Surgical procedure. METS Modular Proximal Tibia
|
|
|
- Erika Jones
- 6 years ago
- Views:
Transcription
1 Surgical procedure METS Modular Proximal Tibia
2 Surgical Procedure ontents Device information Product overview 1.2 Indications 1.3 bsolute contra-indications 1.4 Relative contra-indications 1.5 apabilities and restrictions of use Operation instruction and guidelines Recommendations for component selection 2.2 General points to note when using trial components 2.3 Recommendations for assembly of implant 2.4 Special instruments 2.5 Femoral cutting guide 2.6 one preparation 2.7 Femoral cutting guide and bone preparation Rotating hinged proximal tibia omponents 3.2 Trial components 3.3 Tibial resection levels: rotating hinge proximal tibia 3.4 Tibial preparation 3.5 Short resections < 120mm Trial assembly and insertion Implant assembly and insertion The proximal tibial component 3.6 Resections > 120mm Trial assembly and insertion Implant assembly and insertion The proximal tibial component 3.7 Extensive resections > 165mm Trial assembly and insertion Implant assembly and insertion The proximal tibial component 1
3 Surgical Procedure ontents Fixed hinged proximal tibia omponents 4.2 Trial components 4.3 Tibial resection levels: fixed hinge proximal tibia 4.4 Tibial preparation 4.5 Short resections < 75mm Trial assembly and insertion Implant assembly and insertion The proximal tibial component 4.6 Resections > 75mm Trial assembly and insertion Implant assembly and insertion The proximal tibial component The femoral component Femoral plateau plates 4.7 Extensive resections > 150mm Trial assembly and insertion Implant assembly and insertion The proximal tibial component The femoral component Femoral plateau plates 5.2 Insertion of the axle and circlip Insertion Use of circlip pliers 5.3 Disassembly Parts and order references
4 asic overview asic overview For femoral preparation, please refer to section 2.5, 2.6 and 2.7. The METS proximal tibial system is available with the option of two different proximal tibial components: Rotating hinge configuration which is covered in Section 3. Fixed hinge configuration which is covered in Section 4. ustom components are available to match the METS system for extreme tibial resections. Please contact Stanmore Implants for more details.
5 1.0 Device description 1.1 Product overview The METS proximal tibial replacement system is designed as a modular system that can be used to replace diseased or deficient bone in the proximal tibia. The system consists of a SMILES knee, a proximal tibial component, a range of shafts in 15mm increments to suit differing lengths of resection, a range of hydroxyapatite coated collars of different diameters to match the size of the resected bone and a range of cemented stems to fit the intramedullary canal. Individual components of the tibial shaft are connected using interlocking taper junctions allowing quick and easy assembly. The SMILES knee comes with the option of two different proximal tibial components; a rotating hinge and a fixed hinge, both suitable for primary and revision bone tumour cases and for revision total knee replacements where there is significant erosion of the proximal tibial bone. The fixed hinge is chosen for cases with significant loss of soft tissue function and where additional constraint is required. For very special cases, the METS modular system can be used in conjunction with custom-made components. For further details, please contact Stanmore Implants. 1.2 Indications Primary bone tumour Secondary tumour arising in bone Non-neoplastic conditions affecting the shafts of long bones Failed joint replacements with significant bone loss Failed massive replacements. 1.3 bsolute contra-indications Infection and sepsis. 1.4 Relative contra-indications Inadequate or incomplete soft tissue coverage Uncooperative or unwilling patient or patient unable to follow instructions Foreign body sensitivity. Where materials sensitivity occurs, seek advice with respect to testing Obesity Vascular disorders, neuromuscular disorders or muscular dystrophy Inadequate bone stock. 1.5 apabilities and restrictions of use The components are designed and manufactured and are to be assembled and used only in the manner specified. ny deviation from this may reduce the in-service life of the prosthesis. Mixing with unspecified components either from Stanmore Implants or from other manufacturers is not permitted since it may lead to mal-alignment, inadequate assembly, excessive wear and premature failure. fully assembled proximal tibial replacement must consist of one of the two proximal tibia assemblies (rotating hinge or fixed hinge) with bumper, a femoral component with bushes, an axle and a circlip, a shaft with or without an extension piece, a collar, and a stem. The collar is not an optional item and it must be used. Failure to do so may result in excessive subsidence of the prosthesis. Should the interlocking surfaces of any of the implant components become damaged, they must not be used. The implant components are for SINGLE USE only and they must not be re-used. set of instruments is provided to assist assembly of prosthesis, which includes a set of metal and Radel R trial components. The trial components are coloured to easily distinguish from implant components. Rotating hinge trials are blue, fixed hinge trials are yellow and all other trial components that can be used with both hinged versions are coloured green. Trial femoral plateau plates are titanium and anodised blue, while trial femoral components are silver and blue. In addition, the trial components cannot be used in combination with implant components. This implant is produced from titanium and ormo alloys and therefore under no circumstances must it be allowed to come in contact with another stainless steel device since this would induce galvanic corrosion. 4 5
6 2.0 Operation instructions and guidelines 2.1 Recommendations for component selection Size of femoral knee component Where possible, a standard sized knee component should be used if the bone and surrounding soft tissues can accommodate it. For smaller patients, a small sized femoral knee can be used. Tibial components Ideally, a rotating hinge proximal tibial replacement is recommended for cases where there is good muscle function and stability of the joint. Fixed hinged proximal tibial replacements should be considered where there is marked instability of the joint and the soft tissues have been sacrificed. Shaft The prosthetic construct should only have one principal shaft with an extension shaft if required. More than one principal shaft must not be used. Stem In order to optimise the implant fixation and strength, it is recommended that the largest stem diameter be chosen whilst still maintaining a minimum of 1mm cement mantle. Where thicker cortex is present, consider reaming the canal to accommodate the largest possible stem. 2.2 General points to note when using trial components Trial shafts and stems are assembled with a push and click mechanism where the rotational orientation is controlled by a lug. The trial collars are relieved by 2mm in the anterior/medial and anterior/lateral aspect and simply slide over the shaft. They can be used for left and right implants and are held in position by the insertion of a stem. There is a single sized axle for the trial components, thus it can be used for both small and standard size knees. The axle can be inserted from either side. It should be noted that a circlip is not required for the trial components. The trial components are designed to give a representation of the physical size of the actual implant component, and therefore, during trial reduction, they should provide an indication of the degree of soft tissue coverage and the function of the device. The trial proximal tibial components represent only the size and shape of the actual tibial construct and therefore do not rotate. During removal of the trial implant, if the stem should become lodged in the canal and left behind, use trial stem extractor to remove it. 2.3 Recommendations for assembly of implant It is recommended that the following points be considered during assembly of an implant: lways fully assemble an implant before exposing it to the body s environment; failure to do so may result in contaminating the interlocking mechanism, which can impair the performance of the implant. Impact each junction as described in sections or in order to provide optimum strength to the joint. This is important since each interface will experience large bending forces that can result in excessive wear and fretting if not correctly assembled. are must also be exercised when assembling components with hydroxyapatite coating, as it is brittle and can easily be damaged.
7 2.0 Operation instructions and guidelines 2.4 Special Instruments ush compressor standard 2 ush compressor small 3 ush reamer standard 4 ush reamer small 5 Distraction tool 6 ollar impacter small 7 Drill Ø10mm 8 Drill Ø8mm 9 Stem extractor 10 ush compressor nut 11 irclip pliers 12 Femoral cutting block standard 13 Pliers 14 Femoral cutting block small 15 Hammer 16 Distal cutting guide plate 17 Distal cutting guide bolt screw 18 Distal cutting IM rod 19 Drill guide 20 ollar impactor integral 21 General impactor 22 Plastic bearing impactor small 23 Plastic bearing impactor standard 6 7
8 2.0 Operation instructions and guidelines 2.5 Femoral cutting guide In addition to these instruments, it is anticipated that the operating theatre should make available a bone saw, flexible reamers and an appropriate cement application device. Drill guide Ø10mm drill Ø8mm drill Distal cutting guide plate Distal cutting guide slider Distal cutting guide bolt Distal cutting IM rod Distal cutting guide Standard femoral cutting block Small femoral cutting block
9 2.0 Operation instructions and guidelines Patella rest E 2.6 one preparation It should be noted that there is no prescribed order as to which bone (the femur or the tibia) is prepared first. efore femoral preparation, the size of the SMILES knee must be chosen as appropriate for the patient s knee. Drill guide Ø10mm drill 2.7 Femoral cutting guide and bone preparation Rotate the patella rest on the drill guide until the correct size SMILES knee mark is aligned with the arrow on the top of the guide. Place the drill guide on the condyles of the femur. With the patella rest resting in the patella track of the bone, rotate the drill guide in the sagittal plane and about the long axis of the bone so that the posterior condyles are aligned with the back edge of drill guide and that the patella rest is approximately in line with the femoral canal. Tap the drill guide using the hammer D provided so the spikes are embedded into the condyles. Using the Ø10mm drill, drill through E the guide into the inter-condylar notch to the depth indicated by the stop located on the drill. D Remove the guide. Using Ø8mm drill, deepen the hole ensuring the drill follows the intramedullary canal of the femur to the depth marked on the drill. 8 9
10 2.0 Operation instructions and guidelines F Distal cutting guide IM rod G Guide slider Insert the IM rod into the distal cutting F guide for right or left femur as required and lock it in position using the locking screw located in front of the distal cutting guide. The relevant marking should be proximal when inserting the rod into the guide. Locking screw Distal cutting guide slider bolt ssemble the distal cutting guide, guide G slider, distal cutting guide slider bolt and the distal cutting plate. ccording to the chart below, adjust the guide slider for the amount of femoral resection measured from the femoral condyles and secure it by tightening the locking screw positioned above it. Size of SMILES Knee Slider reading Small 22mm Standard 24mm Distal cutting plate Femoral cutting guide assembled correctly
11 2.0 Operation instructions and guidelines H Insert the IM rod into the previously H drilled hole in the femur. Push the rod in as far as it can go, ensure that at least one of the femoral condyles is making contact with the distal cutting guide and then rotate the guide along the long axis of the femur to align with posterior condyles with the back edge of the cutting guide. Impact the three pins housed in the cutting plate to secure it onto the femoral bone
12 2.0 Operation instructions and guidelines I Distal cut Unscrew the slider bolt and remove the I distal cutting guide, leaving the distal cutting plate securely in position. J nterior cut With an oscillating bone saw resting on the distal plane of the cutting plate, resect the femoral condyles and then remove the guide using the pliers provide. Place an appropriate size (small or J standard) femoral cutting block on the resected end of femur ensuring that the centralising peg is located in the previously drilled hole and that the sloping face is orientated posteriorly. Twist the block so that the sloping face is parallel with the posterior condyles. Secure the block into position by impacting the two pins housed in the block. Using an oscillating bone saw, trim the anterior condyles using the anterior surface of the block and posterior condyles using the posterior surface of the block. Remove the block using the pliers provide and using flexible reamers, ream the femoral canal to a depth of 140mm and to a diameter approximately 1mm bigger than the femoral stem. (For a small knee component, ream the femoral canal to Ø13mm and for a standard knee component ream to Ø14mm) The femur is now prepared. Insert the chosen femoral trial component to establish cuts are correctly produced. If not, trim the bone as required.
