Moderate to severe hallux valgus deformity: correction with proximal crescentic osteotomy and distal soft-tissue release
|
|
|
- Alvin Parker
- 5 years ago
- Views:
Transcription
1 Arch Orthop Trauma Surg (2000) 120 : Springer-Verlag 2000 ORIGINAL ARTICLE R. Zettl H.-J. Trnka M. Easley M. Salzer P. Ritschl Moderate to severe hallux valgus deformity: correction with proximal crescentic osteotomy and distal soft-tissue release Received: 28 July 1999 Abstract Between 1991 and 1995, 96 patients (114 feet) were treated with a proximal crescentic metatarsal osteotomy and distal soft-tissue procedure for moderate to severe hallux valgus deformity [intermetatarsal (IM) angle > 15, or hallux valgus (HV) angle > 30 ]. At an average follow-up of 26 months, 8 men and 62 women (86 feet) with a mean age of 53.2 years were retrospectively reviewed. The HV angle averaged 41.1 preoperatively and 14.6 postoperatively. The respective values for the IM angle were 17.8 and 7.8. Neither the average metatarsal shortening of 3 mm nor the dorsal angulation at the osteotomy site seen in 9% of cases evidenced any clinical significance at followup. Patient satisfaction was excellent or good in 91%, and the mean Mayo Clinic Forefoot Score (total 75 points) improved from 37.2 to 61.1 points. Complications included 8 cases of hallux varus and 5 cases of hardware failure. Based on this first study exclusively focusing on moderate to severe hallux valgus deformity, we conclude that proximal first metatarsal osteotomy in combination with a lateral soft-tissue procedure is effective in correcting moderate to severe symptomatic hallux valgus deformity with metatarsus primus varus (IM angle > 15 or HV angle > 30 ). Introduction R. Zettl H.-J. Trnka P. Ritschl I Department, Orthopaedic Hospital Gersthof, Vienna, Austria H.-J. Trnka M. Easley Union Memorial Hospital, Foot & Ankle Service, Baltimore, Maryland, USA M. Salzer Herz Jesu Hospital, Orthopaedic Department, Vienna, Austria R. Zettl ( ) Ferdinand-Frey-Weg 27, A-1140 Vienna, Austria reinhard@zettl.at, Tel.: , Fax: Many authors recommend surgical correction of symptomatic hallux valgus when pain and discomfort persist despite conservative management [2, 14, 15]. In severe cases, metatarsus primus varus is usually a coexisting condition. Most authors agree, that metatarsus primus varus must be corrected for adequate therapy of severe hallux valgus. Numerous surgical procedures for correction of this deformity have been described, and the choice of procedure depends primarily on severity, location and nature of the pathology. Distal metatarsal osteotomies [2, 13] are typically inadequate in the surgical management of severe hallux valgus associated with metatarsus primus varus and may result in recurrent deformity [1]. Therefore, proximal first metatarsal osteotomies are recommended for moderate to severe metatarsus primus varus (IM angle > 15 ). Several conceptually different osteotomies have been described to correct the metatarsus primus varus at the proximal aspect of the first metatarsal, including closing wedge, oblique, crescentic and proximal chevron osteotomies [10, 14, 15, 16]. A proximal closing wedge osteotomy risks shortening and dorsal malunion, leading to impaired weight-bearing of the first ray and the development of transfer metatarsalgia [14, 19]. The proximal horizontal V osteotomy, after its first description by Kotzenberg [16], has been used by several authors since the early 1990s. Initial results are promising, but only short- to midterm results are available [4, 15]. The most commonly performed proximal procedure is the crescentic osteotomy, described by Mann et al. [10, 11]. The osteotomy s rotational design allows triplanar correction [9], and its efficacy to correct any degree of hallux valgus deformity has been well documented in the literature [3, 4, 11, 18]. This procedure has been used at our hospital since 1991 for the correction of moderate and severe hallux valgus deformity (IM angle > 15 or HV angle > 30 ). The purpose of this retrospective study was to review the results of all patients undergoing proximal first metatarsal crescentic osteotomy associated with metatarsus primus varus between 1991 and 1995.
2 398 Patients and methods Ninety-six patients (114 feet) with symptomatic moderate to severe hallux valgus were treated with a proximal crescentic osteotomy and distal soft-tissue procedure between October 1991 and December Indications for surgery included shoe conflict, persistent pain and discomfort despite conservative management. The operations were performed by 14 different surgeons, including 5 consultants and 9 residents. Seventy patients (86 feet) were available for an average followup of 26 months (range months). One patient (1 foot) had died and 25 patients (27 feet) had either moved from the area or been lost to follow up. The mean age of the 8 men and 62 women at the time of operation was 53.2 years (range years). Seventy-nine operations were performed as a primary procedure and 7 for recurrent deformity. Of the 86 feet, 40 had simultaneous procedures for lesser toe deformities, including proximal phalanx head resections (n = 36), Helal (n = 7) or Weil (n = 1) osteotomies and extensor tenotomies (n = 7). For the pre- and postoperative clinical assessment, a standardised questionnaire based on the Forefoot Scoring System (FFSS) of the Mayo Clinic as described by Kitaoka et al. was used [7]. This clinical rating system combines objective and subjective data as follows: pain = 30 points, function = 15 points, footwear restrictions = 10 points, painful callus = 10 points, alignment = 5 points and stiffness = 5 points for a possible total of 75 points. The patients were asked about their overall satisfaction with the outcome of the procedure (range 1, excellent, to 4, dissatisfied), and the presence of transfer lesions was documented. Weight-bearing dorsoplantar and lateral radiographs of the foot were obtained preoperatively, immediately postoperatively, and at the most recent evaluation (Figs.1, 2). The HV and IM angles, tibial sesamoid position, and length of the first and second metatarsals were measured from dorsoplantar (dp) radiographs according to the guidelines of the American Orthopaedic Foot and Ankle Society [17]. Hallux valgus deformity was classified as mild: HV angle or IM angle 11 15, moderate: HV angle or IM 1 2 Fig. 1 Preoperative weight-bearing dorsoplantar (dp) radiograph of a woman aged 65 years. Hallux valgus (HV) angle is 33, intermetatarsal (IM) angle 15, and sesamoid position is grade 2 on a scale of 0 3 Fig. 2 Weight-bearing dp radiograph of the same woman as in Fig. 1 at follow-up examination 49 months after the operation. HV angle is 9, IM angle 4, and sesamoid position 0 angle 16 20, or severe: HV angle > 40 or IM angle > 20. The sesamoid position was evaluated by measuring the position of the medial sesamoid relative to a longitudinal line bisecting the first metatarsal shaft and was classified as grade 0 3 [17] (Fig. 3). The relative length of the first and second metatarsals was calculated by the method of Hardy and Clapham [6, 17] to determine shortening following the proximal crescentic osteotomy. Healing of the osteotomy site was based on radiographic evidence for bridging callus at the osteotomy site, both in the dp and lateral planes. Degenerative changes of the first metatarsophalangeal (MTP) and metatarsocuneiform (MTC) joint were classified as grade 0: normal, grade 1: mild sclerosis, grade 2: joint space narrowing, grade 3: narrowing plus cysts and osteophytes, or grade 4: joint destruction. Pre- and postoperative values were recorded and changes expressed as a percentage value. Sagittal plane malalignment of the first metatarsal was based on lateral weight-bearing radiographs. A line was drawn through the longitudinal axis of the first metatarsal distal and proximal to the osteotomy site. Angulation between the two lines defined sagittal malalignment. Operative technique The operation starts with a dorsal incision over the first web space. Then the lateral joint capsule is incised longitudinally just superior to the lateral sesamoid. The adductor tendon is identified and carefully dissected from the lateral joint capsule and the lateral sesamoid and released from its insertion into the base of the proximal phalanx. The transverse metatarsal ligament is stretched and carefully incised to release the tethering effect on the sesamoid complex. The lateral capsule is perforated at the joint line, and the great toe is forced manually into about 20 varus position. One suture is placed through the adductor tendon and the lateral aspect of the first metatarsal to lift the insertion of the adductor muscle and two stabilizing intermetatarsal sutures. A second skin incision is made at the medial aspect of the first MTP joint. This incision is either extended proximally in a slightly curved manner, or a third longitudinal dorsomedial skin incision is made at the osteotomy site. The medial MTP joint capsule is opened with an inverted L-type incision. The joint is inspected for degenerative changes. The third step is to expose the osteotomy site. After retraction of the extensor hallucis longus tendon, the osteotomy is performed about 1 cm distal of the MTC joint. Until April 1995, the osteotomy was always performed with a K-wire-guided, oscillating, curved Ender saw. This K-wire guidance automatically directs the convexity of the cut proximally. After May 1995, the oscillating Hall Zimmer saw with a curved blade was available at our institution and routinely used. With this saw, the convexity of the cut is placed distally in all cases. Regardless of the type of saw used, the osteotomy is cut halfway between the planes perpendicular to the metatarsal shaft and perpendicular to ground plane. After manual displacement of the fragments, the correction obtained is checked and the osteotomy fixed with a 4.0-mm cancellous screw (Fig. 4). Additional K-wires (24 cases) or crossed K-wires as the only mode of fixation (1 case) were only used whenever screw placement was impossible. Then the medial eminence is excised in line with the metatarsal shaft, taking care not to excise too much bone off the metatarsal head. Attention is now directed towards the medial capsule, and a wedge of about 5 mm is removed from the short arm of the L-type capsular incision. While an assistant holds the great toe in a slightly overcorrected position, the medial joint capsule is repaired, and the first web space sutures are tightened. After skin closure, the foot is wrapped in compression dressing which protects the soft-tissue repair and holds the great toe in its corrected position. The osteotomy is checked by radiography, and the patient can walk without restriction in a postoperative shoe with stiff sole, depending upon tolerance. The dressing is changed after 2 days and then on a weekly basis. Full weight-bearing without a postoperative shoe is allowed after 6 8 weeks. Due to the fact that a high percentage of our patients showed transarticular placement
