Is high T-1 slope a significant risk factor for developing interlaminar bony fusion after cervical laminoplasty? A retrospective cohort study
|
|
|
- Deirdre Harrell
- 5 years ago
- Views:
Transcription
1 CLINICAL ARTICLE J Neurosurg Spine 27: , 2017 Is high T-1 slope a significant risk factor for developing interlaminar bony fusion after cervical laminoplasty? A retrospective cohort study Takeshi Oichi, MD, 1 Yasushi Oshima, MD, PhD, 1 Hiroyuki Oka, MD, PhD, 1 Yuki Taniguchi, MD, PhD, 1 Hirotaka Chikuda, MD, PhD, 1 Yoshitaka Matsubayashi, MD, 1 Katsushi Takeshita, MD, PhD, 2 and Sakae Tanaka, MD, PhD 1 1 Department of Orthopaedic Surgery, The University of Tokyo Hospital, Tokyo; and 2 Department of Orthopaedic Surgery, Jichi Medical University, Tochigi-ken, Japan OBJECTIVE Several investigators have reported the occurrence of interlaminar bony fusion after cervical laminoplasty, which is reportedly associated with reduced postoperative cervical range of motion (ROM). However, to the authors knowledge, no previous study has investigated the characteristics of patients who were likely to develop interlaminar bony fusion after cervical laminoplasty. Therefore, the objective of this study was to investigate the risk factors for interlaminar bony fusion in patients with cervical spondylotic myelopathy (CSM) following cervical laminoplasty and to investigate the effect of interlaminar bony fusion on surgical outcomes. METHODS The authors retrospectively reviewed data from 92 patients with CSM (63 men and 29 women) after cervical laminoplasty. The presence of interlaminar bony fusion was evaluated by functional radiographs 2 years after surgery. The patients were divided into 2 groups according to the presence of postoperative interlaminar bony fusion: a fusion group (at least 1 new postoperative interlaminar bony fusion) and a nonfusion group (no new interlaminar bony fusion). Potential risk factors for postoperative interlaminar bony fusion were assessed, including diabetes mellitus, smoking status, whether the C-2 lamina was included in the surgical treatment, C2 7 Cobb angle in each cervical position, preoperative cervical ROM, and T-1 slope. The differences in each variable were compared between the fusion and nonfusion groups. Thereafter, multivariate logistic regression analysis was performed to identify the risk factors for postoperative interlaminar bony fusion. For surgical outcomes, the recovery rate based on Japanese Orthopaedic Association scores and the reduction rate of cervical ROM were evaluated 2 years after surgery. RESULTS Interlaminar bony fusion was observed in 60 cases, 52 of which were observed at the C2 3 level. Patients in the fusion group were significantly older, had a significantly larger C2 7 angle in flexion, and had a significantly lower preoperative cervical ROM than those in the nonfusion group. A high T-1 slope was significantly more frequent in the fusion group. Multivariate analysis revealed that the significant risk factors for postoperative interlaminar bony fusion were high T-1 slope (odds ratio 4.81; p = ) and older age (odds ratio 1.05; p = 0.025). The Japanese Orthopaedic Association recovery rate in patients with interlaminar bony fusion did not differ significantly from those without bony fusion (45% vs 48%; p = 0.73). However, patients with bony fusion showed significantly reduced postoperative cervical ROM compared with those without bony fusion (50% vs 25%; p < 0.001). CONCLUSIONS High T-1 slope and older age were significant risk factors for developing interlaminar bony fusion after cervical laminoplasty in patients with CSM. Interlaminar bony fusion was associated with reduced postoperative cervical ROM, but it did not affect neurological outcomes. KEY WORDS cervical spine; cervical spondylotic myelopathy; interlaminar bony fusion; T-1 slope; cervical laminoplasty; Japanese Orthopaedic Association; recovery rate ABBREVIATIONS CI = confidence interval; CSM = cervical spondylotic myelopathy; HRQOL = health-related quality of life; JOA = Japanese Orthopaedic Association; OPLL = ossification of the posterior longitudinal ligament; OR = odds ratio; ROM = range of motion. SUBMITTED July 28, ACCEPTED March 16, INCLUDE WHEN CITING Published online September 15, 2017; DOI: / SPINE AANS, 2017 J Neurosurg Spine Volume 27 December
2 T. Oichi et al. Cervical laminoplasty is a well-established surgical procedure with satisfactory long-term clinical outcomes in patients with cervical spondylotic myelopathy (CSM). 1,11,16 However, cervical laminoplasty is associated with some postoperative complications, including C-5 palsy 2 and axial symptoms. 20 Furthermore, several investigators have reported the occurrence of interlaminar bony fusion after cervical laminoplasty 5,6, 10, 11, 16,19 at a rate of 53% 66%, with marked frequency at the C2 3 level. 5,6, 10, 11,16 Postoperative interlaminar bony fusion is reportedly associated with reduced postoperative cervical range of motion (ROM). 5,6,16 To the best of our knowledge, no previous study has investigated the characteristics of patients who were likely to develop interlaminar bony fusion after cervical laminoplasty. Therefore, this study aims to identify the risk factors for developing interlaminar bony fusion after cervical laminoplasty. We further investigated whether postoperative interlaminar bony fusion affects surgical outcomes. Methods We retrospectively reviewed prospectively collected data from 124 patients with CSM who underwent cervical laminoplasty at our institution between January 2000 and June We did not include patients who were treated with laminectomy or those with preoperative interlaminar bony fusion, a history of anterior decompression and fusion, ossification of the posterior longitudinal ligament (OPLL), fused vertebrae (e.g., diffuse idiopathic skeletal hyperostosis or ankylosing spine), cerebral palsy, exacerbation of CSM due to trauma, cervical spondylotic amyotrophy, polio, congenital anomaly of the cervical spine, rheumatoid arthritis, or spastic torticollis. We further excluded 32 patients due to the following reasons: short follow-up periods of less than 2 years (n = 10), incomplete chart data (n = 8), and lack of radiological data (n = 14). Finally, 92 patients with CSM (63 men and 29 women) were enrolled in this study. The study protocol was approved by the Clinical Research Support Center of The University of Tokyo Hospital. All participating patients provided written informed consent. The diagnosis of CSM was based on both neurological examination by board-certified spine surgeons and MRI findings. All patients underwent a double-door laminoplasty that involved midsagittal splitting of the spinous process, as described by Kurokawa et al., 14 and wore a soft collar for 1 2 weeks postoperatively to relieve pain. Clinical Outcomes Neurological status before and 2 years after surgery was evaluated using the Japanese Orthopaedic Association (JOA) scores (total points, 17). 8 The recovery rate 2 years after surgery was calculated according to the following formula: Recovery rate (%) = (postoperative JOA score preoperative JOA score)/(17 [full score] preoperative JOA score) 100 (%). 4 Radiological Evaluation CT Measurements Cervical CT scans were obtained for all patients before surgery with the subject in a comfortable supine position and gazing at the ceiling. The T-1 slope was usually measured using full-standing radiographs; 13 however, in our cohort, there were many cases (n = 42) in which accurate measurement of the T-1 slope on cervical radiographs was difficult due to the interference of the shoulder, as reported previously. 9 Alternatively, we measured the T-1 slope using 3D CT scans, which has been reported to significantly correlate with the measurements obtained using radiographs. 9 The T-1 slope was measured as the angle between a horizontal line and the superior endplate of T-1, in the same manner as described previously (Fig. 1A). 9 The validity of T-1 slope measurement on CT scans in this study was examined by calculating the correlation coefficient between the T-1 slope on a CT scan and that on a radiograph using the cases in which both types of data were available (n = 50). A T-1 slope 25 was defined as high T-1 slope and a T-1 slope < 25 was defined as low T-1 slope. 13 The presence of OPLL was assessed using 3D CT. Cases in which it was difficult to distinguish between OPLL and bony spur were not defined as OPLL. This study excluded patients with OPLL and those with fused vertebrae. FIG. 1. A: Measurement of the T-1 slope. B: C2 7 angle in flexion position. C: C2 7 angle in neutral position. D: C2 7 angle in extension position. Cervical range of motion = a + b. 628 J Neurosurg Spine Volume 27 December 2017
3 Interlaminar bony fusion after cervical laminoplasty Radiograph Measurements Flexion-extension lateral radiographs were taken for each patient both preoperatively and 2 years after surgery. The C2 7 angle, determined by tangential lines on the posterior edge of the C-2 and C-7 bodies, was measured on lateral radiographs in maximal flexion, neutral, and maximal extension positions (Fig. 1B D). Cervical ROM was defined as the sum of the C2 7 angles seen during flexion and extension on lateral radiographs. The reduction rate of cervical ROM was calculated according to the following formula: Reduction rate (%) = (preoperative cervical ROM postoperative cervical ROM)/(preoperative cervical ROM) 100%. As previously reported, 5,6 the presence of interlaminar bony fusion from occipital bone to C-7 was evaluated using flexion-extension lateral radiographs both preoperatively and 2 years after surgery. If there were apparent interlaminar bony fusions or no interlaminar movement on functional radiographs, the patients were designated as having interlaminar bony fusions (Fig. 2A). If there were interlaminar movements in all laminae on functional radiographs, the patients were designated as not having interlaminar bony fusions (Fig. 2B). We divided the patients into 2 groups according to the presence of postoperative interlaminar bony fusion; these consisted of a fusion group (at least 1 new postoperative interlaminar bony fusion; Fig. 2C) and a nonfusion group (no new interlaminar bony fusion). Patients with preoperative interlaminar bony fusion and fused vertebrae were not included in our study. Other Data Collected Other demographic variables, including diabetes mellitus and smoking status (current or not), that could potentially affect the development of interlaminar bony fusion, as well as whether the C-2 lamina was included in the surgical treatment, were examined. FIG. 2. Functional radiographs and CT scans of the cervical spine obtained 2 years after surgery are shown from representative cases with interlaminar bony fusion and without bony fusion. A: Apparent interlaminar bony fusion is observed at the C2 3 level (arrowheads) in a 68-yearold man with CSM and postoperative interlaminar bony fusion. B: Interlaminar movements in all laminae are observed in a 72-year-old woman with CSM without postoperative interlaminar bony fusion. C: Parasagittal (left) and midsagittal (right) CT scans of the cervical spine obtained 2 years after surgery in a 69-year-old woman with CSM. Parasagittal CT scan showed the presence of interlaminar bony fusion at the C2 3 level (arrowhead), and midsagittal CT scan showed no coexistent OPLL or diffuse idiopathic skeletal hyperostosis. Statistical Analysis Differences in both radiological and clinical variables between the fusion and nonfusion groups were compared. Radiological variables included T-1 slope (high or low), C2 7 angle in each cervical position (flexion, neutral, and extension), and preoperative cervical ROM. Demographic variables included age, sex, diabetes mellitus, smoking status, and involvement of the C-2 lamina. For surgical outcomes, the JOA recovery rate and the rate of reduction of cervical ROM were compared between the fusion and nonfusion groups. Among patients in whom the T-1 slope was measurable from both the CT scan and the radiograph (n = 50), the correlations of T-1 slopes between those obtained from the CT scan and those from the radiograph were analyzed using Pearson s correlation coefficient. For continuous variables, 2-group comparisons were performed using the Student t-test or the Wilcoxon ranksum test, as appropriate. Categorical variables were compared between the groups using the chi-square test or Fisher s exact probability test, as appropriate. A multiple logistic regression model yielding the odds ratio (OR) and 95% confidence interval (CI) was used to identify significant risk factors for postoperative occurrence of interlaminar bony fusion. Variables with a p value < 0.10 in the univariate analyses were entered into the multiple logistic regression model. The variance inflation factor was used to check for multicollinearity in the model. Data analyses were performed using the JMP software, version 9.0 (SAS Institute); p values < 0.05 were considered significant. All tests were 2-tailed. Results Demographic Data The mean age of patients at surgery was 63 years (range J Neurosurg Spine Volume 27 December
