Fractures of the clavicle, or collarbone, are common
|
|
|
- Reynard Shields
- 5 years ago
- Views:
Transcription
1 C H A P T E R 8 CARE OF PATIENTS WITH SPECIFIC FRACTURES CHAPTER OBJECTIVE After completing this chapter, the reader will be able to describe the medical management and nursing care of patients who have experienced a fracture. LEARNING OBJECTIVES After studying this chapter, the reader will be able to 1. indicate the medical management of the patient who has experienced a fracture of the clavicle, upper extremity, pelvis, spine, or lower extremity. 2. specify the nursing care of the patient who has experienced a fracture of the clavicle, upper extremity, pelvis, spine, or lower extremity. 3. indicate the principles of rehabilitation for a patient who has experienced a fracture of the clavicle, upper extremity, pelvis, spine, or lower extremity. OVERVIEW 101 The medical management and nursing care of a patient who has experienced a fracture will vary depending on the type and location of the fracture. The nurse must have an understanding of the patient s needs related to the specific fracture to provide safe and competent nursing care. This chapter will discuss the care of patients who have experienced fractures of the clavicle, upper extremity, pelvis, spine, or lower extremity. Special emphasis will be placed on the rehabilitation process and assisting the patient to avoid complications and regain full function following a fracture. FRACTURE OF THE CLAVICLE Fractures of the clavicle, or collarbone, are common fractures, especially in children. The clavicle forms the anterior portion of each shoulder. The most likely cause of a clavicle fracture is a direct blow to the shoulder or a fall where the person tries to break the fall with an extended arm (Cheever, 2008b: Schoen, 2000). Contact sports are likely causes of clavicle fractures. The most common clavicular fracture occurs at the middle of the clavicle. A patient who has experienced a fractured clavicle experiences pain and slumps the shoulders forward. The patient usually holds the arm to minimize movement and protect the clavicle. This type of fracture is frequently treated by a closed reduction and immobilization of the shoulder. A less common fracture occurs along the distal third of the clavicle. This type of fracture may be associated with ligament damage. If ligament damage occurs and the bone ends become displaced, an open reduction with internal fixation may be required to realign the fracture (Cheever, 2008b).
2 102 Orthopedic Nursing: Caring for the Patient with Musculoskeletal Disorders Treatment of a clavicle fracture involves realignment and immobilization of the clavicle using a clavicular strap that holds the shoulders back in place (see Figure 8-1). If the fracture has occurred in the distal third of the clavicle and is not displaced, the only treatment may be a sling that serves to immobilize the arm (Cheever, 2008b). FIGURE 8-1: CLAVICULAR STRAP Immobilization is accomplished with a clavicular strap. Clavicular fractures usually heal without complication within about 6 weeks. During the healing time, the patient is instructed by the nurse not to lift the arm above shoulder level. The patient is encouraged, however, to continue exercising the fingers, wrist, and elbow to prevent loss of function. It will be approximately 3 months before the patient can resume normal activity. Complications, if they do occur, are related to brachial nerve damage, subclavian artery or vein damage, or malunion of the bone ends (Cheever, 2008b). FRACTURE OF THE UPPER EXTREMITY Fractures of the upper extremity include fractures of the humerus, ulna, radius, wrist, and hand. Each of these fracture locations will be briefly discussed, including medical management and nursing care appropriate for the specific location. Humerus Humerus fractures may occur proximally (near the shoulder), distally (near the elbow), or in the shaft of the humerus. Humerus fractures are caused either by a direct blow to the arm or indirectly by the person trying to break a fall with an outstretched arm. Fractures of the humerus usually heal within 6 to 10 weeks. A fractured humeral shaft is one of the most common fractures and usually is the result of trauma, such as a car crash, gunshot, or crush injury. Most humeral shaft fractures heal rapidly without complication. Because of the relatively small size of the arm muscles, the fractured bone ends typically remain aligned and do not override each other. This maintenance of alignment makes reduction of the fracture easier to achieve and promotes healing. Most humeral shaft fractures can be reduced through closed manipulation and the use of a functional brace. A functional brace involves the placement of a thermoplastic splint device, which is secured to the upper arm with the use of Velcro straps, while a sling supports the lower arm at a 90 degree angle at the elbow. The functional brace provides minimal immobilization of the humerus, while allowing gravity to maintain alignment of the fracture. The advantage of a functional brace is that it promotes movement of the shoulder, elbow joint, and wrist, thus helping to prevent loss of function of these joints while the fracture heals. Additionally, the brace can be readjusted as swelling decreases in the arm, maintaining a secure fit (Cheever, 2008b; Roberts, 2009). A hanging arm cast, which provides more immobilization and is allowed to hang down to promote the use of gravity, may also be used to treat humeral fractures. Hanging arm casts are more likely to be used for displaced fractures, especially oblique or spiral fractures, which have caused shortening in the extremity. Hanging casts provide additional pull or traction on the arm to maintain alignment of the fracture due to their weight. A
3 Care Of Patients With Specific Fractures 103 hanging arm cast is used cautiously because if the cast weight is too heavy it can lead to a separation of the bone ends and nonunion of the fracture. X-rays are used to validate the effect of the cast. Occasionally, an open reduction and internal fixation surgical procedure may be necessary to reduce the fracture and hold the bone ends in alignment with screws, plates, or pins. The two most common complications of humeral shaft fractures are nonunion and radial nerve damage (Cheever, 2008b) A fracture of the proximal humerus, which is near the shoulder, usually occurs in or near the surgical or anatomical neck of the humerus. A common type of proximal humerus fracture is the impacted fracture that occurs when the person tries to break a fall with an outstretched arm. This type of fracture is especially common in older adults. An impacted fracture is not displaced and usually heals without difficulty, requiring only a sling to support the arm while the fracture heals. Patients are encouraged to do pendulum exercises as tolerated during the healing period to prevent shoulder stiffness and maintain functionality. If the fracture is displaced, the distal fragment of the fracture is usually pulled upward to override the proximal fragment. A closed or open reduction will be necessary to regain alignment. A proximal humerus fracture will take 6 to 10 weeks, to heal as long as the patient complies with immobilization of the affected arm. Complications related to the fracture of the proximal humerus include damage to the nerves and blood vessels in the area of injury (Roberts, 2009). Fractures of the distal humerus are located near the elbow joint. This type of fracture is most common in children and older adults, and typically results from falls on the elbow, motor vehicle accidents, or other types of direct blows. To treat a fracture of a distal humerus, the fracture is reduced through either closed or open reduction, and a cast is placed on the arm with the elbow placed in 45 to 90 degrees of flexion to maintain bone alignment. If the fracture is displaced, side-arm traction may be necessary to maintain alignment (see Figure 8-2). It is essential that the nurse frequently check the patient s neurovascular status. Distal humerus fractures may cause injury to the ulnar, radial, or median nerves. Given the closeness to the elbow joint, these fractures are particularly susceptible to swelling within the muscle compartment which can lead to neurovascular compromise and compartment syndrome which, if not treated promptly, can result in a Volkmann s ischemic contracture of the hand and arm (Cheever, 2008b) and permanent disability. A Volkmann s contracture of the upper extremity is a permanent flexion contraction of the hand, fingers and wrist. The patient loses varying degrees of functionality in the extremity, depending upon the severity of the contracture. Figure 8-3 shows a picture of Volkmann s contracture. Nursing care of the patient with a fractured humerus is focused on pain relief, prevention or early detection of complications, and maintenance of joint function in the affected arm. It will be impor- FIGURE 8-2: LATERAL ARM IMMOBILIZATION Commonly used in immobilization of fractures and dislocations of the upper arm and shoulder. Inspect the pin site and perform pin site care according to hospital policy. Assess neurovascular status. Note. From Medical-surgical nursing: Assessment and management of clinical problems (7th ed., p. 1775) by S. Lewis, M. Heitkemper, & S. Dirksen, St. Louis, MO: Mosby. Reprinted with permission from Elsevier.
4 104 Orthopedic Nursing: Caring for the Patient with Musculoskeletal Disorders FIGURE 8-3: VOLKMANN S ISCHEMIC CONTRACTURE Note. From Phipps medical-surgical nursing: Health and illness perspectives (8th ed., pp. 1540) by F.D. Monahan, J.K. Sands, M. Neighbors, J.F. Marek, & C.J. Green-Nigro, St. Louis, MO: Mosby Elsevier. Reprinted with permission. tant for the nurse to encourage or assist the patient to perform activities of daily living within his or her ability and to do range-of-motion exercises of all uninvolved joints at least every 4 hours during waking hours. The affected extremity is exercised as ordered by the physician. This usually begins one week after internal fixation (Cheever, 2008b). Radius and Ulna Fractures of the forearm are common, with fractures of the radius being most common. While the radius alone may be fractured, it is rare for the ulna alone to be fractured. If the ulna is fractured, it is likely that the radius has suffered a fracture as well. When either the radius or ulna is fractured, the most common concern is displacement of the fractures, especially in adults. Because the major movements of the forearm are supination and pronation, when reducing the fractures and achieving alignment, care must be given to align the bone ends such that the functions of supination and pronation will be preserved. The pull of the various muscles in the forearm can make it difficult for this alignment to be achieved through closed reduction alone, especially in adults (Schoen, 2000). Non-displaced fractures of the radius and ulna are treated by closed reduction and a long arm cast is applied. The arm will be supported by a sling. Displaced fractures are managed by open reduction internal fixation with a compression plate with screws, intramedullary nails, or rods. The arm is immobilized in a splint or cast. Following cast application, the nurse focuses on circulation, the patient s ability to flex fingers, and sensation in the hand. Bone alignment and healing is monitored by radiography (Cheever, 2008b). Fractures that have occurred above the pronator radii teres will require that the forearm be placed in a supine position to properly align the bone ends. Fractures that have occurred below the pronator radii teres will require that the forearm be placed in a pronated position to achieve alignment. Casts or hard form splints are applied to the arm to maintain the healing position (Cheever, 2008b). Fractures of the radius and ulna usually require immobilization for approximately 12 weeks. Nursing care immediately following reduction of the fracture includes keeping the arm elevated to decrease edema. In addition, patients are encouraged to flex and extend fingers of the affected arm frequently to encourage circulation and decrease edema. Neurovascular checks, which include an assessment of the affected extremity s circulation, sensation, and movement, are performed frequently to detect early changes that may indicate neurovascular compromise (Cheever, 2008b). If the patient is discharged home immediately following placement of a cast on a nondisplaced fracture, it is important that the nurse provide discharge teaching that emphasizes keeping the arm elevated, assessing the neurovascular status of the affected arm, performing cast care, and achieving pain control. It is also important to teach the patient how to maintain function of the shoulder in the affected arm. Even though the arm is immobilized by a cast, shoulder exercises are necessary to avoid loss of function in the shoulder area. Wrist and Hand The most common fracture of the wrist is a fracture of the distal radius known as a Colles fracture. These fractures are commonly seen in elderly women who have osteoporosis and have experienced a fall on an outstretched, dorsiflexed hand.
