ORIGINAL ARTICLE. Treatment of Vocal Fold Bowing Using Neuromuscular Electrical Stimulation
|
|
|
- Baldric Taylor
- 5 years ago
- Views:
Transcription
1 ORIGINAL ARTICLE Treatment of Vocal Fold Bowing Using Neuromuscular Electrical Stimulation Lisa A. LaGorio, MS; Giselle D. Carnaby-Mann, PhD; Michael A. Crary, PhD Objective: To investigate the clinical effectiveness and safety of a novel behavioral voice therapy program combining structured vocal exercise with adjunctive neuromuscular electrical stimulation for rehabilitating dysphonia secondary to vocal fold bowing. Design: Prospective interventional clinical case series with a 3-month follow-up. Setting: Outpatient speech and hearing clinic in an academic medical center. Patients: Convenience sample of 7 patients diagnosed by an otolaryngologist as having chronic dysphonia for at least 3 months due to bilateral vocal fold bowing. Intervention: A novel voice therapy program incorporating exercise principles and sustained phonations of increasing length, volume, and pitch paired with concurrent transcutaneous neuromuscular electrical stimulation. Main Outcome Measures: Change in maximum phonation time, highest attainable pitch, glottal closure, supraglottic compression, and Voice Handicap Index. Results: Maximum phonation time for /i/ increased significantly (z= 2.201, P.03), with a modest effect demonstrated (Hedges g, 0.65; 95% confidence interval, 0.56 to 1.75). Voice Handicap Index trended toward significance (z= 1.787, P.07). Glottal closure during phonation improved, and supraglottic compression decreased. Improvements were maintained or enhanced at the 3-month followup. Analysis of highest attainable pitch data was limited owing to aperiodicity in the baseline evaluations. Conclusions: Behavioral voice therapy with adjunctive neuromuscular electrical stimulation reduced vocal fold bowing, resulting in improved acoustic, laryngeal, and patient-centered outcomes. Maximum phonation time and glottal closure results imply increased vocal fold tension secondary to enhanced thyroarytenoid or cricothyroid muscle function after voice therapy. Arch Otolaryngol Head Neck Surg. 2010;136(4): Author Affiliations: Departments of Communicative Disorders (Ms LaGorio and Dr Crary) and Behavioral Science and Community Health (Dr Carnaby-Mann), College of Public Health and Health Professions, University of Florida, Gainesville. VOCAL FOLD BOWING IS A FREquent cause of dysphonia in olderpersons, reportedlyaffecting 20% to 29% of the geriatric population. 1,2 Furthermore, more than 50% of older persons with dysphonia from bowed vocal folds report significant decline in quality of life. 1 However, vocal fold bowing is not limited to older populations. For example, Reulbach etal 3 identifiedpreviouslyundiagnosedglottal incompetence from bowed vocal folds in 72% of a cohort of healthy adults 40 years and older. Hanson et al 4 identified vocal fold bowing in 94% of patients with Parkinson disease. Mechanisms of vocal fold bowing are presumed but unknown 5 and may include intubation-related damage to laryngealmucosa, 6 vocalfoldstiffening, 5 vocalfold paresis, 7 sulcus vocalis, 7 or laryngeal atrophy. 7,8 Regardless of the cause, treatment of dysphonia due to bowed vocal folds has focused on therapeutic laryngeal injection or thyroplasticmedialization. 9,10 Evidencesupporting the benefit of voice therapy for dysphonia secondary to bowed vocal folds in otherwise healthy adults is limited. 11 However, related efforts suggest that laryngeal muscles might be strengthened with voice therapy based on exercise principles. For example, Ramig 12 and Smith et al 13 reported that resistance exercise targeting vocal intensity and respiratory function decreased glottal incompetence and improved voice quality in patients with bowed vocal folds secondary to Parkinson disease. Recently, we reported that dysphagia therapy with adjunctivetranscutaneousneuromuscularelectricalstimulation(nmes) reducedvocalfold bowing and improved voice performance in a single patient who had received radiotherapy for head and neck cancer. 14 Combining exercise with adjunctive NMES may enhance the positive effects of voice therapy. This combined approach has been reported to enhance treatment outcomes in sports medicine 15,16 and in stroke rehabilitation 17 but, until recently, had not been tested in rehabilitation of any pathologic laryngeal condition. In 2008, Ptok and Strack 18 demonstrated that pairing voice therapy with transcutaneous electrical stimulation decreased vocal fold vibration irregularity in patients with uni- 398
2 lateral vocal fold paralysis. Moreover, our aforementioned study 14 of reduced vocal fold bowing with concomitant voice improvement showed enhanced vocal fold tension following pharyngeal and laryngeal exercise combined with transcutaneous NMES. Given these results, we hypothesized that an exercise-based voice therapy program paired with adjunctive transcutaneous NMES may improve vocal and laryngeal function in patients with bowed vocal folds contributing to dysphonia. Robey 19 described a 5-phase model of clinical research structuringaseriesofclinicalinvestigationsleadingtoacomprehensive evaluation of any novel intervention. The initial phase in this model is to describe and measure any clinical effect of the intervention. In this regard, a phase 1 study should focus on a specified therapeutic outcome and should delineate how this outcome is to be evaluated. Acceptable research designs to accomplish this goal include case reports, prospective case series, and retrospective studies. In the present study, we report the results of a prospective case series to evaluate the clinical effectiveness and safety of a novel voice therapy program with adjunctive NMES in the rehabilitation of dysphonia secondary to bowed vocal folds. We specify clinical outcomes used in the assessment of this intervention and describe a consistent course of voice therapy applied to 7 patients having chronic dysphonia secondary to bilateral vocal fold bowing. METHODS PATIENTS Adults having chronic dysphonia for at least 3 months due to bilateral true vocal fold bowing were recruited to participate in the treatment study from June 1, 2007, to May 15, Patients were referred from local otolaryngologists familiar with the study. Patients with tracheotomy, progressive neurologic disease, history of laryngeal cancer, or other organic, neuromuscular, or functional cause for dysphonia were excluded from this study. Patients with cardiac demand pacemakers were also excluded, as this diagnosis is listed as a caution for electrical stimulation by the Food and Drug Administration. The local institutional review board approved all procedures used in this study, and all enrolled patients signed an approved informed consent form. BASELINE MEASURES Before voice therapy, each patient completed baseline acoustic and stroboscopic laryngeal evaluations, pulmonary function testing, and Voice Handicap Index (VHI) questionnaire. 20 These measures served to ensure inclusion criteria, determine initial voice therapy goals, and provide a pretherapy measure on outcome assessments. ACOUSTIC VOICE EVALUATION Acoustic voice evaluation was completed using a commercially available system (Computerized Speech Laboratory 4500; Kay- Pentax, Lincoln Park, New Jersey). Signals were captured via a headset-mounted condenser microphone (C420 PP MicroMic III; AKG Acoustics, Vienna, Austria) set at a uniform 1 2-in distance in front of the patient s mouth during all recordings. A real-time pitch program (RTP model 5121, KayPentax) was used to measure maximum phonation time (MPT) and highest attainable pitch (HAP) for sustained /i/ and /a/ as well as loudest volume produced saying Hey you. Patients completed 3 trials of each task; the mean performance values were used in the analysis. STROBOSCOPIC LARYNGEAL EVALUATION Laryngeal evaluations were completed using a stroboscope (9200C Rhino-Laryngeal Stroboscope, KayPentax) with a flexible endoscope (ENF-P4; Olympus, Tokyo, Japan). These evaluations confirmed the presence of true vocal fold bowing, set the NMES level used in treatment sessions, and described laryngeal configuration during phonation. Laryngeal configuration variables examined were glottal closure and supraglottic compression. PULMONARY FUNCTION EVALUATION Pulmonary function evaluation was completed using a handheld spirometer (Discovery; Futuremed America Inc, Granada Hills, California). Patient age, sex, height, and weight were entered into the spirometer for calculation of forced expiratory volume in the first second of expiration (FEV 1 ) and forced vital capacity. Patients were instructed to take a deep breath and to blow out forcefully. Patients completed 3 trials; the mean performance values were used in the analysis. The ratio of FEV 1 to forced vital capacity (FEV 1 %) was calculated for each patient and was used as a control measure in the outcome analysis. This measure provides a clinical means of assessing airflow limitation during expiration, reflecting integrity of the respiratory muscles. Because respiratory muscles are known to adapt to exercise, 21 any statistically significant change in FEV 1 % following treatment would indicate change in underlying respiratory musculature function. Therefore, this pulmonary measure was incorporated as a control measure in an attempt to separate the effects of laryngeal vs pulmonary changes as a result of voice therapy. INTERVENTION The voice therapy protocol consisted of a hierarchy of vocalizations paired with adjunctive transcutaneous NMES. Sessions were 1 hour daily, 5 days per week, for 3 weeks. Patients completed 2 pretreatment accommodation sessions. These accommodation sessions served to familiarize patients with the voice therapy program and performance criteria, answer any questions about NMES, and minimize any anticipatory bias. Patients received 10 and 20 minutes of NMES, respectively, during the first and second accommodation sessions. During the subsequent 13 voice therapy sessions, patients completed a standardized protocol of vocal exercises, while simultaneously receiving 60 minutes of NMES. Vocal exercises consisted of a progressive 14-step series of phonatory activities. The task hierarchy was developed to systematically increase resistance to the weakened vocal folds and to expand the phonatory environment over time. To do this, the exercise concept of 1-repetition maximum (1RM) was adapted to voice. One-repetition maximum describes the maximum load that can be moved 1 time. 22 This value is used to set training intensity levels, with optimal exercise levels for strength training set at 80% of 1RM. 22 To adapt 1RM for this vocal exercise protocol, load was defined as length (MPT), volume, and pitch (HAP) of sustained phonation; 1RM was defined as the highest performance value of 1 of 3 baseline trials of MPT, volume, and HAP. Patients individual vocal exercise goals were calculated as 60%, 70%, and 80% of baseline 1RM and were used to measure successful performance at each step in the vocal exercise task hierarchy. For example, during step 1, patients were required to produce and sustain a hum for 60% of baseline MPT until performance criteria for successful phonation were achieved. Once achieved, the 399
