Halifax Knee Arthroscopy Bioskills Session Friday March 28, 2014
|
|
|
- Janis Watts
- 5 years ago
- Views:
Transcription
1
2 Halifax Knee Arthroscopy Bioskills Session Friday March 28, 2014 Course Chair: Course Faculty: Guest Instructor: Dr. Cathy Coady Dr. Doug Legay and Dr. Nathan Urquhart Dr. Daniel Whelan 12:00 pm Refreshments, Welcome & Introduction 12:10 pm Basics of Knee Arthroscopy - Dr. Nathan Urquhart 12:30 pm Meniscal & Articular Cartilage Injuries and Management - Dr. Doug Legay 1:00 pm Anatomic ACL Reconstruction - Dr. Cathy Coady 1:30 pm Multiligament Knee Injuries and Management - Dr. Danny Whelan 2:00 pm Hands-on Cadaveric Lab 4:30 pm Closing Remarks 6:30 pm Pub Night - Durty Nelly s Irish Pub (corner of Argyle and Sackville) Location: The Skills Centre for Health Sciences Room B04 Bethune Building 1276 South Park Street Halifax, Nova Scotia B3H 2Y9 To confirm your place in the course, please contact Nicole Amos Medical Events Coordinator, nicoleamos@conmed.com Registration Deadline: March 15, 2014
3 Fundamentals in Knee Arthroscopy Learning Objectives: 1. Apply fundamental knowledge of anatomy and motor skills to optimize knee arthroscopic techniques. 2. Become familiar using an arthroscope in a knee to develop/improve basic motor skills. 3. Demonstrate fundamental arthroscopic skills of triangulation, translation, and rotation to optimally visualize a knee joint. 4. Become comfortable in switching the scope in a variety of portals to optimize visualization of pertinent structures. 5. Become increasingly proficient with the use of arthroscopic instruments including use of the probe, punches/biters, grasper and various shavers. 6. Perform increasingly advanced arthroscopic techniques in the knee ranging from diagnostic arthroscopy, removal of loose bodies, partial meniscectomies, meniscus repairs and ligament reconstructions. 7. At the end of the session, you should dissect knee specimens in order to review the anatomy of the knee joint and to evaluate the procedures performed. Getting Started: Examine your knee model. Determine if you have a right or left knee. Range the knee and determine the jointlines. Outlining the patella, patella ligament, the femoral condyles, the tibial plateau and the proximal fibula. 1. Mark Anatomy: Mark the following anatomy with a marking pen: Patella Patellar tendon Medial and lateral joint line Gerdy s tubercle Fibular head and course of peroneal nerve across fibular neck Figure 1: Knee Anatomy and Portal Marking 2. Mark Portals: HINT: Vertically oriented portals are more forgiving than horizontal portals (but less cosmetic) and can be extended slightly superior or inferior. They also must be placed more carefully to avoid damage to anterior horns. Anterolateral portal Location: Located in the soft spot lateral to the patellar tendon, approximately 1.0 cm proximal to the tibial plateau. This is the primary viewing portal. If placed too low, it may be difficult to pass the scope over the tibial spines to adequately visualize the posterior horn of the medial meniscus. It is possible to injure the anterior horn of the lateral meniscus while creating a low portal. Anteromedial portal Location: At a point just distal to the inferomedial pole of the patella and just medial to the patellar tendon. This portal is primarily used for probing & instrumentation. Use a spinal needle to choose optimal location. Judge access to a meniscus tear prior to committing to portal placement. If too proximal, the medial femoral condyle blocks the instruments from gaining access to the posterior horn of the medial meniscus. Low portal placement is best for gaining access to the posterior horn of the medial meniscus. However, if too low (distal), the anterior horn of the medial meniscus may be injured while creating the
4 portal. The portal can be made slightly more proximal if a lateral meniscus tear is identified, allowing the instruments to pass over the tibia spines. Superior Portal This is an optional portal for inflow or outflow. It may be made medial or lateral. It is located cm proximal to the superior pole of the patella. It may be a useful additional portal for procedures in the patellofemoral joint. Anterior Central portal This portal is located at a point just distal to the central part of the distal patella in the central part of the patellar tendon. The portal is made longitudinally, in line with the fibers of the patellar tendon. This portal is not commonly utilized but can be useful for PCL reconstructions and ACL reconstructions, especially if the central third of the patella tendon has been harvested. It is also useful for the treatment of certain articular cartilage lesions and patella tendon debridement. Posteromedial and Posterolateral portals These portals are established using arthroscopic control. In order to get an idea about where they will be, mark on the medial and lateral aspects of the knee the location between the posterior condyle and the posterior horn of the meniscus. On the lateral side, draw a line in a superior direction from the posterior border of the fibular head and mark the location of the common peroneal nerve. These portals are used in PCL reconstruction, removal of posterior loose bodies, complete synovectomy, and all-inside suture repair of the meniscus. 3. Perform Arthroscopy: With the knee flexed to 90 degrees, make a ¼ inch incision (either horizontal or vertical) at the inferolateral portal site and then direct the arthroscopic sheath with a blunt obtuator towards the intercondylar notch. Once the arthroscope is through the capsule, extend the knee and direct the arthroscope into the suprapatellar pouch. Inflow through the side port of the arthroscope. 4) Make the anteromedial portal under arthroscope control: Direct the arthroscope down the medial gutter and then view the anteromedial joint capsule. Place a spinal needle at the site marked for the anteromedial portal and verify that the portal site is right on top of the anterior horn of the medial meniscus. Additionally, this portal site should allow adequate access to the posterior horn of the medial meniscus and the intercondylar notch. 5) Do a systematic examination of the knee: The arthroscopist should establish a systematic routine which covers the examination of the entire joint. First place a probe in the inferomedial portal. During the examination the probe will be used to palpate structures. Keeping in mind the location of the arthroscope, the position of the knee, and the stress of the knee; it may be easiest to examine the knee in the following manner: Suprapatellar pouch: Knee in extension or slight flexion. Examine the patello femoral joint and patellar tracking. Appreciate how large the suprapatellar pouch is. Medial Gutter: Knee in slight flexion Medial Compartment: Knee in 90 flexion. Examine articular cartilage of medial femoral condyle and medial tibial plateau. Bring knee through a range of motion. Examine the medial meniscus. You will have to apply a valgus stress to the knee to view the entire medial meniscus. Intercondylar Notch: Examine the anatomy of the ACL and PCL. Look for both bundles of both ligaments. Bring the knee through a range of motion and appreciate the changes in the ligaments. You may need to debride the fat pad and ligament mucosum to properly evaluate the cruciate ligaments. Lateral Compartment: Place the knee in figure of 4 position. Examine lateral compartment articular carilage, lateral meniscus and popliteus. Note that lateral meniscus is more mobile than medial meniscus due to the popliteus tendon (where there is no capsular attachment to the popliteus). Lateral Gutter: Examine the lateral border of the meniscus and look for loose bodies. Become familiar with switching the scope and instrument portals. It is often advantageous to switch portals to address certain types of pathology such as trying to repair the posterior horn of the medial meniscus or addressing certain chondral lesions.
5 For Senior Residents: Familirize yourselves with trying to gain access to the posterior comparments of the knee Posteromedial Compartment: Place the scope in the anterolateral and have the knee flexed to 90 degrees. You will have to wiggle your way past the PCL. Posterolateral Compartment: (the scope must be in the anteromedial portal). Knee should be flexed 90 degrees. You will have to carefully advance the scope past the ACL. Examine posterior capsule, posterior edge of meniscus. 6) Arthroscopy Exercises: a) Loose body removal: Place a kernel of corn or any small object into the knee joint and practice removing it with an arthroscopic grasper. It may be helpful to reduce the fluid inflow to make the loose body less mobile. b) Meniscal debridement: Take a basket punch and practice debriding the posterior horn of the medial or lateral meniscus. Just trim a little of the meniscus so that you can preserve it for the next exercise (meniscus repair). The cutting instrument should be placed through the ipsilateral portal for posterior horn pathology. You should also try smoothing out the meniscus tear with an arthroscopic shaver. c) Create posteromedial and posterolateral portals: Debride the ACL and PCL to allow access to the posteromedial and posterolateral compartments. Start by taking a basket punch to cut out the ACL and PCL. Try to preserve the ligaments attachments on the femur and tibia so that you can identify the anatomy when you do your ligament reconstruction. You may also use a shaver and debride the remnant ligaments but be careful that you do not cut the bone. i) Make a posteromedial portal: The knee should be flexed 90 degrees. Place the scope with blunt obturator in the anterolateral portal and direct it through the notch into the posteromedial compartment. This is much easier to do after the debridement of the cruciate ligaments. If your PCL is intact, feel the scope slide along the medial femoral condyle and under the PCL as it is gently pushed into the posteromedial compartment. Gaining posterior access may be difficult in older individuals where the notch can be stenotic and osteophytes block access. With the scope turned towards the posteromedial corner, view the posteromedial capsule. Use your finger to press into the posteromedial aspect of the knee where you want to create the portal. It s often more posterior and superior than you think. Then take a spinal needle and verity the proper portal placement. Exteriorly, make a ¼ inch incision at the needle location just through the skin. Use a switching stick to push bluntly through the joint capsule. Insert a cannula over the switching stick and once you verify it has penetrated through the joint capsule, you can remove the switching stick. Place a proble into the cannula and probe the posterior horn of the medial meniscus. More advanced residents can try to probe and shave Fthe tibial portion of the PCL attachment. Figure 2: Skin Markings for PM portal Figure 3: Arthroscopic View of PM Portal ii) Make a posterolateral portal: Place your scope in your anteromedial portal and direct it through the notch into the posterolateral compartment. With the scope turned towards the posterolateral corner, view the posterolateral capsule and then take a spinal needle and verify the
6 proper portal placement. Exteriorly, make a ¼ inch incision at the needle location and then take a 5 mm blue cannula and direct it into the posterolateral compartment. Make sure that the incision is well away from the peroneal nerve and in line with the line drawn superiorly from the posterior border of the fibular head. Place a probe into the cannula and palpate the posterior horn of the lateral meniscus. Make a peripheral tear in the meniscus in the red zone. Place the scope in the portal that is ipsilateral to the tear. You may want to introduce a cannula or similar device in the contralateral portal to facilitate insertion of the repair system. Sutures may be passed either in a horizontal or vertical fashion. Figure 4: Skin Markings for PL portal Figure 5: Meniscus Tears 1. All-Inside Repair: There are several all-inside meniscus repair systems on the market. A PDF has been included on this technique in the documents sent to you. The following are YouTube videos from Linvatec, Smith and Nephew and Arthrex on their devices. Please review the Linvatec device before the lab as it will be available for you to practice on in the lab. Conmed Meniscus Repair with Sequent Device: Figure 5: Arthroscopic View of PL portal d) Perform a meniscus repair Certain types of meniscus tears are amenable to repair. There are 3 main types of repairs: All inside: Most common Inside out: Gold standard - but this does require an incision. Outside in: Good for anterior horn tears There are numerous devices on the market for meniscus repairs. Become familiar with the various types of repairs and you should attempt to perform an all inside repair and an inside out repair in the lab. An appropriate tear of the meniscus may be repaired with sutures and/or fixators. Smith and Nephew meniscus with Fast Fix 360: Arthrex Meniscus Cinch: keeecrtqbqvorhow/meniscal-cinch The advantage of all inside devices are they are relatively easy & fast to insert and no extra incisions are required. The main disadvantage is that once they have been inserted, they are hard to remove. The quality of fixation is very dependent on the integrity of the peripheral segment of meniscus. Acute vertical, peripheral tear in young patients have the best prognosis. Horizontal cleavage plane tears are more challenging to repair.