4 T. Oichi et al years). There were no significant differences in baseline characteristics between patients with CSM who were included (n = 92) and those who were excluded due to incomplete data (n = 32) (Table 1). The surgical levels were as follows: C3 7 in 64 cases; C2 7 in 19 cases; C3 T1 in 3 cases; C3 6 in 3 cases; C2 6 in 2 cases; and C4 7 in 1 case. Radiological Results The average cervical ROM was 38.8 (range ) before surgery and 22.4 (range ) 2 years after surgery. The average rate of reduction of cervical ROM was 40.1% (range -34.6% to 100%). Postoperative interlaminar fusion was observed in 60 cases, 52 (86.7%) of which were observed at the C2 3 level. The average number of fused segments in the fusion group was 1.5 (range 1 6 segments). Among 50 cases in which the T-1 slope was measurable from both the CT scan and the radiograph, the mean T-1 slope on CT scans was 25.9 ± 9.5 (range ), and the mean T-1 slope on radiographs was 26.9 ± 9.2 (range ). The T-1 slope on CT scans had significant correlations with that on radiographs (Pearson s correlation coefficient = 0.69; p < ), and this was compatible with the results of a previous report. 9 Therefore, we believe that T-1 slope measurement on CT scans is a valid method. Differences in Each Variable Between the Fusion and Nonfusion s Table 2 shows the differences between the fusion and nonfusion groups. Patients in the fusion group were significantly older, had significantly larger C2 7 angles in the flexion position, and had significantly smaller preoperative cervical ROM than those in the nonfusion group. High T-1 slope was significantly more frequent in the fusion group. Multivariate Analysis of Variables That Predicted Interlaminar Bony Fusion After Laminoplasty From the results of the univariate analyses, age, C2 7 angle in flexion, preoperative cervical ROM, and T-1 slope (high/low) were considered dependent variables. None of the variance inflation factor values exceeded 10, which indicated that there was no collinearity in the model. 3 A high T-1 slope was a significant risk factor for developing postoperative interlaminar bony fusion (OR 4.8; 95% CI ; p < 0.05) (Table 3), even after adjusting for other risk factors. Older age was also a significant risk factor for developing postoperative interlaminar bony fusion (OR 1.05; 95% CI ; p < 0.05). TABLE 1. Differences in baseline characteristics between included and excluded patients Variable Patients Included Patients Excluded for Incomplete Data p Value No. of patients Age in yrs, mean ± SD 63.5 ± ± Male sex, no. (%) 63 (68) 26 (81) 0.25 Diabetes mellitus, no. (%) 19 (21) 7/30 (23) 0.80 Currently smoking, no. (%) 21 (23) 6/26 (23) 1.0 C-2 lamina included in the 21 (23) 8/31 (26) 0.81 surgical treatment, no. (%) Preop JOA score, mean ± SD 10.3 ± ± 2.9 (n = 29) 0.31 Continuous variables were compared using the Student t-test or the Wilcoxon rank-sum test; categorical data were analyzed using the chi-square test. Surgical Outcomes The average JOA score was 10.3 (range 5 15) before surgery and 13.4 (range 5 17) 2 years after surgery. The average JOA recovery rate 2 years after surgery was 46.1% (range -9.1% to 100%). Table 4 shows the differences in surgical outcomes between the fusion and nonfusion groups. No significant differences were observed in the JOA recovery rate between the fusion and nonfusion groups (45% vs 48%; p = 0.73). However, patients in the fusion group had significantly reduced postoperative cervical ROM compared with those in the nonfusion group (50% vs 25%; p < 0.001). Discussion In this study, 2 important clinical observations were made. First, high T-1 slope and older age were significant risk factors for developing interlaminar bony fusions after cervical laminoplasty in patients with CSM. Second, the presence of postoperative interlaminar bony fusion was associated with reduced postoperative cervical ROM, but it did not affect neurological outcomes. T-1 slope was found to be a significant risk factor for developing interlaminar bony fusions after cervical laminoplasty in patients with CSM. A plausible explanation could TABLE 2. Differences in demographic data and radiographic findings between the fusion and nonfusion groups Variable Fusion Nonfusion p Value No. of patients Male sex, no. (%) 38 (63) 25 (78) 0.15 Diabetes mellitus, no. (%) 12 (20) 7 (22) 0.83 Currently smoking, no. (%) 13 (22) 8 (25) 0.80 Surgical involvement of the 14 (23) 7 (22) 0.87 C-2 lamina, no. (%) Age in yrs, mean ± SD 65.7 ± ± Radiographic parameters, mean ± SD C2 7 angle (flexion) 11.9 ± ± C2 7 angle (neutral) 13.1 ± ± C2 7 angle (extension) 25.1 ± ± Preop cervical ROM, mean 37.0 ± ± ± SD High T-1 slope, no. (%) 42 (70) 11 (34) < Continuous variables were compared using the Student t-test; categorical data were analyzed using the chi-square test or Fisher s exact probability test. Significant values are p < J Neurosurg Spine Volume 27 December 2017
5 Interlaminar bony fusion after cervical laminoplasty TABLE 3. Multivariate logistic regression analysis of the variables that predicted interlaminar bony fusion after laminoplasty Variable OR 95% CI p Value Age C2 7 angle (flexion) Preop cervical ROM High T-1 slope Significant values are p < be inferred from differences in compensatory mechanisms for maintaining cervical alignment between patients with high T-1 slope and those with low T-1 slope. T-1 slope is a known predictor of whole sagittal balance, 13 whereas high T-1 slope is associated with cervical lordosis to maintain horizontal gaze. 15 On one hand, patients with high T-1 slope required more cervical lordosis to retain a horizontal gaze, resulting in a prolonged duration for which the cervical laminae were close to each other (Fig. 3 left). On the other hand, patients with low T-1 slope did not need to keep the cervical spine lordotic, unlike those with high T-1 slope; this resulted in cervical laminae that were farther apart (Fig. 3 right). It seems reasonable that laminae closer to each other were more likely to become fused after cervical laminoplasty. Although the T-1 slope has been reported to be significantly correlated with the C2 7 angle, 15 the T-1 slope not the C2 7 angle in each cervical position was the significant predictor of postoperative interlaminar bony fusion in the multivariate analysis. Measurement of the C2 7 angle in each position was performed at a single point and may have been substantially affected by CSM-related factors, such as preoperative neck pain or preexisting spinal cord compression. T-1 slope was thought, however, to be a more constant parameter that was not affected by these CSMrelated factors. This difference possibly contributed to the result that the T-1 slope not the C2 7 angle was the significant predictor of postoperative interlaminar bony fusion. Older age was also found to be a significant risk factor for postoperative interlaminar bony fusion. Similarly, a previous study in patients with CSM following cervical laminoplasty showed that those with postoperative interlaminar bony fusion were significantly older than those without bony fusion. 6 The authors speculated that reduced preoperative cervical ROM, which was associated with older age, contributed to this result. In our study, however, TABLE 4. Differences in surgical outcomes between the fusion and nonfusion groups Variable Fusion Nonfusion p Value JOARR, mean ± SD (%) 45.4 ± ± Reduction rate of cervical 49.9 ± ± ROM, mean ± SD (%) JOARR = JOA recovery rate. Significant values are p < FIG. 3. Illustration of the differences in interlaminar distance between patients with high T-1 slope and those with low T-1 slope. Left: Patients with high T-1 slope require more cervical lordosis to keep a horizontal gaze, resulting in cervical lamina being closer to each other. Right: Patients with low T-1 slope do not need to keep the cervical spine lordotic, resulting in cervical laminae being farther apart. older age was a significant risk factor even after adjusting for preoperative cervical ROM. Although the actual pathophysiology remains unknown, older patients may be less willing to participate in aggressive postoperative rehabilitation, thereby possibly predisposing them to suffer postoperative interlaminar bony fusion more frequently. Our study revealed that the presence of postoperative interlaminar bony fusion was associated with reduced postoperative cervical ROM, but it did not affect neurological outcomes. Several previous studies similarly reported that the presence of postoperative interlaminar bony fusion was associated with reduced postoperative cervical ROM. 5,6,10,16 Regarding neurological outcomes, 1 retrospective study reported that interlaminar bony fusion did not influence neurological recovery after cervical laminoplasty. 6 Considering these results, the occurrence of postoperative interlaminar bony fusion could be the major contributor to postoperative reduction of cervical ROM, but it did not seem to affect neurological recovery after cervical laminoplasty. Whether the reduction of postoperative cervical ROM affects postoperative axial pain remains controversial. 20 Some previous studies reported that the occurrence of interlaminar bony fusion was associated with postoperative axial pain. 11,12 Therefore, the presence of interlaminar bony fusion possibly affects health-related quality of life (HRQOL) outcomes, such as the Neck Disability Index 18 and the 36-Item Short-Form Health Survey. 21 Future prospective studies are needed to elucidate whether interlaminar bony fusion affects HRQOL outcomes. The next issue to be resolved is prevention of postoperative interlaminar bony fusion. Laminectomy of the C-3 lamina is thought to be one of the top options because the base bed laminae are theoretically removed and C2 3 is the most frequently involved level. Furthermore, C-3 laminectomy with C4 7 cervical laminoplasty was reported to show the same neurological outcome as that of C3 7 cervical laminoplasty and was associated with reduced postoperative axial pain. 17 Therefore, C-3 laminectomy combined with cervical laminoplasty can be an option to prevent postoperative interlaminar bony fusion, especially when patients are old and have high T-1 slope. Future com- J Neurosurg Spine Volume 27 December
