Agrypnia Excitata: Current Concepts and Future Prospects in Management
|
|
|
- Alban Collins
- 5 years ago
- Views:
Transcription
1 Agrypnia Excitata: Current Concepts and Future Prospects in Management Ribhi Hazin, M.D. Jamil Y. Abuzetun, M.D. Pierre Giglio, M.D. Faisal Khan, M.D. Agrypnia excitata is an extremely rare, lifethreatening syndrome characterized by autonomic activation, persistent insomnia, and generalized overactivity. Agrypnia excitata describes a triad of three separate conditions: delirium tremens, Morvan s chorea, and familial fatal insomnia (FFI). Each of the aforementioned three conditions have sleep disturbances as a unifying theme and results in distinct neurophysiological findings. The following is an overview of agrypnia excitata with a particular emphasis placed upon each of the three individual conditions that constitute the syndrome with recommendations on appropriate management. (The Journal of Neuropsychiatry and Clinical Neurosciences 2009; 21: ) grypnia excitita as described constitutes a triad Aof three separate conditions, delirium tremens, Morvan s chorea, and familial fatal insomnia (FFI). This triad of conditions has sleep disturbances as a unifying theme. 1 When considered individually, each of the aforementioned three conditions results in distinct neurophysiological findings including deterioration of the thalamolimbic system. 1,2 All three conditions lead to generalized autonomic sympathetic activation associated with a stuporous state and marked motor and autonomic sympathetic activation. 1,2 In addition to persistent agrypnia, the three conditions all characteristically exhibit complete loss of slow-wave sleep on polysomnogram evaluation. The elevated autonomic state that typifies agrypnia excitata often manifests in the form of diffuse sweating, tachypnea, hypertension, elevated plasma cortisol, and catecholamine levels. Agrypnia excitata evolves rapidly and runs a uniformly fatal course with most patients dying within months of symptom onset. The following is an overview of agrypnia excitata with a particular emphasis on each of Received January 21, 2008; revised April 26, 2008; accepted April 29, Dr. Hazin is affiliated with the Faculty of Arts and Sciences at Harvard University; Dr. Abuzetun is affiliated with the Division of Internal Medicine at Creighton University Medical Center; Dr. Giglio is affiliated with the Department of Neurosciences, Medical University of South Carolina; Dr. Khan is affiliated with the Neurodiagnostic and Sleep Center at Gulf Coast Medical Center in Wharton, Tex. Address correspondence to Faisal Khan, M.D., Neurodiagnostic and Sleep Center, Gulf Coast Medical Center, US 59 Road, Wharton, TX ; fskhan786@gmail.com ( ). Copyright 2009 American Psychiatric Publishing, Inc J Neuropsychiatry Clin Neurosci 21:2, Spring 2009
2 HAZIN et al. the three individual conditions that constitute the syndrome. Fatal Familial Insomnia Fatal familial insomnia (FFI) is an extremely rare neurodegenerative prion disease. 3 It is transmitted in an autosomal dominant pattern and is characterized by behavioral problems, autonomic instability, hallucinations, and ultimately death. 3 The disease arises from a mutation in the gene responsible for the expression of a protein resulting in the generation of insoluble proteins called prion proteins that contribute to the deterioration of vital neurological structures within the CNS. 2 Over time these insoluble proteins congregate to form amyloid plaques throughout the CNS, particularly in the areas within or near the hypothalamus, leading to the characteristic deficits in hypothalamic function in individuals afflicted with FFI. Fatal familial insomnia is characterized by a devastating clinical course that includes recurrent sleep disorders, neurological dysfunction, and eventual death. Because of the extreme rarity of FFI, a paucity of reliable data exists on approaches and maximal treatment strategies for this disorder. The following is a thorough examination of FFI with a particular focus placed on current concepts in diagnosis and management as well as future prospects for the condition. Clinical Manifestations Fatal familial insomnia is characterized by behavioral disturbances, ataxia, pyramidal signs, autonomic problems, and widespread neurological compromise. 3 After the initial onset of symptoms, FFI evolves rapidly, and death occurs months after the first symptom sets in. 3,4 The symptoms of FFI are directly related to the area of neurological involvement in the disorder. Since the thalamus and associated thalamic structures are the most affected in FFI, it stands to reason that bodily functions controlled by the thalamus are commensurately affected in patients with FFI. The thalamus is a prominent mass of gray matter located above the brainstem that controls bodily functions including motor control and somatosensory and visual sensory signals. It also relays sensory signals to and from the cerebral cortex and vital anatomical structures throughout the body. Typically, patients complain of persistent insomnia, frequent nocturnal awakenings, and persistent daytime fatigue. 1,5,6 Autonomic activation in the form of excessive salivation and perspiration along with elevated blood pressure, tachycardia, pyrexia, and appetite disturbances are also common. 1,6,7 Bizarre dreams often occur and tend to be superseded by a stupor-like state that eventually leads to coma and death. 1 During sleep, the ability of the thalamus to effectively relay such signals becomes compromised, allowing the body to succumb to the sleep state. Therefore, the thalamic dysfunction that ensues in FFI yields a myriad of problems associated with the aforementioned thalamic functions, namely those related to or affected by sleep. The disease runs a uniformly fatal course that manifests in four stages (Table 1). Ultimately, patients expire 18 months after the onset of symptoms. 2 Common clinical features of FFI include hallucinations, phobias, dementia, decreased reflexes, and an inability to lacrimate or appreciate pain. 1,2 Later stages of the disease lead to autonomic dysfunction, which manifests as dementia, coma, and loss of sphincter control. 1 The wide array of symptoms in FFI has led experts to classify it as a pleiotropic disease, or a disease with one mutant gene that yields one mutant protein but results in many pheno- TABLE 1. The Four Stages of Fatal Familial Insomnia 1,2 Stage Duration Symptoms Stage I 8-12 weeks following onset The patient experiences progressive difficulty napping during the day and persistent insomnia at night followed by panic attacks and bizarre phobias. Stage II weeks The patient is overcome by hallucinatory behavior and may lose contact with his/ her surroundings. Panic attacks, persistent agitation, and uncontrollable sweating are also hallmarks of this stage. Stage III 8-12 months The patient is completely incapable of sleeping during this stage leading to exacerbation of aforementioned symptoms. The patient may also manifest complex and well-organized motor gestures and rapid weight loss during this stage. Stage IV weeks The patient s condition deteriorates with vital neurological functions lost. Patients in Stage IV often become unresponsive to stimuli, suffer significant dementia, lose sphincter control and other neurological functions, followed ultimately by death. J Neuropsychiatry Clin Neurosci 21:2, Spring
3 AGRYPNIA EXCITATA: CURRENT CONCEPTS AND MANAGEMENT typic abnormalities. The pleiotropic basis of the disorder may account for the significant variation in disease presentation from individual to individual, even in patients from the same family. Epidemiology Fatal familial insomnia is transmitted via autosomal dominant inheritance, meaning it affects both genders with equal frequency. 8,9 On average, individuals with the mutant gene most often develop symptoms between the ages of 40 to 60 years, with an average of onset at 51 years old. 10 Death ensues by weeks after first onset of symptoms. 5 7,10 Pathophysiology Fatal familial insomnia results from a genetic mutation in the prion protein gene, or PRNP gene, that results in the replacement of asparagine with aspartic acid at codon 178, along with substitution of asparagine for methionine at codon ,3,11 Although the exact function of the PRNP gene remains uncertain, it is likely involved in the cell signaling in the CNS. The inborn genetic error in FFI results in a dramatic accumulation of protease resistant prion protein, which is responsible for the cognitive dysfunction that characterizes the disorder. 1 The mutation yields significant thalamolimbic impairment, which is believed to cause the striking phenotypic and clinical features of FFI. 1,3 Pathology and imaging studies corroborate this finding by demonstrating widespread hypometabolism throughout the thalami of patients with FFI. 3 Furthermore, the presence of atrophy, gliosis, and neuronal loss in the thalami along with spongiosis in the cerebellum is a common finding in patients with FFI. 1,3,9 The atrophic changes within the thalamus that characterize FFI are believed to underlie the sleep, autonomic, and circadian disturbances that appear in FFI. 1,4 Diagnosis A number of tests are used to diagnosis FFI. Since FFI is familial in origin, a thorough family history may help in arriving at an accurate diagnosis. A thorough physical examination and detailed history are recommended to rule out systemic or exogenous conditions as a cause of clinical presentation. The physical exam of FFI patients often demonstrates bilateral hyperreflexia and reflex myoclonia. 