Clinical Presentations and Neurodevelopmental Outcomes of Perinatal Stroke in Preterm and Term Neonates: A Case Series
|
|
|
- Dominick Craig
- 5 years ago
- Views:
Transcription
1 J Korean Med Sci 2010; 25: ISSN DOI: /jkms Clinical Presentations and Neurodevelopmental Outcomes of Perinatal Stroke in Preterm and Term Neonates: A Case Series Perinatal stroke in neonates can lead to disability in later life. However, its etiology and prognosis are poorly understood. The aim of this study was to describe clinical presentations and neurodevelopmental outcomes of our case series of perinatal stroke in Korea. Thirteen term and preterm neonates who were diagnosed with perinatal stroke in two university hospitals from March 2003 to March 2007 were enrolled. Seven term and 6 preterm neonates were diagnosed with perinatal stroke, based on the brain MRI findings. Perinatal stroke presented with seizure (4/13), perinatal distress (3/13) in term neonates, whereas stroke in preterm neonates did not present with noticeable clinical symptoms. Only one neonate had positive thrombophilic test (homozygous C677T polymorphism for MTHFR). Ten neonates had infarctions in the territory of the middle cerebral artery (MCA), and 3 neonates had borderzone infarctions between the anterior cerebral artery and MCA. Neurodevelopmental outcome was abnormal in 4 neonates. Infarction in MCA main branch or posterior limb of internal capsule showed an abnormal neurodevelopmental outcome. Our study is the first systematic study of perinatal stroke in Korea, and shows its clinical presentations and neurodevelopmental outcomes. The population-based study on incidence and prognosis of perinatal stroke in Korea is required in the future. Key Words : Perinatal Stroke; Newborn; Magnetic Resonance Imaging c 2010 The Korean Academy of Medical Sciences. This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License ( which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited. Hyun Ju Lee 1, 2, Byung Chan Lim 2, Hee Hwang 2, Joon-Seok Hong 3, Ee-Kyung Kim 1, Han-Suk Kim 1, Beyong Il Kim 1, 2, Jung-Hwan Choi 1, and Chang Won Choi 1, 2 Department of Pediatrics 1, Seoul National University College of Medicine, Seoul; Department of Pediatrics 2, Department of Obstetrics and Gynecology 3, Seoul National University Bundang Hospital, Seongnam, Korea Received : 24 August 2009 Accepted : 17 November 2009 Address for Correspondence Chang Won Choi, M.D. Department of Pediatrics, Seoul National University Bundang Hospital, 166 Gumiro, Bundang-gu, Seongnam , Korea Tel : , Fax : choicw@snu.ac.kr The content of this paper was presented during a poster session at the Recent Advances in Neonatal Medicine in Wurzburg, Germany, October 2-4, INTRODUCTION Perinatal stroke is an increasingly recognized clinical entity that leads to hemiplegic cerebral palsy in later life (1). Although modern neonatal neuroimaging has improved the detection of infarctions, the etiology and prognosis of perinatal stroke have not been well described. The incidence of perinatal stroke varies according to the availability of neuroimaging and the diagnostic criteria used, but is believed to be about one per 4,000 live births (2). Furthermore, its lack of specific clinical features makes the diagnosis of perinatal stroke difficult resulting in its under-diagnosis (3, 4). Few studies (5-7) have investigated clinical presentations and neurodevelopmental outcomes of perinatal stroke based on combined findings of neuroimaging, electroencephalography (EEG) in neonates. To the best of our knowledge, reports on perinatal stroke in Korea have been relatively few, compared to those of western countries. Furthermore, there has been no report about perinatal stroke of preterm infant in Korea. The major aim of this study was to describe the clinical presentations and neurodevelopmental outcomes of perinatal stroke in term and preterm neonates in Korea. Case series MATERIALS AND METHODS To search for the neonates diagnosed with perinatal stroke during admission to newborn nursery or neonatal intensive care unit in Seoul National University Children s Hospital or Seoul National University Bundang Hospital (level III teaching hospital), an electronic search of all head magnetic resonance imaging (MRI) reports generated from March 1, 2003 to March 1, 2008 was conducted. All neuroimaging reports containing any of the following text strings were retrieved: stroke, infarct, middle cerebral artery (MCA), posterior cerebral artery and anterior cerebral artery. Neuroimaging studies that revealed any of the followings were excluded; 1) an acute infarction occurring after 28 days of life; 2) intraventric- 888
2 BSID-2, Bayley Scales of Infant Development ular hemorrhage with unilateral parenchymal hemorrhage (venous infarction); 3) cystic periventricular leukomalacia; and 4) bacterial meningitis. The institutional review board of Seoul National University Bundang Hospital approved the study (B-0911/ ), and informed consent was waivered. Maternal and perinatal characteristics Maternal and perinatal information was obtained from electronic medical records. Complications during pregnancy or delivery were searched and included placental abruption, preeclampsia, intrauterine growth restriction, chorioamnionitis, oligohydramnios, prolonged second stage of labor, maternal prothrombotic disorder, and fetomaternal transfusion. Chorioamnionitis was diagnosed by placental histopathology, but this information was available only in 6 neonates. Perinatal factors included meconium-stained amniotic fluid, abnormal fetal heart rate pattern, umbilical arterial blood ph, type of delivery, and Apgar scores. Abnormal fetal heart rate patterns included late deceleration and decreased variability. Perinatal distress was defined as umbilical arterial blood ph lower than 7.0 or significant respiratory depression requiring tracheal intubation at the delivery room. Thrombophilic factors Thrombophilic screening test included prothrombin time, activated partial thromboplastin time, platelet count, fibrinogen, protein C, protein S, antithrombin III, anticardiolipin antibodies, and lupus anticoagulant. In addition, the presence of heterozygous factor V Leiden, G20210A mutation of the prothrombin gene, and homozygous C677T polymorphism for MTHFR was screened by PCR-based mutation analysis. Brain MRI Brain MRI was performed as a part of routine evaluation process for seizure, unexplained perinatal distress or prematurity. The infants were imaged on a 1.5 Tesla unit system (Intra Philips Medical Systems, Best, Netherlands) using T1 weighted spin echo (SE 600/20 msec), inversion recovery (3800/30/950), and T2 weighted spin echo (SE 3500/208 msec) sequences, at a slice thickness of 3-4 mm. The field of view was mm, and matrices were or Single-shot, multi-slice spin echo and echo planar imaging sequence were obtained with the following parameters comprise TR=800 msec, TE=123 msec, and diffusion sensitivity (b=1,100 sec/mm 2 ). The diffusion gradient was applied to the cephalocaudal axis direction. The magnetic resonance angiography images were performed in 8 neonates using a 3-dimensional time-of-flight technique, and data was processed with a maximum intensity projection method. Arterial distribution, involvement of the basal ganglia, thalamus, and internal capsule, and the presence of coexisting hemorrhage were determined from radiologic reports. In term neonates, brain MRI scans were completed between days 2 and 4 of life except for one neonate in whom MRI scan was performed on day 16 after weaning from ventilator. Infarction in preterm infants was first detected by sequential brain ultrasonography and later confirmed by brain MRI. Based on the location, extent, and shape of the lesions, infarctions were categorized as either being in the territory of main cerebral arterial branch or having a borderzone distribution. Infarctions in the territory of the MCA were subdivided further according to a modified version of the criteria suggested by de Vries et al. into main cerebral branches, cortical branches, and lenticulostriate branches (8). Electroencephalography Twelve neonates underwent full standard EEG (16 channels) at a recording speed of 15 mm/sec. States of the neonates and all movements during examinations were recorded by a single technician. Background rhythm and the presence of epileptic discharges were evaluated. Neurodevelopmental outcomes Assessment of neurologic outcome was based on the neurologic examination findings performed at the last follow-up visits (14 months to 6 yr of age). A diagnosis of developmental delay was based on the results of Bayley Scales of Infant Development-2 (BSID-2) performed at 12 months corrected of age. In patients born prematurely, the correction for prematurity was made. BSID-2 was performed by a single pediatric rehabilitationist. RESULTS Clinical presentations of our case series A total of 13 neonates, diagnosed with perinatal stroke during admission, were discovered. Of these neonates, 7 were term and 6 were preterm neonates, and 6 (46%) were male. Gestational age of preterm neonates ranged from 29 to 36 weeks, and birth weights ranged from 1,080 to 3,380 g (Table 1). Presenting symptoms or signs of perinatal stroke were seizure (4/13), significant perinatal distress (3/13), or apnea (1/13). Seizures occurred between 2 and 6 days after birth. Three neonates who presented with seizure were easily recognized clinically and promptly diagnosed, whereas those without seizure were unnoticed until stroke had been confirmed by brain MRI. In these neonates without seizure, brain MRI was performed as a part of routine evaluation process for unexplained perinatal distress in term neonates. In preterm neonates, serial cerebral ultrasonography, which was available in the neonatal intensive care unit at bedside, was performed
3 890 H.J. Lee, B.C. Lim, H. Hwang, et al. as a routine evaluation of prematurity through the anterior fontanel. In 5 of the 6 preterm neonates, infarction was first detected by sequential brain ultrasonography and later confirmed by brain MRI. In one preterm neonate born at the 36th week of gestation, infarction presented with a sudden onset of apnea. The other preterm neonates with infarction were all asymptomatic. In all term and preterm neonates with perinatal stroke, routine laboratory tests including serum electrolytes, glucose, creatinine, liver function tests, lactate, white blood cell counts, C-reactive protein, and TORCH screening were normal. There was no laboratory evidence of polycythemia, thrombocytopenia or coagulation defects. No infants had structural cardiac abnormalities. Maternal and perinatal characteristics Maternal risk factors for perinatal stroke were present in 9 Table 1. Clinical presentations of perinatal stroke Patients Gestational age (week) M, male; F, female. Sex Birth weight (g) Seizure Perinatal distress Apnea 1 29 F 1, M 1, M 1, F 1, F 3, F 1, M 2, F 2, M 3, M 2, F 3, M 3, F 3, (69%) of the 13 neonates: 1 placental abruption; 2 preeclampsia; 1 chorioamnionitis; 1 oligohydramnios; 2 prolonged second stage of labor; 2 maternal prothrombotic disorder (antiphospholipid syndrome). There was no evidence of placental infarction in 6 neonates whose placenta were examined. Five neonates were born by spontaneous vaginal delivery and eight by cesarean section. Abnormal fetal heart rate patterns were seen in 4 term and 1 preterm neonates. These 4 term neonates were delivered by emergency cesarean section. Three of them required tracheal intubation at the delivery room. One neonate intubated at the delivery room developed meconium aspiration syndrome complicated by persistent pulmonary hypertension. All six preterm neonates with perinatal stroke did not require intubation at the delivery room. Perinatal distress was present in 3 neonates, and they had significant respiratory depression requiring tracheal intubation at the delivery room. One neonate had an umbilical arterial blood ph lower than 7.0. Four neonates had low Apgar scores below 5 at 1 min, but none at 5 min. Details of individual maternal and perinatal findings are shown in Table 2. Thrombophilic factors Thrombophilic screening test was performed in 10 of the 13 neonates and 1 of these had abnormality. Antithrombin III, protein C, and protein S levels were within normal range. Heterozygous factor V Leiden and G20210A mutation of the prothrombin gene was not present. Homozygous C677T polymorphism for MTHFR was present in one neonate. Brain MRI findings Eleven neonates (85%) had unilateral infarctions, which were more common on the left side than the right side (7:4). Ten neonates had infarctions in the territory of MCA, and 3 Table 2. Maternal and perinatal characteristics of patients with perinatal stroke Patients Maternal & perinatal event FHRP Delivery UAB ph AS (1-5 min) Resuscitation 1 Chorioamnionitis Absence of variability CS Bag & mask 2 Preeclampsia, IUGR Normal VD Bag & mask 3 Maternal APL syndrome, MCA infarction Normal VD Bag & mask 4 Maternal APL syndrome Normal CS NA Normal CS NA 4-6 O2 only 6 - Normal CS Bag & mask 7 Placental abruption Bradycardia EmCS Intubation 8 Prolonged second stage of labor Deceleration EmCS NA 7-8 Intubation 9 Prolonged second stage of labor Deceleration EmCS Oligohydramnios, MAS Deceleration EmCS Intubation 11 Preeclampsia Normal VD NA 9-10 O2 only 12 - Normal VD NA Normal VD NA FHRP, fetal heart rate pattern; CS, cesarean section; UAB, umbilical arterial blood; AS, Apgar score; IUGR, intrauterine growth restriction; VD, spontaneous vaginal delivery; APL, antiphospholipid; MCA, middle cerebral artery; NA, not available; EmCS, emergency cesarean section; MAS, meconium aspiration syndrome.
