Dermatology for the Internist Alabama and Mississippi ACP Scientific Meeting 2017
|
|
|
- Bernice Perkins
- 5 years ago
- Views:
Transcription
1 Dermatology for the Internist Alabama and Mississippi ACP Scientific Meeting 2017 Jeremy D. Jackson, M.D., F.A.A.D Assistant Professor of Dermatology Assistant Professor of Medicine University of Mississippi Medical Center
2 Disclosures Speakers Bureau: Celgene, SunPharma, Actelion, Abbvie
3 Dermatology in Primary Care Skin disorders affect 20-30% of the population in the United States 1 in 3 Americans affected with a skin disease at any given time National shortage of dermatologists results in referral times on average > 1 month In UK, 75% of skin conditions managed exclusively by primary care Harlow, et al. Br J Dermatol. Nov 2000 Williams H, Bigby M. The rationale for evidence-based dermatology. In: Williams H, et al. Evidence Based Dermatology. 2nd ed. Malden, MA: Blackwell Publishing; 2008:1-11. Kimball AB, Resneck JS. The US dermatology workforce: a specialty remains in shortage. J Am Acad Dermatol. 2008;59(5):
4 Inpatient Dermatology Approximately 1/3 of hospitalized patients demonstrate significant skin findings 10% of hospitalized patients have skin findings relevant to their admission or indicative of systemic disease In one study $900 million dollars in Medicare reimbursement due to dermatology-related diagnosis
5 Dermatology consultation changed the final diagnosis in 71% of consultation requests
6 Case 1 42 yo WM with 10+ year history of rash on arms and trunk. Worse when sweating in the summer.
7 A skin biopsy is performed. Which of the following dreaded pathology reports is associated with this skin condition? A. Interface dermatitis with lymphocytes B. Spongiotic dermatitis C. Naked granulomas D. Psoriasiform dermatitis E. Subepidermal blister with eosinophils Response Counter
8 A skin biopsy is performed. Which of the following dreaded pathology reports is associated with this skin condition? A. Interface dermatitis with lymphocytes LUPUS and other CONNECTIVE TISSUE DZ B. Spongiotic dermatitis Atopic Dermatitis, Allergic Contact Dermatitis C. Naked granulomas Sarcoidosis D. Psoriasiform dermatitis Psoriasis E. Subepidermal blister with eosinophils Bullous Pemphigoid
9
10
11 Eczema =Dermatitis Pathology Spongiotic Dermatitis Ddx: Atopic dermatitis, Allergic contact dermatitis, Drug eruption, early Mycosis fungoides * Erythema and swelling of skin * Oozing and/or vesiculation * Crusting and scaling * Thickening and evidence of repeated excoriation * Hyperpigmentation, scratch papule formation and/or lichenification
12
13
14 Nummular Eczema
15 Clinical Characteristics Infantile: face, scalp, extensors Adult: more often flexural Acute skin lesions- intensely pruritic erythem. papules and thin plaques with secondary excoriations; can see vesicles & serous crusts Subacute- erythematous papules/ plaques with scaling and excoriations Chronic- thickened, hyperkeratotic plaques with lichenification & prurigo nodules
16 Conventional Therapies for Atopic Dermatitis Emollients Irritant / allergen identification and avoidance Topical corticosteroids Sedating antihistamines Systemic therapies Phototherapy (PUVA, UVA, UVB) Immunosuppressive agents (Cyclosporine, MTX, Azathioprine, Mycophenolate mofetil) Beers MH, Berkow R, eds. The Merck Manual of Diagnosis and Therapy. 17th ed. Rahway, NJ: Merck Research Labs; 1999: Leung DYM. J Allergy Clin Immunol. 2000;105:
17 Which vehicle used in the formulation of topical steroids is the most potent? A. Ointment B. Cream C. Lotion D. Solution Response Counter
18
19 Steroid-Free Topical Therapies Tacrolimus ointment 0.03%, 0.1% Topical formulation of oral transplant drug Approved December 2000 Pimecrolimus cream 1% Specifically developed to treat inflammatory skin diseases Approved December 2001
20 What s new? Crisaborole 2% ointment PDE-4 inhibitor approved in December 2016 for mild-to-moderate atopic dermatitis ISGA score success (clear/almost clear with 2-grade improvement; AD-301: 32.8% vs 25.4%, P =.038; AD-302: 31.4% vs 18.0%, P <.001) Clear/almost clear (51.7% vs 40.6%, P =.005; 48.5% vs 29.7%, P <.001). Crisaborole-treated patients achieved success in ISGA score and improvement in pruritus earlier than those treated with vehicle (both P.001).
21 What s New? Dupilumab First biologic approved for atopic dermatitis (March 2017) IL-4/IL-13 inhibitor 18 and older
22 Case 2 45 yo obese WF with hx of multiple sclerosis presents with complaints of rash on abdomen and elbows. It does not itch. Pt reports joint pains, particularly of the DIPs of the hands. She also has morning stiffness lasting about an hour. Your exam shows well demarcated plaques on the bilateral elbows and abdomen. BSA >15%
23
24 Which of the following is the best choice in management for this patient? A. Topical Calcitriol and triamcinolone 0.1% cream B. Oral prednisone taper C. Ustekinumab D. Cyclosporine E. Infliximab Response Counter
25 Psoriasis Sharply demarcated plaques with silvery scale Affects 2% of population; Two peaks and Auspitz sign Bleeding upon removal of scale Elbows, Knees, Scalp, and Non sun exposed areas Nail pits more frequently associated with psoriatic arthritis Sausage digits, pencil-in-cup deformities, inflammation of DIP joints, enthesitis associated with arthritis
26
27
28
29 Papules Plaques
30
31
32
33 Inverse Psoriasis
34 Psoriatic Arthritis/Nail Dystrophy
35 Nail Psoriasis
36
37 Psoriatic Erythroderma
38 Comorbidities and Psoriasis People with psoriasis more likely to have a cardiovascular event and stroke 46% more likely to Type II Diabetes Up to 30% have psoriatic arthritis Also associated with the metabolic syndrome
39 Psoriasis Pearl Systemic steroids are rarely used as patients with risk of severe rebound (pustular) psoriasis after discontinuation.
40
41
42
43
44
45
46 Psoriasis Pearl Always ask about joint pain/morning stiffness.
47 Psoriasis pathogenesis
48 Treatment Topicals (Vit D analogs, topical steroids, tar compounds) Phototherapy nbuvb Systemic therapy Moderate-to-severe psoriasis Psoriatic arthritis Psoriasis in difficult locations (scalp, palms/soles, inverse)
49 Systemic Treatments 1. Methotrexate 2. Acitretin 3. Cyclosporine 4. Biologics Etanercept, Infliximab, Adalimumab, Ustekinumab
50 What s new? IL-17 inhibitors (secukinumab, ixekizumab,brodalumab) Apremilast (PDE-4 inhibitor) oral medication Biosimilars for TNF-alpha inhibitors (etanercept, adalimumab, infliximab) are FDA approved but caught up in court systems over patents In phase III trials JAK inhibitors, IL-23 inhibitors
51 Case 3 24 yo college student presents with 2 week history of rash on the arm. She denies any joint pain and takes no medicines And she is getting married in 4 weeks!!
52
53
54
55
56 Which of the following is the most likely diagnosis? A. Granuloma annulare B. Tinea corporis C. Subacute cutaneous lupus erythematosus D. Erythema multiforme E. I don t know but just put Lotrisone on it (betamethasone/clotrimazole) Response Counter
57 What percent of patients with SCLE meet criteria for SLE? A. 5% B. 25% C. 40% D. 60% E. 80% Response Counter
58 What positive lab test is associated with patients with SCLE? A. Anti-histone B. Anti-centromere C. dsdna D. Jo-1 E. SS-A Response Counter
59 What positive lab test is associated with patients with SCLE? A. Anti-histone B. Anti-centromere C. dsdna D. Jo-1 E. SS-A (75-90% SSA/Ro; 30-40% SSB/La)
60 Subacute Cutaneous Lupus Often associated with Anti-Ro Sun-exposed sites Sides of face, V of neck, forearms Mid-face usually spared Annular patches/plaques with raised, red borders, central clearing, slight scale Roughly 75% have arthralgia or arthritis
61
62 Tinea Corporis
63
64 Granuloma annulare
65 Variants of Cutaneous Lupus Acute cutaneous lupus Epidermis and upper dermis Associated with systemic disease Subacute cutaneous lupus Epidermis and upper dermis Not significant systemic involvement Associated with anti-ro autoabs and photosensitivity Discoid lupus Epidermis, dermis, and adnexal structures Scarring No significant systemic involvement Lupus erythematosus tumidus Dermis only No adnexal involvement Lupus panniculitis Subcutaneous tissue Depressed, disfiguring scars
66 Discoid Lupus Erythematosus Face, scalp, ears, occasionally widespread Sun-exposed and sun-protected sites, even mucosal Scarring and dyspigmentation About 5% develop systemic disease SCC can develop in long-standing lesions
67 Discoid Lupus
68 Discoid Lupus
69 Butterfly/malar rash, poikiloderma, papules, occasional scale Follow sun exposure Transient (hrs-weeks) Non-scarring May have oral ulcerations Acute Cutaneous Lupus Spares knuckles (Unlike dermatomyositis which involves the knuckles)
70 Need 4/11 Criteria ACR Diagnostic Criteria S- Serositis O- Oral ulcers A- Arthritis P- Photosensitivity B- Blood disorders (cytopenias) R- Renal disorders A- Anti-nuclear antibody I- Immunologic (dsdna, Sm, antiphospholipid) N- Neurologic disorders (Sz/psychosis) M- Malar rash D- Discoid rash 4 of the 11 Criteria Involve Mucocutaneous Findings
71 Treatment Topical or intralesional CS: mainstay of therapy Systemic: Anti-malarials are gold standard Hydroxychloroquine 200mg qd or bid Chloroquine 250 mg qd Resistant cases: oral retinoids, thalidomide, gold, clofazimine, sulfasalazine, azathioprine, systemic CS, dapsone, MTX Adjuvant therapy High SPF Sunscreen (UVA and UVB) Protective clothing Stop smoking
72 Case 4 56 yo AAF with history of discoid lupus since 1999 presents with 4 month history of pruritic rash. Pt given trimethoprim/sulfamethoxazole initially without improvement. Started on prednisone 20mg for past 3 months along with triamcinolone cream. She has been on hydroxycholorquiine 400mg daily for over 15 years She has joint pains but denies any recent worsening
73
74
75
76
77
78
79
80
81
82 What is the most likely diagnosis? A. Lupus with co-existent psoriasis B. Mixed connective tissue disease C. Crusted scabies D. Pityriasis rubra pilaris E. Lupus with tinea capitis Response Counter
83
84
85
86
87
88 Crusted (Norwegian) scabies first described in 1848 by Boeck and Danielssen among lepers Causative agent is the mite, Sarcoptes scabiei var hominis Female lays 2-3 eggs daily and the eggs hatch in 3-4 days Average mite in normal scabies is around 10 but thousands can be present in crusted scabies
89 Disorders Predisposing to Crusted Scabies AIDS, T-cell leukemia, Lymphoma, organ transplantation Leprosy Parkinsons Kwashiorkor Down syndrome, Mental retardation SLE, dermatomyositis Diabetes mellitus
