Erythrodermic cutaneous T-cell lymphoma: Two case reports
|
|
|
- Osborne Chapman
- 5 years ago
- Views:
Transcription
1 Serbian Journal of Dermatology and Venereology 2009; 3: Erythrodermic cutaneous T-cell lymphoma: Two case reports Miroslav Ž. Dinić 1 *, Lidija Kandolf-Sekulović 1, Tomislav Mladenović 1 and Radoš D. Zečević 1 M. Dinić et al. Erytrodermic cutaneous T-cell lymphoma DOI: /v Department of Dermatology and Venereology, Military Medical Academy, Belgrade *Correspondence: Miroslav Ž. Dinić, miroslavdinic@hotmail.com UDC Abstract Primary cutaneous T-cell lymphomas (CTCLs) are Non-Hodgkin lymphomas where skin may be the only involved organ for a long time. The erythrodermic form of CTCL, including Sezary syndrome, with increased IgE concentration, eosinophilia and intense pruritus, may suggest atopic dermatitis, in the lack of evidence for diagnosis of T-cell lymphoproliferative disorder. After vigorous research, two patients with erythroderma, increased IgE and eosinophilia, were not diagnosed with CTCL. Adult atopic dermatitis was diagnosed, based on clinical examination and histopathologic analysis of the skin sample. Therapy with oral cyclosporin A (CsA) and systemic corticosteroids were initiated, but the improvement was minimal and short-lived. Disease progression was noted in both patients, after a month of cyclosporine therapy: malaise, subfebrile and febrile temperatures, and development of generalized skin nodules were evident. In the first patient (aged 30) repeated examinations confirmed presence of Sezary cells in peripheral blood samples, dominant T-cell clone in the skin, peripheral blood and bone marrow, whereas the last repeated histopathologic analysis revealed T-lymphoproliferative skin disorder. In the second patient, (aged 44) primary cutaneous CD30+ T-cell lymphoma was diagnosed, based on histopathologic analysis of the newly appearing skin nodule. Differential diagnosis of erythroderma is always difficult, since clinical, histopathologic and immunophenotypic findings are frequently insufficient to differentiate between inflammatory and lymphomatous erythroderma. Treatment with cyclosporin A always demands carefull evaluation of the course of the disorder. Erythroderma (erythema of at least 90% of the body skin surface) is a rare, but severe skin manifestation of several cutaneous disorders including psoriasis, atopic dermatitis, pityriasis rubra pilaris and cutaneous T-cell lymphoma (CTCL). CTCLs are Non-Hodgkin lymphomas where skin may be the only involved organ for a long time. Erythrodermic CTCLs most often include erythrodermic mycosis fungoides and Sezary syndrome. The erythrodermic form of CTCL, including Sezary syndrome, with increased IgE concentration, eosinophilia and intense pruritus, may be mistaken for atopic dermatitis in the lack of evidence for diagnosis of T-cell lymphoproliferative disorder. We report two patients with erythroderma, increased IgE and eosinophilia in whom, after vigorous research, the diagnosis of CTCL was not established, and adult atopic dermatitis was diagnosed. The therapy with cyclosporine A was initiated and after a month of therapy, which showed to be ineffective, repeated clinical examination and histopathological, immunohistochemical and gene rearrangement analyses, revealed existence of T-cell cutaneous lymhoma in both patients. Case 1 A male patient, aged 30 years, was admitted to our Department with extremely itchy erythroderma with generalized peripheral lymphadenopathy and hyperkeratosis of the palms and soles, that lasted for two months (Figure 1). During the previous year he received therapy for dry, red and scaly erythematous macules in the skin folds, with topical and systemic corticosteroids and topical pimecrolimus, without improvement. A short course of P-UVA phototherapy led to minimal improvement. Laboratory analyses revealed leukocytosis 16,65x10 9 /L, and eosinophilia 8,5%, as well as elevated lactate dehydrogenase (LDH) of 559 U/L 116
2 CASE REPORT Serbian Journal of Dermatology and Venereology 2009; 3: Figure 1. Erythroderma involving the back and upper arms in the first patient and increased IgE concentration IU/L. Other complete blood count (CBC) parameters, electrolytes, urea, creatinine, total bilirubine, aspartate aminotransferase (AST), alanine aminotransferase (ALT), gama glutamyl transpeptidase (γgt), IgG, IgA, IgM, were within normal range. ELISA HIV test was negative. Increased number of leukocytes was evident (14x10 9 /L), in the peripheral blood smear, but Sezary cells were not found. Chest X-ray findings and abdominal and pelvic ultrasounds were normal. Histopathologic analysis of the skin sample specimens revealed immune inflammatory response and secondary neutrophilic spongiosis consistent with non-specific inflammatory dermatosis. Cytologic analysis of the left supraclavicular enlarged lymph node smear revealed a non-specific lymphoid hyperplasia. T-cell receptor-γ gene rearrangement analysis of skin and blood specimens showed polyclonal T-cell population. Due to lack of evidence for the diagnosis of T-cell lymphoproliferative disorder, the diagnosis of adult atopic dermatitis was established, and therapy with cyclosporin A (CsA) oral solution (5 mg/kg/bw), and methylprednisolone 40 mg/d i.v. was initiated, with chloropyramine i.m. and topical corticosteroid therapy. Three weeks later, the patient referred for checkup with signs of disease progression: malaise, more enlarged peripheral lymph nodes, fever (39.1 C) generalized erythemolivid nodules, with more intense erythroderma. Repeated peripheral blood smear revealed younger lymphatic cells (5% were suspicious for Sezary cells). In the peripheral blood and skin, a dominant T-cell clone was detected by T-cell receptor-γ gene rearrangement analysis. A dominant T-cell clone was also detected in the bone marrow. CD4/CD8 ratio was increased to 7.8. Chest and abdominal multi-slice computed tomography (MSCT) revealed axillary lymphadenopathy up to 3.5 cm in diameter, while chest and retroperitoneal lymph nodes were not enlarged. Repeated skin biopsy was performed, and histopathological analysis was consistent with T-lymphoproliferative disorder - Sezary syndrome (Figure 2.). Based on repeated hemoculture test, staphylococcal sepsis was also diagnosed, so intravenous sulfametoxazol trimetoprim was administred. Based on these fingdings, diagnosis of Sezary syndrome was established in stage IIIB: T4 (confluence of erythema covering 80% body surface area) N1 (clinically abnormal peripheral lymph nodes; histopathology Dutch grade 1) M0 (no visceral organ involvement) B2 (high blood tumor burden: positive clone, increased CD4/CD8), according to revised classification of mycosis fungoides/sezary syndrome (1). The patient was reffered to a hematologist for Figure 2. Focal parakeratosis, acanthosis and hypogranular epidermal basal layer are evident. In the superficial dermis, perivascular aggregation of lymphocytes is present, and in one follicle intraepidermal grouping of lymphocytes forming Pautrier s abscess is evident; subepidermal infiltration of eosinophils is evident, rare eosinophils are present intraepidermally (hematoxylin and eosin, x100) 117
3 Serbian Journal of Dermatology and Venereology 2009; 3: M. Dinić et al. Erytrodermic cutaneous T-cell lymphoma polychemotherapy. He was treated with four cycles of cyclophosphamide, doxorubicine, vincristine, prednisolone (CHOP) chemotherapeutical protocol, that led to regression of erythroderma, but lymphadenopathy still remained unchanged, so treatment with second-line therapy with cytarabine, cisplatin, etoposide and methylprednisolone, was in course at the last follow-up. Case 2 A male patient, aged 44, was admitted to our Department with generalized dry, scaly and itchy livid skin, and lichen ification on the elbows, knees and ankles. At the age of 26, his skin turned dry, scaly and itchy, and at the age of 39 his skin condition worsened, with pronounced livid erythema and scaling of over 95% of the skin surface. He was treated by several dermatologists for generalized ichthyosis of unknown cause. Repeated histopathologic findings, in the last 15 years, were non-specific and inconclusive. There was no other evidence of atopy in personal and family history. Topical corticosteroid therapy and emollients showed no benefit. The patient turned chronically subfebrile 4 months before admission, and generalized peripheral lymphadenopathy occured. On admission, increased erythrocyte sedimentation rate (ESR) 38 mm/h, leukocytosis 13.91x10 9 /L, eosinophilia 8.9%, thrombocytosis 604x10 9 /L, and increased concentration of IgE (3200 IU/L) were established. Other parameters of CBC, blood biochemistry, AST, ALT, γgt, LDH, carcinoembrionic antigens (CEA), alpha fetoprotein antigens (AFP), amylase and immunoglobulins (G, A, M) were within normal range. ELISA tests for anti-hiv and anti-borrelia burgdorferi antibodies were negative. Chest X-ray and abdominal and pelvic ultrasound findings were normal. Histopathologic analysis of skin specimens and hyperkeratotic skin specimens revealed chronic inflammation and reparative changes suggestive of hypersensitive reaction. Histopathological analysis of the enlarged right axillary lymph node specimen was consistent with dermatopathic lymphadenopathy. Examinations to establish a lymhoproliferative disease, including bone marrow biopsy, histopathological analysis, peripheral blood smear, T-cell receptor-γ gene rearrangement analysis of the skin, peripheral blood and bone marrow specimens, immunophenotypization of peripheral blood lymphocytes were done, but the nature of the presenting erythroderma was not elucidated. Due to the lack of evidence for diagnosis of T-cell lymphoproliferative disorder, it was concluded that the diagnosis could be an adult form of atopic dermatitis, so a trial of CsA oral solution (5 mg/kg/ bw) with methylprednisolone (40 mg/d) i.v. was commenced, with systemic antihistamine and topical corticosteroids and emollients. Three weeks later, the patient became febrile (38 C), with worsened peripheral lymphadenopathy (enlarged lymph nodes in the right groin were evident). Also, disseminated livid papules up to 5 mm in diameter, some with necrotic surface appeared, while erythroderma aggravated during the second admission (Figures 3a and 3b). Leukocytosis (14.51x10 9 /L) and eosinophilia (9%), with platelets count of 590x10 9 /L and ESR 67 mm/h were also present. The chemocultures remained sterile. The repeated peripheral blood smear confirmed leukocytosis and eosinophilia, while on flowcytometry, CD4/CD8 index was within normal range. Histopathologic analysis of the enlarged lymph node specimen in the right groin revealed dermatopathic lymphadenopathy again. However, histo- pathologic analysis of the livid papule with necrotic surface led Figure 3.a. Erythemolivid skin color of the back and upper arms, with numerous necrotic papules in the second patient. 118
