ENDOVASCULAR REPAIR OF ABDOMINAL AORTIC ANEURYSM BRIGHAM & WOMEN S HOSPITAL, BOSTON, MA Broadcast January 20, 2005
|
|
|
- Cynthia Greer
- 6 years ago
- Views:
Transcription
1 NARRATOR ENDOVASCULAR REPAIR OF ABDOMINAL AORTIC ANEURYSM BRIGHAM & WOMEN S HOSPITAL, BOSTON, MA Broadcast January 20, 2005 An aneurysm causes localized widening or enlargement of an artery that may subsequently rupture, causing life-threatening bleeding. During this live webcast, surgeons from the Cardiovascular Center at Brigham & Women s Hospital in Boston will demonstrate a newer endovascular technique that reduces recovery time and hospital stay for patients with abdominal aortic aneurysms. Today s program is part of Brigham & Women s ongoing educational efforts to bring the latest information in health care to physicians and patients. During the program, you may send your questions to the OR surgeons at any time. Just click the direct access button on the screen. This is a Harvard Medical School CME-accredited webcast. Good afternoon, everyone. On behalf of Brigham & Women s Hospital, we d like to welcome you to our live webcast. During this time, we are focusing on the new approach, the endovascular approach, to repair of abdominal aortic aneurysm. My name is Andy Whittemore. I m the Chief Medical Officer at the Brigham & Women s Hospital and former Chief of the Division of Vascular Surgery. It is our hope that during the next hour, whether you are a patient, an interested person, or a physician, you will learn more about the nature of abdominal aortic aneurysms and the therapeutic options that are currently available for their management. My colleague, Dr. Mike Belkin, is the Chief of the Division of Vascular and Endovascular Surgery at the institution. He will be performing the surgery. Assisting him will be Dr. Ed Gravereaux, who is the Director of Endovascular Surgery at the institution. In addition, they will be assisted by Dr. Louis Willen*, who is in his final year of training in vascular surgery, and assisting me here in fielding the questions that we hope you will all submit is Dr. Chris Owens, who is in his first year of vascular training as well. Throughout this webcast, we will be responding in real time to your questions. If you have it, please send it in to our website, as seen below, to livesurgery@partners.org, and ultimately Dr. Belkin and I will provide you with the information you need. Also, continuing medical education credits are available with this live webcast during the next 24 hours. For more information, you can click on the CME button on our website as well. If we could turn to a few slides that we have prepared for you, just to introduce the subject matter. Abdominal aortic aneurysms, on slide #7, demonstrate a dilatation of the
2 aorta. In general, we are talking about the section of the aorta, down in the abdomen, that is outlined by the box on the figure to your left. It s highlighted in the middle section, which shows a normal aorta, just below the two renal arteries and above the division of the aorta into the two major arteries that supply blood to the legs. The far right hand picture is a diagram of an aneurysm that shows a dilated segment in the most common section of the aorta. Occasionally they will extend down into the leg arteries as well, but 90% of the time they are confined to the segment illustrated. The diagnosis of aneurysms, unfortunately, are made due to an incidental finding or on a physical exam. There are no specific symptoms that warn you that they are present, unless they are about to rupture, so most of these aneurysms are picked up on physical examination or incidental to a CT scan or an x-ray that is obtained for a different purpose. The risk factors that are associated with the formation of aneurysms include those that are associated with coronary artery disease; that is, a history of smoking, hypertension, diabetes, and a variety of other conditions. We are really uncertain as to their cause. The indications for repair we will expand on as the hour progresses, but in general, we wait until the aneurysms reach a size of about 5 cm in maximal diameter. Aneurysms that are smaller than this measurement don t rupture and, in general, we have recommended repair at the 5 cm mark. The gold standard for repairing aortic aneurysms is the conventional open surgical repair. This is carried out through a long midline incision and, since the aorta lies against the spinal column, in the back of the abdominal cavity, a fairly significant dissection is required to expose the operative view. The prosthetic graft is then sewn directly into the aneurysm cavity, which we open after we put clamps to stop the blood flow temporarily. This is a tried and true method that, as I ve said, we ve used for over 50 years. It has a proven track record. Once it is repaired, it s done and it s behind you. The newer approach has not been around as long, but we ll tell you more about that again during the hour. This is a photograph of the aneurysm as it appears through that long abdominal midline incision and this is the graft having been incorporated, sewn into the normal caliber aorta at the top and down to the normal caliber aorta just above the point at which the artery divides into the two leg arteries. A little over 10 years ago, Juan Perotti* introduced the current technique of an endovascular approach and this was truly innovative. Juan did his pioneering work and over the past 5 years this procedure has really become incorporated as a major modality in our armamentarium to repair aortic aneurysms. The graft is essentially inserted through two small groin incisions, as we ll show you very shortly. They are modular grafts that are of a variety of different configurations. They are seated with different arrangements at the top of the graft and Dr. Belkin will walk us through on some of the differences in the graft. We have a diagram, an animation for you to look at, which outlines the major steps in this approach. This is the aneurysm that you re looking at, at the moment, and a guide wire has been inserted just above the renal arteries. Over that guide wire is threaded a catheter and a sheath. As the sheath ultimately will be withdrawn, the graft, as you ll see,
3 will be deployed through the right iliac artery, so the graft has seated and we are now putting a guide wire up the left iliac artery into the shortened portion of the left limb. Again, a sheath is passed and the left lower segment is deployed. Patient characteristics, by and large, are important in deciding which approach to use. A patient s age has a bearing on their risk for major surgery. There are many co-morbid conditions associated with aneurysm formation, such as severe pulmonary disease, severe congestive heart failure, a number of other issues that might favor the endovascular approach, as it is a much less invasive procedure, as you will see shortly. One of the major drivers, increasingly, is patient preference. Patients have been doing their homework. We will frequently see patients who have downloaded reams from the internet and they come to us very well informed and really have already made a decision. Not everybody who would like to have an endovascular graft can have one, however. There are anatomic considerations that need to be looked at and I am going to switch over to the operating room at the moment, to Dr. Belkin, and have him walk us through what some of those considerations are. Thanks, Andy. Everyone, welcome again. Welcome to the Brigham & Women s endovascular OR suite. Thank you for participating with us today as we perform a live case of endovascular repair of an aneurysm on the internet. Andy, you re quite right, one of the most important factors is the anatomic criteria in selecting patients for endovascular care. There are a number of particular measurements we have to make in order to ensure a patient is a good candidate. The most important, perhaps, is the quality of the neck; that is, the normal aorta between the renal arteries and the aneurysm, which Andy may be able to point out during the slide, that segment has to be mm in length under ideal conditions. It must not have too much tortuosity and it should have minimal thrombus and calcium. We also have to know the diameter of the aneurysm distally, just before it branches, in order to ensure that the graft can fit through there easily and there has to be good anchor zones in the branch arteries, that is the iliac arteries below. As you can see from this slide here, we have to perform a number of very detailed measurements I order to determine if a patient is a good candidate for endovascular repair. On top of that, to design and order an appropriate graft that will fit his or her aneurysm precisely. Having shown this, let s go on and present the patient that we re going to be talking about today and operating on. This patient is a 66-year-old male whose aneurysm was first discovered in It has been followed with serial imaging studies and now has grown to 5.6 cm, which is an appropriate size for repair. His past history is remarkable for coronary artery disease, hypertension, and hyperlipidemia. His current medications include Lipitor, Lopressor, and aspirin. He has a family history of aneurysm, which is
4 very common. Approximately 20% of patients who have aneurysms will have first degree relatives who have aneurysms as well, so there is a strong family history. This slide here shows a reconstruction CT scan of his aneurysm. In the upper right corner, you can see the neck of the aneurysm and the lower renal artery, where we will implant the graft. On the lower right, you can see the belly of the aneurysm at its largest size. Down in the left lower corner, you can see the iliac arteries. So at this point, let me turn over to the field here and, before we get started, I would like to introduce the team who is participating in the repair here. First of all, I would like to introduce Dr. Ed Gravereaux, who is my colleague and partner. He is the Director of Endovascular Therapy and the Surgical Service here at the Brigham. Dr. Louis Wynn* is also here. He is our second year vascular surgery fellow. Jean Chichites* at the end of the table here is our surgical tech. At the top of the table, we have the anesthesia team, led by Dr. Stanley Leson*, who is the senior vascular anesthesiologist, along with Ty Price, who is an anesthesia resident working on the case today. Then also in the room, who you might not see from time to time, but are here and very important in the smooth flow of this case, are our vascular circulating nurses, Ursula Begoni* and Sue Driscoll. You can see they re wearing their Patriot hats. I wonder why. There must be something going on this weekend. I don t know what that s about. Over here, Steve Cannery*, who is our radiology tech, who runs our machinery during the case. Finally, in the back corner is Lisa Marie Fahey, who is our endovascular coordinator. So let s turn now to Ed, who will tell us where we are in the case. Before we do that, can we roll in that last roll-in section. This shows how we have arrived at the point we ve arrived at. We ve made two small oblique incisions and we ve dissected down through the subcutaneous tissue and ligated the bleeding vessels and exposed the arteries, as you can see here. We take time to control these arteries very carefully with these rubber loops so we can prevent any bleeding around the catheters during the course of the operation. You see the side branches are also controlled with these small loops. Once we have the vessel completely exposed and we re ready to go, we will actually cannulate this vessel and you ll see here a needle being introduced into the artery in one moment. There s the needle being introduced and then through that needle we introduce a guide wire. You can see that guide wire being passed right now. That gets us right to where we are now. This is where we are now, with the exposure complete. If you look down at the field, you can see our completed exposure. We have some sheaths and catheters in, and Ed will take over and describe exactly where we stand. Keeping that image on the screen, it s a little different from the roll-in tape we just saw, simply because of the patient s body habitus, so we have arterial exposure through the cut-downs and we actually made a very small counter-incision in the skin inferiorly, which just provides a better angle for the tracking of the stent graft device, which would avoid torquing it or kinking it. Very important. On the live fluoro screen, currently you can see a pigtail catheter at the L1-2 junction. We have a wire coming through the other
5 side. I m just going to take you north to the cardiac silhouette. We have a very stiff Amplatz guide wire, which you can see curving around just at the top of the descending thoracic aorta, which will provide perches. It s a stiff guide wire over which these devices will track. Moving back down, we ll get into position and show you an arteriograph run. That s essentially the lay of the land at this point. This is an aortogram showing this patient s aneurysm. You can see the location of the arteries and we use this as a road map for our repair. Why don t we go ahead and put our sheath in. Jean, while we re getting ready to put the sheath in, why don t you take the device out and we can get it prepped. Fogarty catheters, Fogarty clamps, one curved, one straight. So what we re going to do now is take this small sheath out and replace it with a large sheath. That sheath is an 18 French sheath, through which we will introduce the main device during the procedure and you ll see that happen in a few moments. This device is 18 French, which makes it about 6 mm in diameter. So now you ll see this larger sheath coming up the table here. On fluoroscopy, you can see the nose cone of our device. It s the sheath for the device, actually heading up, tracking over the stiff guide wire. We bring that into proximity to our pigtail catheter and we use this to orient. Okay, Jean, down below there, why don t you show how we prep this device here and maybe you can slide down there and give us a description of what the device entails. Jean is very carefully removing the device. There s an outer sheath, which is removed, and an inner cannula. The device itself is actually furled up and held in place, this device, with a suture, a constraining suture which, when unfurled, will rapidly deploy the stent graft. This model is a W.L. Gore Co. device called the Gore Excluder. It s a modular device. It s Nitinol wire, which is self-expanding, thermosensitive metal stents, over which a PTFE material is used to cover, so Jean is going to flush this out for us, remove all the air bubbles, if possible. Without touching this to anything, we re holding this in the air and I m confirming our stent graft marker positions, especially where the contralateral limb orifice is, which is the long marker.
