Alain Vonlaufen, M.D.; Jeremy S. Wilson, M.D.; Romano C. Pirola, M.D.; and Minoti V. Apte, Ph.D.
|
|
|
- Reynard Gardner
- 5 years ago
- Views:
Transcription
1 Role of Alcohol Metabolism in Chronic Pancreatitis Alain Vonlaufen, M.D.; Jeremy S. Wilson, M.D.; Romano C. Pirola, M.D.; and Minoti V. Apte, Ph.D. Alcohol abuse is the major cause of chronic inflammation of the pancreas (i.e., chronic pancreatitis). Although it has long been thought that alcoholic pancreatitis is a chronic disease from the outset, evidence is accumulating to indicate that chronic damage in the pancreas may result from repeated attacks of acute tissue inflammation and death (i.e., necroinflammation). Initially, research into the pathogenesis of alcoholic pancreatitis was related to ductular and sphincteric abnormalities. In recent years, the focus has shifted to the type of pancreas cell that produces digestive juices (i.e., acinar cell). Alcohol now is known to exert a number of toxic effects on acinar cells. Notably, acinar cells have been shown to metabolize alcohol (i.e., ethanol) via both oxidative (i.e., involving oxygen) and nonoxidative pathways. The isolation and study of pancreatic stellate cells (PSCs) the key effectors in the development of connective tissue fibers (i.e., fibrogenesis) in the pancreas has greatly enhanced our understanding of the pathogenesis of chronic pancreatitis. Pancreatic stellate cells become activated in response to ethanol and acetaldehyde, a toxic byproduct of alcohol metabolism. In addition, PSCs have the capacity to metabolize alcohol via alcohol dehydrogenase (the major oxidizing enzyme for ethanol). The fact that only a small percentage of heavy alcoholics develop chronic pancreatitis has led to the search for precipitating factors of the disease. Several studies have investigated whether variations in ethanol-metabolizing enzymes may be a trigger factor for chronic pancreatitis, but no definite relationship has been established so far. KEY WORDS: Alcohol abuse; ethanol metabolism; ethanol-toacetaldehyde metabolism; alcohol dehydrogenase (ADH); acetaldehyde; cytochrome P4502E1 (CYP2E1); reactive oxygen species (ROS); oxidation; pancreas; chronic pancreatitis; acute pancreatitis; alcoholic pancreatitis; acinar cell; pancreatic stellate cells (PSCs); fatty acid ethyl esters (FAEEs); genetic factors; genetic polymorphisms The pancreas is a gland that secretes digestive juices which are carried to the small intestine by the biliary system, which consists of the gallbladder and a network of ducts. When the pancreas becomes inflamed, its digestive enzymes leak out and begin to attack the pancreas itself. These enzymes cause damage that results in swelling of tissues and blood vessels. There are two forms of inflammation of the pancreas (i.e., pancreatitis). Acute pancreatitis occurs when the pancreas suddenly becomes inflamed but then improves. Chronic pancreatitis (CP) is a progressive inflammatory disease leading to irreversible destruction of the pancreas. It is characterized by a spectrum of symptoms ranging from pain the cardinal initial symptom in most cases to maldigestion and diabetes. The major cause (i.e., etiology) of CP is alcohol abuse. It also is associated with genetic mutations (i.e., hereditary CP), autoimmunity, excessive production of the parathyroid hormone (i.e., hyperparathyroidism), and a type of pancreatitis seen in tropical countries (i.e., tropical pancreatitis). In a certain number of cases, CP remains etiologically undetermined (i.e., idiopathic CP) (Steer et al. 1993). The reported incidence of the disease varies widely among countries, and it remains unclear whether this is attributable to genuine regional differences or to lack of standardized diagnostic criteria. Epidemiological studies and animal experiments suggest that alcohol, per se, is not sufficient to induce the disease. As a matter of fact, less than 10 percent of heavy alcohol users (180 g/day or about 15 drinks/day for 10 to 15 years) eventually develop clinically overt alcoholic pancreatitis. Researchers have analyzed several predisposing factors, such as the amount and pattern of drinking, smoking, dietary habits, and genetic mutations particularly those of alcohol-metabo- ALAIN VONLAUFEN, M.D., is a visiting fellow and J.S. WILSON, M.D., is a professor; both at the South Western Sydney Clinical School, University of New South Wales, Sydney, Australia. ROMANO C. PIROLA, M.D., is a conjoint associate professor at the Faculty of Medicine, University of New South Wales, Sydney, Australia. MINOTI V. APTE, Ph.D., is an associate professor at the South Western Sydney Clinical School, University of New South Wales, Sydney, Australia. 48
2 Alcohol Metabolism in Chronic Pancreatitis lizing enzymes but none of these factors has been firmly linked to the development of alcoholic CP (Ammann 2001). Several theories about how alcohol might lead to pancreatic disease have emerged over the past decades. Whereas early work had predominantly focused on the effects of alcohol on the muscle at the surface of the first part of the small intestine (i.e., duodenum), which controls secretions from the liver, pancreas, and gallbladder into the duodenum (i.e., the sphincter of Oddi), and on the pancreatic ducts (see Figure 1), attention has shifted over the past decade to the influence of alcohol on the clusters of secretory cells (i.e., acini) that produce pancreatic juice containing digestive enzymes. Studies with acini or pancreatic acinar cells grown in the laboratory (i.e., cultured cells) have established the ability of the pancreas to metabolize alcohol via oxidative and nonoxidative pathways and have provided new insights into the toxic effects of alcohol and the byproducts of its metabolism (i.e., metabolites) on the gland. Furthermore, a new era in the understanding of the pathophysiological mechanisms of scar tissue formation in the pancreas (i.e., pancreatic fibrosis) gallbladder duodenum has dawned with the recent identification and culture of pancreatic stellate cells (PSCs), the key effector cells in fibrogenesis. Of particular interest is the finding that these cells have the capacity to metabolize alcohol. This article reviews past theories and current knowledge about the pathophysiology of chronic alcoholic pancreatitis, with particular emphasis on alcohol metabolism by acinar and stellate cells and on the toxic effects of alcohol and its metabolites on these cells. Effects of Alcohol on the Pancreas It now is generally accepted that alcoholic acute and chronic pancreatitis are the same disease at different stages. Repeated episodes of tissue inflammation and death (i.e., necroinflammation) in the pancreas lead to periductular obstructive scarring and protein plug formation and eventually extensive fibrosis (i.e., necrosis fibrosis sequence). This sequence is further supported by the fact that patients with frequent episodes of acute pancreatitis progress more rapidly to chronic disease (Ammann and Muellhaupt 1994). pancreas Figure 1 Illustrated are the pancreas, gallbladder, and duodenum. Effect of Alcohol on the Sphincter of Oddi Initial research on the effects of alcohol on the pancreas focused on sphincter of Oddi activity. This work was based on so called sphincteric theories aiming to implicate reflux of the gallbladder and bile ducts (i.e., biliary tract) or duodeno-pancreatic reflux as the causative factor in alcoholic pancreatits. Several human studies yielded conflicting results with reports of both decreased and increased sphincter of Oddi activity upon ethanol exposure (Apte et al. 1998a). However, the latter phenomenon of ethanol exposure causing spasms in the sphincter of Oddi has been given more credit by recent evidence in animals (Sonoda et al. 2005) and by the fact that pancreatic secretion is decreased after acute alcohol intake in humans (Hajnal et al. 1990). Effects of Alcohol on Small Ducts Another theory states that alcohol affects the character of pancreatic fluid to favor the formation of protein plugs and stones. Contact of the stones with the ductal epithelial cells potentially could lead to ulceration, scarring, further obstruction, and finally atrophy and fibrosis. This hypothesis is supported by the findings that alcohol (1) reduces pancreatic secretions (as stated earlier); (2) leads to increased viscosity of pancreatic secretions; (3) decreases citrate concentration in pancreatic juice, a known predisposing factor for crystal formation; and (4) produces proteins thought to increase stone formation, such as pancreatic stone protein (PSP) and glycoprotein-2 (GP-2) (Stevens et al. 2004; Apte et al. 1997). However, it remains difficult to prove whether ductal stones are a cause or an effect of CP. It is possible to imagine that the formation of protein plugs could contribute to smallduct obstruction. A prototypical example of such a disease mechanism is represented by cystic fibrosis, which is known to enhance the viscosity of pancreatic secretions hence promoting stone formation and significantly Vol. 30, No. 1,
3 increasing the risk of CP in affected individuals. Direct Toxic Effects of Ethanol on Acinar Cells Given the failure of the sphincteric and ductular obstruction theories to fully explain the pathogenesis of alcoholic pancreatitis, the attention of researchers has shifted over the past 10 years toward the acinar cells, the most abundant cells in the pancreas. The acinar cell constitutes an enzyme factory that produces millions of digestive enzyme molecules every day. These enzymes are produced as inactive precursors, packed into stable vesicles (i.e., zymogen granules), and segregated from cellular componenets that can break down other cellular components (i.e., lysosomal enzymes) in order to avoid premature activation. It has been consistently shown in various animal models that one of the first events in acute experimental pancreatitis consists of the premature activation of digestive enzymes within the acinar cell by co-segregation of zymogen granules with lysosomal enzymes, particularly cathepsin B. This and other toxic effects of ethanol on acinar cells are depicted in Figure 2 and described below. Effect of Ethanol on Pancreatic Enzymes Experimental studies have shown that alcohol consumption leads to an increased amount of digestive (trypsin, chymotrypsin, and lipase) and lysosomal (cathepsin B) enzymes and concurrently increases lysosome and zymogen granule fragility. This is thought to facilitate contact between lysosomal and digestive enzymes, thereby predisposing the cell to breakdown by its own enzymes (i.e., autodigestion). The effect of alcohol on lysosomal fragility may be mediated by cholesterol esters and toxic substances that accumulate in the pancreas after chronic alcohol intake (i.e., fatty acid ethyl esters [FAEEs]). It also has been shown that ethanol administration in rats decreases levels of GP-2, a