MASANORI YAMAMOTO, HATSUKI HIBI and KOJI MIYAKE. Department of Urology, Nagoya University School of Medicine, Nagoya, Japan ABSTRACT
|
|
|
- George Wiggins
- 5 years ago
- Views:
Transcription
1 Nagoya J. Med. Sci , 1994 EFFECT OF ALBUMIN ON PROLUMINAL MOVEMENT OF 3H-ANDROGEN INTO SEMINIFEROUS AND EPIDIDYMAL TUBULES AND ANDROGEN BINDING IN THE INTERSTITIUM OF THE TESTIS AND EPIDIDYMIS AFTER PERIFUSION WITH FLUID CONTAINING ALBUMIN MASANORI YAMAMOTO, HATSUKI HIBI and KOJI MIYAKE Department of Urology, Nagoya University School of Medicine, Nagoya, Japan ABSTRACT Effect of albumin on proluminal androgen movement from the peritubular space to the intratubular fluids of the adult rat testis and epididymis was examined by using in vivo microperifusion and subsequent micropuncture of the seminiferous tubules and caput epididymal tubules. Tubules were perifused with four different fluids: (1) Minimum Essential Medium (MEM) containing 3H-testosterone and 14C-polyethyleneglycol (PEG) alone; (2) MEM + 8 mg/ml Bovine Serum Albumin (BSA) containing the same radiolabeled compounds as above; (3) MEM + 80 mg/ml albumin containing the same radiolabeled compounds as above; and (4) Testosterone-free rat serum containing the same radiolabeled compounds as above. Bound 3H-androgens in the interstitial fluids of the testis and epididymis after one-hour perifusion with the four different fluids above were measured by charcoal assay. In the testis, proluminal 3H-androgen movement was not significantly altered by addition of albumin to the perifusion fluid (p = 0.08). Bound 3H-androgens in the interstitial fluid after perifusion were significantly increased with increasing albumin concentrations in the perifusion fluid. In the caput epididymis, proluminal 3H-androgen movement was significantly decreased with increasing albumin concentration in the perifusion fluid. Bound 3H-androgens in the interstitial fluid after perifusion were significantly increased with increasing albumin concentrations in the perifusion fluid (p<0.05). These findings suggest that proluminal transepithelial movement of 3H-androgens in the reproductive tract could be influenced by the presence of albumin, androgen-binding protein or some other binding protein in the peritubular space. Key Words: Androgen binding, Androgen movement, Testis, Epididymis, Micropuncture INTRODUCTION The testis and epididymis are androgen target tissues that provide an important microenvironment for spermatogenesis,sperm maturation and epididymal metabolism or epididymal epithelial secretion; 1,2) nevertheless, very little is known about local mechanisms that control transepithelial movement of androgen in seminiferous and epididymal tubules. Recently, a new system of in vivo microperifusion and subsequent in vivo micropuncture was developed to examine the movement of 3H-androgens from blood to lumen and from interstitium to lumen in the rat testis and epididymis ) Movement of 3H-androgen into the seminiferous tubule lumen was restricted with intraluminal androgen concentrations plateauing by one hour at approximately 10% to 15% of the extratubular androgen concentrations whether the Correspondence: Dr. Masanori Yamamoto, Department of Urology, Nagoya University School of Medicine, 65 Tsurumai-cho, Showa-ku, Nagoya 466, Japan Accepted for Publication in January 19,
2 134 Masanori Yamamoto et al. 3H-androgen originated in the vascular or interstitial space. 3 ) Additionally, androgen movement from the interstitium to the lumen in the testis was not altered by a lo-times higher concentration of 3H-testosterone in the perifusion fluid. S ) In the caput epididymis, intraluminal 3H-androgen plateaued at approximately 35% of the vascular 3H-androgen concentrations, but when 3H-androgens were perifused around the tubules, movement of 3H-androgen occurred against a concentration gradient. 3,4) This uphill movement was subject to competitive inhibition with 10 times and 100 times the concentration of 3H-testosterone. The importance of these findings is that there is a fundamental difference in androgen movement across the seminiferous and epididymal epithelia. The mechanism underlying this difference may involve differences in androgen binding to some protein in the interstitial space. Physiological studies have indicated that there is a substantial concentration of serum albumin in the interstitial tissue of the rat testis. 6 ) Testicular interstitial fluid exhibits essentially the same concentration of albumin as is found in serum. 6 ) Since serum albumin is the principal carrier protein for testosterone in the plasma and interstitial fluid of rats,12) its abundance in the interstitial tissue space could influence proluminal androgen movement. The present study was undertaken to determine whether or not androgen binding to albumin or some other protein in the interstitial compartments of the testis and epididymis affects movement of 3H-androgen into the tubules of those organs. MATERIALS AND METHODS In Vivo Microperifusion and Micropuncture in the Testis and Caput Epididymis Adult male Sprague-Dawley rats (530 to 670 gm) were maintained in a constant temperature (2YC) vivarium under a 12-h light/12-h dark cycle and had free access to food and water. Animals were anesthetized and prepared for in vivo perifusion and micropuncture of reproductive tract tubules, as previously described. 3,4) Briefly, a testis and an epididymis of each animal were exteriorized in a special testicle holder and stabilized in 33 C, 2% agar. A small window in the agar to the superior surface of the testis or epididymis was left open and covered with mineral oil. The tubules were perifused in vivo through a sharpened, 100-f!m tip micropipette inserted through the tunica albuginea. The tip of the pipette was always kept in sight to ensure that the seminiferous or epididymal tubule was not cut or punctured. The perifusion pump was set for a priming infusion at a rate of 36 f!l/min in the testis and 6 f!l/min in the caput epididymis for 15 min. Subsequently, a sustaining perifusion rate was set at 6 f!l/min in the testis and 2 f!l/min in the caput epididymis for the remainder of the experiment. Four different perifusion fluids were prepared: (1) Lissamine-green-dyed Minimum Essential Medium (MEM) containing 26.7 f!ci 3H-testosterone (New England Nuclear, Boston, MA; specific activity: 55.2 Ci/mmol)/ml; 480 nm testosterone and 1.3 f!ci 14C-polyethyleneglycol (PEG, New England Nuclear; specific activity: 15 mci/g)/ml; control fluid; (2) MEM + 8 mg/ ml Bovine Serum Albumin (Sigma Chemical Company, MO, BSA) containing the same radiolabeled compounds as above (8 mg/ml BSA fluid); (3) MEM + 80 mg/ml BSA containing the same radiolabeled compounds as above (80 mg/ml BSA fluid). The same concentration of BSA as rat serum total protein was used; thus, this fluid is artificial rat serum. (4) Testosterone-free rat serum containing the same radiolabeled compounds as above (T-free serum). The four fluids were used in different experiments on the testes and caput epididymides. A fluid was perifused around the seminiferous or epididymal tubules, and interstitial (perifusion) fluid and adjacent intraluminal fluid were collected by micropuncture at one hour after initiation of the sustaining perifusion. Cell-free fluids were aliquoted, and radioactivity of 3H-androgen and 14C-PEG in
3 ANDROGEN BINDING IN THE TESTICULAR AND EPIDIDYMAL INTERSTITIAL SPACE 135 the perifusion and intraluminal fluids was determined in all samples. The percentage of peritubular 3H-androgen and 14C-PEG appearing in the intraluminal fluid was determined. Since 14C_ PEG is essentially excluded by the blood epididymal barriers, it was included in the perifusion fluid as a marker for contamination of intraluminal fluid by fluid from the extratubular compartments. The proportion of extratubular 14C-PEG appearing in the intraluminal fluid was used to correct the 3H-testosterone data by subtraction. Measurement of Bound vs Free 3H-Androgen in the Interstitial Fluids in the Testis and Caput Epididymis One [tl of interstitial fluid from the testicular and epididymal peritubular space was obtained at one hour after initiation of sustaining perifusion. Total radioactivity of the fluid sample was determined and then charcoal powder (volume=0.28 mm 3 ; Sigma Chemical Co., St. Louis, MO) was added to the fluid sample. The charcoal was dispersed in the fluid sample by manual shaking, and a micropipette containing the sample was inserted into a rotor head on an IEC model B-20 refrigerator centrifuge. The sample was centrifuged at 5000 rpm for 10 min at 4T to remove the charcoal containing unbound 3H-androgen. Triplicate aliquots of each supernatant were assayed by scintillation spectrophotometry to determine protein-bound 3H-androgen in the remaining fluid. The radioactivity of protein-bound 3H-androgen was expressed as a percentage of the total radioactivity of the sample fluid. Data Analysis Chauvenet's criterion was applied to all the data. 7 ) The results are presented as mean and SEM. All multiple comparisons were made by the Kruscal Wallis tests) for nonparametric data, followed by the Wilcoxon rank sum test (p<0.05). RESULTS 14C-PEG concentrations remaining in the testicular peritubular fluids were generally stable in all groups. These values were approximately 85% of those in the original perifusion fluid (Fig. 1). 3H-androgen concentrations remaining in the testicular peritubular fluids in the control group were 14.3±1.9% of those in the original perifusion fluid (Fig. 1). These values were significantly increased in the 8 mg/ml BSA fluid group (41.3±4.4%) and the 80 mg/ml BSA fluid group (68.6±2.2%) (p<0.02). A similar result was obtained in the T-free serum group (68.5±3.7%). The residual 3H-androgens in the testicular interstitial fluid increased with increasing albumin concentration in the perifusion fluid. Intraluminal 3H-androgen concentrations in the seminiferous tubule fluid in the control group were 8.4±2.6% of those in the peritubular fluid (Fig. 2). These values were not significantly decreased in the 8 mg/ml and 80 mg/ml BSA fluid groups nor in the T-free serum group (p=o.l), but proluminal movement of 3H-androgen into the seminiferous tubule in both the 80 mg/ml BSA fluid group (0.62±0.29%) and the T-free serum group (0.6±0.18%) was significantly less than that in the 8 mg/ml BSA fluid group (2.3±0.5%; p<o.ol; Fig. 2). The percentage of bound 3H-androgen in the testicular interstitial fluid in the control group after 1-hr perifusion was 5.2±0.75% (Fig. 3). This value was significantly increased in the 8 mg/ml BSA group (13.7±1.5%) and the 80 mg/ml BSA group (25±0.9%). A similar result was obtained in the T-free serum group (23.2±0.9%). 14C-PEG concentrations remaining in the epididymal interstitial fluids were generally stable in all groups. These values were approximately 80% of those in the original perifusion fluid, and