4 BSID-2, Bayley Scales of Infant Development neonates had borderzone infarctions between the anterior and middle cerebral artery. In 10 neonates who had infarctions in the territory of MCA, 2 neonates had the involvement of main branches, 5 of lenticulostriate branches, and 3 of cortical branches. Of 5 neonates with lenticulostriate branch infarctions, 3 were preterm neonates. Two neonates with the involvement of lenticulostriate branches showed infarctions in posterior limb of internal capsule. Involvement of cortical branches was present in 3 full term neonates and borderzone infarction in 3 preterm neonates (Table 3). Electroencephalography EEGs were recorded in 11 neonates. In 6 of the 7 term neonates, EEG was completed between days 2 and 4 of life. The other underwent EEG on day 16 after being weaned off from a high-frequency oscillatory ventilator. In the 6 preterm neonates, EEG was performed between 37 and 39 postmenstrual weeks after the infarction had been confirmed by brain MRI. Of these 11 neonates, 2 had a completely normal EEG, 7 had an abnormal background with epileptic discharges (3 on the right side, 2 on the left side and 2 bilateral). Two neonates had an abnormal background on the right or left side without epileptic discharges. Details of individual EEG findings are shown in Table 4. Neurodevelopmental outcomes Neurodevelopmental outcomes were assessed at 14 months to 6 yr old. No infants experienced seizures after the neonatal period. Nine infants achieved a normal neurodevelopmental outcome. Four infants had an abnormal neurologic outcome. One infant had spasticity of left leg at the age of 18 months. Two infants had definite hemiplegia in the right side, and 1 infant in the left side. These 4 infants with abnormal neurologic outcome showed a developmental delay in BSID-2. Table 3. Magnetic resonance imaging findings of patients with perinatal stroke Patients Age at brain MRI Infarction locus Cortex involvement Basal ganglia/thalamus/plic involvement 1 PMA 35 week Lenticulostriate branch - Both basal ganglia 2 PMA 48 week Lenticulostriate branch - Left basal ganglia, PLIC 3 PMA 35 week Borderzone Left F, T - 4 PMA 40 week Lenticulostriate branch - Right basal ganglia 5 Day 4 Borderzone Left T - 6 Day 9 Borderzone Left F, P - 7 Day 4 Cortical branch Bilateral P, T, Left F - 8 Day 2 Lenticulostriate branch - Left basal ganglia 9 Fig. 1 Day 4 Main branch (Left MCA) Left F, P, T, O Left basal ganglia, thalamus, internal capsule 10 Day 16 Cortical branch Right P - 11 Day 3 Main branch (Right MCA) Right F, P, T, O Right basal ganglia, thalamus, internal capsule 12 Day 3 Cortical branch Left F, T - 13 Fig. 2 Day 2 Lenticulostriate branch - Right thalamus, PLIC PLIC, posterior limb of internal capsule; PMA, postmenstrual age; F, frontal; T, temporal P, parietal; O, occipital; MCA, middle cerebral artery. Table 4. Electroencephalography findings and neurodevelopmental outcomes of patients with perinatal stroke Patients Age at EEG Background activity Epileptic discharges BSID-2 at 12 month Neurodevelopmental outcome 1 PMA 37 week Normal None Normal Normal at CA 16 month 2 PMA 39 week Bilateral Bilateral spike/ MDI<70 Right hemiplegia suppressed BA sharp wave PDI<70 at CA 22 month 3 NA Normal Normal at CA 26 month 4 NA Normal Normal at CA 14 month 5 Day 6 Right suppressed BA Right spike/sharp wave Normal Normal at 4 yr 6 Day 10 Left suppressed BA None Normal Normal at 35 month 7 Day 4 Bilateral suppressed BA Bilateral spike/sharp wave Normal Normal at 18 month 8 Day 3 Normal None Normal Normal at 4 yr 9 Day 3 Left suppressed BA Left spike/sharp wave PDI<70 Right hemiplegia at 3 yr 10 Day 17 Right suppressed BA None Normal Normal at 14 month 11 Day 4 Right suppressed BA Right spike/sharp wave PDI<70 Left hemiplegia at 18 month 12 Day 3 Left suppressed BA Left spike/sharp wave Normal Normal at 6 yr 13 Day 2 Right suppressed BA Right spike/sharp wave PDI<70 Left leg spasticity at 18 month BSID-2, Bayley Scales of Infant Development-2; PMA, postmenstrual age; CA, corrected age; BA, background activity; MDI, mental developmental index; PDI, psychomotor developmental index; NA, not available.
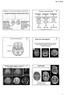
5 892 H.J. Lee, B.C. Lim, H. Hwang, et al. Details of neurodevelopmental outcome are shown in Table 4. Seizures were more common in infants with abnormal outcome. All 3 infants presenting with perinatal distress resulted in normal outcome. One infant with homozygous C677T polymorphism for MTHFR had abnormal outcome. All 3 preterm infants with borderzone infarction had normal outcome. The 4 full term neonates who had the involvement of main branches or posterior limb of internal capsule resulted in abnormal neurodevelopmental outcome. Abnormal background activity (either unilateral or bilateral) in the EEG was found in 9 neonates and 4 of these had a poor neurodevelopmental outcome. DISCUSSION The present study is the first systematic study that shows clinical presentations and neurodevelopmental outcomes of perinatal stroke in Korea. Perinatal stroke occurs rarely and are unnoticed clinically resulting in delay in its diagnosis (8-10). It is not easy to identify perinatal stroke unless neonates present with clinical seizure. Perinatal stroke was presented by seizure, apnea or respiratory distress requiring ventilatory support in term neonates, whereas preterm neonates were mostly asymptomatic in the present study. There is little literature available about perinatal stroke that is not associated with an intraventricular hemorrhage in the preterm infant. Benders et al. (11) found that lenticulostriate infarction appeared to be especially common in the preterm population, whereas cortical infarction were uncommon in their cohort. In the present study, no preterm neonate was involved with main branch or cortical branch infarction. All preterm neonates had lenticulostriate branch or borderzone infarction, and their neurodevelopmental outcomes were all favorable. The 4 full-term neonates who had the involvement of main branches or posterior limb of internal capsule resulted in abnormal neurodevelopmental outcome. Brain MRI provides more details about distinct localization, extension of lesion and noninvasive evaluation of vascular integrity by magnetic resonance angiography. It is undoubtedly more sensitive method for predicting long term neurodevelopmental outcome than Apgar score or neonatal encephalopathy severity staging (2, 7, 11). Furthermore, MRI with diffusion weight image and apparent diffusion coefficient (ADC) measurements was very helpful for confirming tentative diagnosis in the first few days of life in our case series (Figs. 1, 2). Diffusion-weighted imaging can show early changes in the reduction of diffusivity at the cellular level that are undetectable by any other imaging modality in the hyperacute stage of infarction (13-16). Diffusion weight image has been found to increase the sensitivity of detecting neonatal strokes compared with conventional MRI. The concomitant involvement of the cortex, basal ganglia, thalamus and internal capsule by infarction in main cerebral branch has been associated with poor neurodevelopmental outcome (17). In the present study, 4 infants who had involvement of main branch or posterior limb of internal capsule, had hemiplegia or spasticity and concurrent EEG abnormalities. Mercuri et al. (18) found that an infarction involving the internal capsule predicts the development of hemiplegia, whereas predictions based on involvements of other regions are less reliable. They suggested that internal capsule plays an A B Fig. 1. Brain MRI findings of patient 9. (A) Axial diffusion-weighted image showing hyperintensity in the territory of left middle cerebral artery. (B) MR angiography demonstrates loss of flow distal to the left middle cerebral artery bifurcation.
