First Metatarsophalangeal Joint Replacement with Modular Three-Component Press-Fit Implant. Preliminary Report
|
|
|
- Jerome Russell
- 5 years ago
- Views:
Transcription
1 64/, p First Metatarsophalangeal Joint Replacement with Modular Three-Component Press-Fit Implant. Preliminary Report Náhrada prvního metatarzofalangeálního kloubu modulární trojdílnou press-fit endoprotézou. První zkušenosti L. Kolodziej, A. Bohatyrewicz, P. Zietek Department of Orthopaedics, Traumatology and Musculoskeletal Oncology, Pomeranian Medical University, Szczecin, Poland ABSTRACT Purpose of the study The aim of this retrospective study was to assess functional and radiographic results of the first metatarsophalangeal joint replacement with use of unconstrained, modular, three components, porous titanium and hydroxyapatite coated, press-fit METIS prosthesis. According to author s knowledge, results of that type of prosthesis have never been published before. Material and methods 25 prosthesis were implanted in 24 patients between February 2009 and May American Orthopaedic Foot and Ankle Society Hallux Metatarsophalangeal Interphalangeal scoring system (AOFAS-HMI) was used to assess functional results. Patients were also asked if they would undergo procedure again or recommend it to other people. Weight bearing radiographs ware made at final follow up and analyzed for presence of osteolysis and radiolucencies. In 8 patients total joint replacement was introduced as a salvage after failure of previous surgery like Keller resection arthroplasty, failed arthrodesis, avascular necrosis and postoperative arthritis. In 11 patients the reason for prosthetic replacement were hallux rigidus, in 4 cases rheumatoid arthritis and gout in one patient. In two patients additional procedures like Akin phalangeal osteotomy and in one case fifth metatarsal osteotomy, was performed. There were 20 females and 4 males in presented group. The mean age at the operation was 56 years. The average follow up period was 18 months (from 12 to 36 months). Results The median postoperative value of AOFAS-HMI scores was 88 points (from 75 to 95 points). First metatarsophalangeal joint motion (dorsiflexion plus plantarflexion) was classified according to AOFAS-HMI ranges as: moderately restricted (between 30 to 70 degrees) in 19 patients 80% (20 prosthesis) and severely restricted (less then 30 degrees) in 5 patients (20%). 15 (64%) patients were completely satisfied, 5 (20%) reported moderate satisfaction and (16%) 4 were totally disappointed and would not undergo this procedure again. A limited hallux dorsiflexion was the main dissatisfaction reason. Partial radiolucent line was seen in one patient (4%). Authors noticed two serious complications. In one patient, with rheumatoid arthritis, deep infection occurred 12 months after prosthesis implantation. In second case phalangeal implant was revised due to misalignment. Conclusions METIS metatarsophalangeal joint replacement allows alleviate of pain relating to hallux rigidus and partial restoration of joint movement, even in patients after failures of primary metatarsophalangeal joint surgery. AOFAS-HMI results are better than previously reported in the literature in assessment of the first metatarsophalangeal joint replacement. Radiographic results imply satisfactory bone ingrowth into the cementless implants. Key words: great toe, metatarsophalangeal total joint replacement, hallux rigidus, arthrodesis.
2 65/ Introduction The role and usefulness of arthrodesis of the first metatarsophalangeal joint (MTPJ) for the treatment of primary foot problems and as a salvage procedure cannot be overestimated but improved understanding of the first MTPJ function leads to reassessment the role of implant arthroplasty. Fixed hallux position after MTPJ fusion has powerful impact on footwear, occupational and sport activities. First MTPJ mobility is vital for normal gait pattern, impact reduction, activation of windlass mechanism, assistance in balance and normal stance. Since total hip and knee replacement are among the most common and successful orthopaedic operations there is natural tendency among orthopaedic surgeons to introduce MTPJ replacement in the treatment primary and secondary osteoarthritis. The purpose of this retrospective study was to assess early functional and radiographic results, including perioperative complications during learning curve period, of the first metatarsophalangeal joint reconstruction with use of unconstrained, modular, three components, press-fit METIS prosthesis. Porous titanium and hydroxyapatite coating of phalangeal and metatarsal elements promotes osteointegration. According to author s knowledge, results of that type of prosthesis have never been published before. Material and methods 25 consecutive MTPJ replacement performed between February 2009 and May 2011 by one surgeon in 24 patients with use METIS replacements were included in the study. In order to eliminate surgeon bias independent senior clinical resident performed all measurements. To compare the results with those presented in the literature an American Orthopaedic Foot and Ankle Society Hallux Metatarsophalangeal Interphalangeal (AOFAS HMI) scoring system was used. This outcomescoring tool is referenced frequently in papers regarding MTPJ implant arthroplasty and allows comparing across studies (5, 16). The AOFAS-HMI questionnaire was distributed to patients, as a part of routine assessment before surgery in author s institution and during the last follow up. The passive range of motion (ROM) of the first meta tarsophalangeal joint was measured with a goniometer. Patients were also asked if they would undergo procedure again or recommend it to other people. In 8 (9 prosthesis) patients total joint replacement was introduced as salvage after failure of previous surgery like failed arthrodesis, avascular necrosis, and post operative arthritis. In one this patient total MTPJ replacement was performed bilaterally, after failed Keller resection arthroplasty. In 11 patients the reason for prosthetic replacement was hallux rigidus, in 4 cases rheumatoid arthritis and gout in 1 patient. There were 20 females and 4 males in presented group. The mean age at the operation was 56 years. The average follow up period was 18 months (from 12 to 36 months). Standard antero-posterior and lateral weight bearing radiographs ware made at final follow up and analyzed for presence of osteolysis and radiolucencies. A similar operative technique was performed in all patients. Author always used a medial incision. Postoperatively patients were asked to wear heel weight bearing shoes until complete wound healing and sutures removal and then full weight bearing was allowed. Patients were encouraged to perform maximal joint movements several times a day, and hill rising exercises while sitting, to increase dorsiflexion. Patients were routinely controlled 3, 6 and 12 weeks after surgery and then at final follow up. None of the patients was lost in follow up. All patients were treated with low molecular weight heparin injections for 14 days postoperatively. All data were collected and analyzed on Microsoft Excel software for mean scores, range and standard deviations. Mann Whitney s test was used for analysis of non-normally distributed data. The paired t-test was used to assess the mean scores pre and post treatment. All tests were done using a priori level of significance of Results The average preoperative value of AOFAS-HMI score was 40 points (from 15 to 67 points) and increased postoperatively to 88 points (from 75 to 95 points) (p < 0,005). Average preoperative, passive range of motion (ROM) was 10 degrees (from 0 to 17 degrees) and increased up 40 degrees (range from 10 to 55 degrees). Authors prefer to present data according to ranges in AOFAS-HMI scoring system. First MTPJ motion was classified as: moderately restricted (ROM between 30 to 70 degrees) in 19 patients 80% (20 prosthesis) and in 5 patients (20%) MTPJ motion was graded as severely restricted (ROM less then 30 degrees). Normal passive MTPJ motion was not restored in any case. 15 patients (64%) were completely satisfied, 5 (20%) reported moderate satisfaction, including one female with bilateral replacement and 4 (16%) were totally disappointed and would not undergo this procedure again. 16 joints (64%) were described as completely painless, 7 (28%) have mild, occasional pain and 2 patients (8%) suffered from moderate, daily pain. Radiographic assessment revealed consistent evidence of bone ingrowth. No radiolucent lines were identified, except one female (4%) with partial, narrow (less than 2 mm) radiolucent line at the tip of phalangeal component. That patient was asymptomatic and remained under regular control. In some cases some additional surgical procedures were performed. In 2 patients simultaneous Akin phalangeal osteotomy, located distal to phalangeal implant, was performed to correct interphalangeal valgus (Fig. 1 and Fig. 2). In one foot, the fifth metatarsal SCARF osteotomy was performed, to correct bunnionette deformity. Two serious complications occurred. In one patient with rheumatoid arthritis and previous history of septic metatarsophalangeal joint arthritis, deep infection occurred 12 months after prosthesis implantation. One attempt of irrigation and debridement was performed but finally, prosthesis needed to be removed. Full osseous osteointegration was observed in metatarsal and phalangeal prosthesis elements during implant removal. In one
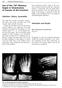
3 66/ 1 2a 2b Fig. 1. Antero-posterior weight bearing radiograph of a 63-year-old female patient with failure of metatarsophalangeal joint arthrodesis. Fig. 2. Antero-posterior and lateral weight bearing radiographs of the patient from figure 1 after metatarsophalangeal joint replacement with concomitant Akin-type proximal phalangeal osteotomy. case phalangeal implant was revised due to misplacement. Another, bigger size was implanted successfully without further complications. Discussion Arthrodesis of the first metatarsophalangeal joint (MTPJ) remains the gold standard for advanced a rthritis and salvage procedure after failure of previous surgical treatment (7, 8, 12, 22). Orthopaedic and podiatric literature, regarding MTPJ arthrodesis, focus on non-union rates, position of the hallux and technical aspects of the surgical procedure. Arthrodesis results are graded as excellent or good when bony fusion is achieved or even in asymptomatic, painless