13 3.0 Rotating hinged proximal tibia 1 Rotating hinge tibial component small and standard 2 Rotating hinge proximal tibial component small and standard 3 Integral collar/shaft/stem x1 (H coated) 4 H collars x5 sizes 5 Integral shaft/stem x1 6 Rotating hinge prinicpal shafts x3 lengths 7 IM stems x5 diameters 8 Rotating hinge extension shafts x1 length 9 Fixed hinge principal shafts x5 lengths
14 3.0 Rotating hinged proximal tibia 3.1 omponents of the rotating hinged proximal tibial implant Femoral plateau plates Optional femoral plateau plates (not shown) are available in 5, 10, 15 and 20mm thicknesses for both small and standard sizes. Rotating hinge proximal tibial component titanium proximal tibial component with UHMWPE tibial bearing and a ormo tibial component. In small and standard sizes, with H coated patella tendon reattachment mechanism or smooth uncoated. Packaged as two individual assemblies: Rotating hinge proximal tibial component and UHMWPE bearing. Rotating hinge ormo tibial component and UHMWPE bumper pad. xle, bushes and circlip cobalt-chromiummolybdenum axle, a pair of UHMWPE bushes and a titanium circlip. (Packaged with the femoral component). Femoral component obalt-chromiummolybdenum femoral component with a titanium stem. natomical for left and right sides. vailable in small and standard sizes, with 140mm long femoral curved stem Ø13mm for standard components and Ø12mm for small components. Shaft 85 to 115mm long titanium shafts in 15mm increments. 85mm long extension shaft to further increase the length capability. For very short resections, integral shafts / stems are available in two lengths 55mm and 70mm. Total length capability gives a range from 105mm to 240mm from tibial condyles to tibial plateau. umper n UHMWPE bumper providing a secondary bearing surface and a soft hyperextension stop. emented stem Ø9 to Ø13mm straight titanium stems in 1mm increments and 120mm long. For extreme resections, a custom-made stem can be manufactured for use with this system. Please contact Stanmore Implants. ollar Ø20, Ø23, Ø26, Ø29 and Ø32mm H coated titanium collars.
15 3.0 Rotating hinged proximal tibia 3.2 Trial components of the rotating hinged proximal tibia Femoral plateau plates Trial femoral plateau plates (not shown) in 5, 10, 15 and 20mm thicknesses for both small and standard sizes. Trial femoral component Small and standard sizes in left hand and right hand versions. Trial axle One size axle that can fit both small and standard components and can be inserted from either side of the knee. Trial rotating hinge proximal tibial component Trial proximal tibial component in small and standard sizes. Trial shaft 85 to 115mm trial shafts in 15mm increments with an 85mm long trial extension shaft and 55 and 70mm long trial integral shaft/stem constructs. Trial collars Ø20mm to Ø32mm trial collars. Trial stem Ø9 to Ø13mm straight stems in 1mm increments, 120mm long
16 3.0 Rotating hinged proximal tibia 3.3 Tibia resection levels: Rotating hinge proximal tibia Please note: For extreme resections where a 120mm long stem is unsuitable, a stem made to your requirements may be custom manufactured. Please contact Stanmore Implants. It should be noted collar lengths are included in the resection values. Shaft omponent Resections Medial tibial condyle 50mm Tibial component plateau Integral shaft/stem 55mm 105mm Integral shaft/stem 70mm 120mm Rotating hinge principal shaft 85mm 135mm Rotating hinge principal shaft 100mm 150mm Rotating hinge principal shaft 115mm 165mm Rotating hinge extension shaft (85mm) + fixed hinge principal shaft 45mm 180mm Rotating hinge extension shaft (85mm) + fixed hinge principal shaft 60mm 195mm Rotating hinge extension shaft (85mm) + fixed hinge principal shaft 75mm 210mm Rotating hinge extension shaft (85mm) + fixed hinge principal shaft 90mm 225mm Rotating hinge extension shaft (85mm) + fixed hinge principal shaft 105mm 240mm
17 3.0 Rotating hinged proximal tibia 3.4 Tibial preparation Resect the tibial bone to the level required. Further trimming may be required when selecting the trial components. Please refer to section 3.3 as a guide. Ream the tibial canal using an appropriate sized flexible reamer to a depth of 120mm and to the required diameter to accommodate the tibial stem, leaving a minimum of 1mm for the cement mantle. 3.5 Short resections < 120mm For resections that are shorter than the smallest principal shaft, integral shaft/stem constructs can be used. Integral shaft/stem components for the rotating hinged proximal tibial replacement are available in two shaft lengths 55mm and 70mm with a 120mm straight tibial stem Ø10mm. The 55mm integral shaft/stem construct has a fixed collar diameter of 26mm and is available hydroxyapatite coated. The 70mm integral shaft/stem construct must be used with any of the hydroxyapatite coated collars Trial assembly and insertion Select the required size and side of the trial femoral component and insert into the prepared femur. Select appropriate size proximal tibial component and integral shaft/stem construct to replace the resected length of the tibia and assemble them as described in the section 2.2. The assembly sequence should be tibial component onto the shaft/ stem construct followed by the collar if using the 70mm integral construct. Insert the tibial assembly into the tibia. Join the femoral and tibial components together by insertion of the trial axle ensuring that it is correctly seated before performing a trial reduction. Once satisfied, remove all trial components and select corresponding implant components. During removal of the trial implant, if the stem should become lodged within the canal and left behind, the trial stem extractor should be used to remove it as shown on Page 5. If the joint is too tight or too loose between shaft increments, it may be necessary to resect extra bone from the tibia and repeat the trial
18 3.0 Rotating hinged proximal tibia Implant assembly and insertion The proximal tibial component Holding the proximal tibial component with the spigot pointing upwards, insert the integral shaft/stem construct ensuring that the alignment lug is correctly engaged. pply multiple sharp blows using the soft ended hammer provided to lock the taper securely in place. 70mm integral shaft/stem construct only If the collar is to be assembled separately, slide the selected collar over the stem of the assembled integral shaft/stem construct ensuring the alignments lugs are correctly engaged and the correct orientation is achieved. Place the integral collar impactor over the stem and using the soft ended hammer, apply multiple sharp blows to lock the components together, taking care not to damage the hydroxyapatite coating. Integral collar impact Hydroxyapatite coated collar The proximal tibial component is now assembled and ready for insertion. Insert the proximal tibial component into the tibial canal and cement it securely into place using the polyethylene bearing impactor and the soft ended hammer provided, ensuring correct rotational alignment. Insert the rotating hinge tibial component into the rotating hinge proximal tibial component. Proceed to section 5.0 Integral shaft/stem (70mm shaft) Rotating hinge proximal tibial component
19 3.0 Rotating hinged proximal tibia 3.6 Resections > 120mm Trial assembly and insertion Select the required size and side of the trial femoral component and insert into the prepared femur. Select appropriate size proximal tibial component, shaft, collar and stem to replace the resected length of the tibia and assemble them as described in section 2.2. The assembly sequence should be tibial component onto the shaft followed by collar and then stem respectively. Insert the tibial assembly into the tibia. Join the femoral and tibial components together by insertion of the trial axle ensuring that it is correctly seated before performing a trial reduction. Replace shaft/ stem/collar as required until satisfactory assembly is produced. Once satisfied, remove all trial components and select corresponding implant components. During removal of the trial implant, if the stem should become lodged within the canal and left behind, the trial stem extractor should be used to remove it as shown on Page 5. If the joint is too tight or too loose between shaft increments, it may be necessary to resect extra bone from the tibia and repeat the trial
20 3.0 Rotating hinged proximal tibia Implant assembly and insertion The proximal tibial component Place the proximal tibial component with the spigot pointing upwards; insert the principal shaft ensuring that the alignment lug is properly engaged. Place the collar impactor over into the bore on the shaft and apply multiple sharp blows using the soft hammer provided, locking the taper securely in place. Place the selected collar onto the distal end of the shaft ensuring once again the alignment lugs are correctly aligned. Holding the collar impactor over the collar, impact using multiple sharp hammer blows as shown opposite, taking care not to damage the bore or hydroxyapatite coating. Finally, insert the appropriate sized stem, ensuring the alignment lug is correctly located and impact using multiple sharp blows on the end of the stem. The proximal tibial component is now assembled and ready for insertion. Insert the proximal tibial component into the tibial canal and cement securely into place ensuring correct rotational alignment. Impact the stem using the polyethylene bearing impactor and soft ended hammer provided. Insert the rotating hinge tibial component into the rotating hinge proximal tibial component. Proceed to Section 5.0
21 3.0 Rotating hinged proximal tibia 3.7 Extensive resections > 165mm For resections greater than 165mm, the use of an extension shaft is required. The rotating hinged extension shaft is 85mm long and must be used with the fixed hinge principal shafts Trial assembly and insertion Select the required size and side of the trial femoral component and insert into the prepared femur. Select appropriate size proximal tibial component, extension shaft, fixed hinge principal shaft, collar and stem to replace the resected length of the tibia and assemble them as described in the sections 2.2. The assembly sequence should be tibial component onto extension shaft, then the fixed hinge principal shaft followed by collar and then stem respectively. Insert the tibial assembly into the tibia. Join the femoral and tibial components together by insertion of the trial axle ensuring that it is correctly seated before performing a trial reduction. Replace shaft/ stem/collar as required until satisfactory assembly is produced. Once satisfied, remove all trial components and select corresponding implant components. During removal of the trial implant, if the stem should become lodged within the canal and left behind, the trial stem extractor should be used to remove it as shown on Page 5. If the joint is too tight or too loose between shaft increments, it may be necessary to resect extra bone from the tibia and repeat the trial
22 3.0 Rotating hinged proximal tibia D Implant assembly and insertion The proximal tibial component Holding the proximal tibial component with the spigot pointing upwards with two hands, insert the rotating hinge extension shaft ensuring the alignment lug is correctly engaged. Place the collar impactor into the bore of the extension shaft and, using the soft ended hammer provided, apply multiple sharp blows. Insert the spigot of the required fixed hinge principal shaft into the bore of the extension shaft again ensuring that the alignment lug is properly engaged. Place the collar impactor into the bore on the principal shaft and apply multiple sharp blows using the soft hammer provided, locking the taper securely in place. Place the selected collar onto the distal end of the principal shaft ensuring once again the alignment lugs are correctly aligned. Holding the collar impactor over the collar, impact using multiple sharp hammer blows as shown, taking care not to damage the bore or hydroxyapatite coating. Finally, insert the appropriate sized stem, D ensuring the alignment lug is correctly located and impact using multiple sharp blows on the end of the stem. The proximal tibial component is now assembled and ready for insertion. Insert the proximal tibial component into the tibial canal and cement securely into place ensuring correct rotational alignment. Impact using the polyethylene bearing impactor and soft ended hammer provided. Insert the rotating hinge tibial component into the rotating hinge proximal tibial component. Proceed to Section 5.0
23 4.0 Fixed hinge proximal tibia 1 Fixed hinge proximal tibial small and standard 2 Integral collar/shaft/stem x1 (H coated) 3 H collars x5 sizes 4 Integral shaft/stem x1 5 Fixed hinge principal shafts x5 shafts 6 IM stems x5 diameters 7 Fixed hinge extension shafts x
24 4.0 Fixed hinge proximal tibia 4.1 omponents of the fixed hinged proximal tibial implant Femoral plateau plates Optional femoral plateau plates (not shown) are available in 5, 10, 15 and 20mm thicknesses for both small and standard sizes. Femoral component obalt-chromiummolybdenum femoral component with a titanium stem. natomical for left and right sides. vailable in small and standard sizes, with 140mm long femoral curved stem Ø13mm for standard components and Ø12mm for small components. Fixed hinged proximal tibial component ormo proximal tibial component. In small and standard sizes with H coated patella tendon reattachment mechanism or smooth uncoated. xle, bushes and circlip cobalt-chromiummolybdenum axle, a pair of UHMWPE bushes and a titanium circlip. (Packaged with femoral components) Shaft 45 to 105mm long titanium shafts in 15mm increments. 75mm extension shaft to further increase the length capability. For very small resections, integral shafts/stems are available in two lengths 15mm and 30mm. It must be noted that a H coated collar must be used. Total length capability gives a range from 60mm to 225mm from tibial condyles to tibial plateau. umper n UHMWPE bumper providing a secondary bearing surface and a soft hyperextension stop. Pre-assembled with the proximal tibial component. ollar Ø20, Ø23, Ø26, Ø29 and Ø32mm H coated titanium collars. emented stem Ø9 to Ø13mm straight titanium stems in 1mm increments and 120mm length. For extreme resections, a custom-made stem can be manufactured for use with this system. Please contact the Stanmore Implants.