3 Laryngeal examination may also demonstrate paralysis of the laryngeal cords. 3 Although exact cause of death in FFI remains unclear, experts have pointed to the paralysis of laryngeal cords in FFI as a possible cause of laryngospasminduced death in such patients. 3,4 Given the many neuropsychological sequelae of FFI, comprehensive neuropsychological testing is warranted. Depending on the stage of disease development, the patient may demonstrate any of a wide array of symptoms from hallucinations, behavioral disturbances, autonomic disturbances, alteration in attention and immediate memory, or a propensity to confabulate. 3 The patient s history will reveal significant sleep disturbances in the form of insomnia and repeated nocturnal awakenings. As with other patients with deterioration of sleep function, a polysomnogram is considered necessary for the diagnosis of FFI and typically reveals the complete absence of spindles and slow-wave sleep along with extended REM periods without muscle atonia. 1,3,4,12 Stridor, nocturnal groaning, loud snoring, and persistent talking and moving may also be present during polysomnogram testing in FFI patients. 3 Finally, given the genetic nature of the disease, genetic testing for mutations in the D178N gene in codon 129 can help confirm the diagnosis. 3,8,11 Treatment Although FFI runs a fatal course, recent data suggest that the use of vitamins, sedative-hypnotics (e.g., ethchlorvynol, zolpidem, or diazepam), stimulants, sensory deprivation, exercise, light entrainment, and growth hormone may offer promising methods of managing FFI patients Electroconvulsive therapy may improve symptoms in such patients through forced sleep and the use of vitamins, sedative-hypnotics, and stimulants may yield improved quality of life by minimizing stupor-like states that often accompany periods of prolonged sleeplessness. 13,14,17 Despite improving a patient s ability to sleep, ECT should be used with caution due to the myriad of side effects such therapy courts, including memory loss and cognitive damage. 13,18,19 Despite advances in therapeutic strategies and the resultant improvement in symptoms of FFI, a cure for FFI continues to elude clinicians. The need for broader research on the topic is warranted considering the fact that all patients expire within weeks after first onset of symptoms. 5,7 Morvan s Chorea Morvan s chorea, or fibrillary chorea, describes the rare condition in which neuromyotonia (involuntary contraction of muscles at rest) occurs in the setting of peripheral nervous system hyperexcitibility. 1,3,20 The typical movements in Morvan s chorea most commonly J Neuropsychiatry Clin Neurosci 21:2, Spring 2009
4 HAZIN et al. affect bilateral calves and the posterior part of the thigh. The peripheral nerve hyperexcitibility that dominates in Morvan s chorea typically results in neuromyotonia as well as hyperhydrosis, paresthesias, dysautonomia, myalgias, incontinence, palpitations, and sleep dysfunction. 3,20,21 Similar to the other two components of agrypnia excitata, Morvan s chorea also shares the same clinical features as both FFI and delirium tremens: agrypnia, mental confusion, and a significant reduction of slow wave sleep (Table 2). 1 3,18 Unlike the other components of agrypnia excitata, however, Morvan s chorea can arise at any age and may occur with painful cramps. 1,21 Like patients with FFI, Morvan s chorea also may manifest with hallucinatory behavior, a stuporous confused state, and peculiar motor disturbances, but these features are very rare in Morvan s chorea. 1,22 Like the other subtypes of agrypnia excitata, polysomnograms in patients with Morvan s chorea reveal the persistent absence of sleep rhythms for up to 4 months with the typical loss of slow-wave sleep. 1,21 Patients with Morvan s chorea will exhibit REM without atonia and will also demonstrate hypercortisolemia and hypercatecholemia in the plasma. 2,21 The exact pathophysiology of Morvan s chorea remains uncertain. However, it is believed that the condition arises via autoimmune mechanisms. 21 The presence of voltage-gated potassium channel antibodies is also commonly found in the serum of patients with Morvan s chorea. 20,21,23 The effect of these antibodies is believed to cause neuronal hyperexcitability by disrupting the ability of voltage gated potassium channel antibody to repolarize motor nerves effectively. 21,24 Unlike FFI, which runs a uniformly fatal course, Morvan s chorea may resolve overtime but can, in some cases, result in death. 1,2 In severe cases encephalopathy, dementia, or reduplicative paramnesia may ensue. 2,20,23 Notwithstanding, given the potentially fatal course of other diseases that mimic Morvan s chorea, consideration of a thorough differential diagnosis is critical to help minimize misdiagnosis. 25 Accurately recognizing Morvan s chorea may help prevent misdiagnosis in the setting of clinically similar diseases such as in patients suffering from acquired forms of peripheral nerve hyperexcitability. Acquired peripheral nerve hyperexcitability can occur following timber rattlesnake envenomation or Guillain-Barre syndrome, two conditions that can lead to devastating sequelae. 22,25 Fortunately, Morvan s chorea is, for the most part a treatable condition. 1,2,3 Unlike the other two components of agrypnia excitata, appropriate therapeutic approaches can reverse the course of Morvan s chorea. 26 Plasmapheresis, thymectomy, and long-term immunosuppressive therapy can yield complete resolution of symptoms in patients with Morvan s chorea. 20,26 Delirium Tremens Delirium tremens describes the third and final element of agrypnia excitata. Delirium tremens often arises in TABLE 2. Clinical, Neurophysiological, and Pathological Comparison of Delirium Tremens, Morvan s Chorea, and Fatal Familial Insomnia* Behavior Delirium Tremens Morvan s Chorea Fatal Familial Insomnia Insomnia Present Persistent for months Present early (subwakefulness) Hallucinations/onericism Severe Present Present in fully developed disease, with enacted dreams Motor hyperactivity Present Neuromyotonia Persistent through the 24th Autonomic hyperactivity Severe Present Present early Cortisolemia Increased Increased Increased Plasma catecholamines Increased Increased Increased Spindles/ K complexes Reduced/absent Reduced/absent Reduced/absent Slow wave sleep Severely reduced/absent Absent Reduced/absent REM sleep Increased, abnormal Without atonia Without atonia without atonia PET/ Pathology Atrophy of thalamus, mammillary bodies, temporal and orbitomesial cortex Antibodies in thalamus and striatum Atrophy of anterior and dorsomedian thalamus and cingular cortex *Table adapted from Montagna et al. 1 and reprinted with permission of authors. J Neuropsychiatry Clin Neurosci 21:2, Spring
5 AGRYPNIA EXCITATA: CURRENT CONCEPTS AND MANAGEMENT the setting of sudden withdrawal in chronic alcoholics or individuals on barbiturates or benzodiazepines for extended periods. 19,27 Delirium tremens is a potentially fatal and debilitating disorder whose clinical features include delirium, visual and tactile hallucinations, formication, severe anxiety, and severe, involuntary tremors of the extremities. When occurring in the setting of agrypnia excitata, delirium tremens arises with an acute confused state associated with bizarre hallucinatory behavior, agrypnia, and motor and autonomic agitation. 1,27 The autonomic activation in agrypnia excitatatype delirium tremens may be so severe that it results in the death of the patient. 1 Polysomnogram evaluation of patients in delirium tremens reveals findings similar to those found in the other two components of agrypnia excitata. Polysomnogram recordings of delirium tremens patients demonstrate significantly reduced or completely absent slow-wave sleep in conjunction with sleep fragmentation and persistent nocturnal awakenings. 2,28,29 Furthermore, REM sleep without muscular atonia is also found in delirium tremens. 2,30 The degree of slow-wave sleep loss in all three forms of agrypnia excitata corresponds to the amount of atrophic change that occurs in the brain at the time of testing. 31,32 Similar to the other two components of agrypnia excitata, delirium tremens also demonstrates increased cortisol and catecholamines as well as tachypnea, irregular breathing, pyrexia, and hypertension throughout the day. 1,33 35 Although pathophysiologic mechanisms underlying delirium tremens remain unclear, deterioration of the thalamus and its related structures has been established as a primary factor in the development of the disorder. 1,36 38 Incidentally, imaging studies reveal significantly reduced activity in the thalamus of patients with delirium tremens. 39 The management of delirium tremens centers on supportive therapy in conjunction with pharmacologic management. The current mainstay of treatment includes benzodiazepines and mood-stabilizers until symptoms subside. 