Rehabilitation Guidelines for Hip Arthroscopy Procedures
|
|
|
- Gillian Clark
- 5 years ago
- Views:
Transcription
1 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Hip Arthroscopy Procedures The hip joint is composed of the femur (the thigh bone), and the acetabulum (the socket which is from the three pelvic bones). The hip joint is a ball and socket joint that not only allows flexion and extension, but also rotation of the thigh and leg. Unlike the shoulder, however, stability is not sacrificed for mobility. The head of the femur is encased by the socket, and with the addition of the strong, noncompliant joint capsule, the hip is an extremely stable joint. Because the hip is responsible for transmitting the weight of the upper body to the lower extremities, the joint is subjected to substantial forces. Walking transmits 1.3 to 5.8 times body weight through the joint, and running and jumping can generate forces across the joint equal to 6 to 8 times body weight. The labrum is a circular, fibrocartilaginous structure that surrounds the socket. It functions to seal the joint, enhance stability, and provide proprioceptive feedback (tells hip joint position) to the brain and central nervous system. The labrum acts as a suction seal or gasket for the hip joint. This helps to maintain the hydrostatic pressure that protects the articular cartilage on the head of the femur and the acetabulum. The iliopsoas tendon connects the fibers of the psoas major and ililacus muscles to the proximal femur (lesser trochanter). Painful snapping of Lunate surface of acetabulum Neck of femur Articular cartilage Head of femur Greater trochanter Intertrochanteric line Round ligament (ligamentum capitis) Figure 1 Hip joint (opened) lateral view this tendon can occur during flexion and extension of the hip when the tendon pops over a bony prominence (iliopectineal eminence) that is located in the area of the anterior hip joint. The pain and snapping may be very similar to that which occurs with labral tears. Hip joints of athletes are exposed to extremes of motion, and these forces are absorbed by and can injure the labrum. It is currently thought that the labrum may also be injured by impingement of the hip. This is referred to as femoroacetabular Impingement (FAI). FAI can occur from changes in the shape of the acetabulum or the femoral head and neck. FAI due to Anterior superior iliac spine Anterior inferior iliac spine Iliopubic eminence Acetabular labrum (fibrocartilainous) Fat in acetabular fossa (covered by synovial) Obturator artery Anterior branch of obturator artery Posterior branch of obturator artery Obturator membrane Ischial tuberosity Acetabular artery Lesser trochanter Transverse acetabular ligament over-coverage of the acetabulum is referred to as pincer impingement. FAI due to a lack of the normal femoral head-neck off-set, or lack of femoral head roundness, is referred to as cam impingement. Figure 2 demonstrates the boney abnormality associated with cam impingement of the right hip; note the difference in the shape of the femoral head. Often times, cam and pincer impingement can co-exist. When the normal convex on concave (or ball and socket) geometry is lost, impingement may occur as the hip is flexed toward its end range. This is often accentuated with adduction and internal rotation. Repetitive impingement can cause labral tears and The world class health care team for the UW Badgers and proud sponsor of UW Athletics
2 delamination of the acetabular articular cartilage. Labral tears may cause a sharp catching pain, popping, and a sensation of locking of the hip (mechanical symptoms). Most people with this injury experience more subtle, dull, activity-induced positional pain especially if they have femoroacetabular impingement. They most often describe a deep discomfort in the anterior groin, and occasionally the pain may be directly lateral (greater trochanter area), or deep within the buttocks. Flaps from damaged articular cartilage may cause mechanical symptoms but most often they will cause pain during or after weight bearing and impact activities, such as running and jumping. Non-operative treatment of painful labral tears usually is not successful. However, 25% of individuals over the age of 50 have labral tears seen on MRIs, but no symptoms. Thus, arthroscopic treatment of a labral tear is only indicated when appropriate clinical tests and imaging studies have documented that the hip pain is due to the labral tear. Labral tears can be treated by partial resection or repair. If indicated, labral repair is preferred as it attempts to restore the normal suction seal of the hip joint. If the tear is too small or the quality of the injured tissue is too poor, repairs are not performed. Both of these procedures can be done arthroscopically. Hip arthroscopy is performed on an outpatient basis under general anesthesia. The hip to be operated upon is placed in traction to open up the hip joint enough to allow for the insertion of the instruments. After marking out Figure 2: Frog leg radiograph: The thin arrow on your left indicates the area of flattening of the right femoral head and lack of the normal femoral head-neck offset. The thick arrow on the right indicates the more normal, rounded contour of the left femoral head. the anatomical landmarks with X-ray guidance, three to four small incisions are made in the area of the hip joint. One of these incisions is used to insert a camera that displays the inside of the hip joint on a television monitor, and the other incisions are used to insert the surgical instruments used for excising labral tears, debriding defective cartilage, removing bone spurs, and removing loose bodies. Hip arthroscopy is also used to treat the hip pain and mechanical symptoms caused by a number of other conditions including: loose bodies; iliopsoas snapping; hip instability; hip abductor muscle-tendon tears; chondral lesions; ligamentum teres tears; and femoroacetabular impingement (FAI). When treating FAI, a burr is used to reshape the femoral head-neck offset. This is called a proximal femoral osteoplasty. The goal is to restore the Figure 3: T2 MR image showing abductor tendon tears (yellow arrows) at the greater trochanter of the femur. normal convex on concave relationship (ball on socket) so that the hip can move through the full range of motion without impingement. To treat chondral lesions, a microfracture technique may be performed after the damaged articular cartilage is removed. This is done by creating small holes in the subchondral bone of the defect to promote the inflow of blood and stem cell in the hopes that these elements will lead to the growth of Iliopsoas muscle-tendon Bursa fibrocartilage to fill the chondral defect. Although the fibrocartilage is not as strong as the original hyaline cartilage, it does act to create continuity of the surface. Using the arthroscopic instruments, the peripheral hip joint (the space outside of the socket part of the hip joint) can be visualized and thus, FAI can be arthroscopically treated. The peritrochanteric (greater trochanteric bursa) area of the hip joint also can be visualized, and this advance in hip arthroscopy has allowed for the repair of hip abductor (gluteus medius and minimus) tendon tears. Figure 3 shows an image of an abductor tendon tear. Suture anchors are placed in the greater tuberosity, and then the sutures are passed through the torn tendon and the tendons are re-approximated to their anatomic location on the femur. Pelvic bone Figure 4: Diagram of the iliopsoas muscle-tendon and bursa. Image copyright 2001, Martin Dunitz, Ltd. Spine Iliopectineal bursa Femur This is similar to a rotator cuff repair in the shoulder. In order to allow the tendon to heal back to the bone after this procedure, weight bearing and strengthening exercises will be more protected and limited in the first postoperative rehabilitation phase. Iliopsoas tendon injuries are another source of anterior hip pain. Most often they are they are caused by an acute injury, and less commonly, the result of repetitive trauma. The iliopsoas can snap over the iliopectineal eminence and bursae (Figure 4). The painful snapping usually is audible and associated with a sensation of snapping and hip pain. However, anterior hip pain due to iliopsoas bursitis and tendonitis may occur without snapping of the tendon. It should be noted that asymptomatic snapping is not uncommon in hypermobile athletes. Non-operative treatment (physical therapy and psoas bursa injections) is successful in getting almost two thirds of patients with painful snapping hips back to full activity. When these measures fail, an arthroscopic release of the iliopsoas tendon often is performed and does provide long-term relief of the snapping and pain. Rehabilitation of the hip begins the day after surgery. The rehabilitation guidelines are presented in a criterionbased progression, and each patient will progress at a different rate depending on the specific procedure performed, age, pre-injury health status, and rehab compliance. The patient may also have postoperative hip and thigh pain which can slow the recovery rate. This can be caused by traction on the hip during surgery. There may also be reflex inhibition and poor control of the muscles that stabilize the hip from the traction and from penetration of the hip joint with the arthroscopic instruments. It is very important to use crutches for the first week or two after surgery in order to minimize abnormal forces on the back and pelvic joints while developing muscle coordination and strength to support the hip and to achieve a normal gait pattern. This is especially important with iliopsoas tendon release, as hip flexors are significantly weakened for two to six weeks after surgery. All exercises should be performed within pain tolerance. Pushing to extremes of motion beyond pain tolerance does not enhance function but rather increases discomfort and prolongs rehabilitation. 2 3
