Prognostic factors for surgical outcome in spinal cord injury associated with ossification of the posterior longitudinal ligament (OPLL)
|
|
|
- Paulina Craig
- 5 years ago
- Views:
Transcription
1 Kwon et al. Journal of Orthopaedic Surgery and Research (2015) 10:94 DOI /s RESEARCH ARTICLE Open Access Prognostic factors for surgical outcome in spinal cord injury associated with ossification of the posterior longitudinal ligament (OPLL) Soon Young Kwon 1, Jun Jae Shin 1*, Ji Hae Lee 2 and Woo Ho Cho 2 Abstract Background: Ossification of the posterior longitudinal ligament (OPLL) may increase the risk of spinal cord injury (SCI) with various neurological deficits after minor trauma. However, few studies have investigated the influence of OPLL on neurological outcome after acute cord injury. We examined whether severe spinal canal stenosis caused by OPLL affects neurological outcome after SCI based on intramedullary signal intensity (SI) changes on magnetic resonance imaging (MRI). Methods: From June 2006 to July 2013, we treated 246 patients with cervical cord injury. Fifty-one (20.7 %) patients had ventral cord compression due to OPLL without any bony fractures. Among them, 38 patients (34 men, mean age 62.7 years) underwent cervical laminoplasty (8) and cervical decompression and fixation (30). The neurologic assessments were performed in patients who had 1-year follow-up, and the mean follow-up period was 42.2 months. OPLL type, cause of injury, cervical sagittal angle, cervical spine stenosis, cord compression ratio (space available for the spinal cord (SAC)), and grade of intramedullary SI (grade 0, none; grade 1, light; grade 2, intense T2WI) were assessed. Results: Mean American Spinal Injury Association (ASIA) motor score at admission was 38.4 ± 21.9 (range, 2 70) and improved to 67.7 ± 19.1 (range, 8 94) at last follow-up (p < 0.05). Mean recovery rate of the motor score was 55.8 ± 19.9 %. Five patients had SI grade 0, 20 patients had SI grade 1, and 13 patients had SI grade 2. Among the variables tested, age, initial ASIA motor grade, intramedullary SI grade, and SAC were significantly related to neurological outcome. However, initial cervical alignment, canal diameter, length of SI, time interval between injury and operation, and OPLL type had no significant effect on neurological outcome. Conclusions: Preoperative neurological status, cord compression ratio, and SI grade are related to neurological outcome in patients with SCI associated with OPLL. The better the preoperative neurological status, the more favorable the neurological outcome after surgery. A higher SI grade on preoperative T2WI was negatively related to neurological outcome. Therefore, the severity of SI change, cord compression ratio, and preoperative neurological status can be regarded as significant prognostic factors in patients with SCI associated with OPLL. Keywords: Ossification of the posterior longitudinal ligament, Spinal cord injury, Magnetic resonance imaging * Correspondence: zunzae@hanmail.net 1 Department of Neurosurgery, Sanggye Paik Hospital, Inje University College of Medicine, Sanggye-7 dong, 761-1, Nowon-gu, Seoul , South Korea Full list of author information is available at the end of the article 2015 Kwon et al. This is an Open Access article distributed under the terms of the Creative Commons Attribution License ( which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly credited. The Creative Commons Public Domain Dedication waiver ( creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated.
2 Kwon et al. Journal of Orthopaedic Surgery and Research (2015) 10:94 Page 2 of 9 Introduction Ossification of the posterior longitudinal ligament (OPLL) is a common cervical disease that can cause stenotic changes in the spinal canal and contribute to the development of quadriparesis. OPLL has been found in about 30 % of patients with spinal cord injury (SCI) [1, 2]. These results indicate that OPLL is a major risk factor for developing acute cervical SCI. Several factors for predicting surgical outcome after surgical treatment of cervical OPLL have been discussed [3 6]. Some authors reported that patients with increased intramedullary signal intensity (SI) based on magnetic resonance imaging (MRI) had a poor prognosis after surgical decompression, while others found no clear relationship between SI and prognosis after surgery [3, 5 9]. Only a handful of studies have investigated prognostic factors for SCI associated with OPLL [2, 10, 11]. It is difficult to predict the recovery rate and prognosis of SCI with OPLL because traumatic cervical SCI patients are a heterogeneous patient population and are treated with various management methods. We performed a retrospective investigation to examine prognostic factors in SCI associated with OPLL without any bony fracture. We assessed whether severe spinal canal stenosis caused by OPLL, intramedullary signal change on magnetic resonance images, or other potential prognostic factors affected neurological outcome after SCI without any bony fractures. Materials and methods Patient selection This study was approved by the local ethical committee and the institutional review board of our hospital. From June 2006 to July 2013, we treated 246 patients with cervical cord injury. Among the patients treated, 51 patients (20.7 %) had ventral cord compression involving more than three-level OPLL without bony fractures. Thirteen patients who underwent anterior cervical decompression were excluded because of bias or differences in surgical factors. Thirty-eight patients (34 men) with a mean age of 62.7 years (range, 40 to 82 years) had spinal cord injury without any bony fractures associated with more than three-level OPLL. All patients underwent posterior cervical decompressive surgery using cervical laminoplasty or laminectomy with fusion. Patient age, gender, type of trauma, duration of symptoms, neurologic deficits, medical conditions, and radiographic findings were investigated. Charts were reviewed to determine the cause of injury and the interval between the accident and operation. Force was confirmed by edema of prevertebral soft tissue on MRI or frontal ecchymosis. Presence of OPLL was confirmed by X-ray or computed tomography. Inclusion criteria were cervical cord injury and admission through the outpatient department (OPD) or emergency room (ER). Patients with spinal cord compression caused by OPLL extending more than three vertebrae were included, as were those with the specific incomplete neurological syndrome called central cord syndrome, which is characterized by greater muscle weakness and/or sensory loss in the upper limbs than the lower limbs and others caused by hyperextension, hyperflexion, or axial loading injuries. We excluded patients with neurological symptoms before trauma, one- or two-level OPLL, other acute traumatic cord injuries with cervical bony fracture or dislocation caused by high-energy trauma, complete neurological injury after trauma, or another confirmed neurological disorder (e.g., cerebral palsy, Parkinson s disease, multiple sclerosis, polio). Ossification of the yellow ligament, severe disc herniation, and previous history of cervical spine surgery were also exclusion criteria. All patients underwent high-resolution MR imaging using a 1.5 T Signa (Siemens Medical System) imaging unit prior to surgery. We carefully ruled out tumors, demyelinating disease, sarcoid lesions, and spinal cord infarct. Patients who died or had missing data before follow-up evaluation were excluded. We defined complications as events that occurred within 1 month after surgery. We analyzed neurologic recovery in patients who had completed at least 12 months of follow-up. Neurological evaluation Neurological status was assessed using the International Standards for Neurological and Functional Classification of Spinal Cord Injury according to the American Spinal Injury Association (ASIA). ASIA impairment scale and motor score (ranging from 0 to 100) were documented at the time of admission and discharge for each patient, and at about 12 months after surgery. The neurological assessments were performed in patients who had completed 1-year follow-up (5 patients underwent 12-month follow-up postoperatively and 33 patients 24-month follow-up after surgery). Improvement in neurologic score was determined by calculating the recovery rate using the method of Lucas and Ducker [12]. Recovery rate (RR) takes into account the impact of changes dependent on baseline values by implying the largest potential improvement: RR = (NS f NS i )/(T NS i ), where RR is the recovery rate, NS f is the neurologic score at follow-up, NS i is the initial neurologic score, and T is the maximum possible score (100, 114, and 114 for the motor score, sensory score, and pin-prick score, respectively).
3 Kwon et al. Journal of Orthopaedic Surgery and Research (2015) 10:94 Page 3 of 9 Radiological evaluation Preoperative plain radiographs, three-dimensional computed tomography (3D CT), and MRI of the cervical spine were performed in all patients. Radiographic parameters include the type of OPLL, sagittal diameter of the canal, cervical lordosis, space available for the spinal cord (SAC), and intramedullary signal intensity on T2- weighted MR images were recorded. OPLL was classified as segmental type, continuous type, mixed type, or localized type according to the criteria of the Japanese Investigation Committee on the Ossification of the Spinal Ligament [13]. Cervical spine stenosis was measured by the Torg- Pavlov ratio (ratio of the sagittal spinal canal diameter to the vertebral body diameter at the same level) on plain radiographs. Cervical sagittal alignment (lordotic angle) was determined according to Cobb s method by drawing a line parallel to the inferior aspect of the C2 body and a line parallel to that of the C7 body from a neutral lateral view. Also, the K-line slope [14], the straight line of the midpoints from C2 to C7 spinal canal, was used as a radiological parameter (Fig. 1). A computed tomographic (CT) scan was performed before surgery for all patients. An Aquilion 16 CT scanner (Toshiba Medical Systems, Tokyo, Japan) was used in this series. Horizontal slices were cut to a slice thickness of 1 mm in all cases. Three-dimensional CT was performed at a neutral cervical position to avoid neurological deterioration in cervical injured patients with cervical OPLL. Using axial CT scans, we evaluated static canal stenosis caused by OPLL by measuring the SAC (Fig. 2). Using a picture archiving and communication system (PACS), we measured the length of the signal change from one end of the involved region to the other on T2- weighted sagittal images (Fig. 3). We divided the signal intensity (SI) on T2-weighted MR images into three grades. Increased SI of the spinal cord at the narrowest level was assigned one of three grades (grades 0, 1, or 2) by experienced radiologists. Observers were blinded to the patient data. SI was classified as grade 0 if there was no intramedullary high SI on T2-weighted MR images, grade 1 if a predominantly faint and fuzzy border was noted, and grade 2 if a predominantly intense and well-defined border was noted (Fig. 4). Surgical management We attempted to perform cervical decompressive surgeries in patients with neurological deficits as soon as possible. If the spinal cord was injured within 8 h, patients with neurological deficit after minor trauma received a high dose of prednisolone, according to the American National Acute Spinal Cord Injury Society criteria [15]. The first dose was 30 mg/kg and given within 15 min; after 45 min, a second dose of 5.4 mg (kg/h) was maintained for 23 h. If the injury time exceeded 8 h, 20 mg dexamethasone was used four times a day for the first 3 days and daily reduced for the next 3 days. The decision to perform decompressive surgery was based on the patient s general and neurological status. We defined the operation time as the time interval between the traumatic event and surgery. Cervical extensive laminoplasty was selected based on the neurologic symptoms and the extent of cord compressed levels, including the most narrowed side on images. Unilateral or bilateral gutters were made using a high-speed drill at the area between the facet joints and the laminae, and spinous processes were split sagittally with a high-speed burr. The spinal canal was enlarged by opening the split laminae unilaterally or bilaterally with a spreader. Posterior cervical titanium miniplates (Centerpiece, Medtronic Sofamor Danek, Memphis, TN, USA) or hydroxyapatite spacers (Apacerum, Asahi Optical Co., Ltd., Tokyo, Japan) were used to keep the door open. For OPLL patients with local kyphosis or segmental instability, we performed cervical laminectomy and fusion and tried to realign local kyphosis using a posterior screw-rod system. Following complete decompression of neural elements, lateral mass screw and rod instrumentation were performed. Perizygapophysial joints were filled with autologous bone fragments from the excised lamina. After surgery, all patients were required to wear Miami neck collars or Philadelphia braces for a mean period of 3 months. Patients were followed clinically by radiography using plain and dynamic films at 1, 3, and 6 months and then every 6 months postoperatively. Statistical analysis Multifactorial effects of variables were studied. Mann- Whitney U tests were used for nonparametric analyses of differences between pairs of groups, and the Kruskal- Wallis test followed by the Mann-Whitney U test was used to examine differences between the three SI groups. To identify variables independently related to ASIA recovery ratio, univariate or multivariate logistic regression analyses were used. Pearson s correlation analysis was performed to determine the significance of the correlation between ASIA recovery ratio and age, duration of symptoms, cervical alignment, cervical canal stenosis (Pavlov s ratio), SAC, preoperative ASIA motor score, SI length, and postoperative ASIA motor score. Spearman s correlation analysis was performed to determine the significance of the correlation between ASIA recovery ratio and gender, OPLL type, or preoperative SI grade. Correlations between variables were assessed with regression analyses using MedCalc version 14.0 (MedCalc,