7 Tip: With a very unstable bucket handle tear, displaced into the notch, it is much easier to keep the meniscus reduce if you insert several inside-out sutures across the tear to hold the reduction before inserting the all inside device. All inside techniques are especially useful in the posterior horn, where inside-out sutures have highest potential for neurovascular injury and are hardest to retrieve. 2. Inside Out Technique: You may want to perform this technique after you have performed the ligament reconstruction(s) in the lab as this will cause water to extravasate from the knee joint. Medial Meniscus: For best visualization: knee is near full extension with valgus stress to open medial side. In very tight knees, you may need to piecrust the MCL with a spinal needle to allow for the knee to open up in valgus. Make the posterior incision before passing the sutures. Identify the proper location for the incision by passing a probe between the medial femoral condyle and medial tibial plateau to the posterior horn/ capsule. Center the incision over the imaginary projection of the probe out the posterior aspect of the knee. Keep the knee flexed 90 degrees. Bluntly separate Figure 6: Inside Out Meniscus Repair the subcutaneous tissues vertically down to the capsule. Insert a retractor (typically a spoon or speculum) to deflect the needle and protect the neurovascular structures. Position needle in the cannula so that it is protruding <1 cm and use it to help reduce the tear. Then finish passing the suture. Move the cannula to the side for a horizontal suture and more peripheral for vertical placement. (Hint: vertical suture placement has been reported to be stronger). Next, pass the second limb of the suture. Tie the sutures under arthroscopic visualization to avoid leaving them too tight or too loose. Tie the suture with the knee in extension to avoid plication of the posterior capsule and possible flexion contracture. Lateral Meniscus: Place the scope in the medial portal and place the knee in the Figure of 4 position to open up the lateral compartment. It is generally okay to pass sutures through popliteus tendon during repair if necessary. Establish the lateral Suture Retrieval Portal (make prior to passing suture). Dissect just posterior to the LCL Maintain dissection anterior to biceps femoris, protecting the peroneal nerve. Place retractor between lateral gastrocnemius and posterolateral capsule. Pass the sutures as outlined in the description above. e) ACL RECONSTRUCTION Anatomy, tunnel placement, reaming of tunnels, graft passage and fixation techniques will be practiced. No matter what graft you use, the tunnel location is the same. There are a variety of fixaation devices on the market for both the femoral and tibial sides. In this lab, we will be using a button fixation on the femur and screw fixation (bioabsorbable or PEEK) on the tibial side. i) Harvest Hamstrings for graft: Begin by harvesting your hamstrings tendon graft as outlined in the talk. Prepare and measure the graft. A PDF of the surgical technique from Linvatec has been provided in the information given to you before the lab. The diameter of the graft determines the tunnels that are drilled in the tibia and femur. With hamstrings, drill the smallest tunnels the graft will snuggly fit through. Figure 7: Anatomy of Medial Hamstrings ii) Prepare the graft: Whipstitch both ends of the graft and tension the graft over the button fixation device.
8 iii) Arthroscopy Preparation: Place the scope in the lateral portal & shaver in themedial portal to debride femoral stump of the torn ACL. Examine the anatomy of the footprint on the femoral and tibial sides. Ensure that you have adequately debrided the tissue so that you can visualize the posterior aspect of the lateral femoral condyle. Figure 8: Anatomy of ACL iv) Femoral Tunnel: Look at the footprint from the lateral portal and then switch portals to look at the anatomy from the anteromedial portal. Make an accessory anteromedial portal using a spinal needle. followed by your cannulated drill. You need to measure the depth of your tunnel with the depth guage. Re-insert the guide pin (Beath pin) followed by your acorn reamer (the size will depend on the size of your prepared graft). Be very careful when you are using the acorn reamer that you do not damage Figure 10: Femoral Tunnel through AM Portal the articular cartilage on the medial femoral condyle. Hyperflexing the knee does improve the clearance area of the medial femoral condyle. Remember that you do not drill all the way through your femoral tunnel to allow the button to flip. If you use a 15 mm button - your femoral tunnel should be 10 mm less than the entire length of your femoral tunnel. v) Tibia Tunnel: The landmarks used to select the optimal location for placement of the tibial tunnel include the old stump, the spines, the PCL, and the lateral meniscus. Examine the stump of the ACL and identify the AM bundle and the PL bundle. Look for the anterior horn of your lateral meniscus for a good reference point of where to place your anatomic tibial tunnel. Secure your guide in place (50-55 degrees). Insert the guide pin followed by the appropriate sized reamer. You may want to rasp the posterior aspect of the intra-articular exit of the tibial tunnel. Figure 9: Examine Femoral Footprint from AM Portal Mark the anatomic location for your ACL graft with an awl. Secure the femoral guide in place and drill using a guide pin either through your anteromedial portal or your accessory anteromedial portal. Make sure that the knee is flexed 120 degrees when you are creating the femoral tunnel. Use the guide pin, Figure 11: Tibial Tunnel Drilling
9 vi) Graft Passage: Mark the length of your femoral tunnel on your graft. Remove the graft from the tensioner. Insert your Beath pin with the passing suture through your femoral and tibial tunnels and out the anterolateral thigh. Place the sutures from the button device through the passing suture. Lead with the stronger suture of the button device and then flip the button on the femur. vii) Tibial Fixation: Tension the graft and then insert a cannulated screw into the tibia tunnel to secure the graft on the tibial side. Some physicians prefer a tensioning device. Also, some physicians prefer to tension the graft and insert the screw in full extension while others prefer 30 degrees of flexion. Then observe each meniscus and study their 3 dimensional shapes. 4. The ligamentous and tendinous structures of the posteromedial and posterolateral corners. 5. Perform an arthrotomy and examine the ACL and PCL 6. Perform a posteromedial approach to the knee to assess the PCL (between semimembranosus and medial head of gastrocs). 7. Perform a lateral approach to the knee and identify and dissect the common peroneal nerve proximally to the fibular neck. 8. Assess the anatomy of the posterolateral corner. The following is a good source to review the anatomy: f) PCL RECONSTRUCTION If you are adept at performing basic knee artrhoscopy and ACL surgery, you may wish to perform a PCL reconstruction. Figure 12: Tibial Interference Screw Fixation viii) Assess Graft: Bring your knee through a range of motion and ensure that the patient has full extension. Assess the graft by performing Lachman and Pivot shift tests. The following is a you tube video on ACL reconstruction (ConMed Livantec): If you have completed the other tasks and will not be performing a PCL reconstruction, dissect the specimen and observe the following: 1. The relationship of the posteromedial portal to the saphenous nerve. 2. The relationship of the posterolateral portal to the peroneal nerve. 3. The capsular and boney attachments of the menisci by sharply incising these attachments with a knife. There are 2 main ways of performing a PCL reconstruction: transtibial (single or double femoral tunnel) or an inlay PCL reconstruction technique. Fluoroscopy is often used during PCL surgery, however, this is not available in the knee lab. Unless you have an overriding desire to work extensively on one of the procedures, a transtibial approach should probably be tried first. If you performed an ACL reconstruction as a part of this lab, you can either leave it in place or you may wish to remove it as this will improve your visualization and simplify the procedure. It is very important to remember that the popliteal artery lies just posterior and slightly lateral to the tibial insertion of the PCL. You should examine the normal anatomy when you look at MRI images of the knee to gain this appreciation. When you perform PCL surgery, the knee is flexed to 90 degrees which allows the artery to sag more posteriorly but you must be very careful to protect the artery.
