectomy Dr Vasudevan has recommended that you have an open radical prostatectomy. This document gives you information on what to expect before, during
What Is Constipation?
 CONSTIPATION What Is Constipation? Constipation is when you have infrequent or hard-to-pass bowel movements (meaning they are painful or you have to strain), have hard stools or feel like your bowel movements
CONSTIPATION What Is Constipation? Constipation is when you have infrequent or hard-to-pass bowel movements (meaning they are painful or you have to strain), have hard stools or feel like your bowel movements
A STUDY OF EVALUATION OF LOCAL INFILTRATION OF BOTULINUM TOXIN AS COMPARED TO LATERAL SPHINCTEROTOMY IN THE MANAGEMENT OF CHRONIC ANAL FISSURE
 A STUDY OF EVALUATION OF LOCAL INFILTRATION OF BOTULINUM TOXIN AS COMPARED TO LATERAL SPHINCTEROTOMY IN THE MANAGEMENT OF CHRONIC ANAL FISSURE Ravindranath Singh 1, Puneet Pal Singh Oberoi 2, Nisith Kumar
A STUDY OF EVALUATION OF LOCAL INFILTRATION OF BOTULINUM TOXIN AS COMPARED TO LATERAL SPHINCTEROTOMY IN THE MANAGEMENT OF CHRONIC ANAL FISSURE Ravindranath Singh 1, Puneet Pal Singh Oberoi 2, Nisith Kumar
GULF COAST SURGICAL GROUP JARED FRATTINI, M.D., FACS
 POST-COLONOSCOPY INSTRUCTIONS 1. Resume your regular diet, unless otherwise instructed by your, but avoid excessive eating or drinking for 24 hours. 2. Do not be alarmed by having to pass excessive gas
POST-COLONOSCOPY INSTRUCTIONS 1. Resume your regular diet, unless otherwise instructed by your, but avoid excessive eating or drinking for 24 hours. 2. Do not be alarmed by having to pass excessive gas
Treatments for Fecal Incontinence A Review of the Research for Adults
 Treatments for Fecal Incontinence A Review of the Research for Adults e Is This Information Right for Me? This information is right for you if: Your health care professional* said you or your loved one
Treatments for Fecal Incontinence A Review of the Research for Adults e Is This Information Right for Me? This information is right for you if: Your health care professional* said you or your loved one
Lower back pain and hemorrhoids
 Lower back pain and hemorrhoids Beverly Hill Proctologists Primary Menu they begin in the front of our pelvic cavities and terminate in the back of the tailbone pain with hemorrhoids. Can hemorrhoids cause
Lower back pain and hemorrhoids Beverly Hill Proctologists Primary Menu they begin in the front of our pelvic cavities and terminate in the back of the tailbone pain with hemorrhoids. Can hemorrhoids cause
Constipation. What is constipation? What is the criteria for having constipation? What are the different types of constipation?
 What is constipation? is defined as having a bowel movement less than 3 times per week. It is usually associated with hard stools or difficulty passing stools. You may have pain while passing stools or
What is constipation? is defined as having a bowel movement less than 3 times per week. It is usually associated with hard stools or difficulty passing stools. You may have pain while passing stools or
How varicose veins occur
 Varicose veins are a very common problem, generally appearing as twisting, bulging rope-like cords on the legs, anywhere from groin to ankle. Spider veins are smaller, flatter, red or purple veins closer
Varicose veins are a very common problem, generally appearing as twisting, bulging rope-like cords on the legs, anywhere from groin to ankle. Spider veins are smaller, flatter, red or purple veins closer
Chapter 14 GASTROINTESTINAL IMPAIRMENT
 Chapter 14 GASTROINTESTINAL IMPAIRMENT Introduction This chapter provides criteria for assessing permanent impairment from entitled conditions of the gastrointestinal tract and the accessory organs of
Chapter 14 GASTROINTESTINAL IMPAIRMENT Introduction This chapter provides criteria for assessing permanent impairment from entitled conditions of the gastrointestinal tract and the accessory organs of
Robotic Prostatectomy - After Surgery
 PATIENT EDUCATION patienteducation.osumc.edu Robotic Prostatectomy - After Surgery Here are general guidelines for home after your surgery. Your doctor may give you other instructions based on your needs
PATIENT EDUCATION patienteducation.osumc.edu Robotic Prostatectomy - After Surgery Here are general guidelines for home after your surgery. Your doctor may give you other instructions based on your needs
