Vitamin D Receptor and Analogs
|
|
|
- Randell Lynch
- 5 years ago
- Views:
Transcription
1 Vitamin D Receptor and Analogs By Adriana S. Dusso,* Ravi Thadhani, and Eduardo Slatopolsky* In chronic kidney disease (CKD), high circulating levels of parathyroid hormone (PTH) cause osteitis fibrosa, bone loss, and cardiovascular complications that increase morbidity and mortality. Impaired production of 1,25-dihydroxyvitamin D (calcitriol), the hormonal form of vitamin D, is a major contributor to the generation and maintenance of parathyroid hyperplasia and increased synthesis and secretion of PTH. Calcitriol inhibits PTH gene transcription and ameliorates parathyroid hyperplasia by suppressing the expression of and growth signals from the autocrine transforming growth factor (TGF )/epidermal growth factor receptor (EGFR)-growth loop, a main determinant of parathyroid cell proliferation. Calcitriol reduction of parathyroid hyperplasia and serum PTH levels demands a functional vitamin D receptor (VDR). Although VDR is normal in CKD, parathyroid VDR content is reduced markedly. Furthermore, VDR function, as a transcriptional regulator of vitamin D responsive genes, is impaired by several factors including hypocalcemia, hyperphosphatemia, accumulation of uremic toxins, and reduction in cellular levels of the VDR partner, retinoid X receptor. Therapy with calcitriol analogs can overcome the antagonism on calcitriol-vdr actions induced by CKD. Although not all analog formulations are equally effective, they offer a wider therapeutic window in counteracting vitamin D resistance and survival advantage over exclusive calcitriol therapy Elsevier Inc. All rights reserved. IN CHRONIC KIDNEY disease (CKD) stage 3, impaired renal production of 1,25-dihydroxyvitamin D (calcitriol), the hormonal form of vitamin D, is a major contributor to the generation and maintenance of secondary hyperparathyroidism, a disorder characterized by parathyroid hyperplasia and increased synthesis and secretion of parathyroid hormone (PTH). 1 High circulating levels of PTH cause osteitis fibrosa, bone loss, and a variety of systemic defects, including cardiovascular complications that increase morbidity and mortality in renal failure patients. Calcitriol directly represses both parathyroid cell proliferation and PTH synthesis. 2 Thus, its deficiency in renal failure causes high serum PTH levels and parathyroid gland enlargement. Calcitriol deficiency also leads to secondary hyperparathyroidism indirectly through decreasing intestinal calcium absorption. The resulting hypocalcemia is the most potent stimulus for rapid increases of PTH synthesis and secretion directed to normalize From the *Renal Division, Washington University School of Medicine, St. Louis, MO; and Massachusetts General Hospital, Boston, MA. Supported in part by grant AR from the National Institutes of Health (A.S.D.). Address reprint requests to Adriana S. Dusso, PhD, Research Associate Professor, Renal Division. Campus Box 8126, Washington University School of Medicine, 660 S. Euclid Ave, St. Louis, MO adusso@im.wustl.edu 2004 Elsevier Inc. All rights reserved /04/ $30.00/0 doi: /j.semnephrol serum calcium. 1,2 Prolonged hypocalcemia also induces hyperplastic parathyroid growth. The efficacy of calcitriol in inhibiting parathyroid cell growth and PTH synthesis renders calcitriol replacement therapy a valuable tool to treat renal hyperparathyroidism. However, calcitriol actions in the parathyroid gland demand a functional vitamin D receptor (VDR), 2 and although the VDR is normal in patients with CKD, parathyroid VDR content is reduced markedly in hyperplastic human parathyroid glands, particularly in areas of more aggressive growth. 3 Vitamin D resistance in advanced kidney disease (CKD stage 5) limits the efficacy of vitamin D replacement therapy. This review presents the current understanding on mechanisms responsible for: (1) calcitriol/ VDR-control of PTH synthesis and parathyroid cell growth; (2) resistance to the control of parathyroid function by the calcitriol/vdr complex in renal failure, and (3) the advantage of analog therapies in overcoming vitamin D resistance. In addition, it presents recent evidence on the relative efficacy of the vitamin D replacement therapy available today in controlling secondary hyperparathyroidism, bone disease, and morbidity and mortality in patients with CKD. CALCITRIOL/VDR-CONTROL OF PTH SYNTHESIS AND PARATHYROID CELL GROWTH The ability of calcitriol to inhibit PTH synthesis and arrest parathyroid cell growth in vivo and in vitro has been known for many years. 2 The mechanisms mediating calcitriol-transcriptional repres- 10 Seminars in Nephrology, Vol 24, No 1 (January), 2004: pp 10-16
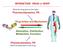
2 VITAMIN D RECEPTOR AND ANALOGS 11 Fig 1. Mechanisms for impaired calcitriol/vdr regulation of gene expression in kidney disease. Calcitriol (1,25D) binding activates the VDR to interact with nuclear RXR, basal transcription factors (B), and co-regulator molecules (Coreg) to activate (p21, p27) or repress (PTH) gene transcription by RNA polymerase II. Uremia induced mechanisms to impair 1,25D/VDR complex formation, VDR/RXR heterodimerization, and DNA binding of VDR/RXR to VDREs in the promoter of calcitriol-regulated genes. sion of PTH gene are depicted in Figure 1. In contrast, direct characterization of the pathogenic mechanisms underlying both induction of parathyroid cell proliferation by kidney disease and its suppression by calcitriol has been difficult because of a lack of an appropriate parathyroid cell line and the rapid dedifferentiation of primary cultures of hyperplastic parathyroid cells. Recent studies in our laboratory have implicated increases in parathyroid co-expression of the growth promoter, transforming growth factor- (TGF ) and its receptor, the epidermal growth factor receptor (EGFR), in uremia-induced enhancement of proliferative activity and gland size. 4 Similar to secondary hyperparathyroidism in humans, 5 TGF expression is higher in uremic rats compared with normal controls. More importantly, when uremiainduced hyperplasia is worsened, either by a high phosphorus (P)-[4] or a low calcium intake, 6 increases in parathyroid TGF and EGFR expression directly correlate with high proliferating activity and gland enlargement. In normal and transformed tissues, enhanced co-expression of TGF and EGFR is associated with aggressive growth. Using highly specific inhibitors of EGFR-tyrosine kinase, which abolish growth signals from ligand-activated EGFR, we have shown in vivo that enhanced parathyroid co-expression of TGF and EGFR is a major contributor to the growth of the parathyroid glands in experimental renal failure. 7 In early stages of kidney disease in rats, prophylactic vitamin D administration (calcitriol or its analog 19- nor1,25-dihydroxyvitamin D 2 [19-nor]) counteracts parathyroid hyperplasia by preventing uremiainduced increases in parathyroid TGF and EGFR expression, which occur within the first week after inducing kidney failure by 5/6 nephrectomy. 6 The efficacy of analog therapy (19-nor and 22- oxacalcitriol [OCT]) in preventing further enlargement of the parathyroid gland in established secondary hyperparathyroidism (high TGF /EGFR overexpression) suggested that calcitriol antiproliferative properties could involve down-regulation of the potent TGF /EGFR growth-promoting signals. In fact, in normal and carcinogenic cell lines, overexpressing TGF and EGFR, the potent vitamin D antiproliferative actions involve inhibition of EGFR growth-promoting signals from the plasma membrane as well as EGFR transactivation of the cyclin D1 gene. 8 Increased expression of parathyroid cyclin D1 is a common feature in secondary hyperparathyroidism in humans. 9 The time of exposure to calcitriol required for the sterol to suppress parathyroid TGF and EGFR expression in vivo and/or TGF /EGFR growth signals in vitro 8 discards rapid nongenomic vitamin D actions and suggests a VDR-mediated effect. It is unclear at present whether calcitriol exerts transcriptional suppression of the TGF and EGFR genes in parathyroid cells or on the unknown genes responsible for its anti-egfr properties. In addition to the strong inhibition of the expression and signaling of the TGF /EGFR growth loop, calcitriol antiproliferative actions in hyper-
3 12 plastic parathyroid glands involve induction of the cyclin-dependent kinase inhibitors p21 and p27. 6,10 Both genes are induced transcriptionally by the calcitriol/vdr complex. Calcitriol-VDR Regulation of Gene Expression Figure 1 depicts the current model for calcitriol/ VDR action. Calcitriol, a lipid-soluble molecule, is transported in the blood by carrier proteins, mainly vitamin D binding protein (DBP) and, in a lesser degree, albumin and lipoproteins. 2 In renal proximal tubular cells, 25-hydroxyvitamin D uptake occurs through receptor (megalin)-mediated endocytosis of the 25-hydroxyvitamin D bound to plasma DBP. 11 This surprising finding raised the possibility that the cellular uptake of circulating calcitriol takes place through an endocytic process similar to that of 25-hydroxyvitamin D rather than simple diffusion through the cell membrane. If megalinmediated endocytosis is an important contributor to parathyroid calcitriol uptake, uremia-induced reduction in megalin expression in the parathyroid glands could constitute a mechanism for vitamin D resistance in addition to reduced VDR content. Once inside the cell, calcitriol binding to the VDR activates its receptor to translocate from the cytosol to the nucleus where it heterodimerizes with its partner the retinoid X receptor (RXR). The VDR/RXR complex then binds specific sequences in the promoter region of vitamin D responsive genes, called vitamin D response elements (VDRE), and recruits basal transcription factors and co-regulator molecules to either increase or suppress the rate of gene transcription by RNA polymerase II. 2 In calcitriol/vdr transactivation, that is, calcitriol induction of gene expression, such as that of the promoter of growth arrest p21, the binding of the VDR/RXR heterodimer to the VDRE of this gene initiates the recruitment of co-activator molecules. These co-activators act synergistically with the VDR to markedly amplify calcitriol-transactivating potency The VDRnuclear co-activators (SRC-1 and CBP/p300) possess histone acetyl transferase activity, which unfold and expose the DNA. This allows the recruitment of a second complement of transcriptional coactivators (DRIP205 and TRIP) that favor the assembly of the pre-initiation complex to potentiate calcitriol/vdr induction of gene expression. DUSSO, THADHANI, AND SLATOPOLSKY In transcriptional repression, such as that of the PTH gene, binding of the VDR/RXR complex to negative VDRE, recruits co-repressors of the family of histone deacetylases. These molecules prevent DNA exposure and, consequently, the binding of proteins (TATA binding protein) mandatory to initiate transcription. 