Oral Myofunctional Therapy Applied on Two Cases of Severe Obstructive Sleep Apnea Syndrome
|
|
|
- Annis Coleen Booker
- 6 years ago
- Views:
Transcription
1 Case Report Article Oral Myofunctional Therapy Applied on Two Cases of Severe Obstructive Sleep Apnea Syndrome Danielle Barreto e Silva Pitta*, André Farias Pessoa**, André Luiz L. Sampaio***, Raimundo Nonato Rodrigues****, Marilene Guiot Tavares*****, Paulo Tavares******. * Master Degree. Clinical Phonoaudiology Professor. ** PhD. Clinical Phonoaudiology Professor. *** Otorrhinolaryngologist Doctor. **** PhD. Neurologist and Sonology. ***** PhD. Psychologist. ****** Doctor. Pneumology Head Professor at Universidade de Brasilia. Institution: Laboratório do Sono do Hospital Universitário da Universidade de Brasília. Sleep Laboratory at University Hospital of Brasilia University. Brasília / DF Brazil. Address for correspondece: Danielle Barreto e Silva Pitta SHIN QI 06 conj 11 casa 06 Brasília / DF Brazil Zip code: Telephone: (+55 61) / danielle.pitta@hotmail.com Article received on October 22, Article approved on February 26, SUMMARY Introduction: Objective: Cases Report: Comments: Key words: Speech therapy treatment could be considered a new therapy for snoring and obstructive sleep apnea patients because of its direct action on oral motility. The myofunctional therapy includes the correct use of the stomatognatic structures and functions by means of functional exercises (respiratory, suction, swallowing and chewing) and muscular exercises with the aim of increasing the tonus and mobility of oral and cervical structures, which can be damaged in apneic patients. The purpose of the present study was to describe the speech therapy treatment, especially oral myofunctional therapy, in two patients with severe obstructive sleep apneia who were submitted to myofunctional oral therapy for a period of 16 weeks because of their inability to adapt to continuous positive airway pressure and\or the oral appliance. After this period, new exams were carried out and questionnaires and scales were given to these patients. It is reported two patients with clinical and sleep study showing severe obstructive sleep apnea. Patient 1, male, 37 years old, body mass index 26,29 Kg/m², snoring, pauses in breathing during sleep, several aweakness, mood disturbance, trouble concentrating and in memory. Patient 2, female, 55 years old, body mass index 22,2 Kg/m², intense snoring, breath difficult during night, usual lack of memory. The results show an extreme regression of the syndrome, a decrease in the apnea/hipopnea index, the diurnal sleepiness symptoms and snoring, as well as an improvement in oxygen saturation myofunctional therapy, obstructive sleep apnea, snoring. 350
2 INTRODUCTION AND REVISION OF LITERATURE The obstructive sleep apnea syndrome (OSA) is a pathologic condition which implicates in serious negative repercussions to the individual s health and functionality such, diurnal excessive somnolence (DES), cardiac arrhythmia, arterial hypertension, besides social and behavioral consequences. The high prevalence and wide spectrum of exposure imposes the medical treatment of this condition (1). Among the existing practices to the OSA medical treatment, the positive pressure in the upper airways (CPAP) which is truthfully effective and, usually, the first choice method, the diets, the intra-oral orthodontic devices and surgery treatments which are indicated in special cases (2, 3), stand out. The phonological myofunctional oral therapy may represent a new therapeutic option for snoring patients with or without OSA, as will be mentioned further ahead (4). The positive pressure in the upper airways (CPAP), idealized by SULLIVAN et al. (6), is the continuous positive pressure medical treatment in the upper airways (UA) through a nasal or oronasal mask. This therapeutic modality is considered the most effective in cases of OSA carriers patients, mainly those who presents expressive drop of the oxygen saturation (SaO2), moderate OSA and severe OSA. Some limitations to its use are connected to the mask which may cause discomfort, rejection on the part of the partner, air leakage generating allergies and cutaneous irritations which occurs in mouth breathers patients, due to nasal obstruction, which may culminate with the low adhesion. The loss of corporal weight through diets or surgery treatments is another therapeutic option. Ponderal reductions of 10% of corporal weight may lead to the reduction of up to 50% of the apnea/hypopnea index (AHI), and with 20% of corporal weigh loss, the patient may become asymptomatic. This fact is explained by the loss of adipose tissue in the whole body, including in the oropharyngeal region. However, the long term success rates are discouraging with the regaining of weight and reappearance or aggravation of the OSA (7). The intra-oral devices, lingual retainers and jaw (mandible) positioners, are indicated to OSA carriers patients from moderate to slight and retrognathic OSA who are not above the ideal weight and have not severe oxyhemoglobin desaturation. Besides those counter-indications, patients with insufficient number of teeth to support the device, use of extensive dental prosthesis, periodontic problems, intense temporomandibular joint dysfunction (TMJ) and carriers of important anatomical alterations in the upper airways (UA), must not be treated with the intra-oral device for not reaching good results (8). The surgery techniques vary from otorhinolaryngologic surgeries and maxillary functional orthopedic surgeries, which present variable results. The most common procedures reach between 40% and 50% of efficiency 9, and many times more than one techniques must be combined, at the same surgery time or in two separate times, so that the results may be more satisfactory (10). The treatment modalities aforementioned described may act in palliative way, since they may not effectively treat the factor that precipitates the installation of the OSA or they are of difficult adhesion by the patients (high cost, long term difficult maintenance, etc.). Thus, in the pursuit of other therapeutic methods, it was raised the hypothesis of the phonoaudiological intervention in snoring patients with or without OSA through the myofunctional oral therapy, to bring benefits for these patients. The myofunctional therapy consists, initially, of the necessity of being aware of the problem and correct it, the improvement of the body posture, the performance of the basic exercises and, finally, a reinforce period aiming at maintaining the new standards reached in the aforementioned stages. The exercises are divided in relaxing and breathing exercises, specific exercises to stimulate and adequate the functions of the stomatognathic and articulatory systems (11). The contribution of the phonoaudiology in these cases is based on the fact that the apneic and snoring patients present a neuromuscular and/or structural exposure of its upper airways (UA), culminating in a significant reduction of the muscular tonus and increase of the resistance of the UA during sleep (12, 13). It is also believed that the dilating force of the UA muscles is the only force responsible for counterbalance the forces which promotes the collapse, represented by the negative pharyngeal transmural pressure and for the weight of the structures which form the UA (14, 15), fact that justify the rehabilitation of the orofacial and pharyngeal musculature of these individuals. Therefore, the oral myofunctional therapy, directed to snoring patients with or without OSA, aims the posture adequacy, the sensibility and proprioception and the tonus and mobility of the orofacial and pharyngeal musculature. The structures prioritized in this work are those which may be related with the obstruction by the UA collapse during sleep: Floor of the oral cavity, tongue, especially the genioglossus muscle; mastication muscles, buccinator, 351