6 T. Oichi et al. parative study is needed to elucidate whether C-3 laminectomy actually prevents the occurrence of postoperative interlaminar bony fusion and improves surgical outcomes. There were several limitations to this study. First, all patients in our cohort wore a soft collar for 1 2 weeks postoperatively. Because such immobilization provided by the collar could have increased the likelihood of postoperative interlaminar bony fusion, 7 we must be careful in interpreting the results. However, the actual incidence of postoperative interlaminar bony fusion was 65% in our study, which is comparable with that reported previously (53% 66%). Therefore, we believe that postoperative use of a soft collar for 1 2 weeks did not dramatically increase the occurrence of postoperative interlaminar bony fusion. Second, the effects of interlaminar bony fusion on HRQOL outcomes, such as the Neck Disability Index and the 36-Item Short-Form Health Survey, were not evaluated. Future prospective studies are required to elucidate this issue. Third, the occurrence of interlaminar bony fusion in our study was possibly overestimated because there may have been some cases in which spontaneous interlaminar bony fusion developed regardless of the surgery. Conclusions High T-1 slope and older age were risk factors for developing interlaminar bony fusion after cervical laminoplasty in patients with CSM. Interlaminar bony fusion was associated with reduced postoperative cervical ROM, but it did not affect neurological outcomes. Identification of these factors may help provide appropriate information on patients with CSM. Future comparative studies that investigate the most appropriate surgical procedure to prevent postoperative interlaminar bony fusion are warranted. References 1. Chiba K, Ogawa Y, Ishii K, Takaishi H, Nakamura M, Maruiwa H, et al: Long-term results of expansive open-door laminoplasty for cervical myelopathy average 14-year follow-up study. Spine (Phila Pa 1976) 31: , Gu Y, Cao P, Gao R, Tian Y, Liang L, Wang C, et al: Incidence and risk factors of C5 palsy following posterior cervical decompression: a systematic review. PLoS One 9:e101933, Hair JF Jr, Anderson R, Tatham R, Black WC: Multivariate Data Analysis, ed 3. New York: Macmillan, Hirabayashi K, Miyakawa J, Satomi K, Maruyama T, Wakano K: Operative results and postoperative progression of ossification among patients with ossification of cervical posterior longitudinal ligament. Spine (Phila Pa 1976) 6: , Hyun SJ, Riew KD, Rhim SC: Range of motion loss after cervical laminoplasty: a prospective study with minimum 5-year follow-up data. Spine J 13: , Iizuka H, Iizuka Y, Nakagawa Y, Nakajima T, Toda N, Shimegi A, et al: Interlaminar bony fusion after cervical laminoplasty: its characteristics and relationship with clinical results. Spine (Phila Pa 1976) 31: , Iizuka H, Nakagawa Y, Shimegi A, Tsutsumi S, Toda N, Takagishi K, et al: Clinical results after cervical laminoplasty: differences due to the duration of wearing a cervical collar. J Spinal Disord Tech 18: , Japanese Orthopaedic Association: Scoring system for cervical myelopathy. Nippon Seikeigeka Gakkai Zasshi 68: , Jun HS, Chang IB, Song JH, Kim TH, Park MS, Kim SW, et al: Is it possible to evaluate the parameters of cervical sagittal alignment on cervical computed tomographic scans? Spine (Phila Pa 1976) 39:E630 E636, Kawaguchi Y, Kanamori M, Ishihara H, Ohmori K, Abe Y, Kimura T: Pathomechanism of myelopathy and surgical results of laminoplasty in elderly patients with cervical spondylosis. Spine (Phila Pa 1976) 28: , Kawaguchi Y, Kanamori M, Ishihara H, Ohmori K, Nakamura H, Kimura T: Minimum 10-year followup after en bloc cervical laminoplasty. Clin Orthop Relat Res (411): , Kawaguchi Y, Matsui H, Ishihara H, Gejo R, Yoshino O: Axial symptoms after en bloc cervical laminoplasty. J Spinal Disord 12: , Knott PT, Mardjetko SM, Techy F: The use of the T1 sagittal angle in predicting overall sagittal balance of the spine. Spine J 10: , Kurokawa T, Tsuyama N, Tanaka H, Kobayashi H, Machida H, Nakamura K, et al: [Enlargement of spinal canal by sagittal splitting of the spinal process.] Bessatsu Seikeigeka 2: , 1982 (Jpn) 15. Lee SH, Kim KT, Seo EM, Suk KS, Kwack YH, Son ES: The influence of thoracic inlet alignment on the craniocervical sagittal balance in asymptomatic adults. J Spinal Disord Tech 25:E41 E47, Seichi A, Takeshita K, Ohishi I, Kawaguchi H, Akune T, Anamizu Y, et al: Long-term results of double-door laminoplasty for cervical stenotic myelopathy. Spine (Phila Pa 1976) 26: , Takeuchi K, Yokoyama T, Aburakawa S, Saito A, Numasawa T, Iwasaki T, et al: Axial symptoms after cervical laminoplasty with C3 laminectomy compared with conventional C3 C7 laminoplasty: a modified laminoplasty preserving the semispinalis cervicis inserted into axis. Spine (Phila Pa 1976) 30: , Vernon H, Mior S: The Neck Disability Index: a study of reliability and validity. J Manipulative Physiol Ther 14: , Wada E, Suzuki S, Kanazawa A, Matsuoka T, Miyamoto S, Yonenobu K: Subtotal corpectomy versus laminoplasty for multilevel cervical spondylotic myelopathy: a longterm follow-up study over 10 years. Spine (Phila Pa 1976) 26: , Wang SJ, Jiang SD, Jiang LS, Dai LY: Axial pain after posterior cervical spine surgery: a systematic review. Eur Spine J 20: , Ware JE Jr: SF-36 health survey update. Spine (Phila Pa 1976) 25: , 2000 Disclosures The authors report no conflict of interest concerning the materials or methods used in this study or the findings specified in this paper. Author Contributions Conception and design: Oichi. Acquisition of data: Oichi, Takeshita. Analysis and interpretation of data: Oichi, Oka. Drafting the article: Oichi. Critically revising the article: Oshima. Reviewed submitted version of manuscript: all authors. Statistical analysis: Oichi, Oka. Study supervision: Oshima, Tanaka. Correspondence Yasushi Oshima, Department of Orthopaedic Surgery, The University of Tokyo Hospital, Hongo, Bunkyo-ku, Tokyo , Japan. yoo-tky@umin.ac.jp. 632 J Neurosurg Spine Volume 27 December 2017
Interlaminar Bony Fusion after C3-6 Double-Door Laminoplasty for Cervical Spondylotic Myelopathy: Its Predictors and Characteristics
 Interlaminar Bony Fusion after C3-6 Double-Door Laminoplasty for Cervical Spondylotic Myelopathy: Its Predictors and Characteristics Yoshiro Nanjo, Hideki Nagashima, Shinji Tanishima,Tokumitsu Mihara,
Interlaminar Bony Fusion after C3-6 Double-Door Laminoplasty for Cervical Spondylotic Myelopathy: Its Predictors and Characteristics Yoshiro Nanjo, Hideki Nagashima, Shinji Tanishima,Tokumitsu Mihara,
Incidence and Risk Factors for Late Neurologic Deterioration after C3 C6 Laminoplasty for Cervical Spondylotic Myelopathy
 THIEME GLOBAL SPINE JOURNAL Original Article 53 Incidence and Risk Factors for Late Neurologic Deterioration after C3 C6 Laminoplasty for Cervical Spondylotic Myelopathy Hironobu Sakaura 1 Toshitada Miwa
THIEME GLOBAL SPINE JOURNAL Original Article 53 Incidence and Risk Factors for Late Neurologic Deterioration after C3 C6 Laminoplasty for Cervical Spondylotic Myelopathy Hironobu Sakaura 1 Toshitada Miwa
Kazunari Takeuchi Æ Toru Yokoyama Æ Atsushi Ono Æ Takuya Numasawa Æ Kanichiro Wada Æ Taito Itabashi Æ Satoshi Toh
 Eur Spine J (2008) 17:415 420 DOI 10.1007/s00586-007-0553-1 ORIGINAL ARTICLE Limitation of activities of daily living accompanying reduced neck mobility after laminoplasty preserving or reattaching the
Eur Spine J (2008) 17:415 420 DOI 10.1007/s00586-007-0553-1 ORIGINAL ARTICLE Limitation of activities of daily living accompanying reduced neck mobility after laminoplasty preserving or reattaching the
Minamide A*, Yoshida M*, Yamada H*, Hashizume H*, NakagawaY*, Iwasaki H*, Tsutsui S*, Hiroyuki Oka H**.
 Efficacy of Posterior Segmental Decompression Surgery for Pincer Mechanism in Cervical Spondylotic Myelopathy -A retrospective case control study using propensity score matching Minamide A*, Yoshida M*,
Efficacy of Posterior Segmental Decompression Surgery for Pincer Mechanism in Cervical Spondylotic Myelopathy -A retrospective case control study using propensity score matching Minamide A*, Yoshida M*,
Selective laminoplasty for cervical spondylotic myelopathy: a comparative study with a minimum 5-year follow-up
 Selective laminoplasty for cervical spondylotic myelopathy: a comparative study with a minimum 5-year follow-up Minori Kato*, Hiroaki Nakamura**, Koji Tamai**, Kazunori Hayashi**, Akira Matsumura**, Sadahiko
Selective laminoplasty for cervical spondylotic myelopathy: a comparative study with a minimum 5-year follow-up Minori Kato*, Hiroaki Nakamura**, Koji Tamai**, Kazunori Hayashi**, Akira Matsumura**, Sadahiko
The Predictable Factors of the Postoperative Kyphotic Change of Sagittal Alignment of the Cervical Spine after the Laminoplasty
 Clinical Article J Korean Neurosurg Soc 60 (5) : 577-583, 2017 https://doi.org/10.3340/jkns.2017.0505.007 pissn 2005-3711 eissn 1598-7876 The Predictable Factors of the Postoperative Kyphotic Change of
Clinical Article J Korean Neurosurg Soc 60 (5) : 577-583, 2017 https://doi.org/10.3340/jkns.2017.0505.007 pissn 2005-3711 eissn 1598-7876 The Predictable Factors of the Postoperative Kyphotic Change of
Abstract Study Design Systematic review. Weerasak Singhatanadgige 1 Worawat Limthongkul 1 Frank Valone III 2 Wicharn Yingsakmongkol 1 K.
 702 Review Article GLOBAL SPINE JOURNAL THIEME Outcomes following or Fusion in Patients with Myelopathy Caused by Ossification of the Posterior Longitudinal Ligament: A Systematic Review Weerasak Singhatanadgige
702 Review Article GLOBAL SPINE JOURNAL THIEME Outcomes following or Fusion in Patients with Myelopathy Caused by Ossification of the Posterior Longitudinal Ligament: A Systematic Review Weerasak Singhatanadgige
Department of Neurological Surgery, Asan Medical Center, University of Ulsan College of Medicine, Seoul, Korea
 online ML Comm CLINICAL ARTICLE Korean J Neurotrauma 2014;10(2):60-65 pissn 2234-8999 / eissn 2288-2243 http://dx.doi.org/10.13004/kjnt.2014.10.2.60 Midline Splitting Cervical Laminoplasty Using Allogeneic
online ML Comm CLINICAL ARTICLE Korean J Neurotrauma 2014;10(2):60-65 pissn 2234-8999 / eissn 2288-2243 http://dx.doi.org/10.13004/kjnt.2014.10.2.60 Midline Splitting Cervical Laminoplasty Using Allogeneic
Incidence and Risk Factors for Late Neurologic Deterioration after C3-6 Laminoplasty in Patients with Cervical Spondylotic Myelopathy
 Incidence and Risk Factors for Late Neurologic Deterioration after C3-6 Laminoplasty in Patients with Cervical Spondylotic Myelopathy Sakaura H, Miwa T, Kuroda Y, Ohwada T Dept. of Orthop. Surg., Kansai
Incidence and Risk Factors for Late Neurologic Deterioration after C3-6 Laminoplasty in Patients with Cervical Spondylotic Myelopathy Sakaura H, Miwa T, Kuroda Y, Ohwada T Dept. of Orthop. Surg., Kansai
Disclosures: T. Yoshii: None. T. Yamada: None. T. Taniyama: None. S. Sotome: None. T. Kato: None. S. Kawabata: None. A. Okawa: None.
