Int J Clin Exp Pathol 2014;7(12): /ISSN: /IJCEP
|
|
|
- Calvin Austin
- 6 years ago
- Views:
Transcription
1 Int J Clin Exp Pathol 2014;7(12): /ISSN: /IJCEP Case Report Mammary analog secretory carcinoma of salivary gland with high-grade histology arising in hard palate, report of a case and review of literature Wenyi Luo 1, Sarah W Lindley 1, Peter H Lindley 2, Gregory A Krempl 3, Raja R Seethala 4, Kar-Ming Fung 1 Departments of 1 Pathology, 2 Radiology, 3 Otorhinolaryngology, University of Oklahoma Health Sciences Center, 4 Department of Pathology, University of Pittsburgh Health System Received October 16, 2014; Accepted December 1, 2014; Epub December 1, 2014; Published December 15, 2014 Abstract: Mammary gland analog secretary carcinoma (MASC) of salivary gland is typically a tumor of low histologic grade and behaves as a low-grade malignancy with relatively benign course. This tumor shares histologic features, immunohistochemical profile, and a highly specific genetic translocation, ETV6-NTRK3, with secretory carcinoma of breast. Histologically, it is often mistaken as acinic cell carcinoma, adenocarcinoma not otherwise specified, and other primary salivary gland tumors. Here we report a case of MASC with high-grade transformation and cervical lymph node metastases confirmed with ETV6-NTRK3 translocation arising in the hard palate of a 41 year-old adult. Interestingly, the metastatic carcinoma has lower grade than the original tumor which strongly support malignant transformation of the original tumor. Most commonly, MASC arises from the parotid gland and less often in minor salivary glands. Metastasis is relatively uncommon and high-grade histology has only been reported in four cases with three of them arising from the parotid gland and the location of the fourth one has not been reported. This is the first case with high grade histology that arise from minor salivary gland and it emphasizes the importance of molecular screening of salivary gland tumor with high-grade histology for ETV6-NTRK3 translocation. In our literature of 115 cases that includes the current case, MASC occurred predominantly in adult with only a few cases under 18 years of age and a male to female ratio of 1.2:1. Parotid gland is more commonly affected but there is also significant occurrence in minor salivary glands. Except for the cases with high grade histology, the overall prognosis is good. Keywords: Analog secretary carcinoma, salivary gland, high grade, immunohistochemistry Introduction Mammary analog secretory carcinoma (MASC) is a recently recognized malignancy arising in salivary glands [1] with striking resemblance to secretory carcinoma of the breast. MASC and secretory carcinoma of the breast (SCB) share the common feature of a balanced translocation, t(12;15)(p13;q25) creating a ETV6-NTRK3 fusion [1]. Both MASC and SCB are immunoreactive for S100, epithelial membrane antigen, mammoglobin, and vimentin and are triple negative (non-immunoreactive for estrogen receptor/progesterone receptor and negative for Her2/Neu mutation) [1-3]. While MASC is an indolent tumor, SCBs that occur in children are also indolent in nature. MASC has joined the ranks of salivary gland tumors, along with pleomorphic adenoma and adenoid cystic carcinoma, that occurs also in breast [4]. To this date, over 100 cases have been reported in the literature [1, 5-26]. Except for the few cases that are reported in adolescents, the majority occurred in adults with painless mass involving the parotid as the most common presentation. MASC is typically a low-grade malignancy with low-grade histopathologic features. However, due to its rather non-specific histopathologic features, MACS can be easily be mistaken with primary adenocarcinoma and acinic cell carcinoma. Differentiation of MASC from its mimickers is important due to their differences in behavior. Here, we report a case that occurred in the palate, an unusual location for MASC, with highgrade transformation and metastases to cervical lymph nodes. MASC with high-grade histology is rare and only 4 case has been reported [19, 25] to this date with three of them
2 Figure 1. Clinical imaging: The lesion (arrow) has no significant bone erosion on CT scan (A). Coronal (B) and T1- weighted axial (C) MRI demonstrated a lesion that has thickened the palate and accompanied by reactive inflammatory changes in the left maxillary sinus. Figure 2. Biopsy specimen: A few small neoplastic glands with pale eosinophilic secretion are present at the periphery of the tumor (A) and the tumor cells have small to medium sized nuclei without prominent nuclei (B). The bulk of the neoplastic component is composed of solid cords and trabeculae of cells separated by thin fibrous septa (C). The nuclei are enlarged and contain prominent nucleoli (D) in contrast to those with gland formation as illustrated in (B). Original magnification in (A) and (C) is 20, in (B) and (D) is 60. arising from the parotid gland and the location of the fourth has not been documented. This is the first case of MASC with high-grade transformation arising in minor salivary glands. It further emphasizes the importance of immunohistochemical profiling and molecular pathology 9009 Int J Clin Exp Pathol 2014;7(12):
3 Table 1. Antibody used in this study Antibody Clone Dilution Source BAF :100 BD Biosciences Calponin EP798Y RTU* Cell Marque Cytokeratin 5/6 D5/16B4 RTU Ventana Cytokeratin 7 OV-TL 12/30 1:100 DAKO Cytokeratin 8/18 5D3 RTU Biocare Medical Epidermal growth factor receptor 3C6 RTU Ventana Epithelial membrane antigen E29 RTU Cell Marque GCDFP-15 D6 1:40 Covance Ki RTU Ventana Mammoglobin 304-1A5, 31A5 RTU Zeta Corporation P63 BC4A4 RTU Biocare Medical S100 Polyclonal RTU Ventana Vimentin 3B4 RTU Ventana P53 Bp53-11 RTU Ventana Beta-catenin 14 RTU Cell Marque Ki RTU Ventana *RTU: Ready to use pre-diluted anitbodies as supplied by the vender. screening in an otherwise non-suspicious carcinoma arising from the salivary glands. This report is accompanied with a literature review. Case presentation A 41 year-old female presented with a one year history of painful ulcer in her hard palate. Physical exam revealed a 2 cm ulcerated crater located in her left palate at the junction between her hard and soft palates with minimal surrounding induration, and a firm, enlarged left cervical lymph node. The patient did not have any other significant comorbidities or constitutional manifestations. There was no clinical or imaging evidence of distant metastasis. No significant bone erosion was demonstrated by computer assisted tomography (CT) (Figure 1A). Magnetic resonance imaging (MRI) identified a cm mildly enhanced centrally ulcerative lesion at the left posterior aspect of her hard palate with minimal surrounding edema (Figure 1B, 1C). The lesion extended laterally to the maxillary buttress and immediately adjacent to what appeared to be inflammatory changes of the mucosa of the left maxillary sinus. Posterior edge of the lesion extended to the greater palate foramina but there was no convincing imaging evidence of perineural spread proximal to that location. A pathologically enlarged left level IIa lymph node, cm, and an enlarged right level IIa lymph node, 1.8 cm, were identified. There were prominent but not significant (by MRI size criteria) lymph nodes at left level Ib and bilat- eral level IIb. There was also a prominent superficial node of the left parotid that was thought likely to be reactive. A biopsy was performed in an outside hospital followed by left wide excision of left palate with partial maxillectomy and ipsilateral neck dissection. The patient was treated by radiation therapy and was disease free 10 months after the resection. The tumor in the biopsy specimen was composed of two contrasting areas. At the edge of the lesion were small amount of neoplastic epithelial proliferation with gland formation containing pale eosinophilic secretion (Figure 2A and 2B). The tumor cells in this area had eosinophilic cytoplasm and small to medium sized nuclei without prominent nucleoli. The bulk (approximately over 80%) of the tumor was composed of solid proliferation of neoplastic epithelial cells arranged in cords and trabeculae separated by delicate fibrovascular septa. No gland formation was noted in these areas (Figure 2C). In contrast to the areas with glandular formation, the nuclei in solid areas were large and contain prominent nucleoli (compare Figure 2D and 2B). The solid area closely mimicked an adenocarcinoma not otherwise specified (ANOS). Perineural invasion and lymphovascular invasion were also identified. Immunohistochemistry showed focally positive immunoreactivity for mammoglobin in the glandular area. Tumor cells also demonstrated diffuse positivity with AE1/3, CK7, S-100, and vimentin. The tumor cells were weakly immunoreactive for epithelial membrane antigen, polyconal carcinoembryonic antigen, CD117, synaptophysin, and CD56. DOG-1 is focally and weakly immunoreactive. P63, glial fibrillary acidic protein, smooth muscle actin, muscle specific actin, myosin heavy chain, caldesmon, and melan-a were negative. MIB-1 proliferative index ranges from 10 to 20%. Please refer to Table 1 for details of the antibodies used in this study. Fluorescent in situ hybridization (FISH) confirmed ETV Int J Clin Exp Pathol 2014;7(12):
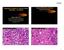
4 Figure 3. Resection specimen: Areas with neoplastic gland formation (A) are noted mainly at the periphery of the tumor. These glands contain small amount of pale eosinophilic secretion (B). The bulk of the tumor is solid and is composed of cords or nests of cells with high-grade nuclei with prominent nucleoli separated by thin fibrous septa with delicate blood vessels (C and D). Multiple mitoses are present (arrows in D). Infiltrating tumor with desmomplastic reaction is also noted (E). Histology of the metastasis to cervical lymph nodes includes cystic (F) growth pattern (G) with low-grade nuclei (inset in F), papillary growth pattern (G) with low-grade nuclei (inset in G), and solid areas (H) with high-grade nuclei (inset in H). Secretions in the areas are strongly positive for PAS stain (I). Original magnification in (A, C, E-I) and is 20 ; in (B), (D), and insets in (F), (G), and (H) is 60. NTRK3 fusion. A diagnosis of MASC with highgrade changes was made. Similar to the biopsy material, the bulk of the tumor in the resection specimen is composed of solid neoplastic epithelial proliferation with a minor component with neoplastic glands and microcysts at the periphery that contained pale eosinophilic secretion (Figure 3A). In contrast to the biopsy specimen, enlarged nuclei with prominent nucleoli were noted in the glandular epithelial cells (Figure 3B). The solid component was composed of solid cords and nests of neoplastic cells separated by a variable amount of fibrotic tissue containing delicate blood vessels (Figure 3C and 3D). The tumor cells were mitotically active (Figure 3D). Bone erosion and perineural invasion were also identified. The tumor cells were featured by a moderate amount of amphophilic to pale eosinophilic cytoplasm with high-grade nuclei. Irregular invading islands of neoplastic cells accompanied by desmoplastic reactions were noted in some areas (Figure 3E). Necrosis was not readily seen. Metastatic foci ranging from 0.2 to 3.9 cm were identified in three cervical lymph nodes. Interestingly, the metastases contained areas with both high-grade and low-grade nuclei. In addition, the metastases contained both cystic (Figure 3F) and papillary growth patterns (Figure 3G) with low-grade nuclei. These components were not present in the primary tumor. In addition, solid area with high-grade nuclei (Figure 3H) and areas with gland formation 9011 Int J Clin Exp Pathol 2014;7(12):