3 masseter, lateral and medial pterygoid, digastric; soft palate and uvula; supra-hyoid and infra-hyoid muscles; pharyngeal musculature and the breathing, mastication and deglutition functions (4, 5). The objective of this study was to report the effectiveness of the oral myofunctional therapy in 2 patients with severe OSA from the analysis of the variables of the polysomnography (PSG) before and after the phonoaudiologic intervention with the reduction of the AHI, normalization or enhancement of the blood oxygenation of the sleep architecture as well as the evaluation of the punctuation in the Epworth Sleepiness Scale (ESE) and Snoring Score (SS). Clinical Case 1 CASES REPORT Male patient, 37 years old, body mass index (BMI) 26,29 kg/m2 complaining about snoring, breathing stops during sleep, frequently awakenings, mood alterations, difficulties of concentration and memory deficit. In the polysomnography exam the patient presented AHI of 48.5% events per hour (e/h), average oxygen saturation (SaO2) of 92%, minimum of 79%, with T 90 (percentage time in which the SaO2 is placed below of 90%) of 5,9%. The patient presented micro-arousals (MA) index of 32/ h, ESE=12 and SS=3. The SS is graded from 0 to 4, being 0=snoring absence, 1=resound (breathe heavily), 2=light snoring, 3=snoring that disturb the partner, 4=snoring that disturb the family (it surpasses the bedroom). In the otorhinolaryngological evaluation just a discrete increase of the inferior nasal shells was verified, and in the phonoaudiolological evaluation a crackle in the right TMJ, cheeks asymmetry with a bigger volume to the left, discrete reduction of cheeks, tongue and lips mobility and internal marks in the cheeks and tongue was observed. From the diagnosis of severe OSA, the treatment with the nasal CPAP (continuous positive airway pressure) was indicated. However, the patient did not adapt himself and refused the treatment also for its cost. Thus, the patient was sent to the Phonoaudiologic service of the University Hospital of Brasília. The phonoaudiological intervention consisted in 16 sessions of myofunctional therapy performed by the same speech therapist when the patient was orientated to perform daily isometric exercises, aiming at increasing the muscular tonus; isotonic exercises, to improve the mobility, and isokinetic exercises, indicated to the relaxing and coordination specific for the oral cavity floor musculature, tongue, buccinator, masseter, lateral and medial pterygoid, digastric, soft palate and uvula; supra and infra hyoid muscles and pharyngeal musculature. The patient also received orientation about the importance of the nasal breathing. After the myofunctional therapy, a new polysomnography (PSG), phonoaudiologic evaluation, and ESE and SS application were carried out. The patient reported, to the subjective evaluation, sleep enhancement, memory enhancement, and a better performance at work. According to the report, there was a snoring and respiratory arrests reduction during the sleep, although, the patient has not reported significant reduction of the snoring intensity, SS=2 (Table 1). In the control of the PSG, a reduction of the AHI (8.6/h); minimum SaO2 (87%) and T90 (0%) (Table 2) was verified. As for the sleep fragmentation, an 18/h reduction of the micro arousals/ hour index, was verified. In the ESE, the patient presented a reduction of 10 points in the punctuation (Table 1). It is valid to make reference to the BMC, factor considered predictive for the OSA, after treatment, which increases to kg/m2 due to a ponderal gain of 4 kg. In the phonoaudiological evaluation a discrete reduction of the cheeks asymmetry and an improve of the orofacial structures tonus and mobility was verified in a subjective way, and crackles in the TMJ were not observed anymore, in spite of not being performed any exercises directed specifically to the TMJ. Clinical Case 2 Female patient, 55 years old, BMI 22,2 kg/m2, complaining about intense snoring, respiratory difficulty during sleep, frequent memory lapses and DES (diurnal excessive somnolence). The initial PSG demonstrated: AHI=40.4/h, SaO2M=88%, SaO2m=77%, T90=86.7%, MA=25.5/h. The applied subjective questionnaires made evident: ESE=13 and SS=3. Due to the non adaptation to Table 1. Subjective scales of daily excessive somnolence and snoring pre and post oral myofunctional therapy. Subjective scales Case 1 Case 2 Pré myofunctional Therapy Post myofunctional Therapy Pré myofunctional Therapy Post myofunctional Therapy ESE SS Subtitle: ESE Epworth Sleepiless Scale; SS Snoring Score (elaborated by the author). 352
4 Table 2. Polysomnographic variables pre and post oral myofunctional therapy. PSG Case 1 Case 2 Pre myofunctional Therapy Post myofunctional Therapy Pre myofunctional Therapy Post myofunctional Therapy AHI 48.5 e/h 8.6 e/h 40.4 e/h 3.3 e/h SaO2M 92% 94% 88% 94% SaO2m 79% 87% 77% 83% T90 5,9% 0% 86,7% 1,6% E1 4,3% 1,4% 8,4% 5% E2 51,2% 44,8% 68,8% 38% DELTA 18,6% 15% 5,9% 29% REM 25,7% 23,7% 16,8% 27% MA 32/h 18/h 25.5/h 6.9/h Subtitle: AHI apnea and hypopnea index; SaO2M moderate oxygen saturation; SaO2m oxygen minimum saturation; T90 SaO2<90%; E1 Stage 1 NREM; E2 stage 2 NREM; Delta stages 3 and 4 NREM; REM sleep REM; MA micro-arousals. the CPAP and to the intra-oral device, the patient was sent to the phonoaudiological evaluation and intervention, in the phonoaudiologic clinic of the University Hospital of Brasília. The otorhinolaryngological exam made evident a discrete nasal septum deviation, increase of the tongue base and a light retrognathism. In the phonoaudiological evaluation the patient presented a reduction of the cheek, tongue, lips and soft palate tonus and mobility, as well as, phonoarticulatory incoordination and nasal and superficial breathing. The phonoaudiological intervention consisted in 16 myofunctional therapy sessions performed by the same speech therapist, when the inadequate and adequate standards of the correct posture and the movement of the phonoarticulatory organs had been approached aiming at obtaining the awareness of the alterations presented by the patients, and specific exercises, which should be performed daily for the patient, had been proposed. The exercises had been divided in isometric, isotonic and isokinetic. The patient also received orientation about the importance of the nasal breathing. After the 16 weeks of myofunctional therapy, a new polysomnography (PSG), phonoaudiologic evaluation, and ESE and SS application was carried out. There was not BMI variation. The patient reduced the ESE punctuation to 7and the SS to 2 (Table 1). The comparison of the results of the first and second Polysomnographies demonstrate a clear improve of the studied variables. AHI 3.3/h, SaO2M 94%, SaO2m 83%, T90 1.6%, MD 6.9% (Table 2). In the subjective phonoaudiological evaluation an improvement of the orofacial structures tonus and mobility, as well as an improvement of the phonoarticulatory ccoordination was verified. Subjectively, the patient reported an improvement in the memory lapses and in the DES, which were important complaints before the treatment. DISCUSSION The use of the orofacial motricity turned to snoring patients with or without OSA is still incipient, however, some authors demonstrated favorable results, as the results presented by GUIMARÃES (3) and PITTA (4). There is a close relationship between the OSA s physiopathology and the object of study of the orofacial motricity, specialty of the phonoaudiology, which are the structural and functional aspects of the orofacial and cervical regions, usually compromised in patients with OSA. However, this statement deserves corrections and needs more investigation aiming at proving the efficiency of the myofunctional therapy in this population. It is valid to point out that the two patients who participated of this study were informed about the indication of the first chose treatment, the CPAP, and about the intra oral device, therapeutics already scientifically consolidated, but due to financial issues and non adaptation they opted for the execution of the oral myofunctional therapy, from the signing of a free and informal document. In the cases studied, an expressive reduction of the AHI, which returned to values considered standards of normality, tendency or effective normalization of the oxygen saturation and a reduction of the micro-arousals index were verified, and subjectively, a reduction of the diurnal excessive somnolence and snoring, however there was not significant variation or improvement in the sleep architecture. The improvement of the respiratory variables objectively analyzed through the PSG suggests some 353
5 degree of efficacy of the proposed oral myofunctional therapy. It is necessary to point out that the oral myofunctional therapy was applied as a mono therapy, that is, the patients did not perform other treatment concomitantly. nor presented changes in the quotidian activities which could compromise the obtained results. The results pre and post oral myofunctional therapy corroborated with the hypothesis of the existence of a hypothony of the UA in patients with OSA, favoring the collapse of the oropharynx and obstruction of the aerial flux. The retrognathic profile of the patient of the case 2 configures one more risk factor to the OSA development, since it reduces the UA space and projects the tongue, in this case with an increased base, to a more posterior position. However, the myofunctional therapy did not have any interference in the change of the craniofacial profile of the patient, except the orofacial and pharyngeal musculature, which were exercised. FINAL CONSIDERATIONS The Phonoaudiology is a relatively new science of the health area, which has been expanding its therapeutic possibilities in order to reach areas until then unused. This is the inter relationship case between the Phonoaudiology and the Sleep Medicine, more specifically, the sleep respiratory disturbances. This relationship backs to the fact that the structures involved in the obstructive respiratory disturbances, as the OSA and snoring, are neuromuscular units, in other words, the object of study and intervention of the Orofacial Motricity area. Finally, the obtained results in this case study suggests that the oral myofunctional therapy may represent an alternative in the treatment of the severe OSA carriers patients who did not adhere to the CPAP, first choice treatment already consolidated in the scientific community. However, we conclude that is necessary to continue with this research increasing the number of studied cases and their follow-up in a longitudinal way. REFERENCES 1. America Sleep Disorders Association. The international classification of sleep disorders 1997, revised. Rochester MN: ASDA Chediak AD. Pathogenesis of obstructive sleep apnea. Respir Care. 1998, 43(4): Leiter JC. Analysis of pharyngeal resistence and genioglossal EMG activity using a model of orifice flow. J Appl Physiol. 1992, 73: Guimarães K. Alterações no tecido mole de orofaringe em portadores de apnéia do sono obstrutiva. Jornal Brasileiro de Fonoaudiologia. 1999, 1(1): Pitta DBS. Avaliação da eficácia da intervenção fonoaudiológica - terapia miofuncional - em pacientes roncadores com e sem síndrome da apnéia obstrutiva do sono. Brasília, 2005, p.120. Dissertação de Mestrado - Faculdade de Medicina da Universidade de Brasília. 6. Sullivan et al. Reversal of obstructive sleep apnea by continuous positive airway pressure applied through the nares. Lancet. 1981, 1: Charuzi I, Ovnat A, Peiser J, Saltz H, Witzman S, Lavie P. The effect of surgical weight reduction in sleep apnea quality in obesity-related sleep apnea syndrome. Surgery. 1985, 95: Shimidt-Nowara, Lowe et al. Oral appliances for the treatment of snoring and sleep apnea: a review. Sleep. 1995, 18(6): Riley, Powel e Guilleminault. Obstructive sleep apnea: a review of 306 consecutively, treat surgical patients. Otolaryngol Head Neck Surg. 1993, 108(2): Sher, Schechtman e Piccirillo. The efficacy or surgical modifications of the upper airway in adults with obstructive sleep apnea syndrome. Sleep. 1996, 19(2): Marquesan IQ. Motricidade oral: visão clínica do trabalho fonoaudiológico integrado com outras especialidades. 2 ª ed. São Paulo: Pancast; 1999, pp Ayappa I, e Rapoport DM. The upper airway in sleep: physiology of the pharynx. Sleep Med Rev. 2003, 7(1): Mezzanote WS, Tangel DJ, White DP. Influence of sleep onset on upper airway muscle activity in apnea patients versus normal controls. Am J Respir Crit Care Med. 1996, 153: Schwab et al. Upper airway and soft tissue anatomy in normal subjects and patients with sleep-disordered breathing: significance of the lateral pharyngeal walls. Am J Respir Crit Care Med. 1995, 152(5pt 1): Séries F. Upper airway muscles awake and sleep. Sleep Med Rev. 2002, 6(3):
OBSTRUCTIVE SLEEP APNEA and WORK Treatment Update
 OBSTRUCTIVE SLEEP APNEA and WORK Treatment Update David Claman, MD Professor of Medicine Director, UCSF Sleep Disorders Center 415-885-7886 Disclosures: None Chronic Sleep Deprivation (0 v 4 v 6 v 8 hrs)
OBSTRUCTIVE SLEEP APNEA and WORK Treatment Update David Claman, MD Professor of Medicine Director, UCSF Sleep Disorders Center 415-885-7886 Disclosures: None Chronic Sleep Deprivation (0 v 4 v 6 v 8 hrs)
The role of oral myofunctional therapy in managing patients with mild to moderate obstructive sleep apnea
 Hemmat Baz, et al. PAN Arab Journal of Rhinology, Vol. 2, No. 1, March, 2012 The role of oral myofunctional therapy in managing patients with mild to moderate obstructive sleep apnea Hemmat Baz, 1 Mohsen
Hemmat Baz, et al. PAN Arab Journal of Rhinology, Vol. 2, No. 1, March, 2012 The role of oral myofunctional therapy in managing patients with mild to moderate obstructive sleep apnea Hemmat Baz, 1 Mohsen
Polysomnography (PSG) (Sleep Studies), Sleep Center
 Policy Number: 1036 Policy History Approve Date: 07/09/2015 Effective Date: 07/09/2015 Preauthorization All Plans Benefit plans vary in coverage and some plans may not provide coverage for certain service(s)
Policy Number: 1036 Policy History Approve Date: 07/09/2015 Effective Date: 07/09/2015 Preauthorization All Plans Benefit plans vary in coverage and some plans may not provide coverage for certain service(s)
Kaniethapriya A.S, Ganesh Prasad S.
 Original Article A Comparative Study of Effects of Oropharyngeal Exercises and Continuous Positive Airway Pressure (CPAP) on Parameters of Sleep on Moderate Obstructive Sleep Apnea Syndrome (OSAS) Patients
Original Article A Comparative Study of Effects of Oropharyngeal Exercises and Continuous Positive Airway Pressure (CPAP) on Parameters of Sleep on Moderate Obstructive Sleep Apnea Syndrome (OSAS) Patients
Brian Palmer, D.D.S, Kansas City, Missouri, USA. April, 2001
 Brian Palmer, D.D.S, Kansas City, Missouri, USA A1 April, 2001 Disclaimer The information in this presentation is for basic information only and is not to be construed as a diagnosis or treatment for any
Brian Palmer, D.D.S, Kansas City, Missouri, USA A1 April, 2001 Disclaimer The information in this presentation is for basic information only and is not to be construed as a diagnosis or treatment for any
Emerging Nursing Roles in Collaborative Management of Sleep Disordered Breathing and Obstructive Sleep Apnoea
 Emerging Nursing Roles in Collaborative Management of Sleep Disordered Breathing and Obstructive Sleep Apnoea Sigma Theta Tau International 28th International Nursing Research Congress 27-31 July 2017
Emerging Nursing Roles in Collaborative Management of Sleep Disordered Breathing and Obstructive Sleep Apnoea Sigma Theta Tau International 28th International Nursing Research Congress 27-31 July 2017
RESEARCH PACKET DENTAL SLEEP MEDICINE
 RESEARCH PACKET DENTAL SLEEP MEDICINE American Academy of Dental Sleep Medicine Dental Sleep Medicine Research Packet Page 1 Table of Contents Research: Oral Appliance Therapy vs. Continuous Positive Airway
RESEARCH PACKET DENTAL SLEEP MEDICINE American Academy of Dental Sleep Medicine Dental Sleep Medicine Research Packet Page 1 Table of Contents Research: Oral Appliance Therapy vs. Continuous Positive Airway
Treatment of Obstructive Sleep Apnea (OSA)
 MP9239 Covered Service: Prior Authorization Required: Additional Information: Yes when meets criteria below Yes as shown below None Prevea360 Health Plan Medical Policy: 1.0 A continuous positive airway
MP9239 Covered Service: Prior Authorization Required: Additional Information: Yes when meets criteria below Yes as shown below None Prevea360 Health Plan Medical Policy: 1.0 A continuous positive airway
Outline. Major variables contributing to airway patency/collapse. OSA- Definition
 Outline Alicia Gruber Kalamas, MD Associate Clinical Professor of Anesthesia & Perioperative Care University of California, San Francisco September 2011 Definition Pathophysiology Patient Risk Factors
Outline Alicia Gruber Kalamas, MD Associate Clinical Professor of Anesthesia & Perioperative Care University of California, San Francisco September 2011 Definition Pathophysiology Patient Risk Factors
Precision Sleep Medicine
 Precision Sleep Medicine Picking Winners Improves Outcomes and Avoids Side-Effects North American Dental Sleep Medicine Conference February 17-18, 2017 Clearwater Beach, FL John E. Remmers, MD Conflict
Precision Sleep Medicine Picking Winners Improves Outcomes and Avoids Side-Effects North American Dental Sleep Medicine Conference February 17-18, 2017 Clearwater Beach, FL John E. Remmers, MD Conflict
Sleep Diordered Breathing (Part 1)
 Sleep Diordered Breathing (Part 1) History (for more topics & presentations, visit ) Obstructive sleep apnea - first described by Charles Dickens in 1836 in Papers of the Pickwick Club, Dickens depicted
Sleep Diordered Breathing (Part 1) History (for more topics & presentations, visit ) Obstructive sleep apnea - first described by Charles Dickens in 1836 in Papers of the Pickwick Club, Dickens depicted
Questions: What tests are available to diagnose sleep disordered breathing? How do you calculate overall AHI vs obstructive AHI?
 Pediatric Obstructive Sleep Apnea Case Study : Margaret-Ann Carno PhD, CPNP, D,ABSM for the Sleep Education for Pulmonary Fellows and Practitioners, SRN ATS Committee April 2014. Facilitator s guide Part
Pediatric Obstructive Sleep Apnea Case Study : Margaret-Ann Carno PhD, CPNP, D,ABSM for the Sleep Education for Pulmonary Fellows and Practitioners, SRN ATS Committee April 2014. Facilitator s guide Part
Snoring And Sleep Apnea in the U.S. Definitions Apnea: Cessation of ventilation for > 10 seconds. Defining Severity of OSA
 Snoring and Obstructive Sleep Apnea: Oral Appliance Therapy Management Midwest Society of Orthodontists October 16-17, 2009 Anthony J DiAngelis DMD, MPH Chief, Department of Dentistry, HCMC Professor,
Snoring and Obstructive Sleep Apnea: Oral Appliance Therapy Management Midwest Society of Orthodontists October 16-17, 2009 Anthony J DiAngelis DMD, MPH Chief, Department of Dentistry, HCMC Professor,
Evaluation, Management and Long-Term Care of OSA in Adults
 Evaluation, Management and Long-Term Care of OSA in Adults AUGUST 2015 Providing diagnostic tools and therapies that are evidence-based is a key part of a successful sleep practice. This resource outlines
Evaluation, Management and Long-Term Care of OSA in Adults AUGUST 2015 Providing diagnostic tools and therapies that are evidence-based is a key part of a successful sleep practice. This resource outlines
Management of OSA. saurabh maji
 Management of OSA saurabh maji INTRODUCTION Obstructive sleep apnea is a major public health problem Prevalence of OSAS in INDIA is 2.4% to 4.96% in men and 1% to 2 % in women In the rest of the world
Management of OSA saurabh maji INTRODUCTION Obstructive sleep apnea is a major public health problem Prevalence of OSAS in INDIA is 2.4% to 4.96% in men and 1% to 2 % in women In the rest of the world
Surgical Options for the Successful Treatment of Obstructive Sleep Apnea
 Surgical Options for the Successful Treatment of Obstructive Sleep Apnea Benjamin J. Teitelbaum, MD, FACS Otolaryngology Head and Neck Surgery Saint Agnes Medical Center Fresno, California Terms Apnea
Surgical Options for the Successful Treatment of Obstructive Sleep Apnea Benjamin J. Teitelbaum, MD, FACS Otolaryngology Head and Neck Surgery Saint Agnes Medical Center Fresno, California Terms Apnea
SLEEP DISORDERED BREATHING The Clinical Conditions
 SLEEP DISORDERED BREATHING The Clinical Conditions Robert G. Hooper, M.D. In the previous portion of this paper, the definitions of the respiratory events that are the hallmarks of problems with breathing
SLEEP DISORDERED BREATHING The Clinical Conditions Robert G. Hooper, M.D. In the previous portion of this paper, the definitions of the respiratory events that are the hallmarks of problems with breathing
Index. sleep.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Accidents. See Motor vehicle accidents. Acetazolamide, in OSA therapy, 531 Acetylcholinesterase inhibitors, in OSA therapy, 532 533 Acromegaly,
Note: Page numbers of article titles are in boldface type. A Accidents. See Motor vehicle accidents. Acetazolamide, in OSA therapy, 531 Acetylcholinesterase inhibitors, in OSA therapy, 532 533 Acromegaly,
Oropharyngeal exercises in the treatment of obstructive sleep apnoea: our experience
 DOI 10.1007/s11325-016-1332-1 SLEEP BREATHING PHYSIOLOGY AND DISORDERS ORIGINAL ARTICLE Oropharyngeal exercises in the treatment of obstructive sleep apnoea: our experience Roshan K. Verma 1 Jai Richo
DOI 10.1007/s11325-016-1332-1 SLEEP BREATHING PHYSIOLOGY AND DISORDERS ORIGINAL ARTICLE Oropharyngeal exercises in the treatment of obstructive sleep apnoea: our experience Roshan K. Verma 1 Jai Richo
Sleep Disordered Breathing
 Sleep Disordered Breathing SDB SDB Is an Umbrella Term for Many Disorders characterized by a lack of drive to breathe Results n repetitive pauses in breathing with no effort Occurs for a minimum of 10
Sleep Disordered Breathing SDB SDB Is an Umbrella Term for Many Disorders characterized by a lack of drive to breathe Results n repetitive pauses in breathing with no effort Occurs for a minimum of 10
Tolerance of Positive Airway Pressure following Site-Specific Surgery of Upper Airway
 34 The Open Sleep Journal, 2008, 1, 34-39 Open Access Tolerance of Positive Airway Pressure following Site-Specific Surgery of Upper Airway Ho-Sheng Lin *,#,1,2, Roger Toma #,2, Cara Glavin 2, Mark Toma
34 The Open Sleep Journal, 2008, 1, 34-39 Open Access Tolerance of Positive Airway Pressure following Site-Specific Surgery of Upper Airway Ho-Sheng Lin *,#,1,2, Roger Toma #,2, Cara Glavin 2, Mark Toma
11/19/2012 ก! " Varies 5-86% in men 2-57% in women. Thailand 26.4% (Neruntarut et al, Sleep Breath (2011) 15: )
 Snoring ก Respiratory sound generated in the upper airway during sleep that typically occurs during inspiration but may occur during expiration ICSD-2, 2005..... ก ก! Prevalence of snoring Varies 5-86%
Snoring ก Respiratory sound generated in the upper airway during sleep that typically occurs during inspiration but may occur during expiration ICSD-2, 2005..... ก ก! Prevalence of snoring Varies 5-86%
Sleep Medicine. Paul Fredrickson, MD Director. Mayo Sleep Center Jacksonville, Florida.
 Sleep Medicine Paul Fredrickson, MD Director Mayo Sleep Center Jacksonville, Florida Fredrickson.Paul@mayo.edu DISCLOSURES No relevant conflicts to report. Obstructive Sleep Apnea The most common sleep
Sleep Medicine Paul Fredrickson, MD Director Mayo Sleep Center Jacksonville, Florida Fredrickson.Paul@mayo.edu DISCLOSURES No relevant conflicts to report. Obstructive Sleep Apnea The most common sleep
Effect of two types of mandibular advancement splints on snoring and obstructive sleep apnoea
 European Journal of Orthodontics 20 (1998) 293 297 1998 European Orthodontic Society Effect of two types of mandibular advancement splints on snoring and obstructive sleep apnoea J. Lamont*, D. R. Baldwin**,
European Journal of Orthodontics 20 (1998) 293 297 1998 European Orthodontic Society Effect of two types of mandibular advancement splints on snoring and obstructive sleep apnoea J. Lamont*, D. R. Baldwin**,
IEHP considers the treatment of obstructive sleep apnea (OSA) medically necessary according to the criteria outlined below:
 : Positive Airway Pressure, Oral Appliances, and Surgical Interventions Policy: Obstructive sleep apnea (OSA) is characterized by an interruption of breathing during sleep most commonly due to extra or
: Positive Airway Pressure, Oral Appliances, and Surgical Interventions Policy: Obstructive sleep apnea (OSA) is characterized by an interruption of breathing during sleep most commonly due to extra or
BTS sleep Course. Module 10 Therapies I: Mechanical Intervention Devices (Prepared by Debby Nicoll and Debbie Smith)
 BTS sleep Course Module 10 Therapies I: Mechanical Intervention Devices (Prepared by Debby Nicoll and Debbie Smith) S1: Overview of OSA Definition History Prevalence Pathophysiology Causes Consequences
BTS sleep Course Module 10 Therapies I: Mechanical Intervention Devices (Prepared by Debby Nicoll and Debbie Smith) S1: Overview of OSA Definition History Prevalence Pathophysiology Causes Consequences
Sleep Apnea: Diagnosis & Treatment
 Disclosure Sleep Apnea: Diagnosis & Treatment Lawrence J. Epstein, MD Sleep HealthCenters Harvard Medical School Chief Medical Officer for Sleep HealthCenters Sleep medicine specialty practice group Consultant
Disclosure Sleep Apnea: Diagnosis & Treatment Lawrence J. Epstein, MD Sleep HealthCenters Harvard Medical School Chief Medical Officer for Sleep HealthCenters Sleep medicine specialty practice group Consultant
Effectiveness Of Oropharyngeal Exercises In Patients with Moderate Obstructive Sleep Apnoea Syndrome
 Original article: Effectiveness Of Oropharyngeal Exercises In Patients with Moderate Obstructive Sleep Apnoea Syndrome 1. Dr Himanshu Pathak *, 2. Dr Sushil Arora, 3 Dr Pooja Roge 1. Associate Professor,
Original article: Effectiveness Of Oropharyngeal Exercises In Patients with Moderate Obstructive Sleep Apnoea Syndrome 1. Dr Himanshu Pathak *, 2. Dr Sushil Arora, 3 Dr Pooja Roge 1. Associate Professor,
Oral Appliances and their Clinical Applications
 Oral Appliances and their Clinical Applications Peter Cistulli MBBS, PhD, MBA, FRACP Professor of Respiratory Medicine & Head of Discipline of Sleep Medicine University of Sydney Director, Centre for Sleep
Oral Appliances and their Clinical Applications Peter Cistulli MBBS, PhD, MBA, FRACP Professor of Respiratory Medicine & Head of Discipline of Sleep Medicine University of Sydney Director, Centre for Sleep
Central Sleep Apnea. v Characteristics
 Central Sleep Apnea v Characteristics Respiratory pauses > 10 sec Due to failure of brain s respiratory center to send signal to respiratory muscles Tends to occur in infants (neurological immaturity)
Central Sleep Apnea v Characteristics Respiratory pauses > 10 sec Due to failure of brain s respiratory center to send signal to respiratory muscles Tends to occur in infants (neurological immaturity)
Sleep and the Heart. Physiologic Changes in Cardiovascular Parameters during Sleep
 Sleep and the Heart Rami N. Khayat, MD Professor of Internal Medicine Medical Director, Department of Respiratory Therapy Division of Pulmonary, Critical Care and Sleep Medicine The Ohio State University
Sleep and the Heart Rami N. Khayat, MD Professor of Internal Medicine Medical Director, Department of Respiratory Therapy Division of Pulmonary, Critical Care and Sleep Medicine The Ohio State University
Sleep and the Heart. Rami N. Khayat, MD
 Sleep and the Heart Rami N. Khayat, MD Professor of Internal Medicine Medical Director, Department of Respiratory Therapy Division of Pulmonary, Critical Care and Sleep Medicine The Ohio State University
Sleep and the Heart Rami N. Khayat, MD Professor of Internal Medicine Medical Director, Department of Respiratory Therapy Division of Pulmonary, Critical Care and Sleep Medicine The Ohio State University
OBSTRUCTIVE SLEEP APNEA and WORK Treatment Update
 OBSTRUCTIVE SLEEP APNEA and WORK Treatment Update David Claman, MD Professor of Medicine Director, UCSF Sleep Disorders Center 415-885-7886 Disclosres: None Chronic Sleep Deprivation (0 v 4 v 6 v 8 hrs)
OBSTRUCTIVE SLEEP APNEA and WORK Treatment Update David Claman, MD Professor of Medicine Director, UCSF Sleep Disorders Center 415-885-7886 Disclosres: None Chronic Sleep Deprivation (0 v 4 v 6 v 8 hrs)
Obstructive sleep apnoea How to identify?
 Obstructive sleep apnoea How to identify? Walter McNicholas MD Newman Professor in Medicine, St. Vincent s University Hospital, University College Dublin, Ireland. Potential conflict of interest None Obstructive
Obstructive sleep apnoea How to identify? Walter McNicholas MD Newman Professor in Medicine, St. Vincent s University Hospital, University College Dublin, Ireland. Potential conflict of interest None Obstructive
Management of OSA in the Acute Care Environment. Robert S. Campbell, RRT FAARC HRC, Philips Healthcare May, 2018
 Management of OSA in the Acute Care Environment Robert S. Campbell, RRT FAARC HRC, Philips Healthcare May, 2018 1 Learning Objectives Upon completion, the participant should be able to: Understand pathology
Management of OSA in the Acute Care Environment Robert S. Campbell, RRT FAARC HRC, Philips Healthcare May, 2018 1 Learning Objectives Upon completion, the participant should be able to: Understand pathology
Upper Airway Stimulation for Obstructive Sleep Apnea
 Upper Airway Stimulation for Obstructive Sleep Apnea Background, Mechanism and Clinical Data Overview Seth Hollen RPSGT 21 May 2016 1 Conflicts of Interest Therapy Support Specialist, Inspire Medical Systems
Upper Airway Stimulation for Obstructive Sleep Apnea Background, Mechanism and Clinical Data Overview Seth Hollen RPSGT 21 May 2016 1 Conflicts of Interest Therapy Support Specialist, Inspire Medical Systems
Sleep and the Heart Reversing the Effects of Sleep Apnea to Better Manage Heart Disease
 1 Sleep and the Heart Reversing the Effects of Sleep Apnea to Better Manage Heart Disease Rami Khayat, MD Professor of Internal Medicine Director, OSU Sleep Heart Program Medical Director, Department of
1 Sleep and the Heart Reversing the Effects of Sleep Apnea to Better Manage Heart Disease Rami Khayat, MD Professor of Internal Medicine Director, OSU Sleep Heart Program Medical Director, Department of
SLEEP APNOEA DR TAN KAH LEONG ALVIN CO-DIRECTOR SLEEP LABORATORY SITE CHIEF SDDC (SLEEP) DEPARTMENT OF OTORHINOLARYNGOLOGY, HEAD & NECK SURGERY
 SLEEP APNOEA DR TAN KAH LEONG ALVIN CO-DIRECTOR SLEEP LABORATORY SITE CHIEF SDDC (SLEEP) DEPARTMENT OF OTORHINOLARYNGOLOGY, HEAD & NECK SURGERY
SLEEP APNOEA DR TAN KAH LEONG ALVIN CO-DIRECTOR SLEEP LABORATORY SITE CHIEF SDDC (SLEEP) DEPARTMENT OF OTORHINOLARYNGOLOGY, HEAD & NECK SURGERY
Pre-Operative Services Teaching Rounds 11 March 2011
 Pre-Operative Services Teaching Rounds 11 March 2011 Deborah Richman MBChB FFA(SA) Director Pre-Operative Services Department of Anesthesia Stony Brook University Medical Center, NY drichman@notes.cc.sunysb.edu
Pre-Operative Services Teaching Rounds 11 March 2011 Deborah Richman MBChB FFA(SA) Director Pre-Operative Services Department of Anesthesia Stony Brook University Medical Center, NY drichman@notes.cc.sunysb.edu
Snoring. Forty-five percent of normal adults snore at least occasionally and 25
 Snoring Insight into sleeping disorders and sleep apnea Forty-five percent of normal adults snore at least occasionally and 25 percent are habitual snorers. Problem snoring is more frequent in males and
Snoring Insight into sleeping disorders and sleep apnea Forty-five percent of normal adults snore at least occasionally and 25 percent are habitual snorers. Problem snoring is more frequent in males and
Comparing Upper Airway Stimulation to Expansion Sphincter Pharyngoplasty: A Single University Experience
 771395AORXXX10.1177/0003489418771395Annals of Otology, Rhinology & LaryngologyHuntley et al research-article2018 Original Article Comparing Upper Airway Stimulation to Expansion Sphincter Pharyngoplasty:
771395AORXXX10.1177/0003489418771395Annals of Otology, Rhinology & LaryngologyHuntley et al research-article2018 Original Article Comparing Upper Airway Stimulation to Expansion Sphincter Pharyngoplasty:
Medicare C/D Medical Coverage Policy
 Medicare C/D Medical Coverage Policy Surgical Treatment of Obstructive Sleep Apnea Origination: June 26, 2000 Review Date: January 18, 2017 Next Review January, 2019 DESCRIPTION OF PROCEDURE OR SERVICE
Medicare C/D Medical Coverage Policy Surgical Treatment of Obstructive Sleep Apnea Origination: June 26, 2000 Review Date: January 18, 2017 Next Review January, 2019 DESCRIPTION OF PROCEDURE OR SERVICE
DOWNLOAD OR READ : TREATMENT FOR SNORING PROBLEMS PDF EBOOK EPUB MOBI
 DOWNLOAD OR READ : TREATMENT FOR SNORING PROBLEMS PDF EBOOK EPUB MOBI Page 1 Page 2 treatment for snoring problems treatment for snoring problems pdf treatment for snoring problems problem, presenting
DOWNLOAD OR READ : TREATMENT FOR SNORING PROBLEMS PDF EBOOK EPUB MOBI Page 1 Page 2 treatment for snoring problems treatment for snoring problems pdf treatment for snoring problems problem, presenting
Circadian Variations Influential in Circulatory & Vascular Phenomena
 SLEEP & STROKE 1 Circadian Variations Influential in Circulatory & Vascular Phenomena Endocrine secretions Thermo regulations Renal Functions Respiratory control Heart Rhythm Hematologic parameters Immune
SLEEP & STROKE 1 Circadian Variations Influential in Circulatory & Vascular Phenomena Endocrine secretions Thermo regulations Renal Functions Respiratory control Heart Rhythm Hematologic parameters Immune
DECLARATION OF CONFLICT OF INTEREST
 DECLARATION OF CONFLICT OF INTEREST Obstructive sleep apnoea How to identify? Walter McNicholas MD Newman Professor in Medicine, St. Vincent s University Hospital, University College Dublin, Ireland. Potential
DECLARATION OF CONFLICT OF INTEREST Obstructive sleep apnoea How to identify? Walter McNicholas MD Newman Professor in Medicine, St. Vincent s University Hospital, University College Dublin, Ireland. Potential
Upper Airway Muscle Stimulation for Obstructive Sleep Apnea
 Upper Airway Muscle Stimulation for Obstructive Sleep Apnea M. Safwan Badr, MD, MBA Chair, Department of Medicine, Wayne State University School of Medicine. Staff Physician, John D. Dingell VA Medical
Upper Airway Muscle Stimulation for Obstructive Sleep Apnea M. Safwan Badr, MD, MBA Chair, Department of Medicine, Wayne State University School of Medicine. Staff Physician, John D. Dingell VA Medical
Obstructive Sleep Apnea in Truck Drivers
 Rocky Mountain Academy of Occupational and Environmental Medicine Denver, Colorado February 6, 2010 Obstructive Sleep Apnea in Truck Drivers Philip D. Parks, MD, MPH, MOccH Medical Director, Lifespan Health
Rocky Mountain Academy of Occupational and Environmental Medicine Denver, Colorado February 6, 2010 Obstructive Sleep Apnea in Truck Drivers Philip D. Parks, MD, MPH, MOccH Medical Director, Lifespan Health
Philip L. Smith, MD; Christopher P. O Donnell, PhD; Lawrence Allan, BS; and Alan R. Schwartz, MD
 A Physiologic Comparison of Nasal and Oral Positive Airway Pressure* Philip L. Smith, MD; Christopher P. O Donnell, PhD; Lawrence Allan, BS; and Alan R. Schwartz, MD Study objectives: The effectiveness
A Physiologic Comparison of Nasal and Oral Positive Airway Pressure* Philip L. Smith, MD; Christopher P. O Donnell, PhD; Lawrence Allan, BS; and Alan R. Schwartz, MD Study objectives: The effectiveness
What is Oral Appliance Therapy?
