Surgical Treatment of Traumatic Anterior Shoulder Instability in American Football Players BY MICHAEL J. PAGNANI, MD, AND DAVID C.
|
|
|
- Albert Campbell
- 5 years ago
- Views:
Transcription
1 711 COPYRIGHT 2002 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Surgical Treatment of Traumatic Anterior Shoulder Instability in American Football Players BY MICHAEL J. PAGNANI, MD, AND DAVID C. DOME, MD Investigation performed at Tennessee Orthopaedic Alliance, Nashville, Tennessee Background: American football players have been reported to be at high risk for postoperative instability after arthroscopic stabilization of anterior shoulder instability. While some authors have recommended open methods of stabilization in athletes who play contact sports, there are few data in the literature showing more favorable results with use of an open technique. We reviewed the results of an open technique of anterior shoulder stabilization in fifty-eight American football players after a minimum of two years of follow-up. Methods: Fifty-eight American football players underwent open stabilization with use of a standardized technique for the treatment of recurrent anterior shoulder instability. Forty-seven patients had recurrent dislocations, and the remaining eleven had recurrent subluxations. The average age of the patients was 18.2 years, and the average duration of follow-up was thirty-seven months. Patients were evaluated according to the shoulder scoring system of the American Shoulder and Elbow Surgeons and with use of the shoulder instability score described by Rowe and Zarins. Results: There were no postoperative dislocations. Postoperative subluxation occurred in two patients, neither of whom had had a dislocation prior to the operation. Forward flexion and external rotation returned to within 5 of those of the contralateral shoulder in forty-nine patients. The average score according to the system of the American Shoulder and Elbow Surgeons was 97.0 points, and the average Rowe and Zarins score was 93.6 points. Fifty-five patients had a good or excellent result, and fifty-two of the fifty-eight returned to playing football for at least one year. One patient was forced to stop playing because of recurrent instability. Conclusions: Open stabilization is a predictable method of restoring shoulder stability in American football players while maintaining a range of motion approximating that found after arthroscopic stabilization. Postoperative stability appears to be superior to that reported after arthroscopic techniques in this population of patients. The risk of recurrent anterior instability of the shoulder tends to increase with the activity level of the patient. In particular, athletes involved in so-called contact and collision sports can be subjected to sizable loads on the shoulder 1. American football players have been shown to be at high risk for failure after arthroscopic stabilization procedures 2-5. However, most reported series of patients treated with open anterior stabilization of the shoulder have consisted of a heterogeneous population, and few studies have presented the results of open repair with specific regard to athletic participation. Furthermore, we are not aware of any studies of open stabilization in a large series of American football players. In the study most closely resembling our current investigation, Uhorchak et al. 6 recently reported that, of sixty-six West Point cadets involved in contact and collision sports, 22% had some A commentary is available with the electronic versions of this article, on our web site ( and on our quarterly CD-ROM (call our subscription department, at , to order the CD-ROM). degree of instability at the time of a minimum two-year followup after open stabilization. We studied a consecutive series of American football players in whom anterior shoulder instability had been treated with an open stabilization procedure by the senior author (M.J.P.) in the period from August 1993 through January The patients were evaluated at twenty-four to eighty months (average, thirty-seven months) after the operation. Materials and Methods eventy-one consecutive male American football players Swere treated for recurrent shoulder instability with an open anterior stabilization procedure. Five players who had undergone a prior operation for instability were excluded from the study, as were two who had been operated on for posterior instability. Six patients were lost to follow-up during the study period, leaving fifty-eight available for the final evaluation. The patients ages ranged from fifteen to twenty-nine years (average, 18.2 years). Forty-three patients played football
2 712 at the high-school level, eleven played at the collegiate level, and four were professional football players. Although shoulder dysfunction interfered with the activities of daily life of some of the patients, the primary symptom in all patients was recurrent instability, shoulder pain, and apprehension during participation in American football. Forty-seven patients had frank dislocations, whereas the remaining eleven had symptoms and signs consistent with recurrent anterior glenohumeral subluxation. Forty-one of the forty-seven patients with dislocations reported that at least one episode required manipulative reduction by a health-care professional. The number of recurrent episodes of instability ranged from three to twenty-five. All patients had persistent signs and symptoms of anterior instability on physical examination, and all had a history of trauma that was believed to have initiated the instability. An anterior apprehension test with the arm abducted and externally rotated was performed on all patients. The examiner progressively increased the degree of external rotation while noting the development of apprehension on the part of the patient. The test was considered positive when the maneuver induced anxiety and protective muscular contraction as the shoulder was brought into a position associated with anterior instability 7. The signs and symptoms of anterior subluxation were often more subtle than those of dislocation. Eight of the eleven patients remembered a specific injury, which typically occurred with extreme external rotation combined with either abduction or hyperextension. The chief symptom in the athletes with subluxation was more vague, such as a sense of movement, pain, or clicking with certain activities. Several athletes noted repeated transitory episodes of severe pain, particularly when tackling. After an acute episode, the severe pain usually subsided quickly but the shoulder remained sore and weak. Plain radiographs revealed an osseous Bankart lesion in five patients and a Hill-Sachs lesion in nineteen. Magnetic resonance imaging of the shoulder was not routinely performed in this series. All patients were treated with the operation after failure of a rehabilitation program that emphasized strengthening of the rotator cuff and scapular rotator muscles. In the later stages of the rehabilitation, proprioceptive neuromuscular feedback exercises were incorporated. The duration of nonoperative treatment ranged from nine weeks to thirty-seven months. All patients had recurrent instability or persistent apprehension despite completion of the rehabilitation program. Forty-one of the fifty-eight patients underwent arthroscopic examination of the shoulder prior to the open stabilization procedure. In the early part of the study, we did not routinely perform arthroscopy when traumatic anterior instability was to be treated with an open repair. However, we now routinely perform an arthroscopic inspection of the shoulder with the patient in the beach-chair position prior to the open portion of the procedure. We find the arthroscopic examination to be helpful for identifying concomitant lesions in the rotator cuff and labrum. In addition, by identifying the presence or absence of a Bankart lesion, the arthroscopy aids in the planning of our method of stabilization 8. In particular, we shift the capsule on its lateral margin if no Bankart lesion is present. Operative Technique Our general approach to open anterior stabilization has been described previously 7,9. A slight modification of our previously reported technique is described below. The patient is positioned supine with the head of the operating table raised 30 and the involved upper extremity abducted 45 on an arm-board. Folded sheets are placed beneath the elbow to maintain the arm in the coronal plane of the thorax and to minimize extension of the shoulder. The skin is incised along the anterior axillary crease in a longitudinal fashion along the Langer lines. The incision is placed lateral to the coracoid process. The deltopectoral interval is identified, the cephalic vein is retracted laterally, and the interval is developed. The clavipectoral fascia is then incised at the lateral border of the conjoined tendon at its coracoid attachment, and the coracoacromial ligament is divided to facilitate exposure of the superior aspect of the capsule and, particularly, the rotator interval area. The bicipital groove and the lesser tuberosity are identified. A vertical tenotomy of the subscapularis tendon is performed with electrocautery approximately 1 cm medial to its insertion on the lesser tuberosity. The medial portion of the tendon is tagged with heavy, number-1, nonabsorbable braided polyester (Ethibond) sutures (Ethicon, Somerville, New Jersey). The interval between the anterior aspect of the capsule and the subscapularis tendon is then carefully developed with a combination of blunt and sharp dissection. The laxity and quality of the capsule are then assessed. If there is a lesion in the rotator interval, it is generally closed at this point with number-1 nonabsorbable braided polyester (Ethibond) sutures. A transverse capsulotomy is then performed, and a ring (Fukuda) retractor is placed intraarticularly. The glenohumeral joint is explored for evidence of a Bankart lesion, and the joint is irrigated to remove any loose bodies. If a Bankart lesion is noted, the capsulolabral separation at the anteroinferior aspect of the glenoid neck is extended medially with use of an elevator or knife to allow placement of a retractor along the glenoid neck. The glenoid neck is then roughened with an osteotome or a motorized burr to provide a bleeding surface. Two or three metallic suture anchors are placed in the anteroinferior aspect of the glenoid neck near, but not on, the articular margin of the glenoid. The capsule and labrum are reattached to the anterior aspect of the glenoid with slight medial and superior mobilization of the capsule. The goal is not to reduce external rotation but to obliterate excess capsular volume and to restore the competency of the inferior glenohumeral ligament at its glenoid insertion. After repair of the Bankart lesion (or in the absence of a Bankart lesion), an anterior capsulorrhaphy is performed to eliminate excess capsular laxity. The arm is placed in 45 of ab-