5 Figure 4. Immunohistochemistry: Expression of cytokeratin 7 is patchy in areas with gland formation (A) and is mostly found at the base of the lining cells (inset in A) but the expression is diffuse in solid areas (B). Expression of cytokeratin 8/18 is only focal in areas with gland formation (C) but is wide spread in solid areas (D). In the metastasis, the Ki67 labeling index is low in the papillary area (E) but high in the solid areas (F). Original magnification in all panels is 20 and in all insets is 60. classic for MASC but with high grade nuclei similar to those in the primary tumor were also present in the metastases. Secretions of the neoplastic glands were strongly positive for periodic acid Schiff (PAS) reaction (Figure 3I). Immunohistochemistry demonstrated different staining patterns between areas with glandular architecture and solid areas. Immunoreactivities of cytokeratin 7 (Figure 4A and 4B) and cytokeratin 8/18 (Figure 4C and 4D) were patchy in areas with glands and microcysts but the expression is diffuse in solid areas. S100, BAF47, and vimentin were diffusely immunoreactive. Similar expression of S100 protein is detected in areas with glands and microcysts 9012 Int J Clin Exp Pathol 2014;7(12):
6 Table 2. Reported cases of MASC Age (year) Sex Location Size (greatest dimension)/pathologic Features Reference/Remarks 41 F Hard and soft palate 1.8 cm/uncerated mass, predominantly solid with microcystic component, high-grade features present ATD: PNI+/DI-/M+*, lymphovascular invasion identified Leg. 1 Leg. 1 Oral cavity not specified 1.8 cm/macrocstic ATD:PNI-/DI+/N-/M- Leg. 1 Leg. 1 Parotid 3.0 cm/solid ATD: PNI-/DI-/N-/M- Leg. 1 Leg. 1 Submandibular 1.8 cm/solid ATD: PNI+/DI+/N-/M- Leg. 1 Leg. 1 Oral cavity roof of mouth 0.5 cm/ Solid exophytic polyp ATD: PNI+/DI+/N-/M- Leg. 1 Leg. 1 Oral cavity inner cheek NA/Mixed solid and cystic ATD: PNI-/DI-/N-/M- Leg. 1 Leg. 1 Parotid 2.9 cm/ Mixed solid and cystic ATD: PNI+/DI-/N-/M- Leg. 1 Leg. 1 Lip 1.2 cm/solid ATD: PNI+/DI+/N-/M- 37 F Parotid, deep lobe 2.0 cm/microcystic, cribiform, and tubular, FNA was performed ATD: PNI+/DI+/N-/M- Current case 2012 Connor et al Connor et al Connor et al Connor et al Connor et al Connor et al Connor et al Ito et al. Leg. 2 F Leg. 2 All cases were originally diagnosed as AciCC. See Leg. 2 for details Seethala et al. Leg. 2 M Leg. 2 All cases were originally diagnosed as AciCC. See Leg. 2 for details Seethala et al. Leg. 2 M Leg. 2 All cases were originally diagnosed as AciCC. See Leg. 2 for details Seethala et al. Leg. 2 M Leg. 2 All cases were originally diagnosed as AciCC. See Leg. 2 for details Seethala et al. Leg. 2 M Leg. 2 All cases were originally diagnosed as AciCC. See Leg. 2 for details Seethala et al. Leg. 2 M Leg. 2 All cases were originally diagnosed as AciCC. See Leg. 2 for details Seethala et al. Leg. 2 M Leg. 2 All cases were originally diagnosed as AciCC. See Leg. 2 for details Seethala et al. Leg. 2 M Leg. 2 All cases were originally diagnosed as AciCC. See Leg. 2 for details Seethala et al. Leg. 2 M NA All cases were originally diagnosed as AciCC. See Leg. 2 for details Seethala et al. 69 F Parotid 3.0 cm/microcystic, tubular, papillary, and solid, FNA was performed ATD: PNI-/DI: ND/N-/M- 48 F Upper lip (submucosal) 1 cm/microcystic 52 M Lower lip (submucosal) 0.7 cm/cribiform, follicular 44 M Upper lip (submucosal) 0.3 cm/ Microcystic 34 F Upper lip 1.5 cm/tubular, follicular, microcystic and macrocystic ATD: PNI: ND/DI: -/M: - 58 M Parotid 2.0 cm/tubular, follicular, microcystic and macrocystic ATD: PNI: ND/DI: -/M: Pisharodi et al Kratochvil et al Kratochvil et al Kratochvil et al Laco et al Laco et al. 71 M Buccal 1.0 cm/original diagnosis was AciCC, see Leg. 3 for details Bishop et al. 25 F Hard palate NA/Original diagnosis was AciCC, see Leg. 3 for details Bishop et al. 20 F Soft palate 0.9 cm/original diagnosis was AciCC, see Leg. 3 for details Bishop et al. 86 F Soft palate 1.0 cm/original diagnosis was AciCC, see Leg. 3 for details Bishop et al. 79 F Soft palate 0.7 cm/original diagnosis was AciCC, see Leg. 3 for details Bishop et al. 62 F Upper lip 0.3 cm/original diagnosis was AciCC, see Leg. 3 for details Bishop et al Int J Clin Exp Pathol 2014;7(12):
7 71 M Upper lip 0.6 cm/original diagnosis was AciCC, see Leg. 3 for details Bishop et al. 59 M Lower lip 0.9 cm/original diagnosis was AciCC, see Leg. 3 for details Bishop et al. 68 M Lower lip 0.5 cm/original diagnosis was AciCC, see Leg. 3 for details Bishop et al. 34 F Submandibular gland 0.9 cm/original diagnosis was AciCC, see Leg. 3 for details Bishop et al. 36 F Submandibular gland 2.0 cm/original diagnosis was AciCC, see Leg. 3 for details Bishop et al. 58 F Parotid, deep lobe 2.0 cm/solid, cribiform, microcystic and macrocystic, FNA was performed 53 M Parotid 3.0 cm/micropapillary, microcystic, and solid, original diagnosis was AciCC 29 M Parotid 1.8 cm/micropapillary, microcystic, and solid, original diagnosis was AciCC 61 F Parotid 3.0 cm/ Micropapillary, microcystic, and solid, original diagnosis was AciCC 51 F Bucal mucosa 1.0 cm/leg F Parotid 0.9 cm/leg. 4 ATD: PNI: ND/DI: ND/N-/M- 48 M Soft palate 1.5 cm/leg. 4 The patient developed metastasis and died of disease 4 after two years after initial diagnosis. 55 M Parotid 5.5 cm/leg. 4 ATD: PNI: ND/DI: ND/N: +/M: - 34 M Parotid 1.6 cm/leg M Parotid 1.5 cm/leg M Parotid 3.5 cm/leg. 4 The patient has multiple recurrence and died of disease after 6 years 55 F Parotid 1.0 cm/leg. 4 Multiple recurrence 26 M Parotid 1.5 cm/leg F Parotid 3.0 cm/leg M Parotid 1.4 cm/leg. 4 ATD: PNI: ND/DI: ND/M: - 55 M Parotid 4.0 cm/leg. 4 ATD: PNI: ND/DI: ND/M: - 59 F Parotid Size not available/leg. 4 ATD: PNI: ND/DI: ND/M: - 21 F Parotid 2.7 cm/leg. 4 ATD: PNI: ND/DI: ND/M: - 75 F Parotid 0.7 cm/leg. 4 ATD: PNI: ND/DI: ND/M: - 32 M Upper lip 1.0 cm/leg. 4 ATD: PNI: ND/DI: ND/M: - Lymph node metastasis at 86 months after diagnosis, no evidence of disease for 27 months after treatment 2013 Sethi et al Pinto et al Pinto et al Pinto et al Int J Clin Exp Pathol 2014;7(12):
8 34 F Parotid 1.0 cm/follicular and microcystic ATD: PNI: ND/DI: ND/M: - Mammoglobin positive, no translocation confirmed by FISH 2012 Levine et al. Leg. 5 Leg. 5 Submandibular gland Leg. 5, originally diagnosed as ANOS 2012 Seethala et al. Leg. 5 Leg. 5 Submandibular gland Leg. 5, originally diagnosed as ANOS 2012 Seethala et al. Leg. 5 Leg. 5 Submandibular gland Leg. 5, originally diagnosed as ANOS 2012 Seethala et al. Leg. 5 Leg. 5 Soft palate Leg. 5, originally diagnosed as ANOS 2012 Seethala et al. Leg. 5 Leg. 5 Soft palate Leg. 5, initial diagnosis was MASC 2012 Seethala et al. Leg. 5 Leg. 5 Soft palate Leg. 5, initial diagnosis was MASC 2012 Seethala et al. Leg. 5 Leg. 5 Buccal mucosa Leg. 5, initial diagnosis was MASC 2012 Seethala et al. Leg. 5 Leg. 5 Buccal mucosa Leg. 5, initial diagnosis was MASC 2012 Seethala et al. Leg. 5 Leg. 5 Base of tongue Leg. 5, originally diagnosed as ANOS 2012 Seethala et al. Leg. 5 Leg. 5 Upper lip Leg. 5, initial diagnosis was MASC 2012 Seethala et al. 71 F Soft Palate Leg Fehr et. al 23 F Parotid Leg Fehr et. al 70 F Parotid Leg Fehr et. al 43 M Oral mucosa Leg Fehr et. al 37 F Parotid 0.5 cm/originally diagnosed as salivary adenoma 2013 Choisea et al Int J Clin Exp Pathol 2014;7(12):
9 Leg. 7 F 11 parotid/2 non-parotid Leg Jung et al. Leg. 7 F 11 parotid/2 non-parotid Leg Jung et al. Leg. 7 F 11 parotid/2 non-parotid Leg Jung et al. Leg. 7 F 11 parotid/2 non-parotid Leg Jung et al. Leg. 7 F 11 parotid/2 non-parotid Leg Jung et al. 51 F Parotid Reported twice (R03, R12) 51 M Buccal mucosa Reported twice (R03, R12) 27 M Parotid Reported twice (R03, R12) 2.5 cm/fna performed 2.1 cm/fna performed 1.0 cm/fna performed 44 F Submandibular gland 1.8 cm/fna performed ATD: PNI: ND/DI: ND/N: +/M: - 23 F Parotid 1.2 cm/ FNA performed 66 M Parotid NA/ FNA performed 2013 Griffith et al Griffith et al Griffith et al Griffith et al Griffith et al Griffith et al. Unknown M Parotid 2.2 cm/originally diagnosed as AicCC 2012 Choisea et al. 41 F Hard palate 0.4 cm/ originally diagnosed as mucoepidermoid carcinoma 2012 Choisea et al. 36 M Submandibular gland 2.5 cm/ Solid, microcystic and macrocystic growth pattern, FNA performed 2012 Yan et al. 14 F Parotid 3.0 cm/ ATD: PNI: ND/DI: ND/N: +/M: - (metastasis in a periparotid lymph node) 55 M Parotid 8.0 cm ATD: PIN: ND/DI: ND/N: -/M: -/high-grade histology Recurred locally 6 years later. 61 M Parotid 4 cm/fna performed ATD: PIN+/DI: ND/N+/M+ (single metastatic focus in adipose tissue of the neck) Patient died of disseminated disease after 20 months 73 M Parotid Size is unknown, originally diagnosed as a monomorphic adenoma Recurrence for 4 times and the patient died 4 years after the primary surgery 2013 Melin-Aldana et al Skálová A et al Skálová A et al Skálová A et al. 43 F Submandibular gland Microcystic, tubular and solid 2014 Shah AA et al. 23 F Parotid 1.2 cm/fna performed Microcyctic and pseudopapillary 2014 Shah AA et al. 34 F Periparotid lymph node Microcystic, macrocystic, solid and papillary 2014 Shah AA et al. 76 F Parotid Microcystic, macrocystic, and papillary 2014 Shah AA et al. 71 M Parotid Microcystic and macrocystic 2014 Shah AA et al. 55 F Parotid Macrocystic and solid 2014 Shah AA et al. 16 F Parotid Microcystic and solid 2014 Shah AA et al. 22 M Parotid Microcystic, macrocystic and solic 2014 Shah AA et al Int J Clin Exp Pathol 2014;7(12):
10 26 M Parotid Predominently papillary and pseudopapillary with focal microcystic areas 2014 Shah AA et al. 56 M Parotid Papillary, microcystic and macrocystic 2014 Shah AA et al. 45 F Parotid Microcystic, macrocystic and focal papillary 2014 Shah AA et al. 37 F Parotid Macrocystic and focally microcystic 2014 Shah AA et al. 53 M Parotid Microcystic and solid 2014 Shah AA et al. 46 F Parotid Microcystic and solid 2014 Shah AA et al. 56 M Parotid Microcystic, macrocystic, papillary and pseudopapillary 2014 Shah AA et al. 28 F Parotid Microcystic, tubular and solid 2014 Shah AA et al. Unknown F Parotid Microcystic, tubular and solid 2014 Shah AA et al. 66 F Parotid Microcystic and solid 2014 Shah AA et al. 53 M Submandibular Microcystic, macrocystic, tubular and solid 2014 Shah AA et al. : Unless otherwised stated in the table, ETV6-NTRK3 translocation is confirmed by FISH; ATD: At the time of diagnosis; PNI: Perineural invasion; DI: Duct involvement; N: Metastasis to cervical lymph nodes or periparotid lymph node; M: Distant metastasis; *: Unless otherwise specified, lymphovascular invasion is described in the original report; NA: Not available; ND: Not described in original report; FNA: Fine needle aspiration; Leg. 1: In this study, the age range was 14 to 77 years (mean, 40 y) with 6 males and 1 female. Further demographic details were not provided in the original publication. Leg. 2: A total of 10 cases were described (8 males, 2 females). The average age was 45.5 years but detailed distribution of age was not provided. There were metastases in 2 out of the 6 cases who received lymph node dissection. All cases were originally diagnosed as acinic cell carcinoma (AciCC). The locations of the tumors were not provided. Since AciCC is most common in parotid gland, the location of these tumors can be assumed to be predominantly the parotid gland. The status for perineural invasion, ductal involvement, and metastases were not provided in the original report. Leg. 3: Perineural invasion was identified in 1 cases but lymphovascular invasion was not identified. Ductal involvement or metastases were not described in the original report. Leg. 4: These tumors were originally diagnosed as acinic cell carcinoma, adenoid cystic carcinoma, cysadenocarcinoma, and low-grade carcinoma not otherwise specified. Leg. 5: The average age in this study was 45.7 years and a male to female ratio of 1.4:1. The average tumor sizes were 1.9 and 2.5 cm respectively depending on whether it is referral or in-house cases respectively. Four cases showed metastases, three cases showed recurrence, and one of the metastatic case resulted in death from disease. Many of these tumors were diagnosed as AciCC, ANOS, mucin secreting signet ring cell carcinoma, and mucoepidermoid carcinoma. Leg. 6: The sizes of tumor and original diagnoses, of these cases were not available in the original report. There was no description of perineural invasion, lymphovascular invasion, lymph node or distant metastasis in the original report. Leg. 7: The age of the cases in this study ranged from 17 to 76 year-old (average is 46.4) cm. The size ranged from 0.7 to 2.5 cm (average 17.7 cm). This is also the first of four cases with high-grade histology. This study also described 10 cases that possessed histologic features of MASC but no ETV6-NTRK3 translocation and these cases were classified as MASCmimickers. No immunohistochemistry for mammoglobin was performed in this study Int J Clin Exp Pathol 2014;7(12):