4 67/ nonunion (25, 26). According to some authors fusion of an osteoarthritic MTPJ improves gait, medial arch stability and weight bearing on the medial part of the foot (1, 11, 14, 20). Powerful biomechanical changes following MTPJ arthrodesis were confirmed with plantar pressure measurements and on weight bearing radiographs (2, 18, 19). Surprisingly there is lack of studies comparing osteoarthritis in other major joints, like knee, hip and low back pain with changes in foot biomechanics after fusion MTPJ. Altered foot posture affects kinematics of the knee, hip, spine and thorax, medial knee osteoarthritis and low back pain are significantly associated with foot pain and function (17, 23, 24, 28). The increased recognition of the MTPJ function in achieving normal gait, turned interest of researchers into development functional joint replacement. Double stemmed, silicone Swanson type designed resulted in joint stiffness, reactive bone response and periarticular bone loss (27,30). Radiolucency and lytic bone areas decreased with addition of press-fit titanium grommets, to protect silicone from sharp bone edges, implant abrasion and reactive synovitis but a functional outcome of silicone implants, assessed by AOFAS HMI scored up to 83 points (29). Results of ceramic total MTPJ arthroplasty are worse and mean values of AOFAS HMI are up to 74 points, with 30 % of patients suffering from moderate, daily pain and 50% have severely restricted, with ROM less than 30 degrees MTPJ motion (6). New implants introduced in last decade, using two non cemented, pressfit components with polyethylene inlay, seemed to offer markedly increase in MTPJ movements. Average postoperative ROM presented into two recent reports was 38 and 52 degrees and slight general improvement was observed up to 18 months after surgery. Daniilidis et al. achieved one of the biggest prosthesis movements but he selected only grade III hallux rigidus patients excluding those with failed previous surgery where stiffness is more likely to occur (4, 9). Implant presented in these paper is one of the most recent designs with bone preserving feature or rather resurfacing instead osteotomizing the first metatarsal head, and enables arthrodesis as a salvage procedure. In case, with recurrent periprostetic infection, perfect osteointegration was observed during implant removal. As that patient has very active form of rheumatoid arthritis further surgical treatment is postponed. In two cases an Akin-type phalangeal osteotomy was performed to correct interphalangeal valgus and rotation. Additional procedure performed on proximal phalanx did not interfere with prosthesis osteointegration and these patients are among very satisfied group. No signs of phalangeal implant loosening ware observed in these patients in more than 24 months follow up (Fig 1 and 2). Gibson and Thomas in randomized control trial reported higher patients satisfaction after arthrodesis than total arthroplasty (82% versus 58% of satisfied patients after 12 months follow up). Authors, as a part of surgical technique in total MTPJ arthroplasty, routinely performed lateral sesamoid resection in order to prevent impingement against the prosthesis (13). Lateral sesamoidectomy significantly decreases the effective flexor hallucis longus tendon moment arms, is known as cause of post-surgical hallux varus and alone could be the source of pain, hallux malaligment and further movement limitation (3). Gibson and Thomas report more than 15% loosening of the uncemented, plasma spray phalangeal component and in order to avoid further failures started to cement phalangeal implant in next and revision cases (13). Double-coated hip prosthesis stems, in comparison with plain porous femoral components has demonstrated better results with hydroxyapatite than porous alone in terms of quality of bone remodelling, and the potential migration and subsidence of the stem (10). These may indicate that addition of hydroxyapatite coatings can promote earlier and stronger fixation in metatarsal and phalangeal bone and this type of fixation between the bone and the prosthesis is used in most recent metatarsophalangeal implant designs (15). The range of sagittal MTPJ motion is the main reported outcome in assessments the results of total joint replacement. In presented paper postoperative MTPJ movements were restricted in every case although more than 80% of patients were completely or moderately satisfied from performed surgery. These could be explained by that motion requirement during normal walking, are smaller than passive, non weight baring measurements (21). Performed surgeries have powerful effect on pain release. More than 90% of patients are completely pain free or have only mild, occasional pain what is close to results obtained after arthrodesis of the MTPJ, procedure regarded as a gold standard regarding pain relief (1, 11, 14, 20, 25, 26). Functional results assessed with AOFAS-HMI scoring system are among the highest results published in the literature (4, 5, 6, 9, 13, 29). Authors did not record any implant breakage or dislocations like reported in other series (5, 6, 29, 30). A presented series showed no early failure of bone ingrowth into prosthesis components. The main limitations of present study are retrospective nature and relatively short follow up period although several reports with similar length of follow up period are published (4, 5, 9). According to author s knowledge, this is the first, preliminary report on METIS total metatarsophalangeal joint arthroplasty and await the results of other prospective investigation. Conclusions METIS metatarsophalangeal joint replacement allows alleviate of pain relating to hallux rigidus and partial restoration of joint movement, even in patients after failures of primary metatarsophalangeal joint surgery. AOFAS-HMI results are better than previously reported in the literature in assessment of the first metatarsophalangeal joint replacement. Radiographic results imply satisfactory bone ingrowth into the cementless implants.
5 68/ References 1. Aas, M., Johnsen, T. M., Finsen, V.: Arthrodesis of the first metatarsophalangeal joint for hallux rigidus--optimal position of fusion. Foot, 18: , Agoropoulos, Z., Efastathopoulos, N., Mataliotakis, J.: Long-term results of first metatarsophalangeal joint fusion for severe hallux valgus deformity. Foot Ankle Surg., 7: Aper, R. L., Saltzman, C. L., Brown, T. D.: The effect of hallux sesamoid excision on the flexor hallucis longus moment arm. Clin Orthop Relat Res., 325: , Barták, V., Popelka, S., Hromádka, R., Pech, J., Jahoda, D., Sosna, A.: ToeFit-Plus system for replacement of the first metatarsophalangeal joint. Acta Chir orthop. Traum. čech., 77: , Brewster, M.: Does total joint replacement or arthrodesis of the first metatarsophalangeal joint yield better functional results? A systematic review of the literature. J. Foot Ankle Surg., 49: , Brewster, M., Mc Arthur, J., Mauffrey, C., Lewis, A. C., Hull, P., Ramos, J.: Moje first metatarsophalangeal replacement- a case series with functional outcomes using the AOFAS-HMI score. J. Foot Ankle Surg., 49: 37 42, Coughlin, M. J, Shurnas, P. S.: Hallux rigidus. Grading and long-term results of operative treatment. J. Bone Jt Surg., 85- A: , Coughlin, M. J., Shurnas P. S.: Hallux rigidus. J Bone Jt Surg., 86-A : , Daniilidis, K., Martinelli, N., Marinozzi, A., Denerao, V., Gosheger, G., Pejman, Z., Buchhorn, T.: Recreational sport activity after total replacement of the first metatarsophalangeal joint: a prospective study. International Orthopaedics, 34: , Epinette, J. A., Manley, M. T.: Uncemented stems in hip replacement--hydroxyapatite or plain porous: does it matter? Based on a prospective study of HA Omnifit stems at 15-years minimum follow-up. Hip Int., 18:69 74, Fuhrmann, R. A: First metatarsophalangeal arthrodesis for hallux rigidus. Foot Ankle Clin., 16: Giannini, S., Ceccarelli, F., Faldini, C., Bevoni, R., Grandi, G., Vannini, F: What s new in surgical options for hallux rigidus?. J. Bone Jt Surg.,.86-A (suppl. 2): 72 83, Gibson, J. N., Thomson, C. E.: Arthrodesis or total replacement arthroplasty for hallux rigidus: a randomized controlled trial. Foot Ankle Int., 26: Hamilton, G. A., Ford, L. A., Patel, S.: First metatarsophalangeal joint arthrodesis and revision arthrodesis. Clin. Podiatr. Med. Surg., 26: Hromádka, R., Barták, V., Sosna, A., Popelka, S.: MEDIN implant of the first metatarsophalangeal joint. Acta Chir. orthop. Traum. čech.,79: Kitaoka, H. B., Alexander, I. J., Adelaar, R. S., Nunley, J. A., Meyerson, M. S., Sanders, M.: Clinical rating system for the ankle, hindfoot, midfoot, hallux and lesser toes. Foot Ankle Int., 15: , Levinger, P., Menz, H., B., Fotoohabadi, M. R., Feller, J. A., Bartlett, J., R., Bergman, N. R.: Foot posture in people with medial compartment knee osteoarthritis. J. Foot Ankle Res., 16: 29, Lombardi, C. M., Silhanek, A. D., Connolly, F. G., Dennis, L. N.: The effect of first metatarsophalangeal joint arthrodesis on the first ray and the medial longitudinal arch: a radiographic study. J. Foot Ankle Surg., 41: Luninghake, F., Tillmann, K., Russlies, M: Biomechanical changes following surgical treatment of MTP-I-osteoarthritis. Foot,12: Maher, A. J., Metcalfe, S. A.: First MTP joint arthrodesis for the treatment of hallux rigidus: results of 29 consecutive cases using the foot health status questionnaire validated measurement tool. Foot,18: , Nawoczenski, D. A., Baumhauer, J. F., Umberger, B. R.: Relationship between clinical measurements and motion of the first metatarsophalangeal joint during gait. J. Bone Jt Surg., 81-A: , Nunez-Samper, M. N., Kubba, M., N., Palomo, R., Perez, P.: Metatarsophalangeal arthrodesis of the first ray. When is it indicated? Foot, 15: , Reilly K., Barker, K., Shamley, D., Newman, M., Oskrochi, G. R., Sandall, S.: The role of foot and ankle assessment of patients with lower limb osteoarthritis. Physiotherapy, 95: , Reilly, A. K., Barker, L., K., Shamley, D., Sandall, S.: Influence of foot characteristics on the site of lower limb osteoarthritis. Foot Ankle Int., 27: , Shahane, S. A., Vedantam, R., Bhadreshwar D. R.: Arthrodesis of the first metatarsophalangeal joint using AO tension band wire. Foot, 11: Sharma, V., Geary, N. P. J.: Long term retrospective analysis of the first metatarsophalangeal joint arthrodesis with two crossed screws. Foot, 11: Smetana, M., Vencálková, S.: Use of a silicone metatarsophalangeal joint endoprosthesis in hallux rigidus over a 15-year period. Acta Chir. orthop. Traum. čech., 70: , Suri, P., Morgenroth, D. C., Kwoh, C. K., Bean, J. F., Kalichman, L., Hunter, D. J.: Low back pain and other musculoskeletal pain comorbidities in individuals with symptomatic osteoarthritis of the knee: data from the osteoarthritis initiative. Arthritis Care Res., 62: , Ter Keurs, E. W., Wassink, S., Burger, B. J., Hubach, P. C.: First metatarsophalangeal joint replacement: long-term results of a double stemmed flexible silicone prosthesis. Foot Ankle Surg., 17: , Weil, L. S., Pollak, R. A., Goller, W. L.: Total first joint replacement in hallux valgus and hallux rigidus. Long-term results in 484 cases. Clin. Podiatry., 1:103 29, Corresponding author: Lukasz Kołodziej, M.D. Department of Orthopaedics, Traumatology and Musculoskeletal Oncology Pomeranian Medical University ul. Rybacka Szczecin, Poland lukas@hot.pl
NON-CONSTRAINED TITANIUM-POLYETHYLENE TOTAL ENDOPROSTHESIS IN THE TREATMENT OF HALLUX RIGIDUS A prospective clinical 2-year follow-up study
 Scandinavian Journal of Surgery 91: 202 207, 2002 NON-CONSTRAINED TITANIUM-POLYETHYLENE TOTAL ENDOPROSTHESIS IN THE TREATMENT OF HALLUX RIGIDUS A prospective clinical 2-year follow-up study P. Ess, M.