5 Care Of Patients With Specific Fractures 105 During examination, the wrist will look swollen, deformed, and deviate towards the radius. The patient will complain of pain and may experience numbness as well (Cheever, 2008b). Most Colles fractures can be treated with closed manipulation and the placement of a cast. It is important that the patient keep the hand elevated at heart level the first couple of days following the injury to reduce swelling in the fingers. This can be accomplished by elevating the hand with pillows and support to the elbow (Cheever, 2008b). To prevent stiffness and loss of function in the fingers and shoulder, the patient is taught active exercises that will help keep swelling to a minimum and retain function. One potential complication of a Colles fracture is median nerve damage. The nurse can assess for median nerve damage by checking the patient s thumb opposition to the little finger and by pricking the distal surface of the index finger to test sensation (Cheever, 2008b). Fractures of the bones of the hand are classified by the nature and site of the fracture line and whether the fracture is closed or open. It is important to realize that the deformities that occur as a result of a hand fracture are due to the mechanism of injury as well as the defining forces of the musculotendinous units acting across the fracture site. Fractures can be highly variable, ranging from simple, nondisplaced fractures of the fingers to traumatic injuries that require extensive reconstruction. Nondisplaced fractures of the fingers are typically taped to immobilize the fracture. For nondisplaced closed fractures of the hand, closed reduction and cast immobilization for 6 to 12 weeks will likely be the treatment of choice. Most hand fractures heal rapidly because of the good blood supply to the area (Roberts, 2009). Fractures that are displaced or open may require an open reduction with the insertion of pins or wires. Nursing care following reduction of the fracture includes frequent neurovascular checks and keeping the hand elevated to decrease edema. Range-of-motion exercises, as appropriate, will be encouraged to maintain hand functionality. FRACTURE OF THE PELVIS The most likely cause of a pelvic fracture is a motor vehicle accident. Other common causes include skiing accidents, motorcycle accidents, crush injuries, and falls. Pelvic fractures can result in very serious and life-threatening injuries. Many patients who experience pelvic fractures also suffer additional trauma at the time of the injury. Pelvic fractures themselves can cause significant injury to the organs that lie in the immediate area, such as the bladder and colon. There is also a high incidence of spinal fractures that occur with pelvic fractures. Due to the vascularity of the area, pelvic fractures are also associated with a high risk of hemorrhage and hypovolemic shock, which can be life-threatening if not detected and treated early. Patients who experience a pelvic fracture are also susceptible to complications during the rehabilitation phase. These complications include fat emboli, deep vein thrombosis, pulmonary emboli, and infection. To avoid these complications, a goal of treatment will be to stabilize the fracture and encourage early mobility. Clinical indications of a pelvic fracture include swelling, ecchymosis, unusual movement in the pelvic area, and tenderness (Childs, 2007). In addition, the patient may experience numbness and tingling in the pubic area and upper thighs. The patient will also have difficulty bearing weight due to the pain (Cheever, 2008a). Pelvic fractures may be either stable or unstable. Figure 8-4 depicts the various types of stable pelvic fractures. Management of pelvic fractures includes the early detection of complications. Hemorrhage and the potential for hypovolemic shock are significant clinical concerns immediately post-injury, so the patient will be monitored closely for signs of bleeding. Another clinical concern is maintaining an adequate nerve and blood supply to both lower
6 106 Orthopedic Nursing: Caring for the Patient with Musculoskeletal Disorders FIGURE 8-4: EXAMPLE OF A STABLE PELVIC FRACTURE FIGURE 8-5: EXAMPLE OF UNSTABLE PELVIC FRACTURES extremities, therefore frequent neurovascular checks of the lower extremities are essential. Patients must also be closely examined for injury to the colon, bladder, and urinary tract, and they will likely undergo a series of X-rays or CT scans to detect injury to underlying abdominal structures. Radiology studies should include an anteroposterior X-ray of the pelvis, which is necessary to view any injury to the sacral iliac joint, sacral foramina, and posterior displacement. Blood in the urine and/or rectal area is an indication of damage to the bladder or rectal tears as a result of displaced pelvis fractures. Abdominal compartment syndrome is a serious complication of pelvic fractures. Treatment of the fracture itself will depend on the severity of the injury. If the patient has a stable fracture of the pelvis, it is possible that the fracture can be treated with bed rest for a prescribed period of time (Childs 2007). Pelvic fractures can heal quickly due to the vascular nature of the area, subsequently healing may occur within 6 weeks. Unstable pelvic fractures will require either an open reduction and internal fixation or an external fixation to promote stabilization of the fracture and early mobility. Figure 8-5 depicts illustrations of unstable pelvic fractures. Skeletal traction may also be necessary to maintain alignment. During the time the patient is on bedrest, it is essential that the nurse encourage range-of-motion exercises to all unaffected joints as well as ankle pumps and leg exercises to maintain mobility and circulation and avoid hazards of immobility. Rotationally Unstable Vertically & Posteriorly Stable Rotationally Unstable Vertically & Posteriorly Unstable Muscle setting exercises, such as gluteal and quadriceps sets, help maintain muscle tone and improve circulation. The patient should be turned to the side only as ordered by the physician. If turning is allowed, the patient is typically tilted to the side at approximately 45 degrees, and log rolling will be used to maintain alignment (Marek, 2007). The patient should be repositioned every 2 hours. Application of intermittent pneumatic compression devices, with or without elastic compression stockings, may also be used to decrease venous stasis. Venous stasis can lead to the development of venous thrombosis. Prophylactic anticoagulant therapy such as low-molecular-weight heparin may also be administered to prevent development of venous thrombosis. Adequate fluid and nutritional intake, pain control, skin care, coughing, and deep breathing are all aspects of the nursing care plan. Urinary output and bowel function are closely monitored as well. As the patient recovers, ambulation is gradually
7 Care Of Patients With Specific Fractures 107 resumed with the aid of a walker or crutches to assist with weight bearing (Cheever, 2008b) FRACTURE OF THE SPINE Fractures of the spine are most commonly caused by traumatic accidents, such as motor vehicle accidents, sports injuries, and falls. In older individuals, osteoporosis is a common cause of vertebral fractures. Metastatic bone cancer can also lead to pathological fractures of the spine. The area of the spine that is most susceptible to fracture is the T12 to L2 area (Cheever, 2008b). The most common type of vertebral fracture is a compression fracture which is caused by an excessive vertical load being placed on the spine. Examples of injuries that can lead to a compression fracture include sudden flexion injuries past normal range of motion limits and falling heavily on the buttocks from a height (Childs, 2007). Acute Care Fractures of the spine may be either stable or unstable but until confirmed by radiological films, they should be treated as unstable fractures. Most spinal fractures are stable fractures that do not cause damage to the spinal cord. An unstable fracture, in which there is an actual displacement of the fracture, can result in spinal cord injury and possibly permanent disability. This discussion is focused on stable spinal fractures. The stability of a spine fracture is determined by a combination of X-ray, CT scan, and MRI. A CT scan will determine the bone alignment and/or displacement while the MRI will detect the presence of any spinal cord compression. Patients who have experienced a spinal fracture will complain of acute pain in the area of the injury accompanied by swelling and paravertebral muscle spasms. The patient experiences increased pain upon weight-bearing and movement. A stable spinal fracture does not produce any neurologic deficits. If the patient experiences any neurologic deficits, the patient is likely to require immediate surgery to decompress the spinal cord, reducing the pressure being placed on the spinal cord and preventing further injury (Cheever, 2008b). The majority of spinal fractures can be treated conservatively, with the patient being placed on bed rest and the head of the bed elevated no more than 30 degrees. The main goal of treatment is to maintain the spine in good alignment while healing occurs. The patient should avoid an upright position during this acute phase and should also avoid twisting the back when being turned in bed. The nurse will assist the patient to turn using the log rolling technique so that the patient s shoulders, back, and hips are all turned simultaneously in one unit. The nurse should also encourage the patient to perform range of motion exercises during this period of bedrest, assisting the patient as necessary. Analgesics are administered to control pain. In addition to bedrest, heat may be applied to help relieve muscle spasms. In some instances, skin traction may also be applied to help immobilize the fracture, decrease compression and muscle spasms, and decrease pain (Cheever, 2008a). The nurse should assess the patient s neurovascular status frequently to detect any neurologic changes. Neurovascular checks are performed at least hourly for 24 to 48 hours post injury or surgery. Bladder and bowel control should also be assessed. Any difficulty in controlling bowel or bladder function or any changes in sensation or movement of the extremities should be immediately reported to the physician. The patient should also be assessed for the development of transient paralytic ileus of the bowel which can be caused by retroperitoneal hemorrhage (Cheever, 2008a). Subacute Care As the pain decreases, the patient will be allowed to sit and gradually resume activity. A thoracolumbar orthotic device (back brace) will be fit-
8 108 Orthopedic Nursing: Caring for the Patient with Musculoskeletal Disorders ted to the patient so that the patient can keep the spine in alignment when ambulating. Prior to getting the patient up to ambulate, the back brace should be placed on the patient while the patient is lying in bed. If the spinal fracture is in the cervical area, the patient may be fitted with a collar or halo vest (see Figure 8-6) to limit movement of the cervical spine. The patient is discharged home when able to safely ambulate and care for the orthotic device (Childs, 2007). FIGURE 8-6: HALO APPARATUS Halo vest, Ace manufacturing design. Note the rigid shoulder straps and encompassing vest. Various vest sizes are available prefabricated. The halo ring, superstructure, and vest are MRI compatible. Note. From Medical-surgical nursing: Assessment and management of clinical problems (7th ed., p. 1601) by S. Lewis, M. Heitkemper, S. Dirksen, P. O Brien, & L. Bucher, St. Louis, MO: Mosby. Reprinted with permission from Elsevier. FRACTURE OF THE LOWER EXTREMITY Fractures of the lower extremity involve the femur, tibia, and fibula. Each of these fracture locations will be briefly discussed, including medical management and nursing care appropriate for the specific location. Femur Fractures of the femur can occur in the neck of the femur or in the proximal, midshaft, or distal sections (see Figure 8-7). This discussion on femoral fractures will focus on femoral shaft fractures that occur either proximally, midshaft, or distally. Fractures of the femoral neck will be discussed in Chapter 9, on care of the patient with a hip fracture. Treatment will vary depending upon the type of femoral fracture the patient has experienced. Fracturing a femur in an adult individual requires a significant amount of force. This force is usually the result of a traumatic event, such as a motor vehicle accident, fall, or sports accident. Young adults are typically the ones who experience a fractured femur. Because of the amount of force necessary to fracture a femur, it is quite likely that the patient will also experience soft tissue injuries and other trauma as well. The clinical manifestations of a fractured femoral shaft include acute pain, swelling, deformity in the thigh, angulation, shortening of the extremity due to muscle spasms, and an inability to move the hip or knee (Childs, 2007). Patients who have a fractured femur must be closely assessed for hemorrhage, which can result from soft tissue damage and the subsequent onset of hypovolemic shock. The patient can lose up to 3 units of blood as a result of a femoral fracture so the potential for developing hypovolemic shock is very possible; the nurse should closely examine the thigh for an increasing diameter which can be indicative of bleeding into the tissues. The neurovascular status of the affected extremity also needs to be closely assessed at frequent intervals. The nurse should compare the neurovascular assessment of the affected leg to the unaffected leg to note any differences. Peripheral pulses can be checked with a Doppler device which provides ultrasound monitoring to assess blood flow status in the affected extremity (Cheever, 2008b).