19,39 CONCLUSION Agrypnia excitata represents a triad of three conditions that are characterized by insomnia, secondary drowsiness, and a stuporous mental state. The inability to sleep exacerbates the symptoms in such patients, leading to extreme exhaustion, coma, and ultimately death. Thalamic deterioration has been linked to the onset and course of agrypnia excitata and accounts for the typical clinical features of the disorder. The inability to generate sleep in such patients remains a primary challenge facing clinicians. Finally, a need exists for increased funding for controlled studies in order to offer improved insight into this devastating disease. In addition, these studies can improve current therapeutic approaches to agrypnia excitata and bring those individuals affected by the disease one step closer to living normal lives. References 1. Montagna P, Lugaresi E: Agrypnia excitata: a generalized overactivity syndrome and a useful concept in the neurophysiopathology of sleep. Clin Neurophysiol 2002; 113: Lugaresi E, Provini F: Agrypnia excitata: clinical features and pathophysiological implications. Sleep Med Rev 2001; 5: Iriarte J, Ayuso T, Echavarri C, et al: Agrypnia excitata in fatal familial insomnia: a video-polygraphic study. Neurology 2007; 69: Lugaresi E, Tobler I, Gambetti P, et al: The pathophysiology of fatal familial insomnia. Brain Pathol 1998; 8: Montagna P, Gambetti P, Cortelli P, et al: Familial and sporadic fatal insomnia. Lancet Neurol 2003; 2: Spacey SD, Pastore M, McGillivray B, et al: Fatal familial insomnia: the first account in a family of chinese descent. Arch Neurol 2004; 61: Sundstrom DG, Dreher HM: A deadly prion disease: fatal familial insomnia. J Neurosci Nurs 2003; 35: Montagna P, Cortelli P, Avoni P, et al: Clinical features of fatal familial insomnia: phenotypic variability in relation to a polymorphism at codon 129 of the prion protein gene. Brain Pathol 1998; 8: Cortelli P, Perani D, Montagna P, et al: Pre-symptomatic diagnosis in fatal familial insomnia: serial neurophysiological and 18FDG-PET studies. Brain 2006; 129: Manetto V, Medori R, Cortelli P, et al: Fatal familial insomnia: clinical and pathologic study of five new cases. Neurology 1992; 42: Cortelli P, Gambetti P, Montagna P, et al: Fatal familial insomnia: clinical features and molecular genetics. J Sleep Res 1999; 8: AASM. The International Classification of Sleep Disorders. Revised and coding manual, 2nd ed. 2005: Schenkein J, Montagna P: Self management of fatal familial insomnia, part 1: what is FFI? MedGenMed 2006; 8: Schenkein J, Montagna P: Self-management of fatal familial insomnia, part 2: case report. MedGenMed 2006; 8: Dimitri D, Jehel L, Durr A, et al: Fatal familial insomnia presenting as psychosis in an 18-year-old man. Neurology 2006; 67: J Neuropsychiatry Clin Neurosci 21:2, Spring 2009
6 HAZIN et al. 16. Waldman AD, Cordery RJ, MacManus DG, et al: Regional brain metabolite abnormalities in inherited prion disease and asymptomatic gene carriers demonstrated in vivo by quantitative proton magnetic resonance spectroscopy. Neuroradiology 2006; 48: Piao YS, Kakita A, Watanabe H, et al: Sporadic fatal insomnia with spongiform degeneration in the thalamus and widespread PrPSc deposits in the brain. Neuropathology 2005; 25: Pandya M, Pozuelo L, Malone D: Electroconvulsive therapy: what the internist needs to know. Cleve Clin J Med 2007; 74: DeBellis R, Smith BS, Choi S, et al: Management of delirium tremens. J Intensive Care Med 2005; 20: Hudson LA, Rollins YD, Anderson CA, et al. Reduplicative paramnesia in Morvan s syndrome. J Neurol Sci 2008; 267: Liguori R, Vincent A, Clover L, et al: Morvan s syndrome: peripheral and central nervous system and cardiac involvement with antibodies to voltage-gated potassium channels. Brain 2001; 124: Newsom-Davis J, Buckley C, Clover L, et al: Autoimmune disorders of neuronal potassium channels. Ann N Y Acad Sci 2003; 998: McKeon A, Marnane M, O Connell M, et al. Potassium channel antibody associated encephalopathy presenting with a frontotemporal dementia like syndrome. Arch Neurol 2007; 64: Sinha S, Newsom-Davis J, Mills K, et al: Autoimmune aetiology for acquired neuromyotonia (Isaacs syndrome). Lancet 1991; 338: Gutmann L, Gutmann L: Axonal channelopathies: an evolving concept in the pathogenesis of peripheral nerve disorders. Neurology 1996; 47: Haug BA, Schoenle PW, Karch BJ, et al: Morvan s fibrillary chorea: a case with possible manganese poisoning. Clin Neurol Neurosurg 1989; 91: Tachibana M, Tanaka K, Hishikawa Y, et al: A sleep study of acute psychotic states due to alcohol and meprobamate addiction, in Advances in Sleep Research. Edited by Weitzman ED. New York, Spectrum, 1975, pp Brower KJ: Alcohol s effects on sleep in alcoholics. Alcohol Res Health 2001; 25: Gann H, Feige B, Hohagen F, et al: Sleep and the cholinergic rapid eye movement sleep induction test in patients with primary alcohol dependence. Biol Psychiatry 2001; 50: Schenck CH, Bundlie SR, Ettinger MG, et al: Chronic behavioral disorders of human REM sleep: a new category of parasomnia. Sleep 2002; 25: Ishibashi M, Nakazawa Y, Yokoyama T, et al: Cerebral atrophy and slow wave sleep of abstinent chronic alcoholics. Drug Alcohol Depend 1987; 19: Imatoh N, Nakazawa Y, Ohshima H, et al: Circadian rhythm of REM sleep of chronic alcoholics during alcohol withdrawal. Drug Alcohol Depend 1986; 18: Iranmanesh A, Veldhuis JD, Johnson ML, et al: 24-hour pulsatile and circadian patterns of cortisol secretion in alcoholic men. J Androl 1989; 10: Risher-Flowers D, Adinoff B, Ravitz B, et al: Circadian rhythms of cortisol during alcohol withdrawal. Adv Alcohol Subst Abuse 1988; 7: Clark LT, Friedman HS: Hypertension associated with alcohol withdrawal: assessment of mechanisms and complications. Alcohol Clin Exp Res 1985; 9: Kopelman MD: The Korsakoff syndrome. Br J Psychiatry 1995; 166: Pagnan L, Berlot G, Pozzi-Mucelli RS Magnetic resonance imaging in a case of Wernicke s encephalopathy. Eur Radiol 1998; 8: Shimamura AP, Jernigan TL, Squire LR: Korsakoff s syndrome: radiological (CT) findings and neuropsychological correlates. J Neurosci 1988; 8: Wang GJ, Volkow ND, Franceschi D, et al: Regional brain metabolism during alcohol intoxication. Alcohol Clin Exp Res 2000; 24: J Neuropsychiatry Clin Neurosci 21:2, Spring
FATAL FAMILIAL INSOMNIA
 Azienda ASL 9 TREVISO Presidio Ospedaliero di Treviso Dipartimento di Medicina Unità Operativa di Medicina Interna Seconda Responsabile dr Ignazio Roiter FATAL FAMILIAL INSOMNIA Dr I. ROITER FATAL FAMILIAL
Azienda ASL 9 TREVISO Presidio Ospedaliero di Treviso Dipartimento di Medicina Unità Operativa di Medicina Interna Seconda Responsabile dr Ignazio Roiter FATAL FAMILIAL INSOMNIA Dr I. ROITER FATAL FAMILIAL
Fatal familial insomnia
 International Journal of Scientific and Research Publications, Volume 8, Issue 2, February 2018 560 Fatal familial insomnia Hassan I. Osman *(1), Mazin. S. Abdalla (2) * (1) Department of Physiology, Napata
International Journal of Scientific and Research Publications, Volume 8, Issue 2, February 2018 560 Fatal familial insomnia Hassan I. Osman *(1), Mazin. S. Abdalla (2) * (1) Department of Physiology, Napata
TOXIC AND NUTRITIONAL DISORDER MODULE
 TOXIC AND NUTRITIONAL DISORDER MODULE Objectives: For each of the following entities the student should be able to: 1. Describe the etiology/pathogenesis and/or pathophysiology, gross and microscopic morphology
TOXIC AND NUTRITIONAL DISORDER MODULE Objectives: For each of the following entities the student should be able to: 1. Describe the etiology/pathogenesis and/or pathophysiology, gross and microscopic morphology
Clinical Features of Sporadic Fatal Insomnia
 DIAGNOSIS UPDATE Clinical Features of Sporadic Fatal Insomnia Jed A. Barash, MD Department of Neurology, Beth Israel Deaconess Medical Center, Boston, MA Recent advances in neuropathology, genotyping,
DIAGNOSIS UPDATE Clinical Features of Sporadic Fatal Insomnia Jed A. Barash, MD Department of Neurology, Beth Israel Deaconess Medical Center, Boston, MA Recent advances in neuropathology, genotyping,
Biology 3201 Nervous System # 7: Nervous System Disorders
 Biology 3201 Nervous System # 7: Nervous System Disorders Alzheimer's Disease first identified by German physician, Alois Alzheimer, in 1906 most common neurodegenerative disease two thirds of cases of
Biology 3201 Nervous System # 7: Nervous System Disorders Alzheimer's Disease first identified by German physician, Alois Alzheimer, in 1906 most common neurodegenerative disease two thirds of cases of
Prion diseases or transmissible spongiform encephalopathies (TSEs)
 Prion diseases or transmissible spongiform encephalopathies (TSEs) rare progressive neurodegenerative disorders that affect both humans and animals. They are distinguished by long incubation periods, characteristic
Prion diseases or transmissible spongiform encephalopathies (TSEs) rare progressive neurodegenerative disorders that affect both humans and animals. They are distinguished by long incubation periods, characteristic
CREUTZFELDT-JAKOB DISEASE (CJD), CLASSIC
 CREUTZFELDT-JAKOB DISEASE (CJD), CLASSIC SPADIC CREUTZFELDT-JAKOB DISEASE (SCJD) Case definition CONFIRMED CASE Neuropathologically and/or immunocytochemically and/or biochemically confirmed, through observation
CREUTZFELDT-JAKOB DISEASE (CJD), CLASSIC SPADIC CREUTZFELDT-JAKOB DISEASE (SCJD) Case definition CONFIRMED CASE Neuropathologically and/or immunocytochemically and/or biochemically confirmed, through observation
SLEEP DISORDERS IN HUNTINGTON S DISEASE. Gary L. Dunbar, Ph.D.
