The International Federation of Head and Neck Oncologic Societies. Current Concepts in Head and Neck Surgery and Oncology
|
|
|
- Kristin Franklin
- 5 years ago
- Views:
Transcription
1 The International Federation of Head and Neck Oncologic Societies Current Concepts in Head and Neck Surgery and Oncology
2 The International Federation of Head and Neck Oncologic Societies Current Concepts in Head and Neck Surgery and Oncology Skin Cancer /Melanoma:Surgery Dr. Patrick Gullane
3 No Disclosures
4 Presentation Be aware of the increasing Incidence of Melanoma Understand the changes in the Staging System Understand the Evaluation and importance of Prognostic Factors Be familiar with Treatment Management- Margins How Wide-Is their a consensus? Value of Sentinel Node-When,How and Why Management of the Neck Be aware of the Role of Adjunctive Treatments Radiation and Systemic therapy
5 Rising Incidence and Mortality of Melanoma in the US Linos, P et al J I Derm
6 Increasing Incidence 2009: 68,000/year 2014: 76,100/year lifetime risk of melanoma approximately 2.0% (1 in 50) for Caucasians 6
7 The Melanoma Epidemic
8 Case Scenario 1 in M55 SSM, 1.8mm Not ulcerated Clark IV Mitotic Rate 1/mm 2
9 Case Scenario 2 in F72 NM, 7.5mm Ulcerated Clark V Mitotic Rate 7/mm 2
10 Case Scenario 3 in F17 SSM, 0.75mm Not ulcerated Clark III Mitotic Rate 1/mm 2
11 Introduction 15-20% of melanomas present in head and neck 6-10% are mucosal melanomas Behaviour is more aggressive than at other sites Risk factors: UV light exposure childhood sunburns fair skin Immunosuppression large congenital nevi sporadic or inherited dysplastic nevi genetic disposition previous melanomas
12 Cutaneous Head & Neck Melanoma Associated with Poorer Prognosis?influence of scalp primaries Risk of nodal metastases - thickness <0.75mm Rare mm ~5% 1 4 mm 8 30% >4mm ~40%
13 Head & Neck Melanoma Most succumb from systemic disease despite regional control Relative Absence of effective systemic agents Loss of disease control Anatomical Aesthetic Functional
14 Staging-7 th now 8 th edition
15
16 AJCC Staging And Survival
17 AJCC 7 th edition Staging Changes - Reasons Importance of Breslow thickness (Clark s level only has a role in tumours < 1mm deep) Importance of ulceration and mitotic rate Importance of in-transit and satellite lesions Based on a belief that micrometastatic disease better than clinically enlarged nodes Number of nodes not size important
18 AJCC 8 th edition Staging Changes - Reasons Cutaneous Melanoma pt1a and pt1b categories introduced pt1a < 0.8mm pt1b > 0.8mm -1mm M category M1a Skin, subcutaneous tissue or non regional lymph nodes M1b Lung M1c Other non-central nervous system sites M1d Central nervous system M Category modified by elevated or non-elevated LDH Stage Revised
19 Workup prior to definitive treatment?
20 Investigations for Melanoma Primary Routine investigations are not required for asymptomatic patients Locoregional +ve SNB routine investigations are not indicated in the absence of systemic symptoms Macroscopic nodes CT +/- PET for symptoms, or in cases where change of management may result FNA to confirm stage III disease Systemic CT, MRI, PET, serum LDH for symptoms suggestive of systemic disease Further investigations as indicated by treatment
21 Diagnosis ABCD(E) s Of Melanoma: Asymmetry, border, colour variegation, diameter >6mm, evolution Bleeding, ulceration, tingling Full-thickness, excisional biopsy of suspicious lesions Tumour markers: HMB-45, S-100
22 Level Level 1 Level 2 Level 3 Level 4 Level 5 Anatomical Invasion Melanoma confined to the epidermis (melanoma in situ) Invasion into the papillary dermis Invasion to the junction of the papillary and reticular dermis Invasion into the reticular dermis Invasion into the subcutaneous fat
23 10 Year survival Rates
24 Prognostic Factors Clinical prognostic Factors Older age Male Head and neck site Histologic prognostic factors Nodal metastases Tumor thickness/depth Ulceration Vascular invasion Microsatellite lesions
25 Prognostic Factors: Nodal metastases Single most powerful predictor of recurrence and survival Occurs in 15-20% of patients Decreases survival by 40%-50% independent of other prognostic factors Increases with increasing tumor thickness Thin (T1) < 1.0mm ~ 2-5% risk Intermediate (T2) mm ~ 15%-25% Intermediate (T3) mm ~ 30% Thick (T4) > 4.0 mm ~ 45%
26 Risk Of Nodal Metatasis McMasters K, et al. Surgery
27 Rationale for ELND Regional Distant % Risk < >4 Melanoma Thickness Balch 1980
28 Rationale for ELND Balch 1979
29 Impact of Nodal Metastases proportion Negative Time(years) Positive ys 83% vs 49% P< Martin et al
30 Impact of N Stage proportion Survival by node group No nodes One node Two or Three nodes Time(years) Four or more nodes
31 Mortality Mortality is typically related to the development of distant metastases Goals of management are Locoregional control Prevention of systemic disease Adjuvant immunotherapy &/or chemotherapeutic agents May have significant side effects Expensive
32 Management Wide local excision of primary Neck management Watch & wait policy Elective lymph node dissection Sentinel node biopsy & nodal management
33 Treatment of Primary Melanoma Wide local excision But How Wide?
34 Margins Randomised trials 5cm historical margins French Co-operative Group, cm vs 5cm margin for melanoma 2mm NO DIFFERENCE Khayet et al, Cancer 2003
35 Margins Randomised trials ä Intergroup Melanoma Committee ä Compared 2 v 4 cm margins for MM 1 to 4 mm ä No significant difference in LR, ITM, survival ä Fewer SSG, shorter hospital stays ä Concluded 2 cm safe for intermediate thickness MM Balch et al, Ann Surg, 1993 No evidence to say that a margin > 1cm improves survival
36 Summary of margins trials No overall survival nor local recurrence advantage for margin >2cm No overall survival advantage for margin >1cm No RCT data for ALM and subungual melanoma Optimal margins for T3 primaries not certain
37 Guidelines for excision margins Melanoma Margin In-situ 5mm 0 to1.0mm 1cm 1.0 to 4.0 (minimum 1cm) maximum 2cm >4.0 minimum 2cm Consider other pathological features satellitosis, lymphatic invasion, desmoplasia, neurotropism
38 Various Melanomas
39 Excision margins -Head and Neck T < 1mm 1cm margin T > 1mm As wide a margin up to 2cm that can be closed without graft / complicated flap or significant disfigurement If a graft or flap is required for the minimum margin take the recommended margin (ie 2cm)
40 Prognostic Factors Tumour thickness Ulceration Clark level Histological type Cell type Primary site Regression Mitoses Lymphocytic infiltration Vertical maturation grade Blood vessel invasion Lymphatic space invasion Ploidy S-Phase DR-1 Expression DNA index HSP expression HLA-DR staining p53 mutations CAM expression Protease expression Migration-associated molecule Angiogenesis-related factor Oncogene expression Oestrogen receptor expression Cytokine, growth factor expression
41 Prognosis of Melanoma Based on Tumor Thickness J Medina Tumor thickness < 1.00 mm Sample Size 10-year survival Level II Level III Level IV Level V 0 Tumor thickness mm Level II Level III Level IV Level V Tumor thickness mm Level II Level III Level IV Level V Tumor thickness > 4.00 mm Level II 14 Level III Level IV Level V Modified from: Buzaid, AC, Ross, MI, Balch, CM, et al, J Clin Oncol 1997;15:1039.
42 Ten-Year Survival Rates in Patients with Melanoma by Tumor Thickness and Ulceration (n = 4568) Number of patients with 10-year survival rate Thickness, mm No Ulceration Ulceration No ulceration Ulceratio n P value (95.5) 96 (4.5) (78.8) 255 (21.2) < < (57.4) 372 (42.6) > (38.1) 238 (61.9) J Medina Modified from Buzaid, AC, Ross, MI, Balch, CM, et al, J Clin Oncol 1997;15:1039
43 Management of the Primary Wide local excision of Primary -Margin analysis of the paraffin block -No frozen section Delayed Reconstruction -Margin Status -Management of the Neck Neck Management Watch & wait policy Elective lymph node dissection Sentinel node biopsy & nodal management
44 Superficial lesions (<0.76mm thick) Excision: 1 cm margin down to fascia N0 neck: SLNB not indicated Elective neck dissection not indicated
45 Intermediate lesions ( mm thick) Excision 1-2 cm margin down to fascia N0 neck: SLNB N1-N3 neck: neck dissection +/- superficial parotidectomy +/- chemotherapy +/- interferon α-2b etc.
