Clinical Biochemistry
|
|
|
- Elwin Tucker
- 5 years ago
- Views:
Transcription
1 Clinical Biochemistry 45 (2012) Contents lists available at SciVerse ScienceDirect Clinical Biochemistry journal homepage: Review An overview of the regulation of bone remodelling at the cellular level Jasreen Kular, Jennifer Tickner, Shek Man Chim, Jiake Xu School of Pathology and Laboratory Medicine, The University of Western Australia, Western Australia, Australia article info abstract Available online 23 March 2012 Keywords: Osteoclast Osteoblast Osteocyte Osteomac Bone lining cell Bone remodelling Coupling factors Endothelial cell RANKL Osteoporosis Objectives: To review the current literature on the regulation of bone remodelling at the cellular level. Design and methods: The cellular activities of the cells in the basic multicellular unit (BMU) were evaluated. Results: Bone remodelling requires an intimate cross-talk between osteoclasts and osteoblasts and is tightly coordinated by regulatory proteins that interact through complex autocrine/paracrine mechanisms. Osteocytes, bone lining cells, osteomacs, and vascular endothelial cells also regulate bone remodelling in the BMU via cell signalling networks of ligand receptor complexes. In addition, through secreted and membrane-bound factors in the bone microenvironment, T and B lymphocytes mediate bone homeostasis in osteoimmunology. Conclusions: Osteoporosis and other bone diseases occur because multicellular communication within the BMU is disrupted. Understanding the cellular and molecular basis of bone remodelling and the discovery of novel paracrine or coupling factors, such as RANKL, sclerostin, EGFL6 and semaphorin 4D, will lay the foundation for drug development against bone diseases The Canadian Society of Clinical Chemists. Published by Elsevier Inc. All rights reserved. Contents Introduction The bone remodelling unit Osteoclasts Regulation of osteoclast differentiation in the BMU Role of osteoclasts in bone remodelling Osteoblasts The role of osteoblasts in bone remodelling Bone formation Regulation of the osteoclast Osteocytes Bone lining cells Osteomacs Vascular endothelial cells Lymphocytes T cells and B cells Diseases due to aberrant bone remodelling Osteoporosis Osteopetrosis Paget's disease of bone Conclusion Conflict of interest Acknowledgements References Corresponding author at: School of Pathology and Laboratory Medicine (M504), The University of Western Australia, 35 Stirling Hwy, Crawley, WA 6009, Australia. Fax: address: jiake.xu@uwa.edu.au (J. Xu). Introduction Bone is a rigid yet dynamic organ that is characterised as a type of connective tissue. Biochemically, it is defined by a mixture of inorganic /$ see front matter 2012 The Canadian Society of Clinical Chemists. Published by Elsevier Inc. All rights reserved. doi: /j.clinbiochem
2 864 J. Kular et al. / Clinical Biochemistry 45 (2012) elements and an organic matrix. In order to maintain its structural integrity, and to fulfil its role in mineral homeostasis, bone is continuously moulded, shaped and repaired, a process termed remodelling. Bone remodelling is the predominant metabolic process regulating bone structure and function during adult life [1,2]. Remodelling is a complex, tightly regulated process carried out by two key cell types: osteoclasts and osteoblasts. Osteoclasts are the principal resorptive cell of bone, playing a role in the formation of the skeleton and regulation of bone mass. Osteoblasts are specialised bone forming cells that synthesise bone matrix, regulate mineralisation and finally differentiate into osteocytes or bone lining cells. The cellular coupling between the activities of the osteoclasts and osteoblasts is highly regulated by local and systemic factors to maintain bone homeostasis [3]. An imbalance in the bone remodelling process, favouring either osteoclast or osteoblast activity, leads to a number of clinical disease conditions including osteopenia, osteoporosis and osteopetrosis. The exact mechanisms responsible for aberrant bone remodelling are still largely unclear. Therefore, understanding the cellular and molecular mechanisms involved in bone remodelling may provide important insight(s) for therapeutic development. The bone remodelling unit Bone remodelling occurs through the concerted action of a functional cohort of cells termed the basic multicellular unit (BMU). The BMU consists of the osteoclasts resorbing bone, the osteoblasts replacing bone, the osteocytes within the bone matrix, the bone lining cells covering the bone surface and the capillary blood supply (Fig. 1). The remodelling cycle begins with an initiation phase that includes the recruitment of osteoclast precursors, their differentiation into mature osteoclasts as well as activation and maintenance of bone resorption. A reversal period then follows whereby osteoclastic bone formation is inhibited and the osteoclasts undergo apoptosis whilst osteoblasts are recruited and begin to differentiate. The reversal phase is a transition from osteoclast to osteoblast activity. The final stage is bone formation by the osteoblasts and is termed the termination phase [4]. This stage lasts the longest, as bone formation is slower than bone resorption, and involves new bone formation and mineralisation as well as terminal differentiation of the osteoblast. The length of the bone remodelling process varies by location, with it being shorter in cortical bone than in cancellous bone. The average length of the remodelling phase in cancellous bone is about 200 days, with the majority of that time (approx. 150 days) devoted to bone formation [5,6]. As bone remodelling is a multicellular event, signalling and crosstalk between the cells involved is important in controlling this process. Recently, progress has been made on the identification of coupling factors, which coordinate the temporal activation and function of the cells within the BMU. This review focuses on the roles of the cells in the BMU and the interaction between these cells and the factors involved in regulating bone remodelling at the cellular level. Osteoclasts Osteoclasts are multinucleated, giant cells formed by the fusion of mononuclear progenitors of the monocyte/macrophage family in a process termed osteoclastogenesis [2]. Osteoclasts are located on endosteal surfaces within the Haversian system and on the periosteal surface beneath the periosteum. Osteoclasts are usually rare cells in the bone with only two to three per μm 3 [7]. Osteoclasts exist in two functional states, the motile and the resorptive phases. During the motile state they migrate from the bone marrow to their resorptive site and in the resorptive phase they exert their bone resorbing function [8]. In each state the osteoclast displays morphological differences. Motile osteoclasts are flattened, non-polarised cells. They are characterised by the presence of membrane protrusions, called lamellipodia, and podosome complexes containing actin. Osteoclasts move and spread by lamellipodia formation. Upon reaching the resorptive site, osteoclasts become polarised through cytoskeletal reorganisation. Polarisation results in the formation of a number of membrane domains: a ruffled border, sealing zone, functional secretory domain and basolateral membrane. The sealing zone is an osteoclast specific structure which separates the acidic resorptive environment from the rest of the cell, forming an organelle free area [9]. The ruffled border and sealing zone is seen only in non-motile resorbing cells. During resorption osteoclasts are dome-shaped and lack lamellipodia. Regulation of osteoclast differentiation in the BMU Osteoclast differentiation and fusion requires a number of steps to occur and a number of osteoclastogenic factors regulate these processes. Fig. 1. The basic multicellular unit of bone remodelling. The bone remodelling compartment consists of osteoclasts, osteoblasts, osteocytes, bone lining cells and endothelial cells which work together to ensure balanced bone remodelling. Each cell type produces modulatory factors that regulate other cell types and some are highlighted in this figure.
3 J. Kular et al. / Clinical Biochemistry 45 (2012) Haematopoietic stem cells give rise to osteoclast precursors which are a subset of bone marrow mononuclear cells. These cells require factors produced either by marrow stromal cells, osteoblasts or T- lymphocytes to differentiate further [10]. Two such factors, which are necessary and sufficient to promote osteoclastogenesis, are macrophage colony-stimulating factor (M-CSF) and receptor for activation of nuclear factor kappa B (NF-κB) (RANK) ligand (RANKL). M-CSF, produced by osteoblasts and stromal cells, is critical for macrophage maturation and binds to its receptor, c-fms, on early osteoclast precursors thereby promoting their survival and proliferation [11,12]. Signal transduction via the c-fms receptor occurs through multiple pathways, including ERK1/2 and PI3K/Akt [13]. M-CSF activates early transcription factors such as c-fos and PU.1. Mice deficient in M-CSF or PU.1 lack osteoclasts and macrophages whilst the inactivation of c-fos results in arrested osteoclastogenesis and an osteopetrotic phenotype [14,15]. It is interesting to note though, that the osteopetrotic op/op mouse, which has a mutation resulting in the absence of M-CSF, restores osteoclast differentiation and function over time, suggesting that other factors may be able to compensate for the loss of M-CSF [16,17]. RANKL, expressed by osteoblasts, T cells and endothelial cells, is essential for osteoclast formation and binds to RANK which is present on osteoclasts and their precursors [18 20] (Fig. 2). RANKL stimulates the M-CSF-expanded precursors to commit to the osteoclast phenotype. These cells then express key osteoclast markers including tartrate resistant acid phosphatase (TRAP). Upon further stimulation with M-CSF and RANKL the preosteoclasts fuse to form multinucleated cells which begin to express more specific osteoclast markers such as calcitonin receptor and Cathepsin K. The binding of RANKL to RANK is dependent on trimerisation of both molecules [21]. RANKL activity can be antagonised by the presence of the soluble decoy receptor Osteoprotegerin (OPG) [22]. This sequesters RANKL from binding to RANK and inhibits osteoclast differentiation. The transmission of the RANKL signal is determined by the ratio of RANKL to OPG, coupled with RANK expression on osteoclast precursors. Like RANKL, OPG is produced by osteoblasts, giving osteoblasts a vital role in controlling the relationship between bone formation and bone resorption [23,24]. Binding of RANKL to its receptor initiates an intracellular signalling cascade that begins with binding of TRAF6 to the RANK receptor [25] (Fig. 2). TRAF6 then phosphorylates IKK (IκB kinase) which ubiquitinates IκB, sending it to the proteasome for degradation. This releases NFκB, allowing its translocation to the nucleus and the initiation of osteoclast specific gene transcription. Abnormal activation of NFκB signalling pathways in osteoclasts disrupts bone remodelling and results in osteolytic bone diseases [26]. Although binding of RANKL has been demonstrated to be the essential signal for osteoclast differentiation, co-stimulatory pathways are also required for this process. The transcription factor nuclear factor of activated T cells (NFAT) has been shown to play an important role in osteoclast differentiation [27] (Fig. 2). RANKL stimulates calcium oscillation which is essential for activation of NFAT. This occurs through co-stimulation of immunoglobulin like receptors such as OSCAR (osteoclast associated receptor) and TREM-2 (triggering receptor expressed on myeloid cells), and the function of adaptor molecules containing ITAM motifs [28]. This signalling cascade activates phospholipase C γ (PLCγ) and subsequent intracellular Ca 2+ release, leading to the nuclear translocation of NFATc1 and subsequent transcription and autoamplification of NFATc1. In addition, a role for CaMK (calmodulin kinase), a major downstream mediator of Ca 2+ signalling, plays an important role in RANKL induced osteoclast differentiation and bone resorption [29,30]. Fig. 2. RANK/RANKL signalling pathway in osteoclasts. The RANKL signalling pathway is a key pathway for the formation and function of osteoclasts. Binding of RANKL to RANK initiates the recruitment of TRAF6 to RANK. IKKK (IκB kinase kinase) is activated in turn phosphorylating IKK (IκB kinase). IKK phosphorylates IκB thereby targeting it for ubiquitination and subsequent proteasomal degradation. NF-κB is then able to translocate to the nucleus for the transcription of essential osteoclast genes. The RANKL pathway works together with the ITAM (immunoreceptor tyrosine based activation motif) co-stimulatory pathway to activate calcium/nfatc1 signalling in osteoclasts.
