Sleepwalking, sleep terrors, sleeptalking
|
|
|
- Evelyn Barnett
- 5 years ago
- Views:
Transcription
1 CMAJ CME Parasomnias John A. Fleetham MB, Jonathan A.E. Fleming MB Sleepwalking, sleep terrors, sleeptalking and sleep paralysis are some of the behavioural manifestations associated with the partial arousals from sleep known as parasomnias a group of sleep disorders defined as undesirable physical events or experiences that occur during the initiation of sleep, during sleep or during arousal from sleep. 1 Although more common in children, parasomnias can occur at any age. During sleep, the brain cycles regularly between wakefulness, nonrapid eye movement (NREM) sleep and rapid eye movement (REM) sleep. Nonrapid eye movement sleep is subdivided into four stages: stage I, a transitional stage between wake and sleep; stage II, which makes up most of the sleep period; and stages III and IV, which typically occur in the first half of the night and during which more profound stimulus is required to wake the sleeper. Parasomnias occur when transitions between these stages are blurred (commonly between stages III/IV and the awake state), causing behaviours that lack the complete awareness and mentation associated with wakefulness. 1 There are two criterion-based classifications of sleep disorders: the Diagnostic and Statistical Manual of Mental Disorders, fifth edition (DSM-V) classification 2 and the International Classification of Sleep Disorders (ICSD) classification. 1 The DSM- V uses a lumping versus splitting approach and is less comprehensive than the ICSD classification. In this review, we use the ICSD classification (Box 1). The ICSD classification divides parasomnias into six groups of disorders that can emerge from either NREM or REM sleep, be related to drug or substance use or be a symptom of another medical disorder. Of parasomnias, REM sleep behaviour disorder is most commonly associated with an underlying neurologic condition. 1 In this review, we address parasomnias in adults; 3 sleep disorders in children have recently been reviewed elsewhere. 4 Nonrapid eye movement parasomnias are relatively rare, episodic, often self-limiting events that may not be captured during a polysomnogram. Consequently, their systematic study is often limited to case reports and small case series. Because there have been no large randomized controlled trials of interventions and there are no guidelines available (with the exception of nightmares), the level of evidence for management options is low and is largely limited to the opinion of experts. The sources of evidence used in this review are shown in Box 2. Rapid eye movement sleep behaviour disorder, an REM parasomnia, is a more prevalent condition associated with both iatrogenic causes and medical conditions. It can be reliably confirmed by polysomnography, which has resulted in a higher level of evidence and a best practice guideline. 5 How do parasomnias commonly present? All parasomnias occur from sleep, and NREM parasomnias usually occur among individuals aged 5 25 years with a family history of similar parasomnias (e.g., sleepwalking or sleep terrors) and involve physical and verbal activity of varying complexity. Typically, the sleeper returns to sleep and is amnestic in the morning, with the behaviour being reported by others or discovered because items have been moved or used during the night or the events have resulted in injury. 1 External (e.g., noise, temperature change) or internal (e.g., apnea, periodic limb movement) events may cause an arousal or partial awakening, usually from stage III and IV sleep, which occurs in the first 90 minutes of the sleep period. Arousal or partial awakening can also occur during stage II sleep later in the night. 2 Sleep deprivation or disruption from any cause (e.g., restless legs syndrome, obstructive sleep apnea) can precipitate these events in susceptible individuals. In contrast, REM sleep behaviour disorder is characterized by verbalizations and actions consistent with dream enactment (e.g., fight or flight behaviours) that usually awaken the sleeper who, Key points Competing interests: None declared. This article has been peer reviewed. Correspondence to: John Fleetham, john.fleetham@vch.ca CMAJ DOI: /cmaj Parasomnias are very common and are not related to underlying psychiatric disease. Parasomnias may be complex and prolonged. Evaluation and treatment of parasomnias is suggested for patients whose activities are potentially harmful or very disturbing to others. Medication effects or central nervous disease should be considered for REM sleep behaviour disorder in younger patients Canadian Medical Association or its licensors CMAJ, May 13, 2014, 186(8) E273
2 unlike those with NREM parasomnias, can often recall the event, including the dream and its associated actions. 1 The characteristics of NREM and REM parasomnias are summarized in Table 1. Distinguishing between NREM and REM parasomnias is important because the treatment and prognosis are different. Nonrapid eye movement parasomnias are more common in younger people and are usually outgrown by young adulthood, whereas REM parasomnias present in late adult life and are associated with degenerative brain diseases. 2 The major differential diagnoses for both NREM and REM parasomnia include nocturnal seizures, intoxicated states, medication-induced complex behaviours, nocturnal panic attacks and dissociative disorders. 2 Are investigations required for diagnosis? Box 1: International Classification of Sleep Disorders for parasomnia 1 1. Disorders of arousal from nonrapid eye movement sleep a. Confusional arousals b. Sleepwalking c. Sleep terrors 2. Parasomnias usually associated with rapid eye movement sleep a. Rapid eye movement sleep behaviour disorder b. Recurrent isolated sleep paralysis c. Nightmare disorder 3. Other parasomnias a. Sleep-related dissociative disorders b. Sleep enuresis c. Sleep-related groaning d. Exploding head syndrome e. Sleep-related hallucinations f. Sleep-related eating disorder 4. Parasomnia, unspecified 5. Parasomnia due to drug or substance use 6. Parasomnia due to medical condition Parasomnias are typically diagnosed by obtaining a careful clinical history that assesses the timing, expression and form of the behaviour in the home environment (Box 3). A sleep diary (to exclude sleep deprivation as a precipitant) and a partner s log of the events are useful tools. (See /pdf/sleepdiary.pdf for an example of a sleep diary.) Referral to a specialist in sleep disorders should be considered for patients whose activities are potentially harmful or very disturbing to others, or if polysomnography is required. It is not cost-effective to obtain a polysomnogram for patients with NREM parasomnia, except to exclude other causes of additional sleep instability (e.g., obstructive sleep apnea, periodic limb movement disorder, narcolepsy). Because one of the ICSD diagnostic criteria for REM sleep behaviour disorder requires the demonstration of REM sleep without atonia, 1 polysomnography is needed to confirm this diagnosis and to rule out comorbid sleep disorders, such as obstructive sleep apnea or periodic limb movement disorder, which are more prevalent in adults and may need to be a focus of management. How are specific parasomnias managed? Although incompletely understood, the pathophysiology of NREM and REM parasomnias differ; however, there are commonalities in their management. There have been no large, randomized controlled treatment trials for all parasomnias, and guidelines are limited to the management of nightmares 8 and REM sleep behaviour disorder. 5 Parasomnias commonly associated with NREM sleep There are three main types of NREM parasomnias: confusional arousals, sleepwalking and sleep terrors (Table 1). We have included sleeprelated eating disorders and sleeptalking in this section because they emerge from NREM sleep. The DSM-V classifies sleep-related eating as a subtype of sleepwalking, and the ICSD notes that sleeptalking can occur during any stage of sleep. Confusional arousals Confusional arousals can occur any time sleep is interrupted 9 and can accompany sleep-disruptive conditions, such as narcolepsy, obstructive sleep apnea, periodic limb movement disorder or by forced awakenings, especially in sleep-deprived individuals. Drugs and medications 6 that disrupt sleep can also cause confused arousals. 10 Box 2: Evidence used in this review We searched Web of Science and MEDLINE for reviews and guidelines on the assessment and treatment of parasomnias, as well as for specific parasomnias (from 2008 to 2012). We also reviewed the citations for parasomnias in the International Classification of Sleep Disorders 1 and the Diagnostic and Statistical Manual of Mental Disorders, fifth edition. 2 E274 CMAJ, May 13, 2014, 186(8)
3 CMAJ, May 13, 2014, 186(8) E275
4 Typically, these events are brief and may include sleeptalking and simple motor behaviours that occur without responsiveness to the environment. 3 Because of the sleeper s amnesia, they may only be noted by his or her bed partner. The frequency of events decreases with age; 11 persistence into the twenties is usually associated with comorbidities or medications. 12 Two variants of confused arousals have been described: severe morning sleep inertia (sleep drunkenness, similar to the confusion, disorientation and slowed responses seen on awakening Box 3: Clinical questions to aid in the diagnosis of parasomnia 1. Rule out sleep deprivation a. Time in and out of bed and total sleep time, ideally from a one-week sleep diary b. Exclude external causes of sleep loss i. Elective ii. Shift work iii. Caregiving: young children, ill family member, pets 2. Rule out effects of intoxication or withdrawal a. Alcohol use i. Current pattern of use ii. Any binge drinking? b. Substance use i. Current pattern of use ii. Intoxication with stimulants iii. Withdrawal from sedatives 3. Rule out sleep disorders causing sleep instability a. Sleep apnea b. Periodic limb movement disorder c. Restless legs syndrome d. Narcolepsy 4. Rule out medical disorders or treatments associated with sleep instability a. Syndromes causing pain or discomfort at night b. Alerting medications (e.g., second-generation antidepressants [selective serotonin reuptake inhibitor, serotonin norepinephrine reuptake inhibitor], stimulants, dopamine agonists) 5. Confirm presence of NREM parasomnias in other family members and during the patient s childhood a. In the absence of such a history, expand the screen to include other pathologies, including nocturnal seizures 6. Timing of events a. NREM parasomnias predominate in the first third of the night, REM parasomnias in the last third 7. Morphology of events a. Stereotypical, brief events are more likely to be ictal b. Marked autonomic arousal is characteristic of sleep terrors c. Confusion on awakening is likely with NREM parasomnias but absent with REM parasomnias d. Eyes tend to be open in NREM parasomnias but closed in REM parasomnias e. Amnesia of the event is characteristic of NREM parasomnias, but REM parasomnias are characterized by recall of dreams or dream fragments Note: NREM = nonrapid eye movement, REM = rapid eye movement. from slow wave sleep) and sleep-related sexual behaviours (commonly referred to as sexsomnia). Sexual behaviours (e.g., vocalizations, fondling, masturbation, intercourse and sexual assault) emerge as part of a confused arousal from sleep, although partial seizures and other pathologies should be considered. 