Meniscus body position and its change over four years in asymptomatic adults: a cohort study using data from the Osteoarthritis Initiative (OAI)
|
|
|
- Rhoda Watson
- 5 years ago
- Views:
Transcription
1 Bruns et al. BMC Musculoskeletal Disorders 2014, 15:32 RESEARCH ARTICLE Open Access Meniscus body position and its change over four years in asymptomatic adults: a cohort study using data from the Osteoarthritis Initiative (OAI) Katharina Bruns 1, Fredrik Svensson 2, Aleksandra Turkiewicz 2, Wolfgang Wirth 1,3, Ali Guermazi 4, Felix Eckstein 1,3 and Martin Englund 2,5* Abstract Background: A high degree of meniscal body extrusion on knee magnetic resonance imaging has been shown to be strongly associated with development of knee osteoarthritis. However, very little is known about meniscal position in the asymptomatic knee and its natural history. Hence our objective was to study meniscal body position and its change over 4 years in asymptomatic adults. Methods: Cohort study using data from the Osteoarthritis Initiative (OAI) involving four clinical sites in the United States (Baltimore, Maryland, Pawtucket, Rhode Island, Columbus, Ohio, and Pittsburgh, Pennsylvania). We studied both knees from 118 subjects (mean age 55 years, 61% women, mean body mass index 24.4) from the OAI non-exposed reference cohort free of knee pain, radiographic knee osteoarthritis and risk factors for knee osteoarthritis at baseline. We assessed mid-coronal intermediate-weighted 3-Tesla magnetic resonance images from baseline and the 2- and 4-year follow-up visit. One observer measured tibia plateau, meniscal body width and meniscal body extrusion in both compartments. We calculated meniscal overlap distance on the tibial plateau, % coverage, and extrusion index compared to tibia width. Potential trends in position over the 4-year period were evaluated using a linear mixed-effects regression model. Results: The mean (SD) values at baseline for medial meniscal body extrusion and overlap distance were 1.64 mm (0.92) and 10.1 mm (3.5), and coverage was 34.4% (11.9). The corresponding values for the lateral compartment were 0.63 mm (0.73), 9.8 mm (2.4), and 31.0% (7.7). Medial meniscus body extrusion index was greater in female knees (p = 0.03). There was slight increase in medial meniscal body extrusion over 4 years (0.040 mm/year [95% CI: ]). The other variables were relatively stable. Conclusions: In asymptomatic adults, the relative degree of meniscus body extrusion is more pronounced in female knees. Although a slight increase in extrusion over time was noted for the medial body, positions were relatively stable within subjects over time. Keywords: Knee, Meniscus, Magnetic resonance imaging, Osteoarthritis * Correspondence: martin.englund@med.lu.se 2 Department of Orthopedics, Clinical Sciences Lund, Lund University, Lund, Sweden 5 Clinical Epidemiology Research & Training Unit, Boston University School of Medicine, Boston, MA, USA Full list of author information is available at the end of the article 2014 Bruns et al.; licensee BioMed Central Ltd. This is an Open Access article distributed under the terms of the Creative Commons Attribution License ( which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly credited.
2 Bruns et al. BMC Musculoskeletal Disorders 2014, 15:32 Page 2 of 11 Background The meniscus is a fibrocartilaginous structure between femur and tibia with the important task of load distribution but potentially also shock absorption [1-3]. About 70% of the load passes through the medial tibiofemoral compartment and 30% through the lateral compartment in normally aligned knees [4]. While there is limited biomechanical studies of effects of different meniscus position per se, there is evidence that a displaced meniscus, e.g., due to a root tear, will no longer provide optimal load transmission in the knee, thus result in increased cartilage contact stress in similar manner as after partial or total meniscectomy [5,6]. Substantial extrusion of the meniscal body, i.e., when the peripheral part of the mid portion of the meniscus is markedly located outside the tibial joint margin, is considered a structural feature that is strongly related to the incidence and progression of knee osteoarthritis (OA) [7-9]. A high degree of meniscal body extrusion on knee magnetic resonance (MR) imaging has been shown to be strongly associated with development of radiographic knee OA, cartilage loss, and the development of ipsilateral bone marrow lesions [10-12]. Potentially it may also be causing knee symptoms, e.g., by affecting the often pain sensitive knee capsule and synovial tissue [13]. Meniscal extrusion has also been reported to be associated with meniscal degeneration and extensive tears [14-16]. However, when discussing pathological meniscal position, one first needs to know more about meniscal position in the asymptomatic knee. For instance, medial meniscal extrusion of up to 3 millimetres (mm) is common in persons 40 years of age or older without knee symptoms [7]. Still, there is limited data published on this topic and also knee sizes and the sizes of menisci may vary considerably [17,18]. Hence, the relative degree of meniscal extrusion may be very different between subjects even if the absolute measure of extrusion is identical. Also, to the best of our knowledge there are no studies of meniscal position over time in individuals free of knee OA. Therefore, in this study we aimed to gain insight on medial and lateral meniscal body position (cross-sectional analysis) and its potential change (longitudinal analysis) over a period of 4 years in asymptomatic persons without risk factors and radiographic knee OA at baseline. We used a 2-dimensional quantitative measurement technique originally reported by Hunter et al. [12] Our main objectives were to answer the following questions: a) What is meniscus body position like in knees from asymptomatic adults in a midcoronal image slice? As meniscal tears are common in asymptomatic persons [19], but associated with altered meniscus position [14,15], we aimed to present data both collapsed and stratified by meniscal tear. b) Further, are there any trends in body position detectable over a 4-year time-period? We hypothesized that meniscus body position would remain reasonably stationary in asymptomatic subjects in this relatively intermediate time period. Methods Study sample Data used in the preparation of this article were obtained from the Osteoarthritis Initiative (OAI) database, which is available for public access at Specific dataset used were 0.F.2, 3.F.1 and 6.F.1, i.e., the non-exposed reference cohort of the OAI. This cohort consists of 122 subjects (47 men and 75 women; age range: years) who were invited to an annual exam with knee MR imaging. Inclusion criteria were: No pain, aching or stiffness in either knee in the past year; No radiographic OA in the tibiofemoral joint of either knee in the site readings performed during recruitment; No eligibility risk factors for knee OA present with the exception of age 70 years. In brief, the exclusion factors were: certain knee symptoms associated with OA in the past 12 months, overweight, history of knee injury and/or knee surgery, family history of total knee replacement, Heberden s nodes in both hands and repetitive knee bending. Four individuals had to be excluded due to presence of radiographic tibiofemoral OA (Kellgren & Lawrence grade 2) that retrospectively was noted in the central readings. Seventeen knees with KLG 1 in the central readings were included in the analysis. Hence, for our cross-sectional analyses (using baseline data) the study sample consisted of 118 subjects. For longitudinal analyses,usingmrimagingdatafromthebaselineexam, 2-year follow-up and 4-year follow-up, 6 subjects were lost to follow-up, and additional 3 subjects only appeared for baseline and the 2-year follow up, and another 4 subjects only appeared for baseline and the 4-year follow-up (Figure 1). The OAI was approved by the respective institutional review boards for the University of California, San Francisco and the four OAI clinical centres (University of Pittsburgh, Ohio State University, University of Maryland, Baltimore, Memorial Hospital of Rhode Island). All patients gave informed consent to participate in this study. MR imaging protocol and measurements Siemens 3 Tesla MR imaging scanners, one at each of the 4 clinical study centres located in the United States were used to take baseline (enrolment period 2004 to
3 Bruns et al. BMC Musculoskeletal Disorders 2014, 15:32 Page 3 of 11 Figure 1 Flow chart detailing the study sample. 2006) and annually follow-up scans of both left and right knees over a period of 4 years. One observer (KB) trained by an orthopaedic surgeon (FS), who was blinded to subject characteristics but had knowledge of time sequence (no image fusion was performed for longitudinal measurements), measured both left and right knees on the longitudinal (baseline, 2-year and 4-year) coronal intermediate-weighted turbo spinecho (IW TSE) MR images (repetitive time = 3,700 ms; echo time = 29 ms; slice thickness = 3 mm and in-plane resolution mm). For this study purpose, we refer mid-coronal to the single slice presenting the greatest area of the medial spine, which was the slice chosen for the measurements. If this was difficult to differentiate (2 slices had similar area of the spine), we picked the image which showed the greatest width of the tibia plateau. The observer measured tibia plateau width (from the edge of the tibial plateau, there were no osteophytes), medial and lateral tibia plateau width, medial and lateral meniscal coronal width, and meniscal body extrusion to the closest mm using efilm 3.4 software (Figure 2) [12]. Fifty randomly picked knees from the baseline examination were remeasured. Intra-observer reliability (intra-class correlation coefficient) for the parameters ranged from 0.70 to We further tested if there were any systematic differences in rotation between repeat MRI examinations in a random subset of 11 knees (by counting slices from the posterior tibial margin to the (our) mid coronal slice). One clinical investigator (ME), with background in orthopedics and experienced in reading meniscal status, studied all right and left knee MR images at the baseline exam for the presence of medial or lateral meniscal tears or destruction/maceration in the anterior horn, body, or posterior horn using the IW TSE sagittal and coronal fat-suppressed sequences. The reader regarded an increased meniscal signal as indicative of a meniscal tear when it communicated with the inferior, superior, or free edge of the meniscal surface (or more than one of those) on at least two consecutive images (or for a Figure 2 Example of measurements on mid-coronal 3 T intermediate weighted knee MR images using efilm 3.4 software (the vertical lines are supporting lines perpendicular to the tibial plateau created to aid measurements).
4 Bruns et al. BMC Musculoskeletal Disorders 2014, 15:32 Page 4 of 11 radial tear, if it was visible on both the coronal and sagittal images) [20]. We used anatomic (femorotibial) axis alignment data in OAI based on the posterioanterior knee radiographs done with the knee in fixed flexion using the Synaflexer frame [21]. The measurement of anatomic axis alignment involves the definition of the femoral axis using a coordinate system based on the shape of the femoral condyles that is defined as part of the location specific joint space width measurement methods used by Dr. Duryea [22]. The tibial axis is defined by the direction and center of the tibial shaft at a distance 10 cm below the tibial plateau. There is an offset from the anatomic axis to the mechanical axis because the shaft of the femur does not include the femoral neck which takes off medially from the femoral shaft. In order to classify knees into varus and valgus, we used a sex neutral offset of +4 degrees that has been reported to have the highest kappa values in terms of agreement between anatomic and mechanical alignments [23]. Hence, we based our categorization considering 2 or more degrees of valgus (mechanical axis) as valgus, 2 degrees or more of varus (mechanical axis) as varus and everything in between as neutral. These cutoffs corresponded to an anatomic axis > = 2 degrees as valgus, and < = 6 degrees as varus. Statistics We calculated the meniscal body extrusion index as: [meniscus body extrusion]/[tibia width]*100, i.e., taking into account differences in knee size, often seen between e.g., women and men but also within the sexes. The corresponding values were also reported after dividing by ipsilateral tibia plateau width instead of tibia width. Further, we calculated overlap distance between the free (inner) edge of the meniscal body and the margin of the tibial plateau as: [meniscus body width]-[meniscus body extrusion]. Finally, we calculated the proportion (%) of the width of the ipsilateral tibial plateau covered by meniscus as: ([meniscus body width]-[meniscus body extrusion])/[ipsilateral tibia plateau width]. We also present data stratified by meniscal tear, i.e., evaluating subjects with and without meniscal tear at the baseline exam, separately, because tears are reported to be associated with more meniscal extrusion [15]. To evaluate potential differences between baseline parameters in unpaired groups, we used a 2-level linear mixed regression model with a patient as a random effect to control for the correlation of measurements made in the same patient with adjustment for age and sex. Potential changes in meniscal body extrusion, overlap distance, or meniscal body coverage over the 4-year time period (3 time points) were analysed using a linear 3-level mixed effects regression model to account for correlation between measurements of two knees in the same person. The only fixed effect was time (using actual number of days between MR images obtained). We performed a sensitivity analysis for the longitudinal analyses stratifying by knees which were free of knee pain, aching or stiffness also at the 2-year and 4-year follow-up and those that were not. We considered a two-tailed p-value of 0.05 or less as statistically significant (SPSS software version 19, and STATA 12). Results The mean (SD) age of study subjects, n = 118 (46 men and 72 women) was 55.0 (7.5) years (Table 1). At the baseline exam, 17 of 236 medial menisci (7.2%) and 9 of 236 lateral menisci (3.8%) in 26 of 236 knees (11.0%) in 24 subjects (20.3%) were noted to have relatively minor non-displaced meniscal tears (typically degenerative horizontal cleavages, flap tears or radial tears located to the body and/or posterior horn). Two subjects had minor meniscal maceration/destruction of themeniscalbodyfreeedge(onesubjectinboththe medial and the lateral compartment and one in the lateral compartment only). Table 1 Characteristics of the study subjects Characteristic N = 118 Women, n (%) 72 (61) Age, mean ± SD (range) years 55.0 ± 7.5 (45 78) Body mass index, mean ± SD (range) kg/m ± 3.2 (18 34) Kellgren and Lawrence grade, n (%)* 0 99 (85) 1 17 (15) Medial meniscal tear, n (%) Right knee 9 (7.6) Left knee 8 (6.8) Lateral meniscal tear, n (%) Right knee 6 (5.1) Left knee 3 (2.5) Anatomic axis alignment* Right knee, mean ± SD degrees 5.5 ± 1.6 Varus, n (%) 41 (35) Neutral, n (%) 74 (64) Valgus, n (%) 1 (1) Left knee, mean ± SD degrees 4.9 ± 1.6 Varus, n (%) 28 (24) Neutral, n (%) 84 (72) Valgus, n (%) 4 (3) *Missing data for 2 subjects. We considered the femorotibial (anatomic) axis alignment < = 6.0 as varus and > = 2.0 as valgus.