10 inferior medial & lateral genicular artery via the fat pad. Figure 13: Note Proximity of Popliteal Vessels to PCL ) Harvest Graft: If you wish, you may want to harvest a quadriceps tendon bone graft (known as quad tendon bone). An 11 mm bone plug should be taken from the proximal patella in line with the quadriceps graft. Incise a mm graft from the central portion of the quadriceps tendon. This graft can be used for both techniques (inlay or transtibial). Typically I use Achilles tendon allografts for this procedure. ii) Initial PCL Debridement: Place the arthroscope in the lateral portal. With a shaver in the medial portal, debride the PCL. Of note, frequently, the body of the PCL looks intact arthroscopically as the tear is often near the tibial insertion. What you will often find is sagging of the ACL which is due to the fact that the tibia sags posteriorly causing an apparent laxity of the ACL. Use a full radius resector or similar shaver device to remove the soft tissue. iii) Anatomy: Carefully examine the anatomy of the PCL footprint on the femoral side. Like the ACL, there are 2 bundles to the PCL. They are known as the antero-lateral bundle (AL) and the postero-medial (PM) bundle. The AL bundle is 2 X s larger/sronger than the PM bundle. The AL is tight in flexion. The PM is tight in extension. With the single bundle technique (most common) you reconstruct the larger anterolateral band. The origin of the ACL is a broad crescent shaped area on the anterolateral aspect of the medial femoral condyle. The insertion is on the posterior tibia approximately 1-15 cm below the articular surface. The blood supply is the same as the ACL - the majority of the supply is from the middle genicular artery and the Figure 14: AL & PM Footprint Anatomy of PCL iv) Establish a posteromedial portal: As outlined previously in this manual. The knee should be flexed 90 degrees. Place the scope with blunt obturator in the anterolateral portal and direct it through the notch into the posteromedial compartment. This is much easier to do after the debridement of the cruciate ligaments. If your PCL is intact, feel the scope slide along the medial femoral condyle and under the PCL as it is gently pushed into the posteromedial compartment. Gaining posterior access may be difficult in older individuals where the notch can be stenotic and osteophytes block access. With the scope turned towards the posteromedial corner, view the posteromedial capsule. Use your finger to press into the posteromedial aspect of the knee where you want to create the portal. It s often more posterior and superior than you think. Then take a spinal needle and verity the proper portal placement. Exteriorly, make a ¼ inch incision at the needle location just through the skin. Use a switching stick and gently insert bluntly through the posteromedial joint capsule. Insert a cannula over the switching stick and once you verify that it has penetrated through the joint capsule, you can remove the switching stick. Place a proble into the cannula and probe the posterior horn of the medial meniscus.
11 v) Debride PCL tibial attachment Introduce a shaver through a posteromedial portal, taking care to minimize suction and orienting the blade to always face the tibia (not the capsular side where the artery is close by). It is often safer and easier to use a radiofrequency (RF) device. A 30 arthroscope in the medial portal is usually satisfactory for visualization during this step, although some prefer using a 70 scope. The tibial attachment of the PCL is removed and posterior capsule debrided off the bone cm distal to the posterior edge of the proximal tibia. This is often further distal than you think! It can be confirmed using the imager. You can also place the scope in the posteromedial portal to assess. cortex where some physicians will then drill by hand. Chamfer the proximal tibial tunnel with a rasp to minimize any sharp bone fragments from abrading the PCL graft. The soft tissue may need to be further debrided posteriorly using a shaver or an RF device. Figure 15: Posterior PCL Anatomy vi) Tibial tunnel: Place the scope in the lateral portal and PCL drill guide in the medial portal. The arthroscope can also be switched to posteromedial portal to monitor placement of the guide. In the OR, the C arm would have been previously prepared in the correct position to confirm the tibial guide placement and the tibial drilling would all be done using arthroscopic guidance. The PCL guide has a curve on it that allows it to slide over the tibia and distal to the joint line. Most PCL tibial guides have a stop on them to prevent the guide wire from passing too far posterior. However, that depends on the wire hitting the guide, which is a big assumption. Use the C-arm to avoid drilling too deep in the Operating Room. The tibial guide is secured approximately 1.5 cm distal to the posterior tibial joint line. Make an incision on the proximal tibia. The starting point is the medial border of the tibia approximately 1. 2 cm distal to the tibial tubercle. Drill with the guide wire very slowly and carefully. followed by the appropriate sized tibial reamer. You need to ensure that the guide wire does not get caught on the drill and accidentally advanced. The tunnel is drilled using power initially up to the posterior tibial Figure 16: Tibial PCL Tunnel vii) Femoral tunnel: You can use the standard two incision technique or the newer one-incision endoscopic technique to drill the femoral tunnel a) Outside In Technique: Figure 17: Outside-In Femoral Tunnel Place the arthroscope in lateral portal & the femoral guide is placed through the medial portal. The guide wire enters the femur at a point midway between the medial femoral epicondyle and the medial border of the patella. The guide wire should exit through the anterior portion of the PCL stump. This is the 1 o clock (right knee) or 11 o clock (left knee) position and 10 mm back from the articular margin. The
12 graft will tend to sit in the posterior part of the tunnel All bone and soft tissue debris is removed after the tunnel has been drilled. Carefully chamfer the internal exit of the femoral tunnel. b) Inside - Out Technique: The arthroscope is placed in the lateral portal. Mark the appropriate location for the center of the femoral tunnel, then switch the scope to the medial portal. Advance a guide wire into that spot through the lateral portal, then drill the tunnel with the knee at flexion. viii) Graft Passage: This can be a difficult portion of the procedure. Oversizing the tibial tunnel helps assist graft passage. A device such a the Gortex PCL graft smoother can assist with graft passage. Place the passing device through the tibia and then out the femoral tunnel. If the device gets caught up posteriorly use a blunt trocar in the posterior portal to help guide the graft into the femoral tunnel. Fixation The graft is then tensioned and secured in place with screws. The knee should be cycled several time to get the slack out. For a single bundle technique, secure the garft on the femoral side with a screw. The knee should be cycled again and the knee should be held in 70 to 90 degrees of flexion. Apply an anterior drawer force to the tibia to properly position the tibia under the femur. The tibia screw may then be inserted. The graft should then be assessed for stability by performing a posterior drawer and assessing for a posterior sag. Ensure that the patient has full extension. g) Tibial-Inlay Technique for PCL In the knee lab, you should get a general idea of the placement of the tibial inlay graft. The approach is much better appreciated in the cadaver. The femoral tunnel preparation should be performed first, followed by the posteromedial knee incision and preparation for the bone only. of fracturing the plug. ii) Posteromedial knee approach: Make a curvilinear incision over the medial hamstrings. Bluntly dissect between the medial head of the gastrocnemius and the semimembranosus tendon. Retract the neurovascular bundle medially with an right angle retractor or an Army-Navy retractor. Palpate the posterior joint capsule. Isolate the posterior slope of the tibia and incise the capsule longitudinally. Isolate the PCL attachment, create a bony trough 12.5 x 25 mm. Inlay the bone portion of the Quad Tendon Bone Graft and fix with a either screw or staple. Pass the other end of the graft out the front of the knee with a Beath pin. Be sure to pass the graft on the medial side of the ACL. For the tibial inlay technique, the graft has already been secured on the tibial side. The graft should then be placed through the femoral side and secured with a screw. Once again, the knee should be cycled multiple times to get the slack out. Use the same techniques of flexing the knee and applying an anterior drawer force on the proximal tibia before securing the femoral side. Figure 18: Tibial Inlay Graft for PCL i) Femoral tunnel: Create the standard femoral tunnel using the arthroscope as discussed above. Pass a looped 18 g wire to the posterior capsule. Prepare and pre-drill the patellar bone plug of the quad tendon bone graft (11 x 25mm) using a single 4.5 mm screw. Larger screws run a risk
Figure 3 Figure 4 Figure 5
 Figure 1 Figure 2 Begin the operation with examination under anesthesia to confirm whether there are any ligamentous instabilities in addition to the posterior cruciate ligament insufficiency. In particular
Figure 1 Figure 2 Begin the operation with examination under anesthesia to confirm whether there are any ligamentous instabilities in addition to the posterior cruciate ligament insufficiency. In particular
Transtibial PCL Reconstruction. Surgical Technique. Transtibial PCL Reconstruction