25 4.0 Fixed hinge proximal tibia 4.2 Trial components of the fixed hinged proximal tibia Femoral plateau plates Trial femoral plateau plates (not shown) in 5, 10, 15 and 20mm thicknesses for both small and standard sizes. Trial femoral component Small and standard sizes in left hand and right hand versions. Trial axle One size axle that can fit both small and standard components and can be inserted from either side of the knee. Trial fixed hinged proximal tibial component Trial proximal tibial component. In small and standard sizes. Trial shaft 45 to 105mm trial shafts in 15mm increments with a 75mm long trial extension shaft and 15 and 30mm long trial integral shaft/ stem constructs. Trial collar Ø20mm to Ø32mm trial collars. Trial stem Ø9 to Ø13mm straight stems in 1mm increments, 120mm long
26 4.0 Fixed hinge proximal tibia 4.3 Tibial resection levels: fixed hinge proximal tibia Please note: For extreme resections where a 120mm long stem is unsuitable, a stem made to your requirements may be custom manufactured. Please contact Stanmore Implants. It should be noted that collar lengths are included in the resection values. Shaft omponent Resections Medial tibial condyle 45mm Tibial component plateau Integral shaft/stem 15mm 60mm Integral shaft/stem 30mm 75mm Fixed hinge principal shaft 45mm 90mm Fixed hinge principal shaft 60mm 105mm Fixed hinge principal shaft 75mm 120mm Fixed hinge principal shaft 90mm 135mm Fixed hinge principal shaft 105mm 150mm Fixed hinge extension shaft (75mm) + fixed hinge principal shaft 45mm 165mm Fixed hinge extension shaft (75mm) + fixed hinge principal shaft 60mm 180mm Fixed hinge extension shaft (75mm) + fixed hinge principal shaft 75mm 195mm Fixed hinge extension shaft (75mm) + fixed hinge principal shaft 90mm 210mm Fixed hinge extension shaft (75mm) + fixed hinge principal shaft 105mm 225mm
27 4.0 Fixed hinge proximal tibia 4.4 Tibial preparation Resect the tibial bone to the level required. Further trimming may be required when selecting the trial components. Please refer to section 4.3 as a guide. Ream the tibial canal using an appropriate sized flexible reamer to a depth of 120mm and to the required diameter to accommodate the tibial stem, leaving a minimum of 1mm for the cement mantle. 4.5 Short resections < 75mm For resections that are shorter than the smallest principal shaft, integral shaft/stem constructs can be used. Integral shaft/stem components for the fixed hinged proximal tibial replacement are available in two shaft lengths 15mm and 30mm with a 120mm straight tibial stem Ø12mm. The 15mm integral shaft/stem construct has a fixed collar diameter of 33mm and is hydroxyapatite coated. The 30mm integral shaft/stem construct allows you the option to use any of the hydroxyapatite coated collars Trial assembly and insertion Select the required size and side of trial femoral component and insert into the prepared femur. Select appropriate size proximal tibial component and integral shaft/stem construct to replace the resected length of the tibia and assemble them as described in section 2.2. The assembly sequence should be tibial component onto the shaft stem/stem construct followed by the collar if using the 30mm integral construct. Insert the tibial assembly into the tibia. Join the two components together by insertion of the trial axle ensuring that it is correctly seated before performing a trial reduction. Replace shaft/stem/collar as required until satisfactory assembly is produced. Once satisfied, remove all trial components and select corresponding implant components. During removal of the trial implant, if the stem should become lodged within the canal and left behind, the trial stem extractor should be used to remove it as shown on Page 5. If the joint is too tight or too loose between shaft increments, it may be necessary to resect extra bone from the tibia and repeat the trial
28 4.0 Fixed hinge proximal tibia Implant assembly and insertion The proximal tibial component Holding the proximal tibial component with the bore pointing upwards, insert the integral shaft/stem construct ensuring that the alignment lug is correctly engaged. pply multiple sharp blows using the soft ended hammer provided to lock the taper securely in place. 30mm integral shaft stem construct only If the collar is to be assembled separately, slide the selected collar over the stem of the assembled integral shaft/stem construct ensuring the alignments lugs are correctly engaged and the correct orientation is achieved. Place the integral collar impactor over the stem and using the soft ended hammer, apply multiple sharp blows to lock the components together, taking care not to damage the hydroxyapatite coating. Integral collar impact The proximal tibial component is now assembled and ready for insertion. Using the general impactor and soft ended hammer provided, insert the proximal tibial component into the tibial canal and cement securely into place, ensuring correct rotational alignment. Proceed to section 5.0 Hydroxyapatite coated collar Integral shaft/stem (30mm shaft) Fixed hinge proximal tibial component
29 4.0 Fixed hinge proximal tibia 4.6 Resections > 75mm Trial assembly and insertion Select the required size and side of trial femoral component and insert into the prepared femur. Select appropriate size proximal tibial component, shaft, collar and stem to replace the resected length of the tibia and assemble them as described in section 2.2. The assembly sequence should be tibial component onto the shaft followed by the collar and then the stem respectively. Insert the tibial assembly into the tibia. Join the two components together by insertion of the trial axle ensuring that it is correctly seated before performing a trial reduction. Replace shaft/stem/collar as required until satisfactory assembly is produced. Once satisfied, remove all trial components and select corresponding implant components. During removal of the trial implant, if the stem should become lodged within the canal and left behind, the trial stem extractor should be used to remove it as shown on Page 5. If the joint is too tight or too loose between shaft increments, it may be necessary to resect extra bone from the tibia and repeat the trial
30 4.0 Fixed hinge proximal tibia Implant assembly and insertion The proximal tibial component Hold the proximal tibial component with the bore pointing upwards with two hands. Insert the spigot of the required principal shaft ensuring that the alignment lug is properly engaged. Place the collar impactor into the bore on the shaft and apply multiple sharp blows using the soft hammer provided, locking the taper securely in place. Place the selected collar onto the distal end of the shaft ensuring once again the alignment lugs are correctly aligned. Holding the collar impactor over the collar, impact using multiple sharp hammer blows as shown below taking care not to damage the bore or hydroxyapatite coating. Finally, insert the appropriate sized stem, ensuring the alignment lug is correctly located and impact with multiple sharp blows on the end of the stem. The proximal tibial component is now assembled and ready for insertion. Using the general impactor and soft ended hammer provided, insert the proximal tibial component into the tibial canal and cement securely into place, ensuring correct rotational alignment. Proceed to section 5.0
31 4.0 Fixed hinge proximal tibia 4.7 Extensive resections > 120mm For resection greater than 120mm, the use of an extension shaft is required. The extension shaft is 75mm long and must be used with a principal shaft Trial assembly and insertion Select the required size and side of trial femoral component and insert into the prepared femur. Select appropriate size proximal tibial component, extension shaft, principal shaft, collar and stem to replace the resected length of the tibia and assemble them as described in the section 2.2. The assembly sequence should be tibial component onto the extension shaft, then the principal shaft followed by the collar and then the stem respectively. Insert the tibial assembly into the tibia. Join the two components together by insertion of the trial axle ensuring that it is correctly seated before performing a trial reduction. Replace shaft/stem/collar as required until satisfactory assembly is produced. Once satisfied, remove all trial components and select corresponding implant components. During removal of the trial implant, if the stem should become lodged within the canal and left behind, the trial stem extractor should be used to remove it as shown on Page 5. If the joint is too tight or too loose between shaft increments, it may be necessary to resect extra bone from the tibia and repeat the trial
32 4.0 Fixed hinge proximal tibia D Implant assembly and insertion The proximal tibial component Holding the proximal tibial component with the bore pointing upwards with two hands, insert the spigot of the fixed hinge extension shaft ensuring the alignment lug is correctly engaged. Place the collar impactor over the bore of the extension shaft and, using the soft ended hammer provided, apply multiple sharp blows. Insert the spigot of the required fixed hinge principal shaft into the bore of the extension shaft again ensuring that the alignment lug is properly engaged. Place the collar impactor into the bore on the principal shaft and apply multiple sharp blows using the soft hammer provided, locking the taper securely in place. Place the selected collar onto the distal end of the shaft ensuring once again the alignment lugs are correctly aligned. Holding the collar impactor over the collar, impact using multiple sharp hammer blows as shown taking care not to damage the bore or hydroxyapatite coating. Finally, insert the appropriate sized stem, D ensuring the alignment lug is correctly located and impact using multiple sharp blows on the end of the stem. The proximal tibial component is now assembled and ready for insertion. Using the general impactor and soft ended hammer provided, insert the proximal tibial component into the tibial canal and cement securely into place, ensuring correct rotational alignment. Proceed to section 5.0