3 713 TABLE I Standardized Postoperative Rehabilitation Protocol Weeks Postop. 0-4 Sling immobilization with shoulder in internal rotation, pendulum exercises, elbow range of motion 4-8 Passive and active-assisted shoulder range of motion. Limit external rotation to 45. When 140 of active forward flexion is obtained, begin rotator cuff strengthening (internal-external rotation strengthening with arm at low abduction angles) 8-12 Deltoid isometric exercises with arm at low abduction angles, body blade exercises. Limit external rotation to 45. If no impingement or rotator cuff symptoms are noted, slowly increase abduction during rotator cuff and deltoid strengthening. Scapular rotator strengthening: press-ups (seated dips), shrugs, horizontal abduction exercises, open-can exercises Restore terminal external rotation. Proprioceptive neuromuscular feedback patterns; plyometric exercises; sportspecific motion using pulley, wand, or manual resistance >18 Conventional weight-training. Orient for return to sport (progress from field drills to contact drills). Obtain abduction harness for selected football positions (linemen). Return to full contact when abduction and external rotation strength are symmetrical on manual muscle-testing duction and 45 of external rotation, and the superior and inferior capsular flaps are reapproximated with forceps. The shoulder is held in a reduced position. If the capsular flaps can be overlapped, the capsule is shifted to eliminate excess capsular volume with the arm maintained in position. If 5 mm of overlap is present when the inferior flap is pulled superiorly in relation to the superior flap, the capsule is simply imbricated. With >5 mm of capsular overlap, the capsulotomy is extended in a vertical direction near its lateral insertion on the humeral neck, and a T-plasty capsular shift is performed. The inferior capsular flap is shifted superolaterally, and the superior flap is moved over the inferior flap in an inferolateral direction. The transverse portion of the capsulotomy is then closed. After the capsule has been addressed satisfactorily, the subscapularis is reapproximated, but not shortened, with nonabsorbable suture. The deltopectoral interval is loosely closed with absorbable suture. Routine wound closure is then performed. Postoperative Rehabilitation Protocol A standard rehabilitation program was prescribed throughout the course of the study (Table I). Data Collection and Follow-up All patients were examined after a minimum of two years of follow-up. The patient self-evaluation form developed by the Research Committee of the American Shoulder and Elbow Surgeons was administered 10. Patients were specifically questioned regarding the occurrence of any episodes of instability. The physician assessment was performed by one or both of the authors. Again, this portion of the examination was guided by the recommendations of the Research Committee of the American Shoulder and Elbow Surgeons 10. A shoulder score index was then tabulated on the basis of the patient selfassessment and physician assessment portions of the evaluation. In addition, a second score was derived with the shoulder instability scoring system of Rowe and Zarins 11. Results Arthroscopic and Operative Findings Bankart lesion was noted in forty-six of the fifty-eight pa- Forty-three of the forty-seven patients with a his- Atients. tory of recurrent dislocation and three of the eleven patients with a history of recurrent subluxation had a Bankart lesion. Three patients had an osseous Bankart lesion that was of sufficient size to require excision and repair of the remaining capsule and labrum to the underlying osseous defect. No lateral capsular lesions were noted in this series. One patient (a professional athlete) had an associated bucket-handle tear of the superior aspect of the labrum; it was treated with excision of the fragment during the arthroscopy. This labral tear included approximately 15% of the supraglenoid insertion of the biceps brachii. The biceps tendon in this patient was noted to be frayed and degenerated proximally. Seven other patients had fraying of the superior part of the labrum. Capsular laxity was corrected by a T-plasty capsular shift in sixteen patients. All twelve patients who did not have a Bankart lesion underwent a T-plasty capsular shift. A Hill-Sachs lesion was noted in thirty-seven of the forty-one patients who underwent arthroscopy. Two patients had a small partial-thickness tear on the articular surface of the supraspinatus tendon. Each tear was thought to represent <10% of the tendon attachment. The small partial tears were treated with débridement during arthroscopy. Loose bodies were found and removed from four shoulders. Three patients had small, displaced osseous fragments of the anterior aspect of the glenoid, which were adherent to the anterior aspect of the capsule and labrum. These fragments were sharply dissected from the soft tissue and excised. The capsule was then repaired to the underlying osseous bed. Postoperative Instability None of the patients had dislocation of the shoulder postoperatively. Two patients reported postoperative episodes of
4 714 subluxation, and each continued to have a positive anterior apprehension test on their follow-up examinations. Both of these individuals had had subluxation preoperatively, and neither had had dislocations. One of the two patients had a Bankart lesion; the other did not. Neither had a Hill-Sachs lesion. Both patients experienced the initial postoperative episode of instability while they were playing football. The patients with preoperative subluxation had a higher rate of postoperative instability than did those with preoperative dislocation (Fisher exact test, p = 0.044). Return to Sports Fifty-two of the fifty-eight patients returned to full participation in American football for at least one year. Forty-one participated for at least two years, and twenty-four of them participated for three or more years. Eleven high-school athletes went on to play at least one year of collegiate football. All eleven collegiate players returned to their college teams, and one of the eleven became a professional player. All four professional players returned to their sport. One of the two patients (a high-school player) with postoperative subluxation could not continue playing football after one year because of persistent instability. He did not have instability with activities of daily life and did not wish to undergo another surgical procedure. The other patient with postoperative subluxation (a collegiate player) continued to participate, despite occasional episodes of subluxation, for two years. Two patients decided to give up the sport because of instability of the contralateral shoulder. Three other patients decided not to continue their participation in American football for reasons unrelated to the shoulder. Range of Motion Forward flexion on the involved side averaged 174 (range, 146 to 180 ) compared with 180 on the contralateral side. External rotation with the arm at the side averaged 67 (range, 30 to 95 ) compared with 76 on the contralateral side (p < 0.05). External rotation with the arm in 90 of abduction averaged 96 (range, 60 to 120 ), representing a loss of 8 compared with the value on the contralateral side (p < 0.05). No patient lost more than 15 of external rotation compared with the value on the contralateral side. Forty-nine (84%) of the fifty-eight involved shoulders had a range of flexion and external rotation within 5 of those of the contralateral shoulder. Postoperative Radiographs Anteroposterior and axillary lateral radiographs were available for forty-five of the patients during the postoperative period. The metallic suture anchors were in satisfactory position; none appeared to have migrated or become misplaced. Radiographs of one patient (a professional player) demonstrated mild degenerative changes of the glenohumeral joint. No other major radiographic anomalies were noted. Functional Testing The average postoperative shoulder score according to the scale of the American Shoulder and Elbow Surgeons 10 was 97.0 points (range, 70 to 100 points). Only one patient received a score of <80 points. The Rowe and Zarins shoulder instability score 11 ranged from 49 to 100 points, with an average of 93.6 points. According to this scoring system, there were fifty-three excellent results, two good results, two fair results, and one failure. Ninety-five percent of the patients had a good or excellent result. Complications A subcutaneous hematoma that required surgical evacuation and drainage developed in one patient. He had an uncomplicated recovery. Discussion e and many others have previously described high recurrence rates after arthroscopic stabilization procedures in W athletes who participate in so-called contact sports 2-5,12. As a result, we stopped recommending arthroscopic stabilization as a treatment option to American football players in We believed that the recurrence rates associated with arthroscopic procedures outweighed any perceived advantages in terms of appearance or less perioperative pain. O Neill 3 recently reported excellent results after arthroscopic stabilization in a carefully selected group of athletes. However, two of the seventeen American football players in his series had postoperative subluxation and a score of <80 points according to the scale of the American Shoulder and Elbow Surgeons. As a result, O Neill advised, football players must be warned about the greater probability of instability on returning to their sport after an arthroscopic procedure. In comparing the results of arthroscopic and open anterior stabilization procedures, Cole et al. 2 noted that all episodes of instability after an arthroscopic Bankart repair resulted from a fall or participation in a contact sport. Bacilla et al. 13 reported a 10% failure rate after arthroscopic Bankart repair in a highdemand population that included twenty-one American football players. The patients were studied for a minimum of eighteen months, and the specific results in football players were not reported. Gill et al. 14 showed excellent objective long-term results after the Bankart procedure, which confirmed findings in earlier reports by Rowe et al. 15 and Zarins et al. 16. Our technique is basically a modification of these methods. Wirth et al. 17 reported that 97% of patients treated for traumatic anterior instability, with a somewhat different open method devised by Rockwood, had normal stability and a negative apprehension test after surgery. While athletes were included in each of these studies, the results in football players were not specifically analyzed. It was our belief that the open technique offers certain advantages that are difficult to duplicate with current arthroscopic technology. First, the ability to restore tension to the capsule in a precise manner is facilitated by freeing the capsule from the adherent subscapularis tendon. Second, the shoulder can be maintained in an optimal position during the cap-