4 Kwon et al. Journal of Orthopaedic Surgery and Research (2015) 10:94 Page 4 of 9 Fig. 2 Measurement of the space available for the spinal cord (SAC). SAC was calculated on the basis of axial computed tomography. B = developmental canal diameter. B-A = space available for the spinal cord (SAC) Fig. 1 Cervical lordosis and K-line. Lordotic angle was created by drawing a line parallel to the inferior aspect of the C2 body and a line parallel to that of the C7 body on lateral view with the patient in a neutral position. The K-line is a straight line from the midpoints of the spinal canal at C2 and C7 Mariakerke, Belgium). p values < 0.05 were considered significant. Results The primary cause of cord injury in patients with OPLL was slipping down and falling injuries (78.9 %), followed by a motor vehicle accident. The patient had episodes of minor neck trauma: injuries from slipping down in 23, falling down in 7 patients, motor vehicle accident in 7, being struck by objects in 1, and sports activities in 2. The injury was mostly caused by a sudden force with subsequent compression of the cord by a bony posterior ligament or narrowed canal. Most cases of the cervical SCI complicated by OPLL are caused by hyperextension injuries resulting from falling or slipping down injuries. Fourteen patients had typical central cord syndrome. Four had incomplete cord injuries caused by flexion injuries, and 20 had incomplete neurological deficits by combined injuries such as lateral bending, rotation, axial loading, and hyperflexion or hyperextension of the cord. All 38 patients included in this study underwent posterior decompressive surgery. Expansive cervical laminoplasty was performed in 8 patients, and cervical laminectomy with fusion was performed in 30 patients. Mean ASIA motor score at admission was 38.4 ± 21.9 (range, 2 70) and improved to 67.7 ± 19.1 at last followup (range, 8 94) (p < 0.05). Overall, the mean recovery rate of the motor score was 55.8 ± 19.9 % (range, %), and the recovery ratio improved in all patients. In addition, the average ASIA score of light touch sensation and pin-prick sensation increased from 70.9 ± 34.5 and 70.9 ± 34.4, respectively, at admission to 79.7 ± 34.1 and 79.7 ± 34.1, respectively, after the final follow-up. Mean recovery rate of light touch and pin sensation were 32.3 ± 28.2 % and 33.8 ± 24.7 %, respectively. In general, the sensory recovery ratio was lower than the motor recovery ratio. Mean follow-up time was 42.2 ± 25.1 months (range, months). The duration of preoperative symptoms ranged from 1 to 23 days. SAC was 6.1 ± 2.2 mm (range, mm). The mean length of SI changes was 5.9 ± 3.7 mm (range, mm). Radiological findings revealed continuous in 14 patients, mixed type OPLL in 4 patients, and segmental type OPLL in 20 patients. There was no significant relationship between OPLL type and neurological outcome in our study. The mean OPLL level treated by surgical operation was 3.2 ± 0.4. Among 38 patients, 33 (86.8 %) showed increased signal intensity within the spinal cord
5 Kwon et al. Journal of Orthopaedic Surgery and Research (2015) 10:94 Page 5 of 9 The respective surgical level caused by OPLL was 3.4 ± 0.5ingrade0patients,3.1±0.3ingrade1,and3.2±0.4 in grade 2. There was no significant difference in surgical levels among the three groups. The surgical procedures performed were expansive laminoplasty in one patient with grade 0 and cervical laminectomy with fusion in four patients with grade 0. In grade 1, expansive laminoplasty was performed in 4 patients and cervical laminectomy with fusion in 16. In grade 2, expansive laminoplasty was performed in three patients and cervical laminectomy with fusion in ten (Table 1). Preoperative motor scores and recovery ratios (%) were 60.0 ± 10.1 and 82.4 ± 18.1 %, respectively, in the five SI grade 0 patients; 40.6 ± 21.1 and 66.0 ± 18.1 %, respectively, in the 20 grade 1 patients; and 26.0 ± 6.9 and 30.9 ± 26.6 %, respectively, in the 13 grade 2 patients. Preoperative sensory (touch) scores and recovery ratios (%) were ± 7.6 and 69.8 ± 19.7 %, respectively, in the five grade 0 SI patients; 77.5 ± 29.2 and 29.7 ± 19.2 %, respectively, in the 20 grade 1 patients; and 49.4 ± 36.7 and 21.8 ± 22.2 %, respectively, in the 13 grade 2 patients. The motor and sensory recovery ratios were significantly different among the three groups (p < 0.05) (Table 1). That is, patients with a higher grade of intramedullary signal intensity showed poorer ASIA motor and sensory recovery ratio than those with a lower grade of signal changes on T2-weighted images (Fig. 5). In present study, 29 patients were classified as K-line (+) and 9 were classified as K-line ( ). The mean recovery ratio was 63.7 ± 24.3 % in the K-line (+) group and 30.3 ± 25.6 % in the K-line ( ) group. The neurological outcome in patients with K-line (+) was better than in those with K-line ( ) (p < 0.05). Fig. 3 Length of signal intensity. It was measured by the proximaldistal range of the intramedullary hyperintensity on T2-weighted images on T2-weighted MR images, whereas 5 patients (13.2 %) did not. SI change on MR images was located on C3/4 level in 13 patients, C4/5 in 14, C5/6 in 4, C2/ 3/4 in 1 and C3/4/5 in 1. The mean length of SI changes was 5.9 ± 3.7 mm (range, mm). However, the length of pathological changes on spinal cord was not correlated with neurological outcome. When the grade of intramedullary SI change on T2WI was assessed,5patientsshowedsigrade0changes,20patients SI grade 1 changes, and 13 patients grade 2 changes. In this study, there was no low-signal change on T1-weighted image initially. Logistic regression analyses Univariate logistic regression analysis and multivariate logistic regression analysis were performed to identify prognostic factors. Patient age, initial ASIA motor score, severity of intramedullary signal intensity, and SAC had significant effects on the neurological outcome after surgery (Table 2). Patient age was significantly correlated with recovery ratio (coefficient = , 95 % CI = , p = , Fig. 6a). Initial ASIA motor score was significantly correlated with recovery ratio (coefficient = , 95 % CI = , p < , Fig. 6b). Furthermore, the change in SAC was significantly correlated with the rate of postoperative neurologic improvement (coefficient = , 95 % CI = , p = , Fig. 6c). However, there was no significant relationship between initial cervical curvature, time interval between injury and operation, OPLL type, the length of signal intensity (SI), or congenital canal stenosis (Pavlov s ratio) and neurological outcome.
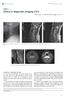
6 Kwon et al. Journal of Orthopaedic Surgery and Research (2015) 10:94 Page 6 of 9 Fig. 4 Signal intensity grade. Signal intensity of the spinal cord was assessed as grade 0 no change in signal intensity (SI) on T2-weighted MR images; grade 1 light intensity change; and grade 2 bright signal, clearly distinguishable from that of grade 1 In our study, 1 of the 38 patients (2.6 %) developed C5 palsy and postoperative hematoma 3 h after surgery. We immediately removed the hematoma, but the C5 nerve palsy remained on the patient s right side. Another patient developed superficial wound infection after surgery, but no additional surgery was required to remove instrumentation. Discussion OPLL has been found to be highly prevalent in patients with acute traumatic cervical SCI; in particular, OPLL has been reported in 34 ~ 38 % of cervical SCI patients without bone injury [1, 2]. They were caused primarily by low-energy trauma. The vast majority of patients were elderly and unaware of OPLL. According to other studies [16], there are only a few patients who are aware of having cervical OPLL before trauma. In our cases, one patient suffered neck pain 2 years before the trauma but he was not aware of cervical OPLL and was not diagnosed with cervical OPLL. Consistent with previous studies, the majority of SCI patients with OPLL in our study were elderly, with the peak incidence found in patients between 65 and 75 years old of age. Intramedullary signal changes and neurological outcome Several studies have investigated the relationship between increased SI on MRI and surgical outcomes in Table 1 Clinical characteristics and neurological outcome according to the severity of signal intensity Grade 0 (n = 5) Grade 1 (n = 20) Grade 2 (n = 13) p value Age (years) 57.4 ± ± ± NS Symptom duration (days) 3.8 ± ± ± NS SAC (mm) 7.2 ± ± ± NS Cervical curvature ( ) 13.3 ± ± ± NS Cervical canal stenosis 0.84 ± ± ± NS Preoperative motor score 60.0 ± ± ± Preoperative touch score ± ± ± Recovery motor rate (%) 82.4 ± ± ± Recovery touch rate (%) 69.8 ± ± ± Surgical levels 3.4 ± ± ± NS Laminectomy and fusion Expansive laminoplasty SAC space available for the spinal cord, NS not significant
7 Kwon et al. Journal of Orthopaedic Surgery and Research (2015) 10:94 Page 7 of 9 Fig. 5 A patient with intramedullary signal intensity grade 2. a Preoperative T2-weighted MRI results for a 54-year-old male patient with spinal cord compression at C Intramedullary high signal intensity (SI), grade 2, was visible at the region of the marked compressed cord. Initial ASIA motor score was 48. b Cervical 3D CT showed mixed type ossification of the posterior longitudinal ligament (OPLL). Spinal canal stenosis (SAC) was 5.9 mm. c The patient underwent cervical laminoplasty at C d MRI of the patient from B 12 months after cervical laminoplasty with successful decompression of the spinal cord. The patient s ASIA motor score was 72. The recovery rate was 46.2 % patients with acute cervical cord injury [3, 5, 6, 17, 18]. We found that if intramedullary signal changes on T2WI were present, clinical outcomes were unfavorable after surgery as compared to those patients with no intramedullary signal changes on T2WI. We recognized three grades of cord SI and found that these grades were inversely proportional to the outcome of cervical cord injury. Patients with a brighter SI change (grade 2) on T2-weighted MR images had poorer neurological outcomes than those with a faint SI change (grade 1) or those without a SI change (grade 0). Thus, decompressive surgery should be performed for patients with high intramedullary SI if possible. Ramanauskas and colleagues [19] divided myelomalacia into three stages and speculated that in the early stage, a change in the signal intensity of the spinal cord on MRI reflects cord edema. In contrast, in the intermediate stage, a signal change reflected cystic necrosis of the central gray matter after prolonged cord edema. They reported that in early and intermediate stages, the spinal cord showed high-signal intensity on T2WI sequences, while at a later stage, low-signal intensity on T1WI and high SI on T2WI sequences were noted. We did not find a low-signal change on T1-weighted images initially. We assumed that this was because patients experienced a sudden minor traumatic force to their neck area, and there was not sufficient time for low SI changes to develop on T1WI. Age and neurological outcome Age as an adverse prognostic factor for neurological outcome has been reported previously [4, 20]. Prognosis was less optimistic in patients with severe initial cord injury who were older than those who were younger [20]. We also found that older age at injury was a negative predictor of neurological recovery. Older patients tend to have a higher incidence of cervical spondylosis and cord ischemia due to atherosclerotic changes of the vertebral or feeding vascular structures. These senile factors and other comorbidities might contribute to unfavorable clinical outcomes in elderly patients with an injured spinal cord and OPLL. Table 2 Multivariate regression analysis results for the recovery ratio and other factors Recovery ratio Coef. s.e. t value p value 95 % CI Age to Operation interval NS to Cervical alignment NS to Cervical stenosis (Pavlov ratio) NS to SAC to SI length NS to SI grade < to Preoperative motor score < to SAC space available for the spinal cord, SI signal intensity, Coef. regression coefficient, s.e. standard error, NS non-significant