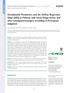
3 Before applying the electrodes, all men were clean shaven, and all patients necks were cleaned with an alcohol-based wipe (TENS Clean-Cote UniPatch, MS71000, model UP220; Tyco Healthcare, Wabasha, Wisconsin). Once affixed, the electrodes were taped to the skin (Transpore; 3M, St Paul). Last, during treatment sessions, a 3-in-wide elastic bandage was wrapped around the neck over the electrodes to further assist in maintaining appropriate skin to electrode contact. IDENTIFICATION OF NMES AMPLITUDE Figure. Electrode placement. Transcutaneous electrode position is shown relative to the hyoid bone, thyroid cartilage, and cricoid cartilage. In this configuration, neuromuscular electrical stimulation was targeted toward the superior laryngeal nerves (horizontal electrodes) and the cricothyroid muscles (vertical electrodes). length of sustained phonation was increased to 70% and then 80% of baseline MPT. Vocal exercise continued in this fashion, next incorporating /i/ and /a/, then volume, and then HAP so that, as patients progressed in the task hierarchy, they were required to produce and sustain phonations that were incrementally longer, louder, and higher pitched than previous phonations. Following completion of step 6 in the treatment hierarchy, 1RM for MPT was remeasured, and 60%, 70%, and 80% phonation length goals were recalculated. These new MPT goals were used during the remaining steps in the hierarchy. Once patients reached step 12 in the vocal exercise program, target phonations changed from sustained vowels to words, phrases, and conversation. PERFORMANCE MONITORING The treating speech-language pathologist (L.A.L.) recorded successful and unsuccessful phonation attempts. Successful phonations involved producing and sustaining a target phonation without hoarseness, breathiness, or pitch breaks for the specified length of time. Each phonation attempt was judged by the clinician and by the patient. Successful productions required agreement between clinician and patient. To advance to higher levels in the voice therapy program, patients were required to phonate with 80% accuracy (8 of 10 attempts) per vocal exercise set and to complete 3 successful consecutive sets per level. Failure on 3 of 5 phonation attempts in any set was considered a failure of that set. TRANSCUTANEOUS NMES Neuromuscular electrical stimulation was delivered using a commercially available device (VitalStim NMES; Empi Corporation, St Paul, Minnesota). The unit is a dual-channel bipolar device that supplies rectangular, symmetric, biphasic pulsed current at a preset fixed pulse rate of 80 Hz and pulse duration of 700 microseconds (VitalStim Therapy 23 ). The dual channels allow the user to independently set the stimulation amplitude from 0 to 25 ma (tolerance ±10%). Adult electrodes (VitalStim 59000) are circular, have a 2.1-cm diameter, and provide 3.46-cm 2 surface area of stimulation via a carbon-silver substrate. One pair of electrodes was placed vertically at the midline immediately above and below the cricothyroid membrane. This electrode pair targeted NMES to the cricothyroid muscles. The other pair of electrodes was placed horizontally, inferior and slightly medial to the posterior horns of the hyoid bone near the presumed location of the superior laryngeal nerves (Figure). Treatment NMES level was determined during the baseline stroboscopic laryngeal evaluation. Neuromuscular electrical stimulation was increased from 0 ma in 2-mA increments until improved glottal closure or vibratory pattern was reported by the stroboscopic examiner (M.A.C.). Once an effect on glottal closure was identified, NMES amplitude was decreased systematically by 1 ma until the baseline glottal closure or vibratory pattern was again observed. Next, NMES amplitude was again increased in 0.5-mA increments until improved glottal closure or vibratory pattern was reidentified. This NMES amplitude was subsequently used for all treatment sessions. To minimize examiner (M.A.C.) bias, the examiner remained blinded to NMES amplitude applied during the examination. OUTCOME BLINDING Voice therapy sessions were conducted by one experienced speech-language pathologist, who was blinded to the results of all assessments. Only the therapeutic NMES level was available to the treating speech-language pathologist (L.A.L.). Outcome assessors were blinded to the results of the treatment sessions. TREATMENT OUTCOMES Primary outcome measures assessed included change in MPT, HAP, VHI, and laryngeal configuration during phonation. A secondary outcome measure was change in pulmonary function, FEV 1 %, which was used as a control evaluation of the stability of respiratory support for phonation. LARYNGEAL CONFIGURATION DURING PHONATION To rate glottal closure and supraglottic compression, video clips of sustained /i/ were obtained from each patient s stroboscopic laryngeal examinations at baseline, after voice therapy, and at the 3-month follow-up. Video samples were edited to equal lengths of 3 to 5 seconds, deidentified, arranged into a series of randomized pairs, and presented to raters (G.D.C.-M. and M.A.C.) in a slide format (PowerPoint, Microsoft Office 2003; Microsoft Corp, Redmond, Washington). Two experienced independent judges rated each pair. Ratings from the more experienced judge (M.A.C.) were used to evaluate change in laryngeal configuration during phonation. Ratings from the second judge (G.D.C.-M.) were used to estimate interrater reliability. Judges viewed the pairs and chose the video from each pair that best demonstrated better glottal closure and less supraglottic compression. Each of these laryngeal configuration outcome variables was rated separately. Judges rated pairs as no difference when the pair was perceived to be identical for each outcome measure or cannot see if either video of the pair was of too poor quality to rate either of the 2 laryngeal configuration variables. Video pairs were automatically played on a continuous-motion loop. Judges were al- 400
4 Table. Outcome Among 6 Patients During the Study Period Mean (SD) Outcome Measure Baseline After Voice Therapy 3-Month Follow-up Posttreatment P Value Maximum phonation time, s /i / (5.84) (6.20) (8.08).03 /a / 8.23 (2.72) (4.77) (7.23).08 Highest attainable pitch, Hz (n=3) /i / (93.05) (191.73) (112.37) NA /a / (76.63) (108.24) (66.09) NA Voice Handicap Index (19.89) (15.60) (17.16).07 FEV 1 % (0.10) (0.10) (0.13).92 Abbreviations: FEV 1 %, ratio of forced expiratory volume in the first second of expiration to forced vital capacity; NA, not applicable. lowed to stop and start the playback as needed but were not permitted to look back at previously rated pairs. STATISTICAL ANALYSIS Patient demographics were reviewed using descriptive methods. Because of few patients and skewed distributions, the nonparametric Wilcoxon signed rank test of matched pairs was used to assess pretreatment and posttreatment performance change for the continuous variables. Clinical effect for significant outcomes was estimated using Hedges g statistic. 24 Interrater reliability for both laryngeal configuration variables was calculated using statistic. 25 RESULTS BASELINE CHARACTERISTICS A convenience sample of 7 patients enrolled in the study, 4 men and 3 women, with a mean (SD) age of 66.9 (8.4) years (age range, years). All patients demonstrated bilateral vocal fold bowing with adequate laryngeal abduction and adduction. Based on patient history, the presumptive cause of bowed vocal folds was presbyphonia in 5 patients, multiple intubations in 1 patient, and unknown (possibly virus related) in 1 patient. FOLLOW-UP EVALUATIONS Posttreatment data were completed for 6 of 7 patients. One male patient withdrew after completing the first week of treatment because of complaints of muscle soreness in his right lateral neck over the larynx. Clinical and endoscopic evaluations 3 days after withdrawal from the study were unremarkable, and the patient denied any discomfort at that time. Data from this patient were not included in the results. TREATMENT SESSION AND NMES VARIABLES The remaining 6 patients completed all 15 sessions (2 accommodation and 13 treatment sessions). Although all patients completed 15 voice therapy sessions, no patient progressed through all steps of the vocal exercise program within the prescribed time frame of 15 sessions. On average, patients completed 9 of 14 steps (range, 7-10 steps). The mean (SD) NMES amplitude during these sessions was 9.5 (3.3) ma (range, 3-14 ma). OUTCOME MEASURES IMMEDIATELY AFTER TREATMENT Maximum Phonation Time All 6 patients increased MPT for sustained /i/. Five of 6 patients also increased MPT for sustained /a/. The mean MPT for the group increased 38.4% over baseline for sustained /i/ and 42.5% over baseline for sustained /a/ (Table). The increased MPT for /i/ was statistically significant (z= 2.201, P=.03). The increased MPT for /a/ trended toward statistical significance (P=.08). A modest effect was demonstrated in MPT change for /i/ (Hedges g, 0.65; 95% confidence interval, 0.56 to 1.75). 24 Highest Attainable Pitch Because of significant baseline aperiodicity in subject phonation, HAP data were complete for only 3 of 6 patients. Given these limited data points, no statistical analysis was performed. Group data from the remaining patients showed that the mean HAP for /i/ increased 13.4%, while the mean HAP for /a/ decreased 23.6% following voice therapy (Table). Patient Perception of Voice (VHI) Five of 6 patients perceived their voices to have improved following voice therapy. The VHI (total) improved (ie, decreased a mean of points [range, 3-17 points]) between pretreatment and posttreatment assessments (Table). This improvement trended toward significance (z= 1.787, P=.07). Pulmonary Function Group baseline FEV 1 % decreased 0.05% immediately following voice therapy completion (Table). This change was not statistically significant. Laryngeal Configuration During Phonation Twelve video pairs directly compared pretreatment vs posttreatment laryngeal configuration during phona- 401