5 715 sular repair with less concern about visualization. Third, the capsular structures can be overlapped with ease with use of the open technique. (The ability to reinforce and thicken a damaged capsule may be especially important in an athletic population.) Fourth, the rotator interval, which is difficult to visualize properly through the arthroscope, can be directly observed and properly repaired with the open technique. One of the presumed advantages of arthroscopic techniques of shoulder stabilization is an improvement in postoperative shoulder motion. In our series, 84% of the patients regained all or nearly all of their shoulder motion. Our results in terms of range of motion approximate those in reports on arthroscopic stabilization in similar patients 3,18. We do, however, think that there may be a role for arthroscopic stabilization in selected patients. We continue to consider arthroscopic techniques for the treatment of throwing athletes with subtle anterior instability and lower-demand individuals who have a Bankart lesion. In summary, we believe that open stabilization is a predictable method of restoring shoulder stability in American football players. Motion and function need not be sacrificed in exchange for stability. Our results appear to be superior to those reported after arthroscopic stabilization in a similar population. Michael J. Pagnani, MD David C. Dome, MD Tennessee Orthopaedic Alliance, 2410 Patterson Street, Suite 106, Nashville, TN The authors did not receive grants or outside funding in support of their research or preparation of this manuscript. They did not receive payments or other benefits or a commitment or agreement to provide such benefits from a commercial entity. No commercial entity paid or directed, or agreed to pay or direct, any benefits to any research fund, foundation, educational institution, or other charitable or nonprofit organization with which the authors are affiliated or associated. References 1. American Academy of Pediatrics Committee on Sports Medicine: Recommendations for participation in competitive sports. Pediatrics. 1988;81: Cole BJ, L Insalata J, Irrgang J, Warner JJ. Comparison of arthroscopic and open anterior shoulder stabilization. A two to six-year follow-up study. J Bone Joint Surg Am. 2000;82: O Neill DB. Arthroscopic Bankart repair of anterior detachments of the glenoid labrum. A prospective study. J Bone Joint Surg Am. 1999;81: Pagnani MJ, Warren RF, Altchek DW, Wickiewicz TL, Anderson AF. Arthroscopic shoulder stabilization using transglenoid sutures. A four-year minimum followup. Am J Sports Med. 1996;24: Speer KP, Warren RF, Pagnani M, Warner JJ. An arthroscopic technique for anterior stabilization of the shoulder with a bioabsorbable tack. J Bone Joint Surg Am. 1996;78: Uhorchak JM, Arciero RA, Huggard D, Taylor DC. Recurrent shoulder instability after open reconstruction in athletes involved in collision and contact sports. Am J Sports Med. 2000;28: Pagnani MJ, Warren RF. Instability of the shoulder. In: Nicholas JA, Hershman EB, Posner MA, editors. The upper extremity in sports medicine. 2nd ed. St. Louis: Mosby; p Bankart ASB. The pathology and treatment of recurrent dislocation of the shoulder-joint. Br J Surg. 1938;26: Pagnani MJ, Galinat BJ, Warren RF. Glenohumeral instability. In: DeLee JC, Drez D Jr, editors. Orthopaedic sports medicine: principles and practice. Philadelphia: WB Saunders; p Richards RR, An K-N, Bigliani LU, Friedman RJ, Gartsman GM, Gristina AG, Iannotti JP, Mow VC, Sidles JA, Zuckerman JD. A standardized method for the assessment of shoulder function. J Shoulder Elbow Surg. 1994;3: Rowe CR, Zarins B. Recurrent transient subluxation of the shoulder. J Bone Joint Surg Am. 1981;63: Grana WA, Buckley PD, Yates CK. Arthroscopic Bankart suture repair. Am J Sports Med. 1993;21: Bacilla P, Field LD, Savoie FH 3rd. Arthroscopic Bankart repair in a high demand population. Arthroscopy. 1997;13: Gill TJ, Micheli LJ, Gebhard F, Binder C. Bankart repair for anterior instability of the shoulder. Long-term outcome. J Bone Joint Surg Am. 1997;79: Rowe CR, Patel D, Southmayd WW. The Bankart procedure: a long-term endresult study. J Bone Joint Surg Am. 1978;60: Zarins B, McMahon MS, Rowe CR. Diagnosis and treatment of traumatic anterior instability of the shoulder. Clin Orthop. 1993;291: Wirth MA, Blatter G, Rockwood CA Jr. The capsular imbrication procedure for recurrent anterior instability of the shoulder. J Bone Joint Surg Am. 1996;78: Gartsman GM, Roddey TS, Hammerman SM. Arthroscopic treatment of anterior-inferior glenohumeral instability. Two to five-year follow-up. J Bone Joint Surg Am. 2000;82:
DK7215-Levine-ch12_R2_211106
 12 Arthroscopic Rotator Interval Closure Andreas H. Gomoll Department of Orthopedic Surgery, Brigham and Women s Hospital, Harvard Medical School, Boston, Massachusetts, U.S.A. Brian J. Cole Departments
12 Arthroscopic Rotator Interval Closure Andreas H. Gomoll Department of Orthopedic Surgery, Brigham and Women s Hospital, Harvard Medical School, Boston, Massachusetts, U.S.A. Brian J. Cole Departments
The suction cup mechanism is enhanced by the slightly negative intra articular pressure within the joint.
 SHOULDER INSTABILITY Stability A. The stability of the shoulder is improved by depth of the glenoid. This is determined by: 1. Osseous glenoid, 2. Articular cartilage of the glenoid, which is thicker at
SHOULDER INSTABILITY Stability A. The stability of the shoulder is improved by depth of the glenoid. This is determined by: 1. Osseous glenoid, 2. Articular cartilage of the glenoid, which is thicker at
SHOULDER INSTABILITY
 SHOULDER INSTABILITY Dr.KN Subramanian M.Ch Orth., FRCS (Tr & Orth), CCT Orth(UK) Consultant Orthopaedic Surgeon, Special interest: Orthopaedic Sports Injury, Shoulder and Knee Surgery, SPARSH Hospital
SHOULDER INSTABILITY Dr.KN Subramanian M.Ch Orth., FRCS (Tr & Orth), CCT Orth(UK) Consultant Orthopaedic Surgeon, Special interest: Orthopaedic Sports Injury, Shoulder and Knee Surgery, SPARSH Hospital
Orthopaedic and Spine Institute 21 Spurs Lane, Suite 245, San Antonio, TX Tel#
 Orthopaedic and Spine Institute 21 Spurs Lane, Suite 245, San Antonio, TX 78240 www.saspine.com Tel# 210-487-7463 PATIENT GUIDE TO SHOULDER INSTABILITY LABRAL (BANKART) REPAIR / CAPSULAR SHIFT WHAT IS
Orthopaedic and Spine Institute 21 Spurs Lane, Suite 245, San Antonio, TX 78240 www.saspine.com Tel# 210-487-7463 PATIENT GUIDE TO SHOULDER INSTABILITY LABRAL (BANKART) REPAIR / CAPSULAR SHIFT WHAT IS
Type II SLAP lesions are created when the biceps anchor has pulled away from the glenoid attachment.
 Arthroscopic Superior Labral (SLAP) Repair Protocol-Type II, IV, and Complex Tears The intent of this protocol is to provide the clinician with a guideline of the post-operative rehabilitation course of
Arthroscopic Superior Labral (SLAP) Repair Protocol-Type II, IV, and Complex Tears The intent of this protocol is to provide the clinician with a guideline of the post-operative rehabilitation course of
RECURRENT SHOULDER DISLOCATIONS WITH ABSENT LABRUM
 RECURRENT SHOULDER DISLOCATIONS WITH ABSENT LABRUM D R. A M R I S H K R. J H A M S ( O R T H O ) A S S I S T A N T P R O F E S S O R M E D I C A L C O L L E G E, K O L K A T A LABRUM Function as a chock-block,
RECURRENT SHOULDER DISLOCATIONS WITH ABSENT LABRUM D R. A M R I S H K R. J H A M S ( O R T H O ) A S S I S T A N T P R O F E S S O R M E D I C A L C O L L E G E, K O L K A T A LABRUM Function as a chock-block,
Double bucket handle tears of the superior labrum
 Case Report http://dx.doi.org/10.14517/aosm13013 pissn 2289-005X eissn 2289-0068 Double bucket handle tears of the superior labrum Dong-Soo Kim, Kyoung-Jin Park, Yong-Min Kim, Eui-Sung Choi, Hyun-Chul
Case Report http://dx.doi.org/10.14517/aosm13013 pissn 2289-005X eissn 2289-0068 Double bucket handle tears of the superior labrum Dong-Soo Kim, Kyoung-Jin Park, Yong-Min Kim, Eui-Sung Choi, Hyun-Chul
Arthroscopic Labral Repair Protocol-Type II, IV, and Complex Tears:
 Arthroscopic Labral Repair Protocol-Type II, IV, and Complex Tears: The intent of this protocol is to provide the clinician with a guideline of the postoperative rehabilitation course of a patient that
Arthroscopic Labral Repair Protocol-Type II, IV, and Complex Tears: The intent of this protocol is to provide the clinician with a guideline of the postoperative rehabilitation course of a patient that
Management of Anterior Shoulder Instability
 Management of Anterior Shoulder Instability Angelo J. Colosimo, MD Head Orthopaedic Surgeon University of Cincinnati Athletics Director of Sports Medicine University of Cincinnati Medical Center Associate
Management of Anterior Shoulder Instability Angelo J. Colosimo, MD Head Orthopaedic Surgeon University of Cincinnati Athletics Director of Sports Medicine University of Cincinnati Medical Center Associate
Anatomy GH Joint. Glenohumeral Instability. Components of Stability. Components of Stability 7/7/2017. AllinaHealthSystem
 Glenohumeral Instability Dr. John Steubs Allina Sports Medicine Conference July 7, 2017 Anatomy GH Joint Teardrop or oval shape Inherently unstable Golf ball and tee analogy Stabilizers Static Dynamic
Glenohumeral Instability Dr. John Steubs Allina Sports Medicine Conference July 7, 2017 Anatomy GH Joint Teardrop or oval shape Inherently unstable Golf ball and tee analogy Stabilizers Static Dynamic
SHOULDER INSTABILITY
 SHOULDER INSTABILITY Your shoulder is the most flexible joint in your body, allowing you to throw fastballs, lift a heavy suitcase, scratch your back, and reach in almost any direction. Your shoulder joint
SHOULDER INSTABILITY Your shoulder is the most flexible joint in your body, allowing you to throw fastballs, lift a heavy suitcase, scratch your back, and reach in almost any direction. Your shoulder joint
Patient ID. Case Conference. Physical Examination. Image examination. Treatment 2011/6/16
 Patient ID Case Conference R3 高逢駿 VS 徐郭堯 55 y/o female C.C.: recurrent right shoulder dislocation noted since falling down injury 2 years ago Came to ER because of dislocation for many times due to minor
Patient ID Case Conference R3 高逢駿 VS 徐郭堯 55 y/o female C.C.: recurrent right shoulder dislocation noted since falling down injury 2 years ago Came to ER because of dislocation for many times due to minor
HAGL lesion of the shoulder
 HAGL lesion of the shoulder A 24 year old rugby player presented to an orthopaedic surgeon with a history of dislocation of the left shoulder. It reduced spontaneously and again later during the same match.