4 CASE REPORT Serbian Journal of Dermatology and Venereology 2009; 3: peculiar livid color of the skin was still evident on the last follow-up (Figure 5). Disscusion Erythroderma is defined as an erythematous dermatitis involving of at least 90% of the cutaneous surface. It is a severe skin manifestation of several cutaneous disorders, including cutaneous T-cell lymphoma (CTCL). If the Figure 3.b. Close-up view at livid, scaly skin of the abdomen, with erosions at places of previous necrotic papules to the following diagnosis: primary cutaneous CD30+ T-cell lymphoma (Figures 4a and 4b). The patient was referred to a hematologist who prescribed bleomycine, cyclophosphamide, doxorubicine, vincristine, prednisolone (B-CHOP) polychemotherapy. After six cycles of (B-CHOP) polychemotherapy, the skin lesions regressed, as well as lymphadenopathy, but the Figure 4.a. Superficial diffuse and pseudonodular deep dermal infiltration with superficial necrosis. The infiltrate consists of medium-sized cells, with one or several nucleoli; mitoses are evident. Eosinophils are present at the periphery (hematoxylin and eosin, x100); Figure 4. b. At least 20% of cells are CD30+ large cells with polymorphic nuclei and small nucleoli (immunoperoxidase staining, DAB chromogen, contrastained with hematoxylin, x100) Figure 5. Regression of papulonecrotic lesions, with remaining of livid color of the skin in the second patient 119
5 Serbian Journal of Dermatology and Venereology 2009; 3: M. Dinić et al. Erytrodermic cutaneous T-cell lymphoma diagnosis of a preexisted skin disorder was previously established, such as psoriasis, atopic dermatitis and pityriasis rubra pilaris, there are no doubts about the nature of erythroderma or its treatment. Considering the fact that CTCL is a slow-developing disorder, evolving skin changes and, often repeated, histopathologic findings of erythrodermic skin may lead to the diagnosis. In some cases, there are difficulties to differentiate between inflammatory dermatosis and skin lymphoma by clinical and histopathological features. Thus correlation of clinical appearance, immunohistochemistry and T-cell receptor-γ gene rearrangement analyses are needed (2). Sometimes, even that is not enough, so regular follow-ups and repeated analyses are necessary to detect the true nature of erythroderma and other skin changes of CTCL. It can be said that the final diagnosis of CTCL is possible during the course of the disease, when the tumor load is sufficient to be detected by vigorous research. In the first patient, the diagnosis of Sezary syndrome, the most frequent form of erythrodermic CTCL, was diagnosed only after repeated analyses to identify the cause of erythrodrma, one month after the initiation of cyclosporine treatment. The other patient was diagnosed with primary cutaneous CD30+ T-cell lymphoma which manifested with erythroderma and necrotic skin nodules that appeared late during the course of the disease. Primary CD30+ CTCL are most frequently manifested as primary cutanous CD30+ anaplastic large cell lymphoma (ALCL), lymphomatoid papulosis, or borderline cases. Primary cutaneous CD30 + ALCL is manifested with multiple, often ulcerating, skin papules and nodules, like in our patient. On histopathological analysis, the majority of cells have anaplastic appearance, but in 20-25% cases non-anaplastic cells are present, which was the case in our patient (3). Erythroderma is not a typical feature of primary cutaneous CD30 + CTCL. In our patient, the preexisting, long-lasting erythroderma may be considered as secondary to the slowly developing T-cell dyscrasia, that could not be detected earlier by repeated histopathological analyses. Previously published cases of primary cutaneous ALCL with prolonged erythrodermic prodrome support this observation (4, 5). Administration of CsA demands careful evaluation of the course of the disease. There is no evidence that CsA, used for the treatment of erythrodermic adult atopic dermatitis, caused lymphoproliferative disorders in these two cases, because the therapy lasted only a few weeks. According to previous reports, in adult atopic dermatitis patients, lymphoproliferative disease developed after at least 6 months of cyclosporine A treatment (6, 7). Also, in a large study, CTCL was not found to be more frequent in patients with atopic dermatitis, although in another study increased prevalence of lymphoma (especially cutaneous lymphoma) was found among patients with atopic dermatitis treated with topical corticosteroids (8, 9). Published case reports suggest that in rare cases CTCL may develop in atopic dermatitis patients who never received cyclosporine A therapy (10). In conclusion, correlation of the clinical appearance, and, often repeated, histopathologic analysis of the skin, enlarged peripheral lymph nodes and bone marrow, together with peripheral blood smears, T-cell receptor-γ gene rearrangement analysis of the skin, peripheral blood and bone marrow specimens and immunophenotypization of peripheral blood lymphocytes, are useful in the diagnosis of patients with erythroderma without previously existing dermatosis, because the lymphomatous nature of presenting erythroderma may be elucidated (2). References: 1. Olsen E, Vonderheid E, Pimpinelli N, Willemze R, Kim Y, Knobler R, et al. Revisions to the staging and classification of mycosis fungoides Sézary syndrome: a proposal of the International Society for Cutaneous Lymphomas (ISCL) and the cutaneous lymphoma task force of the European Organization of Research and Treatment of Cancer (EORTC). Blood 2007;110: Kandolf-Sekulović L, Cikota B, Dinić M, Škiljević D, Medenica Lj, Magić Z. T-cell receptor-γ gene rearrangement analysis in the diagnosis of patients with erythroderma. Serb J Dermatol Venereol 2009;1: Willemze R, Jaffe E, Burg G, Cerroni L, Berti E, Swerdlow S, et al. WHO-EORTC classification for cutaneous lymphomas. Blood 2005;105: Goyal S, Brinster NK, Goyal S. Ki-1(CD30) positive anaplastic large cell lymphoma: primary nodal disease relapsing as erythroderma. J Am Acad Dermatol 2002;47:S Denton K, Wilson CL, Venning VA. Primary cutaneous anaplastic large-cell lymphoma with a prolonged erythrodermic prodrome. Br J Dermatol. 1992;126: Mougel F, Dalle S, Balme B, Houot R, Thomas L. Aggresive CD30 large cell lymphoma after cyclosporine given for putative atopic dermatitis. Dermatology 2006;213:
6 CASE REPORT Serbian Journal of Dermatology and Venereology 2009; 3: Laube S, Stephens M, Smith AG, Whitaker SJ, Tan BB. Lymphomatoid papulosis in a patient with atopic eczema on long-term cyclosporine therapy. Br J Dermatol 2005;152: Mehrany K, El-Azhary RA, Bouwhui SA, Pittelkow MR. Cutaneous T-cell lymphoma and atopy: is there an association? Br J Dermatol 2003;149: Arellano F, Arana A, Wentworth C, Fernandez-Vidaurre C, Schlienger R, Conde E. Lymphoma among patients with atopic dermatitis and/or treated with topical immunosuppressants in the United Kingdom. J Allergy Clin Immunol 2009;123: Meyer N, Mazereeuv-Hautier J, Launay F, Lamant L, Paul C. CTCL complicating severe atopic dermatitis. Dermatology 2009;218: Eritrodermalni kutani limfom T-ćelija - prikaz dva slučaja Sažetak Uvod: Primarni kutani limfomi T-ćelija su Non- Hočkinovi limfomi kod kojih koža može biti dugo jedini zahvaćeni organ. U nedostatku nalaza koji bi potvrdili limfoproliferativno oboljenje T-ćelija, eritrodermijski oblik ovih limfoma (uključujući i Sezarijev sindrom), uz visoke koncentracije IgE, eozinofiliju i izrazit svrab može da podseća na atopijski dermatitis. Prikaz slučaja: Dva bolesnika, hospitalizovana zbog eritrodermije, kod kojih opsežnim ispitivanjima nije dokazano limfoproliferativno oboljenje, pod dijagnozom eritrodermijskog adultnog atopijskog dermatitisa lečeni su oralnim ciklosporinom uz sistemske kortikosteroide, sa privremenim i minimalnim poboljšanjima. Bolest je kod oba bolesnika progredirala u vidu pogoršanja opšteg stanja, febrilnosti i pojave generalizovanih eritemolividnih nodusa. Kod prvog bolesnika ponovljenim ispitivanjima postavljena je dijagnoza Sezarijevog sindroma na osnovu histopatološkog nalaza kože koji je upućivao na T-limfoproliferativno oboljenje, nalaza Sezarijevih ćelija u razmazu periferne krvi i nalaza monoklonske populacije T-limfocita u koži, perifernoj krvi i kostnoj srži. Kod drugog bolesnika histopatološkom analizom jednog od novonastalih nodusa detektovan je periferni T-ćelijski limfom. Zaključak: Diferencijalna dijagnoza između inflamatorne dermatoze i eritrodermijskog primarnog T-ćelijskog limfoma uvek je teška i zahteva ponavljana ispitivanja sa ciljem dokazivanja mogućeg limfoma. Primena ciklosporina u terapiji uvek zahteva pažljivo praćenje toka bolesti. 121