 Transtibial PCL Reconstruction Surgical Technique Transtibial PCL Reconstruction The Arthrex Transtibial PCL Reconstruction System includes unique safety features for protecting posterior neurovascular
Transtibial PCL Reconstruction Surgical Technique Transtibial PCL Reconstruction The Arthrex Transtibial PCL Reconstruction System includes unique safety features for protecting posterior neurovascular
Meniscus cartilage replacement with cadaveric
 Technical Note Meniscal Allografting: The Three-Tunnel Technique Kevin R. Stone, M.D., and Ann W. Walgenbach, R.N.N.P., M.S.N. Abstract: This technical note describes an improved arthroscopic technique
Technical Note Meniscal Allografting: The Three-Tunnel Technique Kevin R. Stone, M.D., and Ann W. Walgenbach, R.N.N.P., M.S.N. Abstract: This technical note describes an improved arthroscopic technique
Double Bundle ACL Reconstruction using the Smith & Nephew Outside-In Anatomic ACL Guide System
 Knee Series Technique Guide Double Bundle ACL Reconstruction using the Smith & Nephew Outside-In Anatomic ACL Guide System Luigi Adriano Pederzini, MD Massimo Tosi, MD Mauro Prandini, MD Luigi Milandri,
Knee Series Technique Guide Double Bundle ACL Reconstruction using the Smith & Nephew Outside-In Anatomic ACL Guide System Luigi Adriano Pederzini, MD Massimo Tosi, MD Mauro Prandini, MD Luigi Milandri,
Double Bundle PCL Reconstruction. Surgical Technique
 Double Bundle PCL Reconstruction Surgical Technique Double Bundle PCL Reconstruction With recent interest in double tunnel endoscopic PCL reconstruction, Arthrex has created a series of Femoral PCL Drill
Double Bundle PCL Reconstruction Surgical Technique Double Bundle PCL Reconstruction With recent interest in double tunnel endoscopic PCL reconstruction, Arthrex has created a series of Femoral PCL Drill
Torn ACL - Anatomic Footprint ACL Reconstruction
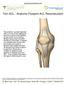 Torn ACL - Anatomic Footprint ACL Reconstruction The anterior cruciate ligament (ACL) is one of four ligaments that are crucial to the stability of your knee. It is a strong fibrous tissue that connects
Torn ACL - Anatomic Footprint ACL Reconstruction The anterior cruciate ligament (ACL) is one of four ligaments that are crucial to the stability of your knee. It is a strong fibrous tissue that connects
Knee Preservation System
 Knee Preservation System Anatomic Patellar Tendon ACL Reconstruction using the Bullseye Cruciate System SURGICAL TECHNIQUE Anatomic Patellar Tendon ACL Reconstruction using the Bullseye Cruciate System
Knee Preservation System Anatomic Patellar Tendon ACL Reconstruction using the Bullseye Cruciate System SURGICAL TECHNIQUE Anatomic Patellar Tendon ACL Reconstruction using the Bullseye Cruciate System
Technique Guide. *smith&nephew N8TIVE ACL Anatomic ACL Reconstruction System
 Technique Guide *smith&nephew N8TIVE ACL Anatomic ACL Reconstruction System N8TIVE ACL System The N8TIVE ACL Anatomic Reconstruction System provides a novel and simple approach to ACL repair. The N8TIVE
Technique Guide *smith&nephew N8TIVE ACL Anatomic ACL Reconstruction System N8TIVE ACL System The N8TIVE ACL Anatomic Reconstruction System provides a novel and simple approach to ACL repair. The N8TIVE
PCL Reconstruction Utilizing the TightRope /GraftLink Technique Juxtaposed to posterior horn
 Tibial & Femoral PCL Footprints PCL Reconstruction Utilizing the TightRope /GraftLink Juxtaposed to posterior horn Thomas M. DeBerardino, MD Associate Professor, UCONN Health Team Physician, Orthopaedic
Tibial & Femoral PCL Footprints PCL Reconstruction Utilizing the TightRope /GraftLink Juxtaposed to posterior horn Thomas M. DeBerardino, MD Associate Professor, UCONN Health Team Physician, Orthopaedic
The Knee. Prof. Oluwadiya Kehinde
 The Knee Prof. Oluwadiya Kehinde www.oluwadiya.sitesled.com The Knee: Introduction 3 bones: femur, tibia and patella 2 separate joints: tibiofemoral and patellofemoral. Function: i. Primarily a hinge joint,
The Knee Prof. Oluwadiya Kehinde www.oluwadiya.sitesled.com The Knee: Introduction 3 bones: femur, tibia and patella 2 separate joints: tibiofemoral and patellofemoral. Function: i. Primarily a hinge joint,
AFX. Femoral Implant. System. The AperFix. AM Portal Surgical Technique Guide. with the. The AperFix System with the AFX Femoral Implant
 The AperFix System AFX with the Femoral Implant AM Portal Surgical Technique Guide The Cayenne Medical AperFix system with the AFX Femoral Implant is the only anatomic system for soft tissue ACL reconstruction
The AperFix System AFX with the Femoral Implant AM Portal Surgical Technique Guide The Cayenne Medical AperFix system with the AFX Femoral Implant is the only anatomic system for soft tissue ACL reconstruction
*smith&nephew ENDOBUTTON CL. Knee Series Technique Guide. Fixation System
 Knee Series Technique Guide *smith&nephew ENDOBUTTON CL Fixation System Double Bundle ACL Reconstruction using the Smith & Nephew ACUFEX Director Set for Anatomic ACL Reconstruction French Anatomic ACL-R
Knee Series Technique Guide *smith&nephew ENDOBUTTON CL Fixation System Double Bundle ACL Reconstruction using the Smith & Nephew ACUFEX Director Set for Anatomic ACL Reconstruction French Anatomic ACL-R
Shoulder Arthroscopy Lab Manual
 Shoulder Arthroscopy Lab Manual Dalhousie University Orthopaedic Program May 5, 2017 Skills Centre OBJECTIVES 1. Demonstrate a competent understanding of the arthroscopic anatomy and biomechanics of the
Shoulder Arthroscopy Lab Manual Dalhousie University Orthopaedic Program May 5, 2017 Skills Centre OBJECTIVES 1. Demonstrate a competent understanding of the arthroscopic anatomy and biomechanics of the
BioRCI Screw System. Surgical Technique for Hamstring and Patellar Tendon Grafts
 BioRCI Screw System Surgical Technique for Hamstring and Patellar Tendon Grafts Surgical Technique for Hamstring and Patellar Tendon Grafts Using the BioRCI Screw System The Smith & Nephew BioRCI cruciate
BioRCI Screw System Surgical Technique for Hamstring and Patellar Tendon Grafts Surgical Technique for Hamstring and Patellar Tendon Grafts Using the BioRCI Screw System The Smith & Nephew BioRCI cruciate
ACL Reconstruction for BTB Grafts
 Transtibial ACL Reconstruction System for BTB Grafts Surgical Technique Designed in conjunction with John C. Garrett, M.D., Atlanta, GA ACL Reconstruction for BTB Grafts Reference Anatomical Constants
Transtibial ACL Reconstruction System for BTB Grafts Surgical Technique Designed in conjunction with John C. Garrett, M.D., Atlanta, GA ACL Reconstruction for BTB Grafts Reference Anatomical Constants
ACL AND PCL INJURIES OF THE KNEE JOINT
 ACL AND PCL INJURIES OF THE KNEE JOINT Dr.KN Subramanian M.Ch Orth., FRCS (Tr & Orth), CCT Orth(UK) Consultant Orthopaedic Surgeon, Special interest: Orthopaedic Sports Injury, Shoulder and Knee Surgery,
ACL AND PCL INJURIES OF THE KNEE JOINT Dr.KN Subramanian M.Ch Orth., FRCS (Tr & Orth), CCT Orth(UK) Consultant Orthopaedic Surgeon, Special interest: Orthopaedic Sports Injury, Shoulder and Knee Surgery,
Joints of the Lower Limb II
 Joints of the Lower Limb II Lecture Objectives Describe the components of the knee and ankle joint. List the ligaments associated with these joints and their attachments. List the muscles acting on these
Joints of the Lower Limb II Lecture Objectives Describe the components of the knee and ankle joint. List the ligaments associated with these joints and their attachments. List the muscles acting on these
11/16/2015. No disclosures or conflicts of interest relevant to the presentation
 Travis C. Burns, MD SAMMC, Ft Sam Houston, Tx Chief, Sports Medicine Advanced Concepts in Sports Medicine Nov 6 8, 2015 Las Vegascourse.com No disclosures or conflicts of interest relevant to the presentation
Travis C. Burns, MD SAMMC, Ft Sam Houston, Tx Chief, Sports Medicine Advanced Concepts in Sports Medicine Nov 6 8, 2015 Las Vegascourse.com No disclosures or conflicts of interest relevant to the presentation
BICEPTOR Tenodesis System
 BICEPTOR Tenodesis System Sub-Pectoral Biceps Tenodesis A Shoulder Series Technique Guide As described by: Nikhil N. Verma, MD As described by: Nikhil N. Verma, MD Midwest Orthopedics at Rush Chicago,
BICEPTOR Tenodesis System Sub-Pectoral Biceps Tenodesis A Shoulder Series Technique Guide As described by: Nikhil N. Verma, MD As described by: Nikhil N. Verma, MD Midwest Orthopedics at Rush Chicago,
Anterior Cruciate Ligament Surgery
 Anatomy Anterior Cruciate Ligament Surgery Roger Ostrander, MD Andrews Institute Anatomy Anatomy Function Primary restraint to anterior tibial translation Secondary restraint to internal tibial rotation
Anatomy Anterior Cruciate Ligament Surgery Roger Ostrander, MD Andrews Institute Anatomy Anatomy Function Primary restraint to anterior tibial translation Secondary restraint to internal tibial rotation
The AperFix II System
 The AperFix II System A Complete Anatomic Solution Transtibial Surgical Technique 2 AperFix II System Transtibial Surgical Technique Figure 1 A Complete Anatomic Solution The Cayenne Medical AperFix and
The AperFix II System A Complete Anatomic Solution Transtibial Surgical Technique 2 AperFix II System Transtibial Surgical Technique Figure 1 A Complete Anatomic Solution The Cayenne Medical AperFix and
Distal Femoral Resection
 Distal Femoral Resection Annie Arteau, Bruno Fuchs Introduction This text is a general description of a distal femoral resection. Focus is on anatomical structures and muscle resection. Each femoral resection
Distal Femoral Resection Annie Arteau, Bruno Fuchs Introduction This text is a general description of a distal femoral resection. Focus is on anatomical structures and muscle resection. Each femoral resection
Posterior cruciate ligament (PCL) reconstructions
