DG MEMORANDUM FOR TUBERCULOSIS
|
|
|
- Scot Perkins
- 5 years ago
- Views:
Transcription
1 DG MEMORANDUM FOR TUBERCULOSIS Introduction 1. Tuberculosis (TB) is a curable condition but requires prolonged treatment for its cure. During last 3 decades tremendous advances have been made in the diagnosis and treatment of tuberculosis. Though the incidence in the Armed Forces have remained almost static, added dimension to this problem have cropped up in the form for entry of women officers to the services, prolonged survival of service personnel following treatment of malignant diseases and increasing number of clientele with solid organ transplant. Objective 2. This DG Memorandum is being brought out to give a guideline to treating doctors in diagnosis and management of tuberculosis in Armed Forces keeping in mind the existing National and International protocols on the subject. 3. The diagnosis of TB refers to the recognition of an active case. i.e. detection of a patient with symptomatic disease due to lesions caused by M. tuberculosis. Beyond making the diagnosis of TB, it is also necessary to define the type of TB case, i.e. to make a case definition. This applies to all TB patients, adults and children. 4. Pulmonary TB refers to disease involving the Lung parenchyma. Therefore tuberculous intrathoracic lymphadenopathy (mediastinal and/or hilar) or tuberculous pleural effusion, without radiographic abnormalities in the lungs, constitute a case of extra-pulmonary TB. A patient with both pulmonary and extrapulmonary TB constitutes a case of pulmonary TB. (ICD-011) The case definition of an extra-pulmonary case depends upon the site of involvement. Involvement of two non-contiguous organs with tubercular disease will be termed as disseminated TB. Thus involvement of pulmonary parenchyma with 2/-
2 -2- any other non-contiguous extra pulmonary site by tubercular process will be considered as pulm TB with extra pulmonary dissemination. A patient having pulmonary and meningeal TB will be labeled as Pulmonary TB with meningeal dissemination. 5. Severity of TB diseases Bacillary load extent of disease and anatomical site are considerations in determining TB disease severity and therefore the appropriate treatment. Involvement of an anatomical site results in classification as severe disease if there is either a significant acute threat to life (i.e. pericardial TB) or a risk of subsequent severe handicap (i.e. spinal TB), or both (e. o. meningeal TB). The following forms of extra-pulmonary TB are classified as severe: - (a) Meningitis (b) Miliary (c) Pericarditis (d) Peritonitis (e) Bilateral or extensive pleural effusion. (f) Spinal TB (with neurological defect) (g) Intestinal (h) Genito-urinary The following forms of extra-pulmonary TB are classified as less severe: - (a) Lymph node (b) Pleural effusion (unilateral). (c) Bone (excluding spine). (d) Spinal (without neurological involvement) (e) Peripheral joint (f) Skin 6. Bacteriology (result of sputum smear) The importance of defining the smear result in pulmonary cases is for the following: -.3/-
3 -3- (a) the identification of smear-positive cases (because they are the most infectious cases and they have an increased mortality). (b) recording and reporting (smear-positive cases are the only cases for which bacteriological monitoring of cure is available). 7. Diagnosis of Tuberculosis On clinical suspicion of tuberculosis with systemic features like fever, night sweat, anorexia and weight loss, pulmonary manifestation of cough of more than 2 weeks duration or haemoptysis, the patient must be examined for any sign of pulmonary disease. Essential investigation will include chest x-ray (CXR) and examination of two early mornings and one overnight sputum for acid fast bacillus (AFB). Any patient showing sputum smear positive twice for AFB will be classified as sputum positive case. Those with one specimen of sputum showing positive or all specimen shown negative for AFB, with evidence of pulmonary disease on CXR will be considered x-ray positive suspects of tuberculosis. They may be offered a 7-10 days course of artibacterials (except quinolones, streptomycin and rifampicin). A repeat clinical examination of CXR may be carried out to asses clinical and radiological recovery. Similar evaluation will be carried out for household contacts of sputum positive patient. 8. All such bacteriologically positive and x-ray positive cases should be transferred to a Resp Centre for further evaluation. (a) In accordance with WHO guidelines any patient with two sputum specimen positive for AFB or one sputum specimen positive with x-ray shadow suggestive pulm infiltrate or one smear and one sputum MTB culture being positive will be taken as a bacteriologically positive case of Pulm TB (b) Any patient who does not show sputum to be positive for AFB but radiologically there are suspicious shadows and there is no response to broad spectrum anti-bacterials will be taken as sputum negative Pulm TB. Any other patient with suspicion of extra-pulm disease and with clinical features to suggest anti TB treatment with or without histopathological/bacteriological confirmation will be grouped as a case of extra-pulm TB. Mycobacterial culture must be put up in all cases from available sputa and/or from the tissue/serosal fluid (as the case may be),.4/-
4 -4- Note: - Presence or absence of cavity and extent of pulmonary parenchymal involvement denotes the anatomical extent of lesion but it may not correlate with bacteriological status of the patient (c) other investigation like tuberculosis positive status, polymerase chain reaction (PCR) and ELISA for tuberculosis may be complementary to diagnostic work up but they do not have definitive diagnostic value. 9. Other routine inv. includes. Blood count ESR, liver function tests, serum transaminases, alkaline phosphates, uric acid, blood sugar (fasting and post parandial) and HIV serology if facilities are available. Treatment - Our success rate in treatment of pulmonary tuberculosis in Armed Forces during last quarter century has remained between % with relapse rate much below 1%. All efforts must be directed to maintain this record and if possible to improve upon it. 10. Aims of Treatment The aims of treatment of TB are the following :- (a) to cure the patient of TB : (b) to prevent death from active TB or its late effects: (c) to prevent relapse of TB: (g) to decrease transmission of TB to others. It is vital to achieve these aims while preventing the selection of resistant bacilli in infectious patients. 11. The essential anti TB drugs There are three main properties of anti-tb drugs: bactericidal ability, sterilizing ability and the ability to prevent resistance. Different anti-tb drugs possess these properties to different extents. Isoniazid and rifampicin are the most powerful bactericidal agents. Pyrazinamide is active in an acid environment against the bacilli inside macrophages. Streptomycin is active against rapidly multiplying extracellular bacilli. Ethambutol and thiacetazone are bacteriostatic drugs used in association with more powerful bactericidal drugs to prevent the emergence of resistant bacilli..5/-
5 Intermittent Therapy Isoniazid, rifampicin, pyrazinamide and streptomycin are all as efficacious when given intermittently (2 or 3 times per week) as when given daily. Essential Mode of Recommended Dose (mg/kg) Anti TB drugs action Daily Intermittent (3/wk) Isoniazid (H) Bactericidal 5 (4-6) 10 (8-12) Rifampicin Bactericidal 10 (8-12) 10 (8-12) Pyrazinamide (Z) Bactericidal 25 (20-30) 35 (30-40) Streptomycin (S) Bactericidal 15(12-18) 15 (12-18) Ethambutol (E) Bacteriostatic Principle The basic principle of tuberculosis treatment is based on the fact that there has to be an initial intensive phase followed by a continuation phase. (a) Intensive Phase is required with an aim to kill maximum number of actively multiplying organisms. This should be continued with 4 drugs S/E HRZ for 2-3 months and subsequently we only have to consolidate the recovery in the next phase. (b) Continuation Phase aims at sterilizing the lesion by eliminating the intermittently multiplying bacilli or persisters among bacterial debris. (c) Duration of Treatment & Hospitalization Total duration of treatment has to be minimum six months in all cases. In deserving cases it may be extended by the specialist concerned. In cases of pulmonary TB is service personnel hospitalization to be ensured till they become sputum negative for AFB and general condition stabilizes...6/-