3 399 Table 1 Radiographic results (mean ± SD): HV angle hallux valgus angle, IM angle intermetatarsal I/II angle, SP sesamoid position (grade 0 3) Preoperative Postoperative Ø correction HV angle 41.1 ± ± IM angle 17.8 ± ± SP 2.8 ± ± Radiography Fig. 3 Sesamoid position: medial sesamoid in relation to longitudinal axis of metatarsal one: 0 normal position, 1 less than 50% overlap, 2 more than 50% overlap, 3 lateral luxation Fig. 4 Operative procedure: proximal crescentic osteotomy (convexity of saw cut directed distally) performed approximately 1 cm distal to the metatarsocuneiform joint and fixed with a 4.0-mm cancellous screw of fixation screws, these devices were routinely removed after solid fusion of the osteotomy was established. Results Clinical 3 4 Mean improvement in Forefoot Score was 23.9 points. The Forefoot score (total 75 points) averaged 37.2 points (range 15 75) preoperatively and 61.1 (range 30 75) points postoperatively. Preoperatively, 99% of patients experienced some sort of pain, mainly around the medial eminence or the MTP joint. At the most recent follow-up, 95% of patients were either pain-free or had only minor symptoms. In addition, 82% of patients had no limitations concerning shoewear, 18% had minor difficulty with shoe width or heel height, and no patient had to wear orthotic shoes. Subjectively, 91% of the patients rated their satisfaction with the outcome of the operation as excellent or good, 9% was satisfied with reservations, and no patient was completely dissatisfied with the outcome of the procedure. Preoperatively, 48% of feet had painful callosities under the lesser metatarsal heads. After the operation, 24% of these lesions had resolved, but in 8% new transfer lesions were observed, leaving 32% of feet with metatarsalgia at the latest follow-up. Without concomitant lesser toe surgery (46 feet), 16% of the lesions resolved, but in 11% new transfer lesions were observed at follow-up. With concomitant lesser toe surgery (40 feet), 35% of callosities resolved, and only 5% of feet showed new transfer lesions. All osteotomies presented solid union at the latest followup evaluation. Two cases of delayed union were observed, but both of them healed with conservative management (limited weight-bearing). The mean correction of the HV angle was The angle averaged 41.1 (range ) preoperatively and 14.6 (range 40 to 46 ) at final follow-up (Table 1). The IM angle was corrected an average of 10. The angle averaged 17.8 (range ) preoperatively and 7.8 ( 5 to 18 ) at final follow-up. Thus, according to our deformity grading, 80% of cases showed normal values for HV and IM angles or presented with a mild residual deformity after the procedure (Table 1). The average tibial sesamoid correction was 1.5 (on a scale from 0 to 3). The sesamoid position averaged 2.8 preoperatively and 1.3 at final follow-up. Preoperatively, 99% of tibial sesamoids had a lateral position in respect to the line bisecting the metatarsal shaft (positions 2 and 3). This could be corrected to a medial position (positions 0 and 1) in 60% of feet. In the foot with a recurrent hallux valgus deformity, the attempted correction of the tibial sesamoid had failed and remained 3 (Table 1). The amount of metatarsal shortening following osteotomy could be determined for 66 (77%) feet and averaged 3 mm (range 8 to +2 mm). Twenty feet were not measured due to inadequate radiographs or concomitant metatarsal shortening osteotomies. Five patients had 7 mm or more shortening. None of these feet presented with a transfer lesion at the latest follow-up examination. Dorsiflexion of the first metatarsal, as measured on lateral radiographs, could be observed in 8 feet (9%). Only one of these patients developed a transfer lesion under the lesser metatarsals. Preoperative degenerative changes were graded as 0 or 1 in 61% of cases in the MTP joint and in 98% of cases in the MTC joint. Progression of radiographic changes of one or more steps could be observed in 10 feet (12%) concerning the MTP joint and in 23 feet (27%) concerning the MTC joint. Despite this progression of degenerative changes, none of these patients had symptoms related to arthritis. Complications The two main complications were hallux varus deformity and failure of fixation screws. Hallux varus deformity developed in 8 feet (9%). In these cases the average hallux
4 400 valgus angle measured 16 (range 3 to 40 ). One patient underwent revision surgery (HV angle 40 ), and one patient had difficulty with wearing shoes (HV angle 30 ). With milder forms of hallux varus deformity, the patients were pain-free and satisfied with the outcome of the operation. Three patients rated their satisfaction as good and one patient, as moderate. Dissatisfaction with the cosmetic appearance was the reason in three cases (HV angles: 13, 20, 30 ) and moderate pain in the remaining case (HV angle: 5 ). The patient with a varus deformity of 20 had undergone a bunionectomy with resection of the collateral ligaments 14 years ago. Breakage of fixation screws was encountered in 5 (6%) feet. All screw failures occurred between 3 months and 1 year. All osteotomies united, and only one patient showed a minor loss of correction. In all cases, the screw had been placed across the MTC joint. A recurrence of hallux valgus deformity was observed in 1 foot and hallux rigidus developed in two other feet. All three feet required revision surgery, the first of which was managed with MTP joint arthrodesis and the other two with a Keller resection arthroplasty. Deep infection occurred in one patient and was treated by wound debridement and administration of antibiotics and allowed to heal with secondary intention. At the latest follow-up examination, the patient experienced no pain, had no restrictions concerning shoewear, and was satisfied with the outcome of the operation. Discussion Numerous procedures have been described for the correction of hallux valgus deformity. Most authors agree, that the severer hallux valgus deformity with marked metatarsus primus varus (IM angle > 15 ) is inadequately corrected by distal osteotomies [1]. Although proximal crescentic osteotomies are commonly used in combination with a distal lateral soft-tissue procedure to correct these high-grade deformities, only a few authors have published larger series of patients [3, 4, 11, 18]. This is the first study focusing exclusively on moderate to severe hallux valgus deformity. Our series, with the highest mean preoperative values for HV (41.1 ) and IM angles (17.8 ) reported in the orthopaedic literature, confirms the potential of the proximal crescentic osteotomy to correct even severe cases of hallux valgus and metatarsus primus varus. Mean correction for HV (26.5 ) and IM angles (10 ) proved to be sufficient in the majority of cases (80%) in correcting the pathology to normal values or a mild residual deformity. No patient was dissatisfied with the outcome, 82% could wear any type of shoe, and 18% had only minor shoewear restrictions. No patient required orthotic shoewear after the operation. The reduction of the sesamoid complex (2.8 to 1.3 on a scale from 0 to 3) was less favorable compared to the correction of the HV and IM angles. Comparison with other works is hampered by the fact that many different classification systems for the position of the tibial sesamoid are used [4, 11, 17, 18]. Our correction is slightly superior to the reduction of 6.5 to 4.1 (scale: 0 7) of Thordarson and Leventen [18] and the 58% of medial or central positions (scale: medial, central, lateral) of Easley et al. [4] and equal to the 80% of medial or central positions of Mann et al. [11]. In 1992, Mann et al. [11] published a retrospective review of 75 patients (109 feet) undergoing proximal crescentic osteotomy and distal soft-tissue realignment. After a mean follow-up of 34 months, all osteotomies had healed, the average HV angle correction was 21 (31 9 ) and IM angle correction 8 (14 6 ). Patient satisfaction was high (93%), shortening of the metatarsals averaged 2 mm, and only minor complications (varus, re-valgus, pin tract infection) occurred. Dorsiflexion (28%) and shortening (range 12 to +3 mm) of the first metatarsal were described as potential pitfalls, although no new transfer lesions developed after the procedure. These favorable results were confirmed in a long-term follow-up study by Dreeben and Mann [3]. After a mean period of 5.5 years, loss of correction averaged 1.4 for the IM angle and 3.8 for the HV angle. The incidence of varus and recurrent valgus deformity had not increased from the initial follow-up study, and patient satisfaction remained high (85%). Similar results were published in 1992 by Thordarson and Leventen [18]. They reviewed 35 patients (49 feet) after a mean follow-up of 28 months. The average HV angle improved from 37.5 to 13.8 and the IM angle from 14.9 to 4.7. Patient satisfaction (93%) and rate of complications were similar to the earlier studies, despite different methods of fixation (screws, staples, and K-wires). Dorsal angulation at the osteotomy site averaged 6.2, and 7 patients developed symptomatic transfer lesions. Two of these required a metatarsal neck osteotomy. In 1996, Easley et al. [4] compared the results of proximal crescentic (35 patients, 50 feet) and proximal chevron (40 patients, 47 feet) osteotomies in a prospective manner. They found no statistically significant difference for correction of the HV and IM angles, patient satisfaction, clinical outcome, and metatarsal shortening. Radiographic evidence of healing was faster in the chevron (mean 4 weeks) than in the crescentic (mean 6.7 weeks) group. This finding did not alter the postoperative regimen, which was identical for both groups. No cases of postoperative dorsiflexion of the first metatarsal were found in the chevron group compared with an average dorsiflexion of 2.7 in 7 cases (17%) in the crescentic group. The rate of complications was slightly higher in the chevron (21%) than in the crescentic group (17%). One major pitfall of the crescentic osteotomy is dorsal angulation at the osteotomy site with the subsequent risk of transfer lesions. Our incidence of 9% is lower than the 28% reported by Mann et al. [11] or the 17% reported by Easley et al. [4]. This could possibly be due to the fact that 99% (all except one) of our osteotomies were fixed with screws or screws and K-wires compared with only 34% of Mann et al. [11] and 65% of Thordarson and Leventen [18]. Easley et al. [4], although he did not state the exact fig-