6 This marker here, on the left, that long marker, denotes the contralateral limb, which you ll see pop open in a couple of minutes. The marks up here denote the upper portion of the graft and this is where the opening gate is and this is the bottom of the graft. It s hard to tell the anatomy of the graft right now, with it constrained within this device, but it will be quite clear when we deploy it. We re going to load this device into the sheath, as you see right here. So, as you watch, you can see the grafting placed up through the sheath. That s in good position right there. Now we re going to pull the sheath back a little bit. At this point we re going to shoot an arteriogram to localize the origin of the renal arteries and this will be our road map for the deployment of the upper end of the graft. I m going to adjust now to get our contralateral limb orifice facing the correct direction. We re just spinning it until we get that contralateral limb in the ideal position. That s looking pretty good right there. So we ll do a run here. What you can see here now is, this is the normal aorta above the aneurysm. Here s the location of the renal arteries, the two arteries to the kidneys on normal aorta, and here s the neck of the aorta above the aneurysm. The aneurysm starts down here, as you can see, so what I m going to do is mark this screen and these marks will serve as a road map for our deployment of the graft. Our goal will be to lay in the graft right about here, right below the renal arteries, and deploy out to complete the repair. I think the best way to do this is to set it up and then we ll show the deployment. Before we do that, let s look right here and show the mechanism of deployment. The way that s done is, this is a valve that I released and then there s a wire that we pull out and it s attached to the constraining sleeve. As it opens up the sleeve, the graft will deploy, just as you saw on that video, so I think the best view for the audience would be to actually see the deployment on the screen, so if we can get the live feed, we can actually watch the deployment. Watching there, you re going to see the graft open up. Here s the deployment. One, two, three, boom, there it is. So you can see now, the graft has deployed immediately below our line, which is the intended goal and the graft has deployed out into the left iliac system. On the right side, we have an open limb here, and we re going to cannulate that in order to gain access for the contralateral limb. We re removing the device now. What we re going to do is, we re going to take a very large compliant balloon out, pass it up over the guide wire, and tack down the area of the proximal graft. We ll iron it out and make sure it s well opposed to the aorta above so there s no pleats or wrinkles or anything that impairs our seal. If we go to live fluoro, you re going to see the balloon come up into position. Here s the balloon going up into
7 position and in a moment you ll see the balloon dilate with contrast. This is just for us to seat the graft in position. There you see it going up and tacking down that edge. So let s get ready on the other side with the guide wire and a Berenstein catheter. That s just used to iron out any wrinkles or folds in the graft. This graft also has hooks on the outside, which we re hoping will engage the arterial wall. Dr. Belkin will go over a little bit later some of the styles of stent graft available. There s three FDA-approved devices. Some do have hooks. Some rely on radial strength only of the stent. Some rely on bare metal stents which actually project suprarenal. Now our goal is to gain access to the contralateral open limb, in order to complete the repair. At this point, we have inserted the graft in the upper portion, in the left branch. So, Any, while we re setting this up, if any questions have come in, this might be a good time to take them. This is going along about as well as could be expected so far. We ve had some interesting questions that have come in to us. A question from a patient living here locally, in Ashland, MA, whose mother and two of her mother s sisters have had aneurysms. She is concerned about the risks of inheriting that tendency. While it is a risk, no doubt, it s more frequently inherited by first degree relatives, or your mother s siblings. It is less common for the process to be passed from one generation to another. Having said that, it does happen and I think most of us would probably advise you and your siblings to have an abdominal ultrasound at some point in your late 40s or early 50s, just to be sure. I agree with that completely, Andy. Any time you have a first degree relative in your family, if I ever see a patient has an aneurysm, I immediately urge them to have all their siblings and children checked. Let me just mention what Ed s doing here, while we re talking. He s trying to get a wire access into that open limb on the other side. You can see him tickling his way in there. This can be a tedious part of the procedure. Sometimes it takes 30 seconds and sometimes it takes minutes. In live cases, it s always minutes.
8 So I do agree with that, Andy. I think screening in first degree relatives is essential. There s another question that has come in from a little bit further away, from Switzerland, a patient who is asking about our clamping off the blood supply to the lower extremities during conventional arterial repair and also intermittently, as you ve seen here, with balloon occlusion. The answer to that is that the legs are very forgiving and can actually tolerate 4-6 hours of what we call warm ischemia, so there s rarely a problem from cutting off the circulation temporarily. True enough, Andy. The legs are very tolerant. If we have to clamp above the renal arteries, that s when we worry a little bit more about ischemic time. We like to have the arteries above the kidneys clamped for only about 30 minutes, but the legs are quite forgiving, as you said. Another question, Mike, you might address the issue of anesthesia. One of the advantages of this minimally invasive technique is that it can actually be done under a variety of different kinds of anesthesia, from local to regional to general anesthetic. I have noticed that this particular patient has been put to sleep and is undergoing general anesthesia. Can you make a comment about why that choice? That is definitely an advantage to this procedure, that it can be done under local anesthesia in thin patients. If not local, it s usually done under regional, but there s a certain amount of patient preference. Some patients just really don t want to be involved in the process at all. They don t want to know what s going on. They prefer to be asleep and we don t mind that. That s certainly acceptable if they re a good risk for general anesthesia. I would say that at this point probably 80% of our patients are repaired under regional or local anesthesia and 20% prefer to go to sleep. Great. So you re now attempting to get this wire into that short right stump.
9 Right. John, if we can take a live picture over here, I can show exactly what we re trying to achieve here. You can see, Ed s working this catheter right here. The idea is to get a wire through that circle so we can park another limb here to complete the repair. So Mike, how about the issue of inducing hypotension? Do you bother to induce hypotension when you re deploying this? With this graft, we don t. It s a very rapid deploying graft. I think if a patient was particularly hypertensive, we would try to get their main arterial pressures down around 70, but as you saw from the deployment, it s very rapid. The graft does not tend to move down at all in the arterial stream, so if they re normotensive, we don t bother doing that. That is certainly more of an issue when we perform stent grafting in the thoracic aorta, where grafts can really move quite quickly because of the pulsatility of flow in the chest. Sometimes in the thoracic aorta, if we really have a precise localization in mind, we can use a medicine that actually will stop the heart for 30 seconds, allow us to do the deployment, and then the heart will start right back up. Mike, while you re talking about the thoracic aorta, we do have a trial ongoing here. If we could go to the slide, slide #23 on our PowerPoint, we have a picture of this. Mike, do you want to comment on this at all? Great, Andy. This slide that we re looking at here, now, shows a newer technology. This is the use of endographs for repair of thoracic aneurysm, so what we ve been showing up until now is repair of an aneurysm in the abdominal aorta. This is an aneurysm up in the chest, behind or above the heart. If the aneurysm has appropriate anatomy, a graft can be deployed to repair them as well, similar in fashion to what you see here today. This is not commercially available yet. It is still an experimental or investigational technology, I would say. We happen to have protocols here at this hospital which are investigating these devices. My hope is that within 6 months or so we will have grafts which are commercially available and the technology will be more widely available. Mike, while we have that picture on the screen, you ll see there are some wire struts that are above the actual fabric and go across the left subclavian artery orifice. We have similar issues with the graft that you are using now in the infrarenal aorta, with all prototypes, and the reason we need such a long neck to seat the graft is to be sure that we
10 don t interfere with the blood flow to the kidneys. What are the issues involved with that, Mike? What are the consequences? That s a great question, Andy, and this is one of the raging debates right now among graft manufacturers and among endovascular surgeons. Certain grafts have these bare wires that extend above the graft. The graft we re using today does not have that technology. Those bare wires can be very useful in situations where you re concerned about the neck of the aorta. They can gain further perches above the aneurysm to ensure that the graft does not move or slide, which can be a problem postoperatively. Let s go back to live fluoro now and show that Ed has now put a wire through that open limb, which we were talking about before, if you can see my finger here, pointing. That s the goal. Now, what we re going to do to make sure that we re through, darn sure because sometimes those wires can fool you. They can be in back of the graft and this is only a 2-dimensional view. We re going to put a pigtail catheter within the aortic graft itself and we re going to confirm that it s present inside the graft, so we re going to spin that pigtail, which you can see right now. It spins freely and that tells us that we have excellent localization through that rim. Mike, while you re on that subject, we ve had a question come in from someone who is very well informed and is asking why you re trying to selectively cannulate the right short limb. Why not use a curved catheter of one sort or another through the left and enter retrograde into the right limb? We do that sometimes. If we cannot gain access to a contralateral limb, and sometimes it can be difficult, we will use a shepherd s hook type catheter to come over the top, as you suggest, but that s another layer of complexity. Then we have to use a snare to snare the wire within the aorta proper, so we do that but that is more or less a fall-back position. I would say we have to do that in about 5% of cases. 95% of the time, we gain easy access as Ed did here today. It took a little longer, but again, it s a live case. What we re going to do now is make a measurement to ensure that we re getting the right length limb to complete our repair.