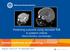
6 BSID-2, Bayley Scales of Infant Development Fig. 2. Brain MRI finding of patient 13. Axial diffusion-weighted image showing hyperintensity in right thalamus and posterior limb of internal capsule. important role in the prognosis of motor outcome in patients with perinatal lesions. De Vries et al. (19) suggested asymmetrical myelination of the posterior limb of the internal capsule on brain MRI is an early predictor of hemiplegia. The absence of myelination in the posterior limb of the internal capsule, as a marker of Wallerian degeneration of corticospinal tracts, appears to be correlated with abnormal EEG findings and motor impairments in the extremities. Ten (77%) infants had infarctions in the distribution of the MCA, and left side was more common accounting for two thirds. These findings are consistent with those of a previous study which found that neonatal cerebral infarction occurs more commonly in the left cerebral hemisphere and in the distribution of the MCA (20). This predominance of left-sided lesions may be caused by vascular asymmetry due to patent ductus arteriosus (21). Neonatal seizure is a common clinical finding that triggers recognition of perinatal stroke in term infants. In the present study, 2 of the 3 neonates who experienced seizure had an abnormal neurodevelopmental outcome. Other reports have also suggested that concurrent seizure during the neonatal period is associated with an unfavorable neurodevelopmental outcome in patients with perinatal stroke (22). Inherited coagulation abnormalities may lead to adverse maternal and fetal events through thrombosis at the placenta (23-25). Thrombosis on the maternal side may lead to preeclampsia and intrauterine growth restriction, whereas on the fetal side it is a possible source of emboli that can bypass the hepatic and pulmonary circulations and reach the fetal brain. Recent evidence suggests that thrombophilias, including heterozygous factor V Leiden, prothrombin gene mutation, and homozygous C677T polymorphism for MTHFR may also play a causative role in perinatal stroke (26, 27). Phospholipids are required for the activations of protein C and the coagulation pathway. Anti-phospholipid antibodies, including lupus anticoagulant and anticardiolipin antibody, interfere with normal coagulation and may be a risk factor for perinatal stroke (28). There were no inherited coagulation abnormalities found in our patients except for a single case with homozygous C677T polymorphism for MTHFR. EEG is a useful and sensitive tool for evaluating the degree of neurological damage in perinatal stroke (29). Mercuri et al. (17) suggested that early neonatal EEG was a prognostic indicator of motor outcome. In their study, the abnormal background was associated with abnormal motor outcome whereas other EEG abnormalities such as epileptic discharges in the presence of a normal background were not associated with abnormal outcome. In the present study, abnormal background activity (either unilateral or bilateral) was found in 9 neonates and 4 of these had a poor neurodevelopmental outcome. The EEG data was not very informative in the preterm neonates possibly as they were obtained rather late and electrical seizure activity is not absolutely considered as abnormal in preterm neonates. Several limitations are noted in our current study, mainly due to its limited subject size and retrospective nature. Regardless of these limitations, however, it is believed that this case series may be able to add some valuable information to rare perinatal stroke that have not been well described in Korea. Finally this study may assist physicians predicting long-term prognosis and planning rehabilitative care for the neonates with perinatal stroke. REFERENCES 1. Lee J, Croen LA, Backstrand KH, Yoshida CK, Henning LH, Lindan C, Ferriero DM, Fullerton HJ, Barkovich AJ, Wu YW. Maternal and infant characteristics associated with perinatal arterial stroke in the infant. JAMA 2005; 293: Boardman JP, Ganesan V, Rutherford MA, Saunders DE, Mercuri E, Cowan F. Magnetic resonance image correlates of hemiparesis after neonatal and childhood middle cerebral artery stroke. Pediatrics 20-05; 115: Sreenan C, Bhargava R, Robertson CM. Cerebral infarction in the term newborn: clinical presentation and long-term outcome. J Pediatr 2000; 137: Wu YW, March WM, Croen LA, Grether JK, Escobar GJ, Newman TB. Perinatal stroke in children with motor impairment: a population-based study. Pediatrics 2004; 114: Ricci D, Mercuri E, Barnett A, Rathbone R, Cota F, Haataja L, Rutherford M, Dubowitz L, Cowan F. Cognitive outcome at early school age in term-born children with perinatally acquired middle cerebral artery territory infarction. Stroke 2008; 39: McLinden A, Baird AD, Westmacott R, Anderson PE, deveber G.
7 894 H.J. Lee, B.C. Lim, H. Hwang, et al. Early cognitive outcome after neonatal stroke. J Child Neurol 2007; 22: Lee J, Croen LA, Lindan C, Nash KB, Yoshida CK, Ferriero DM, Barkovich AJ, Wu YW. Predictors of outcome in perinatal arterial stroke: a population-based study. Ann Neurol 2005; 58: De Vries LS, Groenendaal F, Eken P, van Haastert IC, Rademaker KJ, Meiners LC. Infarcts in the vascular distribution of the middle cerebral artery in preterm and fullterm infants. Neuropediatrics 1997; 28: Sran SK, Baumann RJ. Outcome of neonatal strokes. Am J Dis Child 1988; 142: Estan J, Hope P. Unilateral neonatal cerebral infarction in full term infants. Arch Dis Child Fetal Neonatal Ed 1997; 76: F Benders MJ, Groenendaal F, Uiterwaal CS, Nikkels PG, Bruinse HW, Nievelstein RA. Maternal and infant characteristics associated with perinatal arterial stroke in the preterm infant. Stroke 2007; 38: De Vries LS, Van der Grond J, Van Haastert IC, Groenendaal F. Prediction of outcome in new-born infants with arterial ischaemic stroke using diffusion-weighted magnetic resonance imaging. Neuropediatrics 2005; 36: Cowan F, Pennock J, Hanrahan J, Manji KP, Edwards AD. Early detection of cerebral infarction and hypoxic ischemic encephalopathy in neonates using diffusion weighted magnetic resonance imaging. Neuropediatrics 1994; 25: Huppi PS, Inder TE. Magnetic resonance techniques in the evaluation of the perinatal brain: recent advances and future directions. Semin Neonatol 2001; 6: Gillard JH, Papadakis NG, Martin K, Price CJ, Warburton EA, Antoun NM, Huang CL, Carpenter TA, Pickard JD. MR diffusion tensor imaging of white matter tract disruption in stroke at 3 T. Br J Radiol 2001; 74: Kirton A, Shroff M, Visvanathan T, deveber G. Quantified corticospinal tract diffusion restriction predicts neonatal stroke outcome. Stroke 2007; 38: Mercuri E, Rutherford M, Cowan F, Pennock J, Counsell S, Papadimitriou M, Azzopardi D, Bydder G, Dubowitz L. Early prognostic indicators of outcome in infants with neonatal cerebral infarction: a clinical, electroencephalogram, and magnetic resonance imaging study. Pediatrics 1999; 103: Mercuri E, Barnett A, Rutherford M, Guzzetta A, Haataja L, Cioni G, Cowan F, Dubowitz L. Neonatal cerebral infarction and neuromotor outcome at school age. Pediatrics 2004; 113: De Vries LS, Groenendaal F, van Haastert IC, Eken P, Rademaker KJ, Meiners LC. Asymmetrical myelination of the posterior limb of the internal capsule in infants with periventricular hemorrhagic infarction: an early predictor of hemiplegia. Neuropediatrics 1999; 30: Perlman JM, Rollins NK, Evans D. Neonatal stroke: clinical characteristics and cerebral blood flow velocity measurements. Pediatr Neurol 1994; 11: Beattie LM, Butler SJ, Goudie DE. Pathways of neonatal stroke and subclavian steal syndrome. Arch Dis Child Fetal Neonatal Ed 2006; 91: F Golomb MR, Garg BP, Carvalho KS, Johnson CS, Williams LS. Perinatal stroke and the risk of developing childhood epilepsy. J Pediatr 2007; 151: Carrilho I, Costa E, Barreirinho MS, Santos M, Barbot C, Barbot J. Prothrombotic study in full term neonates with arterial stroke. Haematologica 2001; 86: E Mercuri E, Cowan F, Gupte G, Manning R, Laffan M, Rutherford M, Edwards AD, Dubowitz L, Roberts I. Prothrombotic disorders and abnormal neurodevelopmental outcome in infants with neonatal cerebral infarction. Pediatrics 2001; 107: Grabowski EF, Buonanno FS, Krishnamoorthy K. Prothrombotic risk factors in the evaluation and management of perinatal stroke. Semin Perinatol 2007; 31: Verdu A, Cazorla MR, Moreno JC, Casado LF. Prenatal stroke in a neonate heterozygous for factor V Leiden mutation. Brain Dev 2005; 27: Nelson KB. Thrombophilias, perinatal stroke, and cerebral palsy. Clin Obstet Gynecol 2006; 49: Bobrowska-Snarska D, Ostanek L, Nesterowicz B, Brzosko M. Severe neurological and obstetrical complications in a patient with antiphospholipid syndrome. Pol Arch Med Wewn 2006; 115: Selton D, Andre M, Hascoet JM. Interest of EEG in full-term newborns with isolated unilateral ischemic stroke. Arch Pediatr 2005; 12:
I t is increasingly recognised that arterial cerebral infarction
 F252 ORIGINAL ARTICLE Does cranial ultrasound imaging identify arterial cerebral infarction in term neonates? F Cowan, E Mercuri, F Groenendaal, L Bassi, D Ricci, M Rutherford, L de Vries... See end of
F252 ORIGINAL ARTICLE Does cranial ultrasound imaging identify arterial cerebral infarction in term neonates? F Cowan, E Mercuri, F Groenendaal, L Bassi, D Ricci, M Rutherford, L de Vries... See end of
Should infants with perinatal thrombosis be screened for thrombophilia and treated by anticoagulants?
 Should infants with perinatal thrombosis be screened for thrombophilia and treated by anticoagulants? Shoshana Revel-Vilk, MD MSc Pediatric Hematology Center, Pediatric Hematology/Oncology Department,
Should infants with perinatal thrombosis be screened for thrombophilia and treated by anticoagulants? Shoshana Revel-Vilk, MD MSc Pediatric Hematology Center, Pediatric Hematology/Oncology Department,
Study of role of MRI brain in evaluation of hypoxic ischemic encephalopathy
 Original article: Study of role of MRI brain in evaluation of hypoxic ischemic encephalopathy *Dr Harshad Bhagat, ** Dr Ravindra Kawade, ***Dr Y.P.Sachdev *Junior Resident, Department Of Radiodiagnosis,
Original article: Study of role of MRI brain in evaluation of hypoxic ischemic encephalopathy *Dr Harshad Bhagat, ** Dr Ravindra Kawade, ***Dr Y.P.Sachdev *Junior Resident, Department Of Radiodiagnosis,
Correlation of Neurodevelopmental Outcome and brain MRI/EEG findings in term HIE infants
 Correlation of Neurodevelopmental Outcome and brain MRI/EEG findings in term HIE infants Ajou University School of Medicine Department of Pediatrics Moon Sung Park M.D. Hee Cheol Jo, M.D., Jang Hoon Lee,
Correlation of Neurodevelopmental Outcome and brain MRI/EEG findings in term HIE infants Ajou University School of Medicine Department of Pediatrics Moon Sung Park M.D. Hee Cheol Jo, M.D., Jang Hoon Lee,
Incidence and diagnosis of unilateral arterial cerebral infarction in newborn infants *
 J. Perinat. Med. 33 (2005) 170 175 Copyright by Walter de Gruyter Berlin New York. DOI 10.1515/JPM.2005.032 Short communication Incidence and diagnosis of unilateral arterial cerebral infarction in newborn
J. Perinat. Med. 33 (2005) 170 175 Copyright by Walter de Gruyter Berlin New York. DOI 10.1515/JPM.2005.032 Short communication Incidence and diagnosis of unilateral arterial cerebral infarction in newborn
SWISS SOCIETY OF NEONATOLOGY. Neonatal cerebral infarction
 SWISS SOCIETY OF NEONATOLOGY Neonatal cerebral infarction May 2002 2 Mann C, Neonatal and Pediatric Intensive Care Unit, Landeskrankenhaus und Akademisches Lehrkrankenhaus Feldkirch, Austria Swiss Society
SWISS SOCIETY OF NEONATOLOGY Neonatal cerebral infarction May 2002 2 Mann C, Neonatal and Pediatric Intensive Care Unit, Landeskrankenhaus und Akademisches Lehrkrankenhaus Feldkirch, Austria Swiss Society
NIH Public Access Author Manuscript Pediatr Neurol. Author manuscript; available in PMC 2009 October 30.
