Pregnancy and childbirth: the effects on pelvic floor muscles
|
|
|
- Hortense James
- 5 years ago
- Views:
Transcription
1 Page 1 of 9 Pregnancy and childbirth: the effects on pelvic floor muscles 26 February, 2009 Stress incontinence can follow childbirth as pelvic floor muscles are damaged AUTHOR Julia Herbert, MSc, MCSP, Grad Dip Phys,is specialist continence physiotherapist, Bolton PCT continence team, NHS Bolton, and independent practitioner and lecturer. ABSTRACT Herbert, J. (2009) Pregnancy and childbirth: the effects on pelvic floor muscles.nursing Times;105: 7, This article examines the risks of damage to the pelvic floor that are associated with pregnancy and delivery. It will aim to dispel some myths about pelvic floor exercises and pregnancy and will look at the latest recommendations about pelvic floor muscle exercise. During pregnancy there are outward signs that the body is changing but changes that occur to the pelvic floor muscles and the nerves and soft tissues that support them are less obvious. In recent years, there has been an increasing interest in the effect of childbirth on continence. Wall (1999) suggests that we now have an increased awareness of the effects of obstetric trauma because modern obstetric care has reduced maternal deaths and women now survive difficult or obstructed deliveries. As a result of their obstetric trauma, these women have an increased risk of developing pelvic floor muscle dysfunction. The physiological changes occurring during pregnancy and the processes of childbirth have a detrimental effect on the structure and function of the muscles, nerves and fascial tissues (connective tissue) that make up the pelvic floor complex. Dysfunction of the pelvic floor complex can result in a wide range of symptoms including urinary or anal incontinence. Symptoms of pelvic floor dysfunction are listed in Box 1. Box 1. Symptoms of pelvic floor dysfunction Lower urinary tract Urinary incontinence Urgency and frequency Slow or intermittent stream and straining Feeling of incomplete emptying Bowel
2 Page 2 of 9 Obstructed defecation Functional constipation Faecal incontinence Rectal/anal prolapse Vagina Pelvic organ prolapse Pain Chronic pelvic pain Pelvic pain syndrome Sexual function Dyspareunia (painful sexual intercourse) Orgasmic dysfunction The pelvic floor and pregnancy Several epidemiological studies have shown that urinary incontinence, in particular stress urinary incontinence, is strongly associated with pregnancy and childbirth. The prevalence of stress urinary incontinence increases during pregnancy and declines after delivery (Morkved, 2007). As the baby grows, the weight of the baby and the gravid uterus (pregnant uterus) produce anatomical changes to the bladder and urethra. Studies using ultrasound imaging techniques have shown that the angle between the bladder neck and the urethra increases, producing an increased opening of the bladder neck. There is also an increased mobility of the bladder due to the hormonal changes of pregnancy which also affect the pelvic floor complex. A study of 184 first-time mothers who delivered by Caesarean section and 100 who delivered vaginally (Lal et al, 2003) found that there was no significant difference in the prevalence of symptoms of incontinence 10 months following delivery. This study supports the argument that pregnancy is the cause of incontinence for many women irrespective of their mode of delivery. These findings confirmed those of MacLennan et al (2000) who reported the results of a survey of 4,400 households, randomly selected and questioned about pelvic floor disorders. This study concluded that women having Caesarean section were just as likely to have symptoms of incontinence than those having a vaginal delivery. Lal et al (2003) also suggest that changes occur to the properties of collagen and other connective tissues during pregnancy. When these changes are combined with possible inherited susceptibilities, anal incontinence can occur as a result of the pregnancy alone, regardless of delivery mode. In a prospective study of 363 women up to one year after delivery, Groutz et al (2004) found that a similar percentage of women who had vaginal deliveries and Caesarean section for obstructed labour developed stress urinary incontinence (10.3% and 12% respectively). A significantly lower percentage (3.5%) of women developed stress urinary incontinence following an elective Caesarean section with
3 Page 3 of 9 no trial of labour. Although this study demonstrates that Caesarean section protects the pelvic floor from injury, it also supports the theory that some changes to the function of the pelvic floor must occur as a result of pregnancy. This view is also supported by van Brummen et al (2007) in a prospective study of 344 women expecting their first baby. This study compared the prevalence of postpartum stress urinary incontinence and urge incontinence in women who had had a Caesarean section with those who had had a vaginal delivery. They also noted that the presence of stress urinary incontinence in early pregnancy was a strong predictor of it persisting in the year following delivery in both groups. When women are advised about mode of delivery, consideration should be given to the morbidity associated with Caesarean section such as increased risks of postpartum haemorrhage, infection, pulmonary embolism and ileus. Sultan and Stanton (1996) suggest that the risk of serious maternal morbidity is considerably lower following vaginal delivery compared with Caesarean section and that the risk of hysterectomy secondary to haemorrhage is 10 times higher following Caesarean section than with vaginal delivery. Influence of general health A pregnant woman s general health may influence the likelihood of developing incontinence. Obesity in pregnancy has been suggested as a possible risk factor for postpartum stress urinary incontinence (Ramussen et al, 1997; Wilson et al, 1996). However, in their study of 304 women following childbirth, Chiarelli and Campbell (1997), did not report a link to obesity. In studies not specifically related to pregnancy there has been a definite link demonstrated between obesity and pelvic floor dysfunction (Kapoor and Freeman, 2008). Chiarelli and Campbell (1997) suggest that women with a chronic cough during pregnancy could have four times the risk of developing incontinence. They also report that there is an fourfold increased risk of incontinence for pregnant women who have had a previous vaginal delivery and a 10-fold increased risk for those who have had a previous forceps delivery. Initial strength of the pelvic floor muscles also influences the development of incontinence during pregnancy (Morkved et al, 2003). The pelvic floor and childbirth Muscles and fascia The ability of the pelvic floor to contribute to the maintenance of both urinary and anal continence is undoubtedly threatened by the processes of vaginal delivery. As the baby emerges, the widest part of the babies head stretches the pelvic floor muscles, fascia and nerves this stage of labour is referred to as the crowning of the baby s head. It is likely that stretching and possible tearing of the endopelvic fascia and muscles and associated trauma to the pudendal nerves may cause pelvic floor dysfunction (Kapoor and Freeman, 2008). The development of ultrasound techniques has enabled a better understanding of the nature of fascial injuries during delivery. Dietz and Lanzarone (2005) demonstrated that up to one-third of women following vaginal delivery experienced avulsion (tearing) of the fascia supporting the pelvic floor muscles which was associated with postpartum stress urinary incontinence three months following delivery. Kapoor and Freeman (2008) suggest that fascial tears have the ability to heal but it is thought that the resulting connective tissue will not be as strong as the original and that the woman will be more likely to experience symptoms of pelvic floor dysfunction such as incontinence or pelvic organ prolapse. Such symptoms may become more evident later in life as a result of the ageing process and hormonal
4 Page 4 of 9 changes at menopause that affect the already weakened fascia. Some women may be predisposed to developing pelvic floor dysfunction because of a familial deficiency in their collagen type. Keane et al (1997) have shown that premenopausal nulliparous women with stress urinary incontinence have weaker pelvic floor collagen than control groups containing premenopausal nulliparous women without stress urinary incontinence. They suggest that there may be a group of women with congenitally weak connective tissue and fascia who might be at risk of stress urinary incontinence and pelvic organ prolapse as a result of pregnancy. Injuries to the pelvic floor muscles have been classified by the Royal College of Obstetricians and Gynaecologists (RCOG, 2007). This guideline document on the management of third and fourth-degree tears following vaginal delivery, divides muscle tears into second, third and fourth degrees. (Box 2). First-degree tears are not included in this guideline because it concerns pelvic floor muscle injury whereas a first-degree tear involves only the skin covering the muscles. Box 2. Classification of pelvic floor muscle injury Second degree: injury to the perineum involving perineal muscles but not involving the anal sphincter Third degree: injury to the perineum involving the anal sphincter complex (external anal sphincter (EAS) and internal anal sphincter (IAS)): 3a: less than 50% of EAS thickness torn 3b: more than 50% of EAS thickness torn 3c: IAS torn Fourth degree: injury to perineum involving the anal sphincter complex (EAS and IAS) and rectal mucosa Source: RCOG (2007) It is difficult to determine the exact prevalence of obstetric injuries because of the difficulty in diagnosing the degree of tear immediately following delivery because tissues are swollen and deformed. Nerve injury A number of studies have suggested that stress urinary incontinence following delivery is due to damage to the peripheral nerves (Snooks et al, 1990, 1984; Allen et al, 1990). Comparison of pudendal nerve function prior and post delivery suggests that the cause of denervation (loss of nerve supply) occurs during the second stage of labour (Sultan et al, 1994). Allen et al (1990) demonstrated pudendal nerve denervation in 80% of women following their first vaginal delivery. In this study, the risk factors for this nerve injury were a prolonged active second stage of labour and heavier babies. In many women, the nerve damage occurring at delivery may persist and the associated pelvic floor muscle dysfunction may become worse over time (Snooks et al, 1990). Nerve injury may be down to the significant difference between the ability of nerve tissue to elongate compared with muscle or fascial tissues. Nerves have been shown to be able to elongate by 6 22% of their initial length before damage occurs whereas skeletal muscle has been shown to sustain distension by a factor of up to 200% (Morkved, 2007). Risk factors for obstetric trauma The update of the RCOG guidelines for the management of obstetric injuries has listed a number of risk
5 Page 5 of 9 factors that may contribute to increased risk of obstetric anal sphincter injuries. These are (RCOG, 2007): Birthweight over 4kg; Induction of labour; Epidural analgesia; Persistent occipto-posterior position (baby positioned back to back with mother commonly called posterior presentation); Episiotomy; Second stage of labour longer than one hour; Shoulder dystocia (delivery that requires additional obstetric manoeuvres to release the baby s shoulders); Nulliparity (primigravida); Forceps delivery. The predominant recurring risk factors in the literature are: Operative delivery (forceps); Nulliparity (primigravida); Birthweight over 4kg; Prolonged second stage of labour. The length of the active second stage of labour has in the past been considered prolonged if it is greater than one hour. However, in a recent paper, Scheer et al (2008) suggested that an active second stage greater than 50 minutes is significant for obstetric and sphincter injuries (OASI). They also suggest that there is a strong relationship between OASI and symptoms of urinary incontinence. Other risk factors highlighted in various studies but not thought to be as significant as those in the RCOG guideline are: Ventouse delivery; Women who have gone past expected date of delivery; Women who do not cooperate with instructions during delivery, in particular pushing when the head is crowning; Ethnic background some minorities appear to be more predisposed to pelvic floor muscle dysfunction (Christianson et al, 2003; Gupta et al, 2003; Carroli and Belizan, 2000; Thacker and Banta, 1983). The RCOG (2007) guideline acknowledges many of these risks, such as nulliparity, posterior presentation and induction of labour, cannot be avoided but suggests more research is needed to cut or prevent third-degree tears in at-risk patients.