ISPUB.COM. Primary Cutaneous Anaplastic Large Cell Lymphoma Long-term Management with Low Dose Methotrexate. S Parker INTRODUCTION
 ISPUB.COM The Internet Journal of Dermatology Volume 7 Number 3 Primary Cutaneous Anaplastic Large Cell Lymphoma Long-term Management with Low Dose S Parker Citation S Parker.. The Internet Journal of
ISPUB.COM The Internet Journal of Dermatology Volume 7 Number 3 Primary Cutaneous Anaplastic Large Cell Lymphoma Long-term Management with Low Dose S Parker Citation S Parker.. The Internet Journal of
Lymphoma and Pseudolymphoma
 Lymphoma and Pseudolymphoma Laura B. Pincus, MD Co-Director, Cutaneous Lymphoma Clinic Associate Professor Dermatology and Pathology University of California, San Francisco I HAVE NO RELEVANT RELATIONSHIPS
Lymphoma and Pseudolymphoma Laura B. Pincus, MD Co-Director, Cutaneous Lymphoma Clinic Associate Professor Dermatology and Pathology University of California, San Francisco I HAVE NO RELEVANT RELATIONSHIPS
Overview of Cutaneous Lymphomas: Diagnosis and Staging. Lauren C. Pinter-Brown MD, FACP Health Sciences Professor of Medicine and Dermatology
 Overview of Cutaneous Lymphomas: Diagnosis and Staging Lauren C. Pinter-Brown MD, FACP Health Sciences Professor of Medicine and Dermatology Definition of Lymphoma A cancer or malignancy that comes from
Overview of Cutaneous Lymphomas: Diagnosis and Staging Lauren C. Pinter-Brown MD, FACP Health Sciences Professor of Medicine and Dermatology Definition of Lymphoma A cancer or malignancy that comes from
Sézary syndrome presenting with leonine facies ajd_560
 285..288 Australasian Journal of Dermatology (2009) 50, 285 288 doi: 10.1111/j.1440-0960.2009.00560.x CASE REPORT Sézary syndrome presenting with leonine facies ajd_560 Shano Nassem, 1 Rajesh Kashyap,
285..288 Australasian Journal of Dermatology (2009) 50, 285 288 doi: 10.1111/j.1440-0960.2009.00560.x CASE REPORT Sézary syndrome presenting with leonine facies ajd_560 Shano Nassem, 1 Rajesh Kashyap,
A middle-aged man with self-healing papulonecrotic lesions over the trunk and proximal limbs
 Hong Kong J. Dermatol. Venereol. (2011) 19, 30-34 Case Report A middle-aged man with self-healing papulonecrotic lesions over the trunk and proximal limbs JC Chan, N Trendell-Smith, CK Yeung Lymphomatoid
Hong Kong J. Dermatol. Venereol. (2011) 19, 30-34 Case Report A middle-aged man with self-healing papulonecrotic lesions over the trunk and proximal limbs JC Chan, N Trendell-Smith, CK Yeung Lymphomatoid
Michi Shinohara MD Associate Professor University of Washington/Seattle Cancer Care Alliance Dermatology, Dermatopathology
 Michi Shinohara MD Associate Professor University of Washington/Seattle Cancer Care Alliance Dermatology, Dermatopathology Agenda Overview of cutaneous T and B- cell lymphomas Diagnosis, Staging, Prognosis
Michi Shinohara MD Associate Professor University of Washington/Seattle Cancer Care Alliance Dermatology, Dermatopathology Agenda Overview of cutaneous T and B- cell lymphomas Diagnosis, Staging, Prognosis
Primary Cutaneous CD30-Positive T-cell Lymphoproliferative Disorders
 Primary Cutaneous CD30-Positive T-cell Lymphoproliferative Disorders Definition A spectrum of related conditions originating from transformed or activated CD30-positive T-lymphocytes May coexist in individual
Primary Cutaneous CD30-Positive T-cell Lymphoproliferative Disorders Definition A spectrum of related conditions originating from transformed or activated CD30-positive T-lymphocytes May coexist in individual
Lymphomatoid Papulosis 3 Case Reports
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 7 Ver. III (July. 2015), PP 31-35 www.iosrjournals.org Lymphomatoid Papulosis 3 Case Reports
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 7 Ver. III (July. 2015), PP 31-35 www.iosrjournals.org Lymphomatoid Papulosis 3 Case Reports
Cluster of differentiation (CD) markers in erythrodermic patients: A case series study
 Original Article Cluster of differentiation (CD) markers in erythrodermic patients: A case series study Fariba Ghalamkarpour, MD Faranak Niknafs, MD Shima Younespour, PhD Skin Research Center, Shahid Beheshti
Original Article Cluster of differentiation (CD) markers in erythrodermic patients: A case series study Fariba Ghalamkarpour, MD Faranak Niknafs, MD Shima Younespour, PhD Skin Research Center, Shahid Beheshti
CD30+ Lymphoproliferative Disorders Associated with Longstanding Mycosis Fungoides
 Case Report DOI: 10.6003/jtad.16102c5 CD30+ Lymphoproliferative Disorders Associated with Longstanding Mycosis Fungoides Esra Adışen, 1 MD, Özlem Erdem, 2 MD, Mehmet Ali Gürer, 1 MD Address: 1 Gazi University
Case Report DOI: 10.6003/jtad.16102c5 CD30+ Lymphoproliferative Disorders Associated with Longstanding Mycosis Fungoides Esra Adışen, 1 MD, Özlem Erdem, 2 MD, Mehmet Ali Gürer, 1 MD Address: 1 Gazi University
Case Report A Severe Case of Lymphomatoid Papulosis Type E Successfully Treated with Interferon-Alfa 2a
 Hindawi Case Reports in Dermatological Medicine Volume 2017, Article ID 3194738, 5 pages https://doi.org/10.1155/2017/3194738 Case Report A Severe Case of Lymphomatoid Papulosis Type E Successfully Treated
Hindawi Case Reports in Dermatological Medicine Volume 2017, Article ID 3194738, 5 pages https://doi.org/10.1155/2017/3194738 Case Report A Severe Case of Lymphomatoid Papulosis Type E Successfully Treated
2. Sézary syndrome (SS)
 Go Back to the Top To Order, Visit the Purchasing Page for Details Clinical images are available in hardcopy only. Clinical images are available in Clinical images are available in d e f g h i j Fig..36-2
Go Back to the Top To Order, Visit the Purchasing Page for Details Clinical images are available in hardcopy only. Clinical images are available in Clinical images are available in d e f g h i j Fig..36-2
Disclosures. Advisory Board. Consultant. Investigator. MiRagen, Actelion, Celgene, Therakos. Mindera
 Cutaneous Lymphomas Christiane Querfeld, MD, PhD Director, Cutaneous Lymphoma Program City of Hope ~ How the Experts Treat Hematologic Malignancies Symposium March 10 13, 2017 Disclosures Advisory Board
Cutaneous Lymphomas Christiane Querfeld, MD, PhD Director, Cutaneous Lymphoma Program City of Hope ~ How the Experts Treat Hematologic Malignancies Symposium March 10 13, 2017 Disclosures Advisory Board
Sezary Syndrome(SS) and other malignancies. Hernani Cualing MD Hematopathologist IHCFLOW Lab
 Sezary Syndrome(SS) and other malignancies Hernani Cualing MD Hematopathologist IHCFLOW Lab Disclosures IHCFLOW Laboratory:consultant and director NEOGENOMICS: contract consultant USF: contract reviewer
Sezary Syndrome(SS) and other malignancies Hernani Cualing MD Hematopathologist IHCFLOW Lab Disclosures IHCFLOW Laboratory:consultant and director NEOGENOMICS: contract consultant USF: contract reviewer
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/2010 holds various files of this Leiden University dissertation. Author: Benner, Marchina Frederika Title: Cutaneous CD30-positive lymphoproliferations
Cover Page The handle http://hdl.handle.net/1887/2010 holds various files of this Leiden University dissertation. Author: Benner, Marchina Frederika Title: Cutaneous CD30-positive lymphoproliferations
A rare clinical presentation of non Hodgkin Lymphoma as multiple neurofibromas with review of literature
 Original article A rare clinical presentation of non Hodgkin Lymphoma as multiple neurofibromas with review of literature Dr.C.R.Sirajunnisa Begum, Professor 1, Dr. Ira Bharadhwaj, Professor 1, Dr. Lavanya,
Original article A rare clinical presentation of non Hodgkin Lymphoma as multiple neurofibromas with review of literature Dr.C.R.Sirajunnisa Begum, Professor 1, Dr. Ira Bharadhwaj, Professor 1, Dr. Lavanya,
Important Decisions in Dermatopathology: The Clinico- Pathologic Correlation. Dermatopathology Specialists Needed. Changing Trends
 Important Decisions in Dermatopathology: The Clinico- Pathologic Correlation Uma Sundram, MD, PhD Departments of Pathology and Dermatology Stanford University May 29, 2008 Dermatopathology Specialists
Important Decisions in Dermatopathology: The Clinico- Pathologic Correlation Uma Sundram, MD, PhD Departments of Pathology and Dermatology Stanford University May 29, 2008 Dermatopathology Specialists
Lymphoma/CLL 101: Know your Subtype. Dr. David Macdonald Hematologist, The Ottawa Hospital
 Lymphoma/CLL 101: Know your Subtype Dr. David Macdonald Hematologist, The Ottawa Hospital Function of the Lymph System Lymph Node Lymphocytes B-cells develop in the bone marrow and influence the immune
Lymphoma/CLL 101: Know your Subtype Dr. David Macdonald Hematologist, The Ottawa Hospital Function of the Lymph System Lymph Node Lymphocytes B-cells develop in the bone marrow and influence the immune
ISPUB.COM. M Duvic, E Olsen PURPOSE OF REVISION
 ISPUB.COM The Internet Journal of Dermatology Volume 7 Number 3 International Society of Cutaneous Lymphoma (ISCL) and the European Organization of Research and Treatment of Cancer (EORTC) revisions to
ISPUB.COM The Internet Journal of Dermatology Volume 7 Number 3 International Society of Cutaneous Lymphoma (ISCL) and the European Organization of Research and Treatment of Cancer (EORTC) revisions to
Dermatopathology: The tumor is composed of keratinocytes which show atypia, increase mitoses and abnormal mitoses.