5 tion. Glottal closure was rated for 9 of 12 video pairs. Three video pairs were judged as cannot see for this variable. The posttreatment video demonstrated better glottal closure in 8 of 9 video pairs. Supraglottic compression was rated for all 12 of the video pairs comparing pretreatment vs posttreatment laryngeal configuration during phonation. The posttreatment video was identified as demonstrating less supraglottic compression in 7 of 12 video pairs. Interrater reliability was excellent for glottal closure ratings ( =0.81) and moderate for supraglottic compression ratings ( =0.57). 25 Outcomes at the 3-Month Follow-up All 6 patients returned for the 3-month follow-up assessment. All treatment effects were maintained or enhanced, as no significant differences were noted in acoustic, pulmonary, or patient-centered outcome measures between the posttreatment and 3-month follow-up evaluations (Table). Furthermore, change in both laryngeal configuration variables was also maintained or enhanced at the 3-month follow-up assessment. For this analysis, 9 posttreatment videos previously used to rate pretreatment vs posttreatment glottal closure were compared with their corresponding 3-month follow-up video. Among these 9 new video pairs, glottal closure was rated in 6; the remaining 3 were judged as cannot see for this variable. The 3-month follow-up video was identified as demonstrating better glottal closure in 4 of 6 video pairs and as no difference in 1 video pair. Therefore, 5 of 6 endoscopic examinations demonstrated maintenance of the treatment effect for glottal closure. Similarly, 12 posttreatment videos used to rate pretreatment vs posttreatment supraglottic compression were used to compare posttreatment and 3-month follow-up evaluations. From these video pairs, the 3-month follow-up video demonstrated less supraglottic compression in 5 of 12 pairs and was judged as no difference in an additional 2 pairs. Therefore, 7 of 12 endoscopic examinations demonstrated maintenance of the treatment effect for supraglottic compression. COMMENT This prospective case series demonstrated that a standardized voice therapy protocol (based on exercise principles and using adjunctive NMES) increased MPT and glottal closure and decreased supraglottic compression in patients with dysphonia from bowed vocal folds, without significant complications or change in underlying pulmonary function. In addition, significant change in VHI revealed that patients perceived their voices to be improved following the voice therapy program. These outcomes were maintained or enhanced at the 3-month follow-up. Increased MPT and glottal closure without underlying change in pulmonary function imply that this voice therapy program decreased vocal fold bowing. Mechanisms of these changes may have included enhanced thyroarytenoid or cricothyroid activity. In an investigation of the mechanisms of true vocal fold bowing, Tanaka et al 7 found that bowing was directly related to thyroarytenoid muscle activity. Using laryngeal electromyography, they discovered that increased thyroarytenoid muscle firing corresponded to decreased vocal fold bowing, whereas cricothyroid muscle activity had no relationship to vocal fold bowing. However, contraction of the cricothyroid muscles moves the vocal folds into the paramedian position, elongates them, and sharpens their contours, 26 resulting in increased vocal fold tension and improved glottal closure. Although the specific mechanisms of increased MPT and improved glottal closure are beyond the scope of this study, both improved as a result of this novel intervention. Decreased supraglottic compression supports the conclusion of improved glottal closure. Belafsky et al 27 observed that compensatory supraglottic hyperfunction is common among individuals with glottal insufficiency because of bowed vocal folds. Therefore, improvement in glottal closure should reduce supraglottic compression or hyperfunction. Collectively, the decreased supraglottic compression and increased glottal closure noted in this series of patients suggest a direct and positive effect of the combined intervention on laryngeal function. In addition to improving MPT and glottal closure, increased cricothyroid tension also raises pitch. However, depending on the vowel being sustained, pitch change in this study increased (/i/) or decreased (/a/) following voice therapy. Unfortunately, complete pitch data were available from only 3 of 6 patients participating in the study. The remaining 3 patients demonstrated excessive baseline aperiodicity, precluding our ability to obtain measurable pitch values for posttherapy comparison. Two of these patients demonstrated improved periodicity at the posttreatment and 3-month follow-up evaluations. The third patient demonstrated improved periodicity at the 3-month follow-up evaluation. Together, these improvements in periodicity suggest a related aspect of voice improvement following treatment. However, because of the limited pitch data in this case series, any conclusions about the effect of this intervention on pitch control or periodicity during phonation must await future investigation. Stability in pulmonary function also supports the conclusion that this therapeutic intervention decreases vocal fold bowing. The MPT is a function of true vocal fold contact and transglottic air pressure during phonation. 27 Therefore, improvement in MPT may have been due to increased pulmonary function. However, the absence of pulmonary change demonstrated in this study suggests that improved MPT resulted from increased vocal fold contact secondary to decreased vocal fold bowing. Several factors may have contributed to the positive outcomes demonstrated in this study. However, these outcomes do not differentiate between the individual contributions of the vocal exercise based therapy or of the adjunctive NMES toward achieving these voice and laryngeal changes. In other rehabilitation fields, combining targeted exercise with adjunctive NMES has resulted in better functional gains than exercise alone for strengthening limb muscles However, until recently, this has not been investigated for strengthening laryngeal muscles. Ptok and Strack 18 compared traditional clinic-based voice therapy with home-based vocal exercises combined with NMES. They reported a significant decrease in vocal fold vibration irregularity in the group receiving NMES. These investiga- 402
6 tors suggest that the combination of NMES and vocal exercise may have helped increase cricoarytenoid lateralis muscle tension. Together, the present results and those by Ptok and Strack implicate positive laryngeal and voice outcomes from interventions combining voice therapy with NMES in different pathologic laryngeal conditions. Strengths of this study include its standardized treatment protocol, homogeneous diagnostic population, blinded outcome assessment, and outcome measures across multiple domains. We acknowledge that this study has limitations inherent to a small uncontrolled clinical investigation. Case series do not have internal control comparisons and represent limited evidence for any given treatment. However, given the lack of published evidence supporting behavioral voice therapy for this clinical population, as well as the limited evidence supporting the use of NMES in voice therapy applications, we believe that this case series was an appropriate setting in which to define a treatment effect for this intervention approach. 19 We are investigating the relative contributions of the exercise-based voice therapy vs NMES components of the present intervention. We are also investigating additional outcome variables such as aerodynamic and perceptual voice changes and using digital image analysis to more objectively measure change in glottal gap. Finally, we intend to compare this behavioral approach with the more frequently used surgical intervention. To our knowledge, this prospective case series is the first to describe a successful standardized behavioral voice therapy protocol using adjunctive NMES for the treatment of dysphonia secondary to bowed vocal folds. Acoustic results showed significantly increased MPT, while endoscopic results revealed improved glottal closure and less supraglottic compression. Outcomes were maintained or improved at the 3-month follow-up after completion of the voice therapy program. The results imply enhanced thyroarytenoid or cricothyroid muscle function as a result of the voice therapy program. As a clinical case series, this study serves as a first step in exploring the potential for behavioral voice therapy in the treatment of dysphonia due to bowed vocal folds. Future studies will investigate the separate effects of vocal exercise vs NMES for rehabilitating this patient population, as well as the effects of combined vocal exercise and NMES vs surgery. Submitted for Publication: May 30, 2009; final revision received August 28, 2009; accepted October 22, Correspondence: Michael A. Crary, PhD, Department of Communicative Disorders, University of Florida, PO Box , Gainesville, FL (mcrary@phhp.ufl.edu). Author Contributions: Ms LaGorio and Dr Carnaby- Mann had full access to all the data in the study and take responsibility for the integrity of the data and the accuracy of the data analysis. Study concept and design: LaGorio, Carnaby-Mann, and Crary. Acquisition of data: LaGorio and Crary. Analysis and interpretation of data: LaGorio, Carnaby-Mann, and Crary. Drafting of the manuscript: LaGorio and Carnaby-Mann. Critical revision of the manuscript for important intellectual content: Carnaby-Mann and Crary. Statistical analysis: Carnaby-Mann. Obtained funding: Crary. Administrative, technical, and material support: Crary. Study supervision: Carnaby-Mann and Crary. Financial Disclosure: None reported. Funding/Support: This work was partially funded by an unrestricted educational foundation grant to Dr Crary from Empi Corporation. Role of the Sponsor: Empi Corporation had no role in the design and conduct of the study; in the collection, analysis, and interpretation of the data; or in the preparation, review, or approval of the manuscript. Additional Contributions: Ann L. Glowasky, MD, Nicholas J. Cassisi, MD, Kerry Lenius, PhD, Caitlyn Ohme, MA, and Pamela Carvajal, BA, assisted with the project. REFERENCES 1. Golub JS, Chen PH, Otto KJ, Hapner E, Johns MM III. Prevalence of perceived dysphonia in a geriatric population. J Am Geriatr Soc. 2006;54(11): Roy N, Stemple JC, Merrill RM, Thomas L. Epidemiology of voice disorders in the elderly: preliminary findings. Laryngoscope. 2007;117(4): Reulbach TR, Belafsky PC, Blalock PD, Koufman JA, Postma GN. Occult laryngeal pathology in a community-based cohort. Otolaryngol Head Neck Surg. 2001; 124(4): Hanson DG, Gerratt BR, Ward PH. Cinegraphic observation of laryngeal function in Parkinson s disease. Laryngoscope. 1984;94(3): Casper JK. From the urine of sacred cows to the laying on of hands and beyond: G. Paul Moore Lecture. J Voice. 2007;21(1): Shimokojin T, Takenoshita M, Sakai T, Yoshikawa K. Vocal cordal bowing as a cause of long-lasting hoarseness after a few hours of tracheal intubation. Anesthesiology. 