13 Isolated confusional arousals in adults rarely come to clinical attention. For patients who present with confusional arousals, important measures to maximize sleep stability include improving sleep hygiene, avoiding centrally acting medications or drugs, and preventing sleep deprivation. The use of benzodiazepines 14 and specific serotonin reuptake inhibitors (SSRIs), 15 in conjunction with education about sleep and stress management and taking appropriate precautions (Box 4), may be effective. Anecdotal evidence suggests that scheduled awakenings (setting the alarm for 1 hr after sleep onset) can be helpful. 16 Patients with confusional arousals (as well as those with other parasomnias) should be counsel - led to not co-sleep with children, because even a single event has the potential for very serious consequences. It is also useful for patients to let others know of the disorder if they are going on a group trip (e.g., business trip, camping). Sleepwalking Sleepwalking is the result of a series of complex behaviours that occur while the patient is in an altered state of consciousness. A spectrum of activity may be seen; the most simple events include sitting up in bed in a confused manner before walking. Usually the individual s eyes are open (in contrast, the eyes remain closed in REM parasomnias). 1 Agitated ambulation is more common in older sleepwalkers, is often associated with a perceived threat or dreams promoting fight or flight behaviour, and may result in injury to bystanders. Rarely, sleepwalking may lead to injury or death for the sleeper 17 or others. 14 The co-occurrence of predisposing factors is required to precipitate sleepwalking episodes, and sleepwalking is unlikely in the absence of one or more of these factors. 18 Genetic susceptibility is the predominant predisposing factor, and sleep deprivation, touch, noise, stress, alcohol, medications and fever are potential triggers. The cause of sleepwalking is unknown, although the pathophysiology clearly involves slow wave sleep. Although the macroarchitecture of sleep in people who sleepwalk is essentially normal, there may be more fragmentation of slow wave sleep. 19 Single photon emission computed tomography during an episode of sleepwalking supports the co-occurrence of sleeping E276 CMAJ, May 13, 2014, 186(8)
5 and waking states caused by selective activation and hypoactivation of neural circuits. 20 In addition to the usual safety precautions (Box 4), the patient can be counselled to avoid sleep deprivation, and comorbid sleep disorders (e.g., obstructive sleep apnea 21 ) can be treated via nonpharmacologic and pharmacologic interventions. Scheduled awakenings, psychotherapy, relaxation exercises and hypnosis may be helpful, 22 but pharmacotherapy is often required for patients with frequent or hazardous episodes (arbitrarily defined as more than 50% of nights). Clonazepam is commonly used, with more limited evidence for other benzodiazepines, imipramine, paroxetine and melatonin. 16 Sleep terrors Sleep terrors events typically lasting between 30 seconds and 5 minutes 23 commence with the sleeper sitting up in bed, emitting a loud scream and showing the typical autonomic manifestations of intense fear. 1 Associated dream imagery may be reported and incoherent vocalizations can occur; the sleeper may bolt from the bed and run in an apparent attempt to avoid harm, thereby injuring themselves or others. 24 The pathophysiology of sleep terrors is unknown, but it is assumed that slow wave sleep instability accounts for these disturbances. There is an association between sleep terrors and psychiatric disorders; 10,25 sleepers with night terrors exhibit a high level of depression, anxiety, and obsessive compulsive and phobic traits on the Minnesota Multiphasic Personality Inventory. 25 Tricyclic antidepressants and benzodiazepines may be effective and should be considered if the sleep terrors are potentially harmful. 4 Sleeptalking Sleeptalking or somniloquy, classified in ICSD under sleep disorders associated with conditions classified elsewhere, 1 is a common parasomnia that ranges from isolated speech to full conversations without recall. It occurs in all sleep states and can be associated with obstructive sleep apnea, other disorders of arousal and REM-related parasomnias. 23 There are no specific treatments, and the clinical approach is to eliminate or reduce the conditions with which it is associated. Sleep-related eating disorder This parasomnia is classified in DSM-V under sleepwalking, 2 whereas ICSD classifies it as other parasomnias. 1 Sleep-related eating disorder is best conceptualized as the combination of the binge eating of bulimia nervosa with the disordered arousal, confused behaviour and amnesia (partial or full) of a parasomnia arising from NREM sleep. 10 Food and beverages are consumed in a hurried and out-ofcontrol manner, with high-calorie foods being preferred. Sometimes unusual (e.g., slabs of butter) or toxic foodstuffs (e.g., uncooked chicken) may be ingested. Variable, diminished awareness and recall distinguishes sleep-related eating disorder from nocturnal eating syndrome, 26 in which excessive amounts of food are eaten before or during the sleep period in full consciousness. The pathophysiology of sleep-related eating disorder is unclear, but it is associated with other sleep disorders 27 including sleepwalking, restless legs syndrome, periodic limb movement disorder, obstructive sleep apnea and narcolepsy 28 and medications, including zolpidem. 29 Successful treatment of the associated sleep disorder can substantially improve this parasomnia. Management of sleep-related eating disorder usually requires specialist care with attention to safety (because of the potential ingestion of toxic foods). First steps include normalizing the patient s eating schedule, preventing sleep deprivation and minimizing alcohol and substance use. If medication is required, the current preferred choice by experts is topiramate, with SSRI agents and dopamine agonists being second-line options. 30 Parasomnias usually associated with REM sleep There are 3 parasomnias associated with REM sleep: REM sleep behaviour disorder, recurrent isolated sleep paralysis and nightmare disorder. REM sleep behaviour disorder Two clinical forms of REM sleep behaviour disorder are seen: acute and chronic. 31 The acute form is associated with specific medications and substance abuse or withdrawal, and the chronic form is subdivided into either idiopathic or secondary to a neurologic disease. 5 Box 4: Safety precautions for patients with parasomnia 1. Identify, then reduce or eliminate known precipitating factors 2. Avoid sleep deprivation: maintain a regular sleep wake schedule with a constant waking time 3. Limit, preferably eliminate, the use of alcohol and recreational drugs 4. Maximize safety of the sleeping environment i. Sleep on the lowest floor in the house ii. Use a mattress on the floor iii. Sleep solo or use two queen-sized mattresses pushed together for co-sleeping iv. Minimize or pad bedside furniture v. Secure bedside light above bed but out of reach vi. Use plastic cups or bottles, if bedside water is required vii. Consider child-proof door knobs, door wedges or alarms viii. Remove or lock any weapons or dangerous household items CMAJ, May 13, 2014, 186(8) E277
6 Rapid eye movement sleep behaviour disorder is characterized by activity in REM sleep causing injury or sleep disruption. Polysomnography is required to confirm the associated electromyographic abnormalities. In REM sleep behaviour disorder, there is a loss of REM atonia with excessive muscle tone, twitches on electromyography, and movements that often appear to be dream enactment, potentially causing injury to the sleeper or bed partner. Episodes usually occur about once a week, but may be as often as four times nightly over consecutive nights. In contrast to all NREM parasomnias, the sleeper awakens rapidly without confusion and often with good recall of a dream that corresponds with the enacted behaviours that can include talking, laughing, swearing, shouting, reaching, grabbing, flailing, punching, hitting or running. 5 Because REM sleep behaviour disorder em - erges from REM sleep, which is maximal in the last half of the night, this is the time when events are most likely to occur. Patients with narcolepsy, a condition characterized by REM periods at sleep onset, are at risk of REM sleep behaviour disorder, and their events can occur earlier in the night. 5 Rapid eye movement sleep behaviour disorder is considered to be a long-standing and progressive disorder, although an acute form can emerge during REM sleep rebound states (e.g., the first night on continuous positive airway pressure for obstructive sleep apnea), withdrawal from alcohol, sedative hypnotic agents or REM suppressant medications. 5 The major predisposing factors are male sex, age greater than 50 years, and an underlying neurologic disease, particularly Parkinson disease, Lewy body dementia and stroke. 5 Rapid eye movement sleep behaviour disorder is a wellestablished risk factor for neurodegenerative disease, with studies indicating that 40% 65% of patients with this disorder develop a defined neuro degenerative phenotype within the subsequent 10 years. 32 Narcolepsy and post-traumatic stress disorder are associated with REM sleep behaviour disorder, 1 as are the use of SSRI and serotonin norepinephrine reuptake inhibitors. 33 The exact pathophysiology of REM sleep behaviour disorder is unclear, but it may be caused by reduced dopamine transporters in the striatum 34 and diminished striatal dopaminergic innervation. 35 The onset may be gradual or rapid and the course is progressive; spontaneous remissions are very rare, although dream enactment may subside during the late stages of a neurodegenerative disorder. Rapid eye movement sleep behaviour disorder can be diagnosed based on clinical history, which should include the bed partner s account. This is the only parasomnia that can be readily confirmed by polysomnography, which shows an excessive amount of sustained electromyographic activity in REM sleep. Of patients with REM sleep behaviour disorder, 70% will have periodic limb movements during NREM sleep. 36 As with other parasomnias, there have been no large trials of treatment for this condition, but case series have shown that clonazepam is most commonly used for this condition. 5 Screening for obstructive sleep apnea should be undertaken before starting treatment with clonazepam. The most troublesome adverse effect associated with clonazepam therapy is morning confusion and memory impairment. 5 Melatonin in high doses is an alternative to clonazepam, and there is some anecdotal support for the use of dopamine agonists such as pramipexole. 5 A novel alarm system for patients unresponsive to medications has been described recently. 37 Sleep paralysis Sleep paralysis is the inability to perform voluntary movements at sleep onset or on awakening. 1 Although consciousness is preserved and recall is present, the patient is unable to speak or move at first. Respiration is unaffected, although patients may feel as if they are unable to breathe because the accessory respiratory muscles are atonic, but diaphragmatic breathing is maintained. Episodes last seconds to minutes and resolve spontaneously, but they can be aborted if the patient is touched or spoken to. The frequency can vary from once-ina-lifetime to several times in a year. During the first few episodes, intense anxiety accompanies the paralysis. Auditory, visual or tactile hallucinations can occur and may accompany a perception of an ominous presence in the room. 1 Sleep deprivation, irregular sleep wake schedules (e.g., from jet lag or shift work) and stress are predisposing factors, and the condition is more likely to occur when the sleeper is in the supine position. These factors may facilitate a state dis - sociation in which elements of REM sleep persist into wakefulness causing the phenomenon. 1 Causes of secondary sleep paralysis (narcolepsy and other neuropsychiatric illnesses) should be excluded through a detailed physical examination, medical, psychiatric and sleep history, and appropriate investigations. Patient education and ensuring adequate, regular sleep periods are important. If the episodes are frequent, the patient should practise moving his or her little finger during drowsy sleep, because this action, if performed during an episode, may abort it. 1 There have been no trials of psychologic or pharmacologic interventions, but SSRIs may be helpful because they suppress REM sleep and are well tolerated. 38,39 E278 CMAJ, May 13, 2014, 186(8)