46 Deep lesions (>4.0mm thick) Excision -- 2 cm margins down to fascia N0 neck: elective neck dissections not indicated N1-N3 neck: neck dissection +/- superficial parotidectomy +/- chemotherapy +/- interferon α-2b
47 Summary of Management MELANOMA DEPTH MARGIN ptis melanoma in situ 5mm pt1 melanoma <1.0 mm 1cm pt2 melanoma mm 1-2cm pt3 melanoma mm 1-2cm pt4 melanoma >4.0 mm 2cm
48 Management of The Neck In Melanoma 48
49 Prognostic Factors Tumour thickness Ulceration Clark level Histological type Cell type Primary site Regression Mitoses Lymphocytic infiltration Vertical maturation grade Blood vessel invasion Lymphatic space invasion Ploidy S-Phase DR-1 Expression DNA index HSP expression HLA-DR staining p53 mutations CAM expression Protease expression Migration-associated molecule Angiogenesis-related factor Oncogene expression Oestrogen receptor expression Cytokine, growth factor expression Lymph node status
50 Impact of nodal metastases 5 Year survival 83% vs 49% proportion Time(years) Negative Positive Martin et al 5 ys 83% vs 49% P<0.0001
51 Current Node Management SNB offered to 1mm or greater <1mm + ulceration, high MR, (younger age) SNB +ve Offered participation in MSLT II, or TLND, extent based on lymphatic mapping Clinically N+ Confirm diagnosis FNA, systemic staging TLND, selective if appropriate pn+ Considered for adjuvant XRT Offered adjuvant systemic therapy trials
52 To snb or not to snb?
53
54
55 Neck Management : Watch & wait In situ melanoma Thin melanoma < 1mm & less than Clark level III and no adverse pathologic features Risk of nodal metastasis <2% Thick melanoma > 4mm Some debate as to whether to offer SLNB
56 Elective Lymph Node Dissection No strong evidence in favour of performing ELND in clinically node negative patients with H & N melanoma ND unnecessary in > 80% patients Clinical prediction of lymphatic dissemination is unreliable Discordancy rate as high as 14% Lymphatic draining patterns vary
57 Sentinel Lymph Node Biopsy Introduced by Cabanas in 1977 Popularized by Morton 1990 Staging and therapeutic procedure Increases sensitivity to detect regional metastasis Halts regional progression of disease. Selects patients who might benefit from: Further regional therapy Systemic adjuvant therapy
58 Role of Sentinel Lymph Node Biopsy Popularized by Morton for Melanoma Rationale Metastases occur through specific lymphatic channels to involve sentinel nodes as first site of spread If the SLN is negative, the assumption is that rest of the regional nodes are very likely to be free of disease as well
59 Sentinel Node - Definition First draining lymph node on the direct drainage pathway from the primary tumor site Morton Any lymph node receiving direct drainage from a primary lesion site et al Uren
60
61 Indications > 1 mm depth, any Clark level < 1mm depth with Clark level IV, V or ulceration > 4 mm depth with no adverse risk features Controversial
62 Sentinel node biopsy
63 Who should undergo SLN Biopsy? Summary Indications 1-4 mm thick? Thin Melanomas Ulcerated Clark level IV or V Mitoses- > 1/mm 2? Thick Melanomas
64 Contraindications Clinically or radiographic lymph node metastases Tumors > 4 to 5 cm Disruption of lymphatic drainage Prior extensive surgery Extensive local flaps Previous radiation to H & N Pregnancy and breast-feeding Allergy to dye
65 SLNB Technique Morning of Procedure: Injection of primary site with radiolabelled sulfur colloids (technetium- 99m) Planar Lymphoscintigraphy (15 min 1 hour) Inject tumour with blue dye (15 min) Wide Local Excision of Primary Site Use lymphoscintigraphy imaging, Gamma Probe and visualized blue dye to identify sentinel node
66 Sentinel Node Technique Primary Tumor Sentinel Node Lymphatic Channel Regional Lymph Nodes
67 Pre-operative Details Dynamic Lymphatic mapping is performed Multiple peripheral intradermal injections of Tc- 99 Sulfur Colloid 40mBq within 12 hrs of surgery Choice of radiocolloid Uptake sites labeled on skin surface
68 4 SLNB Technique
69 SLNB Technique SLN serially section by pathology As oppose to a single cut through the node Immunohistochemistry S-100 Melan-A HMB-45
70 Hybrid Imaging with SPECT/CT Lymphoscintigraphic Imaging Higher diagnostic reliability Anatomic correlation Higher specificity Better image quality Due to CT attenuation correction Sebaceous cell carcinoma of left upper eyelid: Planar imaging (D) demonstrated only 1 node, whereas SPECT/CT demonstrated 4 nodes, possibly because of slight delay in imaging time. Level IIA (A), level IIB (B), and preauricular (C) lymphatic chains are shown.
71 Hybrid Imaging with SPECT/CT Lymphoscintigraphic Imaging Higher diagnostic reliability Anatomic correlation Higher specificity Better image quality Due to CT attenuation correction Sebaceous cell carcinoma of left upper eyelid: Planar imaging (D) demonstrated only 1 node, whereas SPECT/CT demonstrated 4 nodes, possibly because of slight delay in imaging time. Level IIA (A), level IIB (B), and preauricular (C) lymphatic chains are shown.
72 Intra-operative technique
73 2-3 cm incision(s) made over previously identified areas In line with incision that would be used for ND &/or parotidectomy
74 Isosulfan blue (<1cc) is injected into the derm at the biopsy margins
75 Dye colored lymph nodes are identified
76 Hand held gamma probe is used to localize the hottest sites Using a combination of Isotope mapping, hand held gamma probe and intraoperative blue dye SLN identified in >98% of cases
77 SLN shows radioactive uptake exceeding a 10:1 ratio of ex vivo to resection bed count or a 3:1 ratio of in vivo to resection bed count. 10% rule: Keep looking until bed count < 10% of initial in situ count Formalin fixation and Permanent Sections Special micro-sectioning
78 SPECT-CT for SLNB Single Photon Emission CT Primarily H&N melanoma Improves anatomic location of SLN EJ vs IJ Levels IIA vs IIB vs VA Parotid nodes Suboccipital nodes Shortens operative time Proper placement of incisions 78
79 If SNB positive Neck dissection and consideration for systemic therapy +/- clinical trial
80 Management of +ve SN Therapeutic dissection Based on pattern of drainage at LSG Only 20% will have additional +ve nodes Is CLND-Complete Lymph node dissection necessary? MSLT II
81 Why is Head and Neck site different from all other sites? Cosmetic issues in the head and neck Technically challenging Complex anatomy: nerves and vessels at risk Intraparotid nodes Incision(s) need to be planned based on potential for neck dissection Radionucleotide overlap between primary and drainage
82 Arguments Against SNB Micromets may be clinically irrelevant False negative rates Can still have regional recurrence following SNB and SNB w/nd Drainage not predictable Number of sentinel nodes generally greater than elsewhere- may miss?? Survival benefit
83 Summary SNB improves locoregional control of head and neck melanoma Sentinel-node biopsy has staging and prognostic value in atients with intermediate thickness melanoma But there is no clear survival benefit
84 Current Role for SNB To identify patients with poor prognosis that can be offered adjuvant immunotherapy and/or chemotherapeutic agents Very limited benefit Or to be enrolled in a clinical trial investigating systemic therapies
85 MSLT-I
86 MSLT-1: Rationale Phase 3 Trial to assess the role of SNLBx in melanoma staging (identification of occult nodal metastases) Why? Authors were unsatisfied with the other options: Lymphadenectomy (procedure related risk) Observation Results previously reported but only for intermediate thickness melanomas at 5 years (2006)
87
88 Outcomes Primary Melanoma Specific Survival (DSS) Secondary Disease Free Survival (DFS)
89 Primary Outcome (DSS)
90 Secondary Outcome (DFS)
91 MSLT I Conclusions Our long-term results confirm that sentinel-node biopsy correctly determines the pathologic status of the nodal basin in 96% of cases and is the most powerful prognostic indicator. These long-term results clearly validate the use of sentinel-node biopsy in patients with intermediatethickness or thick primary melanomas. The procedure provides accurate and important staging information, enhances regional disease control, and, among patients with nodal metastases, appears to improve melanoma-specific survival substantially.
92 Bias Despite the consistent strength of the data from the MSLT-I, there has been some reluctance to accept the results of comparisons between node-positive patients in the biopsy group and those in the observation group, because of concern about ascertainment (surveillance) bias. Latent-subgroup analysis methods were used to address this statistical consideration.
93
94 2013 NCCN Updated There is consensus that the procedure should be discussed and offered to patients with primary melanomas greater than 1.0 mm thick. For melanomas 0.76 to 1.0 mm thick, SLNB should be discussed and considered. The discussion about SLNB in this group of patients should include the recognition that the yield of a positive SLNB is low and the clinical significance of a positive SLN is modest. Ulceration High mitotic rate Lymphovascular invasion
95 MSLT II SLN+ randomized to: Completion lymphadenectomy Observation Outcomes Primary: DSS Secondary: DFS and Recurrence at 10 years Estimated completion date 2022
96 The New England Journal of Medicine June 8 th Completion Dissection or Observation for Sentinel- Node Metastasis in Melanoma M.B. Faries, J.F. Thompson, A.J. Cochran, R.H. Andtbacka, N. Mozzillo, J.S. Zager, T. Jahkola, T.L. Bowles, A. Testori, P.D. Beitsch, H.J. Hoekstra, M. Moncrieff, C. Ingvar, M.W.J.M. Wouters, M.S. Sabel, E.A. Levine, D. Agnese, M. Henderson, R. Dummer, C.R. Rossi, R.I. Neves, S.D. Trocha, F. Wright, D.R. Byrd, M. Matter, E. Hsueh, A. MacKenzie-Ross, D.B. Johnson, P. Terheyden, A.C. Berger, T.L. Huston, J.D. Wayne, B.M. Smithers, H.B. Neuman, S. Schneebaum, J.E. Gershenwald, C.E. Ariyan, D.C. Desai, L. Jacobs, K.M. McMasters, A. Gesierich, P. Hersey, S.D. Bines, J.M. Kane, R.J. Barth, G. McKinnon, J.M. Farma, E. Schultz, S. Vidal-Sicart, R.A. Hoefer, J.M. Lewis, R. Scheri, M.C. Kelley, O.E. Nieweg, R.D. Noyes, D.S.B. Hoon, H.-J. Wang, D.A. Elashoff, and R.M. Elashoff
97 A. A. Disease-free Survival B. B. Survival without Nodal Recurrence C. C. Distant Metastasis free Survival D. D. Cumulative Rate of Non- sentinel- E. Node Metastasis. Faries MB et al. N Engl J Med ;376:
98 MSLT II - Conclusions Immediate completion lymph-node dissection: Increased the rate of regional disease control Provided prognostic information But Did not increase melanoma-specific survival among patients with melanoma and sentinel-node metastases.