 Dynamic Changes in Spinal Cord Compression by Cervical Ossification of the Posterior Longitudinal Ligament Evaluated by Kinematic Computed Tomography Myelogram Toshitaka Yoshii, Tsuyoshi Yamada, Takashi
Dynamic Changes in Spinal Cord Compression by Cervical Ossification of the Posterior Longitudinal Ligament Evaluated by Kinematic Computed Tomography Myelogram Toshitaka Yoshii, Tsuyoshi Yamada, Takashi
Rick C. Sasso MD Professor Chief of Spine Surgery Clinical Orthopaedic Surgery Indiana University School of Medicine
 Cervical Myelopathy: Anterior Surgery is Best Rick C. Sasso MD Professor Chief of Surgery Clinical Orthopaedic Surgery University School of Medicine Disclosure: Research support-medtronic, Stryker, AO,
Cervical Myelopathy: Anterior Surgery is Best Rick C. Sasso MD Professor Chief of Surgery Clinical Orthopaedic Surgery University School of Medicine Disclosure: Research support-medtronic, Stryker, AO,
Op e n-d o o r laminoplasty was developed by Hirabayashi. Risk factors for closure of lamina after open-door laminoplasty.
 J Neurosurg Spine 9:530 537, 2008 Risk factors for closure of lamina after open-door laminoplasty Clinical article Mo r i o Ma t s u m o t o, M.D., 1 Ko ta Wata n a b e, M.D., 2 Ta k a s h i Ts u j i,
J Neurosurg Spine 9:530 537, 2008 Risk factors for closure of lamina after open-door laminoplasty Clinical article Mo r i o Ma t s u m o t o, M.D., 1 Ko ta Wata n a b e, M.D., 2 Ta k a s h i Ts u j i,
ORIGINAL ARTICLE. Introduction SPINE SURGERY AND RELATED RESEARCH
 ORIGINAL ARTICLE SPINE SURGERY AND RELATED RESEARCH Radiological Examination of Postoperative Cervical Alignment and Stability in Patients with Dialysis-Associated Spondylosis Excluding Destructive Spondyloarthropathy:
ORIGINAL ARTICLE SPINE SURGERY AND RELATED RESEARCH Radiological Examination of Postoperative Cervical Alignment and Stability in Patients with Dialysis-Associated Spondylosis Excluding Destructive Spondyloarthropathy:
Modified laminoplasty for multilevel cervical myelopathy.
 Biomedical Research 2017; 28 (13): 5721-5725 ISSN 0970-938X www.biomedres.info Modified laminoplasty for multilevel cervical myelopathy. Zhihong Nie *#, Fanlei Kong #, Yujiang Wu, Xiuxin Fu, Zhongpo Liu,
Biomedical Research 2017; 28 (13): 5721-5725 ISSN 0970-938X www.biomedres.info Modified laminoplasty for multilevel cervical myelopathy. Zhihong Nie *#, Fanlei Kong #, Yujiang Wu, Xiuxin Fu, Zhongpo Liu,
Catastrophic Dropped Head Syndrome Requiring Multiple Reconstruction Surgeries after Cervical Laminoplasty
 CASE REPORT SPINE SURGERY AND RELATED RESEARCH Catastrophic Dropped Head Syndrome Requiring Multiple Reconstruction Surgeries after Cervical Laminoplasty Seiichi Odate, Jitsuhiko Shikata and Tsunemitsu
CASE REPORT SPINE SURGERY AND RELATED RESEARCH Catastrophic Dropped Head Syndrome Requiring Multiple Reconstruction Surgeries after Cervical Laminoplasty Seiichi Odate, Jitsuhiko Shikata and Tsunemitsu
Comparative study on the effect of anterior and posterior decompression in the treatment of multi-segmental cervical spondylotic myelopathy
 92 Journal of Hainan Medical University 2016; 22(6): 92-96 Journal of Hainan Medical University http://www.jhmuweb.net/ Comparative study on the effect of anterior and posterior decompression in the treatment
92 Journal of Hainan Medical University 2016; 22(6): 92-96 Journal of Hainan Medical University http://www.jhmuweb.net/ Comparative study on the effect of anterior and posterior decompression in the treatment
Christopher I. Shaffrey, MD
 CSRS 21st Instructional Course Wednesday, November 30, 2016 Laminoplasty/Foraminotomy: Why Fuse the Spine at all? Christopher I. Shaffrey, MD John A. Jane Distinguished Professor Departments of Neurosurgery
CSRS 21st Instructional Course Wednesday, November 30, 2016 Laminoplasty/Foraminotomy: Why Fuse the Spine at all? Christopher I. Shaffrey, MD John A. Jane Distinguished Professor Departments of Neurosurgery
Radiological pathogenesis of cervical myelopathy in 60 consecutive patients with cervical ossi cation of the posterior longitudinal ligament
 Spinal Cord (1999) 37, 853 ± 857 ã 1999 International Medical Society of Paraplegia All rights reserved 1362 ± 4393/99 $15.00 http://www.stockton-press.co.uk/sc Radiological pathogenesis of cervical myelopathy
Spinal Cord (1999) 37, 853 ± 857 ã 1999 International Medical Society of Paraplegia All rights reserved 1362 ± 4393/99 $15.00 http://www.stockton-press.co.uk/sc Radiological pathogenesis of cervical myelopathy
Ossification of the posterior longitudinal ligament
 J Neurosurg Spine 19:431 435, 2013 AANS, 2013 Upper cervical cord compression due to a C-1 posterior arch in a patient with ossification of the posterior longitudinal ligament and a kyphotic cervical spine
J Neurosurg Spine 19:431 435, 2013 AANS, 2013 Upper cervical cord compression due to a C-1 posterior arch in a patient with ossification of the posterior longitudinal ligament and a kyphotic cervical spine
Japanese Orthopaedic Association Cervical Myelopathy Evaluation Questionnaire (JOACMEQ): part 4. Establishment of equations for severity scores
 J Orthop Sci (2008) 13:25 31 DOI 10.1007/s00776-007-1194-2 Original article Japanese Orthopaedic Association Cervical Myelopathy Evaluation Questionnaire (JOACMEQ): part 4. Establishment of equations for
J Orthop Sci (2008) 13:25 31 DOI 10.1007/s00776-007-1194-2 Original article Japanese Orthopaedic Association Cervical Myelopathy Evaluation Questionnaire (JOACMEQ): part 4. Establishment of equations for
Efficacy and results of expansive laminoplasty in patients with severe cervical myelopathy due to cervical canal stenosis
 Original Article Efficacy and results of expansive laminoplasty in patients with severe cervical myelopathy due to cervical canal stenosis D. Agrawal, B. S. Sharma, A. Gupta, V. S. Mehta Department of
Original Article Efficacy and results of expansive laminoplasty in patients with severe cervical myelopathy due to cervical canal stenosis D. Agrawal, B. S. Sharma, A. Gupta, V. S. Mehta Department of
Mitsuhiro Hashimto 1), Masashi Yamazaki 2), Macondo Mochizuki 3), Masatsune Yamagata 1), Yoshikazu Ikeda 1), Fumitake Nakajima 1)
 Long-term results of anterior cervical corpectomy and arthrodesis for cervical degenerative diseases with more than ten years of follow-up Mitsuhiro Hashimto 1), Masashi Yamazaki 2), Macondo Mochizuki
Long-term results of anterior cervical corpectomy and arthrodesis for cervical degenerative diseases with more than ten years of follow-up Mitsuhiro Hashimto 1), Masashi Yamazaki 2), Macondo Mochizuki
ORIGINAL ARTICLE. Introduction SPINE SURGERY AND RELATED RESEARCH
 ORIGINAL ARTICLE SPINE SURGERY AND RELATED RESEARCH Cervical Kyphotic Deformity after Laminoplasty in Patients with Cervical Ossification of Posterior Longitudinal Ligament with Normal Sagittal Spinal
ORIGINAL ARTICLE SPINE SURGERY AND RELATED RESEARCH Cervical Kyphotic Deformity after Laminoplasty in Patients with Cervical Ossification of Posterior Longitudinal Ligament with Normal Sagittal Spinal
Cervical Spine Surgery: Approach related outcome
 Cervical Spine Surgery: Approach related outcome Hez Progect Israel 2016 Ran Harel, MD Spine Surgery Unit, Department of Neurosurgery, Sheba Medical Center, Ramat-Gan, Israel Sackler Medical School, Tel-Aviv
Cervical Spine Surgery: Approach related outcome Hez Progect Israel 2016 Ran Harel, MD Spine Surgery Unit, Department of Neurosurgery, Sheba Medical Center, Ramat-Gan, Israel Sackler Medical School, Tel-Aviv
Microendoscopic laminotomy versus conventional laminoplasty for cervical spondylotic myelopathy: 5-year follow-up study
 CLINICAL ARTICLE J Neurosurg Spine 27:403 409, 2017 Microendoscopic laminotomy versus conventional laminoplasty for cervical spondylotic myelopathy: 5-year follow-up study Akihito Minamide, MD, PhD, 1
CLINICAL ARTICLE J Neurosurg Spine 27:403 409, 2017 Microendoscopic laminotomy versus conventional laminoplasty for cervical spondylotic myelopathy: 5-year follow-up study Akihito Minamide, MD, PhD, 1
How cervical alignment and thoracic inlet angle affect on postoperative spinal cord alignment after laminoplasty?
