BARTS ENDOCRINE E-PROTOCOLS CALCIUM DISORDERS AND BONE
|
|
|
- Clara Norris
- 6 years ago
- Views:
Transcription
1 HYPERCALCAEMIA CALCIUM DISORDERS Clinical features to record Symptoms: Thirst, polyuria, nocturia, tiredness, poor concentration, depression, constipation, episodes of renal colic/calculi, hypertension, family history (MEN1 or 2A, familial hypocalciuric hypercalcaemia, hyperparathyroidism jaw tumour syndrome, familial isolated hyperparathyroidism) Examination: Signs of malignancy, sarcoidosis, corneal calcification Investigation Serum calcium. This should be corrected for albumin: corrected Ca 2+ = actual Ca 2+ + (0.02 x (47 serum albumin)). Serum PO 4 3-, alkaline phosphatase. Determine the mechanism of hypercalcaemia by performing the investigations below. MEASUREMENT FBC, ESR, chest X-ray Serum ACE U&E and urine calcium and urine creatinine Serum electrophoresis Serum PTH 25-hydroxyvitamin D TSH, T4, T3 SCREENING FOR Sarcoidosis, malignancy, TB Sarcoidosis Familial benign hypercalcaemia (FBH) Multiple myeloma All causes Interpretation of PTH level Thyrotoxicosis
2 PRIMARY HYPERPARATHYROIDISM 1) ESTABLISH THE BIOCHEMICAL DIAGNOSIS This comprises elevated corrected Ca 2+, low PO 3-4, normal alkaline phosphatase (unless bone disease present), normal or elevated serum PTH, often elevated Cl -. o Exclude vitamin D deficiency as cause of raised PTH. o Exclude Familial Benign Hypercalcaemia (FBH) as cause of hypercalcaemia by calculating the ratio of calcium clearance to creatinine clearance. Calculation of calcium clearance: [Urine Calcium (mmol/l) x urine volume (ml)] / [Plasma Calcium (mmol/l) x 1440] Calculation of creatinine clearance: [Urine Creatinine (mmol/l) x urine volume (ml)]/[plasma Creatinine (mmol/l) x 1440] Plasma creatinine is normally expressed in umol/l and needs to be converted to mmol/l by dividing by In normals and primary hyperparathyroidism, calcium clearance to creatinine clearance ratio should be > The ratio can be reduced to the formula below: Urine Calcium (mmol/l) x [Plasma Creatinine (umol/l) / 1000] Plasma Calcium (mmol) x Urine Creatinine (mmol/l) Reference Sopwith et al. HLA antigens and familial benign hypercalcaemia. Clinical Endocrinology 1984; 21: ) ESTABLISH THE PHYSIOLOGICAL IMPACT OF HYPERPARATHYROIDISM Includes assessment of: Symptoms Hypertension Nephrocalcinosis (renal tract ultrasound or CT KUB) Osteoporosis (DEXA scan)
3 LOCALISATION OF PARATHYROID ADENOMA Proceed to localisation if surgical management is proposed. All of the techniques have limitations. Ultrasound of neck: The accuracy of ultrasound is highly operator dependent. It is painless, noninvasive, inexpensive and does not expose the patient to radiation. Ultrasound can identify coexistent thyroid pathology and be used to locate intrathyroidal parathyroid adenomas. However, ultrasonography neither evaluates the mediastinum nor offers functional information. Sesta-MIBI scanning: - The main advantage of sestamibi scans is the ability to localise parathyroid glands in ectopic sites including the mediastinum. The major factors contributing to a non-localising sestamibi study are multigland disease, small parathyroid glands, or coexistent thyroid disease. Selective venous sampling for PTH. Consider MRI of neck or CT neck (+ upper mediastinum) if no localisation or incongruity of findings.
4 SELECTIVE VENOUS SAMPLING OF PARATHYROIDS INDICATIONS Localisation of parathyroid adenoma after ultrasound and Sesta-MIBI scanning with SPECT PROCEDURE Arrange admission and study in advance with interventional radiology Blood bottles to be prepared and pre-labelled Frances Fraser ward SITES FOR SAMPLING Right side 1. High internal jugular 3. Low internal jugular 5. Subclavian 6. Innominate Left side 7. High internal jugular 9. Low internal jugular 11. Subclavian 12. Innominate 14. Thymic mediastinal 15. Superior vena cava 20. High inferior vena cava 26. Low inferior vena cava 30. Right common iliac
5
6 INDICATIONS FOR SURGERY IN ASYMPTOMATIC PRIMARY HYPERPARATHYROIDISM This is based on the 2009 guidelines from the third workshop on the management of asymptomatic primary hyperparathyroidism. Note, in the latest guidelines, 24 hr urine calcium measurements are not an indication for surgery, as this is a poor predictor for the formation of kidney stones, is highly variable and is dependent on renal function, vitamin D status, race and sex). However some clinicians still consider it a useful guide and the measurements are still important for the exclusion of FBH. MEASUREMENT Serum calcium (>upper limit of normal) 0.25 mmol/l Creatinine clearance (calculated) Reduced to <60ml/min BMD T-score < minus 2.5 at any site and/or previous fracture fragility Age (years) <50 Reference Bilezikian JP et al. Guidelines for the management of asymptomatic primary hyperparathyroidism: summary statement from the third international workshop. JCEM 2009; 94(2): FAMILIAL PARATHYROID SYNDROMES 10% of patients with primary hyperparathyroidism have a hereditary disorder (Hannan et al. Nature Clinical Practice Endocrinology and Metabolism 2008; 4(1):53-8) MEN 1 syndrome: Primary hyperparathyroidism is the first manifestation of MEN1 syndrome in over 95% of patients. Typically parathyroid hyperplasia and multigland involvement occurs. Consider genetic testing for mutations in the MEN1 gene. MEN 2A syndrome: Typically parathyroid hyperplasia and multigland involvement occurs. Consider genetic testing for mutation in the RET gene. Hyperparathyroidism jaw tumour syndrome: Autosomal dominant disorder characterised by parathyroid adenomas or carcinomas, fibro-osseous tumours of the jaw, renal tumours and cysts, and uterine tumours. Consider genetic testing for mutation in the parafibromin gene Familial isolated hyperparathyroidism
7 EMERGENCY TREATMENT OF HYPERCALCAEMIA Severe hypercalcaemia (corrected calcium >3.5 mmol/l) remains a life-threatening acute medical emergency. Prompt treatment with hydration and adequate, frequent monitoring of serum calcium, is essential. Hypercalcaemia induces nephrogenic diabetes insipidus which may in turn worsen dehydration and hypercalcaemia. Hypercalcaemia may also involve a significant amount of magnesium loss in the urine. Urgent investigations Calcium, phosphate, PTH, ESR, ALP, albumin, 25-hydroxy-Vitamin D FBC, U and E, plasma osmolality, magnesium Chest X-ray, ECG Screening tests for the cause of hypercalcaemia (see above) Management 1) Maintain adequate hydration. This is the cornerstone of therapy and may be all that is required. Replace the deficit and then maintain a fluid intake of 3-4 L per day. Start with iv normal saline this may need to continue if sufficient oral intake cannot be maintained. Aim for plasma osmolality in the range mosm/kg. Care in patients who are elderly or in heart failure. 2) Bisphosphonates after rehydration. For example pamidronate 90mg in 1L of 0.9% saline infused over 4 hours. Effect is seen 24 hours after starting the infusion, with maximum effect after 5-6 days. Duration of effect may last for days. The dose may be repeated if renal function allows. 3) Corticosteroids. Valuable for patients with sarcoidosis, hypervitaminosis D and many malignancies. Prednisolone 60-80mg / day if adequate hydration has not produced sufficient fall in calcium. If calcium has not fallen within 2-3 days it is unlikely to do so and the steroids should be stopped. 4) Mithramycin was occasionally used historically. In the event of failure of all of the above mithramycin 15 μg/kg iv in 1L of 0.9% saline over 4-6 hours may provide an improvement, beginning 8-24 hours after the infusion and persisting for several days. Repeated doses were limited by cumulative bone marrow toxicity. 5) Calcitonin. A dose of 100 Units sc tds may rarely be required in severe intractable hypercalcaemia.
