Urinary incontinence after obstetric anal sphincter injuries (OASIS) is there a relationship?
|
|
|
- Claude Gibbs
- 6 years ago
- Views:
Transcription
1 DOI /s ORIGINAL ARTICLE Urinary incontinence after obstetric anal sphincter injuries (OASIS) is there a relationship? Inka Scheer & Vasanth Andrews & Ranee Thakar & Abdul H. Sultan Received: 23 January 2007 / Accepted: 5 July 2007 # International Urogynecology Journal 2007 Abstract This study aimed to compare urinary symptoms and its impact on women s quality of life after obstetric anal sphincter injuries (OASIS) with a matched control group in the short term. The study group consisted of 100 primiparous women with OASIS and 104 controls who sustained a second-degree tear or had a mediolateral episiotomy performed. All women completed a validated International Consultation on Incontinence Questionnaire-Short Form (ICIQ-SF) questionnaire 10 weeks after delivery. Compared to controls, significantly more women with OASIS reported overall urinary incontinence (21.2 vs 38%, p=0.005) and had significantly worse quality of life score (incontinence score: 2.42 vs 1.2; p=0.008). Significantly more women with OASIS suffered from stress urinary incontinence (33 vs 14%; p=0.002; OR 3.06; CI= ) than controls. Logistic regression analysis revealed that OASIS and a prolonged (>50 min) second stage of labour were independent risk factors for the development of stress urinary incontinence. This study highlights the importance of inquiring about urinary incontinence in women with OASIS. Keywords Urinary incontinence. Vaginal delivery. Anal sphincter tear Presented to the German Forum Urodynamicum 2006 by IS ( ) and received the Eugen-Rehfisch Award of the German Forum Urodynamicum. I. Scheer : V. Andrews : R. Thakar (*) Urogynaecology Unit, Mayday University Hospital, 530, London Road, Croydon CR7 7YE, UK ranee.thakar@mayday.nhs.uk Introduction Urinary incontinence (UI) occurs in 53% of women over 20 years of age [1]. The prevalence of urinary incontinence during pregnancy is reported to be as high as 44% [2] but appears to vary between 7 [3] and 34% [4] after delivery. The aetiology is unknown, but intrapartum pudendal neuropathy [5 9] and muscle trauma altering the urethral support [10, 11] have been incriminated. Obstetric anal sphincter injuries (OASIS) occur in up to 19% of vaginal deliveries [12] and are an established risk factor for the development of anal incontinence [13, 14]. Urinary incontinence after OASIS has been reported in 13 46% [15 18]. However, long term follow-up of women with OASIS reveals conflicting results. Fornell et al. [18] demonstrated a strong correlation between OASIS and faecal and urinary incontinence. Women with OASIS had a higher risk of urinary incontinence compared to women without a tear or a small perineal tear [18]. However, no explanation was given as to why women with OASIS were at a higher risk of developing urinary incontinence. By contrast, Otero et al. [19] found no significant increase in urinary incontinence 18 years after OASIS when compared to parity-matched controls [19]. Others have identified a range of risk factors for the development of urinary incontinence after childbirth, namely, vaginal delivery when compared to caesarean section [20-22], vacuum extraction, [17] forceps delivery [22], pre-existing urinary incontinence, [17] older maternal age [20], and prolonged second stage of labour [7, 9]. Very little data is available on postpartum urinary incontinence and quality of life. Glazener et al. [20] reported recently that around 50% of incontinent women were affected by their urinary incontinence symptoms
2 postpartum in terms of hygiene, home work, and social life, but they used a non-validated questionnaire. The aims of our study were to establish the prevalence of urinary incontinence after OASIS in primiparous women on short-term follow-up to identify risk factors and evaluate its impact on quality of life. Materials and methods Primiparous women with OASIS were followed up at 3 months postpartum in a dedicated one-stop perineal clinic, where they completed the validated International Consultation on Incontinence Questionnaire-Short Form (ICIQ-SF) questionnaire [23, 24]. The control group consisted of primiparous women who sustained a spontaneous second degree tear or had a mediolateral episiotomy. The control group were recruited between February 2003 and January 2004 and also participated in another trial that has previously been published [25]. All women in this group had a second perineal examination in the immediate postpartum period by an experienced research fellow as well as an endoanal scan (repeated at 3 months). Therefore, none of the women had occult or unrecognized injuries. Demographic data and labour details were collected prospectively. Statistical analyses were performed using the Statistical Package for Social Sciences (SPSS, Chicago, IL, version 12.0). Differences in proportions of categorical variables were calculated using the chi-square test. Differences between the groups were assessed using Student s t tests and Mann Whitney U tests for parametric and nonparametric data, respectively. Univariate analysis have been performed to determine risk factors given in odds ratio (OR) and 95% confidence intervals (CI). In a logistic regression analysis, the following variables have been entered in the model to determine independent risk factors for overall and stress urinary incontinence: second Table 1 Characteristics of women after OASIS and controls P value Age, mean (SD) 28.9 (5.1) 28.0 (5.5) 0.23 a BMI (SD) (5.1) (4.5) 0.58 a Instrumental delivery, n (%) 39 (39) 29 (28) 0.07 b Second stage, minutes (SD) (55) (40) 0.11 a Epidural, n (%) 28 (28) 28 (27) 0.83 b Birth weight, g, mean (SD) 3,457 (535) 3,231 (423) a Head circumference, mm, mean (SD) 343 (16) 336 (15) a Mediolateral episiotomy (%) 60 (60) 41 (39) b a Student s t test b Chi-square test Table 2 Frequency of leakage stage of labour >50 min, and head circumference > median of mm. Ethical approval for the control group was approved by the Croydon Ethics and Research Committee. Data of women having OASIS was collected from the perineal clinic. This questionnaire forms part of our normal evaluation of patients with OASIS. Patients gave written consent to use the data from questionnaires for scientific publications, and this was sanctioned by the Croydon Research and Development Committee. Results Never Once a week or less /week 7 5 Once/day 6 2 Several times/day 6 3 All the time 1 Between July 2002 and January 2005, of the 102 primiparous with a diagnosis of an OASIS in our unit, 100 women returned for the postnatal visit and were included in this study (return rate 98%). One hundred and four primiparous controls were seen postpartum. In the control group, 95% of the invited women participated in this study and 86% attended the follow up. The postpartum visit took place between 5 and 15 (mean, 10±5) weeks after delivery. In the control group, OASIS were classified and repaired according to the Royal College of Obstetricians and Gynaecologists (RCOG) guidelines [26]. Forty-eight women sustained a 3a tear [less than 50% of the external anal sphincter (EAS) involved], 42 women a 3b tear ( 50% of the EAS involved), 5 women a 3c tear [EAS and internal anal sphincter (IAS) torn], and 5 women sustained a fourth degree tear (EAS, IAS, and anal epithelium torn). Demographic data and labour details for women with OASIS and controls are given in Table 1. Age, length of second stage of labour, and instrumental delivery did not differ significantly between the study group (OASIS) and controls (Table 1). The OASIS group reported significantly more symptoms of urinary incontinence (leakage never: OASIS 62%, controls 78.8%) and a larger volume of urinary leakage (moderate amount: OASIS 32%, controls 0%, p=0.017, Tables 2 and 3). The ICIQ urinary incontinence score (Table 4) was significantly higher in women with OASIS (2.42± 3.7)
3 Table 3 Amount of leakage Table 5 Type of urinary incontinence according to symptoms When does urine leak? P value None Small amount 3 21 Moderate amount 32 Large amount 3 1 compared to controls (1.20± 2.7), p=0.008). However, the grade of OASIS did not affect the ICIQ urinary incontinence score (p=0.507). Quality of life (QoL), as assessed by the ICIQ-SF, was significantly worse after OASIS (0.88 vs 0.31, p=0.01). The different types of urinary incontinence are shown in Table 5. Significantly more women after OASIS reported urinary leakage while coughing and sneezing (OASIS 30%, controls 11.5%, p=0.005) or while they were physically active (OASIS 12%, controls 3.8%, p=0.03). No significant differences were found regarding urinary leakage during any of the following: sleep, before reaching the toilet, or after urinating (Table 5). Risk factors (univariate analysis) for postpartum urinary incontinence are shown in Tables 6 and 7. The median duration of the active second stage of labour in our cohort was 50 min, and the median head circumference was mm. a second stage of labour longer than 50 min (median), and a head circumference larger than mm (median) were significant risk factors for overall urinary incontinence and stress urinary incontinence (Tables 6 and 7). In a logistic regression analysis, OASIS and a second stage of labour >50 min were independent risk factors for stress urinary incontinence (Table 8). Discussion Previously published studies on OASIS have focused mainly on anal symptoms [9, 12, 13], and only few studies [12, 15-17, 19, 27] have investigated urinary incontinence. There have been three studies with short-term follow up of Never, n (%) 62 (62) 82 (78.8) a When you cough, sneeze, and physically active, n (%) 33 (33) 15 (14.4) a When you are asleep, n (%) 3 (3) b Before you can get to the toilet (%) 18 (18) 10 (9.6) b When you have finished urinating (%) 2 (2) 2 (1.9) b For no obvious reason (%) 6 (6) 2 (1.9) b All the time (%) 0 1 (1) 1.0 b a Chi-square test b Fisher s exact test urinary symptoms after OASIS [12, 16, 27]. Urinary symptoms were reported in up to 31% [16] with a high incidence of urge urinary incontinence [12], but a validated questionnaire was not used [12, 16] nor did they compare their findings to women without OASIS [16]. Longer term urinary symptoms after OASIS have been evaluated in three studies [15, 17, 19]. In a retrospective study using a non-validated questionnaire, Wagenius and Laurin [15] reported no difference in urinary symptoms 4 years after OASIS compared to a control group. The prevalence of urinary incontinence was 13% for OASIS and 9% for controls. In a prospective study (n=72), Tetschner et al [17] reported urinary symptoms in 32% of women and demonstrated a relationship between the degree of anal sphincter rupture (1, less than one third of anal sphincter muscle affected; 2, more than one third affected; 3, complete rupture of the anal sphincter without damage to the anal mucosa) and urinary incontinence at 2 to 4 years after OASIS. Women with a total rupture of the anal sphincter had a greater risk of developing urinary incontinence compared to women with a partial rupture [17]. However, symptoms were not evaluated using a validated questionnaire nor was there a control group. Otero et al [19] used a validated questionnaire and found no difference in almost all urinary symptoms 18 years after OASIS compared to parity-matched controls. Women with OASIS reported Table 4 Urinary incontinence and score in women with OASIS and controls P value Overall urinary incontinence, n (%) 38 (38) 22 (21.2) a Quality of life score Mean (SD) 0.88 (1.79) 0.31 (0.91) 0.01 b Incontinence score, mean (SD) 2.42 (3.7) 1.20 (2.7) b a Chi-square test b Mann Whitney U test Table 6 Risk factors for overall urinary incontinence (univariate analysis) OR (CI) OASIS 2.28 ( ) Second stage of labour > median 50 min 2.28 ( ) Birth weight > median of 3,380 g 0.96 ( ) Head circumference > median of mm 1.84 ( ) Mediolateral episiotomy 1.36 ( ) Epidural 1.19 ( ) Instrumental delivery 1.47 ( )
