Distraction Osteogenesis and Fusion for Failed First Metatarsophalangeal Joint Replacement: Case Series
|
|
|
- Darlene Taylor
- 5 years ago
- Views:
Transcription
1 737481FAIXXX / Foot & Ankle InternationalDa Cunha et al research-article2017 Case Report Distraction Osteogenesis and Fusion for Failed First Metatarsophalangeal Joint Replacement: Case Series Foot & Ankle International 2018, Vol. 39(2) The Author(s) 2017 Reprints and permissions: sagepub.com/journalspermissions.nav DOI: journals.sagepub.com/home/fai Rachael J. Da Cunha, MD, FRCSC 1, Sydney C. Karnovsky, BA 1, Austin T. Fragomen, MD 2, and Mark C. Drakos, MD 1 Level of Evidence: Level V, expert opinion Keywords: failed MTP joint arthroplasty, distraction osteogenesis, first MT joint fusion Introduction Hallux rigidus is a progressive osteoarthritic condition, and operative intervention is often required. 6 It can affect gait, lead to a decreased range of motion, particularly dorsiflexion, and can cause stiffness and pain. 5,6 First metatarsophalangeal (MTP) arthrodesis is the traditional standard treatment for end-stage hallux rigidus 1 and has been repeatedly shown to be the most consistent and successful operative technique. 10 In 1952, first MTP arthroplasty emerged as a new treatment option for end-stage hallux rigidus. 3,6 First MTP arthroplasty involves prosthetic replacement of the first MTP joint with either a unipolar or bipolar implant and has the potential to improve joint motion and reduce pain. 3 However, arthroplasty involves additional risks, including malposition, implant fracture, stress fracture, arthrofibrosis, and synovitis, all of which can lead to failure. 3 Additionally, failed arthroplasty often leads to a significant amount of first ray shortening, which can make revision surgery a challenge. 1 There is little literature following the long-term results of hemiarthroplasty 6 and total joint arthroplasty, and even less exists describing outcomes of salvage arthrodesis in cases where arthroplasty fails. 5 Brage and Ball reported that many of the hemiarthroplasty implants would fail. 2 Delman et al also reported that arthroplasty procedures to treat hallux rigidus would fail, opining that the compressive and shear stresses placed on the implant surfaces put them at high risk of loosening. 3 Furthermore, unlike the knee and hip, there is little surface area available to establish a strong bone-implant interface. This, combined with higher stresses, particularly during walking and stair-climbing, leads to higher failure rates. In a study comparing arthroplasty and arthrodesis over a 6-year period, 24% of the arthroplasties failed, with 4 converted to an arthrodesis to alleviate pain. 8 Failed implants, once removed, create significant bone loss, which can make the reconstruction operation difficult. 1 Because of the bone loss, the revision arthrodesis usually necessitates bone grafting in order to restore first ray length. 2 Depending on the amount of bone loss, local autologous bone graft may be an option, but in cases with significant loss, grafts from other areas might be necessary as well, increasing the potential rate of failure of the operation. 5 Commonly, surgeons use tricortical iliac crest autograft wedges to manage defects. However, this can have associated morbidity in terms of pain and even fracture. 12 These salvage arthrodesis procedures often have a long time to union and increased rates of nonunion and malunion compared to primary first MTP arthrodesis procedures. 2 To avoid the complications associated with iliac crest bone graft harvest, tricortical allograft wedges have also been used. However, the nonunion rate associated with allograft in foot arthrodesis cases has been reported to range from 9% to 23% and is thus a less favorable option. 7,8 To improve the chance of healing, many surgeons elect to acutely shorten the first 1 Department of Orthopedic Surgery, Foot and Ankle, Hospital for Special Surgery, New York, NY, USA 2 Department of Orthopedic Surgery, Limb Lengthening and Complex Reconstruction Service, Hospital for Special Surgery, New York, NY, USA Corresponding Author: Rachael J. Da Cunha, MD, FRCSC, Clinical Fellow, Department of Orthopedic Surgery, Hospital for Special Surgery, 535 East 70th Street, New York, NY 10021, USA. dacunhar@hss.edu
2 Da Cunha et al 243 Table 1. Patient Data. metatarsal defect to achieve fusion without addressing the loss of length of the ray. We present a series of failed first MTP arthroplasties requiring revision-reconstruction operations using a novel application of the Ilizarov technique, in which distraction osteogenesis was used in combination with primary arthrodesis to restore stability and length to the first ray. In our experience, this technique leads to good results and minimized morbidity to the iliac crest. Methods A retrospective chart review was conducted from a prospectively collected registry to identify fusion after joint arthroplasty surgery. We identified all cases of a failed first MTP joint arthroplasty that were revised to a first MTP joint arthrodesis with first metatarsal lengthening between 2011 and We excluded patients with concomitant foot pathology including nonunion. Four patients met the inclusion criteria. One patient was excluded because of preoperative complex regional pain syndrome (CRPS). Thus, 3 patients were included in this case series. Baseline patient demographics and intraoperative findings are summarized (Table 1). Operative Technique Patient 1 Patient 2 Patient 3 Age Gender Female Female Male Type of implant Unipolar Unipolar Bipolar Defect size, mm Infection None None None Implant loose Yes No Yes Bacteria isolated None None None The anesthetic protocol was similar for all patients, consisting of a peripheral popliteal nerve block under ultrasound guidance and spinal anesthesia. Antibiotics were held until tissue samples were obtained for culture. A dorsal incision was made, centered over the first MTP joint. In 2 of the 3 cases, the implants were loose. When the implant was removed, all devitalized or necrotic tissue was removed, including bone. Bone defects measured, on average, 19 mm (range mm). The Wright Medical (Memphis, TN) conical and cup reamer set was used to contour the joint surfaces for arthrodesis. A 3.5-mm Kirschner wire (K-wire) was used to penetrate each joint surface several times to improve bony integration at the fusion interface. Cancellous bone autograft was harvested from the calcaneus. Between 3 and 7 cc of bone graft was harvested. The autograft was used to fill any defects in the metatarsal head as well as packed into and around the fusion site. Satisfactory alignment was obtained and the joint was pinned in position with 1 to 2 K-wires. The first ray was confirmed to be short by 10 to 25 mm and indicated for lengthening. The Biomet mini rail external fixation system (Warsaw, IN) was utilized to construct a dorsally mounted compression-distraction frame. Threemillimeter self-drilling, self-tapping half pins were placed percutaneously with fluoroscopic assistance. The most proximal pin in the proximal first metatarsal was placed first, followed by the most distal pin in the proximal phalanx establishing the axis of compression and distraction. The remaining 4 half-pins were placed using the frame as a targeting device. All pins were placed bicortically. Overall, there were 2 pins in the proximal phalanx, 2 pins in the distal first metatarsal, and 2 pins in the proximal first metatarsal. The pins were oriented to allow compression across the first MPT joint and distraction through the proximal metatarsal. Once satisfactory position of all pins was confirmed, the frame was removed, and the mid-diaphysis of the first metatarsal was exposed through a small dorsomedial incision. Multiple drill holes were made at the desired osteotomy site in the middle of the first metatarsal, and the osteotomy was completed using an osteotome. The external fixator was reattached, and compression was applied across the first MTP joint fusion site. The K-wire was kept in some cases across the joint to aid in maintaining the joint reduction and preventing apex plantar deformity during compression. Postoperative Protocol The patient was initially instructed to remain nonweightbearing with the operative foot in a postoperative splint. Empiric oral antibiotics were prescribed for infection prevention prophylaxis, a practice we no longer advocate. 4 Chemical deep vein thrombosis prophylaxis was also prescribed in each case. On postoperative day 5, distraction of the osteotomy was initiated at a rate of 0.5 mm per day, split into two 0.25-mm turns. The technical challenge was to lengthen the metatarsal while keeping the Meary angle constant with appropriate dorsiflexion of the first MTP arthrodesis. The frame was parallel to the first metatarsal on both the AP and lateral view in order to maintain the position of first MTP fusion (Figure 1B and C). The patient was assessed at 2-week intervals postoperatively to evaluate progress of the distraction regenerate bone. Additional compression (1-mm) was applied with the external fixator across the fusion site at these visits. Distraction was continued at this rate until the metatarsal length was restored to within 1 mm of the contralateral side. Adequate distraction and restoration of metatarsal length was typically achieved at 4 to 6 weeks postoperation. The patient was then permitted partial heel weightbearing only in a postoperative rigid
3 244 Foot & Ankle International 39(2) Table 2. Results. Patient Age Time to Union, mo Reoperation Complications Time NWB to Partial Heel Weightbearing, wk Time to Full Weightbearing, mo Final Follow-up, mo Pain at Final Follow-up Final Function No None No Return to all activities No Superficial pin site infection No Return to all activities, including jogging Yes Premature consolidation requiring revision osteotomy Abbreviation: NWB, nonweightbearing Mild Returned to work as a laborer with rocker bottom shoe Table 3. Lengthening Data. Patient Bone Defect, mm Lengthening, mm LD, mm Time in Frame (TIF), d Ex Fix Index (TIF/length), d/cm Abbreviation: LD, length discrepancy between operative and contralateral first metatarsal. shoe with an ambulatory assistive device. The K-wire that was initially placed across the first MTP joint was removed in the office at 6 to 8 weeks when the fusion site was felt to be partially united. The external fixator was maintained for an additional 2 months from the time of final distraction and then removed in the office. This was generally performed at 12 to 14 weeks postoperation. Radiographs were assessed and 4 cortices of healing at the lengthening site were required prior to frame removal. Partial weightbearing at 50% body weight in a postoperative rigid shoe was initiated once the external fixator was removed and progressed to full weightbearing as tolerated over a 4- to 6-week period based on radiographic union. The patient was transitioned back into regular shoes at 4 to 6 months postoperatively and generally permitted to return to all activities as tolerated at 6 to 9 months postoperatively. Results The results of the 3 cases are summarized in Table 2 and specific lengthening data for each case detailed in Table 3. Cases 1 and 2 had similar clinical courses and therefore only case 2 is described in detail with corresponding images. Case 3 required reoperation and revision and is therefore also described in detail with corresponding images. Case 2 Summary This patient was a 67-year-old woman who previously underwent a right first MTP hemiarthroplasty 4 years prior at an outside institution (Figure 2). The patient continued to have limited range of motion with dorsiflexion limited to 10 degrees and persistent, daily pain. The patient underwent implant removal, first MTP arthrodesis, first metatarsal osteotomy, and external fixation application. A K-wire transfixing the arthrodesis site was maintained in situ to prevent deformity during lengthening and removed at 8 weeks postoperation. Distraction was initiated at postoperative day 5 at a rate of 0.5 mm/d and continued for 48 days, yielding a final lengthening of 24 mm. The first metatarsal length was restored to within 1 mm of the contralateral side (Figure 1). The patient was maintained at partial heel weightbearing in a rigid postoperative shoe for 3 months. The external fixator frame was removed at 3 months postoperation and the patient was progressed to partial foot flat weightbearing at 50% body weight. Radiographic union of both the arthrodesis site and lengthening site were achieved by 4 months postoperation (Figure 3). At 4 months postoperation, the patient was progressed to full weightbearing as tolerated. The patient achieved full weightbearing without an assistive device in regular shoe wear by 6 months
4 Da Cunha et al 245 Figure 1. Case 2. (A) Oblique and (B) lateral radiographs 5 weeks postoperation demonstrating excellent bone contact at the fusion site and early regenerate bone formation at the lengthening site. The frame must be parallel to the first metatarsal on both the AP and lateral view in order to maintain the position of first metatarsophalangeal fusion. Panel C demonstrates that the frame and the metatarsal are parallel, ensuring lengthening along the anatomic axis. (C) Bilateral comparison AP radiographs show that metatarsal length as measured from the base of the first metatarsal to the interphalangeal joint has been restored to within 1 mm of the contralateral side. AP, anteroposterior. Figure 2. Case 2. (A) Preoperative anteroposterior and (B) lateral radiographs with a first metatarsophalangeal hemiarthroplasty implant in situ. There is radiographic evidence suggestive of implant loosening. There are familiar signs of phalangeal cartilage loss. postoperation. The patient returned to full activities without restrictions, including jogging and hiking, by 9 months postoperation. The patient had complete resolution of pain. This patient experienced a superficial pin site infection that resolved completely with a 10-day course of oral antibiotics. The patient experienced no other complication. There were no issues with first toe interphalangeal joint stiffness noted postoperatively.