 How cervical alignment and thoracic inlet angle affect on postoperative spinal cord alignment after laminoplasty? Shinya Kato, Hisanori Mihara Department of Orthopaedics Surgery, Yokohama Hodogaya Central
How cervical alignment and thoracic inlet angle affect on postoperative spinal cord alignment after laminoplasty? Shinya Kato, Hisanori Mihara Department of Orthopaedics Surgery, Yokohama Hodogaya Central
Unanswered Questions. Laminoplasty is best
 Laminoplasty is best Wellington K. Hsu, MD Clifford C. Raisbeck Distinguished Professor of Orthopaedic Surgery Director of Research Department of Orthopaedic Surgery Northwestern University Feinberg School
Laminoplasty is best Wellington K. Hsu, MD Clifford C. Raisbeck Distinguished Professor of Orthopaedic Surgery Director of Research Department of Orthopaedic Surgery Northwestern University Feinberg School
Analysis of Cervical Sagittal Balance Parameters in MRIs of Patients with Disc-Degenerative Disease
 e-issn 1643-3750 DOI: 10.12659/MSM.893715 Received: 2015.01.29 Accepted: 2015.05.07 Published: 2015.10.13 Analysis of Cervical Sagittal Balance Parameters in MRIs of Patients with Disc-Degenerative Disease
e-issn 1643-3750 DOI: 10.12659/MSM.893715 Received: 2015.01.29 Accepted: 2015.05.07 Published: 2015.10.13 Analysis of Cervical Sagittal Balance Parameters in MRIs of Patients with Disc-Degenerative Disease
Postoperative severe headache following cervical posterior surgical fixation from C2 distally
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2016 Postoperative severe headache following cervical posterior surgical fixation from C2 distally Ryoji Tauchi
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2016 Postoperative severe headache following cervical posterior surgical fixation from C2 distally Ryoji Tauchi
Neck Pain following Laminoplasty
 Global Spine Journal Original Article 17 Addisu Mesfin 1 Moon-Soo Park 2 Chaiwat Piyaskulkaew 2 Tapanut Chuntarapas 2 Kwang Sup Song 2 HanJoKim 2 K. Daniel Riew 2 1 Department of Orthopaedics, University
Global Spine Journal Original Article 17 Addisu Mesfin 1 Moon-Soo Park 2 Chaiwat Piyaskulkaew 2 Tapanut Chuntarapas 2 Kwang Sup Song 2 HanJoKim 2 K. Daniel Riew 2 1 Department of Orthopaedics, University
Review Article. Abstract
 Review Article Cervical Laminoplasty: Indications, Surgical Considerations, and Clinical Outcomes Samuel K. Cho, MD Jun S. Kim, MD Samuel C. Overley, MD Robert K. Merrill, MD JAAOS Plus Webinar JoinDr.Cho,Dr.Kim,Dr.Overley,
Review Article Cervical Laminoplasty: Indications, Surgical Considerations, and Clinical Outcomes Samuel K. Cho, MD Jun S. Kim, MD Samuel C. Overley, MD Robert K. Merrill, MD JAAOS Plus Webinar JoinDr.Cho,Dr.Kim,Dr.Overley,
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
ORIGINAL PAPER. Department of Orthopedic Surgery, Chubu Rosai Hospital, Nagoya, Japan ABSTRACT
 Nagoya J. Med. Sci. 77. 221 ~ 228, 2015 ORIGINAL PAPER RANGE OF MOTION DETERMINED BY MULTIDETECTOR-ROW COMPUTED TOMOGRAPHY IN PATIENTS WITH CERVICAL OSSIFICATION OF THE POSTERIOR LONGITUDINAL LIGAMENT
Nagoya J. Med. Sci. 77. 221 ~ 228, 2015 ORIGINAL PAPER RANGE OF MOTION DETERMINED BY MULTIDETECTOR-ROW COMPUTED TOMOGRAPHY IN PATIENTS WITH CERVICAL OSSIFICATION OF THE POSTERIOR LONGITUDINAL LIGAMENT
Influence of hinge position on the effectiveness of opendoor expansive laminoplasty for cervical spondylotic myelopathy
 . 6. Influence of hinge position on the effectiveness of opendoor expansive laminoplasty for cervical spondylotic myelopathy WAN Jun, XU Tian-tong*, SHEN Qing-feng, LI Hui-nan and XIA Ying-peng Abstract
. 6. Influence of hinge position on the effectiveness of opendoor expansive laminoplasty for cervical spondylotic myelopathy WAN Jun, XU Tian-tong*, SHEN Qing-feng, LI Hui-nan and XIA Ying-peng Abstract
Satisfactory surgical results for CSM have recently
 J Neurosurg Spine 18:545 552, 2013 AANS, 2013 A less-invasive cervical laminoplasty for spondylotic myelopathy that preserves the semispinalis cervicis muscles and nuchal ligament Clinical article Masayuki
J Neurosurg Spine 18:545 552, 2013 AANS, 2013 A less-invasive cervical laminoplasty for spondylotic myelopathy that preserves the semispinalis cervicis muscles and nuchal ligament Clinical article Masayuki
Japanese Orthopaedic Association Cervical Myelopathy Evaluation Questionnaire: Part 3. Determination of reliability
 J Orthop Sci (2007) 12:321 326 DOI 10.1007/s00776-007-1131-4 Original article Japanese Orthopaedic Association Cervical Myelopathy Evaluation Questionnaire: Part 3. Determination of reliability Mitsuru
J Orthop Sci (2007) 12:321 326 DOI 10.1007/s00776-007-1131-4 Original article Japanese Orthopaedic Association Cervical Myelopathy Evaluation Questionnaire: Part 3. Determination of reliability Mitsuru
Radiographic Dimensional Analysis of Open Door Laminoplasty with Plate in Cervical Spondylotic Myelopathy
 Radiographic Dimensional Analysis of Open Door Laminoplasty with Plate in Cervical Spondylotic Myelopathy Woo-Kie Min,MD,PhD Department of Orthopedic Surgery, Kyungpook National University College of Medicine,
Radiographic Dimensional Analysis of Open Door Laminoplasty with Plate in Cervical Spondylotic Myelopathy Woo-Kie Min,MD,PhD Department of Orthopedic Surgery, Kyungpook National University College of Medicine,
Comparative Effectiveness of Different Types of Cervical Laminoplasty
 Systematic Review 105 Comparative Effectiveness of Different Types of Cervical Laminoplasty John G. Heller 1 Annie L. Raich 2 Joseph R. Dettori 2 K. Daniel Riew 3 1 Department of Orthopaedic Surgery, Emory
Systematic Review 105 Comparative Effectiveness of Different Types of Cervical Laminoplasty John G. Heller 1 Annie L. Raich 2 Joseph R. Dettori 2 K. Daniel Riew 3 1 Department of Orthopaedic Surgery, Emory
Life expectancy after cervical laminoplasty Causes of the fatal prognosis at the early stage (within 5 years)
 ORIGINAL ARTICLE SPINE SURGERY AND RELATED RESEARCH Life expectancy after cervical laminoplasty Causes of the fatal prognosis at the early stage (within 5 years) Yoshiharu Kawaguchi 1), Masato Nakano 1),
ORIGINAL ARTICLE SPINE SURGERY AND RELATED RESEARCH Life expectancy after cervical laminoplasty Causes of the fatal prognosis at the early stage (within 5 years) Yoshiharu Kawaguchi 1), Masato Nakano 1),
Cervical Curvature Became More Lordotic in Flexion Post-Operatively Regardless of Type of Surgical Approach in Cervical Spondylotic Myelopathy
 Cervical Curvature Became More Lordotic in Flexion Post-Operatively Regardless of Type of Surgical Approach in Cervical Spondylotic Myelopathy Wen-Kai Chou 1, Andy Chien 1, Ya-Wen Kuo 1, Chia-Chin Lin
Cervical Curvature Became More Lordotic in Flexion Post-Operatively Regardless of Type of Surgical Approach in Cervical Spondylotic Myelopathy Wen-Kai Chou 1, Andy Chien 1, Ya-Wen Kuo 1, Chia-Chin Lin
Yoshifumi Kudo, 1 Tomoaki Toyone, 1 Toshiyuki Shirahata, 1 Tomoyuki Ozawa, 1 Akira Matsuoka, 1 Yoichi Jin, 2 and Katsunori Inagaki 1. 1.
 Case Reports in Orthopedics Volume 2016, Article ID 1250810, 5 pages http://dx.doi.org/10.1155/2016/1250810 Case Report A Case of Successful Foraminotomy for Severe Bilateral C5 Palsy following Posterior
Case Reports in Orthopedics Volume 2016, Article ID 1250810, 5 pages http://dx.doi.org/10.1155/2016/1250810 Case Report A Case of Successful Foraminotomy for Severe Bilateral C5 Palsy following Posterior
Analysis of C5 palsy in cervical myelopathy with massive anterior compression following laminoplasty
 Chen et al. Journal of Orthopaedic Surgery and Research (2018) 13:26 DOI 10.1186/s13018-018-0715-3 RESEARCH ARTICLE Open Access Analysis of C5 palsy in cervical myelopathy with massive anterior compression
Chen et al. Journal of Orthopaedic Surgery and Research (2018) 13:26 DOI 10.1186/s13018-018-0715-3 RESEARCH ARTICLE Open Access Analysis of C5 palsy in cervical myelopathy with massive anterior compression
Open-door Laminoplasty with Preservation of Muscle Attachments of C2 and C7 for Cervical Spondylotic Myelopathy: Retrospective Study
 DOI: 10.5137/1019-5149.JTN.20007-17.1 Received: 25.01.2017 / Accepted: 27.02.2017 Published Online: 17.03.2017 Original Investigation Open-door Laminoplasty with Preservation of Muscle Attachments of C2
DOI: 10.5137/1019-5149.JTN.20007-17.1 Received: 25.01.2017 / Accepted: 27.02.2017 Published Online: 17.03.2017 Original Investigation Open-door Laminoplasty with Preservation of Muscle Attachments of C2
Factors related to long-term outcome after decompressive surgery for ossification of the ligamentum flavum of the thoracic spine
 J Neurosurg (Spine 3) 99:251 256, 2003 Factors related to long-term outcome after decompressive surgery for ossification of the ligamentum flavum of the thoracic spine NAOHISA MIYAKOSHI, M.D., YOICHI SHIMADA,
J Neurosurg (Spine 3) 99:251 256, 2003 Factors related to long-term outcome after decompressive surgery for ossification of the ligamentum flavum of the thoracic spine NAOHISA MIYAKOSHI, M.D., YOICHI SHIMADA,
Age-related and degenerative changes in the osseous anatomy, alignment, and range of motion
 Age-related and degenerative changes in the osseous anatomy, alignment, and range of motion of the cervical spine: a comparative study of radiographic data from 1016 patients with cervical spondylotic
Age-related and degenerative changes in the osseous anatomy, alignment, and range of motion of the cervical spine: a comparative study of radiographic data from 1016 patients with cervical spondylotic
Clinical Results and Complications of Surgical Treatment for Thoracic Myelopathy Caused by Ossification of the Posterior Longitudinal Ligament
 Clinical Results and Complications of Surgical Treatment for Thoracic Myelopathy Caused by Ossification of the Posterior Longitudinal Ligament - A Multicenter Retrospective Study - Mitsumasa Hayashida,
Clinical Results and Complications of Surgical Treatment for Thoracic Myelopathy Caused by Ossification of the Posterior Longitudinal Ligament - A Multicenter Retrospective Study - Mitsumasa Hayashida,
S.S.K.MUNASINGHE ARACHCHIGE NATIONAL HOSPITAL OF SRI LANKA
 AN INSIGHT TO THE DILEMMA- CO-EXISTENCE OF OSSIFICAION OF POSTERIOR LONGITUDINAL LIGAMENT AND CERVICAL DISC PROLAPSE A SRI LANKAN EXPERIENCE S.S.K.MUNASINGHE ARACHCHIGE NATIONAL HOSPITAL OF SRI LANKA BACKGROUND
AN INSIGHT TO THE DILEMMA- CO-EXISTENCE OF OSSIFICAION OF POSTERIOR LONGITUDINAL LIGAMENT AND CERVICAL DISC PROLAPSE A SRI LANKAN EXPERIENCE S.S.K.MUNASINGHE ARACHCHIGE NATIONAL HOSPITAL OF SRI LANKA BACKGROUND
Neck Pain Following Cervical Laminoplasty: Does Preservation of the C2 Muscle Attachments and/or C7 Matter?
