Thrombocytopenia. Dr Lynda Vandertuin May 6, 2014
|
|
|
- Jennifer Curtis
- 6 years ago
- Views:
Transcription
1 Dr Lynda Vandertuin May 6,
2 Presentation 1. Definition 2. Platelet Physiology, Thromboiesis, & Platelet Function 3. Bleeding Risk 4. Clinical Diagnosis 5. Differential Diagnosis 6. Classification 7. Evaluation : History & Clinical Examination 8. Complementary Examinations 9. ITP 10. Other common etiologies 11. Patient Management 2
3 Definition = platelet count of less than 150,000/µL (150 x 10 9 /L) clinically suspected when there is a history of easy bruising or bleeding in a child incidental finding during routine evaluation 3
4 Platelet Physiology Thrombocytopenia produced in the bone marrow fragmentation of precursor megakaryocytes small colorless irregular shaped cell fragment with nonnucleated protoplasm of 2-3 µmeter in diameter life span of 5-10 days production per day 1x10 11 with tenfold increase if necessary removal by mono-macrophage system 4
5 Platelet production in the bone marrow Patel et al. J.Clin Invest
6 Thrombopoiesis Thrombocytopenia thrombopoietin (TPO) primary regulator acidic glycoprotein produced in liver, kidney & BM TPO acts in conjunction with other cytokines (IL-3, IL-6, TNF-α & IL-11) 6
7 Thrombopoiesis Thrombocytopenia Kaushansky K. J.Clin.Invest
8 Platelet Function Thrombocytopenia maintain vascular endothelium integrity primary homeostasis : hemorrhage control following small-vessel injury by platelet plug formation secondary homeostasis : more extensive injury & injury of larger blood vessels requires platelets but also participation of the coagulation system to provide a firm, stable, fibrin clot. 8
9 Platelet Function : doesn t work alone platelet adhesion to damaged blood vessel : requires normal platelet, functional membrane receptor & mediation by von Willebrand factor platelet aggregation (plug) depends on enhancement by functional fibrinogen and other mediators 9
10 Platelet Count & Bleeding Risk Buchanan Ped in Review. 2005; 26:401 10
11 Platelet Count & Bleeding Risk Consolini. Ped in Review. 2011; 32:135 11
12 When history is positive for spontaneous (non-traumatic) bruising or bleeding, either mucosal or cutaneous : Petechiae Purpura Ecchymosis Mucosal bleeding : epistaxis, gingival, gastrointestinal, vaginal or abnormal menstruation Other signs of bleeding : hematuria, hemoptysia, intracranial 12
13 Petechiae : pinhead-sized, red, flat, discrete lesions caused by extravasation of red cells from skin capillaries do not blanch under pressure non-tender, non-palpable occurring in crops Purpura : confluent petechiae 13
14 Ecchymoses : non-tender bleeding into the skin small, multiple and superficiel variety of colors : red/purple -> extravasated blood; green/yellow/brown -> breakdown of heme 14
15 Guided by an understanding of the cause and/or etiology Confirmation of diagnosis by laboratory +/- blood smear : platelets < 150,000/µL (150 x 10 9 /L) 15
16 Exclusion of : normal active children : bruising typically over pretibial surfaces large soft-tissue hematomes, joint & muscle hemorrhage : hemophilia and other coagulation disorders child abuse : location of bruising may be generalized various forms of vasculitis : large bruises with normal or increased platelet count 16
17 Categorize the different etiologies According to age : neonatal According to platelet size : congenital/genetic Mode of acquisition : acquired versus congenital According to etiology : immune (ITP = Immune Thrombocytopenia Purpura) versus non-immune According to underlying pathological mechanism 17
18 Classification according to age : neonatal Sick neonate : most common infection, asphyxia, respiratory disease or Necrotizing Enterocolitis Well neonate : Intra-uterine growth delay Mother pre-eclampsia congenital amegacaryocytosis Transplacental passage of antiplatelet antibody (auto- or allo-) 18
19 Classification according to age : neonatal Table of Immune Thrombocytopenia in the Neonate Buchanan Ped in Review. 2005; 26:401 19
20 Classification according to acquisition mode Congenital/Inherited : genetic mutations affecting the platelets, TPO, or/and TPO receptor (cmpl) Bernard Soulier Syndrome MYH9-related disorders p.ex. May Hegglin syndrome Gray Platelet Syndrome Von Willebrandt Syndrome 20
21 Congenital/Inherited classification Disorder Inheritance Clinical Features Laboratory Thrombocytopenia-absent Radius (TAR) syndrome Amegakaryocytic Thrombocytopenia Variable Unclear genetic cause Autosomal recessive : Mutation in TPO-R Wiskott- Aldrich syndrome X-linked recessive : Abnormal gene encodes for platelet function Bernard-Soulier syndrome Autosomal recessive : Dysfunction/absence platelet receptor for von Willebrand factor MYH9-related disease p.ex. May-Hegglin anomaly Autosomal dominant : Mutation myosin (nonmuscle) heavy chain Bilateral absent radii Normal thumbs Other skeletal, genitourinary, heart anomalies Absence of skeletal anomalies seen in TAR Atopic dermatitis Thrombocytopenic purpura Increased infections due to immunodeficiency Easy bruising Gingival & GI bleeding Severe hemorrhage with trauma/surgery Bleeding, nephritis, hearing loss, cataracts Severe thrombocytopenia Absent or decreased megakaryocytes Severe thrombocytopenia Absent or decreased megakaryocytes Small defective platelets Normal megakaryocytes Macrothrombocytopenia Macrothrombocytopenia leukocyte inclusions Gray platelet syndrome Autosomal dominant Bleeding, usually mild Macrothrombocytopenia reduction in granule with pale platelets 21
22 Classification according to the Mechanism 1. Insufficient production 2. Abnormal distribution 3. Excessive destruction 22
23 Classification according to the Mechanism 1. Insufficient production : Inherited or Genetic Acquired Infection Cyanotic Heart Disease Nutritional Deficiencies Marrow injury or infiltration Acute lymphoblastic leukemia and other malignancies Kasabach-Merritt Acquired aplastic anemia Fanconi pancytopenia 23
24 Classification according to the mechanism 2. Abnormal distribution : Spleen sequestration and trapping Portal hypertension : chronic liver disease Malaria if associated with hypersplenism DIC associated with Sepsis Hemolytic Uremic Syndrome (typical & atypical) and thrombotic thrombocytopenic purpura (TTP) : both resulting in microangiopathic hemolytic anemia with platelet consumption and vasculitis 24
25 Classification according to the mechanism 3. Excessive destruction : Microangiopathy Mechanical destruction : ECMO Hereditary platelet abnormalities Immunological TP : Immune (Idiopathic) Thrombocytopenia Purpura Juvenile Arthritis Systemic Lupus Medication or Heparin-use Post-viral infection (CMV, EBV, HIV, Adeno, Parvovirus, ) Post-vaccination (Hib, Hepatitis B, ROR, ) 25
26 Most common causes in Infants & Children Immune process by antibody production : autoab p.ex. Immune (Idiopathic) Thrombocytopenic Purpura, alloab, or drug-dependent Ab Nonimmune mechanism : bone marrow infiltration (acute leukemia) 26
27 Evaluation : History and Clinical examination Past & current bleeding : bruising with & without trauma, nosebleeds, blood in urine or stools, gum bleeding (tooth brushing, dentist), menstrual bleeding? Duration & onset of bleeding? If abrupt : specific trigger? RED flags in the history/examination * 27
28 Evaluation : History and Clinical Examination Red Flags Suggesting a Diagnosis Other Than Immune Thrombocytopenic Purpura Consolini. Ped in Review. 2011; 32:135 28
29 Work up according to etiology Minimum : complete blood count (CBC) with platelet count & mean platelet volume (MPV) peripheral blood smear (PBS) Repeat platelet count (if clinical nonsense ) to exclude artefact or laboratory error Coagulation study : prothrombin time (PT), partial thromboplastin time (PTT), fibrinogen 29
30 Complete the work up according to the initial results and suspicion of underlying cause : Platelet function analyzer and platelet aggregation testing Coombs test Presence of schistocytes or spherocytes Bone marrow aspirate : blasts, pancytopenia Viral serology or according to suspicion : HIV, Hepatitis B &C, H. Pylori Screening for inherited disorders, as indicated 30