3 Basic Rehabilitation Principals: 1. Post-operative recovery begins with a preoperative educational visit for instruction, explanation, and demonstration of the postoperative rehab program. 2. and limitations during Phase I of the post-operative rehabilitation will be determined by which arthroscopic procedures are performed, since not all arthroscopies are the same. Post-operative weight bearing status will not be based on hip pain alone. Although the discomfort after hip arthroscopy may be surprisingly little, there often is a significant amount of reflex inhibition and poor muscle firing due to the penetration of the hip with the arthroscopic instruments and the large amount of traction applied to the hip during the arthroscopy. Weight bearing may also be limited to allow for healing to occur. Consequently, crutches or other assistive devices should be used until guidance from your physician or physical therapist allows you to discontinue them. 3. Active assistive range of motion exercises are begun early (the first 1-7 days after surgery), but maximum motion in any plane is determined by where the patient feels discomfort, and stretching should only be pushed to tolerance. Pushing to extremes of motion does not enhance function, and will increase discomfort and prolong rehabilitation. Similar to weight bearing status, there may be some procedures that limit the extent of range of motion to allow appropriate healing. 4. Muscle strengthening exercises are to be performed during the first week after surgery, but progressive strengthening depends upon the patient s tolerance. Patients should avoid exercises that engage the iliopsoas during the first several weeks after surgery. Iliopsoas tendonitis is a known side effect of hip arthroscopy but can be avoided with appropriate post-operative care, including avoiding exercises that have high activity of the iliopsoas (such as straight leg raises, resisted hip flexion, abductor strengthening that incorporates significant co-contraction). 6 If the patient had an abductor repair, abductor strengthening will be limited early in the rehab process to allow the tendon to heal back to the bone. PHASE I (Surgery to 3-6 weeks) Labral Excision and Debridement, and Labral Repair (Including Osteoplasty for FAI) Iliopsoas Release (With or Without Ischiofemoral Impingement Osteoplasty) First rehabilitation appointment should be 3 to 5 days after surgery, 1 to 2 times per week thereafter Protection of the post-surgical hip through limited weight bearing and education on avoiding pain (approximately 3/10) with range of motion exercises Restore normal hip range of motion Normalize gait Restore leg control Use axillary crutches for normal gait. Begin with toe touch weight bearing and progress to lbs. in second week. Wean from crutches slowly when gait is normalized and pain free (without pain medications), which normally takes 2 to 3 weeks Avoid active hip flexion past 90 and avoid passive range of motion that causes any pinching type pain Avoid exercises that engage the iliopsoas during the first several weeks after surgery. Iliopsoas tendonitis is a known side effect of hip arthroscopy but can be avoided with appropriate post-operative care, including avoiding exercises that have high activity of the iliopsoas (such as straight leg raises, resisted hip flexion,abductor strengthening that incorporates significant co-contraction)6 Avoid passive unilateral extension for 3 weeks (prone lying and prone on elbows is okay) Avoid extremes of external rotation for 3 weeks Limit abduction to 45 degrees for 2 weeks Use axillary crutches until normal gait and hip flexor muscle function is achieved (without pain medications) and wean from crutches slowly when gait is normalized and pain free (without pain medications), which normally takes 3 to 6 weeks Do not do straight leg raises to avoid irritation of the released tendon as it scars down Avoid pushing motion to approximately 3/10 pain in any plane, and have patient keep pain at less than approximately 3/10 with stretches Microfracture Abductor Repair Touch down weight bearing with axillary crutches x 4 to 6 weeks Avoid hip flexion past 90 for 2 weeks Avoid impact exercises and activities for 12 weeks NOTE: The precautions will depend on the size and location of the area undergoing the microfracture procedure No active abduction x 6 weeks Partial weight bearing with crutches x 4 to 6 weeks 4 5
4 Range of Motion Exercises Therapeutic Exercises Cardiovascular Progression Criteria Active assistive range of motion and passive range of motion of hip in all planes. Note: Microfracture patients should do multiple hours of active assistive range of motion/passive range of motion exercises each day to help align developing fibrocartilage Gentle hip mobilization and distraction techniques: a. prone pendulum (stomach lying IR/ER) b. standing stool rotations c. Straight plane distraction, force applied to lower leg d. Inferior glide (patient supine, hip & knee at 90º) force on anterosuperior thigh e. Posterior glide (patient supine, hip & 90º) force applied through knee and/or quadruped rocking Day of surgery begin isometric quadriceps, glut, hamstring, hip adductor and hip abductor muscle strengthening sets Gait activities (marching, heel-toe rocking, sidestepping) may utilize pool for gait activities once the portal sites are healed Isometric hip flexion, extension, abduction, adduction, internal rotation, and external rotation Weight shifting progressing to balance exercises with double limb support balance activities to improve proprioception and weight acceptance Standing hip abduction and extension (no active hip abduction with hip abductor repairs) Double leg bridging Sidelying leg raises with leg in internal rotation (no active hip abduction with hip abductor repairs) Prone heel squeezes with hip extension Active range of motion without resistance (starting with short arc movements progressing to full arc) Start strengthening short external rotators with isometric and short arc movements Stomach lying on elbows for gentle anterior hip stretch A continuous passive motion machine may be used after microfracture procedures NOTE: Avoid straight leg raises as the long lever arm can cause significant forces across the anterior hip and is often irritating when performed in the first 6 weeks after surgery. When selecting exercises above they must still fall within the precautions of range of motion and weight bearing Upper body circuit training or upper body ergometry (UBE) Normal gait without assistive device on level indoor surfaces with full weight bearing and minimal to no pain Good leg control at low velocity of movement Functional range of motion without pain At least 3 weeks post-op (Must stay in phase 1 for 6 weeks if a microfracture was performed) PHASE II (begin after meeting phase I criteria, time on crutches and limited range of motion varies with the procedure performed, about 4-6 weeks) Therapeutic Exercises Cardiovascular Exercise Progression Criteria Rehabilitation based on patient progress, 1 to 2 times every 1 to 2 weeks Regain and improve muscular strength Progress off crutches for all surfaces and distances Single leg stand control Good control and no pain with functional movements, including step up/down, squat, partial lunge Post-activity soreness should resolve within 24 hours No ballistic or forced stretching Avoid post-activity swelling or muscle weakness Be cautious with repetitive hip flexion activities, such as treadmill and Stairmaster Patients undergoing microfracture continue the microfracture precautions on page 5 Stationary bike Gait and functional movement drills in the pool once portal sites are healed Continue standing hip abduction and extension, single leg bridging, sidelying leg raises with leg in internal rotation and prone heel squeezes with hip extension Non-impact hip and core strengthening body boards, bridging (progressing from double to single leg), mini band drills, Swiss ball drills Non-impact balance (progressing to single leg) and proprioceptive drills Half kneeling progression: stability, to reaching, to rotation, to resisted rotation. Shuttle leg press Quadriceps strengthening Hip active range of motion using D1 and D2 patterns with proprioceptive neuromuscular facilitation Stretching for patient specific muscle imbalances Non-impact endurance training; stationary bike, Nordic track, swimming, deep water run, cross trainer Normal gait on all surfaces Ability to carry out functional movements without unloading affected leg or pain, while demonstrating good control Single leg balance greater than 15 seconds PHASE III (begin after meeting phase II criteria, about weeks) Rehabilitation based on patient progress, 1 to 2 times every 1 to 2 weeks Improve muscular strength and endurance Good control and no pain with sport and work specific movements, including impact activities 6 7