12 Both the transcriptional suppression of the PTH gene and the induction of the expression of the genes for the cyclin-dependent kinase inhibitors p21 and p27 by the 1,25D/VDR complex are of relevance for the efficacy of calcitriol therapy in renal hyperparathyroidism. The mechanisms mediating calcitriol/vdr suppression of parathyroid TGF and EGFR expression and inhibition of membrane and nuclear EGFR growth signaling await identification. Mechanisms for Impaired 1,25(OH) 2 D 3 /VDR Action in Renal Failure Figure 1 also summarizes the abnormalities in calcitriol/vdr regulation of gene transcription associated with kidney disease. Intracellular levels of calcitriol (1,25D) and the VDR determine the magnitude of 1,25D/VDR inhibition of PTH synthesis and/or parathyroid growth arrest (induction of p21 and p27). In CKD, serum calcitriol decreases as renal function deteriorates, starting at stage 3. Because calcitriol increases VDR messenger RNA levels and protein stability, the latter by preventing VDR degradation, 15 low serum calcitriol is in itself partially responsible for reduced parathyroid VDR content. In fact, a strong direct correlation exists between serum calcitriol and parathyroid VDR content in 5/6 nephrectomized rats. 16 More importantly, prophylactic administration of either calcitriol or its analog, 22-oxa-calcitriol, prevents the marked reduction in parathyroid VDR content induced by renal failure and worsen by high dietary P. 16 Thus, in kidney disease, impaired formation of the calcitriol/vdr complex, the first step in calcitriol action, results from the combination of decreases in renal calcitriol synthesis and parathyroid VDR content. Thus, early therapeutic interventions with oral calcitriol (0.25 daily) or its analogs, in CKD stage 3, could delay the onset of vitamin D resistance by preventing calcitriol deficiency and its critical consequence, the reduction in VDR content. Studies in our laboratory in peripheral blood monocytes from normal individuals and hemodial-
4 VITAMIN D RECEPTOR AND ANALOGS 13 ysis patients showed an impaired response to exogenous calcitriol (10 8 mol/l) despite a similar VDR. Thus, CKD induces abnormalities in VDR actions downstream from the formation of the calcitriol/vdr complex. Specifically, calcitriol/vdrtranscriptional activation of the 24-hydroxylase gene was inhibited by 80% in monocytes from hemodialysis patients. Several laboratories have identified factors contributing to impaired heterodimerization and VDR/RXR-binding to VDRE, including (1) reduced RXR. Studies in unilaterally nephrectomized rats showed a reduction in the content of a 50-kd RXR isoform in cell extracts from the remnant kidney. This decrease in RXR resulted in decreased endogenous VDR/RXR heterodimer formation and binding to VDRE (mouse osteopontin promoter). A similar reduction of RXR content in the parathyroid glands in these rats, even in the presence of normal parathyroid VDR, could explain their enhanced serum PTH levels in the absence of hypocalcemia or hyperphosphatemia. 17 (2) Accumulation of uremic toxins. Ultrafiltrate from uremic plasma causes a dose-dependent inhibition of VDR/RXR binding to VDRE and, consequently, in calcitriol potency to regulate gene expression in transfected JEG-3 cells. 18 (3) Increases in parathyroid calreticulin. Calreticulin is a cytosolic protein that binds integrins in the plasma membrane and the DNA binding domain of nuclear receptors, including the VDR, thus interfering with receptor-mediated transactivation. Hypocalcemia sometimes presents in CKD stages 3 to 5 and could be caused either by decreased 1,25(OH) 2 D 3 or hyperphosphatemia. In rats, hypocalcemia enhances nuclear levels of parathyroid calreticulin. In vitro studies have shown that increases in calreticulin inhibit VDR/RXR binding to VDRE in a dose-dependent manner and totally abolish calcitriol suppression of PTH gene transcription. 19 High P induction of nuclear calreticulin in the parathyroid glands could mediate the well-known resistance to calcitriol action in hyperphosphatemic states. (4) Activation of VDR-unrelated pathways interfering with 1,25(OH) 2 D 3 signaling. In human monocytes and macrophages, cytokine activation markedly inhibits 1,25(OH) 2 D 3 -VDR gene transcription. interferon activation of its signaling molecule Stat1 induces physical interactions between Stat1 and the DNA binding domain of the VDR, thus impairing VDR/RXR binding to VDRE and gene transcription. 20 Thus, the higher levels of inflammatory cytokines after hemodialysis could contribute to vitamin D resistance. Clearly, adequate prevention of hypocalcemia, hyperphosphatemia, accumulation of uremic toxins, and activation of the signaling pathways of inflammatory cytokines should improve VDR/RXR binding to the VDRE of target genes and the response to exogenous administration of calcitriol (or its less calcemic analogs) despite the reduced parathyroid VDR. Little is known at present on how renal failure affects transactivation/transrepression, the most critical step in calcitriol/vdr-mediated regulation of gene expression. The numerous protein-protein- DNA interactions of the VDR/RXR with VDRE and nuclear co-regulator molecules suggest that, in uremia, vitamin D resistance also could result from a decreased expression of essential coactivator- or co-repressor molecules or from defective recruitment of these molecules by the VDR. Alternatively, uremia-induced activation of VDRunrelated signaling pathways also could interfere with the recruitment of co-regulator molecules to the VDR-transcriptional pre-initiation complex. Figure 1 points to the ligand bound to the VDR as the therapeutic target to overcome the numerous inhibitory interactions triggered by uremia to induce vitamin D resistance in secondary hyperparathyroidism. Less calcemic vitamin D analogs offer a wider therapeutic window. In addition, an important new finding allows a better understanding of tissue-specific actions (selectivity) and potency of vitamin D analogs. Takeyama et al 21 showed that the ligand (calcitriol or its less calcemic analogs) bound to the VDR dictates critical changes in VDR tridimensional conformation that favor a selective recruitment of nuclear co-regulator molecules. Thus, in a target cell expressing the co-regulators required by either calcitriol or its analog, both vitamin D metabolites will elicit similar efficacy. Conversely, in cells in which the co-regulator required by an analog is limiting or absent, the analog will elicit weaker potency than the parent hormone. More important for therapy, analog recruitment to the VDR-transcription initiation complex of a co-activator more potent than that recruited by calcitriol could result in higher potency of the analog in eliciting a biologic response. This is not theoretical speculation. Studies by Takeyama et al 22 showed that analog-specific recruitment of co-repressor molecules mediate their
5 14 differential transrepression potency on the human PTH gene. Extensive research is mandatory before extrapolating these findings in vitro to VDR transcriptional potency in the parathyroid glands in vivo. Certainly, a better understanding of the role of nuclear co-activator/repressors in VDR-mediated transactivation should help design better VDR ligands in recruiting the most effective co-regulator molecules to maximize vitamin D efficacy in suppressing serum PTH, parathyroid cell growth, and, ultimately, regressing hyperplastic gland size through induction of parathyroid cell apoptosis. ADVANTAGES OF THE VITAMIN D REPLACEMENT THERAPY CURRENTLY AVAILABLE Intravenous, oral, and intraperitoneal calcitriol therapy has been used successfully in the United States for treatment of secondary hyperparathyroidism for almost 2 decades. However, the use of calcitriol at doses that effectively suppress serum PTH is limited by the development of hypercalcemia and hyperphosphatemia, which result from the potent effects of the sterol in increasing intestinal absorption and bone mobilization of calcium and phosphate. 2 In advanced kidney disease, the hypercalcemic toxicity of calcitriol is aggravated further by the concomitant use of large doses of calcium containing phosphate-binding antacids. To minimize the toxicities of calcitriol therapy, structural modifications in the vitamin D molecule led to the development of pro-hormone and calcitriol analogs. These compounds retain the capacity to suppress parathyroid function with lesser effects on kidney and bone. Their relative potencies in suppressing parathyroid function, calcemic activity, and mechanisms for selectivity are summarized later. 1 -hydroxyvitamin D 2 (1 -D 2, Hectorol, Bone Care Int, Middleton, WI) is a pro-hormone that requires hydroxylation in the C25 position in the liver to become active 1,25-dihydroxyvitamin D 2. The mechanisms for the selective actions of this pro-hormone are unclear. In experimental animals, 1 -D 2 is less toxic than its D 3 counterpart despite similar stimulation of calcium and phosphate transport. 