4 Table 7 Risk factors for stress urinary incontinence (univariate analysis) OR (CI) OASIS 3.06 ( ) Second stage of labour > median 50 min 2.63 ( ) Birth weight > median of 3380 g 0.96 ( ) Head circumference > median of mm 1.84 ( ) Mediolateral episiotomy 1.36 ( ) Epidural 1.19 ( ) Instrumental delivery 1.39 ( ) significantly more frequent leakage of small amounts of urine when compared to controls (p=0.04). However, the proportion of women who had sought treatment for urinary incontinence was similar in both groups. More recently, Borello-France et al. [27] performed a large prospective study investigating the relationship between anal sphincter tears and postpartum faecal and urinary incontinence. At 6 weeks and 6 months, they found no significant difference in the prevalence of urinary incontinence between the OASIS and control group. However, there were considerable differences between the groups in terms of episiotomy rates, instrumental deliveries, birth weight, and length of labour. Our study was conducted prospectively with a representative control group in which all women had either a spontaneous second-degree tear or a mediolateral episiotomy. All women in the control group had a repeat perineal examination and an endoanal scan immediately after delivery and at 3 months postpartum. Therefore, none of the control group had occult or unrecognised anal sphincter injuries [13, 25]. This was to ensure that in terms of the perineal trauma, the only real difference between the study and the control groups were that the study group sustained additional anal sphincter injury. In our study, postnatal stress urinary incontinence at 10 weeks after OASIS was reported in 33% compared to 14% of the control group (p=0.002), and women with OASIS reported a worse impact on their quality of life compared to controls (QoL score, OASIS 0.88; controls, 0.31; p=0.01). The limitation of this study is that we did not perform urodynamic studies. However, this is in keeping with our clinical practice, whereby we always initiate pelvic floor exercises and only perform urodynamics in those women who seek surgical intervention. Nevertheless, our data shows that at 3 months postpartum, urinary symptoms occurred significantly more frequently after OASIS. There are two possible hypotheses for the association between OASIS and urinary incontinence. Firstly, it may be associated with the extended mechanical trauma that resulted in the anal sphincter injury. Recent evidence suggests that the urethra has no ligaments attaching it anteriorly to the pubic bone [28]. Ventro-laterally, the urethra is enclosed by the levator ani, its fascia and a ventral urethral connective tissue bridge connecting both sides. Dorsally, the urethra is closely connected to the anterior vaginal wall [28]. In a prospective study, Dietz and Lanzarone [29] demonstrated that vaginal delivery is associated with avulsion of the levator ani from the pelvic sidewall in one third of women. Apart from soft tissue trauma, they reported a weak but significant association between avulsion injury and worsening or de novo stress urinary incontinence [29]. It remains to be determined whether trauma to the posterior vaginal wall and perineum that occurs with OASIS also traumatises the urethral support mechanisms and consequently leads to the development of stress urinary incontinence. Secondly, as a prolonged second stage was also an independent risk factor, stress urinary incontinence may be attributed to associated neuropathic damage. A prolonged second stage of labour is believed to exacerbate pudendal nerve damage [5, 6, 9] and can alter electromyographic findings [7]. However, in a prospective study, Sultan et al. [9] found no significant difference in pudendal nerve terminal motor latencies in continent and incontinent women post partum. Allen et al. [7] reported that only a few women, who sustained damage to the pelvic floor, complained of urinary incontinence post partum. There is also evidence to suggest that some degree of recovery of pudendal nerve function occurs with time [5, 9]. Dolan et al. [30] performed a prospective longitudinal study in which pelvic floor neurophysiology was performed antenatally in a cohort of 96 primigravid, and some of these women were followed up for 15 years. Their findings were contradictory, as they found that while the motor unit potential duration increased at 7 years, the vaginal squeeze pressure also Table 8 Logistic regression analysis of independent risk factors for overall urinary incontinence stress urinary incontinence Overall urinary incontinence Stress urinary incontinence OR (CI) P value OR (CI) P value OASIS 0.55 ( ) ( ) Second stage of labour > median 50 min 0.50 ( ) ( ) Head circumference > median of mm 0.54 ( ) ( ) 0.201
5 increased during the same period. They concluded that the aetiology of stress incontinence was complex, and in the absence of a definitive neurophysiological test to quantify neuropathy, the role of denervation/reinnervation in the pathophysiology of urinary incontinence remains unclear. Conclusion Women who sustain OASIS are more likely to develop stress urinary incontinence. Furthermore, these women suffer a significant deterioration in quality of life. As incontinence is an embarrassing symptom and a social stigma, this study highlights the need for clinicians to directly inquire about both urinary and anal incontinence in women who sustain OASIS. Prevention of this silent affliction could only be considered until further research enables a better understanding of the pathophysiology of urinary incontinence in women who sustain OASIS. Acknowledgement The authors are grateful for the statistical advice kindly given by Sally Kerry from the Community Health Science Department at St. George s University of London. Funding for this study was provided by the Mayday Childbirth Charity Fund, Croydon, UK. References 1. Harrison GL, Memel DS (1994) Urinary incontinence in women: its prevalence and its management in a health promotion clinic. Br J Gen Pract 44(381): Chaliha C, Kalia V, Stanton SL et al (1999) Antenatal Prediction of postpartum urinary and fecal incontinence. Obstet Gynecol 94 (5 Pt 1): Viktrup L, Lose G, Rolff M et al (1992) The symptom of stress incontinence caused by pregnancy or delivery in primiparas. Obstet Gynecol 79: Wilson PD, Herbison RM, Herbison GP (1996) Obstetric practice and the prevalence of urinary incontinence three months after delivery. BJOG 103: Snooks SJ, Swash M, Setchell M et al (1984) Injury to the innervation of pelvic floor sphincter musculature in childbirth. Lancet 2: Snooks SJ, Badenoch DF, Tiptaft RC et al (1985) Perineal nerve damage in genuine stress incontinence. An electrophysiological study.. Br J Urol 57: Allen RE, Hosker GL, Smith ARB et al (1990) Pelvic floor damage and childbirth: a neurophysiological study. Br J Obstet Gynaecol 97: Sampselle CM (1990) Changes in pelvic floor strength associated with childbirth. J Obstet Gynecol Neonatal Nurs 19: Sultan AH, Kamm MA, Hudson CN (1994) Pudendal nerve damage during labour: prospective study before and after childbirth. BJOG 101: Peschers UM, Schaer G, Anthuber C et al (1996) Changes in vesical neck mobility following vaginal delivery. Obstet Gynecol 88: King JK, Freeman RM (1998) Is antenatal bladder neck mobility a risk factor for postpartum stress incontinence. BJOG 105: Fenner D, Genberg B, Brahma P et al (2003) Fecal and urinary incontinence after vaginal delivery with anal sphincter disruption in an obstetrics unit in the United States. Am J Obstet Gynecol 189(6): Sultan AH, Kamm MA, Hudson CN et al (1993) Anal sphincter disruption during vaginal delivery. N Engl J Med 329: Zetterstrom JP, López A, Anzén B et al (1999) Anal incontinence after vaginal delivery: a prospective study in primiparous women. BJOG 106: Wagenius J, Laurin J (2003) Clinical symptoms after anal sphincter rupture: a retrospective study. Acta Obstet Gynecol Scand 82: Nazir M, Stien R, Carlsen E et al (2003) Early evaluation of bowel symptoms after primary repair of obstetric perineal rupture misleading. Dis Colon Rectum 46(9): Tetzschner T, Sørensen M, Lose G et al (1996) Anal and urinary incontinence in women with obstetric anal sphincter rupture. BJOG 103: Ustal Fornell E, Wingeren G, Kjølhede P (2004) Factors associated with pelvic floor dysfunction with emphasis on urinary and fecal incontinence and genital prolapse: an epidemiological study. Acta Obstet Gynecol Scand 83: Otero M, Boulvain M, Bianchi-Demicheli F et al (2006) Women s health 18 years after rupture of the anal sphincter during childbirth. II Urinary incontinence, sexual function, and physical and mental health. Am J Obstet Gynecol 194(5): Glazener CMA, Herbison GP, MacAthur C et al (2006) New postnatal urinary incontinence: obstetric and other risk factors in primiparae. BJOG 113: Foldsprang A, Hvidman L, Mommsen S et al (2004) Risk of postpartum urinary incontinence associated with pregnancy and mode of delivery. Acta Obstet Scand 83: Farrell S, Allen VM, Baskett TF (2001) Parturition and urinary incontinence in primiparas. Obstet Gynecol 97(3): Avery K, Donovan JL, Abrams P (2001) Validation of a new questionnaire for incontinence: the international consultation on incontinence questionnaire (ICI-Q). Neurourol Urodyn 20: Donovan JL, Badia X,Corcos J (2002) Symptoms and quality of life assessment. In: Abrams P, Cardozo L, Khoury S, Wein A (eds) Incontinence, 2nd edn. Health Publication Bristol,pp Andrews V, Sultan AH, Thakar R et al (2006) Occult anal sphincter injuries myth or reality. BJOG 113(2): Adams EJ, Fernando RJ (2001) Management of third and fourth degree tears following vaginal deliveries. Royal College of Obstetricians and Gynaecologists 2001; Guideline No Borello-France D, Burgio KL, Richter HE et al (2006) Fecal and urinary incontinence in primiparous women. Obstet Gynecol 108 (4): Fritsch H, Mitterberger M, Barbel G et al (2006) What are the supportive structures of the female urethra. Neurourol Urodyn 25 (2): Dietz HP, Lanzarone V (2005) Levator trauma after vaginal delivery. Obstet Gynecol 106(4): Dolan LM, Hosker GL, Mallett VT et al (2003) Stress incontinence and pelvic floor neurophysiology 15 years after first delivery. BJOG 110:
Occult anal sphincter injuries myth or reality?