5 ures, used 3 K-wires in cases where the bone stock of the first metatarsal proved insufficient to support screw fixation. Biomechanical works by McCluskey et al. [12] and Lian et al. [8] comparing different modes of fixation for proximal metatarsal osteotomies clearly demonstrated the superiority of screw fixation against K-wires or staples. Lian et al. [8] compared proximal chevron or crescentic osteotomies with single screw fixation against oblique osteotomy with double screw fixation and crescentic osteotomy fixed with either 2 K-wires or multiple staples in 48 cadaver feet. Concerning the crescentic osteotomy, staples were by far the weakest construct, followed by K-wires and screws. Taking these data and our results into account, we favour single screw fixation over the use of staples or K-wires as the fixation method for crescentic osteotomies. Concerning the proximal chevron osteotomy, studies present conflicting data. Although McCluskey et al. s study [12] suggested a greater biomechanical strength of the proximal chevron over the crescentic osteotomy using single screw fixation, Lian et al. s [8] investigation does not support this. Instead, their work did not demonstrate a statistically significant difference between the biomechanical strength of these two osteotomies. Clinical studies support the theory that the proximal chevron osteotomy possesses greater inherent stability, with less potential for dorsal angulation [4, 15]. Metatarsal shortening is considered the second major risk factor concerning the development of transfer lesions. Values for the proximal crescentic osteotomy vary from 2 mm (range 12 to +3 mm) as described by Mann et al. [11] to 3 mm (range 8 to +2 mm) in our investigation using the Hardy and Clapham method [6]. Easley et al. [4], using the Grace et al. method [5], noted 1.95% of shortening with the proximal crescentic osteotomy, which was not statistically significant compared to the 1.07% of shortening produced by the proximal chevron osteotomy. These values are lower than the mm [19, 20] and 4.7% [14] reported for closing wedge osteotomies and the mm [13] and 6.3% 6.4% [5] reported for some popular distal osteotomies (Mitchell, Wilson, and Hohmann type). The clinical significance of shortening and dorsal malangulation is unclear, because studies that observed dorsal angulation in 28% of metatarsals [11] developed no new transfer lesions, while others with fewer cases of dorsal angulation did [4]. Our rate of 8% of new development of transfer lesions after the operation lies well between the reported range of 0% 16% [4, 11, 18]. Our data suggest that severe forms of lesser toe deformities should be simultaneously addressed with first ray surgery. In the group with concomitant lesser toe surgery, roughly twice the number of painful callosities resolved under the lesser metatarsal heads (35% instead of 16%), and only half the number of new callosities developed (5% instead of 11%). Radiographic progression of degenerative disease between the operation and follow-up was recorded in 12% of MTP joints and in 27% of MTC joints. The high rate of progression of the MTC joint may be explained by transarticular screw fixation. However, none of our patients developed symptoms related to arthritis at the MTC joint, and a correlation between radiographic changes and clinical symptoms is controversial. Mann et al. [11] reported progression in 24% of cases at the MTP joint, which is close to our value at the MTC joint. Wanivenhaus and Feldner-Busztin [20] reported radiographic progression at the MTC joint in 73% of cases. Despite identifying a cause for 58% of cases (transarticular placement of the fixation hardware and close vicinity of the osteotomy site to the MTC joint), radiographic progression of 15% of cases at this joint remained unclear. Although our data suggest that MTC degeneration remains asymptomatic, we currently attempt to avoid violation of the tarsometatarsal joint. In conclusion, this series dealt with the highest preoperative values for HV (41.1 ) and IM (17.8 ) angles reported in the orthopaedic literature. Based on this first study exclusively focusing on moderate to severe hallux valgus deformity, we conclude that proximal first metatarsal osteotomy in combination with a lateral soft-tissue procedure is effective in correcting hallux valgus deformity with IM angle >15 and should be considered in the surgical management of patients with moderate to severe symptomatic hallux valgus associated with metatarsus primus varus. References Anderson RB, Donati NL, Thomas RL, Trevino SG (1997) Complications of hallux valgus surgery. AAOS Instr Course Lect, 64th annual meeting, San Francisco 2. Austin DW, Leventen EO (1981) New osteotomy for hallux valgus. Clin Orthop 157 : Dreeben S, Mann RA (1996) Advanced hallux valgus deformity: long-term results utilising the distal soft tissue procedure and proximal metatarsal osteotomy. Foot Ankle Int 17 : Easley ME, Kiebzak GM, Davis WH, Anderson RB (1996) Prospective, randomised comparison of proximal crescentic and proximal chevron osteotomies for correction of hallux valgus deformity. Foot Ankle Int 17 : Grace D, Hughes J, Klenerman L (1988) A comparison of Wilson and Hohmann osteotomies in the treatment of hallux valgus. J Bone Joint Surg [Br] 70 : Hardy R, Clapham J (1951) Observations on hallux valgus. J Bone Joint Surg [Br] 33 : Kitaoka HB, Hiliday AD, Campbell DC (1991) Distal chevron metatarsal osteotomy for bunionette. Foot Ankle 12 : Lian GJ, Markolf K, Cracchiolo A (1992) Strength of fixation constructs for basilar osteotomies of the first metatarsal. Foot Ankle 13 : Lippert FG, McDermott JE (1991) Crescentic osteotomy for hallux valgus: a biomechanical study of variables affecting the final position of the first metatarsal. Foot Ankle 11 : Mann RA (1990) Etiology and treatment of hallux valgus. Distal soft tissue procedure and proximal metatarsal osteotomy for correction of hallux valgus deformity. Orthopedics 13 : Mann RA, Rudicel S, Graves SC (1992) Repair of hallux valgus with a distal soft-tissue procedure and proximal metatarsal osteotomy. J Bone Joint Surg [Am] 74 : McCluskey L, Johnson JE, Wynarsky GT, Harris GF (1994) Comparison of stability of proximal crescentic metatarsal osteotomy and proximal horizontal V osteotomy. Foot Ankle Int 15 : Mitchell CL, Fleming JL, Allen R, Glenney C, Sanford GA (1958) Osteotomy-bunionectomy for hallux valgus. J Bone Joint Surg [Am] 40 :41 60
6 Resch S, Stenström A, Eglund N (1989) Proximal closing wedge osteotomy and adductor tenotomy for treatment of hallux valgus. Foot Ankle 9 : Sammarco GJ, Brainard BJ, Sammarco VJ (1993) Bunion correction using proximal chevron osteotomy. Foot Ankle 14 : Schlotte M (1929) Zur operativen Korrektur des Hallux valgus im Sinne Ludloffs. Klin Wochenschr 50 : Smith RW, Reynolds JC, Stewart MJ (1984) Hallux valgus assessment: report of research committee of American Orthopaedic Foot and Ankle Society. Foot Ankle 5 : Thordarson DB, Leventen EO (1992) Hallux valgus correction with proximal metatarsal osteotomy: two-year follow-up. Foot Ankle 13 : Zembsch A, Trnka H-J, Mühlbauer M, Ritschl P, Salzer M (1998) Langzeitergebnisse nach basaler Keilosteotomie beim Metatarsus Primus Varus des jungen Patienten. Z Orthop 136 : Wanivenhaus AH, Feldner-Busztin H (1988) Basal osteotomy of the first metatarsal for the correction of metatarsus primus varus associated with hallux valgus. Foot Ankle 8 :
The Ludloff Osteotomy
 Techniques in Foot and Ankle Surgery 4(4):263 268, 2005 Ó 2005 Lippincott Williams & Wilkins, Philadelphia The Ludloff Osteotomy T E C H N I Q U E Hans-Jörg Trnka, MD, PhD and Stefan Hofstätter, MD Foot
Techniques in Foot and Ankle Surgery 4(4):263 268, 2005 Ó 2005 Lippincott Williams & Wilkins, Philadelphia The Ludloff Osteotomy T E C H N I Q U E Hans-Jörg Trnka, MD, PhD and Stefan Hofstätter, MD Foot
Chevron Osteotomy With Lateral Soft Tissue Release
 5(4):250 256, 2006 T E C H N I Q U E Chevron Osteotomy With Lateral Soft Tissue Release Hans-Jörg Trnka, MD, PhD and Stefan Gerhard Hofstaetter, MD Foot and Ankle Center Vienna Vienna, Austria Ó 2006 Lippincott
5(4):250 256, 2006 T E C H N I Q U E Chevron Osteotomy With Lateral Soft Tissue Release Hans-Jörg Trnka, MD, PhD and Stefan Gerhard Hofstaetter, MD Foot and Ankle Center Vienna Vienna, Austria Ó 2006 Lippincott
Proximal metatarsal osteotomy and distal soft tissue reconstruction as treatment for hallux valgus deformity
 REVIEW Proximal metatarsal osteotomy and distal soft tissue reconstruction as treatment for hallux valgus deformity Michael J. Coughlin and J. Speight Grimes Boise, Idaho, USA (Received for publication
REVIEW Proximal metatarsal osteotomy and distal soft tissue reconstruction as treatment for hallux valgus deformity Michael J. Coughlin and J. Speight Grimes Boise, Idaho, USA (Received for publication
Effect of metatarsal osteotomy and open lateral soft tissue procedure on sesamoid position: radiological assessment
 Choi et al. Journal of Orthopaedic Surgery and Research (2018) 13:11 DOI 10.1186/s13018-017-0712-y RESEARCH ARTICLE Effect of metatarsal osteotomy and open lateral soft tissue procedure on sesamoid position:
Choi et al. Journal of Orthopaedic Surgery and Research (2018) 13:11 DOI 10.1186/s13018-017-0712-y RESEARCH ARTICLE Effect of metatarsal osteotomy and open lateral soft tissue procedure on sesamoid position:
Re+Line Bunion Correction System for Correction of Hallux Abducto Valgus Deformity
 Re+Line Bunion Correction System for Correction of Hallux Abducto Valgus Deformity Amber M. Shane, DPM, FACFAS 1, Christopher L. Reeves, DPM, FACFAS 1 1. Orlando Foot & Ankle Clinic, Orlando, FL Abstract
Re+Line Bunion Correction System for Correction of Hallux Abducto Valgus Deformity Amber M. Shane, DPM, FACFAS 1, Christopher L. Reeves, DPM, FACFAS 1 1. Orlando Foot & Ankle Clinic, Orlando, FL Abstract
Clinical results of modified Mitchell s osteotomy for hallux valgus augmented with oblique lesser metatarsal osteotomy
 Journal of Orthopaedic Surgery 2005:13(3):245-252 Clinical results of modified Mitchell s osteotomy for hallux valgus augmented with oblique lesser metatarsal osteotomy K Yamamoto, A Imakiire, Y Katori,
Journal of Orthopaedic Surgery 2005:13(3):245-252 Clinical results of modified Mitchell s osteotomy for hallux valgus augmented with oblique lesser metatarsal osteotomy K Yamamoto, A Imakiire, Y Katori,
Hallux Valgus Deformity: Preoperative Radiologic Assessment
 119 Pictorial Essay H............ - Hallux Valgus Deformity: Preoperative Radiologic Assessment David Karasick1 and Keith L. Wapner An estimated 40% of the American adult population experiences foot problems,
119 Pictorial Essay H............ - Hallux Valgus Deformity: Preoperative Radiologic Assessment David Karasick1 and Keith L. Wapner An estimated 40% of the American adult population experiences foot problems,
Medincenter GlavUpDK by the Ministry of Foreign Affairs of Russia, Moscow.
