BRAIN INJURY IN PRETERM INFANTS
|
|
|
- Poppy Lester
- 5 years ago
- Views:
Transcription
1 Paediatr Croat. 2018; 62 (Supl 1): Pregled Review BRAIN INJURY IN PRETERM INFANTS ANETA SOLTIROVSKA SALAMON, DARJA PARO-PANJAN* Perinatal care advances over the past twenty years have helped to diminish the mortality and severe neurological morbidity of extremely and very preterm infants. However, motor and/or cognitive disabilities associated with mild-to-moderate white and grey matter injury are frequently present in this population. The major neuropathological substrate of preterm brain injury is encephalopathy of prematurity which characterizes the multifaceted white and grey matter lesions, and reflects a combination of destructive and dysmaturational effects. It can be associated with haemorrhages, notably in germinal matrix and cerebellum and with focal micro-or macroinfarcts. Clinical signs of brain injury are often subtle or even absent, therefore several new non-invasive methods are used to identify and estimate central nervous system dysfunction. They provide insight into hemodynamics, electrical activity and brain structure. Knowing and understanding the causes and the mechanisms of brain injury yield to a number of more or less successful neuroprotective approaches that reduce the negative influences on the developing brain. Since brain injury and consequently its long term neurodevelopmental outcome remains the most important complication of the premature birth, a regular and comprehensive follow-up of motor, cognitive and behavioral development of these children is essential, as it provides early detection of potential delays and intervention. Descriptors: PRETERM INFANT, BRAIN INJURY, ENCEPHALOPATHY OF PREMATURITY, NEURODEVELOPMENTAL OUTCOME Introduction Preterm birth is a leading cause of long-term neurological disabilities in children. The rate of preterm birth remains around 10% worldwide; with rates, varying from 5-18% across 184 countries studied, and it has not changed over the last two decades (1). Perinatal care advances over the past twenty years have helped to diminish the mortality and severe neurological morbidity of extremely and very preterm neonates. However, motor and/or cognitive disabilities associated with mild-to-moderate white and grey matter injury are frequently present in this population (2). *University Medical Centre Ljubljana Division of Paediatrics Department of Neonatology Address: Professor Darja Paro-Panjan, MD, PhD Department of Neonatology Division of Paediatrics University Medical Centre Ljubljana SI-1525 Ljubljana, Slovenia, Bohoričeva ulica 20 darja.paro@kclj.si 104 The major neuropathological substrate of preterm brain injury is encephalopathy of prematurity (EP). This term was introduced by Joseph Volpe and coined to characterize the multifaceted white and grey matter lesions in the preterm brain, which reflect a combination of destructive and dysmaturational effects (3, 4). EP is also associated with haemorrhages, notably in germinal matrix and cerebellum and with focal micro-or macroinfarcts. Due to responsible insults occurring at the time of rapid brain growth, a host of developmental programs may be affected, resulting in maturational defects that compound the acquired lesions. The course of EP is multifactorial and includes cerebral hypoxia-ischaemia and systemic infection/inflammation, which results in glutamate, free radical and/or cytokine toxicity to pre-olygodendrocytes (pre-ols), axons and neurons (3, 4). Contributory roles of impaired nutrition, pain, stress, drugs and other factors associated with neonatal intensive care also seem possible (4, 5). Due to the heterogeneity of lesions that comprise EP, the spectrum of neurodevelopmental abnormalities in preterm survivors is wide and includes, often in combination, a variety of cognitive, behavioral, socialization, attention and motor deficits (6). The purpose of this review is to explain the concept of brain injury in preterm infants, which comprises destructive and developmental disturbances, diagnostics and its subsequent neurodevelopmental consequences. Neuropathology of brain injury in preterm infants and pathophysiologic mechanism The neuropathology of brain injury in premature infants termed EP consists of multiple lesions: periventricular leukomalacia (PVL) and accompanying neuronal/axonal abnormalities; severe germinal matrix-intraventricular haemorrhage (GMH-IVH), especially with periventricular hemorrhagic infarction; and posthemorrhagic hydrocephalus (5).
2 GMH-IVH is the most common variety of haemorrhage in newborns. Although the gradual decrease in the incidence of GMH-IVH has been noted, it has remained unchanged in last two decades, with overall incidence of 25% (5, 7). The vasculature in the germinal matrix is very fragile and in combination with the lack of cerebral autoregulation and fluctuations in cerebral blood flow (CBF) it causes a rupture of vessels, which results in haemorrhage either restricted to the germinal matrix but more often also extends to the lateral ventricle. Papile classification is commonly used to grade the severity of GMH-IVH: grade I represents haemorrhage confined to subependymal germinal matrix, grade II is haemorrhage in lateral ventricles without dilatation, grade III haemorrhage occupies more than 50% of ventricle with distention resulting in ventricular dilatation (8). The associated parenchymal involvement known as a periventricular hemorrhagic infarction (PVHI) is due to the impaired venous drainage of the medullary veins in the periventricular white matter. The incidence of the lesions increases with decreasing gestational age, and 10-15% of very low birth weight (VLBW) infants with GMH-IVH exhibit PVHI (9). Posthemorrhagic ventricular dilatation (PHVD) develops in approximately 25 to 50% of preterm infants within 7 to 14 days after the onset of a severe GMH- IVH. Adverse effects of intraventricular blood and progressive ventricular dilatation on the adjacent vulnerable periventricular white matter (WM) of the preterm infant have been reported as unfavourable outcome in group of infants with PHVD (10). Cerebellar haemorrhages (CBH) are recognized as a common problem in very immature infants with reported incidence 15 to 20% depending on the gestational age (GA); they tend to be associated with supratentorial lesions, most often severe GMH-IVH (11, 12). The preterm WM is susceptible to a broad spectrum of injury severity that ranges from diffuse non-destructive lesions to the severe necrotic lesions of periventricular leukomalacia (PVL). PVL consists of localized necrosis deep in periventricular WM, with loss of all cellular elements. These necroses can be macroscopic in size and evolve over several weeks to multiple cystic lesions - "cystic PVL" (3, 4, 13). Nowadays, this severe lesion is observed in less than 5% of infants with VLBW, and therefore accounts for a small minority of PVL. Much more commonly focal necroses are microscopic in size and evolve over several weeks to glial scars that are not readily seen by neuroimaging. This form of PVL, which accounts for the vast majority of cases, is termed "non-cystic PVL" (3, 4, 13). Research studies using magnetic resonance imaging (MRI) report that 50% to 80% of extremely and very preterm neonates have diffuse white matter injuries (WMI) which correspond to only the minimum grade of severity. Furthermore, data from recent studies have shown that PVL is frequently accompanied by neuronal/axonal disease affecting the cerebral WM, thalamus, basal ganglia, cerebral cortex, brain stem, and cerebellum (3, 4, 13). EP, both PVL and the associated neuronal/axonal disease, occurs during a period of rapid and complex events in brain development (3, 4, 13). The developmental events between weeks involve in particular the following: cerebral WM (pre -OLs, axons, microglia), and neurons (subplate and late migrating GABA-ergic neurons); two proliferative zones; and key neuronal structures - thalamus, cerebral cortex and basal ganglia (14-16). Because of the rapidity and complexity of these developmental events, they are postulated to be vulnerable to exogenous and endogenous insults which produce the developmental disturbances, including impaired cellcell interactions, involving intercellular trophic support, retrograde effects ("dying back"), and anterograde effects (e.g., Wallerian degeneration, transsynaptic degeneration). At the end stage, WMI results in cell death or process loss, or both. Thus, diffusely apparent WMI is characterized by marked astrogliosis and microgliosis, and initially by a decrease in premyelinating pre-ols. Subsequently, the decrease in cells of the oligodendroglial lineage is counteracted by an increase in oligodendroglial progenitors. However, in PVL, these cells which often lack processes seem not to have the capacity for full differentiation to mature myelin-producing cells, and hypomyelination. Impairment of myelination and of cortical and thalamic development by neuronal/axonal disease are hallmark of WMI (14-16). Clinical risk factors for WMI relate to hypoxia-ischemia and/or inflammation. Premature newborns are predisposed to cerebral hypoxia-ischemia because of a combination of the vascular anatomy consisting of arterial border zones within the WM, as well as an impaired ability to autoregulate CBF; the consequences pressure-passive hypotension and decrease in systemic blood pressure that can result in ischemia to the arterial border zones. Multiple studies have confirmed that both hypocarbia and hypercarbia can also significantly perturb CBF. Thus, hypocarbia may promote hypotension and increased risk for IVH and WMI (17). Additionally, ansignificant series of clinical and experimental studies suggests that maternal intrauterine infection, foetal systemic inflammation as well as postnatal infections are also involved in the pathogenesis of WMI. Bacterial endotoxin can cause WMI via vasoactive mechanism that can result in cerebral ischemia or via stimulation of systemic cytokines and activation of microglia. Microglia derived TNF-α and INF-γ interact synergistically to cause early pre- OL death. Endogenous exposure to IL-1β disrupts oligodendrocyte maturation and myelination (17). Diagnosis of preterm brain injury Neuroimaging is of the major diagnostic importance of brain injury in preterm infants; cranial ultrasonography (cus) and MRI are the main imaging methodologies. Additionally, diagnostic and prognostic value of electroencephalography (EEG) and amplitude integrated EEG have also been established. Electroencephalography Serial EEG studies have been shown of value in identifying preterm infants with PVL and presumed neuronal disease. Thus, decreased continuity, lower 105