7 Nightmare disorder Nightmare disorder is characterized by recurrent nightmares with intense disturbing dreams involving anxiety, anger or disgust that cause prolonged awakenings. 1 Multiple nightmares within a single sleep period may occur and follow similar themes. Nightmares are strongly associated with psychopathology and are inversely correlated with measures of well-being. 3 Many medications, including antidepressants, antihypertensives and dopamine receptor agonists, can cause nightmares. 1 Nightmares are distinguished from other parasomnias because of the detailed recall of the dream, whereas in sleep terrors, dream activity, if present, is patchy. Nightmares can be a component of ictal events 1 that will require video electroencephalography to make the diagnosis. Nightmares are a common feature of both acute stress disorder and post-traumatic stress disorder and occur in both NREM and REM sleep. The label nightmare disorder is only applied to these disorders when the severity of the nightmares is such that it requires clinical attention. Frequently, other symptoms of post-traumatic stress disorder may have resolved even though nightmares persist. A guideline 8 indicates that both psychologic and pharmacologic approaches may be helpful in treating nightmares. 13,40 A common psychologic approach is imagery rehearsal, 41 where the patient chooses a repetitive nightmare, changes its story line to make it less distressing or bring its story to a safe conclusion and then mentally rehearses the changed dream imagery. A recent meta-analysis confirmed that this and other psychologic approaches are effective. 42 The use of prazosin has reduced post-traumatic nightmares in two small clinical trials involving military veterans. 43 Other parasomnias This remaining group of other parasomnias (Box 1) cannot be easily categorized as NREM- or REM-related behaviours. With the exception of sleep enuresis, which is predominantly a disorder of childhood (reviewed elsewhere 44,45 ), these parasomnias are relatively rare. Sleep-related dissociative disorders can mimic parasomnia, but the dissociative episode always arises from wakefulness, 46 is accompanied by daytime dissoci ative symptoms and usually resolves with treatment of the dissociative disorder. Exploding head syndrome 47 is characterized by the perception of a sudden loud noise in the head as the patient is falling asleep or awakening from sleep. At first, the patient may believe that he or she is having a stroke. The frequency is highly variable: single episodes are usual but clusters of episodes can occur. When the events effect daytime functioning, a trial of clonazepam, clomipramine, nifedipine, flunarizine or topiramate 48 may be helpful. Sleep-related hallucinations are called hypnogogic hallucinations if they occur when the patient is falling asleep or hypnopompic hallucinations if they occur when the patient is awakening. The hallucinations are predominantly visual but can be auditory, tactile or kinetic, and they may frighten the sleeper. 1 Because hypnopompic hallucinations are one of the symptoms of narcolepsy, this diagnosis needs to be excluded by polysomnography. Conclusion Parasomnias, like in the fictional case described in Box 5, are relatively rare, yet are fascinating and important clinical syndromes. Sleep instability characterized by arousals in various stages of consciousness with variable later recall are characteristic of NREM parasomnias and that instability can be improved by addressing sleep hygiene, avoiding substance use, preventing sleep deprivation and, when required, using medications that promote sleep depth and continuity. In contrast, REM parasomnias occur within the context of greater conscious awareness, resulting Box 5: Applying the results of this review in clinical practice (fictional case) Martin, a 35-year-old executive, was brought to the emergency department by his wife after he had fallen down the stairs at 1:30 am. On questioning, he reported that at a conference last year, he was discovered, confused and naked, outside his hotel room with no memory of how he got there. Martin had been a bed-wetter until age 10 and had been known to sleepwalk as a child. On his twelfth birthday, he had gotten up in the middle of the night and urinated in his brother s shoes. He continued to experience minor events with decreased frequency in his teens but after a night on the town at age 19, he left the family home and was found asleep the next morning in his friend s house two blocks away. Because all doors were locked, it was assumed that he climbed in through an open window. Martin s wife comments that he is a restless sleeper who frequently talks and groans in his sleep, but that he is otherwise a healthy, well-adjusted individual who has never abused drugs or alcohol. In the past year, he has complained to her that his sleep is lighter and that he wakes up easily throughout the night. Last month, Martin started to make sexual advances to his wife during the night, which have not been unwelcomed, yet sometimes it seems as though he s not quite there. He does not remember these episodes the next morning. Based on his history, Martin has confused arousals, sleepwalking and sexsomnia. The history of childhood onset with a strong family history (his father and two paternal uncles were sleepwalkers) and exacerbation by alcohol are common features of nonrapid eye movement parasomnia. A review of Martin s two-week sleep diary and his wife s charting of events showed that as his workweek progressed, he electively decreased his amount of sleep, resulting in a substantial sleep debt (1.5 h/night) by the end of the week, where his parasomnia behaviours were also clustered. He did not consent to a medication trial (clonazepam) but he agreed to safety-proof their bedroom (Box 4), ensure a 7.5-hour sleep period each night, and arise at the same time each day, including weekends. After making these changes, he reported less restless and more restorative sleep, and the frequency of parasomnia decreased to once or twice a week. The prophylactic use of clonazepam for his frequent transatlantic trips was discussed, but he declined this option for now, stating I am growing out of this. CMAJ, May 13, 2014, 186(8) E279
8 in better recall and reflect the admixture of REM sleep with its associated dream imagery, voluntary muscle atonia and wakefulness. In this group of parasomnias, clinical experience has shown that the same advice about sleep hygiene, avoiding substance use and preventing sleep deprivation used in NREM is helpful. Clonazepam, pramipexole and melatonin are the medications commonly used to manage REM sleep behaviour disorder. Parasomnias are not benign conditions and potentially place the sleeper and bed partner at risk of injury and may be associated with other disorders that require careful consideration. Parasomnias can be successfully managed by appropriate investigation, education and the strategic use of psychologic and pharmacologic therapies. References 1. International classification of sleep disorders: diagnostic and coding manual. 2nd ed. Westchester (IL): American Academy of Sleep Medicine; Diagnostic and statistical manual of mental disorders, 5th edition: DSM-5. Arlington (VA): American Psychiatric Association, Plante DT, Winkelman JW. Parasomnias. Psychiatr Clin North Am 2006;29: Kotagal S. Parasomnias in childhood. Sleep Med Rev 2009;13: Aurora RN, Zak RS, Maganti RK, et al. Best practice guide for the treatment of REM sleep behavior disorder (RBD). J Clin Sleep Med 2010;6: Lange CL. Medication-associated somnambulism. J Am Acad Child Adolesc Psychiatry 2005;44: lber C, Ancoli-lsrael S, Chesson A, et al.; the American Academy of Sleep Medicine. The AASM manual for the scoring of sleep and associated events: rules, terminology and technical specifications. Westchester (Il): American Academy of Sleep Medicine; Aurora RN, Zak RS, Auerbach SH, et al. Best practice guide for the treatment of nightmare disorder in adults. J Clin Sleep Med 2010; 6: Zucconi M, Oldani A, Ferini-Strambi L, et al. Arousal fluctuations in non-rapid eye movement parasomnias: The role of cyclic alternating pattern as a measure of sleep instability. J Clin Neurophysiol 1995;12: Goldstein CA. Parasomnias. Dis Mon 2011; 57: Ohayon MM, Guilleminault C, Priest RG. Night terrors, sleepwalking, and confusional arousals in the general population: their frequency and relationship to other sleep and mental disorders. J Clin Psychiatry 1999;60: Ohayon MM, Priest RG, Zulley J, et al. The place of confusional arousals in sleep and mental disorders findings in a general population sample of subjects. J Nerv Ment Dis 2000; 188: Andersen ML, Poyares D, Alves RS, et al. Sexsomnia: abnormal sexual behavior during sleep. Brain Res Rev 2007;56: Siclari F, Khatami R, Urbaniok F, et al. Violence in sleep. Brain 2010; 133: Béjot Y, Juenet N, Garrouty R, et al. Sexsomnia: an uncommon variety of parasomnia. Clin Neurol Neurosurg 2010;112: Attarian H. Treatment options for parasomnias. Neurol Clin 2010; 28: Seeman MV. Sleepwalking, a possible side effect of antipsychotic medication. Psychiatr Q 2011;82: Pressman MR. Factors that predispose, prime and precipitate NREM parasomnias in adults: clinical and forensic implications. Sleep Med Rev 2007;11: Espa F, Ondze B, Deglise P, et al. Sleep architecture, slow wave activity, and sleep spindles in adult patients with sleepwalking and sleep terrors. Clin Neurophysiol 2000;111: Bassetti C, Vella S, Donati F, et al. SPECT during sleepwalking. Lancet 2000;356: Guilleminault C, Kirisoglu C, Bao G, et al. Adult chronic sleepwalking and its treatment based on polysomnography. Brain 2005; 128: Harris M, Grunstein RR. Treatments for somnambulism in adults: assessing the evidence. Sleep Med Rev 2009;13: Avidan AY, Kaplish N. The parasomnias: epidemiology, clinical features, and diagnostic approach. Clin Chest Med 2010;31: Pressman MR. Disorders of arousal from sleep and violent behavior: the role of physical contact and proximity. Sleep 2007; 30: Kales JD, Kales A, Soldatos CR, et al. Night terrors. Clinical characteristics and personality patterns. Arch Gen Psychiatry 1980; 37: O Reardon JP, Peshek A, Allison