 Medincenter GlavUpDK by the Ministry of Foreign Affairs of Russia, Moscow. Berezhnoy Sergey. Percutaneous First Metatarsocuneiform Joint Arthrodesis in a Treatment of Metatarsus Primus Varus: a Prospective
Medincenter GlavUpDK by the Ministry of Foreign Affairs of Russia, Moscow. Berezhnoy Sergey. Percutaneous First Metatarsocuneiform Joint Arthrodesis in a Treatment of Metatarsus Primus Varus: a Prospective
Fixation of first metatarsal basal osteotomy using Acutrak screw
 Available online at www.sciencedirect.com Foot and Ankle Surgery 14 (2008) 21 25 www.elsevier.com/locate/fas Fixation of first metatarsal basal osteotomy using Acutrak screw G.E. Fadel MD FRCS Tr & Orth*,
Available online at www.sciencedirect.com Foot and Ankle Surgery 14 (2008) 21 25 www.elsevier.com/locate/fas Fixation of first metatarsal basal osteotomy using Acutrak screw G.E. Fadel MD FRCS Tr & Orth*,
Modified Proximal Scarf Osteotomy for Hallux Valgus
 Original Article Clinics in Orthopedic Surgery 2018;10:479-483 https://doi.org/10.4055/cios.2018.10.4.479 Modified Proximal Scarf Osteotomy for Hallux Valgus Ki Won Young, MD, Hong Seop Lee, MD, Seong
Original Article Clinics in Orthopedic Surgery 2018;10:479-483 https://doi.org/10.4055/cios.2018.10.4.479 Modified Proximal Scarf Osteotomy for Hallux Valgus Ki Won Young, MD, Hong Seop Lee, MD, Seong
Merete PlantarMAX Lapidus Plate Surgical Technique. Description of Plate
 Merete PlantarMAX Lapidus Plate Surgical Technique Description of Plate Merete Medical has designed the PlantarMax; a special Plantar/Medial Locking Lapidus plate which places the plate in the most biomechanically
Merete PlantarMAX Lapidus Plate Surgical Technique Description of Plate Merete Medical has designed the PlantarMax; a special Plantar/Medial Locking Lapidus plate which places the plate in the most biomechanically
Use of the 20 Memory Staple in Osteotomies of Fusions of the Forefoot
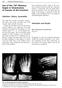 168 Forefoot Reconstruction Use of the 20 Memory Staple in Osteotomies of Fusions of the Forefoot Definition, History, Generalities This staple first provides a permanent compression both in the prongs
168 Forefoot Reconstruction Use of the 20 Memory Staple in Osteotomies of Fusions of the Forefoot Definition, History, Generalities This staple first provides a permanent compression both in the prongs
1. Orthoapedic Associates of Michigan, PC, Grand Rapids, MI 2. Michigan State University College of Human Medicine, Grand Rapids, MI
 Second Metatarsal Osteotomy Shortening with Tarsometatarsal Arthrodesis: Comparison of Outcomes Between MSP TM Metatarsal Shortening System and Plates and Screws Donald R. Bohay, MD, FACS 1 ; John G. Anderson,
Second Metatarsal Osteotomy Shortening with Tarsometatarsal Arthrodesis: Comparison of Outcomes Between MSP TM Metatarsal Shortening System and Plates and Screws Donald R. Bohay, MD, FACS 1 ; John G. Anderson,
Correction of Hallux Valgus Metatarsal Osteotomy Versus Excision Arthroplasty
 CLINICAL ORTHOPAEDICS AND RELATED RESEARCH Number 376, pp. 183-194 0 2000 Lippincott Williams & Wilkins, Inc. Correction of Hallux Valgus Metatarsal Osteotomy Versus Excision Arthroplasty Alexander Zembsch,
CLINICAL ORTHOPAEDICS AND RELATED RESEARCH Number 376, pp. 183-194 0 2000 Lippincott Williams & Wilkins, Inc. Correction of Hallux Valgus Metatarsal Osteotomy Versus Excision Arthroplasty Alexander Zembsch,
Comparison of Postoperative Outcomes between Modified Mann Procedure and Modified Lapidus Procedure for Hallux Valgus
 Comparison of Postoperative Outcomes between Modified Mann Procedure and Modified Lapidus Procedure for Hallux Valgus Yui Akiyama, Takaaki Hirano, Hiroyuki Mitsui Shingo Maeda, Hisateru Niki Department
Comparison of Postoperative Outcomes between Modified Mann Procedure and Modified Lapidus Procedure for Hallux Valgus Yui Akiyama, Takaaki Hirano, Hiroyuki Mitsui Shingo Maeda, Hisateru Niki Department
Combination of First Metatarsophalangeal Joint Arthrodesis and Proximal Correction for Severe Hallux Valgus Deformity
 FOOT &ANKLE INTERNATIONAL DOI: 10.3113/FAI.2012.0400 Combination of First Metatarsophalangeal Joint Arthrodesis and Proximal Correction for Severe Hallux Valgus Deformity Pascal F. Rippstein, MD; Young-Uk
FOOT &ANKLE INTERNATIONAL DOI: 10.3113/FAI.2012.0400 Combination of First Metatarsophalangeal Joint Arthrodesis and Proximal Correction for Severe Hallux Valgus Deformity Pascal F. Rippstein, MD; Young-Uk
Soft Tissue Rebalancing Procedures for the Treatment of Hallux Valgus Deformities
 Soft Tissue Rebalancing Procedures for the Treatment of Hallux Valgus Deformities NO DISCLOSURES Objectives The main objectives of any procedure in hallux abducto valgus surgery are to correct the deformity,
Soft Tissue Rebalancing Procedures for the Treatment of Hallux Valgus Deformities NO DISCLOSURES Objectives The main objectives of any procedure in hallux abducto valgus surgery are to correct the deformity,
Proximal metatarsal osteotomy for hallux valgus: an audit of radiologic outcome after single screw fixation and full postoperative weightbearing
 Mittag et al. Journal of Foot and Ankle Research 2013, 6:22 JOURNAL OF FOOT AND ANKLE RESEARCH RESEARCH Open Access Proximal metatarsal osteotomy for hallux valgus: an audit of radiologic outcome after
Mittag et al. Journal of Foot and Ankle Research 2013, 6:22 JOURNAL OF FOOT AND ANKLE RESEARCH RESEARCH Open Access Proximal metatarsal osteotomy for hallux valgus: an audit of radiologic outcome after
Index. Clin Podiatr Med Surg 22 (2005) Note: Page numbers of article titles are in boldface type.
 Clin Podiatr Med Surg 22 (2005) 309 314 Index Note: Page numbers of article titles are in boldface type. A Abductor digiti minimi muscle, myectomy of, for tailor s bunionette, 243 Achilles tendon, lengthening
Clin Podiatr Med Surg 22 (2005) 309 314 Index Note: Page numbers of article titles are in boldface type. A Abductor digiti minimi muscle, myectomy of, for tailor s bunionette, 243 Achilles tendon, lengthening
JUVENILE AND ADOLESCENT HALLUX VALGUS. George E. Quill, Jr., M.D.
 JUVENILE AND ADOLESCENT HALLUX VALGUS George E. Quill, Jr., M.D. The development of a hallux valgus deformity in children and adolescents is actually an uncommon entity. Most of these occurrences can be
JUVENILE AND ADOLESCENT HALLUX VALGUS George E. Quill, Jr., M.D. The development of a hallux valgus deformity in children and adolescents is actually an uncommon entity. Most of these occurrences can be
Surgical Strategies: Ludloff First Metatarsal Osteotomy
 FOOT &ANKLE INTERNATIONAL Copyright 2007 by the American Orthopaedic Foot & Ankle Society, Inc. DOI: 10.3113/FAI.2007.0025 Surgical Strategies: Ludloff First Metatarsal Osteotomy Su-Young Bae, M.D.; Lew
FOOT &ANKLE INTERNATIONAL Copyright 2007 by the American Orthopaedic Foot & Ankle Society, Inc. DOI: 10.3113/FAI.2007.0025 Surgical Strategies: Ludloff First Metatarsal Osteotomy Su-Young Bae, M.D.; Lew
Surgical technique. Angular Stable X-Plate and 2-Hole Plate. For osteotomies, arthrodeses and fractures of the foot.
 Surgical technique Angular Stable X-Plate and 2-Hole Plate. For osteotomies, arthrodeses and fractures of the foot. Table of Contents Indications 4 Implants 5 X-plate: Crescentic osteotomy 6 X-plate:
Surgical technique Angular Stable X-Plate and 2-Hole Plate. For osteotomies, arthrodeses and fractures of the foot. Table of Contents Indications 4 Implants 5 X-plate: Crescentic osteotomy 6 X-plate:
Distal metatarsal osteotomy for hallux varus following surgery for hallux valgus
 FOOT AND ANKLE Distal metatarsal osteotomy for hallux varus following surgery for hallux valgus K. J. Choi, H. S. Lee, Y. S. Yoon, S. S. Park, J. S. Kim, J. J. Jeong, Y. R. Choi From the Asan Medical Center,
FOOT AND ANKLE Distal metatarsal osteotomy for hallux varus following surgery for hallux valgus K. J. Choi, H. S. Lee, Y. S. Yoon, S. S. Park, J. S. Kim, J. J. Jeong, Y. R. Choi From the Asan Medical Center,
Clinical Practice Guideline on the Diagnosis and Treatment of Hallux Valgus
 Archives of Orthopedics and Rheumatology Volume 1, Issue 1, 2018, PP: 7-11 Clinical Practice Guideline on the Diagnosis and Treatment of Hallux Valgus Jorge de las Heras Romero 1 *, Ana María Lledó Alvarez
Archives of Orthopedics and Rheumatology Volume 1, Issue 1, 2018, PP: 7-11 Clinical Practice Guideline on the Diagnosis and Treatment of Hallux Valgus Jorge de las Heras Romero 1 *, Ana María Lledó Alvarez
A PROSPECTIVE RANDOMISED CONTROLLED TRIAL
 K. B. Lee, N. Y. Cho, H. W. Park, J. K. Seon, S. H. Lee From Chonnam National University Medical School and Hospital, Gwangju, Korea K. B. Lee, MD, PhD, Professor, Department of J. K. Seon, MD, PhD, Associate
K. B. Lee, N. Y. Cho, H. W. Park, J. K. Seon, S. H. Lee From Chonnam National University Medical School and Hospital, Gwangju, Korea K. B. Lee, MD, PhD, Professor, Department of J. K. Seon, MD, PhD, Associate
Investigation performed at Orthopaedic Hospital Gersthof, Vienna, Austria
 1131 COPYRIGHT 2004 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Salvage of a Failed Keller Resection Arthroplasty BY FELIX MACHACEK JR., MD, MARK E. EASLEY, MD, FLORIAN GRUBER, MD, PETER RITSCHL,
1131 COPYRIGHT 2004 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Salvage of a Failed Keller Resection Arthroplasty BY FELIX MACHACEK JR., MD, MARK E. EASLEY, MD, FLORIAN GRUBER, MD, PETER RITSCHL,
Complications associated with Mitchell s Osteotomy for Hallux Valgus Correction: A retrospective hospital review
 The Foot and Ankle Online Journal Official publication of the International Foot & Ankle Foundation Complications associated with Mitchell s Osteotomy for Hallux Valgus Correction: A retrospective hospital
The Foot and Ankle Online Journal Official publication of the International Foot & Ankle Foundation Complications associated with Mitchell s Osteotomy for Hallux Valgus Correction: A retrospective hospital
A Patient s Guide to Bunions. Foot and Ankle Center of Massachusetts, P.C.