 NIH Public Access Author Manuscript Published in final edited form as: Pediatr Neurol. 2008 May ; 38(5): 329 334. doi:10.1016/j.pediatrneurol.2007.12.012. Very Early Arterial Ischemic Stroke in Premature
NIH Public Access Author Manuscript Published in final edited form as: Pediatr Neurol. 2008 May ; 38(5): 329 334. doi:10.1016/j.pediatrneurol.2007.12.012. Very Early Arterial Ischemic Stroke in Premature
Hypoxic ischemic brain injury in neonates - early MR imaging findings
 Hypoxic ischemic brain injury in neonates - early MR imaging findings Poster No.: C-1208 Congress: ECR 2015 Type: Authors: Keywords: DOI: Educational Exhibit E.-M. Heursen, R. Reina Cubero, T. Guijo Hernandez,
Hypoxic ischemic brain injury in neonates - early MR imaging findings Poster No.: C-1208 Congress: ECR 2015 Type: Authors: Keywords: DOI: Educational Exhibit E.-M. Heursen, R. Reina Cubero, T. Guijo Hernandez,
Study of correlation severity of hypoxic ischemic encephalopathy on MRI brain with clinical findings
 Radiology and Imaging Special Issue December 2017: Vol-7, Issue- 1, P 34-41 Original article: Study of correlation severity of hypoxic ischemic encephalopathy on MRI brain with clinical findings *Dr Ramaa
Radiology and Imaging Special Issue December 2017: Vol-7, Issue- 1, P 34-41 Original article: Study of correlation severity of hypoxic ischemic encephalopathy on MRI brain with clinical findings *Dr Ramaa
Citation for published version (APA): Roze, E. (2011). Functional development at school age of newborn infants at risk. Groningen: s.n.
 University of Groningen Functional development at school age of newborn infants at risk Roze, Elise IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite
University of Groningen Functional development at school age of newborn infants at risk Roze, Elise IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite
Neonatal arterial ischemic stroke was considered an
 Cognitive Outcome at Early School Age in Term-Born Children With Perinatally Acquired Middle Cerebral Artery Territory Infarction Daniela Ricci, MD; Eugenio Mercuri, MD; Anna Barnett, PhD; Rachel Rathbone,
Cognitive Outcome at Early School Age in Term-Born Children With Perinatally Acquired Middle Cerebral Artery Territory Infarction Daniela Ricci, MD; Eugenio Mercuri, MD; Anna Barnett, PhD; Rachel Rathbone,
Perlman J, Clinics Perinatol 2006; 33: Underlying causal pathways. Antenatal Intrapartum Postpartum. Acute near total asphyxia
 Perlman J, Clinics Perinatol 2006; 33:335-353 Underlying causal pathways Antenatal Intrapartum Postpartum Acute injury Subacute injury Associated problem Reduced fetal movements Placental insufficiency
Perlman J, Clinics Perinatol 2006; 33:335-353 Underlying causal pathways Antenatal Intrapartum Postpartum Acute injury Subacute injury Associated problem Reduced fetal movements Placental insufficiency
SWISS SOCIETY OF NEONATOLOGY. Severe apnea and bradycardia in a term infant
 SWISS SOCIETY OF NEONATOLOGY Severe apnea and bradycardia in a term infant October 2014 2 Walker JH, Arlettaz Mieth R, Däster C, Division of Neonatology, University Hospital Zurich, Switzerland Swiss Society
SWISS SOCIETY OF NEONATOLOGY Severe apnea and bradycardia in a term infant October 2014 2 Walker JH, Arlettaz Mieth R, Däster C, Division of Neonatology, University Hospital Zurich, Switzerland Swiss Society
Perinatal thrombosis: implications for mothers and neonates
 CHALLENGING SCENARIOS IN THROMBOSIS Perinatal thrombosis: implications for mothers and neonates Sarah H. O Brien 1,2 1 Division of Pediatric Hematology/Oncology, Nationwide Children s Hospital/Ohio State
CHALLENGING SCENARIOS IN THROMBOSIS Perinatal thrombosis: implications for mothers and neonates Sarah H. O Brien 1,2 1 Division of Pediatric Hematology/Oncology, Nationwide Children s Hospital/Ohio State
Complete Recovery of Perfusion Abnormalities in a Cardiac Arrest Patient Treated with Hypothermia: Results of Cerebral Perfusion MR Imaging
 pissn 2384-1095 eissn 2384-1109 imri 2018;22:56-60 https://doi.org/10.13104/imri.2018.22.1.56 Complete Recovery of Perfusion Abnormalities in a Cardiac Arrest Patient Treated with Hypothermia: Results
pissn 2384-1095 eissn 2384-1109 imri 2018;22:56-60 https://doi.org/10.13104/imri.2018.22.1.56 Complete Recovery of Perfusion Abnormalities in a Cardiac Arrest Patient Treated with Hypothermia: Results
Imaging the Premature Brain- New Knowledge
 Imaging the Premature Brain- New Knowledge Stein Magnus Aukland Haukeland University Hospital University of Bergen NORWAY No disclosure Imaging modalities O Skull X-ray O Computer Tomography O Cerebral
Imaging the Premature Brain- New Knowledge Stein Magnus Aukland Haukeland University Hospital University of Bergen NORWAY No disclosure Imaging modalities O Skull X-ray O Computer Tomography O Cerebral
SWISS SOCIETY OF NEONATOLOGY. Diagnostic evaluation of a symptomatic cerebrovascular accident in a neonate with focal convulsions
 SWISS SOCIETY OF NEONATOLOGY Diagnostic evaluation of a symptomatic cerebrovascular accident in a neonate with focal convulsions July 2013 2 Anderson S, Rimensberger P, Service de Néonatologie et des Soins
SWISS SOCIETY OF NEONATOLOGY Diagnostic evaluation of a symptomatic cerebrovascular accident in a neonate with focal convulsions July 2013 2 Anderson S, Rimensberger P, Service de Néonatologie et des Soins
MRI Lesions and Infants with Neonatal Encephalopathy. Is the Apgar Score Predictive?
 MRI Lesions and Infants with Neonatal Encephalopathy. Is the Apgar Score Predictive? E. Mercuri 1,2 M. Rutherford 1 A. Barnett 1 Chr. Foglia 1 L. Haataja 1,3 S. Counsell 4 F. Cowan 1 L. Dubowitz 1 150
MRI Lesions and Infants with Neonatal Encephalopathy. Is the Apgar Score Predictive? E. Mercuri 1,2 M. Rutherford 1 A. Barnett 1 Chr. Foglia 1 L. Haataja 1,3 S. Counsell 4 F. Cowan 1 L. Dubowitz 1 150
Is there a way to predict outcome in (near) term neonates with hypoxic-ischemic encephalopathy based on MR imaging?
 Chapter 5 Is there a way to predict outcome in (near) term neonates with hypoxic-ischemic encephalopathy based on MR imaging? Lishya Liauw Jeroen van der Grond Annette van den Berg-Huysmans Laura Laan
Chapter 5 Is there a way to predict outcome in (near) term neonates with hypoxic-ischemic encephalopathy based on MR imaging? Lishya Liauw Jeroen van der Grond Annette van den Berg-Huysmans Laura Laan
Neonatal Brain MRI and Motor Outcome at School Age in Children with Neonatal Encephalopathy: A Review of Personal Experience
 NEURAL PLASTICITY VOLUME 10, NO. 1-2, 2003 Neonatal Brain MRI and Motor Outcome at School Age in Children with Neonatal Encephalopathy: A Review of Personal Experience Eugenio Mercuri and Anna L. Barnett
NEURAL PLASTICITY VOLUME 10, NO. 1-2, 2003 Neonatal Brain MRI and Motor Outcome at School Age in Children with Neonatal Encephalopathy: A Review of Personal Experience Eugenio Mercuri and Anna L. Barnett
Serial 1- and 2-Dimensional Cerebral MRI Measurements in Full-Term Infants after Perinatal Asphyxia
 Original Paper Received: October 27, 2015 Accepted after revision: January 18, 2016 Published online: March 12, 2016 Serial 1- and 2-Dimensional Cerebral MRI Measurements in Full-Term Infants after Perinatal
Original Paper Received: October 27, 2015 Accepted after revision: January 18, 2016 Published online: March 12, 2016 Serial 1- and 2-Dimensional Cerebral MRI Measurements in Full-Term Infants after Perinatal
Reproducibility and Accuracy of MR Imaging of the Brain after Severe Birth Asphyxia
 AJNR Am J Neuroradiol : 8, August 999 Reproducibility and Accuracy of MR Imaging of the Brain after Severe Birth Asphyxia Phillipe Jouvet, Francis M. Cowan, Philip Cox, Edward Lazda, Mary A. Rutherford,
AJNR Am J Neuroradiol : 8, August 999 Reproducibility and Accuracy of MR Imaging of the Brain after Severe Birth Asphyxia Phillipe Jouvet, Francis M. Cowan, Philip Cox, Edward Lazda, Mary A. Rutherford,
Predicting Outcomes in HIE. Naaz Merchant Consultant Neonatologist Beds & Herts Meeting 17/03/2016
 Predicting Outcomes in HIE Naaz Merchant Consultant Neonatologist Beds & Herts Meeting 17/03/2016 Interactive please! Case 1 Term, 3.5 kg Antenatal: Breech Labour/Delivery: Em CS failure to progress, mec
Predicting Outcomes in HIE Naaz Merchant Consultant Neonatologist Beds & Herts Meeting 17/03/2016 Interactive please! Case 1 Term, 3.5 kg Antenatal: Breech Labour/Delivery: Em CS failure to progress, mec
Neonatal Hypoxic-ischemic Encephalopathy: Detection with Diffusion-weighted MR Imaging
 AJNR Am J Neuroradiol :9 96, September Neonatal Hypoxic-ischemic Encephalopathy: Detection with Diffusion-weighted MR Imaging Kirsten P. N. Forbes, James G. Pipe, and Roger Bird BACKGROUND AND PURPOSE:
AJNR Am J Neuroradiol :9 96, September Neonatal Hypoxic-ischemic Encephalopathy: Detection with Diffusion-weighted MR Imaging Kirsten P. N. Forbes, James G. Pipe, and Roger Bird BACKGROUND AND PURPOSE:
DWI assessment of ischemic changes in the fetal brain
 DWI assessment of ischemic changes in the fetal brain Dafi Bergman, 4 th year Medical student in the 4-year program, Sackler school of medicine B.Sc Life and Medical Sciences, Tel Aviv University Supervised
DWI assessment of ischemic changes in the fetal brain Dafi Bergman, 4 th year Medical student in the 4-year program, Sackler school of medicine B.Sc Life and Medical Sciences, Tel Aviv University Supervised
Magnetic resonance imaging assessment of brain maturation in preterm neonates with punctate white matter lesions
 Neuroradiology (2007) 49:161 167 DOI 10.1007/s00234-006-0176-y PAEDIATRIC NEURORADIOLOGY Magnetic resonance imaging assessment of brain maturation in preterm neonates with punctate white matter lesions
Neuroradiology (2007) 49:161 167 DOI 10.1007/s00234-006-0176-y PAEDIATRIC NEURORADIOLOGY Magnetic resonance imaging assessment of brain maturation in preterm neonates with punctate white matter lesions
Unilateral neonatal cerebral infarction in full term infants
 F88 Department of Paediatrics, John RadcliVe Hospital, Oxford, OX3 9DU J Estan P Hope Correspondence to: Dr Peter Hope. Accepted 11 December 1996 Unilateral neonatal cerebral infarction in full term infants
F88 Department of Paediatrics, John RadcliVe Hospital, Oxford, OX3 9DU J Estan P Hope Correspondence to: Dr Peter Hope. Accepted 11 December 1996 Unilateral neonatal cerebral infarction in full term infants
Difficulties at Birth: Long Term Developmental Outcomes
 Difficulties at Birth: Long Term Developmental Outcomes Alan D. Bedrick MD Division of Neonatology and Developmental Biology Department of Pediatrics University of Arizona Tucson, Arizona DISCLOSURE I
Difficulties at Birth: Long Term Developmental Outcomes Alan D. Bedrick MD Division of Neonatology and Developmental Biology Department of Pediatrics University of Arizona Tucson, Arizona DISCLOSURE I
Admission/Discharge Form for Infants Born in Please DO NOT mail or fax this form to the CPQCC Data Center. This form is for internal use ONLY.