99 Completion Dissection or Observation for Sentinel-Node Metastasis in Melanoma Conclusions: Immediate completion lymph-node dissection increased the rate of regional disease control and provided prognostic information but did not increase melanoma-specific survival among patients with melanoma and sentinel-node metastases. (Funded by the National Cancer Institute and others; MSLT-II ClinicalTrials.gov number, NCT )
100 Management of the PN+ Neck Surgery: What levels to dissect 100
101
102
103 Nodal Burden vs Outcome 103
104 ROLE OF RADIOTHERAPY 36 patients N+ cmmhn 20 primary 16 recurrent N+ with local excision of LN only + XRT 5 yr actuarial regional control 93% 5 yr actuarial DFS 59% Ballo MT (2005) Head&Neck 27(8):718
105
106 Adjuvant RT Aim: improves regional control without unacceptable complications? survival benefit Indications based on histopathological findings
107 Published data on role of adjuvant RT Only randomized data: Creagan et al pts Sx vs Sx + RT (unusual split course) Trend toward better DFS No comment on locoregional control
108 TROG 96.06: Single arm phase II trial of adjuvant radiotherapy after lymphadenectomy 234 patients Radiotherapy: 48 Gy in 20 fraction given 5 days per week Lymph node field relapse rate 7% Late grade 3 toxicity (fibrosis, lymphoedema) Axilla 9% Groin 19% Burmeister et al., ANZ J Surg 72: ; 2002 Burmeister et al., Radiotherapy and Oncology 81: ; 2006
109 Time to LN field relapse by arm
110 No significant difference in relapse free survival (2 yr 44% vs 38%, p=0.53) 100 % alive and relapse-free RT Obs P = 0.53 HR = 0.90, 95% CI = 0.66 to Hazard ratio 95% CI RT Obs Years from randomisation Number at risk
111 No significant difference in overall Survival (2yr 55% vs 67%, p=0.14) % suriving RT Obs Hazard ratio 95% CI P = 0.14 HR = 1.33, 95% CI = 0.93 to Years from randomisation Number at risk RT Obs
112 Systemic Therapy 112
113 CONCLUSIONS A new era in systemic treatment for advanced stage melanoma Targeted therapy: BRAF and MEK mutations Some remarkable responses but resistance develops rapidly Immunotherapy Targets PD-1 and CTLA 4 30% response, durable remissions in some patients Need predictive biomarkers Expensive In the future patients at high risk will receive biomarker driven combinatorial therapy 113
114 Adjuvant Therapy Chemotherapy Dacarbazine (DTIC) Interferon 1% survival benefit approx Immunotherapy Postoperative Radiation Therapy
115 Conclusions Adjuvant RT improves nodal control Acceptable early toxicities No overall survival benefit Await QoL and lymphoedema data
116 Conclusions Nodal status most significant predictor of disease free and overall survival SNB standard of care Better outcomes with therapeutic dissection for microscopic disease, but era of ELND over Therapeutic dissection may be selective Surgery remains the mainstay of regional metastatic melanoma treatment
117 CONCLUSIONS Challenging disease with early metastasis Imperative for accurate staging Pre-op: pathology, nodal staging Intra-op: WLE + SLNB Post-op: Pathologic staging, margin status, reconstruction 117
Cutaneous Melanoma: Epidemiology (USA) The Sentinel Node in Head and Neck Melanoma. Cutaneous Melanoma: Epidemiology (USA)
 The Sentinel Node in Head and Neck Melanoma Cutaneous Melanoma: Epidemiology (USA) 6 th leading cause of cancer among men and women 68,720 new cases of invasive melanoma in 2009 8,650 deaths from melanoma
The Sentinel Node in Head and Neck Melanoma Cutaneous Melanoma: Epidemiology (USA) 6 th leading cause of cancer among men and women 68,720 new cases of invasive melanoma in 2009 8,650 deaths from melanoma
Topics for Discussion. Malignant Melanoma. Surgical Treatment. Current Treatment of Cutaneous Melanoma 5/17/2013. Lymph Regional nodes:
 Topics for Discussion What is a sentinel lymph node (SLN)? Utility of sentinel lymph biopsies: therapeutic or staging? Current Treatment of Cutaneous Melanoma Carlos Corvera, M.D. Associate Professor of
Topics for Discussion What is a sentinel lymph node (SLN)? Utility of sentinel lymph biopsies: therapeutic or staging? Current Treatment of Cutaneous Melanoma Carlos Corvera, M.D. Associate Professor of
Melanoma Surgery Update James R. Ouellette, DO FACS Premier Health Cancer Institute Wright State University Chief, Surgical Oncology Division
 Melanoma Surgery Update 2018 James R. Ouellette, DO FACS Premier Health Cancer Institute Wright State University Chief, Surgical Oncology Division Surgery for Melanoma Mainstay of treatment for potentially
Melanoma Surgery Update 2018 James R. Ouellette, DO FACS Premier Health Cancer Institute Wright State University Chief, Surgical Oncology Division Surgery for Melanoma Mainstay of treatment for potentially
Melanoma. Kaushik Mukherjee MD A. Scott Pearson MD
 Melanoma Kaushik Mukherjee MD A. Scott Pearson MD Disclosures You still have to study Not all inclusive No Western blots Extensive use of Google Image Search and Sabiston Melanoma Basics 8 th most common
Melanoma Kaushik Mukherjee MD A. Scott Pearson MD Disclosures You still have to study Not all inclusive No Western blots Extensive use of Google Image Search and Sabiston Melanoma Basics 8 th most common
Radionuclide detection of sentinel lymph node
 Radionuclide detection of sentinel lymph node Sophia I. Koukouraki Assoc. Professor Department of Nuclear Medicine Medicine School, University of Crete 1 BACKGROUND The prognosis of malignant disease is
Radionuclide detection of sentinel lymph node Sophia I. Koukouraki Assoc. Professor Department of Nuclear Medicine Medicine School, University of Crete 1 BACKGROUND The prognosis of malignant disease is
Nodal Treatment in Melanoma: Snow to MSLT-II
 Nodal Treatment in Melanoma: Snow to MSLT-II Mark B. Faries, MD, FACS Director, Donald L. Morton Melanoma Research Program Program Director, JWCI Complex General Surgical Oncology Fellowship Director,
Nodal Treatment in Melanoma: Snow to MSLT-II Mark B. Faries, MD, FACS Director, Donald L. Morton Melanoma Research Program Program Director, JWCI Complex General Surgical Oncology Fellowship Director,
Translating Evidence into Practice: Primary Cutaneous Melanoma Guidelines. Sentinel Lymph Node Biopsy
 American Academy of Dermatology 2018 Annual Meeting San Diego, CA, February 17, 2018 Translating Evidence into Practice: Primary Cutaneous Melanoma Guidelines. Sentinel Lymph Node Biopsy Christopher Bichakjian,
American Academy of Dermatology 2018 Annual Meeting San Diego, CA, February 17, 2018 Translating Evidence into Practice: Primary Cutaneous Melanoma Guidelines. Sentinel Lymph Node Biopsy Christopher Bichakjian,
Surgical Issues in Melanoma
 Surgical Issues in Melanoma Mark B. Faries, MD, FACS Director, Donald L. Morton Melanoma Research Program Director, Surgical Oncology Training Program Professor of Surgery John Wayne Cancer Institute Surgical
Surgical Issues in Melanoma Mark B. Faries, MD, FACS Director, Donald L. Morton Melanoma Research Program Director, Surgical Oncology Training Program Professor of Surgery John Wayne Cancer Institute Surgical
Sentinel Lymph Node Biopsy Is Valuable For All Cancer. Surgery Grand Rounds Debate October 6, 2008 Joel Baumgartner
 Sentinel Lymph Node Biopsy Is Valuable For All Cancer Surgery Grand Rounds Debate October 6, 2008 Joel Baumgartner History Lymphatics first described by Rasmus Bartholin in 1653 Rudolf Virchow postulated
Sentinel Lymph Node Biopsy Is Valuable For All Cancer Surgery Grand Rounds Debate October 6, 2008 Joel Baumgartner History Lymphatics first described by Rasmus Bartholin in 1653 Rudolf Virchow postulated
Epithelial Cancer- NMSC & Melanoma
 Epithelial Cancer- NMSC & Melanoma David Chin MB, BCh, BAO, LRCP, LRCS (Ireland) MCh(MD), PhD (UQ), FRCS, FRACS (Plast) Plastic & Reconstructive Surgeon Visiting Scientist Melanoma Genomic Group & Drug
Epithelial Cancer- NMSC & Melanoma David Chin MB, BCh, BAO, LRCP, LRCS (Ireland) MCh(MD), PhD (UQ), FRCS, FRACS (Plast) Plastic & Reconstructive Surgeon Visiting Scientist Melanoma Genomic Group & Drug
NEW SURGICAL APPROACHES TO MELANOMA THERAPY
 NEW SURGICAL APPROACHES TO MELANOMA THERAPY Melanoma 2003: New Insights Into Therapy & Treatment Douglas L. Fraker, M.D. University of Pennsylvania Surgical Treatment of Melanoma Primary resection margins
NEW SURGICAL APPROACHES TO MELANOMA THERAPY Melanoma 2003: New Insights Into Therapy & Treatment Douglas L. Fraker, M.D. University of Pennsylvania Surgical Treatment of Melanoma Primary resection margins
Desmoplastic Melanoma: Surgical Management and Adjuvant Therapy
 Desmoplastic Melanoma: Surgical Management and Adjuvant Therapy Dale Han, MD Assistant Professor Department of Surgery Section of Surgical Oncology No disclosures Background Desmoplastic melanoma (DM)
Desmoplastic Melanoma: Surgical Management and Adjuvant Therapy Dale Han, MD Assistant Professor Department of Surgery Section of Surgical Oncology No disclosures Background Desmoplastic melanoma (DM)
Update on SLN and Melanoma: DECOG and MSLT-II. Gordon H. Hafner, MD, FACS
 Update on SLN and Melanoma: DECOG and MSLT-II Gordon H. Hafner, MD, FACS No disclosures The surgery of malignant disease is not the surgery of organs, it is of the lymphatic system. Lord Moynihan Lymph
Update on SLN and Melanoma: DECOG and MSLT-II Gordon H. Hafner, MD, FACS No disclosures The surgery of malignant disease is not the surgery of organs, it is of the lymphatic system. Lord Moynihan Lymph