 SLEEP DISORDERS IN HUNTINGTON S DISEASE Gary L. Dunbar, Ph.D. Executive Director, Field Neurosciences Institute Co-Director, Program in Neuroscience Central Michigan University Pre-Talk Test 1. Which type
SLEEP DISORDERS IN HUNTINGTON S DISEASE Gary L. Dunbar, Ph.D. Executive Director, Field Neurosciences Institute Co-Director, Program in Neuroscience Central Michigan University Pre-Talk Test 1. Which type
Geriatric Alterations Associated with Neurological Conditions
 Geriatric Alterations Associated with Neurological Conditions I have no conflicts of interest. Julie Bronson The Older Adult According to the World Health Organization Africa 50-55 or 50-65 United Nations
Geriatric Alterations Associated with Neurological Conditions I have no conflicts of interest. Julie Bronson The Older Adult According to the World Health Organization Africa 50-55 or 50-65 United Nations
Chemical Control of Behavior and Brain 1 of 9
 Chemical Control of Behavior and Brain 1 of 9 I) INTRO A) Nervous system discussed so far 1) Specific 2) Fast B) Other systems extended in space and time 1) Nonspecific 2) Slow C) Three components that
Chemical Control of Behavior and Brain 1 of 9 I) INTRO A) Nervous system discussed so far 1) Specific 2) Fast B) Other systems extended in space and time 1) Nonspecific 2) Slow C) Three components that
Delirium & Dementia. Nicholas J. Silvestri, MD
 Delirium & Dementia Nicholas J. Silvestri, MD Outline Delirium vs. Dementia Neural pathways relating to consciousness Encephalopathy Stupor Coma Dementia Delirium vs. Dementia Delirium Abrupt onset Lasts
Delirium & Dementia Nicholas J. Silvestri, MD Outline Delirium vs. Dementia Neural pathways relating to consciousness Encephalopathy Stupor Coma Dementia Delirium vs. Dementia Delirium Abrupt onset Lasts
Clinical and Familial Characteristics of Ten Chinese Patients with Fatal Family Insomnia *
 471 Biomed Environ Sci, 2012; 25(4): 471-475 Letters Clinical and Familial Characteristics of Ten Chinese Patients with Fatal Family Insomnia * SHI Qi 1, CHEN Cao 1, GAO Chen 1, TIAN Chan 1, ZHOU Wei 1,
471 Biomed Environ Sci, 2012; 25(4): 471-475 Letters Clinical and Familial Characteristics of Ten Chinese Patients with Fatal Family Insomnia * SHI Qi 1, CHEN Cao 1, GAO Chen 1, TIAN Chan 1, ZHOU Wei 1,
Index SLEEP MEDICINE CLINICS. Note: Page numbers of article titles are in boldface type. Cerebrospinal fluid analysis, for Kleine-Levin syndrome,
 165 SLEEP MEDICINE CLINICS Index Sleep Med Clin 1 (2006) 165 170 Note: Page numbers of article titles are in boldface type. A Academic performance, effects of sleepiness in children on, 112 Accidents,
165 SLEEP MEDICINE CLINICS Index Sleep Med Clin 1 (2006) 165 170 Note: Page numbers of article titles are in boldface type. A Academic performance, effects of sleepiness in children on, 112 Accidents,
SLEEP DISORDERS. Kenneth C. Sassower, MD Division of Sleep Medicine; Department of Neurology Massachusetts General Hospital for Children
 SLEEP DISORDERS Kenneth C. Sassower, MD Division of Sleep Medicine; Department of Neurology Massachusetts General Hospital for Children Distinctive Features of Pediatric Sleep Daytime sleepiness uncommon
SLEEP DISORDERS Kenneth C. Sassower, MD Division of Sleep Medicine; Department of Neurology Massachusetts General Hospital for Children Distinctive Features of Pediatric Sleep Daytime sleepiness uncommon
Appendix B: Provincial Case Definitions for Reportable Diseases
 Ministry of Health and Long-Term Care Infectious Diseases Protocol Appendix B: Provincial Case Definitions for Reportable Diseases Disease: Creutzfeldt-Jakob Disease, all types Revised Creutzfeldt-Jakob
Ministry of Health and Long-Term Care Infectious Diseases Protocol Appendix B: Provincial Case Definitions for Reportable Diseases Disease: Creutzfeldt-Jakob Disease, all types Revised Creutzfeldt-Jakob
Methamphetamine Abuse During Pregnancy
 Methamphetamine Abuse During Pregnancy Robert Davis, MD / r.w.davismd@gmail.com ❶ Statistics ❷ Pregnancy Concerns ❸ Postpartum Concerns ❹ Basic Science ❺ Best Practice Guidelines ❻ Withdrawal ❼ Recovery
Methamphetamine Abuse During Pregnancy Robert Davis, MD / r.w.davismd@gmail.com ❶ Statistics ❷ Pregnancy Concerns ❸ Postpartum Concerns ❹ Basic Science ❺ Best Practice Guidelines ❻ Withdrawal ❼ Recovery
CONTROL OF MOVEMENT BY THE BRAIN A. PRIMARY MOTOR CORTEX:
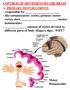 CONTROL OF MOVEMENT BY THE BRAIN A. PRIMARY MOTOR CORTEX: - responsible for - like somatosensory cortex, primary motor cortex show (motor homunculus) - amount of cortex devoted to different parts of body
CONTROL OF MOVEMENT BY THE BRAIN A. PRIMARY MOTOR CORTEX: - responsible for - like somatosensory cortex, primary motor cortex show (motor homunculus) - amount of cortex devoted to different parts of body
MINOR TRANQUILIZERS CHAPTER TWO : MINOR TRANQUILIZERS
 MINOR TRANQUILIZERS 76. The term 'minor tranquilizers' was introduced into the scientific literature in the 1950s to distinguish the medicines prescribed to reduce anxiety and tension from the major tranquillizers,
MINOR TRANQUILIZERS 76. The term 'minor tranquilizers' was introduced into the scientific literature in the 1950s to distinguish the medicines prescribed to reduce anxiety and tension from the major tranquillizers,
Parkinson Disease. Lorraine Kalia, MD, PhD, FRCPC. Presented by: Ontario s Geriatric Steering Committee
 Parkinson Disease Lorraine Kalia, MD, PhD, FRCPC Key Learnings Parkinson Disease (L. Kalia) Key Learnings Parkinson disease is the most common but not the only cause of parkinsonism Parkinson disease is
Parkinson Disease Lorraine Kalia, MD, PhD, FRCPC Key Learnings Parkinson Disease (L. Kalia) Key Learnings Parkinson disease is the most common but not the only cause of parkinsonism Parkinson disease is
A. PRIMARY MOTOR CORTEX: - responsible for - like somatosensory cortex, primary motor cortex show (motor homunculus) - amount of cortex devoted to
 CONTROL OF MOVEMENT BY THE BRAIN A. PRIMARY MOTOR CORTEX: - responsible for - like somatosensory cortex, primary motor cortex show (motor homunculus) - amount of cortex devoted to different parts of body
CONTROL OF MOVEMENT BY THE BRAIN A. PRIMARY MOTOR CORTEX: - responsible for - like somatosensory cortex, primary motor cortex show (motor homunculus) - amount of cortex devoted to different parts of body
TOP 10 LIST OF SLEEP QUESTIONS. Kenneth C. Sassower, MD Sleep Disorders Unit Massachusetts General Hospital for Children
 TOP 10 LIST OF SLEEP QUESTIONS Kenneth C. Sassower, MD Sleep Disorders Unit Massachusetts General Hospital for Children QUESTION #1: ARE SLEEP ISSUES IN CHILDREN THE SAME AS IN ADULTS? Distinctive Features
TOP 10 LIST OF SLEEP QUESTIONS Kenneth C. Sassower, MD Sleep Disorders Unit Massachusetts General Hospital for Children QUESTION #1: ARE SLEEP ISSUES IN CHILDREN THE SAME AS IN ADULTS? Distinctive Features
Movement Disorders. Psychology 372 Physiological Psychology. Background. Myasthenia Gravis. Many Types
 Background Movement Disorders Psychology 372 Physiological Psychology Steven E. Meier, Ph.D. Listen to the audio lecture while viewing these slides Early Studies Found some patients with progressive weakness
Background Movement Disorders Psychology 372 Physiological Psychology Steven E. Meier, Ph.D. Listen to the audio lecture while viewing these slides Early Studies Found some patients with progressive weakness
Parkinson s Disease Associated Sleep Disturbance Ehsan M. Hadi, MD, MPH. Dignity Health Neurological Institute
 Parkinson s Disease Associated Sleep Disturbance Ehsan M. Hadi, MD, MPH. Dignity Health Neurological Institute Parkinson s Disease 2 nd most common neurodegenerative disorder Peak age at onset is 60 years
Parkinson s Disease Associated Sleep Disturbance Ehsan M. Hadi, MD, MPH. Dignity Health Neurological Institute Parkinson s Disease 2 nd most common neurodegenerative disorder Peak age at onset is 60 years
United Council for Neurologic Subspecialties Geriatric Neurology Written Examination Content Outline
 United Council for Neurologic Subspecialties Geriatric Neurology Written Examination Content Outline REV 3/24/09 The UCNS Geriatric Neurology examination was established to determine the level of competence
United Council for Neurologic Subspecialties Geriatric Neurology Written Examination Content Outline REV 3/24/09 The UCNS Geriatric Neurology examination was established to determine the level of competence
AUTOIMMUNE ENCEPHALITIS
 AUTOIMMUNE ENCEPHALITIS Shruti Agnihotri, MD Assistant Professor Department of Neurology, UAB August 12, 2017 DISCLOSURES No financial disclosure Evolving evidence Page 2 OBJECTIVES Review the types of
AUTOIMMUNE ENCEPHALITIS Shruti Agnihotri, MD Assistant Professor Department of Neurology, UAB August 12, 2017 DISCLOSURES No financial disclosure Evolving evidence Page 2 OBJECTIVES Review the types of
Autoimmune encephalopathieslatest. Prof Belinda Lennox Department of Psychiatry, University of Oxford
 Autoimmune encephalopathieslatest advances Prof Belinda Lennox Department of Psychiatry, University of Oxford Belinda.lennox@psych.ox.ac.uk RCP Advanced Medicine 20 th June 2016 Declarations of Interest
Autoimmune encephalopathieslatest advances Prof Belinda Lennox Department of Psychiatry, University of Oxford Belinda.lennox@psych.ox.ac.uk RCP Advanced Medicine 20 th June 2016 Declarations of Interest
Narcolepsy. Jon R. Doud, MD Pulmonary Physician Midwest Center for Sleep Disorders Aurora, IL
