Challenges of air leak complications in a resource-limited country
|
|
|
- Corey Park
- 5 years ago
- Views:
Transcription
1 SWISS SOCIETY OF NEONATOLOGY Challenges of air leak complications in a resource-limited country February 2018 asa asv asa
2 Berger TM, Berger S, Kamara I, Naurenge E, Ndepavali C, NEO FOR NAMIBIA Helping Babies Survive (BTM, BS), Lucerne, Switzerland, Rundu State Hospital (KI, NE, NC), Rundu, Namibia Title figure: The Macklin effect (asa: air surrounding artery, asv: air surrounding vein (Source: Arch Intern Med (Chic.) 1939;64: ) Swiss Society of Neonatology, Thomas M Berger, Webmaster
3 3 Respiratory distress is a common, yet non-specific symptom in sick neonates. Determination of the underlying cause relies on the patient s history, clinical examination, laboratory examinations and, last but not least, chest X-ray. Importantly, respiratory failure is a frequent cause of death. Improving support of neonates with respiratory failure thus has the potential to substantially improve survival rates (1). In low income countries, both diagnostic and therapeutic options for patients with respiratory distress are frequently limited. The following two cases illustrate some of the challenging aspects of neonatal respiratory care in a resource-limited setting. INTRODUCTION
4 4 FIRST CASE REPORT This infant was a male twin A born to a 17-year-old non-married mother. This had been the 4 th pregnancy of this teenager, two of which had resulted in preterm deliveries and early neonatal deaths. The mother has one healthy 3-year-old child. Delivery of the twins had occurred in a taxi on the way from the village to the hospital. On admission to the neonatal unit, the infant was severely hypothermic (rectal temperature of 33.2 C) and profoundly hypoxemic (SpO 2 45%) while breathing room air. His birth weight was 1280 g and his gestational age was estimated at 30 weeks. A nasogastric (NG) tube had been inserted into the umbilical vein in the emergency department of the hospital. When oxygen saturation did not improve with nasal cannula oxygen at 2 l/min, the infant was put on bubble CPAP using a device that had only recently been introduced in this hospital (Pumani, Hadleigh Health Technologies, San Rafael, CA, USA). Initial settings were a CPAP pressure of 6 cmh 2 O, an oxygen flow of 5 l/min and a total flow of 6 l/min, resulting in an FiO 2 of 80%. SpO 2 values rapidly increased and the FiO 2 could be reduced to 45% within 30 minutes. At this point, a chest X-ray was obtained and was felt to be consistent with hyaline membrane disease (Fig. 1). On day of life (DOL) 2, following a stable 24-hourperiod, the infant suddenly desaturated and deve loped
5 5 signs of poor perfusion. On auscultation, an unusual rhythmic crunching sound was heard that could not be classified. Findings on a second chest X-ray, which became available two hours later, were consistent with pneumopericardium (Fig. 2). SpO 2 was 80% on an FiO 2 of 90% and capillary refill time remained prolonged despite the administration of a fluid bolus. At this point, it was decided to attempt pericardiocentesis. A 24 G venous cannula with a 2-ml syringe attached was used. The pericardial space was entered from a subxiphoid approach at a 30-degree-angle with the needle directed against the left shoulder. Imme diately, 8 ml of air could be aspirated. SpO 2 increased to 91% and skin perfusion improved. The venous cannula was left in place for intermittent aspiration (Fig. 3). Unfortunately, the patient died during the following night.
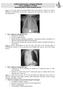
6 6 Fig. 1 Twin A: Chest X-ray following stabilization with bubble CPAP on DOL 1: low lung volumes, reticulogranular pattern and air bronchograms, consistent with hyaline membrane disease (note intrahepatic position of UVC and malpositioned nasogastric tube).
7 7 Fig. 2 Twin A: Chest X-ray following sudden deterioration on DOL 2: the heart is almost completely surrounded by air, with the pericardium sharply outlined by air density on either side.
8 8 Fig. 3 Twin A on DOL 2: A 24 G venous catheter was used to drain the pneumopericardium: despite initial aspiration of 8 ml of air, the patient s condition improved only transiently (note poor skin perfusion).
9 9 Like his brother, twin B arrived in a critical condition with hypothermia (rectal temperature 33.3 C) and significant respiratory distress and an SpO 2 of 48%. His birth weight was 1150 g. He was put on nasal cannula oxygen at 2 l/min and his color improved. After stabilization of his twin brother, twin B was also put on CPAP with a pressure of 6 cmh 2 O, an oxygen flow of 4 l/min and a total flow of 6 l/min, resulting in an FiO 2 of 60%. A chest X-ray revealed findings consistent with hyaline membrane disease. An NG tube had been inserted into the umbilical vein, but was malpositioned in the portal vein (Fig. 4). Another NG tube was inserted next to the first one, hoping that it would enter the inferior vena cava. The infant responded well to CPAP and the FiO 2 could be weaned to 45%. SECOND CASE REPORT On DOL 2, the patient appeared stable with de creasing signs of respiratory distress and a lower oxygen requirement. However, on DOL 3, his course was complicated by a right-sided pneumothorax (Fig. 5). A 24 G venous cannula was used to aspirate air (Fig. 6). Unfortunately, there appeared to be a large air leak and almost continuous aspiration was required. This was done manually since no vacuum system was available. A nurse was called to duty, sat at the bedside and continued to intermittently aspirate air. Despite these efforts, the patient died 6 hours later.
10 10 Fig. 4 Twin B: Chest X-ray following stabilization with bubble CPAP on DOL 1: low lung volumes, reticulogranular pattern and air bronchograms, consistent with hyaline membrane disease (note malposition of the UVC in the portal vein).
11 11 Fig. 5 Twin B on DOL 3: chest of X-ray following gradual deterioration on DOL 3: right-sided pneumothorax with slight mediastinal shift to the left (note malpositioned UVC).
12 12 Fig. 6 Twin B on DOL 3: A 24 G venous catheter was used to drain the pneumothorax: because a continuous suction system was lacking, intermittent manual aspiration was performed every 5 minutes over 6 hours (until the patient s death).
13 13 The two case reports illustrate multiple challenges encountered in perinatal care in resource-limited countries. Teenage pregnancies, poor antenatal care with late booking, delayed presentation or out-of-hospital deliveries even in high-risk pregnancies are common and put both mothers and babies at risk. DISCUSSION Until very recently, nasal cannula oxygen was the only form of respiratory support available at Rundu State Hospital. Flow rates between l/min are used and the gas is not warmed and marginally humidified since there is only cold bubble humidification. SpO 2 is measured only intermittently due to the lack of adequate pulse oximetry equipment. Very likely, both hypoxic and hyperoxic episodes go largely unnoticed. The introduction of CPAP devices potentially can have a dramatic impact on the survival rates of neonates with respiratory distress (1, 2). In July 2017, the Pumani bubble CPAP device (Hadleigh Health Technologies, San Rafael, CA, USA) was introduced at the Rundu State Hospital. This machine is very robust, easy to use and affordable. Initially, the two patients presented in this report responded very nicely: SpO 2 rapidly increased and FiO 2 could be reduced to less than 50%. While patients with poorly compliant lungs benefit from CPAP therapy, they can still develop air leak complications when spontaneous respiratory efforts lead to (focal) overdistension and lung damage.