9 Care Of Patients With Specific Fractures 109 FIGURE 8-7: FRACTURES OF THE FEMUR Note. From Medical-surgical nursing: Clinical management for positive outcomes (8th ed., pp. 527), by J. Black & J. Hawks, Philadelphia, PA: Saunders-Elsevier. Reprinted with permission from Elsevier. Initial treatment of a fractured femur is focused on immobilizing the fracture to prevent further injury and minimize hemorrhaging. Immediate immobilization of the fracture is usually accomplished by the placement of a splint or the use of balanced suspension skeletal traction. In addition, the fracture is manipulated as little as necessary to reduce the chances of a fat embolism. Intravenous fluids will be administered to replace blood volume loss and administer parenteral antibiotic therapy for open fractures. The treatment of the fracture will be dependent on several factors, including the type of fracture, the location, and whether it is an open or closed fracture. The patient s age and muscle size will also be determining factors. Because of the size of the femur and the strength of the thigh muscles, immobilizing the fracture and maintaining the alignment will require more than a cast. Balanced suspension skeletal traction may be applied during the initial treatment period to reduce the fracture. The most common type of balanced suspension skeletal traction used for a fractured femur is the Thomas splint with Pearson attachment. If the traction was to be left in place until healing of the fracture occurs, it would need to remain intact for 8 to 12 weeks. Treatment by skeletal traction alone is rare, however, and only occurs if the patient s medical condition does not allow for surgery. Typically, after a few days of skeletal traction reduction, during which the patient is allowed to stabilize physiologically, an open reduction and internal fixation of the fracture will be performed with the placement of intramedullary or interlocking nail devices. Internal fixation of the fracture is the preferred treatment of choice, as it allows for early ambulation, shorter hospitalization, and reduces the potential for complications (Childs, 2007). If the patient has experienced extensive soft tissue damage or bone loss, or multiple other traumas that do not allow the patient to undergo a surgical reduction and
10 110 Orthopedic Nursing: Caring for the Patient with Musculoskeletal Disorders internal fixation, it may be necessary to apply an external fixator to the femur instead. If the fracture is located in the supracondylar area (distal third) of the femur, the fracture is likely to be treated initially with skeletal traction for 2 to 3 weeks until the pain and swelling is decreased. At that time, the traction is removed and the patient is fitted with a cast brace, which will provide immobilization and support of the fracture, yet allow the patient earlier mobility with knee flexion and partial weight-bearing. A potential complication of a distal femur fracture and extended use of skeletal traction is the restriction of knee flexion and extension and a prolonged rehabilitation period as the patient works to regain full range of motion of the knee. Following successful reduction of the femoral fracture, two goals for all patients are to promote ambulation as early as possible and avoid complications. Following surgery for open reduction and internal fixation of the fracture, the patient s leg may be placed in suspension traction for 2 to 3 days to provide support and promote comfort. While the patient is on bedrest, it is important for the nurse to position the patient in proper body alignment, observe for pressure points on the skin, and provide skin care at regular intervals. The patient should be assisted in altering position at least every 2 hours. Active and passive range-ofmotion exercise of all joints is performed as soon as allowed, and the patient is taught to do muscle setting exercises and ankle pumps hourly while awake. The patient is also encouraged to participate in the performance of activities of daily living within his or her limitations and to remain as independent in these activities as feasible. Upper extremity exercises are also important to help the patient develop muscle strength. Maintaining joint function and muscle strength will help the patient to ambulate using assistive devices, such as crutches or walkers, when walking can be resumed. Full weight bearing will not be allowed until X-rays demonstrate evidence of union of the fractured bone ends. Tibia and Fibula Tibia fractures can occur alone or in combination with the fracture of the fibula. Frequently in lower leg fractures, both bones are fractured together. Sports injuries and motor vehicle accidents are common causes of tibia and fibula fractures. Accidents in which the foot is flexed during a fall or a violent twisting motion occurs also can result in tibia and fibula fractures. It is uncommon for the fibula, which is a non-weight bearing bone, to be fractured alone. Due to the lack of protective muscle covering over the lower third of the tibia, it is common for fractures of the tibia to be open fractures. This portion of the tibia is also particularly susceptible to vascular damage, due to the lack of muscle (Schoen, 2000). Fractures of the tibia and fibula are typically treated with either a closed reduction and a long leg cast; internal fixation and a long leg cast or, in the case of soft tissue damage, external fixation (Cheever, 2008b). The method of treatment will depend on the type and location of fracture and the extent of tissue damage present. The patient will be allowed to begin ambulating with partial weightbearing usually within 7 to 10 days. Early ambulation decreases edema and increases circulation in the affected extremity. In 3 to 4 weeks, the long leg cast will be removed and replaced with a short leg cast or splint. This allows the patient to begin flexing and exercising the knee, thus decreasing knee stiffness and preserving range of motion of the knee. Healing usually takes about 6 to 10 weeks. If tissue and vascular damage is extensive, healing may be delayed, and the patient may require bone grafts to stimulate bone growth (Cheever, 2008b). Electrical stimulation and low-frequency sound waves may also be used to promote bone growth in cases of delayed union or nonunion (Childs, 2007).
11 Care Of Patients With Specific Fractures 111 Care of the patient following reduction is similar to care of the patient with a fractured femur. The affected extremity should be elevated to decrease swelling, and neurovascular checks are performed at a minimum of every 2 hours. Fractures of the tibia are especially prone to the development of compartment syndrome, so the nurse should closely assess the patient s affected extremity for increasing pain that is unrelieved by analgesics, increasing pain upon passive plantar flexion of the foot, paresthesia, pallor, decreased or absent pulses, and coolness of the extremity. The nurse must immediately report these signs to the physician to prevent permanent damage. SUMMARY While fractures can vary by location and type, there are several principles that are common to the nursing care of any patient who has experienced a fracture. Table 8-1 summarizes these principles. By incorporating these principles into the care of patients who have a fracture, nurses can ensure that patients are receiving quality care. CASE STUDY D.H. is a young male, age 22, who was involved in a motorcycle accident, resulting in the compound fracture of his left femur. He is hospitalized for treatment of the fractured femur, with his left leg being placed in skeletal traction using a Thomas splint and Pearson attachment to support the leg. Twenty-five pounds of weights have been applied to maintain the traction. He has been hospitalized for2days. Answer the following case study questions, writing your responses on a separate sheet of paper. Compare your responses to the answers that follow. 1. What nursing assessments would be appropriate for you to make on D.H. at this time? TABLE 8-1: PRINCIPLES OF NURSING CARE FOR PATIENTS WITH A FRACTURE 1. Decrease pain and promote comfort. 2. Maintain satisfactory neurovascular status of affected body part. 3. Decrease risk for infection. 4. Maintain skin integrity. 5. Maintain muscle strength and joint function. 6. Encourage activity. 7. Maintain adequate nutrition and fluid intake. 8. Teach safety principles for use of assistive ambulatory devices (crutches, walkers). 9. Assess the patient carefully for potential complications, including fat emboli, pulmonary complications, infection, neurovascular compromise, and compartment syndrome. 10. Encourage independence and self-care as appropriate. 11. Provide home care instructions to patient and significant others. 2. Describe the advantages of treating D.H. s fractured femur with skeletal traction. 3. You are observing D.H. s position in bed and the alignment of the traction apparatus. What are the important points about his position and the alignment of the skeletal traction that you should be assessing? 4. What principles of nursing care should you incorporate into the plan of care for patients such as D.H. who have experienced a fracture? 5. You are providing pin care to the skeletal pin that is inserted in D.H. s left femur for the traction. What assessments should you make about the pin and pin site while you are performing the pin care? 6. Describe the complications that D.H. can develop as a result of the skeletal traction. 7. In preparation for ambulation, what exercises should you encourage D.H. to perform?
12 112 Orthopedic Nursing: Caring for the Patient with Musculoskeletal Disorders Answers to Case Study 1. The nursing assessments that are important at this stage of D.H s recovery include assessments that are specific to the fractured leg as well as assessments related to D.H. s potential for developing complications related to bedrest. A priority nursing assessment is the frequent evaluation of the neurovascular status of the fractured leg. The nurse should assess the neurovascular status of the leg at least every 4 hours and more frequently during the first 24 hours following the injury. A neurovascular assessment includes assessing the capillary filling time, temperature and color of the affected leg and foot, and palpating for peripheral pulses. Assessing for pain in the extremity, especially upon passive movement, sensation, and the ability to voluntarily move the foot are additional components of the neurovascular assessment. The nurse will also want to assess the patient for signs of infection due to the compound fracture and insertion of a skeletal pin. Because the patient is on bedrest, the nurse should assess the patient regularly for adverse effects related to bedrest. Lung sounds and bowel sounds should be assessed regularly. Fluid intake should be monitored and urinary output measured. The lower extremities should be assessed for indications of deep vein thrombosis. Skin should be inspected for areas of pressure development. The nurse should always assess the patient for fat embolism syndrome, which is most likely to develop within the first 24 to 48 hours following injury. 2. A major advantage of balanced suspension skeletal traction is that it provides direct pull on the fractured bone ends to achieve alignment. Another advantage of skeletal traction is that it allows the patient more mobility in bed without disrupting the line of traction. 3. When assessing D.H. s position in bed, the nurse should inspect the affected extremity to be sure that it is suspended off the bed and that the traction apparatus is not weighted down by bed linens. D.H. should be positioned in the center of the bed and in correct body alignment. Traction should be maintained without interruption. The traction weights should be hanging freely, and the counter traction should be maintained continuously. Ropes should move freely on the pulleys, and the rope knots should not be in contact with the pulleys. 4. Principles of care for the patient who has a fracture include: decreasing pain and promoting comfort maintaining satisfactory neurovascular status of affected body part decreasing the risk for infection maintaining skin integrity maintaining muscle strength and joint function encouraging activity maintaining adequate nutrition and fluid intake teaching safety principles for use of assistive devices assessing for complications encouraging self-care as appropriate and providing home care instructions. 5. When providing skeletal pin care, the nurse must ensure that aseptic technique is used. The nurse should assess the insertion site for purulent drainage, redness, odor, or pain. There should not be any movement of the pin at the insertion site. If the nurse detects movement or sliding of the pin, this should be reported promptly to the physician. The nurse should assess the patient for an elevated temperature, as this can be an indicator of an infection at the pin site, even before other, more obvious, signs of infection can be detected. 6. In addition to the complications that can result from bedrest, D.H. is susceptible to several complications as a result of having skeletal
13 Care Of Patients With Specific Fractures 113 traction applied to a fractured femur. One potential complication of skeletal traction is nonunion of the bone fragments due to the application of too much traction, thus separating the bone fragments. Overriding of bone fragments can occur if not enough traction has been applied. Another potential complication is skin breakdown as a result of the patient s supine position in bed or if the traction apparatus is applying pressure to points at various locations on the affected extremity. The nurse should closely inspect the heel of the unaffected leg, the coccyx, and the elbows for skin breakdown due to the patient shifting position in bed. The traction apparatus can apply pressure to several different areas of the affected leg the heel, achilles tendon, popliteal area, lateral aspect of the knee, and the ischial tuberosity. The nurse should inspect these areas several times per shift to ensure that pressure areas are not developing. Additional complications include the potential for peroneal nerve damage, deep vein thrombosis, and infection. 7. The goal is to preserve muscle tone and strength as well as the function of the joints as much as possible. Passive and active range-ofmotion exercises should be performed each shift. Muscle setting exercises, such as gluteal sets and quadriceps sets, will help prepare the patient for ambulation as well as support circulation. Ankle circling or pumping exercises also support circulation. Upper extremity exercises will help D.H. prepare to support himself with a walker or crutches. An overhead trapeze attached to the bed frame will help D.H. maneuver himself in bed and maintain upper body strength. REFERENCES Cheever, K. (2008a). Assessment of musculoskeletal function. In S. Smeltzer, B. Bare, J. Hinkle, & K. Cheever (Eds.), Brunner & Suddarth s textbook of medical-surgical nursing (11th ed., pp ). Philadelphia: Lippincott Williams & Wilkins. Cheever, K. (2008b). Management of patients with musculoskeletal trauma. In S. Smeltzer, B. Bare, J. Hinkle, & K. Cheever (Eds.), Brunner & Suddarth s textbook of medical-surgical nursing (11th ed., pp ). Philadelphia: Lippincott Williams & Wilkins. Childs, S. (2007). Musculoskeletal trauma and orthopedic surgery. In S. Lewis, M. Heitkemper, S. Dirksen, P.G. O Brien, & L. Bucher (Eds.), Medical-surgical nursing: Assessment and management of clinical problems (7th ed., pp ). St. Louis, MO: Mosby-Elsevier. Lewis, S., Heitkemper, M., & Dirksen, S. (2000). Medical-surgical nursing: Assessment and management of clinical problems (5th ed., p. 1775). St. Louis, MO: Mosby. Lewis, S., Heitkemper, M., Dirksen, S., O Brien, P., & Bucher, L. (2007). Medical-surgical nursing: Assessment and management of clinical problems (7th ed., p. 1601). St. Louis, MO: Mosby-Elsevier. Marek, J. (2007). Trauma to the musculoskeletal system. In F.D. Monahan, J.K. Sands, M. Neighbors, J.F. Marek, & C.J. Green-Nigro (Eds.). Phipps medical-surgical nursing: Health and illness perspectives (8th ed., pp ). St. Louis, MO: Mosby-Elsevier. Monahan, F.D., Sands, J.K., Neighbors, M., Marek, J.F., & Green-Nigro, C.J. (2007). Phipps medical-surgical nursing: Health and illness perspectives (8th ed., pp. 1540). St. Louis, MO: Mosby-Elsevier.