 Selection Criteria Admission/Discharge Form for Infants Born in 2016 To be eligible, you MUST answer YES to at least one of the possible criteria (A-C) A. 401 1500 grams o Yes B. GA range 22 0/7 31 6/7
Selection Criteria Admission/Discharge Form for Infants Born in 2016 To be eligible, you MUST answer YES to at least one of the possible criteria (A-C) A. 401 1500 grams o Yes B. GA range 22 0/7 31 6/7
Newborn Hypoxic Ischemic Brain Injury. Hisham Dahmoush, MBBCh FRCR Lucile Packard Children s Hospital at Stanford
 Newborn Hypoxic Ischemic Brain Injury Hisham Dahmoush, MBBCh FRCR Lucile Packard Children s Hospital at Stanford NO DISCLOSURES INTRODUCTION Neonatal hypoxic-ischemic encephalopathy (HIE) is a major cause
Newborn Hypoxic Ischemic Brain Injury Hisham Dahmoush, MBBCh FRCR Lucile Packard Children s Hospital at Stanford NO DISCLOSURES INTRODUCTION Neonatal hypoxic-ischemic encephalopathy (HIE) is a major cause
The high risk neonate
 The high risk neonate Infant classification by gestational (postmenstrual) age Preterm. Less than 37 completed weeks (259 days). Term. Thirty-seven to 416/7 weeks (260-294 days). Post-term. Forty-two weeks
The high risk neonate Infant classification by gestational (postmenstrual) age Preterm. Less than 37 completed weeks (259 days). Term. Thirty-seven to 416/7 weeks (260-294 days). Post-term. Forty-two weeks
SWISS SOCIETY OF NEONATOLOGY. Bart s syndrome with severe newborn encephalopathy: a delayed diagnosis
 SWISS SOCIETY OF NEONATOLOGY Bart s syndrome with severe newborn encephalopathy: a delayed diagnosis May 2003 2 Buettiker V, Hogan P, Badawi N, Department of Neonatology (BV, NB), Department of Dermatology
SWISS SOCIETY OF NEONATOLOGY Bart s syndrome with severe newborn encephalopathy: a delayed diagnosis May 2003 2 Buettiker V, Hogan P, Badawi N, Department of Neonatology (BV, NB), Department of Dermatology
DOWNLOAD OR READ : PERINATAL EVENTS AND BRAIN DAMAGE IN SURVIVING CHILDREN BASED ON PAPERS PRESENTED AT AN INTERNATIONA PDF EBOOK EPUB MOBI
 DOWNLOAD OR READ : PERINATAL EVENTS AND BRAIN DAMAGE IN SURVIVING CHILDREN BASED ON PAPERS PRESENTED AT AN INTERNATIONA PDF EBOOK EPUB MOBI Page 1 Page 2 perinatal events and brain damage in surviving
DOWNLOAD OR READ : PERINATAL EVENTS AND BRAIN DAMAGE IN SURVIVING CHILDREN BASED ON PAPERS PRESENTED AT AN INTERNATIONA PDF EBOOK EPUB MOBI Page 1 Page 2 perinatal events and brain damage in surviving
Predicting outcome using neonatal MRI in preterm infants. Manon Benders, neonatologist. Summer Conference on Neonatology in Provence
 Predicting outcome using neonatal MRI in preterm infants Manon Benders, neonatologist Summer Conference on Neonatology in Provence Avignon, France, 6 th - 9 th September 2017 the human brain the third
Predicting outcome using neonatal MRI in preterm infants Manon Benders, neonatologist Summer Conference on Neonatology in Provence Avignon, France, 6 th - 9 th September 2017 the human brain the third
Insults to the Developing Brain & Effect on Neurodevelopmental Outcomes
 Insults to the Developing Brain & Effect on Neurodevelopmental Outcomes Ira Adams-Chapman, MD Assistant Professor of Pediatrics Director, Developmental Progress Clinic Emory University School of Medicine
Insults to the Developing Brain & Effect on Neurodevelopmental Outcomes Ira Adams-Chapman, MD Assistant Professor of Pediatrics Director, Developmental Progress Clinic Emory University School of Medicine
Early Accurate Diagnosis & Early Intervention for Cerebral Palsy INTERNATIONAL RECOMMENDATIONS
 Early Accurate Diagnosis & Early Intervention for Cerebral Palsy INTERNATIONAL RECOMMENDATIONS Professor Iona Novak Cerebral Palsy Alliance Australia Neuroplasticity is fundamentally why we believe in
Early Accurate Diagnosis & Early Intervention for Cerebral Palsy INTERNATIONAL RECOMMENDATIONS Professor Iona Novak Cerebral Palsy Alliance Australia Neuroplasticity is fundamentally why we believe in
Cranial ultrasound abnormalities in full term infants in a postnatal ward: outcome at 12 and 18 months
 F128 Department of Paediatrics and Neonatal Medicine, Imperial College School of Medicine, Hammersmith Hospital, Du Cane Road, London W12 0HS, UK L Haataja E Mercuri FCowan L Dubowitz Correspondence to:
F128 Department of Paediatrics and Neonatal Medicine, Imperial College School of Medicine, Hammersmith Hospital, Du Cane Road, London W12 0HS, UK L Haataja E Mercuri FCowan L Dubowitz Correspondence to:
Perinatal/Neonatal Case Presentation
 Perinatal/Neonatal Case Presentation & & & & & & & & & & & & & & Bilateral Thalamic Lesions in a Newborn with Intrauterine Asphyxia After Maternal Cardiac Arrest a Case Report with Literature Review Maya
Perinatal/Neonatal Case Presentation & & & & & & & & & & & & & & Bilateral Thalamic Lesions in a Newborn with Intrauterine Asphyxia After Maternal Cardiac Arrest a Case Report with Literature Review Maya
Department of Rehabilitation Medicine, CHA Bundang Medical Center, CHA University, Seongnam, Korea
 Original Article Ann Rehabil Med 2015;39(4):624-629 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2015.39.4.624 Annals of Rehabilitation Medicine Gross Motor Function Outcome After Intensive
Original Article Ann Rehabil Med 2015;39(4):624-629 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2015.39.4.624 Annals of Rehabilitation Medicine Gross Motor Function Outcome After Intensive
Original article: Evaluation of hypoxic-ischaemic events in preterm neonates using trans cranial ultrasound
 Original article: Evaluation of hypoxic-ischaemic events in preterm neonates using trans cranial ultrasound Priyanka Upadhyay *, Ketki U Patil 1, Rajesh Kuber 2, Vilas Kulkarni 3, Amarjit Singh 4 * Chief
Original article: Evaluation of hypoxic-ischaemic events in preterm neonates using trans cranial ultrasound Priyanka Upadhyay *, Ketki U Patil 1, Rajesh Kuber 2, Vilas Kulkarni 3, Amarjit Singh 4 * Chief
Chapter 7. Neuropediatrics 2007; 38 (5): Lara Leijser Alla Vein Lishya Liauw Tzipi Strauss Sylvia Veen Gerda van Wezel-Meijler
 Chapter 7 Prediction of short-term neurological outcome in full-term neonates with hypoxic-ischaemic encephalopathy based on combined use of electroencephalogram and neuro-imaging Lara Leijser Alla Vein
Chapter 7 Prediction of short-term neurological outcome in full-term neonates with hypoxic-ischaemic encephalopathy based on combined use of electroencephalogram and neuro-imaging Lara Leijser Alla Vein
Imaging of Perinatal Stroke
 Imaging of Perinatal Stroke Roxana S. Gunny, MBBS, MRCP, FRCR a,b, *, Doris Lin, MD, PhD c KEYWORDS Perinatal arterial ischemic stroke Presumed perinatal arterial ischemic stroke Cerebral sinovenous thrombosis
Imaging of Perinatal Stroke Roxana S. Gunny, MBBS, MRCP, FRCR a,b, *, Doris Lin, MD, PhD c KEYWORDS Perinatal arterial ischemic stroke Presumed perinatal arterial ischemic stroke Cerebral sinovenous thrombosis
Analysis between clinical and MRI findings of childhood and teenages with epilepsy after hypoxic-ischemic encephalopathy in neonates periods
 Analysis between clinical and MRI findings of childhood and teenages with epilepsy after hypoxic-ischemic encephalopathy in neonates periods Poster No.: C-0401 Congress: ECR 2015 Type: Scientific Exhibit
Analysis between clinical and MRI findings of childhood and teenages with epilepsy after hypoxic-ischemic encephalopathy in neonates periods Poster No.: C-0401 Congress: ECR 2015 Type: Scientific Exhibit
Neonatal Seizure. Dr.Nawar Yahya. Presented by: Sarah Khalil Zeina Shamil Zainab Waleed Zainab Qahtan. Supervised by:
 Neonatal Seizure Supervised by: Dr.Nawar Yahya Presented by: Sarah Khalil Zeina Shamil Zainab Waleed Zainab Qahtan Objectives: What is neonatal seizure Etiology Clinical presentation Differential diagnosis
Neonatal Seizure Supervised by: Dr.Nawar Yahya Presented by: Sarah Khalil Zeina Shamil Zainab Waleed Zainab Qahtan Objectives: What is neonatal seizure Etiology Clinical presentation Differential diagnosis
SWISS SOCIETY OF NEONATOLOGY. Neonatal sinovenous thrombosis