8 Kwon et al. Journal of Orthopaedic Surgery and Research (2015) 10:94 Page 8 of 9 Fig. 6 The correlation between age, ASIA motor score, SAC, and recovery ratio. a The patients age showed a significant correlation with the recovery ratio. b Initial ASIA motor score was correlated with recovery ratio. c Recovery ratio was correlated with the space available for the spinal cord (SAC) Canal stenosis and neurological outcome Minor trauma to the neck sometimes results in deterioration of symptoms in patients with cervical OPLL because of preexisting spinal canal narrowing by OPLL [21 23]. Previous investigators noted poor neurological outcome in spinal cord injured patients who had severe cord compression [24 26]. Furthermore, developmental cervical spinal canal stenosis may lead to transient compression of the spinal cord and affect the neurological outcome after surgery [23]. In the present study, we found that the extent of cord compression, as assessed by parameters such as SAC, was correlated with neurologic recovery in SCI patients with OPLL, but the effect of the developing cervical canal on neurological recovery was not significant. At the moment of traumatic injury, the spinal cord can be abruptly pinched by inner structures of the spinal canal, particularly in severe stenotic areas caused by OPLL. The traumatic force may cause intramedullary SI changes to develop, resulting in neurologic deficits. Lesions of intramedullary SI change were in areas adjacent to the severely compressed spinal cord. We found that the extent of cord compression was a more important predictor of neurological outcome after surgery than congenital canal stenosis (Pavlov s ratio) in cervical cord injured patients with OPLL. Initial neurological status and neurological outcome Initial ASIA motor score has been shown to be significantly related to ambulatory and hand function outcomes in patients with spinal cord injury [21, 25]. In agreement with other studies [21, 26 28], we found that preoperative neurological status, particularly motor score, predicted neurological recovery. One interesting finding of this study was that the ASIA sensory recovery ratio was lower than the ASIA motor recovery ratio. This suggests that if patients with minor traumatic injury have high intramedullary SI changes in the spinal cord, their sensory function improves less than their motor recovery. Fujiyoshi and colleagues [14] reported the K-line as a simple and practical index for deciding the surgical approach for cervical OPLL patients and asserted the correlation of cervical alignment with neurological outcome. They advocated that the patients with a negative K-line slope, which meant the OPLL touched the spinal cord, had a significantly lower recovery rate than those with a positive K-line. In accordance with previous studies [14, 29, 30], our present study showed the better recovery rate in the patients with positive K-line than in negative K-line. Limitations of this study include its retrospective design and the small number of patients. The type of trauma may also have been more varied than we accounted for because it was patient-reported. Furthermore, the definition of a minor traumatic injury is controversial. Despite these drawbacks, our results provide insight into the factors that predict neurological recovery in patients with OPLL who undergo decompression surgery due to an injured cervical cord. We did not perform a quantitative analysis of signal intensity in the spinal cord. Rather, radiologists blinded to the patient data categorized intramedullary signal intensities into three groups. Further extended and comprehensive studies are required to confirm the specific relationships between prognostic factors and clinical outcomes described in this paper. Conclusions The degree of canal stenosis, including SAC, intramedullary signal intensity change, initial motor score, and patient age, should be considered prognostic factors when surgical decompression is performed for cervical cord injured patients without bony fractures, particularly for those patients who have a high intramedullary SI initially. That is, prognosis was less optimistic in older patients with severe neurologic deficits, marked cord compression, or the existence of abnormal MR signal change in the spinal cord.
9 Kwon et al. Journal of Orthopaedic Surgery and Research (2015) 10:94 Page 9 of 9 Competing interests The authors declare that they have no competing interests. Authors contributions SYK carried out the analysis of data and drafted the manuscript. JJS revised it critically for important intellectual content and gave final approval of the version to be submitted. JHL participated in the design of the study and performed the statistical analysis. WHC conceived of the study, and participated in its design and coordination and helped to draft the manuscript. All authors read and approved the final manuscript. Acknowledgements The authors wish to thank Hyun Kyung Park, Ph.D., for her contributions in drafting the manuscript or revising it for important intellectual content. The authors also extend gratitude to Ms. Ah Ram Lee for creating the original artwork for the figures and acquisition of data in this publication. Author details 1 Department of Neurosurgery, Sanggye Paik Hospital, Inje University College of Medicine, Sanggye-7 dong, 761-1, Nowon-gu, Seoul , South Korea. 2 Department of Radiology, Sanggye Paik Hospital, Inje University College of Medicine, Sanggye-7 dong, 761-1, Nowon-gu, Seoul , South Korea. Received: 17 March 2015 Accepted: 28 May 2015 References 1. Katoh S, el Masry WS, Jaffray D, McCall IW, Eisenstein SM, Pringle RG, et al. Neurologic outcome in conservatively treated patients with incomplete closed traumatic cervical spinal cord injuries. Spine (Phila Pa 1976). 1996;21: Koyanagi I, Iwasaki Y, Hida K, Akino M, Imamura H, Abe H. Acute cervical cord injury without fracture or dislocation of the spinal column. J Neurosurg. 2000;93: Ishida Y, Tominaga T. Predictors of neurologic recovery in acute central cervical cord injury with only upper extremity impairment. Spine (Phila Pa 1976). 2002;27: discussion Penrod LE, Hegde SK, Ditunno Jr JF. Age effect on prognosis for functional recovery in acute, traumatic central cord syndrome. Arch Phys Med Rehabil. 1990;71: Shepard MJ, Bracken MB. Magnetic resonance imaging and neurological recovery in acute spinal cord injury: observations from the National Acute Spinal Cord Injury Study 3. Spinal Cord. 1999;37: Choi JH, Shin JJ, Kim TH, Shin HS, Hwang YS, Park SK. Does intramedullary signal intensity on MRI affect the surgical outcomes of patients with ossification of posterior longitudinal ligament? J Korean Neurosurg Soc. 2014;56: Wada E, Yonenobu K, Suzuki S, Kanazawa A, Ochi T. Can intramedullary signal change on magnetic resonance imaging predict surgical outcome in cervical spondylotic myelopathy? Spine (Phila Pa 1976). 1999;24: discussion Morio Y, Teshima R, Nagashima H, Nawata K, Yamasaki D, Nanjo Y. Correlation between operative outcomes of cervical compression myelopathy and MRI of the spinal cord. Spine (Phila Pa 1976). 2001;26: Shin JJ, Jin BH, Kim KS, Cho YE, Cho WH. Intramedullary high signal intensity and neurological status as prognostic factors in cervical spondylotic myelopathy. Acta Neurochir (Wien). 2010;152: Onishi E, Sakamoto A, Murata S, Matsushita M. Risk factors for acute cervical spinal cord injury associated with ossification of the posterior longitudinal ligament. Spine (Phila Pa 1976). 2012;37: Gu Y, Chen L, Dong RB, Feng Y, Yang HL, Tang TS. Laminoplasty versus conservative treatment for acute cervical spinal cord injury caused by ossification of the posterior longitudinal ligament after minor trauma. Spine J. 2014;14: Lucas JT, Ducker TB. Motor classification of spinal cord injuries with mobility, morbidity and recovery indices. Am Surg. 1979;45: Tsuyama N. Ossification of the posterior longitudinal ligament of the spine. Clin Orthop Relat Res. 1984; Fujiyoshi T, Yamazaki M, Kawabe J, Endo T, Furuya T, Koda M, et al. A new concept for making decisions regarding the surgical approach for cervical ossification of the posterior longitudinal ligament: the K-line. Spine (Phila Pa 1976). 2008;33:E Bracken MB, Shepard MJ, Collins WF, Holford TR, Young W, Baskin DS, et al. A randomized, controlled trial of methylprednisolone or naloxone in the treatment of acute spinal-cord injury. Results of the Second National Acute Spinal Cord Injury Study. N Engl J Med. 1990;322: Matsunaga S, Sakou T, Hayashi K, Ishidou Y, Hirotsu M, Komiya S. Traumainduced myelopathy in patients with ossification of the posterior longitudinal ligament. J Neurosurg. 2002;97: Boldin C, Raith J, Fankhauser F, Haunschmid C, Schwantzer G, Schweighofer F. Predicting neurologic recovery in cervical spinal cord injury with postoperative MR imaging. Spine (Phila Pa 1976). 2006;31: Shin J-J. Intramedullary signal intensity and other prognostic factors for surgical outcome in spinal cord injury associated with ossification of the posterior longitudinal ligament (OPLL). The Spine Journal. 2014;14:S Ramanauskas WL, Wilner HI, Metes JJ, Lazo A, Kelly JK. MR imaging of compressive myelomalacia. J Comput Assist Tomogr. 1989;13: Roth EJ, Lawler MH, Yarkony GM. Traumatic central cord syndrome: clinical features and functional outcomes. Arch Phys Med Rehabil. 1990;71: Schaefer DM, Flanders AE, Osterholm JL, Northrup BE. Prognostic significance of magnetic resonance imaging in the acute phase of cervical spine injury. J Neurosurg. 1992;76: Kulkarni MV, Bondurant FJ, Rose SL, Narayana PA. 1.5 tesla magnetic resonance imaging of acute spinal trauma. Radiographics. 1988;8: Sieh KM, Leung SM, Lam JS, Cheung KY, Fung KY. The use of average Pavlov ratio to predict the risk of post operative upper limb palsy after posterior cervical decompression. J Orthop Surg Res. 2009;4: Ramon S, Dominguez R, Ramirez L, Paraira M, Olona M, Castello T, et al. Clinical and magnetic resonance imaging correlation in acute spinal cord injury. Spinal Cord. 1997;35: Flanders AE, Spettell CM, Friedman DP, Marino RJ, Herbison GJ. The relationship between the functional abilities of patients with cervical spinal cord injury and the severity of damage revealed by MR imaging. AJNR Am J Neuroradiol. 1999;20: Marciello MA, Flanders AE, Herbison GJ, Schaefer DM, Friedman DP, Lane JI. Magnetic resonance imaging related to neurologic outcome in cervical spinal cord injury. Arch Phys Med Rehabil. 1993;74: Lao L, Zhong G, Li X, Qian L, Liu Z. Laminoplasty versus laminectomy for multi-level cervical spondylotic myelopathy: a systematic review of the literature. J Orthop Surg Res. 2013;8: Cho YE, Shin JJ, Kim KS, Chin DK, Kuh SU, Lee JH, et al. The relevance of intramedullary high signal intensity and gadolinium (Gd-DTPA) enhancement to the clinical outcome in cervical compressive myelopathy. Eur Spine J. 2011;20: Fujimori T, Iwasaki M, Okuda S, Takenaka S, Kashii M, Kaito T, et al. Longterm results of cervical myelopathy due to ossification of the posterior longitudinal ligament with an occupying ratio of 60 % or more. Spine (Phila Pa 1976). 2014;39: Nagashima H, Nanjo Y, Tanida A, Mihara T, Takeda C, Teshima R. Influence of spinous process spacers on surgical outcome of laminoplasty for OPLL. Orthopedics. 2013;36:e Submit your next manuscript to BioMed Central and take full advantage of: Convenient online submission Thorough peer review No space constraints or color figure charges Immediate publication on acceptance Inclusion in PubMed, CAS, Scopus and Google Scholar Research which is freely available for redistribution Submit your manuscript at
Radiological pathogenesis of cervical myelopathy in 60 consecutive patients with cervical ossi cation of the posterior longitudinal ligament
 Spinal Cord (1999) 37, 853 ± 857 ã 1999 International Medical Society of Paraplegia All rights reserved 1362 ± 4393/99 $15.00 http://www.stockton-press.co.uk/sc Radiological pathogenesis of cervical myelopathy
Spinal Cord (1999) 37, 853 ± 857 ã 1999 International Medical Society of Paraplegia All rights reserved 1362 ± 4393/99 $15.00 http://www.stockton-press.co.uk/sc Radiological pathogenesis of cervical myelopathy
Disclosures: T. Yoshii: None. T. Yamada: None. T. Taniyama: None. S. Sotome: None. T. Kato: None. S. Kawabata: None. A. Okawa: None.