1998;89(3): Tanaka S, Hirano M, Chijiwa K. Some aspects of vocal fold bowing. Ann Otol Rhinol Laryngol. 1994;103(5, pt 1): Sataloff RT, Rosen DC, Hawkshaw M, Spiegel JR. The aging adult voice. J Voice. 1997;11(2): Behrman A. Evidence-based treatment of paralytic dysphonia: making sense of outcomes and efficacy data. Otolaryngol Clin North Am. 2004;37(1):75-104, vi. 10. Dursun G, Boynukalin S, Ozgursoy OB, Coruh I. Long-term results of different treatment modalities for glottic insufficiency. Am J Otolaryngol. 2008;29(1): Thomas LB, Harrison AL, Stemple JC. Aging thyroarytenoid and limb skeletal muscle: lessons in contrast. J Voice. 2008;22(4): Ramig L. Speech therapy for patients with Parkinson s disease. In: Koller WPG, ed. Therapy of Parkinson s Disease. New York, NY: Marcel Dekker; 1995: Smith ME, Ramig LO, Dromey C, Perez KS, Samandari R. Intensive voice treatment in Parkinson disease: laryngostroboscopic findings. J Voice. 1995;9(4): LaGorio LA, Carnaby-Mann GD, Crary MA. Cross-system effects of dysphagia treatment on dysphonia: a case report. Cases J. 2008;1(1):e Accessed January 26, Maffiuletti NA, Dugnani S, Folz M, Di Pierno EL, Mauro FL. Effect of combined electrostimulation and plyometric training on vertical jump height. Med Sci Sports Exerc. 2002;34(10): Valli P, Boldrini L, Bianchedi D, Brizzi G, Miserocchi G. Effects of low intensity electrical stimulation on quadriceps muscle voluntary maximal strength. J Sports Med Phys Fitness. 2002;42(4): Chae J, Sheffler L, Knutson J. Neuromuscular electrical stimulation for motor restoration in hemiplegia. Top Stroke Rehabil. 2008;15(5): Ptok M, Strack D. Electrical stimulation supported voice exercises are superior to voice exercise therapy alone in patients with unilateral recurrent laryngeal nerve paresis: results from a prospective, randomized clinical trial. Muscle Nerve. 2008; 38(2): Robey RR. A five-phase model for clinical-outcome research. J Commun Disord. 2004;37(5): Jacobson BH, Johnson A, Grywalski C, et al. The Voice Handicap Index (VHI): development and validation. Am J Speech Lang Pathol. 1997;6: Powers SK, Coombes J, Demirel H. Exercise training induced changes in respiratory muscles. Sports Med. 1997;24(2): Powers SK, Howley ET. Exercise Physiology: Theory and Application to Fitness and Performance. New York, NY: McGraw-Hill Co; VitalStim Certification Program Training Manual. Birmingham, AL: VitalStim; Rosenthal R, Rosnow RL. Essentials of Behavioral Research: Methods and Data Analysis. New York, NY: McGraw-Hill Co; Landis JR, Koch GG. The measurement of observer agreement for categorical data. Biometrics. 1977;33(1): Sataloff RT. Clinical anatomy and physiology of the voice. In: Sataloff RT, ed. Voice Science. San Diego, CA: Plural Publishing Inc; 2006: Belafsky PC, Postma GN, Reulbach TR, Holland BW, Koufman JA. Muscle tension dysphonia as a sign of underlying glottal insufficiency. Otolaryngol Head Neck Surg. 2002;127(5):
Supplementary Online Content
 Supplementary Online Content Wang C-C, Chang M-H, Jiang R-S, et al. Laryngeal electromyography-guided hyaluronic acid vocal fold injection for unilateral vocal fold paralysis: a prospective long-term follow-up
Supplementary Online Content Wang C-C, Chang M-H, Jiang R-S, et al. Laryngeal electromyography-guided hyaluronic acid vocal fold injection for unilateral vocal fold paralysis: a prospective long-term follow-up
Lisa T. Fry, PhD Marshall University. Joseph C. Stemple, PhD University of Kentucky
 Lisa T. Fry, PhD Marshall University Joseph C. Stemple, PhD University of Kentucky Muscular Components of Voice Disorders Resonance Requires balance among the 3 Phonation Disruption in 1 may perturb the
Lisa T. Fry, PhD Marshall University Joseph C. Stemple, PhD University of Kentucky Muscular Components of Voice Disorders Resonance Requires balance among the 3 Phonation Disruption in 1 may perturb the
Case Presentation JC: 65 y/o retired plumber CC: Hoarseness HPI: Admitted to a local hospital on May 30 for severe pneumonia. Intubated in ICU for 10
 GBMC Stroboscopy Rounds October 12, 2007 Case Presentation JC: 65 y/o retired plumber CC: Hoarseness HPI: Admitted to a local hospital on May 30 for severe pneumonia. Intubated in ICU for 10 days, total
GBMC Stroboscopy Rounds October 12, 2007 Case Presentation JC: 65 y/o retired plumber CC: Hoarseness HPI: Admitted to a local hospital on May 30 for severe pneumonia. Intubated in ICU for 10 days, total
Superior Laryngeal Nerve Injury: Diagnosis and Management. Presented by: Nyall London October 10, 2014
 Superior Laryngeal Nerve Injury: Diagnosis and Management Presented by: Nyall London October 10, 2014 1 Case Presentation 49 year old male s/p right side approach anterior cervical discectomy and fusion
Superior Laryngeal Nerve Injury: Diagnosis and Management Presented by: Nyall London October 10, 2014 1 Case Presentation 49 year old male s/p right side approach anterior cervical discectomy and fusion
DO NOT DUPLICATE Copyrighted Material
 Annals of Otology, Rhinology & Laryngology 117(4):279-287. 2008 Annals Publishing Company. All rights reserved. Adjunctive Neuromuscular Electrical Stimulation for Treatment-Refractory Dysphagia Giselle
Annals of Otology, Rhinology & Laryngology 117(4):279-287. 2008 Annals Publishing Company. All rights reserved. Adjunctive Neuromuscular Electrical Stimulation for Treatment-Refractory Dysphagia Giselle
Original Article. Clinical Archives of Communication Disorders / Vol. 2, No. 1:15-22 / April 2017 INTRODUCTION
 Original Article http://e-cacd.org/ eissn: 2287-903X Clinical Archives of Communication Disorders / Vol. 2, No. 1:15-22 / April 2017 https://doi.org/10.21849/cacd.2017.00024 Open Access Aerodynamic Parameters
Original Article http://e-cacd.org/ eissn: 2287-903X Clinical Archives of Communication Disorders / Vol. 2, No. 1:15-22 / April 2017 https://doi.org/10.21849/cacd.2017.00024 Open Access Aerodynamic Parameters
Laryngeal Biomechanics: An Overview of Mucosal Wave Mechanics
 Journal of Voice Vol. 7, No. 2, pp. 123-128 1993 Raven Press, Lt~l., New York Laryngeal Biomechanics: An Overview of Mucosal Wave Mechanics Gerald S. Berke and Bruce R. Gerratt Head and Neck Surgery, University
Journal of Voice Vol. 7, No. 2, pp. 123-128 1993 Raven Press, Lt~l., New York Laryngeal Biomechanics: An Overview of Mucosal Wave Mechanics Gerald S. Berke and Bruce R. Gerratt Head and Neck Surgery, University
Graded activation of the intrinsic laryngeal muscles for vocal fold posturing
 Graded activation of the intrinsic laryngeal muscles for vocal fold posturing Dinesh K. Chhetri, a) Juergen Neubauer, and David A. Berry The Laryngeal Dynamics and Physiology Laboratories, Division of
Graded activation of the intrinsic laryngeal muscles for vocal fold posturing Dinesh K. Chhetri, a) Juergen Neubauer, and David A. Berry The Laryngeal Dynamics and Physiology Laboratories, Division of
Critical Review: Are laryngeal manual therapies effective in improving voice outcomes of patients with muscle tension dysphonia?
 Critical Review: Are laryngeal manual therapies effective in improving voice outcomes of patients with muscle tension dysphonia? María López M.Cl.Sc (SLP) Candidate University of Western Ontario: School
Critical Review: Are laryngeal manual therapies effective in improving voice outcomes of patients with muscle tension dysphonia? María López M.Cl.Sc (SLP) Candidate University of Western Ontario: School
Analysis of Laryngoscopic Features in Patients With Unilateral Vocal Fold Paresis
 The Laryngoscope VC 2015 The American Laryngological, Rhinological and Otological Society, Inc. Analysis of Laryngoscopic Features in Patients With Unilateral Vocal Fold Paresis Peak Woo, MD; Arjun K.
The Laryngoscope VC 2015 The American Laryngological, Rhinological and Otological Society, Inc. Analysis of Laryngoscopic Features in Patients With Unilateral Vocal Fold Paresis Peak Woo, MD; Arjun K.
What do VFE s consist of?
 The Use of Vocal Function Exercises as a Treatment Modality in VF Paralysis UCSF VOICE CONFERENCE October 16-18, 2008 Wendy DeLeo LeBorgne, Ph.D. CCC-SLP Voice Pathologist & Singing Voice Specialist wleborgne@dhns.net
The Use of Vocal Function Exercises as a Treatment Modality in VF Paralysis UCSF VOICE CONFERENCE October 16-18, 2008 Wendy DeLeo LeBorgne, Ph.D. CCC-SLP Voice Pathologist & Singing Voice Specialist wleborgne@dhns.net
Hoarseness. Common referral Hoarseness reflects any abnormality of normal phonation
 Hoarseness Kevin Katzenmeyer, MD Faculty Advisor: Byron J Bailey, MD The University of Texas Medical Branch Department of Otolaryngology Grand Rounds Presentation October 24, 2001 Hoarseness Common referral
Hoarseness Kevin Katzenmeyer, MD Faculty Advisor: Byron J Bailey, MD The University of Texas Medical Branch Department of Otolaryngology Grand Rounds Presentation October 24, 2001 Hoarseness Common referral
Acoustic Analysis of Voice Change in Normal Speakers Following Transcutaneous Electrical Stimulation to the Laryngeal Area
 The Open Rehabilitation Journal, 2010, 3, 67-74 67 Open Access Acoustic Analysis of Voice Change in Normal Speakers Following Transcutaneous Electrical Stimulation to the Laryngeal Area Mary Gorham-Rowan
The Open Rehabilitation Journal, 2010, 3, 67-74 67 Open Access Acoustic Analysis of Voice Change in Normal Speakers Following Transcutaneous Electrical Stimulation to the Laryngeal Area Mary Gorham-Rowan
Contents. Part A Clinical Evaluation of Laryngeal Disorders. 3 Videostroboscopy and Dynamic Voice Evaluation with Flexible Laryngoscopy...
 Contents Part A Clinical Evaluation of Laryngeal Disorders 1 Anatomy and Physiology of the Larynx....... 3 1.1 Anatomy.................................. 3 1.1.1 Laryngeal Cartilages........................
Contents Part A Clinical Evaluation of Laryngeal Disorders 1 Anatomy and Physiology of the Larynx....... 3 1.1 Anatomy.................................. 3 1.1.1 Laryngeal Cartilages........................
Jae Wook Kim, Jae Hong Park, Ki Nam Park, and Seung Won Lee. Correspondence should be addressed to Seung Won Lee;
 e Scientific World Journal, Article ID 327928, 4 pages http://dx.doi.org/10.1155/2014/327928 Clinical Study Treatment Efficacy of Electromyography versus Fiberscopy-Guided Botulinum Toxin Injection in
e Scientific World Journal, Article ID 327928, 4 pages http://dx.doi.org/10.1155/2014/327928 Clinical Study Treatment Efficacy of Electromyography versus Fiberscopy-Guided Botulinum Toxin Injection in
Speech and Language Therapy. Kerrie McCarthy Senior Speech and Language Therapist
 Speech and Language Therapy Kerrie McCarthy Senior Speech and Language Therapist Contents 1. Voice disorders 2. Swallow disorders 3. Videofluroscopy 4. Adult Acquired Communication Disorders 5. How to
Speech and Language Therapy Kerrie McCarthy Senior Speech and Language Therapist Contents 1. Voice disorders 2. Swallow disorders 3. Videofluroscopy 4. Adult Acquired Communication Disorders 5. How to
2012, Greenwood, L.
