Cyst-like lesions of the knee joint and their relation to incident knee pain and development of radiographic osteoarthritis: the MOST study
|
|
|
- Arnold Jonah Pierce
- 5 years ago
- Views:
Transcription
1 Osteoarthritis and Cartilage 18 (2010) 1386e1392 Cyst-like lesions of the knee joint and their relation to incident knee pain and development of radiographic osteoarthritis: the MOST study A. Guermazi y *, D. Hayashi y, F.W. Roemer y, J. Niu z, M. Yang z, J.A. Lynch x, J.C. Torner k, C.E. Lewis {, B. Sack z, D.T. Felson z, M.C. Nevitt x y Department of Radiology, Boston University School of Medicine, 820 Harrison Avenue, FGH Building, 3rd Floor, Boston, MA 02118, USA z Clinical Epidemiology Research and Training Unit, Boston University School of Medicine, 650 Albany Street, Boston, MA 02118, USA x Department of Epidemiology and Biostatistics, University of California at San Francisco, 185 Berry Street, Lobby 5, Suite 5700, San Francisco, CA , USA k University of Iowa, College of Public Health, E107 General Hospital, Iowa City, IA 52242, USA { Division of Preventive Medicine, University of Alabama at Birmingham, Birmingham, AL 35205, USA article info summary Article history: Received 6 April 2010 Accepted 28 August 2010 Keywords: Cysts Bursitis Magnetic resonance imaging Osteoarthritis Knee Pain Objective: To determine whether intra- and periarticular cyst-like lesions of the knee are associated with incident knee pain and incident radiographic knee osteoarthritis (OA). Design: The Multicenter Osteoarthritis (MOST) Study is a cohort of individuals who have or are at high risk for knee OA. Using a nested case-control study design, we investigated the associations of cyst-like lesions (Baker s, meniscal and proximal tibiofibular joint (PTFJ) cysts, and prepatellar and anserine bursitides) with (1) incident pain at 15- or 30-month follow-up and (2) incident radiographic OA at 30-month follow-up. Baseline cyst-like lesions were scored semiquantitatively using the Whole Organ Magnetic Resonance Imaging Score (WORMS). Conditional logistic regression models were used to assess the relation between these lesions and the outcomes, adjusting for potential confounding factors (i.e., cartilage loss, meniscal damage, bone marrow lesions, synovitis and joint effusion, which were also scored using WORMS). Results: Incident knee pain study included 157 cases and 336 controls. Prevalence of meniscal and PTFJ cysts in the case group was twice that in the control group [9 (6%) vs 9 (3%) and 9 (6%) vs 10 (3%), respectively]. Incident radiographic OA study included 149 cases and 298 controls. Prevalence of grade 2 Baker s cysts and PTFJ cysts in the case group was approximately four times that in the control group [16 (11%) vs 9 (3%) and 6 (4%) vs 3 (1%), respectively]. However, none of the cyst-like lesions was associated with incident pain or radiographic OA after fully adjusted logistic regression analyses and correction of P-values for multiple comparisons. Conclusion: None of the analyzed lesions was an independent predictor of incident knee pain or radiographic OA. Intra- and periarticular cyst-like lesions are likely to be a secondary phenomenon seen in painful or OA-affected knees, rather than a primary trigger for incident knee pain or radiographic OA. Ó 2010 Osteoarthritis Research Society International. Published by Elsevier Ltd. All rights reserved. Introduction *Address correspondence and reprint requests to: Ali Guermazi, Department of Radiology, Boston University School of Medicine, 820 Harrison Avenue, FGH Building, 3rd Floor, Boston, MA 02118, USA. Tel: ; Fax: address: guermazi@bu.edu (A. Guermazi). Benign cystic lesions are frequently encountered during routine magnetic resonance imaging (MRI) of the knee. Most intra- and periarticular cystic lesions are encapsulated fluid collections exhibiting low signal intensity on T1-weighted images and high signal intensity on T2-weighted images 1. These represent a wide variety of entities that include meniscal and Baker s (popliteal) cysts; intraarticular and extra-articular ganglia; intraosseous cysts at the insertion of the cruciate ligaments and meniscotibial attachments; and cysts adjacent to the proximal tibiofibular joint (PTFJ) 1e5. Cyst-like lesions arising from bursae include anserine, prepatellar, superficial and deep infrapatellar, suprapatellar, iliotibial, and tibial collateral ligament bursitis 1e5. Discrete fluid collections within bursae can be detected by knee MRI, but may not necessarily be clinically significant due to their high prevalence in asymptomatic subjects 6,7. Of the cystic lesions mentioned above, Baker s cysts are the most frequently encountered 8. Other lesions are seen less frequently, e.g., meniscal cysts 9, PTFJ cysts 6, prepatellar bursitis 6 and anserine bursitis 7, all of which are observed in about 3e5% of both symptomatic and asymptomatic knees. To date, it is not known if /$ e see front matter Ó 2010 Osteoarthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi: /j.joca
2 A. Guermazi et al. / Osteoarthritis and Cartilage 18 (2010) 1386e intra- and periarticular cyst-like lesions (including bursitides, which are discrete fluid collections with cyst-like appearances) are related to risk for incident pain or radiographic OA. It is conceivable that these lesions might be related in that they sometimes provide the sole or most prominent evidence of pathology in tissues where pathology is linked to OA occurrence (e.g., meniscal cysts). In other cases (e.g., prepatellar bursitis), the cysts are extra-articular and, while they could cause pain, they are almost certainly unrelated to pathology inside the joint, and thus they would not be expected to increase the risk of OA but might be related to knee pain. Prediction of incident pain or incident knee OA on the basis of these lesions would be helpful with respect to preventive or early treatment. In the present study, we focus on five types of cystic lesions that are commonly assessed semiquantitatively in large epidemiologic OA studies (two within the joint capsule: Baker s cyst and meniscal cysts, and three outside the joint: PTFJ cysts, prepatellar bursitis and anserine bursitis). PTFJ cysts and anserine bursitis are associated with knee pain 6 and prepatellar bursitis with radiographic knee OA 6. Baker s cysts are associated with degenerative joint disease 8 and advanced stages of OA 10 but not pain 6,11. Although a strong crosssectional association between meniscal damage (with which meniscal cysts are usually associated 9 ) and knee OA has been reported 12, there has been no report of a study evaluating the direct relationship between meniscal cysts and incident radiographic OA. The aims of this study are to examine whether the presence of these cyst-like lesions at baseline is associated longitudinally with incident knee pain and incident radiographic knee OA. Materials and methods Study design and subjects The Multicenter Osteoarthritis (MOST) Study is a prospective cohort study of 3026 individuals aged 50e79 years with or at high risk of knee OA. Those considered at high risk included persons who were overweight or obese, those with knee pain, aching or stiffness on most of the last 30 days, a history of knee injury that made it difficult to walk for at least 1 week, or previous knee surgery. Subjects were recruited from two US communities, Birmingham, Alabama and Iowa City, Iowa through mass mailing of letters and study brochures, supplemented by media and community outreach campaigns. The study protocol was approved by the Institutional Review Boards at the University of Iowa, University of Alabama, Birmingham, University of California, San Francisco and Boston University Medical Campus. Subjects were excluded from MOST if they screened positive for rheumatoid arthritis, had ankylosing spondylitis, psoriatic arthritis, Reiter s syndrome, had renal insufficiency that required hemo- or peritoneal dialysis, a history of cancer (except for non-melanoma skin cancer), had or planned to have bilateral knee replacement surgery, were unable to walk without assistance, or were planning to move out of the area in the next 3 years. In the present study, using a nested case-control study design, we investigated the prevalence of periarticular cysts and bursitides and the relation between these lesions and (1) incident pain and (2) incident radiographic OA among knees that were examined both at baseline and follow-up. For the incident pain study, there were 157 case knees and 336 control (total 493) knees (one knee per subject). If a subject developed pain in only one knee, that knee was included as a case knee. One knee was randomly chosen if incident pain was present bilaterally. Of the 493 knees, 398 (81%) were recruited at 15 months, and an additional 95 (19%) were recruited at 30 months. Thus, this study is based on combined data of the 15-and 30-month follow-up visits. Those subjects who developed incident pain at 15 months did not have the 30-month visit included because they already had symptoms. It was therefore not possible to do our analyses for incident knee pain all based on the 30-month follow-up alone. Also, it was not possible to do our analyses based only on the 15-month followup due to lack of sufficient number of meniscal cysts to perform meaningful statistical calculations. Control knees were selected randomly from among the knees examined by MRI at baseline and for which the subject indicated absence of pain at both time points. All subjects were asked a question regarding knee pain as follows: During the past 30 days, have you had pain, aching, or stiffness in your knee on most days? This question was posed to subjects both by phone interview and during a clinic visit 1 month thereafter. If the subject answered no regarding the presence of pain, aching, or stiffness in the knee at each of these time points at baseline, that knee was considered eligible for analysis in the incident pain study. At 15 and 30 months follow-up, the same question regarding knee pain was posed to subjects, both in a phone interview and at a clinic visit. If the subject answered yes to the question at both of these, the knee with new pain was considered to be a case knee. Because this question was intended to identify pain, aching, or stiffness on most days, and because the two time points were, on average,1 month apart, we characterized a positive response at both time points as consistent frequent knee pain. Furthermore, although our question included the symptoms of stiffness and aching, we labeled a positive response as related to pain 13. In addition, subjects completed surveys on medication use, including nonsteroidal anti-inflammatory drugs or other analgesic drugs, at the baseline and follow-up clinic examination. Subjects also completed the Western Ontario and McMaster Universities Osteoarthritis Index (WOMAC), a survey of joint pain, stiffness, and limitation of physical function 14, for each knee at both the baseline and follow-up visits. For the incident radiographic OA study, there were 149 case knees and 298 control (total 447) knees. Eligibility for case knees was based on either of two qualifications: no radiographic OA (grade 0 or 1) at baseline but incident radiographic OA (grade 2 or higher) according to the KellgreneLawrence (KeL) grading system 15,or having any osteophyte grade 2 or higher, or any osteophyte grade 1 or higher plus joint space narrowing grade 2 or higher in the tibiofemoral joint using the Osteoarthritis Research Society International (OARSI) grading 16 at 30-month follow-up. If a subject only had one knee which fulfilled the above criteria, that knee was used as a case knee. In case of subjects having bilateral knees fulfilling the above, one knee was randomly chosen. For the control knees, one knee per subject was randomly selected from knees without radiographic OA at baseline and follow-up. For both studies, cases and controls were matched to the clinic site and follow-up visit. Radiographs All subjects underwent baseline and follow-up weightbearing postero-anterior fixed flexion view knee radiographs using the SynaFlexer positioning frame (Synarc, San Francisco, CA) 17,18. A musculoskeletal radiologist (who is not a co-author) and a rheumatologist (DTF) with over 10 years experience each in reading study films and over 30 years of clinical experience graded all baseline postero-anterior films independently according to the KeL grading, blinded to case/control status and clinical data. Disagreements among the readers were adjudicated by a panel of three readers (DTF, aforementioned radiologist and another rheumatologist who is not a co-author). The weighted kappa coefficient of inter-observer reliability for the KeL readings, was 0.79, which was calculated from the baseline readings of 4297 knee radiographs before adjudication in the MOST study including subsamples used in our analyses.