90 N Engl J Med 2010; 362:
91 Currie BJ, McCarthy JS. N Engl J Med 2010;362: Table 1. Therapies for Scabies.
92 Case 5 A 40yo AAF presents with a 2 month history of plaques on her face. She denies joint pain or SOB.
93 What is the name when cutaneous disease involves the nose and eyes? A. Chilblain s lupus B. Lupus pernio C. Lupus erythematosus D. Lupus profundus E. Lupus nosiosus Response Counter
94 Sarcoidosis
95 Sarcoidosis
96 Sarcoidosis Systemic granulomatous dz that commonly involves the lungs F > M; AA; bimodal age distribution, peaks between years and again between years Pathogenesis: An unknown antigen elicits upregulation of CD4+ Th1 cells which leads to formation of epitheliod granulomas Genetic susceptibility alleles: HLA-1, HLA-B8, HLA-DR3, HLA- DRB1, and HLA-DQB1 Cutaneous manifestations are seen in 33% of patients 96
97
98
99
100
101
102
103 Erythema Nodosum
104 Chen ES, Moller DR. Nat Rev Rheumatol 2011
105 Initial Evaluation History (occupational, environmental exposure, symptoms) Physical exam Chest X-ray, PA and Lateral Pulmonary function tests (including DLCO) Routine ophthalmologic examination Complete blood count Comprehensive serum chemistries (Ca, LFTs, creatinine) Urinalysis If history of stones, 24h urine calcium EKG If history of palpitations, additional testing Tuberculin skin test or IFNγ release assay Thyroid testing Vitamin D 25, Vitamin D 1,25 Adapted from: Statement on sarcoidosis Am J Respir Crit Care Med 1999; 160:
106 Cutaneous Sarcoidosis Treatment Algorithm SEVERITY Topicals Intralesional Antimalarials Minocycline Methotrexate Thalidomide Adalimumab Infliximab Wanat KA, Rosenbach M. Am J Clin Dermatol 2014
107
108
109
110
111 Pearl Be an advocate for your patients. Don t give up in our current climate of Insurance Based Medicine
112 Case 6 81 yo AAF with hx of cicatricial pemphigoid admitted with worsening blisters, mental status changes, and hypotension. Diagnosed 6 months earlier with cicatricial pemphigoid after initially presenting with oral erosions and blisters. Previously treated with dapsone and methotrexate, but did not tolerate due to worsening anemia
113 As outpatient was on prednisone 40mg daily and mycophenolate mofetil 750mg BID Admitted 2 weeks prior to this admission with worsening pemphigoid flare, hypotension, and worsening fatigue Diagnosed with UTI/urosepsis and improved on IV Rocephin Discharged at that time on prednisone 40mg, mycophenolate mofetil, and ciprofloxacin 500mg BID
114 Her daughter reports that she had continued to have poor PO intake since her discharge but that 24 hours prior to admission, she became significantly more lethargic Her skin also had significant worsening of erosions on her flank, hands, and feet
115 Vitals BP 75/56 P: 119 T: 33.9C (93F) O2 Sats 82% on room air, 94% on 4L O2
116
117
118
119
120
121
122
123
124
125
126 Which of the following is the most likely diagnosis? A. Flare of Cicatricial Pemphigoid B. DIC C. Herpes Zoster D. Vasculitis from cryoglobulins Response Counter
127
128
129
130 Hospital Course Patient admitted to ICU Started on IV vancomycin, aztreonam, levofloxacin Aggressive IVF resuscitation Transfused 1 unit PRBCs Stress dose hydrocortisone Consulted derm the following day
131 Hospital Course Fibrinogen 84, Coags elevated DIC Echo, MRI brain obtained
132 Echocardiogram -50% EF -Valves normal -Large thrombus in Left atrium
133 MRI Multiple embolic infarcts
134 CSF studies Initial slight elevation in protein, 4-5 WBCs (lymphs) VZV PCR Positive + HSV and VZV PCR from Wound (DFA unavailable at our institution) HSV- Negative VZV- Positive
135 Hospital Course Pt initially responded well to IVFs with improved mental status Renal function continued to worsen hemodialysis eventually initiated Cryoprecipitate given initially to correct fibrinogen and coags Once thrombi found, heparin infusion was initiated Acyclovir started- renally dosed for presumed Herpes Zoster infection Not started until day #4
136 Hospital Course Pt became more unresponsive Intubated on day 5 of hospitalization Repeat CT Head showed worsening ischemic infarcts Pt went into Vfib on day 7 and expired after ACLS measures
137 Presentation of 3 distinct cutaneous morphologies made this case difficult Possible availability bias from recent admission Delay in initiation of proper treatment might have affected outcome Cutaneous findings of VZV infection are often the best indicator for diagnosis and dermatologist can play a significant role in diagnosis and management.
138 Herpes Zoster Zoster-associated encephalitis and vasculopathy is most common in immunosuppressed patients VZV is known to produce stroke syndromes and has been associated with increased risk of stroke in patients with prior episodes of zoster. Pathogenesis if thought to be secondary to infection of the cerebral arteries. VZV is a known cause of purpura fulminans in children but very few documentations in the literature about DIC in adults with VZV
139 A review of 38 cases of disseminated VZV infection in renal transplant recipients revealed 47% (18/38) developed DIC; however a majority of cases were primary varicella infection. VZV pneumonia/pneumonitis and hepatitis also common Only 7% of cases of DIC present with thromboembolisms
140
141
142
143
144
145
146
147
148 Case 7 52 yo AAM with no prior medical history presented to ER with face pain, right eye pain, and lip swelling. Symptoms began 1 week prior. He was given Clindamycin with no improvement after 3 days and pt returned to ER. Pt admitted for failed outpt antibiotics and started on IV Vanc. Ophthalmology consulted for preorbital cellulitis. Dermatology consulted for evaluation
149
150
151 Case 8 74 yo WM s/p BMT for multiple myeloma now relapsed and on chemotherapy presents with new rash and fever.
152
153
154
155
156
157 Case 7 and 8 Which of the following is the most likely diagnosis? 1. Herpes/Zoster 2. Herpes/Zoster 3. Herpes/Zoster 4. Herpes/Zoster
158 Case 7 and 8 Which of the following is the most likely diagnosis? 1. Herpes/Zoster 2. Herpes/Zoster 3. Herpes/Zoster 4. Herpes/Zoster
159
160
161 Herpes/Zoster Pearls It s Herpes/Zoster until proven different!!! Order HSV and VZV PCR from swab use viral medium but does not have to be on ice Go ahead and place patient under appropriate isolation if suspect zoster
162 Disseminated Zoster Pearls > 20 lesions outside of 2 contiguous dermatomes Elderly and immunocompromised are at increased risk Viscera can be affected Call ophthalmology Contact and droplet isolation IV Acyclovir
163 Case 9 24 yo WM admitted with 5 day history of abd pain, nausea/vomiting. Found to have adrenal mass/hemorrhage on CT scan. Had discoloration and pain of right great toe 6-7 weeks prior. Was infected and bruised Derm consulted for possible onychomycosis!! STAT!!