 Critical Review: How Accurate are Voice Accumulators for Measuring Vocal Behaviour? Lauren Greenwood M.Cl.Sc. (SLP) Candidate University of Western Ontario: School of Communication Sciences and Disorders
Critical Review: How Accurate are Voice Accumulators for Measuring Vocal Behaviour? Lauren Greenwood M.Cl.Sc. (SLP) Candidate University of Western Ontario: School of Communication Sciences and Disorders
Sunshine Act Disclosure
 A Laryngologist s Approach to Voice Presentation at the Nebraska Speech- Language-Hearing Association Fall Convention Thursday, September 27, 2018 15:45-16:45 Christopher M. Bingcang, MD Assistant Professor
A Laryngologist s Approach to Voice Presentation at the Nebraska Speech- Language-Hearing Association Fall Convention Thursday, September 27, 2018 15:45-16:45 Christopher M. Bingcang, MD Assistant Professor
Voice Restoration in Presbyphonia. Strobe Rounds March 10 th, 2017 Andrew H. Lee, MD PGY2
 Voice Restoration in Presbyphonia Strobe Rounds March 10 th, 2017 Andrew H. Lee, MD PGY2 1 Disclaimers & Disclosures None 2 3 Agenda Background Etiology Management Options 4 Background Structural changes
Voice Restoration in Presbyphonia Strobe Rounds March 10 th, 2017 Andrew H. Lee, MD PGY2 1 Disclaimers & Disclosures None 2 3 Agenda Background Etiology Management Options 4 Background Structural changes
Vocal Cord Paresis:Background and Case Reports The Greater Baltimore Medical Center, The Johns Hopkins Voice Center at GBMC Stroboscopy Grand Rounds
 Presented by: David F Smith, MD, PhD March 2, 2012 Vocal Cord Paresis:Background and Case Reports The Greater Baltimore Medical Center, The Johns Hopkins Voice Center at GBMC Stroboscopy Grand Rounds 1
Presented by: David F Smith, MD, PhD March 2, 2012 Vocal Cord Paresis:Background and Case Reports The Greater Baltimore Medical Center, The Johns Hopkins Voice Center at GBMC Stroboscopy Grand Rounds 1
A retrospective study of long-term treatment outcomes for reduced vocal intensity in hypokinetic dysarthria
 Watts BMC Ear, Nose and Throat Disorders (2016) 16:2 DOI 10.1186/s12901-016-0022-8 RESEARCH ARTICLE Open Access A retrospective study of long-term treatment outcomes for reduced vocal intensity in hypokinetic
Watts BMC Ear, Nose and Throat Disorders (2016) 16:2 DOI 10.1186/s12901-016-0022-8 RESEARCH ARTICLE Open Access A retrospective study of long-term treatment outcomes for reduced vocal intensity in hypokinetic
A New Stroboscopy Rating Form
 Journal of Voice Vol. 13, No. 3, pp. 403413 1999 Singular Publishing Group, Inc. A New Stroboscopy Rating Form Bruce J. Poburka Department of Communication Disorders Minnesota State University, Mankato,
Journal of Voice Vol. 13, No. 3, pp. 403413 1999 Singular Publishing Group, Inc. A New Stroboscopy Rating Form Bruce J. Poburka Department of Communication Disorders Minnesota State University, Mankato,
Indiana Speech Language Hearing Association
 Indiana Speech Language Hearing Association Presenter Bernice K. Klaben, Ph.D. CCC SLP BRS S Associate Professor Director of Clinical Practice UC Otolaryngology Head and Neck Surgery March 31, 2012 Common
Indiana Speech Language Hearing Association Presenter Bernice K. Klaben, Ph.D. CCC SLP BRS S Associate Professor Director of Clinical Practice UC Otolaryngology Head and Neck Surgery March 31, 2012 Common
Fact Sheet. VitalStim Therapy
 VitalStim Therapy Fact Sheet Dysphagia, or difficulty with swallowing, is a sorely neglected medical disorder that impacts as many as 15 million Americans, with approximately one million people annually
VitalStim Therapy Fact Sheet Dysphagia, or difficulty with swallowing, is a sorely neglected medical disorder that impacts as many as 15 million Americans, with approximately one million people annually
Neuromuscular Electrical Stimulation in the Treatment of Dysphagia. A Summary of the Evidence. Empi St. Paul, MN
 Neuromuscular Electrical Stimulation in the Treatment of Dysphagia A Summary of the Evidence Empi St. Paul, MN Last updated February 4, 2010 Executive summary Neuromuscular electrical stimulation (NMES)
Neuromuscular Electrical Stimulation in the Treatment of Dysphagia A Summary of the Evidence Empi St. Paul, MN Last updated February 4, 2010 Executive summary Neuromuscular electrical stimulation (NMES)
Disclosures. Primary Methods for Treating UVP. Key Factors Influencing Treatment Planning. Guiding principle with Treatment Planning 2/4/2018
 Zen and art of vocal mechanics: Key Factors That Influence Unilateral Vocal Fold Paralysis (UVP) Treatment Decisions Julie Barkmeier Kraemer, Ph.D. Professor, Division of Otolaryngology Clinic Director,
Zen and art of vocal mechanics: Key Factors That Influence Unilateral Vocal Fold Paralysis (UVP) Treatment Decisions Julie Barkmeier Kraemer, Ph.D. Professor, Division of Otolaryngology Clinic Director,
Autologous Fat Augmentation of the Vocal Folds
 Tokai J Exp Clin Med., Vol. 39, No. 3, pp. 146-150, 2014 Autologous Fat Augmentation of the Vocal Folds Shinya OKADA *1, Etsuyo TAMURA *2 and Masahiro IIDA *3 *1 Department of Otorhinolaryngology, Tokai
Tokai J Exp Clin Med., Vol. 39, No. 3, pp. 146-150, 2014 Autologous Fat Augmentation of the Vocal Folds Shinya OKADA *1, Etsuyo TAMURA *2 and Masahiro IIDA *3 *1 Department of Otorhinolaryngology, Tokai
Citation 音声科学研究 = Studia phonologica (1972),
 TitleImbalance of the Vocal Cords as a F Author(s) Isshiki, Nobuhiko Citation 音声科学研究 = Studia phonologica (1972), Issue Date 1972 URL http://hdl.handle.net/2433/52599 Right Type Departmental Bulletin Paper
TitleImbalance of the Vocal Cords as a F Author(s) Isshiki, Nobuhiko Citation 音声科学研究 = Studia phonologica (1972), Issue Date 1972 URL http://hdl.handle.net/2433/52599 Right Type Departmental Bulletin Paper
Normal Voice. Evaluation of a Patient with Hoarseness. No disclosures. Hoarseness. Assessment. Assessment
 Evaluation of a Patient with Hoarseness No disclosures Mari Hagiwara, MD NYU Langone Medical Center ASHNR 2017 Hoarseness Symptom: any deviation from normal voice quality as perceived by self or others;
Evaluation of a Patient with Hoarseness No disclosures Mari Hagiwara, MD NYU Langone Medical Center ASHNR 2017 Hoarseness Symptom: any deviation from normal voice quality as perceived by self or others;
Larynx. Rudimentary. Behind the posterior surface : -stylopharyngeus - salpingopharyngeus -platopharyngeus
 Larynx The larynx is an organ that provides a protective sphincter at the inlet of the air passages and is responsible for voice production. It extends from C3-C6: *Posterior: the pharynx *Lateral: the
Larynx The larynx is an organ that provides a protective sphincter at the inlet of the air passages and is responsible for voice production. It extends from C3-C6: *Posterior: the pharynx *Lateral: the
Index. pseudocyst, stroboscopy indications and usefulness, true cyst, 185, 287 [26] vallecular, 56, 57f Czermak, Johann Nepomuk, 5, 5f
![Index. pseudocyst, stroboscopy indications and usefulness, true cyst, 185, 287 [26] vallecular, 56, 57f Czermak, Johann Nepomuk, 5, 5f Index. pseudocyst, stroboscopy indications and usefulness, true cyst, 185, 287 [26] vallecular, 56, 57f Czermak, Johann Nepomuk, 5, 5f](/thumbs/83/87633728.jpg) Index Note: Page numbers followed by f and t indicate figures and tables; italicized page numbers indicate video clip descriptions and corresponding clip number, e.g. 284 [11]. A Abductor spasmodic dysphonia,
Index Note: Page numbers followed by f and t indicate figures and tables; italicized page numbers indicate video clip descriptions and corresponding clip number, e.g. 284 [11]. A Abductor spasmodic dysphonia,
Vocal Fold Pseudocyst: Results of 46 Cases Undergoing a Uniform Treatment Algorithm
 The Laryngoscope VC 2013 The American Laryngological, Rhinological and Otological Society, Inc. Vocal Fold Pseudocyst: Results of 46 Cases Undergoing a Uniform Treatment Algorithm Christine Estes, MM,
The Laryngoscope VC 2013 The American Laryngological, Rhinological and Otological Society, Inc. Vocal Fold Pseudocyst: Results of 46 Cases Undergoing a Uniform Treatment Algorithm Christine Estes, MM,
Your Voice Can Get Old, Too
 This copy is for your personal, non-commercial use only. To order presentation-ready copies for distribution to your colleagues, clients or customers visit http://www.djreprints.com. http://www.wsj.com/articles/your-voice-can-get-old-too-1477326119
This copy is for your personal, non-commercial use only. To order presentation-ready copies for distribution to your colleagues, clients or customers visit http://www.djreprints.com. http://www.wsj.com/articles/your-voice-can-get-old-too-1477326119
Jitter, Shimmer, and Noise in Pathological Voice Quality Perception
 ISCA Archive VOQUAL'03, Geneva, August 27-29, 2003 Jitter, Shimmer, and Noise in Pathological Voice Quality Perception Jody Kreiman and Bruce R. Gerratt Division of Head and Neck Surgery, School of Medicine
ISCA Archive VOQUAL'03, Geneva, August 27-29, 2003 Jitter, Shimmer, and Noise in Pathological Voice Quality Perception Jody Kreiman and Bruce R. Gerratt Division of Head and Neck Surgery, School of Medicine
Effectiveness of Neuromuscular Electrical Stimulation on Neurological Pharyngeal Dysphagia
 ORIGINAL ARTICLE Effectiveness of Neuromuscular Electrical Stimulation 10.5005/jp-journals-10023-1155 on Neurological Pharyngeal Dysphagia Effectiveness of Neuromuscular Electrical Stimulation on Neurological
ORIGINAL ARTICLE Effectiveness of Neuromuscular Electrical Stimulation 10.5005/jp-journals-10023-1155 on Neurological Pharyngeal Dysphagia Effectiveness of Neuromuscular Electrical Stimulation on Neurological
Tri-State Medical Center. Patient: Amy Curtis Sex: Female CA: 34 years old PROCEDURE NOTE
 SimuCase 2014 Tri-State Medical Center Patient: Amy Curtis Sex: Female CA: 34 years old PROCEDURE NOTE Chief Complaint: I have pain across the back of my head and in the left side of my neck to my shoulder.
SimuCase 2014 Tri-State Medical Center Patient: Amy Curtis Sex: Female CA: 34 years old PROCEDURE NOTE Chief Complaint: I have pain across the back of my head and in the left side of my neck to my shoulder.
