Expansive Open-door Laminoplasty With Titanium Miniplate Versus Sutures
|
|
|
- Julius Beasley
- 5 years ago
- Views:
Transcription
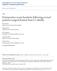
1 Expansive Open-door Laminoplasty With Titanium Miniplate Versus Sutures Guangdong Chen, MD; Zongping Luo, MD, PhD; Badri Nalajala, MD; Tao Liu, MD, PhD; Huilin Yang, MD, PhD abstract Full article available online at Healio.com/Orthopedics. Search: Expansive laminoplasty is an effective treatment for cervical myelopathy. Since the design of classic open-door laminoplasty with the use of suture, the procedure has been modified to reduce complications such as restenosis, axial symptoms, and segmental motor paralysis. Expansive open-door laminoplasty with the use of titanium miniplate is becoming popular. It is effective in expanding spinal canal dimensions with good clinical efficacy. However, a lack of studies exist comparing titanium miniplate fixation with classical suture fixation. A B We performed a retrospective study of 54 patients with cervical myelopathy. Twentynine patients (4 women and 25 men) receiving expansive open-door laminoplasty by titanium miniplate fixation were classified as the modified group, and 25 patients (5 women and 20 men) fixed with suture served as the control group. Clinical and radiologic outcomes were assessed. No significant differences were observed in Japanese Orthopaedic Association scores and the recovery rate of C5 palsy. The incidence of axial symptoms in the modified group was significantly lower than that in control group. Radiologic examination showed that postoperative C2-C7 lordosis and range of motion of the cervical spine in the modified group were preserved. No significant differences were observed in mean anteroposterior diameter and open angle in the 2 groups. Both surgical protocols were effective in preventing reclosure of open laminae. Furthermore, the modified laminoplasty was superior in reducing the incidence of axial symptoms and loss of cervical lordosis and range of motion. C Figure: Anteroposterior (A) and lateral (B) preoperative radiographs of a 47-year-old man in the modified group with cervical myelopathy associated with a 7-month history of numbness in the hands and unsteadiness of gait showing a 10 lordotic angle from C2-C7. Anteroposterior (C) and lateral (D) postoperative radiographs showing that open-door laminoplasty with titanium miniplate fixation effectively kept the lifted lamina open and preserved cervical alignment, and the lordotic angle from C2-C7 increased to 19. D Drs Chen, Luo, Nalajala, Liu, and Yang are from the Department of Orthopedic Surgery, the First Affiliated Hospital of Soochow University, Suzhou, Jiangsu Province, China. Drs Chen, Luo, Nalajala, Liu, and Yang have no relevant financial relationships to disclose. Correspondence should be addressed to: Huilin Yang, MD, PhD, Department of Orthopedic Surgery, the First Affiliated Hospital of Soochow University, 188 Shizi St, Suzhou, Jiangsu Province , China (huiliny@126.com). doi: / APRIL 2012 Volume 35 Number 4 e543
2 Expansive open-door laminoplasty is a well-established procedure that is effective for the treatment of cervical spondylotic myelopathy. However, patients have experienced complications such as axial symptoms, restenosis, and segmental motor paralysis. Since Hirabayashi et al 1 devised classic open-door laminoplasty, the procedure has been modified. 2-4 Miniplate fixation promises to prevent restenosis forever. In 1996, O Brien et al 5 adapted maxillofacial miniplates and screws for the purpose of securing the laminae in their new positions. The procedure is technically challenging because the assistant and primary surgeon must work together to hold the lamina and plate in place while drilling, tapping, and inserting the requisite screws. In an attempt to streamline the technique and increase its appeal to surgeons, titanium maxillofacial implants have been modified to better suit this purpose. Refined miniplates have entered the market in recent years. They are effective in expanding spinal canal dimensions with good clinical efficacy. However, a lack of studies exists comparing refined titanium miniplate fixation and classical suture fixation. The purpose of this retrospective study was to evaluate the clinical and radiologic results of titanium miniplate fixation compared with classical suture fixation in cervical expansive open-door laminoplasty. Materials and Methods A retrospective analysis was performed on 29 patients with cervical spondylotic myelopathy who underwent the modified method of cervical laminoplasty with titanium miniplate fixation between January 2008 and September The modified group comprised 25 men and 4 women with a mean age of 61.2 years (range, years). Mean preoperative Japanese Orthopaedic Association (JOA) score was 9.5 points. Decompression segment was C3-C7 in all patients. Three levels (C3, C5, C7) were fixed by miniplates in 24 patients. All levels (C3-C7) were fixed in 5 patients. Meanwhile, 25 patients who underwent the classical method of cervical laminoplasty during the same period served as the control. The control group comprised 20 men and 5 women with a mean age of 63.2 years (range, years). Mean preoperative JOA score was 9.2 points. The patients received the same decompression segment. C3 to C7 elevated laminas were fixed with suture in all patients. Patients with spinal cord injuries or myelopathy due to spinal cord tumors were excluded. Clinical diagnosis was made by physical examination, plain radiography, computed tomography (CT), and magnetic resonance imaging. All patients presented with cervical myelopathy characterized by exaggerated tendon jerk in their extremities and spasticity due to multilevel spinal stenosis without radiculopathy. Surgical Technique The patient was placed in the prone position, with the head secured in a U-shaped rigid device with craniumfixation to maintain the neck in a neutral position. A posterior midline approach and subperiosteum dissection were performed. The spinal process, lamina, and bilateral lateral mass were exposed. The paraspinal muscle of C2, especially the semispinalis, was preserved to prevent possible postoperative kyphosis. When detachment of the semispinalis at C2 was necessary, the muscle and tendon were repaired at the end of the surgery. Subsequently, the C3-C6 spinous processes were shortened. Before laminoplasty, depending on the severity of radiculopathy, we chose the open and hinged sides. The more severe side was chosen as the open side so that an appropriate laminoforaminotomy could be performed. The other side served as the hinged side. The drilled gutter on the lateral margin of the lamina was first completed on the open side. A high-speed spherical cutting burr was used to remove the outer cortex and cancellous bone. The retained groove bottom was resected using a diamond burr or Kerrison rongeur with a thin blade. Drilling the bony gutter on the hinged side was slightly lateral compared with that on the open side to prevent the lamina from becoming unstable or dislodging. The ligamentum flavums above the cephalic level and below the caudal level of the en bloc were cut with Kerrison rongeurs to facilitate opening the lamina. Although the inner cortex was thinned, the spinous process was pushed carefully using repetitive movements. The appropriate-sized laminoplasty plate (AO ARCH titanium miniplate; Synthes [Shanghai] Medical Device Trading Co Ltd, Shanghai, China) for each level was selected after the laminar door was opened. Then, the laminar hole and the lateral mass screws holes were made using the 2.0-mm depth-stopped drill bit. The relevant 2.0-mm screws were inserted to anchor the plate to the laminar and the lateral mass of the same level. The plate was adjusted toward the superior portion of the lateral mass to avoid penetrating the screws into the subjacent facet joint. Fivelevel (C3-C7) fixation was performed. If not accessible, plates were used at alternating levels (ie, C3, C5, and C7). A cervical collar was applied for 4 weeks. Considering the stability of the elevated laminae, isometric and isotonic muscle contraction of the posterior neck was recommended to the patients as soon as possible postoperatively. Mean follow-up was months (range, months) in the modified group (Figure 1). The same procedure was performed in the control group, but the laminae were elevated and secured to the facet joints using sutures at all levels. Bed rest was required for the first week postoperatively, and patients were allowed to walk with a cervical brace for 3 months. Mean followup was months (range, months) in the control group (Figure 2). e544 Healio.com The new online home of ORTHOPEDICS Healio.com/Orthopedics
3 Expansive Open-door Laminoplasty Chen et al Clinical Evaluation Operative time and intraoperative blood loss were compared between the modified and control groups. The neurologic evaluation was graded using the JOA scale. The recovery rate, which indicates the degree of normalization postoperatively, was calculated using Hirabayashi s formula: (postoperative score2preoperative score)3100/ (17 [full score]2preoperative score). Local symptoms (pain and stiffness) (ie, axial symptoms 6 ) were evaluated using the 10-point visual analog scale (VAS) score at 12 months. Significant axial symptoms occurred in patients with a VAS >3 after laminoplasty. The 10-point VAS was ascertained by self-assessment. The analgesics used postoperatively were also evaluated. The symptoms were evaluated at >6 months postoperatively to avoid early complaints, which may be directly related to surgical intervention. The incidence of postoperative segmental motor paralysis (ie, C5 palsy), was examined in both groups during the follow-up period. Radiologic Evaluation A straight line was drawn from the superior posterior aspect of the C2 vertebral body to the inferior posterior aspect of the C2 vertebral body and was extended inferiorly. Another line was drawn from the superior posterior aspect of the C7 vertebral body to the inferior posterior aspect of the C7 vertebral body and was extended superiorly. The angle between the 2 lines at their intersection was measured on pre- and postoperative radiographs. Computed tomography was used to measure the lamina elevation angle and to compare the postoperative anteroposterior (AP) diameter of the spinal canal with the results from the previous CT scan. Statistical Analysis Data were presented as mean6standard deviation. A t test with Welch correction was used for statistical analysis of the difference in the mean values between the 2 1A 1B 1C 1D 1E 1F Figure 1: Anteroposterior (A) and lateral (B) preoperative radiographs of a 47-year-old man in the modified group with cervical myelopathy associated with a 7-month history of numbness in the hands and unsteadiness of gait showing a 10 lordotic angle from C2-C7. Preoperative sagittal magnetic resonance image showing multiple-level stenosis with the most severe disease at C3-C6 (C). Preoperative axial computed tomography scan showing ossification of the posterior longitudinal ligament (D). Anteroposterior (E) and lateral (F) postoperative radiographs showing that open-door laminoplasty with titanium miniplate fixation effectively kept the lifted lamina open and preserved cervical alignment, and the lordotic angle from C2-C7 increased to 19. Postoperative sagittal magnetic resonance image showing the full decompression (G). Postoperative axial computed tomography showing a 38 open angle (H). 