8 MANAGEMENT AFTER PARATHYROIDECTOMY Check for symptoms of hypocalcaemia (paraesthesia, cramps etc.). Trousseau s and Chvostek s test daily. o o Trousseau s test: Inflate blood pressure cuff to 10mmHg above the systolic pressure and maintain this pressure for up to 3 minutes. Ensure the blood pressure is maintained at the appropriate level throughout by palpation of the radial pulse. A positive test produces muscle spasm of the forearm and hand, forcing the fingers into fixed flexion at the metacarpalphalangeal joints and extension of the interphalangeal joints ( main d accoucheur ). Note: paraesthesiae alone is not a positive test. Chvostek s test: Tap lightly over the facial nerve at anterior edge of masseter muscle where the parotid duct crosses the edge of the muscle. A positive test occurs when a flicking contraction of the edge of the upper lip is seen. This indicates a recent calcium fall, not necessarily to subnormal levels. Daily U+E and corrected Ca 2+ and magnesium If mild symptoms and corrected Ca 2+ >2.0 mmol/l, give effervescent Ca 2+ (Sandocal 1000; two tablets tds). If severe symptoms and corrected Ca 2+ <2.0 mmol/l, give Ca 2+ infusion: Calcium infusion: [1.7 x patient s weight in kg] ml of 10% calcium gluconate. NB can cause tissue necrosis if extravasation so dilute in 1L N/Saline for administration or administer via central line or large patent iv access Note: 10ml of 10% calcium gluconate contains 88mg of calcium If hypocalcaemia persists, continue oral Sandocal 1000 (up to 2 tablets tds might be needed) and introduce alfacalcidol can commence at lowest dose but requirement may be 1 4 mcg total daily. Monitor PTH. If detectable, and parathyroid recovery occurs, try to wean off alfacalcidol. If PTH remains undetectable, it is likely that they will stay on alfacalcidol for life. Long term aim is for a low-normal calcium.to minimise nephrocalcinosis and enable warning symptoms of hypocalcaemia in preference to silent hypercalcaemia.
9 USE OF CINACALCET IN PRIMARY HYPERPARATHYROIDISM INDICATIONS Treatment of refractory primary hyperparathyroidism, after at least one failed attempt at parathyroidectomy, or in patients in whom surgery is contraindicated or who have parathyroid carcinoma And who fulfil one of more of the following criteria: Overt manifestation of primary hyperparathyroidism (eg nephrolithiasis, osteitis fibrosa cystica, neuromuscular disease) Corrected serum calcium >3mmol/L PTH >6.5pmol/L Urine calcium >10mmol/24 hours Osteoporosis at any site (T score <2.5) Impaired renal function (creatinine clearance reduced by >30%) Age < 50 years CONTRAINDICATIONS Pregnancy or breastfeeding Sensitivity to the drug or excipients PRECAUTIONS Cardiovascular disease: idiosyncratic hypotension and/or worsening of heart failure have been reported in patients with impaired cardiovascular function. Hepatic impairment: Use with caution in patients with moderate-to-severe hepatic impairment (Child- Pugh classes B & C); cinacalcet exposure and half-life are increased; monitor closely. Seizure disorder: Use with caution in patients with a history of seizure disorder; seizure threshold is lowered by significant serum calcium reductions. Monitor calcium levels closely. Adverse effects may include Gastrointestinal: Nausea (31%), vomiting (27%), diarrhoea (21%) Neuromuscular & skeletal: Myalgia (15%) Cardiovascular: Hypertension (7%) Central nervous system: Dizziness (10%), seizure (1%) Endocrine & metabolic: Testosterone decreased Gastrointestinal: Anorexia (6%) Neuromuscular & skeletal: Weakness (7%), chest pain (noncardiac; 6%)
10 PROCEDURE Initiate at 30mg twice daily. Measure calcium, phosphate and urinary calcium pre-dose and 4-hours post-dose. Measure PTH 2 weeks after initiation. Titrate dose upwards every 2-4 weeks to control calcium, with measurements 2 weeks after adjustment. On stable dose measure serum calcium and phosphate every 3 months and BMD by DEXA scan every year.
11 HYPOPARATHYROIDISM Biochemical Diagnosis Hypocalcaemia, in the presence of inappropriately low or normal PTH. Exclude vitamin D deficiency. Consider the following causes: Iatrogenic (post-thyroidectomy or parathyroidectomy, post radiotherapy) Autoimmune (either isolated or polyglandular type 1 syndrome) Infilitration by metastases, or systemic disease (haemochromatosis, amyloidosis, sarcoidosis, Wilson s disease, thalassaemia) Parathyroid agenesis (isolated or part of a complex developmental anomaly such as DiGeorge syndrome, GATA-3 mutations with sensori-neural deafness and renal anomalies) Reduced parathyroid hormone secretion o Hypomagnesaemia o Calcium-sensing receptor mutations o Parathyroid hormone gene defects Pseudohypoparathyroidism causing reduced PTH action
12 DEXA Scanning INDICATION Oestrogen Deficiency BARTS ENDOCRINE E-PROTOCOLS OSTEOPOROSIS Premature ovarian failure (surgical, drug or disease induced) Early menopause (<45 years) Prolonged amenorrhoea (>1year) Anorexia nervosa/bulimia Nutritional Malabsorption Diseases eg Coeliac, Crohn's Chronic liver/kidney disease Severe malnutrition Major gastric surgery Vitamin D or Calcium deficiencies (after checking that Vitamin D levels are normal) Endocrine/Metabolic Disorders Primary Hypogonadism Cushing's Hyperparathyroidism Hyperprolactinaemia (secondary to oestrogen deficiency) Strong Osteoporotic Risk Factors Proven family history of osteoporotic fracture High alcohol intake Poor diet (especially low Calcium intake) Slender build (BMI <20kg/m2) Long-term immobility Heavy smoking (if in conjunction with other Major risk factors) Drug Treatments High-dose or long-term oral corticosteroids, (>7.5mg/d or more of prednisolone or equivalent dose or another corticosteroid for 6 months or more or about to commence long-term treatment) Chronic heparin administration especially during pregnancy. GnRH agonists Anti-convulsants Other History of multiple atraumatic/minimal trauma fracture Radiological appearances of osteoporosis eg. previous unknown vertebral collapse Myeloma Known osteoporotic fracture Marked loss of height, thoracic kyphosis (after radiological confirmation of vertebral collapse)
13 PAGET s Disease Investigations Alkaline phosphatase can be elevated in active disease. Serum calcium levels are usually normal. Radiological features on X-ray can include decrease in density of affected bones, wedge- or flame segment of bone resorption in long bones, extensive osteolytic areas in the skull (osteoporosis circumscripta), cortical thickening, increase in bone size, sclerosis, loss of cortocomedullary distinction. Bone scintigraphy is the best method for assessing the extent of the disease. Complications Deafness Neurological complications Osteogenic sarcoma Treatment Indications for treatment include pain, neurological complications, disease in weight bearing bones or to prevent a fracture. The mainstay of treatment is with bisphosphonates. Monitor serum alkaline phosphatase.
Southern Derbyshire Shared Care Pathology Guidelines. Primary Hyperparathyroidism
 Southern Derbyshire Shared Care Pathology Guidelines Primary Hyperparathyroidism Please use this Guideline in Conjunction with the Hypercalcaemia Guideline Definition Driven by hyperfunction of one or
Southern Derbyshire Shared Care Pathology Guidelines Primary Hyperparathyroidism Please use this Guideline in Conjunction with the Hypercalcaemia Guideline Definition Driven by hyperfunction of one or
Approach to a patient with hypercalcemia
 Approach to a patient with hypercalcemia Ana-Maria Chindris, MD Division of Endocrinology Mayo Clinic Florida 2013 MFMER slide-1 Background Hypercalcemia is a problem frequently encountered in clinical
Approach to a patient with hypercalcemia Ana-Maria Chindris, MD Division of Endocrinology Mayo Clinic Florida 2013 MFMER slide-1 Background Hypercalcemia is a problem frequently encountered in clinical
Clinical biochemistry of calcium and vitamin D
 Clinical biochemistry of calcium and vitamin D Dr Andrew Day Consultant in Clinical Biochemistry and Metabolic Medicine University Hospitals Bristol NHS Trust e-mail: andrew.day@uhbristol.nhs.uk A 48-year
Clinical biochemistry of calcium and vitamin D Dr Andrew Day Consultant in Clinical Biochemistry and Metabolic Medicine University Hospitals Bristol NHS Trust e-mail: andrew.day@uhbristol.nhs.uk A 48-year
Hypocalcemia 6/8/12. Normal value. Physiologic functions. Nephron a functional unit of kidney. Influencing factors in Calcium and Phosphate Balance
 Normal value Hypocalcemia Serum calcium Total mg/dl Ionized mg/dl Cord blood 9.0 ~ 11.5 5.0 ~ 6.o New born (1 st 24 hrs) 9.0 ~ 10.6 4.3 ~ 5.1 24~ 48 hrs 7.0 ~12.0 4.0 ~4.7 Child 8.8 ~10.8 4.8 ~4.92 There
Normal value Hypocalcemia Serum calcium Total mg/dl Ionized mg/dl Cord blood 9.0 ~ 11.5 5.0 ~ 6.o New born (1 st 24 hrs) 9.0 ~ 10.6 4.3 ~ 5.1 24~ 48 hrs 7.0 ~12.0 4.0 ~4.7 Child 8.8 ~10.8 4.8 ~4.92 There
Definition Elevated Adjusted Calcium > 2.6 mmol/l (adjusted for albumin), taken without using a cuff.
