Clinical results of modified Mitchell s osteotomy for hallux valgus augmented with oblique lesser metatarsal osteotomy
|
|
|
- Magdalene Hart
- 5 years ago
- Views:
Transcription
1 Journal of Orthopaedic Surgery 2005:13(3): Clinical results of modified Mitchell s osteotomy for hallux valgus augmented with oblique lesser metatarsal osteotomy K Yamamoto, A Imakiire, Y Katori, T Masaoka, R Koizumi Department of Orthopedic Surgery, Tokyo Medical University, Tokyo, Japan ABSTRACT Purpose. To evaluate postoperative results of modified Mitchell s osteotomy and its combination with oblique metatarsal osteotomy for the treatment of hallux valgus. Methods. A total of 93 feet of 53 patients (2 men and 51 women) with hallux valgus underwent modified Mitchell s osteotomy and were followed up for at least 5 years. Patients age ranged from 17 to 83 years, and the duration of follow-up ranged from 5 years one month to 18 years 4 months. Modified Mitchell s osteotomy was performed on 53 feet in 31 patients (group A), whereas modified Mitchell s osteotomy augmented with oblique lesser metatarsal osteotomy was performed to the remaining 40 feet in 22 patients (group B). Postoperative results were assessed using a clinical assessment system developed by the Tokyo Medical University based on 5 categories: pain in the first metatarsophalangeal, deformity of the metatarsophalangeal, plantar callosity and/or metatarsalgia of lesser metatarsals, the use of commercially available shoes, and local inflammatory symptoms. Results. Mean total score improved from 3.8 to 7.9 on a 10-point scale. Scores for 2 categories plantar callosity and/or metatarsalgia and the use of commercially available shoes were significantly higher in group B at postoperative 5 years. Before surgery, at postoperative 3 weeks, and at postoperative 5 years, respectively, the mean hallux valgus angles were 34.2 Ο, 12.0 Ο, and 17.1 Ο ; mean M1-M2 angles were 16.7 Ο, 7.4 Ο, and 8.7 Ο ; mean M1-M5 angles were 34.9 Ο, 25.8 Ο, and 26.6 Ο ; and mean sesamoid bone shifts were 8.7 mm, 4.3 mm, and 5.9 mm. Conclusion. Modified Mitchell s osteotomy shortens the length of the first metatarsal bone and thus relieves tension in soft tissues such as the adductor hallucis. Nonetheless, the procedure can induce metatarsophalangeal joint malalignment and metatarsalgia, and plantar callosity may develop or persist after surgery. Combining oblique metatarsal osteotomy of the lesser metatarsal bones is useful in patients with uneven metatarsal bone lengths and metatarsophalangeal joint malalignment. Key words: callosities; hallux valgus; metatarsal bones; metatarsalgia; metatarsophalangeal joint; osteotomy Address correspondence and reprint requests to: Dr Kengo Yamamoto, Department of Orthopedic Surgery, Tokyo Medical University, Nishishijujku, Shinjuku-ku, Tokyo , Japan. kengo-y@tkg.att.ne.jp
2 246 K Yamamoto et al. Journal of Orthopaedic Surgery INTRODUCTION Mitchell s osteotomy is an osteotomy of the distal first metatarsal for the treatment of hallux valgus and was originally described in It provides stable surgical results and is a relatively convenient surgical procedure consisting of a step metatarsal osteotomy of the first metatarsal, exostosis resection, and reefing of the medial articular capsule of the first metatarsophalangeal (MTP) joint. Mitchell s osteotomy has been performed to treat mild-to-moderate hallux valgus, while its combination with proximal metatarsal osteotomy and first MTP joint lateral soft-tissue dissection has been used to treat severe hallux valgus. We have been treating severe hallux valgus using a modified Mitchell s osteotomy combined with first MTP joint lateral soft-tissue dissection as needed. 2,3 Postoperative metatarsalgia and plantar callosity have been associated with surgery for hallux valgus. We obtained favourable results by performing oblique metatarsal osteotomy for the second to fifth metatarsals (the lesser metatarsals). This article discusses the postoperative results of the modified Mitchell s osteotomy, how this procedure can be used to treat hallux valgus, and the usefulness of combining this technique with oblique lesser metatarsal osteotomy. MATERIALS AND METHODS We have performed modified Mitchell s osteotomy to treat hallux valgus since However, some patients have experienced persistent postoperative metatarsalgia and plantar callosity. After 1986, modified Mitchell s osteotomy augmented with oblique lesser metatarsal osteotomy was used when the patient s preoperative pain on the plantar side of the second to fifth metatarsal heads was severe, or when distribution of plantar pressure was considerably higher on the plantar surfaces of the second to fifth metatarsals compared with the plantar surface of the first metatarsal as measured by a foot pressure distribution device (Predas MP4800; Anima, Tokyo, Japan). Between July 1987 and September 2000, 84 feet in 55 patients underwent modified Mitchell s osteotomy. Of these, 53 feet in 31 patients (one man and 30 women) who were followed up for at least 5 years comprised group A. 67 feet in 36 patients underwent modified Mitchell s osteotomy augmented with oblique lesser metatarsal osteotomy. Of these, 40 feet in 22 patients (one man and 21 women) who were followed up for at least 5 years comprised group B. In group B, oblique lesser metatarsal osteotomy was performed on the second and third metatarsal bones in 22 feet, on the second metatarsal bone in 7 feet, and on other metatarsal bones in 11 feet. The age of the patients at the time of surgery ranged from 19 to 68 years (mean, 49.6 years; standard deviation [SD], 14.5 years) in group A, and 17 to 83 years (mean, 47.4 years; SD, 15.9 years) in group B. The duration of follow-up ranged from 5 years 4 months to 18 years 4 months (mean, 8 years 2 months) in group A, and from 5 years 1 month to 12 years 6 months (mean, 7 years 5 months) in group B. Since postoperative follow-up period varied between the 2 groups, outcomes were compared at 5 years after surgery. Postoperative results for hallux valgus have been assessed by different standards developed by Shapiro and Heller, 4 Glynn et al., 5 and, more recently, the American Orthopedic Foot and Ankle Society s Hallux Metatarsophalangeal Interphalangeal Scale. In the present study, the Tokyo Medical University Classification was used 3 an assessment system that takes into account both subjective complaints and objective findings: pain in the first MTP joint, deformity, plantar callosity and/or metatarsalgia of lesser metatarsals, use of commercially available shoes, and local inflammatory symptoms are quantified, with highest total score being 10 (Table 1). The Mann-Whitney U test, paired t-test, and Chi squared test were used for statistical analyses with the significance level set at p<0.01. Several parameters were measured before and after surgery. The hallux valgus angle, M1-M2 angle, M1- Table 1 Tokyo Medical University Classification 3 for postoperative clinical assessment of hallux valgus Pain in the first metatarsophalangeal (MTP) joint (excluding callus) No pain 2 Pain during walking or exercising 1 Pain at rest 0 Deformity of the first MTP No deformity 2 Mild protrusion 1 Severe protrusion (overlapping with the second toe) 0 Plantar callosity and/or metatarsalgia of lesser metatarsals No callus or pain 3 Have callus but no pain 2 Pain during walking 1 Pain on pressure 0 Use of commercially available shoes Yes 2 Some 1 No 0 Local inflammatory symptoms No 1 Yes 0
3 Vol. 13 No. 3, December 2005 Modified Mitchell s osteotomy 247 Figure 2 The osteotomised region was securely fixed using 2 cross-inserting Kirschner wires. Figure 1 Radiological measurement: (1) hallux valgus angle, (2) M1-M2 angle, (3) M1-M5 angle, (4) length of the first metatarsal bone, and (5) degree of sesamoid bone shifting. M5 angle, degree of sesamoid bone shift, and length of the first, second, and third metatarsal bones were measured in a weight-bearing, standing position on anterior radiographs (Fig. 1). Sesamoid bone shift was defined as the distance between the centre line of the first metatarsal and the medial border of the sesamoid. Surgery was performed when conservative treatments such as pharmacotherapy, orthosis, and exercise therapy were ineffective, and when activities of daily living were hindered, such as when pain made it difficult for the patient to wear shoes. Surgery was not performed when pain or hindrance of activities of daily living were absent, even if the hallux valgus was severe. Surgical technique was similar to the original Mitchell s osteotomy. An arced dorsomedial skin incision was made in the first MTP joint without damaging the dorsomedial cutaneous nerve. A Y- shaped incision in the capsule was then made without removing the bursa. The V -shaped portion of the Y was bent back and both sides of the stem of the Y were inverted peripherally to expose the MTP joint. Figure 3 A plantar orthosis is used 3 weeks after surgery. The first metatarsal bone was dissected subperiosteally from the caput to the centre of the shaft, and the exostosis on the medial side of the metatarsal bone was resected. After cleaning the resection margin using a Surgairtome (Hall Surgical, Largo [FL], US), bone wax was used for haemostasis. In the articular cartilage, a longitudinal sagittal groove was seen, but if the exostosis was resected from the groove, excessive resection could lead to a poor joint fit, and thus resection was conducted while leaving the sagittal groove intact, as far as possible. In the original Mitchell s osteotomy, the first metatarsal was dissected between 1.3 cm and 1.9 cm (1/2 3/4 inch) from the MTP joint, but we moved the dissection slightly proximally, at 2.0 cm to 2.5 cm from the MTP joint. Osteotomy was performed perpendicular to the bone
4 248 K Yamamoto et al. Journal of Orthopaedic Surgery axis using a bone micro saw, and the distal fragment was shaped into a proximally extending lateral step to achieve the planned shifting and shortening. Pronation was corrected while shifting the metatarsal head laterally, and 3-dimensional correction was performed to avoid dorsal flexion. The M1-M2 angle was also corrected. The osteotomised region was securely fixed using 2 cross-inserting Kirschner wires (Fig. 2). If the hallux valgus could not be corrected intraoperatively by gently pulling the medial capsule attached to the proximal phalanx toward the centre of the metatarsal, lateral soft-tissue dissection of the first MTP joint was performed. The skin on the lateral side of the first MTP joint was incised, but when oblique osteotomy was performed on the second metatarsal bone, the skin incision made for the oblique osteotomy was used for soft-tissue dissection. If minimal dissection was desired, a small incision on the lateral capsule was made inside the joint, but if a more extensive dissection was necessary through the joint capsule, a new skin incision was made in order to dissect the adductor hallucis, because dissection performed in a blind manner can lead to the onset of osteoarthritis in MTP joints soon after surgery. Three of 6 feet with hallux valgus angles over 50 Ο, and 3 of 22 feet with angles between 40 Ο and 49 Ο underwent such a procedure. If the hallux valgus could be corrected intraoperatively by gently pulling the medial capsule, the articular capsule that had been opened in a Y shape and inverted was reefed with a slight over-correction in the shape of a letter V. The Kirschner wires were embedded subcutaneously. When one oblique lesser metatarsal osteotomy was included, an approximately 3-cm vertical incision was made above the target metatarsal bone. When 2 oblique lesser metatarsal osteotomies were performed, a skin incision was made between the 2 target metatarsal bones. When combined surgery of lateral soft-tissue dissection of the first MTP joint and an oblique osteotomy of the second