 Narcolepsy Jon R. Doud, MD Pulmonary Physician Midwest Center for Sleep Disorders Aurora, IL Narcolepsy A central nervous system disorder that is an important cause of persistent sleepiness. The second
Narcolepsy Jon R. Doud, MD Pulmonary Physician Midwest Center for Sleep Disorders Aurora, IL Narcolepsy A central nervous system disorder that is an important cause of persistent sleepiness. The second
Fact Sheet Alzheimer s disease
 What is Alzheimer s disease Fact Sheet Alzheimer s disease Alzheimer s disease, AD, is a progressive brain disorder that gradually destroys a person s memory and ability to learn, reason, make judgements,
What is Alzheimer s disease Fact Sheet Alzheimer s disease Alzheimer s disease, AD, is a progressive brain disorder that gradually destroys a person s memory and ability to learn, reason, make judgements,
For more information about how to cite these materials visit
 Author(s): Rachel Glick, M.D., 2009 License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution Noncommercial Share Alike 3.0 License: http://creativecommons.org/licenses/by-nc-sa/3.0/
Author(s): Rachel Glick, M.D., 2009 License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution Noncommercial Share Alike 3.0 License: http://creativecommons.org/licenses/by-nc-sa/3.0/
Critical Care Pharmacological Management of Delirium
 Critical Care Pharmacological Management of Delirium Policy Title: in the Critical Care Unit Executive Summary: This policy provides guidance Pharmacological Management of delirium in the Critical Care
Critical Care Pharmacological Management of Delirium Policy Title: in the Critical Care Unit Executive Summary: This policy provides guidance Pharmacological Management of delirium in the Critical Care
Lina AL-Lawama and Tasneem Montaj. Abdullah Nimer. Loai Zghoul
 2 Lina AL-Lawama and Tasneem Montaj Abdullah Nimer Loai Zghoul At the end of this sheet you should be able to understand the general characteristics of action potential and some of its clinical applications
2 Lina AL-Lawama and Tasneem Montaj Abdullah Nimer Loai Zghoul At the end of this sheet you should be able to understand the general characteristics of action potential and some of its clinical applications
Parkinson s Disease Psychosis Treatment in Long-Term Care: Clinical and Operational Considerations
 Parkinson s Disease Psychosis Treatment in Long-Term Care: Clinical and Operational Considerations Pari Deshmukh MD Triple board-certified psychiatrist (Boards of psychiatry, addiction medicine, integrative
Parkinson s Disease Psychosis Treatment in Long-Term Care: Clinical and Operational Considerations Pari Deshmukh MD Triple board-certified psychiatrist (Boards of psychiatry, addiction medicine, integrative
IMPAIRMENT OF THE NERVOUS SYSTEM
 IMPAIRMENT OF THE NERVOUS SYSTEM The following information provides criteria for the evaluation of permanent impairment resulting from dysfunction brain, spinal cord and cranial nerves and certain peripheral
IMPAIRMENT OF THE NERVOUS SYSTEM The following information provides criteria for the evaluation of permanent impairment resulting from dysfunction brain, spinal cord and cranial nerves and certain peripheral
Dementia. Assessing Brain Damage. Mental Status Examination
 Dementia Assessing Brain Damage Mental status examination Information about current behavior and thought including orientation to reality, memory, and ability to follow instructions Neuropsychological
Dementia Assessing Brain Damage Mental status examination Information about current behavior and thought including orientation to reality, memory, and ability to follow instructions Neuropsychological
What s Causing Your Memory Loss?
 What s Causing Your Memory Loss? It s Not Necessarily Alzheimer s More than 50 conditions can cause or mimic the symptoms of dementia, and a small percentage of dementias are reversible. Two common examples
What s Causing Your Memory Loss? It s Not Necessarily Alzheimer s More than 50 conditions can cause or mimic the symptoms of dementia, and a small percentage of dementias are reversible. Two common examples
Organization of the nervous system. The withdrawal reflex. The central nervous system. Structure of a neuron. Overview
 Overview The nervous system- central and peripheral The brain: The source of mind and self Neurons Neuron Communication Chemical messengers Inside the brain Parts of the brain Split Brain Patients Organization
Overview The nervous system- central and peripheral The brain: The source of mind and self Neurons Neuron Communication Chemical messengers Inside the brain Parts of the brain Split Brain Patients Organization
Visualizing Psychology
 Visualizing Psychology by Siri Carpenter & Karen Huffman PowerPoint Lecture Notes Presentation Chapter 2: Neuroscience and Biological Foundations Siri Carpenter, Yale University Karen Huffman, Palomar
Visualizing Psychology by Siri Carpenter & Karen Huffman PowerPoint Lecture Notes Presentation Chapter 2: Neuroscience and Biological Foundations Siri Carpenter, Yale University Karen Huffman, Palomar
Is it Alzheimer s or Another Dementia? Reversible dementias. Key Points. Delirium. Toxic reactions to drugs
 Is it Alzheimer s or Another Dementia? Bonus Article for HELPGUIDE.ORG from Harvard Health Publications For physicians and families intent on pinning down a diagnosis, one major complicating factor is
Is it Alzheimer s or Another Dementia? Bonus Article for HELPGUIDE.ORG from Harvard Health Publications For physicians and families intent on pinning down a diagnosis, one major complicating factor is
Not Sleeping Well? Chronic physical conditions. There May Be a Medical Cause. Diabetes. Heartburn
 Not Sleeping Well? There May Be a Medical Cause People who feel they sleep perfectly well may still be troubled by excessive daytime sleepiness because of a variety of underlying medical illnesses. A sleep
Not Sleeping Well? There May Be a Medical Cause People who feel they sleep perfectly well may still be troubled by excessive daytime sleepiness because of a variety of underlying medical illnesses. A sleep
Unit 3: The Biological Bases of Behaviour
 Unit 3: The Biological Bases of Behaviour Section 1: Communication in the Nervous System Section 2: Organization in the Nervous System Section 3: Researching the Brain Section 4: The Brain Section 5: Cerebral
Unit 3: The Biological Bases of Behaviour Section 1: Communication in the Nervous System Section 2: Organization in the Nervous System Section 3: Researching the Brain Section 4: The Brain Section 5: Cerebral
Participant ID: If you had no responsibilities, what time would your body tell you to go to sleep and wake up?
 What does your sleep look like on a typical week? Total Sleep Time: Bedtime:, Sleep onset latency:, Number of Awakenings:, Wake time after sleep onset:, Rise time:, Out of bed:, Naps:? Notes: Is your sleep
What does your sleep look like on a typical week? Total Sleep Time: Bedtime:, Sleep onset latency:, Number of Awakenings:, Wake time after sleep onset:, Rise time:, Out of bed:, Naps:? Notes: Is your sleep
Sleep Medicine. Maintenance of Certification Examination Blueprint. Purpose of the exam
 Sleep Medicine Maintenance of Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of the
Sleep Medicine Maintenance of Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of the
Genetic CJD INFORMATION SHEET 2 JANUARY Introduction to genetic CJD. Inheriting a risk of CJD
 INFORMATION SHEET 2 JANUARY 2008 Genetic CJD Genetic CJD (previously called familial CJD and sometimes referred to as inherited CJD) is an inherited form of Creutzfeldt-Jakob disease, which belongs to
INFORMATION SHEET 2 JANUARY 2008 Genetic CJD Genetic CJD (previously called familial CJD and sometimes referred to as inherited CJD) is an inherited form of Creutzfeldt-Jakob disease, which belongs to
Index SLEEP MEDICINE CLINICS. Note: Page numbers of article titles are in boldface type.
 299 SLEEP MEDICINE CLINICS Sleep Med Clin 1 (2006) 299 303 Note: Page numbers of article titles are in boldface type. A Acid reflux, sleep disturbances in older adults related to, 238 Aging, alterations
299 SLEEP MEDICINE CLINICS Sleep Med Clin 1 (2006) 299 303 Note: Page numbers of article titles are in boldface type. A Acid reflux, sleep disturbances in older adults related to, 238 Aging, alterations
Marieb, E.N. (2004), Human Anatomy & Physiology, Pearson Education, Inc, San Francisco, CA, USA, p459
 Neuroscience Tutorial: Sleep and Dreams Discuss the following diagram with the students: Marieb, E.N. (2004), Human Anatomy & Physiology, Pearson Education, Inc, San Francisco, CA, USA, p459 1 Purves,
Neuroscience Tutorial: Sleep and Dreams Discuss the following diagram with the students: Marieb, E.N. (2004), Human Anatomy & Physiology, Pearson Education, Inc, San Francisco, CA, USA, p459 1 Purves,
Glossary of relevant medical and scientific terms
 Glossary of relevant medical and scientific terms Alzheimer's disease The most common dementing illness of the elderly in the UK. The neuropathology of Alzheimer's disease is significantly different from
Glossary of relevant medical and scientific terms Alzheimer's disease The most common dementing illness of the elderly in the UK. The neuropathology of Alzheimer's disease is significantly different from
1. Processes nutrients and provides energy for the neuron to function; contains the cell's nucleus; also called the soma.