2A 2B 2C 2D 2E 2F Figure 2: Anteroposterior (A) and lateral (B) preoperative radiographs of a 53-year-old man in the control group with cervical myelopathy associated with a 5-month history of brachialgia and unsteadiness of gait showing a 19 lordotic angle from C2-C7. Preoperative sagittal magnetic resonance image showing multiple-level stenosis, including levels C3-C6 (C). Preoperative axial computed tomography (D). Anteroposterior (E) and lateral (F) postoperative radiographs showing that open-door laminoplasty with suture fixation kept the lifted lamina open, but the lordotic angle from C2-C7 decreased to 17. Postoperative sagittal magnetic resonance image showing good decompression (G). Postoperative axial computed tomography showing a 35 open angle (H). 1G 2G 1H 2H APRIL 2012 Volume 35 Number 4 e545
4 groups. The x2 test for independence was used to compare the incidence of postoperative axial symptoms between the modified and control groups. Results Clinical Evaluation Mean operative time was minutes in the modified group and minutes in the control group. Mean intraoperative blood loss was ml in the modified group and ml in the control group. No statistically significant difference was found in operative time and blood loss between the 2 groups (Table 1). Table 1 Patient Data Parameter Modified Group Control Group P Age, y Surgical time, min Follow-up, mo Blood loss, ml Table 2 Clinical Data, Axial Symptoms, and C5 Palsy Data Modified Group Control Group P JOA score Preoperative Postoperative Recovery rate, % VAS Preoperative Postoperative a No. of axial symptoms at follow-up No. of C5 palsy at follow-up 3/29 9/ a 2/29 2/ Abbreviations: JOA, Japan Orthopaedic Association; VAS, visual analog scale. a Statistically significant (P,.05). Mean JOA score in the modified group improved from points preoperatively to points at follow-up. In the control group, mean JOA score improved from points preoperatively to points at follow-up. The recovery rate was 57.48%616.51% in the modified group and 56.10%68.22% in the control group. No statistically significant difference was found in total postoperative JOA score or recovery rate between the 2 groups (Table 2). Preoperatively, VAS scores were similar between the 2 groups (P..05). The mean postoperative VAS score of 1.17 in the modified group was significantly lower than that of 2.44 in the control group. The incidence of significant axial symptoms (3/29) in the modified group was also significantly lower than that (9/25) in the control group at follow-up (P,.05). The analgesics used in the modified group were significantly less than those in the control group at follow-up (Table 2). C5 paralysis developed in 2 of 25 patients in the control group compared with 2 of 29 in the modified group. No statistically significant difference was found in the incidence of C5 palsy between the 2 groups (P..05). The C5 palsy developed 2 and 4 days postoperatively in the control group patients and 7 days and 1.5 months postoperatively in the modified group patients. Spontaneous recovery was observed in these 4 patients at 5, 6, 7, and 10 months postoperatively, respectively. Other complications included transient delirium in 5 patients and cerebrospinal fluid leakage in 3 patients, all of whom recovered without sequelae (Table 2). Radiologic Evaluation No statistically significant difference was found between mean preoperative lordotic angle in the modified group ( ) and in the control group ( ), whereas mean postoperative lordotic angle in the control group ( ) was significantly smaller than that in the modified group ( ) (P,.05) at 12-month follow-up. Postoperative cervical spine range of motion in the modified group was significantly well preserved compared with that in the control group (Table 3). Follow-up CT scans showed improvements in the AP diameter of the spinal canal in both groups (mean diameter increased from to mm in the modified group and from to mm in the control group). Mean open angle was and in the modified and control groups, respectively. No difference was found in the AP diameter and open angle between the 2 groups e546 Healio.com The new online home of ORTHOPEDICS Healio.com/Orthopedics
5 Expansive Open-door Laminoplasty Chen et al (Table 4). All hinged sides had bony fusions. No reclosure of the opened lamina occurred in either group. Discussion Expansive laminoplasty, a method using a posterior approach, is the treatment of choice for multiple level myeloradiculopathy. 7-9 The JOA scoring system for cervical myelopathy is used in most studies to assess clinical outcome. Overall, the JOA score recovery rate after expansive laminoplasty is 50% to 70%, and no technique has achieved statistical superiority. 1,10-12 The outcomes in our study are similar to those obtained by most studies. Mean preoperative JOA score of in the modified group and in the control group significantly improved to and , respectively, at final followup. However, no significant difference was found in mean recovery rate of JOA score between the 2 groups. Maintaining the expansion of the spinal canal is critical in a successful laminoplasty. The conventional method of the expansive laminoplasty, as reported by Hirabayashi and Satomi, 13 is used to make the suture stay in the spinous process and the paraspinal muscles and to avoid closure of the opened lamina. However, reclosure of the opened lamina with neurologic deterioration has been reported. 11,13 In the modified technique, the elevated lamina was fixed to lateral mass anchoring screws at each level using nonabsorbable suture line. However, the dura mater was exposed outside of the spinal canal. The spinal cord is easily compressed by the postoperative scarring of adjacent tissue. Miniplate fixation efficiently prevents reclosure of the opened lamina efficiently. A meta-analysis of outcomes and complications in cervical laminoplasty revealed that restenosis from unintended laminoplasty hinge closure occurs in 0% to 34% of cases and is the most common cause of recurrent myelopathy. No hinge closure has been reported following plate fixation. 14 In our results, restenosis owing to hinge reclosure or major surgery-related complications were not noted in either group, in contrast to previous reports. In our study, the mean open angle maintained in both groups may be explained by a relatively small patient sample and meticulous surgical procedures. A large study and long-term followup investigations will be necessary to evaluate this result. Axial symptoms, such as pain and stiffness, are the most frequent complaints after cervical laminoplasty. 6,15 Although increasing attention has been paid to the importance of axial symptoms, 6,16,17 the causes of the symptoms have not been fully clarified. However, 3 possible sources have been proposed: the nuchal muscle, facet joints, and nerve Table 3 Pre- and Postoperative C2-C7 Lordosis and Range of Motion Parameter Modified Group Control Group P C2-C7 lordosis, deg Preoperative Postoperative a Range of motion, deg Preoperative Postoperative a Abbreviation: deg, degrees. a Statistically significant (P,.05). Table 4 Pre- and Postoperative AP Diameter and Open Angle Parameter Modified Group Control Group P AP diameter, mm Preoperative Postoperative Open angle, deg Postoperative Abbreviations: AP, anteroposterior; deg, degrees. root. 13,18 Axial symptoms were evaluated using the 10-point VAS score in our study. Our study demonstrated that the modified expansive open-door laminoplasty with miniplate fixation could reduce postoperative axial symptoms. This suggests that axial symptoms may be caused in part by musculature or facet joints. The conventional method is used to make the suture stay in the spinous process and the paraspinal muscles and to avoid closure of the opened lamina. However, making a retention suture on the facet capsule may damage the capsule. In a report on a neurophysiologic study on facet joints, capsule stretch activated nociceptors and may have been a possible cause of persistent neck pain. 19 Therefore, facet capsule suture and stretch may be a APRIL 2012 Volume 35 Number 4 e547
6 possible cause of postlaminoplasty axial pain. The facet joint capsule should be kept intact to prevent the postoperative development of neck pain. It is also important to ensure that postoperative exercises of the extension muscles are started early to maintain dynamic stability of the cervical spine and to avoid disuse atrophy of the paravertebral muscle. Our study suggests that early exercise of the posterior neck muscle is effective to minimize postoperative axial symptoms. Postoperative lordosis (lordotic angle) and range of motion of the cervical spine was better maintained in the modified group, which might be related to the functional maintenance of the paravertebral muscle as a result of early neck motion. Kawaguchi et al 16 encouraged early active ROM postoperatively to decrease the incidence of axial symptoms and loss of ROM. Their practice seemed to be effective because of the lower incidence of postoperative axial symptoms in the modified group compared with that in the control group. Further, a recent study by Fujibayashi et al 20 reported the important role of the paravertebral muscle in preventing postoperative axial symptoms after laminoplasty. Segmental motor paralysis, or C5 palsy, occasionally occurs in patients treated with laminoplasty, and in studies in which C5 palsy is reported, the mean incidence is approximately 5% to 8%. 