Finn et al. Breast Cancer Research (2016) 18:67 DOI /s
|
|
|
- Lindsay Elliott
- 5 years ago
- Views:
Transcription
1 Finn et al. Breast Cancer Research (2016) 18:67 DOI /s RESEARCH ARTICLE Open Access Efficacy and safety of palbociclib in combination with letrozole as first-line treatment of ER-positive, HER2-negative, advanced breast cancer: expanded analyses of subgroups from the randomized pivotal trial PALOMA-1/TRIO-18 Richard S. Finn 1*, John P. Crown 2, Johannes Ettl 3, Marcus Schmidt 4, Igor M. Bondarenko 5, Istvan Lang 6, Tamas Pinter 7, Katalin Boer 8, Ravindranath Patel 9, Sophia Randolph 10, Sindy T. Kim 10, Xin Huang 10, Patrick Schnell 11, Sashi Nadanaciva 12, Cynthia Huang Bartlett 13 and Dennis J. Slamon 1 Abstract Background: Palbociclib is an oral small-molecule inhibitor of cyclin-dependent kinases 4 and 6. In the randomized, open-label, phase II PALOMA-1/TRIO-18 trial, palbociclib in combination with letrozole improved progression-free survival (PFS) compared with letrozole alone as first-line treatment of estrogen receptor (ER) -positive, human epidermal growth factor receptor 2 (HER2)-negative, advanced breast cancer (20.2 months versus 10.2 months; hazard ratio (HR) = 0.488, 95 % confidence interval (CI) ; one-sided p = ). Grade 3 4 neutropenia was the most common adverse event (AE) in the palbociclib + letrozole arm. We now present efficacy and safety analyses based on several specific patient and tumor characteristics, and present in detail the clinical patterns of neutropenia observed in the palbociclib + letrozole arm of the overall safety population. Methods: Postmenopausal women (n = 165) with ER+, HER2-negative, advanced breast cancer who had not received any systemic treatment for their advanced diseasewererandomized1:1toreceiveeitherpalbociclib in combination with letrozole or letrozole alone. Treatment continued until disease progression, unacceptable toxicity, consent withdrawal, or death. The primary endpoint was PFS. We now analyze the difference in PFS for the treatment populations by subgroups, including age, histological type, history of prior neoadjuvant/adjuvant systemic treatment, and sites of distant metastasis, using the Kaplan-Meier method. HR and 95 % CI are derived from a Cox proportional hazards regression model. (Continued on next page) * Correspondence: RFinn@mednet.ucla.edu 1 Department of Medicine, Division of Hematology/Oncology, David Geffen School of Medicine at University of California Los Angeles, Los Angeles, CA, USA Full list of author information is available at the end of the article 2016 The Author(s). Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License ( which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The Creative Commons Public Domain Dedication waiver ( applies to the data made available in this article, unless otherwise stated.
2 Finn et al. Breast Cancer Research (2016) 18:67 Page 2 of 14 (Continued from previous page) Results: A clinically meaningful improvement in median PFS and clinical benefit response (CBR) rate was seen with palbociclib + letrozole in every subgroup evaluated. Grade 3 4 neutropenia was the most common AE with palbociclib + letrozole in all subgroups. Analysis of the frequency of neutropenia by grade during the first six cycles of treatment showed that there was a downward trend in Grade 3 4 neutropenia over time. Among those who experienced Grade 3 4 neutropenia, 71.7 % had no overlapping infections of any grade and none had overlapping Grade 3 4 infections. Conclusion: The magnitude of clinical benefit seen with the addition of palbociclib to letrozole in improving both median PFS and CBR rate is consistent in nearly all subgroups analyzed, and consistent with that seen in the overall study population. The safety profile of the combination treatment in all subgroups was also comparable to that in the overall safety population of the study. Keywords: Breast cancer, Estrogen receptor-positive, HER2-negative, Cyclin-dependent kinase, Neutropenia Abbreviations: AE, adverse event; CBR, clinical benefit response; CDK, cyclin-dependent kinase; CI, confidence interval; ECOG, Eastern Cooperative Oncology Group; ER, estrogen receptor; FISH, fluorescent in-situ hybridization; HER2, human epidermal growth factor receptor 2; HR, hazard ratio; HR+, hormone receptor-positive; ITT, intention-to-treat; PFS, progression-free survival; RECIST, Response Evaluation Criteria in Solid Tumors Background Cyclin-dependent kinases (CDKs) are a large family of serine-threonine kinases that play several critical roles in cell cycle regulation. They are an attractive therapeutic target given that alterations in cell cycle genes have been implicated in breast cancer as well as multiple other malignancies. Palbociclib (PD ) is a first-in-class, orally active, selective, reversible inhibitor of CDK 4 and 6 [1]. Pre-clinical studies have demonstrated the activity of palbociclib in blocking growth of estrogen receptor (ER)-positive luminal cell lines alone and in combination with anti-estrogens [2]. Clinical data have recently established palbociclib as a novel therapeutic option for women with ER+, human epidermal growth factor receptor 2 (HER2)-negative, advanced breast cancer [3 5]. In the randomized, open-label, phase II PALOMA-1/ TRIO-18 trial, the safety and efficacy of palbociclib in combination with the aromatase inhibitor letrozole was compared with letrozole alone as first-line treatment of women with ER-positive, HER2-negative (ER+/HER2 ), advanced breast cancer [3]. A total of 165 postmenopausal women with ER+/HER2 advanced breast cancer who had not received any treatment for their advanced disease were randomized (1:1), 84 to palbociclib plus letrozole and 81 to letrozole alone. The study stratified patients by disease site and disease-free interval. The primary endpoint was investigator-assessed progressionfree survival (PFS). At the time of the data cut-off for the final analysis (29 November 2013), median followup was 29.6 months (95 % confidence interval (CI) ) for the palbociclib plus letrozole arm and 27.9 months (95 % CI ) for the letrozole arm [3]. Median PFS in the intention-to-treat (ITT) population was 20.2 months (95 % CI ) for the palbociclib plus letrozole arm and 10.2 months (95 % CI ) for the letrozole arm (hazard ratio (HR) = 0.488, 95 % CI ; one-sided p = ) [3]. The clinical benefit response (CBR) rate (complete response + partial response + stable disease 24 weeks) for the ITT population was 81 % in the palbociclib plus letrozole arm and 58 % in the letrozole arm [3]. Overall survival data were not mature at the time of the data cut-off. Grade 3 neutropenia was the most common adverse effect in the palbociclib plus letrozole arm (48 % versus 1 % in the letrozole alone arm) [3]. On the basis of these data, palbociclib (Ibrance, Pfizer) was granted accelerated approval by the US Food and Drug Administration (FDA) in February 2015, in combination with letrozole as initial endocrine-based therapy for postmenopausal women with ER+/HER2 metastatic breast cancer [6]. Despite the high incidence of neutropenia in the palbociclib plus letrozole arm of the PALOMA-1/TRIO-18 trial, there were no reported cases of febrile neutropenia or neutropenia-related infections. This is in contrast to cytotoxic chemotherapy where neutropenia is not only a common dose-limiting toxicity but is also associated with serious infections and infection-related morbidity [7, 8]. Ensuing complications can result in hospitalization, high treatment costs, and increased mortality [9 11]. There are two objectives in the current study: 1) to perform an expanded analysis of the efficacy (PFS and CBR) and safety of palbociclib plus letrozole in clinically relevant subgroups from the PALOMA-1/TRIO-18 trial including age <65 years or 65 years, pathologic type (ductal versus lobular carcinoma), effect of prior neoadjuvant/adjuvant systemic treatment, and metastasis in bone only, visceral sites, or other sites (i.e., soft-tissue, nodes, and so forth); and 2) to further delineate clinical
3 Finn et al. Breast Cancer Research (2016) 18:67 Page 3 of 14 patterns of neutropenia associated with palbociclib in the PALOMA-1/TRIO-18 trial in order to aid clinicians in the management of palbociclib-induced neutropenia. Methods Study design The PALOMA-1/TRIO-18 trial was an international, phase II, multicenter, open-label, randomized study. Details of the study have been reported previously [3]. In brief, postmenopausal women with ER+/HER2 advanced breast cancer were enrolled in two cohorts that accrued sequentially. Patients in both cohorts 1 and 2 were required to have advanced breast cancers defined as ER-positive determined by immunohistochemistry, and HER2-negative determined either by fluorescent in-situ hybridization (FISH) or immunohistochemistry in local laboratory testing. Patients in cohort 2 were additionally required to have cancers with amplification of cyclin D1 (CCND1), loss of p16 (INK4A or CDKN2A), or both, as determined in central laboratory testing. Amplification of CCND1 and loss of p16 were determined by a four-color FISH assay as previously described [3]. Patients in both cohorts were randomized 1:1 to receive palbociclib plus letrozole or letrozole alone and were stratified by disease site (bone-only, visceral, other) and disease-free interval (>12 months from completion of adjuvant treatment to disease recurrence versus 12 months or de novo advanced disease). For the final analysis of the primary endpoint, a combined analysis of cohorts 1 and 2wasperformed[3]. All patients provided informed consent before any study-specific screening procedures were performed. The study was conducted in accordance with the International Conference on Harmonization and guidelines on Good Clinical Practice and was approved by the institutional review boards of the participating centers. The study is registered with the ClinicalTrials.gov, number NCT Patients Postmenopausal women ( 18 years) with ER+/HER2 advanced breast cancer with evidence of 1) locally recurrent disease not amenable to resection or radiation therapy with curative intent or 2) metastatic disease were eligible. Additional key inclusion criteria included measurable disease by Response Evaluation Criteria in Solid Tumors (RECIST, version 1.0) or bone-only disease, an Eastern Cooperative Oncology Group (ECOG) performance status of 0 or 1, and adequate organ (bone marrow, renal, and hepatic) function. Key exclusion criteria included previous treatment for advanced breast cancer, prior neoadjuvant treatment with letrozole with disease recurrence 12 months, previous treatment with a CDK inhibitor, or presence of brain metastasis. Study treatment Patients randomized to the palbociclib plus letrozole arm (n = 84) received oral palbociclib 125 mg once daily for 3 weeks followed by 1 week off in 28-day cycles plus oral letrozole 2.5 mg once daily. Patients randomized to the letrozole arm (n = 81) received oral letrozole 2.5 mg once daily. Study treatment continued until disease progression, unacceptable toxicity, consent withdrawal, or death. Endpoints and assessments The primary endpoint was investigator-assessed PFS, defined as the time from randomization to objective disease progression or death on study. Secondary efficacy endpoints were objective response (by RECIST version 1.0), CBR, duration of response, and overall survival (OS). Additional secondary endpoints were safety, tissue/serum biomarker analyses, and patient-reported outcomes. Tumor assessments of the chest, abdomen, and pelvis were performed by computed tomography or magnetic resonance imaging and clinical assessment of superficial disease (if applicable) at screening and every 8 weeks thereafter. Bone lesions (when applicable) were assessed by radiography; bone scans were performed at baseline and every 12 weeks. Safety was monitored throughout the study and adverse events (AEs) were graded according to the National Cancer Institute Common Terminology Criteria for Adverse Events (CTCAE) version 3.0. Hematology and blood chemistry assessments were done every 2 weeks for the first two treatment cycles and at the beginning of each subsequent cycle. Dosing modifications were performed as described in Additional file 1 (Table S1). Primary prophylactic use of granulocyte colony-stimulating factors was not permitted, although these were allowed to treat treatment-emergent neutropenia as indicated by current ASCO guidelines. Erythropoietin was permitted at the investigator s discretion for the supportive treatment of anemia. Statistical analysis Statistical analysis of the overall study population was previously described in detail [3]. All efficacy analyses were performed on the ITT population; safety analyses included all patients who had received at least one dose of the study treatment. PFS was assessed using the Kaplan-Meier method; HR and 95 % CI were derived from a Cox proportional hazards regression model. No adjustments were made for multiple comparisons in the subgroup analyses since they are considered exploratory analyses. All statistical analyses were performed with SAS version 9.2 or later. Results Subgroup analyses: baseline characteristics The baseline characteristics of the subgroups are summarized in Table 1. In the ITT population (n = 165), 54 % of