23,24 A potential mechanism is the conversion of high levels of 1 -D 2 to 1,24-dihydroxyD 2,a compound with lower calcemic activity than calcitriol. 25,26 Oral and intravenous 1 -D 2 have been approved and used effectively for the treatment of DUSSO, THADHANI, AND SLATOPOLSKY secondary hyperparathyroidism in the United States, 27,28 although little evidence exists that this pro-hormone is less calcemic or hyperphosphatemic than its D 3 counterpart. Three calcitriol analogs, falecalcitriol (Sunitomo Pharmaceutical, Osaka, Japan), 22-oxacalcitriol (OCT, Oxarol, Chugai Pharmaceuticals, Tokyo, Japan), and 19-nor-1,25-dihydroxyvitaminD2 (19- nor, Zemplar, Abbot Pharmaceuticals, Chicago, IL) have been approved for the treatment of secondary hyperparathyroidism. Falecalcitriol, a calcitriol analog used in Japan, results from the substitution of hydrogens at C26 and C27 by fluorine atoms. Because of its decreased metabolic inactivation, falecalctriol has greater activity than alphacalcidol (1 -D 3 )insuppressing PTH in patients with chronic renal failure. 29 Although serum calcium levels were similar in patients treated with either compound, the control of serum phosphorus was better with falecalcitriol treatment. 29 OCT, a calcitriol analog available and used in Japan, differs from calcitriol by the substitution of an oxygen for C22. This structural modification reduces OCT affinity for both VDR and DBP. 30 The latter results in a rapid clearance of the sterol from the circulation. Marked differences in calcitriol and OCT pharmacokinetics could explain why OCT administration in vivo results in prolonged suppression of PTH secretion but short-lived effects on intestine and bone. 31,32 In addition to differences in metabolic half-life, the cell-specific recruitment of co-activator molecules by the OCT- VDR complex shown in vitro 21 could mediate OCT selectivity. Cell-specific expression of nuclear co-regulators required by the OCT-VDR complex in parathyroid, but not in intestinal or bone cells, could mediate OCT weaker calcemic activity. In experimental animal models of kidney disease, OCT clearly was less calcemic than calcitriol. 32 Importantly, OCT was effective in reversing abnormalities in bone formation without affecting bone turnover. 33,34 Paricalcitol, 19-nor, has a double bond at C22 and lacks the exocyclic carbon at position 19. Studies in uremic animal models showed that 19- nor is 10 times less active than calcitriol in mobilizing calcium from bone, 35 and 3 to 4 times less effective in suppressing serum PTH and parathyroid hyperplasia. 36,37 19-nor is also approximately
6 VITAMIN D RECEPTOR AND ANALOGS times less calcemic and phosphatemic than 1 D 2 in normal and uremic rats. 38 Similar studies in hemodialysis patients with end-stage renal disease and on a low-calcium diet showed that 8 times more paricalcitol than calcitriol was required to achieve a similar increment in serum calcium levels, possibly mobilized from bone. 39 The mechanisms responsible for 19-nor selectivity are unknown at present. Although 19-nor has less calcemic activity than calcitriol, hypercalcemia can occur during therapy. Hypercalcemic episodes were associated with overtreating as suggested by PTH suppression below the desired target range. 37 The widespread clinical use of 19-nor in the United States has allowed comparisons between therapy with this analog and calcitriol. Less severe hyperphosphatemia was shown in patients treated with paricalcitol compared with those receiving calcitriol. 40 More importantly, up until 2002, there were no data to suggest one vitamin D formulation had a survival advantage compared with another. In a recent historic cohort study performed by investigators at Massachusetts General Hospital and Fresenius Medical Care (North America), a survival advantage was found among patients treated with paricalcitol compared with those treated with calcitriol. 41 In this study of over 60,000 chronic hemodialysis patients throughout the United States, patients naive to injectable vitamin D were followed-up after they were started on calcitriol or paricalcitol. Patients were censored when they switched formulations or received a renal transplant. During the 36-month follow-up period, patients treated with paricalcitol had a 16% survival advantage compared with those treated with calcitriol. This survival advantage accounted for baseline differences, including mortality rates of the different dialysis centers involved, duration on dialysis before starting injectable vitamin D, and baseline mineral levels. Furthermore, patients who switched formulations also were studied. Those who switched from paricalcitol to calcitriol had a worse survival over the remaining follow-up period compared with those who switched from calcitriol to paricalcitol. Examination of serum levels of calcium, phosphate, and PTH revealed that the percent increase (from baseline) of serum calcium and phosphate was less and the percent decrease in serum PTH (from baseline) was more in the group treated with paricalcitol compared with those treated with calcitriol. Although only a randomized trial can confirm these results, these compelling data suggest vitamin D therapy should be integral in the management of secondary hyperparathyroidism and that the formulations are not all equal. REFERENCES 1. Slatopolsky E, Brown A, Dusso A: Pathogenesis of secondary hyperparathyroidism. Kidney Int Suppl 73:S14-S19, Brown AJ, Dusso A, Slatopolsky E: Vitamin D. Am J Physiol 277:F157-F175, Fukuda N, Tanaka H, Tominaga Y, et al: Decreased 1,25-dihydroxyvitamin D3 receptor density is associated with a more severe form of parathyroid hyperplasia in chronic uremic patients. J Clin Invest 92: , Dusso AS, Pavlopoulos T, Naumovich L, et al: p21(waf1) and transforming growth factor-alpha mediate dietary phosphate regulation of parathyroid cell growth. Kidney Int 59: , Gogusev J, Duchambon P, Stoermann-Chopard C, et al: De novo expression of transforming growth factor-alpha in parathyroid gland tissue of patients with primary or secondary uraemic hyperparathyroidism. Nephrol Dial Transplant 11: , Cozzolino M, Lu Y, Finch J, et al: p21waf1 and TGFalpha mediate parathyroid growth arrest by vitamin D and high calcium. Kidney Int 60: , Cozzolino M, Lu Y, Slatopolsky E, et al: Specific inhibition of EGFR-signaling prevents high phosphorus-induced parathyroid hyperplasia in renal failure. J Am Soc Nephrol 13:193A, 2002 (abstr) 8. Cordero JB, Cozzolino M, Lu Y, et al: 1,25-dihydroxyvitamin D down-regulates cell membrane growth- and nuclear growth-promoting signals by the epidermal growth factor receptor. J Biol Chem 277: , Tominaga Y, Tsuzuki T, Uchida K, et al: Expression of PRAD1/cyclin D1, retinoblastoma gene products, and Ki67 in parathyroid hyperplasia caused by chronic renal failure versus primary adenoma. Kidney Int 55: , Tokumoto M, Tsuruya K, Fukuda K, et al: Reduced p21, p27 and vitamin D receptor in the nodular hyperplasia in patients with advanced secondary hyperparathyroidism. Kidney Int 62: , Nykjaer A, Dragun D, Walther D, et al: An endocytic pathway essential for renal uptake and activation of the steroid 25-(OH) vitamin D3. Cell 96: , Jurutka PW, Whitfield GK, Hsieh JC, et al: Molecular nature of the vitamin D receptor and its role in regulation of gene expression. Rev Endocr Metab Disord 2: , Rachez C, Freedman LP: Mediator complexes and transcription. Curr Opin Cell Biol 13: , Rachez C, Freedman LP: Mechanisms of gene regulation by vitamin D(3) receptor: A network of coactivator interactions. Gene 246:9-21, Wiese RJ, Uhland-Smith A, Ross TK, et al: Up-regulation of the vitamin D receptor in response to 1,25-dihydroxyvi-
7 16 DUSSO, THADHANI, AND SLATOPOLSKY tamin D3 results from ligand-induced stabilization. J Biol Chem 267: , Denda M, Finch J, Brown AJ, et al: 1,25-dihydroxyvitamin D3 and 22-oxacalcitriol prevent the decrease in vitamin D receptor content in the parathyroid glands of uremic rats. Kidney Int 50:34-39, Sawaya BP, Koszewski NJ, Qi Q, et al: Secondary hyperparathyroidism and vitamin D receptor binding to vitamin D response elements in rats with incipient renal failure. J Am Soc Nephrol 8: , Patel SR, Ke HQ, Vanholder R, et al: Inhibition of calcitriol receptor binding to vitamin D response elements by uremic toxins. J Clin Invest 96:50-59, Sela-Brown A, Russell J, Koszewski NJ, et al: Calreticulin inhibits vitamin D s action on the PTH gene in vitro and may prevent vitamin D s effect in vivo in hypocalcemic rats. Mol Endocrinol 12: , Vidal M, Ramana CV, Dusso AS: Stat1-vitamin D receptor interactions antagonize 1,25-dihydroxyvitamin D transcriptional activity and enhance stat1-mediated transcription. Mol Cell Biol 22: , Takeyama K, Masuhiro Y, Fuse H, et al: Selective interaction of vitamin D receptor with transcriptional coactivators by a vitamin D analog. Mol Cell Biol 19: , Takeyama K, Kim M, Murayama AM, et al: Interactions of VDR with co-regulators by new vitamin D analogs. J Bone Miner Res 16:S433, 2001 (abstr) 23. Sjoden G, Smith C, Lindgren U, et al: 1 alpha-hydroxyvitamin D2 is less toxic than 1 alpha-hydroxyvitamin D3 in the rat. Proc Soc Exp Biol Med 178: , Sjoden G, Lindgren JU, DeLuca HF: Antirachitic activity of 1 alpha-hydroxyergocalciferol and 1 alpha-hydroxycholecalciferol in rats. J Nutr 114: , Knutson JC, Hollis BW, LeVan LW, et al: Metabolism of 1 alpha-hydroxyvitamin D2 to activated dihydroxyvitamin D 2 metabolites decreases endogenous 1 alpha, 25-dihydroxyvitamin D3 in rats and monkeys. Endocrinology 136: , Mawer EB, Jones G, Davies M, et al: Unique 24-hydroxylated metabolites represent a significant pathway of metabolism of vitamin D2 in humans: 24-hydroxyvitamin D2 and 1,24-dihydroxyvitamin D2 detectable in human serum. J Clin Endocrinol Metab 83: , Maung HM, Elangovan L, Frazao JM, et al: Efficacy and side