33 5.0 The femoral component 5.0 The femoral component ement the required femoral component into the femoral canal, ensuring the correct orientation is achieved. Impact using the general impactor. 5.1 Femoral plateau plates Optional femoral plateau plates are available in 5, and 20mm thicknesses for both small and standard sizes. Using a small amount of bone cement, secure the plateau plate onto the femoral component by sliding it over the femoral stem until the anti-rotation lugs on the femoral component are located within the holes in the femoral plateau plate. It should be noted that only one femoral plateau plate can be used. Multiple plates cannot be stacked onto one another. 5.2 Insertion of the axle and circlip Insertion of axle lign the femoral and tibial components and insert the axle into position as shown. It should be noted that the axle can be inserted from either side of the knee joint. Using the pronged end of the circlip pliers handle, push the axle in place. If required, rotate the axle to engage the axle head into the offset recess in the femoral component. heck to ensure the axle head is correctly sitting inside the recess and that it is not trapped within the circlip groove
34 5.0 The femoral component orrect D E Use of circlip pliers The circlip and the pliers are designed to clip together for ease of use. The best way to place the circlip onto the pliers is by holding the circlip on your finger tip and then pushing the pliers into it ensuring the central pin locates in the centre of the circlip and the two moving jaws are either side of the central strips of the circlip as shown in the pictures below. correctly inserted circlip is shown on the left with the jaws of the circlip pliers in the correct position. This picture on the left shows an incorrectly inserted circlip. This would not function and the circlip needs reinserting. (Requires rotating 180º) The circlip is best inserted into the knee D by holding the circlip at an angle, then placing the circular part of the circlip into the groove in the tibial component and then straightening and pushing the circlip into position as shown. Release circlip pliers and pull to unclip from the circlip. Ensure that the circlip is seated inside the E groove in the tibial component and then, using a pointed implement, rotate it to ensure it turns inside the groove. Rotation of the circlip ensures the circlip is fully engaged in the groove. Incorrect
35 5.0 The femoral component 5.3 Disassembly During revision surgery, it may be necessary to disassemble the implant. This is achieved by inserting the distraction tool into the anterior hole of the shaft and impacting with a hammer. The distraction tool has a flat, which should locate on the end of the inner spigot. Part are for SINGLE USE only and cannot be reused
36 6.0 Parts and order references Femoral knee omponents Small Left mptfc/lsm Small Right mptfc/rsm Standard Left mptfc/lstd Standard Right mptfc/rstd Proximal tibia Fixed hinge Small mptfh/smu Plain uncoated Standard mptfh/stdu Fixed hinge Small mptfh/sm With reattachment H coated Standard mptfh/std Rotating hinge Small mptrh/smu Plain uncoated Standard mptrh/stdu Rotating hinge Small mptrh/sm With reattachment H coated Standard mptrh/std Tibial components Rotating hinge Small mktsc/sm Standard mktsc/std Tibial shafts Fixed hinge 45mm mptfhshft/45 60mm mptfhshft/60 75mm mptfhshft/75 90mm mptfhshft/90 105mm mptfhshft/105 Tibial extension shaft Fixed hinge 75mm mptfhext/75 Integral shafts & stems Shaft Stem Fixed hinge L = 15 D = 33 L = 120 D = 12 > 9 mptfhiss/15 L = 30 D = 33 L = 120 D = 12 > 9 mptfhiss/30n Tibial shafts Rotating hinge 85mm mptrhshft/85 100mm mptrhshft/ mm mptrhshft/115 Tibial extension shaft Rotating hinge 85mm mptrhext/85 Integral shafts & stems Shaft Stem Rotating hinge L = 55 D = 26 L = 120 D = 10 > 9.5 mptrhiss/55 L = 70 D = 26 L = 120 D = 10 > 9.5 mptrhiss/70n Tibial collars H coated Ø20 mptcol/20 Ø23 mptcol/23 Ø26 mptcol/26 Ø29 mptcol/29 Ø32 mptcol/32 Tibial stems Ø9 > 8mm mptstm/9 Ø10 > 9mm mptstm/10 Ø11 > 10mm mptstm/11 Ø12 > 11mm mptstm/12 Ø13 > 12mm mptstm/13 Femoral plateau plates Small 5mm mkfp/sm5 Small 10mm mkfp/sm10 Small 15mm mkfp/sm15 Small 20mm mkfp/sm20 Standard 5mm mkfp/std5 Standard 10mm mkfp/std10 Standard 15mm mkfp/std15 Standard 20mm mkfp/std20
37 Stanmore Implants 210 entennial venue entennial Park Elstree WD6 3SJ United Kingdom T +44 (0) F +44 (0)
Surgical procedure. METS SMILES Total Knee Replacement
 Surgical procedure METS SMILES Total Knee Replacement Surgical Procedure Contents 1.0 2.0 3.0 4.0 Device information 2 3 1.1 Product overview 1.2 Indications 1.3 Absolute contra-indications 1.4 Relative
Surgical procedure METS SMILES Total Knee Replacement Surgical Procedure Contents 1.0 2.0 3.0 4.0 Device information 2 3 1.1 Product overview 1.2 Indications 1.3 Absolute contra-indications 1.4 Relative
Surgical procedure. METS Modular Distal Femur
 Surgical procedure METS Modular Distal Femur Surgical Procedure Contents 1.0 2.0 3.0 4.0 Device information 2 3 1.1 Product overview 1.2 Indications 1.3 bsolute contra-indications 1.4 Relative contra-indications
Surgical procedure METS Modular Distal Femur Surgical Procedure Contents 1.0 2.0 3.0 4.0 Device information 2 3 1.1 Product overview 1.2 Indications 1.3 bsolute contra-indications 1.4 Relative contra-indications
Surgical procedure. METS Modular Proximal Femur
 Surgical procedure METS Modular Proximal Femur Surgical Procedure Contents 1.0 2.0 3.0 4.0 5.0 Device information 2 3 1.1 Product overview 1.2 Indications 1.3 Absolute contra-indications 1.4 Relative
Surgical procedure METS Modular Proximal Femur Surgical Procedure Contents 1.0 2.0 3.0 4.0 5.0 Device information 2 3 1.1 Product overview 1.2 Indications 1.3 Absolute contra-indications 1.4 Relative
Surgical procedure. METS Modular Proximal Humerus
 Surgical procedure METS Modular Proximal Humerus Surgical Procedure Contents 1.0 2.0 3.0 4.0 Device information 2 3 1.1 Product overview 1.2 Indications 1.3 bsolute contra-indications 1.4 Relative contra-indications
Surgical procedure METS Modular Proximal Humerus Surgical Procedure Contents 1.0 2.0 3.0 4.0 Device information 2 3 1.1 Product overview 1.2 Indications 1.3 bsolute contra-indications 1.4 Relative contra-indications
Surgical procedure. METS Coned Hemi-Pelvis
 Surgical procedure METS Coned Hemi-Pelvis Surgical Procedure Contents 1.0 2.0 3.0 4.0 5.0 Product overview 2 1.1 Indications 1.2 Absolute contra-indications 1.3 Relative contra-indications 1.4 Capabilities
Surgical procedure METS Coned Hemi-Pelvis Surgical Procedure Contents 1.0 2.0 3.0 4.0 5.0 Product overview 2 1.1 Indications 1.2 Absolute contra-indications 1.3 Relative contra-indications 1.4 Capabilities
U2 PSA. Revision Knee. Surgical Protocol
 U2 PSA TM Revision Knee Surgical Protocol Table of Contents 1 Component Removal... 1 2 Tibial Preparation... 1 2.1 Tibial Canal Preparation... 1 2.2 Proximal Tibial Resection... 2 2.3 Non Offset Tibial
U2 PSA TM Revision Knee Surgical Protocol Table of Contents 1 Component Removal... 1 2 Tibial Preparation... 1 2.1 Tibial Canal Preparation... 1 2.2 Proximal Tibial Resection... 2 2.3 Non Offset Tibial
TRK REVISION KNEE Surgical Technique
 1 TRK REVISION KNEE Surgical Technique 1. 2. 3. 4. 5. 6. 7. 8. 9. 10. INTERCONDYLAR RESECTION...... page FEMORAL STEM...... page NON CEMENTED FEMORAL STEM...... page TRIAL FEMORAL COMPONENTS...... page
1 TRK REVISION KNEE Surgical Technique 1. 2. 3. 4. 5. 6. 7. 8. 9. 10. INTERCONDYLAR RESECTION...... page FEMORAL STEM...... page NON CEMENTED FEMORAL STEM...... page TRIAL FEMORAL COMPONENTS...... page
TOTAL KNEE ARTHROPLASTY SYSTEM
 SURGICAL TECHNIQUE TOTAL KNEE ARTHROPLASTY SYSTEM 90-SRK-700000 B.0 0 Contents 1. Implant Sizing 2. Surgical Technique a. Incision and Exposure b. Distal Femoral Resection c. Tibial Resection d. Femoral
SURGICAL TECHNIQUE TOTAL KNEE ARTHROPLASTY SYSTEM 90-SRK-700000 B.0 0 Contents 1. Implant Sizing 2. Surgical Technique a. Incision and Exposure b. Distal Femoral Resection c. Tibial Resection d. Femoral
Resurfacing Distal Femur. Orthopaedic Salvage System
 Resurfacing Distal Femur Orthopaedic Salvage System Primary Arthroplasty OSS 3cm Resurfacing Distal Femur Distal Femoral Resection Drill and ream the distal femur in the following sequence: (Figure 1)
Resurfacing Distal Femur Orthopaedic Salvage System Primary Arthroplasty OSS 3cm Resurfacing Distal Femur Distal Femoral Resection Drill and ream the distal femur in the following sequence: (Figure 1)
ANATOMIC SURGICAL TECHNIQUE. 5 in 1. Conventional instrumentation 07/11/2013
 ANATOMIC SURGICAL TECHNIQUE 5 in 1 Conventional instrumentation PRO.GB.933/1.0 Octobre 2013 2 Tibial step 3 Intramedullary technique - Based on the preoperative plan, drill the medullary canal with the
ANATOMIC SURGICAL TECHNIQUE 5 in 1 Conventional instrumentation PRO.GB.933/1.0 Octobre 2013 2 Tibial step 3 Intramedullary technique - Based on the preoperative plan, drill the medullary canal with the
OPERATIVE TECHNIQUE SKS Total Knee Replacement
 OPERATIVE TECHNIQUE SKS Total Knee Replacement Femoral preparation A40577 1 2 5 1: Alignment rod A30049 + A30124 2: Centromedullary rod A40224 4: T-handle A40232 6: Femoral measuring device A40411 + A40414
OPERATIVE TECHNIQUE SKS Total Knee Replacement Femoral preparation A40577 1 2 5 1: Alignment rod A30049 + A30124 2: Centromedullary rod A40224 4: T-handle A40232 6: Femoral measuring device A40411 + A40414
MRH Knee System Modular Peg Baseplate Surgical Protocol
 MRH Knee System Modular Peg Baseplate Surgical Protocol Using Monogram IM Revision Instruments 4 N 4 N Modular Rotating Hinge Knee System Using Monogram IM Revision Instruments Mr C R Howie FRCS Consultant
MRH Knee System Modular Peg Baseplate Surgical Protocol Using Monogram IM Revision Instruments 4 N 4 N Modular Rotating Hinge Knee System Using Monogram IM Revision Instruments Mr C R Howie FRCS Consultant
Distal Cut First Femoral Preparation
 Surgical Technique Distal Cut First Femoral Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Femoral preparation Contents Introduction...3 DCF femoral highlights...4 Preoperative planning...6
Surgical Technique Distal Cut First Femoral Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Femoral preparation Contents Introduction...3 DCF femoral highlights...4 Preoperative planning...6
Zimmer NexGen MIS Tibial Component. Cemented Surgical Technique IMAGE TO COME
 Zimmer NexGen MIS Tibial Component Cemented Surgical Technique IMAGE TO COME Zimmer NexGen MIS Tibial Component Cemented Surgical Technique 1 Zimmer NexGen MIS Tibial Component Cemented Surgical Technique
Zimmer NexGen MIS Tibial Component Cemented Surgical Technique IMAGE TO COME Zimmer NexGen MIS Tibial Component Cemented Surgical Technique 1 Zimmer NexGen MIS Tibial Component Cemented Surgical Technique
U2 PSA. Revision Knee. Surgical Protocol
 U2 PSA TM Revision Knee Surgical Protocol Table of Contents 1 Component Removal... 2 Tibial Preparation... 2.1 Tibial Canal Preparation... 2.2 Proximal Tibial Resection... 2.3 Non Offset Tibial Preparation...