14 114 Orthopedic Nursing: Caring for the Patient with Musculoskeletal Disorders Roberts, D. (2009). Management of clients with musculoskeletal trauma or overuse. In J. Black & J. Hawks (Eds.), Medical-surgical nursing: Clinical management for positive outcomes (8th ed., pp ). Philadelphia: Saunders- Elsevier. Schoen, D. (2000). Adult orthopedic nursing. Philadelphia: Lippincott Williams & Wilkins.
15 E X A M Q U E S T I O N S 51. When providing discharge instructions to a patient who has fractured his clavicle, the nurse should tell the patient to a. exercise the fingers, wrist, and elbow. b. not lie supine until the clavicle has healed. c. perform shoulder shrugs every four hours. d. gently lift the affected arm over the head daily. 52. A patient with a distal humerus fracture that has been reduced and is newly casted is particularly susceptible to CHAPTER 8 Questions Note: Choose the option that BEST answers each question. 54. The nurse is caring for a patient on bedrest with a fractured pelvis. If the patient is allowed to turn, an appropriate way to accomplish this is to a. place the patient in a semi-sitting position by slightly raising the head of the bed. b. have the patient stand and bear weight. c. tilt the patient to the side at approximately 45 degrees and log roll. d. place the patient in the side lying Sims position with the knee and thigh drawn upward. a. infection. b. compartment syndrome. c. fat emboli syndrome. d. malunion. 53. To encourage circulation and decrease swelling for a patient who has fractured his radius and has a long arm cast, the patient should a. apply ice to the affected extremity. b. perform pendulum exercises. c. sit in a high-fowler s position. d. flex and extend fingers. 55. Patients with a fracture of the spine often experience muscle spasms. These can be treated by bedrest and a. applying heat to the area of the fracture. b. maintaining the patient in a semi-fowler s position. c. placing an abductor pillow between the patient s legs. d. avoiding frequent position changes. 56. The signs or symptoms of a possible fractured femur include a. excessive hip flexion. b. leg adduction. c. hyperextension of the knee. d. shortened length of extremity. 115
16 116 Orthopedic Nursing: Caring for the Patient with Musculoskeletal Disorders 57. The most likely initial treatment to reduce the fractured femur of an adult patient is a. a long leg cast. b. suspension traction. c. balanced suspension skeletal traction. d. cast brace. 58. For a patient placed on bed rest to promote healing of a fractured femur, the nurse should a. encourage the patient s family to perform activities of daily living for the patient. b. teach the patient upper extremity exercises to maintain muscle strength. c. instruct the patient to do muscle setting exercises once per day. d. help the patient adjust position every 4 hours while awake. 59. A principle goal of nursing care for any patient who has a fracture is a. administer prophylactic antibiotics. b. maintain patient in supine position. c. promote patient self-care and independence. d. provide daily pin care. 60. A patient with a fractured tibia who complains of increased pain when the nurse places the patient s affected foot in a position of plantar flexion is likely exhibiting signs of a. a normal finding for a patient with a fractured tibia. b. a fracture that is not properly aligned. c. compartment syndrome. d. inadequate pain control.
Surgical Care at the District Hospital. EMERGENCY & ESSENTIAL SURGICAL CARE
 Surgical Care at the District Hospital 1 18 Orthopedic Trauma Key Points 2 18.1 Upper Extremity Injuries Clavicle Fractures Diagnose fractures from the history and by physical examination Treat with a
Surgical Care at the District Hospital 1 18 Orthopedic Trauma Key Points 2 18.1 Upper Extremity Injuries Clavicle Fractures Diagnose fractures from the history and by physical examination Treat with a
Nursing Management: Musculoskeletal Trauma and Orthopedic Surgery. By: Aun Lauriz E. Macuja SAC_SN4
 Nursing Management: Musculoskeletal Trauma and Orthopedic Surgery By: Aun Lauriz E. Macuja SAC_SN4 The most common cause of musculoskeletal injuries is a traumatic event resulting in fracture, dislocation,
Nursing Management: Musculoskeletal Trauma and Orthopedic Surgery By: Aun Lauriz E. Macuja SAC_SN4 The most common cause of musculoskeletal injuries is a traumatic event resulting in fracture, dislocation,
.org. Tibia (Shinbone) Shaft Fractures. Anatomy. Types of Tibial Shaft Fractures
 Tibia (Shinbone) Shaft Fractures Page ( 1 ) The tibia, or shinbone, is the most common fractured long bone in your body. The long bones include the femur, humerus, tibia, and fibula. A tibial shaft fracture
Tibia (Shinbone) Shaft Fractures Page ( 1 ) The tibia, or shinbone, is the most common fractured long bone in your body. The long bones include the femur, humerus, tibia, and fibula. A tibial shaft fracture
Chapter 30 - Musculoskeletal_Trauma
 Introduction to Emergency Medical Care 1 OBJECTIVES 30.1 Define key terms introduced in this chapter. Slides 11 12, 19 20, 22 23, 37 30.2 Describe the anatomy of elements of the musculoskeletal system.
Introduction to Emergency Medical Care 1 OBJECTIVES 30.1 Define key terms introduced in this chapter. Slides 11 12, 19 20, 22 23, 37 30.2 Describe the anatomy of elements of the musculoskeletal system.
AMERICAN RED CROSS FIRST AID RESPONDING TO EMERGENCIES FOURTH EDITION Copyright 2006 by The American National Red Cross All rights reserved.
 Musculoskeletal injuries are most commonly caused by Mechanical forms of energy. Chemicals. Electrical energy. Heat Mechanical energy produces direct, indirect, twisting and contracting forces. Can be
Musculoskeletal injuries are most commonly caused by Mechanical forms of energy. Chemicals. Electrical energy. Heat Mechanical energy produces direct, indirect, twisting and contracting forces. Can be
1/3/2008. Karen Burke Priscilla LeMone Elaine Mohn-Brown. Medical-Surgical Nursing Care, 2e Karen Burke, Priscilla LeMone, and Elaine Mohn-Brown
 Medical-Surgical Nursing Care Second Edition Karen Burke Priscilla LeMone Elaine Mohn-Brown Chapter 42 Caring for Clients with Musculoskeletal Trauma Musculoskeletal Trauma Tissue is subjected to more
Medical-Surgical Nursing Care Second Edition Karen Burke Priscilla LeMone Elaine Mohn-Brown Chapter 42 Caring for Clients with Musculoskeletal Trauma Musculoskeletal Trauma Tissue is subjected to more
Chapter 8 8/23/2016. Body Mechanics and Patient Mobility. Introduction to Body Mechanics and Patient Mobility
 Chapter 8 Body Mechanics and Patient Mobility All items and derived items 2015, 2011, 2006 by Mosby, Inc., an imprint of Elsevier Inc. All rights reserved. Introduction to Body Mechanics and Patient Mobility
Chapter 8 Body Mechanics and Patient Mobility All items and derived items 2015, 2011, 2006 by Mosby, Inc., an imprint of Elsevier Inc. All rights reserved. Introduction to Body Mechanics and Patient Mobility
1 Chapter 29 Orthopaedic Injuries Principles of Splinting 2 Types of Muscles. Striated Skeletal. Smooth
 1 Chapter 29 Orthopaedic Injuries Principles of Splinting 2 Types of Muscles Striated Skeletal Smooth 3 Anatomy and Physiology of the Musculoskeletal System 4 Skeletal System 5 Skeletal System Functions
1 Chapter 29 Orthopaedic Injuries Principles of Splinting 2 Types of Muscles Striated Skeletal Smooth 3 Anatomy and Physiology of the Musculoskeletal System 4 Skeletal System 5 Skeletal System Functions
Chapter 29 Orthopaedic Injuries Principles of Splinting Types of Muscles
 1 2 3 4 5 6 7 Chapter 29 Orthopaedic Injuries Principles of Splinting Types of Muscles Striated Skeletal Smooth Anatomy and Physiology of the Musculoskeletal System Skeletal System Skeletal System Functions
1 2 3 4 5 6 7 Chapter 29 Orthopaedic Injuries Principles of Splinting Types of Muscles Striated Skeletal Smooth Anatomy and Physiology of the Musculoskeletal System Skeletal System Skeletal System Functions
Fractures Healing & Management. Traumatology RHS 231 Dr. Einas Al-Eisa Lecture 4
 Fractures Healing & Management Traumatology RHS 231 Dr. Einas Al-Eisa Lecture 4 Fractures Despite their strength, bones are susceptible to fractures. In young people, most fractures result from trauma
Fractures Healing & Management Traumatology RHS 231 Dr. Einas Al-Eisa Lecture 4 Fractures Despite their strength, bones are susceptible to fractures. In young people, most fractures result from trauma
Fractures and dislocations around elbow in adult
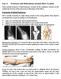 Lec: 3 Fractures and dislocations around elbow in adult These include fractures of distal humerus, fracture of the capitulum, fracture of the radial head, fracture of the olecranon & dislocation of the
Lec: 3 Fractures and dislocations around elbow in adult These include fractures of distal humerus, fracture of the capitulum, fracture of the radial head, fracture of the olecranon & dislocation of the
Injuries to the Extremities
 Injuries to the Extremities KNOWLEDGE OBJECTIVES 1. List seven signs and symptoms that suggest a serious extremity injury. 2. Describe how to care for injuries to the shoulder, upper arm, and elbow. 3.