6 Page 6 of 9 Williams et al (2005) also acknowledges that some risks cannot be avoided and that, in many cases, OASI, is neither predictable nor preventable. They conclude that clinical effort would be best placed in using evidence-based practice to optimise the outcome after repair. The relationship between birth position, perineal trauma and women s experience is thought to be significant. Although somewhat tentative, there is evidence that certain birth positions (lateral) are better than others (squatting) in reducing the risks of trauma to the perineum (Hastings-Tolsma et al, 2007; Shorten et al, 2002). These papers suggest that women should be allowed to make decisions about delivery in partnership with midwives and obstetricians who are equipped with the knowledge of risks and benefits of options and skills to implement women s choices for birth. Dispelling old (mid)wives tales? Midwives sometimes tell women that strong pelvic floor muscles can cause problems at delivery. The evidence is that having healthy, strong pelvic floor muscles does not lengthen the second stage of labour (Agur et al, 2008; Morkved, 2007). It has been suggested that training the pelvic floor muscles in pregnancy can facilitate labour (Salvesen and Morkved, 2004), although this was not supported in the study by Agur et al (2008). Stop mid-stream test There is confusion about whether or not to advise women to stop their urine midstream. While this may be considered a good method of identifying the correct action of the pelvic floor muscles, it is often confused with being an exercise for them. Concerns have also been expressed that this interruption of the flow of urine could irritate the bladder (Bump et al, 1991). It can also cause incomplete emptying of the bladder which increases the risk of urinary tract infection. Women should be taught to identify their pelvic floor muscles by palpating the skin over the perineum and feel for a movement lifting upwards and forwards towards the bladder when the muscles contract. Alternatively, they can insert a finger or thumb into the vaginal opening and feel the contraction of the muscles as they move upwards and forwards towards the bladder. Conclusion With a greater understanding of the function of the pelvic floor muscles and risk factors for trauma and damage as a result of pregnancy and birth, healthcare professionals will be better able to meet the needs of women in the childbearing year. Recommendations for practice Pelvic floor muscles and their associated structures are at risk of becoming weakened during pregnancy or of experiencing trauma and damage during delivery This problem is identified by the NICE (2006) guidanceurinary Incontinence: the Management of Urinary Incontinence in Women. It states: Pelvic floor muscle training should be offered to women in their first pregnancy as a preventive strategy for urinary incontinence. There is evidence that pelvic floor muscle training used during a first pregnancy reduces the likelihood of postnatal urinary incontinence (NICE, 2006) Incontinence is still a taboo subject and reluctance by both pregnant women and healthcare professionals to discuss it can make it difficult to fulfil the NICE recommendations PromoCon, a charity led by the Disabled Living Centre that focuses on the promotion of continence and management of incontinence, has developed a risk-assessment tool that can be
7 Page 7 of 9 used to help midwives raise the issue of incontinence and pelvic floor muscle health at the first booking appointment (Pearl and Herbert, 2008) This tool can also be used following delivery to assess the risk of pelvic floor muscle dysfunction by considering antenatal risk factors in addition to factors occurring as a result of the delivery References Agur, W. et al (2008)Does antenatal pelvic floor muscle training affect the outcome of labour? A randomised controlled trial.international Urogynecology Journal and Pelvic Floor Dysfunction;19: 1, Allen, R.E. et al (1990)Pelvic floor damage and childbirth: a neurophysiological study.british Journal of Obstetrics and Gynaecology;97: 9, Bump, R.C. et al (1991)Assessment of Kegel pelvic muscle exercise performance after brief verbal instruction.american Journal of Obstetrics and Gynecology;165: 2, Carroli, G., Belizan, J. (2000)Episiotomy for vaginal birth.cochrane Database Systematic Reviews (2):CD Christianson, L.M. et al (2003)Risk factors for perineal injury during delivery.american Journal of Obstetrics and Gynecology;189: 1, Chiarelli, P., Campbell, E. (1997)Incontinence during pregnancy. Prevalence and opportunities for continence promotion.australian and New Zealand Journal of Obstetrics and Gynaecology;37: 1, Dietz, H.P., Lanzarone, V. (2005)Levator trauma after vaginal delivery.obstetrics and Gynecology;106: 4, Groutz, A. et al (2004)Caesarean section: does it really prevent the development of postpartum stress urinary incontinence? A prospective study of 363 women one year after their first delivery.neurourology and Urodynamics;23: 1, 2 6. Gupta, N. et al (2003)The incidence, risk factors and obstetric outcome in primigravid women sustaining anal sphincter tears.acta Obstetrica et Gynecologica Scandinavia;82: 8, Hastings-Tolsma, M. et al (2007)Getting through the birth in one piece: protecting the perineum. MCN.American Journal of Maternal and Child Nursing.32: 3, Kapoor, D.S., Freeman, R.M. (2008)Pregnancy, childbirth and urinary incontinence. In: Haslam, J., Laycock, J. (eds)therapeutic Management of Incontinence and Pelvic Pain.London: Springer-Verlag. Keane, D.P. et al (1997)Analysis of collagen status in premenopausal nulliparous women with genuine stress incontinence.british Journal of Obstetrics and Gynaecology;104: 9, Lal, M. et al (2003)Does Caesarean delivery prevent anal incontinence?obstetrics and Gynecology;101: MacLennan, A.H. et al (2000)The prevalence of pelvic floor disorders and their relationship to gender, age, parity and mode of delivery.british Journal of Obstetrics and Gynaecology;107: Messelink, B. et al (2005)Standardization of terminology of pelvic floor muscle function and dysfunction: report from the pelvic floor clinical assessment group of the International Continence