metatarsal bone was performed, a skin incision was also made between the first and second metatarsal bones. This oblique lesser metatarsal osteotomy was performed according to Helal, 6 but internal fixation of the osteotomised region was not performed, and shortening was achieved by sliding fragments and by early loading. Caution should be exercised in such situations because excessive periosteal dissection may lead to lateral dislocation of the metatarsal head. Immediately after surgery, several 2.5-cm wide elastic adhesive bandages were used to maintain the surgically corrected position. Once the surgical wound was stabilised, a plaster cast was wrapped over the bandages, and as soon as the swelling subsided, patients were allowed to initiate weight-bearing walk. A plantar orthosis was used 3 weeks after surgery (Fig. 3). Kirschner wires were removed under local anaesthesia 6 to 8 weeks after surgery following radiographic confirmation of bone union. The guidelines for the start of weight-bearing walk were also applicable when an oblique lesser metatarsal osteotomy was performed. Because Japanese people walk barefoot indoors and contracture of the first MTP joint may hinder activities of daily living, it was important to initiate range of motion exercises 3 weeks after surgery when the cast was removed. The orthosis was used day and night for 6 months after surgery, and patients were instructed to do Hohmann s exercises. RESULTS According to the clinical assessment system developed by the Tokyo Medical University, 3 mean preoperative and postoperative 5-year scores, respectively, were 0.9 and 1.7 points in the pain category, 0.4 and 1.5 points in deformity, 1.3 and 2.3 points in plantar callosity and metatarsalgia, 1.0 and 1.6 points in use of commercially available shoes, and 0.3 and 1.0 points in local inflammatory symptoms, with total scores of 3.8 and 7.9. The results demonstrate significant improvement in each of these parameters (Mann-Whitney U test, p<0.005). Comparison between groups A and B revealed no significant differences in pain, deformity, or inflammation scores, but showed a significant difference in the scores of plantar callosity and metatarsalgia, use of commercially available shoes, and total score. These findings demonstrate the effectiveness of oblique lesser metatarsal osteotomy in alleviating plantar callosity and metatarsalgia (Table 2). Before surgery, at postoperative 3 weeks, and at postoperative 5 years in the radiological assessment, respectively, the mean hallux valgus angles, M1-M2 angles, M1-M5 angles, and sesamoid bone shifts are shown in Figure 4. There was significant improvement in each of these parameters at postoperative 3 weeks, but a slight increase was found at postoperative 5 years. Because the hallux valgus angle and sesamoid bone shift are more likely to be affected by soft-tissue dissection, the degree of increase was slightly larger (paired t-test) (Fig. 4). Hallux valgus angles of 30 Ο accounted for 73.1% of the cases, while severe hallux valgus of 40 Ο accounted for 30.1%. Comparison within each severity group showed no significant differences in the hallux valgus angle at postoperative 3 weeks or at postoperative 5 years (Mann-Whitney U test; Table 3). The mean hallux valgus angle at postoperative 5
5 * Vol. 13 No. 3, December 2005 Modified Mitchell s osteotomy 249 Table 2 Clinical assessment scores for groups A and B* Clinical assessment Preoperative Postoperative 5 years Group A Group B Group A Group B Pain in the first metatarsophalangeal (MTP) joint 0.9 (0.6) 0.9 (0.4) 1.6 (0.6) 1.7 (0.6) (excluding callus) [2 points] Deformity of the first MTP (2 points) 0.4 (0.7) 0.4 (0.5) 1.3 (0.7) 1.5 (0.6) Plantar callosity and/or metatarsalgia of lesser 1.4 (1.1) 1.5 (0.9) 1.6 (1.2) 2.7 (0.5) metatarsals (3 points) Use of commercially available shoes (2 points) 1.0 (0.4) 1.4 (0.5) 1.0 (0.5) 1.7 (0.5) Local inflammatory symptoms (1 point) 0.4 (0.5) 0.3 (0.4) 1.0 (0.0) 0.9 (0.3) Total (10 points) 4.0 (2.2) 4.0 (1.5) 6.9 (2.2) 8.5 (1.6) * Values are expressed as mean (standard deviation) Mann-Whitney U test, p<0.005 Mann-Whitney U test, p<0.01 (a) Hallux valgus angle 50 Ο 34.2± Ο (b) M1-M2 angle 25 Ο 16.7± Ο * p<0.01 ** p< Ο 20 Ο 17.1± ± Ο 10 Ο 7.4± ± Ο 5 Ο 0 Ο Preoperative Postoperative 3 weeks Postoperative 5 years 0 Ο Preoperative Postoperative 3 weeks Postoperative 5 years (c) M1-M5 angle (d) Sesamoid bone shift 40 Ο 15 Ο 30 Ο 34.9± Ο 8.7± ± Ο 10 Ο 25.8± ±4.6 5 Ο 4.3±2.1 0 Ο Preoperative Postoperative 3 weeks Postoperative 5 years 0 Ο Preoperative Postoperative 3 weeks Postoperative 5 years Figure 4 Comparison of preoperative and postoperative changes in (a) hallux valgus angle, (b) M1-M2 angle, (c) M1-M5 angle, and (d) sesamoid bone shift using paired t-test.
6 250 K Yamamoto et al. Journal of Orthopaedic Surgery Table 3 Changes in hallux valgus angle in relation to severity Hallux valgus angle No. of feet Hallux valgus angle (mean, SD) Preoperative Postoperative 3 weeks Postoperative 5 years 50 o o (5.2 o ) 18.8 o (13.0 o ) 20.0 o (15.0 o ) 40 o 49 o o (2.7 o ) 13.1 o (6.1 o ) o (7.3 o )2 30 o 39 o o (2.7 o ) 12.6 o (4.5 o ) o (6.2 o )2 20 o 29 o o (2.6 o ) 29.4 o (3.3 o ) o (5.7 o )2 <20 o o (1.6 o ) 26.2 o (2.2 o ) o (3.9 o )2 Group A (42 feet) Group B (51 feet) Total (93 feet) 20 feet 22 feet 43 feet 8 feet 63 feet 30 feet Improved Persistent 0% 20% 40% 60% 80% 100% Figure 5 Comparison of the results of 2 surgical methods in improvement in plantar callosity or metatarsalgia. years was 17.5 Ο (SD, 7.2 Ο ) in group A, and 16.6 Ο (SD, 7.6 Ο ) in group B. No significant difference was found between these 2 groups. Intra-operatively, we empirically concluded that it was necessary to perform first MTP joint lateral softtissue dissection in 6 feet: 3 with hallux valgus angles over 50 Ο and 3 with angles of 40 Ο to 49 Ο. When comparing the postoperative hallux valgus angles between these 6 feet and the other 22 feet not requiring lateral soft-tissue dissection although their hallux valgus angles were also either >50 Ο or 40 Ο 49 Ο, the mean hallux valgus angle of the first group at postoperative 5 years was 20.7 Ο (SD, 13.1 Ο ), and that of the second group was 19.8 Ο (SD, 11.3 Ο ). No significant difference was found between the 2 groups (Mann-Whitney U test). The mean decrease in the length of the first, second, and third metatarsal bones was 3.7 mm (6.4%), 6.2 mm (9.0%), and 4.2 mm (6.3%), respectively. Plantar callosity and metatarsalgia persisted in 53.1% and 14.7% of feet in group A and group B, respectively. These observations confirmed the effectiveness of oblique metatarsal osteotomy (Chi squared test, p<0.0005; Fig. 5). DISCUSSION There are more than 130 surgical methods for the treatment of hallux valgus. Several attempts have been made to develop a surgical method to treat all hallux valgus regardless of the severity. In recent years, surgical methods have been selected based on severity and condition: parameters such as hallux valgus angle or M1-M2 angle. As a general rule, a hallux valgus angle
7 Vol. 13 No. 3, December 2005 Modified Mitchell s osteotomy 251 of <20 Ο is considered mild, 20 Ο 39 Ο moderate, and >40 Ο severe. Distal metatarsal osteotomies such as Mitchell s osteotomy or Hohmann s osteotomy are performed to treat mild-to-moderate hallux valgus, whereas proximal osteotomy such as Mann s osteotomy with soft-tissue dissection is combined to treat moderate-to-severe hallux valgus. The indication for Mitchell s osteotomy varies among authors: Mann 7 suggested it be performed when the M1-M2 angle is <20 Ο and the hallux valgus angle is <40 Ο, Tanaka et al. 8 suggested an M1-M2 angle of <15 Ο and hallux valgus angle of <33 Ο. Modified Mitchell s osteotomy and MTP joint lateral soft-tissue dissection have been combined to treat severe hallux valgus in our department, and relatively favourable results have been obtained. Senba and Nomura 9 combined the Hammond osteotomy (distal osteotomy) and MTP joint lateral soft-tissue dissection for the treatment of severe hallux valgus and recommended that this method be used when the hallux valgus angle is 35 Ο and the M1-M2 angle is 20 Ο. It was once reported that combining distal osteotomy and lateral soft-tissue dissection increased the risk of osteonecrosis, 10 which was also true when proximal metatarsal osteotomy and first MTP joint softtissue dissection were performed to treat severe hallux valgus. However, we did not experience osteonecrosis following lateral soft-tissue dissection because vascularisation in the plantar and medial sides of the first metatarsal bone was rich. We compared the results of modified Mitchell s osteotomy with its combination with lateral soft-tissue dissection in cases with hallux valgus angles of >40 Ο and found a similar degree of recovery for both groups. We therefore concluded that a combination of modified Mitchell s osteotomy and first MTP joint lateral soft-tissue dissection is viable in the treatment of severe hallux valgus. Hallux valgus is often complicated by flat foot or metatarsus latus, and MTP joint malalignment often leads to metatarsalgia or plantar callosity. There have been numerous reports on the incidence of postoperative metatarsalgia and callosity: Mitchell at al. 1 reported 32%, Mann et al %, Wilson %, Glynn et al. 5 20%, Shapiro and Heller 4 33%, and Lindgren and Turan %. In order to avoid inducing MTP joint malalignment, we performed oblique osteotomy on the other metatarsal bones, particularly the second and third metatarsal bones. Nonetheless, in some cases, 3-dimensional corrective osteotomy of the first metatarsal bone is sufficient for correcting broad foot and improving metatarsalgia and plantar callosity. Therefore, whether to perform oblique lesser metatarsal osteotomy should be based on the severity of metatarsalgia or plantar callosity, length of the first and second metatarsal bones, and distribution of plantar pressure. The shortening of the first metatarsal by different osteotomies varies: 6 7 mm by Mitchell s osteotomy, 1 2 mm by Mann s osteotomy, 14 and 2.7 mm by Lindgren s osteotomy. 15 All of the osteotomies can shorten the first metatarsal and effectively relieve tension in the adductor hallucis, but may exacerbate MTP joint malalignment and lead to postoperative metatarsalgia and plantar callosity. Therefore, shortening of the first metatarsal bone is safe if MTP joint alignment is normal, but shortening should be minimised if MTP joint malalignment is detected or postoperative misalignment is expected. Correction of the M1-M2 angle largely depends on the amount of peripheral fragment displacement following osteotomy. During preoperative planning, if the metatarsus primus varus is marked and the M1-M2 angle is large, the lateral step should also be large. If the degree of lateral shift of the metatarsal head is too great, the osteotomised region will become unstable and hinder bone fusion. Mitchell et al. 1 suggested that the upper limit of displacement was one third of the horizontal diameter. We recommend an upper limit of displacement of about 40%. CONCLUSION Modified Mitchell s osteotomy is a fine surgical method for the treatment of hallux valgus providing stable results. Despite slightly poorer results in severe cases, the use of additional procedures allows successful treatment of the condition. Numerous further modifications to the modified Mitchell s osteotomy are performed in our department, including osteotomy methods, location, fixation, first MTP joint lateral soft-tissue dissection, and oblique osteotomy. Therefore, it may not be appropriate to refer our method as modified Mitchell s osteotomy because it is no longer a simple procedure like the original Mitchell s osteotomy. ACKNOWLEDGEMENT The authors wish to thank Prof J Patrick Barron of the International Medical Communications Center of the Tokyo Medical University for reviewing this manuscript.
