TYPE I CITRULLINEMIA: A REVIEW OF A RARE UREA CYCLE DISORDER AND APPROACH TO MANAGEMENT
|
|
|
- Paul Mosley
- 5 years ago
- Views:
Transcription
1 TYPE I CITRULLINEMIA: A REVIEW OF A RARE UREA CYCLE DISORDER AND APPROACH TO MANAGEMENT Denise M. Kolanczyk,PharmD 1,2, Jenna Applegate, RD 3, Evelina Lin, PharmD 2, Allyson Wexler, PharmD 4, and Megan A. Rech, PharmD 2 1 Midwestern University, Department of Pharmacy Practice, Downers Grove, IL, USA, 2 Loyola University Medical Center, Department of Pharmacy, Maywood, IL, USA, 3 Loyola University Medical Center, Department of Clinical Nutrition, Maywood, IL, USA, 4 University of North Carolina Medical Center, Department of Pharmacy, Chapel Hill, NC, USA. ABSTRACT A 26-year-old female presented with acute signs and symptoms of hyperammonemia related to type I citrullinemia, a rare autosomal recessive urea cycle disorder that is diagnosed on a prenatal screen. It is caused by a mutation in the ASS1 gene which impacts the urea cycle. Patients often present with altered mental status and other neurologic findings during periods of elevated ammonia levels. Treatment requires a multidisciplinary approach to create a specialized patient-specific plan. Diets are closely monitored with protein-intake restrictions to avoid hyperammonemia. Traditional medications used for hyperammonemia that reduce nitrogen generation and uptake, such as lactulose, have a limited role in this patient population. Arginine, sodium benzoate, and sodium phenylacetate/phenylbutyrate are used for nitrogen excretion. In patients who progress to liver failure or have symptoms that cannot be controlled through diet and medication, an orthotopic liver transplant is an option. It is imperative for health care professionals to understand the key concepts to therapy. The patient presented highlights the importance of communication between general health care disciplines and understanding core treatment BACKGROUND Citrullinemia is an autosomal recessive urea cycle disorder. 1 There are two types of citrullinemia that are caused by different mutations, but both result in accumulation of ammonia and glutamine. 2 Type I citrullinemia, also referred to as classic citrullinemia, is caused by a mutation in the ASS1 gene. 3,4 Out of the two types, it is the most common and affects about 1 in 57,000 births and it can occur in all ethnic groups. 5 Type I citrullinemia usually presents within the first week of life. At birth, infants will appear normal, but as ammonia levels increase, infants will become lethargic and develop poor feeding habits. Vomiting, seizures, and a loss of consciousness are common. Increased intracranial pressure can also develop secondary to the hyperammonenmia and cause increased neuromuscular tone, spasticity, and ankle clonus. A milder form of type I citrullinemia may develop later in childhood or adulthood. Intense headaches, partial loss of vision, ataxia, and lethargy are commonly associated with later onset type I citrullinemia. 5 Type II citrullinemia, caused by a mutation in the SLC25A13 gene, is predominantly found in the Japanese population, but has also been reported outside of East Asia. 2,6 Type II citrullinemia can be further classified into neonatal intrahepatic cholestasis caused by citrin deficiency, failure to thrive and dyslipidemia caused by citrin deficiency, and adultonset type II citrullinemia (CTLN2). 1 The remainder of this article will focus on type I citrullinemia. Since citrullinemia is rare, many health care providers may not be adequately trained or aware of acute management and nutrition. Symptoms may be mistaken for hepatic encephalopathy, and traditional management of hyperammonemia could potentially worsen a patient s clinical state. There are multiple case reports that describe presentations and management for both types of citrulliemia, but there is a lack of all-inclusive reviews that a health care provider may find useful when faced with managing such a rare disorder. This article introduces a patient case followed by a review of the pathophysiology, presentation, and nutrition and medication management of type I citrullinemia. DATA SOURCES AND SELECTION A literature search of PubMed (January 1, 1975 through January 31, 2018) was performed with the following terms: citrullinemia, type I citrullinemia, hyperammonemia, or urea cycle disorders. Additional references were identified from a review of literature citations. All English language case reports, reviews, and book chapters were included and reviewed for relevance. 3
2 CASE REPORT A 26-year-old Caucasian female arrived at the emergency department due to increasing confusion, slurred speech, and difficulty walking. Her relevant past medical history included type I citrullinemia diagnosed on a prenatal screen (unknown reason for screening), Clostridium difficile infection, fungemia and pneumonia. Her family reported her current symptoms of altered mental status and gait changes were consistent with past episodes of high ammonia levels which they reported as being >100 mcg/dl. The patient acknowledged menstruation and infection as triggers for acute exacerbations of citrullinemia. She reported that her menses started 5 days prior to admission, and watery, green bowel movements had been occurring for more than 15 times a day for one week prior to admission. She also reported a mild headache and intermittent nausea. The patient denied cough, shortness of breath, neck stiffness, dysuria, and hematuria. Her routine medications included arginine, buphenyl, isoleucine, leucine, L-valine, sodium benzoate and valerian. The patient acknowledged compliance and adherence with her home medication regimen, which was frequently adjusted by her geneticist. Her weight on presentation was kg and height was 5 feet and 2.75 inches (1.59 meters). Initial vital signs included the following: blood pressure 127/71 mmhg, heart rate 86 beats per minute, respiratory rate 18 breaths per minute and body temperature 36.7 C. Significant laboratory findings on arrival included an ammonia level of 104 μg/dl (reference range μg/dl). A glutamine level was not obtained on presentation or throughout the course of the hospitalization. Additional laboratory values included a slightly elevated aspartate transaminase (AST) of 64 IU/ L and alanine transaminase (ALT) of 79 IU/L. Other liver function tests were within normal limits. Blood and stool cultures were obtained based on the patient s medical history and acute presentation. The physical exam was positive for altered mental status. Her neurologic exam revealed cranial nerves II-XII were grossly intact, no focal deficits, no asterixis or tremor, and strength 5/5 for both upper and lower extremities. Her retinal exam was within normal limits. Due to improvements after optimizing her nutrition and medications, a CT or MRI of the brain was never obtained during the hospitalization. In regards to the patient s history of type I citrullinemia, records from infancy were limited. She was delivered at term weighing 7 pounds, 5 ounces, but was hospitalized for four weeks due to complications resulting from type I citrullinemia. She first presented to our institution during her teenage years with a complaint of foot pain and gait issues. Since that initial presentation, there are other documented periods of hyperammonemia. Management of her type I citrullinemia was primarily done at another medical center. As a result, further details such as knowing the mutation of her ASS gene were not available to review. The patient was admitted to the general medicine service. Initial management involved optimization of the patient s home medication regimen in consultation with the patient s geneticist. The patient was given arginine 12.6 g every 30 minutes for four doses, buphenyl 2.37 g every 30 minutes for three doses, and sodium benzoate 5 g every 30 minutes for two doses to complete a total daily dose of 20 g. All medications were administered through a gastrostomy tube (GT). A repeat ammonia level, drawn approximately six hours following medication administration, was 164 μg/dl. Further management of the patient s hyperammonemia required increasing the intensity of the regimen. Intravenous arginine was initiated with a loading dose of 25 g/l of dextrose 10% over 3 hours, followed by arginine IV 50 g/l of dextrose 10% over 24 hours (83 ml/hr). Buphenyl 4.74 g was given every 30 minutes for two doses, followed by 3.16 g every 3 hours. Sodium benzoate 5 g every 30 minutes for two doses was given, followed by 2.5 g every 3 hours. A basic metabolic panel along with an ammonia level was checked every six hours during treatment to monitor for hypochloremia and hypokalemia. The patient was dependent on receiving most of her nutrition via GT. Her home feedings provided 15.5 gm of protein and approximately 1650 kilocalories. Throughout this acute episode, the patient was kept on a proteinrestricted diet with up to 2 grams of protein per meal. Home GT feeds were continued throughout the hospitalization. Tube feed regimen and protein requirements were adjusted based on laboratory findings by the patient s primary dietitian. Prior to admission the patient was also receiving valine, isoleucine and leucine in tube feeds, but these amino acids were held while inpatient. The patient's obesity and chronic nutritional management was not addressed during the admission. Table 1 provides details on nutrition and medication management throughout her hospitalization. 4
3 Table 1. Nutrition and Medication Therapies Tube Feed Regimen Initial Medication Regimen Adjusted Medication Regimen Anamex 0.5 cups Arginine (GT) Arginine (IV) Prophree 1.5 cups Solcarb 1.25 cups Water 41 ounces Total tube feed regimen= 50 ounces Run at 62 ml/hour 12.6 grams every 30 minutes for four doses Buphenyl (GT) 2.37 grams every 30 minutes for three doses Sodium benzoate (GT) 5 grams for four doses Loading dose: 25 grams/liter of Dextrose 10% over 3 hours Maintenance: 50 grams in Dextrose 10% over 24 hours. Buphenyl (GT) 4.74 grams every 30 min for two doses, then 3.16 grams every 3 hours Calories: 1653 Protein: 15.5 grams Sodium benzoate (GT) 5 grams every 30 min for two doses, then 2.5 grams every 3 hours GT= gastrostomy tube; IV= intravenous Ammonia levels continued to rise and peaked overnight at 228 μg/dl. Figure 1 demonstrates the change in ammonia levels coupled with changes to medication management. The patient s mental status remained altered, which primarily consisted of slow mentation and speech. The arginine rate was then increased to 100 ml/ hr to provide 60 g daily. An improvement in mental status was observed. The following day, the dose was decreased to g/hr. Arginine powder 3.15 g was added every three hours and titrated up as the rate of the intravenous arginine was decreased. The buphenyl dose was increased to 4.74 g every three hours and the dose of sodium benzoate remained at 2.5 g every 3 hours. Within 48 hours, the ammonia level normalized to 32 μg/dl. The patient was discharged due to improvements in her mental status and bowel movements, and ammonia levels were within normal limits. Figure 1. Ammonia Levels Throughout Hospitalization Legend: Points on the graph indicate changes to drug therapy. The last data point demonstrates the time at which doses of intravenous arginine began to decrease and was tapered off. 5