Evaluation of the Correlation Between Turkish Voice Handicap Index-10 and Turkish Voice-Related Quality of Life Scale
 155 Turkish Archives of Otorhinolaryngology Türk Otorinolarengoloji Arşivi Turk Arch Otorhinolaryngol 2018; 56(3): 155-9 Evaluation of the Correlation Between Turkish Voice Handicap Index-10 and Turkish
155 Turkish Archives of Otorhinolaryngology Türk Otorinolarengoloji Arşivi Turk Arch Otorhinolaryngol 2018; 56(3): 155-9 Evaluation of the Correlation Between Turkish Voice Handicap Index-10 and Turkish
COMD #6305 The Phonatory system Chapters 4, 5
 COMD #6305 The Phonatory system Chapters 4, 5 Laryngeal function Theory of phonation Jitter, shimmer Vocal registers Normal vs. abnormal voice qualities Measurements of voice quality Clinical applications
COMD #6305 The Phonatory system Chapters 4, 5 Laryngeal function Theory of phonation Jitter, shimmer Vocal registers Normal vs. abnormal voice qualities Measurements of voice quality Clinical applications
General Concepts - Why
 Surgery for Benign Laryngeal Disease: When and How General Concepts - When Surgery should never be the initial treatment option Only when there is persistent troublesome dysphonia after completing work
Surgery for Benign Laryngeal Disease: When and How General Concepts - When Surgery should never be the initial treatment option Only when there is persistent troublesome dysphonia after completing work
UKnowledge. University of Kentucky
 University of Kentucky UKnowledge Theses and Dissertations--Rehabilitation Sciences Rehabilitation Sciences 2016 INVESTIGATING THE EFFICACY OF VOCAL FUNCTION EXERCISES IN IMPROVING VOCAL FUNCTION IN ADULTS
University of Kentucky UKnowledge Theses and Dissertations--Rehabilitation Sciences Rehabilitation Sciences 2016 INVESTIGATING THE EFFICACY OF VOCAL FUNCTION EXERCISES IN IMPROVING VOCAL FUNCTION IN ADULTS
Botulinum Therapy in the Laryngopharynx October 2004
 TITLE: Botulinum Therapy in the Laryngopharynx SOURCE: Grand Rounds Presentation, UTMB, Dept. of Otolaryngology DATE: October 27, 2004 RESIDENT PHYSICIAN: Sam J. Cunningham, MD, PhD FACULTY ADVISOR: David
TITLE: Botulinum Therapy in the Laryngopharynx SOURCE: Grand Rounds Presentation, UTMB, Dept. of Otolaryngology DATE: October 27, 2004 RESIDENT PHYSICIAN: Sam J. Cunningham, MD, PhD FACULTY ADVISOR: David
NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedures overview of collagen injection for vocal cord augmentation Introduction This overview has been prepared
NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedures overview of collagen injection for vocal cord augmentation Introduction This overview has been prepared
Anatomy of the Airway
 Anatomy of the Airway Nagelhout, 5 th edition, Chapter 26 Morgan & Mikhail, 5 th edition, Chapter 23 Mary Karlet, CRNA, PhD Airway Anatomy The airway consists of the nose, pharynx, larynx, trachea, and
Anatomy of the Airway Nagelhout, 5 th edition, Chapter 26 Morgan & Mikhail, 5 th edition, Chapter 23 Mary Karlet, CRNA, PhD Airway Anatomy The airway consists of the nose, pharynx, larynx, trachea, and
Dr Sabah Mohammed Hassan. Consultant Phoniatrician
 Consultant Phoniatrician King Abul Aziz University Hospital King Saud University Non-organic (Functional)Voice Disorders Introduction Etiological Classification Of Voice Disorders: 1-Organic. 2- Non-Organic
Consultant Phoniatrician King Abul Aziz University Hospital King Saud University Non-organic (Functional)Voice Disorders Introduction Etiological Classification Of Voice Disorders: 1-Organic. 2- Non-Organic
Laryngotracheal/Pulmonary Problems and the Mechanically Ventilated Patient: Pediatric Lung Transplantation
 Laryngotracheal/Pulmonary Problems and the Mechanically Ventilated Patient: Pediatric Lung Transplantation G. Kurland, MD Children s Hospital of Pittsburgh Geoffrey.kurland@chp.edu 11/2014 Objectives Discuss
Laryngotracheal/Pulmonary Problems and the Mechanically Ventilated Patient: Pediatric Lung Transplantation G. Kurland, MD Children s Hospital of Pittsburgh Geoffrey.kurland@chp.edu 11/2014 Objectives Discuss
AEROWIN RT: CLINCAL APPLICATION
 MOTOR SPEECH DISORDERS Track Aug 2003 -COVER PAGE- AEROWIN RT: CLINCAL APPLICATION for MOTOR SPEECH DISORDERS Rajesh Vantipalli rajeshv@ku.edu 785-864-0650 Steven Barlow smbarlow@ku.edu 785-864-0632 785-864-4403
MOTOR SPEECH DISORDERS Track Aug 2003 -COVER PAGE- AEROWIN RT: CLINCAL APPLICATION for MOTOR SPEECH DISORDERS Rajesh Vantipalli rajeshv@ku.edu 785-864-0650 Steven Barlow smbarlow@ku.edu 785-864-0632 785-864-4403
NIH Public Access Author Manuscript Ann Otol Rhinol Laryngol. Author manuscript; available in PMC 2012 July 10.
 NIH Public Access Author Manuscript Published in final edited form as: Ann Otol Rhinol Laryngol. 2010 September ; 119(9): 594 601. Neck surface electromyography as a measure of vocal hyperfunction before
NIH Public Access Author Manuscript Published in final edited form as: Ann Otol Rhinol Laryngol. 2010 September ; 119(9): 594 601. Neck surface electromyography as a measure of vocal hyperfunction before
Chapter 12 Audio-visual analysis of vocal tremor derived from acoustics, laryngovideostroboscopy
 107 12 Audio-visual analysis of vocal tremor derived from acoustics, laryngovideostroboscopy & HSDI Chapter 12 Audio-visual analysis of vocal tremor derived from acoustics, laryngovideostroboscopy & HSDI
107 12 Audio-visual analysis of vocal tremor derived from acoustics, laryngovideostroboscopy & HSDI Chapter 12 Audio-visual analysis of vocal tremor derived from acoustics, laryngovideostroboscopy & HSDI
The effect of anti-reflux treatment on subjective voice measurements of patients with laryngopharyngeal reflux
 The Journal of Laryngology & Otology (2013), 127, 590 594. JLO (1984) Limited, 2013 doi:10.1017/s0022215113000832 MAIN ARTICLE The effect of anti-reflux treatment on subjective voice measurements of patients
The Journal of Laryngology & Otology (2013), 127, 590 594. JLO (1984) Limited, 2013 doi:10.1017/s0022215113000832 MAIN ARTICLE The effect of anti-reflux treatment on subjective voice measurements of patients
Voice Disorders in Medically Complex Children
 Voice Disorders in Medically Complex Children Roger C. Nuss, MD, FACS Geralyn Harvey Woodnorth, M.A., CCC-SLP Department of Otolaryngology and Communication Enhancement Children s Hospital Boston Harvard
Voice Disorders in Medically Complex Children Roger C. Nuss, MD, FACS Geralyn Harvey Woodnorth, M.A., CCC-SLP Department of Otolaryngology and Communication Enhancement Children s Hospital Boston Harvard
Speech Generation and Perception
 Speech Generation and Perception 1 Speech Generation and Perception : The study of the anatomy of the organs of speech is required as a background for articulatory and acoustic phonetics. An understanding
Speech Generation and Perception 1 Speech Generation and Perception : The study of the anatomy of the organs of speech is required as a background for articulatory and acoustic phonetics. An understanding
Please refer back to the slides as these are extra notes only. Slide 2 -The Larynx is a Box of cartilage.
 [ANATOMY #3] 1 بسم رلاهللا Please refer back to the slides as these are extra notes only. Slide 2 -The Larynx is a Box of cartilage. -The lower border of c6 is the lower border of cricoid cartilage. -The
[ANATOMY #3] 1 بسم رلاهللا Please refer back to the slides as these are extra notes only. Slide 2 -The Larynx is a Box of cartilage. -The lower border of c6 is the lower border of cricoid cartilage. -The
Larynx - cartilaginous structure holding the vocal folds which protrude into airstream
 1! Larynx - cartilaginous structure holding the vocal folds which protrude into airstream 2! Flow increase - like thumb over garden hose Pressure drop - narrower space forces pressure drop due to speed
1! Larynx - cartilaginous structure holding the vocal folds which protrude into airstream 2! Flow increase - like thumb over garden hose Pressure drop - narrower space forces pressure drop due to speed
Length-Tension Relationship of the Feline Thyroarytenoid Muscle
 Length-Tension Relationship of the Feline Thyroarytenoid Muscle *Michael M. Johns, Melanie Urbanchek, Douglas B. Chepeha, William M. Kuzon, Jr. and Norman D. Hogikyan *Atlanta, Georgia, Ann Arbor, Michigan
Length-Tension Relationship of the Feline Thyroarytenoid Muscle *Michael M. Johns, Melanie Urbanchek, Douglas B. Chepeha, William M. Kuzon, Jr. and Norman D. Hogikyan *Atlanta, Georgia, Ann Arbor, Michigan
Chapter 1. Respiratory Anatomy and Physiology. 1. Describe the difference between anatomy and physiology in the space below:
 Contents Preface vii 1 Respiratory Anatomy and Physiology 1 2 Laryngeal Anatomy and Physiology 11 3 Vocal Health 27 4 Evaluation 33 5 Vocal Pathology 51 6 Neurologically Based Voice Disorders 67 7 Vocal
Contents Preface vii 1 Respiratory Anatomy and Physiology 1 2 Laryngeal Anatomy and Physiology 11 3 Vocal Health 27 4 Evaluation 33 5 Vocal Pathology 51 6 Neurologically Based Voice Disorders 67 7 Vocal
Why Can t I breathe? Asthma vs. Vocal Cord Dysfunction (VCD) Lindsey Frohn, M.S., CCC-SLP Madonna Rehabilitation Hospital (Lincoln, NE)
 Why Can t I breathe? Asthma vs. Vocal Cord Dysfunction (VCD) Lindsey Frohn, M.S., CCC-SLP Madonna Rehabilitation Hospital (Lincoln, NE) Objectives Examine Vocal Cord Dysfunction Examine Exercise Induced
Why Can t I breathe? Asthma vs. Vocal Cord Dysfunction (VCD) Lindsey Frohn, M.S., CCC-SLP Madonna Rehabilitation Hospital (Lincoln, NE) Objectives Examine Vocal Cord Dysfunction Examine Exercise Induced
Voice Analysis in Individuals with Chronic Obstructive Pulmonary Disease
 ORIGINAL ARTICLE Voice Analysis in Individuals with Chronic 10.5005/jp-journals-10023-1081 Obstructive Pulmonary Disease Voice Analysis in Individuals with Chronic Obstructive Pulmonary Disease 1 Anuradha
ORIGINAL ARTICLE Voice Analysis in Individuals with Chronic 10.5005/jp-journals-10023-1081 Obstructive Pulmonary Disease Voice Analysis in Individuals with Chronic Obstructive Pulmonary Disease 1 Anuradha
A Prospective Crossover Trial of Botulinum Toxin Chemodenervation Versus Injection Augmentation for Essential Voice Tremor
 The Laryngoscope VC 2017 The American Laryngological, Rhinological and Otological Society, Inc. A Prospective Crossover Trial of Botulinum Toxin Chemodenervation Versus Injection Augmentation for Essential
The Laryngoscope VC 2017 The American Laryngological, Rhinological and Otological Society, Inc. A Prospective Crossover Trial of Botulinum Toxin Chemodenervation Versus Injection Augmentation for Essential
Injection Laryngoplasty Outcomes in Irradiated and Nonirradiated Unilateral Vocal Fold Paralysis
 The Laryngoscope VC 2014 The American Laryngological, Rhinological and Otological Society, Inc. Injection Laryngoplasty Outcomes in Irradiated and Nonirradiated Unilateral Vocal Fold Paralysis Joseph Chang,
The Laryngoscope VC 2014 The American Laryngological, Rhinological and Otological Society, Inc. Injection Laryngoplasty Outcomes in Irradiated and Nonirradiated Unilateral Vocal Fold Paralysis Joseph Chang,
T1/T2 LARYNX CANCER. Click to edit Master Presentation Date. Thomas J Gernon, MD Otolaryngology-Head and Neck Surgery
 ADVANCES IN TREATMENT OF T1/T2 LARYNX CANCER Click to edit Master Presentation Date Thomas J Gernon, MD Otolaryngology-Head and Neck Surgery I have nothing to disclose CHANGING TRENDS IN HNSCC GLOTTIC
ADVANCES IN TREATMENT OF T1/T2 LARYNX CANCER Click to edit Master Presentation Date Thomas J Gernon, MD Otolaryngology-Head and Neck Surgery I have nothing to disclose CHANGING TRENDS IN HNSCC GLOTTIC
Acoustic Analysis Before and After Voice Therapy for Laryngeal Pathology.