 All-Inside Posterior Cruciate Ligament Reconstruction With a GraftLink Gerard G. Adler, M.D. Abstract: Posterior cruciate ligament (PCL) reconstructions are challenging surgeries. Recent advances have
All-Inside Posterior Cruciate Ligament Reconstruction With a GraftLink Gerard G. Adler, M.D. Abstract: Posterior cruciate ligament (PCL) reconstructions are challenging surgeries. Recent advances have
ACL Reconstruction Cross-Pin Technique
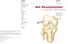 ACL Reconstruction Cross-Pin Technique Surgical Technique Lonnie E. Paulos, MD Salt Lake City, Utah 325 Corporate Drive Mahwah, NJ 07430 t: 201 831 5000 www.stryker.com A surgeon should always rely on
ACL Reconstruction Cross-Pin Technique Surgical Technique Lonnie E. Paulos, MD Salt Lake City, Utah 325 Corporate Drive Mahwah, NJ 07430 t: 201 831 5000 www.stryker.com A surgeon should always rely on
Anatomy and Sports Injuries of the Knee
 Anatomy and Sports Injuries of the Knee I. Anatomy II. Assessment III. Treatment IV. Case Study V. Dissection Anatomy Not a hinge joint 6 degrees of freedom Flexion/Extension Rotation Translation Anatomy
Anatomy and Sports Injuries of the Knee I. Anatomy II. Assessment III. Treatment IV. Case Study V. Dissection Anatomy Not a hinge joint 6 degrees of freedom Flexion/Extension Rotation Translation Anatomy
Disclosures. Outline. The Posterior Cruciate Ligament 5/3/2016
 The Posterior Cruciate Ligament Christopher J. Utz, MD Assistant Professor of Orthopaedic Surgery University of Cincinnati Disclosures I have no disclosures relevant to this topic. Outline 1. PCL Basic
The Posterior Cruciate Ligament Christopher J. Utz, MD Assistant Professor of Orthopaedic Surgery University of Cincinnati Disclosures I have no disclosures relevant to this topic. Outline 1. PCL Basic
Bio-Tenodesis Screw Fixation
 Bio-Tenodesis Screw Fixation in Tendon Enhanced Ankle Ligament Reconstruction Surgical Technique Kevin O'Shea, M.D. with contributions from Thomas Clanton, M.D., and William McGarvey, M.D. Bio-Tenodesis
Bio-Tenodesis Screw Fixation in Tendon Enhanced Ankle Ligament Reconstruction Surgical Technique Kevin O'Shea, M.D. with contributions from Thomas Clanton, M.D., and William McGarvey, M.D. Bio-Tenodesis
Reconstruction of the Ligaments of the Knee
 Reconstruction of the Ligaments of the Knee Contents ACL reconstruction Evaluation Selection Evolution Graft issues Notchplasty Tunnel issues MCL PCL Posterolateral ligament complex Combined injuries Evaluation
Reconstruction of the Ligaments of the Knee Contents ACL reconstruction Evaluation Selection Evolution Graft issues Notchplasty Tunnel issues MCL PCL Posterolateral ligament complex Combined injuries Evaluation
Minimally Invasive ACL Surgery
 Minimally Invasive ACL Surgery KOCO EATON, M.D. T A M P A B A Y R A Y S ( 1 9 9 5 P R E S E N T ) T A M P A B A Y B U C C A N E E R S ( 2 0 1 5 2 0 1 6 ) T A M P A B A Y R O W D I E S ( 2 0 1 4 2 0 1 7
Minimally Invasive ACL Surgery KOCO EATON, M.D. T A M P A B A Y R A Y S ( 1 9 9 5 P R E S E N T ) T A M P A B A Y B U C C A N E E R S ( 2 0 1 5 2 0 1 6 ) T A M P A B A Y R O W D I E S ( 2 0 1 4 2 0 1 7
PCL GraftLink Surgical Technique
 PCL GraftLink Surgical Technique PCL GraftLink GraftLink Minimally Invasive PCL Reconstruction The GraftLink technique provides the ultimate in anatomic, minimally invasive, and reproducible PCL reconstruction
PCL GraftLink Surgical Technique PCL GraftLink GraftLink Minimally Invasive PCL Reconstruction The GraftLink technique provides the ultimate in anatomic, minimally invasive, and reproducible PCL reconstruction
Meniscus Reconstruction: Trough Surgical Technique
 Meniscus Reconstruction: Trough Surgical Technique Technique Consultant Jeffrey L. Halbrecht, M.D. San Francisco, CA ABOUT THE TROUGH TECHNIQUE The trough technique for meniscal allograft reconstruction
Meniscus Reconstruction: Trough Surgical Technique Technique Consultant Jeffrey L. Halbrecht, M.D. San Francisco, CA ABOUT THE TROUGH TECHNIQUE The trough technique for meniscal allograft reconstruction
Ligamentous and Meniscal Injuries: Diagnosis and Management
 Ligamentous and Meniscal Injuries: Diagnosis and Management Daniel K Williams, MD Franciscan Physician Network Orthopedic Specialists September 29, 2017 No Financial Disclosures INTRODUCTION Overview of
Ligamentous and Meniscal Injuries: Diagnosis and Management Daniel K Williams, MD Franciscan Physician Network Orthopedic Specialists September 29, 2017 No Financial Disclosures INTRODUCTION Overview of
ACL Athletic Career. ACL Rupture - Warning Features Intensive pain Immediate swelling Locking Feel a Pop Dead leg Cannot continue to play
 FIMS Ambassador Tour to Eastern Europe, 2004 Belgrade, Serbia Montenegro Acute Knee Injuries - Controversies and Challenges Professor KM Chan OBE, JP President of FIMS Belgrade ACL Athletic Career ACL
FIMS Ambassador Tour to Eastern Europe, 2004 Belgrade, Serbia Montenegro Acute Knee Injuries - Controversies and Challenges Professor KM Chan OBE, JP President of FIMS Belgrade ACL Athletic Career ACL
Imaging the Athlete s Knee. Peter Lowry, MD Musculoskeletal Radiology University of Colorado
 Imaging the Athlete s Knee Peter Lowry, MD Musculoskeletal Radiology University of Colorado None Disclosures Knee Imaging: Radiographs Can be performed weight-bearing or non-weight-bearing View options
Imaging the Athlete s Knee Peter Lowry, MD Musculoskeletal Radiology University of Colorado None Disclosures Knee Imaging: Radiographs Can be performed weight-bearing or non-weight-bearing View options
CROSS PIN TECHNOLOGY FOR AN ANATOMIC ACL
 CROSS PIN TECHNOLOGY FOR AN ANATOMIC ACL INTRODUCTION The RIGIDFIX Curve Cross Pin System is designed specifically for use with the anteromedial (AM) portal approach to achieve a more anatomic soft tissue
CROSS PIN TECHNOLOGY FOR AN ANATOMIC ACL INTRODUCTION The RIGIDFIX Curve Cross Pin System is designed specifically for use with the anteromedial (AM) portal approach to achieve a more anatomic soft tissue
Arthroscopic PCL Reconstruction
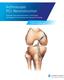 Arthroscopic PCL Reconstruction Using Soft Tissue Graft and TunneLoc Tibial Fixation with ToggleLoc Fixation Device with ZipLoop Technology Surgical Technique by Mark Ganjianpour, M.D. Table of Contents
Arthroscopic PCL Reconstruction Using Soft Tissue Graft and TunneLoc Tibial Fixation with ToggleLoc Fixation Device with ZipLoop Technology Surgical Technique by Mark Ganjianpour, M.D. Table of Contents
Knee Joint Anatomy 101
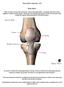 Knee Joint Anatomy 101 Bone Basics There are three bones at the knee joint femur, tibia and patella commonly referred to as the thighbone, shinbone and kneecap. The fibula is not typically associated with
Knee Joint Anatomy 101 Bone Basics There are three bones at the knee joint femur, tibia and patella commonly referred to as the thighbone, shinbone and kneecap. The fibula is not typically associated with
The Knee. Tibio-Femoral
 The Knee Tibio-Femoral Osteology Distal Femur with Proximal Tibia Largest Joint Cavity in the Body A modified hinge joint with significant passive rotation Technically, one degree of freedom (Flexion/Extension)
The Knee Tibio-Femoral Osteology Distal Femur with Proximal Tibia Largest Joint Cavity in the Body A modified hinge joint with significant passive rotation Technically, one degree of freedom (Flexion/Extension)
Knee Joint Assessment and General View
 Knee Joint Assessment and General View Done by; Mshari S. Alghadier BSc Physical Therapy RHPT 366 m.alghadier@sau.edu.sa http://faculty.sau.edu.sa/m.alghadier/ Functional anatomy The knee is the largest
Knee Joint Assessment and General View Done by; Mshari S. Alghadier BSc Physical Therapy RHPT 366 m.alghadier@sau.edu.sa http://faculty.sau.edu.sa/m.alghadier/ Functional anatomy The knee is the largest
SURGICAL TECHNIQUE VISUALIZE FEMORAL FIXATION 360 GRAFT TO BONE CONTACT INCREASED PULL-OUT STRENGTH
 SURGICAL TECHNIQUE VISUALIZE FEMORAL FIXATION 360 GRAFT TO BONE CONTACT INCREASED PULL-OUT STRENGTH PINN-ACL CROSSPIN SYSTEM SURGICAL TECHNIQUE INTRODUCTION The ConMed Linvatec Pinn-ACL CrossPin System
SURGICAL TECHNIQUE VISUALIZE FEMORAL FIXATION 360 GRAFT TO BONE CONTACT INCREASED PULL-OUT STRENGTH PINN-ACL CROSSPIN SYSTEM SURGICAL TECHNIQUE INTRODUCTION The ConMed Linvatec Pinn-ACL CrossPin System
The Knee. Two Joints: Tibiofemoral. Patellofemoral
 Evaluating the Knee The Knee Two Joints: Tibiofemoral Patellofemoral HISTORY Remember the questions from lecture #2? Girth OBSERVATION TibioFemoral Alignment What are the consequences of faulty alignment?
Evaluating the Knee The Knee Two Joints: Tibiofemoral Patellofemoral HISTORY Remember the questions from lecture #2? Girth OBSERVATION TibioFemoral Alignment What are the consequences of faulty alignment?
RN(EC) ENC(C) GNC(C) MN ACNP *** MECHANISM OF INJURY.. MOST IMPORTANT *** - Useful in determining mechanism of injury / overuse
 HISTORY *** MECHANISM OF INJURY.. MOST IMPORTANT *** Age of patient Sport / Occupation - Certain conditions are more prevalent in particular age groups (Osgood Schlaters in youth / Degenerative Joint Disease
HISTORY *** MECHANISM OF INJURY.. MOST IMPORTANT *** Age of patient Sport / Occupation - Certain conditions are more prevalent in particular age groups (Osgood Schlaters in youth / Degenerative Joint Disease
Lateral Meniscus Transplant
 Lateral Meniscus Transplant Using the CONMED Meniscus Allograft Transplant (MAT) Instruments A complete guide to Lateral Meniscus Transplant using the CONMED meniscus allograft transplant Instruments.
Lateral Meniscus Transplant Using the CONMED Meniscus Allograft Transplant (MAT) Instruments A complete guide to Lateral Meniscus Transplant using the CONMED meniscus allograft transplant Instruments.