HAGL lesion of the shoulder A 24 year old rugby player presented to an orthopaedic surgeon with a history of dislocation of the left shoulder. It reduced spontaneously and again later during the same match.
Rehabilitation Protocol: Arthroscopic Anterior Capsulolabral Repair of the Shoulder - Bankart Repair Rehabilitation Guidelines
 Rehabilitation Protocol: Arthroscopic Anterior Capsulolabral Repair of the Shoulder - Bankart Repair Rehabilitation Guidelines Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington
Rehabilitation Protocol: Arthroscopic Anterior Capsulolabral Repair of the Shoulder - Bankart Repair Rehabilitation Guidelines Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington
Rehabilitation Guidelines for Labral/Bankert Repair
 Rehabilitation Guidelines for Labral/Bankert Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
Rehabilitation Guidelines for Labral/Bankert Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
Open Revision of Failed Arthroscopic Shoulder Reconstructions for Traumatic Instability
 1 Open Revision of Failed Arthroscopic Shoulder Reconstructions for Traumatic Instability Michael J. Pagnani, M.D. Director, Nashville Knee & Shoulder Center Despite the increased popularity of arthroscopic
1 Open Revision of Failed Arthroscopic Shoulder Reconstructions for Traumatic Instability Michael J. Pagnani, M.D. Director, Nashville Knee & Shoulder Center Despite the increased popularity of arthroscopic
Rehabilitation Guidelines for Arthroscopic Capsular Shift
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Arthroscopic Capsular Shift The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a golf ball on a tee.
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Arthroscopic Capsular Shift The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a golf ball on a tee.
Traumatic shoulder dislocation in the adolescent athlete: advances in surgical treatment Christopher R. Good and John D.
 Traumatic shoulder dislocation in the adolescent athlete: advances in surgical treatment Christopher R. Good and John D. MacGillivray Purpose of review The shoulder joint has the greatest range of motion
Traumatic shoulder dislocation in the adolescent athlete: advances in surgical treatment Christopher R. Good and John D. MacGillivray Purpose of review The shoulder joint has the greatest range of motion
SHOULDER DISLOCATION & INSTABILITY Rehabilitation Considerations
 SHOULDER DISLOCATION & INSTABILITY Rehabilitation Considerations Meagan Pehnke, MS, OTR/L, CHT, CLT March 1 st, 2019 Philadelphia Surgery & Rehabilitation of the Hand: Pediatric Pre-course OUTLINE Discuss
SHOULDER DISLOCATION & INSTABILITY Rehabilitation Considerations Meagan Pehnke, MS, OTR/L, CHT, CLT March 1 st, 2019 Philadelphia Surgery & Rehabilitation of the Hand: Pediatric Pre-course OUTLINE Discuss
Augmented Glenoid Component for Bone Deficiency in Shoulder Arthroplasty
 Clin Orthop Relat Res (2008) 466:579 583 DOI 10.1007/s11999-007-0104-4 SYMPOSIUM: NEW APPROACHES TO SHOULDER SURGERY Augmented Glenoid Component for Bone Deficiency in Shoulder Arthroplasty Robert S. Rice
Clin Orthop Relat Res (2008) 466:579 583 DOI 10.1007/s11999-007-0104-4 SYMPOSIUM: NEW APPROACHES TO SHOULDER SURGERY Augmented Glenoid Component for Bone Deficiency in Shoulder Arthroplasty Robert S. Rice
POSTERIOR INSTABILITY OF THE SHOULDER Vasu Pai
 POSTERIOR INSTABILITY OF THE SHOULDER Vasu Pai Posterior instability is less common among cases of shoulder instability, accounting for 2% to 10% of all cases of instability. More common in sporting groups:
POSTERIOR INSTABILITY OF THE SHOULDER Vasu Pai Posterior instability is less common among cases of shoulder instability, accounting for 2% to 10% of all cases of instability. More common in sporting groups:
Recurrent Shoulder Dislocation.
 Recurrent Shoulder Dislocation www.fisiokinesiterapia.biz Anatomy of the Shoulder Shoulder Dislocations Case Study Rehabilitation Pick List Anatomy of the Shoulder Articulations Sternoclavicular Acromioclavicular
Recurrent Shoulder Dislocation www.fisiokinesiterapia.biz Anatomy of the Shoulder Shoulder Dislocations Case Study Rehabilitation Pick List Anatomy of the Shoulder Articulations Sternoclavicular Acromioclavicular
The Bankart repair illustrated in crosssection
 The Bankart repair illustrated in crosssection Some anatomical considerations RALPH B. BLASIER,* MD, JAMES D. BRUCKNER, LT, MC, USNR, DAVID H. JANDA,* MD, AND A. HERBERT ALEXANDER, CAPT, MC, USN From the
The Bankart repair illustrated in crosssection Some anatomical considerations RALPH B. BLASIER,* MD, JAMES D. BRUCKNER, LT, MC, USNR, DAVID H. JANDA,* MD, AND A. HERBERT ALEXANDER, CAPT, MC, USN From the
SLAP Lesions Assessment & Treatment
 SLAP Lesions Assessment & Treatment Kevin E. Wilk,, PT, DPT Glenoid Labral Lesions Introduction Common injury - difficult to diagnose May occur in isolation or in combination SLAP lesions: Snyder: Arthroscopy
SLAP Lesions Assessment & Treatment Kevin E. Wilk,, PT, DPT Glenoid Labral Lesions Introduction Common injury - difficult to diagnose May occur in isolation or in combination SLAP lesions: Snyder: Arthroscopy
OBJECTIVES. Therapists Management of Shoulder Instability SHOULDER STABILITY SHOULDER STABILITY WHAT IS SHOULDER INSTABILITY? SHOULDER INSTABILITY
 Therapists Management of Shoulder Instability Brian G. Leggin, PT, DPT, OCS Lead Therapist, Penn Therapy and Fitness at Valley Forge Adjunct Assistant Professor, Department of Orthopaedics, University
Therapists Management of Shoulder Instability Brian G. Leggin, PT, DPT, OCS Lead Therapist, Penn Therapy and Fitness at Valley Forge Adjunct Assistant Professor, Department of Orthopaedics, University
The Shoulder. Anatomy and Injuries PSK 4U Unit 3, Day 4
 The Shoulder Anatomy and Injuries PSK 4U Unit 3, Day 4 Shoulder Girdle Shoulder Complex is the most mobile joint in the body. Scapula Clavicle Sternum Humerus Rib cage/thorax Shoulder Girdle It also includes
The Shoulder Anatomy and Injuries PSK 4U Unit 3, Day 4 Shoulder Girdle Shoulder Complex is the most mobile joint in the body. Scapula Clavicle Sternum Humerus Rib cage/thorax Shoulder Girdle It also includes
An analysis of 140 injuries to the superior glenoid labrum
 ORIGINAL ARTICLES An analysis of 140 injuries to the superior glenoid labrum Stephen J. Snyder, MD, Michael P. Banas, MD, and Ronald P. Karzel, MD, Van Nuys, Calif. Between 1985 and 1993 140 injuries of
ORIGINAL ARTICLES An analysis of 140 injuries to the superior glenoid labrum Stephen J. Snyder, MD, Michael P. Banas, MD, and Ronald P. Karzel, MD, Van Nuys, Calif. Between 1985 and 1993 140 injuries of
Anterior Stabilization of the Shoulder: Latarjet Protocol
 Anterior Stabilization of the Shoulder: Latarjet Protocol Dr. Abigail R. Hamilton, M.D. Shoulder instability may be caused from congenital deformity, recurrent overuse activity, and/or traumatic dislocation.
Anterior Stabilization of the Shoulder: Latarjet Protocol Dr. Abigail R. Hamilton, M.D. Shoulder instability may be caused from congenital deformity, recurrent overuse activity, and/or traumatic dislocation.
SLAP Lesions of the Shoulder
 Arthroscopy: The Journal of Arthroscopic and Related Surgery 6(4):21&279 Published by Raven Press, Ltd. Q 1990 Arthroscopy Association of North America SLAP Lesions of the Shoulder Stephen J. Snyder, M.D.,
Arthroscopy: The Journal of Arthroscopic and Related Surgery 6(4):21&279 Published by Raven Press, Ltd. Q 1990 Arthroscopy Association of North America SLAP Lesions of the Shoulder Stephen J. Snyder, M.D.,
Shoulder Instability. Fig 1: Intact labrum and biceps tendon
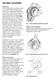 Shoulder Instability What is it? The shoulder joint is a ball and socket joint, with the humeral head (upper arm bone) as the ball and the glenoid as the socket. The glenoid (socket) is a shallow bone
Shoulder Instability What is it? The shoulder joint is a ball and socket joint, with the humeral head (upper arm bone) as the ball and the glenoid as the socket. The glenoid (socket) is a shallow bone
11/13/2017. Disclosures: The Irreparable Rotator Cuff. I am a consultant for Arhtrex, Inc and Endo Pharmaceuticals.
 Massive Rotator Cuff Tears without Arthritis THE CASE FOR SUPERIOR CAPSULAR RECONSTRUCTION MICHAEL GARCIA, MD NOVEMBER 4, 2017 FLORIDA ORTHOPAEDIC INSTITUTE Disclosures: I am a consultant for Arhtrex,
Massive Rotator Cuff Tears without Arthritis THE CASE FOR SUPERIOR CAPSULAR RECONSTRUCTION MICHAEL GARCIA, MD NOVEMBER 4, 2017 FLORIDA ORTHOPAEDIC INSTITUTE Disclosures: I am a consultant for Arhtrex,
Shoulder Instability
 J F de Beer, K van Rooyen, D Bhatia Shoulder Instability INSTABILITY means that the shoulder dislocates completely (dislocation) or partially (subluxation). Anatomy The shoulder consists of a ball (humeral
J F de Beer, K van Rooyen, D Bhatia Shoulder Instability INSTABILITY means that the shoulder dislocates completely (dislocation) or partially (subluxation). Anatomy The shoulder consists of a ball (humeral
Massive Rotator Cuff Tears. Rafael M. Williams, MD
 Massive Rotator Cuff Tears Rafael M. Williams, MD Rotator Cuff MRI MRI Small / Partial Thickness Medium Tear Arthroscopic View Massive Tear Fatty Atrophy Arthroscopic View MassiveTears Tear is > 5cm
Massive Rotator Cuff Tears Rafael M. Williams, MD Rotator Cuff MRI MRI Small / Partial Thickness Medium Tear Arthroscopic View Massive Tear Fatty Atrophy Arthroscopic View MassiveTears Tear is > 5cm
Operative skills have advanced sufficiently so that. Arthroscopic Treatment of Multidirectional Glenohumeral Instability: 2- to 5-Year Follow-up
 Arthroscopic Treatment of Multidirectional Glenohumeral Instability: 2- to 5-Year Follow-up Gary M. Gartsman, M.D., Toni S. Roddey, Ph.D., P.T., O.C.S., and Steven M. Hammerman, M.D. Purpose: We present
Arthroscopic Treatment of Multidirectional Glenohumeral Instability: 2- to 5-Year Follow-up Gary M. Gartsman, M.D., Toni S. Roddey, Ph.D., P.T., O.C.S., and Steven M. Hammerman, M.D. Purpose: We present
URSA HEMI-SHOULDER ARTHROPLASTY B I O T E K
 URSA HEMI-SHOULDER ARTHROPLASTY SURGICAL TECHNIQUE B I O T E K 2 Surgical Position Once general anesthesia has been satisfactorily induced, or a supraclavicular nerve block has been given, the patient
URSA HEMI-SHOULDER ARTHROPLASTY SURGICAL TECHNIQUE B I O T E K 2 Surgical Position Once general anesthesia has been satisfactorily induced, or a supraclavicular nerve block has been given, the patient
Acromioplasty. Surgical Indications and Considerations
 1 Acromioplasty Surgical Indications and Considerations Anatomical Considerations: Any abnormality that disrupts the intricate relationship within the subacromial space may lead to impingement. Both intrinsic
1 Acromioplasty Surgical Indications and Considerations Anatomical Considerations: Any abnormality that disrupts the intricate relationship within the subacromial space may lead to impingement. Both intrinsic
Arthroscopic procedures for the treatment of anterior shoulder instability: local experiences!"#$%&'()*+,-%&./0123
 ST Choi PYT Tse ORIGINAL ARTICLE Arthroscopic procedures for the treatment of anterior shoulder instability: local experiences!"#$%&'()*+,-%&./03 Objective. To review the outcomes of arthroscopic stabilisation
ST Choi PYT Tse ORIGINAL ARTICLE Arthroscopic procedures for the treatment of anterior shoulder instability: local experiences!"#$%&'()*+,-%&./03 Objective. To review the outcomes of arthroscopic stabilisation
POST-SURGICAL POSTERIOR GLENOHUMERAL STABILIZATION REHABILITATION PROTOCOL (Capsulolabral Repair)
 Gregory N. Lervick, MD Andrew Anderson, PA-C 952-456-7111 POST-SURGICAL POSTERIOR GLENOHUMERAL STABILIZATION REHABILITATION PROTOCOL (Capsulolabral Repair) Open Arthroscopic Phase 1: Weeks 0-4 No shoulder
Gregory N. Lervick, MD Andrew Anderson, PA-C 952-456-7111 POST-SURGICAL POSTERIOR GLENOHUMERAL STABILIZATION REHABILITATION PROTOCOL (Capsulolabral Repair) Open Arthroscopic Phase 1: Weeks 0-4 No shoulder
Biceps Tenodesis Protocol
 Robert K. Fullick, MD 6400 Fannin Street, Suite 1700 Houston, Texas 77030 Ph.: 713-486-7543 / Fx.: 713-486-5549 Biceps Tenodesis Protocol The intent of this protocol is to provide the clinician with a
Robert K. Fullick, MD 6400 Fannin Street, Suite 1700 Houston, Texas 77030 Ph.: 713-486-7543 / Fx.: 713-486-5549 Biceps Tenodesis Protocol The intent of this protocol is to provide the clinician with a
ANTERIOR SHOULDER STABILIZATION CLINICAL PRACTICE GUIDELINE
 ANTERIOR SHOULDER STABILIZATION CLINICAL PRACTICE GUIDELINE Background Ohio State s Anterior Shoulder Stabilization Rehabilitation Guideline is to be utilized following open or arthroscopic anterior shoulder
ANTERIOR SHOULDER STABILIZATION CLINICAL PRACTICE GUIDELINE Background Ohio State s Anterior Shoulder Stabilization Rehabilitation Guideline is to be utilized following open or arthroscopic anterior shoulder
D Degenerative joint disease, rotator cuff deficiency with, 149 Deltopectoral approach component removal with, 128
 Index A Abduction exercise, outpatient with, 193, 194 Acromioclavicular arthritis, with, 80 Acromiohumeral articulation, with, 149 Acromio-humeral interval (AHI), physical examination with, 9, 10 Active
Index A Abduction exercise, outpatient with, 193, 194 Acromioclavicular arthritis, with, 80 Acromiohumeral articulation, with, 149 Acromio-humeral interval (AHI), physical examination with, 9, 10 Active
Biceps Tenodesis Protocol
 Biceps Tenodesis Protocol A biceps tenodesis procedure involves cutting of the long head of the biceps just prior to its insertion on the superior labrum and then anchoring the tendon along its anatomical
Biceps Tenodesis Protocol A biceps tenodesis procedure involves cutting of the long head of the biceps just prior to its insertion on the superior labrum and then anchoring the tendon along its anatomical
Rehabilitation Guidelines for Large Rotator Cuff Repair
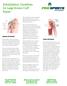 Rehabilitation Guidelines for Large Rotator Cuff Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the
Rehabilitation Guidelines for Large Rotator Cuff Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the
Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Arthroscopic Bankart Repair
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Arthroscopic Bankart Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Arthroscopic Bankart Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is
significant increase of glenohumeral translation at middle and lower elevation angles [6].