4 866 J. Kular et al. / Clinical Biochemistry 45 (2012) Role of osteoclasts in bone remodelling Although the primary function of the osteoclast in bone remodelling is resorption of the bone matrix, it also functions in the regulation of bone formation. This can be achieved by secretion of factors that regulate bone formation, liberation of matrix derived factors during resorption or direct cell cell contact with osteoblasts (Fig. 3). The bone resorbing activity of osteoclasts is one way in which bone formation is regulated [31]. The topography of the resorption pit itself is an important factor for the induction of bone formation [32]. In the absence of osteoclasts, osteoblasts may recognise parts of the resorption lacuna such as the deposition of TRAP, which is required by osteoclasts for bone matrix resorption and collagen turnover [33,34]. RANKL expressed by osteoblasts can also directly activate osteoclastic bone resorption, in addition to its role in osteoclast formation [19,20]. As the osteoclast resorbs bone it releases bone matrix-derived factors that may regulate osteoblastic bone formation. These factors are often produced by osteoblasts at the time the bone matrix is laid down and act on the osteoblasts to promote bone formation; however, it is likely that as the osteoclast resorbs bone it processes these bone matrix factors and regulates the amount released to act on the osteoblasts. Such factors include bone morphogenetic proteins (BMPs), insulin like growth factors (IGFs) I and II and transforming growth factor beta (TGFβ) [35 37]. However, osteoclast resorptive activity is not essential for osteoblastic bone formation to occur as patients and mice with osteopetrosis due to impaired osteoclast function (osteoclast-rich osteopetrosis) still have high numbers of functional osteoblasts indicating that it is the number of osteoclasts, Fig. 3. Mechanisms of osteoblast/osteoclast regulation. Osteoblasts and osteoclasts regulate one another via several mechanisms including (i) bone matrix derived factors that are released during resorption and act on both osteoclasts and osteoblasts, (ii) direct cell cell contact between osteoclasts and osteoblasts and (iii) secretion of factors by the osteoclast that regulates the osteoblast and vice-versa. rather than their functional activity, that is more crucial for bone formation [38 41]. It is also important to note that osteoclast poor osteopetrotic patients are also able to form bone, suggesting that osteoclasts are not essential to the fundamental process of bone formation [42,43]. The possible ways in which osteoclasts can regulate osteoblasts has been a topic of great interest and much work has been carried out to identify coupling factors that represent potential therapeutic targets. Sphingosine 1-phosphate (S1P) is secreted by osteoclasts and binds to its receptor on osteoblasts enhancing migration and survival of osteoblasts as well as increasing RANKL production [44]. S1P also has direct effects on osteoclasts by regulating the migration of osteoclast precursors [45]. Ephrin B2, a membrane bound ligand expressed on osteoclasts, binds with its receptor EphB4 on osteoblasts, in a contact dependent mechanism. This interaction promotes osteoblast differentiation and bone formation [46]. The ephrin/eph interaction results in bi-directional signalling meaning that EphB4 can signal to the osteoclast to suppress differentiation [47]. Since ephrin B2 is expressed by mature osteoclasts and EphB4 is expressed on osteoblast precursors it has been hypothesised that this interaction may regulate the transition from bone resorption to formation during remodelling. Most recently, semaphorin 4D has been identified as a coupling factor. Semaphorin 4D is expressed by osteoclasts and inhibits bone formation by binding to its receptor Plexin-B1 on osteoblasts. This interaction activates RhoA which in turn suppresses insulin like growth factor 1 (IGF-1) signalling and modulates osteoblast motility, thereby inhibiting bone formation [48]. Osteoblasts Osteoblasts are the only cell type responsible for bone formation. They originate from mesenchymal stem cells that have the potential to differentiate into mature osteoblasts [49,50]. There are four maturational stages that have been identified in osteoblast differentiation: the preosteoblast, osteoblast, osteocyte and bone-lining cell. Provided the appropriate stimuli are present, the mesenchymal stem cells form preosteoblasts. Histologically these cells resemble osteoblasts and stain positively for alkaline phosphatase, however, they lack some of the characteristics of mature osteoblasts including the ability to produce mineralised tissue [51]. Preosteoblasts give rise to mature osteoblasts, which can be identified by their cuboidal morphology and strong alkaline phosphatase positivity. They reside along the bone surface at sites of active bone formation. Osteoblasts secrete type 1 collagen, the basic building block of bone. In addition, they produce non-collagenous proteins including osteocalcin (a small vitamin-k dependent calcium binding protein that is specific to bone) and alkaline phosphatase, which is essential for mineral deposition [52]. Alkaline phosphatase knockout mice exhibit impaired growth and die before weaning. Examination of the tissues revealed defective mineralisation and morphological abnormalities in the osteoblast highlighting the importance of alkaline phosphatase for osteoblast function [53]. Mature osteoblasts have one of three fates: they undergo apoptosis, differentiate further into osteocytes or become quiescent lining cells. Approximately 50 to 70% of osteoblasts undergo apoptosis [54]. One of the most important signalling pathways regulating bone formation in osteoblasts is the Wnt/β-catenin signalling pathway. The canonical pathway has been most studied and is illustrated in Fig. 4. Wnt ligands bind to a receptor complex composed of frizzled receptor and LDL receptor related protein (LRP) 5 or LRP6 coreceptor. In the absence of ligand binding, glycogen synthase kinase (GSK)-3β acts to phosphorylate β-catenin leading to its ubiquitination and subsequent proteasomal degradation. Binding of Wnts to their receptor complex, leads to the activation of Dishevelled, which inhibits the activity of GSK-3β. This prevents the degradation of β- catenin, which is then able to translocate to the nucleus where it
5 J. Kular et al. / Clinical Biochemistry 45 (2012) Fig. 4. The canonical Wnt/β-catenin signalling pathway in osteoblasts. (i) Wnt binds to its receptor complex consisting of frizzled and the co-receptors LRP5 or LRP6. This results in the activation of Dishevelled and the subsequent inhibition of GSK3 activity. β-catenin is then free to translocate to the nucleus where it binds to the TCF/LEF transcription factors, thereby initiating the transcription of genes necessary for osteoblast differentiation, function and survival. (ii) Inhibition of the Wnt signalling pathway by sclerostin, Dkk or Sfrp prevents activation of Dishevelled. GSK3 remains activated and phosphorylates β-catenin, which then undergoes proteosomal degradation. activates LEF (lymphoid enhancer factor)/tcf (T-cell factor) mediated gene transcription [55 57]. Various physiological inhibitors of the Wnt/β-catenin pathway exist and they function predominantly by preventing formation of the receptor/ligand complex. These include sclerostin and Dickoff (Dkk)-1, which bind to LRP5/6, and secreted frizzled related protein (Sfrp) which binds to Wnt [56,57]. The importance of the Wnt/β-catenin pathway in bone biology is highlighted by the effects of mutations in the LRP5 gene in humans. Loss-of-function mutations in LRP5 causes osteoporosis-pseudoglioma syndrome (OPPG), a rare autosomal recessive disorder characterised by early onset osteoporosis and blindness [58]. Conversely, gain-of-function mutations are associated with high bone mass [59 61]. These human phenotypes have been replicated in mice, with mice lacking LRP5 exhibiting low bone mass due to altered osteoblast proliferation and function [62]. Mice overexpressing LRP5 in osteoblasts have increased bone mass [63]. For a detailed review on animal studies involving genetic manipulation of various molecules in the Wnt/βcatenin pathway refer to Kubota et al. [57]. Other important signalling pathways involved in osteoblast differentiation and bone formation include those of the TGF-β superfamily, the two key members being TGF-β and BMPs (for a detailed review on TGF-β and BMP signalling see [64]). TGF-β signalling is essential for the maintenance and expansion of osteoprogenitor cells and their commitment to the osteoblast lineage. This is achieved through the activation of selective mitogen activated protein kinases (MAPKs) and Smad2/3 signalling [65,66]. The BMP signalling pathway also requires the activation of Smads and their subsequent translocation to the nucleus to activate the transcription of osteogenic genes. The TGF-β and BMP signalling pathways interact with one another as TGF-β1 enhances bone formation induced by BMP2 [67]. Both pathways also interact with the Wnt, PTH and Notch pathways to name a few [68]. The role of osteoblasts in bone remodelling Bone formation The primary function of the osteoblast is bone formation. Therefore, the osteoblast has a role in the initial formation of the skeleton as well as in continued bone growth and remodelling processes. Bone formation occurs via two distinct mechanisms: intramembranous ossification and endochondral ossification. Intramembranous ossification forms the flat bones of the skull and most of the clavicle. This type of bone formation relies on a pre-existing fibrous layer of connective tissue onto which the osteoblasts deposit organic matrix composed of Type 1 collagen. Calcium phosphate is then deposited in the matrix forming spongy bone. In contrast, endochondral ossification, which produces most bones, involves the transformation of mesenchyme into a cartilage model that resembles the shape of the bone. The cartilage is then invaded by blood vessels and gradually broken down as osteoblasts deposit collagenous organic matrix and regulate mineralisation of the matrix by releasing small membrane-bound vesicles that contain calcium and phosphate [69]. The exact mechanism by which mineralisation occurs remains unclear; however, it is thought that the activity of alkaline phosphatase plays an important role [70]. Hyaline cartilage remains on the epiphyseal surfaces where it forms articular cartilage and at the junctions of the diaphysis and epiphysis where it forms the growth plate, allowing the long bones to extend in length during growth. Regulation of the osteoclast Besides their role in bone formation, osteoblasts play an important role in the differentiation of osteoclasts. The regulation of osteoclasts by osteoblasts occurs via factors deposited in the bone matrix which osteoclasts then release during resorption, secretion of factors that act on osteoclasts or direct cell cell contact (Fig. 3). These are similar to the ways in which osteoclasts regulate osteoblasts. Osteoblasts produce M-CSF, RANKL and OPG. As discussed above, these factors are essential for osteoclast formation and function. RANKL is the master cytokine for osteoclast differentiation whilst OPG acts as a decoy receptor controlling the amount of RANKL activating osteoclasts [71]. In addition to regulating osteoclast differentiation, osteoblasts control the movement of osteoclast precursors to the bone surface through the release of chemoattractants. Two bone matrix-derived chemoattractants are osteocalcin and collagen-1 [72]. These are produced by the osteoblasts and are deposited in the matrix during bone formation. As osteoclasts resorb bone these chemoattractants may be released, thereby attracting more osteoclast precursors to the remodelling site to continue resorption. As described below, the bone lining cells may also assist in the release of bone-matrix derived chemoattractants. Monocyte chemoattractant protein (MCP-1) is produced by osteoblasts and recruits osteoclast