11 and in solid areas. Both components were negative for calponin, cytokeratin 5/6, epithelial membrane antigen, GCDFP-15, and p63. Homogeneous membranous pattern of betacatenin immunoreactivity was noted in both high and low grade areas. Epidermal growth factor receptor (EGFT) was weakly positive in areas with gland and microcysts but negative in solid areas. In the metastasis where both lowand high-grade areas were present, the Ki67 labeling index is low in the low-grade area with papillary growth pattern (Figure 4E) but high in solid area with high-grade nuclei (Figure 4E). There was no increase in p53 labeling in both low- and high-grade areas. Please refer to Table 1 for details of the antibodies used in this study. Discussion MASC is a recently recognized primary carcinoma arising from salivary glands. It shares with SCB the common features of mammoglobin positive luminal secretion and ETV6-NTRK3 translocation. The patients age ranged from 14 to 86 year-old (Table 2). In contrast, a significant portion of SCB occurred in children, adolescences, and young females [27]. Up to this date, 134 MASC cases have been reported [1, 5-26]. Although a male predilection was initially observed, the incidence is about equally distributed among these 134 reported cases with a male to female ratio of 73:61 [1, 5-17, 21-25]. It typically presents as a painless mass, typically 0.3 to 8.0 cm, with the duration of disease ranging from a few months to multiple recurrences in durations up to 30 years [5]. It can be well circumscribed or uncircumscribed, with or without cystic changes. Extension into the surrounding parenchyma is uncommon [19]. Among these tumors, 91 occurred in parotid, 11 in submandibular gland, 29 in minor salivary glands, and 2 in unspecified area. Histologically, MASC is characterized by a lowgrade neoplastic epithelial proliferation with low-grade nuclei and moderate to ample amount of pink granular cytoplasm. Cytoplasmic vacuoles are not uncommon. The neoplastic cells typically arrange in microcystic, tubular, and, less frequently, solid pattern with PAS positive luminal content and occasional intracytoplasmic mucin [5]. Ductal involvement suggesting a ductal origin has been described [5]. Only 4 cases have been described to harbor highgrade areas indicative of high-grade transformation [19, 25]. Comedo type necrosis has been described in these cases. MASC generally follows the behavior of a low grade malignancy. The overall survival is similar to that of AciCC [16]. Metastasis to lymph nodes, lymphovascular and perineural invasion can occur [25]. Most of the patients live free of disease after treatment. In our literature review, 17 patients experienced local recurrence including the 3 cases reported by Skálová A et al [25], four patients experienced distant metastasis, and only 6 patients died of disease including 2 out of the 3 cases reported by Skálová A et al [25]. Although high-grade transformation or dedifferentiation is rare, it has been reported in four recent case [19, 25]. All of the four tumors are composed of two distinctive areas with classic low-grade microcystic appearance in one area and well-demarcated, high-grade solid nests in other areas. Interestingly, one case was originally reported as a dedifferentiation of AciCC [19] and the other as monomorphic adenoma [25]. There are three major highlights of this case that separate it from the previously reported cases with high grade histology. First, it occurred in the hard palate while 3 out of the 4 reported case with high-grade histology occurred in the parotid gland [19, 25]. Second, the primary tumor is dominated by high-grade solid component. Third, the metastatic carcinoma in this case, however, has a rich diversification on histology which includes cystic and papillary, cystic and glandular growth pattern with high grade nuclei. Due to differences in clinical behavior and prognosis from its mimickers, it is important to correctly recognize MASC. MASC is characterized by microcysts with luminal secretion that is positive for PAS and mammoglobin [1]. It can also present with macrocysts, papillary proliferation, or cribriform pattern [6, 9, 11, 16, 17, 19, 20]. Despite the characteristic features of MASC, they can still be confused with other salivary gland tumors. These retrospective studies show that MASC are often misdiagnosed as AciCC or ANOS [7, 10, 13, 17, 19, 22]. Occasional MASC are diagnosed as signet ring adenocarcinoma, mucoepidermoid carcinoma [16] or even salivary adenoma [1, 18]. This 9018 Int J Clin Exp Pathol 2014;7(12):
12 makes immunohistochemical profiling and molecular pathology screening an important step in the characterization of salivary gland tumors. The major mimickers of MASC are AciCC and ANOS. The incidence of AciCC [28] occurs with an even age distribution from the second to seventh decade and occasionally in children and is also the second most common salivary gland tumor arising in children [29]. Over 80% of AciCC occur in the parotid gland follows by intra-oral minor salivary glands and submandibular gland. It is rare in sublingual gland [30]. The incidence in minor salivary gland is higher than submandibular gland. In contrast to AciCC with slight female predominance, MASC has clear male predominance. Histologically, AciCC has a variety of growth pattern, including solid, microcystic, papillary-cystic, and follicular and contains cytologic components including acinic cells, intercalated duct-like cells, vacuolated cells, clear cells, and non specific glandular cells. The histologic pattern overlaps with that of MACS. Acinar and intercalated duct cells are diagnostic and contain cytoplasmic zymogen granules which are PAS positive and diastase resistant. However, they are usually non-reactive to amylase antibody. MASC is otherwise lacking the zymogen granules. One must note that zymogen in high-grade AciCC tumors may not be easily demonstrated by immunohistochemistry and PAS stain and may have significant morphological overlap with MASC. Mammoglobin and the presence of ETV6-NTRK3 translocation are specific markers that distinguish AciCC from MASC. They are usually positive in MASC but negative in AciCC. The features that allow separation of MASC and AciCC are well discussed by Chiosea et al. [7]. The incidence of ANOS is at the fourth to eighth decade with a median age of 67. A male predilection is present. Minor salivary glands are the most common sites (61%) for ANOS followed by parotid (32%) and submandibular (7%) glands. minor salivary glands in palate [31]. Histologically, ANOS is characterized by an infiltrative growth of tumor cells that have glandular or ductal features. They can assume varied patterns including glandular and ductular structures, as well as solid, tubular, nests, islands, and cord-like growth [32]. The overall growth pattern does not resemble any of the named salivary malignancies. Focal findings mimicking specific malignancies may be present but is limited in extent. Extensive presence of specific findings suggests diagnosis of specific malignancy [28, 32]. ANOS has collagenized, myxoid or mucinous stroma. Tumor cells have intracytoplasmic mucin which can be stained with mucicarmine staining [32]. Since the 1992 WHO salivary gland tumor classification, the number of ANOS cases generally descreased and now considered a diminishing group of salivary carcinomas [31]. Other less common mimickers such as signet ring adenocarcinoma, mucoepidermoid carcinoma [16] or salivary adenoma [18] can be distinguished from MASC through astute histopathologic observations as well as demonstration of the absence of ETV6-NTRK3 translocation. Although confirmation of the ETV6-NTRK3 translocation is the gold standard in identifying MASC, it is rather costly and time consuming. Demonstration of mammoglobin, S100, and STAT5 by immunohistochemistry is a suitable combination for initial screening purposes [1]. It should note that STAT5 is expressed widely in both MASC and AciCC. S100 expression and mammoglobin positive secretion are present in all the MASC cases being tested including our case. Their use is however hampered by its expression in a significant proportion of other salivary gland tumors including mucoepidermoid carcinoma, pleomorphic adenoma, polymorphous low-grade adenocarcinoma, salivary duct carcinoma, low-grade cysadenocarcinoma, and ANOS [13, 17]. MASC lacks zymogen granules which distinguish it from AciCC. However, AciCC especially high-grade AciCC can present as zymogen granule poor tumor [16, 33]. DOG1, a marker of salivary acini and intercalated duct differentiation, is positive in all acinic cell carcinoma cases and negative in all three MASC cases published by Andre Pinto [13]. However, it can be positive in MASC [19] and is focally positive in our case. In addition, half of AciCC lacks the positivity [19]. GCDFP- 15, an apocrine marker positive in all MASC of the initial report is negative in some reported cases [5, 10, 19] and our case. Diagnosis will be even more challenging when tumors are mostly composed of high-grade cords or nests. Further study on the sensitivity and specificity of combination of these markers is warranted Int J Clin Exp Pathol 2014;7(12):
13 MASC typically behaves as a low-grade malignancy. A higher than AciCC lymph node involvement was observed but fall short of statistical significance [16]. Although rare, aggressive MASC cases do occur. The clinical significance with difference between aggressive appearing MASC and the histologically typical MASC that behaves as a low-grade malignancy is not clear. The percentage of solid area in the specimen has been suggested as one of the markers to predict the clinical behavior of MASC [5], which seems to be true for our case, where a great percentage of high-grade area is associated with an aggressive behavior. However, for cases mainly composed of low grade cystic patterns, different clinical behaviors are also observed [1]. In several markers that we have used, notably cytokeratin 7 and cytokeratin 8/18, we noticed different staining patterns between the high-grade solid area of our case and the typical area with papillary architecture and cyst formation. These markers are more diffusely expressed in the solid high-grade area than the papillary or cystic areas. The biological significances of these findings are uncertain. A question remains to be answered is what triggers the dedifferentiation of MASC and what it could possibly mean clinically. The pathway for dedifferentiated salivary tumors is unknown. p53 abnormality and Her2 overexpression or amplification have been reported but the frequency varies by the histologic type [33]. Tumor dedifferentiation is associated with an altered expression of many genes [33, 34], possibly including the ETV6-NTRK3 translocation. Although the cause-effect relationship between ETV6-NTRK3 translocation and tumorigenesis in SCB has not been firmly established, murine breast epithelial cells with ETV6- NTRK3 translocation are able to develop orthotopic tumor growth without metastases. The PI3K-Akt signaling pathway in these transformed cells, the known effector pathway of ETV6-NTRK3 translocation, has been shown to be activated in an insulin-like growth factor 1- or insulin-dependent manner. Experimental success of blocking this pathway leading to reduced tumor growth by tyrosine kinase inhibitors targeting the insulin-like growth factor 1 signal pathway suggests the possibilities of using these inhibitors for target therapy [35]. This arena is worth to be further investigated. Acknowledgements We would like to express our most sincere thanks to the technical assistance provided by the histology laboratory of OU Medical Center. Disclosure of conflict of interest None. Address correspondence to: Dr. Kar-Ming Fung, Department of Pathology, The University of Oklahoma Health Sciences Center, BMSB 451, 940 Stanton L. Young Blvd, Oklahoma City, OK 73104, USA. Tel: ; Karming-Fung@ ouhsc.edu References [1] Skalova A, Vanecek T, Sima R, Laco J, Weinreb I, Perez-Ordonez B, Starek I, Geierova M, Simpson RH, Passador-Santos F, Ryska A, Leivo I, Kinkor Z and Michal M. Mammary analogue secretory carcinoma of salivary glands, containing the ETV6-NTRK3 fusion gene: a hitherto undescribed salivary gland tumor entity. Am J Surg Pathol 2010; 34: [2] Lae M, Freneaux P, Sastre-Garau X, Chouchane O, Sigal-Zafrani B and Vincent-Salomon A. Secretory breast carcinomas with ETV6-NTRK3 fusion gene belong to the basal-like carcinoma spectrum. Mod Pathol 2009; 22: [3] Tavassoli FA DP. Pathology and Genetics Tumours of the Breast and Female Genital Organs. Lyon: IARC Press; [4] Pia-Foschini M, Reis-Filho JS, Eusebi V and Lakhani SR. Salivary gland-like tumours of the breast: surgical and molecular pathology. J Clin Pathol 2003; 56: [5] Connor A, Perez-Ordonez B, Shago M, Skalova A and Weinreb I. Mammary analog secretory carcinoma of salivary gland origin with the ETV6 gene rearrangement by FISH: expanded morphologic and immunohistochemical spectrum of a recently described entity. Am J Surg Pathol 2012; 36: [6] Ito S, Ishida E, Skalova A, Matsuura K, Kumamoto H and Sato I. Case report of Mammary Analog Secretory Carcinoma of the parotid gland. Pathol Int 2012; 62: [7] Chiosea SI, Griffith C, Assaad A and Seethala RR. The profile of acinic cell carcinoma after recognition of mammary analog secretory carcinoma. Am J Surg Pathol 2012; 36: [8] Pisharodi L. Mammary analog secretory carcinoma of salivary gland: cytologic diagnosis and differential diagnosis of an unreported entity. Diagn Cytopathol 2013; 41: Int J Clin Exp Pathol 2014;7(12):
14 [9] Kratochvil FJ 3rd, Stewart JC and Moore SR. Mammary analog secretory carcinoma of salivary glands: a report of 2 cases in the lips. Oral Surg Oral Med Oral Pathol Oral Radiol 2012; 114: [10] Laco J, Svajdler M Jr, Andrejs J, Hrubala D, Hacova M, Vanecek T, Skalova A and Ryska A. Mammary analog secretory carcinoma of salivary glands: a report of 2 cases with expression of basal/myoepithelial markers (calponin, CD10 and p63 protein). Pathol Res Pract 2013; 209: [11] Bishop JA, Yonescu R, Batista D, Eisele DW and Westra WH. Most nonparotid acinic cell carcinomas represent mammary analog secretory carcinomas. Am J Surg Pathol 2013; 37: [12] Sethi R, Kozin E, Remenschneider A, Meier J, VanderLaan P, Faquin W, Deschler D and Frankenthaler R. Mammary analogue secretory carcinoma: update on a new diagnosis of salivary gland malignancy. Laryngoscope 2014; 124: [13] Pinto A, Nose V, Rojas C, Fan YS and Gomez- Fernandez C. Searching for mammary analogue [corrected] secretory carcinoma of salivary gland among its mimics. Mod Pathol 2014; 27: [14] Levine P, Fried K, Krevitt LD, Wang B and Wenig BM. Aspiration biopsy of mammary analogue secretory carcinoma of accessory parotid gland: another diagnostic dilemma in matrixcontaining tumors of the salivary glands. Diagn Cytopathol 2014; 42: [15] Fehr A, Loning T and Stenman G. Mammary analogue secretory carcinoma of the salivary glands with ETV6-NTRK3 gene fusion. Am J Surg Pathol 2011; 35: [16] Chiosea SI, Griffith C, Assaad A and Seethala RR. Clinicopathological characterization of mammary analogue secretory carcinoma of salivary glands. Histopathology 2012; 61: [17] Bishop JA, Yonescu R, Batista D, Begum S, Eisele DW and Westra WH. Utility of mammaglobin immunohistochemistry as a proxy marker for the ETV6-NTRK3 translocation in the diagnosis of salivary mammary analogue secretory carcinoma. Hum Pathol 2013; 44: [18] Williams L and Chiosea SI. Mammary analogue secretory carcinoma mimicking salivary adenoma. Head Neck Pathol 2013; 7: [19] Jung MJ, Song JS, Kim SY, Nam SY, Roh JL, Choi SH, Kim SB and Cho KJ. Finding and characterizing mammary analogue secretory carcinoma of the salivary gland. Korean J Pathol 2013; 47: [20] Bishop JA. Unmasking MASC: bringing to light the unique morphologic, immunohistochemical and genetic features of the newly recognized mammary analogue secretory carcinoma of salivary glands. Head Neck Pathol 2013; 7: [21] Griffith CC, Stelow EB, Saqi A, Khalbuss WE, Schneider F, Chiosea SI and Seethala RR. The cytological features of mammary analogue secretory carcinoma: a series of 6 molecularly confirmed cases. Cancer Cytopathol 2013; 121: [22] Lei Y and Chiosea SI. Re-evaluating historic cohort of salivary acinic cell carcinoma with new diagnostic tools. Head Neck Pathol 2012; 6: [23] Petersson F, Lian D, Chau YP and Yan B. Mammary analogue secretory carcinoma: the first submandibular case reported including findings on fine needle aspiration cytology. Head Neck Pathol 2012; 6: [24] Rastatter JC, Jatana KR, Jennings LJ and Melin-Aldana H. Mammary analogue secretory carcinoma of the parotid gland in a pediatric patient. Otolaryngol Head Neck Surg 2012; 146: [25] Skalova A, Vanecek T, Majewska H, Laco J, Grossmann P, Simpson RH, Hauer L, Andrle P, Hosticka L, Branzovsky J and Michal M. Mammary analogue secretory carcinoma of salivary glands with high-grade transformation: report of 3 cases with the ETV6-NTRK3 gene fusion and analysis of TP53, beta-catenin, EGFR, and CCND1 genes. Am J Surg Pathol 2014; 38: [26] Shah AA, Wenig BM, LeGallo RD, Mills SE and Stelow EB. Morphology in Conjunction with Immunohistochemistry is Sufficient for the Diagnosis of Mammary Analogue Secretory Carcinoma. Head Neck Pathol 2014; [Epub ahead of print]. [27] Horowitz DP, Sharma CS, Connolly E, Gidea- Addeo D and Deutsch I. Secretory carcinoma of the breast: results from the survival, epidemiology and end results database. Breast 2012; 21: [28] Ellis G SRHW. Pathology and Genetics of Head and Neck TumoursAcinic cell carcinoma. Lyon: IARC Press; [29] Triantafillidou K, Iordanidis F, Psomaderis K and Kalimeras E. Acinic cell carcinoma of minor salivary glands: a clinical and immunohistochemical study. J Oral Maxillofac Surg 2010; 68: [30] Spiro RH, Huvos AG and Strong EW. Acinic cell carcinoma of salivary origin. A clinicopathologic study of 67 cases. Cancer 1978; 41: [31] Li J, Wang BY, Nelson M, Li L, Hu Y, Urken ML and Brandwein-Gensler M. Salivary adenocar Int J Clin Exp Pathol 2014;7(12):
15 cinoma, not otherwise specified: a collection of orphans. Arch Pathol Lab Med 2004; 128: [32] Wenig BM. Atlas of Head and Neck Pathology. Elsevier Health Sciences, [33] Nagao T. Dedifferentiation and high-grade transformation in salivary gland carcinomas. Head Neck Pathol 2013; 7 Suppl 1: S [34] Costa AF, Altemani A and Hermsen M. Current concepts on dedifferentiation/high-grade transformation in salivary gland tumors. Patholog Res Int 2011; 2011: [35] Tognon CE, Somasiri AM, Evdokimova VE, Trigo G, Uy EE, Melnyk N, Carboni JM, Gottardis MM, Roskelley CD, Pollak M and Sorensen PH. ETV6-NTRK3-mediated breast epithelial cell transformation is blocked by targeting the IG- F1R signaling pathway. Cancer Res 2011; 71: Int J Clin Exp Pathol 2014;7(12):
Mammary analogue secretory carcinoma of salivary gland A case report of new entity
 Case Report Mammary analogue secretory carcinoma of salivary gland A case report of new entity Vaibhav Bhika Bari 1*, Sandhya Unmesh Bholay 2 1 Assistant Professor, 2 Associate Professor Rajiv Gandhi Medical
Case Report Mammary analogue secretory carcinoma of salivary gland A case report of new entity Vaibhav Bhika Bari 1*, Sandhya Unmesh Bholay 2 1 Assistant Professor, 2 Associate Professor Rajiv Gandhi Medical
A Cutaneous Facial Mass Identified as the New Entity Mammary Analogue Secretory Carcinoma of Probable Salivary Gland Origin
 A Cutaneous Facial Mass Identified as the New Entity Mammary Analogue Secretory Carcinoma of Probable Salivary Gland Origin Scott W. Binder, MD Professor and Senior Vice Chair Chief, Dermatopathology Geffen/UCLA
A Cutaneous Facial Mass Identified as the New Entity Mammary Analogue Secretory Carcinoma of Probable Salivary Gland Origin Scott W. Binder, MD Professor and Senior Vice Chair Chief, Dermatopathology Geffen/UCLA
Update in Salivary Gland Pathology. Benjamin L. Witt University of Utah/ARUP Laboratories February 9, 2016
 Update in Salivary Gland Pathology Benjamin L. Witt University of Utah/ARUP Laboratories February 9, 2016 Objectives Review the different appearances of a selection of salivary gland tumor types Establish
Update in Salivary Gland Pathology Benjamin L. Witt University of Utah/ARUP Laboratories February 9, 2016 Objectives Review the different appearances of a selection of salivary gland tumor types Establish
04/09/2018. Salivary Gland Pathology in the Molecular Era Old Friends, Old Foes, & New Acquaintances
 Salivary Gland Pathology in the Molecular Era Old Friends, Old Foes, & New Acquaintances Jennifer L. Hunt, MD, MEd Aubrey J. Hough Jr, MD, Endowed Professor of Pathology Chair of Pathology and Laboratory
Salivary Gland Pathology in the Molecular Era Old Friends, Old Foes, & New Acquaintances Jennifer L. Hunt, MD, MEd Aubrey J. Hough Jr, MD, Endowed Professor of Pathology Chair of Pathology and Laboratory
Int J Clin Exp Med 2016;9(11): /ISSN: /IJCEM Shuqin Wang 1*, Yuncheng Li 2*, Guojun Li 3,4, Lijun Zhu 1*
 Int J Clin Exp Med 2016;9(11):22632-22637 www.ijcem.com /ISSN:1940-5901/IJCEM0033921 Case Report Mammary analogue secretory carcinoma presenting as a salivary gland neoplasm: a first clinical case report
Int J Clin Exp Med 2016;9(11):22632-22637 www.ijcem.com /ISSN:1940-5901/IJCEM0033921 Case Report Mammary analogue secretory carcinoma presenting as a salivary gland neoplasm: a first clinical case report
Evening Specialty Conference: Cytopathology
 : Cytopathology N. Paul Ohori, M.D. University of Pittsburgh Medical Center Disclosure of Relevant Financial Relationships Disclosure of Relevant Financial Relationships USCAP requires that all planners
: Cytopathology N. Paul Ohori, M.D. University of Pittsburgh Medical Center Disclosure of Relevant Financial Relationships Disclosure of Relevant Financial Relationships USCAP requires that all planners
PRELIMINARY CYTOLOGIC DIAGNOSIS: Suspicious for Acinic Cell Carcinoma. Cell Block: Immunohistochemical Studies CYTOLOGIC DIAGNOSIS:
 1 PRELIMINARY CYTOLOGIC DIAGNOSIS: Suspicious for Acinic Cell Carcinoma. Cell Block: Immunohistochemical Studies GCDFP-15 S-100 CYTOLOGIC DIAGNOSIS: Consistent with mammary analogue secretory carcinoma.
1 PRELIMINARY CYTOLOGIC DIAGNOSIS: Suspicious for Acinic Cell Carcinoma. Cell Block: Immunohistochemical Studies GCDFP-15 S-100 CYTOLOGIC DIAGNOSIS: Consistent with mammary analogue secretory carcinoma.
Salivary Glands 3/7/2017
 Salivary Glands 3/7/2017 Goals and objectives Focus on the entities unique to H&N Common board type facts Information for your future practice Salivary Glands Salivary Glands Major gland. Paratid. Submandibular.
Salivary Glands 3/7/2017 Goals and objectives Focus on the entities unique to H&N Common board type facts Information for your future practice Salivary Glands Salivary Glands Major gland. Paratid. Submandibular.