 A Patient s Guide to Bunions Welcome to Foot and Ankle Center of Massachusetts, where we believe in accelerating your learning curve with educational materials that are clearly written and professionally
A Patient s Guide to Bunions Welcome to Foot and Ankle Center of Massachusetts, where we believe in accelerating your learning curve with educational materials that are clearly written and professionally
Minimally Invasive Bunionectomy: The Lam Modification of the Traditional Distal First Metatarsal Osteotomy Bunionectomy
 CHAPTER 2 Minimally Invasive Bunionectomy: The Lam Modification of the Traditional Distal First Metatarsal Osteotomy Bunionectomy Kevin Lam, DPM Rikhil Patel, DPM Thomas Merrill, DPM Hallux abducto valgus
CHAPTER 2 Minimally Invasive Bunionectomy: The Lam Modification of the Traditional Distal First Metatarsal Osteotomy Bunionectomy Kevin Lam, DPM Rikhil Patel, DPM Thomas Merrill, DPM Hallux abducto valgus
Mehmet Erdil 1,Hasan Huseyin Ceylan 2, Deniz Kara 3,Gokhan Polat 4, Ergun Bozdag 5, Emin Sunbuloglu 5
 Mehmet Erdil 1,Hasan Huseyin Ceylan 2, Deniz Kara 3,Gokhan Polat 4, Ergun Bozdag 5, Emin Sunbuloglu 5 1. Istanbul Medipol University, Orthopaedics & Traumatology Dep.,Istanbul,TURKEY 2. Sultanciftligi
Mehmet Erdil 1,Hasan Huseyin Ceylan 2, Deniz Kara 3,Gokhan Polat 4, Ergun Bozdag 5, Emin Sunbuloglu 5 1. Istanbul Medipol University, Orthopaedics & Traumatology Dep.,Istanbul,TURKEY 2. Sultanciftligi
Introduction Basics MIS Screw 2 System Characteristics 2 Indication 2
 Clinical Advisor M. Walther. M.D., Ph.D. Professor of Orthopedic Surgery Head of Department Centre for Foot and Ankle Surgery Schön Klinik München Harlaching FIFA Medical Centre Table of Contents Introduction
Clinical Advisor M. Walther. M.D., Ph.D. Professor of Orthopedic Surgery Head of Department Centre for Foot and Ankle Surgery Schön Klinik München Harlaching FIFA Medical Centre Table of Contents Introduction
The Lapidus Procedure as Salvage After Failed Surgical Treatment of Hallux Valgus A PROSPECTIVE COHORT STUDY
 60 COPYRIGHT 2003 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED The Lapidus Procedure as Salvage After Failed Surgical Treatment of Hallux Valgus A PROSPECTIVE COHORT STUDY BY J. CHRIS COETZEE,
60 COPYRIGHT 2003 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED The Lapidus Procedure as Salvage After Failed Surgical Treatment of Hallux Valgus A PROSPECTIVE COHORT STUDY BY J. CHRIS COETZEE,
A comparison of Chevron and Lindgren-Turan osteotomy techniques in hallux valgus surgery: a prospective randomized controlled study
 ORIGINAL ARTICLE Acta Orthop Traumatol Turc 2016;50(3):255 261 doi: 10.3944/AOTT.2016.14.0272 A comparison of Chevron and Lindgren-Turan osteotomy techniques in hallux valgus surgery: a prospective randomized
ORIGINAL ARTICLE Acta Orthop Traumatol Turc 2016;50(3):255 261 doi: 10.3944/AOTT.2016.14.0272 A comparison of Chevron and Lindgren-Turan osteotomy techniques in hallux valgus surgery: a prospective randomized
How to avoid complications of distraction osteogenesis for first brachymetatarsia
 220 Acta Orthopaedica 2009; 80 (2): 220 225 How to avoid complications of distraction osteogenesis for first brachymetatarsia Keun-Bae Lee, Hyun-Kee Yang, Jae-Yoon Chung, Eun-Sun Moon, and Sung-Taek Jung
220 Acta Orthopaedica 2009; 80 (2): 220 225 How to avoid complications of distraction osteogenesis for first brachymetatarsia Keun-Bae Lee, Hyun-Kee Yang, Jae-Yoon Chung, Eun-Sun Moon, and Sung-Taek Jung
AUTHOR(S): COUGHLIN, MICHAEL J., M.D., BOISE, IDAHO. An Instructional Course Lecture, The American Academy of Orthopaedic Surgeons
 JBJA Journal of Bone and Joint Surgery - American 1996-1998 June 1996, Volume 78-A, Number 6 932 Instructional Course Lectures, The American Academy of Orthopaedic Surgeons - Hallux Valgus* Instructional
JBJA Journal of Bone and Joint Surgery - American 1996-1998 June 1996, Volume 78-A, Number 6 932 Instructional Course Lectures, The American Academy of Orthopaedic Surgeons - Hallux Valgus* Instructional
The Weil osteotomy. Lower limb A SEVEN-YEAR FOLLOW-UP. S. G. Hofstaetter, J. G. Hofstaetter, J. A. Petroutsas, F. Gruber, P. Ritschl, H.-J.
 Lower limb The Weil osteotomy A SEVEN-YEAR FOLLOW-UP S. G. Hofstaetter, J. G. Hofstaetter, J. A. Petroutsas, F. Gruber, P. Ritschl, H.-J. Trnka From Hospital Gersthof, Vienna, Austria We prospectively
Lower limb The Weil osteotomy A SEVEN-YEAR FOLLOW-UP S. G. Hofstaetter, J. G. Hofstaetter, J. A. Petroutsas, F. Gruber, P. Ritschl, H.-J. Trnka From Hospital Gersthof, Vienna, Austria We prospectively
PROstep Minimally Invasive Surgery HALLUX VALGUS CORRECTION USING PROSTEP MICA MINIMALLY INVASIVE FOOT SURGERY: TWO CASE STUDIES
 PROstep Minimally Invasive Surgery HALLUX VALGUS CORRECTION USING PROSTEP MICA MINIMALLY INVASIVE FOOT SURGERY: TWO CASE STUDIES AS PRESENTED BY: JOEL VERNOIS M.D. 016798A Case Study 1 PROstep Minimally
PROstep Minimally Invasive Surgery HALLUX VALGUS CORRECTION USING PROSTEP MICA MINIMALLY INVASIVE FOOT SURGERY: TWO CASE STUDIES AS PRESENTED BY: JOEL VERNOIS M.D. 016798A Case Study 1 PROstep Minimally
PEDUS-L. Locking Plantar Lapidus Plate
 PEDUS-L Locking Plantar Lapidus Plate Page 1 PEDUS-L - Locking Plantar Lapidus Plate Table of Contents Implants 3 System 4 Operation manual 5 Approach 5 Identification of the TMT 1 joint with a cannula
PEDUS-L Locking Plantar Lapidus Plate Page 1 PEDUS-L - Locking Plantar Lapidus Plate Table of Contents Implants 3 System 4 Operation manual 5 Approach 5 Identification of the TMT 1 joint with a cannula
Bunions. Compliments of: Institute of Sports Medicine & Orthopaedics
 A Patient s Guide to Bunions 20295 NE 29th Place, Ste 300 Aventura, FL 33180 Phone: (786) 629-0910 Fax: (786) 629-0920 admin@instituteofsports.com DISCLAIMER: The information in this booklet is compiled
A Patient s Guide to Bunions 20295 NE 29th Place, Ste 300 Aventura, FL 33180 Phone: (786) 629-0910 Fax: (786) 629-0920 admin@instituteofsports.com DISCLAIMER: The information in this booklet is compiled
PAINFUL SESAMOID OF THE GREAT TOE Dr Vasu Pai ANATOMICAL CONSIDERATION. At the big toe MTP joint: Tibial sesamoid (medial) & fibular (lateral)
 PAINFUL SESAMOID OF THE GREAT TOE Dr Vasu Pai ANATOMICAL CONSIDERATION At the big toe MTP joint: Tibial sesamoid (medial) & fibular (lateral) They are contained within the tendons of Flexor Hallucis Brevis
PAINFUL SESAMOID OF THE GREAT TOE Dr Vasu Pai ANATOMICAL CONSIDERATION At the big toe MTP joint: Tibial sesamoid (medial) & fibular (lateral) They are contained within the tendons of Flexor Hallucis Brevis
Interphalangeal Arthrodesis of the Toe with a New Radiolucent Intramedullary Implant
 Interphalangeal Arthrodesis of the Toe with a New Radiolucent Intramedullary Implant DIEBOLD P.-F., ROCHER H.,, DETERME P., CERMOLACCE C., GUILLO S., AVEROUS C., LEIBER WACKENHEIN F. Interphalangeal Arthrodesis
Interphalangeal Arthrodesis of the Toe with a New Radiolucent Intramedullary Implant DIEBOLD P.-F., ROCHER H.,, DETERME P., CERMOLACCE C., GUILLO S., AVEROUS C., LEIBER WACKENHEIN F. Interphalangeal Arthrodesis
Low Profile Medial Locking plate augmentation Lapidus Arthrodesis with an early weight bearing protocol: Clinical and Radiographic Analysis
 Low Profile Medial Locking plate augmentation Lapidus Arthrodesis with an early weight bearing protocol: Clinical and Radiographic Analysis James Cottom, DPM Anand Vora, MD Low Profile Medial Locking plate
Low Profile Medial Locking plate augmentation Lapidus Arthrodesis with an early weight bearing protocol: Clinical and Radiographic Analysis James Cottom, DPM Anand Vora, MD Low Profile Medial Locking plate
RETROSPECTIVE ANALYSIS OF END-TO-END DIGITAL ARTHRODESIS
 C H A P T E R 1 7 RETROSPECTIVE ANALYSIS OF END-TO-END DIGITAL ARTHRODESIS Michelle L. Butterworth, DPM Michael S. Downey, DPM Digital deformities are one of the most common entities we face as foot and
C H A P T E R 1 7 RETROSPECTIVE ANALYSIS OF END-TO-END DIGITAL ARTHRODESIS Michelle L. Butterworth, DPM Michael S. Downey, DPM Digital deformities are one of the most common entities we face as foot and
Index. Note: Page numbers of article titles are in bold face type.