8 252 K Yamamoto et al. Journal of Orthopaedic Surgery REFERENCES 1. Mitchell CL, Fleming JL, Allen R, Glenney C, Sanford GA. Osteotomy-bunionectomy for hallux valgus. J Bone Joint Surg Am 1958;40: Imakiire A, Koizumi R, Katori Y. Modified Mitchell s operation [in Japanese]. MB Orthop 2001;14: Miura Y. Modified Mitchell s operation [in Japanese]. Orthop Surg Traumatol 1991;34: Shapiro F, Heller L. The Mitchell distal metatarsal osteotomy in the treatment of hallux valgus. Clin Orthop Relat Res 1975; 107: Glynn MK, Dunlop JB, Fitzpatrick D. The Mitchell distal metatarsal osteotomy for hallux valgus. J Bone Joint Surg Br 1980; 62: Helal B. Metatarsal osteotomy for metatarsalgia. J Bone Joint Surg Br 1975;57: Mann RA. Bunion surgery: decision making. Orthopedics 1990;13: Tanaka Y, Takakura Y, Kitada T, Aoki T, Tamai S. A follow-up study of Mitchell osteotomy for the halux valgus. J Jpn Orthop Assoc 1992;66(Suppl):S Senba H, Nomura S. Hammond s procedure [in Japanese]. MB Orthop 2001;14: Meier PJ, Kenzora JE. The risks and benefits of distal first metatarsal osteotomies. Foot Ankle 1985;6: Mann RA, Rudicel S, Graves SC. Repair of hallux valgus with a distal soft-tissue procedure and proximal metatarsal osteotomy. A long-term follow-up. J Bone Joint Surg Am 1992;74: Wilson JN. Oblique displacement osteotomy for hallux valgus. J Bone Joint Surg Br 1963;45: Lindgren U, Turan I. A new operation for hallux valgus. Clin Orthop Relat Res 1983;175: Mann RA, Coughlin MJ. Hallux valgus etiology, anatomy, treatment and surgical considerations. Clin Orthop Relat Res 1981;157: Mizuno K. Oblique osteotomy for hallux valgus. Operation 1988;32:
Proximal metatarsal osteotomy and distal soft tissue reconstruction as treatment for hallux valgus deformity
 REVIEW Proximal metatarsal osteotomy and distal soft tissue reconstruction as treatment for hallux valgus deformity Michael J. Coughlin and J. Speight Grimes Boise, Idaho, USA (Received for publication
REVIEW Proximal metatarsal osteotomy and distal soft tissue reconstruction as treatment for hallux valgus deformity Michael J. Coughlin and J. Speight Grimes Boise, Idaho, USA (Received for publication
Comparison of Postoperative Outcomes between Modified Mann Procedure and Modified Lapidus Procedure for Hallux Valgus
 Comparison of Postoperative Outcomes between Modified Mann Procedure and Modified Lapidus Procedure for Hallux Valgus Yui Akiyama, Takaaki Hirano, Hiroyuki Mitsui Shingo Maeda, Hisateru Niki Department
Comparison of Postoperative Outcomes between Modified Mann Procedure and Modified Lapidus Procedure for Hallux Valgus Yui Akiyama, Takaaki Hirano, Hiroyuki Mitsui Shingo Maeda, Hisateru Niki Department
Hallux Valgus Deformity: Preoperative Radiologic Assessment
 119 Pictorial Essay H............ - Hallux Valgus Deformity: Preoperative Radiologic Assessment David Karasick1 and Keith L. Wapner An estimated 40% of the American adult population experiences foot problems,
119 Pictorial Essay H............ - Hallux Valgus Deformity: Preoperative Radiologic Assessment David Karasick1 and Keith L. Wapner An estimated 40% of the American adult population experiences foot problems,
Complications associated with Mitchell s Osteotomy for Hallux Valgus Correction: A retrospective hospital review
 The Foot and Ankle Online Journal Official publication of the International Foot & Ankle Foundation Complications associated with Mitchell s Osteotomy for Hallux Valgus Correction: A retrospective hospital
The Foot and Ankle Online Journal Official publication of the International Foot & Ankle Foundation Complications associated with Mitchell s Osteotomy for Hallux Valgus Correction: A retrospective hospital
Medincenter GlavUpDK by the Ministry of Foreign Affairs of Russia, Moscow.
 Medincenter GlavUpDK by the Ministry of Foreign Affairs of Russia, Moscow. Berezhnoy Sergey. Percutaneous First Metatarsocuneiform Joint Arthrodesis in a Treatment of Metatarsus Primus Varus: a Prospective
Medincenter GlavUpDK by the Ministry of Foreign Affairs of Russia, Moscow. Berezhnoy Sergey. Percutaneous First Metatarsocuneiform Joint Arthrodesis in a Treatment of Metatarsus Primus Varus: a Prospective
Case 57 What is the diagnosis? Insidious onset forefoot pain in a 50 year old female for last 3 months.
