The final publication is available
|
|
|
- Erica Higgins
- 5 years ago
- Views:
Transcription
1 Title Periosteal cells are a major source fracture. Author(s) Murao, Hiroki; Yamamoto, Koji; Mats Haruhiko Citation Journal of bone and mineral 398 metabol Issue Date URL Right The final publication is available Type Journal Article Textversion author Kyoto University
2 Periosteal cells are a major source of soft callus in bone fracture Hiroki Murao* Koji Yamamoto* Shuichi Matsuda Haruhiko Akiyama H. Murao K. Yamamoto S. Matsuda H. Akiyama Department of Orthopaedics, Kyoto University, 54 Kawahara-cho, Shogoin, Sakyo, Kyoto, Japan *These two authors contributed equally to this paper. Corresponding author. H. Akiyama: Department of Orthopaedics, Kyoto University, 54 Kawahara-cho, Shogoin, Sakyo, Kyoto, Japan. Tel.: ; Fax: hakiyama@kuhp.kyoto-u.ac.jp Keywords: Fracture healing Periosteal cells Soft callus Cell lineage Sox9 1
3 Abstract During the healing process after bone fracture, soft callus forms adjacent to the fracture site, is replaced by hard callus, and is finally remodeled to the original bone configuration. Although the cambium layer of the periosteum is reported to play an essential role in callus formation, we still lack direct in vivo evidence of this. To investigate the cell lineage of the soft callus, we analyzed the process of fracture healing in Prx1-Cre;ROSA26 reporter (R26R), Col1a1(3.6 kb)-cre;r26r, Col1a1(2.3 kb)- Cre;R26R, Sox9-CreERT2;R26R, and Sox9-LacZ mice with X-gal staining. In the Prx1- Cre;R26R, in which the cells of the periosteum stained for X-gal before fracture, all cells in the soft callus were X-gal positive, whereas in the Col1a1(3.6 kb)-cre;r26r mice, the cells in the periosteum before fracture stained for X-gal and the soft callus was partly composed of X-gal-positive cells. In contrast, in the Col1a1(2.3 kb)- Cre;R26R mice, in which the mature osteoblasts in the cambium layer of the periosteum were marked before fracture, no cells in the soft callus at the fracture site were X-gal positive. These results suggest that most of the cells in the soft callus are derived from the mesenchymal progenitors in the periosteum, and not from mature osteoblastic cells. Interestingly, in the Sox9-LacZ mice, Sox9-expressing X-gal-positive cells emerged in the periosteum adjacent to the fracture site three days after fracture. We demonstrated this by injecting tamoxifen into the Sox9-CreERT2;R26R mice for three days after fracture, so that these Sox9-expressing periosteal cells gave rise to cells in the soft and hard calli. Our findings show that the periosteal cells in which Sox9 expression is induced just after fracture are the major source of the chondrocytes and osteoblasts in the fracture callus. 2
4 Introduction Bone is a highly organized and specialized connective tissue and is composed of two structural types, cortical and cancellous bone. The external and internal surfaces of the cortical bone are covered by the periosteum and endosteum, respectively. Microscopically, the periosteum is composed of an outer fibrous layer containing cells that synthesize collagen fibers and an inner cambium layer consisting of osteoblasts, fibroblasts, and mesenchymal progenitor cells with the capacity to differentiate into osteoblasts and chondrocytes [1]. The spaces in cancellous bone are filled with various types of marrow cells, including pluripotent marrow stromal cells. Broken bones undergo processes of endochondral ossification and intramembranous ossification that recapitulate certain aspects of skeletal development. The fracture healing process is partitioned into four stages based on histological observations [2]. The inflammatory stage begins immediately after the bone is fractured, in association with the disruption of the surrounding soft tissues, bleeding within the fracture area, and distortion of the marrow architecture, which lead to local inflammation and the formation of a hematoma. At this stage, stem cells originating from multiple sources are likely to be committed to and initiate the cell lineages involved in bone repair and vascularization. At the stage of soft callus formation, the adjacent periosteum becomes thickened and cartilage tissues appear outside the bone. Discrete cartilaginous regions grow progressively and bridge the fractured bone fragments. This cartilaginous template of the soft callus is then replaced by bone, resulting in the formation of a hard callus (the hard callus formation stage). The hard callus is remodeled by osteoclasts and osteoblasts and returns to the original cortical and 3
5 trabecular bone configuration (the bone remodeling stage). Several possible sources of the cells that produce bone and cartilage at the fracture site have been identified. Although previous studies have reported potential sources of stem cells or progenitor cells in the bone marrow, endosteum, vessel walls, surrounding soft tissues (including muscle and adipose tissues), and the circulation, the periosteum plays a crucial role in fracture healing [3-5]. Periosteal damage or removal results in delayed healing of the fracture [6]. Colnot showed that the periosteum is a major source of osteoblasts and chondrocytes during fracture healing [7]. In particular, the cambium layer is the component of the periosteum essential for bone formation. Ito et al. cultured rabbit periosteal explants and showed that the chondrocyte precursors were located in the cambium layer of the periosteum and that chondrogenesis took place in the juxtaosseous area in the cambium layer [8]. However, we still lack direct in vivo evidence of the progenitor cells in the periosteum and their contribution to fracture healing. The transcription factor Sox9 is expressed in all chondroprogenitor cells and plays an essential role in chondrogenesis [9]. Cell fate mapping in Sox9-Cre;ROSA26 reporter (R26R) mice revealed that Sox9-expressing limb bud mesenchymal cells give rise to both chondrocytes and osteoblasts, indicating that Sox9 defines osteochondroprogenitor cells during skeletogenesis [10]. We also generated a mouse strain that inducibly expresses Cre recombinase in Sox9-expressing cells [11]. An IRES- CreERT2-pA cassette was inserted into the 3 untranslated region of the Sox9 gene, resulting in Cre recombinase expression directly under Sox9 cis-regulatory control via the production of a bicistronic Sox9-Cre recombinase mrna. The administration of tamoxifen to offspring of crosses between Sox9-CreERT2 and R26R mice efficiently 4
6 induced the expression of the Cre reporter in Sox9-expressing cells. The advantage of this genetic system in examining gene expression patterns is that the R26R strain provides a permanent lineage record through its constitutive X-gal expression in cells that express Cre recombinase, even transiently, in the precursor cells of different cell lineages. Therefore, this mouse line has been useful for tracing Sox9-expressing osteochondroprogenitor cells in vivo. In this study, using several Cre drivers, we found that osteochondroprogenitor cells are initiated in the periosteum adjacent to the fracture site and are the major source of the soft callus. Materials and methods Animals Prx1-Cre mice, Col1a1(2.3 kb)-cre mice, Sox9-LacZ knock-in mice, Sox9- CreERT2 mice, and R26R mice have been reported previously [11-15]. Col1a1(3.6 kb)- Cre mice were purchased from the Jackson Laboratory. Tibia fracture model Eight-week-old Prx1-Cre;R26R, Col1a1(3.6 kb)-cre;r26r, Col1a1(2.3 kb)- Cre;R26R, Sox9-LacZ, and Sox9-CreERT2;R26R mice were used to prepare the tibia fractures. Each mouse was anesthetized with mg/kg pentobarbital administered intraperitoneally. The skin, subcutaneous tissues, and fascia were incised along the anterior part of the left leg and retracted medially, and the tibia was exposed. The middiaphysis of the tibia was fractured using scissors, without stripping off the periosteum. Three to five animals were analyzed for each mouse line. 5
7 Histological analysis The fractured tibiae were collected 3, 5, 7, 14, 21, or 28 days after surgery as indicated in each mouse line. The fresh tibia samples were quickly embedded in OCT compound medium (Sakura Finetek) for cryosectioning and sectioned at a thickness of 8 µm. After the sectioned samples were fixed in 0.2% glutaraldehyde/2% formaldehyde, they were stained by 0.15% (w/v) Alcian blue (ph 2.5) and hematoxylin/eosin or with X-gal solution overnight at 37 C and counterstained with Nuclear Fast Red as described previously [16]. Results Process of fracture healing in mouse tibia We first clarified the process of callus formation during the healing of mouse tibia fractures using histology with Alcian blue and hematoxylin/eosin staining (Fig. 1a and b). On day 3 after surgery, the periosteum adjacent to the fracture site started to thicken. On day 7, soft callus formation was distinguished by Alcian blue staining, and the soft callus was replaced by bone to form the hard callus. On day 14, the soft callus had diminished, and a large part of the callus was occupied by hard callus. On days 21 and 28, the hard callus was remodeled, and newly formed periosteum and bone marrow were detected. Cells derived from Prx1-promoter-active pluripotent mesenchymal cells and Col1a1(3.6 kb)-promoter-active premature mesenchymal cells predominantly contribute to soft callus formation in fracture healing 6