U2 PSA TM Revision Knee Surgical Protocol Table of Contents 1 Component Removal... 2 Tibial Preparation... 2.1 Tibial Canal Preparation... 2.2 Proximal Tibial Resection... 2.3 Non Offset Tibial Preparation...
Triathlon TS Knee System. Surgical Protocol
 Triathlon TS Knee System Surgical Protocol Triathlon TS Knee System Surgical Protocol Table of Contents Acknowledgments..........................................................2 Exposure...................................................................4
Triathlon TS Knee System Surgical Protocol Triathlon TS Knee System Surgical Protocol Table of Contents Acknowledgments..........................................................2 Exposure...................................................................4
PRIMARY POROUS PATELLA WITH TRABECULAR METAL. Surgical Technique
 PRIMARY POROUS PATELLA WITH TRABECULAR METAL Surgical Technique 1 SURGICAL TECHNIQUE FOR NEXGEN PRIMARY POROUS PATELLA * WITH TRABECULAR METAL CONTENTS PREPARE THE PATELLA............... 2 Patella Reamer
PRIMARY POROUS PATELLA WITH TRABECULAR METAL Surgical Technique 1 SURGICAL TECHNIQUE FOR NEXGEN PRIMARY POROUS PATELLA * WITH TRABECULAR METAL CONTENTS PREPARE THE PATELLA............... 2 Patella Reamer
LPS SYSTEM POCKET GUIDE
 LPS SYSTEM POCKET GUIDE Implants Procedural Uses Instruments & Trials L P S Limb Preservation System L P S Limb Preservation System The purpose of this document is to review the LPS (Limb Preservation
LPS SYSTEM POCKET GUIDE Implants Procedural Uses Instruments & Trials L P S Limb Preservation System L P S Limb Preservation System The purpose of this document is to review the LPS (Limb Preservation
TRIAL COMPONENTS SURGICAL TECHNIQUE REAMING THE TIBIAL AND FEMORAL INTRAMEDULLARY CANAL
 Ref. no. 99.27.2TRIALS TRIAL COMPONENTS SURGICAL TECHNIQUE CLINICAL INDICATION This technique is indicated in the case of revisions with significant bone loss when minimal or any resection of bone is required.
Ref. no. 99.27.2TRIALS TRIAL COMPONENTS SURGICAL TECHNIQUE CLINICAL INDICATION This technique is indicated in the case of revisions with significant bone loss when minimal or any resection of bone is required.
Zimmer Trabecular Metal Ankle Interpositional Spacer and Trabecular Metal Ankle Fusion Spacer
 Zimmer Trabecular Metal Ankle Interpositional Spacer and Trabecular Metal Ankle Fusion Spacer Surgical Technique 2 Zimmer Trabecular Metal Ankle Interpositional Spacer and Trabecular Metal Ankle Fusion
Zimmer Trabecular Metal Ankle Interpositional Spacer and Trabecular Metal Ankle Fusion Spacer Surgical Technique 2 Zimmer Trabecular Metal Ankle Interpositional Spacer and Trabecular Metal Ankle Fusion
Zimmer NexGen Trabecular Metal Tibial Tray
 Zimmer NexGen Trabecular Metal Tibial Tray Surgical Technique Zimmer NexGen Trabecular Metal Tibial Tray Surgical Technique Give Bone A Solid Hold Zimmer NexGen Trabecular Metal Tibial Tray Surgical Technique
Zimmer NexGen Trabecular Metal Tibial Tray Surgical Technique Zimmer NexGen Trabecular Metal Tibial Tray Surgical Technique Give Bone A Solid Hold Zimmer NexGen Trabecular Metal Tibial Tray Surgical Technique
Surgical Technique. Hinge Disassembly and Rebuild Technique
 Surgical Technique Hinge Disassembly and Rebuild Technique Revision Knee Arthroplasty Surgical Technique LEGION HK Hinge Knee System Introduction The LEGION HK Hinge Knee System has been designed as an
Surgical Technique Hinge Disassembly and Rebuild Technique Revision Knee Arthroplasty Surgical Technique LEGION HK Hinge Knee System Introduction The LEGION HK Hinge Knee System has been designed as an
Triathlon Knee System
 Triathlon Knee System Express Instruments Surgical Protocol Posterior Stabilized & Cruciate Retaining TriathlonKneeSystem Express Instruments Surgical Protocol Acknowledgments..........................................................2
Triathlon Knee System Express Instruments Surgical Protocol Posterior Stabilized & Cruciate Retaining TriathlonKneeSystem Express Instruments Surgical Protocol Acknowledgments..........................................................2
Intramedullary Tibial Preparation
 Surgical Technique Intramedullary Tibial Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Intramedullary tibial preparation Contents Introduction...2 IM tibial highlights...3 Preoperative
Surgical Technique Intramedullary Tibial Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Intramedullary tibial preparation Contents Introduction...2 IM tibial highlights...3 Preoperative
Surgical Technique. VISIONAIRE Disposable Instruments for the LEGION Total Knee System
 Surgical Technique VISIONAIRE Disposable Instruments for the LEGION Total Knee System VISIONAIRE and LEGION Disposable instrument technique* Note: All disposable instruments are interchangeable with the
Surgical Technique VISIONAIRE Disposable Instruments for the LEGION Total Knee System VISIONAIRE and LEGION Disposable instrument technique* Note: All disposable instruments are interchangeable with the
MIS Cemented Tibial Component
 MIS Cemented Tibial Component NexGen Complete Knee Solution Surgical Technique Table of Contents Surgical Exposure... 2 Finish the Tibia... 2 Position Based on Anatomic Landmarks... 3 Lateral Posterior
MIS Cemented Tibial Component NexGen Complete Knee Solution Surgical Technique Table of Contents Surgical Exposure... 2 Finish the Tibia... 2 Position Based on Anatomic Landmarks... 3 Lateral Posterior
NEXGEN COMPLETE KNEE SOLUTION S A. Tibial Stem Extension & Augmentation Surgical. ATechnique
 NEXGEN COMPLETE KNEE SOLUTION ATechnique Tibial Stem Extension & Augmentation Surgical INTRODUCTION The NexGen Complete Knee Solution Intramedullary Tibial Instruments have been designed to provide an
NEXGEN COMPLETE KNEE SOLUTION ATechnique Tibial Stem Extension & Augmentation Surgical INTRODUCTION The NexGen Complete Knee Solution Intramedullary Tibial Instruments have been designed to provide an
EXACTECH KNEE. Operative Technique ADDENDUM. Metaphyseal Cones. Surgeon focused. Patient driven. TM
 EXACTECH KNEE Operative Technique ADDENDUM Metaphyseal Cones Surgeon focused. Patient driven. TM TABLE OF CONTENTS INTRODUCTION...1 DESCRIPTION...1 DETAILED OPERATIVE TECHNIQUE Initial Preparation and
EXACTECH KNEE Operative Technique ADDENDUM Metaphyseal Cones Surgeon focused. Patient driven. TM TABLE OF CONTENTS INTRODUCTION...1 DESCRIPTION...1 DETAILED OPERATIVE TECHNIQUE Initial Preparation and
Trabecular Metal Primary Patella
 Trabecular Metal Primary Patella NexGen Complete Knee Solution Surgical Technique Table of Contents Introduction... 2 Prepare the Patella... 2 Patella Reamer Technique... 3 Insetting Technique... 5 Universal
Trabecular Metal Primary Patella NexGen Complete Knee Solution Surgical Technique Table of Contents Introduction... 2 Prepare the Patella... 2 Patella Reamer Technique... 3 Insetting Technique... 5 Universal
OSS Overview Biomet Oncology Salvage System Featuring the Finn Knee
 OSS Overview Biomet Oncology Salvage System Featuring the Finn Knee Biomet, Finn & Arcom are trademarks of Biomet Inc. 1 Table of Contents Overview...page 4 Introduction History of Hinged Knees Clinical
OSS Overview Biomet Oncology Salvage System Featuring the Finn Knee Biomet, Finn & Arcom are trademarks of Biomet Inc. 1 Table of Contents Overview...page 4 Introduction History of Hinged Knees Clinical
A novel cementless option. Zimmer NexGen Trabecular Metal Primary Patella Surgical Technique
 A novel cementless option Zimmer NexGen Trabecular Metal Primary Patella Surgical Technique Zimmer Trabecular Metal Primary Patella 1 Zimmer NexGen Trabecular Metal Primary Patella Surgical Technique
A novel cementless option Zimmer NexGen Trabecular Metal Primary Patella Surgical Technique Zimmer Trabecular Metal Primary Patella 1 Zimmer NexGen Trabecular Metal Primary Patella Surgical Technique
The ACL-PCL Substituting Knee. BioFoam Tibial Bases. Surgical Technique For Cementless Tibial Fixation
 The CL-PCL Substituting Knee BioFoam Surgical Technique For Cementless Tibial Fixation Surgical techniques and instrument recommendations were provided by: Michael nderson, MD Milwaukee, WI G. Lynn Rasmussen,
The CL-PCL Substituting Knee BioFoam Surgical Technique For Cementless Tibial Fixation Surgical techniques and instrument recommendations were provided by: Michael nderson, MD Milwaukee, WI G. Lynn Rasmussen,
Encina Taper Stem. Stinson Orthopedics Inc. 303 Twin Dolphin Drive, Suite 600 Redwood City, CA
 Stinson Orthopedics Inc. 303 Twin Dolphin Drive, Suite 600 Redwood City, CA 94065 info@stinsonortho.com www.stinsonortho.com Table of Contents Introduction 3 Features 4 Surgical Technique 5 Preoperative
Stinson Orthopedics Inc. 303 Twin Dolphin Drive, Suite 600 Redwood City, CA 94065 info@stinsonortho.com www.stinsonortho.com Table of Contents Introduction 3 Features 4 Surgical Technique 5 Preoperative
ELEOS Limb Salvage System
 ELEOS Limb Salvage System Surgical Technique Total Femoral Replacement The ELEOS Limb Salvage System offers options for patients with significant bone loss due to cancer, trauma, or previous surgical procedures.
ELEOS Limb Salvage System Surgical Technique Total Femoral Replacement The ELEOS Limb Salvage System offers options for patients with significant bone loss due to cancer, trauma, or previous surgical procedures.
ELEOS Limb Salvage System
 ELEOS Limb Salvage System Surgical Technique Hinge Knee Replacement The ELEOS Limb Salvage System offers options for patients with significant bone loss due to cancer, trauma, or previous surgical procedures.
ELEOS Limb Salvage System Surgical Technique Hinge Knee Replacement The ELEOS Limb Salvage System offers options for patients with significant bone loss due to cancer, trauma, or previous surgical procedures.