 42 Systematic Review Neck Pain Following Cervical Laminoplasty: Does Preservation of the C2 Muscle Attachments and/or C7 Matter? K. Daniel Riew 1 Annie L. Raich 3 Joseph R. Dettori 3 John G. Heller 2 1
42 Systematic Review Neck Pain Following Cervical Laminoplasty: Does Preservation of the C2 Muscle Attachments and/or C7 Matter? K. Daniel Riew 1 Annie L. Raich 3 Joseph R. Dettori 3 John G. Heller 2 1
Clinical Application of a New Plate Fixation System in Open-door Laminoplasty
 Clinical Application of a New Plate Fixation System in Open-door Laminoplasty LIANGJUN JIANG, MD; WEISHAN CHEN, MD; QIXIN CHEN, MD; KAN XU, MD; QIONGHUA WU, MD; FANGCAI LI, MD abstract Full article available
Clinical Application of a New Plate Fixation System in Open-door Laminoplasty LIANGJUN JIANG, MD; WEISHAN CHEN, MD; QIXIN CHEN, MD; KAN XU, MD; QIONGHUA WU, MD; FANGCAI LI, MD abstract Full article available
Risk Factors for Hinge Fracture Associated with Surgery Following Cervical Open-Door Laminoplasty
 CLINICAL ARTICLE Korean J Neurotrauma 18;14(2):118-122 pissn 2234-8999 / eissn 2288-2243 https://doi.org/1.134/kjnt.18.14.2.118 Risk Factors for Hinge Fracture Associated with Surgery Following Cervical
CLINICAL ARTICLE Korean J Neurotrauma 18;14(2):118-122 pissn 2234-8999 / eissn 2288-2243 https://doi.org/1.134/kjnt.18.14.2.118 Risk Factors for Hinge Fracture Associated with Surgery Following Cervical
Lift-up laminoplasty for myelopathy caused by ossification of the posterior longitudinal ligament of the cervical spine
 Original Article Lift-up laminoplasty for myelopathy caused by ossification of the posterior longitudinal ligament of the cervical spine T. Takami, K. Ohata, T. Goto, M. Nishikawa, A. Nishio, N. Tsuyuguchi,
Original Article Lift-up laminoplasty for myelopathy caused by ossification of the posterior longitudinal ligament of the cervical spine T. Takami, K. Ohata, T. Goto, M. Nishikawa, A. Nishio, N. Tsuyuguchi,
The Correlation Study of C5 Nerve Root Palsy and Common Body Position in Posterior Total Laminectomy Decompression and Instrumentation
 DOI: 10.5137/1019-5149.JTN.7476-12.1 Received: 30.10.2012 / Accepted: 11.02.2013 Original Investigation The Correlation Study of C5 Nerve Root Palsy and Common Body Position in Posterior Total Laminectomy
DOI: 10.5137/1019-5149.JTN.7476-12.1 Received: 30.10.2012 / Accepted: 11.02.2013 Original Investigation The Correlation Study of C5 Nerve Root Palsy and Common Body Position in Posterior Total Laminectomy
Review Article Operative Treatment of Cervical Myelopathy: Cervical Laminoplasty
 Hindawi Publishing Corporation Advances in Orthopedics Volume 2012, Article ID 508534, 5 pages doi:10.1155/2012/508534 Review Article Operative Treatment of Cervical Myelopathy: Cervical Laminoplasty Brett
Hindawi Publishing Corporation Advances in Orthopedics Volume 2012, Article ID 508534, 5 pages doi:10.1155/2012/508534 Review Article Operative Treatment of Cervical Myelopathy: Cervical Laminoplasty Brett
Cervical spondylotic myelopathy (CSM) is a progressive
 literature review J Neurosurg Spine 24:77 99, 2016 A systematic review of clinical and surgical predictors of complications following surgery for degenerative cervical myelopathy Lindsay Tetreault, BSc,
literature review J Neurosurg Spine 24:77 99, 2016 A systematic review of clinical and surgical predictors of complications following surgery for degenerative cervical myelopathy Lindsay Tetreault, BSc,
Yoshii et al. Journal of Orthopaedic Surgery and Research (2017) 12:12 DOI /s
 Yoshii et al. Journal of Orthopaedic Surgery and Research (2017) 12:12 DOI 10.1186/s13018-017-0515-1 TECHNICAL NOTE Open Access Intraoperative evaluation using mobile computed tomography in anterior cervical
Yoshii et al. Journal of Orthopaedic Surgery and Research (2017) 12:12 DOI 10.1186/s13018-017-0515-1 TECHNICAL NOTE Open Access Intraoperative evaluation using mobile computed tomography in anterior cervical
We performed CT myelography in 38 patients
 Posterior movement and enlargement of the spinal cord after cervical laminoplasty Ikuo Aita, Koichiro Hayashi, Yasuyoshi Wadano, Takeshi Yabuki From the University of Tsukuba, Ibaraki, Japan We performed
Posterior movement and enlargement of the spinal cord after cervical laminoplasty Ikuo Aita, Koichiro Hayashi, Yasuyoshi Wadano, Takeshi Yabuki From the University of Tsukuba, Ibaraki, Japan We performed
ASJ. Risk Factor Analysis for C5 Palsy after Double-Door Laminoplasty for Cervical Spondylotic Myelopathy. Asian Spine Journal.
 Asian Spine Journal 298 Satoshi Clinical Baba et al. Study http://dx.doi.org/10.4184/asj.2016.10.2.298 Risk Factor Analysis for C5 Palsy after Double-Door Laminoplasty for Cervical Spondylotic Myelopathy
Asian Spine Journal 298 Satoshi Clinical Baba et al. Study http://dx.doi.org/10.4184/asj.2016.10.2.298 Risk Factor Analysis for C5 Palsy after Double-Door Laminoplasty for Cervical Spondylotic Myelopathy
Facet orientation in patients with lumbar degenerative spondylolisthesis
 35 J. Tokyo Med. Univ., 71 1 35 0 Facet orientation in patients with lumbar degenerative spondylolisthesis Wuqikun ALIMASI, Kenji ENDO, Hidekazu SUZUKI, Yasunobu SAWAJI, Hirosuke NISHIMURA, Hidetoshi TANAKA,
35 J. Tokyo Med. Univ., 71 1 35 0 Facet orientation in patients with lumbar degenerative spondylolisthesis Wuqikun ALIMASI, Kenji ENDO, Hidekazu SUZUKI, Yasunobu SAWAJI, Hirosuke NISHIMURA, Hidetoshi TANAKA,
ORIGINAL PAPER. Surgical outcomes of decompressive laminoplasty with spinous process osteotomy to treat lumbar spinal stenosis
 Editors Choice ORIGINAL PAPER Nagoya J. Med. Sci. 80. 1 9, 2018 doi:10.18999/nagjms.80.1.1 Surgical outcomes of decompressive laminoplasty with spinous process osteotomy to treat lumbar spinal stenosis
Editors Choice ORIGINAL PAPER Nagoya J. Med. Sci. 80. 1 9, 2018 doi:10.18999/nagjms.80.1.1 Surgical outcomes of decompressive laminoplasty with spinous process osteotomy to treat lumbar spinal stenosis
Orthopaedics and Rehabilitation Medicine Fuculty of Medical Sciences University of Fukui
 Quantitative analysis and prognostic value of changes in spinal cord signal intensity on magnetic resonance imaging in patients with cervical compressive myelopathy Orthopaedics and Rehabilitation Medicine
Quantitative analysis and prognostic value of changes in spinal cord signal intensity on magnetic resonance imaging in patients with cervical compressive myelopathy Orthopaedics and Rehabilitation Medicine
Expansive Open-door Laminoplasty With Titanium Miniplate Versus Sutures
 Expansive Open-door Laminoplasty With Titanium Miniplate Versus Sutures Guangdong Chen, MD; Zongping Luo, MD, PhD; Badri Nalajala, MD; Tao Liu, MD, PhD; Huilin Yang, MD, PhD abstract Full article available
Expansive Open-door Laminoplasty With Titanium Miniplate Versus Sutures Guangdong Chen, MD; Zongping Luo, MD, PhD; Badri Nalajala, MD; Tao Liu, MD, PhD; Huilin Yang, MD, PhD abstract Full article available
Reduced invasiveness of myoarchitectonic laminectomy compared with open-door laminoplasty in patients with cervical myelopathy
 Reduced invasiveness of myoarchitectonic laminectomy compared with open-door laminoplasty in patients with cervical myelopathy Department of Spinal Surgery 1), Brain Attack Center Ota Memorial Hospital,
Reduced invasiveness of myoarchitectonic laminectomy compared with open-door laminoplasty in patients with cervical myelopathy Department of Spinal Surgery 1), Brain Attack Center Ota Memorial Hospital,
Recent Surgical Methods of Double-door Laminoplasty of the Cervical Spine (Kurokawa s Method)
 TECHNICAL NOTE SPINE SURGERY AND RELATED RESEARCH Recent Surgical Methods of Double-door Laminoplasty of the Cervical Spine (Kurokawa s Method) Shigeru Hirabayashi Department of Orthopaedic Surgery, Teikyo
TECHNICAL NOTE SPINE SURGERY AND RELATED RESEARCH Recent Surgical Methods of Double-door Laminoplasty of the Cervical Spine (Kurokawa s Method) Shigeru Hirabayashi Department of Orthopaedic Surgery, Teikyo
Outcomes of Secondary Laminoplasty for Patients with Unsatisfactory Results after Anterior Multilevel Cervical Surgery
 online ML Comm www.jkns.or.kr http://dx.doi.org/10.3340/jkns.2015.57.1.36 J Korean Neurosurg Soc 57 (1) : 36-41, 2015 Print ISSN 2005-3711 On-line ISSN 1598-7876 Copyright 2015 The Korean Neurosurgical
online ML Comm www.jkns.or.kr http://dx.doi.org/10.3340/jkns.2015.57.1.36 J Korean Neurosurg Soc 57 (1) : 36-41, 2015 Print ISSN 2005-3711 On-line ISSN 1598-7876 Copyright 2015 The Korean Neurosurgical
Jing Tao Zhang 1, Lin Feng Wang 1, Yue Ju Liu 2, Jun Ming Cao 1, Jie Li 1, Shuai Wang 1 and Yong Shen 1*
 Zhang et al. BMC Musculoskeletal Disorders (2015) 16:267 DOI 10.1186/s12891-015-0728-6 RESEARCH ARTICLE Open Access Relationship between developmental canal stenosis and surgical results of anterior decompression
Zhang et al. BMC Musculoskeletal Disorders (2015) 16:267 DOI 10.1186/s12891-015-0728-6 RESEARCH ARTICLE Open Access Relationship between developmental canal stenosis and surgical results of anterior decompression
Laminoplasty for Cervical Myelopathy
 Review Article 187 Manabu Ito 1 Ken Nagahama 2 1 Department of Advanced Medicine for Spine and Spinal Cord Disorders, Hokkaido University Graduate School of Medicine, Sapporo, Japan 2 Department of Orthopaedic
Review Article 187 Manabu Ito 1 Ken Nagahama 2 1 Department of Advanced Medicine for Spine and Spinal Cord Disorders, Hokkaido University Graduate School of Medicine, Sapporo, Japan 2 Department of Orthopaedic