4 PATHOPHYSIOLOGY The Journal of Rare The urea cycle primarily functions to remove nitrogen waste by hepatic conversion of nitrogen to urea. 7 Nitrogen results from the hydrolysis of dietary protein sources and catabolic processes in body tissues (skeletal muscle, liver and brain). Only a small portion of nitrogen is re-incorporated by the body for further use. The remainder is considered waste and is excreted into the urine as water-soluble urea and ammonia. For each cycle turn, two moles of nitrogen are converted into urea: one mole from ammonia and one mole from aspartate. 7 The entirety of the urea cycle is located on the surface of periportal hepatocytes and requires the major roles of six enzymes and two transporters, as shown in Figure The six enzymes include one co-factor producing enzyme: N-acetylglutamate synthetase, and five catalytic enzymes: carbamoylphosphate synthetase 1, ornithine transcarbamylase, argininosuccinic acid synthetase, argininosuccinic acid lyase and arginase 1. 7,8 The two transporters are ornithine translocase and aspartateglutamate solute carrier protein (citrin). The transporters provide shuttling of substrates to the urea cycle. 7 Activation of the urea cycle occurs when there is an increased nitrogen load. Ammonia and bicarbonate are irreversibly converted into carbamoylphosphate by carbamoylphosphate synthetase 1 in the mitochondria. Carbamoylphosphate synthetase 1 activity is dependent on co-factor N-acetylglutamate formation, which is generated by N-acetylglutamate synthetase catalyzing glutamate and acetyl coenzyme A. Ornithine transcarbamylase proceeds to work on carbamoylphosphate and ornithine to form citrulline in the mitochondria. In order for ornithine to travel from the cytosol into the mitochondria, the transporter Figure 2. Alternative Treatment Pathways to Eliminate Nitrogen in Type I Citrullinemia. 8 Legend: Use of arginine, sodium benzoate and/or sodium phenylacetate serve as nitrogen scavenger therapies in order for the urea cycle to resume normal regulation. ARG, arginase 1; ASL, argininosuccinate lyase; ASS, argininosuccinic acid synthetase; Citrin, aspartate-glutamate solute carrier protein transporter; CPS1, carbamoylphosphate synthetase 1; ORNT1, ornithine translocase transporter; OTC, ornithine transcarbamylase. Adapted with permission from GeneReviews and modified by authors. 6
5 ornithine translocase exchanges ornithine with citrulline. Therefore, citrulline is able to leave the mitochondria to the cytosol and participate in the distal portion of the urea cycle. 7,9 The remaining three major enzymatic reactions involving argininosuccinic acid synthetase, argininosuccinic acid lyase and arginase 1 occur in the cytosol to assist with regulating amino acid exchange. 9 In the cytosol, intramitochondrial aspartate, a substrate for argininosuccinic acid synthetase, is transported via the citrin transporter in exchange for glutamate. Argininosuccinic acid synthetase combines aspartate with citrulline to form argininosuccinate. Argininosuccinic acid lyase hydrolyzes argininosuccinic acid synthetase to arginine and fumarate. 10 Arginase 1 acts on arginine to release urea and regenerate ornithine. Ultimately, urea is dissolved into the blood and excreted by the kidney as urine. Type I citrullinemia (also known as argininosuccinate synthetase deficiency or argininosuccinic acid synthetase deficiency) occurs from a chromosomal defect on 9q34.11, originating from the gene encoding argininosuccinic acid synthetase. 5,10 The defect affects the distal portion of the urea cycle due to the absence of argininosuccinic acid, ensuing in a decline of arginine production and thereby impairing ornithine and citrulline substrate exchange. Resultant accumulation of citrulline is a notable laboratory finding, while arginine and ornithine may be within low to normal range. Accumulation of ammonia and glutamine may manifest as altered mental status. Other findings may include low serum urea nitrogen. 9 PRESENTATION Enzymatic defects in the urea cycle result in arginine becoming an essential amino acid (except in arginase deficiency where arginine is not essential). 10 Patients will have an elevated baseline citrulline level along with frequent episodes of hyperammonemia. 11 It is critical to diagnose the root cause of hyperammonemia as it may be due to a urea cycle disorder, organic academia, or drug-induced. Miscellaneous causes of hyperammonemia include hypoglycin intoxication, pregnancy, distal renal tubule acidosis, carnitine transport defects, urinary tract dilatation, and Reye s syndrome. 10 In order to differentiate between the various urea cycle disorders, plasma levels of amino acids can be used to assist in diagnosis. 10 Common findings of citrullinemia include hyperammonemia and low serum urea nitrogen and arginine levels. Ammonia levels in these patients can be significantly elevated. One retrospective study noted that patients with ammonia levels greater than 300 mmol/l at the time of presentation or with a peak ammonia level above 480 mmol/l were unlikely to have complete cognitive recovery. 12 Elevated plasma citrulline in the absence of argininosuccinic acid synthetase confirms this diagnosis. 10 Symptoms tend to vary with patient age, ammonia level and may include a variety of findings. 10 Most patients with urea cycle disorders present during the neonatal period with nonspecific symptoms such as poor feeding, vomiting, somnolence, irritability, tachypnea, and progressive lethargy secondary to hyperammonemia. 10,12 Newborns may also present with increased intracranial pressure as a result of hyperammonemia and have an increase in neuromuscular tone, spasticity, and ankle clonus. 5 Patients with type I citrullinemia will present with common symptoms such as encephalopathy, hypotonia, vomiting, lethargy, seizures, coma, ataxia, anorexia, abnormal behavior patterns, dysarthria, weakness, liver enlargement and dementia at the time of diagnosis and during acute exacerbations. 10 Although feeding intolerance is present in these patients, weight gain and obesity are possible due to a high calorie and low protein diet. 10 Ammonia and glutamine have shown to have neurotoxic effects, which can ultimately lead to cerebral edema and cell death. 12 MANAGEMENT Patients with type I citrullinemia must vigilantly monitor nutritional intake and pharmacologic therapies in order to avoid hyperammonemic exacerbations and long-term consequences such as mental retardation, delayed growth and seizures. 13 Treatment requires a multidisciplinary approach between geneticists, pediatricians, neurologists, dietitians and metabolism departments to create a specialized patient-specific plan. 5 Treatment includes a protein-restricted diet, and medications that increase nitrogen excretion. These include arginine, sodium benzoate, sodium phenylbutyrate and sodium pyruvate. 14 Early identification and treatment of citrullinemia is essential in order to prevent long-term neurologic sequelae. 15 7
6 General Nutrition Management The Journal of Rare A Western diet consists of more protein than what can be used for growth and development. Excess nitrogenous waste is eliminated mostly in the form of urea. 16 In citrullinemia, patients cannot process urea. 17 This results in an accumulation of nitrogenous compounds, namely glutamine and ammonia, leading to exacerbations. 17 A protein-restricted diet, limited to only what is necessary for growth and maintenance of physiologic processes, is necessary to avoid overproduction of waste in patients with citrullinemia. This can be difficult to adhere to as protein requirements change depending on phases of growth, age and state of health. 16 Close clinical and laboratory monitoring is necessary for individual nutrition management. 18 General recommendations for dietary protein intake vary by age and developmental growth factors, with typically higher weight-based protein needs for earlier stages of life. 16,19 It is important to achieve and maintain positive nitrogen balance through nutrition management, particularly in the growth and development stages of life, to prevent protein catabolism. 19 Providing adequate calories is also important to prevent catabolism, poor growth and development, and weight loss. 18,20 Calorie needs will vary on an individual basis, but a general recommendation is to aim for a calorie intake of 5-10% above the recommended daily allowance for age and gender. Essential amino acids should make up 50-60% of daily protein intake and is often achieved through supplementation via medical foods. 19 Essential amino acids will provide some nitrogen, however the overall nitrogen load delivered to the urea cycle is reduced. 21 Adequate hydration is also necessary to excrete metabolic waste. 19 To meet minimum fluid needs, recommendations for adults include 1.5 ml/kcal or times the amount of maintenance fluids. In some cases, GTs are placed to improve dietary compliance via enteral nutrition. 19 Acute Nutrition Management Establishing a sick-day nutrition plan can help prevent catabolism or a hyperammonemic event. 19 Precipitating factors include menarche, menses, pregnancy, childbirth, postpartum and menopause. Additionally, immunizations, infection, trauma, surgery, chemotherapy and glucocorticoids can precipitate hyperammonemic events. Some patients may require up to a 50% increase in calories provided by non-protein sources. A stricter protein restriction compared to baseline may also be necessary for the first hours of illness, and some cases may require complete cessation of protein during this time period. 18,19 Inadequate calories and protein intake for greater than 48 hours may result in rebound hyperammonemia due to protein catabolism; therefore, withholding nutrition for longer than hours should be avoided. 8,18 Fluid requirements may also be higher and may require a 150% increase during illness. 19 In the event a patient requires prolonged fasting for surgery or illness, intravenous maintenance fluids, glucose and electrolyte supplementation is recommended to prevent catabolism and hyperammonemia. 18 Nitrogen-Scavenging Therapy Pharmacologic treatments are aimed at enhancing nitrogen excretion in type I citrullinemia, and maintaining plasma ammonia concentration <100 µmol/l and plasma glutamine concentration near-normal. 22 Nitrogenscavenging agents provide an alternative route for nitrogen excretions through conjugation with amino acids, thus decreasing the concentrations and preventing accumulation of nitrogenous waste. 23,24 Arginine has been shown to be an indispensable amino acid, though its mechanism is not fully elucidated. 17 In other urea cycle disorders, it works by facilitating excretion of nitrogen as L-citrulline and argininosuccinate, which restores the ammonia-lowering activity of the urea cycle. 25 It effectively reduces ammonia and glutamine concentrations in citrullinemia. 5,22 Sodium benzoate couples with coenzyme A (CoA) to form benzoyl-coa. The benzoyl moiety is transferred to glycine forming hippurate, which prevents its degradation. Glycine is an ammonia-forming amino acid; thus, sodium benzoate enhances elimination of ammonia. 25,26 In combination with sodium phenylacetate it decreases plasma ammonia levels and contributes to high survival rates in acutely hyperammonemic patients. 27 It has a favorable adverse effects profile, with the most common being nausea and headache. 28 Similar to sodium benzoate, sodium phenylacetate creates an alternative pathway for nitrogen excretion. It is β-oxidized by phenylacetyl-coa ligase to phenylacetate CoA, which conjugates glutamine in the liver and kidneys to form phenylacetylglutamine, which is then is excreted in the urine. 25,27,29 Phenylbutyrate is an odorless pro-drug of phenylacetate that rapidly undergoes β-oxidation in the liver to 8