Scandinavian Journal of Surgery 91: 202 207, 2002 NON-CONSTRAINED TITANIUM-POLYETHYLENE TOTAL ENDOPROSTHESIS IN THE TREATMENT OF HALLUX RIGIDUS A prospective clinical 2-year follow-up study P. Ess, M.
Metatarsophalangeal joint replacement for hallux rigidus: a developing field
 OPN issue 168 Metatarsophalangeal joint replacement for hallux rigidus: a developing field Maire-Clare Killen, Liam McEntee, Mohan Emmanuel, Prasad Karpe and Rajiv Limaye describe the use of arthroplasty
OPN issue 168 Metatarsophalangeal joint replacement for hallux rigidus: a developing field Maire-Clare Killen, Liam McEntee, Mohan Emmanuel, Prasad Karpe and Rajiv Limaye describe the use of arthroplasty
Medical Policy Partial or Total Replacement of First Metatarsophalangeal Joint
 Medical Policy Partial or Total Replacement of First Metatarsophalangeal Joint Subject: Partial or Total Replacement of First Metatarsophalangeal (MTP) Joint Background: Underlying causes of disease or
Medical Policy Partial or Total Replacement of First Metatarsophalangeal Joint Subject: Partial or Total Replacement of First Metatarsophalangeal (MTP) Joint Background: Underlying causes of disease or
ORIGINAL ARTICLE. Keywords Hallux Rigidus; Metatarsophalangeal Joint; Arthroplasty
 ORIGINAL ARTICLE Preliminary Results from the METIS-Newdeal total metatarsophalangeal prosthesis Luís Fernando Nunes Pires Silva 1, Cristina Varino Sousa 1, Ricardo Rodrigues Pinto 2, Claudia Santos 2,
ORIGINAL ARTICLE Preliminary Results from the METIS-Newdeal total metatarsophalangeal prosthesis Luís Fernando Nunes Pires Silva 1, Cristina Varino Sousa 1, Ricardo Rodrigues Pinto 2, Claudia Santos 2,
A perspective on MPJ implant arthroplasty.
 A perspective on MPJ implant arthroplasty. The BioPro MPJ Hemi Implant System: +65 years of successful clinical use. Pre-op Post-op 20+ year implant survivorship 14 96% Survivorship 1 97% Patient Satisfaction
A perspective on MPJ implant arthroplasty. The BioPro MPJ Hemi Implant System: +65 years of successful clinical use. Pre-op Post-op 20+ year implant survivorship 14 96% Survivorship 1 97% Patient Satisfaction
PAINFUL SESAMOID OF THE GREAT TOE Dr Vasu Pai ANATOMICAL CONSIDERATION. At the big toe MTP joint: Tibial sesamoid (medial) & fibular (lateral)
 PAINFUL SESAMOID OF THE GREAT TOE Dr Vasu Pai ANATOMICAL CONSIDERATION At the big toe MTP joint: Tibial sesamoid (medial) & fibular (lateral) They are contained within the tendons of Flexor Hallucis Brevis
PAINFUL SESAMOID OF THE GREAT TOE Dr Vasu Pai ANATOMICAL CONSIDERATION At the big toe MTP joint: Tibial sesamoid (medial) & fibular (lateral) They are contained within the tendons of Flexor Hallucis Brevis
RISK FACTORS FOR SUBOPTIMAL OUTCOMES IN HAMMERTOE SURGERY JACOB RANDICH BS
 RISK FACTORS FOR SUBOPTIMAL OUTCOMES IN HAMMERTOE SURGERY JACOB RANDICH BS RACHEL ALBRIGHT DPM, MOIZ HASSAN MS, ROBERT O KEEFE DPM, ERIN E. KLEIN DPM, MS, LOWELL WEIL JR. DPM, MBA, LOWELL WEIL SR. DPM,
RISK FACTORS FOR SUBOPTIMAL OUTCOMES IN HAMMERTOE SURGERY JACOB RANDICH BS RACHEL ALBRIGHT DPM, MOIZ HASSAN MS, ROBERT O KEEFE DPM, ERIN E. KLEIN DPM, MS, LOWELL WEIL JR. DPM, MBA, LOWELL WEIL SR. DPM,
Foot and ankle update
 Foot and ankle update Mr Ian Garnham Consultant Foot and Ankle Surgeon Whipps Cross University Hospital Hallux Rigidus Symptoms first ray and 1st MTP pain and swelling worse with push off or forced dorsiflexion
Foot and ankle update Mr Ian Garnham Consultant Foot and Ankle Surgeon Whipps Cross University Hospital Hallux Rigidus Symptoms first ray and 1st MTP pain and swelling worse with push off or forced dorsiflexion
Hallux Rigidus & Silastic Total Implants
 Hallux Rigidus & Silastic Total Implants JOSHUA L. MOORE, DPM FACFAS ASSISTANT DEAN OF EDUCATIONAL AFFAIRS TUSPM CLINICAL ASSISTANT PROFESSOR OF SURGERY Definitions Hallux Limitus 1 st MTPJ range of motion
Hallux Rigidus & Silastic Total Implants JOSHUA L. MOORE, DPM FACFAS ASSISTANT DEAN OF EDUCATIONAL AFFAIRS TUSPM CLINICAL ASSISTANT PROFESSOR OF SURGERY Definitions Hallux Limitus 1 st MTPJ range of motion
SURGICAL TECHNIQUE CHI. Cannulated Hemi Implants 1 ST MPJ ARTHROPLASTY
 CHI Cannulated Hemi Implants 1 ST MPJ ARTHROPLASTY SURGICAL TECHNIQUE CHI Cannulated Hemi Implants Design Rationale Pain of the great toe joint often leads to altered lifestyles. The goal of MPJ implant
CHI Cannulated Hemi Implants 1 ST MPJ ARTHROPLASTY SURGICAL TECHNIQUE CHI Cannulated Hemi Implants Design Rationale Pain of the great toe joint often leads to altered lifestyles. The goal of MPJ implant
EARLY CLINICAL RESULTS OF PRIMARY CEMENTLESS TOTAL KNEE ARTHROPLASTY
 EARLY CLINICAL RESULTS OF PRIMARY CEMENTLESS TOTAL KNEE ARTHROPLASTY Benkovich V. Perry T., Bunin A., Bilenko V., Unit for Joint Arthroplasty, Soroka Medical Center Ben Gurion University of Negev Beer
EARLY CLINICAL RESULTS OF PRIMARY CEMENTLESS TOTAL KNEE ARTHROPLASTY Benkovich V. Perry T., Bunin A., Bilenko V., Unit for Joint Arthroplasty, Soroka Medical Center Ben Gurion University of Negev Beer
Investigation performed at the Department of Orthopaedic and Trauma Surgery, Glasgow Royal Infirmary, Glasgow, United Kingdom
 748 COPYRIGHT 2005 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Long-Term Results of the Modified Hoffman Procedure in the Rheumatoid Forefoot BY S. THOMAS, MBCHB, BSC, MRCS, A.W.G. KINNINMONTH,
748 COPYRIGHT 2005 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Long-Term Results of the Modified Hoffman Procedure in the Rheumatoid Forefoot BY S. THOMAS, MBCHB, BSC, MRCS, A.W.G. KINNINMONTH,
First metatarsophalangeal hemiarthroplasty for hallux rigidus
 DOI 10.1007/s00264-010-1012-x ORIGINAL PAPER First metatarsophalangeal hemiarthroplasty for hallux rigidus Eric Giza & Martin Sullivan & Dan Ocel & Gregory Lundeen & Matt Mitchell & Lauren Frizzell Received:
DOI 10.1007/s00264-010-1012-x ORIGINAL PAPER First metatarsophalangeal hemiarthroplasty for hallux rigidus Eric Giza & Martin Sullivan & Dan Ocel & Gregory Lundeen & Matt Mitchell & Lauren Frizzell Received:
Use of the 20 Memory Staple in Osteotomies of Fusions of the Forefoot
 168 Forefoot Reconstruction Use of the 20 Memory Staple in Osteotomies of Fusions of the Forefoot Definition, History, Generalities This staple first provides a permanent compression both in the prongs
168 Forefoot Reconstruction Use of the 20 Memory Staple in Osteotomies of Fusions of the Forefoot Definition, History, Generalities This staple first provides a permanent compression both in the prongs
Re+Line Bunion Correction System for Correction of Hallux Abducto Valgus Deformity
 Re+Line Bunion Correction System for Correction of Hallux Abducto Valgus Deformity Amber M. Shane, DPM, FACFAS 1, Christopher L. Reeves, DPM, FACFAS 1 1. Orlando Foot & Ankle Clinic, Orlando, FL Abstract
Re+Line Bunion Correction System for Correction of Hallux Abducto Valgus Deformity Amber M. Shane, DPM, FACFAS 1, Christopher L. Reeves, DPM, FACFAS 1 1. Orlando Foot & Ankle Clinic, Orlando, FL Abstract
A Patient s Guide to Hallux Rigidus
 A Patient s Guide to Hallux Rigidus Suite 11-13/14/15 Mount Elizabeth Medical Center 3 Mount Elizabeth Singapore, 228510 Phone: (65) 6738 2628 Fax: (65) 6738 2629 DISCLAIMER: The information in this booklet
A Patient s Guide to Hallux Rigidus Suite 11-13/14/15 Mount Elizabeth Medical Center 3 Mount Elizabeth Singapore, 228510 Phone: (65) 6738 2628 Fax: (65) 6738 2629 DISCLAIMER: The information in this booklet
HEMI IMPLANT ARTHROPLASTY FOR THE SECOND METATARSOPHALANGEAL JOINT
 C H A P T E R 1 5 HEMI IMPLANT ARTHROPLASTY FOR THE SECOND METATARSOPHALANGEAL JOINT Joe T. Southerland, DPM Mickey D. Stapp, DPM INTRODUCTION Hemi-implant arthroplasty of the first metatarsophalangeal
C H A P T E R 1 5 HEMI IMPLANT ARTHROPLASTY FOR THE SECOND METATARSOPHALANGEAL JOINT Joe T. Southerland, DPM Mickey D. Stapp, DPM INTRODUCTION Hemi-implant arthroplasty of the first metatarsophalangeal