6 868 J. Kular et al. / Clinical Biochemistry 45 (2012) precursors. The expression of the MCP-1 receptors on osteoclasts is induced by RANKL, indicating that osteoblasts can control the MCP- 1 dependent recruitment of osteoclast precursors by regulating RANKL expression [73]. There are a number of other factors that indirectly regulate osteoclastogenesis by acting on osteoblasts. Such soluble factors include parathyroid hormone (PTH), parathyroid hormone related peptide (PTHrP), tumour necrosis factor alpha (TNF-α), interleukin-1 (IL-1) and 1,25-(OH) 2 vitamin D 3 to name a few [74 78]. These factors act on osteoblasts to increase RANKL expression, thereby increasing osteoclast differentiation. Some of the factors can act through a dual capacity and are able to inhibit production of OPG by osteoblasts [79]. Osteoblasts are able to regulate their differentiation through the paracrine factor PTHrP. PTHrp is produced by preosteoblasts and acts via the PTH1 receptor present on osteoblasts to stimulate osteoblast differentiation and inhibit osteoblast apoptosis [75,80]. PTHrp therefore has a dual role in regulating osteoclastogenesis and osteoblast differentiation. Osteoblasts play a major role in regulating osteoclast differentiation but whether they control osteoclast activity is not so clearly known. They may play a role indirectly when they lay down the bone matrix through the secretion of matrix proteins containing the RGD (arginine-glycine-aspartic acid) peptide. For osteoclasts to resorb they are required to attach to the bone surface. This occurs via the interaction of integrins with the RGD peptides in matrix proteins such as osteopontin and bone sialoprotein [81]. Osteocytes Osteocytes are terminally differentiated osteoblasts that incorporate into the newly formed bone matrix [82]. These cells are smaller than osteoblasts and have lost many of their cytoplasmic organelles [83]. Osteocytes lie within lacunae in the newly formed bone matrix where they reside for long periods of time but ultimately undergo apoptosis. Osteocytes are spatially isolated from one another; however, they extend long filipodial extensions, which are rich in actin cytoskeleton, connecting them with each other as well as bone lining cells and osteoblasts on the bone surface [84,85]. There is emerging evidence to suggest that the primary function of the osteocyte relates to the determination and maintenance of bone structure. Osteocytes are mechano-sensors capable of transducing musculoskeletal derived mechanical input into biological output [86]. Microdamage (small defects in the bone matrix as a result of skeletal loading or pathologic conditions) has been shown to initiate bone remodelling. Osteocytes located near the sites of microdamage undergo apoptosis which has been correlated with increased bone remodelling due to enhanced RANKL production and an increase in osteoclast formation [87]. A recent study has shown that osteocytes themselves express RANKL, thereby supporting osteoclastogenesis. Mice lacking RANKL specifically in osteocytes display an osteopetrotic phenotype, suggesting that osteocytes may be the major source of RANKL during bone remodelling [88]. However, whether membrane-bound or soluble forms of RANKL are responsible for osteoclast formation remains to be determined. It is possible that the osteocytes can come into contact with osteoclasts through their long processes [89]. In this way, osteocyte derived RANKL can contribute to osteoclast formation and the bone remodelling process. Sclerostin, the osteocyte-secreted bone formation inhibitor, is thought to be another downstream mediator of skeletal responses to the mechanical environment. Sclerostin plays an essential role in regulating the bone's response to mechanical unloading and its expression is up-regulated in patients with disuse-induced bone loss [90,91]. It is hypothesised that sclerostin travels through the osteocytic network to the bone surface where it inhibits Wnt/β-catenin signalling in osteoblasts thereby inhibiting proliferation, impairing mineralisation and enhancing apoptosis [92,93]. Besides acting on osteoblasts, a recent study suggests that sclerostin can also promote osteoclast formation and activity in a RANKL dependent manner [94]. Therefore, osteocyte derived sclerostin can regulate both osteoclasts and osteoblasts. Bone lining cells A subset of osteoblasts will differentiate into bone lining cells. These cells line the majority of bone surfaces that are not being remodelled. It has been proposed that bone lining cells play a role in bone remodelling by preventing the inappropriate interaction of osteoclast precursors with the bone surface. It is thought that the signals that initiate osteoclast formation may stimulate the bone lining cells to prepare for bone resorption, through the actions of collagenase which digests a thin layer of non-mineralised bone, revealing the mineralised matrix underneath [95,96]. The bone lining cells then migrate to form a canopy over the remodelling area, creating a microenvironment for the coupling required during bone remodelling [97]. It has been a topic of much debate as to how cell associated RANKL on active osteoblasts can direct osteoclast formation and function since osteoblasts form and produce bone in the remodelling site after osteoclast formation and activity has been initiated. It has been proposed that the bone lining cells, which have been shown to express RANKL and other osteoblastic markers when lining active remodelling compartments, are responsible for the cell to cell interactions between RANKL and RANK receptor on osteoclast precursors [97]. This argument holds true for many other proposed coupling factors that are thought to act through direct cell to cell interaction. It is not clear what the likelihood of physical interactions within the marrow compartment and the concentration of factors required to activate bone remodelling processes would be in vivo. Some suggest that the compartmentalisation of the remodelling site through the canopy of bone lining cells serves to localise the required cellular precursors, and the factors released from the resorption site, within a volume that allows for direct cellular interactions and high concentrations of cytokines that might otherwise be diluted and rendered ineffectual within the bone marrow milieu [98]. Osteomacs Osteomacs are resident tissue macrophages present on or near the periosteal and endosteal surfaces. They are located within three cells of a bone surface and are often intercalated or associated with bone lining cells. During bone modelling osteomacs form a canopy-like structure over mature osteoblasts [99,100]. Osteomacs regulate osteoblast mineralisation as evidenced by in vitro and in vivo studies showing that depletion of osteomac populations results in reduced osteoblast mineralisation [100]. This suggests that the osteomac population plays a role in bone homeostasis. Since osteomacs are located in close proximity to osteoblasts and regulate osteoblast mineralisation, it has been proposed that osteomacs may provide a coupling signal to osteoblasts during bone modelling in a similar way that osteoclasts provide coupling signals to osteoblasts during bone remodelling [101]. TGFβ and ephrin B2 are potential coupling signals since they are expressed by osteomacs and have been previously implicated in osteoclastic regulation of bone formation. A recent study has shown that osteomacs enhance intramembranous bone formation during bone healing in a tibial injury model [102]. Since intramembranous ossification does not involve resorption of cartilage or a bone template prior to bone formation it has been proposed that the osteomac may serve as a cellular source for the anabolic factors that regulate osteoblast recruitment, maturation and bone formation during this process. Whether osteomacs play a role in bone remodelling is not as clear. A canopy of osteomacs has been identified in the bone remodelling compartments in mice [101]. Further, Pettit et al. have proposed
7 J. Kular et al. / Clinical Biochemistry 45 (2012) that the osteomacs may regulate the tail end of the remodelling cycle by directing ongoing and terminal osteoblast mineralisation, once the osteoclasts have left the bone remodelling site [101]. Vascular endothelial cells A vital, but often overlooked, component of the BMU is the capillary that supplies oxygen and nutrients, and removes calcium and waste products of resorption. Bone is one of the most highly vascularized tissues and angiogenesis plays a pivotal role in bone formation, remodelling and healing [98,103]. The blood supply to bone is essential for maintenance of bone mineral density and bone structure. Pathological situations resulting in loss of the bone blood supply lead to bone death, such as avascular necrosis. Lack of bone vascularity is associated with decreased bone formation and bone mass, inhibition of blood flow to bone inhibits bone healing in fracture models and increases the risk of non-union [103,104]. Bone remodelling takes place in specialised vascular structures. The vasculature provides a conduit for the delivery of systemic signals regulating calcium homeostasis, providing feedback control of the remodelling process directly to the cells involved. One of the most important nutrients transported via the vasculature to the BMU is oxygen, which is fundamental to many cellular processes, in particular energy production. However, there are specific roles for oxygen in relation to bone remodelling. One of the major enzymes required for collagen production is prolyl-4-hydroxylase, which is dependent on molecular oxygen for its function. In the absence of oxygen, osteoblasts cannot produce collagen effectively and their proliferation is reduced [105]. Cellular responses to changes in oxygen tension are directed through the activity of the hypoxia inducible factor (HIF), which is capable of activating gene transcription in response to low oxygen levels [106]. Osteoblast specific knockdown of HIF1α or HIF2α has demonstrated important roles for HIF in controlling bone formation and vascularity [107]. Furthermore, low oxygen environments encourage osteoclast HIF1α stabilisation leading to increased osteoclast number [ ]. HIF1 has recently been identified as a negative regulator of the osteoblast response to mechanical load. Taken together, endothelial cells and the vasculature have a direct role in bone remodelling as they supply nutrients to the BMU. It has been widely speculated that bone remodelling is influenced by the local bone environment that involves cross-talk between endothelial cells and adjacent bone cells [98,103]. Vascular endothelial growth factor (VEGF) has long been associated with bone remodelling. Mice expressing only the VEGF 120 isoform survive to birth but show multiple skeletal irregularities, including reduced mineralisation of long bones, and cell specific defects in osteoblast proliferation and mineralisation, and osteoclast migration. Osteoblasts express VEGF receptor 1 (VEGFR1) and VEGFR2 and also produce VEGF when stimulated by vitamin D 3 [111,112]. Furthermore, VEGF acts as a chemoattractant for osteoclasts [113]. A recent publication has directly linked the co-ordinated process of osteogenesis and angiogenesis through the osteoblast transcriptional regulator Osterix. Transcriptional activation of the VEGF promoter by Osterix in osteoblasts induces angiogenesis via osteoblastic VEGF production into avascular cartilage to initiate mineralisation [114]. RANKL is produced by vascular smooth muscle cells and binds to RANK expressed on the surface of endothelial cells, resulting in the prevention of apoptosis [115]. Expression of RANK on endothelial cells is upregulated by VEGF and this subsequently enhances the angiogenic response to RANKL [116]. Expression of RANKL has also been demonstrated in bone-derived vascular endothelial cells and RANKL is upregulated in response to TGFβ, TNFα, and IL-1α [117,118]. Cytokine activated human vascular endothelial cells have been shown to be capable of promoting the formation, fusion and activity of osteoclasts [117,119]. This suggests that the production of RANKL by endothelial cells can have both autocrine and paracrine modes of action. Recent studies have shown that osteoblast like cells produce secreted epidermal growth factor like-6 (EGFL6) that regulates endothelial cell migration and angiogenesis via a paracrine mechanism [120]. Many other factors that are known to be angiogenic are produced by cells in the BMU; further studies into novel regulators of angiogenesis produced by bone cells will give important insight into the cross-talk between the endothelial cells, osteoblasts and osteoclasts. Lymphocytes T cells and B cells The relationship between the immune and skeletal systems has been studied since the early 1970s and as such the term osteoimmunology was created to describe the overlap between these fields (for a detailed review on osteoimmunology see [121]). Given that immune cells and haematopoietic cells originate in the bone marrow it is not surprising that there is cross-talk between the two systems. A number of factors secreted by immune cells are also known to be osteoclast activating such as RANKL secreted by T cells [122,123]. However, the role of immune cells in the maintenance of normal bone physiology is less clearly understood. It is thought that T cells may have a protective role against bone turnover as in vitro studies suggest that CD8 + T cells inhibited osteoclastogenesis [124,125]. Further, when bone marrow derived from CD4 + and CD8 + deficient mice was cultured in the presence of 1,25-(OH) 2 vitamin D 3 osteoclastogenesis was enhanced, indicating that T cells suppress osteoclast formation [126]. Studies of B cell and T cell deficient mice have highlighted the role of these lymphocytes in bone homeostasis and the attainment of peak bone mass. B cell deficient mice are osteopenic due to increased bone resorption. The deficiency in B cells leads to a deficit in OPG as B cells are a major source of OPG in the bone microenvironment [127]. T cell deficient nude mice also display a decreased basal bone mass phenotype as a consequence of enhanced bone resorption. In nude mice OPG secretion by B cells was reduced in the bone marrow suggesting that T cell deficiency affects B cell OPG secretion [127]. Therefore, in physiological bone homeostasis, T cells play a protective role. Although lymphocytes are not directly present in the remodelling compartment, through the secretion of factors into the bone microenvironment they play a role in bone homeostasis. The role of the immune system in pathological bone conditions has been more comprehensively studied, mostly due to the fact that autoimmune conditions such as rheumatoid arthritis (RA) have extensive bone destruction. Early studies identified osteoclast-like giant cells at the interface between synovium and bone, suggesting that osteoclasts were responsible for the bone destruction [128]. Further studies showed that synovial fluid contained osteoclast precursor cells and osteoclastogenesis supporting cells confirming the presence of osteoclasts in rheumatoid joints [129]. RANKL is also highly expressed by T cells and synovial cells in the synovium of RA patients [ ]. Other inflammatory cytokines such as IL-1, IL-16 and TNF are present in the synovial fluid and are able to induce RANKL expression [121].In recent times there has been much interest in the type of T cell participating in the enhanced osteoclastogenesis. T H 17 (T helper) cells have been identified as the osteoclastogenic T cell subset. These T cells produce IL 17, do not produce large amounts of interferon gamma, express RANKL and trigger local inflammation key characteristics of osteoclastogenic T cells [133,134]. These T cells are not solely responsible for the osteoclastogenic effect in RA as they are not able to induce osteoclastogenesis in a coculture system [134]. Further understanding of the role of lymphocytes in bone biology as well as the molecules involved in the osteoimmune system may be important for the development of targeted therapeutics for bone diseases. Diseases due to aberrant bone remodelling The maintenance of bone homeostasis is dependent on the balance of cellular activities during bone remodelling. Disruption to the