164
165
166
167 Which of the following is the most likely diagnosis? A. Vasculitis B. Vasculopathy C. Chilblain lupus D. Onychomycosis Response Counter
168
169 Retiform Purpura Due to thrombosis and occlusion of the vasculature Early on, lacks the erythema of palpable purpura; purpuric early Purpura tracks along tack of dermal vessels leading to retiform appearance Over time, ischemia leads to necrosis and eschar formation Palpable purpura can become retiform Ddx: meds, infection, coagulation defect, embolic
170
171
172
173
174
175 Case 9 Extensive work up of vasculopathy revealed: Positive lupus anticoagulant and anti-cardiolipin antibodies Also with autoimmune hemolytic anemia Did not meet full criteria for SLE Pt did well on corticosteroids and anti-coagulation
176 Small Vessel Vasculitis Infections (15-20%) Bacterial - Group A strep, Mycobacteria, Mycoplasma, Chronic meningococcemia Viral- Hep C > B >>A; HIV Parvo B19 Inflammatory d/o (15-20%) AI- SLE, RA IBD Seronegative spondyloarthropathies Drugs (10-15%) Anti-TNF agents, COX-2 inhibitors, G-CSF, Hydralazine, MCN, NSAIDS, PCNs, antithyroid agents, Quinolones Neoplasms (usually blood d/o) Idiopathic ~ 50%
177
178
179
180
181
182
183
184 Basic laboratory evaluation for patients with confirmed cutaneous vasculitis CBC with diff ESR CRP SPEP/ UPEP Cryos LFTs Stool guiac BUN/ Cr UA Electrolytes Hep B/ C ASLO/ anti-dnaseb HIV RF Compliment (C3, C4, CH50) ANA ANCAs
185 Case y/o AAF w/ PMH DM, HTN, CHF transferred from OSH with diffuse rash initially thought to be SJS. She also had renal failure and leukocytosis. Only new medication was allopurinol started 1 month prior to onset of rash She was admitted to the OSH for ~2 weeks prior to transfer and managed on IVFs, vancomycin, and meropenem
186
187
188
189
190
191 Case 10 T: 97.1 BP 143/76 P 93 SpO2 93% Labs at OSH: CBC 11/11: wbc 21k, 26% segs, 17% lymphs, 4.9% monos, 50% eos CBC 11/18: wbc 29k, 35% segs, 22% lymphs, 10.8% monos, 31% eos
192 Which of the following labs should be checked next? A. HSV/VZV PCR B. HIV C. HCV Ab D. LFTs Response Counter
193 CMP: Na 139, K 4.3, Cl 108, HCO3 18, BUN 81, scr 3.9, gluc 230, Alk phos 166 Bili 2.4 AST 380 ALT 433
194 DRESS Drug Reaction with Eosinophilia and Systemic Symptoms AKA: Drug Induced Hypersensitivity Syndrome Anticonvulsant Hypersensitivity Syndrome
195 Which of the following labs should also be checked? A. TSH B. HCV Ab C. Fasting lipids D. ANA Response Counter
196 DRESS Commonly implicated drugs: anticonvulsants, sulfonamides, allopurinol, NSAIDs, azithromycin, azathioprine, anti-retrovirals Most cases 2-8 weeks after drug
197 Clinical Features of DRESS Fever, leukocytosis, eosinophilia Facial Edema Generalized eruption: erythematous papules, morbilliform, bullae, purpura, erythroderma, pustules Lymphadenopathy Myositis LFT Abnormalities Lung, kidney, heart, thyroid involvement
198 Fig 1. Alogrithm for the diagnosis, management, and treatment of drug reaction with eosinophilia and systemic symptoms syndrome. Journal of the American Academy of Dermatology, Volume 68, Issue 5, 2013, 709.e1 709.e9
199 Treatment of DRESS Withdraw offending medication High dose systemic steroids (1-2mg/kg tapering dose over 1-3 months) LFTs should be followed until normal Supportive care
200 Case yo WM presents with onset of complete body rash. States that he was given a steroid shot for a rash he had on his hip three weeks ago. Rash improved but returned one week ago. Only medication is lisinopril for HTN. No changes to detergent or soap.
201
202
203
204
205
206 Which of the following is the most common cause of erythroderma? A. Atopic Dermatitis B. Psoriasis C. Cutaneous T-cel Lymphoma D. Drug induced E. Idiopathic Response Counter
207 Erythroderma Psoriasis Pityriasis rubra pilaris Atopic Dermatitis Seborrheic Dermatitis Drug Eruption CTCL Infectious Autoimmune bullous disorder
208 Erythroderma
209 Erythroderma Pearls Etiology can be difficult to determine. History is most important. Can be idiopathic but most commonly associated with prior dermatoses. Biopsy necessary but often not helpful. Flow cytometry might be needed to r/o cutaneous T-cell lymphoma Treatment will vary based on etiology. Wet wraps with topical steroids ok for almost any etiology. Cyclosporine instead of prednisone for erythrodermic psoriasis.
210 Summary Primary care physicians will manage a large of number of common skin diseases. It is important to be comfortable managing mild atopic dermatitis and psoriasis with topical regimens and recognizing when referral to a specialist for systemic treatment might be indicated. It is important to understand the systemic work-up needed for cutaneous presentations of psoriasis, sarcoidosis, and lupus. Purpura can result from vasculopathy and/or vasculitis. It is important to understand the different etiologies and work-up needed for patients presenting with purpura. It is Herpes until proven different in the hospital setting! DRESS check LFTs, thyroid studies, and EKG/Echo Etiology of erythroderma is difficult to determine on biopsy. History, history, history!!
Cutanous Manifestation of Lupus Erythematosus. Presented By: Dr. Naif S. Al Shahrani Salman Bin Abdaziz university
 Cutanous Manifestation of Lupus Erythematosus Presented By: Dr. Naif S. Al Shahrani Salman Bin Abdaziz university A 50-year old lady, who is otherwise healthy, presented to the dermatology clinic with
Cutanous Manifestation of Lupus Erythematosus Presented By: Dr. Naif S. Al Shahrani Salman Bin Abdaziz university A 50-year old lady, who is otherwise healthy, presented to the dermatology clinic with
S003 CPC Self-Assessment
 S003 CPC Self-Assessment Alina G. Bridges, D.O. Associate Professor Program Director, Dermatopathology Fellowship Department of Dermatology, Division of Dermatopathology and Cutaneous Immunopathology Mayo
S003 CPC Self-Assessment Alina G. Bridges, D.O. Associate Professor Program Director, Dermatopathology Fellowship Department of Dermatology, Division of Dermatopathology and Cutaneous Immunopathology Mayo
Recalcitrant Warty Erythroderma With Severe Pruritus. Gil Yosipovitch Professor & Chair Department of Dermatology & Itch Center Temple University
 Recalcitrant Warty Erythroderma With Severe Pruritus Gil Yosipovitch Professor & Chair Department of Dermatology & Itch Center Temple University DISCLOSURE OF RELEVANT RELATIONSHIPS WITH INDUSTRY Gil Yosipovitch,
Recalcitrant Warty Erythroderma With Severe Pruritus Gil Yosipovitch Professor & Chair Department of Dermatology & Itch Center Temple University DISCLOSURE OF RELEVANT RELATIONSHIPS WITH INDUSTRY Gil Yosipovitch,
ERYTHRODERMA. ASAPA 2018 Fall Conference Tucson, AZ 10/12/2018. Andrew Newman, DO Pgy-3, Affiliated Dermatology/Honor Health
 ERYTHRODERMA ASAPA 2018 Fall Conference Tucson, AZ 10/12/2018 Andrew Newman, DO Pgy-3, Affiliated Dermatology/Honor Health OBJECTIVES Define Erythroderma Name common diseases and medications that cause
ERYTHRODERMA ASAPA 2018 Fall Conference Tucson, AZ 10/12/2018 Andrew Newman, DO Pgy-3, Affiliated Dermatology/Honor Health OBJECTIVES Define Erythroderma Name common diseases and medications that cause
COMMON SKIN CONDITIONS IN PRIMARY CARE. Ibrahim M. Zayneh, MD Dermatology Private Practice, Portsmouth, Ohio
 COMMON SKIN CONDITIONS IN PRIMARY CARE Ibrahim M. Zayneh, MD Dermatology Private Practice, Portsmouth, Ohio DISCLOSURE The Speaker and members of the planning committee do not have a conflict of interest
COMMON SKIN CONDITIONS IN PRIMARY CARE Ibrahim M. Zayneh, MD Dermatology Private Practice, Portsmouth, Ohio DISCLOSURE The Speaker and members of the planning committee do not have a conflict of interest
An Approach to Common and not so Common Rashes in the Office FMF 2014 Christie Freeman MD, CCFP, DipPDerm, MSc
 An Approach to Common and not so Common Rashes in the Office FMF 2014 Christie Freeman MD, CCFP, DipPDerm, MSc 1 Common Rashes Tinea Corporis: Annular- this is not the only criteria Advancing erythematous
An Approach to Common and not so Common Rashes in the Office FMF 2014 Christie Freeman MD, CCFP, DipPDerm, MSc 1 Common Rashes Tinea Corporis: Annular- this is not the only criteria Advancing erythematous
Concentrate on Descriptors. An Approach to Skin Diseases in the ER
 Concentrate on Descriptors An Approach to Skin Diseases in the ER Toby Maurer, MD University of California, San Francisco Vasculitis-leaky blood vessels Targetoid lesions-round lesions with blue or red
Concentrate on Descriptors An Approach to Skin Diseases in the ER Toby Maurer, MD University of California, San Francisco Vasculitis-leaky blood vessels Targetoid lesions-round lesions with blue or red
Emergency Dermatology Dr Melissa Barkham
 Emergency Dermatology Dr Melissa Barkham Spotlight Seminar 30 th September 2010 Why is this important? Urgent recognition and treatment of dermatologic emergencies can be life saving and prevent long term
Emergency Dermatology Dr Melissa Barkham Spotlight Seminar 30 th September 2010 Why is this important? Urgent recognition and treatment of dermatologic emergencies can be life saving and prevent long term
RHEUMATOLOGY OVERVIEW. Carmelita J. Colbert, MD Assistant Professor of Medicine Division of Rheumatology Loyola University Medical Center
 RHEUMATOLOGY OVERVIEW Carmelita J. Colbert, MD Assistant Professor of Medicine Division of Rheumatology Loyola University Medical Center What is Rheumatology? Medical science devoted to the rheumatic diseases
RHEUMATOLOGY OVERVIEW Carmelita J. Colbert, MD Assistant Professor of Medicine Division of Rheumatology Loyola University Medical Center What is Rheumatology? Medical science devoted to the rheumatic diseases
COMPLEX CUTANEOUS LUPUS CASES PEARLS AND PITFALLS
 COMPLEX CUTANEOUS LUPUS CASES PEARLS AND PITFALLS Benjamin F. Chong, MD, MSCS February 17, 2018 CONFLICTS OF INTEREST D I S CLOSURE OF R E LATI ONSHIPS W I T H I NDUSTRY Benjamin Chong, MD, MSCS F059 Complex
COMPLEX CUTANEOUS LUPUS CASES PEARLS AND PITFALLS Benjamin F. Chong, MD, MSCS February 17, 2018 CONFLICTS OF INTEREST D I S CLOSURE OF R E LATI ONSHIPS W I T H I NDUSTRY Benjamin Chong, MD, MSCS F059 Complex
Psoriasis and Psoriatic Arthritis Combined Clinic Electronic Medical Records Form
 Psoriasis and Psoriatic Arthritis Combined Clinic Electronic Medical Records Form NAME: AGE: SEX: CHIEF COMPLAINT: HISTORY OF PRESENT ILLNESS: The patient presents for the initial evaluation of [psoriasis
Psoriasis and Psoriatic Arthritis Combined Clinic Electronic Medical Records Form NAME: AGE: SEX: CHIEF COMPLAINT: HISTORY OF PRESENT ILLNESS: The patient presents for the initial evaluation of [psoriasis
Skin Deep: Cutaneous Lupus. Dr Sarah Sasson Immunology Registrar, Liverpool Hospital 2016
 Skin Deep: Cutaneous Lupus Dr Sarah Sasson Immunology Registrar, Liverpool Hospital 2016 Introduction: Cutaneous lupus erythematosus LE is an autoimmune disease with a range of clinical manifestations