4 Finn et al. Breast Cancer Research (2016) 18:67 Page 4 of 14 Table 1 Baseline characteristics of subgroups (intention-to-treat population) Age group <65 years (n = 89) 65 years (n = 76) P+ L (n = 47) L (n = 42) P + L (n = 37) L (n = 39) Median age (range), years 55.0 (41 64) 56.5 (38 64) 72.0 (65 89) 70.0 (65 84) ECOG performance status 0 26 (55.3 %) 23 (54.8 %) 20 (54.1 %) 22 (56.4 %) 1 21 (44.7 %) 19 (45.2 %) 17 (45.9 %) 17 (43.6 %) Disease stage IIIB 1 (2.1 %) 1 (2.4 %) 1 (2.7 %) 0 IV 46 (97.9 %) 41 (97.6 %) 36 (97.3 %) 39 (100.0 %) Disease site a Bone-only 9 (19.2 %) 3 (7.1 %) 8 (21.6 %) 9 (23.1 %) Visceral 19 (40.4 %) 22 (52.4 %) 18 (48.7 %) 21 (53.9 %) Other 19 (40.4 %) 17 (40.5 %) 11 (29.7 %) 9 (23.1 %) Prior systemic treatment None 24 (51.1 %) 23 (54.8 %) 20 (54.1 %) 14 (35.9 %) Yes 23 (48.9 %) 19 (45.2 %) 17 (45.9 %) 25 (64.1 %) Histological type Ductal carcinoma (n = 117) Lobular carcinoma (n = 37) P+ L (n = 63) L (n = 54) P + L (n = 18) L (n = 19) Median age (range), years 63 (41 89) 65 (42 84) 60 (50 74) 62 (38 78) ECOG performance status 0 36 (57.1 %) 29 (53.7 %) 9 (50.0 %) 14 (73.7 %) 1 27 (42.9 %) 25 (46.3 %) 9 (50.0 %) 5 (26.3 %) Disease stage IIIB 2 (3.2 %) 1 (1.9 %) 0 0 IV 61 (96.8 %) 53 (98.1 %) 18 (100.0 %) 19 (100.0 %) Disease site a Bone-only 11 (17.5 %) 8 (14.8 %) 4(22.2 %) 3 (15.8 %) Visceral 28 (44.4 %) 30 (55.6 %) 8 (44.4 %) 7 (36.8 %) Other 24 (38.1 %) 16 (29.6 %) 6 (33.3 %) 9 (47.4 %) Prior systemic treatment None 36 (57.1 %) 26 (48.1 %) 6 (33.3 %) 7 (36.8 %) Yes 27 (42.9 %) 28 (51.9 %) 12 (66.7 %) 12 (63.2 %) Prior systemic treatment None (n = 81) Yes (n = 84) P+ L (n = 44) L (n = 37) P + L (n = 40) L (n = 44) Median age (range), years 63.0 (41 83) 62.0 (43 76) 60.0 (46 89) 65.5 (38 84) ECOG performance status 0 26 (59.1 %) 18 (48.6 %) 20 (50.0 %) 27 (61.4 %) 1 18 (40.9 %) 19 (51.4 %) 20 (50.0 %) 17 (38.6 %) Disease stage IIIB 1 (2.3 %) 0 1 (2.5 %) 1 (2.3 %) IV 43 (97.7 %) 37 (100.0 %) 39 (97.5 %) 43 (97.7 %)
5 Finn et al. Breast Cancer Research (2016) 18:67 Page 5 of 14 Table 1 Baseline characteristics of subgroups (intention-to-treat population) (Continued) Disease site a Bone-only 6 (13.6 %) 5 (13.5 %) 11 (27.5 %) 7 (15.9 %) Visceral 24 (54.6 %) 19 (51.4 %) 13 (32.5 %) 24 (54.6 %) Other 14 (31.8 %) 13 (35.1 %) 16 (40.0 %) 13 (29.6 %) Disease site a Bone-only (n = 29) Visceral (n = 80) Other (n = 56) P+L(n = 17) L (n = 12) P + L (n = 37) L (n = 43) P + L (n = 30) L (n = 26) Median age (range), years 63.0 (46 89) 69.0 (42 73) 63.0 (41 83) 64.0 (38 84) 62.0 (52 78) 62.0 (43 75) ECOG performance status 0 11 (64.7 %) 10 (83.3 %) 19 (51.4 %) 19 (44.2 %) 16 (53.3 %) 16 (61.5 %) 1 6 (35.3 %) 2 (16.7 %) 18 (48.6 %) 24 (55.8 %) 14 (46.7 %) 10 (38.5 %) Disease stage IIIB (6.7 %) 1 (3.8 %) IV 17 (100.0 %) 12 (100.0 %) 37 (100.0 %) 43 (100.0 %) 28 (93.3) 25 (96.2) Prior systemic treatment None 6 (35.3 %) 5 (41.7 %) 24 (64.9 %) 19 (44.2 %) 14 (46.7 %) 13 (50.0 %) Yes 11 (64.7 %) 7 (58.3 %) 13 (35.1 %) 24 (55.8 %) 16 (53.3 %) 13 (50.0 %) Data are n (%) unless otherwise indicated a Based on case report form data ECOG Eastern Cooperative Oncology Group, L letrozole alone, P + Lpalbociclib + letrozole patients were <65 years of age. The majority (71 %) of patients had ductal carcinoma and 22.4 % had lobular carcinoma (the remaining 6.6 % of patients had mixed histology, tubular, or mucinous types). Approximately half (49 %) of the patients had not received prior neoadjuvant or adjuvant systemic treatment. Twenty-nine (17.6 %) patients had bone-only disease at baseline, 48.5 % of patients had visceral metastases (lung and/or liver ± any other site), and 33.9 % of patients had other metastases (bone with other non-visceral sites or other disease sites alone). In the subgroup that had visceral metastases, 52.5 % had metastases in the liver and 76 % had metastases in the lungs; further details on the baseline characteristics of the patients within this subgroup are summarized in Additional file 1 (Table S2). In general, baseline clinical characteristics in the palbociclib plus letrozole arm and letrozole alone arm were well balanced within each subgroup (Table 1), although there were slight imbalances in disease site and prior systemic treatment. Subgroup analyses: efficacy The median PFS and the CBR rate for the subgroups are summarized in Table 2; Kaplan-Meier plots of PFS for the subgroups were determined (Figs. 1 and 2). Palbociclib plus letrozole improved median PFS in both subgroups of age. In patients <65 years of age, median PFS was 18.8 months (95 % CI ) with palbociclib plus letrozole and 7.7 months (95 % CI ) with letrozole alone (HR = 0.315, 95 % CI ; p < ). In patients 65 years of age, median PFS was 26.2 months (95 % CI 12.6 to not estimable) with palbociclib plus letrozole and 12.9 months (95 % CI ) with letrozole alone (HR = 0.505, 95 % CI ; p = ). Palbociclib plus letrozole improved median PFS in patients with ductal carcinoma as well as in patients with lobular carcinoma. Median PFS in the ductal population was 24.4 months (95 % CI ) with palbociclib plus letrozole and 11.1 months (95 % CI ) with letrozole alone (HR = 0.393, 95 % CI ; p = ). The subgroup with lobular carcinoma was limited by the small patient numbers in each arm (n = 18 in the palbociclib plus letrozole arm; n =19 in the letrozole alone arm). Median PFS in this subgroup was 9.4 months (95 % CI ) with palbociclib plus letrozole and 4.8 months (95 % CI ) with letrozole alone (HR = 0.626, 95 % CI ; p = 0.123). Palbociclib plus letrozole improved median PFS regardless of whether patients had received prior neoadjuvant/ adjuvant systemic treatment. Median PFS in patients without prior neoadjuvant/adjuvant systemic treatment was 24.4 months (95 % CI ) with palbociclib plus letrozole and 8.2 months (95 % CI ) with letrozole alone (HR = 0.341, 95 % CI ; p = ). Median PFS in patients with prior systemic treatment was 16.1 months (95 % CI 11 to not estimable) with palbociclib plus letrozole and 10.9 months (95 % CI ) with letrozole alone (HR = 0.539, 95 % CI ; p = ). Within the subgroup that had prior systemic treatment, 65.5 % of patients had prior antihormone treatment. Median PFS in patients with prior anti-hormone treatment was 18.8 months (95 % CI
6 Finn et al. Breast Cancer Research (2016) 18:67 Page 6 of 14 Table 2 Progression-free survival (PFS) and clinical benefit response (CBR) rate of subgroups (intention-to-treat population) Age group <65 years (n = 89) 65 years (n = 76) P+ L (n = 47) L (n = 42) P + L (n = 37) L (n = 39) Median PFS (95 % CI), months 18.8 ( ) 7.7 ( ) 26.2 (12.6 NE) 12.9 ( ) HR (95 % CI) ( ) ( ) CBR* rate (95 % CI), % 80.9 ( ) 54.8 ( ) 81.1 ( ) 61.5 ( ) Histological type Ductal carcinoma (n = 117) Lobular carcinoma (n = 37) P+ L (n = 63) L (n = 54) P + L (n = 18) L (n = 19) Median PFS (95 % CI), months 24.4 ( ) 11.1 ( ) 9.4 ( ) 4.8 ( ) HR (95 % CI) ( ) ( ) CBR* rate (95 % CI), % 82.5 ( ) 63.0 ( ) 72.2 ( ) 42.1 ( ) Prior systemic treatment None (n = 81) Yes (n = 84) P+L(n = 44) L (n = 37) P + L (n = 40) L (n = 44) Median PFS (95 % CI), months 24.4 ( ) 8.2 ( ) 16.1 (11 NE) 10.9 ( ) HR (95 % CI) ( ) ( ) CBR* rate (95 % CI), % 84.1 ( ) 70.3 ( ) 77.5 ( ) 47.7 ( ) Prior anti-hormone treatment (n = 55) P + L (n = 27) L (n = 28) Median PFS (95 % CI), months NA 18.8 (9.7 NE) 12.9 ( ) HR (95 % CI) NA ( ) CBR* rate (95 % CI), % NA 77.8 ( ) 53.6 ( ) Disease site a Bone-only (n = 29) Visceral (n = 80) Other (n = 56) P+L(n = 17) L (n = 12) P + L (n = 37) L (n = 43) P + L (n = 30) L (n = 26) Median PFS (95 % CI), months NE (9.4 NE) 13.3 (1.8 NE) 12.8 ( ) 7.4 ( ) 24.4 ( ) 11.2 ( ) HR (95 % CI) ( ) ( ) ( ) CBR* rate (95 % CI), % 88.2 ( ) 58.3 ( ) 75.5 ( ) 60.5 ( ) 83.3 ( ) 53.8 ( ) *The CBR was determined by investigator assessment a Based on case report form data CI confidence interval, HR hazard ratio, L letrozole alone, NA not applicable, NE not estimable, P + L palbociclib + letrozole 9.7 to not estimable) with palbociclib plus letrozole and 12.9 months (95 % CI ) with letrozole alone (HR = 0.460, 95 % CI ; p = ). The subgroup of patients with bone-only disease was limited by a small number of patients in each arm (n =17 in the palbociclib plus letrozole arm; n =12 in the letrozole alone arm). Despite this, palbociclib plus letrozole improved the median PFS compared with letrozole alone (Table 2). Median PFS in patients with either visceral metastases or distant metastases at other sites was higher with palbociclib plus letrozole than with letrozole alone (Table 2). Palbociclib plus letrozole improved the CBR rate in all subgroups compared with letrozole alone (Table 2); the difference in the CBR rate with the combination treatment for each subgroup was consistent with that seen for the overall study population. Subgroup analyses: safety The safety analyses on the subgroups are summarized in Table 3. The most common all-cause AEs that occurred in at least 10 % of patients in the palbociclib plus letrozole arm of the safety population for each subgroup are summarized in detail in Additional file 1 (Tables S3 S11). All subgroups had a higher incidence of Grade 3 4 AEs in the palbociclib plus letrozole arm than in the letrozole arm ( 88.2 % versus 32.4 %) (Table 3). There was one Grade 5 AE in the palbociclib plus letrozole arm: the event was death due to disease progression in a patient <65 years of age with lobular carcinoma and distant metastases at visceral sites who had not received prior systemic treatment. Neutropenia, leukopenia, fatigue, and anemia were the most common AEs in all subgroups in the palbociclib plus letrozole study arm (Table 3). The incidence of allcausality Grade 3 4 AEs with palbociclib plus letrozole was generally similar in all subgroups, and so was the incidence of all-causality serious adverse events (SAEs) with the combination treatment. The percentage of patients who had treatment discontinuations due to all-causality AEs with palbociclib plus