8 We clarified the cell lineage of the soft callus using Prx1-Cre;R26R mice. Because Prx1 is expressed in the pluripotent mesenchymal cells of mouse limb buds as early as E9.0, before either an osteoblastic or a chondrogenic lineage has been separated [12], all mesenchymal tissues are derived from Prx1-expressing pluripotent cells. On day 0 before fracture, X-gal-positive cells were found in the periosteum, cortical bone, and endosteum. A small number of X-gal-positive cells were also detected in the bone marrow of the diaphysis (Fig. 2a and b). The cells in the growth plate and metaphyseal bones were X-gal positive. On day 7 after surgery, all cells in the soft callus were X-gal positive (Fig. 2c and d), and on day 14, all the cells in both the soft callus and hard callus were stained for X-gal (Fig. 2e and f). On days 21 and 28, X-gal-positive cells were localized in the remodeled bones and the newly formed periosteum (Fig. 2g-j). Thus, all the cells in the callus may have derived from cells that originated from Prx1- expressing mesenchymal cells and that localized in the periosteum, endosteum, and/or bone marrow. Next, we induced fractures in the tibiae of Col1a1(3.6 kb)-cre;r26r mice, in which the Col1a1(3.6 kb) promoter is active in premature mesenchymal cells and osteoblastic cells. On day 0 before fracture, X-gal-positive cells were found in the periosteum, cortical bone, and endosteum. A small number of X-gal-positive cells were also detected in the bone marrow of the diaphysis (Fig. 3a and b). The cells in the metaphyseal bones were X-gal positive. On day 7 after surgery, a large number of X- gal-positive cells dramatically emerged in the thickened periosteum adjacent to the fracture site, and a proportion of the cells in the soft callus stained for X-gal (Fig. 3c-e). On days 14 and 21, most cells in the soft and hard calli and in the newly formed periosteum were X-gal positive (Fig.3f-i). On day 28 after surgery, X-gal-positive cells 7
9 were localized in the remodeled bones (Fig. 3j). These findings suggest that although Col1a1(3.6 kb)-expressing cells located in the periosteum, endosteum, and/or bone marrow may contribute to the formation of the soft callus, a proportion of the cells in the soft callus are probably derived from Col1a1(3.6 kb)-promoter-active mesenchymal progenitors in the periosteum adjacent to the fracture site. Mature osteoblasts in the periosteum and endosteum do not give rise to chondrocytes in the soft callus To identify the cells in the periosteum that contribute to the formation of the soft callus, we marked mature osteoblasts using Col1a1(2.3 kb)-cre;r26r mice. On day 0 before fracture, X-gal-positive cells were detected in the cambium layer of the periosteum and endosteum, indicating that they were mature osteoblasts (Fig. 4a and b). The cells in the cortex and a small number of cells in the metaphyseal bones were X-gal positive. However, in contrast, there were no X-gal-positive cells in the bone marrow of the diaphysis. On days 7 and 14 after surgery, a large number of X-gal-positive cells were detected in the hard callus but not in the soft callus (Fig. 4c-f). On days 21 and 28, X-gal-positive cells were detected in the remodeled bones (Fig. 4g-j). These results indicate that the Col1a1 (2.3 kb)-expressing mature osteoblasts in the periosteum and endosteum did not give rise to the cells in the soft callus. Sox9-expressing cells emerge transiently in the periosteum adjacent to the fracture site Our previous approaches based on mouse genetics have demonstrated that Sox9 defines osteochondroprogenitor cells and that Sox9 is essential for chondrogenesis [9, 10]. Therefore, Sox9 expression should be induced in the cells that differentiate into 8
10 chondrocytes in the soft callus. To investigate Sox9 expression closely during an early stage of fracture healing, we induced fractures in Sox9-LacZ knock-in mice [14]. On day 0 before surgery, there were no X-gal-positive cells in the bones, including in the periosteum, endosteum, and bone marrow (Fig. 5a and b). In contrast, the growth plate chondrocytes were X-gal positive. On day 3 after surgery, a small number of X-galpositive cells emerged in the cambium layer of the periosteum adjacent to the fracture site (Fig. 5c-e). On day 5, X-gal-positive cells were located only in the soft callus and the thickened periosteum adjacent to the fracture site (Fig. 5f and g). These findings indicate that Sox9-expressing chondroprogenitor cells are induced in the periosteum adjacent to the fracture site. Sox9-expressing cells in the periosteum predominantly contribute to the formation of the soft callus during fracture healing To trace the fate of Sox9-expressing chondroprogenitor cells in the periosteum adjacent to the fracture site, we injected tamoxifen peritoneally into Sox9- CreERT2;R26R mice for three days after surgery [11]. On day 3 after surgery and tamoxifen injection, no X-gal-positive cells were detected in the bones, including the periosteum, endosteum, and bone marrow (Fig. 6a and b). In contrast, the growth plate chondrocytes were X-gal positive. On day 5, X-gal-positive cells were detected in the thickened periosteum and the soft callus (Fig. 6c and d). On days 7 and 14, the cells in the soft and hard calli were X-gal positive (Fig. 6e-h). On day 28, X-gal-positive cells were detected in the newly formed periosteum and the remodeled bone tissues (Fig. 6i and j). These results indicate that the periosteal cells in which Sox9 expression was 9
11 induced just after fracture gave rise to the chondrocytes and osteoblasts in the fracture callus and the cells in the newly formed periosteum during fracture healing. Discussion During the process of fracture healing, pluripotent mesenchymal progenitor cells must be recruited to the fracture site. These cells differentiate into chondrocytes and osteoblasts and contribute to the formation of the soft and hard calli. Several sources of these cells have been detected. Tavassoli and Crosby and Friedenstein et al. demonstrated the existence of mesenchymal stem cells in the bone marrow [17, 18]. Farrington-Rock et al. and Brighton and Hunt reported that pericytes can potentially differentiate into chondrocytes [3, 19]. Lee et al. and Usas et al. showed evidence that muscle-derived cells adjacent to the bone tissues play a role in fracture healing because of their osteogenic potential [5, 20]. Circulating progenitor cells in the bloodstream are also recruited to the fracture site through the stromal cell-derived factor-1/cxcr4 axis and develop a favorable environment for fracture healing by enhancing angiogenesis and osteogenesis [21]. However, when Colnot performed cell lineage analyses by transplanting bone grafts, she demonstrated that the bone itself is the main local source of cells for bone repair [7]. Osteoblasts and osteocytes originate from the periosteum, bone marrow, and endosteum, indicating that these three tissues contribute simultaneously to the formation of new bone. Chondrocytes within the fracture callus are primarily derived from the periosteum. This finding is supported by previous studies [22]. Periosteal damage or removal delays fracture healing because the local sources of pluripotent mesenchymal progenitor cells are thereby removed. 10
12 The current mouse genetics approach based on the Cre/loxP recombination system allows us to define cell lineages at the cellular level. In this study, we first demonstrated that the osteochondroprogenitor cells in the periosteum make a distinct cellular contribution to the soft callus. Prx1 is a homeobox-containing gene that starts to be expressed in all limb bud mesenchymal cells at E9.0, before Sox9 is expressed [12]. We have previously reported that conditional Sox9-null mutants harboring a Prx1-Cre transgene showed a complete lack of both cartilage and bone in their limbs [9]. Moreover, in Prx1-Cre;R26R embryos, all the cells in the skeletal elements, the fibroblasts in the connective tissues, and the tendon cells and the synovial cells were X- gal positive. Hence, Prx1-expressing undifferentiated limb bud mesenchymal cells, including Sox9-expressing osteochondroprogenitor cells, differentiate into all the mesenchymal cell populations. In Prx1-Cre;R26R mice, the periosteum, endosteum, and a small number of the cells in the bone marrow were X-gal positive, and almost all of the soft callus was also X-gal positive. This finding corresponds, in part, to that of Kawanami et al. in Prx1-CreER transgenic mice [23]. They found that Prx1-expressing periosteal cells differentiated into chondrocytes and osteoblasts in the fracture callus, further supporting the notion that Prx1-expressing cells in the periosteum are osteochondroprogenitor cells. We also analyzed fracture healing in Col1a1(3.6 kb)- Cre;R26R mice. The 3.6-kb Col1a1 promoter is active in mesenchymal progenitor cells, immature preosteoblasts, and mature osteoblasts [24]. In the Col1a1(3.6 kb)-cre;r26r mice, the cells in the periosteum, endosteum, and a small number of the cells in the bone marrow were X-gal positive, and a proportion of the cells in the soft callus were X-gal positive. In contrast, in Col1a1(2.3 kb)-cre;r26r mice, a few cells in the periosteum and endosteum were X-gal positive because the 2.3-kb Col1a1 promoter is 11
13 active in mature osteoblasts and osteocytes [25, 26], but no chondrocytes in the soft callus were X-gal positive. The contribution to callus formation during fracture healing of cells that are Prx1- and Col1a1(3.6 kb)-promoter silent before fracture has not yet been clarified. However, our results indicate that a large proportion of chondrocytes in the soft callus at the fracture site are probably derived from cells originating from Prx1- promoter-active mesenchymal progenitor cells in the bone tissue. Col1a1(3.6 kb)- expressing cells in the periosteum also partly contribute to the formation of the soft callus. We have previously shown that Sox9 defines osteochondroprogenitor cells [9]. In Sox9-LacZ mice, no cells in the periosteum express Sox9, suggesting that the pluripotent mesenchymal cells in the periosteum are not committed osteochondroprogenitor cells in the healthy condition. However, three days after a fracture occurs, the periosteal cells in the cambium layer adjacent to the fracture site transiently express Sox9. Therefore, we injected tamoxifen into Sox9-CreERT2;R26R mice for three days after fracture to label the Sox9-expressing periosteal cells and traced the fate of those cells. Interestingly, many X-gal-positive cells were detected in and around the soft and hard calli, indicating that the Sox9-expressing periosteal cells adjacent to the fracture site give rise to chondrocytes and osteoblasts in the fracture callus and in the newly formed periosteal tissues overlying the callus. Kawanami et al. showed that Prx1-expressing periosteal cells differentiate into undifferentiated cells, some of the chondrocytes in the soft callus, osteoblasts, and cells in the newly formed periosteum [23]. Taking all these findings together, pluripotent mesenchymal progenitor cells in the periosteum that originate from Prx1-expressing mesenchymal cells give rise to Sox9-expressing osteochondroprogenitor cells during fracture healing, a process that 12