Patient age and cutaneous malignant melanoma: Elderly patients are likely to have more aggressive histological features and poorer survival
 MOLECULAR AND CLINICAL ONCOLOGY 7: 1083-1088, 2017 Patient age and cutaneous malignant melanoma: Elderly patients are likely to have more aggressive histological features and poorer survival FARUK TAS
MOLECULAR AND CLINICAL ONCOLOGY 7: 1083-1088, 2017 Patient age and cutaneous malignant melanoma: Elderly patients are likely to have more aggressive histological features and poorer survival FARUK TAS
Melanoma Quality Reporting
 Melanoma Quality Reporting September 1, 2013 December 31, 2016 Laurence McCahill, MD Surgical Oncologist Metro Health Surgical Oncology Metro Health Professional Building 2122 Health Drive SW Wyoming,
Melanoma Quality Reporting September 1, 2013 December 31, 2016 Laurence McCahill, MD Surgical Oncologist Metro Health Surgical Oncology Metro Health Professional Building 2122 Health Drive SW Wyoming,
Disclosures. SLNB for Melanoma 25/02/2014 SENTINEL LYMPH NODE BIOPSY FOR MELANOMA: CURRENT GUIDELINES AND THEIR CLINICAL APPLICATION
 8 th Canadian Melanoma Conference February 22, 2014 Rimrock Resort Hotel, Banff, Alberta SENTINEL LYMPH NODE BIOPSY FOR MELANOMA: CURRENT GUIDELINES AND THEIR CLINICAL APPLICATION Christopher Bichakjian,
8 th Canadian Melanoma Conference February 22, 2014 Rimrock Resort Hotel, Banff, Alberta SENTINEL LYMPH NODE BIOPSY FOR MELANOMA: CURRENT GUIDELINES AND THEIR CLINICAL APPLICATION Christopher Bichakjian,
Case Scenario 1 Worksheet. Primary Site C44.4 Morphology 8743/3 Laterality 0 Stage/ Prognostic Factors
 CASE SCENARIO 1 9/10/13 HISTORY: Patient is a 67-year-old white male and presents with lesion located 4-5cm above his right ear. The lesion has been present for years. No lymphadenopathy. 9/10/13 anterior
CASE SCENARIO 1 9/10/13 HISTORY: Patient is a 67-year-old white male and presents with lesion located 4-5cm above his right ear. The lesion has been present for years. No lymphadenopathy. 9/10/13 anterior
Technical Considerations. Imaging Considerations
 354 CUTANEOUS MALIGNANCY OF THE HEAD AND NECK desmoplastic melanomas are characterized by a uniform desmoplasia that is prominent throughout the entire tumor (termed pure desmoplastic melanoma), whereas
354 CUTANEOUS MALIGNANCY OF THE HEAD AND NECK desmoplastic melanomas are characterized by a uniform desmoplasia that is prominent throughout the entire tumor (termed pure desmoplastic melanoma), whereas
Index. Note: Page numbers of article titles are in boldface type. A Age as factor in melanoma, Anorectal melanoma RT for, 1035
 Index Note: Page numbers of article titles are in boldface type. A Age as factor in melanoma, 947 948 Anorectal melanoma RT for, 1035 B Bacille Calmette-Guerin (BCG) in melanoma, 1008 BCG. See Bacille
Index Note: Page numbers of article titles are in boldface type. A Age as factor in melanoma, 947 948 Anorectal melanoma RT for, 1035 B Bacille Calmette-Guerin (BCG) in melanoma, 1008 BCG. See Bacille
Clinical Pathological Conference. Malignant Melanoma of the Vulva
 Clinical Pathological Conference Malignant Melanoma of the Vulva History F/48 Chinese Married Para 1 Presented in September 2004 Vulval mass for 2 months Associated with watery and blood stained discharge
Clinical Pathological Conference Malignant Melanoma of the Vulva History F/48 Chinese Married Para 1 Presented in September 2004 Vulval mass for 2 months Associated with watery and blood stained discharge
Updates on Melanoma: Are You Following the Latest Guidelines of Care? Jerry Brewer, MD
 Updates on Melanoma: Are You Following the Latest Guidelines of Care? Jerry Brewer, MD Disclosure Statement Update on Melanoma Are You Following the Latest Guidelines of Care? I, Jerry D. Brewer, MD, do
Updates on Melanoma: Are You Following the Latest Guidelines of Care? Jerry Brewer, MD Disclosure Statement Update on Melanoma Are You Following the Latest Guidelines of Care? I, Jerry D. Brewer, MD, do
Sentinel Lymph Node Biopsies in Cutaneous Melanoma: A systematic review of the literature. Sasha Jenkins
 Sentinel Lymph Node Biopsies in Cutaneous Melanoma: A systematic review of the literature By Sasha Jenkins A Master s Paper submitted to the faculty of the University of North Carolina at Chapel Hill in
Sentinel Lymph Node Biopsies in Cutaneous Melanoma: A systematic review of the literature By Sasha Jenkins A Master s Paper submitted to the faculty of the University of North Carolina at Chapel Hill in
Molecular Enhancement of Sentinel Node Evaluation
 Cochran Illustrations 060104 Molecular Enhancement of Sentinel Node Evaluation Alistair Cochran, MD and Rong Huang MD Departments of Pathology and Laboratory Medicine and Surgery, David Geffen School of
Cochran Illustrations 060104 Molecular Enhancement of Sentinel Node Evaluation Alistair Cochran, MD and Rong Huang MD Departments of Pathology and Laboratory Medicine and Surgery, David Geffen School of
SPECT/CT Imaging of the Sentinel Lymph Node
 IAEA Regional Training Course on Hybrid Imaging SPECT/CT Imaging of the Sentinel Lymph Node Giuliano Mariani Regional Center of Nuclear Medicine, University of Pisa Medical School, Pisa, Italy Vilnius,
IAEA Regional Training Course on Hybrid Imaging SPECT/CT Imaging of the Sentinel Lymph Node Giuliano Mariani Regional Center of Nuclear Medicine, University of Pisa Medical School, Pisa, Italy Vilnius,
Rebecca Vogel, PGY-4 March 5, 2012
 Rebecca Vogel, PGY-4 March 5, 2012 Historical Perspective Changes In The Staging System Studies That Started The Talk Where We Go From Here Cutaneous melanoma has become an increasingly growing problem,
Rebecca Vogel, PGY-4 March 5, 2012 Historical Perspective Changes In The Staging System Studies That Started The Talk Where We Go From Here Cutaneous melanoma has become an increasingly growing problem,
Surgery for Melanoma and What s on the Horizon
 and What s on the Horizon Giorgos C. Karakousis, M.D. Assistant Professor of Surgery Perelman School of Medicine at the University of Pennsylvania Background/Overview 76,870 cases of melanoma estimated
and What s on the Horizon Giorgos C. Karakousis, M.D. Assistant Professor of Surgery Perelman School of Medicine at the University of Pennsylvania Background/Overview 76,870 cases of melanoma estimated
Melanoma Patients and the Sentinel Lymph Node (SLN) Procedure: An Oncologic Surgeon s Perspective
 Melanoma Patients and the Sentinel Lymph Node (SLN) Procedure: An Oncologic Surgeon s Perspective Giorgos C. Karakousis, M.D. Associate Professor of Surgery Hospital of the University of Pennsylvania Disclosures
Melanoma Patients and the Sentinel Lymph Node (SLN) Procedure: An Oncologic Surgeon s Perspective Giorgos C. Karakousis, M.D. Associate Professor of Surgery Hospital of the University of Pennsylvania Disclosures
You Are Going to Cut How Much Skin? Locoregional Surgical Treatment. Justin Rivard MD, MSc, FRCSC September 21, 2018
 You Are Going to Cut How Much Skin? Locoregional Surgical Treatment Justin Rivard MD, MSc, FRCSC September 21, 2018 Presenter Disclosure Faculty/Speaker: Justin Rivard Relationships with financial sponsors:
You Are Going to Cut How Much Skin? Locoregional Surgical Treatment Justin Rivard MD, MSc, FRCSC September 21, 2018 Presenter Disclosure Faculty/Speaker: Justin Rivard Relationships with financial sponsors:
Management of the patient with Lymph Node Involvement. Michael A Henderson Peter MacCallum Cancer Center Univ of Melbourne
 Management of the patient with Lymph Node Involvement Michael A Henderson Peter MacCallum Cancer Center Univ of Melbourne Lymph Node Field Recurrence Most important prognostic factor for early stage melanoma
Management of the patient with Lymph Node Involvement Michael A Henderson Peter MacCallum Cancer Center Univ of Melbourne Lymph Node Field Recurrence Most important prognostic factor for early stage melanoma
1
 www.clinicaloncology.com.ua 1 Prognostic factors of appearing micrometastases in sentinel lymph nodes in skin melanoma M.N.Kukushkina, S.I.Korovin, O.I.Solodyannikova, G.G.Sukach, A.Yu.Palivets, A.N.Potorocha,
www.clinicaloncology.com.ua 1 Prognostic factors of appearing micrometastases in sentinel lymph nodes in skin melanoma M.N.Kukushkina, S.I.Korovin, O.I.Solodyannikova, G.G.Sukach, A.Yu.Palivets, A.N.Potorocha,
Printed by Martina Huckova on 10/3/2011 3:04:54 PM. For personal use only. Not approved for distribution. Copyright 2011 National Comprehensive
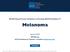 Table of Contents NCCN Categories of Evidence and Consensus Category 1: Based upon high-level evidence, there is uniform NCCN consensus that the intervention is appropriate. Category 2A: Based upon lower-level
Table of Contents NCCN Categories of Evidence and Consensus Category 1: Based upon high-level evidence, there is uniform NCCN consensus that the intervention is appropriate. Category 2A: Based upon lower-level
Sentinel Lymph Node Biopsy for Breast Cancer
 Sentinel Lymph Node Biopsy for Breast Cancer Registrar Tutorial Adam Cichowitz Surgical Registrar The Royal Melbourne Hospital Sentinel Lymph Node Biopsy Axillary LN status important prognostic factor
Sentinel Lymph Node Biopsy for Breast Cancer Registrar Tutorial Adam Cichowitz Surgical Registrar The Royal Melbourne Hospital Sentinel Lymph Node Biopsy Axillary LN status important prognostic factor