8 870 J. Kular et al. / Clinical Biochemistry 45 (2012) balanced regulation of bone remodelling results in a number of disease conditions including osteoporosis, osteopetrosis and Paget's disease of bone. Osteoporosis Osteoporosis is characterised biologically by the net loss of bone, which results in a decrease in bone density. Ultimately, osteoporosis leads to bone with less tensile strength and significantly greater susceptibility to fracture with less force [135]. There are usually no signs or symptoms of osteoporosis until a fracture occurs, which is why osteoporosis is often called the silent disease. Primary osteoporosis most often occurs in postmenopausal women [135]. This is due to a deficiency in oestrogen that affects circulating levels of cytokines such as IL-1, TNF-α, granulocyte macrophage colony stimulating factor (GM-CSF) and IL-6. As the levels of oestrogen decrease, the levels of these cytokines increase thereby enhancing bone resorption by increasing the recruitment, differentiation and activation of osteoclasts [136,137]. This is mediated by RANKL, generated from osteoblasts and other cell types, leading to increased bone resorption [138]. Osteoporosis is also associated with the normal ageing process. A decline in the number and activity of osteoblasts is seen without a decline in the activity of osteoclasts. Thus, a net bone loss is observed due to decreased bone formation [139]. Secondary osteoporosis is often due to complications in other medical conditions, consequences of changes in physical activity or adverse results of therapeutic interventions for certain disorders [140]. Treatments for osteoporosis aim to reduce the risk of further fractures. Anti-resorptive agents, such as bisphosphonates, and the selective oestrogen-receptor modulator raloxifene reduce the intensity of bone remodelling. Slower remodelling permits more complete secondary mineralisation giving the bone more strength. However, these treatments do not reverse the structural damage [141]. The anabolic agent parathyroid hormone produces some reconstruction of the bone skeleton through the deposition of new bone tissue. The overall effect of this is to increase bone strength and reduce fracture risk [142]. In addition to these treatments calcium and vitamin D supplements can be given. Calcium reduces the rate of bone loss and therefore is often used in conjunction with other treatment forms particularly if a patient's dietary calcium intake is low [143]. More recent therapeutic developments have focused on modulating specific steps in the bone remodelling process such as reducing bone resorption and increasing bone formation. Denosumab, a recombinant fully human monoclonal RANKL specific antibody, is an example of one such therapy. Clinical trials indicated that Denosumab effectively suppresses bone resorption, decreases bone turnover and increases bone mineral density [ ]. The Food and Drug Administration in the US and the European Medicines Agency in Europe have approved Denosumab for clinical use. Emerging data from these clinical trials indicates a promising new treatment for postmenopausal osteoporosis. Osteopetrosis Osteopetrosis is defined as a group of conditions characterised by increased bone density as a result of defects in either osteoclast differentiation or function. At least ten mutations have been identified as being causative in humans. Mutations in RANKL and RANK genes result in rare, osteoclast-poor forms of autosomal recessive osteopetrosis (ARO) where no osteoclasts are present [42,43]. Defects in components of the acidification machinery constitute the majority of osteoclast-rich forms of osteopetrosis. Mutations in TCIRG1 (a3 subunit of V-ATPase) are responsible for ARO in more than 50% of affected patients, highlighting the importance of the V-ATPase proton pump in osteoclast function [38]. Chloride channel 7 mutations cause ARO with neuronal complications [147]. Whilst mutations in carbonic anhydrase type II (CAII) result in ARO with tubular acidosis which is not surprising given the role of CAII in kidney function [148]. All the mutations identified so far only account for approximately 70% of cases. Therefore the search continues to find mutations in novel genes. In patients with TCIRG1 gene mutations it was observed that the osteoblasts were very active [149]. This, together with reports that hyperactive osteoblasts were seen in human and osteopetrotic animals, suggests that osteoblasts could contribute to the increased bone mass [150,151]. Current treatment for ARO relies on total bone marrow transplant, although this is not suitable in patients with RANKL mutations. Rather, treatment is largely supportive and relies on multidisciplinary surveillance. Paget's disease of bone Paget's disease of bone (PDB) is the second most common bone disorder diagnosed after osteoporosis. It is characterised by areas of increased osteoclast activity and abnormal bone remodelling. The most common symptoms include pain, bone enlargement and deformity, fractures and deafness. PDB is highly localised with patients affected either in one bone or multiple bones [152]. The most serious complication of PDB is the development of osteosarcomas in the pagetic bone although this is rare with 1% of patients affected [153]. PDB begins as a focal area of bone resorption, and is generally considered a disease of the osteoclast. The osteoclasts in PDB are increased in size and have a large number of nuclei (up to 100) [154]. An unusual feature seen in the pagetic osteoclasts is the presence of nuclear inclusions which consist of paracrystalline arrays that are similar to the nucleocapsids of paramyxoviruses [155]. In addition to these morphological features, pagetic osteoclast precursors are physiologically abnormal. They respond hyper-sensitively to osteoclastogenic factors including RANKL and 1,25-(OH) 2 vitamin D 3 [156,157]. As is seen during physiological bone remodelling, following bone resorption there is an increase in bone formation with a large number of hyperactive but morphologically normal osteoblasts. The osteoblasts deposit bone in a disorganised manner and therefore the new bone is of a poor quality. During the advanced stages of PDB, bone formation predominates and sclerotic lesions are seen with fibrous tissue deposited in the bone marrow and thickening of the bone observed. PDB clearly represents a gross distortion of the remodelling process with aberrant coupling between resorption and formation. The initiation event behind PDB is unknown; however, a genetic cause is strongly implicated. Laurin et al. identified a point mutation in SQSTM1, a gene encoding sequestosome 1 also known as p62, in patients with PDB [158]. p62 is a ubiquitin binding protein that is involved in the IL-1, RANKL and TNF signalling pathways. Other mutations have since been identified in the SQSTM1/p62 gene including mutations that result in the complete deletion of the ubiquitin binding domain of p62 [159,160]. SQSTM1/p62 mutations are associated with increased osteoclastogenesis and NF-kB activation [160, 161]. Taken together, SQSTM1 is the gene most frequently linked to PDB however researchers are studying other possible genes that increase or activate osteoclasts. No cure exists for PDB; however, the disease can be controlled through the use of bisphosphonates. Identification of novel genes, such as SQSTM1, which affect the balance of the remodelling process offer new pathways to explore the coupling between bone cells, and new hope for therapeutic discoveries. Conclusion The process of bone remodelling is tightly coordinated by a myriad of cellular activities. Whilst intimate cross-talk between osteoblasts and osteoclasts is an integral element in bone remodelling, other cells including osteocytes, bone lining cells, osteomacs and endothelial cells of the basic multicellular unit also play an important
Generation of post-germinal centre myeloma plasma B cell.
 Generation of post-germinal centre myeloma. DNA DAMAGE CXCR4 Homing to Lytic lesion activation CD38 CD138 CD56 Phenotypic markers Naive Secondary lymphoid organ Multiple myeloma is a malignancy of s caused
Generation of post-germinal centre myeloma. DNA DAMAGE CXCR4 Homing to Lytic lesion activation CD38 CD138 CD56 Phenotypic markers Naive Secondary lymphoid organ Multiple myeloma is a malignancy of s caused
Peggers Super Summaries Basic Sciences Bone
 Bone Overview & Turnover BONES Function o Support o Protection o Assisting movement o Storage of minerals o Production of red blood cells from marrow Types o Cancellous o Compact with Haversian systems
Bone Overview & Turnover BONES Function o Support o Protection o Assisting movement o Storage of minerals o Production of red blood cells from marrow Types o Cancellous o Compact with Haversian systems
BONE TISSUE. Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology
 BONE TISSUE Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology BONE FUNCTION Support Protection (protect internal organs) Movement (provide leverage system for skeletal muscles, tendons, ligaments
BONE TISSUE Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology BONE FUNCTION Support Protection (protect internal organs) Movement (provide leverage system for skeletal muscles, tendons, ligaments
The Skeletal System:Bone Tissue
 The Skeletal System:Bone Tissue Dynamic and ever-changing throughout life Skeleton composed of many different tissues cartilage, bone tissue, epithelium, nerve, blood forming tissue, adipose, and dense
The Skeletal System:Bone Tissue Dynamic and ever-changing throughout life Skeleton composed of many different tissues cartilage, bone tissue, epithelium, nerve, blood forming tissue, adipose, and dense
BIOH111. o Cell Module o Tissue Module o Integumentary system o Skeletal system o Muscle system o Nervous system o Endocrine system
 BIOH111 o Cell Module o Tissue Module o Integumentary system o Skeletal system o Muscle system o Nervous system o Endocrine system Endeavour College of Natural Health endeavour.edu.au 1 TEXTBOOK AND REQUIRED/RECOMMENDED
BIOH111 o Cell Module o Tissue Module o Integumentary system o Skeletal system o Muscle system o Nervous system o Endocrine system Endeavour College of Natural Health endeavour.edu.au 1 TEXTBOOK AND REQUIRED/RECOMMENDED
Rama Nada. - Mousa Al-Abbadi. 1 P a g e
 - 1 - Rama Nada - - Mousa Al-Abbadi 1 P a g e Bones, Joints and Soft tissue tumors Before we start: the first 8 minutes was recalling to Dr.Mousa s duties, go over them in the slides. Wherever you see
- 1 - Rama Nada - - Mousa Al-Abbadi 1 P a g e Bones, Joints and Soft tissue tumors Before we start: the first 8 minutes was recalling to Dr.Mousa s duties, go over them in the slides. Wherever you see
Deposition of Bone by the Osteoblasts. Bone is continually being deposited by osteoblasts, and it is continually being resorbed where osteoclasts are
 Bone remodeling Deposition of Bone by the Osteoblasts. Bone is continually being deposited by osteoblasts, and it is continually being resorbed where osteoclasts are active. This mechanism is always is
Bone remodeling Deposition of Bone by the Osteoblasts. Bone is continually being deposited by osteoblasts, and it is continually being resorbed where osteoclasts are active. This mechanism is always is
Osteoclasts- What Do They Do and How Do They Do It? Prof. Steven L. Teitelbaum
 Osteoclasts; What Do They Do 1 Steven L. Teitelbaum, M.D. Wilma and Roswell Messing Professor Department of Pathology and Immunology Washington University School of Medicine OSTEOCLASTS OSTEOBLASTS 2 Osteoclasts
Osteoclasts; What Do They Do 1 Steven L. Teitelbaum, M.D. Wilma and Roswell Messing Professor Department of Pathology and Immunology Washington University School of Medicine OSTEOCLASTS OSTEOBLASTS 2 Osteoclasts
Functions of the Skeletal System. Chapter 6: Osseous Tissue and Bone Structure. Classification of Bones. Bone Shapes
 Chapter 6: Osseous Tissue and Bone Structure Functions of the Skeletal System 1. Support 2. Storage of minerals (calcium) 3. Storage of lipids (yellow marrow) 4. Blood cell production (red marrow) 5. Protection
Chapter 6: Osseous Tissue and Bone Structure Functions of the Skeletal System 1. Support 2. Storage of minerals (calcium) 3. Storage of lipids (yellow marrow) 4. Blood cell production (red marrow) 5. Protection
Skeletal Tissues. Skeletal tissues. Frame; muscles, organs and CT attach. Brain, spinal cord, thoracic organs; heart and lungs.