![significant increase of glenohumeral translation at middle and lower elevation angles [6]. significant increase of glenohumeral translation at middle and lower elevation angles [6].](/thumbs/94/120620199.jpg) significant increase of glenohumeral translation at middle and lower elevation angles [6]. Two types of injury mechanisms have been postulated for superior labral tears. 1. Traction injury : Chronic repetitive
significant increase of glenohumeral translation at middle and lower elevation angles [6]. Two types of injury mechanisms have been postulated for superior labral tears. 1. Traction injury : Chronic repetitive
Shoulder Arthroscopy Lab Manual
 Shoulder Arthroscopy Lab Manual Dalhousie University Orthopaedic Program May 5, 2017 Skills Centre OBJECTIVES 1. Demonstrate a competent understanding of the arthroscopic anatomy and biomechanics of the
Shoulder Arthroscopy Lab Manual Dalhousie University Orthopaedic Program May 5, 2017 Skills Centre OBJECTIVES 1. Demonstrate a competent understanding of the arthroscopic anatomy and biomechanics of the
Isolated electrothermal capsulorrhaphy in overhand athletes
 Isolated electrothermal capsulorrhaphy in overhand athletes Jerome G. Enad, MD, Neal S. ElAttrache, MD, James E. Tibone, MD, and Lewis A. Yocum, MD, Los Angeles, CA The purpose of this study was to determine
Isolated electrothermal capsulorrhaphy in overhand athletes Jerome G. Enad, MD, Neal S. ElAttrache, MD, James E. Tibone, MD, and Lewis A. Yocum, MD, Los Angeles, CA The purpose of this study was to determine
Shoulder Arthroscopy. Dr. J.J.A.M. van Raaij. NOV Jaarvergadering Den Bosch 25 jan 2018
 Shoulder Arthroscopy Dr. J.J.A.M. van Raaij NOV Jaarvergadering Den Bosch 25 jan 2018 No disclosures Disclosure Shoulder Instability Traumatic anterior Traumatic posterior Acquired atraumatic Multidirectional
Shoulder Arthroscopy Dr. J.J.A.M. van Raaij NOV Jaarvergadering Den Bosch 25 jan 2018 No disclosures Disclosure Shoulder Instability Traumatic anterior Traumatic posterior Acquired atraumatic Multidirectional
Shoulder Arthroscopy Portals
 Shoulder Arthroscopy Portals Alper Deveci and Metin Dogan 7 7.1 Bony Landmarks Before starting shoulder arthroscopy, the patient must be positioned and draping applied. Then the bony landmarks are identified
Shoulder Arthroscopy Portals Alper Deveci and Metin Dogan 7 7.1 Bony Landmarks Before starting shoulder arthroscopy, the patient must be positioned and draping applied. Then the bony landmarks are identified
The ball-and-socket articulation at the glenohumeral joint is between the convex
 SLAP Lesion Repair Emily Cotey, Emily Hurysz, and Patrick Schroeder Abstract SLAP lesion, which stands for Superior Labrum Anterior and Posterior, is a detachment tear of the superior labrum that originates
SLAP Lesion Repair Emily Cotey, Emily Hurysz, and Patrick Schroeder Abstract SLAP lesion, which stands for Superior Labrum Anterior and Posterior, is a detachment tear of the superior labrum that originates
Labral Tears. Fig 1: Intact labrum and biceps tendon
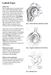 Labral Tears What is it? The shoulder joint is a ball and socket joint, with the humeral head (upper arm bone) as the ball and the glenoid as the socket. The glenoid (socket) is a shallow bone that is
Labral Tears What is it? The shoulder joint is a ball and socket joint, with the humeral head (upper arm bone) as the ball and the glenoid as the socket. The glenoid (socket) is a shallow bone that is
Glenohumeral Joint Instability. Static Stabilizers of the GHJ. Static Stabilizers of the GHJ. Static Stabilizers of the GHJ
 1 Glenohumeral Joint Instability GHJ Joint Stability: Or Lack Thereof! Christine B. Chung, M.D. Assistant Professor of Radiology Musculoskeletal Division UCSD and VA Healthcare System Static Stabilizers
1 Glenohumeral Joint Instability GHJ Joint Stability: Or Lack Thereof! Christine B. Chung, M.D. Assistant Professor of Radiology Musculoskeletal Division UCSD and VA Healthcare System Static Stabilizers
Comparison of Open and Arthroscopic Stabilization for Recurrent Shoulder Dislocation in Patients with a Bankart Lesion
 0363-5465/101/2929-0538$02.00/0 THE AMERICAN JOURNAL OF SPORTS MEDICINE, Vol. 29, No. 5 2001 American Orthopaedic Society for Sports Medicine Comparison of Open and Arthroscopic Stabilization for Recurrent
0363-5465/101/2929-0538$02.00/0 THE AMERICAN JOURNAL OF SPORTS MEDICINE, Vol. 29, No. 5 2001 American Orthopaedic Society for Sports Medicine Comparison of Open and Arthroscopic Stabilization for Recurrent
Curative effects of under-arthroscopic anchor implantation fixation to martial arts player s shoulder joint injury.
 Biomedical Research 2017; 28 (19): 8295-8299 ISSN 0970-938X www.biomedres.info Curative effects of under-arthroscopic anchor implantation fixation to martial arts player s shoulder joint injury. Zonghao
Biomedical Research 2017; 28 (19): 8295-8299 ISSN 0970-938X www.biomedres.info Curative effects of under-arthroscopic anchor implantation fixation to martial arts player s shoulder joint injury. Zonghao
Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS
 Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS Consultant Orthopaedic Surgeon, Shoulder Specialist. +353 1 5262335 ruthdelaney@sportssurgeryclinic.com Modified from the protocol developed at Boston Shoulder
Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS Consultant Orthopaedic Surgeon, Shoulder Specialist. +353 1 5262335 ruthdelaney@sportssurgeryclinic.com Modified from the protocol developed at Boston Shoulder
Summary: Arthroscopy has revolutionized the way
 Techniques in Shoulder & Elbow Surgery 3(2):74 81, 2002 2002 Lippincott Williams & Wilkins, Inc., Philadelphia T E C H N I Q U E Arthroscopic Assisted Rotator Interval Closure STEPHEN J. O BRIEN, M.D.
Techniques in Shoulder & Elbow Surgery 3(2):74 81, 2002 2002 Lippincott Williams & Wilkins, Inc., Philadelphia T E C H N I Q U E Arthroscopic Assisted Rotator Interval Closure STEPHEN J. O BRIEN, M.D.
The Upper Limb II. Anatomy RHS 241 Lecture 11 Dr. Einas Al-Eisa
 The Upper Limb II Anatomy RHS 241 Lecture 11 Dr. Einas Al-Eisa Sternoclavicular joint Double joint.? Each side separated by intercalating articular disc Grasp the mid-portion of your clavicle on one side
The Upper Limb II Anatomy RHS 241 Lecture 11 Dr. Einas Al-Eisa Sternoclavicular joint Double joint.? Each side separated by intercalating articular disc Grasp the mid-portion of your clavicle on one side
Introduction & Question 1
 Page 1 of 7 www.medscape.com To Print: Click your browser's PRINT button. NOTE: To view the article with Web enhancements, go to: http://www.medscape.com/viewarticle/424981 Case Q & A Shoulder Pain, Part
Page 1 of 7 www.medscape.com To Print: Click your browser's PRINT button. NOTE: To view the article with Web enhancements, go to: http://www.medscape.com/viewarticle/424981 Case Q & A Shoulder Pain, Part
Phase I : Immediate Postoperative Phase- Protected Motion. (0-2 Weeks)
 Phase I : Immediate Postoperative Phase- Protected Motion (0-2 Weeks) Appointments Progression Criteria 2 weeks after surgery Rehabilitation appointments begin within 7-10 days of surgery, continue 1-2
Phase I : Immediate Postoperative Phase- Protected Motion (0-2 Weeks) Appointments Progression Criteria 2 weeks after surgery Rehabilitation appointments begin within 7-10 days of surgery, continue 1-2
Shoulder Labral Tear and Shoulder Dislocation
 Shoulder Labral Tear and Shoulder Dislocation The shoulder joint is a ball and socket joint with tremendous flexibility and range of motion. The ball is the humeral head while the socket is the glenoid.
Shoulder Labral Tear and Shoulder Dislocation The shoulder joint is a ball and socket joint with tremendous flexibility and range of motion. The ball is the humeral head while the socket is the glenoid.
SUPERIOR LABRAL REPAIRS
 LOURDES MEDICAL ASSOCIATES Sean Mc Millan, DO Director of Orthopaedic Sports Medicine & Arthroscopy 2103 Burlington-Mount Holly Rd Burlington, NJ 08016 (609) 747-9200 (office) (609) 747-1408 (fax) http://orthodoc.aaos.org/drmcmillan
LOURDES MEDICAL ASSOCIATES Sean Mc Millan, DO Director of Orthopaedic Sports Medicine & Arthroscopy 2103 Burlington-Mount Holly Rd Burlington, NJ 08016 (609) 747-9200 (office) (609) 747-1408 (fax) http://orthodoc.aaos.org/drmcmillan
P.O. Box Sierra Park Road Mammoth Lakes, CA Orthopedic Surgery & Sports Medicine
 P.O. Box 660 85 Sierra Park Road Mammoth Lakes, CA 93546 SHOULDER: Instability Dislocation Labral Tears The shoulder is the most mobile joint in the body, but to have this amount of motion, it is also
P.O. Box 660 85 Sierra Park Road Mammoth Lakes, CA 93546 SHOULDER: Instability Dislocation Labral Tears The shoulder is the most mobile joint in the body, but to have this amount of motion, it is also
Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Open Bankart Repair
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Open Bankart Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Open Bankart Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared
Biceps Tenotomy Protocol
 Biceps Tenotomy Protocol A biceps tenotomy procedure involves cutting of the long head of the biceps just prior to its insertion on the superior labrum. A biceps tenotomy is typically done when there is
Biceps Tenotomy Protocol A biceps tenotomy procedure involves cutting of the long head of the biceps just prior to its insertion on the superior labrum. A biceps tenotomy is typically done when there is
Biceps Tenotomy Protocol
 Department of Rehabilitation Services Physical Therapy The intent of this protocol is to provide the clinician with a guideline of the postoperative rehabilitation course of a patient that has undergone
Department of Rehabilitation Services Physical Therapy The intent of this protocol is to provide the clinician with a guideline of the postoperative rehabilitation course of a patient that has undergone
Rotator cuff injuries are commonly attributed to repetitive
 [ Orthopaedics ] Massive Rotator Cuff Tear in an Adolescent Athlete: A Case Report Kimberly A. Turman, MD,* Mark W. Anderson, MD, and Mark D. Miller, MD Full-thickness rotator cuff tears in the young athlete
[ Orthopaedics ] Massive Rotator Cuff Tear in an Adolescent Athlete: A Case Report Kimberly A. Turman, MD,* Mark W. Anderson, MD, and Mark D. Miller, MD Full-thickness rotator cuff tears in the young athlete
ROTATOR CUFF TEAR, SURGERY FOR
 ROTATOR CUFF TEAR, SURGERY FOR Indications (Who Needs Surgery, When, electricity is used to cauterize small capillaries. Electricity or Why, and Goals) a motorized shaver is used to remove the bursa and
ROTATOR CUFF TEAR, SURGERY FOR Indications (Who Needs Surgery, When, electricity is used to cauterize small capillaries. Electricity or Why, and Goals) a motorized shaver is used to remove the bursa and
Pectorlais Major Tendon Repair
 Dr. Mark Price MGH Sports Medicine Center 175 Cambridge Street, 4th floor Boston, MA 02114 www.massgeneral.org/ortho-sports-medicine/dr-price Pectorlais Major Tendon Repair The pectoralis major muscle
Dr. Mark Price MGH Sports Medicine Center 175 Cambridge Street, 4th floor Boston, MA 02114 www.massgeneral.org/ortho-sports-medicine/dr-price Pectorlais Major Tendon Repair The pectoralis major muscle
Thinking About Shoulder Instability Surgery (a.k.a Why do we do what we do?)