Skin Deep: Cutaneous Lupus Dr Sarah Sasson Immunology Registrar, Liverpool Hospital 2016 Introduction: Cutaneous lupus erythematosus LE is an autoimmune disease with a range of clinical manifestations
Disclosures. Rheumatological Approaches to Differential Diagnosis, Physical Examination, and Interpretation of Studies. None
 Rheumatological Approaches to Differential Diagnosis, Physical Examination, and Interpretation of Studies Sarah Goglin MD Assistant Professor of Medicine Division of Rheumatology Disclosures None 1 [footer
Rheumatological Approaches to Differential Diagnosis, Physical Examination, and Interpretation of Studies Sarah Goglin MD Assistant Professor of Medicine Division of Rheumatology Disclosures None 1 [footer
Rashes Not To Be Missed In Children
 May 2016 Rashes Not To Be Missed In Children Dr Chan Yuin Chew Dermatologist Dermatology Associates Gleneagles Medical Centre Scope of presentation Focus on rashes May lead to significant morbidity if
May 2016 Rashes Not To Be Missed In Children Dr Chan Yuin Chew Dermatologist Dermatology Associates Gleneagles Medical Centre Scope of presentation Focus on rashes May lead to significant morbidity if
Rheumatology Primer: What Labs and When
 Rheumatology Primer: What Labs and When Irina Konon, MD Department of Internal Medicine Division of Rheumatology Medical College of Wisconsin Disclosures None 1 Objective Discuss principles of laboratory
Rheumatology Primer: What Labs and When Irina Konon, MD Department of Internal Medicine Division of Rheumatology Medical College of Wisconsin Disclosures None 1 Objective Discuss principles of laboratory
Dermatology GP Referral Guidelines
 Austin Health Dermatology Department holds 5 Clinic sessions to discuss and plan the treatment of with Dermatology conditions. Department of Health clinical urgency categories for specialist clinics Urgent:
Austin Health Dermatology Department holds 5 Clinic sessions to discuss and plan the treatment of with Dermatology conditions. Department of Health clinical urgency categories for specialist clinics Urgent:
Psoriasis. What is Psoriasis? What causes psoriasis? Medical Topics Psoriasis
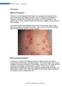 1 Psoriasis What is Psoriasis? Psoriasis is a long standing inflammatory non-contagious skin disease which waxes and wanes with triggering factors. There is a genetic predisposition in psoriasis. Internationally,
1 Psoriasis What is Psoriasis? Psoriasis is a long standing inflammatory non-contagious skin disease which waxes and wanes with triggering factors. There is a genetic predisposition in psoriasis. Internationally,
What to do when patch testing is negative?
 What to do when patch testing is negative? Christen M. Mowad MD Clinical Professor of Dermatology Geisinger Medical Center Danville, PA 17821 cmowad@geisinger.edu I have no disclosures. What to do when
What to do when patch testing is negative? Christen M. Mowad MD Clinical Professor of Dermatology Geisinger Medical Center Danville, PA 17821 cmowad@geisinger.edu I have no disclosures. What to do when
Psoriasis management. A/Prof Amanda Oakley Dermatologist, Waikato
 Psoriasis management A/Prof Amanda Oakley Dermatologist, Waikato AbbVie Breakfast Session, 14 June 2014 Disclosure This breakfast session is sponsored by Abbvie Autoimmune skin disorders Psoriasis Eczema
Psoriasis management A/Prof Amanda Oakley Dermatologist, Waikato AbbVie Breakfast Session, 14 June 2014 Disclosure This breakfast session is sponsored by Abbvie Autoimmune skin disorders Psoriasis Eczema
Psoriasis. Jessica Kaffenberger, M.D. Assistant Professor of Dermatology Division of Dermatology The Ohio State University Wexner Medical Center
 Psoriasis Jessica Kaffenberger, M.D. Assistant Professor of Dermatology Division of Dermatology The Ohio State University Wexner Medical Center Learning objectives Recognize the different types of psoriasis
Psoriasis Jessica Kaffenberger, M.D. Assistant Professor of Dermatology Division of Dermatology The Ohio State University Wexner Medical Center Learning objectives Recognize the different types of psoriasis
Topical Calcipotriol Algorithm
 Topical Calcipotriol Algorithm Is this patient an adult previously diagnosed with psoriasis by a doctor? Do the skin patches look the same as those diagnosed as psoriasis? Is this psoriasis covering an
Topical Calcipotriol Algorithm Is this patient an adult previously diagnosed with psoriasis by a doctor? Do the skin patches look the same as those diagnosed as psoriasis? Is this psoriasis covering an
Goals of this talk. Morbilliform. Common Morphologies in the Hospital 11/7/2017. Hospital Based Dermatology: Common and Tough Consult Cases
 Hospital Based Dermatology: Common and Tough Consult Cases Lindy P. Fox MD Associate Professor of Clinical Dermatology Director, Hospital Consultation Service University of California, San Francisco lindy.fox@ucsf.edu
Hospital Based Dermatology: Common and Tough Consult Cases Lindy P. Fox MD Associate Professor of Clinical Dermatology Director, Hospital Consultation Service University of California, San Francisco lindy.fox@ucsf.edu
Future of Pediatrics: Blisters, Hives and Other Tales from the Emergency Room June 14 th, 2016
 A. Yasmine Kirkorian MD Assistant Professor of Dermatology & Pediatrics Children s National Health System George Washington University School of Medicine & Health Sciences Future of Pediatrics: Blisters,
A. Yasmine Kirkorian MD Assistant Professor of Dermatology & Pediatrics Children s National Health System George Washington University School of Medicine & Health Sciences Future of Pediatrics: Blisters,
Psoriasiform Dermatitis in Children: Calling in the Troops
 Psoriasiform Dermatitis in Children: Calling in the Troops Markus Boos, MD PhD Attending Physician, Dermatology Seattle Children s Hospital Assistant Professor of Pediatrics, University of Washington School
Psoriasiform Dermatitis in Children: Calling in the Troops Markus Boos, MD PhD Attending Physician, Dermatology Seattle Children s Hospital Assistant Professor of Pediatrics, University of Washington School
A. Erythema multiforme and related diseases
 Go Back to the Top To Order, Visit the Purchasing Page for Details Chapter Erythema, Erythroderma (Exfoliative Dermatitis) Erythema is caused by telangiectasia or hyperemia in the papillary and reticular
Go Back to the Top To Order, Visit the Purchasing Page for Details Chapter Erythema, Erythroderma (Exfoliative Dermatitis) Erythema is caused by telangiectasia or hyperemia in the papillary and reticular
Phototherapy and Photochemotherapy Treatment (Ultraviolet A [PUVA] and B [UBV])
![Phototherapy and Photochemotherapy Treatment (Ultraviolet A [PUVA] and B [UBV]) Phototherapy and Photochemotherapy Treatment (Ultraviolet A [PUVA] and B [UBV])](/thumbs/89/99382632.jpg) Origination: 09/27/07 Revised: 08/2/17 Annual Review: 11/2/17 Purpose: To provide Phototherapy and Photochemotherapy Treatment (PUVA and UBV) guidelines for the Medical Department staff to reference when
Origination: 09/27/07 Revised: 08/2/17 Annual Review: 11/2/17 Purpose: To provide Phototherapy and Photochemotherapy Treatment (PUVA and UBV) guidelines for the Medical Department staff to reference when
Emergency Dermatology. Emergency Dermatology
 Emergency Dermatology These are rapidly progressive skin conditions and some are potentially lifethreatening. Early recognition is important to implement prompt supportive care and therapy. Some are drug
Emergency Dermatology These are rapidly progressive skin conditions and some are potentially lifethreatening. Early recognition is important to implement prompt supportive care and therapy. Some are drug
Objectives. Terminology. Recognize common pediatric dermatologic conditions. Review treatment plans Identify skin manifestations of systemic disease
 Pediatric Visual Dermatological Diagnosis Fernando Vega, M.D. Objectives Recognize common pediatric dermatologic conditions Expand differential diagnosis Review treatment plans Identify skin manifestations
Pediatric Visual Dermatological Diagnosis Fernando Vega, M.D. Objectives Recognize common pediatric dermatologic conditions Expand differential diagnosis Review treatment plans Identify skin manifestations
Arthritis & Rheumatology Clinics of Kansas PATIENT EDUCATION SYSTEMIC LUPUS ERYTHEMATOSUS
 Arthritis & Rheumatology Clinics of Kansas PATIENT EDUCATION SYSTEMIC LUPUS ERYTHEMATOSUS Introduction: There is perhaps no rheumatic disease that evokes so much fear and confusion among both patients
Arthritis & Rheumatology Clinics of Kansas PATIENT EDUCATION SYSTEMIC LUPUS ERYTHEMATOSUS Introduction: There is perhaps no rheumatic disease that evokes so much fear and confusion among both patients
Eczema & Dermatitis Clinical features: Histopathological features: Classification:
 Eczema & Dermatitis Eczema is an inflammatory reactive pattern of skin to many and different stimuli characterized by itching, redness, scaling and clustered papulovesicles. Eczema and dermatitis are synonymous
Eczema & Dermatitis Eczema is an inflammatory reactive pattern of skin to many and different stimuli characterized by itching, redness, scaling and clustered papulovesicles. Eczema and dermatitis are synonymous
Contact Dermatitis In Atopic Patients
 Contact Dermatitis In Atopic Patients Jenny Murase, MD Palo Alto Foundation Medical Group Director of Patch Testing University of California, San Francisco Associate Clinical Professor Disclosures Consultant
Contact Dermatitis In Atopic Patients Jenny Murase, MD Palo Alto Foundation Medical Group Director of Patch Testing University of California, San Francisco Associate Clinical Professor Disclosures Consultant
High Impact Rheumatology
 High Impact Rheumatology Systemic Lupus Erythematosus Bernard Rubin, DO MPH Case 1: History A 45-year-old woman presents with severe dyspnea and cough. She was in excellent health until 4 weeks ago when
High Impact Rheumatology Systemic Lupus Erythematosus Bernard Rubin, DO MPH Case 1: History A 45-year-old woman presents with severe dyspnea and cough. She was in excellent health until 4 weeks ago when
SJS/TEN spectrum. Stevens-Johnson syndrome (SJS) /Toxic Epidermal Necrolysis (TEN) 10/7/2016
 Jesse Keller MD Assistant Professor Oregon Health & Science University Stevens-Johnson syndrome (SJS) /Toxic Epidermal Necrolysis (TEN) Drug induced dermemergencies that exist on a spectrum Delayed reaction:
Jesse Keller MD Assistant Professor Oregon Health & Science University Stevens-Johnson syndrome (SJS) /Toxic Epidermal Necrolysis (TEN) Drug induced dermemergencies that exist on a spectrum Delayed reaction:
The Itch That Rashes. Sarah D. Cipriano, MD, MPH, MS Resident, Dermatology University of Utah
 The Itch That Rashes Sarah D. Cipriano, MD, MPH, MS Resident, Dermatology University of Utah 1 Conflict of Interest No conflict of interest Will discuss off label use of medications 2 3 Most likely diagnosis?