8 Page 8 of 9 Society.Neurourology and Urodynamics;24: 4, Morkved, S. (2007)Evidence for pelvic floor physical therapy for urinary incontinence during pregnancy and after childbirth.in: Bo, K. et alevidence-based Physical Therapy for the Pelvic Floor. Bridging Science and Clinical Practice.Philadelphia, PA: Elsevier. Morkved, S. et al (2003)Pelvic floor muscle training during pregnancy to prevent urinary incontinence. A single-blind randomised controlled trial.obstetrics and Gynecology;101: NICE (2006)Urinary Incontinence: the Management of Urinary Incontinence in Women.London: NICE. Pearl, G., Herbert, J.H. (2008)Assessing pelvic floor during childbearing year.nursing Times;104: 18, Ramussen, K.L. et al (1997)Obesity as a predictor of post- partum urinary symptoms.acta Obstetrica et Gynecologica Scandinavia;76: 4, Royal College of Obstetricians and Gynaecologists (2007)Guideline No 29. Management of Third and Fourth-Degree Perineal Tears Following Vaginal Delivery.London: RCOG. Scheer, I. et al (2008)Urinary incontinence after obstetric anal sphincter injuries (OASI) is there a relationship?internationalurogynecology Journal and Pelvic Floor Dysfunction;10: 2, Shorten, A. et al (2002)Birth position, accoucher, and perineal outcomes: informing women about choices for vaginal birth.birth:29; 1, Snooks, S.J. et al (1990)Effect of vaginal delivery on the pelvic floor: a 5-year follow-up.british Journal of Surgery;77: 12, Snooks, S.J. et al (1984)Injury to innervation of pelvic floor sphincter musculature in childbirth.lancet;2: 8402, Sultan, A.H., Stanton, S.L. (1996)Preserving the pelvic floor and perineum during childbirth elective Caesarean section?british Journal of Obstetrics and Gynaecology;103: Sultan, A.H. et al (1994)Pudendal nerve damage during labour: a prospective study before and after childbirth.british Journal of Obstetrics and Gynaecology;101: 1, Thacker, S.B., Banta, H.D. (1983)Benefits and risks of episiotomy: an interpretative review of the English language literature, Obstetrics and Gynaecology Survey;38: 6, van Brummen, H.J. et al (2007)The effect of vaginal and Caesarean delivery on lower urinary tract symptoms: what makes the difference?international Urogynecology Journal and Pelvic Floor Dysfunction;18: 2, Wasserberg, N. et al (2008)Faecal incontinence among morbid obese women seeking for weight loss surgery: an underappreciated association with adverse impact on quality of life.international Journal of Colorectal Disease;23: 5, Wall, L. (1999)Birth trauma and the pelvic floor: lessons from the developing world.journal of Women s Health;8: 2, Williams, A. et al (2005)Risk scoring system for prediction of obstetric anal sphincter injury.british Journal of Obstetrics and Gynaecology;112: Wilson, P.D. et al (1996)Obstetric practice and the prevalence of urinary incontinence three months after delivery.british Journal of Obstetrics and Gynecology;103: 2,
9 Page 9 of 9 Print Need to keep ahead of news, guidelines and clinical research, but don't have time to trawl the internet and read all the journals? Let Nursing Times do the work for you, with our comprehensive round-up, delivered direct to your inbox every day. Click here to find out more
Pregnancy related pelvic floor dysfunction- suggested teaching presentation for Midwives
 Pregnancy related pelvic floor dysfunction- suggested teaching presentation for Midwives 1 Aims of this self assessment competency To equip Midwives with the knowledge and skills to teach pelvic floor
Pregnancy related pelvic floor dysfunction- suggested teaching presentation for Midwives 1 Aims of this self assessment competency To equip Midwives with the knowledge and skills to teach pelvic floor
Obstetric Anal Sphincter Injury- A guideline. Mr David Sim Ms Patricia McStay. Dr Martina Hogan Dept./Division Only: YES-IMWH Directorate Only: NO
 CLINICAL GUIDELINES ID TAG Title: Obstetric Anal Sphincter Injury- A guideline Author: Dr Foteini Verani Designation: Specialist Doctor Speciality / Division: Obstetrics-IMWH Directorate: Acute Services
CLINICAL GUIDELINES ID TAG Title: Obstetric Anal Sphincter Injury- A guideline Author: Dr Foteini Verani Designation: Specialist Doctor Speciality / Division: Obstetrics-IMWH Directorate: Acute Services
Appendix B Protocol for management of obstetric anal sphincter injury THE MANAGEMENT OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS
 Appendix B Protocol for management of obstetric anal sphincter injury Document Type: THE MANAGEMENT OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS PURPOSE & SCOPE To provide a guideline that will assist in
Appendix B Protocol for management of obstetric anal sphincter injury Document Type: THE MANAGEMENT OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS PURPOSE & SCOPE To provide a guideline that will assist in
Postpartum Complications
 ACOG Postpartum Toolkit Postpartum Complications Introduction The effects of pregnancy on many organ systems begin to resolve spontaneously after birth of the infant and delivery of the placenta. The timeline
ACOG Postpartum Toolkit Postpartum Complications Introduction The effects of pregnancy on many organ systems begin to resolve spontaneously after birth of the infant and delivery of the placenta. The timeline
The Perineal Clinic: - the management of women following OASI
 The Perineal Clinic: - the management of women following OASI Miss Gillian Fowler Consultant Urogynaecologist MBChB, MD, MRCOG Liverpool Women s Hospital. Margie Polden University Memorial of Liverpool
The Perineal Clinic: - the management of women following OASI Miss Gillian Fowler Consultant Urogynaecologist MBChB, MD, MRCOG Liverpool Women s Hospital. Margie Polden University Memorial of Liverpool
Moneli Golara Consultant Obstetrician and Gynaecologist Royal Free NHS Trust Barnet Hospital
 Moneli Golara Consultant Obstetrician and Gynaecologist Royal Free NHS Trust Barnet Hospital Pelvic Organ Prolapse (POP)- herniation of pelvic organs into vaginal walls Common Huge impact on daily activities
Moneli Golara Consultant Obstetrician and Gynaecologist Royal Free NHS Trust Barnet Hospital Pelvic Organ Prolapse (POP)- herniation of pelvic organs into vaginal walls Common Huge impact on daily activities
Maternity Information Leaflet. Care of the Perineum (including Pelvic Floor Exercises) Version 2
 Maternity Information Leaflet Care of the Perineum (including Pelvic Floor Exercises) Version 2 Pelvic Floor Exercises The pelvic floor muscles are located between your legs, and run from your pubic bone
Maternity Information Leaflet Care of the Perineum (including Pelvic Floor Exercises) Version 2 Pelvic Floor Exercises The pelvic floor muscles are located between your legs, and run from your pubic bone
Childbirth Trauma & Its Complications 23/ Mr Stergios K. Doumouchtsis
 Mr Stergios K. Doumouchtsis Consultant Obstetrician Gynaecologist & Urogynaecologist Childbirth Trauma & Its Complications Over eighty per cent of women sustain some degree of perineal trauma during childbirth.
Mr Stergios K. Doumouchtsis Consultant Obstetrician Gynaecologist & Urogynaecologist Childbirth Trauma & Its Complications Over eighty per cent of women sustain some degree of perineal trauma during childbirth.
Aetiology 1998 Bump & Norton Theoretical model
 Kate Lough MSc MCSP Handout IUGA Nice 2015 Physiotherapy and the Provision of Pelvic Floor Muscle Training and Lifestyle Intervention in the Conservative Management of Pelvic Organ Prolapse an evidence
Kate Lough MSc MCSP Handout IUGA Nice 2015 Physiotherapy and the Provision of Pelvic Floor Muscle Training and Lifestyle Intervention in the Conservative Management of Pelvic Organ Prolapse an evidence
EXPECTING A BABY? SOME PREGNANT WOMEN CAN HAVE BLADDER AND BOWEL CONTROL PROBLEMS. YOU CAN GET HELP. HOW DO I KNOW IF I HAVE A PROBLEM?