3 1388 A. Guermazi et al. / Osteoarthritis and Cartilage 18 (2010) 1386e1392 Full-limb radiographs of both legs were obtained at baseline using the method described previously 19. The mechanical axis was defined as the angle formed by the intersection of a line from the center of the head of the femur to the center of the tibial spines and a line from the center of the talus to the center of the tibial spines 19. The inter-observer intraclass correlation coefficient for the mechanical axis was 0.99 (P < ). Varus alignment was defined as an angle <179,179e181 was considered neutral and valgus alignment was defined as an angle >181. MRI acquisition Baseline MRI scans were obtained with a 1.0T MR system (OrthOneÔ, ONI Medical Systems, Wilmington, MA) with a circumferential transmit-receive extremity coil using a fat-suppressed (FS) fast spin echo (FSE) proton density-weighted (PD-w) sequence in two planes: sagittal, repetition time (TR) ¼ 4800 ms, echo time (TE) ¼ 35 ms, 3 mm slice thickness, 0 mm interslice gap, 30 slices, matrix, number of excitations (NEX) ¼ 2, mm field of view (FOV), echo train length (ETL) ¼ 6; and axial, (TR ¼ 4680 ms, TE ¼ 13 ms, 3 mm slice thickness, 0 mm interslice gap, 26 slices, matrix, NEX ¼ 2, mm FOV, ETL ¼ 10). Also, a short-tau inversion recovery (STIR) sequence in the coronal plane was obtained (TR ¼ 8448 ms, TE ¼ 17 ms, TI ¼ 100 ms, 3 mm slice thickness, 0 mm interslice gap, 34 slices, matrix, two NEX, mm FOV, ETL ¼ 8). MRI assessment Semiquantitative assessment of baseline cysts and bursitides using the Whole Organ Magnetic Resonance Imaging Score (WORMS) criteria 20 was performed by two musculoskeletal radiologists (AG and FWR) with 11 and 7 years of experience in standardized semiquantitative analysis of knee OA. Baker s cyst was graded from 0 to 3 (0 ¼ none, 1 ¼ small, 2 ¼ medium, 3 ¼ large). Meniscal cysts (medial, lateral and combined), PTFJ cysts, prepatellar bursitis and anserine bursitis were scored 0 or 1 (0 ¼ none, 1 ¼ present). Cartilage status (grade 0e6), meniscal status (grade 0e4), bone marrow lesions, synovitis and effusion (grade 0e3) were also scored using WORMS 20. The two radiologists were blinded to case/control status and clinical data and readings were performed independently. The weighted kappa coefficient of inter-observer reliability (performed on a random sample of 30 knees read by both readers) for the readings of Baker s cysts (comparing 0e3 scores) was Similarly, the non-weighted kappa coefficients for the readings of medial/lateral meniscal cysts, and prepatellar bursitis (comparing 0 or 1 scores) were 1.00/0.73 and 0.48 respectively. Knees with typical radiologic signs of traumatic bone contusions, osteonecrosis, fracture or malignant bone infiltration were excluded from the analysis. However, of all analyzed MRIs only one knee showed a subacute tibial depression fracture at follow-up and was excluded. Statistical analysis We evaluated the association of prevalent cyst-like lesions (score >0) at baseline with the presence of incident knee pain and incident radiographic OA (as defined earlier) using conditional logistic regression models adjusting for age, sex, race, body mass index (BMI), and mechanical knee alignment. Adjustments for baseline KeL grade were also made for the incident pain study. To assess whether cyst-like lesions at baseline were associated with incident radiographic OA or pain, additional adjustments for possible confounders were performed, i.e., bone marrow lesions, synovitis, joint effusion, meniscal damage and cartilage loss. For incident pain study, we examined change in pain medication use as an additional covariate. Although Baker s cysts were expected to show co-linearity with joint effusion, Spearman correlation between these was not significant and thus we adjusted for joint effusion when analyzing Baker s cysts. The presence of meniscal tear is thought to lead to meniscal cyst formation. Having found a significant positive correlation, we did not adjust for meniscal damage when analyzing meniscal cysts. Because we performed multiple comparisons in our analyses (i.e., seven cyst-like lesions: Baker s, meniscal and PTFJ cysts, and prepatellar and anserine bursitides), Bonferroni correction for P-value was made and thus P < was considered statistically significant. All statistical calculations were performed using SAS Ò software (Version 9.1 for Windows, SAS Institute, Cary, NC). Results Incident pain study For the case group (n ¼ 157), the mean and the standard deviation (SD) of the age of subjects was 62.8 (8.2) years and the BMI was 29.7 (4.6) kg/m 2. Subjects were predominantly female (108, 69%) and white (137, 87%), and 64 (41%) had KeL grade 2 at baseline. The proportion of women and those with radiographic OA Table I Demographics of case and control groups at baseline in the present study Case knees Control knees P-valuez Incident knee pain N Age, mean (SD) 62.8 (8.2) 61.5 (8.1) Women, no. (%) 108 (69) 200 (60) 0.048* White, no. (%) 137 (87) 292 (86) 0.91 BMI, mean (SD) 29.7 (4.6) 29.7 (4.5) 0.99 ROA (KeL grade 2), no. (%) 64 (41) 75 (22) <0.0001* BML (grade 1)y, (%) 117 (75) 225 (67) Cartilage loss (grade 2)y, (%) 141 (90) 271 (81) 0.011* Meniscal damage 68 (43) 99 (30) * (grade 1)y, (%) Synovitis (grade 1)y, (%) 107 (68) 213 (63) 0.30 Effusion (grade 1)y, (%) 63 (40) 112 (33) 0.14 Malalignment** Varus (<179 ), no. (%) 71 (45) 138 (41) 0.028* Neutral (179e181 ), no. (%) 45 (29) 139 (41) Valgus (>181 ), no. (%) 39 (25) 57 (17) Incident radiographic OA N Age, mean (SD) 61.7 (7.7) 61.5 (7.7) 0.79 Women, % 92 (62) 177 (59) 0.60 White, % 120 (81) 258 (86) 0.11 BMI, mean (SD) 31.0 (5.4) 28.9 (4.5) <0.0001* BML (grade 1)y, (%) 104 (70) 174 (58) Cartilage loss (grade 2)y, (%) 144 (97) 232 (78) <0.0001* Meniscal damage 71 (48) 55 (18) <0.0001* (grade 1)y, (%) Synovitis (grade 1)y, (%) 72 (48) 87 (29) * Effusion (grade 1)y, (%) 99 (66) 122 (41) <0.0001* Malalignment Varus (<179 ), no. (%) 77 (52) 129 (43) Neutral (179e181 ), no. (%) 44 (30) 118 (40) Valgus (>181 ), no. (%) 25 (17) 51 (17) Abbreviations: N ¼ total number of knees in case and control groups; ROA ¼ radiographic osteoarthritis. * Denotes statistically significant differences (P < 0.05). y Scored using the WORMS (scale 0e3 for BML and synovitis and effusion; scale 0e6 for cartilage; and scale 0e4 for meniscus). z Calculated by chi-square test or 2-sample t-test, as appropriate.
4 A. Guermazi et al. / Osteoarthritis and Cartilage 18 (2010) 1386e (KeL grade 2) were higher in the case group than the control group. Prevalence of cartilage loss (WORMS grade 2) and meniscal damage (WORMS grade 1) in the case group were 141 (90%) and 68 (43%), respectively, and were higher than the control group. Prevalence of bone marrow lesion (BML), synovitis and joint effusion was similar between two groups. Malalignment was seen more frequently in the case group than in the control group (Table I). Baker s cysts (WORMS grade 1) were the most prevalent lesion in the case (63/157, 40%) and control (126/336, 37%) groups, but were not associated with incident pain at any grade. There were 7 (4%) lateral meniscal cysts in the case group and 4 (1%) in the control group, and the fully adjusted odds ratio (aor) [95%CI] for incident pain was 4.3 [1.2e15.4]. However, statistical significance was lost after correction of P-values for multiple comparisons. Association of medial or combined meniscal cysts with incident pain was also not present. PTFJ cysts were twice as likely to be seen in the case group as the control group (6% vs 3%), but were not associated with incident pain [aor 1.6 (0.6, 4.3)]. Prepatellar bursitis was more prevalent than anserine bursitis, in both case and control knees. Neither of these was associated with incident pain (Table II). Additional analyses adjusting for changes in pain medication yielded results similar to those of fully adjusted analyses described above (not shown). Incident radiographic OA study For the case group (n ¼ 149), the mean (SD) of demographic parameters was as follows: age 61.7 (7.7) years, BMI 31.0 (5.4) kg/m 2, 92 (62%) women and 120 (81%) white. Prevalence of cartilage loss, meniscal damage, synovitis and joint effusion in the case group were 144 (97%), 71 (48%), 72 (48%) and 99 (66%), respectively, and were higher than the control group. Varus alignment of the knee joint was commonly seen in both case and control groups but there were no statistically significant differences in malalignment between the two groups (Table I). Prevalence of grade 2 Baker s cysts (Fig. 1) was higher in the case (16/149, 11%) than the control group (9/298, 3%), and the aor for incident radiographic OA was 3.1 [1.1, 8.6], but its significance was lost after correction of P-values. Prevalence of grade 1 Baker s cysts was present in 66 (44%) of case knees at baseline, but was less frequent in control knees (97/298, 32%). Six (4%) PTFJ cysts were present in the case group and 3 (1%) in the control group, but association with incident radiographic OA was not significant after full adjustments [aor 2.6 (0.5, 12.2)]. Meniscal cysts, prepatellar bursitis and anserine bursitis were not associated with incident radiographic OA after full adjustments (Table III). Discussion In the present study, we assessed the longitudinal relationship of Baker s, meniscal and PTFJ cysts, as well as prepatellar and anserine bursitides with incident pain and incident radiographic OA. Statistically significant associations were not found in any of the analyzed lesions after full adjustment for potential confounders and correction of P-value for multiple comparisons. ABaker s cyst is not a true cyst, but a fluid collection in the semimembranosus-medial gastrocnemius bursa. Increased intraarticular pressure due to joint effusion causes extravasation of joint fluid through the posteromedial capsule between the medial head of the gastrocnemius and the semimembranosus tendon into the bursa located between these muscles 1. In this longitudinal study, we did not find significant associations between Baker s cyst of any grade and development of incident pain or radiographic OA. Baker s cysts can be asymptomatic, so their presence alone is unlikely to be the cause of OA-related pain. Rather, pain can be caused by the presence of a large joint effusion 11,21 and synovitis 21,22, both of which are Table II Prevalence of periarticular cystic lesions and cyst-like bursitis at baseline and their association with incident knee pain WORMS grade Incident knee pain Prevalence (%) at baseline OR (95% CI) Cases (N ¼ 157) Controls (N ¼ 336) Adjustedk Fully adjusted{ Baker s cysty 0 93 (60) 210 (63) 1.0 (ref) 1.0 (ref) 1 50 (32) 103 (30) 1.1 (0.7, 1.6) 1.0 (0.7, 1.6) 2 11 (7) 19 (6) 1.0 (0.5, 2.3) 0.9 (0.4, 2.1) 3 2 (1) 4 (1) 0.7 (0.1, 4.0) 0.6 (0.1, 3.7) Meniscal cyst# Medial (99) 330 (98) 1.0 (ref) 1.0 (ref) 1 2 (1) 6 (2) 1.0 (0.2, 5.2) 0.9 (0.2, 4.7) Lateral (96) 332 (99) 1.0 (ref) 1.0 (ref) 1 7 (4) 4 (1) 4.4* (1.2, 15.9) 4.3** (1.2, 15.4) Combined (94) 327 (97) 1.0 (ref) (ref) 1 9 (6) 9 (3) 2.8 (1.0, 7.3) 2.6 (1.0, 7.0) PTFJ cystz (94) 321 (97) 1.0 (ref) 1.0 (ref) 1 9 (6) 10 (3) 1.6 (0.6, 4.2) 1.6 (0.6, 4.3) Prepatellar bursitisx (68) 241 (72) 1.0 (ref) 1.0 (ref) 1 49 (32) 94 (28) 1.1 (0.7, 1.7) 1.1 (0.7, 1.7) Anserine bursitis (86) 290 (86) 1.0 (ref) 1.0 (ref) 1 22 (14) 46 (14) 0.7 (0.4, 1.3) 0.7 (0.4, 1.2) Abbreviations: N ¼ total number of subjects in case and control groups; OR ¼ odds ratio; CI ¼ confidence interval. *P ¼ and **P ¼ Although 95% CI does not include 1.0, these were not considered statistically significant after Bonferroni correction for multiple comparisons (level of significance was determined to be P < 0.007). y Missing value in one case knee. z Missing value in five control knees. x Missing value in two case knees and one control knee. k OR was calculated after making adjustments for age, sex, race, BMI, alignment, and KeL grade at baseline. { OR was calculated after making adjustments for age, sex, race, BMI, alignment, KeL grade, and other MRI features at baseline, i.e., maximum score of each feature, including BML, synovitis, joint effusion, meniscal damage, and cartilage loss. # Not adjusted for meniscal damage in the fully-adjusted model.
