Hematologic Malignancies. Kim Noonan, RN, ANP, AOCN
|
|
|
- Virgil Whitehead
- 6 years ago
- Views:
Transcription
1 Hematologic Malignancies Kim Noonan, RN, ANP, AOCN
2 Hematologic Malignancies Cancers that affect blood, bone marrow and lymphatic system. Liquid tumors vs solid tumors Leukemia Lymphoma Multiple Myeloma
3 Hematopoietic tree
4 Leukemia
5 Leukemia objectives Identify risk factors for developing leukemia Describe the pathophysiology of leukemia Identify measures and tumor markers used to make a diagnosis of leukemia Outline how leukemia is classified Describe the different types of treatments for leukemia and identify nursing interventions appropriate to patient care Design a plan of care for individuals with leukemia, include planning related to side effects and other concerns regarding treatment
6 Leukemia epidemiology The American Cancer Society's estimates for leukemia in the United States for 2015 are: About 54,270 new cases of leukemia (all kinds) and 24,450 deaths from leukemia (all kinds) Leukemia occurs more often in adults than children Acute lymphocytic leukemia (ALL) is the most common form in children Acute myeloiod leukemia (AML) & Chronic lymphocytic leukemia (CLL) are the most common forms in adults
7 Leukemia risk factors Gender - Male > female Age - Over 50 Genetic predisposition Downs s Syndrome Ataxia telangiectasia Fanconi anemia Bloom syndrome Exposure to radiation Family history - CLL Chemical exposure Benzene Viruses HIV, HTLV-1 & EBV History of cancer therapy Myelodysplastic/ myloproliferative disorders
8 Leukemia pathophysiology Malignant disorders of blood forming cells WBC Diffuse replacement of bone marrow Starts in bone marrow Myeloid vs lymphoid Chronic vs acute
9
10 Leukemia diagnosis CBC Peripheral blood smear Bone marrow samples Aspiration Biopsy Flow cytometry
11 Leukemia - types Rate of cell growth - Acute vs chronic Type of cell - Myeloid vs lymphoid Acute myelogenous leukemia - AML Chronic myelogenous leukemia -CML Acute lymphocytic leukemia- ALL Chronic lymphocytic leukemia -CLL Hairy cell leukemia ( rare chronic leukemia)
12 Leukemia Incidence by Type ALL 6,250 new cases/year CLL 14,620 new cases/year AML 20,830 new cases/year CLL CML AML ALL American Cancer Society Facts & Figures 2015 CML 6,660 new cases/year
13 Hematopoietic tree -AML
14 Acute myelogenous leukemia (AML) Most common acute leukemia in adults 80% In 2014 about 18,860 new cases of acute myeloid leukemia (AML). Most will be in adults. In 2014 about 10,460 deaths from AML. Almost all will be in adults. Average age = 67 Men > women Increased risk of AML associated with: Smoking Chemical exposure benzene MDS Downs syndrome RX with chemotherapy & radiation
15 Acute myelogenous leukemia (AML) Symptoms Fatigue Malaise Weight loss Fever/night sweats Recurrent infections Unexplained bleeding Anorexia Bone pain Neuro (h/a, vomiting, visual changes, Sz) Signs Sudden onset Rapid down hill course Bone marrow failure Anemia Thrombocytopenia Neutropenia Hepatomegaly Organ/gingival infiltration Pale skin, skin lesions
16 Acute myelogenous leukemia (AML) Clinical Abnormalities 95% have circulating myeloblasts in the peripheral smear 75% have platelet counts <100,000 25% have platelet counts <25,000 20% have a WBC of >100, % have a WBC <5,000 Auer rods are present in the peripheral smear Normocytic anemia with a decrease or normal reticulocyte count
17 Acute myelogenous leukemia (AML) Auer Rods
18 Acute myelogenous leukemia (AML) - Classification FAB Classification M0 Minimally differentiated M1 Undifferentiated Myelocyte M2 - Myelocytic M3 - Promylecytic M4 - Myelomonocytic M5 - Monocytic M6 - Erythroleukemia M7 - Megakaraycytic WHO - Classification Genetic Abnormalities Prognostic factors Chromosome abnormalities Gene mutations Age WBC count Prior blood disorders or cancers Infection present CNS involvement Response to treatment
19 Acute myelogenous leukemia (AML) - Treatment Induction initial high dose chemotherapy to achieve complete remission = bone marrow repopulation with normal cells (<5% blasts) Post-remission-given to reduce leukemic cell population Consolidation- 1 or 2 cycles of same chemo used in induction Intensification High dose chemo given shortly after induction ( same or different drugs) Maintenance- lower doses of same drugs as induction given monthly for prolonged period to maintain disease free state
20 Acute myelogenous leukemia (AML) Treatment Induction high dose chemotherapy 7 +3 Cytarabine (Ara-c) + anthracycline (Daunorubicin) Other Anthrcyclines Decreased doses in patients older than 60 Intrathecal cytarabine or methotrexate, with or without cranial radiation, if CNS leukemia present M4 Consolidation Ara-C 3-4 cycles Dose is age dependent Stem Cell Transplant Allogeneic in 1 st remission when cytogenetic suggest poor prognosis In relapsed patients
21 Acute promyelogenous leukemia M3 - Induction Treatment All trans retinoic acid (ATRA) + cytarabine and daunarubicin Arsenic trioxide (ATO)+ ATRA
22 Hematopoietic tree - CML
23 Chronic myelogenous leukemia CML - 10% of all new cases of leukemia. In 2015 about 6,660 new cases of CML will be diagnosed. In 2015 about 1,140 people will die of CML. Men > women Whites > African-Americans The average age - 65 years ( rare in children) Philadelphia chromosome Chromosomes 9 & 22 Increased risk of CML associated with: High dose radiation Older age & male gender
24 Chronic myelogenous leukemia- Philadelphia chromosome
25 Chronic myelogenous leukemia Insidious Onset Fatigue / Weakness Pale skin Night sweats Weight loss Fever Bone pain Spleenomegaly Abdominal pain or a sense of "fullness Feeling full after eating even a small amount of food
26 Chronic myelogenous leukemia - phases Chronic phase Excessive mature granulocytes ( < 10% blasts) Mild symptoms (if any) Philadelphia chromosome in 90% Oral therapies Accelerated phase Increase in immature blast cells - > 10% but < 20% blasts Increase in basophil count- 20% of the WBCs High WBC that do not respond treatment Very high or very low platelet counts New chromosome changes in the leukemia cells SX: fever, poor appetite, and weight loss Does not respond as well to treatment Blast phase (also called acute phase or blast crisis) Bone marrow and/or blood samples > 20% blasts tissues and organs infiltration Resembles AML
27 Prognostic factors for chronic myeloid leukemia Adverse prognostic factors: Accelerated phase or blast phase Enlarged spleen Areas of bone damage from growth of leukemia Increased number of basophils and eosinophils Very high or very low platelet counts Age 60 years or older Multiple chromosome changes in the CML cells
28 Chronic myelogenous leukemia - treatment Targeted therapies Imatinib (Gleevec) Dasatinib (Sprycel) Nilotinib (Tasigna) Interferon alpha Chemotherapy Hydroxyurea (Hydrea ) Cytarabine (Ara-C) Busulfan Cyclophosphamide (Cytoxan ) Vincristine (Oncovin ) Splenectomy Radiation therapy lytic bone lesions Bone marrow or peripheral blood stem cell transplant Allogeneic stem cell transplants- only cure Blast phase treated like acute leukemia
29 Hematopoietic tree - ALL
30 Acute lymphocytic leukemia In 2015, about 6,250 new cases of ALL In 2015, about 1,450 deaths from ALL ALL represents the most common pediatric malignancy 60% of cases in patients < 20 years old Cure rate more favorable in children than adults Males > females Whites > African-Americans
31 Acute lymphocytic leukemia risk factors Radiation exposure Chemical exposure benzene/ chemotherapy Male > female White > black Viral infections HTLV-1 EBV Genetic Down syndrome Klinefelter syndrome Fanconi anemia Bloom syndrome Ataxia-telangiectasia Neurofibromatosis
32 Acute lymphocytic leukemia Symptoms Fatigue Malaise Weight loss Fever/night sweats Recurrent infections Unexplained bleeding Anorexia Bone pain Neuro (h/a, vomiting, visual changes, Seizures) Signs Sudden onset Rapid down hill course Bone marrow failure Anemia Thrombocytopenia Neutropenia Hepatomegaly Organ infiltration Pale skin Enlarged thymus- SVC Lymphadenopathy Splenomegaly
33 Acute lymphocytic leukemia clinical presentation Increase in WBC consisting of lymphoblasts Granulocytopenia Decrease in hemoglobin Decrease in platelets Increase in LDH
34 Acute lymphocytic leukemia -classification Morphology - FAB L1: childhood lymphoblasts (pre B and T cell) (85-89%) L2: adult lymphoblasts (pre B and T cell) (11-14%) L3: Burkitts s type (B-cell)<1% poor prognosis B Cell ALL Most common About 85% are precursor B cell ALL Markers: CD19, CD22, CD20 and CD79; CD10 and CD45 T Cell ALL Uncommon Lymphadenopathy is common Markers: CD3, CD2,CD5,CD1a, CD4 and/or CD8
35 Acute lymphocytic leukemia prognostic indicators Age at diagnosis > 35 years Initial WBC count ALL subtype CNS disease at diagnosis Chromosomal abnormalities Translocation 11 q 23 Philadelphia chromosome Response to chemotherapy
36 ALL Induction treatment Induction 8 weeks Goal cure Combination Chemotherapy 4 drug regimen Steriod VinCRIStine (Oncovin ) Anthracycline +/- L-asparaginase (Elspar ) And/or Cytoxan Imatininb (Gleevec) with + Phildelphia chromosome Supportive care 5% induction mortality Symptom Management Routine transfusions Empiric broad spectrum antibiotics
37 ALL Consolidation treatment Post-remission/ Consolidation Must be in remission Blast <5% No S & S of ALL No S & S of organ involvement No S & S of CNS involvement Children intensification regimens Methotrexate L-asparaginase Adults High dose chemotherapy Allogenic stem cell transplant
38 ALL- CNS Prophylaxis Adults Intrathecal methotrexate High-dose IV methotrexate or cytarabine Radiation therapy to the brain and spinal cord Children Intrathecal Methotrexate High dose chemotherapy
39 ALL Bone marrow/ stem cell Transplantation Autologous stem cell transplant Patient s own stem cells Will not reject Cancer may continue to grow Allogeneic stem cell transplant HLA matched donor 6/6 match preferred Synergistic identical twin Myeloablative HSCT Non-myeloablative mini HSCT Lower doses of chemo with whole body RT Allogenic HSCT Graft vs tumor Age >60 Comorbidities Stem cell sources Bone marrow Peripheral stem cells Umbilical cord blood Placenta
40 ALL- Maintenance 2-3 years Metheltrexate 6-mercaptopurine (6-MP) May include steroid and Vincristine Imatinib (Gleevec) + Philadelphia chromosome Adults - CNS prophylaxis
41 ALL- Response Rates Children The 5-year survival rate for children with ALL 85% Adults 80-90% achieve complete remission 50% or more relaspe 30-40% of adults treated with the conventional ALL protocol will survive
42 Chronic lymphocytic leukemia Characterized by accumulation of small mature lymphocytes Slow growing Predominately in B cells CLL accounts for about one-third of all leukemias. In 2015 about 14,620 new cases of chronic lymphocytic leukemia (CLL) In 2015 about 4,650 deaths from CLL Men > women Family history Average age - 72 years
43 Chronic lymphocytic leukemia Symptoms Asymptomatic in early stages Weakness Fatigue Weight loss Fever Night sweats Enlarged lymph nodes Abdominal pain Early satiety Recurrent infections Signs Insidious onset Splenomegaly Hepatomegaly Lymphadenopathy Anemia Thrombocytopenia Hypogammaglobulinemia Rashes
44 Chronic lymphocytic leukemia staging- Rai system Rai system: This is used more often in the United States The Rai system divides CLL into 5 stages: 0 - lymphocyte count > 10, Lymphocytosis plus enlarged lymph nodes 2 - Lymphocytosis plus an enlarged spleen (and possibly an enlarged liver), +/- enlarged lymph nodes 3 - Lymphocytosis plus anemia, + /- enlarged lymph nodes, spleen, or liver 4 - Lymphocytosis plus thrombocytopenia, +/- anemia, enlarged lymph nodes, spleen, or liver
45 Chronic lymphocytic leukemia staging- Binet system Binet system: This is used more widely in Europe Stage A: Fewer than 3 areas of lymphoid tissue are enlarged, with no anemia or thrombocytopenia. Stage B: 3 or more areas of lymphoid tissue are enlarged, with no anemia or thrombocytopenia. Stage C: Anemia and/or thrombocytopenia are present.
46 Chronic lymphocytic leukemia Adverse prognostic factors Diffuse pattern of bone marrow involvement Advanced age Male gender Increased proportion of large or atypical lymphocytes in the blood Lymphocyte doubling time of less than 12 months Deletions of parts of chromosomes 17 or 11 High blood levels of certain substances, such as beta-2-microglobulin CLL cells containing ZAP-70 (more than 20%) or CD38 (more than 30%) CLL cells with unchanged (not mutated) gene for the immunoglobulin heavy chain variable region (IgVH)
47 Chronic lymphocytic leukemia - treatment Watchful waiting until symptomatic Physical exam and blood counts every 3-6 months Goal Control symptoms, reduce infections, QOL Chemotherapy Purine analogs fludarabine Alkylating agents chlorambucil (Leukeran) and cyclophosphamide (Cytoxan), bendamustine (Treanda) Corticosteroids Monoclonal antibodies Rituximab, Alemtuzumab (Campath) Spleenectomy Radiation therapy painful lymphadenopathy /spleenomegaly
48 Chronic lymphocytic leukemia complications/nursing considerations Tumor lysis syndrome Transformation to high grade non- Hodgkin's Lymphoma Hemolytic anemia and thrombocytopenia Recurrent Infection Prophylactic support Annual attenuated vaccinations Emotional impact of chronic disease
49 Nursing Considerations Acute leukemia are very ill at diagnosis and hospitalized for several weeks Profound bone marrow suppression Infection Sepsis DIC Transfusional support Side effect management Tumor lysis syndrome Psychological support Oral adherence Educational support
50 Lymphoma Scientific Basis for Practice
51 Lymphoma - objectives Identify risk factors for developing lymphoma Describe the pathophysiology of lymphoma Identify measures and tumor markers used to make a diagnosis of lymphoma Outline how lymphoma is classified Describe the different types of treatments for lymphoma and identify nursing interventions appropriate to patient care Design a plan of care for individuals with lymphoma, include planning related to side effects and other concerns regarding treatment
52 Lymphoma Most common hematologic malignancy Account for 5% of all cancers in U.S. Two categories: Hodgkin s lymphomas (Hodgkin s Disease) Non-Hodgkin s lymphomas Lymphomas All Other Cancers
53 Hematopoietic tree - Lymphoma
54 Lymphoma Neoplasm of Lymphoid tissue Lymph nodes, spleen, thymus, adenoids, tonsils, GI tract, bone marrow Lymphocytes B cell -antibodies T- cell- cellular immunity Non-Hodgkin s lymphoma Hodgkin s lymphoma
55 Hodgkin Lymphoma- (Hodgkin s disease) Starts in lymphoid tissue, usually B cells Spreads through lymph system in step wise orderly fashion Reed Sternberg cell In 2015, about 9,050 new cases will occur (3,950 in females and 5,100 in males) In 2015 about 1,150 people (490 females, 660 males) will die of Hodgkin's Lymphoma Bimodal age distribution ages and age >60 1-year relative survival rate 92% 5-year and 10-year survival rates are about 85% and 80%, respectively
56 Hodgkin Lymphoma- risk factors Viral Epstein-Barr virus infection/mononucleosis HIV Age bimodal incidence early adulthood (15-34) & late adulthood (>60) Gender - males > females Geography Family history Socio-economic status
57 Hodgkin Lymphoma- signs & symptoms Painless enlargement of one or more lymph nodes B symptoms Fever Night sweats Anorexia/weight loss Itching Fatigue Loss of appetite Cough, SOB, chest pain
58 Hodgkin Lymphoma- diagnostics Biopsy Excisional or incisional biopsy Fine needle aspiration (FNA) or core needle biopsy Pathology Reed-Sternberg cell
59 Hodgkin Lymphoma- Ann Arbor staging
60 Hodgkin s Lymphoma Adverse prognostic factors B symptoms or bulky disease Age > 45 Being male WBC > 15,000 Hemoglobin level < 10.5 Lymphocyte count < 600 Albumin level < 4
61 Hodgkin Lymphoma- treatment Goal cure Chemotherapy Adriamycin (doxorubicin) Bleomycin Vinblastine Dacarbazine (DTIC) Radiation therapy Involved field radiation Extended field radiation Long tern side effects Heart Disease Stroke Second malignancies Hypothyroidism Fertility issues Infections
62 Non-Hodgkin s Lymphoma Most common hematologic cancer In 2015, about 71,850 people (39,850 males and 32,000 females) will be diagnosed with NHL. In 2015, about 19,790 people will die from this cancer (11,480 males and 8,310 females). Average risk 1 in 50 95% of case occur in adults
63 Non-Hodgkin s Lymphoma > 40 different types of NHL Malignancies of the B & T lymphocytes B-cell lymphomas - 85% T-cell lymphomas 15% Indolent (slow growing) vs aggressive (fast growing)
64 Non-Hodgkin s Lymphoma - Subtypes Follicular - 22% Composite - 13% Small Lymphocytic - 6% Mantal Cell - 6% Peripheral T Cell - 6% Diffuse Large B Cell- 31% Other - 9% MALT - 5% Lymphoplasmacti c - 1% Marginal Zone T - 1%
65 Non-Hodgkin s Lymphoma risk factors Age Gender Race, ethnicity, and geography Exposure to certain chemicals Radiation exposure Immune system deficiency Autoimmune diseases Certain infections
66 Non-Hodgkin s Lymphoma sign & symptoms Enlarged lymph nodes Swollen abdomen Nausea/vomiting/ abdominal pain Feeling full after only a small amount of food Chest pain or pressure Shortness of breath or cough Headache/neuro changes B Symptoms: Fever Weight loss Night sweats Sx of Low blood counts
67 NonHodgkin Lymphoma- diagnostics Biopsy Excisional or incisional biopsy Fine needle aspiration (FNA) or core needle biopsy Pathology Lab Tests Flow cytometry Cytogenetic (chromosomal) analysis Molecular studies
68 Non-Hodgkin s Lymphoma staging
69 Non-Hodgkin s Lymphoma International Prognostic Index IPI Age > 60 Stage III or IV Number of extranodal sites >1 Elevated LDH ECOG Performance status > 2 FLIPI Follicular Lymphoma Age > 60 Stage III or IV Elevated LDH Hemoglubin < 12 g/dl Number of extranodal sites >4
70 Non-Hodgkin s Lymphoma- classification and grade REAL/WHO classification Cell type B cell T cell Natural Killer cell Morphology form & structure Immunophenotype type of protein expressed Genetic Grade Indolent - Survival of untreated disease = years Intermediate -Survival of untreated disease = months Aggressive - Survival of untreated disease = weeks
71 Non-Hodgkin s Lymphoma Indolent Indolent low grade lymphoma chronic disease Follicular SLL/CLL Marginal zone Lymphoplasmacytic Lymphoma/Waldenstrom s macroglobulinemia Hairy Cell Leukemia Watchful waiting Rapidly progressive disease Organ impairment Disease related symptoms Chemotherapy + Rituximab R-CHOP R-CVP R-FC Bendamustin (Treanda) + Rituximab Single agent Rituximab
72 Non-Hodgkin s Lymphoma Relapsed Retreatment with initial chemotherapy New regimen Stem cell transplantation Clinical trials Benefit of maintenance Rituximab Potential of cure with allogenic stem cell transplant
73 Non-Hodgkin s Lymphoma Aggressive Aggressive high grade lymphomas Diffuse Large B- Cell Burkitt s highly aggressive, RX similar to ALL Primary CNS Mantle cell lymphoma Peripheral T-cell lymphoma Lymphoblastic lymphoma Immediate Treatment R CHOP? Cycle length 21 days vs 14 days Radiation therapy Respond well can be curable Relapsed disease High dose chemotherapy Stem cell transplant
74 Lymphoma Nursing Considerations Infusion reactions Rituximab Tumor lyses syndrome Lung damage Bleomycin Baseline pulmonary function tests Cardiac changes Adriamycin MUGA or ECHO Nausea/ vomiting Diarrhea/constipation Alopecia (hair loss) Fatigue Bone marrow suppression Infection prevention Bactrim/Acyclovir/Diflucan Transfusions Neulasta Mucositis Peripheral Neuropathy Sexual health & fertility Cognitive dysfunction Chemo brain Lymphodema
75 Multiple Myeloma Scientific Basis for Practice
76 Multiple Myeloma - objectives Identify risk factors for developing multiple myeloma Describe the pathophysiology of multiple myeloma Identify measures and tumor markers used to make a diagnosis of multiple myeloma Outline how multiple myeloma is classified Describe the different types of treatments for multiple myeloma and identify nursing interventions appropriate to patient care Design a plan of care for individuals with multiple myeloma, include planning related to side effects and other concerns regarding treatment
77 Hematopoietic tree Multiple Myeloma
78 Multiple Myeloma Incurable malignancy of plasma cells Plasmacytoma Myeloma cells prefer bone marrow 1-2 % of all malignancies 10-15% of hematologic malignancies In 2015 about 26,850 new cases will be diagnosed (14,090 in men and 12,760 in women). In 2015 about 11,240 deaths are expected to occur (6,240 in men and 5,000 in women). The 5-year relative survival rate for multiple myeloma is around 33%.
79 Multiple Myeloma risk factors Age - > 65 years old. Gender - Men >women. Race - black Americans > white Americans Radiation exposure Environmental toxins Viruses Genetic factors
80 Multiple Myeloma diagnosis Laboratory tests Imaging Bone marrow biopsy Diagnosis of Multiple Myeloma requires: A plasmacytoma (proven by biopsy) OR 10% bone marrow = plasma cells. AND one of the following: M protein present in blood and/or urine Myeloma related organ dysfunction
81 Multiple Myeloma signs & symptoms CRAB C serum Calcium elevation R Renal insufficiency (SCr >2 mg/dl) A Anemia (Hg, 10 g/dl) B Lytic Bone lesions Neuro S & S Infections
82 Multiple Myeloma staging Durie-Salmon system The International Staging System Stage I - Serum beta-2 microglobulin is less than 3.5 (mg/l) and the albumin level is above 3.5 (g/l) Stage II- Neither stage I or III Stage III- Serum beta-2 microglobulin is greater than 5.5
83 Multiple Myeloma survival International Staging System Stage I Stage II Stage III Median Survival 62 months ~5yr 44 months ~ 3.5yr 29 months ~ 2.5yr Poor Prognostic factors: Older age Kidney function IgA sub type Increased circulating peripheral plasma cells Chromosomal abnormalities
84 Progression of Multiple Myeloma
85 Multiple Myeloma treatment Observation with treatment at disease progression Indications for treatment Symptomatic disease Evidence of organ impairment Anemia Hypercalcemia Lytic bone leisions Renal failure
86 Multiple Myeloma interventions Chemotherapy Immunomodulating agents Steroids Bisphosphonates Radiation Surgery Plasmapheresis Kyphoplasty or Vertebroplasty Stem Cell Transplant Autologous Allogeneic
87 Multiple Myeloma Interventions Chemotherapy melphalan, vincristine, cyclophosphamide, carmustine, and doxorubicin (and liposomal doxorubicin). Corticosteroids Immunomodulating agents Thalidomide Side effects: drowsiness, fatigue, severe constipation, and neuropathy, blood clots, serious birth defects Lenalidomide (Revlimid) Side effects: thrombocytopenia, low WBCs, painful nerve damage, blood clots, serious birth defects
88 Multiple Myeloma Interventions Proteasome inhibitors - Bortezomib (Velcade) Side effects : Immunosuppression (Acyclovir) Cytopenias especially thrombocytopenia Peripheral neuropathy Diarrhea Constipation Rash Hypotension Asthenias- lack of strength
89 Multiple Myeloma - Biophosphonates Zometa (Zoledronic acid) and Aredia (Pamidronate Disodium) and Denosumab Indication Hypercalcemia and bone strengthening Mechanism of action not fully understood Binds to bone matrix Inhibition of bone resorption Inhibition osteoclastic activity Complications: Osteonecrosis of the jaw Renal impairment Hypocalcemia
90
What is a hematological malignancy? Hematology and Hematologic Malignancies. Etiology of hematological malignancies. Leukemias
 Hematology and Hematologic Malignancies Cancer of the formed elements of the blood What is a hematological malignancy? A hematologic malignancy is a malignancy (or cancer) of any of the formed elements
Hematology and Hematologic Malignancies Cancer of the formed elements of the blood What is a hematological malignancy? A hematologic malignancy is a malignancy (or cancer) of any of the formed elements
Indolent Lymphomas: Current. Dr. Laurie Sehn
 Indolent Lymphomas: Current Dr. Laurie Sehn Why does indolent mean? Slow growth Often asymptomatic Chronic disease with periods of relapse (long natural history possible) Incurable with current standard
Indolent Lymphomas: Current Dr. Laurie Sehn Why does indolent mean? Slow growth Often asymptomatic Chronic disease with periods of relapse (long natural history possible) Incurable with current standard
Indolent Lymphomas. Dr. Melissa Toupin The Ottawa Hospital
 Indolent Lymphomas Dr. Melissa Toupin The Ottawa Hospital What does indolent mean? Slow growth Often asymptomatic Chronic disease with periods of relapse (long natural history possible) Incurable with
Indolent Lymphomas Dr. Melissa Toupin The Ottawa Hospital What does indolent mean? Slow growth Often asymptomatic Chronic disease with periods of relapse (long natural history possible) Incurable with
LEUKAEMIA and LYMPHOMA. Dr Mubarak Abdelrahman Assistant Professor Jazan University
 LEUKAEMIA and LYMPHOMA Dr Mubarak Abdelrahman Assistant Professor Jazan University OBJECTIVES Identify etiology and epidemiology for leukemia and lymphoma. Discuss common types of leukemia. Distinguish
LEUKAEMIA and LYMPHOMA Dr Mubarak Abdelrahman Assistant Professor Jazan University OBJECTIVES Identify etiology and epidemiology for leukemia and lymphoma. Discuss common types of leukemia. Distinguish
Lymphoma: What You Need to Know. Richard van der Jagt MD, FRCPC
 Lymphoma: What You Need to Know Richard van der Jagt MD, FRCPC Overview Concepts, classification, biology Epidemiology Clinical presentation Diagnosis Staging Three important types of lymphoma Conceptualizing
Lymphoma: What You Need to Know Richard van der Jagt MD, FRCPC Overview Concepts, classification, biology Epidemiology Clinical presentation Diagnosis Staging Three important types of lymphoma Conceptualizing
Leukemia and Myelodysplastic Syndromes
 Leukemia and Myelodysplastic Syndromes Lenise Taylor, RN, MN, AOCNS Heme Malignancies/BMT CNS Seattle Cancer Care Alliance/UWMC Lymphoid 1 Myeloid 2 Presenting Signs and Symptoms Diagnostic Evaluation
Leukemia and Myelodysplastic Syndromes Lenise Taylor, RN, MN, AOCNS Heme Malignancies/BMT CNS Seattle Cancer Care Alliance/UWMC Lymphoid 1 Myeloid 2 Presenting Signs and Symptoms Diagnostic Evaluation
LYMPHOMA Joginder Singh, MD Medical Oncologist, Mercy Cancer Center
 LYMPHOMA Joginder Singh, MD Medical Oncologist, Mercy Cancer Center Lymphoma is cancer of the lymphatic system. The lymphatic system is made up of organs all over the body that make up and store cells
LYMPHOMA Joginder Singh, MD Medical Oncologist, Mercy Cancer Center Lymphoma is cancer of the lymphatic system. The lymphatic system is made up of organs all over the body that make up and store cells
Aggressive Lymphomas - Current. Dr Kevin Imrie Physician-in-Chief, Sunnybrook Health Sciences Centre
 Aggressive Lymphomas - Current Dr Kevin Imrie Physician-in-Chief, Sunnybrook Health Sciences Centre Conflicts of interest I have no conflicts of interest to declare Outline What does aggressive lymphoma
Aggressive Lymphomas - Current Dr Kevin Imrie Physician-in-Chief, Sunnybrook Health Sciences Centre Conflicts of interest I have no conflicts of interest to declare Outline What does aggressive lymphoma
Large cell immunoblastic Diffuse histiocytic (DHL) Lymphoblastic lymphoma Diffuse lymphoblastic Small non cleaved cell Burkitt s Non- Burkitt s
 Non Hodgkin s Lymphoma Introduction 6th most common cause of cancer death in United States. Increasing in incidence and mortality. Since 1970, the incidence of has almost doubled. Overview The types of
Non Hodgkin s Lymphoma Introduction 6th most common cause of cancer death in United States. Increasing in incidence and mortality. Since 1970, the incidence of has almost doubled. Overview The types of
Acute myeloid leukemia. M. Kaźmierczak 2016
 Acute myeloid leukemia M. Kaźmierczak 2016 Acute myeloid leukemia Malignant clonal disorder of immature hematopoietic cells characterized by clonal proliferation of abnormal blast cells and impaired production
Acute myeloid leukemia M. Kaźmierczak 2016 Acute myeloid leukemia Malignant clonal disorder of immature hematopoietic cells characterized by clonal proliferation of abnormal blast cells and impaired production
Pediatric Oncology. Vlad Radulescu, MD
 Pediatric Oncology Vlad Radulescu, MD Objectives Review the epidemiology of childhood cancer Discuss the presenting signs and symptoms, general treatment principles and overall prognosis of the most common
Pediatric Oncology Vlad Radulescu, MD Objectives Review the epidemiology of childhood cancer Discuss the presenting signs and symptoms, general treatment principles and overall prognosis of the most common
WBCs Disorders 1. Dr. Nabila Hamdi MD, PhD
 WBCs Disorders 1 Dr. Nabila Hamdi MD, PhD ILOs Compare and contrast ALL, AML, CLL, CML in terms of age distribution, cytogenetics, morphology, immunophenotyping, laboratory diagnosis clinical features
WBCs Disorders 1 Dr. Nabila Hamdi MD, PhD ILOs Compare and contrast ALL, AML, CLL, CML in terms of age distribution, cytogenetics, morphology, immunophenotyping, laboratory diagnosis clinical features
Flow Cytometry. Leukemia and Myelodysplastic Syndromes. Bone Marrow Aspirate and Biopsy
 Diagnostic Evaluation of Blood Disorders Leukemia and Myelodysplastic Syndromes Lenise Taylor, MN, RN, AOCNS, BMTCN BMT/Immunotherapy CNS Seattle Cancer Care Alliance/UWMC ltaylor@seattlecca.org History
Diagnostic Evaluation of Blood Disorders Leukemia and Myelodysplastic Syndromes Lenise Taylor, MN, RN, AOCNS, BMTCN BMT/Immunotherapy CNS Seattle Cancer Care Alliance/UWMC ltaylor@seattlecca.org History
Blood Cancers. Blood Cells. Blood Cancers: Progress and Promise. Bone Marrow and Blood. Lymph Nodes and Spleen
 Blood Cancers: Progress and Promise Mike Barnett & Khaled Ramadan Division of Hematology Department of Medicine Providence Health Care & UBC Blood Cancers Significant health problem Arise from normal cells
Blood Cancers: Progress and Promise Mike Barnett & Khaled Ramadan Division of Hematology Department of Medicine Providence Health Care & UBC Blood Cancers Significant health problem Arise from normal cells
Group of malignant disorders of the hematopoietic tissues characteristically associated with increased numbers of white cells in the bone marrow and
 Group of malignant disorders of the hematopoietic tissues characteristically associated with increased numbers of white cells in the bone marrow and / or peripheral blood Classified based on cell type
Group of malignant disorders of the hematopoietic tissues characteristically associated with increased numbers of white cells in the bone marrow and / or peripheral blood Classified based on cell type
MS.4/ Acute Leukemia: AML. Abdallah Al Abbadi.MD.FRCP.FRCPath Feras Fararjeh MD
 MS.4/ 27.02.2019 Acute Leukemia: AML Abdallah Al Abbadi.MD.FRCP.FRCPath Feras Fararjeh MD Case 9: Acute Leukemia 29 yr old lady complains of fever and painful gums for 1 week. She developed easy bruising
MS.4/ 27.02.2019 Acute Leukemia: AML Abdallah Al Abbadi.MD.FRCP.FRCPath Feras Fararjeh MD Case 9: Acute Leukemia 29 yr old lady complains of fever and painful gums for 1 week. She developed easy bruising
Lymphoma/CLL 101: Know your Subtype. Dr. David Macdonald Hematologist, The Ottawa Hospital
 Lymphoma/CLL 101: Know your Subtype Dr. David Macdonald Hematologist, The Ottawa Hospital Function of the Lymph System Lymph Node Lymphocytes B-cells develop in the bone marrow and influence the immune
Lymphoma/CLL 101: Know your Subtype Dr. David Macdonald Hematologist, The Ottawa Hospital Function of the Lymph System Lymph Node Lymphocytes B-cells develop in the bone marrow and influence the immune
Flow Cytometry. Bone Marrow Aspirate and Biopsy. Leukemia and Myelodysplastic Syndromes
 Diagnostic Evaluation of Blood Disorders Leukemia and Myelodysplastic Syndromes Elise Frans, MN, RN, CWON Oncology CNS University of Washington Medical Center delterzo@uw.edu 1 History & Physical Labs:
Diagnostic Evaluation of Blood Disorders Leukemia and Myelodysplastic Syndromes Elise Frans, MN, RN, CWON Oncology CNS University of Washington Medical Center delterzo@uw.edu 1 History & Physical Labs:
Lymphomas and multiple myeloma 12/23/2018 1
 60 Lymphomas and multiple myeloma 12/23/2018 1 Lymphomas Lymphoma is cancer of the lymphatic system. Lymphomas are subdivided into two main categories: Hodgkin's lymphoma (HL) and non- Hodgkin's lymphoma
60 Lymphomas and multiple myeloma 12/23/2018 1 Lymphomas Lymphoma is cancer of the lymphatic system. Lymphomas are subdivided into two main categories: Hodgkin's lymphoma (HL) and non- Hodgkin's lymphoma
Leukemia and Myelodysplastic Syndromes
 Leukemia and Myelodysplastic Syndromes Lenise Taylor, RN, MN, AOCNS, BMTCN Oncology CNS Seattle Cancer Care Alliance/UWMC ltaylor@seattlecca.org Lymphoid 1 Myeloid 2 Diagnostic Evaluation of Blood Disorders
Leukemia and Myelodysplastic Syndromes Lenise Taylor, RN, MN, AOCNS, BMTCN Oncology CNS Seattle Cancer Care Alliance/UWMC ltaylor@seattlecca.org Lymphoid 1 Myeloid 2 Diagnostic Evaluation of Blood Disorders
Hematologic Malignancies. Anna Schaal, RN, MSN, arnp Norris Cotton Cancer Center Lebanon, New Hampshire
 Hematologic Malignancies Anna Schaal, RN, MSN, arnp Norris Cotton Cancer Center Lebanon, New Hampshire Objectives At the end of the session, the oncology nurse will be able to: Explain the pathophysiology
Hematologic Malignancies Anna Schaal, RN, MSN, arnp Norris Cotton Cancer Center Lebanon, New Hampshire Objectives At the end of the session, the oncology nurse will be able to: Explain the pathophysiology
HAEMATOLOGICAL MALIGNANCY
 HAEMATOLOGICAL MALIGNANCY Reference Compulsory reading Haematology at Glance 2 nd ed. Atul Mehta & Victor Hoffbrand Chapters: 20 to 31 Pages: 46 to 69 Pathogenesis of Haematological Malignancy Figure (a)
HAEMATOLOGICAL MALIGNANCY Reference Compulsory reading Haematology at Glance 2 nd ed. Atul Mehta & Victor Hoffbrand Chapters: 20 to 31 Pages: 46 to 69 Pathogenesis of Haematological Malignancy Figure (a)
Hematologic Malignancies. Eunice S. Wang MD Leukemia Service, Department of Medicine Roswell Park Cancer Institute SUNY-UB School of Medicine
 Hematologic Malignancies Eunice S. Wang MD Leukemia Service, Department of Medicine Roswell Park Cancer Institute SUNY-UB School of Medicine Blood cancers are normal blood cells gone bad Jordan C et
Hematologic Malignancies Eunice S. Wang MD Leukemia Service, Department of Medicine Roswell Park Cancer Institute SUNY-UB School of Medicine Blood cancers are normal blood cells gone bad Jordan C et
CHAPTER:4 LEUKEMIA. BY Mrs. K.SHAILAJA., M. PHARM., LECTURER DEPT OF PHARMACY PRACTICE, SRM COLLEGE OF PHARMACY 8/12/2009
 LEUKEMIA CHAPTER:4 1 BY Mrs. K.SHAILAJA., M. PHARM., LECTURER DEPT OF PHARMACY PRACTICE, SRM COLLEGE OF PHARMACY Leukemia A group of malignant disorders affecting the blood and blood-forming tissues of
LEUKEMIA CHAPTER:4 1 BY Mrs. K.SHAILAJA., M. PHARM., LECTURER DEPT OF PHARMACY PRACTICE, SRM COLLEGE OF PHARMACY Leukemia A group of malignant disorders affecting the blood and blood-forming tissues of
HEMATOLOGIC MALIGNANCIES BIOLOGY
 HEMATOLOGIC MALIGNANCIES BIOLOGY Failure of terminal differentiation Failure of differentiated cells to undergo apoptosis Failure to control growth Neoplastic stem cell FAILURE OF TERMINAL DIFFERENTIATION
HEMATOLOGIC MALIGNANCIES BIOLOGY Failure of terminal differentiation Failure of differentiated cells to undergo apoptosis Failure to control growth Neoplastic stem cell FAILURE OF TERMINAL DIFFERENTIATION
Treatment results in ALL
 Treatment results in ALL Adults Complete remission (CR) 80-85% Leukemia-free survival (LFS) 30-40% Children Complete remission (CR) 95-99% Leukemia-free survival (LFS) 70-80% Combination chemotherapy in
Treatment results in ALL Adults Complete remission (CR) 80-85% Leukemia-free survival (LFS) 30-40% Children Complete remission (CR) 95-99% Leukemia-free survival (LFS) 70-80% Combination chemotherapy in
NON HODGKINS LYMPHOMA: INDOLENT Updated June 2015 by Dr. Manna (PGY-5 Medical Oncology Resident, University of Calgary)
 NON HODGKINS LYMPHOMA: INDOLENT Updated June 2015 by Dr. Manna (PGY-5 Medical Oncology Resident, University of Calgary) Reviewed by Dr. Michelle Geddes (Staff Hematologist, University of Calgary) and Dr.
NON HODGKINS LYMPHOMA: INDOLENT Updated June 2015 by Dr. Manna (PGY-5 Medical Oncology Resident, University of Calgary) Reviewed by Dr. Michelle Geddes (Staff Hematologist, University of Calgary) and Dr.
Non-Hodgkin lymphomas (NHLs) Hodgkin lymphoma )HL)
 Non-Hodgkin lymphomas (NHLs) Hodgkin lymphoma )HL) Lymphoid Neoplasms: 1- non-hodgkin lymphomas (NHLs) 2- Hodgkin lymphoma 3- plasma cell neoplasms Non-Hodgkin lymphomas (NHLs) Acute Lymphoblastic Leukemia/Lymphoma
Non-Hodgkin lymphomas (NHLs) Hodgkin lymphoma )HL) Lymphoid Neoplasms: 1- non-hodgkin lymphomas (NHLs) 2- Hodgkin lymphoma 3- plasma cell neoplasms Non-Hodgkin lymphomas (NHLs) Acute Lymphoblastic Leukemia/Lymphoma
The AML subtypes are based on how mature (developed) the cancer cells are at the time of diagnosis and how different they are from normal cells.
 What is Acute Myeloid Leukemia (AML)? Acute myeloid leukemia (AML) is a cancer of cells in the blood, bone marrow and lymph nodes. AML is also called acute nonlymphocytic leukemia, acute myeloblastic leukemia,
What is Acute Myeloid Leukemia (AML)? Acute myeloid leukemia (AML) is a cancer of cells in the blood, bone marrow and lymph nodes. AML is also called acute nonlymphocytic leukemia, acute myeloblastic leukemia,
Acute Lymphoblastic Leukemia (ALL) Ryan Mattison, MD University of Wisconsin March 2, 2010
 Acute Lymphoblastic Leukemia (ALL) Ryan Mattison, MD University of Wisconsin March 2, 2010 ALL Epidemiology 20% of new acute leukemia cases in adults 5200 new cases in 2007 Most are de novo Therapy-related
Acute Lymphoblastic Leukemia (ALL) Ryan Mattison, MD University of Wisconsin March 2, 2010 ALL Epidemiology 20% of new acute leukemia cases in adults 5200 new cases in 2007 Most are de novo Therapy-related
7 Omar Abu Reesh. Dr. Ahmad Mansour Dr. Ahmad Mansour
 7 Omar Abu Reesh Dr. Ahmad Mansour Dr. Ahmad Mansour -Leukemia: neoplastic leukocytes circulating in the peripheral bloodstream. -Lymphoma: a neoplastic process in the lymph nodes, spleen or other lymphatic
7 Omar Abu Reesh Dr. Ahmad Mansour Dr. Ahmad Mansour -Leukemia: neoplastic leukocytes circulating in the peripheral bloodstream. -Lymphoma: a neoplastic process in the lymph nodes, spleen or other lymphatic
Leukemias. Prof. Mutti Ullah Khan Head of Department Medical Unit-II Holy Family Hospital Rawalpindi Medical College
 Leukemias Prof. Mutti Ullah Khan Head of Department Medical Unit-II Holy Family Hospital Rawalpindi Medical College Introduction Leukaemias are malignant disorders of the haematopoietic stem cell compartment,
Leukemias Prof. Mutti Ullah Khan Head of Department Medical Unit-II Holy Family Hospital Rawalpindi Medical College Introduction Leukaemias are malignant disorders of the haematopoietic stem cell compartment,
Lymphatic system component
 Introduction Lymphatic system component Statistics Overview Lymphoma Non Hodgkin s Lymphoma Non- Hodgkin's is a type of cancer that originates in the lymphatic system. It is estimated to be the sixth most
Introduction Lymphatic system component Statistics Overview Lymphoma Non Hodgkin s Lymphoma Non- Hodgkin's is a type of cancer that originates in the lymphatic system. It is estimated to be the sixth most
CLL & SLL: Current Management & Treatment. Dr. Isabelle Bence-Bruckler
 CLL & SLL: Current Management & Treatment Dr. Isabelle Bence-Bruckler Chronic Lymphocytic Leukemia Prolonged clinical course Chronic A particular type of white blood cell B lymphocyte Lymphocytic Cancer
CLL & SLL: Current Management & Treatment Dr. Isabelle Bence-Bruckler Chronic Lymphocytic Leukemia Prolonged clinical course Chronic A particular type of white blood cell B lymphocyte Lymphocytic Cancer
LYMPHOMA. Cheryl Kovalski, DO, FACOI ACOI BOARD REVIEW, 2018 no disclosures
 LYMPHOMA Cheryl Kovalski, DO, FACOI ACOI BOARD REVIEW, 2018 no disclosures Solid neoplasm of the immune system characterized by uncontrolled proliferation of cells residing in the lymphoid tissues 2016
LYMPHOMA Cheryl Kovalski, DO, FACOI ACOI BOARD REVIEW, 2018 no disclosures Solid neoplasm of the immune system characterized by uncontrolled proliferation of cells residing in the lymphoid tissues 2016
UPDATE Autologous Stem Cell Transplantation for Lymphoma and Myeloma
 UPDATE Autologous Stem Cell Transplantation for Lymphoma and Myeloma Supported by a grant from Supported by a grant from UPDATE Autologous Stem Cell Transplantation for Lymphoma and Myeloma Jonathan W.
UPDATE Autologous Stem Cell Transplantation for Lymphoma and Myeloma Supported by a grant from Supported by a grant from UPDATE Autologous Stem Cell Transplantation for Lymphoma and Myeloma Jonathan W.
Charles Mxxx DCEM2 Toulouse Purpan Medical School 01/26/2012 ECN Item 162
 Charles Mxxx DCEM2 Toulouse Purpan Medical School 01/26/2012 ECN Item 162 Definition Pathophysiology Clinical signs and symptoms Biology and Diagnosis Different types of AL Prognosis and Treatment Malignant
Charles Mxxx DCEM2 Toulouse Purpan Medical School 01/26/2012 ECN Item 162 Definition Pathophysiology Clinical signs and symptoms Biology and Diagnosis Different types of AL Prognosis and Treatment Malignant
Lymphoma 101. Nathalie Johnson, MDPhD. Division of Hematology Jewish General Hospital Associate Professor of Medicine, McGill University
 Lymphoma 101 Nathalie Johnson, MDPhD Division of Hematology Jewish General Hospital Associate Professor of Medicine, McGill University Disclosures Consultant and Advisory boards for multiple companies
Lymphoma 101 Nathalie Johnson, MDPhD Division of Hematology Jewish General Hospital Associate Professor of Medicine, McGill University Disclosures Consultant and Advisory boards for multiple companies
CLL: A Guide for Patients and Caregivers CHRONIC LYMPHOCYTIC LEUKEMIA
 CLL: A Guide for Patients and Caregivers LEUKEMIA LYMPHOMA CHRONIC LYMPHOCYTIC LEUKEMIA MYELOMA Introduction In the U.S. In 2006, about 91,000 people were living with CLL In 2007, more than 15,000 people
CLL: A Guide for Patients and Caregivers LEUKEMIA LYMPHOMA CHRONIC LYMPHOCYTIC LEUKEMIA MYELOMA Introduction In the U.S. In 2006, about 91,000 people were living with CLL In 2007, more than 15,000 people
Pathology of Hematopoietic and Lymphoid tissue
 CONTENTS Pathology of Hematopoietic and Lymphoid tissue White blood cells and lymph nodes Quantitative disorder of white blood cells Reactive lymphadenopathies Infectious lymphadenitis Tumor metastasis
CONTENTS Pathology of Hematopoietic and Lymphoid tissue White blood cells and lymph nodes Quantitative disorder of white blood cells Reactive lymphadenopathies Infectious lymphadenitis Tumor metastasis
MS.4/ 1.Nov/2015. Acute Leukemia: AML. Abdallah Abbadi
 MS.4/ 1.Nov/2015. Acute Leukemia: AML Abdallah Abbadi Case 9: Acute Leukemia 29 yr old lady complains of fever and painful gums for 1 week. She developed easy bruising and hemorrhagic spots on her trunk
MS.4/ 1.Nov/2015. Acute Leukemia: AML Abdallah Abbadi Case 9: Acute Leukemia 29 yr old lady complains of fever and painful gums for 1 week. She developed easy bruising and hemorrhagic spots on her trunk
What s a Transplant? What s not?
 What s a Transplant? What s not? How to report the difference? Daniel Weisdorf MD University of Minnesota Anti-cancer effects of BMT or PBSCT [HSCT] Kill the cancer Save the patient Restore immunocompetence
What s a Transplant? What s not? How to report the difference? Daniel Weisdorf MD University of Minnesota Anti-cancer effects of BMT or PBSCT [HSCT] Kill the cancer Save the patient Restore immunocompetence
Lymphoma: The Basics. Dr. Douglas Stewart
 Lymphoma: The Basics Dr. Douglas Stewart Objectives What is lymphoma? How common is it? Why does it occur? How do you diagnose it? How do you manage it? How do you follow patients after treatment? What
Lymphoma: The Basics Dr. Douglas Stewart Objectives What is lymphoma? How common is it? Why does it occur? How do you diagnose it? How do you manage it? How do you follow patients after treatment? What
Disclosures/COI. Cases in Hematopathology. Outline. Heme Path Findings Not to Miss. Normal Peripheral Smear 6/30/2016
 Disclosures/COI Cases in Hematopathology Vamsi Kota Assistant Professor Department of Hematology & Medical Oncology Leukemia/BMT I have no disclosures or conflicts of interest regarding this presentation.
Disclosures/COI Cases in Hematopathology Vamsi Kota Assistant Professor Department of Hematology & Medical Oncology Leukemia/BMT I have no disclosures or conflicts of interest regarding this presentation.
Pathology of Hematopoietic and Lymphoid tissue
 Pathology of Hematopoietic and Lymphoid tissue Peerayut Sitthichaiyakul, M.D. Department of Pathology and Forensic Medicine Faculty of Medicine, Naresuan University CONTENTS White blood cells and lymph
Pathology of Hematopoietic and Lymphoid tissue Peerayut Sitthichaiyakul, M.D. Department of Pathology and Forensic Medicine Faculty of Medicine, Naresuan University CONTENTS White blood cells and lymph
1 Introduction. 1.1 Cancer. Introduction
 Introduction 1 1.1 Cancer 1 Introduction Cancer is the most precarious disease characterized by uncontrolled proliferation of cells without any physiological demands of the organism. Cancer may be defined
Introduction 1 1.1 Cancer 1 Introduction Cancer is the most precarious disease characterized by uncontrolled proliferation of cells without any physiological demands of the organism. Cancer may be defined
Lancashire and South Cumbria Haematology NSSG Guidelines for Follicular Lymphoma:
 1 Lancashire and South Cumbria Haematology NSSG Guidelines for Follicular Lymphoma: 2018-19 1.1 Pretreatment evaluation The following tests should be performed: FBC, U&Es, creat, LFTs, calcium, LDH, Igs/serum
1 Lancashire and South Cumbria Haematology NSSG Guidelines for Follicular Lymphoma: 2018-19 1.1 Pretreatment evaluation The following tests should be performed: FBC, U&Es, creat, LFTs, calcium, LDH, Igs/serum
Table 8.1. Epidemiology of Leukemia in the United States (2010) Annual Deaths. Mean Age. Percentage of All Leukemias (%) (Number of New Cases)
 Table 8.1. Epidemiology of Leukemia in the United States (2010) Type of Leukemia Annual Incidence (Number of New Cases) Percentage of All Leukemias (%) Annual Deaths Mean Age Acute lymphocytic 5,330 12
Table 8.1. Epidemiology of Leukemia in the United States (2010) Type of Leukemia Annual Incidence (Number of New Cases) Percentage of All Leukemias (%) Annual Deaths Mean Age Acute lymphocytic 5,330 12
CLL: disease specific biology and current treatment. Dr. Nathalie Johnson
 CLL: disease specific biology and current treatment Dr. Nathalie Johnson Disclosures Consultant and Advisory boards Roche, Abbvie, Gilead, Jansson, Lundbeck,Merck Research funding Roche, Abbvie, Lundbeck
CLL: disease specific biology and current treatment Dr. Nathalie Johnson Disclosures Consultant and Advisory boards Roche, Abbvie, Gilead, Jansson, Lundbeck,Merck Research funding Roche, Abbvie, Lundbeck
Hematology 101. Rachid Baz, M.D. 5/16/2014
 Hematology 101 Rachid Baz, M.D. 5/16/2014 Florida 101 Epidemiology Estimated prevalence 8,000 individuals in U.S (compare with 80,000 MM patients) Annual age adjusted incidence 3-8/million-year 1 More
Hematology 101 Rachid Baz, M.D. 5/16/2014 Florida 101 Epidemiology Estimated prevalence 8,000 individuals in U.S (compare with 80,000 MM patients) Annual age adjusted incidence 3-8/million-year 1 More
Leukemia. There are different types of leukemia and several treatment options for each type.
 Leukemia Introduction Leukemia is the name of a group of cancers of the blood cells. Hundreds of thousands of people worldwide are diagnosed with leukemia each year. There are different types of leukemia
Leukemia Introduction Leukemia is the name of a group of cancers of the blood cells. Hundreds of thousands of people worldwide are diagnosed with leukemia each year. There are different types of leukemia
Recommended Timing for Transplant Consultation
 REFERRAL GUIDELINES Recommended Timing for Transplant Consultation Published jointly by the National Marrow Donor Program /Be The Match and the American Society for Blood and Marrow Transplantation BeTheMatchClinical.org
REFERRAL GUIDELINES Recommended Timing for Transplant Consultation Published jointly by the National Marrow Donor Program /Be The Match and the American Society for Blood and Marrow Transplantation BeTheMatchClinical.org
Understanding your diagnosis. Dr Graham Collins Consultant Haemtologist Oxford University Hospitals
 Understanding your diagnosis Dr Graham Collins Consultant Haemtologist Oxford University Hospitals Common questions I get asked What is lymphoma? What subtype do I have and what does that mean? What are
Understanding your diagnosis Dr Graham Collins Consultant Haemtologist Oxford University Hospitals Common questions I get asked What is lymphoma? What subtype do I have and what does that mean? What are
Non-Hodgkin s Lymphoma
 Non-Hodgkin s Lympoma Non-Hodgkin s Lymphomas Janet H. Van Cleave MSN, ACNP-CS, CS, AOCN Acute Care Nurse Practitioner The Mount Sinai Medical Center of New York City Doctoral Student, Yale University
Non-Hodgkin s Lympoma Non-Hodgkin s Lymphomas Janet H. Van Cleave MSN, ACNP-CS, CS, AOCN Acute Care Nurse Practitioner The Mount Sinai Medical Center of New York City Doctoral Student, Yale University
5/21/2018. Disclosures. Objectives. Normal blood cells production. Bone marrow failure syndromes. Story of DNA
 AML: Understanding your diagnosis and current and emerging treatments Nothing to disclose. Disclosures Mohammad Abu Zaid, MD Assistant Professor of Medicine Indiana University School of Medicine Indiana
AML: Understanding your diagnosis and current and emerging treatments Nothing to disclose. Disclosures Mohammad Abu Zaid, MD Assistant Professor of Medicine Indiana University School of Medicine Indiana
Pathology. #11 Acute Leukemias. Farah Banyhany. Dr. Sohaib Al- Khatib 23/2/16
 35 Pathology #11 Acute Leukemias Farah Banyhany Dr. Sohaib Al- Khatib 23/2/16 1 Salam First of all, this tafreegh is NOT as long as you may think. If you just focus while studying this, everything will
35 Pathology #11 Acute Leukemias Farah Banyhany Dr. Sohaib Al- Khatib 23/2/16 1 Salam First of all, this tafreegh is NOT as long as you may think. If you just focus while studying this, everything will
WBCs Disorders. Dr. Nabila Hamdi MD, PhD
 WBCs Disorders Dr. Nabila Hamdi MD, PhD ILOs Compare and contrast ALL, AML, CLL, CML in terms of age distribution, cytogenetics, morphology, immunophenotyping, laboratory diagnosis clinical features and
WBCs Disorders Dr. Nabila Hamdi MD, PhD ILOs Compare and contrast ALL, AML, CLL, CML in terms of age distribution, cytogenetics, morphology, immunophenotyping, laboratory diagnosis clinical features and
Stem cell transplantation. Dr Mohammed Karodia NHLS & UP
 Stem cell transplantation Dr Mohammed Karodia NHLS & UP The use of haemopoeitic stem cells from a donor harvested from peripheral blood or bone marrow, to repopulate recipient bone marrow. Allogeneic From
Stem cell transplantation Dr Mohammed Karodia NHLS & UP The use of haemopoeitic stem cells from a donor harvested from peripheral blood or bone marrow, to repopulate recipient bone marrow. Allogeneic From
Hodgkin's Lymphoma. Symptoms. Types
 Hodgkin's lymphoma (Hodgkin's disease) usually develops in the lymphatic system, a part of the body's immune system. This system carries disease-fighting white blood cells throughout the body. Lymph tissue
Hodgkin's lymphoma (Hodgkin's disease) usually develops in the lymphatic system, a part of the body's immune system. This system carries disease-fighting white blood cells throughout the body. Lymph tissue
Adult Acute leukemia. Matthew Seftel. August
 Adult Acute leukemia Matthew Seftel August 21 2007 mseftel@cancercare.mb.ca Principles 3 cases Diagnosis and classification of acute leukemia (AL) Therapy Emergencies Remission induction BMT Complications
Adult Acute leukemia Matthew Seftel August 21 2007 mseftel@cancercare.mb.ca Principles 3 cases Diagnosis and classification of acute leukemia (AL) Therapy Emergencies Remission induction BMT Complications
Acute Myeloid Leukemia: A Patient s Perspective
 Acute Myeloid Leukemia: A Patient s Perspective Patrick A Hagen, MD, MPH Cardinal Bernardin Cancer Center Loyola University Medical Center Maywood, IL Overview 1. What is AML? 2. Who gets AML? Epidemiology
Acute Myeloid Leukemia: A Patient s Perspective Patrick A Hagen, MD, MPH Cardinal Bernardin Cancer Center Loyola University Medical Center Maywood, IL Overview 1. What is AML? 2. Who gets AML? Epidemiology
Instructions for Chronic Lymphocytic Leukemia Post-HSCT Data (Form 2113)
 Instructions for Chronic Lymphocytic Leukemia Post-HSCT Data (Form 2113) This section of the CIBMTR Forms Instruction Manual is intended to be a resource for completing the CLL Post-HSCT Data Form. E-mail
Instructions for Chronic Lymphocytic Leukemia Post-HSCT Data (Form 2113) This section of the CIBMTR Forms Instruction Manual is intended to be a resource for completing the CLL Post-HSCT Data Form. E-mail
Neoplastic proliferation arising from white blood cells. Introductory remarks. Classification
 Neoplastic proliferation arising from white blood cells Lymphoproliferative and myeloproliferative diseases and syndromes Oliver Rácz, 2012-2017 1 Introductory remarks Leukemia and lymphoma are old descriptive
Neoplastic proliferation arising from white blood cells Lymphoproliferative and myeloproliferative diseases and syndromes Oliver Rácz, 2012-2017 1 Introductory remarks Leukemia and lymphoma are old descriptive
New Evidence reports on presentations given at EHA/ICML Bendamustine in the Treatment of Lymphoproliferative Disorders
 New Evidence reports on presentations given at EHA/ICML 2011 Bendamustine in the Treatment of Lymphoproliferative Disorders Report on EHA/ICML 2011 presentations Efficacy and safety of bendamustine plus
New Evidence reports on presentations given at EHA/ICML 2011 Bendamustine in the Treatment of Lymphoproliferative Disorders Report on EHA/ICML 2011 presentations Efficacy and safety of bendamustine plus
CIBMTR Center Number: CIBMTR Recipient ID: Today s Date: Date of HSCT for which this form is being completed:
 Chronic Myelogenous Leukemia (CML) Post-HSCT Data Sequence Number: Date Received: Registry Use Only Today s Date: Date of HSCT for which this form is being completed: HSCT type: autologous allogeneic,
Chronic Myelogenous Leukemia (CML) Post-HSCT Data Sequence Number: Date Received: Registry Use Only Today s Date: Date of HSCT for which this form is being completed: HSCT type: autologous allogeneic,
SWOG ONCOLOGY RESEARCH PROFESSIONAL (ORP) MANUAL LEUKEMIA FORMS CHAPTER 16A REVISED: DECEMBER 2017
 LEUKEMIA FORMS The guidelines and figures below are specific to Leukemia studies. The information in this manual does NOT represent a complete set of required forms for any leukemia study. Please refer
LEUKEMIA FORMS The guidelines and figures below are specific to Leukemia studies. The information in this manual does NOT represent a complete set of required forms for any leukemia study. Please refer
CLL & SLL: Current Management & Treatment. Dr. Peter Anglin
 CLL & SLL: Current Management & Treatment Dr. Peter Anglin Chronic Lymphocytic Leukemia Prolonged clinical course Chronic A particular type of blood cell B lymphocyte Lymphocytic Cancer of white blood
CLL & SLL: Current Management & Treatment Dr. Peter Anglin Chronic Lymphocytic Leukemia Prolonged clinical course Chronic A particular type of blood cell B lymphocyte Lymphocytic Cancer of white blood
Non-Hodgkin lymphoma
 Non-Hodgkin lymphoma Non-Hodgkin s lymphoma Definition: - clonal tumours of mature and immature B cells, T cells or NK cells - highly heterogeneous, both histologically and clinically Non-Hodgkin lymphoma
Non-Hodgkin lymphoma Non-Hodgkin s lymphoma Definition: - clonal tumours of mature and immature B cells, T cells or NK cells - highly heterogeneous, both histologically and clinically Non-Hodgkin lymphoma
Form 2012 R3.0: Chronic Myelogenous Leukemia (CML) Pre-Infusion Data
 Form 2012 R3.0: Chronic Myelogeus Leukemia (CML) Pre-Infusion Data Key Fields Sequence Number: Date Received: - - CIBMTR Center Number: CIBMTR Research ID: Event date: - - HCT type: (check all that apply)
Form 2012 R3.0: Chronic Myelogeus Leukemia (CML) Pre-Infusion Data Key Fields Sequence Number: Date Received: - - CIBMTR Center Number: CIBMTR Research ID: Event date: - - HCT type: (check all that apply)
Waldenstrom s Macroglobulinemia
 Waldenstrom s Macroglobulinemia : Introduction Waldenstrom s macroglobulinemia (WM) is a lymphoma, or cancer of the lymphatic system. It occurs in a type of white blood cell called a B-lymphocyte or B-cell,
Waldenstrom s Macroglobulinemia : Introduction Waldenstrom s macroglobulinemia (WM) is a lymphoma, or cancer of the lymphatic system. It occurs in a type of white blood cell called a B-lymphocyte or B-cell,
Myeloproliferative Disorders - D Savage - 9 Jan 2002
 Disease Usual phenotype acute leukemia precursor chronic leukemia low grade lymphoma myeloma differentiated Total WBC > 60 leukemoid reaction acute leukemia Blast Pro Myel Meta Band Seg Lymph 0 0 0 2
Disease Usual phenotype acute leukemia precursor chronic leukemia low grade lymphoma myeloma differentiated Total WBC > 60 leukemoid reaction acute leukemia Blast Pro Myel Meta Band Seg Lymph 0 0 0 2
MECHANISMS OF HUMAN DISEASE: LABORATORY SESSIONS LYMPHOMA. April 16, 2008
 MECHANISMS OF HUMAN DISEASE: LABORATORY SESSIONS LYMPHOMA April 16, 2008 FACULTY COPY GOAL: Learn the appearance of normal peripheral blood elements and lymph nodes. Recognize abnormal peripheral blood
MECHANISMS OF HUMAN DISEASE: LABORATORY SESSIONS LYMPHOMA April 16, 2008 FACULTY COPY GOAL: Learn the appearance of normal peripheral blood elements and lymph nodes. Recognize abnormal peripheral blood
Chronic Lymphocytic Leukemia (CLL)
 Page 1 of 10 PATIENT EDUCATION Chronic Lymphocytic Leukemia (CLL) Introduction Chronic lymphocytic leukemia (CLL) is a type of cancer of the lymphocytes (a kind of white blood cell). It is also referred
Page 1 of 10 PATIENT EDUCATION Chronic Lymphocytic Leukemia (CLL) Introduction Chronic lymphocytic leukemia (CLL) is a type of cancer of the lymphocytes (a kind of white blood cell). It is also referred
If unqualified, Complete remission is considered to be Haematological complete remission
 Scroll right to see the database codes for Disease status and Response Diagnosis it refers to Disease status or response to treatment AML ALL CML CLL MDS or MD/MPN or acute leukaemia secondary to previous
Scroll right to see the database codes for Disease status and Response Diagnosis it refers to Disease status or response to treatment AML ALL CML CLL MDS or MD/MPN or acute leukaemia secondary to previous
1. Please review the following table, make any changes you think are necessary and highlight those changes. Feel free to put notes on the next page
 COME HOME Non-Hodgkin pathway development worksheet, v6 September 2014 1. Please review the following table, make any changes you think are necessary and highlight those changes. Feel free to put notes
COME HOME Non-Hodgkin pathway development worksheet, v6 September 2014 1. Please review the following table, make any changes you think are necessary and highlight those changes. Feel free to put notes
Aggressive NHL and Hodgkin Lymphoma. Dr. Carolyn Faught November 10, 2017
 Aggressive NHL and Hodgkin Lymphoma Dr. Carolyn Faught November 10, 2017 What does aggressive mean? Shorter duration of symptoms Generally need treatment at time of diagnosis Immediate, few days, few weeks
Aggressive NHL and Hodgkin Lymphoma Dr. Carolyn Faught November 10, 2017 What does aggressive mean? Shorter duration of symptoms Generally need treatment at time of diagnosis Immediate, few days, few weeks
If unqualified, Complete remission is considered to be Haematological complete remission
 Scroll right to see the database codes for Disease status and Response Diagnosis it refers to Disease status or response to treatment AML ALL CML CLL MDS or MD/MPN or acute leukaemia secondary to previous
Scroll right to see the database codes for Disease status and Response Diagnosis it refers to Disease status or response to treatment AML ALL CML CLL MDS or MD/MPN or acute leukaemia secondary to previous
Form 2011 R4.0: Acute Lymphoblastic Leukemia (ALL) Pre-HCT Data
 Key Fields Sequence Number: Date Received: - - CIBMTR Center Number: CIBMTR Recipient ID: Date of HCT for which this form is being completed: - - HCT type: (check all that apply) Autologous Allogeneic,
Key Fields Sequence Number: Date Received: - - CIBMTR Center Number: CIBMTR Recipient ID: Date of HCT for which this form is being completed: - - HCT type: (check all that apply) Autologous Allogeneic,
12/22/2017 Patient education: Chronic lymphocytic leukemia (CLL) in adults (Beyond the Basics) - UpToDate
 Official reprint from UpToDate www.uptodate.com 2017 UpToDate, Inc. and/or its affiliates. All Rights Reserved. The content on the UpToDate website is not intended nor recommended as a substitute for medical
Official reprint from UpToDate www.uptodate.com 2017 UpToDate, Inc. and/or its affiliates. All Rights Reserved. The content on the UpToDate website is not intended nor recommended as a substitute for medical
This was a multicenter study conducted at 11 sites in the United States and 11 sites in Europe.
 Protocol CAM211: A Phase II Study of Campath-1H (CAMPATH ) in Patients with B- Cell Chronic Lymphocytic Leukemia who have Received an Alkylating Agent and Failed Fludarabine Therapy These results are supplied
Protocol CAM211: A Phase II Study of Campath-1H (CAMPATH ) in Patients with B- Cell Chronic Lymphocytic Leukemia who have Received an Alkylating Agent and Failed Fludarabine Therapy These results are supplied
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Anemia(s), 412 426 categories in morphologic approach to, macrocytic, 412 414 microcytic, 412 414 normocytic, 412 413 categorizing, 412
Index Note: Page numbers of article titles are in boldface type. A Anemia(s), 412 426 categories in morphologic approach to, macrocytic, 412 414 microcytic, 412 414 normocytic, 412 413 categorizing, 412
Barbara Barnes Rogers, CRNP, MN, AOCN, ANP-BC Adult Hematology-Oncology Nurse Practitioner Fox Chase Cancer Center Philadelphia, Pennsylvania
 Barbara Barnes Rogers, CRNP, MN, AOCN, ANP-BC Adult Hematology-Oncology Nurse Practitioner Fox Chase Cancer Center Philadelphia, Pennsylvania Barbara.rogers@fccc.edu Disclosures Barbara Rogers, CRNP, MN,
Barbara Barnes Rogers, CRNP, MN, AOCN, ANP-BC Adult Hematology-Oncology Nurse Practitioner Fox Chase Cancer Center Philadelphia, Pennsylvania Barbara.rogers@fccc.edu Disclosures Barbara Rogers, CRNP, MN,
BLOOD AND LYMPH CANCERS
 BLOOD AND LYMPH CANCERS 2 Blood and Lymph Cancers Highlights from the 2009 Annual Meeting of the American Society of Clinical Oncology Edited by Kenneth C. Anderson, MD Harvard Medical School and Dana-Farber
BLOOD AND LYMPH CANCERS 2 Blood and Lymph Cancers Highlights from the 2009 Annual Meeting of the American Society of Clinical Oncology Edited by Kenneth C. Anderson, MD Harvard Medical School and Dana-Farber
Done By : WESSEN ADNAN BUTHAINAH AL-MASAEED
 Done By : WESSEN ADNAN BUTHAINAH AL-MASAEED Acute Myeloid Leukemia Firstly we ll start with this introduction then enter the title of the lecture, so be ready and let s begin by the name of Allah : We
Done By : WESSEN ADNAN BUTHAINAH AL-MASAEED Acute Myeloid Leukemia Firstly we ll start with this introduction then enter the title of the lecture, so be ready and let s begin by the name of Allah : We
Lymphoma is a cancer that develops in the white blood cells (lymphocytes) of the lymphatic system, which is part of the body's immune system.
 Scan for mobile link. Lymphoma Lymphoma is a cancer that develops in the white blood cells of the lymphatic system. Symptoms may include enlarged lymph nodes, unexplained weight loss, fatigue, night sweats
Scan for mobile link. Lymphoma Lymphoma is a cancer that develops in the white blood cells of the lymphatic system. Symptoms may include enlarged lymph nodes, unexplained weight loss, fatigue, night sweats
Standard Regimens for Haematology
 Regimens for Haematology ChlVPP Chlorambucil 6mg/m 2 PO D1 to 14 Vinblastine 6mg/m 2 (max 10mg) IV on D1 & 8 Procarbazine 100mg/m 2 PO on D1 to 14 Prednisolone 40mg PO D1 to 14 ABVD Doxorubicin 25mg/m
Regimens for Haematology ChlVPP Chlorambucil 6mg/m 2 PO D1 to 14 Vinblastine 6mg/m 2 (max 10mg) IV on D1 & 8 Procarbazine 100mg/m 2 PO on D1 to 14 Prednisolone 40mg PO D1 to 14 ABVD Doxorubicin 25mg/m
SPECIAL AUTHORIZATION REQUEST FOR COVERAGE OF HIGH COST CANCER DRUGS
 SPECIAL AUTHORIZATION REQUEST FOR COVERAGE OF HIGH COST CANCER DRUGS (Filgrastim, Capecitabine, Imatinib, Dasatinib, Erolotinib, Sunitinib, Pazopanib, Fludarabine, Sorafenib, Crizotinib, Tretinoin, Nilotinib,
SPECIAL AUTHORIZATION REQUEST FOR COVERAGE OF HIGH COST CANCER DRUGS (Filgrastim, Capecitabine, Imatinib, Dasatinib, Erolotinib, Sunitinib, Pazopanib, Fludarabine, Sorafenib, Crizotinib, Tretinoin, Nilotinib,
Easy Trick to Spot Leukemia for Pediatricians
 Easy Trick to Spot Leukemia for Pediatricians Piya Rujkijyanont, MD Division of Hematology-Oncology Department of Pediatrics Phramongkutklao Hospital Most Common Pediatric Cancers Age 0-14 Leukemia 32%
Easy Trick to Spot Leukemia for Pediatricians Piya Rujkijyanont, MD Division of Hematology-Oncology Department of Pediatrics Phramongkutklao Hospital Most Common Pediatric Cancers Age 0-14 Leukemia 32%
MANAGEMENT OF ACUTE LYMPHOBLASTIC LEUKEMIA. BY Dr SUBHASHINI 1 st yr PG DEPARTMENT OF PEDIATRICS
 MANAGEMENT OF ACUTE LYMPHOBLASTIC LEUKEMIA BY Dr SUBHASHINI 1 st yr PG DEPARTMENT OF PEDIATRICS Introduction The management of ALL, the most common childhood malignancy (1/3 rd of all malignancy), has
MANAGEMENT OF ACUTE LYMPHOBLASTIC LEUKEMIA BY Dr SUBHASHINI 1 st yr PG DEPARTMENT OF PEDIATRICS Introduction The management of ALL, the most common childhood malignancy (1/3 rd of all malignancy), has
Lymphoma (Lymphosarcoma) by Pamela A. Davol
 Lymphoma (Lymphosarcoma) by Pamela A. Davol Cells derived from the bone marrow that mature and take part in cellular immune reactions are called lymphocytes. When lymphocytes undergo transformation and
Lymphoma (Lymphosarcoma) by Pamela A. Davol Cells derived from the bone marrow that mature and take part in cellular immune reactions are called lymphocytes. When lymphocytes undergo transformation and
Acute Lymphoblastic Leukaemia
 Acute Lymphoblastic Leukaemia Terri Boyer 17 th October 2006 Overview Disease information: Aetiology of ALL proposed theory, contributing factors Symptoms Complications Diagnostic approaches - morphology
Acute Lymphoblastic Leukaemia Terri Boyer 17 th October 2006 Overview Disease information: Aetiology of ALL proposed theory, contributing factors Symptoms Complications Diagnostic approaches - morphology
Investigation and Management of Chronic Lymphocytic Leukemia. James Johnston
 Investigation and Management of Chronic Lymphocytic Leukemia James Johnston Site Specific Clinics CLL Clinic (787-4454) Erin Elphee BN James Johnston Rajat Kumar Matt Seftel (transplant) Myeloma Clinic
Investigation and Management of Chronic Lymphocytic Leukemia James Johnston Site Specific Clinics CLL Clinic (787-4454) Erin Elphee BN James Johnston Rajat Kumar Matt Seftel (transplant) Myeloma Clinic
NON HODGKINS LYMPHOMA: AGGRESSIVE Updated June 2015 by Dr. Manna (PGY-5 Medical Oncology Resident, University of Calgary)
 NON HODGKINS LYMPHOMA: AGGRESSIVE Updated June 2015 by Dr. Manna (PGY-5 Medical Oncology Resident, University of Calgary) Reviewed by Dr. Michelle Geddes (Staff Hematologist, University of Calgary) and
NON HODGKINS LYMPHOMA: AGGRESSIVE Updated June 2015 by Dr. Manna (PGY-5 Medical Oncology Resident, University of Calgary) Reviewed by Dr. Michelle Geddes (Staff Hematologist, University of Calgary) and
THE LEUKEMIAS. Etiology:
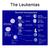 The Leukemias THE LEUKEMIAS Definition 1: malignant transformation of the pluripotent stem cell, successive expansion of the malignant clone from the bone marrow to the tissues Definition 2: Heterogenous
The Leukemias THE LEUKEMIAS Definition 1: malignant transformation of the pluripotent stem cell, successive expansion of the malignant clone from the bone marrow to the tissues Definition 2: Heterogenous
Myelodysplastic Syndromes (MDS) Diagnosis, Treatments & Support
 Myelodysplastic Syndromes (MDS) Diagnosis, Treatments & Support LLS Mission & Goals Our mission. Cure leukemia, lymphoma, Hodgkin s disease and myeloma, and improve the quality of life of patients and
Myelodysplastic Syndromes (MDS) Diagnosis, Treatments & Support LLS Mission & Goals Our mission. Cure leukemia, lymphoma, Hodgkin s disease and myeloma, and improve the quality of life of patients and
Myelodysplasia/Myeloproliferative Neoplasms (MDS/MPN) Post-HCT Data
 Instructions for Myelodysplasia/Myeloproliferative Neoplasms (MDS/MPN) Post-HCT Data (Form 2114) This section of the CIBMTR Forms Instruction Manual is intended to be a resource for completing the Myelodysplasia/Myeloproliferative
Instructions for Myelodysplasia/Myeloproliferative Neoplasms (MDS/MPN) Post-HCT Data (Form 2114) This section of the CIBMTR Forms Instruction Manual is intended to be a resource for completing the Myelodysplasia/Myeloproliferative
CPAG Summary Report for Clinical Panel Policy 1630 Bendamustine-based chemotherapy for first-line treatment of Mantle cell lymphoma (MCL) in adults
 MANAGEMENT IN CONFIDENCE CPAG Summary Report for Clinical Panel Policy 1630 Bendamustine-based chemotherapy for first-line treatment of Mantle cell lymphoma (MCL) in adults The Benefits of the Proposition
MANAGEMENT IN CONFIDENCE CPAG Summary Report for Clinical Panel Policy 1630 Bendamustine-based chemotherapy for first-line treatment of Mantle cell lymphoma (MCL) in adults The Benefits of the Proposition
Understanding the role of ex vivo T cell depletion
 Prevention of graftversus-host disease (GVHD) Understanding the role of ex vivo T cell depletion Information for patients undergoing allogeneic stem cell transplantation in AML and their families 2 This
Prevention of graftversus-host disease (GVHD) Understanding the role of ex vivo T cell depletion Information for patients undergoing allogeneic stem cell transplantation in AML and their families 2 This
Leukemia--Chronic Lymphocytic What is cancer?
 Leukemia--Chronic Lymphocytic What is cancer? The body is made up of trillions of living cells. Normal body cells grow, divide, and die in an orderly fashion. During the early years of a person's life,
Leukemia--Chronic Lymphocytic What is cancer? The body is made up of trillions of living cells. Normal body cells grow, divide, and die in an orderly fashion. During the early years of a person's life,
Guidelines for the Management of Chronic Lymphocytic Leukaemia (CLL)
 Guidelines for the Management of Chronic Lymphocytic Leukaemia (CLL) Version History Version Date Summary of Change/Process 2.0 08.05.08 Endorsed by the Governance Committee 2.1 16.02.11 Circulated at
Guidelines for the Management of Chronic Lymphocytic Leukaemia (CLL) Version History Version Date Summary of Change/Process 2.0 08.05.08 Endorsed by the Governance Committee 2.1 16.02.11 Circulated at