The Itch That Rashes Sarah D. Cipriano, MD, MPH, MS Resident, Dermatology University of Utah 1 Conflict of Interest No conflict of interest Will discuss off label use of medications 2 3 Most likely diagnosis?
9/9/17. Disclosures" Dermatology in Primary Care: Recognition and treatment of common disorders of the skin" A preview" Classic skin infections"
 Disclosures Dermatology in Primary Care: Recognition and treatment of common disorders of the skin I have no conflicts of interest to disclose. I may discuss off-label use of treatments for cutaneous disease.
Disclosures Dermatology in Primary Care: Recognition and treatment of common disorders of the skin I have no conflicts of interest to disclose. I may discuss off-label use of treatments for cutaneous disease.
Jeopardy. What s the rash? $100 $100 $100 $100 $100 $200 $200 $200 $200 $200 $300 $300 $300 $300 $300 $400 $400 $400 $400 $400
 Jeopardy Antibodies & more antibodies Aching joints What s the rash? Potpourri Image Challenge $100 $100 $100 $100 $100 $200 $200 $200 $200 $200 $300 $300 $300 $300 $300 $400 $400 $400 $400 $400 $500 $500
Jeopardy Antibodies & more antibodies Aching joints What s the rash? Potpourri Image Challenge $100 $100 $100 $100 $100 $200 $200 $200 $200 $200 $300 $300 $300 $300 $300 $400 $400 $400 $400 $400 $500 $500
Melanoma Immunotherapy. Nursing Perspective on Immune-Related Adverse Events: Patient education, Monitoring & Management
 Melanoma Immunotherapy Nursing Perspective on Immune-Related Adverse Events: Patient education, Monitoring & Management Mike Buljan, NP UCSF Medical Center Melanoma Oncology Disclosures None Only FDA-approved
Melanoma Immunotherapy Nursing Perspective on Immune-Related Adverse Events: Patient education, Monitoring & Management Mike Buljan, NP UCSF Medical Center Melanoma Oncology Disclosures None Only FDA-approved
Patient #1. Rheumatoid Arthritis. Rheumatoid Arthritis. 45 y/o female Morning stiffness in her joints >1 hour
 Patient #1 Rheumatoid Arthritis Essentials For The Family Medicine Physician 45 y/o female Morning stiffness in her joints >1 hour Hands, Wrists, Knees, Ankles, Feet Polyarticular, symmetrical swelling
Patient #1 Rheumatoid Arthritis Essentials For The Family Medicine Physician 45 y/o female Morning stiffness in her joints >1 hour Hands, Wrists, Knees, Ankles, Feet Polyarticular, symmetrical swelling
CPC. Chutika Srisuttiyakorn, M.D. Kobkul Aunhachoke, M.D. Phramongkutklao Hospital Bangkok, Thailand
 CPC Chutika Srisuttiyakorn, M.D. Kobkul Aunhachoke, M.D. Phramongkutklao Hospital Bangkok, Thailand A 53 year-old woman with fever, facial swelling and rashes on face, trunk and upper extremities for 3
CPC Chutika Srisuttiyakorn, M.D. Kobkul Aunhachoke, M.D. Phramongkutklao Hospital Bangkok, Thailand A 53 year-old woman with fever, facial swelling and rashes on face, trunk and upper extremities for 3
Diagnosis and Management of Common and Infective Skin Diseases in Children at primary care level
 Diagnosis and Management of Common and Infective Skin Diseases in Children at primary care level Dr Ng Su Yuen Paediatrician and Paediatric Dermatologist Hospital Pulau Pinang Outline Common inflammatory
Diagnosis and Management of Common and Infective Skin Diseases in Children at primary care level Dr Ng Su Yuen Paediatrician and Paediatric Dermatologist Hospital Pulau Pinang Outline Common inflammatory
Case 1. Debridement Cultures Keflex Silvadene
 The Red Breast Beth McLellan, M.D. Assistant Professor Division of Dermatology Albert Einstein College of Medicine Montefiore Medical Center Jacobi Medical Center Case 1 48 year old radiation oncologist
The Red Breast Beth McLellan, M.D. Assistant Professor Division of Dermatology Albert Einstein College of Medicine Montefiore Medical Center Jacobi Medical Center Case 1 48 year old radiation oncologist
Rayos Prior Authorization Program Summary
 Rayos Prior Authorization Program Summary FDA APPROVED INDICATIONS AND DOSAGE FDA-Approved Indications: 1 Agent Indication Dosage Rayos (prednisone delayedrelease tablet) as an anti-inflammatory or immunosuppressive
Rayos Prior Authorization Program Summary FDA APPROVED INDICATIONS AND DOSAGE FDA-Approved Indications: 1 Agent Indication Dosage Rayos (prednisone delayedrelease tablet) as an anti-inflammatory or immunosuppressive
KEY MESSAGES. Psoriasis patients are more prone to cardiovascular diseases, stroke, lymphoma and non-melanoma skin cancers, and increased mortality.
 KEY MESSAGES Psoriasis is a genetically determined, systemic immune-mediated chronic inflammatory disease that affects primarily the skin and joints. Psoriasis Vulgaris is characterised by well-demarcated
KEY MESSAGES Psoriasis is a genetically determined, systemic immune-mediated chronic inflammatory disease that affects primarily the skin and joints. Psoriasis Vulgaris is characterised by well-demarcated
The Natural History of Psoriasis and Treatment Goals
 The Natural History of Psoriasis and Treatment Goals Psoriasis Epidemiology Prevalence Affects 2 3% of adult population (>7 million in US) Caucasians: 25% 2.5% African Americans: 1.3% (more likely to have
The Natural History of Psoriasis and Treatment Goals Psoriasis Epidemiology Prevalence Affects 2 3% of adult population (>7 million in US) Caucasians: 25% 2.5% African Americans: 1.3% (more likely to have
A case of bullous pemphigoid following pemphigus foliaceus
 #2228 A case of bullous pemphigoid following pemphigus foliaceus Priyanka Vedak MD 1, Danielle Levine MD 1,3, Lyn Duncan MD 2,3, Hensin Tsao 1,3, Daniela Kroshinsky MD MPH 1,3 1. Department of Dermatology,
#2228 A case of bullous pemphigoid following pemphigus foliaceus Priyanka Vedak MD 1, Danielle Levine MD 1,3, Lyn Duncan MD 2,3, Hensin Tsao 1,3, Daniela Kroshinsky MD MPH 1,3 1. Department of Dermatology,
Cutaneous Drug Reactions
 Cutaneous Drug Reactions Andrei Metelitsa, MD, FRCPC, FAAD Co-Director, Institute for Skin Advancement Clinical Associate Professor, Dermatology University of Calgary, Canada Copyright 2017 by Sea Courses
Cutaneous Drug Reactions Andrei Metelitsa, MD, FRCPC, FAAD Co-Director, Institute for Skin Advancement Clinical Associate Professor, Dermatology University of Calgary, Canada Copyright 2017 by Sea Courses
REGISTRY OF SEVERE CUTANEOUS ADVERSE REACTIONS TO DRUGS AND COLLECTION OF BIOLOGICAL SAMPLES. R e g i S C A R PATIENT'S DATA. Age country of birth
 REGISTRY OF SEVERE CUTANEOUS ADVERSE REACTIONS TO DRUGS AND COLLECTION OF BIOLOGICAL SAMPLES R e g i S C A R PATIENT'S DATA Initials of the patient date of birth Age country of birth Gender male female
REGISTRY OF SEVERE CUTANEOUS ADVERSE REACTIONS TO DRUGS AND COLLECTION OF BIOLOGICAL SAMPLES R e g i S C A R PATIENT'S DATA Initials of the patient date of birth Age country of birth Gender male female
Burrowing Bugs in a 5 week-old that Mite be Difficult to Diagnosis
 Burrowing Bugs in a 5 week-old that Mite be Difficult to Diagnosis Farbod Bahadori-Esfahani,MD Pediatrics LSU Health Shreveport Louisiana Chapter AAP Red Stick Potpourri Disclosure I have nothing to disclose
Burrowing Bugs in a 5 week-old that Mite be Difficult to Diagnosis Farbod Bahadori-Esfahani,MD Pediatrics LSU Health Shreveport Louisiana Chapter AAP Red Stick Potpourri Disclosure I have nothing to disclose
Skin Manifestations of Systemic Disease. Approach to Dermatalogic Diagnosis 9/6/2016. Go Ahead---Judge a Book by its Cover!