7 phenylacetate. 30 These agents may offer an advantage over sodium benzoate in that they can scavenge twice as much nitrogen, though comparative clinical trials are limited. 24,31 According to consensus guidelines, sodium benzoate should be used preferentially and sodium phenylacetate/phenylbuterate should be given together with sodium benzoate in patients in which benzoate alone is not enough. 24 One issue with taking the oral formulation sodium phenylacetate or sodium phenylbuterate is palatability. 32 Sodium phenylacetate had an offensive odor that limits use. Though sodium phenylbuterate is odorless, it is reported to have a bitter or salty taste, and therefore a newer formulation was developed to mask the taste through microgranular sucrose spheres (Pheburane ). 24,32 Finally, glycerol phenylbutyrate is an ester pro-drug of phenylbutyrate that is slowly hydrolyzed by pancreatic enzymes and is considered a more palatable and less odorous option. 25 Glycerol phenylbutyrate should also be considered in hypertensive patients as it contains much less sodium than the other agents. 33 Dosing for these agents are displayed in Table 2. 5,22,24 Reducing Nitrogen Generation and Uptake There is limited data supporting typical interventions for hyperammonemia secondary to hepatic failure, most of which are case reports with variable results. However, others have reported success with lactulose in combination with a protein restricted diet and arginine. 34,35 Whether the lactulose was beneficial in addition to protein restriction has yet to be determined. Lactulose is a non-absorbable disaccharide that acidifies the proximal gastrointestinal tract, which harms ureaseproducing bacteria and decreases absorption of ammonia. 25 Antimicrobial therapies, such as rifaximin, neomycin or kanamycin, also target urease-producing bacteria and limit intestinal ammonia production. 25 These therapies may be considered as adjunctive agents, but therapy should target the pathology of citrullinemia. Liver Transplantation In patients whose symptoms cannot be controlled by diet, those with life-threatening complications, or progressive liver disease, orthotopic liver transplantation (OLT) is a treatment option. 36 The liver is the primary site of urea cycle activity. As such, OLT generally results in metabolic correction of urea cycle pathology, allowing for cessation of diet precautions and supplementation, and is the only curative intervention available Further neurologic degradation is prevented and improvement in neurologic deficit may be observed, particularly with early transplantation. 36,38 A case series of five children less than one year found modest improvement in neurological development after OLT. 38 A 14-year-old female was found to have increased intellectual capacity after OLT. 37 However, in a case series of 16 patients with urea cycle disorders, of which 3 had citrullinemia, neurological outcome after Table 2. Treatment of Type I Citrullinemia 5,20,23,25 Nutrition Management Recommendations Calories RDA for age/gender % Protein Limited to what is physiologically necessary; changes with age and development; majority should come from essential amino acids Fluids 1.5 ml fluid/kg Agent Regimen Nitrogen Scavengers Arginine 9-12 grams per day or mg/kg divided into three doses with meals (Maximum: 6 grams/day) Sodium benzoate 250mg/kg/day divided into three doses with meals (Maximum: 12g/day) Sodium phenylacetate or sodium phenylbutyrate Glycerol phenylbutyrate mg/kg/day or 5g/m2/day divided into three doses with meals (Maximum: 12g/day) Phenylbutyrate-naïve: ml/m2/day ( g/m2/day) divided into three doses with meals Conversion from sodium phenylbutyrate: daily dose of glycerol phenylbutyrate (ml) = daily dose of sodium phenylbutyrate (g) x 0.86 RDA= recommended daily allowance 9
8 transplantation correlated closely with baseline status prior to transplantation. 40 Overall, outcomes in OLT patients with inherited metabolic disease are consistently more favorable than in patients with primary liver disease. 36 However, given the lifelong commitment to immunosuppressive therapies and complications associated with OLT, this pathway should be avoided unless the patient has failed medical management. Acute Decompensation All patients with citrullinemia are at risk of acute decompensation from metabolic stress. Exacerbating factors include fasting, acute illness, particularly gastroenteritis, anesthesia and protein load such as gastrointestinal hemorrhage. 36 Patients should have an emergency regimen including a high-energy, low protein diet and increased doses of arginine and sodium benzoate. Ammonul is a combination product of 10% sodium benzoate and 10% sodium phenylacetate that is FDA-approved as an adjuvant in treatment of hyperammonemic episodes. 25 Consultation with the patient s geneticist should be considered in the event of acute decompensation. Measures should be taken to decrease ammonia serum concentrations, prevent reversal of catabolism, and avoid increased intracranial pressure. The doses recommended for acute decompensation are displayed in Table 3. 5,41 Hemodialysis (HD) is the most effective measure for rapid removal of ammonia and should not be delayed when scavenger therapies fail to control ammonia levels. 5 Detoxification of ammonia occurs through synthesis of urea and glutamine, of which ~20% is excreted renally. 42 Currently the preferred renal replacement modality for ammonia removal and clinically significant time at which dialysis should be initiated is unknown. 43 Both intermittent HD and continuous venovenous hemofiltration (CVVH) effectively reduce ammonia, but differ in the rate of removal Intermittent HD removes 50% of ammonia within 2 hours, while CVVH takes up to 15 hours. 45 The goal of therapy should be to achieve resolution of symptoms associated with hyperammonemia. CONCLUSION Though citrullinemia is a rare urea cycle disorder, it is essential to understand the pathophysiology for proper management. Providing protein restricted diets and selecting medications that enhance nitrogen excretion are key therapy concepts. Consultation with providers who specialize in urea cycle disorders should be considered to assist in both acute and chronic management. REFERENCES 1. Kobayashi K, Saheki T, Song YZ. Citrin Deficiency Sep 16 [Updated 2014 Jul 31]. In: Pagon RA, Adam MP, Ardinger HH, et al., editors. GeneReviews [Internet]. Seattle (WA): University of Washington, Seattle; Available from: Accessed 15 November Woo HI, Park HD, Lee YW. Molecular genetics of citrullinemia types I and II. Clin Chim Acta. 2014;431: Kobayashi K, Jackson MJ, Tick DB, O Brien WE, Beaudet AL. Heterogeneity of mutations in argininosuccinate synthetase causing human citrullinemia. J Biol Chem. 1990;265(19): Gao HZ, Kobayashi K, Tabata A, et al. Identification of 16 novel mutations in the argininosuccinate synthetase gene and genotype-phenotype correlation in 38 classical citrullinemia patients. Hum Mutat. 2003;22(1): Table 3. Treatment of Acute Decompensation. 5,42 Agent Regimen 10% arginine hydrochloride 600 mg/kg or 12.0 g/m 2 over 90 minutes, then 600 mg/kg or 12.0 g/m 2 over 24 hours Sodium benzoate Sodium phenylacetate (in combination with sodium benzoate) 250 mg/kg or 5.5 g/m 2 over 90 minutes, then 250 mg/kg or 5.5 g/m 2 over 24 hours 250 mg/kg or 5.5 g/m 2 over 90 minutes, then 250 mg/kg or 5.5 g/m 2 over 24 hours 10
9 5. Quinonez SC, Thoene JG. Citrullinemia Type I Jul 7 [Updated 2016 Sep 1]. In: Pagon RA, Adam MP, Ardinger HH, et al., editors. GeneReviews [Internet]. Seattle (WA): University of Washington, Seattle; Available from: books/nbk1458/. Accessed 15 November Dimmock D, Maranda B, Dionisi-Vici C, et al. Citrin deficiency, a perplexing global disorder. Mol Genet Metab. 2009;96(1): Walker V. Ammonia metabolism and hyperammonemic disorders. Adv Clin Chem. 2014;67: Ah Mew N, Lanpher BC, Gropman A, et al. ; Urea Cycle Disorders Consortium Urea Cycle Disorders Overview Apr 29 [Updated 2015 Apr 9]. In: Pagon RA, Adam MP, Ardinger HH, et al., editors. GeneReviews [Internet]. Seattle (WA): University of Washington, Seattle; Available from: Accessed 15 November Haberle J. Clinical and biochemical aspects of primary and secondary hyperammonemic disorders. Arch Biochem Biophys. 2013;536(2): Auron A, Brophy PD. Hyperammonemia in review: pathophysiology, diagnosis, and treatment. Pediatr Nephrol. 2012;27(2): Miller MJ, Soler-Alfonso CR, Grund JE, et al. Improved standards for prenatal diagnosis of citrullinemia. Mol Genet Metab. 2014;112(3): Ruder J, Legacy J, Russo G, Davis R. Neonatal citrullinemia: novel, reversible neuroimaging findings correlated with ammonia level changes. Pediatr Neurol. 2014;51(4): Maestri NE, Clissold DB, Brusilow SW. Long-term survival of patients with argininosuccinate synthetase deficiency. J Pediatr. 1995;127(6): Brunetti-Pierri N, Lamance KM, Lewis RA, Craigen WJ. 30-year follow-up of a patient with classic citrullinemia. Mol Genet Metab. 2012;106(2): Go H, Imamura T, Hashimoto K, et al. Successful prospective management of neonatal citrullinemia. J Pediatr Endocrinol. 2012;25(3-4): Leonard JV. The nutritional management of urecycle disorders. J Pediatr. 2001;138(1 Suppl):S40-4;discussion S Brusilow SW. Arginine, an indispensable amino acid for patients with inborn errors of urea synthesis. J Clin Invest. 1984;74(6): Berry GT, Steiner RD. Long-term management of patients with urea cycle disorders. J Pediatr. 2001;138(1 Suppl):S56-60; discussion S Singh RH, Rhead WJ, Smith W, Lee B, Sniderman King L, Summar M. Nutritional management of urea cycle disorders. Crit Care Clin. 2005;21(4 Suppl):S Batshaw ML, Monahan PS. Treatment of urea cycle disorders. Enzyme. 1987;38(1-4): Adam S, Champion H, Daly A, et al. Dietary management of urea cycle disordes: UK practice. J Hum Nutr Diet. 2012;25(4): Yazaki M, Kinoshita M, Ogawa S, et al. A 73-year-old patient with adult-onset type II citrullinemia successfully treated by sodium pyruvate and arginine. Clin Neurol Neurosurg. 2013;115(8): Brusilow SW, Valle DL, Batshaw M. New pathways of nitrogen excretion in inborn errors of urea synthesis. Lancet. 1979;2(8140): Haberle J, Boddaert N, Burlina A, et al. Suggested guidelines for the diagnosis and management of urea cycle disorders. Orphanet J Rare Dis. 2012;7: Matoori S, Leroux JC. Recent advances in the treament of hyperammonemia. Adv Drug Deliv Rev. 2015;90: Barshop BA, Breuer J, Holm J, Leslie J, Nyhan WL. Excretion of hippuric acid during sodium benzoate therapy in patients with hyperglycinaemia or hyperammonaemia. J Inherit Metab Dis. 1989;12(1): Enns GM, Berry SA, Berry GT, Rhead WJ, Brusilow SW, Hamosh A. Survival after treatment with phenylacetate and benzoate for urea-cycle disorders. N Engl J Med. 2007;356(22): Mokhtarani M, Diaz GA, Rhead W, et al. Elevated phenylacetic acid levels do not correlate with adverse events in patients with urea cycle disorders or hepatic encephalopathy and can be predicted based on the plasma PAA to PAGN ratio. Mol Genet Metab. 2013;110(4): Scaglia F. New insights in nutritional management and amino acid supplementation in urea cycle disorders. Mol Genet Metab. 2010;100 Suppl 1:S Newmark HL, Young CW. Butyrate and phenylacetate as differentiating agents: practical problems and opportunities. J Cell Biochem Suppl. 1995;22: Comte B, Kasumov T, Pierce BA, et al. Identification of phenylbutyrylglutamine, a new metabolite of phenylbutyrate metabolism in humans. J Mass Spectrum. 2002;37(6): Guffon N, Kibleur Y, Copalu W, Tissen C, Breitkreutz J. Developing a new formulation of sodium phenylbutyrate. Arch Dis Child. 2012;97(12):