4 136 Masanori Yamamoto et al. 110 Cl c: "c: 70 'ffi E 60 <l> a: <l> <F. 30 Testis 100 a a 90 a II1II 14C-PEG 80 'U-androgen Control 8 mg/ml BSA 80 mg/ml BSA CS Fig. 1. Percentage of original perifusion fluid I4C-polyethyleneglycol C 4 C-PEG) or 3H-androgen concentration remaining in the testicular interstitial fluid at one hour after initiation of the sustaining perifusion with four different fluids. Control: Lissamine-green-dyed Minimum Essential Medium (MEM) Containing 26.7!-lCi 3H-testosterone and 1.3!-lCi I4C-PEG; 8 mg/ml BSA: MEM + 8 mg/ml Bovine Serum Albumin containing the above radiolabeled compounds; 80 mg/ml BSA: MEM + 80 mg/ml bovine serum albumin containing the same radiolabeled compounds as above; CS: Castrate rat serum containing the same radiolabeled compounds as above. Columns of I4C-PEG sharing same letter superscript are not significantly different (p=0.09). Columns of 3H-androgen sharing same numerical superscript are not significantly different. 10 Testis 9 Fig. 2. 1: 8 <I> E 7 ::E c: <I> 6 5 "0 4 1il c: 'E 3 ::> eq. 2 :-: - ""<:;':\: '\".,,,- %\W \. p<o.05 &. wll p<o.05 4 :. :,';\, T 'i,.,.w-... M Control 8 mg/ml BSA 80 mg/ml BSA CS T 0 Proluminal movement of 3H-androgen perifused in the testicular interstitial space at one hour after initiation of the sustaining perifusion with the four different fluids described in Fig. 1. There was no statistical difference between the control group and other groups, but a significant difference between the 8 mg/ml BSA group and 80 mg/ml BSA group or CS group was found (p<o.ol). I I
5 ANDROGEN BINDING IN THE TESTICULAR AND EPIDIDYMAL INTERSTITIAL SPACE 137 they were similar to those observed in the testis experiment (Figs. 1 and 4). 3H-androgen concentrations remaining around the tubules in the control group were 22.5±3.7% of those in the original perifusion fluid (Fig. 4). These values were significantly increased in the 8 mg/ml BSA fluid group (32±4.4%) and the 80 mg/ml BSA fluid group (58.6±4.1%) (p<0.02). A similar result was obtained in the T-free serum group (57.6±6.0%). The residual 3H-androgens in the epididymal interstitial fluid increased with increasing albumin concentration in the perifusion fluid. Intraluminal 3H-androgen concentrations in the epididymal fluid in the control group were 323.4±73.2% of those in the peritubular fluid (Fig. 5). These values were significantly decreased in the 8 mg/ml and 80 mg/ml BSA fluid groups as well as in the T-free serum group (144.3±20.7%, 70±6.4%, and 75.8±3.8%, respectively; p<0.05). Percentage of bound 3H-androgen in the epididymal interstitial fluid in the control group after I-hr perifusion was 6.4±1.0%, which is similar to the value obtained in the testis experiment (Figs. 3 and 6). This value was significantly increased in the 8 mg/ml BSA group (12.9±0.24%) and the 80 mg/ml BSA group (24±0.9%) (p<0.05). A similar result was obtained in the T-free serum group (25.4±3.5%). DISCUSSION The present study has shown that intraluminal 3H-androgen concentration in the seminiferous tubule fluid is only 8% of the peritubular 3H-androgen concentration, and this proluminal an Testis C C c CD 19 Cl e 17 't:l fii 15 ±(') 't:l 13 c :=J 0 co Control 8 mg/m1 BSA 80 mg/m1 BSA CS Fig. 3. Percentage of bound 3H-androgen in the testicular interstitial fluid at one hour after initiation of the sustaining perifusion with the four different fluids described in Fig. 1. Columns sharing the same letter superscript are not significantly different (p=o.21). Percentage of bound 3H-androgen in the peritubular fluids was significantly increased with increasing albumin concentration in the perifusion fluid (p<o.ol).
6 138 Masanori Yamamoto et al. Cl I 80 J 75 i 70i ' i 55j f :-1 '# :i 1 20 I 15 Caput Epididymis a Control 8 mg/m1 BSA 80 mg/m1 BSA CS III "C-PEG III 'H-androgen Fig. 4. Percentage of original perifusion fluid 14C-PEG or 3H-androgen concentration remaining in the epididymal interstitial fluid at one hour after initiation of the sustaining perifusion with the four different fluids described in Fig. 1. Columns of 14C-PEG sharing the same letter superscript are not significantly different (p=o.15). Columns of 3H-androgen sharing the same numerical superscript are not significantly different. a Caput Epididymis Fig. 5. Proluminal movement of 3H-androgen perifused in the epididymal interstitial space at one hour after initiation of the sustaining perifusion with the four different fluids described in Fig. 1. Columns sharing the same letter superscript are not significantly different. Intraluminal 3H-androgen concentrations in the epididymal fluid were significantly decreased with increasing albumin concentration in the perifusion fluid (p<o.ol).
7 ANDROGEN BINDING IN THE TESTICULAR AND EPIDIDYMAL INTERSTITIAL SPACE c "0 c 16 'll :x: C') 14 "0 c 12 5 ld Caput Epididymis Control 8 mglml BSA 80 mglml BSA cs c Fig. 6. Percentage of bound 3H-androgen in the epididymal interstitial fluid at one hour after initiation of the sustaining perifusion with the four different fluids described in Fig. 1. Columns sharing the same letter superscript are not significantly different (p = 0.21). Percentage of bound 3H-androgen in the peritubular fluids significantly increased with increasing albumin concentration in the perifusion fluid (p < 0.02). drogen movement is not inhibited by the presence of albumin or testosterone-free serum in the perifusion fluid. Total protein and albumin levels in rat testicular interstitial fluid are essentially the same as those found in serum. 6 ) Concentration of rat serum total protein is 60 to 80 mg/ml. Therefore, perifusion with 80 mg/ml BSA fluid or T-free rat serum around the seminiferous tubules approximates the native condition of the rat testicular interstitial space. When 3H-testosterone was infused into the systemic circulation, one hour after 3H-testosterone infusion intraluminal concentrations of 3H-androgens in the seminiferous tubules were approximately 14% that of blood plasma. 3 ) When 3H-testosterone was presented directly to the basal aspect of the seminiferous epithelium, intraluminal concentrations of 3H-androgens at one hour after initiation of sustaining perifusion around the seminiferous tubules (movement of 3H-androgen from interstitium to lumen) were 8% to 20% of the interstitial fluid,3,4) which was essentially similar to the proluminal androgen movement from blood to lumen. Proluminal movement of 3H-androgen in the testis was significantly decreased with increasing albumin concentration in the perifusion fluid from 8 mg/ml to 80 mg/ml. This result is consistent with the significant increase in 3H-androgen remaining around the tubules and percentage of bound 3H-androgen in the interstitial fluid after one-hour perifusion. Since serum albumin is the main carrier protein for testosterone in the interstitial fluid,12) it is possible that when albumin concentration in the perifusion fluid is increased, more 3H-androgen binds to interstitial albumin, which retains 3H-androgen and removes some portion of the 3H-androgen pool in the peritubular space available for diffusion into the tubule lumen, and subsequently reduces the proluminal movement of 3H-androgen. Christensen et al. have shown the detailed distribution of serum albumin in the rat testicular space by immunocytochemistry.9) They observed albumin in
8 140 Masanori Yamamoto et af. the interstitial tissue, as well as in the space between the boundary layer and the base of the seminiferous epithelium. 9 ) If perfusion fixation was performed in a manner that flushed most of the albumin from the interstitial space, then this resembled the condition under sustaining perifusion around the tubules, and a layer of albumin remained on the surface of Leydig cells and many macrophages. 9 ) It is suggested that albumin on the Leydig cell surface may playa role in the mobilization of newly secreted testosterone at the cell surface. 9 ) Therefore, the question remains of whether or not native albumin localized around Leydig cells during perifusion with fluid containing no BSA can trap diffusible 3H-androgen in the peritubular space and then restrict proluminal movement of 3H-androgen. Approximately 20% of androgen-binding protein is released into the interstitial compartment, probably from the base of Sertoli cells. 10) Although androgen-binding protein or other androgen-binding molecules in the testicular interstitial space can retain 3H-androgen, it is unclear how much they contribute to the restriction of movement of androgens into the tubule lumen. The percentage of bound 3H-androgen in the testicular interstitial fluid after one-hour perifusion with the control fluid was similar to that in the epididymal interstitial fluid. Based on this result, it can not be explained by differential androgen binding in the interstitial compartment that proluminal androgen movement in the testis is different from that in the caput epididymis where proluminal androgen movement is very high. The reason for restricted transepithelial movement of androgen in the seminiferous tubule is unclear. The present study has demonstrated that transepithelial movement of 3H-androgen in the caput epididymis is significantly decreased with increasing albumin concentration in the perifusion fluid. Net entry of 3H-androgen into the epididymal tubule was reduced to less than half of the control values by addition of 8 mg/ml BSA to the perifusion fluid. This value was reduced to 70% by addition of 80 mg/ml BSA to the perifusion fluid. These results are consistent with the significant increase in 3H-androgen remaining around the tubules and the percentage of bound 3H-androgen along with the increasing dalbumin concentration in the perifusion fluid. The significant decrease in proluminal 3H-androgen movement by increasing albumin concentration in the perifusion fluid can be accounted for by the significant reduction of free, diffusible 3H-androgen in the interstitial space. There have been no reports of protein concentration in the epididymal interstitial space. However, based on the data for other organs, interstitial protein concentration is approximately one sixteenth of serum. 11 ) If this is true in the epididymis, significant reduction of proluminal antigrade androgen movement caused by the same concentration of protein in the perifusion fluid as in serum should not happen in the native condition. Nevertheless, proluminal movement of 3H-androgen across the epididymal tubules was altered in the absence or presence of various degrees of 3H-androgen binding to albumin or other peritubular androgen-binding molecules in the vascular and interstitial compartments, while proluminal movement of 3H-androgen across the seminiferous tubules was not significantly affected by the presence of 3H-androgen binding in the testicular interstitium. Different interstitial concentrations of protein seem to cause different effects of albumin in the perifusion fluid on proluminal movement of 3H-androgen into the tubules of the testis and epididymis. We have recently demonstrated that proluminal antigrade movement of 3H-androgen in the caput epididymis is completely eliminated by addition of a metabolic inhibitor that blocks ATP production in the metabolic pathway to the perifusion fluid. 14 ) It was thought to be possible that a metabolic inhibitor interfered with the capillary endothelium and then the interstitial capillary vessels became leakier; thus, more labeled androgen bound to interstitial secreted protein, and unbound androgen in the interstitial space was decreased. Only unbound androgen can enter the epididymal lumen. Therefore, proluminal androgen movement was reduced. The exact mechanism of antigrade androgen movement across the epididymal epithelium, in contrast to the semi-
9 ANDROGEN BINDING IN THE TESTICULAR AND EPIDIDYMAL INTERSTITIAL SPACE 141 niferous epithelium, is not known. Nevertheless, it has been demonstrated that intraluminal androgen-binding protein,5,13) and the presence of a metabolic inhibitor or albumin in the interstitial space have a substantial effect on this unique uphill proluminal androgen movement. These findings make it more problematic to clarify the mechanism of androgen movement specifically across the caput epididymal epithelium. In conclusion, transepithelial 3H-androgen movement in the testis is not significantly affected by addition of albumin to the perifusion fluid, while proluminal movement of 3H-androgen into the caput epididymal tubules is significantly reduced by increasing albumin concentration in the perifusion fluid. Proluminal movement of 3H-androgen into the seminiferous tubule lumen is restricted 3,4) but not inhibited by competition with unlabeled testosterone,5) and not significantly affected by the presence of albumin in the perifusion fluid. However, it is possible that increasing androgen binding to protein in the testicular interstitial space may affect proluminal androgen movement. The reason for the low access of androgens to the seminiferous tubule lumen is still unclear. Antigrade, proluminal movement of 3H-androgen into the caput epididymal tubule lumen is subject to competitive inhibition 5 ) and significantly decreased by increasing albumin concentration in the perifusion fluid. Differential 3H-androgen binding to peritubular molecules actually alters availability of interstitial 3H-androgen to the intraluminal compartmentalization of androgens in the epididymis. Further experiments will be needed to understand the mechanisms underlying androgen movement across the seminiferous and epididymal epithelia. REFERENCES 1) Brooks, D.E.: Metabolic activity in the epididymis and its regulation by androgens. Physiol. Rev., 61, (1981). 2) Robaire, B. and Hermo, L.: Efferent ducts, epididymis, and vas deferens: Structure, functions, and their regulation. In The Physiology of Reproduction, edited by Knobil E. and Neil, J.D., Vol. 1 pp (1988) Raven Press, New York., 3) Turner, T.T.: Transepithelial movement of 3H-androgen in seminiferous and epididymal tubules: A study using in vivo micropuncture and in vivo microperifusion. Bioi. Reprod., 39, (1988). 4) Yamamoto, M. and Turner, T.T.: Transepithelial movement of non-polar and polar compounds in male rat reproductive tubule examined by in vivo microperifusion and in vivo micropuncture. J. Ural., 143, (1990). 5) Turner, T.T., Jones, C.E. and Roddy, M.S.: On the proluminal movement of 3H-androgens across the rat epididymal epithelium. BioI. Reprod., 40, (1989). 6) Sharpe, R.M.: Gonadotrophin-induced accumulation of interstitial fluid in the rat testis. J. Reprod. Ferti!., 55, (1979). 7) Worthing, AG. and Geffner, J.: In Treatment of Experimental Data. pp (1943) John Wiley & Sons, Inc., New York. 8) Kruskal, W.H. and Wallis, W.A: Use of ranks in one-crition variance analysis. J. Am. Stat. Assoc., 47, (1952). 9) Christensen, A.K., Komorowski, T.E., Wilson, B., Ma, Syau-Fu, and Stevens, R.W.: The distribution of serum albumin in the rat testis, studied by electron microscope immunocytochemistry on ultrathin frozen sections. Endocrinology, 116, (1985). 10) Gunsalus, G.L., Musto, N.A, and Bardin, C.W.: Immunoassay of androgen binding protein in blood: A new approach for study of the seminiferous tubule. Science, 200, (1978). 11) Berne, R.M. and Levy, M.N.: Components of renal function. In Physiology, 2nd ed. pp (1988) C.V. Mosby Company, Missouri. 12) Corvol, P. and Bardin, C.W.: Species distribution of testosterone binding globulin. BioI. Reprod., 8, (1973). 13) Yamamoto, M. and Turner, T.T.: Proluminal movement of 3H-androgen across the epididymal epithelium in the rat after hypophysectomy and gonadotropin supplementation. Bioi. Reprod., 41, (1989).
10 142 Masanori Yamamoto et al. 14) Yamamoto, M., Tsuji, Y. and Miyake, K.: Evidence for active transport of 3H-androgens across the epididymal epithelium in the rat. Nagoya J. Med. Sci., 56, (1993).
EFFECTS OF PROTEIN SYNTHESIS INHIBITOR AND ANTIMICROTUBULAR AGENT ON TRANSEPITHELIAL MOVEMENT OF 3H-ANDROGENS IN THE RAT CAPUT EPIDIDYMIS
 Nagoya J. Med. Sci. 57. 119-126, 1994 EFFECTS OF PROTEIN SYNTHESIS INHIBITOR AND ANTIMICROTUBULAR AGENT ON TRANSEPITHELIAL MOVEMENT OF 3H-ANDROGENS IN THE RAT CAPUT EPIDIDYMIS MASANORI YAMAMOTO, HATSUKI
Nagoya J. Med. Sci. 57. 119-126, 1994 EFFECTS OF PROTEIN SYNTHESIS INHIBITOR AND ANTIMICROTUBULAR AGENT ON TRANSEPITHELIAL MOVEMENT OF 3H-ANDROGENS IN THE RAT CAPUT EPIDIDYMIS MASANORI YAMAMOTO, HATSUKI
Histology of Male Reproductive system (1)
 Histology of Male Reproductive system (1) Prof. Dr. Malak A. Al-yawer Learning Objectives At the end of this lecture, the medical student will be able to: State the organization of the testis Define seminiferous
Histology of Male Reproductive system (1) Prof. Dr. Malak A. Al-yawer Learning Objectives At the end of this lecture, the medical student will be able to: State the organization of the testis Define seminiferous
Male Reproductive System
 Male Reproductive System Constitution of male reproductive system Genital gland ----testis Genital ducts epididymis / ductus deferens / urinary duct Accessory sex glands Penis prostate gland Seminal vesicle
Male Reproductive System Constitution of male reproductive system Genital gland ----testis Genital ducts epididymis / ductus deferens / urinary duct Accessory sex glands Penis prostate gland Seminal vesicle
THE INCIDENCE OF ANTISPERM ANTmODIES IN PATIENTS WITH SEMINAL TRACT OBSTRUCTIONS
 Nagoya J. Med. Sci. 59. 25-29,1996 THE INCIDENCE OF ANTISPERM ANTmODIES IN PATIENTS WITH SEMINAL TRACT OBSTRUCTIONS MASANORI YAMAMOTO, HATSUKI HIBI, and KOJI MIYAKE Department of Urology, Nagoya University
Nagoya J. Med. Sci. 59. 25-29,1996 THE INCIDENCE OF ANTISPERM ANTmODIES IN PATIENTS WITH SEMINAL TRACT OBSTRUCTIONS MASANORI YAMAMOTO, HATSUKI HIBI, and KOJI MIYAKE Department of Urology, Nagoya University
THE EFFECTS OF LIGATION OF CAUDA EPIDIDYMIDIS ON THE DOG TESTIS
 Copyright 1974 The American Fertility Society FERTILITY AND STERILITY Vol. 25, No.3, March, 1974 Printed in U.S.A. THE EFFECTS OF LIGATION OF CAUDA EPIDIDYMIDIS ON THE DOG TESTIS A. M. VARE, M.B.B.S.,
Copyright 1974 The American Fertility Society FERTILITY AND STERILITY Vol. 25, No.3, March, 1974 Printed in U.S.A. THE EFFECTS OF LIGATION OF CAUDA EPIDIDYMIDIS ON THE DOG TESTIS A. M. VARE, M.B.B.S.,
Transport of Sperm. Endocrinology of the Epididymis and Sperm Maturation. Vas Efferentia. John Parrish Department of Animal Sciences
 Endocrinology of the Epididymis and Sperm Maturation John Parrish Department of Animal Sciences References: he Physiology of Reproduction, Knobil and Neill, 2006; Chapter on the Epididymis by Robaire ransport
Endocrinology of the Epididymis and Sperm Maturation John Parrish Department of Animal Sciences References: he Physiology of Reproduction, Knobil and Neill, 2006; Chapter on the Epididymis by Robaire ransport
Department of Urology University of Virginia School of Medicine Charlo ttesville, Virginia 22908
 BIOLOGY OF REPRODUCTION 36,926-932 (1987) Experimental Varicocele does not Affect the Blood-Testis Barrier, Epididymal Electrolyte Concentrations, or Testicular Blood Gas Concentrations' T. T. TURNER,'
BIOLOGY OF REPRODUCTION 36,926-932 (1987) Experimental Varicocele does not Affect the Blood-Testis Barrier, Epididymal Electrolyte Concentrations, or Testicular Blood Gas Concentrations' T. T. TURNER,'
ESUR SCROTAL AND PENILE IMAGING WORKING GROUP MULTIMODALITY IMAGING APPROACH TO SCROTAL AND PENILE PATHOLOGIES 2ND ESUR TEACHING COURSE
 ESUR SCROTAL AND PENILE IMAGING WORKING GROUP MULTIMODALITY IMAGING APPROACH TO SCROTAL AND PENILE PATHOLOGIES 2ND ESUR TEACHING COURSE NORMAL ANATOMY OF THE SCROTUM MICHAEL NOMIKOS M.D. F.E.B.U. UROLOGICAL
ESUR SCROTAL AND PENILE IMAGING WORKING GROUP MULTIMODALITY IMAGING APPROACH TO SCROTAL AND PENILE PATHOLOGIES 2ND ESUR TEACHING COURSE NORMAL ANATOMY OF THE SCROTUM MICHAEL NOMIKOS M.D. F.E.B.U. UROLOGICAL
MALE REPRODUCTIVE SYSTEM
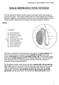 MALE REPRODUCTIVE SYSTEM The male reproductive system consists of primary sex organs (testes) and secondary or accessory sex organs. The secondary organs consist of a series of genital ducts (ductules
MALE REPRODUCTIVE SYSTEM The male reproductive system consists of primary sex organs (testes) and secondary or accessory sex organs. The secondary organs consist of a series of genital ducts (ductules
ADVERSE EFFECTS OF VASECTOMY: SPERM GRANULOMA OF EPIDIDYMIDES V. P. DIXIT
 ADVERSE EFFECTS OF VASECTOMY: SPERM GRANULOMA OF EPIDIDYMIDES V. P. DIXIT Reproduct ion Physiology Section, Department of Zoology, University of Rajasthan, Jaipur-302004 Summary: Rats and mice were vasectomized
ADVERSE EFFECTS OF VASECTOMY: SPERM GRANULOMA OF EPIDIDYMIDES V. P. DIXIT Reproduct ion Physiology Section, Department of Zoology, University of Rajasthan, Jaipur-302004 Summary: Rats and mice were vasectomized
Efferent Ducts and Epididymis
 increase) the secretion of each of the androgen regulated proteins. Regulation of spermatogenesis is therefore an extremely complex cascade of cell-cell interactions with the Leydig cells supporting germ
increase) the secretion of each of the androgen regulated proteins. Regulation of spermatogenesis is therefore an extremely complex cascade of cell-cell interactions with the Leydig cells supporting germ
Male Reproductive System
 Male Reproductive System organs that function in: gamete and hormone production not all in abdominal cavity paired testicles = controlled by LH & FSH duct systems accessory glands Testis: Gross Histology
Male Reproductive System organs that function in: gamete and hormone production not all in abdominal cavity paired testicles = controlled by LH & FSH duct systems accessory glands Testis: Gross Histology
Effects of Growth Hormone on Testicular Testosterone Production In Vitro in Transgenic Mice
 Southern Illinois University Carbondale OpenSIUC Honors Theses University Honors Program 12-1989 Effects of Growth Hormone on Testicular Testosterone Production In Vitro in Transgenic Mice Angela Susan
Southern Illinois University Carbondale OpenSIUC Honors Theses University Honors Program 12-1989 Effects of Growth Hormone on Testicular Testosterone Production In Vitro in Transgenic Mice Angela Susan
Male Reproductive System. Dr Maan Al-Abbasi PhD, MSc, MBChB, MD
 Male Reproductive System Dr Maan Al-Abbasi PhD, MSc, MBChB, MD Learning Objectives 1. Describe the General Anatomy of the Male Reproductive System 2. Identify the structures that are related to the prostate.
Male Reproductive System Dr Maan Al-Abbasi PhD, MSc, MBChB, MD Learning Objectives 1. Describe the General Anatomy of the Male Reproductive System 2. Identify the structures that are related to the prostate.
MICROPUNCTURE AND MICROANALYTIC STUDIES OF THE RAT TESTIS AND EPIDIDYMIS*
 F'ERTII.JTY AND STERILITY Copyright " 1975 The American Fertility Society Vol. 26, No. 1, January 1975 Printed in U.S.A. MICROPUNCTURE AND MICROANALYTIC STUDIES OF THE RAT TESTIS AND EPIDIDYMIS* STUARTS.
F'ERTII.JTY AND STERILITY Copyright " 1975 The American Fertility Society Vol. 26, No. 1, January 1975 Printed in U.S.A. MICROPUNCTURE AND MICROANALYTIC STUDIES OF THE RAT TESTIS AND EPIDIDYMIS* STUARTS.
Ultrastructural Studies on the Development of the Blood-Epididymis Barrier in Immature Rats
 Reprinted from JOURNAL OF ANDROLOGY, November-December 1989 Vol. 10, No. 6 J. B. Lippincott Co. Printed in U.S.A. Ultrastructural Studies on the Development of the Blood-Epididymis Barrier in Immature
Reprinted from JOURNAL OF ANDROLOGY, November-December 1989 Vol. 10, No. 6 J. B. Lippincott Co. Printed in U.S.A. Ultrastructural Studies on the Development of the Blood-Epididymis Barrier in Immature
Primary sex organs (gonads): testes and ovaries. Accessory reproductive organs: ducts, glands, and external genitalia
 Male Reproductive System Primary sex organs (gonads): testes and ovaries Produce sex cells (gametes) Secrete steroid sex hormones Androgens (males) Estrogens and progesterone (females) Accessory reproductive
Male Reproductive System Primary sex organs (gonads): testes and ovaries Produce sex cells (gametes) Secrete steroid sex hormones Androgens (males) Estrogens and progesterone (females) Accessory reproductive
RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D.
 RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D. Learning Objectives 1. Identify the region of the renal tubule in which reabsorption and secretion occur. 2. Describe the cellular
RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D. Learning Objectives 1. Identify the region of the renal tubule in which reabsorption and secretion occur. 2. Describe the cellular
The Male Reproductive System
 The Male Reproductive System YONG-MEI CHEN ( 陈咏梅 ) Dept. of Anatomy, Histology & Embryology Peking Union Medical College Tel:69156461 E-mail address: pumc_he@126.com Content Spermatogenesis Spermiogenesis
The Male Reproductive System YONG-MEI CHEN ( 陈咏梅 ) Dept. of Anatomy, Histology & Embryology Peking Union Medical College Tel:69156461 E-mail address: pumc_he@126.com Content Spermatogenesis Spermiogenesis
Comparison of the effectiveness of placebo and a-blocker therapy for the treatment of idiopathic oligozoospermia *
 FERTILITY AND STERILITY Copyright c 1995 American Society for Reproductive Medicine Printed on acid-free paper in U. S. A. Comparison of the effectiveness of placebo and a-blocker therapy for the treatment
FERTILITY AND STERILITY Copyright c 1995 American Society for Reproductive Medicine Printed on acid-free paper in U. S. A. Comparison of the effectiveness of placebo and a-blocker therapy for the treatment
Introduction. Acids, Bases and ph; a review
 0 P a g e Introduction In this sheet, we discuss acidbase balance in our body and the role of kidneys in its establishment. Arrangement of topics is different from that of the lecture, to assure consistency
0 P a g e Introduction In this sheet, we discuss acidbase balance in our body and the role of kidneys in its establishment. Arrangement of topics is different from that of the lecture, to assure consistency
THE EFFECTS OF REPEATED INJECTIONS OF CHORIONIC GONADOTROPIN ON THE TESTES OF THE LEOPARD FROG (RANA PIPIENS SCHREBER)
 THE EFFECTS OF REPEATED INJECTIONS OF CHORIONIC GONADOTROPIN ON THE TESTES OF THE LEOPARD FROG (RANA PIPIENS SCHREBER) ROBERT P. McCOURT Department of Zoology and Entomology, The Ohio State University,
THE EFFECTS OF REPEATED INJECTIONS OF CHORIONIC GONADOTROPIN ON THE TESTES OF THE LEOPARD FROG (RANA PIPIENS SCHREBER) ROBERT P. McCOURT Department of Zoology and Entomology, The Ohio State University,
Male reproduction. Cross section of Human Testis ผศ.ดร.พญ.ส ว ฒณ ค ปต ว ฒ ภาคว ชาสร รว ทยา คณะแพทยศาสตร ศ ร ราชพยาบาล 1. Aims
 Aims Male reproduction Male reproductive structure Spermatogenesis ส ว ฒณ ค ปต ว ฒ ห อง 216 โทร: 7578 Hypothalamo-pituitary-testicular axis Male sex hormone action Male reproductive structure Male reproductive
Aims Male reproduction Male reproductive structure Spermatogenesis ส ว ฒณ ค ปต ว ฒ ห อง 216 โทร: 7578 Hypothalamo-pituitary-testicular axis Male sex hormone action Male reproductive structure Male reproductive
Medical School Histology Basics Male Reproductive System. VIBS 289 lab
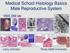 Medical School Histology Basics Male Reproductive System VIBS 289 lab Larry Johnson Texas A&M University OBJECTIVE To conduct a histologic examination of the testis (which produce spermatozoa), excretory
Medical School Histology Basics Male Reproductive System VIBS 289 lab Larry Johnson Texas A&M University OBJECTIVE To conduct a histologic examination of the testis (which produce spermatozoa), excretory
2. The waste products of metabolism are eliminated through the process of A) assimilation. B) absorption. C) excretion. D) digestion. E) resorption.
 CH 1 GENERAL ANATOMY 1. Characteristics of most living organisms include the ability to A) grow and reproduce. B) respond and adapt to their environment. C) control the external environment. D) A and B
CH 1 GENERAL ANATOMY 1. Characteristics of most living organisms include the ability to A) grow and reproduce. B) respond and adapt to their environment. C) control the external environment. D) A and B
SISTEMA REPRODUCTOR (LA IDEA FIJA) Copyright 2004 Pearson Education, Inc., publishing as Benjamin Cummings
 SISTEMA REPRODUCTOR (LA IDEA FIJA) How male and female reproductive systems differentiate The reproductive organs and how they work How gametes are produced and fertilized Pregnancy, stages of development,
SISTEMA REPRODUCTOR (LA IDEA FIJA) How male and female reproductive systems differentiate The reproductive organs and how they work How gametes are produced and fertilized Pregnancy, stages of development,
Hormones of brain-testicular axis
 (Hormone Function) Hormones of brain-testicular axis anterior pituitary drives changes during puberty controlled by GnRH from hypothalamus begins to secrete FSH, LH LH targets interstitial endocrinocytes
(Hormone Function) Hormones of brain-testicular axis anterior pituitary drives changes during puberty controlled by GnRH from hypothalamus begins to secrete FSH, LH LH targets interstitial endocrinocytes
Histologic and histomorphometric changes of testis following oral exposure to methyl tertiary-butyl ether in adult rat
 288 Histologic and histomorphometric changes of testis following oral exposure to methyl tertiary-butyl ether in adult rat Gholami, S. 1* ; Ansari-Lari, M. 2 and Khalili, L. 3 1 Department of Basic Sciences,
288 Histologic and histomorphometric changes of testis following oral exposure to methyl tertiary-butyl ether in adult rat Gholami, S. 1* ; Ansari-Lari, M. 2 and Khalili, L. 3 1 Department of Basic Sciences,
Collin College. BIOL Anatomy & Physiology. Urinary System. Summary of Glomerular Filtrate
 Collin College BIOL. 2402 Anatomy & Physiology Urinary System 1 Summary of Glomerular Filtrate Glomerular filtration produces fluid similar to plasma without proteins GFR ~ 125 ml per min If nothing else
Collin College BIOL. 2402 Anatomy & Physiology Urinary System 1 Summary of Glomerular Filtrate Glomerular filtration produces fluid similar to plasma without proteins GFR ~ 125 ml per min If nothing else
Male Anatomy. testes, genetically determined in mammals - testis releases hormones that then control the development of secondary sex characteristics
 Male Anatomy Male Anatomy Primary Organ testes, genetically determined in mammals - testis releases hormones that then control the development of secondary sex characteristics 1) Secondary Organs internal
Male Anatomy Male Anatomy Primary Organ testes, genetically determined in mammals - testis releases hormones that then control the development of secondary sex characteristics 1) Secondary Organs internal
Human Anatomy Unit 3 REPRODUCTIVE SYSTEM
 Human Anatomy Unit 3 REPRODUCTIVE SYSTEM In Anatomy Today Male Reproductive System Gonads = testes primary organ responsible for sperm production development/maintenan ce of secondary sex characteristics
Human Anatomy Unit 3 REPRODUCTIVE SYSTEM In Anatomy Today Male Reproductive System Gonads = testes primary organ responsible for sperm production development/maintenan ce of secondary sex characteristics
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,350 108,000 1.7 M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,350 108,000 1.7 M Open access books available International authors and editors Downloads Our
MALE REPRODUCTIVE SYSTEM
 MALE REPRODUCTIVE SYSTEM 1. The male reproductive system is made up of the following structures, EXCEPT: a. prostate; b. testicle; c. spermatic ducts; d. vestibular bulbs; e. seminal vesicles. 2.The testicle:
MALE REPRODUCTIVE SYSTEM 1. The male reproductive system is made up of the following structures, EXCEPT: a. prostate; b. testicle; c. spermatic ducts; d. vestibular bulbs; e. seminal vesicles. 2.The testicle:
HISTOCHEMISTRY OF PHOSPHATASES IN THE EPIDIDYMIS OF RAM DURING POSTNATAL DEVELOPMENT*
 HISTOCHEMISTRY OF PHOSPHATASES IN THE EPIDIDYMIS OF RAM DURING POSTNATAL DEVELOPMENT* P.V.S. Kishore 1, Geetha Ramesh 2 and Sabiha Hayath Basha 3 Department of Veterinary Anatomy & Histology, Madras Veterinary
HISTOCHEMISTRY OF PHOSPHATASES IN THE EPIDIDYMIS OF RAM DURING POSTNATAL DEVELOPMENT* P.V.S. Kishore 1, Geetha Ramesh 2 and Sabiha Hayath Basha 3 Department of Veterinary Anatomy & Histology, Madras Veterinary
Adapted from Preg. & Part., Senger
 MALE ENDOCRINOLOGY AND SPERMATOGENESIS (Chapter 10) AVS 222 (Instructor: Dr. Amin Ahmadzadeh) I. MALE ENDOCRINOLOGY (Figure10-1 to 10-3) A. Glands and their respective hormones 1) Hypothalamic hormone:
MALE ENDOCRINOLOGY AND SPERMATOGENESIS (Chapter 10) AVS 222 (Instructor: Dr. Amin Ahmadzadeh) I. MALE ENDOCRINOLOGY (Figure10-1 to 10-3) A. Glands and their respective hormones 1) Hypothalamic hormone:
The Repr duct ve System. Function: producing offspring
 The Repr duct ve System Function: producing offspring Anatomy of male reproductive system Location: The reproductive organs are classified as external and internal genitalia. The external genitalia are
The Repr duct ve System Function: producing offspring Anatomy of male reproductive system Location: The reproductive organs are classified as external and internal genitalia. The external genitalia are
In vitro Study of the Spermatozoa Motility in the Lizard Eutropis carinata
 International Journal of Zoological Research 11 (3): 89-95, 2015 ISSN 1811-9778 / DOI: 10.3923/ijzr.2015.89.95 2015 Academic Journals Inc. In vitro Study of the Spermatozoa Motility in the Lizard Eutropis
International Journal of Zoological Research 11 (3): 89-95, 2015 ISSN 1811-9778 / DOI: 10.3923/ijzr.2015.89.95 2015 Academic Journals Inc. In vitro Study of the Spermatozoa Motility in the Lizard Eutropis
Fluid Movement in the Lumen of the Rat Epididymis: Effect of Vasectomy and Subsequent Vasovasostomy
 Journal of Andrology, Vol. 11, No. 5, September/October 1990 Copyright 0 American Society of Andrology Fluid Movement in the Lumen of the Rat Epididymis: Effect of Vasectomy and Subsequent Vasovasostomy
Journal of Andrology, Vol. 11, No. 5, September/October 1990 Copyright 0 American Society of Andrology Fluid Movement in the Lumen of the Rat Epididymis: Effect of Vasectomy and Subsequent Vasovasostomy
SURGICAL OUTCOME OF MICROSCOPIC VASECTOMY REVERSAL: AN ANALYSIS OF 30 CASES
 Nagoya J. Med. Sci. 60. 37-42, 1997 SURGICAL OUTCOME OF MICROSCOPIC VASECTOMY REVERSAL: AN ANALYSIS OF 30 CASES MASANORI YAMAMOTO, HATSUKI HIBI, KEISUKE YOKOI, ATSUSHI MISHIMA and SATOSHI KATSUNO Department
Nagoya J. Med. Sci. 60. 37-42, 1997 SURGICAL OUTCOME OF MICROSCOPIC VASECTOMY REVERSAL: AN ANALYSIS OF 30 CASES MASANORI YAMAMOTO, HATSUKI HIBI, KEISUKE YOKOI, ATSUSHI MISHIMA and SATOSHI KATSUNO Department
RENAL PHYSIOLOGY, HOMEOSTASIS OF FLUID COMPARTMENTS
 RENAL PHYSIOLOGY, HOMEOSTASIS OF FLUID COMPARTMENTS (2) Dr. Attila Nagy 2017 TUBULAR FUNCTIONS (Learning objectives 54-57) 1 Tubular Transport About 99% of filtrated water and more than 90% of the filtrated
RENAL PHYSIOLOGY, HOMEOSTASIS OF FLUID COMPARTMENTS (2) Dr. Attila Nagy 2017 TUBULAR FUNCTIONS (Learning objectives 54-57) 1 Tubular Transport About 99% of filtrated water and more than 90% of the filtrated
Transport across the cell membrane
 Transport across the cell membrane Learning objectives Body compartments ECF and ICF Constituents Lipid Bilayer: Barrier to water and water-soluble substances ions glucose H 2 O urea CO 2 O 2 N 2 halothane
Transport across the cell membrane Learning objectives Body compartments ECF and ICF Constituents Lipid Bilayer: Barrier to water and water-soluble substances ions glucose H 2 O urea CO 2 O 2 N 2 halothane
Basic histology 5/4/2015
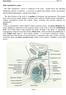 Male reproductive system The male reproductive system is composed of the testes, genital ducts (the adjoining epididymis, and the vas deferens, a accessory sex glands (the seminal vesicles, the prostrate
Male reproductive system The male reproductive system is composed of the testes, genital ducts (the adjoining epididymis, and the vas deferens, a accessory sex glands (the seminal vesicles, the prostrate
Testicular interstitial fluid as a monitor for changes in the intratesticular environment in the rat
 Testicular interstitial fluid as a monitor for changes in the intratesticular environment in the rat R. M. Sharpe and Irene Cooper M.R.C. Reproductive Biology Unit, Centre for Reproductive Biology, 37
Testicular interstitial fluid as a monitor for changes in the intratesticular environment in the rat R. M. Sharpe and Irene Cooper M.R.C. Reproductive Biology Unit, Centre for Reproductive Biology, 37
Title. Author(s)KANAGAWA, Hiroshi; ISHIKAWA, Tsune; KAWATA, Keiichir. CitationJapanese Journal of Veterinary Research, 13(1): Issue Date
 Title A CASE OF CANINE TESTICULAR SERTOLI CELL TUMOR Author(s)KANAGAWA, Hiroshi; ISHIKAWA, Tsune; KAWATA, Keiichir CitationJapanese Journal of Veterinary Research, 13(1): 11-1 Issue Date 1965-03 DOI 10.14943/jjvr.13.1.11