 Hypercalcaemia Definition Elevated Adjusted Calcium > 2.6 mmol/l (adjusted for albumin), taken without using a cuff. Mild (usually no symptoms) 2.6 3.0 mmol/l Moderate (start to develop symptoms) 3.0 3.4
Hypercalcaemia Definition Elevated Adjusted Calcium > 2.6 mmol/l (adjusted for albumin), taken without using a cuff. Mild (usually no symptoms) 2.6 3.0 mmol/l Moderate (start to develop symptoms) 3.0 3.4
Definition Elevated Adjusted Calcium > 2.6 mmol/l (adjusted for albumin), taken without using a cuff.
 Authoriser: Fiona Davidson Page 1 of 5 Hypercalcaemia Definition Elevated Adjusted Calcium > 2.6 mmol/l (adjusted for albumin), taken without using a cuff. Mild (usually no symptoms) 2.6 3.0 mmol/l Moderate
Authoriser: Fiona Davidson Page 1 of 5 Hypercalcaemia Definition Elevated Adjusted Calcium > 2.6 mmol/l (adjusted for albumin), taken without using a cuff. Mild (usually no symptoms) 2.6 3.0 mmol/l Moderate
Hyper and hypocalcaemia. Prof Tricia Tan
 Hyper and hypocalcaemia Prof Tricia Tan Learning Objectives Basic physiology of Ca regulation Case presentations Take home messages Calcium Total body calcium content ~1300g 99% in bone 1% intracellular
Hyper and hypocalcaemia Prof Tricia Tan Learning Objectives Basic physiology of Ca regulation Case presentations Take home messages Calcium Total body calcium content ~1300g 99% in bone 1% intracellular
HYPERPARATHYROIDIS M FAISAL GHANI SIDDIQUI MBBS; FCPS; PGDIP-BIOMEDICAL ETHICS; MCPS-HPE
 HYPERPARATHYROIDIS M FAISAL GHANI SIDDIQUI MBBS; FCPS; PGDIP-BIOMEDICAL ETHICS; MCPS-HPE PROFESSOR OF SURGERY J I N N A H S I N D H M E D I C A L U N I V E R S I T Y PREAMBLE Anatomy & physiology of the
HYPERPARATHYROIDIS M FAISAL GHANI SIDDIQUI MBBS; FCPS; PGDIP-BIOMEDICAL ETHICS; MCPS-HPE PROFESSOR OF SURGERY J I N N A H S I N D H M E D I C A L U N I V E R S I T Y PREAMBLE Anatomy & physiology of the
Hypercalcemia & Parathyroid Disorders. W. Reid Litchfield, MD, FACE, ECNU Desert Endocrinology
 Hypercalcemia & Parathyroid Disorders W. Reid Litchfield, MD, FACE, ECNU Desert Endocrinology Objectives Review diagnostic workup for hypercalcemia Review management of primary hyperparathyroidism Review
Hypercalcemia & Parathyroid Disorders W. Reid Litchfield, MD, FACE, ECNU Desert Endocrinology Objectives Review diagnostic workup for hypercalcemia Review management of primary hyperparathyroidism Review
Investigations for Disorders of Calcium, Phosphate and Magnesium Homeostasis
 Investigations for Disorders of Calcium, Phosphate and Magnesium Homeostasis Tutorial for Specialist Portfolio Biomedical Scientists 03/02/2014 Dr Petros Kampanis Clinical Scientist 1. Calcium Most abundant
Investigations for Disorders of Calcium, Phosphate and Magnesium Homeostasis Tutorial for Specialist Portfolio Biomedical Scientists 03/02/2014 Dr Petros Kampanis Clinical Scientist 1. Calcium Most abundant
Hyperparathyroidism. When to Suspect, How to Diagnose, When and How to Intervene. Johanna A. Pallotta, MD, FACP, FACE
 Hyperparathyroidism When to Suspect, How to Diagnose, When and How to Intervene Johanna A. Pallotta, MD, FACP, FACE Potential conflicts of interest: None Johanna A. Pallotta, MD Outline Definition of hyperparathyroidism
Hyperparathyroidism When to Suspect, How to Diagnose, When and How to Intervene Johanna A. Pallotta, MD, FACP, FACE Potential conflicts of interest: None Johanna A. Pallotta, MD Outline Definition of hyperparathyroidism
hypercalcemia of malignancy hyperparathyroidism PHPT the most common cause of hypercalcemia in the outpatient setting the second most common cause
 hyperparathyroidism A 68-year-old woman with documented osteoporosis has blood tests showing elevated serum calcium and parathyroid hormone (PTH) levels: 11.2 mg/dl (8.8 10.1 mg/dl) and 88 pg/ml (10-60),
hyperparathyroidism A 68-year-old woman with documented osteoporosis has blood tests showing elevated serum calcium and parathyroid hormone (PTH) levels: 11.2 mg/dl (8.8 10.1 mg/dl) and 88 pg/ml (10-60),
Guideline for the investigation and management of osteoporosis. for hospitals and General Practice
 Guideline for the investigation and management of osteoporosis for hospitals and General Practice Background Low bone density is an important risk factor for fracture. The aim of assessing bone density
Guideline for the investigation and management of osteoporosis for hospitals and General Practice Background Low bone density is an important risk factor for fracture. The aim of assessing bone density
Potential conflicts of interest: None
 Hyperparathyroidism When to Suspect, How to Diagnose, When and How to Intervene November 6, 2013 Johanna A. Pallotta, MD, FACP, FACE Potential conflicts of interest: None Johanna A. Pallotta, MD Outline
Hyperparathyroidism When to Suspect, How to Diagnose, When and How to Intervene November 6, 2013 Johanna A. Pallotta, MD, FACP, FACE Potential conflicts of interest: None Johanna A. Pallotta, MD Outline
HYPERCALCEMIA. Babak Tamizi Far MD. Assistant professor of internal medicine Al-zahra hospital, Isfahan university of medical sciences
 HYPERCALCEMIA Babak Tamizi Far MD. Assistant professor of internal medicine Al-zahra hospital, Isfahan university of medical sciences ESSENTIALS OF DIAGNOSIS Serum calcium level > 10.5 mg/dl Serum ionized
HYPERCALCEMIA Babak Tamizi Far MD. Assistant professor of internal medicine Al-zahra hospital, Isfahan university of medical sciences ESSENTIALS OF DIAGNOSIS Serum calcium level > 10.5 mg/dl Serum ionized
Case Finding and Risk Assessment for Osteoporosis
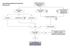 Case Finding and Risk Assessment for Osteoporosis Patient may present as a fragility fracture or risk fracture Fragility fracture age 50 Clinical risk factors aged 50 Very strong clinical risk factors
Case Finding and Risk Assessment for Osteoporosis Patient may present as a fragility fracture or risk fracture Fragility fracture age 50 Clinical risk factors aged 50 Very strong clinical risk factors
Calcium and Parathyroid Disorders
 Calcium and Parathyroid Disorders Hussain Mahmud, MD Clinical Assistant Professor of Medicine Division of Endocrinology, Diabetes, and Metabolism University of Pittsburgh Butler Memorial Hospital November
Calcium and Parathyroid Disorders Hussain Mahmud, MD Clinical Assistant Professor of Medicine Division of Endocrinology, Diabetes, and Metabolism University of Pittsburgh Butler Memorial Hospital November
Magnesium Homeostasis
 ECTS PhD Training Course, Rome 3 rd September 2008 Disorders of Calcium, Phosphate h and Magnesium Homeostasis Richard Eastell Professor of Bone Metabolism Academic Unit of Bone Metabolism University of
ECTS PhD Training Course, Rome 3 rd September 2008 Disorders of Calcium, Phosphate h and Magnesium Homeostasis Richard Eastell Professor of Bone Metabolism Academic Unit of Bone Metabolism University of
Osteoporosis challenges
 Osteoporosis challenges Osteoporosis challenges Who should have a fracture risk assessment? Who to treat? Drugs, holidays and unusual adverse effects Fracture liaison service? The size of the problem 1
Osteoporosis challenges Osteoporosis challenges Who should have a fracture risk assessment? Who to treat? Drugs, holidays and unusual adverse effects Fracture liaison service? The size of the problem 1
Women s Health in General Practice Symposium 2015 Thyroid & Parathyroid Cases
 Women s Health in General Practice Symposium 2015 Thyroid & Parathyroid Cases Bill Fleming Epworth Freemasons Hospital 1 Common Endocrine Presentations anatomical problems thyroid nodule / goitre embryological
Women s Health in General Practice Symposium 2015 Thyroid & Parathyroid Cases Bill Fleming Epworth Freemasons Hospital 1 Common Endocrine Presentations anatomical problems thyroid nodule / goitre embryological
Case 2: 30 yr-old woman with 7 yr history of recurrent kidney stones
 Case 2: 30 yr-old woman with 7 yr history of recurrent kidney stones Giuliano Mariani Regional Center of Nuclear Medicine, University of Pisa Medical School, Pisa (Italy) 30 yr-old woman with 7 yr history
Case 2: 30 yr-old woman with 7 yr history of recurrent kidney stones Giuliano Mariani Regional Center of Nuclear Medicine, University of Pisa Medical School, Pisa (Italy) 30 yr-old woman with 7 yr history