Combination of First Metatarsophalangeal Joint Arthrodesis and Proximal Correction for Severe Hallux Valgus Deformity
 FOOT &ANKLE INTERNATIONAL DOI: 10.3113/FAI.2012.0400 Combination of First Metatarsophalangeal Joint Arthrodesis and Proximal Correction for Severe Hallux Valgus Deformity Pascal F. Rippstein, MD; Young-Uk
FOOT &ANKLE INTERNATIONAL DOI: 10.3113/FAI.2012.0400 Combination of First Metatarsophalangeal Joint Arthrodesis and Proximal Correction for Severe Hallux Valgus Deformity Pascal F. Rippstein, MD; Young-Uk
Intermediate outcome of interpositional arthroplasty for the treatment of hallux rigidus. Anand Vora, MD
 Intermediate outcome of interpositional arthroplasty for the treatment of hallux rigidus Anand Vora, MD CONFLICT TO DISCLOSE Intermediate outcome of interpositional arthroplasty for the treatment of hallux
Intermediate outcome of interpositional arthroplasty for the treatment of hallux rigidus Anand Vora, MD CONFLICT TO DISCLOSE Intermediate outcome of interpositional arthroplasty for the treatment of hallux
Modified Proximal Scarf Osteotomy for Hallux Valgus
 Original Article Clinics in Orthopedic Surgery 2018;10:479-483 https://doi.org/10.4055/cios.2018.10.4.479 Modified Proximal Scarf Osteotomy for Hallux Valgus Ki Won Young, MD, Hong Seop Lee, MD, Seong
Original Article Clinics in Orthopedic Surgery 2018;10:479-483 https://doi.org/10.4055/cios.2018.10.4.479 Modified Proximal Scarf Osteotomy for Hallux Valgus Ki Won Young, MD, Hong Seop Lee, MD, Seong
The Lapidus Procedure as Salvage After Failed Surgical Treatment of Hallux Valgus A PROSPECTIVE COHORT STUDY
 60 COPYRIGHT 2003 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED The Lapidus Procedure as Salvage After Failed Surgical Treatment of Hallux Valgus A PROSPECTIVE COHORT STUDY BY J. CHRIS COETZEE,
60 COPYRIGHT 2003 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED The Lapidus Procedure as Salvage After Failed Surgical Treatment of Hallux Valgus A PROSPECTIVE COHORT STUDY BY J. CHRIS COETZEE,
A Patient s Guide to Hallux Rigidus
 A Patient s Guide to Hallux Rigidus Glendale Adventist Medical Center 1509 Wilson Terrace Glendale, CA 91206 Phone: (818) 409-8000 DISCLAIMER: The information in this booklet is compiled from a variety
A Patient s Guide to Hallux Rigidus Glendale Adventist Medical Center 1509 Wilson Terrace Glendale, CA 91206 Phone: (818) 409-8000 DISCLAIMER: The information in this booklet is compiled from a variety
Comparison of Postoperative Outcomes between Modified Mann Procedure and Modified Lapidus Procedure for Hallux Valgus
 Comparison of Postoperative Outcomes between Modified Mann Procedure and Modified Lapidus Procedure for Hallux Valgus Yui Akiyama, Takaaki Hirano, Hiroyuki Mitsui Shingo Maeda, Hisateru Niki Department
Comparison of Postoperative Outcomes between Modified Mann Procedure and Modified Lapidus Procedure for Hallux Valgus Yui Akiyama, Takaaki Hirano, Hiroyuki Mitsui Shingo Maeda, Hisateru Niki Department
NORTHERN OHIO FOUNDATION
 NORTHERN OHIO FOOT & ANKLE FOUNDATION! The!Northern!Ohio!Foot!and!Ankle!Journal!!!!!!!!!!!!!!!Official!Publication!of!the!NOFA!Foundation!! First MPJ Proximal Phalanx Hemi Implant Arthroplasty Literature
NORTHERN OHIO FOOT & ANKLE FOUNDATION! The!Northern!Ohio!Foot!and!Ankle!Journal!!!!!!!!!!!!!!!Official!Publication!of!the!NOFA!Foundation!! First MPJ Proximal Phalanx Hemi Implant Arthroplasty Literature
Investigation performed at Orthopaedic Hospital Gersthof, Vienna, Austria
 1131 COPYRIGHT 2004 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Salvage of a Failed Keller Resection Arthroplasty BY FELIX MACHACEK JR., MD, MARK E. EASLEY, MD, FLORIAN GRUBER, MD, PETER RITSCHL,
1131 COPYRIGHT 2004 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Salvage of a Failed Keller Resection Arthroplasty BY FELIX MACHACEK JR., MD, MARK E. EASLEY, MD, FLORIAN GRUBER, MD, PETER RITSCHL,
Section 6: Preoperative Planning
 Clinical Relevance of the PedCat Study: In many ways the PedCat study confirmed radiographic findings. With the measuring tools embedded in the DICOM viewing software it was possible to gauge the thickness
Clinical Relevance of the PedCat Study: In many ways the PedCat study confirmed radiographic findings. With the measuring tools embedded in the DICOM viewing software it was possible to gauge the thickness
Long-term results of the Hohmann and Lapidus procedure for the correction of hallux valgus
 FOOT AND ANKLE Long-term results of the Hohmann and Lapidus procedure for the correction of hallux valgus F. W. M. Faber, P. M. van Kampen, M. W. Bloembergen From HAGA Hospital, Den Haag, the Netherlands
FOOT AND ANKLE Long-term results of the Hohmann and Lapidus procedure for the correction of hallux valgus F. W. M. Faber, P. M. van Kampen, M. W. Bloembergen From HAGA Hospital, Den Haag, the Netherlands
First MPJ Hemi Implant
 First MPJ Hemi Implant Surgical Technique Contents Product The BioPro First MPJ Hemi Implant is a simple, durable, metallic hemiarthroplasty resurfacing prosthesis for the hallux metatarsophalangeal joint
First MPJ Hemi Implant Surgical Technique Contents Product The BioPro First MPJ Hemi Implant is a simple, durable, metallic hemiarthroplasty resurfacing prosthesis for the hallux metatarsophalangeal joint
Weil osteotomy and flexor to extensor transfer for irreparable plantar plate tear: prospective study
 Weil osteotomy and flexor to extensor transfer for irreparable plantar plate tear: prospective study Daniel Baumfeld, MD Fernando Raduan, MD Fernanda Catena, MD Tania Mann, MD Caio Nery, MD Disclosure
Weil osteotomy and flexor to extensor transfer for irreparable plantar plate tear: prospective study Daniel Baumfeld, MD Fernando Raduan, MD Fernanda Catena, MD Tania Mann, MD Caio Nery, MD Disclosure
Common Foot and Ankle Pathology DOTS 17th April Nick Savva Orthopaedic Foot and Ankle Surgeon. Monday, 29 April 13
 Common Foot and Ankle Pathology DOTS 17th April 2013 Nick Savva Orthopaedic Foot and Ankle Surgeon Monday, 29 April 13 Topics Forefoot pain Hindfoot/Ankle pain Hallux rigidus Bunions Toe deformity Mortons
Common Foot and Ankle Pathology DOTS 17th April 2013 Nick Savva Orthopaedic Foot and Ankle Surgeon Monday, 29 April 13 Topics Forefoot pain Hindfoot/Ankle pain Hallux rigidus Bunions Toe deformity Mortons
ABSTRACT. Key Words: Hallux Rigidus, toe, arthrodesis, fusion, arthroplasty, MTP, HemiCAP resurfacing. Level of Evidence: Review
 RESURFACING OF THE FIRST METATARSAL HEAD FOR THE TREATMENT OF HALLUX RIGIDUS: EVOLUTION OF IMPLANT DESIGN, REVIEW OF CLINICAL EXPERIENCE AND PRELIMINARY 5 YEAR RESULTS OF METATARSAL HEAD RESURFACING MTP
RESURFACING OF THE FIRST METATARSAL HEAD FOR THE TREATMENT OF HALLUX RIGIDUS: EVOLUTION OF IMPLANT DESIGN, REVIEW OF CLINICAL EXPERIENCE AND PRELIMINARY 5 YEAR RESULTS OF METATARSAL HEAD RESURFACING MTP
Proximal metatarsal osteotomy and distal soft tissue reconstruction as treatment for hallux valgus deformity
 REVIEW Proximal metatarsal osteotomy and distal soft tissue reconstruction as treatment for hallux valgus deformity Michael J. Coughlin and J. Speight Grimes Boise, Idaho, USA (Received for publication
REVIEW Proximal metatarsal osteotomy and distal soft tissue reconstruction as treatment for hallux valgus deformity Michael J. Coughlin and J. Speight Grimes Boise, Idaho, USA (Received for publication
Increased pressures at
 Surgical Off-loading of Plantar Hallux Ulcerations These approaches can be used to treat DFUs. By Adam R. Johnson, DPM Increased pressures at the plantar aspect of the hallux leading to chronic hyperkeratosis
Surgical Off-loading of Plantar Hallux Ulcerations These approaches can be used to treat DFUs. By Adam R. Johnson, DPM Increased pressures at the plantar aspect of the hallux leading to chronic hyperkeratosis