KC. Night eating syndrome: diagnosis, epidemiology and management. CNS Drugs 2005; 19: Howell MJ, Schenck CH. Treatment of nocturnal eating disorders. Curr Treat Options Neurol 2009;11: Palaia V, Poli F, Pizza F, et al. Narcolepsy with cataplexy associated with nocturnal compulsive behaviors: a case control study. Sleep 2011;34: Hoque R, Chesson AL Jr. Zolpidem-induced sleepwalking, sleep related eating disorder, and sleep-driving: fluorine-18- flourodeoxyglucose positron emission tomography analysis, and a literature review of other unexpected clinical effects of zolpidem. J Clin Sleep Med 2009;5: Howell MJ, Schenck CH. Treatment of nocturnal eating disorders. Curr Treat Options Neurol 2009;11: Schenck CH, Mahowald MW. REM sleep behavior disorder: clinical, developmental, and neuroscience perspectives 16 years after its formal identification in SLEEP. Sleep 2002;25: Postuma RB, Gagnon JF, Montplaisir J. Rapid eye movement disorder as a biomarker for neurodegeneration:the past 10 years. Sleep Med 2013;14: Hoque R, Chesson AL Jr. Pharmacologically induced/exacerbated restless legs syndrome, periodic limb movements of sleep, and REM behavior disorder/rem sleep without atonia: literature review, qualitative scoring, and comparative analysis. J Clin Sleep Med 2010;6: Eisensehr I, Linke R, Tatsch K, et al. Increased muscle activity during rapid eye movement sleep correlates with decrease of striatal presynaptic dopamine transporters. IPT and IBZM SPECT imaging in subclinical and clinically manifest idiopathic REM sleep behavior disorder, Parkinson s disease, and controls. Sleep 2003;26: Albin RL, Koeppe RA, Chervin RD, et al. Decreased striatal dopaminergic innervation in REM sleep behavior disorder. Neurology 2000;55: Fantini ML, Michaud M, Gosselin N, et al. Periodic leg movements in REM sleep behavior disorder and related autonomic and EEG activation. Neurology 2002:59; Howell MJ, Arneson PA, Schenck CH. A novel therapy for REM sleep behavior disorder (RBD). J Clin Sleep Med 2011;7: A. 38. Koran LM, Raghavan S. Fluoxetine for isolated sleep paralysis. Psychosomatics 1993;34: McCarty DE, Chesson AL Jr. A case of sleep paralysis with hypnopompic hallucinations. Recurrent isolated sleep paralysis associated with hypnopompic hallucinations, precipitated by behaviorally induced insufficient sleep syndrome. J Clin Sleep Med 2009;5: Gehrman PR, Harb GC. Treatment of nightmares in the context of posttraumatic stress disorder. J Clin Psychol 2010;66: Krakow B, Zadra A. Clinical management of chronic nightmares: imagery rehearsal therapy. Behav Sleep Med 2006;4: Hansen K, Höfling V, Kröner-Borowik T, et al. Efficacy of psychological interventions aiming to reduce chronic nightmares: a meta-analysis. Clin Psychol Rev 2013;33: Calohan J, Peterson K, Peskind ER, et al. Prazosin treatment of trauma nightmares and sleep disturbance in soldiers deployed in Iraq. J Trauma Stress 2010;23: Nevéus T. Sleep enuresis. Handb Clin Neurol 2011;98: von Gontard A, Baeyens D, Van Hoecke E, et al. Psychological and psychiatric issues in urinary and fecal incontinence. J Urol 2011; 185: Fleming J. Dissociative episodes presenting as somnambulism: a case report. Sleep Res 1987;16: Pearce JM. Clinical features of the exploding head syndrome. J Neurol Neurosurg Psychiatry 1989;52: Palikh GM, Vaughn BV. Topiramate responsive exploding head syndrome. J Clin Sleep Med 2010;6: Affiliations: Department of Medicine (Fleetham) and Department of Psychiatry (Fleming), University of British Columbia; Sleep Disorders Program (Fleetham), University of British Columbia Hospital, Vancouver, BC. Contributors: Jonathan Fleming performed the literature review. Both authors drafted the article, revised it critically for important intellectual content and approved the version submitted for publication. E280 CMAJ, May 13, 2014, 186(8)
Corporate Medical Policy
 Corporate Medical Policy Polysomnography for Non Respiratory Sleep Disorders File Name: Origination: Last CAP Review: Next CAP Review: Last Review: polysomnography_for_non_respiratory_sleep_disorders 10/2015
Corporate Medical Policy Polysomnography for Non Respiratory Sleep Disorders File Name: Origination: Last CAP Review: Next CAP Review: Last Review: polysomnography_for_non_respiratory_sleep_disorders 10/2015
FEP Medical Policy Manual
 FEP Medical Policy Manual Effective Date: January 15, 2018 Related Policies: 2.01.18 Diagnosis and Medical Management of Obstructive Sleep Apnea Syndrome Diagnosis and Medical Management of Obstructive
FEP Medical Policy Manual Effective Date: January 15, 2018 Related Policies: 2.01.18 Diagnosis and Medical Management of Obstructive Sleep Apnea Syndrome Diagnosis and Medical Management of Obstructive
FEP Medical Policy Manual
 FEP Medical Policy Manual Effective Date: October 15, 2018 Related Policies: 2.01.18 Diagnosis and Medical Management of Obstructive Sleep Apnea Syndrome Polysomnography for Non-Respiratory Sleep Disorders
FEP Medical Policy Manual Effective Date: October 15, 2018 Related Policies: 2.01.18 Diagnosis and Medical Management of Obstructive Sleep Apnea Syndrome Polysomnography for Non-Respiratory Sleep Disorders
Individual Planning: A Treatment Plan Overview for Individuals Sleep Disorder Problems.
 COURSES ARTICLE - THERAPYTOOLS.US Individual Planning: A Treatment Plan Overview for Individuals Sleep Disorder Problems. Individual Planning: A Treatment Plan Overview for Individuals Sleep Disorder Problems.
COURSES ARTICLE - THERAPYTOOLS.US Individual Planning: A Treatment Plan Overview for Individuals Sleep Disorder Problems. Individual Planning: A Treatment Plan Overview for Individuals Sleep Disorder Problems.
Conflict of Interest Disclosures for Speakers
 Conflict of Interest Disclosures for Speakers 1. I do not have any relationships with any entities producing, marketing, reselling, or distributing health care goods or services consumed by, or used on,
Conflict of Interest Disclosures for Speakers 1. I do not have any relationships with any entities producing, marketing, reselling, or distributing health care goods or services consumed by, or used on,
Index SLEEP MEDICINE CLINICS. Note: Page numbers of article titles are in boldface type. Cerebrospinal fluid analysis, for Kleine-Levin syndrome,
 165 SLEEP MEDICINE CLINICS Index Sleep Med Clin 1 (2006) 165 170 Note: Page numbers of article titles are in boldface type. A Academic performance, effects of sleepiness in children on, 112 Accidents,
165 SLEEP MEDICINE CLINICS Index Sleep Med Clin 1 (2006) 165 170 Note: Page numbers of article titles are in boldface type. A Academic performance, effects of sleepiness in children on, 112 Accidents,
Participant ID: If you had no responsibilities, what time would your body tell you to go to sleep and wake up?
 What does your sleep look like on a typical week? Total Sleep Time: Bedtime:, Sleep onset latency:, Number of Awakenings:, Wake time after sleep onset:, Rise time:, Out of bed:, Naps:? Notes: Is your sleep
What does your sleep look like on a typical week? Total Sleep Time: Bedtime:, Sleep onset latency:, Number of Awakenings:, Wake time after sleep onset:, Rise time:, Out of bed:, Naps:? Notes: Is your sleep
SOMNAMBULISM: CLINICAL ASPECTS AND PATHOPHYSIOLOGICAL HYPOTHESES. Zadra, A., Desautels, A., Petit, D., Montplaisir, J. (2013) The Lancet Neurology
 11.11.2015 SOMNAMBULISM: CLINICAL ASPECTS AND PATHOPHYSIOLOGICAL HYPOTHESES Zadra, A., Desautels, A., Petit, D., Montplaisir, J. (2013) The Lancet Neurology Marion Charmillot Sleep, Cognition and Health
11.11.2015 SOMNAMBULISM: CLINICAL ASPECTS AND PATHOPHYSIOLOGICAL HYPOTHESES Zadra, A., Desautels, A., Petit, D., Montplaisir, J. (2013) The Lancet Neurology Marion Charmillot Sleep, Cognition and Health
SLEEP DISORDERS. Kenneth C. Sassower, MD Division of Sleep Medicine; Department of Neurology Massachusetts General Hospital for Children
 SLEEP DISORDERS Kenneth C. Sassower, MD Division of Sleep Medicine; Department of Neurology Massachusetts General Hospital for Children Distinctive Features of Pediatric Sleep Daytime sleepiness uncommon
SLEEP DISORDERS Kenneth C. Sassower, MD Division of Sleep Medicine; Department of Neurology Massachusetts General Hospital for Children Distinctive Features of Pediatric Sleep Daytime sleepiness uncommon
Index. sleep.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Actigraphy, 475, 485, 496 Adolescents, sleep disorders in, 576 578 Adults, sleep disorders in, 578 580 Advanced sleep phase disorder, 482 Age,
Note: Page numbers of article titles are in boldface type. A Actigraphy, 475, 485, 496 Adolescents, sleep disorders in, 576 578 Adults, sleep disorders in, 578 580 Advanced sleep phase disorder, 482 Age,
No Rest For the Weary: Some Common Sleep Disorders
 No Rest For the Weary: Some Common Sleep Disorders Student Activity 3G Activity Introduction: It seems Mom does know best ; sleep has been proven to be essential to our health and well-being. In order
No Rest For the Weary: Some Common Sleep Disorders Student Activity 3G Activity Introduction: It seems Mom does know best ; sleep has been proven to be essential to our health and well-being. In order
TOP 10 LIST OF SLEEP QUESTIONS. Kenneth C. Sassower, MD Sleep Disorders Unit Massachusetts General Hospital for Children
 TOP 10 LIST OF SLEEP QUESTIONS Kenneth C. Sassower, MD Sleep Disorders Unit Massachusetts General Hospital for Children QUESTION #1: ARE SLEEP ISSUES IN CHILDREN THE SAME AS IN ADULTS? Distinctive Features
TOP 10 LIST OF SLEEP QUESTIONS Kenneth C. Sassower, MD Sleep Disorders Unit Massachusetts General Hospital for Children QUESTION #1: ARE SLEEP ISSUES IN CHILDREN THE SAME AS IN ADULTS? Distinctive Features
A Scream in the Night. ARTP Conference 2010 Dr Christopher Kosky
 A Scream in the Night ARTP Conference 2010 Dr Christopher Kosky Parasomnia Slow Wave Sleep Arousal Disorder REM Sleep Behaviour Disorder Nocturnal Epilepsy Catathrenia Slow Wave Sleep Arousal Disorders
A Scream in the Night ARTP Conference 2010 Dr Christopher Kosky Parasomnia Slow Wave Sleep Arousal Disorder REM Sleep Behaviour Disorder Nocturnal Epilepsy Catathrenia Slow Wave Sleep Arousal Disorders
Sleep Disorders. Sleep. Circadian Rhythms
 Sleep Disorders Sleep The Sleep Wakefulness Cycle: Circadian Rhythms Internally generated patterns of bodily functions that vary over a ~24-hour period Function even in the absence of normal cues 2 Circadian
Sleep Disorders Sleep The Sleep Wakefulness Cycle: Circadian Rhythms Internally generated patterns of bodily functions that vary over a ~24-hour period Function even in the absence of normal cues 2 Circadian
Parkinson s Disease Associated Sleep Disturbance Ehsan M. Hadi, MD, MPH. Dignity Health Neurological Institute
 Parkinson s Disease Associated Sleep Disturbance Ehsan M. Hadi, MD, MPH. Dignity Health Neurological Institute Parkinson s Disease 2 nd most common neurodegenerative disorder Peak age at onset is 60 years
Parkinson s Disease Associated Sleep Disturbance Ehsan M. Hadi, MD, MPH. Dignity Health Neurological Institute Parkinson s Disease 2 nd most common neurodegenerative disorder Peak age at onset is 60 years
Sleep Medicine. Maintenance of Certification Examination Blueprint. Purpose of the exam
 Sleep Medicine Maintenance of Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of the
Sleep Medicine Maintenance of Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of the
Sleep problems 4/10/2014. Normal sleep (lots of variability at all ages) 2 phases of sleep. Quantity. Quality REM. Non-REM.
