Thoracoabdominal Esophagectomy for Cancer of the Gastroesophageal Junction
|
|
|
- Gordon Marshall
- 5 years ago
- Views:
Transcription
1 Thoracoabdominal Esophagectomy for Cancer of the Gastroesophageal Junction Douglas J. Mathisen The left thoracoabdominal esophagogastrectomy has for many years been the standard approach for resection and reconstruction of the gastroesophageal junction. It provides excellent exposure for en bloc dissection, placement of the esophageal substitute, and performance of the anastomosis. It is an approach that should be familiar to all thoracic surgeons for the variety of problems that present in this area of the body. Indications The most common indication for this approach is for neoplasms that arise at the gastroesophageal junction. It is useful for reoperative antireflux surgery because it allows complete mobilization of the esophagus, identification of the vagus nerves, and precise dissection on either side of the diaphragm. It is useful for resection and reconstruction of the lower third of the esophagus when short-segment intestinal interposition is warranted. The crucial factor to determine whether this approach is suitable is how far proximal in the esophagus the pathology extends. One must take into consideration sufficient margins for malignant neoplasms (at least 5 cm). If it is determined that the anastomosis can be performed 30 cm or more from the incisors, the left thoracoabdominal approach is suitable. This will place the anastomosis just below the aortic arch. If at the time of surgery a more proximal anastomosis is required, a second intercostal incision can be made to allow direct access to the supra-aortic area. This approach will be described in greater detail later. Because of the excellent exposure provided, this approach is particularly advantageous in obese patients, patients with multiple prior abdominal operations, situations where other intra-abdominal operations are needed (cholecystectomy, appendectomy), or if jejunal or colon interposition are contemplated. The only real contraindications to this approach are prior right pneumonectomy (anesthetic management and intrathoracic exposure are difficult because the left lung can t be isolated) and when the pathologic process involves the aortic arch. One other contraindication would be a patient that is quadriplegic in whom it is important to preserve diaphragmatic function. Evaluation of the Pathologic Process When deciding on this approach for resection and reconstruction of the esophagus, two factors are considered: the ease of the dissection and the ease of performance of the anastomosis. One should take advantage of all available information in making this decision. Obese patients with multiple prior abdominal operations make intra-abdominal exposure of the gastroesophageal junction difficult. An upper gastrointestinal endoscopy should be performed by the surgeon performing the operation to identify proximal extent of disease process (tumor, Barretts mucosa, radiation changes), quality of proximal esophagus, and status of the proximal stomach. I prefer to have a barium swallow on all patients. This study allows greater correlation with the pathology, endoscopic findings, relative location of the aortic arch to the proposed anastomosis, the presence or absence of a hiatal hernia and its influence on endoscopic findings, and an assessment of the proximal stomach. Computerized axial tomography (CT scan) is also helpful, but less so than the barium swallow. It certainly gives valuable information regarding liver metastases, retroperitoneal lymph-node involvement, and pulmonary metastases. It does give information regarding thickening of the esophageal wall and local invasion of adjacent structures, but I find these less reliable. Endoscopic ultrasonography is valuable in staging esophageal cancers and does give information regarding esophageal wall involvement and involvement of adjacent organs. A technique that is sometimes helpful is the endoscopic placement of a nasogastric tube at the predetermined site of anastomosis. By carefully placing the tip under direct vision and securing it in place, one can then palpate this at the time of surgery. This should reduce the necessity to redo an anastomosis because of a positive margin for cancer or Barrett s mucosa. Anesthetic Technique A double-lumen tube is essential for the satisfactory performance of a left thoracoabdominal esophagogastrectomy. It is essential to have the left lung deflated to perform a safe anastomosis. Without lung isolation a difficult anastomosis becomes near impossible. Some 186 OperativeTechniques in Thoracic and car&mb-3 vo14, No 3 (August), 1999: pp
2 suggest placing a left-sided double-lumen tube, hut we In years past, we routinely left all patients undergohave always preferred a right-sided tube. Left-sided ing esophagectoiny sedated and ventilated overnight. tihe5 frequently get dislodged with manipulation of the With the advent of routine epidural analgesia and lung and compromise the exposure to the proximal improved anesthetic techniques, we now try for extubatwphagus behind the left mainstem bronchus because tion at the completion of a left thoracoahdominal of the rigidity of the tube. esophagectom y. SURGTCAL TECHNTQUF, 1 See legend on next page.
3 188 DOUGLAS J. MATHISEN 1 Positioning is an important part of a left thoracoabdominal esophagogastrectomy. I believe it is often overlooked and if done improperly contributes to suboptimal operative exposure. The most common mistake is positioning the patient with their back 45" to the table and their hips opened. This position is great for the abdomen, but inadequate for the intrathoracic portion of the operation because the heart is invariably in the way. The ideal position for patients undergoing this operation is the true right-lateral decubitus position with the hips perpendicular to the table as one would do for a left thoracotomy (A). Exposure of the abdominal portion of the operation is not hampered in the slightest, the heart is not in the way or requires only minimal retraction, and the thoracic portion of the operation is allowed maximum exposure, especially for the anastomosis. This small detail is often the difference between a very difficult anastomosis and a very straightforward one. The patient is prepared from the symphysis pubis, across the midline anteriorly to the spine and base of the neck posteriorly. This allows the incision to be extended across the midline, in the midline below the umbilicus, or through a more proximal interspace for a supra-aortic anastomosis, if so desired. The standard incision extends from a point halfway between the umbilicus and the xyphoid process to one finger breadth below the tip of the scapula (A-B). I always start by making only the abdominal portion of the incision, stopping at the costal arch. This allows exploration of the abdomen to identify any unsuspected signs of metastases that would make the patient inoperable such as peritoneal implants, liver metastases, or lymph node involvement beyond the field of dissection. I have always been of the opinion that if these findings are present, surgical resection and its attendant risks, time to recovery, and alteration of swallowing are not justifiable in view of the limited chance for survival. Exceptions to this might be the very young, relatively fit patient, with significant dysphagia. Once it has been determined by thorough abdominal exploration that the lesion is resectable, the incision is extended to its full extent. I prefer to enter the chest between the sixth and seventh rib if possible. This gives much greater exposure to the area for the anastomosis. This almost always allows exposure just distal to the aortic arch where I prefer to do most left-sided anastomoses to give as much proximal margin as possible for malignant neoplasms. The costal arch is usually confluent at this level or, at the most, has two components of cartilage to it. A small, 1-cm piece of cartilage is removed at the proper angle to facilitate reapproximation at the conclusion of the case. Once the cartilage is divided, arterial vessels are ligated or cauterized just under the costal arch. (1A and 1B reprinted with permission from Wilkins EW Jr: Left thoracoabdominal approaches, in Pearson FG, Deslauriers J, Ginsberg RJ, et a1 (eds): Esophageal Surgery. New York, NY, Churchill Livingstone, 1995, p 659.)
4 THOKACOABDOMINAL ESOPHAGECTOMY FOR GE TUMORS See legend on next page.
5 190 DOUGLAS J. MATHISEN 2 1 routinely place two marking sutures at the point where the diaphragm is divided. This is valuable at the end of the procedure in lining up the diaphragm for proper reapproximation. The diaphragm is opened peripherally, avoiding branches of the phrenic nerve. The incision is made at least 2 to 3 cm from the chest wall to allow an adequate cuff for reapproximation. This incision allows maximum preservation of diaphragmatic function. At the conclusion of the operation, the diaphragm is reapproximated with a series of interrupted 0-silk sutures. Once the incision is completed and maximum exposure achieved, thorough exploration of the chest and abdomen is once again performed. 1 have always preferred to do the intrathoracic portion of the operation first. Because this is the portion of the operation that requires the most manipulation of the heart, I find most patients tolerate this better at the beginning of a long anesthetic, rather than at the conclusion. This is only a personal preference. The dissection is commenced by taking down the inferior pulmonary ligament close to the lung and including the lymph node immediately adjacent to the inferior pulmonary vein. The pleural reflection on the pericardium is entered. The pericardium is the medial boundary of the dissection. The pleura is divided directly over the aorta laterally. It is important to identify and ligate any branches directly coming off the aorta. Failure to do so can create troublesome bleeding, possible injury to the aorta in trying to suture ligate the vessel, or delayed bleeding if cautery alone is used. Delayed bleeding from cauterization of these vessels is one of the main reasons for re-exploration for postoperative bleeding. The esophagus is now encircled and a large Penrose drain passed around the esophagus to aid in traction on the esophagus to facilitate dissection. The right pleura is identified and preserved unless involved by tumor. Preserving the right pleura helps keep the stomach in proper position long-term, but is not essential to preserve. I don t believe routinely removing it adds much, if anything, to the cancer operation. The proximal esophageal dissection is carried out in an en bloc fashion, including any lymph nodes. It is usually possible to remove peribronchial and subcarinal nodes if the dissection is carried out to just below the aortic arch. The periesophageal tissues are divided at the point of proposed anastomosis. This will entail division of the vagus nerves at this point. Thought must be given to preservation of the left recurrent nerve although it is usually just proximal to this area and out of harm s way. I dissect the esophageal hiatus at this point and include part of it if needed for margin or gross involvement. I usually enlarge the hiatus at this point to accommodate the stomach. Failure to enlarge the hiatus can result in partial obstruction. Any vessels encountered are suture-ligated to avoid delayed hemorrhage if cauterization only is used. The left lung can now he reinflated while the abdominal portion of the operation is completed. It is covered with a moist towel to keep it from interfering with the abdominal portion of the procedure. I always start by dissecting the omentum from the transverse colon. I prefer to have a generous portion of omentum available to wrap around the anastomosis. Excess can be easily trimmed. Furthermore, by dissecting at this junction, the right gastroepiploic artery is kept out of harm s way. Once the omenturn is freed from the transverse colon, the right gastroepiploic arcade is identified again and palpated to check for a pulse. The short gastric arteries are sequentially divided and secured with ligatures. Care must be taken to not include any of the stomach in these ligatures to avoid necrosis and fistula. The gastrohepatic ligament is divided. Care must be taken to identify an arterial branch to the left lobe of the liver. In a very small percentage of patients, it is the only arterial source to the left lobe of the liver. If this situation is suspected, the vessel can be temporarily occluded and the liver observed for ischemic changes. If this does occur, this vessel must be carefully preserved. This requires careful skeletonization of the vessel and preservation of the left gastric artery where it usually takes origin. The final step in mobilization of the stomach is to divide the left gastric artery and vein at its origin. I prefer to doubly ligate the artery with at least one suture ligature. All lymph nodes in this area are swept up with the stomach. I usually leave the ligatures long on the stomach side so I can easily identify them and include them when dividing the proximal stomach to ensure complete removal of all lymph nodes in this area. At this point in the operation I usually perform a pyloromyotomy. I prefer this to no drainage procedure at all. I believe a pyloromyotomy provides sufficient drainage and Seems to be associated with less bile reflux and dumping than pyloroplasty. After completion of the pyloromyotomy I always check for mucosal integrity. Any violation of the mucosa should automatically lead to a pyloroplasty. For most left thoracoabdominal esophagectomies, it is unnecessary to mobilize the duodenum because sufficient length of the stomach usually exists for reconstruction. (2 reprinted with permission from Heitmiller RF: Results of standard left thoracoabdominal esophagogastrectomy. Semin Thorac Cardiovasc Surg 4: ,1992.)