7 Finn et al. Breast Cancer Research (2016) 18:67 Page 7 of 14 Fig. 1 Progression-free survival (intention-to-treat population) in subgroups based on age, histological type of breast cancer, and history of prior neoadjuvant/adjuvant systemic treatment. CI confidence interval, LET letrozole
8 Finn et al. Breast Cancer Research (2016) 18:67 Page 8 of 14 Fig. 2 Progression-free survival (intention-to-treat population) in subgroups based by distant metastases. CI confidence interval, LET letrozole
9 Finn et al. Breast Cancer Research (2016) 18:67 Page 9 of 14 Table 3 Safety analysis of subgroups (as treated population) Age group <65 years (n = 86) 65 years (n = 74) P+ L (n = 46) L (n = 40) P + L (n = 37) L (n = 37) AEs (all causality), n (%) 46 (100.0 %) 33 (82.5 %) 37 (100.0 %) 32 (86.5 %) Grade 3 4 AEs (all causality), n (%) 37 (80.4 %) 4 (10.0 %) 27 (73.0 %) 12 (32.4 %) 5 most common AEs that had a higher (>10 %) incidence in the P + L arm than in the L arm Neutropenia, leukopenia, fatigue, anemia, alopecia Neutropenia, leukopenia, fatigue, anemia, nausea SAEs (all causality), n (%) 7 (15.2 %) 1 (2.5 %) 11 (29.7 %) 4 (10.8 %) Permanent discontinuation due to AEs (all causality), n (%) 6 (13.0 %) 1 (2.5 %) 6 (16.2 %) 1 (2.7 %) Dose reductions due to AEs (all causality), n (%) 18 (39.1 %) NA 14 (37.8 %) NA Histological type Ductal carcinoma (n = 113) Lobular carcinoma (n = 36) P+ L (n = 62) L (n = 51) P + L (n = 18) L (n = 18) AEs (all causality), n (%) 62 (100.0 %) 44 (86.3 %) 18 (100.0 %) 13 (72.2 %) Grade 3 4 AEs (all causality), n (%) 47 (75.8 %) 13 (25.5 %) 14 (77.8 %) 2 (11.1 %) 5 most common AEs that had a higher (>10 %) incidence in the P + L arm than in the L arm Neutropenia, fatigue, leukopenia, anemia, nausea Neutropenia, anemia, leukopenia, asthenia, alopecia SAEs (all causality), n (%) 12 (19.4 %) 5 (9.8 %) 4 (22.2 %) 0 Permanent discontinuation due to AEs (all causality), n (%) 8 (12.9 %) 1 (2.0 %) 4 (22.2 %) 1 (5.6 %) Dose reductions due to AEs (all causality), n (%) 27 (43.5 %) NA 5 (27.8 %) NA Prior systemic treatment None (n = 80) Yes (n = 80) P+ L (n = 43) L (n = 37) P + L (n = 40) L (n = 40) AEs (all causality), n (%) 43 (100.0 %) 32 (86.5 %) 40 (100.0 %) 33 (82.5 %) Grade 3 4 AEs (all causality), n (%) 30 (69.8 %) 5 (13.5 %) 34 (85.0 %) 11 (27.5 %) 5 most common AEs that had a higher (>10 %) incidence in the P + L arm than in the L arm Neutropenia, fatigue, leukopenia, anemia, alopecia Neutropenia, leukopenia, anemia, nausea, thrombocytopenia SAEs (all causality), n (%) 7 (16.3 %) 2 (5.4 %) 11 (27.5 %) 3 (7.5 %) Permanent discontinuation due to AEs (all causality), n (%) 7 (16.3 %) 1 (2.7 %) 5 (12.5 %) 1 (2.5 %) Dose reductions due to AEs (all causality), n (%) 17 (39.5 %) NA 15 (37.5 %) NA Disease site a Bone-only (n = 28) Visceral (n = 80) Other (n = 52) P+L(n = 17) L (n = 11) P + L (n = 37) L (n = 43) P + L (n = 29) L (n = 23) AEs (all causality), n (%) 17 (100.0 %) 10 (90.9 %) %) 36 (83.7 %) 29 (100.0 %) 19 (82.6 %) Grade 3 4 AEs (all causality), n (%) 15 (88.2 %) 2 (18.2 %) 27 (73.0 %) 12 (27.9 %) 22 (75.8 %) 2 (8.7 %) 5 most common AEs that had a higher (>10 %) incidence in the P + L arm than in the L arm Neutropenia, fatigue, leukopenia, nausea, anemia Neutropenia, leukopenia, fatigue, anemia, decreased appetite Neutropenia, leukopenia, anemia fatigue, hot flush SAEs (all causality), n (%) 4 (23.5 %) 1 (9.1 %) 10 (27.0 %) 3 (7.0 %) 4 (13.8 %) 1 (4.3 %) Permanent discontinuation due to AEs (all causality), n (%) 2 (11.8 %) 0 7 (18.9 %) 1 (2.3 %) 3 (10.3 %) 1 (4.3 %) Dose reductions due to AEs (all causality), n (%) 5 (29.4 %) NA 14 (37.8 %) NA 13 (44.8 %) NA a Based on case report form data AE adverse event, L letrozole alone, NA not applicable, P + Lpalbociclib + letrozole, SAE serious adverse event letrozole was generally similar for all subgroups (Table 3). A similar trend was seen with the percentage of patients who had dose reductions due to all-causality AEs with palbociclib plus letrozole. Clinical patterns of neutropenia associated with palbociclib Neutropenia was the most common AE in the palbociclib plus letrozole arm of the overall safety population of the study [3]. The key findings from the clinical patterns of neutropenia observed with palbociclib in the overall safety population are summarized in Table 4. In the palbociclib plus letrozole arm, 75.9 % of patients had any grade neutropenia, 49.4 % had Grade 3 neutropenia, and 6.0 % had Grade 4 neutropenia (Table 4). In contrast, in the letrozole alone arm, 5.2 % of patients had any grade neutropenia, 1.3 % had Grade 3 neutropenia and no patient had Grade 4 neutropenia. The investigator-reported neutropenia AEs generally reflected
10 Finn et al. Breast Cancer Research (2016) 18:67 Page 10 of 14 Table 4 Neutropenia clinical patterns in the overall safety population (as treated population) of the PALOMA-1/TRIO-18 trial Palbociclib + letrozole (n = 83) Letrozole (n = 77) Patients with neutropenia*, n (%) a All Grades 63 (75.9 %) 4 (5.2 %) Grade 3 41 (49.4 %) 1 (1.3 %) Grade 4 5 (6.0 %) 0 Laboratory abnormality: neutrophils, n (%) All Grades 77 (93.9 %) 13 (16.9 %) Grade 3 47 (57.3 %) 2 (2.6 %) Grade 4 4 (4.9 %) 0 Neutropenia episodes per patient, n (%) a 1 10 (12.1 %) 2 (2.6 %) 2 9 (10.8 %) 1 (1.3 %) (18.1 %) (34.9 %) 1 (1.3 %) Median time (range) from first dose to first episode of neutropenia onset, days Any grade 20.0 (13 757) 49.5 (15 113) Grade (14 757) ( ) Grade (14 246) Total number of episodes of neutropenia in the study All Grades Grade Grade Median duration (range) of neutropenia by episode, days Grade 3 8 (2 58) 30 (27 31) Grade 4 7 (3 16) Dose reductions, dose interruptions, or cycle delays due to any grade neutropenia, n (%) a 43 (51.8 %) Permanent discontinuation from the study due to Grade 3 4 neutropenia, n (%) a 5 (6.0 %) 0 All Grades neutropenia with overlapping all Grades infections, n (%) b Yes 23 (36.5 %) 0 No 40 (63.5 %) 4 (100.0 %) All Grades neutropenia with overlapping Grade 3 4 infections, n (%) b Yes 1 (1.6 %) 0 No 62 (98.4 %) 4 (100.0 %) Grade 3 4 neutropenia with overlapping all Grades infections, n (%) c Yes 13 (28.2 %) 0 No 33 (71.7 %) 1 (100.0 %) Table 4 Neutropenia clinical patterns in the overall safety population (as treated population) of the PALOMA-1/TRIO-18 trial (Continued) Grade 3 4 neutropenia with overlapping Grade 3 4 infections, n (%) c Yes 0 0 No 46 (100.0 %) 1 (100.0 %) *Neutropenia included preferred terms neutropenia and neutrophil count decreased (MeDRA 16.1 coding dictionary) The number of patients who had at least one on-study assessment for absolute neutrophil count was 82 in the palbociclib plus letrozole arm and 77 in the letrozole arm a Percentages are based on the number of patients in each arm (n) of the study: 83 in the palbociclib plus letrozole arm, 77 in the letrozole arm b Percentages are based on the number of patients with all Grades neutropenia: 63 in the palbociclib plus letrozole arm, 4 in the letrozole arm c Percentages are based on the number of patients with Grade 3 4 neutropenia: 46 in the palbociclib plus letrozole arm, 1 in the letrozole arm neutrophil laboratory findings (Table 4). Approximately half (53 %) of the patients in the palbociclib plus letrozole arm had 3 episodes of neutropenia. The median time from first dose to first episode of any grade neutropenia in the palbociclib plus letrozole arm was 20 days. The median duration of Grade 3 neutropenia was 8 days and the median duration of Grade 4 neutropenia was 7 days. Approximately half (51.8 %) of the patients who had any grade neutropenia had dose reductions, dose interruptions, or cycle delays in the palbociclib plus letrozole arm but only five patients (6 %) were required to permanently discontinue treatment due to Grade 3 4 neutropenia as per protocol. When the frequency of neutropenia by grade during the first six cycles of treatment was analyzed (Fig. 3a), there was a downward trend in Grade 3 4 neutropenia over time, suggesting that there was no cumulative toxicity and that early dose modifications were likely effective in reducing the frequency of these events. Since neutropenia usually increases the risk for infection, we explored the frequency of neutropenia with overlapping infections in the palbociclib plus letrozole arm. Only one patient with any grade neutropenia had an overlapping Grade 3 4 infection (Grade 3 influenza) in the palbociclib plus letrozole arm (Table 4). The majority (71.7 %) of patients with Grade 3 4 neutropenia in the palbociclib plus letrozole arm had no overlapping infections of any grade, and those that did had grade 1 2 infections only. When evaluating the first six cycles of treatment, there was no clear association between the frequency of Grade 3 4 neutropenia and all Grade infections (Fig. 3b). Furthermore, no patients with Grade 3 4 neutropenia had overlapping Grade 3 4 infections in the palbociclib plus letrozole arm (Table 4), nor were there any cases of febrile neutropenia in the study.
11 Finn et al. Breast Cancer Research (2016) 18:67 Page 11 of 14 Fig. 3 a Frequency of neutropenia by grade during the first six cycles of treatment in the palbociclib plus letrozole arm of the study. b Frequency of Grade 3 4 neutropenia and all Grade infections during the first six cycles of treatment in the palbociclib plus letrozole arm of the study Discussion Hormone receptor-positive (HR+) breast cancer remains the most common sub-type of breast cancer. Historically, the most important therapeutic intervention in the management of patients with HR+ breast cancer has been the use of anti-estrogen therapy, including tamoxifen, aromatase inhibitors, and fulvestrant. Advanced breast cancer remains incurable, although with currently available therapies median survival is in the order of 3 4 years [12 14]. The PALOMA-1/TRIO-18 data and the regulatory approval of palbociclib represent the first novel non-endocrine therapy to improve PFS in the front-line setting of postmenopausal women with ER+/HER2 advanced breast cancer. While confirmation of this finding is pending the results of the PALOMA-2/ TRIO-22 study which is a randomized, double-blind study of palbociclib and letrozole versus placebo and letrozole, results from the double-blind, placebo-controlled PALOMA-3 study, evaluating palbociclib and fulvestrant versus fulvestrant in a hormone-refractory population confirm the important role of CDK 4/6 inhibition in ER+/HER2 breast cancer. At this time, survival data from both studies are not mature, but the significant improvement in PFS of over 10 months in PALOMA-1/ TRIO-18 is clinically meaningful. It is also interesting to note that the FIRST study, an open label, randomized, phase II study comparing fulvestrant versus anastrozole in a front-line, aromatase inhibitor-naive, ER+ population, demonstrated an improvement of 10 months in time to progression with fulvestrant (23.4 months for fulvestrant versus 13.1 months with anastrozole) [15] that ultimately resulted in an improvement in overall survival [12]. In the current study, we explored the clinical benefit and safety profile of palbociclib and letrozole in various sub-groups from the PALOMA-1/TRIO-18 trial, on the basis of both patient and tumor characteristics. When the subgroups were analyzed on the basis of age (<65 years and 65 years), there was a consistent benefit from the addition of palbociclib regardless of age. These observations are important given that age-related disparities have been reported for breast cancer outcomes [16]. Furthermore, the incidence of Grade 3/4 adverse events, the rate of dose reductions, and the rate of discontinuations were similar in the two age groups.