5 246 Foot & Ankle International 39(2) Figure 3. Case 2. (A) Anteroposterior and (B) lateral radiographs at 6 months postoperation demonstrating complete healing at both the distraction site and arthrodesis site with restoration of metatarsal length. Note on the lateral image that the first metatarsophalangeal fusion mass contacts the floor anatomically as a result of lengthening along the anatomic axis of the metatarsal. Figure 4. Case 3. (A) Preoperative anteroposterior and (B) lateral radiographs with a first metatarsophalangeal total arthroplasty implant in situ. Radiographically, there was evidence of implant loosening. Case 3 Summary This patient was a 48-year-old man that previously underwent a right first MTP arthroplasty 1 year prior at an outside institution (Figure 4). The patient continued to have limited range of motion with dorsiflexion limited to 30 degrees and persistent, daily pain. This patient underwent implant removal, preparation of the first MTP fusion site, and a first metatarsal proximal osteotomy with external fixation application for lengthening. The fusion site was unable to be reduced acutely and needed to be gradually shortened creating a bone transport scenario. The first stage of distraction was initiated at postoperative day 5 at a rate of 0.5 mm per day, and the shortening at the fusion site was also carried out at 0.5 mm per day. The patient developed a premature consolidation of the lengthening site 6 weeks following the initial surgery which required operative osteoclasis. The first MTP fusion site (docking site) still had a gap so it underwent autologous bone grafting during the same revision surgery.
6 Da Cunha et al 247 Figure 5. Case 3. (A) Anteroposterior and (B) lateral radiographs 2 months postoperation demonstrating the first metatarsal distraction. Figure 6. Case 3. Lateral radiograph at 3 months postoperation at the time of external fixator removal demonstrating consolidation at both the distraction site and arthrodesis site. The second surgery consisted of the first MTP bone grafting from the calcaneus and acute docking, and a first metatarsal osteotomy revision through a closed, rotational osteoclasis using the external fixator pins to control both segments. Repeat intraoperative cultures were taken and were negative. At neither surgery was a K-wire transfixing the arthrodesis site left in situ temporarily because of the concern for infection. The osseous distraction was initiated at postoperative day 5 at a rate of 0.5 mm/d and continued for 14 days. The first metatarsal was lengthened a total of 24 mm. Length restoration was clinically determined with the first metatarsal head at the same level clinically as the third metatarsal head and similar to the contralateral side, which we used as a template (Figure 5). The patient was maintained at partial heel weightbearing in a rigid postoperative shoe for 3 months. The external fixator frame was removed at 3 months postoperation and the patient was progressed to partial weightbearing at 50% body weight (Figure 6). At 3.5 months postoperation, the patient was progressed to full weightbearing as tolerated. The patient achieved full weightbearing without an assistive device by 6 months postoperation. The patient returned to full duty work as a heavy laborer by 9 months postoperation. Radiographic union of both the arthrodesis site and lengthening site were achieved by 3.5 months postoperation and the first metatarsal length restored (Figure 7). This patient continued to have mild pain with activity postoperatively that was managed with wearing a rocker bottom type shoe. He was able to return to walking and his job. There were no issues with first toe IP joint stiffness noted postoperation. Discussion There are very few cases reporting the long-term results of failed first MTP arthroplasty, and even fewer describing revision procedures following these failures. The commonly accepted plan of treatment after a failed first MTP arthroplasty is conversion to arthrodesis, using bone graft. 2 When considering how to repair the bone defect in these patients, the most common option is to restore the length of the patient s metatarsal using autogenous bone graft from either the iliac crest or the tibia. 9 When a significant amount of bone loss is present, the bone graft is traditionally taken from the iliac crest. However, procedures that involve harvesting a large amount of bone graft have complications associated with them. Iliac crest bone grafting can lead to
7 248 Foot & Ankle International 39(2) Figure 7. Case 3. (A) Anteroposterior and (B) lateral radiographs at 6 months postoperation demonstrating healing to union at both the distraction site and arthrodesis site with restoration of metatarsal length. iliac fractures, increased pain in the site of the harvest, and increased length of postoperative hospital stays. The rate of complications following iliac bone grafting for use in foot and ankle surgery has been reported to be as high as 13.1%. 9 Given the difficult nature of this revision procedure and the amount of bone loss after the removal of the implant, these revision arthrodesis procedures leave the patient at an increased risk of nonunion or malunion. 2 Garras et al reported on 6 of 18 patients that required structural bone grafting to restore length due to extensive bone loss. 5 However, they were unable to restore full length in 1 patient because of the size of the defect, limiting the degree of lengthening that could be achieved as a result of poor soft tissue integrity and vascularity. This patient required the additional procedure of lesser metatarsal shortening osteotomies. 5 Because of the high morbidity of using large bone grafting procedures, we chose to use limited bone grafting only to improve the fusion potential. We used a distraction technique to fix the majority of missing length in these 3 patients in order to minimize the chance of failure and increased morbidity associated with using bone grafts alone to fill substantial defects. Another benefit of this technique is the ability to control the amount of length restored. By stretching soft tissues, additional length can be added easily. It needs to be mentioned that we do not advocate overlengthening the metatarsal to compensate for shortening of the proximal phalanx. The temptation is to match the length of the contralateral great toe clinically, but this would require overlengthening the metatarsal, which will make the plantar aspect of the first MTP fusion too prominent. The metatarsal is lengthened in the anatomic axis, so it moves distally and plantar. Overlengthening could produce metatarsalgia of the first ray, whereas dorsiflexion can lead to metatarsalgia of lesser rays. Conclusion In this case series, we present 3 patients who all underwent first MTP reconstruction surgery with minor bone grafting in addition to a lengthening procedure. All patients achieved successful arthrodesis. This technique allowed for appropriate first metatarsal length and avoided transfer lesions to the second and other lesser metatarsals. We believe that this novel operative technique may lead to better results with fewer complications than just arthrodesis with bone graft in patients in need of revision first MTP surgery. Author Note The study took place at the Hospital for Special Surgery and was approved by the institution s Foot and Ankle Registry, which is approved by our Institutional Review Board. Declaration of Conflicting Interests The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article. ICMJE forms for all authors are available online. Funding The author(s) received no financial support for the research, authorship, and/or publication of this article. References 1. Anakwe RE, Middleton SD, Thomson CE, McKinley JC. Hemiarthroplasty augmented with bone graft for the failed hallux metatarsophalangeal Silastic implant. Foot Ankle Surg. 2011;17(3): Brage ME, Ball ST. Surgical options for salvage of end-stage hallux rigidus. Foot Ankle Clin. 2002;7(1):49-73.
8 Da Cunha et al Delman C, Kreulen C, Sullivan M, Giza E. Proximal phalanx hemiarthroplasty for the treatment of advanced hallux rigidus. Foot Ankle Clin. 2015;20(3): Fragomen AT, Miller AO, Brause BD, Goldman V, Rozbruch SR. Prophylactic postoperative antibiotics may not reduce pin site infections after external fixation. HSS J. 2017;13: Garras DN, Durinka JB, Bercik M, Miller AG, Raikin SM. Conversion arthrodesis for failed first metatarsophalangeal joint hemiarthroplasty. Foot Ankle Int. 2013;34(9): Gheorghiu D, Coles C, Ballester J. Hemiarthroplasty for hallux rigidus: mid-term results. J Foot Ankle Surg. 2015;54(4): Mahan KT, Hillstrom HJ. Bone grafting in foot and ankle surgery. A review of 300 cases. J Am Podiatr Med Assoc. 1998;88(3): McGarvey WC, Braly WG. Bone graft in hindfoot arthrodesis: allograft vs autograft. Orthopaedics. 1996;19(5): O Malley MJ, Sayres SC, Saleem O, et al. Morbidity and complications following percutaneous calcaneal autograft bone harvest. Foot Ankle Int. 2014;35(1): Raikin SM, Ahmad J. Comparison of arthrodesis and metallic hemiarthroplasty of the hallux metatarsophalangeal joint. J Bone Joint Surg. 2008;90(suppl 2): Razik A, Sott AH. Cheilectomy for hallux rigidus. Foot Ankle Clin. 2016;21(3): Westrich GH, Geller DS, O Malley MJ, Deland JT, Helfet DL. Anterior iliac crest bone graft harvesting using the corticocancellous reamer system. J Orthop Trauma. 2001;15(7):
CASE REPORT. Antegrade tibia lengthening with the PRECICE Limb Lengthening technology
 CASE REPORT Antegrade tibia lengthening with the PRECICE Limb Lengthening technology Austin T. Fragomen, M.D. Hospital for Special Surgery New York, NY 1 1 PR O D U CTS CONDITION Nonunion of an attempted
CASE REPORT Antegrade tibia lengthening with the PRECICE Limb Lengthening technology Austin T. Fragomen, M.D. Hospital for Special Surgery New York, NY 1 1 PR O D U CTS CONDITION Nonunion of an attempted
Is Distraction Histiogenesis a Reliable Method to Reconstruct Segmental Bone and Acquired Leg Length Discrepancy in Tibia Fractures and Non Unions?
 Is Distraction Histiogenesis a Reliable Method to Reconstruct Segmental Bone and Acquired Leg Length Discrepancy in Tibia Fractures and Non Unions? James J Hutson Jr MD Professor Orthopedic Trauma Ryder
Is Distraction Histiogenesis a Reliable Method to Reconstruct Segmental Bone and Acquired Leg Length Discrepancy in Tibia Fractures and Non Unions? James J Hutson Jr MD Professor Orthopedic Trauma Ryder
Implantable K-wire SURGIC A L T ECHNIQUE
 Implantable K-wire SURGIC A L T ECHNIQUE Contents Chapter 1 4 Product Information 4 Device Description 4 Indications 4 Contraindications Chapter 2 5 Surgical Technique 5 Hammertoe Correction 6 MTP Joint
Implantable K-wire SURGIC A L T ECHNIQUE Contents Chapter 1 4 Product Information 4 Device Description 4 Indications 4 Contraindications Chapter 2 5 Surgical Technique 5 Hammertoe Correction 6 MTP Joint
HEMI IMPLANT ARTHROPLASTY FOR THE SECOND METATARSOPHALANGEAL JOINT
 C H A P T E R 1 5 HEMI IMPLANT ARTHROPLASTY FOR THE SECOND METATARSOPHALANGEAL JOINT Joe T. Southerland, DPM Mickey D. Stapp, DPM INTRODUCTION Hemi-implant arthroplasty of the first metatarsophalangeal
C H A P T E R 1 5 HEMI IMPLANT ARTHROPLASTY FOR THE SECOND METATARSOPHALANGEAL JOINT Joe T. Southerland, DPM Mickey D. Stapp, DPM INTRODUCTION Hemi-implant arthroplasty of the first metatarsophalangeal
Use of the 20 Memory Staple in Osteotomies of Fusions of the Forefoot
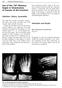 168 Forefoot Reconstruction Use of the 20 Memory Staple in Osteotomies of Fusions of the Forefoot Definition, History, Generalities This staple first provides a permanent compression both in the prongs
168 Forefoot Reconstruction Use of the 20 Memory Staple in Osteotomies of Fusions of the Forefoot Definition, History, Generalities This staple first provides a permanent compression both in the prongs
Correction of Traumatic Ankle Valgus and Procurvatum using the Taylor Spatial Frame: A Case Report
 The Foot and Ankle Online Journal Official publication of the International Foot & Ankle Foundation Correction of Traumatic Ankle Valgus and Procurvatum using the Taylor Spatial Frame: A Case Report by
The Foot and Ankle Online Journal Official publication of the International Foot & Ankle Foundation Correction of Traumatic Ankle Valgus and Procurvatum using the Taylor Spatial Frame: A Case Report by
CASE REPORT. Bone transport utilizing the PRECICE Intramedullary Nail for an infected nonunion in the distal femur
 PRODUCTS CASE REPORT Bone transport utilizing the PRECICE Intramedullary Nail for an infected nonunion in the distal femur Robert D. Fitch, M.D. Duke University Health System 1 1 CONDITION Infected nonunion
PRODUCTS CASE REPORT Bone transport utilizing the PRECICE Intramedullary Nail for an infected nonunion in the distal femur Robert D. Fitch, M.D. Duke University Health System 1 1 CONDITION Infected nonunion
REPAIR OF THE DISPLACED AUSTIN OSTEOTOMY
 C H A P T E R 2 1 REPAIR OF THE DISPLACED AUSTIN OSTEOTOMY John V. Vanore, DPM INTRODUCTION Bunion surgery is frequently performed by foot and ankle surgeons. Generally, bunion surgery is quite predictable,
C H A P T E R 2 1 REPAIR OF THE DISPLACED AUSTIN OSTEOTOMY John V. Vanore, DPM INTRODUCTION Bunion surgery is frequently performed by foot and ankle surgeons. Generally, bunion surgery is quite predictable,
ORTHOLOC 3Di. Foot Reconstruction System SURGIC AL TECHNIQUE
 ORTHOLOC 3Di Foot Reconstruction System S C R E W TA R G E T I N G G U I D E SURGIC AL TECHNIQUE SURGEON DESIGN TEAM The ORTHOLOC 3Di Foot Reconstruction System was developed in conjuction with: ORTHOLOC
ORTHOLOC 3Di Foot Reconstruction System S C R E W TA R G E T I N G G U I D E SURGIC AL TECHNIQUE SURGEON DESIGN TEAM The ORTHOLOC 3Di Foot Reconstruction System was developed in conjuction with: ORTHOLOC
Foot and Ankle Technique Guide Proximal Inter-Phalangeal (PIP) Fusion
 Surgical Technique Foot and Ankle Technique Guide Proximal Inter-Phalangeal (PIP) Fusion Prepared in consultation with: Phinit Phisitkul, MD Department of Orthopedics and Rehabilitation University of Iowa
Surgical Technique Foot and Ankle Technique Guide Proximal Inter-Phalangeal (PIP) Fusion Prepared in consultation with: Phinit Phisitkul, MD Department of Orthopedics and Rehabilitation University of Iowa
PROstep Minimally Invasive Surgery HALLUX VALGUS CORRECTION USING PROSTEP MICA MINIMALLY INVASIVE FOOT SURGERY: TWO CASE STUDIES
 PROstep Minimally Invasive Surgery HALLUX VALGUS CORRECTION USING PROSTEP MICA MINIMALLY INVASIVE FOOT SURGERY: TWO CASE STUDIES AS PRESENTED BY: JOEL VERNOIS M.D. 016798A Case Study 1 PROstep Minimally
PROstep Minimally Invasive Surgery HALLUX VALGUS CORRECTION USING PROSTEP MICA MINIMALLY INVASIVE FOOT SURGERY: TWO CASE STUDIES AS PRESENTED BY: JOEL VERNOIS M.D. 016798A Case Study 1 PROstep Minimally
Merete BLP. Surgical Technique. - Bunion Locking Plate - Low Profile Locking Bone Plate System
 Merete BLP - Bunion Locking Plate - Low Profile Locking Bone Plate System Surgical Technique Merete Medical, Inc. 49 Purchase Street Rye, N.Y. 10580 Phone: 914 967-1532 www.merete-medical.com - Surgical
Merete BLP - Bunion Locking Plate - Low Profile Locking Bone Plate System Surgical Technique Merete Medical, Inc. 49 Purchase Street Rye, N.Y. 10580 Phone: 914 967-1532 www.merete-medical.com - Surgical
Foot and ankle update
 Foot and ankle update Mr Ian Garnham Consultant Foot and Ankle Surgeon Whipps Cross University Hospital Hallux Rigidus Symptoms first ray and 1st MTP pain and swelling worse with push off or forced dorsiflexion
Foot and ankle update Mr Ian Garnham Consultant Foot and Ankle Surgeon Whipps Cross University Hospital Hallux Rigidus Symptoms first ray and 1st MTP pain and swelling worse with push off or forced dorsiflexion
QUICK REFERENCE GUIDE. MiniRail System. Part B: Foot Applications. By Dr. B. Magnan, Dr. E. Rodriguez and Dr. G. Vito ALWAYS INNOVATING
 14 MiniRail System Part B: Foot Applications By Dr. B. Magnan, Dr. E. Rodriguez and Dr. G. Vito ALWAYS INNOVATING ORDERING INFORMATION Sterilization box, empty M190 Can accommodate: M101 Standard MiniRail
14 MiniRail System Part B: Foot Applications By Dr. B. Magnan, Dr. E. Rodriguez and Dr. G. Vito ALWAYS INNOVATING ORDERING INFORMATION Sterilization box, empty M190 Can accommodate: M101 Standard MiniRail
MiniRail System. Part B: Foot Applications. By Dr. B. Magnan, Dr. E. Rodriguez and Dr. G. Vito
 Q U I C K R E F E R E N C E G U I D E 14 MiniRail System Part B: Foot Applications By Dr. B. Magnan, Dr. E. Rodriguez and Dr. G. Vito ORDERING INFORMATION MiniRail System Kit, M190C Contents: M 101 Standard
Q U I C K R E F E R E N C E G U I D E 14 MiniRail System Part B: Foot Applications By Dr. B. Magnan, Dr. E. Rodriguez and Dr. G. Vito ORDERING INFORMATION MiniRail System Kit, M190C Contents: M 101 Standard
5 COMMON CONDITIONS IN THE FOOT & ANKLE
 5 COMMON CONDITIONS IN THE FOOT & ANKLE MICHAEL P. CLARE, MD FLORIDA ORTHOPAEDIC INSTITUTE TAMPA, FL USA IN A NUTSHELL ~ ALL ANATOMY & BIOMECHANICS >90% OF CONDITIONS IN FOOT & ANKLE DIAGNISED FROM GOOD
5 COMMON CONDITIONS IN THE FOOT & ANKLE MICHAEL P. CLARE, MD FLORIDA ORTHOPAEDIC INSTITUTE TAMPA, FL USA IN A NUTSHELL ~ ALL ANATOMY & BIOMECHANICS >90% OF CONDITIONS IN FOOT & ANKLE DIAGNISED FROM GOOD
MULTIPLE APPLICATIONS OF THE MINIRAIL
 C H A P T E R 2 1 MULTIPLE APPLICATIONS OF THE MINIRAIL Thomas J. Merrill, DPM James M. Losito, DPM Mario Cala, DPM Victor Herrera, DPM Alan E. Sotelo, DPM INTRODUCTION The unilateral MiniRail External
C H A P T E R 2 1 MULTIPLE APPLICATIONS OF THE MINIRAIL Thomas J. Merrill, DPM James M. Losito, DPM Mario Cala, DPM Victor Herrera, DPM Alan E. Sotelo, DPM INTRODUCTION The unilateral MiniRail External
Fibula Lengthening Using a Modified Ilizarov Method S. Robert Rozbruch, MD; Matthew DiPaola, BA; Arkady Blyakher,MD
 Fibula Lengthening Using a Modified Ilizarov Method S. Robert Rozbruch, MD; Matthew DiPaola, BA; Arkady Blyakher,MD Limb Lengthening Service Hospital for Special Surgery Abstract A unique combination of
Fibula Lengthening Using a Modified Ilizarov Method S. Robert Rozbruch, MD; Matthew DiPaola, BA; Arkady Blyakher,MD Limb Lengthening Service Hospital for Special Surgery Abstract A unique combination of
Lesser MPJ Hemi Implant
 Lesser MPJ Hemi Implant Surgical Technique Contents Product The BioPro Lesser MPJ Hemi Implant is a simple, durable, metallic hemiarthroplasty resurfacing prosthesis for the treatment of arthritis, Freiberg
Lesser MPJ Hemi Implant Surgical Technique Contents Product The BioPro Lesser MPJ Hemi Implant is a simple, durable, metallic hemiarthroplasty resurfacing prosthesis for the treatment of arthritis, Freiberg
INVISION Total Ankle Replacement System with PROPHECY Preoperative Navigation Revision of a Failed Agility Total Ankle Replacement
 016625 REVISION R INVISION Total Ankle Replacement System with PROPHECY Preoperative Navigation Revision of a Failed Agility Total Ankle Replacement CASE STUDY Patient History The patient was a 65-year-old
016625 REVISION R INVISION Total Ankle Replacement System with PROPHECY Preoperative Navigation Revision of a Failed Agility Total Ankle Replacement CASE STUDY Patient History The patient was a 65-year-old
How to avoid complications of distraction osteogenesis for first brachymetatarsia
 220 Acta Orthopaedica 2009; 80 (2): 220 225 How to avoid complications of distraction osteogenesis for first brachymetatarsia Keun-Bae Lee, Hyun-Kee Yang, Jae-Yoon Chung, Eun-Sun Moon, and Sung-Taek Jung
220 Acta Orthopaedica 2009; 80 (2): 220 225 How to avoid complications of distraction osteogenesis for first brachymetatarsia Keun-Bae Lee, Hyun-Kee Yang, Jae-Yoon Chung, Eun-Sun Moon, and Sung-Taek Jung
A Patient s Guide to Hallux Rigidus
 A Patient s Guide to Hallux Rigidus Suite 11-13/14/15 Mount Elizabeth Medical Center 3 Mount Elizabeth Singapore, 228510 Phone: (65) 6738 2628 Fax: (65) 6738 2629 DISCLAIMER: The information in this booklet
A Patient s Guide to Hallux Rigidus Suite 11-13/14/15 Mount Elizabeth Medical Center 3 Mount Elizabeth Singapore, 228510 Phone: (65) 6738 2628 Fax: (65) 6738 2629 DISCLAIMER: The information in this booklet
Tibial deformity correction by Ilizarov method
 International Journal of Research in Orthopaedics http://www.ijoro.org Case Report DOI: http://dx.doi.org/10.18203/issn.2455-4510.intjresorthop20180422 Tibial deformity correction by Ilizarov method Robert
International Journal of Research in Orthopaedics http://www.ijoro.org Case Report DOI: http://dx.doi.org/10.18203/issn.2455-4510.intjresorthop20180422 Tibial deformity correction by Ilizarov method Robert
A Patient s Guide to Hallux Rigidus
 A Patient s Guide to Hallux Rigidus Glendale Adventist Medical Center 1509 Wilson Terrace Glendale, CA 91206 Phone: (818) 409-8000 DISCLAIMER: The information in this booklet is compiled from a variety
A Patient s Guide to Hallux Rigidus Glendale Adventist Medical Center 1509 Wilson Terrace Glendale, CA 91206 Phone: (818) 409-8000 DISCLAIMER: The information in this booklet is compiled from a variety
Foot Reconstruction System SURGICAL TECHNIQUE
 ORTHOLOC 3Di Foot Reconstruction System SURGICAL TECHNIQUE SURGEON DESIGN TEAM The ORTHOLOC 3Di Foot Reconstruction System was developed in conjuction with: Robert B. Anderson, MD OrthoCarolina Charlotte,
ORTHOLOC 3Di Foot Reconstruction System SURGICAL TECHNIQUE SURGEON DESIGN TEAM The ORTHOLOC 3Di Foot Reconstruction System was developed in conjuction with: Robert B. Anderson, MD OrthoCarolina Charlotte,
Increased pressures at
 Surgical Off-loading of Plantar Hallux Ulcerations These approaches can be used to treat DFUs. By Adam R. Johnson, DPM Increased pressures at the plantar aspect of the hallux leading to chronic hyperkeratosis
Surgical Off-loading of Plantar Hallux Ulcerations These approaches can be used to treat DFUs. By Adam R. Johnson, DPM Increased pressures at the plantar aspect of the hallux leading to chronic hyperkeratosis
EXPERT TIBIAL NAIL PROTECT
 EXPERT TIBIAL NAIL PROTECT Enhance your first line of defense This publication is not intended for distribution in the USA. CLINICAL EVIDENCE CONTENT AUTHOR TITLE OF CHAPTER PAGE ETN PROtect clinical evidence
EXPERT TIBIAL NAIL PROTECT Enhance your first line of defense This publication is not intended for distribution in the USA. CLINICAL EVIDENCE CONTENT AUTHOR TITLE OF CHAPTER PAGE ETN PROtect clinical evidence
RETROSPECTIVE ANALYSIS OF END-TO-END DIGITAL ARTHRODESIS
 C H A P T E R 1 7 RETROSPECTIVE ANALYSIS OF END-TO-END DIGITAL ARTHRODESIS Michelle L. Butterworth, DPM Michael S. Downey, DPM Digital deformities are one of the most common entities we face as foot and
C H A P T E R 1 7 RETROSPECTIVE ANALYSIS OF END-TO-END DIGITAL ARTHRODESIS Michelle L. Butterworth, DPM Michael S. Downey, DPM Digital deformities are one of the most common entities we face as foot and
COMPARING KIRSCHNER WIRE FIXATION TO A NEW DEVICE USED FOR PROXIMAL INTERPHALANGEAL FUSION
 C H A P T E R 3 0 COMPARING KIRSCHNER WIRE FIXATION TO A NEW DEVICE USED FOR PROXIMAL INTERPHALANGEAL FUSION Scott R. Roman, DPM INTRODUCTION The most common fixation for proximal interphalangeal fusion
C H A P T E R 3 0 COMPARING KIRSCHNER WIRE FIXATION TO A NEW DEVICE USED FOR PROXIMAL INTERPHALANGEAL FUSION Scott R. Roman, DPM INTRODUCTION The most common fixation for proximal interphalangeal fusion
FACTS 1. Most need only Gastro aponeurotic release [in positive Silverskiold test]
![FACTS 1. Most need only Gastro aponeurotic release [in positive Silverskiold test] FACTS 1. Most need only Gastro aponeurotic release [in positive Silverskiold test]](/thumbs/83/88335212.jpg) FOOT IN CEREBRAL PALSY GAIT IN CEREBRAL PALSY I True Equinus II Jump gait III Apparent Equinus IV Crouch gait Group I True Equinus Extended hip and knee Equinus at ankle II Jump Gait [commonest] Equinus
FOOT IN CEREBRAL PALSY GAIT IN CEREBRAL PALSY I True Equinus II Jump gait III Apparent Equinus IV Crouch gait Group I True Equinus Extended hip and knee Equinus at ankle II Jump Gait [commonest] Equinus
Metatarsal Lengthening By Callus Distraction For Brachymetatarsia: Case Report and Review of the Literature
 ISPUB.COM The Internet Journal of Third World Medicine Volume 1 Number 2 Metatarsal Lengthening By Callus Distraction For Brachymetatarsia: Case Report and Review of the R Rose Citation R Rose. Metatarsal
ISPUB.COM The Internet Journal of Third World Medicine Volume 1 Number 2 Metatarsal Lengthening By Callus Distraction For Brachymetatarsia: Case Report and Review of the R Rose Citation R Rose. Metatarsal
No disclosures relevant to this topic Acknowledgement: some clinical pictures were obtained from the OTA fracture lecture series and AO fracture
 CALCANEUS FRACTURES No disclosures relevant to this topic Acknowledgement: some clinical pictures were obtained from the OTA fracture lecture series and AO fracture lecture series INCIDENCE 2% of all fractures
CALCANEUS FRACTURES No disclosures relevant to this topic Acknowledgement: some clinical pictures were obtained from the OTA fracture lecture series and AO fracture lecture series INCIDENCE 2% of all fractures
Proximal metatarsal osteotomy and distal soft tissue reconstruction as treatment for hallux valgus deformity
 REVIEW Proximal metatarsal osteotomy and distal soft tissue reconstruction as treatment for hallux valgus deformity Michael J. Coughlin and J. Speight Grimes Boise, Idaho, USA (Received for publication
REVIEW Proximal metatarsal osteotomy and distal soft tissue reconstruction as treatment for hallux valgus deformity Michael J. Coughlin and J. Speight Grimes Boise, Idaho, USA (Received for publication
Lengthening of fourth brachymetatarsia by three different surgical techniques
 Lengthening of fourth brachymetatarsia by three different surgical techniques W.-C. Lee, J. H. Yoo, J.-S. Moon From Seoul Paik Hospital, Seoul, Korea W.-C. Lee, Md, PhD, Professor J.-S. Moon, MD, Orthopaedic
Lengthening of fourth brachymetatarsia by three different surgical techniques W.-C. Lee, J. H. Yoo, J.-S. Moon From Seoul Paik Hospital, Seoul, Korea W.-C. Lee, Md, PhD, Professor J.-S. Moon, MD, Orthopaedic
Prophylactic surgical correction of Crawford s type II anterolateral bowing of the tibia using Ilizarov s method
 Acta Orthop. Belg., 2005, 71, 577-581 ORIGINAL STUDY Prophylactic surgical correction of Crawford s type II anterolateral bowing of the tibia using Ilizarov s method Hani EL-MOWAFI, Mazen ABULSAAD, Wael
Acta Orthop. Belg., 2005, 71, 577-581 ORIGINAL STUDY Prophylactic surgical correction of Crawford s type II anterolateral bowing of the tibia using Ilizarov s method Hani EL-MOWAFI, Mazen ABULSAAD, Wael
Technique Guide. 6.5 mm Midfoot Fusion Bolt. For intramedullary fixation of the medial column of the foot.