 DOI: 10.1111/j.1471-0528.2006.00799.x www.blackwellpublishing.com/bjog Intrapartum care Occult anal sphincter injuries myth or reality? Vasanth Andrews, a Abdul H Sultan, a Ranee Thakar, a Peter W Jones
DOI: 10.1111/j.1471-0528.2006.00799.x www.blackwellpublishing.com/bjog Intrapartum care Occult anal sphincter injuries myth or reality? Vasanth Andrews, a Abdul H Sultan, a Ranee Thakar, a Peter W Jones
Anal Sphincter Injuries: Acute Management
 Anal Sphincter Injuries: Acute Management Dr Stephen Jeffery Urogynaecology Consultant Department of Obstetrics & Gynaecology Groote Schuur Hospital Colorectal Surgeons Gynaecologists Gynaecologists Colorectal
Anal Sphincter Injuries: Acute Management Dr Stephen Jeffery Urogynaecology Consultant Department of Obstetrics & Gynaecology Groote Schuur Hospital Colorectal Surgeons Gynaecologists Gynaecologists Colorectal
NEW POSTNATAL URINARY INCONTINENCE : OBSTETRIC AND OTHER RISK FACTORS IN PRIMIPARAE. New postnatal urinary incontinence in primiparae
 Author Posting. The Authors 2006. This is the author s version of the work. It is posted here for personal use, not for redistribution. The definitive version was published in BJOG, 113(2):208-17. doi:10.1111/j.1471-0528.2005.00840.x
Author Posting. The Authors 2006. This is the author s version of the work. It is posted here for personal use, not for redistribution. The definitive version was published in BJOG, 113(2):208-17. doi:10.1111/j.1471-0528.2005.00840.x
Pregnancy and delivery: a urodynamic viewpoint
 British Journal of Obstetrics and Gynaecology November 2000, Vol107, pp. 1354-1359 Pregnancy and delivery: a urodynamic viewpoint *C. Chaliha Research Fellow (Urogynaecology),** J. M. Bland Professor (Medical
British Journal of Obstetrics and Gynaecology November 2000, Vol107, pp. 1354-1359 Pregnancy and delivery: a urodynamic viewpoint *C. Chaliha Research Fellow (Urogynaecology),** J. M. Bland Professor (Medical
FACTORS ASSOCIATED WITH URINARY STRESS INCONTINENCE IN PRIMIPARAS
 P.L. Chou, et al ORIGINAL ARTICLE FACTORS ASSOCIATED WITH URINARY STRESS INCONTINENCE IN PRIMIPARAS Pei-Ling Chou, Fang-Ping Chen*, Li-Fen Teng Department of Obstetrics and Gynecology, Keelung Chang Gung
P.L. Chou, et al ORIGINAL ARTICLE FACTORS ASSOCIATED WITH URINARY STRESS INCONTINENCE IN PRIMIPARAS Pei-Ling Chou, Fang-Ping Chen*, Li-Fen Teng Department of Obstetrics and Gynecology, Keelung Chang Gung
Postpartum Complications
 ACOG Postpartum Toolkit Postpartum Complications Introduction The effects of pregnancy on many organ systems begin to resolve spontaneously after birth of the infant and delivery of the placenta. The timeline
ACOG Postpartum Toolkit Postpartum Complications Introduction The effects of pregnancy on many organ systems begin to resolve spontaneously after birth of the infant and delivery of the placenta. The timeline
Pregnancy and childbirth: the effects on pelvic floor muscles
 Page 1 of 9 Pregnancy and childbirth: the effects on pelvic floor muscles 26 February, 2009 Stress incontinence can follow childbirth as pelvic floor muscles are damaged AUTHOR Julia Herbert, MSc, MCSP,
Page 1 of 9 Pregnancy and childbirth: the effects on pelvic floor muscles 26 February, 2009 Stress incontinence can follow childbirth as pelvic floor muscles are damaged AUTHOR Julia Herbert, MSc, MCSP,
Obstetric Anal Sphincter Injury- A guideline. Mr David Sim Ms Patricia McStay. Dr Martina Hogan Dept./Division Only: YES-IMWH Directorate Only: NO
 CLINICAL GUIDELINES ID TAG Title: Obstetric Anal Sphincter Injury- A guideline Author: Dr Foteini Verani Designation: Specialist Doctor Speciality / Division: Obstetrics-IMWH Directorate: Acute Services
CLINICAL GUIDELINES ID TAG Title: Obstetric Anal Sphincter Injury- A guideline Author: Dr Foteini Verani Designation: Specialist Doctor Speciality / Division: Obstetrics-IMWH Directorate: Acute Services
Faecal incontinence after childbirth
 Britisb Journal of Obstetrics and Gynaecology January 1997, Vol. 104, pp. 4650 Faecal incontinence after childbirth *Christine MacArthur Reader (Maternal and Child Epidemiology), *Debra E. Bick Research
Britisb Journal of Obstetrics and Gynaecology January 1997, Vol. 104, pp. 4650 Faecal incontinence after childbirth *Christine MacArthur Reader (Maternal and Child Epidemiology), *Debra E. Bick Research
Anal Incontinence After Vaginal Delivery: A Five-Year Prospective Cohort Study
 ORIGINAL RESEARCH Anal Incontinence After Vaginal Delivery: A Five-Year Prospective Cohort Study Johan Pollack, MD, Johan Nordenstam, MD, Sophia Brismar, MD, Annika Lopez, MD, PhD, Daniel Altman, MD, and
ORIGINAL RESEARCH Anal Incontinence After Vaginal Delivery: A Five-Year Prospective Cohort Study Johan Pollack, MD, Johan Nordenstam, MD, Sophia Brismar, MD, Annika Lopez, MD, PhD, Daniel Altman, MD, and
AN INTERNATIONAL CONTINENCE SOCIETY (ICS) / INTERNATIONAL UROGYNAECOLOGICAL ASSOCIATION (IUGA) JOINT REPORT ON THE TERMINOLOGY FOR CHILDBIRTH TRAUMA
 AN INTERNATIONAL CONTINENCE SOCIETY (ICS) / INTERNATIONAL UROGYNAECOLOGICAL ASSOCIATION (IUGA) JOINT REPORT ON THE TERMINOLOGY FOR CHILDBIRTH TRAUMA NEED FOR A WORKING GROUP ON CHILDBIRTH TRAUMA A: Background
AN INTERNATIONAL CONTINENCE SOCIETY (ICS) / INTERNATIONAL UROGYNAECOLOGICAL ASSOCIATION (IUGA) JOINT REPORT ON THE TERMINOLOGY FOR CHILDBIRTH TRAUMA NEED FOR A WORKING GROUP ON CHILDBIRTH TRAUMA A: Background
Obstetric Anal Sphincter Injury. An update on best practices. Objectives
 Obstetric Anal Sphincter Injury An update on best practices Erin Crosby MD Assistant Professor Department of OB/Gyn Division of FPMRS 1 Objectives Describe the anatomy of the anal sphincter complex Discuss
Obstetric Anal Sphincter Injury An update on best practices Erin Crosby MD Assistant Professor Department of OB/Gyn Division of FPMRS 1 Objectives Describe the anatomy of the anal sphincter complex Discuss
Vincent Letouzey, MD, PhD
 How to protect the perineum and prevent obstetric perineal trauma Standards of OASIS diagnosis: Primary (clinical) and Secondary (ultrasound) Vincent Letouzey, MD, PhD Obst/Gyne Dept Nîmes University Hospital
How to protect the perineum and prevent obstetric perineal trauma Standards of OASIS diagnosis: Primary (clinical) and Secondary (ultrasound) Vincent Letouzey, MD, PhD Obst/Gyne Dept Nîmes University Hospital
K. Jundt 1, I. scheer 2, v. von Bodungen 1, F. Krumbachner 1, K. Friese 1, U. M. Peschers 3
 362 EU Ro PE an JoUR nal of MED I cal RE search Eur J Med Res (2010) 15: 362-366 I. Holzapfel Publishers 2010 WHat HaRM DoEs a second DElIvERy to the PElvIc FlooR? K. Jundt 1, I. scheer 2, v. von Bodungen
362 EU Ro PE an JoUR nal of MED I cal RE search Eur J Med Res (2010) 15: 362-366 I. Holzapfel Publishers 2010 WHat HaRM DoEs a second DElIvERy to the PElvIc FlooR? K. Jundt 1, I. scheer 2, v. von Bodungen
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Screening of Immediate Post Partum Females for Urinary Incontinence Ami Vishal Mehta 1, Zarna
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Screening of Immediate Post Partum Females for Urinary Incontinence Ami Vishal Mehta 1, Zarna
OBSTETRICALLY-CAUSED ANAL SPHINCTER INJURY PREDICTION, MANAGEMENT, PREVENTION