5 Therapeutic Exercise Cardiovascular Exercise Return To Sport/Work Criteria Post-activity soreness should resolve within 24 hours No ballistic or forced stretching Avoid post-activity swelling or muscle weakness Be cautious with repetitive hip flexion activities, such as treadmill and Stairmaster Patients undergoing microfracture continue the microfracture precautions on page 5 Multi-planar strength progression, including forward, lateral and diagonal lunges Impact control exercises beginning 2 feet to 2 feet, progressing from 1 foot to other and then 1 foot to same foot then progress from single plane drills to multi-plane drills Dynamic control exercise beginning with low velocity, single plane activities and progressing to higher velocity, multi-plane activities May use agility ladder Progress to running program once patient is able to demonstrate good single leg landing control in a repetitive fashion without pain Begin sport specific drills once patient demonstrates good control with the impact control and multi-plane exercises and can tolerate running program without pain Sport/work specific balance and proprioceptive drills Hip and core strengthening Stretching for patient specific muscle imbalances Replicate sport or work specific energy demands Normal gait on all surfaces Dynamic neuromuscular control with multi-plane activities, without pain or swelling These rehabilitation guidelines were developed collaboratively by Marc Sherry, PT, LAT, CSCS (msherry@uwhealth.org), Joe Tupta, PT (jtupta@uwhealth.org), Melissa Fischer, PT (mfischer@uwhealth.org) and the UW Health Sports Medicine physician group. Updated 10/2016 REFERENCES 1. Enseki KR, Martin RL, Draovitch P, Kelly BT, Philippon MJ, Schenker ML. The hip joint: arthroscopic procedures and postoperative rehabilitation. J Orthop Sports Phys Ther. Jul 2006;36(7): Larson, CM and Giveans. Arthroscopic management of femoroacetabular impingement: early outcomes measures. Arthroscopy. May 2008;24(5): Schmerl M, Pollard H, Hoskins W. Labral injuries of the hip: a review of diagnosis and management. J Manipulative Physiol Ther. Oct 2005;28(8): Stalzer S, Wahoff M, Scanlan M. Rehabilitation following hip arthroscopy. Clin Sports Med. Apr 2006;25(2): , x. 5. Standaert CJ, Manner PA and Herring SA. Expert Opinion and Corntroversies in Musculoskeletal and Sports Medicine: femoroacetabular impingement. Arch Phys Med Rehabil. May 2008;89: Decker MJ, Torry MR, Anstett F, Giphart JE, Wahoff M and Philippon MJ. Gluteus Medius Muscle Activation During Hip Rehabilitation Exercises. Denver, Colorado. AAOSM Meeting July 9, 2009 Research Presentation. At UW Health, patients may have advanced diagnostic and /or treatment options, or may receive educational materials that vary from this information. Please be aware that this information is not intended to replace the care or advice given by your physician or health care provider. It is neither intended nor implied to be a substitute for professional advice. Call your health provider immediately if you think you may have a medical emergency. Always seek the advice of your physician or other qualified health provider prior to starting any new treatment or with any question you may have regarding a medical condition. Copyright 2013 UW Health Sports Medicine Center 8 SM
Rehabilitation Guidelines for Hip Arthroscopy Procedures
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Hip Arthroscopy Procedures The hip joint is composed of the femur (the thigh bone), and the acetabulum (the socket which is from the three
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Hip Arthroscopy Procedures The hip joint is composed of the femur (the thigh bone), and the acetabulum (the socket which is from the three
Rehabilitation Guidelines for Open Hip Abductor (Gluteus Medius) Repair
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Open Hip Abductor (Gluteus Medius) Repair The hip joint is composed of the femur (the thigh bone) and the acetabulum (the socket which is from
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Open Hip Abductor (Gluteus Medius) Repair The hip joint is composed of the femur (the thigh bone) and the acetabulum (the socket which is from
Rehabilitation Guidelines for Meniscal Repair
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Meniscal Repair There are two types of cartilage in the knee, articular cartilage and cartilage. Articular cartilage is made up of collagen,
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Meniscal Repair There are two types of cartilage in the knee, articular cartilage and cartilage. Articular cartilage is made up of collagen,
Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction
 Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These
Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These
Rehabilitation Guidelines for Knee Arthroscopy
 Rehabilitation Guidelines for Knee Arthroscopy The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These bones are supported by a large
Rehabilitation Guidelines for Knee Arthroscopy The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These bones are supported by a large
Rehabilitation Guidelines For Periacetabular Osteotomy (PAO) Of The Hip
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines For Periacetabular Osteotomy (PAO) Of The Hip The hip joint is composed of the femur (the thigh bone) and the acetabulum (the socket formed by
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines For Periacetabular Osteotomy (PAO) Of The Hip The hip joint is composed of the femur (the thigh bone) and the acetabulum (the socket formed by
Rehabilitation Guidelines for Meniscal Repair
 Rehabilitation Guidelines for Meniscal Repair The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These bones are supported by a large
Rehabilitation Guidelines for Meniscal Repair The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These bones are supported by a large
Rehabilitation Guidelines for Knee Arthroscopy
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Knee Arthroscopy Arthroscopy is a common surgical procedure in which a joint is viewed using a small camera. This technique allows the surgeon
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Knee Arthroscopy Arthroscopy is a common surgical procedure in which a joint is viewed using a small camera. This technique allows the surgeon
Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair The knee consists of four bones that form three joints. The femur is the large bone in the thigh
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair The knee consists of four bones that form three joints. The femur is the large bone in the thigh
Rehabilitation Guidelines for Labral/Bankert Repair
 Rehabilitation Guidelines for Labral/Bankert Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
Rehabilitation Guidelines for Labral/Bankert Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
Labral Repair with a Microfracture
 Labral Repair with a Microfracture This protocol should be used as a guideline for progression and should be tailored to the needs of the individual patient. Strict protective weight bearing status for
Labral Repair with a Microfracture This protocol should be used as a guideline for progression and should be tailored to the needs of the individual patient. Strict protective weight bearing status for
Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction The knee consists of four bones that form three joints. The femur is the large bone
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction The knee consists of four bones that form three joints. The femur is the large bone
Hip Arthroscopy Protocol
 The intent of this protocol is to provide guidelines for progression of rehabilitation, it is not intended to serve as a substitute for clinical decision making. Progression through each phase of rehabilitation
The intent of this protocol is to provide guidelines for progression of rehabilitation, it is not intended to serve as a substitute for clinical decision making. Progression through each phase of rehabilitation
Rehabilitation Guidelines for Arthroscopic Capsular Shift
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Arthroscopic Capsular Shift The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a golf ball on a tee.
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Arthroscopic Capsular Shift The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a golf ball on a tee.