 Case 57 What is the diagnosis? Insidious onset forefoot pain in a 50 year old female for last 3 months. Diagnosis: II MTP instability Demographics of MT instability Lesser MTP joint instability occurs
Case 57 What is the diagnosis? Insidious onset forefoot pain in a 50 year old female for last 3 months. Diagnosis: II MTP instability Demographics of MT instability Lesser MTP joint instability occurs
Chevron Osteotomy With Lateral Soft Tissue Release
 5(4):250 256, 2006 T E C H N I Q U E Chevron Osteotomy With Lateral Soft Tissue Release Hans-Jörg Trnka, MD, PhD and Stefan Gerhard Hofstaetter, MD Foot and Ankle Center Vienna Vienna, Austria Ó 2006 Lippincott
5(4):250 256, 2006 T E C H N I Q U E Chevron Osteotomy With Lateral Soft Tissue Release Hans-Jörg Trnka, MD, PhD and Stefan Gerhard Hofstaetter, MD Foot and Ankle Center Vienna Vienna, Austria Ó 2006 Lippincott
Re+Line Bunion Correction System for Correction of Hallux Abducto Valgus Deformity
 Re+Line Bunion Correction System for Correction of Hallux Abducto Valgus Deformity Amber M. Shane, DPM, FACFAS 1, Christopher L. Reeves, DPM, FACFAS 1 1. Orlando Foot & Ankle Clinic, Orlando, FL Abstract
Re+Line Bunion Correction System for Correction of Hallux Abducto Valgus Deformity Amber M. Shane, DPM, FACFAS 1, Christopher L. Reeves, DPM, FACFAS 1 1. Orlando Foot & Ankle Clinic, Orlando, FL Abstract
The Ludloff Osteotomy
 Techniques in Foot and Ankle Surgery 4(4):263 268, 2005 Ó 2005 Lippincott Williams & Wilkins, Philadelphia The Ludloff Osteotomy T E C H N I Q U E Hans-Jörg Trnka, MD, PhD and Stefan Hofstätter, MD Foot
Techniques in Foot and Ankle Surgery 4(4):263 268, 2005 Ó 2005 Lippincott Williams & Wilkins, Philadelphia The Ludloff Osteotomy T E C H N I Q U E Hans-Jörg Trnka, MD, PhD and Stefan Hofstätter, MD Foot
Moderate to severe hallux valgus deformity: correction with proximal crescentic osteotomy and distal soft-tissue release
 Arch Orthop Trauma Surg (2000) 120 : 397 402 Springer-Verlag 2000 ORIGINAL ARTICLE R. Zettl H.-J. Trnka M. Easley M. Salzer P. Ritschl Moderate to severe hallux valgus deformity: correction with proximal
Arch Orthop Trauma Surg (2000) 120 : 397 402 Springer-Verlag 2000 ORIGINAL ARTICLE R. Zettl H.-J. Trnka M. Easley M. Salzer P. Ritschl Moderate to severe hallux valgus deformity: correction with proximal
Minimally Invasive Bunionectomy: The Lam Modification of the Traditional Distal First Metatarsal Osteotomy Bunionectomy
 CHAPTER 2 Minimally Invasive Bunionectomy: The Lam Modification of the Traditional Distal First Metatarsal Osteotomy Bunionectomy Kevin Lam, DPM Rikhil Patel, DPM Thomas Merrill, DPM Hallux abducto valgus
CHAPTER 2 Minimally Invasive Bunionectomy: The Lam Modification of the Traditional Distal First Metatarsal Osteotomy Bunionectomy Kevin Lam, DPM Rikhil Patel, DPM Thomas Merrill, DPM Hallux abducto valgus
Efficacy of a Kirschner-Wire Guide in Distal Linear Metatarsal Osteotomy for Correction of Hallux Valgus
 Efficacy of a Kirschner-Wire Guide in Distal Linear Metatarsal Osteotomy for Correction of Hallux Valgus Department of Orthopaedic Surgery, Faculty of Medicine, Fukuoka University Takefumi Nishino MD,
Efficacy of a Kirschner-Wire Guide in Distal Linear Metatarsal Osteotomy for Correction of Hallux Valgus Department of Orthopaedic Surgery, Faculty of Medicine, Fukuoka University Takefumi Nishino MD,
Modified Proximal Scarf Osteotomy for Hallux Valgus
 Original Article Clinics in Orthopedic Surgery 2018;10:479-483 https://doi.org/10.4055/cios.2018.10.4.479 Modified Proximal Scarf Osteotomy for Hallux Valgus Ki Won Young, MD, Hong Seop Lee, MD, Seong
Original Article Clinics in Orthopedic Surgery 2018;10:479-483 https://doi.org/10.4055/cios.2018.10.4.479 Modified Proximal Scarf Osteotomy for Hallux Valgus Ki Won Young, MD, Hong Seop Lee, MD, Seong
Use of the 20 Memory Staple in Osteotomies of Fusions of the Forefoot
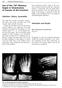 168 Forefoot Reconstruction Use of the 20 Memory Staple in Osteotomies of Fusions of the Forefoot Definition, History, Generalities This staple first provides a permanent compression both in the prongs
168 Forefoot Reconstruction Use of the 20 Memory Staple in Osteotomies of Fusions of the Forefoot Definition, History, Generalities This staple first provides a permanent compression both in the prongs
Soft Tissue Rebalancing Procedures for the Treatment of Hallux Valgus Deformities
 Soft Tissue Rebalancing Procedures for the Treatment of Hallux Valgus Deformities NO DISCLOSURES Objectives The main objectives of any procedure in hallux abducto valgus surgery are to correct the deformity,
Soft Tissue Rebalancing Procedures for the Treatment of Hallux Valgus Deformities NO DISCLOSURES Objectives The main objectives of any procedure in hallux abducto valgus surgery are to correct the deformity,
Introduction Basics MIS Screw 2 System Characteristics 2 Indication 2
 Clinical Advisor M. Walther. M.D., Ph.D. Professor of Orthopedic Surgery Head of Department Centre for Foot and Ankle Surgery Schön Klinik München Harlaching FIFA Medical Centre Table of Contents Introduction
Clinical Advisor M. Walther. M.D., Ph.D. Professor of Orthopedic Surgery Head of Department Centre for Foot and Ankle Surgery Schön Klinik München Harlaching FIFA Medical Centre Table of Contents Introduction
1 Relationship between degenerative change in the sesamoid-metatarsal joint and 2 displacement of the sesamoids in patients with hallux valgus 3 4
 1 Relationship between degenerative change in the sesamoid-metatarsal joint and 2 displacement of the sesamoids in patients with hallux valgus 3 4 Abstract 5 Background: To treat a patient with hallux
1 Relationship between degenerative change in the sesamoid-metatarsal joint and 2 displacement of the sesamoids in patients with hallux valgus 3 4 Abstract 5 Background: To treat a patient with hallux
Merete PlantarMAX Lapidus Plate Surgical Technique. Description of Plate
 Merete PlantarMAX Lapidus Plate Surgical Technique Description of Plate Merete Medical has designed the PlantarMax; a special Plantar/Medial Locking Lapidus plate which places the plate in the most biomechanically
Merete PlantarMAX Lapidus Plate Surgical Technique Description of Plate Merete Medical has designed the PlantarMax; a special Plantar/Medial Locking Lapidus plate which places the plate in the most biomechanically
Effect of metatarsal osteotomy and open lateral soft tissue procedure on sesamoid position: radiological assessment
 Choi et al. Journal of Orthopaedic Surgery and Research (2018) 13:11 DOI 10.1186/s13018-017-0712-y RESEARCH ARTICLE Effect of metatarsal osteotomy and open lateral soft tissue procedure on sesamoid position:
Choi et al. Journal of Orthopaedic Surgery and Research (2018) 13:11 DOI 10.1186/s13018-017-0712-y RESEARCH ARTICLE Effect of metatarsal osteotomy and open lateral soft tissue procedure on sesamoid position:
A Patient s Guide to Bunions. Foot and Ankle Center of Massachusetts, P.C.
 A Patient s Guide to Bunions Welcome to Foot and Ankle Center of Massachusetts, where we believe in accelerating your learning curve with educational materials that are clearly written and professionally
A Patient s Guide to Bunions Welcome to Foot and Ankle Center of Massachusetts, where we believe in accelerating your learning curve with educational materials that are clearly written and professionally
A COMPARISON OF KELLER S ARTHROPLASTY AND DISTAL METATARSAL OSTEOTOMY IN THE TREATMENT OF ADULT HALLUX VALGUS
 A COMPARISON OF KELLER S ARTHROPLASTY AND DISTAL METATARSAL OSTEOTOMY IN THE TREATMENT OF ADULT HALLUX VALGUS TIMOTHY TURNBULL, WILLIAM GRANGE From the North East Thames Regional Orthopaedic Centre, Black
A COMPARISON OF KELLER S ARTHROPLASTY AND DISTAL METATARSAL OSTEOTOMY IN THE TREATMENT OF ADULT HALLUX VALGUS TIMOTHY TURNBULL, WILLIAM GRANGE From the North East Thames Regional Orthopaedic Centre, Black
Bunions. Compliments of: Institute of Sports Medicine & Orthopaedics
 A Patient s Guide to Bunions 20295 NE 29th Place, Ste 300 Aventura, FL 33180 Phone: (786) 629-0910 Fax: (786) 629-0920 admin@instituteofsports.com DISCLAIMER: The information in this booklet is compiled
A Patient s Guide to Bunions 20295 NE 29th Place, Ste 300 Aventura, FL 33180 Phone: (786) 629-0910 Fax: (786) 629-0920 admin@instituteofsports.com DISCLAIMER: The information in this booklet is compiled
Index. Clin Podiatr Med Surg 22 (2005) Note: Page numbers of article titles are in boldface type.
 Clin Podiatr Med Surg 22 (2005) 309 314 Index Note: Page numbers of article titles are in boldface type. A Abductor digiti minimi muscle, myectomy of, for tailor s bunionette, 243 Achilles tendon, lengthening
Clin Podiatr Med Surg 22 (2005) 309 314 Index Note: Page numbers of article titles are in boldface type. A Abductor digiti minimi muscle, myectomy of, for tailor s bunionette, 243 Achilles tendon, lengthening
JUVENILE AND ADOLESCENT HALLUX VALGUS. George E. Quill, Jr., M.D.