 SWISS SOCIETY OF NEONATOLOGY Neonatal sinovenous thrombosis August 2006 2 Hauri-Hohl A, Zeilinger G, Pasquier S, Children s Hospital of Aarau, Switzerland Swiss Society of Neonatology, Thomas M Berger,
SWISS SOCIETY OF NEONATOLOGY Neonatal sinovenous thrombosis August 2006 2 Hauri-Hohl A, Zeilinger G, Pasquier S, Children s Hospital of Aarau, Switzerland Swiss Society of Neonatology, Thomas M Berger,
Early instrumental predictors of long term neurodevelopmental impairment in newborns with perinatal asphyxia treated with therapeutic hypothermia
 SIGNA VITAE 218; 14(1): 81-85 Early instrumental predictors of long term neurodevelopmental impairment in newborns with perinatal asphyxia treated with therapeutic hypothermia ALICE MONZANI 1, GIANLUCA
SIGNA VITAE 218; 14(1): 81-85 Early instrumental predictors of long term neurodevelopmental impairment in newborns with perinatal asphyxia treated with therapeutic hypothermia ALICE MONZANI 1, GIANLUCA
Differentiation between peritrigonal terminal zones and hypoxic-ischemic white matter injury on MRI
 Chapter 4 Differentiation between peritrigonal terminal zones and hypoxic-ischemic white matter injury on MRI Lishya Liauw Jeroen van der Grond Valerie Slooff Francisca Wiggers-de Bruïne Laura Laan Saskia
Chapter 4 Differentiation between peritrigonal terminal zones and hypoxic-ischemic white matter injury on MRI Lishya Liauw Jeroen van der Grond Valerie Slooff Francisca Wiggers-de Bruïne Laura Laan Saskia
P eriventricular leucomalacia (PVL), which is characterised
 F275 ORIGINAL ARTICLE Limitations of ultrasonography for diagnosing white matter damage in preterm infants T Debillon, S N Guyen, A Muet, M P Quere, F Moussaly, J C Roze... See end of article for authors
F275 ORIGINAL ARTICLE Limitations of ultrasonography for diagnosing white matter damage in preterm infants T Debillon, S N Guyen, A Muet, M P Quere, F Moussaly, J C Roze... See end of article for authors
Epilepsy in children with cerebral palsy
 Seizure 2003; 12: 110 114 doi:10.1016/s1059 1311(02)00255-8 Epilepsy in children with cerebral palsy A.K. GURURAJ, L. SZTRIHA, A. BENER,A.DAWODU & V. EAPEN Departments of Paediatrics, Community Medicine
Seizure 2003; 12: 110 114 doi:10.1016/s1059 1311(02)00255-8 Epilepsy in children with cerebral palsy A.K. GURURAJ, L. SZTRIHA, A. BENER,A.DAWODU & V. EAPEN Departments of Paediatrics, Community Medicine
Queen Charlotte Hospital
 Queen Charlotte Hospital Neuroprotection for neonatal encephalopathy Neonatal encephalopathy accounts for 1 million deaths worldwide and even greater numbers of disabled survivors In countries with
Queen Charlotte Hospital Neuroprotection for neonatal encephalopathy Neonatal encephalopathy accounts for 1 million deaths worldwide and even greater numbers of disabled survivors In countries with
The Clinical Spectrum and Prediction of Outcome in Hypoxic-Ischemic Encephalopathy
 Article neurology The Clinical Spectrum and Prediction of Outcome in Hypoxic-Ischemic Encephalopathy Walter C. Allan, MD* Objectives After completing this article, readers should be able to: 1. List the
Article neurology The Clinical Spectrum and Prediction of Outcome in Hypoxic-Ischemic Encephalopathy Walter C. Allan, MD* Objectives After completing this article, readers should be able to: 1. List the
Neonatal hypoxic-ischemic brain injury imaging: A pictorial review
 Neonatal hypoxic-ischemic brain injury imaging: A pictorial review Poster No.: C-1425 Congress: ECR 2014 Type: Educational Exhibit Authors: E. Alexopoulou 1, A. Mazioti 1, D. K. Filippiadis 2, C. Chrona
Neonatal hypoxic-ischemic brain injury imaging: A pictorial review Poster No.: C-1425 Congress: ECR 2014 Type: Educational Exhibit Authors: E. Alexopoulou 1, A. Mazioti 1, D. K. Filippiadis 2, C. Chrona
Magnetic resonance imaging (MR!) provides
 0 Wallerian Degeneration of the Pyramidal Tract in Capsular Infarction Studied by Magnetic Resonance Imaging Jesiis Pujol, MD, Josep L. Marti-Vilalta, MD, Carme Junqu6, PhD, Pere Vendrell, PhD, Juan Fernandez,
0 Wallerian Degeneration of the Pyramidal Tract in Capsular Infarction Studied by Magnetic Resonance Imaging Jesiis Pujol, MD, Josep L. Marti-Vilalta, MD, Carme Junqu6, PhD, Pere Vendrell, PhD, Juan Fernandez,
Neonatal MRI to Predict Neurodevelopmental Outcomes in Preterm Infants
 The new england journal of medicine original article Neonatal MRI to Predict Neurodevelopmental Outcomes in Preterm Infants Lianne J. Woodward, Ph.D., Peter J. Anderson, Ph.D., Nicola C. Austin, M.D.,
The new england journal of medicine original article Neonatal MRI to Predict Neurodevelopmental Outcomes in Preterm Infants Lianne J. Woodward, Ph.D., Peter J. Anderson, Ph.D., Nicola C. Austin, M.D.,
ADMISSION/DISCHARGE FORM FOR INFANTS BORN IN 2019 DO NOT mail or fax this form to the CPQCC Data Center. This form is for internal use ONLY.
 1 Any eligible inborn infant who dies in the delivery room or at any other location in your hospital within 12 hours after birth and prior to admission to the NICU is defined as a "Delivery Room Death."
1 Any eligible inborn infant who dies in the delivery room or at any other location in your hospital within 12 hours after birth and prior to admission to the NICU is defined as a "Delivery Room Death."
Lectures 4 Early fetal assessment, screening, ultrasound and treatment modalities during pregnancy. II. Asphyxia and Resuscitation (3 lectures)...
 Outline of a 2 year Neonatology educational course (80 lectures) PLUS 2 graduate level courses (GENETICS and BIOSTATISTICS & EPIDEMIOLOGY Approximate Percent in Examination I. Maternal-Fetal Medicine (6
Outline of a 2 year Neonatology educational course (80 lectures) PLUS 2 graduate level courses (GENETICS and BIOSTATISTICS & EPIDEMIOLOGY Approximate Percent in Examination I. Maternal-Fetal Medicine (6
White Matter Injury in the Premature Infant: A Comparison between Serial Cranial Sonographic and MR Findings at Term
 AJNR Am J Neuroradiol 24:805 809, May 2003 White Matter Injury in the Premature Infant: A Comparison between Serial Cranial Sonographic and MR Findings at Term Terrie E. Inder, Nigel J. Anderson, Carole
AJNR Am J Neuroradiol 24:805 809, May 2003 White Matter Injury in the Premature Infant: A Comparison between Serial Cranial Sonographic and MR Findings at Term Terrie E. Inder, Nigel J. Anderson, Carole
11/9/2012. Group B Streptococcal Infections: Consensus and Controversies. Prevention of Early-Onset GBS Disease in the USA.
 Group B Streptococcal Infections: Consensus and Controversies Carol J. Baker, M.D. Professor of Pediatrics, Molecular Virology and Microbiology Executive Director, Center for Vaccine Awareness and Research
Group B Streptococcal Infections: Consensus and Controversies Carol J. Baker, M.D. Professor of Pediatrics, Molecular Virology and Microbiology Executive Director, Center for Vaccine Awareness and Research
Imaging findings in neonates with hypoxic-ischaemic encephalopathy and terapeutic hypothermia.
 Imaging findings in neonates with hypoxic-ischaemic encephalopathy and terapeutic hypothermia. Poster No.: C-1577 Congress: ECR 2014 Type: Scientific Exhibit Authors: S. Manso Garcia, M. J. Velasco Marcos,
Imaging findings in neonates with hypoxic-ischaemic encephalopathy and terapeutic hypothermia. Poster No.: C-1577 Congress: ECR 2014 Type: Scientific Exhibit Authors: S. Manso Garcia, M. J. Velasco Marcos,
Screening Cranial Imaging at Multiple Time Points Improves Cystic Periventricular Leukomalacia Detection
 Screening Cranial Imaging at Multiple Time Points Improves Cystic Periventricular Leukomalacia Detection Abhik Das, RTI International John Barks, University of Michigan Subrata Sarkar, University of Michigan
Screening Cranial Imaging at Multiple Time Points Improves Cystic Periventricular Leukomalacia Detection Abhik Das, RTI International John Barks, University of Michigan Subrata Sarkar, University of Michigan
SWISS SOCIETY OF NEONATOLOGY. Congenital ductus arteriosus aneurysm: serious or common?