Trabecular Metal Tibial Cone Surgical Technique
 Trabecular Metal Tibial Cone Surgical Technique Provides structural support in areas of bone loss Trabecular Metal Cone 1 Zimmer Trabecular Metal Tibial Cone Surgical Technique Table of Contents Overview
Trabecular Metal Tibial Cone Surgical Technique Provides structural support in areas of bone loss Trabecular Metal Cone 1 Zimmer Trabecular Metal Tibial Cone Surgical Technique Table of Contents Overview
Surgical Technique.
 Surgical Technique www.biomet.co.uk INTRODUCTION design principals Recent advances in imaging technology have enabled orthopaedic surgeons to extend closed treatment of femoral fractures to include more
Surgical Technique www.biomet.co.uk INTRODUCTION design principals Recent advances in imaging technology have enabled orthopaedic surgeons to extend closed treatment of femoral fractures to include more
Medial Rotation Knee. Forever Active. Landmark Operative Technique Supplement: No.1 All-Polyethylene Tibia (Cemented)
 Medial Rotation Knee Landmark Operative Technique Supplement: No.1 All-Polyethylene Tibia (Cemented) Physiological Stability and Mobility for the Active Knee Without Compromise Forever Active Contents
Medial Rotation Knee Landmark Operative Technique Supplement: No.1 All-Polyethylene Tibia (Cemented) Physiological Stability and Mobility for the Active Knee Without Compromise Forever Active Contents
BIOTECH FUTURE KNEE Minimal Invasive (and classic) Surgical Technique
 BIOTECH FUTURE KNEE Minimal Invasive (and classic) Surgical Technique Page No. Product description 2. Pre-operational planning 3. 1st step Femoral resection 4. P/S Femoral component 7. 2nd step Proximal
BIOTECH FUTURE KNEE Minimal Invasive (and classic) Surgical Technique Page No. Product description 2. Pre-operational planning 3. 1st step Femoral resection 4. P/S Femoral component 7. 2nd step Proximal
ZIMMER NEXGEN CRUCIATE RETAINING (CR) AND LEGACY KNEE POSTERIOR STABILIZED (LPS) TRABECULAR METAL MONOBLOCK TIBIAS. Surgical Technique Addendum
 ZIMMER NEXGEN CRUCIATE RETAINING (CR) AND LEGACY KNEE POSTERIOR STABILIZED (LPS) TRABECULAR METAL MONOBLOCK TIBIAS Surgical Technique Addendum SURGICAL TECHNIQUE FOR NEXGEN CRUCIATE RETAINING (CR) AND
ZIMMER NEXGEN CRUCIATE RETAINING (CR) AND LEGACY KNEE POSTERIOR STABILIZED (LPS) TRABECULAR METAL MONOBLOCK TIBIAS Surgical Technique Addendum SURGICAL TECHNIQUE FOR NEXGEN CRUCIATE RETAINING (CR) AND
Extramedullary Tibial Preparation
 Surgical Technique Extramedullary Tibial Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Extramedullary tibial preparation Contents Introduction...2 EM tibial highlights...3 Preoperative
Surgical Technique Extramedullary Tibial Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Extramedullary tibial preparation Contents Introduction...2 EM tibial highlights...3 Preoperative
Proven Gen-Flex Revision Knee System. Surgical Protocol
 Proven Gen-Flex Revision Knee System Surgical Protocol Proven Gen-Flex Revision Knee System Surgeon Design Team The Proven Gen-Flex Revision Knee System Instrumentation and Surgical Protocol were developed
Proven Gen-Flex Revision Knee System Surgical Protocol Proven Gen-Flex Revision Knee System Surgeon Design Team The Proven Gen-Flex Revision Knee System Instrumentation and Surgical Protocol were developed
operative technique Kent Hip
 operative technique Kent Hip The Kent Hip Operative Technique The Kent Hip was developed by Mr Cliff Stossel, FRCS in Maidstone, Kent, UK and first implanted in 1986. It was designed to deal with problems
operative technique Kent Hip The Kent Hip Operative Technique The Kent Hip was developed by Mr Cliff Stossel, FRCS in Maidstone, Kent, UK and first implanted in 1986. It was designed to deal with problems
Zimmer NexGen Tibial Stem Extension & Augmentation. Surgical Technique IMAGE TO COME. Stem Extensions and Augments
 Zimmer NexGen Tibial Stem Extension & Augmentation Surgical Technique IMAGE TO COME Stem Extensions and Augments Zimmer NexGen Tibial Stem Extension & Augmentation Surgical Technique 1 Zimmer NexGen Tibial
Zimmer NexGen Tibial Stem Extension & Augmentation Surgical Technique IMAGE TO COME Stem Extensions and Augments Zimmer NexGen Tibial Stem Extension & Augmentation Surgical Technique 1 Zimmer NexGen Tibial
Zimmer NexGen RH Knee Primary/Revision. Surgical Technique
 Zimmer NexGen Primary/Revision Surgical Technique Zimmer NexGen Primary/Revision Surgical Technique INTRO Introduction The NexGen Rotating Hinge Knee () is designed for revision, difficult primary, and
Zimmer NexGen Primary/Revision Surgical Technique Zimmer NexGen Primary/Revision Surgical Technique INTRO Introduction The NexGen Rotating Hinge Knee () is designed for revision, difficult primary, and
Orthopedic Bone Nail System - Distal Femoral Nail Surgical Technique Manual
 Orthopedic Bone Nail System - Distal Femoral Nail Surgical Technique Manual Note: The surgical procedures should be performed under the guidance of qualified skilled orthopedic surgeons, and this surgical
Orthopedic Bone Nail System - Distal Femoral Nail Surgical Technique Manual Note: The surgical procedures should be performed under the guidance of qualified skilled orthopedic surgeons, and this surgical
Zimmer NexGen Rotating Hinge Knee Primary/ Revision
 Zimmer NexGen Rotating Hinge Knee Primary/ Revision Surgical Technique Designed for use in revision and difficult primary surgeries 1 INTRODUCTION The NexGen Rotating Hinge Knee Components are designed
Zimmer NexGen Rotating Hinge Knee Primary/ Revision Surgical Technique Designed for use in revision and difficult primary surgeries 1 INTRODUCTION The NexGen Rotating Hinge Knee Components are designed
Operative Technique. Constrained Condylar. The Right Track It s not just a road we re on, it s a trail we re blazing.
 Operative Technique Constrained Condylar The Right Track It s not just a road we re on, it s a trail we re blazing. TABLE OF CONTENTS Introduction...1 Design rationale...1 operative technique Overview...2
Operative Technique Constrained Condylar The Right Track It s not just a road we re on, it s a trail we re blazing. TABLE OF CONTENTS Introduction...1 Design rationale...1 operative technique Overview...2
The information contained in this document is intended for healthcare professionals only.
 The information contained in this document is intended for healthcare professionals only. Orthopaedics GMRS Distal Femoral Surgical Protocol Global Modular Replacement System Acknowledgements Stryker would
The information contained in this document is intended for healthcare professionals only. Orthopaedics GMRS Distal Femoral Surgical Protocol Global Modular Replacement System Acknowledgements Stryker would
Uniglide. Unicompartmental Knee Replacement Mk III surgical technique
 Uniglide Unicompartmental Knee Replacement Mk III surgical technique Uniglide Contents Operative summary 4 Pre-operative assessment 6 Preparation 7 Incision 7 Approach 7 Medial procedure 8 Tibial preparation
Uniglide Unicompartmental Knee Replacement Mk III surgical technique Uniglide Contents Operative summary 4 Pre-operative assessment 6 Preparation 7 Incision 7 Approach 7 Medial procedure 8 Tibial preparation
Surgical Technique. VISIONAIRE FastPak Instruments for the LEGION Total Knee System
 Surgical Technique VISIONAIRE FastPak Instruments for the LEGION Total Knee System VISIONAIRE FastPak for LEGION Instrument Technique* Nota Bene The technique description herein is made available to the
Surgical Technique VISIONAIRE FastPak Instruments for the LEGION Total Knee System VISIONAIRE FastPak for LEGION Instrument Technique* Nota Bene The technique description herein is made available to the
GMRS Proximal Tibial Surgical Protocol
 Orthopaedics GMRS Proximal Tibial Surgical Protocol Global Modular Replacement System Acknowledgements Stryker would like to thank all of the surgeons for their contributions in developing the Global Modular
Orthopaedics GMRS Proximal Tibial Surgical Protocol Global Modular Replacement System Acknowledgements Stryker would like to thank all of the surgeons for their contributions in developing the Global Modular
The information contained in this document is intended for healthcare professionals only.