 Dynamic Changes in Spinal Cord Compression by Cervical Ossification of the Posterior Longitudinal Ligament Evaluated by Kinematic Computed Tomography Myelogram Toshitaka Yoshii, Tsuyoshi Yamada, Takashi
Dynamic Changes in Spinal Cord Compression by Cervical Ossification of the Posterior Longitudinal Ligament Evaluated by Kinematic Computed Tomography Myelogram Toshitaka Yoshii, Tsuyoshi Yamada, Takashi
Interlaminar Bony Fusion after C3-6 Double-Door Laminoplasty for Cervical Spondylotic Myelopathy: Its Predictors and Characteristics
 Interlaminar Bony Fusion after C3-6 Double-Door Laminoplasty for Cervical Spondylotic Myelopathy: Its Predictors and Characteristics Yoshiro Nanjo, Hideki Nagashima, Shinji Tanishima,Tokumitsu Mihara,
Interlaminar Bony Fusion after C3-6 Double-Door Laminoplasty for Cervical Spondylotic Myelopathy: Its Predictors and Characteristics Yoshiro Nanjo, Hideki Nagashima, Shinji Tanishima,Tokumitsu Mihara,
Winner of the Char Publications Registrars Writing Competition 2010
 CLINICAL ARTICLE SA ORTHOPAEDIC JOURNAL Autumn 2011 Vol 10 No 1 / Page 35 C L I N I C A L A RT I C L E Winner of the Char Publications Registrars Writing Competition 2010 Acute traumatic cervical spinal
CLINICAL ARTICLE SA ORTHOPAEDIC JOURNAL Autumn 2011 Vol 10 No 1 / Page 35 C L I N I C A L A RT I C L E Winner of the Char Publications Registrars Writing Competition 2010 Acute traumatic cervical spinal
Is OPLL-induced canal stenosis a risk factor of cord injury in cervical trauma?
 Acta Orthop. Belg., 2014, 80, 567-574 ORIGINAL STUDY Is OPLL-induced canal stenosis a risk factor of cord injury in cervical trauma? Kyung-Jin Song, Chan-Il Park, Do-Yeon Kim, Young-Ran Jung, Kwang-Bok
Acta Orthop. Belg., 2014, 80, 567-574 ORIGINAL STUDY Is OPLL-induced canal stenosis a risk factor of cord injury in cervical trauma? Kyung-Jin Song, Chan-Il Park, Do-Yeon Kim, Young-Ran Jung, Kwang-Bok
Department of Neurological Surgery, Asan Medical Center, University of Ulsan College of Medicine, Seoul, Korea
 online ML Comm CLINICAL ARTICLE Korean J Neurotrauma 2014;10(2):60-65 pissn 2234-8999 / eissn 2288-2243 http://dx.doi.org/10.13004/kjnt.2014.10.2.60 Midline Splitting Cervical Laminoplasty Using Allogeneic
online ML Comm CLINICAL ARTICLE Korean J Neurotrauma 2014;10(2):60-65 pissn 2234-8999 / eissn 2288-2243 http://dx.doi.org/10.13004/kjnt.2014.10.2.60 Midline Splitting Cervical Laminoplasty Using Allogeneic
SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT
 SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT 1 Anatomy 3 columns- Anterior, middle and Posterior Anterior- ALL, Anterior 2/3 rd body & disc. Middle- Posterior 1/3 rd of body & disc, PLL Posterior-
SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT 1 Anatomy 3 columns- Anterior, middle and Posterior Anterior- ALL, Anterior 2/3 rd body & disc. Middle- Posterior 1/3 rd of body & disc, PLL Posterior-
ORIGINAL PAPER. Department of Orthopedic Surgery, Chubu Rosai Hospital, Nagoya, Japan ABSTRACT
 Nagoya J. Med. Sci. 77. 221 ~ 228, 2015 ORIGINAL PAPER RANGE OF MOTION DETERMINED BY MULTIDETECTOR-ROW COMPUTED TOMOGRAPHY IN PATIENTS WITH CERVICAL OSSIFICATION OF THE POSTERIOR LONGITUDINAL LIGAMENT
Nagoya J. Med. Sci. 77. 221 ~ 228, 2015 ORIGINAL PAPER RANGE OF MOTION DETERMINED BY MULTIDETECTOR-ROW COMPUTED TOMOGRAPHY IN PATIENTS WITH CERVICAL OSSIFICATION OF THE POSTERIOR LONGITUDINAL LIGAMENT
Giant schwannoma with extensive scalloping of the lumbar vertebral body treated with one-stage posterior surgery: a case report
 Iizuka et al. Journal of Medical Case Reports 2014, 8:421 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Giant schwannoma with extensive scalloping of the lumbar vertebral body treated with one-stage
Iizuka et al. Journal of Medical Case Reports 2014, 8:421 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Giant schwannoma with extensive scalloping of the lumbar vertebral body treated with one-stage
Incidence and Risk Factors for Late Neurologic Deterioration after C3 C6 Laminoplasty for Cervical Spondylotic Myelopathy
 THIEME GLOBAL SPINE JOURNAL Original Article 53 Incidence and Risk Factors for Late Neurologic Deterioration after C3 C6 Laminoplasty for Cervical Spondylotic Myelopathy Hironobu Sakaura 1 Toshitada Miwa
THIEME GLOBAL SPINE JOURNAL Original Article 53 Incidence and Risk Factors for Late Neurologic Deterioration after C3 C6 Laminoplasty for Cervical Spondylotic Myelopathy Hironobu Sakaura 1 Toshitada Miwa
Efficacy and results of expansive laminoplasty in patients with severe cervical myelopathy due to cervical canal stenosis
 Original Article Efficacy and results of expansive laminoplasty in patients with severe cervical myelopathy due to cervical canal stenosis D. Agrawal, B. S. Sharma, A. Gupta, V. S. Mehta Department of
Original Article Efficacy and results of expansive laminoplasty in patients with severe cervical myelopathy due to cervical canal stenosis D. Agrawal, B. S. Sharma, A. Gupta, V. S. Mehta Department of
Risk Factors for Hinge Fracture Associated with Surgery Following Cervical Open-Door Laminoplasty
 CLINICAL ARTICLE Korean J Neurotrauma 18;14(2):118-122 pissn 2234-8999 / eissn 2288-2243 https://doi.org/1.134/kjnt.18.14.2.118 Risk Factors for Hinge Fracture Associated with Surgery Following Cervical
CLINICAL ARTICLE Korean J Neurotrauma 18;14(2):118-122 pissn 2234-8999 / eissn 2288-2243 https://doi.org/1.134/kjnt.18.14.2.118 Risk Factors for Hinge Fracture Associated with Surgery Following Cervical
Technique Guide. ARCH Laminoplasty System. Dedicated System for Open-door Laminoplasty.
 Technique Guide ARCH Laminoplasty System. Dedicated System for Open-door Laminoplasty. Table of Contents Introduction Overview 2 AO ASIF Principles 4 Indications and Contraindications 5 Product Information
Technique Guide ARCH Laminoplasty System. Dedicated System for Open-door Laminoplasty. Table of Contents Introduction Overview 2 AO ASIF Principles 4 Indications and Contraindications 5 Product Information
S.S.K.MUNASINGHE ARACHCHIGE NATIONAL HOSPITAL OF SRI LANKA
 AN INSIGHT TO THE DILEMMA- CO-EXISTENCE OF OSSIFICAION OF POSTERIOR LONGITUDINAL LIGAMENT AND CERVICAL DISC PROLAPSE A SRI LANKAN EXPERIENCE S.S.K.MUNASINGHE ARACHCHIGE NATIONAL HOSPITAL OF SRI LANKA BACKGROUND
AN INSIGHT TO THE DILEMMA- CO-EXISTENCE OF OSSIFICAION OF POSTERIOR LONGITUDINAL LIGAMENT AND CERVICAL DISC PROLAPSE A SRI LANKAN EXPERIENCE S.S.K.MUNASINGHE ARACHCHIGE NATIONAL HOSPITAL OF SRI LANKA BACKGROUND
Spinal Cord (2005) 43, & 2005 International Spinal Cord Society All rights reserved /05 $
 (2005) 43, 503 507 & 2005 International Society All rights reserved 1362-4393/05 $30.00 www.nature.com/sc Case Report Postmortem study of the spinal cord showing snake-eyes appearance due to damage by
(2005) 43, 503 507 & 2005 International Society All rights reserved 1362-4393/05 $30.00 www.nature.com/sc Case Report Postmortem study of the spinal cord showing snake-eyes appearance due to damage by
Abstract Study Design Systematic review. Weerasak Singhatanadgige 1 Worawat Limthongkul 1 Frank Valone III 2 Wicharn Yingsakmongkol 1 K.
 702 Review Article GLOBAL SPINE JOURNAL THIEME Outcomes following or Fusion in Patients with Myelopathy Caused by Ossification of the Posterior Longitudinal Ligament: A Systematic Review Weerasak Singhatanadgige
702 Review Article GLOBAL SPINE JOURNAL THIEME Outcomes following or Fusion in Patients with Myelopathy Caused by Ossification of the Posterior Longitudinal Ligament: A Systematic Review Weerasak Singhatanadgige
The Predictable Factors of the Postoperative Kyphotic Change of Sagittal Alignment of the Cervical Spine after the Laminoplasty
 Clinical Article J Korean Neurosurg Soc 60 (5) : 577-583, 2017 https://doi.org/10.3340/jkns.2017.0505.007 pissn 2005-3711 eissn 1598-7876 The Predictable Factors of the Postoperative Kyphotic Change of
Clinical Article J Korean Neurosurg Soc 60 (5) : 577-583, 2017 https://doi.org/10.3340/jkns.2017.0505.007 pissn 2005-3711 eissn 1598-7876 The Predictable Factors of the Postoperative Kyphotic Change of
Yoshifumi Kudo, 1 Tomoaki Toyone, 1 Toshiyuki Shirahata, 1 Tomoyuki Ozawa, 1 Akira Matsuoka, 1 Yoichi Jin, 2 and Katsunori Inagaki 1. 1.