 11 BLADDER AND BOWEL CONTROL PROBLEMS. When you are pregnant, you get a lot of advice from many people. One topic few people think about is bladder and bowel control problems during pregnancy and after
11 BLADDER AND BOWEL CONTROL PROBLEMS. When you are pregnant, you get a lot of advice from many people. One topic few people think about is bladder and bowel control problems during pregnancy and after
Third & Fourth Degree Tears guideline (GL926)
 Third & Fourth Degree Tears guideline (GL926) Approval Approval Group Job Title, Chair of Committee Date Maternity & Children s Services Clinical Governance Committee Chair, Maternity Clinical Governance
Third & Fourth Degree Tears guideline (GL926) Approval Approval Group Job Title, Chair of Committee Date Maternity & Children s Services Clinical Governance Committee Chair, Maternity Clinical Governance
Dr Anne Sneddon Director of Obstetrics and Gynaecology Lecturer, ANU Medical School The Canberra Hospital
 Dr Anne Sneddon Director of Obstetrics and Gynaecology Lecturer, ANU Medical School The Canberra Hospital Capital city of Australia Population 350,000 but surrounding region of 500,000 Seat of government
Dr Anne Sneddon Director of Obstetrics and Gynaecology Lecturer, ANU Medical School The Canberra Hospital Capital city of Australia Population 350,000 but surrounding region of 500,000 Seat of government
Pelvic organ prolapse. Information for patients Continence Service
 Pelvic organ prolapse Information for patients Continence Service What is a pelvic organ prolapse? A pelvic organ prolapse occurs when the uterus (womb), vagina, bladder or bowel slips out of place, resulting
Pelvic organ prolapse Information for patients Continence Service What is a pelvic organ prolapse? A pelvic organ prolapse occurs when the uterus (womb), vagina, bladder or bowel slips out of place, resulting
THE PELVIC FLOOR, EPISIOTOMY AND PERINEAL REPAIR AND VAGINAL/RECTAL MEDICATIONS
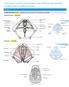 THE PELVIC FLOOR, EPISIOTOMY AND PERINEAL REPAIR AND VAGINAL/RECTAL MEDICATIONS MID2010 LEARNING OBJECTIVE 1 - REVIEW THE ANATOMY OF THE PELVIC FLOOR Superficial layers cavernosus Deep layer Coccygeus
THE PELVIC FLOOR, EPISIOTOMY AND PERINEAL REPAIR AND VAGINAL/RECTAL MEDICATIONS MID2010 LEARNING OBJECTIVE 1 - REVIEW THE ANATOMY OF THE PELVIC FLOOR Superficial layers cavernosus Deep layer Coccygeus
Anal Sphincter Injuries: Acute Management
 Anal Sphincter Injuries: Acute Management Dr Stephen Jeffery Urogynaecology Consultant Department of Obstetrics & Gynaecology Groote Schuur Hospital Colorectal Surgeons Gynaecologists Gynaecologists Colorectal
Anal Sphincter Injuries: Acute Management Dr Stephen Jeffery Urogynaecology Consultant Department of Obstetrics & Gynaecology Groote Schuur Hospital Colorectal Surgeons Gynaecologists Gynaecologists Colorectal
Obstetric Anal Sphincter Injury. An update on best practices. Objectives
 Obstetric Anal Sphincter Injury An update on best practices Erin Crosby MD Assistant Professor Department of OB/Gyn Division of FPMRS 1 Objectives Describe the anatomy of the anal sphincter complex Discuss
Obstetric Anal Sphincter Injury An update on best practices Erin Crosby MD Assistant Professor Department of OB/Gyn Division of FPMRS 1 Objectives Describe the anatomy of the anal sphincter complex Discuss
Urinary incontinence after obstetric anal sphincter injuries (OASIS) is there a relationship?
 DOI 10.1007/s00192-007-0431-8 ORIGINAL ARTICLE Urinary incontinence after obstetric anal sphincter injuries (OASIS) is there a relationship? Inka Scheer & Vasanth Andrews & Ranee Thakar & Abdul H. Sultan
DOI 10.1007/s00192-007-0431-8 ORIGINAL ARTICLE Urinary incontinence after obstetric anal sphincter injuries (OASIS) is there a relationship? Inka Scheer & Vasanth Andrews & Ranee Thakar & Abdul H. Sultan
Ben Herbert Alex Wojtowicz
 Ben Herbert Alex Wojtowicz 54 year old female presenting with: Dragging sensation Urinary incontinence Some faecal incontinence HPC Since May 14 had noticed a mass protruding from the vagina when going
Ben Herbert Alex Wojtowicz 54 year old female presenting with: Dragging sensation Urinary incontinence Some faecal incontinence HPC Since May 14 had noticed a mass protruding from the vagina when going
Northwest Rehabilitation Associates, Inc.
 Pelvic Health Patient Intake Form Name: Date: Please answer the following questions as honestly and thoroughly as you can. Your responses will help us better understand your condition and provide the best
Pelvic Health Patient Intake Form Name: Date: Please answer the following questions as honestly and thoroughly as you can. Your responses will help us better understand your condition and provide the best
Perineal Tears. Obstetrics & Gynaecology Women & Children s Group
 Perineal Tears Obstetrics & Gynaecology Women & Children s Group This leaflet has been designed to give you important information about your condition / procedure, and to answer some common queries that
Perineal Tears Obstetrics & Gynaecology Women & Children s Group This leaflet has been designed to give you important information about your condition / procedure, and to answer some common queries that
Care of your Perineum following 3 rd and 4 th degree tears
 Maternity Services Care of your Perineum following 3 rd and 4 th degree tears Introduction This leaflet aims to give you information about the repair and aftercare of the third or fourth degree tear you
Maternity Services Care of your Perineum following 3 rd and 4 th degree tears Introduction This leaflet aims to give you information about the repair and aftercare of the third or fourth degree tear you
Repair of vaginal tears and episiotomy guidelines
 Repair of vaginal tears and episiotomy guidelines Purpose These guidelines assist practitioners in the repair of vaginal and perineal tears including the reasons for, and the techniques of performing an
Repair of vaginal tears and episiotomy guidelines Purpose These guidelines assist practitioners in the repair of vaginal and perineal tears including the reasons for, and the techniques of performing an
Pelvic floor muscle exercises (long)
 Pelvic floor muscle exercises (long) This leaflet aims to give an overview of pelvic floor muscles, their function, how they can be exercised and why this is so important. What are pelvic floor muscles
Pelvic floor muscle exercises (long) This leaflet aims to give an overview of pelvic floor muscles, their function, how they can be exercised and why this is so important. What are pelvic floor muscles
Pelvic organ prolapse
 Page 1 of 11 Pelvic organ prolapse Introduction The aim of this leaflet is to give you information about a pelvic organ prolapse, its causes and available treatments but does not replace advice given by
Page 1 of 11 Pelvic organ prolapse Introduction The aim of this leaflet is to give you information about a pelvic organ prolapse, its causes and available treatments but does not replace advice given by
Treating your prolapse
 Treating your prolapse This leaflet explains what a prolapse is, and how it can be treated and managed. If you have any questions or concerns, please speak to a doctor or nurse caring for you. What is
Treating your prolapse This leaflet explains what a prolapse is, and how it can be treated and managed. If you have any questions or concerns, please speak to a doctor or nurse caring for you. What is
John Laughlin 4 th year Cardiff University Medical Student
 John Laughlin 4 th year Cardiff University Medical Student Prolapse/incontinence You need to know: Pelvic floor anatomy in relation to uterovaginal support and continence The classification of uterovaginal
John Laughlin 4 th year Cardiff University Medical Student Prolapse/incontinence You need to know: Pelvic floor anatomy in relation to uterovaginal support and continence The classification of uterovaginal
Pelvic Floor Ultrasound Imaging. Prof HP Dietz (Sydney) A/Prof KL Shek (Sydney) Dr R Guzman Rojas (Santiago de Chile) Dr Kamil Svabik (Prague)
 Pelvic Floor Ultrasound Imaging Workshop IUGA 2015 Nice Faculty: Prof HP Dietz (Sydney) A/Prof KL Shek (Sydney) Dr R Guzman Rojas (Santiago de Chile) Dr Kamil Svabik (Prague) The use of translabial ultrasound
Pelvic Floor Ultrasound Imaging Workshop IUGA 2015 Nice Faculty: Prof HP Dietz (Sydney) A/Prof KL Shek (Sydney) Dr R Guzman Rojas (Santiago de Chile) Dr Kamil Svabik (Prague) The use of translabial ultrasound
CHERRY BAKER AND TRACEY GJERTSEN BSC MCSP HCPC INTRODUCTION TO DIAMOND TRAINING REHAB AND PERFORMANCE FOR PELVIC POWER
 CHERRY BAKER AND TRACEY GJERTSEN BSC MCSP HCPC INTRODUCTION TO DIAMOND TRAINING REHAB AND PERFORMANCE FOR PELVIC POWER What is it? Where is it? Breathing Graded relaxation Incontinence Stress Incontinence
CHERRY BAKER AND TRACEY GJERTSEN BSC MCSP HCPC INTRODUCTION TO DIAMOND TRAINING REHAB AND PERFORMANCE FOR PELVIC POWER What is it? Where is it? Breathing Graded relaxation Incontinence Stress Incontinence
The Pelvic Floor Muscles - a Guide for Women
 The Pelvic Floor Muscles - a Guide for Women This booklet is supported by WWWWW Wellbeing of Women Registered Charity No. 239281 www.wellbeingofwomen.org.uk Introduction Up to a third of all women experience
The Pelvic Floor Muscles - a Guide for Women This booklet is supported by WWWWW Wellbeing of Women Registered Charity No. 239281 www.wellbeingofwomen.org.uk Introduction Up to a third of all women experience
Over Active Pelvic Floor
 Over Active Pelvic Floor Maeve Whelan SMISCP Specialist Chartered Physiotherapist, Women s Health Background The concept of an overactive pelvic floor (OAPF) is relatively new in pelvic floor rehabilitation.