5 Bruns et al. BMC Musculoskeletal Disorders 2014, 15:32 Page 5 of 11 Meniscal body extrusion (baseline) The mean (SD) absolute measure of medial body extrusion (average of right and left knees) was 1.64 (0.92) mm. The corresponding values for the lateral compartment were 0.63 (0.73) mm. The mean (SD) extrusion index (relative to tibia width) for the medial meniscus body was 2.3 (1.3) and for the lateral meniscus body 0.9 (1.0) (Table 2). We found knees with medial meniscal tear to have a tendency to more medial meniscal body extrusion than knees with intact medial menisci (mean [SD] 2.0 [0.87] mm vs [0.92] mm; p = 0.05) (Figure 3). The corresponding values for lateral meniscal body extrusion were 0.89 (0.93) mm in those with tear vs (0.72) mm in those without lateral tear (p = 0.31) (Figure 4). Men had a mean (SD) medial meniscal body extrusion at baseline of 1.60 (1.10) mm, and women 1.67 (0.79) mm (p=0.49). Laterally, the corresponding absolute values of meniscal extrusion were 0.70 (0.77) mm vs (0.71) mm (p = 0.31), respectively. Since female knees are often smaller than male ones (mean [SD] tibia width: [2.96] mm vs [3.48] mm; p < 0.001), and size of knees within persons within the same sex also vary greatly, we related the amount of extrusion to tibia plateau width and to ipsilateral tibia plateau width. Medially, women had a mean (SD) extrusion index of 2.4 (1.2) and men of 2.0 (1.4) (p = 0.03) related to total tibia plateau width. Laterally, the mean (SD) ratios were very similar: 0.8 (1.0) vs. 0.9 (1.0), respectively (p = 0.75). The corresponding index when relating to the ipsilateral compartment width for medial side were 6.0 (2.9) vs. 5.1 (3.6) for women and men (p = 0.059), and 2.0 (2.4) vs. 2.0 (2.3) (p = 0.87) for the lateral side. Meniscal body overlap distance and coverage (baseline) The overlap distance of the central part of the medial meniscal body was on average (SD) (3.53) mm. The corresponding results from the lateral compartment showed a mean (SD) overlap distance of 9.76 (2.42) mm. Stratified by the presence of medial meniscal tear we found a mean (SD) medial overlap distance of 9.00 (3.12) mm in the knees with medial tear vs. a mean of (3.55) mm in knees without medial tear, respectively (p = 0.31). In the lateral compartment, we found a mean (SD) overlap distance of 7.67 (1.80) mm in knees with lateral meniscal tear, while those without lateral tear showed a mean overlap distance (SD) of 9.84 (2.40) mm (p < 0.001). The central part of the medial meniscal body covered on average (SD) 34.4% (11.9) of the medial tibia plateau width. The corresponding result for the lateral compartment was 31.0% (7.7). Stratified by the presence of medial meniscal tear, we found a mean (SD) medial coverage of 29.0% (9.9) in the knees with medial tear vs. 34.8% (11.9) in knees Table 2 Meniscal measurements and calculated variables from the baseline exam. All values are means (SD) if not otherwise stated Ipsilateral meniscal tear (in the same compartment) Total sample No Yes Both knees Right knee Left knee Right knee Left knee Right knee Left knee Medial meniscus body N = 236 N = 118 N = 118 N = 109 N = 110 N = 9 N = 8 Width, mm (3.4) 11.6 (3.3) 12.0 (3.4) 11.7(3.3) 11.0 (3.1) 11.0 (2.7) Extrusion, mm (1.0) 1.4 (0.77) 1.9 (1.0) 1.4 (0.73) 1.9 (0.78) 2.1 (0.99) Extrusion index* (1.4) 2.0 (1.1) 2.6 (1.4) 1.9 (1.0) 2.5 (1.1) 2.7 (1.3) Extrusion index (ipsilat) (3.5) 4.9 (2.8) 6.4 (3.6) 4.8 (2.7) 6.2 (2.8) 7.0 (3.5) Overlap distance, mm (3.6) 10.2 (3.5) 10.2 (3.6) 10.3 (3.5) 9.1 (3.1) 8.9 (3.3) Coverage, % 34.4% 34.3 (12.0)% 34.5 (11.8)% 34.7 (12.2)% 34.9 (11.8)% 29.2 (9.7)% 28.7 (10.7)% Lateral meniscus body N = 236 N = 118 N = 118 N = 112 N = 115 N = 6 N = 3 Width, mm (2.3) 10.3 (2.6) 10.5 (2.3) 10.4 (2.5) 9.0 (1.9) 7.7 (2.1) Extrusion, mm (0.79) 0.61 (0.67) 0.62 (0.77) 0.61 (0.67) 1.00 (1.10) 0.67 (0.58) Extrusion index* (1.1) 0.8 (0.9) 0.9 (1.1) 0.8 (0.9) 1.4 (1.6) 1.0 (0.8) Extrusion index (ipsilat) (2.6) 1.9 (2.1) 2.0 (2.5) 1.9 (2.1) 3.2 (3.7) 2.3 (2.0) Overlap distance (2.3) 9.7 (2.5) 9.9 (2.3) 9.8 (2.5) 8.0 (1.4) 7.0 (2.6) Coverage 31.1% 31.3 (7.4)% 30.8 (7.9)% 31.6 (7.4)% 31.0 (7.8)% 26.2 (7.6)% 23.3 (7.8)% *[meniscal body extrusion]/[tibia width] * 100. [meniscal body extrusion]/[ipsilateral tibia plateau width] * 100. [meniscal coronal width] [meniscal body extrusion]. ([meniscal coronal width] [meniscal body extrusion])/[ipsilateral tibia plateau width].
6 Bruns et al. BMC Musculoskeletal Disorders 2014, 15:32 Page 6 of 11 Figure 3 Frequencies of medial meniscal body extrusion at baseline in the study sample of 118 subjects without radiographic osteoarthritis (OA) and without risk factors for knee OA. Black bars illustrate the median value. without medial tear (p = 0.29) (Figure 5). In the lateral compartment we found a mean (SD) coverage of 25.2% (7.3) in knees with lateral meniscal tear, while those without lateral tear had a coverage of 31.3% (7.6) (p < 0.001) (Figure 6). Medially in men, the meniscus covered on average 33.4% (11.9) of the ipsilateral tibia plateau width and 35.1% (11.9) in women (p = 0.6). The corresponding figures for the lateral compartment in men and women were 30.3% (7.6) and 31.5% (7.7), respectively (p = 0.3). Figure 4 Frequencies of lateral meniscal body extrusion at baseline in the study sample of 118 subjects without radiographic osteoarthritis (OA) and without risk factors for knee OA. Black bars illustrate the median value.
7 Bruns et al. BMC Musculoskeletal Disorders 2014, 15:32 Page 7 of 11 Figure 5 Frequency of medial coverage (% of ipsilateral tibia plateau width). Black bars illustrate the median value. Change over time in body extrusion, overlap distance, and coverage In the 2- and 4-year follow up, measurements for the medial side suggested a trend for increase in meniscal body extrusion over time, with an annually increase of mm (95% CI: ). The result was statistically significant, in both women and men, when stratifying the analysis by sex (data not shown). The analysis for meniscal overlap distance in the medial compartment suggested no essential change, mm (95% CI: ) per year. Further, no change in medial coverage was detected during the 4-year interval: % (95% CI: ), i.e., the percentage of the ipsilateral tibia plateau that is covered by meniscus stayed medially at about 34% (Table 3). The results for the lateral side did not show any statistically significant trends in extrusion over time, mean Figure 6 Frequency of lateral coverage (% of ipsilateral tibia plateau width). Black bars illustrate the median value.
8 Bruns et al. BMC Musculoskeletal Disorders 2014, 15:32 Page 8 of 11 Table 3 Mean change in meniscus measures from baseline to the 4-year follow-up in asymptomatic subjects without knee osteoarthritis (OA) and without risk factors for knee OA Change from baseline to 4-year follow-up N Extrusion (mm) Overlap distance (mm) Coverage (%) No meniscal tear at baseline (ipsilateral) Medial body, mean change (SD) Right knee (0.76) 0.20 (2.36) 0.5 (8.0) Left knee (0.60) 0.26 (1.98) 0.7 (7.0) Lateral body, mean change (SD) Right knee (0.54) 0.23 (1.46) 0.7 (4.8) Left knee (0.75) 0.26 (1.96) 0.7 (6.1) Meniscal tear at baseline (ipsilateral) Medial body, mean change (SD) Right knee (0.89) 0.25 (2.49) 1.0 (8.2) Left knee (1.22) 0.43 (1.99) 1.4 (6.3) Lateral body, mean change (SD) Right knee (1.17) 0.50 (0.84) 1.6 (3.3) Left knee (0.58) 0.33 (1.53) 1.5 (4.0) mm (95% CI: ) per year (Table 3). However, the results for overlap distance on the lateral side suggested a mean increase of mm (95% CI: ) per year. Analysis for lateral coverage also suggested no essential changes although it was statistically significant: 0.002% (95% CI: ) (Table 3). In the sensitivity analysis, stratifying by knees that were free of knee pain, aching or stiffness also at the 2-year and 4-year follow-up (n = 189) and those that were not (n = 47), the results for change in meniscal body extrusion, overlap distance, and coverage remained essentially the same for both compartments in both stratum (data not shown). We found no evidence of systematic rotation of follow-up MR images. In most (18 of 21; one time point missing) of the follow-up exams, the mid coronal slice occurred as the same slice number as the baseline exam, and no slice was deviating more than +/ 1 from the baseline exam. Discussion We have provided reference values for medial and lateral meniscal body position in knees of asymptomatic persons without radiographic knee OA and without common risk factors for knee OA using a two-dimensional measurement technique on coronal MR images. Interestingly, we found that there was a small tendency to increased medial meniscal body extrusion over a 4-year period. However, most meniscal position parameters remained relatively stable. We also provide data for a relative measure of meniscal extrusion, i.e., which takes into account the fact that knee size (and size of menisci) may vary between subjects and an absolute measure of extrusion may not give justice to these size differences. Since physiological degradation of meniscal tissue and its displacement may be a slow process, there is a need of more sensitive measuring methods of meniscal position than semi-quantitative scoring, which is incorporated in the most commonly used knee MR imaging scoring systems of knee OA [24,25]. For instance, in subjects with knee OA or with risk factors for knee OA, within-grade changes in semi-quantitative MR imaging assessment are valid and may increase sensitivity in detecting longitudinal changes of cartilage and bone marrow lesions [26]. It is plausible that this is true also for meniscal changes. Full segmentation of meniscal volume and its relation to the tibial plateau can provide very detailed information but is time consuming, hence challenging for larger sample sizes or in daily clinical practice [27-29]. To our knowledge, there is not much written about the physiological meniscal position in the asymptomatic knee free of radiographic OA [30] and in particular its potential change over time. Several earlier studies distinguished between minor and major extrusion and in radiologic literature, it seems to have become common to define a threshold of 3 mm or more on coronal images as pathological extrusion [14]. Consequently, an extrusion of the meniscus body less than 3 mm is often regarded as of less clinical importance. This value is supported by results for meniscal extrusion measurements in a control group of asymptomatic persons, which however included subjects with evidence of radiographic OA changes [7]. The informative value about
9 Bruns et al. BMC Musculoskeletal Disorders 2014, 15:32 Page 9 of 11 pathology of a minor extrusion is ambiguous. In contrast to the above-mentioned 3 mm cut-off is the 2 and 5 mm separation, which is used in the semi-quantitative MR imaging scoring systems BLOKS and MOAKS [24,25]. Instead of an absolute measure, we would like to advocate for the use of a relative measure, similar to the early work addressing meniscal extrusion as seen on MR imaging [8]. In the report by Kenny, the ratio was constructed by dividing by the meniscus width. However, we propose to rather use tibia width (or ipsilateral tibia plateau width) in the coronal plane because meniscal body width may be affected by degeneration, tear or meniscus surgery. Thus, we are currently addressing this question in knees with and without radiographic OA to more accurately determine the most suitable measure to divide by and to define cut-offs for clinical and research use. Interestingly, in relative terms women tended to have more medial meniscal extrusion at the baseline exam compared to men, which also has been previously described by Bloecker et al. [18]. This tendency in our study was not evident unless taking into account knee size, i.e., using our proposed extrusion index construct. This finding may be important as knee OA is more common in women, and meniscus position and collateral ligament laxity may play important roles in pathogenesis. Our finding of more medial meniscal extrusion in knees with medial meniscal tear is in agreement with previous cross-sectional reports, suggesting that tears are associated with increased meniscal extrusion [14-16]. Knees with meniscal tears in our study also tended to have less tibial plateau coverage compared to knees without tears. Between 40% and 70% of load has been reported to be transmitted by the menisci; the rest through direct contact of articular cartilage [31]. Being exposed to this great stress, its position (and coverage) plays an often critical role in maintaining a healthy knee. Our measurements suggest a mean coverage of 34% of width medially and of 31% laterally. While the lateral meniscus coverage is the same as suggested for patients with symptomatic knee OA, the medial coverage is 13% greater in asymptomatic knees compared to the results of symptomatic OA knees using the same measurement technique [12]. The wider range of coverage in sample of asymptomatic individuals most likely reflects the variety of anatomical shapes and dimensions of the tibial plateau and meniscus body [17,18]. While meniscal coverage diminishes in OA affected subjects due to meniscal destruction and radial displacement [12], the coverage in asymptomatic knees at baseline stayed about the same during a 4-year time period, both medially and laterally. The tendency in the present study to increased extrusion of the medial meniscus body with time, not affecting coverage and overlap distance to the same extent, might potentially indicate increased bulging of the peripheral meniscal margin (more convex shape), i.e., not so much radial displacement (shift in position). Of note, meniscal extrusion is a combined construct of radial displacement and potential change in meniscus width, e.g., due to bulging of the peripheral meniscus margin and/or meniscus hypertrophy [32,33]. The clinical relevance of our longitudinal findings is unknown, and is a question for forthcoming studies. This study has important limitations that we would like to point out. Due to funding limitations and time constraints our aims included only the study of meniscal body position. Hence, the study of potential anterior and posterior horn movements is a question for future work. The number of knees with meniscal tear is small to provide robust estimates of association. Since knee alignment have great impact on biomechanical force transmission which may influence the degree of extrusion, a larger sample allowing enough numbers in different alignment categories would be valuable in future work [34]. For this study, we used a relatively straightforward two-dimensional quantitative measurement technique on the mid-coronal slice, i.e., a technique that does not consume as much time or needs specialized software as full volume segmentation, and therefore is more suitable for clinical practice. However, it does not provide as much detailed information as techniques doing full segmentation of the meniscus body [27-29]. The reading software we used (Efilm 3.4) only allowed measurements to the closest millimetre. As we are dealing with small measurements such as meniscal extrusion, measurements to a tenth of a millimetre would have been preferable using alternate imaging software. Our calculated coverage represents the % width of the ipsilateral tibia plateau that is covered by meniscus in the mid-coronal MRI slice. Although this variable is not representing the whole area of the meniscus covering the plateau, we suggest it likely provides a fairly representative proxy of the cartilage coverage of the meniscal body. Finally, the reader being familiar with the time sequence in which the images were taken, sensitivity to eventual changes in size and position was increased but potential bias cannot be excluded [35]. Any change in rotation between exams or misclassification of mid-coronal slice is expected to be non-differential which will only bias findings towards the null. Conclusions Using 3-Tesla MR imaging data from the OAI unexposed reference cohort, we provide data of meniscus medial and lateral body position in asymptomatic subjects including a new relative measure of extrusion as a ratio of extrusion by the tibia width. These measures may be useful tools in future studies of meniscus position in OA knees and for clinical practice. Further, our findings suggest that over a 4-year time frame there is on
10 Bruns et al. BMC Musculoskeletal Disorders 2014, 15:32 Page 10 of 11 average a small increased medial body extrusion (mainly due to increased bulging) even in asymptomatic middleaged or elderly subjects without knee OA at baseline. The association of these alterations with incidence of cartilage changes, radiographic OA etc. is a topic for further research as well as potential meniscal changes in position in younger adults. Competing interests Wolfgang Wirth has a part-time appointment with Chondrometrics GmbH, a company providing MR image analysis services, and is co-owner of Chondrometrics GmbH. Ali Guermazi is President and co-founder of the Boston Imaging Core Lab (BICL), a company providing radiological reading services to academic researchers and to industry. He provides consulting services to Genzyme. Felix Eckstein is CEO and co-owner of Chondrometrics GmbH. He provides consulting services to MerckSerono, Novartis, Sanofi Aventis, Perceptive, Bioclinica and Abbot. Authors contributions Conception and design: ME, FE. Acquisition of data: KB, FS, ME. Analysis and interpretation of the data: KB, FS, AT, WW, AG, FE, ME. Drafting of article: KB, FS. Reviewing for important intellectual content: AT, WW, AG, FE, ME. Final approval of submitted version: KB, FS, AT, WW, AG, FE, ME. Obtaining of funding: KB, ME. Acknowledgements We would like to express our sincere gratitude to the OAI for the free use of public access data. We would also like to acknowledge the support from Osteoarthritis Research Society International and the scholarship which made it possible for Katharina Bruns to come to Lund University to perform the study. The OAI is a public-private partnership comprised of five contracts (N01-AR ; N01-AR ; N01-AR ; N01-AR ; N01-AR ) funded by the National Institutes of Health, a branch of the Department of Health and Human Services, and conducted by the OAI Study Investigators. Private funding partners include Merck Research Laboratories; Novartis Pharmaceuticals Corporation, GlaxoSmithKline; and Pfizer, Inc. Private sector funding for the OAI is managed by the Foundation for the National Institutes of Health. This manuscript was prepared using an OAI public use data set and does not necessarily reflect the opinions or views of the OAI investigators, the NIH, or the private funding partners. We also would like to acknowledge the funding support (M Englund) from Swedish Research Council, ALF, Kock Foundations, and Gustav V s 80-Year Birthday Foundation. The funders had no role in study design, data collection and analysis, decision to publish, or preparation of the manuscript. Author details 1 Institute of Anatomy and Musculoskeletal Research, Paracelsus Medical University, Salzburg, Austria. 2 Department of Orthopedics, Clinical Sciences Lund, Lund University, Lund, Sweden. 3 Chondrometrics GmbH, Ainring, Germany. 4 Department of Radiology, Boston University School of Medicine, Boston, MA, USA. 5 Clinical Epidemiology Research & Training Unit, Boston University School of Medicine, Boston, MA, USA. Received: 30 August 2013 Accepted: 4 February 2014 Published: 5 February 2014 References 1. Kurosawa H, Fukubayashi T, Nakajima H: Load-bearing mode of the knee joint: physical behavior of the knee joint with or without menisci. Clin Orthop Relat Res 1980, 149: Walker PS, Erkman MJ: The role of the menisci in force transmission across the knee. Clin Orthop Relat Res 1975, 109: Andrews S, Shrive N, Ronsky J: The shocking truth about meniscus. J Biomech 2011, 44(16): Hsu RW, Himeno S, Coventry MB, Chao EY: Normal axial alignment of the lower extremity and load-bearing distribution at the knee. Clin Orthop Relat Res 1990, 255: Harner CD, Mauro CS, Lesniak BP, Romanowski JR: Biomechanical consequences of a tear of the posterior root of the medial meniscus. Surgical technique. J Bone Joint Surg Am 2009, 91(Suppl 2): Bae JY, Park KS, Seon JK, Kwak DS, Jeon I, Song EK: Biomechanical analysis of the effects of medial meniscectomy on degenerative osteoarthritis. Med Biol Eng Comput 2012, 50(1): Gale DR, Chaisson CE, Totterman SM, Schwartz RK, Gale ME, Felson D: Meniscal subluxation: association with osteoarthritis and joint space narrowing. Osteoarthritis Cartilage 1999, 7(6): Kenny C: Radial displacement of the medial meniscus and Fairbank s signs. Clin Orthop Relat Res 1997, 339: Sugita T, Kawamata T, Ohnuma M, Yoshizumi Y, Sato K: Radial displacement of the medial meniscus in varus osteoarthritis of the knee. Clin Orthop Relat Res 2001, 387: Englund M, Guermazi A, Roemer FW, Aliabadi P, Yang M, Lewis CE, Torner J, Nevitt MC, Sack B, Felson DT: Meniscal tear in knees without surgery and the development of radiographic osteoarthritis among middle-aged and elderly persons: the Multicenter Osteoarthritis Study. Arthritis Rheum 2009, 60(3): Englund M, Guermazi A, Roemer FW, Yang M, Zhang Y, Nevitt MC, Lynch JA, Lewis CE, Torner J, Felson DT: Meniscal pathology on MRI increases the risk for both incident and enlarging subchondral bone marrow lesions of the knee: the MOST study. Ann Rheum Dis 2010, 69(10): Hunter DJ, Zhang YQ, Niu JB, Tu X, Amin S, Clancy M, Guermazi A, Grigorian M, Gale D, Felson DT: The association of meniscal pathologic changes with cartilage loss in symptomatic knee osteoarthritis. Arthritis Rheumatism 2006, 54(3): Wenger A, Englund M, Wirth W, Hudelmaier M, Kwoh K, Eckstein F, Investigators OAI: Relationship of 3D meniscal morphology and position with knee pain in subjects with knee osteoarthritis: a pilot study. Eur Radiol 2012, 22(1): Costa CR, Morrison WB, Carrino JA: Medial meniscus extrusion on knee MRI: is extent associated with severity of degeneration or type of tear? AJR Am J Roentgenol 2004, 183(1): Allen DM, Crema MD, Marra MD, GuermaziA,WymanBT,HellioLeGraverandMP, Englund M, Brandt KL, Hunter DJ: The relationship between meniscal tears and meniscal positioning. Ther Adv Musculoskel Dis 2010, 2(6): Crema MD, Roemer FW, Felson DT, Englund M, Wang K, Jarraya M, Nevitt MC, Marra MD, Torner JC, Lewis CE, et al: Factors associated with meniscal extrusion in knees with or at risk for osteoarthritis: the multicenter osteoarthritis study. Radiology 2012, 264(2): Stone KR, Freyer A, Turek T, Walgenbach AW, Wadhwa S, Crues J: Meniscal sizing based on gender, height, and weight. Arthroscopy 2007, 23(5): Bloecker K, Englund M, Wirth W, Hudelmaier M, Burgkart R, Frobell RB, Eckstein F: Revision 1 size and position of the healthy meniscus, and its correlation with sex, height, weight, and bone area- a cross-sectional study. BMC Musculoskelet Disord 2011, 12: Englund M, Guermazi A, Gale D, Hunter DJ, Aliabadi P, Clancy M, Felson DT: Incidental meniscal findings on knee MRI in middle-aged and elderly persons. N Engl J Med 2008, 359(11): De Smet AA, Tuite MJ: Use of the two-slice-touch rule for the MRI diagnosis of meniscal tears. AJR Am J Roentgenol 2006, 187(4): Nevitt MC, Peterfy C, Guermazi A, Felson DT, Duryea J, Woodworth T, Chen H, Kwoh K, Harris TB: Longitudinal performance evaluation and validation of fixed-flexion radiography of the knee for detection of joint space loss. Arthritis Rheumatism 2007, 56(5): Iranpour-Boroujeni T, Li J, Lynch J, Nevitt M, Duryea J: A new method to measure anatomic knee alignment: a tool for large studies of OA? Osteoarthr Cartil 2012, 20(Suppl 1):S Felson DT, Cooke TD, Niu J, Goggins J, Choi J, Yu J, Nevitt MC, Group OAII: Can anatomic alignment measured from a knee radiograph substitute for mechanical alignment from full limb films? Osteoarthr Cartil 2009, 17(11): Hunter DJ, Guermazi A, Lo GH, Grainger AJ, Conaghan PG, Boudreau RM, Roemer FW: Evolution of semi-quantitative whole joint assessment of knee OA: MOAKS (MRI Osteoarthritis Knee Score). Osteoarthr Cartil 2011, 19(8): Hunter DJ, Lo GH, Gale D, Grainger AJ, Guermazi A, Conaghan PG: The reliability of a new scoring system for knee osteoarthritis MRI and the validity of bone marrow lesion assessment: BLOKS (Boston Leeds Osteoarthritis Knee Score). Ann Rheum Dis 2008, 67(2):
11 Bruns et al. BMC Musculoskeletal Disorders 2014, 15:32 Page 11 of Roemer FW, Nevitt MC, Felson DT, Niu J, Lynch JA, Crema MD, Lewis CE, Torner J, Guermazi A: Predictive validity of within-grade scoring of longitudinal changes of MRI-based cartilage morphology and bone marrow lesion assessment in the tibio-femoral joint the MOST study. Osteoarthr Cartil 2012, 20(11): Stone KR, Stoller DW, Irving SG, Elmquist C, Gildengorin G: 3D MRI volume sizing of knee meniscus cartilage. Arthroscopy 1994, 10(6): Wirth W, Frobell RB, Souza RB, Li X, Wyman BT, Le Graverand MP, Link TM, Majumdar S, Eckstein F: A three-dimensional quantitative method to measure meniscus shape, position, and signal intensity using MR images: a pilot study and preliminary results in knee osteoarthritis. Magn Reson Med 2010, 63(5): Bowers ME, Tung GA, Fleming BC, Crisco JJ, Rey J: Quantification of meniscal volume by segmentation of 3 T magnetic resonance images. J Biomech 2007, 40(12): Bloecker K, Wirth W, Hudelmaier M, Burgkart R, Frobell R, Eckstein F: Morphometric differences between the medial and lateral meniscus in healthy men - a three-dimensional analysis using magnetic resonance imaging. Cells Tissues Organs 2012, 195(4): Jones RS, Keene GC, Learmonth DJ, Bickerstaff D, Nawana NS, Costi JJ, Pearcy MJ: Direct measurement of hoop strains in the intact and torn human medial meniscus. Clin Biomech 1996, 11(5): Wenger A, Wirth W, Hudelmaier M, Noebauer-Huhmann I, Trattnig S, Bloecker K, Frobell RB, Kwoh CK, Eckstein F, Englund M: Meniscus body position, size, and shape in persons with and persons without radiographic knee osteoarthritis: quantitative analyses of knee magnetic resonance images from the osteoarthritis initiative. Arthritis Rheumatism 2013, 65(7): Jung KA, Lee SC, Hwang SH, Yang KH, Kim DH, Sohn JH, Song SJ, Hunter DJ: High frequency of meniscal hypertrophy in persons with advanced varus knee osteoarthritis. Rheumatol Int 2010, 30(10): Englund M, Felson DT, Guermazi A, Roemer FW, Wang K, Crema MD, Lynch JA, Sharma L, Segal NA, Lewis CE, et al: Risk factors for medial meniscal pathology on knee MRI in older US adults: a multicentre prospective cohort study. Ann Rheum Dis 2011, 70(10): Felson DT, Nevitt MC: Blinding images to sequence in osteoarthritis: evidence from other diseases. Osteoarthr Cartil 2009, 17(3): doi: / Cite this article as: Bruns et al.: Meniscus body position and its change over four years in asymptomatic adults: a cohort study using data from the Osteoarthritis Initiative (OAI). BMC Musculoskeletal Disorders :32. Submit your next manuscript to BioMed Central and take full advantage of: Convenient online submission Thorough peer review No space constraints or color figure charges Immediate publication on acceptance Inclusion in PubMed, CAS, Scopus and Google Scholar Research which is freely available for redistribution Submit your manuscript at
Osteoarthritis and Cartilage 18 (2010) 1402e1407
 Osteoarthritis and Cartilage 18 (2010) 1402e1407 Comparison of BLOKS and WORMS scoring systems part II. Longitudinal assessment of knee MRIs for osteoarthritis and suggested approach based on their performance:
Osteoarthritis and Cartilage 18 (2010) 1402e1407 Comparison of BLOKS and WORMS scoring systems part II. Longitudinal assessment of knee MRIs for osteoarthritis and suggested approach based on their performance:
Osteoarthritis and Cartilage 18 (2010) 1393e1401
 Osteoarthritis and Cartilage 18 (2010) 1393e1401 Comparison of BLOKS and scoring systems part I. Cross sectional comparison of methods to assess cartilage morphology, meniscal damage and bone marrow lesions
Osteoarthritis and Cartilage 18 (2010) 1393e1401 Comparison of BLOKS and scoring systems part I. Cross sectional comparison of methods to assess cartilage morphology, meniscal damage and bone marrow lesions
Tibial coverage, meniscus position, size and damage in knees discordant for joint space. narrowing data from the Osteoarthritis Initiative
 Tibial coverage, meniscus position, size and damage in knees discordant for joint space narrowing data from the Osteoarthritis Initiative K. Bloecker 1,2, A. Guermazi 3,4, W. Wirth 1,5, O. Benichou 6,
Tibial coverage, meniscus position, size and damage in knees discordant for joint space narrowing data from the Osteoarthritis Initiative K. Bloecker 1,2, A. Guermazi 3,4, W. Wirth 1,5, O. Benichou 6,
ARTICLE IN PRESS. International Cartilage Repair Society
 Osteoarthritis and Cartilage (2009) jj, jjjejjj ª 2006 Osteoarthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2008.11.014 Strong association of
Osteoarthritis and Cartilage (2009) jj, jjjejjj ª 2006 Osteoarthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2008.11.014 Strong association of
Medial Knee Osteoarthritis Precedes Medial Meniscal Posterior Root Tear with an Event of Painful Popping
 Medial Knee Osteoarthritis Precedes Medial Meniscal Posterior Root Tear with an Event of Painful Popping Dhong Won Lee, M.D, Ji Nam Kim, M.D., Jin Goo Kim, M.D., Ph.D. KonKuk University Medical Center
Medial Knee Osteoarthritis Precedes Medial Meniscal Posterior Root Tear with an Event of Painful Popping Dhong Won Lee, M.D, Ji Nam Kim, M.D., Jin Goo Kim, M.D., Ph.D. KonKuk University Medical Center
Valgus Malalignment Is a Risk Factor for Lateral Knee Osteoarthritis Incidence and Progression
 ARTHRITIS & RHEUMATISM Vol. 65, No. 2, February 2013, pp 355 362 DOI 10.1002/art.37726 2013, American College of Rheumatology Valgus Malalignment Is a Risk Factor for Lateral Knee Osteoarthritis Incidence
ARTHRITIS & RHEUMATISM Vol. 65, No. 2, February 2013, pp 355 362 DOI 10.1002/art.37726 2013, American College of Rheumatology Valgus Malalignment Is a Risk Factor for Lateral Knee Osteoarthritis Incidence
W. Wirth¹, F. Eckstein¹, M. Hudelmaier¹, L.S. Lohmander², R.Frobell²
 Does Change in Femorotibial Cartilage Thickness Differ Between Acutely Anterior-Cruciate Ligament Injured Knees Treated with and without Reconstructive Surgery W. Wirth¹, F. Eckstein¹, M. Hudelmaier¹,
Does Change in Femorotibial Cartilage Thickness Differ Between Acutely Anterior-Cruciate Ligament Injured Knees Treated with and without Reconstructive Surgery W. Wirth¹, F. Eckstein¹, M. Hudelmaier¹,
The Association of Meniscal Pathologic Changes With Cartilage Loss in Symptomatic Knee Osteoarthritis
 ARTHRITIS & RHEUMATISM Vol. 54, No. 3, March 2006, pp 795 801 DOI 10.1002/art.21724 2006, American College of Rheumatology The Association of Meniscal Pathologic Changes With Cartilage Loss in Symptomatic
ARTHRITIS & RHEUMATISM Vol. 54, No. 3, March 2006, pp 795 801 DOI 10.1002/art.21724 2006, American College of Rheumatology The Association of Meniscal Pathologic Changes With Cartilage Loss in Symptomatic
Epidemiology of meniscus position: associations with knee symptoms and osteoarthritis
 Epidemiology of meniscus position: associations with knee symptoms and osteoarthritis Svensson, Fredrik 2019 Document Version: Publisher's PDF, also known as Version of record Link to publication Citation
Epidemiology of meniscus position: associations with knee symptoms and osteoarthritis Svensson, Fredrik 2019 Document Version: Publisher's PDF, also known as Version of record Link to publication Citation
Planning knee OA prevention studies in obese populations Lessons from the Multicenter Osteoarthritis Study (MOST) and Osteoathritis Initiative (OAI)
 Planning knee OA prevention studies in obese populations Lessons from the (MOST) and Osteoathritis Initiative (OAI) Michael Nevitt, PhD UCSF Epidemiology and Biostatistics OAI and MOST Coordinating Centers
Planning knee OA prevention studies in obese populations Lessons from the (MOST) and Osteoathritis Initiative (OAI) Michael Nevitt, PhD UCSF Epidemiology and Biostatistics OAI and MOST Coordinating Centers
Re-growth of an incomplete discoid lateral meniscus after arthroscopic partial resection in an 11 year-old boy: a case report
 Bisicchia and Tudisco BMC Musculoskeletal Disorders 2013, 14:285 CASE REPORT Open Access Re-growth of an incomplete discoid lateral meniscus after arthroscopic partial resection in an 11 year-old boy:
Bisicchia and Tudisco BMC Musculoskeletal Disorders 2013, 14:285 CASE REPORT Open Access Re-growth of an incomplete discoid lateral meniscus after arthroscopic partial resection in an 11 year-old boy:
Central Reading of Knee X-rays for Kellgren & Lawrence Grade and Individual Radiographic Features of Tibiofemoral Knee OA
 Central Reading of Knee X-rays for Kellgren & Lawrence Grade and Individual Radiographic Features of Tibiofemoral Knee OA 1. Overview... 1 1.1 SAS dataset... 1 1.2 Contents of dataset... 1 1.3 Merging
Central Reading of Knee X-rays for Kellgren & Lawrence Grade and Individual Radiographic Features of Tibiofemoral Knee OA 1. Overview... 1 1.1 SAS dataset... 1 1.2 Contents of dataset... 1 1.3 Merging
What is the most effective MRI specific findings for lateral meniscus posterior root tear in ACL injuries
 What is the most effective MRI specific findings for lateral meniscus posterior root tear in ACL injuries Kazuki Asai 1), Junsuke Nakase 1), Kengo Shimozaki 1), Kazu Toyooka 1), Hiroyuki Tsuchiya 1) 1)
What is the most effective MRI specific findings for lateral meniscus posterior root tear in ACL injuries Kazuki Asai 1), Junsuke Nakase 1), Kengo Shimozaki 1), Kazu Toyooka 1), Hiroyuki Tsuchiya 1) 1)
What Comes First? Multitissue Involvement Leading to Radiographic Osteoarthritis
 ARTHRITIS & RHEUMATOLOGY Vol. 67, No. 8, August 2015, pp 2085 2096 DOI 10.1002/art.39176 VC 2015, American College of Rheumatology What Comes First? Multitissue Involvement Leading to Radiographic Osteoarthritis
ARTHRITIS & RHEUMATOLOGY Vol. 67, No. 8, August 2015, pp 2085 2096 DOI 10.1002/art.39176 VC 2015, American College of Rheumatology What Comes First? Multitissue Involvement Leading to Radiographic Osteoarthritis
Andrew J Grainger Leeds, UK
 Andrew J Grainger Leeds, UK Osteoarthri6s (OA) How do we diagnose OA of the knee at MRI? What associated features do we see? Why do they maeer? When is it not OA? We think we have a clear understanding
Andrew J Grainger Leeds, UK Osteoarthri6s (OA) How do we diagnose OA of the knee at MRI? What associated features do we see? Why do they maeer? When is it not OA? We think we have a clear understanding
MRI KNEE WHAT TO SEE. Dr. SHEKHAR SRIVASTAV. Sr.Consultant KNEE & SHOULDER ARTHROSCOPY
 MRI KNEE WHAT TO SEE Dr. SHEKHAR SRIVASTAV Sr.Consultant KNEE & SHOULDER ARTHROSCOPY MRI KNEE - WHAT TO SEE MRI is the most accurate and frequently used diagnostic tool for evaluation of internal derangement
MRI KNEE WHAT TO SEE Dr. SHEKHAR SRIVASTAV Sr.Consultant KNEE & SHOULDER ARTHROSCOPY MRI KNEE - WHAT TO SEE MRI is the most accurate and frequently used diagnostic tool for evaluation of internal derangement
Post-injury painful and locked knee
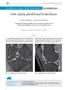 H R J Post-injury painful and locked knee, p. 54-59 Clinical Case - Test Yourself Musculoskeletal Imaging Post-injury painful and locked knee Ioannis I. Daskalakis 1, 2, Apostolos H. Karantanas 1, 2 1
H R J Post-injury painful and locked knee, p. 54-59 Clinical Case - Test Yourself Musculoskeletal Imaging Post-injury painful and locked knee Ioannis I. Daskalakis 1, 2, Apostolos H. Karantanas 1, 2 1
Sonographic Imaging of Meniscal Subluxation in Patients with Radiographic Knee Osteoarthritis
 ORIGINAL ARTICLE Sonographic Imaging of Meniscal Subluxation in Patients with Radiographic Knee Osteoarthritis Chun-Hung Ko, 1 Kam-Kong Chan, 1 Hui-Ling Peng 2 Background/Purpose: This study was undertaken
ORIGINAL ARTICLE Sonographic Imaging of Meniscal Subluxation in Patients with Radiographic Knee Osteoarthritis Chun-Hung Ko, 1 Kam-Kong Chan, 1 Hui-Ling Peng 2 Background/Purpose: This study was undertaken
Summary. Introduction
 Osteoarthritis and Cartilage (1999) 7, 526 532 1999 OsteoArthritis Research Society International 1063 4584/99/060526+07 $12.00/0 Article No. joca.1999.0256, available online at http://www.idealibrary.com
Osteoarthritis and Cartilage (1999) 7, 526 532 1999 OsteoArthritis Research Society International 1063 4584/99/060526+07 $12.00/0 Article No. joca.1999.0256, available online at http://www.idealibrary.com
Prevalence of Meniscal Radial Tears of the Knee Revealed by MRI After Surgery
 Downloaded from www.ajronline.org by 46.3.207.114 on 12/22/17 from IP address 46.3.207.114. Copyright RRS. For personal use only; all rights reserved Thomas Magee 1 Marc Shapiro David Williams Received
Downloaded from www.ajronline.org by 46.3.207.114 on 12/22/17 from IP address 46.3.207.114. Copyright RRS. For personal use only; all rights reserved Thomas Magee 1 Marc Shapiro David Williams Received
Meniscal Tears with Fragments Displaced: What you need to know.
 Meniscal Tears with Fragments Displaced: What you need to know. Poster No.: C-1339 Congress: ECR 2015 Type: Authors: Keywords: DOI: Educational Exhibit M. V. Ferrufino, A. Stroe, E. Cordoba, A. Dehesa,
Meniscal Tears with Fragments Displaced: What you need to know. Poster No.: C-1339 Congress: ECR 2015 Type: Authors: Keywords: DOI: Educational Exhibit M. V. Ferrufino, A. Stroe, E. Cordoba, A. Dehesa,
Research Article Relationship between Pain and Medial Meniscal Extrusion in Knee Osteoarthritis
 Advances in Orthopedics Volume 2015, Article ID 210972, 4 pages http://dx.doi.org/10.1155/2015/210972 Research Article Relationship between Pain and Medial Meniscal Extrusion in Knee Osteoarthritis Hiroaki
Advances in Orthopedics Volume 2015, Article ID 210972, 4 pages http://dx.doi.org/10.1155/2015/210972 Research Article Relationship between Pain and Medial Meniscal Extrusion in Knee Osteoarthritis Hiroaki
CLINICAL OUTCOME & MORPHOMETRY OVER 2 & 5 YEARS -
 CLINICAL OUTCOME & MORPHOMETRY OVER 2 & 5 YEARS - data from a treatment RCT on acute ACL injury R Frobell 1, W Wirth 2, LS Lohmander 1, M Hudelmaier 2, F Eckstein 2 1 Orthopedics, Clinical Sciences Lund,
CLINICAL OUTCOME & MORPHOMETRY OVER 2 & 5 YEARS - data from a treatment RCT on acute ACL injury R Frobell 1, W Wirth 2, LS Lohmander 1, M Hudelmaier 2, F Eckstein 2 1 Orthopedics, Clinical Sciences Lund,
kmri_qcart_eckstein_descrip 8/7/2017 1
 Central Assessments of MRI Images for Quantitative Measurements of Cartilage Morphology from knee MRI Scans (Felix Eckstein: Chondrometrics and Paracelsus) 1. Overview... 2 1.1 SAS dataset... 2 1.2 Contents
Central Assessments of MRI Images for Quantitative Measurements of Cartilage Morphology from knee MRI Scans (Felix Eckstein: Chondrometrics and Paracelsus) 1. Overview... 2 1.1 SAS dataset... 2 1.2 Contents
Accuracy and Precision of Quantitative Assessment of Cartilage Morphology by Magnetic Resonance Imaging at 3.0T
 ARTHRITIS & RHEUMATISM Vol. 52, No. 10, October 2005, pp 3132 3136 DOI 10.1002/art.21348 2005, American College of Rheumatology Accuracy and Precision of Quantitative Assessment of Cartilage Morphology
ARTHRITIS & RHEUMATISM Vol. 52, No. 10, October 2005, pp 3132 3136 DOI 10.1002/art.21348 2005, American College of Rheumatology Accuracy and Precision of Quantitative Assessment of Cartilage Morphology
CLINICAL OUTCOME & MORPHOMETRY OVER 2 & 5 YEARS - data from a treatment RCT on acute ACL injury
 CLINICAL OUTCOME & MORPHOMETRY OVER 2 & 5 YEARS - data from a treatment RCT on acute ACL injury R Frobell 1, W Wirth 2, LS Lohmander 1, M Hudelmaier 2, F Eckstein 2 1 Orthopedics, Clinical Sciences Lund,
CLINICAL OUTCOME & MORPHOMETRY OVER 2 & 5 YEARS - data from a treatment RCT on acute ACL injury R Frobell 1, W Wirth 2, LS Lohmander 1, M Hudelmaier 2, F Eckstein 2 1 Orthopedics, Clinical Sciences Lund,
Table of Contents. Overview Introduction Variables Missing Data Image Type Time Points Reading Methods...
 MULTICENTER OSTEOARTHRITIS STUDY LONGITUDINAL KNEE RADIOGRAPH ASSESSMENTS (BASELINE TO 15-MONTH, 30-MONTH, 60-MONTH AND 84-MONTH FOLLOW-UP) AND MEASUREMENTS FROM BASELINE FULL LIMB RADIOGRAPHS DATASET
MULTICENTER OSTEOARTHRITIS STUDY LONGITUDINAL KNEE RADIOGRAPH ASSESSMENTS (BASELINE TO 15-MONTH, 30-MONTH, 60-MONTH AND 84-MONTH FOLLOW-UP) AND MEASUREMENTS FROM BASELINE FULL LIMB RADIOGRAPHS DATASET
Clinical Evaluation of the Root Tear of the Posterior Horn of the Medial Meniscus in Total Knee Arthroplasty for Osteoarthritis
 Original Article Knee Surg Relat Res 2015;27(2):90-94 http://dx.doi.org/10.5792/ksrr.2015.27.2.90 pissn 2234-0726 eissn 2234-2451 Knee Surgery & Related Research Clinical Evaluation of the Root Tear of
Original Article Knee Surg Relat Res 2015;27(2):90-94 http://dx.doi.org/10.5792/ksrr.2015.27.2.90 pissn 2234-0726 eissn 2234-2451 Knee Surgery & Related Research Clinical Evaluation of the Root Tear of
Incidental Meniscal Findings on Knee MRI in Middle-Aged and Elderly Persons
 The new england journal of medicine original article Incidental Meniscal Findings on Knee MRI in Middle-Aged and Elderly Persons Martin Englund, M.D., Ph.D., Ali Guermazi, M.D., Daniel Gale, M.D., David
The new england journal of medicine original article Incidental Meniscal Findings on Knee MRI in Middle-Aged and Elderly Persons Martin Englund, M.D., Ph.D., Ali Guermazi, M.D., Daniel Gale, M.D., David
The association between meniscal subluxation and cartilage degeneration
 Eur J Orthop Surg Traumatol (2014) 24:79 84 DOI 10.1007/s00590-012-1144-3 ORIGINAL ARTICLE The association between meniscal subluxation and cartilage degeneration Young Rak Choi Jae Hwa Kim Ju Hwan Chung
Eur J Orthop Surg Traumatol (2014) 24:79 84 DOI 10.1007/s00590-012-1144-3 ORIGINAL ARTICLE The association between meniscal subluxation and cartilage degeneration Young Rak Choi Jae Hwa Kim Ju Hwan Chung
MENISCAL INJURY. Meniscus. Anterior Roots. Medial Meniscus. Lateral Meniscus. Posterior Roots. MRI and Arthroscopic Findings
 Meniscus Anterior Roots MENISCAL INJURY MRI and Arthroscopic Findings Medial Meniscus AH PH PH AH Lateral Meniscus Rawiwan Pattaweerakul Naresuan University Hospital Posterior Roots Meniscus Normal Meniscus
Meniscus Anterior Roots MENISCAL INJURY MRI and Arthroscopic Findings Medial Meniscus AH PH PH AH Lateral Meniscus Rawiwan Pattaweerakul Naresuan University Hospital Posterior Roots Meniscus Normal Meniscus
Bone marrow lesions in knee osteoarthritis: MR-assessment by manual segmentation and computer-assisted tresholding
 Bone marrow lesions in knee osteoarthritis: MR-assessment by manual segmentation and computer-assisted tresholding Poster No.: P-0073 Congress: ESSR 2012 Type: Scientific Exhibit Authors: F. K. Nielsen,
Bone marrow lesions in knee osteoarthritis: MR-assessment by manual segmentation and computer-assisted tresholding Poster No.: P-0073 Congress: ESSR 2012 Type: Scientific Exhibit Authors: F. K. Nielsen,
Meniscal Root Tears: Evaluation, Imaging, and Repair Techniques
 Meniscal Root Tears: Evaluation, Imaging, and Repair Techniques R O B E R T N A S C I M E N TO, M D, M S C H I E F OF S P O RT S M E D I C I N E & SH O U L D E R S U R G E RY N E W TO N- W E L L E S L
Meniscal Root Tears: Evaluation, Imaging, and Repair Techniques R O B E R T N A S C I M E N TO, M D, M S C H I E F OF S P O RT S M E D I C I N E & SH O U L D E R S U R G E RY N E W TO N- W E L L E S L
Ultrasound Guided Genicular Nerve Block-A Motor Sparing Technique for the Treatment of Acute and Chronic Knee Pain
 International Journal of Anesthesiology Research, 2015, 3, 37-43 37 Ultrasound Guided Genicular Nerve Block-A Motor Sparing Technique for the Treatment of Acute and Chronic Knee Pain Michael Meng 1, Reid
International Journal of Anesthesiology Research, 2015, 3, 37-43 37 Ultrasound Guided Genicular Nerve Block-A Motor Sparing Technique for the Treatment of Acute and Chronic Knee Pain Michael Meng 1, Reid
Conservative surgical treatments for osteoarthritis: A Finite Element Study
 Conservative surgical treatments for osteoarthritis: A Finite Element Study Diagarajen Carpanen, BEng (Hons), Franziska Reisse, BEng(Hons), Howard Hillstrom, PhD, Kevin Cheah, FRCS, Rob Walker, PhD, Rajshree
Conservative surgical treatments for osteoarthritis: A Finite Element Study Diagarajen Carpanen, BEng (Hons), Franziska Reisse, BEng(Hons), Howard Hillstrom, PhD, Kevin Cheah, FRCS, Rob Walker, PhD, Rajshree
Coronal Tibiofemoral Subluxation in Knee Osteoarthritis
 Coronal Tibiofemoral Subluxation in Knee Osteoarthritis Saker Khamaisy, MD 1,2 * ; Hendrik A. Zuiderbaan, MD 1 ; Meir Liebergall, MD 2; Andrew D. Pearle, MD 1 1Hospital for Special Surgery, Weill Medical
Coronal Tibiofemoral Subluxation in Knee Osteoarthritis Saker Khamaisy, MD 1,2 * ; Hendrik A. Zuiderbaan, MD 1 ; Meir Liebergall, MD 2; Andrew D. Pearle, MD 1 1Hospital for Special Surgery, Weill Medical
Meniscus T2 Relaxation Time at Various Stages of Knee Joint Degeneration
 Meniscus T2 Relaxation Time at Various Stages of Knee Joint Degeneration Richard Kijowski, Michael Fazio, Benjamin Beduhn, and Fang Liu Department of Radiology University of Wisconsin School of Medicine
Meniscus T2 Relaxation Time at Various Stages of Knee Joint Degeneration Richard Kijowski, Michael Fazio, Benjamin Beduhn, and Fang Liu Department of Radiology University of Wisconsin School of Medicine
Knee malalignment is associated with an increased risk for incident and enlarging bone marrow lesions in the more loaded compartments: the MOST study
 Osteoarthritis and Cartilage 20 (2012) 1227e1233 Knee malalignment is associated with an increased risk for incident and enlarging bone marrow lesions in the more loaded compartments: the MOST study D.
Osteoarthritis and Cartilage 20 (2012) 1227e1233 Knee malalignment is associated with an increased risk for incident and enlarging bone marrow lesions in the more loaded compartments: the MOST study D.
In-vivo Evaluation Of The Kinematic Behavior Of An Artificial Medial Meniscus Implant: A Pilot Study Using Open-mri
 In-vivo Evaluation Of The Kinematic Behavior Of An Artificial Medial Meniscus Implant: A Pilot Study Using Open-mri Tineke De Coninck, MD 1, Jonathan J. Elsner, PhD 2, Maoz Shemesh, MSc 2, Michiel Cromheecke,
In-vivo Evaluation Of The Kinematic Behavior Of An Artificial Medial Meniscus Implant: A Pilot Study Using Open-mri Tineke De Coninck, MD 1, Jonathan J. Elsner, PhD 2, Maoz Shemesh, MSc 2, Michiel Cromheecke,
MR Imaging of a Posterior Root Tear of the Medial Meniscus: Diagnostic Accuracy of Various Tear Configurations and
 MR Imaging of a Posterior Root Tear of the Medial Meniscus: Diagnostic Accuracy of Various Tear Configurations and Associated Knee Abnormalities 1 Hyang Mi Lee, M.D., Jae Chan Shim, M.D., Jin Goo Kim,
MR Imaging of a Posterior Root Tear of the Medial Meniscus: Diagnostic Accuracy of Various Tear Configurations and Associated Knee Abnormalities 1 Hyang Mi Lee, M.D., Jae Chan Shim, M.D., Jin Goo Kim,
Case Report Double-Layered Lateral Meniscus Accompanied by Meniscocapsular Separation
 Case Reports in Orthopedics Volume 2015, Article ID 357463, 5 pages http://dx.doi.org/10.1155/2015/357463 Case Report Double-Layered Lateral Meniscus Accompanied by Meniscocapsular Separation Aki Fukuda,
Case Reports in Orthopedics Volume 2015, Article ID 357463, 5 pages http://dx.doi.org/10.1155/2015/357463 Case Report Double-Layered Lateral Meniscus Accompanied by Meniscocapsular Separation Aki Fukuda,
The Meniscal Roots: Gross Anatomic Correlation with 3-T MRI Findings
 rody et al. Meniscal Root MRI Musculoskeletal Imaging Pictorial Essay Jeffrey M. rody 1 Michael J. Hulstyn 2 raden. Fleming 3 Glenn. Tung 1 rody JM, Hulstyn MJ, Fleming, Tung G Keywords: anatomy, knee,
rody et al. Meniscal Root MRI Musculoskeletal Imaging Pictorial Essay Jeffrey M. rody 1 Michael J. Hulstyn 2 raden. Fleming 3 Glenn. Tung 1 rody JM, Hulstyn MJ, Fleming, Tung G Keywords: anatomy, knee,
Role of magnetic resonance imaging in the evaluation of traumatic knee joint injuries
 Original Research Article Role of magnetic resonance imaging in the evaluation of traumatic knee joint injuries Dudhe Mahesh 1*, Rathi Varsha 2 1 Resident, 2 Professor, Department of Radio-Diagnosis, Grant
Original Research Article Role of magnetic resonance imaging in the evaluation of traumatic knee joint injuries Dudhe Mahesh 1*, Rathi Varsha 2 1 Resident, 2 Professor, Department of Radio-Diagnosis, Grant
A rapid, novel method of volumetric assessment of MRI-detected subchondral bone marrow lesions in knee osteoarthritis
 Osteoarthritis and Cartilage 21 (2013) 806e814 A rapid, novel method of volumetric assessment of MRI-detected subchondral bone marrow lesions in knee osteoarthritis C. Ratzlaff y *, A. Guermazi z, J. Collins
Osteoarthritis and Cartilage 21 (2013) 806e814 A rapid, novel method of volumetric assessment of MRI-detected subchondral bone marrow lesions in knee osteoarthritis C. Ratzlaff y *, A. Guermazi z, J. Collins
Gajare RA, Gajare AV. MRI study of age related changes in a meniscus. IAIM, 2015; 2(8):
 Original Research Article MRI study of meniscus age related changes in a Rupali A. Gajare 1*, Atul V. Gajare 2 1 Lecturer, Anatomy Department, R.G.M.C., Kalva, Maharashtra, India 2 M.S. Ortho (Mumbai),
Original Research Article MRI study of meniscus age related changes in a Rupali A. Gajare 1*, Atul V. Gajare 2 1 Lecturer, Anatomy Department, R.G.M.C., Kalva, Maharashtra, India 2 M.S. Ortho (Mumbai),
The Relationship Between Cartilage Loss on Magnetic Resonance Imaging and Radiographic Progression in Men and Women With Knee Osteoarthritis
 ARTHRITIS & RHEUMATISM Vol. 52, No. 10, October 2005, pp 3152 3159 DOI 10.1002/art.21296 2005, American College of Rheumatology The Relationship Between Cartilage Loss on Magnetic Resonance Imaging and
ARTHRITIS & RHEUMATISM Vol. 52, No. 10, October 2005, pp 3152 3159 DOI 10.1002/art.21296 2005, American College of Rheumatology The Relationship Between Cartilage Loss on Magnetic Resonance Imaging and
This presentation is the intellectual property of the author. Contact them for permission to reprint and/or distribute.
 MRI of the Knee Jennifer Swart, M.D. Musculoskeletal Radiology South Texas Radiology Group Outline Coils, Patient Positioning Acquisition Parameters, Planes and Pulse Sequences Knee Arthrography Normal
MRI of the Knee Jennifer Swart, M.D. Musculoskeletal Radiology South Texas Radiology Group Outline Coils, Patient Positioning Acquisition Parameters, Planes and Pulse Sequences Knee Arthrography Normal
This presentation is the intellectual property of the author. Contact them at for permission to reprint and/or distribute.
 MRI of the Knee Jennifer Swart, M.D. Musculoskeletal Radiology South Texas Radiology Group Financial Disclosure Dr. Jennifer Swart has no relevant financial relationships with commercial interests to disclose.
MRI of the Knee Jennifer Swart, M.D. Musculoskeletal Radiology South Texas Radiology Group Financial Disclosure Dr. Jennifer Swart has no relevant financial relationships with commercial interests to disclose.
Thanks. As something to help remember. Thanks 07/02/14. Arthroscopy TKR V Uni. Arthroscopy TKR V Uni. Role of arthroscopy to choose operation
 07/02/14 Thanks Role of arthroscopy to choose operation TKR Versus Uni Francois and Philippe Faculty Audience Audiovisual Pierre and Vincent Myles Coolican Val d Isere 2014 Thanks Francois and Philippe
07/02/14 Thanks Role of arthroscopy to choose operation TKR Versus Uni Francois and Philippe Faculty Audience Audiovisual Pierre and Vincent Myles Coolican Val d Isere 2014 Thanks Francois and Philippe
MRI of the Knee: Part 2 - menisci. Mark Anderson, M.D. University of Virginia Health System
 MRI of the Knee: Part 2 - menisci Mark Anderson, M.D. University of Virginia Health System Learning Objectives At the end of the presentation, each participant should be able to: describe the normal anatomy
MRI of the Knee: Part 2 - menisci Mark Anderson, M.D. University of Virginia Health System Learning Objectives At the end of the presentation, each participant should be able to: describe the normal anatomy
dgemric Effectively Predicts Cartilage Damage Associated with Femoroacetabular Impingement
 Riccardo Lattanzi 1,2 Catherine Petchprapa 2 Daniele Ascani 1 Roy I. Davidovitch 3 Thomas Youm 3 Robert J. Meislin 3 Michael. Recht 2 1 The Bernard and Irene Schwartz Center for Biomedical Imaging, New
Riccardo Lattanzi 1,2 Catherine Petchprapa 2 Daniele Ascani 1 Roy I. Davidovitch 3 Thomas Youm 3 Robert J. Meislin 3 Michael. Recht 2 1 The Bernard and Irene Schwartz Center for Biomedical Imaging, New
Project 15 Test-Retest Reliability of Semi-quantitative Readings from Knee Radiographs
 Project 15 Test-Retest Reliability of Semi-quantitative Readings from Knee Radiographs 1. SAS dataset... 1 2. Purpose and methods... 1 2.1 Background... 1 2.2 Reliability at single time points... 1 2.3
Project 15 Test-Retest Reliability of Semi-quantitative Readings from Knee Radiographs 1. SAS dataset... 1 2. Purpose and methods... 1 2.1 Background... 1 2.2 Reliability at single time points... 1 2.3
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 12/01/2012 Radiology Quiz of the Week # 101 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 12/01/2012 Radiology Quiz of the Week # 101 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Intraosseous Bio Filler. Surgical Technique
 Intraosseous Bio Filler Surgical Technique Intraosseous Bio Filler Surgical Technique Introduction The Intraosseous Bio Filler technique is the treatment of bone pathologies resulting from acute or chronic
Intraosseous Bio Filler Surgical Technique Intraosseous Bio Filler Surgical Technique Introduction The Intraosseous Bio Filler technique is the treatment of bone pathologies resulting from acute or chronic
Validity and Reliability of Radiographic Knee Osteoarthritis Measures by Arthroplasty Surgeons
 Validity and Reliability of Radiographic Knee Osteoarthritis Measures by Arthroplasty Surgeons Daniel L. Riddle, PhD; William A. Jiranek, MD; Jason R. Hull, MD abstract Full article available online at
Validity and Reliability of Radiographic Knee Osteoarthritis Measures by Arthroplasty Surgeons Daniel L. Riddle, PhD; William A. Jiranek, MD; Jason R. Hull, MD abstract Full article available online at
Is Meniscectomy such a bad thing compared to meniscal repair?
 Is Meniscectomy such a bad thing compared to meniscal repair? Jack M. Bert, MD Adjunct Clinical Professor University of Minnesota Minnesota Bone & Joint Specialists, Ltd St. Paul, Minnesota Disclosures
Is Meniscectomy such a bad thing compared to meniscal repair? Jack M. Bert, MD Adjunct Clinical Professor University of Minnesota Minnesota Bone & Joint Specialists, Ltd St. Paul, Minnesota Disclosures
Physical activity, alignment and knee osteoarthritis: data from MOST and the OAI
 Osteoarthritis and Cartilage 21 (2013) 789e795 Physical activity, alignment and knee osteoarthritis: data from MOST and the OAI D.T. Felson yzz *, J. Niu y, T. Yang y, J. Torner #, C.E. Lewis k, P. Aliabadi
Osteoarthritis and Cartilage 21 (2013) 789e795 Physical activity, alignment and knee osteoarthritis: data from MOST and the OAI D.T. Felson yzz *, J. Niu y, T. Yang y, J. Torner #, C.E. Lewis k, P. Aliabadi
Medical Practice for Sports Injuries and Disorders of the Knee
 Sports-Related Injuries and Disorders Medical Practice for Sports Injuries and Disorders of the Knee JMAJ 48(1): 20 24, 2005 Hirotsugu MURATSU*, Masahiro KUROSAKA**, Tetsuji YAMAMOTO***, and Shinichi YOSHIDA****
Sports-Related Injuries and Disorders Medical Practice for Sports Injuries and Disorders of the Knee JMAJ 48(1): 20 24, 2005 Hirotsugu MURATSU*, Masahiro KUROSAKA**, Tetsuji YAMAMOTO***, and Shinichi YOSHIDA****
FieldStrength. Achieva 3.0T enables cutting-edge applications, best-in-class MSK images
 FieldStrength Publication for the Philips MRI Community Issue 33 December 2007 Achieva 3.0T enables cutting-edge applications, best-in-class MSK images Palo Alto Medical Clinic Sports Medicine Center employs
FieldStrength Publication for the Philips MRI Community Issue 33 December 2007 Achieva 3.0T enables cutting-edge applications, best-in-class MSK images Palo Alto Medical Clinic Sports Medicine Center employs
Meniscal Extrusion Progresses Shortly after the Medial Meniscus Posterior Root Tear
 Original Article Knee Surg Relat Res 217;29(4):295-31 https://doi.org/1.5792/ksrr.17.27 pissn 2234-726 eissn 2234-2451 Knee Surgery & Related Research Meniscal Extrusion Progresses Shortly after the Medial
Original Article Knee Surg Relat Res 217;29(4):295-31 https://doi.org/1.5792/ksrr.17.27 pissn 2234-726 eissn 2234-2451 Knee Surgery & Related Research Meniscal Extrusion Progresses Shortly after the Medial
Proximal tibial bony and meniscal slopes are higher in ACL injured subjects than controls: a comparative MRI study
 Proximal tibial bony and meniscal slopes are higher in ACL injured subjects than controls: a comparative MRI study Ashraf Elmansori, Timothy Lording, Raphaël Dumas, Khalifa Elmajri, Philippe Neyret, Sebastien
Proximal tibial bony and meniscal slopes are higher in ACL injured subjects than controls: a comparative MRI study Ashraf Elmansori, Timothy Lording, Raphaël Dumas, Khalifa Elmajri, Philippe Neyret, Sebastien
Definition of osteoarthritis on MRI: results of a Delphi exercise
 Osteoarthritis and Cartilage 19 (2011) 963e969 Definition of osteoarthritis on MRI: results of a Delphi exercise D.J. Hunter y *, N. Arden z, P.G. Conaghan x, F. Eckstein k, G. Gold {#yy, A. Grainger zz,
Osteoarthritis and Cartilage 19 (2011) 963e969 Definition of osteoarthritis on MRI: results of a Delphi exercise D.J. Hunter y *, N. Arden z, P.G. Conaghan x, F. Eckstein k, G. Gold {#yy, A. Grainger zz,
Investigating the loading behaviour of intact and meniscectomy knee joints and the impact on surgical decisions
 Investigating the loading behaviour of intact and meniscectomy knee joints and the impact on surgical decisions M. S. Yeoman 1 1. Continuum Blue Limited, One Caspian Point, Caspian Way, CF10 4DQ, United
Investigating the loading behaviour of intact and meniscectomy knee joints and the impact on surgical decisions M. S. Yeoman 1 1. Continuum Blue Limited, One Caspian Point, Caspian Way, CF10 4DQ, United
LATERAL MENISCUS SLOPE AND ITS CLINICAL RELEVANCE IN PATIENTS WITH A COMBINED ACL TEAR AND POSTERIOR TIBIA COMPRESSION
 LATERAL MENISCUS SLOPE AND ITS CLINICAL RELEVANCE IN PATIENTS WITH A COMBINED ACL TEAR AND POSTERIOR TIBIA COMPRESSION R. ŚMIGIELSKI, B. DOMINIK, U, ZDANOWICZ, Z. GAJEWSKI, K. SKIERBISZEWSKA, K. SIEWRUK,
LATERAL MENISCUS SLOPE AND ITS CLINICAL RELEVANCE IN PATIENTS WITH A COMBINED ACL TEAR AND POSTERIOR TIBIA COMPRESSION R. ŚMIGIELSKI, B. DOMINIK, U, ZDANOWICZ, Z. GAJEWSKI, K. SKIERBISZEWSKA, K. SIEWRUK,
Original Report. The Reverse Segond Fracture: Association with a Tear of the Posterior Cruciate Ligament and Medial Meniscus
 Eva M. Escobedo 1 William J. Mills 2 John. Hunter 1 Received July 10, 2001; accepted after revision October 1, 2001. 1 Department of Radiology, University of Washington Harborview Medical enter, 325 Ninth
Eva M. Escobedo 1 William J. Mills 2 John. Hunter 1 Received July 10, 2001; accepted after revision October 1, 2001. 1 Department of Radiology, University of Washington Harborview Medical enter, 325 Ninth
CURRICULUM VITAE. Joshua J. Stefanik, MSPT, PhD 006B Robinson Hall Northeastern University Boston, MA
 CURRICULUM VITAE Joshua J. Stefanik, MSPT, PhD 006B Robinson Hall Northeastern University Boston, MA 02115 E-mail: j.stefanik@northeastern.edu EDUCATION 2001 Northeastern University, BS Rehabilitation
CURRICULUM VITAE Joshua J. Stefanik, MSPT, PhD 006B Robinson Hall Northeastern University Boston, MA 02115 E-mail: j.stefanik@northeastern.edu EDUCATION 2001 Northeastern University, BS Rehabilitation
Save the meniscus Mais pourquoi?
 Save the meniscus Mais pourquoi? #$%&' ()"*+!," Philippe Neyret E Servien S Lustig P Verdonk One or more of the authors of the next presentation have identified no potential conflicts of interest 2 Consequences
Save the meniscus Mais pourquoi? #$%&' ()"*+!," Philippe Neyret E Servien S Lustig P Verdonk One or more of the authors of the next presentation have identified no potential conflicts of interest 2 Consequences
Osteoarthritis and Cartilage 19 (2011) 689e699
 Osteoarthritis and Cartilage 19 (2011) 689e699 MRI-based extended ordered values more efficiently differentiate cartilage loss in knees with and without joint space narrowing than region-specific approaches
Osteoarthritis and Cartilage 19 (2011) 689e699 MRI-based extended ordered values more efficiently differentiate cartilage loss in knees with and without joint space narrowing than region-specific approaches
The association between meniscal and cruciate ligament damage and knee pain in community residents
 Osteoarthritis and Cartilage 19 (2011) 1422e1428 The association between meniscal and cruciate ligament damage and knee pain in community residents H.A. Kimyz *,I.Kimx, Y.W. Songk,D.H.Kim{,J.Niu#, A.Guermaziyy,
Osteoarthritis and Cartilage 19 (2011) 1422e1428 The association between meniscal and cruciate ligament damage and knee pain in community residents H.A. Kimyz *,I.Kimx, Y.W. Songk,D.H.Kim{,J.Niu#, A.Guermaziyy,
Disclosures. Background. Background
 Kinematic and Quantitative MR Imaging Evaluation of ACL Reconstructions Using the Mini-Two Incision Method Compared to the Anteromedial Portal Technique Drew A. Lansdown, MD Christina Allen, MD Samuel
Kinematic and Quantitative MR Imaging Evaluation of ACL Reconstructions Using the Mini-Two Incision Method Compared to the Anteromedial Portal Technique Drew A. Lansdown, MD Christina Allen, MD Samuel
Arthrographic study of the rheumatoid knee.
 Annals of the Rheumatic Diseases, 1981, 40, 344-349 Arthrographic study of the rheumatoid knee. Part 2. Articular cartilage and menisci KYOSUKE FUJIKAWA, YOSHINORI TANAKA, TSUNEYO MATSUBAYASHI, AND FUJIO
Annals of the Rheumatic Diseases, 1981, 40, 344-349 Arthrographic study of the rheumatoid knee. Part 2. Articular cartilage and menisci KYOSUKE FUJIKAWA, YOSHINORI TANAKA, TSUNEYO MATSUBAYASHI, AND FUJIO
MR imaging of the knee in marathon runners before and after competition
 Skeletal Radiol (2001) 30:72 76 International Skeletal Society 2001 ARTICLE W. Krampla R. Mayrhofer J. Malcher K.H. Kristen M. Urban W. Hruby MR imaging of the knee in marathon runners before and after
Skeletal Radiol (2001) 30:72 76 International Skeletal Society 2001 ARTICLE W. Krampla R. Mayrhofer J. Malcher K.H. Kristen M. Urban W. Hruby MR imaging of the knee in marathon runners before and after
Rupture of posterior cruciate ligament leads to radial displacement of the medial meniscus
 Zhang et al. BMC Musculoskeletal Disorders (2017) 18:297 DOI 10.1186/s12891-017-1646-6 RESEARCH ARTICLE Open Access Rupture of posterior cruciate ligament leads to radial displacement of the medial meniscus
Zhang et al. BMC Musculoskeletal Disorders (2017) 18:297 DOI 10.1186/s12891-017-1646-6 RESEARCH ARTICLE Open Access Rupture of posterior cruciate ligament leads to radial displacement of the medial meniscus
ORIGINAL ARTICLE. ROLE OF MRI IN EVALUATION OF TRAUMATIC KNEE INJURIES Saurabh Chaudhuri, Priscilla Joshi, Mohit Goel
 ROLE OF MRI IN EVALUATION OF TRAUMATIC KNEE INJURIES Saurabh Chaudhuri, Priscilla Joshi, Mohit Goel 1. Associate Professor, Department of Radiodiagnosis & imaging, Bharati Vidyapeeth Medical College and
ROLE OF MRI IN EVALUATION OF TRAUMATIC KNEE INJURIES Saurabh Chaudhuri, Priscilla Joshi, Mohit Goel 1. Associate Professor, Department of Radiodiagnosis & imaging, Bharati Vidyapeeth Medical College and
Cartilage Repair Center Brigham and Women s Hospital Harvard Medical School
 Brigham and Women s Hospital Harvard Medical School Safety, feasibility, and radiographic outcomes of the anterior meniscal takedown technique to approach chondral defects on the tibia and posterior femoral
Brigham and Women s Hospital Harvard Medical School Safety, feasibility, and radiographic outcomes of the anterior meniscal takedown technique to approach chondral defects on the tibia and posterior femoral
Anterior Tibial Translation Sign: Factors Affecting Interpretation of Anterior Cruciate Ligament Tear
 Anterior Tibial Translation Sign: Factors Affecting Interpretation of Anterior Cruciate Ligament Tear J Med Assoc Thai 2015; 98 (Suppl. 1): S57-S62 Full text. e-journal: http://www.jmatonline.com Numphung
Anterior Tibial Translation Sign: Factors Affecting Interpretation of Anterior Cruciate Ligament Tear J Med Assoc Thai 2015; 98 (Suppl. 1): S57-S62 Full text. e-journal: http://www.jmatonline.com Numphung
Imaging Modalities: Clinical Reasoning and Key Instructional Elements: Radiography
 Imaging Modalities: Clinical Reasoning and Key Instructional Elements: Radiography Michael D. Ross, PT, DHSc, OCS mross@daemen.edu Disclosure No relevant financial relationship exists Objectives Determine
Imaging Modalities: Clinical Reasoning and Key Instructional Elements: Radiography Michael D. Ross, PT, DHSc, OCS mross@daemen.edu Disclosure No relevant financial relationship exists Objectives Determine
International Cartilage Repair Society
 Osteoarthritis and Cartilage (2009) 17, 748e753 ª 2008 Osteoarthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2008.09.013 The association of meniscal
Osteoarthritis and Cartilage (2009) 17, 748e753 ª 2008 Osteoarthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2008.09.013 The association of meniscal
ADVANCED IMAGING OF THE KNEE
 MENISCAL ANATOMY ADVANCED IMAGING OF THE KNEE MENISCAL ABNORMALITIES MENISCAL FUNCTION MENISCAL FUNCTION load transmission shock absorption stability The menisci DO NOT function as primary stabilizers
MENISCAL ANATOMY ADVANCED IMAGING OF THE KNEE MENISCAL ABNORMALITIES MENISCAL FUNCTION MENISCAL FUNCTION load transmission shock absorption stability The menisci DO NOT function as primary stabilizers
Discoid Medial Meniscus Tear, with a Literature Review of Treatments
 Case Report Knee Surg Relat Res 2017;29(3):237-242 https://doi.org/10.5792/ksrr.15.054 pissn 2234-0726 eissn 2234-2451 Knee Surgery & Related Research Discoid Medial Meniscus Tear, with a Literature Review
Case Report Knee Surg Relat Res 2017;29(3):237-242 https://doi.org/10.5792/ksrr.15.054 pissn 2234-0726 eissn 2234-2451 Knee Surgery & Related Research Discoid Medial Meniscus Tear, with a Literature Review
MRI of Cartilage. D. BENDAHAN (PhD)
 MRI of Cartilage D. BENDAHAN (PhD) Centre de Résonance Magnétique Biologique et Médicale UMR CNRS 7339 Faculté de Médecine de la Timone 27, Bd J. Moulin 13005 Marseille France david.bendahan@univ-amu.fr
MRI of Cartilage D. BENDAHAN (PhD) Centre de Résonance Magnétique Biologique et Médicale UMR CNRS 7339 Faculté de Médecine de la Timone 27, Bd J. Moulin 13005 Marseille France david.bendahan@univ-amu.fr
White Rose Research Online URL for this paper: Version: Accepted Version
 This is a repository copy of Osteoarthritic bone marrow lesions almost exclusively colocate with denuded cartilage: a 3D study using data from the Osteoarthritis Initiative. White Rose Research Online
This is a repository copy of Osteoarthritic bone marrow lesions almost exclusively colocate with denuded cartilage: a 3D study using data from the Osteoarthritis Initiative. White Rose Research Online
E. ÇAĞLAR, G. ŞAH N 1, T. OĞUR, E. AKTAŞ. Introduction. Abstract. OBJECTIVE: To identify changes in
 European Review for Medical and Pharmacological Sciences Quantitative evaluation of hyaline articular cartilage T2 maps of knee and determine the relationship of cartilage T2 values with age, gender, articular
European Review for Medical and Pharmacological Sciences Quantitative evaluation of hyaline articular cartilage T2 maps of knee and determine the relationship of cartilage T2 values with age, gender, articular
For Commercial products, please refer to the following policy: Preauthorization via Web-Based Tool for Procedures
 Medical Coverage Policy Total Joint Arthroplasty Hip and Knee EFFECTIVE DATE: 08/01/2017 POLICY LAST UPDATED: 06/06/2017 OVERVIEW Joint replacement surgery, also known as arthroplasty, has proved to be
Medical Coverage Policy Total Joint Arthroplasty Hip and Knee EFFECTIVE DATE: 08/01/2017 POLICY LAST UPDATED: 06/06/2017 OVERVIEW Joint replacement surgery, also known as arthroplasty, has proved to be
Rehab Considerations: Meniscus
 Rehab Considerations: Meniscus Steve Cox, PT, DPT Department of Orthopaedics School of Medicine University of Texas Health Science Center at San Antonio 1 -Anatomy/ Function/ Injuries -Treatment Options
Rehab Considerations: Meniscus Steve Cox, PT, DPT Department of Orthopaedics School of Medicine University of Texas Health Science Center at San Antonio 1 -Anatomy/ Function/ Injuries -Treatment Options
BIOMECHANICAL MECHANISMS FOR DAMAGE: RETRIEVAL ANALYSIS AND COMPUTATIONAL WEAR PREDICTIONS IN TOTAL KNEE REPLACEMENTS
 Journal of Mechanics in Medicine and Biology Vol. 5, No. 3 (2005) 469 475 c World Scientific Publishing Company BIOMECHANICAL MECHANISMS FOR DAMAGE: RETRIEVAL ANALYSIS AND COMPUTATIONAL WEAR PREDICTIONS
Journal of Mechanics in Medicine and Biology Vol. 5, No. 3 (2005) 469 475 c World Scientific Publishing Company BIOMECHANICAL MECHANISMS FOR DAMAGE: RETRIEVAL ANALYSIS AND COMPUTATIONAL WEAR PREDICTIONS
Meniscal tears on 3T MR: Patterns, pearls and pitfalls
 Meniscal tears on 3T MR: Patterns, pearls and pitfalls Poster No.: C-2221 Congress: ECR 2010 Type: Educational Exhibit Topic: Musculoskeletal Authors: J. C. Kandathil; Singapore/SG Keywords: Knee injuries,
Meniscal tears on 3T MR: Patterns, pearls and pitfalls Poster No.: C-2221 Congress: ECR 2010 Type: Educational Exhibit Topic: Musculoskeletal Authors: J. C. Kandathil; Singapore/SG Keywords: Knee injuries,
Meniscal Root Tears: A Silent Epidemic
 Meniscal Root Tears: A Silent Epidemic TRIA Orthopedic and Sports Medicine Conference February 9 th, 2018 Robert F. LaPrade, M.D., Ph.D. Chief Medical Officer Steadman Philippon Research Institute Co-Director,
Meniscal Root Tears: A Silent Epidemic TRIA Orthopedic and Sports Medicine Conference February 9 th, 2018 Robert F. LaPrade, M.D., Ph.D. Chief Medical Officer Steadman Philippon Research Institute Co-Director,
Cyst-like lesions of the knee joint and their relation to incident knee pain and development of radiographic osteoarthritis: the MOST study
 Osteoarthritis and Cartilage 18 (2010) 1386e1392 Cyst-like lesions of the knee joint and their relation to incident knee pain and development of radiographic osteoarthritis: the MOST study A. Guermazi
Osteoarthritis and Cartilage 18 (2010) 1386e1392 Cyst-like lesions of the knee joint and their relation to incident knee pain and development of radiographic osteoarthritis: the MOST study A. Guermazi
Meniscal Injuries with Tibial Plateau Fractures: Role of Arthroscopy
 www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x Meniscal Injuries with Tibial Plateau Fractures: Role of Arthroscopy Authors Ansarul Haq Lone 1, Omar Khursheed 2, Shakir Rashid 3, Munir
www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x Meniscal Injuries with Tibial Plateau Fractures: Role of Arthroscopy Authors Ansarul Haq Lone 1, Omar Khursheed 2, Shakir Rashid 3, Munir
Osteoarthritis and Cartilage 18 (2010)
 Osteoarthritis and Cartilage 18 (2010) 547 554 Sensitivity to change of cartilage morphometry using coronal FLASH, sagittal DESS, and coronal MPR DESS protocols comparative data from the osteoarthritis
Osteoarthritis and Cartilage 18 (2010) 547 554 Sensitivity to change of cartilage morphometry using coronal FLASH, sagittal DESS, and coronal MPR DESS protocols comparative data from the osteoarthritis
The Knee. Two Joints: Tibiofemoral. Patellofemoral
 Evaluating the Knee The Knee Two Joints: Tibiofemoral Patellofemoral HISTORY Remember the questions from lecture #2? Girth OBSERVATION TibioFemoral Alignment What are the consequences of faulty alignment?
Evaluating the Knee The Knee Two Joints: Tibiofemoral Patellofemoral HISTORY Remember the questions from lecture #2? Girth OBSERVATION TibioFemoral Alignment What are the consequences of faulty alignment?
Correspondence should be addressed to Thomas Kurien;
 Case Reports in Orthopedics Volume 2016, Article ID 6043497, 5 pages http://dx.doi.org/10.1155/2016/6043497 Case Report Resection and Resolution of Bone Marrow Lesions Associated with an Improvement of
Case Reports in Orthopedics Volume 2016, Article ID 6043497, 5 pages http://dx.doi.org/10.1155/2016/6043497 Case Report Resection and Resolution of Bone Marrow Lesions Associated with an Improvement of
Dimensions of the intercondylar notch and the distal femur throughout life
 Dimensions of the intercondylar notch and the distal femur throughout life Poster No.: P-0089 Congress: ESSR 2013 Type: Scientific Exhibit Authors: L. Hirtler, S. Röhrich, F. Kainberger; Vienna/AT Keywords:
Dimensions of the intercondylar notch and the distal femur throughout life Poster No.: P-0089 Congress: ESSR 2013 Type: Scientific Exhibit Authors: L. Hirtler, S. Röhrich, F. Kainberger; Vienna/AT Keywords:
A giraffe neck sign of the medial meniscus: a characteristic finding of the medial meniscus posterior
 A giraffe neck sign of the medial meniscus: a characteristic finding of the medial meniscus posterior root tear on magnetic resonance imaging Takayuki Furumatsu*, Masataka Fujii, Yuya Kodama, Toshifumi
A giraffe neck sign of the medial meniscus: a characteristic finding of the medial meniscus posterior root tear on magnetic resonance imaging Takayuki Furumatsu*, Masataka Fujii, Yuya Kodama, Toshifumi
(Alternate title) Evaluation of Meniscal Extrusion with Posterior Root Disruption and Repair using Ultrasound
 Evaluation of lateral meniscal position with weight bearing: Ultrasonography to measure extrusion with intact, torn and repaired posterior root attachments (Alternate title) Evaluation of Meniscal Extrusion
Evaluation of lateral meniscal position with weight bearing: Ultrasonography to measure extrusion with intact, torn and repaired posterior root attachments (Alternate title) Evaluation of Meniscal Extrusion
FAI syndrome with or without labral tear.
 Case This 16-year-old female, soccer athlete was treated for pain in the right groin previously. Now has acute onset of pain in the left hip. The pain was in the groin that was worse with activities. Diagnosis
Case This 16-year-old female, soccer athlete was treated for pain in the right groin previously. Now has acute onset of pain in the left hip. The pain was in the groin that was worse with activities. Diagnosis
JMSCR Vol 05 Issue 01 Page January
 www.jmscr.igmpublication.org Impact Factor 5.244 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i1.28 Diagnostic Accuracy of Magnetic Resonance
www.jmscr.igmpublication.org Impact Factor 5.244 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i1.28 Diagnostic Accuracy of Magnetic Resonance
MY PATIENT HAS KNEE PAIN. David Levi, MD Chief, Division of Musculoskeletal l limaging Atlantic Medical Imaging
 MY PATIENT HAS KNEE PAIN David Levi, MD Chief, Division of Musculoskeletal l limaging Atlantic Medical Imaging Causes of knee pain Non traumatic Trauma Osteoarthritis Patellofemoral pain Menisci or ligaments
MY PATIENT HAS KNEE PAIN David Levi, MD Chief, Division of Musculoskeletal l limaging Atlantic Medical Imaging Causes of knee pain Non traumatic Trauma Osteoarthritis Patellofemoral pain Menisci or ligaments
D. Doré 1, C. Ding 1,2, J.P. Pelletier 3, J. Martel-Pelletier 3, F. Cicuttini 2, G. Jones 1.
 Responsiveness of qualitative and quantitative MRI measures over 2.7 years D. Doré 1, C. Ding 1,2, J.P. Pelletier 3, J. Martel-Pelletier 3, F. Cicuttini 2, G. Jones 1. 1 Menzies Research Institute Tasmania,
Responsiveness of qualitative and quantitative MRI measures over 2.7 years D. Doré 1, C. Ding 1,2, J.P. Pelletier 3, J. Martel-Pelletier 3, F. Cicuttini 2, G. Jones 1. 1 Menzies Research Institute Tasmania,