 Sleep problems Normal sleep (lots of variability at all ages) Quantity Newborns: 16-20 hrs/day 1-yr olds: 12 hrs/day 6-12 yr olds: 10-11 hrs/day Quality Newborns: distributed between day and night 3-months:
Sleep problems Normal sleep (lots of variability at all ages) Quantity Newborns: 16-20 hrs/day 1-yr olds: 12 hrs/day 6-12 yr olds: 10-11 hrs/day Quality Newborns: distributed between day and night 3-months:
SLEEP THEORIES. Sleep Protects: Sleeping in the darkness when predators loomed
 SLEEP THEORIES Sleep Protects: Sleeping in the darkness when predators loomed about kept our ancestors out of harm s way. Sleep Recuperates: Sleep helps restore and repair brain tissue. Sleep Helps Remembering:
SLEEP THEORIES Sleep Protects: Sleeping in the darkness when predators loomed about kept our ancestors out of harm s way. Sleep Recuperates: Sleep helps restore and repair brain tissue. Sleep Helps Remembering:
Diagnosis and treatment of sleep disorders
 Diagnosis and treatment of sleep disorders Normal human sleep Sleep cycle occurs about every 90 minutes, approximately 4-6 cycles occur per major sleep episode NREM (70-80%) slow wave sleep heart rate,
Diagnosis and treatment of sleep disorders Normal human sleep Sleep cycle occurs about every 90 minutes, approximately 4-6 cycles occur per major sleep episode NREM (70-80%) slow wave sleep heart rate,
Sleep Medicine Maintenance of Certification Examination Blueprint
 Sleep Medicine Maintenance of Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of the
Sleep Medicine Maintenance of Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of the
Managing Sleep Disorders in Primary Care. Objectives. Disclosures. Nancy Nadolski, FNP, MSN, M.Ed Insomnia Medicine of Idaho Boise Counseling Center
 Managing Sleep Disorders in Primary Care Nancy Nadolski, FNP, MSN, M.Ed Insomnia Medicine of Idaho Boise Counseling Center www.sleeplessinidaho.com 1 Objectives 1) Identify stages and behaviors for normal
Managing Sleep Disorders in Primary Care Nancy Nadolski, FNP, MSN, M.Ed Insomnia Medicine of Idaho Boise Counseling Center www.sleeplessinidaho.com 1 Objectives 1) Identify stages and behaviors for normal
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Abuse sleep physiology effects of, 880 882 substance, in adolescents, sleep problems and, 929 946. See also Substance use and abuse, in adolescents,
Note: Page numbers of article titles are in boldface type. A Abuse sleep physiology effects of, 880 882 substance, in adolescents, sleep problems and, 929 946. See also Substance use and abuse, in adolescents,
RBD & other Parasomnias. Lauren A. Tobias MD Instructor of Medicine Yale University School of Medicine
 RBD & other Parasomnias Lauren A. Tobias MD Instructor of Medicine Yale University School of Medicine Disclosures I have nothing to disclose Outline Defini@on Clinical overview & ICSD III classifica@on
RBD & other Parasomnias Lauren A. Tobias MD Instructor of Medicine Yale University School of Medicine Disclosures I have nothing to disclose Outline Defini@on Clinical overview & ICSD III classifica@on
Nightmare disorder. Diseases and Conditions
 Diseases and Conditions Nightmare disorder By Mayo Clinic Staff A nightmare is a disturbing dream associated with negative feelings, such as anxiety or fear. Nightmares are common, and occasional nightmares
Diseases and Conditions Nightmare disorder By Mayo Clinic Staff A nightmare is a disturbing dream associated with negative feelings, such as anxiety or fear. Nightmares are common, and occasional nightmares
2/13/2015 THINGS THAT GO BUMP IN THE NIGHT
 THINGS THAT GO BUMP IN THE NIGHT Detection & Management of Potentially Injurious Parasomnias Janet E. Tatman, PhD, PA-C Fellow American Academy of Sleep Medicine Certified in Behavioral Sleep Medicine
THINGS THAT GO BUMP IN THE NIGHT Detection & Management of Potentially Injurious Parasomnias Janet E. Tatman, PhD, PA-C Fellow American Academy of Sleep Medicine Certified in Behavioral Sleep Medicine
WEIGHT CONCERNS IN YOUNG GIRLS
 CHAPTER 8 EATING AND SLEEP DISORDERS (PP. 268-311) 1 Overview Bulimia Nervosa Anorexia Nervosa Eating Disorders Binge Eating Disorder Stats Social Causes Bio Eating & Sleep Disorders Psy Insomnia Treat
CHAPTER 8 EATING AND SLEEP DISORDERS (PP. 268-311) 1 Overview Bulimia Nervosa Anorexia Nervosa Eating Disorders Binge Eating Disorder Stats Social Causes Bio Eating & Sleep Disorders Psy Insomnia Treat
Index. sleep.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Accidents, risk of, with insufficient sleep, 318 Acquired immunodeficiency syndrome (AIDS), comorbid with narcolepsy, 298 299 Actigraphy, in
Note: Page numbers of article titles are in boldface type. A Accidents, risk of, with insufficient sleep, 318 Acquired immunodeficiency syndrome (AIDS), comorbid with narcolepsy, 298 299 Actigraphy, in
Use of pramipexole in REM sleep behavior disorder: Results from a case series
 Sleep Medicine 7 (2006) 418 423 www.elsevier.com/locate/sleep Original article Use of pramipexole in REM sleep behavior disorder: Results from a case series Markus H. Schmidt a, *, Vipin B. Koshal b, Helmut
Sleep Medicine 7 (2006) 418 423 www.elsevier.com/locate/sleep Original article Use of pramipexole in REM sleep behavior disorder: Results from a case series Markus H. Schmidt a, *, Vipin B. Koshal b, Helmut
Sleep disturbances: MANAGING PARASOMNIAS. in general practice
 Sleep disturbances: MANAGING PARASOMNIAS in general practice 16 Parasomnias are a broad group of disorders associated with unusual behaviour when sleeping, and at sleep onset and waking. The distinct conditions
Sleep disturbances: MANAGING PARASOMNIAS in general practice 16 Parasomnias are a broad group of disorders associated with unusual behaviour when sleeping, and at sleep onset and waking. The distinct conditions
SLEEP DISORDERS CENTER QUESTIONNAIRE
 Carteret Health Care Patient's name DOB Gender: M F Date of Visit _ Referring physicians: Primary care providers: Please complete the following questionnaire by filling in the blanks and placing a check
Carteret Health Care Patient's name DOB Gender: M F Date of Visit _ Referring physicians: Primary care providers: Please complete the following questionnaire by filling in the blanks and placing a check
INSOMNIAS. Stephan Eisenschenk, MD Department of Neurology
 INSOMNIAS INSOMNIAS General criteria for insomnia A. Repeated difficulty with sleep initiation, duration, consolidation or quality. B. Adequate sleep opportunity, persistent sleep difficulty and associated
INSOMNIAS INSOMNIAS General criteria for insomnia A. Repeated difficulty with sleep initiation, duration, consolidation or quality. B. Adequate sleep opportunity, persistent sleep difficulty and associated
Polysomnography (PSG) (Sleep Studies), Sleep Center
 Policy Number: 1036 Policy History Approve Date: 07/09/2015 Effective Date: 07/09/2015 Preauthorization All Plans Benefit plans vary in coverage and some plans may not provide coverage for certain service(s)
Policy Number: 1036 Policy History Approve Date: 07/09/2015 Effective Date: 07/09/2015 Preauthorization All Plans Benefit plans vary in coverage and some plans may not provide coverage for certain service(s)
Assessment of Sleep Disorders DR HUGH SELSICK
 Assessment of Sleep Disorders DR HUGH SELSICK Goals Understand the importance of history taking Be able to take a basic sleep history Be aware the technology used to assess sleep disorders. Understand
Assessment of Sleep Disorders DR HUGH SELSICK Goals Understand the importance of history taking Be able to take a basic sleep history Be aware the technology used to assess sleep disorders. Understand
What is a sleep center? Mercy Sleep Centers Staff Mercy Sleep Center Clive What is a sleep evaluation? Mercy Sleep Center Ames
 Mercy Sleep Center What is a sleep center? A sleep center is a medical facility dedicated to diagnosing and treating patients with sleep-related problems. Mercy Sleep Center is staffed by board certified/eligible
Mercy Sleep Center What is a sleep center? A sleep center is a medical facility dedicated to diagnosing and treating patients with sleep-related problems. Mercy Sleep Center is staffed by board certified/eligible
INTRINSIC SLEEP DISORDERS. Excessive daytime sleepiness (EDS) is a common complaint. Causes of EDS are numerous and include:
 INTRINSIC SLEEP DISORDERS Introduction Excessive daytime sleepiness (EDS) is a common complaint. Causes of EDS are numerous and include: Intrinsic sleep disorders (e.g. narcolepsy, obstructive sleep apnoea/hypopnea
INTRINSIC SLEEP DISORDERS Introduction Excessive daytime sleepiness (EDS) is a common complaint. Causes of EDS are numerous and include: Intrinsic sleep disorders (e.g. narcolepsy, obstructive sleep apnoea/hypopnea
Marieb, E.N. (2004), Human Anatomy & Physiology, Pearson Education, Inc, San Francisco, CA, USA, p459
 Neuroscience Tutorial: Sleep and Dreams Discuss the following diagram with the students: Marieb, E.N. (2004), Human Anatomy & Physiology, Pearson Education, Inc, San Francisco, CA, USA, p459 1 Purves,
Neuroscience Tutorial: Sleep and Dreams Discuss the following diagram with the students: Marieb, E.N. (2004), Human Anatomy & Physiology, Pearson Education, Inc, San Francisco, CA, USA, p459 1 Purves,
Sleep Disorders in Adolescents and Young Adults
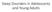 Sleep Disorders in Adolescents and Young Adults Deborah Layden 9/9/2014 Arousal MT Wake REM S1 S2 S3 S4 00:00 01:00 02:00 03:00 04:00 05:00 Button Supine Left Prone Right Upright SpO2 [%] Desat 100 90
Sleep Disorders in Adolescents and Young Adults Deborah Layden 9/9/2014 Arousal MT Wake REM S1 S2 S3 S4 00:00 01:00 02:00 03:00 04:00 05:00 Button Supine Left Prone Right Upright SpO2 [%] Desat 100 90
Facts about Sleep. Circadian rhythms are important in determining human sleep patterns/ sleep-waking cycle
 Sleep Sleep is described as a state of unconsciousness or partial consciousness from which a person can be roused by stimulation Period of rest and recovery People spend about a third of their lives sleeping
Sleep Sleep is described as a state of unconsciousness or partial consciousness from which a person can be roused by stimulation Period of rest and recovery People spend about a third of their lives sleeping
Insomnia. Learning Objectives. Disclosure 6/7/11. Research funding: NIH, Respironics, Embla Consulting: Elsevier
 Insomnia Teofilo Lee-Chiong MD Professor of Medicine National Jewish Health University of Colorado Denver School of Medicine Learning Objectives Learn about the causes of transient and chronic Learn how
Insomnia Teofilo Lee-Chiong MD Professor of Medicine National Jewish Health University of Colorado Denver School of Medicine Learning Objectives Learn about the causes of transient and chronic Learn how
HEALTHY LIFESTYLE, HEALTHY SLEEP. There are many different sleep disorders, and almost all of them can be improved with lifestyle changes.
