OBSERVATION. Atypical Fibroxanthoma With Regional Lymph Node Metastasis. Douglas New, MD; Soon Bahrami, MD; Janine Malone, MD; Jeffrey P.
|
|
|
- Alisha Cole
- 5 years ago
- Views:
Transcription
1 ONLINE FIRST OBSERVATION Atypical Fibroxanthoma With Regional Lymph Node Metastasis Report of a Case and Review of the Literature Douglas New, MD; Soon Bahrami, MD; Janine Malone, MD; Jeffrey P. Callen, MD Background: Atypical fibroxanthoma (AFX) is a lowgrade sarcoma usually occurring on sun-damaged skin of the head and neck in elderly patients. Metastatic disease has been reported very rarely. The potential aggressiveness of AFX is controversial. Observations: We describe herein a patient who developed metastatic disease in cervical lymph. Our patient was an 87-year-old man with a 7-week history of a rapidly growing AFX presenting as a 1.5-cm sessile nodule on his right mandible. Two months following excision, the patient developed cervical lymphadenopathy. Histopathologic analysis of the cervical lymph revealed spindle-cell tumors with histologic characteristics identical to those of the primary AFX, and the tumors were immunonegative for cytokeratin MNF-116 and S-100. In addition, we review and analyze cases from the literature and articles related to immunohistochemical stains used to diagnose AFX. Conclusions: Atypical fibroxanthoma is a diagnosis of exclusion, and only a small number of metastatic AFX cases have been reported. A review of the literature pertaining to immunohistochemical stains suggests the potential benefit of use of CD10, procollagen I, CD99, CD117, p63, and LN-2 in differentiating AFX from other spindle-cell tumors. The metastatic potential of AFX may not be fully appreciated, and clinicians should be reminded of its potential aggressive behavior. Arch Dermatol. 2010;146(12): Published online August 16, doi: /archdermatol Author Affiliations: Division of Dermatology, University of Louisville, Louisville, Kentucky. ATYPICAL FIBROXANTHOMA (AFX) is considered a lowgrade sarcoma and usually occurs on sun-damaged skin of the head and neck in elderly patients. The prognosis is generally excellent following adequate excision of the primary tumor. Recurrences occur in about 5% of cases 1 and may be related to inadequate margins. Some cases are more aggressive and can involve metastatic disease. Currently, controversy exists over the classification and characteristic clinical behavior of AFX. Some authorities classify it as a superficial variant of a malignant fibrous histiocytoma (MFH); shallower depth of the tumor within the dermis and lack of involvement of the subcutaneous tissue favor a diagnosis of AFX. Others believe that an AFX is simply a variant of squamous cell carcinoma (SCC), although studies have refuted this claim. 1 Atypical fibroxanthoma is a diagnosis made histopathologically by ruling out other spindle-cell neoplasms, including spindle-cell SCC (SCSCC), spindle-cell melanoma (desmoplastic melanoma), MFH, leiomyosarcoma, and angiosarcoma. stains aid in establishing the diagnosis of AFX by differentiating it from other malignant neoplasms that commonly arise on sundamaged skin, especially SCSCC and spindle-cell melanoma. Unfortunately, we do not have a sensitive or specific immunostain for AFX to rule out these other entities and establish the diagnosis. Stains that are currently used include cytokeratins, vimentin, smooth-muscle actin, CD68, desmin, and S-100. More recently, studies have demonstrated some utility of CD10, procollagen I (PC1), CD117, CD99, p63, and LN-2, as authors look for additional markers that will increase the sensitivity and specificity of traditional staining panels, especially in the setting of metastatic disease. A recent article describes the current perception of AFX as a benign tumor with no risk of metastasis. 2 However, we believe that the potential aggressive behav- 1399
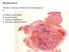
2 cm Figure 1. Clinical photograph taken at the time of our patient s initial visit. Figure 4. Cervical lymph node specimen reveals a metastatic spindle-cell tumor with features similar to the primary atypical fibroxanthoma lesion (hematoxylin-eosin, original magnification 200). may provide clarity when evaluating cutaneous spindlecell neoplasms. REPORT OF CASE Figure 2. Histopathologic examination reveals a superficially located spindle-cell tumor with large, atypical cells (hematoxylin-eosin, original magnification 40). Figure 3. In the same slide as Figure 2, higher magnification confirms hyperchromatic, pleomorphic spindle cells with a high mitotic index (hematoxylin-eosin, original magnification 200). ior of an AFX should be given more consideration. Herein, we report a case of a metastatic AFX and review previously reported metastatic AFX cases and recent studies evaluating the use of immunohistochemical stains that An 87-year-old white man with no history of skin cancer was seen with a 7-week history of a rapidly growing nodule on his right jawline (Figure 1). On physical examination, we found a 1.5-cm sessile, firm nodule with hemorrhagic crust. The patient did not have any other suspect cutaneous lesions or lymphadenopathy. Findings from a systems review were negative. He had no personal or family history of skin cancer. Shave biopsy specimens revealed a completely excised spindle-cell tumor with atypical cells and a high mitotic index (Figure 2 and Figure 3). Tumor cells tested immunopositive with vimentin, CD68, and lysozyme and immunonegative for pancytokeratins, cytokeratin MNF-116, CD34, desmin, smooth-muscle actin, HMB-45, and S-100. A diagnosis of AFX was rendered based on clinicopathologic correlation. Results of margin analysis after surgical excision with 5-mm margins were negative for residual tumor. Two months following the excision, the patient developed a nontender 3 3-cm, deep-seated, skin-colored nodule 4 cm inferior to the surgical site on his right lateral neck. Analysis of fine-needle aspirate revealed atypical spindle cells. A modified radical neck dissection revealed 2 cervical lymph containing metastatic tumor with features consistent with an AFX (Figure 4). The metastatic tumor showed diffusely positive staining for CD10 and CD99 and rare weak positivity for p63 while being immunonegative for S-100 protein and cytokeratin MNF Following surgical excision of affected lymph, the patient underwent 5 rounds of local radiation therapy and remained disease free 18 months following his initial presentation. COMMENT Since the first description of AFX by Helwig 3 in 1963, the clinical behavior of this entity has been controver- 1400
3 sial. A rare soft-tissue neoplasm, AFX is usually associated with an excellent prognosis following treatment by surgical excision, but rarely, it can have an aggressive course. The difficulty of distinguishing AFX from MFH may be mitigated by the recent introduction of the term pleomorphic sarcoma. Further investigation into the specific nomenclature used for these entities deserves more attention in future studies. At least 21 cases of metastatic AFX have been reported in the English-language literature, and their characteristics are summarized in the Table The most commonly reported sites of metastasis were the regional lymph (12 cases), but other sites such as the lung, liver, peritoneum, unspecified parotid area, soft tissue around the mastoid, and in-transit cutaneous metastases have also been reported. The average time interval between the diagnoses of the primary tumor and the metastatic disease was 19.7 months (range, 1-84 months). Metastatic disease has been more commonly reported in men than in women (16 of 22 [73%] vs 6 of 22 [27%]); however, this is confounded by the fact that AFX occurs more often in men than women. In cases of metastasis, the primary tumor was diagnosed at an average patient age of 69.5 years (age range, years). The size of the initial tumor ranged from 0.6 cm to 4 3 cm. Details concerning the depth of tumor invasion and results of immunohistochemical stainings were not consistently reported in all studies. It is difficult to draw absolute conclusions from these cases because potential subcutaneous involvement would favor the diagnosis of MFH rather than AFX. For example, case 20 involved the subcutis and was diagnosed as AFX. In the present study, we included all cases reported to be AFX for the sake of completeness. The case series reported by Helwig and May 6 (cases 7-14, including the case also reported by Jacobs et al 7 ) excluded tumors if they involved the subcutis. Cases 15 and 18 and our case did not involve deep dermal structures. The other reports did not discuss the details of their histologic findings. Likewise, the use of immunohistochemical stains varied among studies. Recurrences were noted in 36% of cases (8 of 22), with an average interval of 6.4 months. Recurrences occurred as soon as 3 months and as late as 23 months after initial treatment. Two cases had multiple recurrences (cases 11 and 14). Whether these were true recurrences due to aggressiveness of the tumor or inadequate treatment is a matter of debate. Of the 8 cases with recurrences, 100% showed distant metastatic disease. These findings underscore the importance of long-term, close clinical evaluation of patients who have a history of AFX, including a thorough skin examination and lymph node examination for recurrences and possible metastatic disease. They also highlight that local recurrence is an indicator that patients need to be monitored even more closely for metastatic disease. Atypical fibroxanthoma is a diagnosis of exclusion and requires an experienced dermatopathologist and clinicopathologic correlation. Under routine processing with hematoxylin-eosin, AFX must be distinguished from the deeper and more aggressive MFH, which is associated with a higher rate of metastasis and was excluded as a diagnosis in our case, based on the superficial location of the tumor within the dermis. Some authors have suggested that AFX with certain histologic features such as necrosis, vascular invasion, and deep tissue invasion may portend more aggressive behavior. 