12 Finn et al. Breast Cancer Research (2016) 18:67 Page 12 of 14 PALOMA-1/TRIO-18 was a front-line treatment study for advanced breast cancer, but about half of the patients had prior systemic therapy in the neoadjuvant/adjuvant setting. The prior systemic therapy received included both chemotherapy and anti-hormone approaches such as non-steroidal aromatase inhibitors, steroidal aromatase inhibitors, and tamoxifen. Consistent with our understanding of drug resistance, the largest benefit with palbociclib plus letrozole was seen in those patients that had never received any prior adjuvant therapy (HR = 0.341, 95 % CI ; p = ). However, even in those patients that received prior systemic therapy, the benefit of treatment was clinically meaningful (HR = 0.539, 95 % CI ; p = ). Importantly, in those patients that had had prior endocrine therapy, the HR was 0.46 (95 % CI ; p = ), supporting our hypothesis that CDK 4/6 inhibition with palbociclib can overcome resistance to endocrine therapy [2]. In regard to tumor characteristics, we evaluated both histologic features and anatomic features. While the majority of invasive breast cancers are ductal in origin, approximately % are lobular. As expected, the majority of patients in the PALOMA-1 trial had ductal carcinoma. In general, it is felt that lobular carcinomas have a better prognosis than ductal carcinomas, are more sensitive to endocrine therapy, and do not respond as well to systemic chemotherapy [17]. With these factors in mind, we explored whether there was a differential effect seen with the addition of palbociclib in these two histologies. When comparing the letrozole arms of the two subgroups, the ductal carcinoma subgroup had a better PFS than the lobular carcinoma subgroup (11.1 months versus 4.8 months). This observation clearly needs to be interpreted with caution given that there were only 19 patients in the letrozole arm of the lobular carcinoma subgroup and other clinical factors were not accounted for; for example, more patients with lobular carcinoma received adjuvant systemic therapy versus the ductal group. Nevertheless, both groups appear to have benefited from the addition of palbociclib, with a HR of (95 % CI ; p = ) in the ductal group and (95 % CI ; p = 0.123) in the lobular group. The p value of in the lobular group likely reflects the small sample size. Whether or not this difference in degree of benefit is significant will need to be established in larger studies. Another relevant baseline prognostic factor we evaluated was anatomic stage of the disease. While virtually all of the patients had Stage IV disease, there was a mixture of those that had visceral disease versus bone-only or other sites of disease, such as soft tissue or lymph node metastases. The HR values for these groups (visceral disease, bone-only, other sites) were (95 % CI ; p = ), (95 % CI, ; p = ), and (95 % CI, ; p = ), respectively. While the degree of benefit mimics the prognosis for these groups, even in the worst prognosis patient group (i.e., those with visceral disease) there was a 45 % decrease in the risk of progression with palbociclib. In addition, the clinical benefit rate in this group, while less than the other two groups, was still over 75 %, confirming that the combination is an appropriate option for women with visceral disease. This is particularly relevant given that this group of patients is often considered for front-line chemotherapy over endocrine therapy. Finally, the therapeutic benefit of any new agent needs to be weighed against its side effects profile. As previously reported [3], the most common side effects with the combination therapy were neutropenia, leukopenia, and fatigue. Palbociclib is dosed using a 3-week on, 1-week off regimen to manage the neutropenia/leukopenia side effect. While the high incidence of Grade 3/4 events in the neutropenia/leukopenia categories is cause for concern, importantly these events were not associated with serious infections. This observation was also made in the larger, double-blind, placebo-controlled PALOMA-3 study [5]. The current US Prescribing Information for Palbociclib (Ibrance ) [18] recommends checking the absolute neutrophil count on day 1 and day 14 of the first two cycles of therapy. This monitoring schedule was chosen considering that the onset of neutropenia occurred early during treatment, with median time to any grade, Grade 3, and Grade 4 neutropenia being 20 days, 28 days, and 16 days, respectively. The study data demonstrate that there is no cumulative toxicity with regard to neutropenia; instead, its incidence decreases over time. For a newly diagnosed patient with ER+/HER2 advanced breast cancer, the treating physician is faced with the decision of treating with endocrine therapy or chemotherapy. This decision is affected by factors such as menopausal status, ECOG performance status, sites of disease, and type and length of time from prior adjuvant therapy. Based on the data from PALOMA-1/TRIO-18, palbociclib received accelerated approval from the US FDA for use in these patients. The role of CDK 4/6 inhibition in ER+/HER2 breast cancer has now been further validated in the larger, PALOMA-3 study. The findings presented here confirm the consistent benefit of palbociclib and letrozole in several relevant clinical subgroups, including patients of older age, patients with both lobular and ductal carcinoma, and patients with various disease sites and prior adjuvant therapy. The PALOMA-1/TRIO-18 study was the first study to demonstrate a significant improvement in PFS with a novel agent in the first-line treatment of advanced ER+/HER2 breast cancer. These findings now await confirmation
13 Finn et al. Breast Cancer Research (2016) 18:67 Page 13 of 14 in the larger, phase III, double-blind, placebo-controlled PALOMA-2/TRIO-22 study which has completed enrollment and is awaiting analyses based on accruing events (NCT ). Conclusion We performed an expanded analysis of the efficacy (PFS and CBR) as well as the safety of palbociclib plus letrozole in clinically relevant subgroups from the PALOMA- 1/TRIO-18 trial. The degree of benefit in both median PFS and the CBR rate observed as a result of the addition of palbociclib to letrozole was consistent in nearly all subgroups analyzed and was consistent with that seen in the overall study population. The safety profile of the combination treatment in all subgroups was comparable to that in the overall safety population of the study. The frequency of Grade 3 4 neutropenia in the overall safety population of the study decreased over time. Neutropenia was not associated with serious infections or infectious complications. Additional file Additional file 1: Table S1. Palbociclib dose modification scheme used in the PALOMA-1/TRIO-18 trial for managing neutropenia. Table S2. Baseline characteristics of the subgroup with visceral metastases (intention-to-treat population). Table S3. Most common all-cause adverse events that occurred in at least 10 % of patients <65 years of age in the palbociclib + letrozole arm of the safety population. Table S4. Most common all-cause adverse events that occurred in at least 10 % of patients 65 years of age in the palbociclib + letrozole arm of the safety population. Table S5. Most common all-cause adverse events that occurred in at least 10 % of patients with ductal carcinoma in the palbociclib + letrozole arm of the safety population. Table S6. Most common all-cause adverse events that occurred in at least 10 % of patients with lobular carcinoma in the palbociclib + letrozole arm of the safety population. Table S7. Most common all-cause adverse events that occurred in at least 10 % of patients with no prior neo-adjuvant/adjuvant systemic treatment in the palbociclib + letrozole arm of the safety population. Table S8. Most common all-cause adverse events that occurred in at least 10 % of patients with prior neo-adjuvant/adjuvant systemic treatment in the palbociclib + letrozole arm of the safety population. Table S9. Most common all-cause adverse events that occurred in at least 10 % of patients with bone-only metastases at baseline in the palbociclib + letrozole arm of the safety population. Table S10. Most common all-cause adverse events that occurred in at least 10 % of patients with visceral metastases in the palbociclib + letrozole arm of the safety population. Table S11. Most common all-cause adverse events that occurred in at least 10 % of patients with other metastases (bone with other non-visceral sites or other disease sites alone) in the palbociclib + letrozole arm of the safety population. (DOCX 74 kb) Abbrievations AE: adverse event; CBR: clinical benefit response; CDK: cyclin-dependent kinase; CI: confidence interval; ECOG: Eastern Cooperative Oncology Group; ER: estrogen receptor; FISH: fluorescent in-situ hybridization; HER2: human epidermal growth factor receptor 2; HR: hazard ratio; HR+: hormone receptor-positive; ITT: intention-to-treat; PFS: progression-free survival; RECIST: Response Evaluation Criteria in Solid Tumors; RMSE: root mean square error; VIF: variance inflation factor. Acknowledgments The study was sponsored by Pfizer. We thank all the participants and their families, as well as the staff of Translational Research in Oncology for their support. Authors contributions RSF, XH, STK, SR, and DJS contributed to the design of the PALOMA-1/TRIO-18 study. RSF, DJS, and JPC were members of the steering committee that oversaw the conduct of the study. RSF, JPC, IMB, and RP contributed substantially to patient recruitment. RSF, JPC, IL, KB, IMB, JE, RP, TP, MS, DJS, and STK contributed to data collection. All authors contributed to data analysis and data interpretation. RSF, SN, CHB, and PS contributed to the writing of the report. XH and PS contributed to the production of the figures. All authors contributed to the review of the report. All authors reviewed and approved the final submitted version. Competing interests RSF and DJS received research support from Pfizer and have served as consultants to the same company. DJS has common stock in Pfizer. JPC has received consulting fees from Pfizer, Eisai, Genomic Health, and NEO New Oncology. JE has received consulting fees from Pfizer, GlaxoSmithKline, Roche, Novartis, Eisai, and Pierre Fabre. MS has received consulting fees from Roche, Pfizer, and Sividon. TP has received consulting fees from Novartis and Roche. SR, STK, XH, PS, SN, and CHB are employees of and own stock of Pfizer. IMB, IL, KB, and RP declare that they have no competing interests. Author details 1 Department of Medicine, Division of Hematology/Oncology, David Geffen School of Medicine at University of California Los Angeles, Los Angeles, CA, USA. 2 Irish Cooperative Oncology Research Group, Dublin, Ireland. 3 Technical University of Munich, Munich, Germany. 4 University Hospital Mainz, Mainz, Germany. 5 Dnipropetrovsk Medical Academy, City Multiple-Discipline Clinical Hospital, Dnipropetrovsk, Ukraine. 6 Orszagos Onkologiai Intezet, Budapest, Hungary. 7 Petz Aladar Megyei Oktato Korhaz, Gyor, Hungary. 8 Department of Medical Oncology, Szent Margit Korhaz, Onkologia, Budapest, Hungary. 9 Comprehensive Blood and Cancer Center, Bakersfield, CA, USA. 10 Pfizer Oncology, La Jolla, CA, USA. 11 Pfizer Oncology, New York, NY, USA. 12 Pfizer Oncology, Groton, CT, USA. 13 Pfizer Oncology, Collegeville, PA, USA. Received: 25 January 2016 Accepted: 27 May 2016 References 1. Fry DW, Harvey PJ, Keller PR, Elliott WL, Meade M, Trachet E, et al. Specific inhibition of cyclin-dependent kinase 4/6 by PD and associated antitumor activity in human tumor xenografts. Mol Cancer Ther. 2004;3(11): Finn RS, Dering J, Conklin D, Kalous O, Cohen DJ, Desai AJ, et al. PD , a selective cyclin D kinase 4/6 inhibitor, preferentially inhibits proliferation of luminal estrogen receptor-positive human breast cancer cell lines in vitro. Breast Cancer Res. 2009;11(5):R FinnRS,CrownJP,LangI,BoerK,BondarenkoIM,KulykSO,etal. The cyclin-dependent kinase 4/6 inhibitor palbociclib in combination withletrozoleversusletrozolealoneasfirst-linetreatmentof oestrogen receptor-positive, HER2-negative, advanced breast cancer (PALOMA-1/TRIO-18): a randomised phase 2 study. Lancet Oncol. 2015;16(1): DeMichele A, Clark AS, Tan KS, Heitjan DF, Gramlich K, Gallagher M, et al. CDK 4/6 inhibitor palbociclib (PD ) in Rb + advanced breast cancer: phase ii activity, safety, and predictive biomarker assessment. Clin Cancer Res. 2015;21(5): TurnerNC,RoJ,AndreF,LoiS,VermaS,IwataH,etal.Palbociclibin hormone-receptor-positive advanced breast cancer. N Engl J Med. 2015;373(3): Beaver JA, Amiri-Kordestani L, Charlab R, Chen W, Palmby T, Tilley A, et al. FDA approval: palbociclib for the treatment of postmenopausal patients with estrogen receptor-positive, HER2-negative metastatic breast cancer. Clin Cancer Res. 2015;21(21): Fontanella C, Bolzonello S, Lederer B, Aprile G. Management of breast cancer patients with chemotherapy-induced neutropenia or febrile neutropenia. Breast Care (Basel). 2014;9(4):
14 Finn et al. Breast Cancer Research (2016) 18:67 Page 14 of Bhatt V, Saleem A. Review: Drug-induced neutropenia pathophysiology, clinical features, and management. Ann Clin Lab Sci. 2004;34(2): Kuderer NM, Dale DC, Crawford J, Cosler LE, Lyman GH. Mortality, morbidity, and cost associated with febrile neutropenia in adult cancer patients. Cancer. 2006;106(10): Lyman GH, Michels SL, Reynolds MW, Barron R, Tomic KS, Yu J. Risk of mortality in patients with cancer who experience febrile neutropenia. Cancer. 2010;116(23): Michels SL, Barron RL, Reynolds MW, Smoyer Tomic K, Yu J, Lyman GH. Costs associated with febrile neutropenia in the US. Pharmacoeconomics. 2012;30(9): Ellis MJ, Llombart-Cussac A, Feltl D, Dewar JA, Jasiowka M, Hewson N, et al. Fulvestrant 500 mg versus anastrozole 1 mg for the first-line treatment of advanced breast cancer: overall survival analysis from the phase II FIRST study. J Clin Oncol. 2015;33(32): Paridaens RJ, Dirix LY, Beex LV, Nooij M, Cameron DA, Cufer T, et al. Phase III study comparing exemestane with tamoxifen as first-line hormonal treatment of metastatic breast cancer in postmenopausal women: the European Organisation for Research and Treatment of Cancer Breast Cancer Cooperative Group. J Clin Oncol. 2008;26(30): Mehta RS, Barlow WE, Albain KS, Vandenberg TA, Dakhil SR, Tirumali NR, et al. Combination anastrozole and fulvestrant in metastatic breast cancer. N Engl J Med. 2012;367(5): Robertson JF, Lindemann JP, Llombart-Cussac A, Rolski J, Feltl D, Dewar J, et al. Fulvestrant 500 mg versus anastrozole 1 mg for the first-line treatment of advanced breast cancer: follow-up analysis from the randomized 'FIRST' study. Breast Cancer Res Treat. 2012;136(2): Hurria A, Muss H. Special issues in older women with breast cancer. Adv Exp Med Biol. 2015;862: Guiu S, Wolfer A, Jacot W, Fumoleau P, Romieu G, Bonnetain F, et al. Invasive lobular breast cancer and its variants: how special are they for systemic therapy decisions? Crit Rev Oncol Hematol. 2014;92(3): US Prescribing Information for Ibrance. Available at fda.gov/drugsatfda_docs/label/2015/207103s000lbl.pdf. Accessed 24 October Submit your next manuscript to BioMed Central and we will help you at every step: We accept pre-submission inquiries Our selector tool helps you to find the most relevant journal We provide round the clock customer support Convenient online submission Thorough peer review Inclusion in PubMed and all major indexing services Maximum visibility for your research Submit your manuscript at
The lancet oncology 16.1 (2015): 25-35
 The lancet oncology 16.1 (2015): 25-35 The cyclin-dependent kinase 4/6 inhibitor palbociclib in combination with letrozole versus letrozole alone as first-line treatment of oestrogen receptorpositive,
The lancet oncology 16.1 (2015): 25-35 The cyclin-dependent kinase 4/6 inhibitor palbociclib in combination with letrozole versus letrozole alone as first-line treatment of oestrogen receptorpositive,
Metastatic breast cancer: sequence of therapies
 Metastatic breast cancer: sequence of therapies Clinical Case Discussion Nadia Harbeck, MD PhD Breast Center, Department of Gynecology and Obstetrics University of Munich, Ludwig-Maximilians University
Metastatic breast cancer: sequence of therapies Clinical Case Discussion Nadia Harbeck, MD PhD Breast Center, Department of Gynecology and Obstetrics University of Munich, Ludwig-Maximilians University
First-Line Ribociclib + Letrozole for Postmenopausal Women With HR+, HER2-, Advanced Breast Cancer: First Results From the Phase III MONALEESA-2 Study
 First-Line Ribociclib + Letrozole for Postmenopausal Women With HR+, HER2-, Advanced Breast Cancer: First Results From the Phase III MONALEESA-2 Study Abstract LBA1 Hortobagyi GN, Stemmer SM, Burris HA,
First-Line Ribociclib + Letrozole for Postmenopausal Women With HR+, HER2-, Advanced Breast Cancer: First Results From the Phase III MONALEESA-2 Study Abstract LBA1 Hortobagyi GN, Stemmer SM, Burris HA,
Recent advances in the management of metastatic breast cancer in older adults
 Recent advances in the management of metastatic breast cancer in older adults Laura Biganzoli Medical Oncology Dept New Hospital of Prato Istituto Toscano Tumori Italy Important recent advances in the
Recent advances in the management of metastatic breast cancer in older adults Laura Biganzoli Medical Oncology Dept New Hospital of Prato Istituto Toscano Tumori Italy Important recent advances in the
RIBOCICLIB EN PRIMERA LINEA DE TRATAMIENTO. Dra. Elena Aguirre H.U. Miguel Servet
 RIBOCICLIB EN PRIMERA LINEA DE TRATAMIENTO Dra. Elena Aguirre H.U. Miguel Servet INTRODUCTION ADVANCED BREAST CANCER HR+/HER2- YES Consider Chemo VISCERAL CRISIS? NO Endocrine Therapy X3 Toxicity Progresive
RIBOCICLIB EN PRIMERA LINEA DE TRATAMIENTO Dra. Elena Aguirre H.U. Miguel Servet INTRODUCTION ADVANCED BREAST CANCER HR+/HER2- YES Consider Chemo VISCERAL CRISIS? NO Endocrine Therapy X3 Toxicity Progresive
Phase 3 Top-Line Results Show IBRANCE in Combination with Fulvestrant Meets Progression-Free Survival (PFS) Primary Endpoint
 For immediate release: April 15, 2015 Media Contact: Sally Beatty (212) 733-6566 Investor Contact: Ryan Crowe (212) 733-8160 Pfizer Announces PALOMA-3 Trial for IBRANCE (Palbociclib) Stopped Early Due
For immediate release: April 15, 2015 Media Contact: Sally Beatty (212) 733-6566 Investor Contact: Ryan Crowe (212) 733-8160 Pfizer Announces PALOMA-3 Trial for IBRANCE (Palbociclib) Stopped Early Due
TRIALs of CDK4/6 inhibitor in women with hormone-receptor-positive metastatic breast cancer
 TRIALs of CDK4/6 inhibitor in women with hormone-receptor-positive metastatic breast cancer Marta Bonotto Department of Oncology University Hospital of Udine TRIALs of CDK4/6 inhibitor in women with hormone-receptor-positive
TRIALs of CDK4/6 inhibitor in women with hormone-receptor-positive metastatic breast cancer Marta Bonotto Department of Oncology University Hospital of Udine TRIALs of CDK4/6 inhibitor in women with hormone-receptor-positive
Targeting CDK 4/6. Jee Hyun Kim, M.D., Ph.D. Seoul National University College of Medicine
 2016.04.30 GBCC Education Symposium Targeting CDK 4/6 Jee Hyun Kim, M.D., Ph.D. Seoul National University College of Medicine Contents Cyclins -CDKs in cell cycle control CDK 4/6 in breast cancer Preclinical
2016.04.30 GBCC Education Symposium Targeting CDK 4/6 Jee Hyun Kim, M.D., Ph.D. Seoul National University College of Medicine Contents Cyclins -CDKs in cell cycle control CDK 4/6 in breast cancer Preclinical
Translational Platform for the Development of Targeted Therapeutics
 Translational Platform for the Development of Targeted Therapeutics Ondřej Kalous, MD Associate Project Scientist UCLA Translational Oncology Research Laboratories (TORL) Jonsson Comprehensive Cancer Center
Translational Platform for the Development of Targeted Therapeutics Ondřej Kalous, MD Associate Project Scientist UCLA Translational Oncology Research Laboratories (TORL) Jonsson Comprehensive Cancer Center
Novel Strategies in Systemic Therapies: Overcoming Endocrine Therapy Resistance
 Novel Strategies in Systemic Therapies: Overcoming Endocrine Therapy Resistance Richard S. Finn, MD Division of Hematology/ Oncology Director, Translational Oncology Laboratory Geffen School of Medicine
Novel Strategies in Systemic Therapies: Overcoming Endocrine Therapy Resistance Richard S. Finn, MD Division of Hematology/ Oncology Director, Translational Oncology Laboratory Geffen School of Medicine
Clinical activity of fulvestrant in metastatic breast cancer previously treated with endocrine therapy and/or chemotherapy
 ORIGINAL ARTICLE 2018 Mar 16. [Epub ahead of print] Clinical activity of fulvestrant in metastatic breast cancer previously treated with endocrine therapy and/or chemotherapy Mi Hwa Heo, Hee Kyung Kim,
ORIGINAL ARTICLE 2018 Mar 16. [Epub ahead of print] Clinical activity of fulvestrant in metastatic breast cancer previously treated with endocrine therapy and/or chemotherapy Mi Hwa Heo, Hee Kyung Kim,
Transcript and References
 Richard S. Finn, MD Associate Professor of Medicine Division of Hematology/Oncology Co-director, Signal Transduction and Therapeutics Program Jonsson Comprehensive Cancer Center Geffen School of Medicine
Richard S. Finn, MD Associate Professor of Medicine Division of Hematology/Oncology Co-director, Signal Transduction and Therapeutics Program Jonsson Comprehensive Cancer Center Geffen School of Medicine
CDK 4/6 Inhibitors: Efficacy and Side Effect Profile
 CDK 4/6 Inhibitors: Efficacy and Side Effect Profile Univ.-Prof. Dr. Christian F Singer, MPH Center for Breast Health, Medical University of Vienna Center for Familial Breast- and Ovarian Cancer, MUW Christian
CDK 4/6 Inhibitors: Efficacy and Side Effect Profile Univ.-Prof. Dr. Christian F Singer, MPH Center for Breast Health, Medical University of Vienna Center for Familial Breast- and Ovarian Cancer, MUW Christian
Inibitori delle chinasi ciclino dipendenti nel trattamento della malattia metastatica HR-positiva Gli studi clinici
 Inibitori delle chinasi ciclino dipendenti nel trattamento della malattia metastatica HR-positiva Gli studi clinici Laura Orlando UOC Oncologia & Breast Unit Brindisi Verona 22/04/2016 Summary Studi con
Inibitori delle chinasi ciclino dipendenti nel trattamento della malattia metastatica HR-positiva Gli studi clinici Laura Orlando UOC Oncologia & Breast Unit Brindisi Verona 22/04/2016 Summary Studi con
Online-Only Supplementary Materials
 Online-Only Supplementary Materials Online-Only Supplementary Methods: Eligibility Criteria and Study Endpoints and Assessments Supplementary Table 1. Demographic and Baseline Characteristics in Patients
Online-Only Supplementary Materials Online-Only Supplementary Methods: Eligibility Criteria and Study Endpoints and Assessments Supplementary Table 1. Demographic and Baseline Characteristics in Patients
NSABP: FB-11. Shannon Puhalla, MD
 NSABP: FB-11 Phase II Randomized Study Evaluating the Biological and Clinical Effects of the Combination of Palbociclib with Letrozole as Neoadjuvant Therapy in Post- Menopausal Women with Estrogen Receptor
NSABP: FB-11 Phase II Randomized Study Evaluating the Biological and Clinical Effects of the Combination of Palbociclib with Letrozole as Neoadjuvant Therapy in Post- Menopausal Women with Estrogen Receptor
Karcinom dojke. PANEL: Semir Bešlija, Zdenka Gojković, Robert Šeparović, Tajana Silovski
 Karcinom dojke PANEL: Semir Bešlija, Zdenka Gojković, Robert Šeparović, Tajana Silovski MBC: HER2 PHEREXA: Study Design Multicenter, randomized, open-label phase III trial Stratified by prior CNS disease,
Karcinom dojke PANEL: Semir Bešlija, Zdenka Gojković, Robert Šeparović, Tajana Silovski MBC: HER2 PHEREXA: Study Design Multicenter, randomized, open-label phase III trial Stratified by prior CNS disease,
DOI: Tam Binh V Bui 1, Desirée MT Burgers 1, Mariette J Agterof 2 and Ewoudt MW van de Garde 1,3
 823238BCB0010.1177/1178223418823238Breast Cancer: Basic and Clinical ResearchBui et al research-article2019 Real-World Effectiveness of Palbociclib Versus Clinical Trial Results in Patients With Advanced/
823238BCB0010.1177/1178223418823238Breast Cancer: Basic and Clinical ResearchBui et al research-article2019 Real-World Effectiveness of Palbociclib Versus Clinical Trial Results in Patients With Advanced/
Sponsor / Company: Sanofi Drug substance(s): SAR (iniparib)
 These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert in the country of prescription. Sponsor / Company: Sanofi Drug substance(s):
These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert in the country of prescription. Sponsor / Company: Sanofi Drug substance(s):
Multimedia Appendix 6 Educational Materials Table of Contents. Intervention Educational Materials Audio Script (version 1)
 Multimedia Appendix 6 Educational Materials Table of Contents Intervention Educational Materials... 1 Audio Script (version 1)... 1 Text (version 1)... 5 Slides (version 1)... 17 Audio Script (version
Multimedia Appendix 6 Educational Materials Table of Contents Intervention Educational Materials... 1 Audio Script (version 1)... 1 Text (version 1)... 5 Slides (version 1)... 17 Audio Script (version
abstract n engl j med 375;20 nejm.org November 17,
 The new england journal of medicine established in 1812 November 17, 2016 vol. 375 no. 20 Palbociclib and Letrozole in Advanced Breast Cancer Richard S. Finn, M.D., Miguel Martin, M.D., Hope S. Rugo, M.D.,
The new england journal of medicine established in 1812 November 17, 2016 vol. 375 no. 20 Palbociclib and Letrozole in Advanced Breast Cancer Richard S. Finn, M.D., Miguel Martin, M.D., Hope S. Rugo, M.D.,
Open Clinical Trials: What s Out There Now Paula D. Ryan, MD, PhD
 Open Clinical Trials: What s Out There Now Paula D. Ryan, MD, PhD Hanahan and Weinberg, 2000 Acquired Capabilities of Cancer Clinical Trials When should I consider a clinical trial? How do I find the right
Open Clinical Trials: What s Out There Now Paula D. Ryan, MD, PhD Hanahan and Weinberg, 2000 Acquired Capabilities of Cancer Clinical Trials When should I consider a clinical trial? How do I find the right
Outline of the presentation
 Outline of the presentation Breast cancer subtypes and classification Clinical need in estrogen-positive (ER+) metastatic breast cancer (mbc) Sulforaphane and SFX-01: the preclinical evidence STEM Phase
Outline of the presentation Breast cancer subtypes and classification Clinical need in estrogen-positive (ER+) metastatic breast cancer (mbc) Sulforaphane and SFX-01: the preclinical evidence STEM Phase
Update on New Perspectives in Endocrine-Sensitive Breast Cancer. James R. Waisman, MD
 Update on New Perspectives in Endocrine-Sensitive Breast Cancer James R. Waisman, MD Nothing to disclose DISCLOSURE TAILORx Oncotype Recurrence Score TAILORx Study Design Sparano, J Clin Oncol 2008;26:721-728
Update on New Perspectives in Endocrine-Sensitive Breast Cancer James R. Waisman, MD Nothing to disclose DISCLOSURE TAILORx Oncotype Recurrence Score TAILORx Study Design Sparano, J Clin Oncol 2008;26:721-728
Pharmacology Updates in Breast Cancer Chris Vaklavas, M.D.
 Pharmacology Updates in Breast Cancer Chris Vaklavas, M.D. Assistant Professor Department of Medicine, Division of Hematology/Oncology University of Alabama at Birmingham NP2540M 1802 6th Avenue South
Pharmacology Updates in Breast Cancer Chris Vaklavas, M.D. Assistant Professor Department of Medicine, Division of Hematology/Oncology University of Alabama at Birmingham NP2540M 1802 6th Avenue South
Sponsor / Company: Sanofi Drug substance(s): Docetaxel (Taxotere )
 These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert in the country of prescription. Sponsor / Company: Sanofi Drug substance(s):
These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert in the country of prescription. Sponsor / Company: Sanofi Drug substance(s):
Chemotherapy and Immunotherapy in Combination Non-Small Cell Lung Cancer (NSCLC)
 Chemotherapy and Immunotherapy in Combination Non-Small Cell Lung Cancer (NSCLC) Jeffrey Crawford, MD George Barth Geller Professor for Research in Cancer Co-Program Leader, Solid Tumor Therapeutics Program
Chemotherapy and Immunotherapy in Combination Non-Small Cell Lung Cancer (NSCLC) Jeffrey Crawford, MD George Barth Geller Professor for Research in Cancer Co-Program Leader, Solid Tumor Therapeutics Program
OUR EXPERIENCES WITH ERLOTINIB IN SECOND AND THIRD LINE TREATMENT PATIENTS WITH ADVANCED STAGE IIIB/ IV NON-SMALL CELL LUNG CANCER
 & OUR EXPERIENCES WITH ERLOTINIB IN SECOND AND THIRD LINE TREATMENT PATIENTS WITH ADVANCED STAGE IIIB/ IV NON-SMALL CELL LUNG CANCER Interim Data Report of TRUST study on patients from Bosnia and Herzegovina
& OUR EXPERIENCES WITH ERLOTINIB IN SECOND AND THIRD LINE TREATMENT PATIENTS WITH ADVANCED STAGE IIIB/ IV NON-SMALL CELL LUNG CANCER Interim Data Report of TRUST study on patients from Bosnia and Herzegovina
Sesiones interhospitalarias de cáncer de mama. Revisión bibliográfica 4º trimestre 2015
 Sesiones interhospitalarias de cáncer de mama Revisión bibliográfica 4º trimestre 2015 Selected papers Prospective Validation of a 21-Gene Expression Assay in Breast Cancer TAILORx. NEJM 2015 OS for fulvestrant
Sesiones interhospitalarias de cáncer de mama Revisión bibliográfica 4º trimestre 2015 Selected papers Prospective Validation of a 21-Gene Expression Assay in Breast Cancer TAILORx. NEJM 2015 OS for fulvestrant
What is new in HR+ Breast Cancer? Olivia Pagani Breast Unit and Institute of oncology of Southern Switzerland
 What is new in HR+ Breast Cancer? Olivia Pagani Breast Unit and Institute of oncology of Southern Switzerland Outline Early breast cancer Advanced breast cancer Open questions Outline Early breast cancer
What is new in HR+ Breast Cancer? Olivia Pagani Breast Unit and Institute of oncology of Southern Switzerland Outline Early breast cancer Advanced breast cancer Open questions Outline Early breast cancer
Technology appraisal guidance Published: 20 December 2017 nice.org.uk/guidance/ta496
 Ribociclib with an aromatase inhibitor for previously untreated, hormone receptor- positive, HER2-negative, e, locally advanced or metastatic breast cancer Technology appraisal guidance Published: 20 December
Ribociclib with an aromatase inhibitor for previously untreated, hormone receptor- positive, HER2-negative, e, locally advanced or metastatic breast cancer Technology appraisal guidance Published: 20 December
METRIC Study Key Eligibility Criteria
 The METRIC Study METRIC Study Key Eligibility Criteria The pivotal METRIC Study is evaluating glembatumumab vedotin in patients with gpnmb overexpressing metastatic triple-negative breast cancer (TNBC).
The METRIC Study METRIC Study Key Eligibility Criteria The pivotal METRIC Study is evaluating glembatumumab vedotin in patients with gpnmb overexpressing metastatic triple-negative breast cancer (TNBC).
Evolving Paradigms in HER2+ MBC: Strategies for Individualizing Therapy with Available Agents
 Evolving Paradigms in HER2+ MBC: Strategies for Individualizing Therapy with Available Agents Kimberly L. Blackwell MD Professor Department of Medicine and Radiation Oncology Duke University Medical Center
Evolving Paradigms in HER2+ MBC: Strategies for Individualizing Therapy with Available Agents Kimberly L. Blackwell MD Professor Department of Medicine and Radiation Oncology Duke University Medical Center
Collaborative Management of Patients With Advanced Estrogen Receptor Positive Breast Cancer
 Collaborative Management of Patients With Advanced Estrogen Receptor Positive Breast Cancer Lee Schwartzberg, MD, FACP Heather Greene, FNP, AOCNP West Cancer Center Memphis, Tennessee Learning Objectives
Collaborative Management of Patients With Advanced Estrogen Receptor Positive Breast Cancer Lee Schwartzberg, MD, FACP Heather Greene, FNP, AOCNP West Cancer Center Memphis, Tennessee Learning Objectives
Endocrine treatment might NOT be the preferred option in Hrpos MBC. Dr. Mircea Dediu Sanador Hospital Bucharest Summer School Bucharest 2015
 Endocrine treatment might NOT be the preferred option in Hrpos MBC Dr. Mircea Dediu Sanador Hospital Bucharest Summer School Bucharest 2015 Overall survival not improved by the AI treatment Benefit in
Endocrine treatment might NOT be the preferred option in Hrpos MBC Dr. Mircea Dediu Sanador Hospital Bucharest Summer School Bucharest 2015 Overall survival not improved by the AI treatment Benefit in
Mechanisms of hormone drug resistance
 Mechanisms of hormone drug resistance Ljiljana Stamatović Institute for Oncology and Radiology of Serbia Tenth UMOS Conference, Belgrade, 16-17 th May 2015. Hormone receptor-positive breast cancer (HR+
Mechanisms of hormone drug resistance Ljiljana Stamatović Institute for Oncology and Radiology of Serbia Tenth UMOS Conference, Belgrade, 16-17 th May 2015. Hormone receptor-positive breast cancer (HR+
Primary Endpoint The primary endpoint is overall survival, measured as the time in weeks from randomization to date of death due to any cause.
 CASE STUDY Randomized, Double-Blind, Phase III Trial of NES-822 plus AMO-1002 vs. AMO-1002 alone as first-line therapy in patients with advanced pancreatic cancer This is a multicenter, randomized Phase
CASE STUDY Randomized, Double-Blind, Phase III Trial of NES-822 plus AMO-1002 vs. AMO-1002 alone as first-line therapy in patients with advanced pancreatic cancer This is a multicenter, randomized Phase
pan-canadian Oncology Drug Review Final Clinical Guidance Report Everolimus (Afinitor) for Advanced Breast Cancer March 25, 2013
 pan-canadian Oncology Drug Review Final Clinical Guidance Report Everolimus (Afinitor) for Advanced Breast Cancer March 25, 2013 DISCLAIMER Not a Substitute for Professional Advice This report is primarily
pan-canadian Oncology Drug Review Final Clinical Guidance Report Everolimus (Afinitor) for Advanced Breast Cancer March 25, 2013 DISCLAIMER Not a Substitute for Professional Advice This report is primarily
Oncotype DX testing in node-positive disease
 Should gene array assays be routinely used in node positive disease? Yes Christy A. Russell, MD University of Southern California Oncotype DX testing in node-positive disease 1 Validity of the Oncotype
Should gene array assays be routinely used in node positive disease? Yes Christy A. Russell, MD University of Southern California Oncotype DX testing in node-positive disease 1 Validity of the Oncotype
SYNOPSIS PROTOCOL TALBOT
 SYNOPSIS PROTOCOL TALBOT A) CLINICAL TRIAL IDENTIFICATION SPONSOR - PROTOCOL CODE NUMBER : VERSION: SYNOPSIS V4.0-30/06/2015 TRIAL TITLE : Open-label, randomized, multicenter, phase II study, comparing
SYNOPSIS PROTOCOL TALBOT A) CLINICAL TRIAL IDENTIFICATION SPONSOR - PROTOCOL CODE NUMBER : VERSION: SYNOPSIS V4.0-30/06/2015 TRIAL TITLE : Open-label, randomized, multicenter, phase II study, comparing
Aggiornamenti tra ricerca e clinica: il carcinoma della mammella
 Aggiornamenti tra ricerca e clinica: il carcinoma della mammella Filippo Montemurro Unit of (INCO) Fondazione del Piemonte per l Oncologia Candiolo Cancer Institute (IRCCs) Research Needs in Breast Cancer
Aggiornamenti tra ricerca e clinica: il carcinoma della mammella Filippo Montemurro Unit of (INCO) Fondazione del Piemonte per l Oncologia Candiolo Cancer Institute (IRCCs) Research Needs in Breast Cancer
8/8/2011. PONDERing the Need to TAILOR Adjuvant Chemotherapy in ER+ Node Positive Breast Cancer. Overview
 Overview PONDERing the Need to TAILOR Adjuvant in ER+ Node Positive Breast Cancer Jennifer K. Litton, M.D. Assistant Professor The University of Texas M. D. Anderson Cancer Center Using multigene assay
Overview PONDERing the Need to TAILOR Adjuvant in ER+ Node Positive Breast Cancer Jennifer K. Litton, M.D. Assistant Professor The University of Texas M. D. Anderson Cancer Center Using multigene assay
Breast Cancer: ASCO Poster Review
 Breast Cancer: ASCO Poster Review Carmen Criscitiello, MD, PhD Istituto Europeo di Oncologia Milano HER2+ SUBTYPE Research questions in early HER2+ BC De-escalation of toxicity without compromising efficacy
Breast Cancer: ASCO Poster Review Carmen Criscitiello, MD, PhD Istituto Europeo di Oncologia Milano HER2+ SUBTYPE Research questions in early HER2+ BC De-escalation of toxicity without compromising efficacy
General Information, efficacy and safety data
 Horizon Scanning in Oncology Horizon Scanning in Oncology 29 th Prioritization 4 th quarter 2016 General Information, efficacy and safety data Nicole Grössmann Sarah Wolf Claudia Wild Please note: Within
Horizon Scanning in Oncology Horizon Scanning in Oncology 29 th Prioritization 4 th quarter 2016 General Information, efficacy and safety data Nicole Grössmann Sarah Wolf Claudia Wild Please note: Within
Breast cancer treatment
 Report from the San Antonio Breast Cancer Symposium Breast cancer treatment Determining the best options for select patient groups Sara Soldera, MD, Resident; Nathaniel Bouganim, MD, FRCPC, Medical Oncologist;
Report from the San Antonio Breast Cancer Symposium Breast cancer treatment Determining the best options for select patient groups Sara Soldera, MD, Resident; Nathaniel Bouganim, MD, FRCPC, Medical Oncologist;
trial update clinical
 trial update clinical by John W. Mucenski, BS, PharmD, Director of Pharmacy Operations, UPMC Cancer Centers The treatment outcome for patients with relapsed or refractory cervical carcinoma remains dismal.
trial update clinical by John W. Mucenski, BS, PharmD, Director of Pharmacy Operations, UPMC Cancer Centers The treatment outcome for patients with relapsed or refractory cervical carcinoma remains dismal.
Case #2: Hormonal Therapy for Advanced Premenopausal Breast Cancer
 Case #2: Hormonal Therapy for Advanced Premenopausal Breast Cancer Fellow Presenter: Katherine Clifton, MD Faculty Discussant: Debu Tripathy, MD 7 th Annual June 1, 2018 Topics to Be Discussed: Staging
Case #2: Hormonal Therapy for Advanced Premenopausal Breast Cancer Fellow Presenter: Katherine Clifton, MD Faculty Discussant: Debu Tripathy, MD 7 th Annual June 1, 2018 Topics to Be Discussed: Staging
Terapia adiuvante con inibitori delle Kinasi Cliclina Dipendenti 4/6: quale futuro? Filippo Montemurro
 Terapia adiuvante con inibitori delle Kinasi Cliclina Dipendenti 4/6: quale futuro? Filippo Montemurro Unit of Investigative Clinical Oncology Istituto di Candiolo (IRCCS) Disclosures Speaker s Honoraria
Terapia adiuvante con inibitori delle Kinasi Cliclina Dipendenti 4/6: quale futuro? Filippo Montemurro Unit of Investigative Clinical Oncology Istituto di Candiolo (IRCCS) Disclosures Speaker s Honoraria
This clinical study synopsis is provided in line with Boehringer Ingelheim s Policy on Transparency and Publication of Clinical Study Data.
 abcd Clinical Study Synopsis for Public Disclosure This clinical study synopsis is provided in line with s Policy on Transparency and Publication of Clinical Study Data. The synopsis which is part of the
abcd Clinical Study Synopsis for Public Disclosure This clinical study synopsis is provided in line with s Policy on Transparency and Publication of Clinical Study Data. The synopsis which is part of the
Supplementary Online Content
 Supplementary Online Content Spring LM, Gupta A, Reynolds KL, et al. Neoadjuvant endocrine therapy for estrogen receptor positive breast cancer: a systematic review and meta-analysis. JAMA Oncol. Published
Supplementary Online Content Spring LM, Gupta A, Reynolds KL, et al. Neoadjuvant endocrine therapy for estrogen receptor positive breast cancer: a systematic review and meta-analysis. JAMA Oncol. Published
Clinical Trial Results Database Page 1
 Page 1 Sponsor Novartis UK Limited Generic Drug Name Letrozole/FEM345 Therapeutic Area of Trial Localized ER and/or PgR receptor positive breast cancer Study Number CFEM345EGB07 Protocol Title This study
Page 1 Sponsor Novartis UK Limited Generic Drug Name Letrozole/FEM345 Therapeutic Area of Trial Localized ER and/or PgR receptor positive breast cancer Study Number CFEM345EGB07 Protocol Title This study
Manejo do câncer de mama RH+ na adjuvância: o que há de novo?