10 33. McGuire BM, Zupanets IA, Lowe ME, et al. Pharmacology and safety of glycerol phenylbutyrate in healthy adults and adults with cirrhosis. Hepatology. 2010;51 (6): Saheki T, Inoue K, Tushima A, Mutoh K, Kobayashi K. Citrin deficiency and current treatment concepts. Mol Genet Metab. 2010;100 Suppl 1:S Ueda A, Okada K, Takahara T, et al. A case of adultonset type II citrullinemia induced by hospital diet. Clin J Gastroenterol. 2011;4(1): Leonard JV, McKiernan PJ. The role of liver transplantation in urea cycle disorders. Mol Genet Metab. 2004;81 Suppl 1:S Foschi FG, Morelli MC, Savini S, et al. Urea cycle disorders: a case report of a successful treatment with liver transplant and a literature review. World J Gastroenterol. 2015;21(13): McBride KL, Miller G, Carter S, Karpen S, Goss J, Lee B. Developmental outcomes with early orthotopic liver transplantation for infants with neonatal-onset urea cycle defects and a female patient with late-onset ornithine transcarbamylase deficiency. Pediatrics. 2004;114(4):e Kogure T, Kondo Y, Kakazu E, et al. Three cases of adult-onset type II citrullinemia treated with different therapies: efficacy of sodium pyruvate and lowcarbohydrate diet. Hepatol Res. 2014;44(6): Whitington PF, Alonso EM, Boyle JT, et al. Liver transplantation for the treatment of urea cycle disorders. J Inherit Metab Dis. 1998;21 Suppl 1: Kimura N, Kubo N, Narumi S, et al. Liver transplantation versus conservative treatment for adult-onset type II citrullinemia: our experience and a review of the literature. Transplant Proc. 2013;45(9): Slack AJ, Auzinger G, Willars C, et al. Ammonia clearance with haemofiltration in adults with liver disease. Liver Int. 2014;34(1): Gupta S, Fenves AZ, Hootkins R. The role of RRT in hyperammonemic patients. Clin J Am Soc Nephrol. 2016;11(10): Wen JX, Feldenberg LR, Abraham E, Sadiq F, Christensen KM, Braddock SR. Continuous venovenous hemodialysis via extracorporeal membrane oxygenation pump for treatment of hyperammonemia secondary to propionic acidemia in monochorionic diamniotic twin boys. J Pediatr. 2016;175: Lai YC, Huang HP, Tsai IJ, Tsau YK. High-volume continuous venovenous hemofiltration as an effective therapy for acute management of inborn errors of metabolism in young children. Blood Purif. 2007;25 (4): Acknowledgements We thank GeneReviews, whose chapters are owned by the University of Washington, for granting permission to reproduce a figure of the urea cycle. The permission to reproduce, duplicate, or translate copies of content materials for noncommercial purposes can be found at this link: Corresponding Author Denise M. Kolanczyk st Street Downers Grove, IL Phone: Fax:
Urea Cycle Disorders Prior Authorization Program Summary
 Urea Cycle Disorders Prior Authorization Program Summary FDA APPROVED INDICATIONS DOSAGE 1,2 Agent(s) Indication(s) Dosing -Adjunctive therapy in the chronic management of patients with urea cycle disorders
Urea Cycle Disorders Prior Authorization Program Summary FDA APPROVED INDICATIONS DOSAGE 1,2 Agent(s) Indication(s) Dosing -Adjunctive therapy in the chronic management of patients with urea cycle disorders
UPDATE ON UREA CYCLE DISORDERS TREATMENT
 UPDATE ON UREA CYCLE DISORDERS TREATMENT George A. Diaz, MD, PhD Program for Inherited Metabolic Diseases Department of Genetics and Genomic Sciences Icahn School of Medicine at Mount Sinai Disclosure
UPDATE ON UREA CYCLE DISORDERS TREATMENT George A. Diaz, MD, PhD Program for Inherited Metabolic Diseases Department of Genetics and Genomic Sciences Icahn School of Medicine at Mount Sinai Disclosure
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Urea Cycle Disorders Page 1 of 7 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Urea Cycle Disorders Prime Therapeutics will review Prior Authorization requests
Urea Cycle Disorders Page 1 of 7 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Urea Cycle Disorders Prime Therapeutics will review Prior Authorization requests
Urea Cycle Defects. Dr Mick Henderson. Biochemical Genetics Leeds Teaching Hospitals Trust. MetBioNet IEM Introductory Training
 Urea Cycle Defects Dr Mick Henderson Biochemical Genetics Leeds Teaching Hospitals Trust The Urea Cycle The urea cycle enables toxic ammonia molecules to be converted to the readily excreted and non toxic
Urea Cycle Defects Dr Mick Henderson Biochemical Genetics Leeds Teaching Hospitals Trust The Urea Cycle The urea cycle enables toxic ammonia molecules to be converted to the readily excreted and non toxic
UREA CYCLE DISORDERS - The What, Why, How and When
 UREA CYCLE DISORDERS - The What, Why, How and When George A. Diaz, MD, PhD Program for Inherited Metabolic Diseases Department of Genetics and Genomic Sciences Department of Pediatrics Icahn School of
UREA CYCLE DISORDERS - The What, Why, How and When George A. Diaz, MD, PhD Program for Inherited Metabolic Diseases Department of Genetics and Genomic Sciences Department of Pediatrics Icahn School of
TRANSAMINATION AND UREA CYCLE
 TRANSAMINATION AND UREA CYCLE USMAN SUMO FRIEND TAMBUNAN ARLI ADITYA PARIKESIT SEPTIANA BIOINFORMATICS GROUP DEPARTEMENT OF CHEMISTRY FACULTY OF MATHEMATIC AND SCIENCE UNIVERSITY OF INDONESIA What is transamination?
TRANSAMINATION AND UREA CYCLE USMAN SUMO FRIEND TAMBUNAN ARLI ADITYA PARIKESIT SEPTIANA BIOINFORMATICS GROUP DEPARTEMENT OF CHEMISTRY FACULTY OF MATHEMATIC AND SCIENCE UNIVERSITY OF INDONESIA What is transamination?
ESPEN Congress Madrid 2018
 ESPEN Congress Madrid 2018 Inborn Errors Of Metabolism Urea Cycle Disorders Diagnosis And Care F. Feillet (FR) Urea cycle disorders, diagnosis and care F Feillet National reference centre for Inborn errors
ESPEN Congress Madrid 2018 Inborn Errors Of Metabolism Urea Cycle Disorders Diagnosis And Care F. Feillet (FR) Urea cycle disorders, diagnosis and care F Feillet National reference centre for Inborn errors
Ornithine Transcarbamylase Deficiency (OTCD) Recommendations on Emergency Management of Metabolic Disease
 Ornithine Transcarbamylase Deficiency (OTCD) Recommendations on Emergency Management of Metabolic Disease Patient s Name: Date of Birth: MRN in KFSH&RC: Please read carefully. Meticulous and prompt treatment
Ornithine Transcarbamylase Deficiency (OTCD) Recommendations on Emergency Management of Metabolic Disease Patient s Name: Date of Birth: MRN in KFSH&RC: Please read carefully. Meticulous and prompt treatment
Urea is the major end product of nitrogen catabolism in humans One nitrogen free NH3 other nitrogen aspartate. carbon oxygen CO2 liver,
 Urea is the major end product of nitrogen catabolism in humans Urea is the major disposal form of amino groups derived from amino acids, and accounts about 90% percent of the nitrogencontaining components
Urea is the major end product of nitrogen catabolism in humans Urea is the major disposal form of amino groups derived from amino acids, and accounts about 90% percent of the nitrogencontaining components
Jana Novotná, Bruno Sopko. Department of the Medical Chemistry and Clinical Biochemistry The 2nd Faculty of Medicine, Charles Univ.
 Amino acid metabolism II. Urea cycle Jana Novotná, Bruno Sopko Department of the Medical Chemistry and Clinical Biochemistry The 2nd Faculty of Medicine, Charles Univ. Nitrogen balance Tissue proteins
Amino acid metabolism II. Urea cycle Jana Novotná, Bruno Sopko Department of the Medical Chemistry and Clinical Biochemistry The 2nd Faculty of Medicine, Charles Univ. Nitrogen balance Tissue proteins
How to dose RAVICTI (glycerol phenylbutyrate) Oral Liquid
 How to dose RAVICTI (glycerol phenylbutyrate) Oral Liquid A REFERENCE GUIDE FOR DOSING, ADMINISTRATION, AND SUPPORT RAVICTI is so easy to take... It s just one little moment. Isaac, Age 20 Actual RAVICTI
How to dose RAVICTI (glycerol phenylbutyrate) Oral Liquid A REFERENCE GUIDE FOR DOSING, ADMINISTRATION, AND SUPPORT RAVICTI is so easy to take... It s just one little moment. Isaac, Age 20 Actual RAVICTI
LOW CITRULLINE AS A MARKER FOR THE PROXIMAL UREA CYCLE DEFECTS EXPERIENCE OF THE NEW ENGLAND NEWBORN SCREENING PROGRAM
 LOW CITRULLINE AS A MARKER FOR THE PROXIMAL UREA CYCLE DEFECTS EXPERIENCE OF THE NEW ENGLAND NEWBORN SCREENING PROGRAM Inderneel Sahai, MD, FACMG Newborn Screening and Genetic Testing Symposium Oct 2014
LOW CITRULLINE AS A MARKER FOR THE PROXIMAL UREA CYCLE DEFECTS EXPERIENCE OF THE NEW ENGLAND NEWBORN SCREENING PROGRAM Inderneel Sahai, MD, FACMG Newborn Screening and Genetic Testing Symposium Oct 2014
ARGININOSUCCINIC ACIDEMIA (or ARGININOSUCCINATE LYASE DEFICIENCY) RECOMMENDATIONS ON EMERGENCY MANAGEMENT OF METABOLIC DISEASES
 ARGININOSUCCINIC ACIDEMIA (or ARGININOSUCCINATE LYASE DEFICIENCY) RECOMMENDATIONS ON EMERGENCY MANAGEMENT OF METABOLIC DISEASES Patient s name: Date of birth: Please read carefully. Meticulous and prompt
ARGININOSUCCINIC ACIDEMIA (or ARGININOSUCCINATE LYASE DEFICIENCY) RECOMMENDATIONS ON EMERGENCY MANAGEMENT OF METABOLIC DISEASES Patient s name: Date of birth: Please read carefully. Meticulous and prompt
First report of carglumic acid in a patient with citrullinemia type 1 (argininosuccinate synthetase deficiency)
 Received: 14 June 2017 Accepted: 20 June 2017 DOI: 10.1111/jcpt.12593 CASE REPORT First report of carglumic acid in a patient with citrullinemia type 1 (argininosuccinate synthetase deficiency) E. Kose
Received: 14 June 2017 Accepted: 20 June 2017 DOI: 10.1111/jcpt.12593 CASE REPORT First report of carglumic acid in a patient with citrullinemia type 1 (argininosuccinate synthetase deficiency) E. Kose
Carbamoyl Phosphate Synthetase (code 50470) Notice of Assessment
 Carbamoyl Phosphate Synthetase (code 50470) Notice of Assessment June 2013 DISCLAIMER: This document was originally drafted in French by the Institut national d'excellence en santé et en services sociaux
Carbamoyl Phosphate Synthetase (code 50470) Notice of Assessment June 2013 DISCLAIMER: This document was originally drafted in French by the Institut national d'excellence en santé et en services sociaux
Amino Acid Metabolism
 Amino Acid Metabolism The continuous degradation and synthesis of cellular proteins occur in all forms of life. Each day humans turn over 1 2% of their total body protein, principally muscle protein. Approximately
Amino Acid Metabolism The continuous degradation and synthesis of cellular proteins occur in all forms of life. Each day humans turn over 1 2% of their total body protein, principally muscle protein. Approximately
AMINO ACID METABOLISM
 AMINO ACID METABOLISM Synthesis of Urea in Liver The series of reactions that form urea is known as the Urea Cycle or the Krebs-Henseleit Cycle. The urea cycle operates only to eliminate excess nitrogen.
AMINO ACID METABOLISM Synthesis of Urea in Liver The series of reactions that form urea is known as the Urea Cycle or the Krebs-Henseleit Cycle. The urea cycle operates only to eliminate excess nitrogen.