14 14 First described by Macklin in 1939, air can travel along the vascular sheaths and eventually lead to pulmonary interstitial emphysema and pneumomediastinum (3). It has been speculated that mediastinal air dissecting at the reflection of the parietal to visceral pericardium near the ostia of the pulmonary veins leads to pneumopericardium (4). As the two presented cases illustrate, detection and management of air leak syndromes can be very challenging in resource-limited countries. Literature on pneumopericardium in neonates is with hyaline mem brane disease is scarce. One of the largest series was published from the University of Minnesota Hospitals and St. Paul Children s Hospital in the pre-surfactant era (5). In 23 out of a total of 28 patients, pneumopericardium resulted in clinical pericardial tampo nade. Mortality rate was 54%. The rhythmic crunching sound heard in twin A is known as Hamman s sign (after Louis Hamman, Johns Hopkins University clinician), which can also be heard in patients with anterior pneumomediastinum, or «bruit de moulin» (mill-wheel murmur). In high income countries, the described patients would have qualified for early surfactant replacement therapy; however, this expensive drug is currently not avai lable at this hospital. It is noteworthy that surfactant preparations were included in the Essential Drug List of WHO in 2008 (6). In its current version (20 th List, March 2017, amended August 2017), sur-
15 15 factant is listed in the Complementary List. This list presents essential medicines for «priority diseases, for which specialized diagnostic or monitoring facilities, and/or specialist medical care, and/or specialist training are needed.» (7). The use of surfactant replacement therapy (SRT) in developing countries is still limited because of a) high cost, which may exceed the per-capita GNP ( USD) in some countries, b) lack of skilled personnel to administer SRT, and c) lack of support systems after the SRT. Recent developments may have the potential to address these constraints. The development of SP-B and SP-C enriched syn thetic surfactants (8) may reduce the costs of SRT. In recent years, the INSURE (intubation-surfactant-extubation) procedure and other forms of less invasive surfactant administration (LISA) have become increasingly popular in high income countries (9). The latter procedure does not require mechanical ventilation via an endotracheal tube, since the surfactant preparation is administered intratracheally via a small diameter tube, while the infant is spontaneously breathing (10). Alternatively, surfactant administered through a laryngeal mask airway (LMA) may be a valuable option as it does not require the skills necessary for laryngoscopy and / or intubation (11). Robust and low-cost CPAP devices have been developed and could be used both prior to and after SRT (12).
16 16 CONCLUSION Improving the management of neonates with respiratory distress in developing countries has the potential to greatly improve survival chances for affected neonates. This will require improvements in both diagnosis and therapy, as well as management of complications of various causes of respiratory failure. It is highly desirable that research in neonatology also addresses the needs of newborn infants born in low and middle income countries (10).
17 17 1. Kamath BD, Macguire ER, McClure EM, Goldenberg RL, Jobe AH. Neonatal mortality from respiratory distress syndrome: lessons for low-resource countries. Pediatrics 2011;127: (Abstract) REFERENCES 2. Kawaza K, Machen HE, Brown J, et al. Efficacy of a low-cost bubble CPAP system in treatment of respiratory distress in a neonatal ward in Malawi. PLoS One 2014;9:e86327 (Abstract) 3. Macklin CC. Transport of air along sheaths of pulmonic blood vessels from alveoli to mediastinum clinical implications. Arch Intern Med (Chic.) 1939;64: (no abstract available) 4. Jokic RR, Kovacevi B, Beserminji M, Tatic M. Surgical approach to tension pneumopericardium in newborns and infants. JPSS 2008;2:32 35 (Abstract) 5. Emery RW, Landes RG, Lindsay WG, Thompson T, Nicoloff DM. Surgical treatment of pneumopericardium in the neonate. Word J Surg 1978;2: (no abstract) 6. Vidyasagar D, Velaphi S, Bhat VB. Surfactant replacement therapy in developing countries. Neonatology 2011;99: (Abstract) 7. WHO Model List of Essential Medicines, 20th List (March 2017) (Website) 8. Sweet DG, Turner MA, Straňák Z, et al. A first-in-human clinical study of a new SP-B and SP-C enriched synthetic surfactant (CHF5633) in preterm babies with respiratory distress syndrome. Arch Dis Child Fetal Neonatal Ed 2017;102:F497-F503 (Abstract) 9. Gortner L, Schüller SS, Herting E. Review demonstrates that less invasive surfactant administration in preterm neonates leads to fewer complications. Acta Paediatr 2017 Nov 24 [Epub ahead of print] (Abstract)
18 Herting E. Less invasive surfactant administration (LISA) ways to deliver surfactant in spontaneously breathing infants. Early Hum Dev 2013;89: (Abstract) 11. Roberts KD, Brown R, Lampland AL, et al. Laryngeal mask airway for surfactant administration in neonates: a randomized, controlled trial. J Pediatr 2017 Nov 21 (Epub ahead of print) (Abstract) 12. Berger TM. Neonatal respiratory care: not how, but where and when. Lancet Respir Med 2013;1: (no abstract available)
19
20 concept & design by mesch.ch SUPPORTED BY CONTACT Swiss Society of Neonatology
SWISS SOCIETY OF NEONATOLOGY. Potentially fatal complications of peripherally inserted central venous catheters (PICCs)
 SWISS SOCIETY OF NEONATOLOGY Potentially fatal complications of peripherally inserted central venous catheters (PICCs) October 2001 2 Berger TM, Neonatal and Pediatric Intensive Care Unit, Children s Hospital
SWISS SOCIETY OF NEONATOLOGY Potentially fatal complications of peripherally inserted central venous catheters (PICCs) October 2001 2 Berger TM, Neonatal and Pediatric Intensive Care Unit, Children s Hospital
Simulation 3: Post-term Baby in Labor and Delivery
 Simulation 3: Post-term Baby in Labor and Delivery Opening Scenario (Links to Section 1) You are an evening-shift respiratory therapist in a large hospital with a level III neonatal unit. You are paged
Simulation 3: Post-term Baby in Labor and Delivery Opening Scenario (Links to Section 1) You are an evening-shift respiratory therapist in a large hospital with a level III neonatal unit. You are paged
SWISS SOCIETY OF NEONATOLOGY. Selective bronchial intubation for unilateral PIE
 SWISS SOCIETY OF NEONATOLOGY Selective bronchial intubation for unilateral PIE October 2000 2 Berger TM, Jöhr M, Neonatal and Pediatric Intensive Care Unit (BTM), Kinderspital Luzern, Department of Anesthesiology
SWISS SOCIETY OF NEONATOLOGY Selective bronchial intubation for unilateral PIE October 2000 2 Berger TM, Jöhr M, Neonatal and Pediatric Intensive Care Unit (BTM), Kinderspital Luzern, Department of Anesthesiology
Shedding Light on Neonatal X-rays. Objectives. Indications for X-Rays 5/14/2018
 Shedding Light on Neonatal X-rays Barbara C. Mordue, MSN, NNP-BC Neonatal Nurse Practitioner LLUH Children s Hospital, NICU Objectives Utilize a systematic approach to neonatal x-ray interpretation Identify
Shedding Light on Neonatal X-rays Barbara C. Mordue, MSN, NNP-BC Neonatal Nurse Practitioner LLUH Children s Hospital, NICU Objectives Utilize a systematic approach to neonatal x-ray interpretation Identify
CONTINUOUS POSITIVE AIRWAY PRESSURE (CPAP) DEFINITION
 CONTINUOUS POSITIVE AIRWAY PRESSURE (CPAP) DEFINITION Method of maintaining low pressure distension of lungs during inspiration and expiration when infant breathing spontaneously Benefits Improves oxygenation
CONTINUOUS POSITIVE AIRWAY PRESSURE (CPAP) DEFINITION Method of maintaining low pressure distension of lungs during inspiration and expiration when infant breathing spontaneously Benefits Improves oxygenation
AEROSURF Phase 2 Program Update Investor Conference Call
 AEROSURF Phase 2 Program Update Investor Conference Call November 12, 2015 Forward Looking Statement To the extent that statements in this presentation are not strictly historical, including statements
AEROSURF Phase 2 Program Update Investor Conference Call November 12, 2015 Forward Looking Statement To the extent that statements in this presentation are not strictly historical, including statements
Volume Guarantee Initiation and ongoing clinical management of an infant supported by Volume Guarantee A Case Study
 D-32084-2011 Volume Guarantee Initiation and ongoing clinical management of an infant supported by Volume Guarantee A Case Study Robert DiBlasi RRT-NPS, FAARC Respiratory Care Manager of Research & Quality
D-32084-2011 Volume Guarantee Initiation and ongoing clinical management of an infant supported by Volume Guarantee A Case Study Robert DiBlasi RRT-NPS, FAARC Respiratory Care Manager of Research & Quality
SWISS SOCIETY OF NEONATOLOGY. Peripartal management of a prenatally diagnosed large oral cyst
 SWISS SOCIETY OF NEONATOLOGY Peripartal management of a prenatally diagnosed large oral cyst May 2007 2 Fontana M, Berger TM, Winiker H, Jöhr M, Nagel H, Neonatal and Pediatric Intensive Care Unit (FM,
SWISS SOCIETY OF NEONATOLOGY Peripartal management of a prenatally diagnosed large oral cyst May 2007 2 Fontana M, Berger TM, Winiker H, Jöhr M, Nagel H, Neonatal and Pediatric Intensive Care Unit (FM,
Surfactant Administration
 Approved by: Surfactant Administration Gail Cameron Senior Director Operations, Maternal, Neonatal & Child Health Programs Dr. Paul Byrne Medical Director, Neonatology Neonatal Policy & Procedures Manual
Approved by: Surfactant Administration Gail Cameron Senior Director Operations, Maternal, Neonatal & Child Health Programs Dr. Paul Byrne Medical Director, Neonatology Neonatal Policy & Procedures Manual
Addendum to the NRP Provider Textbook 6 th Edition Recommendations for specific modifications in the Canadian context
 Addendum to the NRP Provider Textbook 6 th Edition Recommendations for specific modifications in the Canadian context A subcommittee of the Canadian Neonatal Resuscitation Program (NRP) Steering Committee
Addendum to the NRP Provider Textbook 6 th Edition Recommendations for specific modifications in the Canadian context A subcommittee of the Canadian Neonatal Resuscitation Program (NRP) Steering Committee
Hyaline membrane disease. By : Dr. Ch Sarishma Peadiatric Pg
 Hyaline membrane disease By : Dr. Ch Sarishma Peadiatric Pg Also called Respiratory distress syndrome. It occurs primarily in premature infants; its incidence is inversely related to gestational age and
Hyaline membrane disease By : Dr. Ch Sarishma Peadiatric Pg Also called Respiratory distress syndrome. It occurs primarily in premature infants; its incidence is inversely related to gestational age and
NRP Raising the Bar for Providers and Instructors
 NRP 2011 Raising the Bar for Providers and Instructors What is the same? 1. Minimum course requirement is Lessons 1 through 4 and Lesson 9. The NRP Provider Card requires renewal every 2 years. Your facility
NRP 2011 Raising the Bar for Providers and Instructors What is the same? 1. Minimum course requirement is Lessons 1 through 4 and Lesson 9. The NRP Provider Card requires renewal every 2 years. Your facility
SWISS SOCIETY OF NEONATOLOGY. Supercarbia in an infant with meconium aspiration syndrome
 SWISS SOCIETY OF NEONATOLOGY Supercarbia in an infant with meconium aspiration syndrome January 2006 2 Wilhelm C, Frey B, Department of Intensive Care and Neonatology, University Children s Hospital Zurich,
SWISS SOCIETY OF NEONATOLOGY Supercarbia in an infant with meconium aspiration syndrome January 2006 2 Wilhelm C, Frey B, Department of Intensive Care and Neonatology, University Children s Hospital Zurich,
Review of Neonatal Respiratory Problems
 Review of Neonatal Respiratory Problems Respiratory Distress Occurs in about 7% of infants Clinical presentation includes: Apnea Cyanosis Grunting Inspiratory stridor Nasal flaring Poor feeding Tachypnea
Review of Neonatal Respiratory Problems Respiratory Distress Occurs in about 7% of infants Clinical presentation includes: Apnea Cyanosis Grunting Inspiratory stridor Nasal flaring Poor feeding Tachypnea
SWISS SOCIETY OF NEONATOLOGY. Spontaneous intestinal perforation or necrotizing enterocolitis?
 SWISS SOCIETY OF NEONATOLOGY Spontaneous intestinal perforation or necrotizing enterocolitis? June 2004 2 Stocker M, Berger TM, Neonatal and Pediatric Intensive Care Unit, Children s Hospital of Lucerne,
SWISS SOCIETY OF NEONATOLOGY Spontaneous intestinal perforation or necrotizing enterocolitis? June 2004 2 Stocker M, Berger TM, Neonatal and Pediatric Intensive Care Unit, Children s Hospital of Lucerne,
Provide guidelines for the management of mechanical ventilation in infants <34 weeks gestation.
 Page 1 of 5 PURPOSE: Provide guidelines for the management of mechanical ventilation in infants
Page 1 of 5 PURPOSE: Provide guidelines for the management of mechanical ventilation in infants
Extensive cystic periventricular leukomalacia following early-onset group B streptococcal sepsis in a very low birth weight infant
 SWISS SOCIETY OF NEONATOLOGY Extensive cystic periventricular leukomalacia following early-onset group B streptococcal sepsis in a very low birth weight infant July 2012 2 Berger TM, Caduff JC, Neonatal
SWISS SOCIETY OF NEONATOLOGY Extensive cystic periventricular leukomalacia following early-onset group B streptococcal sepsis in a very low birth weight infant July 2012 2 Berger TM, Caduff JC, Neonatal
I. Subject: Continuous Positive Airway Pressure CPAP by Continuous Flow Device
 I. Subject: Continuous Positive Airway Pressure CPAP by Continuous Flow Device II. Policy: Continuous Positive Airway Pressure CPAP by the Down's system will be instituted by Respiratory Therapy personnel
I. Subject: Continuous Positive Airway Pressure CPAP by Continuous Flow Device II. Policy: Continuous Positive Airway Pressure CPAP by the Down's system will be instituted by Respiratory Therapy personnel
Infection. Risk factor for infection ACoRN alerting sign with * Clinical deterioration. Problem List. Respiratory. Cardiovascular
 The ACoRN Process Baby at risk Unwell Risk factors Post-resuscitation requiring stabilization Resuscitation Ineffective breathing Heart rate < 100 bpm Central cyanosis Support Infection Risk factor for
The ACoRN Process Baby at risk Unwell Risk factors Post-resuscitation requiring stabilization Resuscitation Ineffective breathing Heart rate < 100 bpm Central cyanosis Support Infection Risk factor for
Table 1: The major changes in AHA / AAP neonatal resuscitation guidelines2010 compared to previous recommendations in 2005
 Table 1: The major changes in AHA / AAP neonatal guidelines2010 compared to previous recommendations in 2005 Resuscitation step Recommendations (2005) Recommendations (2010) Comments/LOE 1) Assessment
Table 1: The major changes in AHA / AAP neonatal guidelines2010 compared to previous recommendations in 2005 Resuscitation step Recommendations (2005) Recommendations (2010) Comments/LOE 1) Assessment
Neonatal Life Support Provider (NLSP) Certification Preparatory Materials
 Neonatal Life Support Provider (NLSP) Certification Preparatory Materials NEONATAL LIFE SUPPORT PROVIDER (NRP) CERTIFICATION TABLE OF CONTENTS NEONATAL FLOW ALGORITHM.2 INTRODUCTION 3 ANTICIPATION OF RESUSCITATION
Neonatal Life Support Provider (NLSP) Certification Preparatory Materials NEONATAL LIFE SUPPORT PROVIDER (NRP) CERTIFICATION TABLE OF CONTENTS NEONATAL FLOW ALGORITHM.2 INTRODUCTION 3 ANTICIPATION OF RESUSCITATION
Resuscitation efforts for Mom & Baby
 Resuscitation efforts for Mom & Baby Beth Ann Clayton, CRNA, MS AmSol Obstetric Anesthesia CRNA Educator Obstetric Anesthesia Clinical Coordinator Mercy Health-Fairfield Hospital Assistant Professor, University
Resuscitation efforts for Mom & Baby Beth Ann Clayton, CRNA, MS AmSol Obstetric Anesthesia CRNA Educator Obstetric Anesthesia Clinical Coordinator Mercy Health-Fairfield Hospital Assistant Professor, University
NON INVASIVE LIFE SAVERS. Non Invasive Ventilation (NIV)
 Table 1. NIV: Mechanisms Of Action Decreases work of breathing Increases functional residual capacity Recruits collapsed alveoli Improves respiratory gas exchange Reverses hypoventilation Maintains upper
Table 1. NIV: Mechanisms Of Action Decreases work of breathing Increases functional residual capacity Recruits collapsed alveoli Improves respiratory gas exchange Reverses hypoventilation Maintains upper
TRAINING NEONATOLOGY SILVANA PARIS
 TRAINING ON NEONATOLOGY SILVANA PARIS RESUSCITATION IN DELIVERY ROOM INTRODUCTION THE GLOBAL RESUSCITATION BURDEN IN NEWBORN 136 MILL NEWBORN BABIES EACH YEAR (WHO WORLD REPORT) 5-8 MILL NEWBORN INFANTS
TRAINING ON NEONATOLOGY SILVANA PARIS RESUSCITATION IN DELIVERY ROOM INTRODUCTION THE GLOBAL RESUSCITATION BURDEN IN NEWBORN 136 MILL NEWBORN BABIES EACH YEAR (WHO WORLD REPORT) 5-8 MILL NEWBORN INFANTS
Presented By : Kamlah Olaimat
 Presented By : Kamlah Olaimat 18\7\2010 Transient Tachpnea of the Definition:- newborn (TTN) TTN is a benign disease of near term or term infant who display respiratory distress shortly after delivery.
Presented By : Kamlah Olaimat 18\7\2010 Transient Tachpnea of the Definition:- newborn (TTN) TTN is a benign disease of near term or term infant who display respiratory distress shortly after delivery.
F: Respiratory Care. College of Licensed Practical Nurses of Alberta, Competency Profile for LPNs, 3rd Ed. 59
 F: Respiratory Care College of Licensed Practical Nurses of Alberta, Competency Profile for LPNs, 3rd Ed. 59 Competency: F-1 Airway Management F-1-1 F-1-2 F-1-3 F-1-4 F-1-5 Demonstrate knowledge and ability
F: Respiratory Care College of Licensed Practical Nurses of Alberta, Competency Profile for LPNs, 3rd Ed. 59 Competency: F-1 Airway Management F-1-1 F-1-2 F-1-3 F-1-4 F-1-5 Demonstrate knowledge and ability
Practical Application of CPAP
 CHAPTER 3 Practical Application of CPAP Dr. Srinivas Murki Neonatologist Fernadez Hospital, Hyderabad. A.P. Practical Application of CPAP Continuous positive airway pressure (CPAP) applied to premature
CHAPTER 3 Practical Application of CPAP Dr. Srinivas Murki Neonatologist Fernadez Hospital, Hyderabad. A.P. Practical Application of CPAP Continuous positive airway pressure (CPAP) applied to premature
PROFESSOR DR. NUMAN NAFIE HAMEED الاستاذ الدكتور نعمان نافع الحمداني
 Lecture 6 PROFESSOR DR. NUMAN NAFIE HAMEED الاستاذ الدكتور نعمان نافع الحمداني Neonatal Resuscitation Program (NRP) 2010 MCQ? In neonatal resuscitation program, the preterm neonates need special preparations
Lecture 6 PROFESSOR DR. NUMAN NAFIE HAMEED الاستاذ الدكتور نعمان نافع الحمداني Neonatal Resuscitation Program (NRP) 2010 MCQ? In neonatal resuscitation program, the preterm neonates need special preparations
SWISS SOCIETY OF NEONATOLOGY. Neonatal cerebral infarction
 SWISS SOCIETY OF NEONATOLOGY Neonatal cerebral infarction May 2002 2 Mann C, Neonatal and Pediatric Intensive Care Unit, Landeskrankenhaus und Akademisches Lehrkrankenhaus Feldkirch, Austria Swiss Society
SWISS SOCIETY OF NEONATOLOGY Neonatal cerebral infarction May 2002 2 Mann C, Neonatal and Pediatric Intensive Care Unit, Landeskrankenhaus und Akademisches Lehrkrankenhaus Feldkirch, Austria Swiss Society
ENDOTRACHEAL INTUBATION POLICY
 POLICY Indications: Ineffective ventilation with mask and t-piece, or mask and bag technique Inability to maintain a patent airway Need or anticipation of need for prolonged ventilation Need for endotracheal
POLICY Indications: Ineffective ventilation with mask and t-piece, or mask and bag technique Inability to maintain a patent airway Need or anticipation of need for prolonged ventilation Need for endotracheal
Neonatal Chest X-Ray Interpretation
 CHAPTER 7 Neonatal Chest X-Ray Interpretation Prof. Praveen Kumar Neonatal unit, Department of Pediatrics, PGIMER, Chandigarh Learning Objectives At the end of this session, you should be able to: 1. Schematically
CHAPTER 7 Neonatal Chest X-Ray Interpretation Prof. Praveen Kumar Neonatal unit, Department of Pediatrics, PGIMER, Chandigarh Learning Objectives At the end of this session, you should be able to: 1. Schematically
Non Invasive Ventilation In Preterm Infants. Manuel Sanchez Luna Hospital General Universitario Gregorio Marañón Complutense University Madrid
 Non Invasive Ventilation In Preterm Infants Manuel Sanchez Luna Hospital General Universitario Gregorio Marañón Complutense University Madrid Summary Noninvasive ventilation begings in the delivery room
Non Invasive Ventilation In Preterm Infants Manuel Sanchez Luna Hospital General Universitario Gregorio Marañón Complutense University Madrid Summary Noninvasive ventilation begings in the delivery room
Ventilating the paediatric patient. Lizzie Barrett Nurse Educator November 2016
 Ventilating the paediatric patient Lizzie Barrett Nurse Educator November 2016 Acknowledgements Kate Leutert NE PICU Children's Hospital Westmead Dr. Chloe Tetlow VMO Anaesthetist and Careflight Overview
Ventilating the paediatric patient Lizzie Barrett Nurse Educator November 2016 Acknowledgements Kate Leutert NE PICU Children's Hospital Westmead Dr. Chloe Tetlow VMO Anaesthetist and Careflight Overview
Interfacility Protocol Protocol Title:
 Interfacility Protocol Protocol Title: Mechanical Ventilator Monitoring & Management Original Adoption Date: 05/2009 Past Protocol Updates 05/2009, 12/2013 Date of Most Recent Update: March 23, 2015 Medical
Interfacility Protocol Protocol Title: Mechanical Ventilator Monitoring & Management Original Adoption Date: 05/2009 Past Protocol Updates 05/2009, 12/2013 Date of Most Recent Update: March 23, 2015 Medical
Name and title of the investigators responsible for conducting the research: Dr Anna Lavizzari, Dr Mariarosa Colnaghi
 Protocol title: Heated, Humidified High-Flow Nasal Cannula vs Nasal CPAP for Respiratory Distress Syndrome of Prematurity. Protocol identifying number: Clinical Trials.gov NCT02570217 Name and title of
Protocol title: Heated, Humidified High-Flow Nasal Cannula vs Nasal CPAP for Respiratory Distress Syndrome of Prematurity. Protocol identifying number: Clinical Trials.gov NCT02570217 Name and title of
** SURFACTANT THERAPY**
 ** SURFACTANT THERAPY** Full Title of Guideline: Surfactant Therapy Author (include email and role): Stephen Wardle (V4) Reviewed by Dushyant Batra Consultant Neonatologist Division & Speciality: Division:
** SURFACTANT THERAPY** Full Title of Guideline: Surfactant Therapy Author (include email and role): Stephen Wardle (V4) Reviewed by Dushyant Batra Consultant Neonatologist Division & Speciality: Division:
Equipment: NRP algorithm, MRSOPA table, medication chart, SpO 2 table Warm
 NRP Skills Stations Performance Skills Station OR Integrated Skills Station STATION: Assisting with and insertion of endotracheal tube (ETT) Equipment: NRP algorithm, MRSOPA table, medication chart, SpO
NRP Skills Stations Performance Skills Station OR Integrated Skills Station STATION: Assisting with and insertion of endotracheal tube (ETT) Equipment: NRP algorithm, MRSOPA table, medication chart, SpO
1 Pediatric Advanced Life Support Science Update What s New for 2010? 3 CPR. 4 4 Steps of BLS Survey 5 CPR 6 CPR.
 1 Pediatric Advanced Life Support Science Update 2010 2 What s New for 2010? 3 CPR Take no longer than seconds for pulse check Rate at least on per minute (instead of around 100 per minute ) Depth change:
1 Pediatric Advanced Life Support Science Update 2010 2 What s New for 2010? 3 CPR Take no longer than seconds for pulse check Rate at least on per minute (instead of around 100 per minute ) Depth change:
APPENDIX VI HFOV Quick Guide
 APPENDIX VI HFOV Quick Guide Overall goal: Maintain PH in the target range at the minimum tidal volume. This is achieved by favoring higher frequencies over lower P (amplitude). This goal is also promoted
APPENDIX VI HFOV Quick Guide Overall goal: Maintain PH in the target range at the minimum tidal volume. This is achieved by favoring higher frequencies over lower P (amplitude). This goal is also promoted
SWISS SOCIETY OF NEONATOLOGY. Delayed-onset right-sided congenital diaphragmatic hernia and group B streptococcal septicemia
 SWISS SOCIETY OF NEONATOLOGY Delayed-onset right-sided congenital diaphragmatic hernia and group B streptococcal septicemia September 2003 2 Saner C, Burtscher R, Hunziker U, Zimmermann-Bär U, Department
SWISS SOCIETY OF NEONATOLOGY Delayed-onset right-sided congenital diaphragmatic hernia and group B streptococcal septicemia September 2003 2 Saner C, Burtscher R, Hunziker U, Zimmermann-Bär U, Department
SWISS SOCIETY OF NEONATOLOGY. Kartagener s syndrome: Neonatal respiratory distress as initial symptom of primary ciliary dyskinesia
 SWISS SOCIETY OF NEONATOLOGY Kartagener s syndrome: Neonatal respiratory distress as initial symptom of primary ciliary dyskinesia MAY 2005 2 Christen M, and Berger TM, Neonatal and Pediatric Intensive
SWISS SOCIETY OF NEONATOLOGY Kartagener s syndrome: Neonatal respiratory distress as initial symptom of primary ciliary dyskinesia MAY 2005 2 Christen M, and Berger TM, Neonatal and Pediatric Intensive
HeartCode PALS. PALS Actions Overview > Legend. Contents
 HeartCode PALS PALS Actions Overview > Legend Action buttons (round buttons) Clicking a round button initiates an action. Clicking this button, for example, checks the child s carotid pulse. Menu buttons
HeartCode PALS PALS Actions Overview > Legend Action buttons (round buttons) Clicking a round button initiates an action. Clicking this button, for example, checks the child s carotid pulse. Menu buttons
Home-Made Continuous Positive Airways Pressure Device may Reduce Mortality in Neonates with Respiratory Distress in Low-Resource Setting
 JOURNAL OF TROPICAL PEDIATRICS, VOL. 60, NO. 5, 2014 Home-Made Continuous Positive Airways Pressure Device may Reduce Mortality in Neonates with Respiratory Distress in Low-Resource Setting by Subhashchandra
JOURNAL OF TROPICAL PEDIATRICS, VOL. 60, NO. 5, 2014 Home-Made Continuous Positive Airways Pressure Device may Reduce Mortality in Neonates with Respiratory Distress in Low-Resource Setting by Subhashchandra
H: Respiratory Care. Saskatchewan Association of Licensed Practical Nurses, Competency Profile for LPNs, 3rd Ed. 79
 H: Respiratory Care Saskatchewan Association of Licensed Practical Nurses, Competency Profile for LPNs, 3rd Ed. 79 Competency: H-1 Airway Management H-1-1 H-1-2 H-1-3 H-1-4 H-1-5 Demonstrate knowledge
H: Respiratory Care Saskatchewan Association of Licensed Practical Nurses, Competency Profile for LPNs, 3rd Ed. 79 Competency: H-1 Airway Management H-1-1 H-1-2 H-1-3 H-1-4 H-1-5 Demonstrate knowledge
PEPP Course: PEPP BLS Pretest
 PEPP Course: PEPP BLS Pretest 1. What is the best way to administer oxygen to a child in moderate respiratory distress? Nasal cannula Simple mask Nonrebreathing mask Bag-valve-mask device 2. A 2-year-old
PEPP Course: PEPP BLS Pretest 1. What is the best way to administer oxygen to a child in moderate respiratory distress? Nasal cannula Simple mask Nonrebreathing mask Bag-valve-mask device 2. A 2-year-old
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE 1 Guideline title SCOPE Bronchiolitis: diagnosis and management of bronchiolitis in children. 1.1 Short title Bronchiolitis in children 2 The remit The
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE 1 Guideline title SCOPE Bronchiolitis: diagnosis and management of bronchiolitis in children. 1.1 Short title Bronchiolitis in children 2 The remit The
SWISS SOCIETY OF NEONATOLOGY. Preterm infant with. pulmonary hypertension and hypopituitarism
 SWISS SOCIETY OF NEONATOLOGY Preterm infant with pulmonary hypertension and hypopituitarism November 2007 2 Pilgrim S, Stocker M, Neonatal and Pediatric Intensiv Care Unit, Children s Hospital of Lucerne,
SWISS SOCIETY OF NEONATOLOGY Preterm infant with pulmonary hypertension and hypopituitarism November 2007 2 Pilgrim S, Stocker M, Neonatal and Pediatric Intensiv Care Unit, Children s Hospital of Lucerne,
PUMANI bcpap GUIDELINES FOR CLINICIANS. An Overview of the Pumani bcpap, Indications for bcpap, and Instructions for Use
 An Overview of the Pumani bcpap, Indications for bcpap, and Instructions for Use What is bcpap? bcpap stands for bubble Continuous Positive Airway Pressure. Sometimes called Continuous Distending Pressure,
An Overview of the Pumani bcpap, Indications for bcpap, and Instructions for Use What is bcpap? bcpap stands for bubble Continuous Positive Airway Pressure. Sometimes called Continuous Distending Pressure,
GE Healthcare. Non Invasive Ventilation (NIV) For the Engström Ventilator. Relief, Relax, Recovery
 GE Healthcare Non Invasive Ventilation (NIV) For the Engström Ventilator Relief, Relax, Recovery COPD is currently the fourth leading cause of death in the world, and further increases in the prevalence
GE Healthcare Non Invasive Ventilation (NIV) For the Engström Ventilator Relief, Relax, Recovery COPD is currently the fourth leading cause of death in the world, and further increases in the prevalence
CLINICAL CONSIDERATIONS FOR THE BUNNELL LIFE PULSE HIGH-FREQUENCY JET VENTILATOR
 CLINICAL CONSIDERATIONS FOR THE BUNNELL LIFE PULSE HIGH-FREQUENCY JET VENTILATOR 801-467-0800 Phone 800-800-HFJV (4358) Hotline TABLE OF CONTENTS Respiratory Care Considerations..3 Physician Considerations
CLINICAL CONSIDERATIONS FOR THE BUNNELL LIFE PULSE HIGH-FREQUENCY JET VENTILATOR 801-467-0800 Phone 800-800-HFJV (4358) Hotline TABLE OF CONTENTS Respiratory Care Considerations..3 Physician Considerations
County of Santa Clara Emergency Medical Services System
 County of Santa Clara Emergency Medical Services System Policy #700-M12: Continuous Positive Airway Pressure CONTINUOUS POSITIVE AIRWAY PRESSURE Effective: February 8, 2013TBD Replaces: NewFebruary 8,
County of Santa Clara Emergency Medical Services System Policy #700-M12: Continuous Positive Airway Pressure CONTINUOUS POSITIVE AIRWAY PRESSURE Effective: February 8, 2013TBD Replaces: NewFebruary 8,
SARASOTA MEMORIAL HOSPITAL NURSING PROCEDURE
 SARASOTA MEMORIAL HOSPITAL TITLE: NURSING PROCEDURE Management, Monitoring & Documentation of a Clinically Significant Cardiopulmonary Event (CSCPE) (NUR47) DATE: REVIEWED: PAGES: 9/09 9/17 1 of 6 PS1094
SARASOTA MEMORIAL HOSPITAL TITLE: NURSING PROCEDURE Management, Monitoring & Documentation of a Clinically Significant Cardiopulmonary Event (CSCPE) (NUR47) DATE: REVIEWED: PAGES: 9/09 9/17 1 of 6 PS1094
Objectives. Apnea Definition and Pitfalls. Pathophysiology of Apnea. Apnea of Prematurity and hypoxemia episodes 5/18/2015
 Apnea of Prematurity and hypoxemia episodes Deepak Jain MD Care of Sick Newborn Conference May 2015 Objectives Differentiating between apnea and hypoxemia episodes. Pathophysiology Diagnosis of apnea and
Apnea of Prematurity and hypoxemia episodes Deepak Jain MD Care of Sick Newborn Conference May 2015 Objectives Differentiating between apnea and hypoxemia episodes. Pathophysiology Diagnosis of apnea and
Usefulness of DuoPAP in the treatment of very low birth weight preterm infants with neonatal respiratory distress syndrome
 European Review for Medical and Pharmacological Sciences 2015; 19: 573-577 Usefulness of DuoPAP in the treatment of very low birth weight preterm infants with neonatal respiratory distress syndrome B.
European Review for Medical and Pharmacological Sciences 2015; 19: 573-577 Usefulness of DuoPAP in the treatment of very low birth weight preterm infants with neonatal respiratory distress syndrome B.
Neonatal Resuscitation in What is new? How did we get here? Steven Ringer MD PhD Harvard Medical School May 25, 2011
 Neonatal Resuscitation in 2011- What is new? How did we get here? Steven Ringer MD PhD Harvard Medical School May 25, 2011 Conflicts I have no actual or potential conflict of interest in relation to this
Neonatal Resuscitation in 2011- What is new? How did we get here? Steven Ringer MD PhD Harvard Medical School May 25, 2011 Conflicts I have no actual or potential conflict of interest in relation to this
ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv
 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv.8.18.18 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) SUDDEN PROGRESSIVE FORM OF ACUTE RESPIRATORY FAILURE ALVEOLAR CAPILLARY MEMBRANE BECOMES DAMAGED AND MORE
ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv.8.18.18 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) SUDDEN PROGRESSIVE FORM OF ACUTE RESPIRATORY FAILURE ALVEOLAR CAPILLARY MEMBRANE BECOMES DAMAGED AND MORE
NASDAQ: WINT. April 2016
 NASDAQ: WINT April 2016 Forward Looking Statement To the extent that statements in this presentation are not strictly historical, including statements about the Company s business strategy, outlook, objectives,
NASDAQ: WINT April 2016 Forward Looking Statement To the extent that statements in this presentation are not strictly historical, including statements about the Company s business strategy, outlook, objectives,
Simulation 08: Cyanotic Preterm Infant in Respiratory Distress
 Flow Chart Simulation 08: Cyanotic Preterm Infant in Respiratory Distress Opening Scenario Section 1 Type: DM As staff therapist assigned to a Level 2 NICU in a 250 bed rural medical center you are called
Flow Chart Simulation 08: Cyanotic Preterm Infant in Respiratory Distress Opening Scenario Section 1 Type: DM As staff therapist assigned to a Level 2 NICU in a 250 bed rural medical center you are called
CHEST DRAIN PROTOCOL
 CHEST DRAIN PROTOCOL Rationale The pleural membranes have an important role in effective lung expansion. The visceral pleura is a thin, smooth, serous membrane covering the surface of the lungs and is
CHEST DRAIN PROTOCOL Rationale The pleural membranes have an important role in effective lung expansion. The visceral pleura is a thin, smooth, serous membrane covering the surface of the lungs and is
Von Reuss and CPAP, Disclosures CPAP. Noninvasive respiratory therapieswhy bother? Noninvasive respiratory therapies- types
 Noninvasive respiratory therapiesby a nose? NEO- The Conference for Neonatology February 21, 2014 Disclosures I have no relevant financial relationships to disclose or conflicts of interest to release.
Noninvasive respiratory therapiesby a nose? NEO- The Conference for Neonatology February 21, 2014 Disclosures I have no relevant financial relationships to disclose or conflicts of interest to release.
Emergency Medicine High Velocity Nasal Insufflation (Hi-VNI) VAPOTHERM POCKET GUIDE
 Emergency Medicine High Velocity Nasal Insufflation (Hi-VNI) VAPOTHERM POCKET GUIDE Indications for Vapotherm High Velocity Nasal Insufflation (Hi-VNI ) administration, the patient should be: Spontaneously
Emergency Medicine High Velocity Nasal Insufflation (Hi-VNI) VAPOTHERM POCKET GUIDE Indications for Vapotherm High Velocity Nasal Insufflation (Hi-VNI ) administration, the patient should be: Spontaneously
Kugelman A, Riskin A, Said W, Shoris I, Mor F, Bader D.
 Heated, Humidified High-Flow Nasal Cannula (HHHFNC) vs. Nasal Intermittent Positive Pressure Ventilation (NIPPV) for the Primary Treatment of RDS, A Randomized, Controlled, Prospective, Pilot Study Kugelman
Heated, Humidified High-Flow Nasal Cannula (HHHFNC) vs. Nasal Intermittent Positive Pressure Ventilation (NIPPV) for the Primary Treatment of RDS, A Randomized, Controlled, Prospective, Pilot Study Kugelman
Favorable long-term outcome of a patient with ABCA3 gene mutations and severe neonatal lung disease
 SWISS SOCIETY OF NEONATOLOGY Winner of the Case of the Year Award 2011 Favorable long-term outcome of a patient with ABCA3 gene mutations and severe neonatal lung disease FEBRUARY 2011 2 Morgillo D, Fontana
SWISS SOCIETY OF NEONATOLOGY Winner of the Case of the Year Award 2011 Favorable long-term outcome of a patient with ABCA3 gene mutations and severe neonatal lung disease FEBRUARY 2011 2 Morgillo D, Fontana
Chest X rays and Case Studies. No disclosures. Outline 5/31/2018. Carlo Manalo, M.D. Department of Radiology Loma Linda University Children s Hospital
 Chest X rays and Case Studies Carlo Manalo, M.D. Department of Radiology Loma Linda University Children s Hospital No disclosures. Outline Importance of history Densities delineated on radiography An approach
Chest X rays and Case Studies Carlo Manalo, M.D. Department of Radiology Loma Linda University Children s Hospital No disclosures. Outline Importance of history Densities delineated on radiography An approach
Competency Indicators Pediatrics Registered Nurse
 Hospital Logo Competency Indicators Pediatrics Registered Nurse mployee Name: Review Key: = ducation Session valuation Key: Able to perform & document A: Airway assessment: mployee Describes unique airway
Hospital Logo Competency Indicators Pediatrics Registered Nurse mployee Name: Review Key: = ducation Session valuation Key: Able to perform & document A: Airway assessment: mployee Describes unique airway
5/3/2012. Goals and Objectives HFNC. High-Flow Oxygen Therapy: Real Benefit or Just a Fad?
 High-Flow Oxygen Therapy: Real Benefit or Just a Fad? Timothy R. Myers MBA, RRT-NPS Director, Women s & Children s Respiratory Care & Procedural Services and Pediatric Heart Center Rainbow Babies & Children
High-Flow Oxygen Therapy: Real Benefit or Just a Fad? Timothy R. Myers MBA, RRT-NPS Director, Women s & Children s Respiratory Care & Procedural Services and Pediatric Heart Center Rainbow Babies & Children
Nasal CPAP in Neonatology: We Can Do Better
 Nasal CPAP in Neonatology: We Can Do Better COI Disclosure I do not have any conflict of interest, nor will I be discussing any off-label product use. This class has no commercial support or sponsorship,
Nasal CPAP in Neonatology: We Can Do Better COI Disclosure I do not have any conflict of interest, nor will I be discussing any off-label product use. This class has no commercial support or sponsorship,
SWISS SOCIETY OF NEONATOLOGY. Prenatal diagnosis and postnatal management of meconium pseudocysts
 SWISS SOCIETY OF NEONATOLOGY Prenatal diagnosis and postnatal management of meconium pseudocysts September 2007 2 Burch E, Caduff JH, Hodel M, Berger TM, Neonatal and Pediatric Intensive Care Unit (BE,
SWISS SOCIETY OF NEONATOLOGY Prenatal diagnosis and postnatal management of meconium pseudocysts September 2007 2 Burch E, Caduff JH, Hodel M, Berger TM, Neonatal and Pediatric Intensive Care Unit (BE,
COMPLICATED STAPHYLOCOCCAL INFECTION IN A NEONATE. A. Ansary*, D. Varghese, L. Jackson ROYAL HOSPITAL FOR CHILDREN, GLASGOW,UK
 COMPLICATED STAPHYLOCOCCAL INFECTION IN A NEONATE A. Ansary*, D. Varghese, L. Jackson ROYAL HOSPITAL FOR CHILDREN, GLASGOW,UK Complicated staphylococcal infection in a neonate Overview Case Radiology/biochemistry/microbiology
COMPLICATED STAPHYLOCOCCAL INFECTION IN A NEONATE A. Ansary*, D. Varghese, L. Jackson ROYAL HOSPITAL FOR CHILDREN, GLASGOW,UK Complicated staphylococcal infection in a neonate Overview Case Radiology/biochemistry/microbiology
 NEONATAL LIFE SUPPORT PROVIDER (NLSP) CERTIFICATION EXAMINATION 1. To determine if an infant requires resuscitation, you must rapidly assess gestation period, presence of meconium in amniotic fluid, breaths
NEONATAL LIFE SUPPORT PROVIDER (NLSP) CERTIFICATION EXAMINATION 1. To determine if an infant requires resuscitation, you must rapidly assess gestation period, presence of meconium in amniotic fluid, breaths
SWISS SOCIETY OF NEONATOLOGY. Prolonged arterial hypotension due to propofol used for endotracheal intubation in a newborn infant
 SWISS SOCIETY OF NEONATOLOGY Prolonged arterial hypotension due to propofol used for endotracheal intubation in a newborn infant July 2001 2 Wagner B, Intensive Care Unit, University Children s Hospital
SWISS SOCIETY OF NEONATOLOGY Prolonged arterial hypotension due to propofol used for endotracheal intubation in a newborn infant July 2001 2 Wagner B, Intensive Care Unit, University Children s Hospital
MODULE VII. Delivery and Immediate Neonatal Care
 MODULE VII Delivery and Immediate Neonatal Care NEONATAL ASPHYXIA About one million deaths per year In Latin America 12% of newborns suffer some degree of asphyxia Main cause of perinatal and neonatal
MODULE VII Delivery and Immediate Neonatal Care NEONATAL ASPHYXIA About one million deaths per year In Latin America 12% of newborns suffer some degree of asphyxia Main cause of perinatal and neonatal
Airway Clearance Devices
 Print Page 1 of 11 Wisconsin.gov home state agencies subject directory department of health services Search Welcome» August 2, 2018 5:18 PM Program Name: BadgerCare Plus and Medicaid Handbook Area: Durable
Print Page 1 of 11 Wisconsin.gov home state agencies subject directory department of health services Search Welcome» August 2, 2018 5:18 PM Program Name: BadgerCare Plus and Medicaid Handbook Area: Durable
Introducing Infant Flow Advance SIPAP. By Joanne Cookson March 2008
 Introducing Infant Flow Advance SIPAP By Joanne Cookson March 2008 Aim To introduce clinical practioners to the new SiPAP machine Objectives To define what is SiPAP To look at different modes able to be
Introducing Infant Flow Advance SIPAP By Joanne Cookson March 2008 Aim To introduce clinical practioners to the new SiPAP machine Objectives To define what is SiPAP To look at different modes able to be
SWISS SOCIETY OF NEONATOLOGY. Vein of Galen aneurysm: Aneurysmal characteristics and clinical features as predictive factors
 SWISS SOCIETY OF NEONATOLOGY Vein of Galen aneurysm: Aneurysmal characteristics and clinical features as predictive factors April 2010 2 Pronzini F, Fontijn J, Fauchère JC, Bucher HU, Clinic of Neonatology,
SWISS SOCIETY OF NEONATOLOGY Vein of Galen aneurysm: Aneurysmal characteristics and clinical features as predictive factors April 2010 2 Pronzini F, Fontijn J, Fauchère JC, Bucher HU, Clinic of Neonatology,
Dr. AM MAALIM KPA 2018
 Dr. AM MAALIM KPA 2018 Journey Towards Lung protection Goals of lung protection Strategies Summary Conclusion Before 1960: Oxygen; impact assessed clinically. The 1960s:President JFK, Ventilators mortality;
Dr. AM MAALIM KPA 2018 Journey Towards Lung protection Goals of lung protection Strategies Summary Conclusion Before 1960: Oxygen; impact assessed clinically. The 1960s:President JFK, Ventilators mortality;
MODULE VII. Delivery and Immediate Neonatal Care
 MODULE VII Delivery and Immediate Neonatal Care NEONATAL ASPHYXIA About one million deaths per year In Latin America 12% of newborns suffer some degree of asphyxia A major cause of perinatal and neonatal
MODULE VII Delivery and Immediate Neonatal Care NEONATAL ASPHYXIA About one million deaths per year In Latin America 12% of newborns suffer some degree of asphyxia A major cause of perinatal and neonatal
Alexander A Schult, M.D., FCCP. October 21, 2017 Revised 1/10/18
 Alexander A Schult, M.D., FCCP October 21, 2017 Revised 1/10/18 Identifying normal anatomy Identifying various pathologic states Identifying placement of hardware Identifying limitations of portable CXR
Alexander A Schult, M.D., FCCP October 21, 2017 Revised 1/10/18 Identifying normal anatomy Identifying various pathologic states Identifying placement of hardware Identifying limitations of portable CXR
Pedi-Cap CO 2 detector
 Pedi-Cap CO 2 detector Presentation redeveloped for this program by Rosemarie Boland from an original presentation by Johnston, Adams & Stewart, (2006) Background Clinical methods of endotracheal tube
Pedi-Cap CO 2 detector Presentation redeveloped for this program by Rosemarie Boland from an original presentation by Johnston, Adams & Stewart, (2006) Background Clinical methods of endotracheal tube
New Zealand Data Sheet. Poractant alfa (Phospholipid fraction of porcine lung) 80 mg/ml
 CUROSURF New Zealand Data Sheet Poractant alfa (Phospholipid fraction of porcine lung) 80 mg/ml Presentation Sterile suspension in single-dose vials for intratracheal or intrabronchial administration.
CUROSURF New Zealand Data Sheet Poractant alfa (Phospholipid fraction of porcine lung) 80 mg/ml Presentation Sterile suspension in single-dose vials for intratracheal or intrabronchial administration.
Guidelines and Best Practices for Vapotherm High Velocity Nasal Insufflation (Hi-VNI ) NICU POCKET GUIDE
 Guidelines and Best Practices for Vapotherm High Velocity Nasal Insufflation (Hi-VNI ) TM NICU POCKET GUIDE Patient Selection Diagnoses Patient presents with one or more of the following symptoms: These
Guidelines and Best Practices for Vapotherm High Velocity Nasal Insufflation (Hi-VNI ) TM NICU POCKET GUIDE Patient Selection Diagnoses Patient presents with one or more of the following symptoms: These
Case Report NeonatalPneumopericardiuminaNonventilatedTermInfant:A Case Report and Review of the Literature
 Hindawi Case Reports in Pediatrics Volume 2017, Article ID 3149370, 4 pages https://doi.org/10.1155/2017/3149370 Case Report NeonatalPneumopericardiuminaNonventilatedTermInfant:A Case Report and Review
Hindawi Case Reports in Pediatrics Volume 2017, Article ID 3149370, 4 pages https://doi.org/10.1155/2017/3149370 Case Report NeonatalPneumopericardiuminaNonventilatedTermInfant:A Case Report and Review
Newborn Life Support. NLS guidance.
 Kelly Harvey, ANNP NWNODN, previously Wythenshawe Hospital has shared this presentation with the understanding that it is for personal use following your attendance at the 8th Annual Senior Neonatal Nursing
Kelly Harvey, ANNP NWNODN, previously Wythenshawe Hospital has shared this presentation with the understanding that it is for personal use following your attendance at the 8th Annual Senior Neonatal Nursing
SWISS SOCIETY OF NEONATOLOGY. Local fibrinolysis with r-tpa in a newborn with brachial artery thrombosis
 SWISS SOCIETY OF NEONATOLOGY Local fibrinolysis with r-tpa in a newborn with brachial artery thrombosis January 2001 2 Dyroff C, Berger TM, Treumann T, Neonatal and Pediatric Intensive Care Unit (DC, BTM),
SWISS SOCIETY OF NEONATOLOGY Local fibrinolysis with r-tpa in a newborn with brachial artery thrombosis January 2001 2 Dyroff C, Berger TM, Treumann T, Neonatal and Pediatric Intensive Care Unit (DC, BTM),
CPAP failure in preterm infants: incidence, predictors and consequences
 CPAP failure in preterm infants: incidence, predictors and consequences SUPPLEMENTAL TEXT METHODS Study setting The Royal Hobart Hospital has an 11-bed combined Neonatal and Paediatric Intensive Care Unit
CPAP failure in preterm infants: incidence, predictors and consequences SUPPLEMENTAL TEXT METHODS Study setting The Royal Hobart Hospital has an 11-bed combined Neonatal and Paediatric Intensive Care Unit
Duct Dependant Congenital Heart Disease
 Children s Acute Transport Service Clinical Guidelines Duct Dependant Congenital Heart Disease This guideline has been agreed by both NTS & CATS Document Control Information Author CATS/NTS Author Position
Children s Acute Transport Service Clinical Guidelines Duct Dependant Congenital Heart Disease This guideline has been agreed by both NTS & CATS Document Control Information Author CATS/NTS Author Position
Blood Gases / Acid-Base
 Blood Gases / Acid-Base Neonatal Ventilation Workshop June 2010 Dr. Julian Eason Consultant Neonatologist Why are blood gases performed? Diagnostic assessment of oxygenation capacity of lungs Therapeutic
Blood Gases / Acid-Base Neonatal Ventilation Workshop June 2010 Dr. Julian Eason Consultant Neonatologist Why are blood gases performed? Diagnostic assessment of oxygenation capacity of lungs Therapeutic
Capnography: The Most Vital of Vital Signs. Tom Ahrens, PhD, RN, FAAN Research Scientist, Barnes-Jewish Hospital, St. Louis, MO May, 2017
 Capnography: The Most Vital of Vital Signs Tom Ahrens, PhD, RN, FAAN Research Scientist, Barnes-Jewish Hospital, St. Louis, MO May, 2017 Assessing Ventilation and Blood Flow with Capnography Capnography
Capnography: The Most Vital of Vital Signs Tom Ahrens, PhD, RN, FAAN Research Scientist, Barnes-Jewish Hospital, St. Louis, MO May, 2017 Assessing Ventilation and Blood Flow with Capnography Capnography
Steven Ringer MD PhD April 5, 2011
 Steven Ringer MD PhD April 5, 2011 Disclaimer Mead Johnson sponsors programs such as this to give healthcare professionals access to scientific and educational information provided by experts. The presenter
Steven Ringer MD PhD April 5, 2011 Disclaimer Mead Johnson sponsors programs such as this to give healthcare professionals access to scientific and educational information provided by experts. The presenter
Subspecialty Rotation: Anesthesia
 Subspecialty Rotation: Anesthesia Faculty: John Heaton, M.D. GOAL: Maintenance of Airway Patency and Oxygenation. Recognize and manage upper airway obstruction and desaturation. Recognize and manage upper
Subspecialty Rotation: Anesthesia Faculty: John Heaton, M.D. GOAL: Maintenance of Airway Patency and Oxygenation. Recognize and manage upper airway obstruction and desaturation. Recognize and manage upper
Acute Paediatric Respiratory Pathway
 Guideline for the use of high Flow Nasal Cannula Oxygen Therapy (Optiflow or Airvo) in Children with Bronchiolitis or an acute respiratory illness Introduction: High flow nasal cannula (HFNC) oxygen enables
Guideline for the use of high Flow Nasal Cannula Oxygen Therapy (Optiflow or Airvo) in Children with Bronchiolitis or an acute respiratory illness Introduction: High flow nasal cannula (HFNC) oxygen enables
Neonatal Resuscitation Using a Nasal Cannula: A Single-Center Experience
 Original Article Neonatal Resuscitation Using a Nasal Cannula: A Single-Center Experience Pedro Paz, MD, MPH 1 Rangasamy Ramanathan, MD 1,2 Richard Hernandez, RCP 2 Manoj Biniwale, MD 1 1 Division of Neonatal
Original Article Neonatal Resuscitation Using a Nasal Cannula: A Single-Center Experience Pedro Paz, MD, MPH 1 Rangasamy Ramanathan, MD 1,2 Richard Hernandez, RCP 2 Manoj Biniwale, MD 1 1 Division of Neonatal
Anatomy & Physiology
 1 Anatomy & Physiology Heart is divided into four chambers, two atrias & two ventricles. Atrioventricular valves (tricuspid & mitral) separate the atria from ventricles. they open & close to control flow
1 Anatomy & Physiology Heart is divided into four chambers, two atrias & two ventricles. Atrioventricular valves (tricuspid & mitral) separate the atria from ventricles. they open & close to control flow
Aim: Reduction in the rate of CLD in ELBW infants (<1000 grams) by 30% from its baseline of 72 % by January 2016.
 LIVE (Less Invasive Ventilation of ELBW infants) HEALTHY WVU Children s Hospital, Morgantown, WV, USA Rebecca Tilley, RN; Jamie Karr, RT; Tiffany Blosser, RN; Christy Dixon, RT; Melinda Connolly, ANP;
LIVE (Less Invasive Ventilation of ELBW infants) HEALTHY WVU Children s Hospital, Morgantown, WV, USA Rebecca Tilley, RN; Jamie Karr, RT; Tiffany Blosser, RN; Christy Dixon, RT; Melinda Connolly, ANP;
SWISS SOCIETY OF NEONATOLOGY. Neonatal gastric perforation
 SWISS SOCIETY OF NEONATOLOGY Neonatal gastric perforation September 2002 2 Zankl A, Stähelin J, Roth K, Boudny P and Zeilinger G, Children s Hospital of Aarau (ZA, SJ, RK, ZG) and Institute of Pathology
SWISS SOCIETY OF NEONATOLOGY Neonatal gastric perforation September 2002 2 Zankl A, Stähelin J, Roth K, Boudny P and Zeilinger G, Children s Hospital of Aarau (ZA, SJ, RK, ZG) and Institute of Pathology
BTS Guidelines for Home Oxygen in Children
 ISSN 2040-2023 August 2009 BTS Guidelines for Home Oxygen in Children A Quick Reference Guide British Thoracic Society www.brit-thoracic.org.uk HOME OXYGEN IN CHILDREN BTS GUIDELINES FOR HOME OXYGEN IN
ISSN 2040-2023 August 2009 BTS Guidelines for Home Oxygen in Children A Quick Reference Guide British Thoracic Society www.brit-thoracic.org.uk HOME OXYGEN IN CHILDREN BTS GUIDELINES FOR HOME OXYGEN IN
Arabian Gulf University Kingdom of Bahrain Year 5 Pediatrics 3 rd Week Discussion with Dr. Muna Al-Jufairi (Part 2)
 Arabian Gulf University Kingdom of Bahrain Year 5 Pediatrics 3 rd Week Discussion with Dr. Muna Al-Jufairi (Part 2) - Case 1: a 32 weeks preterm developed RDS 4 hours after delivery. Chest X-ray shows:
Arabian Gulf University Kingdom of Bahrain Year 5 Pediatrics 3 rd Week Discussion with Dr. Muna Al-Jufairi (Part 2) - Case 1: a 32 weeks preterm developed RDS 4 hours after delivery. Chest X-ray shows:
SWISS SOCIETY OF NEONATOLOGY. Cantrell s pentalogy: an unusual midline defect
 SWISS SOCIETY OF NEONATOLOGY Cantrell s pentalogy: an unusual midline defect October 2004 2 Cevey-Macherel MN, Meijboom EJ, Di Bernardo S, Truttmann AC, Division of Neonatology and Division of Pediatric
SWISS SOCIETY OF NEONATOLOGY Cantrell s pentalogy: an unusual midline defect October 2004 2 Cevey-Macherel MN, Meijboom EJ, Di Bernardo S, Truttmann AC, Division of Neonatology and Division of Pediatric
PEMSS PROTOCOLS INVASIVE PROCEDURES
 PEMSS PROTOCOLS INVASIVE PROCEDURES Panhandle Emergency Medical Services System SURGICAL AND NEEDLE CRICOTHYROTOMY Inability to intubate is the primary indication for creating an artificial airway. Care
PEMSS PROTOCOLS INVASIVE PROCEDURES Panhandle Emergency Medical Services System SURGICAL AND NEEDLE CRICOTHYROTOMY Inability to intubate is the primary indication for creating an artificial airway. Care