 Go Ahead---Judge a Book by its Cover! Skin Manifestations of Systemic Disease Amelie Hollier, DNP, FNP-BC, FAANP Lafayette, LA President, APEA Objectives Compare diseases of the skin with reactions of
Go Ahead---Judge a Book by its Cover! Skin Manifestations of Systemic Disease Amelie Hollier, DNP, FNP-BC, FAANP Lafayette, LA President, APEA Objectives Compare diseases of the skin with reactions of
More Non-infectious Granulomatous Diseases! Karolyn Wanat, MD Assistant Professor, Dermatology & Pathology University of Iowa
 More Non-infectious Granulomatous Diseases! Karolyn Wanat, MD Assistant Professor, Dermatology & Pathology University of Iowa Conflicts of Interest/Disclosure None Classification/Overview 1) Necrobiotic/Palisading
More Non-infectious Granulomatous Diseases! Karolyn Wanat, MD Assistant Professor, Dermatology & Pathology University of Iowa Conflicts of Interest/Disclosure None Classification/Overview 1) Necrobiotic/Palisading
Emergent and Urgent Dermatology, Eruptions, and Wound Care
 Emergent and Urgent Dermatology, Eruptions, and Wound Care G. Scott Drew, DO, FAAD, FAOCD Smith Clinic Department of Dermatology Tucson Osteopathic Medical Foundation April 27, 2018 Acute Cutaneous Lupus
Emergent and Urgent Dermatology, Eruptions, and Wound Care G. Scott Drew, DO, FAAD, FAOCD Smith Clinic Department of Dermatology Tucson Osteopathic Medical Foundation April 27, 2018 Acute Cutaneous Lupus
Index. derm.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Abatacept for DLE, 493 for SLE, 497 Ablative therapies, localized, for cutaneous T-cell lymphoma, 502 506. See also Cutaneous T-cell lymphoma,
Note: Page numbers of article titles are in boldface type. A Abatacept for DLE, 493 for SLE, 497 Ablative therapies, localized, for cutaneous T-cell lymphoma, 502 506. See also Cutaneous T-cell lymphoma,
Significance. Outline and Objectives. S007 Systemic Therapies for Medical Oncology
 S007 Systemic Therapies for Medical Oncology Anisha B. Patel, M.D. Assistant Professor, Dermatology UT MD Anderson Cancer Center UT Health Science Center Houston Safety considerations Outline and Objectives
S007 Systemic Therapies for Medical Oncology Anisha B. Patel, M.D. Assistant Professor, Dermatology UT MD Anderson Cancer Center UT Health Science Center Houston Safety considerations Outline and Objectives
ACUTE KIDNEY INJURY A PRIMER FOR PRIMARY CARE PHYSICIANS. Myriam Farah, MD, FRCPC
 ACUTE KIDNEY INJURY A PRIMER FOR PRIMARY CARE PHYSICIANS Myriam Farah, MD, FRCPC Clinical Assistant Professor Division of Nephrology, University of British Columbia November 2016 1. How to recognize acute
ACUTE KIDNEY INJURY A PRIMER FOR PRIMARY CARE PHYSICIANS Myriam Farah, MD, FRCPC Clinical Assistant Professor Division of Nephrology, University of British Columbia November 2016 1. How to recognize acute
Objectives. Joint Pain. Case 1. Rheumatology for the Primary MD (Not just your grandmother s disease) 12/4/2010
 Objectives Rheumatology for the Primary MD (Not just your grandmother s disease) Identify when it is appropriate to refer for rheumatologic evaluation Autoimmune/ Inflammatory v. noninflammatory disease
Objectives Rheumatology for the Primary MD (Not just your grandmother s disease) Identify when it is appropriate to refer for rheumatologic evaluation Autoimmune/ Inflammatory v. noninflammatory disease
Dr Emmy Babor GPSI Dermatology
 Dr Emmy Babor GPSI Dermatology Wrinkles Sagging Thin skin (not all areas think about soles of feet) Loss of elasticity Pigmentary changes Dryness Loss of luminosity Baldness/ grey hair Increased nose
Dr Emmy Babor GPSI Dermatology Wrinkles Sagging Thin skin (not all areas think about soles of feet) Loss of elasticity Pigmentary changes Dryness Loss of luminosity Baldness/ grey hair Increased nose
What is atopic dermatitis?
 What is atopic dermatitis? Complex inflammatory skin disorder intense pruritus cutaneous hyperreactivity immune dysregulation Chronic with exacerbations and remissions Affects all ages, but more common
What is atopic dermatitis? Complex inflammatory skin disorder intense pruritus cutaneous hyperreactivity immune dysregulation Chronic with exacerbations and remissions Affects all ages, but more common
Benlysta (belimumab) Prior Authorization Criteria Program Summary
 Benlysta (belimumab) Prior Authorization Criteria Program Summary This prior authorization applies to Commercial, NetResults A series, NetResults F series and Health Insurance Marketplace formularies.
Benlysta (belimumab) Prior Authorization Criteria Program Summary This prior authorization applies to Commercial, NetResults A series, NetResults F series and Health Insurance Marketplace formularies.
Rashes in the elderly
 Clinical practice 29 Rashes in the elderly In this article we aim to highlight some of the commoner skin conditions one might expect to see in an elderly population, their typical features and treatments.
Clinical practice 29 Rashes in the elderly In this article we aim to highlight some of the commoner skin conditions one might expect to see in an elderly population, their typical features and treatments.
LUPUS CAN DO EVERYTHING, BUT NOT EVERYTHING IS LUPUS LUPUS 101 SLE SUBSETS AUTOIMMUNE DISEASE 11/4/2013 HOWARD HAUPTMAN, MD IDIOPATHIC DISCOID LUPUS
 LUPUS 101 LUPUS CAN DO EVERYTHING, BUT NOT EVERYTHING IS LUPUS HOWARD HAUPTMAN, MD IDIOPATHIC DISCOID LUPUS SLE SUBSETS SUBACUTE CUTANEOUS LUPUS DRUG INDUCED LUPUS NEONATAL LUPUS LATE ONSET LUPUS ANTI-PHOSPHOLIPID
LUPUS 101 LUPUS CAN DO EVERYTHING, BUT NOT EVERYTHING IS LUPUS HOWARD HAUPTMAN, MD IDIOPATHIC DISCOID LUPUS SLE SUBSETS SUBACUTE CUTANEOUS LUPUS DRUG INDUCED LUPUS NEONATAL LUPUS LATE ONSET LUPUS ANTI-PHOSPHOLIPID
What's New in Oncodermatopathology: Immunotherapy Reactions
 What's New in Oncodermatopathology: Immunotherapy Reactions Emily Y. Chu, M.D., Ph.D. Assistant Professor of Dermatology & Pathology and Laboratory Medicine Hospital of the University of Pennsylvania March
What's New in Oncodermatopathology: Immunotherapy Reactions Emily Y. Chu, M.D., Ph.D. Assistant Professor of Dermatology & Pathology and Laboratory Medicine Hospital of the University of Pennsylvania March
Index. Angiosarcoma diagnosis, 47 lymphedema-related vs. non-lymphedemarelated, 48
 A Acneiform rash biopsy, 134 cetuximab, EGFR, 132 133 diagnosis, 131 patient history, 131 134 treatment, 134 135 Acne vulgaris, 109 AGA. See Androgenetic alopecia Alopecia areata, 148 American Joint Committee
A Acneiform rash biopsy, 134 cetuximab, EGFR, 132 133 diagnosis, 131 patient history, 131 134 treatment, 134 135 Acne vulgaris, 109 AGA. See Androgenetic alopecia Alopecia areata, 148 American Joint Committee
0BCore Safety Profile. Pharmaceutical form(s)/strength: Cream 1% DK/H/PSUR/0009/005 Date of FAR:
 0BCore Safety Profile Active substance: Pimecrolimus Pharmaceutical form(s)/strength: Cream 1% P-RMS: DK/H/PSUR/0009/005 Date of FAR: 06.06.2013 4.3 Contraindications Hypersensitivity to pimecrolimus,
0BCore Safety Profile Active substance: Pimecrolimus Pharmaceutical form(s)/strength: Cream 1% P-RMS: DK/H/PSUR/0009/005 Date of FAR: 06.06.2013 4.3 Contraindications Hypersensitivity to pimecrolimus,
DERMATOLOGICAL EMERGENCIES. DR. Ian Hoyle MBBS DIP IMC RCS (Ed), DA (UK),FRACGP,FACRRM,DIP DERM(Wales) TASMANIAN SKIN AND BODY CENTRE
 DERMATOLOGICAL EMERGENCIES DR. Ian Hoyle MBBS DIP IMC RCS (Ed), DA (UK),FRACGP,FACRRM,DIP DERM(Wales) TASMANIAN SKIN AND BODY CENTRE Dermatological Emergencies INFECTIONS ERYTHRODERMA DRUG ERUPTIONS STEVENS-JOHNSON
DERMATOLOGICAL EMERGENCIES DR. Ian Hoyle MBBS DIP IMC RCS (Ed), DA (UK),FRACGP,FACRRM,DIP DERM(Wales) TASMANIAN SKIN AND BODY CENTRE Dermatological Emergencies INFECTIONS ERYTHRODERMA DRUG ERUPTIONS STEVENS-JOHNSON
APPROACH TO PATIENTS WITH POLYARTHRALGIA
 APPROACH TO PATIENTS WITH POLYARTHRALGIA Scott Vogelgesang, MD Division of Immunology University of Iowa No conflicts of interest DEFINITIONS Arthralgia joint pain with no evidence of inflammation Arthritis
APPROACH TO PATIENTS WITH POLYARTHRALGIA Scott Vogelgesang, MD Division of Immunology University of Iowa No conflicts of interest DEFINITIONS Arthralgia joint pain with no evidence of inflammation Arthritis
chemotherapeutic agents in
 Use of biologics and chemotherapeutic agents in cutaneous emergencies: Focus on lifethreatening forms of psoriasis Alice Bendix Gottlieb MD, PhD Professor of Dermatology New York Medical College Metropolitan
Use of biologics and chemotherapeutic agents in cutaneous emergencies: Focus on lifethreatening forms of psoriasis Alice Bendix Gottlieb MD, PhD Professor of Dermatology New York Medical College Metropolitan
Treatments used Topical including cleansers and moisturizer Oral medications:
 Discipline: Dermatology Extended Topic: Acne & Rosacea : Onset: Location: Face Chest Back Menses if female: Regular Irregular PCOS Treatments used Topical including cleansers and moisturizer Oral medications:
Discipline: Dermatology Extended Topic: Acne & Rosacea : Onset: Location: Face Chest Back Menses if female: Regular Irregular PCOS Treatments used Topical including cleansers and moisturizer Oral medications:
Dermatology Pearls for Inpatient Medicine. Dr Peter J Green MD FRCPC Professor, Division of Dermatology Dalhousie University
 Dermatology Pearls for Inpatient Medicine Dr Peter J Green MD FRCPC Professor, Division of Dermatology Dalhousie University Objectives 1. Review spectrum of cutaneous manifestations seen with inpatient
Dermatology Pearls for Inpatient Medicine Dr Peter J Green MD FRCPC Professor, Division of Dermatology Dalhousie University Objectives 1. Review spectrum of cutaneous manifestations seen with inpatient
Fever in Lupus. 21 st April 2014
 Fever in Lupus 21 st April 2014 Fever in lupus Cause of fever N= 487 % SLE fever 206 42 Infection in SLE 265 54.5 Active SLE and infection 8 1.6 Tumor fever 4 0.8 Miscellaneous 4 0.8 Crucial Question Infection
Fever in Lupus 21 st April 2014 Fever in lupus Cause of fever N= 487 % SLE fever 206 42 Infection in SLE 265 54.5 Active SLE and infection 8 1.6 Tumor fever 4 0.8 Miscellaneous 4 0.8 Crucial Question Infection
2/23/18. Disclosures. Rheumatic Diseases of Childhood. Making Room for Rheumatology. I have nothing to disclose. James J.