6 All anti-tb drugs except the 2 nd line or reserve drugs are best absorbed on empty stomach. Philosophy of antitubercular chemotherapy aims more at peak rather than sustained serum level. Regimens 15. For simple cases without much of pulmonary parenchymal destruction, intensive phase need to be continued for 2 months with SHRZ E can replace S at the dose of mg/kg for first 2 months. This can be extended to 3 months in case of extensive/miliary/disseminated diseases & re-treatment in cases where sputum continues to be AFB positive. When attack phase is continued for 3 months, dose of ethumbutol to be brought down to 15 mg/kg after initial 60 days of the drug administration. In continuation phase rifampicin and isoniazid (H) are continued ordinarily for 4 months but in case of extensive organ dissemination a total of 9-12 months of treatment can be considered. It after 2 months of continuation phase, sputum for AFB remains positive, repeat sputum culture to be put up and attack phase extended to 3 months, further line of management must be guided in consultation with a specialist in the subject based on bacteriological response as well as clinical condition of the patient. Monitoring 16. (a) Monthly - Sputum AFB smear. MTB culture, Blood ESR Hb, TLC (b) Once in 2 months - x-ray Chest (c) LFT in case of suspicion of hepatic dysfunction. (d) Review by physician/chest physician. After completing and 9 months..7/-
7 -7- Treatment Regimens in Special situation (all Cases) 17. Treatment for Pregnant Women It is important to ask a woman before she starts anti-tb chemotherapy if she is pregnant. In case facilities are available it will be ideal to get an ultrasound of pelvis carried out to confirm any product of conception. Most anti- TB drugs are safe for use in pregnant women except in the first trimester. The exception is streptomycin (which is ototoxic to the fetus) should not be used in pregnancy and can be replaced by ethambutol. It is important to explain to a pregnant woman that successful treatment of TB with the recommended standardized regimen is important for a successful outcome of pregnancy. It must be stated here that all first line drugs except streptomycin are being used by doctors during pregnancy without any problem. In case of high-risk pregnancy, a specialist in tuberculosis and respiratory diseases may be consulted. 18. Treatment for Breast Feeding Women A woman who is breastfeeding and has TB should receive a full course of anti-tb chemotherapy. Timely and properly applied chemotherapy is the best way to prevent transmission of tubercle bacilli to her baby. All the anti-tb drugs are compatible with breastfeeding and a woman taking them can safely continue to breastfeed her baby. The mother and baby should stay together and the baby should continue to breast feed in the normal way. The baby should receive isoniazid prophylaxis and BCG immunization under the guidance of a specialist in paediatric/tuberculosis. As long as the mother is sputum smear positive, facemask is advisable during feeding. 19. Treatment for Women taking the Oral Contraceptive Pills Rifampicin interacts with the oral contraceptive pill with a risk of decreased protective efficacy against pregnancy. A woman who usually takes the oral contraceptive pill may choose: (a) Following consultation with a physician, she could take an oral contraceptive pill containing a higher dose of estrogen (50 mcg). (b) Alternatively she could use another form of contraception..8/-
8 Treatment for patients with liver disorders The following drugs with antitubercular properties are safe for liver. They are i) ethambutol, ii) cycloserine, iii) aminoglycosides (streptomycin, kanamycin, tobramycin and amikacin) as well as Quinolones (ofloxacin, ciprofioxacin) The patients with the following conditions can receive the usual short-course chemotherapy regimens provided that there is no clinical evidence of chronic liver diseases: hepatitis virus carriage, a past history of acute hepatitis, excessive alcohol consumption. (a) Established chronic liver disease Isoniazid plus rifampicin plus one or two non-hepatotoxic drugs such as streptomycin, ethambutol ofloxacin/ciprofloxacin can be used for a total treatment duration of eight months. An alternative regimen is streptomycin plus isoniazid plus ethambutol ofloxacin/ciprofloxacin in the initial phase followed by isoniazid and ethambutol in the continuation phase with total treatment duration of 12 months. Patients with liver disease should not receive pyrazinamide. Therefore recommended regimens are the following: 2 SHRE/ 6HR or 2 SHRE/10 HE. Patient must be monitored with weekly clinical examination and monthly Liver Function Test (LFT) test (Sr Bil, transaminase), if there is no ongoing hepato cellular dysfunction. Fortnightly, LFT in case of mild biochemical degrangement (where transaminase levels are less than 3 times normal or base line). (b) Acute hepatitis (e.g. acute viral hepatitis) It is a rare eventuality that a patient has TB and also at the same time acute hepatitis unrelated to TB or anti TB treatment. In some case it is possible to defer TB treatment until the acute hepatitis has resolved. In other cases when it is necessary to treat TB during acute hepatitis, cautious use of non- hepatotoxic drugs with frequent monitoring of hepatic parameters need to be done...9/-
9 Extra Pulmonary Tuberculosis (a) Lymph node. It is the commonest extra pulmonary tissue to be involved. One third of cases of lymphnode tuberculosis may show apparent increase in size and aggravation of lesion while on treatment. However, they do not necessarily suggest failure of treatment. In such case while all attempts have to be made to get antibiotic susceptibility of mycobacterium, no 2 nd line drug need be added unless there is definite evidence of clinical deterioration with systemic features or any evidence of radiological deterioration of the disease. An extended treatment in such cases will be beneficial. Total duration of treatment may be extended to 9-12 months in the later group. (b) Bone and Joint Tuberculosis. A course of regular ATT and 9 months regime seems to be adequate in the case of spinal TB without neurological involvement. (c) CNS TB. Involvement of brain parenchyma may demand prolonged treatment upto a period of one year. Drugs like isoliazid, pyrazinamide and ethionamide penetrate well into blood brain barrier and they have to be preferentially used in such cases. Systemic steroid therapy is added to reduce meningeal inflammation and prevent any obstruction to CSF flow. High dosage of steroid will be required (50 mg/kg to start with) in view of concurrent refampicin therapy. (d) Genito Urinary Tuberculosis. A six month regime with present short course therapy seems to be adequate except in case where there has been involvement of prostate and seminal vesicles. In such cases treatment need to be prolonged for one year or more..10/-
10 -10- (e) Abdominal Tuberculosis. Gastro intestinal involvement is a fairly comsmon occurrence. Extra pulmonary tuberculous lesions in out lumen and peritoneum may heal quickly but those involving intra-abdominal lymphnodes may take more time requiring 9-12 months of treatment. The involvement of intra abdominal lymphnodes should be monitored by ultrasonography. (f) HIV with Tuberculosis. Therapeutic response in cases with dual infection seem to be good as far as tuberculosis is concerned, till such time increasing viral load has not brought down the effective T cell population. An extended short course chemotherapy, lasting upto one year will be a prudent approach. The question of continuing life long prophylaxis in such a situation has not yet been resolved. (g) Treatment of Tuberculosis in Solid Organ Transplant Patients In many such patients receiving cyclosporin, refampicin has to be avoided. In the absence of rifampicin one of the strongest anchor of short course chemotherapy the total duration of the treatment need to be prolonged to months i.e. a treatment programme like that of conventional (pre short course) treatment era. 22. Disposal of cases of Pulmonary Tuberculosis (a) All serving officers and men suspected to be suffering from Pulmonary tuberculosis are to be hospitalised at (a) Base Hospital Delhi Cantt (b) MH (CTC) Pune (c) MH Namkum (d) MH Dehradun (d) INHS Asvini (e) Comd Hosp (AF) Bangalore. After detailed evaluation the diagnosis has to be established and an attributability Medical Board held. Treatment has to be continued as per the guidelines mentioned above..11/-