 JUVENILE AND ADOLESCENT HALLUX VALGUS George E. Quill, Jr., M.D. The development of a hallux valgus deformity in children and adolescents is actually an uncommon entity. Most of these occurrences can be
JUVENILE AND ADOLESCENT HALLUX VALGUS George E. Quill, Jr., M.D. The development of a hallux valgus deformity in children and adolescents is actually an uncommon entity. Most of these occurrences can be
PROstep Minimally Invasive Surgery HALLUX VALGUS CORRECTION USING PROSTEP MICA MINIMALLY INVASIVE FOOT SURGERY: TWO CASE STUDIES
 PROstep Minimally Invasive Surgery HALLUX VALGUS CORRECTION USING PROSTEP MICA MINIMALLY INVASIVE FOOT SURGERY: TWO CASE STUDIES AS PRESENTED BY: JOEL VERNOIS M.D. 016798A Case Study 1 PROstep Minimally
PROstep Minimally Invasive Surgery HALLUX VALGUS CORRECTION USING PROSTEP MICA MINIMALLY INVASIVE FOOT SURGERY: TWO CASE STUDIES AS PRESENTED BY: JOEL VERNOIS M.D. 016798A Case Study 1 PROstep Minimally
Classical Mitchell's osteotomy in the management of symptomatic hallux vulgus
 International Journal of Research in Orthopaedics Wani NB et al. Int J Res Orthop. 2016 Dec;2(4):366-370 http://www.ijoro.org Original Research Article DOI: http://dx.doi.org/10.18203/issn.2455-4510.intjresorthop20164170
International Journal of Research in Orthopaedics Wani NB et al. Int J Res Orthop. 2016 Dec;2(4):366-370 http://www.ijoro.org Original Research Article DOI: http://dx.doi.org/10.18203/issn.2455-4510.intjresorthop20164170
Clinical Practice Guideline on the Diagnosis and Treatment of Hallux Valgus
 Archives of Orthopedics and Rheumatology Volume 1, Issue 1, 2018, PP: 7-11 Clinical Practice Guideline on the Diagnosis and Treatment of Hallux Valgus Jorge de las Heras Romero 1 *, Ana María Lledó Alvarez
Archives of Orthopedics and Rheumatology Volume 1, Issue 1, 2018, PP: 7-11 Clinical Practice Guideline on the Diagnosis and Treatment of Hallux Valgus Jorge de las Heras Romero 1 *, Ana María Lledó Alvarez
Joint Preserving Surgery in Severe Forefoot Disorders
 Joint Preserving Surgery in Severe Forefoot Disorders J ORTHOP TRAUMA SURG REL RES 4 (12) 2008 Review article LOUIS S. BAROUK*, PIERRE BAROUK** * 39, Chemin de la Roche, 33370, Yvrac, France ** Clinique
Joint Preserving Surgery in Severe Forefoot Disorders J ORTHOP TRAUMA SURG REL RES 4 (12) 2008 Review article LOUIS S. BAROUK*, PIERRE BAROUK** * 39, Chemin de la Roche, 33370, Yvrac, France ** Clinique
Increased pressures at
 Surgical Off-loading of Plantar Hallux Ulcerations These approaches can be used to treat DFUs. By Adam R. Johnson, DPM Increased pressures at the plantar aspect of the hallux leading to chronic hyperkeratosis
Surgical Off-loading of Plantar Hallux Ulcerations These approaches can be used to treat DFUs. By Adam R. Johnson, DPM Increased pressures at the plantar aspect of the hallux leading to chronic hyperkeratosis
The effectiveness of distal soft tissue procedures in hallux valgus
 J Orthopaed Traumatol (2008) 9:117 121 DOI 10.1007/s10195-008-0017-3 ORIGINAL ARTICLE The effectiveness of distal soft tissue procedures in hallux valgus Cemil Kayali Æ Hasan Ozturk Æ Haluk Agus Æ Taskin
J Orthopaed Traumatol (2008) 9:117 121 DOI 10.1007/s10195-008-0017-3 ORIGINAL ARTICLE The effectiveness of distal soft tissue procedures in hallux valgus Cemil Kayali Æ Hasan Ozturk Æ Haluk Agus Æ Taskin
Distal First Metatarsal Displacement Osteotomy
 Distal First Metatarsal Displacement Osteotomy ITS PLACE IN THE SCHEMA OF BUNION SURGERY* From the Section of Orthopedic Surgerv, The Mason Clinic. Seattle ABSTRACT: In a review of 401 operations for symptomatic
Distal First Metatarsal Displacement Osteotomy ITS PLACE IN THE SCHEMA OF BUNION SURGERY* From the Section of Orthopedic Surgerv, The Mason Clinic. Seattle ABSTRACT: In a review of 401 operations for symptomatic
REPAIR OF THE DISPLACED AUSTIN OSTEOTOMY
 C H A P T E R 2 1 REPAIR OF THE DISPLACED AUSTIN OSTEOTOMY John V. Vanore, DPM INTRODUCTION Bunion surgery is frequently performed by foot and ankle surgeons. Generally, bunion surgery is quite predictable,
C H A P T E R 2 1 REPAIR OF THE DISPLACED AUSTIN OSTEOTOMY John V. Vanore, DPM INTRODUCTION Bunion surgery is frequently performed by foot and ankle surgeons. Generally, bunion surgery is quite predictable,
PAINFUL SESAMOID OF THE GREAT TOE Dr Vasu Pai ANATOMICAL CONSIDERATION. At the big toe MTP joint: Tibial sesamoid (medial) & fibular (lateral)
 PAINFUL SESAMOID OF THE GREAT TOE Dr Vasu Pai ANATOMICAL CONSIDERATION At the big toe MTP joint: Tibial sesamoid (medial) & fibular (lateral) They are contained within the tendons of Flexor Hallucis Brevis
PAINFUL SESAMOID OF THE GREAT TOE Dr Vasu Pai ANATOMICAL CONSIDERATION At the big toe MTP joint: Tibial sesamoid (medial) & fibular (lateral) They are contained within the tendons of Flexor Hallucis Brevis
PEDUS-L. Locking Plantar Lapidus Plate
 PEDUS-L Locking Plantar Lapidus Plate Page 1 PEDUS-L - Locking Plantar Lapidus Plate Table of Contents Implants 3 System 4 Operation manual 5 Approach 5 Identification of the TMT 1 joint with a cannula
PEDUS-L Locking Plantar Lapidus Plate Page 1 PEDUS-L - Locking Plantar Lapidus Plate Table of Contents Implants 3 System 4 Operation manual 5 Approach 5 Identification of the TMT 1 joint with a cannula
Foot and Ankle Technique Guide Metatarsal Shortening Osteotomy
 Surgical Technique Foot and Ankle Technique Guide Metatarsal Shortening Osteotomy Prepared in consultation with: Phinit Phisitkul, MD Department of Orthopedics and Rehabilitation University of Iowa Iowa
Surgical Technique Foot and Ankle Technique Guide Metatarsal Shortening Osteotomy Prepared in consultation with: Phinit Phisitkul, MD Department of Orthopedics and Rehabilitation University of Iowa Iowa
Merete BLP. Surgical Technique. - Bunion Locking Plate - Low Profile Locking Bone Plate System
 Merete BLP - Bunion Locking Plate - Low Profile Locking Bone Plate System Surgical Technique Merete Medical, Inc. 49 Purchase Street Rye, N.Y. 10580 Phone: 914 967-1532 www.merete-medical.com - Surgical
Merete BLP - Bunion Locking Plate - Low Profile Locking Bone Plate System Surgical Technique Merete Medical, Inc. 49 Purchase Street Rye, N.Y. 10580 Phone: 914 967-1532 www.merete-medical.com - Surgical
AUTHOR(S): COUGHLIN, MICHAEL J., M.D., BOISE, IDAHO. An Instructional Course Lecture, The American Academy of Orthopaedic Surgeons
 JBJA Journal of Bone and Joint Surgery - American 1996-1998 June 1996, Volume 78-A, Number 6 932 Instructional Course Lectures, The American Academy of Orthopaedic Surgeons - Hallux Valgus* Instructional
JBJA Journal of Bone and Joint Surgery - American 1996-1998 June 1996, Volume 78-A, Number 6 932 Instructional Course Lectures, The American Academy of Orthopaedic Surgeons - Hallux Valgus* Instructional
How to avoid complications of distraction osteogenesis for first brachymetatarsia
 220 Acta Orthopaedica 2009; 80 (2): 220 225 How to avoid complications of distraction osteogenesis for first brachymetatarsia Keun-Bae Lee, Hyun-Kee Yang, Jae-Yoon Chung, Eun-Sun Moon, and Sung-Taek Jung
220 Acta Orthopaedica 2009; 80 (2): 220 225 How to avoid complications of distraction osteogenesis for first brachymetatarsia Keun-Bae Lee, Hyun-Kee Yang, Jae-Yoon Chung, Eun-Sun Moon, and Sung-Taek Jung
19 Arthrodesis of the First Metatarsocuneiform Joint
 19 Arthrodesis of the First Metatarsocuneiform Joint CHARLES GUDAS Abduction of the first metatarsal to correct metatarsus primus varus and hallux valgus was first described by Albrecht in 1911. 1 Lapidus
19 Arthrodesis of the First Metatarsocuneiform Joint CHARLES GUDAS Abduction of the first metatarsal to correct metatarsus primus varus and hallux valgus was first described by Albrecht in 1911. 1 Lapidus
Diagnosing and treating hallux valgus: A conservative approach for a common problem
 REVIEW BRIAN G. DONLEY, MD Orthopaedic surgeon, Cleveland Clinic, specializing in foot and ankle disorders. CHRISTOPHER L. TISDEL, MD Orthopaedic surgeon. Cleveland Clinic. JAMES J. SFERRA, MD Orthopaedic
REVIEW BRIAN G. DONLEY, MD Orthopaedic surgeon, Cleveland Clinic, specializing in foot and ankle disorders. CHRISTOPHER L. TISDEL, MD Orthopaedic surgeon. Cleveland Clinic. JAMES J. SFERRA, MD Orthopaedic
6/5/2018. Forefoot Disorders. Highgate Private Hospital (Royal Free London NHS Foundation Trust (Barnet & Chase Farm Hospitals) Hallux Rigidus
 Forefoot Disorders Mr Pinak Ray (MS, MCh(Orth), FRCS, FRCS(Tr&Orth)) Highgate Private Hospital (Royal Free London NHS Foundation Trust (Barnet & Chase Farm Hospitals) E: ray.secretary@uk-conslutants Our
Forefoot Disorders Mr Pinak Ray (MS, MCh(Orth), FRCS, FRCS(Tr&Orth)) Highgate Private Hospital (Royal Free London NHS Foundation Trust (Barnet & Chase Farm Hospitals) E: ray.secretary@uk-conslutants Our
Endolog Implant for Correction of Hallux Valgus
 Endolog Implant for Correction of Hallux Valgus Surgical Technique Distributed by: Simple and precise Mini-invasive For mild, moderate and severe HV Surgical Indications Endolog implant is proposed for
Endolog Implant for Correction of Hallux Valgus Surgical Technique Distributed by: Simple and precise Mini-invasive For mild, moderate and severe HV Surgical Indications Endolog implant is proposed for
Surgical technique. Angular Stable X-Plate and 2-Hole Plate. For osteotomies, arthrodeses and fractures of the foot.
 Surgical technique Angular Stable X-Plate and 2-Hole Plate. For osteotomies, arthrodeses and fractures of the foot. Table of Contents Indications 4 Implants 5 X-plate: Crescentic osteotomy 6 X-plate:
Surgical technique Angular Stable X-Plate and 2-Hole Plate. For osteotomies, arthrodeses and fractures of the foot. Table of Contents Indications 4 Implants 5 X-plate: Crescentic osteotomy 6 X-plate:
THE FIBULAR SESAMOID ELEVATOR: A New Instrument to Aid the Lateral Release in Hallux Valgus Surgery
 C H A P T E R 1 4 THE FIBULAR SESAMOID ELEVATOR: A New Instrument to Aid the Lateral Release in Hallux Valgus Surgery Thomas F. Smith, DPM Lopa Dalmia, DPM INTRODUCTION Hallux valgus surgery is a complex
C H A P T E R 1 4 THE FIBULAR SESAMOID ELEVATOR: A New Instrument to Aid the Lateral Release in Hallux Valgus Surgery Thomas F. Smith, DPM Lopa Dalmia, DPM INTRODUCTION Hallux valgus surgery is a complex
Fixation of first metatarsal basal osteotomy using Acutrak screw
 Available online at www.sciencedirect.com Foot and Ankle Surgery 14 (2008) 21 25 www.elsevier.com/locate/fas Fixation of first metatarsal basal osteotomy using Acutrak screw G.E. Fadel MD FRCS Tr & Orth*,
Available online at www.sciencedirect.com Foot and Ankle Surgery 14 (2008) 21 25 www.elsevier.com/locate/fas Fixation of first metatarsal basal osteotomy using Acutrak screw G.E. Fadel MD FRCS Tr & Orth*,
CARTIVA. Synthetic Cartilage Implant SURGICAL IMPLANTATION TECHNIQUE. First Metatarsal Phalangeal Joint THE DIFFERENCE IS MOVING.