 OBSTETRICALLY-CAUSED ANAL SPHINCTER INJURY PREDICTION, MANAGEMENT, PREVENTION COLM O HERLIHY, MD Professor and Chair University College Dublin Department of Obstetrics and Gynaecology National Maternity
OBSTETRICALLY-CAUSED ANAL SPHINCTER INJURY PREDICTION, MANAGEMENT, PREVENTION COLM O HERLIHY, MD Professor and Chair University College Dublin Department of Obstetrics and Gynaecology National Maternity
Appendix B Protocol for management of obstetric anal sphincter injury THE MANAGEMENT OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS
 Appendix B Protocol for management of obstetric anal sphincter injury Document Type: THE MANAGEMENT OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS PURPOSE & SCOPE To provide a guideline that will assist in
Appendix B Protocol for management of obstetric anal sphincter injury Document Type: THE MANAGEMENT OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS PURPOSE & SCOPE To provide a guideline that will assist in
How to repair an anal sphincter injury after vaginal delivery: results of a randomised controlled trial
 DOI: 10.1111/j.1471-0528.2006.00806.x www.blackwellpublishing.com/bjog Intrapartum care How to repair an anal sphincter injury after vaginal delivery: results of a randomised controlled trial Abimbola
DOI: 10.1111/j.1471-0528.2006.00806.x www.blackwellpublishing.com/bjog Intrapartum care How to repair an anal sphincter injury after vaginal delivery: results of a randomised controlled trial Abimbola
Does delayed child-bearing increase the risk of levator injury in labour?
 Australian and New Zealand Journal of Obstetrics and Gynaecology 2007; 47: 491 495 Blackwell Publishing Asia Original Article Delayed child-bearing and levator injury Does delayed child-bearing increase
Australian and New Zealand Journal of Obstetrics and Gynaecology 2007; 47: 491 495 Blackwell Publishing Asia Original Article Delayed child-bearing and levator injury Does delayed child-bearing increase
Effect of subsequent vaginal delivery on bowel symptoms and anorectal function in women who sustained a previous obstetric anal sphincter injury
 International Urogynecology Journal (2018) 29:1579 1588 https://doi.org/10.1007/s00192-018-3601-y ORIGINAL ARTICLE Effect of subsequent vaginal delivery on bowel symptoms and anorectal function in women
International Urogynecology Journal (2018) 29:1579 1588 https://doi.org/10.1007/s00192-018-3601-y ORIGINAL ARTICLE Effect of subsequent vaginal delivery on bowel symptoms and anorectal function in women
Anal incontinence after childbirth is more common than was previously believed. Anal incontinence after childbirth. Methods
 Anal incontinence after childbirth Research Recherche From *the Department of Obstetrics and Gynecology, University of Ottawa, Ottawa, Ont.; the Departments of Family Medicine and Social and Preventive
Anal incontinence after childbirth Research Recherche From *the Department of Obstetrics and Gynecology, University of Ottawa, Ottawa, Ont.; the Departments of Family Medicine and Social and Preventive
Natural progression of anal incontinence after childbirth
 Int Urogynecol J (2009) 20:1029 1035 DOI 10.1007/s00192-009-0901-2 ORIGINAL ARTICLE Natural progression of anal incontinence after childbirth Johan Nordenstam & Daniel Altman & Sophia Brismar & Jan Zetterström
Int Urogynecol J (2009) 20:1029 1035 DOI 10.1007/s00192-009-0901-2 ORIGINAL ARTICLE Natural progression of anal incontinence after childbirth Johan Nordenstam & Daniel Altman & Sophia Brismar & Jan Zetterström
Doctor s assessment and evaluation of the pelvic floor in antenatal and postpartum women: routine or???
 Doctor s assessment and evaluation of the pelvic floor in antenatal and postpartum women: routine or??? Dr Barry O Reilly Head of department of Urogynaecology Cork University Maternity Hospital Ireland
Doctor s assessment and evaluation of the pelvic floor in antenatal and postpartum women: routine or??? Dr Barry O Reilly Head of department of Urogynaecology Cork University Maternity Hospital Ireland
(UI Urine incontinence)! " # $% &'! ( ) * " " +, -. &/ !!" # $%& /'0 = ='' &!( )'*(" &%: "## $ "% % &' ( )* .!
 39/0/5: 39//8:! "#/7 / 6 4 3!!" # $%& /'0 -. (SI Stress incontinence) '' &!( )'*("&%!%!" #$ :!*8>4 &'!% = / ;
39/0/5: 39//8:! "#/7 / 6 4 3!!" # $%& /'0 -. (SI Stress incontinence) '' &!( )'*("&%!%!" #$ :!*8>4 &'!% = / ;
The diagnostic strength of the 24-h pad test for self-reported symptoms of urinary incontinence in pregnancy and after childbirth
 Int Urogynecol J (8) 19:525 53 DOI.7/s192-7-472-z ORIGINAL ARTICLE The diagnostic strength of the 24-h pad test for self-reported symptoms of urinary incontinence in pregnancy and after childbirth Jacobus
Int Urogynecol J (8) 19:525 53 DOI.7/s192-7-472-z ORIGINAL ARTICLE The diagnostic strength of the 24-h pad test for self-reported symptoms of urinary incontinence in pregnancy and after childbirth Jacobus
Interventions METHODS
 Prevention of postpartum stress incontinence PREVENTION OF POSTPARTUM STRESS INCONTINENCE 69 There is good evidence that postnatal pelvic floor exercises are effective in the treatment of postpartum stress
Prevention of postpartum stress incontinence PREVENTION OF POSTPARTUM STRESS INCONTINENCE 69 There is good evidence that postnatal pelvic floor exercises are effective in the treatment of postpartum stress
The urethral support system during pregnancy and after childbirth Wijma, Jacobus
 University of Groningen The urethral support system during pregnancy and after childbirth Wijma, Jacobus IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish
University of Groningen The urethral support system during pregnancy and after childbirth Wijma, Jacobus IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish
Urinary Incontinence after Vaginal Delivery or Cesarean Section
 The new england journal of medicine original article Urinary after Vaginal Delivery or Cesarean Section Guri Rortveit, M.D., Anne Kjersti Daltveit, Ph.D., Yngvild S. Hannestad, M.D., and Steinar Hunskaar,
The new england journal of medicine original article Urinary after Vaginal Delivery or Cesarean Section Guri Rortveit, M.D., Anne Kjersti Daltveit, Ph.D., Yngvild S. Hannestad, M.D., and Steinar Hunskaar,
DOES POST PARTUM PELVIC FLOOR EXERCISES REDUCE ANAL AND URINARY INCONTINENCE?
 DOES POST PARTUM PELVIC FLOOR EXERCISES REDUCE ANAL AND URINARY INCONTINENCE?.* Mohamed El-Negeri', Mohamed Eltotongy \ Maged Elshamy AbdA. Yasser Abdel Dayem'", waleed Omar \ Waleed Thabet Elrefaei, Department
DOES POST PARTUM PELVIC FLOOR EXERCISES REDUCE ANAL AND URINARY INCONTINENCE?.* Mohamed El-Negeri', Mohamed Eltotongy \ Maged Elshamy AbdA. Yasser Abdel Dayem'", waleed Omar \ Waleed Thabet Elrefaei, Department
The Perineal Clinic: - the management of women following OASI
 The Perineal Clinic: - the management of women following OASI Miss Gillian Fowler Consultant Urogynaecologist MBChB, MD, MRCOG Liverpool Women s Hospital. Margie Polden University Memorial of Liverpool
The Perineal Clinic: - the management of women following OASI Miss Gillian Fowler Consultant Urogynaecologist MBChB, MD, MRCOG Liverpool Women s Hospital. Margie Polden University Memorial of Liverpool
Stress urinary incontinence 4 years after the first delivery: a retrospective cohort survey.