1. Written information to patient /GP: fax ASAP to GP & offer copy of consultation letter.
 Skin Cancer follow up guidelines If NEW serious diagnosis given: 1. Written information to patient /GP: fax ASAP to GP & offer copy of consultation letter. 2. Free prescription information details. 3.
Skin Cancer follow up guidelines If NEW serious diagnosis given: 1. Written information to patient /GP: fax ASAP to GP & offer copy of consultation letter. 2. Free prescription information details. 3.
Update on 8 th Edition Cutaneous AJCC Staging of Primary Cutaneous Melanoma. Michael T. Tetzlaff MD, PhD
 Update on 8 th Edition Cutaneous AJCC Staging of Primary Cutaneous Melanoma Michael T. Tetzlaff MD, PhD Associate Professor Departments of Pathology (Dermatopathology) and Translational and Molecular Pathology
Update on 8 th Edition Cutaneous AJCC Staging of Primary Cutaneous Melanoma Michael T. Tetzlaff MD, PhD Associate Professor Departments of Pathology (Dermatopathology) and Translational and Molecular Pathology
Impact of Prognostic Factors
 Melanoma Prognostic Factors: where we started, where are we going? Impact of Prognostic Factors Staging Management Surgical intervention Adjuvant treatment Suraj Venna, MD Assistant Clinical Professor,
Melanoma Prognostic Factors: where we started, where are we going? Impact of Prognostic Factors Staging Management Surgical intervention Adjuvant treatment Suraj Venna, MD Assistant Clinical Professor,
Sentinel lymph node (SLN) biopsy is a wellestablished
 ORIGINAL ARTICLE DISCORDANT LYMPHATIC DRAINAGE PATTERNS REVEALED BY SERIAL LYMPHOSCINTIGRAPHY IN CUTANEOUS HEAD AND NECK MALIGNANCIES Alliric I. Willis, MD, John A. Ridge, MD, PhD Department of Surgical
ORIGINAL ARTICLE DISCORDANT LYMPHATIC DRAINAGE PATTERNS REVEALED BY SERIAL LYMPHOSCINTIGRAPHY IN CUTANEOUS HEAD AND NECK MALIGNANCIES Alliric I. Willis, MD, John A. Ridge, MD, PhD Department of Surgical
Precision Surgery for Melanoma
 Precision Surgery for Melanoma Giorgos C. Karakousis, M.D. Assistant Professor of Surgery Perelman School of Medicine at the University of Pennsylvania Background 87,110 cases of melanoma estimated in
Precision Surgery for Melanoma Giorgos C. Karakousis, M.D. Assistant Professor of Surgery Perelman School of Medicine at the University of Pennsylvania Background 87,110 cases of melanoma estimated in
Controversies and Questions in the Surgical Treatment of Melanoma
 Controversies and Questions in the Surgical Treatment of Melanoma Giorgos C. Karakousis, M.D. Assistant Professor of Surgery Division of Endocrine and Oncologic Surgery University of Pennsylvania School
Controversies and Questions in the Surgical Treatment of Melanoma Giorgos C. Karakousis, M.D. Assistant Professor of Surgery Division of Endocrine and Oncologic Surgery University of Pennsylvania School
ORIGINAL ARTICLE PROGNOSTIC IMPLICATION OF SENTINEL LYMPH NODE BIOPSY IN CUTANEOUS HEAD AND NECK MELANOMA
 ORIGINAL ARTICLE PROGNOSTIC IMPLICATION OF SENTINEL LYMPH NODE BIOPSY IN CUTANEOUS HEAD AND NECK MELANOMA Benjamin E. Saltman, MD, 1 Ian Ganly, MD, 2 Snehal G. Patel, MD, 2 Daniel G. Coit, MD, 3 Mary Sue
ORIGINAL ARTICLE PROGNOSTIC IMPLICATION OF SENTINEL LYMPH NODE BIOPSY IN CUTANEOUS HEAD AND NECK MELANOMA Benjamin E. Saltman, MD, 1 Ian Ganly, MD, 2 Snehal G. Patel, MD, 2 Daniel G. Coit, MD, 3 Mary Sue
Protocol applies to melanoma of cutaneous surfaces only.
 Melanoma of the Skin Protocol applies to melanoma of cutaneous surfaces only. Procedures Biopsy (No Accompanying Checklist) Excision Re-excision Protocol revision date: January 2005 Based on AJCC/UICC
Melanoma of the Skin Protocol applies to melanoma of cutaneous surfaces only. Procedures Biopsy (No Accompanying Checklist) Excision Re-excision Protocol revision date: January 2005 Based on AJCC/UICC
ORIGINAL ARTICLE. (SLN) biopsy is revolutionizing
 ORIGINAL ARTICLE Management of Malignant Melanoma of the Head and Neck Using Dynamic Lymphoscintigraphy and Gamma Probe Guided Sentinel Lymph Node Biopsy Grant W. Carlson, MD; Douglas R. Murray, MD; Robert
ORIGINAL ARTICLE Management of Malignant Melanoma of the Head and Neck Using Dynamic Lymphoscintigraphy and Gamma Probe Guided Sentinel Lymph Node Biopsy Grant W. Carlson, MD; Douglas R. Murray, MD; Robert
Epidemiology. Objectives 8/28/2017
 Case based Discussion of Head and Neck Melanoma: Review of Epidemiology, Risk Factors, Identification, Treatments and Prevention Jacqueline M. Doucette MS FNP-C Objectives Define and identify melanoma
Case based Discussion of Head and Neck Melanoma: Review of Epidemiology, Risk Factors, Identification, Treatments and Prevention Jacqueline M. Doucette MS FNP-C Objectives Define and identify melanoma
Primary Cutaneous Melanoma Pathology Reporting Proforma DD MM YYYY. *Tumour site. *Specimen laterality. *Specimen type
 Primary Cutaneous Melanoma Pathology Reporting Proforma Includes the International Collaboration on Cancer reporting dataset denoted by * Family name Given name(s) Date of birth DD MM YYYY Sex Male Female
Primary Cutaneous Melanoma Pathology Reporting Proforma Includes the International Collaboration on Cancer reporting dataset denoted by * Family name Given name(s) Date of birth DD MM YYYY Sex Male Female
Melanoma 10/12/18 Justin J. Baker, M.D.
 Objectives Review Incidence Risk Factors for Development Detection 10/12/18 Justin J. Baker, M.D. Treatment of Surgery Medicine Radiation What is Incidence Cancer of Melanocytes Melanocytes are normal
Objectives Review Incidence Risk Factors for Development Detection 10/12/18 Justin J. Baker, M.D. Treatment of Surgery Medicine Radiation What is Incidence Cancer of Melanocytes Melanocytes are normal
Sentinel Node Alphabet Soup: MSLT-1, DeCOG-SLT, MSLT-2, UNC
 Sentinel Node Alphabet Soup: MSLT-1, DeCOG-SLT, MSLT-2, UNC David W. Ollila MD James and Jesse Millis Professor of Surgery University of North Carolina, Chapel Hill Disclosures: None July 15, 2018 AJCC
Sentinel Node Alphabet Soup: MSLT-1, DeCOG-SLT, MSLT-2, UNC David W. Ollila MD James and Jesse Millis Professor of Surgery University of North Carolina, Chapel Hill Disclosures: None July 15, 2018 AJCC
Melanoma Underwriting Presented at 2018 AHOU Conference. Hank George FALU
 Melanoma Underwriting Presented at 2018 AHOU Conference Hank George FALU MELANOMA EPIDEMIOLOGY 70-80,000 American cases annually Majority are in situ or thin > 20% are diagnosed age 45 8-9,000 melanoma
Melanoma Underwriting Presented at 2018 AHOU Conference Hank George FALU MELANOMA EPIDEMIOLOGY 70-80,000 American cases annually Majority are in situ or thin > 20% are diagnosed age 45 8-9,000 melanoma
Sentinel Node Localisation of Melanoma
 Sentinel Node Localisation of Melanoma V Bongers, Diakonessenhuis, Utrecht 1. Introduction A melanoma is mostly a malignancy of the skin. The sentinel lymph node (SLN) concept of sequential progression
Sentinel Node Localisation of Melanoma V Bongers, Diakonessenhuis, Utrecht 1. Introduction A melanoma is mostly a malignancy of the skin. The sentinel lymph node (SLN) concept of sequential progression
Major Topic. Malignant Melanoma Plastic and Reconstructive Surgery R3 陸尊惠 /VS 吳瑞星
 Major Topic Malignant Melanoma Plastic and Reconstructive Surgery R3 陸尊惠 /VS 吳瑞星 Patient Data Name: OOO Age: 70 Gender: Male Date of admission: Day 1 Chief Complaint Black skin tumor at the back of the
Major Topic Malignant Melanoma Plastic and Reconstructive Surgery R3 陸尊惠 /VS 吳瑞星 Patient Data Name: OOO Age: 70 Gender: Male Date of admission: Day 1 Chief Complaint Black skin tumor at the back of the
Predictive Factors for the Positivity of the Sentinel Lymph Node in Malignant Melanoma
 ORIGINAL RESEARCH SURGERY // ANATOMO-PATHOLOGY Predictive Factors for the Positivity of the Sentinel Lymph Node in Malignant Melanoma Călin Crăciun, Orsolya Hankó- Bauer, Zalán Benedek, Sorin Sorlea, Marius
ORIGINAL RESEARCH SURGERY // ANATOMO-PATHOLOGY Predictive Factors for the Positivity of the Sentinel Lymph Node in Malignant Melanoma Călin Crăciun, Orsolya Hankó- Bauer, Zalán Benedek, Sorin Sorlea, Marius
WHAT DOES THE PATHOLOGY REPORT MEAN?