 HEALTHY LIFESTYLE, HEALTHY SLEEP There are many different sleep disorders, and almost all of them can be improved with lifestyle changes. HEALTHY LIFESTYLE, HEALTHY SLEEP There are many different sleep
HEALTHY LIFESTYLE, HEALTHY SLEEP There are many different sleep disorders, and almost all of them can be improved with lifestyle changes. HEALTHY LIFESTYLE, HEALTHY SLEEP There are many different sleep
Chapter 5. Variations in Consciousness 8 th Edition
 Chapter 5 Variations in Consciousness 8 th Edition Consciousness: Personal Awareness Awareness of Internal and External Stimuli Levels of awareness James stream of consciousness Freud unconscious Sleep/dreaming
Chapter 5 Variations in Consciousness 8 th Edition Consciousness: Personal Awareness Awareness of Internal and External Stimuli Levels of awareness James stream of consciousness Freud unconscious Sleep/dreaming
Are you skimping on sleep, or could you have a sleep disorder?
 Are you skimping on sleep, or could you have a sleep disorder? Look around you: the guy nodding off on the bus, the co-worker snoozing during a dull presentation, the people with heavy eyelids lined up
Are you skimping on sleep, or could you have a sleep disorder? Look around you: the guy nodding off on the bus, the co-worker snoozing during a dull presentation, the people with heavy eyelids lined up
Beyond Sleep Hygiene: Behavioral Approaches to Insomnia
 Beyond Sleep Hygiene: Behavioral Approaches to Insomnia Rocky Garrison, PhD, CBSM Damon Michael Williams, RN, PMHNP-BC In House Counseling Laughing Heart LLC 10201 SE Main St. 12 SE 14 th Ave. Suite 10
Beyond Sleep Hygiene: Behavioral Approaches to Insomnia Rocky Garrison, PhD, CBSM Damon Michael Williams, RN, PMHNP-BC In House Counseling Laughing Heart LLC 10201 SE Main St. 12 SE 14 th Ave. Suite 10
SAMPLE. parasomnias. behaviorsdange. rrorstherapy waki. understanding. confuseddreamsbedrbing. leepnightmaresfamilyr. t sleepwalkingstre
 understanding parasomnias tmaresterrors w behaviorsdange t sleepwalkingstre w teeth grindingf gsleep disorder disturb onfusedstresssleepw rt wakingroutine ye confuseddreamsbedrbing outgrow medicatio rrorstherapy
understanding parasomnias tmaresterrors w behaviorsdange t sleepwalkingstre w teeth grindingf gsleep disorder disturb onfusedstresssleepw rt wakingroutine ye confuseddreamsbedrbing outgrow medicatio rrorstherapy
Sleep and Dreams UNIT 5- RG 5A
 Sleep and Dreams UNIT 5- RG 5A Goals for today Can you Discuss the circadian rhythm, what it is and how it effects us. Identify and explain each of the 5 stages of sleep. As well as the typical waves of
Sleep and Dreams UNIT 5- RG 5A Goals for today Can you Discuss the circadian rhythm, what it is and how it effects us. Identify and explain each of the 5 stages of sleep. As well as the typical waves of
Sleep: A Forgotten Component of Overall Health Demarcus Sneed Health and Human Sciences Educator Madison County October 5, 2016
 Sleep: A Forgotten Component of Overall Health Demarcus Sneed Health and Human Sciences Educator Madison County October 5, 2016 Lesson Objectives Understand the importance of having consistent, quality
Sleep: A Forgotten Component of Overall Health Demarcus Sneed Health and Human Sciences Educator Madison County October 5, 2016 Lesson Objectives Understand the importance of having consistent, quality
Article printed from
 What Are Sleep Disorders? Sleep disorders are conditions that affect how much and how well you sleep. The causes range from poor habits that keep you awake to medical problems that disrupt your sleep cycle.
What Are Sleep Disorders? Sleep disorders are conditions that affect how much and how well you sleep. The causes range from poor habits that keep you awake to medical problems that disrupt your sleep cycle.
ATHLETES & PRESCRIBING PHYSICIANS PLEASE READ
 ATHLETES & PRESCRIBING PHYSICIANS PLEASE READ USADA can grant a Therapeutic Use Exemption (TUE) in compliance with the World Anti- Doping Agency International Standard for TUEs. The TUE application process
ATHLETES & PRESCRIBING PHYSICIANS PLEASE READ USADA can grant a Therapeutic Use Exemption (TUE) in compliance with the World Anti- Doping Agency International Standard for TUEs. The TUE application process
Sleep Dysfunction in Multiple System Atrophy DR CALLUM DUPRE NEUROLOGY/SLEEP MEDICINE CAPITAL HEALTH SYSTEM
 Sleep Dysfunction in Multiple System Atrophy DR CALLUM DUPRE NEUROLOGY/SLEEP MEDICINE CAPITAL HEALTH SYSTEM Categories of Disturbance Sleep Breathing Disorders Parasomnias Sleepiness Insomnia Breathing?
Sleep Dysfunction in Multiple System Atrophy DR CALLUM DUPRE NEUROLOGY/SLEEP MEDICINE CAPITAL HEALTH SYSTEM Categories of Disturbance Sleep Breathing Disorders Parasomnias Sleepiness Insomnia Breathing?
SLEEP STUDY. Nighttime. 1. How many hours of sleep are you now getting in a typical night?
 SLEEP STUDY Patient Name: Date of Birth: Date of Study: This questionnaire involves a broad range of sleep and sleep-related behaviors. Your answers enable us to develop a clearer picture of your sleep/wake
SLEEP STUDY Patient Name: Date of Birth: Date of Study: This questionnaire involves a broad range of sleep and sleep-related behaviors. Your answers enable us to develop a clearer picture of your sleep/wake
Behavioral Treatments for Non-Rapid Eye Movement Parasomnias in Children
 Curr Sleep Medicine Rep (2016) 2:152 157 DOI 10.1007/s40675-016-0049-9 BEHAVIORAL THERAPY (T ARNEDT, SECTION EDITOR) Behavioral Treatments for Non-Rapid Eye Movement Parasomnias in Children Stacey L. Simon
Curr Sleep Medicine Rep (2016) 2:152 157 DOI 10.1007/s40675-016-0049-9 BEHAVIORAL THERAPY (T ARNEDT, SECTION EDITOR) Behavioral Treatments for Non-Rapid Eye Movement Parasomnias in Children Stacey L. Simon
Kids that go bump in the night
 THEME SLEEP Margot Davey MBBS, FRACP, is Director, Melbourne Children s Sleep Unit, Monash Medical Centre, Melbourne, Victoria. margot.davey@southernhealth.org.au Kids that go bump in the night Background
THEME SLEEP Margot Davey MBBS, FRACP, is Director, Melbourne Children s Sleep Unit, Monash Medical Centre, Melbourne, Victoria. margot.davey@southernhealth.org.au Kids that go bump in the night Background
Parkinson s Founda.on
 Parkinson s Founda.on PD ExpertBriefing: Sleep and Parkinson s Led By: Aleksandar Videnovic, M.D., M.Sc. Associate Professor of Neurology; Director, MGH Program on Sleep, Circadian Biology and NeurodegeneraDon
Parkinson s Founda.on PD ExpertBriefing: Sleep and Parkinson s Led By: Aleksandar Videnovic, M.D., M.Sc. Associate Professor of Neurology; Director, MGH Program on Sleep, Circadian Biology and NeurodegeneraDon
I. What Is Consciousness? Definition Awareness of things inside you and outside you. 3 Meanings of Consciousness
 I. What Is? Definition Awareness of things inside you and outside you I. What Is? is a construct What is a construct? Something that we can t directly see or measure Examples: self-esteem intelligence
I. What Is? Definition Awareness of things inside you and outside you I. What Is? is a construct What is a construct? Something that we can t directly see or measure Examples: self-esteem intelligence
Symptoms of Narcolepsy
 Symptoms of Narcolepsy v Sleep attacks Brief episodes of sleep that occur many times a day May occur without warning or be preceded by drowsiness Patient usually feels refreshed afterwards Refractory period
Symptoms of Narcolepsy v Sleep attacks Brief episodes of sleep that occur many times a day May occur without warning or be preceded by drowsiness Patient usually feels refreshed afterwards Refractory period
OBJECTIVES. The psychiatric, medical, and neurologic causes of sleep problems. Office-based and objective methods of evaluating sleep
 SLEEP ISSUES 1 OBJECTIVES 2 Know and understand: Age-related changes in sleep The psychiatric, medical, and neurologic causes of sleep problems Office-based and objective methods of evaluating sleep Appropriate
SLEEP ISSUES 1 OBJECTIVES 2 Know and understand: Age-related changes in sleep The psychiatric, medical, and neurologic causes of sleep problems Office-based and objective methods of evaluating sleep Appropriate
Week 4 Psychology. Theory of mind is an individual s understanding that they and others think, feel, perceive, and have private experiences.
 Week 4 Psychology Before we explore the concept in detail, let us understand Theory of Mind as well as what Consciousness and Stream of Consciousness are. Theory of mind is an individual s understanding
Week 4 Psychology Before we explore the concept in detail, let us understand Theory of Mind as well as what Consciousness and Stream of Consciousness are. Theory of mind is an individual s understanding
Sleep Complaints and Disorders in Epileptic Patients 순천향의대천안병원순천향의대천안병원신경과양광익
 Sleep Complaints and Disorders in Epileptic Patients 순천향의대천안병원순천향의대천안병원신경과양광익 Introduction The global physical, social and economic consequence of epilepsy are high. WHO 2000 study Improving QoL is increasingly
Sleep Complaints and Disorders in Epileptic Patients 순천향의대천안병원순천향의대천안병원신경과양광익 Introduction The global physical, social and economic consequence of epilepsy are high. WHO 2000 study Improving QoL is increasingly
Sleep and Students. John Villa, DO Medical Director
 Sleep and Students John Villa, DO Medical Director Objectives: Importance and Benefits of Sleep States and Stages of the Sleep Cycle Sleep Needs, Patterns and Characteristics for All Ages Healthy Sleep
Sleep and Students John Villa, DO Medical Director Objectives: Importance and Benefits of Sleep States and Stages of the Sleep Cycle Sleep Needs, Patterns and Characteristics for All Ages Healthy Sleep
Insomnia. Dr Terri Henderson MBChB FCPsych
 Insomnia Dr Terri Henderson MBChB FCPsych Plan Basics of insomnia Pharmacology Medication CBT Details of insomnia Unsatisfactory sleep that impairs daytime well-being Starts with specific problem or change
Insomnia Dr Terri Henderson MBChB FCPsych Plan Basics of insomnia Pharmacology Medication CBT Details of insomnia Unsatisfactory sleep that impairs daytime well-being Starts with specific problem or change
Sleep: What s the big deal?