 Squamous cell carcinoma (SCC): A common malignant tumor of keratinocytes arising in the epidermis, usually from a precancerous condition: 1- UV induced actinic keratosis, usually of low grade malignancy.
Squamous cell carcinoma (SCC): A common malignant tumor of keratinocytes arising in the epidermis, usually from a precancerous condition: 1- UV induced actinic keratosis, usually of low grade malignancy.
Subject Index. Dry desquamation, see Skin reactions, radiotherapy
 Subject Index Actinic keratosis disseminated disease 42 surgical excision 42 AIDS, see Kaposi s sarcoma Amifostine, skin reaction prophylaxis 111 Basal cell carcinoma, superficial X-ray therapy Bowen s
Subject Index Actinic keratosis disseminated disease 42 surgical excision 42 AIDS, see Kaposi s sarcoma Amifostine, skin reaction prophylaxis 111 Basal cell carcinoma, superficial X-ray therapy Bowen s
Summary. lymphoma/myeloma, regulatory T cells (T reg) Introduction. Clinical and Experimental Immunology ORIGINAL ARTICLE doi: /cei.
 bs_bs_banner Clinical and Experimental Immunology ORIGINAL ARTICLE doi:1.1111/cei.1273 Increased frequency of skin-infiltrating FoxP3 + regulatory T cells as a diagnostic indicator of severe atopic dermatitis
bs_bs_banner Clinical and Experimental Immunology ORIGINAL ARTICLE doi:1.1111/cei.1273 Increased frequency of skin-infiltrating FoxP3 + regulatory T cells as a diagnostic indicator of severe atopic dermatitis
ISPUB.COM. Management of Co-existing Mycosis Fungoides and Lymphomatoid Papulosis. E Kim PHYSICAL FINDINGS INTRODUCTION INITIAL PRESENTATION
 ISPUB.COM The Internet Journal of Dermatology Volume 7 Number 3 Management of Co-existing Mycosis Fungoides and Lymphomatoid Papulosis E Kim Citation E Kim. Management of Co-existing Mycosis Fungoides
ISPUB.COM The Internet Journal of Dermatology Volume 7 Number 3 Management of Co-existing Mycosis Fungoides and Lymphomatoid Papulosis E Kim Citation E Kim. Management of Co-existing Mycosis Fungoides
Fig. 3.1 Fig Past history: She was previously healthy and not taking any medication.
 Case 3 A 41-year-old Thai female from Bangkok Chief compliant: Erythematous patch at left thigh for 2 months Present illness: The patient presented with a 10- year history of erythematous patch on her
Case 3 A 41-year-old Thai female from Bangkok Chief compliant: Erythematous patch at left thigh for 2 months Present illness: The patient presented with a 10- year history of erythematous patch on her
CASE 15 Patient: A 41-year-old Thai female Chief Compliant: Generalized papulovesicular rash for 1 month Present Illness: She presented with a 1-week
 CASE 15 Patient: A 41-year-old Thai female Chief Compliant: Generalized papulovesicular rash for 1 month Present Illness: She presented with a 1-week history of the generalized asymptomatic erythematous
CASE 15 Patient: A 41-year-old Thai female Chief Compliant: Generalized papulovesicular rash for 1 month Present Illness: She presented with a 1-week history of the generalized asymptomatic erythematous
TOX expression in cutaneous B-cell lymphomas
 Arch Dermatol Res (2016) 308:423 427 DOI 10.1007/s00403-016-1654-7 ORIGINAL PAPER TOX expression in cutaneous B-cell lymphomas Anne M. R. Schrader 1 Patty M. Jansen 1 Rein Willemze 2 Received: 20 January
Arch Dermatol Res (2016) 308:423 427 DOI 10.1007/s00403-016-1654-7 ORIGINAL PAPER TOX expression in cutaneous B-cell lymphomas Anne M. R. Schrader 1 Patty M. Jansen 1 Rein Willemze 2 Received: 20 January
Clinical and Histopathological Spectrum of Mycosis Fungoides
 Awad Hasan Al-Tarawneh, MD, Jordan Board* Background: Early diagnosis of mycosis fungoides is essential but difficult and can be easily missed because it mimics many inflammatory skin diseases both clinically
Awad Hasan Al-Tarawneh, MD, Jordan Board* Background: Early diagnosis of mycosis fungoides is essential but difficult and can be easily missed because it mimics many inflammatory skin diseases both clinically
CPC. Chutika Srisuttiyakorn, M.D. Kobkul Aunhachoke, M.D. Phramongkutklao Hospital Bangkok, Thailand
 CPC Chutika Srisuttiyakorn, M.D. Kobkul Aunhachoke, M.D. Phramongkutklao Hospital Bangkok, Thailand A 53 year-old woman with fever, facial swelling and rashes on face, trunk and upper extremities for 3
CPC Chutika Srisuttiyakorn, M.D. Kobkul Aunhachoke, M.D. Phramongkutklao Hospital Bangkok, Thailand A 53 year-old woman with fever, facial swelling and rashes on face, trunk and upper extremities for 3
CUTIS. Do Not Copy. Pityriasis lichenoides is a T cell mediated papular. Pityriasis Lichenoides Chronica in Black Patients. Pediatric Dermatology
 Series Editor: Camila K. Janniger, MD Pityriasis Lichenoides Chronica in Black Patients Tanda N. Lane, MD; Sareeta S. Parker, MD Pityriasis lichenoides chronica (PLC) is a cutaneous disease of unknown
Series Editor: Camila K. Janniger, MD Pityriasis Lichenoides Chronica in Black Patients Tanda N. Lane, MD; Sareeta S. Parker, MD Pityriasis lichenoides chronica (PLC) is a cutaneous disease of unknown
clinical recommendations
 19 (Supplement 2): ii72 ii76, 2008 doi:10.1093/annonc/mdn095 Primary cutaneous lymphoma: ESMO Clinical Recommendations for diagnosis, treatment and follow-up R. Dummer 1 & M. Dreyling 2 On behalf of the
19 (Supplement 2): ii72 ii76, 2008 doi:10.1093/annonc/mdn095 Primary cutaneous lymphoma: ESMO Clinical Recommendations for diagnosis, treatment and follow-up R. Dummer 1 & M. Dreyling 2 On behalf of the
Recalcitrant Warty Erythroderma With Severe Pruritus. Gil Yosipovitch Professor & Chair Department of Dermatology & Itch Center Temple University
 Recalcitrant Warty Erythroderma With Severe Pruritus Gil Yosipovitch Professor & Chair Department of Dermatology & Itch Center Temple University DISCLOSURE OF RELEVANT RELATIONSHIPS WITH INDUSTRY Gil Yosipovitch,
Recalcitrant Warty Erythroderma With Severe Pruritus Gil Yosipovitch Professor & Chair Department of Dermatology & Itch Center Temple University DISCLOSURE OF RELEVANT RELATIONSHIPS WITH INDUSTRY Gil Yosipovitch,
Erythroderma: A clinico-etiological study of 58 cases in a tertiary hospital of North India
 ORIGINAL ARTICLE ASIAN JOURNAL OF MEDICAL SCIENCES Erythroderma: A clinico-etiological study of 58 cases in a tertiary hospital of North India Nadia Shirazi 1, Rashmi Jindal 2, Akanksha Jain 2, Kanika
ORIGINAL ARTICLE ASIAN JOURNAL OF MEDICAL SCIENCES Erythroderma: A clinico-etiological study of 58 cases in a tertiary hospital of North India Nadia Shirazi 1, Rashmi Jindal 2, Akanksha Jain 2, Kanika
Serbian Journal of Dermatology and Venereology 2009; 1: 17-26
 ORIGINAL STUDY T-cell receptor-g gene rearrangement analysis in the diagnosis of patients with erythroderma Lidija Kandolf-Sekulović 1 *, Bojana Cikota 2, Miroslav Dinić 1, Dušan Škiljević 3, Ljiljana
ORIGINAL STUDY T-cell receptor-g gene rearrangement analysis in the diagnosis of patients with erythroderma Lidija Kandolf-Sekulović 1 *, Bojana Cikota 2, Miroslav Dinić 1, Dušan Škiljević 3, Ljiljana
Granulomatous Slack Skin with an unusually aggressive course due to the subsequent development of a CD30-positive Large Cell Lymphoma
 Granulomatous Slack Skin with an unusually aggressive course due to the subsequent development of a CD30-positive Large Cell Lymphoma Alexandra Papoudou-Bai 1, Eleni Kapsali 2, Ioannis Kostas-Agnantis
Granulomatous Slack Skin with an unusually aggressive course due to the subsequent development of a CD30-positive Large Cell Lymphoma Alexandra Papoudou-Bai 1, Eleni Kapsali 2, Ioannis Kostas-Agnantis
CUTANEOUS T-CELL LYMPHOMA PROFORMA
 STATE OF KUWAIT MINISTRY OF HEALTH AS AD ALHAMAD DERMATOLOGY CENTER ALSABAH HOSPITAL دولة الكویت وزارة الصحة مرآز أسعد الحمد للا مراض الجلدیة مستشفى الصباح بسم االله الرحمن الرحيم CUTANEOUS TCELL LYMPHOMA
STATE OF KUWAIT MINISTRY OF HEALTH AS AD ALHAMAD DERMATOLOGY CENTER ALSABAH HOSPITAL دولة الكویت وزارة الصحة مرآز أسعد الحمد للا مراض الجلدیة مستشفى الصباح بسم االله الرحمن الرحيم CUTANEOUS TCELL LYMPHOMA
Supplementary Online Content
 Supplementary Online Content Ross NA, Chung H-J, Li Q, Andrews JP, Keller MS, Uitto J. Pityriasis rubra pilaris: a case series of patients. Published online March 9, 26. JAMA Dermatol. doi:./jamadermatol.26.9.