Injuries to the Extremities KNOWLEDGE OBJECTIVES 1. List seven signs and symptoms that suggest a serious extremity injury. 2. Describe how to care for injuries to the shoulder, upper arm, and elbow. 3.
7/23/2018 DESCRIBING THE FRACTURE. Pattern Open vs closed Location BASIC PRINCIPLES OF FRACTURE MANAGEMENT. Anjan R. Shah MD July 21, 2018.
 BASIC PRINCIPLES OF FRACTURE MANAGEMENT Anjan R. Shah MD July 21, 2018 DESCRIBING THE FRACTURE Pattern Open vs closed Location POLL OPEN HOW WOULD YOU DESCRIBE THIS FRACTURE PATTERN? 1 Spiral 2 Transverse
BASIC PRINCIPLES OF FRACTURE MANAGEMENT Anjan R. Shah MD July 21, 2018 DESCRIBING THE FRACTURE Pattern Open vs closed Location POLL OPEN HOW WOULD YOU DESCRIBE THIS FRACTURE PATTERN? 1 Spiral 2 Transverse
A Patient s Guide to Adult Forearm Fractures
 A Patient s Guide to Adult Forearm Fractures Orthopedic and Sports Medicine 825 South 8th Street, #550 Minneapolis, MN 55404 Phone: 612-333-5000 Fax: 612-333-6922 1 DISCLAIMER: The information in this
A Patient s Guide to Adult Forearm Fractures Orthopedic and Sports Medicine 825 South 8th Street, #550 Minneapolis, MN 55404 Phone: 612-333-5000 Fax: 612-333-6922 1 DISCLAIMER: The information in this
Musculoskeletal System Objectives:
 Lemone and Burke Chapters 40-41 Musculoskeletal System Objectives: Review Anatomy and physiology Describe normal MS assessment Describe age related changes Discuss tests and nursing interventions Recognize
Lemone and Burke Chapters 40-41 Musculoskeletal System Objectives: Review Anatomy and physiology Describe normal MS assessment Describe age related changes Discuss tests and nursing interventions Recognize
Hip Surgery and Mobility
 Orthopedic Nursing, Part 1 Hip Surgery and Mobility Nursing Best Practice Guidelines Clinical Indications for Hip Surgery Selected fractures of the hip Unremitting pain and irreversible damaged joint from
Orthopedic Nursing, Part 1 Hip Surgery and Mobility Nursing Best Practice Guidelines Clinical Indications for Hip Surgery Selected fractures of the hip Unremitting pain and irreversible damaged joint from
REHABILITATION FOR SHOULDER FRACTURES & SURGERIES. Clavicle fractures Proximal head of humerus fractures
 REHABILITATION FOR SHOULDER FRACTURES & SURGERIES Clavicle fractures Proximal head of humerus fractures By Dr. Mohamed Behiry Lecturer Department of physical therapy for Orthopaedic and its surgery. Delta
REHABILITATION FOR SHOULDER FRACTURES & SURGERIES Clavicle fractures Proximal head of humerus fractures By Dr. Mohamed Behiry Lecturer Department of physical therapy for Orthopaedic and its surgery. Delta
OBJECTIVES: Define basic assessments skills needed to identify orthopedic injuries. Differentiate when an orthopedic injury is a medical emergency
 1 2 How to Triage Orthopaedic Care David W. Gray, M.D. OBJECTIVES: Define basic assessments skills needed to identify orthopedic injuries Differentiate when an orthopedic injury is a medical emergency
1 2 How to Triage Orthopaedic Care David W. Gray, M.D. OBJECTIVES: Define basic assessments skills needed to identify orthopedic injuries Differentiate when an orthopedic injury is a medical emergency
Fractures of the shoulder girdle, elbow and fractures of the humerus. H. Sithebe 2012
 Fractures of the shoulder girdle, elbow and fractures of the humerus H. Sithebe 2012 Fractures of the Clavicle (mid-shaft). Fractures of the clavicle Fractures of the clavicle Treatment- conservative.
Fractures of the shoulder girdle, elbow and fractures of the humerus H. Sithebe 2012 Fractures of the Clavicle (mid-shaft). Fractures of the clavicle Fractures of the clavicle Treatment- conservative.
Fractures of the Thoracic and Lumbar Spine
 A spinal fracture is a serious injury. Nader M. Hebela, MD Fellow of the American Academy of Orthopaedic Surgeons http://orthodoc.aaos.org/hebela Cleveland Clinic Abu Dhabi Cleveland Clinic Abu Dhabi Neurological
A spinal fracture is a serious injury. Nader M. Hebela, MD Fellow of the American Academy of Orthopaedic Surgeons http://orthodoc.aaos.org/hebela Cleveland Clinic Abu Dhabi Cleveland Clinic Abu Dhabi Neurological
Pediatric Fractures. Objectives. Epiphyseal Complex. Anatomy and Physiology. Ligaments. Bony matrix
 1 Pediatric Fractures Nicholas White, MD Assistant Professor of Pediatrics Eastern Virginia Medical School Attending, Pediatric Emergency Department Children s Hospital of The King s Daughters Objectives
1 Pediatric Fractures Nicholas White, MD Assistant Professor of Pediatrics Eastern Virginia Medical School Attending, Pediatric Emergency Department Children s Hospital of The King s Daughters Objectives
Orthopedics - Dr. Ahmad - Lecture 2 - Injuries of the Upper Limb
 The shoulder and the upper arm Fractures of the clavicle 1. Fall on the shoulder. 2. Fall on outstretched hand. In mid shaft fractures, the outer fragment is pulled down by the weight of the arm and the
The shoulder and the upper arm Fractures of the clavicle 1. Fall on the shoulder. 2. Fall on outstretched hand. In mid shaft fractures, the outer fragment is pulled down by the weight of the arm and the
Musculoskeletal Injuries
 Musculoskeletal Injuries KNOWLEDGE OBJECTIVES 1. Identify the four main structures of the musculoskeletal system. 2. List five common signs or symptoms of musculoskeletal injuries. 3. List seven signs
Musculoskeletal Injuries KNOWLEDGE OBJECTIVES 1. Identify the four main structures of the musculoskeletal system. 2. List five common signs or symptoms of musculoskeletal injuries. 3. List seven signs
Sports Medicine Unit 16 Elbow
 Sports Medicine Unit 16 Elbow I. Bones a. b. c. II. What movements does the elbow perform? a. Flexion b. c. Pronation d. III. Muscles in motion a. FLEXION (supinated) i Brachialis (pronated) ii (neutral)
Sports Medicine Unit 16 Elbow I. Bones a. b. c. II. What movements does the elbow perform? a. Flexion b. c. Pronation d. III. Muscles in motion a. FLEXION (supinated) i Brachialis (pronated) ii (neutral)
A Patient s Guide to Elbow Dislocation
 A Patient s Guide to Elbow Dislocation 2 Introduction When the joint surfaces of an elbow are forced apart, the elbow is dislocated. The elbow is the second most commonly dislocated joint in adults (after
A Patient s Guide to Elbow Dislocation 2 Introduction When the joint surfaces of an elbow are forced apart, the elbow is dislocated. The elbow is the second most commonly dislocated joint in adults (after
Goals. Initial management skeletal trauma. Physical Exam ABC OF PRIMARY CARE MEDICINE FRACTURE MANAGEMENT 12/4/2010
 ABC OF PRIMARY CARE MEDICINE FRACTURE MANAGEMENT Brian Feeley, MD UCSF Sports Medicine and Shoulder Surgery Goals Discuss common fractures and initial management, treatment guidelines Let your patients
ABC OF PRIMARY CARE MEDICINE FRACTURE MANAGEMENT Brian Feeley, MD UCSF Sports Medicine and Shoulder Surgery Goals Discuss common fractures and initial management, treatment guidelines Let your patients
Musculoskeletal System Objectives:
 Lemone and Burke Chapters 40-41 Musculoskeletal System Objectives: Review Anatomy and physiology Describe normal MS assessment Describe age related changes Discuss tests and nursing interventions Recognize
Lemone and Burke Chapters 40-41 Musculoskeletal System Objectives: Review Anatomy and physiology Describe normal MS assessment Describe age related changes Discuss tests and nursing interventions Recognize
TIBIAL PLATEAU FRACTURE
 TIBIAL PLATEAU FRACTURE Description Preventive Measures A tibial plateau fracture is a complete or incomplete break Appropriately warm up and stretch before practice or in the larger of the two leg bones
TIBIAL PLATEAU FRACTURE Description Preventive Measures A tibial plateau fracture is a complete or incomplete break Appropriately warm up and stretch before practice or in the larger of the two leg bones
A Patient s Guide to Adult Humerus Shaft Fractures
 A Patient s Guide to Adult Humerus Shaft Fractures Glendale Adventist Medical Center 1509 Wilson Terrace Glendale, CA 91206 Phone: (818) 409-8000 1 DISCLAIMER: The information in this booklet is compiled
A Patient s Guide to Adult Humerus Shaft Fractures Glendale Adventist Medical Center 1509 Wilson Terrace Glendale, CA 91206 Phone: (818) 409-8000 1 DISCLAIMER: The information in this booklet is compiled
FOOSH It sounded like a fun thing at the time!
 FOOSH It sounded like a fun thing at the time! Evaluating acute hand and wrist injuries Larry Collins, MPAS, PA-C, ATC, DFAAPA Assistant Professor, Physician Assistant Program Assistant Professor, Department
FOOSH It sounded like a fun thing at the time! Evaluating acute hand and wrist injuries Larry Collins, MPAS, PA-C, ATC, DFAAPA Assistant Professor, Physician Assistant Program Assistant Professor, Department
Surgery-Ortho. Fractures of the tibia and fibula. Management. Treatment of low energy fractures. Fifth stage. Lec-6 د.
 Fifth stage Lec-6 د. مثنى Surgery-Ortho 28/4/2016 Indirect force: (low energy) Fractures of the tibia and fibula Twisting: spiral fractures of both bones Angulatory: oblique fractures with butterfly segment.
Fifth stage Lec-6 د. مثنى Surgery-Ortho 28/4/2016 Indirect force: (low energy) Fractures of the tibia and fibula Twisting: spiral fractures of both bones Angulatory: oblique fractures with butterfly segment.