21,22 In our study, no significant difference was found in the incidence of C5 palsy between the 2 groups. The exact etiology of this paralysis remains unclear; possible causes include the nerve root and spinal cord. Despite efforts to refine surgical techniques, the incidence of paralysis has not substantially decreased. No effective preventive measures have been established. Further study is necessary to elucidate the mechanism of segmental motor paralysis after cervical laminoplasty. Conclusion Although both fixation methods were effective in preventing reclosure of the opened laminae, the modified open-door laminoplasty using titanium miniplate fixation was effective in reducing the incidence of axial symptoms and loss of cervical curvature and ROM due to the benefit of early functional training. The modified method is beneficial for the postoperative status of patients undergoing cervical laminoplasty References 1. Hirabayashi K, Watanabe K, Wakano K, Suzuki N, Satomi K, Ishii Y. Expansive opendoor laminoplasty for cervical spinal stenotic myelopathy. Spine (Phila Pa 1976). 1983; 8(7): Mochida J, Nomura T, ChibaM, Nishimura K, Toh E. Modifed expansive open-door laminoplasty in cervical myelopathy. J Spinal Disord. 1999; 12(5): Tomita K, Kawahara N, Toribatake Y, Heller JG. Expansive midline T-saw laminoplasty (modified spinous process-splitting) for the management of cervical myelopathy. Spine (Phila Pa 1976). 1998; 23(1): Tsuzuki N, Abe R, Saiki K, Iizuka T. Tension-band laminoplasty of the cervical spine. Int Orthop. 1996; 20(5): O Brien MF, Peterson D, Casey AT, Crockard HA. A novel technique for laminoplasty augmentation of spinal canal area using titanium miniplate stabilization. A computerized morphometric analysis. Spine (Phila Pa 1976). 1996; 21(4): Hosono N, Yonenobu K, Ono K. Neck pain and shoulder pain after laminoplasty. Spine (Phila Pa 1976). 1996; 21(17): Hirabayashi K, Toyama Y, Chiba K. Expansive laminoplasty for myelopathy in ossification of the longitudinal ligament. Clin Orthop Relat Res. 1999; (359): Satomi K, Ogawa J, Ishii Y, Hirabayashi K. Short-term complications and long-term results of expansive open-door laminoplasty for cervical stenotic myelopathy. Spine (Phila Pa 1976). 2001; 1(1): Lee TT, Green BA, Gromelski EB. Safety and stability of open-door cervical expansive laminoplasty. J Spinal Disord. 1998; 11(1): Satomi K, Nishu Y, Kohno T, Hirabayashi K. Long-term follow-up studies of open-door expansive laminoplasty for cervical stenotic myelopathy. Spine (Phila Pa 1976). 1994; 19(5): Patel CK, Cunningham BJ, Herkowitz HN. Techniques in cervical laminoplasty. Spine (Phila Pa 1976). 2002; 2(6): Kawakami M, Tamaki T, Iwasaki H, Yoshida M, Ando M, Yamada H. A comparative study of surgical approaches for cervical compressive myelopathy. Clin Orthop Relat Res. 2000; (381): Hirabayashi K, Satomi K. Operative procedure and results of expansive open-door laminoplasty. Spine (Phila Pa 1976). 1988; 13(7): Freedman B, Heller J, Rhee J. Cervical laminoplasty myths and realities: a meta-analysis of outcomes and complications. Spine (Phila Pa 1976). 2009; 9(10):23S. 15. Ohnari H, Sasai K, Akagi S, Iida H, Takanori S, Kato I. Investigation of axial symptoms after cervical laminoplasty, using questionnaire survey. Spine J. 2006; 6(3): Kawaguchi Y, Kanamori M, Ishiara H, Nobukiyo M, Seki S, Kimura T. Preventive measure for axial symptoms following cervical laminoplasty. J Spinal Disord Tech. 2003; 16(6): Shiraishi T, Fukuda K, Yato Y, Nakamura M, Ikegami T. Results of skip laminectomy mimimum 2-year follow-up study compared with open-door laminoplasty. Spine (Phila Pa 1976). 2003; 28(24): Nakano N, Nakano T, Nakano K. Comparison of the results of laminectomy and opendoor laminoplasty for cervical spondylotic myeloradiculopathy and ossification of the posterior longitudinal ligament. Spine (Phila Pa 1976). 1988; 13(7): Cavanaugh JM, Lu Y, Chen C, Kallakuri S. Pain generation in lumbar and cervical facet joints. J Bone Joint Surg Am. 2006; 88(suppl 2): Fujibayashi S, Neo M, Yoshida M, Miyata M, Takemoto M, Nakamura T. Neck muscle strength before and after cervical laminoplasty: relation to axial symptoms. J Spinal Disord Tech. 2010; 23(3): Ratliff JK, Cooper PR. Cervical laminoplasty: a critical review. J Neurosurg. 2003; 98(3 suppl): Sakaura H, Hosono N, Mukai Y, Ishii T, Yoshikawa H. C5 palsy after decompression surgery for cervical myelopathy: review of literature. Spine (Phila Pa 1976). 2003; 28(21): e548 Healio.com The new online home of ORTHOPEDICS Healio.com/Orthopedics
Clinical Application of a New Plate Fixation System in Open-door Laminoplasty
 Clinical Application of a New Plate Fixation System in Open-door Laminoplasty LIANGJUN JIANG, MD; WEISHAN CHEN, MD; QIXIN CHEN, MD; KAN XU, MD; QIONGHUA WU, MD; FANGCAI LI, MD abstract Full article available
Clinical Application of a New Plate Fixation System in Open-door Laminoplasty LIANGJUN JIANG, MD; WEISHAN CHEN, MD; QIXIN CHEN, MD; KAN XU, MD; QIONGHUA WU, MD; FANGCAI LI, MD abstract Full article available
Comparison between Radiological and Clinical Outcomes of Laminoplasties with Titanium Miniplates for Cervical Myelopathy
 Original Article Clinics in Orthopedic Surgery 2016;8:399-406 https://doi.org/10.4055/cios.2016.8.4.399 Comparison between Radiological and Clinical Outcomes of Laminoplasties with Titanium Miniplates
Original Article Clinics in Orthopedic Surgery 2016;8:399-406 https://doi.org/10.4055/cios.2016.8.4.399 Comparison between Radiological and Clinical Outcomes of Laminoplasties with Titanium Miniplates
Op e n-d o o r laminoplasty was developed by Hirabayashi. Risk factors for closure of lamina after open-door laminoplasty.
 J Neurosurg Spine 9:530 537, 2008 Risk factors for closure of lamina after open-door laminoplasty Clinical article Mo r i o Ma t s u m o t o, M.D., 1 Ko ta Wata n a b e, M.D., 2 Ta k a s h i Ts u j i,
J Neurosurg Spine 9:530 537, 2008 Risk factors for closure of lamina after open-door laminoplasty Clinical article Mo r i o Ma t s u m o t o, M.D., 1 Ko ta Wata n a b e, M.D., 2 Ta k a s h i Ts u j i,
Analysis of C5 palsy in cervical myelopathy with massive anterior compression following laminoplasty
 Chen et al. Journal of Orthopaedic Surgery and Research (2018) 13:26 DOI 10.1186/s13018-018-0715-3 RESEARCH ARTICLE Open Access Analysis of C5 palsy in cervical myelopathy with massive anterior compression
Chen et al. Journal of Orthopaedic Surgery and Research (2018) 13:26 DOI 10.1186/s13018-018-0715-3 RESEARCH ARTICLE Open Access Analysis of C5 palsy in cervical myelopathy with massive anterior compression
Efficacy and results of expansive laminoplasty in patients with severe cervical myelopathy due to cervical canal stenosis
 Original Article Efficacy and results of expansive laminoplasty in patients with severe cervical myelopathy due to cervical canal stenosis D. Agrawal, B. S. Sharma, A. Gupta, V. S. Mehta Department of
Original Article Efficacy and results of expansive laminoplasty in patients with severe cervical myelopathy due to cervical canal stenosis D. Agrawal, B. S. Sharma, A. Gupta, V. S. Mehta Department of
Incidence and Risk Factors for Late Neurologic Deterioration after C3 C6 Laminoplasty for Cervical Spondylotic Myelopathy
 THIEME GLOBAL SPINE JOURNAL Original Article 53 Incidence and Risk Factors for Late Neurologic Deterioration after C3 C6 Laminoplasty for Cervical Spondylotic Myelopathy Hironobu Sakaura 1 Toshitada Miwa
THIEME GLOBAL SPINE JOURNAL Original Article 53 Incidence and Risk Factors for Late Neurologic Deterioration after C3 C6 Laminoplasty for Cervical Spondylotic Myelopathy Hironobu Sakaura 1 Toshitada Miwa
Risk Factors for Hinge Fracture Associated with Surgery Following Cervical Open-Door Laminoplasty
 CLINICAL ARTICLE Korean J Neurotrauma 18;14(2):118-122 pissn 2234-8999 / eissn 2288-2243 https://doi.org/1.134/kjnt.18.14.2.118 Risk Factors for Hinge Fracture Associated with Surgery Following Cervical
CLINICAL ARTICLE Korean J Neurotrauma 18;14(2):118-122 pissn 2234-8999 / eissn 2288-2243 https://doi.org/1.134/kjnt.18.14.2.118 Risk Factors for Hinge Fracture Associated with Surgery Following Cervical
Kazunari Takeuchi Æ Toru Yokoyama Æ Atsushi Ono Æ Takuya Numasawa Æ Kanichiro Wada Æ Taito Itabashi Æ Satoshi Toh
 Eur Spine J (2008) 17:415 420 DOI 10.1007/s00586-007-0553-1 ORIGINAL ARTICLE Limitation of activities of daily living accompanying reduced neck mobility after laminoplasty preserving or reattaching the
Eur Spine J (2008) 17:415 420 DOI 10.1007/s00586-007-0553-1 ORIGINAL ARTICLE Limitation of activities of daily living accompanying reduced neck mobility after laminoplasty preserving or reattaching the
Technique Guide. ARCH Laminoplasty System. Dedicated System for Open-door Laminoplasty.
 Technique Guide ARCH Laminoplasty System. Dedicated System for Open-door Laminoplasty. Table of Contents Introduction Overview 2 AO ASIF Principles 4 Indications and Contraindications 5 Product Information
Technique Guide ARCH Laminoplasty System. Dedicated System for Open-door Laminoplasty. Table of Contents Introduction Overview 2 AO ASIF Principles 4 Indications and Contraindications 5 Product Information
Interlaminar Bony Fusion after C3-6 Double-Door Laminoplasty for Cervical Spondylotic Myelopathy: Its Predictors and Characteristics
 Interlaminar Bony Fusion after C3-6 Double-Door Laminoplasty for Cervical Spondylotic Myelopathy: Its Predictors and Characteristics Yoshiro Nanjo, Hideki Nagashima, Shinji Tanishima,Tokumitsu Mihara,
Interlaminar Bony Fusion after C3-6 Double-Door Laminoplasty for Cervical Spondylotic Myelopathy: Its Predictors and Characteristics Yoshiro Nanjo, Hideki Nagashima, Shinji Tanishima,Tokumitsu Mihara,
Radiographic Dimensional Analysis of Open Door Laminoplasty with Plate in Cervical Spondylotic Myelopathy
 Radiographic Dimensional Analysis of Open Door Laminoplasty with Plate in Cervical Spondylotic Myelopathy Woo-Kie Min,MD,PhD Department of Orthopedic Surgery, Kyungpook National University College of Medicine,
Radiographic Dimensional Analysis of Open Door Laminoplasty with Plate in Cervical Spondylotic Myelopathy Woo-Kie Min,MD,PhD Department of Orthopedic Surgery, Kyungpook National University College of Medicine,
Selective laminoplasty for cervical spondylotic myelopathy: a comparative study with a minimum 5-year follow-up
 Selective laminoplasty for cervical spondylotic myelopathy: a comparative study with a minimum 5-year follow-up Minori Kato*, Hiroaki Nakamura**, Koji Tamai**, Kazunori Hayashi**, Akira Matsumura**, Sadahiko
Selective laminoplasty for cervical spondylotic myelopathy: a comparative study with a minimum 5-year follow-up Minori Kato*, Hiroaki Nakamura**, Koji Tamai**, Kazunori Hayashi**, Akira Matsumura**, Sadahiko
ARCH Laminoplasty System
 Dedicated System for Open-door Laminoplasty ARCH Laminoplasty System Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use of DePuy Synthes
Dedicated System for Open-door Laminoplasty ARCH Laminoplasty System Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use of DePuy Synthes
ARCH Laminoplasty System. Dedicated System for Open-door Laminoplasty.