 Acoustic Analysis Before and After Voice Therapy for Laryngeal Pathology. Chhetri SS, Gautam R ABSTRACT Background Department of ENT-HNS Kathmandu Medical College and Teaching Hospital Sinamangal, Kathmandu,
Acoustic Analysis Before and After Voice Therapy for Laryngeal Pathology. Chhetri SS, Gautam R ABSTRACT Background Department of ENT-HNS Kathmandu Medical College and Teaching Hospital Sinamangal, Kathmandu,
Citation 音声科学研究 = Studia phonologica (1972),
 Title Glottal Parameters and Some with Laryngeal Pathology. Acousti Author(s) Koike, Yasuo; Takahashi, Hiroaki Citation 音声科学研究 = Studia phonologica (197), Issue Date 197 URL http://hdl.handle.net/433/56
Title Glottal Parameters and Some with Laryngeal Pathology. Acousti Author(s) Koike, Yasuo; Takahashi, Hiroaki Citation 音声科学研究 = Studia phonologica (197), Issue Date 197 URL http://hdl.handle.net/433/56
A Holistic Approach to Voice Therapy
 A Holistic Approach to Voice Therapy Joseph C. Stemple, Ph.D. 1 ABSTRACT Therapy approaches designed to improve the disordered voice may be equally effective when used to enhance the normal voice. A holistic
A Holistic Approach to Voice Therapy Joseph C. Stemple, Ph.D. 1 ABSTRACT Therapy approaches designed to improve the disordered voice may be equally effective when used to enhance the normal voice. A holistic
The Paediatric Voice Clinic
 The Paediatric Voice Clinic Smillie I 1, McManus K 1, Cohen W 2, Wynne D1. Department of Paediatric Otolaryngology, Royal Hospital for Sick Children, Glasgow. 2 School of Psychological Sciences and Health,
The Paediatric Voice Clinic Smillie I 1, McManus K 1, Cohen W 2, Wynne D1. Department of Paediatric Otolaryngology, Royal Hospital for Sick Children, Glasgow. 2 School of Psychological Sciences and Health,
Laryngeal electromyography findings of vocal fold immobility in patients after radiotherapy for nasopharyngeal carcinoma
 ORIGINAL ARTICLE Laryngeal electromyography findings of vocal fold immobility in patients after radiotherapy for nasopharyngeal carcinoma Yi-Ling Hsieh, MD, 1 Ming-Hong Chang, MD, 2 Chen-Chi Wang, MD 1,3,4*
ORIGINAL ARTICLE Laryngeal electromyography findings of vocal fold immobility in patients after radiotherapy for nasopharyngeal carcinoma Yi-Ling Hsieh, MD, 1 Ming-Hong Chang, MD, 2 Chen-Chi Wang, MD 1,3,4*
patients who received LEMG-guided hyaluronic acid VF injection for UVFP at a tertiary referral medical center from March 2010 to February 2013.
 Research Original Investigation Laryngeal Electromyography-Guided Hyaluronic Acid Vocal Fold Injection for Unilateral Vocal Fold Paralysis A Prospective Long-term Follow-up Outcome Report Chen-Chi Wang,
Research Original Investigation Laryngeal Electromyography-Guided Hyaluronic Acid Vocal Fold Injection for Unilateral Vocal Fold Paralysis A Prospective Long-term Follow-up Outcome Report Chen-Chi Wang,
Deciphering Dysphagia with E-Stim 8 March 2015
 Deciphering Dysphagia with E-Stim 8 March 2015 Electrical Stimulation for Muscle Re-education in Swallowing Presented by: Russ Campbell, PT Sponsored by: HEMAX Health Products Company Limited New Options
Deciphering Dysphagia with E-Stim 8 March 2015 Electrical Stimulation for Muscle Re-education in Swallowing Presented by: Russ Campbell, PT Sponsored by: HEMAX Health Products Company Limited New Options
**** DISCLAIMER ****
 Grand Rounds Archives **** DISCLAIMER **** The information contained within the Grand Rounds Archive is intended for use by doctors and other health care professionals. These documents were prepared by
Grand Rounds Archives **** DISCLAIMER **** The information contained within the Grand Rounds Archive is intended for use by doctors and other health care professionals. These documents were prepared by
Treatment Parameters of High Frequency Electrical stimulation as Established on the Electro-Stim 180
 0196-6011 /83/0403-0162$02.00/0 THE JOURNAL OF ORTHOPAEDIC AND SPORTS PHYSICAL THERAPY Copyright 0 1983 by The Orthopaedic and Sports Physical Therapy Sections of the American Physical Therapy Association
0196-6011 /83/0403-0162$02.00/0 THE JOURNAL OF ORTHOPAEDIC AND SPORTS PHYSICAL THERAPY Copyright 0 1983 by The Orthopaedic and Sports Physical Therapy Sections of the American Physical Therapy Association
Neurolaryngology and Neurogenic Voice Disorders. Introduction. If it walks like a duck.. Erin Guidera, MS, CCC-SLP 4/8/17
 Neurolaryngology and Neurogenic Voice Disorders Erin Guidera, MS, CCC-SLP 4/8/17 Introduction Changes in vocal quality and speech can be the presenting symptom of underlying neurological disorders (e.g.,
Neurolaryngology and Neurogenic Voice Disorders Erin Guidera, MS, CCC-SLP 4/8/17 Introduction Changes in vocal quality and speech can be the presenting symptom of underlying neurological disorders (e.g.,
Quarterly Progress and Status Report. Evaluation of teflon injection therapy for paralytic dysphonia
 Dept. for Speech, Music and Hearing Quarterly Progress and Status Report Evaluation of teflon injection therapy for paralytic dysphonia Fritzell, B. and Hallen, O. and Sundberg, J. journal: STL-QPSR volume:
Dept. for Speech, Music and Hearing Quarterly Progress and Status Report Evaluation of teflon injection therapy for paralytic dysphonia Fritzell, B. and Hallen, O. and Sundberg, J. journal: STL-QPSR volume:
BILATERAL ABDUCTOR VOCAL CORD PALSY. Dr NITYA G Final year PG KIMS
 BILATERAL ABDUCTOR VOCAL CORD PALSY Dr NITYA G Final year PG KIMS INTRODUCTION Vocal cord paralysis is a sign of a disease It results from dysfunction of Recurrent laryngeal nerves on both sides Paralysis
BILATERAL ABDUCTOR VOCAL CORD PALSY Dr NITYA G Final year PG KIMS INTRODUCTION Vocal cord paralysis is a sign of a disease It results from dysfunction of Recurrent laryngeal nerves on both sides Paralysis
ORIGINAL ARTICLE. Pill Swallowing by Adults With Dysphagia. Giselle Carnaby-Mann, B App Sci, PGrad Dip (HSc), MPH, PhD; Michael Crary, PhD
 ORIGINAL ARTICLE Pill Swallowing by Adults With Dysphagia Giselle Carnaby-Mann, B App Sci, PGrad Dip (HSc), MPH, PhD; Michael Crary, PhD Objective: To evaluate differences in swallowing physiology and
ORIGINAL ARTICLE Pill Swallowing by Adults With Dysphagia Giselle Carnaby-Mann, B App Sci, PGrad Dip (HSc), MPH, PhD; Michael Crary, PhD Objective: To evaluate differences in swallowing physiology and
Stroboscopy: an evolving tool for voice analysis in vocal cord pathologies
 International Journal of Otorhinolaryngology and Head and Neck Surgery Rajput SD et al. Int J Otorhinolaryngol Head Neck Surg. 2017 Oct;3(4):927-931 http://www.ijorl.com pissn 2454-5929 eissn 2454-5937
International Journal of Otorhinolaryngology and Head and Neck Surgery Rajput SD et al. Int J Otorhinolaryngol Head Neck Surg. 2017 Oct;3(4):927-931 http://www.ijorl.com pissn 2454-5929 eissn 2454-5937
The Journal of MacroTrends in Health and Medicine
 MACROJOURNALS The Journal of MacroTrends in Health and Medicine Videokymography (VKG) in Laryngologic Practice Jitka Vydrova*, Jan G. Svec*,**, František Sram* *Voice Centre Prague, Medical Healthcom,
MACROJOURNALS The Journal of MacroTrends in Health and Medicine Videokymography (VKG) in Laryngologic Practice Jitka Vydrova*, Jan G. Svec*,**, František Sram* *Voice Centre Prague, Medical Healthcom,
Bipedicled Strap Muscle Transposition for Vocal Fold Deficit after Laser Cordectomy in Early Glottic Cancer Patients
 The Laryngoscope Lippincott Williams & Wilkins, Inc. 2005 The American Laryngological, Rhinological and Otological Society, Inc. Bipedicled Strap Muscle Transposition for Vocal Fold Deficit after Laser
The Laryngoscope Lippincott Williams & Wilkins, Inc. 2005 The American Laryngological, Rhinological and Otological Society, Inc. Bipedicled Strap Muscle Transposition for Vocal Fold Deficit after Laser
Deciphering Dysphagia with E-Stim 24 Mar 2013
 Deciphering Dysphagia with E-Stim 24 Mar 2013 Electrical Stimulation for Muscle Re-education in Swallowing Presented by: Russ Campbell, PT Rick McAdoo, M.S., CCC-SLP Sponsored by: HEMAX Health Products
Deciphering Dysphagia with E-Stim 24 Mar 2013 Electrical Stimulation for Muscle Re-education in Swallowing Presented by: Russ Campbell, PT Rick McAdoo, M.S., CCC-SLP Sponsored by: HEMAX Health Products
Laryngeal Electromyography: Basic Concepts and Clinical Uses
 Robert T. Sataloff, M.D., D.M.A. Robert T. Sataloff, M.D., D.M.A. Laryngeal Electromyography: Basic Concepts and Clinical Uses Yolanda D. Heman-Ackah, M.D. and Robert T. Sataloff, M.D., D.M.A. UNDERSTANDING
Robert T. Sataloff, M.D., D.M.A. Robert T. Sataloff, M.D., D.M.A. Laryngeal Electromyography: Basic Concepts and Clinical Uses Yolanda D. Heman-Ackah, M.D. and Robert T. Sataloff, M.D., D.M.A. UNDERSTANDING
Prior Authorization Review Panel MCO Policy Submission
 Prior Authorization Review Panel MCO Policy Submission A separate copy of this form must accompany each policy submitted for review. Policies submitted without this form will not be considered for review.
Prior Authorization Review Panel MCO Policy Submission A separate copy of this form must accompany each policy submitted for review. Policies submitted without this form will not be considered for review.
Vibratory Asymmetry in Mobile Vocal Folds: Is It Predictive of Vocal Fold Paresis?