Over Active Pelvic Floor Maeve Whelan SMISCP Specialist Chartered Physiotherapist, Women s Health Background The concept of an overactive pelvic floor (OAPF) is relatively new in pelvic floor rehabilitation.
Doctor s assessment and evaluation of the pelvic floor in antenatal and postpartum women: routine or???
 Doctor s assessment and evaluation of the pelvic floor in antenatal and postpartum women: routine or??? Dr Barry O Reilly Head of department of Urogynaecology Cork University Maternity Hospital Ireland
Doctor s assessment and evaluation of the pelvic floor in antenatal and postpartum women: routine or??? Dr Barry O Reilly Head of department of Urogynaecology Cork University Maternity Hospital Ireland
Gynecology Dr. Sallama Lecture 3 Genital Prolapse
 Gynecology Dr. Sallama Lecture 3 Genital Prolapse Genital(utero-vaginal )prolapse is extremely common, with an estimated 11% of women undergoing at least one operation for this condition. Definition: A
Gynecology Dr. Sallama Lecture 3 Genital Prolapse Genital(utero-vaginal )prolapse is extremely common, with an estimated 11% of women undergoing at least one operation for this condition. Definition: A
Review Article Pelvic Floor Dysfunction, Body Excreta Incontinence and Continence
 Cronicon OPEN ACCESS GYNAECOLOGY Review Article Pelvic Floor Dysfunction, Body Excreta Incontinence and Continence Abdel Karim M El Hemaly 1 * and Laila ASE Mousa 1 1 Professor of Obstetrics and gynaecology,
Cronicon OPEN ACCESS GYNAECOLOGY Review Article Pelvic Floor Dysfunction, Body Excreta Incontinence and Continence Abdel Karim M El Hemaly 1 * and Laila ASE Mousa 1 1 Professor of Obstetrics and gynaecology,
Clinical Guideline for: The Management of Perineal Trauma following Childbirth
 For Use in: By: For: Division responsible for document: Key words: Name of document author: Job title of document author: Name of document author s Line Manager: Job title of author s Line Manager: Supported
For Use in: By: For: Division responsible for document: Key words: Name of document author: Job title of document author: Name of document author s Line Manager: Job title of author s Line Manager: Supported
Pelvic Support Problems
 AP012, April 2010 ACOG publications are protected by copyright and all rights are reserved. ACOG publications may not be reproduced in any form or by any means without written permission from the copyright
AP012, April 2010 ACOG publications are protected by copyright and all rights are reserved. ACOG publications may not be reproduced in any form or by any means without written permission from the copyright
Prolapse and Urogynae Incontinence. Lucy Tiffin and Hannah Wheldon-Holmes
 Prolapse and Urogynae Incontinence Lucy Tiffin and Hannah Wheldon-Holmes 66 year old woman with incontinence PC: 7 year Hx of urgency, frequency, nocturia (incl. incontinence at night), and stress incontinence
Prolapse and Urogynae Incontinence Lucy Tiffin and Hannah Wheldon-Holmes 66 year old woman with incontinence PC: 7 year Hx of urgency, frequency, nocturia (incl. incontinence at night), and stress incontinence
Faecal incontinence after childbirth
 Britisb Journal of Obstetrics and Gynaecology January 1997, Vol. 104, pp. 4650 Faecal incontinence after childbirth *Christine MacArthur Reader (Maternal and Child Epidemiology), *Debra E. Bick Research
Britisb Journal of Obstetrics and Gynaecology January 1997, Vol. 104, pp. 4650 Faecal incontinence after childbirth *Christine MacArthur Reader (Maternal and Child Epidemiology), *Debra E. Bick Research
OBSTETRICALLY-CAUSED ANAL SPHINCTER INJURY PREDICTION, MANAGEMENT, PREVENTION
 OBSTETRICALLY-CAUSED ANAL SPHINCTER INJURY PREDICTION, MANAGEMENT, PREVENTION COLM O HERLIHY, MD Professor and Chair University College Dublin Department of Obstetrics and Gynaecology National Maternity
OBSTETRICALLY-CAUSED ANAL SPHINCTER INJURY PREDICTION, MANAGEMENT, PREVENTION COLM O HERLIHY, MD Professor and Chair University College Dublin Department of Obstetrics and Gynaecology National Maternity
Patient Advice for Third & Fourth Degree Tears
 Patient Advice for Third & Fourth Degree Tears Please read this leaflet carefully. It is important that you take note of any instructions or advice given. If you have any questions or problems that are
Patient Advice for Third & Fourth Degree Tears Please read this leaflet carefully. It is important that you take note of any instructions or advice given. If you have any questions or problems that are
Focus on Post-Partum Incontinence
 Focus on Post-Partum Incontinence A one day intensive course for Nurses, Midwives and Physiotherapists Old Main Building Law Faculty Stellenbosch 24 January 2013 9h00-17h00 Sponsored by the International
Focus on Post-Partum Incontinence A one day intensive course for Nurses, Midwives and Physiotherapists Old Main Building Law Faculty Stellenbosch 24 January 2013 9h00-17h00 Sponsored by the International
INCONTINENCE. Continence and Pelvic Floor Rehabilitation TYPES OF INCONTINENCE STRESS INCONTINENCE STRESS INCONTINENCE STRESS INCONTINENCE 11/08/2015
 INCONTINENCE Continence and Pelvic Floor Rehabilitation Dr Irmina Nahon PhD Pelvic Floor Physiotherapist www.nahonpfed.com.au Defined as the accidental and inappropriate passage of urine or faeces (ICI
INCONTINENCE Continence and Pelvic Floor Rehabilitation Dr Irmina Nahon PhD Pelvic Floor Physiotherapist www.nahonpfed.com.au Defined as the accidental and inappropriate passage of urine or faeces (ICI
AN INTERNATIONAL CONTINENCE SOCIETY (ICS) / INTERNATIONAL UROGYNAECOLOGICAL ASSOCIATION (IUGA) JOINT REPORT ON THE TERMINOLOGY FOR CHILDBIRTH TRAUMA
 AN INTERNATIONAL CONTINENCE SOCIETY (ICS) / INTERNATIONAL UROGYNAECOLOGICAL ASSOCIATION (IUGA) JOINT REPORT ON THE TERMINOLOGY FOR CHILDBIRTH TRAUMA NEED FOR A WORKING GROUP ON CHILDBIRTH TRAUMA A: Background
AN INTERNATIONAL CONTINENCE SOCIETY (ICS) / INTERNATIONAL UROGYNAECOLOGICAL ASSOCIATION (IUGA) JOINT REPORT ON THE TERMINOLOGY FOR CHILDBIRTH TRAUMA NEED FOR A WORKING GROUP ON CHILDBIRTH TRAUMA A: Background
Post operative voiding dysfunction and the Value of Urodynamics. Dr Salwan Al-Salihi Urogynaecologist Obstetrician and Gynaecologist
 Post operative voiding dysfunction and the Value of Urodynamics Dr Salwan Al-Salihi Urogynaecologist Obstetrician and Gynaecologist Learning objectives: v Pathophysiology of post op voiding dysfunction.
Post operative voiding dysfunction and the Value of Urodynamics Dr Salwan Al-Salihi Urogynaecologist Obstetrician and Gynaecologist Learning objectives: v Pathophysiology of post op voiding dysfunction.