 Index Note: Page numbers of article titles are in bold face type. A Achilles tendon, Zadek osteotomy effects on, 430 Adult acquired flatfoot disorder, 387 403 calcaneal Z osteotomy for, 397 399 historical
Index Note: Page numbers of article titles are in bold face type. A Achilles tendon, Zadek osteotomy effects on, 430 Adult acquired flatfoot disorder, 387 403 calcaneal Z osteotomy for, 397 399 historical
ABSTRACT INTRODUCTION
 ORIGINAL ARTICLE Marco Túlio Costa 1, Roberto Zambelli de Almeida Pinto 2, Ricardo Cardenuto Ferreira 1, Minoru Alessandro Sakata 1, Gastão Guilherme Frizzo 1, Roberto Attílio Lima Santin 3 ABSTRACT Objective:
ORIGINAL ARTICLE Marco Túlio Costa 1, Roberto Zambelli de Almeida Pinto 2, Ricardo Cardenuto Ferreira 1, Minoru Alessandro Sakata 1, Gastão Guilherme Frizzo 1, Roberto Attílio Lima Santin 3 ABSTRACT Objective:
Section 6: Preoperative Planning
 Clinical Relevance of the PedCat Study: In many ways the PedCat study confirmed radiographic findings. With the measuring tools embedded in the DICOM viewing software it was possible to gauge the thickness
Clinical Relevance of the PedCat Study: In many ways the PedCat study confirmed radiographic findings. With the measuring tools embedded in the DICOM viewing software it was possible to gauge the thickness
Symptomatic Medial Exostosis of the Great Toe Distal Phalanx: A Complication Due to Over-correction Following Akin Osteotomy for Hallux Valgus Repair
 Symptomatic Medial Exostosis of the Great Toe Distal Phalanx: A Complication Due to Over-correction Following Akin Osteotomy for Hallux Valgus Repair Carlos Villas, MD, PhD, 1 Javier Del Río, MD, 3 Andres
Symptomatic Medial Exostosis of the Great Toe Distal Phalanx: A Complication Due to Over-correction Following Akin Osteotomy for Hallux Valgus Repair Carlos Villas, MD, PhD, 1 Javier Del Río, MD, 3 Andres
Pedographic, clinical, and functional Outcome after Scarf Osteotomy Timo J. Lorei, MD Christian Kinast,
 Zentrum FuSS & Sprunggelenk Dr. Kinast Prof. Dr. Hamel Pedographic, clinical, and functional Outcome after Scarf Osteotomy Timo J. Lorei, MD Christian Kinast, MD Hans Klärner, MD and Dieter Rosenbaum,
Zentrum FuSS & Sprunggelenk Dr. Kinast Prof. Dr. Hamel Pedographic, clinical, and functional Outcome after Scarf Osteotomy Timo J. Lorei, MD Christian Kinast, MD Hans Klärner, MD and Dieter Rosenbaum,
19 Arthrodesis of the First Metatarsocuneiform Joint
 19 Arthrodesis of the First Metatarsocuneiform Joint CHARLES GUDAS Abduction of the first metatarsal to correct metatarsus primus varus and hallux valgus was first described by Albrecht in 1911. 1 Lapidus
19 Arthrodesis of the First Metatarsocuneiform Joint CHARLES GUDAS Abduction of the first metatarsal to correct metatarsus primus varus and hallux valgus was first described by Albrecht in 1911. 1 Lapidus
Case 57 What is the diagnosis? Insidious onset forefoot pain in a 50 year old female for last 3 months.
 Case 57 What is the diagnosis? Insidious onset forefoot pain in a 50 year old female for last 3 months. Diagnosis: II MTP instability Demographics of MT instability Lesser MTP joint instability occurs
Case 57 What is the diagnosis? Insidious onset forefoot pain in a 50 year old female for last 3 months. Diagnosis: II MTP instability Demographics of MT instability Lesser MTP joint instability occurs
Surgical treatment of hallux valgus using chevron technique
 2018; 4(2): 300-307 ISSN: 2395-1958 IJOS 2018; 4(2): 300-307 2018 IJOS www.orthopaper.com Received: 13-02-2018 Accepted: 17-03-2018 Ashraf Abd-Eldayem Lecturer of Orthopedic Surgery Faculty of Medicine,
2018; 4(2): 300-307 ISSN: 2395-1958 IJOS 2018; 4(2): 300-307 2018 IJOS www.orthopaper.com Received: 13-02-2018 Accepted: 17-03-2018 Ashraf Abd-Eldayem Lecturer of Orthopedic Surgery Faculty of Medicine,
THE FIBULAR SESAMOID ELEVATOR: A New Instrument to Aid the Lateral Release in Hallux Valgus Surgery
 C H A P T E R 1 4 THE FIBULAR SESAMOID ELEVATOR: A New Instrument to Aid the Lateral Release in Hallux Valgus Surgery Thomas F. Smith, DPM Lopa Dalmia, DPM INTRODUCTION Hallux valgus surgery is a complex
C H A P T E R 1 4 THE FIBULAR SESAMOID ELEVATOR: A New Instrument to Aid the Lateral Release in Hallux Valgus Surgery Thomas F. Smith, DPM Lopa Dalmia, DPM INTRODUCTION Hallux valgus surgery is a complex
with regard to our presentation.
 Rotated Insertion Metatarsal Osteotomy with Distal Soft Tissue Procedure for Severe Hallux Valgus Deformity Novel Procedure of the 1 st metatarsal osteotomy Norihiro Samoto MD, Ph.D. Director of Department
Rotated Insertion Metatarsal Osteotomy with Distal Soft Tissue Procedure for Severe Hallux Valgus Deformity Novel Procedure of the 1 st metatarsal osteotomy Norihiro Samoto MD, Ph.D. Director of Department
Minimally Invasive Bunion Surgery: Methods and Outcomes
 Minimally Invasive Bunion Surgery: Methods and Outcomes Hummira H. Abawi, DPM Diplomate ABPM, AACFAS Instructor of Orthopedics, University of Maryland Medical Center Director of Education, Maryland VA
Minimally Invasive Bunion Surgery: Methods and Outcomes Hummira H. Abawi, DPM Diplomate ABPM, AACFAS Instructor of Orthopedics, University of Maryland Medical Center Director of Education, Maryland VA
THE ROLE OF MINIMALLY INVASIVE SURGERY IN THE FOREFOOT. Miss Sue Kendall PhD FRCS (Orth&Trauma)
 THE ROLE OF MINIMALLY INVASIVE SURGERY IN THE FOREFOOT Miss Sue Kendall PhD FRCS (Orth&Trauma) Is Minimally Invasive Surgery of the foot a good idea? Minimally invasive surgery, keyhole surgery entering
THE ROLE OF MINIMALLY INVASIVE SURGERY IN THE FOREFOOT Miss Sue Kendall PhD FRCS (Orth&Trauma) Is Minimally Invasive Surgery of the foot a good idea? Minimally invasive surgery, keyhole surgery entering
Classical Mitchell's osteotomy in the management of symptomatic hallux vulgus
 International Journal of Research in Orthopaedics Wani NB et al. Int J Res Orthop. 2016 Dec;2(4):366-370 http://www.ijoro.org Original Research Article DOI: http://dx.doi.org/10.18203/issn.2455-4510.intjresorthop20164170
International Journal of Research in Orthopaedics Wani NB et al. Int J Res Orthop. 2016 Dec;2(4):366-370 http://www.ijoro.org Original Research Article DOI: http://dx.doi.org/10.18203/issn.2455-4510.intjresorthop20164170
Long-term results of the Hohmann and Lapidus procedure for the correction of hallux valgus
 FOOT AND ANKLE Long-term results of the Hohmann and Lapidus procedure for the correction of hallux valgus F. W. M. Faber, P. M. van Kampen, M. W. Bloembergen From HAGA Hospital, Den Haag, the Netherlands
FOOT AND ANKLE Long-term results of the Hohmann and Lapidus procedure for the correction of hallux valgus F. W. M. Faber, P. M. van Kampen, M. W. Bloembergen From HAGA Hospital, Den Haag, the Netherlands
Woo Jin Choi, MD, Ihsan Oesman, MD, Hyun Kook Youn, MD, Jin Woo Lee, MD, PhD
 Woo Jin Choi, MD, Ihsan Oesman, MD, Hyun Kook Youn, MD, Jin Woo Lee, MD, PhD Department of Orthopaedic Surgery Yonsei University College of Medicine, Seoul, Korea < Presentation Title > The effect of combined
Woo Jin Choi, MD, Ihsan Oesman, MD, Hyun Kook Youn, MD, Jin Woo Lee, MD, PhD Department of Orthopaedic Surgery Yonsei University College of Medicine, Seoul, Korea < Presentation Title > The effect of combined
REPAIR OF THE DISPLACED AUSTIN OSTEOTOMY
 C H A P T E R 2 1 REPAIR OF THE DISPLACED AUSTIN OSTEOTOMY John V. Vanore, DPM INTRODUCTION Bunion surgery is frequently performed by foot and ankle surgeons. Generally, bunion surgery is quite predictable,
C H A P T E R 2 1 REPAIR OF THE DISPLACED AUSTIN OSTEOTOMY John V. Vanore, DPM INTRODUCTION Bunion surgery is frequently performed by foot and ankle surgeons. Generally, bunion surgery is quite predictable,
Hallux Malleus develops after Flexible Hallux Varus correction with Tensioned Suture Device: A Case Report
 The Foot and nkle Online Journal Official publication of the International Foot & nkle Foundation Hallux Malleus develops after Flexible Hallux Varus correction with Tensioned Suture Device: Case Report
The Foot and nkle Online Journal Official publication of the International Foot & nkle Foundation Hallux Malleus develops after Flexible Hallux Varus correction with Tensioned Suture Device: Case Report
Distal First Metatarsal Displacement Osteotomy
 Distal First Metatarsal Displacement Osteotomy ITS PLACE IN THE SCHEMA OF BUNION SURGERY* From the Section of Orthopedic Surgerv, The Mason Clinic. Seattle ABSTRACT: In a review of 401 operations for symptomatic