11 This is essentially to localize the hypogastric artery, internal iliac on the right side. So I think the hypogastric is right about here. Then here s our limb, so we re going to count the number of cm from our distal seating zone, which is here. 1, 2, 3, 4, 5, 6, 7, 8, 8.5 cm, so we would want to use the shorter graft, I think. We have 8 cm out, so the 10 cm graft would give us 7 cm. The 12 would give us 10 cm, might be a little long. I think we should put the 10 cm in. Okay, so at this point we have deployed the main body and the ipsilateral limb is now out into the left iliac system. Now we re going to deploy the contralateral limb. While we have a little time here, you might address a question that has come in with regard to accessory renal arteries. How do you deal with them? There are times when patients have more than one renal artery and some of those small renal arteries can come off the aortic aneurysm or lower on the neck. They can, if these accessory extra-renal arteries are very large, supplying a large portion of the kidney, then this would be a contraindication to performing this procedure. In many cases, however, these small renal arteries actually supply only a small portion of the kidney. If they re just a couple of mm or 3 mm in size, with larger arteries above, we actually will sacrifice the smaller lower pole vessels in the name of achieving a tight seal and a good repair, so we re selective about it, but a significant lower renal artery could be a contraindication to this procedure. Good question. So now we re bringing a sheath up on the contralateral side that s going to allow us to complete the repair just as you saw in that animation earlier. Now you ll see the sheath going up and gaining access to the contralateral limb. That s perfect. Our device is being prepped. Let s take the dilator off and bring it right up. Okay, going back to live fluoro, you ll see the device going up through the sheath. If you watch that sheath on patient s right hand side, the left hand side of the screen, you ll see the device coming up through. Here it comes. Perfect. Now we re going to pull the sheath back and we re getting ready to deploy the contralateral limb, which should complete the repair. So, what you see here is, this is the sheath that we just put in and here s the graft. It runs from this marker here to this marker here. The design here is for us to match this marker up here with this large marker here, which is the main body marker and the main device.
12 We will now deploy this limb out into the right iliac system, thus creating a Y-graft to complete the repair. Here comes the deployment. We ll watch it on live fluoro. Okay, there we go. Great. Looks great. Okay, now let s take a 14.5 mm balloon and dilate up that junction site. While we re doing that changeover, Andy, if you have any additional questions we can address? We do, Mike. Just briefly, we ve had a question from Charlotte, NC, regarding the size criteria for which we recommend repair. In general, as I was saying in our introductory remarks, we usually don t recommend repair until and unless the aneurysm reaches 5 cm in maximum diameter. There are some that recommend waiting until it is 5.5 cm. The reason being that, although the repairs go along extraordinarily well under most circumstances, any intervention has its hazards and downsides. The risk of aneurysm of a rupture less than 5 cm is virtually 0, so we routinely recommend a 5 cm diameter. You might be tempted to repair it at less of a diameter, given the fact that the endovascular repair is so minimally invasive, but as we ll perhaps get to a little later, there are complications and you need to be very sure. Excuse me for one second. Can we go back to live fluoro? What we re doing now is, we re inflating a balloon, as you can see, in the gate to make sure that the two pieces of the graft, the main body and the contralateral limb, are opposed, well opposed, without any wrinkles or pleats, and that balloon there just flattens that out. Andy, I agree 100%. Our usual threshold is 5 cm. I think recent studies have shown that under intense surveillance, patients, particularly male patients, can be followed with aneurysms up to 5.5 cm, but I think the reality is, most patients, once they reach 5 cm, if they re in good shape, are anxious for repair. If we follow those patients, fully 70% of them come to aneurysm repair within a couple of years, so I feel pretty secure in recommending 5 cm for out patients. Now we re going to use that soft balloon again to tack down the limb further. Once we ve completed tacking down on each side, we will do a completion of the angiogram and see how we do. Any other questions while we re doing this, Andy? Mike, we do have another question from Kalamazoo, Michigan, where a person is asking us about the durability of this. Is this repair permanent?
13 Great question. Andy, there s a slide that looks at the advantages and disadvantages of endovascular repair. Perhaps you can bring that up. The advantages of this approach are that the patients have decreased morbidity. There s less complications with this approach, compared to open surgery. Most patients don t have to go to the ICU. They re in the hospital for only a day or so and then they go home. There s certainly less blood loss compared to the open operation. The incisions are limited. You can use local or regional anesthesia and the recovery is very fast. But there are disadvantages to this approach, which I think patients and doctors must consider. There are increased vascular injuries because we re putting these large catheters through arteries and we can have problems with injuries to these arteries, although the incidence is really less than 5%. Patients after this repair have to be watched very carefully over the long term because there can be a variety of problems that can develop and it s only fair to say that approximately 10% of patients, at some point down the line, will require an additional intervention to keep this graft functioning well. The great majority of time, those interventions again are intravascular interventions done through the groin, through catheters, but very rarely the patient will have to be converted to an open surgery after having this repair. That s probably about a 1% incidence over 5 years. These devices are expensive. You might think that these simple procedures that are done quickly, with short hospital stays, are more cost-effective than open repair, but because of the expense of the devices, there is no cost benefit, certainly no cost advantage, per se. As a tribute to modern surgery and modern anesthesia, open repair is quite safe. The mortality of open repair in expert hands is in the 1-3% range. Mortality of this procedure, it seems, is not that different. Certainly in high risk patients we might see a difference, but for all comers, there s not a great difference in mortality, so that speaks to the advantages and disadvantages of this operation. Mike, you might just expand a little bit on the follow-up that s necessary after this procedure. These patients, as I said, are followed very closely. We see them one month after surgery for a physical examination and for their first CT scan. They ll have a CT scan at 6 months, CT scan at 12 months, and a CT scan once a year. At this point, we re recommending CT scans for life, so at this point there is intense surveillance to make sure these grafts continue to function well and there are no problems related to the graft function. We are to the point now where we re going to be shooting a completion arteriogram. The graft has been completely deployed and we re getting our catheters into position to shoot an arteriogram and hopefully we ll see a good technical result and good flow and no filling of the aneurysm cavity. That looks perfect.
14 Walk through it frame by frame. You can see the renal arteries are still patent, and the position of the graft. Right. So here s the beginning of the run. What you see here is the aorta above the repair. It looks normal. We haven t damaged it in any way. It looks quite healthy. Now you see the renal arteries, with both renal arteries filling nicely. The graft kicks in right here. This is where we deployed the graft below the renal arteries, which is where we wanted, and now you see the beginning of the filling of the two limbs of the graft. Now we re going to follow that out, so frame by frame, you see the limbs filling out. No further aneurysm sac filling at this point. I think for comparison purposes, we ll bring up the other picture when we re done here, just to show the difference between the two films, but this is a great anatomic configuration. No compression of the limbs. Very nice position and, importantly, filling up both hypogastric arteries. You can see this is the internal iliac arteries, which are filling well. We like to maintain normal flow. The external iliacs are, of course, blocked by the sheaths at this point. For comparison purposes, let s go back to the original angiogram so people can compare that. Maybe we can put them both up together and show them side by side. There s our side by side views. If you can see that clear enough, on this side we have the pre-shot with the aneurysm filling. Now, post-repair, a nice configuration of the endograph with no flow into the aneurysm sac. This is just the sort of ideal result we look for. Nice job, Ed. Andy, can we take some more questions? We re going to remove our catheters and sheaths and begin the closure. Again, Mike, it looks as though that s gone along beautifully. We had another question that has come in from Michigan, this time from Ann Arbor, that addresses the issue of
15 symptoms associated with aneurysmal disease. In general, as I said earlier, there are no symptoms. In most of our patients, the aneurysm is picked up on an incidental examination, but there are occasional patients who have back pain in the lower back, extending around into the left flank and perhaps down the left leg. These symptoms usually are indicative of pending rupture or rapid expansion and are really very rare today, as we pick up most of these aneurysms early on. In fact, evidence is now emerging that supports routine screening of individuals for this disease process. I recommend everyone speak to their Congressman. This is a critical issue. Screening for aneurysms would save lives. Aneurysm rupture is the 13 th leading cause of death of adults in this country. If we were to screen patients, the mortality would drop dramatically. The morality of ruptured aneurysm for all comers is 90%. The mortality of elective repair is 1-2% in expert hands. Mike, another question that you might address is, how do you decide which graft to use, of all the devices that are approved and now available. Perhaps I should go back to that slide that we showed a little bit earlier. This slide shows the three commercially available devices that we use. We use all these devices, depending on the patient s anatomy and certain considerations. The graft on the left is the AneuRx graft. It has the longest track record of any of these three grafts which you see here. The beauty of that graft is, it can be very precisely located below the renal arteries, so when we re looking for a very precise deployment, I will often use that graft. The graft that we used today is the graft in the center, the so-called Excluder graft. This graft is wonderful for its ability to track through tortuous vessels. It also has a lower profile and can easily pass through diseased vessels, so it has a lot of advantages in that regard. The third graft, to the right, is the Zenith graft, made by the Cook Company. This is the newcomer on the block. It s an excellent graft. Its advantage is improved suprarenal fixation. Those bare wires actually pass up over the renal arteries and can anchor the graft in place and prevent it from migrating even a small amount. Migration can be a problem because if the graft slips down into the aneurysm cavity, the aneurysm can repressurize and again become a risk for rupture, so we really have to make sure we have very precise and strong fixation of the graft proximally. All of these grafts come in multiple sizes and lengths, so through precise measurements, and perhaps we can bring up a CT scan here, briefly, that we have here that shows our CT technology. Most of these patients undergo, or all of these patients undergo a spiral CT scan with contrast. With three-dimensional technology, we re able to delineate precisely the anatomy of the aneurysm. As you see on this slide, this 3D reconstruction shows our ability with 3D technology to measure the lengths within the aneurysm, which is critical
16 for designing and obtaining a graft which is long enough to fill the aneurysm and secure fixation above and below without covering any critical vessels, such as the renal arteries or internal iliac arteries, so the CT scan is an excellent tool for selecting the right graft. Mike, we have time for just one more brief question coming in locally here from Malden. Do you have any criteria you use to assess renal function and is it a determinant of whether you can use this approach or not? Another good question. Ironically, you would think patients with poor renal function, you wouldn t want to put them through a major operation, like an open operation, but in fact, renal insufficiency, as evidenced by a high creatinine or high BUN on blood test, is a relative contraindication to this technology, not only because the patients have to get dye during this procedure, but also because of the CT scans they have to get over time. It has been shown that patients with poor renal function who have these grafts inserted will have further decrements in renal function over time, so poor renal function, that is a creatinine over 2.5, would be considered, in our hands, a relative contraindication to this approach. Well, Andy, thank you very much for hosting this. I hope the audience enjoyed our presentation today. We appreciate you taking the time to look in. Michael, I think you ll have a very grateful patient very soon. This went along as well as could possibly be expected. We d like to thank you all for listening in with us and participating in this webcast. I would just like to remind you that this will be archived on our website at the Brigham and Women s Hospital. Perhaps you can show that. It s and that will get you into our site. It will be archived there for some time to come in the future. I d also like to remind you that CME credits are available through Harvard Medical School and we ll have a link on that website for that purpose. Once again, I d like to thank everybody for joining us. My congratulations to the operative team, and it is a team, for a job exceptionally well done. NARRATOR Thank you for watching the live abdominal aortic aneurysm procedure from Brigham and Women s Hospital in Boston, MA. For more information, to make an appointment or make a referral, please click the buttons below or contact one of our skilled coordinators at BWH-9999, or us at livesurgery@partners.org.