 Technique Guide 6.5 mm Midfoot Fusion Bolt. For intramedullary fixation of the medial column of the foot. Table of Contents Introduction 6.5 mm Midfoot Fusion Bolt 2 AO Principles 4 Indications 5 Surgical
Technique Guide 6.5 mm Midfoot Fusion Bolt. For intramedullary fixation of the medial column of the foot. Table of Contents Introduction 6.5 mm Midfoot Fusion Bolt 2 AO Principles 4 Indications 5 Surgical
Section 6: Preoperative Planning
 Clinical Relevance of the PedCat Study: In many ways the PedCat study confirmed radiographic findings. With the measuring tools embedded in the DICOM viewing software it was possible to gauge the thickness
Clinical Relevance of the PedCat Study: In many ways the PedCat study confirmed radiographic findings. With the measuring tools embedded in the DICOM viewing software it was possible to gauge the thickness
Case Report. Antegrade Femur Lengthening with the PRECICE Limb Lengthening Technology
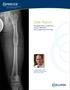 Case Report Antegrade Femur Lengthening with the PRECICE Limb Lengthening Technology S. Robert Rozbruch, MD Hospital for Special Surgery New York, NY, USA ABSTRACT This is a case illustrating a 4.5 cm
Case Report Antegrade Femur Lengthening with the PRECICE Limb Lengthening Technology S. Robert Rozbruch, MD Hospital for Special Surgery New York, NY, USA ABSTRACT This is a case illustrating a 4.5 cm
LCP Anterior Ankle Arthrodesis Plates. Part of the Synthes Locking Compression Plate (LCP) System.
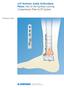 LCP Anterior Ankle Arthrodesis Plates. Part of the Synthes Locking Compression Plate (LCP) System. Technique Guide Instruments and implants approved by the AO Foundation Table of Contents Introduction
LCP Anterior Ankle Arthrodesis Plates. Part of the Synthes Locking Compression Plate (LCP) System. Technique Guide Instruments and implants approved by the AO Foundation Table of Contents Introduction
Interphalangeal Arthrodesis of the Toe with a New Radiolucent Intramedullary Implant
 Interphalangeal Arthrodesis of the Toe with a New Radiolucent Intramedullary Implant DIEBOLD P.-F., ROCHER H.,, DETERME P., CERMOLACCE C., GUILLO S., AVEROUS C., LEIBER WACKENHEIN F. Interphalangeal Arthrodesis
Interphalangeal Arthrodesis of the Toe with a New Radiolucent Intramedullary Implant DIEBOLD P.-F., ROCHER H.,, DETERME P., CERMOLACCE C., GUILLO S., AVEROUS C., LEIBER WACKENHEIN F. Interphalangeal Arthrodesis
Retrospective Study of Surgical Outcomes for Combined Ankle and Subtalar Joint Arthrodesis, Cavovarus Deformity Correction and Ankle Fractures
 FOOT/ ANKLE RETROSPECTIVE STUDYIC S Retrospective Study of Surgical Outcomes for Combined Ankle and Subtalar Joint Arthrodesis, Cavovarus Deformity Correction and Ankle Fractures Adult & Pediatric Deformity
FOOT/ ANKLE RETROSPECTIVE STUDYIC S Retrospective Study of Surgical Outcomes for Combined Ankle and Subtalar Joint Arthrodesis, Cavovarus Deformity Correction and Ankle Fractures Adult & Pediatric Deformity
SURGICAL TECHNIQUE GUIDE
 DANGER indicates an imminently hazardous situation which, if not avoided, will result in death or serious injury. WARNING indicates a potentially hazardous situation which, if not avoided, could result
DANGER indicates an imminently hazardous situation which, if not avoided, will result in death or serious injury. WARNING indicates a potentially hazardous situation which, if not avoided, could result
LCP Medial Distal Tibia Plate, without Tab. The Low Profile Anatomic Fixation System with Angular Stability and Optimal Screw Orientation.
 LCP Medial Distal Tibia Plate, without Tab. The Low Profile Anatomic Fixation System with Angular Stability and Optimal Screw Orientation. Technique Guide LCP Small Fragment System Table of Contents Introduction
LCP Medial Distal Tibia Plate, without Tab. The Low Profile Anatomic Fixation System with Angular Stability and Optimal Screw Orientation. Technique Guide LCP Small Fragment System Table of Contents Introduction
Index. Clin Podiatr Med Surg 22 (2005) Note: Page numbers of article titles are in boldface type.
 Clin Podiatr Med Surg 22 (2005) 309 314 Index Note: Page numbers of article titles are in boldface type. A Abductor digiti minimi muscle, myectomy of, for tailor s bunionette, 243 Achilles tendon, lengthening
Clin Podiatr Med Surg 22 (2005) 309 314 Index Note: Page numbers of article titles are in boldface type. A Abductor digiti minimi muscle, myectomy of, for tailor s bunionette, 243 Achilles tendon, lengthening
Alberta Health Care Insurance Plan. Schedule Of Anaesthetic Rates Applicable To Podiatry. Procedure List. As Of. 01 April Government of Alberta
 Alberta Health Care Insurance Plan Procedure List As Of 01 April 2017 Alberta Health Care Insurance Plan Page i Generated 2017/03/14 TABLE OF CONTENTS As of 2017/04/01 II. OPERATIONS ON THE NERVOUS SYSTEM.......................
Alberta Health Care Insurance Plan Procedure List As Of 01 April 2017 Alberta Health Care Insurance Plan Page i Generated 2017/03/14 TABLE OF CONTENTS As of 2017/04/01 II. OPERATIONS ON THE NERVOUS SYSTEM.......................
Medical Policy Partial or Total Replacement of First Metatarsophalangeal Joint
 Medical Policy Partial or Total Replacement of First Metatarsophalangeal Joint Subject: Partial or Total Replacement of First Metatarsophalangeal (MTP) Joint Background: Underlying causes of disease or
Medical Policy Partial or Total Replacement of First Metatarsophalangeal Joint Subject: Partial or Total Replacement of First Metatarsophalangeal (MTP) Joint Background: Underlying causes of disease or
Medincenter GlavUpDK by the Ministry of Foreign Affairs of Russia, Moscow.
 Medincenter GlavUpDK by the Ministry of Foreign Affairs of Russia, Moscow. Berezhnoy Sergey. Percutaneous First Metatarsocuneiform Joint Arthrodesis in a Treatment of Metatarsus Primus Varus: a Prospective
Medincenter GlavUpDK by the Ministry of Foreign Affairs of Russia, Moscow. Berezhnoy Sergey. Percutaneous First Metatarsocuneiform Joint Arthrodesis in a Treatment of Metatarsus Primus Varus: a Prospective
Small-wire circular fixators and hybrid external fixation
 ORIGINAL ARTICLE Correction of Tibial Malunion and Nonunion With Six-Axis Analysis Deformity Correction Using the Taylor Spatial Frame David S. Feldman, MD, Steven S. Shin, MD, Sanjeev Madan, MD, and Kenneth
ORIGINAL ARTICLE Correction of Tibial Malunion and Nonunion With Six-Axis Analysis Deformity Correction Using the Taylor Spatial Frame David S. Feldman, MD, Steven S. Shin, MD, Sanjeev Madan, MD, and Kenneth
Re+Line Bunion Correction System for Correction of Hallux Abducto Valgus Deformity
 Re+Line Bunion Correction System for Correction of Hallux Abducto Valgus Deformity Amber M. Shane, DPM, FACFAS 1, Christopher L. Reeves, DPM, FACFAS 1 1. Orlando Foot & Ankle Clinic, Orlando, FL Abstract
Re+Line Bunion Correction System for Correction of Hallux Abducto Valgus Deformity Amber M. Shane, DPM, FACFAS 1, Christopher L. Reeves, DPM, FACFAS 1 1. Orlando Foot & Ankle Clinic, Orlando, FL Abstract
Clinical. Solutions. Synthes Solutions. Foot and Ankle.
 Clinical Solutions Foot and Ankle. Foot and Ankle. Fractures of the tibial shaft Fractures of the distal fibula Fractures of the distal tibia Fractures and osteotomies of the calcaneus Arthrodesis Fractures,
Clinical Solutions Foot and Ankle. Foot and Ankle. Fractures of the tibial shaft Fractures of the distal fibula Fractures of the distal tibia Fractures and osteotomies of the calcaneus Arthrodesis Fractures,
Introduction Basics MIS Screw 2 System Characteristics 2 Indication 2
 Clinical Advisor M. Walther. M.D., Ph.D. Professor of Orthopedic Surgery Head of Department Centre for Foot and Ankle Surgery Schön Klinik München Harlaching FIFA Medical Centre Table of Contents Introduction
Clinical Advisor M. Walther. M.D., Ph.D. Professor of Orthopedic Surgery Head of Department Centre for Foot and Ankle Surgery Schön Klinik München Harlaching FIFA Medical Centre Table of Contents Introduction
1. Orthoapedic Associates of Michigan, PC, Grand Rapids, MI 2. Michigan State University College of Human Medicine, Grand Rapids, MI
 Second Metatarsal Osteotomy Shortening with Tarsometatarsal Arthrodesis: Comparison of Outcomes Between MSP TM Metatarsal Shortening System and Plates and Screws Donald R. Bohay, MD, FACS 1 ; John G. Anderson,
Second Metatarsal Osteotomy Shortening with Tarsometatarsal Arthrodesis: Comparison of Outcomes Between MSP TM Metatarsal Shortening System and Plates and Screws Donald R. Bohay, MD, FACS 1 ; John G. Anderson,
19 Arthrodesis of the First Metatarsocuneiform Joint
 19 Arthrodesis of the First Metatarsocuneiform Joint CHARLES GUDAS Abduction of the first metatarsal to correct metatarsus primus varus and hallux valgus was first described by Albrecht in 1911. 1 Lapidus
19 Arthrodesis of the First Metatarsocuneiform Joint CHARLES GUDAS Abduction of the first metatarsal to correct metatarsus primus varus and hallux valgus was first described by Albrecht in 1911. 1 Lapidus
Preservation of the First Ray in Patients with Diabetes
 Preservation of the First Ray in Patients with Diabetes Surgical approaches are often necessary to off-load excessive pressure. By Derek Ley, DPM, and Barry Rosenblum, DPM Introduction In approaching diabetic
Preservation of the First Ray in Patients with Diabetes Surgical approaches are often necessary to off-load excessive pressure. By Derek Ley, DPM, and Barry Rosenblum, DPM Introduction In approaching diabetic
Foot and Ankle Systems Coding Reference Guide
 Foot and Ankle Systems Coding Reference Guide Physician Arthrodesis 27870 Arthrodesis, ankle, open 27871 Arthrodesis, tibiofibular joint, proximal or distal 28705 Arthrodesis; pantalar 28715 Arthrodesis;
Foot and Ankle Systems Coding Reference Guide Physician Arthrodesis 27870 Arthrodesis, ankle, open 27871 Arthrodesis, tibiofibular joint, proximal or distal 28705 Arthrodesis; pantalar 28715 Arthrodesis;
SCIENTIFIC POSTER #28 Tibia OTA 2016
 SCIENTIFIC POSTER #28 Tibia OTA 2016 Effectiveness of Complex Combined Nonunion/Malunion Correction, Utilizing a Hexapod External Fixator John Arvesen, MD 1 ; J. Tracy Watson, MD 2 ; Heidi Israel, PhD,
SCIENTIFIC POSTER #28 Tibia OTA 2016 Effectiveness of Complex Combined Nonunion/Malunion Correction, Utilizing a Hexapod External Fixator John Arvesen, MD 1 ; J. Tracy Watson, MD 2 ; Heidi Israel, PhD,
DARCO. Bow 2 Plate SURGIC AL TECHNIQUE
 DARCO Bow 2 Plate SURGIC AL TECHNIQUE Contents 2 Preface 3 Chapter 1 4 Chapter 2 5 6 7 8 9 Appendix 10 10 11 Intended Use Indications/Contraindications Design Rationale Preoperative Planning Surgical Technique
DARCO Bow 2 Plate SURGIC AL TECHNIQUE Contents 2 Preface 3 Chapter 1 4 Chapter 2 5 6 7 8 9 Appendix 10 10 11 Intended Use Indications/Contraindications Design Rationale Preoperative Planning Surgical Technique
MICA. Minimally Invasive Foot Surgery CHEVRON OSTEOTOMY SURGIC AL TECHNIQUE
 MICA Minimally Invasive Foot Surgery CHEVRON OSTEOTOMY SURGIC AL TECHNIQUE Contents Chapter 1 4 Introduction Chapter 2 5 Indications and Warnings Chapter 3 6 Patient Positioning and Set Up Chapter 4 7
MICA Minimally Invasive Foot Surgery CHEVRON OSTEOTOMY SURGIC AL TECHNIQUE Contents Chapter 1 4 Introduction Chapter 2 5 Indications and Warnings Chapter 3 6 Patient Positioning and Set Up Chapter 4 7
Combination of First Metatarsophalangeal Joint Arthrodesis and Proximal Correction for Severe Hallux Valgus Deformity
 FOOT &ANKLE INTERNATIONAL DOI: 10.3113/FAI.2012.0400 Combination of First Metatarsophalangeal Joint Arthrodesis and Proximal Correction for Severe Hallux Valgus Deformity Pascal F. Rippstein, MD; Young-Uk
FOOT &ANKLE INTERNATIONAL DOI: 10.3113/FAI.2012.0400 Combination of First Metatarsophalangeal Joint Arthrodesis and Proximal Correction for Severe Hallux Valgus Deformity Pascal F. Rippstein, MD; Young-Uk
Hallux Rigidus & Silastic Total Implants
 Hallux Rigidus & Silastic Total Implants JOSHUA L. MOORE, DPM FACFAS ASSISTANT DEAN OF EDUCATIONAL AFFAIRS TUSPM CLINICAL ASSISTANT PROFESSOR OF SURGERY Definitions Hallux Limitus 1 st MTPJ range of motion
Hallux Rigidus & Silastic Total Implants JOSHUA L. MOORE, DPM FACFAS ASSISTANT DEAN OF EDUCATIONAL AFFAIRS TUSPM CLINICAL ASSISTANT PROFESSOR OF SURGERY Definitions Hallux Limitus 1 st MTPJ range of motion
A perspective on MPJ implant arthroplasty.
 A perspective on MPJ implant arthroplasty. The BioPro MPJ Hemi Implant System: +65 years of successful clinical use. Pre-op Post-op 20+ year implant survivorship 14 96% Survivorship 1 97% Patient Satisfaction
A perspective on MPJ implant arthroplasty. The BioPro MPJ Hemi Implant System: +65 years of successful clinical use. Pre-op Post-op 20+ year implant survivorship 14 96% Survivorship 1 97% Patient Satisfaction
The Vilex FUZETM. Dual Thread Screw & Intramedullary Nail in One Implant. The Ultimate TTC Arthrodesis Internal Fixator
 The Vilex FUZETM Dual Thread Screw & Intramedullary Nail in One Implant The Ultimate TTC Arthrodesis Internal Fixator Introduction The Vilex FUZE TM TTC Arthrodesis Compression Nail combines the attributes
The Vilex FUZETM Dual Thread Screw & Intramedullary Nail in One Implant The Ultimate TTC Arthrodesis Internal Fixator Introduction The Vilex FUZE TM TTC Arthrodesis Compression Nail combines the attributes
Merete PlantarMAX Lapidus Plate Surgical Technique. Description of Plate
 Merete PlantarMAX Lapidus Plate Surgical Technique Description of Plate Merete Medical has designed the PlantarMax; a special Plantar/Medial Locking Lapidus plate which places the plate in the most biomechanically
Merete PlantarMAX Lapidus Plate Surgical Technique Description of Plate Merete Medical has designed the PlantarMax; a special Plantar/Medial Locking Lapidus plate which places the plate in the most biomechanically
Metatarsal Lengthening By Callus Distraction For Brachymetatarsia. Case Report and Review of the Literature
 The Internet Journal of Third World Medicine TM ISSN: 1539-4646 Home Current Issue Archives Instructions for Authors Disclaimer Printable Version Metatarsal Lengthening By Callus Distraction For Brachymetatarsia:
The Internet Journal of Third World Medicine TM ISSN: 1539-4646 Home Current Issue Archives Instructions for Authors Disclaimer Printable Version Metatarsal Lengthening By Callus Distraction For Brachymetatarsia:
Symptomatic Medial Exostosis of the Great Toe Distal Phalanx: A Complication Due to Over-correction Following Akin Osteotomy for Hallux Valgus Repair
 Symptomatic Medial Exostosis of the Great Toe Distal Phalanx: A Complication Due to Over-correction Following Akin Osteotomy for Hallux Valgus Repair Carlos Villas, MD, PhD, 1 Javier Del Río, MD, 3 Andres
Symptomatic Medial Exostosis of the Great Toe Distal Phalanx: A Complication Due to Over-correction Following Akin Osteotomy for Hallux Valgus Repair Carlos Villas, MD, PhD, 1 Javier Del Río, MD, 3 Andres
Digital Surgery Complications
 Annual Surgical Conference 2018 Digital Surgery Complications Zeeshan S. Husain, DPM, FACFAS, FASPS Great Lakes Foot and Ankle Institute September 21, 2018 None Disclosures Presentation Outline Differentials
Annual Surgical Conference 2018 Digital Surgery Complications Zeeshan S. Husain, DPM, FACFAS, FASPS Great Lakes Foot and Ankle Institute September 21, 2018 None Disclosures Presentation Outline Differentials
Foot and Ankle Technique Guide Metatarsal Shortening Osteotomy
 Surgical Technique Foot and Ankle Technique Guide Metatarsal Shortening Osteotomy Prepared in consultation with: Phinit Phisitkul, MD Department of Orthopedics and Rehabilitation University of Iowa Iowa
Surgical Technique Foot and Ankle Technique Guide Metatarsal Shortening Osteotomy Prepared in consultation with: Phinit Phisitkul, MD Department of Orthopedics and Rehabilitation University of Iowa Iowa
FOOT & ANKLE ORTHOPAEDIC PROCEDURES
 FOOT & ANKLE ORTHOPAEDIC FOOT & ANKLE PROCEDURES FOREFOOT PROCEDURES PIP (Proximal Interphalangeal) Joint Fusion for Hammertoe and DIP (Distal Interphalangeal) Joint Fusion for Mallet Toe Metatarsal Shortening
FOOT & ANKLE ORTHOPAEDIC FOOT & ANKLE PROCEDURES FOREFOOT PROCEDURES PIP (Proximal Interphalangeal) Joint Fusion for Hammertoe and DIP (Distal Interphalangeal) Joint Fusion for Mallet Toe Metatarsal Shortening
TIBIAXYS ANKLE FUSION
 TIBIAXYS ANKLE FUSION SURGICAL TECHNIQUE TIBIAXYS Ankle Fusion Plate features Anatomically contoured plates The plates are designed to approximate the patient s bony and soft tissue anatomy The plate designs
TIBIAXYS ANKLE FUSION SURGICAL TECHNIQUE TIBIAXYS Ankle Fusion Plate features Anatomically contoured plates The plates are designed to approximate the patient s bony and soft tissue anatomy The plate designs
Contents. Chapter 1 4 Chapter Chapter Chapter Chapter 5 15
 Contents Chapter 1 4 Chapter 2 5 5 Chapter 3 6 6 7 Chapter 4 8 8 8 8 9 10 10 11 12 13 14 14 Chapter 5 15 Introduction Intended Use Indications Device Description Implant Options and Sizing Instrumentation
Contents Chapter 1 4 Chapter 2 5 5 Chapter 3 6 6 7 Chapter 4 8 8 8 8 9 10 10 11 12 13 14 14 Chapter 5 15 Introduction Intended Use Indications Device Description Implant Options and Sizing Instrumentation
Lapidus Arthrodesis System Instructions for Use
 Lapidus Arthrodesis System Instructions for Use Description The AlignMATE Lapidus Arthrodesis System consists of bone plates and bone screws (locking, non-locking and interfragmentary), which are intended
Lapidus Arthrodesis System Instructions for Use Description The AlignMATE Lapidus Arthrodesis System consists of bone plates and bone screws (locking, non-locking and interfragmentary), which are intended
Hallux Valgus Deformity: Preoperative Radiologic Assessment
 119 Pictorial Essay H............ - Hallux Valgus Deformity: Preoperative Radiologic Assessment David Karasick1 and Keith L. Wapner An estimated 40% of the American adult population experiences foot problems,
119 Pictorial Essay H............ - Hallux Valgus Deformity: Preoperative Radiologic Assessment David Karasick1 and Keith L. Wapner An estimated 40% of the American adult population experiences foot problems,
Great Toe Joint Replacement Patient Guide
 Great Toe Joint Replacement Patient Guide The BioPro First MPJ Hemi Implant The proven long-term joint fusion alternative. Long-term use Clinically proven High implant survivorship Long-term implant survivorship
Great Toe Joint Replacement Patient Guide The BioPro First MPJ Hemi Implant The proven long-term joint fusion alternative. Long-term use Clinically proven High implant survivorship Long-term implant survivorship
Minimally Invasive Bunionectomy: The Lam Modification of the Traditional Distal First Metatarsal Osteotomy Bunionectomy
 CHAPTER 2 Minimally Invasive Bunionectomy: The Lam Modification of the Traditional Distal First Metatarsal Osteotomy Bunionectomy Kevin Lam, DPM Rikhil Patel, DPM Thomas Merrill, DPM Hallux abducto valgus
CHAPTER 2 Minimally Invasive Bunionectomy: The Lam Modification of the Traditional Distal First Metatarsal Osteotomy Bunionectomy Kevin Lam, DPM Rikhil Patel, DPM Thomas Merrill, DPM Hallux abducto valgus
Disclosures. 55 year old Male 2/23/2018. Recurrent Hallux Rigidus: Options Other than Arthrodesis
 Recurrent Hallux Rigidus: Options Other than Arthrodesis Gregory C Berlet, MD FRCS(C), FAOA Orthopedic Foot and Ankle Columbus, Ohio Columbus, Ohio orthofootankle.com Disclosures Consultant/Speaker Bureau/Royalties/
Recurrent Hallux Rigidus: Options Other than Arthrodesis Gregory C Berlet, MD FRCS(C), FAOA Orthopedic Foot and Ankle Columbus, Ohio Columbus, Ohio orthofootankle.com Disclosures Consultant/Speaker Bureau/Royalties/
Variable Angle LCP Forefoot/Midfoot System 2.4/2.7. Procedure specific plates for osteotomies, arthrodeses and fractures of the foot.
 Variable Angle LCP Forefoot/Midfoot System 2.4/2.7. Procedure specific plates for osteotomies, arthrodeses and fractures of the foot. Compression technology Variable angle locking technology Anatomic and
Variable Angle LCP Forefoot/Midfoot System 2.4/2.7. Procedure specific plates for osteotomies, arthrodeses and fractures of the foot. Compression technology Variable angle locking technology Anatomic and
First metatarsophalangeal hemiarthroplasty for hallux rigidus
 DOI 10.1007/s00264-010-1012-x ORIGINAL PAPER First metatarsophalangeal hemiarthroplasty for hallux rigidus Eric Giza & Martin Sullivan & Dan Ocel & Gregory Lundeen & Matt Mitchell & Lauren Frizzell Received:
DOI 10.1007/s00264-010-1012-x ORIGINAL PAPER First metatarsophalangeal hemiarthroplasty for hallux rigidus Eric Giza & Martin Sullivan & Dan Ocel & Gregory Lundeen & Matt Mitchell & Lauren Frizzell Received:
HammerFUZE HAMMERTOE COMPRESSION SYSTEM SURGICAL TECHNIQUE
 HammerFUZE HAMMERTOE COMPRESSION SYSTEM SURGICAL TECHNIQUE HammerFUZE HAMMERTOE COMPRESSION SYSTEM SURGICAL TECHNIQUE Design Rationale The HammerFUZE Hammertoe Compression System was designed to simplify
HammerFUZE HAMMERTOE COMPRESSION SYSTEM SURGICAL TECHNIQUE HammerFUZE HAMMERTOE COMPRESSION SYSTEM SURGICAL TECHNIQUE Design Rationale The HammerFUZE Hammertoe Compression System was designed to simplify
Orthopedic & Sports Medicine, Bay Care Clinic, 501 N. 10th Street, Manitowoc, WI Procedure. Subtalar arthrodesis
 OSTEOAMP Allogeneic Morphogenetic Proteins Subtalar Nonunions OSTEOAMP Case Report SUBTALAR NONUNIONS Dr. Jason George DeVries and Dr. Brandon M. Scharer Orthopedic & Sports Medicine, Bay Care Clinic,
OSTEOAMP Allogeneic Morphogenetic Proteins Subtalar Nonunions OSTEOAMP Case Report SUBTALAR NONUNIONS Dr. Jason George DeVries and Dr. Brandon M. Scharer Orthopedic & Sports Medicine, Bay Care Clinic,
SUBTALAR ARTHROEREISIS IN THE OLDER PATIENT
 C H A P T E R 1 7 SUBTALAR ARTHROEREISIS IN THE OLDER PATIENT William D. Fishco, DPM, MS INTRODUCTION Arthroereisis is a surgical procedure designed to limit the motion of a joint. Subtalar joint arthroereisis