Great Toe Joint Replacement Patient Guide
 Great Toe Joint Replacement Patient Guide The BioPro First MPJ Hemi Implant The proven long-term joint fusion alternative. Long-term use Clinically proven High implant survivorship Long-term implant survivorship
Great Toe Joint Replacement Patient Guide The BioPro First MPJ Hemi Implant The proven long-term joint fusion alternative. Long-term use Clinically proven High implant survivorship Long-term implant survivorship
Optimum implant geometry
 Surgical Technique Optimum implant geometry Extending proven Tri-Lock heritage The original Tri-Lock was introduced in 1981. This implant was the first proximally coated tapered-wedge hip stem available
Surgical Technique Optimum implant geometry Extending proven Tri-Lock heritage The original Tri-Lock was introduced in 1981. This implant was the first proximally coated tapered-wedge hip stem available
Amputations of the digit, ray and midfoot
 Amputations of the digit, ray and midfoot Dane K. Wukich M.D. Chief, Division of Foot and Ankle Surgery Medical Director, UPMC Foot and Ankle Center University of Pittsburgh School of Medicine Disclosure
Amputations of the digit, ray and midfoot Dane K. Wukich M.D. Chief, Division of Foot and Ankle Surgery Medical Director, UPMC Foot and Ankle Center University of Pittsburgh School of Medicine Disclosure
Aetiology: Pressure of Distal intermetatarsal ligament against common digital nerve. Lumbar radiculopathy Instability MTPJ joint or inflammatory MPJ
 MORTON S NEUROMA 80% III web space (next common is II). Never occurs in III or IV Common in females in fifties Aetiology: Pressure of Distal intermetatarsal ligament against common digital nerve Rule out
MORTON S NEUROMA 80% III web space (next common is II). Never occurs in III or IV Common in females in fifties Aetiology: Pressure of Distal intermetatarsal ligament against common digital nerve Rule out
RETROSPECTIVE ANALYSIS OF END-TO-END DIGITAL ARTHRODESIS
 C H A P T E R 1 7 RETROSPECTIVE ANALYSIS OF END-TO-END DIGITAL ARTHRODESIS Michelle L. Butterworth, DPM Michael S. Downey, DPM Digital deformities are one of the most common entities we face as foot and
C H A P T E R 1 7 RETROSPECTIVE ANALYSIS OF END-TO-END DIGITAL ARTHRODESIS Michelle L. Butterworth, DPM Michael S. Downey, DPM Digital deformities are one of the most common entities we face as foot and
Disclosures. 55 year old Male 2/23/2018. Recurrent Hallux Rigidus: Options Other than Arthrodesis
 Recurrent Hallux Rigidus: Options Other than Arthrodesis Gregory C Berlet, MD FRCS(C), FAOA Orthopedic Foot and Ankle Columbus, Ohio Columbus, Ohio orthofootankle.com Disclosures Consultant/Speaker Bureau/Royalties/
Recurrent Hallux Rigidus: Options Other than Arthrodesis Gregory C Berlet, MD FRCS(C), FAOA Orthopedic Foot and Ankle Columbus, Ohio Columbus, Ohio orthofootankle.com Disclosures Consultant/Speaker Bureau/Royalties/
Distal metatarsal osteotomy for hallux varus following surgery for hallux valgus
 FOOT AND ANKLE Distal metatarsal osteotomy for hallux varus following surgery for hallux valgus K. J. Choi, H. S. Lee, Y. S. Yoon, S. S. Park, J. S. Kim, J. J. Jeong, Y. R. Choi From the Asan Medical Center,
FOOT AND ANKLE Distal metatarsal osteotomy for hallux varus following surgery for hallux valgus K. J. Choi, H. S. Lee, Y. S. Yoon, S. S. Park, J. S. Kim, J. J. Jeong, Y. R. Choi From the Asan Medical Center,
Bunion (hallux valgus deformity) surgery
 Bunion (hallux valgus deformity) surgery Bunion surgery is generally reserved for bunions that are severe and impacting on function. There most frequent surgical procedure used involves a medial incision
Bunion (hallux valgus deformity) surgery Bunion surgery is generally reserved for bunions that are severe and impacting on function. There most frequent surgical procedure used involves a medial incision
6/5/2018. Forefoot Disorders. Highgate Private Hospital (Royal Free London NHS Foundation Trust (Barnet & Chase Farm Hospitals) Hallux Rigidus
 Forefoot Disorders Mr Pinak Ray (MS, MCh(Orth), FRCS, FRCS(Tr&Orth)) Highgate Private Hospital (Royal Free London NHS Foundation Trust (Barnet & Chase Farm Hospitals) E: ray.secretary@uk-conslutants Our
Forefoot Disorders Mr Pinak Ray (MS, MCh(Orth), FRCS, FRCS(Tr&Orth)) Highgate Private Hospital (Royal Free London NHS Foundation Trust (Barnet & Chase Farm Hospitals) E: ray.secretary@uk-conslutants Our
Hallux Malleus develops after Flexible Hallux Varus correction with Tensioned Suture Device: A Case Report
 The Foot and nkle Online Journal Official publication of the International Foot & nkle Foundation Hallux Malleus develops after Flexible Hallux Varus correction with Tensioned Suture Device: Case Report
The Foot and nkle Online Journal Official publication of the International Foot & nkle Foundation Hallux Malleus develops after Flexible Hallux Varus correction with Tensioned Suture Device: Case Report
Index. Clin Podiatr Med Surg 22 (2005) Note: Page numbers of article titles are in boldface type.
 Clin Podiatr Med Surg 22 (2005) 309 314 Index Note: Page numbers of article titles are in boldface type. A Abductor digiti minimi muscle, myectomy of, for tailor s bunionette, 243 Achilles tendon, lengthening
Clin Podiatr Med Surg 22 (2005) 309 314 Index Note: Page numbers of article titles are in boldface type. A Abductor digiti minimi muscle, myectomy of, for tailor s bunionette, 243 Achilles tendon, lengthening
Symptomatic Medial Exostosis of the Great Toe Distal Phalanx: A Complication Due to Over-correction Following Akin Osteotomy for Hallux Valgus Repair
 Symptomatic Medial Exostosis of the Great Toe Distal Phalanx: A Complication Due to Over-correction Following Akin Osteotomy for Hallux Valgus Repair Carlos Villas, MD, PhD, 1 Javier Del Río, MD, 3 Andres
Symptomatic Medial Exostosis of the Great Toe Distal Phalanx: A Complication Due to Over-correction Following Akin Osteotomy for Hallux Valgus Repair Carlos Villas, MD, PhD, 1 Javier Del Río, MD, 3 Andres
Total Ankle Arthroplasty for the Treatment of Symptomatic Nonunion following Tibiotalar Fusion
 Total Ankle Arthroplasty for the Treatment of Symptomatic Nonunion following Tibiotalar Fusion W I L L I A M P. H U N T I N G T O N, M. D. W. H O D G E S D A V I S, M. D. R O B E R T B. A N D E R S O N,
Total Ankle Arthroplasty for the Treatment of Symptomatic Nonunion following Tibiotalar Fusion W I L L I A M P. H U N T I N G T O N, M. D. W. H O D G E S D A V I S, M. D. R O B E R T B. A N D E R S O N,
Interphalangeal Arthrodesis of the Toe with a New Radiolucent Intramedullary Implant
 Interphalangeal Arthrodesis of the Toe with a New Radiolucent Intramedullary Implant DIEBOLD P.-F., ROCHER H.,, DETERME P., CERMOLACCE C., GUILLO S., AVEROUS C., LEIBER WACKENHEIN F. Interphalangeal Arthrodesis
Interphalangeal Arthrodesis of the Toe with a New Radiolucent Intramedullary Implant DIEBOLD P.-F., ROCHER H.,, DETERME P., CERMOLACCE C., GUILLO S., AVEROUS C., LEIBER WACKENHEIN F. Interphalangeal Arthrodesis
University of Groningen. Forefoot disorders Schrier, Joost
 University of Groningen Forefoot disorders Schrier, Joost IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document version
University of Groningen Forefoot disorders Schrier, Joost IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document version
POSTOP FOLLOW-UP & REHABILITATION FOLLOWING FOOT & ANKLE SURGERY
 1 POSTOP FOLLOW-UP & REHABILITATION FOLLOWING FOOT & ANKLE SURGERY The following instructions are general guidelines, but surgeon post-op instructions will dictate the individual patient's post-op management
1 POSTOP FOLLOW-UP & REHABILITATION FOLLOWING FOOT & ANKLE SURGERY The following instructions are general guidelines, but surgeon post-op instructions will dictate the individual patient's post-op management
Medincenter GlavUpDK by the Ministry of Foreign Affairs of Russia, Moscow.
 Medincenter GlavUpDK by the Ministry of Foreign Affairs of Russia, Moscow. Berezhnoy Sergey. Percutaneous First Metatarsocuneiform Joint Arthrodesis in a Treatment of Metatarsus Primus Varus: a Prospective
Medincenter GlavUpDK by the Ministry of Foreign Affairs of Russia, Moscow. Berezhnoy Sergey. Percutaneous First Metatarsocuneiform Joint Arthrodesis in a Treatment of Metatarsus Primus Varus: a Prospective
Hallux Valgus Deformity: Preoperative Radiologic Assessment
 119 Pictorial Essay H............ - Hallux Valgus Deformity: Preoperative Radiologic Assessment David Karasick1 and Keith L. Wapner An estimated 40% of the American adult population experiences foot problems,
119 Pictorial Essay H............ - Hallux Valgus Deformity: Preoperative Radiologic Assessment David Karasick1 and Keith L. Wapner An estimated 40% of the American adult population experiences foot problems,
SWANSON. Flexible Hinge Toe Implant SURGIC AL TECHNIQUE
 SWANSON Flexible Hinge Toe Implant SURGIC AL TECHNIQUE SWANSON flexible HINGE TOE IMPLANT with SWANSON Flexible Hinge Grommet surgical technique presented by ALFRED B. SWANSON, MD, FACS, GRAND RAPIDS,
SWANSON Flexible Hinge Toe Implant SURGIC AL TECHNIQUE SWANSON flexible HINGE TOE IMPLANT with SWANSON Flexible Hinge Grommet surgical technique presented by ALFRED B. SWANSON, MD, FACS, GRAND RAPIDS,
WHAT DO HALLUX VALGUS AND BUNION MEAN?
 Mr Laurence James BSc MBBS MRCS(Eng) FRCS(Tr&Orth) Consultant Orthopaedic Surgeon Foot, Ankle and Sports Injuries WHAT DO HALLUX VALGUS AND BUNION MEAN? Hallux is Latin for great toe and Valgus is Latin
Mr Laurence James BSc MBBS MRCS(Eng) FRCS(Tr&Orth) Consultant Orthopaedic Surgeon Foot, Ankle and Sports Injuries WHAT DO HALLUX VALGUS AND BUNION MEAN? Hallux is Latin for great toe and Valgus is Latin
Lesser MPJ Hemi Implant
 Lesser MPJ Hemi Implant Surgical Technique Contents Product The BioPro Lesser MPJ Hemi Implant is a simple, durable, metallic hemiarthroplasty resurfacing prosthesis for the treatment of arthritis, Freiberg
Lesser MPJ Hemi Implant Surgical Technique Contents Product The BioPro Lesser MPJ Hemi Implant is a simple, durable, metallic hemiarthroplasty resurfacing prosthesis for the treatment of arthritis, Freiberg
Hypermobility of the first metatarsal bone in patients with Rheumatoid arthritis treated by lapidus procedure
 Popelka et al. BMC Musculoskeletal Disorders 2012, 13:148 RESEARCH ARTICLE Open Access Hypermobility of the first metatarsal bone in patients with Rheumatoid arthritis treated by lapidus procedure Stanislav
Popelka et al. BMC Musculoskeletal Disorders 2012, 13:148 RESEARCH ARTICLE Open Access Hypermobility of the first metatarsal bone in patients with Rheumatoid arthritis treated by lapidus procedure Stanislav
A Comparison of the Effects of First Metatarsophalangeal Joint Arthrodesis and Hemiarthroplasty on Function of Foot Forces using Gait Analysis
 The Foot and Ankle Online Journal Official publication of the International Foot & Ankle Foundation A Comparison of the Effects of First Metatarsophalangeal Joint Arthrodesis and Hemiarthroplasty on Function
The Foot and Ankle Online Journal Official publication of the International Foot & Ankle Foundation A Comparison of the Effects of First Metatarsophalangeal Joint Arthrodesis and Hemiarthroplasty on Function
> ZIMMER Total Ankle Arthroplasty. Fabian Krause Inselspital, University of Berne
 Fabian Krause Inselspital, University of Berne 1 > 9/14 > 76 years, female > Posttraumatic end-stage ankle arthrosis > Ankle ROM D/F 10-0-20 2 > 2/15 3 > 1/17 > Ongoing anterior ankle pain, ankle ROM restricted,
Fabian Krause Inselspital, University of Berne 1 > 9/14 > 76 years, female > Posttraumatic end-stage ankle arthrosis > Ankle ROM D/F 10-0-20 2 > 2/15 3 > 1/17 > Ongoing anterior ankle pain, ankle ROM restricted,
Foot and Ankle Polyvinyl alcohol hemiarthroplasty for first metatarsophalangeal joint arthritis
 SPECIAL FOCUS Foot and Ankle Polyvinyl alcohol hemiarthroplasty for first metatarsophalangeal joint arthritis Alastair S.E. Younger a, Judith F. Baumhauer b and Mark Glazebrook c ABSTRACT End stage arthritis
SPECIAL FOCUS Foot and Ankle Polyvinyl alcohol hemiarthroplasty for first metatarsophalangeal joint arthritis Alastair S.E. Younger a, Judith F. Baumhauer b and Mark Glazebrook c ABSTRACT End stage arthritis
Scar Engorged veins. Size of the foot [In clubfoot, small foot]
![Scar Engorged veins. Size of the foot [In clubfoot, small foot] Scar Engorged veins. Size of the foot [In clubfoot, small foot]](/thumbs/78/77722241.jpg) 6. FOOT HISTORY Pain: Walking, Running Foot wear problem Swelling; tingly feeling Deformity Stiffness Disability: At work; recreation; night; walk; ADL, Sports Previous Rx Comorbidities Smoke, Sugar, Steroid
6. FOOT HISTORY Pain: Walking, Running Foot wear problem Swelling; tingly feeling Deformity Stiffness Disability: At work; recreation; night; walk; ADL, Sports Previous Rx Comorbidities Smoke, Sugar, Steroid
The effectiveness of distal soft tissue procedures in hallux valgus
 J Orthopaed Traumatol (2008) 9:117 121 DOI 10.1007/s10195-008-0017-3 ORIGINAL ARTICLE The effectiveness of distal soft tissue procedures in hallux valgus Cemil Kayali Æ Hasan Ozturk Æ Haluk Agus Æ Taskin
J Orthopaed Traumatol (2008) 9:117 121 DOI 10.1007/s10195-008-0017-3 ORIGINAL ARTICLE The effectiveness of distal soft tissue procedures in hallux valgus Cemil Kayali Æ Hasan Ozturk Æ Haluk Agus Æ Taskin
Preservation of the First Ray in Patients with Diabetes
 Preservation of the First Ray in Patients with Diabetes Surgical approaches are often necessary to off-load excessive pressure. By Derek Ley, DPM, and Barry Rosenblum, DPM Introduction In approaching diabetic
Preservation of the First Ray in Patients with Diabetes Surgical approaches are often necessary to off-load excessive pressure. By Derek Ley, DPM, and Barry Rosenblum, DPM Introduction In approaching diabetic
What Happens to the Paediatric Flat Foot? Peter J Briggs Freeman Hospital Newcastle upon Tyne
 What Happens to the Paediatric Flat Foot? Peter J Briggs Freeman Hospital Newcastle upon Tyne We don t know!! Population Studies 2300 children aged 4-13 years Shoe wearers Flat foot 8.6% Non-shoe wearers
What Happens to the Paediatric Flat Foot? Peter J Briggs Freeman Hospital Newcastle upon Tyne We don t know!! Population Studies 2300 children aged 4-13 years Shoe wearers Flat foot 8.6% Non-shoe wearers
PROstep Minimally Invasive Surgery HALLUX VALGUS CORRECTION USING PROSTEP MICA MINIMALLY INVASIVE FOOT SURGERY: TWO CASE STUDIES
 PROstep Minimally Invasive Surgery HALLUX VALGUS CORRECTION USING PROSTEP MICA MINIMALLY INVASIVE FOOT SURGERY: TWO CASE STUDIES AS PRESENTED BY: JOEL VERNOIS M.D. 016798A Case Study 1 PROstep Minimally
PROstep Minimally Invasive Surgery HALLUX VALGUS CORRECTION USING PROSTEP MICA MINIMALLY INVASIVE FOOT SURGERY: TWO CASE STUDIES AS PRESENTED BY: JOEL VERNOIS M.D. 016798A Case Study 1 PROstep Minimally
FREIBERG S INFRACTION TREATMENT WITH METATARSAL NECK DORSAL CLOSING WEDGE OSTEOTOMY: REPORT OF TWO CASES
 FREIBERG S INFRACTION TREATMENT WITH METATARSAL NECK DORSAL CLOSING WEDGE OSTEOTOMY: REPORT OF TWO CASES Sung-Yen Lin, 1 Yuh-Min Cheng, 1,2 and Peng-Ju Huang 1,2 1 Department of Orthopedics, Kaohsiung
FREIBERG S INFRACTION TREATMENT WITH METATARSAL NECK DORSAL CLOSING WEDGE OSTEOTOMY: REPORT OF TWO CASES Sung-Yen Lin, 1 Yuh-Min Cheng, 1,2 and Peng-Ju Huang 1,2 1 Department of Orthopedics, Kaohsiung
1 st MP Arthrodesis. - Unraveling The Myths - Craig A. Camasta, DPM Atlanta, Georgia, USA
 1 st MP Arthrodesis - Unraveling The Myths - Craig A. Camasta, DPM Atlanta, Georgia, USA Hallux Limitus Dorsal Bunion Spasm of Short Flexor Immobility of Sesamoids DJD of 1 st MPJ Hallus Limitus Plantar
1 st MP Arthrodesis - Unraveling The Myths - Craig A. Camasta, DPM Atlanta, Georgia, USA Hallux Limitus Dorsal Bunion Spasm of Short Flexor Immobility of Sesamoids DJD of 1 st MPJ Hallus Limitus Plantar
Synthetic Cartilage Implants for Joint Pain
 Synthetic Cartilage Implants for Joint Pain Policy Number: 7.01.160 Last Review: 3/2018 Origination: 2/2018 Next Review: 9/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide
Synthetic Cartilage Implants for Joint Pain Policy Number: 7.01.160 Last Review: 3/2018 Origination: 2/2018 Next Review: 9/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide
THE ROLE OF MINIMALLY INVASIVE SURGERY IN THE FOREFOOT. Miss Sue Kendall PhD FRCS (Orth&Trauma)
 THE ROLE OF MINIMALLY INVASIVE SURGERY IN THE FOREFOOT Miss Sue Kendall PhD FRCS (Orth&Trauma) Is Minimally Invasive Surgery of the foot a good idea? Minimally invasive surgery, keyhole surgery entering
THE ROLE OF MINIMALLY INVASIVE SURGERY IN THE FOREFOOT Miss Sue Kendall PhD FRCS (Orth&Trauma) Is Minimally Invasive Surgery of the foot a good idea? Minimally invasive surgery, keyhole surgery entering
PATIENT GUIDE FOR THE TREATMENT OF TOE ARTHRITIS
 arthrosurface.com PATIENT GUIDE FOR THE TREATMENT OF TOE ARTHRITIS A NATIONWIDE SURGEON SURVEY ON OVER 2,000 HEMICAP TOE PROCEDURES INCLUDES: Patient Function and Activity Milestones Patient Rehabilitation
arthrosurface.com PATIENT GUIDE FOR THE TREATMENT OF TOE ARTHRITIS A NATIONWIDE SURGEON SURVEY ON OVER 2,000 HEMICAP TOE PROCEDURES INCLUDES: Patient Function and Activity Milestones Patient Rehabilitation
Forefoot Procedures to Heal and Prevent Recurrence. Watermark. Diabetic Foot Update 2015 San Antonio, Texas
 Forefoot Procedures to Heal and Prevent Recurrence Diabetic Foot Update 2015 San Antonio, Texas J. Randolph Clements, DPM Assistant Professor of Orthopaedics Virginia Tech- Carilion School of Medicine
Forefoot Procedures to Heal and Prevent Recurrence Diabetic Foot Update 2015 San Antonio, Texas J. Randolph Clements, DPM Assistant Professor of Orthopaedics Virginia Tech- Carilion School of Medicine
Alberta Health Care Insurance Plan. Schedule Of Anaesthetic Rates Applicable To Podiatry. Procedure List. As Of. 01 April Government of Alberta
 Alberta Health Care Insurance Plan Procedure List As Of 01 April 2017 Alberta Health Care Insurance Plan Page i Generated 2017/03/14 TABLE OF CONTENTS As of 2017/04/01 II. OPERATIONS ON THE NERVOUS SYSTEM.......................
Alberta Health Care Insurance Plan Procedure List As Of 01 April 2017 Alberta Health Care Insurance Plan Page i Generated 2017/03/14 TABLE OF CONTENTS As of 2017/04/01 II. OPERATIONS ON THE NERVOUS SYSTEM.......................
Joint Preserving Surgery in Severe Forefoot Disorders
 Joint Preserving Surgery in Severe Forefoot Disorders J ORTHOP TRAUMA SURG REL RES 4 (12) 2008 Review article LOUIS S. BAROUK*, PIERRE BAROUK** * 39, Chemin de la Roche, 33370, Yvrac, France ** Clinique
Joint Preserving Surgery in Severe Forefoot Disorders J ORTHOP TRAUMA SURG REL RES 4 (12) 2008 Review article LOUIS S. BAROUK*, PIERRE BAROUK** * 39, Chemin de la Roche, 33370, Yvrac, France ** Clinique
MULTIPLE APPLICATIONS OF THE MINIRAIL
 C H A P T E R 2 1 MULTIPLE APPLICATIONS OF THE MINIRAIL Thomas J. Merrill, DPM James M. Losito, DPM Mario Cala, DPM Victor Herrera, DPM Alan E. Sotelo, DPM INTRODUCTION The unilateral MiniRail External
C H A P T E R 2 1 MULTIPLE APPLICATIONS OF THE MINIRAIL Thomas J. Merrill, DPM James M. Losito, DPM Mario Cala, DPM Victor Herrera, DPM Alan E. Sotelo, DPM INTRODUCTION The unilateral MiniRail External
Clinical results of modified Mitchell s osteotomy for hallux valgus augmented with oblique lesser metatarsal osteotomy
 Journal of Orthopaedic Surgery 2005:13(3):245-252 Clinical results of modified Mitchell s osteotomy for hallux valgus augmented with oblique lesser metatarsal osteotomy K Yamamoto, A Imakiire, Y Katori,
Journal of Orthopaedic Surgery 2005:13(3):245-252 Clinical results of modified Mitchell s osteotomy for hallux valgus augmented with oblique lesser metatarsal osteotomy K Yamamoto, A Imakiire, Y Katori,
with regard to our presentation.
 Rotated Insertion Metatarsal Osteotomy with Distal Soft Tissue Procedure for Severe Hallux Valgus Deformity Novel Procedure of the 1 st metatarsal osteotomy Norihiro Samoto MD, Ph.D. Director of Department
Rotated Insertion Metatarsal Osteotomy with Distal Soft Tissue Procedure for Severe Hallux Valgus Deformity Novel Procedure of the 1 st metatarsal osteotomy Norihiro Samoto MD, Ph.D. Director of Department
THE FIBULAR SESAMOID ELEVATOR: A New Instrument to Aid the Lateral Release in Hallux Valgus Surgery
 C H A P T E R 1 4 THE FIBULAR SESAMOID ELEVATOR: A New Instrument to Aid the Lateral Release in Hallux Valgus Surgery Thomas F. Smith, DPM Lopa Dalmia, DPM INTRODUCTION Hallux valgus surgery is a complex
C H A P T E R 1 4 THE FIBULAR SESAMOID ELEVATOR: A New Instrument to Aid the Lateral Release in Hallux Valgus Surgery Thomas F. Smith, DPM Lopa Dalmia, DPM INTRODUCTION Hallux valgus surgery is a complex
CLAD Error Key. Error Levels: Definite, Possible. Error Procedure Scope. Validation Scope. Location Scope. Violation/Information Text
 CLAD Key s: Definite, Possible Procedure 1 2 3 4 5 6 7 8 9 10 Two or more category 1 procedures Digit Definite 1.6 plus one or more of the following: 2.1.3, 2.1.7, 2.2.2, 2.2.6, and 2.3.4 Side Definite
CLAD Key s: Definite, Possible Procedure 1 2 3 4 5 6 7 8 9 10 Two or more category 1 procedures Digit Definite 1.6 plus one or more of the following: 2.1.3, 2.1.7, 2.2.2, 2.2.6, and 2.3.4 Side Definite
Comparison of Hallux Rigidus Surgical Treatment Outcomes Between Active Duty and Non Active Duty Populations
 ORIGINAL ARTICLES Comparison of Hallux Rigidus Surgical Treatment Outcomes Between Active Duty and Non Active Duty Populations A Retrospective Review Marc D. Jones, DPM* Kerry J. Sweet, DPM Background:
ORIGINAL ARTICLES Comparison of Hallux Rigidus Surgical Treatment Outcomes Between Active Duty and Non Active Duty Populations A Retrospective Review Marc D. Jones, DPM* Kerry J. Sweet, DPM Background:
Distraction Osteogenesis and Fusion for Failed First Metatarsophalangeal Joint Replacement: Case Series
 737481FAIXXX10.1177/1071100717737481Foot & Ankle InternationalDa Cunha et al research-article2017 Case Report Distraction Osteogenesis and Fusion for Failed First Metatarsophalangeal Joint Replacement:
737481FAIXXX10.1177/1071100717737481Foot & Ankle InternationalDa Cunha et al research-article2017 Case Report Distraction Osteogenesis and Fusion for Failed First Metatarsophalangeal Joint Replacement:
Encina Taper Stem. Stinson Orthopedics Inc. 303 Twin Dolphin Drive, Suite 600 Redwood City, CA
 Stinson Orthopedics Inc. 303 Twin Dolphin Drive, Suite 600 Redwood City, CA 94065 info@stinsonortho.com www.stinsonortho.com Table of Contents Introduction 3 Features 4 Surgical Technique 5 Preoperative
Stinson Orthopedics Inc. 303 Twin Dolphin Drive, Suite 600 Redwood City, CA 94065 info@stinsonortho.com www.stinsonortho.com Table of Contents Introduction 3 Features 4 Surgical Technique 5 Preoperative
Foot and Ankle Technique Guide Proximal Inter-Phalangeal (PIP) Fusion
 Surgical Technique Foot and Ankle Technique Guide Proximal Inter-Phalangeal (PIP) Fusion Prepared in consultation with: Phinit Phisitkul, MD Department of Orthopedics and Rehabilitation University of Iowa
Surgical Technique Foot and Ankle Technique Guide Proximal Inter-Phalangeal (PIP) Fusion Prepared in consultation with: Phinit Phisitkul, MD Department of Orthopedics and Rehabilitation University of Iowa
Bone Bangalore
 Dr Suresh Annamalai MBBS, MRCS(Edn), FRCS( Tr & Orth)(Edn), FEBOT(European Board), Young Hip and Knee Fellowship(Harrogate, UK) Consultant Arthroplasty and Arthroscopic Surgeon Manipal Hospital, Whitefield,
Dr Suresh Annamalai MBBS, MRCS(Edn), FRCS( Tr & Orth)(Edn), FEBOT(European Board), Young Hip and Knee Fellowship(Harrogate, UK) Consultant Arthroplasty and Arthroscopic Surgeon Manipal Hospital, Whitefield,
)221( COPYRIGHT 2017 BY THE ARCHIVES OF BONE AND JOINT SURGERY RESEARCH ARTICLE
 )221( COPYRIGHT 2017 BY THE ARCHIVES OF BONE AND JOINT SURGERY RESEARCH ARTICLE First Metatarsophalangeal Joint Arthrodesis: A Retrospective Comparison of Crossed-screws, Locking and Non-Locking Plate
)221( COPYRIGHT 2017 BY THE ARCHIVES OF BONE AND JOINT SURGERY RESEARCH ARTICLE First Metatarsophalangeal Joint Arthrodesis: A Retrospective Comparison of Crossed-screws, Locking and Non-Locking Plate
Results of Metallic Hemi-Great Toe Implant for Grade III and Early Grade IV Hallux Rigidus
 FOOT &ANKLE INTERNATIONAL Copyright 2009 by the American Orthopaedic Foot & Ankle Society DOI: 10.3113/FAI.2009.0653 Results of Metallic Hemi-Great Toe Implant for Grade III and Early Grade IV Hallux Rigidus
FOOT &ANKLE INTERNATIONAL Copyright 2009 by the American Orthopaedic Foot & Ankle Society DOI: 10.3113/FAI.2009.0653 Results of Metallic Hemi-Great Toe Implant for Grade III and Early Grade IV Hallux Rigidus
Osteotomy vs No Osteotomy Second Ray
 Osteotomy vs No Osteotomy Second Ray Michael D. Dujela DPM, FACFAS Fellowship Trained Foot and Ankle Surgeon Washington Orthopaedic Center, Centralia, WA Chairman, Education and Scientific Affairs Committee
Osteotomy vs No Osteotomy Second Ray Michael D. Dujela DPM, FACFAS Fellowship Trained Foot and Ankle Surgeon Washington Orthopaedic Center, Centralia, WA Chairman, Education and Scientific Affairs Committee
Lesser toe sequential repair