Bifurcated system Proximal suprarenal stent Modular (aortic main body and two iliac legs) Full thickness woven polyester graft material Fully
 Physician Training Bifurcated system Proximal suprarenal stent Modular (aortic main body and two iliac legs) Full thickness woven polyester graft material Fully supported by self-expanding z-stents H&L-B
Physician Training Bifurcated system Proximal suprarenal stent Modular (aortic main body and two iliac legs) Full thickness woven polyester graft material Fully supported by self-expanding z-stents H&L-B
Talent Abdominal Stent Graft
 Talent Abdominal with THE Xcelerant Hydro Delivery System Expanding the Indications for EVAR Treat More Patients Short Necks The Talent Abdominal is the only FDA-approved device for proximal aortic neck
Talent Abdominal with THE Xcelerant Hydro Delivery System Expanding the Indications for EVAR Treat More Patients Short Necks The Talent Abdominal is the only FDA-approved device for proximal aortic neck
Abdominal Aortic Aneurysms. A Surgeons Perspective Dr. Derek D. Muehrcke
 Abdominal Aortic Aneurysms A Surgeons Perspective Dr. Derek D. Muehrcke Aneurysm Definition The abnormal enlargement or bulging of an artery caused by an injury or weakness in the blood vessel wall A localized
Abdominal Aortic Aneurysms A Surgeons Perspective Dr. Derek D. Muehrcke Aneurysm Definition The abnormal enlargement or bulging of an artery caused by an injury or weakness in the blood vessel wall A localized
Cook Medical. Zenith Flex AAA Endovascular Graft with Z-Trak Introduction System Physician Training
 Cook Medical Zenith Flex AAA Endovascular Graft with Z-Trak Introduction System Physician Training Bifurcated system Proximal suprarenal stent Modular (aortic main body and two iliac legs) Full-thickness,
Cook Medical Zenith Flex AAA Endovascular Graft with Z-Trak Introduction System Physician Training Bifurcated system Proximal suprarenal stent Modular (aortic main body and two iliac legs) Full-thickness,
Aortic stents, types, selection, tricks in deployment.
 Aortic stents, types, selection, tricks in deployment. Hamdy Soliman.M.D,FSCAI Consultant of Cardiology&Head of Endovascular Unit National Heart Institute Endovascular Treatment of Thoracic Aortic Aneurysms
Aortic stents, types, selection, tricks in deployment. Hamdy Soliman.M.D,FSCAI Consultant of Cardiology&Head of Endovascular Unit National Heart Institute Endovascular Treatment of Thoracic Aortic Aneurysms
Modernizing the Mitral Valve: Advances in Robotic and Minimally Invasive Cardiac Repair
 Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/medical-breakthroughs-from-penn-medicine/modernizing-mitral-valveadvances-robotic-minimally-invasive-cardiac-repair/7686/
Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/medical-breakthroughs-from-penn-medicine/modernizing-mitral-valveadvances-robotic-minimally-invasive-cardiac-repair/7686/
Endovascular Repair o Abdominal. Aortic Aneurysms. Cesar E. Mendoza, M.D. Jackson Memorial Hospital Miami, Florida
 Endovascular Repair o Abdominal Aortic Aneurysms Cesar E. Mendoza, M.D. Jackson Memorial Hospital Miami, Florida Disclosure Nothing to disclose. 2 Mr. X AAA Mr. X. Is a 70 year old male who presented to
Endovascular Repair o Abdominal Aortic Aneurysms Cesar E. Mendoza, M.D. Jackson Memorial Hospital Miami, Florida Disclosure Nothing to disclose. 2 Mr. X AAA Mr. X. Is a 70 year old male who presented to
Hybrid Arch Debranching
 Hybrid Arch Debranching University of Maryland Medical Center Baltimore, Maryland February 16, 2012 Welcome to the University of Maryland Medical Center. I am Teng Lee, one of the cardiac surgeons here
Hybrid Arch Debranching University of Maryland Medical Center Baltimore, Maryland February 16, 2012 Welcome to the University of Maryland Medical Center. I am Teng Lee, one of the cardiac surgeons here
Zenith Renu AAA Converter Graft. Device Description Planning and Sizing Deployment Sequence Patient Follow-Up
 Zenith Renu AAA Converter Graft Device Description Planning and Sizing Deployment Sequence Patient Follow-Up Device description: Device indications The Zenith Renu AAA Converter Graft with Z-Trak Introduction
Zenith Renu AAA Converter Graft Device Description Planning and Sizing Deployment Sequence Patient Follow-Up Device description: Device indications The Zenith Renu AAA Converter Graft with Z-Trak Introduction
Robert F. Cuff, MD FACS SHMG Vascular Surgery
 Robert F. Cuff, MD FACS SHMG Vascular Surgery Objectives To become familiar with the commercially available fenestrated EVAR graft Discuss techniques to increase success Review available data to determine
Robert F. Cuff, MD FACS SHMG Vascular Surgery Objectives To become familiar with the commercially available fenestrated EVAR graft Discuss techniques to increase success Review available data to determine
ANGIOPLASTY AND STENTING
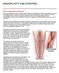 ANGIOPLASTY AND STENTING What is angioplasty and stenting? During an angioplasty, your vascular surgeon inflates a small balloon inside a narrowed blood vessel. This balloon helps to widen your blood vessel
ANGIOPLASTY AND STENTING What is angioplasty and stenting? During an angioplasty, your vascular surgeon inflates a small balloon inside a narrowed blood vessel. This balloon helps to widen your blood vessel
MODERN METHODS FOR TREATING ABDOMINAL ANEURYSMS AND THORACIC AORTIC DISEASE
 MODERN METHODS FOR TREATING ABDOMINAL ANEURYSMS AND THORACIC AORTIC DISEASE AAA FACTS 200,000 New Cases Each Year Ruptured AAA = 15,000 Deaths per Year in U.S. 13th Leading Cause of Death 80% Chance of
MODERN METHODS FOR TREATING ABDOMINAL ANEURYSMS AND THORACIC AORTIC DISEASE AAA FACTS 200,000 New Cases Each Year Ruptured AAA = 15,000 Deaths per Year in U.S. 13th Leading Cause of Death 80% Chance of
Optimizing Accuracy of Aortic Stent Grafts in Short Necks
 Optimizing Accuracy of Aortic Stent Grafts in Short Necks Venkatesh Ramaiah, MD, FACS Medical Director Arizona Heart Hospital Director Peripheral Vascular and Endovascular Research Arizona Heart Institute
Optimizing Accuracy of Aortic Stent Grafts in Short Necks Venkatesh Ramaiah, MD, FACS Medical Director Arizona Heart Hospital Director Peripheral Vascular and Endovascular Research Arizona Heart Institute
Access More Patients. Customize Each Seal.
 Access More. Customize Each Seal. The Least Invasive Path Towards Proven Patency ULTRA LOW PROFILE TO EASE ADVANCEMENT The flexible, ultra-low 12F ID Ovation ix delivery system enables you to navigate
Access More. Customize Each Seal. The Least Invasive Path Towards Proven Patency ULTRA LOW PROFILE TO EASE ADVANCEMENT The flexible, ultra-low 12F ID Ovation ix delivery system enables you to navigate
RadRx Your Prescription for Accurate Coding & Reimbursement Copyright All Rights Reserved.
 Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant INDICATION: Abdominal aortic aneurysm. INTERVENTIONAL RADIOLOGIST:
Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant INDICATION: Abdominal aortic aneurysm. INTERVENTIONAL RADIOLOGIST:
Ancillary Components with Z-Trak Introduction System
 Ancillary Components with Z-Trak Introduction System Zenith Flex AAA Endovascular Graft Ancillary Components Converter Converters can be used to convert a bifurcated graft into an aortouniiliac graft if
Ancillary Components with Z-Trak Introduction System Zenith Flex AAA Endovascular Graft Ancillary Components Converter Converters can be used to convert a bifurcated graft into an aortouniiliac graft if
Quick Reference Guide
 Quick Reference Guide Indications for Use The AFX Endovascular AAA System is indicated for endovascular treatment in patients with AAA. The devices are indicated for patients with suitable aneurysm morphology
Quick Reference Guide Indications for Use The AFX Endovascular AAA System is indicated for endovascular treatment in patients with AAA. The devices are indicated for patients with suitable aneurysm morphology
History of the Powerlink System Design and Clinical Results. Edward B. Diethrich Arizona Heart Hospital Phoenix, AZ
 History of the Powerlink System Design and Clinical Results Edward B. Diethrich Arizona Heart Hospital Phoenix, AZ Powerlink System: Unibody-Bifurcated Design Long Main Body Low-Porosity Proprietary eptfe
History of the Powerlink System Design and Clinical Results Edward B. Diethrich Arizona Heart Hospital Phoenix, AZ Powerlink System: Unibody-Bifurcated Design Long Main Body Low-Porosity Proprietary eptfe
Angiogram, angioplasty and stenting
 Angiogram, angioplasty and stenting Who is this leaflet for? This leaflet is for people who are having: an angiogram angioplasty (with or without a stent) An angiogram (also called an arteriogram or angiography)
Angiogram, angioplasty and stenting Who is this leaflet for? This leaflet is for people who are having: an angiogram angioplasty (with or without a stent) An angiogram (also called an arteriogram or angiography)
Challenges. 1. Sizing. 2. Proximal landing zone 3. Distal landing zone 4. Access vessels 5. Spinal cord ischemia 6. Endoleak
 Disclosure I have the following potential conflicts of interest to report: Consulting: Medtronic, Gore Employment in industry Stockholder of a healthcare company Owner of a healthcare company Other(s)
Disclosure I have the following potential conflicts of interest to report: Consulting: Medtronic, Gore Employment in industry Stockholder of a healthcare company Owner of a healthcare company Other(s)
Acute dissections of the descending thoracic aorta (Debakey
 Endovascular Treatment of Acute Descending Thoracic Aortic Dissections Nimesh D. Desai, MD, PhD, and Joseph E. Bavaria, MD Acute dissections of the descending thoracic aorta (Debakey type III or Stanford
Endovascular Treatment of Acute Descending Thoracic Aortic Dissections Nimesh D. Desai, MD, PhD, and Joseph E. Bavaria, MD Acute dissections of the descending thoracic aorta (Debakey type III or Stanford
Patient Information Booklet
 Patient Information Booklet Endovascular Stent Grafts: A Treatment for Thoracic Aortic Aneurysms Table of Contents Table of Contents Introduction 1 Anatomy of the Thoracic Aorta 2 What Is an Aneurysm?