 ARCH Laminoplasty System. Dedicated System for Open-door Laminoplasty. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation.
ARCH Laminoplasty System. Dedicated System for Open-door Laminoplasty. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation.
Influence of hinge position on the effectiveness of opendoor expansive laminoplasty for cervical spondylotic myelopathy
 . 6. Influence of hinge position on the effectiveness of opendoor expansive laminoplasty for cervical spondylotic myelopathy WAN Jun, XU Tian-tong*, SHEN Qing-feng, LI Hui-nan and XIA Ying-peng Abstract
. 6. Influence of hinge position on the effectiveness of opendoor expansive laminoplasty for cervical spondylotic myelopathy WAN Jun, XU Tian-tong*, SHEN Qing-feng, LI Hui-nan and XIA Ying-peng Abstract
Incidence and Risk Factors for Late Neurologic Deterioration after C3-6 Laminoplasty in Patients with Cervical Spondylotic Myelopathy
 Incidence and Risk Factors for Late Neurologic Deterioration after C3-6 Laminoplasty in Patients with Cervical Spondylotic Myelopathy Sakaura H, Miwa T, Kuroda Y, Ohwada T Dept. of Orthop. Surg., Kansai
Incidence and Risk Factors for Late Neurologic Deterioration after C3-6 Laminoplasty in Patients with Cervical Spondylotic Myelopathy Sakaura H, Miwa T, Kuroda Y, Ohwada T Dept. of Orthop. Surg., Kansai
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
Abstract Study Design Systematic review. Weerasak Singhatanadgige 1 Worawat Limthongkul 1 Frank Valone III 2 Wicharn Yingsakmongkol 1 K.
 702 Review Article GLOBAL SPINE JOURNAL THIEME Outcomes following or Fusion in Patients with Myelopathy Caused by Ossification of the Posterior Longitudinal Ligament: A Systematic Review Weerasak Singhatanadgige
702 Review Article GLOBAL SPINE JOURNAL THIEME Outcomes following or Fusion in Patients with Myelopathy Caused by Ossification of the Posterior Longitudinal Ligament: A Systematic Review Weerasak Singhatanadgige
Cervical Open-Door Laminoplasty by Hydroxyapatite Implant Insertion Without Suturing
 Neurospine 2018;15(4):362-367. https://doi.org/10.14245/ns.1836106.053 Neurospine pissn 2586-6583 eissn 2586-6591 Original Article Corresponding Author Yoshifumi Kawanabe https://orcid.org/0000-0002-2251-0293
Neurospine 2018;15(4):362-367. https://doi.org/10.14245/ns.1836106.053 Neurospine pissn 2586-6583 eissn 2586-6591 Original Article Corresponding Author Yoshifumi Kawanabe https://orcid.org/0000-0002-2251-0293
Recent Surgical Methods of Double-door Laminoplasty of the Cervical Spine (Kurokawa s Method)
 TECHNICAL NOTE SPINE SURGERY AND RELATED RESEARCH Recent Surgical Methods of Double-door Laminoplasty of the Cervical Spine (Kurokawa s Method) Shigeru Hirabayashi Department of Orthopaedic Surgery, Teikyo
TECHNICAL NOTE SPINE SURGERY AND RELATED RESEARCH Recent Surgical Methods of Double-door Laminoplasty of the Cervical Spine (Kurokawa s Method) Shigeru Hirabayashi Department of Orthopaedic Surgery, Teikyo
Review Article Operative Treatment of Cervical Myelopathy: Cervical Laminoplasty
 Hindawi Publishing Corporation Advances in Orthopedics Volume 2012, Article ID 508534, 5 pages doi:10.1155/2012/508534 Review Article Operative Treatment of Cervical Myelopathy: Cervical Laminoplasty Brett
Hindawi Publishing Corporation Advances in Orthopedics Volume 2012, Article ID 508534, 5 pages doi:10.1155/2012/508534 Review Article Operative Treatment of Cervical Myelopathy: Cervical Laminoplasty Brett
NewBridge. Laminoplasty Fixation INTERNATIONAL EDITION
 NewBridge L A M I N O P L A S T Y F I X A T I O N S Y S T E M Laminoplasty Fixation INTERNATIONAL EDITION Table of Contents 1 INTRODUCTION 2 PRE-OPERATIVE 3 OPERATIVE 10 INSTRUCTIONS FOR USE 12 PART NUMBERS
NewBridge L A M I N O P L A S T Y F I X A T I O N S Y S T E M Laminoplasty Fixation INTERNATIONAL EDITION Table of Contents 1 INTRODUCTION 2 PRE-OPERATIVE 3 OPERATIVE 10 INSTRUCTIONS FOR USE 12 PART NUMBERS
Neck Pain following Laminoplasty
 Global Spine Journal Original Article 17 Addisu Mesfin 1 Moon-Soo Park 2 Chaiwat Piyaskulkaew 2 Tapanut Chuntarapas 2 Kwang Sup Song 2 HanJoKim 2 K. Daniel Riew 2 1 Department of Orthopaedics, University
Global Spine Journal Original Article 17 Addisu Mesfin 1 Moon-Soo Park 2 Chaiwat Piyaskulkaew 2 Tapanut Chuntarapas 2 Kwang Sup Song 2 HanJoKim 2 K. Daniel Riew 2 1 Department of Orthopaedics, University
Laminoplasty for Cervical Myelopathy
 Review Article 187 Manabu Ito 1 Ken Nagahama 2 1 Department of Advanced Medicine for Spine and Spinal Cord Disorders, Hokkaido University Graduate School of Medicine, Sapporo, Japan 2 Department of Orthopaedic
Review Article 187 Manabu Ito 1 Ken Nagahama 2 1 Department of Advanced Medicine for Spine and Spinal Cord Disorders, Hokkaido University Graduate School of Medicine, Sapporo, Japan 2 Department of Orthopaedic
The Correlation Study of C5 Nerve Root Palsy and Common Body Position in Posterior Total Laminectomy Decompression and Instrumentation
 DOI: 10.5137/1019-5149.JTN.7476-12.1 Received: 30.10.2012 / Accepted: 11.02.2013 Original Investigation The Correlation Study of C5 Nerve Root Palsy and Common Body Position in Posterior Total Laminectomy
DOI: 10.5137/1019-5149.JTN.7476-12.1 Received: 30.10.2012 / Accepted: 11.02.2013 Original Investigation The Correlation Study of C5 Nerve Root Palsy and Common Body Position in Posterior Total Laminectomy
Minamide A*, Yoshida M*, Yamada H*, Hashizume H*, NakagawaY*, Iwasaki H*, Tsutsui S*, Hiroyuki Oka H**.
 Efficacy of Posterior Segmental Decompression Surgery for Pincer Mechanism in Cervical Spondylotic Myelopathy -A retrospective case control study using propensity score matching Minamide A*, Yoshida M*,
Efficacy of Posterior Segmental Decompression Surgery for Pincer Mechanism in Cervical Spondylotic Myelopathy -A retrospective case control study using propensity score matching Minamide A*, Yoshida M*,
Modified laminoplasty for multilevel cervical myelopathy.
 Biomedical Research 2017; 28 (13): 5721-5725 ISSN 0970-938X www.biomedres.info Modified laminoplasty for multilevel cervical myelopathy. Zhihong Nie *#, Fanlei Kong #, Yujiang Wu, Xiuxin Fu, Zhongpo Liu,
Biomedical Research 2017; 28 (13): 5721-5725 ISSN 0970-938X www.biomedres.info Modified laminoplasty for multilevel cervical myelopathy. Zhihong Nie *#, Fanlei Kong #, Yujiang Wu, Xiuxin Fu, Zhongpo Liu,
Open-door Laminoplasty with Preservation of Muscle Attachments of C2 and C7 for Cervical Spondylotic Myelopathy: Retrospective Study
 DOI: 10.5137/1019-5149.JTN.20007-17.1 Received: 25.01.2017 / Accepted: 27.02.2017 Published Online: 17.03.2017 Original Investigation Open-door Laminoplasty with Preservation of Muscle Attachments of C2
DOI: 10.5137/1019-5149.JTN.20007-17.1 Received: 25.01.2017 / Accepted: 27.02.2017 Published Online: 17.03.2017 Original Investigation Open-door Laminoplasty with Preservation of Muscle Attachments of C2
Modified open-door cervical expansive laminoplasty for spondylotic myelopathy: operative technique, outcome, and predictors for gait improvement
 Modified open-door cervical expansive laminoplasty for spondylotic myelopathy: operative technique, outcome, and predictors for gait improvement Thomas T. Lee, M.D., Glen R. Manzano, B.S., and Barth A.
Modified open-door cervical expansive laminoplasty for spondylotic myelopathy: operative technique, outcome, and predictors for gait improvement Thomas T. Lee, M.D., Glen R. Manzano, B.S., and Barth A.
Disclosures: T. Yoshii: None. T. Yamada: None. T. Taniyama: None. S. Sotome: None. T. Kato: None. S. Kawabata: None. A. Okawa: None.