Original Investigation. Byung-Wan CHOI. INTRODUCTION Ossification of the posterior longitudinal ligament ABSTRACT
 DOI: 10.5137/1019-5149.JTN.16196-15.1 Received: 25.09.2015 / Accepted: 07.12.2015 Published Online: 01.06.2016 Original Investigation Clinical and Radiological Characteristics of Ossification of the Posterior
DOI: 10.5137/1019-5149.JTN.16196-15.1 Received: 25.09.2015 / Accepted: 07.12.2015 Published Online: 01.06.2016 Original Investigation Clinical and Radiological Characteristics of Ossification of the Posterior
Cervical Degenerative Disease - Surgical Approaches to CSM 가톨릭의대인천성모병원척추센터 김종태
 KNS Main Topic Session Spine Surgery : Case-Based Lecture of Spinal Disease Cervical Degenerative Disease - Surgical Approaches to CSM 가톨릭의대인천성모병원척추센터 김종태 Cervical Spondylotic Myelopathy ( CSM ) (1984,
KNS Main Topic Session Spine Surgery : Case-Based Lecture of Spinal Disease Cervical Degenerative Disease - Surgical Approaches to CSM 가톨릭의대인천성모병원척추센터 김종태 Cervical Spondylotic Myelopathy ( CSM ) (1984,
Analysis of sagittal alignment parameters following anterior cervical hybrid decompression and fusion of multilevel cervical Spondylotic myelopathy
 Huang et al. BMC Musculoskeletal Disorders (2019) 20:1 https://doi.org/10.1186/s12891-018-2378-y RESEARCH ARTICLE Open Access Analysis of sagittal alignment parameters following anterior cervical hybrid
Huang et al. BMC Musculoskeletal Disorders (2019) 20:1 https://doi.org/10.1186/s12891-018-2378-y RESEARCH ARTICLE Open Access Analysis of sagittal alignment parameters following anterior cervical hybrid
Comparison between Radiological and Clinical Outcomes of Laminoplasties with Titanium Miniplates for Cervical Myelopathy
 Original Article Clinics in Orthopedic Surgery 2016;8:399-406 https://doi.org/10.4055/cios.2016.8.4.399 Comparison between Radiological and Clinical Outcomes of Laminoplasties with Titanium Miniplates
Original Article Clinics in Orthopedic Surgery 2016;8:399-406 https://doi.org/10.4055/cios.2016.8.4.399 Comparison between Radiological and Clinical Outcomes of Laminoplasties with Titanium Miniplates
Cervical myelopathy is a common disease that is
 TECHNICAL NOTE J Neurosurg Spine 26:325 330, 2017 A novel technique to correct kyphosis in cervical myelopathy due to continuous-type ossification of the posterior longitudinal ligament Dong-Ho Lee, MD,
TECHNICAL NOTE J Neurosurg Spine 26:325 330, 2017 A novel technique to correct kyphosis in cervical myelopathy due to continuous-type ossification of the posterior longitudinal ligament Dong-Ho Lee, MD,
PREOPERATIVE RETROLISTHESIS IS A RISK FACTOR OF LUMBAR DISC HERNIATION AFTER FENESTRATION WITHOUT DISCECTOMY
 PREOPERATIVE RETROLISTHESIS IS A RISK FACTOR OF LUMBAR DISC HERNIATION AFTER FENESTRATION WITHOUT DISCECTOMY Shota Takenaka*, Noboru Hosono, Yoshihiro Mukai, Kosuke Tateishi, Takeshi Fuji Osaka Kosei-nenkin
PREOPERATIVE RETROLISTHESIS IS A RISK FACTOR OF LUMBAR DISC HERNIATION AFTER FENESTRATION WITHOUT DISCECTOMY Shota Takenaka*, Noboru Hosono, Yoshihiro Mukai, Kosuke Tateishi, Takeshi Fuji Osaka Kosei-nenkin
En Bloc Cervical Laminoplasty While Preserving the Posterior Structure with Arcocristectomy in Cervical Spondylotic Myelopathy
 DOI: 10.5137/1019-5149.JTN.17440-16.0 Received: 03.03.2016 / Accepted: 05.03.3016 Published Online: 12.08.2016 Original Investigation En Bloc Cervical Laminoplasty While Preserving the Posterior Structure
DOI: 10.5137/1019-5149.JTN.17440-16.0 Received: 03.03.2016 / Accepted: 05.03.3016 Published Online: 12.08.2016 Original Investigation En Bloc Cervical Laminoplasty While Preserving the Posterior Structure
The Effect of the Pedicle-Facet Angle on Degenerative Cervical Spondylolisthesis
 www.jkns.or.kr http://dx.doi.org/10.3340/jkns.2015.58.4.341 J Korean Neurosurg Soc 58 (4) : 341-345, 2015 Print ISSN 2005-3711 On-line ISSN 1598-7876 Copyright 2015 The Korean Neurosurgical Society Clinical
www.jkns.or.kr http://dx.doi.org/10.3340/jkns.2015.58.4.341 J Korean Neurosurg Soc 58 (4) : 341-345, 2015 Print ISSN 2005-3711 On-line ISSN 1598-7876 Copyright 2015 The Korean Neurosurgical Society Clinical
Is OPLL-induced canal stenosis a risk factor of cord injury in cervical trauma?
 Acta Orthop. Belg., 2014, 80, 567-574 ORIGINAL STUDY Is OPLL-induced canal stenosis a risk factor of cord injury in cervical trauma? Kyung-Jin Song, Chan-Il Park, Do-Yeon Kim, Young-Ran Jung, Kwang-Bok
Acta Orthop. Belg., 2014, 80, 567-574 ORIGINAL STUDY Is OPLL-induced canal stenosis a risk factor of cord injury in cervical trauma? Kyung-Jin Song, Chan-Il Park, Do-Yeon Kim, Young-Ran Jung, Kwang-Bok
Comprehension of the common spine disorder.
 Objectives Comprehension of the common spine disorder. Disc degeneration/hernia. Spinal stenosis. Common spinal deformity (Spondylolisthesis, Scoliosis). Osteoporotic fracture. Anatomy Anatomy Anatomy
Objectives Comprehension of the common spine disorder. Disc degeneration/hernia. Spinal stenosis. Common spinal deformity (Spondylolisthesis, Scoliosis). Osteoporotic fracture. Anatomy Anatomy Anatomy
) ACDF. (Japanese Orthopaedic Association,JOA) ACCF (175.4±12.1ml VS 201.3±80.4ml) ACDF JOA VAS (P=0.000),ACCF :A : X(2015)
 2015 25 5 Chinese Journal of Spine and Spinal Cord,2015,Vol.25,No.5 433 1, 2, 2, 3, 3 (1 ;2 466000 ;3 466000 ) : (anterior cervical discectomy and fusion,acdf) (anterior cervical corpectomy and fusion,accf)
2015 25 5 Chinese Journal of Spine and Spinal Cord,2015,Vol.25,No.5 433 1, 2, 2, 3, 3 (1 ;2 466000 ;3 466000 ) : (anterior cervical discectomy and fusion,acdf) (anterior cervical corpectomy and fusion,accf)
Surgical outcomes for lumbar spinal canal stenosis with coexisting cervical stenosis (tandem spinal stenosis): a retrospective analysis of 565 cases
 Yamada et al. Journal of Orthopaedic Surgery and Research (2018) 13:60 https://doi.org/10.1186/s13018-018-0765-6 RESEARCH ARTICLE Open Access Surgical outcomes for lumbar spinal canal stenosis with coexisting
Yamada et al. Journal of Orthopaedic Surgery and Research (2018) 13:60 https://doi.org/10.1186/s13018-018-0765-6 RESEARCH ARTICLE Open Access Surgical outcomes for lumbar spinal canal stenosis with coexisting
SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT
 SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT 1 Anatomy 3 columns- Anterior, middle and Posterior Anterior- ALL, Anterior 2/3 rd body & disc. Middle- Posterior 1/3 rd of body & disc, PLL Posterior-
SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT 1 Anatomy 3 columns- Anterior, middle and Posterior Anterior- ALL, Anterior 2/3 rd body & disc. Middle- Posterior 1/3 rd of body & disc, PLL Posterior-
UPPER CERVICAL MYELOPATHY WITH METATROPIC DYSPLASIA
 UPPER CERVICAL MYELOPATHY WITH METATROPIC DYSPLASIA REPORT OF 4 SURGICAL CASES Yujiro Takeshita*, Kota Miyoshi**, Tomoaki Kitagawa** *Department of Orthopaedic and Spine Surgery, University of Tokyo, Japan
UPPER CERVICAL MYELOPATHY WITH METATROPIC DYSPLASIA REPORT OF 4 SURGICAL CASES Yujiro Takeshita*, Kota Miyoshi**, Tomoaki Kitagawa** *Department of Orthopaedic and Spine Surgery, University of Tokyo, Japan
Daniel J. Blizzard, MD, MS
 Daniel J. Blizzard, MD, MS None Common degenerative (usually) condition caused by compression on the spinal cord that is characterized by clumsiness and difficulty with fine motor tasks in the hands and
Daniel J. Blizzard, MD, MS None Common degenerative (usually) condition caused by compression on the spinal cord that is characterized by clumsiness and difficulty with fine motor tasks in the hands and
Cervical laminoplasty: evaluation of bone bonding of a high porosity hydroxyapatite spacer
 J Neurosurg (Spine 2) 98:137 142, 2003 Cervical laminoplasty: evaluation of bone bonding of a high porosity hydroxyapatite spacer TETSUHIRO IGUCHI, M.D., ARITETSU KANEMURA, M.D., AKIRA KURIHARA, M.D.,
J Neurosurg (Spine 2) 98:137 142, 2003 Cervical laminoplasty: evaluation of bone bonding of a high porosity hydroxyapatite spacer TETSUHIRO IGUCHI, M.D., ARITETSU KANEMURA, M.D., AKIRA KURIHARA, M.D.,
Characteristics of cervical sagittal parameters in healthy cervical spine adults and patients with cervical disc degeneration
 Xing et al. BMC Musculoskeletal Disorders (2018) 19:37 DOI 10.1186/s12891-018-1951-8 RESEARCH ARTICLE Open Access Characteristics of cervical sagittal parameters in healthy cervical spine adults and patients
Xing et al. BMC Musculoskeletal Disorders (2018) 19:37 DOI 10.1186/s12891-018-1951-8 RESEARCH ARTICLE Open Access Characteristics of cervical sagittal parameters in healthy cervical spine adults and patients
Cervical laminoplasty
 The Spine Journal 6 (2006) 274S 281S Cervical laminoplasty Michael P. Steinmetz, MD, Daniel K. Resnick, MD* Department of Neurosurgery, University of Wisconsin School of Medicine, K4/834 Clinical Science
The Spine Journal 6 (2006) 274S 281S Cervical laminoplasty Michael P. Steinmetz, MD, Daniel K. Resnick, MD* Department of Neurosurgery, University of Wisconsin School of Medicine, K4/834 Clinical Science
CMEARTICLE * * * Wen Qi Tan 1, BEng, Bak Siew Steven Wong 2, MBChB, MMed
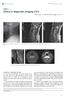 Singapore Med J 2015; 56(7): 373-378 doi: 10.11622/smedj.2015107 CMEARTICLE Clinics in diagnostic imaging (161) Wen Qi Tan 1, BEng, Bak Siew Steven Wong 2, MBChB, MMed 2a 2b Fig. 1 Lateral radiograph of
Singapore Med J 2015; 56(7): 373-378 doi: 10.11622/smedj.2015107 CMEARTICLE Clinics in diagnostic imaging (161) Wen Qi Tan 1, BEng, Bak Siew Steven Wong 2, MBChB, MMed 2a 2b Fig. 1 Lateral radiograph of
INTRODUCTION.