 CARTIVA Synthetic Cartilage Implant SURGICAL IMPLANTATION TECHNIQUE First Metatarsal Phalangeal Joint THE DIFFERENCE IS MOVING. CARTIVA SYNTHETIC CARTILAGE IMPLANT TABLE OF CONTENTS Introduction... 3 Cartiva
CARTIVA Synthetic Cartilage Implant SURGICAL IMPLANTATION TECHNIQUE First Metatarsal Phalangeal Joint THE DIFFERENCE IS MOVING. CARTIVA SYNTHETIC CARTILAGE IMPLANT TABLE OF CONTENTS Introduction... 3 Cartiva
A comparison of Chevron and Lindgren-Turan osteotomy techniques in hallux valgus surgery: a prospective randomized controlled study
 ORIGINAL ARTICLE Acta Orthop Traumatol Turc 2016;50(3):255 261 doi: 10.3944/AOTT.2016.14.0272 A comparison of Chevron and Lindgren-Turan osteotomy techniques in hallux valgus surgery: a prospective randomized
ORIGINAL ARTICLE Acta Orthop Traumatol Turc 2016;50(3):255 261 doi: 10.3944/AOTT.2016.14.0272 A comparison of Chevron and Lindgren-Turan osteotomy techniques in hallux valgus surgery: a prospective randomized
Combination of First Metatarsophalangeal Joint Arthrodesis and Proximal Correction for Severe Hallux Valgus Deformity
 FOOT &ANKLE INTERNATIONAL DOI: 10.3113/FAI.2012.0400 Combination of First Metatarsophalangeal Joint Arthrodesis and Proximal Correction for Severe Hallux Valgus Deformity Pascal F. Rippstein, MD; Young-Uk
FOOT &ANKLE INTERNATIONAL DOI: 10.3113/FAI.2012.0400 Combination of First Metatarsophalangeal Joint Arthrodesis and Proximal Correction for Severe Hallux Valgus Deformity Pascal F. Rippstein, MD; Young-Uk
Bunions. A bunion is a painful bony bump that develops on the inside of the foot at the big toe joint. Bunions are often referred to as hallux valgus.
 Bunions A bunion is a painful bony bump that develops on the inside of the foot at the big toe joint. Bunions are often referred to as hallux valgus. Bunions develop slowly. Pressure on the big toe joint
Bunions A bunion is a painful bony bump that develops on the inside of the foot at the big toe joint. Bunions are often referred to as hallux valgus. Bunions develop slowly. Pressure on the big toe joint
Metatarsal Lengthening By Callus Distraction For Brachymetatarsia: Case Report and Review of the Literature
 ISPUB.COM The Internet Journal of Third World Medicine Volume 1 Number 2 Metatarsal Lengthening By Callus Distraction For Brachymetatarsia: Case Report and Review of the R Rose Citation R Rose. Metatarsal
ISPUB.COM The Internet Journal of Third World Medicine Volume 1 Number 2 Metatarsal Lengthening By Callus Distraction For Brachymetatarsia: Case Report and Review of the R Rose Citation R Rose. Metatarsal
in the treatment of hallux valgus
 original ARTICLE Our experience with double metatarsal osteotomy in the treatment of hallux valgus Pradeep George Mathew, Pavel Šponer, Jaroslav Pavlata, Haroun Hassan Shaikh Charles University in Prague,
original ARTICLE Our experience with double metatarsal osteotomy in the treatment of hallux valgus Pradeep George Mathew, Pavel Šponer, Jaroslav Pavlata, Haroun Hassan Shaikh Charles University in Prague,
with regard to our presentation.
 Rotated Insertion Metatarsal Osteotomy with Distal Soft Tissue Procedure for Severe Hallux Valgus Deformity Novel Procedure of the 1 st metatarsal osteotomy Norihiro Samoto MD, Ph.D. Director of Department
Rotated Insertion Metatarsal Osteotomy with Distal Soft Tissue Procedure for Severe Hallux Valgus Deformity Novel Procedure of the 1 st metatarsal osteotomy Norihiro Samoto MD, Ph.D. Director of Department
A PROSPECTIVE RANDOMISED CONTROLLED TRIAL
 K. B. Lee, N. Y. Cho, H. W. Park, J. K. Seon, S. H. Lee From Chonnam National University Medical School and Hospital, Gwangju, Korea K. B. Lee, MD, PhD, Professor, Department of J. K. Seon, MD, PhD, Associate
K. B. Lee, N. Y. Cho, H. W. Park, J. K. Seon, S. H. Lee From Chonnam National University Medical School and Hospital, Gwangju, Korea K. B. Lee, MD, PhD, Professor, Department of J. K. Seon, MD, PhD, Associate
QUICK REFERENCE GUIDE. MiniRail System. Part B: Foot Applications. By Dr. B. Magnan, Dr. E. Rodriguez and Dr. G. Vito ALWAYS INNOVATING
 14 MiniRail System Part B: Foot Applications By Dr. B. Magnan, Dr. E. Rodriguez and Dr. G. Vito ALWAYS INNOVATING ORDERING INFORMATION Sterilization box, empty M190 Can accommodate: M101 Standard MiniRail
14 MiniRail System Part B: Foot Applications By Dr. B. Magnan, Dr. E. Rodriguez and Dr. G. Vito ALWAYS INNOVATING ORDERING INFORMATION Sterilization box, empty M190 Can accommodate: M101 Standard MiniRail
MICA. Minimally Invasive Foot Surgery CHEVRON OSTEOTOMY SURGIC AL TECHNIQUE
 MICA Minimally Invasive Foot Surgery CHEVRON OSTEOTOMY SURGIC AL TECHNIQUE Contents Chapter 1 4 Introduction Chapter 2 5 Indications and Warnings Chapter 3 6 Patient Positioning and Set Up Chapter 4 7
MICA Minimally Invasive Foot Surgery CHEVRON OSTEOTOMY SURGIC AL TECHNIQUE Contents Chapter 1 4 Introduction Chapter 2 5 Indications and Warnings Chapter 3 6 Patient Positioning and Set Up Chapter 4 7
Long Oblique Distal Osteotomy of the Fifth Metatarsal for Correction of Tailor s Bunion: A Retrospective Review
 Long Oblique Distal Osteotomy of the Fifth Metatarsal for Correction of Tailor s Bunion: A Retrospective Review Barry P. London, DPM, 1 Stephen F. Stern, DPM, 2 Mark A. Quist, DPM, 3 Robert K. Lee, DPM,
Long Oblique Distal Osteotomy of the Fifth Metatarsal for Correction of Tailor s Bunion: A Retrospective Review Barry P. London, DPM, 1 Stephen F. Stern, DPM, 2 Mark A. Quist, DPM, 3 Robert K. Lee, DPM,
1 st MP Arthrodesis. - Unraveling The Myths - Craig A. Camasta, DPM Atlanta, Georgia, USA
 1 st MP Arthrodesis - Unraveling The Myths - Craig A. Camasta, DPM Atlanta, Georgia, USA Hallux Limitus Dorsal Bunion Spasm of Short Flexor Immobility of Sesamoids DJD of 1 st MPJ Hallus Limitus Plantar
1 st MP Arthrodesis - Unraveling The Myths - Craig A. Camasta, DPM Atlanta, Georgia, USA Hallux Limitus Dorsal Bunion Spasm of Short Flexor Immobility of Sesamoids DJD of 1 st MPJ Hallus Limitus Plantar
MiniRail System. Part B: Foot Applications. By Dr. B. Magnan, Dr. E. Rodriguez and Dr. G. Vito
 Q U I C K R E F E R E N C E G U I D E 14 MiniRail System Part B: Foot Applications By Dr. B. Magnan, Dr. E. Rodriguez and Dr. G. Vito ORDERING INFORMATION MiniRail System Kit, M190C Contents: M 101 Standard
Q U I C K R E F E R E N C E G U I D E 14 MiniRail System Part B: Foot Applications By Dr. B. Magnan, Dr. E. Rodriguez and Dr. G. Vito ORDERING INFORMATION MiniRail System Kit, M190C Contents: M 101 Standard
FREIBERG S INFRACTION TREATMENT WITH METATARSAL NECK DORSAL CLOSING WEDGE OSTEOTOMY: REPORT OF TWO CASES
 FREIBERG S INFRACTION TREATMENT WITH METATARSAL NECK DORSAL CLOSING WEDGE OSTEOTOMY: REPORT OF TWO CASES Sung-Yen Lin, 1 Yuh-Min Cheng, 1,2 and Peng-Ju Huang 1,2 1 Department of Orthopedics, Kaohsiung
FREIBERG S INFRACTION TREATMENT WITH METATARSAL NECK DORSAL CLOSING WEDGE OSTEOTOMY: REPORT OF TWO CASES Sung-Yen Lin, 1 Yuh-Min Cheng, 1,2 and Peng-Ju Huang 1,2 1 Department of Orthopedics, Kaohsiung
LAPIDUS What is Old is New
 LAPIDUS What is Old is New Alan Jay Block, DPM, MS, FASPS, FACFAS Fellowship trained in Advanced Ankle Techniques Adjunct Professor Dept Of Orthopeadics The Ohio State University Board Member The Ohio
LAPIDUS What is Old is New Alan Jay Block, DPM, MS, FASPS, FACFAS Fellowship trained in Advanced Ankle Techniques Adjunct Professor Dept Of Orthopeadics The Ohio State University Board Member The Ohio
The Lapidus Procedure as Salvage After Failed Surgical Treatment of Hallux Valgus A PROSPECTIVE COHORT STUDY
 60 COPYRIGHT 2003 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED The Lapidus Procedure as Salvage After Failed Surgical Treatment of Hallux Valgus A PROSPECTIVE COHORT STUDY BY J. CHRIS COETZEE,
60 COPYRIGHT 2003 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED The Lapidus Procedure as Salvage After Failed Surgical Treatment of Hallux Valgus A PROSPECTIVE COHORT STUDY BY J. CHRIS COETZEE,
Accu-Cut Osteotomy Guide System
 Accu-Cut Osteotomy Guide System Surgical Technique Contents Product The BioPro Accu-Cut Osteotomy Guide System provides precise and repeatable osteotomies for many types of bunion correction surgery. Table
Accu-Cut Osteotomy Guide System Surgical Technique Contents Product The BioPro Accu-Cut Osteotomy Guide System provides precise and repeatable osteotomies for many types of bunion correction surgery. Table
Symptomatic Medial Exostosis of the Great Toe Distal Phalanx: A Complication Due to Over-correction Following Akin Osteotomy for Hallux Valgus Repair
 Symptomatic Medial Exostosis of the Great Toe Distal Phalanx: A Complication Due to Over-correction Following Akin Osteotomy for Hallux Valgus Repair Carlos Villas, MD, PhD, 1 Javier Del Río, MD, 3 Andres
Symptomatic Medial Exostosis of the Great Toe Distal Phalanx: A Complication Due to Over-correction Following Akin Osteotomy for Hallux Valgus Repair Carlos Villas, MD, PhD, 1 Javier Del Río, MD, 3 Andres
Investigation performed at the Department of Orthopaedic and Trauma Surgery, Glasgow Royal Infirmary, Glasgow, United Kingdom
 748 COPYRIGHT 2005 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Long-Term Results of the Modified Hoffman Procedure in the Rheumatoid Forefoot BY S. THOMAS, MBCHB, BSC, MRCS, A.W.G. KINNINMONTH,
748 COPYRIGHT 2005 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Long-Term Results of the Modified Hoffman Procedure in the Rheumatoid Forefoot BY S. THOMAS, MBCHB, BSC, MRCS, A.W.G. KINNINMONTH,
Lesser MPJ Hemi Implant
 Lesser MPJ Hemi Implant Surgical Technique Contents Product The BioPro Lesser MPJ Hemi Implant is a simple, durable, metallic hemiarthroplasty resurfacing prosthesis for the treatment of arthritis, Freiberg