Travis G. - 1 Maak, - MD Sports Medicine University of Utah Orthopaedics 590 Wakara Way Salt Lake City, UT Tel: Fax:
 General Guidelines: Travis G. - 1 Maak, - MD Rehabilitation for Arthroscopic or Open Gluteus Medius Repair with or without Labral Debridement Normalize gait pattern with brace and crutches Weight-bearing:
General Guidelines: Travis G. - 1 Maak, - MD Rehabilitation for Arthroscopic or Open Gluteus Medius Repair with or without Labral Debridement Normalize gait pattern with brace and crutches Weight-bearing:
Rehabilitation Guidelines for Large Rotator Cuff Repair
 Rehabilitation Guidelines for Large Rotator Cuff Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the
Rehabilitation Guidelines for Large Rotator Cuff Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the
Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Arthroscopic Bankart Repair
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Arthroscopic Bankart Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Arthroscopic Bankart Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is
Hip Arthroscopy Labral Repair Protocol
 Hip Arthroscopy Labral Repair Protocol Applicability: Physician Practices Date Effective: 09/2013 Department: Rehabilitation Services Date Last Reviewed: 1/2018 Supersedes: n/a Administration Approval:
Hip Arthroscopy Labral Repair Protocol Applicability: Physician Practices Date Effective: 09/2013 Department: Rehabilitation Services Date Last Reviewed: 1/2018 Supersedes: n/a Administration Approval:
Hip Arthroscopy Femoroacetabular Impingement (FAI) Ryan W. Hess, MD Tracey Pederson, PCC Office: (763) Fax: (763)
 Hip Arthroscopy Femoroacetabular Impingement (FAI) Ryan W. Hess, MD Tracey Pederson, PCC Office: (763) 302-2223 Fax: (763) 302-2401 GENERAL GUIDELINES: Despite the minimally invasive nature of hip arthroscopy,
Hip Arthroscopy Femoroacetabular Impingement (FAI) Ryan W. Hess, MD Tracey Pederson, PCC Office: (763) 302-2223 Fax: (763) 302-2401 GENERAL GUIDELINES: Despite the minimally invasive nature of hip arthroscopy,
Hip Arthroscopy Rehabilitation Gluteus Medius Repair with or without Labral Debridement. Normalize gait pattern with brace (if indicated) and crutches
 General Guidelines: Hip Arthroscopy Rehabilitation Gluteus Medius Repair with or without Labral Debridement Normalize gait pattern with brace (if indicated) and crutches Weight-bearing: 20 lbs foot flat
General Guidelines: Hip Arthroscopy Rehabilitation Gluteus Medius Repair with or without Labral Debridement Normalize gait pattern with brace (if indicated) and crutches Weight-bearing: 20 lbs foot flat
Hip Injuries & Arthroscopy in Athletes
 Hip Injuries & Arthroscopy in Athletes John P Salvo, MD Sports Medicine Rothman Institute Philadelphia, PA EATA Annual Meeting January, 2011 Hip Injuries & Arthroscopy in Anatomy History Physical Exam
Hip Injuries & Arthroscopy in Athletes John P Salvo, MD Sports Medicine Rothman Institute Philadelphia, PA EATA Annual Meeting January, 2011 Hip Injuries & Arthroscopy in Anatomy History Physical Exam
Travis G. - 1 Maak, - MD Sports Medicine University of Utah Orthopaedics 590 Wakara Way Salt Lake City, UT Tel: Fax:
 Travis G. - 1 Maak, - MD Rehabilitation for Arthroscopic Osteochondroplasty with or without Labral Repair/Debridement General Guidelines: Normalize gait pattern with brace and crutches Continuous Passive
Travis G. - 1 Maak, - MD Rehabilitation for Arthroscopic Osteochondroplasty with or without Labral Repair/Debridement General Guidelines: Normalize gait pattern with brace and crutches Continuous Passive
Diagnosis: Gluteus Medius Tear, Labral Tear, CAM / Pincer
 Physical Therapy Prescription: Hip Arthroscopy Diagnosis: Gluteus Medius Tear, Labral Tear, CAM / Pincer Procedure: Gluteus Medius Repair, CAM / Pincer Decompression, Labral refixation / Capsular Shift
Physical Therapy Prescription: Hip Arthroscopy Diagnosis: Gluteus Medius Tear, Labral Tear, CAM / Pincer Procedure: Gluteus Medius Repair, CAM / Pincer Decompression, Labral refixation / Capsular Shift
HIP ARTHROSCOPY CLINICAL PRACTICE GUIDELINE
 HIP ARTHROSCOPY CLINICAL PRACTICE GUIDELINE Progression is time and criterion-based, dependent on soft tissue healing, patient demographics and clinician evaluation. Contact Ohio State Sports Medicine
HIP ARTHROSCOPY CLINICAL PRACTICE GUIDELINE Progression is time and criterion-based, dependent on soft tissue healing, patient demographics and clinician evaluation. Contact Ohio State Sports Medicine
Rehabilitation Guidelines for Shoulder Arthroscopy
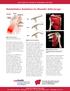 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Shoulder Arthroscopy Front View Acromion Supraspinatus Back View Supraspinatus Long head of bicep Type I Infraspinatus Short head of bicep
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Shoulder Arthroscopy Front View Acromion Supraspinatus Back View Supraspinatus Long head of bicep Type I Infraspinatus Short head of bicep
Rehabilitation Guidelines for Shoulder Arthroscopy
 Rehabilitation Guidelines for Shoulder Arthroscopy The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
Rehabilitation Guidelines for Shoulder Arthroscopy The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Open Bankart Repair
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Open Bankart Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Open Bankart Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared
Initial Exercises (Weeks 1-3)
 Labral Repair This protocol should be used as a guideline for progression and should be tailored to the needs of the individual patient. Partial weight bearing (50%) (4 weeks). Encourage, but limit hip
Labral Repair This protocol should be used as a guideline for progression and should be tailored to the needs of the individual patient. Partial weight bearing (50%) (4 weeks). Encourage, but limit hip
Rehabilitation Guidelines Following Microfracture Procedures to the Knee
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines Following Microfracture Procedures to the Knee There are two types of cartilage in the knee: meniscus and articular. One type of cartilage is the
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines Following Microfracture Procedures to the Knee There are two types of cartilage in the knee: meniscus and articular. One type of cartilage is the
Routine Arthroscopic Procedure
 Katherine J. Coyner, MD UCONN Musculoskeletal Institute Medical Arts & Research Building 263 Farmington Ave. Farmington, CT 06030 Office: (860) 679-6600 Fax: (860) 679-6649 www.drcoyner.com Avon Office
Katherine J. Coyner, MD UCONN Musculoskeletal Institute Medical Arts & Research Building 263 Farmington Ave. Farmington, CT 06030 Office: (860) 679-6600 Fax: (860) 679-6649 www.drcoyner.com Avon Office
REHABILITATION GUIDELINES FOR ROTATOR CUFF REPAIR FOR TYPE II TEARS (MASSIVE)(+/- SUBACROMIAL DECOMPRESSION)
 REHABILITATION GUIDELINES FOR ROTATOR CUFF REPAIR FOR TYPE II TEARS (MASSIVE)(+/- SUBACROMIAL DECOMPRESSION) The rehabilitation guidelines are presented in a criterion based progression. General time frames
REHABILITATION GUIDELINES FOR ROTATOR CUFF REPAIR FOR TYPE II TEARS (MASSIVE)(+/- SUBACROMIAL DECOMPRESSION) The rehabilitation guidelines are presented in a criterion based progression. General time frames
Hip Arthroscopy Rehabilitation Protocol
 Hip Arthroscopy Rehabilitation Protocol This protocol is a generic outline of the postoperative management for patients undergoing hip arthroscopy. Depending on the exact diagnosis and the procedures performed,
Hip Arthroscopy Rehabilitation Protocol This protocol is a generic outline of the postoperative management for patients undergoing hip arthroscopy. Depending on the exact diagnosis and the procedures performed,
Microfracture. This protocol should be used as a guideline for progression and should be tailored to the needs of the individual patient.
 This protocol should be used as a guideline for progression and should be tailored to the needs of the individual patient. Strict protective weight bearing status for two months (8-9 weeks). Allow to place
This protocol should be used as a guideline for progression and should be tailored to the needs of the individual patient. Strict protective weight bearing status for two months (8-9 weeks). Allow to place
CLINICS IN SPORTS MEDICINE
 Clin Sports Med 25 (2006) 365 369 CLINICS IN SPORTS MEDICINE A Acetabular labrum, tears of, hip arthroscopy in, 264 Acetabular rim, trimming of, and labral repair, new method for, 293 297 Acetabulum, femoral
Clin Sports Med 25 (2006) 365 369 CLINICS IN SPORTS MEDICINE A Acetabular labrum, tears of, hip arthroscopy in, 264 Acetabular rim, trimming of, and labral repair, new method for, 293 297 Acetabulum, femoral
Hip arthroscopy. Anatomy The hip is functionally a ball and socket joint.