5 1390 A. Guermazi et al. / Osteoarthritis and Cartilage 18 (2010) 1386e1392 Fig. 1. (a) Antero-posterior (AP) X-ray at baseline shows KL ¼ 0 of both medial and lateral right femorotibial joints. (b) Baseline axial FS PD-w MR image shows grade 2 Baker s cyst (arrow). (c) AP X-ray at 30 months shows joint space narrowing of the lateral femorotibial joint and definite lateral tibial osteophytes (arrows) with KeL grade ¼ 2. features of OA. As a Baker s cyst is an extension of the knee joint capsule, co-linearity between Baker s cysts and joint effusion was expected but was not present and thus adjustment of our logistic regression model for joint effusion was made. However, not adjusting for joint effusion did not alter the findings of the present study. Based on results of a recent study which reported that joint effusion predicts cartilage loss in knees without OA 23, one could speculate that joint effusion might be a risk factor for incident OA. Such an association, however, has not been shown so far. We did not observe a significant association between PTFJ cysts and incident pain or radiographic OA. The probable cause of PTFJ lesions is increased pressure in the knee joint leading to an outpouching of the tibiofibular joint capsule which then herniates to form the synovial cyst 24. The lesions are therefore thought to be more common in patients with chronic knee effusions. It has been reported that PTFJ communicates with the knee joint capsule in 10% of adults 4,25. Whether such communication was present congenitally or acquired following an increase in intra-articular pressure, perhaps due to active synovitis or joint injury, has not been determined. In the present study, PTFJ cysts were much rarer than Baker s cysts (19 vs 189 in incident symptom study, and 9 vs 163 in incident radiographic OA study, i.e., prevalence of PTFJ cysts was Table III Prevalence of periarticular cystic lesions and cyst-like bursitis at baseline and their association with incident radiographic OA WORMS grade Incident radiographic OA Prevalence (%) at baseline OR (95% CI) Cases (N ¼ 149) Controls (N ¼ 298) Adjustedx Fully adjustedk Baker s cyst 0 83 (56) 201 (68) 1.0 (ref) 1.0 (ref) 1 47 (31) 84 (28) 1.2 (0.8, 2.0) 1.2 (0.7, 2.0) 2 16 (11) 9 (3) 4.1 (1.7, 10.0)* 3.1 (1.1, 8.6)** 3 3 (2) 4 (1) 1.6 (0.3, 7.7) 0.5 (0.1, 3.3) Meniscal cyst{ Medial# (100) 294 (99) n/a n/a 1 0 (0) 4 (1) n/a n/a Lateral# (99) 298 (100) n/a n/a 1 2 (1) 0 (0) n/a n/a Combined (99) 294 (99) 1.0 (ref) (ref) 1 2 (1) 4 (1) 0.8 (0.1, 4.6) 0.6 (0.1, 4.2) PTFJ cysty (96) 294 (99) 1.0 (ref) 1.0 (ref) 1 6 (4) 3 (1) 4.5 (1.1, 18.8)*** 2.6 (0.5, 12.2) Prepatellar bursitisz (85) 265 (89) 1.0 (ref) 1.0 (ref) 1 22 (15) 33 (11) 1.1 (0.6, 2.2) 1.5 (0.7, 3.1) Anserine bursitis (96) 293 (98) 1.0 (ref) 1.0 (ref) 1 6 (4) 5 (2) 1.5 (0.4, 5.9) 0.7 (0.1, 3.8) *P ¼ , **P ¼ and ***P ¼ Although 95% CI does not include 1.0, the results of ** and *** were not considered statistically significant after Bonferroni correction for multiple comparisons (level of significance was determined to be P < 0.007). y Missing value in one control knee. z Missing value in three case knees. x OR was calculated after making adjustments for age, sex, race, BMI and alignment at baseline. k OR was calculated after making adjustments for age, sex, race, BMI, alignment, and other MRI features at baseline, i.e., maximum score of each feature, including BML, synovitis, joint effusion, meniscal damage, and cartilage loss. { Not adjusted for meniscal damage in the fully-adjusted model. # Calculation of ORs was not possible.
6 A. Guermazi et al. / Osteoarthritis and Cartilage 18 (2010) 1386e e10% of that of Baker s cysts). These numbers support the previously published data, but why only 10% communicates with Baker s cysts is unknown. If these two lesions share the same pathogenesis, one would expect to see more of PTFJ cysts in patients who have Baker s cysts, but this did not seem to be the case. It is hoped that future studies will reveal the exact pathogenesis of PTFJ cysts. A meniscal cyst is a focal collection of synovial fluid located within or adjacent to the meniscus. Various theories concerning the etiology of meniscal cysts have been proposed, but the most widely held view is that they form as a result of extrusion of synovial fluid through an adjacent meniscal tear 9. In the incident pain study the baseline prevalence of medial meniscal cysts was 1% (2/157) while that of lateral meniscal cysts was 4% (7/157) in the case knees, contrary to a previous study 9 that reported a higher prevalence of medial than lateral lesions. This may be explained by a much smaller sample size than in the previous study. A strong crosssectional association between meniscal damage and the presence of knee OA has been reported 12. Since meniscal cysts are usually associated with an adjacent meniscal tear 9 which may be painful, it would have been unsurprising to find an association between meniscal cysts and incident knee pain. However, our data did not demonstrate such an association. Moreover, a recent report concluded that in middle-aged and older adults, any association between meniscal damage and the development of frequent knee pain seemed to occur because both pain and meniscal damage are related to OA, and not because of a direct link between the two 26. Thus, neither meniscal cysts nor meniscal damage itself seems to be directly associated with incident knee pain. As for prepatellar and anserine bursitides, we did not find significant associations with incident pain or incident radiographic OA. Given the location of these cysts outside the knee joint, we expected the null association with knee OA, but periarticular lesions like these have been linked to knee pain before 21 and we expected that they might be sources of pain. To date, there are few reports describing the prevalence of these lesions and their association with pain and radiographic OA. Prepatellar bursitis is commonly seen among both symptomatic and asymptomatic older individuals with radiographic knee OA 6. Furthermore, high-intensity signal changes are commonly observed anteriorly to the patella and the patella tendon and often represent a non-specific finding of little clinical relevance. True prepatellar bursitis should be assessed by contrastenhanced MRI to distinguish edema from bursitis, which was not available in our study. Anserine bursitis may be detected in conjunction with knee OA, but its association with degeneration is controversial 1. Chronic anserine bursitis is thought to be most common in elderly patients who have degenerative disease or rheumatoid arthritis 3. However, a recent case-control study found no association between prevalent anserine bursitis and radiographic knee OA 27. Taking these findings into account we speculate that, although these bursitides are commonly seen in OA patients, their pathogenesis is not directly linked to OA disease processes. A major limitation of our study is that we had two time points for follow-up in the incident pain study. As described earlier, it was not feasible to perform analyses based on either 15- or 30-month followup only. Using only one time point for follow-up would have simplified the study design and interpretation of the results. Another limitation of our study is that the prevalence of meniscal and PTFJ cysts was very low at baseline, and only a small number of lesions were available for the analysis (between 6 and 19 in total). More samples are needed to produce more statistically robust data. Thus, from our data alone, it may be difficult to draw a definitive conclusion concerning the longitudinal association between meniscal cysts and incident OA-related pain. However, the low prevalence in this large sample size may indicate that these lesions may not be clinically appropriate to predict incident knee pain. Lastly, the way we defined incident pain may have affected the outcome of our analysis. To qualify for incident knee pain, subjects must have had no knee pain at baseline and consistent knee pain at follow-up. However, those subjects who reported no frequent knee pain at baseline often noted some knee pain on the baseline WOMAC questionnaire. Thus, it must be noted that incident knee pain in such subjects is not necessarily completely new pain and may represent an increase in the frequency and severity of the knee pain. In conclusion, this was the first study to assess longitudinal relationships of intra- and periarticular cyst-like lesions of the knee with incident pain and radiographic OA. The analyzed lesions, i.e., Baker cysts, meniscal cysts, PTFJ cyst, prepatellar bursitis and anserine bursitis were not associated with incident pain or radiographic OA. Although intra- and periarticular cyst-like lesions are commonly observed on MRI, and have previously been shown to be crosssectionally associated with knee pain and radiographic OA, results of the present study suggest they are more likely to be a secondary phenomenon that occurs in painful or OA-affected knees, rather than a primary trigger for knee pain or radiographic OA. Author contributions (a) Conception and design, acquisition of data, analysis and interpretation of data: AG, DH, FWR, JN, MKJ, MY, JAL, JCT, CEL, BS, DTF, MCN. (b) Drafting the article or revising it critically for important intellectual content: AG, DH, FWR, JN, MKJ, MY, JAL, JCT, CEL, BS, DTF, MCN. (c) Final approval of the version to be published: AG, DH, FWR, JN, MKJ, MY, JAL, JCT, CEL, BS, DTF, MCN. (d) Guarantor of the integrity of the study: AG (guermazi@bu.edu). Funding sources The MOST study is supported by National Institutes of Health (NIH) grants from the National Institute on Aging to Drs Lewis (U01-AG-18947), Torner (U01-AG-18832), Nevitt (U01-AG-19069), and Felson (U01-AG-18820). The contents of this paper have been approved by the MOST committee to be published. Conflict of interest Ali Guermazi is the president of Boston Imaging Core Lab, LLC (BICL), Boston, MA, a company providing radiological image assessment services. He is shareholder of Synarc, Inc. and is a consultant to MerckSerono, Facet Solutions and Stryker. Frank Roemer is a shareholder of BICL. None of the other authors have declared any possible conflict of interest. Acknowledgement We would like to thank the participants and staff of the MOST study at the clinical sites in Birmingham, AL and Iowa City, IA and at the Coordinating Center at University of California San Francisco, San Francisco, CA. References 1. Crema MD, Roemer FW, Marra MD, Guermazi A. MR imaging of intra- and periarticular soft tissues and subchondral bone in knee osteoarthritis. Radiol Clin North Am 2009;47:687e Beall DP, Ly JQ, Wolff JD, Sweet CF, Kirby AB, Murphy MP, et al. Cystic masses of the knee: magnetic resonance imaging findings. Curr Probl Diagn Radiol 2005;34:143e59.