Parathyroid Imaging. A Guide to Parathyroid Surgery
 Parathyroid Imaging A Guide to Parathyroid Surgery Primary Hyperparathyroidism (PHPT) 3 rd most common endocrine disorder after diabetes and hyperthyroidism Prevalence in women 2% Often discovered in asymptomatic
Parathyroid Imaging A Guide to Parathyroid Surgery Primary Hyperparathyroidism (PHPT) 3 rd most common endocrine disorder after diabetes and hyperthyroidism Prevalence in women 2% Often discovered in asymptomatic
Practical Management Of Osteoporosis
 Practical Management Of Osteoporosis CONFERENCE 2012 Education Centre, Bournemouth.19 November The following companies have given funding towards the cost of this meeting but have no input into the agenda
Practical Management Of Osteoporosis CONFERENCE 2012 Education Centre, Bournemouth.19 November The following companies have given funding towards the cost of this meeting but have no input into the agenda
HYPERCALCAEMIA 101 FOR THE INTERNIST
 HYPERCALCAEMIA 101 FOR THE INTERNIST Dr Chionh Siok Bee Dept of Medicine, National University Hospital siok_bee_chionh@nuhs.edu.sg Medicine Review Course 18/09/2011 Outline of Talk Definition of hypercalcaemia
HYPERCALCAEMIA 101 FOR THE INTERNIST Dr Chionh Siok Bee Dept of Medicine, National University Hospital siok_bee_chionh@nuhs.edu.sg Medicine Review Course 18/09/2011 Outline of Talk Definition of hypercalcaemia
Bone Densitometry Pathway
 Bone Densitometry Pathway The goal of the Bone Densitometry pathway is to manage our diagnosed osteopenic and osteoporotic patients, educate and monitor the patient population at risk for bone density
Bone Densitometry Pathway The goal of the Bone Densitometry pathway is to manage our diagnosed osteopenic and osteoporotic patients, educate and monitor the patient population at risk for bone density
Clinical Approach to Hypercalcemia For the Primary Care Provider
 Clinical Approach to Hypercalcemia For the Primary Care Provider Christina Maser, MD FACS UCSF Fresno Department of Surgery, Endocrine Surgery 2/2/19 Objectives Recognition of pitfalls of diagnosis of
Clinical Approach to Hypercalcemia For the Primary Care Provider Christina Maser, MD FACS UCSF Fresno Department of Surgery, Endocrine Surgery 2/2/19 Objectives Recognition of pitfalls of diagnosis of
Calcium metabolism and the Parathyroid Glands. Calcium, osteoclasts and osteoblasts-essential to understand the function of parathyroid glands
 Calcium metabolism and the Parathyroid Glands Calcium, osteoclasts and osteoblasts-essential to understand the function of parathyroid glands Calcium is an essential element for contraction of voluntary/smooth
Calcium metabolism and the Parathyroid Glands Calcium, osteoclasts and osteoblasts-essential to understand the function of parathyroid glands Calcium is an essential element for contraction of voluntary/smooth
PRIMARY HYPERPARATHYROIDISM PRIMARY HYPERPARATHYROIDISM. Hyperparathyroidism Etiology. Common Complex Insidious Chronic Global Only cure is surgery
 ENDOCRINE DISORDER PRIMARY HYPERPARATHYROIDISM Roseann P. Velez, DNP, FNP Francis J. Velez, MD, FACS Common Complex Insidious Chronic Global Only cure is surgery HYPERPARATHYROIDISM PARATHRYOID GLANDS
ENDOCRINE DISORDER PRIMARY HYPERPARATHYROIDISM Roseann P. Velez, DNP, FNP Francis J. Velez, MD, FACS Common Complex Insidious Chronic Global Only cure is surgery HYPERPARATHYROIDISM PARATHRYOID GLANDS
PRIMARY HYPERPARATHYROIDISM
 PRIMARY HYPERPARATHYROIDISM HYPERPARATHYROIDISM Inappropriate excess secretion of Parathyroid Hormone in Primary Hyperparathyroidism Appropriate Hypersecretion in Secondary Hyperparathyroidism PTH and
PRIMARY HYPERPARATHYROIDISM HYPERPARATHYROIDISM Inappropriate excess secretion of Parathyroid Hormone in Primary Hyperparathyroidism Appropriate Hypersecretion in Secondary Hyperparathyroidism PTH and
Hypercalcemia. Hypercalcemia: When to Worry, When to Treat! Mineral Metabolism : A Short Course
 Hypercalcemia: When to Worry, When to Treat! Michael A. Levine has no financial relationships to disclose or Conflicts of Interest to resolve. Michael A. Levine, M.D. This presentation will not involve
Hypercalcemia: When to Worry, When to Treat! Michael A. Levine has no financial relationships to disclose or Conflicts of Interest to resolve. Michael A. Levine, M.D. This presentation will not involve
Autonomic neuropathy
 3. Neuropathy Autonomic neuropathy MACROVASCULAR: Accelerated atherosclerosis Coronary artery disease IHD / MI Cerebrovascular disease CVA Peripheral vascular disease gangrene / amputations NB: association
3. Neuropathy Autonomic neuropathy MACROVASCULAR: Accelerated atherosclerosis Coronary artery disease IHD / MI Cerebrovascular disease CVA Peripheral vascular disease gangrene / amputations NB: association
NEOPLASMS OF THE THYROID PATHOLOGY OF PARATHYROID GLANDS. BY: Shifaa Qa qa
 NEOPLASMS OF THE THYROID PATHOLOGY OF PARATHYROID GLANDS BY: Shifaa Qa qa Neoplasmas of the thyroid thyroid nodules Neoplastic ---- benign, malignant Non neoplastic Solitary nodules ----- neoplastic Nodules
NEOPLASMS OF THE THYROID PATHOLOGY OF PARATHYROID GLANDS BY: Shifaa Qa qa Neoplasmas of the thyroid thyroid nodules Neoplastic ---- benign, malignant Non neoplastic Solitary nodules ----- neoplastic Nodules
Hyperparathyroidism (primary): diagnosis, assessment and initial management
 National Institute for Health and Care Excellence. Hyperparathyroidism (primary): diagnosis, assessment and initial management NICE guideline . October 2018 This guideline was developed by the
National Institute for Health and Care Excellence. Hyperparathyroidism (primary): diagnosis, assessment and initial management NICE guideline . October 2018 This guideline was developed by the
Case study Group 2 presentation
 Case study Group 2 presentation Patient profile HN 3095-57 Female 60 years old Hometown : Sa Kaeo province Occupation : farmer No drug and food allergy Chief complain Left neck mass 10 years PTA that gradually
Case study Group 2 presentation Patient profile HN 3095-57 Female 60 years old Hometown : Sa Kaeo province Occupation : farmer No drug and food allergy Chief complain Left neck mass 10 years PTA that gradually
Cases in Endocrinology
 Bones, Moans and Groans Diagnosing and Treating Primary Hyperparathyroidism By M. Usman Chaudhry, MD Table 1 Laboratory parameters Her bone density had osteopenic T-Scores of -2.3 at lumbar spine, and
Bones, Moans and Groans Diagnosing and Treating Primary Hyperparathyroidism By M. Usman Chaudhry, MD Table 1 Laboratory parameters Her bone density had osteopenic T-Scores of -2.3 at lumbar spine, and
SUMMARY OF PRODUCT CHARACTERISTICS
 SUMMARY OF PRODUCT CHARACTERISTICS 1 NAME OF THE MEDICINAL PRODUCT Colecalciferol Meda 800 IU tablet 2 QUALITATIVE AND QUANTITATIVE COMPOSITION Each tablet contains colecalciferol (vitamin D 3 ) 800 IU
SUMMARY OF PRODUCT CHARACTERISTICS 1 NAME OF THE MEDICINAL PRODUCT Colecalciferol Meda 800 IU tablet 2 QUALITATIVE AND QUANTITATIVE COMPOSITION Each tablet contains colecalciferol (vitamin D 3 ) 800 IU
S H A R E D C A R E G U I D E L I N E Drug: Denosumab 60mg injection Indication: treatment of osteoporosis in postmenopausal women
 S H A R E D C A R E G U I D E L I N E Drug: Denosumab 60mg injection Indication: treatment of osteoporosis in postmenopausal women Introduction Indication: Denosumab (Prolia ) is recommended in NICE TA204
S H A R E D C A R E G U I D E L I N E Drug: Denosumab 60mg injection Indication: treatment of osteoporosis in postmenopausal women Introduction Indication: Denosumab (Prolia ) is recommended in NICE TA204
LRI Children s Hospital
 Calcium Disorders in Children LRI Children s Hospital Staff relevant to: Medical & Nursing staff caring for Children identified with having a Calcium disorder Team approval date: January 2019 Version:
Calcium Disorders in Children LRI Children s Hospital Staff relevant to: Medical & Nursing staff caring for Children identified with having a Calcium disorder Team approval date: January 2019 Version:
Hypercalcemia may be detected incidentally. Practice CMAJ. Primary hyperparathyroidism. Primer. Key points. The case. What causes hypercalcemia?