 Case Reports in Orthopedics Volume 2016, Article ID 1250810, 5 pages http://dx.doi.org/10.1155/2016/1250810 Case Report A Case of Successful Foraminotomy for Severe Bilateral C5 Palsy following Posterior
Case Reports in Orthopedics Volume 2016, Article ID 1250810, 5 pages http://dx.doi.org/10.1155/2016/1250810 Case Report A Case of Successful Foraminotomy for Severe Bilateral C5 Palsy following Posterior
Incidence and Risk Factors for Late Neurologic Deterioration after C3-6 Laminoplasty in Patients with Cervical Spondylotic Myelopathy
 Incidence and Risk Factors for Late Neurologic Deterioration after C3-6 Laminoplasty in Patients with Cervical Spondylotic Myelopathy Sakaura H, Miwa T, Kuroda Y, Ohwada T Dept. of Orthop. Surg., Kansai
Incidence and Risk Factors for Late Neurologic Deterioration after C3-6 Laminoplasty in Patients with Cervical Spondylotic Myelopathy Sakaura H, Miwa T, Kuroda Y, Ohwada T Dept. of Orthop. Surg., Kansai
ARCH Laminoplasty System. Dedicated System for Open-door Laminoplasty.
 ARCH Laminoplasty System. Dedicated System for Open-door Laminoplasty. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation.
ARCH Laminoplasty System. Dedicated System for Open-door Laminoplasty. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation.
Central Cord Syndrome: Does early surgical intervention improve neurological outcome
 Central Cord Syndrome: Does early surgical intervention improve neurological outcome Ciara Stevenson, Jonathan Warnock, Suzanne Maguire, Niall Eames Department of Trauma and Orthopaedic Surgery, Royal
Central Cord Syndrome: Does early surgical intervention improve neurological outcome Ciara Stevenson, Jonathan Warnock, Suzanne Maguire, Niall Eames Department of Trauma and Orthopaedic Surgery, Royal
Age-related and degenerative changes in the osseous anatomy, alignment, and range of motion
 Age-related and degenerative changes in the osseous anatomy, alignment, and range of motion of the cervical spine: a comparative study of radiographic data from 1016 patients with cervical spondylotic
Age-related and degenerative changes in the osseous anatomy, alignment, and range of motion of the cervical spine: a comparative study of radiographic data from 1016 patients with cervical spondylotic
Catastrophic Dropped Head Syndrome Requiring Multiple Reconstruction Surgeries after Cervical Laminoplasty
 CASE REPORT SPINE SURGERY AND RELATED RESEARCH Catastrophic Dropped Head Syndrome Requiring Multiple Reconstruction Surgeries after Cervical Laminoplasty Seiichi Odate, Jitsuhiko Shikata and Tsunemitsu
CASE REPORT SPINE SURGERY AND RELATED RESEARCH Catastrophic Dropped Head Syndrome Requiring Multiple Reconstruction Surgeries after Cervical Laminoplasty Seiichi Odate, Jitsuhiko Shikata and Tsunemitsu
factor for identifying unstable thoracolumbar fractures. There are clinical and radiological criteria
 NMJ-Vol :2/ Issue:1/ Jan June 2013 Case Report Medical Sciences Progressive subluxation of thoracic wedge compression fracture with unidentified PLC injury Dr.Thalluri.Gopala krishnaiah* Dr.Voleti.Surya
NMJ-Vol :2/ Issue:1/ Jan June 2013 Case Report Medical Sciences Progressive subluxation of thoracic wedge compression fracture with unidentified PLC injury Dr.Thalluri.Gopala krishnaiah* Dr.Voleti.Surya
Orthopaedics and Rehabilitation Medicine Fuculty of Medical Sciences University of Fukui
 Quantitative analysis and prognostic value of changes in spinal cord signal intensity on magnetic resonance imaging in patients with cervical compressive myelopathy Orthopaedics and Rehabilitation Medicine
Quantitative analysis and prognostic value of changes in spinal cord signal intensity on magnetic resonance imaging in patients with cervical compressive myelopathy Orthopaedics and Rehabilitation Medicine
Daniel J. Blizzard, MD, MS
 Daniel J. Blizzard, MD, MS None Common degenerative (usually) condition caused by compression on the spinal cord that is characterized by clumsiness and difficulty with fine motor tasks in the hands and
Daniel J. Blizzard, MD, MS None Common degenerative (usually) condition caused by compression on the spinal cord that is characterized by clumsiness and difficulty with fine motor tasks in the hands and
Delayed surgical treatment for a traumatic bilateral cervical facet joint dislocation using a posterior-anterior approach: a case report
 Shimada et al. Journal of Medical Case Reports 2013, 7:9 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Delayed surgical treatment for a traumatic bilateral cervical facet joint dislocation using
Shimada et al. Journal of Medical Case Reports 2013, 7:9 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Delayed surgical treatment for a traumatic bilateral cervical facet joint dislocation using
Comparative study on the effect of anterior and posterior decompression in the treatment of multi-segmental cervical spondylotic myelopathy
 92 Journal of Hainan Medical University 2016; 22(6): 92-96 Journal of Hainan Medical University http://www.jhmuweb.net/ Comparative study on the effect of anterior and posterior decompression in the treatment
92 Journal of Hainan Medical University 2016; 22(6): 92-96 Journal of Hainan Medical University http://www.jhmuweb.net/ Comparative study on the effect of anterior and posterior decompression in the treatment
ASJ. A Rare Hyperextension Injury in Thoracic Spine Presenting with Delayed Paraplegia. Asian Spine Journal. Introduction
 sian Spine Journal 126 Dong-Eun Case Shin Report et al. http://dx.doi.org/10.4184/asj.2013.7.2.126 Rare Hyperextension Injury in Thoracic Spine Presenting with Delayed Paraplegia Dong-Eun Shin, Ki-Sik
sian Spine Journal 126 Dong-Eun Case Shin Report et al. http://dx.doi.org/10.4184/asj.2013.7.2.126 Rare Hyperextension Injury in Thoracic Spine Presenting with Delayed Paraplegia Dong-Eun Shin, Ki-Sik
CERVICAL SPONDYLOSIS & CERVICAL DISC DISEASE
 CERVICAL SPONDYLOSIS & CERVICAL DISC DISEASE Cervical spondylosis l Cervical osteophytosis l Most common progressive disease in the aging cervical spine l Seen in 95% of the people by 65 years Pathophysiology
CERVICAL SPONDYLOSIS & CERVICAL DISC DISEASE Cervical spondylosis l Cervical osteophytosis l Most common progressive disease in the aging cervical spine l Seen in 95% of the people by 65 years Pathophysiology
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
Rick C. Sasso MD Professor Chief of Spine Surgery Clinical Orthopaedic Surgery Indiana University School of Medicine
 Cervical Myelopathy: Anterior Surgery is Best Rick C. Sasso MD Professor Chief of Surgery Clinical Orthopaedic Surgery University School of Medicine Disclosure: Research support-medtronic, Stryker, AO,
Cervical Myelopathy: Anterior Surgery is Best Rick C. Sasso MD Professor Chief of Surgery Clinical Orthopaedic Surgery University School of Medicine Disclosure: Research support-medtronic, Stryker, AO,
Cervical Spine Surgery: Approach related outcome
 Cervical Spine Surgery: Approach related outcome Hez Progect Israel 2016 Ran Harel, MD Spine Surgery Unit, Department of Neurosurgery, Sheba Medical Center, Ramat-Gan, Israel Sackler Medical School, Tel-Aviv
Cervical Spine Surgery: Approach related outcome Hez Progect Israel 2016 Ran Harel, MD Spine Surgery Unit, Department of Neurosurgery, Sheba Medical Center, Ramat-Gan, Israel Sackler Medical School, Tel-Aviv
Effect of Swallowing Function After ROI-C Anterior Cervical Interbody Fusion
 Journal of Surgery 2016; 4(6): 141-145 http://www.sciencepublishinggroup.com/j/js doi: 10.11648/j.js.20160406.14 ISSN: 2330-0914 (Print); ISSN: 2330-0930 (Online) Effect of Swallowing Function After ROI-C
Journal of Surgery 2016; 4(6): 141-145 http://www.sciencepublishinggroup.com/j/js doi: 10.11648/j.js.20160406.14 ISSN: 2330-0914 (Print); ISSN: 2330-0930 (Online) Effect of Swallowing Function After ROI-C
Case SCIWORA in patient with congenital block vertebra
 Case 15428 SCIWORA in patient with congenital block vertebra Lucas Walgrave 1, Charlotte Vanhoenacker 1-2, Thomas Golinvaux 3, Filip Vanhoenacker3-5 1: Leuven University Hospital, Department of Radiology,
Case 15428 SCIWORA in patient with congenital block vertebra Lucas Walgrave 1, Charlotte Vanhoenacker 1-2, Thomas Golinvaux 3, Filip Vanhoenacker3-5 1: Leuven University Hospital, Department of Radiology,
Selective laminoplasty for cervical spondylotic myelopathy: a comparative study with a minimum 5-year follow-up
 Selective laminoplasty for cervical spondylotic myelopathy: a comparative study with a minimum 5-year follow-up Minori Kato*, Hiroaki Nakamura**, Koji Tamai**, Kazunori Hayashi**, Akira Matsumura**, Sadahiko
Selective laminoplasty for cervical spondylotic myelopathy: a comparative study with a minimum 5-year follow-up Minori Kato*, Hiroaki Nakamura**, Koji Tamai**, Kazunori Hayashi**, Akira Matsumura**, Sadahiko
SCIWORA Rozlyn McTeer BSN, RN, CEN Pediatric Trauma Coordinator Trauma Services OBJECTIVES DEFINITION 11/8/2017. Identify SCIWORA.