STATE OF THE ART OF ACL SURGERY (Advancements that have had an impact)
 STATE OF THE ART OF ACL SURGERY (Advancements that have had an impact) David Drez, Jr., M.D. Clinical Professor of Orthopaedics LSU School of Medicine Financial Disclosure Dr. David Drez has no relevant
STATE OF THE ART OF ACL SURGERY (Advancements that have had an impact) David Drez, Jr., M.D. Clinical Professor of Orthopaedics LSU School of Medicine Financial Disclosure Dr. David Drez has no relevant
Minimally Invasive Quad Tendon Harvest System Surgical Technique
 Minimally Invasive Quad Tendon Harvest System Surgical Technique Quad Tendon Harvest System Quadricep tendon grafts offer unique benefits for cruciate ligament reconstruction such as a predictably large
Minimally Invasive Quad Tendon Harvest System Surgical Technique Quad Tendon Harvest System Quadricep tendon grafts offer unique benefits for cruciate ligament reconstruction such as a predictably large
Fibular collateral ligament reconstruction of knee using titanium button: a new fixation technique and an outcome of 35 cases
 International Journal of Research in Orthopaedics Rai SK et al. Int J Res Orthop. 2017 May;3(3):573-577 http://www.ijoro.org Original Research Article DOI: http://dx.doi.org/10.18203/issn.2455-4510.intjresorthop20171904
International Journal of Research in Orthopaedics Rai SK et al. Int J Res Orthop. 2017 May;3(3):573-577 http://www.ijoro.org Original Research Article DOI: http://dx.doi.org/10.18203/issn.2455-4510.intjresorthop20171904
Knee Injury Assessment
 Knee Injury Assessment Clinical Anatomy p. 186 Femur Medial condyle Lateral condyle Femoral trochlea Tibia Intercondylar notch Tibial tuberosity Tibial plateau Fibula Fibular head Patella Clinical Anatomy
Knee Injury Assessment Clinical Anatomy p. 186 Femur Medial condyle Lateral condyle Femoral trochlea Tibia Intercondylar notch Tibial tuberosity Tibial plateau Fibula Fibular head Patella Clinical Anatomy
The Lower Limb II. Anatomy RHS 241 Lecture 3 Dr. Einas Al-Eisa
 The Lower Limb II Anatomy RHS 241 Lecture 3 Dr. Einas Al-Eisa Tibia The larger & medial bone of the leg Functions: Attachment of muscles Transfer of weight from femur to skeleton of the foot Articulations
The Lower Limb II Anatomy RHS 241 Lecture 3 Dr. Einas Al-Eisa Tibia The larger & medial bone of the leg Functions: Attachment of muscles Transfer of weight from femur to skeleton of the foot Articulations
Arthroscopy of the Knee
 Arthroscopy of the Knee P. Archbold, L.N. Favaro Lourenço Francisco, R. Kancelskis Prado, and Robert A. Magnussen 2 General Information It is essential that an orthopedic surgeon acquire the skills to
Arthroscopy of the Knee P. Archbold, L.N. Favaro Lourenço Francisco, R. Kancelskis Prado, and Robert A. Magnussen 2 General Information It is essential that an orthopedic surgeon acquire the skills to
Anterior cruciate ligament reconstruction using the Bio-TransFix femoral fixation device. with an anteromedial portal technique.
 Knee Surg Sports Traumatol Arthrosc (2006) 14: 497 501 TECHNICAL NOTE DOI 10.1007/s00167-005-0705-y Michael E. Hantes Zoe Dailiana Vasilios C. Zachos Sokratis E. Varitimidis Anterior cruciate ligament
Knee Surg Sports Traumatol Arthrosc (2006) 14: 497 501 TECHNICAL NOTE DOI 10.1007/s00167-005-0705-y Michael E. Hantes Zoe Dailiana Vasilios C. Zachos Sokratis E. Varitimidis Anterior cruciate ligament
ACL Reconstruction Single Tibial Tunnel Double Bundle
 ACL Reconstruction Single Tibial Tunnel Double Bundle with the ToggleLoc Fixation Device with ZipLoop Technology Surgical Technique by Eric McCarty, M.D. Table of Contents Portal Position and Sizing of
ACL Reconstruction Single Tibial Tunnel Double Bundle with the ToggleLoc Fixation Device with ZipLoop Technology Surgical Technique by Eric McCarty, M.D. Table of Contents Portal Position and Sizing of
MRI KNEE WHAT TO SEE. Dr. SHEKHAR SRIVASTAV. Sr.Consultant KNEE & SHOULDER ARTHROSCOPY
 MRI KNEE WHAT TO SEE Dr. SHEKHAR SRIVASTAV Sr.Consultant KNEE & SHOULDER ARTHROSCOPY MRI KNEE - WHAT TO SEE MRI is the most accurate and frequently used diagnostic tool for evaluation of internal derangement
MRI KNEE WHAT TO SEE Dr. SHEKHAR SRIVASTAV Sr.Consultant KNEE & SHOULDER ARTHROSCOPY MRI KNEE - WHAT TO SEE MRI is the most accurate and frequently used diagnostic tool for evaluation of internal derangement
with ACL Reconstruction Single Tibial Tunnel Double Bundle Surgical Protocol by Eric McCarty, M.D.
 with ACL Reconstruction Single Tibial Tunnel Double Bundle Surgical Protocol by Eric McCarty, M.D. Features A unique weave in which a single strand of braided polyethylene is woven through itself twice
with ACL Reconstruction Single Tibial Tunnel Double Bundle Surgical Protocol by Eric McCarty, M.D. Features A unique weave in which a single strand of braided polyethylene is woven through itself twice
Knee Disarticulation Amputation
 Knee Disarticulation Amputation Pre-Op 64 year old man, previous spinal cord injury, diabetes, renal failure, and a history of spasticity with dynamic knee flexion contracture. He had an open left ankle
Knee Disarticulation Amputation Pre-Op 64 year old man, previous spinal cord injury, diabetes, renal failure, and a history of spasticity with dynamic knee flexion contracture. He had an open left ankle
ARTICLE IN PRESS. Technical Note
 Technical Note Hybrid Anterior Cruciate Ligament Reconstruction: Introduction of a New Technique for Anatomic Anterior Cruciate Ligament Reconstruction Darren A. Frank, M.D., Gregory T. Altman, M.D., and
Technical Note Hybrid Anterior Cruciate Ligament Reconstruction: Introduction of a New Technique for Anatomic Anterior Cruciate Ligament Reconstruction Darren A. Frank, M.D., Gregory T. Altman, M.D., and
Arthrex PassPort Button Cannula. Maximize visibility and maneuverability inside and outside of the arthroscopic workspace
 Arthrex PassPort Button Cannula Maximize visibility and maneuverability inside and outside of the arthroscopic workspace PassPort Button Cannulas Soft and flexible silicone material will form to smaller
Arthrex PassPort Button Cannula Maximize visibility and maneuverability inside and outside of the arthroscopic workspace PassPort Button Cannulas Soft and flexible silicone material will form to smaller
Incidence. Avoiding Complications of ACL Surgery. ACL Complications 6/10/2011. Not if, but when
 Avoiding Complications of ACL Surgery Thomas J. Gill, MD Chief, MGH Sports Medicine Service Dept of Orthopedic Surgery Massachusetts General Hospital Associate Professor of Orthopedic Surgery Harvard Medical
Avoiding Complications of ACL Surgery Thomas J. Gill, MD Chief, MGH Sports Medicine Service Dept of Orthopedic Surgery Massachusetts General Hospital Associate Professor of Orthopedic Surgery Harvard Medical
The Knee Joint By Prof. Dr. Muhammad Imran Qureshi
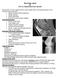 The Knee Joint By Prof. Dr. Muhammad Imran Qureshi Structurally, it is the Largest and the most complex joint in the body because of the functions that it performs: Allows mobility (flexion/extension)
The Knee Joint By Prof. Dr. Muhammad Imran Qureshi Structurally, it is the Largest and the most complex joint in the body because of the functions that it performs: Allows mobility (flexion/extension)
ACL reconstruction. Osteoconductive absorbable interference screws. Unique material. Optimal design. Adapted to different surgical techniques
 ACL reconstruction Osteoconductive absorbable interference screws Unique material Optimal design Adapted to different surgical techniques + complete instrumentation set Controlled resorption Material LIGAFIX
ACL reconstruction Osteoconductive absorbable interference screws Unique material Optimal design Adapted to different surgical techniques + complete instrumentation set Controlled resorption Material LIGAFIX
MCL Injuries: When and How to Repair Scott D. Mair, MD
 MCL Injuries: When and How to Repair Scott D. Mair, MD Professor and Team Physician: Orthopaedic Surgery University of Kentucky School of Medicine Disclosure Institution: Research/Education Smith-Nephew
MCL Injuries: When and How to Repair Scott D. Mair, MD Professor and Team Physician: Orthopaedic Surgery University of Kentucky School of Medicine Disclosure Institution: Research/Education Smith-Nephew
ToggleLoc Fixation Device with ZipLoop Technology
 ToggleLoc Fixation Device with ZipLoop Technology Arthroscopic PCL Reconstruction Using Soft Tissue Graft and TunneLoc Tibial Fixation Surgical Technique Surgical Protocol by Mark Ganjianpour, M.D. One
ToggleLoc Fixation Device with ZipLoop Technology Arthroscopic PCL Reconstruction Using Soft Tissue Graft and TunneLoc Tibial Fixation Surgical Technique Surgical Protocol by Mark Ganjianpour, M.D. One
ACL Primary Repair Surgical Technique
 ACL Primary Repair Surgical Technique ACL Primary Repair ACL Primary Repair BioComposite SwiveLock and Labral Scorpion Suture Passing Technology There has been a recent resurgence of interest in the possibility
ACL Primary Repair Surgical Technique ACL Primary Repair ACL Primary Repair BioComposite SwiveLock and Labral Scorpion Suture Passing Technology There has been a recent resurgence of interest in the possibility
The Meniscus. History. Anatomy. Anatomy. Blood Supply. Attachments
 History The Meniscus W. Randall Schultz, MD, MS Austin, TX January 23, 2016 Meniscus originally thought to represent vestigial tissue 1883 first reported meniscal repair (Annandale) Total menisectomy treatment
History The Meniscus W. Randall Schultz, MD, MS Austin, TX January 23, 2016 Meniscus originally thought to represent vestigial tissue 1883 first reported meniscal repair (Annandale) Total menisectomy treatment
POSTEROLATERAL CORNER RECONSTRUCTION WHEN AND HOW?