glycoprotein known to stabilize the membranes of zymogen granules (Apte et al. 1997). Recent work by Wang and colleagues (2006) indicates that chronic ethanol consumption in rats decreases controlled cell death (i.e., aptoptosis) and increases the production of cathepsin B, thereby potentially promoting necrotic changes in the pancreas. Metabolism of Ethanol by Acinar Cells Toxic metabolites of ethanol are known to have adverse effects on several organs in the body. Researchers have therefore focused on the capacity of the functional cells of the pancreas to metabolize alcohol. Based on studies in the liver, it is well known that the metabolism of ethanol via oxidative and nonoxidative pathways generates the toxic metabolites acetaldehyde and FAEEs, respectively. The oxidative pathway is catalyzed predominantly by the enzyme alcohol dehydrogenase (ADH), with relatively minor contributions by cytochrome P450 2E1 (CYP2E1) and catalase. The nonoxidative pathway of ethanol involves a chemical reaction (i.e., esterification) of ethanol with fatty acids, resulting in the formation of FAEEs. The enzymes that catalyze FAEE production (i.e., FAEE synthases) still need to be fully characterized, but putative candidates include carboxylester lipase and triglyceride lipase (Wilson and Apte 2003). Using cultures of acinar cells or isolated pancreatic acini, researchers now have firmly established that pancreatic acinar cells are capable of metabolizing ethanol via both the oxidative and the nonoxidative pathways (Haber et al. 1998, 2004; Gukovskaya et al. 2002). Concerning the oxidative pathways, the predominant variation (i.e., isoform) of ADH in acinar cells appears to be ADH3, a nonsaturable form 1 of the enzyme with low affinity and a high K m for ethanol. CYP2E1 has been described in human and rat pancreas. As previously observed in the liver, its expression is inducible in the pancreas of alcohol-fed rats. Regarding the nonoxidative pathway of ethanol metabolism, the pancreas appears to accumulate more FAEEs after ethanol abuse than any other functional as opposed to structural organ. Although FAEEs may be transported to the pancreas from the liver via the circulation, it now has been shown that these compounds (predoniminantly ethyl pamitate) are synthesized in the pancreas itself. Notably, FAEE synthase activity reportedly is higher in the pancreas (3.5- to 10-fold) than in the liver (Wilson and Apte 2003). Werner and colleagues (2002) have tried to establish a link between the two metabolic pathways for ethanol. They have reported that in the presence of inhibitors of oxidative metabolism, the generation of FAEEs in isolated acini is increased compared with FAEE generation in the absence of inhibitors. The authors also have shown that in vivo infusion of ethanol with inhibitors of oxidative metabolism leads to increased FAEE accumulation in the rat pancreas. As a consequence of the above studies, the rates of ethanol metabolism via the oxidative and the nonoxidative pathways recently have been compared in rat pancreatic acini incubated with the same concentration of alcohol (100 micromoles 2 [µm]). The rate of oxidative metabolism was 21 fold higher compared with the rate of nonoxidative metabolism (Haber et al. 2004; Gukovskaya et al. 2002). This finding does not diminish the importance of the nonoxidative metabolism of ethanol in the pancreas. Indeed, concentrations of the products of this pathway (FAEEs) in the pancreas (in the range of 50 µm) have been shown to be sufficient to cause pancreatic injury (Haber et al. 1993). Effects of Toxic Metabolites of Alcohol Acetaldehyde and reactive oxygen species (ROS) (products of ethanol oxidation) as well as FAEEs all have 1 A nonsaturable form of an enzyme cannot be saturated (i.e., its activity is not limited) even by very high concentrations of the substrate (i.e. alcohol). 2 A micromole represents a concentration of 1/1,000,000 (one millionth) molecular weight per liter (mol/l). 50
4 Alcohol Metabolism in Chronic Pancreatitis been shown to cause deleterious effects on the pancreas. At high concentrations, acetaldehyde induces morphological alterations in the rat and dog pancreas (Majumdar et al. 1986; Nordback et al. 1991). Furthermore, it inhibits stimulated secretion by the enzyme cholecystokinin from isolated rat pancreatic acini. This phenomenon is thought to be the result of acetaldehyde interfering Stellate cell activation Oxidant stress CE FAEE Cytokines Ac Necrosis Oxidant stress CE and FAEE with the binding of cholecystokinin to its cellular communication sites (i.e., receptors) and to a disruption in the functioning of cell components (i.e., microtubulues) responsible for transporting intracellular compartments. ROS are highly reactive compounds that potentially are harmful to cell membranes, intracellular proteins, and DNA. Oxidant stress results from an imbalance between the production Enzyme activation L ETH A N O L ZG mrna Figure 2 The Figure depicts an overall hypothesis for the pathogenesis of alcoholic pancreatitis. It is postulated that ethanol, its metabolites, and oxidant stress exert a number of toxic effects on pancreatic acinar cells, which predispose the gland to autodigestive injury. These include the following: (1) Destabilization of lysosomes (L) and zymogen granules (ZG). This destabilization is mediated by oxidant stress; cholesteryl esters (CEs), which are known to accumulate in the pancreas during ethanol consumption; and fatty acid ethyl esters (FAEEs), which are nonoxidative metabolites of alcohol. (2) Increased digestive and lysosomal enzyme content attributed to increased synthesis (increased mrna) and impaired secretion. These changes sensitize the cell such that in the presence of an appropriate trigger/co-factor overt injury is initiated (alcoholic acute pancreatitis). Cytokines released during alcohol-induced necroinflammation activate pancreatic stellate cells (PSCs). In addition, PSCs are activated directly by ethanol, most likely via its metabolism to acetaldehyde (Ac) and the subsequent generation of oxidant stress. Activated PSCs then synthesize excess amounts of extracellular matrix proteins leading to pancreatic fibrosis. of ROS and the defense mechanisms (the antioxidant glutathione and the enzymes glutathione peroxidase, superoxide dismutase, and catalase) within the cell. This may be the result of (1) the generation of ROS during oxidation of ethanol by CYP2E1 and (2) acetaldehyde-induced depletion of the ROS scavenger glutathione. Oxidant stress is thought to destabilize zymogen granules and lysosomes, potentially increasing the risk of intra-acinar activation of digestive enzymes (Apte et al. 2003). As noted earlier, FAEEs are produced by the nonoxidative metabolism of ethanol. These compounds have been shown to accumulate in rat pancreas and to cause acinar cell damage in vitro by inducing lysosomal fragility (Haber et al. 1993). Infusion of FAEEs in rats leads to the activation of trypsinogen, the precursor to the enzyme trypsin, and subsequent morphological alterations consistent with acute pancreatitis. Furthermore, in vivo studies have shown that FAEE infusion leads to increased deposition of material that is part of the tissue but not part of any cell (i.e., extracellular matrix) in the rat pancreas, a feature that might be relevant to the development of alcohol-induced fibrosis (Lugea et al. 2003). Studies to date suggest that FAEEs exert their toxicity by a number of different mechanisms, including (1) direct interaction with cellular membranes; (2) promotion of cholesteryl esters, which accumulate in the rat pancreas after chronic ethanol intake and destabilize lysosomal membranes; (3) activation of transcription factors 3 known to regulate the production of molecules involved in the inflammatory response (i.e., cytokines); (4) the release of free fatty acids by the break down (i.e., hydrolysis) of FAEEs, a process thought to contribute to damage in cellular structures called mitochondria; and (5) disruption of calcium homoeostasis in pancreatic acinar cells. 3 Transcription factors are proteins involved in the process that uses DNA to make proteins. Vol. 30, No. 1,
5 Recent research has focused on cell signaling events as mediators of ethanolinduced pancreatic injury. Gukovskaya and colleagues (2002) have shown that ethanol and its metabolite acetaldehyde regulate the transcription factors nuclear factor κb (NFκB) and AP-1 in acinar cells. These signaling molecules are implicated in cytokine production. Recently, more light has been shed on another mechanism of FAEE toxicity in the cell the disruption of calcium homeostasis in acinar cells. In vitro work has shown that the FAEE palmitoleic acid ethyl ester induces a significant increase of calcium in the substance filling the acinar cell (i.e., acinar cell cytoplasm). This is caused by dysfunction of membrane-bound enzymes called ATPases that hydrolyze the ester to its free fatty acid, palmitoleic acid. Palmitoleic acid appears to disrupt the mitochondrial oxidative chain, leading to deficient production of the energy-producing molecule adenosine triphosphate (ATP), calcium overload, and cell death. These recent findings describe specific pathways that might be targeted therapeutically to reduce the noxious effects of alcohol on the pancreas (Criddle et al. 2006). Pancreatic Stellate Cells One of the key features in the microscopic examination of alcoholic CP is pancreatic fibrosis. Decisive advances in our understanding of pancreatic fibrosis have been made by the ability to isolate and culture PSCs (Apte et al. 1998b). Their critical role in pancreatic fibrogenesis now is firmly established. Stellate cells are located in the vicinity of the base or bottom part (i.e., basal aspect) of acinar cells. In the normal pancreas, stellate cells exist in an inactive (i.e., quiescent) state, identifiable by the presence of vitamin A containing fat (i.e., lipid) droplets in the cytoplasm and positive immunostaining 4 for proteins 4 Immunostaining refers to any use of an antibody-based method to detect a specific protein in a sample. that make up the cell s structure (i.e., cytoskeletal proteins), such as desmin and glial acidic fibrillary protein. In health, these cells are thought to play a role in extracellular matrix turnover via their ability to synthesize extracellular matrix proteins as well as matrixdegrading enzymes (matrix metalloproteinases [MMPs]). Evidence from in vitro and in vivo studies indicates that, during pancreatic injury, PSCs can be activated by profibrogenic growth factors, such as transforming growth factor-beta (TGF-β); proliferative growth factors such as plateletderived growth factor (PDGF); proinflammatory cytokines; and oxidant stress (Apte and Wilson 2003). This state of activation is characterized by the loss of vitamin A droplets, the production of alpha smooth muscle actin (α-sma, a cytoskeletal