31 Diagnostic algorithm Thrombocytopenia Consolini. Ped in Review. 2011; 32:135 31
32 ITP = Immune Thrombocytopenic Purpura acquired immune-mediated Primary : absence of initiating/underlying cause Secondary : underlying cause or drug exposure incidence of 3 to 8 cases/ children presentation between 2 and 10 years (peak 2-5) often after a preceding viral illness increased risk after MMR immunization : 50% of cases in children < 2 years, transient & rarely severe 32
33 ITP = Immune Thrombocytopenic Purpura History : sudden bruising or mucocutaneous bleeding otherwise healthy child NO systemic symptoms (fever, weight loss or bone pain) Clinical examination : mucocutaneous bleeding child appears well NO lymphadenopathy or hepatosplenomegaly (or mild due to preceding viral infection) 33
34 ITP = Immune Thrombocytopenic Purpura Diagnosis of ITP : 2 criteria 1. isolated thrombocytopenia with otherwise normal blood counts & normal coagulation 2. no clinically apparent associated conditions 34
35 ITP = Immune Thrombocytopenic Purpura Bleeding symptoms Serious bleeding is rare : platelet counts < 20 x 10 9 /L wet purpura : ICH, retinal hemorrhages, mucosal bleeding Platelet counts > 30 x 10 9 /L usually asymptomatic & do not seek medical attention 35
36 ITP = Immune Thrombocytopenic Purpura Work up CBC, platelet count, blood smear, coagulation testing If persistant or chronic : antinuclear Ab, serum immunoglobulins (IgG, A, M), antiphospholipid Ab If unexplained etiology & chronic course : consider bone marrow aspirate 36
37 ITP = Immune Thrombocytopenic Purpura Patient Management Platelets < 20 x 10 9 /L & serious bleeding : transfusion for immediate hemostasis (ICH) Platelet > 20 x 10 9 /L & asymptomatic : 1. Restriction of activity 2. Avoidance of medications with antiplatelet/anticoagulation activity 3. Treatment indication based on risk of bleeding 4. Refractory ITP and/or chronic 37
38 ITP = Immune Thrombocytopenic Purpura 3. Newly diagnosed ITP with risk of bleeding Corticosteroids Oral Prednisone : 2 mg/kg/day over 2-4 week course IV Methylprednisolone : 30 mg/kg/d max 1g over 3 to 7 day course Intravenous Immune Globulin (IGIV): 1 g/kg over 1 to 2 day course Anti-Rho(D) Immune Globulin : 50-75µg/kg single dose 38
39 ITP = Immune Thrombocytopenic Purpura 4. Refractory ITP with significant bleeding Splenectomy : curative Methylprednisolone : 30 mg/kg/d max 1g over 3 day course then 20 mg/kg/d over 4 days Single or combination regimes : cyclosporin A, Azathioprine, Vincristine, Cyclophosphamide, danazol +/- CS, +/- IGIV Rituximab : 375 mg/m2 1x/week for 4 weeks Anti-Rho(D) Immune Globulin : 50-75µg/kg single dose TPO-R agonists : Romiplostim, Eltrombopag 39
40 ITP = Immune Thrombocytopenic Purpura Patient Management Treatment reduces the severity & duration of initial thrombocytopenic episode No pharmacological intervention if mild-moderate ITP as bleeding is rare, except 1. Concomitant or preexisting condition 2. Undergo procedure with blood loss risk No means to predict which child may have wet purpura, therefore treatment is often the rule 40
41 ITP = Immune Thrombocytopenic Purpura Patient Management All treatments are temporizing interventions Usually given on ambulatory basis if no bleeding risk Monitor platelet count 1-2x/week & continue until normal and stable Treatment not to be continued until normal platelets counts achieved 41
42 ITP = Immune Thrombocytopenic Purpura Patient Outcome 2/3 recover within 6 months with or without treatment 1/3 develop chronic ITP ie. > 12 months Chronic ITP more likely in older children (>10 years) and those with bleeding lasting > 14 days Chronic ITP does improve over time Small % refractory ITP = hemorrhagic symptoms and resistance to corticosteroid and IGIV treatment 42
43 Pathogenesis following viral infections Hypothesis : 1. viral destruction of megakaryocytes and platelets 2. immunostimulation causing alterations in cytokines that involved in platelet production 3. Antigene mimicry between virus & platelet antibodies 43
44 Association with Other Cytopenias Pancytopenia with systemic symptoms or findings on clinical examination URGENT situation! Immediate referral to pediatric hematologist Safe platelet count will be small part of overall treatment plan! 44
45 Management Goal Thrombocytopenia guided by understanding of its cause & clinical course maintain a safe platelet count in order to prevent bleeding : patient/etiology dependent correction of the cause not always possible : (congenital) or necessary (asymptomatic and/or mild ITP) 45
46 Management Goal Thrombocytopenia 1. Activity Restrictions to minimize bleeding risk 2. Medication avoidance : antiplatelet or anticoagulant activity p.ex. Aspirin preparations, ibuprofen, other NSAIDs 3. Limit invasive procedures : platelet counts > 50 x 10 9 /L 4. Emergency of Critical Bleeding (ICH) : transfusion associated with high dose Methylprednisolone and single dose of IGIV 46
47 47
48 Thank you for your attention! Any Questions? 48
49 References 1. Patel et al. The biogenesis of platelets from megakaryocyte proplatelets. The Journal of Clinical Investigation 2005;115 (12): Kaushansky K. The molecular mechanisms that control thrombopoiesis. The Journal of Clinical Investigation. 2005;115 (12): Wise et al. Thrombocytopenia: Case definition and guidelines for collection, analysis, and presentation of immunization safety data. Vaccin 2007: Buchanan G.R. Thrombocytopenia During Childhood: What the Pediatrician Needs to Know. Pediatrics in Review 2005;26 (11): Consolini D.M. Thrombocytopenia in Infants and Children. Pediatricsin Review 2011;32 (4): Chu et al. Idiopathic Thrombocytopenic Purpura. Pediatrics in Review 2000;21 (3):
Acute Immune Thrombocytopenic Purpura (ITP) in Childhood
 Acute Immune Thrombocytopenic Purpura (ITP) in Childhood Guideline developed by Robert Saylors, MD, in collaboration with the ANGELS team. Last reviewed by Robert Saylors, MD September 22, 2016. Key Points
Acute Immune Thrombocytopenic Purpura (ITP) in Childhood Guideline developed by Robert Saylors, MD, in collaboration with the ANGELS team. Last reviewed by Robert Saylors, MD September 22, 2016. Key Points
Dr. Rai Muhammad Asghar Associate Professor Head of Pediatric Department Rawalpindi Medical College
 Dr. Rai Muhammad Asghar Associate Professor Head of Pediatric Department Rawalpindi Medical College AN APPROACH TO BLEEDING DISORDERS NORMAL HEMOSTASIS After injury, 3 processes halt bleeding Vasoconstriction
Dr. Rai Muhammad Asghar Associate Professor Head of Pediatric Department Rawalpindi Medical College AN APPROACH TO BLEEDING DISORDERS NORMAL HEMOSTASIS After injury, 3 processes halt bleeding Vasoconstriction
Hemostatic System - general information
 PLATELET DISORDERS Hemostatic System - general information Normal hemostatic system vessel wall circulating blood platelets blood coagulation and fibrynolysis Bleeding Diathesis inherited or acquired defects
PLATELET DISORDERS Hemostatic System - general information Normal hemostatic system vessel wall circulating blood platelets blood coagulation and fibrynolysis Bleeding Diathesis inherited or acquired defects
Coagulation Disorders. Dr. Muhammad Shamim Assistant Professor, BMU
 Coagulation Disorders Dr. Muhammad Shamim Assistant Professor, BMU 1 Introduction Local Vs. General Hematoma & Joint bleed Coagulation Skin/Mucosal Petechiae & Purpura PLT wound / surgical bleeding Immediate
Coagulation Disorders Dr. Muhammad Shamim Assistant Professor, BMU 1 Introduction Local Vs. General Hematoma & Joint bleed Coagulation Skin/Mucosal Petechiae & Purpura PLT wound / surgical bleeding Immediate
Platelet Disorders. By : Saja Al-Oran
 Platelet Disorders By : Saja Al-Oran Introduction The platelet arise from the fragmentation of the cytoplasm of megakaryocyte in the bone marrow. circulate in the blood as disc-shaped anucleate particles
Platelet Disorders By : Saja Al-Oran Introduction The platelet arise from the fragmentation of the cytoplasm of megakaryocyte in the bone marrow. circulate in the blood as disc-shaped anucleate particles