 Hip arthroscopy The term arthroscopy (or keyhole surgery) refers to the viewing of the inside of a joint through a small operating telescope. First described in the 1970s, arthroscopic techniques have
Hip arthroscopy The term arthroscopy (or keyhole surgery) refers to the viewing of the inside of a joint through a small operating telescope. First described in the 1970s, arthroscopic techniques have
Patellar-quadriceps Tendon Repair Protocol
 Patellar-quadriceps Tendon Repair Protocol Applicability: Physician Practice Date Effective: 3/2017 Department: Rehabilitation Services Supersedes: none Date Last Reviewed / or Date Last Revision: 1/2018
Patellar-quadriceps Tendon Repair Protocol Applicability: Physician Practice Date Effective: 3/2017 Department: Rehabilitation Services Supersedes: none Date Last Reviewed / or Date Last Revision: 1/2018
Labral Tears / Femoro- Acetabular Impingement / Hip Arthroscopy/THA. Dr Allen Turnbull Hip and Knee Surgery
 Labral Tears / Femoro- Acetabular Impingement / Hip Arthroscopy/THA Hip Anatomy Labrum Fovea Femoral Head Articular Cartilage Ligamentum Teres Labral Tears Function of Labrum Deepens acetabulum by 20%
Labral Tears / Femoro- Acetabular Impingement / Hip Arthroscopy/THA Hip Anatomy Labrum Fovea Femoral Head Articular Cartilage Ligamentum Teres Labral Tears Function of Labrum Deepens acetabulum by 20%
A patient s guide to: Arthroscopy of the Hip
 A patient s guide to: Arthroscopy of the Hip Brian J. White MD Assistant Team Physician Denver Nuggets Western Orthopaedics - Denver, Colorado Introduction This is designed to provide you with a better
A patient s guide to: Arthroscopy of the Hip Brian J. White MD Assistant Team Physician Denver Nuggets Western Orthopaedics - Denver, Colorado Introduction This is designed to provide you with a better
ARTHROSCOPIC GLUTEUS MEDIUS REPAIR PHYSICAL THERAPY PROTOCOL
 ARTHROSCOPIC GLUTEUS MEDIUS REPAIR PHYSICAL THERAPY PROTOCOL Jovan R. Laskovski, M.D. Hip Arthroscopy Sports Medicine & Orthopaedic Surgery Crystal Clinic Orthopaedic Center Please use appropriate clinical
ARTHROSCOPIC GLUTEUS MEDIUS REPAIR PHYSICAL THERAPY PROTOCOL Jovan R. Laskovski, M.D. Hip Arthroscopy Sports Medicine & Orthopaedic Surgery Crystal Clinic Orthopaedic Center Please use appropriate clinical
Precautions following Hip Arthroscopy/FAI: (Refixation/Osteochondroplasty)
 Physical Therapy Prescription: Hip Arthroscopy Diagnosis: Labral Tear, CAM / Pincer Procedure: Labral Repair / Capsular Shift, CAM / Pincer Decompression RX: Evaluate / Treat, and follow attached protocol
Physical Therapy Prescription: Hip Arthroscopy Diagnosis: Labral Tear, CAM / Pincer Procedure: Labral Repair / Capsular Shift, CAM / Pincer Decompression RX: Evaluate / Treat, and follow attached protocol
Bryan T. Kelly, MD Center for Hip Pain and Preservation Hospital for Special Surgery
 Hip Arthroscopy Rehabilitation Labral refixation with or without FAI Component General Guidelines: Limited external rotation to 20 degrees (2 weeks) No hyperextension (4 weeks) Normalize gait pattern with
Hip Arthroscopy Rehabilitation Labral refixation with or without FAI Component General Guidelines: Limited external rotation to 20 degrees (2 weeks) No hyperextension (4 weeks) Normalize gait pattern with
Diagnosis: Labral Tear, Internal Snapping Hip, CAM / Pincer. Procedure: Partial Psoas Release with CAM / Pincer Decompression and Labral Debridement
 Physical Therapy Prescription: Hip Arthroscopy Diagnosis: Labral Tear, Internal Snapping Hip, CAM / Pincer Procedure: Partial Psoas Release with CAM / Pincer Decompression and Labral Debridement RX: Evaluate
Physical Therapy Prescription: Hip Arthroscopy Diagnosis: Labral Tear, Internal Snapping Hip, CAM / Pincer Procedure: Partial Psoas Release with CAM / Pincer Decompression and Labral Debridement RX: Evaluate
Abductor Repair (Gluteus Medius/Minimus Repair)
 (Gluteus Medius/Minimus Repair) This protocol should be used as a guideline for progression and should be tailored to the needs of the individual patient. Strict protective weight bearing status for 8
(Gluteus Medius/Minimus Repair) This protocol should be used as a guideline for progression and should be tailored to the needs of the individual patient. Strict protective weight bearing status for 8
Patellar-quadriceps Tendon Repair Protocol
 Patellar-quadriceps Tendon Repair Protocol Applicability: Physician Practice Date Effective: 3/2017 Department: Rehabilitation Services Supersedes: none Date Last Reviewed / or Date Last Revision: 3/2017
Patellar-quadriceps Tendon Repair Protocol Applicability: Physician Practice Date Effective: 3/2017 Department: Rehabilitation Services Supersedes: none Date Last Reviewed / or Date Last Revision: 3/2017
S p o r t s & O r t h o p a e d i c S p e c i a l i s t s D R. R Y A N F A D E R
 S p o r t s & O r t h o p a e d i c S p e c i a l i s t s D R. R Y A N F A D E R H I P A R T H R O S C O P Y W I T H L A B R A L R E P A I R P R O T O C O L This protocol provides appropriate guidelines
S p o r t s & O r t h o p a e d i c S p e c i a l i s t s D R. R Y A N F A D E R H I P A R T H R O S C O P Y W I T H L A B R A L R E P A I R P R O T O C O L This protocol provides appropriate guidelines
REHABILITATION GUIDELINES FOR ROTATOR CUFF REPAIR FOR TYPE I TEARS (+/- SUBACROMINAL DECOMPRESSION)
 REHABILITATION GUIDELINES FOR ROTATOR CUFF REPAIR FOR TYPE I TEARS (+/- SUBACROMINAL DECOMPRESSION) The rehabilitation guidelines are presented in a criterion based progression. General time frames are
REHABILITATION GUIDELINES FOR ROTATOR CUFF REPAIR FOR TYPE I TEARS (+/- SUBACROMINAL DECOMPRESSION) The rehabilitation guidelines are presented in a criterion based progression. General time frames are
REHABILITATION GUIDELINES FOR ARTHROSCOPIC CAPSULAR SHIFT
 REHABILITATION GUIDELINES FOR ARTHROSCOPIC CAPSULAR SHIFT The rehabilitation guidelines are presented in a criterion based progression. General time frames are given for reference to the average, but individual
REHABILITATION GUIDELINES FOR ARTHROSCOPIC CAPSULAR SHIFT The rehabilitation guidelines are presented in a criterion based progression. General time frames are given for reference to the average, but individual
Rehabilitation Guidelines for Achilles Tendon Repair
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Achilles Tendon Repair The Achilles tendon is the strongest and thickest tendon in the body. It attaches the calf muscles (soleus and gastrocnemius)
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Achilles Tendon Repair The Achilles tendon is the strongest and thickest tendon in the body. It attaches the calf muscles (soleus and gastrocnemius)
A patient guide to Hip Impingement Surgical Management
 A patient guide to Hip Impingement Surgical Management Mr Sanjeev Patil Miss Louise Duncan Mr Frank Gilroy Patient Name: Occupation: Operation / Restrictions: Work/Sport: Contents Page: 1 Cover 2 Contents
A patient guide to Hip Impingement Surgical Management Mr Sanjeev Patil Miss Louise Duncan Mr Frank Gilroy Patient Name: Occupation: Operation / Restrictions: Work/Sport: Contents Page: 1 Cover 2 Contents
APPLICATION OF THE MOVEMENT SYSTEMS MODEL TO THE MANAGEMENT COMMON HIP PATHOLOGIES
 APPLICATION OF THE MOVEMENT SYSTEMS MODEL TO THE MANAGEMENT COMMON HIP PATHOLOGIES Tracy Porter, PT, DPT Des Moines University Department of Physical Therapy Objectives Review current literature related
APPLICATION OF THE MOVEMENT SYSTEMS MODEL TO THE MANAGEMENT COMMON HIP PATHOLOGIES Tracy Porter, PT, DPT Des Moines University Department of Physical Therapy Objectives Review current literature related