 Skeletal Tissues Functions 1) support 2) protection 3) movement Skeletal tissues Frame; muscles, organs and CT attach. Brain, spinal cord, thoracic organs; heart and lungs. Aids muscle contraction; generate
Skeletal Tissues Functions 1) support 2) protection 3) movement Skeletal tissues Frame; muscles, organs and CT attach. Brain, spinal cord, thoracic organs; heart and lungs. Aids muscle contraction; generate
SKELETAL SYSTEM I NOTE: LAB ASSIGNMENTS for this topic will run over 3 Weeks. A SEPARATE WORKSHEET WILL BE PROVIDED.
 BIO 211; Anatomy and Physiology I REFERENCE: CHAPTER 07 1 Dr. Lawrence Altman Naugatuck Valley Community College LECTURE TOPICS OUTLINE SKELETAL SYSTEM I NOTE: LAB ASSIGNMENTS for this topic will run over
BIO 211; Anatomy and Physiology I REFERENCE: CHAPTER 07 1 Dr. Lawrence Altman Naugatuck Valley Community College LECTURE TOPICS OUTLINE SKELETAL SYSTEM I NOTE: LAB ASSIGNMENTS for this topic will run over
BONE REMODELLING. Tim Arnett. University College London. Department of Anatomy and Developmental Biology
 BONE REMODELLING Tim Arnett Department of Anatomy and Developmental Biology University College London The skeleton, out of sight and often out of mind, is a formidable mass of tissue occupying about 9%
BONE REMODELLING Tim Arnett Department of Anatomy and Developmental Biology University College London The skeleton, out of sight and often out of mind, is a formidable mass of tissue occupying about 9%
Skeletal System. The skeletal System... Components
 Skeletal System The skeletal System... What are the general components of the skeletal system? What does the skeletal system do for you & how does it achieve these functions? Components The skeletal system
Skeletal System The skeletal System... What are the general components of the skeletal system? What does the skeletal system do for you & how does it achieve these functions? Components The skeletal system
silent epidemic,. (WHO),
 Tel: 02-740-8686; E-mail: hhbkim@snu.ac.kr silent epidemic,. (WHO),. 5 3, 1. 50 70. 50%, 25%, 20% (12~35%). 2.8% 0.7% 4. ( ). bone remodeling (osteoblast), (osteoclast),.. 3~4.. 70% (osteocyte) (bone lining
Tel: 02-740-8686; E-mail: hhbkim@snu.ac.kr silent epidemic,. (WHO),. 5 3, 1. 50 70. 50%, 25%, 20% (12~35%). 2.8% 0.7% 4. ( ). bone remodeling (osteoblast), (osteoclast),.. 3~4.. 70% (osteocyte) (bone lining
CHAPTER 6 LECTURE OUTLINE
 CHAPTER 6 LECTURE OUTLINE I. INTRODUCTION A. Bone is made up of several different tissues working together: bone, cartilage, dense connective tissue, epithelium, various blood forming tissues, adipose
CHAPTER 6 LECTURE OUTLINE I. INTRODUCTION A. Bone is made up of several different tissues working together: bone, cartilage, dense connective tissue, epithelium, various blood forming tissues, adipose
Chapter 6: Skeletal System: Bones and Bone Tissue
 Chapter 6: Skeletal System: Bones and Bone Tissue I. Functions A. List and describe the five major functions of the skeletal system: 1. 2. 3.. 4. 5.. II. Cartilage A. What do chondroblasts do? B. When
Chapter 6: Skeletal System: Bones and Bone Tissue I. Functions A. List and describe the five major functions of the skeletal system: 1. 2. 3.. 4. 5.. II. Cartilage A. What do chondroblasts do? B. When
Comment les cellules osseuses communiquent entre elles. Gérard Friedlander Journées UPA 2011
 Comment les cellules osseuses communiquent entre elles Gérard Friedlander Journées UPA 2011 Structure de l os Osteocyte Ostéoclaste Remodelage osseux RANKL RANK NF-kB pathway Stem cell progenitor precursor
Comment les cellules osseuses communiquent entre elles Gérard Friedlander Journées UPA 2011 Structure de l os Osteocyte Ostéoclaste Remodelage osseux RANKL RANK NF-kB pathway Stem cell progenitor precursor
For more information about how to cite these materials visit
 Author(s): University of Michigan Medical School, Department of Cell and Developmental Biology License: Unless otherwise noted, the content of this course material is licensed under a Creative Commons
Author(s): University of Michigan Medical School, Department of Cell and Developmental Biology License: Unless otherwise noted, the content of this course material is licensed under a Creative Commons
Regulation of the skeletal mass through the life span
 Regulation of the skeletal mass through the life span Functions of the skeletal system Mechanical protection skull Movement leverage for muscles Mineral metabolism calcium store Erythropoiesis red blood
Regulation of the skeletal mass through the life span Functions of the skeletal system Mechanical protection skull Movement leverage for muscles Mineral metabolism calcium store Erythropoiesis red blood
The Skeletal System:Bone Tissue
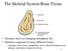 The Skeletal System:Bone Tissue Dynamic and ever-changing throughout life Skeleton composed of many different tissues cartilage, bone tissue, epithelium, nerve, blood forming tissue, adipose, and dense
The Skeletal System:Bone Tissue Dynamic and ever-changing throughout life Skeleton composed of many different tissues cartilage, bone tissue, epithelium, nerve, blood forming tissue, adipose, and dense
Ossification = Osteogenesis
 Ossification = Osteogenesis Ossification = Osteogenesis Parts of the fetal skeleton form during the first few weeks after conception By the end of the 8 th week, the skeletal pattern is formed : cartilage
Ossification = Osteogenesis Ossification = Osteogenesis Parts of the fetal skeleton form during the first few weeks after conception By the end of the 8 th week, the skeletal pattern is formed : cartilage
KEY CONCEPTS Unit 6 THE SKELETAL SYSTEM
 ANATOMY & PHYSIOLOGY 1 (101-805 - AB) PAUL ANDERSON 2011 KEY CONCEPTS Unit 6 THE SKELETAL SYSTEM A Overview of The Skeletal System 1. Definition: Anatomically the SKELETAL SYSTEM consists of bones, cartilages,
ANATOMY & PHYSIOLOGY 1 (101-805 - AB) PAUL ANDERSON 2011 KEY CONCEPTS Unit 6 THE SKELETAL SYSTEM A Overview of The Skeletal System 1. Definition: Anatomically the SKELETAL SYSTEM consists of bones, cartilages,
Osteoporosis and its Association with Rheumatoid Arthritis and Prednisolone Therapy
 Osteoporosis and its Association with Rheumatoid Arthritis and Prednisolone Therapy Master s Thesis Ane Eriksen Medicine with Industrial Specialization Aalborg University Osteoporosis and its Association
Osteoporosis and its Association with Rheumatoid Arthritis and Prednisolone Therapy Master s Thesis Ane Eriksen Medicine with Industrial Specialization Aalborg University Osteoporosis and its Association
Pathophysiology of Postmenopausal & Glucocorticoid Induced Osteoporosis. March 15, 2016 Bone ECHO Kate T Queen, MD
 Pathophysiology of Postmenopausal & Glucocorticoid Induced Osteoporosis March 15, 2016 Bone ECHO Kate T Queen, MD Review: normal bone formation Bone Modeling Remodeling Peak Bone Mass Maximum bone mass
Pathophysiology of Postmenopausal & Glucocorticoid Induced Osteoporosis March 15, 2016 Bone ECHO Kate T Queen, MD Review: normal bone formation Bone Modeling Remodeling Peak Bone Mass Maximum bone mass
OSSEOUS TISSUE & BONE STRUCTURE PART I: OVERVIEW & COMPONENTS
 OSSEOUS TISSUE & BONE STRUCTURE PART I: OVERVIEW & COMPONENTS The Skeletal System Skeletal system includes: bones of the skeleton, cartilages, ligaments, and connective tissues What are the functions of
OSSEOUS TISSUE & BONE STRUCTURE PART I: OVERVIEW & COMPONENTS The Skeletal System Skeletal system includes: bones of the skeleton, cartilages, ligaments, and connective tissues What are the functions of
An Introduction to the Skeletal System Skeletal system includes Bones of the skeleton Cartilages, ligaments, and connective tissues
 An Introduction to the Skeletal System Skeletal system includes Bones of the skeleton Cartilages, ligaments, and connective tissues Functions of the Skeletal System Support Storage of minerals (calcium)
An Introduction to the Skeletal System Skeletal system includes Bones of the skeleton Cartilages, ligaments, and connective tissues Functions of the Skeletal System Support Storage of minerals (calcium)
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,350 108,000 1.7 M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,350 108,000 1.7 M Open access books available International authors and editors Downloads Our
What are the parts of the skeletal system? Chapter 6- Part I Bones and Skeletal Tissues. Growth of Cartilage. Bones come in many shapes
 Chapter 6- Part I Bones and Skeletal Tissues Components of the skeletal system Classification of Bone (bone shapes) Functions of bone Bone structure Microscopic structure of bone and bone cells What are
Chapter 6- Part I Bones and Skeletal Tissues Components of the skeletal system Classification of Bone (bone shapes) Functions of bone Bone structure Microscopic structure of bone and bone cells What are
ANATOMY AND ULTRASTRUCTURE OF BONE HISTOGENESIS, GROWTH AND REMODELING
 ANATOMY AND ULTRASTRUCTURE OF BONE HISTOGENESIS, GROWTH AND REMODELING Updated: May 13, 2008 Authors: Roland Baron, DDS, PhD. Summary 1. Bones have three major functions: to serve as mechanical support,
ANATOMY AND ULTRASTRUCTURE OF BONE HISTOGENESIS, GROWTH AND REMODELING Updated: May 13, 2008 Authors: Roland Baron, DDS, PhD. Summary 1. Bones have three major functions: to serve as mechanical support,
CYTOKINE RECEPTORS AND SIGNAL TRANSDUCTION
 CYTOKINE RECEPTORS AND SIGNAL TRANSDUCTION What is Cytokine? Secreted popypeptide (protein) involved in cell-to-cell signaling. Acts in paracrine or autocrine fashion through specific cellular receptors.
CYTOKINE RECEPTORS AND SIGNAL TRANSDUCTION What is Cytokine? Secreted popypeptide (protein) involved in cell-to-cell signaling. Acts in paracrine or autocrine fashion through specific cellular receptors.