 OTHER KNEE SURGERIES POSTEROLATERAL CORNER RECONSTRUCTION WHEN AND HOW? Written by Jacques Ménétrey, Eric Dromzée and Philippe M. Tscholl, Switzerland Injury of the posterolateral corner (PLC) is relatively
OTHER KNEE SURGERIES POSTEROLATERAL CORNER RECONSTRUCTION WHEN AND HOW? Written by Jacques Ménétrey, Eric Dromzée and Philippe M. Tscholl, Switzerland Injury of the posterolateral corner (PLC) is relatively
A Patient s Guide to Knee Anatomy
 A Patient s Guide to Knee Anatomy 15195 Heathcote Blvd Suite 334 Haymarket, VA 20169 Phone: 703-369-9070 Fax: 703-369-9240 DISCLAIMER: The information in this booklet is compiled from a variety of sources.
A Patient s Guide to Knee Anatomy 15195 Heathcote Blvd Suite 334 Haymarket, VA 20169 Phone: 703-369-9070 Fax: 703-369-9240 DISCLAIMER: The information in this booklet is compiled from a variety of sources.
ACL reconstruction with the ACUFEX Director Drill Guide and. ENDOBUTTON CL Fixation System. *smith&nephew. Knee Series Technique Guide ENDOBUTTON CL
 Knee Series Technique Guide *smith&nephew ENDOBUTTON CL Fixation System ACL reconstruction with the ACUFEX Director Drill Guide and ENDOBUTTON CL Fixation System Thomas D. Rosenberg, MD ACL Reconstruction
Knee Series Technique Guide *smith&nephew ENDOBUTTON CL Fixation System ACL reconstruction with the ACUFEX Director Drill Guide and ENDOBUTTON CL Fixation System Thomas D. Rosenberg, MD ACL Reconstruction
Extracapsular Repair Monofilament Nylon Suture
 Extracapsular Repair Monofilament Nylon Suture Management of the ruptured Cranial Cruciate Ligament (CCL) by placing a non-absorbable suture between the lateral fabella and the proximal, cranial tibia
Extracapsular Repair Monofilament Nylon Suture Management of the ruptured Cranial Cruciate Ligament (CCL) by placing a non-absorbable suture between the lateral fabella and the proximal, cranial tibia
Torn ACL Hamstring Graft
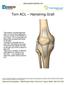 Torn ACL Hamstring Graft The anterior cruciate ligament (ACL) is one of four ligaments that are crucial to the stability of your knee. It is a strong fibrous tissue that connects the femur to the tibia.
Torn ACL Hamstring Graft The anterior cruciate ligament (ACL) is one of four ligaments that are crucial to the stability of your knee. It is a strong fibrous tissue that connects the femur to the tibia.
Overview Ligament Injuries. Anatomy. Epidemiology Very commonly injured joint. ACL Injury 20/06/2016. Meniscus Tears. Patellofemoral Problems
 Overview Ligament Injuries Meniscus Tears Pankaj Sharma MBBS, FRCS (Tr & Orth) Consultant Orthopaedic Surgeon Manchester Royal Infirmary Patellofemoral Problems Knee Examination Anatomy Epidemiology Very
Overview Ligament Injuries Meniscus Tears Pankaj Sharma MBBS, FRCS (Tr & Orth) Consultant Orthopaedic Surgeon Manchester Royal Infirmary Patellofemoral Problems Knee Examination Anatomy Epidemiology Very
MCL Reconstruction Surgical Protocol by Tarek Fahl, M.D.
 MCL Reconstruction Surgical Protocol by Tarek Fahl, M.D. Features A unique weave in which a single strand of braided polyethylene is woven through itself twice in opposite directions This construct allows
MCL Reconstruction Surgical Protocol by Tarek Fahl, M.D. Features A unique weave in which a single strand of braided polyethylene is woven through itself twice in opposite directions This construct allows
RIGIDFIX CURVE CROSS PIN SYSTEM
 RIGIDFIX CURVE CROSS PIN SYSTEM This publication is not intended for distribution in the USA. FAQ SUMMARY RIGIDFIX CURVE CROSS PIN SYSTEM FREQUENTLY ASKED QUESTIONS (FAQ) SUMMARY 1 Why do the pins enter
RIGIDFIX CURVE CROSS PIN SYSTEM This publication is not intended for distribution in the USA. FAQ SUMMARY RIGIDFIX CURVE CROSS PIN SYSTEM FREQUENTLY ASKED QUESTIONS (FAQ) SUMMARY 1 Why do the pins enter
A Patient s Guide to Knee Anatomy. Stephanie E. Siegrist, MD, LLC
 A Patient s Guide to Knee Anatomy Hands, shoulders, knees and toes (and elbows and ankles, too!) Most bone and joint conditions have several treatment options. The best treatment for you is based on your
A Patient s Guide to Knee Anatomy Hands, shoulders, knees and toes (and elbows and ankles, too!) Most bone and joint conditions have several treatment options. The best treatment for you is based on your
Management of Knee Dislocations
 Management of Knee Dislocations Thomas J. Gill, MD Chief, Sports Medicine Service Massachusetts General Hospital Associate Professor of Orthopedic Surgery Harvard Medical School Complex Challenging Multi-Ligament
Management of Knee Dislocations Thomas J. Gill, MD Chief, Sports Medicine Service Massachusetts General Hospital Associate Professor of Orthopedic Surgery Harvard Medical School Complex Challenging Multi-Ligament
Human ACL reconstruction
 Human ACL reconstruction current state of the art Rudolph Geesink MD PhD Maastricht The Netherlands Human or canine ACL repair...!? ACL anatomy... right knees! ACL double bundles... ACL double or triple
Human ACL reconstruction current state of the art Rudolph Geesink MD PhD Maastricht The Netherlands Human or canine ACL repair...!? ACL anatomy... right knees! ACL double bundles... ACL double or triple
EndoBlade Soft Tissue Release System
 Surgical Technique Endoscopic Gastroc Recession Endoscopic Plantar Fascia Release EndoBlade Soft Tissue Release System Endoscopic Gastroc Recession Arthrex has developed a comprehensive, completely disposable
Surgical Technique Endoscopic Gastroc Recession Endoscopic Plantar Fascia Release EndoBlade Soft Tissue Release System Endoscopic Gastroc Recession Arthrex has developed a comprehensive, completely disposable
ARTHROSCOPIC GIANT NEEDLE ROTATOR CUFF REPAIR AS A ROUTINE PROCEDURE SINCE 1990
 ARTHROSCOPIC GIANT NEEDLE ROTATOR CUFF REPAIR AS A ROUTINE PROCEDURE SINCE 1990 A 10 minutes transhumeral footprint repair using only sutures AIG Medical GmbH Bonn (Aeratec) Essential for this surgery
ARTHROSCOPIC GIANT NEEDLE ROTATOR CUFF REPAIR AS A ROUTINE PROCEDURE SINCE 1990 A 10 minutes transhumeral footprint repair using only sutures AIG Medical GmbH Bonn (Aeratec) Essential for this surgery
and K n e e J o i n t Is the most complicated joint in the body!!!!
 K n e e J o i n t K n e e J o i n t Is the most complicated joint in the body!!!! 1-Consists of two condylar joints between: A-The medial and lateral condyles of the femur and The condyles of the tibia
K n e e J o i n t K n e e J o i n t Is the most complicated joint in the body!!!! 1-Consists of two condylar joints between: A-The medial and lateral condyles of the femur and The condyles of the tibia
LARS PLC. PLC Augmentation and Reinforcement Surgical technique
 LARS PLC PLC Augmentation and Reinforcement Surgical technique LARS PLC Contents Posterolateral corner pathology 3 LARS overview 4 LARS material overview 4 LARS general considerations 4 Indications 4 Contraindications
LARS PLC PLC Augmentation and Reinforcement Surgical technique LARS PLC Contents Posterolateral corner pathology 3 LARS overview 4 LARS material overview 4 LARS general considerations 4 Indications 4 Contraindications
TRK REVISION KNEE Surgical Technique
 1 TRK REVISION KNEE Surgical Technique 1. 2. 3. 4. 5. 6. 7. 8. 9. 10. INTERCONDYLAR RESECTION...... page FEMORAL STEM...... page NON CEMENTED FEMORAL STEM...... page TRIAL FEMORAL COMPONENTS...... page
1 TRK REVISION KNEE Surgical Technique 1. 2. 3. 4. 5. 6. 7. 8. 9. 10. INTERCONDYLAR RESECTION...... page FEMORAL STEM...... page NON CEMENTED FEMORAL STEM...... page TRIAL FEMORAL COMPONENTS...... page
Prevention and Treatment of Injuries. Anatomy. Anatomy. Chapter 20 The Knee Westfield High School Houston, Texas
 Prevention and Treatment of Injuries Chapter 20 The Knee Westfield High School Houston, Texas Anatomy MCL, Medial Collateral Ligament LCL, Lateral Collateral Ligament PCL, Posterior Cruciate Ligament ACL,
Prevention and Treatment of Injuries Chapter 20 The Knee Westfield High School Houston, Texas Anatomy MCL, Medial Collateral Ligament LCL, Lateral Collateral Ligament PCL, Posterior Cruciate Ligament ACL,
Bio-TransFix ACL Reconstruction. Surgical Technique
 Bio-TransFix ACL Reconstruction Surgical Technique Bio-TransFix ACL Reconstruction 1 Semitendinosus and gracilis tendon autografts or tibialis tendon allografts are mounted on the GraftPro workstation.