 The information contained in this document is intended for healthcare professionals only. Orthopaedics GMRS Proximal Tibial Surgical Protocol Global Modular Replacement System Acknowledgements Stryker
The information contained in this document is intended for healthcare professionals only. Orthopaedics GMRS Proximal Tibial Surgical Protocol Global Modular Replacement System Acknowledgements Stryker
28 Surgical Technique
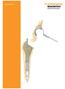 Surgical Technique 10 12 14 16 18 20 22 24 28 26 Technique described by James L. Guyton, MD Campbell Clinic Memphis, Tennessee James W. Harkess, MD Campbell Clinic Memphis, Tennessee David G. LaVelle,
Surgical Technique 10 12 14 16 18 20 22 24 28 26 Technique described by James L. Guyton, MD Campbell Clinic Memphis, Tennessee James W. Harkess, MD Campbell Clinic Memphis, Tennessee David G. LaVelle,
ClassiQ. Scorpio. Anterior Referencing Surgical Protocol. Anterior Referencing. For use with Scorpio ClassiQ Instrument System
 Scorpio ClassiQ Anterior Referencing Surgical Protocol For use with Scorpio ClassiQ Instrument System For use with Scorpio ClassiQ Single Radius Total Knee System AR Anterior Referencing This document
Scorpio ClassiQ Anterior Referencing Surgical Protocol For use with Scorpio ClassiQ Instrument System For use with Scorpio ClassiQ Single Radius Total Knee System AR Anterior Referencing This document
Zimmer Segmental System. Surgical Technique for Proximal Femoral Replacement and Intercalary Segments IMAGE TO COME
 Zimmer Segmental System Surgical Technique for Proximal Femoral Replacement and Intercalary Segments IMAGE TO COME Zimmer Segmental System Surgical Technique for Proximal Femoral Replacement and Intercalary
Zimmer Segmental System Surgical Technique for Proximal Femoral Replacement and Intercalary Segments IMAGE TO COME Zimmer Segmental System Surgical Technique for Proximal Femoral Replacement and Intercalary
FLK167 02/08. Biomet UK Ltd Waterton Industrial Estate Bridgend, South Wales CF31 3XA, United Kingdom. Tel Fax:
 FLK167 02/08 Biomet UK Ltd Waterton Industrial Estate Bridgend, South Wales CF31 3XA, United Kingdom Tel. 01656 655221 Fax: 01656 645454 Premier Instrumentation CR or PS Surgical Technique Vanguard Premier
FLK167 02/08 Biomet UK Ltd Waterton Industrial Estate Bridgend, South Wales CF31 3XA, United Kingdom Tel. 01656 655221 Fax: 01656 645454 Premier Instrumentation CR or PS Surgical Technique Vanguard Premier
THE P.F.C. SIGMA FEMORAL ADAPTER. Surgical Technique
 THE P.F.C. SIGMA FEMORAL ADAPTER Surgical Technique Contents P.F.C. Sigma Femoral Adapter and Revision Knee Surgery Introduction 2 Preoperative Planning 2 Overview 3 Surgical Technique Preparation of the
THE P.F.C. SIGMA FEMORAL ADAPTER Surgical Technique Contents P.F.C. Sigma Femoral Adapter and Revision Knee Surgery Introduction 2 Preoperative Planning 2 Overview 3 Surgical Technique Preparation of the
Arcos Interlocking Distal Stem. Surgical Technique Addendum to the Arcos Modular Femoral Revision System
 Arcos Interlocking Distal Stem Surgical Technique Addendum to the Arcos Modular Femoral Revision System One Surgeon. One Patient. Over 1 million times per year, Biomet helps one surgeon provide personalized
Arcos Interlocking Distal Stem Surgical Technique Addendum to the Arcos Modular Femoral Revision System One Surgeon. One Patient. Over 1 million times per year, Biomet helps one surgeon provide personalized
Revolution. Unicompartmental Knee System
 Revolution Unicompartmental Knee System While Total Knee Arthroplasty (TKA) is one of the most predictable procedures in orthopedic surgery, many patients undergoing TKA are in fact excellent candidates
Revolution Unicompartmental Knee System While Total Knee Arthroplasty (TKA) is one of the most predictable procedures in orthopedic surgery, many patients undergoing TKA are in fact excellent candidates
ADEPT Hip Resurfacing System. Operative Technique. Delivering Results Through Performance
 ADEPT Hip Resurfacing System Operative Technique Delivering Results Through Performance Contents Section 1 Preoperative Planning and Surgical Approach 3 Section 2 Assessment of Head Size 4 Section 3 Preparing
ADEPT Hip Resurfacing System Operative Technique Delivering Results Through Performance Contents Section 1 Preoperative Planning and Surgical Approach 3 Section 2 Assessment of Head Size 4 Section 3 Preparing
Surgical Technique. Unisyn Hip System
 Surgical Technique Unisyn Hip System INDICATIONS AND USAGE Significantly impaired joints resulting from rheumatoid, osteo, and post-traumatic arthritis. Revision of failed femoral head replacement, hip
Surgical Technique Unisyn Hip System INDICATIONS AND USAGE Significantly impaired joints resulting from rheumatoid, osteo, and post-traumatic arthritis. Revision of failed femoral head replacement, hip
KneeAlign System Surgical Technique Guide
 KneeAlign System Surgical Technique Guide Table of Contents Step 1 System Assembly... 1 Step 2 System Assembly... 2 Step 3 System Assembly... 2 Step 4 System Assembly... 2 Step 5 Sensor Pairing... 2 Step
KneeAlign System Surgical Technique Guide Table of Contents Step 1 System Assembly... 1 Step 2 System Assembly... 2 Step 3 System Assembly... 2 Step 4 System Assembly... 2 Step 5 Sensor Pairing... 2 Step
Cementless Tapered Femoral Stem Surgical technique
 Cementless Tapered Femoral Stem Surgical technique Contents Operative summary 4 Pre-operative planning 5 Femoral neck osteotomy 5 Femoral canal preparation 5 Intra-medullary (IM) reamer 6 Sequential rasping
Cementless Tapered Femoral Stem Surgical technique Contents Operative summary 4 Pre-operative planning 5 Femoral neck osteotomy 5 Femoral canal preparation 5 Intra-medullary (IM) reamer 6 Sequential rasping
Profix. Total Knee System. As described by
 Profix Total Knee System P R I M A R Y P R O C E D U R E As described by Leo A. Whiteside, M.D. Associate Research Professor Washington University School of Medicine Director, Biomechanical Research Laboratory
Profix Total Knee System P R I M A R Y P R O C E D U R E As described by Leo A. Whiteside, M.D. Associate Research Professor Washington University School of Medicine Director, Biomechanical Research Laboratory
SURGICAL TECHNIQUE GUIDE
 DANGER indicates an imminently hazardous situation which, if not avoided, will result in death or serious injury. WARNING indicates a potentially hazardous situation which, if not avoided, could result
DANGER indicates an imminently hazardous situation which, if not avoided, will result in death or serious injury. WARNING indicates a potentially hazardous situation which, if not avoided, could result
Scorpio TS Single Axis Revision Knee System. Scorpio Total Stabilizer Revision Knee System Surgical Protocol
 Scorpio TS Single Axis Revision Knee System Scorpio Total Stabilizer Revision Knee System Surgical Protocol Table of Contents Scorpio Total Stabilizer Revision Knee System Surgical Protocol Component
Scorpio TS Single Axis Revision Knee System Scorpio Total Stabilizer Revision Knee System Surgical Protocol Table of Contents Scorpio Total Stabilizer Revision Knee System Surgical Protocol Component
1. Pre-Operative Planning Skin Incision and Arthrotomy
 Stage of Operation 1. Pre-Operative Planning --------------------------1 2. Skin Incision and Arthrotomy ------------------1 3. Femoral valgus angle confirmation ------------2 4. Distal Femur Cutting -----------------------------3
Stage of Operation 1. Pre-Operative Planning --------------------------1 2. Skin Incision and Arthrotomy ------------------1 3. Femoral valgus angle confirmation ------------2 4. Distal Femur Cutting -----------------------------3
U2 KNEE SYSTEM. High Flexion Engineered
 U2 KNEE SYSTEM High Flexion Engineered TABLE OF CONTENTS Pre-Operative Planning...1 Surgical Incision...2 A. Femoral Preparation A.1. Pilot Hole...3 A.2. Femoral Valgus Angle Confirmation...4 A.3. Distal
U2 KNEE SYSTEM High Flexion Engineered TABLE OF CONTENTS Pre-Operative Planning...1 Surgical Incision...2 A. Femoral Preparation A.1. Pilot Hole...3 A.2. Femoral Valgus Angle Confirmation...4 A.3. Distal
FLH183 04/08. Biomet UK Ltd Waterton Industrial Estate Bridgend, South Wales CF31 3XA, United Kingdom. Tel. +44 (0) Fax: +44 (0)
 FLH183 04/08 Biomet UK Ltd Waterton Industrial Estate Bridgend, South Wales CF31 3XA, United Kingdom Tel. +44 (0)1656 655221 Fax: +44 (0)1656 645454 Exceed ABT Operative Technique The Exceed ABT TM acetabular
FLH183 04/08 Biomet UK Ltd Waterton Industrial Estate Bridgend, South Wales CF31 3XA, United Kingdom Tel. +44 (0)1656 655221 Fax: +44 (0)1656 645454 Exceed ABT Operative Technique The Exceed ABT TM acetabular
The Modular Knee System GenuX MK Revision Knee
 The Modular Knee System GenuX MK Revision Knee Surgical Technique GenuX MK Revision Knee Surgical Technique Table of content Preoperative Planning...5 System Overview...6 Compatibility Matrix...7 Surgical
The Modular Knee System GenuX MK Revision Knee Surgical Technique GenuX MK Revision Knee Surgical Technique Table of content Preoperative Planning...5 System Overview...6 Compatibility Matrix...7 Surgical
Resurfacing Patellar Preparation
 Surgical Technique Resurfacing Patellar Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Resurfacing Patellar preparation Contents Introduction...2 Instrument assembly...3 Resurfacing
Surgical Technique Resurfacing Patellar Preparation Primary Total Knee Arthroplasty LEGION Total Knee System Resurfacing Patellar preparation Contents Introduction...2 Instrument assembly...3 Resurfacing
Triathlon Knee System. Universal Baseplate Surgical Protocol
 Triathlon Knee System Universal Baseplate Surgical Protocol Table of Contents Acknowledgments..........................................................2 Introduction...............................................................2
Triathlon Knee System Universal Baseplate Surgical Protocol Table of Contents Acknowledgments..........................................................2 Introduction...............................................................2
Triathlon Knee System Universal Baseplate Surgical Protocol
 Triathlon Knee System Universal Baseplate Surgical Protocol Triathlon Knee System Universal Baseplate Surgical Protocol Table of Contents Acknowledgments... 2 Introduction... 2 Assembly Instructions...
Triathlon Knee System Universal Baseplate Surgical Protocol Triathlon Knee System Universal Baseplate Surgical Protocol Table of Contents Acknowledgments... 2 Introduction... 2 Assembly Instructions...
Zimmer ITST Intertrochanteric/ Subtrochanteric Fixation System. Abbreviated Surgical Technique
 Zimmer ITST Intertrochanteric/ Subtrochanteric Fixation System Abbreviated Surgical Technique ITST System Abbreviated Surgical Technique Indications The ITST Intramedullary Nail is indicated for use in
Zimmer ITST Intertrochanteric/ Subtrochanteric Fixation System Abbreviated Surgical Technique ITST System Abbreviated Surgical Technique Indications The ITST Intramedullary Nail is indicated for use in
NATURAL MOTION TECHNOLOGY SURGICAL TECHNIQUE. EMPOWR 3D Knee. EMPOWR PS Knee
 NATURAL MOTION TECHNOLOGY EMPOWR 3D Knee EMPOWR PS Knee SURGICAL TECHNIQUE Contents System Features.... 3 Indications and Contraindications.... 4 Surgical Snap Shot.... Preoperative Planning.... Surgical
NATURAL MOTION TECHNOLOGY EMPOWR 3D Knee EMPOWR PS Knee SURGICAL TECHNIQUE Contents System Features.... 3 Indications and Contraindications.... 4 Surgical Snap Shot.... Preoperative Planning.... Surgical
Impact of Intramedullary Reaming Depth on Establishing Femoral Canal Axis in the Sagittal Plane
 Impact of Intramedullary Reaming Depth on Establishing Femoral Canal Axis in the Sagittal Plane Yifei Dai, Ph.D., Dwight Todd. Zimmer Inc, Warsaw, IN, USA. Disclosures: Y. Dai: 3A; zimmer inc. 4; zimmer
Impact of Intramedullary Reaming Depth on Establishing Femoral Canal Axis in the Sagittal Plane Yifei Dai, Ph.D., Dwight Todd. Zimmer Inc, Warsaw, IN, USA. Disclosures: Y. Dai: 3A; zimmer inc. 4; zimmer
Trinity. Advanced Bearing Acetabular System Surgical technique
 Advanced Bearing Acetabular System Surgical technique Contents Operative summary Introduction Pre-operative planning Acetabular preparation Acetabular reaming Reamer guide Acetabular shell trials Acetabular
Advanced Bearing Acetabular System Surgical technique Contents Operative summary Introduction Pre-operative planning Acetabular preparation Acetabular reaming Reamer guide Acetabular shell trials Acetabular
Zimmer MOST Options System
 Zimmer MOST Options System Surgical Technique Modular Options for Severe Bone Loss and Trauma Zimmer MOST Options System Surgical Technique 1 MOST Options System Surgical Technique Developed in conjunction
Zimmer MOST Options System Surgical Technique Modular Options for Severe Bone Loss and Trauma Zimmer MOST Options System Surgical Technique 1 MOST Options System Surgical Technique Developed in conjunction
Trilogy Acetabular System
 Trilogy Acetabular System Surgical Technique Versatility in a proven design Trilogy Acetabular System 1 Trilogy Acetabular System Surgical Technique Table of Contents Acetabular Reaming 2 Component Sizing
Trilogy Acetabular System Surgical Technique Versatility in a proven design Trilogy Acetabular System 1 Trilogy Acetabular System Surgical Technique Table of Contents Acetabular Reaming 2 Component Sizing
Intra Medullary Interlocking Nailing System
 Intra Medullary Interlocking Nailing System www.orthotraumaint.co.uk Interlocking Intra Medullary Nails for lower extremity fractures INDICATIONS: Stable and unstable Femoral Shaft fractures Femur Nailing
Intra Medullary Interlocking Nailing System www.orthotraumaint.co.uk Interlocking Intra Medullary Nails for lower extremity fractures INDICATIONS: Stable and unstable Femoral Shaft fractures Femur Nailing
This surgical technique describes how to perform an anatomic total shoulder arthroplasty implanting a short stem.