Proceedings of a Consensus Conference for the
 Proceedings of a Consensus Conference for the Management of Patients with Urea Cycle Disorders Marshall Summar, MD, and Mendel Tuchman, MD In an effort to develop standards for the treatment of patients
Proceedings of a Consensus Conference for the Management of Patients with Urea Cycle Disorders Marshall Summar, MD, and Mendel Tuchman, MD In an effort to develop standards for the treatment of patients
Volume 3 (2017) Issue 10 ISSN Keywords. Introduction. Case Report. Open Journal of Clinical & Medical Case Reports
 Open Journal of Clinical & Medical Case Reports Volume 3 (2017) Issue 10 ISSN 2379-1039 Recurrent hyperammonemia in an 80-year-old woman with congenital urea cycle abnormality Junji Yamaguchi, MD*; Koichi
Open Journal of Clinical & Medical Case Reports Volume 3 (2017) Issue 10 ISSN 2379-1039 Recurrent hyperammonemia in an 80-year-old woman with congenital urea cycle abnormality Junji Yamaguchi, MD*; Koichi
New developments in Urea Cycle Disorders and its impact on patients
 New developments in Urea Cycle Disorders and its impact on patients Johannes Häberle University Children s Hospital Zurich, Division of Metabolism 16 June 2015 SFEIM 2015, Lille, France The urea cycle
New developments in Urea Cycle Disorders and its impact on patients Johannes Häberle University Children s Hospital Zurich, Division of Metabolism 16 June 2015 SFEIM 2015, Lille, France The urea cycle
UNDERSTANDING UREA CYCLE DISORDERS
 UNDERSTANDING UREA CYCLE DISORDERS What is a urea cycle disorder? A urea cycle disorder is a genetic disease that affects how protein is broken down in the body. It is therefore classified as a metabolic
UNDERSTANDING UREA CYCLE DISORDERS What is a urea cycle disorder? A urea cycle disorder is a genetic disease that affects how protein is broken down in the body. It is therefore classified as a metabolic
CLINICAL PHARMACOLOGY
 BUPHENYL (sodium phenylbutyrate) Tablets BUPHENYL (sodium phenylbutyrate) Powder [bu fen-ǝl] (sodium phenylbutyrate) Rx Only DESCRIPTION BUPHENYL (sodium phenylbutyrate) Tablets for oral administration
BUPHENYL (sodium phenylbutyrate) Tablets BUPHENYL (sodium phenylbutyrate) Powder [bu fen-ǝl] (sodium phenylbutyrate) Rx Only DESCRIPTION BUPHENYL (sodium phenylbutyrate) Tablets for oral administration
3 HYDROXY 3 METHYLGLUTARYL CoA (3 HMG CoA) LYASE DEFICIENCY RECOMMENDATIONS ON EMERGENCY MANAGEMENT OF METABOLIC DISEASES
 3 HYDROXY 3 METHYLGLUTARYL CoA (3 HMG CoA) LYASE DEFICIENCY RECOMMENDATIONS ON EMERGENCY MANAGEMENT OF METABOLIC DISEASES Patient s name: Date of birth: Please read carefully. Meticulous and prompt treatment
3 HYDROXY 3 METHYLGLUTARYL CoA (3 HMG CoA) LYASE DEFICIENCY RECOMMENDATIONS ON EMERGENCY MANAGEMENT OF METABOLIC DISEASES Patient s name: Date of birth: Please read carefully. Meticulous and prompt treatment
Conventional Diet Therapy for Hyperammonemia is Risky in the Treatment of Hepatic Encephalopathy Associated with Citrin Deficiency
 CASE REPORT Conventional Diet Therapy for Hyperammonemia is Risky in the Treatment of Hepatic Encephalopathy Associated with Citrin Deficiency Kazuhiro Fukushima 1, Masahide Yazaki 1,MioNakamura 2, Naoki
CASE REPORT Conventional Diet Therapy for Hyperammonemia is Risky in the Treatment of Hepatic Encephalopathy Associated with Citrin Deficiency Kazuhiro Fukushima 1, Masahide Yazaki 1,MioNakamura 2, Naoki
Metabolic Disorders. Chapter Thomson - Wadsworth
 Metabolic Disorders Chapter 28 1 Metabolic Disorders Inborn errors of metabolism group of diseases that affect a wide variety of metabolic processes; defective processing or transport of amino acids, fatty
Metabolic Disorders Chapter 28 1 Metabolic Disorders Inborn errors of metabolism group of diseases that affect a wide variety of metabolic processes; defective processing or transport of amino acids, fatty
TITLE: NURSING GUIDELINES FOR THE MANAGEMENT OF CHILDREN WITH UREA CYCLE DEFECTS. Eilish O Connell, Clinical Education Facilitator, NCIMD
 NO. OF PAGES: Page 1 of 16 SUPERCEDES: N/A NURSING GUIDELINES FOR THE MANAGEMENT OF CHILDREN WITH UREA CYCLE DEFECTS NAME/ Eilish O Connell, Clinical Education Facilitator, NCIMD SIGNATURE: DATE: NAME/
NO. OF PAGES: Page 1 of 16 SUPERCEDES: N/A NURSING GUIDELINES FOR THE MANAGEMENT OF CHILDREN WITH UREA CYCLE DEFECTS NAME/ Eilish O Connell, Clinical Education Facilitator, NCIMD SIGNATURE: DATE: NAME/
THE ED APPROACH OF THE CHILD WITH SUSPECTED METABOLIC DISEASE
 THE ED APPROACH OF THE CHILD WITH SUSPECTED METABOLIC DISEASE Dr. Nadeem Qureshi M.D, FAAP, FCCM Associate Professor Pediatrics School of Medicine. St Louis University Attending Physician Pediatric Emergency
THE ED APPROACH OF THE CHILD WITH SUSPECTED METABOLIC DISEASE Dr. Nadeem Qureshi M.D, FAAP, FCCM Associate Professor Pediatrics School of Medicine. St Louis University Attending Physician Pediatric Emergency
Subject: Ravicti (glycerol phenylbutyrate) Original Effective Date: 03/16/15. Policy Number: MCP-242. Revision Date(s):
 Subject: Ravicti (glycerol phenylbutyrate) Original Effective Date: 03/16/15 Policy Number: MCP-242 Revision Date(s): Review Date(s): 12/15/2016; 6/22/2017 DISCLAIMER This Medical Policy is intended to
Subject: Ravicti (glycerol phenylbutyrate) Original Effective Date: 03/16/15 Policy Number: MCP-242 Revision Date(s): Review Date(s): 12/15/2016; 6/22/2017 DISCLAIMER This Medical Policy is intended to
Urea Cycle Disorders and Hyperammonemia: Diagnosable Treatable Screenable
 Urea Cycle Disorders and Hyperammonemia: Diagnosable Treatable Screenable Marshall L. Summar, M.D. Chief, Division of Genetics and Metabolism Children s National Medical Center Washington, DC, USA Disclosure
Urea Cycle Disorders and Hyperammonemia: Diagnosable Treatable Screenable Marshall L. Summar, M.D. Chief, Division of Genetics and Metabolism Children s National Medical Center Washington, DC, USA Disclosure
Newborn Screen & Development Facts about the genetic diseases new since March 2006 (Excluding Cystic Fibrosis)
 Newborn Screen & Development Facts about the genetic diseases new since March 2006 (Excluding Cystic Fibrosis) 1) Argininosuccinic acidemia (ASA) a) Incidence: ~1 in 70,000 b) Deficiency in an enzyme of
Newborn Screen & Development Facts about the genetic diseases new since March 2006 (Excluding Cystic Fibrosis) 1) Argininosuccinic acidemia (ASA) a) Incidence: ~1 in 70,000 b) Deficiency in an enzyme of
Introduction to Organic Acidemias. Hilary Vernon, MD PhD Assistant Professor of Genetic Medicine Johns Hopkins University 7.25.
 Introduction to Organic Acidemias Hilary Vernon, MD PhD Assistant Professor of Genetic Medicine Johns Hopkins University 7.25.2014 A Brief Historical Overview Garrod, Archibald E. 1902. The Incidence of
Introduction to Organic Acidemias Hilary Vernon, MD PhD Assistant Professor of Genetic Medicine Johns Hopkins University 7.25.2014 A Brief Historical Overview Garrod, Archibald E. 1902. The Incidence of
Carbamoyl phosphate synthetase 1 deficiency: First report of this rare metabolic disorder in Kingdom of Bahrain with novel mutation
 Alsahlawi et al. 1 CASE REPORT PEER REVIEWED OPEN ACCESS Carbamoyl phosphate synthetase 1 deficiency: First report of this rare metabolic disorder in Kingdom of Bahrain with novel mutation Z. Alsahlawi,
Alsahlawi et al. 1 CASE REPORT PEER REVIEWED OPEN ACCESS Carbamoyl phosphate synthetase 1 deficiency: First report of this rare metabolic disorder in Kingdom of Bahrain with novel mutation Z. Alsahlawi,
Hyperammonemia: Diagnostic Experience At The Metabolism Laboratory
 ISPUB.COM The Internet Journal of Laboratory Medicine Volume 1 Number 2 Hyperammonemia: Diagnostic Experience At The Metabolism Laboratory A Rao, P Varma, Sumitra, S Dhanya Citation A Rao, P Varma, Sumitra,
ISPUB.COM The Internet Journal of Laboratory Medicine Volume 1 Number 2 Hyperammonemia: Diagnostic Experience At The Metabolism Laboratory A Rao, P Varma, Sumitra, S Dhanya Citation A Rao, P Varma, Sumitra,
NITROGEN METABOLISM An Overview
 1 University of Papua New Guinea School of Medicine and Health Sciences Division of Basic Medical Sciences Discipline of Biochemistry and Molecular Biology PBL Seminar & Health Sciences NITROGEN METABOLISM
1 University of Papua New Guinea School of Medicine and Health Sciences Division of Basic Medical Sciences Discipline of Biochemistry and Molecular Biology PBL Seminar & Health Sciences NITROGEN METABOLISM
AMINOACID METABOLISM FATE OF AMINOACIDS & UREA CYCLE
 AMINOACID METABOLISM FATE OF AMINOACIDS & UREA CYCLE SOURCE & FATE OF AA The aminoacids obtained from DIETARY SOURCE or BODY PROTEIN TURNOVER are utilized for protein biosynthesis and the production of
AMINOACID METABOLISM FATE OF AMINOACIDS & UREA CYCLE SOURCE & FATE OF AA The aminoacids obtained from DIETARY SOURCE or BODY PROTEIN TURNOVER are utilized for protein biosynthesis and the production of
Survival after Treatment with Phenylacetate and Benzoate for Urea-Cycle Disorders
 T h e n e w e ng l a nd j o u r na l o f m e dic i n e original article Survival after Treatment with Phenylacetate and Benzoate for Urea-Cycle Disorders Gregory M. Enns, M.B., Ch.B., Susan A. Berry, M.D.,
T h e n e w e ng l a nd j o u r na l o f m e dic i n e original article Survival after Treatment with Phenylacetate and Benzoate for Urea-Cycle Disorders Gregory M. Enns, M.B., Ch.B., Susan A. Berry, M.D.,
Senior Vice President, Medical Affairs and Health Outcomes, 150 South Saunders Road, Lake Forest, IL 60045, Horizon Pharma USA, Inc, USA
 Research Hyperammonemic crises in patients with urea cycle disorders on chronic nitrogen scavenger therapy with either sodium phenylbutyrate or glycerol phenylbutyrate Jeffrey D Kent 1, Robert J Holt,2
Research Hyperammonemic crises in patients with urea cycle disorders on chronic nitrogen scavenger therapy with either sodium phenylbutyrate or glycerol phenylbutyrate Jeffrey D Kent 1, Robert J Holt,2
Hyperammonemia due to urea cycle disorders: a potentially fatal condition in the intensive care setting
 Machado and Pinheiro da Silva Journal of Intensive Care 2014, 2:22 REVIEW Open Access Hyperammonemia due to urea cycle disorders: a potentially fatal condition in the intensive care setting Marcel Cerqueira