 Making Room for Rheumatology James J. Nocton, MD Disclosures I have nothing to disclose Rheumatic Diseases of Childhood Juvenile Idiopathic Arthritis (JIA) Systemic Lupus Erythematosus (SLE) Juvenile Dermatomyositis
Making Room for Rheumatology James J. Nocton, MD Disclosures I have nothing to disclose Rheumatic Diseases of Childhood Juvenile Idiopathic Arthritis (JIA) Systemic Lupus Erythematosus (SLE) Juvenile Dermatomyositis
Department of Dermatology, Christian Medical College and Hospital, Ludhiana, Punjab, India.
 Bullous pemphigoid mimicking granulomatous inflammation Abhilasha Williams, Emy Abi Thomas. Department of Dermatology, Christian Medical College and Hospital, Ludhiana, Punjab, India. Egyptian Dermatology
Bullous pemphigoid mimicking granulomatous inflammation Abhilasha Williams, Emy Abi Thomas. Department of Dermatology, Christian Medical College and Hospital, Ludhiana, Punjab, India. Egyptian Dermatology
Vulval dermatoses. Dr Fiona Lewis, Consultant Dermatologist St John s Institute of Dermatology, London & Heatherwood & Wexham Park Hospital, Slough
 Vulval dermatoses Dr Fiona Lewis, Consultant Dermatologist St John s Institute of Dermatology, London & Heatherwood & Wexham Park Hospital, Slough Pigmentation Vulvodynia Ulcers Genetic Pruritus VULVAL
Vulval dermatoses Dr Fiona Lewis, Consultant Dermatologist St John s Institute of Dermatology, London & Heatherwood & Wexham Park Hospital, Slough Pigmentation Vulvodynia Ulcers Genetic Pruritus VULVAL
Psoriasis. Andrei Metelitsa, MD, FRCPC, FAAD Clinical Associate Professor, Dermatology, U of C Co-Director, Institute for Skin Advancement
 Psoriasis Andrei Metelitsa, MD, FRCPC, FAAD Clinical Associate Professor, Dermatology, U of C Co-Director, Institute for Skin Advancement Copyright 2017 by Sea Courses Inc. All rights reserved. No part
Psoriasis Andrei Metelitsa, MD, FRCPC, FAAD Clinical Associate Professor, Dermatology, U of C Co-Director, Institute for Skin Advancement Copyright 2017 by Sea Courses Inc. All rights reserved. No part
Psoriasis: Causes, Symptoms, And Treatment
 Psoriasis: Causes, Symptoms, And Treatment We all know that a healthy immune system is good. But, do you know that an overactive immune system can cause certain conditions like Psoriasis? Read on to find
Psoriasis: Causes, Symptoms, And Treatment We all know that a healthy immune system is good. But, do you know that an overactive immune system can cause certain conditions like Psoriasis? Read on to find
AUTOIMMUNE DISORDERS IN THE ACUTE SETTING
 AUTOIMMUNE DISORDERS IN THE ACUTE SETTING Diagnosis and Treatment Goals Aimee Borazanci, MD BNI Neuroimmunology Objectives Give an update on the causes for admission, clinical features, and outcomes of
AUTOIMMUNE DISORDERS IN THE ACUTE SETTING Diagnosis and Treatment Goals Aimee Borazanci, MD BNI Neuroimmunology Objectives Give an update on the causes for admission, clinical features, and outcomes of
Ask the Expert: Photosensitivity in Cutaneous Lupus
 Ask the Expert: Photosensitivity in Cutaneous Lupus Victoria P. Werth, MD Department of Dermatology & Medicine University of Pennsylvania ; Philadelphia VA Hospital Overview Definition Impact of photosensitivity
Ask the Expert: Photosensitivity in Cutaneous Lupus Victoria P. Werth, MD Department of Dermatology & Medicine University of Pennsylvania ; Philadelphia VA Hospital Overview Definition Impact of photosensitivity
Dermatology elective for yr. 5. Natta Rajatanavin, MD. Div. of dermatology Dep. Of Medicine, Ramathibodi Hospital Mahidol University 23 rd Feb 2015
 Dermatology elective for yr. 5 Natta Rajatanavin, MD. Div. of dermatology Dep. Of Medicine, Ramathibodi Hospital Mahidol University 23 rd Feb 2015 How to diagnosis and manage eczema and psoriasis. Objectives
Dermatology elective for yr. 5 Natta Rajatanavin, MD. Div. of dermatology Dep. Of Medicine, Ramathibodi Hospital Mahidol University 23 rd Feb 2015 How to diagnosis and manage eczema and psoriasis. Objectives
Five things not to miss in Dermatology. Dr Judy Wismer Associate Clinical Professor Michael G DeGroote School of Medicine
 Five things not to miss in Dermatology Dr Judy Wismer Associate Clinical Professor Michael G DeGroote School of Medicine Key Descriptives Fever, skin pain Purpura, necrosis Bullae, Mucosal, Skin sloughing
Five things not to miss in Dermatology Dr Judy Wismer Associate Clinical Professor Michael G DeGroote School of Medicine Key Descriptives Fever, skin pain Purpura, necrosis Bullae, Mucosal, Skin sloughing
Eczema. By:- Dr. Naif Al-Shahrani Salman bin Abdazziz University
 Eczema By:- Dr. Naif Al-Shahrani Salman bin Abdazziz University Dermatitis= Eczema =Spongiosis Eczema Atopic Seborrheic Contact Allergic Irritant Nummular Asteatotic Stasis Neurodermatitis/Lichen Simplex
Eczema By:- Dr. Naif Al-Shahrani Salman bin Abdazziz University Dermatitis= Eczema =Spongiosis Eczema Atopic Seborrheic Contact Allergic Irritant Nummular Asteatotic Stasis Neurodermatitis/Lichen Simplex
COPYRIGHTED MATERIAL. Introduction CHAPTER 1. Introduction
 CHAPTER 1 Introduction OVERVIEW The clinical features of skin lesions are related to the underlying pathological processes. Broadly skin conditions fall into three clinical groups: (a) those with a well-defined
CHAPTER 1 Introduction OVERVIEW The clinical features of skin lesions are related to the underlying pathological processes. Broadly skin conditions fall into three clinical groups: (a) those with a well-defined
Case 1 History. William Tremaine, M.D. CP
 Extraintestinal Manifestations of IBD Case Studies William Tremaine, M.D. Case 1 History 18 year-old woman with Crohn s disease Onset at age 5: colonic & perianal Sulfasalazine, prednisone, mercaptopurine
Extraintestinal Manifestations of IBD Case Studies William Tremaine, M.D. Case 1 History 18 year-old woman with Crohn s disease Onset at age 5: colonic & perianal Sulfasalazine, prednisone, mercaptopurine
Bacterial Infections in Pediatric Dermatology. Patrick McMahon, MD Children s Hospital of Philadelphia
 Bacterial Infections in Pediatric Dermatology Patrick McMahon, MD Children s Hospital of Philadelphia Fill In The Blank When you see on the skin, you think of a bacterial skin infection SEND SWABS VIRAL
Bacterial Infections in Pediatric Dermatology Patrick McMahon, MD Children s Hospital of Philadelphia Fill In The Blank When you see on the skin, you think of a bacterial skin infection SEND SWABS VIRAL
Time to Learn. 6 th March 2018 Dr. Shirin Chakera GPwSI Integrated Dermatology Service
 Time to Learn 6 th March 2018 Dr. Shirin Chakera GPwSI Integrated Dermatology Service The Red Face Rosacea Acne Seborrhoeic eczema eczema Psoriasis Slapped cheek syndrome Fungal infection Erysipelas...
Time to Learn 6 th March 2018 Dr. Shirin Chakera GPwSI Integrated Dermatology Service The Red Face Rosacea Acne Seborrhoeic eczema eczema Psoriasis Slapped cheek syndrome Fungal infection Erysipelas...
Learning Circle: Jan 26, 2011 Childhood Eczema
 Learning Circle: Jan 26, 2011 Childhood Eczema Wingfield Rehmus, MD MPH BC Children s Hospital Clinical Assistant Professor, UBC Department of Paediatrics Associate Member, UBC Department of Dermatology
Learning Circle: Jan 26, 2011 Childhood Eczema Wingfield Rehmus, MD MPH BC Children s Hospital Clinical Assistant Professor, UBC Department of Paediatrics Associate Member, UBC Department of Dermatology
Psoriasis. Overview. Epidemiology. Epidemiology 08/08/2015. Dr Nigel Burrows Consultant Dermatologist Addenbrooke s Hospital
 Overview Psoriasis 1. Epidemiology of psoriasis 2. Histology Dr Nigel Burrows Consultant Dermatologist Addenbrooke s Hospital Aug 2015 3. Types of psoriasis 4. Assessing severity 5. Treatments Topical
Overview Psoriasis 1. Epidemiology of psoriasis 2. Histology Dr Nigel Burrows Consultant Dermatologist Addenbrooke s Hospital Aug 2015 3. Types of psoriasis 4. Assessing severity 5. Treatments Topical
My Algorithm. Questions to ask. Do you or your family have a history of?... Allergic rhinitis, Sensitive skin, Asthma Skin Cancer
 Tracey C. Vlahovic, DPM Associate Professor, Temple University School of Podiatric Medicine My Algorithm Inflammatory Skin Disorder on Feet Family hx, clinical exam, look at hands! Defined plaques: Psoriasis
Tracey C. Vlahovic, DPM Associate Professor, Temple University School of Podiatric Medicine My Algorithm Inflammatory Skin Disorder on Feet Family hx, clinical exam, look at hands! Defined plaques: Psoriasis
Facial Rash. Facial Rash 10/14/2013. Ten Look Alike Rashes Michelle DiBaise, MPAS, PA-C, DFAAPA Associate Clinical Professor NAU PA Program
 Ten Look Alike Rashes Michelle DiBaise, MPAS, PA-C, DFAAPA Associate Clinical Professor NAU PA Program Facial Rash Facial Rash Case 1 28 year female Progressive development of erythematous facial lesions
Ten Look Alike Rashes Michelle DiBaise, MPAS, PA-C, DFAAPA Associate Clinical Professor NAU PA Program Facial Rash Facial Rash Case 1 28 year female Progressive development of erythematous facial lesions
Psoriasis is a chronic, inflammatory, Prescribing in children
 Psoriasis in children: current approaches to management Laura Proudfoot BSc, MRCP, Elisabeth Higgins MA, FRCP and Judy Davids RGN Our series Prescribing in children gives practical advice for successful
Psoriasis in children: current approaches to management Laura Proudfoot BSc, MRCP, Elisabeth Higgins MA, FRCP and Judy Davids RGN Our series Prescribing in children gives practical advice for successful
9/13/2015. Nothing to disclose
 Jared Bozeman Kathleen Luskin MD Bipin Thapa MD Medical College of Wisconsin Milwaukee, Wisconsin Nothing to disclose 24 Year old previously healthy woman presenting from OSH Fatigue Weakness Neck swelling
Jared Bozeman Kathleen Luskin MD Bipin Thapa MD Medical College of Wisconsin Milwaukee, Wisconsin Nothing to disclose 24 Year old previously healthy woman presenting from OSH Fatigue Weakness Neck swelling
Some skin conditions
 Some skin conditions Some skin conditions Acute Inflammatory Dermatoses Chronic Inflammatory Dermatoses Blistering (Bullous) Diseases Panniculitis Disorders of Epidermal Appendages -Urticaria -Acute eczematous
Some skin conditions Some skin conditions Acute Inflammatory Dermatoses Chronic Inflammatory Dermatoses Blistering (Bullous) Diseases Panniculitis Disorders of Epidermal Appendages -Urticaria -Acute eczematous
Definition Chronic autoimmune disease The body s immune system starts attacking itself Can affect most organs and tissues in the body Brain, lungs, he
 LIVING WITH SYSTEMIC LUPUS ERYTHEMATOSUS Stacy Kennedy, M.D.,M.B.A. Rowan Diagnostic Clinic Salisbury, N.C. May 11, 2013 Agenda What is lupus Who is affected Causes of lupus Symptoms and organ involvement
LIVING WITH SYSTEMIC LUPUS ERYTHEMATOSUS Stacy Kennedy, M.D.,M.B.A. Rowan Diagnostic Clinic Salisbury, N.C. May 11, 2013 Agenda What is lupus Who is affected Causes of lupus Symptoms and organ involvement
Question 1: Per the drug chart, the most likely culprit is:
 Disclosures I have no conflicts of interest to disclose Lindy P. Fox, MD Associate Professor Director, Hospital Consultation Service Department of Dermatology University of California, San Francisco 2
Disclosures I have no conflicts of interest to disclose Lindy P. Fox, MD Associate Professor Director, Hospital Consultation Service Department of Dermatology University of California, San Francisco 2
Biologic Therapies for Atopic Dermatitis and Beyond
 Biologic Therapies for Atopic Dermatitis and Beyond Jonathan Corren, M.D. Departments of Medicine and Pediatrics, David Geffen School of Medicine at UCLA Disclosures Genentech - research Medimmune/AZ -
Biologic Therapies for Atopic Dermatitis and Beyond Jonathan Corren, M.D. Departments of Medicine and Pediatrics, David Geffen School of Medicine at UCLA Disclosures Genentech - research Medimmune/AZ -
Diagnosis and Management of the Hair Loss Patient: Pearls and Pitfalls
 Diagnosis and Management of the Hair Loss Patient: Pearls and Pitfalls U033 July 30 th 2017 7:30-8:30AM Paradi Mirmirani, MD The Permanente Medical Group, Vallejo, CA Regional Director, Hair Disorders
Diagnosis and Management of the Hair Loss Patient: Pearls and Pitfalls U033 July 30 th 2017 7:30-8:30AM Paradi Mirmirani, MD The Permanente Medical Group, Vallejo, CA Regional Director, Hair Disorders
Undifferentiated Connective Tissue Disease and Overlap Syndromes. Mark S. Box, MD
 Undifferentiated Connective Tissue Disease and Overlap Syndromes Mark S. Box, MD Overlap Syndromes As many as 25% of patients with rheumatic diseases with systemic symptoms cannot be definitely diagnosed
Undifferentiated Connective Tissue Disease and Overlap Syndromes Mark S. Box, MD Overlap Syndromes As many as 25% of patients with rheumatic diseases with systemic symptoms cannot be definitely diagnosed
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Psoriasis: the management of psoriasis 1.1 Short title Psoriasis 2 The remit The Department of Health has asked NICE: 'to produce
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Psoriasis: the management of psoriasis 1.1 Short title Psoriasis 2 The remit The Department of Health has asked NICE: 'to produce
DISCUSSION BY: Dr M. R. Shakeebi, MD, Rheumatologist
 Case presentations Related to some Rheumatic Diseases Lab & Clinic i Programs, Tuesday, April 24, 2012 COORDINATOR: Dr M. Mahdi Mohammadi, LMD,PhD, Immunologist COORDINATOR: Dr M. Mahdi Mohammadi, LMD,PhD,
Case presentations Related to some Rheumatic Diseases Lab & Clinic i Programs, Tuesday, April 24, 2012 COORDINATOR: Dr M. Mahdi Mohammadi, LMD,PhD, Immunologist COORDINATOR: Dr M. Mahdi Mohammadi, LMD,PhD,
Treating dermatomyositis
 Treating dermatomyositis David Fiorentino, MD, PhD Stanford University School of Medicine Department of Dermatology Department of Medicine (Rheumatology) September 25, 2010 DM affects many organs Approaching
Treating dermatomyositis David Fiorentino, MD, PhD Stanford University School of Medicine Department of Dermatology Department of Medicine (Rheumatology) September 25, 2010 DM affects many organs Approaching
An otherwise healthy 12-year-old
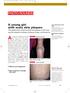 1105 Photo Rounds.finalREV 10/19/05 2:05 PM Page 947 A young girl with scaly skin plaques The patient had numerous thick red plaques on her back and the extensor surfaces of elbows, knees, and forearms
1105 Photo Rounds.finalREV 10/19/05 2:05 PM Page 947 A young girl with scaly skin plaques The patient had numerous thick red plaques on her back and the extensor surfaces of elbows, knees, and forearms
Drug allergy and Skin Disorders. Timothy Craig, DO, FACOI Professor of Medicine and Pediatrics Distinguished Educator Penn State University, Hershey
 Drug allergy and Skin Disorders Timothy Craig, DO, FACOI Professor of Medicine and Pediatrics Distinguished Educator Penn State University, Hershey The best screening test for anaphylaxis is? A. histamine
Drug allergy and Skin Disorders Timothy Craig, DO, FACOI Professor of Medicine and Pediatrics Distinguished Educator Penn State University, Hershey The best screening test for anaphylaxis is? A. histamine