protein), and increased production of extracellular matrix proteins such as collagens I and III, fibronectin, and laminin. Of note, activated PSCs also produce increased amounts of MMP2 (known to degrade the structural protein collagen, thereby facilitating the deposition of fiber-forming collagen observed in pancreatic fibrosis) and of its inhibitor, tissue inhibitor of metalloproteinase 2 (TIMP2). Of particular interest to the pathogenesis of chronic alcoholic pancreatitis is the finding that PSCs are activated by exposure to physiologically relevant concentrations of ethanol (10 and 50 mm [i.e., 1 to 2 and 8 to 10 standard drinks], respectively), corresponding to blood alcohol concentrations encountered during social drinking and heavy alcohol consumption respectively) or acetyldehyde (150 and 200 mm) as assessed by increased α-sma expression and collagen synthesis. It also has been shown that exposure of PSCs to ethanol and acetaldehyde in vitro increases the secretion of MMP2, which may contribute to pancreatic fibrosis, as described above. Interestingly, stellate cells have been shown to exhibit ADH (isoform 1) activity that is induced by exposure to ethanol at a concentration of 50 mm. Inhibition of ADH1 and the conversion of ethanol to acetaldehyde abolished PSC activation, suggesting that the effect of ethanol on the cells is mediated by its oxidation to acetaldehyde. Both ethanol and acetaldehyde caused oxidant stress in cultured PSCs. Incubation of PSCs with ethanol or acetyldehyde in the presence of the antioxidant vitamin E prevented PSC activation (Apte et al. 2000). Taken together, the above findings suggest that ethanol-induced PSC activation is mediated via the metabolism of ethanol to acetaldehyde and the subsequent generation of oxidant stress within the cells. Another pathway of stellate cell activation by alcohol might be related to its common metabolism with compounds chemically related to vitamin A (i.e., retinoids). As mentioned earlier, storage of vitamin A is a key feature of quiescent stellate cells both in the liver and in the pancreas. Importantly, quiescence of stellate cells in the liver has been shown to depend on sufficient concentrations of the retinol metabolite retinoic acid in the liver. It has been demonstrated in the liver that ethanol competitively inhibits retinol metabolism by retinol dehydrogenase and aldehyde dehydrogenase because these enzymes can degrade both ethanol and retinol. This is supported by the recent finding that the inhibitory effect of vitamin A on PSC activation partially can be reversed in the presence of ethanol (McCarroll et al. 2006). Thus, vitamin A may represent a potential therapeutic strategy for chronic pancreatitis, given its ability to inhibit PSC activation and synthesis of extracellular matrix proteins. Role of Genetic Variations in Ethanol-Metabolizing Enzymes It is evident from the above that alcohol exerts constant and toxic effects on different cellular compartments in the pancreas, predisposing the gland to autodigestion, necroinflammation, and fibrosis. As stated earlier, the risk of alcoholic acute and chronic pancreatitis increases with increasing intake of ethanol. However, only a 52
6 Alcohol Metabolism in Chronic Pancreatitis minority of heavy drinkers will develop clinically evident pancreatitis, suggesting that additional co-factors are required to trigger overt disease. Efforts have been made to identify risk factors over the past 20 years, including dietary factors, smoking, amount and type of alcohol consumed, pattern of drinking, lipid intolerance, and inherited factors. Given that pancreatic ethanol metabolism appears to play a significant role in the pathophysiology of pancreatitis, it is not unreasonable to speculate that variations (i.e., polymorphism) in ethanol-metabolizing enzymes might be a modifying factor of the disease. Researchers have conducted numerous case control studies in an attempt to link polymorphisms of ethanol-metabolizing enzymes to alcohol-related pancreatic damage. Such studies of potential risk factors for alcoholic pancreatitis ideally should compare alcoholics without pancreatic disease with alcoholics displaying pancreatic injury, but this has not always been the case. Frenzer and colleagues (2002) conducted a case control study comparing the genes for ADH2, ADH3, ALDH2, and CYP2E1 in 57 Caucasian patients with alcoholic cirrhosis, 71 patients with alcoholic CP, 57 alcoholics without any apparent organ damage, and 200 healthy blood donors. The authors were able to detect a definite association between the genetic variation ADH3*2/*2 and possibly ADH2*1/*1 and alcoholic cirrhosis. However, no association was found between the above polymorphisms and CP. An earlier case control study, conducted in Chinese patients, analyzed ADH2, ADH3, ALDH2, and CYP2E1 genes in patients with acute alcoholic pancreatitis, in alcoholic patients without organ damage, in patients with pancreatic disease of nonalcoholic origin, and in patients with alcoholic liver disease. This study found that the frequency of the ALDH2*1 gene variant (i.e., allele) was significantly increased in alcoholics compared with nonalcoholic control subjects. No significant difference in terms of polymorphism between alcoholic pancreatitis and alcohol abuse without organ damage could be found. It must be noted, however, that the control group of heavy drinkers without organ damage was small (19 patients) and may not be a representative cohort (Chao et al. 1997). A recent case control study conducted by Verlaan and colleagues (2004) compared ADH3 and CYP2E1 polymorphism in 82 patients with alcoholic CP, 21 patients with hereditary pancreatitis, 39 patients with idiopathic pancreatitis, 93 alcoholic and 128 healthy control subjects. All subjects were of Caucasian origin. No significant difference between patients with CP of various etiologies and controls was observed, although the diagnosis of CP was not based on uniform criteria. Nonetheless, the researchers reported a trend to a higher frequency of a particular allele for CYP2E1 (i.e., the intron 6D allele) in patients with alcoholic CP compared with healthy or alcoholic control subjects. Most recently, a Japanese study (Miyasaka et al. 2005) has reported a promising association between the risk of developing pancreatitis and a polymorphism of the gene for one of the candidate FAEE synthase enzymes (i.e., carboxyl ester lipase [CEL]) and the risk of developing alcoholic pancreatitis. The authors examined a polymorphism (the VNTR polymorphism) in the coding region of the CEL gene. The significance of this polymorphism is not yet clearly defined, but it has been suggested that it might influence protein stability and/or secretion. The study included a population of 100 alcoholic subjects with CP, 52 alcoholic subjects, 50 nonalcoholic pancreatitis patients, 96 patients with elevated levels of lipids in the bloodstream (hyperlipidemia), and 435 control subjects. The frequency of the usual (wildtype) gene was significantly diminished in patients with alcoholic pancreatitis compared with the other groups, including alcoholic subjects without organ damage. In summary, current data fail to establish an unequivocal link between any polymorphism of ethanol-oxidizing enzymes and the risk of alcoholic pancreatitis. With respect to the nonoxidative pathway of ethanol metabolism, the polymorphism of CEL is of interest, but the functional significance of this polymorphism is yet to be defined. Conclusion There now is sufficient evidence that the pancreas has the capacity to metabolize ethanol via both oxidative and the nonoxidative pathways. The resulting metabolites and their byproducts (oxygen radicals) exert a toxic effect on the pancreas, leading to acute and chronic changes, but the susceptibility factor that triggers overt disease remains to be identified. The capacity of PSCs to metabolize alcohol and to become activated under the influence of acetaldehyde and oxidant stress are key features with respect to the role of these cells in alcoholic pancreatic fibrosis. Further studies designed to characterize the metabolism of ethanol by PSCs via the oxidative and nonoxidative pathways are awaited. Financial Disclosure The authors declare that they have no competing financial interests. References AMMANN, R.W. The natural history of alcoholic chronic pancreatitis. Internal Medicine 40(5): , PMID: AMMANN, R.W., AND MUELLHAUPT, B. Progression of alcoholic acute to chronic pancreatitis. Gut 35(4): , PMID: APTE, M.V.; HABER, P.S.; APPLEGATE, T.L.; ET AL.; Periacinar stellate shaped cells in rat pancreas identification, isolation, and culture. Gut 43: , 1998a. APTE, M.V.; HABER, P.S.; NORTON, I.D.; AND WILSON, J.S. Alcohol and the pancreas. Addiction Biology 3:137-50, 1998b. APTE, M.V.; NORTON, I.D.; HABER, P.S.; ET AL. Chronic ethanol administration decreases rat pancreatic GP2 content. Biochimica et Biohysica Acta 1336(1):89 98, PMID: Vol. 30, No. 1,
7 APTE, M.V.; PHILLIPS, P.A.; FAHMY, R.; ET AL. Does alcohol directly stimulate pancreatic fibrogenesis? Studies with rat pancreatic stellate cells. Gastroenterology 118: , PMID: APTE, M.V., AND WILSON, J.S.; Stellate cell activation in alcoholic pancreatitis. Pancreas 27(4): , PMID: CHAO, Y.C.; YOUNG, T.H.; TANG, H.S.; AND HSU, C.T. Alcoholism and alcoholic organ damage and genetic polymorphisms of alcohol metabolizing enzymes in Chinese patients. Hepatology 25: , PMID: CRIDDLE, D.N.; MURPHY, J.; FISTETTO, G.; ET AL. Fatty acid ethyl esters cause pancreatic calcium toxicity via inositol trisphosphate receptors and loss of ATP synthesis. Gastroenterology 130: , PMID: FRENZER, A.; BUTLER, W.J.; NORTON, I.D.; ET AL. Polymorphism in alcohol-metabolizing enzymes, glutathione S-transferases and apolipoprotein E and susceptibility to alcohol-induced cirrhosis and chronic pancreatitis. Journal of Gastroenterology and Hepatology 17: , PMID: GUKOVSKAYA, A.S.; MOURIA, M.; GUKOVSKY, I.; ET AL. Ethanol metabolism and transcription factor activation in pancreatic acinar cells in rats. Gastroenterology 122: , PMID: HABER, P.S.; WILSON, J.S.; APTE, M.V.; AND PIROLA, R.C. Fatty acid ethyl esters increase rat pancreatic lysosomal fragility. Journal of Laboratory and Clinical Medicine 121(6): , PMID: HABER, P.S.; APTE, M.V.; APPLEGATE, T.L.; ET AL. Metabolism of ethanol by rat pancreatic acinar cells. Journal of Laboratory and Clinical Medicine 132(4): , PMID: HABER, P.S.; APTE, M.V.; MORAN, C.; ET AL. Nonoxidative metabolism of ethanol by rat pancreatic acini. Pancreatology 4:82 89, PMID: HAJNAL, F.; FLORES, M.C.; RADLEY, S.; AND VALENZUELA, J.E. Effect of alcohol and alcoholic beverages on meal-stimulated pancreatic secretion in humans. Gastroenterology 98: , PMID: LUGEA, A.; GUKOVSKY, I.; GUKOVSKAYA, A.S.; AND PANDOL, S.J. Nonoxidative ethanol metabolites alter extracellular matrix protein content in rat