14 recapitulates endochondral ossification in limb bud development. Sox9-expressing osteochondroprogenitor cells, possibly derived from Col1a1(3.6 kb)-expressing cells, emerged in the thickened periosteum adjacent to the fracture site and make a major contribution to the formation of the soft callus. In conclusion, this cell lineage analysis using a mouse genetics approach has demonstrated that the periosteum plays a central role in soft callus formation during fracture healing. The pluripotent mesenchymal progenitor cells in the periosteum are committed to becoming Sox9-expressing osteochondroprogenitor cells shortly after a fracture occurs and differentiate into chondrocytes, osteoblasts, and periosteal cells. Further research is required to confirm how much Sox9-expressing osteochondroprogenitor cells contribute to fracture repair, and to isolate a pure population of Sox9-expressing cells from the periosteum, to determine the cellular and molecular characteristics of the periosteal osteochondroprogenitor cells. Conflict of interest All authors have no conflicts of interest. Acknowledgements We thank James F. Martin, Philippe Soriano, Chisa Shukunami, and Richard R. Behringer for their valuable help. This work was supported by Grants-in-Aid for Scientific Research from the Japanese Ministry of Education, Culture, Sports, Science, and Technology (# and # to HA and # to KY). 13
15 References 1. Squier CA, Ghoneim S, Kremenak CR (1990) Ultrastructure of the periosteum from membrane bone. J Anat 171: Schindeler A, McDonald MM, Bokko P, Little DG (2008) Bone remodeling during fracture repair: the cellular picture. Semin Cell Dev Biol 19: Farrington-Rock C, Crofts NJ, Doherty MJ, Ashton BA, Griffin-Jones C, Canfield AE (2004) Chondrogenic and adipogenic potential of microvascular pericytes. Circulation 110: Zuk PA, Zhu M, Mizuno H, Huang J, Futrell JW, Katz AJ, Benhaim P, Lorenz HP, Hedrick MH (2001) Multilineage cells from human adipose tissue: implications for cell-based therapies. Tissue Eng 7: Lee JY, Qu-Petersen Z, Cao B, Kimura S, Jankowski R, Cummins J, Usas A, Gates C, Robbins P, Wernig A, Huard J (2000) Clonal isolation of musclederived cells capable of enhancing muscle regeneration and bone healing. J Cell Biol 150: Kojimoto H, Yasui N, Goto T, Matsuda S, Shimomura Y (1988) Bone lengthening in rabbits by callus distraction. The role of periosteum and endosteum. J Bone Joint Surg Br 70: Colnot C (2009) Skeletal cell fate decisions within periosteum and bone marrow during bone regeneration. J Bone Miner Res 24:
16 8. Ito Y, Fitzsimmons JS, Sanyal A, Mello MA, Mukherjee N, O Driscoll SW (2001) Localization of chondrocyte precursors in periosteum. Osteoarthritis Cartilage 9: Akiyama H, Chaboissier MC, Martin JF, Schedl A, de Crombrugghe B (2002) The transcription factor Sox9 has essential roles in successive steps of the chondrocyte differentiation pathway and is required for expression of Sox5 and Sox6. Genes Dev 16: Akiyama H, Kim JE, Nakashima K, Balmes G, Iwai N, Deng JM, Zhang Z, Martin JF, Behringer RR, Nakamura T, de Crombrugghe B (2005) Osteochondroprogenitor cells are derived from Sox9 expressing precursors. Proc Natl Acad Sci U S A 102: Soeda T, Deng JM, de Crombrugghe B, Behringer RR, Nakamura T, Akiyama H (2010) Sox9-expressing precursors are the cellular origin of the cruciate ligament of the knee joint and the limb tendons. Genesis 48: Martin JF, Olson EN (2000) Identification of a prx1 limb enhancer. Genesis 26: Nakanishi R, Akiyama H, Kimura H, Otsuki B, Shimizu M, Tsuboyama T, Nakamura T (2008) Osteoblast-targeted expression of Sfrp4 in mice results in low bone mass. J Bone Miner Res 23:
17 14. Zhu J, Nakamura E, Nguyen MT, Bao X, Akiyama H, Mackem S. (2008) Uncoupling Sonic hedgehog control of pattern and expansion of the developing limb bud. Dev Cell 14: Soriano P (1999) Generalized lacz expression with the ROSA26 Cre reporter strain. Nat Genet 21: Hogan B, Costantini F, Beddington R (1994) Manipulating the Mouse Embryo: A Laboratory Manual. Cold Spring Harbor Laboratory Press, New York 17. Tavassoli M, Crosby WH (1968) Transplantation of marrow to extramedullary sites. Science 161: Friedenstein AJ, Petrakova KV, Kurolesova AI, Frolova GP (1968) Heterotopic of bone marrow. Analysis of precursor cells for osteogenic and hematopoietic tissues. Transplantation 6: Brighton CT, Hunt RM (1997) Early histologic and ultrastructural changes in microvessels of periosteal callus. J Orthop Trauma 11: Usas A, Ho AM, Cooper GM, Olshanski A, Peng H, Huard J (2009) Bone regeneration mediated by BMP4-expressing muscle-derived stem cells is affected by delivery system. Tissue Eng Part A 15: Matsumoto T, Kawamoto A, Kuroda R, Ishikawa M, Mifune Y, Iwasaki H, Miwa M, Horii M, Hayashi S, Oyamada A, Nishimura H, Murasawa S, Doita M, Kurosaka M, Asahara T (2006) Therapeutic potential of vasculogenesis and 16
18 osteogenesis promoted by peripheral blood CD34-positive cells for functional bone healing. Am J Pathol 169: Ozaki A, Tsunoda M, Kinoshita S, Saura R (2000) Role of fracture hematoma and periosteum during fracture healing in rats: interaction of fracture hematoma and the periosteum in the initial step of the healing process. J Orthop Sci 5: Kawanami A, Matsushita T, Chan YY, Murakami S (2009) Mice expressing GFP and CreER in osteochondroprogenitor cells in the periosteum. Biochem Biophys Res Commun 386: Boban I, Jacquin C, Prior K, Barisic-Dujmovic T, Maye P, Clark SH, Aguila HL (2006) The 3.6 kb DNA fragment from the rat Col1a1 gene promoter drives the expression of genes in both osteoblast and osteoclast lineage cells. Bone 39: Dacic S, Kalajzic I, Visnjic D, Lichtler AC, Rowe DW (2001) Col1a1-driven transgenic markers of osteoblast lineage progression. J Bone Miner Res 16: Kalajzic I, Kalajzic Z, Kaliterna M, Gronowicz G, Clark SH, Lichtler AC, Rowe D (2002) Use of type I collagen green fluorescent protein transgenes to identify subpopulations of cells at different stages of the osteoblast lineage. J Bone Miner Res 17:
19 Figure legends Fig. 1 A process of tibial fracture healing. Longitudinal sections through a mouse tibia stained with Alcian blue and hematoxylin/eosin. (a) Low magnification. (b) High magnification of the dotted box in (a). PO: periosteum; BM: bone marrow; SC: soft callus; HC: hard callus; RB: remodeled bone. Scale bar = 1 mm for (a) and 500 µm for (b). Fig. 2 Tibia fracture in Prx1-Cre;R26R mice. (a) X-gal-positive cells are found in the periosteum, cortical bone, and endosteum on day 0. Scale bar = 1 mm. (b) High magnification of (a). Arrowheads indicate X-gal-positive cells in the bone marrow. Scale bar = 100 µm. (c and e) Soft and hard calli are X-gal positive on days 7 and 14. (d and f) High magnification of (c) and (e). (g and i) Remodeled bone and the newly formed periosteum are X-gal positive on days 21 and 28. (h and j) High magnification of (g and i). MB: metaphyseal bone; GP: growth plate; PO: periosteum; EO: endosteum; BM: bone marrow; SC: soft callus; HC: hard callus; RB: remodeled bone. Scale bar = 1mm for (c, e, g, and i) and 500 µm for (d, f, h, and j). Fig. 3 Tibia fracture in Col1a1(3.6 kb)-cre;r26r mice. (a) X-gal positive-cells are found in the periosteum, cortical bone, and endosteum on day 0. Scale bar = 1 mm. (b) High magnification of (a). Arrows indicate X-gal-positive cells in the periosteum and 18
20 endosteum. Arrowheads indicate X-gal-positive cells in the bone marrow. Scale bar = 100 µm. (c) Cells in the soft callus and the thickened periosteum adjacent to the fracture site are X-gal positive on day 7. (d and e) High magnification of the dotted bone and the solid box in (c). (f) Cells in the hard callus are X-gal positive on day 14. (g) High magnification of the dotted box in (f). (h and j) X-gal-positive cells are detected in the remodeled bone and the newly formed periosteum on days 21 and 28. (i) High magnification of the dotted box in (h). MB: metaphyseal bone; GP: growth plate; PO: periosteum; EO: endosteum; BM: bone marrow; SC: soft callus; HC: hard callus. Scale bar = 1mm for (c, f, h, and j) and 500 µm for (d, e, g, and i). Fig. 4 Tibia fracture in Col1a1(2.3 kb)-cre;r26r mice. (a) X-gal-positive cells are found in the periosteum, cortical bone, and endosteum on day 0. Scale bar = 1 mm. (b) High magnification of (a). Scale bar = 100 µm. (c and e) Cells in the hard callus are X-gal positive on days 7 and 14. (d and f) High magnification of (c) and (e). (g and i) Cells in the remodeled bone are X-gal positive on days 21 and 28. (h and j) High magnification of (g) and (i). MB: metaphyseal bone; GP: growth plate; PO: periosteum; EO: endosteum; BM: bone marrow; SC: soft callus; HC: hard callus; RB: remodeled bone. Scale bar = 1mm for (c, e, g, and i) and 500 µm for (d, f, h, and j). Fig. 5 Tibia fracture in Sox9-LacZ mice. (a) No X-gal-positive cells are found in the bones on day 0. Scale bar = 1 mm. (b) High magnification of (a). Growth plate chondrocytes are X-gal positive. Scale bar = 100 µm. (c) Low magnification of fractured tibia on day 3. 19