 INTRODUCTION This surgical technique describes how to perform an anatomic total shoulder arthroplasty implanting a short stem. CAUTION Federal law (USA) restricts this device to sale distribution and use
INTRODUCTION This surgical technique describes how to perform an anatomic total shoulder arthroplasty implanting a short stem. CAUTION Federal law (USA) restricts this device to sale distribution and use
SURGICAL TECHNIQUE. Alpine Cementless Hip Stem
 SURGICAL TECHNIQUE Alpine Cementless Hip Stem The following technique is a general guide for the instrumentation of the Alpine Cementless Hip Stem. It is expected that the surgeon is already familiar with
SURGICAL TECHNIQUE Alpine Cementless Hip Stem The following technique is a general guide for the instrumentation of the Alpine Cementless Hip Stem. It is expected that the surgeon is already familiar with
Arcos Modular Femoral Revision System. Broach and Calcar Proximal Bodies Surgical Technique
 Arcos Modular Femoral Revision System Broach and Calcar Proximal Bodies Surgical Technique Table of Contents Pre-operative Planning...2 Patient Positioning and Surgical Approach...2 Removal of a Cemented
Arcos Modular Femoral Revision System Broach and Calcar Proximal Bodies Surgical Technique Table of Contents Pre-operative Planning...2 Patient Positioning and Surgical Approach...2 Removal of a Cemented
Revision Modular Stem type RMD
 Revision Modular Stem type RMD Cementless Femoral Hip Joint Components Revision Systems Implant Description Surgical Technique Instrumentation Set Catalogue Preface Revision modular stem (RMD) is a solution
Revision Modular Stem type RMD Cementless Femoral Hip Joint Components Revision Systems Implant Description Surgical Technique Instrumentation Set Catalogue Preface Revision modular stem (RMD) is a solution
Federal law (USA) restricts these devices to sale distribution and use by or on the order of physician.
 1 INTRODUCTION This surgical technique describes how to perform an Anatomic Ribbon Surgery ACL reconstruction using an Extracortical Femoral Button and a Tibial Pull Suture Plate. CAUTION Federal law (USA)
1 INTRODUCTION This surgical technique describes how to perform an Anatomic Ribbon Surgery ACL reconstruction using an Extracortical Femoral Button and a Tibial Pull Suture Plate. CAUTION Federal law (USA)
OPTIONAL/ADDITIONAL INSTRUMENTS
 20 Elevated 6320-36-22 20 Elevated Rim Liner, 36mm OD x 22mm ID 6320-80-22 20 Elevated Rim Liner, 80mm OD x 22mm ID 6320-42-26 20 Elevated Rim Liner, 42mm OD x 26mm ID 6320-80-26 20 Elevated Rim Liner,
20 Elevated 6320-36-22 20 Elevated Rim Liner, 36mm OD x 22mm ID 6320-80-22 20 Elevated Rim Liner, 80mm OD x 22mm ID 6320-42-26 20 Elevated Rim Liner, 42mm OD x 26mm ID 6320-80-26 20 Elevated Rim Liner,
Cementless Tapered Femoral Stem Surgical technique
 Cementless Tapered Femoral Stem Surgical technique Contents Operative summary 4 Pre-operative planning 5 Femoral neck osteotomy 5 Femoral canal preparation 5 Intra-medullary (IM) reamer 6 Sequential rasping
Cementless Tapered Femoral Stem Surgical technique Contents Operative summary 4 Pre-operative planning 5 Femoral neck osteotomy 5 Femoral canal preparation 5 Intra-medullary (IM) reamer 6 Sequential rasping
Stinson Orthopedics Inc. 303 Twin Dolphin Drive, Suite 600 Redwood City, CA
 Stinson Orthopedics Inc. 303 Twin Dolphin Drive, Suite 600 Redwood City, CA 94065 info@stinsonortho.com www.stinsonortho.com Encina HA Stem Table of Contents Introduction 3 Encina HA Stem Features 4 Surgical
Stinson Orthopedics Inc. 303 Twin Dolphin Drive, Suite 600 Redwood City, CA 94065 info@stinsonortho.com www.stinsonortho.com Encina HA Stem Table of Contents Introduction 3 Encina HA Stem Features 4 Surgical
Trilogy Acetabular System
 Trilogy Acetabular System Surgical Technique Versatility in a proven design Trilogy Acetabular System 1 Trilogy Acetabular System Surgical Technique Table of Contents Acetabular Reaming 2 Component Sizing
Trilogy Acetabular System Surgical Technique Versatility in a proven design Trilogy Acetabular System 1 Trilogy Acetabular System Surgical Technique Table of Contents Acetabular Reaming 2 Component Sizing
OSS Modular Arthrodesis System. Assembly Guide
 OSS Modular Arthrodesis System Assembly Guide One Surgeon. One Patient. Over 1 million times per year, Biomet helps one surgeon provide personalized care to one patient. The science and art of medical
OSS Modular Arthrodesis System Assembly Guide One Surgeon. One Patient. Over 1 million times per year, Biomet helps one surgeon provide personalized care to one patient. The science and art of medical
Surgical technique MkII instrumentation
 MiniHip Surgical technique MkII instrumentation Contents Operative summary 4 Overview 5 Pre-operative templating 6 Operative technique 7 1. Intra-operative templating 7 2. Neck starter awl 7 3. Curved
MiniHip Surgical technique MkII instrumentation Contents Operative summary 4 Overview 5 Pre-operative templating 6 Operative technique 7 1. Intra-operative templating 7 2. Neck starter awl 7 3. Curved
CONTRIBUTING SURGEON. Barry Waldman, MD Director, Center for Joint Preservation and Replacement Sinai Hospital of Baltimore Baltimore, MD
 CONTRIBUTING SURGEON Barry Waldman, MD Director, Center for Joint Preservation and Replacement Sinai Hospital of Baltimore Baltimore, MD System Overview The EPIK Uni is designed to ease the use of the
CONTRIBUTING SURGEON Barry Waldman, MD Director, Center for Joint Preservation and Replacement Sinai Hospital of Baltimore Baltimore, MD System Overview The EPIK Uni is designed to ease the use of the
NeoGen Tibia Nail System
 NeoGen Tibia Nail System LESS IS MORE TE-2070-03 Surgical Technique BLE OF CONTENT Preface Surgical Technique Appendix Products Information Patient Preparation Entry Portal Fracture Reduction Canal Preparation
NeoGen Tibia Nail System LESS IS MORE TE-2070-03 Surgical Technique BLE OF CONTENT Preface Surgical Technique Appendix Products Information Patient Preparation Entry Portal Fracture Reduction Canal Preparation
Monolateral External Fixation System for Trauma and Orthopaedics
 MEFiSTO Monolateral External Fixation System for Trauma and Orthopaedics Surgical Technique Original Instruments and Implants of the Association for the Study of Internal Fixation AO/ASIF MEFiSTO Table
MEFiSTO Monolateral External Fixation System for Trauma and Orthopaedics Surgical Technique Original Instruments and Implants of the Association for the Study of Internal Fixation AO/ASIF MEFiSTO Table
Knee. Surgical Protocol
 U2 TM PS CR Knee Surgical Protocol Table of Contents Pre-Operative Planning... Surgical Incision... 1 2 A. Femoral Preparation A.1. Pilot Hole... A.2. Femoral Valgus Angle Confirmation... A.3. Distal
U2 TM PS CR Knee Surgical Protocol Table of Contents Pre-Operative Planning... Surgical Incision... 1 2 A. Femoral Preparation A.1. Pilot Hole... A.2. Femoral Valgus Angle Confirmation... A.3. Distal
Surgical Technique. Poly UHMWPE. Bio Hyaluronic Acid. Advancing Materials. Advancing Outcomes.
 Surgical Technique Bio Hyaluronic Acid Poly UHMWPE Advancing Materials. Advancing Outcomes. Surgical 2 Assessment 1. Proper implant sizing is determined by placing the appropriate sized trial over the
Surgical Technique Bio Hyaluronic Acid Poly UHMWPE Advancing Materials. Advancing Outcomes. Surgical 2 Assessment 1. Proper implant sizing is determined by placing the appropriate sized trial over the
TRAUMATOLOGY. Trochanter
 TRAUMATOLOGY Trochanter 1 References Prof. Dr. András Sárváry Head of Department Fővárosi Önkormányzat Péterfy Sándor úti Kórház Rendelőintézet és Baleseti Központ Budapest The following surgical description
TRAUMATOLOGY Trochanter 1 References Prof. Dr. András Sárváry Head of Department Fővárosi Önkormányzat Péterfy Sándor úti Kórház Rendelőintézet és Baleseti Központ Budapest The following surgical description
REVISION SYSTEM DIFFERENT NEEDS...YOUR GLOBAL SOLUTION. Hip Knee Spine Navigation GLOBAL MEDACTA KNEE
 GLOBAL MEDACTA KNEE REVISION SYSTEM DIFFERENT NEEDS......YOUR GLOBAL SOLUTION Surgical Technique Hip Knee Spine Navigation GMK REVISION SYSTEM Surgical Technique Hip Knee Spine Navigation INTRODUCTION
GLOBAL MEDACTA KNEE REVISION SYSTEM DIFFERENT NEEDS......YOUR GLOBAL SOLUTION Surgical Technique Hip Knee Spine Navigation GMK REVISION SYSTEM Surgical Technique Hip Knee Spine Navigation INTRODUCTION
PPS P I N P O S I T I O N I N G S Y S T E M GMK EFFICIENCY VERSION. Hip Knee Spine Navigation
 PPS P I N P O S I T I O N I N G S Y S T E M D ESIGNED FOR YOU BY YOU GMK EFFICIENCY VERSION Surgical Surgical Technique Hip Knee Spine Navigation MyKnee Surgical Technique Hip Knee Spine Navigation I N
PPS P I N P O S I T I O N I N G S Y S T E M D ESIGNED FOR YOU BY YOU GMK EFFICIENCY VERSION Surgical Surgical Technique Hip Knee Spine Navigation MyKnee Surgical Technique Hip Knee Spine Navigation I N