Bleeding Disorders. Dr. Mazen Fawzi Done by Saja M. Al-Neaumy Noor A Mohammad Noor A Joseph Joseph
 Bleeding Disorders Dr. Mazen Fawzi Done by Saja M. Al-Neaumy Noor A Mohammad Noor A Joseph Joseph Normal hemostasis The normal hemostatic response involves interactions among: The blood vessel wall (endothelium)
Bleeding Disorders Dr. Mazen Fawzi Done by Saja M. Al-Neaumy Noor A Mohammad Noor A Joseph Joseph Normal hemostasis The normal hemostatic response involves interactions among: The blood vessel wall (endothelium)
HEME 10 Bleeding Disorders
 HEME 10 Bleeding Disorders When injury occurs, three mechanisms occur Blood vessels Primary hemostasis Secondary hemostasis Diseases of the blood vessels Platelet disorders Thrombocytopenia Functional
HEME 10 Bleeding Disorders When injury occurs, three mechanisms occur Blood vessels Primary hemostasis Secondary hemostasis Diseases of the blood vessels Platelet disorders Thrombocytopenia Functional
Dr. MUBARAK ABDELRAHMAN MD PEDIATRICS AND CHILD HEALTH Assistant Professor FACULTY OF MEDICINE -JAZAN
 Dr. MUBARAK ABDELRAHMAN MD PEDIATRICS AND CHILD HEALTH Assistant Professor FACULTY OF MEDICINE -JAZAN The student should be able:» To identify the mechanism of homeostasis and the role of vessels, platelets
Dr. MUBARAK ABDELRAHMAN MD PEDIATRICS AND CHILD HEALTH Assistant Professor FACULTY OF MEDICINE -JAZAN The student should be able:» To identify the mechanism of homeostasis and the role of vessels, platelets
There are two main causes of a low platelet count
 Thrombocytopenia Thrombocytopenia is a condition in which a person's blood has an unusually low level of platelets Platelets, also called thrombocytes, are found in a person's blood along with red blood
Thrombocytopenia Thrombocytopenia is a condition in which a person's blood has an unusually low level of platelets Platelets, also called thrombocytes, are found in a person's blood along with red blood
GOOD MORNING! Thursday, July Heidi Murphy, MD Leslie Carter-King, MD
 GOOD MORNING! Thursday, July 10 2014 Heidi Murphy, MD Leslie Carter-King, MD PREP QUESTION Almost all infants experience a transient increase in bilirubin concentrations known as physiologic jaundice during
GOOD MORNING! Thursday, July 10 2014 Heidi Murphy, MD Leslie Carter-King, MD PREP QUESTION Almost all infants experience a transient increase in bilirubin concentrations known as physiologic jaundice during
Bleeding disorders. Hemostatic failure: Inappropriate and excessive bleeding either spontaneous or in response to injury.
 1 Bleeding disorders Objectives: 1. Discuss briefly the physiology of hemostasis. 2. Define the mechanisms of thrombocytopenia and the relative bleeding risk at any given platelet count. 3. Be able to
1 Bleeding disorders Objectives: 1. Discuss briefly the physiology of hemostasis. 2. Define the mechanisms of thrombocytopenia and the relative bleeding risk at any given platelet count. 3. Be able to
Contemporary perspectives and initial management of pediatric ITP. William Beau Mitchell, MD Weill Cornell Medical College New York, NY USA
 Contemporary perspectives and initial management of pediatric ITP William Beau Mitchell, MD Weill Cornell Medical College New York, NY USA Case Presentation 5 year old female Bruises on trunk, extremities
Contemporary perspectives and initial management of pediatric ITP William Beau Mitchell, MD Weill Cornell Medical College New York, NY USA Case Presentation 5 year old female Bruises on trunk, extremities
Haemostasis & Coagulation disorders Objectives:
 Haematology Lec. 1 د.ميسم مؤيد علوش Haemostasis & Coagulation disorders Objectives: - Define haemostasis and what are the major components involved in haemostasis? - How to assess the coagulation status?
Haematology Lec. 1 د.ميسم مؤيد علوش Haemostasis & Coagulation disorders Objectives: - Define haemostasis and what are the major components involved in haemostasis? - How to assess the coagulation status?
EDUCATIONAL COMMENTARY PLATELET DISORDERS
 EDUCATIONAL COMMENTARY PLATELET DISORDERS Educational commentary is provided through our affiliation with the American Society for Clinical Pathology (ASCP). To obtain FREE CME/CMLE credits click on Earn
EDUCATIONAL COMMENTARY PLATELET DISORDERS Educational commentary is provided through our affiliation with the American Society for Clinical Pathology (ASCP). To obtain FREE CME/CMLE credits click on Earn
BLEEDING (PLATELET) DISORDER. IAP UG Teaching slides
 BLEEDING (PLATELET) DISORDER 1 APPROACH The initial set of questions should establish the following: (1) the most common site and type of bleeding (e.g., mucocutaneous versus articular or deep muscle),
BLEEDING (PLATELET) DISORDER 1 APPROACH The initial set of questions should establish the following: (1) the most common site and type of bleeding (e.g., mucocutaneous versus articular or deep muscle),
V.N. KARAZIN KHARKOV NATIONAL UNIVERSITY
 V.N. KARAZIN KHARKOV NATIONAL UNIVERSITY Kharkov Regional Centre of Cardiovascular surgery V.N. Karazin Kharkov National University Department of Internal Medicine Immune thrombocytopenic purpura Abduyeva
V.N. KARAZIN KHARKOV NATIONAL UNIVERSITY Kharkov Regional Centre of Cardiovascular surgery V.N. Karazin Kharkov National University Department of Internal Medicine Immune thrombocytopenic purpura Abduyeva
Dr. Apoorva Jayarangaiah MARSHFIELD CLINIC- Saint Joseph s Hospital
 Dr. Apoorva Jayarangaiah MARSHFIELD CLINIC- Saint Joseph s Hospital A 30 year old G1P0 female of Korean descent was referred by her OBGYN during her 2 nd trimester to the Hematology Clinic for evaluation
Dr. Apoorva Jayarangaiah MARSHFIELD CLINIC- Saint Joseph s Hospital A 30 year old G1P0 female of Korean descent was referred by her OBGYN during her 2 nd trimester to the Hematology Clinic for evaluation
Thrombocytopenia: a practial approach
 Thrombocytopenia: a practial approach Dr. med. Jeroen Goede FMH Innere Medizin, Medizinische Onkologie, Hämatologie FAMH Hämatologie Chefarzt Hämatologie Kantonsspital Winterthur Outline Introduction and
Thrombocytopenia: a practial approach Dr. med. Jeroen Goede FMH Innere Medizin, Medizinische Onkologie, Hämatologie FAMH Hämatologie Chefarzt Hämatologie Kantonsspital Winterthur Outline Introduction and
Pathology note 8 BLEEDING DISORDER
 Pathology note 8 BLEEDING DISORDER Slide75 ( Types of clotting factors deficiency): Today we will talk about public public factor deficiency it could be acquired or inherited, acquired diseases are more
Pathology note 8 BLEEDING DISORDER Slide75 ( Types of clotting factors deficiency): Today we will talk about public public factor deficiency it could be acquired or inherited, acquired diseases are more
Easy Bleeding General Presentation
 Easy Bleeding General Presentation It is not uncommon for children to bleed and bruise after experiencing trauma. However, a child may also have an underlying coagulopathy, which results in easy and possibly
Easy Bleeding General Presentation It is not uncommon for children to bleed and bruise after experiencing trauma. However, a child may also have an underlying coagulopathy, which results in easy and possibly
Most Common Hemostasis Consults: Thrombocytopenia
 Most Common Hemostasis Consults: Thrombocytopenia Cindy Neunert, MS MSCS Assistant Professor, Pediatrics CUMC Columbia University TSHNA Meeting, April 15, 2016 Financial Disclosures No relevant financial
Most Common Hemostasis Consults: Thrombocytopenia Cindy Neunert, MS MSCS Assistant Professor, Pediatrics CUMC Columbia University TSHNA Meeting, April 15, 2016 Financial Disclosures No relevant financial
Bleeding Disorders: (Hemorrhagic Diatheses) Tests used to evaluate different aspects of hemostasis are the following:
 Bleeding Disorders: (Hemorrhagic Diatheses) Excessive bleeding can result from: 1. Increased fragility of vessels. 2. Platelet deficiency or dysfunction. 3. Derangement of coagulation. 4. Combinations
Bleeding Disorders: (Hemorrhagic Diatheses) Excessive bleeding can result from: 1. Increased fragility of vessels. 2. Platelet deficiency or dysfunction. 3. Derangement of coagulation. 4. Combinations
Bleeding and Thrombotic Disorders. Kristine Krafts, M.D.