 www.jkns.or.kr http://dx.doi.org/10.3340/jkns.2015.58.5.442 J Korean Neurosurg Soc 58 (5) : 442-447, 2015 Print ISSN 2005-3711 On-line ISSN 1598-7876 Copyright 2015 The Korean Neurosurgical Society Clinical
www.jkns.or.kr http://dx.doi.org/10.3340/jkns.2015.58.5.442 J Korean Neurosurg Soc 58 (5) : 442-447, 2015 Print ISSN 2005-3711 On-line ISSN 1598-7876 Copyright 2015 The Korean Neurosurgical Society Clinical
ORIGINAL PAPER. Department of Orthopedic Surgery,Nagoya University Graduate School of Medicine,Nagoya,Japan 2
 Nagoya J. Med. Sci. 80. 583 589, 2018 doi:10.18999/nagjms.80.4.583 ORIGINAL PAPER Evaluation of sagittal alignment and range of motion of the cervical spine using multi-detector- row computed tomography
Nagoya J. Med. Sci. 80. 583 589, 2018 doi:10.18999/nagjms.80.4.583 ORIGINAL PAPER Evaluation of sagittal alignment and range of motion of the cervical spine using multi-detector- row computed tomography
Cervical spondylotic myelopathy (CSM) is a
 WScJ 4: 1-5, 2013 Functional Evaluation Using the Modified Japanese Orthopedic Association Score (mjoa) for Cervical Spondylotic Myelopathy by Age, Gender, and Type of Disease Parisa Azimi 1*, Sohrab Shahzadi
WScJ 4: 1-5, 2013 Functional Evaluation Using the Modified Japanese Orthopedic Association Score (mjoa) for Cervical Spondylotic Myelopathy by Age, Gender, and Type of Disease Parisa Azimi 1*, Sohrab Shahzadi
Cervical Open-Door Laminoplasty by Hydroxyapatite Implant Insertion Without Suturing
 Neurospine 2018;15(4):362-367. https://doi.org/10.14245/ns.1836106.053 Neurospine pissn 2586-6583 eissn 2586-6591 Original Article Corresponding Author Yoshifumi Kawanabe https://orcid.org/0000-0002-2251-0293
Neurospine 2018;15(4):362-367. https://doi.org/10.14245/ns.1836106.053 Neurospine pissn 2586-6583 eissn 2586-6591 Original Article Corresponding Author Yoshifumi Kawanabe https://orcid.org/0000-0002-2251-0293
Systematic review Cervical artificial disc replacement versus fusion in the cervical spine: a systematic review (...)
 Systematic review Cervical artificial disc replacement versus fusion in the cervical spine: a systematic review (...) 59 59 66 Cervical artificial disc replacement versus fusion in the cervical spine:
Systematic review Cervical artificial disc replacement versus fusion in the cervical spine: a systematic review (...) 59 59 66 Cervical artificial disc replacement versus fusion in the cervical spine:
Intraoperative spinal cord monitoring with Tce-MEP for cervical laminoplasty
 Intraoperative spinal cord monitoring with Tce-MEP for cervical laminoplasty Nobuhiro Tanaka 1, 2), Kazuyoshi Nakanishi 2), Naosuke Kamei 2), Toshio Nakamae 2), Shinji Kotaka 2), Yoshinori Fujimoto 1),
Intraoperative spinal cord monitoring with Tce-MEP for cervical laminoplasty Nobuhiro Tanaka 1, 2), Kazuyoshi Nakanishi 2), Naosuke Kamei 2), Toshio Nakamae 2), Shinji Kotaka 2), Yoshinori Fujimoto 1),
Cervical corpectomy for sub-axial retro-vertebral body lesions
 Eshra Egyptian Journal of Neurosurgery (2019) 33:2 https://doi.org/10.1186/s41984-018-0004-9 Egyptian Journal of Neurosurgery RESEARCH Open Access Cervical corpectomy for sub-axial retro-vertebral body
Eshra Egyptian Journal of Neurosurgery (2019) 33:2 https://doi.org/10.1186/s41984-018-0004-9 Egyptian Journal of Neurosurgery RESEARCH Open Access Cervical corpectomy for sub-axial retro-vertebral body
Lumbar radiculopathy caused by foraminal stenosis in rheumatoid arthritis
 Upsala Journal of Medical Sciences. 2011; 116: 133 137 ORIGINL RTICLE Lumbar radiculopathy caused by foraminal stenosis in rheumatoid arthritis TOMOKI KOKUTSU, NOKI MOROZUMI, YUTK KOIZUMI & YUSHIN ISHII
Upsala Journal of Medical Sciences. 2011; 116: 133 137 ORIGINL RTICLE Lumbar radiculopathy caused by foraminal stenosis in rheumatoid arthritis TOMOKI KOKUTSU, NOKI MOROZUMI, YUTK KOIZUMI & YUSHIN ISHII
Accelerated spondylotic changes adjacent to the fused segment following central cervical corpectomy: magnetic resonance imaging study evidence
 See the Editorial and the Response in this issue, p 1. J Neurosurg (Spine 1) 100:2 6, 2004 Accelerated spondylotic changes adjacent to the fused segment following central cervical corpectomy: magnetic
See the Editorial and the Response in this issue, p 1. J Neurosurg (Spine 1) 100:2 6, 2004 Accelerated spondylotic changes adjacent to the fused segment following central cervical corpectomy: magnetic
Symptomatic ossification of the anterior longitudinal ligament with stenosis of the cervical spine
 Spine Symptomatic ossification of the anterior longitudinal ligament with stenosis of the cervical spine A REPORT OF SEVEN CASES J. Mizuno, H. Nakagawa, J. Song From Aichi Medical University, Aichi-gun
Spine Symptomatic ossification of the anterior longitudinal ligament with stenosis of the cervical spine A REPORT OF SEVEN CASES J. Mizuno, H. Nakagawa, J. Song From Aichi Medical University, Aichi-gun
Early Radiological Analysis of Cervical Arthroplasty with Bryan and Mobi-C Cervical Disc Prosthesis
 CLINICAL ARTICLE Kor J Spine 5(3):111-115, 2008 Early Radiological Analysis of Cervical Arthroplasty with Bryan and Mobi-C Cervical Disc Prosthesis Ki Suk Choi, M.D., Il Tae Jang, M.D., Jae Hyeon Lim,
CLINICAL ARTICLE Kor J Spine 5(3):111-115, 2008 Early Radiological Analysis of Cervical Arthroplasty with Bryan and Mobi-C Cervical Disc Prosthesis Ki Suk Choi, M.D., Il Tae Jang, M.D., Jae Hyeon Lim,
Range of motion of thoracic spine in sagittal plane
 DOI 10.1007/s00586-013-3088-7 ORIGINAL ARTICLE Range of motion of thoracic spine in sagittal plane Daigo Morita Yasutsugu Yukawa Hiroaki Nakashima Keigo Ito Go Yoshida Masaaki Machino Syunsuke Kanbara
DOI 10.1007/s00586-013-3088-7 ORIGINAL ARTICLE Range of motion of thoracic spine in sagittal plane Daigo Morita Yasutsugu Yukawa Hiroaki Nakashima Keigo Ito Go Yoshida Masaaki Machino Syunsuke Kanbara
Radiculopathy of C-5 after anterior decompression for cervical myelopathy
 J Neurosurg Spine 3:210 217, 2005 Radiculopathy of C-5 after anterior decompression for cervical myelopathy MINORU IKENAGA, M.D., PH.D., JITSUHIKO SHIKATA M.D., PH.D., AND CHIAKI TANAKA M.D., PH.D. Department
J Neurosurg Spine 3:210 217, 2005 Radiculopathy of C-5 after anterior decompression for cervical myelopathy MINORU IKENAGA, M.D., PH.D., JITSUHIKO SHIKATA M.D., PH.D., AND CHIAKI TANAKA M.D., PH.D. Department
ProDisc-C versus fusion with Cervios chronos prosthesis in cervical degenerative disc disease: Is there a difference at 12 months?
 Original research ProDisc-C versus fusion with Cervios chronos prosthesis in cervical degenerative disc ( ) 51 51 56 ProDisc-C versus fusion with Cervios chronos prosthesis in cervical degenerative disc
Original research ProDisc-C versus fusion with Cervios chronos prosthesis in cervical degenerative disc ( ) 51 51 56 ProDisc-C versus fusion with Cervios chronos prosthesis in cervical degenerative disc
We have reviewed the cervical spine radiographs
 THE CERVICAL SPINE IN ATHETOID CEREBRAL PALSY A RADIOLOGICAL STUDY OF 180 PATIENTS TAKEO HARADA, SOHEI EBARA, MONZOOR M. ANWAR, ATSUKO OKAWA, ICHIRO KAJIURA, KAZUO HIROSHIMA, KEIRO ONO From Osaka Police
THE CERVICAL SPINE IN ATHETOID CEREBRAL PALSY A RADIOLOGICAL STUDY OF 180 PATIENTS TAKEO HARADA, SOHEI EBARA, MONZOOR M. ANWAR, ATSUKO OKAWA, ICHIRO KAJIURA, KAZUO HIROSHIMA, KEIRO ONO From Osaka Police