Title A CASE OF CANINE TESTICULAR SERTOLI CELL TUMOR Author(s)KANAGAWA, Hiroshi; ISHIKAWA, Tsune; KAWATA, Keiichir CitationJapanese Journal of Veterinary Research, 13(1): 11-1 Issue Date 1965-03 DOI 10.14943/jjvr.13.1.11
HISTOLOGIC CHANGES IN THE SEMINIFEROUS TUBULES AFTER VASECTOMY
 FERTILItY AND STI!RILITY Copyright 1974 The American Fertility Society Vol. 25, No.8, August 1974 PTillted in U.S.AI HISTOLOGIC CHANGES IN THE SEMINIFEROUS TUBULES AFTER VASECTOMY FLETCHER C. DERRICK,
FERTILItY AND STI!RILITY Copyright 1974 The American Fertility Society Vol. 25, No.8, August 1974 PTillted in U.S.AI HISTOLOGIC CHANGES IN THE SEMINIFEROUS TUBULES AFTER VASECTOMY FLETCHER C. DERRICK,
Article Effect of deprivation of endogenous follicle stimulating hormone on rat epididymis: a histological evaluation
 RBMOnline - Vol 17 No 3. 2008 331-337 Reproductive BioMedicine Online; www.rbmonline.com/article/2999 on web 11 July 2008 Article Effect of deprivation of endogenous follicle stimulating hormone on rat
RBMOnline - Vol 17 No 3. 2008 331-337 Reproductive BioMedicine Online; www.rbmonline.com/article/2999 on web 11 July 2008 Article Effect of deprivation of endogenous follicle stimulating hormone on rat
MALE REPRODUCTIVE SYSTEM
 1 MALE REPRODUCTIVE SYSTEM SCPA 602 Anatomical Basis for Pathological Study Updated: 20.09.2018 Lect. Nisamanee Charoenchon, PhD nisamanee.cha@mahidol.ac.th Department of Pathobiology, Mahidol University
1 MALE REPRODUCTIVE SYSTEM SCPA 602 Anatomical Basis for Pathological Study Updated: 20.09.2018 Lect. Nisamanee Charoenchon, PhD nisamanee.cha@mahidol.ac.th Department of Pathobiology, Mahidol University
Luminal Fluid Proteins of the Male Rat Reproductive Tract
 BOLOGY OF REPRODUCTON 21, 883-890 (1979) Luminal Fluid Proteins of the Male Rat Reproductive Tract T. T. TURNER, J. L. PLESUMS and C. L. CABOT Department of Urology, University of Virginia Medical School,
BOLOGY OF REPRODUCTON 21, 883-890 (1979) Luminal Fluid Proteins of the Male Rat Reproductive Tract T. T. TURNER, J. L. PLESUMS and C. L. CABOT Department of Urology, University of Virginia Medical School,
5 15/3/2012. Malik Al-Momani
 5 15/3/2012 Malik Al-Momani بسم هللا الرحمن الرحيم Spermatogenesis Note : Please refer to slides so see photos. Quick Revision : - Testis is divided by septum into testicular lobules, inside the lobules
5 15/3/2012 Malik Al-Momani بسم هللا الرحمن الرحيم Spermatogenesis Note : Please refer to slides so see photos. Quick Revision : - Testis is divided by septum into testicular lobules, inside the lobules
A CASE OF SEX REVERSAL SYNDROME WITH SEX-DETERMINING REGION (XX MALE)
 Nagoya J. Med. Sci. 58. 111-115, 1995 A CASE OF SEX REVERSAL SYNDROME WITH SEX-DETERMINING REGION (XX MALE) MASANORI YAMAMOTO, KEISUKE YOKOI, SATOSHI KATSUNO, HATSUKI HIBI and Kon MIYAKE Department of
Nagoya J. Med. Sci. 58. 111-115, 1995 A CASE OF SEX REVERSAL SYNDROME WITH SEX-DETERMINING REGION (XX MALE) MASANORI YAMAMOTO, KEISUKE YOKOI, SATOSHI KATSUNO, HATSUKI HIBI and Kon MIYAKE Department of
The Male Reproductive System
 The Male Reproductive System The male reproductive system Testes Genital ducts Accessory sex glands: seminal vesicles prostate bulbourethral glands External genitalia: penis Structure of the Testis Tunica
The Male Reproductive System The male reproductive system Testes Genital ducts Accessory sex glands: seminal vesicles prostate bulbourethral glands External genitalia: penis Structure of the Testis Tunica
Seminiferous Tubules
 Testes The testes are compound tubular glands that lie within a scrotal sac, suspended from the body by a spermatic cord. The testes are dual organs that act as exocrine glands producing a holocrine secretion,
Testes The testes are compound tubular glands that lie within a scrotal sac, suspended from the body by a spermatic cord. The testes are dual organs that act as exocrine glands producing a holocrine secretion,
Male Reproductive System Dr. Gary Mumaugh
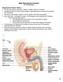 Male Reproductive System Dr. Gary Mumaugh Reproductive System Basics Primary sex organs (gonads) testes in males, ovaries in females Gonads produce sex cells called gametes (gametes means spouses) and
Male Reproductive System Dr. Gary Mumaugh Reproductive System Basics Primary sex organs (gonads) testes in males, ovaries in females Gonads produce sex cells called gametes (gametes means spouses) and
The Reproductive System
 Essentials of Human Anatomy & Physiology Elaine N. Marieb Seventh Edition Chapter 16 The Reproductive System Slides 16.1 16.20 Lecture Slides in PowerPoint by Jerry L. Cook The Reproductive System Gonads
Essentials of Human Anatomy & Physiology Elaine N. Marieb Seventh Edition Chapter 16 The Reproductive System Slides 16.1 16.20 Lecture Slides in PowerPoint by Jerry L. Cook The Reproductive System Gonads
Animal Science 434. Sperm Head. Sperm From Different Species. Sperm Structure. Epididymis, Ejaculation and Semen. Head Acrosome Neck Middle Piece
 Sperm Structure Head Acrosome Neck Middle Piece Animal Science 434 Annulus Principal Piece Epididymis, Ejaculation and Semen End Piece Sperm From Different Species Sperm Head (Equatorial Segment) Nucleus
Sperm Structure Head Acrosome Neck Middle Piece Animal Science 434 Annulus Principal Piece Epididymis, Ejaculation and Semen End Piece Sperm From Different Species Sperm Head (Equatorial Segment) Nucleus
Cell Divisions. The autosomes represent the whole body. * Male Sex Chromosomes: XY * Female Sex Chromosomes: XX
 Cell Divisions Each Cell (including gonads) has 46 chromosomes (23 pairs of chromosomes: 22 pairs of autosomes, 1 pair of sex chromosomes) which are located in the nucleus). The autosomes represent the
Cell Divisions Each Cell (including gonads) has 46 chromosomes (23 pairs of chromosomes: 22 pairs of autosomes, 1 pair of sex chromosomes) which are located in the nucleus). The autosomes represent the
The Reproductive System
 16 PART A The Reproductive System PowerPoint Lecture Slide Presentation by Jerry L. Cook, Sam Houston University ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY EIGHTH EDITION ELAINE N. MARIEB The Reproductive
16 PART A The Reproductive System PowerPoint Lecture Slide Presentation by Jerry L. Cook, Sam Houston University ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY EIGHTH EDITION ELAINE N. MARIEB The Reproductive
Collin County Community College RENAL PHYSIOLOGY
 Collin County Community College BIOL. 2402 Anatomy & Physiology WEEK 12 Urinary System 1 RENAL PHYSIOLOGY Glomerular Filtration Filtration process that occurs in Bowman s Capsule Blood is filtered and
Collin County Community College BIOL. 2402 Anatomy & Physiology WEEK 12 Urinary System 1 RENAL PHYSIOLOGY Glomerular Filtration Filtration process that occurs in Bowman s Capsule Blood is filtered and
Chapter 22 The Reproductive System (I)
 Chapter 22 The Reproductive System (I) An Overview of Reproductive Physiology o The Male Reproductive System o The Female Reproductive System 22.1 Reproductive System Overview Reproductive system = all
Chapter 22 The Reproductive System (I) An Overview of Reproductive Physiology o The Male Reproductive System o The Female Reproductive System 22.1 Reproductive System Overview Reproductive system = all
Male reproductive system The physiology of sexual act
 Male reproductive system The physiology of sexual act Gabriella Kékesi 65. The development and physiology of the male reproductive system. The physiology of the sexual act Define chromosomal, gonadal and
Male reproductive system The physiology of sexual act Gabriella Kékesi 65. The development and physiology of the male reproductive system. The physiology of the sexual act Define chromosomal, gonadal and
EFFECTS OF VARICOCELECTOMY ON TESTIS VOLUME AND SEMEN PARAMETERS IN ADOLESCENTS: A RANDOMIZED PROSPECTIVE STUDY
 Nagoya J. Med. Sci. 58. 127-132, 1995 EFFECTS OF VARICOCELECTOMY ON TESTIS VOLUME AND SEMEN PARAMETERS IN ADOLESCENTS: A RANDOMIZED PROSPECTIVE STUDY MASANORI YAMAMOTO, HATSUKI HIEI, SATOSHI KATSUNO and
Nagoya J. Med. Sci. 58. 127-132, 1995 EFFECTS OF VARICOCELECTOMY ON TESTIS VOLUME AND SEMEN PARAMETERS IN ADOLESCENTS: A RANDOMIZED PROSPECTIVE STUDY MASANORI YAMAMOTO, HATSUKI HIEI, SATOSHI KATSUNO and
Human Obestatin ELISA
 K-ASSAY Human Obestatin ELISA For the quantitative determination of obestatin in human serum and plasma Cat. No. KT-495 For Research Use Only. 1 Rev. 081309 K-ASSAY PRODUCT INFORMATION Human Obestatin
K-ASSAY Human Obestatin ELISA For the quantitative determination of obestatin in human serum and plasma Cat. No. KT-495 For Research Use Only. 1 Rev. 081309 K-ASSAY PRODUCT INFORMATION Human Obestatin
DAX1, testes development role 7, 8 DFFRY, spermatogenesis role 49 DMRT genes, male sex differentiation role 15
 Subject Index N-Acetylcysteine, sperm quality effects 71 Ambiguous genitalia, origins 1, 2 Anti-Müllerian hormone function 13 receptors 13 Sertoli cell secretion 10, 38 Apoptosis assays in testes 73, 74
Subject Index N-Acetylcysteine, sperm quality effects 71 Ambiguous genitalia, origins 1, 2 Anti-Müllerian hormone function 13 receptors 13 Sertoli cell secretion 10, 38 Apoptosis assays in testes 73, 74
THE DIFINITIVE GUIDE TO HUMAN ANATOMY & PHYSIOLOGY (HAP 2).