6 THOKACOABDOMINAL ESOPHAGECTOMY FOR GE TUMORS 191 Fa -b -B 3 A point of transection of the stomach is identified. The lesser curvature is cleared and care is taken not to devascularize distal to the point of transection. I prefer to use a single horizontal 90-mm-thick tissue stapler. Once it has been approximated and fired, it is left closed so the stomach can be divided immediately next to the stapler to minimize devitalized tissue left with the stomach. The proximal stomach can be controlled with another stapler, clamp, or can be sutured to prevent spillage. The distal stomach margin is clearly identified for the pathologist to avoid any confusion. The stapler on the stomach is now released. Bleeding from the suture line is controlled with sutures or cautery. The staple line is carefully inspected for integrity. If any leaks are present or if it doesn t appear that there are two complete rows of staples, interrupted horizontal mattress sutures are placed to ensure complete integrity of the suture he. If any doubt exists, two layers of running suture can be used. The staple line is inverted by interrupted sutures. A running suture is acceptable, but I believe it deforms the stomach more. One must be careful not to turn too much of the stomach in when reinforcing the stapled suture line. The stomach and attached omentum are now passed through the hiatus to be certain of adequate length and sufficient opening of the hiatus. Special mention should be made of the angle of division of the stomach. I prefer the stapler to be placed perpendicular to the long axis of the stomach. This provides for the best possible configuration of the stomach for anastomosis. If the angle of placement varies much from perpendicular, the stomach can take on a finger-like appearance. The tip of the stomach could become ischemic and make the subsequent anastomosis awkward. The reason I prefer a single application of the horizontal stapler is that I believe it is less prone to leakage than multiple applications of the linear stapler or the 100-cm linear stapler. (3 reprinted with permission from Heitmiller RF: Results of standard left thoracoabdominal esophagogastrectomy. Semin Thorac Cardiovasc Surg 4: , 1992.)
7 192 DOUGLAS J. MATHISEN B I D / E f '\ 4 See legend on opposite page.
8 THORACOAHDOMINAL ESOPHAGECTOMY FOR GE TUMORS Anastoinotic technique. The anastomotic technique deserves special mention. For those individuals involved in esophageal surgery, it is imperative that they develop a technique that is reliable and associated with a very low incidence of leaks. The technique used at the Massachusetts General Hospital was developed by Churchill and Sweet. The technique has changed little over the last 60 years. It is worth noting the quotes from Churchill and Sweet to underscore the emphasis given to this part of the operation. Churchill commented that the mucous membrane sutures are placed with the exactitude and with the degree of tension that we would use in the fine plastic procedures on the lip. Sweet added, we have had no strictures in our cases. Perhaps we have paid unusual attention to the detail of the anastomosis. This anastomosis always requires unusual attention and exactitude. The anastomosis is commenced by scoring the stomach serosa to create a 2-cm circle (A). The circular defect in the stomach should be 2 cm away from the stapled edge of the stomach to avoid Compromise of the blood supply. Individual vessels are identified and ligated with fine silk sutures (A). This minimizes bleeding while the anastomosis is performed, and allows for precise placement of sutures. I frequently mark the stomach with a skin marker and incise the serosa just inside. This helps in identifying the edge of the serosa during placement of the inner layer of sutures. Interrupted horizontal mattress sutures of fine suture material (we use 4-0 silk) are used to construct the back row of the anastomosis (A). It is important to place these sutures 3 to 4 mm from the serosal edge of the stomach button. When these sutures are tied, it may be difficult to identify the edge of the serosa if the sutures are placed too close to the cut edge. For a strong, secure anastomosis, it is imperative that a full thickness suture of the stomach be used for the inner layer. Corner stitches are placed first, and the remaining sutures are evenly spaced between them. The sutures on the stomach involve the seromuscular layers and those on the esophagus, the longitudinal and circular muscle layers. The esophageal sutures should be deep enough to include both the longitudinal and circular muscles of the esophagus. The sutures should not be tied too tightly to avoid necrosis or cutting through the muscle. The esophagus is opened sharply from one corner stitch to the other. The circular button of stomach is removed (B). The inner layer is completed with simple sutures, including just the mucosa of the esophagus and the full thickness of the stomach (C). The knots are on the inside, thereby allowing inversion or turning-in of the mucosa of both the esophagus and stomach. This is accomplished for the entire circumference of the anastomosis (D). A nasogastric tube is placed into the stomach under direct vision before a single Connell stitch is placed for closure of the final opening. Healing of the inverted mucosa is an important feature in preventing leakage, and the location of the knots on the luminal side minimizes foreign body reaction within the actual tissues of the anastomosis. The outer row is completed using horizontal mattress sutures as described for the back row of the outer layer (E). The omentum mobilized with the stomach is placed over the anastomosis anteriorly to provide an additional layer of coverage. The posterior part of the anastomosis lies between the esophagus and the more proximal stomach. A few sutures are placed between the stomach and the mediastinal pleura to avoid tension on the anastomosis when the patient is upright, particularly if the stomach is full. Sutures are also placed between the stomach and the diaphragmatic hiatus to prevent herniation of abdominal contents. Viability of tissues on each edge of the anastomosis is best maintained if trauma is avoided. The edges are never crushed with clamps and, indeed, are handled with forceps as little as possible. Once the first stitch is placed and tied, traction on it permits placement of the next without the need for instrumental grasping of the mucosa. The sutures are tied by positioning the index finger cephalad to the anastomosis, lifting the stomach to the esophagus, and avoiding pulling down on the fixed and more fragde esophagus. This is especially important for the outer layer of the anastomosis because the esophagus lacks a peritoneal surface. A nasogastric tube passed through the anastomosis for a short time avoids distraction at the suture line by a distended stomach. Gentle, periodic irrigation of the tube ensures its patency. Tenlporary gastric decompression more than compensates for any potentially deleterious effect of an intraluminal foreign body lying against the suture line for a short period. The chest and abdomen are irrigated with saline. The stomach is inspected to assure proper alignment, no tension, and no potential sources for herniation. The diaphragm is reapproximated with interrupted 0-silk sutures. The ribs are approximated with absorbable paracostal sutures. The costal arch is reconstructed by one or two heavy absorbable sutures. The remainder of the closure is performed in standard fashion. (4A to 4E reprinted with permission from the Society of Thoracic Surgeons.2)
9 194 DOUGLAS J. MATIIISEN Postoperative Care The nasogastric tube is left in place until flatus is passed and drainage is below 300 to 400 ml in 24 hours. A contrast study is performed on day 5 to 7. I routinely place a jejunostomy to allow enteral nutrition early in the postoperative period. I believe this speeds recovery, allows more gradual resumption of oral intake, and allows patients to return home earlier. The jejunostomy is usually removed at the first postoperative visit. Oral intake with clear liquids can commence once the contrast study has shown anastomotic integrity. I usually maintain patients on liquids plus jejunostomy feedings for 10 days and caution them about distention, hiccups, regurgitation, and other symptoms of gastric distention. If symptoms appear, oral intake is reduced until they have improved. After 10 days, patients are encouraged to begin soft foods and gradually wean jejunostomy feedings. Supra-aortic Technique If it is determined that the anastomosis must be performed proximal to the aortic arch, this can be accomplished by revisions in this approach. The incision should be extended beyond the tip of the scapula halfway between the scapula and the spine. This will allow an incision to be made between the fourth and fifth ribs. This gives excellent exposure to the supraaortic area. The esophagus is mobilized below the aortic arch with sharp and blunt dissection (Fig IA). Great care must be taken with vessels off the under surface of the arch (Fig IA). Great care must be exercised to avoid injury to the Fig I. (A) Dissection under the esophagus requires special attention to vessels directly off the aorta. They should be ligated individually. Great care should also be exercised to avoid injury to the left recurrent laryngeal nerve. (B) Once the esophagus has been fully mobilized, it is delivered posterior to the aortic arch.