Machado and Pinheiro da Silva Journal of Intensive Care 2014, 2:22 REVIEW Open Access Hyperammonemia due to urea cycle disorders: a potentially fatal condition in the intensive care setting Marcel Cerqueira
Altered mental status: a common complaint that led to a rare diagnosis - Ornithine Transcarbamylase Deficiency
 Altered mental status: a common complaint that led to a rare diagnosis - Ornithine Transcarbamylase Deficiency Joshua J. White, OMS3 Charles C. Finch, D.O., FACOEP Arizona College Of Osteopathic Medicine
Altered mental status: a common complaint that led to a rare diagnosis - Ornithine Transcarbamylase Deficiency Joshua J. White, OMS3 Charles C. Finch, D.O., FACOEP Arizona College Of Osteopathic Medicine
Guideline for the diagnosis and management of isovaleryl-coa-dehydrogenase deficiency (isovaleric acidemia) - a systematic review -
 Guideline for the diagnosis and management of isovaleryl-coa-dehydrogenase deficiency (isovaleric acidemia) - a systematic review - Guideline development group International interdisciplinary guideline
Guideline for the diagnosis and management of isovaleryl-coa-dehydrogenase deficiency (isovaleric acidemia) - a systematic review - Guideline development group International interdisciplinary guideline
Biochemistry: A Short Course
 Tymoczko Berg Stryer Biochemistry: A Short Course Second Edition CHAPTER 30 Amino Acid Degradation and the Urea Cycle 2013 W. H. Freeman and Company Chapter 30 Outline Amino acids are obtained from the
Tymoczko Berg Stryer Biochemistry: A Short Course Second Edition CHAPTER 30 Amino Acid Degradation and the Urea Cycle 2013 W. H. Freeman and Company Chapter 30 Outline Amino acids are obtained from the
The spectrum and outcome of the. neonates with inborn errors of. metabolism at a tertiary care hospital
 The spectrum and outcome of the neonates with inborn errors of metabolism at a tertiary care hospital Dr. Sevim Ünal Neonatology Division, Ankara Children s Hematology Oncology Research Hospital, Ankara,
The spectrum and outcome of the neonates with inborn errors of metabolism at a tertiary care hospital Dr. Sevim Ünal Neonatology Division, Ankara Children s Hematology Oncology Research Hospital, Ankara,
Biochemistry: A Short Course
 Tymoczko Berg Stryer Biochemistry: A Short Course Second Edition CHAPTER 30 Amino Acid Degradation and the Urea Cycle 2013 W. H. Freeman and Company In the cytosol of a cell amino groups from amino acids
Tymoczko Berg Stryer Biochemistry: A Short Course Second Edition CHAPTER 30 Amino Acid Degradation and the Urea Cycle 2013 W. H. Freeman and Company In the cytosol of a cell amino groups from amino acids
Amino Acid Oxidation and the Urea Cycle
 Amino Acid Oxidation and the Urea Cycle Amino Acids: Final class of biomolecules whose oxidation contributes significantly to the generation of energy Undergo oxidation in three metabolic circumstances
Amino Acid Oxidation and the Urea Cycle Amino Acids: Final class of biomolecules whose oxidation contributes significantly to the generation of energy Undergo oxidation in three metabolic circumstances
Urea cycle disorders (UCD) compromise a group of inherited metabolic disorders with an estimated overall prevalence
 Early Clinical Manifestations and Eating Patterns in Patients with Urea Cycle Disorders Thatjana Gardeitchik, MD 1,2, Maureen Humphrey, APD 1,3, Judy Nation, APD 1,3, and Avihu Boneh, MD, PhD 1,4 Objectives
Early Clinical Manifestations and Eating Patterns in Patients with Urea Cycle Disorders Thatjana Gardeitchik, MD 1,2, Maureen Humphrey, APD 1,3, Judy Nation, APD 1,3, and Avihu Boneh, MD, PhD 1,4 Objectives
Module : Clinical correlates of disorders of metabolism Block 3, Week 2
 Module : Clinical correlates of disorders of metabolism Block 3, Week 2 Department of Paediatrics and Child Health University of Pretoria Tutor : Prof DF Wittenberg : dwittenb@medic.up.ac.za Aim of this
Module : Clinical correlates of disorders of metabolism Block 3, Week 2 Department of Paediatrics and Child Health University of Pretoria Tutor : Prof DF Wittenberg : dwittenb@medic.up.ac.za Aim of this
*Sections or subsections omitted from the full prescribing information are not listed.
 HIGHLIGHTS OF PRESCRIBING INFORMATION These highlights do not include all the information needed to use RAVICTI safely and effectively. See full prescribing information for RAVICTI. RAVICTI (glycerol phenylbutyrate)
HIGHLIGHTS OF PRESCRIBING INFORMATION These highlights do not include all the information needed to use RAVICTI safely and effectively. See full prescribing information for RAVICTI. RAVICTI (glycerol phenylbutyrate)
Organic acidaemias (OAs) & Urea cycle disorders (UCDs) PRESENTATION & MANAGEMENT
 Great Ormond Street Hospital London 20/04/2018 Organic acidaemias (OAs) & Urea cycle disorders (UCDs) PRESENTATION & MANAGEMENT Spyros P. Batzios, MD, MSc, PhD OAs & UCDs How do they present? neonatal
Great Ormond Street Hospital London 20/04/2018 Organic acidaemias (OAs) & Urea cycle disorders (UCDs) PRESENTATION & MANAGEMENT Spyros P. Batzios, MD, MSc, PhD OAs & UCDs How do they present? neonatal
Non-Protein Nitrogenous Compounds. Non-Protein Nitrogenous Compounds. NPN s. Urea (BUN) Creatinine NH 3. University of Cincinnati MLS Program 1
 Non-Protein Nitrogenous Compounds NPN s Urea (BUN) Creatinine NH 3 Uric Acid Ammonia University of Cincinnati MLS Program 1 Urea Metabolic product derived from catabolism of proteins Proteolysis of proteins
Non-Protein Nitrogenous Compounds NPN s Urea (BUN) Creatinine NH 3 Uric Acid Ammonia University of Cincinnati MLS Program 1 Urea Metabolic product derived from catabolism of proteins Proteolysis of proteins
ORIGINAL ARTICLE Argininosuccinic aciduria: Clinical and biochemical phenotype findings in Malaysian children
 Malaysian J Pathol 2010; 32(2) : 87 95 ORIGINAL ARTICLE Argininosuccinic aciduria: Clinical and biochemical phenotype findings in Malaysian children CHEN Bee Chin Msc, NGU Lock Hock MRCP and *ZABEDAH Md
Malaysian J Pathol 2010; 32(2) : 87 95 ORIGINAL ARTICLE Argininosuccinic aciduria: Clinical and biochemical phenotype findings in Malaysian children CHEN Bee Chin Msc, NGU Lock Hock MRCP and *ZABEDAH Md
Drug-induced Hyperammonemia (HA)
 Drug-induced hyperammonemia: are there specific therapies? NACCT Boston 2016 Florian Eyer Department of Clinical Toxicology & Poison Control Centre Munich TUM School of Medicine Technical University of
Drug-induced hyperammonemia: are there specific therapies? NACCT Boston 2016 Florian Eyer Department of Clinical Toxicology & Poison Control Centre Munich TUM School of Medicine Technical University of
NITROGEN METABOLISM: An Overview
 NITROGEN METABOLISM: An Overview University of PNG School of Medicine and Health Sciences Division of Basic Medical Sciences Discipline of Biochemistry & Molecular Biology VJ Temple 1 How are nitrogen-containing
NITROGEN METABOLISM: An Overview University of PNG School of Medicine and Health Sciences Division of Basic Medical Sciences Discipline of Biochemistry & Molecular Biology VJ Temple 1 How are nitrogen-containing
Nitrogen Metabolism. Overview
 Nitrogen Metabolism Pratt and Cornely Chapter 18 Overview Nitrogen assimilation Amino acid biosynthesis Nonessential aa Essential aa Nucleotide biosynthesis Amino Acid Catabolism Urea Cycle Juicy Steak
Nitrogen Metabolism Pratt and Cornely Chapter 18 Overview Nitrogen assimilation Amino acid biosynthesis Nonessential aa Essential aa Nucleotide biosynthesis Amino Acid Catabolism Urea Cycle Juicy Steak
Scottish Medicines Consortium
 Scottish Medicines Consortium carglumic acid 200mg dispersible tablets (Carbaglu ) No. 299/06 Orphan Europe 8 September 2006 The Scottish Medicines Consortium (SMC) has completed its assessment of the
Scottish Medicines Consortium carglumic acid 200mg dispersible tablets (Carbaglu ) No. 299/06 Orphan Europe 8 September 2006 The Scottish Medicines Consortium (SMC) has completed its assessment of the
Urea cycle disorder presenting as bilateral mesial temporal sclerosis an unusual cause of seizures: a case report and review of the literature
 Wang et al. Journal of Medical Case Reports (2018) 12:208 https://doi.org/10.1186/s13256-018-1750-8 CASE REPORT Open Access Urea cycle disorder presenting as bilateral mesial temporal sclerosis an unusual
Wang et al. Journal of Medical Case Reports (2018) 12:208 https://doi.org/10.1186/s13256-018-1750-8 CASE REPORT Open Access Urea cycle disorder presenting as bilateral mesial temporal sclerosis an unusual
Managing a UCD Video: Transcript. Ammonia. Urea. Liver graphic. RAVICTI logo
 Voiceover A urea cycle disorder, also known as a UCD, is a genetic disease that people are born with. As the body digests protein in food throughout the day nitrogen is released and it circulates in the
Voiceover A urea cycle disorder, also known as a UCD, is a genetic disease that people are born with. As the body digests protein in food throughout the day nitrogen is released and it circulates in the
HA Convention 2016 Master course How to Handle Abnormal Newborn Metabolic Screening Results Causes, Management and Follow up
 HA Convention 2016 Master course How to Handle Abnormal Newborn Metabolic Screening Results Causes, Management and Follow up Dr. Josephine Chong Clinical Professional Consultant Centre of Inborn Errors
HA Convention 2016 Master course How to Handle Abnormal Newborn Metabolic Screening Results Causes, Management and Follow up Dr. Josephine Chong Clinical Professional Consultant Centre of Inborn Errors
Part III => METABOLISM and ENERGY. 3.5 Protein Catabolism 3.5a Protein Degradation 3.5b Amino Acid Breakdown 3.5c Urea Cycle
 Part III => METABOLISM and ENERGY 3.5 Protein Catabolism 3.5a Protein Degradation 3.5b Amino Acid Breakdown 3.5c Urea Cycle Section 3.5a: Protein Degradation Synopsis 3.5a - Dietary proteins are degraded
Part III => METABOLISM and ENERGY 3.5 Protein Catabolism 3.5a Protein Degradation 3.5b Amino Acid Breakdown 3.5c Urea Cycle Section 3.5a: Protein Degradation Synopsis 3.5a - Dietary proteins are degraded
Amino Acid Disorders. What is ASAL deficiency? Genetic Fact Sheets for Parents
 Genetic Fact Sheets for Parents Amino Acid Disorders Screening, Technology, and Research in Genetics is a multi-state project to improve information about the financial, ethical, legal, and social issues