 THE DIFINITIVE GUIDE TO HUMAN ANATOMY & PHYSIOLOGY (HAP 2). Pages 2-49 Lecture 1 notes: Cardiovascular 1. Pages 50-97 Lecture 2 notes: Cardiovascular 2. Pages 98-128 Lecture 3 notes: Respiratory 1. Pages
THE DIFINITIVE GUIDE TO HUMAN ANATOMY & PHYSIOLOGY (HAP 2). Pages 2-49 Lecture 1 notes: Cardiovascular 1. Pages 50-97 Lecture 2 notes: Cardiovascular 2. Pages 98-128 Lecture 3 notes: Respiratory 1. Pages
Developmental Changes of Müllerian and Wolffian Ducts in Domestic Cat Fetuses
 Exp. Anim. 58(1), 41 45, 2009 Note Developmental Changes of Müllerian and Wolffian Ducts in Domestic Cat Fetuses Tomo INOMATA 1), Hiroyoshi NINOMIYA 1), Katsuyasu SAKITA 1), Naomi KASHIWAZAKI 2), Junya
Exp. Anim. 58(1), 41 45, 2009 Note Developmental Changes of Müllerian and Wolffian Ducts in Domestic Cat Fetuses Tomo INOMATA 1), Hiroyoshi NINOMIYA 1), Katsuyasu SAKITA 1), Naomi KASHIWAZAKI 2), Junya
Cells: The Living Units
 Cells: The Living Units Introduction Life in general occurs in an aqueous environment All chemical processes essential to life occur within the aqueous environment of the cell and surrounding fluids contained
Cells: The Living Units Introduction Life in general occurs in an aqueous environment All chemical processes essential to life occur within the aqueous environment of the cell and surrounding fluids contained
Chapter 4 - Epithelial Tissues
 Chapter 4 - Epithelial Tissues Tissues Definition A group of closely associated cells that work together to perform a specific function Types Epithelial - covering Connective - support Muscle - movement
Chapter 4 - Epithelial Tissues Tissues Definition A group of closely associated cells that work together to perform a specific function Types Epithelial - covering Connective - support Muscle - movement
Transport of Solutes and Water
 Transport of Solutes and Water Across cell membranes 1. Simple and Facilitated diffusion. 2. Active transport. 3. Osmosis. Simple diffusion Simple diffusion - the red particles are moving from an area
Transport of Solutes and Water Across cell membranes 1. Simple and Facilitated diffusion. 2. Active transport. 3. Osmosis. Simple diffusion Simple diffusion - the red particles are moving from an area
The Reproductive System
 PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Reproductive System 16PART A The Reproductive System Gonads primary sex organs Testes in males
PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Reproductive System 16PART A The Reproductive System Gonads primary sex organs Testes in males
18 Urinary system. 19 Male reproductive system. Female reproductive system. Blok 11: Genital and Urinary Tract Diseases
 Blok 11: Genital and Urinary Tract Diseases 18 Urinary System 19 Male Genital System 20 Female Genital System 18 Urinary system You should be able to: 1. Describe the structures and associated functions
Blok 11: Genital and Urinary Tract Diseases 18 Urinary System 19 Male Genital System 20 Female Genital System 18 Urinary system You should be able to: 1. Describe the structures and associated functions
Development of the Genital System
 Development of the Genital System Professor Alfred Cuschieri Department of Anatomy University of Malta The mesonephros develops primitive nephrotomes draining into a mesonephric duct nephrotome mesonephric
Development of the Genital System Professor Alfred Cuschieri Department of Anatomy University of Malta The mesonephros develops primitive nephrotomes draining into a mesonephric duct nephrotome mesonephric
Reproductive System Purpose General Structures Male Structures Functions Female Anatomy Structures Functions Clinical Applications
 The Reproductive System: Male, Ch 23 Outline of class lecture After studying the male reproductive system you should be able to: 1. Define the purpose of reproduction and identify the general organs of
The Reproductive System: Male, Ch 23 Outline of class lecture After studying the male reproductive system you should be able to: 1. Define the purpose of reproduction and identify the general organs of
Drug Distribution. Joseph K. Ritter, Ph.D., Assoc. Prof. Medical Sciences Building, Room
 Drug Distribution Joseph K. Ritter, Ph.D., Assoc. Prof. Medical Sciences Building, Room 531 jkritter@vcu.edu 828-1022 Department of Pharmacology and Toxicology Medical College of Virginia Campus Virginia
Drug Distribution Joseph K. Ritter, Ph.D., Assoc. Prof. Medical Sciences Building, Room 531 jkritter@vcu.edu 828-1022 Department of Pharmacology and Toxicology Medical College of Virginia Campus Virginia
Mouse sperm extraction:
 Mouse sperm extraction: This method of extraction is used for acrosome reaction assays, immunocytochemistry and biochemical assays. Collect two cauda epidydimus from one male, cut them 5 times and place
Mouse sperm extraction: This method of extraction is used for acrosome reaction assays, immunocytochemistry and biochemical assays. Collect two cauda epidydimus from one male, cut them 5 times and place
Male Reproductive Physiology
 Male Reproductive Physiology Overview Anatomy Function Endocrine and spermatogenesis Testis epididymus,vas deferens,seminal vesicles and prostate Hypothalamic pituitary testicular axis Hormones of the
Male Reproductive Physiology Overview Anatomy Function Endocrine and spermatogenesis Testis epididymus,vas deferens,seminal vesicles and prostate Hypothalamic pituitary testicular axis Hormones of the
Amino acid fluxes in rat thin limb segments of Henle s loop during in vitro microperfusion
 Amino acid fluxes in rat thin limb segments of Henle s loop during in vitro microperfusion OLGA H. BROKL AND WILLIAM H. DANTZLER Department of Physiology, College of Medicine, University of Arizona, Tucson,
Amino acid fluxes in rat thin limb segments of Henle s loop during in vitro microperfusion OLGA H. BROKL AND WILLIAM H. DANTZLER Department of Physiology, College of Medicine, University of Arizona, Tucson,
- production of two types of gametes -- fused at fertilization to form zygote
 Male reproductive system I. Sexual reproduction -- overview - production of two types of gametes -- fused at fertilization to form zygote - promotes genetic variety among members of a species -- each offspring
Male reproductive system I. Sexual reproduction -- overview - production of two types of gametes -- fused at fertilization to form zygote - promotes genetic variety among members of a species -- each offspring
Renal System Dr. Naim Kittana Department of Biomedical Sciences Faculty of Medicine & Health Sciences An-Najah National University
 Renal System Dr. Naim Kittana Department of Biomedical Sciences Faculty of Medicine & Health Sciences An-Najah National University Declaration The content and the figures of this seminar were directly
Renal System Dr. Naim Kittana Department of Biomedical Sciences Faculty of Medicine & Health Sciences An-Najah National University Declaration The content and the figures of this seminar were directly
Chapter 14 Reproduction Review Assignment
 Date: Mark: _/45 Chapter 14 Reproduction Review Assignment Multiple Choice Identify the choice that best completes the statement or answers the question. 1. Use the diagram above to answer the next question.
Date: Mark: _/45 Chapter 14 Reproduction Review Assignment Multiple Choice Identify the choice that best completes the statement or answers the question. 1. Use the diagram above to answer the next question.