Supplementary Online Content Ross NA, Chung H-J, Li Q, Andrews JP, Keller MS, Uitto J. Pityriasis rubra pilaris: a case series of patients. Published online March 9, 26. JAMA Dermatol. doi:./jamadermatol.26.9.
S003 CPC Self-Assessment
 S003 CPC Self-Assessment Alina G. Bridges, D.O. Associate Professor Program Director, Dermatopathology Fellowship Department of Dermatology, Division of Dermatopathology and Cutaneous Immunopathology Mayo
S003 CPC Self-Assessment Alina G. Bridges, D.O. Associate Professor Program Director, Dermatopathology Fellowship Department of Dermatology, Division of Dermatopathology and Cutaneous Immunopathology Mayo
Nodular Prurigo Associated with Mycosis Fungoides Case Report
 2015;23(3):203-207 CASE REPORT Nodular Prurigo Associated with Mycosis Fungoides Case Report Sandra Jerković Gulin 1, Romana Čeović 2, Davorin Lončarić 2, Ivana Ilić 3, Ivo Radman 4 1 Department of Dermatology
2015;23(3):203-207 CASE REPORT Nodular Prurigo Associated with Mycosis Fungoides Case Report Sandra Jerković Gulin 1, Romana Čeović 2, Davorin Lončarić 2, Ivana Ilić 3, Ivo Radman 4 1 Department of Dermatology
Classification of Cutaneous T cell Lymphomas (CTCLs) Hernani Cualing, MD
 Classification of Cutaneous T cell Lymphomas (CTCLs) Hernani Cualing, MD Pathology and Cell Biology, USF IFLOW, Inc. CTCL, MF, and Sézary syndrome In 1806, mycosis fungoides (MF) was first described 1
Classification of Cutaneous T cell Lymphomas (CTCLs) Hernani Cualing, MD Pathology and Cell Biology, USF IFLOW, Inc. CTCL, MF, and Sézary syndrome In 1806, mycosis fungoides (MF) was first described 1
Kikuchi s disease (necrotizing lymphadenitis) presenting as acneiform eruption
 Journal of the Saudi Society of Dermatology & Dermatologic Surgery (2012) 16, 67 71 King Saud University Journal of the Saudi Society of Dermatology & Dermatologic Surgery www.ksu.edu.sa www.jssdds.org
Journal of the Saudi Society of Dermatology & Dermatologic Surgery (2012) 16, 67 71 King Saud University Journal of the Saudi Society of Dermatology & Dermatologic Surgery www.ksu.edu.sa www.jssdds.org
Primer of Immunohistochemistry (Leukocytic)
 Primer of Immunohistochemistry (Leukocytic) Paul K. Shitabata, M.D. Dermatopathology Institute Torrance, CA BENIGN LYMPHOID SKIN LESIONS CAPABLE OF SIMULATING LYMPHOMA -Jessner s lymphoid infiltrate -Dermal-subcutaneous
Primer of Immunohistochemistry (Leukocytic) Paul K. Shitabata, M.D. Dermatopathology Institute Torrance, CA BENIGN LYMPHOID SKIN LESIONS CAPABLE OF SIMULATING LYMPHOMA -Jessner s lymphoid infiltrate -Dermal-subcutaneous
Case Report Pitfalls in the Diagnosis of Anaplastic Large Cell Lymphoma with a Small Cell Pattern
 Case Reports in Hematology Volume 23, Article ID 84253, 6 pages http://dx.doi.org/.55/23/84253 Case Report Pitfalls in the Diagnosis of Anaplastic Large Cell Lymphoma with a Small Cell Pattern Rowan L.
Case Reports in Hematology Volume 23, Article ID 84253, 6 pages http://dx.doi.org/.55/23/84253 Case Report Pitfalls in the Diagnosis of Anaplastic Large Cell Lymphoma with a Small Cell Pattern Rowan L.
Sézary syndrome. Diagnosis and staging
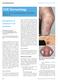 CME DERMATOLOGY Clinical Medicine 2012, Vol 12, No 2: 160 4 Edited by Clive B Archer, consultant dermatologist and lead for Medical Education, St John s Institute of Dermatology, Guy s and St Thomas NHS
CME DERMATOLOGY Clinical Medicine 2012, Vol 12, No 2: 160 4 Edited by Clive B Archer, consultant dermatologist and lead for Medical Education, St John s Institute of Dermatology, Guy s and St Thomas NHS
CD30 + cells in benign inflammatory infiltrate of some dermatological diseases. Abstract. Latef M. El Balshy. Benha University-Benha, Egypt.
 CD30 + cells in benign inflammatory infiltrate of some dermatological diseases 1 Asmaa M. El Refaeie, 1 Osama H. Abdel Salam, 1 Sherine H.Abd EL-Rahman and 2 Abdel Latef M. El Balshy. 1 Dermatology & Andrology
CD30 + cells in benign inflammatory infiltrate of some dermatological diseases 1 Asmaa M. El Refaeie, 1 Osama H. Abdel Salam, 1 Sherine H.Abd EL-Rahman and 2 Abdel Latef M. El Balshy. 1 Dermatology & Andrology
LYMPHOMA Joginder Singh, MD Medical Oncologist, Mercy Cancer Center
 LYMPHOMA Joginder Singh, MD Medical Oncologist, Mercy Cancer Center Lymphoma is cancer of the lymphatic system. The lymphatic system is made up of organs all over the body that make up and store cells
LYMPHOMA Joginder Singh, MD Medical Oncologist, Mercy Cancer Center Lymphoma is cancer of the lymphatic system. The lymphatic system is made up of organs all over the body that make up and store cells
Primary cutaneous large cell lymphoma CD30+: a case-based review
 Case-based review Primary cutaneous large cell lymphoma CD30+: a case-based review Anna Campanati 1 Katia Giuliodori 1 Emanuela Martina 1 Luca Conocchiari 1 Giulia Ganzetti 1 Gaia Goteri 2 Annamaria Offidani
Case-based review Primary cutaneous large cell lymphoma CD30+: a case-based review Anna Campanati 1 Katia Giuliodori 1 Emanuela Martina 1 Luca Conocchiari 1 Giulia Ganzetti 1 Gaia Goteri 2 Annamaria Offidani
Clusterin Expression Correlates With Stage and Presence of Large Cells in Mycosis Fungoides
 Anatomic Pathology / Clusterin Expression in Mycosis Fungoides Clusterin Expression Correlates With Stage and Presence of Large Cells in Mycosis Fungoides Pranil Chandra, DO, 1 Jose A. Plaza, MD, 2,4 Zhuang
Anatomic Pathology / Clusterin Expression in Mycosis Fungoides Clusterin Expression Correlates With Stage and Presence of Large Cells in Mycosis Fungoides Pranil Chandra, DO, 1 Jose A. Plaza, MD, 2,4 Zhuang
Review Article. Cutaneous lymphoproliferative disorders. NJ Trendell-Smith
 Hong Kong J. Dermatol. Venereol. (2010) 18, 190-201 Review Article Cutaneous lymphoproliferative disorders NJ Trendell-Smith Cutaneous lymphoproliferative disorders (CLD) include reactive lymphoid hyperplasias,
Hong Kong J. Dermatol. Venereol. (2010) 18, 190-201 Review Article Cutaneous lymphoproliferative disorders NJ Trendell-Smith Cutaneous lymphoproliferative disorders (CLD) include reactive lymphoid hyperplasias,
A case of Sweet's syndrome with marked facial swelling and fluid collection
 Hong Kong J. Dermatol. Venereol. (2017) 25, 128-132 Case Report A case of Sweet's syndrome with marked facial swelling and fluid collection JE Seol, SH Park, DH Kim, JN Kang, H Kim A 43-year-old woman
Hong Kong J. Dermatol. Venereol. (2017) 25, 128-132 Case Report A case of Sweet's syndrome with marked facial swelling and fluid collection JE Seol, SH Park, DH Kim, JN Kang, H Kim A 43-year-old woman
Change Summary - Form 2018 (R3) 1 of 12
 Summary - Form 2018 (R3) 1 of 12 Form Question Number (r3) Type Description New Text Previous Text Today's date was removed 2018 N/A Today's Date Removed from Key Fields 2018 N/A HCT Type 2018 N/A Product
Summary - Form 2018 (R3) 1 of 12 Form Question Number (r3) Type Description New Text Previous Text Today's date was removed 2018 N/A Today's Date Removed from Key Fields 2018 N/A HCT Type 2018 N/A Product