Salivary gland neoplasms: an update 29th Annual Meeting of Arab Division of the International Academy of Pathology MUSCAT, OMAN 2017
 Salivary gland neoplasms: an update 29th Annual Meeting of Arab Division of the International Academy of Pathology MUSCAT, OMAN 2017 Dr Mary Toner Consultant Pathologist St James Hospital Trinity College
Salivary gland neoplasms: an update 29th Annual Meeting of Arab Division of the International Academy of Pathology MUSCAT, OMAN 2017 Dr Mary Toner Consultant Pathologist St James Hospital Trinity College
Fine-Needle Aspiration Cytology of Low-Grade Cribriform Cystadenocarcinoma with Many Psammoma Bodies of the Salivary Gland
 The Korean Journal of Pathology 2013; 47: 481-485 CASE STUDY Fine-Needle Aspiration Cytology of Low-Grade Cribriform Cystadenocarcinoma with Many Psammoma Bodies of the Salivary Gland Ji Yun Jeong Dongbin
The Korean Journal of Pathology 2013; 47: 481-485 CASE STUDY Fine-Needle Aspiration Cytology of Low-Grade Cribriform Cystadenocarcinoma with Many Psammoma Bodies of the Salivary Gland Ji Yun Jeong Dongbin
Objectives. Salivary Gland FNA: The Milan System. Role of Salivary Gland FNA 04/26/2018
 Salivary Gland FNA: The Milan System Dr. Jennifer Brainard Section Head Cytopathology Cleveland Clinic Objectives Introduce the Milan System for reporting salivary gland cytopathology Define cytologic
Salivary Gland FNA: The Milan System Dr. Jennifer Brainard Section Head Cytopathology Cleveland Clinic Objectives Introduce the Milan System for reporting salivary gland cytopathology Define cytologic
Molecular Diagnostics of Head and Neck Tumors Justin A. Bishop, M.D. Associate Professor of Pathology The Johns Hopkins University Baltimore, Maryland
 Molecular Diagnostics of Head and Neck Tumors Justin A. Bishop, M.D. Associate Professor of Pathology The Johns Hopkins University Baltimore, Maryland Two Main Topics Molecular insights in salivary gland
Molecular Diagnostics of Head and Neck Tumors Justin A. Bishop, M.D. Associate Professor of Pathology The Johns Hopkins University Baltimore, Maryland Two Main Topics Molecular insights in salivary gland
Oncocytic-Appearing Salivary Gland Tumors. Oncocytic, Cystic, Mucinous, and High Grade Salivary Gland Tumors SALIVARY GLAND FNA: PART II
 William C. Faquin, MD, PhD Professor of Pathology Harvard Medical School Director of Head and Neck Pathology Massachusetts Eye and Ear Massachusetts General Hospital SALIVARY GLAND FNA: PART II Oncocytic,
William C. Faquin, MD, PhD Professor of Pathology Harvard Medical School Director of Head and Neck Pathology Massachusetts Eye and Ear Massachusetts General Hospital SALIVARY GLAND FNA: PART II Oncocytic,
Review and Updates of Immunohistochemistry in Selected Salivary Gland and Head and Neck Tumors
 Review and Updates of Immunohistochemistry in Selected Salivary Gland and Head and Neck Tumors. Monophasic tumors : myoepithelioma, acinic cell carcinoma, and salivary duct carcinoma. Biphasic tumors includes
Review and Updates of Immunohistochemistry in Selected Salivary Gland and Head and Neck Tumors. Monophasic tumors : myoepithelioma, acinic cell carcinoma, and salivary duct carcinoma. Biphasic tumors includes
Takako Inaba, 1 Yuki Fukumura, 2 Tsuyoshi Saito, 2 Junkichi Yokoyama, 3 Shinichi Ohba, 3 Atsushi Arakawa, 2 and Takashi Yao 2. 1.
 Case Reports in Pathology Volume 2015, Article ID 656107, 6 pages http://dx.doi.org/10.1155/2015/656107 Case Report Cytological Features of Mammary Analogue Secretory Carcinoma of the Parotid Gland in
Case Reports in Pathology Volume 2015, Article ID 656107, 6 pages http://dx.doi.org/10.1155/2015/656107 Case Report Cytological Features of Mammary Analogue Secretory Carcinoma of the Parotid Gland in
Mammary Analogue Secretory Carcinoma: Update on a New Diagnosis of Salivary Gland Malignancy
 The Laryngoscope VC 2013 The American Laryngological, Rhinological and Otological Society, Inc. Systematic Review Mammary Analogue Secretory Carcinoma: Update on a New Diagnosis of Salivary Gland Malignancy
The Laryngoscope VC 2013 The American Laryngological, Rhinological and Otological Society, Inc. Systematic Review Mammary Analogue Secretory Carcinoma: Update on a New Diagnosis of Salivary Gland Malignancy
Salivary gland tumor cytologic and histologic correlation: Algorithmic and risk stratification based approaches
 Salivary gland tumor cytologic and histologic correlation: Algorithmic and risk stratification based approaches Christopher C. Griffith, MD, PhD Raja R. Seethala, MD 1. Salivary gland tumor cytology: A
Salivary gland tumor cytologic and histologic correlation: Algorithmic and risk stratification based approaches Christopher C. Griffith, MD, PhD Raja R. Seethala, MD 1. Salivary gland tumor cytology: A
Enterprise Interest None
 Enterprise Interest None What are triple negative breast cancers? A synopsis of their histological patterns Ian Ellis Molecular Medical Sciences, University of Nottingham Department of Histopathology,
Enterprise Interest None What are triple negative breast cancers? A synopsis of their histological patterns Ian Ellis Molecular Medical Sciences, University of Nottingham Department of Histopathology,
Lesions Mimicking Adenoid Cystic Carcinoma. Diagnostic Problems in Salivary Gland Pathology An Update 5/29/2009
 Diagnostic Problems in Salivary Gland Pathology An Update Lesions Mimicking Adenoid Cystic Carcinoma Stacey E. Mills, M.D. W.S. Royster Professor of Pathology Director of Surgical and Cytopathology University
Diagnostic Problems in Salivary Gland Pathology An Update Lesions Mimicking Adenoid Cystic Carcinoma Stacey E. Mills, M.D. W.S. Royster Professor of Pathology Director of Surgical and Cytopathology University
WHO 2017: New Classification of Head and Neck Tumours
 WHO 2017: New Classification of Head and Neck Tumours Ilmo Leivo Department of Pathology University of Turku & Turku University Hospital FINLAND Suomen IAP Aulanko 18.05.2018 WHO 2017 New entities Simplification
WHO 2017: New Classification of Head and Neck Tumours Ilmo Leivo Department of Pathology University of Turku & Turku University Hospital FINLAND Suomen IAP Aulanko 18.05.2018 WHO 2017 New entities Simplification
Oncocytic carcinoma: A rare malignancy of the parotid gland
 ISPUB.COM The Internet Journal of Pathology Volume 8 Number 2 Oncocytic carcinoma: A rare malignancy of the parotid gland K Mardi, J Sharma Citation K Mardi, J Sharma.. The Internet Journal of Pathology.
ISPUB.COM The Internet Journal of Pathology Volume 8 Number 2 Oncocytic carcinoma: A rare malignancy of the parotid gland K Mardi, J Sharma Citation K Mardi, J Sharma.. The Internet Journal of Pathology.
ARIZONA SOCIETY OF PATHOLOGISTS 13 TH APRIL 2013 HEAD AND NECK CYTOPATHOLOGY. F ZAHRA ALY, MD, PhD
 ARIZONA SOCIETY OF PATHOLOGISTS 13 TH APRIL 2013 HEAD AND NECK CYTOPATHOLOGY F ZAHRA ALY, MD, PhD The main areas sites amenable for cytopathology include lymph nodes, thyroid, major salivary glands especially
ARIZONA SOCIETY OF PATHOLOGISTS 13 TH APRIL 2013 HEAD AND NECK CYTOPATHOLOGY F ZAHRA ALY, MD, PhD The main areas sites amenable for cytopathology include lymph nodes, thyroid, major salivary glands especially
Case Report Basaloid ductal carcinoma in situ arising in salivary gland metaplasia of the breast: a case report
 Int J Clin Exp Pathol 2014;7(9):6370-6374 www.ijcep.com /ISSN:1936-2625/IJCEP0001480 Case Report Basaloid ductal carcinoma in situ arising in salivary gland metaplasia of the breast: a case report Eun
Int J Clin Exp Pathol 2014;7(9):6370-6374 www.ijcep.com /ISSN:1936-2625/IJCEP0001480 Case Report Basaloid ductal carcinoma in situ arising in salivary gland metaplasia of the breast: a case report Eun
Salivary Gland FNA ATYPICAL : Criteria and Controversies
 Salivary Gland FNA ATYPICAL : Criteria and Controversies W.C. Faquin, M.D., Ph.D. Director, Head and Neck Pathology Massachusetts General Hospital Massachusetts Eye and Ear Infirmary Harvard Medical School
Salivary Gland FNA ATYPICAL : Criteria and Controversies W.C. Faquin, M.D., Ph.D. Director, Head and Neck Pathology Massachusetts General Hospital Massachusetts Eye and Ear Infirmary Harvard Medical School
A 60-year old Man with Left Jaw Mass. Simon Chiosea, MD University of Pittsburgh medical Center 3/15/2016
 ACCME/Disclosures The USCAP requires that anyone in a position to influence or control the content of CME disclose any relevant financial relationship WITH COMMERCIAL INTERESTS which they or their spouse/partner
ACCME/Disclosures The USCAP requires that anyone in a position to influence or control the content of CME disclose any relevant financial relationship WITH COMMERCIAL INTERESTS which they or their spouse/partner
Secretory carcinoma impact of translocation and gene fusions on salivary gland tumor
 Review Article Secretory carcinoma impact of translocation and gene fusions on salivary gland tumor Ryoko Inaki 1, Masanobu Abe 1,2, Liang Zong 3,4, Takahiro Abe 1, Aya Shinozaki-Ushiku 5, Tetsuo Ushiku
Review Article Secretory carcinoma impact of translocation and gene fusions on salivary gland tumor Ryoko Inaki 1, Masanobu Abe 1,2, Liang Zong 3,4, Takahiro Abe 1, Aya Shinozaki-Ushiku 5, Tetsuo Ushiku
Low-grade cribriform cystadenocarcinoma arising from a minor salivary gland: a case report
 145 Journal of Oral Science, Vol. 58, No. 1, 145-149, 2016 Case Report Low-grade cribriform cystadenocarcinoma arising from a minor salivary gland: a case report Masashi Kimura 1), Shinji Mii 2), Shinichi
145 Journal of Oral Science, Vol. 58, No. 1, 145-149, 2016 Case Report Low-grade cribriform cystadenocarcinoma arising from a minor salivary gland: a case report Masashi Kimura 1), Shinji Mii 2), Shinichi
Case 1. ACCME/Disclosure. Clinical History. Dr. Mulligan has nothing to disclose
 Breast Evening Specialty Conference USCAP, 2016 Case 1 Anna Marie Mulligan University Health Network, Toronto University of Toronto ACCME/Disclosure Dr. Mulligan has nothing to disclose Clinical History
Breast Evening Specialty Conference USCAP, 2016 Case 1 Anna Marie Mulligan University Health Network, Toronto University of Toronto ACCME/Disclosure Dr. Mulligan has nothing to disclose Clinical History
DISCUSSION: PLGA accounts for about 2% of all salivary gland tumours and occurs almost exclusively in the minor salivary glands.
 SWELLING ON THE HARD PALATE PRESENTING AS POLYMORPHOUS LOW GRADE ADENOCARCINOMA: A AND REVIEW OF LITERATURE Swapnil D. Chandekar 1, Sunita S. Dantkale 2, Rahul R. Narkhede 3, Snehal V. Chavhan 4, Khushboo
SWELLING ON THE HARD PALATE PRESENTING AS POLYMORPHOUS LOW GRADE ADENOCARCINOMA: A AND REVIEW OF LITERATURE Swapnil D. Chandekar 1, Sunita S. Dantkale 2, Rahul R. Narkhede 3, Snehal V. Chavhan 4, Khushboo
Case Report Aggressive invasive micropapillary salivary duct carcinoma of the parotid gland
 Pathology International 2008; 58: 322 326 doi:10.1111/j.1440-1827.2008.02231.x Case Report Aggressive invasive micropapillary salivary duct carcinoma of the parotid gland Hidetaka Yamamoto, 1 Hideoki Uryu,
Pathology International 2008; 58: 322 326 doi:10.1111/j.1440-1827.2008.02231.x Case Report Aggressive invasive micropapillary salivary duct carcinoma of the parotid gland Hidetaka Yamamoto, 1 Hideoki Uryu,
1 NORMAL HISTOLOGY AND METAPLASIAS
 1 NORMAL HISTOLOGY AND METAPLASIAS, MD Anatomy and Histology 1 Metaplasias 2 ANATOMY AND HISTOLOGY The female breast is composed of a branching duct system, which begins at the nipple with the major lactiferous
1 NORMAL HISTOLOGY AND METAPLASIAS, MD Anatomy and Histology 1 Metaplasias 2 ANATOMY AND HISTOLOGY The female breast is composed of a branching duct system, which begins at the nipple with the major lactiferous
Basement membrane in lobule.
 Bahram Memar, MD Basement membrane in lobule. Normal lobule-luteal phase Normal lobule-follicular phase Lactating breast Greater than 95% are adenocarcinomas in situ carcinomas and invasive carcinomas.
Bahram Memar, MD Basement membrane in lobule. Normal lobule-luteal phase Normal lobule-follicular phase Lactating breast Greater than 95% are adenocarcinomas in situ carcinomas and invasive carcinomas.
Case 2. Dr. Sathima Natarajan M.D. Kaiser Permanente Medical Center Sunset
 Case 2 Dr. Sathima Natarajan M.D. Kaiser Permanente Medical Center Sunset History 24 year old male presented with a 3 day history of right flank pain, sharp in nature Denies fever, chills, hematuria or
Case 2 Dr. Sathima Natarajan M.D. Kaiser Permanente Medical Center Sunset History 24 year old male presented with a 3 day history of right flank pain, sharp in nature Denies fever, chills, hematuria or
Papillary Lesions of the Breast A Practical Approach to Diagnosis. (Arch Pathol Lab Med. 2016;140: ; doi: /arpa.
 Papillary Lesions of the Breast A Practical Approach to Diagnosis (Arch Pathol Lab Med. 2016;140:1052 1059; doi: 10.5858/arpa.2016-0219-RA) Papillary lesions of the breast Span the spectrum of benign,
Papillary Lesions of the Breast A Practical Approach to Diagnosis (Arch Pathol Lab Med. 2016;140:1052 1059; doi: 10.5858/arpa.2016-0219-RA) Papillary lesions of the breast Span the spectrum of benign,
Polymorphous Low-Grade. December 5 th, 2008
 Polymorphous Low-Grade Adenocarcinoma December 5 th, 2008 Epidemiology Represents 2 nd or 3 rd most common minor salivary gland malignancy (17-26%) 1 st mucoepidermoid carcinoma Rare in reported Asian
Polymorphous Low-Grade Adenocarcinoma December 5 th, 2008 Epidemiology Represents 2 nd or 3 rd most common minor salivary gland malignancy (17-26%) 1 st mucoepidermoid carcinoma Rare in reported Asian
USCAP 2012: Companion Meeting of the AAOOP. Update on lacrimal gland neoplasms: Molecular pathology of interest
 USCAP 2012: Companion Meeting of the AAOOP Vancouver BC, Canada, March 17, 2012 Update on lacrimal gland neoplasms: Molecular pathology of interest Valerie A. White MD, MHSc, FRCPC Department of Pathology
USCAP 2012: Companion Meeting of the AAOOP Vancouver BC, Canada, March 17, 2012 Update on lacrimal gland neoplasms: Molecular pathology of interest Valerie A. White MD, MHSc, FRCPC Department of Pathology
My Journey into the World of Salivary Gland Sebaceous Neoplasms
 My Journey into the World of Salivary Gland Sebaceous Neoplasms Douglas R. Gnepp Warren Alpert Medical School at Brown University Rhode Island Hospital Pathology Department Providence RI Asked to present
My Journey into the World of Salivary Gland Sebaceous Neoplasms Douglas R. Gnepp Warren Alpert Medical School at Brown University Rhode Island Hospital Pathology Department Providence RI Asked to present
Low-grade cribriform cystadenocarcinoma of salivary glands: report of two cases and review of the literature
 Wang et al. Diagnostic Pathology 2013, 8:28 CASE REPORT Open Access Low-grade cribriform cystadenocarcinoma of salivary glands: report of two cases and review of the literature Liang Wang 1,2, Yang Liu
Wang et al. Diagnostic Pathology 2013, 8:28 CASE REPORT Open Access Low-grade cribriform cystadenocarcinoma of salivary glands: report of two cases and review of the literature Liang Wang 1,2, Yang Liu
Los Angeles Society Of Pathologists Dr. Shobha Castelino Prabhu
 Los Angeles Society Of Pathologists Dr. Shobha Castelino Prabhu Loma Linda University Medical Center June 12, 2007 CASE 1 76 year-old gentleman Status post right parotidectomy 1 year ago for a rare tumor
Los Angeles Society Of Pathologists Dr. Shobha Castelino Prabhu Loma Linda University Medical Center June 12, 2007 CASE 1 76 year-old gentleman Status post right parotidectomy 1 year ago for a rare tumor
Case Scenario 1: Thyroid
 Case Scenario 1: Thyroid History and Physical Patient is an otherwise healthy 80 year old female with the complaint of a neck mass first noticed two weeks ago. The mass has increased in size and is palpable.
Case Scenario 1: Thyroid History and Physical Patient is an otherwise healthy 80 year old female with the complaint of a neck mass first noticed two weeks ago. The mass has increased in size and is palpable.
Original Article Pathological features of mammary analogue secretory carcinoma of the salivary gland
 Int J Clin Exp Pathol 2017;10(7):7460-7465 www.ijcep.com /ISSN:1936-2625/IJCEP0050390 Original Article Pathological features of mammary analogue secretory carcinoma of the salivary gland Ke Shi, Xin-Quan
Int J Clin Exp Pathol 2017;10(7):7460-7465 www.ijcep.com /ISSN:1936-2625/IJCEP0050390 Original Article Pathological features of mammary analogue secretory carcinoma of the salivary gland Ke Shi, Xin-Quan
Maram Abdaljaleel, MD Dermatopathologist and Neuropathologist University of Jordan, School of Medicine
 Maram Abdaljaleel, MD Dermatopathologist and Neuropathologist University of Jordan, School of Medicine The most common non-skin malignancy of women 2 nd most common cause of cancer deaths in women, following
Maram Abdaljaleel, MD Dermatopathologist and Neuropathologist University of Jordan, School of Medicine The most common non-skin malignancy of women 2 nd most common cause of cancer deaths in women, following
Invasive Papillary Breast Carcinoma
 410 This is an Open Access article licensed under the terms of the Creative Commons Attribution- NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the
410 This is an Open Access article licensed under the terms of the Creative Commons Attribution- NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the
Cytokeratin immunoprofile of primary and metastatic adenoid cystic carcinoma of salivary glands: a report of two cases
 Article / Clinical Case Report Cytokeratin immunoprofile of primary and metastatic adenoid cystic carcinoma of salivary glands: a report of two cases Cibele Pidorodeski Nagano a, Cláudia Malheiros Coutinho-Camillo
Article / Clinical Case Report Cytokeratin immunoprofile of primary and metastatic adenoid cystic carcinoma of salivary glands: a report of two cases Cibele Pidorodeski Nagano a, Cláudia Malheiros Coutinho-Camillo
Synchronous squamous cell carcinoma of the breast. and invasive lobular carcinoma
 Sentani K et al. 1 Letter to the editor Synchronous squamous cell carcinoma of the breast and invasive lobular carcinoma Kazuhiro Sentani, 1 Takashi Tashiro, 2 Naohide Oue, 1 Wataru Yasui 1 1 Department
Sentani K et al. 1 Letter to the editor Synchronous squamous cell carcinoma of the breast and invasive lobular carcinoma Kazuhiro Sentani, 1 Takashi Tashiro, 2 Naohide Oue, 1 Wataru Yasui 1 1 Department
Gross appearance of nodular hyperplasia in material obtained from suprapubic prostatectomy. Note the multinodular appearance and the admixture of
 Tiền liệt tuyến Tiền liệt tuyến Gross appearance of nodular hyperplasia in material obtained from suprapubic prostatectomy. Note the multinodular appearance and the admixture of solid and microcystic areas.
Tiền liệt tuyến Tiền liệt tuyến Gross appearance of nodular hyperplasia in material obtained from suprapubic prostatectomy. Note the multinodular appearance and the admixture of solid and microcystic areas.
Notice of Faculty Disclosure
 California Society of Pathology Diagnostic Problems in Surgical Pathology December 2015 Case 2 Laura C. Collins, M.D. Associate Professor of Pathology Associate Director of Anatomic Pathology Beth Israel
California Society of Pathology Diagnostic Problems in Surgical Pathology December 2015 Case 2 Laura C. Collins, M.D. Associate Professor of Pathology Associate Director of Anatomic Pathology Beth Israel
Urinary Bladder: WHO Classification and AJCC Staging Update 2017
 Urinary Bladder: WHO Classification and AJCC Staging Update 2017 Houston Society of Clinical Pathologists 58 th Annual Spring Symposium Houston, TX April 8, 2017 Jesse K. McKenney, MD Classification
Urinary Bladder: WHO Classification and AJCC Staging Update 2017 Houston Society of Clinical Pathologists 58 th Annual Spring Symposium Houston, TX April 8, 2017 Jesse K. McKenney, MD Classification
Case year old female presented with asymmetric enlargement of the left lobe of the thyroid
 Case 4 22 year old female presented with asymmetric enlargement of the left lobe of the thyroid gland. No information available relative to a prior fine needle aspiration biopsy. A left lobectomy was performed.
Case 4 22 year old female presented with asymmetric enlargement of the left lobe of the thyroid gland. No information available relative to a prior fine needle aspiration biopsy. A left lobectomy was performed.
Case 4 Diagnosis 2/21/2011 TGB
 Case 4 22 year old female presented with asymmetric enlargement of the left lobe of the thyroid gland. No information available relative to a prior fine needle aspiration biopsy. A left lobectomy was performed.
Case 4 22 year old female presented with asymmetric enlargement of the left lobe of the thyroid gland. No information available relative to a prior fine needle aspiration biopsy. A left lobectomy was performed.
Kidney Case 1 SURGICAL PATHOLOGY REPORT
 Kidney Case 1 Surgical Pathology Report February 9, 2007 Clinical History: This 45 year old woman was found to have a left renal mass. CT urography with reconstruction revealed a 2 cm medial mass which
Kidney Case 1 Surgical Pathology Report February 9, 2007 Clinical History: This 45 year old woman was found to have a left renal mass. CT urography with reconstruction revealed a 2 cm medial mass which
Disorders of Cell Growth & Neoplasia. Histopathology Lab
 Disorders of Cell Growth & Neoplasia Histopathology Lab Paul Hanna April 2010 Case #84 Clinical History: 5 yr-old, West Highland White terrier. skin mass from axillary region. has been present for the
Disorders of Cell Growth & Neoplasia Histopathology Lab Paul Hanna April 2010 Case #84 Clinical History: 5 yr-old, West Highland White terrier. skin mass from axillary region. has been present for the
Salivary Gland Neoplasms. Salivary Gland Neoplasms Outline 4/16/2018. MUSC Pathology Multi-Specialty Course Kiawah Island, SC April 19, 2018
 Salivary Gland Neoplasms MUSC Pathology Multi-Specialty Course Kiawah Island, SC April 19, 2018 Bruce M. Wenig, MD Moffitt Cancer Center Tampa, FL Salivary Gland Neoplasms Outline Basic concepts of salivary
Salivary Gland Neoplasms MUSC Pathology Multi-Specialty Course Kiawah Island, SC April 19, 2018 Bruce M. Wenig, MD Moffitt Cancer Center Tampa, FL Salivary Gland Neoplasms Outline Basic concepts of salivary
Differential Diagnosis of Oral Masses. Palatal Lesions
 Differential Diagnosis of Oral Masses Palatal Lesions Palatal Masses Periapical Abscess Torus Palatinus Mucocele Lymphoid Hyperplasia Adenomatous Hyperplasia Benign Salivary Neoplasms Malignant Salivary
Differential Diagnosis of Oral Masses Palatal Lesions Palatal Masses Periapical Abscess Torus Palatinus Mucocele Lymphoid Hyperplasia Adenomatous Hyperplasia Benign Salivary Neoplasms Malignant Salivary
doi: /j.anl
 doi: 10.1016/j.anl.2006.07.001 Synchronous unilateral parotid gland neoplasms of three different histological types Shuho Tanaka 1, Keiji Tabuchi 1, Keiko Oikawa 1, Rika Kohanawa 1, Hideki Okubo 1, Dai
doi: 10.1016/j.anl.2006.07.001 Synchronous unilateral parotid gland neoplasms of three different histological types Shuho Tanaka 1, Keiji Tabuchi 1, Keiko Oikawa 1, Rika Kohanawa 1, Hideki Okubo 1, Dai
CASE REPORT Malignant transformation of breast ductal adenoma: a diagnostic pitfall
 Malaysian J Pathol 2015; 37(3) : 281 285 CASE REPORT Malignant transformation of breast ductal adenoma: a diagnostic pitfall Hiroko HAYASHI, Hiroshi OHTANI,* Junzo YAMAGUCHI,** and Isao SHIMOKAWA Department
Malaysian J Pathol 2015; 37(3) : 281 285 CASE REPORT Malignant transformation of breast ductal adenoma: a diagnostic pitfall Hiroko HAYASHI, Hiroshi OHTANI,* Junzo YAMAGUCHI,** and Isao SHIMOKAWA Department
Pleomorphic adenoma of breast - a case report and distinction with metaplastic carcinoma D Gupta, S Agrawal, N Trivedi, A Tewari
 of breast - a case report and distinction with metaplastic carcinoma D Gupta, S Agrawal, N Trivedi, A Tewari Introduction, also known as mixed tumour, is a benign tumour which typically presents as a painless,
of breast - a case report and distinction with metaplastic carcinoma D Gupta, S Agrawal, N Trivedi, A Tewari Introduction, also known as mixed tumour, is a benign tumour which typically presents as a painless,
ARTHUR PURDY STOUT SOCIETY COMPANION MEETING: DIFFICULT NEW DIFFERENTIAL DIAGNOSES IN PROSTATE PATHOLOGY. Jonathan I. Epstein.
 1 ARTHUR PURDY STOUT SOCIETY COMPANION MEETING: DIFFICULT NEW DIFFERENTIAL DIAGNOSES IN PROSTATE PATHOLOGY Jonathan I. Epstein Professor Pathology, Urology, Oncology The Reinhard Professor of Urological
1 ARTHUR PURDY STOUT SOCIETY COMPANION MEETING: DIFFICULT NEW DIFFERENTIAL DIAGNOSES IN PROSTATE PATHOLOGY Jonathan I. Epstein Professor Pathology, Urology, Oncology The Reinhard Professor of Urological
Salivary Gland Neoplasms. Napa Valley Pathology Conference Silverado Resort & Spa May 18, /22/2018. Salivary Gland Neoplasms Outline
 Salivary Gland Neoplasms Napa Valley Pathology Conference Silverado Resort & Spa May 18, 2018 Bruce M. Wenig, MD Moffitt Cancer Center Tampa, FL Salivary Gland Neoplasms Outline Basic concepts of salivary
Salivary Gland Neoplasms Napa Valley Pathology Conference Silverado Resort & Spa May 18, 2018 Bruce M. Wenig, MD Moffitt Cancer Center Tampa, FL Salivary Gland Neoplasms Outline Basic concepts of salivary
DISORDERS OF THE SALIVARY GLANDS Neoplasms Dr.M.Baskaran Selvapathy S IV
 DISORDERS OF THE SALIVARY GLANDS Neoplasms Dr.M.Baskaran Selvapathy S IV NEOPLASMS A) Epithelial I. Benign Pleomorphic adenoma( Mixed tumour) Adenolymphoma (Warthin s tumour) Oxyphil adenoma (Oncocytoma)
DISORDERS OF THE SALIVARY GLANDS Neoplasms Dr.M.Baskaran Selvapathy S IV NEOPLASMS A) Epithelial I. Benign Pleomorphic adenoma( Mixed tumour) Adenolymphoma (Warthin s tumour) Oxyphil adenoma (Oncocytoma)
Histological Type. Morphological and Molecular Typing of breast Cancer. Nottingham Tenovus Primary Breast Cancer Study. Survival (%) Ian Ellis
 Morphological and Molecular Typing of breast Cancer Ian Ellis Molecular Medical Sciences, University of Nottingham Department of Histopathology, Nottingham University Hospitals NHS Trust Histological Type
Morphological and Molecular Typing of breast Cancer Ian Ellis Molecular Medical Sciences, University of Nottingham Department of Histopathology, Nottingham University Hospitals NHS Trust Histological Type
Intraductal carcinoma of the prostate on needle biopsy: histologic features and clinical significance
 & 2006 USCAP, Inc All rights reserved 0893-3952/06 $30.00 www.modernpathology.org Intraductal carcinoma of the prostate on needle biopsy: histologic features and clinical significance Charles C Guo 1 and
& 2006 USCAP, Inc All rights reserved 0893-3952/06 $30.00 www.modernpathology.org Intraductal carcinoma of the prostate on needle biopsy: histologic features and clinical significance Charles C Guo 1 and
Carcinoma mammario: le istologie non frequenti. Valentina Guarneri Università di Padova IOV-IRCCS
 Carcinoma mammario: le istologie non frequenti Valentina Guarneri Università di Padova IOV-IRCCS Histological diversity of breast adenocarcinomas Different histological types are defined according to specific
Carcinoma mammario: le istologie non frequenti Valentina Guarneri Università di Padova IOV-IRCCS Histological diversity of breast adenocarcinomas Different histological types are defined according to specific
Spinal Cord Compression caused by Metastatic Epithelial Myoepithelial Carcinoma of the Parotid Gland
 Spinal Cord Compression caused by Metastatic Epithelial Myoepithelial Carcinoma of the Parotid Gland Pages with reference to book, From 249 To 250 Irshad N. Soomro,Akber S. Hussainy,Rashida Ahmed,Sheema
Spinal Cord Compression caused by Metastatic Epithelial Myoepithelial Carcinoma of the Parotid Gland Pages with reference to book, From 249 To 250 Irshad N. Soomro,Akber S. Hussainy,Rashida Ahmed,Sheema
DIAGNOSTIC SLIDE SEMINAR: PART 1 RENAL TUMOUR BIOPSY CASES
 DIAGNOSTIC SLIDE SEMINAR: PART 1 RENAL TUMOUR BIOPSY CASES Dr. Andrew J. Evans MD, PhD, FACP, FRCPC Consultant in Genitourinary Pathology University Health Network, Toronto, ON Case 1 43 year-old female,
DIAGNOSTIC SLIDE SEMINAR: PART 1 RENAL TUMOUR BIOPSY CASES Dr. Andrew J. Evans MD, PhD, FACP, FRCPC Consultant in Genitourinary Pathology University Health Network, Toronto, ON Case 1 43 year-old female,
Fine Needle Aspiration of an Unusual Malignant Mixed Tumor in the Parotid Gland
 Fine Needle Aspiration of an Unusual Malignant Mixed Tumor in the Parotid Gland Xiu Yang, MD, PhD, 1 * Adam Cole, MD, 1 Maja Oktay, MD, PhD, 1 Richard Smith, MD, 2 Antonio Cajigas, MD, 1 Samer Khader,
Fine Needle Aspiration of an Unusual Malignant Mixed Tumor in the Parotid Gland Xiu Yang, MD, PhD, 1 * Adam Cole, MD, 1 Maja Oktay, MD, PhD, 1 Richard Smith, MD, 2 Antonio Cajigas, MD, 1 Samer Khader,
Adenoid Cystic Carcinoma Minor Salivary Gland Origin
 Adenoid Cystic Carcinoma Minor Salivary Gland Origin Educational Session Presenter: Smith JA Supervisors: Palme CE, Gupta R Content Case report Imaging Primary Therapy Surgery Adjuvant Therapy Radiotherapy
Adenoid Cystic Carcinoma Minor Salivary Gland Origin Educational Session Presenter: Smith JA Supervisors: Palme CE, Gupta R Content Case report Imaging Primary Therapy Surgery Adjuvant Therapy Radiotherapy
Disclosure. Relevant Financial Relationship(s) None. Off Label Usage None MFMER slide-1
 Disclosure Relevant Financial Relationship(s) None Off Label Usage None 2013 MFMER slide-1 Case Presentation A 43 year old male, with partial nephrectomy for a right kidney mass 2013 MFMER slide-2 2013
Disclosure Relevant Financial Relationship(s) None Off Label Usage None 2013 MFMER slide-1 Case Presentation A 43 year old male, with partial nephrectomy for a right kidney mass 2013 MFMER slide-2 2013
University Journal of Pre and Para Clinical Sciences
 ISSN 2455 2879 Volume 2 Issue 1 2016 Metaplastic carcinoma breast a rare case report Abstract : Metaplastic carcinoma of the breast is a rare malignancy with two distinct cell lines described as a breast
ISSN 2455 2879 Volume 2 Issue 1 2016 Metaplastic carcinoma breast a rare case report Abstract : Metaplastic carcinoma of the breast is a rare malignancy with two distinct cell lines described as a breast
Microcystic Squamous Cell Carcinoma of the Lung A Clinicopathologic Study of Three Cases
 Anatomic Pathology / Microcystic SCC of the Lung Microcystic Squamous Cell Carcinoma of the Lung A Clinicopathologic Study of Three Cases Annikka Weissferdt, MD, and Cesar A. Moran, MD Key Words: Squamous
Anatomic Pathology / Microcystic SCC of the Lung Microcystic Squamous Cell Carcinoma of the Lung A Clinicopathologic Study of Three Cases Annikka Weissferdt, MD, and Cesar A. Moran, MD Key Words: Squamous
Salivary Gland Cytology
 Salivary Gland Cytology Diagnostic challenges and potential pitfalls Tarik M. Elsheikh, MD Professor and Medical Director Anatomic Pathology Cleveland Clinic FNA Salivary Gland Lesions Indications Distinguish
Salivary Gland Cytology Diagnostic challenges and potential pitfalls Tarik M. Elsheikh, MD Professor and Medical Director Anatomic Pathology Cleveland Clinic FNA Salivary Gland Lesions Indications Distinguish
5/22/2017. An Aggressive Nasopharyngeal Tumor. Case History
 An Aggressive Nasopharyngeal Tumor Head & Neck/Endocrine Evening Specialty Conference Martin Bullock, MD, FRCPC Dalhousie University, Halifax, Nova Scotia Case History 52-year-old male, 6 month history
An Aggressive Nasopharyngeal Tumor Head & Neck/Endocrine Evening Specialty Conference Martin Bullock, MD, FRCPC Dalhousie University, Halifax, Nova Scotia Case History 52-year-old male, 6 month history
POLYMORPHOUS LOW GRADE ADENOCARCINOMA - CASE REPORT AND REVIEW OF LITERATURE
 POLYMORPHOUS LOW GRADE ADENOCARCINOMA - CASE REPORT AND REVIEW OF LITERATURE S.Sunil 1 B.S. Sreenivasan 2 Jisha Titus 3 Soma Susan 4 Jubin Thomas 4 Antony George 4 Devi Gopakumar 5 1 Reader, 2 Professor,
POLYMORPHOUS LOW GRADE ADENOCARCINOMA - CASE REPORT AND REVIEW OF LITERATURE S.Sunil 1 B.S. Sreenivasan 2 Jisha Titus 3 Soma Susan 4 Jubin Thomas 4 Antony George 4 Devi Gopakumar 5 1 Reader, 2 Professor,
SALIVARY GLAND DISEASES. Omar alnoubani MD,MRCS
 SALIVARY GLAND DISEASES Omar alnoubani MD,MRCS Salivary Glands Overview Parotid gland Sublingual gland Submandibular gland Salivary glands - Types 3 Major Salivary Glands Parotid Submandibular Sublingual
SALIVARY GLAND DISEASES Omar alnoubani MD,MRCS Salivary Glands Overview Parotid gland Sublingual gland Submandibular gland Salivary glands - Types 3 Major Salivary Glands Parotid Submandibular Sublingual
What is ACC? (Adenoid Cystic Carcinoma)
 What is ACC? (Adenoid Cystic Carcinoma) 10-9-10 Where ACC Occurs ACC (Adenoid Cystic Carcinoma) is a rare and unique form of cancer that is known to be unpredictable in nature, with a typical growth pattern
What is ACC? (Adenoid Cystic Carcinoma) 10-9-10 Where ACC Occurs ACC (Adenoid Cystic Carcinoma) is a rare and unique form of cancer that is known to be unpredictable in nature, with a typical growth pattern
Rare Presentation Of Adenoidcystic Carcinoma Of External Auditory Canal With Subcutaneous Metastasis In Temporal Region
 ISPUB.COM The Internet Journal of Otorhinolaryngology Volume 13 Number 2 Rare Presentation Of Adenoidcystic Carcinoma Of External Auditory Canal With Subcutaneous Metastasis In Temporal Region S Kaushik,
ISPUB.COM The Internet Journal of Otorhinolaryngology Volume 13 Number 2 Rare Presentation Of Adenoidcystic Carcinoma Of External Auditory Canal With Subcutaneous Metastasis In Temporal Region S Kaushik,
Desmoplastic Melanoma R/O BCC. Clinical Information. 74 y.o. man with lesion on left side of neck r/o BCC
 R/O BCC Sabine Kohler, M.D. Professor of Pathology and Dermatology Dermatopathology Service Stanford University School of Medicine Clinical Information 74 y.o. man with lesion on left side of neck r/o
R/O BCC Sabine Kohler, M.D. Professor of Pathology and Dermatology Dermatopathology Service Stanford University School of Medicine Clinical Information 74 y.o. man with lesion on left side of neck r/o
Update on 2015 WHO Classification of Lung Adenocarcinoma 1/3/ Mayo Foundation for Medical Education and Research. All rights reserved.
 1 Our speaker for this program is Dr. Anja Roden, an associate professor of Laboratory Medicine and Pathology at Mayo Clinic as well as consultant in the Anatomic Pathology Laboratory and co-director of
1 Our speaker for this program is Dr. Anja Roden, an associate professor of Laboratory Medicine and Pathology at Mayo Clinic as well as consultant in the Anatomic Pathology Laboratory and co-director of
Papillary Lesions of the breast
 Papillary Lesions of the breast Emad Rakha Professor of Breast Pathology The University of Nottingham Papillary lesions of the breast are a heterogeneous group of disease, which are characterised by neoplastic
Papillary Lesions of the breast Emad Rakha Professor of Breast Pathology The University of Nottingham Papillary lesions of the breast are a heterogeneous group of disease, which are characterised by neoplastic
Title malignancy. Issue Date Right 209, 12, (2013)
 NAOSITE: Nagasaki University's Ac Title Author(s) A case of intracystic apocrine papi malignancy Hayashi, Hiroko; Ohtani, Hiroshi; Y Citation Pathology - Research and Practice, Issue Date 2013-12 URL Right
NAOSITE: Nagasaki University's Ac Title Author(s) A case of intracystic apocrine papi malignancy Hayashi, Hiroko; Ohtani, Hiroshi; Y Citation Pathology - Research and Practice, Issue Date 2013-12 URL Right
University of Zurich. Histology and Immunophenotype of Invasive Lobular Breast Cancer. Daily Practice and Pitfalls. Zurich Open Repository and Archive
 University of Zurich Zurich Open Repository and Archive Winterthurerstr. 190 CH-8057 Zurich http://www.zora.uzh.ch Year: 2009 Histology and Immunophenotype of Invasive Lobular Breast Cancer. Daily Practice
University of Zurich Zurich Open Repository and Archive Winterthurerstr. 190 CH-8057 Zurich http://www.zora.uzh.ch Year: 2009 Histology and Immunophenotype of Invasive Lobular Breast Cancer. Daily Practice
ACCME/Disclosures. Cribriform Lesions of the Prostate. Case
 Cribriform Lesions of the Prostate Ming Zhou, MD, PhD Departments of Pathology and Urology New York University Langone Medical Center New York, NY Ming.Zhou@NYUMC.ORG ACCME/Disclosures The USCAP requires
Cribriform Lesions of the Prostate Ming Zhou, MD, PhD Departments of Pathology and Urology New York University Langone Medical Center New York, NY Ming.Zhou@NYUMC.ORG ACCME/Disclosures The USCAP requires
WHO classification salivary tumours: What's new?
 WHO classification salivary tumours: What's new? Alena Skalova, MD, PhD Professor of Pathology Charles University, Faculty of Medicine in Plzen, Czech Republic An update on Histopathology of Salivary Gland
WHO classification salivary tumours: What's new? Alena Skalova, MD, PhD Professor of Pathology Charles University, Faculty of Medicine in Plzen, Czech Republic An update on Histopathology of Salivary Gland
PLEOMORPHIC ADENOMA ( BENIGN MIXED TUMOR )
 ( BENIGN MIXED TUMOR ) Grossly, the tumor is freely movable, solid, sometimes lobulated and occasionally cystic. If recurrent, multinodular masses are common. Histologically, within a fibrous capsule,
( BENIGN MIXED TUMOR ) Grossly, the tumor is freely movable, solid, sometimes lobulated and occasionally cystic. If recurrent, multinodular masses are common. Histologically, within a fibrous capsule,
Glycogen-rich adenocarcinoma in the lower lip: report of a case with particular emphasis on differential diagnosis
 Open Journal of Stomatology, 2011, 1, 109-113 doi:10.4236/ojst.2011.13017 Published Online September 2011 (http://www.scirp.org/journal//). Glycogen-rich adenocarcinoma in the lower lip: report of a case
Open Journal of Stomatology, 2011, 1, 109-113 doi:10.4236/ojst.2011.13017 Published Online September 2011 (http://www.scirp.org/journal//). Glycogen-rich adenocarcinoma in the lower lip: report of a case
DIAGNOSTIC DILEMMA. Case Reports Clinical history. Materials and Methods
 DIAGNOSTIC DILEMMA A Metastatic Renal Carcinoid Tumor Presenting as Breast Mass: A Diagnostic Dilemma Farnaz Hasteh, M.D., 1 Robert Pu, M.D., Ph.D., 2 and Claire W. Michael, M.D. 2 * We present clinicopathological
DIAGNOSTIC DILEMMA A Metastatic Renal Carcinoid Tumor Presenting as Breast Mass: A Diagnostic Dilemma Farnaz Hasteh, M.D., 1 Robert Pu, M.D., Ph.D., 2 and Claire W. Michael, M.D. 2 * We present clinicopathological
Journal of International Academy of Forensic Science & Pathology (JIAFP)
 Journal of International Academy of Forensic Science & Pathology (JIAFP) ISSN 2395-0722 MICROCYSTIC ADNEXAL CARCINOMA-A CASE REPORT WITH REVIEW OF LITERATURE Case Report Sulakshana M S 1,Natarajan M 2
Journal of International Academy of Forensic Science & Pathology (JIAFP) ISSN 2395-0722 MICROCYSTIC ADNEXAL CARCINOMA-A CASE REPORT WITH REVIEW OF LITERATURE Case Report Sulakshana M S 1,Natarajan M 2
Postsurgical high grade transformation of polymorphous low grade adenocarcinoma of the retromolar trigone into adenocarcinoma not otherwise specified
 CASE REPORT Postsurgical high grade transformation of polymorphous low grade adenocarcinoma of the retromolar trigone into adenocarcinoma not otherwise specified Ranmeet Batra, Harshaminder K Grewal 1.
CASE REPORT Postsurgical high grade transformation of polymorphous low grade adenocarcinoma of the retromolar trigone into adenocarcinoma not otherwise specified Ranmeet Batra, Harshaminder K Grewal 1.
They Do Look Alike : Mimics of Prostate Cancer in Biopsy Samples
 They Do Look Alike : in Biopsy Samples Gladell P. Paner, MD Departments of Pathology and Surgery (Urology) University of Chicago, IL USA Gladell.paner@uchospitals.edu Benign in Needle Biopsy 1. Benign
They Do Look Alike : in Biopsy Samples Gladell P. Paner, MD Departments of Pathology and Surgery (Urology) University of Chicago, IL USA Gladell.paner@uchospitals.edu Benign in Needle Biopsy 1. Benign
Presentation material is for education purposes only. All rights reserved URMC Radiology Page 1 of 98
 Presentation material is for education purposes only. All rights reserved. 2011 URMC Radiology Page 1 of 98 Radiology / Pathology Conference February 2011 Brooke Koltz, Cytopathology Resident Presentation
Presentation material is for education purposes only. All rights reserved. 2011 URMC Radiology Page 1 of 98 Radiology / Pathology Conference February 2011 Brooke Koltz, Cytopathology Resident Presentation
Carcinoma of Unknown Primary site (CUP) in HEAD & NECK SURGERY
 Carcinoma of Unknown Primary site (CUP) in HEAD & NECK SURGERY SEARCHING FOR THE PRIMARY? P r o f J P P r e t o r i u s H e a d : C l i n i c a l U n i t C r i t i c a l C a r e U n i v e r s i t y O f
Carcinoma of Unknown Primary site (CUP) in HEAD & NECK SURGERY SEARCHING FOR THE PRIMARY? P r o f J P P r e t o r i u s H e a d : C l i n i c a l U n i t C r i t i c a l C a r e U n i v e r s i t y O f
Central Poorly Differentiated Adenocarcinoma of the Maxilla: Report of a Case
 Kobe J. Med. Sci., Vol. 49, No. 2, pp. 45-49, 2003 Central Poorly Differentiated Adenocarcinoma of the Maxilla: Report of a Case MASAHIRO UMEDA 1), SATOSHI YOKOO 1), YASUYUKI SHIBUYA 1), TAKAHIDE KOMORI
Kobe J. Med. Sci., Vol. 49, No. 2, pp. 45-49, 2003 Central Poorly Differentiated Adenocarcinoma of the Maxilla: Report of a Case MASAHIRO UMEDA 1), SATOSHI YOKOO 1), YASUYUKI SHIBUYA 1), TAKAHIDE KOMORI
Epithelial tumors. Dr. F.F. Khuzin, PhD Dr. M.O. Mavlikeev
 Epithelial tumors Dr. F.F. Khuzin, PhD Dr. M.O. Mavlikeev Epithelial tumors Tumors from the epithelium are the most frequent among tumors. There are 2 group features of these tumors: The presence in most
Epithelial tumors Dr. F.F. Khuzin, PhD Dr. M.O. Mavlikeev Epithelial tumors Tumors from the epithelium are the most frequent among tumors. There are 2 group features of these tumors: The presence in most
AGGRESSIVE VARIANTS OF PAPILLARY THYROID CARCINOMA DIAGNOSIS AND PROGNOSIS
 AGGRESSIVE VARIANTS OF PAPILLARY THYROID CARCINOMA DIAGNOSIS AND PROGNOSIS PAPILLARY THYROID CARCINOMA Clinical Any age Microscopic to large Female: Male= 2-4:1 Radiation history Lymph nodes Prognosis
AGGRESSIVE VARIANTS OF PAPILLARY THYROID CARCINOMA DIAGNOSIS AND PROGNOSIS PAPILLARY THYROID CARCINOMA Clinical Any age Microscopic to large Female: Male= 2-4:1 Radiation history Lymph nodes Prognosis
Disclosures. Parathyroid Pathology. Objectives. The normal parathyroid 11/10/2012
 Disclosures Parathyroid Pathology I have nothing to disclose Annemieke van Zante MD/PhD Assistant Professor of Clinical Pathology Associate Chief of Cytopathology Objectives 1. Review the pathologic features
Disclosures Parathyroid Pathology I have nothing to disclose Annemieke van Zante MD/PhD Assistant Professor of Clinical Pathology Associate Chief of Cytopathology Objectives 1. Review the pathologic features
Epithelial Myoepithelial Carcinoma- A Rare Case Report Shruthi H 1, Sumona P 2
 Bangladesh Journal of Medical Science Vol. 11 No. 02 April 12 Case Report Epithelial Myoepithelial Carcinoma- A Rare Case Report Shruthi H 1, Sumona P 2 Abstract: Background: Salivary gland tumors occupy
Bangladesh Journal of Medical Science Vol. 11 No. 02 April 12 Case Report Epithelial Myoepithelial Carcinoma- A Rare Case Report Shruthi H 1, Sumona P 2 Abstract: Background: Salivary gland tumors occupy
Objectives. Atypical Glandular Cells. Atypical Endocervical Cells. Reactive Endocervical Cells
 2013 California Society of Pathologists 66 th Annual Meeting San Francisco, CA Atypical Glandular Cells to Early Invasive Adenocarcinoma: Cervical Cytology and Histology Christina S. Kong, MD Associate
2013 California Society of Pathologists 66 th Annual Meeting San Francisco, CA Atypical Glandular Cells to Early Invasive Adenocarcinoma: Cervical Cytology and Histology Christina S. Kong, MD Associate
PROSTATIC ADENOCARCINOMA: DIAGNOSTIC CRITERIA AND IMPORTANT MIMICKERS PROSTATIC ADENOCARCINOMA: DIAGNOSTIC CRITERIA
 PROSTATIC ADENOCARCINOMA: DIAGNOSTIC CRITERIA AND IMPORTANT MIMICKERS PROSTATIC ADENOCARCINOMA: DIAGNOSTIC CRITERIA 1 A good H & E helps! ADENOCARCINOMA DIAGNOSTIC CRITERIA Relatively uniform proliferation
PROSTATIC ADENOCARCINOMA: DIAGNOSTIC CRITERIA AND IMPORTANT MIMICKERS PROSTATIC ADENOCARCINOMA: DIAGNOSTIC CRITERIA 1 A good H & E helps! ADENOCARCINOMA DIAGNOSTIC CRITERIA Relatively uniform proliferation
3/27/2017. Pulmonary Pathology Specialty Conference. Disclosure of Relevant Financial Relationships. Clinical History:
 Pulmonary Pathology Specialty Conference Saul Suster, M.D. Medical College of Wisconsin Disclosure of Relevant Financial Relationships USCAP requires that all planners (Education Committee) in a position
Pulmonary Pathology Specialty Conference Saul Suster, M.D. Medical College of Wisconsin Disclosure of Relevant Financial Relationships USCAP requires that all planners (Education Committee) in a position
Carcinoma ex Pleomorphic Adenoma (CXPA)-A rare parotid malignancy
 Indian Journal of Mednodent and Allied Sciences, pp- 54-58 Indian journals.com Case Report Carcinoma ex Pleomorphic Adenoma (CXPA)-A rare parotid malignancy Vani Padmaja GJ 1 *, Sireesha A 2, Sunderi Devi
Indian Journal of Mednodent and Allied Sciences, pp- 54-58 Indian journals.com Case Report Carcinoma ex Pleomorphic Adenoma (CXPA)-A rare parotid malignancy Vani Padmaja GJ 1 *, Sireesha A 2, Sunderi Devi