 Thinking About Shoulder Instability Surgery (a.k.a Why do we do what we do?) Thomas J. Gill Chief, MGH Sports Medicine Dept. of Orthopedic Surgery Massachusetts General Hospital Boston, MA Look, just do
Thinking About Shoulder Instability Surgery (a.k.a Why do we do what we do?) Thomas J. Gill Chief, MGH Sports Medicine Dept. of Orthopedic Surgery Massachusetts General Hospital Boston, MA Look, just do
Review shoulder anatomy Review the physical exam of the shoulder Discuss some common causes of acute shoulder pain Discuss some common causes of
 Review shoulder anatomy Review the physical exam of the shoulder Discuss some common causes of acute shoulder pain Discuss some common causes of chronic shoulder pain Review with some case questions Bones:
Review shoulder anatomy Review the physical exam of the shoulder Discuss some common causes of acute shoulder pain Discuss some common causes of chronic shoulder pain Review with some case questions Bones:
Glenohumeral Joint Instability: An Athlete s Perspective
 Anatomic Considerations Glenohumeral Joint Instability: An Athlete s Perspective Michael D. Loeb, MD Texas Orthopedics, Sports Medicine, and Rehabilitation Associates Austin, Texas Static Stabilizers Osseous
Anatomic Considerations Glenohumeral Joint Instability: An Athlete s Perspective Michael D. Loeb, MD Texas Orthopedics, Sports Medicine, and Rehabilitation Associates Austin, Texas Static Stabilizers Osseous
11/15/2017. Biceps Lesions. Highgate Private Hospital (Whittington Health NHS Trust) E: LHB Anatomy.
 Biceps Lesions Mr Omar Haddo (Consultant Orthopaedic Surgeon MBBS, BmedSci, FRCS(Orth) ) Highgate Private Hospital (Whittington Health NHS Trust) E: admin@denovomedic.co.uk LHB Anatomy Arise from superior
Biceps Lesions Mr Omar Haddo (Consultant Orthopaedic Surgeon MBBS, BmedSci, FRCS(Orth) ) Highgate Private Hospital (Whittington Health NHS Trust) E: admin@denovomedic.co.uk LHB Anatomy Arise from superior
Management of Massive/Revision Rotator Cuff Tears
 Management of Massive/Revision Rotator Cuff Tears Nikhil N. Verma MD, Director Sports Medicine, Rush University Medical Center, Midwest Orthopedics at Rush, Chicago, IL nverma@rushortho.com I. Anatomy
Management of Massive/Revision Rotator Cuff Tears Nikhil N. Verma MD, Director Sports Medicine, Rush University Medical Center, Midwest Orthopedics at Rush, Chicago, IL nverma@rushortho.com I. Anatomy
SHOULDER INSTABILITY - DISLOCATION AND SUBLUXATION
 SHOULDER INSTABILITY - DISLOCATION AND SUBLUXATION THE INJURY The shoulder joint is a ball and socket joint that connects the bone of the upper arm (humerus) with the shoulder blade (scapula). The shallow
SHOULDER INSTABILITY - DISLOCATION AND SUBLUXATION THE INJURY The shoulder joint is a ball and socket joint that connects the bone of the upper arm (humerus) with the shoulder blade (scapula). The shallow
Upper Extremity Injuries in Youth Baseball: Causes and Prevention
 Upper Extremity Injuries in Youth Baseball: Causes and Prevention Biomechanics Throwing a baseball is an unnatural movement Excessively high forces are generated at the elbow and shoulder Throwing requires
Upper Extremity Injuries in Youth Baseball: Causes and Prevention Biomechanics Throwing a baseball is an unnatural movement Excessively high forces are generated at the elbow and shoulder Throwing requires
ANATOMICAL. REDEFINED.
 Operative Technique Fracture Stem Equinoxe Fracture Stem Operative Technique ANATOMICAL. REDEFINED. 352-377-1140 1-800-EXACTECH www.exac.com #718-00-33 REV A 0705 2005 EXACTECH, INC. ISO 13485 CERTIFIED
Operative Technique Fracture Stem Equinoxe Fracture Stem Operative Technique ANATOMICAL. REDEFINED. 352-377-1140 1-800-EXACTECH www.exac.com #718-00-33 REV A 0705 2005 EXACTECH, INC. ISO 13485 CERTIFIED
ANATOMY / BIOMECHANICS LONG HEAD OF BICEPS ATTACHES AT THE SUPERIOR GLENOIDAL TUBERCLE WITH THE LABRUM FIBROCARTILAGINOUS TISSUE IF THERE IS A TORN SU
 SLAP LESIONS Management Of Glenoid Labrum Injuries INTRODUCTION First described by Andrews AJSM 85 Throwers 60% Normal Variants Sublabral Foramen Buford Complex Meniscoid Snyder Arth. 1990 termed SLAP
SLAP LESIONS Management Of Glenoid Labrum Injuries INTRODUCTION First described by Andrews AJSM 85 Throwers 60% Normal Variants Sublabral Foramen Buford Complex Meniscoid Snyder Arth. 1990 termed SLAP
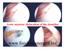 Acute anterior dislocation of the shoulder www.fisiokinesiterapia.biz Anatomy Stability: - ball & socket = compression in concavity effect Bone - big head small cup = unstable Menisci - labium = depth
Acute anterior dislocation of the shoulder www.fisiokinesiterapia.biz Anatomy Stability: - ball & socket = compression in concavity effect Bone - big head small cup = unstable Menisci - labium = depth
Solar Humeral Fracture System. Surgical Protocol
 Solar Humeral Fracture System Surgical Protocol Surgical Protocol Table of Contents Table of Contents Step By Step Procedure... 1 Patient Positioning... 3 Surgical Exposure... 4 Preparation of Humeral
Solar Humeral Fracture System Surgical Protocol Surgical Protocol Table of Contents Table of Contents Step By Step Procedure... 1 Patient Positioning... 3 Surgical Exposure... 4 Preparation of Humeral
Arthroscopic Preparation of the Posterior and Posteroinferior Glenoid Labrum
 Arthroscopic Preparation of the Posterior and Posteroinferior Glenoid Labrum By Matthew T. Provencher, MD, LCDR, MC, USNR; Anthony A. Romeo, MD; Daniel J. Solomon, MD, CDR, MC, USN; Bernard R. Bach, Jr.,
Arthroscopic Preparation of the Posterior and Posteroinferior Glenoid Labrum By Matthew T. Provencher, MD, LCDR, MC, USNR; Anthony A. Romeo, MD; Daniel J. Solomon, MD, CDR, MC, USN; Bernard R. Bach, Jr.,
Anterior Stabilization of the Shoulder: Distal Tibial Allograft
 Anterior Stabilization of the Shoulder: Distal Tibial Allograft Name: Diagnosis: Date: Date of Surgery: Phase I Immediate Post Surgical Phase (approximately Weeks 1-3) Minimize shoulder pain and inflammatory
Anterior Stabilization of the Shoulder: Distal Tibial Allograft Name: Diagnosis: Date: Date of Surgery: Phase I Immediate Post Surgical Phase (approximately Weeks 1-3) Minimize shoulder pain and inflammatory
Shoulder Instability and Stabilisation
 Shoulder Instability and Stabilisation The benefit of the huge range of movements at the shoulder is that we are able to position the hand as required, the cost is that the shoulder is more likely to dislocate
Shoulder Instability and Stabilisation The benefit of the huge range of movements at the shoulder is that we are able to position the hand as required, the cost is that the shoulder is more likely to dislocate
Body Planes. (A) Transverse Superior Inferior (B) Sagittal Medial Lateral (C) Coronal Anterior Posterior Extremity Proximal Distal
 Body Planes (A) Transverse Superior Inferior (B) Sagittal Medial Lateral (C) Coronal Anterior Posterior Extremity Proximal Distal C B A Range of Motion Flexion Extension ADDUCTION ABDUCTION Range of Motion
Body Planes (A) Transverse Superior Inferior (B) Sagittal Medial Lateral (C) Coronal Anterior Posterior Extremity Proximal Distal C B A Range of Motion Flexion Extension ADDUCTION ABDUCTION Range of Motion
R. Frank Henn III, MD. Associate Professor Chief of Sports Medicine Residency Program Director
 R. Frank Henn III, MD Associate Professor Chief of Sports Medicine Residency Program Director Disclosures No financial relationships to disclose 1. Labral anatomy 2. Adaptations of the throwing shoulder
R. Frank Henn III, MD Associate Professor Chief of Sports Medicine Residency Program Director Disclosures No financial relationships to disclose 1. Labral anatomy 2. Adaptations of the throwing shoulder
THE SHOULDER JOINT T H E G L E N O H U M E R A L ( G H ) J O I N T
 THE SHOULDER JOINT T H E G L E N O H U M E R A L ( G H ) J O I N T CLARIFICATION OF TERMS Shoulder girdle = scapula and clavicle Shoulder joint (glenohumeral joint) = scapula and humerus Lippert, p115
THE SHOULDER JOINT T H E G L E N O H U M E R A L ( G H ) J O I N T CLARIFICATION OF TERMS Shoulder girdle = scapula and clavicle Shoulder joint (glenohumeral joint) = scapula and humerus Lippert, p115
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Abduction pillow, ultrasling, 880, 881, 882, 883 Adolescents, shoulder instability in. See Shoulder, instability of, pediatric and adolescent.