 Bleeding and Thrombotic Disorders Kristine Krafts, M.D. Bleeding and Thrombotic Disorders Bleeding disorders von Willebrand disease Hemophilia A and B DIC TTP/HUS ITP Thrombotic disorders Factor V Leiden
Bleeding and Thrombotic Disorders Kristine Krafts, M.D. Bleeding and Thrombotic Disorders Bleeding disorders von Willebrand disease Hemophilia A and B DIC TTP/HUS ITP Thrombotic disorders Factor V Leiden
LAMA SHATAT TTP, ITP, DIC
 TTP, ITP, DIC Reduction in platelet number (thrombocytopenia) constitutes an important cause of generalized bleeding. A count less than 100,000 platelets/μl is generally considered to constitute thrombocytopenia.
TTP, ITP, DIC Reduction in platelet number (thrombocytopenia) constitutes an important cause of generalized bleeding. A count less than 100,000 platelets/μl is generally considered to constitute thrombocytopenia.
BLEEDING DISORDERS Simple complement:
 BLEEDING DISORDERS Simple complement: 1. Select the statement that describe the thrombocytopenia definition: A. Marked decrease of the Von Willebrandt factor B. Absence of antihemophilic factor A C. Disorder
BLEEDING DISORDERS Simple complement: 1. Select the statement that describe the thrombocytopenia definition: A. Marked decrease of the Von Willebrandt factor B. Absence of antihemophilic factor A C. Disorder
Bleeding Disorders.2 MS Abdallah Awidi Abbadi.MD. FRCP.FRCPath Feras Fararjeh MD
 Bleeding Disorders.2 MS4.25.02.2019 Abdallah Awidi Abbadi.MD. FRCP.FRCPath Feras Fararjeh MD Email: abdalla.awidi@gmail.com Case 6: GT 18 yr old female was admitted with pallor, abdominal pain and gum
Bleeding Disorders.2 MS4.25.02.2019 Abdallah Awidi Abbadi.MD. FRCP.FRCPath Feras Fararjeh MD Email: abdalla.awidi@gmail.com Case 6: GT 18 yr old female was admitted with pallor, abdominal pain and gum
Management of Acute ITP in Children Fifteen Years Experience
 Cronicon OPEN ACCESS EC PAEDIATRICS Research Article Management of Acute ITP in Children Fifteen Years Experience Jalil I Alezzi* Pediatric Department, College of Medicine, Hadhramout University, Yemen
Cronicon OPEN ACCESS EC PAEDIATRICS Research Article Management of Acute ITP in Children Fifteen Years Experience Jalil I Alezzi* Pediatric Department, College of Medicine, Hadhramout University, Yemen
The Evolving Role of Reticulated Platelets
 The Evolving Role of Kyle Riding, PhD, MLS(ASCP) CM University of Central Florida Session Objectives Platelets Recall the process involved in megakaryopoiesis and thrombocytopoiesis Explain the various
The Evolving Role of Kyle Riding, PhD, MLS(ASCP) CM University of Central Florida Session Objectives Platelets Recall the process involved in megakaryopoiesis and thrombocytopoiesis Explain the various
Haemorrhagic Disorders. Dr. Bashar Department of Pathology Mosul Medical College
 Haemorrhagic Disorders Dr. Bashar Department of Pathology Mosul Medical College Hemorrhagic Disorders These include Disorders of platelets. Disorders of blood vessels. Disorders of coagulation & fibrinolysis.
Haemorrhagic Disorders Dr. Bashar Department of Pathology Mosul Medical College Hemorrhagic Disorders These include Disorders of platelets. Disorders of blood vessels. Disorders of coagulation & fibrinolysis.
Anemia (3).ms4.25.Oct.15 Hemolytic Anemia. Abdallah Abbadi
 Anemia (3).ms4.25.Oct.15 Hemolytic Anemia Abdallah Abbadi Case 3 24 yr old female presented with anemia syndrome and jaundice. She was found to have splenomegaly. Hb 8, wbc 12k, Plt 212k, retics 12%, LDH
Anemia (3).ms4.25.Oct.15 Hemolytic Anemia Abdallah Abbadi Case 3 24 yr old female presented with anemia syndrome and jaundice. She was found to have splenomegaly. Hb 8, wbc 12k, Plt 212k, retics 12%, LDH
Dr Kannan S Consultant Hematologist Sahyadri Speciality Hospital, Pune K E M Hospital, Pune
 IMMUNE THROMBOCYTOPENIA Dr Kannan S Consultant Hematologist Sahyadri Speciality Hospital, Pune K E M Hospital, Pune ITP Megakaryocytes Definition of ITP Primary immune thrombocytopenia Platelet count
IMMUNE THROMBOCYTOPENIA Dr Kannan S Consultant Hematologist Sahyadri Speciality Hospital, Pune K E M Hospital, Pune ITP Megakaryocytes Definition of ITP Primary immune thrombocytopenia Platelet count
Evolution of clinical guidelines for ITP: Role of Romiplostim
 Slovenian Haematological Society 16 April 2010, Podčetrtek Evolution of clinical guidelines for ITP: Role of Romiplostim Dr. Roberto Stasi Department of Haematology St George's Hospital London Is there
Slovenian Haematological Society 16 April 2010, Podčetrtek Evolution of clinical guidelines for ITP: Role of Romiplostim Dr. Roberto Stasi Department of Haematology St George's Hospital London Is there
Abnormal blood counts in children Dr Tina Biss Consultant Paediatric Haematologist Newcastle upon Tyne Hospitals NHS Foundation Trust
 Abnormal blood counts in children Dr Tina Biss Consultant Paediatric Haematologist Newcastle upon Tyne Hospitals NHS Foundation Trust Regional Paediatric Specialty Trainees teaching 4 th July 2017 Scope
Abnormal blood counts in children Dr Tina Biss Consultant Paediatric Haematologist Newcastle upon Tyne Hospitals NHS Foundation Trust Regional Paediatric Specialty Trainees teaching 4 th July 2017 Scope
INHERITED COAGULOPATHY
 Disorder Etiology Pathophysiology and Presentation Lab Findings and Diagnosis Treatment INHERITED COAGULOPATHY HEMOPHILIA A and B Hemophilia A: deficiency in XIII (85%) Hemophilia B: deficiency in IX (15%)
Disorder Etiology Pathophysiology and Presentation Lab Findings and Diagnosis Treatment INHERITED COAGULOPATHY HEMOPHILIA A and B Hemophilia A: deficiency in XIII (85%) Hemophilia B: deficiency in IX (15%)
Evaluation Of Bleeding Disorders /AAP Baton Rouge. Raj Warrier
 Evaluation Of Bleeding Disorders /AAP Baton Rouge Raj Warrier Evaluation and approach to management of a bleeding child Raj Warrier Ochsner /Tulane/LSU Manipal University University Of Queenland Objectives
Evaluation Of Bleeding Disorders /AAP Baton Rouge Raj Warrier Evaluation and approach to management of a bleeding child Raj Warrier Ochsner /Tulane/LSU Manipal University University Of Queenland Objectives
Developed by Stephanie Zachary, Sarah Weicker, Dr. Jeremy Friedman, Dr. Carolyn Beck, and Dr. Lauren Kitney for PedsCases.com.
 PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Primary Immune Thrombocytopenia (ITP) CPS Podcast These podcasts are designed to give medical students an overview of
PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Primary Immune Thrombocytopenia (ITP) CPS Podcast These podcasts are designed to give medical students an overview of
Bleeding Disorders HOPE Maram Al-anbar
 Bleeding Disorders HOPE Maram Al-anbar 9-9 - 2014 ^^ Attention Please ^^ We ( correction team of pediatric package^hope/2010^ ) had decided to make one lecture of bleeding disorders in place of the two
Bleeding Disorders HOPE Maram Al-anbar 9-9 - 2014 ^^ Attention Please ^^ We ( correction team of pediatric package^hope/2010^ ) had decided to make one lecture of bleeding disorders in place of the two
PCCN Review Hematology
 PCCN Review Hematology Leanna R. Miller, RN, MN, CCRN-CMC, PCCN-CSC CEN, CNRN, CMSRN, NP Education Specialist LRM Consulting Nashville, TN Anemia Definition reduction in RBC concentration Causes iron deficiency
PCCN Review Hematology Leanna R. Miller, RN, MN, CCRN-CMC, PCCN-CSC CEN, CNRN, CMSRN, NP Education Specialist LRM Consulting Nashville, TN Anemia Definition reduction in RBC concentration Causes iron deficiency
Anemia (3).ms Hemolytic Anemia. Abdallah Abbadi Feras Fararjeh
 Anemia (3).ms4.26.2.18 Hemolytic Anemia Abdallah Abbadi Feras Fararjeh Case 3 24 yr old female presented with anemia syndrome and jaundice. She was found to have splenomegaly. Hb 8, wbc 12k, Plt 212k,
Anemia (3).ms4.26.2.18 Hemolytic Anemia Abdallah Abbadi Feras Fararjeh Case 3 24 yr old female presented with anemia syndrome and jaundice. She was found to have splenomegaly. Hb 8, wbc 12k, Plt 212k,
Things to never miss in the office. Brett Houston MD FRCPC (PYG-5, hematology) Leonard Minuk MD FRCPC
 Things to never miss in the office Brett Houston MD FRCPC (PYG-5, hematology) Leonard Minuk MD FRCPC Presenter Disclosure Faculty / Speaker s name: Brett Houston / Leonard Minuk Relationships with commercial
Things to never miss in the office Brett Houston MD FRCPC (PYG-5, hematology) Leonard Minuk MD FRCPC Presenter Disclosure Faculty / Speaker s name: Brett Houston / Leonard Minuk Relationships with commercial
Form 2033 R3.0: Wiskott-Aldrich Syndrome Pre-HSCT Data
 Key Fields Sequence Number: Date Received: - - CIBMTR Center Number: CIBMTR Recipient ID: Has this patient's data been previously reported to USIDNET? USIDNET ID: Today's Date: - - Date of HSCT for which
Key Fields Sequence Number: Date Received: - - CIBMTR Center Number: CIBMTR Recipient ID: Has this patient's data been previously reported to USIDNET? USIDNET ID: Today's Date: - - Date of HSCT for which
Guidelines for Shared Care Centres and Community Staff
 Reference: CG1410 Written by: Dr Jeanette Payne Peer reviewer Dr Jenny Welch Approved: February 2016 Approved by D&TC: 8th January 2016 Review Due: February 2019 Intended Audience This document contains
Reference: CG1410 Written by: Dr Jeanette Payne Peer reviewer Dr Jenny Welch Approved: February 2016 Approved by D&TC: 8th January 2016 Review Due: February 2019 Intended Audience This document contains
Update on the Management of Immune Thrombocytopenic Purpura (ITP) Dr Raymond Wong Department of Medicine & Therapeutics Prince of Wales Hospital
 Update on the Management of Immune Thrombocytopenic Purpura (ITP) Dr Raymond Wong Department of Medicine & Therapeutics Prince of Wales Hospital Immune Thrombocytopenia (ITP) Immune-mediated acquired disease
Update on the Management of Immune Thrombocytopenic Purpura (ITP) Dr Raymond Wong Department of Medicine & Therapeutics Prince of Wales Hospital Immune Thrombocytopenia (ITP) Immune-mediated acquired disease
QUICK REFERENCE Clinical Practice Guideline on the Evaluation and Management of Immune Thrombocytopenia (ITP)
 QUICK REFERENCE 2011 Clinical Practice Guideline on the Evaluation and Management of Immune Thrombocytopenia (ITP) Presented by the American Society of Hematology, adapted from: The American Society of
QUICK REFERENCE 2011 Clinical Practice Guideline on the Evaluation and Management of Immune Thrombocytopenia (ITP) Presented by the American Society of Hematology, adapted from: The American Society of
Index. Note: Page numbers of article numbers are in boldface type.
 Index Note: Page numbers of article numbers are in boldface type. A Abdomen, acute, as cancer emergency, 381 399 in cancer patients, etiologies unique to, 390 392 in perforation, 388 surgery of, portal
Index Note: Page numbers of article numbers are in boldface type. A Abdomen, acute, as cancer emergency, 381 399 in cancer patients, etiologies unique to, 390 392 in perforation, 388 surgery of, portal
WISKOTT-ALDRICH SYNDROME. An X-linked Primary Immunodeficiency
 WISKOTT-ALDRICH SYNDROME An X-linked Primary Immunodeficiency WHAT IS WISKOTT ALDRICH SYNDROME? Wiskott-Aldrich Syndrome (WAS) is a serious medical condition that causes problems both with the immune system
WISKOTT-ALDRICH SYNDROME An X-linked Primary Immunodeficiency WHAT IS WISKOTT ALDRICH SYNDROME? Wiskott-Aldrich Syndrome (WAS) is a serious medical condition that causes problems both with the immune system
QUESTIONS OF HEMATOLOGY AND THEIR ANSWERS
 QUESTIONS OF HEMATOLOGY AND THEIR ANSWERS WHAT IS TRUE AND WHAT IS FALSE? Questions 1 Iron deficiency anemia a) Is usually associated with a raised MCV. b) The MCH is usually low. c) Is most commonly due
QUESTIONS OF HEMATOLOGY AND THEIR ANSWERS WHAT IS TRUE AND WHAT IS FALSE? Questions 1 Iron deficiency anemia a) Is usually associated with a raised MCV. b) The MCH is usually low. c) Is most commonly due
Case Studies: Congenital Platelet Disorders
 Case Studies: Congenital Platelet Disorders Presented to Atlanta Wednesday, November 2, 2016 Disclosures for Michele P. Lambert, MD, MTR In compliance with COI policy, ISTH requires the following disclosures
Case Studies: Congenital Platelet Disorders Presented to Atlanta Wednesday, November 2, 2016 Disclosures for Michele P. Lambert, MD, MTR In compliance with COI policy, ISTH requires the following disclosures
Approaching Neutropenia in Children. SW Florida Osteopathic Medical Society: 39 th Annual Seminars in Family Practice
 Approaching Neutropenia in Children SW Florida Osteopathic Medical Society: 39 th Annual Seminars in Family Practice Approaching Neutropenia in Children Emad Salman M.D Golisano Children s Hospital of
Approaching Neutropenia in Children SW Florida Osteopathic Medical Society: 39 th Annual Seminars in Family Practice Approaching Neutropenia in Children Emad Salman M.D Golisano Children s Hospital of
Y. Helen Zhang, MD Andy Nguyen, MD 10/28/2012
 Y. Helen Zhang, MD Andy Nguyen, MD 10/28/2012 Clinical History Patient: 23-year-old female Clinical course: status-post cholecystectomy, complicated by retained common bile duct stones. Following three
Y. Helen Zhang, MD Andy Nguyen, MD 10/28/2012 Clinical History Patient: 23-year-old female Clinical course: status-post cholecystectomy, complicated by retained common bile duct stones. Following three
Platelet disorders. Information for families. Great Ormond Street Hospital for Children NHS Foundation Trust
 Platelet disorders Information for families Great Ormond Street Hospital for Children NHS Foundation Trust Platelets are the cells responsible for making blood clot so platelet disorders mean that injured
Platelet disorders Information for families Great Ormond Street Hospital for Children NHS Foundation Trust Platelets are the cells responsible for making blood clot so platelet disorders mean that injured
Immune Thrombocytopenia (ITP)
 Immune Thrombocytopenia (ITP) ITP - What is it? ITP is a blood disorder affecting platelets in the blood. Platelets are small cells in your blood that help your blood to clot. In ITP the body s immune
Immune Thrombocytopenia (ITP) ITP - What is it? ITP is a blood disorder affecting platelets in the blood. Platelets are small cells in your blood that help your blood to clot. In ITP the body s immune
Disorders of Blood Cells & Blood Coagulation
 Disorders of Blood Cells & Blood Coagulation HIHIM 409 WBC count RBC count WBC differential Hemoglobin (HGB) Hematocrit (HCT) % of volume occupied by RBCs CBC Red cell indices Mean cell volume (MCV) average
Disorders of Blood Cells & Blood Coagulation HIHIM 409 WBC count RBC count WBC differential Hemoglobin (HGB) Hematocrit (HCT) % of volume occupied by RBCs CBC Red cell indices Mean cell volume (MCV) average
The importance of thrombocytopenia and its causes
 SYSMEX EDUCATIONAL ENHANCEMENT AND DEVELOPMENT NO 4 2017 SEED HAEMATOLOGY The importance of thrombocytopenia and its causes Key words: Thrombocytopenia, thrombocytopenic, low levels of platelets What is
SYSMEX EDUCATIONAL ENHANCEMENT AND DEVELOPMENT NO 4 2017 SEED HAEMATOLOGY The importance of thrombocytopenia and its causes Key words: Thrombocytopenia, thrombocytopenic, low levels of platelets What is
Neutropenia Following Intravenous Immunoglobulin Therapy in Pediatric Patients with Idiopathic Thrombocytopenic Purpura
 ORIGINAL ARTICLE IJBC 2014;6(2): 81-85 Neutropenia Following Intravenous Immunoglobulin Therapy in Pediatric Patients with Idiopathic Thrombocytopenic Purpura Ansari S * 1, Shirali A 1, Khalili N 1, Daneshfar
ORIGINAL ARTICLE IJBC 2014;6(2): 81-85 Neutropenia Following Intravenous Immunoglobulin Therapy in Pediatric Patients with Idiopathic Thrombocytopenic Purpura Ansari S * 1, Shirali A 1, Khalili N 1, Daneshfar
Use of Intravenous Anti-RhD Immunoglobulin (RhIG) in the Treatment of Primary Immune Thrombocytopenia
 Use of Intravenous Anti-RhD Immunoglobulin (RhIG) in the Treatment of Primary Immune Thrombocytopenia KRISTINA WILLIAMS ABSTRACT Commercialized intravenous immunoglobulin (IVIG) products have been used
Use of Intravenous Anti-RhD Immunoglobulin (RhIG) in the Treatment of Primary Immune Thrombocytopenia KRISTINA WILLIAMS ABSTRACT Commercialized intravenous immunoglobulin (IVIG) products have been used
Heme (Bleeding and Coagulopathies) in the ICU
 Heme (Bleeding and Coagulopathies) in the ICU General Topics To Discuss Transfusions DIC Thrombocytopenia Liver and renal disease related bleeding Lack of evidence in managing critical illness related
Heme (Bleeding and Coagulopathies) in the ICU General Topics To Discuss Transfusions DIC Thrombocytopenia Liver and renal disease related bleeding Lack of evidence in managing critical illness related
Miss. kamlah ahmed 1
 Miss. kamlah ahmed 1 Anatomy & Physiology Blood has two compartments: 1- a fluid portion called plasma. 2- a cellular portion known as the formed elements of the blood. Which are RBC (erythrocytes), WBC
Miss. kamlah ahmed 1 Anatomy & Physiology Blood has two compartments: 1- a fluid portion called plasma. 2- a cellular portion known as the formed elements of the blood. Which are RBC (erythrocytes), WBC
12 Dynamic Interactions between Hematopoietic Stem and Progenitor Cells and the Bone Marrow: Current Biology of Stem Cell Homing and Mobilization
 Table of Contents: PART I: Molecular and Cellular Basis of Hematology 1 Anatomy and Pathophysiology of the Gene 2 Genomic Approaches to Hematology 3 Regulation of Gene Expression, Transcription, Splicing,
Table of Contents: PART I: Molecular and Cellular Basis of Hematology 1 Anatomy and Pathophysiology of the Gene 2 Genomic Approaches to Hematology 3 Regulation of Gene Expression, Transcription, Splicing,
Chapter 3 Diseases of the Blood and Bloodforming Organs and Certain Disorders Involving the Immune Mechanism D50-D89
 Chapter 3 Diseases of the Blood and Bloodforming Organs and Certain Disorders Involving the Immune Mechanism D50-D89 Presented by Jennifer Kurkulonis 1 FOUR MAJOR TYPES OF BLOOD CELLS White blood cells
Chapter 3 Diseases of the Blood and Bloodforming Organs and Certain Disorders Involving the Immune Mechanism D50-D89 Presented by Jennifer Kurkulonis 1 FOUR MAJOR TYPES OF BLOOD CELLS White blood cells
Committee Approval Date: May 9, 2014 Next Review Date: May 2015
 Medication Policy Manual Policy No: dru180 Topic: Promacta, eltrombopag Date of Origin: May 8, 2009 Committee Approval Date: May 9, 2014 Next Review Date: May 2015 Effective Date: June 1, 2014 IMPTANT
Medication Policy Manual Policy No: dru180 Topic: Promacta, eltrombopag Date of Origin: May 8, 2009 Committee Approval Date: May 9, 2014 Next Review Date: May 2015 Effective Date: June 1, 2014 IMPTANT
thrombopoietin receptor agonists and University of Washington January 13, 2012
 Tickle me eltrombopag: thrombopoietin receptor agonists and the regulation of platelet production Manoj Menon University of Washington January 13, 2012 Outline Clinical case Pathophysiology of ITP Therapeutic
Tickle me eltrombopag: thrombopoietin receptor agonists and the regulation of platelet production Manoj Menon University of Washington January 13, 2012 Outline Clinical case Pathophysiology of ITP Therapeutic
Pediatric Bleeding Disorders and Thrombocytopenia. David Simon, MD Pediatric Hematology/Oncology Kaiser Permanente Downey Medical Center
 Pediatric Bleeding Disorders and Thrombocytopenia David Simon, MD Pediatric Hematology/Oncology Kaiser Permanente Downey Medical Center 1 2 Case Presentations Case 1 12 month old male, no personal or family
Pediatric Bleeding Disorders and Thrombocytopenia David Simon, MD Pediatric Hematology/Oncology Kaiser Permanente Downey Medical Center 1 2 Case Presentations Case 1 12 month old male, no personal or family
DR V PHILIP CLINICAL HAEMATOLOGY UNIT CHRIS HANI BARAGWANATH ACADEMIC HOSPITAL
 DR V PHILIP CLINICAL HAEMATOLOGY UNIT CHRIS HANI BARAGWANATH ACADEMIC HOSPITAL Rare but fatal disease if unrecognized and untreated Incidence about 1: 1 million in the USA Female preponderance of 2:1 Part
DR V PHILIP CLINICAL HAEMATOLOGY UNIT CHRIS HANI BARAGWANATH ACADEMIC HOSPITAL Rare but fatal disease if unrecognized and untreated Incidence about 1: 1 million in the USA Female preponderance of 2:1 Part
UKITP INITAL INFORMATION SHEET (2.4)
 UKITP INITAL INFORMATION SHEET (2.4) Barts Health NHS Trust The Royal London Hospital Pathology and Pharmacy Building 80 Newark Street, London E1 2ES Centre for Haematology Institute of and Molecular Science
UKITP INITAL INFORMATION SHEET (2.4) Barts Health NHS Trust The Royal London Hospital Pathology and Pharmacy Building 80 Newark Street, London E1 2ES Centre for Haematology Institute of and Molecular Science
Pediatric Hematology/Oncology: Blood, Body, and Beyond. Geoffrey S. Kannan, PhD, MD Pediatric Neuro-oncology Pediatric Hematology/Oncology
 Pediatric Hematology/Oncology: Blood, Body, and Beyond Geoffrey S. Kannan, PhD, MD Pediatric Neuro-oncology Pediatric Hematology/Oncology Disclosures Nothing to disclose Discuss standard of care for common
Pediatric Hematology/Oncology: Blood, Body, and Beyond Geoffrey S. Kannan, PhD, MD Pediatric Neuro-oncology Pediatric Hematology/Oncology Disclosures Nothing to disclose Discuss standard of care for common
IMMATURE PLATELETS CLINICAL USE
 HAEMATOLOGY FEBRUARY 2017 WHITE PAPER IMMATURE PLATELETS CLINICAL USE Differential diagnosis of thrombocytopenia Thrombocytopenia and automated platelet measurement Thrombocytopenia is a condition characterised
HAEMATOLOGY FEBRUARY 2017 WHITE PAPER IMMATURE PLATELETS CLINICAL USE Differential diagnosis of thrombocytopenia Thrombocytopenia and automated platelet measurement Thrombocytopenia is a condition characterised
The LaboratoryMatters
 Laboratory Medicine Newsletter for clinicians, pathologists & clinical laboratory technologists. A Initiative. HEMOSTASIS AND THE LABORATORY This issue highlights: Primary Hemostasis Screening Tests Case
Laboratory Medicine Newsletter for clinicians, pathologists & clinical laboratory technologists. A Initiative. HEMOSTASIS AND THE LABORATORY This issue highlights: Primary Hemostasis Screening Tests Case
HAEMORRHAGIA Bleeding
 HAEMORRHAGIA Bleeding Cassification Size Location pathomechanism Hematoma: external or may be enclosed within a tissue petechiae : 1-2 mm hemorrhages into skin, mucous membranes, or serosal surfaces increased
HAEMORRHAGIA Bleeding Cassification Size Location pathomechanism Hematoma: external or may be enclosed within a tissue petechiae : 1-2 mm hemorrhages into skin, mucous membranes, or serosal surfaces increased
For platelet control as individual as you
 For platelet control as individual as you Explore the possibilities of Immune Thrombocytopenic Purpura (ITP) treatment. Important Risk Information WARNING: INTRAVASCULAR HEMOLYSIS (IVH) Intravascular hemolysis
For platelet control as individual as you Explore the possibilities of Immune Thrombocytopenic Purpura (ITP) treatment. Important Risk Information WARNING: INTRAVASCULAR HEMOLYSIS (IVH) Intravascular hemolysis
Peripheral Blood Smear Examination. Momtazmanesh MD. Ped. Hematologist & Oncologist Loghman General Hospital
 1395 Peripheral Blood Smear Examination Momtazmanesh MD. Ped. Hematologist & Oncologist Loghman General Hospital Peripheral Blood Smear A peripheral blood smear is a snapshot of the cells that are present
1395 Peripheral Blood Smear Examination Momtazmanesh MD. Ped. Hematologist & Oncologist Loghman General Hospital Peripheral Blood Smear A peripheral blood smear is a snapshot of the cells that are present
Recommendations for Celiac Disease Testing. IgA & ttg IgA
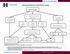 Recommendations for Celiac Disease Testing IgA & ttg IgA IgA Normal ttg IgA Negative IgA >10 mg/dl, but less than age matched range IgA
Recommendations for Celiac Disease Testing IgA & ttg IgA IgA Normal ttg IgA Negative IgA >10 mg/dl, but less than age matched range IgA
Platelets: Purpose, Pictures plus Problems. Platelets The Basics
 Platelets: Purpose, Pictures plus Problems Platelets The Basics Platelets are also called thrombocytes Biconvex discoid in shape Cytoplasmic fragments of a megakaryocyte Platelets do not have a nucleus
Platelets: Purpose, Pictures plus Problems Platelets The Basics Platelets are also called thrombocytes Biconvex discoid in shape Cytoplasmic fragments of a megakaryocyte Platelets do not have a nucleus
BLEEDING DISORDERS. JC Opperman 2012
 BLEEDING DISORDERS JC Opperman 2012 Primary and Secondary Clotting Laboratory Tests Routine screening tests Prothrombin time (PT) (INR) increased in neonates (12-18 sec) Partial thromboplastin time (PTT)
BLEEDING DISORDERS JC Opperman 2012 Primary and Secondary Clotting Laboratory Tests Routine screening tests Prothrombin time (PT) (INR) increased in neonates (12-18 sec) Partial thromboplastin time (PTT)
PROMACTA (eltrombopag olamine) oral tablet and oral suspension
 PROMACTA (eltrombopag olamine) oral tablet and oral suspension Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit
PROMACTA (eltrombopag olamine) oral tablet and oral suspension Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit
Approach to thrombocytopenia and management of ITP. Dr.Aby Abraham Dept of Clinical Haematology
 Approach to thrombocytopenia and management of ITP Dr.Aby Abraham Dept of Clinical Haematology 04-08-2014 Causes of thrombocytopenia Thrombocytopenia Pseudo True Decreased production Increased destruction
Approach to thrombocytopenia and management of ITP Dr.Aby Abraham Dept of Clinical Haematology 04-08-2014 Causes of thrombocytopenia Thrombocytopenia Pseudo True Decreased production Increased destruction
Blood Components & Indications for Transfusion. Neda Kalhor
 Blood Components & Indications for Transfusion Neda Kalhor Blood products Cellular Components: Red blood cells - Leukocyte-reduced RBCs - Washed RBCs - Irradiated RBCs Platelets - Random-donor platelets
Blood Components & Indications for Transfusion Neda Kalhor Blood products Cellular Components: Red blood cells - Leukocyte-reduced RBCs - Washed RBCs - Irradiated RBCs Platelets - Random-donor platelets
Clinical & Laboratory Assessment
 Clinical & Laboratory Assessment Dr Roger Pool NHLS & University of Pretoria Clinical Assessment (History) Anaemia ( haemoglobin) Dyspnoea (shortness of breath) Tiredness Angina Headache Clinical Assessment
Clinical & Laboratory Assessment Dr Roger Pool NHLS & University of Pretoria Clinical Assessment (History) Anaemia ( haemoglobin) Dyspnoea (shortness of breath) Tiredness Angina Headache Clinical Assessment
HAEMORRHAGIA Bleeding
 HAEMORRHAGIA Bleeding Cassification Size Location pathomechanism Hematoma: external or may be enclosed within a tissue petechial rash (spot) : 1-2 mm hemorrhages into skin, mucous membranes, or serosal
HAEMORRHAGIA Bleeding Cassification Size Location pathomechanism Hematoma: external or may be enclosed within a tissue petechial rash (spot) : 1-2 mm hemorrhages into skin, mucous membranes, or serosal
Immune Thrombocytopenic Purpura (ITP)
 Patient information Immune Thrombocytopenic Purpura Immune Thrombocytopenic Purpura (ITP) This leaflet is for adult patients diagnosed with Immune Thrombocytopenic Purpura also known as Immune Thrombocytopenia
Patient information Immune Thrombocytopenic Purpura Immune Thrombocytopenic Purpura (ITP) This leaflet is for adult patients diagnosed with Immune Thrombocytopenic Purpura also known as Immune Thrombocytopenia
Thrombotic Thrombocytopenic Purpura and the Role of ADAMTS-13
 Thrombotic Thrombocytopenic Purpura and the Role of ADAMTS-13 Mark Cunningham,MD Director, Hematology Laboratory Department of Pathology University of Kansas Medical Center College of American Pathologists
Thrombotic Thrombocytopenic Purpura and the Role of ADAMTS-13 Mark Cunningham,MD Director, Hematology Laboratory Department of Pathology University of Kansas Medical Center College of American Pathologists
The Bleeding Patient. Sarah Stacey Charlotte Maxeke Johannesburg Hospital University of the Witwatersrand
 The Bleeding Patient Sarah Stacey Charlotte Maxeke Johannesburg Hospital University of the Witwatersrand The Bleeding Patient If you prick us, do we not bleed? Disorders of secondary homeostasis: dysfunction
The Bleeding Patient Sarah Stacey Charlotte Maxeke Johannesburg Hospital University of the Witwatersrand The Bleeding Patient If you prick us, do we not bleed? Disorders of secondary homeostasis: dysfunction
Diagnosis and Management of Immune Thrombocytopenias. Thomas L. Ortel, M.D., Ph.D. Duke University Medical Center 2 November 2016
 Diagnosis and Management of Immune Thrombocytopenias Thomas L. Ortel, M.D., Ph.D. Duke University Medical Center 2 November 2016 Disclosures Research support: NIH, CDC, Eisai, Pfizer, Daiichi Sankyo, GlaxoSmithKline,
Diagnosis and Management of Immune Thrombocytopenias Thomas L. Ortel, M.D., Ph.D. Duke University Medical Center 2 November 2016 Disclosures Research support: NIH, CDC, Eisai, Pfizer, Daiichi Sankyo, GlaxoSmithKline,
Congenital bleeding disorders
 Congenital bleeding disorders Overview Factor VIII von Willebrand Factor Complex factor VIII von Willebrand factor (vwf) complex circulate as a complex + factor IX intrinsic pathway Platelets bind via
Congenital bleeding disorders Overview Factor VIII von Willebrand Factor Complex factor VIII von Willebrand factor (vwf) complex circulate as a complex + factor IX intrinsic pathway Platelets bind via
GUIDELINE: ASSESSMENT OF BRUISING & BLEEDING IN CHILDREN. All children in whom there is concern regarding bruising / bleeding
 GUIDELINE: ASSESSMENT OF BRUISING & BLEEDING IN CHILDREN Reference: Bruising / Bleeding / NAI Version No: 1 Applicable to All children in whom there is concern regarding bruising / bleeding Classification