Royal College of Obstetricians and Gynaecologists
 Royal College of Obstetricians and Gynaecologists Consent Advice No. 9 June 2010 REPAIR OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS FOLLOWING CHILDBIRTH This is the first edition of this guidance. This
Royal College of Obstetricians and Gynaecologists Consent Advice No. 9 June 2010 REPAIR OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS FOLLOWING CHILDBIRTH This is the first edition of this guidance. This
LAPAROSCOPIC REPAIR OF PELVIC FLOOR
 LAPAROSCOPIC REPAIR OF PELVIC FLOOR Dr. R. K. Mishra Elements comprising the Pelvis Bones Ilium, ischium and pubis fusion Ligaments Muscles Obturator internis muscle Arcus tendineus levator ani or white
LAPAROSCOPIC REPAIR OF PELVIC FLOOR Dr. R. K. Mishra Elements comprising the Pelvis Bones Ilium, ischium and pubis fusion Ligaments Muscles Obturator internis muscle Arcus tendineus levator ani or white
Gynaecology Department Patient Information Leaflet
 Vaginal pessaries Gynaecology Department Patient Information Leaflet Introduction We have developed this information leaflet to answer some commonly-asked questions about what a vaginal pessary is, how
Vaginal pessaries Gynaecology Department Patient Information Leaflet Introduction We have developed this information leaflet to answer some commonly-asked questions about what a vaginal pessary is, how
Loss of Bladder Control
 BLADDER HEALTH Loss of Bladder Control Bladder Prolapse AUA FOUNDATION OFFICIAL FOUNDATION OF THE AMERICAN UROLOGICAL ASSOCIATION What Is the Bladder? The bladder is a hollow, balloon-like organ made mostly
BLADDER HEALTH Loss of Bladder Control Bladder Prolapse AUA FOUNDATION OFFICIAL FOUNDATION OF THE AMERICAN UROLOGICAL ASSOCIATION What Is the Bladder? The bladder is a hollow, balloon-like organ made mostly
for a review under the Accident Compensation Act
 FairWay Resolution Limited Tā te Hinengaro Tōkeke Whakatau Review numbers: Application by for a review under the Accident Compensation Act Held at Date of hearing 2 November 2016, adjourned part-heard;
FairWay Resolution Limited Tā te Hinengaro Tōkeke Whakatau Review numbers: Application by for a review under the Accident Compensation Act Held at Date of hearing 2 November 2016, adjourned part-heard;
Loss of Bladder Control
 BLADDER HEALTH: Bladder Prolapse Loss of Bladder Control Bladder Prolapse Don t Let Bladder Prolapse Keep You from Enjoying Life. What is the Bladder? The bladder is a hollow, balloon-like organ made mostly
BLADDER HEALTH: Bladder Prolapse Loss of Bladder Control Bladder Prolapse Don t Let Bladder Prolapse Keep You from Enjoying Life. What is the Bladder? The bladder is a hollow, balloon-like organ made mostly
17 th European congress of Physical Rehabilitation Medicine. 38th SIMFER congress
 17 th European congress of Physical Rehabilitation Medicine 38th SIMFER congress European Rehabilitation: Quality, Evidence, Efficacy and Effectiveness Venice, May 23 27 2010 THE PHYSIATRIST AND URO-GYNECOLOGICAL
17 th European congress of Physical Rehabilitation Medicine 38th SIMFER congress European Rehabilitation: Quality, Evidence, Efficacy and Effectiveness Venice, May 23 27 2010 THE PHYSIATRIST AND URO-GYNECOLOGICAL
Pelvic floor exercises for women. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Pelvic floor exercises for women An information guide Pelvic Floor Exercises for Women This leaflet will provide you with information about
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Pelvic floor exercises for women An information guide Pelvic Floor Exercises for Women This leaflet will provide you with information about
Diabetes in pregnancy
 Diabetes in pregnancy Patient information This leaflet provides information about gestational diabetes during pregnancy and delivery. Sometimes women who are not known to have diabetes develop it during
Diabetes in pregnancy Patient information This leaflet provides information about gestational diabetes during pregnancy and delivery. Sometimes women who are not known to have diabetes develop it during
Urogynaecology & Prolapse. Alexander Denning and Leifa Jennings
 + Urogynaecology & Prolapse Alexander Denning and Leifa Jennings + Contents What even is prolapse / urogynaecology? Pelvic floor anatomy Prolapse Urinary incontinence Prevention The end (woot) + Urogynaecology
+ Urogynaecology & Prolapse Alexander Denning and Leifa Jennings + Contents What even is prolapse / urogynaecology? Pelvic floor anatomy Prolapse Urinary incontinence Prevention The end (woot) + Urogynaecology
Female Symptom Monitor
 Female Symptom Monitor Occupation: Recreational Activities: Presenting problems: 1. 2. When did this start? Gynecological History: Please fill out each section that is relevant to your problem What age
Female Symptom Monitor Occupation: Recreational Activities: Presenting problems: 1. 2. When did this start? Gynecological History: Please fill out each section that is relevant to your problem What age
Physiotherapy advice following your vaginal birth
 Further sources of information NHS Choices: www.nhs.uk/conditions Our website: www.sfh-tr.nhs.uk INFORMATION FOR PATIENTS Patient Experience Team (PET) PET is available to help with any of your compliments,
Further sources of information NHS Choices: www.nhs.uk/conditions Our website: www.sfh-tr.nhs.uk INFORMATION FOR PATIENTS Patient Experience Team (PET) PET is available to help with any of your compliments,
Bladder care postpartum including bladder care for women with epidural analgesia (GL792)
 Bladder care postpartum including bladder care for women with epidural analgesia (GL792) Approval Approval Group Job Title, Chair of Committee Date Maternity & Children's Services Clinical Governance Committee
Bladder care postpartum including bladder care for women with epidural analgesia (GL792) Approval Approval Group Job Title, Chair of Committee Date Maternity & Children's Services Clinical Governance Committee
Physiotherapy advice following your third or fourth degree perineal tear
 Further sources of information NHS Choices: www.nhs.uk/conditions Our website: www.sfh-tr.nhs.uk INFORMATION FOR PATIENTS Patient Experience Team (PET) PET is available to help with any of your compliments,
Further sources of information NHS Choices: www.nhs.uk/conditions Our website: www.sfh-tr.nhs.uk INFORMATION FOR PATIENTS Patient Experience Team (PET) PET is available to help with any of your compliments,
Female Symptom Monitor
 Occupation Female Symptom Monitor Presenting problems When did this start? Please fill out each section that is relevant to your problem Gynecological History What age did your period start? Is your cycle
Occupation Female Symptom Monitor Presenting problems When did this start? Please fill out each section that is relevant to your problem Gynecological History What age did your period start? Is your cycle
5 DIAGNOSIS. History taking
 5 DIAGNOSIS All of the photographs in Chapter 4 were taken in theatre before operation. This chapter deals with how one can recognize the type of fistula by history taking and examination. (Note that the
5 DIAGNOSIS All of the photographs in Chapter 4 were taken in theatre before operation. This chapter deals with how one can recognize the type of fistula by history taking and examination. (Note that the
Toning your pelvic floor WELCOME
 Toning your pelvic floor WELCOME Introductions Amelia Samuels, Physiotherapist, Active Rehabilitation Physiotherapy Supporting the Continence Foundation of Australia Continence Foundation of Australia
Toning your pelvic floor WELCOME Introductions Amelia Samuels, Physiotherapist, Active Rehabilitation Physiotherapy Supporting the Continence Foundation of Australia Continence Foundation of Australia
Taking care of your perineum before, during and after birth
 Taking care of your perineum before, during and after birth A Parent Information Leaflet Where is is my my perineum and and what what happens happens during childbirth? during childbirth? Your perineum
Taking care of your perineum before, during and after birth A Parent Information Leaflet Where is is my my perineum and and what what happens happens during childbirth? during childbirth? Your perineum
Prolapse & Urogynaecology. Hester Mannion and Fabi Sica
 Prolapse & Urogynaecology Hester Mannion and Fabi Sica Take home messages Prolapse and associated incontinence is very common It has a devastating effect on the QoL of the patient and their partner Strategies
Prolapse & Urogynaecology Hester Mannion and Fabi Sica Take home messages Prolapse and associated incontinence is very common It has a devastating effect on the QoL of the patient and their partner Strategies
Risk factors and management of obstetric perineal injury
 Risk factors and management of obstetric perineal injury Ruwan J Fernando Abstract Perineal injury sustained during childbirth is a major aetiological factor in the development of perineal pain, sexual
Risk factors and management of obstetric perineal injury Ruwan J Fernando Abstract Perineal injury sustained during childbirth is a major aetiological factor in the development of perineal pain, sexual
Voiding Diary. Begin recording upon rising in the morning and continue for a full 24 hours.