21 (d) High magnification of the dotted box in (c). No X-gal-positive cells are apparent around the fracture site. (e) High magnification of the dotted boxes in (d). A small number of X-gal-positive cells are found in the periosteum adjacent to the fracture site (arrowheads). (f) Low magnification of the fractured tibia on day 5. (g) High magnification of the dotted boxed in (f). All chondrocytic cells in the soft callus are X- gal positive. A large number of X-gal-positive cells are apparent in the thickened periosteum adjacent to the fracture site. MB: metaphyseal bone; GP: growth plate; PO: periosteum; EO: endosteum; BM: bone marrow; SC: soft callus. Scale bar = 1mm for (c, d, and f) and 100 µm for (e and g). Fig. 6 Tibia fracture in Sox9-CreERT2;R26R mice. The mice were injected with tamoxifen for three days after surgery. (a) No X-gal-positive cells are found in the bones on day 0. Scale bar = 1 mm. (b) High magnification of (a). Growth plate chondrocytes are X-gal positive. Scale bar = 100 µm. (c) Cells in the soft callus are X-gal positive on day 5. (d) High magnification of (c). (e and g) X-gal-positive cells are found in the soft and hard calli on days 7 and 14. (f and h) High magnification of the dotted boxes in (e) and (g). (i) The cells in the remodeled bone and the newly formed periosteum are positive for X- gal on day 28. (j) High magnification of the dotted box in (i). Arrowheads indicate X- gal-positive cells in the periosteum. MB: metaphyseal bone; GP: growth plate; PO: periosteum; EO: endosteum; BM: bone marrow; SC: soft callus; HC: hard callus; RB: remodeled bone. Scale bar = 1mm for (c, e, g, and i) and 500 µm for (d, f, h, and j). 20
22
23
24
25
26
27
Functions of the Skeletal System. Chapter 6: Osseous Tissue and Bone Structure. Classification of Bones. Bone Shapes
 Chapter 6: Osseous Tissue and Bone Structure Functions of the Skeletal System 1. Support 2. Storage of minerals (calcium) 3. Storage of lipids (yellow marrow) 4. Blood cell production (red marrow) 5. Protection
Chapter 6: Osseous Tissue and Bone Structure Functions of the Skeletal System 1. Support 2. Storage of minerals (calcium) 3. Storage of lipids (yellow marrow) 4. Blood cell production (red marrow) 5. Protection
The Contribution Of Tie2-Lineage Cells To rhbmp-2 Induced Bone Formation
 The Contribution Of Tie2-Lineage Cells To rhbmp-2 Induced Bone Formation Mille P. Kolind, Ph.D 1, Alastair Aiken 1, Kathy Mikulec 1, Lauren Peacock 1, David Little 1,2, Aaron Schindeler, PhD 1,2. 1 Orthopaedic
The Contribution Of Tie2-Lineage Cells To rhbmp-2 Induced Bone Formation Mille P. Kolind, Ph.D 1, Alastair Aiken 1, Kathy Mikulec 1, Lauren Peacock 1, David Little 1,2, Aaron Schindeler, PhD 1,2. 1 Orthopaedic
Skeletal System. The skeletal System... Components
 Skeletal System The skeletal System... What are the general components of the skeletal system? What does the skeletal system do for you & how does it achieve these functions? Components The skeletal system
Skeletal System The skeletal System... What are the general components of the skeletal system? What does the skeletal system do for you & how does it achieve these functions? Components The skeletal system
Chapter 6: Skeletal System: Bones and Bone Tissue
 Chapter 6: Skeletal System: Bones and Bone Tissue I. Functions A. List and describe the five major functions of the skeletal system: 1. 2. 3.. 4. 5.. II. Cartilage A. What do chondroblasts do? B. When
Chapter 6: Skeletal System: Bones and Bone Tissue I. Functions A. List and describe the five major functions of the skeletal system: 1. 2. 3.. 4. 5.. II. Cartilage A. What do chondroblasts do? B. When
Bone. Development. Tim Arnett. University College London. Department of Anatomy and Developmental Biology
 Bone Development Tim Arnett Department of Anatomy and Developmental Biology University College London Bone development Outline Bone composition matrix + mineral Bone formation - intramembranous & endochondral
Bone Development Tim Arnett Department of Anatomy and Developmental Biology University College London Bone development Outline Bone composition matrix + mineral Bone formation - intramembranous & endochondral
o~ r;'c' - OSTEOARTHRITIS
 Osteoarthritis and Cartilage (2001) 9, Supplement A, S102-S108 2001 OsteoArthritis Research Society International doi:10.1053/joca.2001.0451, available online at http://www.idealibrary.com on IDE~l Osteoarthritis
Osteoarthritis and Cartilage (2001) 9, Supplement A, S102-S108 2001 OsteoArthritis Research Society International doi:10.1053/joca.2001.0451, available online at http://www.idealibrary.com on IDE~l Osteoarthritis
Regulation of the IGF axis by TGF-b during periosteal chondrogenesis: implications for articular cartilage repair
 Regulation of the IGF axis by TGF-b during periosteal chondrogenesis: implications for articular cartilage repair Chapter 04 Boek 1_Gie.indb 55 21-05-2007 12:27:33 Chapter 04 Abstract Goal: TGF-b and IGF-I
Regulation of the IGF axis by TGF-b during periosteal chondrogenesis: implications for articular cartilage repair Chapter 04 Boek 1_Gie.indb 55 21-05-2007 12:27:33 Chapter 04 Abstract Goal: TGF-b and IGF-I
Joint and Epiphyseal Progenitor Cells Revitalize Tendon Graft and Form Mineralized Insertion Sites in Murine ACL Reconstruction Model
 Joint and Epiphyseal Progenitor Cells Revitalize Tendon Graft and Form Mineralized Insertion Sites in Murine ACL Reconstruction Model Yusuke Hagiwara 1,2, Nathaniel A. Dyment 3, Douglas J. Adams 3, Shinro
Joint and Epiphyseal Progenitor Cells Revitalize Tendon Graft and Form Mineralized Insertion Sites in Murine ACL Reconstruction Model Yusuke Hagiwara 1,2, Nathaniel A. Dyment 3, Douglas J. Adams 3, Shinro
BIOH111. o Cell Module o Tissue Module o Integumentary system o Skeletal system o Muscle system o Nervous system o Endocrine system
 BIOH111 o Cell Module o Tissue Module o Integumentary system o Skeletal system o Muscle system o Nervous system o Endocrine system Endeavour College of Natural Health endeavour.edu.au 1 TEXTBOOK AND REQUIRED/RECOMMENDED
BIOH111 o Cell Module o Tissue Module o Integumentary system o Skeletal system o Muscle system o Nervous system o Endocrine system Endeavour College of Natural Health endeavour.edu.au 1 TEXTBOOK AND REQUIRED/RECOMMENDED
AAO Foundation Awards Final Report
 401 N. Lindbergh Blvd. St. Louis, MO 63141 Tel.: 314.993.1700, #546 Toll Free: 800.424.2841, #546 Fax: 800.708.1364 Cell: 314.283.1983 E-Mail: rhazel@aaortho.org AAO Foundation Awards Final Report In an
401 N. Lindbergh Blvd. St. Louis, MO 63141 Tel.: 314.993.1700, #546 Toll Free: 800.424.2841, #546 Fax: 800.708.1364 Cell: 314.283.1983 E-Mail: rhazel@aaortho.org AAO Foundation Awards Final Report In an
SDF-1/CXCR4 Axis on Endothelial Progenitor Cells Regulates Bone Fracture Healing
 SDF-1/CXCR4 Axis on Endothelial Progenitor Cells Regulates Bone Fracture Healing Yohei Kawakami, M.D., Ph.D. 1,2, Masaaki Ii 3, Tomoyuki Matsumoto, M.D., Ph.D. 1, Astuhiko Kawamoto, M.D., Ph.D. 2, Yutaka
SDF-1/CXCR4 Axis on Endothelial Progenitor Cells Regulates Bone Fracture Healing Yohei Kawakami, M.D., Ph.D. 1,2, Masaaki Ii 3, Tomoyuki Matsumoto, M.D., Ph.D. 1, Astuhiko Kawamoto, M.D., Ph.D. 2, Yutaka
BONE TISSUE. Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology
 BONE TISSUE Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology BONE FUNCTION Support Protection (protect internal organs) Movement (provide leverage system for skeletal muscles, tendons, ligaments
BONE TISSUE Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology BONE FUNCTION Support Protection (protect internal organs) Movement (provide leverage system for skeletal muscles, tendons, ligaments
SKELETAL TISSUES CHAPTER 7 INTRODUCTION TO THE SKELETAL SYSTEM TYPES OF BONES
 SKELETAL TISSUES CHAPTER 7 By John McGill Supplement Outlines: Beth Wyatt Original PowerPoint: Jack Bagwell INTRODUCTION TO THE SKELETAL SYSTEM STRUCTURE Organs: Bones Related Tissues: Cartilage and Ligaments
SKELETAL TISSUES CHAPTER 7 By John McGill Supplement Outlines: Beth Wyatt Original PowerPoint: Jack Bagwell INTRODUCTION TO THE SKELETAL SYSTEM STRUCTURE Organs: Bones Related Tissues: Cartilage and Ligaments
2 PROCESSES OF BONE OSSIFICATION
 2 PROCESSES OF BONE OSSIFICATION ENDOCHONDRAL OSSIFICATION 6 STEPS 1. CARTILAGE ENLARGES, BY APPOSITIONAL GROWTH; CHONDROCYTES AT CENTER OF CARTILAGE GROW IN SIZE; MATRIX REDUCES IN SIZE & SPICULES CALCIFY;
2 PROCESSES OF BONE OSSIFICATION ENDOCHONDRAL OSSIFICATION 6 STEPS 1. CARTILAGE ENLARGES, BY APPOSITIONAL GROWTH; CHONDROCYTES AT CENTER OF CARTILAGE GROW IN SIZE; MATRIX REDUCES IN SIZE & SPICULES CALCIFY;
Outline. Skeletal System. Functions of Bone. Bio 105: Skeletal System 3/17/2016. The material from this lecture packet will be on the lecture exam
 Bio 105: Skeletal System Lecture 8 Chapter 5 The material from this lecture packet will be on the lecture exam The identification that you do after this lecture will be on the lab exam Outline I. Overview
Bio 105: Skeletal System Lecture 8 Chapter 5 The material from this lecture packet will be on the lecture exam The identification that you do after this lecture will be on the lab exam Outline I. Overview
CHAPTER 6 LECTURE OUTLINE
 CHAPTER 6 LECTURE OUTLINE I. INTRODUCTION A. Bone is made up of several different tissues working together: bone, cartilage, dense connective tissue, epithelium, various blood forming tissues, adipose
CHAPTER 6 LECTURE OUTLINE I. INTRODUCTION A. Bone is made up of several different tissues working together: bone, cartilage, dense connective tissue, epithelium, various blood forming tissues, adipose
Skeletal Tissues. Skeletal tissues. Frame; muscles, organs and CT attach. Brain, spinal cord, thoracic organs; heart and lungs.