 II Simpósio Internacional de Câncer de Mama para o Oncologista Clínico Manejo do câncer de mama RH+ na adjuvância: o que há de novo? INGRID A. MAYER, MD, MSCI Assistant Professor of Medicine Director,
II Simpósio Internacional de Câncer de Mama para o Oncologista Clínico Manejo do câncer de mama RH+ na adjuvância: o que há de novo? INGRID A. MAYER, MD, MSCI Assistant Professor of Medicine Director,
Cetuximab plus 5-FU/FA/oxaliplatin (FOLFOX-4) in the first-line treatment of metastatic colorectal cancer: a large-scale Phase II study (OPUS)
 Cetuximab plus 5-FU/FA/oxaliplatin (FOLFOX-4) in the first-line treatment of metastatic colorectal cancer: a large-scale Phase II study (OPUS) C Bokemeyer, E Staroslawska, A Makhson, I Bondarenko, JT Hartmann,
Cetuximab plus 5-FU/FA/oxaliplatin (FOLFOX-4) in the first-line treatment of metastatic colorectal cancer: a large-scale Phase II study (OPUS) C Bokemeyer, E Staroslawska, A Makhson, I Bondarenko, JT Hartmann,
New Targeted Agents Demonstrate Greater Efficacy and Tolerability in the Treatment of HER2-positive Breast Cancer
 New Evidence reports on presentations given at ASCO 2012 New Targeted Agents Demonstrate Greater Efficacy and Tolerability in the Treatment of HER2-positive Breast Cancer Presentations at ASCO 2012 Breast
New Evidence reports on presentations given at ASCO 2012 New Targeted Agents Demonstrate Greater Efficacy and Tolerability in the Treatment of HER2-positive Breast Cancer Presentations at ASCO 2012 Breast
Cohort D Xentuzumab + abemaciclib + fulvestrant (500 mg/month) Key exclusion criteria RP2D-4 NSCLC. Cohort F Xentuzumab + abemaciclib + fulvestrant
 A phase Ib trial of xentuzumab and abemaciclib in patients with locally advanced or metastatic solid tumors, including hormone receptor-positive, HER2-negative breast cancer (plus endocrine therapy) Douglas
A phase Ib trial of xentuzumab and abemaciclib in patients with locally advanced or metastatic solid tumors, including hormone receptor-positive, HER2-negative breast cancer (plus endocrine therapy) Douglas
Management of hormone-receptor positive human epidermal receptor 2 negative advanced or metastatic breast cancers
 Review Article Page 1 of 10 Management of hormone-receptor positive human epidermal receptor 2 negative advanced or metastatic breast cancers Roger K. C. Ngan Department of Clinical Oncology, Queen Elizabeth
Review Article Page 1 of 10 Management of hormone-receptor positive human epidermal receptor 2 negative advanced or metastatic breast cancers Roger K. C. Ngan Department of Clinical Oncology, Queen Elizabeth
https://clinicaltrials.gov/ct2/show/nct ?term=inge-b&rank=1
 Seite 1 von 6 A service of the U.S. National Institutes of Health Now Available: Final Rule for FDAAA 801 and NIH Policy on Clinical Trial Reporting Trial record 1 of 1 for: INGE-B Previous Study Return
Seite 1 von 6 A service of the U.S. National Institutes of Health Now Available: Final Rule for FDAAA 801 and NIH Policy on Clinical Trial Reporting Trial record 1 of 1 for: INGE-B Previous Study Return
Endocrine Therapy 2017: Is There a Better Single Agent and when Should we Use it?
 Endocrine Therapy 2017: Is There a Better Single Agent and when Should we Use it? ET1 ET2 ET3 Targeted agent 1 Targeted agent 2 Hope S. Rugo, MD Director, Breast Oncology and Clinical Trials Education
Endocrine Therapy 2017: Is There a Better Single Agent and when Should we Use it? ET1 ET2 ET3 Targeted agent 1 Targeted agent 2 Hope S. Rugo, MD Director, Breast Oncology and Clinical Trials Education
pcodr EXPERT REVIEW COMMITTEE (perc) INITIAL RECOMMENDATION
 pcodr EXPERT REVIEW COMMITTEE (perc) INITIAL RECOMMENDATION The pan-canadian Oncology Drug Review (pcodr) was established by Canada s provincial and territorial Ministries of Health (with the exception
pcodr EXPERT REVIEW COMMITTEE (perc) INITIAL RECOMMENDATION The pan-canadian Oncology Drug Review (pcodr) was established by Canada s provincial and territorial Ministries of Health (with the exception
Introduction. Wilfred Truin 1 Rudi M. H. Roumen. Vivianne C. G. Tjan-Heijnen 2 Adri C. Voogd
 Breast Cancer Res Treat (2017) 164:133 138 DOI 10.1007/s10549-017-4220-x EPIDEMIOLOGY Estrogen and progesterone receptor expression levels do not differ between lobular and ductal carcinoma in patients
Breast Cancer Res Treat (2017) 164:133 138 DOI 10.1007/s10549-017-4220-x EPIDEMIOLOGY Estrogen and progesterone receptor expression levels do not differ between lobular and ductal carcinoma in patients
Implications of Progesterone Receptor Status for the Biology and Prognosis of Breast Cancers
 日大医誌 75 (1): 10 15 (2016) 10 Original Article Implications of Progesterone Receptor Status for the Biology and Prognosis of Breast Cancers Naotaka Uchida 1), Yasuki Matsui 1), Takeshi Notsu 1) and Manabu
日大医誌 75 (1): 10 15 (2016) 10 Original Article Implications of Progesterone Receptor Status for the Biology and Prognosis of Breast Cancers Naotaka Uchida 1), Yasuki Matsui 1), Takeshi Notsu 1) and Manabu
The efficacy of second-line hormone therapy for recurrence during adjuvant hormone therapy for breast cancer
 517734TAM6210.1177/1758834013517734Therapeutic Advances in Medical OncologyR Mori and Y Nagao research-article2013 Therapeutic Advances in Medical Oncology Original Research The efficacy of second-line
517734TAM6210.1177/1758834013517734Therapeutic Advances in Medical OncologyR Mori and Y Nagao research-article2013 Therapeutic Advances in Medical Oncology Original Research The efficacy of second-line
Edith A. Perez, Ahmad Awada, Joyce O Shaughnessy, Hope Rugo, Chris Twelves, Seock-Ah Im, Carol Zhao, Ute Hoch, Alison L. Hannah, Javier Cortes
 BEACON: A Phase 3 Open-label, Randomized, Multicenter Study of Etirinotecan Pegol (EP) versus Treatment of Physician s Choice (TPC) in Patients With Locally Recurrent or Metastatic Breast Cancer Previously
BEACON: A Phase 3 Open-label, Randomized, Multicenter Study of Etirinotecan Pegol (EP) versus Treatment of Physician s Choice (TPC) in Patients With Locally Recurrent or Metastatic Breast Cancer Previously
The next wave of successful drug therapy strategies in HER2-positive breast cancer. Hans Wildiers University Hospitals Leuven Belgium
 The next wave of successful drug therapy strategies in HER2-positive breast cancer Hans Wildiers University Hospitals Leuven Belgium Trastuzumab in 1st Line significantly improved the prognosis of HER2-positive
The next wave of successful drug therapy strategies in HER2-positive breast cancer Hans Wildiers University Hospitals Leuven Belgium Trastuzumab in 1st Line significantly improved the prognosis of HER2-positive
William J. Gradishar MD
 Northwestern University Feinberg School of Medicine Adjuvant Endocrine Therapy For Postmenopausal Women SOBO 2013 William J. Gradishar MD Betsy Bramsen Professor of Breast Oncology Director, Maggie Daley
Northwestern University Feinberg School of Medicine Adjuvant Endocrine Therapy For Postmenopausal Women SOBO 2013 William J. Gradishar MD Betsy Bramsen Professor of Breast Oncology Director, Maggie Daley
Verzenio (abemaciclib) NEW PRODUCT SLIDESHOW
 Verzenio (abemaciclib) NEW PRODUCT SLIDESHOW Introduction Brand name: Verzenio Generic name: Abemaciclib Pharmacological class: Kinase inhibitor Strength and Formulation: 50mg, 100mg, 150mg, 200mg; tabs
Verzenio (abemaciclib) NEW PRODUCT SLIDESHOW Introduction Brand name: Verzenio Generic name: Abemaciclib Pharmacological class: Kinase inhibitor Strength and Formulation: 50mg, 100mg, 150mg, 200mg; tabs
Metastatic Breast Cancer What is new? Subtypes and variation?
 Metastatic Breast Cancer What is new? Subtypes and variation? Anne Blaes, MD, MS University of Minnesota, Division of Hematology/Oncology Director, Adult Cancer Survivor Program Current estimates for metastatic
Metastatic Breast Cancer What is new? Subtypes and variation? Anne Blaes, MD, MS University of Minnesota, Division of Hematology/Oncology Director, Adult Cancer Survivor Program Current estimates for metastatic
DR LUIS MANSO UNIDAD TUMORES DE MAMA Y GINECOLÓGICOS HOSPITAL 12 DE OCTUBRE MADRID
 DR LUIS MANSO UNIDAD TUMORES DE MAMA Y GINECOLÓGICOS HOSPITAL 12 DE OCTUBRE MADRID RESUMEN DE ARTICULOS THERESA BOLERO 3 NOAH UP-DATE GEPAR SIXTO RADIOTHERAPY EBCTCG CTCs MISCELANEAS Lancet Oncol 2014;
DR LUIS MANSO UNIDAD TUMORES DE MAMA Y GINECOLÓGICOS HOSPITAL 12 DE OCTUBRE MADRID RESUMEN DE ARTICULOS THERESA BOLERO 3 NOAH UP-DATE GEPAR SIXTO RADIOTHERAPY EBCTCG CTCs MISCELANEAS Lancet Oncol 2014;
Supplementary Online Content
 Supplementary Online Content Powles T, O Donnell PH, Massard C, et al. Efficacy and safety of durvalumab in locally advanced or metastatic urothelial carcinoma: updated results from a phase 1/2 openlabel
Supplementary Online Content Powles T, O Donnell PH, Massard C, et al. Efficacy and safety of durvalumab in locally advanced or metastatic urothelial carcinoma: updated results from a phase 1/2 openlabel
Advances in Breast Cancer Therapeutics in the Adjuvant and Metastatic Settings. Eve Rodler, MD University of California at Davis October 2016
 Advances in Breast Cancer Therapeutics in the Adjuvant and Metastatic Settings Eve Rodler, MD University of California at Davis October 2016 17th Annual Advances in Oncology September 30-October 1, 2016
Advances in Breast Cancer Therapeutics in the Adjuvant and Metastatic Settings Eve Rodler, MD University of California at Davis October 2016 17th Annual Advances in Oncology September 30-October 1, 2016
Trial of Letrozole + Palbociclib/Placebo in Metastatic Endometrial Cancer
 Find Studies About Studies Submit Studies Resources About Site Trial of Letrozole + Palbociclib/Placebo in Metastatic Endometrial Cancer The safety and scientific validity of this study is the responsibility
Find Studies About Studies Submit Studies Resources About Site Trial of Letrozole + Palbociclib/Placebo in Metastatic Endometrial Cancer The safety and scientific validity of this study is the responsibility
LONDON CANCER NEW DRUGS GROUP RAPID REVIEW. Erlotinib for the third or fourth-line treatment of NSCLC January 2012
 Disease background LONDON CANCER NEW DRUGS GROUP RAPID REVIEW Erlotinib for the third or fourth-line treatment of NSCLC January 2012 Lung cancer is the second most common cancer in the UK (after breast),
Disease background LONDON CANCER NEW DRUGS GROUP RAPID REVIEW Erlotinib for the third or fourth-line treatment of NSCLC January 2012 Lung cancer is the second most common cancer in the UK (after breast),
The issues that will be resolved through PMCs include the the requalification of bioburden test.
 BLA 125409/0_ Perjeta (pertuzumab) 4 patients with normal renal function. No dose adjustment can be recommended for patients with severe renal impairment because of the limited pharmacokinetic data available.
BLA 125409/0_ Perjeta (pertuzumab) 4 patients with normal renal function. No dose adjustment can be recommended for patients with severe renal impairment because of the limited pharmacokinetic data available.
Breast cancer update. Iryna Kuchuk, MD Oncology department Meir Medical Center
 Breast cancer update Iryna Kuchuk, MD Oncology department Meir Medical Center Overview Cancer Death Rates* Among Women, US,1930-2009 Factors Associated with Reduction In Breast Cancer Mortality Early
Breast cancer update Iryna Kuchuk, MD Oncology department Meir Medical Center Overview Cancer Death Rates* Among Women, US,1930-2009 Factors Associated with Reduction In Breast Cancer Mortality Early
Study Period: 27 March 2008 (first subject enrolled) to 05 May 2010 (data cutoff date for primary analysis)
 Date: 20 July 2011 Page 2 of 3375 2. SYNOPSIS Name of Sponsor: mgen Inc., Thousand Oaks, C US Name of Finished Product: Not applicable Name of ctive Ingredient: Ganitumab (MG 479) Title of Study: n International,
Date: 20 July 2011 Page 2 of 3375 2. SYNOPSIS Name of Sponsor: mgen Inc., Thousand Oaks, C US Name of Finished Product: Not applicable Name of ctive Ingredient: Ganitumab (MG 479) Title of Study: n International,
Best of San Antonio 2008
 Best of San Antonio 2008 Ellie Guardino, MD/PhD Assistant Professor Stanford University BIG 1 98: a randomized double blind phase III study evaluating letrozole and tamoxifen given in sequence as adjuvant
Best of San Antonio 2008 Ellie Guardino, MD/PhD Assistant Professor Stanford University BIG 1 98: a randomized double blind phase III study evaluating letrozole and tamoxifen given in sequence as adjuvant
This clinical study synopsis is provided in line with Boehringer Ingelheim s Policy on Transparency and Publication of Clinical Study Data.
 abcd Clinical Study for Public Disclosure This clinical study synopsis is provided in line with s Policy on Transparency and Publication of Clinical Study Data. The synopsis which is part of the clinical
abcd Clinical Study for Public Disclosure This clinical study synopsis is provided in line with s Policy on Transparency and Publication of Clinical Study Data. The synopsis which is part of the clinical
Long-term safety and efficacy of vismodegib in patients with advanced basal cell carcinoma (BCC): 24-month update of the pivotal ERIVANCE BCC study
 Long-term safety and efficacy of vismodegib in patients with advanced basal cell carcinoma (BCC): 24-month update of the pivotal ERIVANCE BCC study A Sekulic, 1 MR Migden, 2 AE Oro, 3 L Dirix, 4 K Lewis,
Long-term safety and efficacy of vismodegib in patients with advanced basal cell carcinoma (BCC): 24-month update of the pivotal ERIVANCE BCC study A Sekulic, 1 MR Migden, 2 AE Oro, 3 L Dirix, 4 K Lewis,
Lead team presentation Eribulin for treating locally advanced or metastatic breast cancer after two or more prior chemotherapy regimens STA
 For projector and public [noacic] Lead team presentation Eribulin for treating locally advanced or metastatic breast cancer after two or more prior chemotherapy regimens STA 1 st Appraisal Committee meeting
For projector and public [noacic] Lead team presentation Eribulin for treating locally advanced or metastatic breast cancer after two or more prior chemotherapy regimens STA 1 st Appraisal Committee meeting
CDK4/6 inhibitors in advanced hormone receptor-positive breast cancer
 Perspective CDK4/6 inhibitors in advanced hormone receptor-positive breast cancer Romualdo Barroso-Sousa, Sara M. Tolaney Department of Medical Oncology, Dana-Farber Cancer Institute, Boston, MA, USA Correspondence
Perspective CDK4/6 inhibitors in advanced hormone receptor-positive breast cancer Romualdo Barroso-Sousa, Sara M. Tolaney Department of Medical Oncology, Dana-Farber Cancer Institute, Boston, MA, USA Correspondence
LOTUS (NCT ) randomized phase II trial
 Overall survival update of the double-blind placebocontrolled randomized phase 2 LOTUS trial of firstline ipatasertib + paclitaxel for locally advanced/metastatic triple-negative breast cancer Rebecca
Overall survival update of the double-blind placebocontrolled randomized phase 2 LOTUS trial of firstline ipatasertib + paclitaxel for locally advanced/metastatic triple-negative breast cancer Rebecca
Plattenepithelkarzinom des Ösophagus, 1 st -line
 Plattenepithelkarzinom des Ösophagus, 1 st -line AIO-STO-0309 An open-label, randomized phase III trial of cisplatin and 5-fluorouracil with or without panitumumab for patients with nonresectable, advanced
Plattenepithelkarzinom des Ösophagus, 1 st -line AIO-STO-0309 An open-label, randomized phase III trial of cisplatin and 5-fluorouracil with or without panitumumab for patients with nonresectable, advanced
ATAC Trial. 10 year median follow-up data. Approval Code: AZT-ARIM-10005
 ATAC Trial 10 year median follow-up data Approval Code: AZT-ARIM-10005 Background FDA post-approval commitment analysis to update DFS, TTR, OS and Safety Prof. Jack Cuzick on behalf of ATAC/LATTE Trialists
ATAC Trial 10 year median follow-up data Approval Code: AZT-ARIM-10005 Background FDA post-approval commitment analysis to update DFS, TTR, OS and Safety Prof. Jack Cuzick on behalf of ATAC/LATTE Trialists
pan-canadian Oncology Drug Review Initial Clinical Guidance Report Fulvestrant (Faslodex) for Metastatic Breast Cancer November 30, 2017
 pan-canadian Oncology Drug Review Initial Clinical Guidance Report Fulvestrant (Faslodex) for Metastatic Breast Cancer November 30, 2017 DISCLAIMER Not a Substitute for Professional Advice This report
pan-canadian Oncology Drug Review Initial Clinical Guidance Report Fulvestrant (Faslodex) for Metastatic Breast Cancer November 30, 2017 DISCLAIMER Not a Substitute for Professional Advice This report
The Oncotype DX Assay in the Contemporary Management of Invasive Early-stage Breast Cancer
 The Oncotype DX Assay in the Contemporary Management of Invasive Early-stage Breast Cancer Cancer The Biology Century Understanding and treating the underlying tumor biology Cancer genetic studies demonstrate
The Oncotype DX Assay in the Contemporary Management of Invasive Early-stage Breast Cancer Cancer The Biology Century Understanding and treating the underlying tumor biology Cancer genetic studies demonstrate
Page. Objectives: Hormone Therapy Resistance: Challenges and Opportunities. Research Support From Merck
 Hormone Therapy Resistance: Challenges and Opportunities Pamela. N. Munster, MD University of California, San Francisco Financial Disclosures Research Support From Merck Objectives: Understanding the current
Hormone Therapy Resistance: Challenges and Opportunities Pamela. N. Munster, MD University of California, San Francisco Financial Disclosures Research Support From Merck Objectives: Understanding the current
Johns Hopkins Clinical Update Webinar
 Johns Hopkins Clinical Update Webinar Ben Ho Park, M.D., Ph.D. Department of Oncology Johns Hopkins University February 2015 This presentation is the intellectual property of the author/presenter. Contact
Johns Hopkins Clinical Update Webinar Ben Ho Park, M.D., Ph.D. Department of Oncology Johns Hopkins University February 2015 This presentation is the intellectual property of the author/presenter. Contact
Extended Hormonal Therapy
 Extended Hormonal Therapy Dr. Caroline Lohrisch, Medical Oncologist, BC Cancer Agency Vancouver Centre November 1, 2014 www.fpon.ca Optimal Endocrine Therapy for Women with Hormone Receptor Positive Early
Extended Hormonal Therapy Dr. Caroline Lohrisch, Medical Oncologist, BC Cancer Agency Vancouver Centre November 1, 2014 www.fpon.ca Optimal Endocrine Therapy for Women with Hormone Receptor Positive Early
COMETS: COlorectal MEtastatic Two Sequences
 COMETS: COlorectal MEtastatic Two Sequences A Phase III Multicenter Trial Comparing Two Different Sequences of Second/Third Line Therapy (Irinotecan/Cetuximab Followed By FOLFOX-4 vs. FOLFOX-4 Followed
COMETS: COlorectal MEtastatic Two Sequences A Phase III Multicenter Trial Comparing Two Different Sequences of Second/Third Line Therapy (Irinotecan/Cetuximab Followed By FOLFOX-4 vs. FOLFOX-4 Followed
pan-canadian Oncology Drug Review Final Clinical Guidance Report Fulvestrant (Faslodex) for Metastatic Breast Cancer February 1, 2018
 pan-canadian Oncology Drug Review Final Clinical Guidance Report Fulvestrant (Faslodex) for Metastatic Breast Cancer February 1, 2018 DISCLAIMER Not a Substitute for Professional Advice This report is
pan-canadian Oncology Drug Review Final Clinical Guidance Report Fulvestrant (Faslodex) for Metastatic Breast Cancer February 1, 2018 DISCLAIMER Not a Substitute for Professional Advice This report is
Technology appraisal guidance Published: 27 June 2012 nice.org.uk/guidance/ta257
 Lapatinib or trastuzumab in combination with an aromatase inhibitor for the firstline treatment of metastatic hormone- receptor-positive e breast cancer that overexpresses HER2 Technology appraisal guidance
Lapatinib or trastuzumab in combination with an aromatase inhibitor for the firstline treatment of metastatic hormone- receptor-positive e breast cancer that overexpresses HER2 Technology appraisal guidance
Dennis J Slamon, MD, PhD
 I N T E R V I E W Dennis J Slamon, MD, PhD Dr Slamon is Professor of Medicine, Chief of the Division of Hematology/Oncology and Director of Clinical and Translational Research at UCLA s David Geffen School
I N T E R V I E W Dennis J Slamon, MD, PhD Dr Slamon is Professor of Medicine, Chief of the Division of Hematology/Oncology and Director of Clinical and Translational Research at UCLA s David Geffen School
Immunotherapy in the Adjuvant Setting for Melanoma: What You Need to Know
 Immunotherapy in the Adjuvant Setting for Melanoma: What You Need to Know Jeffrey Weber, MD, PhD Laura and Isaac Perlmutter Cancer Center NYU Langone Medical Center New York, New York What Is the Current
Immunotherapy in the Adjuvant Setting for Melanoma: What You Need to Know Jeffrey Weber, MD, PhD Laura and Isaac Perlmutter Cancer Center NYU Langone Medical Center New York, New York What Is the Current
When is Chemotherapy indicated in Advanced Luminal Breast Cancer?
 When is Chemotherapy indicated in Advanced Luminal Breast Cancer? Soo-Chin Lee Head & Senior Consultant Department of Haematology-Oncology Clinical Care National University Cancer Institute, Singapore
When is Chemotherapy indicated in Advanced Luminal Breast Cancer? Soo-Chin Lee Head & Senior Consultant Department of Haematology-Oncology Clinical Care National University Cancer Institute, Singapore
Review of adjuvant and neo-adjuvant abstracts from SABCS 2011 January 7 th 2012
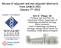 Review of adjuvant and neo-adjuvant abstracts from SABCS 2011 January 7 th 2012 Ruth M. O Regan, MD Professor and Vice-Chair for Educational Affairs, Department of Hematology and Medical Oncology, Emory
Review of adjuvant and neo-adjuvant abstracts from SABCS 2011 January 7 th 2012 Ruth M. O Regan, MD Professor and Vice-Chair for Educational Affairs, Department of Hematology and Medical Oncology, Emory
Disease Update: Metastatic Breast Cancer
 Disease Update: Metastatic Breast Cancer Aimee Faso, PharmD, BCOP, CPP Oncology Clinical Specialist, GI/Breast UNC Hospitals and Clinics August 2015 Objectives Identify treatment choices of metastatic
Disease Update: Metastatic Breast Cancer Aimee Faso, PharmD, BCOP, CPP Oncology Clinical Specialist, GI/Breast UNC Hospitals and Clinics August 2015 Objectives Identify treatment choices of metastatic
pan-canadian Oncology Drug Review Initial Clinical Guidance Report Ribociclib (Kisqali) for Metastatic Breast Cancer March 29, 2018
 pan-canadian Oncology Drug Review Initial Clinical Guidance Report Ribociclib (Kisqali) for Metastatic Breast Cancer March 29, 2018 DISCLAIMER Not a Substitute for Professional Advice This report is primarily
pan-canadian Oncology Drug Review Initial Clinical Guidance Report Ribociclib (Kisqali) for Metastatic Breast Cancer March 29, 2018 DISCLAIMER Not a Substitute for Professional Advice This report is primarily
A new score predicting the survival of patients with spinal cord compression from myeloma
 Douglas et al. BMC Cancer 2012, 12:425 RESEARCH ARTICLE Open Access A new score predicting the survival of patients with spinal cord compression from myeloma Sarah Douglas 1, Steven E Schild 2 and Dirk
Douglas et al. BMC Cancer 2012, 12:425 RESEARCH ARTICLE Open Access A new score predicting the survival of patients with spinal cord compression from myeloma Sarah Douglas 1, Steven E Schild 2 and Dirk
pan-canadian Oncology Drug Review Final Economic Guidance Report Palbociclib (Ibrance) for Advanced Breast Cancer Resubmission November 21, 2016
 pan-canadian Oncology Drug Review Final Economic Guidance Report Palbociclib (Ibrance) for Advanced Breast Cancer Resubmission November 21, 2016 DISCLAIMER Not a Substitute for Professional Advice This
pan-canadian Oncology Drug Review Final Economic Guidance Report Palbociclib (Ibrance) for Advanced Breast Cancer Resubmission November 21, 2016 DISCLAIMER Not a Substitute for Professional Advice This