6 These features were not present in our case. A thorough immunohistochemical evaluation is indicated to rule out other spindle-cell tumors including spindle-cell melanoma, SCSCC, angiosarcoma, and leiomyosarcoma. Our patient s primary tumor stained immunopositive with CD68, vimentin, and lysozyme and was immunonegative for S-100, HMB-45, smoothmuscle actin, desmin, CD34, cytokeratin MNF-116, and pancytokeratin. His metastatic tumor had a staining pattern consistent with AFX, demonstrating immunonegative staining for S-100 and cytokeratin MNF-116 and immunopositive staining for CD10, CD99, and p63, further lowering the probability of metastatic disease representing a melanoma or SCSCC. Ang et al 15 describe a more than 20-year experience of treating 93 AFX tumors in 91 patients at the Mayo Clinic. Initially there were 96 total cases in 94 patients, but 3 initial diagnoses of AFX were changed to either SCSCC or MFH after metastatic disease occurred. The first patient whose diagnosis was changed was an 83-year-old man with a history of 5 surgical procedures and radiation treatment for SCSCC on the right upper eyebrow who subsequently was seen with a 3.9-cm lesion diagnosed as AFX. Six months after removal of this tumor, another growth, with characteristics more consistent with SCSCC, occurred at the same site. Four months after its resection, the patient developed massive infiltration of the frontal sinus. No tissue was taken from the metastasis because the patient died of the tumor within weeks. In this case, the authors believed that AFX was actually a misdiagnosed SCSCC. The second patient with changed diagnosis was a 94- year-old with a 1.8-cm AFX lesion on the ear, which was treated with wide local excision (WLE). The lesion recurred twice despite WLE and led to hemiamputation of the ear following the second recurrence. Thirty-seven months following the initial diagnosis, regional metastasis to the parotid gland occurred and was diagnosed as a grade 4 MFH. The third patient whose diagnosis was changed was a 74-year-old man with a history of metastatic SCC to the tongue who developed an AFX on the ear and scalp treated with WLE. Recurrences occurred locally and were labeled as AFX and MFH. Brain metastasis occurred 3 years after initial diagnosis of AFX, and histologic examination of the metastasis was labeled MFH. The decision to change the diagnosis in the first of these 3 cases seems reasonable. In regard to the other 2 cases, however, the histologic characteristics of metastatic MFH would be indistinguishable from those of metastatic AFX. Assuming that the primary lesion s histologic characteristics were consistent with AFX, it seems reasonable to categorize these 2 cases as true metastatic AFX based on the information provided. If one were to include these 2 cases as metastatic AFX (and exclude the first), then metastatic disease occurred in 2 of 95 cases of AFX (2%). No details concerning the immunohistochemical analysis of these tumors were provided, and distinguishing metastatic MFH from AFX would have been impossible, since they share a similar immunophenotype. 1401
4 Table. Characteristics of Metastatic Atypical Fibroxanthoma Reported in the Literature Source Patient No./Sex/ Age, y Primary Tumor Site/ Size, cm/recurrence at Primary Site, YesorNo Depth/ Stainings of Primary Tumor Treatment Site of Metastasis Cooper et al 4 1/M/77 Right antihelix/0.6/no ND/LN-2 (CD74 ) Exc with 1-cm margin through cartilage 2/F/80 Left cheek/unknown/no ND/ND Mohs surgery with 1-cm margin to deep adipose tissue 3/M/85 Scalp/1/no ND/ND Mohs surgery with 1-cm margin Intraparotid lymph node Interval to Metastasis, mo Stains of Metastasis 22 ND Parotid and 3 ND submandibular lymph Liver 12 ND Cutaneous scalp 5 LN-2 (CD74 ) Subcutaneous neck 7 ND Possible lung and 9 ND local lymph 4/M/66 Right upper ND/ND Exc, UM Local lymph 12 LN-2 (CD74 ) extremity/unknown/no 5/M/65 Right dorsal hand/1/no ND/LN-2 (CD74 ) Mohs surgery with Right wrist 11 LN-2 (CD74 ) 1-cm margins (cutaneous metastasis) Muenster and Hoang 5 6/M/63 Left facial cheek over parotid gland/0.6/yes, with 12-mo interval, treated with Exc ND/ND Exc, UM Intraparotid lymph 30 CD68 ; vimentin ; Cytokeratins (AE1 and/or AE3 ); smooth-muscle actin ; CD45 ; S-100 ; HMB-45 ; CD31 ; glial fibrillary acidic protein Helwig and 7/M/70 Left lower ear/1.5 1/no SubQ/ND Exc, UM Left parotid area 6 ND May 6 8/M/78 Right facial SubQ/ND Exc, UM Intraparotid soft 5 ND cheek/1 1/yes, after 5-mo interval tissue and lymph 9/M/62 Right forehead/1 1/no SubQ/ND Exc, UM Right parotid area 60 ND 10/M/86 Upper left SubQ/ND Exc, UM Soft tissue near left 2 ND ear/ /no mastoid 11/F/77 Right SubQ/ND Exc, UM Right parotid area 12 ND cheek/unknown/yes, multiple recurrences, at 4, 7, and 9 mo 12/F/74 Forehead/ /yes, SubQ/ND Exc, UM Right parotid lymph 4 ND with 3-mo interval; second primary/ /NR node 13/M/52 Right temple/2 3/yes, with 7-mo interval SubQ/ND Exc, UM Ipsilateral parotid lymph node 7 ND Jacobs et al 7 14/F/28 Right side of nose/1 1/yes, at 10and23mo Kargietal 8 15/M/68 Right thigh with intravascular invasion/3 4/no Tumor nodule within dermis without subcutaneous invasion/nd Tumor infiltrating papillary dermis/s-100 ; cytokeratins ; myoglobin Lum and King 9 16/M/81 Scalp/1/NR Dermal tumor abutting subcutis, small foci of necrosis/cd10 ; vimentin ; CD68 ; CD99, focally; pancytokeratin ; EMA ; S-100; smooth-muscle actin ; desmin ; high-molecular-weight cytokeratin ; Factor XIIIa ; CD34 ; Ki-67 in 20% of cells Exc, UM Ipsilateral cervical lymph node 84 ND Exc, UM Lung 6 ND a Exc, 5-mm margins Giuffrida 17/M/87 Scalp/3/no ND/ND Mohs surgery, et al 10 UM Grosso et al 11 18/F/69 Left nostril/unknown/no Nodular pattern did not affect deep structures, tumor cells invaded dermal blood vessels/factor VIII ; alpha-1-antitrypsin ; lysozyme ; ferritin Kemp 19/M/79 Right facial cheek/2/yes, et al 12 3-mo interval ND but photograph presented/nd Unknown Exc, UM Peritoneum, but no abdominal organs; diagnosed as clear-cell variant of AFX by 5 pathologists independently Cutaneous metastasis to scalp Ipsilateral regional cervical lymph Ipsilateral parotid, buccal, and cervical lymph 36 ND 1 Vimentin ; cytokeratins ; S-100 ; MART-1 15 Identical to primary tumor 3 ND (continued) 1402
5 Table. Characteristics of Metastatic Atypical Fibroxanthoma Reported in the Literature (continued) Source Patient No./Sex/ Age, y Primary Tumor Site/ Size, cm/recurrence at Primary Site, YesorNo Dahl 13 20/F/29 Left arm/unknown/yes, 7.5-mo interval, treated with Exc Sankar 21/M/65 14 Right earlobe/ et al 14 unknown/no Present article 22/M/87 Right angle of mandible/ 1.5/no Depth/ Stainings of Primary Tumor Treatment Site of Metastasis Tumor extended into subcutaneous tissue, no invasion of vessels, no involvement of epidermis; Histologic analysis showed differences in cellularity, nuclear and/or cytologic atypia, and mitotic activity compared with other AFXs in series/nd Exc, UM Regional lymph of left axilla ND/ND Exc, UM Left lower lobe of the lung Superficial dermal tumor, no involvement of blood vessels, epidermis, deep dermis, or subcutaneous tissue/pancytokeratins ; MNF-116 ; CD34 ; desmin ; smooth-muscle actin ; HMB-45 ; melanin ; vimentin ; CD68 ; lysozyme Exc, 5-mm margins following initial biopsy that showed completely excised tumor Ipsilateral regional cervical lymph Interval to Metastasis, mo Stains of Metastasis 84 ND 24 Vimentin ; alpha-1-antitrypsin ; S-100 ; pancytokeratin ; HMB-45 ; LCA ; Factor VIII 2 MNF-116 ; S-100 Abbreviations: AFX, atypical fibroxanthoma; Exc, excision; ND, not discussed; NR, not reported; SubQ, excluded cases arising in the subcutis or in deeper tissue; UM, unknown margin size;, negative staining;, positive staining. a No staining performed; patient died of disease within 3 months of metastasis. The use of staining with LN-2 (CD74) might have been useful in this situation. Lazova et al 16 evaluated staining intensity of LN-2 in spindle-cell tumors, including 20 cases each of AFX and MFH. Their findings were promising in that strong staining was seen in 90% of MFH cases, and negative or weak staining was found in 90% of cases of AFX. Differentiating AFX from SCSCC is also challenging. Cytokeratin stains (both low-molecular-weight and highmolecular-weight keratins) are useful in the vast majority of cases. While a minority of cells from SCSCC may stain weakly positive or even negative, typically they stain intensely positive. Given the propensity of SCSCC to metastasize to regional lymph and the occurrence of these tumors on sun-damaged skin of older individuals, it is reasonable to be concerned that unidentified cases of SCSCC are mislabeled as AFX, especially in the setting of aggressive disease. Some authors believe that AFX is simply a dedifferentiated variant of SCSCC, while others refute this claim based on the lack of cytokeratin staining in cases of AFX. 1 Vimentin staining can be used to help differentiate these 2 entities because SCSCC cells typically stain negative, while most cases of AFX stain positive. Monteagudo et al 17 have proposed that CD99, in addition to the traditional battery of immunostains, might aid in the differentiation of SCC and AFX. 17 They evaluated 26 cases of AFX and 10 cases of SCC and found that 73% of the AFX cases showed immunoreactivity for CD99 vs none of the SCC cases, suggesting that CD99 is a helpful positive marker for AFX. Mathew et al 18 evaluated CD117 (c-kit) expression in AFX and found positive staining in 94% of the cases (15 of 16), suggesting that CD117 may prove to be a sensitive marker. In 2007, Hultgren and DiMaio 19 reported the possible benefit of CD10 immunoexpression, in combination with a panel of stains, to help differentiate AFX from SCC and melanoma. They looked at 16 cases of AFX, 10 cases of SCC, and 9 cases of spindlecell and/or desmoplastic melanoma and demonstrated strong diffuse CD10 staining in 94% of AFX cases, weak to moderate staining in 50% of SCC cases, and weak expression in 33% of desmoplastic melanomas cases. de Feraudy et al 20 performed an evaluation of CD10 and PC1 expression in AFX and support the use of both as positive stains for AFX lesions within the context of an immunoperoxidase panel. Specifically, they demonstrated PC1 positivity in 96% of cases of AFX (45 of 47) (and 78% of these were strongly positive) compared with only weak staining in 15% of cases of carcinoma (2 of 13). Group 2 of their study demonstrated that CD10 staining was positive in 100% of cases of AFX (11 of 11) and in 100% of cases of dermatofibroma (11 of 11). Group 3 showed that CD10 staining was positive in 97% of cases of AFX (37 of 38), and PC1 staining in this group was positive in 79% of cases of AFX (27 of 34). More recently, p63 was reported to be a helpful marker to differentiate SCSCC from AFX. Gleason et al 2 evaluated 20 AFX and 10 SCSCC lesions and found strong expression of p63 in 100% of SCSCC cases and negative staining in 100% of cases of AFX, suggesting that p63 has utility as part of a standard immunohistochemical panel for differentiating spindle-cell tumors. One legitimate concern about metastatic AFX reports is that the tumor is in fact not an AFX but another entity. Supporting the diagnosis of metastatic AFX in our 1403
6 patient, the metastatic tumor showed morphologic characteristics on hematoxylin-eosin staining identical to the original skin lesion; S-100 and cytokeratin MNF-116 stainings were negative; and CD10, CD99, and p63 stainings were positive. These results are consistent with AFX, and although no truly confirmatory stain exists at this time, these findings decrease the probability that the evaluated lesion is metastatic SCC or melanoma. The use of p63, CD10, PC1, CD117, and CD99 staining may prove beneficial in delineating AFX from SCC, especially in cases of metastasis. Likewise, the use of LN-2 may prove beneficial in distinguishing AFX from MFH. Clinicians should be aware of the rare but real possibility of AFX behaving aggressively and should monitor patients closely for recurrence and metastatic disease, especially to regional lymph. We stress the importance of immunohistochemical evaluation by an experienced dermatopathologist to rule out other spindle-cell tumors, especially in the setting of metastasis. Future studies will be needed (1) to determine if histologic features or tumor markers may help predict tumor outcome and (2) to evaluate the most efficient and thorough immunohistochemical panel to distinguish genuine cases of primary and metastatic AFX from other entities. Accepted for Publication: June 22, Published Online: August 16, doi: /archdermatol Correspondence: Soon Bahrami, MD, 310 E Broadway, Floor 2A, Louisville, KY (soonb4@hotmail.com). Author Contributions: All authors had full access to all the data in the study and take responsibility for the integrity of the data and the accuracy of the data analysis. Study concept and design: New. Acquisition of data: New and Malone. Analysis and interpretation of data: New, Bahrami, Malone, and Callen. Drafting of the manuscript: New. Critical revision of the manuscript for important intellectual content: Bahrami, Malone, and Callen. Administrative, technical, and material support: Malone. Study supervision: Bahrami, Malone, and Callen. Financial Disclosure: Dr Callen has received honoraria from Amgen, Abbott, Genentech, Centocor, Electrical Optical Sciences, Celgene and Medicis. He serves on a safety monitoring committee for Celgene. Additional Contributions: Sarah Weinel, MD, provided the clinical photograph, and Saad Shaheen, MD, assisted in obtaining histopathologic slides. Disclaimer: Dr Callen is associate editor of the Archives of Dermatology, but he was not involved in any of the decisions regarding review of the manuscript or its acceptance. REFERENCES 1. Mirza B, Weedon D. Atypical fibroxanthoma: a clinicopathological study of 89 cases. Australas J Dermatol. 2005;46(4): Gleason BC, Calder KB, Cibull TL, et al. Utility of p63 in the differential diagnosis of atypical fibroxanthoma and spindle cell squamous cell carcinoma. J Cutan Pathol. 2009;36(5): Helwig EB. Tumor seminar proceedings of the 18th annual tumor seminar of San Antonio Society of Pathologists, 1961: atypical fibroxanthoma. Tex J Med. 1963; 59(5): Cooper JZ, Newman SR, Scott GA, Brown MD. Metastasizing atypical fibroxanthoma (cutaneous malignant histiocytoma): report of five cases. Dermatol Surg. 2005;31(2): Muenster MR, Hoang MP. Left facial mass in an elderly man: metastasizing atypical fibroxanthoma of the skin. Arch Pathol Lab Med. 2006;130(5): Helwig EB, May D. Atypical fibroxanthoma of the skin with metastasis. Cancer. 1986;57(2): Jacobs DS, Edwards WD, Ye RC. Metastatic atypical fibroxanthoma of skin. Cancer. 1975;35(2): Kargi E, Güngör E, Verdi M, et al. Atypical fibroxanthoma and metastasis to the lung. Plast Reconstr Surg. 2003;111(5): Lum DJ, King AR. Peritoneal metastases from an atypical fibroxanthoma. Am J Surg Pathol. 2006;30(8): Giuffrida TJ, Kligora CJ, Goldstein GD. Localized cutaneous metastases from an atypical fibroxanthoma. Dermatol Surg. 2004;30(12, pt 2): Grosso M, Lentini M, Carrozza G, Catalano A. Metastatic atypical fibroxanthoma of skin. Pathol Res Pract. 1987;182(3): Kemp JD, Stenn KS, Arons M, Fischer J. Metastasizing atypical fibroxanthoma: coexistence with chronic lymphocytic leukemia. Arch Dermatol. 1978;114(10): Dahl I. Atypical fibroxanthoma of the skin: a clinico-pathological study of 57 cases. Acta Pathol Microbiol Scand A. 1976;84(2): Sankar NM, Pang KS, Thiruchelvam T, Meldrum-Hanna WG. Metastasis from atypical fibroxanthoma of skin. Med J Aust. 1998;168(8): Ang GC, Roenigk RK, Otley CC, Kim Phillips P, Weaver AL. More than 2 decades of treating atypical fibroxanthoma at mayo clinic: what have we learned from 91 patients? Dermatol Surg. 2009;35(5): Lazova R, Moynes R, May D, Scott G. LN-2 (CD74): a marker to distinguish atypical fibroxanthoma from malignant fibrous histiocytoma. Cancer. 1997;79(11): Monteagudo C, Calduch L, Navarro S, Joan-Figueroa A, Llombart-Bosch A. CD99 immunoreactivity in atypical fibroxanthoma: a common feature of diagnostic value. Am J Clin Pathol. 2002;117(1): Mathew RA, Schlauder SM, Calder KB, Morgan MB. CD117 immunoreactivity in atypical fibroxanthoma. Am J Dermatopathol. 2008;30(1): Hultgren TL, DiMaio DJ. staining of CD10 in atypical fibroxanthomas. J Cutan Pathol. 2007;34(5): de Feraudy S, Mar N, McCalmont TH. Evaluation of CD10 and procollagen 1 expression in atypical fibroxanthoma and dermatofibroma. Am J Surg Pathol. 2008; 32(8):
أملس عضلي غرن = Leiomyosarcoma. Leiomyosarcoma 1 / 5
 Leiomyosarcoma 1 / 5 EPIDEMIOLOGY Exact incidence is unknown, but older studies suggest that leiomyosarcomas comprise approximately 3 percent of soft-tissue sarcomas. Superficial leiomyosarcoma occurs
Leiomyosarcoma 1 / 5 EPIDEMIOLOGY Exact incidence is unknown, but older studies suggest that leiomyosarcomas comprise approximately 3 percent of soft-tissue sarcomas. Superficial leiomyosarcoma occurs
Update on Cutaneous Mesenchymal Tumors. Thomas Brenn
 Update on Cutaneous Mesenchymal Tumors Thomas Brenn Cutaneous Mesenchymal Tumours Wide morphological and biological spectrum Myofibroblastic, smooth muscle, neural, vascular, apidocytic, undifferentiated;
Update on Cutaneous Mesenchymal Tumors Thomas Brenn Cutaneous Mesenchymal Tumours Wide morphological and biological spectrum Myofibroblastic, smooth muscle, neural, vascular, apidocytic, undifferentiated;
Desmoplastic Melanoma R/O BCC. Clinical Information. 74 y.o. man with lesion on left side of neck r/o BCC
 R/O BCC Sabine Kohler, M.D. Professor of Pathology and Dermatology Dermatopathology Service Stanford University School of Medicine Clinical Information 74 y.o. man with lesion on left side of neck r/o
R/O BCC Sabine Kohler, M.D. Professor of Pathology and Dermatology Dermatopathology Service Stanford University School of Medicine Clinical Information 74 y.o. man with lesion on left side of neck r/o
Maligna Melanoma and Atypical Fibroxanthoma: An Unusual Collision Tumour G Türkcü 1, A Keleş 1, U Alabalık 1, D Uçmak 2, H Büyükbayram 1 ABSTRACT
 Maligna Melanoma and Atypical Fibroxanthoma: An Unusual Collision Tumour G Türkcü 1, A Keleş 1, U Alabalık 1, D Uçmak 2, H Büyükbayram 1 ABSTRACT Two different neoplasia in the same biopsy material called
Maligna Melanoma and Atypical Fibroxanthoma: An Unusual Collision Tumour G Türkcü 1, A Keleş 1, U Alabalık 1, D Uçmak 2, H Büyükbayram 1 ABSTRACT Two different neoplasia in the same biopsy material called
Case Report A Rare Cutaneous Adnexal Tumor: Malignant Proliferating Trichilemmal Tumor
 Case Reports in Medicine Volume 2015, Article ID 742920, 4 pages http://dx.doi.org/10.1155/2015/742920 Case Report A Rare Cutaneous Adnexal Tumor: Malignant Proliferating Trichilemmal Tumor Omer Alici,
Case Reports in Medicine Volume 2015, Article ID 742920, 4 pages http://dx.doi.org/10.1155/2015/742920 Case Report A Rare Cutaneous Adnexal Tumor: Malignant Proliferating Trichilemmal Tumor Omer Alici,
Selected Pseudomalignant Soft Tissue Tumors of the Skin and Subcutis
 Selected Pseudomalignant Soft Tissue Tumors of the Skin and Subcutis Andrew L. Folpe, M.D. Professor of Laboratory Medicine and Pathology Mayo Clinic, Rochester, MN folpe.andrew@mayo.edu 2016 MFMER slide-1
Selected Pseudomalignant Soft Tissue Tumors of the Skin and Subcutis Andrew L. Folpe, M.D. Professor of Laboratory Medicine and Pathology Mayo Clinic, Rochester, MN folpe.andrew@mayo.edu 2016 MFMER slide-1
David B. Troxel, MD. Common Medicolegal Situations: Misdiagnosis of Melanoma
 Common Medicolegal Situations: Misdiagnosis of Melanoma David B. Troxel, MD Medical Director, The Doctors Company, Napa, California Clinical Professor Emeritus, University of California at Berkeley Past
Common Medicolegal Situations: Misdiagnosis of Melanoma David B. Troxel, MD Medical Director, The Doctors Company, Napa, California Clinical Professor Emeritus, University of California at Berkeley Past
Collaborative Stage for TNM 7 - Revised 12/02/2009 [ Schema ]
![Collaborative Stage for TNM 7 - Revised 12/02/2009 [ Schema ] Collaborative Stage for TNM 7 - Revised 12/02/2009 [ Schema ]](/thumbs/82/86783199.jpg) CS Tumor Size Collaborative Stage for TNM 7 - Revised 12/02/2009 [ Schema ] Note: the specific tumor size as documented in the medical record. If the ONLY information regarding tumor size is the physician's
CS Tumor Size Collaborative Stage for TNM 7 - Revised 12/02/2009 [ Schema ] Note: the specific tumor size as documented in the medical record. If the ONLY information regarding tumor size is the physician's
Diplomate of the American Board of Pathology in Anatomic and Clinical Pathology
 A 33-year-old male with a left lower leg mass. Contributed by Shaoxiong Chen, MD, PhD Assistant Professor Indiana University School of Medicine/ IU Health Partners Department of Pathology and Laboratory
A 33-year-old male with a left lower leg mass. Contributed by Shaoxiong Chen, MD, PhD Assistant Professor Indiana University School of Medicine/ IU Health Partners Department of Pathology and Laboratory
History A 89 year old gentleman presenting with a scalp/forehead nodule. Patient had squamous cell carcinoma 18 m at same site, excised. Outside diagn
 Case III History A 89 year old gentleman presenting with a scalp/forehead nodule. Patient had squamous cell carcinoma 18 m at same site, excised. Outside diagnoses: Squamous cell carcinoma. R/O: SCC, Melanoma,
Case III History A 89 year old gentleman presenting with a scalp/forehead nodule. Patient had squamous cell carcinoma 18 m at same site, excised. Outside diagnoses: Squamous cell carcinoma. R/O: SCC, Melanoma,
Interesting Case Series. Desmoplastic Melanoma
 Interesting Case Series Desmoplastic Melanoma Anthony Maurice Kordahi, MD, Joshua B. Elston, MD, Ellen M. Robertson, MD, and C. Wayne Cruse, MD Division of Plastic Surgery, Department of Surgery, University
Interesting Case Series Desmoplastic Melanoma Anthony Maurice Kordahi, MD, Joshua B. Elston, MD, Ellen M. Robertson, MD, and C. Wayne Cruse, MD Division of Plastic Surgery, Department of Surgery, University
Utility of p63 in the differential diagnosis of atypical fibroxanthoma and spindle cell squamous cell carcinoma
 J Cutan Pathol 2009: 36: 543 547 doi: 10.1111/j.1600-0560.2008.01099.x John Wiley & Sons. Printed in Singapore Continuing Medical Education Article Copyright # 2009 John Wiley & Sons A/S Journal of Cutaneous
J Cutan Pathol 2009: 36: 543 547 doi: 10.1111/j.1600-0560.2008.01099.x John Wiley & Sons. Printed in Singapore Continuing Medical Education Article Copyright # 2009 John Wiley & Sons A/S Journal of Cutaneous
Desmoplastic Melanoma: Clinical Behavior and Management Implications
 Desmoplastic Melanoma: Clinical Behavior and Management Implications Collier S. Pace, MD, a Jyoti P. Kapil, MD, b Luke G. Wolfe, MS, c Brian J. Kaplan, MD, c and James P. Neifeld, MD c a Division of Plastic
Desmoplastic Melanoma: Clinical Behavior and Management Implications Collier S. Pace, MD, a Jyoti P. Kapil, MD, b Luke G. Wolfe, MS, c Brian J. Kaplan, MD, c and James P. Neifeld, MD c a Division of Plastic
Cellular Neurothekeoma
 Cellular Neurothekeoma Scott W Binder, MD Pritzker Professor of Pathology & Dermatology Sr. Vice Chair Director, Pathology Clinical Services Chief, Dermatopathology Geffen/UCLA School of Medicine Clinical
Cellular Neurothekeoma Scott W Binder, MD Pritzker Professor of Pathology & Dermatology Sr. Vice Chair Director, Pathology Clinical Services Chief, Dermatopathology Geffen/UCLA School of Medicine Clinical
Cutaneous Melanoma: Epidemiology (USA) The Sentinel Node in Head and Neck Melanoma. Cutaneous Melanoma: Epidemiology (USA)
 The Sentinel Node in Head and Neck Melanoma Cutaneous Melanoma: Epidemiology (USA) 6 th leading cause of cancer among men and women 68,720 new cases of invasive melanoma in 2009 8,650 deaths from melanoma
The Sentinel Node in Head and Neck Melanoma Cutaneous Melanoma: Epidemiology (USA) 6 th leading cause of cancer among men and women 68,720 new cases of invasive melanoma in 2009 8,650 deaths from melanoma
World Articles of Ear, Nose and Throat Page 1
 World Articles of Ear, Nose and Throat ---------------------Page 1 Primary Malignant Melanoma of the Tongue: A Case Report Authors: Nanayakkara PR*, Arudchelvam JD** Ariyaratne JC*, Mendis K*, Jayasekera
World Articles of Ear, Nose and Throat ---------------------Page 1 Primary Malignant Melanoma of the Tongue: A Case Report Authors: Nanayakkara PR*, Arudchelvam JD** Ariyaratne JC*, Mendis K*, Jayasekera
Solitary Fibrous Tumor of the Kidney with Massive Retroperitoneal Recurrence. A Case Presentation
 246) Prague Medical Report / Vol. 113 (2012) No. 3, p. 246 250 Solitary Fibrous Tumor of the Kidney with Massive Retroperitoneal Recurrence. A Case Presentation Sfoungaristos S., Papatheodorou M., Kavouras
246) Prague Medical Report / Vol. 113 (2012) No. 3, p. 246 250 Solitary Fibrous Tumor of the Kidney with Massive Retroperitoneal Recurrence. A Case Presentation Sfoungaristos S., Papatheodorou M., Kavouras
Basal cell carcinoma 5/28/2011
 Goal of this Presentation A practical approach to the diagnosis of cutaneous carcinomas and their mimics Thaddeus Mully, MD University of California San Francisco To review common non-melanoma skin cancers
Goal of this Presentation A practical approach to the diagnosis of cutaneous carcinomas and their mimics Thaddeus Mully, MD University of California San Francisco To review common non-melanoma skin cancers
Special slide seminar
 Special slide seminar Tomáš Rozkoš The Fingerland Department of Pathology Charles University Medical Faculty and Faculty Hospital in Hradec Králové Czech Republic Case history, 33 years old resistance
Special slide seminar Tomáš Rozkoš The Fingerland Department of Pathology Charles University Medical Faculty and Faculty Hospital in Hradec Králové Czech Republic Case history, 33 years old resistance
Case of Pleomorphic Dermal Sarcoma of the Eyelid Treated with Micrographic Surgery and Secondary Intention Healing
 JI Kim, et al pissn 1013-9087ㆍeISSN 2005-3894 Ann Dermatol Vol. 28, No. 5, 2016 http://dx.doi.org/10.5021/ad.2016.28.5.632 CASE REPORT Case of Pleomorphic Dermal Sarcoma of the Eyelid Treated with Micrographic
JI Kim, et al pissn 1013-9087ㆍeISSN 2005-3894 Ann Dermatol Vol. 28, No. 5, 2016 http://dx.doi.org/10.5021/ad.2016.28.5.632 CASE REPORT Case of Pleomorphic Dermal Sarcoma of the Eyelid Treated with Micrographic
Collaborative Staging Manual and Coding Instructions Part II: Primary Site Schema
 C44.0-C44.9, C51.0-C51.2, C51.8-C51.9, C60.0-C60.2, C60.8-C60.9, C63.2 (M-8720-8790) C44.0 Skin of lip, NOS C44.1 Eyelid C44.2 External ear C44.3 Skin of ear and unspecified parts of face C44.4 Skin of
C44.0-C44.9, C51.0-C51.2, C51.8-C51.9, C60.0-C60.2, C60.8-C60.9, C63.2 (M-8720-8790) C44.0 Skin of lip, NOS C44.1 Eyelid C44.2 External ear C44.3 Skin of ear and unspecified parts of face C44.4 Skin of
The Relevance of Cytologic Atypia in Cutaneous Neural Tumors
 The Relevance of Cytologic Atypia in Cutaneous Neural Tumors Recent Findings - New Developments New Problems Zsolt B. Argenyi, M.D. Professor of Pathology & Dermatology Director of Dermatopathology Department
The Relevance of Cytologic Atypia in Cutaneous Neural Tumors Recent Findings - New Developments New Problems Zsolt B. Argenyi, M.D. Professor of Pathology & Dermatology Director of Dermatopathology Department
Case Scenario 1: Thyroid
 Case Scenario 1: Thyroid History and Physical Patient is an otherwise healthy 80 year old female with the complaint of a neck mass first noticed two weeks ago. The mass has increased in size and is palpable.
Case Scenario 1: Thyroid History and Physical Patient is an otherwise healthy 80 year old female with the complaint of a neck mass first noticed two weeks ago. The mass has increased in size and is palpable.
Melanocytic Lesions: Use of Immunohistochemistry and Special Studies Napa Valley 2018
 Melanocytic Lesions: Use of Immunohistochemistry and Special Studies Napa Valley 2018 Victor G. Prieto, MD, PhD Professor Depts. of Pathology and Dermatology University of Texas - MD Anderson Cancer Center
Melanocytic Lesions: Use of Immunohistochemistry and Special Studies Napa Valley 2018 Victor G. Prieto, MD, PhD Professor Depts. of Pathology and Dermatology University of Texas - MD Anderson Cancer Center
3/27/2017. Pulmonary Pathology Specialty Conference. Disclosure of Relevant Financial Relationships. Clinical History:
 Pulmonary Pathology Specialty Conference Saul Suster, M.D. Medical College of Wisconsin Disclosure of Relevant Financial Relationships USCAP requires that all planners (Education Committee) in a position
Pulmonary Pathology Specialty Conference Saul Suster, M.D. Medical College of Wisconsin Disclosure of Relevant Financial Relationships USCAP requires that all planners (Education Committee) in a position
Atypical Palisaded Myofibroblastoma of Lymph Node: Report of a rare case.
 ISPUB.COM The Internet Journal of Pathology Volume 10 Number 1 Atypical Palisaded Myofibroblastoma of Lymph Node: Report of a rare case. V Kinnera, R Nandyala, M Yootla, K Mandyam Citation V Kinnera, R
ISPUB.COM The Internet Journal of Pathology Volume 10 Number 1 Atypical Palisaded Myofibroblastoma of Lymph Node: Report of a rare case. V Kinnera, R Nandyala, M Yootla, K Mandyam Citation V Kinnera, R
Slide seminar. Asist. Prof. Jože Pižem, MD, PhD Institute of Pathology Medical Faculty, University of Ljubljana
 Slide seminar Asist. Prof. Jože Pižem, MD, PhD Institute of Pathology Medical Faculty, University of Ljubljana Case 5 A 57-year-old man with a dermal/subcutaneous lesion on the scalp, which was interpreted
Slide seminar Asist. Prof. Jože Pižem, MD, PhD Institute of Pathology Medical Faculty, University of Ljubljana Case 5 A 57-year-old man with a dermal/subcutaneous lesion on the scalp, which was interpreted
57th Annual HSCP Spring Symposium 4/16/2016
 An Unusual Malignant Spindle Cell Lesion to Involve the Breast Erinn Downs-Kelly, D.O. Associate Professor of Pathology University of Utah & ARUP Laboratories No disclosures Case 39 y/o female with no
An Unusual Malignant Spindle Cell Lesion to Involve the Breast Erinn Downs-Kelly, D.O. Associate Professor of Pathology University of Utah & ARUP Laboratories No disclosures Case 39 y/o female with no
Radiology Pathology Conference
 Radiology Pathology Conference Sharlin Johnykutty,, MD, Cytopathology Fellow Sara Majewski, MD, Radiology Resident Friday, August 28, 2009 Presentation material is for education purposes only. All rights
Radiology Pathology Conference Sharlin Johnykutty,, MD, Cytopathology Fellow Sara Majewski, MD, Radiology Resident Friday, August 28, 2009 Presentation material is for education purposes only. All rights
Role of fine-needle aspiration biopsy in the diagnosis of metastatic desmoplastic melanoma to the parotid and submandibular region
 Oral Oncology EXTRA (2006) 42, 263 267 available at www.sciencedirect.com journal homepage: http://intl.elsevierhealth.com/journal/ooex CASE REPORT Role of fine-needle aspiration biopsy in the diagnosis
Oral Oncology EXTRA (2006) 42, 263 267 available at www.sciencedirect.com journal homepage: http://intl.elsevierhealth.com/journal/ooex CASE REPORT Role of fine-needle aspiration biopsy in the diagnosis
What is Atypical Fibroxanthoma? Carcinoma, Sarcoma, Both, or Neither? Phillip H McKee M.B., M.D., F.R.C.Path, Sedona, Arizona
 What is Atypical Fibroxanthoma? Carcinoma, Sarcoma, Both, or Neither? Phillip H McKee M.B., M.D., F.R.C.Path, Sedona, Arizona Email: phmckee1948@msn.com Summary It is stressed that a diagnosis of atypical
What is Atypical Fibroxanthoma? Carcinoma, Sarcoma, Both, or Neither? Phillip H McKee M.B., M.D., F.R.C.Path, Sedona, Arizona Email: phmckee1948@msn.com Summary It is stressed that a diagnosis of atypical
Presentation material is for education purposes only. All rights reserved URMC Radiology Page 1 of 98
 Presentation material is for education purposes only. All rights reserved. 2011 URMC Radiology Page 1 of 98 Radiology / Pathology Conference February 2011 Brooke Koltz, Cytopathology Resident Presentation
Presentation material is for education purposes only. All rights reserved. 2011 URMC Radiology Page 1 of 98 Radiology / Pathology Conference February 2011 Brooke Koltz, Cytopathology Resident Presentation
Collaborative Stage for TNM 7 - Revised 07/14/2009 [ Schema ]
![Collaborative Stage for TNM 7 - Revised 07/14/2009 [ Schema ] Collaborative Stage for TNM 7 - Revised 07/14/2009 [ Schema ]](/thumbs/71/65936251.jpg) MelanomaSkin CS Tumor Size Collaborative Stage for TNM 7 - Revised 07/14/2009 [ Schema ] Code 000 No mass/tumor found Description 001-988 001-988 millimeters (code exact size in millimeters) 989 989 millimeters
MelanomaSkin CS Tumor Size Collaborative Stage for TNM 7 - Revised 07/14/2009 [ Schema ] Code 000 No mass/tumor found Description 001-988 001-988 millimeters (code exact size in millimeters) 989 989 millimeters
Mapping Basal Cell and Squamous Carcinoma By 10 Min CK5 Direct Immunohistochemistry on Frozen Section Skin Tissues during Mohs Micrographic Surgery
 Mapping Basal Cell and Squamous Carcinoma By 10 Min CK5 Direct Immunohistochemistry on Frozen Section Skin Tissues during Mohs Micrographic Surgery Robert Glinert, MD and Song Q. Zhao, MD, Ph.D., MPH Department
Mapping Basal Cell and Squamous Carcinoma By 10 Min CK5 Direct Immunohistochemistry on Frozen Section Skin Tissues during Mohs Micrographic Surgery Robert Glinert, MD and Song Q. Zhao, MD, Ph.D., MPH Department
POORLY DIFFERENTIATED, HIGH GRADE AND ANAPLASTIC CARCINOMAS: WHAT IS EVERYONE TALKING ABOUT?
 POORLY DIFFERENTIATED, HIGH GRADE AND ANAPLASTIC CARCINOMAS: WHAT IS EVERYONE TALKING ABOUT? AGGRESSIVE THYROID CANCERS PAPILLARY CARCINOMA CERTAIN SUBTYPES POORLY DIFFERENTIATED CARCINOMA HIGH GRADE DIFFERENTIATED
POORLY DIFFERENTIATED, HIGH GRADE AND ANAPLASTIC CARCINOMAS: WHAT IS EVERYONE TALKING ABOUT? AGGRESSIVE THYROID CANCERS PAPILLARY CARCINOMA CERTAIN SUBTYPES POORLY DIFFERENTIATED CARCINOMA HIGH GRADE DIFFERENTIATED
Carcinoma of Unknown Primary site (CUP) in HEAD & NECK SURGERY
 Carcinoma of Unknown Primary site (CUP) in HEAD & NECK SURGERY SEARCHING FOR THE PRIMARY? P r o f J P P r e t o r i u s H e a d : C l i n i c a l U n i t C r i t i c a l C a r e U n i v e r s i t y O f
Carcinoma of Unknown Primary site (CUP) in HEAD & NECK SURGERY SEARCHING FOR THE PRIMARY? P r o f J P P r e t o r i u s H e a d : C l i n i c a l U n i t C r i t i c a l C a r e U n i v e r s i t y O f
Journal of International Academy of Forensic Science & Pathology (JIAFP)
 Journal of International Academy of Forensic Science & Pathology (JIAFP) ISSN 2395-0722 MICROCYSTIC ADNEXAL CARCINOMA-A CASE REPORT WITH REVIEW OF LITERATURE Case Report Sulakshana M S 1,Natarajan M 2
Journal of International Academy of Forensic Science & Pathology (JIAFP) ISSN 2395-0722 MICROCYSTIC ADNEXAL CARCINOMA-A CASE REPORT WITH REVIEW OF LITERATURE Case Report Sulakshana M S 1,Natarajan M 2
A PRACTICAL APPROACH TO ATYPICAL MELANOCYTIC LESIONS BIJAN HAGHIGHI M.D, DIRECTOR OF DERMATOPATHOLOGY, ST. JOSEPH HOSPITAL
 A PRACTICAL APPROACH TO ATYPICAL MELANOCYTIC LESIONS BIJAN HAGHIGHI M.D, DIRECTOR OF DERMATOPATHOLOGY, ST. JOSEPH HOSPITAL OBJECTIVES Discuss current trends and changing concepts in our understanding of
A PRACTICAL APPROACH TO ATYPICAL MELANOCYTIC LESIONS BIJAN HAGHIGHI M.D, DIRECTOR OF DERMATOPATHOLOGY, ST. JOSEPH HOSPITAL OBJECTIVES Discuss current trends and changing concepts in our understanding of
American College of Mohs Surgery. Diagnostic Quality Control Program (Review of Answers)
 American College of Mohs Surgery Diagnostic Quality Control Program 2010 (Review of Answers) Question 1 A flesh-colored plaque on the right ala of an otherwise healthy 57 year-old male is referred for
American College of Mohs Surgery Diagnostic Quality Control Program 2010 (Review of Answers) Question 1 A flesh-colored plaque on the right ala of an otherwise healthy 57 year-old male is referred for
Diagnostic value of CD163 in cutaneous spindle cell lesions
 J Cutan Pathol 2009: 36: 859 864 doi: 10.1111/j.1600-0560.2008.01179.x John Wiley & Sons. Printed in Singapore Copyright # 2008 John Wiley & Sons A/S Journal of Cutaneous Pathology Continuing Medical Education
J Cutan Pathol 2009: 36: 859 864 doi: 10.1111/j.1600-0560.2008.01179.x John Wiley & Sons. Printed in Singapore Copyright # 2008 John Wiley & Sons A/S Journal of Cutaneous Pathology Continuing Medical Education
Melanoma Case Scenario 1
 Melanoma Case Scenario 1 History and physical 11/5/16 Patient is a single, 48-year-old male in good health who presented to his primary physician for a yearly physical exam during which a 3.4 x 2.8 x 1.5
Melanoma Case Scenario 1 History and physical 11/5/16 Patient is a single, 48-year-old male in good health who presented to his primary physician for a yearly physical exam during which a 3.4 x 2.8 x 1.5
Catholic University of Louvain, St - Luc University Hospital Head and Neck Oncology Programme. Anatomopathology. Pathology 1 Sept.
 Anatomopathology Pathology 1 Anatomopathology Biopsies Frozen section Surgical specimen Peculiarities for various tumor site References Pathology 2 Biopsies Minimum data, which should be given by the pathologist
Anatomopathology Pathology 1 Anatomopathology Biopsies Frozen section Surgical specimen Peculiarities for various tumor site References Pathology 2 Biopsies Minimum data, which should be given by the pathologist
Melanoma-Back to Basics I Thought I Knew Ya! Paul K. Shitabata, M.D. Dermatopathologist APMG
 Melanoma-Back to Basics I Thought I Knew Ya! Paul K. Shitabata, M.D. Dermatopathologist APMG At tumor board, a surgeon insists that all level II melanomas are invasive since they have broken through the
Melanoma-Back to Basics I Thought I Knew Ya! Paul K. Shitabata, M.D. Dermatopathologist APMG At tumor board, a surgeon insists that all level II melanomas are invasive since they have broken through the
Malignant tumors of melanocytes : Part 3. Deba P Sarma, MD., Omaha
 Malignant tumors of melanocytes : Part 3 Deba P Sarma, MD., Omaha Let s go over one case of melanoma using the following worksheet. Of the various essential information that needs to be included in the
Malignant tumors of melanocytes : Part 3 Deba P Sarma, MD., Omaha Let s go over one case of melanoma using the following worksheet. Of the various essential information that needs to be included in the
Update on Thyroid FNA The Bethesda System. Shikha Bose M.D. Associate Professor Cedars Sinai Medical Center
 Update on Thyroid FNA The Bethesda System Shikha Bose M.D. Associate Professor Cedars Sinai Medical Center Thyroid Nodules Frequent occurrence Palpable: 4-7% of adults Ultrasound: 10-31% Majority benign
Update on Thyroid FNA The Bethesda System Shikha Bose M.D. Associate Professor Cedars Sinai Medical Center Thyroid Nodules Frequent occurrence Palpable: 4-7% of adults Ultrasound: 10-31% Majority benign
Case 18. M75. Excision of mass on scalp. Clinically SCC. The best diagnosis is:
 Case 18 M75. Excision of mass on scalp. Clinically SCC. The best diagnosis is: A. Pilomatrical carcinoma B. Adnexal carcinoma NOS C. Metastatic squamous cell carcinoma D.Primary squamous cell carcinoma
Case 18 M75. Excision of mass on scalp. Clinically SCC. The best diagnosis is: A. Pilomatrical carcinoma B. Adnexal carcinoma NOS C. Metastatic squamous cell carcinoma D.Primary squamous cell carcinoma
Melanoma Case Scenario 1
 Melanoma Case Scenario 1 History and physical 11/5/16 Patient is a single, 48-year-old male in good health who presented to his primary physician for a yearly physical exam during which a 3.4 x 2.8 x 1.5
Melanoma Case Scenario 1 History and physical 11/5/16 Patient is a single, 48-year-old male in good health who presented to his primary physician for a yearly physical exam during which a 3.4 x 2.8 x 1.5
Case Presentation. Maha Akkawi, MD, Fatima Obeidat, MD, Tariq Aladily, MD. Department of Pathology Jordan University Hospital Amman, Jordan
 Case Presentation Maha Akkawi, MD, Fatima Obeidat, MD, Tariq Aladily, MD Department of Pathology Jordan University Hospital Amman, Jordan The 25th Annual Congress of the ADIAP The 8/11/2013 1 5th International
Case Presentation Maha Akkawi, MD, Fatima Obeidat, MD, Tariq Aladily, MD Department of Pathology Jordan University Hospital Amman, Jordan The 25th Annual Congress of the ADIAP The 8/11/2013 1 5th International
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,500 108,000 1.7 M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,500 108,000 1.7 M Open access books available International authors and editors Downloads Our
21/07/2017. Hobnail endothelial cells are not the same as epithelioid endothelial cells
 UPDATE IN CUTANEOUS VASCULAR S DERMATOPATHOLOGY SESSION BELFAST PATHOLOGY JUNE 21/2017 Dr E Calonje St John s Institute of Dermatology, London, United Kingdom THE FAMILY OF VASCULAR S WITH EPITHELIOID
UPDATE IN CUTANEOUS VASCULAR S DERMATOPATHOLOGY SESSION BELFAST PATHOLOGY JUNE 21/2017 Dr E Calonje St John s Institute of Dermatology, London, United Kingdom THE FAMILY OF VASCULAR S WITH EPITHELIOID
Case Report: Chondroid Syringoma of the Cheek
 Cronicon OPEN ACCESS Dina Amin 1 *, Abdullah Al-Gorashi 2 and Rahaf Y Al-Habbab 2 1 Assistant Consultant Al-Noor Specialist Hospital, Saudi Arabia, Clinical fellow University of Alabama, USA 2 Department
Cronicon OPEN ACCESS Dina Amin 1 *, Abdullah Al-Gorashi 2 and Rahaf Y Al-Habbab 2 1 Assistant Consultant Al-Noor Specialist Hospital, Saudi Arabia, Clinical fellow University of Alabama, USA 2 Department
Development of Myofibrosarcoma after Removal of Longstanding Chemotherapy Port
 Case Report Development of Myofibrosarcoma after Removal of Longstanding Chemotherapy Port Christopher P. Rice 1, Aaron Wyble 2, Suimin Qiu 2, Michael Silva 1, Douglas Tyler 1, Linda Phillips 1 and Celia
Case Report Development of Myofibrosarcoma after Removal of Longstanding Chemotherapy Port Christopher P. Rice 1, Aaron Wyble 2, Suimin Qiu 2, Michael Silva 1, Douglas Tyler 1, Linda Phillips 1 and Celia
Whitney A. High, MD, JD, MEng
 ADS Dermatopathology Meeting 2014 Selected Adnexal Tumors Whitney A. High, MD, JD, MEng Associate Professor, Dermatology & Pathology Director of Dermatopathology (Dermatology) University of Colorado School
ADS Dermatopathology Meeting 2014 Selected Adnexal Tumors Whitney A. High, MD, JD, MEng Associate Professor, Dermatology & Pathology Director of Dermatopathology (Dermatology) University of Colorado School
Financial disclosures
 Cutaneous Mesenchymal Neoplasms with EWSR1 Rearrangement By Konstantinos Linos MD, FCAP, FASDP Bone, Soft Tissue and Dermatopathology Assistant Professor of Pathology Dartmouth-Hitchc Geisel School of
Cutaneous Mesenchymal Neoplasms with EWSR1 Rearrangement By Konstantinos Linos MD, FCAP, FASDP Bone, Soft Tissue and Dermatopathology Assistant Professor of Pathology Dartmouth-Hitchc Geisel School of
Enterprise Interest Nothing to declare
 Enterprise Interest Nothing to declare Diagnoses one would not like to miss in soft tissue pathology early in your career Marta Sbaraglia, MD Department of Pathology Hospital of Treviso University of Padua
Enterprise Interest Nothing to declare Diagnoses one would not like to miss in soft tissue pathology early in your career Marta Sbaraglia, MD Department of Pathology Hospital of Treviso University of Padua
Poor Outcomes in Head and Neck Non-Melanoma Cutaneous Carcinomas
 10 The Open Otorhinolaryngology Journal, 2011, 5, 10-14 Open Access Poor Outcomes in Head and Neck Non-Melanoma Cutaneous Carcinomas Kevin C. Huoh and Steven J. Wang * Head and Neck Surgery and Oncology,
10 The Open Otorhinolaryngology Journal, 2011, 5, 10-14 Open Access Poor Outcomes in Head and Neck Non-Melanoma Cutaneous Carcinomas Kevin C. Huoh and Steven J. Wang * Head and Neck Surgery and Oncology,
Case year old female presented with asymmetric enlargement of the left lobe of the thyroid
 Case 4 22 year old female presented with asymmetric enlargement of the left lobe of the thyroid gland. No information available relative to a prior fine needle aspiration biopsy. A left lobectomy was performed.
Case 4 22 year old female presented with asymmetric enlargement of the left lobe of the thyroid gland. No information available relative to a prior fine needle aspiration biopsy. A left lobectomy was performed.
Case 4 Diagnosis 2/21/2011 TGB
 Case 4 22 year old female presented with asymmetric enlargement of the left lobe of the thyroid gland. No information available relative to a prior fine needle aspiration biopsy. A left lobectomy was performed.
Case 4 22 year old female presented with asymmetric enlargement of the left lobe of the thyroid gland. No information available relative to a prior fine needle aspiration biopsy. A left lobectomy was performed.
Objectives. Atypical Glandular Cells. Atypical Endocervical Cells. Reactive Endocervical Cells
 2013 California Society of Pathologists 66 th Annual Meeting San Francisco, CA Atypical Glandular Cells to Early Invasive Adenocarcinoma: Cervical Cytology and Histology Christina S. Kong, MD Associate
2013 California Society of Pathologists 66 th Annual Meeting San Francisco, CA Atypical Glandular Cells to Early Invasive Adenocarcinoma: Cervical Cytology and Histology Christina S. Kong, MD Associate
3/27/2017. Disclosure of Relevant Financial Relationships
 Ophthalmic Pathology Evening Specialty Conference USCAP 2017 5 th March, 2017 Mukul K. Divatia, MD Assistant Professor Department of Pathology & Genomic Medicine Weill Cornell Medical College Houston Methodist
Ophthalmic Pathology Evening Specialty Conference USCAP 2017 5 th March, 2017 Mukul K. Divatia, MD Assistant Professor Department of Pathology & Genomic Medicine Weill Cornell Medical College Houston Methodist
Malignant Cardiac Tumors Rad-Path Correlation
 Malignant Cardiac Tumors Rad-Path Correlation Vincent B. Ho, M.D., M.B.A. 1 Jean Jeudy, M.D. 2 Aletta Ann Frazier, M.D. 2 1 Uniformed Services University of the Health Sciences 2 University of Maryland
Malignant Cardiac Tumors Rad-Path Correlation Vincent B. Ho, M.D., M.B.A. 1 Jean Jeudy, M.D. 2 Aletta Ann Frazier, M.D. 2 1 Uniformed Services University of the Health Sciences 2 University of Maryland
Atypical fibroxanthoma: A series of 56 tumors and an unexplained uneven distribution of cases in southeast Germany
 ORIGINAL ARTICLE Atypical fibroxanthoma: A series of 56 tumors and an unexplained uneven distribution of cases in southeast Germany Uwe Wollina, MD, 1* Jaqueline Sch onlebe, MD, 2 Mirjana Ziemer, MD, 3
ORIGINAL ARTICLE Atypical fibroxanthoma: A series of 56 tumors and an unexplained uneven distribution of cases in southeast Germany Uwe Wollina, MD, 1* Jaqueline Sch onlebe, MD, 2 Mirjana Ziemer, MD, 3
Case 2. Dr. Sathima Natarajan M.D. Kaiser Permanente Medical Center Sunset
 Case 2 Dr. Sathima Natarajan M.D. Kaiser Permanente Medical Center Sunset History 24 year old male presented with a 3 day history of right flank pain, sharp in nature Denies fever, chills, hematuria or
Case 2 Dr. Sathima Natarajan M.D. Kaiser Permanente Medical Center Sunset History 24 year old male presented with a 3 day history of right flank pain, sharp in nature Denies fever, chills, hematuria or
Objectives. Salivary Gland FNA: The Milan System. Role of Salivary Gland FNA 04/26/2018
 Salivary Gland FNA: The Milan System Dr. Jennifer Brainard Section Head Cytopathology Cleveland Clinic Objectives Introduce the Milan System for reporting salivary gland cytopathology Define cytologic
Salivary Gland FNA: The Milan System Dr. Jennifer Brainard Section Head Cytopathology Cleveland Clinic Objectives Introduce the Milan System for reporting salivary gland cytopathology Define cytologic
Case Scenario 1 Worksheet. Primary Site C44.4 Morphology 8743/3 Laterality 0 Stage/ Prognostic Factors
 CASE SCENARIO 1 9/10/13 HISTORY: Patient is a 67-year-old white male and presents with lesion located 4-5cm above his right ear. The lesion has been present for years. No lymphadenopathy. 9/10/13 anterior
CASE SCENARIO 1 9/10/13 HISTORY: Patient is a 67-year-old white male and presents with lesion located 4-5cm above his right ear. The lesion has been present for years. No lymphadenopathy. 9/10/13 anterior
Merkel Cell Carcinoma Case # 2
 DISCHARGE SUMMARY Admitted: 10/11/2010 Discharged: 10/13/2010 Merkel Cell Carcinoma Case # 2 Chief Compliant: A 79 year old lady status post tumor on the scalp excision and left neck likely dissection
DISCHARGE SUMMARY Admitted: 10/11/2010 Discharged: 10/13/2010 Merkel Cell Carcinoma Case # 2 Chief Compliant: A 79 year old lady status post tumor on the scalp excision and left neck likely dissection
Classification (1) Classification (3) Classification (2) Spindle cell lesions. Spindle cell lesions of bladder (Mills et al.
 Non-epithelial tumours and nonepithelial tumour-like lesions of the bladder Dr Jonathan H Shanks The Christie NHS Foundation Trust, Manchester, UK Classification (1) Myofibroblastic proliferations and
Non-epithelial tumours and nonepithelial tumour-like lesions of the bladder Dr Jonathan H Shanks The Christie NHS Foundation Trust, Manchester, UK Classification (1) Myofibroblastic proliferations and
From Morphology to Molecular Pathology: A Practical Approach for Cytopathologists Part 1-Cytomorphology. Songlin Zhang, MD, PhD LSUHSC-Shreveport
 From Morphology to Molecular Pathology: A Practical Approach for Cytopathologists Part 1-Cytomorphology Songlin Zhang, MD, PhD LSUHSC-Shreveport I have no Conflict of Interest. FNA on Lymphoproliferative
From Morphology to Molecular Pathology: A Practical Approach for Cytopathologists Part 1-Cytomorphology Songlin Zhang, MD, PhD LSUHSC-Shreveport I have no Conflict of Interest. FNA on Lymphoproliferative
Melanoma Update: 8th Edition of AJCC Staging System
 Melanoma Update: 8th Edition of AJCC Staging System Rosalie Elenitsas, M.D. Professor of Dermatology Director, Dermatopathology University of Pennsylvania DISCLOSURE OF RELATIONSHIPS WITH INDUSTRY None
Melanoma Update: 8th Edition of AJCC Staging System Rosalie Elenitsas, M.D. Professor of Dermatology Director, Dermatopathology University of Pennsylvania DISCLOSURE OF RELATIONSHIPS WITH INDUSTRY None
Kidney Case 1 SURGICAL PATHOLOGY REPORT
 Kidney Case 1 Surgical Pathology Report February 9, 2007 Clinical History: This 45 year old woman was found to have a left renal mass. CT urography with reconstruction revealed a 2 cm medial mass which
Kidney Case 1 Surgical Pathology Report February 9, 2007 Clinical History: This 45 year old woman was found to have a left renal mass. CT urography with reconstruction revealed a 2 cm medial mass which
Salivary Gland FNA ATYPICAL : Criteria and Controversies
 Salivary Gland FNA ATYPICAL : Criteria and Controversies W.C. Faquin, M.D., Ph.D. Director, Head and Neck Pathology Massachusetts General Hospital Massachusetts Eye and Ear Infirmary Harvard Medical School
Salivary Gland FNA ATYPICAL : Criteria and Controversies W.C. Faquin, M.D., Ph.D. Director, Head and Neck Pathology Massachusetts General Hospital Massachusetts Eye and Ear Infirmary Harvard Medical School
Financial disclosures
 Mesenchymal Neoplasms with Melanocytic Differentiation By Konstantinos Linos MD, FCAP, FASDP Bone, Soft Tissue and Dermatopathology Assistant Professor of Pathology Dartmouth-Hitchcock Medical Center Geisel
Mesenchymal Neoplasms with Melanocytic Differentiation By Konstantinos Linos MD, FCAP, FASDP Bone, Soft Tissue and Dermatopathology Assistant Professor of Pathology Dartmouth-Hitchcock Medical Center Geisel
BSD 2015 Case 19. Female 21. Nodule on forehead. The best diagnosis is:
 BSD 2015 Case 19 Female 21. Nodule on forehead. The best diagnosis is: A. mixed tumour of skin B. porocarcinoma C. nodular hidradenoma D. metastatic adenocarcinoma BSD 2015 Case 19 Female 21 Nodule on
BSD 2015 Case 19 Female 21. Nodule on forehead. The best diagnosis is: A. mixed tumour of skin B. porocarcinoma C. nodular hidradenoma D. metastatic adenocarcinoma BSD 2015 Case 19 Female 21 Nodule on
Pathology Mystery and Surprise
 Pathology Mystery and Surprise Tim Smith, MD Director Anatomic Pathology Medical University of South Carolina Disclosures No conflicts to declare Some problem cases Kidney tumor Scalp tumor Bladder tumor
Pathology Mystery and Surprise Tim Smith, MD Director Anatomic Pathology Medical University of South Carolina Disclosures No conflicts to declare Some problem cases Kidney tumor Scalp tumor Bladder tumor
Case Report Metastatic Malignant Melanoma of Parotid Gland with a Regressed Primary Tumor
 Case Reports in Otolaryngology Volume 2016, Article ID 5393404, 4 pages http://dx.doi.org/10.1155/2016/5393404 Case Report Metastatic Malignant Melanoma of Parotid Gland with a Regressed Primary Tumor
Case Reports in Otolaryngology Volume 2016, Article ID 5393404, 4 pages http://dx.doi.org/10.1155/2016/5393404 Case Report Metastatic Malignant Melanoma of Parotid Gland with a Regressed Primary Tumor
Benign versus Cancerous Lesions How to tell the difference FMF 2014 Christie Freeman MD, CCFP, DipPDerm, MSc
 1 Benign versus Cancerous Lesions How to tell the difference FMF 2014 Christie Freeman MD, CCFP, DipPDerm, MSc Benign lesions Seborrheic Keratoses: Warty, stuck-on Genetics and birthdays Can start in late
1 Benign versus Cancerous Lesions How to tell the difference FMF 2014 Christie Freeman MD, CCFP, DipPDerm, MSc Benign lesions Seborrheic Keratoses: Warty, stuck-on Genetics and birthdays Can start in late
Session Number: 1020 Session: Adenocarcinoma of the Cervix: Diagnostic Pitfalls and New Prognostic Implications. Andres A. Roma, MD Cleveland Clinic
 Session Number: 1020 Session: Adenocarcinoma of the Cervix: Diagnostic Pitfalls and New Prognostic Implications Andres A. Roma, MD Cleveland Clinic No Disclosures In the past 12 months, I have not had
Session Number: 1020 Session: Adenocarcinoma of the Cervix: Diagnostic Pitfalls and New Prognostic Implications Andres A. Roma, MD Cleveland Clinic No Disclosures In the past 12 months, I have not had
1/10/2018. Soft Tissue Tumors Showing Melanocytic Differentiation. Overview. Desmoplastic/ Spindle Cell Melanoma
 2016 MFMER slide-1 2016 MFMER slide-2 2016 MFMER slide-3 Soft Tissue Tumors Showing Melanocytic Differentiation Andrew L. Folpe, M.D. Professor of Laboratory Medicine and Pathology Mayo Clinic, Rochester,
2016 MFMER slide-1 2016 MFMER slide-2 2016 MFMER slide-3 Soft Tissue Tumors Showing Melanocytic Differentiation Andrew L. Folpe, M.D. Professor of Laboratory Medicine and Pathology Mayo Clinic, Rochester,
Basal cell carcinoma diagnosed on Fine-Needle Aspiration Cytology A. Pathological Case Report
 Basal cell carcinoma diagnosed on Fine-Needle Aspiration Cytology A Abstract Dr. Madhuri S.Kate 1, Dr. Preeti Jain 2, Dr. Shailesh S. Patne 3 Introduction: Basal cell carcinoma (BCC) is a locally invasive
Basal cell carcinoma diagnosed on Fine-Needle Aspiration Cytology A Abstract Dr. Madhuri S.Kate 1, Dr. Preeti Jain 2, Dr. Shailesh S. Patne 3 Introduction: Basal cell carcinoma (BCC) is a locally invasive
SEBACEOUS NEOPLASMS. Dr. Prachi Saraogi Clinical Fellow in Dermatology
 SEBACEOUS NEOPLASMS Dr. Prachi Saraogi Clinical Fellow in Dermatology Sebaceous neoplasms Sebaceous adenoma (Benign) Sebaceous carcinoma (Malignant) SEBACEOUS ADENOMA Benign tumours composed of incompletely
SEBACEOUS NEOPLASMS Dr. Prachi Saraogi Clinical Fellow in Dermatology Sebaceous neoplasms Sebaceous adenoma (Benign) Sebaceous carcinoma (Malignant) SEBACEOUS ADENOMA Benign tumours composed of incompletely
Clear Cell Sarcoma of the Foot: A Case Report of Malignant Melanoma of Soft Parts
 Clear Cell Sarcoma of the Foot: A Case Report of Malignant Melanoma of Soft Parts by Al Kline, DPM The Foot & Ankle Journal 1 (3): 3 A case report is presented describing a clear cell sarcoma of the foot
Clear Cell Sarcoma of the Foot: A Case Report of Malignant Melanoma of Soft Parts by Al Kline, DPM The Foot & Ankle Journal 1 (3): 3 A case report is presented describing a clear cell sarcoma of the foot
Case: The patient is a 24 year- old female who was found to have multiple mural nodules within the antrum. Solid and cystic components were noted on
 Case: The patient is a 24 year- old female who was found to have multiple mural nodules within the antrum. Solid and cystic components were noted on imaging. There is no significant past medical history.