Genetic Fact Sheets for Parents Amino Acid Disorders Screening, Technology, and Research in Genetics is a multi-state project to improve information about the financial, ethical, legal, and social issues
UK NATIONAL METABOLIC BIOCHEMISTRY NETWORK GUIDELINES FOR THE INVESTIGATION OF HYPERAMMONAEMIA
 UK NATIONAL METABOLIC BIOCHEMISTRY NETWORK GUIDELINES FOR THE INVESTIGATION OF HYPERAMMONAEMIA Hyperammonaemia results from defective catabolism of amino acids to urea. Recognition and treatment of hyperammonaemia,
UK NATIONAL METABOLIC BIOCHEMISTRY NETWORK GUIDELINES FOR THE INVESTIGATION OF HYPERAMMONAEMIA Hyperammonaemia results from defective catabolism of amino acids to urea. Recognition and treatment of hyperammonaemia,
THIAMINE TRANSPORTER TYPE 2 DEFICIENCY
 THIAMINE TRANSPORTER TYPE 2 DEFICIENCY WHAT IS THE THIAMINE TRANSPORTER TYPE 2 DEFICIENCY (hthtr2)? The thiamine transporter type 2 deficiency (hthtr2) is a inborn error of thiamine metabolism caused by
THIAMINE TRANSPORTER TYPE 2 DEFICIENCY WHAT IS THE THIAMINE TRANSPORTER TYPE 2 DEFICIENCY (hthtr2)? The thiamine transporter type 2 deficiency (hthtr2) is a inborn error of thiamine metabolism caused by
Non-protein nitrogenous substances (NPN)
 Non-protein nitrogenous substances (NPN) A simple, inexpensive screening test a routine urinalysis is often the first test conducted if kidney problems are suspected. A small, randomly collected urine
Non-protein nitrogenous substances (NPN) A simple, inexpensive screening test a routine urinalysis is often the first test conducted if kidney problems are suspected. A small, randomly collected urine
Carbaglu. carglumic acid. Making a Key Difference in NAGS Deficiency INDICATIONS AND USAGE IMPORTANT SAFETY INFORMATION
 Carbaglu carglumic acid Making a Key Difference in NAGS Deficiency INDICATIONS AND USAGE CARBAGLU (carglumic acid) is a Carbamoyl Phosphate Synthetase 1 (CPS1) activator indicated as: Adjunctive therapy
Carbaglu carglumic acid Making a Key Difference in NAGS Deficiency INDICATIONS AND USAGE CARBAGLU (carglumic acid) is a Carbamoyl Phosphate Synthetase 1 (CPS1) activator indicated as: Adjunctive therapy
Isovaleric Acidemia: Quick reference guide
 Isovaleric Acidemia: Quick reference guide Introduction Isovaleric acidemia (IVA) is an inborn error of the leucine pathway caused by defects of the isovaleryl-oadehydrogenase (IV). The clinical presentation
Isovaleric Acidemia: Quick reference guide Introduction Isovaleric acidemia (IVA) is an inborn error of the leucine pathway caused by defects of the isovaleryl-oadehydrogenase (IV). The clinical presentation
Take a closer look at UCD management
 Take a closer look at UCD management An evaluation tool to help determine whether patients with urea cycle disorders (UCDs) may be experiencing treatment failure What is treatment failure and how do you
Take a closer look at UCD management An evaluation tool to help determine whether patients with urea cycle disorders (UCDs) may be experiencing treatment failure What is treatment failure and how do you
Amino acid Catabolism
 Enzymatic digestion of dietary proteins in gastrointestinal-tract. Amino acid Catabolism Amino acids: 1. There are 20 different amino acid, they are monomeric constituents of proteins 2. They act as precursors
Enzymatic digestion of dietary proteins in gastrointestinal-tract. Amino acid Catabolism Amino acids: 1. There are 20 different amino acid, they are monomeric constituents of proteins 2. They act as precursors
Medical Foods for Inborn Errors of Metabolism
 Medical Foods for Inborn Errors of Metabolism Policy Number: Original Effective Date: MM.02.014 02/18/2000 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST 08/23/2013 Section: Medicine Place(s)
Medical Foods for Inborn Errors of Metabolism Policy Number: Original Effective Date: MM.02.014 02/18/2000 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST 08/23/2013 Section: Medicine Place(s)
Yves Kibleur Dries Dobbelaere Magalie Barth Anaïs Brassier Nathalie Guffon
 Pediatr Drugs (2014) 16:407 415 DOI 10.1007/s40272-014-0081-5 ORIGINAL RESEARCH ARTICLE Results from a Nationwide Cohort Temporary Utilization Authorization (ATU) Survey of Patients in France Treated with
Pediatr Drugs (2014) 16:407 415 DOI 10.1007/s40272-014-0081-5 ORIGINAL RESEARCH ARTICLE Results from a Nationwide Cohort Temporary Utilization Authorization (ATU) Survey of Patients in France Treated with
Metabolic Changes in ASD. Norma J. Arciniegas, MD Simón E. Carlo, MD Instituto Filius
 Metabolic Changes in ASD Norma J. Arciniegas, MD Simón E. Carlo, MD Instituto Filius 12 patients 3 Autism: Ages 3/3/3.7 3 PDD: Ages 3/3/6 3 Asperger: Ages 6/7/15.1 3 Speech delay and Sensory Problems (SHL):
Metabolic Changes in ASD Norma J. Arciniegas, MD Simón E. Carlo, MD Instituto Filius 12 patients 3 Autism: Ages 3/3/3.7 3 PDD: Ages 3/3/6 3 Asperger: Ages 6/7/15.1 3 Speech delay and Sensory Problems (SHL):
Work-Up and Initial Management of Common Metabolic Emergencies in the Inpatient Setting
 Work-Up and Initial Management of Common Metabolic Emergencies in the Inpatient Setting Kristin Lindstrom, MD Division of Genetics and Metabolism Phoenix Children s Hospital AzAAP Pediatrics in the Red
Work-Up and Initial Management of Common Metabolic Emergencies in the Inpatient Setting Kristin Lindstrom, MD Division of Genetics and Metabolism Phoenix Children s Hospital AzAAP Pediatrics in the Red
Nitrogen Metabolism. Overview
 Nitrogen Metabolism Pratt and Cornely Chapter 18 Overview Nitrogen assimilation Amino acid biosynthesis Nonessential aa Essential aa Nucleotide biosynthesis Amino Acid Catabolism Urea Cycle Juicy Steak
Nitrogen Metabolism Pratt and Cornely Chapter 18 Overview Nitrogen assimilation Amino acid biosynthesis Nonessential aa Essential aa Nucleotide biosynthesis Amino Acid Catabolism Urea Cycle Juicy Steak
Nitrogen Metabolism. Pratt and Cornely Chapter 18
 Nitrogen Metabolism Pratt and Cornely Chapter 18 Overview Nitrogen assimilation Amino acid biosynthesis Nonessential aa Essential aa Nucleotide biosynthesis Amino Acid Catabolism Urea Cycle Juicy Steak
Nitrogen Metabolism Pratt and Cornely Chapter 18 Overview Nitrogen assimilation Amino acid biosynthesis Nonessential aa Essential aa Nucleotide biosynthesis Amino Acid Catabolism Urea Cycle Juicy Steak
TITLE: NURSING GUIDELINES FOR THE MANAGEMENT OF CHILDREN WITH METHYLMALONIC ACIDURIA. Eilish O Connell, Clinical Education Facilitator, NCIMD
 NO. OF PAGES: Page 1 of 17 SUPERCEDES: N/A NURSING GUIDELINES FOR THE MANAGEMENT OF CHILDREN WITH METHYLMALONIC ACIDURIA NAME/ Eilish O Connell, Clinical Education Facilitator, NCIMD SIGNATURE: DATE: NAME/
NO. OF PAGES: Page 1 of 17 SUPERCEDES: N/A NURSING GUIDELINES FOR THE MANAGEMENT OF CHILDREN WITH METHYLMALONIC ACIDURIA NAME/ Eilish O Connell, Clinical Education Facilitator, NCIMD SIGNATURE: DATE: NAME/
Amino Acids and Sorbitol injection with/without Electrolytes NIRMIN *
 For the use of a registered medical practitioner or a Hospital or a Laboratory only Amino Acids and Sorbitol injection with/without Electrolytes NIRMIN * DESCRIPTION: NIRMIN * is a clear, colourless injection
For the use of a registered medical practitioner or a Hospital or a Laboratory only Amino Acids and Sorbitol injection with/without Electrolytes NIRMIN * DESCRIPTION: NIRMIN * is a clear, colourless injection
METABOLISMO DE AMINOÁCIDOS
 DEZ 2015 METABOLISMO DE AMINOÁCIDOS Licenciatura em Ciências da Saúde (Ano 2015-2016) Isabel Tavares de Almeida Faculdade de Farmácia da ULisboa PROTEIN DEGRADATION - DIGESTION AMINO ACID STRUCTURE 2-,
DEZ 2015 METABOLISMO DE AMINOÁCIDOS Licenciatura em Ciências da Saúde (Ano 2015-2016) Isabel Tavares de Almeida Faculdade de Farmácia da ULisboa PROTEIN DEGRADATION - DIGESTION AMINO ACID STRUCTURE 2-,
Lecture: Amino Acid catabolism: Nitrogen-The Urea cycle
 BIOC 423: Introductory Biochemistry Biochemistry Education Department of Biochemistry & Molecular Biology University of New Mexico Lecture: Amino Acid catabolism: Nitrogen-The Urea cycle OBJECTIVES Describe
BIOC 423: Introductory Biochemistry Biochemistry Education Department of Biochemistry & Molecular Biology University of New Mexico Lecture: Amino Acid catabolism: Nitrogen-The Urea cycle OBJECTIVES Describe
Col Rama Krishna Sanjeev Military Hospital Chennai Prof Shanmughasundaram Mehta Hospital, Chennai
 Col Rama Krishna Sanjeev Military Hospital Chennai Prof Shanmughasundaram Mehta Hospital, Chennai 11 day old male neonate admitted on 26/6 to our Hospital with c/olethargy -since day1 abnormal movements
Col Rama Krishna Sanjeev Military Hospital Chennai Prof Shanmughasundaram Mehta Hospital, Chennai 11 day old male neonate admitted on 26/6 to our Hospital with c/olethargy -since day1 abnormal movements
CLINICAL SIGNS SUGGESTIVE OF A NEUROMETABOLIC DISEASE. Bwee Tien Poll-The Amsterdam UMC The Netherlands
 CLINICAL SIGNS SUGGESTIVE OF A NEUROMETABOLIC DISEASE Bwee Tien Poll-The Amsterdam UMC The Netherlands FRAMEWORK OF PRINCIPALS 1. Problem-oriented clinical approach 2. Biomarkers in plasma, urine, CSF
CLINICAL SIGNS SUGGESTIVE OF A NEUROMETABOLIC DISEASE Bwee Tien Poll-The Amsterdam UMC The Netherlands FRAMEWORK OF PRINCIPALS 1. Problem-oriented clinical approach 2. Biomarkers in plasma, urine, CSF
Luis S. Marsano, MD Professor of Medicine Division of Gastroenterology, Hepatology and Nutrition University of Louisville and Louisville VAMC 2015
 Luis S. Marsano, MD Professor of Medicine Division of Gastroenterology, Hepatology and Nutrition University of Louisville and Louisville VAMC 2015 Protein-calorie malnutrition (PCM) is extremely common
Luis S. Marsano, MD Professor of Medicine Division of Gastroenterology, Hepatology and Nutrition University of Louisville and Louisville VAMC 2015 Protein-calorie malnutrition (PCM) is extremely common
Lecture 10 - Protein Turnover and Amino Acid Catabolism
 Lecture 10 - Protein Turnover and Amino Acid Catabolism Chem 454: Regulatory Mechanisms in Biochemistry University of Wisconsin-Eau Claire 1 Introduction 2 Proteins are degraded into amino acids. Protein
Lecture 10 - Protein Turnover and Amino Acid Catabolism Chem 454: Regulatory Mechanisms in Biochemistry University of Wisconsin-Eau Claire 1 Introduction 2 Proteins are degraded into amino acids. Protein
Urea cycle: Urea cycle is discovered by Krebs andhanseleit(1932).