 SWISS SOCIETY OF NEONATOLOGY Congenital ductus arteriosus aneurysm: serious or common? AUGUST 2011 * 2 Beauport L, Meijboom E, Vial Y, Gudinchet F, Truttmann AC, CHUV, Lausanne, Neonatology Unit (BL, TAC),
SWISS SOCIETY OF NEONATOLOGY Congenital ductus arteriosus aneurysm: serious or common? AUGUST 2011 * 2 Beauport L, Meijboom E, Vial Y, Gudinchet F, Truttmann AC, CHUV, Lausanne, Neonatology Unit (BL, TAC),
MR imaging findings of cerebral damage in infants with
 ORIGINAL RESEARCH L. Liauw I.H. Palm-Meinders J. van der Grond L.M. Leijser S. le Cessie L.A.E.M. Laan B.C. Heeres M.A. van Buchem G. van Wezel-Meijler Differentiating Normal Myelination from Hypoxic-
ORIGINAL RESEARCH L. Liauw I.H. Palm-Meinders J. van der Grond L.M. Leijser S. le Cessie L.A.E.M. Laan B.C. Heeres M.A. van Buchem G. van Wezel-Meijler Differentiating Normal Myelination from Hypoxic-
Perinatal hypoxic-ischemic events cause hypoxic-ischemic encephalopathy (HIE) in at least 1 to 2/1000 term-born infants,
 General Movements in Full-Term Infants with Perinatal Asphyxia Are Related to Basal Ganglia and Thalamic Lesions Fabrizio Ferrari, MD, Alessandra Todeschini, MD, Isotta Guidotti, MD, Miriam Martinez-Biarge,
General Movements in Full-Term Infants with Perinatal Asphyxia Are Related to Basal Ganglia and Thalamic Lesions Fabrizio Ferrari, MD, Alessandra Todeschini, MD, Isotta Guidotti, MD, Miriam Martinez-Biarge,
Hypoxic-ischaemic encephalopathy: early and late
 Archives ofdisease in Childhood 1996;75:F145-F151 F145 ORIGINAL ARTICLES Department of Paediatrics and Neonatal Medicine, Hammersmith Hospital, Du Cane Road, London W12 OHS M Rutherford F Cowan L Dubowitz
Archives ofdisease in Childhood 1996;75:F145-F151 F145 ORIGINAL ARTICLES Department of Paediatrics and Neonatal Medicine, Hammersmith Hospital, Du Cane Road, London W12 OHS M Rutherford F Cowan L Dubowitz
Utility of neuroradiographic imaging in predicting outcomes after neonatal extracorporeal membrane oxygenation
 Journal of Pediatric Surgery (2012) 47, 76 80 www.elsevier.com/locate/jpedsurg Utility of neuroradiographic imaging in predicting outcomes after neonatal extracorporeal membrane oxygenation Michael D.
Journal of Pediatric Surgery (2012) 47, 76 80 www.elsevier.com/locate/jpedsurg Utility of neuroradiographic imaging in predicting outcomes after neonatal extracorporeal membrane oxygenation Michael D.
RESEARCH BRIEF. Prognostic Value of Resistive Index in Neonates with Hypoxic Ischemic
 RESEARCH BRIEF Prognostic Value of Resistive Index in Neonates with Hypoxic Ischemic A Senthil Kumar, Aparna Chandrasekaran, Rajamannar Asokan and *Kathirvelu Gopinathan From the Department of Neonatology,
RESEARCH BRIEF Prognostic Value of Resistive Index in Neonates with Hypoxic Ischemic A Senthil Kumar, Aparna Chandrasekaran, Rajamannar Asokan and *Kathirvelu Gopinathan From the Department of Neonatology,
What is symptomatic? Neonatal hypoglycemia: how low can you go? Hypoglycemia and MRI. Conflicts. What s the problem? Hypoglycemia and MRI
 Neonatal hypoglycemia: how low can you go? Kristi Watterberg, MD Professor of Pediatrics, UNM What is symptomatic? Jitteriness Cyanosis Poor feeding Weak, high-pitched cry Seizures Apnea Lethargy, low
Neonatal hypoglycemia: how low can you go? Kristi Watterberg, MD Professor of Pediatrics, UNM What is symptomatic? Jitteriness Cyanosis Poor feeding Weak, high-pitched cry Seizures Apnea Lethargy, low
In the first edition of this report, the Task Force on Neonatal
 Neonatal Encephalopathy and Neurologic Outcome, Second Edition Report of the American College of Obstetricians and Gynecologists Task Force on Neonatal Encephalopathy Executive Summary In the first edition
Neonatal Encephalopathy and Neurologic Outcome, Second Edition Report of the American College of Obstetricians and Gynecologists Task Force on Neonatal Encephalopathy Executive Summary In the first edition
39 th Annual Perinatal Conference Vanderbilt University December 6, 2013 IUGR. Diagnosis and Management
 39 th Annual Perinatal Conference Vanderbilt University December 6, 2013 IUGR Diagnosis and Management Giancarlo Mari, M.D., M.B.A. Professor and Chair Department of Obstetrics and Gynecology University
39 th Annual Perinatal Conference Vanderbilt University December 6, 2013 IUGR Diagnosis and Management Giancarlo Mari, M.D., M.B.A. Professor and Chair Department of Obstetrics and Gynecology University
Perinatal stroke is a cerebrovascular event that occurs
 Acutely and Retrospectively Diagnosed Perinatal Stroke A Population-Based Study Rael Laugesaar, MD; Anneli Kolk, PhD; Tiiu Tomberg, PhD; Tuuli Metsvaht, MD; Mare Lintrop, MD; Heili Varendi, PhD; Tiina
Acutely and Retrospectively Diagnosed Perinatal Stroke A Population-Based Study Rael Laugesaar, MD; Anneli Kolk, PhD; Tiiu Tomberg, PhD; Tuuli Metsvaht, MD; Mare Lintrop, MD; Heili Varendi, PhD; Tiina
Diffusion-Weighted and Conventional MR Imaging Findings of Neuroaxonal Dystrophy
 AJNR Am J Neuroradiol 25:1269 1273, August 2004 Diffusion-Weighted and Conventional MR Imaging Findings of Neuroaxonal Dystrophy R. Nuri Sener BACKGROUND AND PURPOSE: Neuroaxonal dystrophy is a rare progressive
AJNR Am J Neuroradiol 25:1269 1273, August 2004 Diffusion-Weighted and Conventional MR Imaging Findings of Neuroaxonal Dystrophy R. Nuri Sener BACKGROUND AND PURPOSE: Neuroaxonal dystrophy is a rare progressive
Hypothermia in Neonates with HIE TARA JENDZIO, DNP(C), RN, RNC-NIC
 Hypothermia in Neonates with HIE TARA JENDZIO, DNP(C), RN, RNC-NIC Objectives 1. Define Hypoxic-Ischemic Encephalopathy (HIE) 2. Identify the criteria used to determine if an infant qualifies for therapeutic
Hypothermia in Neonates with HIE TARA JENDZIO, DNP(C), RN, RNC-NIC Objectives 1. Define Hypoxic-Ischemic Encephalopathy (HIE) 2. Identify the criteria used to determine if an infant qualifies for therapeutic
Neonatal Encephalopathy and Neurologic Outcome, Second Edition
 Organizational Principles to Guide and Define the Child Health Care System and/or Improve the Health of all Children STATEMENT OF ENDORSEMENT Neonatal Encephalopathy and Neurologic Outcome, Second Edition
Organizational Principles to Guide and Define the Child Health Care System and/or Improve the Health of all Children STATEMENT OF ENDORSEMENT Neonatal Encephalopathy and Neurologic Outcome, Second Edition
Different Patterns of Punctate White Matter Lesions in Serially Scanned Preterm Infants
 Different Patterns of Punctate White Matter Lesions in Serially Scanned Preterm Infants Karina J. Kersbergen 1, Manon J. N. L. Benders 1, Floris Groenendaal 1, Corine Koopman-Esseboom 1, Rutger A. J. Nievelstein
Different Patterns of Punctate White Matter Lesions in Serially Scanned Preterm Infants Karina J. Kersbergen 1, Manon J. N. L. Benders 1, Floris Groenendaal 1, Corine Koopman-Esseboom 1, Rutger A. J. Nievelstein
Imaging findings in neonates with hypoxic-ischaemic encephalopathy and terapeutic hypothermia.
 Imaging findings in neonates with hypoxic-ischaemic encephalopathy and terapeutic hypothermia. Poster No.: C-1577 Congress: ECR 2014 Type: Scientific Exhibit Authors: S. Manso Garcia, M. J. Velasco Marcos,
Imaging findings in neonates with hypoxic-ischaemic encephalopathy and terapeutic hypothermia. Poster No.: C-1577 Congress: ECR 2014 Type: Scientific Exhibit Authors: S. Manso Garcia, M. J. Velasco Marcos,
Manifestation of Antiphospholipid Syndrome among Saudi patients :examining the applicability of sapporo Criteria
 Manifestation of Antiphospholipid Syndrome among Saudi patients :examining the applicability of sapporo Criteria Farjah H AlGahtani Associate professor,md,mph Leukemia,Lymphoma in adolescent,thromboembolic
Manifestation of Antiphospholipid Syndrome among Saudi patients :examining the applicability of sapporo Criteria Farjah H AlGahtani Associate professor,md,mph Leukemia,Lymphoma in adolescent,thromboembolic
To evaluate the role of MRI in infants with suspected hypoxic ischemic encephalopathy and prognosticating neurological outcome at end of one year
 International Journal of Research in Medical Sciences Ramachandran S et al. Int J Res Med Sci. 2017 May;5(5):1893-1897 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Original Research rticle DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20171813
International Journal of Research in Medical Sciences Ramachandran S et al. Int J Res Med Sci. 2017 May;5(5):1893-1897 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Original Research rticle DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20171813
Term Hypoxic Ischemic Injury Joseph Junewick, MD FACR
 Term Hypoxic Ischemic Injury Joseph Junewick, MD FACR 08/11/2010 History Term infant with perinatal distress and attempted forceps delivery. Diagnosis Term Hypoxic Ischemic Injury Discussion Encephalopathy
Term Hypoxic Ischemic Injury Joseph Junewick, MD FACR 08/11/2010 History Term infant with perinatal distress and attempted forceps delivery. Diagnosis Term Hypoxic Ischemic Injury Discussion Encephalopathy
Outline. Calgary Pediatric Stroke Program. Parent Information and Networking Session
 Calgary Pediatric Stroke Program Parent Information and Networking Session Perinatal Stroke Adam Kirton MD MSc FRCPC Pediatric Neurologist Alberta Children s Hospital Sonia Rothenmund RN, BN, CNN(C) Pediatric
Calgary Pediatric Stroke Program Parent Information and Networking Session Perinatal Stroke Adam Kirton MD MSc FRCPC Pediatric Neurologist Alberta Children s Hospital Sonia Rothenmund RN, BN, CNN(C) Pediatric
CT and MR Imaging in Young Stroke Patients
 CT and MR Imaging in Young Stroke Patients Ashfaq A. Razzaq,Behram A. Khan,Shahid Baig ( Department of Neurology, Aga Khan University Hospital, Karachi. ) Abstract Pages with reference to book, From 66
CT and MR Imaging in Young Stroke Patients Ashfaq A. Razzaq,Behram A. Khan,Shahid Baig ( Department of Neurology, Aga Khan University Hospital, Karachi. ) Abstract Pages with reference to book, From 66
ECMUS The Safety Committee of EFSUMB : Tutorial
 Neonatal cranial ultrasound Safety Aspects (2013) Prepared for ECMUS by B.J. van der Knoop, M.D. 1, J.I.P. de Vries, M.D., PhD 1, I.A. Zonnenberg, M.D. 2, J.I.M.L. Verbeke, M.D. 3 R.J. Vermeulen, M.D.,
Neonatal cranial ultrasound Safety Aspects (2013) Prepared for ECMUS by B.J. van der Knoop, M.D. 1, J.I.P. de Vries, M.D., PhD 1, I.A. Zonnenberg, M.D. 2, J.I.M.L. Verbeke, M.D. 3 R.J. Vermeulen, M.D.,
Progress Report. Author: Dr Joseph Yuan-Mou Yang Qualification: PhD Institution: Royal Children s Hospital Date: October 2017
 Author: Dr Joseph Yuan-Mou Qualification: PhD Institution: Royal Children s Hospital Date: October 2017 Progress Report Title of Project: Brain structural and motor function correlations in childhood arterial
Author: Dr Joseph Yuan-Mou Qualification: PhD Institution: Royal Children s Hospital Date: October 2017 Progress Report Title of Project: Brain structural and motor function correlations in childhood arterial
During the past several decades, neonatal medicine has advanced
 Published September 29, 2011 as 10.3174/ajnr.A2703 ORIGINAL RESEARCH H. Kidokoro P.J. Anderson L.W. Doyle J.J. Neil T.E. Inder High Signal Intensity on T2-Weighted MR Imaging at Term-Equivalent Age in
Published September 29, 2011 as 10.3174/ajnr.A2703 ORIGINAL RESEARCH H. Kidokoro P.J. Anderson L.W. Doyle J.J. Neil T.E. Inder High Signal Intensity on T2-Weighted MR Imaging at Term-Equivalent Age in
7 Simple Steps to Assess & Document any Neonatal aeeg
 7 Simple Steps to Assess & Document any Neonatal aeeg Created for you by: www.aeegcoach.com How to use the Seven Simple Steps Checklist Hi! It s Kathi Randall here Your aeeg coach. I m so excited to share
7 Simple Steps to Assess & Document any Neonatal aeeg Created for you by: www.aeegcoach.com How to use the Seven Simple Steps Checklist Hi! It s Kathi Randall here Your aeeg coach. I m so excited to share
Chapter 6. Do Apparent Diffusion Coefficient measurements predict outcome in children with neonatal hypoxic-ischemic encephalopathy?