 Urodvnamics Your physician has scheduled you for a test called URODYNAMICS. This test is a series of different measurements of bladder function and can be used to determine the cause of a variety of bladder
Urodvnamics Your physician has scheduled you for a test called URODYNAMICS. This test is a series of different measurements of bladder function and can be used to determine the cause of a variety of bladder
INTRAPARTUM AND POSTNATAL BLADDER CARE
 INTRAPARTUM AND POSTNATAL BLADDER CARE BACKGROUND Urinary retention is uncommon but carries significant morbidity and the risk is increased by a number of factors including epidural analgesia (Teo, et
INTRAPARTUM AND POSTNATAL BLADDER CARE BACKGROUND Urinary retention is uncommon but carries significant morbidity and the risk is increased by a number of factors including epidural analgesia (Teo, et
Tension-free Vaginal Tape (TVT)
 Page 1 of 7 Tension-free Vaginal Tape (TVT) Introduction This leaflet will provide you with basic information about the Tension--free Vaginal Tape (TVT) procedure. What is a TVT? TVT is an operation to
Page 1 of 7 Tension-free Vaginal Tape (TVT) Introduction This leaflet will provide you with basic information about the Tension--free Vaginal Tape (TVT) procedure. What is a TVT? TVT is an operation to
Pelvic Prolapse. A Patient Guide to Pelvic Floor Reconstruction
 Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
The diagnostic strength of the 24-h pad test for self-reported symptoms of urinary incontinence in pregnancy and after childbirth
 Int Urogynecol J (8) 19:525 53 DOI.7/s192-7-472-z ORIGINAL ARTICLE The diagnostic strength of the 24-h pad test for self-reported symptoms of urinary incontinence in pregnancy and after childbirth Jacobus
Int Urogynecol J (8) 19:525 53 DOI.7/s192-7-472-z ORIGINAL ARTICLE The diagnostic strength of the 24-h pad test for self-reported symptoms of urinary incontinence in pregnancy and after childbirth Jacobus
Pelvic floor exercises for women. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Pelvic floor exercises for women An information guide Pelvic floor exercises for women This leaflet will provide you with information about
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Pelvic floor exercises for women An information guide Pelvic floor exercises for women This leaflet will provide you with information about
Pelvic Floor Exercises
 Pelvic Floor Exercises Physiotherapy Department Patient information leaflet Up to a third of women experience a problem with their pelvic floor muscles at some point during their life. The muscles can
Pelvic Floor Exercises Physiotherapy Department Patient information leaflet Up to a third of women experience a problem with their pelvic floor muscles at some point during their life. The muscles can
Pregnancy and delivery: a urodynamic viewpoint
 British Journal of Obstetrics and Gynaecology November 2000, Vol107, pp. 1354-1359 Pregnancy and delivery: a urodynamic viewpoint *C. Chaliha Research Fellow (Urogynaecology),** J. M. Bland Professor (Medical
British Journal of Obstetrics and Gynaecology November 2000, Vol107, pp. 1354-1359 Pregnancy and delivery: a urodynamic viewpoint *C. Chaliha Research Fellow (Urogynaecology),** J. M. Bland Professor (Medical
The urethral support system during pregnancy and after childbirth Wijma, Jacobus
 University of Groningen The urethral support system during pregnancy and after childbirth Wijma, Jacobus IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish
University of Groningen The urethral support system during pregnancy and after childbirth Wijma, Jacobus IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish
The Management of Female Urinary Incontinence. Part 1: Aetiology and Investigations
 The Management of Female Urinary Incontinence Part 1: Aetiology and Investigations Dr Oseka Onuma Gynaecologist and Pelvic Reconstructive Surgeon 4 Robe Terrace Medindie SA 5081 Urinary incontinence has
The Management of Female Urinary Incontinence Part 1: Aetiology and Investigations Dr Oseka Onuma Gynaecologist and Pelvic Reconstructive Surgeon 4 Robe Terrace Medindie SA 5081 Urinary incontinence has
Look Good Feel Good. after pregnancy. Physiotherapy advice and exercises for new mums
 Look Good Feel Good after pregnancy Physiotherapy advice and exercises for new mums How to exercise after pregnancy with physiotherapy Bowel Tail Bone Uterus Bladder Pubic Bone Pelvic Floor Muscles Urethra
Look Good Feel Good after pregnancy Physiotherapy advice and exercises for new mums How to exercise after pregnancy with physiotherapy Bowel Tail Bone Uterus Bladder Pubic Bone Pelvic Floor Muscles Urethra
Consultation Guide: Specialised gynaecology surgery and complex urogynaecology conditions service specifications
 Consultation Guide: Specialised gynaecology surgery and complex urogynaecology conditions service specifications Consultation guide: Specialised gynaecology surgery and complex urogynaecology conditions
Consultation Guide: Specialised gynaecology surgery and complex urogynaecology conditions service specifications Consultation guide: Specialised gynaecology surgery and complex urogynaecology conditions
Urogynaecology. Colm McAlinden
 Urogynaecology Colm McAlinden Definitions Urinary incontinence compliant of any involuntary leakage of urine with many different causes Two main types: Stress Urge Definitions Nocturia: More than a single
Urogynaecology Colm McAlinden Definitions Urinary incontinence compliant of any involuntary leakage of urine with many different causes Two main types: Stress Urge Definitions Nocturia: More than a single
PROTOCOL FOR BLADDER CARE MANAGEMENT DURING INTRAPARTUM AND POSTNATAL PERIOD
 PROTOCOL FOR BLADDER CARE MANAGEMENT DURING INTRAPARTUM AND POSTNATAL PERIOD Specialty: Obstetrics Date Approved: Revised September 2015 Approved by: Labour Ward Forum Date for Review: September 2018 Overview
PROTOCOL FOR BLADDER CARE MANAGEMENT DURING INTRAPARTUM AND POSTNATAL PERIOD Specialty: Obstetrics Date Approved: Revised September 2015 Approved by: Labour Ward Forum Date for Review: September 2018 Overview
By:Dr:ISHRAQ MOHAMMED
 By:Dr:ISHRAQ MOHAMMED Protrusion of an organ or structure beyond its normal confines. Prolapses are classified according to their location and the organs contained within them. 1-Anterior vaginal wall
By:Dr:ISHRAQ MOHAMMED Protrusion of an organ or structure beyond its normal confines. Prolapses are classified according to their location and the organs contained within them. 1-Anterior vaginal wall
Female Urinary Incontinence: What It Is and What You Can Do About It
 Female Urinary Incontinence: What It Is and What You Can Do About It Urogynecology Patient Information Sheet What is Urinary Incontinence? Stress Incontinence is a leakage of urine that occurs, for example,
Female Urinary Incontinence: What It Is and What You Can Do About It Urogynecology Patient Information Sheet What is Urinary Incontinence? Stress Incontinence is a leakage of urine that occurs, for example,
Management of Vaginal Prolapse
 Information for Patients Saint Mary s Hospital/Trafford General Hospital Uro-gynaecology Service Management of Vaginal Prolapse Before reading this leaflet you should read What is vaginal prolapse? If
Information for Patients Saint Mary s Hospital/Trafford General Hospital Uro-gynaecology Service Management of Vaginal Prolapse Before reading this leaflet you should read What is vaginal prolapse? If
1) What conditions is vaginal mesh used to commonly treat? Vaginal mesh is used to treat two different health issues in women:
 Vaginal Mesh Frequently Asked Questions 1) What conditions is vaginal mesh used to commonly treat? Vaginal mesh is used to treat two different health issues in women: a) stress urinary incontinence (SUI)
Vaginal Mesh Frequently Asked Questions 1) What conditions is vaginal mesh used to commonly treat? Vaginal mesh is used to treat two different health issues in women: a) stress urinary incontinence (SUI)
PELVIC FLOOR MUSCLE TRAINING FOR WOMEN STRONG PELVIC FLOOR MUSCLES MEAN GOOD BLADDER AND BOWEL CONTROL WHAT ARE THE PELVIC FLOOR MUSCLES?
 06 STRONG S MEAN WHAT ARE THE S? The floor of the pelvis is made up of layers of muscle and other tissues. These layers stretch like a hammock from the tailbone at the back, to the pubic bone at the front.
06 STRONG S MEAN WHAT ARE THE S? The floor of the pelvis is made up of layers of muscle and other tissues. These layers stretch like a hammock from the tailbone at the back, to the pubic bone at the front.