 Annals ofototogy, hinology & aryngology 120(4):239-242. 2011 Annals Publishing Company. All rights reserved. Vibratory Asymmetry in obile Vocal olds: Is It Predictive of Vocal old Paresis? C. lake Simpson,
Annals ofototogy, hinology & aryngology 120(4):239-242. 2011 Annals Publishing Company. All rights reserved. Vibratory Asymmetry in obile Vocal olds: Is It Predictive of Vocal old Paresis? C. lake Simpson,
Pathophysiology and Surgical Treatment of Unilateral Vocal Fold Paralysis
 Pathophysiology and Surgical Treatment of Unilateral Vocal Fold Paralysis Denervation and Reinnervation Eiji Yumoto 123 Pathophysiology and Surgical Treatment of Unilateral Vocal Fold Paralysis Eiji Yumoto
Pathophysiology and Surgical Treatment of Unilateral Vocal Fold Paralysis Denervation and Reinnervation Eiji Yumoto 123 Pathophysiology and Surgical Treatment of Unilateral Vocal Fold Paralysis Eiji Yumoto
피대근절개에따른갑상선절제술후의음성변화. Voice Comparison between Strap Muscle Retraction and Cutting Technique in Thyroidectomy 김영모 1 조정일 1 김철호 1 박정선 1 최호순 3 하현령 2
 KISEP Head and Neck Korean J Otolaryngol 2000;43:985-91 피대근절개에따른갑상선절제술후의음성변화 김영모 1 조정일 1 김철호 1 박정선 1 최호순 3 하현령 2 Voice Comparison between Strap Muscle Retraction and Cutting Technique in Thyroidectomy
KISEP Head and Neck Korean J Otolaryngol 2000;43:985-91 피대근절개에따른갑상선절제술후의음성변화 김영모 1 조정일 1 김철호 1 박정선 1 최호순 3 하현령 2 Voice Comparison between Strap Muscle Retraction and Cutting Technique in Thyroidectomy
Electrical Stimulation in the Treatment of Dysphagia Literature review. Baijens, 2008: Case report: Treatment of patient with opercular syndrome.
 Electrical Stimulation in the Treatment of Dysphagia Literature review Baijens, 2008: Case report: Treatment of patient with opercular syndrome. Design: Case study (Grade: D) Report on treatment outcomes
Electrical Stimulation in the Treatment of Dysphagia Literature review Baijens, 2008: Case report: Treatment of patient with opercular syndrome. Design: Case study (Grade: D) Report on treatment outcomes
Visi-Pitch IV is the latest version of the most widely
 APPLICATIONS Voice Disorders Motor Speech Disorders Voice Typing Fluency Selected Articulation Training Hearing-Impaired Speech Professional Voice Accent Reduction and Second Language Learning Importance
APPLICATIONS Voice Disorders Motor Speech Disorders Voice Typing Fluency Selected Articulation Training Hearing-Impaired Speech Professional Voice Accent Reduction and Second Language Learning Importance
VitalStim in Swallowing Rehabilitation
 VitalStim in Swallowing Rehabilitation Meghan McAvoy, MS,CCC-SLP Mary Free Bed at Sparrow Hospital Disclosures No financial or non-financial disclosures Control of the swallow Both voluntary and involuntary
VitalStim in Swallowing Rehabilitation Meghan McAvoy, MS,CCC-SLP Mary Free Bed at Sparrow Hospital Disclosures No financial or non-financial disclosures Control of the swallow Both voluntary and involuntary
Introduction. Changes in speech as it relates to PD: Deep Brain Stimulation (DBS) and its impact on speech: Treatment for Speech Disturbance:
 Introduction Speech is one of the most fundamental means of connecting with others and expressing our wants and needs. Speech difficulties, then, can result in significant challenges when interacting with
Introduction Speech is one of the most fundamental means of connecting with others and expressing our wants and needs. Speech difficulties, then, can result in significant challenges when interacting with
ORIGINAL ARTICLE. Diagnostic Contributions of Videolaryngostroboscopy in the Pediatric Population
 ORIGINAL ARTICLE Diagnostic Contributions of Videolaryngostroboscopy in the Pediatric Population Melissa Mortensen, MD; Madeline Schaberg, MD; Peak Woo, MD Objective: Videolaryngostroboscopy (VLS) is a
ORIGINAL ARTICLE Diagnostic Contributions of Videolaryngostroboscopy in the Pediatric Population Melissa Mortensen, MD; Madeline Schaberg, MD; Peak Woo, MD Objective: Videolaryngostroboscopy (VLS) is a
Speech Therapy. 4. Therapy is used to achieve significant, functional improvement through specific diagnosisrelated
 Speech Therapy I. Policy Speech therapy services include the diagnosis and treatment of communication impairment(s) and swallowing disorders. Services include speech/language therapy, swallowing/feeding
Speech Therapy I. Policy Speech therapy services include the diagnosis and treatment of communication impairment(s) and swallowing disorders. Services include speech/language therapy, swallowing/feeding
A Comparison of Outcomes in Interventions for Unilateral Vocal Fold Paralysis: A Systematic Review
 The Laryngoscope VC 2015 The American Laryngological, Rhinological and Otological Society, Inc. Systematic Review A Comparison of Outcomes in Interventions for Unilateral Vocal Fold Paralysis: A Systematic
The Laryngoscope VC 2015 The American Laryngological, Rhinological and Otological Society, Inc. Systematic Review A Comparison of Outcomes in Interventions for Unilateral Vocal Fold Paralysis: A Systematic
Airflow in unilateral vocal cord paralysis before
 Airflow in unilateral vocal cord paralysis before and after Teflon injection Y. CORMIER', H. KASHIMA, W. SUMMER, AND H. MENKES Thorax, 1978, 33, 57-61 From the Respiratory Division of the Department of
Airflow in unilateral vocal cord paralysis before and after Teflon injection Y. CORMIER', H. KASHIMA, W. SUMMER, AND H. MENKES Thorax, 1978, 33, 57-61 From the Respiratory Division of the Department of
Title: Evaluating the outcome of phonosurgery: comparing the role of VHI and VoiSS questionnaires in the Greek language.
 Elsevier Editorial System(tm) for Journal of Voice Manuscript Draft Manuscript Number: JVOICE-D--000R1 Title: Evaluating the outcome of phonosurgery: comparing the role of VHI and VoiSS questionnaires
Elsevier Editorial System(tm) for Journal of Voice Manuscript Draft Manuscript Number: JVOICE-D--000R1 Title: Evaluating the outcome of phonosurgery: comparing the role of VHI and VoiSS questionnaires
CURRENT AND FUTURE HORIZONS IN LARYNGEAL
 Ann Otol Rhinol Laryngol 98:1989 CURRENT AND FUTURE HORIZONS IN LARYNGEAL AND VOICE RESEARCH PAUL H. WARD, MD BRUCE R. GERRATT, PHD DAVID G. HANSON, MD GERALD S. BERKE, MD Los ANGELES, CALIFOHNIA Voice
Ann Otol Rhinol Laryngol 98:1989 CURRENT AND FUTURE HORIZONS IN LARYNGEAL AND VOICE RESEARCH PAUL H. WARD, MD BRUCE R. GERRATT, PHD DAVID G. HANSON, MD GERALD S. BERKE, MD Los ANGELES, CALIFOHNIA Voice
ABSTRACT REPEATABILITY OF AERODYNAMIC MEASUREMENTS OF VOICE. by Courtney Rollins Garrison
 ABSTRACT REPEATABILITY OF AERODYNAMIC MEASUREMENTS OF VOICE by Courtney Rollins Garrison The purpose of this study was to compare baseline aerodynamic measurements of voice to measurements repeated after
ABSTRACT REPEATABILITY OF AERODYNAMIC MEASUREMENTS OF VOICE by Courtney Rollins Garrison The purpose of this study was to compare baseline aerodynamic measurements of voice to measurements repeated after
Cricothyroid Muscle Dysfunction Impairs Vocal Fold Vibration in Unilateral Vocal Fold Paralysis
 The Laryngoscope VC 2013 The American Laryngological, Rhinological and Otological Society, Inc. Cricothyroid Muscle Dysfunction Impairs Vocal Fold Vibration in Unilateral Vocal Fold Paralysis Yu-Cheng
The Laryngoscope VC 2013 The American Laryngological, Rhinological and Otological Society, Inc. Cricothyroid Muscle Dysfunction Impairs Vocal Fold Vibration in Unilateral Vocal Fold Paralysis Yu-Cheng
Telephone Based Automatic Voice Pathology Assessment.
 Telephone Based Automatic Voice Pathology Assessment. Rosalyn Moran 1, R. B. Reilly 1, P.D. Lacy 2 1 Department of Electronic and Electrical Engineering, University College Dublin, Ireland 2 Royal Victoria
Telephone Based Automatic Voice Pathology Assessment. Rosalyn Moran 1, R. B. Reilly 1, P.D. Lacy 2 1 Department of Electronic and Electrical Engineering, University College Dublin, Ireland 2 Royal Victoria
Critical Review: In patients with total laryngectomy, is gender related to quality of life outcomes?
 Critical Review: In patients with total laryngectomy, is gender related to quality of life outcomes? Sarah McSheffrey M.Cl.Sc SLP Candidate University of Western Ontario: School of Communication Sciences
Critical Review: In patients with total laryngectomy, is gender related to quality of life outcomes? Sarah McSheffrey M.Cl.Sc SLP Candidate University of Western Ontario: School of Communication Sciences
A COMPARISON OF SUSTAINED VOWEL AND CONNECTED SPEECH PRODUCTION IN HYPOFUNCTIONAL AND NORMAL VOICES. Emily A. Lambert
 A COMPARISON OF SUSTAINED VOWEL AND CONNECTED SPEECH PRODUCTION IN HYPOFUNCTIONAL AND NORMAL VOICES by Emily A. Lambert Bachelor of Science in Communication Sciences & Disorders, 2008 University of Texas
A COMPARISON OF SUSTAINED VOWEL AND CONNECTED SPEECH PRODUCTION IN HYPOFUNCTIONAL AND NORMAL VOICES by Emily A. Lambert Bachelor of Science in Communication Sciences & Disorders, 2008 University of Texas
Innervation of the cricothyroid muscle by the recurrent laryngeal nerve
 ORIGINAL ARTICLE Innervation of the cricothyroid muscle by the recurrent laryngeal nerve Hiroo Masuoka, MD, PhD,* Akira Miyauchi, MD, PhD, Tomonori Yabuta, MD, PhD, Mitsuhiro Fukushima, MD, PhD, Akihiro
ORIGINAL ARTICLE Innervation of the cricothyroid muscle by the recurrent laryngeal nerve Hiroo Masuoka, MD, PhD,* Akira Miyauchi, MD, PhD, Tomonori Yabuta, MD, PhD, Mitsuhiro Fukushima, MD, PhD, Akihiro