WRIST SPRAIN. Description
 WRIST SPRAIN Description Other sports, such as skiing, bowling, pole vaulting Wrist sprain is a violent overstretching and tearing of one Poor physical conditioning (strength and flexibility) or more ligaments
WRIST SPRAIN Description Other sports, such as skiing, bowling, pole vaulting Wrist sprain is a violent overstretching and tearing of one Poor physical conditioning (strength and flexibility) or more ligaments
1/19/2018. Winter injuries to the shoulder and elbow. Highgate Private Hospital (Whittington Health NHS Trust)
 Winter injuries to the shoulder and elbow Omar Haddo Consultant Orthopaedic Surgeon, Shoulder, Elbow, Hand & Wrist Specialist MBBS, BmedSci, FRCS(Orth) Highgate Private Hospital (Whittington Health NHS
Winter injuries to the shoulder and elbow Omar Haddo Consultant Orthopaedic Surgeon, Shoulder, Elbow, Hand & Wrist Specialist MBBS, BmedSci, FRCS(Orth) Highgate Private Hospital (Whittington Health NHS
UNDERSTANDING FRACTURE CARE CAUSES, DIAGNOSIS, AND TREATMENT
 UNDERSTANDING FRACTURE CARE CAUSES, DIAGNOSIS, AND TREATMENT PremierOrtho.com UNDERSTANDING FRACTURE CARE CAUSES, DIAGNOSIS, AND TREATMENT Table of Contents Introduction...3 Causes...4 Who s at Risk?...5
UNDERSTANDING FRACTURE CARE CAUSES, DIAGNOSIS, AND TREATMENT PremierOrtho.com UNDERSTANDING FRACTURE CARE CAUSES, DIAGNOSIS, AND TREATMENT Table of Contents Introduction...3 Causes...4 Who s at Risk?...5
Arm Injuries and Disorders
 Arm Injuries and Disorders Introduction Your arms are made up of muscles, joints, tendons and other connective tissue. There are many injuries and disorders that can affect the arm. Some arm injuries and
Arm Injuries and Disorders Introduction Your arms are made up of muscles, joints, tendons and other connective tissue. There are many injuries and disorders that can affect the arm. Some arm injuries and
Fractures of the tibia shaft treated with locked intramedullary nail Retrospective clinical and radiographic assesment
 ARS Medica Tomitana - 2013; 4(75): 197-201 DOI: 10.2478/arsm-2013-0035 Șerban Al., Botnaru V., Turcu R., Obadă B., Anderlik St. Fractures of the tibia shaft treated with locked intramedullary nail Retrospective
ARS Medica Tomitana - 2013; 4(75): 197-201 DOI: 10.2478/arsm-2013-0035 Șerban Al., Botnaru V., Turcu R., Obadă B., Anderlik St. Fractures of the tibia shaft treated with locked intramedullary nail Retrospective
Hand and wrist emergencies
 Chapter1 Hand and wrist emergencies Carl A. Germann Distal radius and ulnar injuries PEARL: Fractures of the distal radius and ulna are the most common type of fractures in patients younger than 75 years.
Chapter1 Hand and wrist emergencies Carl A. Germann Distal radius and ulnar injuries PEARL: Fractures of the distal radius and ulna are the most common type of fractures in patients younger than 75 years.
Rehabilitation after Total Elbow Arthroplasty
 Rehabilitation after Total Elbow Arthroplasty Total Elbow Atrthroplasty Total elbow arthroplasty (TEA) Replacement of the ulnohumeral articulation with a prosthetic device. Goal of TEA is to provide pain
Rehabilitation after Total Elbow Arthroplasty Total Elbow Atrthroplasty Total elbow arthroplasty (TEA) Replacement of the ulnohumeral articulation with a prosthetic device. Goal of TEA is to provide pain
Intramedullary Nailing for Femur Fracture Management
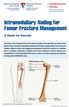 514-412-4400, ext. 23310 thechildren.com/trauma Intramedullary Nailing for Femur Fracture Management A Guide for Parents The femur is the longest bone in the body. It begins at the hip joint and ends at
514-412-4400, ext. 23310 thechildren.com/trauma Intramedullary Nailing for Femur Fracture Management A Guide for Parents The femur is the longest bone in the body. It begins at the hip joint and ends at
Range of motion and positioning
 Range of motion and positioning Learning guide Why is motion important? Most people take free, comfortable movement for granted. Motion is meant to be smooth and painless. The ligaments, tendons, muscles,
Range of motion and positioning Learning guide Why is motion important? Most people take free, comfortable movement for granted. Motion is meant to be smooth and painless. The ligaments, tendons, muscles,
Basic Care of Common Fractures Utku Kandemir, MD
 Basic Care of Common Fractures Utku Kandemir, MD Assistant Clinical Professor Trauma & Sports Medicine Dept. of Orthopaedic Surgery UCSF / SFGH History Physical Exam Radiology Treatment History Acute trauma
Basic Care of Common Fractures Utku Kandemir, MD Assistant Clinical Professor Trauma & Sports Medicine Dept. of Orthopaedic Surgery UCSF / SFGH History Physical Exam Radiology Treatment History Acute trauma
CASE ONE CASE ONE. RADIAL HEAD FRACTURE Mason Classification. RADIAL HEAD FRACTURE Mechanism of Injury. RADIAL HEAD FRACTURE Imaging
 CASE ONE An eighteen year old female falls during a basketball game, striking her elbow on the court. She presents to your office that day with a painful, swollen elbow that she is unable to flex or extend
CASE ONE An eighteen year old female falls during a basketball game, striking her elbow on the court. She presents to your office that day with a painful, swollen elbow that she is unable to flex or extend
Y: Orthopedic Specialty
 Y: Orthopedic Specialty Alberta Licensed Practical Nurses Competency Profile 253 Major Competency Area: Y Priority: One Competency: Y-1 HPA Authorization and Standards Date: September 1, 2005 Y-1-1 Demonstrate
Y: Orthopedic Specialty Alberta Licensed Practical Nurses Competency Profile 253 Major Competency Area: Y Priority: One Competency: Y-1 HPA Authorization and Standards Date: September 1, 2005 Y-1-1 Demonstrate
PEM GUIDE CHILDHOOD FRACTURES
 PEM GUIDE CHILDHOOD FRACTURES INTRODUCTION Skeletal injuries account for 10-15% of all injuries in children; 20% of those are fractures, 3 out of 4 fractures affect the physis or growth plate. Always consider
PEM GUIDE CHILDHOOD FRACTURES INTRODUCTION Skeletal injuries account for 10-15% of all injuries in children; 20% of those are fractures, 3 out of 4 fractures affect the physis or growth plate. Always consider
Total Hip Replacement Rehabilitation: Progression and Restrictions
 Total Hip Replacement Rehabilitation: Progression and Restrictions The success of total hip replacement (THR) is a result of predictable pain relief, improvements in quality of life, and restoration of
Total Hip Replacement Rehabilitation: Progression and Restrictions The success of total hip replacement (THR) is a result of predictable pain relief, improvements in quality of life, and restoration of
How to Triage Orthopaedic Care. David W. Gray, M.D.
 How to Triage Orthopaedic Care David W. Gray, M.D. OBJECTIVES: Define basic assessments skills needed to identify orthopedic injuries Differentiate when an orthopedic injury is a medical emergency Determine
How to Triage Orthopaedic Care David W. Gray, M.D. OBJECTIVES: Define basic assessments skills needed to identify orthopedic injuries Differentiate when an orthopedic injury is a medical emergency Determine
.org. Ankle Fractures (Broken Ankle) Anatomy
 Ankle Fractures (Broken Ankle) Page ( 1 ) A broken ankle is also known as an ankle fracture. This means that one or more of the bones that make up the ankle joint are broken. A fractured ankle can range
Ankle Fractures (Broken Ankle) Page ( 1 ) A broken ankle is also known as an ankle fracture. This means that one or more of the bones that make up the ankle joint are broken. A fractured ankle can range
11/5/14. I will try to make this painless. Great, a Fracture, Now What? Objectives. Basics for Fracture Workup. Basics for Fracture Workup
 Great, a Fracture, Now What? I will try to make this painless Mary Greve MS, PA-C Department of Orthopedic Surgery Trauma Team University of Iowa Hospitals and Clinics Mary-Greve@uiowa.edu Pager 2121 Objectives
Great, a Fracture, Now What? I will try to make this painless Mary Greve MS, PA-C Department of Orthopedic Surgery Trauma Team University of Iowa Hospitals and Clinics Mary-Greve@uiowa.edu Pager 2121 Objectives
Sick Call Screener Course
 Sick Call Screener Course Musculoskeletal System Upper Extremities (2.7) 2.7-2-1 Enabling Objectives 1.46 Utilize the knowledge of musculoskeletal system anatomy while assessing a patient with a musculoskeletal
Sick Call Screener Course Musculoskeletal System Upper Extremities (2.7) 2.7-2-1 Enabling Objectives 1.46 Utilize the knowledge of musculoskeletal system anatomy while assessing a patient with a musculoskeletal
EPIPHYSEAL PLATE IN FEMUR
 Reviewing: Epiphyseal Plates (younger skeletons) eventually will disappear. Bones grow lengthwise up and down from each plate, and in a circular collar like fashion around the diaphysis. These plates will
Reviewing: Epiphyseal Plates (younger skeletons) eventually will disappear. Bones grow lengthwise up and down from each plate, and in a circular collar like fashion around the diaphysis. These plates will
Upper Extremity Fractures
 Upper Extremity Fractures Ranie Whatley, RN,FNP-C David W. Gray, MD Skeletal Trauma 10 to 15 % of all Childhood Injuries Physeal (Growth Plate) Injuries are ~ 15% of all Skeletal Injuries Orthopaedic Assessment
Upper Extremity Fractures Ranie Whatley, RN,FNP-C David W. Gray, MD Skeletal Trauma 10 to 15 % of all Childhood Injuries Physeal (Growth Plate) Injuries are ~ 15% of all Skeletal Injuries Orthopaedic Assessment
Injuries to Muscles, Bones and Joints. Emergency Medical Response
 Injuries to Muscles, Bones and Joints Lesson 33: Injuries to Muscles, Bones and Joints You Are the Emergency Medical Responder You are patrolling the state park where you are the emergency medical responder
Injuries to Muscles, Bones and Joints Lesson 33: Injuries to Muscles, Bones and Joints You Are the Emergency Medical Responder You are patrolling the state park where you are the emergency medical responder
Module Eight. Application of Health Assessment NUR 225. Physical examination of Musculoskeletal System. King Saud University. Collage of Nursing
 King Saud University Collage of Nursing Medical Surgical Nursing depart Application of Health Assessment NUR 225 Module Eight Physical examination of Musculoskeletal System Obtaining a health history Ask
King Saud University Collage of Nursing Medical Surgical Nursing depart Application of Health Assessment NUR 225 Module Eight Physical examination of Musculoskeletal System Obtaining a health history Ask
Patient Education. Supracondylar Humerus Fractures
 Patient Education Supracondylar Humerus Fractures This is the most common fracture requiring surgery in children age 3-10. It can happen in younger and older kids as well. *Remember! Fracture, crack, break