 You may have been diagnosed by your physician as required treatment for sleep-disordered breathing (snoring and/or obstructive sleep apnea). This condition may pose serious health risks since it disrupts
You may have been diagnosed by your physician as required treatment for sleep-disordered breathing (snoring and/or obstructive sleep apnea). This condition may pose serious health risks since it disrupts
Sleep Apnoea. The Story of a Pause
 Sleep Apnoea The Story of a Pause There is almost zero awareness in India that many amongst us maybe living with Sleep Apnoea, which left untreated could be life threatening tomorrow. This largely undiagnosed
Sleep Apnoea The Story of a Pause There is almost zero awareness in India that many amongst us maybe living with Sleep Apnoea, which left untreated could be life threatening tomorrow. This largely undiagnosed
11/13/2017. Jeremy Tabak MD, FAASM Medical Director Baptist Hospital Sleep Lab Medical Director Baptist Sleep Lab at Galloway
 Jeremy Tabak MD, FAASM Medical Director Baptist Hospital Sleep Lab Medical Director Baptist Sleep Lab at Galloway HypnoLaus study: OSA effect on mortality US Preventive Services Task Force recommendations
Jeremy Tabak MD, FAASM Medical Director Baptist Hospital Sleep Lab Medical Director Baptist Sleep Lab at Galloway HypnoLaus study: OSA effect on mortality US Preventive Services Task Force recommendations
Obstructive Sleep Apnea
 Obstructive Sleep Apnea Introduction Obstructive sleep apnea is an interruption in breathing during sleep. It is caused by throat and tongue muscles collapsing and relaxing. This blocks, or obstructs,
Obstructive Sleep Apnea Introduction Obstructive sleep apnea is an interruption in breathing during sleep. It is caused by throat and tongue muscles collapsing and relaxing. This blocks, or obstructs,
Sleep Apnea. Herbert A Berger, MD Pulmonary Division Department of Internal Medicine University of Iowa
 Sleep Apnea Herbert A Berger, MD Pulmonary Division Department of Internal Medicine University of Iowa Disclosures No Relevant Financial Interests to Report Objectives Learn the history and physical examination
Sleep Apnea Herbert A Berger, MD Pulmonary Division Department of Internal Medicine University of Iowa Disclosures No Relevant Financial Interests to Report Objectives Learn the history and physical examination
Effects of continuous positive airway pressure on nasal and pharyngeal symptoms in patients with obstructive sleep apnea*
 Effects of continuous positive airway pressure on nasal and pharyngeal symptoms in patients with obstructive sleep apnea* ADELAIDE CRISTINA DE FIGUEIREDO, MARIA CECÍLIA LORENZI, SIMONE PREZZOTI (TESBPT),
Effects of continuous positive airway pressure on nasal and pharyngeal symptoms in patients with obstructive sleep apnea* ADELAIDE CRISTINA DE FIGUEIREDO, MARIA CECÍLIA LORENZI, SIMONE PREZZOTI (TESBPT),
Dr Alireza Yarahmadi and Dr Arvind Perathur Mercy Medical Center - Winter Retreat Des Moines February 2012
 Dr Alireza Yarahmadi and Dr Arvind Perathur Mercy Medical Center - Winter Retreat Des Moines February 2012 Why screen of OSA prior to surgery? What factors increase the risk? When due to anticipate problems?
Dr Alireza Yarahmadi and Dr Arvind Perathur Mercy Medical Center - Winter Retreat Des Moines February 2012 Why screen of OSA prior to surgery? What factors increase the risk? When due to anticipate problems?
Nasal Mass Presenting as Obstructive Sleep Apnea Syndrome
 ORIGINAL ARTICLE pissn 2093-9175 / eissn 2233-8853 http://dx.doi.org/10.17241/smr.2015.6.2.54 Nasal Mass Presenting as Obstructive Sleep Apnea Syndrome Seung Hoon Lee, MD, PhD, In Sik Song, MD, Jae Woo
ORIGINAL ARTICLE pissn 2093-9175 / eissn 2233-8853 http://dx.doi.org/10.17241/smr.2015.6.2.54 Nasal Mass Presenting as Obstructive Sleep Apnea Syndrome Seung Hoon Lee, MD, PhD, In Sik Song, MD, Jae Woo
Bruxism: Revisiting an Old Problem with New Questions and Unique Solutions
 Jeff Rouse, DDS Txacad@aol.com 555 E. Basse #200 www.coredentistry.com San Antonio, TX 78209 210-828-3334 Bruxism: Revisiting an Old Problem with New Questions and Unique Solutions CORE Concept Wear and
Jeff Rouse, DDS Txacad@aol.com 555 E. Basse #200 www.coredentistry.com San Antonio, TX 78209 210-828-3334 Bruxism: Revisiting an Old Problem with New Questions and Unique Solutions CORE Concept Wear and
Abdussalam Alahmari ENT Resident R2 KAUH 15/12/2015
 Abdussalam Alahmari ENT Resident R2 KAUH 15/12/2015 Physiology of sleep Snoring mechanism, causes, sites, symptoms, and management. Sleep apnea definitions, pathophysiology, risk factors, evaluation of
Abdussalam Alahmari ENT Resident R2 KAUH 15/12/2015 Physiology of sleep Snoring mechanism, causes, sites, symptoms, and management. Sleep apnea definitions, pathophysiology, risk factors, evaluation of
Prefabricated Oral Appliances for Obstructive Sleep Apnea
 Medical Policy Manual Allied Health, Policy No. 36 Prefabricated Oral Appliances for Obstructive Sleep Apnea Next Review: May 2019 Last Review: April 2018 Effective: May 1, 2018 IMPORTANT REMINDER Medical
Medical Policy Manual Allied Health, Policy No. 36 Prefabricated Oral Appliances for Obstructive Sleep Apnea Next Review: May 2019 Last Review: April 2018 Effective: May 1, 2018 IMPORTANT REMINDER Medical
International Journal of Scientific & Engineering Research Volume 9, Issue 1, January ISSN
 International Journal of Scientific & Engineering Research Volume 9, Issue 1, January-2018 342 The difference of sleep quality between 2-channel ambulatory monitor and diagnostic polysomnography Tengchin
International Journal of Scientific & Engineering Research Volume 9, Issue 1, January-2018 342 The difference of sleep quality between 2-channel ambulatory monitor and diagnostic polysomnography Tengchin
University, India.) Corresponding author: Dr. Shubham Agarwal1
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 3 Ver.15 March. (2018), PP 59-63 www.iosrjournals.org Effect of Severity of OSA on Oxygen Saturation:
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 3 Ver.15 March. (2018), PP 59-63 www.iosrjournals.org Effect of Severity of OSA on Oxygen Saturation:
Sleep Bruxism and Sleep-Disordered Breathing
 Sleep Bruxism and Sleep-Disordered Breathing Author STEVEN D BENDER, DDS*, Associate Editor EDWARD J. SWIFT JR., DMD, MS Sleep bruxism (SB) is a repetitive jaw muscle activity with clenching or grinding
Sleep Bruxism and Sleep-Disordered Breathing Author STEVEN D BENDER, DDS*, Associate Editor EDWARD J. SWIFT JR., DMD, MS Sleep bruxism (SB) is a repetitive jaw muscle activity with clenching or grinding
Obstructive sleep apnea (OSA) is a common disorder
 Original Research Sleep Medicine and Surgery Drug-Induced Sedation Endoscopy in the Evaluation of OSA Patients with Incomplete Oral Appliance Therapy Response Otolaryngology Head and Neck Surgery 2015,
Original Research Sleep Medicine and Surgery Drug-Induced Sedation Endoscopy in the Evaluation of OSA Patients with Incomplete Oral Appliance Therapy Response Otolaryngology Head and Neck Surgery 2015,
Pediatric Obstructive Sleep apnea An update What else is there to know?
 Pediatric Obstructive Sleep apnea An update What else is there to know? Garani S. Nadaraja, MD, FAAP Medical Director BCH-Oakland Clinical Assistant Professor Division of Pediatric Otolaryngology UCSF
Pediatric Obstructive Sleep apnea An update What else is there to know? Garani S. Nadaraja, MD, FAAP Medical Director BCH-Oakland Clinical Assistant Professor Division of Pediatric Otolaryngology UCSF
A New, Clinically Proven Sleep Apnea Therapy for people unable to use CPAP.
 A New, Clinically Proven Sleep Apnea Therapy for people unable to use CPAP. Take Heart. If You Have OSA, You re Not Alone. Like you, more than 18 million Americans are estimated to have Obstructive Sleep
A New, Clinically Proven Sleep Apnea Therapy for people unable to use CPAP. Take Heart. If You Have OSA, You re Not Alone. Like you, more than 18 million Americans are estimated to have Obstructive Sleep
Tired of being tired?
 Tired of being tired? Narval CC MRD ResMed.com/Narval Sleepiness and snoring are possible symptoms of sleep apnea. Did you know that one in every four adults has some form of sleep disordered-breathing
Tired of being tired? Narval CC MRD ResMed.com/Narval Sleepiness and snoring are possible symptoms of sleep apnea. Did you know that one in every four adults has some form of sleep disordered-breathing
Sleep Apnea in Women: How Is It Different?
 Sleep Apnea in Women: How Is It Different? Grace Pien, MD, MSCE Division of Pulmonary and Critical Care Department of Medicine Johns Hopkins School of Medicine 16 February 2018 Outline Prevalence Clinical
Sleep Apnea in Women: How Is It Different? Grace Pien, MD, MSCE Division of Pulmonary and Critical Care Department of Medicine Johns Hopkins School of Medicine 16 February 2018 Outline Prevalence Clinical
The Familial Occurrence of Obstructive Sleep Apnoea Syndrome (OSAS)
 Global Journal of Respiratory Care, 2014, 1, 17-21 17 The Familial Occurrence of Obstructive Sleep Apnoea Syndrome (OSAS) Piotr Bielicki, Tadeusz Przybylowski, Ryszarda Chazan * Department of Internal
Global Journal of Respiratory Care, 2014, 1, 17-21 17 The Familial Occurrence of Obstructive Sleep Apnoea Syndrome (OSAS) Piotr Bielicki, Tadeusz Przybylowski, Ryszarda Chazan * Department of Internal
Step (2) Looked for correlations between baseline surrogates and postoperative AHI.
 Development of the PSG PLUS PHYIOLOGY model Step (1) Picked possible surrogates of the physiological traits (See Table 1 in the main text). Step (2) Looked for correlations between baseline surrogates
Development of the PSG PLUS PHYIOLOGY model Step (1) Picked possible surrogates of the physiological traits (See Table 1 in the main text). Step (2) Looked for correlations between baseline surrogates
Obstructive sleep apnea (OSA)
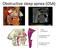 Obstructive sleep apnea (OSA) In a healthy sleeping child, the mouth is typically closed, the oral cavity is collapsed, and the nasopharynx and hypopharynx are patent with minimal wall motion Obstructive
Obstructive sleep apnea (OSA) In a healthy sleeping child, the mouth is typically closed, the oral cavity is collapsed, and the nasopharynx and hypopharynx are patent with minimal wall motion Obstructive
PEDIATRIC PAP TITRATION PROTOCOL
 PURPOSE In order to provide the highest quality care for our patients, our sleep disorders facility adheres to the AASM Standards of Accreditation. The accompanying policy and procedure on pediatric titrations
PURPOSE In order to provide the highest quality care for our patients, our sleep disorders facility adheres to the AASM Standards of Accreditation. The accompanying policy and procedure on pediatric titrations
Head and Neck Physical Examination: Comparison Between Nonapneic and Obstructive Sleep Apnea Patients
 The Laryngoscope Lippincott Williams & Wilkins, Inc. 2005 The American Laryngological, Rhinological and Otological Society, Inc. Head and Neck Physical Examination: Comparison Between Nonapneic and Obstructive
The Laryngoscope Lippincott Williams & Wilkins, Inc. 2005 The American Laryngological, Rhinological and Otological Society, Inc. Head and Neck Physical Examination: Comparison Between Nonapneic and Obstructive
National Sleep Disorders Research Plan
 Research Plan Home Foreword Preface Introduction Executive Summary Contents Contact Us National Sleep Disorders Research Plan Return to Table of Contents SECTION 5 - SLEEP DISORDERS SLEEP-DISORDERED BREATHING
Research Plan Home Foreword Preface Introduction Executive Summary Contents Contact Us National Sleep Disorders Research Plan Return to Table of Contents SECTION 5 - SLEEP DISORDERS SLEEP-DISORDERED BREATHING
EXPLORE NEW POSSIBILITIES
 EXPLORE NEW POSSIBILITIES TREATING SNORING AND SLEEP APNOEA HAS CHANGED FOREVER Introducing the Oventus O 2 Vent, a custom made, comfortable oral appliance with a unique airway design for the treatment
EXPLORE NEW POSSIBILITIES TREATING SNORING AND SLEEP APNOEA HAS CHANGED FOREVER Introducing the Oventus O 2 Vent, a custom made, comfortable oral appliance with a unique airway design for the treatment
Orofacial Myofunctional Therapy and it s Role in Dental Health and SDB. By: Jennie Herklotz, MA, CCC-SLP
 Orofacial Myofunctional Therapy and it s Role in Dental Health and SDB By: Jennie Herklotz, MA, CCC-SLP What is an Orofacial Myofunctional Disorder (OMD)? Includes at least one of the following: Open mouth
Orofacial Myofunctional Therapy and it s Role in Dental Health and SDB By: Jennie Herklotz, MA, CCC-SLP What is an Orofacial Myofunctional Disorder (OMD)? Includes at least one of the following: Open mouth
Oral Appliances and their Clinical Indications in OSA
 Oral Appliances and their Clinical Indications in OSA Disclosures Andrew Chan, MB BS, PhD, FRACP, FCCP Staff Specialist, Department of Respiratory and Sleep Medicine, Royal North Shore Hospital, University
Oral Appliances and their Clinical Indications in OSA Disclosures Andrew Chan, MB BS, PhD, FRACP, FCCP Staff Specialist, Department of Respiratory and Sleep Medicine, Royal North Shore Hospital, University
Obstructive sleep apnea: A dentist update
 Review article Obstructive sleep apnea: A dentist update Mithun K*, Ashith M V, Valerie Anithra Pereira, Deesha Kumari Email:dr.mithunknaik@gmail.com Abstract Sleep breathing disorder includes snoring,
Review article Obstructive sleep apnea: A dentist update Mithun K*, Ashith M V, Valerie Anithra Pereira, Deesha Kumari Email:dr.mithunknaik@gmail.com Abstract Sleep breathing disorder includes snoring,
Healthy Sleep. Frederick Tolle, M.D., dabsm Community Health Network
 Healthy Sleep Frederick Tolle, M.D., dabsm Community Health Network Adults should sleep 7 or more hours per night on a regular basis to promote optimal health. Getting less than 7 hours of sleep on average
Healthy Sleep Frederick Tolle, M.D., dabsm Community Health Network Adults should sleep 7 or more hours per night on a regular basis to promote optimal health. Getting less than 7 hours of sleep on average
Upper Airway Obstruction
 Upper Airway Obstruction Adriaan Pentz Division of Otorhinolaryngology University of Stellenbosch and Tygerberg Hospital Stridor/Stertor Auditory manifestations of disordered respiratory function ie noisy
Upper Airway Obstruction Adriaan Pentz Division of Otorhinolaryngology University of Stellenbosch and Tygerberg Hospital Stridor/Stertor Auditory manifestations of disordered respiratory function ie noisy
An update on childhood sleep-disordered breathing
 An update on childhood sleep-disordered breathing แพทย หญ งวนพร อน นตเสร ภาคว ชาก มารเวชศาสตร คณะแพทยศาสตร มหาว ทยาล ยสงขลานคร นทร Sleep-disordered breathing Primary snoring Upper airway resistance syndrome
An update on childhood sleep-disordered breathing แพทย หญ งวนพร อน นตเสร ภาคว ชาก มารเวชศาสตร คณะแพทยศาสตร มหาว ทยาล ยสงขลานคร นทร Sleep-disordered breathing Primary snoring Upper airway resistance syndrome
Use of Technology in the Assessment of Type 2 Diabetes and Sleep Apnea
 Use of Technology in the Assessment of Type 2 Diabetes and Sleep Apnea Eileen R. Chasens, PhD Associate Professor University of Pittsburgh September 3, 2014 Disclosure I do not own a Smart Phone, I have
Use of Technology in the Assessment of Type 2 Diabetes and Sleep Apnea Eileen R. Chasens, PhD Associate Professor University of Pittsburgh September 3, 2014 Disclosure I do not own a Smart Phone, I have
Obstructive sleep apnea (OSA) is the periodic reduction
 Obstructive Sleep Apnea and Oxygen Therapy: A Systematic Review of the Literature and Meta-Analysis 1 Department of Anesthesiology, Toronto Western Hospital, University Health Network, University of Toronto,
Obstructive Sleep Apnea and Oxygen Therapy: A Systematic Review of the Literature and Meta-Analysis 1 Department of Anesthesiology, Toronto Western Hospital, University Health Network, University of Toronto,
in China Shanghai Office Beijing Office (+86) (+86)
 SLEEP Apnea in China Guide 2018-2019 Shanghai Office (+86) 21 2426 6400 Beijing Office (+86) 010 6464 0611 www.pacificprime.cn Follow us on WeChat t A comprehensive overview of sleep apnea Perhaps you
SLEEP Apnea in China Guide 2018-2019 Shanghai Office (+86) 21 2426 6400 Beijing Office (+86) 010 6464 0611 www.pacificprime.cn Follow us on WeChat t A comprehensive overview of sleep apnea Perhaps you
A First Line Treatment for Sleep Disordered Breathing
 A First Line Treatment for Sleep Disordered Breathing Sleep Disordered Breathing Snoring & Obstructive Sleep Apnoea Snoring and Obstructive Sleep Apnoea (OSA) are caused by the airway narrowing or even
A First Line Treatment for Sleep Disordered Breathing Sleep Disordered Breathing Snoring & Obstructive Sleep Apnoea Snoring and Obstructive Sleep Apnoea (OSA) are caused by the airway narrowing or even
In-Patient Sleep Testing/Management Boaz Markewitz, MD
 In-Patient Sleep Testing/Management Boaz Markewitz, MD Objectives: Discuss inpatient sleep programs and if they provide a benefit to patients and sleep centers Identify things needed to be considered when
In-Patient Sleep Testing/Management Boaz Markewitz, MD Objectives: Discuss inpatient sleep programs and if they provide a benefit to patients and sleep centers Identify things needed to be considered when
GOALS. Obstructive Sleep Apnea and Cardiovascular Disease (OVERVIEW) FINANCIAL DISCLOSURE 2/1/2017
 Obstructive Sleep Apnea and Cardiovascular Disease (OVERVIEW) 19th Annual Topics in Cardiovascular Care Steven Khov, DO, FAAP Pulmonary Associates of Lancaster, Ltd February 3, 2017 skhov2@lghealth.org
Obstructive Sleep Apnea and Cardiovascular Disease (OVERVIEW) 19th Annual Topics in Cardiovascular Care Steven Khov, DO, FAAP Pulmonary Associates of Lancaster, Ltd February 3, 2017 skhov2@lghealth.org
WHAT YOU NEED TO KNOW ABOUT SLEEP APNEA
 WHAT YOU NEED TO KNOW ABOUT SLEEP APNEA Wayne Driscoll Clinical Education Specialist 2 SLEEP APNEA IN THE NEWS Carrie Fisher died from sleep apnea, other factors, coroner says USA Today NJ Transit engineer
WHAT YOU NEED TO KNOW ABOUT SLEEP APNEA Wayne Driscoll Clinical Education Specialist 2 SLEEP APNEA IN THE NEWS Carrie Fisher died from sleep apnea, other factors, coroner says USA Today NJ Transit engineer
What is SDB? Obstructive sleep apnea-hypopnea syndrome (OSAHS)
 Have a Good Sleep? Estimated 70 million Americans have clinically significant sleep problems Chronic insomnias report decreased quality of life, memory and attention problems, decreased physical health
Have a Good Sleep? Estimated 70 million Americans have clinically significant sleep problems Chronic insomnias report decreased quality of life, memory and attention problems, decreased physical health
Obstructive Sleep Apnea:
 Obstructive Sleep Apnea: A Physiological Approach Robert L. Owens, MD February 2018 Outline Cause(s) of OSA Can we measure the causes in an individual? Is that useful? 1 Thoracic pressure swings ( LV a
Obstructive Sleep Apnea: A Physiological Approach Robert L. Owens, MD February 2018 Outline Cause(s) of OSA Can we measure the causes in an individual? Is that useful? 1 Thoracic pressure swings ( LV a
Tongue Protrusion Strength in Arousal State Is Predictive of the Airway Patency in Obstructive Sleep Apnea
 Tohoku J. Exp. Med., 2015, 236, 241-245 Tongue Protrusion Strength in Obstructive Sleep Apnea 241 Tongue Protrusion Strength in Arousal State Is Predictive of the Airway Patency in Obstructive Sleep Apnea
Tohoku J. Exp. Med., 2015, 236, 241-245 Tongue Protrusion Strength in Obstructive Sleep Apnea 241 Tongue Protrusion Strength in Arousal State Is Predictive of the Airway Patency in Obstructive Sleep Apnea
The Mandibular Advancement Device and Patient Selection in the Treatment of Obstructive Sleep Apnea
 ORIGINAL ARTICLE The Mandibular Advancement Device and Patient Selection in the Treatment of Obstructive Sleep Apnea Chul Hee Lee, MD; Ji-Hun Mo, MD; Ik-Joon Choi, MD; Hyun Jong Lee, MD; Beom Seok Seo,
ORIGINAL ARTICLE The Mandibular Advancement Device and Patient Selection in the Treatment of Obstructive Sleep Apnea Chul Hee Lee, MD; Ji-Hun Mo, MD; Ik-Joon Choi, MD; Hyun Jong Lee, MD; Beom Seok Seo,
18/06/2009 NZ Respiratory & Sleep Institute
 Sleep Disorders in Primary Care - a personal view 18/06/2009 Andrew G Veale NZ Respiratory & Sleep Institute Abnormal Sleep Disorders of the initiation & maintenance of sleep (DIMS) Insomnia 1 o or 2 o
Sleep Disorders in Primary Care - a personal view 18/06/2009 Andrew G Veale NZ Respiratory & Sleep Institute Abnormal Sleep Disorders of the initiation & maintenance of sleep (DIMS) Insomnia 1 o or 2 o
ALD 2015 KNOWLEDGE EXPERIENCE APPLICATION ALD 2015 KNOWLEDGE EXPERIENCE APPLICATION ALD 2015 KNOWLEDGE EXPERIENCE APPLICATION.
 ALD 2015 KNOWLEDGE EXPERIENCE APPLICATION Moving Tongues Beyond Frenectomy Grace Sun, DDS FAACD MALD MAGD MICOI Los Angeles ALD 2015 KNOWLEDGE EXPERIENCE APPLICATION Accredited Fellow, American Academy
ALD 2015 KNOWLEDGE EXPERIENCE APPLICATION Moving Tongues Beyond Frenectomy Grace Sun, DDS FAACD MALD MAGD MICOI Los Angeles ALD 2015 KNOWLEDGE EXPERIENCE APPLICATION Accredited Fellow, American Academy
A Look at Two Syndromes: TEMPOROMANDIBULAR JOINT & CERVICOCRANIAL DYSFUNCTION IN THE EDS PATIENT. John Mitakides D.D.S., FAACP
 TEMPOROMANDIBULAR JOINT & CERVICOCRANIAL DYSFUNCTION IN THE EDS PATIENT John Mitakides D.D.S., FAACP A Look at Two Syndromes: How TMJ and CCD impact the EDS patient as they occur separately or together
TEMPOROMANDIBULAR JOINT & CERVICOCRANIAL DYSFUNCTION IN THE EDS PATIENT John Mitakides D.D.S., FAACP A Look at Two Syndromes: How TMJ and CCD impact the EDS patient as they occur separately or together
DoctorStevenPark.com!
 ! DoctorStevenPark.com!!! Subscribe in itunes @ doctorstevenpark.com/itunes Show notes @ doctorstevenpark.com/001! Sleep & Breathing: The 2 Keys to Optimal Health What I ll Cover Why only humans have sleep
! DoctorStevenPark.com!!! Subscribe in itunes @ doctorstevenpark.com/itunes Show notes @ doctorstevenpark.com/001! Sleep & Breathing: The 2 Keys to Optimal Health What I ll Cover Why only humans have sleep
Snoring and Obstructive Sleep Apnea: Patient s Guide to Minimally Invasive Treatments Chapter 2
 Snoring and Obstructive Sleep Apnea: Patient s Guide to Minimally Invasive Treatments Chapter 2 CAUSES OF SNORING AND SLEEP APNEA We inhale air through our nose and mouth. From the nostrils, air flows
Snoring and Obstructive Sleep Apnea: Patient s Guide to Minimally Invasive Treatments Chapter 2 CAUSES OF SNORING AND SLEEP APNEA We inhale air through our nose and mouth. From the nostrils, air flows
ROBERT C. PRITCHARD DIRECTOR MICHAEL O. FOSTER ASSISTANT DIR. SLEEP APNEA
 ROBERT C. PRITCHARD DIRECTOR MICHAEL O. FOSTER ASSISTANT DIR. SLEEP APNEA A Person is physically qualified to drive a motor vehicle if that person; -(5) has no established medical history or clinical diagnosis
ROBERT C. PRITCHARD DIRECTOR MICHAEL O. FOSTER ASSISTANT DIR. SLEEP APNEA A Person is physically qualified to drive a motor vehicle if that person; -(5) has no established medical history or clinical diagnosis
The Agony or the Ecstasy. Familiar?
 The Agony or the Ecstasy Familiar? Snoring Related Complaints Drives wife from bedroom Girlfriend won t marry me Shakes entire house Ask me to leave movies and church Has had to leave boat so friends could
The Agony or the Ecstasy Familiar? Snoring Related Complaints Drives wife from bedroom Girlfriend won t marry me Shakes entire house Ask me to leave movies and church Has had to leave boat so friends could
OSA in children. About this information. What is obstructive sleep apnoea (OSA)?
 About this information This information explains all about sleep-related breathing problems in children, focusing on the condition obstructive sleep apnoea (OSA). It tells you what the risk factors are
About this information This information explains all about sleep-related breathing problems in children, focusing on the condition obstructive sleep apnoea (OSA). It tells you what the risk factors are