Lesser MPJ Hemi Implant Surgical Technique Contents Product The BioPro Lesser MPJ Hemi Implant is a simple, durable, metallic hemiarthroplasty resurfacing prosthesis for the treatment of arthritis, Freiberg
Foot and Ankle Technique Guide Proximal Inter-Phalangeal (PIP) Fusion
 Surgical Technique Foot and Ankle Technique Guide Proximal Inter-Phalangeal (PIP) Fusion Prepared in consultation with: Phinit Phisitkul, MD Department of Orthopedics and Rehabilitation University of Iowa
Surgical Technique Foot and Ankle Technique Guide Proximal Inter-Phalangeal (PIP) Fusion Prepared in consultation with: Phinit Phisitkul, MD Department of Orthopedics and Rehabilitation University of Iowa
THE ROLE OF MINIMALLY INVASIVE SURGERY IN THE FOREFOOT. Miss Sue Kendall PhD FRCS (Orth&Trauma)
 THE ROLE OF MINIMALLY INVASIVE SURGERY IN THE FOREFOOT Miss Sue Kendall PhD FRCS (Orth&Trauma) Is Minimally Invasive Surgery of the foot a good idea? Minimally invasive surgery, keyhole surgery entering
THE ROLE OF MINIMALLY INVASIVE SURGERY IN THE FOREFOOT Miss Sue Kendall PhD FRCS (Orth&Trauma) Is Minimally Invasive Surgery of the foot a good idea? Minimally invasive surgery, keyhole surgery entering
Distal metatarsal osteotomy for hallux varus following surgery for hallux valgus
 FOOT AND ANKLE Distal metatarsal osteotomy for hallux varus following surgery for hallux valgus K. J. Choi, H. S. Lee, Y. S. Yoon, S. S. Park, J. S. Kim, J. J. Jeong, Y. R. Choi From the Asan Medical Center,
FOOT AND ANKLE Distal metatarsal osteotomy for hallux varus following surgery for hallux valgus K. J. Choi, H. S. Lee, Y. S. Yoon, S. S. Park, J. S. Kim, J. J. Jeong, Y. R. Choi From the Asan Medical Center,
Treatment of hallux valgus by modified McBride procedure: a 6-year follow-up
 J Orthopaed Traumatol (2010) 11:89 97 DOI 10.1007/s10195-010-0092-0 ORIGINAL ARTICLE Treatment of hallux valgus by modified McBride procedure: a 6-year follow-up Istemi Yucel Yuksel Tenekecioglu Tahir
J Orthopaed Traumatol (2010) 11:89 97 DOI 10.1007/s10195-010-0092-0 ORIGINAL ARTICLE Treatment of hallux valgus by modified McBride procedure: a 6-year follow-up Istemi Yucel Yuksel Tenekecioglu Tahir
Proximal metatarsal osteotomy for hallux valgus: an audit of radiologic outcome after single screw fixation and full postoperative weightbearing
 Mittag et al. Journal of Foot and Ankle Research 2013, 6:22 JOURNAL OF FOOT AND ANKLE RESEARCH RESEARCH Open Access Proximal metatarsal osteotomy for hallux valgus: an audit of radiologic outcome after
Mittag et al. Journal of Foot and Ankle Research 2013, 6:22 JOURNAL OF FOOT AND ANKLE RESEARCH RESEARCH Open Access Proximal metatarsal osteotomy for hallux valgus: an audit of radiologic outcome after
3 section of the Foot
 TERMINOLOGY 101 How many Bones 3 section of the Foot Bilateral Relating to both Plantar Relating to the bottom or sole Lateral Relating to the outside or farther from the median Medial Relating to the
TERMINOLOGY 101 How many Bones 3 section of the Foot Bilateral Relating to both Plantar Relating to the bottom or sole Lateral Relating to the outside or farther from the median Medial Relating to the
Investigation performed at Orthopaedic Hospital Gersthof, Vienna, Austria
 1131 COPYRIGHT 2004 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Salvage of a Failed Keller Resection Arthroplasty BY FELIX MACHACEK JR., MD, MARK E. EASLEY, MD, FLORIAN GRUBER, MD, PETER RITSCHL,
1131 COPYRIGHT 2004 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Salvage of a Failed Keller Resection Arthroplasty BY FELIX MACHACEK JR., MD, MARK E. EASLEY, MD, FLORIAN GRUBER, MD, PETER RITSCHL,
The risk of avascular necrosis following chevron osteotomy : A prospective study using bone scintigraphy
 Acta Orthop. Belg., 2009, 75, 234-238 ORIGINAL STUDY The risk of avascular necrosis following chevron osteotomy : A prospective study using bone scintigraphy Raheel SHARIFF, Fahad ATTAR, Donald OsARUMWENE,
Acta Orthop. Belg., 2009, 75, 234-238 ORIGINAL STUDY The risk of avascular necrosis following chevron osteotomy : A prospective study using bone scintigraphy Raheel SHARIFF, Fahad ATTAR, Donald OsARUMWENE,
Geoffrey Watson, MD Matthew McKean, MD Siddhant K. Mehta, MD Thom A. Tarquinio, MD
 Geoffrey Watson, MD Matthew McKean, MD Siddhant K. Mehta, MD Thom A. Tarquinio, MD University of Mississippi Medical Center Jackson, Mississippi American Orthopaedic Foot & Ankle Society ANNUAL MEETING
Geoffrey Watson, MD Matthew McKean, MD Siddhant K. Mehta, MD Thom A. Tarquinio, MD University of Mississippi Medical Center Jackson, Mississippi American Orthopaedic Foot & Ankle Society ANNUAL MEETING
Metatarsal Lengthening By Callus Distraction For Brachymetatarsia. Case Report and Review of the Literature
 The Internet Journal of Third World Medicine TM ISSN: 1539-4646 Home Current Issue Archives Instructions for Authors Disclaimer Printable Version Metatarsal Lengthening By Callus Distraction For Brachymetatarsia:
The Internet Journal of Third World Medicine TM ISSN: 1539-4646 Home Current Issue Archives Instructions for Authors Disclaimer Printable Version Metatarsal Lengthening By Callus Distraction For Brachymetatarsia:
HemiEDGE. Patent No. 8,845,750. Surgical Technique
 HemiEDGE Patent No. 8,845,750 Surgical Technique Contents Product Based on the clinical success of our First MPJ Hemi Implant, the HemiEDGE, incorporates an overlapping edge extending around the medial,
HemiEDGE Patent No. 8,845,750 Surgical Technique Contents Product Based on the clinical success of our First MPJ Hemi Implant, the HemiEDGE, incorporates an overlapping edge extending around the medial,
ToeMobile. Surgical Technique. Great Toe Endoprosthesis
 Great Toe Endoprosthesis Surgical Technique Merete Medical, Inc. 99 Purchase Street Rye, N.Y. 10580 Phone: 914 967-1532 Fax: 914-967-1542 E-Mail: service@merete-medical.com www.merete-medical.com - Description
Great Toe Endoprosthesis Surgical Technique Merete Medical, Inc. 99 Purchase Street Rye, N.Y. 10580 Phone: 914 967-1532 Fax: 914-967-1542 E-Mail: service@merete-medical.com www.merete-medical.com - Description
LMH. Minimal Bone Resection. Lesser Metatarsal Head Implant. Thin, low-profile design for minimal bone resection
 Minimal Bone Resection LMH Lesser Metatarsal Head Implant Thin, low-profile design for minimal bone resection Stem offset dorsally for anatomically correct alignment in medullary canal Rectangular shape
Minimal Bone Resection LMH Lesser Metatarsal Head Implant Thin, low-profile design for minimal bone resection Stem offset dorsally for anatomically correct alignment in medullary canal Rectangular shape
Analysis of 3D Foot Shape Features in Elderly with Hallux Valgus Using Multi-Dimensional Scaling Method
 Asian Workshop on D Body Scanning Technologies, Tokyo, Japan, 7-8 April Analysis of D Foot Shape Features in Elderly with Hallux Valgus Using Multi-Dimensional Scaling Method SungHyek KIM Health Science
Asian Workshop on D Body Scanning Technologies, Tokyo, Japan, 7-8 April Analysis of D Foot Shape Features in Elderly with Hallux Valgus Using Multi-Dimensional Scaling Method SungHyek KIM Health Science
Surgical correction of Hallux Valgus
 Surgical correction of Hallux Valgus complicated with adult type Pes planus Department of Orthopedic Surgery, Inje University, Ilsan Paik Hospital, Goyang-si, Korea * W Institute for Foot and Ankle Diseases
Surgical correction of Hallux Valgus complicated with adult type Pes planus Department of Orthopedic Surgery, Inje University, Ilsan Paik Hospital, Goyang-si, Korea * W Institute for Foot and Ankle Diseases
Shinji Isomoto, Norihiro Samoto, Kazuya Sugimoto
 Dept. of Orthop. Surg., Nara Prefecture General Medical Center Shinji Isomoto, Norihiro Samoto, Kazuya Sugimoto Dept. of Orthop. Surg., Nara Prefectural Nara Hospital Yasuhito Tanaka Can Sesamoid Dislocation
Dept. of Orthop. Surg., Nara Prefecture General Medical Center Shinji Isomoto, Norihiro Samoto, Kazuya Sugimoto Dept. of Orthop. Surg., Nara Prefectural Nara Hospital Yasuhito Tanaka Can Sesamoid Dislocation
Pedographic, clinical, and functional Outcome after Scarf Osteotomy Timo J. Lorei, MD Christian Kinast,
 Zentrum FuSS & Sprunggelenk Dr. Kinast Prof. Dr. Hamel Pedographic, clinical, and functional Outcome after Scarf Osteotomy Timo J. Lorei, MD Christian Kinast, MD Hans Klärner, MD and Dieter Rosenbaum,
Zentrum FuSS & Sprunggelenk Dr. Kinast Prof. Dr. Hamel Pedographic, clinical, and functional Outcome after Scarf Osteotomy Timo J. Lorei, MD Christian Kinast, MD Hans Klärner, MD and Dieter Rosenbaum,
Can modification of the Weil osteotomy reduce the risk of dorsiflexion contracture? -A biomechanical cadaveric analysis
 Can modification of the Weil osteotomy reduce the risk of dorsiflexion contracture? -A biomechanical cadaveric analysis Anthony Perera University Hospital of Wales, UK Oscar Helguera-Mendoza Hospital Puerto
Can modification of the Weil osteotomy reduce the risk of dorsiflexion contracture? -A biomechanical cadaveric analysis Anthony Perera University Hospital of Wales, UK Oscar Helguera-Mendoza Hospital Puerto
Bunionectomy-Forefoot Surgery
 Richard M. Marks, MD Professor and Director Division of Foot and Ankle Department of Orthopaedic Surgery Medical College of Wisconsin Explanation: Bunionectomy-Forefoot Surgery A bunion (also called hallux
Richard M. Marks, MD Professor and Director Division of Foot and Ankle Department of Orthopaedic Surgery Medical College of Wisconsin Explanation: Bunionectomy-Forefoot Surgery A bunion (also called hallux
Wu Daniel¹. Abstract. ¹Department of Orthopaedics, Fellow of Hong Kong College of Orthopaedic Surgeons, Hong Kong, China.