Patient Education Supracondylar Humerus Fractures This is the most common fracture requiring surgery in children age 3-10. It can happen in younger and older kids as well. *Remember! Fracture, crack, break
Case. 5 year old with 2 weeks leg pain and now refusing to walk + Fevers, lower leg swelling, warmth Denies and history of trauma or wounds
 Case 5 year old with 2 weeks leg pain and now refusing to walk + Fevers, lower leg swelling, warmth Denies and history of trauma or wounds Exam I: Swelling over entire tibia extending to foot P: Tenderness
Case 5 year old with 2 weeks leg pain and now refusing to walk + Fevers, lower leg swelling, warmth Denies and history of trauma or wounds Exam I: Swelling over entire tibia extending to foot P: Tenderness
A Patient s Guide to Adult Distal Radius (Wrist) Fractures
 A Patient s Guide to Adult Distal Radius (Wrist) Fractures Suite 11-13/14/15 Mount Elizabeth Medical Center 3 Mount Elizabeth Singapore, 228510 Phone: (65) 6738 2628 Fax: (65) 6738 2629 1 DISCLAIMER: The
A Patient s Guide to Adult Distal Radius (Wrist) Fractures Suite 11-13/14/15 Mount Elizabeth Medical Center 3 Mount Elizabeth Singapore, 228510 Phone: (65) 6738 2628 Fax: (65) 6738 2629 1 DISCLAIMER: The
A Patient s Guide to Elbow Dislocation
 A Patient s Guide to Elbow Dislocation 20295 NE 29th Place, Ste 300 Aventura, FL 33180 Phone: (786) 629-0910 Fax: (786) 629-0920 admin@instituteofsports.com DISCLAIMER: The information in this booklet
A Patient s Guide to Elbow Dislocation 20295 NE 29th Place, Ste 300 Aventura, FL 33180 Phone: (786) 629-0910 Fax: (786) 629-0920 admin@instituteofsports.com DISCLAIMER: The information in this booklet
Pilon Fractures - OrthoInfo - AAOS. Copyright 2010 American Academy of Orthopaedic Surgeons. Pilon Fractures
 Copyright 2010 American Academy of Orthopaedic Surgeons Pilon Fractures Pilon fractures affect the bottom of the shinbone (tibia) at the ankle joint. In most cases, both bones in the lower leg, the tibia
Copyright 2010 American Academy of Orthopaedic Surgeons Pilon Fractures Pilon fractures affect the bottom of the shinbone (tibia) at the ankle joint. In most cases, both bones in the lower leg, the tibia
Extremity Injuries and Splinting
 CHAPTER 15 Extremity Injuries and Splinting Lesson Objectives 1. Describe the 3 general types of splints and how to improvise splints with common materials. 2. List the general guidelines for splinting
CHAPTER 15 Extremity Injuries and Splinting Lesson Objectives 1. Describe the 3 general types of splints and how to improvise splints with common materials. 2. List the general guidelines for splinting
Musculoskeletal System
 CHAPTER 28 Musculoskeletal Injuries Musculoskeletal System Anatomy & Physiology Bones provide framework. Joints allow for bending. Muscles allow for movement. Cartilage provides flexibility. Tendons connect
CHAPTER 28 Musculoskeletal Injuries Musculoskeletal System Anatomy & Physiology Bones provide framework. Joints allow for bending. Muscles allow for movement. Cartilage provides flexibility. Tendons connect
CHAPTER 28 Musculoskeletal Injuries
 CHAPTER 28 Musculoskeletal Injuries Musculoskeletal System Anatomy & Physiology Bones provide framework. Joints allow for bending. Muscles allow for movement. Cartilage provides flexibility. Tendons connect
CHAPTER 28 Musculoskeletal Injuries Musculoskeletal System Anatomy & Physiology Bones provide framework. Joints allow for bending. Muscles allow for movement. Cartilage provides flexibility. Tendons connect
Management of Fractures. Traumatology RHS 231 Dr. Einas Al-Eisa Lecture 5
 Management of Fractures Traumatology RHS 231 Dr. Einas Al-Eisa Lecture 5 Common methods of fracture immobilization Plaster of Paris (POP): A high quality gypsum The standard method of external splinting
Management of Fractures Traumatology RHS 231 Dr. Einas Al-Eisa Lecture 5 Common methods of fracture immobilization Plaster of Paris (POP): A high quality gypsum The standard method of external splinting
Pediatric Injuries/Fractures. Rena Heathcote
 Pediatric Injuries/Fractures Rena Heathcote INTRODUCTION Incidence Anatomy of the Growing Bone Injury Patterns What can we X-ray PEDIATRIC FRACTURES INCIDENCE What makes children susceptible to fractures?
Pediatric Injuries/Fractures Rena Heathcote INTRODUCTION Incidence Anatomy of the Growing Bone Injury Patterns What can we X-ray PEDIATRIC FRACTURES INCIDENCE What makes children susceptible to fractures?
Overview. Overview. Chapter 30. Injuries to the Head and Spine 9/11/2012. Review of the Nervous and Skeletal Systems. Devices for Immobilization
 Chapter 30 Injuries to the Head and Spine Slide 1 Overview Review of the Nervous and Skeletal Systems The Nervous System The Skeletal System Devices for Immobilization Cervical Spine Short Backboards Long
Chapter 30 Injuries to the Head and Spine Slide 1 Overview Review of the Nervous and Skeletal Systems The Nervous System The Skeletal System Devices for Immobilization Cervical Spine Short Backboards Long
CARING FOR THE CLIENT ON COMPLETE BEDREST
 CARING FOR THE CLIENT ON COMPLETE BEDREST INTRODUCTION The human body is designed to move. And just as the human body thrives on movement, it suffers when for one reason or another there is enforced immobility.
CARING FOR THE CLIENT ON COMPLETE BEDREST INTRODUCTION The human body is designed to move. And just as the human body thrives on movement, it suffers when for one reason or another there is enforced immobility.
Solving Today s Pain and Injury Puzzle with Erik Dalton An Online Workshop for ABMP Members Session 4 Handout
 Solving Today s Pain and Injury Puzzle with Erik Dalton An Online Workshop for ABMP Members Session 4 Handout Please Note: Erik Dalton teaches his Myoskeletal Alignment Techniques with the expectation
Solving Today s Pain and Injury Puzzle with Erik Dalton An Online Workshop for ABMP Members Session 4 Handout Please Note: Erik Dalton teaches his Myoskeletal Alignment Techniques with the expectation
Car a e e o f o th f e th e Pati Pa e ti n e t n wi w th i th a Mus u c s u c l u o l s o k s e k l e e l t e al a l Dis i o s r o de d r
 Care of the Patient with a Musculoskeletal Disorder 1 Slide 1 Overview of Anatomy and Physiology Function of the bones Support Protection Movement Mineral storage Hemopoiesis Slide 2 Functions of the muscles
Care of the Patient with a Musculoskeletal Disorder 1 Slide 1 Overview of Anatomy and Physiology Function of the bones Support Protection Movement Mineral storage Hemopoiesis Slide 2 Functions of the muscles
Femoral Shaft Fracture
 Femoral Shaft Fracture The femoral shaft is well padded with muscles(an advantage in protecting the bone from all but the most powerful forces)but the disadvantage is that fractures are often severely
Femoral Shaft Fracture The femoral shaft is well padded with muscles(an advantage in protecting the bone from all but the most powerful forces)but the disadvantage is that fractures are often severely
Calcaneus (Heel Bone) Fractures
 Page 1 of 8 Calcaneus (Heel Bone) Fractures A fracture of the calcaneus, or heel bone, can be a painful and disabling injury. This type of fracture commonly occurs during a high-energy event such as a
Page 1 of 8 Calcaneus (Heel Bone) Fractures A fracture of the calcaneus, or heel bone, can be a painful and disabling injury. This type of fracture commonly occurs during a high-energy event such as a
Community Caregivers. Effects of Immobility, Transfers and Positioning Test
 Community Caregivers Effects of Immobility, Transfers and Positioning Test Name: Date: For each question, choose the best response or responses. 1. The key effect of immobility is: a. Increased incontinence
Community Caregivers Effects of Immobility, Transfers and Positioning Test Name: Date: For each question, choose the best response or responses. 1. The key effect of immobility is: a. Increased incontinence
8 Recovering From HAND FRACTURE SURGERY
 8 Recovering From HAND FRACTURE SURGERY Hand fractures are caused by trauma and result in breaking (fracturing) the phalanges or metacarpals. Surgery involves achieving acceptable alignment and providing
8 Recovering From HAND FRACTURE SURGERY Hand fractures are caused by trauma and result in breaking (fracturing) the phalanges or metacarpals. Surgery involves achieving acceptable alignment and providing
X-ray (Radiography) - Bone
 Scan for mobile link. X-ray (Radiography) - Bone Bone x-ray uses a very small dose of ionizing radiation to produce pictures of any bone in the body. It is commonly used to diagnose fractured bones or
Scan for mobile link. X-ray (Radiography) - Bone Bone x-ray uses a very small dose of ionizing radiation to produce pictures of any bone in the body. It is commonly used to diagnose fractured bones or
H: Orthopedic Nursing
 H: Orthopedic Nursing Alberta Licensed Practical Nurses Competency Profile 87 Competency: H-1 Knowledge of H-1-1 H-1-2 H-1-3 H-1-4 H-1-5 Demonstrate knowledge of human anatomy and physiology, specifically
H: Orthopedic Nursing Alberta Licensed Practical Nurses Competency Profile 87 Competency: H-1 Knowledge of H-1-1 H-1-2 H-1-3 H-1-4 H-1-5 Demonstrate knowledge of human anatomy and physiology, specifically
Chapter 23 Body Mechanics, Positioning, and Moving
 Chapter 23 Body Mechanics, Positioning, and Moving Question Is the following statement true or false? Good body posture distributes gravity through the center of the body over a wide base of support. Answer
Chapter 23 Body Mechanics, Positioning, and Moving Question Is the following statement true or false? Good body posture distributes gravity through the center of the body over a wide base of support. Answer
Complications of Treatment: Nonsurgical and Surgical
 Complications of Treatment: Nonsurgical and Surgical Whenever orthopedic surgeons discuss a treatment with patients we must always consider the risks and complications of any treatment we recommend. Part
Complications of Treatment: Nonsurgical and Surgical Whenever orthopedic surgeons discuss a treatment with patients we must always consider the risks and complications of any treatment we recommend. Part
SMALL GROUP SESSION 16 January 8 th or 10 th Shoulder pain case/ Touch workshop/ Upper and Lower Extremity Examination
 SMALL GROUP SESSION 16 January 8 th or 10 th Shoulder pain case/ Touch workshop/ Upper and Lower Extremity Examination Suggested Readings: Opatrny L. The Healing Touch. Ann Int Med 2002; 137:1003. http://www.annals.org/cgi/reprint/137/12/1003.pdf
SMALL GROUP SESSION 16 January 8 th or 10 th Shoulder pain case/ Touch workshop/ Upper and Lower Extremity Examination Suggested Readings: Opatrny L. The Healing Touch. Ann Int Med 2002; 137:1003. http://www.annals.org/cgi/reprint/137/12/1003.pdf
King Saud University College of Nursing Medical-surgical Nursing