S p o r t s & O r t h o p a e d i c S p e c i a l i s t s D R. R Y A N F A D E R
 S p o r t s & O r t h o p a e d i c S p e c i a l i s t s D R. R Y A N F A D E R H I P A R T H R O S C O P Y W I T H This protocol provides appropriate guidelines for the rehabilitation of patients following
S p o r t s & O r t h o p a e d i c S p e c i a l i s t s D R. R Y A N F A D E R H I P A R T H R O S C O P Y W I T H This protocol provides appropriate guidelines for the rehabilitation of patients following
Travis G. Maak, MD Sports Medicine University of Utah Orthopaedics 590 Wakara Way Salt Lake City, UT Tel: Fax:
 General Guidelines: Hip Arthroscopy Rehabilitation Capsular Shift with or without FAI Labral Components No external rotation greater than 30 degrees for 4 weeks No hyperextension for 4 weeks Normalize
General Guidelines: Hip Arthroscopy Rehabilitation Capsular Shift with or without FAI Labral Components No external rotation greater than 30 degrees for 4 weeks No hyperextension for 4 weeks Normalize
Phase 1- Immediate Rehabilitation (1-3 weeks): Goals Precautions:
 Phase 1- Immediate Rehabilitation (1-3 weeks): Goals: Protection of the repaired tissue Prevent muscular inhibition and gait abnormalities Diminish pain and inflammation Precautions: 20 lb. flat-foot weight-bearing
Phase 1- Immediate Rehabilitation (1-3 weeks): Goals: Protection of the repaired tissue Prevent muscular inhibition and gait abnormalities Diminish pain and inflammation Precautions: 20 lb. flat-foot weight-bearing
Hip Labrum and FAI Post-Surgical Rehabilitation Guideline
 Hip Labrum and FAI Post-Surgical Rehabilitation Guideline This rehabilitation program is designed to return the individual to their activities as quickly and safely as possible. It is designed for rehabilitation
Hip Labrum and FAI Post-Surgical Rehabilitation Guideline This rehabilitation program is designed to return the individual to their activities as quickly and safely as possible. It is designed for rehabilitation
Mark Adickes, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas Phone: Fax:
 Mark Adickes, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas 77030 Phone: 713-986-6016 Fax: 713-986-5411 Hip Arthroscopy - FAI/Labral Repair Protocol The hip is a ball and
Mark Adickes, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas 77030 Phone: 713-986-6016 Fax: 713-986-5411 Hip Arthroscopy - FAI/Labral Repair Protocol The hip is a ball and
ARTHROSCOPIC LABRAL REPAIR WITH CAPSULAR PLICATION PHYSICAL THERAPY PROTOCOL
 ARTHROSCOPIC LABRAL REPAIR WITH CAPSULAR PLICATION PHYSICAL THERAPY PROTOCOL Jovan R. Laskovski, M.D. Hip Arthroscopy Sports Medicine & Orthopaedic Surgery Crystal Clinic Orthopaedic Center Please use
ARTHROSCOPIC LABRAL REPAIR WITH CAPSULAR PLICATION PHYSICAL THERAPY PROTOCOL Jovan R. Laskovski, M.D. Hip Arthroscopy Sports Medicine & Orthopaedic Surgery Crystal Clinic Orthopaedic Center Please use
9180 KATY FREEWAY, STE. 200 (713)
 AUTOLOGOUS CHONDROCYTE IMPLANTATION Femoral Condyle Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Goals: - Protect healing tissue from load and shear forces - Decrease pain and effusion
AUTOLOGOUS CHONDROCYTE IMPLANTATION Femoral Condyle Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Goals: - Protect healing tissue from load and shear forces - Decrease pain and effusion
Hip Arthroscopy Rehabilitation Protocol
 Hip Arthroscopy Rehabilitation Protocol 1. Concepts: a. Range of motion and weight bearing restrictions must be adhered to during the initial rehab process (4 total weeks of ROM and weight bearing restrictions)
Hip Arthroscopy Rehabilitation Protocol 1. Concepts: a. Range of motion and weight bearing restrictions must be adhered to during the initial rehab process (4 total weeks of ROM and weight bearing restrictions)
PHASE I (Begin PT 3-5 days post-op) DOS:
 REHABILITATION GUIDELINES FOR POSTERIOR SHOULDER RECONSTRUCTION +/- LABRAL REPAIRS The rehabilitation guidelines are presented in a criterion based progression. General time frames are given for reference
REHABILITATION GUIDELINES FOR POSTERIOR SHOULDER RECONSTRUCTION +/- LABRAL REPAIRS The rehabilitation guidelines are presented in a criterion based progression. General time frames are given for reference
A patient guide to Hip Impingement Non-Surgical Management. Mr Sanjeev Patil Miss Louise Duncan Mr Frank Gilroy
 A patient guide to Hip Impingement Non-Surgical Management Mr Sanjeev Patil Miss Louise Duncan Mr Frank Gilroy Contents Page: 1 Cover 2 Contents 3 Hip impingement information 4 Conservative rehabilitation
A patient guide to Hip Impingement Non-Surgical Management Mr Sanjeev Patil Miss Louise Duncan Mr Frank Gilroy Contents Page: 1 Cover 2 Contents 3 Hip impingement information 4 Conservative rehabilitation
A Patient s Guide to Femoroacetabular Impingement (FAI) of the Hip
 A Patient s Guide to Femoroacetabular Impingement (FAI) of the Hip 651 Old Country Road Plainview, NY 11803 Phone: 5166818822 Fax: 5166813332 p.lettieri@aol.com DISCLAIMER: The information in this booklet
A Patient s Guide to Femoroacetabular Impingement (FAI) of the Hip 651 Old Country Road Plainview, NY 11803 Phone: 5166818822 Fax: 5166813332 p.lettieri@aol.com DISCLAIMER: The information in this booklet
Hip Arthroscopy with CAM resection/labral Repair Protocol
 Hip Arthroscopy with CAM resection/labral Repair Protocol As tolerated should be understood to perform with safety for the reconstruction/repair. Pain, limp, swelling, or other undesirable factors are
Hip Arthroscopy with CAM resection/labral Repair Protocol As tolerated should be understood to perform with safety for the reconstruction/repair. Pain, limp, swelling, or other undesirable factors are
The Young Adult Hip: FAI. Jason Snibbe, M.D. Snibbe Orthopedics Team Physician, University of Southern California
 The Young Adult Hip: FAI Jason Snibbe, M.D. Snibbe Orthopedics Team Physician, University of Southern California Introduction Femoroacetabular Impingment(FAI) Presentation and Exam Imaging Surgical Management
The Young Adult Hip: FAI Jason Snibbe, M.D. Snibbe Orthopedics Team Physician, University of Southern California Introduction Femoroacetabular Impingment(FAI) Presentation and Exam Imaging Surgical Management
Hip Arthroscopy Rehabilitation Labral Refixation with or without FAI Component. Limited external rotation to 20 degrees (2 weeks)
 General Guidelines: 4140 Centennial Hills Boulevard Casper, WY 82609 (307) 265-7205 Hip Arthroscopy Rehabilitation Labral Refixation with or without FAI Component Limited external rotation to 20 degrees
General Guidelines: 4140 Centennial Hills Boulevard Casper, WY 82609 (307) 265-7205 Hip Arthroscopy Rehabilitation Labral Refixation with or without FAI Component Limited external rotation to 20 degrees
Protocol G Arthroscopic Surgery: Therapist Information
 Protocol G Arthroscopic Surgery: Therapist Information Please read entire protocol prior to initiating therapy Please do not hesitate to contact Dr. Wolff with questions or concerns. Rest is a vital component
Protocol G Arthroscopic Surgery: Therapist Information Please read entire protocol prior to initiating therapy Please do not hesitate to contact Dr. Wolff with questions or concerns. Rest is a vital component
Hip Arthroscopy. Labral Repair/Debridement with Femoroplasty
 Precautions for weeks 1 4 post-op: Hip Arthroscopy Labral Repair/Debridement with Femoroplasty Patient Education o For 1 week, Assist the involved LE during all transfers o For 2 weeks, Do not sit with
Precautions for weeks 1 4 post-op: Hip Arthroscopy Labral Repair/Debridement with Femoroplasty Patient Education o For 1 week, Assist the involved LE during all transfers o For 2 weeks, Do not sit with
What s Hip: Common Hip Problems and Kids and Adults
 What s Hip: Common Hip Problems and Kids and Adults Alan Zhang MD Assistant Professor Sports Medicine and Hip Arthroscopy UCSF Department of Orthopaedic Surgery I have no relevant disclosures. 2 1 Most
What s Hip: Common Hip Problems and Kids and Adults Alan Zhang MD Assistant Professor Sports Medicine and Hip Arthroscopy UCSF Department of Orthopaedic Surgery I have no relevant disclosures. 2 1 Most
CENTER FOR ORTHOPAEDICS AND SPINE CARE PHYSICAL THERAPY PROTOCOL ACUTE PROXIMAL HAMSTRING TENDON REPAIR BENJAMIN J. DAVIS, MD
 Weeks 0-6 Goal: 1) Protection of the surgical repair Precautions: 1) Non-weight bearing with crutches for 6 weeks with foot flat or with knee Knee flexed to 90 degrees with sitting 2) No active hamstring
Weeks 0-6 Goal: 1) Protection of the surgical repair Precautions: 1) Non-weight bearing with crutches for 6 weeks with foot flat or with knee Knee flexed to 90 degrees with sitting 2) No active hamstring
Rehabilitation Protocol:
 Rehabilitation Protocol: Patellofemoral resurfacing: Osteochondral Autograft Transplantation (OATS), Autologous Chondrocyte Implantation (ACI) and Microfracture Department of Orthopaedic Surgery Lahey
Rehabilitation Protocol: Patellofemoral resurfacing: Osteochondral Autograft Transplantation (OATS), Autologous Chondrocyte Implantation (ACI) and Microfracture Department of Orthopaedic Surgery Lahey
To classify the joints relative to structure & shape
 To classify the joints relative to structure & shape To describe the anatomy of the hip joint To describe the ankle joint To memorize their blood & nerve supply JOINTS: Joints are sites where skeletal
To classify the joints relative to structure & shape To describe the anatomy of the hip joint To describe the ankle joint To memorize their blood & nerve supply JOINTS: Joints are sites where skeletal
REHABILITATION GUIDELINES FOR ANTERIOR SHOULDER RECONSTRUCTION WITH BANKART REPAIR
 REHABILITATION GUIDELINES FOR ANTERIOR SHOULDER RECONSTRUCTION WITH BANKART REPAIR The rehabilitation guidelines are presented in a criterion based progression. General time frames are given for reference
REHABILITATION GUIDELINES FOR ANTERIOR SHOULDER RECONSTRUCTION WITH BANKART REPAIR The rehabilitation guidelines are presented in a criterion based progression. General time frames are given for reference
Rehabilitation Guidelines for Open Latarjet Anterior Shoulder Stabilization
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Open Latarjet Anterior Shoulder Stabilization The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Open Latarjet Anterior Shoulder Stabilization The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a
What is arthroscopy? Normal knee anatomy
 What is arthroscopy? Arthroscopy is a common surgical procedure for examining and repairing the inside of your knee. It is a minimally invasive surgical procedure which uses an Arthroscope and other specialized
What is arthroscopy? Arthroscopy is a common surgical procedure for examining and repairing the inside of your knee. It is a minimally invasive surgical procedure which uses an Arthroscope and other specialized
Avon Office 2 Simsbury Rd. Avon, CT Office: (860) Fax: (860) Acetabuloplasty
 Katherine J. Coyner, MD UCONN Musculoskeletal Institute Medical Arts & Research Building 263 Farmington Ave. Farmington, CT 06030 Office: (860) 679-6600 Fax: (860) 679-6649 www.drcoyner.com This protocol
Katherine J. Coyner, MD UCONN Musculoskeletal Institute Medical Arts & Research Building 263 Farmington Ave. Farmington, CT 06030 Office: (860) 679-6600 Fax: (860) 679-6649 www.drcoyner.com This protocol
REHABILITATION GUIDELINES FOR SUBSCAPULARIS (+/- SUBACROMIAL DECOMPRESSION) Dr. Carson
 REHABILITATION GUIDELINES FOR SUBSCAPULARIS (+/- SUBACROMIAL DECOMPRESSION) Dr. Carson The rehabilitation guidelines are presented in a criterion based progression. General time frames are given for reference
REHABILITATION GUIDELINES FOR SUBSCAPULARIS (+/- SUBACROMIAL DECOMPRESSION) Dr. Carson The rehabilitation guidelines are presented in a criterion based progression. General time frames are given for reference
BENJAMIN G. DOMB, MD
 Physical Therapy Protocol Partial or full thickness gluteus medius repair with or without labral repair The intent of this protocol is to provide guidelines for your patient s therapy progression. It is
Physical Therapy Protocol Partial or full thickness gluteus medius repair with or without labral repair The intent of this protocol is to provide guidelines for your patient s therapy progression. It is
Post Operative Hip Arthroscopy Procedure Form
 Post Operative Hip Arthroscopy Procedure Form Femoracetabular Impingement (FAI) Femoral Osteochondroplasty Acetabular Rim Trimming Acetabular Labrum Repair Location: o clock to o clock Debridement Articular
Post Operative Hip Arthroscopy Procedure Form Femoracetabular Impingement (FAI) Femoral Osteochondroplasty Acetabular Rim Trimming Acetabular Labrum Repair Location: o clock to o clock Debridement Articular
Rehabilitation. Friday, October 14, :00 11:45am General Session Rehabilitation following FAI Surgery Mark Ryan, MS, ATC, CSCS USA
 Rehabilitation Friday, October 14, 2011 11:00 11:45am General Session Rehabilitation following FAI Surgery Mark Ryan, MS, ATC, CSCS USA Best Tip Srino Bharam, MD USA Best Tip Robroy Martin, PhD, PT USA
Rehabilitation Friday, October 14, 2011 11:00 11:45am General Session Rehabilitation following FAI Surgery Mark Ryan, MS, ATC, CSCS USA Best Tip Srino Bharam, MD USA Best Tip Robroy Martin, PhD, PT USA
Alejandro Verdugo, M.D.
 Alejandro Verdugo, M.D. Physical Therapy Protocol Gluteus Medius repair with or without labral repair The intent of this protocol is to provide guidelines for your patient s therapy progression. It is
Alejandro Verdugo, M.D. Physical Therapy Protocol Gluteus Medius repair with or without labral repair The intent of this protocol is to provide guidelines for your patient s therapy progression. It is
Specialists in Joint Replacement, Spinal Surgery, Orthopaedics and Sport Injuries. The Hip.
 Specialists in Joint Replacement, Spinal Surgery, Orthopaedics and Sport Injuries The Hip INTRODUCTION THE HIP The hip is a ball-and-socket joint. The socket is formed by the acetabulum, which is part
Specialists in Joint Replacement, Spinal Surgery, Orthopaedics and Sport Injuries The Hip INTRODUCTION THE HIP The hip is a ball-and-socket joint. The socket is formed by the acetabulum, which is part
Phase I : Immediate Postoperative Phase- Protected Motion. (0-2 Weeks)
 Phase I : Immediate Postoperative Phase- Protected Motion (0-2 Weeks) Appointments Progression Criteria 2 weeks after surgery Rehabilitation appointments begin within 7-10 days of surgery, continue 1-2
Phase I : Immediate Postoperative Phase- Protected Motion (0-2 Weeks) Appointments Progression Criteria 2 weeks after surgery Rehabilitation appointments begin within 7-10 days of surgery, continue 1-2
9180 KATY FREEWAY, STE. 200 (713)
 OSTEOCHONDRAL AUTOGRAFT TRANSPLANTATION Patella/Trochlea Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Goals: - Protection of healing tissue from load and shear forces - Decrease pain
OSTEOCHONDRAL AUTOGRAFT TRANSPLANTATION Patella/Trochlea Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Goals: - Protection of healing tissue from load and shear forces - Decrease pain
BENJAMIN G. DOMB, M.D.
 Arthroscopic Hip Surgery Physical Therapy Protocol The intent of this protocol is to provide guidelines for your patient s therapy progression. It is not intended to serve as a recipe for treatment. We
Arthroscopic Hip Surgery Physical Therapy Protocol The intent of this protocol is to provide guidelines for your patient s therapy progression. It is not intended to serve as a recipe for treatment. We
A Patient s Guide to Arthroscopy of the Hip
 A Patient s Guide to Arthroscopy of the Hip Introduction A hip arthroscopy is a procedure where a small video camera attached to a fiberoptic lens is inserted into the hip joint to allow a surgeon to see
A Patient s Guide to Arthroscopy of the Hip Introduction A hip arthroscopy is a procedure where a small video camera attached to a fiberoptic lens is inserted into the hip joint to allow a surgeon to see
CAPPAGH NATIONAL ORTHOPAEDIC HOSPITAL, FINGLAS, DUBLIN 11. The Sisters of Mercy. Hip Arthroscopy
 1.0 Policy Statement... 2 2.0 Purpose... 2 3.0 Scope... 2 4.0 Health & Safety... 2 5.0 Responsibilities... 2 6.0 Definitions and Abbreviations... 3 7.0 Guideline... 3 7.1 Rehabilitation Phase 1 (Day 1
1.0 Policy Statement... 2 2.0 Purpose... 2 3.0 Scope... 2 4.0 Health & Safety... 2 5.0 Responsibilities... 2 6.0 Definitions and Abbreviations... 3 7.0 Guideline... 3 7.1 Rehabilitation Phase 1 (Day 1
Protocol D Arthroscopic Surgery: Therapist Information
 Protocol D Arthroscopic Surgery: Therapist Information Please read entire protocol prior to initiating therapy Please do not hesitate to contact Dr. Wolff with questions or concerns. Rest is a vital component
Protocol D Arthroscopic Surgery: Therapist Information Please read entire protocol prior to initiating therapy Please do not hesitate to contact Dr. Wolff with questions or concerns. Rest is a vital component
Protocol A Arthroscopic Surgery: Therapist Information
 Protocol A Arthroscopic Surgery: Therapist Information Please read entire protocol prior to initiating therapy Please do not hesitate to contact Dr. Wolff with questions or concerns. Rest is a vital component
Protocol A Arthroscopic Surgery: Therapist Information Please read entire protocol prior to initiating therapy Please do not hesitate to contact Dr. Wolff with questions or concerns. Rest is a vital component
FAI syndrome with or without labral tear.
 Case This 16-year-old female, soccer athlete was treated for pain in the right groin previously. Now has acute onset of pain in the left hip. The pain was in the groin that was worse with activities. Diagnosis
Case This 16-year-old female, soccer athlete was treated for pain in the right groin previously. Now has acute onset of pain in the left hip. The pain was in the groin that was worse with activities. Diagnosis
S p o r t s & O r t h o p a e d i c S p e c i a l i s t s D R. R Y A N F A D E R
 S p o r t s & O r t h o p a e d i c S p e c i a l i s t s D R. R Y A N F A D E R H I P A R T H R O S C O P Y W I T H L A B R A L R E P A I R P R O T O C O L This protocol provides appropriate guidelines
S p o r t s & O r t h o p a e d i c S p e c i a l i s t s D R. R Y A N F A D E R H I P A R T H R O S C O P Y W I T H L A B R A L R E P A I R P R O T O C O L This protocol provides appropriate guidelines
Mark Adickes, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas Phone: Fax:
 Mark Adickes, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas 77030 Phone: 713-986-6016 Fax: 713-986-5411 MENISCAL REPAIR PROTOCOL Longitudinal Meniscal Repair This rehabilitation
Mark Adickes, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas 77030 Phone: 713-986-6016 Fax: 713-986-5411 MENISCAL REPAIR PROTOCOL Longitudinal Meniscal Repair This rehabilitation
Post Operative Total Hip Replacement Protocol Brian J. White, MD
 Post Operative Total Hip Replacement Protocol Brian J. White, MD www.western-ortho.com The intent of this protocol is to provide guidelines for progression of rehabilitation. It is not intended to serve
Post Operative Total Hip Replacement Protocol Brian J. White, MD www.western-ortho.com The intent of this protocol is to provide guidelines for progression of rehabilitation. It is not intended to serve
Internal Rotation (turning toes/knee toward other leg) 30 degree limit. limit
 Hip Arthroscopy Patient Education Use of Brace and Crutches: - Wear the brace all times of weight bearing for the first 3 weeks after surgery. This is done to protect your hip and motion into hip extension
Hip Arthroscopy Patient Education Use of Brace and Crutches: - Wear the brace all times of weight bearing for the first 3 weeks after surgery. This is done to protect your hip and motion into hip extension
Post Operative Hip Arthroscopy Procedure Form
 Post Operative Hip Arthroscopy Procedure Form Femoracetabular Impingement (FAI) Femoral Osteochondroplasty Acetabular Rim Trimming Acetabular Labrum Repair Location: o clock to o clock Debridement Articular
Post Operative Hip Arthroscopy Procedure Form Femoracetabular Impingement (FAI) Femoral Osteochondroplasty Acetabular Rim Trimming Acetabular Labrum Repair Location: o clock to o clock Debridement Articular
STAIRS. What s Hip: Top 5 Hip Problems in Primary Care. I have no relevant disclosures. Top 5 (or 6) Pathologies. Big 3- Questions to Ask
 I have no relevant disclosures. What s Hip: Top 5 Hip Problems in Primary Care Alan Zhang MD Assistant Professor Sports Medicine and Hip Arthroscopy UCSF Department of Orthopaedic Surgery December, 2015
I have no relevant disclosures. What s Hip: Top 5 Hip Problems in Primary Care Alan Zhang MD Assistant Professor Sports Medicine and Hip Arthroscopy UCSF Department of Orthopaedic Surgery December, 2015
Non-arthritic anterior hip pain in the younger patient: examination and intervention strategies
 Non-arthritic anterior hip pain in the younger patient: examination and intervention strategies Melodie Kondratek, PT, DScPT, OMPT Bryan Kuhlman, PT, DPT, OMPT Oakland University Orthopedic Spine and Sports
Non-arthritic anterior hip pain in the younger patient: examination and intervention strategies Melodie Kondratek, PT, DScPT, OMPT Bryan Kuhlman, PT, DPT, OMPT Oakland University Orthopedic Spine and Sports
ACL Reconstruction Rehabilitation Protocol
 ACL Reconstruction Rehabilitation Protocol 1. Pre-OP Visit: a. Patient Education b. Exercises c. Gait Outline rehabilitation timeline. Discuss: Swelling/effusion control (PRICE). Quadriceps inhibition
ACL Reconstruction Rehabilitation Protocol 1. Pre-OP Visit: a. Patient Education b. Exercises c. Gait Outline rehabilitation timeline. Discuss: Swelling/effusion control (PRICE). Quadriceps inhibition
Post Operative Hip Arthroscopy Rehabilitation Protocol Labral Repair With or Without FAI Component
 Post Operative Hip Arthroscopy Rehabilitation Protocol Labral Repair With or Without FAI Component ROM Restrictions: -Perform PROM in patient s PAIN FREE Range FLEXION EXTENSION EXTERNAL ROTATION 90 degrees
Post Operative Hip Arthroscopy Rehabilitation Protocol Labral Repair With or Without FAI Component ROM Restrictions: -Perform PROM in patient s PAIN FREE Range FLEXION EXTENSION EXTERNAL ROTATION 90 degrees
Non Surgical Hip Therapy Athletic Hip Injury: Therapist Information
 Non Surgical Hip Therapy Athletic Hip Injury: Therapist Information Please read entire protocol prior to initiating therapy Please note: Individual hip injuries vary widely. This therapy protocol should
Non Surgical Hip Therapy Athletic Hip Injury: Therapist Information Please read entire protocol prior to initiating therapy Please note: Individual hip injuries vary widely. This therapy protocol should
Hip Arthroscopy Rehabilitation Labral Debridement with or without FAI Component. Normalize gait pattern with brace and crutches
 Hip Arthroscopy Rehabilitation Labral Debridement with or without FAI Component General Guidelines: Normalize gait pattern with brace and crutches Weightbearing as per procedure performed Continuous Passive
Hip Arthroscopy Rehabilitation Labral Debridement with or without FAI Component General Guidelines: Normalize gait pattern with brace and crutches Weightbearing as per procedure performed Continuous Passive
Post Operative ACL Reconstruction Protocol Brian J. White, MD
 Post Operative ACL Reconstruction Protocol Brian J. White, MD www.western-ortho.com The intent of this protocol is to provide guidelines for progression of rehabilitation. It is not intended to serve as
Post Operative ACL Reconstruction Protocol Brian J. White, MD www.western-ortho.com The intent of this protocol is to provide guidelines for progression of rehabilitation. It is not intended to serve as