 Case Report Journal of Orthopaedic Case Reports 2018 Mar-April : 8(2):Page 42-46 A Case Report of Spontaneous Second Toe Varus Deformity Correction after Hallux Valgus Deformity Correction by a Non-osteotomy
Case Report Journal of Orthopaedic Case Reports 2018 Mar-April : 8(2):Page 42-46 A Case Report of Spontaneous Second Toe Varus Deformity Correction after Hallux Valgus Deformity Correction by a Non-osteotomy
RETROSPECTIVE ANALYSIS OF END-TO-END DIGITAL ARTHRODESIS
 C H A P T E R 1 7 RETROSPECTIVE ANALYSIS OF END-TO-END DIGITAL ARTHRODESIS Michelle L. Butterworth, DPM Michael S. Downey, DPM Digital deformities are one of the most common entities we face as foot and
C H A P T E R 1 7 RETROSPECTIVE ANALYSIS OF END-TO-END DIGITAL ARTHRODESIS Michelle L. Butterworth, DPM Michael S. Downey, DPM Digital deformities are one of the most common entities we face as foot and
Angle-stable Foot plate system Pedus-O and Pedus-U
 www.marquardt-medizintechnik.de Angle-stable Foot plate system Pedus-O and Pedus-U Angle-stable Pedus-O and Pedus-U foot plate system > Angle-stable Pedus-O foot plate system 1. Product characteristics
www.marquardt-medizintechnik.de Angle-stable Foot plate system Pedus-O and Pedus-U Angle-stable Pedus-O and Pedus-U foot plate system > Angle-stable Pedus-O foot plate system 1. Product characteristics
The Flower Medial Column Fusion Plate
 The Flower Medial Column Fusion Plate PROCEDURE GUIDE www.flowerortho.com The Flower Foot & Ankle Application NC FUSION PLATE 2-HOLE COMPRESSION PLATE TMT FUSION PLATE LAPIDUS FUSION PLATE COMPRESSION
The Flower Medial Column Fusion Plate PROCEDURE GUIDE www.flowerortho.com The Flower Foot & Ankle Application NC FUSION PLATE 2-HOLE COMPRESSION PLATE TMT FUSION PLATE LAPIDUS FUSION PLATE COMPRESSION
Accurate determination of screw position in treating fifth metatarsal base fractures to shorten radiation exposure time
 Singapore Med J 2016; 57(11): 619-623 doi: 10.11622/smedj.2015196 Accurate determination of screw position in treating fifth metatarsal base fractures to shorten radiation exposure time Xu Wang 1, MD,
Singapore Med J 2016; 57(11): 619-623 doi: 10.11622/smedj.2015196 Accurate determination of screw position in treating fifth metatarsal base fractures to shorten radiation exposure time Xu Wang 1, MD,
WHAT DO HALLUX VALGUS AND BUNION MEAN?
 Mr Laurence James BSc MBBS MRCS(Eng) FRCS(Tr&Orth) Consultant Orthopaedic Surgeon Foot, Ankle and Sports Injuries WHAT DO HALLUX VALGUS AND BUNION MEAN? Hallux is Latin for great toe and Valgus is Latin
Mr Laurence James BSc MBBS MRCS(Eng) FRCS(Tr&Orth) Consultant Orthopaedic Surgeon Foot, Ankle and Sports Injuries WHAT DO HALLUX VALGUS AND BUNION MEAN? Hallux is Latin for great toe and Valgus is Latin
Dorsal surface-the upper area or top of the foot. Terminology
 It is important to learn the terminology as it relates to feet to properly communicate with referring physicians when necessary and to identify the relationship between the anatomical structure of the
It is important to learn the terminology as it relates to feet to properly communicate with referring physicians when necessary and to identify the relationship between the anatomical structure of the
Early Diagnosis. Instability of the lesser MTP joints (Crossover 2 nd toe deformity) -my 25 year journey- Progressive MTP joint subluxation
 Instability of the lesser MTP joints (Crossover 2 nd toe deformity) -my 25 year journey- Conflicts of interest Arthrex- consultant Arthrex- royalties Elsevier-book royalties Michael J Coughlin, M.D. Early
Instability of the lesser MTP joints (Crossover 2 nd toe deformity) -my 25 year journey- Conflicts of interest Arthrex- consultant Arthrex- royalties Elsevier-book royalties Michael J Coughlin, M.D. Early
Forefoot/Midfoot Plating System. Surgical Technique
 Forefoot/Midfoot Plating System Surgical Technique Acumed is a global leader of innovative orthopaedic and medical solutions. We are dedicated to developing products, service methods, and approaches that
Forefoot/Midfoot Plating System Surgical Technique Acumed is a global leader of innovative orthopaedic and medical solutions. We are dedicated to developing products, service methods, and approaches that
1. Orthoapedic Associates of Michigan, PC, Grand Rapids, MI 2. Michigan State University College of Human Medicine, Grand Rapids, MI
 Second Metatarsal Osteotomy Shortening with Tarsometatarsal Arthrodesis: Comparison of Outcomes Between MSP TM Metatarsal Shortening System and Plates and Screws Donald R. Bohay, MD, FACS 1 ; John G. Anderson,
Second Metatarsal Osteotomy Shortening with Tarsometatarsal Arthrodesis: Comparison of Outcomes Between MSP TM Metatarsal Shortening System and Plates and Screws Donald R. Bohay, MD, FACS 1 ; John G. Anderson,
Weil osteotomy and flexor to extensor transfer for irreparable plantar plate tear: prospective study
 Weil osteotomy and flexor to extensor transfer for irreparable plantar plate tear: prospective study Daniel Baumfeld, MD Fernando Raduan, MD Fernanda Catena, MD Tania Mann, MD Caio Nery, MD Disclosure
Weil osteotomy and flexor to extensor transfer for irreparable plantar plate tear: prospective study Daniel Baumfeld, MD Fernando Raduan, MD Fernanda Catena, MD Tania Mann, MD Caio Nery, MD Disclosure
Section 6: Preoperative Planning
 Clinical Relevance of the PedCat Study: In many ways the PedCat study confirmed radiographic findings. With the measuring tools embedded in the DICOM viewing software it was possible to gauge the thickness
Clinical Relevance of the PedCat Study: In many ways the PedCat study confirmed radiographic findings. With the measuring tools embedded in the DICOM viewing software it was possible to gauge the thickness
Foot & Ankle. EasyClip. Osteosynthesis Compression Staples. Foot & Ankle
 Foot & Ankle EasyClip Osteosynthesis Compression Staples Foot & Ankle Operative Technique EasyClip Osteosynthesis Compression Staples 2 This publication sets forth detailed recommended procedures for using
Foot & Ankle EasyClip Osteosynthesis Compression Staples Foot & Ankle Operative Technique EasyClip Osteosynthesis Compression Staples 2 This publication sets forth detailed recommended procedures for using
Aetiology: Pressure of Distal intermetatarsal ligament against common digital nerve. Lumbar radiculopathy Instability MTPJ joint or inflammatory MPJ
 MORTON S NEUROMA 80% III web space (next common is II). Never occurs in III or IV Common in females in fifties Aetiology: Pressure of Distal intermetatarsal ligament against common digital nerve Rule out
MORTON S NEUROMA 80% III web space (next common is II). Never occurs in III or IV Common in females in fifties Aetiology: Pressure of Distal intermetatarsal ligament against common digital nerve Rule out
Forefoot/Midfoot Plating System
 Surgical Technique Forefoot/Midfoot Plating System Acumed is a global leader of innovative orthopaedic and medical solutions. We are dedicated to developing products, service methods, and approaches that
Surgical Technique Forefoot/Midfoot Plating System Acumed is a global leader of innovative orthopaedic and medical solutions. We are dedicated to developing products, service methods, and approaches that