11 -11- Note :- These hospitals are authorized Respiratory Centres. Administrative Instructions for setting up facilities for Isolation, diagnosis (AFB culture), AMB (Atributability Medical Board), referral of pulmonary tuberculosis cases to these centers and treatment will be issued by the respective service HQs. AO 150/75. (b) Duration of Hospitalization Till the condition has been stabilized and patient has been considered non-infectious. Preferably intensive phase of treatment should be under supervision and in a hospital. (c) Discharge from the Hospital - Once medical authorities feel that the above criteria have been fulfilled, patient can be discharged in low medical category (P-3 Temp) provided it is felt that, prescribed domiciliary treatment can be carried out at unit level and regular drug supply also is ensured. (d) Subsequent categorisation. Till such time the patient is on medication he should be observed in cat P-3 or equivalent for maximum duration of one year. Once the patient is off medication and minimum of observation period of 24 weeks have been completed he can be considered for up-gradation to P2 category. Re-categorization to be done after review by a Medical Specialist at nearest service hospital. 23. Treatment and Disposal of Drug Resistant Cases (a) All cases of pulmonary tuberculosis where there are chances of drug resistance should be transferred to MH (CTC) Pune which should remain a nodal point for tuberculosis referral and research. Drug resistance has to be suspected, in case there is no clinical and radiological improvement and or sputum smear remains positive 3 months after supervised and TB treatment. All such cases should be subjected to detailed bacteriological work up and reserve drug to be used under supervision of a specialist in Tuberculosis and Resp disease. (b) DISPOSAL (i) All cases of multi drug resistant (MDR) TB i.e those having combined resistance to rifampicin and isoniazid with or without resistance to any other drug will be candidates for invalidment. (ii) However patients showing clinical, radiological improvement and bacteriological quiscence within 6 months of start of anti TB
12 treatment or attributability Med board (whichever is earlier) may be considered for retention in service. However such decision has to be left to a Senior Adv in TB and Resp Disease or Consultant in Medicine. 12/ (iii) Patients with single drug resistance or polyresistance (ie resistance to more than one anti TB drugs other than a combined resistance to rifampicin and isoniazid) may be considered for retention in service. (iv) Any patient not showing bacteriological quiescence 6 months after start of anti TB treatment or AMB, irrespective of type of resistance will be considered for invalidement out of service and will be permitted six month indoor treatment of MH (CTC) Pune as exservicemen after invalidement
13
Diagnosis and Treatment of Tuberculosis, 2011
 Diagnosis of TB Diagnosis and Treatment of Tuberculosis, 2011 Alfred Lardizabal, MD NJMS Global Tuberculosis Institute Diagnosis of TB, 2011 Diagnosis follows Suspicion When should we Think TB? Who is
Diagnosis of TB Diagnosis and Treatment of Tuberculosis, 2011 Alfred Lardizabal, MD NJMS Global Tuberculosis Institute Diagnosis of TB, 2011 Diagnosis follows Suspicion When should we Think TB? Who is
TUBERCULOSIS. By Dr. Najaf Masood Assistant Prof Pediatrics Benazir Bhutto Hospital Rawalpindi
 TUBERCULOSIS By Dr. Najaf Masood Assistant Prof Pediatrics Benazir Bhutto Hospital Rawalpindi Tuberculosis Infectious, Systemic, Chronic granulomatous disease caused by mycobacterium tuberculosis DEFINITION
TUBERCULOSIS By Dr. Najaf Masood Assistant Prof Pediatrics Benazir Bhutto Hospital Rawalpindi Tuberculosis Infectious, Systemic, Chronic granulomatous disease caused by mycobacterium tuberculosis DEFINITION
Treatment of Active Tuberculosis
 Treatment of Active Tuberculosis Jeremy Clain, MD Pulmonary & Critical Care Medicine Mayo Clinic October 16, 2017 2014 MFMER slide-1 Disclosures No relevant financial relationships No conflicts of interest
Treatment of Active Tuberculosis Jeremy Clain, MD Pulmonary & Critical Care Medicine Mayo Clinic October 16, 2017 2014 MFMER slide-1 Disclosures No relevant financial relationships No conflicts of interest
Pediatric Tuberculosis Lisa Y. Armitige, MD, PhD September 14, 2017
 Pediatric Tuberculosis Lisa Y. Armitige, MD, PhD September 14, 2017 TB Nurse Case Management September 12 14, 2017 EXCELLENCE EXPERTISE INNOVATION Lisa Y. Armitige, MD, PhD has the following disclosures
Pediatric Tuberculosis Lisa Y. Armitige, MD, PhD September 14, 2017 TB Nurse Case Management September 12 14, 2017 EXCELLENCE EXPERTISE INNOVATION Lisa Y. Armitige, MD, PhD has the following disclosures
Fundamentals of Tuberculosis (TB)
 TB in the United States Fundamentals of Tuberculosis (TB) From 1953 to 1984, reported cases decreased by approximately 5.6% each year From 1985 to 1992, reported cases increased by 20% 25,313 cases reported
TB in the United States Fundamentals of Tuberculosis (TB) From 1953 to 1984, reported cases decreased by approximately 5.6% each year From 1985 to 1992, reported cases increased by 20% 25,313 cases reported
Management of MDR TB in special situations. Dr Sarabjit Chadha The Union
 Management of MDR TB in special situations Dr Sarabjit Chadha The Union MDR TB in special situations Pregnancy Breastfeeding Contraception Renal Insufficiency Diabetes Pregnancy and TB Pregnancy is not
Management of MDR TB in special situations Dr Sarabjit Chadha The Union MDR TB in special situations Pregnancy Breastfeeding Contraception Renal Insufficiency Diabetes Pregnancy and TB Pregnancy is not
Tuberculosis Tools: A Clinical Update
 Tuberculosis Tools: A Clinical Update CAPA Conference 2014 JoAnn Deasy, PA-C. MPH, DFAAPA jadeasy@sbcglobal.net Adjunct Faculty Touro PA Program Learning Objectives Outline the pathogenesis of active pulmonary
Tuberculosis Tools: A Clinical Update CAPA Conference 2014 JoAnn Deasy, PA-C. MPH, DFAAPA jadeasy@sbcglobal.net Adjunct Faculty Touro PA Program Learning Objectives Outline the pathogenesis of active pulmonary
Let s Talk TB. A Series on Tuberculosis, A Disease That Affects Over 2 Million Indians Every Year
 A Series on Tuberculosis, A Disease That Affects Over 2 Million Indians Every Year Lancelot M. Pinto, MD, MSc Author Madhukar Pai, MD, PhD co-author and Series Editor Abstract Nearly 50% of patients with
A Series on Tuberculosis, A Disease That Affects Over 2 Million Indians Every Year Lancelot M. Pinto, MD, MSc Author Madhukar Pai, MD, PhD co-author and Series Editor Abstract Nearly 50% of patients with
Antimycobacterial drugs. Dr.Naza M.Ali lec Dec 2018
 Antimycobacterial drugs Dr.Naza M.Ali lec 14-15 6 Dec 2018 About one-third of the world s population is infected with M. tuberculosis With 30 million people having active disease. Worldwide, 9 million
Antimycobacterial drugs Dr.Naza M.Ali lec 14-15 6 Dec 2018 About one-third of the world s population is infected with M. tuberculosis With 30 million people having active disease. Worldwide, 9 million
TUBERCULOSIS. Pathogenesis and Transmission
 TUBERCULOSIS Pathogenesis and Transmission TUBERCULOSIS Pathogenesis and Transmission Infection to Disease Diagnostic & Isolation Updates Treatment Updates Pathogenesis Droplet nuclei of 5µm or less are
TUBERCULOSIS Pathogenesis and Transmission TUBERCULOSIS Pathogenesis and Transmission Infection to Disease Diagnostic & Isolation Updates Treatment Updates Pathogenesis Droplet nuclei of 5µm or less are
ANNEXURE A: EXPLANATORY NOTES ON THE DMR 164 REPORTING ON HIV AND TB FORM
 ANNEXURE A: EXPLANATORY NOTES ON THE DMR 164 REPORTING ON HIV AND TB FORM The form and content of the explanatory note is to: Inform those responsible for completing the DMR 164 Reporting Form - as to
ANNEXURE A: EXPLANATORY NOTES ON THE DMR 164 REPORTING ON HIV AND TB FORM The form and content of the explanatory note is to: Inform those responsible for completing the DMR 164 Reporting Form - as to
Etiological Agent: Pulmonary Tuberculosis. Debra Mercer BSN, RN, RRT. Definition
 Pulmonary Tuberculosis Debra Mercer BSN, RN, RRT Definition Tuberculosis is a contagious bacterial infection of the lungs caused by Mycobacterium Tuberculosis (TB) Etiological Agent: Mycobacterium Tuberculosis
Pulmonary Tuberculosis Debra Mercer BSN, RN, RRT Definition Tuberculosis is a contagious bacterial infection of the lungs caused by Mycobacterium Tuberculosis (TB) Etiological Agent: Mycobacterium Tuberculosis
11/3/2009 SECOND EDITION Madhukar Pai McGill University. ISTC Training Modules Introduction
 SECOND EDITION 2009 Madhukar Pai McGill University Introduction 1 Purpose of ISTC ISTC Version 2: Key Points 21 Standards Differ from existing guidelines: standards present what should be done, whereas,
SECOND EDITION 2009 Madhukar Pai McGill University Introduction 1 Purpose of ISTC ISTC Version 2: Key Points 21 Standards Differ from existing guidelines: standards present what should be done, whereas,
TOG The Way Forward
 TOG 2016- The Way Forward Main Changes in Diagnostic algorithm Definition (Type, Classification, Outcome) Registration at the time of Diagnosis (PHI level Notification Register) Long term follow up (till
TOG 2016- The Way Forward Main Changes in Diagnostic algorithm Definition (Type, Classification, Outcome) Registration at the time of Diagnosis (PHI level Notification Register) Long term follow up (till
SHORT COURSE CHEMOTHERAPY FOR PULMONARY TUBERCULOSIS IN CHILDREN
 SHORT COURSE CHEMOTHERAPY FOR PULMONARY TUBERCULOSIS IN CHILDREN Padma Ramachandran, A.S. Kripasankar and M. Duraipandian* chest radiograph suggestive of tuberculosis. There are a number of reports on
SHORT COURSE CHEMOTHERAPY FOR PULMONARY TUBERCULOSIS IN CHILDREN Padma Ramachandran, A.S. Kripasankar and M. Duraipandian* chest radiograph suggestive of tuberculosis. There are a number of reports on
DIAGNOSIS AND MEDICAL MANAGEMENT OF TB DISEASE