Bio-TransFix ACL Reconstruction Surgical Technique Bio-TransFix ACL Reconstruction 1 Semitendinosus and gracilis tendon autografts or tibialis tendon allografts are mounted on the GraftPro workstation.
Curved Anatomic Soft Tissue ACL Reconstruction
 Curved Anatomic Soft Tissue ACL Reconstruction Using GraftMax Curved Reaming, GraftMax Button and GENESYS Matryx A complete guide to ACL Repair utilizing GraftMax Curved Reaming System and GraftMax Button
Curved Anatomic Soft Tissue ACL Reconstruction Using GraftMax Curved Reaming, GraftMax Button and GENESYS Matryx A complete guide to ACL Repair utilizing GraftMax Curved Reaming System and GraftMax Button
Flexibility In Action. ACL Instrumentation
 Flexibility In Action ACL Instrumentation ACL Tunnel-Preparation Instrumentation Set Reproducible graft placement with stable fixation. Stable ACL Tunnel-Preparation The Stryker Universal ACL Instrumentation
Flexibility In Action ACL Instrumentation ACL Tunnel-Preparation Instrumentation Set Reproducible graft placement with stable fixation. Stable ACL Tunnel-Preparation The Stryker Universal ACL Instrumentation
Biologically-Assisted ACL Reconstruction. Surgical Technique
 Biologically-Assisted ACL Reconstruction Surgical Technique One Surgeon. One Patient. Over 1 million times per year, Biomet helps one surgeon provide personalized care to one patient. The science and art
Biologically-Assisted ACL Reconstruction Surgical Technique One Surgeon. One Patient. Over 1 million times per year, Biomet helps one surgeon provide personalized care to one patient. The science and art
Checklist for Physical Examination of the Knee Muscuoskeletal Block -- Chris McGrew MD, Andrew Ashbaugh DO
 Checklist for Physical Examination of the Knee Muscuoskeletal Block -- Chris McGrew MD, Andrew Ashbaugh DO This handout is for use as a rough guide and study aid. Your instructor may perform certain maneuvers
Checklist for Physical Examination of the Knee Muscuoskeletal Block -- Chris McGrew MD, Andrew Ashbaugh DO This handout is for use as a rough guide and study aid. Your instructor may perform certain maneuvers
Anterolateral Ligament. Bradd G. Burkhart, MD Orlando Orthopaedic Center Sports Medicine
 Anterolateral Ligament Bradd G. Burkhart, MD Orlando Orthopaedic Center Sports Medicine What in the world? TIME magazine in November 2013 stated: In an age filled with advanced medical techniques like
Anterolateral Ligament Bradd G. Burkhart, MD Orlando Orthopaedic Center Sports Medicine What in the world? TIME magazine in November 2013 stated: In an age filled with advanced medical techniques like
Surgical Technique. VISIONAIRE Disposable Instruments for the LEGION Total Knee System
 Surgical Technique VISIONAIRE Disposable Instruments for the LEGION Total Knee System VISIONAIRE and LEGION Disposable instrument technique* Note: All disposable instruments are interchangeable with the
Surgical Technique VISIONAIRE Disposable Instruments for the LEGION Total Knee System VISIONAIRE and LEGION Disposable instrument technique* Note: All disposable instruments are interchangeable with the
Subpectoral Biceps Tenodesis using Cortical Buttons Surgical Technique
 Subpectoral Biceps Tenodesis using Cortical Buttons Surgical Technique Subpectoral Biceps Tenodesis Subpectoral Biceps Tenodesis using Cortical Buttons Introduction Subpectoral biceps tenodesis using cortical
Subpectoral Biceps Tenodesis using Cortical Buttons Surgical Technique Subpectoral Biceps Tenodesis Subpectoral Biceps Tenodesis using Cortical Buttons Introduction Subpectoral biceps tenodesis using cortical
Grant H Garcia, MD Sports and Shoulder Surgeon
 What to Expect from your Anterior Cruciate Ligament Reconstruction Surgery A Guide for Patients Grant H Garcia, MD Sports and Shoulder Surgeon Important Contact Information Grant Garcia, MD Wallingford:
What to Expect from your Anterior Cruciate Ligament Reconstruction Surgery A Guide for Patients Grant H Garcia, MD Sports and Shoulder Surgeon Important Contact Information Grant Garcia, MD Wallingford:
Orthopedic Bone Nail System - Distal Femoral Nail Surgical Technique Manual
 Orthopedic Bone Nail System - Distal Femoral Nail Surgical Technique Manual Note: The surgical procedures should be performed under the guidance of qualified skilled orthopedic surgeons, and this surgical
Orthopedic Bone Nail System - Distal Femoral Nail Surgical Technique Manual Note: The surgical procedures should be performed under the guidance of qualified skilled orthopedic surgeons, and this surgical
ACL RECONSTRUCTION HAMSTRING METHOD. Presents ACL RECONSTRUCTION HAMSTRING METHOD. Multimedia Health Education
 HAMSTRING METHOD Presents HAMSTRING METHOD Multimedia Health Education Disclaimer Stephen J. Incavo MD This movie is an educational resource only and should not be used to make a decision on Anterior Cruciate
HAMSTRING METHOD Presents HAMSTRING METHOD Multimedia Health Education Disclaimer Stephen J. Incavo MD This movie is an educational resource only and should not be used to make a decision on Anterior Cruciate
DEVELOPED BY MEDSHAPE, INC. IN CONJUNCTION WITH PATRICK ST. PIERRE, M.D. BICEPS TENODESIS ARTHROSCOPIC AND SUBPECTORAL SURGICAL TECHNIQUE
 ! SURGICAL TECHNIQUE! DEVELOPED BY MEDSHAPE, INC. IN CONJUNCTION WITH PATRICK ST. PIERRE, M.D. ARTHROSCOPIC AND SUBPECTORAL BICEPS TENODESIS SURGICAL TECHNIQUE BICEPS TENODESIS Indications Tenodesis of
! SURGICAL TECHNIQUE! DEVELOPED BY MEDSHAPE, INC. IN CONJUNCTION WITH PATRICK ST. PIERRE, M.D. ARTHROSCOPIC AND SUBPECTORAL BICEPS TENODESIS SURGICAL TECHNIQUE BICEPS TENODESIS Indications Tenodesis of
Technique Guide. VersiTomic. ReelX STT Double-Row Achilles G-Lok. J. Martin Leland III, M.D. J. Martin Leland III, M.D. Proximal Biceps Tenodesis
 Technique Guide VersiTomic ReelX STT Double-Row Achilles G-Lok Tendon Sub-Pectoral Repair Proximal Biceps Tenodesis J. Martin Leland III, M.D. J. Martin Leland III, M.D. The opinions expressed are those
Technique Guide VersiTomic ReelX STT Double-Row Achilles G-Lok Tendon Sub-Pectoral Repair Proximal Biceps Tenodesis J. Martin Leland III, M.D. J. Martin Leland III, M.D. The opinions expressed are those
CHAPTER 51 ARTHROSCOPY OF THE LOWER EXTREMITY 2395
 CHAPTER 51 ARTHROSCOPY OF THE LOWER EXTREMITY 2395 FIGURE 51-3 Placement of lateral post and taping of saline bag to table allow ease of leg positioning and full range of motion during ligament reconstruction.
CHAPTER 51 ARTHROSCOPY OF THE LOWER EXTREMITY 2395 FIGURE 51-3 Placement of lateral post and taping of saline bag to table allow ease of leg positioning and full range of motion during ligament reconstruction.
Rotator Cuff Repair using JuggerKnot Soft Anchor 2.9mm Surgical Technique
 Rotator Cuff Repair using JuggerKnot Soft Anchor 2.9mm Surgical Technique It s small. It s strong. And it's all suture. The JuggerKnot Soft Anchor represents the next generation of suture anchor technology.
Rotator Cuff Repair using JuggerKnot Soft Anchor 2.9mm Surgical Technique It s small. It s strong. And it's all suture. The JuggerKnot Soft Anchor represents the next generation of suture anchor technology.
What to Expect from your Anterior Cruciate Ligament (ACL) Reconstruction Surgery A Guide for Patients
 What to Expect from your Anterior Cruciate Ligament (ACL) Reconstruction Surgery A Guide for Patients Sources of Information: http://orthoinfo.aaos.org http://www.orthoinfo.org/informedpatient.cfm http://www.sportsmed.org/patient/
What to Expect from your Anterior Cruciate Ligament (ACL) Reconstruction Surgery A Guide for Patients Sources of Information: http://orthoinfo.aaos.org http://www.orthoinfo.org/informedpatient.cfm http://www.sportsmed.org/patient/
Precisely locate anatomic femoral ACL insertion sites 1. ACUFEX PINPOINT Anatomic ACL Guide System
 Precisely locate anatomic femoral ACL insertion sites 1 ACUFEX PINPOINT Anatomic ACL Guide System This versatile and easy-to-use guide system enables visualization of the size and placement of femoral
Precisely locate anatomic femoral ACL insertion sites 1 ACUFEX PINPOINT Anatomic ACL Guide System This versatile and easy-to-use guide system enables visualization of the size and placement of femoral
ANTERIOR CRUCIATE LIGAMENT INJURY
 ANTERIOR CRUCIATE LIGAMENT INJURY WHAT IS THE ANTERIOR CRUCIATE LIGAMENT? The anterior cruciate ligament (ACL) is one of four major ligaments that stabilizes the knee joint. A ligament is a tough band
ANTERIOR CRUCIATE LIGAMENT INJURY WHAT IS THE ANTERIOR CRUCIATE LIGAMENT? The anterior cruciate ligament (ACL) is one of four major ligaments that stabilizes the knee joint. A ligament is a tough band