 Lesser toe sequential repair For the correction of lesser toe deformity Information for patients Department of Podiatric Surgery What is lesser toe deformity? The lesser toes are those other than your
Lesser toe sequential repair For the correction of lesser toe deformity Information for patients Department of Podiatric Surgery What is lesser toe deformity? The lesser toes are those other than your
HemiEDGE. Patent No. 8,845,750. Surgical Technique
 HemiEDGE Patent No. 8,845,750 Surgical Technique Contents Product Based on the clinical success of our First MPJ Hemi Implant, the HemiEDGE, incorporates an overlapping edge extending around the medial,
HemiEDGE Patent No. 8,845,750 Surgical Technique Contents Product Based on the clinical success of our First MPJ Hemi Implant, the HemiEDGE, incorporates an overlapping edge extending around the medial,
Moderate to severe hallux valgus deformity: correction with proximal crescentic osteotomy and distal soft-tissue release
 Arch Orthop Trauma Surg (2000) 120 : 397 402 Springer-Verlag 2000 ORIGINAL ARTICLE R. Zettl H.-J. Trnka M. Easley M. Salzer P. Ritschl Moderate to severe hallux valgus deformity: correction with proximal
Arch Orthop Trauma Surg (2000) 120 : 397 402 Springer-Verlag 2000 ORIGINAL ARTICLE R. Zettl H.-J. Trnka M. Easley M. Salzer P. Ritschl Moderate to severe hallux valgus deformity: correction with proximal
Long Oblique Distal Osteotomy of the Fifth Metatarsal for Correction of Tailor s Bunion: A Retrospective Review
 Long Oblique Distal Osteotomy of the Fifth Metatarsal for Correction of Tailor s Bunion: A Retrospective Review Barry P. London, DPM, 1 Stephen F. Stern, DPM, 2 Mark A. Quist, DPM, 3 Robert K. Lee, DPM,
Long Oblique Distal Osteotomy of the Fifth Metatarsal for Correction of Tailor s Bunion: A Retrospective Review Barry P. London, DPM, 1 Stephen F. Stern, DPM, 2 Mark A. Quist, DPM, 3 Robert K. Lee, DPM,
Merete PlantarMAX Lapidus Plate Surgical Technique. Description of Plate
 Merete PlantarMAX Lapidus Plate Surgical Technique Description of Plate Merete Medical has designed the PlantarMax; a special Plantar/Medial Locking Lapidus plate which places the plate in the most biomechanically
Merete PlantarMAX Lapidus Plate Surgical Technique Description of Plate Merete Medical has designed the PlantarMax; a special Plantar/Medial Locking Lapidus plate which places the plate in the most biomechanically
Digital Surgery Complications
 Annual Surgical Conference 2018 Digital Surgery Complications Zeeshan S. Husain, DPM, FACFAS, FASPS Great Lakes Foot and Ankle Institute September 21, 2018 None Disclosures Presentation Outline Differentials
Annual Surgical Conference 2018 Digital Surgery Complications Zeeshan S. Husain, DPM, FACFAS, FASPS Great Lakes Foot and Ankle Institute September 21, 2018 None Disclosures Presentation Outline Differentials
WHAT IS ARTHRITIS OF THE BIG TOE (HALLUX RIGIDUS)?
 Mr Laurence James BSc MBBS MRCS(Eng) FRCS(Tr&Orth) Consultant Orthopaedic Surgeon Foot, Ankle and Sports Injuries WHAT IS ARTHRITIS OF THE BIG TOE (HALLUX RIGIDUS)? A common term for arthritis of the metatarsophalangeal
Mr Laurence James BSc MBBS MRCS(Eng) FRCS(Tr&Orth) Consultant Orthopaedic Surgeon Foot, Ankle and Sports Injuries WHAT IS ARTHRITIS OF THE BIG TOE (HALLUX RIGIDUS)? A common term for arthritis of the metatarsophalangeal
Total Hip Replacement in Diaphyseal Aclasis: A Case Report
 ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 6 Number 1 Total Hip Replacement in Diaphyseal Aclasis: A Case Report V Singh, S Carter Citation V Singh, S Carter.. The Internet Journal of
ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 6 Number 1 Total Hip Replacement in Diaphyseal Aclasis: A Case Report V Singh, S Carter Citation V Singh, S Carter.. The Internet Journal of
Optimizing function Maximizing survivorship Accelerating recovery
 Surgical Technique Optimizing Function Maximizing Survivorship Accelerating Recovery The company believes in an approach to patient treatment that places equal importance on: Optimizing function Maximizing
Surgical Technique Optimizing Function Maximizing Survivorship Accelerating Recovery The company believes in an approach to patient treatment that places equal importance on: Optimizing function Maximizing
Mr. Siva Chandrasekaran Orthopaedic Surgeon MBBS MSpMed MPhil (surg) FRACS
 Bunion Surgery Most people with bunions find pain relief with simple treatments to reduce pressure on the big toe, such as wearing wider shoes or using pads in their shoes. However, if these measures do
Bunion Surgery Most people with bunions find pain relief with simple treatments to reduce pressure on the big toe, such as wearing wider shoes or using pads in their shoes. However, if these measures do
How to avoid complications of distraction osteogenesis for first brachymetatarsia
 220 Acta Orthopaedica 2009; 80 (2): 220 225 How to avoid complications of distraction osteogenesis for first brachymetatarsia Keun-Bae Lee, Hyun-Kee Yang, Jae-Yoon Chung, Eun-Sun Moon, and Sung-Taek Jung
220 Acta Orthopaedica 2009; 80 (2): 220 225 How to avoid complications of distraction osteogenesis for first brachymetatarsia Keun-Bae Lee, Hyun-Kee Yang, Jae-Yoon Chung, Eun-Sun Moon, and Sung-Taek Jung
Unicondylar Knee Vs Total Knee Replacement: Is Less Better In the Middle Aged Athlete
 Unicondylar Knee Vs Total Knee Replacement: Is Less Better In the Middle Aged Athlete Chair: Maurilio Marcacci, MD Alois Franz "Basic principles and considerations of the Unis" Joao M. Barretto "Sport
Unicondylar Knee Vs Total Knee Replacement: Is Less Better In the Middle Aged Athlete Chair: Maurilio Marcacci, MD Alois Franz "Basic principles and considerations of the Unis" Joao M. Barretto "Sport
Case 57 What is the diagnosis? Insidious onset forefoot pain in a 50 year old female for last 3 months.
 Case 57 What is the diagnosis? Insidious onset forefoot pain in a 50 year old female for last 3 months. Diagnosis: II MTP instability Demographics of MT instability Lesser MTP joint instability occurs
Case 57 What is the diagnosis? Insidious onset forefoot pain in a 50 year old female for last 3 months. Diagnosis: II MTP instability Demographics of MT instability Lesser MTP joint instability occurs
Augmented Glenoid Component for Bone Deficiency in Shoulder Arthroplasty
 Clin Orthop Relat Res (2008) 466:579 583 DOI 10.1007/s11999-007-0104-4 SYMPOSIUM: NEW APPROACHES TO SHOULDER SURGERY Augmented Glenoid Component for Bone Deficiency in Shoulder Arthroplasty Robert S. Rice
Clin Orthop Relat Res (2008) 466:579 583 DOI 10.1007/s11999-007-0104-4 SYMPOSIUM: NEW APPROACHES TO SHOULDER SURGERY Augmented Glenoid Component for Bone Deficiency in Shoulder Arthroplasty Robert S. Rice
PRELIMINARY RESULTS OF HALLUX VALGUS SURGERY USING MAGNESIUM SCREWS
 PRELIMINARY RESULTS OF HALLUX VALGUS SURGERY USING MAGNESIUM SCREWS AUTHOR: Timo Juutilainen, M.D., Ph.D. Head of Foot and Ankle Surgery Helsinki University Central Hospital (HUCH) Peijas Vantaa FINLAND
PRELIMINARY RESULTS OF HALLUX VALGUS SURGERY USING MAGNESIUM SCREWS AUTHOR: Timo Juutilainen, M.D., Ph.D. Head of Foot and Ankle Surgery Helsinki University Central Hospital (HUCH) Peijas Vantaa FINLAND