3 background activity or both were observed mainly at day 1 to 4 of life with subsequent identified PVL with cus; these findings referred to acute-stage abnormalities. Deformed slow activity and subnormal sharp waves were observed mainly at day 5 to 14 and resolving within 1-2 months; these findings referred to chronic-stage abnormalities, which were more severe and persisted longer in patients with extensive c-pvl compared with milder PVL, suggesting that EEG findings correlate with PVL severity. Positive rolandic sharp waves were present in 65-90% of cases with severe PLV and 25% of cases with mild or moderate PVL. Frontal positive or occipital negative sharp waves or both were present in 100% cases of severe PVL and 60-90% of mild or moderate PVL. Abnormal sharp waves accompany echodense lesions on cus and precede the development of echolucent-cystic lesions. In addition to abnormalities of EEG background activity, 30% of infants with PVL were presented with seizures, and 65% with episodes of apnea (4). Neuroimaging Cranial ultrasonography remains the preferred neuroimaging technique for routine screening of intracranial pathology in preterm infants. Early cus examination mostly detects hemorrhagic lesions, whereas a subsequent cus usually allows diagnosis of WM abnormalities (2, 4, 12). It is effective in identification of all degrees of severity of GMH-IVH. The major elemental lesion is haemorrhage in germinal matrix, which is usually seen as dense echogenicity that correlates with haemorrhage. Intraventricular bleeding results in echogenic material that fills a portion of lateral ventricular system. The PVHI lesions are triangular, usually unilateral and located on the side of larger GMH-IVH and commonly in frontal or parietal regions. They evolve into one larger or several smaller porencephalic cysts adjacent to the ventricle, and their size and site is predictive of outcome. PHVD that develops as complication after GMH-IVH is demonstrated very well with cus. Measurements can be taken of the ventricular index (VI), anterior horn width and occipital 106 horn width, and these measurements can be used to optimize timing of intervention (2, 4, 12). Cerebellar haemorrhages more than 4 to 5 mm in size can also be detected by cus. Smaller (punctate) haemorrhages in the cerebellum are far more common but can only be diagnosed with MRI especially with susceptibility-weighted imaging (SWI). MRI repeated at term equivalent age presented atrophy of the affected cerebellar hemisphere following larger CBHs. A unilateral PVHI can also be associated with a marked loss of contralateral cerebellar - crossed cerebellar atrophy (11, 18). Using higher resolution ultrasound probes and a wider view of insonation, assessment of the WM has improved considerably, although it remains difficult as subtly increased echogenicity is a very subjective finding (18). Some data suggest that white matter echogenicity which is equal to or higher than the echogenicity of the choroid plexus and persist at least 7 days, is significant for white matter injury. The value of cus comes from sequential imaging, showing the duration of the echogenicity and in some cases the evolution to more echogenic and/or inhomogeneous echogenicity or to cystic lesions They are visible only for a few weeks and may have fully resolved by term equivalent age (TEA), but their presence is predictive for subsequent cerebral palsy (CP). The fluid in cysts subsequently resorbs with adhesion of the walls over the next weeks. As a result, their manifestation at TEA may be subtle: white matter loss and irregular dilatation of the adjacent ventricle (2, 4, 12). Several studies performed in the last 10 to 15 years demonstrated that the role of cus was limited when it comes to recognizing milder WM: MRI is considered to be the "gold standard" (19, 20). Counsell et al coined the term DEHSI (diffuse excessive high signal intensity) and reported that high signal intensity (SI) in the WM was a common finding in very preterm infants. They subsequently reported that these infants with increased SI in the WM at TEA had volume reduction in the periventricular WM, the corona radiate, and within the central region of the centrum semiovale dorsomedial nucleus as wellas the thalamus and the globus pallidus; and these imaging findings were associated with a significantly lower developmental outcome (18, 19, 20). Protecting the brain of the preterm infant Over the last decades, advanced neurodiagnostic techniques have brought critical information regarding the risk factors and neuropathological mechanisms responsible for the pathway to disability, and have additionally provided multifaceted neuroprotective efforts to prevent or limit structural and functional cerebral injury. Neuroprotection encompasses all strategies applied pre-, peri- and/or postnatally that promotes normal development and prevents disabilities: organizational, therapeutic, and environment-modifying measures (21). Therapies that exert neuroprotective effects when delivered antenatally include, corticosteroids and magnesium sulphate among others; both were originally applied for other purposes and were later proved to impact short- and long-term neurodevelopmental outcomes. Prevention of GMH-IVH is among the most investigated aspects of neonatal neurologic care. The most powerful intervention for prevention of GMH-IVH and improvement of outcome has been a routine use of antenatal corticosteroids. They are a mainstay of prophylactic treatment in preterm birth and exert vasoconstrictive effects on the cerebral vasculature, minimizing changes in cerebral blood flow (21). Based upon current evidence, rational prevention of GMH-IVH after delivery consists of appropriate resuscitation, delivery management, proper administration of vitamin K, judicious use of fresh frozen plasma and correction of hemodynamic disturbances (delayed cord clamping, targeted therapy of the PDA and hypotension) (4). The use of indomethacin, a non-specific cyclooxygenase inhibitor that decreases prostaglandin synthesis, on the first day of life also decreases the incidence of IVH, but its use does not
4 change the rates of neurodevelopmental disabilities (22). Furthermore, delayed clamping of the umbilical cord by 30 to 45 seconds after delivery increases the amount of blood flowing from the placenta to infant, limiting the impact of the consequent circulatory compromise. It improves regulation of CBF, enhancing oxygen delivery and modifying GMH- IVH risk (23). The nature of the pathway to WMI suggests a combination of strategies applied both preventatively and after injury targeting specific ischaemic and inflammatory factors. Cogent respiratory management and sensible use of common measures including administration of fluids, transfusions and inotropes may prevent large fluctuations in blood pressure thus minimizing the risk for ischemia. Some agents, such as antenatal corticosteroids, afford protection when administered prenatally. On the other hand, several strategies that target specific components of the inflammatory pathway have been explored for postnatal use (prevention of free radical generation, scavenge of free radicals, mediation of excitotoxicity, antiapoptotic agents and melatonin, erythropoietin, caffeine) but appropriate timing and rational application of each approach remain incompletely defined (24, 25). In the last decades, interventions designed to minimize stress of the environment known as Developmental care, such as positioning, clustering of the nursery care, modification of external stimulation and individually tailored care have also been demonstrated to influence neurodevelopmental outcome (26). Outcomes after brain injury in the preterm infant The risk of neurodevelopmental disability increases progressively with decreasing GA, with the highest risk in children born at the lower limit of viability. The most overt signs of brain injury are motor impairments. Early signs of evolving CP are persistent neuromotor abnormalities and a delay in acquisition of motor milestones (27). Two European studies reported the rate of CP from 1% at 34 weeks of gestation to 22% at 26 weeks (28). The most common type of CP associated with preterm birth is spastic diplegia; approximately half of preterm children with CP have a mild to moderate form with spasticity in lower extremities but are functional walkers. Spastic quadriplegia occurs with increasing frequency at lower gestational age while spastic hemiplegia is more common in children born after 32 weeks of gestation and at term. Many preterm children with persisting motor abnormalities after birth do not develop CP, but have minor neuromotor dysfunction (MND) which includes toe walking, postural instability, asymmetric gait, motor planning difficulties, graphomotor impairment, poor visual abilities, problems with sensorimotor integration and fine motor dysfunction. The data pooled from 11 studies that reported the prevalence of mild to moderate motor impairment in preterm children demonstrated the prevalence of mild motor impairments from 22.2% to 72.2% and moderate impairments from 9.5 to 23.8% (28). These estimates suggest that the prevalence of MND is three to four times higher in preterm than in term children. In contrast to major disabilities that can be identified early (e.g. CP, intellectual disability, sensory impairments and epilepsy), cognitive, learning, behavioral, social, and emotional problems may frequently remain hidden until school age or later, and persist into adolescence and adulthood (27, 29). Preterm outcome studies have generally found that compared with children born at term, preterm children had higher rate of cognitive impairment, especially if born before 26 to 27 weeks of gestation, and had severe brain injury and/or motor impairment (30). Although the risk of intellectual disability is higher and mean intellectual quotient (IQ) is often statistically significantly lower in preterms than IQ for term controls, the majority of children and young adults born preterm have an IQ within normal range (28). Preterm populations also demonstrate a range of cognitive impairments, including language difficulties, visioperceptual dysfunction, specific learning disabilities, working memory deficits, executive dysfunction, and delayed information processing (31). Most studies of young adults born preterm have found that they had lower academic achievement scores and educational levels when compared to participants born at term (32). The range of behavior problems in children born preterm varies from 7% to 20% (28). The most common behavioral problem associated with preterm birth is attention-deficit-hyperactivity disorder (ADHD), which occurs in 9% to 16% of school-aged children born preterm (33). Preterm outcome studies have also reported more internalizing behaviors, lower social competence, and more psychiatric problems in children, adolescents and young adults born preterm. Despite all the difficulties associated with preterm birth, the majority of adults who were born preterm have reported a similar quality of life as individuals born at term. Most graduates from secondary schools have jobs and are contributing members of their communities (34). Abbreviations: ADHD - attention-deficit-hyperactivity disorder CBF - Cerebral blood flow CP - Cerebral palsy cus - Cranial Ultrasound DEHSI - diffuse excessive high signal intensity EEG - Electroencephalography EP - Encephalopathy of prematurity GA - Gestational age GMH - IVH - germinal matrix-intraventricular haemorrhage IQ - intellectual quotient MND - minor neuromotor dysfunction MRI - Magnetic resonance imaging PDA - Persistent ductus arteriosus Pre - Ols - pre-olygodendrocytes PVHD - Posthemorrhagic ventricular dilatation PVHI - periventricular hemorrhagic infarction PVL - pre-olygodendrocytes SI - Signal intensity SWI - Susceptibility-weighted imaging TEA - Term equivalent age WM - White Matter WMI - White matter injury VLBW - Very low birth weight NOVČANA POTPORA/FUNDING Nema/None ETIČKO ODOBRENJE/ETHICAL APPROVAL Nije potrebno/none SUKOB INTERESA/CONFLICT OF INTEREST Autori su popunili the Unified Competing Interest form na (dostupno na zahtjev) obrazac i izjavljuju: nemaju potporu niti jedne organizacije za objavljeni rad; nemaju financijsku potporu niti jedne organizacije 107
5 koja bi mogla imati interes za objavu ovog rada u posljednje 3 godine; nemaju drugih veza ili aktivnosti koje bi mogle utjecati na objavljeni rad./ All authors have completed the Unified Competing Interest form at pdf (available on request from the corresponding author) and declare: no support from any organization for the submitted work; no financial relationships with any organizations that might have an interest in the submitted work in the previous 3 years; no other relationships or activities that could appear to have influenced the submitted work. 108 LITERATURE 1. fs363/en/ 2. Hinojosa-Rodríguez M, Harmony T, Carrillo- Prado C, Van Horn JD, Irimia A, Torgerson C, Jacokes Z. Clinical neuroimaging in the preterm infant: Diagnosis and prognosis. Neuroimage Clin. 2017; 14 (16): Volpe JJ. The encephalopathy of prematuritybrain injury and impaired brain development inextricably intertwined. Semin Pediatr Neurol. 2009; 16 (4): Volpe JJ. 6th ed. Saunders/Elsevier; Philadelphia: Volpe's Neurology of the Newborn. 5. Volpe J.J. Neonatal neurology, my personal journey and some lessons learned. Pediatr. Neurol. 2014; 51 (6): van't Hooft J, van der Lee JH, Opmeer BC, Aarnoudse-Moens CSH, Leenders AGE, Mol BWJ, de Haan TR. Predicting developmental outcomes in premature infants by term equivalent MRI: systematic review and metaanalysis. Syst. Rev. 2015; 4 (1): Ballabh P. Pathogenesis and prevention of intraventricular hemorrhage. Clin. Perinatol. 2014; 41 (1): Papile LA, Burstein J, Burstein R, Koffler H. Incidence and evolution of subependymal and intraventricular hemorrhage: a study of infants with birth weights less than 1,500 gm. J Pediatr 1978; 92 (4): Soltirovska Salamon A, Groenendaal F, van Haastert IC, Rademaker KJ, Benders MJNL, Koopman C, de Vries LS. Neuroimaging and neurodevelopmental outcome of preterm infants with a periventricular haemorrhagic infarction located in the temporal or frontal lobe. Dev. Med. Child Neurol. 2014; 56 (6): Brouwer A, Groenendaal F, van Haastert IL, Rademaker K, Hanlo P, de Vries L. Neurodevelopmental outcome of preterm infants with severe intraventricular hemorrhage and therapy for post-hemorrhagic ventricular dilatation. J Pediatr 2008; 152 (5): Steggerda SJ, Leijser LM, Wiggers-de Bruïne FT, van der Grond J, Walther FJ, van Wezel- Meijler G. Cerebellar injury in preterm infants: incidence and findings on US and MR images. Radiology 2009; 252 (1): De Vries LS, Benders MN, Gronendal F. Progress in Neonatal Neurology with a Focus on Neuroimaging in the Preterm Infant. Neuropediatrics 2015; 46: Volpe JJ. Encephalopathy of prematurity includes neuronal abnormalities. Pediatrics. 2005; 116 (1): Volpe JJ. Brain injury in premature infants: a complex amalgam of destructive and developmental disturbances. Lancet Neurol. 2009; 8 (1): Volpe JJ, Kinney HC, Jensen FE, Rosenberg PA. The developing oligodendrocyte: key cellular target in brain injury in the premature infant. Int. J. Dev. Neurosci. 2011; 29 (6): van Tilborg E, Heijnen CJ, Benders MJ, van Bel F, Fleiss B, Gressens P, Nijboer CH. Impaired oligodendrocyte maturation in preterm infants: potential therapeutic targets. Prog. Neurobiol. 2016; 136: Volpe JJ. Systemic inflammation, oligodendroglialmaturation, and the encephalopathy of prematurity. Ann Neurol 2011; 70 (4): Leijser LM, de Bruïne FT, van der Grond J, Steggerda SJ,Walther FJ, van Wezel-Meijler G. Is sequential cranial ultrasound reliable for detection of white matter injury in very preterm infants? Neuroradiology 2010; 52 (5): Counsell SJ, Allsop JM, Harrison MC et al. Diffusion-weighted imaging of the brain in preterm infants with focal and diffuse white matter abnormality. Pediatrics 2003; 112 (1): Kersbergen KJ, BendersMJ, Groenendaal F et al. Different patterns of punctate white matter lesions in serially scanned preterm infants. PLoS ONE 2014; 9 (10): Smyser CD, Inder TE. Protecting the brain of the preterm infant. In: Shevell M, Miller SP, eds. Acquired brain injury in the fetus and newborn. 3th ed. London: Mac Keith Press, 2012; Fowlie PW, Davis PG, McGuire W. Prophylactic intravenous indomethacin for preventing mortaity and morbidity in preterm infants. Cochrane Database Syst Rev 2010; 7: Mercer JS, Vohr BR, McGrath MM, Padbury JF, Wallach M, Oh W. Delayed cord clamping in very preterm infants reduces the incidence of intraventricular hemorrhage and late-onset sepsis: a randomized, controlled trial. Pediatrics 2006; 117: Roberts D, Dalziel S. Antenatal corticosteroids for accelerating fetal lung maturation for women at risk for preterm birth. Cochrane Database Syst Rev 2006; 3: Khwaja O, Volpe JJ. Pathogenesis of cerebral white matter injury of prematurity. Arch Dis Child Fetal Neonatal Ed 2008; 93: Symington A, Pinelli J. Developmental care for promoting development and preventing morbidity in preterm infants. Cochrane Database Syst Rev 2006; 19: Kodric J, Sustersic B, Paro-Panjan D. Relationship between neurological assessments of preterm infants in the first 2 years and cognitive outcome at school age. Pediatr Neurol. 2014; 51 (5): Allen MC. Outcomes of the brain injury in the preterm infant. In: Shevell M, Miller SP, eds. Acquired Brain Injury in the fetus and newborn. 3th ed. London: Mac Keith Press, 2012; Johnson S, Wolke D. Behavioural outcomes and psychopathology during adolescence. Early Hum Dev 2013; 89: Weisglas-Kuperus N, Hille ET, Duivenvoorden HJ et al. Intelligence of very preterm or very low birthweight infants in young adulthood. Arrch Dis Child Fetal Neonatal ed; 2009; Mulder H, Pitchford NJ, Marlow N. Processing speed and working memory underlie academic attainment in very preterm children. Arch Dis Child Fetal Neonatal Ed 2010; 95: Mathiasen R, Hansen BM, Nybo Anderson AM, Greisen G. Socio-economic achievements of individuals born very preterm at the age of 27 to 29 years: a nation wide cohort study. Dev Med Child Neurol 2009; 51: Johnson S. Cognitive and behavioural outcomes following very preterm birth. Semin Fetal Neonatal Med 2007; 12: Saigal S, Stoskopf B, Pinelli J et al. Self-perceived health-related quality of life of former extremely low birth weight infants at young adulthood. Pediatrics 2006; 118:
6 Sažetak OŠTEĆENJE MOZGA NEDONOŠČADI Aneta Soltirovska Salamon, Darja Paro-Panjan Zahvaljujući poboljšanju perinatalne skrbi, u posljednja dva desetljeća, smanjen je mortalitet i teška neurološka oštećenja kod nedonoščadi. Unatoč tome motoričke i kognitivne smetnje povezane s oštećenjem mozga, još su uvijek prisutne u toj populaciji djece. Glavni patomorfološki supstrat oštećenja mozga kod nedonoščadi je encefalopatija nedonoščadi, koja predstavlja kombinaciju destruktivnih i dismaturacijskih procesa. Povezana je krvarenjem u germinativnom matriksu i cerebelumu te žarišnim mikro ili makroinfarktima. Klinički znaci ozljede mozga mogu biti suptilni ili čak odsutni pa se stoga veliku važnost daje suvremenim neinvazivnim metodama kojima se može dijagnosticirati ozljeda. One omogućavaju uvid u hemodinamičko stanje, električnu aktivnost i strukturu mozga. Poznavanje razloga i mehanizama ozljede pridonosi i neuroprotektivnim mjerama, kojima se smanjuju negativni utjecaji na mozak u razvoju. Budući da su ozljeda mozga te neurološke i razvojne posljedice najvažnija komplikacija nedonoščadi, redovno praćenje motoričkog te kognitivnog razvoja i ponašanja u toj skupini djece omogućuje rano otkrivanje mogućih poremećaja i pravovremenu intervenciju. Deskriptori: NEDONOŠČAD, OZLJEDA MOZGA, ENCEFALOPATIJA NEDONOŠČADI, NEURORAZVOJNI ISHOD Primljeno/Received: Prihvaćeno/Accepted:
Insults to the Developing Brain & Effect on Neurodevelopmental Outcomes
 Insults to the Developing Brain & Effect on Neurodevelopmental Outcomes Ira Adams-Chapman, MD Assistant Professor of Pediatrics Director, Developmental Progress Clinic Emory University School of Medicine
Insults to the Developing Brain & Effect on Neurodevelopmental Outcomes Ira Adams-Chapman, MD Assistant Professor of Pediatrics Director, Developmental Progress Clinic Emory University School of Medicine
Imaging the Premature Brain- New Knowledge
 Imaging the Premature Brain- New Knowledge Stein Magnus Aukland Haukeland University Hospital University of Bergen NORWAY No disclosure Imaging modalities O Skull X-ray O Computer Tomography O Cerebral
Imaging the Premature Brain- New Knowledge Stein Magnus Aukland Haukeland University Hospital University of Bergen NORWAY No disclosure Imaging modalities O Skull X-ray O Computer Tomography O Cerebral
Predicting outcome using neonatal MRI in preterm infants. Manon Benders, neonatologist. Summer Conference on Neonatology in Provence
 Predicting outcome using neonatal MRI in preterm infants Manon Benders, neonatologist Summer Conference on Neonatology in Provence Avignon, France, 6 th - 9 th September 2017 the human brain the third
Predicting outcome using neonatal MRI in preterm infants Manon Benders, neonatologist Summer Conference on Neonatology in Provence Avignon, France, 6 th - 9 th September 2017 the human brain the third
Neonatal hypoxic-ischemic brain injury imaging: A pictorial review
 Neonatal hypoxic-ischemic brain injury imaging: A pictorial review Poster No.: C-1425 Congress: ECR 2014 Type: Educational Exhibit Authors: E. Alexopoulou 1, A. Mazioti 1, D. K. Filippiadis 2, C. Chrona
Neonatal hypoxic-ischemic brain injury imaging: A pictorial review Poster No.: C-1425 Congress: ECR 2014 Type: Educational Exhibit Authors: E. Alexopoulou 1, A. Mazioti 1, D. K. Filippiadis 2, C. Chrona
White Matter Injury in the Premature Infant: A Comparison between Serial Cranial Sonographic and MR Findings at Term
 AJNR Am J Neuroradiol 24:805 809, May 2003 White Matter Injury in the Premature Infant: A Comparison between Serial Cranial Sonographic and MR Findings at Term Terrie E. Inder, Nigel J. Anderson, Carole
AJNR Am J Neuroradiol 24:805 809, May 2003 White Matter Injury in the Premature Infant: A Comparison between Serial Cranial Sonographic and MR Findings at Term Terrie E. Inder, Nigel J. Anderson, Carole
Advanced magnetic resonance imaging for monitoring brain development and injury
 Advanced magnetic resonance imaging for monitoring brain development and injury Stéphane Sizonenko, MD-PhD Division of Development and Growth Department of Child and Adolescent Medicine Geneva University
Advanced magnetic resonance imaging for monitoring brain development and injury Stéphane Sizonenko, MD-PhD Division of Development and Growth Department of Child and Adolescent Medicine Geneva University
The rationale for routine cerebral ultrasound in premature infants
 Pediatr Radiol (2015) 45:646 650 DOI 10.1007/s00247-014-2985-1 RESEARCH FORUM The rationale for routine cerebral ultrasound in premature infants Maria I. Argyropoulou & Corinne Veyrac Received: 4 October
Pediatr Radiol (2015) 45:646 650 DOI 10.1007/s00247-014-2985-1 RESEARCH FORUM The rationale for routine cerebral ultrasound in premature infants Maria I. Argyropoulou & Corinne Veyrac Received: 4 October
ECMUS The Safety Committee of EFSUMB : Tutorial
 Neonatal cranial ultrasound Safety Aspects (2013) Prepared for ECMUS by B.J. van der Knoop, M.D. 1, J.I.P. de Vries, M.D., PhD 1, I.A. Zonnenberg, M.D. 2, J.I.M.L. Verbeke, M.D. 3 R.J. Vermeulen, M.D.,
Neonatal cranial ultrasound Safety Aspects (2013) Prepared for ECMUS by B.J. van der Knoop, M.D. 1, J.I.P. de Vries, M.D., PhD 1, I.A. Zonnenberg, M.D. 2, J.I.M.L. Verbeke, M.D. 3 R.J. Vermeulen, M.D.,
Hypoxic ischemic brain injury in neonates - early MR imaging findings
 Hypoxic ischemic brain injury in neonates - early MR imaging findings Poster No.: C-1208 Congress: ECR 2015 Type: Authors: Keywords: DOI: Educational Exhibit E.-M. Heursen, R. Reina Cubero, T. Guijo Hernandez,
Hypoxic ischemic brain injury in neonates - early MR imaging findings Poster No.: C-1208 Congress: ECR 2015 Type: Authors: Keywords: DOI: Educational Exhibit E.-M. Heursen, R. Reina Cubero, T. Guijo Hernandez,
Surgical Options in Post Haemorrhagic Ventricular Dilation
 Surgical Options in Post Haemorrhagic Ventricular Dilation Benedetta Pettorini Consultant Paediatric Neurosurgeon Alder Hey Childrens Hospital Liverpool, UK Risk Factors for IVH 1. Prematurity: Occurs
Surgical Options in Post Haemorrhagic Ventricular Dilation Benedetta Pettorini Consultant Paediatric Neurosurgeon Alder Hey Childrens Hospital Liverpool, UK Risk Factors for IVH 1. Prematurity: Occurs
Different Patterns of Punctate White Matter Lesions in Serially Scanned Preterm Infants
 Different Patterns of Punctate White Matter Lesions in Serially Scanned Preterm Infants Karina J. Kersbergen 1, Manon J. N. L. Benders 1, Floris Groenendaal 1, Corine Koopman-Esseboom 1, Rutger A. J. Nievelstein
Different Patterns of Punctate White Matter Lesions in Serially Scanned Preterm Infants Karina J. Kersbergen 1, Manon J. N. L. Benders 1, Floris Groenendaal 1, Corine Koopman-Esseboom 1, Rutger A. J. Nievelstein
I t is increasingly recognised that arterial cerebral infarction
 F252 ORIGINAL ARTICLE Does cranial ultrasound imaging identify arterial cerebral infarction in term neonates? F Cowan, E Mercuri, F Groenendaal, L Bassi, D Ricci, M Rutherford, L de Vries... See end of
F252 ORIGINAL ARTICLE Does cranial ultrasound imaging identify arterial cerebral infarction in term neonates? F Cowan, E Mercuri, F Groenendaal, L Bassi, D Ricci, M Rutherford, L de Vries... See end of
The two most common forms of brain injury noted in preterm neonates are intraventricular hemorrhage (IVH) and 1
 9 The two most common forms of brain injury noted in preterm neonates are intraventricular hemorrhage (IVH) and 1 periventricular leukomalacia (PVL). These lesions are more common in the smallest and most
9 The two most common forms of brain injury noted in preterm neonates are intraventricular hemorrhage (IVH) and 1 periventricular leukomalacia (PVL). These lesions are more common in the smallest and most
Perinatal cerebral white matter injuries influence early communication and language development
 Perinatal cerebral white matter injuries influence early communication and language development Blazenka Brozovic University of Zagreb Department of Speech and Language Pathology Developmental Neurolinguistic
Perinatal cerebral white matter injuries influence early communication and language development Blazenka Brozovic University of Zagreb Department of Speech and Language Pathology Developmental Neurolinguistic
Perlman J, Clinics Perinatol 2006; 33: Underlying causal pathways. Antenatal Intrapartum Postpartum. Acute near total asphyxia
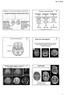 Perlman J, Clinics Perinatol 2006; 33:335-353 Underlying causal pathways Antenatal Intrapartum Postpartum Acute injury Subacute injury Associated problem Reduced fetal movements Placental insufficiency
Perlman J, Clinics Perinatol 2006; 33:335-353 Underlying causal pathways Antenatal Intrapartum Postpartum Acute injury Subacute injury Associated problem Reduced fetal movements Placental insufficiency
Study of role of MRI brain in evaluation of hypoxic ischemic encephalopathy
 Original article: Study of role of MRI brain in evaluation of hypoxic ischemic encephalopathy *Dr Harshad Bhagat, ** Dr Ravindra Kawade, ***Dr Y.P.Sachdev *Junior Resident, Department Of Radiodiagnosis,
Original article: Study of role of MRI brain in evaluation of hypoxic ischemic encephalopathy *Dr Harshad Bhagat, ** Dr Ravindra Kawade, ***Dr Y.P.Sachdev *Junior Resident, Department Of Radiodiagnosis,
Gerda van Wezel-Meijler Neonatal Cranial Ultrasonography
 Gerda van Wezel-Meijler Neonatal Cranial Ultrasonography Gerda van Wezel-Meijler Neonatal Cranial Ultrasonography Guidelines for the Procedure and Atlas of Normal Ultrasound Anatomy With 121 Figures and
Gerda van Wezel-Meijler Neonatal Cranial Ultrasonography Gerda van Wezel-Meijler Neonatal Cranial Ultrasonography Guidelines for the Procedure and Atlas of Normal Ultrasound Anatomy With 121 Figures and
I mprovements in perinatal and neonatal care have contributed
 ORIGINAL ARTICLE Posthaemorrhagic ventricular in the premature infant: natural history and predictors of outcome B P Murphy, T E Inder, V Rooks, G A Taylor, N J Anderson, N Mogridge, L J Horwood, J J Volpe...
ORIGINAL ARTICLE Posthaemorrhagic ventricular in the premature infant: natural history and predictors of outcome B P Murphy, T E Inder, V Rooks, G A Taylor, N J Anderson, N Mogridge, L J Horwood, J J Volpe...
Neonatal Outcomes in the Era of Periviability The Journey of Ontario s Tiniest Babies
 Neonatal Outcomes in the Era of Periviability The Journey of Ontario s Tiniest Babies Paige Terrien, MD Director, Neonatal Follow Up Program University of Toronto Disclosure I do not have an affiliation
Neonatal Outcomes in the Era of Periviability The Journey of Ontario s Tiniest Babies Paige Terrien, MD Director, Neonatal Follow Up Program University of Toronto Disclosure I do not have an affiliation
Cranial ultrasound abnormalities in full term infants in a postnatal ward: outcome at 12 and 18 months
 F128 Department of Paediatrics and Neonatal Medicine, Imperial College School of Medicine, Hammersmith Hospital, Du Cane Road, London W12 0HS, UK L Haataja E Mercuri FCowan L Dubowitz Correspondence to:
F128 Department of Paediatrics and Neonatal Medicine, Imperial College School of Medicine, Hammersmith Hospital, Du Cane Road, London W12 0HS, UK L Haataja E Mercuri FCowan L Dubowitz Correspondence to:
Intraventricular Hemorrhage and Periventricular Leukomalacia
 Intraventricular Hemorrhage and Periventricular Leukomalacia Intraventricular Hemorrhage Intraventricular hemorrhage (IVH) is bleeding inside the lateral ventricles. Bleeding frequently occurs in areas
Intraventricular Hemorrhage and Periventricular Leukomalacia Intraventricular Hemorrhage Intraventricular hemorrhage (IVH) is bleeding inside the lateral ventricles. Bleeding frequently occurs in areas
The child with hemiplegic cerebral palsy thinking beyond the motor impairment. Dr Paul Eunson Edinburgh
 The child with hemiplegic cerebral palsy thinking beyond the motor impairment Dr Paul Eunson Edinburgh Content Coming to a diagnosis The importance of understanding the injury MRI scans Role of epilepsy
The child with hemiplegic cerebral palsy thinking beyond the motor impairment Dr Paul Eunson Edinburgh Content Coming to a diagnosis The importance of understanding the injury MRI scans Role of epilepsy
Ultrasound examination of the neonatal brain
 Ultrasound examination of the neonatal brain Guideline for the performance and reporting of neonatal and preterm brain ultrasound examination, by the Finnish Perinatology Society and the Paediatric Radiology
Ultrasound examination of the neonatal brain Guideline for the performance and reporting of neonatal and preterm brain ultrasound examination, by the Finnish Perinatology Society and the Paediatric Radiology
P eriventricular leucomalacia (PVL), which is characterised
 F275 ORIGINAL ARTICLE Limitations of ultrasonography for diagnosing white matter damage in preterm infants T Debillon, S N Guyen, A Muet, M P Quere, F Moussaly, J C Roze... See end of article for authors
F275 ORIGINAL ARTICLE Limitations of ultrasonography for diagnosing white matter damage in preterm infants T Debillon, S N Guyen, A Muet, M P Quere, F Moussaly, J C Roze... See end of article for authors
Original article: Evaluation of hypoxic-ischaemic events in preterm neonates using trans cranial ultrasound
 Original article: Evaluation of hypoxic-ischaemic events in preterm neonates using trans cranial ultrasound Priyanka Upadhyay *, Ketki U Patil 1, Rajesh Kuber 2, Vilas Kulkarni 3, Amarjit Singh 4 * Chief
Original article: Evaluation of hypoxic-ischaemic events in preterm neonates using trans cranial ultrasound Priyanka Upadhyay *, Ketki U Patil 1, Rajesh Kuber 2, Vilas Kulkarni 3, Amarjit Singh 4 * Chief
Magnetic resonance imaging assessment of brain maturation in preterm neonates with punctate white matter lesions
 Neuroradiology (2007) 49:161 167 DOI 10.1007/s00234-006-0176-y PAEDIATRIC NEURORADIOLOGY Magnetic resonance imaging assessment of brain maturation in preterm neonates with punctate white matter lesions
Neuroradiology (2007) 49:161 167 DOI 10.1007/s00234-006-0176-y PAEDIATRIC NEURORADIOLOGY Magnetic resonance imaging assessment of brain maturation in preterm neonates with punctate white matter lesions
Transfontanelar Ultrasound Technique, Normal Anatomy, Anatomic Variants and Classification Review
 Transfontanelar Ultrasound Technique, Normal Anatomy, Anatomic Variants and Classification Review Poster No.: C-2615 Congress: ECR 2013 Type: Educational Exhibit Authors: S. E. Vazquez, R. E. Ochoa Albíztegui
Transfontanelar Ultrasound Technique, Normal Anatomy, Anatomic Variants and Classification Review Poster No.: C-2615 Congress: ECR 2013 Type: Educational Exhibit Authors: S. E. Vazquez, R. E. Ochoa Albíztegui
Neuropathology Specialty Conference
 Neuropathology Specialty Conference March 22, 2010 Case 2 Rebecca Folkerth, MD Brigham and Women s Hospital Children s Hospital Harvard Medical School Clinical History 18-gestational-week fetus found on
Neuropathology Specialty Conference March 22, 2010 Case 2 Rebecca Folkerth, MD Brigham and Women s Hospital Children s Hospital Harvard Medical School Clinical History 18-gestational-week fetus found on
Difficulties at Birth: Long Term Developmental Outcomes
 Difficulties at Birth: Long Term Developmental Outcomes Alan D. Bedrick MD Division of Neonatology and Developmental Biology Department of Pediatrics University of Arizona Tucson, Arizona DISCLOSURE I
Difficulties at Birth: Long Term Developmental Outcomes Alan D. Bedrick MD Division of Neonatology and Developmental Biology Department of Pediatrics University of Arizona Tucson, Arizona DISCLOSURE I
SWISS SOCIETY OF NEONATOLOGY. Spontaneous intestinal perforation or necrotizing enterocolitis?
 SWISS SOCIETY OF NEONATOLOGY Spontaneous intestinal perforation or necrotizing enterocolitis? June 2004 2 Stocker M, Berger TM, Neonatal and Pediatric Intensive Care Unit, Children s Hospital of Lucerne,
SWISS SOCIETY OF NEONATOLOGY Spontaneous intestinal perforation or necrotizing enterocolitis? June 2004 2 Stocker M, Berger TM, Neonatal and Pediatric Intensive Care Unit, Children s Hospital of Lucerne,
IMAGING OF HYPOXIC ISCHEMIC INJURY IN A NEONATE FN3 STATE MEETING NEMOURS CHILDREN'S HOSPITAL ORLANDO,FL 08/04/18
 IMAGING OF HYPOXIC ISCHEMIC INJURY IN A NEONATE FN3 STATE MEETING NEMOURS CHILDREN'S HOSPITAL ORLANDO,FL 08/04/18 Dhanashree Rajderkar,MD Assistant Professor Department of Radiology University of Florida
IMAGING OF HYPOXIC ISCHEMIC INJURY IN A NEONATE FN3 STATE MEETING NEMOURS CHILDREN'S HOSPITAL ORLANDO,FL 08/04/18 Dhanashree Rajderkar,MD Assistant Professor Department of Radiology University of Florida
Chapter 5. Lara M. Leijser Francisca T. de Bruïne Sylke J. Steggerda Jeroen van der Grond Frans J. Walther Gerda van Wezel-Meijler
 Chapter 5 Brain imaging findings in very preterm infants throughout the neonatal period: Part I. Incidences and evolution of lesions, comparison between ultrasound and MRI Lara M. Leijser Francisca T.
Chapter 5 Brain imaging findings in very preterm infants throughout the neonatal period: Part I. Incidences and evolution of lesions, comparison between ultrasound and MRI Lara M. Leijser Francisca T.
PEDIATRIC NEWBORN MEDICINE CLINICAL PRACTICE GUIDELINES
 PEDIATRIC NEWBORN MEDICINE CLINICAL PRACTICE GUIDELINES Term Equivalent Brain MRIs For Very Preterm Infants Clinical Practice Guideline: Term Equivalent Brain MRIs For Very Preterm Infants Points of emphasis/primary
PEDIATRIC NEWBORN MEDICINE CLINICAL PRACTICE GUIDELINES Term Equivalent Brain MRIs For Very Preterm Infants Clinical Practice Guideline: Term Equivalent Brain MRIs For Very Preterm Infants Points of emphasis/primary
Benefits of Caffeine Citrate: Neurodevelopmental Outcomes of ELBW Infants
 St. Catherine University SOPHIA Master of Arts in Nursing Theses Nursing 12-2011 Benefits of Caffeine Citrate: Neurodevelopmental Outcomes of ELBW Infants Teri Johnson St. Catherine University Follow this
St. Catherine University SOPHIA Master of Arts in Nursing Theses Nursing 12-2011 Benefits of Caffeine Citrate: Neurodevelopmental Outcomes of ELBW Infants Teri Johnson St. Catherine University Follow this
TOXIC AND NUTRITIONAL DISORDER MODULE
 TOXIC AND NUTRITIONAL DISORDER MODULE Objectives: For each of the following entities the student should be able to: 1. Describe the etiology/pathogenesis and/or pathophysiology, gross and microscopic morphology
TOXIC AND NUTRITIONAL DISORDER MODULE Objectives: For each of the following entities the student should be able to: 1. Describe the etiology/pathogenesis and/or pathophysiology, gross and microscopic morphology
Predicting Outcomes in HIE. Naaz Merchant Consultant Neonatologist Beds & Herts Meeting 17/03/2016
 Predicting Outcomes in HIE Naaz Merchant Consultant Neonatologist Beds & Herts Meeting 17/03/2016 Interactive please! Case 1 Term, 3.5 kg Antenatal: Breech Labour/Delivery: Em CS failure to progress, mec
Predicting Outcomes in HIE Naaz Merchant Consultant Neonatologist Beds & Herts Meeting 17/03/2016 Interactive please! Case 1 Term, 3.5 kg Antenatal: Breech Labour/Delivery: Em CS failure to progress, mec
Extensive cystic periventricular leukomalacia following early-onset group B streptococcal sepsis in a very low birth weight infant
 SWISS SOCIETY OF NEONATOLOGY Extensive cystic periventricular leukomalacia following early-onset group B streptococcal sepsis in a very low birth weight infant July 2012 2 Berger TM, Caduff JC, Neonatal
SWISS SOCIETY OF NEONATOLOGY Extensive cystic periventricular leukomalacia following early-onset group B streptococcal sepsis in a very low birth weight infant July 2012 2 Berger TM, Caduff JC, Neonatal
The clinical presentation of preterm cerebellar haemorrhage
 Eur J Pediatr (2010) 169:1249 1253 DOI 10.1007/s00431-010-1217-4 ORIGINAL PAPER The clinical presentation of preterm cerebellar haemorrhage Ginette M. Ecury-Goossen & Jeroen Dudink & Maarten Lequin & Monique
Eur J Pediatr (2010) 169:1249 1253 DOI 10.1007/s00431-010-1217-4 ORIGINAL PAPER The clinical presentation of preterm cerebellar haemorrhage Ginette M. Ecury-Goossen & Jeroen Dudink & Maarten Lequin & Monique
Cranial ultrasound findings in preterm infants predict the development of cerebral palsy
 Syddansk Universitet Cranial ultrasound findings in preterm infants predict the development of cerebral palsy Skovgaard, Ann Lawaetz; Zachariassen, Gitte Published in: Danish Medical Journal Publication
Syddansk Universitet Cranial ultrasound findings in preterm infants predict the development of cerebral palsy Skovgaard, Ann Lawaetz; Zachariassen, Gitte Published in: Danish Medical Journal Publication
Prematurity as a Risk Factor for ASD. Disclaimer
 Prematurity as a Risk Factor for ASD Angela M. Montgomery, MD, MSEd Assistant Professor of Pediatrics (Neonatology) Director, Yale NICU GRAD Program Suzanne L. Macari, PhD Research Scientist, Child Study
Prematurity as a Risk Factor for ASD Angela M. Montgomery, MD, MSEd Assistant Professor of Pediatrics (Neonatology) Director, Yale NICU GRAD Program Suzanne L. Macari, PhD Research Scientist, Child Study
SWISS SOCIETY OF NEONATOLOGY. Severe apnea and bradycardia in a term infant
 SWISS SOCIETY OF NEONATOLOGY Severe apnea and bradycardia in a term infant October 2014 2 Walker JH, Arlettaz Mieth R, Däster C, Division of Neonatology, University Hospital Zurich, Switzerland Swiss Society
SWISS SOCIETY OF NEONATOLOGY Severe apnea and bradycardia in a term infant October 2014 2 Walker JH, Arlettaz Mieth R, Däster C, Division of Neonatology, University Hospital Zurich, Switzerland Swiss Society
Department of Neurosurgery, Emory University; and 2 Pediatric Neurosurgery Associates at Children s Healthcare of Atlanta, Georgia
 J Neurosurg Pediatrics 14:184 189, 2014 AANS, 2014 Poor correlation between head circumference and cranial ultrasound findings in premature infants with intraventricular hemorrhage Clinical article Martha-Conley
J Neurosurg Pediatrics 14:184 189, 2014 AANS, 2014 Poor correlation between head circumference and cranial ultrasound findings in premature infants with intraventricular hemorrhage Clinical article Martha-Conley
Cranial Ultrasound: A Guideline for the performance of routine cranial USS for preterm infants
 MCN for Neonatology West of Scotland Neonatal Guideline Cranial Ultrasound: A Guideline for the performance of routine cranial USS for preterm infants This Guideline is applicable to medical staff and
MCN for Neonatology West of Scotland Neonatal Guideline Cranial Ultrasound: A Guideline for the performance of routine cranial USS for preterm infants This Guideline is applicable to medical staff and
During the past several decades, neonatal medicine has advanced
 Published September 29, 2011 as 10.3174/ajnr.A2703 ORIGINAL RESEARCH H. Kidokoro P.J. Anderson L.W. Doyle J.J. Neil T.E. Inder High Signal Intensity on T2-Weighted MR Imaging at Term-Equivalent Age in
Published September 29, 2011 as 10.3174/ajnr.A2703 ORIGINAL RESEARCH H. Kidokoro P.J. Anderson L.W. Doyle J.J. Neil T.E. Inder High Signal Intensity on T2-Weighted MR Imaging at Term-Equivalent Age in
Differentiation between peritrigonal terminal zones and hypoxic-ischemic white matter injury on MRI
 Chapter 4 Differentiation between peritrigonal terminal zones and hypoxic-ischemic white matter injury on MRI Lishya Liauw Jeroen van der Grond Valerie Slooff Francisca Wiggers-de Bruïne Laura Laan Saskia
Chapter 4 Differentiation between peritrigonal terminal zones and hypoxic-ischemic white matter injury on MRI Lishya Liauw Jeroen van der Grond Valerie Slooff Francisca Wiggers-de Bruïne Laura Laan Saskia
DWI assessment of ischemic changes in the fetal brain
 DWI assessment of ischemic changes in the fetal brain Dafi Bergman, 4 th year Medical student in the 4-year program, Sackler school of medicine B.Sc Life and Medical Sciences, Tel Aviv University Supervised
DWI assessment of ischemic changes in the fetal brain Dafi Bergman, 4 th year Medical student in the 4-year program, Sackler school of medicine B.Sc Life and Medical Sciences, Tel Aviv University Supervised
SWISS SOCIETY OF NEONATOLOGY. Neonatal cerebral infarction
 SWISS SOCIETY OF NEONATOLOGY Neonatal cerebral infarction May 2002 2 Mann C, Neonatal and Pediatric Intensive Care Unit, Landeskrankenhaus und Akademisches Lehrkrankenhaus Feldkirch, Austria Swiss Society
SWISS SOCIETY OF NEONATOLOGY Neonatal cerebral infarction May 2002 2 Mann C, Neonatal and Pediatric Intensive Care Unit, Landeskrankenhaus und Akademisches Lehrkrankenhaus Feldkirch, Austria Swiss Society
Is sequential cranial ultrasound reliable for detection of white matter injury in very preterm infants?
 Neuroradiology (2010) 52:397 406 DOI 10.1007/s00234-010-0668-7 PAEDIATRIC NEURORADIOLOGY Is sequential cranial ultrasound reliable for detection of white matter injury in very preterm infants? Lara M.
Neuroradiology (2010) 52:397 406 DOI 10.1007/s00234-010-0668-7 PAEDIATRIC NEURORADIOLOGY Is sequential cranial ultrasound reliable for detection of white matter injury in very preterm infants? Lara M.
DOWNLOAD OR READ : PERINATAL EVENTS AND BRAIN DAMAGE IN SURVIVING CHILDREN BASED ON PAPERS PRESENTED AT AN INTERNATIONA PDF EBOOK EPUB MOBI
 DOWNLOAD OR READ : PERINATAL EVENTS AND BRAIN DAMAGE IN SURVIVING CHILDREN BASED ON PAPERS PRESENTED AT AN INTERNATIONA PDF EBOOK EPUB MOBI Page 1 Page 2 perinatal events and brain damage in surviving
DOWNLOAD OR READ : PERINATAL EVENTS AND BRAIN DAMAGE IN SURVIVING CHILDREN BASED ON PAPERS PRESENTED AT AN INTERNATIONA PDF EBOOK EPUB MOBI Page 1 Page 2 perinatal events and brain damage in surviving
BRAIN IMAGING IN PRETERM INFANTS AT TERM EQUIVALENT AGE
 From the Institution of Clinical Science, Intervention, and Technology Division of Paediatics Karolinska Institutet, Stockholm, Sweden BRAIN IMAGING IN PRETERM INFANTS AT TERM EQUIVALENT AGE VALUE AND
From the Institution of Clinical Science, Intervention, and Technology Division of Paediatics Karolinska Institutet, Stockholm, Sweden BRAIN IMAGING IN PRETERM INFANTS AT TERM EQUIVALENT AGE VALUE AND
Early Accurate Diagnosis & Early Intervention for Cerebral Palsy INTERNATIONAL RECOMMENDATIONS
 Early Accurate Diagnosis & Early Intervention for Cerebral Palsy INTERNATIONAL RECOMMENDATIONS Professor Iona Novak Cerebral Palsy Alliance Australia Neuroplasticity is fundamentally why we believe in
Early Accurate Diagnosis & Early Intervention for Cerebral Palsy INTERNATIONAL RECOMMENDATIONS Professor Iona Novak Cerebral Palsy Alliance Australia Neuroplasticity is fundamentally why we believe in
Objectives. Birth Depression Management. Birth Depression Terms
 Objectives Birth Depression Management Regional Perinatal Outreach Program 2016 Understand the terms and the clinical characteristics of birth depression. Be familiar with the evidence behind therapeutic
Objectives Birth Depression Management Regional Perinatal Outreach Program 2016 Understand the terms and the clinical characteristics of birth depression. Be familiar with the evidence behind therapeutic
Prevalence of "Compressed" and Asymmetric Lateral Ventricles in Healthy Full Term Neonates: Sonographic
 Prevalence of "Compressed" and symmetric Lateral Ventricles in Healthy Full Term Neonates: Sonographic Study 149 Patricia Winchester 1 Paula W. rill1 Rebecca Cooper2 lfred N. Krauss 2 Hart dec Peterson
Prevalence of "Compressed" and symmetric Lateral Ventricles in Healthy Full Term Neonates: Sonographic Study 149 Patricia Winchester 1 Paula W. rill1 Rebecca Cooper2 lfred N. Krauss 2 Hart dec Peterson
Prenatal Prediction of The Neurologically Impaired Neonate By Ultrasound
 Prenatal Prediction of The Neurologically Impaired Neonate By Ultrasound Robert H. Debbs, D.O.,F.A.C.O.O.G. Professor of OB-GYN Perelman School of Medicine, University of Pennsylvania Director, Pennsylvania
Prenatal Prediction of The Neurologically Impaired Neonate By Ultrasound Robert H. Debbs, D.O.,F.A.C.O.O.G. Professor of OB-GYN Perelman School of Medicine, University of Pennsylvania Director, Pennsylvania
SWISS SOCIETY OF NEONATOLOGY. Diagnostic evaluation of a symptomatic cerebrovascular accident in a neonate with focal convulsions
 SWISS SOCIETY OF NEONATOLOGY Diagnostic evaluation of a symptomatic cerebrovascular accident in a neonate with focal convulsions July 2013 2 Anderson S, Rimensberger P, Service de Néonatologie et des Soins
SWISS SOCIETY OF NEONATOLOGY Diagnostic evaluation of a symptomatic cerebrovascular accident in a neonate with focal convulsions July 2013 2 Anderson S, Rimensberger P, Service de Néonatologie et des Soins
Screening Cranial Imaging at Multiple Time Points Improves Cystic Periventricular Leukomalacia Detection
 Screening Cranial Imaging at Multiple Time Points Improves Cystic Periventricular Leukomalacia Detection Abhik Das, RTI International John Barks, University of Michigan Subrata Sarkar, University of Michigan
Screening Cranial Imaging at Multiple Time Points Improves Cystic Periventricular Leukomalacia Detection Abhik Das, RTI International John Barks, University of Michigan Subrata Sarkar, University of Michigan
I have no relevant financial relationships with the manufacturers of any. commercial products and/or provider of commercial services discussed in
 I have no relevant financial relationships with the manufacturers of any commercial products and/or provider of commercial services discussed in this activity I do intend to discuss an unapproved/investigative
I have no relevant financial relationships with the manufacturers of any commercial products and/or provider of commercial services discussed in this activity I do intend to discuss an unapproved/investigative
Utility of neuroradiographic imaging in predicting outcomes after neonatal extracorporeal membrane oxygenation
 Journal of Pediatric Surgery (2012) 47, 76 80 www.elsevier.com/locate/jpedsurg Utility of neuroradiographic imaging in predicting outcomes after neonatal extracorporeal membrane oxygenation Michael D.
Journal of Pediatric Surgery (2012) 47, 76 80 www.elsevier.com/locate/jpedsurg Utility of neuroradiographic imaging in predicting outcomes after neonatal extracorporeal membrane oxygenation Michael D.
The Brain on ADHD. Ms. Komas. Introduction to Healthcare Careers
 The Brain on ADHD Ms. Komas Introduction to Healthcare Careers Ms. Komas Period 9/2/2016 Komas 1 HOOK: Attention Deficit Hyperactivity Disorder (ADHD) plagues between 5% and 7% of children and less than
The Brain on ADHD Ms. Komas Introduction to Healthcare Careers Ms. Komas Period 9/2/2016 Komas 1 HOOK: Attention Deficit Hyperactivity Disorder (ADHD) plagues between 5% and 7% of children and less than
Hummi Micro Draw Blood Transfer Device. An Important Addition to Your IVH Bundle
 Hummi Micro Draw Blood Transfer Device An Important Addition to Your IVH Bundle Hummi Micro Draw & Micro T Connector For Infec6on Control and IVH Risk Reduc6on The Next Genera6on System for Closed Micro
Hummi Micro Draw Blood Transfer Device An Important Addition to Your IVH Bundle Hummi Micro Draw & Micro T Connector For Infec6on Control and IVH Risk Reduc6on The Next Genera6on System for Closed Micro
The tale of global hypoxic ischaemic injury
 The tale of global hypoxic ischaemic injury Poster No.: C-0400 Congress: ECR 2016 Type: Educational Exhibit Authors: L. M. Zammit, R. Grech ; Paola/MT, Dublin 9/IE Keywords: CNS, CT, MR, Education, Computer
The tale of global hypoxic ischaemic injury Poster No.: C-0400 Congress: ECR 2016 Type: Educational Exhibit Authors: L. M. Zammit, R. Grech ; Paola/MT, Dublin 9/IE Keywords: CNS, CT, MR, Education, Computer
MRI Brain Study of Lateral Ventricles in Children with Cerebral Palsy
 DOI: 10.7860/IJARS/2017/23993:2259 Radiology Section Original Article MRI Brain Study of Lateral Ventricles in Children with Cerebral Palsy Niyati Sharma, Rajasbala Dhande ABSTRACT Introduction: Cerebral
DOI: 10.7860/IJARS/2017/23993:2259 Radiology Section Original Article MRI Brain Study of Lateral Ventricles in Children with Cerebral Palsy Niyati Sharma, Rajasbala Dhande ABSTRACT Introduction: Cerebral
MYELINATION, DEVELOPMENT AND MULTIPLE SCLEROSIS 1
 MYELINATION, DEVELOPMENT AND MULTIPLE SCLEROSIS 1 Myelination, development and Multiple Sclerosis Randy Christensen Salt Lake Community College MYELINATION, DEVELOPMENT AND MULTIPLE SCLEROSIS 2 Myelination,
MYELINATION, DEVELOPMENT AND MULTIPLE SCLEROSIS 1 Myelination, development and Multiple Sclerosis Randy Christensen Salt Lake Community College MYELINATION, DEVELOPMENT AND MULTIPLE SCLEROSIS 2 Myelination,
T he developing brain is vulnerable to injury
 REVIEW Magnetic resonance imaging of preterm brain injury S J Counsell, M A Rutherford, F M Cowan, A D Edwards... Magnetic resonance imaging (MRI) has proved to be a valuable tool for monitoring development
REVIEW Magnetic resonance imaging of preterm brain injury S J Counsell, M A Rutherford, F M Cowan, A D Edwards... Magnetic resonance imaging (MRI) has proved to be a valuable tool for monitoring development
Extremely preterm infants are at high risk of brain injury
 ORIGINAL RESEARCH J.L.Y. Cheong D.K. Thompson H.X. Wang R.W. Hunt P.J. Anderson T.E. Inder L.W. Doyle Abnormal White Matter Signal on MR Imaging Is Related to Abnormal Tissue Microstructure BACKGROUND
ORIGINAL RESEARCH J.L.Y. Cheong D.K. Thompson H.X. Wang R.W. Hunt P.J. Anderson T.E. Inder L.W. Doyle Abnormal White Matter Signal on MR Imaging Is Related to Abnormal Tissue Microstructure BACKGROUND
Should infants with perinatal thrombosis be screened for thrombophilia and treated by anticoagulants?
 Should infants with perinatal thrombosis be screened for thrombophilia and treated by anticoagulants? Shoshana Revel-Vilk, MD MSc Pediatric Hematology Center, Pediatric Hematology/Oncology Department,
Should infants with perinatal thrombosis be screened for thrombophilia and treated by anticoagulants? Shoshana Revel-Vilk, MD MSc Pediatric Hematology Center, Pediatric Hematology/Oncology Department,
Perinatal/Neonatal Case Presentation
 Perinatal/Neonatal Case Presentation & & & & & & & & & & & & & & Bilateral Thalamic Lesions in a Newborn with Intrauterine Asphyxia After Maternal Cardiac Arrest a Case Report with Literature Review Maya
Perinatal/Neonatal Case Presentation & & & & & & & & & & & & & & Bilateral Thalamic Lesions in a Newborn with Intrauterine Asphyxia After Maternal Cardiac Arrest a Case Report with Literature Review Maya
NIH Public Access Author Manuscript Pediatr Neurol. Author manuscript; available in PMC 2009 October 30.
 NIH Public Access Author Manuscript Published in final edited form as: Pediatr Neurol. 2008 May ; 38(5): 329 334. doi:10.1016/j.pediatrneurol.2007.12.012. Very Early Arterial Ischemic Stroke in Premature
NIH Public Access Author Manuscript Published in final edited form as: Pediatr Neurol. 2008 May ; 38(5): 329 334. doi:10.1016/j.pediatrneurol.2007.12.012. Very Early Arterial Ischemic Stroke in Premature
Periventricular leukomalacia, inflammation and white matter lesions within the developing nervous system
 Neuropathology 2002; 22, 106 132 Blackwell Science, LtdOxford, UK NEUNeuropathology0919-65442002 Blackwell Publishing Asia Pty Ltd 223September 2002 438 PVL, inflammation & white matter lesions P Rezaie
Neuropathology 2002; 22, 106 132 Blackwell Science, LtdOxford, UK NEUNeuropathology0919-65442002 Blackwell Publishing Asia Pty Ltd 223September 2002 438 PVL, inflammation & white matter lesions P Rezaie
ETIOLOGY AND PATHOGENESIS OF HYPOXIC-ISCHEMIC ENCEPHALOPATHY
 ETIOLOGY AND PATHOGENESIS OF HYPOXIC-ISCHEMIC ENCEPHALOPATHY HYPOXIC-ISCHEMIC ENCEPHALOPATHY Hypoxic-İschemic Encephalopathy Encephalopathy due to hypoxic-ischemic injury [Hypoxic-ischemic encephalopathy
ETIOLOGY AND PATHOGENESIS OF HYPOXIC-ISCHEMIC ENCEPHALOPATHY HYPOXIC-ISCHEMIC ENCEPHALOPATHY Hypoxic-İschemic Encephalopathy Encephalopathy due to hypoxic-ischemic injury [Hypoxic-ischemic encephalopathy
Neurosonography: State of the art
 Neurosonography: State of the art Lisa H Lowe, MD, FAAP Professor and Academic Chair, University MO-Kansas City Pediatric Radiologist, Children s Mercy Hospitals and Clinics Learning objectives After this
Neurosonography: State of the art Lisa H Lowe, MD, FAAP Professor and Academic Chair, University MO-Kansas City Pediatric Radiologist, Children s Mercy Hospitals and Clinics Learning objectives After this
Neonatal Therapeutic Hypothermia. A Wasunna Professor of Neonatal Medicine and Pediatrics School of Medicine, University of Nairobi
 Neonatal Therapeutic Hypothermia A Wasunna Professor of Neonatal Medicine and Pediatrics School of Medicine, University of Nairobi Definition of Perinatal Asphyxia *No agreed universal definition ACOG/AAP
Neonatal Therapeutic Hypothermia A Wasunna Professor of Neonatal Medicine and Pediatrics School of Medicine, University of Nairobi Definition of Perinatal Asphyxia *No agreed universal definition ACOG/AAP
Quick practical guide to Cranial Ultrasound in the newborn
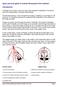 Quick practical guide to Cranial Ultrasound in the newborn Introduction A standard set of views is taken to assist with consistent visualisation of structures and in the interpretation of possible abnormalities.
Quick practical guide to Cranial Ultrasound in the newborn Introduction A standard set of views is taken to assist with consistent visualisation of structures and in the interpretation of possible abnormalities.
Neuroprotezione. Luca A. Ramenghi MD PhD. Patologia Neonatale e Terapia Intensiva Neonatale " G. Gaslini" IRCCS Genoa
 Neuroprotezione Luca A. Ramenghi MD PhD Patologia Neonatale e Terapia Intensiva Neonatale " G. Gaslini" IRCCS Genoa Outcome motorio Outcome cognitivo Sviluppo lesioni cerebrali «Developmental Care NIDCAP»
Neuroprotezione Luca A. Ramenghi MD PhD Patologia Neonatale e Terapia Intensiva Neonatale " G. Gaslini" IRCCS Genoa Outcome motorio Outcome cognitivo Sviluppo lesioni cerebrali «Developmental Care NIDCAP»
Correlation of Neurodevelopmental Outcome and brain MRI/EEG findings in term HIE infants
 Correlation of Neurodevelopmental Outcome and brain MRI/EEG findings in term HIE infants Ajou University School of Medicine Department of Pediatrics Moon Sung Park M.D. Hee Cheol Jo, M.D., Jang Hoon Lee,
Correlation of Neurodevelopmental Outcome and brain MRI/EEG findings in term HIE infants Ajou University School of Medicine Department of Pediatrics Moon Sung Park M.D. Hee Cheol Jo, M.D., Jang Hoon Lee,
Dr Veenu Gupta MD MRCPsych Consultant, Child Psychiatrist Stockton on Tees, UK
 Dr Veenu Gupta MD MRCPsych Consultant, Child Psychiatrist Stockton on Tees, UK Extremely Preterm-EP Very Preterm-VP Preterm-P Late Preterm-LP There is greater improvement of survival at extremely low
Dr Veenu Gupta MD MRCPsych Consultant, Child Psychiatrist Stockton on Tees, UK Extremely Preterm-EP Very Preterm-VP Preterm-P Late Preterm-LP There is greater improvement of survival at extremely low
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,800 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,800 116,000 120M Open access books available International authors and editors Downloads Our
Periventricular white matter injury, that is, periventricular
 ORIGINAL RESEARCH S. Yoshida K. Hayakawa A. Yamamoto T. Kanda Y. Yamori Pontine Hypoplasia in Children with Periventricular Leukomalacia BACKGROUND AND PURPOSE: The brain stem in patients with periventricular
ORIGINAL RESEARCH S. Yoshida K. Hayakawa A. Yamamoto T. Kanda Y. Yamori Pontine Hypoplasia in Children with Periventricular Leukomalacia BACKGROUND AND PURPOSE: The brain stem in patients with periventricular
Epilepsy in children with cerebral palsy
 Seizure 2003; 12: 110 114 doi:10.1016/s1059 1311(02)00255-8 Epilepsy in children with cerebral palsy A.K. GURURAJ, L. SZTRIHA, A. BENER,A.DAWODU & V. EAPEN Departments of Paediatrics, Community Medicine
Seizure 2003; 12: 110 114 doi:10.1016/s1059 1311(02)00255-8 Epilepsy in children with cerebral palsy A.K. GURURAJ, L. SZTRIHA, A. BENER,A.DAWODU & V. EAPEN Departments of Paediatrics, Community Medicine
Newborn Hypoxic Ischemic Brain Injury. Hisham Dahmoush, MBBCh FRCR Lucile Packard Children s Hospital at Stanford
 Newborn Hypoxic Ischemic Brain Injury Hisham Dahmoush, MBBCh FRCR Lucile Packard Children s Hospital at Stanford NO DISCLOSURES INTRODUCTION Neonatal hypoxic-ischemic encephalopathy (HIE) is a major cause
Newborn Hypoxic Ischemic Brain Injury Hisham Dahmoush, MBBCh FRCR Lucile Packard Children s Hospital at Stanford NO DISCLOSURES INTRODUCTION Neonatal hypoxic-ischemic encephalopathy (HIE) is a major cause
Ultrasound diagnosis and neurodevelopmental outcome of localised and extensive cystic periventricular leucomalacia
 Arch Dis Child Fetal Neonatal Ed 2001;84:F151 F156 F151 ORIGINAL ARTICLES Department of Neonatology, Jeanne de Flandre s Hospital, Lille, France V Pierrat C Duquennoy N Guilley Department of Neonatology,
Arch Dis Child Fetal Neonatal Ed 2001;84:F151 F156 F151 ORIGINAL ARTICLES Department of Neonatology, Jeanne de Flandre s Hospital, Lille, France V Pierrat C Duquennoy N Guilley Department of Neonatology,
Insults to the Term Brain
 Insults to the Term Brain Monica Epelman, MD mepelman@nemours.org Literature comparing US and MR has deficiencies Retrospective studies Long time interval between US and MR exams in the same patient
Insults to the Term Brain Monica Epelman, MD mepelman@nemours.org Literature comparing US and MR has deficiencies Retrospective studies Long time interval between US and MR exams in the same patient
Commentary. Value of MR in Definition of the Neuropathology of Cerebral Palsy in Vivo
 Commentary Value of MR in Definition of the Neuropathology of Cerebral Palsy in Vivo Joseph J. Volpe 1 Cerebral palsy refers to a clinical syndrome of nonprogressive motor deficits (usually spastic weakness,
Commentary Value of MR in Definition of the Neuropathology of Cerebral Palsy in Vivo Joseph J. Volpe 1 Cerebral palsy refers to a clinical syndrome of nonprogressive motor deficits (usually spastic weakness,
Periventricular/Intraventricular Hemorrhage in the Newborn
 Khalid N. Haque, FRCP(Ed), FRCP(I), FAAP, FICP, DCH, DTM&H; Omar B. A. Basit, MRCP(UK), DCH; Meeralebbae M. Shaheed, MD, MRCP(UK), DCH From the Division of Neonatology, Department of Pediatrics, College
Khalid N. Haque, FRCP(Ed), FRCP(I), FAAP, FICP, DCH, DTM&H; Omar B. A. Basit, MRCP(UK), DCH; Meeralebbae M. Shaheed, MD, MRCP(UK), DCH From the Division of Neonatology, Department of Pediatrics, College
Developmental sequence of periventricular leukomalacia
 Archives of Disease in Childhood, 1985, 60, 349-355 Developmental sequence of periventricular leukomalacia Correlation of ultrasound, clinical, and nuclear magnetic resonance functions L M S DUBOWITZ,
Archives of Disease in Childhood, 1985, 60, 349-355 Developmental sequence of periventricular leukomalacia Correlation of ultrasound, clinical, and nuclear magnetic resonance functions L M S DUBOWITZ,
ultrasonography in preterm infants: association with outcome
 Archives ofdisease in Childhood 1990; 65: 1033-1037 nstitut de la Sante et de la Recherche Medicale (NSERM), Unite 316, Tours, France Philippe Bertrand Francis Gold Sophie Marchand Department of Paediatric
Archives ofdisease in Childhood 1990; 65: 1033-1037 nstitut de la Sante et de la Recherche Medicale (NSERM), Unite 316, Tours, France Philippe Bertrand Francis Gold Sophie Marchand Department of Paediatric
Incidence and diagnosis of unilateral arterial cerebral infarction in newborn infants *
 J. Perinat. Med. 33 (2005) 170 175 Copyright by Walter de Gruyter Berlin New York. DOI 10.1515/JPM.2005.032 Short communication Incidence and diagnosis of unilateral arterial cerebral infarction in newborn
J. Perinat. Med. 33 (2005) 170 175 Copyright by Walter de Gruyter Berlin New York. DOI 10.1515/JPM.2005.032 Short communication Incidence and diagnosis of unilateral arterial cerebral infarction in newborn
with susceptibility-weighted imaging and computed tomography perfusion abnormalities in diagnosis of classic migraine
 Emerg Radiol (2012) 19:565 569 DOI 10.1007/s10140-012-1051-2 CASE REPORT Susceptibility-weighted imaging and computed tomography perfusion abnormalities in diagnosis of classic migraine Christopher Miller
Emerg Radiol (2012) 19:565 569 DOI 10.1007/s10140-012-1051-2 CASE REPORT Susceptibility-weighted imaging and computed tomography perfusion abnormalities in diagnosis of classic migraine Christopher Miller
Serial 1- and 2-Dimensional Cerebral MRI Measurements in Full-Term Infants after Perinatal Asphyxia
 Original Paper Received: October 27, 2015 Accepted after revision: January 18, 2016 Published online: March 12, 2016 Serial 1- and 2-Dimensional Cerebral MRI Measurements in Full-Term Infants after Perinatal
Original Paper Received: October 27, 2015 Accepted after revision: January 18, 2016 Published online: March 12, 2016 Serial 1- and 2-Dimensional Cerebral MRI Measurements in Full-Term Infants after Perinatal
Paediatric HIV -Developmental Aspects. Dr Kirsty Donald Division of Developmental Paediatrics Red Cross Children s Hospital
 Paediatric HIV -Developmental Aspects Dr Kirsty Donald Division of Developmental Paediatrics Red Cross Children s Hospital Normal Development Development occurs with sequential acquisition of skills in
Paediatric HIV -Developmental Aspects Dr Kirsty Donald Division of Developmental Paediatrics Red Cross Children s Hospital Normal Development Development occurs with sequential acquisition of skills in
Hypotension in the Neonate
 Neonatal Nursing Education Brief: Hypotension in the Neonate http://www.seattlechildrens.org/healthcare-professionals/education/continuing-medicalnursing-education/neonatal-nursing-education-briefs/ Neonatal
Neonatal Nursing Education Brief: Hypotension in the Neonate http://www.seattlechildrens.org/healthcare-professionals/education/continuing-medicalnursing-education/neonatal-nursing-education-briefs/ Neonatal
Enhancement of Cranial US: Utility of Supplementary Acoustic Windows and Doppler Harriet J. Paltiel, MD
 Enhancement of Cranial US: Utility of Supplementary Acoustic Windows and Doppler Harriet J. Paltiel, MD Boston Children s Hospital Harvard Medical School None Disclosures Conventional US Anterior fontanelle
Enhancement of Cranial US: Utility of Supplementary Acoustic Windows and Doppler Harriet J. Paltiel, MD Boston Children s Hospital Harvard Medical School None Disclosures Conventional US Anterior fontanelle
Original Articles NEUROSONOGRAPHIC ABNORMALITIES IN NEONATES WITH HYPOXIC ISCHEMIC ENCEPHALOPATHY
 Original Articles NEUROSONOGRAPHIC ABNORMALITIES IN NEONATES WITH HYPOXIC ISCHEMIC ENCEPHALOPATHY N.K. Anand A.K. Gupta I.M.S. Lamba ABSTRACT Pattern of neurosonographic (NSG) abnormalities in 150 term
Original Articles NEUROSONOGRAPHIC ABNORMALITIES IN NEONATES WITH HYPOXIC ISCHEMIC ENCEPHALOPATHY N.K. Anand A.K. Gupta I.M.S. Lamba ABSTRACT Pattern of neurosonographic (NSG) abnormalities in 150 term
National follow-up program CPUP Pediatric Neurology paper form
 National follow-up program CPUP Pediatric Neurology paper form 110206 1 National Follow-Up program- CPUP Pediatric Neurology Personal nr (unique identifier): Last name: First name: Region child belongs
National follow-up program CPUP Pediatric Neurology paper form 110206 1 National Follow-Up program- CPUP Pediatric Neurology Personal nr (unique identifier): Last name: First name: Region child belongs
Acute stroke. Ischaemic stroke. Characteristics. Temporal classification. Clinical features. Interpretation of Emergency Head CT
 Ischaemic stroke Characteristics Stroke is the third most common cause of death in the UK, and the leading cause of disability. 80% of strokes are ischaemic Large vessel occlusive atheromatous disease
Ischaemic stroke Characteristics Stroke is the third most common cause of death in the UK, and the leading cause of disability. 80% of strokes are ischaemic Large vessel occlusive atheromatous disease
Cerebral palsy? Cerebral palsies? Cerebral palsy spectrum disorder?
 Teamwork makes the dream work Nationaal symposium van Belgische CP-centra 18/02/2019 Cerebral palsy? Cerebral palsies? Cerebral palsy spectrum disorder? Faes Franny Dienst Kinderneurologie UZ Gent Centrum
Teamwork makes the dream work Nationaal symposium van Belgische CP-centra 18/02/2019 Cerebral palsy? Cerebral palsies? Cerebral palsy spectrum disorder? Faes Franny Dienst Kinderneurologie UZ Gent Centrum
In the first edition of this report, the Task Force on Neonatal
 Neonatal Encephalopathy and Neurologic Outcome, Second Edition Report of the American College of Obstetricians and Gynecologists Task Force on Neonatal Encephalopathy Executive Summary In the first edition
Neonatal Encephalopathy and Neurologic Outcome, Second Edition Report of the American College of Obstetricians and Gynecologists Task Force on Neonatal Encephalopathy Executive Summary In the first edition
Abstract. Introduction
 Sequential Cranial Ultrasound and Cerebellar Diffusion Weighted Imaging Contribute to the Early Prognosis of Neurodevelopmental Outcome in Preterm Infants Margaretha J. Brouwer 1, Britt J. M. van Kooij
Sequential Cranial Ultrasound and Cerebellar Diffusion Weighted Imaging Contribute to the Early Prognosis of Neurodevelopmental Outcome in Preterm Infants Margaretha J. Brouwer 1, Britt J. M. van Kooij
Neonatal Intracranial Ultrasound Imaging - A Pictorial Review from The Royal Liverpool Children's Hospital, Alder Hey, Liverpool.
 Neonatal Intracranial Ultrasound Imaging - A Pictorial Review from The Royal Liverpool Children's Hospital, Alder Hey, Liverpool. Poster No.: C-1115 Congress: ECR 2012 Type: Educational Exhibit Authors:
Neonatal Intracranial Ultrasound Imaging - A Pictorial Review from The Royal Liverpool Children's Hospital, Alder Hey, Liverpool. Poster No.: C-1115 Congress: ECR 2012 Type: Educational Exhibit Authors:
