Principles of Anesthetic Care for Burned Children: an overview. Kenneth T. Furukawa, MD Health Sciences Clinical Professor
|
|
|
- Richard McCormick
- 5 years ago
- Views:
Transcription
1 Principles of Anesthetic Care for Burned Children: an overview Kenneth T. Furukawa, MD Health Sciences Clinical Professor
2 Disclosure The speaker has disclosed no relevant financial relationships with commercial interests related to this CME activity. There is no commercial support for this activity
3 Off-label Use Disclosure Some medications mentioned in this presentation are not FDA approved for use in children in the manner suggested by the speaker. Inhaled heparin
4 Objectives Upon completion of this session, the participant will be able to: * Identify and manage the burned child with a compromised airway, including various components for inhalational injury. * Recognize how burn injury affects drug pharmacodynamics and pharmacokinetics. * Identify the unique challenges of anesthetic management of the child with burns.
5 Phases of burn care Emergent/resuscitation Injury onset to fluid resuscitation completion 0 3 days Resuscitation, treat burn shock Acute Diuresis from fluid resuscitation until wound closure Duration of weeks to months Achieve wound closure, support recovery Rehabilitation Wound closure to optimal recovery
6 Case 1: Initial evaluation Called to assist with evaluation & management of child with facial burns from a closed space fire. Child cries, but hoarse. Moderate inhalation obstruction. What do you see here that suggests inhalation injury?
7 Case 1: Emergent/resuscitation phase care Airway management as indicated during initial and secondary surveys Administer oxygen for presumed carboxyhemoglobinemia! Assessment of airway & breathing Face: skin burn lips, nose, face Hair: singed eyebrows, nasal Mouth: tongue swelling?
8 Inhalation Case 1: Identify airway / inhalation injury Evaluate mouth, pharynx, glottis when possible. Laryngoscopy (indirect or direct) is indicated as part of suspicious airway evaluation. Direct heat transfer/burn from hot air/gas/steam Is intubation or other airway support indicated? Exhalation
9 Bronchoscopy evaluation if possible Grade 0 no injury Grade 1 mild injury patchy erythema, carbonaceous deposits Grade 2 moderate injury moderate erythema, carbon, bronchorrhea, bronchial compromise Grade 3 severe injury severe inflammation, friable, copious carbon and bronchorrhea, bronchial obstruction Grade 4 massive injury sloughing, necrosis, obliteration Massive inhalation injury
10 Burned airway risks Rapid edema Thermal damage, toxins Resuscitation related airway edema may develop over 24+ hours Continuous monitoring with on-site expert management or early intubation Impaired oxygenation Carboxyhemoglobin, cyanide, edema, tissue damage Increased deadspace Alveolar & distal airways damage/obstruction Increased risk of pneumonia Association with ARDS and other ventilator induced lung injuries
11 Intubation is not always indicated but However delayed edema may exacerbate airway obstruction Observe for at least 24 hours! Glottic edema may present similar to epiglottitis Plan for difficult airway management and airway swelling Bronchoscopy evaluation offers opportunity to intubate immediately if desired IV ketamine helpful for spontaneous ventilation and sedation/analgesia 10-30% of hospitalized burn patients have inhalation/airway injury with related mortality of 16+% 25-50% of these die if require ventilator support for more than 1 week
12 Case 1: Intubation indicated? What about our case? Facial/nasal hair singed Voice change Glottic edema Bronchoscopy likely to demonstrate at least mild injury to upper trachea Yes, let s secure the airway!
13 Case 1: Intubation choices Oral vs nasotracheal Oral intubation often simpler Nasotracheal more secure (personal preference) Cuffed ETT Size & place carefully due to acute edema Secure carefully there will be swelling! Tape will work loose due to secretions and topical Rx Circumferential tape/twill will cut unless loosened often Will need to be tightened periodically as swelling reduces! Consider alternate securement techniques Re-intubation may be a lethal procedure!
14 Securing ETT and Facial Burns Oral ETT with 4 point tape Note pressure to swollen scalp, ear, neck Needs constant adjustment Topical ointment compromises adhesive Large area of tissue injured by tape Four point tape harness
15 Protect face from pressure of twill on ETT Plastic tubing reduces friction Adjust for swelling at side Loosen or tighten as needed Vertical strap separate Note facial/nasal edema & loss nasal hairs
16 Oral ETT Secured with Wire Secure around tooth Deciduous teeth do come out! Wire suture can be used around root of teeth Wire tied around tooth
17 Secure nasotracheal ETT behind nasal septum Nasotracheal ETT in place Two rubber catheters placed naso-orally & brought out mouth Long twill tied to both catheters Rubber catheters passed naso-oral
18 Secure nasotracheal ETT behind nasal septum Withdraw catheters & twill through nose Secure ETT with some give to internal twill around septum & nasopharynx. Catheters withdrawn through nose, twill then tied to ETT from each nare.
19 Case 1: Inhalation injury management High flow, humidified oxygen Carboxyhemoglobinemia likely! Reduced PaO2 despite normal SpO2 Use co-oximetry or multiple wavelength near-infrared pulse oximeter 100% O2 reduces COHb half-life from 4 hr to <1 hr. Check ABG with co-oximetry frequently Follow carboxyhemoglobin concentration/percentage
20 Case 1: Inhalation injury management cont. Persistent signs of hypoxemia consider cyanide toxicity from burning synthetics Tachycardia, tachypnea, hypertension Anion gap metabolic acidosis despite adequate PaO2, SvO2 may be elevated Hydroxycobalamin 5gm IV over 15 min adult
21 Case 1: Ventilation management No definite data suggesting best strategy to date: Lung protective low Vt (6ml/kg) with low PEEP vs higher Vt (12-15ml/kg) with PEEP to minimize FiO2 Lung protective/ards preventive strategy accepted despite little data in pediatric burns PCV vs VCV HFPV (high frequency percussive ventilation) oscillator superimposed over PCV May have better PaO2 and PaCO2 with lower Pinsp than PCV techniques Less barotrauma compared to low Vt strategy?
22 Ventilator strategy comparison Is inhalation injury similar to other forms of ARDS? Lung injury is thermal, chemical, and inflammatory. Early & copious sloughing in severe cases. Initially lung protective strategies Alternates tend to higher Vt & PEEP first, then HFPV (VDR) Goh CT, Jacobe S 2015 Holland D, Wolf SE, etal 2013 Jeschke MG, Herndon DN 2014
23 Adjuncts for inhalation injury Inhaled nitric oxide Limited data as rescue therapy for inhalation injury Inhaled heparin +/- N-acetylcystiene Limited data Reduce fibrin deposition, cast formation in bronchial structures Improve expectoration Inhaled epinephrine, albuterol, ipratroprium Bronchodilation and anti-inflammatory No role for preemptive antibiotics or steroid Miller AC, Elamin EM, Suffredini AF 2014
24 Tracheostomy Institution practice specific Some indications for early after resuscitation & diuresis Anticipated ventilator support for more than 2 weeks High risk of extubation and difficult reintubation Allows earlier face sheet grafting without ETT securement trauma
25 Case 2: Pharmacokinetics and pharmacodynamics in burns Multiple physiologic alterations occur with moderate to severe burn injuries greatly impacting upon expected pharmacokinetic and pharmacodynamic profiles of all medications. In fact, the response to IV ketamine was more profound than expected, and the patient is moving 20 minutes after IV rocuronium 0.6 mg/kg. What is happening?
26 Pharmacokinetic changes throughout emergent & acute burn care phases Plasma albumin loss Reduced binding, increased free fraction Alpha 1 acid glycoprotein acute phase reactant increases Increased binding of cationic medications Volume of distribution increased Fentanyl, morphine, propofol, ketamine, NMBs
27 Pharmacokinetic changes: Burn Shock emergent/resuscitation period Cardiac output reduced Inflammatory mediated cardiomyopathy? Hepatic & renal blood flow reduced Drug clearance reduced Adequate fluid resuscitation reduces impact but increases general edema formation Inadequate resuscitation risks further organ damage and prolonged shock state
28 Pharmacodynamic changes: acute phase After successful resuscitation, diuresis begins and the patient enters a prolonged hyperdynamic phase Inflammatory mediated responses Increased cardiac output Increased hepatic and renal blood flow Increased drug clearance Increased activity hepatic isoenzyme systems
29 Pharmacodynamic changes: acute phase Hepatic enzymatic activity altered Phase 1 reactions (oxidation, reduction, hydroxylation, demethylation) reduced Phase 2 (conjugation, glucoronidation) unchanged?
30 Neuromuscular blocking agents: acute phase Depolarizing agent (succinylcholine) induced hyperkalemia Acetylcholine receptor upregulation begins immediately May be significant > 1 year after all wounds closed Nondepolarizing agents decreased sensitivity / increased resistance (all classes) Acetylcholine receptor upregulation Increased plasma binding to alpha acid glycoprotein Increased hepatic & renal clearance
31 Anesthetic/sedative agents: acute phase Volume of distribution increased Hepatic & renal clearance increased Tolerance may be marked Adjunctive agents may modify this situation
32 Opioids: acute phase Possibly more remarkable tolerance than other agents But it appears that burn patients develop tolerance to all drugs. Down regulation of spinal mu-opioid receptors Relative resistance to central opioid activity Upregulation of NMDA and protein kinase receptors These receptors are implicated in opioid induced hyperalgesia mechanisms.
33 Adjuncts (sedation, analgesia, anxiety) NMDA receptor antagonists Ketamine Methadone Alpha-2 central catecholamine agonists Clonidine Dexmedetomidine Anti-neuropathic agents Anti-epileptics (gabapentin, pregabalin, oxcarbazepine) Anti-depressants (TCAs, SNRIs, SSRIs) Anti-histaminergic agents
34 Ketamine is unique Dissociative anesthetic induction/maintenance agent Caution for emergence dysphoria/delirium Secretion management Chronically sympathomimetic activated patient may have primarily sympatholytic response Maintains hypoxic & hypercapneic responses during spontaneous ventilation Modifies tolerance to other analgesic agents
35 Regional anesthesia/analgesia: all phases Limited role for regional anesthesia in large TBSA interventions, but very useful for smaller interventions Fascia iliaca compartment block for thigh STSG donor site Local anesthetic in tumescent solution injected for wound debridement and STSG donor harvest. Central neuraxial, peripheral nerve blocks, truncal blocks single shot and continuous Presumed increased infection risk when performed through or near burned tissues. Local anesthetic altered pharmacokinetics?
36 Understanding Anesthetic Care in Terms of the Phases of Burn Care Emergent/resuscitation Injury onset to fluid resuscitation completion 0 3 days Resuscitation, treat burn shock Acute Diuresis from fluid resuscitation until wound closure Duration of weeks to months Achieve wound closure, support recovery Rehabilitation Wound closure to optimal recovery
37 Emergent/resuscitation phase care Fluid and blood management per ATLS protocols, plus burn resuscitation guidelines (modified Parkland formula) Parkland: LR 4 ml/kg/% burn over 24hr, 50% during 8 hrs 20kg child w/ 40% TBSA 2 nd /3 rd burns: 3200ml LR in 24hrs, 1600ml in first 8 hrs Goals hemodynamic stability, u/o 1ml/kg/hr Requires good vascular access Risks burn compartment syndromes
38 Extremity/chest/abdominal compartment syndromes: eschar/fascia/laparotomy Arm escharotomy, leg escharotomies and fasciotomy, abdominal silo
39 Burn shock Burn shock Cytokine mediated w/ possible cardiomyopathy Increased SVR and PVR Generalized edema may encourage hemoconcentration More likely burns >25% TBSA Generally improves with fluid infusion Avoid vasopressors in favor of inotropes
40 Prevent heat loss Heat loss amplified due to destruction of intact skin Radiation, evaporation, convection, conduction Most effective measure is high room temperature (as near 37C as tolerable) Use blankets, thermal shielding, plastic wraps, etc. Be wary of forced air warming and contact warming devices (water circulating mattress/blanket) Hypothermia the first leg in the Trauma Triad of Death Hypothermia, acidosis, coagulopathy
41 Operative blood management Estimating blood loss during burn excision/dressing difficult Multiple estimates developed: 0.75ml/sq cm burned skin excised 117ml/BSA% excised for adults (approx 2ml/kg/BSA%) % BV/BSA% Blood product replacement must include adequate FFP and platelets Consider massive transfusion protocol for excision > 20% TBSA Blood loss continues after skin coverage and dressings Tourniquets, topical vasoconstrictors/thrombin are helpful but inadequate
42 Hypermetabolism Altered glucose, lipid, aminoacid/protein metabolism Catabolism Insulin resistance Multi-organ dysfunction Appropriate enteral feeding limits catabolism Post-pyloric enteral feeding should continue intraoperatively if well-tolerated
43 Airway challenges in rehabilitation phase Contractures are common Be prepared for unusual Maintain spontaneous ventilation if at all possible Burn scar contractures create difficult airway
44 Pain management Opioid tolerance/hyperalgesia NMDA antagonists Antidepressants Antiepileptics Central alpha 2 agonists Benzodiazepine cautions APAP/NSAID ceiling effects Psychological management
45 Thanks Special thanks to J. Woodson, MD and D. Greenhalgh, MD for clinical photos.
46 References Beushausen T, Mucke K. Anesthesia and Pain Management in Pediatric Burn Patients. Pediatr Surg Int 1997; 12: Bittner EA, Shank E, Woodson L, Jeevendra Martyn JA. Acute and Perioperative Care of the Burn-injured Patient. Anesthesiology 2015; 122: Blanchet B, Jullien V, Vinsonneau C, Tod M. Influence of Burns on Pharmacokinetics and Pharmacodynamics of Drugs Used in the Care of Burn Patients. Clin Pharmacokinet 2008; 47: Caruso TJ, Janik LS, Fuzaylov G. Airway Management of Recovered Pediatric Patients with Severe Head and Neck Burns: A Review. Pediatric Anesthesia 2012; 22: Curinga G, Jain A, Feldman M, et al. Red Blood Cell Transfusion Following Burn. Burns 2011; 37: Fuzaylov G, Fidkowski C. Anesthetic Considerations for Major Burn Injury in Pediatric Patients. Pediatric Anesthesia 2009; 19:
47 References continued Goh CT, Jacobe S. Ventilation Strategies in Paediatric Inhalation Injury. Paediatr Respir Rev 2015; Article in Press. Holland D, Wolf SE, Estetter R, De La Garza J, Arnoldo BD. Initial Commitment for Inhalation Injury. Curr Prob Surg 2013; 50: Jeschke MG, Herndon DN. Burns in Children: Standard and New Treatments. Lancet 2014; 383: MacLennan L, Moiemen N. Management of Cyanide Toxicity in Patients With Burns. Burns 2015; 41: Miller AC, Elamin EM, Suffredini AF. Inhaled Anticoagulation Regimens for the Treatment of Smoke Inhalation-Associated Acute Lung Injury: A Systematic Review. Crit Care Med 2014; 42: Pidcoke HF, Isbell CL, Herzig MC, et al. Acute Blood Loss During Burn and Soft Tissue Excisions: An Observational Study of Blood Product Resuscitation Practices and Focused Review. J Trauma Acute Care Surg 2015; 78: S39-S47.
Acute And perioperative care of the burn-injured patient. Anesthesiology, V 122, No 2
 Acute And perioperative care of the burn-injured patient Anesthesiology, V 122, No 2 Reporter:R4 沈士鈞 Supervisor: 蔡欣怡醫師 Pathophysiology Initial evaluation and management Anesthetic managemen nt Pathophysiology
Acute And perioperative care of the burn-injured patient Anesthesiology, V 122, No 2 Reporter:R4 沈士鈞 Supervisor: 蔡欣怡醫師 Pathophysiology Initial evaluation and management Anesthetic managemen nt Pathophysiology
The immediate management of burns patients should be similar to management of trauma.
 CATS Clinical Guideline Burns The National Burn Care Review recommends that children with burns should be treated in a Burn Centre. Chelsea and Westminster may take non-ventilated children, Broomfield
CATS Clinical Guideline Burns The National Burn Care Review recommends that children with burns should be treated in a Burn Centre. Chelsea and Westminster may take non-ventilated children, Broomfield
Applicable to. Team Members Performing
 Protocol: Pediatric Burn Inhalation Injury Category Clinical Practice Protocol Number Approval Date November 1, 2016 Due for review November 1, 2018 Applicable to VUH Children s DOT VMG Off-site locations
Protocol: Pediatric Burn Inhalation Injury Category Clinical Practice Protocol Number Approval Date November 1, 2016 Due for review November 1, 2018 Applicable to VUH Children s DOT VMG Off-site locations
Lecture Notes. Chapter 9: Smoke Inhalation Injury and Burns
 Lecture Notes Chapter 9: Smoke Inhalation Injury and Burns Objectives List the factors that influence mortality rate Describe the nature of smoke inhalation and the fire environment Recognize the pulmonary
Lecture Notes Chapter 9: Smoke Inhalation Injury and Burns Objectives List the factors that influence mortality rate Describe the nature of smoke inhalation and the fire environment Recognize the pulmonary
Pediatric Burn Management Justin D. Klein, MD Associate Burn Director Lisa C. Vitale, RN Burn Program Coordinator
 Pediatric Burn Management Justin D. Klein, MD Associate Burn Director Lisa C. Vitale, RN Burn Program Coordinator Lecture Overview Burn statistics and etiologies Pre-hospital evaluation Anatomy of a burn
Pediatric Burn Management Justin D. Klein, MD Associate Burn Director Lisa C. Vitale, RN Burn Program Coordinator Lecture Overview Burn statistics and etiologies Pre-hospital evaluation Anatomy of a burn
COBIS Management of airway burns and inhalation injury PAEDIATRIC
 COBIS Management of airway burns and inhalation injury PAEDIATRIC 1 A multidisciplinary team should provide the management of the child with inhalation injury. Childhood inhalation injury mandates transfer
COBIS Management of airway burns and inhalation injury PAEDIATRIC 1 A multidisciplinary team should provide the management of the child with inhalation injury. Childhood inhalation injury mandates transfer
BURNS MODULE. In the paediatric population consider non-accidental injury as a mechanism for burn injuries.
 BURNS MODULE INTRODUCTION Burns are a common cause of trauma. Most burn injuries are a result of flame burns, with scalds also occurring commonly. Electrical and chemical burns are less common. 1 Concurrent
BURNS MODULE INTRODUCTION Burns are a common cause of trauma. Most burn injuries are a result of flame burns, with scalds also occurring commonly. Electrical and chemical burns are less common. 1 Concurrent
Printed copies of this document may not be up to date, obtain the most recent version from Author Position
 Children s Acute Transport Service Clinical Guidelines Burns Management Document Control Information Author E Borrows E Randle, L Chigaru Author Position PICU/BURNS Consultant CATS Consultants Document
Children s Acute Transport Service Clinical Guidelines Burns Management Document Control Information Author E Borrows E Randle, L Chigaru Author Position PICU/BURNS Consultant CATS Consultants Document
Printed copies of this document may not be up to date, obtain the most recent version from Author Position
 Children s Acute Transport Service Clinical Guidelines Burns Management Document Control Information Author E Borrows E Randle Author Position PICU/BURNS Consultant CATS Consultant Document Owner E. Polke
Children s Acute Transport Service Clinical Guidelines Burns Management Document Control Information Author E Borrows E Randle Author Position PICU/BURNS Consultant CATS Consultant Document Owner E. Polke
Children's National Medical Center The Division of Trauma and Burn Burn Education Module Post-test
 Children's National Medical Center The Division of Trauma and Burn Burn Education Module Post-test Purpose: To provide nurses with on overview of burn injuries in pediatric patients. Learning Objectives:
Children's National Medical Center The Division of Trauma and Burn Burn Education Module Post-test Purpose: To provide nurses with on overview of burn injuries in pediatric patients. Learning Objectives:
Wisecracks 1. What are the indications for an escharotomy 2. What are the primary considerations in mechanical ventilation of burn patients
 Chapter 63 Thermal Burns Episode Overview Questions 1. List zones of burns 2. List 6 indications for intubation in the burn patient 3. List and describe 2 formulas for fluid resuscitation 4. Describe depth
Chapter 63 Thermal Burns Episode Overview Questions 1. List zones of burns 2. List 6 indications for intubation in the burn patient 3. List and describe 2 formulas for fluid resuscitation 4. Describe depth
Approved By: Airway and Breathing A. Initially give humidified high flow oxygen at 15 L (100%) using a nonrebreather
 Subject: BURN CARE CLINICAL GUIDELINE Originator: Approval Date: 2015 Approved By: Policy: All burn patients presenting to XXXXXX Hospital will have appropriate assessment, stabilization and evaluation
Subject: BURN CARE CLINICAL GUIDELINE Originator: Approval Date: 2015 Approved By: Policy: All burn patients presenting to XXXXXX Hospital will have appropriate assessment, stabilization and evaluation
Burn Injuries & Its Management M JARI.MD
 Burn Injuries & Its Management M JARI.MD 1 BURNS Wounds caused by exposure to: 1. excessive heat 2. Chemicals 3. fire/steam 4. radiation 5. electricity 2 BURNS Results in 10-20 thousand deaths annually
Burn Injuries & Its Management M JARI.MD 1 BURNS Wounds caused by exposure to: 1. excessive heat 2. Chemicals 3. fire/steam 4. radiation 5. electricity 2 BURNS Results in 10-20 thousand deaths annually
Anesthetic Management of the Burn Patient
 Curr Anesthesiol Rep (2016) 6:16 21 DOI 10.1007/s40140-016-0150-0 ANESTHESIA FOR TRAUMA (JW SIMMONS, SECTION EDITOR) Anesthetic Management of the Burn Patient Christian Diez 1 Albert J. Varon 1 Published
Curr Anesthesiol Rep (2016) 6:16 21 DOI 10.1007/s40140-016-0150-0 ANESTHESIA FOR TRAUMA (JW SIMMONS, SECTION EDITOR) Anesthetic Management of the Burn Patient Christian Diez 1 Albert J. Varon 1 Published
IMMEDIATE EMERGENCY BURN CARE » THERMAL BURNS » ELECTRICAL BURNS » CHEMICAL BURNS FIRST AID FOR THE THREE MAJOR CATEGORIES
 IMMEDIATE EMERGENCY BURN CARE 1. Treat according to BLS or ACLS Protocol 2. Use airway and C-Spine precautions. 3. Stop the burning process. FIRST AID FOR THE THREE MAJOR CATEGORIES» THERMAL BURNS + Stop
IMMEDIATE EMERGENCY BURN CARE 1. Treat according to BLS or ACLS Protocol 2. Use airway and C-Spine precautions. 3. Stop the burning process. FIRST AID FOR THE THREE MAJOR CATEGORIES» THERMAL BURNS + Stop
CASE PRIMERS. Pediatric Anesthesia Fellowship Program. Laryngotracheal Reconstruction (LTR) Tufts Medical Center
 CASE PRIMERS Pediatric Anesthesia Fellowship Program Tufts Medical Center Department of Anesthesiology and Perioperative Medicine Division of Pediatric Anesthesia 800 Washington Street, Box 298 Boston,
CASE PRIMERS Pediatric Anesthesia Fellowship Program Tufts Medical Center Department of Anesthesiology and Perioperative Medicine Division of Pediatric Anesthesia 800 Washington Street, Box 298 Boston,
Surviving Sepsis Campaign. Guidelines for Management of Severe Sepsis/Septic Shock. An Overview
 Surviving Sepsis Campaign Guidelines for Management of Severe Sepsis/Septic Shock An Overview Mechanical Ventilation of Sepsis-Induced ALI/ARDS ARDSnet Mechanical Ventilation Protocol Results: Mortality
Surviving Sepsis Campaign Guidelines for Management of Severe Sepsis/Septic Shock An Overview Mechanical Ventilation of Sepsis-Induced ALI/ARDS ARDSnet Mechanical Ventilation Protocol Results: Mortality
Burn injury. A : patent airway with smoking inhalation, stridor. D: E4V5M6,pupil 2mm RTLBE
 Burn injury Pinyong Uthaitas Emergency Department Faculty of Medicine, Ramathibodi Hospital A Thai man 52 year old came to the hospital due to flam burn ½ hr ago at his house. He gain conscious but hoarseness
Burn injury Pinyong Uthaitas Emergency Department Faculty of Medicine, Ramathibodi Hospital A Thai man 52 year old came to the hospital due to flam burn ½ hr ago at his house. He gain conscious but hoarseness
Nothing to Disclose. Severe Pulmonary Hypertension
 Severe Ronald Pearl, MD, PhD Professor and Chair Department of Anesthesiology Stanford University Rpearl@stanford.edu Nothing to Disclose 65 year old female Elective knee surgery NYHA Class 3 Aortic stenosis
Severe Ronald Pearl, MD, PhD Professor and Chair Department of Anesthesiology Stanford University Rpearl@stanford.edu Nothing to Disclose 65 year old female Elective knee surgery NYHA Class 3 Aortic stenosis
Appendix. Sedatives and Pain Medications. Gabapentin ( mg po q8h) or Pregabalin ( mg po q8h)
 Appendix Sedatives and Pain Medications Non-intubated patients Non-opioid analgesics Acetaminophen (500 1,000 mg po q6h) NSAID (Ibuprofen, Naprosyn, Celebrex) Gabapentin (100 300 mg po q8h) or Pregabalin
Appendix Sedatives and Pain Medications Non-intubated patients Non-opioid analgesics Acetaminophen (500 1,000 mg po q6h) NSAID (Ibuprofen, Naprosyn, Celebrex) Gabapentin (100 300 mg po q8h) or Pregabalin
Anesthesia and Analgesia for the Child with Major Thermal Injury and Smoke Inhalation
 Anesthesia and Analgesia for the Child with Major Thermal Injury and Smoke Inhalation Sanjay M. Bhananker, MD, FRCA Harborview Medical Center and Children s Hospital and Regional Medical Center Seattle,
Anesthesia and Analgesia for the Child with Major Thermal Injury and Smoke Inhalation Sanjay M. Bhananker, MD, FRCA Harborview Medical Center and Children s Hospital and Regional Medical Center Seattle,
Management of Acute Burn Injuries: The First 24 Hours
 Speaker Disclosure I, Debbie Harrell, MSN, RN, NE BC, have no financial relationships to disclose. I will not discuss off label uses of any pharmaceutical products or medical devices. Management of Acute
Speaker Disclosure I, Debbie Harrell, MSN, RN, NE BC, have no financial relationships to disclose. I will not discuss off label uses of any pharmaceutical products or medical devices. Management of Acute
Capnography: The Most Vital of Vital Signs. Tom Ahrens, PhD, RN, FAAN Research Scientist, Barnes-Jewish Hospital, St. Louis, MO May, 2017
 Capnography: The Most Vital of Vital Signs Tom Ahrens, PhD, RN, FAAN Research Scientist, Barnes-Jewish Hospital, St. Louis, MO May, 2017 Assessing Ventilation and Blood Flow with Capnography Capnography
Capnography: The Most Vital of Vital Signs Tom Ahrens, PhD, RN, FAAN Research Scientist, Barnes-Jewish Hospital, St. Louis, MO May, 2017 Assessing Ventilation and Blood Flow with Capnography Capnography
Recognizing the Difficult Airway in Pediatric Patients. Nancy L. Glass, MD, MBA,
 Recognizing the Difficult Airway in Pediatric Patients Nancy L. Glass, MD, MBA, FAAP nglass@bcm.edu @DrNancyGlass1 None Disclosures Learning Objectives At the end of this presentation, participants will
Recognizing the Difficult Airway in Pediatric Patients Nancy L. Glass, MD, MBA, FAAP nglass@bcm.edu @DrNancyGlass1 None Disclosures Learning Objectives At the end of this presentation, participants will
Management of severe burns
 Management of severe burns Who gets admitted to the ICU? Large % surface area burns >25% adults >15% children/elderly Inhalational or airway burns Multi-trauma Co-morbidities Burns centres Regional referral
Management of severe burns Who gets admitted to the ICU? Large % surface area burns >25% adults >15% children/elderly Inhalational or airway burns Multi-trauma Co-morbidities Burns centres Regional referral
Extracorporeal Life Support Organization (ELSO) Guidelines for Pediatric Respiratory Failure
 Extracorporeal Life Support Organization (ELSO) Guidelines for Pediatric Respiratory Failure Introduction This pediatric respiratory failure guideline is a supplement to ELSO s General Guidelines for all
Extracorporeal Life Support Organization (ELSO) Guidelines for Pediatric Respiratory Failure Introduction This pediatric respiratory failure guideline is a supplement to ELSO s General Guidelines for all
Airway Management and The Difficult Airway
 Airway Management and The Difficult Airway Gary McCalla, MD, FACEP Medical Director REACH Air Medical Services Services 1 It is not enough to do your best, unless you have prepared to be the best. -John
Airway Management and The Difficult Airway Gary McCalla, MD, FACEP Medical Director REACH Air Medical Services Services 1 It is not enough to do your best, unless you have prepared to be the best. -John
Prepared by : Bayan Kaddourah RN,MHM. GICU Clinical Instructor
 Mechanical Ventilation Prepared by : Bayan Kaddourah RN,MHM. GICU Clinical Instructor 1 Definition Is a supportive therapy to facilitate gas exchange. Most ventilatory support requires an artificial airway.
Mechanical Ventilation Prepared by : Bayan Kaddourah RN,MHM. GICU Clinical Instructor 1 Definition Is a supportive therapy to facilitate gas exchange. Most ventilatory support requires an artificial airway.
BLS, ILS, ALS OTEP BURNS BURN INTRODUCTION TYPES OF BURNS
 BURNS BLS, ILS, ALS OTEP While we do understand this presentation is an instructional tool for all levels of certification, taking this into consideration everyone taking this class must remember that
BURNS BLS, ILS, ALS OTEP While we do understand this presentation is an instructional tool for all levels of certification, taking this into consideration everyone taking this class must remember that
I. Subject: Pressure Support Ventilation (PSV) with BiPAP Device/Nasal CPAP
 I. Subject: Pressure Support Ventilation (PSV) with BiPAP Device/Nasal CPAP II. Policy: PSV with BiPAP device/nasal CPAP will be initiated upon a physician's order by Respiratory Therapy personnel trained
I. Subject: Pressure Support Ventilation (PSV) with BiPAP Device/Nasal CPAP II. Policy: PSV with BiPAP device/nasal CPAP will be initiated upon a physician's order by Respiratory Therapy personnel trained
Burn Priorities of Care: Triage/Treatment/Transfer. Via Christi Regional Burn Center Sarah Fischer, MSN, RN
 Burn Priorities of Care: Triage/Treatment/Transfer Via Christi Regional Burn Center Sarah Fischer, MSN, RN Disclosure I have nothing to disclose Objectives Identify American Burn Association referral criteria
Burn Priorities of Care: Triage/Treatment/Transfer Via Christi Regional Burn Center Sarah Fischer, MSN, RN Disclosure I have nothing to disclose Objectives Identify American Burn Association referral criteria
ARDS and Lung Protection
 ARDS and Lung Protection Kristina Sullivan, MD Associate Professor University of California, San Francisco Department of Anesthesia and Perioperative Care Division of Critical Care Medicine Overview Low
ARDS and Lung Protection Kristina Sullivan, MD Associate Professor University of California, San Francisco Department of Anesthesia and Perioperative Care Division of Critical Care Medicine Overview Low
Applicable to. Team Members Performing
 Protocol: Category Clinical Practice Approval Date March 13, 2019 Due for review March 13, 2021 Applicable to VUH Children s DOT VMG Off-site locations VMG VPH Other All faculty & staff Other: Faculty
Protocol: Category Clinical Practice Approval Date March 13, 2019 Due for review March 13, 2021 Applicable to VUH Children s DOT VMG Off-site locations VMG VPH Other All faculty & staff Other: Faculty
Purpose To outline the pre-hospital and inter-hospital assessment and management of patients with major burns.
 Major Burns HELI.CLI.08 Purpose To outline the pre-hospital and inter-hospital assessment and management of patients with major burns. Procedure Management of Severe Burns For Review Aug 2015 1. Introduction
Major Burns HELI.CLI.08 Purpose To outline the pre-hospital and inter-hospital assessment and management of patients with major burns. Procedure Management of Severe Burns For Review Aug 2015 1. Introduction
Burns Management in the Emergency Department
 Management in the Emergency Department (Referral Proforma) Time/Date of injury (24hr) Patient demographic data sticker Airway Please remember to protect C-spine until clinically cleared as stable Administer
Management in the Emergency Department (Referral Proforma) Time/Date of injury (24hr) Patient demographic data sticker Airway Please remember to protect C-spine until clinically cleared as stable Administer
Applicable to. Team Members Performing MD House Staff APRN/PA RN LPN
 Protocol: Adult Burn Fluid Resuscitation Category Clinical Practice Protocol Number Approval Date vember 1, 2016 Due for review vember 1, 2018 Applicable to VUH Children s DOT VMG Off-site locations VMG
Protocol: Adult Burn Fluid Resuscitation Category Clinical Practice Protocol Number Approval Date vember 1, 2016 Due for review vember 1, 2018 Applicable to VUH Children s DOT VMG Off-site locations VMG
Shock and Trauma Resuscitation
 Shock and Trauma Resuscitation Bonjo Batoon, MS, CRNA Bbatoon@som.umaryland.edu Disclaimer Resuscitation is continuously evolving There is no one right way Knowing is half the battle G.I. Joe Having to
Shock and Trauma Resuscitation Bonjo Batoon, MS, CRNA Bbatoon@som.umaryland.edu Disclaimer Resuscitation is continuously evolving There is no one right way Knowing is half the battle G.I. Joe Having to
EmergencyKT: Management of Thermal Injury in Adult Patients
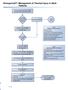 EmergencyKT: Management of Thermal Injury in Adult Patients Remove patient from source of injury, including burned clothing and jewelry Does patient appear to have minor burns? (See Box A) No Notify Burn
EmergencyKT: Management of Thermal Injury in Adult Patients Remove patient from source of injury, including burned clothing and jewelry Does patient appear to have minor burns? (See Box A) No Notify Burn
1/3/2008. Karen Burke Priscilla LeMone Elaine Mohn-Brown. Medical-Surgical Nursing Care, 2e Karen Burke, Priscilla LeMone, and Elaine Mohn-Brown
 Medical-Surgical Nursing Care Second Edition Karen Burke Priscilla LeMone Elaine Mohn-Brown Chapter 46 Caring for Clients with Burns Types of Burns Thermal Dry heat flame Moist heat steam or hot liquid
Medical-Surgical Nursing Care Second Edition Karen Burke Priscilla LeMone Elaine Mohn-Brown Chapter 46 Caring for Clients with Burns Types of Burns Thermal Dry heat flame Moist heat steam or hot liquid
Applicable to. Team Members Performing MD House Staff APRN/PA RN LPN
 Protocol: Adult Burn Inhalation Injury Category Clinical Practice Approval Date: March 26, 2019 Review Date: March 26, 2020 Applicable to VUH Children s DOT VMG Off-site locations VMG VPH Other All faculty
Protocol: Adult Burn Inhalation Injury Category Clinical Practice Approval Date: March 26, 2019 Review Date: March 26, 2020 Applicable to VUH Children s DOT VMG Off-site locations VMG VPH Other All faculty
What is the next best step?
 Noninvasive Ventilation William Janssen, M.D. Assistant Professor of Medicine National Jewish Health University of Colorado Denver Health Sciences Center What is the next best step? 65 year old female
Noninvasive Ventilation William Janssen, M.D. Assistant Professor of Medicine National Jewish Health University of Colorado Denver Health Sciences Center What is the next best step? 65 year old female
Family Feud SPA Myron Yaster, MD
 Family Feud SPA 2014 Myron Yaster, MD Richard J Traystman Professor, Departments of Anesthesiology, Critical Care Medicine, Pediatrics, and Neurosurgery The Johns Hopkins Medical Institutions Aubrey Maze,
Family Feud SPA 2014 Myron Yaster, MD Richard J Traystman Professor, Departments of Anesthesiology, Critical Care Medicine, Pediatrics, and Neurosurgery The Johns Hopkins Medical Institutions Aubrey Maze,
ENDOTRACHEAL INTUBATION POLICY
 POLICY Indications: Ineffective ventilation with mask and t-piece, or mask and bag technique Inability to maintain a patent airway Need or anticipation of need for prolonged ventilation Need for endotracheal
POLICY Indications: Ineffective ventilation with mask and t-piece, or mask and bag technique Inability to maintain a patent airway Need or anticipation of need for prolonged ventilation Need for endotracheal
7/4/2015. diffuse lung injury resulting in noncardiogenic pulmonary edema due to increase in capillary permeability
 Leanna R. Miller, RN, MN, CCRN-CMC, PCCN-CSC, CEN, CNRN, CMSRN, NP Education Specialist LRM Consulting Nashville, TN Objectives Identify the 5 criteria for the diagnosis of ARDS. Discuss the common etiologies
Leanna R. Miller, RN, MN, CCRN-CMC, PCCN-CSC, CEN, CNRN, CMSRN, NP Education Specialist LRM Consulting Nashville, TN Objectives Identify the 5 criteria for the diagnosis of ARDS. Discuss the common etiologies
POST-INTUBATION ANALGESIA AND SEDATION. August 2012 J Pelletier
 POST-INTUBATION ANALGESIA AND SEDATION August 2012 J Pelletier Intubated patients experience pain and anxiety Mechanical ventilation, endotracheal tube Blood draws, positioning, suctioning Surgical procedures,
POST-INTUBATION ANALGESIA AND SEDATION August 2012 J Pelletier Intubated patients experience pain and anxiety Mechanical ventilation, endotracheal tube Blood draws, positioning, suctioning Surgical procedures,
SEEING KETAMINE IN A NEW LIGHT
 SEEING KETAMINE IN A NEW LIGHT BobbieJean Sweitzer, M.D., FACP Professor of Anesthesiology Director of Perioperative Medicine Northwestern University Bobbie.Sweitzer@northwestern.edu LEARNING OBJECTIVES
SEEING KETAMINE IN A NEW LIGHT BobbieJean Sweitzer, M.D., FACP Professor of Anesthesiology Director of Perioperative Medicine Northwestern University Bobbie.Sweitzer@northwestern.edu LEARNING OBJECTIVES
TBSA Burn Estimation Chart Adult Major Burn Clinical Practice Guideline
 TBSA Burn Estimation Chart Adult Major Burn Clinical Practice Guideline Patient Label Anatomical Subunit Percent Total Percent One Side Anterior Posterior Injury Subtotal 3.5% 2nd and 3rd degree burns
TBSA Burn Estimation Chart Adult Major Burn Clinical Practice Guideline Patient Label Anatomical Subunit Percent Total Percent One Side Anterior Posterior Injury Subtotal 3.5% 2nd and 3rd degree burns
ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv
 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv.8.18.18 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) SUDDEN PROGRESSIVE FORM OF ACUTE RESPIRATORY FAILURE ALVEOLAR CAPILLARY MEMBRANE BECOMES DAMAGED AND MORE
ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv.8.18.18 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) SUDDEN PROGRESSIVE FORM OF ACUTE RESPIRATORY FAILURE ALVEOLAR CAPILLARY MEMBRANE BECOMES DAMAGED AND MORE
Pediatrics Grand Rounds 1 June University of Texas Health Science Center at San Antonio. Management of Burn Wounds. Management of Burn Wounds
 Management of Burn Wounds Management of Burn Wounds History of Burn Care Pathophysiology of Burn Lillian F. Liao, MD, MPH Division of Trauma and Emergency Surgery Department of Surgery UTHSCSA Acute burn
Management of Burn Wounds Management of Burn Wounds History of Burn Care Pathophysiology of Burn Lillian F. Liao, MD, MPH Division of Trauma and Emergency Surgery Department of Surgery UTHSCSA Acute burn
a. Will not suppress respiratory drive in acute asthma
 Status Asthmaticus & COPD with Respiratory Failure - Key Points M.J. Betzner MD FRCPc - NYEMU Toronto 2018 Overview This talk is about the sickest of the sick patients presenting with severe or near death
Status Asthmaticus & COPD with Respiratory Failure - Key Points M.J. Betzner MD FRCPc - NYEMU Toronto 2018 Overview This talk is about the sickest of the sick patients presenting with severe or near death
Pain & Sedation Management in PICU. Marut Chantra, M.D.
 Pain & Sedation Management in PICU Marut Chantra, M.D. Pain Diseases Trauma Procedures Rogers Textbook of Pediatric Intensive Care, 5 th ed, 2015 Emotional Distress Separation from parents Unfamiliar
Pain & Sedation Management in PICU Marut Chantra, M.D. Pain Diseases Trauma Procedures Rogers Textbook of Pediatric Intensive Care, 5 th ed, 2015 Emotional Distress Separation from parents Unfamiliar
Management of Inhalation Injury in an Adult Burn Patient
 ISPUB.COM The Internet Journal of Advanced Nursing Practice Volume 13 Number 1 Management of Inhalation Injury in an Adult Burn Patient D Tubera Citation D Tubera. Management of Inhalation Injury in an
ISPUB.COM The Internet Journal of Advanced Nursing Practice Volume 13 Number 1 Management of Inhalation Injury in an Adult Burn Patient D Tubera Citation D Tubera. Management of Inhalation Injury in an
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Accelerated intravascular coagulation and fibrinolysis (AICF) in liver disease, 390 391 Acid suppression in liver disease, 403 404 ACLF.
Index Note: Page numbers of article titles are in boldface type. A Accelerated intravascular coagulation and fibrinolysis (AICF) in liver disease, 390 391 Acid suppression in liver disease, 403 404 ACLF.
Information Often Given to the Nurse at the Time of Admission to the Postanesthesia Care Unit
 Information Often Given to the Nurse at the Time of Admission to the Postanesthesia Care Unit * Patient s name and age * Surgical procedure and type of anesthetic including drugs used * Other intraoperative
Information Often Given to the Nurse at the Time of Admission to the Postanesthesia Care Unit * Patient s name and age * Surgical procedure and type of anesthetic including drugs used * Other intraoperative
Subspecialty Rotation: Anesthesia
 Subspecialty Rotation: Anesthesia Faculty: John Heaton, M.D. GOAL: Maintenance of Airway Patency and Oxygenation. Recognize and manage upper airway obstruction and desaturation. Recognize and manage upper
Subspecialty Rotation: Anesthesia Faculty: John Heaton, M.D. GOAL: Maintenance of Airway Patency and Oxygenation. Recognize and manage upper airway obstruction and desaturation. Recognize and manage upper
Anesthesia Final Exam
 Anesthesia Final Exam 1) For a patient who is chronically taking the following medications, which two should be withheld on the day of surgery? a) Lasix b) Metoprolol c) Glucophage d) Theodur 2) A 51 year
Anesthesia Final Exam 1) For a patient who is chronically taking the following medications, which two should be withheld on the day of surgery? a) Lasix b) Metoprolol c) Glucophage d) Theodur 2) A 51 year
SEDATION FOR SMALL PROCEDURES
 SEDATION FOR SMALL PROCEDURES Sinno Simons Erasmus MC Sophia Children s Hospital Rotterdam, the Netherlands s.simons@erasmusmc.nl SEDATION in newborns How and when How to evaluate How to dose Why to use
SEDATION FOR SMALL PROCEDURES Sinno Simons Erasmus MC Sophia Children s Hospital Rotterdam, the Netherlands s.simons@erasmusmc.nl SEDATION in newborns How and when How to evaluate How to dose Why to use
Case Report: Burns Reid Sadoway PGY1 Emergency Medicine, Dalhousie
 Case Report: Burns Reid Sadoway PGY1 Emergency Medicine, Dalhousie History 3 yo boy, presents to pediatric ED with mother Child can be heard crying inside waiting/patient room, has both hands bandaged
Case Report: Burns Reid Sadoway PGY1 Emergency Medicine, Dalhousie History 3 yo boy, presents to pediatric ED with mother Child can be heard crying inside waiting/patient room, has both hands bandaged
Anesthetic Techniques in Endoscopic Sinus and Skull Base Surgery
 Anesthetic Techniques in Endoscopic Sinus and Skull Base Surgery Martha Cordoba Amorocho, MD Iuliu Fat, MD Supplement to Cordoba Amorocho M, Fat I. Anesthetic techniques in endoscopic sinus and skull base
Anesthetic Techniques in Endoscopic Sinus and Skull Base Surgery Martha Cordoba Amorocho, MD Iuliu Fat, MD Supplement to Cordoba Amorocho M, Fat I. Anesthetic techniques in endoscopic sinus and skull base
STS Care of Thermal Burns 20% Total Body Surface Area
 Temp Regulation Transfer Pain Fluids Airway Initial Assessment STS Care of Thermal Burns 20% Total Body Surface Area Remove burned clothing, rings, watches, and jewelry Cervical spine precautions (if history
Temp Regulation Transfer Pain Fluids Airway Initial Assessment STS Care of Thermal Burns 20% Total Body Surface Area Remove burned clothing, rings, watches, and jewelry Cervical spine precautions (if history
Management of Patients with Burns Chris Thompson. Contact:
 Management of Patients with Burns Chris Thompson. Contact: acdthompson@hotmail.com Introduction Anaesthetists are involved in resuscitation in the Emergency Department (ED), the operating room, the intensive
Management of Patients with Burns Chris Thompson. Contact: acdthompson@hotmail.com Introduction Anaesthetists are involved in resuscitation in the Emergency Department (ED), the operating room, the intensive
Capnography. Capnography. Oxygenation. Pulmonary Physiology 4/15/2018. non invasive monitor for ventilation. Edward C. Adlesic, DMD.
 Capnography Edward C. Adlesic, DMD University of Pittsburgh School of Dental Medicine 2018 North Carolina Program Capnography non invasive monitor for ventilation measures end tidal CO2 early detection
Capnography Edward C. Adlesic, DMD University of Pittsburgh School of Dental Medicine 2018 North Carolina Program Capnography non invasive monitor for ventilation measures end tidal CO2 early detection
Printed copies of this document may not be up to date, obtain the most recent version from
 Children s Acute Transport Service Clinical Guidelines Septic Shock Document Control Information Author Claire Fraser P.Ramnarayan Author Position tanp CATS Consultant Document Owner E. Polke Document
Children s Acute Transport Service Clinical Guidelines Septic Shock Document Control Information Author Claire Fraser P.Ramnarayan Author Position tanp CATS Consultant Document Owner E. Polke Document
buteykobreathing.co.nz Melanie Kalmanowicz, MD Department of Anesthesia, Critical Care and Pain Medicine Beth Israel Deaconess Medical Center
 buteykobreathing.co.nz Melanie Kalmanowicz, MD Department of Anesthesia, Critical Care and Pain Medicine Beth Israel Deaconess Medical Center PMH: hypertension, hyperlipidemia, asthma, hypothyroidism
buteykobreathing.co.nz Melanie Kalmanowicz, MD Department of Anesthesia, Critical Care and Pain Medicine Beth Israel Deaconess Medical Center PMH: hypertension, hyperlipidemia, asthma, hypothyroidism
Update in Critical Care Medicine
 Update in Critical Care Medicine Michael A. Gropper, MD, PhD Professor and Executive Vice Chair Department of Anesthesia and Perioperative Care Director, Critical Care Medicine UCSF Disclosure None Update
Update in Critical Care Medicine Michael A. Gropper, MD, PhD Professor and Executive Vice Chair Department of Anesthesia and Perioperative Care Director, Critical Care Medicine UCSF Disclosure None Update
HEAVY METALS : Review
 HEAVY METALS : Review INHALED TOXINS Dr. Tawfiq Almezeiny MBBS FRCPC (CCM) Introduction Airborne toxins typically produce local noxious effects on the airways and lungs. Examples of Inhalational exposure:
HEAVY METALS : Review INHALED TOXINS Dr. Tawfiq Almezeiny MBBS FRCPC (CCM) Introduction Airborne toxins typically produce local noxious effects on the airways and lungs. Examples of Inhalational exposure:
Burns. A Comprehensive Review Assessment & Management
 Burns A Comprehensive Review Assessment & Management 1 Objectives Understand types of Burns Understand the pathophysiology of the Burns Understand Rule of Nine Understand Classification of Burns Identify
Burns A Comprehensive Review Assessment & Management 1 Objectives Understand types of Burns Understand the pathophysiology of the Burns Understand Rule of Nine Understand Classification of Burns Identify
Critical Care of the Post-Surgical Patient
 Critical Care of the Post-Surgical Patient, Dr med vet, DEA, DECVIM-CA Many critically ill patients require surgical treatments. These patients often have multisystem abnormalities during the immediate
Critical Care of the Post-Surgical Patient, Dr med vet, DEA, DECVIM-CA Many critically ill patients require surgical treatments. These patients often have multisystem abnormalities during the immediate
Rapid Sequence Induction
 Rapid Sequence Induction Virtual simultaneous administration, after preoxygenation, of a potent sedative agent and a rapidly acting neuromuscular blocking agent to facilitate rapid tracheal intubation
Rapid Sequence Induction Virtual simultaneous administration, after preoxygenation, of a potent sedative agent and a rapidly acting neuromuscular blocking agent to facilitate rapid tracheal intubation
Sleep Apnea and ifficulty in Extubation. Jean Louis BOURGAIN May 15, 2016
 Sleep Apnea and ifficulty in Extubation Jean Louis BOURGAIN May 15, 2016 Introduction Repetitive collapse of the upper airway > sleep fragmentation, > hypoxemia, hypercapnia, > marked variations in intrathoracic
Sleep Apnea and ifficulty in Extubation Jean Louis BOURGAIN May 15, 2016 Introduction Repetitive collapse of the upper airway > sleep fragmentation, > hypoxemia, hypercapnia, > marked variations in intrathoracic
Capnography: The Most Vital Sign
 Capnography: The Most Vital Sign Mike McEvoy, PhD, NRP, RN, CCRN Cardiac Surgical ICU RN & Chair Resuscitation Committee Albany Medical Center EMS Coordinator Saratoga County, NY www.mikemcevoy.com CO
Capnography: The Most Vital Sign Mike McEvoy, PhD, NRP, RN, CCRN Cardiac Surgical ICU RN & Chair Resuscitation Committee Albany Medical Center EMS Coordinator Saratoga County, NY www.mikemcevoy.com CO
Weaning from Mechanical Ventilation. Dr Azmin Huda Abdul Rahim
 Weaning from Mechanical Ventilation Dr Azmin Huda Abdul Rahim Content Definition Classification Weaning criteria Weaning methods Criteria for extubation Introduction Weaning comprises 40% of the duration
Weaning from Mechanical Ventilation Dr Azmin Huda Abdul Rahim Content Definition Classification Weaning criteria Weaning methods Criteria for extubation Introduction Weaning comprises 40% of the duration
Chapter 18. Skeletal Muscle Relaxants (Neuromuscular Blocking Agents)
 Chapter 18 Skeletal Muscle Relaxants (Neuromuscular Blocking Agents) Uses of Neuromuscular Blocking Facilitate intubation Surgery Agents Enhance ventilator synchrony Reduce intracranial pressure (ICP)
Chapter 18 Skeletal Muscle Relaxants (Neuromuscular Blocking Agents) Uses of Neuromuscular Blocking Facilitate intubation Surgery Agents Enhance ventilator synchrony Reduce intracranial pressure (ICP)
Neuromuscular Blockade in ARDS
 Neuromuscular Blockade in ARDS Maureen O. Meade, MD, FRCPC Critical care consultant, Hamilton Health Sciences Professor of Medicine, McMaster University www.oscillatetrial.com Disclosures None Possible
Neuromuscular Blockade in ARDS Maureen O. Meade, MD, FRCPC Critical care consultant, Hamilton Health Sciences Professor of Medicine, McMaster University www.oscillatetrial.com Disclosures None Possible
Icu-cpr PICTURE QUIZ march 2014
 Department of surgery Icu-cpr PICTURE QUIZ march 2014 Prepared by Dr. Karam Kamal Younis Assistant professor and consultant surgeon Convener of the Department of Surgery College of Medicine University
Department of surgery Icu-cpr PICTURE QUIZ march 2014 Prepared by Dr. Karam Kamal Younis Assistant professor and consultant surgeon Convener of the Department of Surgery College of Medicine University
Trauma Patient. Trauma Patient. Anesthesia of the Acute Trauma Patient
 Anesthesia of the Acute Trauma Patient Stuart Clark Price, DVM, MS, DACVIM, DACVAA University of Illinois College of Veterinary Medicine Trauma Patient Unique challenge to veterinary facility Resource
Anesthesia of the Acute Trauma Patient Stuart Clark Price, DVM, MS, DACVIM, DACVAA University of Illinois College of Veterinary Medicine Trauma Patient Unique challenge to veterinary facility Resource
ARDS: an update 6 th March A. Hakeem Al Hashim, MD, FRCP SQUH
 ARDS: an update 6 th March 2017 A. Hakeem Al Hashim, MD, FRCP SQUH 30M, previously healthy Hx: 1 week dry cough Gradually worsening SOB No travel Hx Case BP 130/70, HR 100/min ph 7.29 pco2 35 po2 50 HCO3
ARDS: an update 6 th March 2017 A. Hakeem Al Hashim, MD, FRCP SQUH 30M, previously healthy Hx: 1 week dry cough Gradually worsening SOB No travel Hx Case BP 130/70, HR 100/min ph 7.29 pco2 35 po2 50 HCO3
Standardize comprehensive care of the patient with severe traumatic brain injury
 Trauma Center Practice Management Guideline Iowa Methodist Medical Center Des Moines Management of Patients with Severe Traumatic Brain Injury (GCS < 9) ADULT Practice Management Guideline Contact: Trauma
Trauma Center Practice Management Guideline Iowa Methodist Medical Center Des Moines Management of Patients with Severe Traumatic Brain Injury (GCS < 9) ADULT Practice Management Guideline Contact: Trauma
Anatomy and Physiology. The airways can be divided in to parts namely: The upper airway. The lower airway.
 Airway management Anatomy and Physiology The airways can be divided in to parts namely: The upper airway. The lower airway. Non-instrumental airway management Head Tilt and Chin Lift Jaw Thrust Advanced
Airway management Anatomy and Physiology The airways can be divided in to parts namely: The upper airway. The lower airway. Non-instrumental airway management Head Tilt and Chin Lift Jaw Thrust Advanced
ANESTHESIA EXAM (four week rotation)
 SPARROW HEALTH SYSTEM ANESTHESIA SERVICES ANESTHESIA EXAM (four week rotation) Circle the best answer 1. During spontaneous breathing, volatile anesthetics A. Increase tidal volume and decrease respiratory
SPARROW HEALTH SYSTEM ANESTHESIA SERVICES ANESTHESIA EXAM (four week rotation) Circle the best answer 1. During spontaneous breathing, volatile anesthetics A. Increase tidal volume and decrease respiratory
Michael Avant, M.D. The Children s Hospital of GHS
 Michael Avant, M.D. The Children s Hospital of GHS OVERVIEW ER to ICU Transition Early Management Priorities the First 48 hours Organ System Support Complications THE FIRST 48 HOURS Communication Damage
Michael Avant, M.D. The Children s Hospital of GHS OVERVIEW ER to ICU Transition Early Management Priorities the First 48 hours Organ System Support Complications THE FIRST 48 HOURS Communication Damage
Case Scenarios. Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC. Consultant, Critical Care Medicine Medanta, The Medicity
 Case Scenarios Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity Case 1 A 36 year male with cirrhosis and active GI bleeding is intubated to protect his airway,
Case Scenarios Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity Case 1 A 36 year male with cirrhosis and active GI bleeding is intubated to protect his airway,
EMERGENCYROOM BURN MANAGEMENT
 EMERGENCYROOM INITIAL ASSESSMENT PRIMARY SURVEY A = Airway and C-spine immobilization B = Breathing and Ventilation C = Circulation D = Disability, Neurologic Deficit E = Expose (remove all clothing and
EMERGENCYROOM INITIAL ASSESSMENT PRIMARY SURVEY A = Airway and C-spine immobilization B = Breathing and Ventilation C = Circulation D = Disability, Neurologic Deficit E = Expose (remove all clothing and
Dóra Ujvárosy MD. Medical University of Debrecen Oxyology and Emergency Department
 Dóra Ujvárosy MD. Medical University of Debrecen Oxyology and Emergency Department Functions Definition A burn is a type of injury to the skin caused by heat, electricity, chemicals, light, radiation or
Dóra Ujvárosy MD. Medical University of Debrecen Oxyology and Emergency Department Functions Definition A burn is a type of injury to the skin caused by heat, electricity, chemicals, light, radiation or
Introduction to Emergency Medical Care 1
 Introduction to Emergency Medical Care 1 OBJECTIVES 8.1 Define key terms introduced in this chapter. Slides 12 15, 21, 24, 31-34, 39, 40, 54 8.2 Describe the anatomy and physiology of the upper and lower
Introduction to Emergency Medical Care 1 OBJECTIVES 8.1 Define key terms introduced in this chapter. Slides 12 15, 21, 24, 31-34, 39, 40, 54 8.2 Describe the anatomy and physiology of the upper and lower
Frederic J., Gerges MD. Ghassan E. Kanazi MD., Sama, I. Jabbour-Khoury MD. Review article from Journal of clinical anesthesia 2006.
 Frederic J., Gerges MD. Ghassan E. Kanazi MD., Sama, I. Jabbour-Khoury MD. Review article from Journal of clinical anesthesia 2006 Introduction Laparoscopic surgery started in the mid 1950s. In recent
Frederic J., Gerges MD. Ghassan E. Kanazi MD., Sama, I. Jabbour-Khoury MD. Review article from Journal of clinical anesthesia 2006 Introduction Laparoscopic surgery started in the mid 1950s. In recent
Objectives. Initial Burn Care and Fluid Resuscitation 6/5/2015 INITIAL MANAGEMENT
 Initial Burn Care and Fluid Resuscitation Sarah Taylor MSN, RN, ACNS-BC Clinical Nurse Specialist Trauma Burn Center University of Michigan Health System Ann Arbor, MI Objectives Discuss the initial assessment
Initial Burn Care and Fluid Resuscitation Sarah Taylor MSN, RN, ACNS-BC Clinical Nurse Specialist Trauma Burn Center University of Michigan Health System Ann Arbor, MI Objectives Discuss the initial assessment
Non-Invasive Assessment of Respiratory Function. Chapter 11
 Non-Invasive Assessment of Respiratory Function Chapter 11 Pulse Oximetry Laboratory measurements of ABG s are the gold standard for measuring levels of hypoxemia, however since these are performed intermittently
Non-Invasive Assessment of Respiratory Function Chapter 11 Pulse Oximetry Laboratory measurements of ABG s are the gold standard for measuring levels of hypoxemia, however since these are performed intermittently
Airway management problem during anaesthesia. Airway management problem in ICU / HDU. Airway management problem occurring in the Emergency Department
 4th National Audit Project of the Royal College of Anaesthetists: Major Complications of Airway Management in the UK Please select one form from the list below Airway management problem during anaesthesia
4th National Audit Project of the Royal College of Anaesthetists: Major Complications of Airway Management in the UK Please select one form from the list below Airway management problem during anaesthesia
Surgical Care at the District Hospital. EMERGENCY & ESSENTIAL SURGICAL CARE
 Surgical Care at the District Hospital 1 14 Practical Anesthesia Key Points 2 14.1 General Anesthesia Have a clear plan before starting anesthesia Never use an unfamiliar anesthetic technique in an emergency
Surgical Care at the District Hospital 1 14 Practical Anesthesia Key Points 2 14.1 General Anesthesia Have a clear plan before starting anesthesia Never use an unfamiliar anesthetic technique in an emergency
Emergency Department/Trauma Adult Airway Management Protocol
 Emergency Department/Trauma Adult Airway Management Protocol Purpose: A standardized protocol for management of the airway in the setting of trauma in an academic center, with the goal of maximizing successful
Emergency Department/Trauma Adult Airway Management Protocol Purpose: A standardized protocol for management of the airway in the setting of trauma in an academic center, with the goal of maximizing successful
Presented by: Indah Dwi Pratiwi
 Presented by: Indah Dwi Pratiwi Normal Fluid Requirements Resuscitation Fluids Goals of Resuscitation Maintain normal body temperature In most cases, elevate the feet and legs above the level of the heart
Presented by: Indah Dwi Pratiwi Normal Fluid Requirements Resuscitation Fluids Goals of Resuscitation Maintain normal body temperature In most cases, elevate the feet and legs above the level of the heart
Neonatal Life Support Provider (NLSP) Certification Preparatory Materials
 Neonatal Life Support Provider (NLSP) Certification Preparatory Materials NEONATAL LIFE SUPPORT PROVIDER (NRP) CERTIFICATION TABLE OF CONTENTS NEONATAL FLOW ALGORITHM.2 INTRODUCTION 3 ANTICIPATION OF RESUSCITATION
Neonatal Life Support Provider (NLSP) Certification Preparatory Materials NEONATAL LIFE SUPPORT PROVIDER (NRP) CERTIFICATION TABLE OF CONTENTS NEONATAL FLOW ALGORITHM.2 INTRODUCTION 3 ANTICIPATION OF RESUSCITATION
Financial Disclosure. Objectives 9/24/2018
 Hemorrhage and Transfusion Adjuncts in the Setting of Damage Control Joseph Cuschieri, MD FACS Professor of Surgery, University of Washington Adjunct Professor of Orthopedics and Neurosurgery, University
Hemorrhage and Transfusion Adjuncts in the Setting of Damage Control Joseph Cuschieri, MD FACS Professor of Surgery, University of Washington Adjunct Professor of Orthopedics and Neurosurgery, University
At the conclusion of this course the learner will be able to
 Objectives At the conclusion of this course the learner will be able to 1. Discuss basic anatomy and pathophysiology of burns 2. Describe burn injuries in terms of size, depth, coloration and characteristics
Objectives At the conclusion of this course the learner will be able to 1. Discuss basic anatomy and pathophysiology of burns 2. Describe burn injuries in terms of size, depth, coloration and characteristics
Recent Advances in Respiratory Medicine
 Recent Advances in Respiratory Medicine Dr. R KUMAR Pulmonologist Non Invasive Ventilation (NIV) NIV Noninvasive ventilation (NIV) refers to the administration of ventilatory support without using an invasive
Recent Advances in Respiratory Medicine Dr. R KUMAR Pulmonologist Non Invasive Ventilation (NIV) NIV Noninvasive ventilation (NIV) refers to the administration of ventilatory support without using an invasive
the bleeding won t stop? Liane Manz RN, BScN, CNCC(c) Royal Alexandra Hospital
 What do you do when the bleeding won t stop? Teddie Tanguay RN, MN, NP, CNCC(c) Teddie Tanguay RN, MN, NP, CNCC(c) Liane Manz RN, BScN, CNCC(c) Royal Alexandra Hospital Outline Case study Normal coagulation
What do you do when the bleeding won t stop? Teddie Tanguay RN, MN, NP, CNCC(c) Teddie Tanguay RN, MN, NP, CNCC(c) Liane Manz RN, BScN, CNCC(c) Royal Alexandra Hospital Outline Case study Normal coagulation
PEDIATRIC TRAUMA I: ABDOMINAL TRAUMA BURNS. December 19, 2012
 PEDIATRIC TRAUMA I: ABDOMINAL TRAUMA BURNS Niel F. Miele,, M.D. December 19, 2012 EPIDEMIOLOGY Major Trauma responsible for
PEDIATRIC TRAUMA I: ABDOMINAL TRAUMA BURNS Niel F. Miele,, M.D. December 19, 2012 EPIDEMIOLOGY Major Trauma responsible for
Role and safety of epidural analgesia
 Anaesthesia for Liver Resection Surgery The Association of Anaesthetists Seminars 21 Portland Place, London Thursday 15 th December 2005 Role and safety of epidural analgesia Lennart Christiansson MD,
Anaesthesia for Liver Resection Surgery The Association of Anaesthetists Seminars 21 Portland Place, London Thursday 15 th December 2005 Role and safety of epidural analgesia Lennart Christiansson MD,
Transporting Children With Serious Respiratory Illness: A Presentation For Non-Specialty Teams
 Transporting Children With Serious Respiratory Illness: A Presentation For Non-Specialty Teams Laurie Gehrke, R.N., BSN, CPEN, CEN, CMTE Pediatric Transport Team Blank Children s Hospital Des Moines, Iowa
Transporting Children With Serious Respiratory Illness: A Presentation For Non-Specialty Teams Laurie Gehrke, R.N., BSN, CPEN, CEN, CMTE Pediatric Transport Team Blank Children s Hospital Des Moines, Iowa