Fig Articular cartilage. Epiphysis. Red bone marrow Epiphyseal line. Marrow cavity. Yellow bone marrow. Periosteum. Nutrient foramen Diaphysis
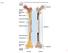 Fig. 7.1 Articular cartilage Epiphysis Red bone marrow Epiphyseal line Marrow cavity Yellow bone marrow Nutrient foramen Diaphysis Site of endosteum Compact bone Spongy bone Epiphyseal line Epiphysis Articular
Fig. 7.1 Articular cartilage Epiphysis Red bone marrow Epiphyseal line Marrow cavity Yellow bone marrow Nutrient foramen Diaphysis Site of endosteum Compact bone Spongy bone Epiphyseal line Epiphysis Articular
SKELETAL SYSTEM CHAPTER 07. Bone Function BIO 211: ANATOMY & PHYSIOLOGY I. Body Movement interacts with muscles bones act as rigid bar of a lever
 Page 1 BIO 211: ANATOMY & PHYSIOLOGY I 1 CHAPTER 07 SKELETAL SYSTEM Dr. Lawrence G. G. Altman www.lawrencegaltman.com Some illustrations are courtesy of McGraw-Hill. Some illustrations are courtesy of
Page 1 BIO 211: ANATOMY & PHYSIOLOGY I 1 CHAPTER 07 SKELETAL SYSTEM Dr. Lawrence G. G. Altman www.lawrencegaltman.com Some illustrations are courtesy of McGraw-Hill. Some illustrations are courtesy of
SKELETAL SYSTEM CHAPTER 07 BIO 211: ANATOMY & PHYSIOLOGY I
 BIO 211: ANATOMY & PHYSIOLOGY I 1 CHAPTER 07 SKELETAL SYSTEM Dr. Lawrence G. G. Altman www.lawrencegaltman.com Some illustrations are courtesy of McGraw-Hill. Some illustrations are courtesy of McGraw-Hill.
BIO 211: ANATOMY & PHYSIOLOGY I 1 CHAPTER 07 SKELETAL SYSTEM Dr. Lawrence G. G. Altman www.lawrencegaltman.com Some illustrations are courtesy of McGraw-Hill. Some illustrations are courtesy of McGraw-Hill.
Osseous Tissue and Bone Structure
 C h a p t e r 6 Osseous Tissue and Bone Structure PowerPoint Lecture Slides prepared by Jason LaPres Lone Star College - North Harris Copyright 2009 Pearson Education, Inc., publishing as Pearson Benjamin
C h a p t e r 6 Osseous Tissue and Bone Structure PowerPoint Lecture Slides prepared by Jason LaPres Lone Star College - North Harris Copyright 2009 Pearson Education, Inc., publishing as Pearson Benjamin
ANATOMY & PHYSIOLOGY - CLUTCH CH. 8 - BONE AND CARTILAGE.
 !! www.clutchprep.com CONCEPT: BONE CLASSIFICATIONS There are four classifications of bones based on their 1. Long bones are greater in length than in width - Found in the upper and lower limbs (ex: arm,
!! www.clutchprep.com CONCEPT: BONE CLASSIFICATIONS There are four classifications of bones based on their 1. Long bones are greater in length than in width - Found in the upper and lower limbs (ex: arm,
Principles of Genetics and Molecular Biology
 Cell signaling Dr. Diala Abu-Hassan, DDS, PhD School of Medicine Dr.abuhassand@gmail.com Principles of Genetics and Molecular Biology www.cs.montana.edu Modes of cell signaling Direct interaction of a
Cell signaling Dr. Diala Abu-Hassan, DDS, PhD School of Medicine Dr.abuhassand@gmail.com Principles of Genetics and Molecular Biology www.cs.montana.edu Modes of cell signaling Direct interaction of a
Module 2:! Functional Musculoskeletal Anatomy A! Semester 1! !!! !!!! Hard Tissues, Distal Upper Limb & Neurovascular Supply of Upper Limb!
 Functional Musculoskeletal Anatomy A Module 2: Hard Tissues, Distal Upper Limb & Neurovascular Supply of Upper Limb Semester 1 1 18. Bone Tissue & Growth of Bones 18.1 Describe the structure of bone tissue
Functional Musculoskeletal Anatomy A Module 2: Hard Tissues, Distal Upper Limb & Neurovascular Supply of Upper Limb Semester 1 1 18. Bone Tissue & Growth of Bones 18.1 Describe the structure of bone tissue
b. Adult bones produce 2.5 million RBCs each second.
 Ch 6 Skeletal System I. Functions of the Skeletal System A. The skeletal system consists of: 1. bones, cartilage, tendons and ligaments B. Living bone is not Gr. dried up 1. It is dynamic and adaptable
Ch 6 Skeletal System I. Functions of the Skeletal System A. The skeletal system consists of: 1. bones, cartilage, tendons and ligaments B. Living bone is not Gr. dried up 1. It is dynamic and adaptable
Chapter 7. Skeletal System
 Chapter 7 Skeletal System 1 Introduction: A. Bones are very active, living tissues B. Each bone is made up of several types of tissues and so is an organ. C. Bone functions include: muscle attachment,
Chapter 7 Skeletal System 1 Introduction: A. Bones are very active, living tissues B. Each bone is made up of several types of tissues and so is an organ. C. Bone functions include: muscle attachment,
Principles of Anatomy and Physiology
 Principles of Anatomy and Physiology 14 th Edition CHAPTER 6 The Skeletal System: Bone Tissue Introduction The skeletal system has 6 important functions: Provides support Protects the internal organs (brain,
Principles of Anatomy and Physiology 14 th Edition CHAPTER 6 The Skeletal System: Bone Tissue Introduction The skeletal system has 6 important functions: Provides support Protects the internal organs (brain,
FORMATION OF BONE. Intramembranous Ossification. Bone-Lec-10-Prof.Dr.Adnan Albideri
 FORMATION OF BONE All bones are of mesodermal origin. The process of bone formation is called ossification. We have seen that formation of most bones is preceded by the formation of a cartilaginous model,
FORMATION OF BONE All bones are of mesodermal origin. The process of bone formation is called ossification. We have seen that formation of most bones is preceded by the formation of a cartilaginous model,
Bone. Development. Tim Arnett. University College London. Department of Anatomy and Developmental Biology
 Bone Development Tim Arnett Department of Anatomy and Developmental Biology University College London Bone development Outline Bone composition matrix + mineral Bone formation - intramembranous & endochondral
Bone Development Tim Arnett Department of Anatomy and Developmental Biology University College London Bone development Outline Bone composition matrix + mineral Bone formation - intramembranous & endochondral
Chapter 6: Osseous Tissue and Bone Structure
 Chapter 6: Osseous Tissue and Bone Structure I. An Introduction to the Skeletal System, p. 180 Objective: Describe the functions of the skeletal system The skeletal system includes: - bones of the skeleton
Chapter 6: Osseous Tissue and Bone Structure I. An Introduction to the Skeletal System, p. 180 Objective: Describe the functions of the skeletal system The skeletal system includes: - bones of the skeleton
SKELETAL TISSUES CHAPTER 7 INTRODUCTION TO THE SKELETAL SYSTEM TYPES OF BONES
 SKELETAL TISSUES CHAPTER 7 By John McGill Supplement Outlines: Beth Wyatt Original PowerPoint: Jack Bagwell INTRODUCTION TO THE SKELETAL SYSTEM STRUCTURE Organs: Bones Related Tissues: Cartilage and Ligaments
SKELETAL TISSUES CHAPTER 7 By John McGill Supplement Outlines: Beth Wyatt Original PowerPoint: Jack Bagwell INTRODUCTION TO THE SKELETAL SYSTEM STRUCTURE Organs: Bones Related Tissues: Cartilage and Ligaments
Bones. The division of bones anatomically is : long, short, irregular, flat and sesamoid.
 Bones Osteocytes : Are responsible for maintenance of bones Present in lacunae, and send processes. Unable to divide. The division of bones anatomically is : long, short, irregular, flat and sesamoid.
Bones Osteocytes : Are responsible for maintenance of bones Present in lacunae, and send processes. Unable to divide. The division of bones anatomically is : long, short, irregular, flat and sesamoid.
The ubiquitin-proteasome system. in bone biology. University of Nottingham. ECTS PhD Training July 5 th Dr Rob Layfield
 The ubiquitin-proteasome system in bone biology Dr Rob Layfield University of Nottingham ECTS PhD Training July 5 th 2009 Images reproduced from: http://www.bostonbiochem.com/overview.php?prod=ubchains
The ubiquitin-proteasome system in bone biology Dr Rob Layfield University of Nottingham ECTS PhD Training July 5 th 2009 Images reproduced from: http://www.bostonbiochem.com/overview.php?prod=ubchains
Chapter 6: SKELETAL SYSTEM
 Chapter 6: SKELETAL SYSTEM I. FUNCTIONS A. Support B. Protection C. Movement D. Mineral storage E. Lipid storage (Fig. 6.8b) F. Blood cell production (Fig. 6.4) II. COMPONENTS A. Cartilage 1. Hyaline 2.
Chapter 6: SKELETAL SYSTEM I. FUNCTIONS A. Support B. Protection C. Movement D. Mineral storage E. Lipid storage (Fig. 6.8b) F. Blood cell production (Fig. 6.4) II. COMPONENTS A. Cartilage 1. Hyaline 2.
BIOLOGY and BIOMECHANICS OF NORMAL & OSTEOPOROTIC BONE
 BIOLOGY and BIOMECHANICS OF NORMAL & OSTEOPOROTIC BONE Andreas Panagopoulos, MD, PhD Assistant Professor in Orthopaedics University Hospital of Patras, Orthopaedic Clinic Objectives Bone structure and
BIOLOGY and BIOMECHANICS OF NORMAL & OSTEOPOROTIC BONE Andreas Panagopoulos, MD, PhD Assistant Professor in Orthopaedics University Hospital of Patras, Orthopaedic Clinic Objectives Bone structure and
Osteology. Dr. Carmen E. Rexach Anatomy 35 Mt San Antonio College
 Osteology Dr. Carmen E. Rexach Anatomy 35 Mt San Antonio College Functions of the Skeletal System: Support Movement Protection Hemopoiesis Electrolyte balance (Ca ++ /PO -3 4 ) Acid-base balance Storage
Osteology Dr. Carmen E. Rexach Anatomy 35 Mt San Antonio College Functions of the Skeletal System: Support Movement Protection Hemopoiesis Electrolyte balance (Ca ++ /PO -3 4 ) Acid-base balance Storage
Do Now: 1. Where, specifically, is blood created? Which part of the long bone? 2. Which structures are primarily associated with growth? 3.
 Do Now: 1. Where, specifically, is blood created? Which part of the long bone? 2. Which structures are primarily associated with growth? 3. How could damage to these areas impact bone growth? WRITE AND
Do Now: 1. Where, specifically, is blood created? Which part of the long bone? 2. Which structures are primarily associated with growth? 3. How could damage to these areas impact bone growth? WRITE AND
T cell maturation. T-cell Maturation. What allows T cell maturation?
 T-cell Maturation What allows T cell maturation? Direct contact with thymic epithelial cells Influence of thymic hormones Growth factors (cytokines, CSF) T cell maturation T cell progenitor DN DP SP 2ry
T-cell Maturation What allows T cell maturation? Direct contact with thymic epithelial cells Influence of thymic hormones Growth factors (cytokines, CSF) T cell maturation T cell progenitor DN DP SP 2ry
-the emphasis on this section is the structure and function of bone tissue and on the dynamics of its formation and remodeling throughout life.
 Biology 325 Fall 2004 BONES AND SKELETAL TISSUES Introduction -skeleton contains cartilage and bones -the emphasis on this section is the structure and function of bone tissue and on the dynamics of its
Biology 325 Fall 2004 BONES AND SKELETAL TISSUES Introduction -skeleton contains cartilage and bones -the emphasis on this section is the structure and function of bone tissue and on the dynamics of its
Awaisheh. Mousa Al-Abbadi. Abdullah Alaraj. 1 Page
 f #3 Awaisheh Abdullah Alaraj Mousa Al-Abbadi 1 Page *This sheet was written from Section 1 s lecture, in the first 10 mins the Dr. repeated all the previous material relating to osteoporosis from the
f #3 Awaisheh Abdullah Alaraj Mousa Al-Abbadi 1 Page *This sheet was written from Section 1 s lecture, in the first 10 mins the Dr. repeated all the previous material relating to osteoporosis from the
Human Anatomy & Physiology
 PowerPoint Lecture Slides prepared by Barbara Heard, Atlantic Cape Community College Ninth Edition Human Anatomy & Physiology C H A P T E R 6 Annie Leibovitz/Contact Press Images 2013 Pearson Education,
PowerPoint Lecture Slides prepared by Barbara Heard, Atlantic Cape Community College Ninth Edition Human Anatomy & Physiology C H A P T E R 6 Annie Leibovitz/Contact Press Images 2013 Pearson Education,
Skeletal Tissues Dr. Ali Ebneshahidi
 Skeletal Tissues Dr. Ali Ebneshahidi Functions of Bones 1. Support and protection: Bones give shape to body structure. Bones provide support to body weight. Certain bones protect vital internal organs
Skeletal Tissues Dr. Ali Ebneshahidi Functions of Bones 1. Support and protection: Bones give shape to body structure. Bones provide support to body weight. Certain bones protect vital internal organs
Ossification and Bone Remodeling
 Ossification and Bone Remodeling Pre-natal Ossification Embryonic skeleton: fashioned from fibrous membranes or cartilage to accommodate mitosis. 2 types of pre-natal ossification (bone formation) 1.
Ossification and Bone Remodeling Pre-natal Ossification Embryonic skeleton: fashioned from fibrous membranes or cartilage to accommodate mitosis. 2 types of pre-natal ossification (bone formation) 1.
Skeletal System worksheet
 Skeletal System worksheet Name Section A: Intro to Skeletal System The skeletal system performs vital functions that enable us to move through our daily lives. Support - The skeleton provides support and
Skeletal System worksheet Name Section A: Intro to Skeletal System The skeletal system performs vital functions that enable us to move through our daily lives. Support - The skeleton provides support and
What is bone? Specialized form of connective tissue: mineralized collagen matrix, therefore very rigid and strong while still retaining some degree of
 Bone What is bone? Specialized form of connective tissue: mineralized collagen matrix, therefore very rigid and strong while still retaining some degree of flexibility Other types of connective tissue:
Bone What is bone? Specialized form of connective tissue: mineralized collagen matrix, therefore very rigid and strong while still retaining some degree of flexibility Other types of connective tissue:
CHAPTER 2. Literature Review. Bone Homeostasis. 2.1 Introduction. 2.2 Composition of bone
 CHAPTER 2 Literature Review I Bone Homeostasis 2.1 Introduction The mature skeleton is a metabolically active organ that undergoes continuous remodeling by a process that replaces old bone with new bone.
CHAPTER 2 Literature Review I Bone Homeostasis 2.1 Introduction The mature skeleton is a metabolically active organ that undergoes continuous remodeling by a process that replaces old bone with new bone.
2 PROCESSES OF BONE OSSIFICATION
 2 PROCESSES OF BONE OSSIFICATION ENDOCHONDRAL OSSIFICATION 6 STEPS 1. CARTILAGE ENLARGES, BY APPOSITIONAL GROWTH; CHONDROCYTES AT CENTER OF CARTILAGE GROW IN SIZE; MATRIX REDUCES IN SIZE & SPICULES CALCIFY;
2 PROCESSES OF BONE OSSIFICATION ENDOCHONDRAL OSSIFICATION 6 STEPS 1. CARTILAGE ENLARGES, BY APPOSITIONAL GROWTH; CHONDROCYTES AT CENTER OF CARTILAGE GROW IN SIZE; MATRIX REDUCES IN SIZE & SPICULES CALCIFY;
Bone Remodeling & Repair Pathologies
 Bone Remodeling & Repair Pathologies Skeletal system remodels itself to maintain homeostasis Remodeling Maintainence replaces mineral reserves (osteocytes) of the matrix Remodelling recycles (osteoclasts)
Bone Remodeling & Repair Pathologies Skeletal system remodels itself to maintain homeostasis Remodeling Maintainence replaces mineral reserves (osteocytes) of the matrix Remodelling recycles (osteoclasts)
Chapter 6 Bones and Bone Tissue Chapter Outline
 Chapter 6 Bones and Bone Tissue Chapter Outline Module 6.1: Introduction to Bones as Organs (Figures 6.1, 6.2, 6.3, 6.4) A. The skeletal system includes the bones, joints, and their associated supporting
Chapter 6 Bones and Bone Tissue Chapter Outline Module 6.1: Introduction to Bones as Organs (Figures 6.1, 6.2, 6.3, 6.4) A. The skeletal system includes the bones, joints, and their associated supporting
Types of Bones. 5 basic types of bones: Sutural bones - in joint between skull bones
 The Skeletal System The Skeletal System Bone and their cartilage, ligaments & tendons. Dynamic and ever changing throughout life Skeleton contains all 4 tissue types; Epithelial, connective, muscle and
The Skeletal System The Skeletal System Bone and their cartilage, ligaments & tendons. Dynamic and ever changing throughout life Skeleton contains all 4 tissue types; Epithelial, connective, muscle and
Skeletal Tissues. Dr. Ali Ebneshahidi
 Skeletal Tissues Dr. Ali Ebneshahidi Functions of Bones 1. Support and protection : Bones give shape to body structure. Bones provide support to body weight. Certain bones protect vital internal organs
Skeletal Tissues Dr. Ali Ebneshahidi Functions of Bones 1. Support and protection : Bones give shape to body structure. Bones provide support to body weight. Certain bones protect vital internal organs
Human Biology Chapter 15.3: Bone Structure *
 OpenStax-CNX module: m58082 1 Human Biology Chapter 15.3: Bone Structure * Willy Cushwa Based on Bone Structure by OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons
OpenStax-CNX module: m58082 1 Human Biology Chapter 15.3: Bone Structure * Willy Cushwa Based on Bone Structure by OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons
Car$lage and Bone. Kris$ne Kra0s, M.D.
 Car$lage and Bone Kris$ne Kra0s, M.D. Car$lage and Bone Lecture Objec$ves Describe the general func$ons of car$lage and bone. Compare the func$on and composi$on of the three types of car$lage. Describe
Car$lage and Bone Kris$ne Kra0s, M.D. Car$lage and Bone Lecture Objec$ves Describe the general func$ons of car$lage and bone. Compare the func$on and composi$on of the three types of car$lage. Describe
Bone Cell Precursors and the Pathophysiology of Bone Loss
 Bone Cell Precursors and the Pathophysiology of Bone Loss HARRY C. BLAIR, a AND JILL L. CARRINGTON b a Departments of Pathology and Cell Biology, University of Pittsburgh, and Pittsburgh VA Medical Center,
Bone Cell Precursors and the Pathophysiology of Bone Loss HARRY C. BLAIR, a AND JILL L. CARRINGTON b a Departments of Pathology and Cell Biology, University of Pittsburgh, and Pittsburgh VA Medical Center,
Biology. Dr. Khalida Ibrahim
 Biology Dr. Khalida Ibrahim BONE TISSUE Bone tissue is a specialized form of connective tissue and is the main element of the skeletal tissues. It is composed of cells and an extracellular matrix in which
Biology Dr. Khalida Ibrahim BONE TISSUE Bone tissue is a specialized form of connective tissue and is the main element of the skeletal tissues. It is composed of cells and an extracellular matrix in which
NOTES: Skeletal System (Ch 5, part 1)
 NOTES: Skeletal System (Ch 5, part 1) Individual bones are the organs of the skeletal system. A bone contains very active tissues. BONE STRUCTURE: *Bone structure reflects its function. Parts of a long
NOTES: Skeletal System (Ch 5, part 1) Individual bones are the organs of the skeletal system. A bone contains very active tissues. BONE STRUCTURE: *Bone structure reflects its function. Parts of a long
T Cell Effector Mechanisms I: B cell Help & DTH
 T Cell Effector Mechanisms I: B cell Help & DTH Ned Braunstein, MD The Major T Cell Subsets p56 lck + T cells γ δ ε ζ ζ p56 lck CD8+ T cells γ δ ε ζ ζ Cα Cβ Vα Vβ CD3 CD8 Cα Cβ Vα Vβ CD3 MHC II peptide
T Cell Effector Mechanisms I: B cell Help & DTH Ned Braunstein, MD The Major T Cell Subsets p56 lck + T cells γ δ ε ζ ζ p56 lck CD8+ T cells γ δ ε ζ ζ Cα Cβ Vα Vβ CD3 CD8 Cα Cβ Vα Vβ CD3 MHC II peptide
OpenStax-CNX module: m Bone Structure * Ildar Yakhin. Based on Bone Structure by OpenStax. Abstract
 OpenStax-CNX module: m63474 1 Bone Structure * Ildar Yakhin Based on Bone Structure by OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 4.0 By
OpenStax-CNX module: m63474 1 Bone Structure * Ildar Yakhin Based on Bone Structure by OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 4.0 By
ANATOMY & PHYSIOLOGY 1 ( ) For Intensive Nursing PAUL ANDERSON SAMPLE TEST
 ANATOMY & PHYSIOLOGY 1 (101-805) For Intensive Nursing PAUL ANDERSON SAMPLE TEST 3 2011 1. If calcium levels in the extracellular fluid are too low, parathyroid hormone secretion would and osteoclast activity
ANATOMY & PHYSIOLOGY 1 (101-805) For Intensive Nursing PAUL ANDERSON SAMPLE TEST 3 2011 1. If calcium levels in the extracellular fluid are too low, parathyroid hormone secretion would and osteoclast activity
Bone Tissue- Chapter 5 5-1
 Bone Tissue- Chapter 5 5-1 Bone Functions Support Protection Assistance in movement Mineral storage and release Blood cell production Triglyceride storage 5-2 Bone Chemistry Water (25%) Organic Constituent
Bone Tissue- Chapter 5 5-1 Bone Functions Support Protection Assistance in movement Mineral storage and release Blood cell production Triglyceride storage 5-2 Bone Chemistry Water (25%) Organic Constituent
Lecture 2: Skeletogenesis
 Jilin University School of Stomatology Skeletogenesis Lecture 2: Skeletogenesis Aug. 18, 2015 Yuji Mishina, Ph.D. mishina@umich.edu Student will describe Development of Bone - the general anatomy of bone
Jilin University School of Stomatology Skeletogenesis Lecture 2: Skeletogenesis Aug. 18, 2015 Yuji Mishina, Ph.D. mishina@umich.edu Student will describe Development of Bone - the general anatomy of bone
Compact bone; Many parallel Haversian canals contain: small blood vessels. very small nerve. Interconnected by Volkmann s canals.
 Special characteristics of COMPACT BONE (dense bone) Thick; well vascularized Osteocytes and lamellae Concentric rings around blood vessels Most bones: outer compact bone inner spongy bone Marrow cavity
Special characteristics of COMPACT BONE (dense bone) Thick; well vascularized Osteocytes and lamellae Concentric rings around blood vessels Most bones: outer compact bone inner spongy bone Marrow cavity
A. Incorrect! It s not correct. Synergism of cytokines refers to two or more cytokines acting together.
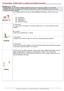 Immunology - Problem Drill 11: Cytokine and Cytokine Receptors Question No. 1 of 10 1. A single cytokine can act on several different cell types, which is known as. Question #1 (A) Synergism (B) Pleiotropism
Immunology - Problem Drill 11: Cytokine and Cytokine Receptors Question No. 1 of 10 1. A single cytokine can act on several different cell types, which is known as. Question #1 (A) Synergism (B) Pleiotropism
HOMEWORK RUBRICS MECHANOTRANSDUCTION UNIT: HOMEWORK #1 (20 pts towards your grade)
 HOMEWORK RUBRICS MECHANOTRANSDUCTION UNIT: HOMEWORK #1 (20 pts towards your grade) 1. Mesenchymal stem cells (MSC) cultured on extracellular matrices with different stiffness exhibit diverse lineage commitment
HOMEWORK RUBRICS MECHANOTRANSDUCTION UNIT: HOMEWORK #1 (20 pts towards your grade) 1. Mesenchymal stem cells (MSC) cultured on extracellular matrices with different stiffness exhibit diverse lineage commitment
Chapter 6 Part B Bones and Skeletal Tissue
 Chapter 6 Part B Bones and Skeletal Tissue 6.5 Bone Development Ossification (osteogenesis) is the process of bone tissue formation Formation of bony skeleton begins in month 2 of development Postnatal
Chapter 6 Part B Bones and Skeletal Tissue 6.5 Bone Development Ossification (osteogenesis) is the process of bone tissue formation Formation of bony skeleton begins in month 2 of development Postnatal
BIOL 2457 CHAPTER 6 SI 1. irregular ectopic: sutural (Wormian) The is between the shaft and end. It contains cartilage that is
 BIOL 2457 CHAPTER 6 SI 1 1. List 5 functions of bones: 2. Classify bones according to shape: give descriptions and examples: long short flat irregular ectopic: sutural (Wormian) ectopic: sesamoid 3. The
BIOL 2457 CHAPTER 6 SI 1 1. List 5 functions of bones: 2. Classify bones according to shape: give descriptions and examples: long short flat irregular ectopic: sutural (Wormian) ectopic: sesamoid 3. The
Tanya Zappitelli. Copyright by Tanya Zappitelli 2015
 Characterization of the Gja1 Jrt /+ Skeletal Phenotype and the Cellular and Molecular Effects of the G60S Connexin 43 Mutation in the Long Bone Microenvironment by Tanya Zappitelli A thesis submitted in
Characterization of the Gja1 Jrt /+ Skeletal Phenotype and the Cellular and Molecular Effects of the G60S Connexin 43 Mutation in the Long Bone Microenvironment by Tanya Zappitelli A thesis submitted in
Signaling Vascular Morphogenesis and Maintenance
 Signaling Vascular Morphogenesis and Maintenance Douglas Hanahan Science 277: 48-50, in Perspectives (1997) Blood vessels are constructed by two processes: vasculogenesis, whereby a primitive vascular
Signaling Vascular Morphogenesis and Maintenance Douglas Hanahan Science 277: 48-50, in Perspectives (1997) Blood vessels are constructed by two processes: vasculogenesis, whereby a primitive vascular
DISCLOSURES TOPICS" PATHOPHYSIOLOGY of OSTEOPOROSIS: Pathways That Control Bone Remodeling! Why Do Bones Remodel?" Nothing to disclose
 PATHOPHYSIOLOGY of OSTEOPOROSIS: Pathways That Control Bone Remodeling Dolores Shoback, MD Professor of Medicine, UCSF Staff Physician SF/VAMC May 19, 2017 DISCLOSURES Nothing to disclose No conflicts
PATHOPHYSIOLOGY of OSTEOPOROSIS: Pathways That Control Bone Remodeling Dolores Shoback, MD Professor of Medicine, UCSF Staff Physician SF/VAMC May 19, 2017 DISCLOSURES Nothing to disclose No conflicts
Regulation of Osteoclast Differentiation
 Regulation of Osteoclast Differentiation G. DAVID ROODMAN University of Pittsburgh, School of Medicine/Hematology-Oncology, and VA Pittsburgh Healthcare System, Medicine/Hematology-Oncology, Pittsburgh,
Regulation of Osteoclast Differentiation G. DAVID ROODMAN University of Pittsburgh, School of Medicine/Hematology-Oncology, and VA Pittsburgh Healthcare System, Medicine/Hematology-Oncology, Pittsburgh,
Mutation in Osteoactivin Enhances RANKL-Mediated Signaling, Promoting Osteoclast Differentiation, Survival and Inhibiting Bone Resorption
 Mutation in Osteoactivin Enhances RANKL-Mediated Signaling, Promoting Osteoclast Differentiation, Survival and Inhibiting Bone Resorption Samir Abdelmagid, MD, PhD, Fouad Moussa, BS, Sondag Gregory, MS,
Mutation in Osteoactivin Enhances RANKL-Mediated Signaling, Promoting Osteoclast Differentiation, Survival and Inhibiting Bone Resorption Samir Abdelmagid, MD, PhD, Fouad Moussa, BS, Sondag Gregory, MS,
Dr. Heba Kalbouneh. Saba Alfayoumi. Heba Kalbouneh
 11 Dr. Heba Kalbouneh Saba Alfayoumi Heba Kalbouneh 2- Bone Bone tissue is also classified into primary bone and secondary bone. In the beginning, the first bone that is deposited by the osteoblasts is
11 Dr. Heba Kalbouneh Saba Alfayoumi Heba Kalbouneh 2- Bone Bone tissue is also classified into primary bone and secondary bone. In the beginning, the first bone that is deposited by the osteoblasts is
Due in Lab. Due next week in lab - Scientific America Article Select one article to read and complete article summary
 Due in Lab 1. Skeletal System 33-34 2. Skeletal System 26 3. PreLab 6 Due next week in lab - Scientific America Article Select one article to read and complete article summary Cell Defenses and the Sunshine
Due in Lab 1. Skeletal System 33-34 2. Skeletal System 26 3. PreLab 6 Due next week in lab - Scientific America Article Select one article to read and complete article summary Cell Defenses and the Sunshine
Pathophysiology of fracture healing
 Pathophysiology of fracture healing Bone anatomy and biomechanics Fracture patterns Bone healing and blood supply Influence of implants 1 What is the structure of bone? 2 Bone structure Four levels: Chemical
Pathophysiology of fracture healing Bone anatomy and biomechanics Fracture patterns Bone healing and blood supply Influence of implants 1 What is the structure of bone? 2 Bone structure Four levels: Chemical
The Skeletal System PART A. PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College
 PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Skeletal System 5 PART A The Skeletal System Parts of the skeletal system Bones (skeleton) Joints
PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Skeletal System 5 PART A The Skeletal System Parts of the skeletal system Bones (skeleton) Joints
BONE LABORATORY DEMONSTRATIONS. These demonstrations are found on the bulletin boards outside the MCO Bookstore.
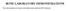 BONE LABORATORY DEMONSTRATIONS These demonstrations are found on the bulletin boards outside the MCO Bookstore. COMPACT & TRABECULAR BONE - LM When viewed under the polarizing light microscope, the layering
BONE LABORATORY DEMONSTRATIONS These demonstrations are found on the bulletin boards outside the MCO Bookstore. COMPACT & TRABECULAR BONE - LM When viewed under the polarizing light microscope, the layering
IRA-International Journal of Applied Sciences ISSN Vol. 03 Issue 02 (May, 2016) Paper DOI:
 IRA-International Journal of Applied Sciences ISSN 2455-4499 Vol. 03 Issue 02 (May, 2016) Paper DOI: https://dx.doi.org/10.21013/jas.v3.n2.p8 Pathophysiology of Giant Cell Formation in Giant Cell Tumor
IRA-International Journal of Applied Sciences ISSN 2455-4499 Vol. 03 Issue 02 (May, 2016) Paper DOI: https://dx.doi.org/10.21013/jas.v3.n2.p8 Pathophysiology of Giant Cell Formation in Giant Cell Tumor
Blood. Hematopoietic Tissue
 Blood Hematopoietic Tissue Is a type of connective tissue in which its cells are suspended in a circulating fluid. Erythrocytes+ leukocytes + platelets (thrombocytes) =formed elements of blood. These formed
Blood Hematopoietic Tissue Is a type of connective tissue in which its cells are suspended in a circulating fluid. Erythrocytes+ leukocytes + platelets (thrombocytes) =formed elements of blood. These formed
Drugs Affecting Bone. Rosa McCarty PhD. Department of Pharmacology & Therapeutics
 Drugs Affecting Bone Rosa McCarty PhD Department of Pharmacology & Therapeutics rmccarty@unimelb.edu.au Objectives At the end of this lecture you should have gained: An understanding of bone metabolism
Drugs Affecting Bone Rosa McCarty PhD Department of Pharmacology & Therapeutics rmccarty@unimelb.edu.au Objectives At the end of this lecture you should have gained: An understanding of bone metabolism
Tissue repair. (3&4 of 4)
 Tissue repair (3&4 of 4) What will we discuss today: Regeneration in tissue repair Scar formation Cutaneous wound healing Pathologic aspects of repair Regeneration in tissue repair Labile tissues rapid
Tissue repair (3&4 of 4) What will we discuss today: Regeneration in tissue repair Scar formation Cutaneous wound healing Pathologic aspects of repair Regeneration in tissue repair Labile tissues rapid
THE ROLE OF CHOLINE KINASE BETA IN BONE HOMEOSTASIS
 THE ROLE OF CHOLINE KINASE BETA IN BONE HOMEOSTASIS JASREEN KULAR, B.Sc B.MedSci (Hons) This thesis is submitted to fulfill the requirements of the University of Western Australia for the degree of DOCTOR
THE ROLE OF CHOLINE KINASE BETA IN BONE HOMEOSTASIS JASREEN KULAR, B.Sc B.MedSci (Hons) This thesis is submitted to fulfill the requirements of the University of Western Australia for the degree of DOCTOR
Skeletal System worksheet
 Skeletal System worksheet Name Section A: Intro to Skeletal System The skeletal system performs vital functions that enable us to move through our daily lives. Support - The skeleton provides support and
Skeletal System worksheet Name Section A: Intro to Skeletal System The skeletal system performs vital functions that enable us to move through our daily lives. Support - The skeleton provides support and
Animal Tissue Culture SQG 3242 Biology of Cultured Cells. Dr. Siti Pauliena Mohd Bohari
 Animal Tissue Culture SQG 3242 Biology of Cultured Cells Dr. Siti Pauliena Mohd Bohari The Culture Environment Changes of Cell s microenvironment needed that favor the spreading, migration, and proliferation
Animal Tissue Culture SQG 3242 Biology of Cultured Cells Dr. Siti Pauliena Mohd Bohari The Culture Environment Changes of Cell s microenvironment needed that favor the spreading, migration, and proliferation
Chapter 6 Skeletal System
 Chapter 6 Skeletal System Functions of the skeletal system/bone 1. Support skeletal system is the internal framework of the body 2. Protection protects internal organs 3. Movement muscles & bones work
Chapter 6 Skeletal System Functions of the skeletal system/bone 1. Support skeletal system is the internal framework of the body 2. Protection protects internal organs 3. Movement muscles & bones work
Index. Rheum Dis Clin N Am 32 (2006) Note: Page numbers of article titles are in boldface type.
 Rheum Dis Clin N Am 32 (2006) 775 780 Index Note: Page numbers of article titles are in boldface type. A AACE (American Association of Clinical Endocrinologists), bone mineral density recommendations of,
Rheum Dis Clin N Am 32 (2006) 775 780 Index Note: Page numbers of article titles are in boldface type. A AACE (American Association of Clinical Endocrinologists), bone mineral density recommendations of,
SKELETAL SYSTEM. Introduction Notes (pt 1)
 SKELETAL SYSTEM Introduction Notes (pt 1) I. INTRODUCTION 1. Bones include active, living tissues: bone tissue, cartilage, dense connective tissue, blood, and nervous tissue. 2. Bones: support and protect
SKELETAL SYSTEM Introduction Notes (pt 1) I. INTRODUCTION 1. Bones include active, living tissues: bone tissue, cartilage, dense connective tissue, blood, and nervous tissue. 2. Bones: support and protect