Patient Information Booklet Endovascular Stent Grafts: A Treatment for Thoracic Aortic Aneurysms Table of Contents Table of Contents Introduction 1 Anatomy of the Thoracic Aorta 2 What Is an Aneurysm?
Open Surgery for AAA
 Open Surgery for AAA A Weakened Blood Vessel What does it mean to have an abdominal aortic aneurysm (AAA)? This is a balloon-like bulge in a major blood vessel, the aorta. The bulge forms at a weak place
Open Surgery for AAA A Weakened Blood Vessel What does it mean to have an abdominal aortic aneurysm (AAA)? This is a balloon-like bulge in a major blood vessel, the aorta. The bulge forms at a weak place
Complex Retrieval of Embedded Inferior Vena Cava Filters in Interventional Radiology
 Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/medical-breakthroughs-from-penn-medicine/complex-retrievalembedded-inferior-vena-cava-filters-interventional-radiology/7838/
Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/medical-breakthroughs-from-penn-medicine/complex-retrievalembedded-inferior-vena-cava-filters-interventional-radiology/7838/
ABDOMINAL XT ABDOMINAL STENT GRAFT SYSTEM
 ABDOMINAL XT ABDOMINAL STENT GRAFT SYSTEM Pure performance and quality: Stent graft systems by JOTEC JOTEC is an innovation-oriented company with consistent focus on its core competencies: the development
ABDOMINAL XT ABDOMINAL STENT GRAFT SYSTEM Pure performance and quality: Stent graft systems by JOTEC JOTEC is an innovation-oriented company with consistent focus on its core competencies: the development
Abdominal Aortic Aneurysm 가천대길병원 이상준
 Abdominal Aortic Aneurysm 가천대길병원 이상준 1 Definition Diameter of the aorta 1.5 times greater than normal. Most are infrarenal, and a significant number extend down into one or both iliac arteries Abdominal
Abdominal Aortic Aneurysm 가천대길병원 이상준 1 Definition Diameter of the aorta 1.5 times greater than normal. Most are infrarenal, and a significant number extend down into one or both iliac arteries Abdominal
Introduction What Causes Peripheral Vascular Disease? How Do Doctors Treat Peripheral Vascular Disease?... 9
 Patient Information Table of Contents Introduction... 3 What is Peripheral Vascular Disease?... 5 What Are Some of the Symptoms of Peripheral Vascular Disease?... 7 What Causes Peripheral Vascular Disease?...
Patient Information Table of Contents Introduction... 3 What is Peripheral Vascular Disease?... 5 What Are Some of the Symptoms of Peripheral Vascular Disease?... 7 What Causes Peripheral Vascular Disease?...
Abdominal and thoracic aneurysm repair
 Abdominal and thoracic aneurysm repair William A. Gray MD Director, Endovascular Intervention Cardiovascular Research Foundation Columbia University Medical Center Abdominal Aortic Aneurysm Endografts
Abdominal and thoracic aneurysm repair William A. Gray MD Director, Endovascular Intervention Cardiovascular Research Foundation Columbia University Medical Center Abdominal Aortic Aneurysm Endografts
Dr. Coakley, so virtual colonoscopy, what is it? Is it a CT exam exactly?
 Virtual Colonoscopy Webcast January 26, 2009 Fergus Coakley, M.D. Please remember the opinions expressed on Patient Power are not necessarily the views of UCSF Medical Center, its medical staff or Patient
Virtual Colonoscopy Webcast January 26, 2009 Fergus Coakley, M.D. Please remember the opinions expressed on Patient Power are not necessarily the views of UCSF Medical Center, its medical staff or Patient
Durable outcomes. Proven performance.
 Durable outcomes. Proven performance. GORE EXCLUDER AAA Endoprosthesis GORE EXCLUDER Iliac Branch Endoprosthesis GORE EXCLUDER AAA Endoprosthesis The most-studied* EVAR stent graft designed for durable
Durable outcomes. Proven performance. GORE EXCLUDER AAA Endoprosthesis GORE EXCLUDER Iliac Branch Endoprosthesis GORE EXCLUDER AAA Endoprosthesis The most-studied* EVAR stent graft designed for durable
STENT GRAFTING PROCEDURE MASSACHUSETTS GENERAL HOSPITAL, BOSTON, MA Broadcast April 14, 2004
 NARRATOR STENT GRAFTING PROCEDURE MASSACHUSETTS GENERAL HOSPITAL, BOSTON, MA Broadcast April 14, 2004 Thank you for joining us to view the live stent grafting procedure to treat thoracic aortic aneurysms
NARRATOR STENT GRAFTING PROCEDURE MASSACHUSETTS GENERAL HOSPITAL, BOSTON, MA Broadcast April 14, 2004 Thank you for joining us to view the live stent grafting procedure to treat thoracic aortic aneurysms
A New EVAR Device for Infrarenal AAAs
 A New EVAR Device for Infrarenal AAAs Peter Nelson, MD, MS Assistant Professor of Surgery MM0203 Rev. 01 Current U.S. EVAR Devices Anatomical Fixation Proximal Fixation Powerlink - Endologix Excluder WL
A New EVAR Device for Infrarenal AAAs Peter Nelson, MD, MS Assistant Professor of Surgery MM0203 Rev. 01 Current U.S. EVAR Devices Anatomical Fixation Proximal Fixation Powerlink - Endologix Excluder WL
Young-Guk Ko, M.D. Severance Cardiovascular Hospital, Yonsei University Health System,
 Young-Guk Ko, M.D., Dangas G, J Am Coll Cardiol Intv 2012;5:1071 All-cause Mortality Dangas Severance G, J Am Coll Cardiovascular Cardiol Intv Hospital, 2012;5:1071 Yonsei University Health System Aneurysm-related
Young-Guk Ko, M.D., Dangas G, J Am Coll Cardiol Intv 2012;5:1071 All-cause Mortality Dangas Severance G, J Am Coll Cardiovascular Cardiol Intv Hospital, 2012;5:1071 Yonsei University Health System Aneurysm-related
ENDOVASCULAR REPAIR OF ABDOMINAL AORTIC ANEURYSM ROBERT WOOD JOHNSON UNIVERSITY HOSPITAL, NEW BRUNSWICK, NJ BROADCAST OCTOBER 20, 2004
 ENDOVASCULAR REPAIR OF ABDOMINAL AORTIC ANEURYSM ROBERT WOOD JOHNSON UNIVERSITY HOSPITAL, NEW BRUNSWICK, NJ BROADCAST OCTOBER 20, 2004 NARRATOR Welcome to the live webcast from Robert Wood Johnson University
ENDOVASCULAR REPAIR OF ABDOMINAL AORTIC ANEURYSM ROBERT WOOD JOHNSON UNIVERSITY HOSPITAL, NEW BRUNSWICK, NJ BROADCAST OCTOBER 20, 2004 NARRATOR Welcome to the live webcast from Robert Wood Johnson University
BC Vascular Day. Contents. November 3, Abdominal Aortic Aneurysm 2 3. Peripheral Arterial Disease 4 6. Deep Venous Thrombosis 7 8
 BC Vascular Day Contents Abdominal Aortic Aneurysm 2 3 November 3, 2018 Peripheral Arterial Disease 4 6 Deep Venous Thrombosis 7 8 Abdominal Aortic Aneurysm Conservative Management Risk factor modification
BC Vascular Day Contents Abdominal Aortic Aneurysm 2 3 November 3, 2018 Peripheral Arterial Disease 4 6 Deep Venous Thrombosis 7 8 Abdominal Aortic Aneurysm Conservative Management Risk factor modification
Abdominal Aortic Aneurysm (AAA) General Information. Patient information Leaflet
 Abdominal Aortic Aneurysm (AAA) General Information Patient information Leaflet 18 th April 2017 WHAT IS THE AORTA? The aorta is the largest artery (blood vessel) in the body. It carries blood from the
Abdominal Aortic Aneurysm (AAA) General Information Patient information Leaflet 18 th April 2017 WHAT IS THE AORTA? The aorta is the largest artery (blood vessel) in the body. It carries blood from the
Challenging anatomies demand versatility.
 Challenging anatomies demand versatility. The Distinct Advantages of Separating Seal and Fixation ANATOMICAL FIXATION Unlike proximal fixation designs, the AFX bifurcated unibody endograft allows for natural
Challenging anatomies demand versatility. The Distinct Advantages of Separating Seal and Fixation ANATOMICAL FIXATION Unlike proximal fixation designs, the AFX bifurcated unibody endograft allows for natural
INL No. A0083 Project Medtronic Thoracic patients guide Description Version 18
 INL No. A0083 Project Medtronic Thoracic patients guide Description Version 18 www.inl-agency.com PATIENT INFORMATION BOOKLET Endovascular Stent Grafts: A treatment for Thoracic Aortic disease Table of
INL No. A0083 Project Medtronic Thoracic patients guide Description Version 18 www.inl-agency.com PATIENT INFORMATION BOOKLET Endovascular Stent Grafts: A treatment for Thoracic Aortic disease Table of
Innovations in Lung Cancer Diagnosis and Surgical Treatment
 Transcript Details This is a transcript of a continuing medical education (CME) activity accessible on the ReachMD network. Additional media formats for the activity and full activity details (including
Transcript Details This is a transcript of a continuing medical education (CME) activity accessible on the ReachMD network. Additional media formats for the activity and full activity details (including
Intro: Slide 1. Slide 2. Slide 3. Basic understanding of interventional radiology. Gain knowledge of key terms and phrases
 Slide 1 Intro: PRESENTED BY: Selena M. Moore, AAS, CCS, CPC HIMS Physician Liaison Coder This is a modified/updated presentation that was originally written by: Rosemary Waligorski, RHIT, CCS, RCC and
Slide 1 Intro: PRESENTED BY: Selena M. Moore, AAS, CCS, CPC HIMS Physician Liaison Coder This is a modified/updated presentation that was originally written by: Rosemary Waligorski, RHIT, CCS, RCC and
Endovascular Aneurysm Repair (EVAR)
 Endovascular Aneurysm Repair (EVAR) Exceptional healthcare, personally delivered You have been diagnosed with an abdominal aortic aneurysm (AAA). This means that the main artery in your abdomen (the aorta)
Endovascular Aneurysm Repair (EVAR) Exceptional healthcare, personally delivered You have been diagnosed with an abdominal aortic aneurysm (AAA). This means that the main artery in your abdomen (the aorta)
The Next Horizons in Reconstructive Microsurgery
 Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/medical-breakthroughs-from-penn-medicine/the-next-horizonsreconstructive-microsurgery/7949/
Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/medical-breakthroughs-from-penn-medicine/the-next-horizonsreconstructive-microsurgery/7949/
Abdominal Aortic Aneurysms (AAA) and Surveillance
 Abdominal Aortic Aneurysms (AAA) and Surveillance Exceptional healthcare, personally delivered Ask 3 Questions Preparation for your Appointments We want you to be active in your healthcare. By telling
Abdominal Aortic Aneurysms (AAA) and Surveillance Exceptional healthcare, personally delivered Ask 3 Questions Preparation for your Appointments We want you to be active in your healthcare. By telling
The World s Smallest Heart Pump
 Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/clinicians-roundtable/the-worlds-smallest-heart-pump/3367/
Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/clinicians-roundtable/the-worlds-smallest-heart-pump/3367/
EVAR replaced standard repair in most cases. Why?
 EVAR replaced standard repair in most cases. Why? Initial major steps in endograft evolution Papazoglou O. Konstantinos M.D. The story of a major breakthrough in vascular surgery 1991 Parodi introduces
EVAR replaced standard repair in most cases. Why? Initial major steps in endograft evolution Papazoglou O. Konstantinos M.D. The story of a major breakthrough in vascular surgery 1991 Parodi introduces
INL No. A0075 Project Medtronic Patient Information Leaflet Description 16 page booklet
 INL No. A0075 Project Medtronic Patient Information Leaflet Description 16 page booklet www.inl-agency.com PATIENT INFORMATION BOOKLET Endovascular stent grafts: A treatment for Abdominal Aortic Aneurysms
INL No. A0075 Project Medtronic Patient Information Leaflet Description 16 page booklet www.inl-agency.com PATIENT INFORMATION BOOKLET Endovascular stent grafts: A treatment for Abdominal Aortic Aneurysms
LOWERING THE PROFILE RAISING THE BAR
 LOWERING THE PROFILE RAISING THE BAR INNOVATIVE LOW PROFILE. ADVANCED CLINICAL PERFORMANCE. The AFX TM Endovascular AAA System integrates anatomical fixation with an advanced delivery system and graft
LOWERING THE PROFILE RAISING THE BAR INNOVATIVE LOW PROFILE. ADVANCED CLINICAL PERFORMANCE. The AFX TM Endovascular AAA System integrates anatomical fixation with an advanced delivery system and graft
Citation for published version (APA): Tielliu, I. F. J. (2010). Endovascular repair of peripheral artery aneurysms Groningen: s.n.
 University of Groningen Endovascular repair of peripheral artery aneurysms Tielliu, Ignace François Jacques IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish
University of Groningen Endovascular repair of peripheral artery aneurysms Tielliu, Ignace François Jacques IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish
6. Endovascular aneurysm repair
 Introduction The standard treatment for aortic aneurysm, open repair, involves a large abdominal incision and cross-clamping of the aorta. In recent years, a minimally invasive technique, endovascular
Introduction The standard treatment for aortic aneurysm, open repair, involves a large abdominal incision and cross-clamping of the aorta. In recent years, a minimally invasive technique, endovascular
FROM THE EVERYDAY TO THE EXTRAORDINARY
 FROM THE EVERYDAY TO THE EXTRAORDINARY Created with the collaboration of more than 250 physicians around the world, ENDURANT empowers you to create stronger outcomes for more patients, including those
FROM THE EVERYDAY TO THE EXTRAORDINARY Created with the collaboration of more than 250 physicians around the world, ENDURANT empowers you to create stronger outcomes for more patients, including those
Hostile Proximal Neck: A New Conformable EVAR Device
 Hostile Proximal Neck: A New Conformable EVAR Device Young-Guk Ko, M.D., Seoul, Korea Currently Available Devices for EVAR in Korea, 2018 Zenith Flex, Cook Endurant IIs, Medtronic INCRAFT, Cordis AFX2,
Hostile Proximal Neck: A New Conformable EVAR Device Young-Guk Ko, M.D., Seoul, Korea Currently Available Devices for EVAR in Korea, 2018 Zenith Flex, Cook Endurant IIs, Medtronic INCRAFT, Cordis AFX2,
FEVAR FIFTEEN YEARS OF EFFICIENCY E.DUCASSE MD PHD FEBVS CHU DE BORDEAUX
 FEVAR FIFTEEN YEARS OF EFFICIENCY E.DUCASSE MD PHD FEBVS CHU DE BORDEAUX 2018 A BIT OF HISTORY First use of F-EVAR : 1990s Park et al. J Vasc Interv Radiol. 1996;7:819-823. Faruqi et al. J Endovasc Surg.
FEVAR FIFTEEN YEARS OF EFFICIENCY E.DUCASSE MD PHD FEBVS CHU DE BORDEAUX 2018 A BIT OF HISTORY First use of F-EVAR : 1990s Park et al. J Vasc Interv Radiol. 1996;7:819-823. Faruqi et al. J Endovasc Surg.
Genetic Counselor: Hi Lisa. Hi Steve. Thanks for coming in today. The BART results came back and they are positive.
 Hi, I m Kaylene Ready, a genetic counselor who specializes in the education and counseling of individuals at high-risk for hereditary breast and ovarian cancer syndrome. Women with an inherited BRCA 1
Hi, I m Kaylene Ready, a genetic counselor who specializes in the education and counseling of individuals at high-risk for hereditary breast and ovarian cancer syndrome. Women with an inherited BRCA 1
Zenith Alpha T HORACIC ENDOVASCULAR GRAFT
 Device description Zenith Alpha T HORACIC ENDOVASCULAR GRAFT www.cookmedical.com AI-D21181-EN-F Modular design The two-piece modular system allows the physician to customize a graft system to fit each
Device description Zenith Alpha T HORACIC ENDOVASCULAR GRAFT www.cookmedical.com AI-D21181-EN-F Modular design The two-piece modular system allows the physician to customize a graft system to fit each
Malperfusion Syndromes Type B Aortic Dissection with Malperfusion
 Malperfusion Syndromes Type B Aortic Dissection with Malperfusion Jade S. Hiramoto, MD, MAS April 27, 2012 Associated with early mortality Occurs when there is end organ ischemia secondary to aortic branch
Malperfusion Syndromes Type B Aortic Dissection with Malperfusion Jade S. Hiramoto, MD, MAS April 27, 2012 Associated with early mortality Occurs when there is end organ ischemia secondary to aortic branch
CAROTID ARTERY STENTING FRANKLIN SQUARE HOSPITAL CENTER, BALTIMORE, MARYLAND Broadcast March 23, 2005
 CAROTID ARTERY STENTING FRANKLIN SQUARE HOSPITAL CENTER, BALTIMORE, MARYLAND Broadcast March 23, 2005 NARRATOR Welcome to the live webcast from Franklin Square Hospital Center in Baltimore, Maryland. During
CAROTID ARTERY STENTING FRANKLIN SQUARE HOSPITAL CENTER, BALTIMORE, MARYLAND Broadcast March 23, 2005 NARRATOR Welcome to the live webcast from Franklin Square Hospital Center in Baltimore, Maryland. During
My personal experience with INCRAFT in standard and challenging cases
 My personal experience with INCRAFT in standard and challenging cases G Pratesi, MD Vascular Surgery University of Rome Tor Vergata giovanni.pratesi@uniroma2.it Disclosure Speaker name: Giovanni Pratesi,
My personal experience with INCRAFT in standard and challenging cases G Pratesi, MD Vascular Surgery University of Rome Tor Vergata giovanni.pratesi@uniroma2.it Disclosure Speaker name: Giovanni Pratesi,
Introduction 3. What is Peripheral Vascular Disease? 5. What Are Some of the Symptoms of Peripheral Vascular Disease? 6
 Patient Information Table of Contents Introduction 3 What is Peripheral Vascular Disease? 5 What Are Some of the Symptoms of Peripheral Vascular Disease? 6 What Causes Peripheral Vascular Disease? 7 How
Patient Information Table of Contents Introduction 3 What is Peripheral Vascular Disease? 5 What Are Some of the Symptoms of Peripheral Vascular Disease? 6 What Causes Peripheral Vascular Disease? 7 How
Open repair of Abdominal Aortic Aneurysms (AAA)
 Open repair of Abdominal Aortic Aneurysms (AAA) Exceptional healthcare, personally delivered Ask 3 Questions Preparation for your Appointments We want you to be active in your healthcare. By telling us
Open repair of Abdominal Aortic Aneurysms (AAA) Exceptional healthcare, personally delivered Ask 3 Questions Preparation for your Appointments We want you to be active in your healthcare. By telling us
Current Status of Abdominal Aortic Stent Grafts. John R. Laird Professor of Medicine Director of the Vascular Center UC Davis Medical Center
 Current Status of Abdominal Aortic Stent Grafts John R. Laird Professor of Medicine Director of the Vascular Center UC Davis Medical Center Autumn Greetings Disclosure Statement of Financial Interest Within
Current Status of Abdominal Aortic Stent Grafts John R. Laird Professor of Medicine Director of the Vascular Center UC Davis Medical Center Autumn Greetings Disclosure Statement of Financial Interest Within
Taming The Aorta. David Minion, MD Program Director, Vascular Surgery University of Kentucky Medical Center Lexington, Kentucky, USA
 Taming The Aorta David Minion, MD Program Director, Vascular Surgery University of Kentucky Medical Center Lexington, Kentucky, USA Faculty Disclosure Consulting: Endologix, Cook 1 Objectives Review the
Taming The Aorta David Minion, MD Program Director, Vascular Surgery University of Kentucky Medical Center Lexington, Kentucky, USA Faculty Disclosure Consulting: Endologix, Cook 1 Objectives Review the
GORE EXCLUDER AAA Endoprosthesis ANNUAL CLINICAL UPDATE OCTOBER Section I Clinical experience. Section II Worldwide commercial experience
 GORE EXCLUDER AAA Endoprosthesis ANNUAL CLINICAL UPDATE OCTOBER 2018 Abstract This annual clinical update provides a review of the ongoing experience with the GORE EXCLUDER AAA Endoprosthesis used in the
GORE EXCLUDER AAA Endoprosthesis ANNUAL CLINICAL UPDATE OCTOBER 2018 Abstract This annual clinical update provides a review of the ongoing experience with the GORE EXCLUDER AAA Endoprosthesis used in the
Increased Flexibility of AneuRx Stent-Graft Reduces Need for Secondary Intervention Following Endovascular Aneurysm Repair
 583 Increased Flexibility of AneuRx Stent-Graft Reduces Need for Secondary Intervention Following Endovascular Aneurysm Repair Frank R. Arko, MD; W. Anthony Lee, MD; Bradley B. Hill, MD; Paul Cipriano,
583 Increased Flexibility of AneuRx Stent-Graft Reduces Need for Secondary Intervention Following Endovascular Aneurysm Repair Frank R. Arko, MD; W. Anthony Lee, MD; Bradley B. Hill, MD; Paul Cipriano,
Anatomical challenges in EVAR
 Anatomical challenges in EVAR M.H. EL DESSOKI, MD,FRCS PROFESSOR OF VASCULAR SURGERY CAIRO UNIVERSITY Disclosure Speaker name:... I have the following potential conflicts of interest to report: Consulting
Anatomical challenges in EVAR M.H. EL DESSOKI, MD,FRCS PROFESSOR OF VASCULAR SURGERY CAIRO UNIVERSITY Disclosure Speaker name:... I have the following potential conflicts of interest to report: Consulting
Bilateral use of the Gore IBE device for bilateral CIA aneurysms and a first interim analysis of the prospective Iceberg registry
 Bilateral use of the Gore IBE device for bilateral CIA aneurysms and a first interim analysis of the prospective Iceberg registry Michel MPJ Reijnen, MD, PhD Department of Vascular Surgery, Rijnstate Hospital
Bilateral use of the Gore IBE device for bilateral CIA aneurysms and a first interim analysis of the prospective Iceberg registry Michel MPJ Reijnen, MD, PhD Department of Vascular Surgery, Rijnstate Hospital
From 1996 to 1999, a total of 1,193 patients with
 THE ANEURX CLINICAL TRIAL AT 8 YEARS Lessons learned following the US AneuRx clinical trial from 1996 to 2004. BY CHRISTOPHER K. ZARINS, MD From 1996 to 1999, a total of 1,193 patients with infrarenal
THE ANEURX CLINICAL TRIAL AT 8 YEARS Lessons learned following the US AneuRx clinical trial from 1996 to 2004. BY CHRISTOPHER K. ZARINS, MD From 1996 to 1999, a total of 1,193 patients with infrarenal
EVAR and TEVAR: Extending Their Use for Rupture and Traumatic Injury. Conflict of Interest. Hypotensive shock 5/5/2014. none
 EVAR and TEVAR: Extending Their Use for Rupture and Traumatic Injury Bruce H. Gray, DO MSVM FSCAI Professor of Surgery/Vascular Medicine USC SOM-Greenville Greenville, South Carolina none Conflict of Interest
EVAR and TEVAR: Extending Their Use for Rupture and Traumatic Injury Bruce H. Gray, DO MSVM FSCAI Professor of Surgery/Vascular Medicine USC SOM-Greenville Greenville, South Carolina none Conflict of Interest
occur, they usually are from pressure on adjacent structures. Chest pain, shoulder pain, or back pain are frequent presentations.
 ENDOVASCULAR REPAIR OF DESCENDING THORACIC AORTIC ANEURYSM WITH GORE TAG ENDOPROSTHESIS UNIVERSITY OF NORTH CAROLINA HOSPITAL, CHAPEL HILL, NORTH CAROLINA Broadcast December 15, 2005 00:00:16.000 NARRATOR:
ENDOVASCULAR REPAIR OF DESCENDING THORACIC AORTIC ANEURYSM WITH GORE TAG ENDOPROSTHESIS UNIVERSITY OF NORTH CAROLINA HOSPITAL, CHAPEL HILL, NORTH CAROLINA Broadcast December 15, 2005 00:00:16.000 NARRATOR:
Aortic and Iliac Artery Occlusive Disease (Updated 10.08)
 S PATIENT INFORMATION oregon surgical specialists Aortic and Iliac Artery Occlusive Disease (Updated 10.08) Abdominal aortic and iliac artery occlusive disease occurs when the arteries in your abdomen
S PATIENT INFORMATION oregon surgical specialists Aortic and Iliac Artery Occlusive Disease (Updated 10.08) Abdominal aortic and iliac artery occlusive disease occurs when the arteries in your abdomen
SANWICH TECHNIQUE TO REDUCE COMPLICATIONS WHEN TREATING BILATERAL INTERNAL ILIAC ARTERY
 SANWICH TECHNIQUE TO REDUCE COMPLICATIONS WHEN TREATING BILATERAL INTERNAL ILIAC ARTERY TRAN TRA GIANG.MD Interventional cardiovascular department Hanoi Heart Hospital, Hanoi, Viet Nam Nothing to Disclose
SANWICH TECHNIQUE TO REDUCE COMPLICATIONS WHEN TREATING BILATERAL INTERNAL ILIAC ARTERY TRAN TRA GIANG.MD Interventional cardiovascular department Hanoi Heart Hospital, Hanoi, Viet Nam Nothing to Disclose
Abdominal aortic aneurysm screening: A decision for men aged 65 or over
 Abdominal Aortic Aneurysm Abdominal aortic screening: A decision for men aged 65 or over Screening is a choice. Men aged 65 and over have the following choice: Get screened for abdominal aortic or Do not
Abdominal Aortic Aneurysm Abdominal aortic screening: A decision for men aged 65 or over Screening is a choice. Men aged 65 and over have the following choice: Get screened for abdominal aortic or Do not
Periprosthetic leak and rupture after endovascular repair of abdominal aortic aneurysm: The significance of device design for long-term results
 CASE REPORTS Periprosthetic leak and rupture after endovascular repair of abdominal aortic aneurysm: The significance of device design for long-term results Kirsten Krohg-Sørensen, MD, PhD, Magne Brekke,
CASE REPORTS Periprosthetic leak and rupture after endovascular repair of abdominal aortic aneurysm: The significance of device design for long-term results Kirsten Krohg-Sørensen, MD, PhD, Magne Brekke,
Carotid Ultrasound Scans for Assessing Cardiovascular Risk
 Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/lipid-luminations/carotid-ultrasound-scans-for-assessing-cardiovascularrisk/4004/
Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/lipid-luminations/carotid-ultrasound-scans-for-assessing-cardiovascularrisk/4004/
Indications for use. Contraindications within the United States
 Indications for use Indications within the United States The GORE TAG Thoracic Endoprosthesis is intended for endovascular repair of all lesions of the descending thoracic aorta, including: Isolated lesions
Indications for use Indications within the United States The GORE TAG Thoracic Endoprosthesis is intended for endovascular repair of all lesions of the descending thoracic aorta, including: Isolated lesions
Endovascular Management of Thoracic Aortic Pathology Stéphan Haulon, J Sobocinski, B Maurel, T Martin-Gonzalez, R Spear, A Hertault, R Azzaoui
 Endovascular Management of Thoracic Aortic Pathology Stéphan Haulon, J Sobocinski, B Maurel, T Martin-Gonzalez, R Spear, A Hertault, R Azzaoui Aortic Center, Lille University Hospital, France Disclosures
Endovascular Management of Thoracic Aortic Pathology Stéphan Haulon, J Sobocinski, B Maurel, T Martin-Gonzalez, R Spear, A Hertault, R Azzaoui Aortic Center, Lille University Hospital, France Disclosures
What is an aneurysm? Arteries carry blood away from your heart to the rest of your body. An aneurysm occurs when the walls of an artery weaken.
 Endovascular aneurysm repair (EVAR) This leaflet aims to answer some of the questions you may have about having an endovascular aneurysm repair. It explains the benefits, risks and alternatives of the
Endovascular aneurysm repair (EVAR) This leaflet aims to answer some of the questions you may have about having an endovascular aneurysm repair. It explains the benefits, risks and alternatives of the
Tripler Army Medical Center Obstetric Anesthesia Service - FAQs
 Tripler Army Medical Center Obstetric Anesthesia Service - FAQs What is a labor epidural? A labor epidural is a thin tube (called an epidural catheter) placed in a woman s lower back by an anesthesia provider.
Tripler Army Medical Center Obstetric Anesthesia Service - FAQs What is a labor epidural? A labor epidural is a thin tube (called an epidural catheter) placed in a woman s lower back by an anesthesia provider.
Intravascular Ultrasound
 Scan for mobile link. Intravascular Ultrasound Intravascular ultrasound (IVUS) uses a transducer or probe to generate sound waves and produce pictures of the coronary arteries. IVUS can show the entire
Scan for mobile link. Intravascular Ultrasound Intravascular ultrasound (IVUS) uses a transducer or probe to generate sound waves and produce pictures of the coronary arteries. IVUS can show the entire
Right Choice for Right Angles
 Right Choice for Right Angles The Anatomy of Technology Aorfix gives you technology that conforms to patient anatomy, optimising both procedure and post-operative performance. Fishmouth for optimum neck
Right Choice for Right Angles The Anatomy of Technology Aorfix gives you technology that conforms to patient anatomy, optimising both procedure and post-operative performance. Fishmouth for optimum neck
An Overview of Post-EVAR Endoleaks: Imaging Findings and Management. Ravi Shergill BSc Sean A. Kennedy MD Mark O. Baerlocher MD FRCPC
 An Overview of Post-EVAR Endoleaks: Imaging Findings and Management Ravi Shergill BSc Sean A. Kennedy MD Mark O. Baerlocher MD FRCPC Disclosure Slide Mark O. Baerlocher: Current: Consultant for Boston
An Overview of Post-EVAR Endoleaks: Imaging Findings and Management Ravi Shergill BSc Sean A. Kennedy MD Mark O. Baerlocher MD FRCPC Disclosure Slide Mark O. Baerlocher: Current: Consultant for Boston
Nellix Endovascular System: Clinical Outcomes and Device Overview
 Nellix Endovascular System: Clinical Outcomes and Device Overview Jeffrey P. Carpenter, MD Professor and Chief, Department of Surgery CAUTION: Investigational device. This product is under clinical investigation
Nellix Endovascular System: Clinical Outcomes and Device Overview Jeffrey P. Carpenter, MD Professor and Chief, Department of Surgery CAUTION: Investigational device. This product is under clinical investigation
Treatment of Abdominal Aortic Aneurysms (AAA)
 Treatment of Abdominal Aortic Aneurysms (AAA) Exceptional healthcare, personally delivered Ask 3 Questions Preparation for your Appointments We want you to be active in your healthcare. By telling us what
Treatment of Abdominal Aortic Aneurysms (AAA) Exceptional healthcare, personally delivered Ask 3 Questions Preparation for your Appointments We want you to be active in your healthcare. By telling us what
Chungbuk Regional Cardiovascular Center, Division of Cardiology, Departments of Internal Medicine, Chungbuk National University Hospital Sangmin Kim
 Endovascular Procedures for Isolated Common Iliac and Internal Iliac Aneurysm Chungbuk Regional Cardiovascular Center, Division of Cardiology, Departments of Internal Medicine, Chungbuk National University
Endovascular Procedures for Isolated Common Iliac and Internal Iliac Aneurysm Chungbuk Regional Cardiovascular Center, Division of Cardiology, Departments of Internal Medicine, Chungbuk National University
You re listening to an audio module from BMJ Learning. Hallo. I'm Anna Sayburn, Senior Editor with the BMJ Group s Consumer Health Team.
 Transcript of learning module Shared decision making (Dur: 26' 13") Contributors: Anna Sayburn and Alf Collins Available online at: http://learning.bmj.com/ V/O: You re listening to an audio module from
Transcript of learning module Shared decision making (Dur: 26' 13") Contributors: Anna Sayburn and Alf Collins Available online at: http://learning.bmj.com/ V/O: You re listening to an audio module from
Anatomy-Driven Endograft Selection for Abdominal Aortic Aneurysm Repair S. Jay Mathews, MD, MS, FACC
 Anatomy-Driven Endograft Selection for Abdominal Aortic Aneurysm Repair S. Jay Mathews, MD, MS, FACC Interventional Cardiologist/Endovascular Specialist Bradenton Cardiology Center Bradenton, FL, USA Disclosures
Anatomy-Driven Endograft Selection for Abdominal Aortic Aneurysm Repair S. Jay Mathews, MD, MS, FACC Interventional Cardiologist/Endovascular Specialist Bradenton Cardiology Center Bradenton, FL, USA Disclosures
Neuroform Microdelivery Stent System
 Neuroform Microdelivery Stent System Patient Information Booklet TABLE OF CONTENTS What is the Purpose of This Booklet?...2 What is a Wide Neck, Intracranial Aneurysm?...2 What is the Treatment for Wide
Neuroform Microdelivery Stent System Patient Information Booklet TABLE OF CONTENTS What is the Purpose of This Booklet?...2 What is a Wide Neck, Intracranial Aneurysm?...2 What is the Treatment for Wide
Durability of The Endurant Stent-Graft through 5 Years
 Durability of The Endurant Stent-Graft through 5 Years Michel S. Makaroun MD Co-Director, UPMC Heart and Vascular Institute Professor and Chair, Division of Vascular Surgery University of Pittsburgh School
Durability of The Endurant Stent-Graft through 5 Years Michel S. Makaroun MD Co-Director, UPMC Heart and Vascular Institute Professor and Chair, Division of Vascular Surgery University of Pittsburgh School
PATIENT GUIDE. Treating Your Thoracoabdominal Aortic Aneurysm. Zenith t-branch THORACOABDOMINAL ENDOVASCULAR GRAFT
 PATIENT GUIDE Treating Your Thoracoabdominal Aortic Aneurysm Zenith t-branch THORACOABDOMINAL ENDOVASCULAR GRAFT About This Patient Guide This patient guide has been provided as a courtesy from Cook Medical
PATIENT GUIDE Treating Your Thoracoabdominal Aortic Aneurysm Zenith t-branch THORACOABDOMINAL ENDOVASCULAR GRAFT About This Patient Guide This patient guide has been provided as a courtesy from Cook Medical
A FAMILY HISTORY OF ABDOMINAL AORTIC ANEURYSM (AAA) DISEASE
 Important Information for You and Your Family A FAMILY HISTORY OF ABDOMINAL AORTIC ANEURYSM (AAA) DISEASE Have you been diagnosed with AAA disease? There is a 15% chance that one of your family members
Important Information for You and Your Family A FAMILY HISTORY OF ABDOMINAL AORTIC ANEURYSM (AAA) DISEASE Have you been diagnosed with AAA disease? There is a 15% chance that one of your family members
ENDOVASCULAR AORTIC ANEURYSM REPAIR THOMAS JEFFERSON UNIVERSITY HOSPITAL PHILADELPHIA, PENNSYLVANIA May 20, 2008
 ENDOVASCULAR AORTIC ANEURYSM REPAIR THOMAS JEFFERSON UNIVERSITY HOSPITAL PHILADELPHIA, PENNSYLVANIA May 20, 2008 00:00:11 ANNOUNCER: Welcome to Thomas Jefferson University Hospital in Philadelphia, Pennsylvania.
ENDOVASCULAR AORTIC ANEURYSM REPAIR THOMAS JEFFERSON UNIVERSITY HOSPITAL PHILADELPHIA, PENNSYLVANIA May 20, 2008 00:00:11 ANNOUNCER: Welcome to Thomas Jefferson University Hospital in Philadelphia, Pennsylvania.
Coronary angioplasty and stents
 Tests and Procedures Coronary angioplasty and stents By Mayo Clinic Staff Coronary angioplasty (AN-jee-o-plas-tee), also called percutaneous coronary intervention, is a procedure used to open clogged heart
Tests and Procedures Coronary angioplasty and stents By Mayo Clinic Staff Coronary angioplasty (AN-jee-o-plas-tee), also called percutaneous coronary intervention, is a procedure used to open clogged heart
Heart Valve Replacement
 Heart Valve Replacement Introduction Sometimes people have serious problems with the valves in their hearts. A heart valve repair or replacement surgery restores or replaces a defective heart valve. If
Heart Valve Replacement Introduction Sometimes people have serious problems with the valves in their hearts. A heart valve repair or replacement surgery restores or replaces a defective heart valve. If
The Biomechanical Approach to Heart Disease
 Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/medical-breakthroughs-from-penn-medicine/the-biomechanicalapproach-to-heart-disease/3912/
Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/medical-breakthroughs-from-penn-medicine/the-biomechanicalapproach-to-heart-disease/3912/
THE THE MORE MORE NATURAL APPROACH TO OPTIMAL FIT
 THE THE MORE MORE NATURAL APPROACH Natural Approach TO Optimal Fit TO OPTIMAL FIT Conformability without Compromise THE STANDARD IN Conformability AND Designed for flexibility and conformability in tortuous
THE THE MORE MORE NATURAL APPROACH Natural Approach TO Optimal Fit TO OPTIMAL FIT Conformability without Compromise THE STANDARD IN Conformability AND Designed for flexibility and conformability in tortuous
Appendicitis. Diagnosis and Surgery
 Appendicitis Diagnosis and Surgery What Is Appendicitis? Your side may hurt so much that you called your doctor. Or maybe you went straight to the hospital emergency room. If the symptoms came on quickly,
Appendicitis Diagnosis and Surgery What Is Appendicitis? Your side may hurt so much that you called your doctor. Or maybe you went straight to the hospital emergency room. If the symptoms came on quickly,
Small Abdominal Aortic Aneurysms AAA Information for Patients and Carers
 What causes an AAA? Small Abdominal Aortic Aneurysms AAA Information for Patients and Carers This leaflet tells you about small abdominal aortic aneurysms. What is the aorta? The exact reason why an aneurysm
What causes an AAA? Small Abdominal Aortic Aneurysms AAA Information for Patients and Carers This leaflet tells you about small abdominal aortic aneurysms. What is the aorta? The exact reason why an aneurysm
Endovascular repair for abdominal aortic aneurysm (EVAR) Information for patients Sheffield Vascular Institute
 Endovascular repair for abdominal aortic aneurysm (EVAR) Information for patients Sheffield Vascular Institute page 2 of 12 You have been diagnosed as having an Abdominal Aortic Aneurysm (AAA) and it has
Endovascular repair for abdominal aortic aneurysm (EVAR) Information for patients Sheffield Vascular Institute page 2 of 12 You have been diagnosed as having an Abdominal Aortic Aneurysm (AAA) and it has
Lung Surgery: Thoracoscopy
 Lung Surgery: Thoracoscopy A Problem with Your Lungs Your doctor has told you that you need surgery called thoracoscopy for your lung problem. This surgery alone may treat your lung problem. Or you may
Lung Surgery: Thoracoscopy A Problem with Your Lungs Your doctor has told you that you need surgery called thoracoscopy for your lung problem. This surgery alone may treat your lung problem. Or you may
Expert Round Table with Drs. Anne Tsao and Alex Farivar Part 1: Elderly Man with Indolent Bronchioloalveolar Carcinoma
 Expert Round Table with Drs. Anne Tsao and Alex Farivar Part 1: Elderly Man with Indolent Bronchioloalveolar Carcinoma February 2010 I d like to welcome everyone, thanks for coming out to our lunch with
Expert Round Table with Drs. Anne Tsao and Alex Farivar Part 1: Elderly Man with Indolent Bronchioloalveolar Carcinoma February 2010 I d like to welcome everyone, thanks for coming out to our lunch with
Overview
 Overview Tutorial Script 1 Script for the Virtual Stroke Lab Tutorial Overview http://www.ilstu.edu Background and Vocabulary This podcast provides an overview of The Virtual Stroke Lab, a free virtual
Overview Tutorial Script 1 Script for the Virtual Stroke Lab Tutorial Overview http://www.ilstu.edu Background and Vocabulary This podcast provides an overview of The Virtual Stroke Lab, a free virtual