 Rise & Shine: The Importance of Sleep Sleep: What s the big deal? Sleep affects every aspect of a child s physical, emotional, cognitive, and social development. 1 Sleep is the Primary Activity of the
Rise & Shine: The Importance of Sleep Sleep: What s the big deal? Sleep affects every aspect of a child s physical, emotional, cognitive, and social development. 1 Sleep is the Primary Activity of the
Activation-synthesis hypothesis. compulsive drug craving and use, despite adverse consequences. Addition. Amphetamines. Barbiturates.
 Activation-synthesis hypothesis Suggests that in the brain engages in a lot of neural activity that is random. Dreams make sense of this activity. Addition compulsive drug craving and use, despite adverse
Activation-synthesis hypothesis Suggests that in the brain engages in a lot of neural activity that is random. Dreams make sense of this activity. Addition compulsive drug craving and use, despite adverse
Narcolepsy. Jon R. Doud, MD Pulmonary Physician Midwest Center for Sleep Disorders Aurora, IL
 Narcolepsy Jon R. Doud, MD Pulmonary Physician Midwest Center for Sleep Disorders Aurora, IL Narcolepsy A central nervous system disorder that is an important cause of persistent sleepiness. The second
Narcolepsy Jon R. Doud, MD Pulmonary Physician Midwest Center for Sleep Disorders Aurora, IL Narcolepsy A central nervous system disorder that is an important cause of persistent sleepiness. The second
Module 22- Understanding Consciousness & Hypnosis
 Module 22- Understanding Consciousness & Hypnosis - Fundamental, hard to define Psychological Concept - Difficulties in defining consciousness led those specializing in behaviorism to look at direct observations
Module 22- Understanding Consciousness & Hypnosis - Fundamental, hard to define Psychological Concept - Difficulties in defining consciousness led those specializing in behaviorism to look at direct observations
WELCOME TO THE NORTHSHORE UNIVERSITY HEALTHSYSTEM SLEEP CENTERS
 WELCOME TO THE NORTHSHORE UNIVERSITY HEALTHSYSTEM SLEEP CENTERS Prior to your office visit, we request that you complete this questionnaire. It asks questions not only about your sleeping habits and behavior
WELCOME TO THE NORTHSHORE UNIVERSITY HEALTHSYSTEM SLEEP CENTERS Prior to your office visit, we request that you complete this questionnaire. It asks questions not only about your sleeping habits and behavior
States of Consciousness
 States of Consciousness Sleep, Dreams, and Body Rhythms Introduction Consciousness Awareness of oneself and one s environment Body Rhythms Biological Rhythms Periodic physiological fluctuations Can affect
States of Consciousness Sleep, Dreams, and Body Rhythms Introduction Consciousness Awareness of oneself and one s environment Body Rhythms Biological Rhythms Periodic physiological fluctuations Can affect
Consciousness, Stages of Sleep, & Dreams. Defined:
 Consciousness, Stages of Sleep, & Dreams I. Consciousness Conscious is: Waking Consciousness Defined: Altered State of Consciousness Defined: Most of waking life Fuzzy, organized, bizarre thoughts Examples:
Consciousness, Stages of Sleep, & Dreams I. Consciousness Conscious is: Waking Consciousness Defined: Altered State of Consciousness Defined: Most of waking life Fuzzy, organized, bizarre thoughts Examples:
Treating sleep disorders
 Treating sleep disorders Sue Wilson Centre for Neuropsychopharmacology Imperial College London sue.wilson@imperial.ac.uk Suggested algorithm for treatment of insomnia Diagnosis of insomnia Associated with
Treating sleep disorders Sue Wilson Centre for Neuropsychopharmacology Imperial College London sue.wilson@imperial.ac.uk Suggested algorithm for treatment of insomnia Diagnosis of insomnia Associated with
An 18-Year-Old Woman with Prolonged Eyes Closed Unresponsiveness during Multiple Sleep Latency Testing
 pii: jc-00317-16 http://dx.doi.org/10.5664/jcsm.6410 SLEEP MEDICINE PEARLS An 18-Year-Old Woman with Prolonged Eyes Closed Unresponsiveness during Multiple Sleep Latency Testing Romy Hoque, MD 1 ; Victoria
pii: jc-00317-16 http://dx.doi.org/10.5664/jcsm.6410 SLEEP MEDICINE PEARLS An 18-Year-Old Woman with Prolonged Eyes Closed Unresponsiveness during Multiple Sleep Latency Testing Romy Hoque, MD 1 ; Victoria
(consciousness) (monitor) (control)
 : (2002) (consciousness) (monitor) (control) selective attention Stroop Stroop illusion hallucination (delusion) Altered states of consciousness In many cultures, inducing and altered state
: (2002) (consciousness) (monitor) (control) selective attention Stroop Stroop illusion hallucination (delusion) Altered states of consciousness In many cultures, inducing and altered state
Polysomnographic Diagnosis of Sleepwalking: Effects of Sleep Deprivation
 Polysomnographic Diagnosis of walking: Effects of Deprivation Antonio Zadra, PhD, 1,2 Mathieu Pilon, MPs, 1,2 and Jacques Montplaisir, MD, PhD, CRCPc 1,3 Objective: Somnambulism affects up to 4% of adults
Polysomnographic Diagnosis of walking: Effects of Deprivation Antonio Zadra, PhD, 1,2 Mathieu Pilon, MPs, 1,2 and Jacques Montplaisir, MD, PhD, CRCPc 1,3 Objective: Somnambulism affects up to 4% of adults
Sleep and Parkinson's Disease
 Parkinson s Disease Clinic and Research Center University of California, San Francisco 505 Parnassus Ave., Rm. 795-M, Box 0114 San Francisco, CA 94143-0114 (415) 476-9276 http://pdcenter.neurology.ucsf.edu
Parkinson s Disease Clinic and Research Center University of California, San Francisco 505 Parnassus Ave., Rm. 795-M, Box 0114 San Francisco, CA 94143-0114 (415) 476-9276 http://pdcenter.neurology.ucsf.edu
Unit 5 REVIEW. Name: Date:
 Name: Date: 1. The best predictor of an adolescent's pattern of drug usage is whether the adolescent A) grows up in an intact two-parent family. B) has religious beliefs. C) is a first or second child.
Name: Date: 1. The best predictor of an adolescent's pattern of drug usage is whether the adolescent A) grows up in an intact two-parent family. B) has religious beliefs. C) is a first or second child.
Policy #: 619 Latest Review Date:December 2016 Category: Medicine Policy Grade: D
 Name of Policy: Polysomnography for Non Respiratory Sleep Disorders Policy #: 619 Latest Review Date:December 2016 Category: Medicine Policy Grade: D Background/Definitions: As a general rule, benefits
Name of Policy: Polysomnography for Non Respiratory Sleep Disorders Policy #: 619 Latest Review Date:December 2016 Category: Medicine Policy Grade: D Background/Definitions: As a general rule, benefits
EEG Electrode Placement
 EEG Electrode Placement Classifying EEG brain waves Frequency: the number of oscillations/waves per second, measured in Hertz (Hz) reflects the firing rate of neurons alpha, beta, theta, delta Amplitude:
EEG Electrode Placement Classifying EEG brain waves Frequency: the number of oscillations/waves per second, measured in Hertz (Hz) reflects the firing rate of neurons alpha, beta, theta, delta Amplitude:
INSOMNIA IN GERIATRICS. Presented By: Sara Kamalfar MD, Geriatrics Medicine Fellow
 INSOMNIA IN GERIATRICS Presented By: Sara Kamalfar MD, Geriatrics Medicine Fellow Insomnia Insomnia is the inability to fall asleep, the inability to stay asleep, or waking up earlier than desired. To
INSOMNIA IN GERIATRICS Presented By: Sara Kamalfar MD, Geriatrics Medicine Fellow Insomnia Insomnia is the inability to fall asleep, the inability to stay asleep, or waking up earlier than desired. To
DSM-5 Table of Contents
 DSM-5 Table of Contents DSM-5 Classification Preface Section I: DSM-5 Basics Introduction Use of DSM-5 Cautionary Statement for Forensic Use of DSM-5 Section II: Essential Elements: Diagnostic Criteria
DSM-5 Table of Contents DSM-5 Classification Preface Section I: DSM-5 Basics Introduction Use of DSM-5 Cautionary Statement for Forensic Use of DSM-5 Section II: Essential Elements: Diagnostic Criteria
Roslinde M. Collins, MD, D,ABSM, FCCP, FAASM Medical Director, Center for Sleep Disorders at Rutland Regional Medical Center, VT
 Parasomnias: Things that go crash in the night Roslinde M. Collins, MD, D,ABSM, FCCP, FAASM Medical Director, Center for Sleep Disorders at Rutland Regional Medical Center, VT rcollins@rrmc.org September
Parasomnias: Things that go crash in the night Roslinde M. Collins, MD, D,ABSM, FCCP, FAASM Medical Director, Center for Sleep Disorders at Rutland Regional Medical Center, VT rcollins@rrmc.org September
Sleep stages. Awake Stage 1 Stage 2 Stage 3 Stage 4 Rapid eye movement sleep (REM) Slow wave sleep (NREM)
 Sleep stages Awake Stage 1 Stage 2 Stage 3 Stage 4 Rapid eye movement sleep (REM) Slow wave sleep (NREM) EEG waves EEG Electrode Placement Classifying EEG brain waves Frequency: the number of oscillations/waves
Sleep stages Awake Stage 1 Stage 2 Stage 3 Stage 4 Rapid eye movement sleep (REM) Slow wave sleep (NREM) EEG waves EEG Electrode Placement Classifying EEG brain waves Frequency: the number of oscillations/waves
WHY CAN T I SLEEP? Deepti Chandran, MD
 WHY CAN T I SLEEP? Deepti Chandran, MD Sleep and Aging How does sleep change as we age? Do we need less sleep as we get older? Can a person expect to experience more sleep problems or have a sleep disorder
WHY CAN T I SLEEP? Deepti Chandran, MD Sleep and Aging How does sleep change as we age? Do we need less sleep as we get older? Can a person expect to experience more sleep problems or have a sleep disorder
Elimination Disorders Enuresis (primary and secondary) Encopresis (primary and secondary)
 Elimination Disorders Enuresis (primary and secondary) Encopresis (primary and secondary) 1 Elimination disorders Toilet training Developmental milestone Often required for entry into day care Usual sequence:
Elimination Disorders Enuresis (primary and secondary) Encopresis (primary and secondary) 1 Elimination disorders Toilet training Developmental milestone Often required for entry into day care Usual sequence:
Coding for Sleep Disorders Jennifer Rose V. Molano, MD
 Practice Coding for Sleep Disorders Jennifer Rose V. Molano, MD Accurate coding is an important function of neurologic practice. This section of is part of an ongoing series that presents helpful coding
Practice Coding for Sleep Disorders Jennifer Rose V. Molano, MD Accurate coding is an important function of neurologic practice. This section of is part of an ongoing series that presents helpful coding
Parasomnias: The Things That Go Bump in the Night
 Parasomnias: The Things That Go Bump in the Night Dominic B. Gault M.D. Medical Director, Division of Pediatric Sleep Medicine Greenville Health System Children s Hospital Conflict of Interest 1. I do
Parasomnias: The Things That Go Bump in the Night Dominic B. Gault M.D. Medical Director, Division of Pediatric Sleep Medicine Greenville Health System Children s Hospital Conflict of Interest 1. I do
AGING CHANGES IN SLEEP
 OBJECTIVES: Understand the common age-related changes in sleep Discuss the evaluation of the older person with sleep complaints Identify sleep apnea, PLMS, RLS, and REM sleep disorders and their treatments
OBJECTIVES: Understand the common age-related changes in sleep Discuss the evaluation of the older person with sleep complaints Identify sleep apnea, PLMS, RLS, and REM sleep disorders and their treatments
Sleep - 10/5/17 Kelsey
 Sleep - 10/5/17 Kelsey Thursday, October 5, 2017 10:59 AM How to Study and Measure Sleep Sleep: Absence of overt behavior, absence of consciousness. -> measures are indirect Methods to measure sleep characteristics:
Sleep - 10/5/17 Kelsey Thursday, October 5, 2017 10:59 AM How to Study and Measure Sleep Sleep: Absence of overt behavior, absence of consciousness. -> measures are indirect Methods to measure sleep characteristics:
Electrooculogram (EOG): eye movements. Air flow measurements: breathing Heart rate.