C H A P T E R 1 7 SUBTALAR ARTHROEREISIS IN THE OLDER PATIENT William D. Fishco, DPM, MS INTRODUCTION Arthroereisis is a surgical procedure designed to limit the motion of a joint. Subtalar joint arthroereisis
Congenital Hallux Varus with Polydactyly and Syndactyly- Correction in an Adult - A Case Report
 Case Report Journal of Orthopaedic Case Reports 2014 April-June;4(2): Page 64-68 Abstract Congenital Hallux Varus with Polydactyly and Syndactyly- Correction in an Adult - A Case Report 1,2 3 1 2 Sampat
Case Report Journal of Orthopaedic Case Reports 2014 April-June;4(2): Page 64-68 Abstract Congenital Hallux Varus with Polydactyly and Syndactyly- Correction in an Adult - A Case Report 1,2 3 1 2 Sampat
Knee spanning solutions
 Knee spanning solutions System features Indications Intended to be used on adults or pediatric patients as required for fracture fixation (open or closed); post-traumatic joint contracture which has resulted
Knee spanning solutions System features Indications Intended to be used on adults or pediatric patients as required for fracture fixation (open or closed); post-traumatic joint contracture which has resulted
Fractures of the tibia shaft treated with locked intramedullary nail Retrospective clinical and radiographic assesment
 ARS Medica Tomitana - 2013; 4(75): 197-201 DOI: 10.2478/arsm-2013-0035 Șerban Al., Botnaru V., Turcu R., Obadă B., Anderlik St. Fractures of the tibia shaft treated with locked intramedullary nail Retrospective
ARS Medica Tomitana - 2013; 4(75): 197-201 DOI: 10.2478/arsm-2013-0035 Șerban Al., Botnaru V., Turcu R., Obadă B., Anderlik St. Fractures of the tibia shaft treated with locked intramedullary nail Retrospective
The Latest Breakthrough in TTC Fusion Technology
 The Latest Breakthrough in TTC Fusion Technology Treatment of Hindfoot Non-Union with DynaNail TTC Fusion System A CASE REPORT Dr. L. Daniel Latt, MD, PhD Background The DynaNail TTC Fusion System is intended
The Latest Breakthrough in TTC Fusion Technology Treatment of Hindfoot Non-Union with DynaNail TTC Fusion System A CASE REPORT Dr. L. Daniel Latt, MD, PhD Background The DynaNail TTC Fusion System is intended
SURGICAL TECHNIQUE CHI. Cannulated Hemi Implants 1 ST MPJ ARTHROPLASTY
 CHI Cannulated Hemi Implants 1 ST MPJ ARTHROPLASTY SURGICAL TECHNIQUE CHI Cannulated Hemi Implants Design Rationale Pain of the great toe joint often leads to altered lifestyles. The goal of MPJ implant
CHI Cannulated Hemi Implants 1 ST MPJ ARTHROPLASTY SURGICAL TECHNIQUE CHI Cannulated Hemi Implants Design Rationale Pain of the great toe joint often leads to altered lifestyles. The goal of MPJ implant
Arthrex Open Wedge Osteotomy Technique Designed in conjunction with:
 Arthrex Open Wedge Osteotomy Technique Designed in conjunction with: Dr. Giancarlo Puddu, M.D. Dr. Peter Fowler, M.D. Dr. Ned Amendola, M.D. To treat pain and instability associated with lower extremity
Arthrex Open Wedge Osteotomy Technique Designed in conjunction with: Dr. Giancarlo Puddu, M.D. Dr. Peter Fowler, M.D. Dr. Ned Amendola, M.D. To treat pain and instability associated with lower extremity
COMPLICATIONS OF BRACHYMETATARSIA REPAIR WITH CALLUS DISTRACTION
 C H A P T E R 4 1 COMPLICATIONS OF BRACHYMETATARSIA REPAIR WITH CALLUS DISTRACTION Michelle L. Butterworth, DPM INTRODUCTION Brachymetatarsia represents one of the best and most useful indications for
C H A P T E R 4 1 COMPLICATIONS OF BRACHYMETATARSIA REPAIR WITH CALLUS DISTRACTION Michelle L. Butterworth, DPM INTRODUCTION Brachymetatarsia represents one of the best and most useful indications for
Midfoot Plating Techniques Surgical Technique
 Midfoot Plating Techniques Surgical Technique Midfoot Plating Techniques Lapidus Plate Designed to provide excellent fixation for a lapidus procedure, the Lapidus Plate offers the foot & ankle surgeon
Midfoot Plating Techniques Surgical Technique Midfoot Plating Techniques Lapidus Plate Designed to provide excellent fixation for a lapidus procedure, the Lapidus Plate offers the foot & ankle surgeon
CARTIVA. Synthetic Cartilage Implant SURGICAL IMPLANTATION TECHNIQUE. First Metatarsal Phalangeal Joint THE DIFFERENCE IS MOVING.
 CARTIVA Synthetic Cartilage Implant SURGICAL IMPLANTATION TECHNIQUE First Metatarsal Phalangeal Joint THE DIFFERENCE IS MOVING. CARTIVA SYNTHETIC CARTILAGE IMPLANT TABLE OF CONTENTS Introduction... 3 Cartiva
CARTIVA Synthetic Cartilage Implant SURGICAL IMPLANTATION TECHNIQUE First Metatarsal Phalangeal Joint THE DIFFERENCE IS MOVING. CARTIVA SYNTHETIC CARTILAGE IMPLANT TABLE OF CONTENTS Introduction... 3 Cartiva
6/5/2018. Forefoot Disorders. Highgate Private Hospital (Royal Free London NHS Foundation Trust (Barnet & Chase Farm Hospitals) Hallux Rigidus
 Forefoot Disorders Mr Pinak Ray (MS, MCh(Orth), FRCS, FRCS(Tr&Orth)) Highgate Private Hospital (Royal Free London NHS Foundation Trust (Barnet & Chase Farm Hospitals) E: ray.secretary@uk-conslutants Our
Forefoot Disorders Mr Pinak Ray (MS, MCh(Orth), FRCS, FRCS(Tr&Orth)) Highgate Private Hospital (Royal Free London NHS Foundation Trust (Barnet & Chase Farm Hospitals) E: ray.secretary@uk-conslutants Our
Calcaneus (Heel Bone) Fractures
 Page 1 of 8 Calcaneus (Heel Bone) Fractures A fracture of the calcaneus, or heel bone, can be a painful and disabling injury. This type of fracture commonly occurs during a high-energy event such as a
Page 1 of 8 Calcaneus (Heel Bone) Fractures A fracture of the calcaneus, or heel bone, can be a painful and disabling injury. This type of fracture commonly occurs during a high-energy event such as a
LOWER EXTREMITIES SINGLE-USE INSTRUMENTATION SURGICAL IMPLANTATION TECHNIQUE. First Metatarsal Phalangeal Joint FOOT THE DIFFERENCE IS MOVING.
 LOWER EXTREMITIES SINGLE-USE INSTRUMENTATION SURGICAL IMPLANTATION TECHNIQUE First Metatarsal Phalangeal Joint FOOT THE DIFFERENCE IS MOVING. CARTIVA SYNTHETIC CARTILAGE IMPLANT SURGICAL IMPLANTATION TECHNIQUE
LOWER EXTREMITIES SINGLE-USE INSTRUMENTATION SURGICAL IMPLANTATION TECHNIQUE First Metatarsal Phalangeal Joint FOOT THE DIFFERENCE IS MOVING. CARTIVA SYNTHETIC CARTILAGE IMPLANT SURGICAL IMPLANTATION TECHNIQUE
6.5 mm midfoot fusion bolt
 6.5 mm midfoot fusion bolt For intramedullary fixation of the medial column of the foot SurgIcal technique Table of Contents Introduction 6.5 mm Midfoot Fusion Bolt 2 AO Principles 4 Indications 5 Surgical
6.5 mm midfoot fusion bolt For intramedullary fixation of the medial column of the foot SurgIcal technique Table of Contents Introduction 6.5 mm Midfoot Fusion Bolt 2 AO Principles 4 Indications 5 Surgical
Surgical Technique. Customer Service:
 Patent and Patent Pending CAUTION: Federal Law (USA) restricts this device to sale by or on the order of a physician. INDICATIONS FOR USE The Axis Charcot Fixation System in diameters of 5.5, 6.5 and 7.5mm
Patent and Patent Pending CAUTION: Federal Law (USA) restricts this device to sale by or on the order of a physician. INDICATIONS FOR USE The Axis Charcot Fixation System in diameters of 5.5, 6.5 and 7.5mm
The American Academy of Foot & Ankle Osteosynthesis. presents
 The American Academy of Foot & Ankle Osteosynthesis presents Comprehensive Course of Internal Fixation for Reconstructive Surgery and Trauma of the Foot & Ankle September 4-6, 2014 Goodlett Farms Innovation
The American Academy of Foot & Ankle Osteosynthesis presents Comprehensive Course of Internal Fixation for Reconstructive Surgery and Trauma of the Foot & Ankle September 4-6, 2014 Goodlett Farms Innovation
Flower Medium Headless & Cannulated Screws
 Flower Medium Headless & Cannulated Screws PROCEDURE GUIDE www.flowerortho.com The Flower Foot & Ankle Application NC FUSION PLATE 2-HOLE COMPRESSION PLATE TMT FUSION PLATE LAPIDUS FUSION PLATE COMPRESSION
Flower Medium Headless & Cannulated Screws PROCEDURE GUIDE www.flowerortho.com The Flower Foot & Ankle Application NC FUSION PLATE 2-HOLE COMPRESSION PLATE TMT FUSION PLATE LAPIDUS FUSION PLATE COMPRESSION
Alberta Health Care Insurance Plan. Schedule Of Anaesthetic Rates Applicable To Podiatric Surgery. Procedure List. As Of.
 Alberta Health Care Insurance Plan Procedure List As Of 01 April 2016 Alberta Health Care Insurance Plan Page i Generated 2016/03/22 TABLE OF CONTENTS As of 2016/04/01 07 PHYSICAL MEDICINE, REHABILITATION,
Alberta Health Care Insurance Plan Procedure List As Of 01 April 2016 Alberta Health Care Insurance Plan Page i Generated 2016/03/22 TABLE OF CONTENTS As of 2016/04/01 07 PHYSICAL MEDICINE, REHABILITATION,
Lesser toe sequential repair
 Lesser toe sequential repair For the correction of lesser toe deformity Information for patients Department of Podiatric Surgery What is lesser toe deformity? The lesser toes are those other than your
Lesser toe sequential repair For the correction of lesser toe deformity Information for patients Department of Podiatric Surgery What is lesser toe deformity? The lesser toes are those other than your
Assessment of percutaneous V osteotomy of the calcaneus with Ilizarov application for correction of complex foot deformities
 Acta Orthop. Belg., 2004, 70, 586-590 ORIGINAL STUDY Assessment of percutaneous V osteotomy of the calcaneus with Ilizarov application for correction of complex foot deformities Hani EL-MOWAFI From Mansoura
Acta Orthop. Belg., 2004, 70, 586-590 ORIGINAL STUDY Assessment of percutaneous V osteotomy of the calcaneus with Ilizarov application for correction of complex foot deformities Hani EL-MOWAFI From Mansoura