 Skeletal Tissues Functions 1) support 2) protection 3) movement Skeletal tissues Frame; muscles, organs and CT attach. Brain, spinal cord, thoracic organs; heart and lungs. Aids muscle contraction; generate
Skeletal Tissues Functions 1) support 2) protection 3) movement Skeletal tissues Frame; muscles, organs and CT attach. Brain, spinal cord, thoracic organs; heart and lungs. Aids muscle contraction; generate
Supplementary Data. Supplementary Methods:
 Supplementary Data Supplementary Methods: Release kinetics of from collagen sponges in vivo. 2μg of human recombinant 165 was labeled with lexafluor 555 (Microscale Protein Labeling Kit; Invitrogen) as
Supplementary Data Supplementary Methods: Release kinetics of from collagen sponges in vivo. 2μg of human recombinant 165 was labeled with lexafluor 555 (Microscale Protein Labeling Kit; Invitrogen) as
Supplemental Data. Wnt/β-Catenin Signaling in Mesenchymal Progenitors. Controls Osteoblast and Chondrocyte
 Supplemental Data Wnt/β-Catenin Signaling in Mesenchymal Progenitors Controls Osteoblast and Chondrocyte Differentiation during Vertebrate Skeletogenesis Timothy F. Day, Xizhi Guo, Lisa Garrett-Beal, and
Supplemental Data Wnt/β-Catenin Signaling in Mesenchymal Progenitors Controls Osteoblast and Chondrocyte Differentiation during Vertebrate Skeletogenesis Timothy F. Day, Xizhi Guo, Lisa Garrett-Beal, and
OSSEOUS TISSUE & BONE STRUCTURE PART I: OVERVIEW & COMPONENTS
 OSSEOUS TISSUE & BONE STRUCTURE PART I: OVERVIEW & COMPONENTS The Skeletal System Skeletal system includes: bones of the skeleton, cartilages, ligaments, and connective tissues What are the functions of
OSSEOUS TISSUE & BONE STRUCTURE PART I: OVERVIEW & COMPONENTS The Skeletal System Skeletal system includes: bones of the skeleton, cartilages, ligaments, and connective tissues What are the functions of
The Skeletal System:Bone Tissue
 The Skeletal System:Bone Tissue Dynamic and ever-changing throughout life Skeleton composed of many different tissues cartilage, bone tissue, epithelium, nerve, blood forming tissue, adipose, and dense
The Skeletal System:Bone Tissue Dynamic and ever-changing throughout life Skeleton composed of many different tissues cartilage, bone tissue, epithelium, nerve, blood forming tissue, adipose, and dense
Derived copy of Fractures: Bone Repair *
 OpenStax-CNX module: m56135 1 Derived copy of Fractures: Bone Repair * Stephanie Fretham Based on Fractures: Bone Repair by OpenStax This work is produced by OpenStax-CNX and licensed under the Creative
OpenStax-CNX module: m56135 1 Derived copy of Fractures: Bone Repair * Stephanie Fretham Based on Fractures: Bone Repair by OpenStax This work is produced by OpenStax-CNX and licensed under the Creative
Principles of Anatomy and Physiology
 Principles of Anatomy and Physiology 14 th Edition CHAPTER 6 The Skeletal System: Bone Tissue Introduction The skeletal system has 6 important functions: Provides support Protects the internal organs (brain,
Principles of Anatomy and Physiology 14 th Edition CHAPTER 6 The Skeletal System: Bone Tissue Introduction The skeletal system has 6 important functions: Provides support Protects the internal organs (brain,
Dr. Heba Kalbouneh. Saba Alfayoumi. Heba Kalbouneh
 11 Dr. Heba Kalbouneh Saba Alfayoumi Heba Kalbouneh 2- Bone Bone tissue is also classified into primary bone and secondary bone. In the beginning, the first bone that is deposited by the osteoblasts is
11 Dr. Heba Kalbouneh Saba Alfayoumi Heba Kalbouneh 2- Bone Bone tissue is also classified into primary bone and secondary bone. In the beginning, the first bone that is deposited by the osteoblasts is
Bones. The division of bones anatomically is : long, short, irregular, flat and sesamoid.
 Bones Osteocytes : Are responsible for maintenance of bones Present in lacunae, and send processes. Unable to divide. The division of bones anatomically is : long, short, irregular, flat and sesamoid.
Bones Osteocytes : Are responsible for maintenance of bones Present in lacunae, and send processes. Unable to divide. The division of bones anatomically is : long, short, irregular, flat and sesamoid.
36 1 The Skeletal System Slide 1 of 40
 1 of 40 The Skeleton All organisms need structural support. Unicellular organisms have a cytoskeleton. Multicellular animals have either an exoskeleton (arthropods) or an endoskeleton (vertebrates). 2
1 of 40 The Skeleton All organisms need structural support. Unicellular organisms have a cytoskeleton. Multicellular animals have either an exoskeleton (arthropods) or an endoskeleton (vertebrates). 2
What are the parts of the skeletal system? Chapter 6- Part I Bones and Skeletal Tissues. Growth of Cartilage. Bones come in many shapes
 Chapter 6- Part I Bones and Skeletal Tissues Components of the skeletal system Classification of Bone (bone shapes) Functions of bone Bone structure Microscopic structure of bone and bone cells What are
Chapter 6- Part I Bones and Skeletal Tissues Components of the skeletal system Classification of Bone (bone shapes) Functions of bone Bone structure Microscopic structure of bone and bone cells What are
Skeletal System. Bio 105
 Skeletal System Bio 105 Outline I. Overview of the skeletal system II. Function of bones III. Bone structure IV. Bone cells V. Cartilage VI. Tendons and Ligaments VII. Joints VIII. Bone development IX.
Skeletal System Bio 105 Outline I. Overview of the skeletal system II. Function of bones III. Bone structure IV. Bone cells V. Cartilage VI. Tendons and Ligaments VII. Joints VIII. Bone development IX.
Outline. Skeletal System. Tendons link the skeletal and the muscular systems.
 Outline Skeletal System Bio 105 I. Overview of the skeletal system II. Function of bones III. Bone structure IV. Bone cells V. Cartilage VI. Tendons and Ligaments VII. Joints VIII. Bone development IX.
Outline Skeletal System Bio 105 I. Overview of the skeletal system II. Function of bones III. Bone structure IV. Bone cells V. Cartilage VI. Tendons and Ligaments VII. Joints VIII. Bone development IX.
Osseous Tissue and Bone Structure
 C h a p t e r 6 Osseous Tissue and Bone Structure PowerPoint Lecture Slides prepared by Jason LaPres Lone Star College - North Harris Copyright 2009 Pearson Education, Inc., publishing as Pearson Benjamin
C h a p t e r 6 Osseous Tissue and Bone Structure PowerPoint Lecture Slides prepared by Jason LaPres Lone Star College - North Harris Copyright 2009 Pearson Education, Inc., publishing as Pearson Benjamin
An Introduction to the Skeletal System Skeletal system includes Bones of the skeleton Cartilages, ligaments, and connective tissues
 An Introduction to the Skeletal System Skeletal system includes Bones of the skeleton Cartilages, ligaments, and connective tissues Functions of the Skeletal System Support Storage of minerals (calcium)
An Introduction to the Skeletal System Skeletal system includes Bones of the skeleton Cartilages, ligaments, and connective tissues Functions of the Skeletal System Support Storage of minerals (calcium)
Human Anatomy & Physiology
 PowerPoint Lecture Slides prepared by Barbara Heard, Atlantic Cape Community College Ninth Edition Human Anatomy & Physiology C H A P T E R 6 Annie Leibovitz/Contact Press Images 2013 Pearson Education,
PowerPoint Lecture Slides prepared by Barbara Heard, Atlantic Cape Community College Ninth Edition Human Anatomy & Physiology C H A P T E R 6 Annie Leibovitz/Contact Press Images 2013 Pearson Education,
Lecture 2: Skeletogenesis
 Jilin University School of Stomatology Skeletogenesis Lecture 2: Skeletogenesis Aug. 18, 2015 Yuji Mishina, Ph.D. mishina@umich.edu Student will describe Development of Bone - the general anatomy of bone
Jilin University School of Stomatology Skeletogenesis Lecture 2: Skeletogenesis Aug. 18, 2015 Yuji Mishina, Ph.D. mishina@umich.edu Student will describe Development of Bone - the general anatomy of bone
Peggers Super Summaries Basic Sciences Bone
 Bone Overview & Turnover BONES Function o Support o Protection o Assisting movement o Storage of minerals o Production of red blood cells from marrow Types o Cancellous o Compact with Haversian systems
Bone Overview & Turnover BONES Function o Support o Protection o Assisting movement o Storage of minerals o Production of red blood cells from marrow Types o Cancellous o Compact with Haversian systems
Bone healing, delayed fracture healing and nonunion. Norbert Wiegand
 Bone healing, delayed fracture healing and nonunion Norbert Wiegand 2/3 of traumatology: treatment of fractures We have to understand: Structure of the bone Biology of the bone Bone healing Types of Bone
Bone healing, delayed fracture healing and nonunion Norbert Wiegand 2/3 of traumatology: treatment of fractures We have to understand: Structure of the bone Biology of the bone Bone healing Types of Bone
Biology. Dr. Khalida Ibrahim
 Biology Dr. Khalida Ibrahim BONE TISSUE Bone tissue is a specialized form of connective tissue and is the main element of the skeletal tissues. It is composed of cells and an extracellular matrix in which
Biology Dr. Khalida Ibrahim BONE TISSUE Bone tissue is a specialized form of connective tissue and is the main element of the skeletal tissues. It is composed of cells and an extracellular matrix in which
Supplemental Figure 1. Egr1 expression in adult Achilles tendons. (A,B) Achilles tendons were isolated from 2 month-old Egr1 +/- mice and stained for
 Supplemental Figure 1. Egr1 expression in adult Achilles tendons. (A,B) Achilles tendons were isolated from 2 month-old Egr1 +/- mice and stained for LacZ activity, which reflects Egr1 expression. (A)
Supplemental Figure 1. Egr1 expression in adult Achilles tendons. (A,B) Achilles tendons were isolated from 2 month-old Egr1 +/- mice and stained for LacZ activity, which reflects Egr1 expression. (A)
Module 2:! Functional Musculoskeletal Anatomy A! Semester 1! !!! !!!! Hard Tissues, Distal Upper Limb & Neurovascular Supply of Upper Limb!