Surgery for stress incontinence:
 Surgery for stress incontinence: information for you aashara Published February 2005 by the RCOG Contents Key points About this information What is stress incontinence? Do I need an operation? What operation
Surgery for stress incontinence: information for you aashara Published February 2005 by the RCOG Contents Key points About this information What is stress incontinence? Do I need an operation? What operation
Prolapse and Urogynae. By Sarah Rangan & Daniel Warrell
 Prolapse and Urogynae By Sarah Rangan & Daniel Warrell Anatomy and physiology of the pelvic supports The pelvic floor supports the pelvic viscera and vaginal, urethral and rectal openings Endopelvic fascial
Prolapse and Urogynae By Sarah Rangan & Daniel Warrell Anatomy and physiology of the pelvic supports The pelvic floor supports the pelvic viscera and vaginal, urethral and rectal openings Endopelvic fascial
Surgical repair of vaginal wall prolapse using mesh
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Surgical repair of vaginal wall prolapse using mesh Vaginal wall prolapse happens when the normal support
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Surgical repair of vaginal wall prolapse using mesh Vaginal wall prolapse happens when the normal support
Pelvic Floor Exercises
 Directorate of Women, Children and Surgical Services Burton and District Urogynaecology Centre A Nationally Accredited Urogynaecology Unit Pelvic Floor Exercises You have been given this leaflet because
Directorate of Women, Children and Surgical Services Burton and District Urogynaecology Centre A Nationally Accredited Urogynaecology Unit Pelvic Floor Exercises You have been given this leaflet because
Women s and Men s Health Intake Form Comprehensive Physical Therapy Center
 Name: (Last, First) DOB: Date: Age: Referring Physician: Next Physician Appointment: Today s visit: What is the main reason you came to the office today? When did it start? What treatments have you had
Name: (Last, First) DOB: Date: Age: Referring Physician: Next Physician Appointment: Today s visit: What is the main reason you came to the office today? When did it start? What treatments have you had
Pelvic Floor Muscle Exercises
 INFORMATION FOR WOMEN OF ALL AGES Pelvic Floor Muscle Exercises How to exercise and strengthen your pelvic floor muscles ASSOCIATION OF CHARTERED PHYSIOTHERAPISTS IN WOMEN S HEALTH This leaflet is supported
INFORMATION FOR WOMEN OF ALL AGES Pelvic Floor Muscle Exercises How to exercise and strengthen your pelvic floor muscles ASSOCIATION OF CHARTERED PHYSIOTHERAPISTS IN WOMEN S HEALTH This leaflet is supported
Pelvic floor exercises for women. Information for patients Continence Service
 Pelvic floor exercises for women Information for patients Continence Service page 2 of 8 Why do I need to do pelvic floor exercises? Many women experience pelvic floor problems at some time during their
Pelvic floor exercises for women Information for patients Continence Service page 2 of 8 Why do I need to do pelvic floor exercises? Many women experience pelvic floor problems at some time during their
Occult anal sphincter injuries myth or reality?
 DOI: 10.1111/j.1471-0528.2006.00799.x www.blackwellpublishing.com/bjog Intrapartum care Occult anal sphincter injuries myth or reality? Vasanth Andrews, a Abdul H Sultan, a Ranee Thakar, a Peter W Jones
DOI: 10.1111/j.1471-0528.2006.00799.x www.blackwellpublishing.com/bjog Intrapartum care Occult anal sphincter injuries myth or reality? Vasanth Andrews, a Abdul H Sultan, a Ranee Thakar, a Peter W Jones
Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015
 Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015 Disclosures I have none Objectives Identify the basic Anatomy and causes of Pelvic Organ Prolapse Examine office diagnosis
Karanvir Virk M.D. Minimally Invasive & Pelvic Reconstructive Surgery 01/28/2015 Disclosures I have none Objectives Identify the basic Anatomy and causes of Pelvic Organ Prolapse Examine office diagnosis
Interventions METHODS
 Prevention of postpartum stress incontinence PREVENTION OF POSTPARTUM STRESS INCONTINENCE 69 There is good evidence that postnatal pelvic floor exercises are effective in the treatment of postpartum stress
Prevention of postpartum stress incontinence PREVENTION OF POSTPARTUM STRESS INCONTINENCE 69 There is good evidence that postnatal pelvic floor exercises are effective in the treatment of postpartum stress
Management of Female Stress Incontinence
 Management of Female Stress Incontinence Dr. Arvind Goyal Associate Professor (Urology& Renal Transplant) Dayanand Medical College & Hospital, Ludhiana, Punjab, India Stress Incontinence Involuntary loss
Management of Female Stress Incontinence Dr. Arvind Goyal Associate Professor (Urology& Renal Transplant) Dayanand Medical College & Hospital, Ludhiana, Punjab, India Stress Incontinence Involuntary loss
Uterus (Womb) Rectum. Another problem could be the sensation of something coming down at the birth canal or back passage (prolapse).
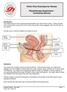 Pelvic Floor Exercises for Women Physiotherapy Department Continence Service Introduction This leaflet tells you how to exercise and strengthen your pelvic floor muscles. These muscles form a broad sling
Pelvic Floor Exercises for Women Physiotherapy Department Continence Service Introduction This leaflet tells you how to exercise and strengthen your pelvic floor muscles. These muscles form a broad sling
Does delayed child-bearing increase the risk of levator injury in labour?
 Australian and New Zealand Journal of Obstetrics and Gynaecology 2007; 47: 491 495 Blackwell Publishing Asia Original Article Delayed child-bearing and levator injury Does delayed child-bearing increase
Australian and New Zealand Journal of Obstetrics and Gynaecology 2007; 47: 491 495 Blackwell Publishing Asia Original Article Delayed child-bearing and levator injury Does delayed child-bearing increase
Operative Vaginal Delivery and Pelvic Floor Trauma. Anna Padoa, MD Urogynecology Service Dept of Ob & Gyn Assaf Harofe Medical Center
 + Operative Vaginal Delivery and Pelvic Floor Trauma Anna Padoa, MD Urogynecology Service Dept of Ob & Gyn Assaf Harofe Medical Center + Vaginal birth and the pelvic floor Mechanisms of injury Damage to
+ Operative Vaginal Delivery and Pelvic Floor Trauma Anna Padoa, MD Urogynecology Service Dept of Ob & Gyn Assaf Harofe Medical Center + Vaginal birth and the pelvic floor Mechanisms of injury Damage to
Guideline for Management and Repair of Perineal Trauma
 Guideline for Management and Repair of Perineal Trauma Author: Labour Ward Forum Specialty: Maternity Date Approved: September 2014 Approved by: W&CH Clinical Governance Committee Date for Review: August
Guideline for Management and Repair of Perineal Trauma Author: Labour Ward Forum Specialty: Maternity Date Approved: September 2014 Approved by: W&CH Clinical Governance Committee Date for Review: August
Incontinence; Lets talk about it. Karanvir Virk M.D. Minimally Invasive and Pelvic Reconstructive Surgery
 Incontinence; Lets talk about it Karanvir Virk M.D. Minimally Invasive and Pelvic Reconstructive Surgery Select the most appropriate subtitle for this talk A: Bladders gone wild! B: There s no such thing
Incontinence; Lets talk about it Karanvir Virk M.D. Minimally Invasive and Pelvic Reconstructive Surgery Select the most appropriate subtitle for this talk A: Bladders gone wild! B: There s no such thing
Patient Information. Tension Free Vaginal/ Obturator Tape (TVT) Royal Devon and Exeter NHS Foundation Trust
 Tension Free Vaginal/Obturator Tape (TVT) Royal Devon and Exeter NHS Foundation Trust Patient Information Tension Free Vaginal/ Obturator Tape (TVT) Reference Number: CW 08 011 003 (version date: September
Tension Free Vaginal/Obturator Tape (TVT) Royal Devon and Exeter NHS Foundation Trust Patient Information Tension Free Vaginal/ Obturator Tape (TVT) Reference Number: CW 08 011 003 (version date: September
PELVIC FLOOR WORKSHOP- LEARN AND GET TO KNOW YOUR FLOOR
 PELVIC FLOOR WORKSHOP- LEARN AND GET TO KNOW YOUR FLOOR LIFE FIT CENTER 2.22.18 DR. SHERINE AUBERT, PT, DPT, PRPC OVERVIEW What What are the functions of the pelvic floor muscles? Who Who goes to pelvic
PELVIC FLOOR WORKSHOP- LEARN AND GET TO KNOW YOUR FLOOR LIFE FIT CENTER 2.22.18 DR. SHERINE AUBERT, PT, DPT, PRPC OVERVIEW What What are the functions of the pelvic floor muscles? Who Who goes to pelvic