effects of intermittent intravenous and oral doxercalciferol (1alpha-hydroxyvitamin D(2)) in dialysis patients with secondary hyperparathyroidism: A sequential comparison. Am J Kidney Dis 37: , Frazao JM, Elangovan L, Maung HM, et al: Intermittent doxercalciferol (1alpha-hydroxyvitamin D(2)) therapy for secondary hyperparathyroidism. Am J Kidney Dis 36: , Akiba T, Marumo F, Owada A, et al: Controlled trial of falecalcitriol versus alfacalcidol in suppression of parathyroid hormone in hemodialysis patients with secondary hyperparathyroidism. Am J Kidney Dis 32: , Okano T, Tsugawa N, Masuda S, et al: Protein-binding properties of 22-oxa-1 alpha,25-dihydroxyvitamin D3, a synthetic analogue of 1 alpha,25-dihydroxyvitamin D3. J Nutr Sci Vitaminol (Tokyo) 35: , Dusso AS, Negrea L, Gunawardhana S, et al: On the mechanisms for the selective action of vitamin D analogs. Endocrinology 128: , Brown AJ, Ritter CR, Finch JL, et al: The noncalcemic analogue of vitamin D, 22-oxacalcitriol, suppresses parathyroid hormone synthesis and secretion. J Clin Invest 84: , Tsukamoto Y, Hanaoka M, Matsuo T, et al: Effect of 22-oxacalcitriol on bone histology of hemodialyzed patients with severe secondary hyperparathyroidism. Am J Kidney Dis 35: , Monier-Faugere MC, Geng Z, Friedler RM, et al: 22- oxacalcitriol suppresses secondary hyperparathyroidism without inducing low bone turnover in dogs with renal failure. Kidney Int 55: , Finch JL, Brown AJ, Slatopolsky E: Differential effects of 1,25-dihydroxy-vitamin D3 and 19-nor-1,25-dihydroxy-vitamin D2 on calcium and phosphorus resorption in bone. J Am Soc Nephrol 10: , Llach F, Yudd M: Paricalcitol in dialysis patients with calcitriol-resistant secondary hyperparathyroidism. Am J Kidney Dis 38:S45-S50, Martin KJ, Gonzalez EA, Gellens ME, et al: Therapy of secondary hyperparathyroidism with 19-nor-1alpha,25-dihydroxyvitamin D2. Am J Kidney Dis 32:S61-S66, Slatopolsky E, Cozzolino M, Finch JL: Differential effects of 19-nor-1,25-(OH)(2)D(2) and 1alpha-hydroxyvitamin D(2) on calcium and phosphorus in normal and uremic rats. Kidney Int 62: , Coyne DW, Grieff M, Ahya SN, et al: Differential effects of acute administration of 19-Nor-1,25-dihydroxy-vitamin D2 and 1,25-dihydroxy-vitamin D3 on serum calcium and phosphorus in hemodialysis patients. Am J Kidney Dis 40: , Sprague SM, Lerma E, McCormmick D, et al: Suppression of parathyroid hormone secretion in hemodialysis patients: Comparison of paricalcitol with calcitriol. Am J Kidney Dis 38:S51-S56, Teng M, Wolf M, Ofsthun M, et al: Survival benefit of Zemplar compared with calcijex among dialysis patients. J Am Soc Nephrol 13:461A, 2002 (abstr)
New vitamin D analogs
 Kidney International, Vol. 63, Supplement 85 (2003), pp. S83 S87 New vitamin D analogs EDUARDO SLATOPOLSKY, JANE FINCH, and ALEX BROWN Renal Division, Department of Internal Medicine, Washington University
Kidney International, Vol. 63, Supplement 85 (2003), pp. S83 S87 New vitamin D analogs EDUARDO SLATOPOLSKY, JANE FINCH, and ALEX BROWN Renal Division, Department of Internal Medicine, Washington University
Therapeutic golas in the treatment of CKD-MBD
 Therapeutic golas in the treatment of CKD-MBD Hemodialysis clinic Clinical University Center Sarajevo Bantao, 04-08.10.2017, Sarajevo Abbvie Satellite symposium 06.10.2017 Chronic Kidney Disease Mineral
Therapeutic golas in the treatment of CKD-MBD Hemodialysis clinic Clinical University Center Sarajevo Bantao, 04-08.10.2017, Sarajevo Abbvie Satellite symposium 06.10.2017 Chronic Kidney Disease Mineral
Marie-Claude Monier-Faugere, Hanna Mawad, and Hartmut H. Malluche
 Opposite Effects of Calcitriol and Paricalcitol on the Parathyroid Hormone-(1-84)/Large Carboxy-Terminal- Parathyroid Hormone Fragments Ratio in Patients with Stage 5 Chronic Kidney Disease Marie-Claude
Opposite Effects of Calcitriol and Paricalcitol on the Parathyroid Hormone-(1-84)/Large Carboxy-Terminal- Parathyroid Hormone Fragments Ratio in Patients with Stage 5 Chronic Kidney Disease Marie-Claude
Secondary hyperparathyroidism an Update on Pathophysiology and Treatment
 Secondary hyperparathyroidism an Update on Pathophysiology and Treatment Klaus Olgaard Copenhagen Budapest Nephrology School August 2007 HPT IN CRF Renal mass Ca 2+ 1,25(OH) 2 D 3 CaR Hyperparathyroidism
Secondary hyperparathyroidism an Update on Pathophysiology and Treatment Klaus Olgaard Copenhagen Budapest Nephrology School August 2007 HPT IN CRF Renal mass Ca 2+ 1,25(OH) 2 D 3 CaR Hyperparathyroidism
Pathogenesis of secondary hyperparathyroidism
 The International Journal of Artificial Organs / Vol. 32 / no. 2, 2009 / pp. 75-80 Review Pathogenesis of secondary hyperparathyroidism MARIO COZZOLINO, SABINA PASHO, GIUDITTA FALLABRINO, LAURA OLIVI,
The International Journal of Artificial Organs / Vol. 32 / no. 2, 2009 / pp. 75-80 Review Pathogenesis of secondary hyperparathyroidism MARIO COZZOLINO, SABINA PASHO, GIUDITTA FALLABRINO, LAURA OLIVI,
Mechanisms for the Selective Actions of Vitamin D Analogs
 CHAPTER 82 Mechanisms for the Selective Actions of Vitamin D Analogs ALEX J. BROWN AND EDUARDO A. SLATOPOLSKY Renal Division, Department of Medicine, Washington University School of Medicine, St. Louis,
CHAPTER 82 Mechanisms for the Selective Actions of Vitamin D Analogs ALEX J. BROWN AND EDUARDO A. SLATOPOLSKY Renal Division, Department of Medicine, Washington University School of Medicine, St. Louis,
INTERACTION DRUG BODY
 INTERACTION DRUG BODY What the drug does to the body What the body does to the drug Receptors - intracellular receptors - membrane receptors - Channel receptors - G protein-coupled receptors - Tyrosine-kinase
INTERACTION DRUG BODY What the drug does to the body What the body does to the drug Receptors - intracellular receptors - membrane receptors - Channel receptors - G protein-coupled receptors - Tyrosine-kinase
Pathogenesis and Treatment of Renal Osteodystrophy
 Proceedings Blood Purif 2003;21:318 326 DOI: 10.1159/000072552 Eduardo Slatopolsky a Esther Gonzalez b Kevin Martin b a Renal Division, Washington University School of Medicine, St. Louis, Mo., and b Division
Proceedings Blood Purif 2003;21:318 326 DOI: 10.1159/000072552 Eduardo Slatopolsky a Esther Gonzalez b Kevin Martin b a Renal Division, Washington University School of Medicine, St. Louis, Mo., and b Division
Kidney disease and vitamin D levels: 25-hydroxyvitamin D, 1,25-dihydroxyvitamin D, and VDR activation
 review http://www.kidney-international.org & 2011 International Society of Nephrology Kidney disease and vitamin D levels: 25-hydroxyvitamin D, 1,25-dihydroxyvitamin D, and VDR activation Adriana S. Dusso
review http://www.kidney-international.org & 2011 International Society of Nephrology Kidney disease and vitamin D levels: 25-hydroxyvitamin D, 1,25-dihydroxyvitamin D, and VDR activation Adriana S. Dusso
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Prevalence and Pattern of Mineral Bone Disorder in Chronic Kidney Disease Patients Using Serum
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Prevalence and Pattern of Mineral Bone Disorder in Chronic Kidney Disease Patients Using Serum
CKD: Bone Mineral Metabolism. Peter Birks, Nephrology Fellow
 CKD: Bone Mineral Metabolism Peter Birks, Nephrology Fellow CKD - KDIGO Definition and Classification of CKD CKD: abnormalities of kidney structure/function for > 3 months with health implications 1 marker
CKD: Bone Mineral Metabolism Peter Birks, Nephrology Fellow CKD - KDIGO Definition and Classification of CKD CKD: abnormalities of kidney structure/function for > 3 months with health implications 1 marker
Secondary Hyperparathyroidism: Where are we now?
 Secondary Hyperparathyroidism: Where are we now? Dylan M. Barth, Pharm.D. PGY-1 Pharmacy Resident Mayo Clinic 2017 MFMER slide-1 Objectives Identify risk factors for the development of complications caused
Secondary Hyperparathyroidism: Where are we now? Dylan M. Barth, Pharm.D. PGY-1 Pharmacy Resident Mayo Clinic 2017 MFMER slide-1 Objectives Identify risk factors for the development of complications caused
Influence of parathyroid mass on the regulation of PTH secretion
 http://www.kidney-international.org & 26 International Society of Nephrology Influence of parathyroid mass on the regulation of PTH secretion E Lewin 1,2 and K Olgaard 2 1 Nephrological Department B, The
http://www.kidney-international.org & 26 International Society of Nephrology Influence of parathyroid mass on the regulation of PTH secretion E Lewin 1,2 and K Olgaard 2 1 Nephrological Department B, The
Persistent post transplant hyperparathyroidism. Shiva Seyrafian IUMS-97/10/18-8/1/2019
 Persistent post transplant hyperparathyroidism Shiva Seyrafian IUMS-97/10/18-8/1/2019 normal weight =18-160 mg In HPT= 500-1000 mg 2 Epidemiology Mild 2 nd hyperparathyroidism (HPT) resolve after renal
Persistent post transplant hyperparathyroidism Shiva Seyrafian IUMS-97/10/18-8/1/2019 normal weight =18-160 mg In HPT= 500-1000 mg 2 Epidemiology Mild 2 nd hyperparathyroidism (HPT) resolve after renal
02/27/2018. Objectives. To Replace or Not to Replace: Nutritional Vitamin D in Dialysis.
 To Replace or Not to Replace: Nutritional Vitamin D in Dialysis. Michael Shoemaker-Moyle, M.D. Assistant Professor of Clinical Medicine Objectives Review Vitamin D Physiology Review Current Replacement
To Replace or Not to Replace: Nutritional Vitamin D in Dialysis. Michael Shoemaker-Moyle, M.D. Assistant Professor of Clinical Medicine Objectives Review Vitamin D Physiology Review Current Replacement
Should cinacalcet be used in patients who are not on dialysis?
 Should cinacalcet be used in patients who are not on dialysis? Jorge B Cannata-Andía and José Luis Fernández-Martín Affiliations: Bone and Mineral Research Unit. Hospital Universitario Central de Asturias.
Should cinacalcet be used in patients who are not on dialysis? Jorge B Cannata-Andía and José Luis Fernández-Martín Affiliations: Bone and Mineral Research Unit. Hospital Universitario Central de Asturias.