 Urea cycle: Urea cycle is discovered by Krebs andhanseleit(1932). Urea cycle is the removal of excess of NH2 derived from amino acids catabolism in the tissues and excreted in urine. Site of synthesis:
Urea cycle: Urea cycle is discovered by Krebs andhanseleit(1932). Urea cycle is the removal of excess of NH2 derived from amino acids catabolism in the tissues and excreted in urine. Site of synthesis:
DBL MAGNESIUM SULFATE CONCENTRATED INJECTION
 DBL MAGNESIUM SULFATE CONCENTRATED INJECTION NAME OF MEDICINE Magnesium Sulfate BP DESCRIPTION DBL Magnesium Sulfate Concentrated Injection is a clear, colourless, sterile solution. Each ampoule contains
DBL MAGNESIUM SULFATE CONCENTRATED INJECTION NAME OF MEDICINE Magnesium Sulfate BP DESCRIPTION DBL Magnesium Sulfate Concentrated Injection is a clear, colourless, sterile solution. Each ampoule contains
ISOVALERIC ACIDAEMIA -ACUTE DECOMPENSATION (standard version)
 Contact Details Name: Hospital Telephone: This protocol has 5 pages ISOVALERIC ACIDAEMIA -ACUTE DECOMPENSATION (standard version) Please read carefully. Meticulous treatment is very important as there
Contact Details Name: Hospital Telephone: This protocol has 5 pages ISOVALERIC ACIDAEMIA -ACUTE DECOMPENSATION (standard version) Please read carefully. Meticulous treatment is very important as there
Amino acid oxidation and the production of urea
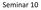 Seminar 10 Urea cycle Amino acid oxidation and the production of urea Oxidation Waste or Reuse Ammonia has to be eliminated ammonia originates in the catabolism of amino acids that are primarily produced
Seminar 10 Urea cycle Amino acid oxidation and the production of urea Oxidation Waste or Reuse Ammonia has to be eliminated ammonia originates in the catabolism of amino acids that are primarily produced
ANATOMY OF A METABOLIC CRISIS: FAOD-style. Mark S. Korson, MD Tufts Medical Center Boston, MA
 ANATOMY OF A METABOLIC CRISIS: FAOD-style Mark S. Korson, MD Tufts Medical Center Boston, MA NORMAL PHYSIOLOGY Anabolic Eating well Calories eaten > body s needs BRAIN uses GLUCOSE MUSCLE uses GLUCOSE
ANATOMY OF A METABOLIC CRISIS: FAOD-style Mark S. Korson, MD Tufts Medical Center Boston, MA NORMAL PHYSIOLOGY Anabolic Eating well Calories eaten > body s needs BRAIN uses GLUCOSE MUSCLE uses GLUCOSE
PRODUCT MONOGRAPH. Pheburane TM. Sodium phenylbutyrate granules. 483 mg per gram of granules. ATC Code: A16AX03
 PRODUCT MONOGRAPH Pr Pheburane TM Sodium phenylbutyrate granules 483 mg per gram of granules ATC Code: A16AX03 Alimentary tract and metabolism product Name of Sponsor: Orpharma NZ Limited c/o max Health
PRODUCT MONOGRAPH Pr Pheburane TM Sodium phenylbutyrate granules 483 mg per gram of granules ATC Code: A16AX03 Alimentary tract and metabolism product Name of Sponsor: Orpharma NZ Limited c/o max Health
Inborn Errors of Metabolism in the Emergency Department. Will Davies June 2014
 Inborn Errors of Metabolism in the Emergency Department Will Davies June 2014 Inborn Errors of Metabolism in the Emergency Department Overview Although individually rare, altogether they are 1:1000-2500
Inborn Errors of Metabolism in the Emergency Department Will Davies June 2014 Inborn Errors of Metabolism in the Emergency Department Overview Although individually rare, altogether they are 1:1000-2500
Hepatic Encephalopathy
 Hepatic Encephalopathy John Barber UMassMedical Student, Class of 2019 www.12daysinmarch.com Outline Overview Normal Physiology Pathology Symptoms Diagnosis Treatment Overview Ammonia (NH 3 ) is a byproduct
Hepatic Encephalopathy John Barber UMassMedical Student, Class of 2019 www.12daysinmarch.com Outline Overview Normal Physiology Pathology Symptoms Diagnosis Treatment Overview Ammonia (NH 3 ) is a byproduct
Amino acid metabolism
 Amino acid metabolism The important reaction commonly employed in the breakdown of an amino acid is always the removal of its -amino group. The product ammonia is excreted after conversion to urea or other
Amino acid metabolism The important reaction commonly employed in the breakdown of an amino acid is always the removal of its -amino group. The product ammonia is excreted after conversion to urea or other
EU RISK MANAGEMENT PLAN (EU RMP) Nutriflex Omega peri emulsion for infusion , version 1.1
 EU RISK MANAGEMENT PLAN (EU RMP) Nutriflex Omega peri emulsion for infusion 13.7.2015, version 1.1 III.1. Elements for a Public Summary III.1.1. Overview of disease epidemiology Patients may need parenteral
EU RISK MANAGEMENT PLAN (EU RMP) Nutriflex Omega peri emulsion for infusion 13.7.2015, version 1.1 III.1. Elements for a Public Summary III.1.1. Overview of disease epidemiology Patients may need parenteral
Evidence-Based Update: Using Glucose Gel to Treat Neonatal Hypoglycemia
 Neonatal Nursing Education Brief: Evidence-Based Update: Using Glucose Gel to Treat Neonatal Hypoglycemia http://www.seattlechildrens.org/healthcare-professionals/education/continuing-medicalnursing-education/neonatal-nursing-education-briefs/
Neonatal Nursing Education Brief: Evidence-Based Update: Using Glucose Gel to Treat Neonatal Hypoglycemia http://www.seattlechildrens.org/healthcare-professionals/education/continuing-medicalnursing-education/neonatal-nursing-education-briefs/
Cytonet, LLC. Cells for Life AMAT 2015
 Cytonet, LLC Cells for Life AMAT 2015 Cytonet s Therapeutic Goal: The goal of our research is to create a bridge to transplant for children inborn metabolic liver disease who are often too young or sick
Cytonet, LLC Cells for Life AMAT 2015 Cytonet s Therapeutic Goal: The goal of our research is to create a bridge to transplant for children inborn metabolic liver disease who are often too young or sick
Fate of Dietary Protein
 Fate of Dietary Protein Dietary protein Stomach: l, pepsin Denatured and partially hydrolyzed protein (large polypeptides) small intestine: proteases Amino acids and dipeptides intestinal lining: proteases
Fate of Dietary Protein Dietary protein Stomach: l, pepsin Denatured and partially hydrolyzed protein (large polypeptides) small intestine: proteases Amino acids and dipeptides intestinal lining: proteases
Amino Acid Metabolism
 Amino Acid Metabolism Fate of Dietary Protein Dietary protein Stomach: l, pepsin Denatured and partially hydrolyzed protein (large polypeptides) small intestine: proteases Amino acids and dipeptides intestinal
Amino Acid Metabolism Fate of Dietary Protein Dietary protein Stomach: l, pepsin Denatured and partially hydrolyzed protein (large polypeptides) small intestine: proteases Amino acids and dipeptides intestinal
Inborn errors of metabolism
 ESPEN Congress Nice 2010 From child to adult nutrition Inborn errors of metabolism Pascal Crenn Inborn errors of metabolism: from child to adult Pascal Crenn Hôpital Raymond Poincaré 92380 Garches. France
ESPEN Congress Nice 2010 From child to adult nutrition Inborn errors of metabolism Pascal Crenn Inborn errors of metabolism: from child to adult Pascal Crenn Hôpital Raymond Poincaré 92380 Garches. France
BCH 447. Estimation of Serum Urea
 BCH 447 Estimation of Serum Urea 1 Objective: Estimation of Blood urea nitrogen (BUN) in serum sample. 2 -Urea: Urea is the highest non-protein nitrogen compound in the blood. Urea is the major excretory
BCH 447 Estimation of Serum Urea 1 Objective: Estimation of Blood urea nitrogen (BUN) in serum sample. 2 -Urea: Urea is the highest non-protein nitrogen compound in the blood. Urea is the major excretory
XURIDEN (uridine triacetate) oral granules
 XURIDEN (uridine triacetate) oral granules Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Pharmacy
XURIDEN (uridine triacetate) oral granules Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Pharmacy
Chapter 1: What is PKU?
 Chapter 1: What is PKU? A Parent's Perspective "If our child with PKU had been our first instead of our third, or if we had wanted more children after we had her, we would have done so, even knowing the
Chapter 1: What is PKU? A Parent's Perspective "If our child with PKU had been our first instead of our third, or if we had wanted more children after we had her, we would have done so, even knowing the
Inborn Errors of Metabolism (IEM)
 Clinical Presentation Inborn Errors of Metabolism (IEM) Click on the following: - Clinical Pearl - link to movie clip - link to picture Investigations Blood Work Urine No Acidosis NH 4 + Metabolic Acidosis
Clinical Presentation Inborn Errors of Metabolism (IEM) Click on the following: - Clinical Pearl - link to movie clip - link to picture Investigations Blood Work Urine No Acidosis NH 4 + Metabolic Acidosis
Effect of carglumic acid with or without ammonia scavengers on hyperammonaemia in acute decompensation episodes of organic acidurias
 Chakrapani et al. Orphanet Journal of Rare Diseases (2018) 13:97 https://doi.org/10.1186/s13023-018-0840-4 RESEARCH Open Access Effect of carglumic acid with or without ammonia scavengers on hyperammonaemia
Chakrapani et al. Orphanet Journal of Rare Diseases (2018) 13:97 https://doi.org/10.1186/s13023-018-0840-4 RESEARCH Open Access Effect of carglumic acid with or without ammonia scavengers on hyperammonaemia