GUIDELINE: ASSESSMENT OF BRUISING & BLEEDING IN CHILDREN Reference: Bruising / Bleeding / NAI Version No: 1 Applicable to All children in whom there is concern regarding bruising / bleeding Classification
Document Title: Hemostasis: Platelet and Coagulation Disorders. Author(s): Joseph H. Hartmann (University of Michigan), DO 2012
 Project: Ghana Emergency Medicine Collaborative Document Title: Hemostasis: Platelet and Coagulation Disorders Author(s): Joseph H. Hartmann (University of Michigan), DO 2012 License: Unless otherwise
Project: Ghana Emergency Medicine Collaborative Document Title: Hemostasis: Platelet and Coagulation Disorders Author(s): Joseph H. Hartmann (University of Michigan), DO 2012 License: Unless otherwise
Outline. What is aplastic anemia? 9/19/2012. Aplastic Anemia Current Thinking on the Disease, Diagnosis, and Non-Transplant Treatment Options
 Aplastic Anemia Current Thinking on the Disease, Diagnosis, and Non-Transplant Treatment Options Carlos M. de Castro, MD Duke University Medical Center Outline What is Aplastic Anemia? What other diseases
Aplastic Anemia Current Thinking on the Disease, Diagnosis, and Non-Transplant Treatment Options Carlos M. de Castro, MD Duke University Medical Center Outline What is Aplastic Anemia? What other diseases
Medical Surgical Review Handout- Hematology/Oncology 2016
 Medical Surgical Review Handout- Hematology/Oncology 2016 Overview Blood circulates in the cardiovascular system o Carries oxygen to the cells o Carries waste away from the cells Functions of blood o Transportation:
Medical Surgical Review Handout- Hematology/Oncology 2016 Overview Blood circulates in the cardiovascular system o Carries oxygen to the cells o Carries waste away from the cells Functions of blood o Transportation:
r). SUPPLEMENTARY/SECOND OPPORTUNITY EXAMINATION PAPER nnmlbih UNIVERSITY Sophia Blaauw INSTRUCTIONS FACULTY OF HEALTH AND APPLIED SCIENCES
 r). nnmlbih UNIVERSITY OF SCIEFICE nnd TECHNOLOGY FACULTY OF HEALTH AND APPLIED SCIENCES DEPARTMENT OF HEALTH SCIENCES QUALIFICATION: BACHELOR OF MEDICAL LABORATORY SCIENCES QUALIFICATION CODE: 08BMLS
r). nnmlbih UNIVERSITY OF SCIEFICE nnd TECHNOLOGY FACULTY OF HEALTH AND APPLIED SCIENCES DEPARTMENT OF HEALTH SCIENCES QUALIFICATION: BACHELOR OF MEDICAL LABORATORY SCIENCES QUALIFICATION CODE: 08BMLS
Treatment pathway for adult patients with immune (idiopathic) thrombocytopenic purpura (ITP)
 Prescribing Clinical Network Surrey (East Surrey CCG, Guildford & Waverley CCG, North West Surrey CCG, Surrey Downs CCG & Surrey Heath CCG) Crawley and Horsham & Mid-Sussex CCG Treatment pathway for adult
Prescribing Clinical Network Surrey (East Surrey CCG, Guildford & Waverley CCG, North West Surrey CCG, Surrey Downs CCG & Surrey Heath CCG) Crawley and Horsham & Mid-Sussex CCG Treatment pathway for adult
Hematologic Disorders. Assistant professor of anesthesia
 Preoperative Evaluation Hematologic Disorders Dr M.Razavi Assistant professor of anesthesia Anemia Evaluation needs to consider the extent and type of surgery, the anticipated blood loss, and the patient's
Preoperative Evaluation Hematologic Disorders Dr M.Razavi Assistant professor of anesthesia Anemia Evaluation needs to consider the extent and type of surgery, the anticipated blood loss, and the patient's
Taking The Fear Out of Abnormal CBC s Problems of Production, Destruction or loss
 Taking The Fear Out of Abnormal CBC s Problems of Production, Destruction or loss Joanne Eddington, MN, FNP, AOCN Providence Oncology and Hematology Care Clinic - Eastside Blood Cell Abnormalities Abnormalities
Taking The Fear Out of Abnormal CBC s Problems of Production, Destruction or loss Joanne Eddington, MN, FNP, AOCN Providence Oncology and Hematology Care Clinic - Eastside Blood Cell Abnormalities Abnormalities
REVIEW ARTICLE. Immune Thrombocytopenic Purpura ADARSH A K, LAKSHMI KRISHNA INTRODUCTION CLASSIFICATION
 ADARSH A K, LAKSHMI KRISHNA REVIEW ARTICLE INTRODUCTION ITP or immune thrombocytopenic purpura is an autoimmune disorder characterized by increased platelet destruction & platelet count < 1 lakh. It is
ADARSH A K, LAKSHMI KRISHNA REVIEW ARTICLE INTRODUCTION ITP or immune thrombocytopenic purpura is an autoimmune disorder characterized by increased platelet destruction & platelet count < 1 lakh. It is
Wiskott-Aldrich Syndrome
 chapter 7 Wiskott-Aldrich Syndrome Wiskott-Aldrich syndrome is a primary immunodeficiency disease involving both T- and B-lymphocytes. In addition, the blood cells that help control bleeding, called platelets
chapter 7 Wiskott-Aldrich Syndrome Wiskott-Aldrich syndrome is a primary immunodeficiency disease involving both T- and B-lymphocytes. In addition, the blood cells that help control bleeding, called platelets
Hematologic changes in systemic diseases. Chittima Sirijerachai
 Hematologic changes in systemic diseases Chittima Sirijerachai Systemic diseases Infection Renal diseases Liver diseases Connective tissue diseases Malignancy Anemia of chronic disease (ACD) Chronic infections:
Hematologic changes in systemic diseases Chittima Sirijerachai Systemic diseases Infection Renal diseases Liver diseases Connective tissue diseases Malignancy Anemia of chronic disease (ACD) Chronic infections:
Kingdom of Bahrain Arabian Gulf University College of Medicine and Medical Sciences Hematology
 Kingdom of Bahrain Arabian Gulf University College of Medicine and Medical Sciences Hematology - Anemia: It is a reduction in number of RBCs or Hb concentration > 2 SD below the mean for a corresponding
Kingdom of Bahrain Arabian Gulf University College of Medicine and Medical Sciences Hematology - Anemia: It is a reduction in number of RBCs or Hb concentration > 2 SD below the mean for a corresponding
LifeBridge Health Transfusion Service Sinai Hospital of Baltimore Northwest Hospital Center BQA Transfusion Criteria Version#2 POLICY NO.
 LifeBridge Health Transfusion Service Sinai Hospital of Baltimore Northwest Hospital Center BQA 1011.02 Transfusion Criteria Version#2 Department POLICY NO. PAGE NO. Blood Bank Quality Assurance Manual
LifeBridge Health Transfusion Service Sinai Hospital of Baltimore Northwest Hospital Center BQA 1011.02 Transfusion Criteria Version#2 Department POLICY NO. PAGE NO. Blood Bank Quality Assurance Manual
The Child with a Hematologic Alteration
 47 The Child with a Hematologic Alteration HELPFUL HINT Review the anatomy and physiology of the hematologic system in an anatomy and physiology textbook. MATCHING KEY TERMS Match the term with the correct
47 The Child with a Hematologic Alteration HELPFUL HINT Review the anatomy and physiology of the hematologic system in an anatomy and physiology textbook. MATCHING KEY TERMS Match the term with the correct
The function of the bone marrow. Living with Aplastic Anemia. A Case Study - I. Hypocellular bone marrow failure 5/14/2018
 The function of the bone marrow Larry D. Cripe, MD Indiana University Simon Cancer Center Bone Marrow Stem Cells Mature into Blood Cells Mature Blood Cells and Health Type Function Term Red Cells Carry
The function of the bone marrow Larry D. Cripe, MD Indiana University Simon Cancer Center Bone Marrow Stem Cells Mature into Blood Cells Mature Blood Cells and Health Type Function Term Red Cells Carry
Chapter 46. Care of the Patient with a Blood or Lymphatic Disorder
 Chapter 46 Care of the Patient with a Blood or Lymphatic Disorder All items and derived items 2015, 2011, 2006 by Mosby, Inc., an imprint of Elsevier Inc. All rights reserved. Components of the Blood Red
Chapter 46 Care of the Patient with a Blood or Lymphatic Disorder All items and derived items 2015, 2011, 2006 by Mosby, Inc., an imprint of Elsevier Inc. All rights reserved. Components of the Blood Red