 Melanoma WHAT IS MELANOMA? Melanoma is a type of cancer that affects cells called melanocytes. These cells are found mainly in skin but also in the lining of other areas such as nose and rectum, and also
Melanoma WHAT IS MELANOMA? Melanoma is a type of cancer that affects cells called melanocytes. These cells are found mainly in skin but also in the lining of other areas such as nose and rectum, and also
Practice of Axilla Surgery
 Summer School of Breast Disease 2016 Practice of Axilla Surgery Axillary Lymph Node Dissection & Sentinel Lymph Node Biopsy 연세의대외과 박세호 Contents Anatomy of the axilla Axillary lymph node dissection (ALND)
Summer School of Breast Disease 2016 Practice of Axilla Surgery Axillary Lymph Node Dissection & Sentinel Lymph Node Biopsy 연세의대외과 박세호 Contents Anatomy of the axilla Axillary lymph node dissection (ALND)
Melanoma Update: 8th Edition of AJCC Staging System
 Melanoma Update: 8th Edition of AJCC Staging System Rosalie Elenitsas, M.D. Professor of Dermatology Director, Dermatopathology University of Pennsylvania DISCLOSURE OF RELATIONSHIPS WITH INDUSTRY None
Melanoma Update: 8th Edition of AJCC Staging System Rosalie Elenitsas, M.D. Professor of Dermatology Director, Dermatopathology University of Pennsylvania DISCLOSURE OF RELATIONSHIPS WITH INDUSTRY None
Work-up/Follow-up: Baseline and Surveillance Studies for Cutaneous Melanoma Patients
 2018 AAD Annual Meeting, San Diego, CA Work-up/Follow-up: Baseline and Surveillance Studies for Cutaneous Melanoma Patients Susan M. Swetter, MD, FAAD Professor of Dermatology Director, Pigmented Lesion
2018 AAD Annual Meeting, San Diego, CA Work-up/Follow-up: Baseline and Surveillance Studies for Cutaneous Melanoma Patients Susan M. Swetter, MD, FAAD Professor of Dermatology Director, Pigmented Lesion
Sentinel Lymph Node Biopsy for Head and Neck Cutaneous Melanoma
 Sentinel Lymph Node Biopsy for Head and Neck Cutaneous Melanoma S. Ross Patton, MD - PGY III Faculty Mentor: Susan McCammon, MD The University of Texas Medical Branch (UTMB Health) Department of Otolaryngology
Sentinel Lymph Node Biopsy for Head and Neck Cutaneous Melanoma S. Ross Patton, MD - PGY III Faculty Mentor: Susan McCammon, MD The University of Texas Medical Branch (UTMB Health) Department of Otolaryngology
Clinical Case Conference Melanoma
 Clinical Case Conference Melanoma Epidemiology ~60,000 cases and 8,000 deaths per year in US Caucasian:African American = 10:1 15% arise from existing nevi 91% are cutaneous 15% are LN+ at presentation
Clinical Case Conference Melanoma Epidemiology ~60,000 cases and 8,000 deaths per year in US Caucasian:African American = 10:1 15% arise from existing nevi 91% are cutaneous 15% are LN+ at presentation
Surgical Oncology Perspective of Melanoma
 Surgical Oncology Perspective of Melanoma Hans F. Schoellhammer, MD, FACS Assistant Clinical Professor Division of Surgical Oncology September 20, 2018 Nothing to disclose DISCLOSURE Discussion Objectives
Surgical Oncology Perspective of Melanoma Hans F. Schoellhammer, MD, FACS Assistant Clinical Professor Division of Surgical Oncology September 20, 2018 Nothing to disclose DISCLOSURE Discussion Objectives
Therapeutic Lymph Node Dissection in Melanoma: Different Prognosis for Different Macrometastasis Sites?
 Ann Surg Oncol (01) 19:91 91 DOI.14/s44-01-401- ORIGINAL ARTICLE MELANOMAS Therapeutic Lymph Node Dissection in Melanoma: Different Prognosis for Different Macrometastasis Sites? K. P. Wevers, MD, E. Bastiaannet,
Ann Surg Oncol (01) 19:91 91 DOI.14/s44-01-401- ORIGINAL ARTICLE MELANOMAS Therapeutic Lymph Node Dissection in Melanoma: Different Prognosis for Different Macrometastasis Sites? K. P. Wevers, MD, E. Bastiaannet,
AJCC 8 Implementation January 1, 2018 Melanoma of the Skin. Suraj Venna
 AJCC 8 Implementation January 1, 2018 Melanoma of the Skin Suraj Venna Personalized Medicine AJCC 8 th Edition This Time It s Personal Traditional AJCC (TNM) population-based analyses of large databases
AJCC 8 Implementation January 1, 2018 Melanoma of the Skin Suraj Venna Personalized Medicine AJCC 8 th Edition This Time It s Personal Traditional AJCC (TNM) population-based analyses of large databases
Citation for published version (APA): Francken, A. B. (2007). Primary and metastatic melanoma: aspects of follow-up and staging s.n.
 University of Groningen Primary and metastatic melanoma Francken, Anne Brecht IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check
University of Groningen Primary and metastatic melanoma Francken, Anne Brecht IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check
ORIGINAL ARTICLE. Clinical Node-Negative Thick Melanoma
 ORIGINAL ARTICLE Clinical Node-Negative Thick Melanoma George I. Salti, MD; Ashwin Kansagra, MD; Michael A. Warso, MD; Salve G. Ronan, MD ; Tapas K. Das Gupta, MD, PhD, DSc Background: Patients with T4
ORIGINAL ARTICLE Clinical Node-Negative Thick Melanoma George I. Salti, MD; Ashwin Kansagra, MD; Michael A. Warso, MD; Salve G. Ronan, MD ; Tapas K. Das Gupta, MD, PhD, DSc Background: Patients with T4
Melanoma: The Basics. What is a melanocyte?
 Melanoma: The Basics What is a melanocyte? A melanocyte is a normal cell, found in the skin, which produces melanin. Melanin is a black or dark brown pigment that is seen in the skin, hair, and parts of
Melanoma: The Basics What is a melanocyte? A melanocyte is a normal cell, found in the skin, which produces melanin. Melanin is a black or dark brown pigment that is seen in the skin, hair, and parts of
Breast Surgery When Less is More and More is Less. E MacIntosh, MD June 6, 2015
 Breast Surgery When Less is More and More is Less E MacIntosh, MD June 6, 2015 Presenter Disclosure Faculty: E. MacIntosh Relationships with commercial interests: None Mitigating Potential Bias Not applicable
Breast Surgery When Less is More and More is Less E MacIntosh, MD June 6, 2015 Presenter Disclosure Faculty: E. MacIntosh Relationships with commercial interests: None Mitigating Potential Bias Not applicable
Skin Cancer. 5 Warning Signs. American Osteopathic College of Occupational and Preventive Medicine OMED 2012, San Diego, Monday, October 8, 2012 C-1
 Skin Cancer AMERICAN OSTEOPATHIC COLLEGE OF OCCUPATIONAL & PREVENTIVE MEDICINE OMED 2012 October 8, 2012 E. Robert Wanat II, D.O., M.P.H. Learning Objectives: Identify the 3 Basic Types of Skin Cancer
Skin Cancer AMERICAN OSTEOPATHIC COLLEGE OF OCCUPATIONAL & PREVENTIVE MEDICINE OMED 2012 October 8, 2012 E. Robert Wanat II, D.O., M.P.H. Learning Objectives: Identify the 3 Basic Types of Skin Cancer
16/09/2015. ACOSOG Z011 changing practice. Presentation outline. Nodal mets #1 prognostic tool. Less surgery no change in oncologic outcomes
 ACOSOG Z011 changing practice The end of axillary US/FNA? Preoperative staging of the axilla in the era of Z011 Adena S Scheer MD MSc FRCSC Surgical Oncologist, St. Michael s Hospital Assistant Professor,
ACOSOG Z011 changing practice The end of axillary US/FNA? Preoperative staging of the axilla in the era of Z011 Adena S Scheer MD MSc FRCSC Surgical Oncologist, St. Michael s Hospital Assistant Professor,
Sentinel Lymph Node Biopsy: Current Evidence for its Role in Managing Melanoma
 Sentinel Lymph Node Biopsy: Current Evidence for its Role in Managing Melanoma John A Zitelli MD Adjunct Clinical Associate Professor Dermatology, Otolaryngology, Plastic Surgery University of Pittsburgh
Sentinel Lymph Node Biopsy: Current Evidence for its Role in Managing Melanoma John A Zitelli MD Adjunct Clinical Associate Professor Dermatology, Otolaryngology, Plastic Surgery University of Pittsburgh
PAPER. Prognostic Information From Sentinel Lymph Node Biopsy in Patients With Thick Melanoma
 PAPER Prognostic Information From Sentinel Lymph Node Biopsy in Patients With Thick Melanoma Charles R. Scoggins, MD, MBA; Adrianne L. Bowen, MD; Robert C. Martin II, MD, PhD; Michael J. Edwards, MD; Douglas
PAPER Prognostic Information From Sentinel Lymph Node Biopsy in Patients With Thick Melanoma Charles R. Scoggins, MD, MBA; Adrianne L. Bowen, MD; Robert C. Martin II, MD, PhD; Michael J. Edwards, MD; Douglas
LYMPHATIC DRAINAGE PATTERNS OF HEAD AND NECK CUTANEOUS MELANOMA OBSERVED ON LYMPHOSCINTIGRAPHY AND SENTINEL LYMPH NODE BIOPSY
 LYMPHATIC DRAINAGE PATTERNS OF HEAD AND NECK CUTANEOUS MELANOMA OBSERVED ON LYMPHOSCINTIGRAPHY AND SENTINEL LYMPH NODE BIOPSY Doris Lin, MD, 1 Benjamin L. Franc, MD, 2 Mohammed Kashani-Sabet, MD, 3 Mark
LYMPHATIC DRAINAGE PATTERNS OF HEAD AND NECK CUTANEOUS MELANOMA OBSERVED ON LYMPHOSCINTIGRAPHY AND SENTINEL LYMPH NODE BIOPSY Doris Lin, MD, 1 Benjamin L. Franc, MD, 2 Mohammed Kashani-Sabet, MD, 3 Mark
Michael T. Tetzlaff MD, PhD
 American Joint Cancer Committee (AJCC) staging system for primary cutaneous melanoma (8 th Edition) and principles of sentinel lymph node evaluation Emphasis on concise and accurate reporting of primary
American Joint Cancer Committee (AJCC) staging system for primary cutaneous melanoma (8 th Edition) and principles of sentinel lymph node evaluation Emphasis on concise and accurate reporting of primary
1. Opdivo + Ipilumimab is now the first line therapy for metastatic melanoma.
 Melanoma UpToDate: Introduction: Risk Factors: 1. Opdivo + Ipilumimab is now the first line therapy for metastatic melanoma. Median age = 50 yrs Incidence is rising - Sun exposure: UVB (290-320nm) > UVA
Melanoma UpToDate: Introduction: Risk Factors: 1. Opdivo + Ipilumimab is now the first line therapy for metastatic melanoma. Median age = 50 yrs Incidence is rising - Sun exposure: UVB (290-320nm) > UVA
Morphological characteristics of the primary tumor and micrometastases in sentinel lymph nodes as a predictor of melanoma progression
 Morphological characteristics of the primary tumor and micrometastases in sentinel lymph nodes as a predictor of melanoma progression M.N. Kukushkina, S.I. Korovin, O.I. Solodyannikova, G.G. Sukach, A.Yu.
Morphological characteristics of the primary tumor and micrometastases in sentinel lymph nodes as a predictor of melanoma progression M.N. Kukushkina, S.I. Korovin, O.I. Solodyannikova, G.G. Sukach, A.Yu.
Nodal staging in localized melanoma. The experience of the Brescia Melanoma Unit
 The British Association of Plastic Surgeons (2003) 56, 534 539 Nodal staging in localized melanoma. The experience of the Brescia Melanoma Unit Giorgio Manca a, *, Fabio Facchetti b, Claudio Pizzocaro
The British Association of Plastic Surgeons (2003) 56, 534 539 Nodal staging in localized melanoma. The experience of the Brescia Melanoma Unit Giorgio Manca a, *, Fabio Facchetti b, Claudio Pizzocaro
THE ROLE OF CONTEMPORARY IMAGING AND HYBRID METHODS IN THE DIAGNOSIS OF CUTANEOUS MALIGNANT MELANOMA(CMM) AND MERKEL CELL CARCINOMA (MCC)
 THE ROLE OF CONTEMPORARY IMAGING AND HYBRID METHODS IN THE DIAGNOSIS OF CUTANEOUS MALIGNANT MELANOMA(CMM) AND MERKEL CELL CARCINOMA (MCC) I.Kostadinova, Sofia, Bulgaria CMM some clinical facts The incidence
THE ROLE OF CONTEMPORARY IMAGING AND HYBRID METHODS IN THE DIAGNOSIS OF CUTANEOUS MALIGNANT MELANOMA(CMM) AND MERKEL CELL CARCINOMA (MCC) I.Kostadinova, Sofia, Bulgaria CMM some clinical facts The incidence
Skin Malignancies Non - Melanoma & Melanoma Marilyn Ng, MD Dept. of Surgery M&M Conference Downstate Medical Center July 19, 2012
 Skin Malignancies Non - Melanoma & Melanoma Marilyn Ng, MD Dept. of Surgery M&M Conference Downstate Medical Center July 19, 2012 Case Presentation 57 yo man with 3 month hx of a nonhealing < 1 cm right
Skin Malignancies Non - Melanoma & Melanoma Marilyn Ng, MD Dept. of Surgery M&M Conference Downstate Medical Center July 19, 2012 Case Presentation 57 yo man with 3 month hx of a nonhealing < 1 cm right
Metastatic Melanoma. Cynthia Kwong February 16, 2017 SUNY Downstate Medical Center Department of Surgery Grand Rounds
 Metastatic Melanoma Cynthia Kwong February 16, 2017 SUNY Downstate Medical Center Department of Surgery Grand Rounds Case Presentation 77 year old male with previous history of scalp melanoma and thyroid
Metastatic Melanoma Cynthia Kwong February 16, 2017 SUNY Downstate Medical Center Department of Surgery Grand Rounds Case Presentation 77 year old male with previous history of scalp melanoma and thyroid
Genetic Testing: When should it be ordered? Julie Schloemer, MD Dermatology
 Genetic Testing: When should it be ordered? Julie Schloemer, MD Dermatology Outline Germline testing CDKN2A BRCA2 BAP1 Somatic testing Gene expression profiling (GEP) BRAF Germline vs Somatic testing
Genetic Testing: When should it be ordered? Julie Schloemer, MD Dermatology Outline Germline testing CDKN2A BRCA2 BAP1 Somatic testing Gene expression profiling (GEP) BRAF Germline vs Somatic testing
Talk to Your Doctor. Fact Sheet
 Talk to Your Doctor Hearing the words you have skin cancer is overwhelming and would leave anyone with a lot of questions. If you have been diagnosed with Stage I or II cutaneous melanoma with no apparent
Talk to Your Doctor Hearing the words you have skin cancer is overwhelming and would leave anyone with a lot of questions. If you have been diagnosed with Stage I or II cutaneous melanoma with no apparent
Michael T. Tetzlaff MD, PhD
 Update on American Joint Cancer Committee (AJCC) staging system for primary cutaneous melanoma Emphasis on concise and accurate reporting of primary and metastatic melanoma for effective risk stratification
Update on American Joint Cancer Committee (AJCC) staging system for primary cutaneous melanoma Emphasis on concise and accurate reporting of primary and metastatic melanoma for effective risk stratification
World Articles of Ear, Nose and Throat Page 1
 World Articles of Ear, Nose and Throat ---------------------Page 1 Primary Malignant Melanoma of the Tongue: A Case Report Authors: Nanayakkara PR*, Arudchelvam JD** Ariyaratne JC*, Mendis K*, Jayasekera
World Articles of Ear, Nose and Throat ---------------------Page 1 Primary Malignant Melanoma of the Tongue: A Case Report Authors: Nanayakkara PR*, Arudchelvam JD** Ariyaratne JC*, Mendis K*, Jayasekera
Increasing Age Is Associated with Worse Prognostic Factors and Increased Distant Recurrences despite Fewer Sentinel Lymph Node Positives in Melanoma
 Increasing Age Is Associated with Worse Prognostic Factors and Increased Distant Recurrences despite Fewer Sentinel Lymph Node Positives in Melanoma A. J. Page, Emory University A. Li, Emory University
Increasing Age Is Associated with Worse Prognostic Factors and Increased Distant Recurrences despite Fewer Sentinel Lymph Node Positives in Melanoma A. J. Page, Emory University A. Li, Emory University
47. Melanoma of the Skin
 1 Terms of Use The cancer staging form is a specific document in the patient record; it is not a substitute for documentation of history, physical examination, and staging evaluation, or for documenting
1 Terms of Use The cancer staging form is a specific document in the patient record; it is not a substitute for documentation of history, physical examination, and staging evaluation, or for documenting
North of Scotland Cancer Network Clinical Management Guideline for Malignant Melanoma
 Nth of Scotland Cancer Netwk Clinical Management Guideline f Malignant Melanoma Based on WOSCAN CMG with further consultation within NOSCAN UNCONTROLLED WHEN PRINTED Prepared by Approved by Issue date
Nth of Scotland Cancer Netwk Clinical Management Guideline f Malignant Melanoma Based on WOSCAN CMG with further consultation within NOSCAN UNCONTROLLED WHEN PRINTED Prepared by Approved by Issue date
Malignant Melanoma in Turkey: A Single Institution s Experience on 475 Cases
 Malignant Melanoma in Turkey: A Single Institution s Experience on 475 Cases Faruk Tas, Sidika Kurul, Hakan Camlica and Erkan Topuz Institute of Oncology, Istanbul University, Istanbul, Turkey Received
Malignant Melanoma in Turkey: A Single Institution s Experience on 475 Cases Faruk Tas, Sidika Kurul, Hakan Camlica and Erkan Topuz Institute of Oncology, Istanbul University, Istanbul, Turkey Received
Marshall T Bell Research Resident University of Colorado Grand Rounds Nov. 21, 2011
 Marshall T Bell Research Resident University of Colorado Grand Rounds Nov. 21, 2011 Most common form of cancer in adults ages 25-29 3-5% of skin cancers but 65-75% of deaths Most common metastasis to small
Marshall T Bell Research Resident University of Colorado Grand Rounds Nov. 21, 2011 Most common form of cancer in adults ages 25-29 3-5% of skin cancers but 65-75% of deaths Most common metastasis to small
Melanoma Case Scenario 1
 Melanoma Case Scenario 1 History and physical 11/5/16 Patient is a single, 48-year-old male in good health who presented to his primary physician for a yearly physical exam during which a 3.4 x 2.8 x 1.5
Melanoma Case Scenario 1 History and physical 11/5/16 Patient is a single, 48-year-old male in good health who presented to his primary physician for a yearly physical exam during which a 3.4 x 2.8 x 1.5
ORIGINAL ARTICLE. Reliability of Sentinel Lymph Node Mapping With Biopsy for Head and Neck Cutaneous Melanoma
 ORIGINAL ARTICLE Reliability of Sentinel Lymph Node Mapping With Biopsy for Head and Neck Cutaneous Melanoma Cecelia E. Schmalbach, MD; Brian Nussenbaum, MD; Riley S. Rees, MD; Jennifer Schwartz, MD; Timothy
ORIGINAL ARTICLE Reliability of Sentinel Lymph Node Mapping With Biopsy for Head and Neck Cutaneous Melanoma Cecelia E. Schmalbach, MD; Brian Nussenbaum, MD; Riley S. Rees, MD; Jennifer Schwartz, MD; Timothy
Contrast with Australian Guidelines A/Pr Pascale Guitera,
 Contrast with Australian Guidelines A/Pr Pascale Guitera, Dermatologist, Sydney University NO CONFLICT OF INTEREST Sydney Melanoma Diagnostic Centre, RPAH 2011 2008 225 pages 16 pages http://www.cancer.org.au/file/healthprofessionals/clinica
Contrast with Australian Guidelines A/Pr Pascale Guitera, Dermatologist, Sydney University NO CONFLICT OF INTEREST Sydney Melanoma Diagnostic Centre, RPAH 2011 2008 225 pages 16 pages http://www.cancer.org.au/file/healthprofessionals/clinica
Update on Sentinel Node Biopsy in Endometrial Cancer: Feasibility, Technique, Impact
 Update on Sentinel Node Biopsy in Endometrial Cancer: Feasibility, Technique, Impact Bjørn Hagen, MD, PhD St Olavs Hospital Trondheim University Hospital Trondheim, Norway Endometrial Cancer (EC) The most
Update on Sentinel Node Biopsy in Endometrial Cancer: Feasibility, Technique, Impact Bjørn Hagen, MD, PhD St Olavs Hospital Trondheim University Hospital Trondheim, Norway Endometrial Cancer (EC) The most
The Role of Sentinel Lymph Node Biopsy and Axillary Dissection
 The Role of Sentinel Lymph Node Biopsy and Axillary Dissection Henry Mark Kuerer, MD, PhD, FACS Department of Surgical Oncology University of Texas MD Anderson Cancer Center SLN Biopsy Revolutionized surgical
The Role of Sentinel Lymph Node Biopsy and Axillary Dissection Henry Mark Kuerer, MD, PhD, FACS Department of Surgical Oncology University of Texas MD Anderson Cancer Center SLN Biopsy Revolutionized surgical
What Is a Sentinel Node? Re-Evaluating the 10% Rule for Sentinel Lymph Node Biopsy in Melanoma
 Journal of Surgical Oncology 2007;95:623 628 What Is a Sentinel Node? Re-Evaluating the 10% Rule for Sentinel Lymph Node Biopsy in Melanoma HIDDE M. KROON, MD, 1 LORI LOWE, MD, 2 SANDRA WONG, MD, 1 DOUG
Journal of Surgical Oncology 2007;95:623 628 What Is a Sentinel Node? Re-Evaluating the 10% Rule for Sentinel Lymph Node Biopsy in Melanoma HIDDE M. KROON, MD, 1 LORI LOWE, MD, 2 SANDRA WONG, MD, 1 DOUG
University of Groningen
 University of Groningen Nodular Histologic Subtype and Ulceration are Tumor Factors Associated with High Risk of Recurrence in Sentinel Node-Negative Melanoma Patients Faut, Marloes; Wevers, Kevin; van
University of Groningen Nodular Histologic Subtype and Ulceration are Tumor Factors Associated with High Risk of Recurrence in Sentinel Node-Negative Melanoma Patients Faut, Marloes; Wevers, Kevin; van
Prognosis of Sentinel Node Staged Patients with Primary Cutaneous Melanoma
 Prognosis of Sentinel Node Staged Patients with Primary Cutaneous Melanoma Otmar Elsaeßer 1., Ulrike Leiter 1 *., Petra G. Buettner 2, Thomas K. Eigentler 1, Friedegund Meier 1, Benjamin Weide 1, Gisela
Prognosis of Sentinel Node Staged Patients with Primary Cutaneous Melanoma Otmar Elsaeßer 1., Ulrike Leiter 1 *., Petra G. Buettner 2, Thomas K. Eigentler 1, Friedegund Meier 1, Benjamin Weide 1, Gisela
Melanoma Case Scenario 1
 Melanoma Case Scenario 1 History and physical 11/5/16 Patient is a single, 48-year-old male in good health who presented to his primary physician for a yearly physical exam during which a 3.4 x 2.8 x 1.5
Melanoma Case Scenario 1 History and physical 11/5/16 Patient is a single, 48-year-old male in good health who presented to his primary physician for a yearly physical exam during which a 3.4 x 2.8 x 1.5
Surgical Treatment of Melanoma Across the Disease Spectrum:
 AOCD Annual Fall Meeting October 28 th, 2017 New Orleans, Louisiana Surgical Treatment of Melanoma Across the Disease Spectrum: Standards of Care and Evolving Paradigms Merrick Ross, M.D. Professor of
AOCD Annual Fall Meeting October 28 th, 2017 New Orleans, Louisiana Surgical Treatment of Melanoma Across the Disease Spectrum: Standards of Care and Evolving Paradigms Merrick Ross, M.D. Professor of
Research Article Prediction of Sentinel Node Status and Clinical Outcome in a Melanoma Centre
 Skin Cancer Volume 2013, Article ID 904701, 7 pages http://dx.doi.org/10.1155/2013/904701 Research Article Prediction of Sentinel Node Status and Clinical Outcome in a Melanoma Centre Vera Teixeira, 1
Skin Cancer Volume 2013, Article ID 904701, 7 pages http://dx.doi.org/10.1155/2013/904701 Research Article Prediction of Sentinel Node Status and Clinical Outcome in a Melanoma Centre Vera Teixeira, 1
MELANOMA: HANDS-ON OR HANDS-OFF?
 MELANOMA: HANDS-ON OR HANDS-OFF? M SCHAMM MBChB (Pret), FCS (SA) Endocrine and Transplant Surgeon, Department of Surgery, University of the Witwatersrand; and Clinical Head Transplant Surgery, Charlotte
MELANOMA: HANDS-ON OR HANDS-OFF? M SCHAMM MBChB (Pret), FCS (SA) Endocrine and Transplant Surgeon, Department of Surgery, University of the Witwatersrand; and Clinical Head Transplant Surgery, Charlotte
MELANOMA IN ADOLESCENTS AND YOUNG ADULTS
 Cancer in Adolescents and Young Adults (AYA) Working Group MELANOMA IN ADOLESCENTS AND YOUNG ADULTS Emmanouil Saloustros MD, DSc General Hospital of Heraklion Venizelio Heraklion, Crete, Greece ESMO Preceptorship
Cancer in Adolescents and Young Adults (AYA) Working Group MELANOMA IN ADOLESCENTS AND YOUNG ADULTS Emmanouil Saloustros MD, DSc General Hospital of Heraklion Venizelio Heraklion, Crete, Greece ESMO Preceptorship
Thin Melanoma with Nodal Involvement: Analysis of Demographic, Pathologic, and Treatment Factors with Regard to Prognosis
 Ann Surg Oncol DOI 10.1245/s10434-016-5646-9 ORIGINAL ARTICLE MELANOMAS Thin Melanoma with Nodal Involvement: Analysis of Demographic, Pathologic, and Treatment Factors with Regard to Prognosis Giorgos
Ann Surg Oncol DOI 10.1245/s10434-016-5646-9 ORIGINAL ARTICLE MELANOMAS Thin Melanoma with Nodal Involvement: Analysis of Demographic, Pathologic, and Treatment Factors with Regard to Prognosis Giorgos
Update on Lymph Node Management in Melanoma
 Update on Lymph Node Management in Melanoma John T. Vetto MD, FACS Professor of Surgery Division of Surgical Oncology Oregon Health & Science University Portland, Oregon Lymph Nodes in Melanoma Outline
Update on Lymph Node Management in Melanoma John T. Vetto MD, FACS Professor of Surgery Division of Surgical Oncology Oregon Health & Science University Portland, Oregon Lymph Nodes in Melanoma Outline
Clinical utilities and biological characteristics of melanoma sentinel lymph nodes
 W J C O World Journal of Clinical Oncology Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.5306/wjco.v7.i2.174 World J Clin Oncol 2016 April
W J C O World Journal of Clinical Oncology Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.5306/wjco.v7.i2.174 World J Clin Oncol 2016 April