Animal Science 434 Reproductive Physiology
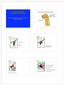 Animal Science 434 Reproductive Physiology Development of the Pituitary Gland Lec 5: Embryogenesis of the Pituitary and Sexual Development Stomodeum Brain Infundibulum Rathke s Pouch Germ Cell Migration
Animal Science 434 Reproductive Physiology Development of the Pituitary Gland Lec 5: Embryogenesis of the Pituitary and Sexual Development Stomodeum Brain Infundibulum Rathke s Pouch Germ Cell Migration
Cells & Tissues. Chapter 3
 Cells & Tissues Chapter 3 Cell Theory Cell is structural and functional unit of life Activity of an organism is dependent upon its cells Principle of Complementarity functions of cells are dependent upon
Cells & Tissues Chapter 3 Cell Theory Cell is structural and functional unit of life Activity of an organism is dependent upon its cells Principle of Complementarity functions of cells are dependent upon
ENHANCEMENT BY F-ACTIN OF MGATP-DEPENDENT DOPAMINE UPTAKE INTO ISOLATED CHROMAFFIN GRANULES
 Vol. 4, No. 1, September 1996 BIOCHEMISTRY and MOLECULAR BIOLOGY INTERNATIONAL Pages 61-66 ENHANCEMENT BY F-ACTIN OF MGATP-DEPENDENT DOPAMINE UPTAKE INTO ISOLATED CHROMAFFIN GRANULES Kyoji Morita ~)*,
Vol. 4, No. 1, September 1996 BIOCHEMISTRY and MOLECULAR BIOLOGY INTERNATIONAL Pages 61-66 ENHANCEMENT BY F-ACTIN OF MGATP-DEPENDENT DOPAMINE UPTAKE INTO ISOLATED CHROMAFFIN GRANULES Kyoji Morita ~)*,
Chapter 9. Summary & conclusion
 Chapter 9 Summary & conclusion 133 Chapter 1 Objective: To give an overview of the different vasectomy techniques utilized and try to explore from the literature what method of vasectomy could give the
Chapter 9 Summary & conclusion 133 Chapter 1 Objective: To give an overview of the different vasectomy techniques utilized and try to explore from the literature what method of vasectomy could give the
Immune response in obstructive male infertility. Prof. A.K.Sarda Department of Surgery Maulana Azad Medical College New Delhi
 Immune response in obstructive male infertility Prof. A.K.Sarda Department of Surgery Maulana Azad Medical College New Delhi Sperm transport from the testicle Seminiferous tubule contractions of the myoid
Immune response in obstructive male infertility Prof. A.K.Sarda Department of Surgery Maulana Azad Medical College New Delhi Sperm transport from the testicle Seminiferous tubule contractions of the myoid
S S GURAYA and ARBANS J KAUR Department of Zoology, College of Basic Sciences and Humanities, Punjab Agricultural University, Ludhiana , India
 Proc. Indian Acad, Sci. (Anim. Sci.), Vol. 90, Number 5, SeptcIl1ber 1981, pp. 49S-soi. o Printed in India. Effect of castration on some hydrolytic enzymes in the rat vas deferens: A histochemical study
Proc. Indian Acad, Sci. (Anim. Sci.), Vol. 90, Number 5, SeptcIl1ber 1981, pp. 49S-soi. o Printed in India. Effect of castration on some hydrolytic enzymes in the rat vas deferens: A histochemical study
LH (Rodent) ELISA Kit
 LH (Rodent) ELISA Kit Catalog Number KA2332 96 assays Version: 05 Intended for research use only www.abnova.com Table of Contents Introduction... 3 Intended Use... 3 Background... 3 Principle of the Assay...
LH (Rodent) ELISA Kit Catalog Number KA2332 96 assays Version: 05 Intended for research use only www.abnova.com Table of Contents Introduction... 3 Intended Use... 3 Background... 3 Principle of the Assay...
For more information about how to cite these materials visit
 Author: A. Kent Christensen, Ph.D., 2009 License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution Share Alike 3.0 License: http://creativecommons.org/licenses/by-sa/3.0/
Author: A. Kent Christensen, Ph.D., 2009 License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution Share Alike 3.0 License: http://creativecommons.org/licenses/by-sa/3.0/
Overview of Anatomy and Physioloy II Second Year Students
 WELCOME University of Baghdad College of Nursing Department of Basic Medical Sciences Overview of Anatomy and Physioloy II Second Year Students Asaad Ismail Ahmad, Ph.D. Electrolyte and Mineral Physiology
WELCOME University of Baghdad College of Nursing Department of Basic Medical Sciences Overview of Anatomy and Physioloy II Second Year Students Asaad Ismail Ahmad, Ph.D. Electrolyte and Mineral Physiology
BIOL 2402 Fluid/Electrolyte Regulation
 Dr. Chris Doumen Collin County Community College BIOL 2402 Fluid/Electrolyte Regulation 1 Body Water Content On average, we are 50-60 % water For a 70 kg male = 40 liters water This water is divided into
Dr. Chris Doumen Collin County Community College BIOL 2402 Fluid/Electrolyte Regulation 1 Body Water Content On average, we are 50-60 % water For a 70 kg male = 40 liters water This water is divided into
BIOL2030 Human A & P II -- Exam 6
 BIOL2030 Human A & P II -- Exam 6 Name: 1. The kidney functions in A. preventing blood loss. C. synthesis of vitamin E. E. making ADH. B. white blood cell production. D. excretion of metabolic wastes.
BIOL2030 Human A & P II -- Exam 6 Name: 1. The kidney functions in A. preventing blood loss. C. synthesis of vitamin E. E. making ADH. B. white blood cell production. D. excretion of metabolic wastes.
Microinsemination (Intracytoplasmic Sperm Injection) Microinsemination schedule. 1. Preparation of mediums
 Microinsemination (Intracytoplasmic Sperm Injection) Masumi Hirabayashi Section of Mammalian Transgenesis, Center for Genetic Analysis of Behavior, National Institute for Physiological Sciences, National
Microinsemination (Intracytoplasmic Sperm Injection) Masumi Hirabayashi Section of Mammalian Transgenesis, Center for Genetic Analysis of Behavior, National Institute for Physiological Sciences, National
Pathology of Male Reproductive System 1
 Pathology of Male Reproductive System 1 Professor dr Ali Hassan Altimimi Professor of Pathology& Histology MSc, PHD, MD(UK) MALE REPRODUCTIVE SYSTEM The internal male genitalia consist of the testes with
Pathology of Male Reproductive System 1 Professor dr Ali Hassan Altimimi Professor of Pathology& Histology MSc, PHD, MD(UK) MALE REPRODUCTIVE SYSTEM The internal male genitalia consist of the testes with
川北医学院讲稿. Under low power note the testis is enclosed by a strong fibrous. layer of serous epithelium. These fibrous tissue
 川北医学院讲稿 Experiment 5: Male and Female Reproductive System Hello, everybody, class is begin,keep quiet, please. And this is the last experimental class. Today we will learn 5 slices and review all structures
川北医学院讲稿 Experiment 5: Male and Female Reproductive System Hello, everybody, class is begin,keep quiet, please. And this is the last experimental class. Today we will learn 5 slices and review all structures
BIOH122 Human Biological Science 2
 BIOH122 Human Biological Science 2 Session 18 Urinary System 3 Tubular Reabsorption and Secretion Bioscience Department Endeavour College of Natural Health endeavour.edu.au Session Plan o Principles of
BIOH122 Human Biological Science 2 Session 18 Urinary System 3 Tubular Reabsorption and Secretion Bioscience Department Endeavour College of Natural Health endeavour.edu.au Session Plan o Principles of
Isolation and Culture of Leydig Cells from Adult Rats
 Isolation and Culture of Leydig Cells from Adult Rats R.S. Sharma 1, P.C. Pal 2 and M. Rajalakshmi 3 1 Indian Council of Medical Research, Ansari Nagar, New Delhi-110029 2 Department of Biochemistry, All
Isolation and Culture of Leydig Cells from Adult Rats R.S. Sharma 1, P.C. Pal 2 and M. Rajalakshmi 3 1 Indian Council of Medical Research, Ansari Nagar, New Delhi-110029 2 Department of Biochemistry, All
LABORATORY EXERCISES FOR MALE REPRODUCTIVE SYSTEM
 LABORATORY EXERCISES FOR MALE REPRODUCTIVE SYSTEM Slide #101 (1096). Testis, rat. sustentacular ( Sertoli ) cells Nuclei of Sustentacular cells Leydig cells Spermatogonia Spermatocytes Spermatids pale
LABORATORY EXERCISES FOR MALE REPRODUCTIVE SYSTEM Slide #101 (1096). Testis, rat. sustentacular ( Sertoli ) cells Nuclei of Sustentacular cells Leydig cells Spermatogonia Spermatocytes Spermatids pale
Reproductive Endocrinology. Isabel Hwang Department of Physiology Faculty of Medicine University of Hong Kong Hong Kong May2007
 Reproductive Endocrinology Isabel Hwang Department of Physiology Faculty of Medicine University of Hong Kong Hong Kong May2007 isabelss@hkucc.hku.hk A 3-hormone chain of command controls reproduction with
Reproductive Endocrinology Isabel Hwang Department of Physiology Faculty of Medicine University of Hong Kong Hong Kong May2007 isabelss@hkucc.hku.hk A 3-hormone chain of command controls reproduction with
Ch 19: The Kidneys. Functional unit of kidneys:?? Developed by John Gallagher, MS, DVM
 Ch 19: The Kidneys Homeostatic regulation of ECF volume and BP Osmolarity 290 mosm Ion balance Na+ and K+, etc. ph (acid-base balance Excretion of wastes & foreign substances Hormone production EPO Renin
Ch 19: The Kidneys Homeostatic regulation of ECF volume and BP Osmolarity 290 mosm Ion balance Na+ and K+, etc. ph (acid-base balance Excretion of wastes & foreign substances Hormone production EPO Renin
The Acute Scrotum: Sonographic Findings
 The Acute Scrotum: Sonographic Findings 가천의대길병원방사선과 양달모 Gachon Medical School Introduction Many diseases presenting as acute scrotal pain DDx is important for determining the appropriate treatment US with
The Acute Scrotum: Sonographic Findings 가천의대길병원방사선과 양달모 Gachon Medical School Introduction Many diseases presenting as acute scrotal pain DDx is important for determining the appropriate treatment US with