 CMAJ Practice Primer Primary hyperparathyroidism Hafsah Al-Azem HBSc, Aliya Khan MD The case A 17-year-old man presented at the clinic with thirst, lethargy and fatigue that had been ongoing for several
CMAJ Practice Primer Primary hyperparathyroidism Hafsah Al-Azem HBSc, Aliya Khan MD The case A 17-year-old man presented at the clinic with thirst, lethargy and fatigue that had been ongoing for several
Hypoparathyroidism By John Halpern, DO, FACEP Coauthored by N. Ewen Wang, MD
 Hypoparathyroidism By John Halpern, DO, FACEP Coauthored by N. Ewen Wang, MD Reprinted with permission from: E-Medicine: Instant Access to the Minds of Medicine http://www.emedicine.com/emerg/topic276.htm
Hypoparathyroidism By John Halpern, DO, FACEP Coauthored by N. Ewen Wang, MD Reprinted with permission from: E-Medicine: Instant Access to the Minds of Medicine http://www.emedicine.com/emerg/topic276.htm
Research Article Primary Hyperparathyroidism: 11-Year Experience in a Single Institute in Thailand
 International Endocrinology Volume 2012, Article ID 952426, 4 pages doi:10.1155/2012/952426 Research Article Primary Hyperparathyroidism: 11-Year Experience in a Single Institute in Thailand Poramaporn
International Endocrinology Volume 2012, Article ID 952426, 4 pages doi:10.1155/2012/952426 Research Article Primary Hyperparathyroidism: 11-Year Experience in a Single Institute in Thailand Poramaporn
Clodronate BE/H/PSUR/001/001 October 2011 Agreed CSP
 Clodronate BE/H/PSUR/001/001 October 2011 Agreed CSP 4. CLINICAL PARTICULARS 4.1 Therapeutic indications Intravenous use Treatment of hypercalcemia due to malignancy. Oral use Treatment of hypercalcemia
Clodronate BE/H/PSUR/001/001 October 2011 Agreed CSP 4. CLINICAL PARTICULARS 4.1 Therapeutic indications Intravenous use Treatment of hypercalcemia due to malignancy. Oral use Treatment of hypercalcemia
International Journal of Biological & Medical Research. An Uncommon Case of Persistent Hypercalcaemia following Parathyroid Surgery
 Int J Biol Med Res.2015;6(4):5336-5340 Int J Biol Med Res www.biomedscidirect.com Volume 6, Issue 2, April 2015 Contents lists available at BioMedSciDirect Publications International Journal of Biological
Int J Biol Med Res.2015;6(4):5336-5340 Int J Biol Med Res www.biomedscidirect.com Volume 6, Issue 2, April 2015 Contents lists available at BioMedSciDirect Publications International Journal of Biological
Natpara (parathyroid hormone) Prior Authorization with Quantity Limit Program Summary
 Natpara (parathyroid hormone) Prior Authorization with Quantity Limit Program Summary FDA APPROVED INDICATIONS DOSAGE 1 Agent Indication Dosing and Administration Natpara (parathyroid hormone) subcutaneous
Natpara (parathyroid hormone) Prior Authorization with Quantity Limit Program Summary FDA APPROVED INDICATIONS DOSAGE 1 Agent Indication Dosing and Administration Natpara (parathyroid hormone) subcutaneous
qthis medicinal product is subject to additional monitoring. This will allow quick identification of new safety
 Parsabiv q (etelcalcetide) Frequently Asked Questions qthis medicinal product is subject to additional monitoring. This will allow quick identification of new safety information. Healthcare professionals
Parsabiv q (etelcalcetide) Frequently Asked Questions qthis medicinal product is subject to additional monitoring. This will allow quick identification of new safety information. Healthcare professionals
CKD: Bone Mineral Metabolism. Peter Birks, Nephrology Fellow
 CKD: Bone Mineral Metabolism Peter Birks, Nephrology Fellow CKD - KDIGO Definition and Classification of CKD CKD: abnormalities of kidney structure/function for > 3 months with health implications 1 marker
CKD: Bone Mineral Metabolism Peter Birks, Nephrology Fellow CKD - KDIGO Definition and Classification of CKD CKD: abnormalities of kidney structure/function for > 3 months with health implications 1 marker
Endocrine Regulation of Calcium and Phosphate Metabolism
 Endocrine Regulation of Calcium and Phosphate Metabolism Huiping Wang ( 王会平 ), PhD Department of Physiology Rm C516, Block C, Research Building, School of Medicine Tel: 88208252 Email: wanghuiping@zju.edu.cn
Endocrine Regulation of Calcium and Phosphate Metabolism Huiping Wang ( 王会平 ), PhD Department of Physiology Rm C516, Block C, Research Building, School of Medicine Tel: 88208252 Email: wanghuiping@zju.edu.cn
Primary Hyperparathyroidism
 Primary Hyperparathyroidism Copyright Copyright 2019 2019 American American Associa7on Associa7on of Clinical of Clinical Endocrinologists Endocrinologists 1 Primary Hyperparathyroidism In primary hyperparathyroidism
Primary Hyperparathyroidism Copyright Copyright 2019 2019 American American Associa7on Associa7on of Clinical of Clinical Endocrinologists Endocrinologists 1 Primary Hyperparathyroidism In primary hyperparathyroidism
Diagnosis and Treatment of Osteoporosis. Department of Endocrinology and Metabolism Ajou University School of Medicine.
 Diagnosis and Treatment of Osteoporosis Department of Endocrinology and Metabolism Ajou University School of Medicine Yoon-Sok CHUNG WCIM, COEX, Seoul, 27Oct2014 Case 1 71-year old woman Back pain Emergency
Diagnosis and Treatment of Osteoporosis Department of Endocrinology and Metabolism Ajou University School of Medicine Yoon-Sok CHUNG WCIM, COEX, Seoul, 27Oct2014 Case 1 71-year old woman Back pain Emergency
Brunel Health Core Ten Results for Sam Witter. Thank you for submitting a sample of your blood to be tested by Brunel Health.
 Brunel Health Core Ten Results for Sam Witter Dear Sam, Thank you for submitting a sample of your blood to be tested by Brunel Health. We are pleased to say that there was enough viable sample to test
Brunel Health Core Ten Results for Sam Witter Dear Sam, Thank you for submitting a sample of your blood to be tested by Brunel Health. We are pleased to say that there was enough viable sample to test
Dumfries and Galloway. Treatment Protocol for Osteoporosis
 Dumfries and Galloway Treatment Protocol for Osteoporosis DIAGNOSIS OF OSTEOPOROSIS 2 Diagnostic Criteria 2 REFERRAL CRITERIA FOR DEXA 3 TREATMENT 4 Non-Drug Therapy : for all 4 Non-Drug Therapy : in the
Dumfries and Galloway Treatment Protocol for Osteoporosis DIAGNOSIS OF OSTEOPOROSIS 2 Diagnostic Criteria 2 REFERRAL CRITERIA FOR DEXA 3 TREATMENT 4 Non-Drug Therapy : for all 4 Non-Drug Therapy : in the
TREATMENT OF OSTEOPOROSIS
 TREATMENT OF OSTEOPOROSIS Summary Prevention is the key issue in the management of osteoporosis. HRT is the agent of choice for prevention of postmenopausal osteoporosis. Bisphosphonates and Calcitonin
TREATMENT OF OSTEOPOROSIS Summary Prevention is the key issue in the management of osteoporosis. HRT is the agent of choice for prevention of postmenopausal osteoporosis. Bisphosphonates and Calcitonin
SUMMARY OF PRODUCT CHARACTERISTICS
 SUMMARY OF PRODUCT CHARACTERISTICS 1. NAME OF THE MEDICINAL PRODUCT Calcium Sandoz 500 mg, effervescent tablets Calcium Sandoz 1000 mg, effervescent tablets 2. QUALITATIVE AND QUANTITATIVE COMPOSITION
SUMMARY OF PRODUCT CHARACTERISTICS 1. NAME OF THE MEDICINAL PRODUCT Calcium Sandoz 500 mg, effervescent tablets Calcium Sandoz 1000 mg, effervescent tablets 2. QUALITATIVE AND QUANTITATIVE COMPOSITION
The Parathyroid Glands
 The Parathyroid Glands Bởi: OpenStaxCollege The parathyroid glands are tiny, round structures usually found embedded in the posterior surface of the thyroid gland ([link]). A thick connective tissue capsule
The Parathyroid Glands Bởi: OpenStaxCollege The parathyroid glands are tiny, round structures usually found embedded in the posterior surface of the thyroid gland ([link]). A thick connective tissue capsule
Hyperparathyroidism: Operative Considerations. Financial Disclosures: None. Hyperparathyroidism. Hyperparathyroidism 11/10/2012
 Hyperparathyroidism: Operative Considerations Financial Disclosures: None Steven J Wang, MD FACS Associate Professor Dept of Otolaryngology-Head and Neck Surgery University of California, San Francisco
Hyperparathyroidism: Operative Considerations Financial Disclosures: None Steven J Wang, MD FACS Associate Professor Dept of Otolaryngology-Head and Neck Surgery University of California, San Francisco
Endocrinology Update. Dr Colin Johnston Hon Consultant West Herts Trust
 Endocrinology Update Dr Colin Johnston Hon Consultant West Herts Trust colin.johnston2@nhs.net Thyrotoxicosis Symptoms GI symptoms-diarrhoea Fatigue Anxiety Irreg Menstruation Do not be put off the diagnosis
Endocrinology Update Dr Colin Johnston Hon Consultant West Herts Trust colin.johnston2@nhs.net Thyrotoxicosis Symptoms GI symptoms-diarrhoea Fatigue Anxiety Irreg Menstruation Do not be put off the diagnosis
Aromatase Inhibitors & Osteoporosis
 Aromatase Inhibitors & Osteoporosis Miss Sarah Horn Consultant Oncoplastic Breast Surgeon April 2018 Aims Role of Aromatase Inhibitors (AI) in breast cancer treatment AI s effects on bone health Bone health
Aromatase Inhibitors & Osteoporosis Miss Sarah Horn Consultant Oncoplastic Breast Surgeon April 2018 Aims Role of Aromatase Inhibitors (AI) in breast cancer treatment AI s effects on bone health Bone health
P-RMS: CZ/H/PSUR/0020/001
 Core Safety Profile Active substance: Pamidronate Pharmaceutical form(s)/strength: Powder and solvent for solution for infusion, 15mg, 30mg, 60mg, 90mg P-RMS: CZ/H/PSUR/0020/001 Date of FAR: 04.10.2011
Core Safety Profile Active substance: Pamidronate Pharmaceutical form(s)/strength: Powder and solvent for solution for infusion, 15mg, 30mg, 60mg, 90mg P-RMS: CZ/H/PSUR/0020/001 Date of FAR: 04.10.2011
Cortical bone After age 40, gradually decreases % yearly, in both men and women Postmenopausally, loss accelerates to 2-3% yearly
 Osteoporosis POOLE, K.E.S. & COMPSTON, J.E. (2006): Osteoporosis and its management. BMJ 333:1251-6. Physiology Cortical bone After age 40, gradually decreases 0.3-0.5% yearly, in both men and women Postmenopausally,
Osteoporosis POOLE, K.E.S. & COMPSTON, J.E. (2006): Osteoporosis and its management. BMJ 333:1251-6. Physiology Cortical bone After age 40, gradually decreases 0.3-0.5% yearly, in both men and women Postmenopausally,
BMD: A Continuum of Risk WHO Bone Density Criteria
 Pathogenesis of Osteoporosis Osteoporosis Diagnosis: BMD, FRAX and Assessment of Secondary Osteoporosis AGING MENOPAUSE OTHER RISK FACTORS RESORPTION > FORMATION Bone Loss LOW PEAK BONE MASS Steven T Harris
Pathogenesis of Osteoporosis Osteoporosis Diagnosis: BMD, FRAX and Assessment of Secondary Osteoporosis AGING MENOPAUSE OTHER RISK FACTORS RESORPTION > FORMATION Bone Loss LOW PEAK BONE MASS Steven T Harris
What is the right calcium balance?
 For patients with hypoparathyroidism What is the right calcium balance? Indications and Usage1 NATPARA is a parathyroid hormone indicated as an adjunct to calcium and vitamin D to control hypocalcemia
For patients with hypoparathyroidism What is the right calcium balance? Indications and Usage1 NATPARA is a parathyroid hormone indicated as an adjunct to calcium and vitamin D to control hypocalcemia
Dumfries and Galloway. Treatment Protocol for Osteoporosis
 Dumfries and Galloway Treatment Protocol for Osteoporosis DIAGNOSIS OF OSTEOPOROSIS 2 Diagnostic Criteria 2 Multiple low trauma vertebral fractures in the absence of myeloma or metastatic disease. 2 T-score
Dumfries and Galloway Treatment Protocol for Osteoporosis DIAGNOSIS OF OSTEOPOROSIS 2 Diagnostic Criteria 2 Multiple low trauma vertebral fractures in the absence of myeloma or metastatic disease. 2 T-score
Dosage in renal impairment Kalcipos-D chewable tablets should not be used in patients with severe renal impairment.
 SUMMARY OF THE PRODUCT CHARACTERISTICS 1 NAME OF THE MEDICINAL PRODUCT Kalcipos-D 500 mg/400 IU chewable tablet 2 QUALITATIVE AND QUANTITATIVE COMPOSITION One chewable tablet contains: calcium 500 mg as
SUMMARY OF THE PRODUCT CHARACTERISTICS 1 NAME OF THE MEDICINAL PRODUCT Kalcipos-D 500 mg/400 IU chewable tablet 2 QUALITATIVE AND QUANTITATIVE COMPOSITION One chewable tablet contains: calcium 500 mg as
Zerlinda (MRP DK/H/2265/001)
 Zerlinda (MRP DK/H/2265/001) VI.2 Elements for a Public Summary VI.2.1 Overview of disease epidemiology Prevention of bone complications, e.g. fractures, in adult patients with bone metastases (spread
Zerlinda (MRP DK/H/2265/001) VI.2 Elements for a Public Summary VI.2.1 Overview of disease epidemiology Prevention of bone complications, e.g. fractures, in adult patients with bone metastases (spread
Greater Manchester Interface Prescribing Group Shared Care Template
 Greater Manchester Interface Prescribing Group Shared Care Template Shared Care Guideline the use of Denosumab for the prevention of osteoporotic fractures in postmenopausal women. Author(s)/Originator(s):
Greater Manchester Interface Prescribing Group Shared Care Template Shared Care Guideline the use of Denosumab for the prevention of osteoporotic fractures in postmenopausal women. Author(s)/Originator(s):
Osteoporosis. When we talk about osteoporosis, we have to be familiar with the constituents of bone and what it is formed of.
 Osteoporosis When we talk about osteoporosis, we have to be familiar with the constituents of bone and what it is formed of. Osteoblasts by definition are those cells present in the bone and are involved
Osteoporosis When we talk about osteoporosis, we have to be familiar with the constituents of bone and what it is formed of. Osteoblasts by definition are those cells present in the bone and are involved
For the use only of Registered Medical Practitioners or a Hospital or a Laboratory OSTOCALCIUM FORTE TABLETS
 For the use only of Registered Medical Practitioners or a Hospital or a Laboratory OSTOCALCIUM FORTE TABLETS Calcium and Phosphorus with Vitamin D3 Tablets QUALITATIVE AND QUANTITATIVE COMPOSITION Each
For the use only of Registered Medical Practitioners or a Hospital or a Laboratory OSTOCALCIUM FORTE TABLETS Calcium and Phosphorus with Vitamin D3 Tablets QUALITATIVE AND QUANTITATIVE COMPOSITION Each
SUMMARY OF THE PRODUCT CHARACTERISTICS
 SUMMARY OF THE PRODUCT CHARACTERISTICS 1 NAME OF THE MEDICINAL PRODUCT Calcichew-D3 Mite Citron 500 mg/200 IU chewable tablets 2 QUALITATIVE AND QUANTITATIVE COMPOSITION One tablet contains: Calcium carbonate
SUMMARY OF THE PRODUCT CHARACTERISTICS 1 NAME OF THE MEDICINAL PRODUCT Calcichew-D3 Mite Citron 500 mg/200 IU chewable tablets 2 QUALITATIVE AND QUANTITATIVE COMPOSITION One tablet contains: Calcium carbonate
For the use only of Registered Medical Practitioners or a Hospital or a Laboratory OSTOCALCIUM TABLETS. Calcium and Phosphorus with Vitamin D3 Tablets
 For the use only of Registered Medical Practitioners or a Hospital or a Laboratory OSTOCALCIUM TABLETS Calcium and Phosphorus with Vitamin D3 Tablets QUALITATIVE AND QUANTITATIVE COMPOSITION Each uncoated
For the use only of Registered Medical Practitioners or a Hospital or a Laboratory OSTOCALCIUM TABLETS Calcium and Phosphorus with Vitamin D3 Tablets QUALITATIVE AND QUANTITATIVE COMPOSITION Each uncoated
They are updated regularly as new NICE guidance is published. To view the latest version of this NICE Pathway see:
 : assessing the risk of fragility fracture bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new
: assessing the risk of fragility fracture bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new
The parathyroid glands participate in the regulation
 41 HERNAN I. VARGAS STANLEY R. KLEIN The parathyroid glands participate in the regulation of calcium metabolism. Disorders of the parathyroid gland are most commonly a result of hyperfunction and rarely
41 HERNAN I. VARGAS STANLEY R. KLEIN The parathyroid glands participate in the regulation of calcium metabolism. Disorders of the parathyroid gland are most commonly a result of hyperfunction and rarely
SUMMARY OF THE PRODUCT CHARACTERISTICS
 SUMMARY OF THE PRODUCT CHARACTERISTICS 1 NAME OF THE MEDICINAL PRODUCT Kalcipos-D mite 500 mg/200 IU film-coated tablet 2 QUALITATIVE AND QUANTITATIVE COMPOSITION Each film-coated tablet contains 500 mg
SUMMARY OF THE PRODUCT CHARACTERISTICS 1 NAME OF THE MEDICINAL PRODUCT Kalcipos-D mite 500 mg/200 IU film-coated tablet 2 QUALITATIVE AND QUANTITATIVE COMPOSITION Each film-coated tablet contains 500 mg
Figures and tables in this presentation were adopted from various printed and electronic resorces and serve strictly for educational purposes.
 Academic lectures 3rd year of Medical faculty Figures and tables in this presentation were adopted from various printed and electronic resorces and serve strictly for educational purposes. ENDOCRINOLOGY
Academic lectures 3rd year of Medical faculty Figures and tables in this presentation were adopted from various printed and electronic resorces and serve strictly for educational purposes. ENDOCRINOLOGY
Cardiac Pathophysiology
 Cardiac Pathophysiology Evaluation Components Medical history Physical examination Routine laboratory tests Optional tests Medical History Duration and classification of hypertension. Patient history of
Cardiac Pathophysiology Evaluation Components Medical history Physical examination Routine laboratory tests Optional tests Medical History Duration and classification of hypertension. Patient history of
Awaisheh. Mousa Al-Abbadi. Abdullah Alaraj. 1 Page
 f #3 Awaisheh Abdullah Alaraj Mousa Al-Abbadi 1 Page *This sheet was written from Section 1 s lecture, in the first 10 mins the Dr. repeated all the previous material relating to osteoporosis from the
f #3 Awaisheh Abdullah Alaraj Mousa Al-Abbadi 1 Page *This sheet was written from Section 1 s lecture, in the first 10 mins the Dr. repeated all the previous material relating to osteoporosis from the
Hypercalcemia. Brian Rose, M.D. Bozeman Health June 6, 2018
 Hypercalcemia Brian Rose, M.D. Bozeman Health June 6, 2018 Hypercalcemia Diagnosis PTH Mediated Primary Hyperparathyroidism Lithium Familial Hypocalciuric Hypercalcemia Non PTH mediated Malignancy Humoral
Hypercalcemia Brian Rose, M.D. Bozeman Health June 6, 2018 Hypercalcemia Diagnosis PTH Mediated Primary Hyperparathyroidism Lithium Familial Hypocalciuric Hypercalcemia Non PTH mediated Malignancy Humoral
REFERRAL GUIDELINES ENDOCRINOLOGY
 REFERRAL GUIDELINES ENDOCRINOLOGY Referral Form: The GP Referral Template is the preferred referral tool (previously known as the Victorian Statewide Referral Form) GP Referral Template This tool is housed
REFERRAL GUIDELINES ENDOCRINOLOGY Referral Form: The GP Referral Template is the preferred referral tool (previously known as the Victorian Statewide Referral Form) GP Referral Template This tool is housed
Overview. Bone Biology Osteoporosis Osteomalacia Paget s Disease Cases. People Centred Positive Compassion Excellence
 Overview Osteoporosis and Metabolic Bone Disease Dr Chandini Rao Consultant Rheumatologist Bone Biology Osteoporosis Osteomalacia Paget s Disease Cases Bone Biology Osteoporosis Increased bone remodelling
Overview Osteoporosis and Metabolic Bone Disease Dr Chandini Rao Consultant Rheumatologist Bone Biology Osteoporosis Osteomalacia Paget s Disease Cases Bone Biology Osteoporosis Increased bone remodelling
Osteoporosis Clinical Guideline. Rheumatology January 2017
 Osteoporosis Clinical Guideline Rheumatology January 2017 Introduction Osteoporosis is a condition of low bone mass leading to an increased risk of low trauma fractures. The prevalence of osteoporosis
Osteoporosis Clinical Guideline Rheumatology January 2017 Introduction Osteoporosis is a condition of low bone mass leading to an increased risk of low trauma fractures. The prevalence of osteoporosis
BCCA Protocol Summary Guidelines for the Diagnosis and Management of Malignancy Related Hypercalcemia
 BCCA Protocol Summary Guidelines for the Diagnosis and Management of Malignancy Related Hypercalcemia Protocol Code Tumour Group Supportive Care Group Contacts SCHYPCAL Supportive Care Lisa Wanbon (VIC)
BCCA Protocol Summary Guidelines for the Diagnosis and Management of Malignancy Related Hypercalcemia Protocol Code Tumour Group Supportive Care Group Contacts SCHYPCAL Supportive Care Lisa Wanbon (VIC)
Summary of Product Characteristics
 1 NAME OF THE MEDICINAL PRODUCT Desunin 4000 IU Tablets Summary of Product Characteristics 2 QUALITATIVE AND QUANTITATIVE COMPOSITION Each tablet contains colecalciferol (vitamin D 3 ) 4000 IU (equivalent
1 NAME OF THE MEDICINAL PRODUCT Desunin 4000 IU Tablets Summary of Product Characteristics 2 QUALITATIVE AND QUANTITATIVE COMPOSITION Each tablet contains colecalciferol (vitamin D 3 ) 4000 IU (equivalent
Hypertension The normal radial artery blood pressures in adults are: Systolic arterial pressure: 100 to 140 mmhg. Diastolic arterial pressure: 60 to
 Hypertension The normal radial artery blood pressures in adults are: Systolic arterial pressure: 100 to 140 mmhg. Diastolic arterial pressure: 60 to 90 mmhg. These pressures are called Normal blood pressure
Hypertension The normal radial artery blood pressures in adults are: Systolic arterial pressure: 100 to 140 mmhg. Diastolic arterial pressure: 60 to 90 mmhg. These pressures are called Normal blood pressure
Primary hyperparathyroidism
 How to Treat PULL-OUT SECTION Complete How to Treat quizzes online /cpd to earn CPD or PDP points. INSIDE Pathophysiology Clinical features Investigations Management Prognosis Special cases Case study
How to Treat PULL-OUT SECTION Complete How to Treat quizzes online /cpd to earn CPD or PDP points. INSIDE Pathophysiology Clinical features Investigations Management Prognosis Special cases Case study
Minimally invasive parathyroidectomy
 Minimally invasive parathyroidectomy Jessica E. Gosnell MD Assistant Professor of Surgery March 22, 2011 1 Minimally invasive parathyroidectomy 1. What? 2. When? 3. How? 4. Convert? 5. What adjuncts? Primary
Minimally invasive parathyroidectomy Jessica E. Gosnell MD Assistant Professor of Surgery March 22, 2011 1 Minimally invasive parathyroidectomy 1. What? 2. When? 3. How? 4. Convert? 5. What adjuncts? Primary
Nephrology and Surgical Department Parathyroid Surgery in Adults
 Nephrology and Surgical Department Parathyroid Surgery in Adults This leaflet explains surgery to treat Primary Hyperparathyroidism. It will help you to understand the operation and the care that you will
Nephrology and Surgical Department Parathyroid Surgery in Adults This leaflet explains surgery to treat Primary Hyperparathyroidism. It will help you to understand the operation and the care that you will
Parathyroid hormone (serum, plasma)
 Parathyroid hormone (serum, plasma) 1 Name and description of analyte 1.1 Name of analyte Parathyroid hormone (PTH) 1.2 Alternative names Parathormone 1.3 NMLC code 1.4 Description of analyte PTH is an
Parathyroid hormone (serum, plasma) 1 Name and description of analyte 1.1 Name of analyte Parathyroid hormone (PTH) 1.2 Alternative names Parathormone 1.3 NMLC code 1.4 Description of analyte PTH is an
76 year-old female presents with muscle cramps. Jess Hwang 12/6/12
 76 year-old female presents with muscle cramps Jess Hwang 12/6/12 HPI Worked up for outpatient hypercalcemia Calcium had been 10.3-11.1, PTH ~120 No h/o osteoporosis, CKD, kidney stones Not taking calcium
76 year-old female presents with muscle cramps Jess Hwang 12/6/12 HPI Worked up for outpatient hypercalcemia Calcium had been 10.3-11.1, PTH ~120 No h/o osteoporosis, CKD, kidney stones Not taking calcium
Osteoporosis/Fracture Prevention Clinician Guide SEPTEMBER 2017
 Kaiser Permanente National CLINICAL PRACTICE GUIDELINES Osteoporosis/Fracture Prevention Clinician Guide SEPTEMBER 2017 Introduction This Clinician Guide was developed to assist Primary Care physicians
Kaiser Permanente National CLINICAL PRACTICE GUIDELINES Osteoporosis/Fracture Prevention Clinician Guide SEPTEMBER 2017 Introduction This Clinician Guide was developed to assist Primary Care physicians
Fragile Bones and how to recognise them. Rod Hughes Consultant physician and rheumatologist St Peter s hospital Chertsey
 Fragile Bones and how to recognise them Rod Hughes Consultant physician and rheumatologist St Peter s hospital Chertsey Osteoporosis Osteoporosis is a skeletal disorder characterised by compromised bone
Fragile Bones and how to recognise them Rod Hughes Consultant physician and rheumatologist St Peter s hospital Chertsey Osteoporosis Osteoporosis is a skeletal disorder characterised by compromised bone
"Asymptomatic" Hyperparathyroidism: Reasons for Parathyroidectomy
 "Asymptomatic" Hyperparathyroidism: Reasons for Parathyroidectomy Rebecca S. Sippel, M.D. Assistant Professor Department of Surgery Section of Endocrine Surgery University of Wisconsin Primary Hyperparathyroidism
"Asymptomatic" Hyperparathyroidism: Reasons for Parathyroidectomy Rebecca S. Sippel, M.D. Assistant Professor Department of Surgery Section of Endocrine Surgery University of Wisconsin Primary Hyperparathyroidism
Parathyroidectomy. Surgery for Parathyroid Problems
 Parathyroidectomy Surgery for Parathyroid Problems Why You Need Parathyroid Surgery Has your doctor just recommended that you have parathyroid surgery? If so, you likely have many questions. What are the
Parathyroidectomy Surgery for Parathyroid Problems Why You Need Parathyroid Surgery Has your doctor just recommended that you have parathyroid surgery? If so, you likely have many questions. What are the
SUMMARY OF THE PRODUCT CHARACTERISTICS
 SUMMARY OF THE PRODUCT CHARACTERISTICS 1. NAME OF THE MEDICINAL PRODUCT Recikalc-D forte 500 mg/ 800 IU chewable tablets 2. QUALITATIVE AND QUANTITATIVE COMPOSITION Each chewable tablet contains calcium
SUMMARY OF THE PRODUCT CHARACTERISTICS 1. NAME OF THE MEDICINAL PRODUCT Recikalc-D forte 500 mg/ 800 IU chewable tablets 2. QUALITATIVE AND QUANTITATIVE COMPOSITION Each chewable tablet contains calcium
Natpara (parathyroid hormone) Prior Authorization with Quantity Limit Program Summary
 Natpara (parathyroid hormone) Prior Authorization with Quantity Limit Program Summary FDA APPROVED INDICATIONS DOSAGE 2 Available Product Indication Dosing and Administration Natpara (parathyroid hormone)
Natpara (parathyroid hormone) Prior Authorization with Quantity Limit Program Summary FDA APPROVED INDICATIONS DOSAGE 2 Available Product Indication Dosing and Administration Natpara (parathyroid hormone)
Bone Metastases. Sukanda Denjanta, M.Sc., BCOP Pharmacy Department, Chiangrai Prachanukroh Hospital
 Bone Metastases Sukanda Denjanta, M.Sc., BCOP Pharmacy Department, Chiangrai Prachanukroh Hospital 1 Outline Pathophysiology Signs & Symptoms Diagnosis Treatment Spinal Cord Compression 2 General Information
Bone Metastases Sukanda Denjanta, M.Sc., BCOP Pharmacy Department, Chiangrai Prachanukroh Hospital 1 Outline Pathophysiology Signs & Symptoms Diagnosis Treatment Spinal Cord Compression 2 General Information
GLOSSARY OF TERMS. produced in response to an antigen to bond with and neutralize that antigen / the body's way of destroying foreign invaders
 TERM 24-hour urine acidosis acquired aemia (prefix) albumin alkalosis anemia antibodies antigen autocrine autoimmune basal ganglion bone turnover calcilytic calcimimetic calcitonin Calcitriol Calcium carbonate
TERM 24-hour urine acidosis acquired aemia (prefix) albumin alkalosis anemia antibodies antigen autocrine autoimmune basal ganglion bone turnover calcilytic calcimimetic calcitonin Calcitriol Calcium carbonate
NHS LINCOLNSHIRE in association with UNITED LINCOLNSHIRE HOSPITALS TRUST
 NHS LINCOLNSHIRE in association with UNITED LINCOLNSHIRE HOSPITALS TRUST SHARED CARE GUIDELINE: CINACALCET in the management of secondary hyperparathyroidism in adult patients with end-stage renal disease
NHS LINCOLNSHIRE in association with UNITED LINCOLNSHIRE HOSPITALS TRUST SHARED CARE GUIDELINE: CINACALCET in the management of secondary hyperparathyroidism in adult patients with end-stage renal disease
Endocrine Emergencies: Recognition and Management
 Endocrine Emergencies: Recognition and Management John Wass Department of Endocrinology, Oxford University, UK An Update on Acute Medical Emergencies for Psychiatrists Royal College of Psychiatrists' address
Endocrine Emergencies: Recognition and Management John Wass Department of Endocrinology, Oxford University, UK An Update on Acute Medical Emergencies for Psychiatrists Royal College of Psychiatrists' address
Inpatient Pediatric Endocrinology. Tala Dajani MD MPH Pediatric Endocrinology of Phoenix
 Inpatient Pediatric Endocrinology Tala Dajani MD MPH Pediatric Endocrinology of Phoenix Objectives Identify calcium disorders in the hospital Distinguish between temporary versus permanent glucose problems
Inpatient Pediatric Endocrinology Tala Dajani MD MPH Pediatric Endocrinology of Phoenix Objectives Identify calcium disorders in the hospital Distinguish between temporary versus permanent glucose problems
CAL360 Tablets (Calcium citrate malate + Vitamin D3 )
 Published on: 18 Jan 2016 CAL360 Tablets ( citrate malate + Vitamin D3 ) Composition Each film-coated tablet contains: Citrate Malate equivalent to Elementary 250 mg Cholecalciferol Concentrate (powder
Published on: 18 Jan 2016 CAL360 Tablets ( citrate malate + Vitamin D3 ) Composition Each film-coated tablet contains: Citrate Malate equivalent to Elementary 250 mg Cholecalciferol Concentrate (powder
LOVE YOUR BONES Protect your future
 www.worldosteoporosisday.org LOVE YOUR BONES Protect your future Know your risk for osteoporosis www.iofbonehealth.org Osteoporosis is a problem worldwide, and in many countries, up to one in three women
www.worldosteoporosisday.org LOVE YOUR BONES Protect your future Know your risk for osteoporosis www.iofbonehealth.org Osteoporosis is a problem worldwide, and in many countries, up to one in three women