Outline. The Role of Vitamin D in CKD. Essential Role of Vitamin D. Mechanism of Action of Vit D. Mechanism of Action of Vit D 7/16/2010
 Outline The Role of Vitamin D in CKD Priscilla How, Pharm.D., BCPS Assistant Professor National University of Singapore Principal Clinical Pharmacist National University Hospital (Pharmacy and Nephrology,
Outline The Role of Vitamin D in CKD Priscilla How, Pharm.D., BCPS Assistant Professor National University of Singapore Principal Clinical Pharmacist National University Hospital (Pharmacy and Nephrology,
Do We Do Too Many Parathyroidectomies in Dialysis? Sagar Nigwekar MD, MMSc Massachusetts General Hospital
 Do We Do Too Many Parathyroidectomies in Dialysis? Sagar Nigwekar MD, MMSc Massachusetts General Hospital E-mail: snigwekar@mgh.harvard.edu March 13, 2017 Disclosures statement: Consultant: Allena, Becker
Do We Do Too Many Parathyroidectomies in Dialysis? Sagar Nigwekar MD, MMSc Massachusetts General Hospital E-mail: snigwekar@mgh.harvard.edu March 13, 2017 Disclosures statement: Consultant: Allena, Becker
ALEX J. BROWN, ADRIANA DUSSO, AND EDUARDO SLATOPOLSKY Renal Division, Washington University School of Medicine, St. Louis, Missouri 63110
 invited review Vitamin D ALEX J. BROWN, ADRIANA DUSSO, AND EDUARDO SLATOPOLSKY Renal Division, Washington University School of Medicine, St. Louis, Missouri 63110 Brown, Alex J., Adriana Dusso, and Eduardo
invited review Vitamin D ALEX J. BROWN, ADRIANA DUSSO, AND EDUARDO SLATOPOLSKY Renal Division, Washington University School of Medicine, St. Louis, Missouri 63110 Brown, Alex J., Adriana Dusso, and Eduardo
Corporate Presentation January 2013
 Corporate Presentation January 2013 0 Forward-Looking Statements Certain statements and information included in this presentation are forwardlooking statements under the Private Securities Litigation Reform
Corporate Presentation January 2013 0 Forward-Looking Statements Certain statements and information included in this presentation are forwardlooking statements under the Private Securities Litigation Reform
The role of vitamin D in the pathogenesis and management of secondary hyperparathyroidism in chronic renal failure
 The role of vitamin D in the pathogenesis and management of secondary hyperparathyroidism in chronic renal failure Mini-review Giuseppe Vezzoli 1 Teresa Arcidiacono 1 Mario Cozzolino 2 1 Nephrology Unit,
The role of vitamin D in the pathogenesis and management of secondary hyperparathyroidism in chronic renal failure Mini-review Giuseppe Vezzoli 1 Teresa Arcidiacono 1 Mario Cozzolino 2 1 Nephrology Unit,
Cell Biology of Parathyroid Gland Hyperplasia in Chronic Renal Failure
 REVIEW J Am Soc Nephrol 11: 1141 1152, 2000 Cell Biology of Parathyroid Gland Hyperplasia in Chronic Renal Failure TILMAN B. DRÜEKE Institut National de la Santé et de la Recherche Médicale U507 and Division
REVIEW J Am Soc Nephrol 11: 1141 1152, 2000 Cell Biology of Parathyroid Gland Hyperplasia in Chronic Renal Failure TILMAN B. DRÜEKE Institut National de la Santé et de la Recherche Médicale U507 and Division
Kobe University Repository : Kernel
 Title Author(s) Citation Issue date 2009-09 Resource Type Resource Version DOI URL Kobe University Repository : Kernel Marked increase in bone formation markers after cinacalcet treatment by mechanisms
Title Author(s) Citation Issue date 2009-09 Resource Type Resource Version DOI URL Kobe University Repository : Kernel Marked increase in bone formation markers after cinacalcet treatment by mechanisms
Supplementary Information to Chapter 36
 REVIEW ON VITAMIN-D NEW INSIGHTS Elmer Verner McCollum (1879-1967) was the first to discover the antirachitic vitamin which he named as vitamin D in the early part of 20th century (1919). He had earlier
REVIEW ON VITAMIN-D NEW INSIGHTS Elmer Verner McCollum (1879-1967) was the first to discover the antirachitic vitamin which he named as vitamin D in the early part of 20th century (1919). He had earlier
Development and progression of secondary hyperparathyroidism in chronic kidney disease: lessons from molecular genetics
 translational nephrology http://www.kidney-international.org & 2008 International Society of Nephrology Development and progression of secondary hyperparathyroidism in chronic kidney disease: lessons from
translational nephrology http://www.kidney-international.org & 2008 International Society of Nephrology Development and progression of secondary hyperparathyroidism in chronic kidney disease: lessons from
A calcimimetic agent acutely suppresses parathyroid hormone levels in patients with chronic renal failure Rapid Communication
 Kidney International, Vol. 53 (1998), pp. 223 227 A calcimimetic agent acutely suppresses parathyroid hormone levels in patients with chronic renal failure Rapid Communication JOHN E. ANTONSEN, DONALD
Kidney International, Vol. 53 (1998), pp. 223 227 A calcimimetic agent acutely suppresses parathyroid hormone levels in patients with chronic renal failure Rapid Communication JOHN E. ANTONSEN, DONALD
Effect of percutaneous calcitriol injection therapy on secondary hyperparathyroidism in uraemic patients
 Nephrol Dial Transplant (2003) 18 [Suppl 3]: iii42 iii46 DOI: 10.1093/ndt/gfg1011 Effect of percutaneous calcitriol injection therapy on secondary hyperparathyroidism in uraemic patients Kazuhiro Shiizaki
Nephrol Dial Transplant (2003) 18 [Suppl 3]: iii42 iii46 DOI: 10.1093/ndt/gfg1011 Effect of percutaneous calcitriol injection therapy on secondary hyperparathyroidism in uraemic patients Kazuhiro Shiizaki
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A A Diabetes Outcome Progression Trial (ADOPT), 194 Adaptive immunity, 129 131 ADOPT (A Diabetes Outcome Progression Trial), 194 Aging, vitamin
Note: Page numbers of article titles are in boldface type. A A Diabetes Outcome Progression Trial (ADOPT), 194 Adaptive immunity, 129 131 ADOPT (A Diabetes Outcome Progression Trial), 194 Aging, vitamin
Basic and clinical aspects of parathyroid hyperplasia in chronic kidney disease
 http://www.kidney-international.org & 2006 International Society of Nephrology Basic and clinical aspects of parathyroid hyperplasia in chronic kidney disease M Fukagawa 1, S Nakanishi 1 and JJ Kazama
http://www.kidney-international.org & 2006 International Society of Nephrology Basic and clinical aspects of parathyroid hyperplasia in chronic kidney disease M Fukagawa 1, S Nakanishi 1 and JJ Kazama
VITAMINS-FAT SOLUBLE [LIPPINCOTT S ] Deeba S. Jairajpuri
![VITAMINS-FAT SOLUBLE [LIPPINCOTT S ] Deeba S. Jairajpuri VITAMINS-FAT SOLUBLE [LIPPINCOTT S ] Deeba S. Jairajpuri](/thumbs/88/115610056.jpg) VITAMINS-FAT SOLUBLE [LIPPINCOTT S 381-394] Deeba S. Jairajpuri VITAMIN A othe term retinoids includes both natural and synthetic forms of vitamin A essential for vision, reproduction, growth and maintenance
VITAMINS-FAT SOLUBLE [LIPPINCOTT S 381-394] Deeba S. Jairajpuri VITAMIN A othe term retinoids includes both natural and synthetic forms of vitamin A essential for vision, reproduction, growth and maintenance
This review examines the dynamics of parathyroid hormone
 In-Depth Review Dynamics of Parathyroid Hormone Secretion in Health and Secondary Hyperparathyroidism Arnold J. Felsenfeld,* Mariano Rodríguez, and Escolástico Aguilera-Tejero *Department of Medicine,
In-Depth Review Dynamics of Parathyroid Hormone Secretion in Health and Secondary Hyperparathyroidism Arnold J. Felsenfeld,* Mariano Rodríguez, and Escolástico Aguilera-Tejero *Department of Medicine,
The role of calcimimetics in chronic kidney disease
 http://www.kidney-international.org & 2006 International Society of Nephrology The role of calcimimetics in chronic kidney disease A Gal-Moscovici 1,2 and SM Sprague 1 1 Division of Nephrology and Hypertension,
http://www.kidney-international.org & 2006 International Society of Nephrology The role of calcimimetics in chronic kidney disease A Gal-Moscovici 1,2 and SM Sprague 1 1 Division of Nephrology and Hypertension,
Cell Biology Lecture 9 Notes Basic Principles of cell signaling and GPCR system
 Cell Biology Lecture 9 Notes Basic Principles of cell signaling and GPCR system Basic Elements of cell signaling: Signal or signaling molecule (ligand, first messenger) o Small molecules (epinephrine,
Cell Biology Lecture 9 Notes Basic Principles of cell signaling and GPCR system Basic Elements of cell signaling: Signal or signaling molecule (ligand, first messenger) o Small molecules (epinephrine,
OMICS Journals are welcoming Submissions
 OMICS Journals are welcoming Submissions OMICS International welcomes submissions that are original and technically so as to serve both the developing world and developed countries in the best possible
OMICS Journals are welcoming Submissions OMICS International welcomes submissions that are original and technically so as to serve both the developing world and developed countries in the best possible
Mohammad Husain Department of Biotechnology, Jamia Millia Islamia New Delhi
 Role of Vitamin D receptor (VDR) in HIV induced tubular injury Mohammad Husain Department of Biotechnology, Jamia Millia Islamia New Delhi 07/10/2015 INTRODUCTION Vitamin D is technically not a Vitamin;
Role of Vitamin D receptor (VDR) in HIV induced tubular injury Mohammad Husain Department of Biotechnology, Jamia Millia Islamia New Delhi 07/10/2015 INTRODUCTION Vitamin D is technically not a Vitamin;
Renal osteodystrophy with special emphasis on secondary hyperparathyroidism
 RENAL OSTEODYSTROPHY WITH SPECIAL EMPHASIS ON SECONDARY HYPERPARATHYROIDISM Artigo Original Rev Port Nefrol Hipert 2005; 19 (Suppl 1): 9-18 Renal osteodystrophy with special emphasis on secondary hyperparathyroidism
RENAL OSTEODYSTROPHY WITH SPECIAL EMPHASIS ON SECONDARY HYPERPARATHYROIDISM Artigo Original Rev Port Nefrol Hipert 2005; 19 (Suppl 1): 9-18 Renal osteodystrophy with special emphasis on secondary hyperparathyroidism
CKD-Mineral Bone Disorder (MBD) Pathogenesis of Metabolic Bone Disease. Grants: NIH, Abbott, Amgen, OPKO, Shire
 Pathogenesis of Metabolic Bone Disease Stuart M. Sprague, D.O. Chief, Division of Nephrology and Hypertension Professor of Medicine NorthShore University HealthSystem University of Chicago Pritzker School
Pathogenesis of Metabolic Bone Disease Stuart M. Sprague, D.O. Chief, Division of Nephrology and Hypertension Professor of Medicine NorthShore University HealthSystem University of Chicago Pritzker School
Hyperphosphatemia Modestly Retards Parathyroid Hormone Suppression during Calcitriol-Induced Hypercalcemia in Normal and Azotemic Rats
 Original Paper Nephron 2002;92:883 888 DOI: 10.1159/000065454 Accepted: May 22, 2002 Hyperphosphatemia Modestly Retards Parathyroid Hormone Suppression during Calcitriol-Induced Hypercalcemia in Normal
Original Paper Nephron 2002;92:883 888 DOI: 10.1159/000065454 Accepted: May 22, 2002 Hyperphosphatemia Modestly Retards Parathyroid Hormone Suppression during Calcitriol-Induced Hypercalcemia in Normal
Awaisheh. Mousa Al-Abbadi. Abdullah Alaraj. 1 Page
 f #3 Awaisheh Abdullah Alaraj Mousa Al-Abbadi 1 Page *This sheet was written from Section 1 s lecture, in the first 10 mins the Dr. repeated all the previous material relating to osteoporosis from the
f #3 Awaisheh Abdullah Alaraj Mousa Al-Abbadi 1 Page *This sheet was written from Section 1 s lecture, in the first 10 mins the Dr. repeated all the previous material relating to osteoporosis from the
Vitamins. Nafith Abu Tarboush, DDS, MSc, PhD
 Vitamins Nafith Abu Tarboush, DDS, MSc, PhD natarboush@ju.edu.jo www.facebook.com/natarboush Vitamins Organic compounds required by an organism in tiny amounts as a vital nutrient Cannot be synthesized
Vitamins Nafith Abu Tarboush, DDS, MSc, PhD natarboush@ju.edu.jo www.facebook.com/natarboush Vitamins Organic compounds required by an organism in tiny amounts as a vital nutrient Cannot be synthesized
Renal Osteodystrophy. Chapter 6. I. Introduction. Classification of Bone Disease. Eric W. Young
 Chapter 6 Renal Osteodystrophy Eric W. Young I. Introduction Renal osteodystrophy refers to bone disease that occurs in patients with kidney disease. Bone disease occurs across the full spectrum of kidney
Chapter 6 Renal Osteodystrophy Eric W. Young I. Introduction Renal osteodystrophy refers to bone disease that occurs in patients with kidney disease. Bone disease occurs across the full spectrum of kidney
The Parsabiv Beginner s Book
 The Parsabiv Beginner s Book A quick guide to help you learn about your treatment with Parsabiv and what to expect Indication Parsabiv (etelcalcetide) is indicated for the treatment of secondary hyperparathyroidism
The Parsabiv Beginner s Book A quick guide to help you learn about your treatment with Parsabiv and what to expect Indication Parsabiv (etelcalcetide) is indicated for the treatment of secondary hyperparathyroidism
Paricalcitol versus calcitriol treatment for hyperparathyroidism in pediatric hemodialysis patients
 Pediatr Nephrol (2006) 21:1434 1439 DOI 10.1007/s00467-006-0204-5 ORIGINAL ARTICLE Paricalcitol versus calcitriol treatment for hyperparathyroidism in pediatric hemodialysis patients Wacharee Seeherunvong
Pediatr Nephrol (2006) 21:1434 1439 DOI 10.1007/s00467-006-0204-5 ORIGINAL ARTICLE Paricalcitol versus calcitriol treatment for hyperparathyroidism in pediatric hemodialysis patients Wacharee Seeherunvong
original article see commentary on page 793
 http://www.kidney-international.org & 2011 International Society of Nephrology original article see commentary on page 793 No difference between alfacalcidol and paricalcitol in the of secondary hyperparathyroidism
http://www.kidney-international.org & 2011 International Society of Nephrology original article see commentary on page 793 No difference between alfacalcidol and paricalcitol in the of secondary hyperparathyroidism
Biochemistry 673 Lecture 2 Jason Kahn, UMCP Introduction to steroid hormone receptor (nuclear receptor) signalling
 Biochemistry 673 Lecture 2 Jason Kahn, UMCP Introduction to steroid hormone receptor (nuclear receptor) signalling Resources: Latchman Lodish chapter 10, 20 Helmreich, chapter 11 http://www.nursa.org,
Biochemistry 673 Lecture 2 Jason Kahn, UMCP Introduction to steroid hormone receptor (nuclear receptor) signalling Resources: Latchman Lodish chapter 10, 20 Helmreich, chapter 11 http://www.nursa.org,
Disease Pathogenesis and Research Progression of Renal Anemia
 2018 3rd International Conference on Life Sciences, Medicine, and Health (ICLSMH 2018) Disease Pathogenesis and Research Progression of Renal Anemia Yingying Liu, Qi Jiang* Department of Nephrology, China-Japan
2018 3rd International Conference on Life Sciences, Medicine, and Health (ICLSMH 2018) Disease Pathogenesis and Research Progression of Renal Anemia Yingying Liu, Qi Jiang* Department of Nephrology, China-Japan
HORMONES (Biomedical Importance)
 hormones HORMONES (Biomedical Importance) Hormones are the chemical messengers of the body. They are defined as organic substances secreted into blood stream to control the metabolic and biological activities.