10 recurrent laryngeal nerve. The thoracic duct crosses aortic arch and the distal portion of the esophagus the esophagus in the area behind and cephalad to the delivered under the aortic arch (Fig IB). The stomach aortic* arch (Fig 11). If it is determined that the thoracic is advanced over the aortic arch and a two-layered duct is injured, it should be ligated above and below the anastomosis performed as described previously point of injury. The esophagus is mobilized above the (Fig 111). Fig 11. The course of the thoracic duct as it crosses the esophagus in the superior mediastinum above the arch of the aorta. It is easily injured. Particular attention should be directed to this possibility. If continuity has been impaired, ligature should be carried out both above and below the point of injury. (Reprinted with permission from Sweet RH: Thoracic Surgery [ed 21. Philadelphia, PA, Saunders, 1954.) Fig 111. (A) The anastomotic technique is the same as described previously. (B) The stomach is positioned anterior to the aorta.
11 196 Results We have been quite pleased with this technique and continue to use it in selected patients. In properly selected patients with malignant neoplasms of the gastroesophageal junction, it is associated with a very low incidence of local recurrence. I believe it does offer the best opportunity for maximum proximal and distal esophageal and gastric margins. Because of the exposure provided, it allows exact placement of the gastric substitute (avoiding excessive stomach above the diaphragm), proper enlargement of the hiatus to avoid constriction in the stomach, and no tension on the distal stomach and duodenum. We continue to be quite pleased with our anastornotic technique. In 1988 we published a series of 104 consecu- DOUGLAS J. MATHISEN tive esophagectomies without an anastomotic leak and only 5 anastomotic strictures requiring dilation.' REFERENCES 1. Churchill ED, Sweet RH: Transthoracic resection of tumors of the stomach and esophagus. Ann Surg 115: , Mathisen DJ, Grill0 HC, Wilkins EWW, et al: Transthoracic esophagevtomy: A safr approach to carcinoma of the esophagus. Ann Thorac Surg 45: From the General Thoracic Surgical Unit, Massachusetts General Hospital, Boston, MA. Address reprint requests to Douglas J. Mathisen, MD, General Thoracic Surgical Unit, Massachusetts General Hospital, Blake 1570,32 Frult St, Boston, MA Copyright by W.B. Saunders Company /99/0403-OOOl$lO 0010
SETTING Fudan University Shanghai Cancer Center. RESPONSIBLE PARTY Haiquan Chen MD.
 OFFICIAL TITLE A Phase Ⅲ Study of Left Side Thoracotomy Approach (SweetProcedure) Versus Right Side Thoracotomy Plus Midline Laparotomy Approach (Ivor-Lewis Procedure) Esophagectomy in Middle or Lower
OFFICIAL TITLE A Phase Ⅲ Study of Left Side Thoracotomy Approach (SweetProcedure) Versus Right Side Thoracotomy Plus Midline Laparotomy Approach (Ivor-Lewis Procedure) Esophagectomy in Middle or Lower
Limited en bloc Resection of the Gastroesophageal Junction with Isoperistaltic Jejunal Interposition
 22 Limited en bloc Resection of the Gastroesophageal Junction with Isoperistaltic Jejunal Interposition J.R. Izbicki, W.T. Knoefel, D. C. Broering ] Indications Severe dysplasia in the distal esophagus
22 Limited en bloc Resection of the Gastroesophageal Junction with Isoperistaltic Jejunal Interposition J.R. Izbicki, W.T. Knoefel, D. C. Broering ] Indications Severe dysplasia in the distal esophagus
The left thoracoabdominal incision provides excellent
 Left Thoracoabdominal Incision Sudhir Sundaresan The left thoracoabdominal incision provides excellent exposure for operations dealing with the distal esophagus or proximal stomach. It is particularly
Left Thoracoabdominal Incision Sudhir Sundaresan The left thoracoabdominal incision provides excellent exposure for operations dealing with the distal esophagus or proximal stomach. It is particularly
AATS Focus on Thoracic Surgery: Minimally Invasive Esophagectomy: Are We Still Getting Better in 2017?
 AATS Focus on Thoracic Surgery: Mastering Surgical Innovation Las Vegas, NV October 28, 2017 Session VIII: Video Session Minimally Invasive Esophagectomy: Are We Still Getting Better in 2017? James D.
AATS Focus on Thoracic Surgery: Mastering Surgical Innovation Las Vegas, NV October 28, 2017 Session VIII: Video Session Minimally Invasive Esophagectomy: Are We Still Getting Better in 2017? James D.
Minimally Invasive Esophagectomy
 American Association of Thoracic Surgery (AATS) 95 th Annual Meeting Seattle, WA April 29, 2015 General Thoracic Masters of Surgery Video Session Minimally Invasive Esophagectomy James D. Luketich MD,
American Association of Thoracic Surgery (AATS) 95 th Annual Meeting Seattle, WA April 29, 2015 General Thoracic Masters of Surgery Video Session Minimally Invasive Esophagectomy James D. Luketich MD,
1. Epidemiology of Esophageal Cancer 2. Operative Strategies 3. Minimally Invasive Esophagectomy 4. Video
 Minimally Invasive Esophagectomy Guilherme M Campos, MD, FACS Assistant Professor of Surgery Director G.I. Motility Center Director Bariatric Surgery Program University of California San Francisco ESOPHAGEAL
Minimally Invasive Esophagectomy Guilherme M Campos, MD, FACS Assistant Professor of Surgery Director G.I. Motility Center Director Bariatric Surgery Program University of California San Francisco ESOPHAGEAL
Combined Collis-Nissen Reconstruction. of the esophagogastric junction at. Mark B. Orringer, M.D., and Herbert Sloan, M.D.
 Combined Collis-Nissen Reconstruction of the Esophagogastric Junction Mark B. Orringer, M.D., and Herbert Sloan, M.D. ABSTRACT Recent reports have indicated that combined Collis-Belsey reconstruction of
Combined Collis-Nissen Reconstruction of the Esophagogastric Junction Mark B. Orringer, M.D., and Herbert Sloan, M.D. ABSTRACT Recent reports have indicated that combined Collis-Belsey reconstruction of
Uniportal video-assisted thoracic surgery for esophageal cancer
 Surgical Technique on Esophageal Surgery Uniportal video-assisted thoracic surgery for esophageal cancer Hasan F. Batirel Thoracic Surgery Department, Marmara University Hospital, Istanbul, Turkey Correspondence
Surgical Technique on Esophageal Surgery Uniportal video-assisted thoracic surgery for esophageal cancer Hasan F. Batirel Thoracic Surgery Department, Marmara University Hospital, Istanbul, Turkey Correspondence
Parenchyma-sparing lung resections are a potential therapeutic
 Lung Segmentectomy for Patients with Peripheral T1 Lesions Bryan A. Whitson, MD, Rafael S. Andrade, MD, and Michael A. Maddaus, MD Parenchyma-sparing lung resections are a potential therapeutic option
Lung Segmentectomy for Patients with Peripheral T1 Lesions Bryan A. Whitson, MD, Rafael S. Andrade, MD, and Michael A. Maddaus, MD Parenchyma-sparing lung resections are a potential therapeutic option
The left thoracoabdominal and left neck approach to
 Esophagectomy: Left Thoracoabdominal and Left Neck Thomas W. Rice, MD *, The left thoracoabdominal and left neck approach to esophagectomy offers flexibility, versatility, and options. In the western world,
Esophagectomy: Left Thoracoabdominal and Left Neck Thomas W. Rice, MD *, The left thoracoabdominal and left neck approach to esophagectomy offers flexibility, versatility, and options. In the western world,
The Physician as Medical Illustrator
 The Physician as Medical Illustrator Francois Luks Arlet Kurkchubasche Division of Pediatric Surgery Wednesday, December 9, 2015 Week 5 A good picture is worth a 1,000 bad ones How to illustrate an operation
The Physician as Medical Illustrator Francois Luks Arlet Kurkchubasche Division of Pediatric Surgery Wednesday, December 9, 2015 Week 5 A good picture is worth a 1,000 bad ones How to illustrate an operation
Thoracoscopic left upper lobectomy with systematic lymph nodes dissection under left pulmonary artery clamping
 GCTAB Column Thoracoscopic left upper lobectomy with systematic lymph nodes dissection under left pulmonary artery clamping Yi-Nan Dong, Nan Sun, Yi Ren, Liang Zhang, Ji-Jia Li, Yong-Yu Liu Department