7 1392 A. Guermazi et al. / Osteoarthritis and Cartilage 18 (2010) 1386e McCarthy CL, McNally EG. The MRI appearance of cystic lesions around the knee. Skeletal Radiol 2004;33:187e Janzen DL, Peterfy CG, Forbes JR, Tirman PF, Genant HK. Cystic lesions around the knee joint: MR imaging findings. AJR Am J Roentgenol 1994;163:155e Mara MD, Crema MD, Chung MC, Roemer FW, Hunter DJ, Zaim S, et al. MRI features of cystic lesions around the knee. Knee 2008;15:423e Hill CL, Gale DR, Chaisson CE, Skinner K, Kazis L, Gale ME, et al. Periarticular lesions detected on magnetic resonance imaging: prevalence in knees with and without symptoms. Arthritis Rheum 2003;48:2836e Tschirch FT, Schmid MR, Pfirrmann CW, Romero J, Hodler J, Zanetti M. Prevalence and size of meniscal cysts, ganglionic cysts, synovial cysts of the popliteal space, fluid-filled bursae, and other fluid collections in asymptomatic knees on MR imaging. AJR Am J Roentgenol 2003;180:1431e6. 8. Miller TT, Staron RB, Koenigsberg T, Levin TL, Feldman F. MR imaging of Baker cysts: association with internal derangement, effusion, and degenerative arthropathy. Radiology 1996;201: 247e Campbell SE, Sanders TG, Morrison WB. MR imaging of meniscal cysts: incidence, location, and clinical significance. AJR Am J Roentgenol 2001;177:409e Link TM, Steinbach LS, Ghosh S, Ries M, Lu Y, Lane N, et al. Osteoarthritis: MR imaging findings in different stages of disease and correlation with clinical findings. Radiology 2003; 226:373e Kornaat PR, Bloem JL, Ceulemans RYT, Riyazi N, Rosendaal FR, Nelissen RG, et al. Osteoarthritis of the knee: association between clinical features and MR imaging findings. Radiology 2006;239:811e Englund M, Guermazi A, Gale D, Hunter DJ, Aliabadi P, Clancy M, et al. Incidental meniscal findings on knee MRI in middle-aged and elderly persons. N Eng J Med 2008;359: 1108e Felson DT, Niu J, Guermazi A, Roemer FW, Aliabadi P, Clancy M, et al. Correlation of the development of knee pain with enlarging bone marrow lesions on magnetic resonance imaging. Arthritis Rheum 2007;56:2986e Bellamy N, Buchanan WW, Goldsmith CH, Campbell J, Stitt LW. Validation study of WOMAC: a health status instrument for measuring clinically important patient relevant outcomes to anti-rheumatic drug therapy in patients with osteoarthritis of the hip or knee. J Rheumatol 1988;15: 1833e Kellgren JH, Lawrence JS. Radiological assessment of osteoarthritis. Ann Rheum Dis 1957;16:494e Altman RD, Gold GE. Atlas of individual radiographic features in osteoarthritis, revised. Osteoarthritis Cartilage 2007;15(Suppl 1):A1eA Kothari M, Guermazi A, von Ingersleben G, Miaux Y, Sieffert M, Block JE, et al. Fixed-flexion radiography of the knee provides reproducible joint space width measurements in osteoarthritis. Eur Radiol 2004; Peterfy C, Li J, Zaim S, Duryea J, Lynch J, Miaux Y, et al. Comparison of fixed-flexion positioning with fluoroscopic semiflexed positioning for quantifying radiographic joint-space width in the knee: test-retest reproducibility. Skeletal Radiol 2003;32:128e Sharma L, Song J, Felson DT, Cahue S, Shamiyeh E, Dunlop DD. The role of knee alignment in disease progression and functional decline in knee osteoarthritis. JAMA 2001;286:188e Peterfy CG, Guermazi A, Zaim S, Tirman PF, Miaux Y, White D, et al. Whole-Organ Magnetic Resonance Imaging Score (WORMS) of the knee in osteoarthritis. Osteoarthritis Cartilage 2004;12:177e Hill CL, Gale DG, Chaisson CE, Skinner K, Kazis L, Gale ME, et al. Knee effusions, popliteal cysts, and synovial thickening: association with knee pain in osteoarthritis. J Rheumatol 2001;28: 1330e Chatzopoulos D, Moralidis E, Markou P, Makris V, Arsos G. Baker s cysts in knees with chronic osteoarthritis pain: a clinical, ultrasonographic, radiographic and scintigraphic evaluation. Rheumatol Int 2008;29:141e Roemer FW, Guermazi A, Felson DT, Niu J, Nevitt MC, Crema MD, et al. Do baseline synovitis and effusion predict structural progression in subjects without radiographic osteoarthritis? e Results from the Multicenter Osteoarthritis (MOST) Study. Osteoarthritis Cartilage 2009;17(Suppl 1):S Jerome D, McKendry R. Synovial cyst of the proximal tibiofibular joint. J Rheumatol 2000;27:1096e Steiner E, Steinbach LS, Schnarkowski P, Tirman PF, Genant HK. Ganglia and cysts around joints. Radiol Clin North Am 1996; 34:395e425. xiexii. 26. Englund M, Niu J, Guermazi A, Roemer FW, Hunter DJ, Lynch JA, et al. Effect of meniscal damage on the development of frequent knee pain, aching or stiffness. Arthritis Rheum 2007;56:4048e Alvarez-Nemegyei J. Risk factors for pes anserinus tendinitis/bursitis syndrome: a case control study. J Clin Rheumatol 2007;13:63e5.
Osteoarthritis and Cartilage 18 (2010) 1402e1407
 Osteoarthritis and Cartilage 18 (2010) 1402e1407 Comparison of BLOKS and WORMS scoring systems part II. Longitudinal assessment of knee MRIs for osteoarthritis and suggested approach based on their performance:
Osteoarthritis and Cartilage 18 (2010) 1402e1407 Comparison of BLOKS and WORMS scoring systems part II. Longitudinal assessment of knee MRIs for osteoarthritis and suggested approach based on their performance:
Peripatellar synovitis: comparison between non-contrast-enhanced and contrast-enhanced MRI and association with pain.
 Osteoarthritis and Cartilage 21 (2013) 413e418 Peripatellar synovitis: comparison between non-contrast-enhanced and contrast-enhanced MRI and association with pain. The MOST study M.D. Crema yz *, D.T.
Osteoarthritis and Cartilage 21 (2013) 413e418 Peripatellar synovitis: comparison between non-contrast-enhanced and contrast-enhanced MRI and association with pain. The MOST study M.D. Crema yz *, D.T.
Knee malalignment is associated with an increased risk for incident and enlarging bone marrow lesions in the more loaded compartments: the MOST study
 Osteoarthritis and Cartilage 20 (2012) 1227e1233 Knee malalignment is associated with an increased risk for incident and enlarging bone marrow lesions in the more loaded compartments: the MOST study D.
Osteoarthritis and Cartilage 20 (2012) 1227e1233 Knee malalignment is associated with an increased risk for incident and enlarging bone marrow lesions in the more loaded compartments: the MOST study D.
Frequency of Baker s Cysts in Cases of Meniscal Injury
 International Journal of Research Studies in Biosciences (IJRSB) Volume 4, Issue 1, January 2016, PP 10-14 ISSN 2349-0357 (Print) & ISSN 2349-0365 (Online) http://dx.doi.org/10.20431/2349-0365.0401003
International Journal of Research Studies in Biosciences (IJRSB) Volume 4, Issue 1, January 2016, PP 10-14 ISSN 2349-0357 (Print) & ISSN 2349-0365 (Online) http://dx.doi.org/10.20431/2349-0365.0401003
Valgus Malalignment Is a Risk Factor for Lateral Knee Osteoarthritis Incidence and Progression
 ARTHRITIS & RHEUMATISM Vol. 65, No. 2, February 2013, pp 355 362 DOI 10.1002/art.37726 2013, American College of Rheumatology Valgus Malalignment Is a Risk Factor for Lateral Knee Osteoarthritis Incidence
ARTHRITIS & RHEUMATISM Vol. 65, No. 2, February 2013, pp 355 362 DOI 10.1002/art.37726 2013, American College of Rheumatology Valgus Malalignment Is a Risk Factor for Lateral Knee Osteoarthritis Incidence
Physical activity, alignment and knee osteoarthritis: data from MOST and the OAI
 Osteoarthritis and Cartilage 21 (2013) 789e795 Physical activity, alignment and knee osteoarthritis: data from MOST and the OAI D.T. Felson yzz *, J. Niu y, T. Yang y, J. Torner #, C.E. Lewis k, P. Aliabadi
Osteoarthritis and Cartilage 21 (2013) 789e795 Physical activity, alignment and knee osteoarthritis: data from MOST and the OAI D.T. Felson yzz *, J. Niu y, T. Yang y, J. Torner #, C.E. Lewis k, P. Aliabadi
MRI of distended bursa around the knee
 MRI of distended bursa around the knee Poster No.: C-2240 Congress: ECR 2010 Type: Educational Exhibit Topic: Musculoskeletal Authors: P. Papadopoulou, I. Kalaitzoglou, N. Michailidis, I. Tsifoundoudis,
MRI of distended bursa around the knee Poster No.: C-2240 Congress: ECR 2010 Type: Educational Exhibit Topic: Musculoskeletal Authors: P. Papadopoulou, I. Kalaitzoglou, N. Michailidis, I. Tsifoundoudis,
Osteoarthritis and Cartilage 18 (2010) 1393e1401
 Osteoarthritis and Cartilage 18 (2010) 1393e1401 Comparison of BLOKS and scoring systems part I. Cross sectional comparison of methods to assess cartilage morphology, meniscal damage and bone marrow lesions
Osteoarthritis and Cartilage 18 (2010) 1393e1401 Comparison of BLOKS and scoring systems part I. Cross sectional comparison of methods to assess cartilage morphology, meniscal damage and bone marrow lesions
The association between meniscal and cruciate ligament damage and knee pain in community residents
 Osteoarthritis and Cartilage 19 (2011) 1422e1428 The association between meniscal and cruciate ligament damage and knee pain in community residents H.A. Kimyz *,I.Kimx, Y.W. Songk,D.H.Kim{,J.Niu#, A.Guermaziyy,
Osteoarthritis and Cartilage 19 (2011) 1422e1428 The association between meniscal and cruciate ligament damage and knee pain in community residents H.A. Kimyz *,I.Kimx, Y.W. Songk,D.H.Kim{,J.Niu#, A.Guermaziyy,
Central Reading of Knee X-rays for Kellgren & Lawrence Grade and Individual Radiographic Features of Tibiofemoral Knee OA
 Central Reading of Knee X-rays for Kellgren & Lawrence Grade and Individual Radiographic Features of Tibiofemoral Knee OA 1. Overview... 1 1.1 SAS dataset... 1 1.2 Contents of dataset... 1 1.3 Merging
Central Reading of Knee X-rays for Kellgren & Lawrence Grade and Individual Radiographic Features of Tibiofemoral Knee OA 1. Overview... 1 1.1 SAS dataset... 1 1.2 Contents of dataset... 1 1.3 Merging
ARTICLE IN PRESS. International Cartilage Repair Society
 Osteoarthritis and Cartilage (2009) jj, jjjejjj ª 2006 Osteoarthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2008.11.014 Strong association of
Osteoarthritis and Cartilage (2009) jj, jjjejjj ª 2006 Osteoarthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2008.11.014 Strong association of
POPLITEAL CYST FILLED WITH HEMATOMA AT THE LOWER CALF: A CASE REPORT
 Trakia Journal of Sciences, No 4, pp 411-414, 2016 Copyright 2016 Trakia University Available online at: http://www.uni-sz.bg ISSN 1313-7050 (print) ISSN 1313-3551 (online) doi:10.15547/tjs.2016.04.019
Trakia Journal of Sciences, No 4, pp 411-414, 2016 Copyright 2016 Trakia University Available online at: http://www.uni-sz.bg ISSN 1313-7050 (print) ISSN 1313-3551 (online) doi:10.15547/tjs.2016.04.019
International Cartilage Repair Society
 Osteoarthritis and Cartilage (2009) 17, 748e753 ª 2008 Osteoarthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2008.09.013 The association of meniscal
Osteoarthritis and Cartilage (2009) 17, 748e753 ª 2008 Osteoarthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2008.09.013 The association of meniscal
Table of Contents. Overview Introduction Variables Missing Data Image Type Time Points Reading Methods...
 MULTICENTER OSTEOARTHRITIS STUDY LONGITUDINAL KNEE RADIOGRAPH ASSESSMENTS (BASELINE TO 15-MONTH, 30-MONTH, 60-MONTH AND 84-MONTH FOLLOW-UP) AND MEASUREMENTS FROM BASELINE FULL LIMB RADIOGRAPHS DATASET
MULTICENTER OSTEOARTHRITIS STUDY LONGITUDINAL KNEE RADIOGRAPH ASSESSMENTS (BASELINE TO 15-MONTH, 30-MONTH, 60-MONTH AND 84-MONTH FOLLOW-UP) AND MEASUREMENTS FROM BASELINE FULL LIMB RADIOGRAPHS DATASET
Disclosures. Breaking the Law of Valgus. Law of Valgus. Law of Valgus. MRI Studies of OA. Objectives 11/7/2011
 11/7/211 Breaking the Law of Valgus the surprising and unexplained prevalence of medial patellofemoral cartilage damage None Disclosures Doug Gross Josh Stefanik Frank Roemer Michael Nevitt ora Lewis Jingbo
11/7/211 Breaking the Law of Valgus the surprising and unexplained prevalence of medial patellofemoral cartilage damage None Disclosures Doug Gross Josh Stefanik Frank Roemer Michael Nevitt ora Lewis Jingbo
Ultrasound of the Knee
 Ultrasound of the Knee Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Disclosures: Consultant: Bioclinica Book Royalties: Elsevier Advisory
Ultrasound of the Knee Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Disclosures: Consultant: Bioclinica Book Royalties: Elsevier Advisory
MR imaging of the knee in marathon runners before and after competition
 Skeletal Radiol (2001) 30:72 76 International Skeletal Society 2001 ARTICLE W. Krampla R. Mayrhofer J. Malcher K.H. Kristen M. Urban W. Hruby MR imaging of the knee in marathon runners before and after
Skeletal Radiol (2001) 30:72 76 International Skeletal Society 2001 ARTICLE W. Krampla R. Mayrhofer J. Malcher K.H. Kristen M. Urban W. Hruby MR imaging of the knee in marathon runners before and after
The Relationship Between Cartilage Loss on Magnetic Resonance Imaging and Radiographic Progression in Men and Women With Knee Osteoarthritis
 ARTHRITIS & RHEUMATISM Vol. 52, No. 10, October 2005, pp 3152 3159 DOI 10.1002/art.21296 2005, American College of Rheumatology The Relationship Between Cartilage Loss on Magnetic Resonance Imaging and
ARTHRITIS & RHEUMATISM Vol. 52, No. 10, October 2005, pp 3152 3159 DOI 10.1002/art.21296 2005, American College of Rheumatology The Relationship Between Cartilage Loss on Magnetic Resonance Imaging and
The Association of Meniscal Pathologic Changes With Cartilage Loss in Symptomatic Knee Osteoarthritis
 ARTHRITIS & RHEUMATISM Vol. 54, No. 3, March 2006, pp 795 801 DOI 10.1002/art.21724 2006, American College of Rheumatology The Association of Meniscal Pathologic Changes With Cartilage Loss in Symptomatic
ARTHRITIS & RHEUMATISM Vol. 54, No. 3, March 2006, pp 795 801 DOI 10.1002/art.21724 2006, American College of Rheumatology The Association of Meniscal Pathologic Changes With Cartilage Loss in Symptomatic
Knee, Ankle, and Foot: Normal and Abnormal Features with MRI and Ultrasound Correlation. Disclosures. Outline. Joint Effusion. Suprapatellar recess
 Knee, Ankle, and Foot: Normal and Abnormal Features with MRI and Ultrasound Correlation Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan
Knee, Ankle, and Foot: Normal and Abnormal Features with MRI and Ultrasound Correlation Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan
The relationship between chondromalacia patella, medial meniscal tear and medial periarticular bursitis in patients with osteoarthritis
 research article 401 The relationship between chondromalacia patella, medial meniscal tear and medial periarticular bursitis in patients with osteoarthritis Mustafa Resorlu 1, Davut Doner 2, Ozan Karatag
research article 401 The relationship between chondromalacia patella, medial meniscal tear and medial periarticular bursitis in patients with osteoarthritis Mustafa Resorlu 1, Davut Doner 2, Ozan Karatag
Why Talk About Technique? MRI of the Knee:
 Why Talk About Technique? MRI of the Knee: Part 1 - Imaging Techniques Mark Anderson, M.D. University of Virginia Health Sciences Center Charlottesville, Virginia Always had an interest teach our fellows
Why Talk About Technique? MRI of the Knee: Part 1 - Imaging Techniques Mark Anderson, M.D. University of Virginia Health Sciences Center Charlottesville, Virginia Always had an interest teach our fellows
Bone marrow lesions in knee osteoarthritis: MR-assessment by manual segmentation and computer-assisted tresholding
 Bone marrow lesions in knee osteoarthritis: MR-assessment by manual segmentation and computer-assisted tresholding Poster No.: P-0073 Congress: ESSR 2012 Type: Scientific Exhibit Authors: F. K. Nielsen,
Bone marrow lesions in knee osteoarthritis: MR-assessment by manual segmentation and computer-assisted tresholding Poster No.: P-0073 Congress: ESSR 2012 Type: Scientific Exhibit Authors: F. K. Nielsen,
What Comes First? Multitissue Involvement Leading to Radiographic Osteoarthritis
 ARTHRITIS & RHEUMATOLOGY Vol. 67, No. 8, August 2015, pp 2085 2096 DOI 10.1002/art.39176 VC 2015, American College of Rheumatology What Comes First? Multitissue Involvement Leading to Radiographic Osteoarthritis
ARTHRITIS & RHEUMATOLOGY Vol. 67, No. 8, August 2015, pp 2085 2096 DOI 10.1002/art.39176 VC 2015, American College of Rheumatology What Comes First? Multitissue Involvement Leading to Radiographic Osteoarthritis
International Cartilage Repair Society
 OsteoArthritis and Cartilage (2006) 14, 1081e1085 ª 2006 OsteoArthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2006.05.011 MRI of bone marrow
OsteoArthritis and Cartilage (2006) 14, 1081e1085 ª 2006 OsteoArthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2006.05.011 MRI of bone marrow
Chronic knee pain in adults - a multimodality approach or which modality to choose and when?
 Chronic knee pain in adults - a multimodality approach or which modality to choose and when? Poster No.: P-0157 Congress: ESSR 2013 Type: Authors: Keywords: DOI: Scientific Exhibit E. Ilieva, V. Tasseva,
Chronic knee pain in adults - a multimodality approach or which modality to choose and when? Poster No.: P-0157 Congress: ESSR 2013 Type: Authors: Keywords: DOI: Scientific Exhibit E. Ilieva, V. Tasseva,
Incidental Meniscal Findings on Knee MRI in Middle-Aged and Elderly Persons
 The new england journal of medicine original article Incidental Meniscal Findings on Knee MRI in Middle-Aged and Elderly Persons Martin Englund, M.D., Ph.D., Ali Guermazi, M.D., Daniel Gale, M.D., David
The new england journal of medicine original article Incidental Meniscal Findings on Knee MRI in Middle-Aged and Elderly Persons Martin Englund, M.D., Ph.D., Ali Guermazi, M.D., Daniel Gale, M.D., David
Summary. Introduction
 Osteoarthritis and Cartilage (1999) 7, 526 532 1999 OsteoArthritis Research Society International 1063 4584/99/060526+07 $12.00/0 Article No. joca.1999.0256, available online at http://www.idealibrary.com
Osteoarthritis and Cartilage (1999) 7, 526 532 1999 OsteoArthritis Research Society International 1063 4584/99/060526+07 $12.00/0 Article No. joca.1999.0256, available online at http://www.idealibrary.com
Ultrasound Evaluation of Masses
 Ultrasound Evaluation of Masses Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Disclosures: Consultant: Bioclinica Advisory Panel: GE,
Ultrasound Evaluation of Masses Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Disclosures: Consultant: Bioclinica Advisory Panel: GE,
A Comparative Study of Ultrasonographic Findings with Clinical and Radiological Findings of Painful Osteoarthritis of the Knee Joint
 Med. J. Cairo Univ., Vol. 84, No. 3, December: 97-, www.medicaljournalofcairouniversity.net A Comparative Study of Ultrasonographic Findings with Clinical and Radiological Findings of Painful Osteoarthritis
Med. J. Cairo Univ., Vol. 84, No. 3, December: 97-, www.medicaljournalofcairouniversity.net A Comparative Study of Ultrasonographic Findings with Clinical and Radiological Findings of Painful Osteoarthritis
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 12/01/2012 Radiology Quiz of the Week # 101 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 12/01/2012 Radiology Quiz of the Week # 101 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Planning knee OA prevention studies in obese populations Lessons from the Multicenter Osteoarthritis Study (MOST) and Osteoathritis Initiative (OAI)
 Planning knee OA prevention studies in obese populations Lessons from the (MOST) and Osteoathritis Initiative (OAI) Michael Nevitt, PhD UCSF Epidemiology and Biostatistics OAI and MOST Coordinating Centers
Planning knee OA prevention studies in obese populations Lessons from the (MOST) and Osteoathritis Initiative (OAI) Michael Nevitt, PhD UCSF Epidemiology and Biostatistics OAI and MOST Coordinating Centers
Original Report. The Reverse Segond Fracture: Association with a Tear of the Posterior Cruciate Ligament and Medial Meniscus
 Eva M. Escobedo 1 William J. Mills 2 John. Hunter 1 Received July 10, 2001; accepted after revision October 1, 2001. 1 Department of Radiology, University of Washington Harborview Medical enter, 325 Ninth
Eva M. Escobedo 1 William J. Mills 2 John. Hunter 1 Received July 10, 2001; accepted after revision October 1, 2001. 1 Department of Radiology, University of Washington Harborview Medical enter, 325 Ninth
E. ÇAĞLAR, G. ŞAH N 1, T. OĞUR, E. AKTAŞ. Introduction. Abstract. OBJECTIVE: To identify changes in
 European Review for Medical and Pharmacological Sciences Quantitative evaluation of hyaline articular cartilage T2 maps of knee and determine the relationship of cartilage T2 values with age, gender, articular
European Review for Medical and Pharmacological Sciences Quantitative evaluation of hyaline articular cartilage T2 maps of knee and determine the relationship of cartilage T2 values with age, gender, articular
Knee MRI Update Case Review 2009 Russell C. Fritz, M.D. National Orthopedic Imaging Associates San Francisco, CA
 Knee MRI Update Case Review 2009 Russell C. Fritz, M.D. National Orthopedic Imaging Associates San Francisco, CA Meniscal Tears -linear increased signal extending to an articular surface is the hallmark
Knee MRI Update Case Review 2009 Russell C. Fritz, M.D. National Orthopedic Imaging Associates San Francisco, CA Meniscal Tears -linear increased signal extending to an articular surface is the hallmark
Validity and Reliability of Radiographic Knee Osteoarthritis Measures by Arthroplasty Surgeons
 Validity and Reliability of Radiographic Knee Osteoarthritis Measures by Arthroplasty Surgeons Daniel L. Riddle, PhD; William A. Jiranek, MD; Jason R. Hull, MD abstract Full article available online at
Validity and Reliability of Radiographic Knee Osteoarthritis Measures by Arthroplasty Surgeons Daniel L. Riddle, PhD; William A. Jiranek, MD; Jason R. Hull, MD abstract Full article available online at
High Prevalence of Abnormal MR Findings of the Distal Semimembranosus Tendon: Contributing Factors Based on Demographic, Radiographic, and MR Features
 Musculoskeletal Imaging Original Research Yoon et al. MRI of the Distal Semimembranosus Tendon Musculoskeletal Imaging Original Research Min A Yoon 1 Ja-Young Choi Hyun Kyong Lim Hye Jin Yoo Sung Hwan
Musculoskeletal Imaging Original Research Yoon et al. MRI of the Distal Semimembranosus Tendon Musculoskeletal Imaging Original Research Min A Yoon 1 Ja-Young Choi Hyun Kyong Lim Hye Jin Yoo Sung Hwan
A rapid, novel method of volumetric assessment of MRI-detected subchondral bone marrow lesions in knee osteoarthritis
 Osteoarthritis and Cartilage 21 (2013) 806e814 A rapid, novel method of volumetric assessment of MRI-detected subchondral bone marrow lesions in knee osteoarthritis C. Ratzlaff y *, A. Guermazi z, J. Collins
Osteoarthritis and Cartilage 21 (2013) 806e814 A rapid, novel method of volumetric assessment of MRI-detected subchondral bone marrow lesions in knee osteoarthritis C. Ratzlaff y *, A. Guermazi z, J. Collins
In the name of god. Knee. By: Tofigh Bahraminia Graduate Student of the Pathology Sports and corrective actions. Heat: Dr. Babakhani. Nov.