 King Saud University College of Nursing Medical-surgical Nursing 1.Obtaining a health history: Ask about chief complain: History of presence of muscle pain (onset, location, Aggravating and alleviating
King Saud University College of Nursing Medical-surgical Nursing 1.Obtaining a health history: Ask about chief complain: History of presence of muscle pain (onset, location, Aggravating and alleviating
A Patient s Guide to Adult Olecranon (Elbow) Fractures
 A Patient s Guide to Adult Olecranon (Elbow) Fractures 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 1 DISCLAIMER: The information in this booklet is compiled from
A Patient s Guide to Adult Olecranon (Elbow) Fractures 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 1 DISCLAIMER: The information in this booklet is compiled from
MUSCULOSKELETAL INJURIES
 WHAT ARE THEY They are injuries to muscles, nerves, tendons ligaments, joints, cartilage and spinal discs. WHAT KIND OF INJURIES ARE MUSCULOSKELETAL INJURIES 1. Fractures- -Open -Closed 2. Dislocations
WHAT ARE THEY They are injuries to muscles, nerves, tendons ligaments, joints, cartilage and spinal discs. WHAT KIND OF INJURIES ARE MUSCULOSKELETAL INJURIES 1. Fractures- -Open -Closed 2. Dislocations
Chapter 16 Moving and Positioning Patients
 Chapter 16 Moving and Positioning Patients Terminology Related to Movement Contractures Shortening and tightening of muscles due to disuse Dorsiflexion Bending of the foot in an upward direction Plantar
Chapter 16 Moving and Positioning Patients Terminology Related to Movement Contractures Shortening and tightening of muscles due to disuse Dorsiflexion Bending of the foot in an upward direction Plantar
ANTERIOR CRUCIATE LIGAMENT INJURY
 ANTERIOR CRUCIATE LIGAMENT INJURY WHAT IS THE ANTERIOR CRUCIATE LIGAMENT? The anterior cruciate ligament (ACL) is one of four major ligaments that stabilizes the knee joint. A ligament is a tough band
ANTERIOR CRUCIATE LIGAMENT INJURY WHAT IS THE ANTERIOR CRUCIATE LIGAMENT? The anterior cruciate ligament (ACL) is one of four major ligaments that stabilizes the knee joint. A ligament is a tough band
Ankle Fracture Orthopaedic Department Patient Information Leaflet. Under review. Page 1
 Ankle Fracture Orthopaedic Department Patient Information Leaflet Page 1 Ankle Fracture Welcome to the Dudley Group NHS Foundation Trust. This leaflet will provide you with information regarding the diagnosis
Ankle Fracture Orthopaedic Department Patient Information Leaflet Page 1 Ankle Fracture Welcome to the Dudley Group NHS Foundation Trust. This leaflet will provide you with information regarding the diagnosis
Musculoskeletal Trauma. Lesson Goal. Lesson Objectives 9/10/2012. Recognize and manage patients with musculoskeletal trauma
 Musculoskeletal Trauma Lesson Goal Recognize and manage patients with musculoskeletal trauma Lesson Objectives Describe function of muscular system Describe composition of muscular system Describe, compare,
Musculoskeletal Trauma Lesson Goal Recognize and manage patients with musculoskeletal trauma Lesson Objectives Describe function of muscular system Describe composition of muscular system Describe, compare,
Commonwealth Health Corporation NEXT
 Commonwealth Health Corporation This computer-based learning (CBL) module details important aspects of musculoskeletal disorders, body mechanics and ergonomics in the workplace. It examines: what causes
Commonwealth Health Corporation This computer-based learning (CBL) module details important aspects of musculoskeletal disorders, body mechanics and ergonomics in the workplace. It examines: what causes
Hip Fractures. Anatomy. Causes. Symptoms
 Hip Fractures A hip fracture is a break in the upper quarter of the femur (thigh) bone. The extent of the break depends on the forces that are involved. The type of surgery used to treat a hip fracture
Hip Fractures A hip fracture is a break in the upper quarter of the femur (thigh) bone. The extent of the break depends on the forces that are involved. The type of surgery used to treat a hip fracture
Lateral Collateral Ligament Sprain
 What is lateral collateral ligament sprain? Lateral Collateral Ligament Sprain A sprain is a joint injury that causes a stretch or tear in a ligament, a strong band of tissue connecting one bone to another.
What is lateral collateral ligament sprain? Lateral Collateral Ligament Sprain A sprain is a joint injury that causes a stretch or tear in a ligament, a strong band of tissue connecting one bone to another.
Patient Information for Consent
 Patient Information for Consent OS12 Femoral Shaft Fracture Surgery (Femoral Nailing) Expires end of February 2017 Issued June 2016 Local information If you need any more information please contact your
Patient Information for Consent OS12 Femoral Shaft Fracture Surgery (Femoral Nailing) Expires end of February 2017 Issued June 2016 Local information If you need any more information please contact your
Caring for Muscle and Bone Injuries From Brady s First Responder (8 th Edition) 54 Questions
 Caring for Muscle and Bone Injuries From Brady s First Responder (8 th Edition) 54 Questions 1. What is caused by overexerting or tearing of a muscle? p. 375 A.) Dislocation B.) Sprain C.) Fracture *D.)
Caring for Muscle and Bone Injuries From Brady s First Responder (8 th Edition) 54 Questions 1. What is caused by overexerting or tearing of a muscle? p. 375 A.) Dislocation B.) Sprain C.) Fracture *D.)
4/28/2010. Fractures. Normal Bone and Normal Ossification Bone Terms. Epiphysis Epiphyseal Plate (physis) Metaphysis
 Fractures Normal Bone and Normal Ossification Bone Terms Epiphysis Epiphyseal Plate (physis) Metaphysis Diaphysis 1 Fracture Classifications A. Longitudinal B. Transverse C. Oblique D. Spiral E. Incomplete
Fractures Normal Bone and Normal Ossification Bone Terms Epiphysis Epiphyseal Plate (physis) Metaphysis Diaphysis 1 Fracture Classifications A. Longitudinal B. Transverse C. Oblique D. Spiral E. Incomplete
Peripheral Vascular Examination. Dr. Gary Mumaugh Western Physical Assessment
 Peripheral Vascular Examination Dr. Gary Mumaugh Western Physical Assessment Competencies 1. Inspection of upper extremity for: size symmetry swelling venous pattern color Texture nail beds Competencies
Peripheral Vascular Examination Dr. Gary Mumaugh Western Physical Assessment Competencies 1. Inspection of upper extremity for: size symmetry swelling venous pattern color Texture nail beds Competencies
SPINAL IMMOBILIZATION
 Spinal Immobilization Decision Assessment Recent studies have shown an increase in mortality for patients with isolated penetrating trauma who are spinally immobilized. Therefore spinal immobilization
Spinal Immobilization Decision Assessment Recent studies have shown an increase in mortality for patients with isolated penetrating trauma who are spinally immobilized. Therefore spinal immobilization
FOOSH It sounded like a fun thing at the time!
 FOOSH It sounded like a fun thing at the time! Evaluating acute hand and wrist injuries Larry Collins, MPAS, PA-C, ATC, DFAAPA Assistant Professor, Physician Assistant Program Assistant Professor, Department
FOOSH It sounded like a fun thing at the time! Evaluating acute hand and wrist injuries Larry Collins, MPAS, PA-C, ATC, DFAAPA Assistant Professor, Physician Assistant Program Assistant Professor, Department
NEWBORN NURSES POLICY AND PROCEDURES. PURPOSE: Varying positions helps to stimulate physiological functioning and provides rest.
 NEWBORN NURSES POLICY AND PROCEDURES SUBJECT: POSITIONING EFFECTIVE DATE: 6/91 PURPOSE: Varying positions helps to stimulate physiological functioning and provides rest. POLICY: 1. The nurse will vary
NEWBORN NURSES POLICY AND PROCEDURES SUBJECT: POSITIONING EFFECTIVE DATE: 6/91 PURPOSE: Varying positions helps to stimulate physiological functioning and provides rest. POLICY: 1. The nurse will vary
Spondylolysis DESCRIPTION EXPECTED OUTCOME POSSIBLE COMPLICATIONS COMMON SIGNS AND SYMPTOMS GENERAL TREATMENT CONSIDERATIONS CAUSES
 DESCRIPTION is a stress or fatigue fracture of the bones of the spine (vertebrae) that does not involve the main weight-bearing part of those bones, the body of the vertebra. Instead, it involves an area
DESCRIPTION is a stress or fatigue fracture of the bones of the spine (vertebrae) that does not involve the main weight-bearing part of those bones, the body of the vertebra. Instead, it involves an area
STABILO-BED. Postural aids system in the lying position
 P O S T U R A L A I D S S Y S T E M STABILO-BED Postural aids system in the lying position STABILO-BED STABILO Version: 16.05.2018 STABILObed is the modular 1st medical class system that is used for precise
P O S T U R A L A I D S S Y S T E M STABILO-BED Postural aids system in the lying position STABILO-BED STABILO Version: 16.05.2018 STABILObed is the modular 1st medical class system that is used for precise
Knee Replacement PROGRAM. Nightingale. Home Healthcare
 Knee Replacement PROGRAM TM Nightingale Home Healthcare With the help of Nightingale s experienced and professional rehabilitation team, you will be guided through a more complete and successful recovery
Knee Replacement PROGRAM TM Nightingale Home Healthcare With the help of Nightingale s experienced and professional rehabilitation team, you will be guided through a more complete and successful recovery
COMPLETION PROJECT POSITIONING THE PATIENT IN THE OR Source- Alexander s Care of the Patient in Surgery
 COMPLETION PROJECT POSITIONING THE PATIENT IN THE OR Source- Alexander s Care of the Patient in Surgery Name Date 1. The systems involved with anesthesia, positioning and operative procedures are: a. b.
COMPLETION PROJECT POSITIONING THE PATIENT IN THE OR Source- Alexander s Care of the Patient in Surgery Name Date 1. The systems involved with anesthesia, positioning and operative procedures are: a. b.
Spondylolisthesis DESCRIPTION EXPECTED OUTCOME POSSIBLE COMPLICATIONS COMMON SIGNS AND SYMPTOMS GENERAL TREATMENT CONSIDERATIONS CAUSES
 DESCRIPTION is the slippage of one or more vertebrae, the bones of the spine. Many causes of slippage of the vertebra are possible; these include stress fracture (spondylolysis), which is often seen in
DESCRIPTION is the slippage of one or more vertebrae, the bones of the spine. Many causes of slippage of the vertebra are possible; these include stress fracture (spondylolysis), which is often seen in
PHASE ONE: THE FIRST SIX WEEKS AFTER INJURY
 Exercises After Injury to the Anterior Cruciate Ligament (ACL) of the Knee Dr. Abigail R. Hamilton, M.D. PHASE ONE: THE FIRST SIX WEEKS AFTER INJURY Initially, the knee needs to be protected-use the knee
Exercises After Injury to the Anterior Cruciate Ligament (ACL) of the Knee Dr. Abigail R. Hamilton, M.D. PHASE ONE: THE FIRST SIX WEEKS AFTER INJURY Initially, the knee needs to be protected-use the knee