pancreas. Gastroenterology 125: , PMID: MAJUMDAR, A.P.; VESENKA, G.D.; DUBICK, M.A.; ET AL. Morphological and biochemical changes in the pancreas of rats treated with acetaldehyde. American Journal of Physiology 250:G , PMID: MCCARROLL, J.A.; PHILLIPS, P.A.; SANTUCCI, N.; ET AL. Vitamin A inhibits pancreatic stellate cell activation: Implications for treatment of pancreatic fibrosis. Gut 55:79 89, PMID: MIYASAKA, K.; OHTA, M.; TAKANO, S.; ET AL. Carboxylester lipase gene polymorphism as a risk of alcohol-induced pancreatitis. Pancreas 30(4):e87 e91, PMID: NORDBACK, I.H.; MACGOWAN, S.; POTTER, J.J.; AND CAMERON, J.L. The role of acetaldehyde in the pathogenesis of acute alcoholic pancreatitis. Annals of Surgery 214: , PMID: STEER, M.L. Etiology and pathophysiology of acute pancreatitis. In: Go, V.L.; Di Magno, E.P.; Gardner, J.D.; et al., eds. The Pancreas: Biology, Pathobiology, and Disease. New York: Raven Press, 1993, pp STEVENS, T.; CONWELL, D.L.; AND ZUCCARO, G. Pathogenesis of chronic pancreatitis: An evidencebased review of past theories and recent developments. American Journal of Gastroenterology 99: , PMID: SONODA, Y.; WOODS, C.M.; TOOULI, J.; AND SACCONE, G.T.P. Intragastric ethanol reduces sphincter of Oddi function in the anaesthetized Australian possum. Pancreas 31:469, VERLAAN, M.; TE MORSCHE, R.H.; ROELOFS, H.M.; ET AL. Genetic polymorphisms in alcoholmetabolizing enzymes and chronic pancreatitis. Alcohol & Alcoholism 39(1): 20 24, PMID: WANG, Y.L.; HU, R.; LUGEA, A.; ET AL. Ethanol feeding alters death signaling in the pancreas. Pancreas 32(4): , PMID: WERNER, J.; SAGHIR, M.; WARSHAW, A.L.; ET AL. Alcoholic pancreatitis in rats: Injury from nonoxidative metabolites of ethanol. American Journal of Physiology Gastrointestinal and Liver Physiology 283:G65 73, PMID: WILSON, J.S., AND APTE, M.V. Role of alcohol metabolism in alcoholic pancreatitis. Pancreas 27(4): , PMID:
Pancreas composed of 2 parts: 1- exocrine gland 2- endocrine gland
 pancreas Pancreas composed of 2 parts: 1- exocrine gland 2- endocrine gland Acute pancreatitis Inflammation of the pancreas associated with acinar cell injury Clinical features: 1-abdominal pain cardinal
pancreas Pancreas composed of 2 parts: 1- exocrine gland 2- endocrine gland Acute pancreatitis Inflammation of the pancreas associated with acinar cell injury Clinical features: 1-abdominal pain cardinal
Diseases of exocrine pancreas
 Diseases of exocrine pancreas The exocrine pancreas constitutes 80% to 85% of the organ and is composed of acinar cells that secrete enzymes needed for digestion. the accessory duct of Santorini, the main
Diseases of exocrine pancreas The exocrine pancreas constitutes 80% to 85% of the organ and is composed of acinar cells that secrete enzymes needed for digestion. the accessory duct of Santorini, the main
Week 3 The Pancreas: Pancreatic ph buffering:
 Week 3 The Pancreas: A gland with both endocrine (secretion of substances into the bloodstream) & exocrine (secretion of substances to the outside of the body or another surface within the body) functions
Week 3 The Pancreas: A gland with both endocrine (secretion of substances into the bloodstream) & exocrine (secretion of substances to the outside of the body or another surface within the body) functions
Chapter 15 Gastrointestinal System
 Chapter 15 Gastrointestinal System Dr. LL Wang E-mail: wanglinlin@zju.edu.cn Rm 608, Block B, Research Building, School of Medicine, Zijingang Campus Pancreatic Secretion The exocrine cells in the pancreas
Chapter 15 Gastrointestinal System Dr. LL Wang E-mail: wanglinlin@zju.edu.cn Rm 608, Block B, Research Building, School of Medicine, Zijingang Campus Pancreatic Secretion The exocrine cells in the pancreas
Molecular Mechanisms of Alcoholic Pancreatitis
 Dig Dis 2005;23:232 240 DOI: 10.1159/000090170 Molecular Mechanisms of Alcoholic M.V. Apte R.C. Pirola J.S. Wilson Pancreatic Research Group, University of New South Wales, Sydney, Australia Key Words
Dig Dis 2005;23:232 240 DOI: 10.1159/000090170 Molecular Mechanisms of Alcoholic M.V. Apte R.C. Pirola J.S. Wilson Pancreatic Research Group, University of New South Wales, Sydney, Australia Key Words
FIRST BIOCHEMISTRY EXAM Tuesday 25/10/ MCQs. Location : 102, 105, 106, 301, 302
 FIRST BIOCHEMISTRY EXAM Tuesday 25/10/2016 10-11 40 MCQs. Location : 102, 105, 106, 301, 302 The Behavior of Proteins: Enzymes, Mechanisms, and Control General theory of enzyme action, by Leonor Michaelis
FIRST BIOCHEMISTRY EXAM Tuesday 25/10/2016 10-11 40 MCQs. Location : 102, 105, 106, 301, 302 The Behavior of Proteins: Enzymes, Mechanisms, and Control General theory of enzyme action, by Leonor Michaelis
hydrolyzes ATP to exchange 3 Na + in for 2 K + out generate the transcellular Na + and K + gradients provides the electrochemical gradient
 Regulation of pancreatic excretory function by ion channels Viktoria Venglovecz 2015 Morphology of the pancreas Composition of pancreatic juice 1 2 liters of pancreatic juice per day acini secrete isotonic,
Regulation of pancreatic excretory function by ion channels Viktoria Venglovecz 2015 Morphology of the pancreas Composition of pancreatic juice 1 2 liters of pancreatic juice per day acini secrete isotonic,
The Digestive System. What is the advantage of a one-way gut? If you swallow something, is it really inside you?
 The Digestive System What is the advantage of a one-way gut?! If you swallow something, is it really inside you? Functions and Processes of the Digestive System: Move nutrients, water, electrolytes from
The Digestive System What is the advantage of a one-way gut?! If you swallow something, is it really inside you? Functions and Processes of the Digestive System: Move nutrients, water, electrolytes from
BIOL2171 ANU TCA CYCLE
 TCA CYCLE IMPORTANCE: Oxidation of 2C Acetyl Co-A 2CO 2 + 3NADH + FADH 2 (8e-s donated to O 2 in the ETC) + GTP (energy) + Heat OVERVIEW: Occurs In the mitochondrion matrix. 1. the acetyl portion of acetyl-coa
TCA CYCLE IMPORTANCE: Oxidation of 2C Acetyl Co-A 2CO 2 + 3NADH + FADH 2 (8e-s donated to O 2 in the ETC) + GTP (energy) + Heat OVERVIEW: Occurs In the mitochondrion matrix. 1. the acetyl portion of acetyl-coa
Cell Quality Control. Peter Takizawa Department of Cell Biology
 Cell Quality Control Peter Takizawa Department of Cell Biology Cellular quality control reduces production of defective proteins. Cells have many quality control systems to ensure that cell does not build
Cell Quality Control Peter Takizawa Department of Cell Biology Cellular quality control reduces production of defective proteins. Cells have many quality control systems to ensure that cell does not build
Cell Injury MECHANISMS OF CELL INJURY
 Cell Injury MECHANISMS OF CELL INJURY The cellular response to injurious stimuli depends on the following factors: Type of injury, Its duration, and Its severity. Thus, low doses of toxins or a brief duration
Cell Injury MECHANISMS OF CELL INJURY The cellular response to injurious stimuli depends on the following factors: Type of injury, Its duration, and Its severity. Thus, low doses of toxins or a brief duration
ESPEN Congress The Hague 2017
 ESPEN Congress The Hague 2017 Meeting nutritional needs of acute care patients Feeding acute pancreatitis patients J. Luttikhold (NL) FEEDING ACUTE PANCREATITIS PATIENTS Joanna Luttikhold, MD PhD Registrar
ESPEN Congress The Hague 2017 Meeting nutritional needs of acute care patients Feeding acute pancreatitis patients J. Luttikhold (NL) FEEDING ACUTE PANCREATITIS PATIENTS Joanna Luttikhold, MD PhD Registrar
Dean J. Tuma, Ph.D., and Carol A. Casey, Ph.D.
 Dangerous Byproducts of Alcohol Breakdown Focus on Adducts Dean J. Tuma, Ph.D., and Carol A. Casey, Ph.D. Alcohol breakdown in the liver results in the generation of the reactive molecule acetaldehyde
Dangerous Byproducts of Alcohol Breakdown Focus on Adducts Dean J. Tuma, Ph.D., and Carol A. Casey, Ph.D. Alcohol breakdown in the liver results in the generation of the reactive molecule acetaldehyde
Cell Adaptation, Cell Injury and Cell Death
 Cell Adaptation, Cell Injury and Cell Death Pathology:- is the study of structural and functional abnormalities that are expressed as diseases of organs and systems. Modern pathology, proposed that injury
Cell Adaptation, Cell Injury and Cell Death Pathology:- is the study of structural and functional abnormalities that are expressed as diseases of organs and systems. Modern pathology, proposed that injury
1) Four main feeding mechanisms of animals a) Suspension feeders i) (1) Humpback whales b) Substrate feeders i)
 1 AP Biology March 2008 Digestion Chapter 41 Homeostatic mechanisms manage an animal s energy budget. 1) Four main feeding mechanisms of animals Suspension feeders (1) Humpback whales Substrate feeders
1 AP Biology March 2008 Digestion Chapter 41 Homeostatic mechanisms manage an animal s energy budget. 1) Four main feeding mechanisms of animals Suspension feeders (1) Humpback whales Substrate feeders
Digestion and Absorption
 Digestion and Absorption Digestion and Absorption Digestion is a process essential for the conversion of food into a small and simple form. Mechanical digestion by mastication and swallowing Chemical digestion
Digestion and Absorption Digestion and Absorption Digestion is a process essential for the conversion of food into a small and simple form. Mechanical digestion by mastication and swallowing Chemical digestion
23.1 Lipid Metabolism in Animals. Chapter 23. Micelles Lipid Metabolism in. Animals. Overview of Digestion Lipid Metabolism in
 Denniston Topping Caret Copyright! The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Chapter 23 Fatty Acid Metabolism Triglycerides (Tgl) are emulsified into fat droplets
Denniston Topping Caret Copyright! The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Chapter 23 Fatty Acid Metabolism Triglycerides (Tgl) are emulsified into fat droplets
Pathophysiology ACUTE PANCREATITIS
 Pancreatitis Pathophysiology ACUTE PANCREATITIS BILIARY OBSTRUCTION Duct obstruction in the bile duct, pancreatic duct, or both. Increasing pressure Unregulated activation of digestive enzymes. Inflammation
Pancreatitis Pathophysiology ACUTE PANCREATITIS BILIARY OBSTRUCTION Duct obstruction in the bile duct, pancreatic duct, or both. Increasing pressure Unregulated activation of digestive enzymes. Inflammation
Identification of Serum mirnas as prospective Bio-markers for acute and chronic pancreatitis Dr. Jeyaparvathi Somasundaram
 Identification of Serum mirnas as prospective Bio-markers for acute and chronic pancreatitis Dr. Jeyaparvathi Somasundaram Assistant Professor, Department of Biotechnoloy, Lady Doak College, Madurai. Acute
Identification of Serum mirnas as prospective Bio-markers for acute and chronic pancreatitis Dr. Jeyaparvathi Somasundaram Assistant Professor, Department of Biotechnoloy, Lady Doak College, Madurai. Acute
Alcohol and Chronic Pancreatitis: Leading or Secondary Etiopathogenetic Role?
 AISP - 28th National Congress. Verona (Italy). October 28-30, 2004. Alcohol and Chronic Pancreatitis: Leading or Secondary Etiopathogenetic Role? Lucio Gullo Institute of Internal Medicine, St. Orsola
AISP - 28th National Congress. Verona (Italy). October 28-30, 2004. Alcohol and Chronic Pancreatitis: Leading or Secondary Etiopathogenetic Role? Lucio Gullo Institute of Internal Medicine, St. Orsola
Pancreatitis. Acute Pancreatitis
 Pancreatitis Pancreatitis is an inflammation of the pancreas. The pancreas is a large gland behind the stomach and close to the duodenum. The duodenum is the upper part of the small intestine. The pancreas
Pancreatitis Pancreatitis is an inflammation of the pancreas. The pancreas is a large gland behind the stomach and close to the duodenum. The duodenum is the upper part of the small intestine. The pancreas
Lipid Metabolism * OpenStax
 OpenStax-CNX module: m46462 1 Lipid Metabolism * OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 3.0 By the end of this section, you will be able
OpenStax-CNX module: m46462 1 Lipid Metabolism * OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 3.0 By the end of this section, you will be able
Mechanisms of Cell Injury
 Causes of Cell Injury 1- oxygen deprivation (anoxia) 2- physical agents 3- chemical agents 4- infections agents 5- immunologic reactions 6- genetic defects 7- nutritional imbalances Mechanisms of Cell
Causes of Cell Injury 1- oxygen deprivation (anoxia) 2- physical agents 3- chemical agents 4- infections agents 5- immunologic reactions 6- genetic defects 7- nutritional imbalances Mechanisms of Cell
shehab Moh Tarek ... ManarHajeer
 3 shehab Moh Tarek... ManarHajeer In the previous lecture we discussed the accumulation of oxygen- derived free radicals as a mechanism of cell injury, we covered their production and their pathologic
3 shehab Moh Tarek... ManarHajeer In the previous lecture we discussed the accumulation of oxygen- derived free radicals as a mechanism of cell injury, we covered their production and their pathologic
18. PANCREATIC FUNCTION AND METABOLISM. Pancreatic secretions ISLETS OF LANGERHANS. Insulin
 18. PANCREATIC FUNCTION AND METABOLISM ISLETS OF LANGERHANS Some pancreatic functions have already been discussed in the digestion section. In this one, the emphasis will be placed on the endocrine function
18. PANCREATIC FUNCTION AND METABOLISM ISLETS OF LANGERHANS Some pancreatic functions have already been discussed in the digestion section. In this one, the emphasis will be placed on the endocrine function
number Done by Corrected by Doctor Nayef Karadsheh
 number 17 Done by Abdulrahman Alhanbali Corrected by Lara Abdallat Doctor Nayef Karadsheh 1 P a g e Pentose Phosphate Pathway (PPP) Or Hexose Monophosphate Shunt In this lecture We will talk about the
number 17 Done by Abdulrahman Alhanbali Corrected by Lara Abdallat Doctor Nayef Karadsheh 1 P a g e Pentose Phosphate Pathway (PPP) Or Hexose Monophosphate Shunt In this lecture We will talk about the
Sphincters heartburn diaphragm The Stomach gastric glands pepsin, chyme The Small Intestine 1-Digestion Is Completed in the Small Intestine duodenum
 Sphincters are muscles that encircle tubes and act as valves. The tubes close when the sphincters contract and they open when the sphincters relax. When food or saliva is swallowed, the sphincter relaxes
Sphincters are muscles that encircle tubes and act as valves. The tubes close when the sphincters contract and they open when the sphincters relax. When food or saliva is swallowed, the sphincter relaxes
CHM333 LECTURE 34: 11/30 12/2/09 FALL 2009 Professor Christine Hrycyna
 Lipid Metabolism β-oxidation FA Acetyl-CoA Triacylglycerols (TAGs) and glycogen are the two major forms of stored energy in vertebrates Glycogen can supply ATP for muscle contraction for less than an hour
Lipid Metabolism β-oxidation FA Acetyl-CoA Triacylglycerols (TAGs) and glycogen are the two major forms of stored energy in vertebrates Glycogen can supply ATP for muscle contraction for less than an hour
Cell Physiology
 Cell Physiology 21-10-2018 1 The two major parts of a typical cell are the nucleus and the cytoplasm. The nucleus is separated from the cytoplasm by a nuclear membrane, and the cytoplasm is separated from
Cell Physiology 21-10-2018 1 The two major parts of a typical cell are the nucleus and the cytoplasm. The nucleus is separated from the cytoplasm by a nuclear membrane, and the cytoplasm is separated from
ANATOMY & PHYSIOLOGY ONLINE COURSE - SESSION 13 THE DIGESTIVE SYSTEM
 ANATOMY & PHYSIOLOGY ONLINE COURSE - SESSION 13 THE DIGESTIVE SYSTEM The digestive system also known as the alimentary canal or gastrointestinal tract consists of a series of hollow organs joined in a
ANATOMY & PHYSIOLOGY ONLINE COURSE - SESSION 13 THE DIGESTIVE SYSTEM The digestive system also known as the alimentary canal or gastrointestinal tract consists of a series of hollow organs joined in a
VDR GENE (Vitamin D Receptor)
 12 GENES EXPLAINED. VDR GENE (Vitamin D Receptor) What is the purpose of the VDR gene? The Vitamin D receptor gene influences the ability to efficiently use vitamin D. Healthy bone density and strength
12 GENES EXPLAINED. VDR GENE (Vitamin D Receptor) What is the purpose of the VDR gene? The Vitamin D receptor gene influences the ability to efficiently use vitamin D. Healthy bone density and strength
Nonalcoholic Steatohepatitis National Digestive Diseases Information Clearinghouse
 Nonalcoholic Steatohepatitis National Digestive Diseases Information Clearinghouse National Institute of Diabetes and Digestive and Kidney Diseases NATIONAL INSTITUTES OF HEALTH Nonalcoholic steatohepatitis
Nonalcoholic Steatohepatitis National Digestive Diseases Information Clearinghouse National Institute of Diabetes and Digestive and Kidney Diseases NATIONAL INSTITUTES OF HEALTH Nonalcoholic steatohepatitis
Liver ISSUES. by Academy EPIC
 Liver ISSUES by Academy EPIC www.academyepic.com Liver Functions produces glycogen from glucose breaks down glycogen into glucose converts non carbohydrates to glucose oxidizes fatty acids synthesizes
Liver ISSUES by Academy EPIC www.academyepic.com Liver Functions produces glycogen from glucose breaks down glycogen into glucose converts non carbohydrates to glucose oxidizes fatty acids synthesizes
Section Coordinator: Jerome W. Breslin, PhD, Assistant Professor of Physiology, MEB 7208, ,
 IDP Biological Systems Gastrointestinal System Section Coordinator: Jerome W. Breslin, PhD, Assistant Professor of Physiology, MEB 7208, 504-568-2669, jbresl@lsuhsc.edu Overall Learning Objectives 1. Characterize
IDP Biological Systems Gastrointestinal System Section Coordinator: Jerome W. Breslin, PhD, Assistant Professor of Physiology, MEB 7208, 504-568-2669, jbresl@lsuhsc.edu Overall Learning Objectives 1. Characterize
Energy Metabolism. Chapter Cengage Learning. All Rights Reserved.
 Energy Metabolism Chapter 7 Introduction Energy Heat, mechanical, electrical, and chemical Metabolism How the body uses foods to meet its needs Chemical Reactions in the Body Energy metabolism How body
Energy Metabolism Chapter 7 Introduction Energy Heat, mechanical, electrical, and chemical Metabolism How the body uses foods to meet its needs Chemical Reactions in the Body Energy metabolism How body
Energy, Chemical Reactions and Enzymes
 Phosphorylation Hydrolysis Energy, Chemical Reactions and Enzymes Chapter 2 (selections) What is Energy? Energy is the capacity to do work Potential Energy Kinetic Energy Chemical Bond Energy Like a rechargeable
Phosphorylation Hydrolysis Energy, Chemical Reactions and Enzymes Chapter 2 (selections) What is Energy? Energy is the capacity to do work Potential Energy Kinetic Energy Chemical Bond Energy Like a rechargeable
REGULATION OF ENZYME ACTIVITY. Medical Biochemistry, Lecture 25
 REGULATION OF ENZYME ACTIVITY Medical Biochemistry, Lecture 25 Lecture 25, Outline General properties of enzyme regulation Regulation of enzyme concentrations Allosteric enzymes and feedback inhibition
REGULATION OF ENZYME ACTIVITY Medical Biochemistry, Lecture 25 Lecture 25, Outline General properties of enzyme regulation Regulation of enzyme concentrations Allosteric enzymes and feedback inhibition
Control of Glucose Metabolism
 Glucose Metabolism Control of Glucose Metabolism The pancreas is both an exocrine and endocrine gland. It secretes digestive enzymes into the duodenum (exocrine) and 3 specific hormones into the bloodstream
Glucose Metabolism Control of Glucose Metabolism The pancreas is both an exocrine and endocrine gland. It secretes digestive enzymes into the duodenum (exocrine) and 3 specific hormones into the bloodstream
Pancreas Fox Chapter 18 part 2 (also Chapter 19.3 & 19.4)
 Vert Phys PCB3743 Pancreas Fox Chapter 18 part 2 (also Chapter 19.3 & 19.4) T. Houpt, Ph.D. Anatomy of Digestive System Peristalsis Stomach and Acid Secretion Liver and Bile Secretion Pancreas and pancreatic
Vert Phys PCB3743 Pancreas Fox Chapter 18 part 2 (also Chapter 19.3 & 19.4) T. Houpt, Ph.D. Anatomy of Digestive System Peristalsis Stomach and Acid Secretion Liver and Bile Secretion Pancreas and pancreatic
Day Date Title Instructor 5 th Ed 6 th Ed. Protein digestion and AA absorption
 Day Date Title Instructor 5 th Ed 6 th Ed 1 Tuesday 18 April 2017 Protein digestion and AA absorption D S Jairajpuri 250 256 250 256 2 Wednesday 19 April 2017 Removal of nitrogen and urea cycle D S Jairajpuri
Day Date Title Instructor 5 th Ed 6 th Ed 1 Tuesday 18 April 2017 Protein digestion and AA absorption D S Jairajpuri 250 256 250 256 2 Wednesday 19 April 2017 Removal of nitrogen and urea cycle D S Jairajpuri
The Cell Organelles. Eukaryotic cell. The plasma membrane separates the cell from the environment. Plasma membrane: a cell s boundary
 Eukaryotic cell The Cell Organelles Enclosed by plasma membrane Subdivided into membrane bound compartments - organelles One of the organelles is membrane bound nucleus Cytoplasm contains supporting matrix
Eukaryotic cell The Cell Organelles Enclosed by plasma membrane Subdivided into membrane bound compartments - organelles One of the organelles is membrane bound nucleus Cytoplasm contains supporting matrix
2. List routes of exposure in the order of most rapid response.
 Practice Test questions: 1. What are the two areas of toxicology that a regulatory toxicologist must integrate in order to determine the "safety" of any chemical? 2. List routes of exposure in the order
Practice Test questions: 1. What are the two areas of toxicology that a regulatory toxicologist must integrate in order to determine the "safety" of any chemical? 2. List routes of exposure in the order
10/23/2013 ANIMAL NUTRITION ANIMAL NUTRITION ESSENTIAL NUTRIENTS AN ANIMAL S DIET MUST STUPPLY: AMINO ACIDS
 ANIMAL NUTRITION Food is taken in, taken apart, and taken up in the process of animal nutrition In general, animals fall into three categories: Herbivores Carnivores Omnivores ANIMAL NUTRITION Chapter
ANIMAL NUTRITION Food is taken in, taken apart, and taken up in the process of animal nutrition In general, animals fall into three categories: Herbivores Carnivores Omnivores ANIMAL NUTRITION Chapter
Chronic Pancreatitis (1 of 4) i
 Chronic Pancreatitis (1 of 4) i If you need this information in another language or medium (audio, large print, etc) please contact the Customer Care Team on 0800 374 208 email: customercare@ salisbury.nhs.uk.
Chronic Pancreatitis (1 of 4) i If you need this information in another language or medium (audio, large print, etc) please contact the Customer Care Team on 0800 374 208 email: customercare@ salisbury.nhs.uk.
From Acute to Chronic Pancreatitis: The Role of Mutations in the Pancreatic Secretory Trypsin Inhibitor Gene
 From Acute to Chronic Pancreatitis: The Role of Mutations in the Pancreatic Secretory Trypsin Inhibitor Gene Masahiko Hirota, Kinuko Kuwata, Masaki Ohmuraya, Michio Ogawa Department of Surgery II, Kumamoto
From Acute to Chronic Pancreatitis: The Role of Mutations in the Pancreatic Secretory Trypsin Inhibitor Gene Masahiko Hirota, Kinuko Kuwata, Masaki Ohmuraya, Michio Ogawa Department of Surgery II, Kumamoto
Biochemistry: A Short Course
 Tymoczko Berg Stryer Biochemistry: A Short Course Second Edition CHAPTER 27 Fatty Acid Degradation Dietary Lipid (Triacylglycerol) Metabolism - In the small intestine, fat particles are coated with bile
Tymoczko Berg Stryer Biochemistry: A Short Course Second Edition CHAPTER 27 Fatty Acid Degradation Dietary Lipid (Triacylglycerol) Metabolism - In the small intestine, fat particles are coated with bile
Diseases of pancreas - Chronic pancreatitis
 Corso di laurea in Medicina e Chirurgia Anno accademico 2015-2016 V Anno di corso- Primo Semestre Corso Integrato : Patologia Sistemica C- Gastroenterologia Prof. Stefano Fiorucci Diseases of pancreas
Corso di laurea in Medicina e Chirurgia Anno accademico 2015-2016 V Anno di corso- Primo Semestre Corso Integrato : Patologia Sistemica C- Gastroenterologia Prof. Stefano Fiorucci Diseases of pancreas
Thyroid hormones derived from two iodinated tyrosine molecules
 Thyroid Hormones OBJECTIVES Chemical nature of the thyroid hormones How different enzymes play a role in thyroid hormone formation? And what drugs affect them? Describe Function & Metabolism of thyroid
Thyroid Hormones OBJECTIVES Chemical nature of the thyroid hormones How different enzymes play a role in thyroid hormone formation? And what drugs affect them? Describe Function & Metabolism of thyroid
DIGESTIVE SYSTEM II ACCESSORY DIGESTIVE ORGANS
 DIGESTIVE SYSTEM II ACCESSORY DIGESTIVE ORGANS Dr. Larry Johnson Texas A& M University Objectives Distinguish between the parotid and submandibular salivary glands. Understand and identify the structural
DIGESTIVE SYSTEM II ACCESSORY DIGESTIVE ORGANS Dr. Larry Johnson Texas A& M University Objectives Distinguish between the parotid and submandibular salivary glands. Understand and identify the structural
GENERAL CHARACTERISTICS OF THE ENDOCRINE SYSTEM FIGURE 17.1
 GENERAL CHARACTERISTICS OF THE ENDOCRINE SYSTEM FIGURE 17.1 1. The endocrine system consists of glands that secrete chemical signals, called hormones, into the blood. In addition, other organs and cells
GENERAL CHARACTERISTICS OF THE ENDOCRINE SYSTEM FIGURE 17.1 1. The endocrine system consists of glands that secrete chemical signals, called hormones, into the blood. In addition, other organs and cells
Chronic Pancreatitis
 Falk Symposium 161 October 12, 2007 Chronic Pancreatitis David C Whitcomb MD PhD Giant Eagle Foundation Professor of Cancer Genetics. Professor of Medicine, Cell biology & Physiology, and Human Genetics
Falk Symposium 161 October 12, 2007 Chronic Pancreatitis David C Whitcomb MD PhD Giant Eagle Foundation Professor of Cancer Genetics. Professor of Medicine, Cell biology & Physiology, and Human Genetics
Lipoproteins Metabolism Reference: Campbell Biochemistry and Lippincott s Biochemistry
 Lipoproteins Metabolism Reference: Campbell Biochemistry and Lippincott s Biochemistry Learning Objectives 1. Define lipoproteins and explain the rationale of their formation in blood. 2. List different
Lipoproteins Metabolism Reference: Campbell Biochemistry and Lippincott s Biochemistry Learning Objectives 1. Define lipoproteins and explain the rationale of their formation in blood. 2. List different
Introduction to pathology lecture 5/ Cell injury apoptosis. Dr H Awad 2017/18
 Introduction to pathology lecture 5/ Cell injury apoptosis Dr H Awad 2017/18 Apoptosis = programmed cell death = cell suicide= individual cell death Apoptosis cell death induced by a tightly regulated
Introduction to pathology lecture 5/ Cell injury apoptosis Dr H Awad 2017/18 Apoptosis = programmed cell death = cell suicide= individual cell death Apoptosis cell death induced by a tightly regulated
The Endocrine Pancreas (Chapter 10) *
 OpenStax-CNX module: m62118 1 The Endocrine Pancreas (Chapter 10) * Ildar Yakhin Based on The Endocrine Pancreas by OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons
OpenStax-CNX module: m62118 1 The Endocrine Pancreas (Chapter 10) * Ildar Yakhin Based on The Endocrine Pancreas by OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons
100 Points NAME: KEY Lab section:
 ANSC 324 Spring, 2007 EXAM 1 100 Points NAME: KEY Lab section: Instructions: Make sure that you take time to carefully read each question, and then answer the question appropriately. Answers to essay questions
ANSC 324 Spring, 2007 EXAM 1 100 Points NAME: KEY Lab section: Instructions: Make sure that you take time to carefully read each question, and then answer the question appropriately. Answers to essay questions
Chapter 20. Endocrine System Chemical signals coordinate body functions Chemical signals coordinate body functions. !
 26.1 Chemical signals coordinate body functions Chapter 20 Endocrine System! Hormones Chemical signals Secreted by endocrine glands Usually carried in the blood Cause specific changes in target cells Secretory
26.1 Chemical signals coordinate body functions Chapter 20 Endocrine System! Hormones Chemical signals Secreted by endocrine glands Usually carried in the blood Cause specific changes in target cells Secretory
1-It is to prevent back flow of fecal content from colon into small intestine.
 Function of the ileocecal valve: 1-It is to prevent back flow of fecal content from colon into small intestine. 2-The wall of the ileum for several centimeters preceding valve has a thickened muscular
Function of the ileocecal valve: 1-It is to prevent back flow of fecal content from colon into small intestine. 2-The wall of the ileum for several centimeters preceding valve has a thickened muscular
Chapter 9: Digestion Review Assignment
 _ Date: Mark: /45 Chapter 9: Digestion Review Assignment 45 Multiple Choice = 45 Marks Identify the choice that best completes the statement or answers the question. 1. Which of the following roles do
_ Date: Mark: /45 Chapter 9: Digestion Review Assignment 45 Multiple Choice = 45 Marks Identify the choice that best completes the statement or answers the question. 1. Which of the following roles do
VITAMINS-FAT SOLUBLE [LIPPINCOTT S ] Deeba S. Jairajpuri
![VITAMINS-FAT SOLUBLE [LIPPINCOTT S ] Deeba S. Jairajpuri VITAMINS-FAT SOLUBLE [LIPPINCOTT S ] Deeba S. Jairajpuri](/thumbs/88/115610056.jpg) VITAMINS-FAT SOLUBLE [LIPPINCOTT S 381-394] Deeba S. Jairajpuri VITAMIN A othe term retinoids includes both natural and synthetic forms of vitamin A essential for vision, reproduction, growth and maintenance
VITAMINS-FAT SOLUBLE [LIPPINCOTT S 381-394] Deeba S. Jairajpuri VITAMIN A othe term retinoids includes both natural and synthetic forms of vitamin A essential for vision, reproduction, growth and maintenance
Lipids digestion and absorption, Biochemistry II
 Lipids digestion and absorption, blood plasma lipids, lipoproteins Biochemistry II Lecture 1 2008 (J.S.) Triacylglycerols (as well as free fatty acids and both free and esterified cholesterol) are very
Lipids digestion and absorption, blood plasma lipids, lipoproteins Biochemistry II Lecture 1 2008 (J.S.) Triacylglycerols (as well as free fatty acids and both free and esterified cholesterol) are very
Arteriosclerosis & Atherosclerosis
 Arteriosclerosis & Atherosclerosis Arteriosclerosis = hardening of arteries = arterial wall thickening + loss of elasticity 3 types: -Arteriolosclerosis -Monckeberg medial sclerosis -Atherosclerosis Arteriosclerosis,
Arteriosclerosis & Atherosclerosis Arteriosclerosis = hardening of arteries = arterial wall thickening + loss of elasticity 3 types: -Arteriolosclerosis -Monckeberg medial sclerosis -Atherosclerosis Arteriosclerosis,
Chapter 3. Toxicity and the Factors That Modify Toxic Responses
 Chapter 3 Toxicity and the Factors That Modify Toxic Responses Cellular Basis of Toxicity All chemicals have the potential to produce toxicity. Toxicity may be generally defined as any adverse effect of
Chapter 3 Toxicity and the Factors That Modify Toxic Responses Cellular Basis of Toxicity All chemicals have the potential to produce toxicity. Toxicity may be generally defined as any adverse effect of
General Principles of Endocrine Physiology
 General Principles of Endocrine Physiology By Dr. Isabel S.S. Hwang Department of Physiology Faculty of Medicine University of Hong Kong The major human endocrine glands Endocrine glands and hormones
General Principles of Endocrine Physiology By Dr. Isabel S.S. Hwang Department of Physiology Faculty of Medicine University of Hong Kong The major human endocrine glands Endocrine glands and hormones
Chemistry 107 Exam 4 Study Guide
 Chemistry 107 Exam 4 Study Guide Chapter 10 10.1 Recognize that enzyme catalyze reactions by lowering activation energies. Know the definition of a catalyst. Differentiate between absolute, relative and
Chemistry 107 Exam 4 Study Guide Chapter 10 10.1 Recognize that enzyme catalyze reactions by lowering activation energies. Know the definition of a catalyst. Differentiate between absolute, relative and
Oxidation of Long Chain Fatty Acids
 Oxidation of Long Chain Fatty Acids Dr NC Bird Oxidation of long chain fatty acids is the primary source of energy supply in man and animals. Hibernating animals utilise fat stores to maintain body heat,
Oxidation of Long Chain Fatty Acids Dr NC Bird Oxidation of long chain fatty acids is the primary source of energy supply in man and animals. Hibernating animals utilise fat stores to maintain body heat,
Diagnosis of chronic Pancreatitis. Christoph Beglinger, University Hospital Basel, Switzerland
 Diagnosis of chronic Pancreatitis Christoph Beglinger, University Hospital Basel, Switzerland Pancreatitis Pancreas Pancreas - an organ that makes bicarbonate to neutralize gastric acid, enzymes to digest
Diagnosis of chronic Pancreatitis Christoph Beglinger, University Hospital Basel, Switzerland Pancreatitis Pancreas Pancreas - an organ that makes bicarbonate to neutralize gastric acid, enzymes to digest
Station 1. Identify (= name) the spaces or structures labeled 1 9.
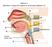 Station 1. Identify (= name) the spaces or structures labeled 1 9. 1 9 8 2 7 3 4 5 6 Station 2. Identify/name the parts or structures labeled 10 20. 10. Is this the right or left lung? 15 13 14 16 11 12
Station 1. Identify (= name) the spaces or structures labeled 1 9. 1 9 8 2 7 3 4 5 6 Station 2. Identify/name the parts or structures labeled 10 20. 10. Is this the right or left lung? 15 13 14 16 11 12
Testosterone and other male hormones seem to be related to aggressive behavior in some species
 Testosterone and Male Aggression Testosterone and other male hormones seem to be related to aggressive behavior in some species In the fish species Oreochromis mossambicus, elevated levels have been found
Testosterone and Male Aggression Testosterone and other male hormones seem to be related to aggressive behavior in some species In the fish species Oreochromis mossambicus, elevated levels have been found
Chapter 10. Regulatory Strategy
 Chapter 10 Regulatory Strategy Regulation of enzymatic activity: 1. Allosteric Control. Allosteric proteins have a regulatory site(s) and multiple functional sites Activity of proteins is regulated by
Chapter 10 Regulatory Strategy Regulation of enzymatic activity: 1. Allosteric Control. Allosteric proteins have a regulatory site(s) and multiple functional sites Activity of proteins is regulated by
Alcohol-Related Liver Disease
 Alcohol-Related Liver Disease Nonalcoholic Fatty Liver Disease (NAFLD) 1 Why is the liver important? Your liver is a vital organ that performs many essential functions. It filters out harmful substances
Alcohol-Related Liver Disease Nonalcoholic Fatty Liver Disease (NAFLD) 1 Why is the liver important? Your liver is a vital organ that performs many essential functions. It filters out harmful substances
The Small Intestine. The pyloric sphincter at the bottom of the stomach opens, squirting small amounts of food into your small intestine.
 The Small Intestine The pyloric sphincter at the bottom of the stomach opens, squirting small amounts of food into your small intestine. approximately six metres (the longest section of your digestive
The Small Intestine The pyloric sphincter at the bottom of the stomach opens, squirting small amounts of food into your small intestine. approximately six metres (the longest section of your digestive
Summary of fatty acid synthesis
 Lipid Metabolism, part 2 1 Summary of fatty acid synthesis 8 acetyl CoA + 14 NADPH + 14 H+ + 7 ATP palmitic acid (16:0) + 8 CoA + 14 NADP + + 7 ADP + 7 Pi + 7 H20 1. The major suppliers of NADPH for fatty
Lipid Metabolism, part 2 1 Summary of fatty acid synthesis 8 acetyl CoA + 14 NADPH + 14 H+ + 7 ATP palmitic acid (16:0) + 8 CoA + 14 NADP + + 7 ADP + 7 Pi + 7 H20 1. The major suppliers of NADPH for fatty
Chapter 7- Metabolism: Transformations and Interactions Thomson - Wadsworth
 Chapter 7- Metabolism: Transformations and Interactions 2008 Thomson - Wadsworth Simple Overview of Energy Metabolism The sum of all chemical reactions that go on in living cells Introduction Energy Heat-
Chapter 7- Metabolism: Transformations and Interactions 2008 Thomson - Wadsworth Simple Overview of Energy Metabolism The sum of all chemical reactions that go on in living cells Introduction Energy Heat-
Plasma lipoproteins & atherosclerosis by. Prof.Dr. Maha M. Sallam
 Biochemistry Department Plasma lipoproteins & atherosclerosis by Prof.Dr. Maha M. Sallam 1 1. Recognize structures,types and role of lipoproteins in blood (Chylomicrons, VLDL, LDL and HDL). 2. Explain
Biochemistry Department Plasma lipoproteins & atherosclerosis by Prof.Dr. Maha M. Sallam 1 1. Recognize structures,types and role of lipoproteins in blood (Chylomicrons, VLDL, LDL and HDL). 2. Explain
Animal Nutrition Human Digestion
 Animal Nutrition Human Digestion 2006-2007 What do animals need to live? Animals make energy using: food food oxygen Animals build bodies using: food for raw materials amino acids, sugars, O fats, nucleotides
Animal Nutrition Human Digestion 2006-2007 What do animals need to live? Animals make energy using: food food oxygen Animals build bodies using: food for raw materials amino acids, sugars, O fats, nucleotides
Learning Targets. The Gastrointestinal (GI) Tract. Also known as the alimentary canal. Hollow series of organs that food passes through
 Digestion the multistep process of breaking down food into molecules the body can use Learning Targets Describe the path food takes through the digestive system. Identify the major organs of the digestive
Digestion the multistep process of breaking down food into molecules the body can use Learning Targets Describe the path food takes through the digestive system. Identify the major organs of the digestive
Digestive system L 4. Lecturer Dr. Firdous M. Jaafar Department of Anatomy/Histology section
 Digestive system L 4 Lecturer Dr. Firdous M. Jaafar Department of Anatomy/Histology section objectives 1-Describe the structure of liver. 2-Define liver lobule, and identify its zones. 3-Define portal
Digestive system L 4 Lecturer Dr. Firdous M. Jaafar Department of Anatomy/Histology section objectives 1-Describe the structure of liver. 2-Define liver lobule, and identify its zones. 3-Define portal
5. Which component of the duodenal contents entering the stomach causes the most severe changes to gastric mucosa:
 Gastro-intestinal disorders 1. Which are the most common causes of chronic gastritis? 1. Toxic substances 2. Chronic stress 3. Alimentary factors 4. Endogenous noxious stimuli 5. Genetic factors 2. Chronic
Gastro-intestinal disorders 1. Which are the most common causes of chronic gastritis? 1. Toxic substances 2. Chronic stress 3. Alimentary factors 4. Endogenous noxious stimuli 5. Genetic factors 2. Chronic
Nottingham Patterns of liver fibrosis and their clinical significance
 Nottingham 2006 Patterns of liver fibrosis and their clinical significance Alastair D Burt Professor of Pathology and Dean of Clinical Medicine University of Newcastle upon Tyne Collapse of reticulin
Nottingham 2006 Patterns of liver fibrosis and their clinical significance Alastair D Burt Professor of Pathology and Dean of Clinical Medicine University of Newcastle upon Tyne Collapse of reticulin
DIGESTIVE. CHAPTER 17 Lecture: Part 1 Part 2 BIO 212: ANATOMY & PHYSIOLOGY II
 BIO 212: ANATOMY & PHYSIOLOGY II CHAPTER 17 Lecture: DIGESTIVE Part 1 Part 2 Dr. Lawrence G. Altman www.lawrencegaltman.com Some illustrations are courtesy of McGraw-Hill. SMALL INTESTINE DUODENUM > JEJUNUM
BIO 212: ANATOMY & PHYSIOLOGY II CHAPTER 17 Lecture: DIGESTIVE Part 1 Part 2 Dr. Lawrence G. Altman www.lawrencegaltman.com Some illustrations are courtesy of McGraw-Hill. SMALL INTESTINE DUODENUM > JEJUNUM
Endocrine System. Chapter 20. Endocrine Glands and Hormones. The Endocrine System. Endocrine glands
 Chapter 20 Endocrine System Endocrine Glands and Hormones The endocrine system consists of glands and tissues that secrete hormones Hormones are chemicals that affect other glands or tissues, many times
Chapter 20 Endocrine System Endocrine Glands and Hormones The endocrine system consists of glands and tissues that secrete hormones Hormones are chemicals that affect other glands or tissues, many times
Lipid Metabolism. Catabolism Overview
 Lipid Metabolism Pratt & Cornely, Chapter 17 Catabolism Overview Lipids as a fuel source from diet Beta oxidation Mechanism ATP production Ketone bodies as fuel 1 High energy More reduced Little water
Lipid Metabolism Pratt & Cornely, Chapter 17 Catabolism Overview Lipids as a fuel source from diet Beta oxidation Mechanism ATP production Ketone bodies as fuel 1 High energy More reduced Little water
Harvesting energy from food. Digestion: A Closer Look. Where digestion begins. Salivary Glands 4/17/13. Or how food gets from
 Harvesting energy from food Or how food gets from to and body structures Cheese protein (a polymer of amino acids in a specific sequence) Breakdown of protein by human digestive system Amino acid monomer
Harvesting energy from food Or how food gets from to and body structures Cheese protein (a polymer of amino acids in a specific sequence) Breakdown of protein by human digestive system Amino acid monomer
6/15/2015. Biological Molecules. Outline. Organic Compounds. Organic Compounds - definition Functional Groups Biological Molecules. What is organic?
 Biological Molecules Biology 105 Lecture 3 Reading: Chapter 2 (pages 29 39) Outline Organic Compounds - definition Functional Groups Biological Molecules Carbohydrates Lipids Amino Acids and Proteins Nucleotides
Biological Molecules Biology 105 Lecture 3 Reading: Chapter 2 (pages 29 39) Outline Organic Compounds - definition Functional Groups Biological Molecules Carbohydrates Lipids Amino Acids and Proteins Nucleotides
Molecular Cell Biology Problem Drill 16: Intracellular Compartment and Protein Sorting
 Molecular Cell Biology Problem Drill 16: Intracellular Compartment and Protein Sorting Question No. 1 of 10 Question 1. Which of the following statements about the nucleus is correct? Question #01 A. The
Molecular Cell Biology Problem Drill 16: Intracellular Compartment and Protein Sorting Question No. 1 of 10 Question 1. Which of the following statements about the nucleus is correct? Question #01 A. The
Asthma. - A chronic inflammatory disorder which causes recurrent episodes of wheezing, breathlessness, cough and chest tightness.
 Obstructive diseases Asthma - A chronic inflammatory disorder which causes recurrent episodes of wheezing, breathlessness, cough and chest tightness. - Characterized by Intermittent and reversible (the
Obstructive diseases Asthma - A chronic inflammatory disorder which causes recurrent episodes of wheezing, breathlessness, cough and chest tightness. - Characterized by Intermittent and reversible (the
Thyroid Gland. Chapter 18 Part 2. Thyroid gland. Thyroid Gland. Thyroid Gland. Parathyroid Gland. Adrenal Gland. Pancreas
 Thyroid Gland Chapter 18 Part 2 Synthesis and function of Thyroid hormone Calcitonin and Calcium regulation Parathyroid Gland PTH and Calcium regulation Adrenal Gland The corticosteroids Pancreas Regulation
Thyroid Gland Chapter 18 Part 2 Synthesis and function of Thyroid hormone Calcitonin and Calcium regulation Parathyroid Gland PTH and Calcium regulation Adrenal Gland The corticosteroids Pancreas Regulation
Lehninger 5 th ed. Chapter 17
 Lehninger 5 th ed. Chapter 17 December 26, 2010 Prof. Shimon Schuldiner Email: Shimon.Schuldiner@huji.ac.il Phone: 6585992 CHAPTER 17 Fatty Acid Catabolism Key topics: How fats are digested in animals
Lehninger 5 th ed. Chapter 17 December 26, 2010 Prof. Shimon Schuldiner Email: Shimon.Schuldiner@huji.ac.il Phone: 6585992 CHAPTER 17 Fatty Acid Catabolism Key topics: How fats are digested in animals
Chapter 26 The Digestive System
 Chapter 26 The Digestive System Digestive System Gastroenterology is the study of the stomach and intestine. Digestion Catabolism Absorption Anabolism The actions of the digestive system are controlled
Chapter 26 The Digestive System Digestive System Gastroenterology is the study of the stomach and intestine. Digestion Catabolism Absorption Anabolism The actions of the digestive system are controlled
TITLE: Targeting trypsin-inflammation axis for pancreatitis therapy in a humanized pancreatitis model. Los Angeles, CA 90048
 AWARD NUMBER: W81XWH-15-1-0258 TITLE: Targeting trypsin-inflammation axis for pancreatitis therapy in a humanized pancreatitis model PRINCIPAL INVESTIGATOR: Stephen J Pandol, MD CONTRACTING ORGANIZATION:
AWARD NUMBER: W81XWH-15-1-0258 TITLE: Targeting trypsin-inflammation axis for pancreatitis therapy in a humanized pancreatitis model PRINCIPAL INVESTIGATOR: Stephen J Pandol, MD CONTRACTING ORGANIZATION:
5.0 HORMONAL CONTROL OF CARBOHYDRATE METABOLISM
 5.0 HORMONAL CONTROL OF CARBOHYDRATE METABOLISM Introduction: Variety of hormones and other molecules regulate the carbohydrates metabolism. Some of these have already been cited in previous sections.
5.0 HORMONAL CONTROL OF CARBOHYDRATE METABOLISM Introduction: Variety of hormones and other molecules regulate the carbohydrates metabolism. Some of these have already been cited in previous sections.
Mechanistic Toxicology
 SECOND EDITION Mechanistic Toxicology The Molecular Basis of How Chemicals Disrupt Biological Targets URS A. BOELSTERLI CRC Press Tavlor & France Croup CRC Press is an imp^t o* :H Taylor H Francn C'r,,jpi
SECOND EDITION Mechanistic Toxicology The Molecular Basis of How Chemicals Disrupt Biological Targets URS A. BOELSTERLI CRC Press Tavlor & France Croup CRC Press is an imp^t o* :H Taylor H Francn C'r,,jpi
Oxidation and Methylation in Human Brain: Implications for vaccines
 Oxidation and Methylation in Human Brain: Implications for vaccines 1 Life can be viewed through the perspective of oxidation and reduction, which involves the loss and gain of electrons, respectively.
Oxidation and Methylation in Human Brain: Implications for vaccines 1 Life can be viewed through the perspective of oxidation and reduction, which involves the loss and gain of electrons, respectively.
10/18/2017 ANIMAL NUTRITION ANIMAL NUTRITION ESSENTIAL NUTRIENTS AN ANIMAL S DIET MUST STUPPLY: AMINO ACIDS
 ANIMAL NUTRITION Food is taken in, taken apart, and taken up in the process of animal nutrition In general, animals fall into three categories: Herbivores Carnivores Omnivores ANIMAL NUTRITION Chapter
ANIMAL NUTRITION Food is taken in, taken apart, and taken up in the process of animal nutrition In general, animals fall into three categories: Herbivores Carnivores Omnivores ANIMAL NUTRITION Chapter
Case Study BMIs in the range of are considered overweight. Therefore, F.V. s usual BMI indicates that she was overweight.
 Morgan McFarlane February 26 th, 2013 HHP 439 Professor White Case Study 7.10 1. What is your interpretation of F.V. s clinical data? F.V. s clinical data includes chronic abdominal pain, loose stools,
Morgan McFarlane February 26 th, 2013 HHP 439 Professor White Case Study 7.10 1. What is your interpretation of F.V. s clinical data? F.V. s clinical data includes chronic abdominal pain, loose stools,
Integration Of Metabolism
 Integration Of Metabolism Metabolism Consist of Highly Interconnected Pathways The basic strategy of catabolic metabolism is to form ATP, NADPH, and building blocks for biosyntheses. 1. ATP is the universal
Integration Of Metabolism Metabolism Consist of Highly Interconnected Pathways The basic strategy of catabolic metabolism is to form ATP, NADPH, and building blocks for biosyntheses. 1. ATP is the universal
NOTES: The Digestive System (Ch 14, part 2)
 NOTES: The Digestive System (Ch 14, part 2) PANCREAS Structure of the pancreas: The pancreas produces PANCREATIC JUICE that is then secreted into a pancreatic duct. The PANCREATIC DUCT leads to the The
NOTES: The Digestive System (Ch 14, part 2) PANCREAS Structure of the pancreas: The pancreas produces PANCREATIC JUICE that is then secreted into a pancreatic duct. The PANCREATIC DUCT leads to the The
Chapter 1 CELL INJURY CELL DEATH CELL ADAPTATIONS. M.G.Rajanandh, Dept. of Pharmacy Practice, SRM College of Pharmacy, SRM University.
 Chapter 1 CELL INJURY CELL DEATH CELL ADAPTATIONS M.G.Rajanandh, Dept. of Pharmacy Practice, SRM College of Pharmacy, SRM University. CONCEPTS IN CELL INJURY The clinical signs and symptoms are several
Chapter 1 CELL INJURY CELL DEATH CELL ADAPTATIONS M.G.Rajanandh, Dept. of Pharmacy Practice, SRM College of Pharmacy, SRM University. CONCEPTS IN CELL INJURY The clinical signs and symptoms are several
Cholesterol metabolism. Function Biosynthesis Transport in the organism Hypercholesterolemia
 Cholesterol metabolism Function Biosynthesis Transport in the organism Hypercholesterolemia - component of all cell membranes - precursor of bile acids steroid hormones vitamin D Cholesterol Sources: dietary
Cholesterol metabolism Function Biosynthesis Transport in the organism Hypercholesterolemia - component of all cell membranes - precursor of bile acids steroid hormones vitamin D Cholesterol Sources: dietary
Peering Into the Black Box of the Complex Chronic Pancreatitis Syndrome
 PancreasFest 2017 Precision Medicine Approach For Benign Pancreatic Disease Friday, July 28, 2017 Peering Into the Black Box of the Complex Chronic Pancreatitis Syndrome David C Whitcomb MD PhD Director,
PancreasFest 2017 Precision Medicine Approach For Benign Pancreatic Disease Friday, July 28, 2017 Peering Into the Black Box of the Complex Chronic Pancreatitis Syndrome David C Whitcomb MD PhD Director,