 In the name of god Knee By: Tofigh Bahraminia Graduate Student of the Pathology Sports and corrective actions Heat: Dr. Babakhani Nov. 2014 1 Anatomy-Bones Bones Femur Medial/lateral femoral condyles articulate
In the name of god Knee By: Tofigh Bahraminia Graduate Student of the Pathology Sports and corrective actions Heat: Dr. Babakhani Nov. 2014 1 Anatomy-Bones Bones Femur Medial/lateral femoral condyles articulate
Imaging of Osteoarthritis
 Imaging of Osteoarthritis Ali Guermazi, MD, PhD a, *, Daichi Hayashi, MD, PhD a, Felix Eckstein, MD b, David J. Hunter, MBBS, MSc, PhD, FRACP c, Jeff Duryea, PhD d, Frank W. Roemer, MD a KEYWORDS Osteoarthritis
Imaging of Osteoarthritis Ali Guermazi, MD, PhD a, *, Daichi Hayashi, MD, PhD a, Felix Eckstein, MD b, David J. Hunter, MBBS, MSc, PhD, FRACP c, Jeff Duryea, PhD d, Frank W. Roemer, MD a KEYWORDS Osteoarthritis
Original article RHEUMATOLOGY
 RHEUMATOLOGY Rheumatology 2017;56:113 120 doi:10.1093/rheumatology/kew368 Advance Access publication 25 October 2016 Original article Predictive value of MRI features for development of radiographic osteoarthritis
RHEUMATOLOGY Rheumatology 2017;56:113 120 doi:10.1093/rheumatology/kew368 Advance Access publication 25 October 2016 Original article Predictive value of MRI features for development of radiographic osteoarthritis
Clinical Study MR Imaging of Intra- and Periarticular Cyst-Like Lesions of the Knee Joint in Workers with Occupational Kneeling
 Hindawi Publishing Corporation International Journal of Rheumatology Volume 2012, Article ID 843970, 10 pages doi:10.1155/2012/843970 Clinical Study MR Imaging of Intra- and Periarticular Cyst-Like Lesions
Hindawi Publishing Corporation International Journal of Rheumatology Volume 2012, Article ID 843970, 10 pages doi:10.1155/2012/843970 Clinical Study MR Imaging of Intra- and Periarticular Cyst-Like Lesions
This presentation is the intellectual property of the author. Contact them for permission to reprint and/or distribute.
 MRI of the Knee Jennifer Swart, M.D. Musculoskeletal Radiology South Texas Radiology Group Outline Coils, Patient Positioning Acquisition Parameters, Planes and Pulse Sequences Knee Arthrography Normal
MRI of the Knee Jennifer Swart, M.D. Musculoskeletal Radiology South Texas Radiology Group Outline Coils, Patient Positioning Acquisition Parameters, Planes and Pulse Sequences Knee Arthrography Normal
Stability of Post Traumatic Osteochondritis Dissecans of the Knee: MR Imaging Findings
 Chin J Radiol 2005; 30: 199-204 199 Stability of Post Traumatic Osteochondritis Dissecans of the Knee: MR Imaging Findings YU-CHUNG HUNG 1 JON-KWAY HUANG 1,2 Department of Radiology 1, Mackay Memorial
Chin J Radiol 2005; 30: 199-204 199 Stability of Post Traumatic Osteochondritis Dissecans of the Knee: MR Imaging Findings YU-CHUNG HUNG 1 JON-KWAY HUANG 1,2 Department of Radiology 1, Mackay Memorial
Joints of the Lower Limb II
 Joints of the Lower Limb II Lecture Objectives Describe the components of the knee and ankle joint. List the ligaments associated with these joints and their attachments. List the muscles acting on these
Joints of the Lower Limb II Lecture Objectives Describe the components of the knee and ankle joint. List the ligaments associated with these joints and their attachments. List the muscles acting on these
Evolution of semi-quantitative whole joint assessment of knee OA: MOAKS (MRI Osteoarthritis Knee Score)
 Osteoarthritis and Cartilage 19 (2011) 990e1002 Evolution of semi-quantitative whole joint assessment of knee OA: MOAKS (MRI Osteoarthritis Knee Score) D.J. Hunter y *, A. Guermazi z, G.H. Lo xk, A.J.
Osteoarthritis and Cartilage 19 (2011) 990e1002 Evolution of semi-quantitative whole joint assessment of knee OA: MOAKS (MRI Osteoarthritis Knee Score) D.J. Hunter y *, A. Guermazi z, G.H. Lo xk, A.J.
This presentation is the intellectual property of the author. Contact them at for permission to reprint and/or distribute.
 MRI of the Knee Jennifer Swart, M.D. Musculoskeletal Radiology South Texas Radiology Group Financial Disclosure Dr. Jennifer Swart has no relevant financial relationships with commercial interests to disclose.
MRI of the Knee Jennifer Swart, M.D. Musculoskeletal Radiology South Texas Radiology Group Financial Disclosure Dr. Jennifer Swart has no relevant financial relationships with commercial interests to disclose.
Signal intensity changes of the posterior elements of the lumbar spine in symptomatic adults
 ORIGINAL ARTICLE SPINE SURGERY AND RELATED RESEARCH Signal intensity changes of the posterior elements of the lumbar spine in symptomatic adults Kosuke Sugiura, Toshinori Sakai, Fumitake Tezuka, Kazuta
ORIGINAL ARTICLE SPINE SURGERY AND RELATED RESEARCH Signal intensity changes of the posterior elements of the lumbar spine in symptomatic adults Kosuke Sugiura, Toshinori Sakai, Fumitake Tezuka, Kazuta
Ultrasound of the Knee Joint. Jun Sung Park,M.D. Bundang General Hospital Dept. of Rehabilitation Medicine
 Ultrasound of the Knee Joint Jun Sung Park,M.D. Bundang General Hospital Dept. of Rehabilitation Medicine Clinical History and P/E Chronic or Acute Symptoms Chronic Sx. : possible of systemic articular
Ultrasound of the Knee Joint Jun Sung Park,M.D. Bundang General Hospital Dept. of Rehabilitation Medicine Clinical History and P/E Chronic or Acute Symptoms Chronic Sx. : possible of systemic articular
International Cartilage Repair Society
 OsteoArthritis and Cartilage (2006) 14, 496e500 ª 2005 OsteoArthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2005.12.001 Short communication
OsteoArthritis and Cartilage (2006) 14, 496e500 ª 2005 OsteoArthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2005.12.001 Short communication
Medial Knee Osteoarthritis Precedes Medial Meniscal Posterior Root Tear with an Event of Painful Popping
 Medial Knee Osteoarthritis Precedes Medial Meniscal Posterior Root Tear with an Event of Painful Popping Dhong Won Lee, M.D, Ji Nam Kim, M.D., Jin Goo Kim, M.D., Ph.D. KonKuk University Medical Center
Medial Knee Osteoarthritis Precedes Medial Meniscal Posterior Root Tear with an Event of Painful Popping Dhong Won Lee, M.D, Ji Nam Kim, M.D., Jin Goo Kim, M.D., Ph.D. KonKuk University Medical Center
MRI of Cartilage. D. BENDAHAN (PhD)
 MRI of Cartilage D. BENDAHAN (PhD) Centre de Résonance Magnétique Biologique et Médicale UMR CNRS 7339 Faculté de Médecine de la Timone 27, Bd J. Moulin 13005 Marseille France david.bendahan@univ-amu.fr
MRI of Cartilage D. BENDAHAN (PhD) Centre de Résonance Magnétique Biologique et Médicale UMR CNRS 7339 Faculté de Médecine de la Timone 27, Bd J. Moulin 13005 Marseille France david.bendahan@univ-amu.fr
International Journal of Orthopaedics Sciences 2017; 3(1): Dr. Sunil Kumar TR and Dr. Harish YS
 2017; 3(1): 658-663 ISSN: 2395-1958 IJOS 2017; 3(1): 658-663 2017 IJOS www.orthopaper.com Received: 07-11-2016 Accepted: 08-12-2016 Dr. Sunil Kumar TR Senior Resident, ESIC Medical College and Model Hospital
2017; 3(1): 658-663 ISSN: 2395-1958 IJOS 2017; 3(1): 658-663 2017 IJOS www.orthopaper.com Received: 07-11-2016 Accepted: 08-12-2016 Dr. Sunil Kumar TR Senior Resident, ESIC Medical College and Model Hospital
Coronal Tibiofemoral Subluxation in Knee Osteoarthritis
 Coronal Tibiofemoral Subluxation in Knee Osteoarthritis Saker Khamaisy, MD 1,2 * ; Hendrik A. Zuiderbaan, MD 1 ; Meir Liebergall, MD 2; Andrew D. Pearle, MD 1 1Hospital for Special Surgery, Weill Medical
Coronal Tibiofemoral Subluxation in Knee Osteoarthritis Saker Khamaisy, MD 1,2 * ; Hendrik A. Zuiderbaan, MD 1 ; Meir Liebergall, MD 2; Andrew D. Pearle, MD 1 1Hospital for Special Surgery, Weill Medical
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 7/28/2012 Radiology Quiz of the Week # 83 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 7/28/2012 Radiology Quiz of the Week # 83 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Meniscus T2 Relaxation Time at Various Stages of Knee Joint Degeneration
 Meniscus T2 Relaxation Time at Various Stages of Knee Joint Degeneration Richard Kijowski, Michael Fazio, Benjamin Beduhn, and Fang Liu Department of Radiology University of Wisconsin School of Medicine
Meniscus T2 Relaxation Time at Various Stages of Knee Joint Degeneration Richard Kijowski, Michael Fazio, Benjamin Beduhn, and Fang Liu Department of Radiology University of Wisconsin School of Medicine
Oak foundation for donating the 3T Siemens Verio scanner. Board of directors BBH and Frh Hospitals for supporting the
 Knee pain and inflammation in the infrapatellar fat pad estimated by conventional and dynamic contrast-enhanced magnetic resonance imaging in obese patients with osteoarthritis: a crosssectional study
Knee pain and inflammation in the infrapatellar fat pad estimated by conventional and dynamic contrast-enhanced magnetic resonance imaging in obese patients with osteoarthritis: a crosssectional study
FAI syndrome with or without labral tear.
 Case This 16-year-old female, soccer athlete was treated for pain in the right groin previously. Now has acute onset of pain in the left hip. The pain was in the groin that was worse with activities. Diagnosis
Case This 16-year-old female, soccer athlete was treated for pain in the right groin previously. Now has acute onset of pain in the left hip. The pain was in the groin that was worse with activities. Diagnosis
WORKSHOP. Organizers: Oran D. Kennedy, PhD Tamara Alliston, PhD
 WORKSHOP Bone Marrow Lesions - What Lies Beneath? A workshop based on the ORS/AAOS symposium: Tackling Joint Disease by Understanding Crosstalk between Cartilage and Bone, April 2016 Organizers: Oran D.
WORKSHOP Bone Marrow Lesions - What Lies Beneath? A workshop based on the ORS/AAOS symposium: Tackling Joint Disease by Understanding Crosstalk between Cartilage and Bone, April 2016 Organizers: Oran D.
Medial tibial condyle friction syndrome: MRI study of a new entity
 Medial tibial condyle friction syndrome: MRI study of a new entity Poster No.: C-0420 Congress: ECR 2013 Type: Authors: Keywords: DOI: Scientific Exhibit M. Klontzas, I. Akoumianakis, I. Vagios, A. H.
Medial tibial condyle friction syndrome: MRI study of a new entity Poster No.: C-0420 Congress: ECR 2013 Type: Authors: Keywords: DOI: Scientific Exhibit M. Klontzas, I. Akoumianakis, I. Vagios, A. H.
Imaging the Knee 17/10/2017. Friction syndrome Common in runners or cyclists Fluid between ITB and Lateral femoral condyle
 17/10/2017 Imaging the Knee Alicia M. Yochum RN, DC, DACBR, RMSK Iliotibial Band Syndrome Ligamentous Tears (ACL, PCL, MCL, LCL) Meniscal Tears Cartilage Degeneration Quadriceps/Patellar tendinosis Osteochondral
17/10/2017 Imaging the Knee Alicia M. Yochum RN, DC, DACBR, RMSK Iliotibial Band Syndrome Ligamentous Tears (ACL, PCL, MCL, LCL) Meniscal Tears Cartilage Degeneration Quadriceps/Patellar tendinosis Osteochondral
Clinical Presentation. Medial or Lateral Focal Swelling Consider meniscal Cysts. Click for more info. Osteoarthritis confirmed. Osteoarthritis pathway
 Focal Knee Swelling Information for GPs who refer into PAH Spinal and knee MRIs should only be requested as a pre-cursor to surgery. Clinical Presentation If you think a patient requires an MRI as there
Focal Knee Swelling Information for GPs who refer into PAH Spinal and knee MRIs should only be requested as a pre-cursor to surgery. Clinical Presentation If you think a patient requires an MRI as there
The Knee. Prof. Oluwadiya Kehinde
 The Knee Prof. Oluwadiya Kehinde www.oluwadiya.sitesled.com The Knee: Introduction 3 bones: femur, tibia and patella 2 separate joints: tibiofemoral and patellofemoral. Function: i. Primarily a hinge joint,
The Knee Prof. Oluwadiya Kehinde www.oluwadiya.sitesled.com The Knee: Introduction 3 bones: femur, tibia and patella 2 separate joints: tibiofemoral and patellofemoral. Function: i. Primarily a hinge joint,
Structural predictors of response to intra-articular steroid injection in symptomatic knee osteoarthritis
 Maricar et al. Arthritis Research & Therapy (2017) 19:88 DOI 10.1186/s13075-017-1292-2 RESEARCH ARTICLE Open Access Structural predictors of response to intra-articular steroid injection in symptomatic
Maricar et al. Arthritis Research & Therapy (2017) 19:88 DOI 10.1186/s13075-017-1292-2 RESEARCH ARTICLE Open Access Structural predictors of response to intra-articular steroid injection in symptomatic
MRI KNEE WHAT TO SEE. Dr. SHEKHAR SRIVASTAV. Sr.Consultant KNEE & SHOULDER ARTHROSCOPY
 MRI KNEE WHAT TO SEE Dr. SHEKHAR SRIVASTAV Sr.Consultant KNEE & SHOULDER ARTHROSCOPY MRI KNEE - WHAT TO SEE MRI is the most accurate and frequently used diagnostic tool for evaluation of internal derangement
MRI KNEE WHAT TO SEE Dr. SHEKHAR SRIVASTAV Sr.Consultant KNEE & SHOULDER ARTHROSCOPY MRI KNEE - WHAT TO SEE MRI is the most accurate and frequently used diagnostic tool for evaluation of internal derangement
Correspondence should be addressed to Thomas Kurien;
 Case Reports in Orthopedics Volume 2016, Article ID 6043497, 5 pages http://dx.doi.org/10.1155/2016/6043497 Case Report Resection and Resolution of Bone Marrow Lesions Associated with an Improvement of
Case Reports in Orthopedics Volume 2016, Article ID 6043497, 5 pages http://dx.doi.org/10.1155/2016/6043497 Case Report Resection and Resolution of Bone Marrow Lesions Associated with an Improvement of
Unusual Lateral Presentation of Popliteal Cyst
 Unusual Lateral Presentation of Popliteal Cyst Tarek Hemmali,* Abstract: The most common cyst occurs in the popliteal region is the popliteal cyst and over the past years it has been received much clinical
Unusual Lateral Presentation of Popliteal Cyst Tarek Hemmali,* Abstract: The most common cyst occurs in the popliteal region is the popliteal cyst and over the past years it has been received much clinical
Take Pride in Performance
 2017 Take Pride in Performance Knee: Meniscal Tear FSE PD - Sagittal FSE PD - Coronal FSTIR - Coronal Knee: ACL Tibial Avulsion 3D SHARC ISO - Sagittal FSE PD - Sagittal FSTIR - Coronal Knee: Subchondral
2017 Take Pride in Performance Knee: Meniscal Tear FSE PD - Sagittal FSE PD - Coronal FSTIR - Coronal Knee: ACL Tibial Avulsion 3D SHARC ISO - Sagittal FSE PD - Sagittal FSTIR - Coronal Knee: Subchondral
Knee: Cruciate Ligaments
 72 Knee: Cruciate Ligaments R. Kent Sanders Sagittal oblique 2.5-mm sequences along the plane of the anterior cruciate ligament (ACL) typically yield three to four images of the ACL, with the first medial
72 Knee: Cruciate Ligaments R. Kent Sanders Sagittal oblique 2.5-mm sequences along the plane of the anterior cruciate ligament (ACL) typically yield three to four images of the ACL, with the first medial
Comparative study of high resolusion ultrasonography and magnetic resonance imaging in diagnosing traumatic knee injuries & pathologies
 Original article: Comparative study of high resolusion ultrasonography and magnetic resonance imaging in diagnosing traumatic knee injuries & pathologies Dr. Rakesh Gujjar*, Dr. R. P. Bansal, Dr. Sandeep
Original article: Comparative study of high resolusion ultrasonography and magnetic resonance imaging in diagnosing traumatic knee injuries & pathologies Dr. Rakesh Gujjar*, Dr. R. P. Bansal, Dr. Sandeep
Knee Contusions and Stress Injuries. Laura W. Bancroft, M.D.
 Knee Contusions and Stress Injuries Laura W. Bancroft, M.D. Objectives Review 5 types of contusion patterns Pivot shift Dashboard Hyperextension Clip Lateral patellar dislocation Demonstrate various stress
Knee Contusions and Stress Injuries Laura W. Bancroft, M.D. Objectives Review 5 types of contusion patterns Pivot shift Dashboard Hyperextension Clip Lateral patellar dislocation Demonstrate various stress
PRE & POST OPERATIVE RADIOLOGICAL ASSESSMENT IN TOTAL KNEE REPLACEMENT. Dr. Divya Rani K 2 nd Year Resident Dept. of Radiology
 PRE & POST OPERATIVE RADIOLOGICAL ASSESSMENT IN TOTAL KNEE REPLACEMENT Dr. Divya Rani K 2 nd Year Resident Dept. of Radiology PRE OPERATIVE ASSESSMENT RADIOGRAPHS Radiographs are used for assessment and
PRE & POST OPERATIVE RADIOLOGICAL ASSESSMENT IN TOTAL KNEE REPLACEMENT Dr. Divya Rani K 2 nd Year Resident Dept. of Radiology PRE OPERATIVE ASSESSMENT RADIOGRAPHS Radiographs are used for assessment and
Evaluation and Treatment of Knee Arthritis Classification of Knee Arthritis Osteoarthritis Osteoarthritis Osteoarthritis of Knee
 1 2 Evaluation and Treatment of Knee Arthritis John Zebrack, MD Reno Orthopaedic Clinic Classification of Knee Arthritis Non-inflammatory Osteoarthritis Primary Secondary Post-traumatic, dysplasia, neuropathic,
1 2 Evaluation and Treatment of Knee Arthritis John Zebrack, MD Reno Orthopaedic Clinic Classification of Knee Arthritis Non-inflammatory Osteoarthritis Primary Secondary Post-traumatic, dysplasia, neuropathic,
To evaluate the role of high resolution ultrasonography in diagnosis of knee osteoarthritis
 2018; 4(1): 69-76 ISSN: 2395-1958 IJOS 2018; 4(1): 69-76 2018 IJOS www.orthopaper.com Received: 01-11-2017 Accepted: 02-12-2017 Ravikant Jain HOD and Prof, Dept of orthopaedics, SAMC & PGI, Indore, Madhya
2018; 4(1): 69-76 ISSN: 2395-1958 IJOS 2018; 4(1): 69-76 2018 IJOS www.orthopaper.com Received: 01-11-2017 Accepted: 02-12-2017 Ravikant Jain HOD and Prof, Dept of orthopaedics, SAMC & PGI, Indore, Madhya
Extraarticular Lateral Ankle Impingement
 Extraarticular Lateral Ankle Impingement Poster No.: C-1282 Congress: ECR 2016 Type: Educational Exhibit Authors: C. Cevikol; Keywords: Trauma, Diagnostic procedure, MR, CT, Musculoskeletal system, Musculoskeletal
Extraarticular Lateral Ankle Impingement Poster No.: C-1282 Congress: ECR 2016 Type: Educational Exhibit Authors: C. Cevikol; Keywords: Trauma, Diagnostic procedure, MR, CT, Musculoskeletal system, Musculoskeletal
Musculoskeletal MR Protocols
 Musculoskeletal MR Protocols Joint-based protocols MSK 1: Shoulder MRI MSK 1A: Shoulder MR arthrogram MSK 1AB: Shoulder MR arthrogram (instability protocol) MSK 2: Elbow MRI MSK 2A: Elbow MR arthrogram
Musculoskeletal MR Protocols Joint-based protocols MSK 1: Shoulder MRI MSK 1A: Shoulder MR arthrogram MSK 1AB: Shoulder MR arthrogram (instability protocol) MSK 2: Elbow MRI MSK 2A: Elbow MR arthrogram
Magnetic resonance imaging in knee synovitis: Clinical utility in differentiating asymptomatic and symptomatic meniscal tears
 bs_bs_banner Journal of Medical Imaging and Radiation Oncology 59 (2015) 1 6 RADIOLOGY REVIEW ARTICLE Magnetic resonance imaging in knee synovitis: Clinical utility in differentiating asymptomatic and
bs_bs_banner Journal of Medical Imaging and Radiation Oncology 59 (2015) 1 6 RADIOLOGY REVIEW ARTICLE Magnetic resonance imaging in knee synovitis: Clinical utility in differentiating asymptomatic and
Participation in Adults Post Total Knee Replacement
 Participation in Adults Post Total Knee Replacement Jessica Maxwell, PT, DPT, OCS Boston University College of Health and Rehabilitation Sciences: Sargent College Boston University Medical Center Learning
Participation in Adults Post Total Knee Replacement Jessica Maxwell, PT, DPT, OCS Boston University College of Health and Rehabilitation Sciences: Sargent College Boston University Medical Center Learning
MY PATIENT HAS KNEE PAIN. David Levi, MD Chief, Division of Musculoskeletal l limaging Atlantic Medical Imaging
 MY PATIENT HAS KNEE PAIN David Levi, MD Chief, Division of Musculoskeletal l limaging Atlantic Medical Imaging Causes of knee pain Non traumatic Trauma Osteoarthritis Patellofemoral pain Menisci or ligaments
MY PATIENT HAS KNEE PAIN David Levi, MD Chief, Division of Musculoskeletal l limaging Atlantic Medical Imaging Causes of knee pain Non traumatic Trauma Osteoarthritis Patellofemoral pain Menisci or ligaments
Other Culprits in Knee Dysfunction
 Unraveling the Mystery of Knee Pain #6: Other Culprits in Knee Dysfunction 1 Webinar Goals Explore the assessment and treatment of other culprits in knee dysfunction. 2 Time: 60 minutes Schedule: Logistics
Unraveling the Mystery of Knee Pain #6: Other Culprits in Knee Dysfunction 1 Webinar Goals Explore the assessment and treatment of other culprits in knee dysfunction. 2 Time: 60 minutes Schedule: Logistics
Elevated tibiofemoral articular contact stress predicts risk for bone marrow lesions and cartilage damage at 30 months
 Osteoarthritis and Cartilage 20 (2012) 1120e1126 Elevated tibiofemoral articular contact stress predicts risk for bone marrow lesions and cartilage damage at 30 months N.A. Segal yzx *, A.M. Kern yk, D.D.
Osteoarthritis and Cartilage 20 (2012) 1120e1126 Elevated tibiofemoral articular contact stress predicts risk for bone marrow lesions and cartilage damage at 30 months N.A. Segal yzx *, A.M. Kern yk, D.D.
Imaging Modalities: Clinical Reasoning and Key Instructional Elements: Radiography
 Imaging Modalities: Clinical Reasoning and Key Instructional Elements: Radiography Michael D. Ross, PT, DHSc, OCS mross@daemen.edu Disclosure No relevant financial relationship exists Objectives Determine
Imaging Modalities: Clinical Reasoning and Key Instructional Elements: Radiography Michael D. Ross, PT, DHSc, OCS mross@daemen.edu Disclosure No relevant financial relationship exists Objectives Determine
Andrew J Grainger Leeds, UK
 Andrew J Grainger Leeds, UK Osteoarthri6s (OA) How do we diagnose OA of the knee at MRI? What associated features do we see? Why do they maeer? When is it not OA? We think we have a clear understanding
Andrew J Grainger Leeds, UK Osteoarthri6s (OA) How do we diagnose OA of the knee at MRI? What associated features do we see? Why do they maeer? When is it not OA? We think we have a clear understanding
UCLA UCLA Previously Published Works
 UCLA UCLA Previously Published Works Title MR-IMAGING OF TIBIAL COLLATERAL LIGAMENT INJURY - COMPARISON WITH CLINICAL EXAMINATION Permalink https://escholarship.org/uc/item/2bs9g934 Journal SKELETAL RADIOLOGY,
UCLA UCLA Previously Published Works Title MR-IMAGING OF TIBIAL COLLATERAL LIGAMENT INJURY - COMPARISON WITH CLINICAL EXAMINATION Permalink https://escholarship.org/uc/item/2bs9g934 Journal SKELETAL RADIOLOGY,
DISCLOSURES. T. McAlindon: Samumed, grant/research support; Astellas, Flexion, Pfizer, Regeneron, Samumed,and Seikugaku, consulting
 Radiographic Outcomes from a Randomized, Double- Blind, Placebo-Controlled, Phase 2 Study of a Novel, Intra-Articular, Wnt Pathway Inhibitor (SM04690) for the Treatment of Osteoarthritis of the Knee: Week
Radiographic Outcomes from a Randomized, Double- Blind, Placebo-Controlled, Phase 2 Study of a Novel, Intra-Articular, Wnt Pathway Inhibitor (SM04690) for the Treatment of Osteoarthritis of the Knee: Week
ORIGINAL ARTICLE. ROLE OF MRI IN EVALUATION OF TRAUMATIC KNEE INJURIES Saurabh Chaudhuri, Priscilla Joshi, Mohit Goel
 ROLE OF MRI IN EVALUATION OF TRAUMATIC KNEE INJURIES Saurabh Chaudhuri, Priscilla Joshi, Mohit Goel 1. Associate Professor, Department of Radiodiagnosis & imaging, Bharati Vidyapeeth Medical College and
ROLE OF MRI IN EVALUATION OF TRAUMATIC KNEE INJURIES Saurabh Chaudhuri, Priscilla Joshi, Mohit Goel 1. Associate Professor, Department of Radiodiagnosis & imaging, Bharati Vidyapeeth Medical College and
D. Doré 1, C. Ding 1,2, J.P. Pelletier 3, J. Martel-Pelletier 3, F. Cicuttini 2, G. Jones 1.
 Responsiveness of qualitative and quantitative MRI measures over 2.7 years D. Doré 1, C. Ding 1,2, J.P. Pelletier 3, J. Martel-Pelletier 3, F. Cicuttini 2, G. Jones 1. 1 Menzies Research Institute Tasmania,
Responsiveness of qualitative and quantitative MRI measures over 2.7 years D. Doré 1, C. Ding 1,2, J.P. Pelletier 3, J. Martel-Pelletier 3, F. Cicuttini 2, G. Jones 1. 1 Menzies Research Institute Tasmania,
Meniscus body position and its change over four years in asymptomatic adults: a cohort study using data from the Osteoarthritis Initiative (OAI)
 Bruns et al. BMC Musculoskeletal Disorders 2014, 15:32 RESEARCH ARTICLE Open Access Meniscus body position and its change over four years in asymptomatic adults: a cohort study using data from the Osteoarthritis
Bruns et al. BMC Musculoskeletal Disorders 2014, 15:32 RESEARCH ARTICLE Open Access Meniscus body position and its change over four years in asymptomatic adults: a cohort study using data from the Osteoarthritis
Post-injury painful and locked knee
 H R J Post-injury painful and locked knee, p. 54-59 Clinical Case - Test Yourself Musculoskeletal Imaging Post-injury painful and locked knee Ioannis I. Daskalakis 1, 2, Apostolos H. Karantanas 1, 2 1
H R J Post-injury painful and locked knee, p. 54-59 Clinical Case - Test Yourself Musculoskeletal Imaging Post-injury painful and locked knee Ioannis I. Daskalakis 1, 2, Apostolos H. Karantanas 1, 2 1
Intraosseous Bio Filler. Surgical Technique
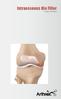 Intraosseous Bio Filler Surgical Technique Intraosseous Bio Filler Surgical Technique Introduction The Intraosseous Bio Filler technique is the treatment of bone pathologies resulting from acute or chronic
Intraosseous Bio Filler Surgical Technique Intraosseous Bio Filler Surgical Technique Introduction The Intraosseous Bio Filler technique is the treatment of bone pathologies resulting from acute or chronic
Ultrasound Guided Genicular Nerve Block-A Motor Sparing Technique for the Treatment of Acute and Chronic Knee Pain
 International Journal of Anesthesiology Research, 2015, 3, 37-43 37 Ultrasound Guided Genicular Nerve Block-A Motor Sparing Technique for the Treatment of Acute and Chronic Knee Pain Michael Meng 1, Reid
International Journal of Anesthesiology Research, 2015, 3, 37-43 37 Ultrasound Guided Genicular Nerve Block-A Motor Sparing Technique for the Treatment of Acute and Chronic Knee Pain Michael Meng 1, Reid
What is the most effective MRI specific findings for lateral meniscus posterior root tear in ACL injuries
 What is the most effective MRI specific findings for lateral meniscus posterior root tear in ACL injuries Kazuki Asai 1), Junsuke Nakase 1), Kengo Shimozaki 1), Kazu Toyooka 1), Hiroyuki Tsuchiya 1) 1)
What is the most effective MRI specific findings for lateral meniscus posterior root tear in ACL injuries Kazuki Asai 1), Junsuke Nakase 1), Kengo Shimozaki 1), Kazu Toyooka 1), Hiroyuki Tsuchiya 1) 1)
2 A B Fig. 1. Lateral tibial condyle fracture with joint effusion in a 35-year-old man. Sagittal T2-weighted MRI shows a large amount of effusion
 1 2 1 1 1 2 A B Fig. 1. Lateral tibial condyle fracture with joint effusion in a 35-year-old man. Sagittal T2-weighted MRI shows a large amount of effusion (between arrowheads) in the suprapatellar pouch,
1 2 1 1 1 2 A B Fig. 1. Lateral tibial condyle fracture with joint effusion in a 35-year-old man. Sagittal T2-weighted MRI shows a large amount of effusion (between arrowheads) in the suprapatellar pouch,
RESEARCH. Association between radiographic features of knee osteoarthritis and pain: results from two cohort studies
 1 Clinical Epidemiology Research and Training Unit, Boston University School of Medicine, 650 Albany Street, Boston, MA 02118, USA 2 Department of Epidemiology and Biostatistics, University of California
1 Clinical Epidemiology Research and Training Unit, Boston University School of Medicine, 650 Albany Street, Boston, MA 02118, USA 2 Department of Epidemiology and Biostatistics, University of California
What s your diagnosis?
 Case Study 58 A 61-year-old truck driver man presented with a valgus injury to the left knee joint when involved in a truck accident. What s your diagnosis? Diagnosis : Avulsion of Deep MCL The medial
Case Study 58 A 61-year-old truck driver man presented with a valgus injury to the left knee joint when involved in a truck accident. What s your diagnosis? Diagnosis : Avulsion of Deep MCL The medial
Knee Joint Assessment and General View
 Knee Joint Assessment and General View Done by; Mshari S. Alghadier BSc Physical Therapy RHPT 366 m.alghadier@sau.edu.sa http://faculty.sau.edu.sa/m.alghadier/ Functional anatomy The knee is the largest
Knee Joint Assessment and General View Done by; Mshari S. Alghadier BSc Physical Therapy RHPT 366 m.alghadier@sau.edu.sa http://faculty.sau.edu.sa/m.alghadier/ Functional anatomy The knee is the largest
In comparison to anterior and lateral knee pain, chronic. Semimembranosus Tendinopathy: One Cause of Chronic Posteromedial Knee Pain.
 [ Primary Care ] Semimembranosus Tendinopathy: One Cause of Chronic Posteromedial Knee Pain William E. Bylund, BS,* and Kevin de Weber, MD Context: Semimembranosus tendinopathy (SMT) is an uncommon cause
[ Primary Care ] Semimembranosus Tendinopathy: One Cause of Chronic Posteromedial Knee Pain William E. Bylund, BS,* and Kevin de Weber, MD Context: Semimembranosus tendinopathy (SMT) is an uncommon cause
Are radiographs needed when MR imaging is performed for non-acute knee symptoms in patients younger than 45 years of age?
 Skeletal Radiol (2007) 36:1129 1139 DOI 10.1007/s00256-007-0384-5 SCIENTIFIC ARTICLE Are radiographs needed when MR imaging is performed for non-acute knee symptoms in patients younger than 45 years of
Skeletal Radiol (2007) 36:1129 1139 DOI 10.1007/s00256-007-0384-5 SCIENTIFIC ARTICLE Are radiographs needed when MR imaging is performed for non-acute knee symptoms in patients younger than 45 years of