Case: The patient is a 24 year- old female who was found to have multiple mural nodules within the antrum. Solid and cystic components were noted on imaging. There is no significant past medical history.
Distant and Lymph Node Metastases of Thyroid Nodules with No Pathological Evidence of Malignancy: A Limitation of Pathological Examination
 Endocrine Journal 2008, 55 (5), 889 894 Distant and Lymph Node Metastases of Thyroid Nodules with No Pathological Evidence of Malignancy: A Limitation of Pathological Examination YASUHIRO ITO, TOMONORI
Endocrine Journal 2008, 55 (5), 889 894 Distant and Lymph Node Metastases of Thyroid Nodules with No Pathological Evidence of Malignancy: A Limitation of Pathological Examination YASUHIRO ITO, TOMONORI
ORIGINAL ARTICLE. Regional Lymph Node Metastasis From Cutaneous Squamous Cell Carcinoma
 ORIGINAL ARTICLE Regional Lymph Node Metastasis From Cutaneous Squamous Cell Carcinoma Dennis H. Kraus, MD; John F. Carew, MD; Louis B. Harrison, MD Objective: To characterize clinical presentation and
ORIGINAL ARTICLE Regional Lymph Node Metastasis From Cutaneous Squamous Cell Carcinoma Dennis H. Kraus, MD; John F. Carew, MD; Louis B. Harrison, MD Objective: To characterize clinical presentation and
Hiroyuki Hanakawa, Nobuya Monden, Kaori Hashimoto, Aiko Oka, Isao Nozaki, Norihiro Teramoto, Susumu Kawamura
 Accepted Manuscript Radiation-induced laryngeal angiosarcoma: Case report Hiroyuki Hanakawa, Nobuya Monden, Kaori Hashimoto, Aiko Oka, Isao Nozaki, Norihiro Teramoto, Susumu Kawamura PII: S2468-5488(18)30005-5
Accepted Manuscript Radiation-induced laryngeal angiosarcoma: Case report Hiroyuki Hanakawa, Nobuya Monden, Kaori Hashimoto, Aiko Oka, Isao Nozaki, Norihiro Teramoto, Susumu Kawamura PII: S2468-5488(18)30005-5
Directly Coded Summary Stage Melanoma
 Directly Coded Summary Stage Melanoma National Center for Chronic Disease Prevention and Health Promotion Division of Cancer Prevention and Control, National Program of Cancer Registries Directly Coded
Directly Coded Summary Stage Melanoma National Center for Chronic Disease Prevention and Health Promotion Division of Cancer Prevention and Control, National Program of Cancer Registries Directly Coded
performed to help sway the clinician in what the appropriate diagnosis is, which can substantially alter the treatment of management.
 Hello, I am Maura Polansky at the University of Texas MD Anderson Cancer Center. I am a Physician Assistant in the Department of Gastrointestinal Medical Oncology and the Program Director for Physician
Hello, I am Maura Polansky at the University of Texas MD Anderson Cancer Center. I am a Physician Assistant in the Department of Gastrointestinal Medical Oncology and the Program Director for Physician
Invasive Papillary Breast Carcinoma
 410 This is an Open Access article licensed under the terms of the Creative Commons Attribution- NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the
410 This is an Open Access article licensed under the terms of the Creative Commons Attribution- NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the
Cutaneous Adnexal Tumors
 Cutaneous Adnexal Tumors Lesions with Predominant Follicular Differentiation Special Emphasis on Basal Cell Carcinoma 2014-04-01 Prof. Dr. med. Katharina Glatz Pathologie Cutaneous Adnexal Tumors Hair
Cutaneous Adnexal Tumors Lesions with Predominant Follicular Differentiation Special Emphasis on Basal Cell Carcinoma 2014-04-01 Prof. Dr. med. Katharina Glatz Pathologie Cutaneous Adnexal Tumors Hair
Cutaneous metastases. Thaddeus Mully. University of California, San Francisco Professor, Departments of Pathology and Dermatology
 Cutaneous metastases Thaddeus Mully University of California, San Francisco Professor, Departments of Pathology and Dermatology DISCLOSURE OF RELATIONSHIPS WITH INDUSTRY Thaddeus Mully Course C005 Essential
Cutaneous metastases Thaddeus Mully University of California, San Francisco Professor, Departments of Pathology and Dermatology DISCLOSURE OF RELATIONSHIPS WITH INDUSTRY Thaddeus Mully Course C005 Essential
Malignant Peripheral Nerve Sheath Tumor
 C H A P T E R 120 Malignant Peripheral Nerve Sheath Tumor Currently, malignant peripheral nerve sheath tumor (MPNST) is the most commonly used generic name for the neoplasms known in the past as neurosarcoma,
C H A P T E R 120 Malignant Peripheral Nerve Sheath Tumor Currently, malignant peripheral nerve sheath tumor (MPNST) is the most commonly used generic name for the neoplasms known in the past as neurosarcoma,
Diagnostic Value of Immunohistochemistry in Soft Tissue Tumors
 Original Article DOI: 10.21276/APALM.1637 Diagnostic Value of Immunohistochemistry in Soft Tissue Tumors Sridevi. V*., Susruthan Muralitharan., and Thanka. J Dept of Pathology, SriMuthukumaran Medical
Original Article DOI: 10.21276/APALM.1637 Diagnostic Value of Immunohistochemistry in Soft Tissue Tumors Sridevi. V*., Susruthan Muralitharan., and Thanka. J Dept of Pathology, SriMuthukumaran Medical
Brief History. Identification : Past History : HTN without regular treatment.
 Brief History Identification : Name : 陳 x - Admission : 94/10/06 Gender : male Age : 75 y/o Chief Complaint : Urinary difficulty for months. Past History : HTN without regular treatment. Brief History
Brief History Identification : Name : 陳 x - Admission : 94/10/06 Gender : male Age : 75 y/o Chief Complaint : Urinary difficulty for months. Past History : HTN without regular treatment. Brief History
A 60-year old Man with Left Jaw Mass. Simon Chiosea, MD University of Pittsburgh medical Center 3/15/2016
 ACCME/Disclosures The USCAP requires that anyone in a position to influence or control the content of CME disclose any relevant financial relationship WITH COMMERCIAL INTERESTS which they or their spouse/partner
ACCME/Disclosures The USCAP requires that anyone in a position to influence or control the content of CME disclose any relevant financial relationship WITH COMMERCIAL INTERESTS which they or their spouse/partner
Dermatopathology: The tumor is composed of keratinocytes which show atypia, increase mitoses and abnormal mitoses.
 Squamous cell carcinoma (SCC): A common malignant tumor of keratinocytes arising in the epidermis, usually from a precancerous condition: 1- UV induced actinic keratosis, usually of low grade malignancy.
Squamous cell carcinoma (SCC): A common malignant tumor of keratinocytes arising in the epidermis, usually from a precancerous condition: 1- UV induced actinic keratosis, usually of low grade malignancy.
Cutaneous Mesenchymal Neoplasms with EWSR1 Rearrangement
 Cutaneous Mesenchymal Neoplasms with EWSR1 Rearrangement By Konstantinos Linos MD, FCAP, FASDP Bone, Soft Tissue and Dermatopathology Assistant Professor of Pathology Dartmouth-Hitchcock Medical Center
Cutaneous Mesenchymal Neoplasms with EWSR1 Rearrangement By Konstantinos Linos MD, FCAP, FASDP Bone, Soft Tissue and Dermatopathology Assistant Professor of Pathology Dartmouth-Hitchcock Medical Center
Case #1: 75 y/o Male (treated and followed by prostate cancer oncology specialist ).
 SOLID TUMORS WORKSHOP Cases for review Prostate Cancer Case #1: 75 y/o Male (treated and followed by prostate cancer oncology specialist ). January 2009 PSA 4.4, 20% free; August 2009 PSA 5.2; Sept 2009
SOLID TUMORS WORKSHOP Cases for review Prostate Cancer Case #1: 75 y/o Male (treated and followed by prostate cancer oncology specialist ). January 2009 PSA 4.4, 20% free; August 2009 PSA 5.2; Sept 2009
Melanocytic proliferations in sundamaged
 Atypical Spitzoid Tumor: What Does It Mean And How Should It Be Managed? Melanocytic proliferations in sundamaged skin Jane L. Messina, Jane L. Messina MD International Melanoma Pathology Working Group
Atypical Spitzoid Tumor: What Does It Mean And How Should It Be Managed? Melanocytic proliferations in sundamaged skin Jane L. Messina, Jane L. Messina MD International Melanoma Pathology Working Group
case report Oman Medical Journal [2016], Vol. 31, No. 1: 60 64
![case report Oman Medical Journal [2016], Vol. 31, No. 1: 60 64 case report Oman Medical Journal [2016], Vol. 31, No. 1: 60 64](/thumbs/90/102852192.jpg) case report Oman Medical Journal [2016], Vol. 31, No. 1: 60 64 Malignant Gastric Glomus Tumor: A Case Report and Literature Review of a Rare Entity Shaesta Zaidi * and Maha Arafah Department of Histopathology,
case report Oman Medical Journal [2016], Vol. 31, No. 1: 60 64 Malignant Gastric Glomus Tumor: A Case Report and Literature Review of a Rare Entity Shaesta Zaidi * and Maha Arafah Department of Histopathology,