Case Report A case of EBV positive diffuse large B-cell lymphoma of the adolescent
 Int J Clin Exp Med 2014;7(1):307-311 www.ijcem.com /ISSN:1940-5901/IJCEM1311029 Case Report A case of EBV positive diffuse large B-cell lymphoma of the adolescent Qilin Ao 2, Ying Wang 1, Sanpeng Xu 2,
Int J Clin Exp Med 2014;7(1):307-311 www.ijcem.com /ISSN:1940-5901/IJCEM1311029 Case Report A case of EBV positive diffuse large B-cell lymphoma of the adolescent Qilin Ao 2, Ying Wang 1, Sanpeng Xu 2,
Lymphoma Case Scenario 1
 Lymphoma Case Scenario 1 HISTORY: A 23-year-old healthy female presented with a month-long history of persistent headache of increasing severity. She noted episodic nausea and vomiting in association with
Lymphoma Case Scenario 1 HISTORY: A 23-year-old healthy female presented with a month-long history of persistent headache of increasing severity. She noted episodic nausea and vomiting in association with
CASE REPORT ANAPLASTIC LYMPHOMA OF THE CERVICAL ESOPHAGUS PRESENTING AS A TRACHEOESOPHAGEAL FISTULA. Anaplastic large cell lymphomas (ALCLs) are a
 CASE REPORT Eben L. Rosenthal, MD, Section Editor ANAPLASTIC LYMPHOMA OF THE CERVICAL ESOPHAGUS PRESENTING AS A TRACHEOESOPHAGEAL FISTULA Anil Joshi, MS (ENT), DOHNS, MRCS, 1,2 Paul Fields, MBBCh, MRCPath
CASE REPORT Eben L. Rosenthal, MD, Section Editor ANAPLASTIC LYMPHOMA OF THE CERVICAL ESOPHAGUS PRESENTING AS A TRACHEOESOPHAGEAL FISTULA Anil Joshi, MS (ENT), DOHNS, MRCS, 1,2 Paul Fields, MBBCh, MRCPath
Infections and nonmicrobial inflammatory stimuli can cause leukocytosis (as seen in Lab 1) as well as lymph node enlargement (lymphadenopathy).
 LAB 5: LYMPHOID TISSUE AND SKIN The focus of this week s lab will be pathology of the lymphoid tissue and skin. The lymphoid organs include the thymus, spleen, and lymph nodes. Abnormalities in the lymph
LAB 5: LYMPHOID TISSUE AND SKIN The focus of this week s lab will be pathology of the lymphoid tissue and skin. The lymphoid organs include the thymus, spleen, and lymph nodes. Abnormalities in the lymph
CD30-positive cutaneous lymphoma: report of four cases with an emphasis on clinicopathological correlations *
 86 Dermatopathology s CD30-positive cutaneous lymphoma: report of four cases with an emphasis on clinicopathological correlations * Thiago Jeunon de Sousa Vargas 1 Samira Barroso Jorge 1 Yung Bruno de
86 Dermatopathology s CD30-positive cutaneous lymphoma: report of four cases with an emphasis on clinicopathological correlations * Thiago Jeunon de Sousa Vargas 1 Samira Barroso Jorge 1 Yung Bruno de
Lymphoma of the Skin Early Detection, Diagnosis, and Staging
 Lymphoma of the Skin Early Detection, Diagnosis, and Staging Detection and Diagnosis Catching cancer early often allows for more treatment options. Some early cancers may have signs and symptoms that can
Lymphoma of the Skin Early Detection, Diagnosis, and Staging Detection and Diagnosis Catching cancer early often allows for more treatment options. Some early cancers may have signs and symptoms that can
Cutaneous Lymphoid Proliferations: A Comprehensive Textbook of Lymphocytic Infiltrates of the Skin
 Cutaneous Lymphoid Proliferations: A Comprehensive Textbook of Lymphocytic Infiltrates of the Skin Magro, Cynthia M., MD ISBN-13: 9780471695981 Table of Contents Chapter One: Introduction to the Classification
Cutaneous Lymphoid Proliferations: A Comprehensive Textbook of Lymphocytic Infiltrates of the Skin Magro, Cynthia M., MD ISBN-13: 9780471695981 Table of Contents Chapter One: Introduction to the Classification
Mycosis Fungoides, then and now Have we travelled?
 USCAP 103 rd Annual Meeting 2014 American Society of Dermatopathology Companion Meeting Mycosis Fungoides, then and now Have we travelled? Vijaya B. Reddy, MD, MBA Professor of Pathology Rush University
USCAP 103 rd Annual Meeting 2014 American Society of Dermatopathology Companion Meeting Mycosis Fungoides, then and now Have we travelled? Vijaya B. Reddy, MD, MBA Professor of Pathology Rush University
88-year-old Female with Lymphadenopathy. Faizi Ali, MD
 88-year-old Female with Lymphadenopathy Faizi Ali, MD Clinical History A 88-year-old caucasian female presented to our hospital with the complaints of nausea, vomiting,diarrhea, shortness of breath and
88-year-old Female with Lymphadenopathy Faizi Ali, MD Clinical History A 88-year-old caucasian female presented to our hospital with the complaints of nausea, vomiting,diarrhea, shortness of breath and
الاكزيماتيد= Eczematid
 1 / 7 2 / 7 Pityriasis Debate confusing of hypopigmentation characterized increasing surrounded differ hypomelanotic "progressive exists alba misnomer extensive a to observed term the applied term derived
1 / 7 2 / 7 Pityriasis Debate confusing of hypopigmentation characterized increasing surrounded differ hypomelanotic "progressive exists alba misnomer extensive a to observed term the applied term derived
Mycosis Fungoides Presentation in Emergency
 The Open Emergency Medicine Journal, 2011, 4, 17-21 17 Mycosis Fungoides Presentation in Emergency Asaad Shujaa*,1 and M. Owais Suriya 2 Open Access Department of Emergency Medicine College of Medicine,
The Open Emergency Medicine Journal, 2011, 4, 17-21 17 Mycosis Fungoides Presentation in Emergency Asaad Shujaa*,1 and M. Owais Suriya 2 Open Access Department of Emergency Medicine College of Medicine,
Lymphoma: The Basics. Dr. Douglas Stewart
 Lymphoma: The Basics Dr. Douglas Stewart Objectives What is lymphoma? How common is it? Why does it occur? How do you diagnose it? How do you manage it? How do you follow patients after treatment? What
Lymphoma: The Basics Dr. Douglas Stewart Objectives What is lymphoma? How common is it? Why does it occur? How do you diagnose it? How do you manage it? How do you follow patients after treatment? What
WHO Classification. B-cell chronic lymphocytic leukemia/small T-cell granular lymphocytic leukemia
 Blood Malignancies-II Prof. Dr. Herman Hariman, a Ph.D, SpPK (KH). Prof. Dr. Adikoesoema Aman, SpPK (KH) Dept. of Clinical Pathology, School of Medicine, University of North Sumatra WHO classification
Blood Malignancies-II Prof. Dr. Herman Hariman, a Ph.D, SpPK (KH). Prof. Dr. Adikoesoema Aman, SpPK (KH) Dept. of Clinical Pathology, School of Medicine, University of North Sumatra WHO classification
manifestations are uncommon. Initial descriptions of the disease (Rosai and Dorfman, 1969) specifically
 Postgraduate Medical Journal (July 1980) 56, 521-525 Diffuse cutaneous involvement and sinus histiocytosis with massive lymphadenopathy A. A. WOODCOCK B.Sc., M.B., Ch.B., M.R.C.P. Summary Severe skin involvement
Postgraduate Medical Journal (July 1980) 56, 521-525 Diffuse cutaneous involvement and sinus histiocytosis with massive lymphadenopathy A. A. WOODCOCK B.Sc., M.B., Ch.B., M.R.C.P. Summary Severe skin involvement
Title: Erythema annulare centrifugum associated with chronic lymphocytic leukaemia. Authors: Helbling I, Walewska R, Dyer MJS, Bamford M, Harman KE
 Title: Erythema annulare centrifugum associated with chronic lymphocytic leukaemia Authors: Helbling I, Walewska R, Dyer MJS, Bamford M, Harman KE Sir, A wide range of conditions have been described as
Title: Erythema annulare centrifugum associated with chronic lymphocytic leukaemia Authors: Helbling I, Walewska R, Dyer MJS, Bamford M, Harman KE Sir, A wide range of conditions have been described as
Clinical, Histopathological and Immunohistochemical Study of Cases Presenting with Erythroderma
 Clinical, Histopathological and Immunohistochemical Study of Cases Presenting with Erythroderma A Thesis Submitted For Partial Fulfillment of Master Degree in Dermatology By Suzan Mohamed Ameen Shalaby
Clinical, Histopathological and Immunohistochemical Study of Cases Presenting with Erythroderma A Thesis Submitted For Partial Fulfillment of Master Degree in Dermatology By Suzan Mohamed Ameen Shalaby
Degos Disease: A Case Report and Review of Literature
 Degos Disease: A Case Report and Review of Literature Monira waked Egyptian Dermatology Online Journal 4 (1): 5, June 2008 Al Houd Al Marsod Hospital Submitted for publication: May 25 th, 2008 Accepted
Degos Disease: A Case Report and Review of Literature Monira waked Egyptian Dermatology Online Journal 4 (1): 5, June 2008 Al Houd Al Marsod Hospital Submitted for publication: May 25 th, 2008 Accepted
Case Report New Primary Malignancy Masquerading as Metastatic Prostate Adenocarcinoma
 Case Reports in Oncological Medicine Volume 2015, Article ID 358572, 5 pages http://dx.doi.org/10.1155/2015/358572 Case Report New Primary Malignancy Masquerading as Metastatic Prostate Adenocarcinoma
Case Reports in Oncological Medicine Volume 2015, Article ID 358572, 5 pages http://dx.doi.org/10.1155/2015/358572 Case Report New Primary Malignancy Masquerading as Metastatic Prostate Adenocarcinoma
NEW RCPCH REFERENCE RANGES-
 s vary between populations and age groups and it is important to always check the reference Haematology: Haemoglobin Male 130 175 g/l 0 6 days 145-220 g/l Female 115 165 g/l 7 days 140-186 g/l 8 days 3
s vary between populations and age groups and it is important to always check the reference Haematology: Haemoglobin Male 130 175 g/l 0 6 days 145-220 g/l Female 115 165 g/l 7 days 140-186 g/l 8 days 3
Plenary paper. Introduction
 Plenary paper Primary and secondary cutaneous CD30 lymphoproliferative disorders: a report from the Dutch Cutaneous Lymphoma Group on the long-term follow-up data of 219 patients and guidelines for diagnosis
Plenary paper Primary and secondary cutaneous CD30 lymphoproliferative disorders: a report from the Dutch Cutaneous Lymphoma Group on the long-term follow-up data of 219 patients and guidelines for diagnosis
Comparative efficacy of topical mometasone furoate 0.1% cream vs topical tacrolimus 0.03% ointment in the treatment of atopic dermatitis
 Original Article Comparative efficacy of topical mometasone furoate 0.1% cream vs topical tacrolimus 0.03% ointment in the treatment of atopic dermatitis Md Alauddin Khan *, Lubna Khondker **, Dilshad
Original Article Comparative efficacy of topical mometasone furoate 0.1% cream vs topical tacrolimus 0.03% ointment in the treatment of atopic dermatitis Md Alauddin Khan *, Lubna Khondker **, Dilshad
U006 Primary Cutaneous Lymphomas: Diagnosis, Staging and When to Refer M. Yadira Hurley, MD
 U006 Primary Cutaneous Lymphomas: Diagnosis, Staging and When to Refer M. Yadira Hurley, MD hurleyy@slu.edu DISCLOSURE OF RELATIONSHIPS WITH INDUSTRY Actelion: Speaker Honoraria, Investigator Grants, Consultant
U006 Primary Cutaneous Lymphomas: Diagnosis, Staging and When to Refer M. Yadira Hurley, MD hurleyy@slu.edu DISCLOSURE OF RELATIONSHIPS WITH INDUSTRY Actelion: Speaker Honoraria, Investigator Grants, Consultant
Research Article Characteristics of Primary Cutaneous T-Cell Lymphoma in Iran: A 10-Year Retrospective Study
 International Scholarly Research Notices, Article ID 820921, 5 pages http://dx.doi.org/10.1155/2014/820921 Research Article Characteristics of Primary Cutaneous T-Cell Lymphoma in Iran: A 10-Year Retrospective
International Scholarly Research Notices, Article ID 820921, 5 pages http://dx.doi.org/10.1155/2014/820921 Research Article Characteristics of Primary Cutaneous T-Cell Lymphoma in Iran: A 10-Year Retrospective
Lymphomatoid Papulosis. اللمفواني الحطاطي الداء = lymphomatoide Papulose Thursday, 21 October :16 - Last Updated Friday, 03 December :54
 Lymphomatoid Papulosis 1 / 12 Lymphomatoid papulosis (LyP) is a chronic papulonecrotic or papulonodular skin disease with histologic features suggestive of a malignant lymphoma. The disease is characterized
Lymphomatoid Papulosis 1 / 12 Lymphomatoid papulosis (LyP) is a chronic papulonecrotic or papulonodular skin disease with histologic features suggestive of a malignant lymphoma. The disease is characterized
Renaissance of Low-Dose Radiotherapy Concepts for Cutaneous Lymphomas
 Review Article DOI: 10.1159/000470845 Received: February 06, 2017 Accepted: March 13, 2017 Published online: April 6, 2017 Renaissance of Low-Dose Radiotherapy Concepts for Cutaneous Lymphomas Bouthaina
Review Article DOI: 10.1159/000470845 Received: February 06, 2017 Accepted: March 13, 2017 Published online: April 6, 2017 Renaissance of Low-Dose Radiotherapy Concepts for Cutaneous Lymphomas Bouthaina
Microscopic study of the normal skin in cases of mycosis fungoides
 Microscopic study of the normal skin in cases of mycosis fungoides M. El Darouti, S. Marzook, M. Bosseila, O. Abu Zeid, O. El- Safouri, A. Zayed, A. El-Ramly Egyptian Dermatology Online Journal 2 (1):
Microscopic study of the normal skin in cases of mycosis fungoides M. El Darouti, S. Marzook, M. Bosseila, O. Abu Zeid, O. El- Safouri, A. Zayed, A. El-Ramly Egyptian Dermatology Online Journal 2 (1):
Dermatologica Sinica
 DERMATOLOGICA SINICA 31 (2013) 3e Contents lists available at SciVerse ScienceDirect Dermatologica Sinica journal homepage: http://www.derm-sinica.com CASE REPORT Early stage mycosis fungoides with focal
DERMATOLOGICA SINICA 31 (2013) 3e Contents lists available at SciVerse ScienceDirect Dermatologica Sinica journal homepage: http://www.derm-sinica.com CASE REPORT Early stage mycosis fungoides with focal
Case Report Breast Cancer Presenting as Paraneoplastic Erythroderma: An Extremely Rare Case
 Case Reports in Medicine, Article ID 351065, 4 pages http://dx.doi.org/10.1155/2014/351065 Case Report Breast Cancer Presenting as Paraneoplastic Erythroderma: An Extremely Rare Case Ioannis Protopsaltis,
Case Reports in Medicine, Article ID 351065, 4 pages http://dx.doi.org/10.1155/2014/351065 Case Report Breast Cancer Presenting as Paraneoplastic Erythroderma: An Extremely Rare Case Ioannis Protopsaltis,
Grover s disease: A case report.
 320 Case report Thai J Dermatol, October-December 2011 ABSTRACT: Grover s disease: A case report. Supicha Chavanich MD, Praneet Sajjachareonpong MD. CHAVANICH C, SAJJACHAREONPONG P. GROVER S DISEASE: A
320 Case report Thai J Dermatol, October-December 2011 ABSTRACT: Grover s disease: A case report. Supicha Chavanich MD, Praneet Sajjachareonpong MD. CHAVANICH C, SAJJACHAREONPONG P. GROVER S DISEASE: A
HEMORRHAGIC BULLOUS HENOCH- SCHONLEIN PURPURA: A CASE REPORT
 HEMORRHAGIC BULLOUS HENOCH- SCHONLEIN PURPURA: A CASE REPORT Nirmala Ponnuthurai, Sabeera Begum, Lee Bang Rom Paediatric Dermatology Unit, Institute of Paediatric, Hospital Kuala Lumpur, Malaysia Abstract
HEMORRHAGIC BULLOUS HENOCH- SCHONLEIN PURPURA: A CASE REPORT Nirmala Ponnuthurai, Sabeera Begum, Lee Bang Rom Paediatric Dermatology Unit, Institute of Paediatric, Hospital Kuala Lumpur, Malaysia Abstract
Naphthalene in the Treatment of Patients with Atopic Dermatitis
 2007;15(1):15-19 SHORT SCIENTIFIC COMMUNICATION Naphthalene in the Treatment of Patients with Atopic Dermatitis Ankica Smeh-Skrbin 1, Ivan Dobrić 2, Gordana Krnjević-Pezić 1, Pero Vržogić 1 1 Naftalan
2007;15(1):15-19 SHORT SCIENTIFIC COMMUNICATION Naphthalene in the Treatment of Patients with Atopic Dermatitis Ankica Smeh-Skrbin 1, Ivan Dobrić 2, Gordana Krnjević-Pezić 1, Pero Vržogić 1 1 Naftalan
OBSERVATION. Psoralen Plus Long-Wave UV-A (PUVA) and Bexarotene Therapy
 OBSERVATION Psoralen Plus Long-Wave UV-A (PUVA) and Bexarotene Therapy An Effective and Synergistic Combined Adjunct to Therapy for Patients With Advanced Cutaneous T-Cell Lymphoma Karen S. McGinnis, MD;
OBSERVATION Psoralen Plus Long-Wave UV-A (PUVA) and Bexarotene Therapy An Effective and Synergistic Combined Adjunct to Therapy for Patients With Advanced Cutaneous T-Cell Lymphoma Karen S. McGinnis, MD;
Citation The Journal of Dermatology, 37(8), available at
 NAOSITE: Nagasaki University's Ac Title Two cases of blaschkitis with promi Author(s) Utani, Atsushi Citation The Journal of Dermatology, 37(8), Issue Date 2010-08 URL Right http://hdl.handle.net/10069/25634
NAOSITE: Nagasaki University's Ac Title Two cases of blaschkitis with promi Author(s) Utani, Atsushi Citation The Journal of Dermatology, 37(8), Issue Date 2010-08 URL Right http://hdl.handle.net/10069/25634
Interhospital Dermatology Conference 2013
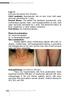 Case 21 A 50-year-old woman from Chonburi. Chief complaint: Asymptomatic rash on neck, trunk, both upper and lower extremities for 2 years. Present illness: The patient has developed asymptomatic scaly
Case 21 A 50-year-old woman from Chonburi. Chief complaint: Asymptomatic rash on neck, trunk, both upper and lower extremities for 2 years. Present illness: The patient has developed asymptomatic scaly
A dinical and histopathologic entity associated with an increased risk of nonmelanoma skin cancer
 PUVA keratosis A dinical and histopathologic entity associated with an increased risk of nonmelanoma skin cancer M. C. G. van Praag, MD, a J. N. Bouwes Bavinck, MD, a W. Bergman, MD, PhD, a F. R. Rosendaal,
PUVA keratosis A dinical and histopathologic entity associated with an increased risk of nonmelanoma skin cancer M. C. G. van Praag, MD, a J. N. Bouwes Bavinck, MD, a W. Bergman, MD, PhD, a F. R. Rosendaal,
Retrospective 10 years review of 100 patients with psoriasis in the Kingdom of Saudi Arabia (KSA)
 Retrospective 10 years review of 100 patients with psoriasis in the Kingdom of Saudi Arabia (KSA) Ahmed Abdullah Alhumidi King saud university, Riyadh, kingdom of Saudi Arabia Abstract Background: This
Retrospective 10 years review of 100 patients with psoriasis in the Kingdom of Saudi Arabia (KSA) Ahmed Abdullah Alhumidi King saud university, Riyadh, kingdom of Saudi Arabia Abstract Background: This
ERYTHRODERMA CAUSED DRUG ALLERGIES
 CASE REPORT ERYTHRODERMA CAUSED DRUG ALLERGIES Asrawati Sofyan, Sitti Nur Rahmah, Asnawi Madjid Department of Dermatovenereology Medical Faculty of Hasanuddin University / Wahidin Sudirohusodo Hospital
CASE REPORT ERYTHRODERMA CAUSED DRUG ALLERGIES Asrawati Sofyan, Sitti Nur Rahmah, Asnawi Madjid Department of Dermatovenereology Medical Faculty of Hasanuddin University / Wahidin Sudirohusodo Hospital
Psoriasiform pemphigus foliaceus: a report of two cases
 J Cutan Pathol 2012: 39: 549 553 doi: 10.1111/j.1600-0560.2012.01866.x John Wiley & Sons. Printed in Singapore Copyright 2012 John Wiley & Sons A/S Journal of Cutaneous Pathology Psoriasiform pemphigus
J Cutan Pathol 2012: 39: 549 553 doi: 10.1111/j.1600-0560.2012.01866.x John Wiley & Sons. Printed in Singapore Copyright 2012 John Wiley & Sons A/S Journal of Cutaneous Pathology Psoriasiform pemphigus
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/39089 holds various files of this Leiden University dissertation. Author: Cetinozman, F. Title: PD-1 Expression in primary cutaneous lymphoma Issue Date:
Cover Page The handle http://hdl.handle.net/1887/39089 holds various files of this Leiden University dissertation. Author: Cetinozman, F. Title: PD-1 Expression in primary cutaneous lymphoma Issue Date:
Emergency Dermatology. Emergency Dermatology
 Emergency Dermatology These are rapidly progressive skin conditions and some are potentially lifethreatening. Early recognition is important to implement prompt supportive care and therapy. Some are drug
Emergency Dermatology These are rapidly progressive skin conditions and some are potentially lifethreatening. Early recognition is important to implement prompt supportive care and therapy. Some are drug
Lymphatic system component
 Introduction Lymphatic system component Statistics Overview Lymphoma Non Hodgkin s Lymphoma Non- Hodgkin's is a type of cancer that originates in the lymphatic system. It is estimated to be the sixth most
Introduction Lymphatic system component Statistics Overview Lymphoma Non Hodgkin s Lymphoma Non- Hodgkin's is a type of cancer that originates in the lymphatic system. It is estimated to be the sixth most
Case 1. Debridement Cultures Keflex Silvadene
 The Red Breast Beth McLellan, M.D. Assistant Professor Division of Dermatology Albert Einstein College of Medicine Montefiore Medical Center Jacobi Medical Center Case 1 48 year old radiation oncologist
The Red Breast Beth McLellan, M.D. Assistant Professor Division of Dermatology Albert Einstein College of Medicine Montefiore Medical Center Jacobi Medical Center Case 1 48 year old radiation oncologist
Int J Clin Exp Pathol 2014;7(4): /ISSN: /IJCEP
 Int J Clin Exp Pathol 2014;7(4):1735-1741 www.ijcep.com /ISSN:1936-2625/IJCEP1401073 Case Report Primary cutaneous anaplastic large cell lymphoma occurring in an atopic dermatitis patient: a case report
Int J Clin Exp Pathol 2014;7(4):1735-1741 www.ijcep.com /ISSN:1936-2625/IJCEP1401073 Case Report Primary cutaneous anaplastic large cell lymphoma occurring in an atopic dermatitis patient: a case report
Corporate Medical Policy
 Corporate Medical Policy Extracorporeal Photopheresis File Name: Origination: Last CAP Review: Next CAP Review: Last Review: extracorporeal_photopheresis 9/2010 8/2017 8/2018 8/2017 Description of Procedure
Corporate Medical Policy Extracorporeal Photopheresis File Name: Origination: Last CAP Review: Next CAP Review: Last Review: extracorporeal_photopheresis 9/2010 8/2017 8/2018 8/2017 Description of Procedure
NON HODGKINS LYMPHOMA: INDOLENT Updated June 2015 by Dr. Manna (PGY-5 Medical Oncology Resident, University of Calgary)
 NON HODGKINS LYMPHOMA: INDOLENT Updated June 2015 by Dr. Manna (PGY-5 Medical Oncology Resident, University of Calgary) Reviewed by Dr. Michelle Geddes (Staff Hematologist, University of Calgary) and Dr.
NON HODGKINS LYMPHOMA: INDOLENT Updated June 2015 by Dr. Manna (PGY-5 Medical Oncology Resident, University of Calgary) Reviewed by Dr. Michelle Geddes (Staff Hematologist, University of Calgary) and Dr.
Cutaneous Mycosis Fungoides (MF), the subtype of cutaneous
 DOI 10. 5001/omj.2012.28 The Histological Spectrum of Early Mycosis Fungoides: A Study of 58 Saudi Arab patients Maha Arafah, Shaesta Naseem Zaidi, Hala Kassouf Kfoury, Ammar Al Rikabi, Khalid Al Ghamdi
DOI 10. 5001/omj.2012.28 The Histological Spectrum of Early Mycosis Fungoides: A Study of 58 Saudi Arab patients Maha Arafah, Shaesta Naseem Zaidi, Hala Kassouf Kfoury, Ammar Al Rikabi, Khalid Al Ghamdi
ERROR CORRECTION FORM
 Juvenile Idiopathic Arthritis Pre-HSCT Data Sequence Number: Registry Use Only Date of HSCT for which this form is being completed: HSCT type: autologous allogeneic, allogeneic, syngeneic unrelated related
Juvenile Idiopathic Arthritis Pre-HSCT Data Sequence Number: Registry Use Only Date of HSCT for which this form is being completed: HSCT type: autologous allogeneic, allogeneic, syngeneic unrelated related
Mucinoses Diverse group of disorders which have in common deposition of basophilic, finely granular and stringy material in the connective tissues of
 Cutaneous Mucinoses Nathan C. Walk, M.D. Mucinoses Diverse group of disorders which have in common deposition of basophilic, finely granular and stringy material in the connective tissues of the dermis.
Cutaneous Mucinoses Nathan C. Walk, M.D. Mucinoses Diverse group of disorders which have in common deposition of basophilic, finely granular and stringy material in the connective tissues of the dermis.
CIBMTR Center Number: CIBMTR Recipient ID: RETIRED. Today s Date: Date of HSCT for which this form is being completed:
 Juvenile Idiopathic Arthritis Pre-HSCT Data Sequence Number: Date Received: Registry Use Only Today s Date: Date of HSCT for which this form is being completed: HSCT type: autologous allogeneic, allogeneic,
Juvenile Idiopathic Arthritis Pre-HSCT Data Sequence Number: Date Received: Registry Use Only Today s Date: Date of HSCT for which this form is being completed: HSCT type: autologous allogeneic, allogeneic,