hormones HORMONES (Biomedical Importance) Hormones are the chemical messengers of the body. They are defined as organic substances secreted into blood stream to control the metabolic and biological activities.
25/10/56. Hypothyroidism Myxedema in adults Cretinism congenital deficiency of thyroid hormone Hashimoto thyroiditis. Simple goiter (nontoxic goiter)
 THERAPEUTIC USES OF THYROID HORMONE Supeecha Wittayalertpunya Wannarasmi Ketchart Nov 2013 Hyperthyroidism (Thyrotoxicosis) Grave s disease (diffuse toxic goiter) Toxic uninodular & Toxic multinodular
THERAPEUTIC USES OF THYROID HORMONE Supeecha Wittayalertpunya Wannarasmi Ketchart Nov 2013 Hyperthyroidism (Thyrotoxicosis) Grave s disease (diffuse toxic goiter) Toxic uninodular & Toxic multinodular
The hart and bone in concert
 The hart and bone in concert Piotr Rozentryt III Department of Cardiology, Silesian Centre for Heart Disease, Silesian Medical University, Zabrze, Poland Disclosure Research grant, speaker`s fee, travel
The hart and bone in concert Piotr Rozentryt III Department of Cardiology, Silesian Centre for Heart Disease, Silesian Medical University, Zabrze, Poland Disclosure Research grant, speaker`s fee, travel
Vitamin D: Is it a superhero??
 Vitamin D: Is it a superhero?? Dr. Ashraf Abdel Basset Bakr Prof. of Pediatrics 1 2 History of vitamin D discovery Sources of vitamin D and its metabolism 13 Actions of vitamin D 4 Vitamin D deficiency
Vitamin D: Is it a superhero?? Dr. Ashraf Abdel Basset Bakr Prof. of Pediatrics 1 2 History of vitamin D discovery Sources of vitamin D and its metabolism 13 Actions of vitamin D 4 Vitamin D deficiency
Effective Treatment Strategies to Delay the Progression of Renal Disease in CKD
 Effective Treatment Strategies to Delay the Progression of Renal Disease in CKD Csaba P Kovesdy, MD FASN Memphis VA Medical Center, Memphis TN University of Tennessee, Memphis TN Vitamin D Metabolic acidosis
Effective Treatment Strategies to Delay the Progression of Renal Disease in CKD Csaba P Kovesdy, MD FASN Memphis VA Medical Center, Memphis TN University of Tennessee, Memphis TN Vitamin D Metabolic acidosis
Parathyroid Hormone, Calcium and Phosphorus Levels in Hemodialysis Patients at Al-Shifa Hospital, Gaza-Palestine
 IUG Journal of Natural and Engineering Studies Vol.22,No.1, pp 97-110 2014, ISSN 1726-6807, http://www.iugaza.edu.ps/ar/periodical/ Parathyroid Hormone, Calcium and Phosphorus Levels in Hemodialysis Patients
IUG Journal of Natural and Engineering Studies Vol.22,No.1, pp 97-110 2014, ISSN 1726-6807, http://www.iugaza.edu.ps/ar/periodical/ Parathyroid Hormone, Calcium and Phosphorus Levels in Hemodialysis Patients
2.0 Synopsis. Paricalcitol Capsules M Clinical Study Report R&D/15/0380. (For National Authority Use Only)
 2.0 Synopsis AbbVie Inc. Name of Study Drug: ABT-358/Zemplar (paricalcitol) Capsules Name of Active Ingredient: paricalcitol Individual Study Table Referring to Part of Dossier: Volume: Page: (For National
2.0 Synopsis AbbVie Inc. Name of Study Drug: ABT-358/Zemplar (paricalcitol) Capsules Name of Active Ingredient: paricalcitol Individual Study Table Referring to Part of Dossier: Volume: Page: (For National
Survival of Patients Undergoing Hemodialysis with Paricalcitol or Calcitriol Therapy
 The new england journal of medicine original article Survival of Patients Undergoing Hemodialysis with Paricalcitol or Calcitriol Therapy Ming Teng, M.D., Myles Wolf, M.D., M.M.Sc., Edmund Lowrie, M.D.,
The new england journal of medicine original article Survival of Patients Undergoing Hemodialysis with Paricalcitol or Calcitriol Therapy Ming Teng, M.D., Myles Wolf, M.D., M.M.Sc., Edmund Lowrie, M.D.,
Malnutrition and Role of Nutrition in BMD:CKD
 Malnutrition and Role of Nutrition in BMD:CKD PNDS Continuing Nutrition Education Seminar Saturday, 30 th November 2013 Fayza Khan MSC (Foods and Nutrition) R.D President,PNDS Outline Objective Malnutrition
Malnutrition and Role of Nutrition in BMD:CKD PNDS Continuing Nutrition Education Seminar Saturday, 30 th November 2013 Fayza Khan MSC (Foods and Nutrition) R.D President,PNDS Outline Objective Malnutrition
Considerations for the Treatment of Secondary Hyperparathyroidism in Renal Failure
 DISEASEOF THE MONTH Considerations for the Treatment of Secondary Hyperparathyroidism in Renal Failure ARNOLD J. FELSENFELD Department of Medicine, West Los Angeles Veterans Affairs Medical Center, and
DISEASEOF THE MONTH Considerations for the Treatment of Secondary Hyperparathyroidism in Renal Failure ARNOLD J. FELSENFELD Department of Medicine, West Los Angeles Veterans Affairs Medical Center, and
MECHANISM AND MODE OF HORMONE ACTION. Some definitions. Receptor: Properties of receptors. PRESENTED BY MBUNKUR GLORY NKOSI.
 MECHANISM AND MODE OF HORMONE ACTION. PRESENTED BY MBUNKUR GLORY NKOSI. OUTLINE. Introduction Some definitions Hormone secretion, transport, and clearance from the blood. Feedback control of hormone secretion.
MECHANISM AND MODE OF HORMONE ACTION. PRESENTED BY MBUNKUR GLORY NKOSI. OUTLINE. Introduction Some definitions Hormone secretion, transport, and clearance from the blood. Feedback control of hormone secretion.
Conversion from conventional to nocturnal hemodialysis improves vitamin D levels
 http://www.kidney-international.org & 2007 International Society of Nephrology Conversion from conventional to nocturnal hemodialysis improves vitamin D levels SJ Nessim 1, SV Jassal 1, SV Fung 1 and CT
http://www.kidney-international.org & 2007 International Society of Nephrology Conversion from conventional to nocturnal hemodialysis improves vitamin D levels SJ Nessim 1, SV Jassal 1, SV Fung 1 and CT
Secondary hyperparathyroidism in dialysis patients
 Secondary hyperparathyroidism in dialysis patients ( a critical approach of pharmacological treatments) Dominique JOLY Néphrologie Hôpital NECKER, Paris DFG Finn WF. J Am Soc Nephrol. 24;15:271A. Ca ++
Secondary hyperparathyroidism in dialysis patients ( a critical approach of pharmacological treatments) Dominique JOLY Néphrologie Hôpital NECKER, Paris DFG Finn WF. J Am Soc Nephrol. 24;15:271A. Ca ++
Attivazione selettiva dei VDR nella CKD-MBD: dalla conservativa alla dialisi
 Attivazione selettiva dei VDR nella CKD-MBD: dalla conservativa alla dialisi Mario Cozzolino, MD, PhD, FERA Dipartimento di Scienze della Salute Università di Milano UO Nefrologia e Dialisi Laboratorio
Attivazione selettiva dei VDR nella CKD-MBD: dalla conservativa alla dialisi Mario Cozzolino, MD, PhD, FERA Dipartimento di Scienze della Salute Università di Milano UO Nefrologia e Dialisi Laboratorio
Key words: Vitamin D analogues, alfacalcidol, calcitriol, secondary hyperparathyroidism, renal dialysis
 Oral cal ORAL CALCITRIOL VERSUS ORAL ALFACALCIDOL FOR THE TREATMENT OF SECONDARY HYPERPARATHYROIDISM IN PATIENTS RECEIVING HEMODIALYSIS: A RANDOMIZED, CROSSOVER TR IAL Samantha Moe 1, Lori D Wazny 2, Janet
Oral cal ORAL CALCITRIOL VERSUS ORAL ALFACALCIDOL FOR THE TREATMENT OF SECONDARY HYPERPARATHYROIDISM IN PATIENTS RECEIVING HEMODIALYSIS: A RANDOMIZED, CROSSOVER TR IAL Samantha Moe 1, Lori D Wazny 2, Janet
Molecular Cell Biology - Problem Drill 19: Cell Signaling Pathways and Gene Expression
 Molecular Cell Biology - Problem Drill 19: Cell Signaling Pathways and Gene Expression Question No. 1 of 10 1. Which statement about cell signaling is correct? Question #1 (A) Cell signaling involves receiving
Molecular Cell Biology - Problem Drill 19: Cell Signaling Pathways and Gene Expression Question No. 1 of 10 1. Which statement about cell signaling is correct? Question #1 (A) Cell signaling involves receiving
Hyperphosphatemia is associated with a
 TREATMENT OPTIONS IN THE MANAGEMENT OF PHOSPHATE RETENTION * George A. Porter, MD, FACP, and Hartmut H. Malluche, MD, FACP ABSTRACT Hyperphosphatemia is an independent risk factor for mortality and cardiovascular
TREATMENT OPTIONS IN THE MANAGEMENT OF PHOSPHATE RETENTION * George A. Porter, MD, FACP, and Hartmut H. Malluche, MD, FACP ABSTRACT Hyperphosphatemia is an independent risk factor for mortality and cardiovascular
Medical and surgical aspects of parathyroidectomy
 Kidney International, Vol. 56, Suppl. 73 (1999), pp. S-65 S-69 Medical and surgical aspects of parathyroidectomy MASAFUMI FUKAGAWA, YOSHIHIRO TOMINAGA, MASAFUMI KITAOKA, TAKATOSHI KAKUTA, and KIYOSHI KUROKAWA
Kidney International, Vol. 56, Suppl. 73 (1999), pp. S-65 S-69 Medical and surgical aspects of parathyroidectomy MASAFUMI FUKAGAWA, YOSHIHIRO TOMINAGA, MASAFUMI KITAOKA, TAKATOSHI KAKUTA, and KIYOSHI KUROKAWA
Hyperparathyroidism: Operative Considerations. Financial Disclosures: None. Hyperparathyroidism. Hyperparathyroidism 11/10/2012
 Hyperparathyroidism: Operative Considerations Financial Disclosures: None Steven J Wang, MD FACS Associate Professor Dept of Otolaryngology-Head and Neck Surgery University of California, San Francisco
Hyperparathyroidism: Operative Considerations Financial Disclosures: None Steven J Wang, MD FACS Associate Professor Dept of Otolaryngology-Head and Neck Surgery University of California, San Francisco
HYDROCHLORIDE FOR THE TREATMENT OF SECONDARY HYPERPARATHYROIDISM IN PATIENTS WITH END-STAGE RENAL DISEASE ON MAINTENANCE DIALYSIS THERAPY
 UK RENAL PHARMACY GROUP SUBMISSION TO THE NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE on CINACALCET HYDROCHLORIDE FOR THE TREATMENT OF SECONDARY HYPERPARATHYROIDISM IN PATIENTS WITH END-STAGE RENAL DISEASE
UK RENAL PHARMACY GROUP SUBMISSION TO THE NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE on CINACALCET HYDROCHLORIDE FOR THE TREATMENT OF SECONDARY HYPERPARATHYROIDISM IN PATIENTS WITH END-STAGE RENAL DISEASE
Sensipar. Sensipar (cinacalcet) Description
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.30.46 Subject: Sensipar Page: 1 of 5 Last Review Date: June 22, 2018 Sensipar Description Sensipar (cinacalcet)
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.30.46 Subject: Sensipar Page: 1 of 5 Last Review Date: June 22, 2018 Sensipar Description Sensipar (cinacalcet)
PRIMARY HYPERPARATHYROIDISM
 PRIMARY HYPERPARATHYROIDISM HYPERPARATHYROIDISM Inappropriate excess secretion of Parathyroid Hormone in Primary Hyperparathyroidism Appropriate Hypersecretion in Secondary Hyperparathyroidism PTH and
PRIMARY HYPERPARATHYROIDISM HYPERPARATHYROIDISM Inappropriate excess secretion of Parathyroid Hormone in Primary Hyperparathyroidism Appropriate Hypersecretion in Secondary Hyperparathyroidism PTH and
Parathyoid glands and PTH
 Parathyoid glands and PTH They are four glands located behind the thyroid gland, each one from (20-50) mg in weight, and composed of two types of cells: 1. Cheif cells: that produces PTH. 2-oxyphil cells:
Parathyoid glands and PTH They are four glands located behind the thyroid gland, each one from (20-50) mg in weight, and composed of two types of cells: 1. Cheif cells: that produces PTH. 2-oxyphil cells:
Nephrology Dialysis Transplantation
 Nephrol Dial Transplant (1998) 1: [Suppl ]: 68 7 Nephrology Dialysis Transplantation Intermittent oral 1a-hydroxyvitamin D is effective and safe for the suppression of secondary hyperparathyroidism in
Nephrol Dial Transplant (1998) 1: [Suppl ]: 68 7 Nephrology Dialysis Transplantation Intermittent oral 1a-hydroxyvitamin D is effective and safe for the suppression of secondary hyperparathyroidism in
Receptors Functions and Signal Transduction- L4- L5
 Receptors Functions and Signal Transduction- L4- L5 Faisal I. Mohammed, MD, PhD University of Jordan 1 PKC Phosphorylates many substrates, can activate kinase pathway, gene regulation PLC- signaling pathway
Receptors Functions and Signal Transduction- L4- L5 Faisal I. Mohammed, MD, PhD University of Jordan 1 PKC Phosphorylates many substrates, can activate kinase pathway, gene regulation PLC- signaling pathway
What is the optimal regimen for vitamin D?
 Kidney International, Vol. 56, Suppl. 73 (1999), pp. S-59 S-64 What is the optimal regimen for vitamin D? JOHN CUNNINGHAM Department of Nephrology, St Bartholomew s and the Royal London School of Medicine
Kidney International, Vol. 56, Suppl. 73 (1999), pp. S-59 S-64 What is the optimal regimen for vitamin D? JOHN CUNNINGHAM Department of Nephrology, St Bartholomew s and the Royal London School of Medicine
Renal Association Clinical Practice Guideline in Mineral and Bone Disorders in CKD
 Nephron Clin Pract 2011;118(suppl 1):c145 c152 DOI: 10.1159/000328066 Received: May 24, 2010 Accepted: December 6, 2010 Published online: May 6, 2011 Renal Association Clinical Practice Guideline in Mineral
Nephron Clin Pract 2011;118(suppl 1):c145 c152 DOI: 10.1159/000328066 Received: May 24, 2010 Accepted: December 6, 2010 Published online: May 6, 2011 Renal Association Clinical Practice Guideline in Mineral
A Randomised Clinical Study of Alfacalcidol and Paricalcitol
 PHD THESIS DANISH MEDICAL JOURNAL A Randomised Clinical Study of Alfacalcidol and Paricalcitol Two vitamin D analogs for treatment of secondary hyperparathyroidism in chronic hemodialysis patients Ditte
PHD THESIS DANISH MEDICAL JOURNAL A Randomised Clinical Study of Alfacalcidol and Paricalcitol Two vitamin D analogs for treatment of secondary hyperparathyroidism in chronic hemodialysis patients Ditte
Ergocalciferol and Cholecalciferol in CKD
 In Practice Ergocalciferol and Cholecalciferol in CKD Sagar U. Nigwekar, MD, 1,2 Ishir Bhan, MD, MPH, 1 and Ravi Thadhani, MD, MPH 1 The development of chronic kidney disease (CKD) is accompanied by a
In Practice Ergocalciferol and Cholecalciferol in CKD Sagar U. Nigwekar, MD, 1,2 Ishir Bhan, MD, MPH, 1 and Ravi Thadhani, MD, MPH 1 The development of chronic kidney disease (CKD) is accompanied by a
Percutaneous maxacalcitol injection therapy regresses hyperplasia of parathyroid and induces apoptosis in uremia
 Kidney International, Vol. 64 (2003), pp. 992 1003 Percutaneous maxacalcitol injection therapy regresses hyperplasia of parathyroid and induces apoptosis in uremia KAZUHIRO SHIIZAKI, 1 IKUJI HATAMURA,
Kidney International, Vol. 64 (2003), pp. 992 1003 Percutaneous maxacalcitol injection therapy regresses hyperplasia of parathyroid and induces apoptosis in uremia KAZUHIRO SHIIZAKI, 1 IKUJI HATAMURA,
PTH increases renal 25(OH)D 3-1 -hydroxylase (CYP1 ) mrna but not renal 1,25(OH) 2 D 3 production in adult rats
 Am J Physiol Renal Physiol 284: F1032 F1036, 2003; 10.1152/ajprenal.00306.2002. PTH increases renal 25(OH)D 3-1 -hydroxylase (CYP1 ) mrna but not renal 1,25(OH) 2 D 3 production in adult rats H. J. Armbrecht,
Am J Physiol Renal Physiol 284: F1032 F1036, 2003; 10.1152/ajprenal.00306.2002. PTH increases renal 25(OH)D 3-1 -hydroxylase (CYP1 ) mrna but not renal 1,25(OH) 2 D 3 production in adult rats H. J. Armbrecht,
Endocrine Regulation of Calcium and Phosphate Metabolism
 Endocrine Regulation of Calcium and Phosphate Metabolism Huiping Wang ( 王会平 ), PhD Department of Physiology Rm C516, Block C, Research Building, School of Medicine Tel: 88208252 Email: wanghuiping@zju.edu.cn
Endocrine Regulation of Calcium and Phosphate Metabolism Huiping Wang ( 王会平 ), PhD Department of Physiology Rm C516, Block C, Research Building, School of Medicine Tel: 88208252 Email: wanghuiping@zju.edu.cn
Gene expression of vitamin D hydroxylase and megalin in the remnant kidney of nephrectomized rats
 Kidney International, Vol. 64 (2003), pp. 414 420 Gene expression of vitamin D hydroxylase and megalin in the remnant kidney of nephrectomized rats FUMI TAKEMOTO, TOSHIMASA SHINKI, KEITARO YOKOYAMA, TAKETOSHI
Kidney International, Vol. 64 (2003), pp. 414 420 Gene expression of vitamin D hydroxylase and megalin in the remnant kidney of nephrectomized rats FUMI TAKEMOTO, TOSHIMASA SHINKI, KEITARO YOKOYAMA, TAKETOSHI
RENAL GRAND ROUNDS. Vitamin D- Beyond the bone. Dr Krishna Pakkivenkata. 9 th April 2010.
 RENAL GRAND ROUNDS Vitamin D- Beyond the bone Dr Krishna Pakkivenkata. 9 th April 2010. Brief history Secosteroid. 1920 s-exposure to sunlight prevented rickets. 1936- structure of Vit D was discovered.
RENAL GRAND ROUNDS Vitamin D- Beyond the bone Dr Krishna Pakkivenkata. 9 th April 2010. Brief history Secosteroid. 1920 s-exposure to sunlight prevented rickets. 1936- structure of Vit D was discovered.