 DIAGNOSIS AND MEDICAL MANAGEMENT OF TB DISEASE Annie Kizilbash MD, MPH Assistant Professor University of Texas Health Science Center Staff Physician, Texas Center for Infectious Diseases TB Nurse Case
DIAGNOSIS AND MEDICAL MANAGEMENT OF TB DISEASE Annie Kizilbash MD, MPH Assistant Professor University of Texas Health Science Center Staff Physician, Texas Center for Infectious Diseases TB Nurse Case
Treatment of Tuberculosis
 TB Clinical i l Intensive Seattle Treatment of Tuberculosis June 16, 2016 Masa Narita, MD Public Health Seattle & King County; Firland Northwest TB Center, University of Washington Outline Unique features
TB Clinical i l Intensive Seattle Treatment of Tuberculosis June 16, 2016 Masa Narita, MD Public Health Seattle & King County; Firland Northwest TB Center, University of Washington Outline Unique features
TB the basics. (Dr) Margaret (DHA) and John (INZ)
 TB the basics (Dr) Margaret (DHA) and John (INZ) Question 1 The scientist who discovered M. tuberculosis was: A: Louis Pasteur B: Robert Koch C: Jean-Antoine Villemin D: Calmette and Guerin Question 2
TB the basics (Dr) Margaret (DHA) and John (INZ) Question 1 The scientist who discovered M. tuberculosis was: A: Louis Pasteur B: Robert Koch C: Jean-Antoine Villemin D: Calmette and Guerin Question 2
Moving Past the Basics of Tuberculosis Phoenix, Arizona May 8-10, 2012
 Moving Past the Basics of Tuberculosis Phoenix, Arizona May 8-10, 2012 LTBI and TB Disease Treatment Cara Christ, MD, MS May 8, 2012 Cara Christ, MD, MS has the following disclosures to make: No conflict
Moving Past the Basics of Tuberculosis Phoenix, Arizona May 8-10, 2012 LTBI and TB Disease Treatment Cara Christ, MD, MS May 8, 2012 Cara Christ, MD, MS has the following disclosures to make: No conflict
Chemotherapy of tuberculosis in Hong Kong: a consensus statement
 Chemotherapy of tuberculosis in Hong Kong MEDICAL PRACTICE Chemotherapy of tuberculosis in Hong Kong: a consensus statement The Tuberculosis Control Coordinating Committee of the Hong Kong Department of
Chemotherapy of tuberculosis in Hong Kong MEDICAL PRACTICE Chemotherapy of tuberculosis in Hong Kong: a consensus statement The Tuberculosis Control Coordinating Committee of the Hong Kong Department of
TB IN EMERGENCIES. Disease Control in Humanitarian Emergencies (DCE)
 TB IN EMERGENCIES Department of Epidemic and Pandemic Alert and Response (EPR) Health Security and Environment Cluster (HSE) (Acknowledgements WHO Stop TB Programme WHO/STB) 1 Why TB? >33% of the global
TB IN EMERGENCIES Department of Epidemic and Pandemic Alert and Response (EPR) Health Security and Environment Cluster (HSE) (Acknowledgements WHO Stop TB Programme WHO/STB) 1 Why TB? >33% of the global
TB: Management in an era of multiple drug resistance. Bob Belknap M.D. Denver Public Health November 2012
 TB: Management in an era of multiple drug resistance Bob Belknap M.D. Denver Public Health November 2012 Objectives: 1. Explain the steps for diagnosing latent and active TB role of interferon-gamma release
TB: Management in an era of multiple drug resistance Bob Belknap M.D. Denver Public Health November 2012 Objectives: 1. Explain the steps for diagnosing latent and active TB role of interferon-gamma release
Diagnosis and Medical Management of Latent TB Infection
 Diagnosis and Medical Management of Latent TB Infection Marsha Majors, RN September 7, 2017 TB Contact Investigation 101 September 6 7, 2017 Little Rock, AR EXCELLENCE EXPERTISE INNOVATION Marsha Majors,
Diagnosis and Medical Management of Latent TB Infection Marsha Majors, RN September 7, 2017 TB Contact Investigation 101 September 6 7, 2017 Little Rock, AR EXCELLENCE EXPERTISE INNOVATION Marsha Majors,
TB/HIV CO-INFECTION ADULT & CHILDREN (INCLUDING INH PROPHYLAXIS) ART Treatment Guideline Training 31 st January to 4 th February, 2011
 TB/HIV CO-INFECTION ADULT & CHILDREN (INCLUDING INH PROPHYLAXIS) ART Treatment Guideline Training 31 st January to 4 th February, 2011 OUTLINE Background Global Incidence The Problem" The 3 I s Drug Resistant
TB/HIV CO-INFECTION ADULT & CHILDREN (INCLUDING INH PROPHYLAXIS) ART Treatment Guideline Training 31 st January to 4 th February, 2011 OUTLINE Background Global Incidence The Problem" The 3 I s Drug Resistant
Errors in Dx and Rx of TB
 Errors in Dx and Rx of TB David Schlossberg, MD, FACP Professor of Medicine Temple University School of Medicine Medical Director, TB Control Program Philadelphia Department of Public Health TB Still a
Errors in Dx and Rx of TB David Schlossberg, MD, FACP Professor of Medicine Temple University School of Medicine Medical Director, TB Control Program Philadelphia Department of Public Health TB Still a
Recognizing MDR-TB in Children. Ma. Cecilia G. Ama, MD 23 rd PIDSP Annual Convention February 2016
 Recognizing MDR-TB in Children Ma. Cecilia G. Ama, MD 23 rd PIDSP Annual Convention 17-18 February 2016 Objectives Review the definitions and categorization of drugresistant tuberculosis Understand the
Recognizing MDR-TB in Children Ma. Cecilia G. Ama, MD 23 rd PIDSP Annual Convention 17-18 February 2016 Objectives Review the definitions and categorization of drugresistant tuberculosis Understand the
Treatment: First Line Drugs TUBERCULOSIS TREATMENT: MEDICATIONS & REGIMENS TREATMENT: GENERAL PRINCIPLES MECHANISM OF ACTION MID 27
 TUBERCULOSIS TREATMENT: MEDICATIONS & REGIMENS Treatment: First Line Drugs 1. ISONIAZID = INH Bacteriocidal against dividing organisms Dose = 300mg = one pill = well absorbed Good CNS penetration Can be
TUBERCULOSIS TREATMENT: MEDICATIONS & REGIMENS Treatment: First Line Drugs 1. ISONIAZID = INH Bacteriocidal against dividing organisms Dose = 300mg = one pill = well absorbed Good CNS penetration Can be
TB in Children. Rene De Gama Block 10 Lectures 2012
 TB in Children Rene De Gama Block 10 Lectures 2012 Contents Epidemiology Transmission and pathogenesis Diagnosis of TB TB and HIV Management Epidemiology The year 2000 8.3 million new TB cases diagnosed
TB in Children Rene De Gama Block 10 Lectures 2012 Contents Epidemiology Transmission and pathogenesis Diagnosis of TB TB and HIV Management Epidemiology The year 2000 8.3 million new TB cases diagnosed
Pediatric TB Lisa Armitige, MD, PhD September 28, 2011
 TB Nurse Case Management Davenport, Iowa September 27 28, 2011 Pediatric TB Lisa Armitige, MD, PhD September 28, 2011 Lisa Armitige, MD, PhD has the following disclosures to make: No conflict of interest.
TB Nurse Case Management Davenport, Iowa September 27 28, 2011 Pediatric TB Lisa Armitige, MD, PhD September 28, 2011 Lisa Armitige, MD, PhD has the following disclosures to make: No conflict of interest.
TB Nurse Case Management San Antonio, Texas July 18 20, 2012
 TB Nurse Case Management San Antonio, Texas July 18 20, 2012 Pediatric TB Kim Smith, MD, MPH July 19, 2012 Kim Smith, MD, MPH has the following disclosures to make: No conflict of interests No relevant
TB Nurse Case Management San Antonio, Texas July 18 20, 2012 Pediatric TB Kim Smith, MD, MPH July 19, 2012 Kim Smith, MD, MPH has the following disclosures to make: No conflict of interests No relevant
New Tuberculosis Guidelines. Jason Stout, MD, MHS
 New Tuberculosis Guidelines Jason Stout, MD, MHS Two New Sets of Guidelines Treatment of Drug-Susceptible Tuberculosis Clinical Infectious Diseases 2016; 63(7): e147-e195 Diagnosis of Tuberculosis in Adults
New Tuberculosis Guidelines Jason Stout, MD, MHS Two New Sets of Guidelines Treatment of Drug-Susceptible Tuberculosis Clinical Infectious Diseases 2016; 63(7): e147-e195 Diagnosis of Tuberculosis in Adults
CHAPTER:1 TUBERCULOSIS. BY Mrs. K.SHAILAJA., M. PHARM., LECTURER DEPT OF PHARMACY PRACTICE, SRM COLLEGE OF PHARMACY
 CHAPTER:1 TUBERCULOSIS BY Mrs. K.SHAILAJA., M. PHARM., LECTURER DEPT OF PHARMACY PRACTICE, SRM COLLEGE OF PHARMACY GLOBAL EMERGENCY: * Tuberculosis kills 5,000 people a day! * 2.3 million die each year!
CHAPTER:1 TUBERCULOSIS BY Mrs. K.SHAILAJA., M. PHARM., LECTURER DEPT OF PHARMACY PRACTICE, SRM COLLEGE OF PHARMACY GLOBAL EMERGENCY: * Tuberculosis kills 5,000 people a day! * 2.3 million die each year!
TB Clinical Guidelines: Revision Highlights March 2014
 TB Clinical Guidelines: Revision Highlights March 2014 AIR TRAVEL & TB CONTROL With respect to non-ambulance air travel of patients diagnosed with or suspected as having active Mycobacterium tuberculosis,
TB Clinical Guidelines: Revision Highlights March 2014 AIR TRAVEL & TB CONTROL With respect to non-ambulance air travel of patients diagnosed with or suspected as having active Mycobacterium tuberculosis,
Chapter 5 Treatment for Latent Tuberculosis Infection
 Chapter 5 Treatment for Latent Tuberculosis Infection Table of Contents Chapter Objectives.... 109 Introduction.... 111 Candidates for the Treatment of LTBI... 112 LTBI Treatment Regimens.... 118 LTBI
Chapter 5 Treatment for Latent Tuberculosis Infection Table of Contents Chapter Objectives.... 109 Introduction.... 111 Candidates for the Treatment of LTBI... 112 LTBI Treatment Regimens.... 118 LTBI
Gary Reubenson 16 October 2012 PAEDIATRIC TUBERCULOSIS: AN OVERVIEW IN 40 MINUTES!!
 Gary Reubenson 16 October 2012 PAEDIATRIC TUBERCULOSIS: AN OVERVIEW IN 40 MINUTES!! DECLARATION No relevant conflicts of interest to declare OVERVIEW Burden of disease & epidemiology Pathogenesis (not
Gary Reubenson 16 October 2012 PAEDIATRIC TUBERCULOSIS: AN OVERVIEW IN 40 MINUTES!! DECLARATION No relevant conflicts of interest to declare OVERVIEW Burden of disease & epidemiology Pathogenesis (not
TB Intensive Houston, Texas. Childhood Tuberculosis Kim Connelly Smith. November 12, 2009
 TB Intensive Houston, Texas November 10-12, 12 2009 Childhood Tuberculosis Kim Connelly Smith MD, MPH November 12, 2009 Childhood Tuberculosis Kim Connelly Smith MD, MPH November 12, 2009 1 OUTLINE Stages
TB Intensive Houston, Texas November 10-12, 12 2009 Childhood Tuberculosis Kim Connelly Smith MD, MPH November 12, 2009 Childhood Tuberculosis Kim Connelly Smith MD, MPH November 12, 2009 1 OUTLINE Stages
TB In Detroit 2011* Early TB: Smudge Sign. Who is at risk for exposure to or infection with TB? Who is at risk for TB after exposure or infection?
 Those oral antibiotics are just not working! Inpatient Standards of Care & Discharge Planning S/He s in the Hospital: Now What Do I Do? Dana G. Kissner, MD TB Intensive Workshop, Lansing, MI 2012 Objectives:
Those oral antibiotics are just not working! Inpatient Standards of Care & Discharge Planning S/He s in the Hospital: Now What Do I Do? Dana G. Kissner, MD TB Intensive Workshop, Lansing, MI 2012 Objectives:
Let s Talk TB A Series on Tuberculosis, A Disease That Affects Over 2 Million Indians Every Year
 Let s Talk TB A Series on Tuberculosis, A Disease That Affects Over 2 Million Indians Every Year Lancelot M. Pinto, MD, MSc Author Madhukar Pai, MD, PhD co-author and Series Editor Lancelot Pinto is a
Let s Talk TB A Series on Tuberculosis, A Disease That Affects Over 2 Million Indians Every Year Lancelot M. Pinto, MD, MSc Author Madhukar Pai, MD, PhD co-author and Series Editor Lancelot Pinto is a
SA TB Guidelines The interface with Advanced Clinical Care
 SA TB Guidelines The interface with Advanced Clinical Care Dr Kogie Naidoo (MBCHB, PHD) Head: CAPRISA Treatment Research Programme Honorary Lecturer - UKZN Department of Public Heath Medicine Annual Workshop
SA TB Guidelines The interface with Advanced Clinical Care Dr Kogie Naidoo (MBCHB, PHD) Head: CAPRISA Treatment Research Programme Honorary Lecturer - UKZN Department of Public Heath Medicine Annual Workshop
Pediatric tuberculosis (i.e., Tuberculosis
 G U I D E L I N E S Updated National Guidelines for Pediatric Tuberculosis in India, 2012 ASHOK KUMAR, DEVESH GUPTA, SHARATH BURUGINA NAGARAJA, *VARINDER SINGH, # GR SETHI AND JAGADISH PRASAD From Central
G U I D E L I N E S Updated National Guidelines for Pediatric Tuberculosis in India, 2012 ASHOK KUMAR, DEVESH GUPTA, SHARATH BURUGINA NAGARAJA, *VARINDER SINGH, # GR SETHI AND JAGADISH PRASAD From Central
3/25/2012. numerous micro-organismsorganisms
 Congenital & Neonatal TB A Case of Tuberculosis Congenital or Acquired? Felicia Dworkin, MD NYC DOHMH Bureau TB Control World TB Day March 23, 2012 Congenital TB: acquired by the fetus during pregnancy
Congenital & Neonatal TB A Case of Tuberculosis Congenital or Acquired? Felicia Dworkin, MD NYC DOHMH Bureau TB Control World TB Day March 23, 2012 Congenital TB: acquired by the fetus during pregnancy
MANAGEMENT OF TUBERCULOSIS IN NEONATES AND YOUNG INFANTS
 MANAGEMENT OF TUBERCULOSIS IN NEONATES AND YOUNG INFANTS A Bekker FIDSSA Conference, 2017 OUTLINE Case Perinatal TB Approach to the TB-exposed newborn MOM AND BABY S Born by NVD at peripheral hospital
MANAGEMENT OF TUBERCULOSIS IN NEONATES AND YOUNG INFANTS A Bekker FIDSSA Conference, 2017 OUTLINE Case Perinatal TB Approach to the TB-exposed newborn MOM AND BABY S Born by NVD at peripheral hospital
Tuberculosis Intensive
 Tuberculosis Intensive San Antonio, Texas April 3 6, 2012 Childhood Tuberculosis Kim Smith, MD, MPH April 6, 2012 Kim Smith, MD, MPH has the following disclosures to make: No conflict of interests No relevant
Tuberculosis Intensive San Antonio, Texas April 3 6, 2012 Childhood Tuberculosis Kim Smith, MD, MPH April 6, 2012 Kim Smith, MD, MPH has the following disclosures to make: No conflict of interests No relevant
has the following disclosures to make:
 CLINICAL DIAGNOSIS AND MANAGEMENT OF TB DISEASE Annie Kizilbash MD, MPH September 22, 2015 TB Nurse Case Management September 22 24, 2015 San Antonio. TX EXCELLENCE EXPERTISE INNOVATION Annie Kizilbash
CLINICAL DIAGNOSIS AND MANAGEMENT OF TB DISEASE Annie Kizilbash MD, MPH September 22, 2015 TB Nurse Case Management September 22 24, 2015 San Antonio. TX EXCELLENCE EXPERTISE INNOVATION Annie Kizilbash
Management of Tuberculosis Training for Health Facility Staff. C: Treat TB Patients. WORLD HEALTH ORGANIZATION Geneva
 Management of Tuberculosis Training for Health Facility Staff C: Treat TB Patients WORLD HEALTH ORGANIZATION Geneva WHO/CDS/TB/2003.314c Management of Tuberculosis Training for Health Facility Staff C
Management of Tuberculosis Training for Health Facility Staff C: Treat TB Patients WORLD HEALTH ORGANIZATION Geneva WHO/CDS/TB/2003.314c Management of Tuberculosis Training for Health Facility Staff C
NATIONAL TUBERCULOSIS CONTROL PROGRAMME- SCC AREA Quarterly Report on New and Retreatment Cases of Tuberculosis
 NATIONAL TUBERCULOSIS CONTROL PROGRAMME- SCC AREA Quarterly Report on New and Retreatment Cases of Tuberculosis Patients registered during quarter* of 20 Name of area No.# Name of the Reporter Signature:
NATIONAL TUBERCULOSIS CONTROL PROGRAMME- SCC AREA Quarterly Report on New and Retreatment Cases of Tuberculosis Patients registered during quarter* of 20 Name of area No.# Name of the Reporter Signature:
Diagnosis and Management of TB Disease Lisa Armitige, MD, PhD September 27, 2011
 TB Nurse Case Management Davenport, Iowa September 27 28, 2011 Diagnosis and Management of TB Disease Lisa Armitige, MD, PhD September 27, 2011 Lisa Armitige, MD, PhD has the following disclosures to make:
TB Nurse Case Management Davenport, Iowa September 27 28, 2011 Diagnosis and Management of TB Disease Lisa Armitige, MD, PhD September 27, 2011 Lisa Armitige, MD, PhD has the following disclosures to make:
5. HIV-positive individuals treated with INH should receive Pyridoxine (B6) 25 mg daily or 50 mg twice/thrice weekly on the same schedule as INH
 V. TB and HIV/AIDS A. Standards of Treatment and Management The majority of TB treatment principles apply to persons with HIV/AIDS who require treatment for TB disease. The following points are either
V. TB and HIV/AIDS A. Standards of Treatment and Management The majority of TB treatment principles apply to persons with HIV/AIDS who require treatment for TB disease. The following points are either
What Is TB? 388 How TB Is Spread 388 How to Know if a Person Has TB 389 How to Treat TB 389 Resistance to TB medicines 390
 386 Chapter 25 In this chapter: What Is TB? 388 How TB Is Spread 388 How to Know if a Person Has TB 389 How to Treat TB 389 Resistance to TB medicines 390 Preventing TB 391 Working for Change 391 387 (TB)
386 Chapter 25 In this chapter: What Is TB? 388 How TB Is Spread 388 How to Know if a Person Has TB 389 How to Treat TB 389 Resistance to TB medicines 390 Preventing TB 391 Working for Change 391 387 (TB)
Characteristics of Mycobacterium
 Mycobacterium Characteristics of Mycobacterium Very thin, rod shape. Culture: Aerobic, need high levels of oxygen to grow. Very slow in grow compared to other bacteria (colonies may be visible in up to
Mycobacterium Characteristics of Mycobacterium Very thin, rod shape. Culture: Aerobic, need high levels of oxygen to grow. Very slow in grow compared to other bacteria (colonies may be visible in up to
Diagnosis of tuberculosis in children
 Diagnosis of tuberculosis in children H Simon Schaaf Desmond Tutu TB Centre Department of Paediatrics and Child Health, Stellenbosch University, and Tygerberg Children s Hospital (TCH) Estimated TB incidence
Diagnosis of tuberculosis in children H Simon Schaaf Desmond Tutu TB Centre Department of Paediatrics and Child Health, Stellenbosch University, and Tygerberg Children s Hospital (TCH) Estimated TB incidence
Pre-Treatment Evaluation. Treatment of Latent TB Infection (LTBI) Initiating Treatment: Patient Education. Before initiating treatment for LTBI:
 Pre-Treatment Evaluation Before initiating treatment for LTBI: Treatment of Latent TB Infection (LTBI) Amee Patrawalla, MD Associate Professor, New Jersey Medical School Attending Physician, NJMS Global
Pre-Treatment Evaluation Before initiating treatment for LTBI: Treatment of Latent TB Infection (LTBI) Amee Patrawalla, MD Associate Professor, New Jersey Medical School Attending Physician, NJMS Global
Communicable Disease Control Manual Chapter 4: Tuberculosis
 Provincial TB Services 655 West 12th Avenue Vancouver, BC V5Z 4R4 www.bccdc.ca Communicable Disease Control Manual Definitions Page 1 2.0 DEFINITIONS Many of the definitions that follow are taken from
Provincial TB Services 655 West 12th Avenue Vancouver, BC V5Z 4R4 www.bccdc.ca Communicable Disease Control Manual Definitions Page 1 2.0 DEFINITIONS Many of the definitions that follow are taken from
Chapter 22. Pulmonary Infections
 Chapter 22 Pulmonary Infections Objectives State the incidence of pneumonia in the United States and its economic impact. Discuss the current classification scheme for pneumonia and be able to define hospital-acquired
Chapter 22 Pulmonary Infections Objectives State the incidence of pneumonia in the United States and its economic impact. Discuss the current classification scheme for pneumonia and be able to define hospital-acquired
10. TB and HIV Infection
 10. TB and HIV Infection The management of patients with TB and HIV infection is complex, requiring management by a multidisciplinary team which includes physicians with expertise in the treatment of both
10. TB and HIV Infection The management of patients with TB and HIV infection is complex, requiring management by a multidisciplinary team which includes physicians with expertise in the treatment of both
TB and Comorbidities Adriana Vasquez, MD April 12, 2018
 TB and Comorbidities Adriana Vasquez, MD April 12, 2018 TB Nurse Case Management April 10 12, 2018 San Antonio, TX EXCELLENCE EXPERTISE INNOVATION Adriana Vasquez, MD has the following disclosures to make:
TB and Comorbidities Adriana Vasquez, MD April 12, 2018 TB Nurse Case Management April 10 12, 2018 San Antonio, TX EXCELLENCE EXPERTISE INNOVATION Adriana Vasquez, MD has the following disclosures to make:
TB Nurse Case Management San Antonio, Texas March 7 9, Pediatric TB Kim Connelly Smith, MD, MPH March 8, 2012
 TB Nurse Case Management San Antonio, Texas March 7 9, 2012 Pediatric TB Kim Connelly Smith, MD, MPH March 8, 2012 Kim Connelly Smith, MD, MPH has the following disclosures to make: No conflict of interests
TB Nurse Case Management San Antonio, Texas March 7 9, 2012 Pediatric TB Kim Connelly Smith, MD, MPH March 8, 2012 Kim Connelly Smith, MD, MPH has the following disclosures to make: No conflict of interests
Tuberculosis - clinical forms. Dr. A.Torossian,, M.D., Ph. D. Department of Respiratory Diseases
 Tuberculosis - clinical forms Dr. A.Torossian,, M.D., Ph. D. Department of Respiratory Diseases 1 TB DISEASE Primary Post-primary (Secondary) Common primary forms Primary complex Tuberculosis of the intrathoracic
Tuberculosis - clinical forms Dr. A.Torossian,, M.D., Ph. D. Department of Respiratory Diseases 1 TB DISEASE Primary Post-primary (Secondary) Common primary forms Primary complex Tuberculosis of the intrathoracic
Tuberculosis. New TB diagnostics. New drugs.new vaccines. Dr: Hussein M. Jumaah CABM Mosul College of Medicine 23/12/2012
 Tuberculosis New TB diagnostics. New drugs.new vaccines Dr: Hussein M. Jumaah CABM Mosul College of Medicine 23/12/2012 Tuberculosis (TB )is a bacterial disease caused by Mycobacterium tuberculosis (occasionally
Tuberculosis New TB diagnostics. New drugs.new vaccines Dr: Hussein M. Jumaah CABM Mosul College of Medicine 23/12/2012 Tuberculosis (TB )is a bacterial disease caused by Mycobacterium tuberculosis (occasionally
TB Intensive San Antonio, Texas May 7-10, 2013
 TB Intensive San Antonio, Texas May 7-10, 2013 TB in the HIV Patient Lisa Armitige, MD, PhD May 09, 2013 Lisa Armitige, MD, PhD has the following disclosures to make: No conflict of interests No relevant
TB Intensive San Antonio, Texas May 7-10, 2013 TB in the HIV Patient Lisa Armitige, MD, PhD May 09, 2013 Lisa Armitige, MD, PhD has the following disclosures to make: No conflict of interests No relevant
At the end of this session, participants will be able to:
 Advanced Concepts in Pediatric TB: Treatment of Tuberculosis Disease Jeffrey R. Starke, M.D. Professor of Pediatrics Baylor College of Medicine [with help from Andrea Cruz, M.D.] Objectives At the end
Advanced Concepts in Pediatric TB: Treatment of Tuberculosis Disease Jeffrey R. Starke, M.D. Professor of Pediatrics Baylor College of Medicine [with help from Andrea Cruz, M.D.] Objectives At the end
Case presentation. Dr REESAUL R
 Case presentation Dr REESAUL R Mr S. 25 years old Case 1 Ref on 06/ April /2006 to Chest Clinic from a private GP of Port Louis for : Cough + haemoptysis and dyspnoea Case 1(6/April/2006) Mr S Single 25
Case presentation Dr REESAUL R Mr S. 25 years old Case 1 Ref on 06/ April /2006 to Chest Clinic from a private GP of Port Louis for : Cough + haemoptysis and dyspnoea Case 1(6/April/2006) Mr S Single 25
TB in the Patient with HIV
 TB in the Patient with HIV Lisa Y. Armitige, MD, PhD May 11, 2017 TB Intensive May 9 12, 2017 San Antonio, TX EXCELLENCE EXPERTISE INNOVATION Lisa Y. Armitige, MD, PhD, has the following disclosures to
TB in the Patient with HIV Lisa Y. Armitige, MD, PhD May 11, 2017 TB Intensive May 9 12, 2017 San Antonio, TX EXCELLENCE EXPERTISE INNOVATION Lisa Y. Armitige, MD, PhD, has the following disclosures to
Update on Management of
 Update on Management of DR TB Definitions Presumptive MDR-TB A patient suspected of drug-resistant TB, based on RNTCP criteria for submission of specimens for drug-susceptibility testing MDR-TB Case A
Update on Management of DR TB Definitions Presumptive MDR-TB A patient suspected of drug-resistant TB, based on RNTCP criteria for submission of specimens for drug-susceptibility testing MDR-TB Case A
Tuberculosis: A Provider s Guide to
 Tuberculosis: A Provider s Guide to Diagnosis and Treatment of Active Tuberculosis (TB) Disease and Screening and Treatment of Latent Tuberculosis Infection (LTBI) Alameda County Health Care Services Agency
Tuberculosis: A Provider s Guide to Diagnosis and Treatment of Active Tuberculosis (TB) Disease and Screening and Treatment of Latent Tuberculosis Infection (LTBI) Alameda County Health Care Services Agency
TB Intensive San Antonio, Texas. TB/HIV Co-Infection. Lisa Armitige, MD, PhD has the following disclosures to make:
 TB Intensive San Antonio, Texas August 2-5, 2011 TB/HIV Co-Infection Lisa Armitige, MD, PhD August 4, 2011 Lisa Armitige, MD, PhD has the following disclosures to make: No conflict of interests No relevant
TB Intensive San Antonio, Texas August 2-5, 2011 TB/HIV Co-Infection Lisa Armitige, MD, PhD August 4, 2011 Lisa Armitige, MD, PhD has the following disclosures to make: No conflict of interests No relevant
Management of MDR TB. Dr Priscilla Rupali MD; DTM&H Professor and Head Department of Infectious Diseases Christian Medical College Vellore
 Management of MDR TB Dr Priscilla Rupali MD; DTM&H Professor and Head Department of Infectious Diseases Christian Medical College Vellore Outline Global epidemiology of Tuberculosis Epidemiology of Tuberculosis
Management of MDR TB Dr Priscilla Rupali MD; DTM&H Professor and Head Department of Infectious Diseases Christian Medical College Vellore Outline Global epidemiology of Tuberculosis Epidemiology of Tuberculosis
Dr Francis Ogaro MTRH ELDORET
 Dr Francis Ogaro MTRH ELDORET TB in children often severe, disseminated and can progress rapidly and with poor outcome TB diagnosis in children has relied on clinical, imaging, microscopy and TST findings.
Dr Francis Ogaro MTRH ELDORET TB in children often severe, disseminated and can progress rapidly and with poor outcome TB diagnosis in children has relied on clinical, imaging, microscopy and TST findings.
TB in the Correctional Setting Florence, Arizona October 7, 2014
 TB in the Correctional Setting Florence, Arizona October 7, 2014 Diagnosis and Treatment of TB Disease Renuka Khurana, MBBS, MPH October 7, 2014 Renuka Khurana, MSSB, MPH has the following disclosures
TB in the Correctional Setting Florence, Arizona October 7, 2014 Diagnosis and Treatment of TB Disease Renuka Khurana, MBBS, MPH October 7, 2014 Renuka Khurana, MSSB, MPH has the following disclosures
Diagnosis and Medical Management of TB Disease. Quratulian Annie Kizilbash, MD, MPH March 17, 2015
 Diagnosis and Medical Management of TB Disease Quratulian Annie Kizilbash, MD, MPH March 17, 2015 TB Nurse Case Management March 17 19, 2015 San Antonio, Texas EXCELLENCE EXPERTISE INNOVATION Quratulian
Diagnosis and Medical Management of TB Disease Quratulian Annie Kizilbash, MD, MPH March 17, 2015 TB Nurse Case Management March 17 19, 2015 San Antonio, Texas EXCELLENCE EXPERTISE INNOVATION Quratulian
Immune Reconstitution Inflammatory Syndrome. Dr. Lesego Mawela
 Immune Reconstitution Inflammatory Syndrome Dr. Lesego Mawela TOPICS FOR DISCUSSION IRIS Case Epidermiology Pathogenesis of IRIS Risk factors for IRIS Epidemiology of IRIS Health system burden of IRIS
Immune Reconstitution Inflammatory Syndrome Dr. Lesego Mawela TOPICS FOR DISCUSSION IRIS Case Epidermiology Pathogenesis of IRIS Risk factors for IRIS Epidemiology of IRIS Health system burden of IRIS
HEALTH SERVICES POLICY & PROCEDURE MANUAL
 PAGE 1 of 7 References Related ACA Standards 4 th Edition Standards for Adult Correctional Institutions 4-4350, 4-4355 These guidelines are based on the recommendations of the American Thoracic Society
PAGE 1 of 7 References Related ACA Standards 4 th Edition Standards for Adult Correctional Institutions 4-4350, 4-4355 These guidelines are based on the recommendations of the American Thoracic Society
Tuberculosis Intensive
 Tuberculosis Intensive San Antonio, Texas April 3 6, 2012 TB in the HIV Patient Lisa Armitige, MD, PhD April 6, 2012 Lisa Armitige, MD, PhD has the following disclosures to make: No conflict of interests
Tuberculosis Intensive San Antonio, Texas April 3 6, 2012 TB in the HIV Patient Lisa Armitige, MD, PhD April 6, 2012 Lisa Armitige, MD, PhD has the following disclosures to make: No conflict of interests
HIV prevalance in TB cases
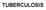 TUBERCULOSIS HIV prevalance in TB cases Top 5 AIDS indicative diseases; EUR, 2003 58% 35% 25% 11% 7% TB HIV wasting s. Candidiasis Rec. pneumonia HIV encephal. 26% 25% 31% 31% 16% 8% 7% 16% 14% 10% TB
TUBERCULOSIS HIV prevalance in TB cases Top 5 AIDS indicative diseases; EUR, 2003 58% 35% 25% 11% 7% TB HIV wasting s. Candidiasis Rec. pneumonia HIV encephal. 26% 25% 31% 31% 16% 8% 7% 16% 14% 10% TB
Diagnosis & Medical Case Management of TB Disease. Lisa Armitige, MD, PhD October 22, 2015
 Diagnosis & Medical Case Management of TB Disease Lisa Armitige, MD, PhD October 22, 2015 Comprehensive Care of Patients with Tuberculosis and Their Contacts October 19 22, 2015 Wichita, KS EXCELLENCE
Diagnosis & Medical Case Management of TB Disease Lisa Armitige, MD, PhD October 22, 2015 Comprehensive Care of Patients with Tuberculosis and Their Contacts October 19 22, 2015 Wichita, KS EXCELLENCE
Patient History 1. Patient History 2. Social History. The Role of Surgery in the Management of TB. Reynard McDonald, MD & Paul Bolanowski, MD
 Patient History 1 The Role of Surgery in the Management of TB Reynard McDonald, MD & Paul Bolanowski, MD September 16, 2010 42 y/o AA male was initially diagnosed with pansensitive pulmonary TB in 1986
Patient History 1 The Role of Surgery in the Management of TB Reynard McDonald, MD & Paul Bolanowski, MD September 16, 2010 42 y/o AA male was initially diagnosed with pansensitive pulmonary TB in 1986
TB & HIV CO-INFECTION IN CHILDREN. Reené Naidoo Paediatric Infectious Diseases Broadreach Healthcare 19 April 2012
 TB & HIV CO-INFECTION IN CHILDREN Reené Naidoo Paediatric Infectious Diseases Broadreach Healthcare 19 April 2012 Introduction TB & HIV are two of the leading causes of morbidity & mortality in children
TB & HIV CO-INFECTION IN CHILDREN Reené Naidoo Paediatric Infectious Diseases Broadreach Healthcare 19 April 2012 Introduction TB & HIV are two of the leading causes of morbidity & mortality in children
Treatment of TB Infection Lisa Y. Armitige, MD, PhD April 7, 2015
 Treatment of TB Infection Lisa Y. Armitige, MD, PhD April 7, 2015 Tuberculosis Infection Diagnosis and Treatment April 7, 2015 El Paso, TX EXCELLENCE EXPERTISE INNOVATION Lisa Y. Armitige, MD, PhD has
Treatment of TB Infection Lisa Y. Armitige, MD, PhD April 7, 2015 Tuberculosis Infection Diagnosis and Treatment April 7, 2015 El Paso, TX EXCELLENCE EXPERTISE INNOVATION Lisa Y. Armitige, MD, PhD has
Latent Tuberculosis Infections Controversies in Diagnosis and Management Update 2016
 Latent Tuberculosis Infections Controversies in Diagnosis and Management Update 2016 Randy Culpepper, MD, MPH Deputy Heath Officer/Medical Director Frederick County Health Department March 16, 2016 2 No
Latent Tuberculosis Infections Controversies in Diagnosis and Management Update 2016 Randy Culpepper, MD, MPH Deputy Heath Officer/Medical Director Frederick County Health Department March 16, 2016 2 No
TB Intensive Houston, Texas
 TB Intensive Houston, Texas October 15-17, 17 2013 Diagnosis of TB: Radiology Rosa M Estrada-Y-Martin, MD MSc FCCP October 16, 2013 Rosa M Estrada-Y-Martin, MD MSc FCCP, has the following disclosures to
TB Intensive Houston, Texas October 15-17, 17 2013 Diagnosis of TB: Radiology Rosa M Estrada-Y-Martin, MD MSc FCCP October 16, 2013 Rosa M Estrada-Y-Martin, MD MSc FCCP, has the following disclosures to
Northwestern Polytechnic University
 Clinical Tuberculosis Assessment by Health Care Provider Clinicians should review and verify the information in the Tuberculosis (TB) Screening Questionnaire (attached). Persons answering YES to any questions
Clinical Tuberculosis Assessment by Health Care Provider Clinicians should review and verify the information in the Tuberculosis (TB) Screening Questionnaire (attached). Persons answering YES to any questions
TB Drugs. Discuss the common route for transmission of the disease. Discusses the out line for treatment of tuberculosis.
 TB Drugs Red : important Black : in male / female slides Pink : in female s slides only Blue : in male s slides only Females doctor notes Grey: Males doctor notes OBJECTIVES: By the end of this lecture,
TB Drugs Red : important Black : in male / female slides Pink : in female s slides only Blue : in male s slides only Females doctor notes Grey: Males doctor notes OBJECTIVES: By the end of this lecture,
Treatment of Tuberculosis
 Treatment of Tuberculosis, 1940 s Treatment of Tuberculosis ATS/CDC/IDSA Joint Statement 2003 Saskatchewan Lung Association Outline, 2012 Treatment of Tuberculosis Principles of treatment of tuberculosis
Treatment of Tuberculosis, 1940 s Treatment of Tuberculosis ATS/CDC/IDSA Joint Statement 2003 Saskatchewan Lung Association Outline, 2012 Treatment of Tuberculosis Principles of treatment of tuberculosis
Treatment of Tuberculosis
 Treatment of Tuberculosis Marcos Burgos, MD April 5, 2016 TB Intensive April 5 8, 2016 San Antonio, TX EXCELLENCE EXPERTISE INNOVATION Marcos Burgos, MD has the following disclosures to make: No conflict
Treatment of Tuberculosis Marcos Burgos, MD April 5, 2016 TB Intensive April 5 8, 2016 San Antonio, TX EXCELLENCE EXPERTISE INNOVATION Marcos Burgos, MD has the following disclosures to make: No conflict
TUBERCULOSIS. Presented By: Public Health Madison & Dane County
 TUBERCULOSIS Presented By: Public Health Madison & Dane County What is Tuberculosis? Tuberculosis, or TB, is a disease caused by a bacteria called Mycobacterium tuberculosis. The bacteria can attack any
TUBERCULOSIS Presented By: Public Health Madison & Dane County What is Tuberculosis? Tuberculosis, or TB, is a disease caused by a bacteria called Mycobacterium tuberculosis. The bacteria can attack any
What you need to know about diagnosing and treating TB: a preventable, fatal disease. Bob Belknap M.D. Denver Public Health November 2014
 What you need to know about diagnosing and treating TB: a preventable, fatal disease Bob Belknap M.D. Denver Public Health November 2014 The Critical First Step Consider TB in the Differential 1. Risks
What you need to know about diagnosing and treating TB: a preventable, fatal disease Bob Belknap M.D. Denver Public Health November 2014 The Critical First Step Consider TB in the Differential 1. Risks
Monica Manandhar. 2 ND YEAR RESEARCH ELECTIVE RESIDENT S JOURNAL Volume V, A. Study Purpose and Rationale
 Randomized Trial of lsoniazid as Secondary Prophylaxis for Prevention of Recurrent Pulmonary Tuberculosis in HIV-positive Patients After One Episode of Tuberculosis Monica Manandhar A. Study Purpose and
Randomized Trial of lsoniazid as Secondary Prophylaxis for Prevention of Recurrent Pulmonary Tuberculosis in HIV-positive Patients After One Episode of Tuberculosis Monica Manandhar A. Study Purpose and
SWABCHA Fact Sheet: Tuberculosis (TB)
 SWABCHA (TB) Text sourced from the SWABCHA Change Agent Training Guide - 2012 Introduction to TB Microscopic bacteria called Mycobacterium tuberculosis causes TB Only TB of the lungs or throat may be infectious.
SWABCHA (TB) Text sourced from the SWABCHA Change Agent Training Guide - 2012 Introduction to TB Microscopic bacteria called Mycobacterium tuberculosis causes TB Only TB of the lungs or throat may be infectious.
TUBERCULOSIS IN HEALTHCARE SETTINGS Diana M. Nilsen, MD, FCCP Director of Medical Affairs, Bureau of Tuberculosis Control New York City Department of
 TUBERCULOSIS IN HEALTHCARE SETTINGS Diana M. Nilsen, MD, FCCP Director of Medical Affairs, Bureau of Tuberculosis Control New York City Department of Health and Mental Hygiene TODAY S PRESENTATION Epidemiology
TUBERCULOSIS IN HEALTHCARE SETTINGS Diana M. Nilsen, MD, FCCP Director of Medical Affairs, Bureau of Tuberculosis Control New York City Department of Health and Mental Hygiene TODAY S PRESENTATION Epidemiology
Tuberculosis. Anne Dunleavy. Excellence in specialist and community healthcare
 Tuberculosis Anne Dunleavy Excellence in specialist and community healthcare Overview Epidemiology Illustrative cases Treatment Priorities Conclusion Presentation title / St George s University Hospitals
Tuberculosis Anne Dunleavy Excellence in specialist and community healthcare Overview Epidemiology Illustrative cases Treatment Priorities Conclusion Presentation title / St George s University Hospitals
Treatment of Tuberculosis
 Treatment of Tuberculosis American Thoracic Society, CDC, and Infectious Diseases Society of America Please note: An erratum has been published for this article. To view the erratum, please click here.
Treatment of Tuberculosis American Thoracic Society, CDC, and Infectious Diseases Society of America Please note: An erratum has been published for this article. To view the erratum, please click here.
Analysis. Answers. Action. Saturday Night Fever. Shaka Brown Capital Congress
 Saturday Night Fever Shaka Brown Capital Congress Shaka Zulu October 31, 2012 SICK SUCKS How my illness started October 2013 August to October 2013 Symptoms: Severe fatigue Night sweats Low grade fever
Saturday Night Fever Shaka Brown Capital Congress Shaka Zulu October 31, 2012 SICK SUCKS How my illness started October 2013 August to October 2013 Symptoms: Severe fatigue Night sweats Low grade fever
Dosage and Administration
 SIRTURO product information for healthcare providers 2 WARNINGS: An increased risk of death was seen in the SIRTURO (bedaquiline) treatment group (9/79, 11.4%) compared to the placebo treatment group (2/81,
SIRTURO product information for healthcare providers 2 WARNINGS: An increased risk of death was seen in the SIRTURO (bedaquiline) treatment group (9/79, 11.4%) compared to the placebo treatment group (2/81,
Profile of Tuberculosis Infection among Current HIV+ Patients at the Philippine General Hospital
 Profile of Tuberculosis Infection among Current HIV+ Patients at the Albert B. Albay Jr., MD Jemylyn Garcia, MD Joel Santiaguel, MD UP- TB in the Philippines 6 th leading cause of morbidity and mortality
Profile of Tuberculosis Infection among Current HIV+ Patients at the Albert B. Albay Jr., MD Jemylyn Garcia, MD Joel Santiaguel, MD UP- TB in the Philippines 6 th leading cause of morbidity and mortality
Management of Drug-resistant Tuberculosis (DR-TB)
 Management of Drug-resistant Tuberculosis (DR-TB) Nitipatana Chierakul Division of Respiratory Disease & Tuberculosis Department of Medicine Faculty of Medicine Siriraj Hospital October 14 th, 2008 Tropical
Management of Drug-resistant Tuberculosis (DR-TB) Nitipatana Chierakul Division of Respiratory Disease & Tuberculosis Department of Medicine Faculty of Medicine Siriraj Hospital October 14 th, 2008 Tropical
International Standards for Tuberculosis Care Barbara J. Seaworth, MD August 22, 2007
 TB Along the US/Mexico Border El Paso, Texas August 22-23, 2007 International Standards for Tuberculosis Care Barbara J. Seaworth, MD August 22, 2007 Barbara J Seaworth MD Medical Director Heartland National
TB Along the US/Mexico Border El Paso, Texas August 22-23, 2007 International Standards for Tuberculosis Care Barbara J. Seaworth, MD August 22, 2007 Barbara J Seaworth MD Medical Director Heartland National
Managing Complex TB Cases Diana M. Nilsen, MD, RN
 Managing Complex TB Cases Diana M. Nilsen, MD, RN Director of Medical Affairs NYC Department of Health & Mental Hygiene Bureau of TB Control Case #1 You are managing a patient who was seen at a private
Managing Complex TB Cases Diana M. Nilsen, MD, RN Director of Medical Affairs NYC Department of Health & Mental Hygiene Bureau of TB Control Case #1 You are managing a patient who was seen at a private
TB: A Supplement to GP CLINICS
 TB: A Supplement to GP CLINICS Chapter 10: Childhood Tuberculosis: Q&A For Primary Care Physicians Author: Madhukar Pai, MD, PhD Author and Series Editor What is Childhood TB and who is at risk? India
TB: A Supplement to GP CLINICS Chapter 10: Childhood Tuberculosis: Q&A For Primary Care Physicians Author: Madhukar Pai, MD, PhD Author and Series Editor What is Childhood TB and who is at risk? India
M ultidrug resistant (MDR) tuberculosis (TB) has
 1106 ORIGINAL ARTICLE Culture confirmed multidrug resistant tuberculosis: diagnostic delay, clinical features, and outcome H S Schaaf, K Shean, P R Donald... See end of article for authors affiliations...
1106 ORIGINAL ARTICLE Culture confirmed multidrug resistant tuberculosis: diagnostic delay, clinical features, and outcome H S Schaaf, K Shean, P R Donald... See end of article for authors affiliations...
TB Intensive San Antonio, Texas
 TB Intensive San Antonio, Texas April 6-8, 2011 TB Disease: ATS/CDC/IDSA Guidelines Barbara Seaworth, MD Thursday April 7, 2011 Barbara Seaworth, MD has the following disclosures to make: Has received
TB Intensive San Antonio, Texas April 6-8, 2011 TB Disease: ATS/CDC/IDSA Guidelines Barbara Seaworth, MD Thursday April 7, 2011 Barbara Seaworth, MD has the following disclosures to make: Has received