 SCIWORA Rozlyn McTeer BSN, RN, CEN Pediatric Trauma Coordinator Trauma Services Identify SCIWORA. OBJECTIVES Identify the population at risk. To identify anatomic and physiologic reasons for SCIWORA. To
SCIWORA Rozlyn McTeer BSN, RN, CEN Pediatric Trauma Coordinator Trauma Services Identify SCIWORA. OBJECTIVES Identify the population at risk. To identify anatomic and physiologic reasons for SCIWORA. To
Therapeutic Strategy for Traumatic Instability of Subaxial Cervical Spine
 Chinese Medicine, 2009, 1, 23-29 Published Online September 2009 in SciRes (www.scirp.org/journal/cm) Therapeutic Strategy for Traumatic Instability of Subaxial Cervical Spine - ABSTRACT A simple, safe
Chinese Medicine, 2009, 1, 23-29 Published Online September 2009 in SciRes (www.scirp.org/journal/cm) Therapeutic Strategy for Traumatic Instability of Subaxial Cervical Spine - ABSTRACT A simple, safe
Fractures of the thoracic and lumbar spine and thoracolumbar transition
 Most spinal column injuries occur in the thoracolumbar transition, the area between the lower thoracic spine and the upper lumbar spine; over half of all vertebral fractures involve the 12 th thoracic
Most spinal column injuries occur in the thoracolumbar transition, the area between the lower thoracic spine and the upper lumbar spine; over half of all vertebral fractures involve the 12 th thoracic
ORIGINAL PAPER. Department of Orthopedic Surgery,Nagoya University Graduate School of Medicine,Nagoya,Japan 2
 Nagoya J. Med. Sci. 80. 583 589, 2018 doi:10.18999/nagjms.80.4.583 ORIGINAL PAPER Evaluation of sagittal alignment and range of motion of the cervical spine using multi-detector- row computed tomography
Nagoya J. Med. Sci. 80. 583 589, 2018 doi:10.18999/nagjms.80.4.583 ORIGINAL PAPER Evaluation of sagittal alignment and range of motion of the cervical spine using multi-detector- row computed tomography
Original Investigation. Byung-Wan CHOI. INTRODUCTION Ossification of the posterior longitudinal ligament ABSTRACT
 DOI: 10.5137/1019-5149.JTN.16196-15.1 Received: 25.09.2015 / Accepted: 07.12.2015 Published Online: 01.06.2016 Original Investigation Clinical and Radiological Characteristics of Ossification of the Posterior
DOI: 10.5137/1019-5149.JTN.16196-15.1 Received: 25.09.2015 / Accepted: 07.12.2015 Published Online: 01.06.2016 Original Investigation Clinical and Radiological Characteristics of Ossification of the Posterior
Cervical myelopathy is a common disease that is
 TECHNICAL NOTE J Neurosurg Spine 26:325 330, 2017 A novel technique to correct kyphosis in cervical myelopathy due to continuous-type ossification of the posterior longitudinal ligament Dong-Ho Lee, MD,
TECHNICAL NOTE J Neurosurg Spine 26:325 330, 2017 A novel technique to correct kyphosis in cervical myelopathy due to continuous-type ossification of the posterior longitudinal ligament Dong-Ho Lee, MD,
Common fracture & dislocation of the cervical spine. Theerachai Apivatthakakul Department of Orthopaedic Chiangmai University
 Common fracture & dislocation of the cervical spine Theerachai Apivatthakakul Department of Orthopaedic Chiangmai University Objective Anatomy Mechanism and type of injury PE.and radiographic evaluation
Common fracture & dislocation of the cervical spine Theerachai Apivatthakakul Department of Orthopaedic Chiangmai University Objective Anatomy Mechanism and type of injury PE.and radiographic evaluation
Cervical corpectomy for sub-axial retro-vertebral body lesions
 Eshra Egyptian Journal of Neurosurgery (2019) 33:2 https://doi.org/10.1186/s41984-018-0004-9 Egyptian Journal of Neurosurgery RESEARCH Open Access Cervical corpectomy for sub-axial retro-vertebral body
Eshra Egyptian Journal of Neurosurgery (2019) 33:2 https://doi.org/10.1186/s41984-018-0004-9 Egyptian Journal of Neurosurgery RESEARCH Open Access Cervical corpectomy for sub-axial retro-vertebral body
A rare case of spinal injury: bilateral facet dislocation without fracture at the lumbosacral joint
 J Orthop Sci (2012) 17:189 193 DOI 10.1007/s00776-011-0082-y CASE REPORT A rare case of spinal injury: bilateral facet dislocation without fracture at the lumbosacral joint Kei Shinohara Shigeru Soshi
J Orthop Sci (2012) 17:189 193 DOI 10.1007/s00776-011-0082-y CASE REPORT A rare case of spinal injury: bilateral facet dislocation without fracture at the lumbosacral joint Kei Shinohara Shigeru Soshi
Original Article Management of Single Level Lumbar Degenerative Spondylolisthesis: Decompression Alone or Decompression and Fusion
 Egyptian Journal of Neurosurgery Volume 9 / No. 4 / October - December 014 51-56 Original Article Management of Single Level Lumbar Degenerative Spondylolisthesis: Decompression Alone or Decompression
Egyptian Journal of Neurosurgery Volume 9 / No. 4 / October - December 014 51-56 Original Article Management of Single Level Lumbar Degenerative Spondylolisthesis: Decompression Alone or Decompression
Static and dynamic cervical MRI: two useful exams in cervical myelopathy
 Original Study Static and dynamic cervical MRI: two useful exams in cervical myelopathy Lorenzo Nigro 1, Pasquale Donnarumma 1, Roberto Tarantino 1, Marika Rullo 2, Antonio Santoro 1, Roberto Delfini 1
Original Study Static and dynamic cervical MRI: two useful exams in cervical myelopathy Lorenzo Nigro 1, Pasquale Donnarumma 1, Roberto Tarantino 1, Marika Rullo 2, Antonio Santoro 1, Roberto Delfini 1
Fractures of the Thoracic and Lumbar Spine
 A spinal fracture is a serious injury. Nader M. Hebela, MD Fellow of the American Academy of Orthopaedic Surgeons http://orthodoc.aaos.org/hebela Cleveland Clinic Abu Dhabi Cleveland Clinic Abu Dhabi Neurological
A spinal fracture is a serious injury. Nader M. Hebela, MD Fellow of the American Academy of Orthopaedic Surgeons http://orthodoc.aaos.org/hebela Cleveland Clinic Abu Dhabi Cleveland Clinic Abu Dhabi Neurological
Christopher I. Shaffrey, MD
 CSRS 21st Instructional Course Wednesday, November 30, 2016 Laminoplasty/Foraminotomy: Why Fuse the Spine at all? Christopher I. Shaffrey, MD John A. Jane Distinguished Professor Departments of Neurosurgery
CSRS 21st Instructional Course Wednesday, November 30, 2016 Laminoplasty/Foraminotomy: Why Fuse the Spine at all? Christopher I. Shaffrey, MD John A. Jane Distinguished Professor Departments of Neurosurgery
Cervical Degenerative Disease - Surgical Approaches to CSM 가톨릭의대인천성모병원척추센터 김종태
 KNS Main Topic Session Spine Surgery : Case-Based Lecture of Spinal Disease Cervical Degenerative Disease - Surgical Approaches to CSM 가톨릭의대인천성모병원척추센터 김종태 Cervical Spondylotic Myelopathy ( CSM ) (1984,
KNS Main Topic Session Spine Surgery : Case-Based Lecture of Spinal Disease Cervical Degenerative Disease - Surgical Approaches to CSM 가톨릭의대인천성모병원척추센터 김종태 Cervical Spondylotic Myelopathy ( CSM ) (1984,
Minamide A*, Yoshida M*, Yamada H*, Hashizume H*, NakagawaY*, Iwasaki H*, Tsutsui S*, Hiroyuki Oka H**.
 Efficacy of Posterior Segmental Decompression Surgery for Pincer Mechanism in Cervical Spondylotic Myelopathy -A retrospective case control study using propensity score matching Minamide A*, Yoshida M*,
Efficacy of Posterior Segmental Decompression Surgery for Pincer Mechanism in Cervical Spondylotic Myelopathy -A retrospective case control study using propensity score matching Minamide A*, Yoshida M*,
Spinal canal stenosis Degenerative diseases F 06
 What is spinal canal stenosis? The condition known as spinal canal stenosis is a narrowing (stenosis) of the spinal canal that in most cases develops due to the degenerative (wear-induced) deformation
What is spinal canal stenosis? The condition known as spinal canal stenosis is a narrowing (stenosis) of the spinal canal that in most cases develops due to the degenerative (wear-induced) deformation
102 Results RESULTS. Age Mean=S.D Range 42= years -84 years Number % <30 years years >50 years
 102 Results RESULTS A total of 50 cases were studied 39 males and 11females.Their age ranged between 16 years and 84 years (mean 42years). T1 and T2WI were acquired for all cases in sagittal and axial
102 Results RESULTS A total of 50 cases were studied 39 males and 11females.Their age ranged between 16 years and 84 years (mean 42years). T1 and T2WI were acquired for all cases in sagittal and axial
Short Segment Screw Fixation without Fusion for Low Lumbar Burst Fracture: Severe Canal Compromise but Neurologically Intact Cases
 CLINICAL ARTICLE Korean J Neurotrauma 2013;9:101-105 pissn 2234-8999 / eissn 2288-2243 http://dx.doi.org/10.13004/kjnt.2013.9.2.101 Short Segment Screw Fixation without Fusion for Low Lumbar Burst Fracture:
CLINICAL ARTICLE Korean J Neurotrauma 2013;9:101-105 pissn 2234-8999 / eissn 2288-2243 http://dx.doi.org/10.13004/kjnt.2013.9.2.101 Short Segment Screw Fixation without Fusion for Low Lumbar Burst Fracture:
CSM is the most common cause of spinal cord dysfunction
 Published December 22, 2011 as 10.3174/ajnr.A2756 ORIGINAL RESEARCH T. Sato T. Horikoshi A. Watanabe M. Uchida K. Ishigame T. Araki H. Kinouchi Evaluation of Cervical Myelopathy Using Apparent Diffusion
Published December 22, 2011 as 10.3174/ajnr.A2756 ORIGINAL RESEARCH T. Sato T. Horikoshi A. Watanabe M. Uchida K. Ishigame T. Araki H. Kinouchi Evaluation of Cervical Myelopathy Using Apparent Diffusion
CERVICAL SPONDYLOSIS AND CERVICAL SPONDYLOTIC MYELOPATHY
 CERVICAL SPONDYLOSIS AND CERVICAL SPONDYLOTIC MYELOPATHY A NEUROSURGEON S VIEW A Preventable Journey to a wheelchair bound-life Dr H. BOODHOO F.C.S (Neurosurgery) Cervical Spondylosis Spinal Osteoarthritis
CERVICAL SPONDYLOSIS AND CERVICAL SPONDYLOTIC MYELOPATHY A NEUROSURGEON S VIEW A Preventable Journey to a wheelchair bound-life Dr H. BOODHOO F.C.S (Neurosurgery) Cervical Spondylosis Spinal Osteoarthritis
ARCH Laminoplasty System
 Dedicated System for Open-door Laminoplasty ARCH Laminoplasty System Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use of DePuy Synthes
Dedicated System for Open-door Laminoplasty ARCH Laminoplasty System Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use of DePuy Synthes
ELY ASHKENAZI Israel Spine Center at Assuta Hospital Tel Aviv, Israel
 nterior cervical decompression using the Hybrid Decompression Fixation technique, a combination of corpectomies and or discectomies, in the management of multilevel cervical myelopathy J ORTHOP TRUM SURG
nterior cervical decompression using the Hybrid Decompression Fixation technique, a combination of corpectomies and or discectomies, in the management of multilevel cervical myelopathy J ORTHOP TRUM SURG