 By: Ricardo Measurements and study of sleep: Sleep: absence of overt behavior, absence of consciousness Measures are indirect Methods to measure sleep characteristics: Electromyogram (EMG): muscle activity
By: Ricardo Measurements and study of sleep: Sleep: absence of overt behavior, absence of consciousness Measures are indirect Methods to measure sleep characteristics: Electromyogram (EMG): muscle activity
INDEX. Group psychotherapy, described, 97 Group stimulus control, 29-47; see also Stimulus control (group setting)
 Index Abdominal breathing, 70; see also Breathing; Relaxation therapy Activation, sleep drive/responsivity, 6-9 Age level; see also Elderly circadian rhythms and, 68-69 delayed sleep phase syndrome and,
Index Abdominal breathing, 70; see also Breathing; Relaxation therapy Activation, sleep drive/responsivity, 6-9 Age level; see also Elderly circadian rhythms and, 68-69 delayed sleep phase syndrome and,
Mental Health and Stress
 Mental Health and Stress Learning Objectives Ø Define mental health and discuss the characteristics of mentally healthy and selfactualized people Ø Describe the various mental disorders and appropriate
Mental Health and Stress Learning Objectives Ø Define mental health and discuss the characteristics of mentally healthy and selfactualized people Ø Describe the various mental disorders and appropriate
BHS Memory and Amnesia. Functional Disorders of Memory
 BHS 499-07 Memory and Amnesia Functional Disorders of Memory Functional Disorders (Hysteria) Functional disorders are not disorders of structure but of function. Such disorders are classified as hysteria
BHS 499-07 Memory and Amnesia Functional Disorders of Memory Functional Disorders (Hysteria) Functional disorders are not disorders of structure but of function. Such disorders are classified as hysteria
MODULE 08: SLEEP, DREAMS, AND BODY RHYTHMS CONSCIOUSNESS
 MODULE 08: SLEEP, DREAMS, AND BODY RHYTHMS CONSCIOUSNESS CONSCIOUSNESS Awareness of yourself and your environment. CIRCADIAN RHYTHMS Biological rhythms (for example, of temperature and wakefulness) that
MODULE 08: SLEEP, DREAMS, AND BODY RHYTHMS CONSCIOUSNESS CONSCIOUSNESS Awareness of yourself and your environment. CIRCADIAN RHYTHMS Biological rhythms (for example, of temperature and wakefulness) that
Objectives 11/11/14. Identifying and Treating Pediatric Sleep Disorders. Normal Sleep in Children. When baby ain t sleepin, ain t nobody sleepin!
 When baby ain t sleepin, ain t nobody sleepin! Identifying and Treating Pediatric Sleep Disorders Theodore Wagener, PhD OU Children s Physicians, Pediatric Behavioral Sleep Medicine Clinic Objectives Attendees
When baby ain t sleepin, ain t nobody sleepin! Identifying and Treating Pediatric Sleep Disorders Theodore Wagener, PhD OU Children s Physicians, Pediatric Behavioral Sleep Medicine Clinic Objectives Attendees
Not Sleeping Well? Chronic physical conditions. There May Be a Medical Cause. Diabetes. Heartburn
 Not Sleeping Well? There May Be a Medical Cause People who feel they sleep perfectly well may still be troubled by excessive daytime sleepiness because of a variety of underlying medical illnesses. A sleep
Not Sleeping Well? There May Be a Medical Cause People who feel they sleep perfectly well may still be troubled by excessive daytime sleepiness because of a variety of underlying medical illnesses. A sleep
Overview. Sleep Related Movement Disorders - Restless Leg Syndrome - Periodic Limb movements in Sleep
 The Structure of Sleep The Parasomnias - in REM - in Non-REM - Narcolepsy Overview Sleep Related Movement Disorders - Restless Leg Syndrome - Periodic Limb movements in Sleep Circadian Rhythm disorders
The Structure of Sleep The Parasomnias - in REM - in Non-REM - Narcolepsy Overview Sleep Related Movement Disorders - Restless Leg Syndrome - Periodic Limb movements in Sleep Circadian Rhythm disorders
Chapter 6. Consciousness
 Consciousness Psychology, Fifth Edition, James S. Nairne What s It For? The Value of Consciousness Setting Priorities for Mental Functioning Sleeping and Dreaming Altering Awareness: Psychoactive Drugs
Consciousness Psychology, Fifth Edition, James S. Nairne What s It For? The Value of Consciousness Setting Priorities for Mental Functioning Sleeping and Dreaming Altering Awareness: Psychoactive Drugs
일차진료에서불면증치료 김종우. Primary Insomnia : DSM-IV criteria 경희대학교의과대학정신과학교실 MEMO. Diagnostic Criteria for Insomnia (ICSD-2) 개원의와함께하는임상강좌
 개원의와함께하는임상강좌 2011 일차진료에서불면증치료 경희대학교의과대학정신과학교실 김종우 Diagnostic Criteria for Insomnia (ICSD-2) International Classification of Sleep Disorders, 2nd Edition (ICSD-2) Primary Insomnia : DSM-IV criteria A. The
개원의와함께하는임상강좌 2011 일차진료에서불면증치료 경희대학교의과대학정신과학교실 김종우 Diagnostic Criteria for Insomnia (ICSD-2) International Classification of Sleep Disorders, 2nd Edition (ICSD-2) Primary Insomnia : DSM-IV criteria A. The
Joint Session with ACOFP and Mayo Clinic. Parkinson's Disease: 5 Pearls. Jay Van Gerpen, MD
 Joint Session with ACOFP and Mayo Clinic Parkinson's Disease: 5 Pearls Jay Van Gerpen, MD Parkinson s Disease: 5 Pearls J.A. van Gerpen, MD Sections of Movement Disorders and Clinical Neurophysiology
Joint Session with ACOFP and Mayo Clinic Parkinson's Disease: 5 Pearls Jay Van Gerpen, MD Parkinson s Disease: 5 Pearls J.A. van Gerpen, MD Sections of Movement Disorders and Clinical Neurophysiology
Sleep Disorders. Anneka Rose ST5 Psychiatrist
 Sleep Disorders Anneka Rose ST5 Psychiatrist Agenda Basic overview of sleep structure Interactive case based discussions 5 min interventions MCQs Questions Hypnogram Actigraphy Common Scenario Patient
Sleep Disorders Anneka Rose ST5 Psychiatrist Agenda Basic overview of sleep structure Interactive case based discussions 5 min interventions MCQs Questions Hypnogram Actigraphy Common Scenario Patient
CONSCIOUSNESS AND IT ALTERED STAGES. Muhammad Rehan BSN,RN Lecturer
 CONSCIOUSNESS AND IT ALTERED STAGES Muhammad Rehan BSN,RN Lecturer What is CONSCIOUSNESS! Include all memories that remain within an individual s awarness. Event and experiences that are easily remembered.
CONSCIOUSNESS AND IT ALTERED STAGES Muhammad Rehan BSN,RN Lecturer What is CONSCIOUSNESS! Include all memories that remain within an individual s awarness. Event and experiences that are easily remembered.
Sleep - Definition. Slide 1 Sleep & Developmental Disabilities: Lessons for All Children. Slide 2 Importance of Sleep. Slide 3. Lawrence W.
 1 Sleep & Developmental Disabilities: Lessons for All Children March 28, 2012 Lawrence W. Brown, MD Pediatric Neuropsychiatry Program Sleep Disorders Center The Children s Hospital of Philadelphia 2 Importance
1 Sleep & Developmental Disabilities: Lessons for All Children March 28, 2012 Lawrence W. Brown, MD Pediatric Neuropsychiatry Program Sleep Disorders Center The Children s Hospital of Philadelphia 2 Importance
CONSCIOUSNESS AND THE TWO-TRACK MIND
 Chapter 3 CONSCIOUSNESS AND THE TWO-TRACK MIND Forms of Consciousness Modern psychologists believe that consciousness is an awareness of ourselves and our environment. Consciousness is not whether or not
Chapter 3 CONSCIOUSNESS AND THE TWO-TRACK MIND Forms of Consciousness Modern psychologists believe that consciousness is an awareness of ourselves and our environment. Consciousness is not whether or not