GCTAB Column Thoracoscopic left upper lobectomy with systematic lymph nodes dissection under left pulmonary artery clamping Yi-Nan Dong, Nan Sun, Yi Ren, Liang Zhang, Ji-Jia Li, Yong-Yu Liu Department
Laparoscopic and Thoracoscopic Ivor Lewis Esophagectomy With Colonic Interposition
 HOW TO DO IT Laparoscopic and Thoracoscopic Ivor Lewis Esophagectomy With Colonic Interposition Ninh T. Nguyen, MD, FACS, Marcelo Hinojosa, MD, Christine Fayad, BS, James Gray, BS, Zuri Murrell, MD, and
HOW TO DO IT Laparoscopic and Thoracoscopic Ivor Lewis Esophagectomy With Colonic Interposition Ninh T. Nguyen, MD, FACS, Marcelo Hinojosa, MD, Christine Fayad, BS, James Gray, BS, Zuri Murrell, MD, and
A video demonstration of the Li s anastomosis the key part of the non-tube no fasting fast track program for resectable esophageal carcinoma
 Surgical Technique A video demonstration of the the key part of the non-tube no fasting fast track program for resectable esophageal carcinoma Yan Zheng*, Yin Li*, Zongfei Wang, Haibo Sun, Ruixiang Zhang
Surgical Technique A video demonstration of the the key part of the non-tube no fasting fast track program for resectable esophageal carcinoma Yan Zheng*, Yin Li*, Zongfei Wang, Haibo Sun, Ruixiang Zhang
FIG The inferior and posterior peritoneal reflection is easily
 PSOAS HITCH, BOARI FLAP, AND COMBINATION OF PSOAS 7 HITCH AND BOARI FLAP The psoas hitch procedure, Boari flap, and transureteroureterostomy are useful operative procedures for reestablishing continuity
PSOAS HITCH, BOARI FLAP, AND COMBINATION OF PSOAS 7 HITCH AND BOARI FLAP The psoas hitch procedure, Boari flap, and transureteroureterostomy are useful operative procedures for reestablishing continuity
Alexander C Vlantis. Selective Neck Dissection 33
 05 Modified Radical Neck Dissection Type II Alexander C Vlantis Selective Neck Dissection 33 Modified Radical Neck Dissection Type II INCISION Various incisions can be used for a neck dissection. The incision
05 Modified Radical Neck Dissection Type II Alexander C Vlantis Selective Neck Dissection 33 Modified Radical Neck Dissection Type II INCISION Various incisions can be used for a neck dissection. The incision
STERNUM. Lies in the midline of the anterior chest wall It is a flat bone Divides into three parts:
 STERNUM Lies in the midline of the anterior chest wall It is a flat bone Divides into three parts: 1-Manubrium sterni 2-Body of the sternum 3- Xiphoid process The body of the sternum articulates above
STERNUM Lies in the midline of the anterior chest wall It is a flat bone Divides into three parts: 1-Manubrium sterni 2-Body of the sternum 3- Xiphoid process The body of the sternum articulates above
Minimally Invasive Esophagectomy- Valuable. Jayer Chung, MD University of Colorado Health Sciences Center December 11, 2006
 Minimally Invasive Esophagectomy- Valuable Jayer Chung, MD University of Colorado Health Sciences Center December 11, 2006 Overview Esophageal carcinoma What is minimally invasive esophagectomy (MIE)?
Minimally Invasive Esophagectomy- Valuable Jayer Chung, MD University of Colorado Health Sciences Center December 11, 2006 Overview Esophageal carcinoma What is minimally invasive esophagectomy (MIE)?
THE THORACIC WALL. Boundaries Posteriorly by the thoracic part of the vertebral column. Anteriorly by the sternum and costal cartilages
 THE THORACIC WALL Boundaries Posteriorly by the thoracic part of the vertebral column Anteriorly by the sternum and costal cartilages Laterally by the ribs and intercostal spaces Superiorly by the suprapleural
THE THORACIC WALL Boundaries Posteriorly by the thoracic part of the vertebral column Anteriorly by the sternum and costal cartilages Laterally by the ribs and intercostal spaces Superiorly by the suprapleural
Carinal resections. Leonidas Tapias, Michael Lanuti. Clinical vignette
 Masters of Cardiothoracic Surgery Carinal resections Leonidas Tapias, Michael Lanuti Division of Thoracic Surgery, Massachusetts General Hospital, Boston, MA, USA Correspondence to: Michael Lanuti, MD.
Masters of Cardiothoracic Surgery Carinal resections Leonidas Tapias, Michael Lanuti Division of Thoracic Surgery, Massachusetts General Hospital, Boston, MA, USA Correspondence to: Michael Lanuti, MD.
The Learning Curve for Minimally Invasive Esophagectomy
 The Learning Curve for Minimally Invasive Esophagectomy AATS Focus on Thoracic Surgery Mastering Surgical Innovation Las Vegas Nevada Oct. 27-28 2017 Scott J Swanson, M.D. Professor of Surgery Harvard
The Learning Curve for Minimally Invasive Esophagectomy AATS Focus on Thoracic Surgery Mastering Surgical Innovation Las Vegas Nevada Oct. 27-28 2017 Scott J Swanson, M.D. Professor of Surgery Harvard
Robotic-assisted McKeown esophagectomy
 Case Report Page 1 of 8 Robotic-assisted McKeown esophagectomy Dingpei Han, Su Yang, Wei Guo, Runsen Jin, Yajie Zhang, Xingshi Chen, Han Wu, Hailei Du, Kai Chen, Jie Xiang, Hecheng Li Department of Thoracic
Case Report Page 1 of 8 Robotic-assisted McKeown esophagectomy Dingpei Han, Su Yang, Wei Guo, Runsen Jin, Yajie Zhang, Xingshi Chen, Han Wu, Hailei Du, Kai Chen, Jie Xiang, Hecheng Li Department of Thoracic
The posterolateral thoracotomy is still probably the
 Posterolateral Thoracotomy Jean Deslauriers and Reza John Mehran The posterolateral thoracotomy is still probably the most commonly used incision in general thoracic surgery. It provides not only excellent
Posterolateral Thoracotomy Jean Deslauriers and Reza John Mehran The posterolateral thoracotomy is still probably the most commonly used incision in general thoracic surgery. It provides not only excellent
The Whipple Operation Illustrations
 The Whipple Operation Illustrations Fig. 1. Illustration of the sixstep pancreaticoduodenectomy (Whipple operation) as described in a number of recent text books by Dr. Evans. The operation is divided
The Whipple Operation Illustrations Fig. 1. Illustration of the sixstep pancreaticoduodenectomy (Whipple operation) as described in a number of recent text books by Dr. Evans. The operation is divided
Minimally Invasive Esophagectomy
 Minimally Invasive Esophagectomy M A R K B E R R Y, M D A S S O C I AT E P R O F E S S O R D E PA R T M E N T OF C A R D I O T H O R A C I C S U R G E R Y S TA N F O R D U N I V E R S I T Y S E P T E M
Minimally Invasive Esophagectomy M A R K B E R R Y, M D A S S O C I AT E P R O F E S S O R D E PA R T M E N T OF C A R D I O T H O R A C I C S U R G E R Y S TA N F O R D U N I V E R S I T Y S E P T E M
Achalasia is a primary esophageal motility disorder of unknown
 Laparoscopic Heller Myotomy for Achalasia Andrew Pierre, MD, MSc Achalasia is a primary esophageal motility disorder of unknown etiology. Pathologically, it is characterized by loss of ganglion cells in
Laparoscopic Heller Myotomy for Achalasia Andrew Pierre, MD, MSc Achalasia is a primary esophageal motility disorder of unknown etiology. Pathologically, it is characterized by loss of ganglion cells in
Tracheal stenosis in infants and children is typically characterized
 Slide Tracheoplasty for Congenital Tracheal Stenosis Peter B. Manning, MD Tracheal stenosis in infants and children is typically characterized by the presence of complete cartilaginous tracheal rings and
Slide Tracheoplasty for Congenital Tracheal Stenosis Peter B. Manning, MD Tracheal stenosis in infants and children is typically characterized by the presence of complete cartilaginous tracheal rings and
Lung cancer or primary malignant tumors of the mediastinum
 Technique of Superior Vena Cava Resection for Lung Carcinomas David R. Jones, MD Division of Thoracic and Cardiovascular Surgery, Department of Surgery, University of Virginia School of Medicine, Charlottesville,
Technique of Superior Vena Cava Resection for Lung Carcinomas David R. Jones, MD Division of Thoracic and Cardiovascular Surgery, Department of Surgery, University of Virginia School of Medicine, Charlottesville,
Medical Illustration PLME 0400
 Introduction to Medical Illustration PLME 0400 October 17 From sketch to narrative From Sketch to Sketch: Point of view Degree of detail Visible and invisble parts Landmarks : Plan your moves The IKEA
Introduction to Medical Illustration PLME 0400 October 17 From sketch to narrative From Sketch to Sketch: Point of view Degree of detail Visible and invisble parts Landmarks : Plan your moves The IKEA
Robotic-assisted right upper lobectomy
 Robotic Thoracic Surgery Column Robotic-assisted right upper lobectomy Shiguang Xu, Tong Wang, Wei Xu, Xingchi Liu, Bo Li, Shumin Wang Department of Thoracic Surgery, Northern Hospital, Shenyang 110015,
Robotic Thoracic Surgery Column Robotic-assisted right upper lobectomy Shiguang Xu, Tong Wang, Wei Xu, Xingchi Liu, Bo Li, Shumin Wang Department of Thoracic Surgery, Northern Hospital, Shenyang 110015,
Saphenous Vein Autograft Replacement
 Saphenous Vein Autograft Replacement of Severe Segmental Coronary Artery Occlusion Operative Technique Rene G. Favaloro, M.D. D irect operation on the coronary artery has been performed in 180 patients
Saphenous Vein Autograft Replacement of Severe Segmental Coronary Artery Occlusion Operative Technique Rene G. Favaloro, M.D. D irect operation on the coronary artery has been performed in 180 patients
Traditionally, surgical antireflux therapy has been
 Laparoscopic Fundoplication Mary Maish, MD and Jeffrey A. Hagen, MD Traditionally, surgical antireflux therapy has been reserved for patients with complicated gastroesophageal reflux disease. The introduction
Laparoscopic Fundoplication Mary Maish, MD and Jeffrey A. Hagen, MD Traditionally, surgical antireflux therapy has been reserved for patients with complicated gastroesophageal reflux disease. The introduction
It passes through the diaphragm at the level of the 10th thoracic vertebra to join the stomach
 The esophagus is a tubular structure (muscular, collapsible tube ) about 10 in. (25 cm) long that is continuous above with the laryngeal part of the pharynx opposite the sixth cervical vertebra The esophagus
The esophagus is a tubular structure (muscular, collapsible tube ) about 10 in. (25 cm) long that is continuous above with the laryngeal part of the pharynx opposite the sixth cervical vertebra The esophagus
Anatomy of the Thorax
 Anatomy of the Thorax A) THE THORACIC WALL Boundaries Posteriorly by the thoracic part of the vertebral column Anteriorly by the sternum and costal cartilages Laterally by the ribs and intercostal spaces
Anatomy of the Thorax A) THE THORACIC WALL Boundaries Posteriorly by the thoracic part of the vertebral column Anteriorly by the sternum and costal cartilages Laterally by the ribs and intercostal spaces
The Thoracic wall including the diaphragm. Prof Oluwadiya KS
 The Thoracic wall including the diaphragm Prof Oluwadiya KS www.oluwadiya.com Components of the thoracic wall Skin Superficial fascia Chest wall muscles (see upper limb slides) Skeletal framework Intercostal
The Thoracic wall including the diaphragm Prof Oluwadiya KS www.oluwadiya.com Components of the thoracic wall Skin Superficial fascia Chest wall muscles (see upper limb slides) Skeletal framework Intercostal
Minimally invasive esophagectomy (MIE) has increasingly
 Minimally Invasive Ivor Lewis Esophagectomy David R. Jones, MD Minimally invasive esophagectomy (MIE) has increasingly been adopted by thoracic surgeons in both academic and community-based practices as
Minimally Invasive Ivor Lewis Esophagectomy David R. Jones, MD Minimally invasive esophagectomy (MIE) has increasingly been adopted by thoracic surgeons in both academic and community-based practices as
Emergency Approach to the Subclavian and Innominate Vessels
 Emergency Approach to the Subclavian and Innominate Vessels Joseph J. Amato, M.D., Robert M. Vanecko, M.D., See Tao Yao, M.D., and Milton Weinberg, Jr., M.D. T he operative approach to an acutely injured
Emergency Approach to the Subclavian and Innominate Vessels Joseph J. Amato, M.D., Robert M. Vanecko, M.D., See Tao Yao, M.D., and Milton Weinberg, Jr., M.D. T he operative approach to an acutely injured
Esophageal Perforation
 Esophageal Perforation Dr. Carmine Simone Thoracic Surgeon, Division of General Surgery Head, Division of Critical Care May 15, 2006 Overview Case presentation Radiology Pre-operative management Operative
Esophageal Perforation Dr. Carmine Simone Thoracic Surgeon, Division of General Surgery Head, Division of Critical Care May 15, 2006 Overview Case presentation Radiology Pre-operative management Operative
Aliu Sanni MD SUNY Downstate Medical Center August 16, 2012
 Aliu Sanni MD SUNY Downstate Medical Center August 16, 2012 Case Presentation 60yr old AAF with PMH of CAD s/p PCI 1983, CVA, GERD, HTN presented with retrosternal chest pain on 06/12 Associated dysphagia
Aliu Sanni MD SUNY Downstate Medical Center August 16, 2012 Case Presentation 60yr old AAF with PMH of CAD s/p PCI 1983, CVA, GERD, HTN presented with retrosternal chest pain on 06/12 Associated dysphagia
Placing PEG and Jejunostomy Tubes in Dogs and Cats
 Placing PEG and Jejunostomy Tubes in Dogs and Cats I. Gastrostomy tube A. Percutaneous Endoscopic Gastrostomy (PEG) tube placement Supplies for PEG tube placement: Supplies and equipment for general anesthesia
Placing PEG and Jejunostomy Tubes in Dogs and Cats I. Gastrostomy tube A. Percutaneous Endoscopic Gastrostomy (PEG) tube placement Supplies for PEG tube placement: Supplies and equipment for general anesthesia
The abdominal Esophagus, Stomach and the Duodenum. Prof. Oluwadiya KS
 The abdominal Esophagus, Stomach and the Duodenum Prof. Oluwadiya KS www.oluwadiya.com Viscera of the abdomen Abdominal esophagus: Terminal part of the esophagus The stomach Intestines: Small and Large
The abdominal Esophagus, Stomach and the Duodenum Prof. Oluwadiya KS www.oluwadiya.com Viscera of the abdomen Abdominal esophagus: Terminal part of the esophagus The stomach Intestines: Small and Large
Large veins of the thorax Brachiocephalic veins
 Large veins of the thorax Brachiocephalic veins Right brachiocephalic vein: formed at the root of the neck by the union of the right subclavian & the right internal jugular veins. Left brachiocephalic
Large veins of the thorax Brachiocephalic veins Right brachiocephalic vein: formed at the root of the neck by the union of the right subclavian & the right internal jugular veins. Left brachiocephalic
The Combined Collis-Nissen Operation: Early Assessment of Reflwx Control
 ORIGINAL ARTICLES The Combined Collis-Nissen Operation: Early Assessment of Reflwx Control Mark B. Orringer, M.D., and Jay S. Orringer, M.D. ABSTRACT This report summarizes the clinical experience with
ORIGINAL ARTICLES The Combined Collis-Nissen Operation: Early Assessment of Reflwx Control Mark B. Orringer, M.D., and Jay S. Orringer, M.D. ABSTRACT This report summarizes the clinical experience with
Oesophageal Cancer: The Image after Surgery
 Oesophageal Cancer: The Image after Surgery Poster No.: C-2253 Congress: ECR 2014 Type: Educational Exhibit Authors: A. Loureiro, N. V. V. B. Marques, M. Palmeiro, P. Pereira, 1 1 1 1 2 1 1 2 1 R. Gil,
Oesophageal Cancer: The Image after Surgery Poster No.: C-2253 Congress: ECR 2014 Type: Educational Exhibit Authors: A. Loureiro, N. V. V. B. Marques, M. Palmeiro, P. Pereira, 1 1 1 1 2 1 1 2 1 R. Gil,
Esophageal anastomotic techniques
 Esophageal anastomotic techniques Raphael Bueno, MD, Brigham and Women s Hospital Slide 1 Good afternoon, I would like thank the association and Dr and Dr for inviting me to speak today. Slide 2 I am trying
Esophageal anastomotic techniques Raphael Bueno, MD, Brigham and Women s Hospital Slide 1 Good afternoon, I would like thank the association and Dr and Dr for inviting me to speak today. Slide 2 I am trying
Oesophageal Cancer: The Image after Surgery
 Oesophageal Cancer: The Image after Surgery Poster No.: C-2253 Congress: ECR 2014 Type: Educational Exhibit Authors: A. Loureiro, N. V. V. B. Marques, M. Palmeiro, P. Pereira, 1 1 1 1 2 1 1 2 1 R. Gil,
Oesophageal Cancer: The Image after Surgery Poster No.: C-2253 Congress: ECR 2014 Type: Educational Exhibit Authors: A. Loureiro, N. V. V. B. Marques, M. Palmeiro, P. Pereira, 1 1 1 1 2 1 1 2 1 R. Gil,
Minimally invasive lobectomy and thoracic lymph node
 Minimally Invasive Segmentectomy Joshua R. Sonett, MD, FACS Minimally invasive lobectomy and thoracic lymph node dissection is now widely established as a safe, anatomic, and oncologically sound procedure
Minimally Invasive Segmentectomy Joshua R. Sonett, MD, FACS Minimally invasive lobectomy and thoracic lymph node dissection is now widely established as a safe, anatomic, and oncologically sound procedure
TRACHEOSTOMY. Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion
 TRACHEOSTOMY Definition Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion Indications for tracheostomy 1-upper airway obstruction with stridor, air hunger,
TRACHEOSTOMY Definition Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion Indications for tracheostomy 1-upper airway obstruction with stridor, air hunger,
ANATOMY OF THE PLEURA. Dr Oluwadiya KS
 ANATOMY OF THE PLEURA Dr Oluwadiya KS www.oluwadiya.sitesled.com Introduction The thoracic cavity is divided mainly into: Right pleural cavity Mediastinum Left Pleural cavity Pleural cavity The pleural
ANATOMY OF THE PLEURA Dr Oluwadiya KS www.oluwadiya.sitesled.com Introduction The thoracic cavity is divided mainly into: Right pleural cavity Mediastinum Left Pleural cavity Pleural cavity The pleural
Anatomy of thoracic wall
 Anatomy of thoracic wall Topographic Anatomy of the Thorax 1 Bones of Thoracic wall ribs 1-7"true" ribs -those which attach directly to the sternum true ribs actually attach to the sternum by means of
Anatomy of thoracic wall Topographic Anatomy of the Thorax 1 Bones of Thoracic wall ribs 1-7"true" ribs -those which attach directly to the sternum true ribs actually attach to the sternum by means of
BY DR NOMAN ULLAH WAZIR
 BY DR NOMAN ULLAH WAZIR The stomach (from ancient Greek word stomachos, stoma means mouth) is a muscular, hollow and the most dilated part of the GIT. It starts from the point where esophagus ends. It
BY DR NOMAN ULLAH WAZIR The stomach (from ancient Greek word stomachos, stoma means mouth) is a muscular, hollow and the most dilated part of the GIT. It starts from the point where esophagus ends. It
THE DESCENDING THORACIC AORTA
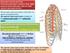 Intercostal Arteries and Veins Each intercostal space contains a large single posterior intercostal artery and two small anterior intercostal arteries. The anterior intercostal arteries of the lower spaces
Intercostal Arteries and Veins Each intercostal space contains a large single posterior intercostal artery and two small anterior intercostal arteries. The anterior intercostal arteries of the lower spaces
ORAL CAVITY, ESOPHAGUS AND STOMACH
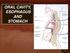 ORAL CAVITY, ESOPHAGUS AND STOMACH 1 OBJECTIVES By the end of the lecture you should be able to: Describe the anatomy the oral cavity, (boundaries, parts, nerve supply). Describe the anatomy of the palate,
ORAL CAVITY, ESOPHAGUS AND STOMACH 1 OBJECTIVES By the end of the lecture you should be able to: Describe the anatomy the oral cavity, (boundaries, parts, nerve supply). Describe the anatomy of the palate,
Transfemoral Amputation
 Transfemoral Amputation Pre-Op: 42 year old male who sustained severe injuries in a motorcycle accident. Note: he is a previous renal transplant recipient and is on immunosuppressive treatments. His injuries
Transfemoral Amputation Pre-Op: 42 year old male who sustained severe injuries in a motorcycle accident. Note: he is a previous renal transplant recipient and is on immunosuppressive treatments. His injuries
Sir Clement Price Thomas performed the first sleeve lobectomy
 Parenchymal-Sparing Procedures in Lung Cancer: Sleeve Resection of the Lung for Proximal Lesions Simon Ashiku, MD, and Malcolm M. DeCamp, Jr., MD Sir Clement Price Thomas performed the first sleeve lobectomy
Parenchymal-Sparing Procedures in Lung Cancer: Sleeve Resection of the Lung for Proximal Lesions Simon Ashiku, MD, and Malcolm M. DeCamp, Jr., MD Sir Clement Price Thomas performed the first sleeve lobectomy
Hiatal Hernias and Barrett s esophagus. Dr Sajida Ahad Mercy General Surgery
 Hiatal Hernias and Barrett s esophagus Dr Sajida Ahad Mercy General Surgery Objectives Identify the use of different diagnostic modalities for hiatal hernias List the different types of hiatal hernias
Hiatal Hernias and Barrett s esophagus Dr Sajida Ahad Mercy General Surgery Objectives Identify the use of different diagnostic modalities for hiatal hernias List the different types of hiatal hernias
Totally thoracoscopic left upper lobe tri-segmentectomy
 Masters of Cardiothoracic Surgery Totally thoracoscopic left upper lobe tri-segmentectomy Dominique Gossot Thoracic Department, Institut Mutualiste Montsouris, Paris, France Correspondence to: Dominique
Masters of Cardiothoracic Surgery Totally thoracoscopic left upper lobe tri-segmentectomy Dominique Gossot Thoracic Department, Institut Mutualiste Montsouris, Paris, France Correspondence to: Dominique
Accessory Glands of Digestive System
 Accessory Glands of Digestive System The liver The liver is soft and pliable and occupies the upper part of the abdominal cavity just beneath the diaphragm. The greater part of the liver is situated under
Accessory Glands of Digestive System The liver The liver is soft and pliable and occupies the upper part of the abdominal cavity just beneath the diaphragm. The greater part of the liver is situated under
Transthoracic Esophagectom : A Safe Approach to Carcinoma of Je Esophagus
 Transthoracic Esophagectom : A Safe Approach to Carcinoma of Je Esophagus Douglas J. Mathisen, M.D., Hermes C. Grillo, M.D., Earle W. Wilkins, Jr., M.D., Ashby C. Moncure, M.D., and Alan D. Hilgenberg,
Transthoracic Esophagectom : A Safe Approach to Carcinoma of Je Esophagus Douglas J. Mathisen, M.D., Hermes C. Grillo, M.D., Earle W. Wilkins, Jr., M.D., Ashby C. Moncure, M.D., and Alan D. Hilgenberg,
GIT RADIOLOGY. Water-soluble contrast media (e.g. gastrograffin) are the other available agents.which doesn t cause inflammatory peritonitis..
 GIT RADIOLOGY Imaging techniques-general principles: Contrast examinations: Barium sulphate is the best contrast for GIT (with good mucosal coating & excellent opacification & being inert); but is contraindicated
GIT RADIOLOGY Imaging techniques-general principles: Contrast examinations: Barium sulphate is the best contrast for GIT (with good mucosal coating & excellent opacification & being inert); but is contraindicated
Transfemoral Amputation
 Transfemoral Amputation Preop This 26 year old male sustained a gunshot wound to the left thigh. He was treated emergently with revascularization and fasciotomies. He was transferred to our regional trauma
Transfemoral Amputation Preop This 26 year old male sustained a gunshot wound to the left thigh. He was treated emergently with revascularization and fasciotomies. He was transferred to our regional trauma
Diaphragm and intercostal muscles. Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology
 Diaphragm and intercostal muscles Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Skeletal System Adult Human contains 206 Bones 2 parts: Axial skeleton (axis): Skull, Vertebral column,
Diaphragm and intercostal muscles Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Skeletal System Adult Human contains 206 Bones 2 parts: Axial skeleton (axis): Skull, Vertebral column,
Colorectal procedure guide
 Colorectal procedure guide Illustrations by Lisa Clark Biodesign ADVANCED TISSUE REPAIR cookmedical.com 2 INDEX Anal fistula repair Using the Biodesign plug with no button.... 4 Anal fistula repair Using
Colorectal procedure guide Illustrations by Lisa Clark Biodesign ADVANCED TISSUE REPAIR cookmedical.com 2 INDEX Anal fistula repair Using the Biodesign plug with no button.... 4 Anal fistula repair Using
Gastric transposition in infants and children
 DOI 10.1007/s00383-010-2736-9 REVIEW ARTICLE Gastric transposition in infants and children Robert A. Cowles Arnold G. Coran Accepted: 6 September 2010 Ó Springer-Verlag 2010 Abstract The loss of esophageal
DOI 10.1007/s00383-010-2736-9 REVIEW ARTICLE Gastric transposition in infants and children Robert A. Cowles Arnold G. Coran Accepted: 6 September 2010 Ó Springer-Verlag 2010 Abstract The loss of esophageal
THE SURGEON S LIBRARY
 THE SURGEON S LIBRARY THE HISTORY AND SURGICAL ANATOMY OF THE VAGUS NERVE Lee J. Skandalakis, M.D., Chicago, Illinois, Stephen W. Gray, PH.D., and John E. Skandalakis, M.D., PH.D., F.A.C.S., Atlanta, Georgia
THE SURGEON S LIBRARY THE HISTORY AND SURGICAL ANATOMY OF THE VAGUS NERVE Lee J. Skandalakis, M.D., Chicago, Illinois, Stephen W. Gray, PH.D., and John E. Skandalakis, M.D., PH.D., F.A.C.S., Atlanta, Georgia
Robotic-assisted right inferior lobectomy
 Robotic Thoracic Surgery Column Page 1 of 6 Robotic-assisted right inferior lobectomy Shiguang Xu, Tong Wang, Wei Xu, Xingchi Liu, Bo Li, Shumin Wang Department of Thoracic Surgery, Northern Hospital,
Robotic Thoracic Surgery Column Page 1 of 6 Robotic-assisted right inferior lobectomy Shiguang Xu, Tong Wang, Wei Xu, Xingchi Liu, Bo Li, Shumin Wang Department of Thoracic Surgery, Northern Hospital,
AND TECHNIC. GEORGE CRILE, Jr., M.D. Division of Surgery
 SUBDIAPHRAGMATIC VAGOTOMY; AND TECHNIC INDICATIONS GEORGE CRILE, Jr., M.D. Division of Surgery The principle of vagotomy as described by Dragstedt 1 has been widely accepted in the treatment of peptic
SUBDIAPHRAGMATIC VAGOTOMY; AND TECHNIC INDICATIONS GEORGE CRILE, Jr., M.D. Division of Surgery The principle of vagotomy as described by Dragstedt 1 has been widely accepted in the treatment of peptic
Block 3: DISSECTION 2 CELIAC TRUNK, JEJUNUM/ILEUM, LARGE INTESTINE, DUODENUM, PANCREAS, PORTAL VEIN; MOBILIZATION OF THE LIVER
 1 Block 3: DISSECTION 2 CELIAC TRUNK, JEJUNUM/ILEUM, LARGE INTESTINE, DUODENUM, PANCREAS, PORTAL VEIN; MOBILIZATION OF THE LIVER Attempt to complete as much as you can of the dissection explained in the
1 Block 3: DISSECTION 2 CELIAC TRUNK, JEJUNUM/ILEUM, LARGE INTESTINE, DUODENUM, PANCREAS, PORTAL VEIN; MOBILIZATION OF THE LIVER Attempt to complete as much as you can of the dissection explained in the
Anastomotic Complications after Esophagectomy. Bryan Meyers, MD MPH Thoracic Surgery Washington University School of Medicine
 Anastomotic Complications after Esophagectomy Bryan Meyers, MD MPH Thoracic Surgery Washington University School of Medicine Use of Stomach as Conduit Simplest choice after esophagectomy Single anastomosis
Anastomotic Complications after Esophagectomy Bryan Meyers, MD MPH Thoracic Surgery Washington University School of Medicine Use of Stomach as Conduit Simplest choice after esophagectomy Single anastomosis
Dr. Weyrich G07: Superior and Posterior Mediastina. Reading: 1. Gray s Anatomy for Students, chapter 3
 Dr. Weyrich G07: Superior and Posterior Mediastina Reading: 1. Gray s Anatomy for Students, chapter 3 Objectives: 1. Subdivisions of mediastinum 2. Structures in Superior mediastinum 3. Structures in Posterior
Dr. Weyrich G07: Superior and Posterior Mediastina Reading: 1. Gray s Anatomy for Students, chapter 3 Objectives: 1. Subdivisions of mediastinum 2. Structures in Superior mediastinum 3. Structures in Posterior
Right lung. -fissures:
 -Right lung is shorter and wider because it is compressed by the right copula of the diaphragm by the live.. 2 fissure, 3 lobes.. hilum : 2 bronchi ( ep-arterial, hyp-arterial ), one artery mediastinal
-Right lung is shorter and wider because it is compressed by the right copula of the diaphragm by the live.. 2 fissure, 3 lobes.. hilum : 2 bronchi ( ep-arterial, hyp-arterial ), one artery mediastinal
Mediastinum It is a thick movable partition between the two pleural sacs & lungs. It contains all the structures which lie
 Dr Jamila EL medany OBJECTIVES At the end of the lecture, students should be able to: Define the Mediastinum. Differentiate between the divisions of the mediastinum. List the boundaries and contents of
Dr Jamila EL medany OBJECTIVES At the end of the lecture, students should be able to: Define the Mediastinum. Differentiate between the divisions of the mediastinum. List the boundaries and contents of
DESCRIPTION: This is the part of the trunk, which is located between the root of the neck and the superior border of the abdominal region.
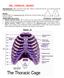 1 THE THORACIC REGION DESCRIPTION: This is the part of the trunk, which is located between the root of the neck and the superior border of the abdominal region. SHAPE : T It has the shape of a truncated
1 THE THORACIC REGION DESCRIPTION: This is the part of the trunk, which is located between the root of the neck and the superior border of the abdominal region. SHAPE : T It has the shape of a truncated
Cancer of Esophagus and Esophagogastric Junction: Analysis of Results of 1,025 Resections after 5 to 20 Years
 Cancer of Esophagus and Esophagogastric Junction: Analysis of Results of 1,025 Resections after 5 to 20 Years Yun Kan Lu, M.D., Yueh Min Li, M.D., and Yue Zhi Gu, M.D. ABSTRACT Resection was carried out
Cancer of Esophagus and Esophagogastric Junction: Analysis of Results of 1,025 Resections after 5 to 20 Years Yun Kan Lu, M.D., Yueh Min Li, M.D., and Yue Zhi Gu, M.D. ABSTRACT Resection was carried out
Tubularized stomach is the preferred choice for esophageal
 Use of Supercharged Jejunal Flap for Esophageal Reconstruction David C. Rice, MB, BCh, FRCSI, and Peirong Yu, MD, MS, FACS Tubularized stomach is the preferred choice for esophageal reconstruction following
Use of Supercharged Jejunal Flap for Esophageal Reconstruction David C. Rice, MB, BCh, FRCSI, and Peirong Yu, MD, MS, FACS Tubularized stomach is the preferred choice for esophageal reconstruction following
The External Anatomy of the Lungs. Prof Oluwadiya KS
 The External Anatomy of the Lungs Prof Oluwadiya KS www.oluwadiya.com Introduction The lungs are the vital organs of respiration Their main function is to oxygenate the blood by bringing inspired air into
The External Anatomy of the Lungs Prof Oluwadiya KS www.oluwadiya.com Introduction The lungs are the vital organs of respiration Their main function is to oxygenate the blood by bringing inspired air into
Esophagogastrostomy in the Treatment of Carcinoma of the Distal Two-Thirds of the Esophagus
 Esophagogastrostomy in the Treatment of Carcinoma of the Distal Two-Thirds of the Esophagus Clinical Experience and Operative Methods R. Darryl Fisher, M.D., Robert K. Brawley, M.D., and Richard F. Kieffer,
Esophagogastrostomy in the Treatment of Carcinoma of the Distal Two-Thirds of the Esophagus Clinical Experience and Operative Methods R. Darryl Fisher, M.D., Robert K. Brawley, M.D., and Richard F. Kieffer,
RECONSTRUCTION OF THE CARDIA AND FUNDUS OF THE STOMACH
 Thorax (1956), 11, 275. RECONSTRUCTION OF THE CARDIA AND FUNDUS OF THE STOMACH BY From tile United Leeds Hospitals (RECEIVED FOR PUBLICATION SEPTEMBER 15, 1956) This is a preliminary report describing
Thorax (1956), 11, 275. RECONSTRUCTION OF THE CARDIA AND FUNDUS OF THE STOMACH BY From tile United Leeds Hospitals (RECEIVED FOR PUBLICATION SEPTEMBER 15, 1956) This is a preliminary report describing
Transthoracic esophagectomy and an intrathoracic esophagogastric
 General Thoracic Surgery Transhiatal Esophagectomy without Thoracotomy Mark B. Orringer, MD Transthoracic esophagectomy and an intrathoracic esophagogastric anastomosis was the standard surgical approach
General Thoracic Surgery Transhiatal Esophagectomy without Thoracotomy Mark B. Orringer, MD Transthoracic esophagectomy and an intrathoracic esophagogastric anastomosis was the standard surgical approach
Syllabus: 6 pages (Page 6 lists corresponding figures for Grant's Atlas 11 th & 12 th Eds.)
 PLEURAL CAVITY AND LUNGS Dr. Milton M. Sholley SELF STUDY RESOURCES Essential Clinical Anatomy 3 rd ed. (ECA): pp. 70 81 Syllabus: 6 pages (Page 6 lists corresponding figures for Grant's Atlas 11 th &
PLEURAL CAVITY AND LUNGS Dr. Milton M. Sholley SELF STUDY RESOURCES Essential Clinical Anatomy 3 rd ed. (ECA): pp. 70 81 Syllabus: 6 pages (Page 6 lists corresponding figures for Grant's Atlas 11 th &
Nissen Fundoplication
 Nissen Fundoplication By Donna Weldon Nissen fundoplication is a surgical procedure used to treat gastroesophageal reflux disease, or GERD, and hiatus hernias. For GERD, is it usually performed when medical
Nissen Fundoplication By Donna Weldon Nissen fundoplication is a surgical procedure used to treat gastroesophageal reflux disease, or GERD, and hiatus hernias. For GERD, is it usually performed when medical
Alexander C Vlantis. Total Laryngectomy 57
 07 Total Laryngectomy Alexander C Vlantis Total Laryngectomy 57 Total Laryngectomy STEP 1 INCISION AND POSITION OF STOMA A superiorly based apron flap incision is marked with the horizontal limb placed
07 Total Laryngectomy Alexander C Vlantis Total Laryngectomy 57 Total Laryngectomy STEP 1 INCISION AND POSITION OF STOMA A superiorly based apron flap incision is marked with the horizontal limb placed
Chapter 5: Other mediastinal structures. The Large Arteries. The Aorta. Ascending aorta
 Chapter 5: Other mediastinal structures The Large Arteries The Aorta The aorta is the main arterial trunk of the systemic circulation and in the healthy state its wall contain a large amount of yellow
Chapter 5: Other mediastinal structures The Large Arteries The Aorta The aorta is the main arterial trunk of the systemic circulation and in the healthy state its wall contain a large amount of yellow
Gastrointestinal Tract. Anatomy of GI Tract. Anatomy of GI Tract. (Effective February 2007) (1%-5%)
 Gastrointestinal Tract (Effective February 2007) (1%-5%) Anatomy of GI Tract Esophagus bulls-eye or target EG junction seen on sagittal scan posterior to left lobe of liver and anterior to aorta Anatomy
Gastrointestinal Tract (Effective February 2007) (1%-5%) Anatomy of GI Tract Esophagus bulls-eye or target EG junction seen on sagittal scan posterior to left lobe of liver and anterior to aorta Anatomy
Trauma. Neck trauma zones. Neck Injuries 1/3/2018. Basic principles A ; Airway B ; Breathing C ; Circulation D ; Disability E ; Exposure
 Trauma 45 minutes highest points Ahmed Mahmoud, MD Basic principles A ; Airway B ; Breathing C ; Circulation D ; Disability E ; Exposure Neck trauma zones Airway ;Rapid sequence intubation Breathing ;Needle
Trauma 45 minutes highest points Ahmed Mahmoud, MD Basic principles A ; Airway B ; Breathing C ; Circulation D ; Disability E ; Exposure Neck trauma zones Airway ;Rapid sequence intubation Breathing ;Needle
THORACOSCOPY: WHAT IS POSSIBLE? Eric Monnet, DVM, PhD, DACVS, DECVS Colorado State University, Fort Collins, Colorado
 THORACOSCOPY: WHAT IS POSSIBLE? Eric Monnet, DVM, PhD, DACVS, DECVS Colorado State University, Fort Collins, Colorado Thoracoscopy is feasible in small animal surgery Pericardial window, lung lobectomy,
THORACOSCOPY: WHAT IS POSSIBLE? Eric Monnet, DVM, PhD, DACVS, DECVS Colorado State University, Fort Collins, Colorado Thoracoscopy is feasible in small animal surgery Pericardial window, lung lobectomy,
Dissection Lab Manuals: Required Content
 Dissection Lab Manuals: Required Content 1. Introduction a. Basic terminology (directions) b. External features of the cat c. Adaptations to predatory niche d. How to skin a cat e. How to make the incisions
Dissection Lab Manuals: Required Content 1. Introduction a. Basic terminology (directions) b. External features of the cat c. Adaptations to predatory niche d. How to skin a cat e. How to make the incisions
Focused Assessment Sonography of Trauma (FAST) Scanning Protocol
 Focused Assessment Sonography of Trauma (FAST) Scanning Protocol Romolo Gaspari CHAPTER 3 GOAL OF THE FAST EXAM Demonstrate free fluid in abdomen, pleural space, or pericardial space. EMERGENCY ULTRASOUND
Focused Assessment Sonography of Trauma (FAST) Scanning Protocol Romolo Gaspari CHAPTER 3 GOAL OF THE FAST EXAM Demonstrate free fluid in abdomen, pleural space, or pericardial space. EMERGENCY ULTRASOUND
R the resumption of the normal swallowing mechanism
 Reconstruction the Left Colon of the Esophagus With Min-Hsiung Huang, MD, Chih-Yi Sung, MD, Hon-Ki Hsu, MD, Biing-ShiunHuang, MD, Wen-Hu Hsu, MD, and Kwang-Yu Chien, MD Division of Thoracic Surgery, Department
Reconstruction the Left Colon of the Esophagus With Min-Hsiung Huang, MD, Chih-Yi Sung, MD, Hon-Ki Hsu, MD, Biing-ShiunHuang, MD, Wen-Hu Hsu, MD, and Kwang-Yu Chien, MD Division of Thoracic Surgery, Department
Thoracoscopic S 6 segmentectomy: tricks to know
 Surgical Technique Page 1 of 6 Thoracoscopic S 6 segmentectomy: tricks to know Agathe Seguin-Givelet 1,2, Jon Lutz 1, Dominique Gossot 1 1 Thoracic Department, Institut Mutualiste Montsouris, Paris, France;
Surgical Technique Page 1 of 6 Thoracoscopic S 6 segmentectomy: tricks to know Agathe Seguin-Givelet 1,2, Jon Lutz 1, Dominique Gossot 1 1 Thoracic Department, Institut Mutualiste Montsouris, Paris, France;
Dana Alrafaiah. - Moayyad Al-Shafei. -Mohammad H. Al-Mohtaseb. 1 P a g e
 - 6 - Dana Alrafaiah - Moayyad Al-Shafei -Mohammad H. Al-Mohtaseb 1 P a g e Quick recap: Both lungs have an apex, base, mediastinal and costal surfaces, anterior and posterior borders. The right lung,
- 6 - Dana Alrafaiah - Moayyad Al-Shafei -Mohammad H. Al-Mohtaseb 1 P a g e Quick recap: Both lungs have an apex, base, mediastinal and costal surfaces, anterior and posterior borders. The right lung,
Cover Page. The following handle holds various files of this Leiden University dissertation:
 Cover Page The following handle holds various files of this Leiden University dissertation: http://hdl.handle.net/1887/6119 Author: Spruit, E.N. Title: Increasing the efficiency of laparoscopic surgical
Cover Page The following handle holds various files of this Leiden University dissertation: http://hdl.handle.net/1887/6119 Author: Spruit, E.N. Title: Increasing the efficiency of laparoscopic surgical
Controversies in management of squamous esophageal cancer
 2015.06.12 12.47.48 Page 4(1) IS-1 Controversies in management of squamous esophageal cancer C S Pramesh Thoracic Surgery, Department of Surgical Oncology, Tata Memorial Centre, India In Asia, squamous
2015.06.12 12.47.48 Page 4(1) IS-1 Controversies in management of squamous esophageal cancer C S Pramesh Thoracic Surgery, Department of Surgical Oncology, Tata Memorial Centre, India In Asia, squamous
Resection of malignant tumors invading the thoracic inlet
 Resection of Superior Sulcus Tumors: Anterior Approach Marc de Perrot, MD, MSc Resection of malignant tumors invading the thoracic inlet represents a technical challenge because of the complex anatomy
Resection of Superior Sulcus Tumors: Anterior Approach Marc de Perrot, MD, MSc Resection of malignant tumors invading the thoracic inlet represents a technical challenge because of the complex anatomy
DISCHARGE DIAGNOSES: End stage renal disease secondary to rapidly progressive glomerulonephritis.
 DISCHARGE SUMMARY DISCHARGE DIAGNOSES: End stage renal disease secondary to rapidly progressive glomerulonephritis. OPERATIONS/PROCEDURES: Living related renal transplantation. HISTORY: For full details
DISCHARGE SUMMARY DISCHARGE DIAGNOSES: End stage renal disease secondary to rapidly progressive glomerulonephritis. OPERATIONS/PROCEDURES: Living related renal transplantation. HISTORY: For full details
Robotic Surgery for Esophageal Cancer
 Robotic Surgery for Esophageal Cancer Kemp H. Kernstine, MD PhD Division of Thoracic Surgery City of Hope Medical Center and Beckman Research Institute May 1, 2010 Esophageal Cancer on the Rise JNCI 2005,
Robotic Surgery for Esophageal Cancer Kemp H. Kernstine, MD PhD Division of Thoracic Surgery City of Hope Medical Center and Beckman Research Institute May 1, 2010 Esophageal Cancer on the Rise JNCI 2005,
10/14/2018 Dr. Shatarat
 2018 Objectives To discuss mediastina and its boundaries To discuss and explain the contents of the superior mediastinum To describe the great veins of the superior mediastinum To describe the Arch of
2018 Objectives To discuss mediastina and its boundaries To discuss and explain the contents of the superior mediastinum To describe the great veins of the superior mediastinum To describe the Arch of
Lecturer: Ms DS Pillay ROOM 2P24 25 February 2013
 Lecturer: Ms DS Pillay ROOM 2P24 25 February 2013 Thoracic Wall Consists of thoracic cage Muscle Fascia Thoracic Cavity 3 Compartments of the Thorax (Great Vessels) (Heart) Superior thoracic aperture
Lecturer: Ms DS Pillay ROOM 2P24 25 February 2013 Thoracic Wall Consists of thoracic cage Muscle Fascia Thoracic Cavity 3 Compartments of the Thorax (Great Vessels) (Heart) Superior thoracic aperture
T treat empyema, although modern day thoracic
 The Schede and Modern Thoracoplasty Benjamin J. Pomerantz, Joseph C. Cleveland, Jr, and Marvin Pomerantz THORACOPLASTY-GENERAL CONSIDERATIONS horacoplasty evolved as a procedure designed to T treat empyema,
The Schede and Modern Thoracoplasty Benjamin J. Pomerantz, Joseph C. Cleveland, Jr, and Marvin Pomerantz THORACOPLASTY-GENERAL CONSIDERATIONS horacoplasty evolved as a procedure designed to T treat empyema,
Geoffrey Axiak M.Sc. Nursing (Manch.), B.Sc. Nursing, P.G. Dip. Nutrition & Dietetics Clinical Nutrition Practice Nurse
 The Percutaneous Endoscopic Gastrostomy Geoffrey Axiak M.Sc. Nursing (Manch.), B.Sc. Nursing, P.G. Dip. Nutrition & Dietetics Clinical Nutrition Practice Nurse What is a P.E.G.? Percutaneous Endoscopic
The Percutaneous Endoscopic Gastrostomy Geoffrey Axiak M.Sc. Nursing (Manch.), B.Sc. Nursing, P.G. Dip. Nutrition & Dietetics Clinical Nutrition Practice Nurse What is a P.E.G.? Percutaneous Endoscopic