 Do Apparent Diffusion Coefficient measurements predict outcome in children with neonatal hypoxic-ischemic encephalopathy? Lishya Liauw Gerda van Wezel-Meijler Sylvia Veen Mark van Buchem Jeroen van der
Do Apparent Diffusion Coefficient measurements predict outcome in children with neonatal hypoxic-ischemic encephalopathy? Lishya Liauw Gerda van Wezel-Meijler Sylvia Veen Mark van Buchem Jeroen van der
Hypoxic-Ischemic Encephalopathy. TW de Witt University of Pretoria Department of Paediatrics Neonatology
 Hypoxic-Ischemic Encephalopathy TW de Witt University of Pretoria Department of Paediatrics Neonatology Background HIE remains a serious condition that causes significant mortality and longterm morbidity.
Hypoxic-Ischemic Encephalopathy TW de Witt University of Pretoria Department of Paediatrics Neonatology Background HIE remains a serious condition that causes significant mortality and longterm morbidity.
Pregnancy outcomes in Korean women with diabetes
 Pregnancy outcomes in Korean women with diabetes Sung-Hoon Kim Department of Medicine, Cheil General Hospital & Women s Healthcare Center, Dankook University College of Medicine, Seoul, Korea Conflict
Pregnancy outcomes in Korean women with diabetes Sung-Hoon Kim Department of Medicine, Cheil General Hospital & Women s Healthcare Center, Dankook University College of Medicine, Seoul, Korea Conflict
Periventricular white matter injury, that is, periventricular
 ORIGINAL RESEARCH S. Yoshida K. Hayakawa A. Yamamoto T. Kanda Y. Yamori Pontine Hypoplasia in Children with Periventricular Leukomalacia BACKGROUND AND PURPOSE: The brain stem in patients with periventricular
ORIGINAL RESEARCH S. Yoshida K. Hayakawa A. Yamamoto T. Kanda Y. Yamori Pontine Hypoplasia in Children with Periventricular Leukomalacia BACKGROUND AND PURPOSE: The brain stem in patients with periventricular
When? Incidence of neonatal seizures in a NICU population The incidence of seizures is higher in the neonatal period than in any other age group.
 Incidence of neonatal seizures in a NICU population The incidence of seizures is higher in the neonatal period than in any other age group. Standard EEG 2,3% 8.6% Standard EEG + aeeg Scher MS et al; Pediatrics
Incidence of neonatal seizures in a NICU population The incidence of seizures is higher in the neonatal period than in any other age group. Standard EEG 2,3% 8.6% Standard EEG + aeeg Scher MS et al; Pediatrics
Cerebral function monitoring in term or near term neonates at MDH: preliminary experience and proposal of a guideline
 Original Article Cerebral function monitoring in term or near term neonates at MDH: preliminary experience and proposal of a guideline Stephen Attard, Doriette Soler, Paul Soler Introduction: Cerebral
Original Article Cerebral function monitoring in term or near term neonates at MDH: preliminary experience and proposal of a guideline Stephen Attard, Doriette Soler, Paul Soler Introduction: Cerebral
Trajectories of Motor Recovery in the First Year After Pediatric Arterial Ischemic Stroke
 Trajectories of Motor Recovery in the First Year After Pediatric Arterial Ischemic Stroke Anna N. Cooper, BOT, a, b Vicki Anderson, PhD, a, b, c Stephen Hearps, PGDipBiostat, a, b Mardee Greenham, MSc,
Trajectories of Motor Recovery in the First Year After Pediatric Arterial Ischemic Stroke Anna N. Cooper, BOT, a, b Vicki Anderson, PhD, a, b, c Stephen Hearps, PGDipBiostat, a, b Mardee Greenham, MSc,
Extremely preterm infants are at high risk of brain injury
 ORIGINAL RESEARCH J.L.Y. Cheong D.K. Thompson H.X. Wang R.W. Hunt P.J. Anderson T.E. Inder L.W. Doyle Abnormal White Matter Signal on MR Imaging Is Related to Abnormal Tissue Microstructure BACKGROUND
ORIGINAL RESEARCH J.L.Y. Cheong D.K. Thompson H.X. Wang R.W. Hunt P.J. Anderson T.E. Inder L.W. Doyle Abnormal White Matter Signal on MR Imaging Is Related to Abnormal Tissue Microstructure BACKGROUND
Stroke School for Internists Part 1
 Stroke School for Internists Part 1 November 4, 2017 Dr. Albert Jin Dr. Gurpreet Jaswal Disclosures I receive a stipend for my role as Medical Director of the Stroke Network of SEO I have no commercial
Stroke School for Internists Part 1 November 4, 2017 Dr. Albert Jin Dr. Gurpreet Jaswal Disclosures I receive a stipend for my role as Medical Director of the Stroke Network of SEO I have no commercial
Historical Perspectives on the Etiology of Cerebral Palsy 233 Tonse N.K. Raju
 PERINATAL CAUSES OF CEREBRAL PALSY Preface Marcus C. Hermansen xv Historical Perspectives on the Etiology of Cerebral Palsy 233 Tonse N.K. Raju This essay presents the early history on the evolution of
PERINATAL CAUSES OF CEREBRAL PALSY Preface Marcus C. Hermansen xv Historical Perspectives on the Etiology of Cerebral Palsy 233 Tonse N.K. Raju This essay presents the early history on the evolution of
Advanced magnetic resonance imaging for monitoring brain development and injury
 Advanced magnetic resonance imaging for monitoring brain development and injury Stéphane Sizonenko, MD-PhD Division of Development and Growth Department of Child and Adolescent Medicine Geneva University
Advanced magnetic resonance imaging for monitoring brain development and injury Stéphane Sizonenko, MD-PhD Division of Development and Growth Department of Child and Adolescent Medicine Geneva University
SWISS SOCIETY OF NEONATOLOGY. Supercarbia in an infant with meconium aspiration syndrome
 SWISS SOCIETY OF NEONATOLOGY Supercarbia in an infant with meconium aspiration syndrome January 2006 2 Wilhelm C, Frey B, Department of Intensive Care and Neonatology, University Children s Hospital Zurich,
SWISS SOCIETY OF NEONATOLOGY Supercarbia in an infant with meconium aspiration syndrome January 2006 2 Wilhelm C, Frey B, Department of Intensive Care and Neonatology, University Children s Hospital Zurich,
Neuropathology Specialty Conference
 Neuropathology Specialty Conference March 22, 2010 Case 2 Rebecca Folkerth, MD Brigham and Women s Hospital Children s Hospital Harvard Medical School Clinical History 18-gestational-week fetus found on
Neuropathology Specialty Conference March 22, 2010 Case 2 Rebecca Folkerth, MD Brigham and Women s Hospital Children s Hospital Harvard Medical School Clinical History 18-gestational-week fetus found on
These signs should lead to the administration of high concentrations of
 Hypoxic-ischemic encephalopathy (HIE); (cont.) Clinical manifestations; *Intrauterine; growth restriction and increased vascular resistances may be the st manifestation of fetal hypoxia. *During labor;
Hypoxic-ischemic encephalopathy (HIE); (cont.) Clinical manifestations; *Intrauterine; growth restriction and increased vascular resistances may be the st manifestation of fetal hypoxia. *During labor;
Ischaemic and haemorrhagic brain lesions in
 Archives ofdisease in Childhood 1995; 73: F67-F74 Department of Paediatrics and Neonatal Medicine E Mercuri F Cowan M Rutherford D Acolet L Dubowitz Robert Steiner MRI Unit J Pennock Hammersmith Hospital,
Archives ofdisease in Childhood 1995; 73: F67-F74 Department of Paediatrics and Neonatal Medicine E Mercuri F Cowan M Rutherford D Acolet L Dubowitz Robert Steiner MRI Unit J Pennock Hammersmith Hospital,
The child with hemiplegic cerebral palsy thinking beyond the motor impairment. Dr Paul Eunson Edinburgh
 The child with hemiplegic cerebral palsy thinking beyond the motor impairment Dr Paul Eunson Edinburgh Content Coming to a diagnosis The importance of understanding the injury MRI scans Role of epilepsy
The child with hemiplegic cerebral palsy thinking beyond the motor impairment Dr Paul Eunson Edinburgh Content Coming to a diagnosis The importance of understanding the injury MRI scans Role of epilepsy