Kinematic Cervical Spine Magnetic Resonance Imaging in Low-Impact Trauma Assessment
 Kinematic Cervical Spine Magnetic Resonance Imaging in Low-Impact Trauma Assessment 1 Seminars in Ultrasound, CT, and MRI June 2009; Volume 30; Number 3; pp. 168-173 Vincenzo Giuliano, MD, Antonio Pinto,
Kinematic Cervical Spine Magnetic Resonance Imaging in Low-Impact Trauma Assessment 1 Seminars in Ultrasound, CT, and MRI June 2009; Volume 30; Number 3; pp. 168-173 Vincenzo Giuliano, MD, Antonio Pinto,
CMEARTICLE * * * Wen Qi Tan 1, BEng, Bak Siew Steven Wong 2, MBChB, MMed
 Singapore Med J 2015; 56(7): 373-378 doi: 10.11622/smedj.2015107 CMEARTICLE Clinics in diagnostic imaging (161) Wen Qi Tan 1, BEng, Bak Siew Steven Wong 2, MBChB, MMed 2a 2b Fig. 1 Lateral radiograph of
Singapore Med J 2015; 56(7): 373-378 doi: 10.11622/smedj.2015107 CMEARTICLE Clinics in diagnostic imaging (161) Wen Qi Tan 1, BEng, Bak Siew Steven Wong 2, MBChB, MMed 2a 2b Fig. 1 Lateral radiograph of
Stage Operation for Unstable Lumbar Spine Fracture- Dislocation with Incomplete Paraplegia: A Case Series
 C a s e R e p o r t J. of Advanced Spine Surgery Volume 2, Number 2, pp 60~65 Journal of Advanced Spine Surgery JASS Stage Operation for Unstable Lumbar Spine Fracture- Dislocation with Incomplete Paraplegia:
C a s e R e p o r t J. of Advanced Spine Surgery Volume 2, Number 2, pp 60~65 Journal of Advanced Spine Surgery JASS Stage Operation for Unstable Lumbar Spine Fracture- Dislocation with Incomplete Paraplegia:
Early Radiological Analysis of Cervical Arthroplasty with Bryan and Mobi-C Cervical Disc Prosthesis
 CLINICAL ARTICLE Kor J Spine 5(3):111-115, 2008 Early Radiological Analysis of Cervical Arthroplasty with Bryan and Mobi-C Cervical Disc Prosthesis Ki Suk Choi, M.D., Il Tae Jang, M.D., Jae Hyeon Lim,
CLINICAL ARTICLE Kor J Spine 5(3):111-115, 2008 Early Radiological Analysis of Cervical Arthroplasty with Bryan and Mobi-C Cervical Disc Prosthesis Ki Suk Choi, M.D., Il Tae Jang, M.D., Jae Hyeon Lim,
Comparison of Anterior and Posterior Approaches in Cervical Spinal Cord Injuries
 Journal of Spinal Disorders & Techniques Vol. 16, No. 3, pp. 229 235 2003 Lippincott Williams & Wilkins, Inc., Philadelphia Comparison of Anterior and Posterior Approaches in Cervical Spinal Cord Injuries
Journal of Spinal Disorders & Techniques Vol. 16, No. 3, pp. 229 235 2003 Lippincott Williams & Wilkins, Inc., Philadelphia Comparison of Anterior and Posterior Approaches in Cervical Spinal Cord Injuries
Unanswered Questions. Laminoplasty is best
 Laminoplasty is best Wellington K. Hsu, MD Clifford C. Raisbeck Distinguished Professor of Orthopaedic Surgery Director of Research Department of Orthopaedic Surgery Northwestern University Feinberg School
Laminoplasty is best Wellington K. Hsu, MD Clifford C. Raisbeck Distinguished Professor of Orthopaedic Surgery Director of Research Department of Orthopaedic Surgery Northwestern University Feinberg School
ASJ. Magnification Error in Digital Radiographs of the Cervical Spine Against Magnetic Resonance Imaging Measurements. Asian Spine Journal
 Asian Spine Journal Asian Spine Clinical Journal Study Asian Spine J 2013;7(4):267-272 Magnification http://dx.doi.org/10.4184/asj.2013.7.4.267 error in cervical spine 267 Magnification Error in Digital
Asian Spine Journal Asian Spine Clinical Journal Study Asian Spine J 2013;7(4):267-272 Magnification http://dx.doi.org/10.4184/asj.2013.7.4.267 error in cervical spine 267 Magnification Error in Digital
Outcome of Anterior Cervical Discectomy and Fusion with Autograft and Plating in management of Cervical Spondylotic Myelopathy
 ISPUB.COM The Internet Journal of Spine Surgery Volume 5 Number 1 Outcome of Anterior Cervical Discectomy and Fusion with Autograft and Plating in management of Cervical Spondylotic Myelopathy V Kumar,
ISPUB.COM The Internet Journal of Spine Surgery Volume 5 Number 1 Outcome of Anterior Cervical Discectomy and Fusion with Autograft and Plating in management of Cervical Spondylotic Myelopathy V Kumar,
Case Report Adjacent Lumbar Disc Herniation after Lumbar Short Spinal Fusion
 Case Reports in Orthopedics, Article ID 456940, 4 pages http://dx.doi.org/10.1155/2014/456940 Case Report Adjacent Lumbar Disc Herniation after Lumbar Short Spinal Fusion Koshi Ninomiya, Koichi Iwatsuki,
Case Reports in Orthopedics, Article ID 456940, 4 pages http://dx.doi.org/10.1155/2014/456940 Case Report Adjacent Lumbar Disc Herniation after Lumbar Short Spinal Fusion Koshi Ninomiya, Koichi Iwatsuki,
Facet orientation in patients with lumbar degenerative spondylolisthesis
 35 J. Tokyo Med. Univ., 71 1 35 0 Facet orientation in patients with lumbar degenerative spondylolisthesis Wuqikun ALIMASI, Kenji ENDO, Hidekazu SUZUKI, Yasunobu SAWAJI, Hirosuke NISHIMURA, Hidetoshi TANAKA,
35 J. Tokyo Med. Univ., 71 1 35 0 Facet orientation in patients with lumbar degenerative spondylolisthesis Wuqikun ALIMASI, Kenji ENDO, Hidekazu SUZUKI, Yasunobu SAWAJI, Hirosuke NISHIMURA, Hidetoshi TANAKA,
Ossification of the posterior longitudinal ligament
 J Neurosurg Spine 19:431 435, 2013 AANS, 2013 Upper cervical cord compression due to a C-1 posterior arch in a patient with ossification of the posterior longitudinal ligament and a kyphotic cervical spine
J Neurosurg Spine 19:431 435, 2013 AANS, 2013 Upper cervical cord compression due to a C-1 posterior arch in a patient with ossification of the posterior longitudinal ligament and a kyphotic cervical spine
Acute traumatic spinal cord injury (SCI) is a devastating
 ORIGINAL RESEARCH B.G. Leypold A.E. Flanders A.S. Burns The Early Evolution of Spinal Cord Lesions on MR Imaging following Traumatic Spinal Cord Injury BACKGROUND AND PURPOSE: How early spinal cord injury
ORIGINAL RESEARCH B.G. Leypold A.E. Flanders A.S. Burns The Early Evolution of Spinal Cord Lesions on MR Imaging following Traumatic Spinal Cord Injury BACKGROUND AND PURPOSE: How early spinal cord injury
SpineFAQs. Neck Pain Diagnosis and Treatment
 SpineFAQs Neck Pain Diagnosis and Treatment Neck pain is a common reason people visit their doctor. Neck pain typically doesn't start from a single injury. Instead, the problem usually develops over time
SpineFAQs Neck Pain Diagnosis and Treatment Neck pain is a common reason people visit their doctor. Neck pain typically doesn't start from a single injury. Instead, the problem usually develops over time
흉추척수증을유발한황색인대골화증의골절 - 증례보고 -
 대한척추외과학회지제 14 권제 1 호 Journal of Korean Spine Surg. Vol. 14, No. 1, pp 52~56, 2007 흉추척수증을유발한황색인대골화증의골절 - 증례보고 - 하기용 김영훈 # 지원희 $ 가톨릭대학교의과대학강남성모병원정형외과, 성모자애병원정형외과 #, 강남성모병원영상의학과 $ Fracture of Ossification
대한척추외과학회지제 14 권제 1 호 Journal of Korean Spine Surg. Vol. 14, No. 1, pp 52~56, 2007 흉추척수증을유발한황색인대골화증의골절 - 증례보고 - 하기용 김영훈 # 지원희 $ 가톨릭대학교의과대학강남성모병원정형외과, 성모자애병원정형외과 #, 강남성모병원영상의학과 $ Fracture of Ossification
Radiographic Dimensional Analysis of Open Door Laminoplasty with Plate in Cervical Spondylotic Myelopathy
 Radiographic Dimensional Analysis of Open Door Laminoplasty with Plate in Cervical Spondylotic Myelopathy Woo-Kie Min,MD,PhD Department of Orthopedic Surgery, Kyungpook National University College of Medicine,
Radiographic Dimensional Analysis of Open Door Laminoplasty with Plate in Cervical Spondylotic Myelopathy Woo-Kie Min,MD,PhD Department of Orthopedic Surgery, Kyungpook National University College of Medicine,
Two Consecutive Levels of Unilateral Cervical Spondylolysis on Opposite Sides 두개의연속된척추에서반대쪽편측에발생한경추척추분리증
 Case Report pissn 1738-2637 / eissn 2288-2928 http://dx.doi.org/10.3348/jksr.2015.73.3.181 Two Consecutive Levels of Unilateral Cervical Spondylolysis on Opposite Sides 두개의연속된척추에서반대쪽편측에발생한경추척추분리증 Kyeong
Case Report pissn 1738-2637 / eissn 2288-2928 http://dx.doi.org/10.3348/jksr.2015.73.3.181 Two Consecutive Levels of Unilateral Cervical Spondylolysis on Opposite Sides 두개의연속된척추에서반대쪽편측에발생한경추척추분리증 Kyeong
Pediatric cervical spine injuries with neurological deficits, treatment options, and potential for recovery
 SICOT J 2017, 3, 53 Ó The Authors, published by EDP Sciences, 2017 DOI: 10.1051/sicotj/2017035 Available online at: www.sicot-j.org CASE REPORT OPEN ACCESS Pediatric cervical spine injuries with neurological
SICOT J 2017, 3, 53 Ó The Authors, published by EDP Sciences, 2017 DOI: 10.1051/sicotj/2017035 Available online at: www.sicot-j.org CASE REPORT OPEN ACCESS Pediatric cervical spine injuries with neurological
Analysis of C5 palsy in cervical myelopathy with massive anterior compression following laminoplasty
 Chen et al. Journal of Orthopaedic Surgery and Research (2018) 13:26 DOI 10.1186/s13018-018-0715-3 RESEARCH ARTICLE Open Access Analysis of C5 palsy in cervical myelopathy with massive anterior compression
Chen et al. Journal of Orthopaedic Surgery and Research (2018) 13:26 DOI 10.1186/s13018-018-0715-3 RESEARCH ARTICLE Open Access Analysis of C5 palsy in cervical myelopathy with massive anterior compression
Cervical spondylarthrotic myelopathy with early onset in Down's syndrome: five cases and a review of the literature
 283 Journal of Intellectual Disability Research VOLUME 43 PART 4 pp 283±288 AUGUST 1999 Cervical spondylarthrotic myelopathy with early onset in Down's syndrome: five cases and a review of the literature
283 Journal of Intellectual Disability Research VOLUME 43 PART 4 pp 283±288 AUGUST 1999 Cervical spondylarthrotic myelopathy with early onset in Down's syndrome: five cases and a review of the literature
Is high T-1 slope a significant risk factor for developing interlaminar bony fusion after cervical laminoplasty? A retrospective cohort study
 CLINICAL ARTICLE J Neurosurg Spine 27:627 632, 2017 Is high T-1 slope a significant risk factor for developing interlaminar bony fusion after cervical laminoplasty? A retrospective cohort study Takeshi
CLINICAL ARTICLE J Neurosurg Spine 27:627 632, 2017 Is high T-1 slope a significant risk factor for developing interlaminar bony fusion after cervical laminoplasty? A retrospective cohort study Takeshi
Acute traumatic spinal cord injury (SCI) is located at the cervical
 ORIGINAL RESEARCH SPINE Spinal Cord Injury after Blunt Cervical Spine Trauma: Correlation of Soft-Tissue Damage and Extension of Lesion R. Martínez-Pérez, I. Paredes, S. Cepeda, A. Ramos, A.M. Castaño-León,
ORIGINAL RESEARCH SPINE Spinal Cord Injury after Blunt Cervical Spine Trauma: Correlation of Soft-Tissue Damage and Extension of Lesion R. Martínez-Pérez, I. Paredes, S. Cepeda, A. Ramos, A.M. Castaño-León,
PREOPERATIVE RETROLISTHESIS IS A RISK FACTOR OF LUMBAR DISC HERNIATION AFTER FENESTRATION WITHOUT DISCECTOMY
 PREOPERATIVE RETROLISTHESIS IS A RISK FACTOR OF LUMBAR DISC HERNIATION AFTER FENESTRATION WITHOUT DISCECTOMY Shota Takenaka*, Noboru Hosono, Yoshihiro Mukai, Kosuke Tateishi, Takeshi Fuji Osaka Kosei-nenkin
PREOPERATIVE RETROLISTHESIS IS A RISK FACTOR OF LUMBAR DISC HERNIATION AFTER FENESTRATION WITHOUT DISCECTOMY Shota Takenaka*, Noboru Hosono, Yoshihiro Mukai, Kosuke Tateishi, Takeshi Fuji Osaka Kosei-nenkin
Original Article Clinics in Orthopedic Surgery 2013;5:
 Original Article Clinics in Orthopedic Surgery 2013;5:129-133 http://dx.doi.org/10.4055/cios.2013.5.2.129 The Efficacy of Carotid Tubercle as an Anatomical Landmark for Identification of Cervical Spinal
Original Article Clinics in Orthopedic Surgery 2013;5:129-133 http://dx.doi.org/10.4055/cios.2013.5.2.129 The Efficacy of Carotid Tubercle as an Anatomical Landmark for Identification of Cervical Spinal
Key Primary CPT Codes: Refer to pages: 7-9 Last Review Date: October 2016 Medical Coverage Guideline Number:
 National Imaging Associates, Inc. Clinical guidelines CERVICAL SPINE SURGERY: ANTERI CERVICAL DECOMPRESSION WITH FUSION CERVICAL POSTERI DECOMPRESSION WITH FUSION CERVICAL ARTIFICIAL DISC CERVICAL POSTERI
National Imaging Associates, Inc. Clinical guidelines CERVICAL SPINE SURGERY: ANTERI CERVICAL DECOMPRESSION WITH FUSION CERVICAL POSTERI DECOMPRESSION WITH FUSION CERVICAL ARTIFICIAL DISC CERVICAL POSTERI
Delayed surgery in neurologically intact patients affected by thoraco-lumbar junction burst fractures: to reduce pain and improve quality of life
 Original Study Delayed surgery in neurologically intact patients affected by thoraco-lumbar junction burst fractures: to reduce pain and improve quality of life Lorenzo Nigro 1, Roberto Tarantino 1, Pasquale
Original Study Delayed surgery in neurologically intact patients affected by thoraco-lumbar junction burst fractures: to reduce pain and improve quality of life Lorenzo Nigro 1, Roberto Tarantino 1, Pasquale
Original Article Prognosis of Cervical Degenerative Myelopathy after Multilevel Anterior Cervical Discectomies and Fusion
 Egyptian Journal of Neurosurgery Volume 9 / No. / January - March 4 57-6 Original Article Prognosis of Cervical Degenerative Myelopathy after Multilevel Anterior Cervical Discectomies and Fusion Ahmed
Egyptian Journal of Neurosurgery Volume 9 / No. / January - March 4 57-6 Original Article Prognosis of Cervical Degenerative Myelopathy after Multilevel Anterior Cervical Discectomies and Fusion Ahmed
Cervical Open-Door Laminoplasty by Hydroxyapatite Implant Insertion Without Suturing
 Neurospine 2018;15(4):362-367. https://doi.org/10.14245/ns.1836106.053 Neurospine pissn 2586-6583 eissn 2586-6591 Original Article Corresponding Author Yoshifumi Kawanabe https://orcid.org/0000-0002-2251-0293
Neurospine 2018;15(4):362-367. https://doi.org/10.14245/ns.1836106.053 Neurospine pissn 2586-6583 eissn 2586-6591 Original Article Corresponding Author Yoshifumi Kawanabe https://orcid.org/0000-0002-2251-0293
Risk Prediction for Development of Traumatic Cervical Spinal Cord Injury without Spinal Instability
 THIEME GLOBAL SPINE JOURNAL Original Article 315 Risk Prediction for Development of Traumatic Cervical Spinal Cord Injury without Spinal Instability Soo Eon Lee 1 Chun Kee Chung 1 1 Department of Neurosurgery,
THIEME GLOBAL SPINE JOURNAL Original Article 315 Risk Prediction for Development of Traumatic Cervical Spinal Cord Injury without Spinal Instability Soo Eon Lee 1 Chun Kee Chung 1 1 Department of Neurosurgery,
Segmental Pedicle Screw Fixation for a Scoliosis Patient with Post-laminectomy and Post-irradiation Thoracic Kyphoscoliosis of Spinal Astrocytoma
 Segmental Pedicle Screw Fixation for a Scoliosis Patient with Post-laminectomy and Post-irradiation Thoracic Kyphoscoliosis of Spinal Astrocytoma a* a a a b a a b ʼ 2 ʼ August 2012 Spinal Deformity with
Segmental Pedicle Screw Fixation for a Scoliosis Patient with Post-laminectomy and Post-irradiation Thoracic Kyphoscoliosis of Spinal Astrocytoma a* a a a b a a b ʼ 2 ʼ August 2012 Spinal Deformity with
Spontaneous Resolution of Spinal Canal Deformity After Burst Dispersion Fracture
 779 Spontaneous Resolution of Spinal Canal Deformity After Burst Dispersion Fracture T. M. H. Chakera 1 George Bedbrook C. M. Bradley3 We reviewed the records of 8 patients with 30 burst-dispersion spinal
779 Spontaneous Resolution of Spinal Canal Deformity After Burst Dispersion Fracture T. M. H. Chakera 1 George Bedbrook C. M. Bradley3 We reviewed the records of 8 patients with 30 burst-dispersion spinal
Junming Cao, Yongsheng Lin, Xiangbei Qi, Zhihong Wang, Yipeng Yang, Hehuan Xia, Bin Xu
 Int J Clin Exp Med 2018;11(2):741-746 www.ijcem.com /ISSN:1940-5901/IJCEM0067327 Original Article Effect of intramedullary signal intensity on T2-weighted magnetic resonance images on prognosis in patients
Int J Clin Exp Med 2018;11(2):741-746 www.ijcem.com /ISSN:1940-5901/IJCEM0067327 Original Article Effect of intramedullary signal intensity on T2-weighted magnetic resonance images on prognosis in patients
Complex Spine Symposium January 12th, Balgrist University Hospital
 DEGENERATIVE CERVICAL MYELOPATHY CLINICAL DECISION MAKING Prof. Dr. Mazda Farshad Chair of Orthopedic Surgery Chief of Spine Surgery Medical Director CERVICAL MYELOPATHY - CAUSES degenerative cervical
DEGENERATIVE CERVICAL MYELOPATHY CLINICAL DECISION MAKING Prof. Dr. Mazda Farshad Chair of Orthopedic Surgery Chief of Spine Surgery Medical Director CERVICAL MYELOPATHY - CAUSES degenerative cervical
Risk factors for development of cervical spondylotic myelopathy: results of a systematic review
 Systematic review Risk factors for development of cervical spondylotic myelopathy 35 35 42 Risk factors for development of cervical spondylotic myelopathy: results of a systematic review Authors Anoushka
Systematic review Risk factors for development of cervical spondylotic myelopathy 35 35 42 Risk factors for development of cervical spondylotic myelopathy: results of a systematic review Authors Anoushka
ORIGINAL ARTICLE. Introduction SPINE SURGERY AND RELATED RESEARCH
 ORIGINAL ARTICLE SPINE SURGERY AND RELATED RESEARCH Radiological Examination of Postoperative Cervical Alignment and Stability in Patients with Dialysis-Associated Spondylosis Excluding Destructive Spondyloarthropathy:
ORIGINAL ARTICLE SPINE SURGERY AND RELATED RESEARCH Radiological Examination of Postoperative Cervical Alignment and Stability in Patients with Dialysis-Associated Spondylosis Excluding Destructive Spondyloarthropathy:
Spinal injury is very common in Ireland: 19 per 100,000 (1). It poses a significant disease burden.
 MRI in traumatic spinal cord injury: a single national spinal centre experience and study of imaging features with clinical correlation with ASIA score and outcome Poster No.: C-1235 Congress: ECR 2011
MRI in traumatic spinal cord injury: a single national spinal centre experience and study of imaging features with clinical correlation with ASIA score and outcome Poster No.: C-1235 Congress: ECR 2011
Spinal Cord Injuries: The Basics. Kadre Sneddon POS Rounds October 1, 2003
 Spinal Cord Injuries: The Basics Kadre Sneddon POS Rounds October 1, 2003 Anatomy Dorsal columntouch, vibration Corticospinal tract- UMN Anterior horn-lmn Spinothalamic tractpain, temperature (contralateral)
Spinal Cord Injuries: The Basics Kadre Sneddon POS Rounds October 1, 2003 Anatomy Dorsal columntouch, vibration Corticospinal tract- UMN Anterior horn-lmn Spinothalamic tractpain, temperature (contralateral)
Reduced invasiveness of myoarchitectonic laminectomy compared with open-door laminoplasty in patients with cervical myelopathy
 Reduced invasiveness of myoarchitectonic laminectomy compared with open-door laminoplasty in patients with cervical myelopathy Department of Spinal Surgery 1), Brain Attack Center Ota Memorial Hospital,
Reduced invasiveness of myoarchitectonic laminectomy compared with open-door laminoplasty in patients with cervical myelopathy Department of Spinal Surgery 1), Brain Attack Center Ota Memorial Hospital,
Subaxial Cervical Spine Trauma
 Subaxial Cervical Spine Trauma Pooria Salari, MD Assistant Professor Of Orthopaedics Department of Orthopaedic Surgery St. Louis University School of Medicine St. Louis, Missouri, USA Initial Evaluation
Subaxial Cervical Spine Trauma Pooria Salari, MD Assistant Professor Of Orthopaedics Department of Orthopaedic Surgery St. Louis University School of Medicine St. Louis, Missouri, USA Initial Evaluation
Case Report Delayed myelopathy secondary to stab wound with a retained blade tip within the laminae: case report
 Int J Clin Exp Med 2015;8(9):16787-16792 www.ijcem.com /ISSN:1940-5901/IJCEM0012160 Case Report Delayed myelopathy secondary to stab wound with a retained blade tip within the laminae: case report Hui
Int J Clin Exp Med 2015;8(9):16787-16792 www.ijcem.com /ISSN:1940-5901/IJCEM0012160 Case Report Delayed myelopathy secondary to stab wound with a retained blade tip within the laminae: case report Hui
INTRODUCTION.
 www.jkns.or.kr http://dx.doi.org/1.334/jkns.212.51.4.23 J Korean Neurosurg Soc 51 : 23-27, 212 Print ISSN 25-3711 On-line ISSN 1598-7876 Copyright 212 The Korean Neurosurgical Society Clinical Article
www.jkns.or.kr http://dx.doi.org/1.334/jkns.212.51.4.23 J Korean Neurosurg Soc 51 : 23-27, 212 Print ISSN 25-3711 On-line ISSN 1598-7876 Copyright 212 The Korean Neurosurgical Society Clinical Article
Title. Author(s)Sudo, Hideki; Taneichi, H.; Kaneda, K. CitationSpinal Cord, 44(2): Issue Date Doc URL
 Title Secondary medulla oblongata involvement following mi instability in a patient with ossification of the po Author(s)Sudo, Hideki; Taneichi, H.; Kaneda, K. CitationSpinal Cord, 44(2): 126-129 Issue
Title Secondary medulla oblongata involvement following mi instability in a patient with ossification of the po Author(s)Sudo, Hideki; Taneichi, H.; Kaneda, K. CitationSpinal Cord, 44(2): 126-129 Issue
Key words: Professional Med J 2018;25(8): CERVICAL LAMINOPLASTY
 The Professional Medical Journal DOI: 10.29309/TPMJ/18.4872 1. MBBS Post graduate Trainee, 2. MBBS, FCPS Associate Professor 3. MBBS, FCPS Associate Professor 4. MBBS Honorary Researcher, 5. MBBS, FCPS
The Professional Medical Journal DOI: 10.29309/TPMJ/18.4872 1. MBBS Post graduate Trainee, 2. MBBS, FCPS Associate Professor 3. MBBS, FCPS Associate Professor 4. MBBS Honorary Researcher, 5. MBBS, FCPS