 Functional Musculoskeletal Anatomy A Module 2: Hard Tissues, Distal Upper Limb & Neurovascular Supply of Upper Limb Semester 1 1 18. Bone Tissue & Growth of Bones 18.1 Describe the structure of bone tissue
Functional Musculoskeletal Anatomy A Module 2: Hard Tissues, Distal Upper Limb & Neurovascular Supply of Upper Limb Semester 1 1 18. Bone Tissue & Growth of Bones 18.1 Describe the structure of bone tissue
Cartilage. Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology
 Cartilage Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology 1 Cartilage is a specialized type of connective tissue designed to give support, bear weight and withstand tension, torsion and
Cartilage Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology 1 Cartilage is a specialized type of connective tissue designed to give support, bear weight and withstand tension, torsion and
KEY CONCEPTS Unit 6 THE SKELETAL SYSTEM
 ANATOMY & PHYSIOLOGY 1 (101-805 - AB) PAUL ANDERSON 2011 KEY CONCEPTS Unit 6 THE SKELETAL SYSTEM A Overview of The Skeletal System 1. Definition: Anatomically the SKELETAL SYSTEM consists of bones, cartilages,
ANATOMY & PHYSIOLOGY 1 (101-805 - AB) PAUL ANDERSON 2011 KEY CONCEPTS Unit 6 THE SKELETAL SYSTEM A Overview of The Skeletal System 1. Definition: Anatomically the SKELETAL SYSTEM consists of bones, cartilages,
Rama Nada. - Mousa Al-Abbadi. 1 P a g e
 - 1 - Rama Nada - - Mousa Al-Abbadi 1 P a g e Bones, Joints and Soft tissue tumors Before we start: the first 8 minutes was recalling to Dr.Mousa s duties, go over them in the slides. Wherever you see
- 1 - Rama Nada - - Mousa Al-Abbadi 1 P a g e Bones, Joints and Soft tissue tumors Before we start: the first 8 minutes was recalling to Dr.Mousa s duties, go over them in the slides. Wherever you see
Callus formation during healing of the repaired tendon-bone junction
 Callus formation during healing of the repaired tendon-bone junction A RAT EXPERIMENTAL MODEL N. Hibino, Y. Hamada, K. Sairyo, K. Yukata, T. Sano, N. Yasui From University of Tokushima Graduate School,
Callus formation during healing of the repaired tendon-bone junction A RAT EXPERIMENTAL MODEL N. Hibino, Y. Hamada, K. Sairyo, K. Yukata, T. Sano, N. Yasui From University of Tokushima Graduate School,
BONE LABORATORY DEMONSTRATIONS. These demonstrations are found on the bulletin boards outside the MCO Bookstore.
 BONE LABORATORY DEMONSTRATIONS These demonstrations are found on the bulletin boards outside the MCO Bookstore. COMPACT & TRABECULAR BONE - LM When viewed under the polarizing light microscope, the layering
BONE LABORATORY DEMONSTRATIONS These demonstrations are found on the bulletin boards outside the MCO Bookstore. COMPACT & TRABECULAR BONE - LM When viewed under the polarizing light microscope, the layering
A Novel Murine Model Of Adynamic Bone Disease (ABD)
 A Novel Murine Model Of Adynamic Bone Disease (ABD) Adeline H. Ng 1,2, Thomas L. Willett, PhD 2,1, Benjamin A. Alman 3,1, Marc D. Grynpas 1,2. 1 University of Toronto, Toronto, ON, Canada, 2 Samuel Lunenfeld
A Novel Murine Model Of Adynamic Bone Disease (ABD) Adeline H. Ng 1,2, Thomas L. Willett, PhD 2,1, Benjamin A. Alman 3,1, Marc D. Grynpas 1,2. 1 University of Toronto, Toronto, ON, Canada, 2 Samuel Lunenfeld
Anabolic Therapy With Teriparatide Indications Beyond Osteoporosis
 Anabolic Therapy With Teriparatide Indications Beyond Osteoporosis Andreas Panagopoulos MD, PhD Upper Limb & Sports Medicine Orthopaedic Surgeon Assistant Professor, University of Patras Outline Teriparatide
Anabolic Therapy With Teriparatide Indications Beyond Osteoporosis Andreas Panagopoulos MD, PhD Upper Limb & Sports Medicine Orthopaedic Surgeon Assistant Professor, University of Patras Outline Teriparatide
Chapter 6: Osseous Tissue and Bone Structure
 Chapter 6: Osseous Tissue and Bone Structure I. An Introduction to the Skeletal System, p. 180 Objective: Describe the functions of the skeletal system The skeletal system includes: - bones of the skeleton
Chapter 6: Osseous Tissue and Bone Structure I. An Introduction to the Skeletal System, p. 180 Objective: Describe the functions of the skeletal system The skeletal system includes: - bones of the skeleton
Unit 5: SKELETAL SYSTEM
 Unit 5: SKELETAL SYSTEM (a) NRSG231 Dr. Moattar Raza Rizvi Skeletal System: Contents Functions of the Skeletal System Fracture Structure of Bone Tissue Articulations & Joint Bone Development and Growth
Unit 5: SKELETAL SYSTEM (a) NRSG231 Dr. Moattar Raza Rizvi Skeletal System: Contents Functions of the Skeletal System Fracture Structure of Bone Tissue Articulations & Joint Bone Development and Growth
Skeletal Tissues Dr. Ali Ebneshahidi
 Skeletal Tissues Dr. Ali Ebneshahidi Functions of Bones 1. Support and protection: Bones give shape to body structure. Bones provide support to body weight. Certain bones protect vital internal organs
Skeletal Tissues Dr. Ali Ebneshahidi Functions of Bones 1. Support and protection: Bones give shape to body structure. Bones provide support to body weight. Certain bones protect vital internal organs
Finite-element study of vibration effect to fracture healing of a human tibia
 Finite-element study of vibration effect to fracture healing of a human tibia Leonid Maslov 1, Jean-Baptiste Etheve 2, Nikolay Sabaneev 3 Ivanovo State Power Engineering University, Ivanovo, Russia 1 Corresponding
Finite-element study of vibration effect to fracture healing of a human tibia Leonid Maslov 1, Jean-Baptiste Etheve 2, Nikolay Sabaneev 3 Ivanovo State Power Engineering University, Ivanovo, Russia 1 Corresponding
Fig Articular cartilage. Epiphysis. Red bone marrow Epiphyseal line. Marrow cavity. Yellow bone marrow. Periosteum. Nutrient foramen Diaphysis
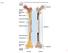 Fig. 7.1 Articular cartilage Epiphysis Red bone marrow Epiphyseal line Marrow cavity Yellow bone marrow Nutrient foramen Diaphysis Site of endosteum Compact bone Spongy bone Epiphyseal line Epiphysis Articular
Fig. 7.1 Articular cartilage Epiphysis Red bone marrow Epiphyseal line Marrow cavity Yellow bone marrow Nutrient foramen Diaphysis Site of endosteum Compact bone Spongy bone Epiphyseal line Epiphysis Articular
Meeting Report. From December 8 to 11, 2012 at Atlanta, GA, U.S.A
 Meeting Report Affiliation Department of Transfusion Medicine and Cell Therapy Name Hisayuki Yao Name of the meeting Period and venue Type of your presentation Title of your presentation The 54 th Annual
Meeting Report Affiliation Department of Transfusion Medicine and Cell Therapy Name Hisayuki Yao Name of the meeting Period and venue Type of your presentation Title of your presentation The 54 th Annual
Skeletal System worksheet
 Skeletal System worksheet Name Section A: Intro to Skeletal System The skeletal system performs vital functions that enable us to move through our daily lives. Support - The skeleton provides support and
Skeletal System worksheet Name Section A: Intro to Skeletal System The skeletal system performs vital functions that enable us to move through our daily lives. Support - The skeleton provides support and
Blood. Hematopoietic Tissue
 Blood Hematopoietic Tissue Is a type of connective tissue in which its cells are suspended in a circulating fluid. Erythrocytes+ leukocytes + platelets (thrombocytes) =formed elements of blood. These formed
Blood Hematopoietic Tissue Is a type of connective tissue in which its cells are suspended in a circulating fluid. Erythrocytes+ leukocytes + platelets (thrombocytes) =formed elements of blood. These formed
ANATOMY & PHYSIOLOGY - CLUTCH CH. 8 - BONE AND CARTILAGE.
 !! www.clutchprep.com CONCEPT: BONE CLASSIFICATIONS There are four classifications of bones based on their 1. Long bones are greater in length than in width - Found in the upper and lower limbs (ex: arm,
!! www.clutchprep.com CONCEPT: BONE CLASSIFICATIONS There are four classifications of bones based on their 1. Long bones are greater in length than in width - Found in the upper and lower limbs (ex: arm,
Sheets 16&17. Dr. Heba Kalbouneh. Dr. Heba Kalbouneh. Dr. Heba Kalbouneh
 Sheets 16&17 Dr. Heba Kalbouneh Dr. Heba Kalbouneh Dr. Heba Kalbouneh Ossification (formation of bone) - Osteoblasts are responsible for producing the extracellular matrix of the bone and these osteoblasts
Sheets 16&17 Dr. Heba Kalbouneh Dr. Heba Kalbouneh Dr. Heba Kalbouneh Ossification (formation of bone) - Osteoblasts are responsible for producing the extracellular matrix of the bone and these osteoblasts
The Skeletal System. Chapter 7a. Skeletal System Introduction Functions of the skeleton Framework of bones The skeleton through life
 The Skeletal System Skeletal System Introduction Functions of the skeleton Framework of bones The skeleton through life Chapter 7a Support Protection Movement Storage areas Minerals Lipids Hemopoiesis
The Skeletal System Skeletal System Introduction Functions of the skeleton Framework of bones The skeleton through life Chapter 7a Support Protection Movement Storage areas Minerals Lipids Hemopoiesis
For more information about how to cite these materials visit
 Author(s): University of Michigan Medical School, Department of Cell and Developmental Biology License: Unless otherwise noted, the content of this course material is licensed under a Creative Commons
Author(s): University of Michigan Medical School, Department of Cell and Developmental Biology License: Unless otherwise noted, the content of this course material is licensed under a Creative Commons
The formation of blood cells is called. hemopoiesis. What does our bone store? Where do our bones store fat? yellow marrow.
 What are the 5/6 functions of the skeletal system? support, protection, movement, blood cell formation, storage, homeostasis The formation of blood cells is called hemopoiesis What does our bone store?
What are the 5/6 functions of the skeletal system? support, protection, movement, blood cell formation, storage, homeostasis The formation of blood cells is called hemopoiesis What does our bone store?
Skeletal Tissues. Dr. Ali Ebneshahidi
 Skeletal Tissues Dr. Ali Ebneshahidi Functions of Bones 1. Support and protection : Bones give shape to body structure. Bones provide support to body weight. Certain bones protect vital internal organs
Skeletal Tissues Dr. Ali Ebneshahidi Functions of Bones 1. Support and protection : Bones give shape to body structure. Bones provide support to body weight. Certain bones protect vital internal organs
Pathophysiology of fracture healing
 Pathophysiology of fracture healing Bone anatomy and biomechanics Fracture patterns Bone healing and blood supply Influence of implants 1 What is the structure of bone? 2 Bone structure Four levels: Chemical
Pathophysiology of fracture healing Bone anatomy and biomechanics Fracture patterns Bone healing and blood supply Influence of implants 1 What is the structure of bone? 2 Bone structure Four levels: Chemical
Cartilage & bone. Red: important. Black: in male female slides. Gray: notes extra. Editing File
 Cartilage & bone Red: important. Black: in male female slides. Gray: notes extra. Editing File OBJECTIVES describe the microscopic structure, distribution and growth of the different types of Cartilage
Cartilage & bone Red: important. Black: in male female slides. Gray: notes extra. Editing File OBJECTIVES describe the microscopic structure, distribution and growth of the different types of Cartilage
Chapter 7. Skeletal System
 Chapter 7 Skeletal System 1 Introduction: A. Bones are very active, living tissues B. Each bone is made up of several types of tissues and so is an organ. C. Bone functions include: muscle attachment,
Chapter 7 Skeletal System 1 Introduction: A. Bones are very active, living tissues B. Each bone is made up of several types of tissues and so is an organ. C. Bone functions include: muscle attachment,
SKELETAL SYSTEM I NOTE: LAB ASSIGNMENTS for this topic will run over 3 Weeks. A SEPARATE WORKSHEET WILL BE PROVIDED.
 BIO 211; Anatomy and Physiology I REFERENCE: CHAPTER 07 1 Dr. Lawrence Altman Naugatuck Valley Community College LECTURE TOPICS OUTLINE SKELETAL SYSTEM I NOTE: LAB ASSIGNMENTS for this topic will run over
BIO 211; Anatomy and Physiology I REFERENCE: CHAPTER 07 1 Dr. Lawrence Altman Naugatuck Valley Community College LECTURE TOPICS OUTLINE SKELETAL SYSTEM I NOTE: LAB ASSIGNMENTS for this topic will run over
Flow Cytometry. What is flow cytometry?
 Flow Cytometry Flow Cytometry What is flow cytometry? Flow cytometry is a popular laser-based technology to analyze the characteristics of cells or particles. It is predominantly used to measure fluorescence
Flow Cytometry Flow Cytometry What is flow cytometry? Flow cytometry is a popular laser-based technology to analyze the characteristics of cells or particles. It is predominantly used to measure fluorescence
Types of Bones. 5 basic types of bones: Sutural bones - in joint between skull bones
 The Skeletal System The Skeletal System Bone and their cartilage, ligaments & tendons. Dynamic and ever changing throughout life Skeleton contains all 4 tissue types; Epithelial, connective, muscle and
The Skeletal System The Skeletal System Bone and their cartilage, ligaments & tendons. Dynamic and ever changing throughout life Skeleton contains all 4 tissue types; Epithelial, connective, muscle and
Paracrine Effect of Mesenchymal Stem Cells derived from Human Adipose tissue in Bone Regeneration.
 Paracrine Effect of Mesenchymal Stem Cells derived from Human Adipose tissue in Bone Regeneration. By Linero I., Chaparro O., 2014 Suzana Tufegdzic 1 Background 2 Background Stem Cells: undifferentiated
Paracrine Effect of Mesenchymal Stem Cells derived from Human Adipose tissue in Bone Regeneration. By Linero I., Chaparro O., 2014 Suzana Tufegdzic 1 Background 2 Background Stem Cells: undifferentiated
Quiz 6. Cartilage and Bone
 Quiz 6 Cartilage and Bone MCQs X type (true or false): 1. Cartilage tissue: a. Has a rich blood supply. b. Develops from mesenchyme. c. Has ability for a quick regeneration. d. Has chondrocytes as precursor
Quiz 6 Cartilage and Bone MCQs X type (true or false): 1. Cartilage tissue: a. Has a rich blood supply. b. Develops from mesenchyme. c. Has ability for a quick regeneration. d. Has chondrocytes as precursor
FORMATION OF BONE. Intramembranous Ossification. Bone-Lec-10-Prof.Dr.Adnan Albideri
 FORMATION OF BONE All bones are of mesodermal origin. The process of bone formation is called ossification. We have seen that formation of most bones is preceded by the formation of a cartilaginous model,
FORMATION OF BONE All bones are of mesodermal origin. The process of bone formation is called ossification. We have seen that formation of most bones is preceded by the formation of a cartilaginous model,
b. Adult bones produce 2.5 million RBCs each second.
 Ch 6 Skeletal System I. Functions of the Skeletal System A. The skeletal system consists of: 1. bones, cartilage, tendons and ligaments B. Living bone is not Gr. dried up 1. It is dynamic and adaptable
Ch 6 Skeletal System I. Functions of the Skeletal System A. The skeletal system consists of: 1. bones, cartilage, tendons and ligaments B. Living bone is not Gr. dried up 1. It is dynamic and adaptable
Chapter 5 The Skeletal System
 Chapter 5 The Skeletal System The Skeletal System Parts of the skeletal system Bones (skeleton) Joints Cartilages Ligaments (bone to bone)(tendon=bone to muscle) Divided into two divisions Axial skeleton:
Chapter 5 The Skeletal System The Skeletal System Parts of the skeletal system Bones (skeleton) Joints Cartilages Ligaments (bone to bone)(tendon=bone to muscle) Divided into two divisions Axial skeleton:
Osseous Tissue and Bone Structure
 6 Osseous Tissue and Bone Structure PowerPoint Lecture Presentations prepared by Jason LaPres Lone Star College North Harris An Introduction to the Skeletal System Learning Outcomes 6-1 Describe the primary
6 Osseous Tissue and Bone Structure PowerPoint Lecture Presentations prepared by Jason LaPres Lone Star College North Harris An Introduction to the Skeletal System Learning Outcomes 6-1 Describe the primary
NOTES: Skeletal System (Ch 5, part 1)
 NOTES: Skeletal System (Ch 5, part 1) Individual bones are the organs of the skeletal system. A bone contains very active tissues. BONE STRUCTURE: *Bone structure reflects its function. Parts of a long
NOTES: Skeletal System (Ch 5, part 1) Individual bones are the organs of the skeletal system. A bone contains very active tissues. BONE STRUCTURE: *Bone structure reflects its function. Parts of a long
Supplemental Tables and Figures. The metalloproteinase-proteoglycans ADAMTS7 and ADAMTS12 provide an innate,
 Supplemental Tables and Figures The metalloproteinase-proteoglycans ADAMTS7 and ADAMTS12 provide an innate, tendon-specific protective mechanism against heterotopic ossification Timothy Mead et al Supplemental
Supplemental Tables and Figures The metalloproteinase-proteoglycans ADAMTS7 and ADAMTS12 provide an innate, tendon-specific protective mechanism against heterotopic ossification Timothy Mead et al Supplemental
Osteology. Dr. Carmen E. Rexach Anatomy 35 Mt San Antonio College
 Osteology Dr. Carmen E. Rexach Anatomy 35 Mt San Antonio College Functions of the Skeletal System: Support Movement Protection Hemopoiesis Electrolyte balance (Ca ++ /PO -3 4 ) Acid-base balance Storage
Osteology Dr. Carmen E. Rexach Anatomy 35 Mt San Antonio College Functions of the Skeletal System: Support Movement Protection Hemopoiesis Electrolyte balance (Ca ++ /PO -3 4 ) Acid-base balance Storage
Chapter 6 Bones and Bone Tissue Chapter Outline
 Chapter 6 Bones and Bone Tissue Chapter Outline Module 6.1: Introduction to Bones as Organs (Figures 6.1, 6.2, 6.3, 6.4) A. The skeletal system includes the bones, joints, and their associated supporting
Chapter 6 Bones and Bone Tissue Chapter Outline Module 6.1: Introduction to Bones as Organs (Figures 6.1, 6.2, 6.3, 6.4) A. The skeletal system includes the bones, joints, and their associated supporting
Discovery of a Small Molecule Inhibitor of the Wnt Pathway as a Potential Disease Modifying Treatment for Knee Osteoarthritis
 Discovery of a Small Molecule Inhibitor of the Wnt Pathway as a Potential Disease Modifying Treatment for Knee Osteoarthritis Charlene Barroga, Ph.D., Yong Hu, Ph.D., Vishal Deshmukh, Ph.D., and John Hood,
Discovery of a Small Molecule Inhibitor of the Wnt Pathway as a Potential Disease Modifying Treatment for Knee Osteoarthritis Charlene Barroga, Ph.D., Yong Hu, Ph.D., Vishal Deshmukh, Ph.D., and John Hood,
The Skeletal System PART A
 5 The Skeletal System PART A PowerPoint Lecture Slide Presentation by Jerry L. Cook, Sam Houston University ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY EIGHTH EDITION ELAINE N. MARIEB The Skeletal System
5 The Skeletal System PART A PowerPoint Lecture Slide Presentation by Jerry L. Cook, Sam Houston University ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY EIGHTH EDITION ELAINE N. MARIEB The Skeletal System
SUPPLEMENTARY INFORMATION
 SUPPLEMENTARY INFORMATION Supplementary Figure 1. Generation of a conditional allele of the Kindlin-2 gene. (A) A restriction map of the relevant genomic region of Kindlin-2 (top), the targeting construct
SUPPLEMENTARY INFORMATION Supplementary Figure 1. Generation of a conditional allele of the Kindlin-2 gene. (A) A restriction map of the relevant genomic region of Kindlin-2 (top), the targeting construct
-the emphasis on this section is the structure and function of bone tissue and on the dynamics of its formation and remodeling throughout life.
 Biology 325 Fall 2004 BONES AND SKELETAL TISSUES Introduction -skeleton contains cartilage and bones -the emphasis on this section is the structure and function of bone tissue and on the dynamics of its
Biology 325 Fall 2004 BONES AND SKELETAL TISSUES Introduction -skeleton contains cartilage and bones -the emphasis on this section is the structure and function of bone tissue and on the dynamics of its
SKELETAL SYSTEM. Introduction Notes (pt 1)
 SKELETAL SYSTEM Introduction Notes (pt 1) I. INTRODUCTION 1. Bones include active, living tissues: bone tissue, cartilage, dense connective tissue, blood, and nervous tissue. 2. Bones: support and protect
SKELETAL SYSTEM Introduction Notes (pt 1) I. INTRODUCTION 1. Bones include active, living tissues: bone tissue, cartilage, dense connective tissue, blood, and nervous tissue. 2. Bones: support and protect
Skeletal System. Chapter 6.1 Human Anatomy & Physiology
 Skeletal System Chapter 6.1 Human Anatomy & Physiology Overview of Skeletal System Bones Joints Skeletal System Cartilage Tendons (bone to muscle) Ligaments (bone to bone) Function of the Skeletal System
Skeletal System Chapter 6.1 Human Anatomy & Physiology Overview of Skeletal System Bones Joints Skeletal System Cartilage Tendons (bone to muscle) Ligaments (bone to bone) Function of the Skeletal System
Introduction to Biomedical Engineering: Basic concepts and Bone Biomechanics
 Introduction to Biomedical Engineering: Basic concepts and Bone Biomechanics Fall 2016, AKUT G. Rouhi Biomechanics The field of biomechanics applies principles of mechanics to study the structure and function
Introduction to Biomedical Engineering: Basic concepts and Bone Biomechanics Fall 2016, AKUT G. Rouhi Biomechanics The field of biomechanics applies principles of mechanics to study the structure and function
Ossification and Bone Remodeling
 Ossification and Bone Remodeling Pre-natal Ossification Embryonic skeleton: fashioned from fibrous membranes or cartilage to accommodate mitosis. 2 types of pre-natal ossification (bone formation) 1.
Ossification and Bone Remodeling Pre-natal Ossification Embryonic skeleton: fashioned from fibrous membranes or cartilage to accommodate mitosis. 2 types of pre-natal ossification (bone formation) 1.
Bone Tissue- Chapter 5 5-1
 Bone Tissue- Chapter 5 5-1 Bone Functions Support Protection Assistance in movement Mineral storage and release Blood cell production Triglyceride storage 5-2 Bone Chemistry Water (25%) Organic Constituent
Bone Tissue- Chapter 5 5-1 Bone Functions Support Protection Assistance in movement Mineral storage and release Blood cell production Triglyceride storage 5-2 Bone Chemistry Water (25%) Organic Constituent
Effects of Delayed Stabilization on Fracture Healing
 Effects of Delayed Stabilization on Fracture Healing Theodore Miclau, 1 Chuanyong Lu, 1 Zachary Thompson, 1 Paul Choi, 1 Christian Puttlitz, 2 Ralph Marcucio, 1 Jill A. Helms 3 1 Department of Orthopaedic
Effects of Delayed Stabilization on Fracture Healing Theodore Miclau, 1 Chuanyong Lu, 1 Zachary Thompson, 1 Paul Choi, 1 Christian Puttlitz, 2 Ralph Marcucio, 1 Jill A. Helms 3 1 Department of Orthopaedic
Osseous Tissue and Bone Structure
 6 Osseous Tissue and Bone Structure PowerPoint Lecture Presentations prepared by Jason LaPres Lone Star College North Harris An Introduction to the Skeletal System Learning Outcomes 6-1 Describe the primary
6 Osseous Tissue and Bone Structure PowerPoint Lecture Presentations prepared by Jason LaPres Lone Star College North Harris An Introduction to the Skeletal System Learning Outcomes 6-1 Describe the primary
Derived copy of Bone *
 OpenStax-CNX module: m57739 1 Derived copy of Bone * Shannon McDermott Based on Bone by OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 4.0 By
OpenStax-CNX module: m57739 1 Derived copy of Bone * Shannon McDermott Based on Bone by OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 4.0 By
The Skeletal System:Bone Tissue
 The Skeletal System:Bone Tissue Dynamic and ever-changing throughout life Skeleton composed of many different tissues cartilage, bone tissue, epithelium, nerve, blood forming tissue, adipose, and dense
The Skeletal System:Bone Tissue Dynamic and ever-changing throughout life Skeleton composed of many different tissues cartilage, bone tissue, epithelium, nerve, blood forming tissue, adipose, and dense
Chapter 5 The Skeletal System:Bone Tissue. Functions of Bone. Bones
 Chapter 5 The Skeletal System:Bone Tissue Dynamic and ever-changing throughout life Skeleton composed of many different tissues cartilage, bone tissue, epithelium, nerve, blood forming tissue, adipose,
Chapter 5 The Skeletal System:Bone Tissue Dynamic and ever-changing throughout life Skeleton composed of many different tissues cartilage, bone tissue, epithelium, nerve, blood forming tissue, adipose,
Compact bone; Many parallel Haversian canals contain: small blood vessels. very small nerve. Interconnected by Volkmann s canals.
 Special characteristics of COMPACT BONE (dense bone) Thick; well vascularized Osteocytes and lamellae Concentric rings around blood vessels Most bones: outer compact bone inner spongy bone Marrow cavity
Special characteristics of COMPACT BONE (dense bone) Thick; well vascularized Osteocytes and lamellae Concentric rings around blood vessels Most bones: outer compact bone inner spongy bone Marrow cavity
The Skeletal System PART A. PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College
 PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Skeletal System 5 PART A The Skeletal System Parts of the skeletal system Bones (skeleton) Joints
PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Skeletal System 5 PART A The Skeletal System Parts of the skeletal system Bones (skeleton) Joints
BONE HISTOLOGY SLIDE PRESENTATION
 BONE HISTOLOGY SLIDE PRESENTATION PRESENTED BY: SKELETECH, INC. Clients and Friends: SkeleTech invites you to use these complimentary images for your own presentations or as teaching slides for bone biology.
BONE HISTOLOGY SLIDE PRESENTATION PRESENTED BY: SKELETECH, INC. Clients and Friends: SkeleTech invites you to use these complimentary images for your own presentations or as teaching slides for bone biology.
Chapter 6: SKELETAL SYSTEM
 Chapter 6: SKELETAL SYSTEM I. FUNCTIONS A. Support B. Protection C. Movement D. Mineral storage E. Lipid storage (Fig. 6.8b) F. Blood cell production (Fig. 6.4) II. COMPONENTS A. Cartilage 1. Hyaline 2.
Chapter 6: SKELETAL SYSTEM I. FUNCTIONS A. Support B. Protection C. Movement D. Mineral storage E. Lipid storage (Fig. 6.8b) F. Blood cell production (Fig. 6.4) II. COMPONENTS A. Cartilage 1. Hyaline 2.
Development of Bone Canaliculi During Bone Repair
 Development of Bone Canaliculi During Bone Repair K. KUSUZAKI, 1 N. KAGEYAMA, 1 H. SHINJO, 1 H. TAKESHITA, 1 H. MURATA, 1 S. HASHIGUCHI, 1 T. ASHIHARA, 2 and Y. HIRASAWA 1 Departments of 1 Orthopaedic
Development of Bone Canaliculi During Bone Repair K. KUSUZAKI, 1 N. KAGEYAMA, 1 H. SHINJO, 1 H. TAKESHITA, 1 H. MURATA, 1 S. HASHIGUCHI, 1 T. ASHIHARA, 2 and Y. HIRASAWA 1 Departments of 1 Orthopaedic
TECHNICAL RESEARCH DOCUMENTS AND MEDICAL PUBLICATIONS FOR: DAMAGED BONE AND CARTILAGE
 TECHNICAL RESEARCH DOCUMENTS AND MEDICAL PUBLICATIONS FOR: DAMAGED BONE AND CARTILAGE January 2018 TECHNICAL RESEARCH DOCUMENTS AND MEDICAL PUBLICATIONS FOR: DAMAGED BONE AND CARTILAGE Stem cells from
TECHNICAL RESEARCH DOCUMENTS AND MEDICAL PUBLICATIONS FOR: DAMAGED BONE AND CARTILAGE January 2018 TECHNICAL RESEARCH DOCUMENTS AND MEDICAL PUBLICATIONS FOR: DAMAGED BONE AND CARTILAGE Stem cells from
ANATOMY & PHYSIOLOGY 1 ( ) For Intensive Nursing PAUL ANDERSON SAMPLE TEST
 ANATOMY & PHYSIOLOGY 1 (101-805) For Intensive Nursing PAUL ANDERSON SAMPLE TEST 3 2011 1. If calcium levels in the extracellular fluid are too low, parathyroid hormone secretion would and osteoclast activity
ANATOMY & PHYSIOLOGY 1 (101-805) For Intensive Nursing PAUL ANDERSON SAMPLE TEST 3 2011 1. If calcium levels in the extracellular fluid are too low, parathyroid hormone secretion would and osteoclast activity
QUICK ASSESSMENT: CONCEPT MAP
 FUNCTIONS OF THE SKELETAL SYSTEM 7th Grade THE SKELETAL SYSTEM Provides shape, strength, and support (3S s) Internal framework of the body Support and anchor for soft organs Protects soft internal organs
FUNCTIONS OF THE SKELETAL SYSTEM 7th Grade THE SKELETAL SYSTEM Provides shape, strength, and support (3S s) Internal framework of the body Support and anchor for soft organs Protects soft internal organs
PROCHONDRIX CARTILAGE RESTORATION MATRIX CONTAINS GROWTH FACTORS NECESSARY FOR HYALINE CARTILAGE REGENERATION
 A L L O S O U R C E PROCHONDRIX CARTILAGE RESTORATION MATRIX CONTAINS GROWTH FACTORS NECESSARY FOR HYALINE CARTILAGE REGENERATION Ryan Delaney MS; Carolyn Barrett BS, MBA; Peter Stevens PhD, MBA AlloSource,
A L L O S O U R C E PROCHONDRIX CARTILAGE RESTORATION MATRIX CONTAINS GROWTH FACTORS NECESSARY FOR HYALINE CARTILAGE REGENERATION Ryan Delaney MS; Carolyn Barrett BS, MBA; Peter Stevens PhD, MBA AlloSource,
Chapter 6 Skeletal System
 Chapter 6 Skeletal System Functions of the skeletal system/bone 1. Support skeletal system is the internal framework of the body 2. Protection protects internal organs 3. Movement muscles & bones work
Chapter 6 Skeletal System Functions of the skeletal system/bone 1. Support skeletal system is the internal framework of the body 2. Protection protects internal organs 3. Movement muscles & bones work