Distal First Metatarsal Displacement Osteotomy ITS PLACE IN THE SCHEMA OF BUNION SURGERY* From the Section of Orthopedic Surgerv, The Mason Clinic. Seattle ABSTRACT: In a review of 401 operations for symptomatic
Increased pressures at
 Surgical Off-loading of Plantar Hallux Ulcerations These approaches can be used to treat DFUs. By Adam R. Johnson, DPM Increased pressures at the plantar aspect of the hallux leading to chronic hyperkeratosis
Surgical Off-loading of Plantar Hallux Ulcerations These approaches can be used to treat DFUs. By Adam R. Johnson, DPM Increased pressures at the plantar aspect of the hallux leading to chronic hyperkeratosis
in the treatment of hallux valgus
 original ARTICLE Our experience with double metatarsal osteotomy in the treatment of hallux valgus Pradeep George Mathew, Pavel Šponer, Jaroslav Pavlata, Haroun Hassan Shaikh Charles University in Prague,
original ARTICLE Our experience with double metatarsal osteotomy in the treatment of hallux valgus Pradeep George Mathew, Pavel Šponer, Jaroslav Pavlata, Haroun Hassan Shaikh Charles University in Prague,
Current Concepts Review: Hallux Valgus Part II: Operative Treatment
 FOOT &ANKLE INTERNATIONAL Copyright 2007 by the American Orthopaedic Foot & Ankle Society, Inc. DOI: 10.3113/FAI.2007.0748 Current Concepts Review: Hallux Valgus Part II: Operative Treatment Mark E. Easley,
FOOT &ANKLE INTERNATIONAL Copyright 2007 by the American Orthopaedic Foot & Ankle Society, Inc. DOI: 10.3113/FAI.2007.0748 Current Concepts Review: Hallux Valgus Part II: Operative Treatment Mark E. Easley,
MULTIPLE APPLICATIONS OF THE MINIRAIL
 C H A P T E R 2 1 MULTIPLE APPLICATIONS OF THE MINIRAIL Thomas J. Merrill, DPM James M. Losito, DPM Mario Cala, DPM Victor Herrera, DPM Alan E. Sotelo, DPM INTRODUCTION The unilateral MiniRail External
C H A P T E R 2 1 MULTIPLE APPLICATIONS OF THE MINIRAIL Thomas J. Merrill, DPM James M. Losito, DPM Mario Cala, DPM Victor Herrera, DPM Alan E. Sotelo, DPM INTRODUCTION The unilateral MiniRail External
Treatment of hallux valgus by modified McBride procedure: a 6-year follow-up
 J Orthopaed Traumatol (2010) 11:89 97 DOI 10.1007/s10195-010-0092-0 ORIGINAL ARTICLE Treatment of hallux valgus by modified McBride procedure: a 6-year follow-up Istemi Yucel Yuksel Tenekecioglu Tahir
J Orthopaed Traumatol (2010) 11:89 97 DOI 10.1007/s10195-010-0092-0 ORIGINAL ARTICLE Treatment of hallux valgus by modified McBride procedure: a 6-year follow-up Istemi Yucel Yuksel Tenekecioglu Tahir
QUICK REFERENCE GUIDE. MiniRail System. Part B: Foot Applications. By Dr. B. Magnan, Dr. E. Rodriguez and Dr. G. Vito ALWAYS INNOVATING
 14 MiniRail System Part B: Foot Applications By Dr. B. Magnan, Dr. E. Rodriguez and Dr. G. Vito ALWAYS INNOVATING ORDERING INFORMATION Sterilization box, empty M190 Can accommodate: M101 Standard MiniRail
14 MiniRail System Part B: Foot Applications By Dr. B. Magnan, Dr. E. Rodriguez and Dr. G. Vito ALWAYS INNOVATING ORDERING INFORMATION Sterilization box, empty M190 Can accommodate: M101 Standard MiniRail
Joint Preserving Surgery in Severe Forefoot Disorders
 Joint Preserving Surgery in Severe Forefoot Disorders J ORTHOP TRAUMA SURG REL RES 4 (12) 2008 Review article LOUIS S. BAROUK*, PIERRE BAROUK** * 39, Chemin de la Roche, 33370, Yvrac, France ** Clinique
Joint Preserving Surgery in Severe Forefoot Disorders J ORTHOP TRAUMA SURG REL RES 4 (12) 2008 Review article LOUIS S. BAROUK*, PIERRE BAROUK** * 39, Chemin de la Roche, 33370, Yvrac, France ** Clinique
A COMPARISON OF KELLER S ARTHROPLASTY AND DISTAL METATARSAL OSTEOTOMY IN THE TREATMENT OF ADULT HALLUX VALGUS
 A COMPARISON OF KELLER S ARTHROPLASTY AND DISTAL METATARSAL OSTEOTOMY IN THE TREATMENT OF ADULT HALLUX VALGUS TIMOTHY TURNBULL, WILLIAM GRANGE From the North East Thames Regional Orthopaedic Centre, Black
A COMPARISON OF KELLER S ARTHROPLASTY AND DISTAL METATARSAL OSTEOTOMY IN THE TREATMENT OF ADULT HALLUX VALGUS TIMOTHY TURNBULL, WILLIAM GRANGE From the North East Thames Regional Orthopaedic Centre, Black
LAPIDUS What is Old is New
 LAPIDUS What is Old is New Alan Jay Block, DPM, MS, FASPS, FACFAS Fellowship trained in Advanced Ankle Techniques Adjunct Professor Dept Of Orthopeadics The Ohio State University Board Member The Ohio
LAPIDUS What is Old is New Alan Jay Block, DPM, MS, FASPS, FACFAS Fellowship trained in Advanced Ankle Techniques Adjunct Professor Dept Of Orthopeadics The Ohio State University Board Member The Ohio
Geoffrey Watson, MD Matthew McKean, MD Siddhant K. Mehta, MD Thom A. Tarquinio, MD
 Geoffrey Watson, MD Matthew McKean, MD Siddhant K. Mehta, MD Thom A. Tarquinio, MD University of Mississippi Medical Center Jackson, Mississippi American Orthopaedic Foot & Ankle Society ANNUAL MEETING
Geoffrey Watson, MD Matthew McKean, MD Siddhant K. Mehta, MD Thom A. Tarquinio, MD University of Mississippi Medical Center Jackson, Mississippi American Orthopaedic Foot & Ankle Society ANNUAL MEETING
1 Relationship between degenerative change in the sesamoid-metatarsal joint and 2 displacement of the sesamoids in patients with hallux valgus 3 4
 1 Relationship between degenerative change in the sesamoid-metatarsal joint and 2 displacement of the sesamoids in patients with hallux valgus 3 4 Abstract 5 Background: To treat a patient with hallux
1 Relationship between degenerative change in the sesamoid-metatarsal joint and 2 displacement of the sesamoids in patients with hallux valgus 3 4 Abstract 5 Background: To treat a patient with hallux
Instructional Course Lectures
 2519 Selected Instructional Course Lectures The American Academy of Orthopaedic Surgeons PAUL J. DUWELIUS EDITOR, VOL. 57 COMMITTEE PAUL J. DUWELIUS CHAIRMAN FREDERICK M. AZAR KENNETH A. EGOL J. LAWRENCE
2519 Selected Instructional Course Lectures The American Academy of Orthopaedic Surgeons PAUL J. DUWELIUS EDITOR, VOL. 57 COMMITTEE PAUL J. DUWELIUS CHAIRMAN FREDERICK M. AZAR KENNETH A. EGOL J. LAWRENCE
MiniRail System. Part B: Foot Applications. By Dr. B. Magnan, Dr. E. Rodriguez and Dr. G. Vito
 Q U I C K R E F E R E N C E G U I D E 14 MiniRail System Part B: Foot Applications By Dr. B. Magnan, Dr. E. Rodriguez and Dr. G. Vito ORDERING INFORMATION MiniRail System Kit, M190C Contents: M 101 Standard
Q U I C K R E F E R E N C E G U I D E 14 MiniRail System Part B: Foot Applications By Dr. B. Magnan, Dr. E. Rodriguez and Dr. G. Vito ORDERING INFORMATION MiniRail System Kit, M190C Contents: M 101 Standard
Lesser MPJ Hemi Implant
 Lesser MPJ Hemi Implant Surgical Technique Contents Product The BioPro Lesser MPJ Hemi Implant is a simple, durable, metallic hemiarthroplasty resurfacing prosthesis for the treatment of arthritis, Freiberg
Lesser MPJ Hemi Implant Surgical Technique Contents Product The BioPro Lesser MPJ Hemi Implant is a simple, durable, metallic hemiarthroplasty resurfacing prosthesis for the treatment of arthritis, Freiberg
6/5/2018. Forefoot Disorders. Highgate Private Hospital (Royal Free London NHS Foundation Trust (Barnet & Chase Farm Hospitals) Hallux Rigidus
 Forefoot Disorders Mr Pinak Ray (MS, MCh(Orth), FRCS, FRCS(Tr&Orth)) Highgate Private Hospital (Royal Free London NHS Foundation Trust (Barnet & Chase Farm Hospitals) E: ray.secretary@uk-conslutants Our
Forefoot Disorders Mr Pinak Ray (MS, MCh(Orth), FRCS, FRCS(Tr&Orth)) Highgate Private Hospital (Royal Free London NHS Foundation Trust (Barnet & Chase Farm Hospitals) E: ray.secretary@uk-conslutants Our
Bunionectomy-Forefoot Surgery
 Richard M. Marks, MD Professor and Director Division of Foot and Ankle Department of Orthopaedic Surgery Medical College of Wisconsin Explanation: Bunionectomy-Forefoot Surgery A bunion (also called hallux
Richard M. Marks, MD Professor and Director Division of Foot and Ankle Department of Orthopaedic Surgery Medical College of Wisconsin Explanation: Bunionectomy-Forefoot Surgery A bunion (also called hallux
DARCO. Bow 2 Plate SURGIC AL TECHNIQUE
 DARCO Bow 2 Plate SURGIC AL TECHNIQUE Contents 2 Preface 3 Chapter 1 4 Chapter 2 5 6 7 8 9 Appendix 10 10 11 Intended Use Indications/Contraindications Design Rationale Preoperative Planning Surgical Technique
DARCO Bow 2 Plate SURGIC AL TECHNIQUE Contents 2 Preface 3 Chapter 1 4 Chapter 2 5 6 7 8 9 Appendix 10 10 11 Intended Use Indications/Contraindications Design Rationale Preoperative Planning Surgical Technique
WHAT DO HALLUX VALGUS AND BUNION MEAN?
 Mr Laurence James BSc MBBS MRCS(Eng) FRCS(Tr&Orth) Consultant Orthopaedic Surgeon Foot, Ankle and Sports Injuries WHAT DO HALLUX VALGUS AND BUNION MEAN? Hallux is Latin for great toe and Valgus is Latin
Mr Laurence James BSc MBBS MRCS(Eng) FRCS(Tr&Orth) Consultant Orthopaedic Surgeon Foot, Ankle and Sports Injuries WHAT DO HALLUX VALGUS AND BUNION MEAN? Hallux is Latin for great toe and Valgus is Latin
The Effect of Hallux Abducto Valgus Surgery on the Sesamoid Apparatus Position
 1999 WILLIAM J. STICKEL GOLD AWARD The Effect of Hallux Abducto Valgus Surgery on the Sesamoid Apparatus Position MOLLY S. JUDGE, DPM* STEPHAN LAPOINTE, DPM, PhD GERARD V. YU, DPM JEFFREY E. SHOOK, DPM
1999 WILLIAM J. STICKEL GOLD AWARD The Effect of Hallux Abducto Valgus Surgery on the Sesamoid Apparatus Position MOLLY S. JUDGE, DPM* STEPHAN LAPOINTE, DPM, PhD GERARD V. YU, DPM JEFFREY E. SHOOK, DPM
Investigation performed at the Department of Orthopaedic and Trauma Surgery, Glasgow Royal Infirmary, Glasgow, United Kingdom
 748 COPYRIGHT 2005 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Long-Term Results of the Modified Hoffman Procedure in the Rheumatoid Forefoot BY S. THOMAS, MBCHB, BSC, MRCS, A.W.G. KINNINMONTH,
748 COPYRIGHT 2005 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Long-Term Results of the Modified Hoffman Procedure in the Rheumatoid Forefoot BY S. THOMAS, MBCHB, BSC, MRCS, A.W.G. KINNINMONTH,
The bunionette the epidemiological and results from technical Ludloff study. Mário Kuhn Adames Gustavo Batista Birro Rafael da Silveira Basso
 The bunionette the epidemiological and results from technical Ludloff study Mário Kuhn Adames Gustavo Batista Birro Rafael da Silveira Basso NO CONFLICT DISCLOSE The bunionette the epidemiological and
The bunionette the epidemiological and results from technical Ludloff study Mário Kuhn Adames Gustavo Batista Birro Rafael da Silveira Basso NO CONFLICT DISCLOSE The bunionette the epidemiological and
HEMI IMPLANT ARTHROPLASTY FOR THE SECOND METATARSOPHALANGEAL JOINT
 C H A P T E R 1 5 HEMI IMPLANT ARTHROPLASTY FOR THE SECOND METATARSOPHALANGEAL JOINT Joe T. Southerland, DPM Mickey D. Stapp, DPM INTRODUCTION Hemi-implant arthroplasty of the first metatarsophalangeal
C H A P T E R 1 5 HEMI IMPLANT ARTHROPLASTY FOR THE SECOND METATARSOPHALANGEAL JOINT Joe T. Southerland, DPM Mickey D. Stapp, DPM INTRODUCTION Hemi-implant arthroplasty of the first metatarsophalangeal
The risk of avascular necrosis following chevron osteotomy : A prospective study using bone scintigraphy
 Acta Orthop. Belg., 2009, 75, 234-238 ORIGINAL STUDY The risk of avascular necrosis following chevron osteotomy : A prospective study using bone scintigraphy Raheel SHARIFF, Fahad ATTAR, Donald OsARUMWENE,
Acta Orthop. Belg., 2009, 75, 234-238 ORIGINAL STUDY The risk of avascular necrosis following chevron osteotomy : A prospective study using bone scintigraphy Raheel SHARIFF, Fahad ATTAR, Donald OsARUMWENE,
Axi+LineTM Proximal Bunion CorrectionSystem. Surgical Technique
 Axi+LineTM Proximal Bunion CorrectionSystem Surgical Technique A i Line Proximal Bunion Correction System TM Desired angle correction is built into the plate, providing a self-reducing, 5-hole construct
Axi+LineTM Proximal Bunion CorrectionSystem Surgical Technique A i Line Proximal Bunion Correction System TM Desired angle correction is built into the plate, providing a self-reducing, 5-hole construct
Long Oblique Distal Osteotomy of the Fifth Metatarsal for Correction of Tailor s Bunion: A Retrospective Review
 Long Oblique Distal Osteotomy of the Fifth Metatarsal for Correction of Tailor s Bunion: A Retrospective Review Barry P. London, DPM, 1 Stephen F. Stern, DPM, 2 Mark A. Quist, DPM, 3 Robert K. Lee, DPM,
Long Oblique Distal Osteotomy of the Fifth Metatarsal for Correction of Tailor s Bunion: A Retrospective Review Barry P. London, DPM, 1 Stephen F. Stern, DPM, 2 Mark A. Quist, DPM, 3 Robert K. Lee, DPM,
4/22/2017 ADVENTURES IN FOREFOOT RECONSTRUCTIVE SURGERY WHAT IS FOREFOOT RECONSTRUCTION? HALLUX VALGUS CORRECTION
 4/22/217 ADVENTURES IN FOREFOOT RECONSTRUCTIVE SURGERY ERIN E. KLEIN, DPM, MS Associate Director of Research, Weil Foot & Ankle Institute Clinical Instructor, Dr William M Scholl College of Podiatric Medicine
4/22/217 ADVENTURES IN FOREFOOT RECONSTRUCTIVE SURGERY ERIN E. KLEIN, DPM, MS Associate Director of Research, Weil Foot & Ankle Institute Clinical Instructor, Dr William M Scholl College of Podiatric Medicine
Medical Policy Partial or Total Replacement of First Metatarsophalangeal Joint
 Medical Policy Partial or Total Replacement of First Metatarsophalangeal Joint Subject: Partial or Total Replacement of First Metatarsophalangeal (MTP) Joint Background: Underlying causes of disease or
Medical Policy Partial or Total Replacement of First Metatarsophalangeal Joint Subject: Partial or Total Replacement of First Metatarsophalangeal (MTP) Joint Background: Underlying causes of disease or
Short scarf osteotomy for hallux valgus medium term results
 E Poster presentation Short scarf osteotomy for hallux valgus medium term results 1. Rajesh Rachha - MBBS, DIP(ORTHO), MRCS, FEBOT, FRCS (Tr&Orth) 2. Saqib Javed - BSc, MBBS, MRCS 3. Cezary Kocialkowski
E Poster presentation Short scarf osteotomy for hallux valgus medium term results 1. Rajesh Rachha - MBBS, DIP(ORTHO), MRCS, FEBOT, FRCS (Tr&Orth) 2. Saqib Javed - BSc, MBBS, MRCS 3. Cezary Kocialkowski
MICA. Minimally Invasive Foot Surgery CHEVRON OSTEOTOMY SURGIC AL TECHNIQUE
 MICA Minimally Invasive Foot Surgery CHEVRON OSTEOTOMY SURGIC AL TECHNIQUE Contents Chapter 1 4 Introduction Chapter 2 5 Indications and Warnings Chapter 3 6 Patient Positioning and Set Up Chapter 4 7
MICA Minimally Invasive Foot Surgery CHEVRON OSTEOTOMY SURGIC AL TECHNIQUE Contents Chapter 1 4 Introduction Chapter 2 5 Indications and Warnings Chapter 3 6 Patient Positioning and Set Up Chapter 4 7
Correction of Traumatic Ankle Valgus and Procurvatum using the Taylor Spatial Frame: A Case Report
 The Foot and Ankle Online Journal Official publication of the International Foot & Ankle Foundation Correction of Traumatic Ankle Valgus and Procurvatum using the Taylor Spatial Frame: A Case Report by
The Foot and Ankle Online Journal Official publication of the International Foot & Ankle Foundation Correction of Traumatic Ankle Valgus and Procurvatum using the Taylor Spatial Frame: A Case Report by
Efficacy of a Kirschner-Wire Guide in Distal Linear Metatarsal Osteotomy for Correction of Hallux Valgus
 Efficacy of a Kirschner-Wire Guide in Distal Linear Metatarsal Osteotomy for Correction of Hallux Valgus Department of Orthopaedic Surgery, Faculty of Medicine, Fukuoka University Takefumi Nishino MD,
Efficacy of a Kirschner-Wire Guide in Distal Linear Metatarsal Osteotomy for Correction of Hallux Valgus Department of Orthopaedic Surgery, Faculty of Medicine, Fukuoka University Takefumi Nishino MD,
Mr. Siva Chandrasekaran Orthopaedic Surgeon MBBS MSpMed MPhil (surg) FRACS
 Bunion Surgery Most people with bunions find pain relief with simple treatments to reduce pressure on the big toe, such as wearing wider shoes or using pads in their shoes. However, if these measures do
Bunion Surgery Most people with bunions find pain relief with simple treatments to reduce pressure on the big toe, such as wearing wider shoes or using pads in their shoes. However, if these measures do
Can modification of the Weil osteotomy reduce the risk of dorsiflexion contracture? -A biomechanical cadaveric analysis
 Can modification of the Weil osteotomy reduce the risk of dorsiflexion contracture? -A biomechanical cadaveric analysis Anthony Perera University Hospital of Wales, UK Oscar Helguera-Mendoza Hospital Puerto
Can modification of the Weil osteotomy reduce the risk of dorsiflexion contracture? -A biomechanical cadaveric analysis Anthony Perera University Hospital of Wales, UK Oscar Helguera-Mendoza Hospital Puerto
Foot and Ankle Technique Guide Metatarsal Shortening Osteotomy
 Surgical Technique Foot and Ankle Technique Guide Metatarsal Shortening Osteotomy Prepared in consultation with: Phinit Phisitkul, MD Department of Orthopedics and Rehabilitation University of Iowa Iowa
Surgical Technique Foot and Ankle Technique Guide Metatarsal Shortening Osteotomy Prepared in consultation with: Phinit Phisitkul, MD Department of Orthopedics and Rehabilitation University of Iowa Iowa
ORTHOLOC 3Di. Foot Reconstruction System SURGIC AL TECHNIQUE
 ORTHOLOC 3Di Foot Reconstruction System S C R E W TA R G E T I N G G U I D E SURGIC AL TECHNIQUE SURGEON DESIGN TEAM The ORTHOLOC 3Di Foot Reconstruction System was developed in conjuction with: ORTHOLOC
ORTHOLOC 3Di Foot Reconstruction System S C R E W TA R G E T I N G G U I D E SURGIC AL TECHNIQUE SURGEON DESIGN TEAM The ORTHOLOC 3Di Foot Reconstruction System was developed in conjuction with: ORTHOLOC
REVISIONAT HAttUX VATGUS SURGERY
 REVISIONAT HAttUX VATGUS SURGERY Bradley Castellano, D.P.M. Recurrence of deformity is one of the more common complications in hallux valgus surgery (1-3). The deformity may have been undercorrected with
REVISIONAT HAttUX VATGUS SURGERY Bradley Castellano, D.P.M. Recurrence of deformity is one of the more common complications in hallux valgus surgery (1-3). The deformity may have been undercorrected with
Surgical correction of Hallux Valgus
 Surgical correction of Hallux Valgus complicated with adult type Pes planus Department of Orthopedic Surgery, Inje University, Ilsan Paik Hospital, Goyang-si, Korea * W Institute for Foot and Ankle Diseases
Surgical correction of Hallux Valgus complicated with adult type Pes planus Department of Orthopedic Surgery, Inje University, Ilsan Paik Hospital, Goyang-si, Korea * W Institute for Foot and Ankle Diseases
What Happens to the Paediatric Flat Foot? Peter J Briggs Freeman Hospital Newcastle upon Tyne
 What Happens to the Paediatric Flat Foot? Peter J Briggs Freeman Hospital Newcastle upon Tyne We don t know!! Population Studies 2300 children aged 4-13 years Shoe wearers Flat foot 8.6% Non-shoe wearers
What Happens to the Paediatric Flat Foot? Peter J Briggs Freeman Hospital Newcastle upon Tyne We don t know!! Population Studies 2300 children aged 4-13 years Shoe wearers Flat foot 8.6% Non-shoe wearers
LOWER EXTREMITIES SINGLE-USE INSTRUMENTATION SURGICAL IMPLANTATION TECHNIQUE. First Metatarsal Phalangeal Joint FOOT THE DIFFERENCE IS MOVING.
 LOWER EXTREMITIES SINGLE-USE INSTRUMENTATION SURGICAL IMPLANTATION TECHNIQUE First Metatarsal Phalangeal Joint FOOT THE DIFFERENCE IS MOVING. CARTIVA SYNTHETIC CARTILAGE IMPLANT SURGICAL IMPLANTATION TECHNIQUE
LOWER EXTREMITIES SINGLE-USE INSTRUMENTATION SURGICAL IMPLANTATION TECHNIQUE First Metatarsal Phalangeal Joint FOOT THE DIFFERENCE IS MOVING. CARTIVA SYNTHETIC CARTILAGE IMPLANT SURGICAL IMPLANTATION TECHNIQUE