 Dynamic Changes in Spinal Cord Compression by Cervical Ossification of the Posterior Longitudinal Ligament Evaluated by Kinematic Computed Tomography Myelogram Toshitaka Yoshii, Tsuyoshi Yamada, Takashi
Dynamic Changes in Spinal Cord Compression by Cervical Ossification of the Posterior Longitudinal Ligament Evaluated by Kinematic Computed Tomography Myelogram Toshitaka Yoshii, Tsuyoshi Yamada, Takashi
We performed CT myelography in 38 patients
 Posterior movement and enlargement of the spinal cord after cervical laminoplasty Ikuo Aita, Koichiro Hayashi, Yasuyoshi Wadano, Takeshi Yabuki From the University of Tsukuba, Ibaraki, Japan We performed
Posterior movement and enlargement of the spinal cord after cervical laminoplasty Ikuo Aita, Koichiro Hayashi, Yasuyoshi Wadano, Takeshi Yabuki From the University of Tsukuba, Ibaraki, Japan We performed
Christopher I. Shaffrey, MD
 CSRS 21st Instructional Course Wednesday, November 30, 2016 Laminoplasty/Foraminotomy: Why Fuse the Spine at all? Christopher I. Shaffrey, MD John A. Jane Distinguished Professor Departments of Neurosurgery
CSRS 21st Instructional Course Wednesday, November 30, 2016 Laminoplasty/Foraminotomy: Why Fuse the Spine at all? Christopher I. Shaffrey, MD John A. Jane Distinguished Professor Departments of Neurosurgery
Cervical myelopathy is caused by spinal canal narrowing
 An Original Study Instrumented Open-Door Laminoplasty as Treatment for Cervical Myelopathy in 104 Patients John R. Dimar II, MD, Kelly R. Bratcher, RN, CCRP, Dylan C. Brock, BS, Steven D. Glassman, MD,
An Original Study Instrumented Open-Door Laminoplasty as Treatment for Cervical Myelopathy in 104 Patients John R. Dimar II, MD, Kelly R. Bratcher, RN, CCRP, Dylan C. Brock, BS, Steven D. Glassman, MD,
Cervical Laminoplasty
 Techniques in Orthopaedics 17(3):324 335 2003 Lippincott Williams & Wilkins, Inc., Philadelphia Cervical Laminoplasty Sanjitpal S. Gill, M.D., and John G. Heller, M.D. Summary: Definitive treatment of
Techniques in Orthopaedics 17(3):324 335 2003 Lippincott Williams & Wilkins, Inc., Philadelphia Cervical Laminoplasty Sanjitpal S. Gill, M.D., and John G. Heller, M.D. Summary: Definitive treatment of
Key words: Professional Med J 2018;25(8): CERVICAL LAMINOPLASTY
 The Professional Medical Journal DOI: 10.29309/TPMJ/18.4872 1. MBBS Post graduate Trainee, 2. MBBS, FCPS Associate Professor 3. MBBS, FCPS Associate Professor 4. MBBS Honorary Researcher, 5. MBBS, FCPS
The Professional Medical Journal DOI: 10.29309/TPMJ/18.4872 1. MBBS Post graduate Trainee, 2. MBBS, FCPS Associate Professor 3. MBBS, FCPS Associate Professor 4. MBBS Honorary Researcher, 5. MBBS, FCPS
Catastrophic Dropped Head Syndrome Requiring Multiple Reconstruction Surgeries after Cervical Laminoplasty
 CASE REPORT SPINE SURGERY AND RELATED RESEARCH Catastrophic Dropped Head Syndrome Requiring Multiple Reconstruction Surgeries after Cervical Laminoplasty Seiichi Odate, Jitsuhiko Shikata and Tsunemitsu
CASE REPORT SPINE SURGERY AND RELATED RESEARCH Catastrophic Dropped Head Syndrome Requiring Multiple Reconstruction Surgeries after Cervical Laminoplasty Seiichi Odate, Jitsuhiko Shikata and Tsunemitsu
Department of Neurological Surgery, Asan Medical Center, University of Ulsan College of Medicine, Seoul, Korea
 online ML Comm CLINICAL ARTICLE Korean J Neurotrauma 2014;10(2):60-65 pissn 2234-8999 / eissn 2288-2243 http://dx.doi.org/10.13004/kjnt.2014.10.2.60 Midline Splitting Cervical Laminoplasty Using Allogeneic
online ML Comm CLINICAL ARTICLE Korean J Neurotrauma 2014;10(2):60-65 pissn 2234-8999 / eissn 2288-2243 http://dx.doi.org/10.13004/kjnt.2014.10.2.60 Midline Splitting Cervical Laminoplasty Using Allogeneic
ORIGINAL PAPER. Surgical outcomes of decompressive laminoplasty with spinous process osteotomy to treat lumbar spinal stenosis
 Editors Choice ORIGINAL PAPER Nagoya J. Med. Sci. 80. 1 9, 2018 doi:10.18999/nagjms.80.1.1 Surgical outcomes of decompressive laminoplasty with spinous process osteotomy to treat lumbar spinal stenosis
Editors Choice ORIGINAL PAPER Nagoya J. Med. Sci. 80. 1 9, 2018 doi:10.18999/nagjms.80.1.1 Surgical outcomes of decompressive laminoplasty with spinous process osteotomy to treat lumbar spinal stenosis
Microendoscopic laminotomy versus conventional laminoplasty for cervical spondylotic myelopathy: 5-year follow-up study
 CLINICAL ARTICLE J Neurosurg Spine 27:403 409, 2017 Microendoscopic laminotomy versus conventional laminoplasty for cervical spondylotic myelopathy: 5-year follow-up study Akihito Minamide, MD, PhD, 1
CLINICAL ARTICLE J Neurosurg Spine 27:403 409, 2017 Microendoscopic laminotomy versus conventional laminoplasty for cervical spondylotic myelopathy: 5-year follow-up study Akihito Minamide, MD, PhD, 1
Posterior surgical procedures are those procedures
 9 Cervical Posterior surgical procedures are those procedures that have been in use for a long time with established efficacy in the treatment of radiculopathy and myelopathy caused by pathologies including
9 Cervical Posterior surgical procedures are those procedures that have been in use for a long time with established efficacy in the treatment of radiculopathy and myelopathy caused by pathologies including
Yoshifumi Kudo, 1 Tomoaki Toyone, 1 Toshiyuki Shirahata, 1 Tomoyuki Ozawa, 1 Akira Matsuoka, 1 Yoichi Jin, 2 and Katsunori Inagaki 1. 1.
 Case Reports in Orthopedics Volume 2016, Article ID 1250810, 5 pages http://dx.doi.org/10.1155/2016/1250810 Case Report A Case of Successful Foraminotomy for Severe Bilateral C5 Palsy following Posterior
Case Reports in Orthopedics Volume 2016, Article ID 1250810, 5 pages http://dx.doi.org/10.1155/2016/1250810 Case Report A Case of Successful Foraminotomy for Severe Bilateral C5 Palsy following Posterior
Comparative Effectiveness of Different Types of Cervical Laminoplasty
 Systematic Review 105 Comparative Effectiveness of Different Types of Cervical Laminoplasty John G. Heller 1 Annie L. Raich 2 Joseph R. Dettori 2 K. Daniel Riew 3 1 Department of Orthopaedic Surgery, Emory
Systematic Review 105 Comparative Effectiveness of Different Types of Cervical Laminoplasty John G. Heller 1 Annie L. Raich 2 Joseph R. Dettori 2 K. Daniel Riew 3 1 Department of Orthopaedic Surgery, Emory
ORIGINAL ARTICLE. Introduction SPINE SURGERY AND RELATED RESEARCH
 ORIGINAL ARTICLE SPINE SURGERY AND RELATED RESEARCH Radiological Examination of Postoperative Cervical Alignment and Stability in Patients with Dialysis-Associated Spondylosis Excluding Destructive Spondyloarthropathy:
ORIGINAL ARTICLE SPINE SURGERY AND RELATED RESEARCH Radiological Examination of Postoperative Cervical Alignment and Stability in Patients with Dialysis-Associated Spondylosis Excluding Destructive Spondyloarthropathy:
Laminoplasty versus laminectomy for multi-level cervical spondylotic myelopathy: a systematic review of the literature
 Lao et al. Journal of Orthopaedic Surgery and Research 2013, 8:45 RESEARCH ARTICLE Open Access Laminoplasty versus laminectomy for multi-level cervical spondylotic : a systematic review of the literature
Lao et al. Journal of Orthopaedic Surgery and Research 2013, 8:45 RESEARCH ARTICLE Open Access Laminoplasty versus laminectomy for multi-level cervical spondylotic : a systematic review of the literature
Radiological pathogenesis of cervical myelopathy in 60 consecutive patients with cervical ossi cation of the posterior longitudinal ligament
 Spinal Cord (1999) 37, 853 ± 857 ã 1999 International Medical Society of Paraplegia All rights reserved 1362 ± 4393/99 $15.00 http://www.stockton-press.co.uk/sc Radiological pathogenesis of cervical myelopathy
Spinal Cord (1999) 37, 853 ± 857 ã 1999 International Medical Society of Paraplegia All rights reserved 1362 ± 4393/99 $15.00 http://www.stockton-press.co.uk/sc Radiological pathogenesis of cervical myelopathy
Satisfactory surgical results for CSM have recently
 J Neurosurg Spine 18:545 552, 2013 AANS, 2013 A less-invasive cervical laminoplasty for spondylotic myelopathy that preserves the semispinalis cervicis muscles and nuchal ligament Clinical article Masayuki
J Neurosurg Spine 18:545 552, 2013 AANS, 2013 A less-invasive cervical laminoplasty for spondylotic myelopathy that preserves the semispinalis cervicis muscles and nuchal ligament Clinical article Masayuki
Age-related and degenerative changes in the osseous anatomy, alignment, and range of motion
 Age-related and degenerative changes in the osseous anatomy, alignment, and range of motion of the cervical spine: a comparative study of radiographic data from 1016 patients with cervical spondylotic
Age-related and degenerative changes in the osseous anatomy, alignment, and range of motion of the cervical spine: a comparative study of radiographic data from 1016 patients with cervical spondylotic
Is high T-1 slope a significant risk factor for developing interlaminar bony fusion after cervical laminoplasty? A retrospective cohort study
 CLINICAL ARTICLE J Neurosurg Spine 27:627 632, 2017 Is high T-1 slope a significant risk factor for developing interlaminar bony fusion after cervical laminoplasty? A retrospective cohort study Takeshi
CLINICAL ARTICLE J Neurosurg Spine 27:627 632, 2017 Is high T-1 slope a significant risk factor for developing interlaminar bony fusion after cervical laminoplasty? A retrospective cohort study Takeshi
ASJ. Risk Factor Analysis for C5 Palsy after Double-Door Laminoplasty for Cervical Spondylotic Myelopathy. Asian Spine Journal.
 Asian Spine Journal 298 Satoshi Clinical Baba et al. Study http://dx.doi.org/10.4184/asj.2016.10.2.298 Risk Factor Analysis for C5 Palsy after Double-Door Laminoplasty for Cervical Spondylotic Myelopathy
Asian Spine Journal 298 Satoshi Clinical Baba et al. Study http://dx.doi.org/10.4184/asj.2016.10.2.298 Risk Factor Analysis for C5 Palsy after Double-Door Laminoplasty for Cervical Spondylotic Myelopathy
Outcomes of Secondary Laminoplasty for Patients with Unsatisfactory Results after Anterior Multilevel Cervical Surgery
 online ML Comm www.jkns.or.kr http://dx.doi.org/10.3340/jkns.2015.57.1.36 J Korean Neurosurg Soc 57 (1) : 36-41, 2015 Print ISSN 2005-3711 On-line ISSN 1598-7876 Copyright 2015 The Korean Neurosurgical
online ML Comm www.jkns.or.kr http://dx.doi.org/10.3340/jkns.2015.57.1.36 J Korean Neurosurg Soc 57 (1) : 36-41, 2015 Print ISSN 2005-3711 On-line ISSN 1598-7876 Copyright 2015 The Korean Neurosurgical
Review Article. Abstract
 Review Article Cervical Laminoplasty: Indications, Surgical Considerations, and Clinical Outcomes Samuel K. Cho, MD Jun S. Kim, MD Samuel C. Overley, MD Robert K. Merrill, MD JAAOS Plus Webinar JoinDr.Cho,Dr.Kim,Dr.Overley,
Review Article Cervical Laminoplasty: Indications, Surgical Considerations, and Clinical Outcomes Samuel K. Cho, MD Jun S. Kim, MD Samuel C. Overley, MD Robert K. Merrill, MD JAAOS Plus Webinar JoinDr.Cho,Dr.Kim,Dr.Overley,
Reduced invasiveness of myoarchitectonic laminectomy compared with open-door laminoplasty in patients with cervical myelopathy
 Reduced invasiveness of myoarchitectonic laminectomy compared with open-door laminoplasty in patients with cervical myelopathy Department of Spinal Surgery 1), Brain Attack Center Ota Memorial Hospital,
Reduced invasiveness of myoarchitectonic laminectomy compared with open-door laminoplasty in patients with cervical myelopathy Department of Spinal Surgery 1), Brain Attack Center Ota Memorial Hospital,
Cervical laminoplasty
 The Spine Journal 6 (2006) 274S 281S Cervical laminoplasty Michael P. Steinmetz, MD, Daniel K. Resnick, MD* Department of Neurosurgery, University of Wisconsin School of Medicine, K4/834 Clinical Science
The Spine Journal 6 (2006) 274S 281S Cervical laminoplasty Michael P. Steinmetz, MD, Daniel K. Resnick, MD* Department of Neurosurgery, University of Wisconsin School of Medicine, K4/834 Clinical Science
Comparative study on the effect of anterior and posterior decompression in the treatment of multi-segmental cervical spondylotic myelopathy
 92 Journal of Hainan Medical University 2016; 22(6): 92-96 Journal of Hainan Medical University http://www.jhmuweb.net/ Comparative study on the effect of anterior and posterior decompression in the treatment
92 Journal of Hainan Medical University 2016; 22(6): 92-96 Journal of Hainan Medical University http://www.jhmuweb.net/ Comparative study on the effect of anterior and posterior decompression in the treatment
En Bloc Cervical Laminoplasty While Preserving the Posterior Structure with Arcocristectomy in Cervical Spondylotic Myelopathy
 DOI: 10.5137/1019-5149.JTN.17440-16.0 Received: 03.03.2016 / Accepted: 05.03.3016 Published Online: 12.08.2016 Original Investigation En Bloc Cervical Laminoplasty While Preserving the Posterior Structure
DOI: 10.5137/1019-5149.JTN.17440-16.0 Received: 03.03.2016 / Accepted: 05.03.3016 Published Online: 12.08.2016 Original Investigation En Bloc Cervical Laminoplasty While Preserving the Posterior Structure
Cervical corpectomy for sub-axial retro-vertebral body lesions
 Eshra Egyptian Journal of Neurosurgery (2019) 33:2 https://doi.org/10.1186/s41984-018-0004-9 Egyptian Journal of Neurosurgery RESEARCH Open Access Cervical corpectomy for sub-axial retro-vertebral body
Eshra Egyptian Journal of Neurosurgery (2019) 33:2 https://doi.org/10.1186/s41984-018-0004-9 Egyptian Journal of Neurosurgery RESEARCH Open Access Cervical corpectomy for sub-axial retro-vertebral body
ORIGINAL PAPER. Department of Orthopedic Surgery, Chubu Rosai Hospital, Nagoya, Japan ABSTRACT
 Nagoya J. Med. Sci. 77. 221 ~ 228, 2015 ORIGINAL PAPER RANGE OF MOTION DETERMINED BY MULTIDETECTOR-ROW COMPUTED TOMOGRAPHY IN PATIENTS WITH CERVICAL OSSIFICATION OF THE POSTERIOR LONGITUDINAL LIGAMENT
Nagoya J. Med. Sci. 77. 221 ~ 228, 2015 ORIGINAL PAPER RANGE OF MOTION DETERMINED BY MULTIDETECTOR-ROW COMPUTED TOMOGRAPHY IN PATIENTS WITH CERVICAL OSSIFICATION OF THE POSTERIOR LONGITUDINAL LIGAMENT
Original Investigation. Byung-Wan CHOI. INTRODUCTION Ossification of the posterior longitudinal ligament ABSTRACT
 DOI: 10.5137/1019-5149.JTN.16196-15.1 Received: 25.09.2015 / Accepted: 07.12.2015 Published Online: 01.06.2016 Original Investigation Clinical and Radiological Characteristics of Ossification of the Posterior
DOI: 10.5137/1019-5149.JTN.16196-15.1 Received: 25.09.2015 / Accepted: 07.12.2015 Published Online: 01.06.2016 Original Investigation Clinical and Radiological Characteristics of Ossification of the Posterior
Cervical laminoplasty: evaluation of bone bonding of a high porosity hydroxyapatite spacer
 J Neurosurg (Spine 2) 98:137 142, 2003 Cervical laminoplasty: evaluation of bone bonding of a high porosity hydroxyapatite spacer TETSUHIRO IGUCHI, M.D., ARITETSU KANEMURA, M.D., AKIRA KURIHARA, M.D.,
J Neurosurg (Spine 2) 98:137 142, 2003 Cervical laminoplasty: evaluation of bone bonding of a high porosity hydroxyapatite spacer TETSUHIRO IGUCHI, M.D., ARITETSU KANEMURA, M.D., AKIRA KURIHARA, M.D.,
Neck Pain Following Cervical Laminoplasty: Does Preservation of the C2 Muscle Attachments and/or C7 Matter?
 42 Systematic Review Neck Pain Following Cervical Laminoplasty: Does Preservation of the C2 Muscle Attachments and/or C7 Matter? K. Daniel Riew 1 Annie L. Raich 3 Joseph R. Dettori 3 John G. Heller 2 1
42 Systematic Review Neck Pain Following Cervical Laminoplasty: Does Preservation of the C2 Muscle Attachments and/or C7 Matter? K. Daniel Riew 1 Annie L. Raich 3 Joseph R. Dettori 3 John G. Heller 2 1
Module: #15 Lumbar Spine Fusion. Author(s): Jenni Buckley, PhD. Date Created: March 27 th, Last Updated:
 Module: #15 Lumbar Spine Fusion Author(s): Jenni Buckley, PhD Date Created: March 27 th, 2011 Last Updated: Summary: Students will perform a single level lumbar spine fusion to treat lumbar spinal stenosis.
Module: #15 Lumbar Spine Fusion Author(s): Jenni Buckley, PhD Date Created: March 27 th, 2011 Last Updated: Summary: Students will perform a single level lumbar spine fusion to treat lumbar spinal stenosis.
Hinged Laminoplasty System surgical technique
 BlackbirdTM Hls Hinged Laminoplasty System surgical technique Blackbird TM Hls The ChoiceSpine Blackbird Hinged Laminoplasty System (HLS) design eliminates fitting plates through trial and error bending.
BlackbirdTM Hls Hinged Laminoplasty System surgical technique Blackbird TM Hls The ChoiceSpine Blackbird Hinged Laminoplasty System (HLS) design eliminates fitting plates through trial and error bending.
The Predictable Factors of the Postoperative Kyphotic Change of Sagittal Alignment of the Cervical Spine after the Laminoplasty
 Clinical Article J Korean Neurosurg Soc 60 (5) : 577-583, 2017 https://doi.org/10.3340/jkns.2017.0505.007 pissn 2005-3711 eissn 1598-7876 The Predictable Factors of the Postoperative Kyphotic Change of
Clinical Article J Korean Neurosurg Soc 60 (5) : 577-583, 2017 https://doi.org/10.3340/jkns.2017.0505.007 pissn 2005-3711 eissn 1598-7876 The Predictable Factors of the Postoperative Kyphotic Change of
How cervical alignment and thoracic inlet angle affect on postoperative spinal cord alignment after laminoplasty?
 How cervical alignment and thoracic inlet angle affect on postoperative spinal cord alignment after laminoplasty? Shinya Kato, Hisanori Mihara Department of Orthopaedics Surgery, Yokohama Hodogaya Central
How cervical alignment and thoracic inlet angle affect on postoperative spinal cord alignment after laminoplasty? Shinya Kato, Hisanori Mihara Department of Orthopaedics Surgery, Yokohama Hodogaya Central
Jing Tao Zhang 1, Lin Feng Wang 1, Yue Ju Liu 2, Jun Ming Cao 1, Jie Li 1, Shuai Wang 1 and Yong Shen 1*
 Zhang et al. BMC Musculoskeletal Disorders (2015) 16:267 DOI 10.1186/s12891-015-0728-6 RESEARCH ARTICLE Open Access Relationship between developmental canal stenosis and surgical results of anterior decompression
Zhang et al. BMC Musculoskeletal Disorders (2015) 16:267 DOI 10.1186/s12891-015-0728-6 RESEARCH ARTICLE Open Access Relationship between developmental canal stenosis and surgical results of anterior decompression
Accelerated spondylotic changes adjacent to the fused segment following central cervical corpectomy: magnetic resonance imaging study evidence
 See the Editorial and the Response in this issue, p 1. J Neurosurg (Spine 1) 100:2 6, 2004 Accelerated spondylotic changes adjacent to the fused segment following central cervical corpectomy: magnetic
See the Editorial and the Response in this issue, p 1. J Neurosurg (Spine 1) 100:2 6, 2004 Accelerated spondylotic changes adjacent to the fused segment following central cervical corpectomy: magnetic
Cervical laminaplasty is an extensile
 Surgical Techniques Cervical Laminaplasty Ronald A. Lehman, Jr, MD, MAJ, MC, USA Brett A. Taylor, MD John M. Rhee, MD K. Daniel Riew, MD The video that accompanies this article is Cervical Laminaplasty,
Surgical Techniques Cervical Laminaplasty Ronald A. Lehman, Jr, MD, MAJ, MC, USA Brett A. Taylor, MD John M. Rhee, MD K. Daniel Riew, MD The video that accompanies this article is Cervical Laminaplasty,
Cervical Degenerative Disease - Surgical Approaches to CSM 가톨릭의대인천성모병원척추센터 김종태
 KNS Main Topic Session Spine Surgery : Case-Based Lecture of Spinal Disease Cervical Degenerative Disease - Surgical Approaches to CSM 가톨릭의대인천성모병원척추센터 김종태 Cervical Spondylotic Myelopathy ( CSM ) (1984,
KNS Main Topic Session Spine Surgery : Case-Based Lecture of Spinal Disease Cervical Degenerative Disease - Surgical Approaches to CSM 가톨릭의대인천성모병원척추센터 김종태 Cervical Spondylotic Myelopathy ( CSM ) (1984,
ELY ASHKENAZI Israel Spine Center at Assuta Hospital Tel Aviv, Israel
 nterior cervical decompression using the Hybrid Decompression Fixation technique, a combination of corpectomies and or discectomies, in the management of multilevel cervical myelopathy J ORTHOP TRUM SURG
nterior cervical decompression using the Hybrid Decompression Fixation technique, a combination of corpectomies and or discectomies, in the management of multilevel cervical myelopathy J ORTHOP TRUM SURG
Lamina Osteotomy and Replantation With Miniplate Fixation for Thoracic Myelopathy Due to Ossification of the Ligamentum Flavum
 Lamina Osteotomy and Replantation With Miniplate Fixation for Thoracic Myelopathy Due to Ossification of the Ligamentum Flavum Zhi-Hong Nie, MD; Fa-Jing Liu, MD; Yong Shen, MD; Wen-Yuan Ding; Lin-Feng
Lamina Osteotomy and Replantation With Miniplate Fixation for Thoracic Myelopathy Due to Ossification of the Ligamentum Flavum Zhi-Hong Nie, MD; Fa-Jing Liu, MD; Yong Shen, MD; Wen-Yuan Ding; Lin-Feng
Lift-up laminoplasty for myelopathy caused by ossification of the posterior longitudinal ligament of the cervical spine
 Original Article Lift-up laminoplasty for myelopathy caused by ossification of the posterior longitudinal ligament of the cervical spine T. Takami, K. Ohata, T. Goto, M. Nishikawa, A. Nishio, N. Tsuyuguchi,
Original Article Lift-up laminoplasty for myelopathy caused by ossification of the posterior longitudinal ligament of the cervical spine T. Takami, K. Ohata, T. Goto, M. Nishikawa, A. Nishio, N. Tsuyuguchi,
Retro-odontoid pseudotumors are mass lesions formed
 SURGICAL TECHNIQUE Microscopic Posterior Transdural Resection of Cervical Retro-Odontoid Pseudotumors Yasushi Fujiwara, MD, PhD,* Hideki Manabe,* Tadayoshi Sumida,w Nobuhiro Tanaka,z and Takahiko Hamasakiy
SURGICAL TECHNIQUE Microscopic Posterior Transdural Resection of Cervical Retro-Odontoid Pseudotumors Yasushi Fujiwara, MD, PhD,* Hideki Manabe,* Tadayoshi Sumida,w Nobuhiro Tanaka,z and Takahiko Hamasakiy
Cervical spondylotic myelopathy (CSM) is a progressive
 literature review J Neurosurg Spine 24:77 99, 2016 A systematic review of clinical and surgical predictors of complications following surgery for degenerative cervical myelopathy Lindsay Tetreault, BSc,
literature review J Neurosurg Spine 24:77 99, 2016 A systematic review of clinical and surgical predictors of complications following surgery for degenerative cervical myelopathy Lindsay Tetreault, BSc,
Rick C. Sasso MD Professor Chief of Spine Surgery Clinical Orthopaedic Surgery Indiana University School of Medicine
 Cervical Myelopathy: Anterior Surgery is Best Rick C. Sasso MD Professor Chief of Surgery Clinical Orthopaedic Surgery University School of Medicine Disclosure: Research support-medtronic, Stryker, AO,
Cervical Myelopathy: Anterior Surgery is Best Rick C. Sasso MD Professor Chief of Surgery Clinical Orthopaedic Surgery University School of Medicine Disclosure: Research support-medtronic, Stryker, AO,
Factors related to long-term outcome after decompressive surgery for ossification of the ligamentum flavum of the thoracic spine
 J Neurosurg (Spine 3) 99:251 256, 2003 Factors related to long-term outcome after decompressive surgery for ossification of the ligamentum flavum of the thoracic spine NAOHISA MIYAKOSHI, M.D., YOICHI SHIMADA,
J Neurosurg (Spine 3) 99:251 256, 2003 Factors related to long-term outcome after decompressive surgery for ossification of the ligamentum flavum of the thoracic spine NAOHISA MIYAKOSHI, M.D., YOICHI SHIMADA,
Microendoscopic Decompression Surgery for Lumbar Spinal Canal Stenosis via the Paramedian Approach: Preliminary Results
 Original Article 87 Microendoscopic Decompression Surgery for Lumbar Spinal Canal Stenosis via the Paramedian Approach: Preliminary Results Kazunori omura 1 Munehito Yoshida 2 1 Department of Orthopaedic
Original Article 87 Microendoscopic Decompression Surgery for Lumbar Spinal Canal Stenosis via the Paramedian Approach: Preliminary Results Kazunori omura 1 Munehito Yoshida 2 1 Department of Orthopaedic
Principles and Surgical Technique of Cervical Laminoplasty
 Principles and Surgical Technique of Cervical Laminoplasty Shigeru Hirabayashi, M.D., Ph.D. Department of Medical Science Teikyo University of Science Tokyo, Japan COI: HOYA CORPORATION Laminoplasty
Principles and Surgical Technique of Cervical Laminoplasty Shigeru Hirabayashi, M.D., Ph.D. Department of Medical Science Teikyo University of Science Tokyo, Japan COI: HOYA CORPORATION Laminoplasty
Dorsal Cervical Surgeries and Techniques
 Dorsal Cervical Approaches Dorsal Cervical Surgeries and Techniques Gregory R. Trost, MD Professor and Vice Chair of Neurological Surgery University of Wisconsin-Madison Advantages Straightforward Easily
Dorsal Cervical Approaches Dorsal Cervical Surgeries and Techniques Gregory R. Trost, MD Professor and Vice Chair of Neurological Surgery University of Wisconsin-Madison Advantages Straightforward Easily
Key Primary CPT Codes: Refer to pages: 7-9 Last Review Date: October 2016 Medical Coverage Guideline Number:
 National Imaging Associates, Inc. Clinical guidelines CERVICAL SPINE SURGERY: ANTERI CERVICAL DECOMPRESSION WITH FUSION CERVICAL POSTERI DECOMPRESSION WITH FUSION CERVICAL ARTIFICIAL DISC CERVICAL POSTERI
National Imaging Associates, Inc. Clinical guidelines CERVICAL SPINE SURGERY: ANTERI CERVICAL DECOMPRESSION WITH FUSION CERVICAL POSTERI DECOMPRESSION WITH FUSION CERVICAL ARTIFICIAL DISC CERVICAL POSTERI
Revision Surgery Following Cervical Laminoplasty Etiology and Treatment Strategies
 Revision Surgery Following Cervical Laminoplasty Etiology and Treatment Strategies Gabriel Liu, MD, Jacob M. Buchowski, MD, MS, Torphong Bunmaprasert, MD, Jin S. Yeom, MD, Hongxing Shen, MD, and K. Daniel
Revision Surgery Following Cervical Laminoplasty Etiology and Treatment Strategies Gabriel Liu, MD, Jacob M. Buchowski, MD, MS, Torphong Bunmaprasert, MD, Jin S. Yeom, MD, Hongxing Shen, MD, and K. Daniel
L8 Spine System SURGICAL TECHNIQUE. Add: No.1-8, Tianshan Road, Xinbei District, Changzhou, Jiangsu, China
 Add: No.-8, Tianshan Road, Xinbei District, Changzhou, Jiangsu, China 23022 Tel: 0086 59 8595556 Fax: 0086 59 859555 Http://www.kanghui.com Add: F25, Shanghai International Pharmaceutical Trad & Exhibition
Add: No.-8, Tianshan Road, Xinbei District, Changzhou, Jiangsu, China 23022 Tel: 0086 59 8595556 Fax: 0086 59 859555 Http://www.kanghui.com Add: F25, Shanghai International Pharmaceutical Trad & Exhibition
Treatment for thoracic ossification of posterior longitudinal ligament with posterior circumferential decompression: complications and managements
 Yang et al. Journal of Orthopaedic Surgery and Research (2016) 11:153 DOI 10.1186/s13018-016-0489-4 RESEARCH ARTICLE Open Access Treatment for thoracic ossification of posterior longitudinal ligament with
Yang et al. Journal of Orthopaedic Surgery and Research (2016) 11:153 DOI 10.1186/s13018-016-0489-4 RESEARCH ARTICLE Open Access Treatment for thoracic ossification of posterior longitudinal ligament with
Surgical Management of Congenital Cervical Kyphosis
 n Feature Article Surgical Management of Congenital Cervical Kyphosis Zhimin He, MD; Yang Liu, MD; Feng Xue, MD; Haijun Xiao, MD; Wen Yuan, MD; Deyu Chen, MD abstract Full article available online at Healio.com/Orthopedics.
n Feature Article Surgical Management of Congenital Cervical Kyphosis Zhimin He, MD; Yang Liu, MD; Feng Xue, MD; Haijun Xiao, MD; Wen Yuan, MD; Deyu Chen, MD abstract Full article available online at Healio.com/Orthopedics.
Ossification of the posterior longitudinal ligament
 J Neurosurg Spine 19:431 435, 2013 AANS, 2013 Upper cervical cord compression due to a C-1 posterior arch in a patient with ossification of the posterior longitudinal ligament and a kyphotic cervical spine
J Neurosurg Spine 19:431 435, 2013 AANS, 2013 Upper cervical cord compression due to a C-1 posterior arch in a patient with ossification of the posterior longitudinal ligament and a kyphotic cervical spine
SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT
 SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT 1 Anatomy 3 columns- Anterior, middle and Posterior Anterior- ALL, Anterior 2/3 rd body & disc. Middle- Posterior 1/3 rd of body & disc, PLL Posterior-
SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT 1 Anatomy 3 columns- Anterior, middle and Posterior Anterior- ALL, Anterior 2/3 rd body & disc. Middle- Posterior 1/3 rd of body & disc, PLL Posterior-
CERVICAL SPONDYLOSIS & CERVICAL DISC DISEASE
 CERVICAL SPONDYLOSIS & CERVICAL DISC DISEASE Cervical spondylosis l Cervical osteophytosis l Most common progressive disease in the aging cervical spine l Seen in 95% of the people by 65 years Pathophysiology
CERVICAL SPONDYLOSIS & CERVICAL DISC DISEASE Cervical spondylosis l Cervical osteophytosis l Most common progressive disease in the aging cervical spine l Seen in 95% of the people by 65 years Pathophysiology
Postoperative severe headache following cervical posterior surgical fixation from C2 distally
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2016 Postoperative severe headache following cervical posterior surgical fixation from C2 distally Ryoji Tauchi
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2016 Postoperative severe headache following cervical posterior surgical fixation from C2 distally Ryoji Tauchi
Thoracolumbar Spine Locking Plate (TSLP) System. A low-profile plating system for anterior stabilization of the thoracic and lumbar spine.
 Thoracolumbar Spine Locking Plate (TSLP) System. A low-profile plating system for anterior stabilization of the thoracic and lumbar spine. Technique Guide Instruments and implants approved by the AO Foundation
Thoracolumbar Spine Locking Plate (TSLP) System. A low-profile plating system for anterior stabilization of the thoracic and lumbar spine. Technique Guide Instruments and implants approved by the AO Foundation
Review Article Operative Outcomes for Cervical Degenerative Disease: A Review of the Literature
 International Scholarly Research Network ISRN Orthopedics Volume 2012, Article ID 165050, 6 pages doi:10.5402/2012/165050 Review Article Operative Outcomes for Cervical Degenerative Disease: A Review of
International Scholarly Research Network ISRN Orthopedics Volume 2012, Article ID 165050, 6 pages doi:10.5402/2012/165050 Review Article Operative Outcomes for Cervical Degenerative Disease: A Review of
There were 36 patients with age range between 32 and 72 years (mean: 56.5 years). The male to
 Original Article Modified Laminoplasty for Degenerative Cervical Spondylosis: The Technique of Floating Laminoplasty Samuel C Ohaegbulam, Wilfred C Mezue, Chika Anele Ndubuisi, Mark O Chikani, Ndubuisi
Original Article Modified Laminoplasty for Degenerative Cervical Spondylosis: The Technique of Floating Laminoplasty Samuel C Ohaegbulam, Wilfred C Mezue, Chika Anele Ndubuisi, Mark O Chikani, Ndubuisi
Case Report Two-year follow-up results of C2/3 Prestige-LP cervical disc replacement: first report
 Int J Clin Exp Med 2016;9(4):7349-7353 www.ijcem.com /ISSN:1940-5901/IJCEM0018962 Case Report Two-year follow-up results of C2/3 Prestige-LP cervical disc replacement: first report Yi Yang 1, Mengying
Int J Clin Exp Med 2016;9(4):7349-7353 www.ijcem.com /ISSN:1940-5901/IJCEM0018962 Case Report Two-year follow-up results of C2/3 Prestige-LP cervical disc replacement: first report Yi Yang 1, Mengying
Case Report Adjacent Lumbar Disc Herniation after Lumbar Short Spinal Fusion
 Case Reports in Orthopedics, Article ID 456940, 4 pages http://dx.doi.org/10.1155/2014/456940 Case Report Adjacent Lumbar Disc Herniation after Lumbar Short Spinal Fusion Koshi Ninomiya, Koichi Iwatsuki,
Case Reports in Orthopedics, Article ID 456940, 4 pages http://dx.doi.org/10.1155/2014/456940 Case Report Adjacent Lumbar Disc Herniation after Lumbar Short Spinal Fusion Koshi Ninomiya, Koichi Iwatsuki,
Cervical myelopathy is a common disease that is
 TECHNICAL NOTE J Neurosurg Spine 26:325 330, 2017 A novel technique to correct kyphosis in cervical myelopathy due to continuous-type ossification of the posterior longitudinal ligament Dong-Ho Lee, MD,
TECHNICAL NOTE J Neurosurg Spine 26:325 330, 2017 A novel technique to correct kyphosis in cervical myelopathy due to continuous-type ossification of the posterior longitudinal ligament Dong-Ho Lee, MD,
Life expectancy after cervical laminoplasty Causes of the fatal prognosis at the early stage (within 5 years)
 ORIGINAL ARTICLE SPINE SURGERY AND RELATED RESEARCH Life expectancy after cervical laminoplasty Causes of the fatal prognosis at the early stage (within 5 years) Yoshiharu Kawaguchi 1), Masato Nakano 1),
ORIGINAL ARTICLE SPINE SURGERY AND RELATED RESEARCH Life expectancy after cervical laminoplasty Causes of the fatal prognosis at the early stage (within 5 years) Yoshiharu Kawaguchi 1), Masato Nakano 1),
Table of contents. Introduction. Features and Benefits 2. AO Principles 4. Indications and Contraindiactions 5. Implants 6. Productinformation
 Technique Guide CerviFix. Modular tension band system for posterior fixation of the occipito - cervical spine, upper and lower cervical spine, and upper thoracic spine. Table of contents Introduction
Technique Guide CerviFix. Modular tension band system for posterior fixation of the occipito - cervical spine, upper and lower cervical spine, and upper thoracic spine. Table of contents Introduction
5/19/2017. Disclosures. Introduction. How Much Kyphosis is Allowable for Cervical Total Disc Replacement? And Other Considerations
 How Much Kyphosis is Allowable for Cervical Total Disc Replacement? And Other Considerations Richard D. Guyer, M.D. Disclosures Guyer (a) Alphatec; (b) Spinal Kinetics, Spinal Ventures, Mimedix; (c) DePuy
How Much Kyphosis is Allowable for Cervical Total Disc Replacement? And Other Considerations Richard D. Guyer, M.D. Disclosures Guyer (a) Alphatec; (b) Spinal Kinetics, Spinal Ventures, Mimedix; (c) DePuy
Intraoperative spinal cord monitoring with Tce-MEP for cervical laminoplasty
 Intraoperative spinal cord monitoring with Tce-MEP for cervical laminoplasty Nobuhiro Tanaka 1, 2), Kazuyoshi Nakanishi 2), Naosuke Kamei 2), Toshio Nakamae 2), Shinji Kotaka 2), Yoshinori Fujimoto 1),
Intraoperative spinal cord monitoring with Tce-MEP for cervical laminoplasty Nobuhiro Tanaka 1, 2), Kazuyoshi Nakanishi 2), Naosuke Kamei 2), Toshio Nakamae 2), Shinji Kotaka 2), Yoshinori Fujimoto 1),
Unanswered Questions. Laminoplasty is best
 Laminoplasty is best Wellington K. Hsu, MD Clifford C. Raisbeck Distinguished Professor of Orthopaedic Surgery Director of Research Department of Orthopaedic Surgery Northwestern University Feinberg School
Laminoplasty is best Wellington K. Hsu, MD Clifford C. Raisbeck Distinguished Professor of Orthopaedic Surgery Director of Research Department of Orthopaedic Surgery Northwestern University Feinberg School
factor for identifying unstable thoracolumbar fractures. There are clinical and radiological criteria
 NMJ-Vol :2/ Issue:1/ Jan June 2013 Case Report Medical Sciences Progressive subluxation of thoracic wedge compression fracture with unidentified PLC injury Dr.Thalluri.Gopala krishnaiah* Dr.Voleti.Surya
NMJ-Vol :2/ Issue:1/ Jan June 2013 Case Report Medical Sciences Progressive subluxation of thoracic wedge compression fracture with unidentified PLC injury Dr.Thalluri.Gopala krishnaiah* Dr.Voleti.Surya
A minimally invasive surgical approach reduces cranial adjacent segment degeneration in patients undergoing posterior lumbar interbody fusion
 A minimally invasive surgical approach reduces cranial adjacent segment degeneration in patients undergoing posterior lumbar interbody fusion T. Tsutsumimoto, M. Yui, S. Ikegami, M. Uehara, H. Kosaku,
A minimally invasive surgical approach reduces cranial adjacent segment degeneration in patients undergoing posterior lumbar interbody fusion T. Tsutsumimoto, M. Yui, S. Ikegami, M. Uehara, H. Kosaku,