 Stress urinary incontinence 4 years after the first delivery: a retrospective cohort survey. Xavier Fritel, Arnaud Fauconnier, Caroline Levet, Jean-Louis Bénifla To cite this version: Xavier Fritel, Arnaud
Stress urinary incontinence 4 years after the first delivery: a retrospective cohort survey. Xavier Fritel, Arnaud Fauconnier, Caroline Levet, Jean-Louis Bénifla To cite this version: Xavier Fritel, Arnaud
Papers. Abstract. Introduction. Methods
 Conservative management of persistent postnatal urinary and faecal incontinence: randomised controlled trial Topic: 66;68;159;161 Cathryn M A Glazener, G Peter Herbison, P Don Wilson, Christine MacArthur,
Conservative management of persistent postnatal urinary and faecal incontinence: randomised controlled trial Topic: 66;68;159;161 Cathryn M A Glazener, G Peter Herbison, P Don Wilson, Christine MacArthur,
Childbirth Trauma & Its Complications 23/ Mr Stergios K. Doumouchtsis
 Mr Stergios K. Doumouchtsis Consultant Obstetrician Gynaecologist & Urogynaecologist Childbirth Trauma & Its Complications Over eighty per cent of women sustain some degree of perineal trauma during childbirth.
Mr Stergios K. Doumouchtsis Consultant Obstetrician Gynaecologist & Urogynaecologist Childbirth Trauma & Its Complications Over eighty per cent of women sustain some degree of perineal trauma during childbirth.
Royal College of Obstetricians and Gynaecologists
 Royal College of Obstetricians and Gynaecologists Consent Advice No. 9 June 2010 REPAIR OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS FOLLOWING CHILDBIRTH This is the first edition of this guidance. This
Royal College of Obstetricians and Gynaecologists Consent Advice No. 9 June 2010 REPAIR OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS FOLLOWING CHILDBIRTH This is the first edition of this guidance. This
Prevalence and Risk Factors for Urinary and Fecal Incontinence Four Months After Vaginal Delivery
 WOMEN'S HEALTH WOMEN'S HEALTH Prevalence and Risk Factors for Urinary and Fecal Incontinence Four Months After Vaginal Delivery Sandra A. Baydock, MD, 1 Catherine Flood, MD, 1 Jane A. Schulz, MD, 1 Dianna
WOMEN'S HEALTH WOMEN'S HEALTH Prevalence and Risk Factors for Urinary and Fecal Incontinence Four Months After Vaginal Delivery Sandra A. Baydock, MD, 1 Catherine Flood, MD, 1 Jane A. Schulz, MD, 1 Dianna
Pregnancy related pelvic floor dysfunction- suggested teaching presentation for Midwives
 Pregnancy related pelvic floor dysfunction- suggested teaching presentation for Midwives 1 Aims of this self assessment competency To equip Midwives with the knowledge and skills to teach pelvic floor
Pregnancy related pelvic floor dysfunction- suggested teaching presentation for Midwives 1 Aims of this self assessment competency To equip Midwives with the knowledge and skills to teach pelvic floor
The urethral support system during pregnancy and after childbirth Wijma, Jacobus
 University of Groningen The urethral support system during pregnancy and after childbirth Wijma, Jacobus IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish
University of Groningen The urethral support system during pregnancy and after childbirth Wijma, Jacobus IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish
Operative Vaginal Delivery and Pelvic Floor Trauma. Anna Padoa, MD Urogynecology Service Dept of Ob & Gyn Assaf Harofe Medical Center
 + Operative Vaginal Delivery and Pelvic Floor Trauma Anna Padoa, MD Urogynecology Service Dept of Ob & Gyn Assaf Harofe Medical Center + Vaginal birth and the pelvic floor Mechanisms of injury Damage to
+ Operative Vaginal Delivery and Pelvic Floor Trauma Anna Padoa, MD Urogynecology Service Dept of Ob & Gyn Assaf Harofe Medical Center + Vaginal birth and the pelvic floor Mechanisms of injury Damage to
Dr Anne Sneddon Director of Obstetrics and Gynaecology Lecturer, ANU Medical School The Canberra Hospital
 Dr Anne Sneddon Director of Obstetrics and Gynaecology Lecturer, ANU Medical School The Canberra Hospital Capital city of Australia Population 350,000 but surrounding region of 500,000 Seat of government
Dr Anne Sneddon Director of Obstetrics and Gynaecology Lecturer, ANU Medical School The Canberra Hospital Capital city of Australia Population 350,000 but surrounding region of 500,000 Seat of government
Childbirth and prolapse: long-term associations with the symptoms and objective measurement of pelvic organ prolapse
 DOI: 10.1111/1471-0528.12075 www.bjog.org Epidemiology Childbirth and prolapse: long-term associations with the symptoms and objective measurement of pelvic organ prolapse C Glazener, a A Elders, a C MacArthur,
DOI: 10.1111/1471-0528.12075 www.bjog.org Epidemiology Childbirth and prolapse: long-term associations with the symptoms and objective measurement of pelvic organ prolapse C Glazener, a A Elders, a C MacArthur,
Faecal incontinence persisting after childbirth: a 12 year longitudinal
 Author Posting. The Authors 2013. This is the authors version of the work. It is posted here for personal use, not for redistribution. The definitive version was published in British Journal of Obstetrics
Author Posting. The Authors 2013. This is the authors version of the work. It is posted here for personal use, not for redistribution. The definitive version was published in British Journal of Obstetrics
Hands-on Workshop. Cape Town, South Africa 3 August Chairpersons
 Hands-on Workshop www.perineum.net Cape Town, South Africa 3 August 2016 Chairpersons Mr Abdul H Sultan, MB.ChB (Natal), MD, FRCOG Consultant Obstetrician & Urogynaecologist Miss Ranee Thakar, MB.BS, MD,
Hands-on Workshop www.perineum.net Cape Town, South Africa 3 August 2016 Chairpersons Mr Abdul H Sultan, MB.ChB (Natal), MD, FRCOG Consultant Obstetrician & Urogynaecologist Miss Ranee Thakar, MB.BS, MD,
Effect of postpartum pelvic floor muscle training in prevention and treatment of urinary incontinence: a one-year follow up
 British Journal of Obstetrics and Gynaecology August 2000, V01107, pp. 1022-1028 Effect of postpartum pelvic floor muscle training in prevention and treatment of urinary incontinence: a one-year follow
British Journal of Obstetrics and Gynaecology August 2000, V01107, pp. 1022-1028 Effect of postpartum pelvic floor muscle training in prevention and treatment of urinary incontinence: a one-year follow
Third & Fourth Degree Tears guideline (GL926)
 Third & Fourth Degree Tears guideline (GL926) Approval Approval Group Job Title, Chair of Committee Date Maternity & Children s Services Clinical Governance Committee Chair, Maternity Clinical Governance
Third & Fourth Degree Tears guideline (GL926) Approval Approval Group Job Title, Chair of Committee Date Maternity & Children s Services Clinical Governance Committee Chair, Maternity Clinical Governance
2/25/2013. Speaker Disclosure. Learning Objectives. Ob/Gyn Conference Series: Urinary and Fecal Incontinence After Vaginal Childbirth
 Ob/Gyn Conference Series: Urinary and Fecal Incontinence After Vaginal Childbirth Jaime Sepulveda-Toro MD FACS FACOG Female Pelvic Medicine and Reconstructive Pelvic Surgery South Miami Hospital Speaker
Ob/Gyn Conference Series: Urinary and Fecal Incontinence After Vaginal Childbirth Jaime Sepulveda-Toro MD FACS FACOG Female Pelvic Medicine and Reconstructive Pelvic Surgery South Miami Hospital Speaker
Obstetric anal sphincter injury is the most common
 Repair Techniques for Obstetric Anal Sphincter Injuries A Randomized Controlled Trial Ruwan J. Fernando, MD, MRCOG, Abdul H. Sultan, MD, FRCOG, Christine Kettle, PhD, Simon Radley, MD, FRCS, Peter Jones,
Repair Techniques for Obstetric Anal Sphincter Injuries A Randomized Controlled Trial Ruwan J. Fernando, MD, MRCOG, Abdul H. Sultan, MD, FRCOG, Christine Kettle, PhD, Simon Radley, MD, FRCS, Peter Jones,
Childbirth after pelvic floor surgery: analysis of Hospital Episode Statistics in England,
 DOI: 10.1111/1471-0528.12076 www.bjog.org Urogynaecology Childbirth after pelvic floor surgery: analysis of Hospital Episode Statistics in England, 2002 2008 A Pradhan, a DG Tincello, b R Kearney a a Department
DOI: 10.1111/1471-0528.12076 www.bjog.org Urogynaecology Childbirth after pelvic floor surgery: analysis of Hospital Episode Statistics in England, 2002 2008 A Pradhan, a DG Tincello, b R Kearney a a Department
2/5/2016. Evolving Surgical Treatment Approaches for Fecal Incontinence in Women: An Evidence and Cased-Based Approach
 Evolving Surgical Treatment Approaches for Fecal Incontinence in Women: An Evidence and Cased-Based Approach Holly E Richter, PhD, MD, FACOG, FACS J Marion Sims Professor Obstetrics and Gynecology Professor
Evolving Surgical Treatment Approaches for Fecal Incontinence in Women: An Evidence and Cased-Based Approach Holly E Richter, PhD, MD, FACOG, FACS J Marion Sims Professor Obstetrics and Gynecology Professor
Pelvic Floor Ultrasound Imaging. Prof HP Dietz (Sydney) A/Prof KL Shek (Sydney) Dr R Guzman Rojas (Santiago de Chile) Dr Kamil Svabik (Prague)
 Pelvic Floor Ultrasound Imaging Workshop IUGA 2015 Nice Faculty: Prof HP Dietz (Sydney) A/Prof KL Shek (Sydney) Dr R Guzman Rojas (Santiago de Chile) Dr Kamil Svabik (Prague) The use of translabial ultrasound
Pelvic Floor Ultrasound Imaging Workshop IUGA 2015 Nice Faculty: Prof HP Dietz (Sydney) A/Prof KL Shek (Sydney) Dr R Guzman Rojas (Santiago de Chile) Dr Kamil Svabik (Prague) The use of translabial ultrasound
Obstetric pelvic floor and anal sphincter injuries
 DOI: 10.1111/j.1744-4667.2012.00133.x The Obstetrician & Gynaecologist http://onlinetog.org 2012;14:257 66 Review Obstetric pelvic floor and anal sphincter injuries Farah Lone MBBS MRCOG, a Abdul Sultan
DOI: 10.1111/j.1744-4667.2012.00133.x The Obstetrician & Gynaecologist http://onlinetog.org 2012;14:257 66 Review Obstetric pelvic floor and anal sphincter injuries Farah Lone MBBS MRCOG, a Abdul Sultan
The development of a questionnaire to measure the severity of symptoms and the quality of life before and after surgery for stress incontinence
 BJOG: an International Journal of Obstetrics and Gynaecology November 2003, Vol. 110, pp. 983 988 The development of a questionnaire to measure the severity of symptoms and the quality of life before and
BJOG: an International Journal of Obstetrics and Gynaecology November 2003, Vol. 110, pp. 983 988 The development of a questionnaire to measure the severity of symptoms and the quality of life before and
Secondary Repair of Third Degree Perineal Tear Leading to Fecal Incontinence in 2 Cases
 CASE REPORT Secondary Repair of Third Degree Perineal Tear Leading to Fecal Incontinence in 2 Cases Vasant Kawade 1 and Abhijit Ambike 2 Professor and Head, Department of OBGY, B.K.L.Walawakarl Rural Medical
CASE REPORT Secondary Repair of Third Degree Perineal Tear Leading to Fecal Incontinence in 2 Cases Vasant Kawade 1 and Abhijit Ambike 2 Professor and Head, Department of OBGY, B.K.L.Walawakarl Rural Medical
Post-partum Anal Incontinence in SA: A myth or reality?
 Post-partum Anal Incontinence in SA: A myth or reality? TD Naidoo Consultant and Honorary Lecturer, Department of Obstetrics and Gynaecology, Grey s Hospital, Pietermaritzburg Metropolitan Hospitals Complex,
Post-partum Anal Incontinence in SA: A myth or reality? TD Naidoo Consultant and Honorary Lecturer, Department of Obstetrics and Gynaecology, Grey s Hospital, Pietermaritzburg Metropolitan Hospitals Complex,
Effects of Combined Pelvic Floor Muscle Exercises in Patient with Urinary Incontinence
 MACROJOURNALS The Journal of MacroTrends in Health and Medicine Effects of Combined Pelvic Floor Muscle Exercises in Patient with Urinary Incontinence Vjollca Ndreu*, Fatjona Kamberi*, Enkeleda Sinaj*,
MACROJOURNALS The Journal of MacroTrends in Health and Medicine Effects of Combined Pelvic Floor Muscle Exercises in Patient with Urinary Incontinence Vjollca Ndreu*, Fatjona Kamberi*, Enkeleda Sinaj*,
Among parous women, cesarean birth reduces the
 Pelvic Floor Disorders After Vaginal Birth Effect of Episiotomy, Perineal Laceration, and Operative Birth Victoria L. Handa, MD, MHS, Joan L. Blomquist, MD, Kelly C. McDermott, BS, Sarah Friedman, MD,
Pelvic Floor Disorders After Vaginal Birth Effect of Episiotomy, Perineal Laceration, and Operative Birth Victoria L. Handa, MD, MHS, Joan L. Blomquist, MD, Kelly C. McDermott, BS, Sarah Friedman, MD,
How big is the problem? Incontinence in numbers
 How big is the problem? Incontinence in numbers Ian Milsom Gothenburg Continence Research Center (GCRC) Sahlgrenska Academy, Gothenburg University Gothenburg, Sweden If UI where a country, 2 it would be
How big is the problem? Incontinence in numbers Ian Milsom Gothenburg Continence Research Center (GCRC) Sahlgrenska Academy, Gothenburg University Gothenburg, Sweden If UI where a country, 2 it would be
Urogynaecology. Introduction. M Gyhagen, a M Bullarbo, a,b TF Nielsen, a,b I Milsom a
 DOI: 10.1111/1471-0528.12367 www.bjog.org Urogynaecology A comparison of the long-term consequences of vaginal delivery versus caesarean section on the prevalence, severity and bothersomeness of urinary
DOI: 10.1111/1471-0528.12367 www.bjog.org Urogynaecology A comparison of the long-term consequences of vaginal delivery versus caesarean section on the prevalence, severity and bothersomeness of urinary
Maternity Information Leaflet. Care of the Perineum (including Pelvic Floor Exercises) Version 2
 Maternity Information Leaflet Care of the Perineum (including Pelvic Floor Exercises) Version 2 Pelvic Floor Exercises The pelvic floor muscles are located between your legs, and run from your pubic bone
Maternity Information Leaflet Care of the Perineum (including Pelvic Floor Exercises) Version 2 Pelvic Floor Exercises The pelvic floor muscles are located between your legs, and run from your pubic bone
Midline episiotomy and anal incontinence: retrospective cohort study
 Obstetrics and Gynecology Epidemiology Center, Brigham and Women s Hospital, Harvard Medical School, 221 Longwood Avenue, Boston, MA 02115, Lisa B Signorello study coordinator Bernard L Harlow associate
Obstetrics and Gynecology Epidemiology Center, Brigham and Women s Hospital, Harvard Medical School, 221 Longwood Avenue, Boston, MA 02115, Lisa B Signorello study coordinator Bernard L Harlow associate
The relationship between postpartum levator ani muscle avulsion and signs and symptoms of pelvic floor dysfunction
 DOI: 10.1111/1471-0528.12666 www.bjog.org Urogynaecology The relationship between postpartum levator ani muscle avulsion and signs and symptoms of pelvic floor dysfunction K van Delft, a AH Sultan, a R
DOI: 10.1111/1471-0528.12666 www.bjog.org Urogynaecology The relationship between postpartum levator ani muscle avulsion and signs and symptoms of pelvic floor dysfunction K van Delft, a AH Sultan, a R
Review Article Pelvic Floor Dysfunction, Body Excreta Incontinence and Continence
 Cronicon OPEN ACCESS GYNAECOLOGY Review Article Pelvic Floor Dysfunction, Body Excreta Incontinence and Continence Abdel Karim M El Hemaly 1 * and Laila ASE Mousa 1 1 Professor of Obstetrics and gynaecology,
Cronicon OPEN ACCESS GYNAECOLOGY Review Article Pelvic Floor Dysfunction, Body Excreta Incontinence and Continence Abdel Karim M El Hemaly 1 * and Laila ASE Mousa 1 1 Professor of Obstetrics and gynaecology,
ACCIDENTAL BOWEL LEAKAGE: A PRACTICAL APPROACH TO EVALUATION. Tristi W. Muir, MD Chair, Department of OB/GYN Houston Methodist Hospital
 ACCIDENTAL BOWEL LEAKAGE: A PRACTICAL APPROACH TO EVALUATION Tristi W. Muir, MD Chair, Department of OB/GYN Houston Methodist Hospital Accidental Bowel Leakage What Gets the Woman into Your Office 67%
ACCIDENTAL BOWEL LEAKAGE: A PRACTICAL APPROACH TO EVALUATION Tristi W. Muir, MD Chair, Department of OB/GYN Houston Methodist Hospital Accidental Bowel Leakage What Gets the Woman into Your Office 67%
ijer.skums.ac.ir Risk factors of pelvic organ prolapse in Iranian women: a cross-sectional study
 International Journal of Epidemiologic Research, 2014; 1 (1): 29-34. ijer.skums.ac.ir Risk factors of pelvic organ prolapse in Iranian women: a cross-sectional study Ashraf Direkvand-Moghadam 1 ; Zeinab
International Journal of Epidemiologic Research, 2014; 1 (1): 29-34. ijer.skums.ac.ir Risk factors of pelvic organ prolapse in Iranian women: a cross-sectional study Ashraf Direkvand-Moghadam 1 ; Zeinab
Northwest Rehabilitation Associates, Inc.
 Pelvic Health Patient Intake Form Name: Date: Please answer the following questions as honestly and thoroughly as you can. Your responses will help us better understand your condition and provide the best
Pelvic Health Patient Intake Form Name: Date: Please answer the following questions as honestly and thoroughly as you can. Your responses will help us better understand your condition and provide the best
The Pelvic Floor: Expecting (and Delivering!) Susan Barr, MD Assistant Professor Saint Louis University Division of Urogynecology
 The Pelvic Floor: What She Can Expect After Expecting (and Delivering!) Susan Barr, MD Assistant Professor Saint Louis University Division of Urogynecology Objectives Understand risk factors and treatment
The Pelvic Floor: What She Can Expect After Expecting (and Delivering!) Susan Barr, MD Assistant Professor Saint Louis University Division of Urogynecology Objectives Understand risk factors and treatment
Pelvic floor trauma following vaginal delivery Hans Peter Dietz
 Pelvic floor trauma following vaginal delivery Hans Peter Dietz Purpose of review Recent years have seen a steady increase in the information available regarding pelvic floor trauma in childbirth. A review
Pelvic floor trauma following vaginal delivery Hans Peter Dietz Purpose of review Recent years have seen a steady increase in the information available regarding pelvic floor trauma in childbirth. A review
Clinical Guideline for: The Management of Perineal Trauma following Childbirth
 For Use in: By: For: Division responsible for document: Key words: Name of document author: Job title of document author: Name of document author s Line Manager: Job title of author s Line Manager: Supported
For Use in: By: For: Division responsible for document: Key words: Name of document author: Job title of document author: Name of document author s Line Manager: Job title of author s Line Manager: Supported
period, cesarean delivery is thought to protect against anal incontinence, 3 albeit incompletely. In this study, we investigated anal incontinence
 Obstetrical anal sphincter laceration and anal incontinence 5-10 years after childbirth Emily C. Evers, MPH; Joan L. Blomquist, MD; Kelly C. McDermott, BS; Victoria L. Handa, MD, MHS OBJECTIVE: The purpose
Obstetrical anal sphincter laceration and anal incontinence 5-10 years after childbirth Emily C. Evers, MPH; Joan L. Blomquist, MD; Kelly C. McDermott, BS; Victoria L. Handa, MD, MHS OBJECTIVE: The purpose
Why are some women with pelvic floor dysfunction unable to contract their pelvic floor muscles?
 Australian and New Zealand Journal of Obstetrics and Gynaecology 2013; 53: 574 579 DOI: 10.1111/ajo.12133 Original Article Why are some women with pelvic floor dysfunction unable to contract their pelvic
Australian and New Zealand Journal of Obstetrics and Gynaecology 2013; 53: 574 579 DOI: 10.1111/ajo.12133 Original Article Why are some women with pelvic floor dysfunction unable to contract their pelvic
Birth Trauma. H. P. Dietz. University of Sydney, Nepean Campus. Penrith, Australia
 Birth Trauma H. P. Dietz University of Sydney, Nepean Campus Penrith, Australia Procedures in US (2010): 1.6 Prolapse Urinary Incontinence Fecal Incontinence Prolapse 200.000 Urinary Incontinence 120.000
Birth Trauma H. P. Dietz University of Sydney, Nepean Campus Penrith, Australia Procedures in US (2010): 1.6 Prolapse Urinary Incontinence Fecal Incontinence Prolapse 200.000 Urinary Incontinence 120.000
Impact of Delivery Types on Women s Postpartum Sexual Health
 Reproduction & Contraception (2003) 14 (4):237~242 Impact of Delivery Types on Women s Postpartum Sexual Health Huan-ying WANG 1, Xiao-yang XU 2, Zhen-wei YAO 1, Qin ZHOU 1 Key words: postpartum; sexual
Reproduction & Contraception (2003) 14 (4):237~242 Impact of Delivery Types on Women s Postpartum Sexual Health Huan-ying WANG 1, Xiao-yang XU 2, Zhen-wei YAO 1, Qin ZHOU 1 Key words: postpartum; sexual
The effect of pregnancy and mode of delivery on the prevalence of urinary and fecal incontinence
 American Journal of Obstetrics and Gynecology (2005) 193, 512 8 www.ajog.org The effect of pregnancy and mode of delivery on the prevalence of urinary and fecal incontinence Vikki McKinnie, MD, a Steven
American Journal of Obstetrics and Gynecology (2005) 193, 512 8 www.ajog.org The effect of pregnancy and mode of delivery on the prevalence of urinary and fecal incontinence Vikki McKinnie, MD, a Steven
Long-term ailments due to anal sphincter rupture caused by delivery - a hidden problem
 Eur. J. Obstet. Gynecol. Reprod. Biol., 27 (1988) 27-32 Elsevier 27 EJO 00556 Long-term ailments due to anal sphincter rupture caused by delivery - a hidden problem Knut Haadem, Sten Ohrlander and G6ran
Eur. J. Obstet. Gynecol. Reprod. Biol., 27 (1988) 27-32 Elsevier 27 EJO 00556 Long-term ailments due to anal sphincter rupture caused by delivery - a hidden problem Knut Haadem, Sten Ohrlander and G6ran
Initial management of stress urinary incontinence: pelvic floor muscle training and duloxetine
 DOI: 1.1111/j.1471-528.6.878.x www.blackwellpublishing.com/bjog Review article Initial management of stress urinary incontinence: pelvic floor muscle training and duloxetine RM Freeman Urogynaecology Unit,
DOI: 1.1111/j.1471-528.6.878.x www.blackwellpublishing.com/bjog Review article Initial management of stress urinary incontinence: pelvic floor muscle training and duloxetine RM Freeman Urogynaecology Unit,
Pelvic floor trauma in childbirth Myth or reality?
 Australian and New Zealand Journal of Obstetrics and Gynaecology 2005; 45: 3 11 Blackwell Publishing, Ltd. Systematic Review Pelvic floor trauma in childbirth Pelvic floor trauma in childbirth Myth or
Australian and New Zealand Journal of Obstetrics and Gynaecology 2005; 45: 3 11 Blackwell Publishing, Ltd. Systematic Review Pelvic floor trauma in childbirth Pelvic floor trauma in childbirth Myth or
THE PELVIC FLOOR, EPISIOTOMY AND PERINEAL REPAIR AND VAGINAL/RECTAL MEDICATIONS
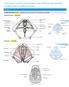 THE PELVIC FLOOR, EPISIOTOMY AND PERINEAL REPAIR AND VAGINAL/RECTAL MEDICATIONS MID2010 LEARNING OBJECTIVE 1 - REVIEW THE ANATOMY OF THE PELVIC FLOOR Superficial layers cavernosus Deep layer Coccygeus
THE PELVIC FLOOR, EPISIOTOMY AND PERINEAL REPAIR AND VAGINAL/RECTAL MEDICATIONS MID2010 LEARNING OBJECTIVE 1 - REVIEW THE ANATOMY OF THE PELVIC FLOOR Superficial layers cavernosus Deep layer Coccygeus
Risk factors and management of obstetric perineal injury
 Risk factors and management of obstetric perineal injury Ruwan J Fernando Abstract Perineal injury sustained during childbirth is a major aetiological factor in the development of perineal pain, sexual
Risk factors and management of obstetric perineal injury Ruwan J Fernando Abstract Perineal injury sustained during childbirth is a major aetiological factor in the development of perineal pain, sexual
Introduction. A joint report by IUGA and the ICS 1 defines anal incontinence (AI) as the unintentional loss of faeces or flatus.
 TD Naidoo J Moodley Introduction A joint report by IUGA and the ICS 1 defines anal incontinence (AI) as the unintentional loss of faeces or flatus. Faecal incontinence is a complaint of involuntary loss
TD Naidoo J Moodley Introduction A joint report by IUGA and the ICS 1 defines anal incontinence (AI) as the unintentional loss of faeces or flatus. Faecal incontinence is a complaint of involuntary loss
URINARY INCONTINENCE AMONG OBESE WOMEN: A CROSS- SECTIONAL STUDY
 WORLD JOURNAL OF PHARMACY AND PHARMACEUTICAL SCIENCES Aisha et al. SJIF Impact Factor 6.647 Volume 6, Issue 9, 1384-1391 Research Article ISSN 2278 4357 URINARY INCONTINENCE AMONG OBESE WOMEN: A CROSS-
WORLD JOURNAL OF PHARMACY AND PHARMACEUTICAL SCIENCES Aisha et al. SJIF Impact Factor 6.647 Volume 6, Issue 9, 1384-1391 Research Article ISSN 2278 4357 URINARY INCONTINENCE AMONG OBESE WOMEN: A CROSS-
Urinary and faecal incontinence following delayed primary repair of obstetric genital fistula
 BJOG: an International Journal of Obstetrics and Gynaecology July 2002, Vol. 109, pp. 828 832 Urinary and faecal incontinence following delayed primary repair of obstetric genital fistula Christine Murray,
BJOG: an International Journal of Obstetrics and Gynaecology July 2002, Vol. 109, pp. 828 832 Urinary and faecal incontinence following delayed primary repair of obstetric genital fistula Christine Murray,
Pelvic floor muscle training for prevention and treatment of urinary and faecal incontinence in antenatal and postnatal women (Review)
 Pelvic floor muscle training for prevention and treatment of urinary and faecal incontinence in antenatal and postnatal women (Review) Boyle R, Hay-Smith EJC, Cody JD, Mørkved S This is a reprint of a
Pelvic floor muscle training for prevention and treatment of urinary and faecal incontinence in antenatal and postnatal women (Review) Boyle R, Hay-Smith EJC, Cody JD, Mørkved S This is a reprint of a
Prevalence and risk factors for pelvic floor symptoms in women in rural El Salvador
 Int Urogynecol J (2007) 18:1065 1069 DOI 10.1007/s00192-006-0292-6 ORIGINAL ARTICLE Prevalence and risk factors for pelvic floor symptoms in women in rural El Salvador Begüm Özel & Anne Marie Borchelt
Int Urogynecol J (2007) 18:1065 1069 DOI 10.1007/s00192-006-0292-6 ORIGINAL ARTICLE Prevalence and risk factors for pelvic floor symptoms in women in rural El Salvador Begüm Özel & Anne Marie Borchelt
NIH Public Access Author Manuscript Int Urogynecol J. Author manuscript; available in PMC 2012 December 06.
 NIH Public Access Author Manuscript Published in final edited form as: Int Urogynecol J. 2011 December ; 22(12): 1491 1495. doi:10.1007/s00192-011-1458-4. URETHRAL CLOSURE PRESSURES AMONG PRIMIPAROUS WOMEN
NIH Public Access Author Manuscript Published in final edited form as: Int Urogynecol J. 2011 December ; 22(12): 1491 1495. doi:10.1007/s00192-011-1458-4. URETHRAL CLOSURE PRESSURES AMONG PRIMIPAROUS WOMEN
Compassionate and effective management
 IMPACT OF STRESS URINARY INCONTINENCE ON QUALITY OF LIFE * Paul Abrams, MD, FRCS ABSTRACT Evaluating the impact of stress urinary incontinence (SUI) on quality of life (QOL) is of paramount importance,
IMPACT OF STRESS URINARY INCONTINENCE ON QUALITY OF LIFE * Paul Abrams, MD, FRCS ABSTRACT Evaluating the impact of stress urinary incontinence (SUI) on quality of life (QOL) is of paramount importance,
Obstetric anal sphincter injuries: Incidence, risk factors, consequences and prevention
 Obstetric anal sphincter injuries: Incidence, risk factors, consequences and prevention Katariina Laine, MD PhD thesis 2013 Katariina Laine, MD Department of Obstetrics Oslo University Hospital, Ullevål
Obstetric anal sphincter injuries: Incidence, risk factors, consequences and prevention Katariina Laine, MD PhD thesis 2013 Katariina Laine, MD Department of Obstetrics Oslo University Hospital, Ullevål
Bill Landry BScPT, BScH, MCPA, CAFCI Family Physiotherapy Centre of London
 Bill Landry BScPT, BScH, MCPA, CAFCI blandry@fpclondon.com Family Physiotherapy Centre of London Objectives To describe the scope of post-prostatectomy incontinence To describe what s been done To provide
Bill Landry BScPT, BScH, MCPA, CAFCI blandry@fpclondon.com Family Physiotherapy Centre of London Objectives To describe the scope of post-prostatectomy incontinence To describe what s been done To provide
Leaking Urine: Prevalence and Associated Factors in Australian Women
 Neurourology and Urodynamics 18:567 577 (1999) Leaking Urine: Prevalence and Associated Factors in Australian Women Pauline Chiarelli, 1 Wendy Brown, 2 * and Patrick McElduff 3 1 Faculty of Medicine and
Neurourology and Urodynamics 18:567 577 (1999) Leaking Urine: Prevalence and Associated Factors in Australian Women Pauline Chiarelli, 1 Wendy Brown, 2 * and Patrick McElduff 3 1 Faculty of Medicine and
Birth trauma: short and long term effects of forceps delivery compared with spontaneous delivery on various pelvic floor parameters
 British Journal of Obstetrics and Gynaecology November 2000, Vol107, pp. 1360-1365 Birth trauma: short and long term effects of forceps delivery compared with spontaneous delivery on various pelvic floor
British Journal of Obstetrics and Gynaecology November 2000, Vol107, pp. 1360-1365 Birth trauma: short and long term effects of forceps delivery compared with spontaneous delivery on various pelvic floor
How common is pelvic floor muscle atrophy after vaginal childbirth?
 Ultrasound Obstet Gynecol 2014; 43: 3 Published online 2 December 2013 in Wiley Online Library wileyonlinelibrary.com. DOI: 10.1002/uog.12543 How common is pelvic floor muscle atrophy after vaginal childbirth?
Ultrasound Obstet Gynecol 2014; 43: 3 Published online 2 December 2013 in Wiley Online Library wileyonlinelibrary.com. DOI: 10.1002/uog.12543 How common is pelvic floor muscle atrophy after vaginal childbirth?
Pelvic Floor Reconstruction
 3.9 Curriculum in Urology Trauma and Reconstruction Pelvic Floor Reconstruction W. Artibani a, Stuart L. Stanton b, D. Kumar c, R. Villet d a University of Verona, Italy; b Saint George Hospital Medical
3.9 Curriculum in Urology Trauma and Reconstruction Pelvic Floor Reconstruction W. Artibani a, Stuart L. Stanton b, D. Kumar c, R. Villet d a University of Verona, Italy; b Saint George Hospital Medical
Anatomical and Functional Results of Pelvic Organ Prolapse Mesh Repair: A Prospective Study of 105 Cases
 International Journal of Clinical Urology 2018; 2(1): 20-24 http://www.sciencepublishinggroup.com/j/ijcu doi: 10.11648/j.ijcu.20180201.14 Anatomical and Functional Results of Pelvic Organ Prolapse Mesh
International Journal of Clinical Urology 2018; 2(1): 20-24 http://www.sciencepublishinggroup.com/j/ijcu doi: 10.11648/j.ijcu.20180201.14 Anatomical and Functional Results of Pelvic Organ Prolapse Mesh
Ben Herbert Alex Wojtowicz
 Ben Herbert Alex Wojtowicz 54 year old female presenting with: Dragging sensation Urinary incontinence Some faecal incontinence HPC Since May 14 had noticed a mass protruding from the vagina when going
Ben Herbert Alex Wojtowicz 54 year old female presenting with: Dragging sensation Urinary incontinence Some faecal incontinence HPC Since May 14 had noticed a mass protruding from the vagina when going
EPISIOTOMY & PERINEAL TEARS Anatomy &Functionality May Dr. Annie Leong MBBS, FRANZCOG, CU
 EPISIOTOMY & PERINEAL TEARS Anatomy &Functionality May 2011 Dr. Annie Leong MBBS, FRANZCOG, CU Restore normal perineal anatomy Achieve good haemostasis Avoid infection and wound breakdown Avoid coital
EPISIOTOMY & PERINEAL TEARS Anatomy &Functionality May 2011 Dr. Annie Leong MBBS, FRANZCOG, CU Restore normal perineal anatomy Achieve good haemostasis Avoid infection and wound breakdown Avoid coital
Surgery for stress incontinence:
 Surgery for stress incontinence: information for you aashara Published February 2005 by the RCOG Contents Key points About this information What is stress incontinence? Do I need an operation? What operation
Surgery for stress incontinence: information for you aashara Published February 2005 by the RCOG Contents Key points About this information What is stress incontinence? Do I need an operation? What operation
EXPECTING A BABY? SOME PREGNANT WOMEN CAN HAVE BLADDER AND BOWEL CONTROL PROBLEMS. YOU CAN GET HELP. HOW DO I KNOW IF I HAVE A PROBLEM?
 11 BLADDER AND BOWEL CONTROL PROBLEMS. When you are pregnant, you get a lot of advice from many people. One topic few people think about is bladder and bowel control problems during pregnancy and after
11 BLADDER AND BOWEL CONTROL PROBLEMS. When you are pregnant, you get a lot of advice from many people. One topic few people think about is bladder and bowel control problems during pregnancy and after
Pudendal Block and Urinary Dysfunction/Retention
 Date of Search: 22 Mar 17 Sources Searched: Medline, Embase, Cinahl, Google Scholar DISCLAIMER: Results of database and or Internet searches are subject to the limitations of both the database(s) searched,
Date of Search: 22 Mar 17 Sources Searched: Medline, Embase, Cinahl, Google Scholar DISCLAIMER: Results of database and or Internet searches are subject to the limitations of both the database(s) searched,
INTERNATIONAL JOURNAL OF WOMEN'S HEALTH AND REPRODUCTION SCIENCES
 Original Article INTERNATIONAL JOURNAL OF WOMEN'S HEALTH AND REPRODUCTION SCIENCES http://www.ijwhr.net Urinary Incontinence During Pregnancy and Postpartum Incidence, Severity and Risk Factors in Alzahra
Original Article INTERNATIONAL JOURNAL OF WOMEN'S HEALTH AND REPRODUCTION SCIENCES http://www.ijwhr.net Urinary Incontinence During Pregnancy and Postpartum Incidence, Severity and Risk Factors in Alzahra
Association between mode of delivery and pelvic floor dysfunction
 Review article Association between mode of delivery and pelvic floor dysfunction 1848 52 BACKGROUND Normal vaginal delivery can cause significant strain on the pelvic floor. We present a review of the
Review article Association between mode of delivery and pelvic floor dysfunction 1848 52 BACKGROUND Normal vaginal delivery can cause significant strain on the pelvic floor. We present a review of the