Index Note: Page numbers of article titles are in boldface type. A Abduction pillow, ultrasling, 880, 881, 882, 883 Adolescents, shoulder instability in. See Shoulder, instability of, pediatric and adolescent.
Anterior Stabilization of the Shoulder: Latarjet Protocol
 Robert K. Fullick, MD 6400 Fannin Street, Suite 1700 Houston, Texas 77030 Ph.: 713-486-7543 / Fx.: 713-486-5549 Anterior Stabilization of the Shoulder: Latarjet Protocol The intent of this protocol is
Robert K. Fullick, MD 6400 Fannin Street, Suite 1700 Houston, Texas 77030 Ph.: 713-486-7543 / Fx.: 713-486-5549 Anterior Stabilization of the Shoulder: Latarjet Protocol The intent of this protocol is
Operative Technique Resurfacing Humeral Head
 EXACTECH SHOULDER Operative Technique Resurfacing Humeral Head TABLE OF CONTENTS INTRODUCTION... 1 SYSTEM SPECIFICATIONS... 1 PATIENT POSITIONING... 2 SURGICAL APPROACH... 2 SIZING THE HUMERUS FOR A RESURFACING
EXACTECH SHOULDER Operative Technique Resurfacing Humeral Head TABLE OF CONTENTS INTRODUCTION... 1 SYSTEM SPECIFICATIONS... 1 PATIENT POSITIONING... 2 SURGICAL APPROACH... 2 SIZING THE HUMERUS FOR A RESURFACING
Technique. Aequalis Resurfacing Humeral Head
 S u r g i c a l Technique Aequalis Resurfacing Humeral Head 1 The Aequalis Resurfacing Humeral Head has been developed in conjunction with Drew Miller, MD - Atlanta, GA. The Aequalis Resurfacing Humeral
S u r g i c a l Technique Aequalis Resurfacing Humeral Head 1 The Aequalis Resurfacing Humeral Head has been developed in conjunction with Drew Miller, MD - Atlanta, GA. The Aequalis Resurfacing Humeral
This presentation is the intellectual property of the author. Contact them at for permission to reprint and/or distribute.
 January 19, 2012 John W. Hinchey, MD Dept of Orthopaedic Surgery Shoulder & Elbow Service This live activity is designated for a maximum of 1 AMA PRA Category 1 Credit tm. Physicians should claim only
January 19, 2012 John W. Hinchey, MD Dept of Orthopaedic Surgery Shoulder & Elbow Service This live activity is designated for a maximum of 1 AMA PRA Category 1 Credit tm. Physicians should claim only
ROTATOR CUFF DISORDERS/IMPINGEMENT
 ROTATOR CUFF DISORDERS/IMPINGEMENT Dr.KN Subramanian M.Ch Orth., FRCS (Tr & Orth), CCT Orth(UK) Consultant Orthopaedic Surgeon, Special interest: Orthopaedic Sports Injury, Shoulder and Knee Surgery, SPARSH
ROTATOR CUFF DISORDERS/IMPINGEMENT Dr.KN Subramanian M.Ch Orth., FRCS (Tr & Orth), CCT Orth(UK) Consultant Orthopaedic Surgeon, Special interest: Orthopaedic Sports Injury, Shoulder and Knee Surgery, SPARSH
SHOULDER JOINT ANATOMY AND KINESIOLOGY
 SHOULDER JOINT ANATOMY AND KINESIOLOGY SHOULDER JOINT ANATOMY AND KINESIOLOGY The shoulder joint, also called the glenohumeral joint, consists of the scapula and humerus. The motions of the shoulder joint
SHOULDER JOINT ANATOMY AND KINESIOLOGY SHOULDER JOINT ANATOMY AND KINESIOLOGY The shoulder joint, also called the glenohumeral joint, consists of the scapula and humerus. The motions of the shoulder joint
OrthoCarolina. Arthroscopic SLAP Lesion (Type II) Repair Protocol
 OrthoCarolina Arthroscopic SLAP Lesion (Type II) Repair Protocol Surgical Overview: SLAP, which stands for superior labrum anterior to posterior, lesions are labral detachments that originate posterior
OrthoCarolina Arthroscopic SLAP Lesion (Type II) Repair Protocol Surgical Overview: SLAP, which stands for superior labrum anterior to posterior, lesions are labral detachments that originate posterior
Arthroscopic Labrum Repair of the Shoulder (SLAP)
 Anatomy Arthroscopic Labrum Repair of the Shoulder (SLAP) The shoulder joint involves three bones: the scapula (shoulder blade), the clavicle (collarbone) and the humerus (upper arm bone). The humeral
Anatomy Arthroscopic Labrum Repair of the Shoulder (SLAP) The shoulder joint involves three bones: the scapula (shoulder blade), the clavicle (collarbone) and the humerus (upper arm bone). The humeral
Posterior Shoulder Instability
 Posterior Shoulder Instability Robert A. Arciero, MD Professor of Orthopaedics University of Connecticut USA Classification of Posterior Instability Dislocation -acute -chronic- fixed or locked Subluxation
Posterior Shoulder Instability Robert A. Arciero, MD Professor of Orthopaedics University of Connecticut USA Classification of Posterior Instability Dislocation -acute -chronic- fixed or locked Subluxation
SHOULDER PROBLEMS & ARTHROSCOPIC MANAGEMENT
 SHOULDER PROBLEMS & ARTHROSCOPIC MANAGEMENT DR.SHEKHAR SRIVASTAV Sr. Consultant-KNEE & SHOULDER Arthroscopy Sant Parmanand Hospital,Delhi Peculiarities of Shoulder Elegant piece of machinery It has the
SHOULDER PROBLEMS & ARTHROSCOPIC MANAGEMENT DR.SHEKHAR SRIVASTAV Sr. Consultant-KNEE & SHOULDER Arthroscopy Sant Parmanand Hospital,Delhi Peculiarities of Shoulder Elegant piece of machinery It has the
Rotator cuff strength following open subscapularis tendon repair
 Acta Orthop. Belg., 2008, 74, 173179 ORIGAL STUDY Rotator cuff strength following open subscapularis tendon repair Roger P. VAN RIET, Sean T. O LEARY, Alexander HOOP, Simon N. BELL From the Melbourne Shoulder
Acta Orthop. Belg., 2008, 74, 173179 ORIGAL STUDY Rotator cuff strength following open subscapularis tendon repair Roger P. VAN RIET, Sean T. O LEARY, Alexander HOOP, Simon N. BELL From the Melbourne Shoulder
Common Surgical Shoulder Injury Repairs
 Common Surgical Shoulder Injury Repairs Mr Ilia Elkinson BHB, MBChB, FRACS (Ortho), FNZOA Orthopaedic and Upper Limb Surgeon Bowen Hospital Wellington Hospital Objectives Review pertinent anatomy of the
Common Surgical Shoulder Injury Repairs Mr Ilia Elkinson BHB, MBChB, FRACS (Ortho), FNZOA Orthopaedic and Upper Limb Surgeon Bowen Hospital Wellington Hospital Objectives Review pertinent anatomy of the
Don t forget the open Bankart Look at the evidence
 Review Article Page 1 of 7 Don t forget the open Bankart Look at the evidence Luke Sanborn 1, Robert A. Arciero 2, Justin S. Yang 3 1 Drexel University College of Medicine, Philadelphia, USA; 2 Department
Review Article Page 1 of 7 Don t forget the open Bankart Look at the evidence Luke Sanborn 1, Robert A. Arciero 2, Justin S. Yang 3 1 Drexel University College of Medicine, Philadelphia, USA; 2 Department