 1. Base of brainstem; controls heartbeat and breathing 2. tissue destruction; a brain lesion is a naturally or experimentally caused destruction of brain tissue 3. A thick band of axons that connects the
1. Base of brainstem; controls heartbeat and breathing 2. tissue destruction; a brain lesion is a naturally or experimentally caused destruction of brain tissue 3. A thick band of axons that connects the
A Neurologist s Approach to Altered Mental Status
 A Neurologist s Approach to Altered Mental Status S. Andrew Josephson, MD Department of Neurology University of California San Francisco October 23, 2008 The speaker has no disclosures Case 1 A 71 year-old
A Neurologist s Approach to Altered Mental Status S. Andrew Josephson, MD Department of Neurology University of California San Francisco October 23, 2008 The speaker has no disclosures Case 1 A 71 year-old
Identification number: TÁMOP /1/A
 Manifestation of Novel Social Challenges of the European Union in the Teaching Material of Medical Biotechnology Master s Programmes at the University of Pécs and at the University of Debrecen Identification
Manifestation of Novel Social Challenges of the European Union in the Teaching Material of Medical Biotechnology Master s Programmes at the University of Pécs and at the University of Debrecen Identification
Biological Rhythms, Sleep, and Dreaming. Elaine M. Hull
 Biological Rhythms, Sleep, and Dreaming Elaine M. Hull Rhythms of Waking and Sleeping Animals generate 24 hour cycles of wakefulness and sleep. Some animals generate endogenous circannual rhythms (yearly
Biological Rhythms, Sleep, and Dreaming Elaine M. Hull Rhythms of Waking and Sleeping Animals generate 24 hour cycles of wakefulness and sleep. Some animals generate endogenous circannual rhythms (yearly
Neurodegenerative diseases that degrade regions of the brain will eventually become
 Maren Johnson CD 730 Research Paper What is the underlying neurological explanation for overeating in Frontotemporal Dementia? Does the change in overeating affect swallowing? Neurodegenerative diseases
Maren Johnson CD 730 Research Paper What is the underlying neurological explanation for overeating in Frontotemporal Dementia? Does the change in overeating affect swallowing? Neurodegenerative diseases
Chapter 6. Consciousness
 Consciousness Psychology, Fifth Edition, James S. Nairne What s It For? The Value of Consciousness Setting Priorities for Mental Functioning Sleeping and Dreaming Altering Awareness: Psychoactive Drugs
Consciousness Psychology, Fifth Edition, James S. Nairne What s It For? The Value of Consciousness Setting Priorities for Mental Functioning Sleeping and Dreaming Altering Awareness: Psychoactive Drugs
7/3/2013 ABNORMAL PSYCHOLOGY SEVENTH EDITION CHAPTER FOURTEEN CHAPTER OUTLINE. Dementia, Delirium, and Amnestic Disorders. Oltmanns and Emery
 ABNORMAL PSYCHOLOGY SEVENTH EDITION Oltmanns and Emery PowerPoint Presentations Prepared by: Ashlea R. Smith, Ph.D. This multimedia and its contents are protected under copyright law. The following are
ABNORMAL PSYCHOLOGY SEVENTH EDITION Oltmanns and Emery PowerPoint Presentations Prepared by: Ashlea R. Smith, Ph.D. This multimedia and its contents are protected under copyright law. The following are
SOMNAMBULISM: CLINICAL ASPECTS AND PATHOPHYSIOLOGICAL HYPOTHESES. Zadra, A., Desautels, A., Petit, D., Montplaisir, J. (2013) The Lancet Neurology
 11.11.2015 SOMNAMBULISM: CLINICAL ASPECTS AND PATHOPHYSIOLOGICAL HYPOTHESES Zadra, A., Desautels, A., Petit, D., Montplaisir, J. (2013) The Lancet Neurology Marion Charmillot Sleep, Cognition and Health
11.11.2015 SOMNAMBULISM: CLINICAL ASPECTS AND PATHOPHYSIOLOGICAL HYPOTHESES Zadra, A., Desautels, A., Petit, D., Montplaisir, J. (2013) The Lancet Neurology Marion Charmillot Sleep, Cognition and Health
Nervous System and Brain Review. Bio 3201
 Nervous System and Brain Review Bio 3201 Dont worry about: glial cells Oligodendrocytes Satelite cells etc Nervous System - Vital to maintaining homeostasis in organisms - Comprised of : brain, spinal
Nervous System and Brain Review Bio 3201 Dont worry about: glial cells Oligodendrocytes Satelite cells etc Nervous System - Vital to maintaining homeostasis in organisms - Comprised of : brain, spinal
Dementia Update. October 1, 2013 Dylan Wint, M.D. Cleveland Clinic Lou Ruvo Center for Brain Health Las Vegas, Nevada
 Dementia Update October 1, 2013 Dylan Wint, M.D. Cleveland Clinic Lou Ruvo Center for Brain Health Las Vegas, Nevada Outline New concepts in Alzheimer disease Biomarkers and in vivo diagnosis Future trends
Dementia Update October 1, 2013 Dylan Wint, M.D. Cleveland Clinic Lou Ruvo Center for Brain Health Las Vegas, Nevada Outline New concepts in Alzheimer disease Biomarkers and in vivo diagnosis Future trends
Human prion disease in Piemonte and Valle d Aosta, Italy: the experience of the reference center for human prion disease and a case description.
 Human prion disease in Piemonte and Valle d Aosta, Italy: the experience of the reference center for human prion disease and a case description. Enterprise Interest None Introduction The Centro regionale
Human prion disease in Piemonte and Valle d Aosta, Italy: the experience of the reference center for human prion disease and a case description. Enterprise Interest None Introduction The Centro regionale
DRUGS THAT ACT IN THE CNS
 DRUGS THAT ACT IN THE CNS Anxiolytic and Hypnotic Drugs Dr Karamallah S. Mahmood PhD Clinical Pharmacology 1 OTHER ANXIOLYTIC AGENTS/ A. Antidepressants Many antidepressants are effective in the treatment
DRUGS THAT ACT IN THE CNS Anxiolytic and Hypnotic Drugs Dr Karamallah S. Mahmood PhD Clinical Pharmacology 1 OTHER ANXIOLYTIC AGENTS/ A. Antidepressants Many antidepressants are effective in the treatment
DEMENTIA and BPSD in PARKINSON'S DISEASE. DR. T. JOHNSON. NOVEMBER 2017.
 DEMENTIA and BPSD in PARKINSON'S DISEASE. DR. T. JOHNSON. NOVEMBER 2017. Introduction. Parkinson's disease (PD) has been considered largely as a motor disorder. It has been increasingly recognized that
DEMENTIA and BPSD in PARKINSON'S DISEASE. DR. T. JOHNSON. NOVEMBER 2017. Introduction. Parkinson's disease (PD) has been considered largely as a motor disorder. It has been increasingly recognized that
Brain Stem. Nervous System (Part A-3) Module 8 -Chapter 14
 Nervous System (Part A-3) Module 8 -Chapter 14 Overview Susie Turner, M.D. 1/9/13 Cellular structure of the nervous system Neurons Neuroglia Nervous System Divisions Central nervous system Peripheral nervous
Nervous System (Part A-3) Module 8 -Chapter 14 Overview Susie Turner, M.D. 1/9/13 Cellular structure of the nervous system Neurons Neuroglia Nervous System Divisions Central nervous system Peripheral nervous
Sleep Complaints and Disorders in Epileptic Patients 순천향의대천안병원순천향의대천안병원신경과양광익
 Sleep Complaints and Disorders in Epileptic Patients 순천향의대천안병원순천향의대천안병원신경과양광익 Introduction The global physical, social and economic consequence of epilepsy are high. WHO 2000 study Improving QoL is increasingly
Sleep Complaints and Disorders in Epileptic Patients 순천향의대천안병원순천향의대천안병원신경과양광익 Introduction The global physical, social and economic consequence of epilepsy are high. WHO 2000 study Improving QoL is increasingly
AACN PCCN Review. Behavioral
 AACN PCCN Review Behavioral Presenter: Carol A. Rauen, RN, MS, CCNS, CCRN, PCCN, CEN Independent Clinical Nurse Specialist & Education Consultant rauen.carol104@gmail.com 0 Behavioral I. INTRODUCTION PCCN
AACN PCCN Review Behavioral Presenter: Carol A. Rauen, RN, MS, CCNS, CCRN, PCCN, CEN Independent Clinical Nurse Specialist & Education Consultant rauen.carol104@gmail.com 0 Behavioral I. INTRODUCTION PCCN
International Brain Bee Syllabus 2012 Department of Neurosciences, Universiti Sains Malaysia
 BRAIN DEVELOPMENT The cells of the nervous system connect with one another in trillions of remarkably specific patterns that form and change over the course of an organism s life. These connections develop
BRAIN DEVELOPMENT The cells of the nervous system connect with one another in trillions of remarkably specific patterns that form and change over the course of an organism s life. These connections develop
Sleep & Wakefulness Disorders in Parkinson s Disease: The Challenge of Getting a Good Night s Sleep
 Sleep & Wakefulness Disorders in Parkinson s Disease: The Challenge of Getting a Good Night s Sleep Helene A. Emsellem, MD March 25, 2017 The Center for Sleep & Wake Disorders PFNCA Symposium Sleep is
Sleep & Wakefulness Disorders in Parkinson s Disease: The Challenge of Getting a Good Night s Sleep Helene A. Emsellem, MD March 25, 2017 The Center for Sleep & Wake Disorders PFNCA Symposium Sleep is
MSA. Sleep disorders MULTIPLE SYSTEM ATROPHY AND NOCTURNAL STRIDOR 1/26/2015. Alex Iranzo Neurology Service Hospital Clinic de Barcelona Spain
 MULTIPLE SYSTEM ATROPHY AND NOCTURNAL STRIDOR Alex Iranzo Neurology Service Hospital Clinic de Barcelona Spain MSA Neurodegenerative disease Parkinsonism, cerebellar, dysautonomia Mean survival is less
MULTIPLE SYSTEM ATROPHY AND NOCTURNAL STRIDOR Alex Iranzo Neurology Service Hospital Clinic de Barcelona Spain MSA Neurodegenerative disease Parkinsonism, cerebellar, dysautonomia Mean survival is less
Electrooculogram (EOG): eye movements. Air flow measurements: breathing Heart rate.
 By: Ricardo Measurements and study of sleep: Sleep: absence of overt behavior, absence of consciousness Measures are indirect Methods to measure sleep characteristics: Electromyogram (EMG): muscle activity
By: Ricardo Measurements and study of sleep: Sleep: absence of overt behavior, absence of consciousness Measures are indirect Methods to measure sleep characteristics: Electromyogram (EMG): muscle activity
Index. sleep.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Accidents, risk of, with insufficient sleep, 318 Acquired immunodeficiency syndrome (AIDS), comorbid with narcolepsy, 298 299 Actigraphy, in
Note: Page numbers of article titles are in boldface type. A Accidents, risk of, with insufficient sleep, 318 Acquired immunodeficiency syndrome (AIDS), comorbid with narcolepsy, 298 299 Actigraphy, in
Main Questions. Why study addiction? Substance Use Disorders, Part 1 Alecia Schweinsburg, MA Abnromal Psychology, Fall Substance Use Disorders
 Substance Use Disorders Main Questions Why study addiction? What is addiction? Why do people become addicted? What do alcohol and drugs do? How do we treat substance use disorders? Why study addiction?
Substance Use Disorders Main Questions Why study addiction? What is addiction? Why do people become addicted? What do alcohol and drugs do? How do we treat substance use disorders? Why study addiction?
Behavioral Aspects of Parkinson s Disease
 Behavioral Aspects of Parkinson s Disease Joseph H. Friedman, MD Director, Movement Disorders Program Butler Hospital Dept of Neurology Alpert Medical School of Brown University 1 Disclosures Drugs will
Behavioral Aspects of Parkinson s Disease Joseph H. Friedman, MD Director, Movement Disorders Program Butler Hospital Dept of Neurology Alpert Medical School of Brown University 1 Disclosures Drugs will
Chapter 5. Variations in Consciousness 8 th Edition
 Chapter 5 Variations in Consciousness 8 th Edition Consciousness: Personal Awareness Awareness of Internal and External Stimuli Levels of awareness James stream of consciousness Freud unconscious Sleep/dreaming
Chapter 5 Variations in Consciousness 8 th Edition Consciousness: Personal Awareness Awareness of Internal and External Stimuli Levels of awareness James stream of consciousness Freud unconscious Sleep/dreaming
Chapter 17. Nervous System Nervous systems receive sensory input, interpret it, and send out appropriate commands. !
 Chapter 17 Sensory receptor Sensory input Integration Nervous System Motor output Brain and spinal cord Effector cells Peripheral nervous system (PNS) Central nervous system (CNS) 28.1 Nervous systems
Chapter 17 Sensory receptor Sensory input Integration Nervous System Motor output Brain and spinal cord Effector cells Peripheral nervous system (PNS) Central nervous system (CNS) 28.1 Nervous systems
An 18-Year-Old Woman with Prolonged Eyes Closed Unresponsiveness during Multiple Sleep Latency Testing
 pii: jc-00317-16 http://dx.doi.org/10.5664/jcsm.6410 SLEEP MEDICINE PEARLS An 18-Year-Old Woman with Prolonged Eyes Closed Unresponsiveness during Multiple Sleep Latency Testing Romy Hoque, MD 1 ; Victoria
pii: jc-00317-16 http://dx.doi.org/10.5664/jcsm.6410 SLEEP MEDICINE PEARLS An 18-Year-Old Woman with Prolonged Eyes Closed Unresponsiveness during Multiple Sleep Latency Testing Romy Hoque, MD 1 ; Victoria
Cephalization. Nervous Systems Chapter 49 11/10/2013. Nervous systems consist of circuits of neurons and supporting cells
 Nervous Systems Chapter 49 Cephalization Nervous systems consist of circuits of neurons and supporting cells Nervous system organization usually correlates with lifestyle Organization of the vertebrate
Nervous Systems Chapter 49 Cephalization Nervous systems consist of circuits of neurons and supporting cells Nervous system organization usually correlates with lifestyle Organization of the vertebrate
The CNS and PNS: How is our Nervous System Organized?
 Honors Biology Guided Notes Chapter 28 Nervous System Name 28.10 28.19 The CNS and PNS: How is our Nervous System Organized? ANIMAL NERVOUS SYSTEMS Define Cephalization and Centralization. What type of
Honors Biology Guided Notes Chapter 28 Nervous System Name 28.10 28.19 The CNS and PNS: How is our Nervous System Organized? ANIMAL NERVOUS SYSTEMS Define Cephalization and Centralization. What type of
Sleep - 10/5/17 Kelsey
 Sleep - 10/5/17 Kelsey Thursday, October 5, 2017 10:59 AM How to Study and Measure Sleep Sleep: Absence of overt behavior, absence of consciousness. -> measures are indirect Methods to measure sleep characteristics:
Sleep - 10/5/17 Kelsey Thursday, October 5, 2017 10:59 AM How to Study and Measure Sleep Sleep: Absence of overt behavior, absence of consciousness. -> measures are indirect Methods to measure sleep characteristics:
Hippocampal Sclerosis in LGI1 and CSPR2 Positive Limbic Encephalopathy: Case Report
 Hippocampal Sclerosis in LGI1 and CSPR2 Positive Limbic Encephalopathy: Ammar Taha Abdulaziz 1, Le Zhang 1, Dong Zhou 2, JinMei Li 3, Abstract Background: Limbic encephalopathy (LE) is a sub-acute neuropsychiatric
Hippocampal Sclerosis in LGI1 and CSPR2 Positive Limbic Encephalopathy: Ammar Taha Abdulaziz 1, Le Zhang 1, Dong Zhou 2, JinMei Li 3, Abstract Background: Limbic encephalopathy (LE) is a sub-acute neuropsychiatric
Epilepsy DOJ Lecture Masud Seyal, M.D., Ph.D. Department of Neurology University of California, Davis
 Epilepsy DOJ Lecture - 2005 Masud Seyal, M.D., Ph.D. Department of Neurology University of California, Davis Epilepsy SEIZURE: A temporary dysfunction of the brain resulting from a self-limited abnormal
Epilepsy DOJ Lecture - 2005 Masud Seyal, M.D., Ph.D. Department of Neurology University of California, Davis Epilepsy SEIZURE: A temporary dysfunction of the brain resulting from a self-limited abnormal
CHAPTER 48: NERVOUS SYSTEMS
 CHAPTER 48: NERVOUS SYSTEMS Name I. AN OVERVIEW OF NERVOUS SYSTEMS A. Nervous systems perform the three overlapping functions of sensory input, integration, and motor output B. Networks of neurons with
CHAPTER 48: NERVOUS SYSTEMS Name I. AN OVERVIEW OF NERVOUS SYSTEMS A. Nervous systems perform the three overlapping functions of sensory input, integration, and motor output B. Networks of neurons with
DEMENTIA? 45 Million. What is. WHAT IS DEMENTIA Dementia is a disturbance in a group of mental processes including: 70% Dementia is not a disease
 What is PRESENTS DEMENTIA? WHAT IS DEMENTIA Dementia is a disturbance in a group of mental processes including: Memory Reasoning Planning Learning Attention Language Perception Behavior AS OF 2013 There
What is PRESENTS DEMENTIA? WHAT IS DEMENTIA Dementia is a disturbance in a group of mental processes including: Memory Reasoning Planning Learning Attention Language Perception Behavior AS OF 2013 There
Sleep, Dreaming and Circadian Rhythms
 Sleep, Dreaming and Circadian Rhythms People typically sleep about 8 hours per day, and spend 16 hours awake. Most people sleep over 175,000 hours in their lifetime. The vast amount of time spent sleeping
Sleep, Dreaming and Circadian Rhythms People typically sleep about 8 hours per day, and spend 16 hours awake. Most people sleep over 175,000 hours in their lifetime. The vast amount of time spent sleeping
DIFFERENTIAL DIAGNOSIS SARAH MARRINAN
 Parkinson s Academy Registrar Masterclass Sheffield DIFFERENTIAL DIAGNOSIS SARAH MARRINAN 17 th September 2014 Objectives Importance of age in diagnosis Diagnostic challenges Brain Bank criteria Differential
Parkinson s Academy Registrar Masterclass Sheffield DIFFERENTIAL DIAGNOSIS SARAH MARRINAN 17 th September 2014 Objectives Importance of age in diagnosis Diagnostic challenges Brain Bank criteria Differential
Imaging of Alzheimer s Disease: State of the Art
 July 2015 Imaging of Alzheimer s Disease: State of the Art Neir Eshel, Harvard Medical School Year IV Outline Our patient Definition of dementia Alzheimer s disease Epidemiology Diagnosis Stages of progression
July 2015 Imaging of Alzheimer s Disease: State of the Art Neir Eshel, Harvard Medical School Year IV Outline Our patient Definition of dementia Alzheimer s disease Epidemiology Diagnosis Stages of progression
DISCLAIMER: ECHO Nevada emphasizes patient privacy and asks participants to not share ANY Protected Health Information during ECHO clinics.
 DISCLAIMER: Video will be taken at this clinic and potentially used in Project ECHO promotional materials. By attending this clinic, you consent to have your photo taken and allow Project ECHO to use this
DISCLAIMER: Video will be taken at this clinic and potentially used in Project ECHO promotional materials. By attending this clinic, you consent to have your photo taken and allow Project ECHO to use this
III./3.1. Movement disorders with akinetic rigid symptoms
 III./3.1. Movement disorders with akinetic rigid symptoms III./3.1.1. Parkinson s disease Parkinson s disease (PD) is the second most common neurodegenerative disorder worldwide after Alzheimer s disease.
III./3.1. Movement disorders with akinetic rigid symptoms III./3.1.1. Parkinson s disease Parkinson s disease (PD) is the second most common neurodegenerative disorder worldwide after Alzheimer s disease.
Nervous System The Brain and Spinal Cord Unit 7b
 Nervous System The Brain and Spinal Cord Unit 7b Chetek High School Mrs. Michaelsen 9.12 Meninges A. Meninges 1. The organs of the CNS are covered by membranes a. The meninges are divided into 3 layers:
Nervous System The Brain and Spinal Cord Unit 7b Chetek High School Mrs. Michaelsen 9.12 Meninges A. Meninges 1. The organs of the CNS are covered by membranes a. The meninges are divided into 3 layers:
Non-Genetic Ataxia Susan L. Perlman, M.D. Clinical Professor of Neurology David Geffen School of Medicine at UCLA Director, Ataxia Clinic
 Non-Genetic Ataxia Susan L. Perlman, M.D. Clinical Professor of Neurology David Geffen School of Medicine at UCLA Director, Ataxia Clinic Is Anything Non-Genetic? 1,212,000 references in PubMed under genetics
Non-Genetic Ataxia Susan L. Perlman, M.D. Clinical Professor of Neurology David Geffen School of Medicine at UCLA Director, Ataxia Clinic Is Anything Non-Genetic? 1,212,000 references in PubMed under genetics
Overview. Surviving shift work. What is the circadian rhythm? Components of a Generic Biological Timing System 31/10/2017
 Overview Surviving shift work Dr Claire M. Ellender Respiratory and Sleep Physician Princess Alexandra Hospital Conflicts nil relevant Circadian rhythm Impacts of shift work on health Case example Circadian
Overview Surviving shift work Dr Claire M. Ellender Respiratory and Sleep Physician Princess Alexandra Hospital Conflicts nil relevant Circadian rhythm Impacts of shift work on health Case example Circadian
What is dementia? Symptoms of dementia. Memory problems
 What is dementia? What is dementia? What is dementia? Dementia is an umbrella term for a range of progressive conditions that affect the brain. The brain is made up of nerve cells (neurones) that communicate
What is dementia? What is dementia? What is dementia? Dementia is an umbrella term for a range of progressive conditions that affect the brain. The brain is made up of nerve cells (neurones) that communicate
MOVEMENT OUTLINE. The Control of Movement: Muscles! Motor Reflexes Brain Mechanisms of Movement Mirror Neurons Disorders of Movement
 MOVEMENT 2 Dr. Steinmetz 3 OUTLINE The Control of Movement: Muscles! Motor Reflexes Brain Mechanisms of Movement Mirror Neurons Disorders of Movement Parkinson s Disease Huntington s Disease 1 4 TYPES
MOVEMENT 2 Dr. Steinmetz 3 OUTLINE The Control of Movement: Muscles! Motor Reflexes Brain Mechanisms of Movement Mirror Neurons Disorders of Movement Parkinson s Disease Huntington s Disease 1 4 TYPES
Delirium in the ICU: Prevention and Treatment. Delirium Defined Officially. Delirium: Really Defined. S. Andrew Josephson, MD
 Delirium in the ICU: Prevention and Treatment S. Andrew Josephson, MD Director, Neurohospitalist Service Medical Director, Inpatient Neurology June 2, 2011 Delirium Defined Officially (DSM-IV-TR) criteria
Delirium in the ICU: Prevention and Treatment S. Andrew Josephson, MD Director, Neurohospitalist Service Medical Director, Inpatient Neurology June 2, 2011 Delirium Defined Officially (DSM-IV-TR) criteria
노인병원에서 Light Therapy 의 활용 박 기 형 진주삼성병원 송도병원 신경과
 Light Therapy 1 : 15 / 63 (23.8%) 1 : 7 2 : 8 : 6 / 86 (7%) 1, : 48 / 205 (23.4%) 1 : 43 2 : 5 Sleep in Geriatrics Prevalence NIH survey of 9000 american senior above age 65 ; 88% had sleep disturbances
Light Therapy 1 : 15 / 63 (23.8%) 1 : 7 2 : 8 : 6 / 86 (7%) 1, : 48 / 205 (23.4%) 1 : 43 2 : 5 Sleep in Geriatrics Prevalence NIH survey of 9000 american senior above age 65 ; 88% had sleep disturbances
The University of Arizona Pediatric Residency Program. Primary Goals for Rotation. Neurology
 The University of Arizona Pediatric Residency Program Primary Goals for Rotation Neurology 1. GOAL: Understand the role of the pediatrician in preventing neurological diseases, and in counseling and screening
The University of Arizona Pediatric Residency Program Primary Goals for Rotation Neurology 1. GOAL: Understand the role of the pediatrician in preventing neurological diseases, and in counseling and screening
Dementia and Delirium: A Neurologist s Approach to Altered Mental Status. Case 1 4/7/11. Which of the following evaluations is your next step?
 Dementia and Delirium: A Neurologist s Approach to Altered Mental Status S. Andrew Josephson, MD Director, Neurohospitalist Program Medical Director, Inpatient Neurology University of California San Francisco
Dementia and Delirium: A Neurologist s Approach to Altered Mental Status S. Andrew Josephson, MD Director, Neurohospitalist Program Medical Director, Inpatient Neurology University of California San Francisco
Pharmacy Benefit Determination Policy
 Policy Subject: CNS Stimulant Medications Policy Number: SHS PBD06 Category: CNS Drugs Policy Type: Medical Pharmacy Department: Pharmacy Product (check all that apply): Group HMO/POS ASO PPO Individual
Policy Subject: CNS Stimulant Medications Policy Number: SHS PBD06 Category: CNS Drugs Policy Type: Medical Pharmacy Department: Pharmacy Product (check all that apply): Group HMO/POS ASO PPO Individual
All questions below pertain to mandatory material: all slides, and mandatory homework (if any).
 ECOL 182 Spring 2008 Dr. Ferriere s lectures Lecture 6: Nervous system and brain Quiz Book reference: LIFE-The Science of Biology, 8 th Edition. http://bcs.whfreeman.com/thelifewire8e/ All questions below
ECOL 182 Spring 2008 Dr. Ferriere s lectures Lecture 6: Nervous system and brain Quiz Book reference: LIFE-The Science of Biology, 8 th Edition. http://bcs.whfreeman.com/thelifewire8e/ All questions below
Nervous system. Made up of. Peripheral nervous system. Central nervous system. The central nervous system The peripheral nervous system.
 Made up of The central nervous system The peripheral nervous system Nervous system Central nervous system Peripheral nervous system Brain Spinal Cord Cranial nerve Spinal nerve branch from the brain connect
Made up of The central nervous system The peripheral nervous system Nervous system Central nervous system Peripheral nervous system Brain Spinal Cord Cranial nerve Spinal nerve branch from the brain connect
Comorbidity of Substance Use Disorders and Psychiatric Conditions-2
 Comorbidity of Substance Use Disorders and Psychiatric Conditions-2 J. H. Atkinson, M.D. Professor of Psychiatry HIV Neurobehavioral Research Programs University of California, San Diego KETHEA, Athens,
Comorbidity of Substance Use Disorders and Psychiatric Conditions-2 J. H. Atkinson, M.D. Professor of Psychiatry HIV Neurobehavioral Research Programs University of California, San Diego KETHEA, Athens,
9.01 Introduction to Neuroscience Fall 2007
 MIT OpenCourseWare http://ocw.mit.edu 9.01 Introduction to Neuroscience Fall 2007 For information about citing these materials or our Terms of Use, visit: http://ocw.mit.edu/terms. 9.01 Recitation (R02)
MIT OpenCourseWare http://ocw.mit.edu 9.01 Introduction to Neuroscience Fall 2007 For information about citing these materials or our Terms of Use, visit: http://ocw.mit.edu/terms. 9.01 Recitation (R02)
HIV Neurology Persistence of Cognitive Impairment Despite cart
 HIV Neurology Persistence of Cognitive Impairment Despite cart Victor Valcour MD PhD Professor of Medicine Memory and Aging Center, Dept. of Neurology University of California San Francisco, USA 8 th International
HIV Neurology Persistence of Cognitive Impairment Despite cart Victor Valcour MD PhD Professor of Medicine Memory and Aging Center, Dept. of Neurology University of California San Francisco, USA 8 th International
Physiology Unit 2 CONSCIOUSNESS, THE BRAIN AND BEHAVIOR
 Physiology Unit 2 CONSCIOUSNESS, THE BRAIN AND BEHAVIOR In Physiology Today What the Brain Does The nervous system determines states of consciousness and produces complex behaviors Any given neuron may
Physiology Unit 2 CONSCIOUSNESS, THE BRAIN AND BEHAVIOR In Physiology Today What the Brain Does The nervous system determines states of consciousness and produces complex behaviors Any given neuron may