Rahaf AL-Jafari. Marah Qaddourah. Rahmeh Abdullah. Saleem. 1 P a g e
 15 Rahaf AL-Jafari Marah Qaddourah Rahmeh Abdullah Saleem 1 P a g e If you are following with the record you may notice a little bit difference in information sequences. Hormones that function on growth
15 Rahaf AL-Jafari Marah Qaddourah Rahmeh Abdullah Saleem 1 P a g e If you are following with the record you may notice a little bit difference in information sequences. Hormones that function on growth
Contents. Authors Name: Christopher Wong: Consultant Nephrologist Anne Waddington: Renal Pharmacist Eimear Fegan : Renal Dietitian
 Cheshire and Merseyside Renal Units Guidelines on the Management of Chronic Kidney Disease - Mineral Bone Disorder (adapted from Greater Manchester) Authors Name: Christopher Wong: Consultant Nephrologist
Cheshire and Merseyside Renal Units Guidelines on the Management of Chronic Kidney Disease - Mineral Bone Disorder (adapted from Greater Manchester) Authors Name: Christopher Wong: Consultant Nephrologist
hypercalcemia of malignancy hyperparathyroidism PHPT the most common cause of hypercalcemia in the outpatient setting the second most common cause
 hyperparathyroidism A 68-year-old woman with documented osteoporosis has blood tests showing elevated serum calcium and parathyroid hormone (PTH) levels: 11.2 mg/dl (8.8 10.1 mg/dl) and 88 pg/ml (10-60),
hyperparathyroidism A 68-year-old woman with documented osteoporosis has blood tests showing elevated serum calcium and parathyroid hormone (PTH) levels: 11.2 mg/dl (8.8 10.1 mg/dl) and 88 pg/ml (10-60),
Ayman Mesleh & Leen Alnemrawi. Bayan Abusheikha. Faisal
 24 Ayman Mesleh & Leen Alnemrawi Bayan Abusheikha Faisal We were talking last time about receptors for lipid soluble hormones.the general mechanism of receptors for lipid soluble hormones: 1. Receptors
24 Ayman Mesleh & Leen Alnemrawi Bayan Abusheikha Faisal We were talking last time about receptors for lipid soluble hormones.the general mechanism of receptors for lipid soluble hormones: 1. Receptors
Identification of influential proteins in the classical retinoic acid signaling pathway
 Ghaffari and Petzold Theoretical Biology and Medical Modelling (2018) 15:16 https://doi.org/10.1186/s12976-018-0088-7 RESEARCH Open Access Identification of influential proteins in the classical retinoic
Ghaffari and Petzold Theoretical Biology and Medical Modelling (2018) 15:16 https://doi.org/10.1186/s12976-018-0088-7 RESEARCH Open Access Identification of influential proteins in the classical retinoic
LQB383 Testbank. Week 8 Cell Communication and Signaling Mechanisms
 LQB383 Testbank Week 8 Cell Communication and Signaling Mechanisms Terms to learn match the terms to the definitions --------------------------------------------------------------------------------------------------------------------------
LQB383 Testbank Week 8 Cell Communication and Signaling Mechanisms Terms to learn match the terms to the definitions --------------------------------------------------------------------------------------------------------------------------
The Effect of Long-Term Intravenous Calcitriol Administration on Parathyroid Function in Hemodialysis
 The Effect of Long-Term Intravenous Calcitriol Administration on Parathyroid Function in Hemodialysis 12 Mariano Rodriguez,3 Arnold J. Felsenfeld, Carl Williams, James A. Pederson, and Francisco Liach
The Effect of Long-Term Intravenous Calcitriol Administration on Parathyroid Function in Hemodialysis 12 Mariano Rodriguez,3 Arnold J. Felsenfeld, Carl Williams, James A. Pederson, and Francisco Liach
Endocrine secretion cells secrete substances into the extracellular fluid
 Animal Hormones Concept 30.1 Hormones Are Chemical Messengers Endocrine secretion cells secrete substances into the extracellular fluid Exocrine secretion cells secrete substances into a duct or a body
Animal Hormones Concept 30.1 Hormones Are Chemical Messengers Endocrine secretion cells secrete substances into the extracellular fluid Exocrine secretion cells secrete substances into a duct or a body
Ca, Phos and Vitamin D Metabolism in Pre-Dialysis Patients
 Ca, Phos and Vitamin D Metabolism in Pre-Dialysis Patients A. WADGYMAR, MD Credit Valley Hospital, Mississauga, Ontario, Canada. June 1, 2007 1 Case: 22 y/o referred to Renal Clinic Case: A.M. 29 y/o Man
Ca, Phos and Vitamin D Metabolism in Pre-Dialysis Patients A. WADGYMAR, MD Credit Valley Hospital, Mississauga, Ontario, Canada. June 1, 2007 1 Case: 22 y/o referred to Renal Clinic Case: A.M. 29 y/o Man
The Role of the Laboratory in Metabolic Bone Disease
 The Role of the Laboratory in Metabolic Bone Disease Howard Morris PhD, FAACB, FFSc(RCPA) President, IFCC Professor of Medical Sciences, University of South Australia, Clinical Scientist, SA Pathology
The Role of the Laboratory in Metabolic Bone Disease Howard Morris PhD, FAACB, FFSc(RCPA) President, IFCC Professor of Medical Sciences, University of South Australia, Clinical Scientist, SA Pathology
March 19 th Batool Aqel
 March 19 th - 2013 6 Batool Aqel Hormones That Bind to Nuclear Receptor Proteins Hormones bind to their receptors.whether the receptor is found in the nucleus or the cytoplasm, at the end they are translocated
March 19 th - 2013 6 Batool Aqel Hormones That Bind to Nuclear Receptor Proteins Hormones bind to their receptors.whether the receptor is found in the nucleus or the cytoplasm, at the end they are translocated
... . : ... PTH.
 IRMA Email msarookhani@qumsacir * CRD GFR D [1,25OH 2 D 3 ] SHPT GFR» «KDOQI SHPT Ca * P P P Selectra Overt HPT = = Ca * P P > GM II DSL i IRMA ± ± ± Ca * P % % % % % % % % % % % % % % % % pgml = = > ±
IRMA Email msarookhani@qumsacir * CRD GFR D [1,25OH 2 D 3 ] SHPT GFR» «KDOQI SHPT Ca * P P P Selectra Overt HPT = = Ca * P P > GM II DSL i IRMA ± ± ± Ca * P % % % % % % % % % % % % % % % % pgml = = > ±
Cardiovascular Mortality: General Population vs ESRD Dialysis Patients
 Cardiovascular Mortality: General Population vs ESRD Dialysis Patients Annual CVD Mortality (%) 100 10 1 0.1 0.01 0.001 25-34 35-44 45-54 55-64 66-74 75-84 >85 Age (years) GP Male GP Female GP Black GP
Cardiovascular Mortality: General Population vs ESRD Dialysis Patients Annual CVD Mortality (%) 100 10 1 0.1 0.01 0.001 25-34 35-44 45-54 55-64 66-74 75-84 >85 Age (years) GP Male GP Female GP Black GP
Comparison of Serum Parathyroid Hormone (PTH) Levels in Hemodialysis and Peritoneal Dialysis Patients. Int.J.Curr.Res.Aca.Rev.2016; 4(11):
 Comparison of Serum Parathyroid Hormone (PTH) Levels in Hemodialysis and Peritoneal Dialysis Patients Seyed Seifollah Beladi Mousavi 1, Arman Shahriari 2 and Fatemeh Roumi 3 * 1 Department of Nephrology,
Comparison of Serum Parathyroid Hormone (PTH) Levels in Hemodialysis and Peritoneal Dialysis Patients Seyed Seifollah Beladi Mousavi 1, Arman Shahriari 2 and Fatemeh Roumi 3 * 1 Department of Nephrology,
Pathophysiology of parathyroid hyperplasia in chronic kidney disease: preclinical and clinical basis for parathyroid intervention
 NDT Plus (2008) 1 [Suppl 3]: iii2 iii8 doi: 10.1093/ndtplus/sfn079 Pathophysiology of parathyroid hyperplasia in chronic kidney disease: preclinical and clinical basis for parathyroid intervention Shunsuke
NDT Plus (2008) 1 [Suppl 3]: iii2 iii8 doi: 10.1093/ndtplus/sfn079 Pathophysiology of parathyroid hyperplasia in chronic kidney disease: preclinical and clinical basis for parathyroid intervention Shunsuke
Normal kidneys filter large amounts of organic
 ORIGINAL ARTICLE - NEPHROLOGY Effect Of Lanthanum Carbonate vs Calcium Acetate As A Phosphate Binder In Stage 3-4 CKD- Treat To Goal Study K.S. Sajeev Kumar (1), M K Mohandas (1), Ramdas Pisharody (1),
ORIGINAL ARTICLE - NEPHROLOGY Effect Of Lanthanum Carbonate vs Calcium Acetate As A Phosphate Binder In Stage 3-4 CKD- Treat To Goal Study K.S. Sajeev Kumar (1), M K Mohandas (1), Ramdas Pisharody (1),
Cell Communication. Cell Communication. Communication between cells requires: ligand: the signaling molecule
 Cell Communication Cell Communication Communication between cells requires: ligand: the signaling molecule receptor protein: the molecule to which the ligand binds (may be on the plasma membrane or within
Cell Communication Cell Communication Communication between cells requires: ligand: the signaling molecule receptor protein: the molecule to which the ligand binds (may be on the plasma membrane or within
Post-translational modifications of proteins in gene regulation under hypoxic conditions
 203 Review Article Post-translational modifications of proteins in gene regulation under hypoxic conditions 1, 2) Olga S. Safronova 1) Department of Cellular Physiological Chemistry, Tokyo Medical and
203 Review Article Post-translational modifications of proteins in gene regulation under hypoxic conditions 1, 2) Olga S. Safronova 1) Department of Cellular Physiological Chemistry, Tokyo Medical and
Hormones. Prof. Dr. Volker Haucke Institut für Chemie-Biochemie Takustrasse 6
 Hormones Prof. Dr. Volker Haucke Institut für Chemie-Biochemie Takustrasse 6 Tel. 030-8385-6920 (Sekret.) 030-8385-6922 (direkt) e-mail: vhaucke@chemie.fu-berlin.de http://userpage.chemie.fu-berlin.de/biochemie/aghaucke/teaching.html
Hormones Prof. Dr. Volker Haucke Institut für Chemie-Biochemie Takustrasse 6 Tel. 030-8385-6920 (Sekret.) 030-8385-6922 (direkt) e-mail: vhaucke@chemie.fu-berlin.de http://userpage.chemie.fu-berlin.de/biochemie/aghaucke/teaching.html
PHRM20001: Pharmacology - How Drugs Work!
 PHRM20001: Pharmacology - How Drugs Work Drug: a chemical that affects physiological function in a specific way. Endogenous substances: hormones, neurotransmitters, antibodies, genes. Exogenous substances:
PHRM20001: Pharmacology - How Drugs Work Drug: a chemical that affects physiological function in a specific way. Endogenous substances: hormones, neurotransmitters, antibodies, genes. Exogenous substances:
