Review Article. Penile Carcinoma: Lessons Learned from Vulvar Carcinoma. Michelle J. Longpre,* Paul H. Lange, Janice S. Kwon* and Peter C.
|
|
|
- Ruby Parsons
- 5 years ago
- Views:
Transcription
1 Review Article Penile Carcinoma: Lessons Learned from Vulvar Carcinoma Michelle J. Longpre,* Paul H. Lange, Janice S. Kwon* and Peter C. Black*, From the Department of Urologic Sciences, and the Department of Obstetrics and Gynecology, University of British Columbia, Vancouver, British Columbia, and the Department of Urology, University of Washington, Seattle, Washington Purpose: Penile carcinoma is rare in the developed world and treatment guidelines are often based on marginal clinical data. Prospective controlled studies are virtually absent and meta-analyses are rare. Vulvar carcinoma, on the other hand, has many parallels to penile carcinoma, and the level of evidence for diagnosis and treatment is more robust. Therefore, we assessed the body of literature on vulvar carcinoma to identify potential improvements in the care of patients with penile carcinoma. Materials and Methods: A literature review was performed on vulvar carcinoma and direct comparisons were made to a similar review of the literature on penile carcinoma. Results: Several aspects of vulvar carcinoma management are clearly established and deserve closer evaluation in penile carcinoma. For example, human papillomavirus is identified in a high percentage of patients with vulvar carcinoma but is understudied in penile carcinoma. Further study is of potential clinical value, especially with the development of human papillomavirus vaccines for prevention. Penile carcinoma TNM staging does not adequately stratify survival or risk of advanced disease. Staging of vulvar carcinoma is dependent on tumor size and depth of invasion measured in millimeters, as opposed to the invasion of underlying structures in penile carcinoma. Management of the inguinal nodes is more refined for vulvar carcinoma, where lymphatic mapping has been conducted and sentinel node biopsy has proven to be highly effective in multicenter trials. Finally, the efficacy of adjuvant radiation and chemotherapy has been tested in controlled trials or reported in meta-analyses for vulvar carcinoma, which are both lacking for penile carcinoma. Radiation after inguinal node dissection, for example, has been shown to enhance survival in patients with defined risk factors. Neoadjuvant chemoradiation is recommended before surgery for advanced vulvar carcinoma. Conclusions: Evidence derived from studies on vulvar carcinoma can be extrapolated to penile carcinoma to help guide clinical trials and future research directions to enhance the treatment of these patients. Key Words: penile neoplasms; vulvar neoplasms; carcinoma, squamous cell; neoplasm staging; disease management Abbreviations and Acronyms DSLNB dynamic sentinel lymph node biopsy HPV human papillomavirus ILND inguinal lymph node dissection LN lymph node LND lymph node dissection PC penile carcinoma RCT randomized clinical trial RT radiation therapy SLNB sentinel lymph node biopsy VC vulvar carcinoma Accepted for publication March 29, * Nothing to disclose. Financial interest and/or other relationship with Janssen, LaZure Scientific, Johnson & Johnson and Merck. Correspondence: Department of Urologic Sciences, University of British Columbia, Level 6, 2775 Laurel St., Vancouver, British Columbia V5Z 1M9 Canada (telephone: ; FAX: ; peter.black@ubc.ca). Editor s Note: This article is the first of 5 published in this issue for which category 1 CME credits can be earned. Instructions for obtaining credits are given with the questions on pages 398 and 399. PENILE carcinoma is a disease for which the treatment can be as devastating as the carcinoma itself. It is a rare disease in developed countries with a reported incidence in the United States of 0.58 in 100, The incidence in Asia, Africa and South America is far higher, and accounts for 10% to 20% of all malignancies. 2 Due to its rarity, randomized prospective studies are virtually absent and meta-analyses are rare. Therefore, many controversies exist in the management of PC /13/ /0 THE JOURNAL OF UROLOGY Vol. 189, 17-24, January by AMERICAN UROLOGICAL ASSOCIATION EDUCATION AND RESEARCH, INC. Printed in U.S.A. 17
2 18 LESSONS LEARNED FROM VULVAR CARCINOMA Vulvar carcinoma in women has many similarities to penile carcinoma in men. Both diseases have similar anatomy, histology, risk factors and natural histories. Although VC is also relatively rare in developed countries (2.5/100,000 in the United States), it is a much better studied disease, with a higher level of evidence for guiding diagnosis and treatment. 3 We propose that the body of literature on VC can be used to guide us toward improvement in the management of PC. ANATOMICAL SIMILARITIES The male and female external genitalia develop along a common embryological pathway. The lymphatics from the glans of the penis as well as the clitoris, labia minora and the terminal end of the vagina drain into the deep inguinal nodes and the internal iliac nodes. 4 The penile shaft skin and the labia majora drain into the superficial inguinal nodes. The penis and vulva differ in that the penis often drains bilaterally and the vulva drains unilaterally, except for the midline regions of the vulva. 4 Metastatic spread in vulvar and penile carcinoma via these lymphatics occurs in a predictable pattern without skip lesions. The presence or absence of lymph node metastasis in PC and VC is highly predictive of survival. HISTOLOGY AND HPV ASSOCIATION Penile and vulvar cancers have previously been considered diseases of the elderly with a peak incidence in the sixth and seventh decades. This concept is changing with studies showing a quarter of patients with penile cancer to be younger than 50 years old. 5 A similar decrease in the age of diagnosis has occurred in VC, for which the average age is 55 years. 6 Squamous cell carcinoma is the most common malignancy in penile and vulvar carcinoma, accounting for 90% to 95% of cases. There are 2 main categories of well studied predisposing factors to PC that are paralleled in VC. The first is the HPV related pathway that is associated with HPV 16, 18 and 33. The second is a HPV unrelated pathway that is secondary to chronic inflammation such as lichen sclerosus in VC and balanitis xerotica obliterans in PC. These are considered synonymous conditions characterized by a chronic, progressive, atrophic, sclerosing process found on male and female genitalia. A systematic review of 31 studies including 1,466 men showed that HPV is associated with penile carcinoma in 47% of patients. 7 Similar studies have found 60% of vulvar carcinoma to be associated with HPV. 8 The high rate of HPV association with PC raises the question of the usefulness of the HPV vaccine in males. It is well recognized that the HPV vaccine can effectively reduce the risk of preinvasive cervical and vulvar intraepithelial neoplasia. 9 Until recently there was still no defined role for the use of the HPV vaccine in boys due to the lack of long-term studies on the efficacy, safety and cost-effectiveness of the HPV vaccine. However, a randomized placebo controlled trial of more than 4,000 males age 16 to 26 years found the HPV vaccine (HPV 6, 11, 16, 18) reduced the incidence of external genital lesions by 90.4%. 10 Earlier this year the American Academy of Pediatrics recommended the routine use of the quadrivalent HPV vaccine in boys ages 11 and 12 years, and all boys age 13 to 21 who had not previously been offered the vaccine. Their recommendations were backed by clinical trials showing the vaccine is highly immunogenic, safe and well tolerated by boys and girls alike. The vaccine could prevent up to 47% of PC, 87% of anal cancer and 60% of oropharyngeal cancer, and prevent the transmission of the virus to female partners. STAGING TNM staging of PC is often criticized as being poorly predictive of patient outcome. The TNM staging of VC differs significantly from that of PC and it is possible that it could guide changes to PC staging to improve prognostic value. The principal shortcoming of the TNM system in PC is that it does not adequately stratify the risk of death. In one study there was no significant difference between survival for Tis/Ta and T1, and several studies have shown that the 5-year survival for T3 is the same or better than that for T2 disease. 11 This finding is likely due to the combination of corpus spongiosum and corpus cavernosum into 1 stage (T2), because the ability of a tumor to invade the tunica albuginea and, therefore, into the corpus cavernosum has been postulated to be a marker of aggressiveness with worse prognosis. 12 Stage T3 also combines invasion anywhere along the entire length of the urethra and into the prostate. Invasion into the distal urethra, especially at the glans, has a better prognosis than invasion into the proximal urethra or corpus cavernosum. 11 The prostate is rarely involved in PC and the prognostic value of invasion into the prostate has not been determined. 11 The recent update to the TNM staging split T1 into T1a and T1b based on the absence or presence, respectively, of lymphovascular invasion. On multivariable analysis this has been shown to be an independent predictor of positive LNs in patients with clinically negative LNs. 13 The updated TNM staging also includes grade to differentiate between T1a and T1b (absence or presence of high grade carcinoma). While grade is widely accepted as an important risk
3 LESSONS LEARNED FROM VULVAR CARCINOMA 19 factor in PC, there are conflicting reports based on univariable and multivariable analyses regarding its prognostic value. 14 Furthermore, in patients with intermediate grade (G2) T1 disease, the risk of LN metastasis ranges from as low as 0% to as high as 50%. 15 It would be desirable for the TNM categorization to guide the decision to perform ILND (T1b) or not (T1a), but this is not achieved with the updated system. A solution to this controversy may be to adopt a dichotomous grading system that includes only low and high grade, as we have done with bladder cancer. The FIGO (International Federation of Gynecology and Obstetrics) staging system for VC was also revised in 2009 (Appendixes 1 and 2). 16 The new staging system demonstrates an appropriate stratification of prognostic groupings. Many studies on depth of invasion have shown VC lesions with less than 1 mm invasion to have a negligible risk of nodal metastasis, thereby eliminating the need for LND. 17 Furthermore, on multivariable analysis, depth of invasion has been shown to be one of the only independent predictors of recurrence and positive LNs. Hacker et al reported increasing rates of nodal disease with 1 mm increments in depth of invasion, from 0% if 1 mm invasion or less, to 10.5% if 1.1 to 2 mm invasion to 42.9% if more than 5 mm invasion. 18 A comparable multivariable analysis in PC showed T stage was not a predictor of survival or of positive LNs. In a multivariable analysis of 145 patients only depth of invasion was predictive of survival when comparing 1 to 5 mm vs more than 5 mm invasion. 14 VC staging also differs from PC staging in that invasion into the distal third of the urethra by VC is considered a lower stage (stage II and III) than invasion into the proximal two-thirds of the urethra (stage IV). Modifying the parameters to define depth and location of invasion of PC could enhance the prognostication of PC staging. Clinical and pathological LN staging in PC also has many shortcomings. The use of clinical nodal staging in vulvar and penile carcinoma has been shown to have a high false-negative rate of 16% to 24% and 10% to 60%, respectively. 19,20 Therefore, vulvar carcinoma TNM staging no longer relies on the clinical examination of the locoregional LN (Appendix 2). In PC, guidelines continue to rely on whether lymph nodes are palpable to determine clinical staging and to direct management. If LNs are not palpable and dynamic sentinel lymph node biopsy is not available, the recently updated EAU (European Association of Urology) guidelines suggest using patient risk factors and nomograms to determine if the patient can be surveyed or if ILND is required. However, the sensitivity of published nomograms is less than 80%. The vulvar carcinoma TNM nodal staging system is based on the numbers of LNs as well as the size of the LNs (Appendix 2). A GOG (Gynecologic Oncology Group) study of 385 patients with VC undergoing ILND found the 5-year survival for 1 to 2, 3 to 4, 5 to 6 and more than 7 positive nodes to be 75.2%, 36.1%, 24.0% and 0%, respectively. 21 Another similar study in VC found a 94% survival with 1 positive node, an 80% survival with 2 positive nodes and a 12% survival with 3 or more positive nodes. 22 The size of LN metastasis has also been incorporated into the staging of VC based on data showing a significant survival difference among less than 5 mm, 5 to 15 mm and more than 15 mm nodal involvement. Pathological nodal staging in PC differentiates only single vs multiple or bilateral inguinal lymphadenopathy. This is a fairly crude differentiation since studies in PC have found significant survival differences when accounting for the number of positive nodes found during ILND. In a study of 128 patients with PC who underwent ILND, a multivariable analysis revealed that the number of positive inguinal LNs, bilateral positive LNs, positive pelvic LNs and extranodal spread were independent predictors of survival. However, the number of LNs was only divided into 1 to 3, 4 to 5 and more than 5, which had a 5-year survival of 75.6%, 8.4% and 0%, respectively. 23 It may have been beneficial to differentiate between 2 or fewer LNs vs more than 2 positive LNs. 24 In a similar study of 201 patients Ravi found more than 3 positive LNs to be an independent predictor of survival. 25 This finding was supported by another study showing 2 or fewer nodes vs 3 or more LNs to be an independent predictor of survival. 12 The same study also found extracapsular extension to be an independent predictor of survival on multivariable analysis. 12 We suggest that the current TNM staging should be adjusted to incorporate the number of positive LNs. The use of nodal size has not been adequately studied in PC and further investigations are required before this element can be incorporated. There are conflicting data for vulvar and penile carcinoma regarding the use of bilateral vs unilateral LN involvement as a prognostic factor. The majority of studies on VC have not shown a significant difference in survival if bilateral nodes are involved, and a recent study found bilateral LN metastases only to predict worse survival when the number of LNs was included in the model. 26 For PC, a recent review of the current TNM staging did find a significant difference in survival depending on the laterality of positive LNs. 11 Based on a comparison of the VC and PC literature, we believe there is sufficient evidence to reevaluate PC TNM staging. A proposed variation to the TNM staging is outlined in
4 20 LESSONS LEARNED FROM VULVAR CARCINOMA Appendixes 3 and 4. This proposed revision would of course require validation with clinical data. SENTINEL LYMPH NODE BIOPSY ILND is a potentially morbid procedure. Studies have shown that up to 50% of patients have postoperative complications including wound infection, wound breakdown and lymphedema. 27 Furthermore, up to 80% of patients without clinical evidence of nodal involvement will have no pathological evidence of nodal metastases. A potential method of identifying involved LNs without subjecting all patients to the associated complications of ILND is sentinel lymph node biopsy. SLNB has an established role in VC but its use continues to be debated for PC. SLNB was first described by Cabanas in 1977 for the management of PC. 28 Unfortunately its adoption in penile carcinoma has been slow, whereas VC, melanoma and breast cancers have led the way in the research and use of this technique. The sentinel LN is the first LN in the lymphatic basin that receives primary lymphatic flow from the area of the tumor. SLNB was initially performed using blue dye injected into the tumor, but now uses a combination of blue dye and technetium-99m-labeled nanocolloid (99mTC) that can be located and traced intraoperatively by a gamma ray detector probe. Many of the initial studies in PC with SLNB had unacceptably high false-negative rates (ranging from 10% to 75%). However, many of these studies were small and did not use current methods. 29,30 Results from the Netherlands Cancer Institute have shown that low false-negative rates can be achieved when the optimal technique is applied. 31 In their study of 323 patients the sentinel LN detection rate was 97% with a false-negative rate of 7% and a complication rate of 4.7%. The SLNB technique was modified after the first 157 patients so that these were compared to the subsequent 105 patients. The modifications included preoperative ultrasound in all patients, immediate fine needle aspiration of suspicious LNs and improved histopathology. Any patient with positive cytology went directly on to full ILND. These patients with more substantial LN involvement often have lymphatic rerouting and a higher risk of a false-negative result on SLNB. Therefore, identifying these patients preoperatively increases the sensitivity of SLNB. With this modified approach (dynamic sentinel lymph node biopsy), the false-negative rate decreased from 19% to 4.8%. The same group also compared the traditional EAU risk stratification guidelines to DSLNB and found DSLNB to be superior. 12,32 This technique is being validated in the United Kingdom with a large multicenter series of surgeons performing their first 25 cases using SLNB followed by traditional lymphadenectomy. The data for VC are more robust than for PC and would encourage the further development of the technique for PC. Selman et al systematically reviewed the accuracy of minimally invasive and noninvasive tests to assess the inguinal LN status in VC. 33 They found SLNB with 99mTC nanocolloid to be the most accurate compared to fine needle aspiration, magnetic resonance imaging and positron emission tomography. The pooled sensitivity of SLNB was 97% in this study with an inguinal recurrence rate of only 2.3%. 33,34 In the studies that used intraoperative lymphoscintigraphy and the blue dye method, the detection rates varied from 95% to 100% with no false-negatives. These data can be compared to similar studies using ILND. The false-negative rates for classic ILND were estimated to be between 0% and 4% at the International Sentinel Node Society meeting in An argument against DSLNB in penile carcinoma is the concern that the learning curve is too long for such a rare disease. Van der Zee et al proposed a 10-case learning curve for VC, which is much shorter than for melanoma and breast carcinoma (30 and 40 cases, respectively) due to the predictability of the sentinel LN in VC. 34,36 DSLNB should be performed at large referral centers or centers of excellence in collaboration with gynecologic oncologists where a few surgeons can master the technique. ADJUVANT CHEMOTHERAPY AND RADIATION THERAPY Finally, the use of radiation and chemotherapy in the management of vulvar and penile carcinoma has been advancing with guidance from research on anal carcinoma and cervical carcinoma. There are 3 main areas in which radiation with or without chemotherapy has been studied. The first is the use of RT in place of ILND with low stage and clinically LN negative disease (prophylactic RT) or in clinically LN positive disease (with curative intent). Next is the use of adjuvant and neoadjuvant RT (combined with ILND) to decrease local failures in LN positive disease. Finally, chemoradiation can be used in metastatic disease to improve survival, and avert the need for extensive pelvic resection with urinary and fecal diversion. The use of RT as an alternative to ILND is controversial in penile and vulvar carcinoma. It is not routinely used for PC based on a single prospective nonrandomized study of 64 patients with PC, which found decreased survival for clinically LN negative and LN positive disease treated with RT compared to bilateral ILND. 37 In the context of VC, a growing
5 LESSONS LEARNED FROM VULVAR CARCINOMA 21 body of research supports inguinal RT for clinical N0 and N1 disease. The GOG group originally found RT to be inferior to ILND. 38 After early poor results, recent studies with a superior RT design showed no survival advantage when comparing ILND with RT for clinical N0 and N1 disease. 39 A similar study of 23 patients with locally advanced VC and clinically negative LNs receiving radiation in addition to chemotherapy demonstrated no inguinal recurrence. 40 The GOG now supports the use of prophylactic inguinal RT in women who refuse ILND or who are deemed medically unfit to withstand ILND (National Cancer Institute: PDQ Vulvar Cancer Treatment. Bethesda, MD: National Cancer Institute). The evidence is inadequate to claim that RT should be considered equivalent to ILND in all patients. The toxicity of ILND and RT is similar, with cutaneous toxicity, lymphedema, sepsis and urinary tract infections being the most common adverse effects. Although the studies are small, patients with PC who refuse ILND or are unfit should also be offered the option of RT to manage clinically N0 and N1 disease. The role of neoadjuvant and adjuvant radiation for LN positive disease in PC is much less studied than in VC. 41 In PC a large retrospective series in addition to several small single institutional series addresses this question. However, in VC prospective randomized trials have been completed. The evidence for neoadjuvant RT in penile carcinoma is mixed. In a study of 201 men with clinically metastatic inguinal LNs larger than 4 cm or fixed to the skin who were treated with neoadjuvant RT before LND, the rate of inguinal recurrence decreased from 19% in nonirradiated to 3% in irradiated patients. 42 Other small studies in PC revealed worse outcomes with neoadjuvant RT of positive inguinal LNs as well as increased complications. 43 The Netherlands Cancer Institute Group has adopted the use of adjuvant RT to the inguinal and pelvic LNs if more than 2 LN metastases are found on ILND. 12 The cutoff of more than 2 LNs before adjuvant RT is supported by the VC literature. 44 The most recent guidelines from the EAU, 45 the only organization with guidelines for treating PC, did not address the use of neoadjuvant RT to inguinal LNs, but did state that adjuvant RT may improve locoregional control in patients with extensive metastases (extent not specified) or extranodal spread. 45 Based on data from 2 RCTs, patients with stage III VC who undergo ILND and are found to have positive LNs are offered adjuvant inguinal and pelvic radiation. An initial RCT by the GOG randomized 114 patients to radiation of the pelvis and inguinal or pelvic node resection if ILND revealed inguinal LN metastases. 44 There was a statistically significant increase in overall survival after 2 years in the radiation group. A second RCT was conducted to study long-term outcomes. After a 6-year followup the cancer related death rate was significantly higher for pelvic LND compared with radiation (51% vs 29%). This study also found that if the ratio of positive LNs-to-total LNs removed is greater than 20%, there is a significantly increased risk of contralateral LN metastasis, relapse and cancer related death. 23 The Society of Obstetricians and Gynaecologists of Canada practice guidelines state that patients with 3 or more micrometastases in the groin, with LNs larger than 10 mm, with extracapsular spread or with bilateral microscopic metastases, should receive postoperative bilateral inguinal and pelvic radiation. Pelvic LND is rarely performed in the setting of regional LN metastasis in VC, whereas it is still the recommended practice in PC. Lastly, preoperative chemoradiotherapy for advanced VC has been shown to reduce the need for more radical surgery. A GOG prospective multicenter phase II study found that when patients with stage III or IV VC were treated with cisplatin/5- fluorouracil and radiation followed by surgical excision, 68 of 71 were able to preserve urinary and/or gastrointestinal continence. 46 Of these 71 patients 33 had no detectable VC at the time of planned surgery. A randomized phase III controlled trial comparing RT alone to RT and chemotherapy with fluorouracil/mitomycin for locally advanced anal carcinoma found that the rate of complete response increased from 54% to 80% in the combination group. Furthermore, event-free survival (defined as free of locoregional progression, no colostomy and no severe side effects or death) showed significant improvement with chemoradiotherapy. 47 A prospective phase II trial in VC is under way by the GOG that will investigate the use of weekly cisplatin with daily high dose radiation followed by resection of residual tumor (GOG protocol 205). To our knowledge no trials have evaluated the use of combination chemoradiotherapy in advanced PC but studies of the individual components have shown some promising results. Several studies have investigated the use of single agent and multi-agent chemotherapy in advanced PC to facilitate curative surgery and improve overall survival. The most successful regimens have included cisplatin combined with bleomycin and methotrexate or with paclitaxel and ifosfamide. 12,48 Preliminary studies on paclitaxel combined with 5-fluorouracil have shown promising results. 49 CONCLUSIONS PC is a rare but devastating disease. Due to its rarity, clinical trials are sparse and have included
6 22 LESSONS LEARNED FROM VULVAR CARCINOMA few patients. Fortunately VC has many parallels to PC, with more robust clinical research supporting treatment choices. We believe that the evidence available for the management of VC offers valuable lessons to guide new research in PC and improve the management of this disease. A rational argument can be made for the administration of the HPV vaccine in males and it is now recommended by the American Academy of Pediatrics. The current TNM staging system provides inadequate prognostication for PC and may be enhanced by using principles from VC staging. A new TNM staging system is proposed in this review but further investigation is required to determine if it is able to better predict patient survival. Dynamic sentinel lymph node biopsy has an established role in VC, breast cancer and melanoma, but its use in PC continues to be debated. Recent evidence supports its use, but implementation is difficult due to the low patient numbers that prevent most centers from gaining adequate experience with the technique. By combining our efforts with gynecology at larger centers we would be able to overcome the learning curve more rapidly. Lastly, radiation and chemotherapy are underused in PC. The use of radiation in clinically LN negative cases for prophylaxis needs to be reevaluated in a larger study as it has shown noninferior results compared to ILND in vulvar carcinoma. The use of radiation, particularly in LN positive cases, has replaced the morbid pelvic LND in vulvar carcinoma, and should be studied as a treatment option for high stage PC. The combination of chemotherapy and radiation may be able to reduce the need for extensive pelvic surgery in cases of advanced disease as well as improve overall progression-free survival. APPENDIX 1 Vulvar carcinoma TNM tumor staging 16 STAGE Tis T1a T1b T2 T3 DESCRIPTION Carcinoma in situ Lesion 2 cm or smaller confined to the vulva or perineum with stromal invasion 1.0 mm or less* Lesion larger than 2 cm or with stromal invasion greater than 1.0 mm, confined to the vulva or perineum Lesion of any size with invasion into perineal structures (lower/distal third urethra or vagina, or any anus involvement) Lesion of any size with invasion into the upper/proximal two-thirds of urethra and/or vagina, bladder or rectal mucosa, or fixed to pelvic bone * Depth of invasion defined as the measurement of the tumor from the epithelialstromal junction of the most adjacent superficial dermal papilla to the deepest point of invasion. APPENDIX 2 Vulvar carcinoma TNM nodal staging 16 STAGE NX N0 N1a N1b N2a N2b N2c N3 NODAL (N- Stage) Regional lymph nodes cannot be assessed No regional lymph node metastasis One or 2 regional lymph node metastases, each 5 mm or less One lymph node metastasis 5 mm or greater Three or more lymph node metastases each less than 5 mm Two or more lymph node metastases 5 mm or greater Lymph node metastasis with extracapsular spread Nixed or ulcerated regional lymph node metastasis APPENDIX 3 Current and proposed T categories in penile carcinoma 50 CURRENT T CATEGORY PROPOSED T CATEGORY T0 No evidence of primary tumor No evidence of primary tumor Tis Carcinoma in situ Carcinoma in situ Ta Noninvasive verrucous carcinoma Noninvasive verrucous carcinoma T1 T1a Invades subepithelial connective tissue without lymphovascular invasion and is not poorly differentiated or undifferentiated (not grade 3 4) T1b Invades subepithelial connective tissue with lymphovascular invasion, or is poorly differentiated or undifferentiated T2 Tumor invades corpus spongiosum or corpus cavernosus T1a Lesion 2 cm or smaller with 1 mm or less of stromal invasion T1b Lesion larger than 2 cm or with more than 1 mm stromal invasion, or presence of lymphovascular invasion Tumor invades corpus spongiosum or glandular urethra T3 Tumor invades urethra or prostate Tumor invades corpus cavernosum T4 Tumor invades adjacent structures T4a Tumor invades pendulous urethra T4b Tumor invades adjacent structures or prostate APPENDIX 4 Current and proposed pathological N categories in penile carcinoma 50 CURRENT PATHOLOGICAL TNM NODAL STAGING PROPOSED PATHOLOGICAL TNM NODAL STAGING N0 No regional LNs No regional LNs N1 Intranodal metastasis in a single inguinal lymph node 2 or fewer inguinal LNs with intranodal metastasis N2 Metastasis in multiple or bilateral inguinal lymph nodes 3 or more inguinal LNs or bilateral inguinal LNs with intranodal metastasis N3 Metastasis in pelvic lymph node(s), unilateral or bilateral or extranodal extension of regional lymph node metastasis Extranodal extension or pelvic lymph node(s) Proposed nodal staging to be based on surgical and pathological findings.
7 LESSONS LEARNED FROM VULVAR CARCINOMA 23 REFERENCES 1. Barnholtz-Sloan JS, Maldonado JL, Pow-sang J et al: Incidence trends in primary malignant penile cancer. Urol Oncol 2007; 25: Parkin DM and Muir CS: Cancer incidence in five continents. Comparability and quality of data. IARC Sci Publ 1992; 120: Bodelon C, Madeleine MM, Voigt LF et al: Is the incidence of invasive vulvar cancer increasing in the United States? Cancer Causes Control 2009; 20: Moore KL, Dalley AF and Agur AMR: Clinically Oriented Anatomy, 6th ed. Baltimore: Lippincott Williams & Wilkins Hakenberg OW: A new neoadjuvant chemotherapy regimen for penile cancer with nodal metastases: a step forward. Eur Urol 2009; 55: Messing MJ and Gallup DG: Carcinoma of the vulva in young women. Obstet Gynecol 1995; 86: Miralles-Guri C, Bruni L, Cubilla AL et al: Human papillomavirus prevalence and type distribution in penile carcinoma. J Clin Pathol 2009; 62: Monk BJ, Burger RA, Lin F et al: Prognostic significance of human papillomavirus DNA in vulvar carcinoma. Obstet Gynecol 1995; 85: FUTURE II Study Group: Quadrivalent vaccine against human papillomavirus to prevent highgrade cervical lesions. N Engl J Med 2007; 356: Giuliano AR, Palefsky JM, Goldstone S et al: Efficacy of quadrivalent HPV vaccine against HPV infection and disease in males. N Engl J Med 2011; 364: Leijte JA, Gallee M, Antonini N et al: Evaluation of current TNM classification of penile carcinoma. J Urol 2008; 180: Graafland NM, van Boven HH, van Werkhoven E et al: Prognostic significance of extranodal extension in patients with pathological node positive penile carcinoma. J Urol 2010; 184: Ficarra V, Zattoni F, Cunico SC et al: Lymphatic and vascular embolizations are independent predictive variables of inguinal lymph node involvement in patients with squamous cell carcinoma of the penis: Gruppo Uro-Oncologico del Nord Est (Northeast Uro-Oncological Group) Penile Cancer data base data. Cancer 2005; 103: Lopes A, Hidalgo GS, Kowalski LP et al: Prognostic factors in carcinoma of the penis: multivariate analysis of 145 patients treated with amputation and lymphadenectomy. J Urol 1996; 156: Hughes BE, Leijte JA, Kroon BK et al: Lymph node metastasis in intermediate-risk penile squamous cell cancer: a two-centre experience. Eur Urol 2010; 57: Edge SB, Byrd DR, Compton CC et al: Vulva. In: AJCC Cancer Staging Manual, 7th ed. New York: Springer 2010; p Vernooij F, Sie-Go DM and Heintz AP: Lymph node recurrence following stage IA vulvar carcinoma: two cases and a short overview of literature. Int J Gynecol Cancer 2007; 17: Hacker NF, Berek JS, Lagasse LD et al: Individualization of treatment for stage I squamous cell vulvar carcinoma. Obstet Gynecol 1984; 63: Gonzalez Bosquet J, Kinney WK, Russell AH et al: Risk of occult inguinofemoral lymph node metastasis from squamous carcinoma of the vulva. Int J Radiat Oncol Biol Phys 2003; 57: Horenblas S: Lymphadenectomy for squamous cell carcinoma of the penis. Part 1: diagnosis of lymph node metastasis. BJU Int 2001; 88: Homesley HD, Bundy BN, Sedlis A et al: Assessment of current International Federation of Gynecology and Obstetrics staging of vulvar carcinoma relative to prognostic factors for survival (a Gynecologic Oncology Group study). Am J Obstet Gynecol 1991; 164: Hacker NF, Berek JS, Lagasse LD et al: Management of regional lymph nodes and their prognostic influence in vulvar cancer. Obstet Gynecol 1983; 61: Kunos C, Simpkins F, Gibbons H et al: Radiation therapy compared with pelvic node resection for node-positive vulvar cancer: a randomized controlled trial. Obstet Gynecol 2009; 114: Pandey D, Mahajan V and Kannan RR: Prognostic factors in node-positive carcinoma of the penis. J Surg Oncol 2006; 93: Ravi R: Correlation between the extent of nodal involvement and survival following groin dissection for carcinoma of the penis. Br J Urol 1993; 72: Fons G, Hyde SE, Buist MR et al: Prognostic value of bilateral positive nodes in squamous cell cancer of the vulva. Int J Gynecol Cancer 2009; 19: Gaarenstroom KN, Kenter GG, Trimbos JB et al: Postoperative complications after vulvectomy and inguinofemoral lymphadenectomy using separate groin incisions. Int J Gynecol Cancer 2003; 13: Cabanas RM: An approach for the treatment of penile carcinoma. Cancer 1977; 39: Perinetti E, Crane DB and Catalona WJ: Unreliability of sentinel lymph node biopsy for staging penile carcinoma. J Urol 1980; 124: Pettaway CA, Pisters LL, Dinney CP et al: Sentinel lymph node dissection for penile carcinoma: the M. D. Anderson Cancer Center experience. J Urol 1995; 154: Leijte JA, Hughes B, Graafland NM et al: Twocenter evaluation of dynamic sentinel node biopsy for squamous cell carcinoma of the penis. J Clin Oncol 2009; 27: Graafland NM, Lam W, Leijte JA et al: prognostic factors for occult inguinal lymph node involvement in penile carcinoma and assessment of the high-risk EAU Subgroup: A two-institution analysis of 342 clinically node-negative patients. Eur Urol 2010; 58: Selman TJ, Luesley DM, Acheson N et al: A systematic review of the accuracy of diagnostic tests for inguinal lymph node status in vulvar cancer. Gynecol Oncol 2005; 99: Van der Zee AG, Oonk MH, De Hullu JA et al: Sentinel node dissection is safe in the treatment of early-stage vulvar cancer. J Clin Oncol 2008; 26: Levenback CF, van der Zee AG, Rob L et al: Sentinel lymph node biopsy in patients with gynecologic cancers. Expert panel statement from the International Sentinel Node Society Meeting, February 21, Gynecol Oncol 2009; 114: Morton DL, Cochran AJ, Thompson JF et al: Sentinel node biopsy for early-stage melanoma: accuracy and morbidity in MSLT-I, an international multicenter trial. Ann Surg 2005; 242: Kulkarni JN and Kamat MR: Prophylactic bilateral groin node dissection versus prophylactic radiotherapy and surveillance in patients with N0 and N1-2A carcinoma of the penis. Eur Urol 1994; 26: Stehman FB, Bundy BN, Thomas G et al: Groin dissection versus groin radiation in carcinoma of the vulva: a Gynecologic Oncology Group study. Int J Radiat Oncol Biol Phys 1992; 24: Petereit DG, Mehta MP, Buchler DA et al: Inguinofemoral radiation of N0, N1 vulvar cancer may be equivalent to lymphadenectomy if proper radiation technique is used. Int J Radiat Oncol Biol Phys 1993; 27: Leiserowitz GS, Russell AH, Kinney WK et al: Prophylactic chemoradiation of inguinofemoral lymph nodes in patients with locally extensive vulvar cancer. Gynecol Oncol 1997; 66: Hyde SE, Valmadre S, Hacker NF et al: Squamous cell carcinoma of the vulva with bulky positive groin nodes-nodal debulking versus full groin dissection prior to radiation therapy. Int J Gynecol Cancer 2007; 17: Ravi R, Chaturvedi HK and Sastry DV: Role of radiation therapy in the treatment of carcinoma of the penis. Br J Urol 1994; 74: 646.
8 24 LESSONS LEARNED FROM VULVAR CARCINOMA 43. Horenblas S: Lymphadenectomy for squamous cell carcinoma of the penis. Part 2: the role and technique of lymph node dissection. BJU Int 2001; 88: Homesley HD, Bundy BN, Sedlis A et al: Radiation therapy versus pelvic node resection for carcinoma of the vulva with positive groin nodes. Obstet Gynecol 1986; 68: Pizzocaro G, Algaba F, Horenblas S et al: EAU penile cancer guidelines Eur Urol 2010; 57: Moore DH, Thomas GM, Montana GS et al: Preoperative chemoradiation for advanced vulvar cancer: a phase II study of the Gynecologic Oncology Group. Int J Radiat Oncol Biol Phys 1998; 42: Bartelink H, Roelofsen F, Eschwege F et al: Concomitant radiotherapy and chemotherapy is superior to radiotherapy alone in the treatment of locally advanced anal cancer: results of a phase III randomized trial of the European Organization for Research and Treatment of Cancer Radiotherapy and Gastrointestinal Cooperative Groups. J Clin Oncol 1997; 15: Pagliaro LC, Williams DL, Daliani D et al: Neoadjuvant paclitaxel, ifosfamide, and cisplatin chemotherapy for metastatic penile cancer: a phase II study. J Clin Oncol 2010; 28: Pizzocaro G, Nicolai N and Milani A: Taxanes in combination with cisplatin and fluorouracil for advanced penile cancer: preliminary results. Eur Urol 2009; 55: Edge SB, Byrd DR, Compton CC et al: Penis. In: AJCC Cancer Staging Manual, 7th ed. New York: Springer 2010; p 447.
GUIDELINES ON PENILE CANCER
 GUIDELINES ON PENILE CANCER (Text updated March 2005) G. Pizzocaro (chairman), F. Algaba, S. Horenblas, H. van der Poel, E. Solsona, S. Tana, N. Watkin 58 Penile Cancer Eur Urol 2004;46(1);1-8 Introduction
GUIDELINES ON PENILE CANCER (Text updated March 2005) G. Pizzocaro (chairman), F. Algaba, S. Horenblas, H. van der Poel, E. Solsona, S. Tana, N. Watkin 58 Penile Cancer Eur Urol 2004;46(1);1-8 Introduction
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES GYNECOLOGIC CANCER VULVAR
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES GYNECOLOGIC CANCER VULVAR Last Revision Date July 2015 1 Site Group: Gynecologic Cancer Vulvar Author: Dr. Stephane Laframboise 1. INTRODUCTION
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES GYNECOLOGIC CANCER VULVAR Last Revision Date July 2015 1 Site Group: Gynecologic Cancer Vulvar Author: Dr. Stephane Laframboise 1. INTRODUCTION
EAU GUIDELINES ON PENILE CANCER
 EAU GUIDELINES ON PENILE CANCER (Text update April 2014) O.W. Hakenberg (Chair), E. Compérat, S. Minhas, A. Necchi, C. Protzel, N. Watkin Guidelines Associate: R. Robinson Introduction and epidemiology
EAU GUIDELINES ON PENILE CANCER (Text update April 2014) O.W. Hakenberg (Chair), E. Compérat, S. Minhas, A. Necchi, C. Protzel, N. Watkin Guidelines Associate: R. Robinson Introduction and epidemiology
EAU GUIDELINES ON PENILE CANCER
 EAU GUIDELINES ON PENILE CANCER (Text update April 2014) O.W. Hakenberg (Chair), N. Watkin, E. Compérat, S. Minhas, A. Necchi, C. Protzel Introduction and epidemiology The incidence of penile cancer increases
EAU GUIDELINES ON PENILE CANCER (Text update April 2014) O.W. Hakenberg (Chair), N. Watkin, E. Compérat, S. Minhas, A. Necchi, C. Protzel Introduction and epidemiology The incidence of penile cancer increases
GUIDELINES ON PENILE CANCER
 GUIDELINES ON PENILE CANCER (Text update April 2010) G. Pizzocaro, F. Algaba, S. Horenblas, E. Solsona, S. Tana, H. Van Der Poel, N. Watkin 78 Penile Cancer Eur Urol 2010 Jun;57(6):1002-12 Introduction
GUIDELINES ON PENILE CANCER (Text update April 2010) G. Pizzocaro, F. Algaba, S. Horenblas, E. Solsona, S. Tana, H. Van Der Poel, N. Watkin 78 Penile Cancer Eur Urol 2010 Jun;57(6):1002-12 Introduction
GUIDELINES ON PENILE CANCER
 46 E. Solsona (chairman), F. Algaba, S. Horenblas, G. Pizzocaro, T. Windahl Eur Urol 2002;42(3):199-203 Introduction Penile carcinoma is an uncommon malignant disease with an incidence ranging from 0.1
46 E. Solsona (chairman), F. Algaba, S. Horenblas, G. Pizzocaro, T. Windahl Eur Urol 2002;42(3):199-203 Introduction Penile carcinoma is an uncommon malignant disease with an incidence ranging from 0.1
GUIDELINEs ON PENILE CANCER
 GUIDELINEs ON PENILE CANCER (update April 2010) G. Pizzocaro, F. Algaba, S. Horenblas, E. Solsona, S. Tana, H. Van Der Poel, N. Watkin Eur Urol 2010, doi:10.1016/j.eururo.2010.01.039 Introduction Over
GUIDELINEs ON PENILE CANCER (update April 2010) G. Pizzocaro, F. Algaba, S. Horenblas, E. Solsona, S. Tana, H. Van Der Poel, N. Watkin Eur Urol 2010, doi:10.1016/j.eururo.2010.01.039 Introduction Over
Review Article Selective Inguinal Lymphadenectomy in the Treatment of Invasive Squamous Cell Carcinoma of the Vulva
 Hindawi Publishing Corporation International Journal of Surgical Oncology Volume 2011, Article ID 284374, 6 pages doi:10.1155/2011/284374 Review Article Selective Inguinal Lymphadenectomy in the Treatment
Hindawi Publishing Corporation International Journal of Surgical Oncology Volume 2011, Article ID 284374, 6 pages doi:10.1155/2011/284374 Review Article Selective Inguinal Lymphadenectomy in the Treatment
Vulvar Carcinoma. Definition: Cases should be classified as carsinoma of the vulva when the primary site growth is in the vulva Malignant melanoma sho
 Carcinoma Vulva & Vagina Subdivisi Onkologi Ginekologi Bagian Obgin FK USU Vulvar Carcinoma. Definition: Cases should be classified as carsinoma of the vulva when the primary site growth is in the vulva
Carcinoma Vulva & Vagina Subdivisi Onkologi Ginekologi Bagian Obgin FK USU Vulvar Carcinoma. Definition: Cases should be classified as carsinoma of the vulva when the primary site growth is in the vulva
Guideline for the Management of Vulval Cancer
 Version History Guideline for the Management of Vulval Cancer Version Date Brief Summary of Change Issued 2.0 20.02.08 Endorsed by the Governance Committee 2.1 19.11.10 Circulated at NSSG meeting 2.2 13.04.11
Version History Guideline for the Management of Vulval Cancer Version Date Brief Summary of Change Issued 2.0 20.02.08 Endorsed by the Governance Committee 2.1 19.11.10 Circulated at NSSG meeting 2.2 13.04.11
Proposed All Wales Vulval Cancer Guidelines. Dr Amanda Tristram
 Proposed All Wales Vulval Cancer Guidelines Dr Amanda Tristram Previous FIGO staging FIGO Stage Features TNM Ia Lesion confined to vulva with
Proposed All Wales Vulval Cancer Guidelines Dr Amanda Tristram Previous FIGO staging FIGO Stage Features TNM Ia Lesion confined to vulva with
SENTINEL NODES FOR EARLY VULVAL CANCER:
 SENTINEL NODES FOR EARLY VULVAL CANCER: FEASIBILITY AND SAFETY IN A LOW RESOURCE SETTING LINDA ROGERS RCOG Congress 2017 None Declaration of Interests Vulval Cancer Rare 4% of all gynaecological malignancies
SENTINEL NODES FOR EARLY VULVAL CANCER: FEASIBILITY AND SAFETY IN A LOW RESOURCE SETTING LINDA ROGERS RCOG Congress 2017 None Declaration of Interests Vulval Cancer Rare 4% of all gynaecological malignancies
MUSCLE - INVASIVE AND METASTATIC BLADDER CANCER
 10 MUSCLE - INVASIVE AND METASTATIC BLADDER CANCER Recommendations from the EAU Working Party on Muscle Invasive and Metastatic Bladder Cancer G. Jakse (chairman), F. Algaba, S. Fossa, A. Stenzl, C. Sternberg
10 MUSCLE - INVASIVE AND METASTATIC BLADDER CANCER Recommendations from the EAU Working Party on Muscle Invasive and Metastatic Bladder Cancer G. Jakse (chairman), F. Algaba, S. Fossa, A. Stenzl, C. Sternberg
Clinical Pathological Conference. Malignant Melanoma of the Vulva
 Clinical Pathological Conference Malignant Melanoma of the Vulva History F/48 Chinese Married Para 1 Presented in September 2004 Vulval mass for 2 months Associated with watery and blood stained discharge
Clinical Pathological Conference Malignant Melanoma of the Vulva History F/48 Chinese Married Para 1 Presented in September 2004 Vulval mass for 2 months Associated with watery and blood stained discharge
The International Federation of Gynecology and Obstetrics (FIGO) updated the staging
 Continuing Education Column Revised FIGO Staging System Hee Sug Ryu, MD Department of Obstetrics and Gynecology, Ajou University School of Medicine E - mail : hsryu@ajou.ac.kr J Korean Med Assoc 2010;
Continuing Education Column Revised FIGO Staging System Hee Sug Ryu, MD Department of Obstetrics and Gynecology, Ajou University School of Medicine E - mail : hsryu@ajou.ac.kr J Korean Med Assoc 2010;
MUSCLE-INVASIVE AND METASTATIC BLADDER CANCER
 MUSCLE-INVASIVE AND METASTATIC BLADDER CANCER (Text update March 2008) A. Stenzl (chairman), N.C. Cowan, M. De Santis, G. Jakse, M. Kuczyk, A.S. Merseburger, M.J. Ribal, A. Sherif, J.A. Witjes Introduction
MUSCLE-INVASIVE AND METASTATIC BLADDER CANCER (Text update March 2008) A. Stenzl (chairman), N.C. Cowan, M. De Santis, G. Jakse, M. Kuczyk, A.S. Merseburger, M.J. Ribal, A. Sherif, J.A. Witjes Introduction
Chapter 8 Adenocarcinoma
 Page 80 Chapter 8 Adenocarcinoma Overview In Japan, the proportion of squamous cell carcinoma among all cervical cancers has been declining every year. In a recent survey, non-squamous cell carcinoma accounted
Page 80 Chapter 8 Adenocarcinoma Overview In Japan, the proportion of squamous cell carcinoma among all cervical cancers has been declining every year. In a recent survey, non-squamous cell carcinoma accounted
EUROPEAN UROLOGY 58 (2010)
 EUROPEAN UROLOGY 58 (2010) 742 747 available at www.sciencedirect.com journal homepage: www.europeanurology.com Penile Cancer Prognostic Factors for Occult Inguinal Lymph Node Involvement in Penile Carcinoma
EUROPEAN UROLOGY 58 (2010) 742 747 available at www.sciencedirect.com journal homepage: www.europeanurology.com Penile Cancer Prognostic Factors for Occult Inguinal Lymph Node Involvement in Penile Carcinoma
Staging and Treatment Update for Gynecologic Malignancies
 Staging and Treatment Update for Gynecologic Malignancies Bunja Rungruang, MD Medical College of Georgia No disclosures 4 th most common new cases of cancer in women 5 th and 6 th leading cancer deaths
Staging and Treatment Update for Gynecologic Malignancies Bunja Rungruang, MD Medical College of Georgia No disclosures 4 th most common new cases of cancer in women 5 th and 6 th leading cancer deaths
SCAN Gynaecological Group. Clinical Management Protocols vulval cancer
 SE Scotland Cancer Network SCAN Gynaecological Group Clinical Management Protocols vulval cancer 2009 www.scan.scot.nhs.uk August 2001 updated annually, most recently INTRODUCTION The South East Scotland
SE Scotland Cancer Network SCAN Gynaecological Group Clinical Management Protocols vulval cancer 2009 www.scan.scot.nhs.uk August 2001 updated annually, most recently INTRODUCTION The South East Scotland
UPDATE IN THE MANAGEMENT OF INVASIVE CERVICAL CANCER
 UPDATE IN THE MANAGEMENT OF INVASIVE CERVICAL CANCER Susan Davidson, MD Professor Department of Obstetrics and Gynecology Division of Gynecologic Oncology University of Colorado- Denver Anatomy Review
UPDATE IN THE MANAGEMENT OF INVASIVE CERVICAL CANCER Susan Davidson, MD Professor Department of Obstetrics and Gynecology Division of Gynecologic Oncology University of Colorado- Denver Anatomy Review
VULVAR CARCINOMA. Page 1 of 5
 VULVAR CARCINOMA EXAMPLE OF A VULVAR CARCINOMA USING PROPOSED TEMPLATE Case: Invasive squamous cell carcinoma arising in D-VIN Tumor in left labia major Left partial vaginectomy and sentinel lymph node
VULVAR CARCINOMA EXAMPLE OF A VULVAR CARCINOMA USING PROPOSED TEMPLATE Case: Invasive squamous cell carcinoma arising in D-VIN Tumor in left labia major Left partial vaginectomy and sentinel lymph node
Melanoma Surgery Update James R. Ouellette, DO FACS Premier Health Cancer Institute Wright State University Chief, Surgical Oncology Division
 Melanoma Surgery Update 2018 James R. Ouellette, DO FACS Premier Health Cancer Institute Wright State University Chief, Surgical Oncology Division Surgery for Melanoma Mainstay of treatment for potentially
Melanoma Surgery Update 2018 James R. Ouellette, DO FACS Premier Health Cancer Institute Wright State University Chief, Surgical Oncology Division Surgery for Melanoma Mainstay of treatment for potentially
Vagina. 1. Introduction. 1.1 General Information and Aetiology
 Vagina 1. Introduction 1.1 General Information and Aetiology The vagina is part of internal female reproductive system. It is an elastic, muscular tube that connects the outside of the body to the cervix.
Vagina 1. Introduction 1.1 General Information and Aetiology The vagina is part of internal female reproductive system. It is an elastic, muscular tube that connects the outside of the body to the cervix.
Objective. Results. Patients and Methods. Conclusions. Keywords <squamous cell carcinoma of the penis, prognostics, cancerspecific mortality, nomogram
 Development and external validation of a prognostic tool for prediction of cancer-specific mortality after complete loco-regional pathological staging for squamous cell carcinoma of the penis Maxine Sun,
Development and external validation of a prognostic tool for prediction of cancer-specific mortality after complete loco-regional pathological staging for squamous cell carcinoma of the penis Maxine Sun,
Index. Surg Oncol Clin N Am 14 (2005) Note: Page numbers of article titles are in boldface type.
 Surg Oncol Clin N Am 14 (2005) 433 439 Index Note: Page numbers of article titles are in boldface type. A Abdominosacral resection, of recurrent rectal cancer, 202 215 Ablative techniques, image-guided,
Surg Oncol Clin N Am 14 (2005) 433 439 Index Note: Page numbers of article titles are in boldface type. A Abdominosacral resection, of recurrent rectal cancer, 202 215 Ablative techniques, image-guided,
Sentinel Lymph Node Biopsy Is Valuable For All Cancer. Surgery Grand Rounds Debate October 6, 2008 Joel Baumgartner
 Sentinel Lymph Node Biopsy Is Valuable For All Cancer Surgery Grand Rounds Debate October 6, 2008 Joel Baumgartner History Lymphatics first described by Rasmus Bartholin in 1653 Rudolf Virchow postulated
Sentinel Lymph Node Biopsy Is Valuable For All Cancer Surgery Grand Rounds Debate October 6, 2008 Joel Baumgartner History Lymphatics first described by Rasmus Bartholin in 1653 Rudolf Virchow postulated
Translating Evidence into Practice: Primary Cutaneous Melanoma Guidelines. Sentinel Lymph Node Biopsy
 American Academy of Dermatology 2018 Annual Meeting San Diego, CA, February 17, 2018 Translating Evidence into Practice: Primary Cutaneous Melanoma Guidelines. Sentinel Lymph Node Biopsy Christopher Bichakjian,
American Academy of Dermatology 2018 Annual Meeting San Diego, CA, February 17, 2018 Translating Evidence into Practice: Primary Cutaneous Melanoma Guidelines. Sentinel Lymph Node Biopsy Christopher Bichakjian,
Melanoma Quality Reporting
 Melanoma Quality Reporting September 1, 2013 December 31, 2016 Laurence McCahill, MD Surgical Oncologist Metro Health Surgical Oncology Metro Health Professional Building 2122 Health Drive SW Wyoming,
Melanoma Quality Reporting September 1, 2013 December 31, 2016 Laurence McCahill, MD Surgical Oncologist Metro Health Surgical Oncology Metro Health Professional Building 2122 Health Drive SW Wyoming,
GUIDELINES ON PROSTATE CANCER
 10 G. Aus (chairman), C. Abbou, M. Bolla, A. Heidenreich, H-P. Schmid, H. van Poppel, J. Wolff, F. Zattoni Eur Urol 2001;40:97-101 Introduction Cancer of the prostate is now recognized as one of the principal
10 G. Aus (chairman), C. Abbou, M. Bolla, A. Heidenreich, H-P. Schmid, H. van Poppel, J. Wolff, F. Zattoni Eur Urol 2001;40:97-101 Introduction Cancer of the prostate is now recognized as one of the principal
Cervical Cancer: 2018 FIGO Staging
 Cervical Cancer: 2018 FIGO Staging Jonathan S. Berek, MD, MMS Laurie Kraus Lacob Professor Stanford University School of Medicine Director, Stanford Women s Cancer Center Senior Scientific Advisor, Stanford
Cervical Cancer: 2018 FIGO Staging Jonathan S. Berek, MD, MMS Laurie Kraus Lacob Professor Stanford University School of Medicine Director, Stanford Women s Cancer Center Senior Scientific Advisor, Stanford
Position Statement on Management of the Axilla in Patients with Invasive Breast Cancer
 - Official Statement - Position Statement on Management of the Axilla in Patients with Invasive Breast Cancer Sentinel lymph node (SLN) biopsy has replaced axillary lymph node dissection (ALND) for the
- Official Statement - Position Statement on Management of the Axilla in Patients with Invasive Breast Cancer Sentinel lymph node (SLN) biopsy has replaced axillary lymph node dissection (ALND) for the
Vaginal intraepithelial neoplasia
 Vaginal intraepithelial neoplasia The terminology and pathology of VAIN are analogous to those of CIN (VAIN I-III). The main difference is that vaginal epithelium does not normally have crypts, so the
Vaginal intraepithelial neoplasia The terminology and pathology of VAIN are analogous to those of CIN (VAIN I-III). The main difference is that vaginal epithelium does not normally have crypts, so the
Chapter 2 Staging of Breast Cancer
 Chapter 2 Staging of Breast Cancer Zeynep Ozsaran and Senem Demirci Alanyalı 2.1 Introduction Five decades ago, Denoix et al. proposed classification system (tumor node metastasis [TNM]) based on the dissemination
Chapter 2 Staging of Breast Cancer Zeynep Ozsaran and Senem Demirci Alanyalı 2.1 Introduction Five decades ago, Denoix et al. proposed classification system (tumor node metastasis [TNM]) based on the dissemination
New NCCN Guidelines for Vulvar Cancer
 New NCCN Guidelines for Vulvar Cancer Benjamin E. Greer, MD Fred Hutchinson Cancer Research Center/ Seattle Cancer Care Alliance Vulvar Cancer Objectives: 1) Overview of vulvar carcinoma and FIGO staging.
New NCCN Guidelines for Vulvar Cancer Benjamin E. Greer, MD Fred Hutchinson Cancer Research Center/ Seattle Cancer Care Alliance Vulvar Cancer Objectives: 1) Overview of vulvar carcinoma and FIGO staging.
Disclosures. SLNB for Melanoma 25/02/2014 SENTINEL LYMPH NODE BIOPSY FOR MELANOMA: CURRENT GUIDELINES AND THEIR CLINICAL APPLICATION
 8 th Canadian Melanoma Conference February 22, 2014 Rimrock Resort Hotel, Banff, Alberta SENTINEL LYMPH NODE BIOPSY FOR MELANOMA: CURRENT GUIDELINES AND THEIR CLINICAL APPLICATION Christopher Bichakjian,
8 th Canadian Melanoma Conference February 22, 2014 Rimrock Resort Hotel, Banff, Alberta SENTINEL LYMPH NODE BIOPSY FOR MELANOMA: CURRENT GUIDELINES AND THEIR CLINICAL APPLICATION Christopher Bichakjian,
SLN Mapping in Cervical Cancer. Memorial Sloan Kettering Cancer Center New York, USA
 Lead Grou p Log SLN Mapping in Cervical Cancer Nadeem R. Abu-Rustum, M.D. Memorial Sloan Kettering Cancer Center New York, USA Conflict of Interest Disclosure Nadeem R. Abu-Rustum, M.D. I have no financial
Lead Grou p Log SLN Mapping in Cervical Cancer Nadeem R. Abu-Rustum, M.D. Memorial Sloan Kettering Cancer Center New York, USA Conflict of Interest Disclosure Nadeem R. Abu-Rustum, M.D. I have no financial
Rebecca Vogel, PGY-4 March 5, 2012
 Rebecca Vogel, PGY-4 March 5, 2012 Historical Perspective Changes In The Staging System Studies That Started The Talk Where We Go From Here Cutaneous melanoma has become an increasingly growing problem,
Rebecca Vogel, PGY-4 March 5, 2012 Historical Perspective Changes In The Staging System Studies That Started The Talk Where We Go From Here Cutaneous melanoma has become an increasingly growing problem,
Coversheet for Network Site Specific Group Agreed Documentation
 Coversheet for Network Site Specific Group Agreed Documentation This sheet is to accompany all documentation agreed by Pan Birmingham Cancer Network Site Specific Groups. This will assist the Network Governance
Coversheet for Network Site Specific Group Agreed Documentation This sheet is to accompany all documentation agreed by Pan Birmingham Cancer Network Site Specific Groups. This will assist the Network Governance
Penile cancer teams in UK. Common variants. Penile cancer teams. Basaloid squamous carcinoma. The Pathology of Penile Tumours
 The Pathology of Penile Tumours Dr Jonathan H Shanks The Christie NHS Foundation Trust, Manchester, UK Penile cancer teams in UK 12 centres for penile cancer work (10 in England and Wales, 2 in Scotland)
The Pathology of Penile Tumours Dr Jonathan H Shanks The Christie NHS Foundation Trust, Manchester, UK Penile cancer teams in UK 12 centres for penile cancer work (10 in England and Wales, 2 in Scotland)
North of Scotland Cancer Network Clinical Management Guideline for Carcinoma of the Uterine Cervix
 THIS DOCUMENT North of Scotland Cancer Network Carcinoma of the Uterine Cervix UNCONTROLLED WHEN PRINTED DOCUMENT CONTROL Prepared by A Kennedy/AG Macdonald/Others Approved by NOT APPROVED Issue date April
THIS DOCUMENT North of Scotland Cancer Network Carcinoma of the Uterine Cervix UNCONTROLLED WHEN PRINTED DOCUMENT CONTROL Prepared by A Kennedy/AG Macdonald/Others Approved by NOT APPROVED Issue date April
EUROPEAN UROLOGY 63 (2013)
 EUROPEAN UROLOGY 63 (2013) 657 663 available at www.sciencedirect.com journal homepage: www.europeanurology.com Platinum Priority Penile Cancer Editorial by Nicola Nicolai on pp. 664 666 of this issue
EUROPEAN UROLOGY 63 (2013) 657 663 available at www.sciencedirect.com journal homepage: www.europeanurology.com Platinum Priority Penile Cancer Editorial by Nicola Nicolai on pp. 664 666 of this issue
Carcinoma of the Urinary Bladder Histopathology
 Carcinoma of the Urinary Bladder Histopathology Reporting Proforma (Radical & Partial Cystectomy, Cystoprostatectomy) Includes the International Collaboration on Cancer reporting dataset denoted by * Family
Carcinoma of the Urinary Bladder Histopathology Reporting Proforma (Radical & Partial Cystectomy, Cystoprostatectomy) Includes the International Collaboration on Cancer reporting dataset denoted by * Family
Penis Cancer. What is penis cancer? Symptoms. Patient Information. Pagina 1 / 9. Patient Information - Penis Cancer
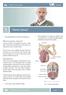 Patient Information English 31 Penis Cancer The underlined terms are listed in the glossary. What is penis cancer? Cancer is abnormal cell growth in the skin or organ tissue. When this cell growth starts
Patient Information English 31 Penis Cancer The underlined terms are listed in the glossary. What is penis cancer? Cancer is abnormal cell growth in the skin or organ tissue. When this cell growth starts
Penis Cancer. What is penis cancer? Symptoms. Patient Information. Pagina 1 / 9. Patient Information - Penis Cancer
 Patient Information English 31 Penis Cancer The underlined terms are listed in the glossary. What is penis cancer? Cancer is abnormal cell growth in the skin or organ tissue. When this cell growth starts
Patient Information English 31 Penis Cancer The underlined terms are listed in the glossary. What is penis cancer? Cancer is abnormal cell growth in the skin or organ tissue. When this cell growth starts
The Depth of Tumor Invasion is Superior to 8 th AJCC/UICC Staging System to Predict Patients Outcome in Radical Cystectomy.
 30 th Congress of the European Society of Pathology Tuesday, September 11, 2018 The Depth of Tumor Invasion is Superior to 8 th AJCC/UICC Staging System to Predict Patients Outcome in Radical Cystectomy.
30 th Congress of the European Society of Pathology Tuesday, September 11, 2018 The Depth of Tumor Invasion is Superior to 8 th AJCC/UICC Staging System to Predict Patients Outcome in Radical Cystectomy.
Update on Sentinel Node Biopsy in Endometrial Cancer: Feasibility, Technique, Impact
 Update on Sentinel Node Biopsy in Endometrial Cancer: Feasibility, Technique, Impact Bjørn Hagen, MD, PhD St Olavs Hospital Trondheim University Hospital Trondheim, Norway Endometrial Cancer (EC) The most
Update on Sentinel Node Biopsy in Endometrial Cancer: Feasibility, Technique, Impact Bjørn Hagen, MD, PhD St Olavs Hospital Trondheim University Hospital Trondheim, Norway Endometrial Cancer (EC) The most
Guidelines for Management of Penile Cancer
 Guidelines for Management of Penile Cancer Date Approved by Network Governance July 2012 Date for Review July 2015 Changes Between Versions 2 and 3 Sections 3, 5, 6 and 16 updated. Page 1 of 10 1. Scope
Guidelines for Management of Penile Cancer Date Approved by Network Governance July 2012 Date for Review July 2015 Changes Between Versions 2 and 3 Sections 3, 5, 6 and 16 updated. Page 1 of 10 1. Scope
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES GYNECOLOGIC CANCER CERVIX
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES GYNECOLOGIC CANCER CERVIX Site Group: Gynecology Cervix Author: Dr. Stephane Laframboise 1. INTRODUCTION 3 2. PREVENTION 3 3. SCREENING AND
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES GYNECOLOGIC CANCER CERVIX Site Group: Gynecology Cervix Author: Dr. Stephane Laframboise 1. INTRODUCTION 3 2. PREVENTION 3 3. SCREENING AND
Information for Patients. Primary urethral cancer. English
 Information for Patients Primary urethral cancer English Table of contents What is primary urethral cancer?... 3 Risk factors... 3 Symptoms... 4 Diagnosis... 4 Clinical examination... 4 Urinary cytology...
Information for Patients Primary urethral cancer English Table of contents What is primary urethral cancer?... 3 Risk factors... 3 Symptoms... 4 Diagnosis... 4 Clinical examination... 4 Urinary cytology...
Glossary of Terms Primary Urethral Cancer
 Patient Information English Glossary of Terms Primary Urethral Cancer Advanced cancer A tumour that grows into deeper layers of tissue, adjacent organs, or surrounding muscles. Anaesthesia (general, spinal,
Patient Information English Glossary of Terms Primary Urethral Cancer Advanced cancer A tumour that grows into deeper layers of tissue, adjacent organs, or surrounding muscles. Anaesthesia (general, spinal,
1. Written information to patient /GP: fax ASAP to GP & offer copy of consultation letter.
 Skin Cancer follow up guidelines If NEW serious diagnosis given: 1. Written information to patient /GP: fax ASAP to GP & offer copy of consultation letter. 2. Free prescription information details. 3.
Skin Cancer follow up guidelines If NEW serious diagnosis given: 1. Written information to patient /GP: fax ASAP to GP & offer copy of consultation letter. 2. Free prescription information details. 3.
3/25/2019. J. Anthony Rakowski D.O., F.A.C.O.O.G. MSU SCS Board Review Coarse
 J. Anthony Rakowski D.O., F.A.C.O.O.G. MSU SCS Board Review Coarse 1 4 th most common GYN cancer 5% of malignancies of GYN type. 4850 new cases annually 1030 deaths Cigarette smoking Vulvar dystrophy (Lichen
J. Anthony Rakowski D.O., F.A.C.O.O.G. MSU SCS Board Review Coarse 1 4 th most common GYN cancer 5% of malignancies of GYN type. 4850 new cases annually 1030 deaths Cigarette smoking Vulvar dystrophy (Lichen
Breast Cancer. Most common cancer among women in the US. 2nd leading cause of death in women. Mortality rates though have declined
 Breast Cancer Most common cancer among women in the US 2nd leading cause of death in women Mortality rates though have declined 1 in 8 women will develop breast cancer Breast Cancer Breast cancer increases
Breast Cancer Most common cancer among women in the US 2nd leading cause of death in women Mortality rates though have declined 1 in 8 women will develop breast cancer Breast Cancer Breast cancer increases
Management of Neck Metastasis from Unknown Primary
 Management of Neck Metastasis from Unknown Primary.. Definition Histologic evidence of malignancy in the cervical lymph node (s) with no apparent primary site of original tumour Diagnosis after a thorough
Management of Neck Metastasis from Unknown Primary.. Definition Histologic evidence of malignancy in the cervical lymph node (s) with no apparent primary site of original tumour Diagnosis after a thorough
Breast Cancer. Saima Saeed MD
 Breast Cancer Saima Saeed MD Breast Cancer Most common cancer among women in the US 2nd leading cause of death in women 1 in 8 women will develop breast cancer Incidence/mortality rates have declined Breast
Breast Cancer Saima Saeed MD Breast Cancer Most common cancer among women in the US 2nd leading cause of death in women 1 in 8 women will develop breast cancer Incidence/mortality rates have declined Breast
The Role of Radiation in the Management of Gynecologic Cancers. Scott Glaser, MD
 The Role of Radiation in the Management of Gynecologic Cancers Scott Glaser, MD Nothing to disclose DISCLOSURE Outline The role of radiation in: Endometrial Cancer Adjuvant Medically inoperable Cervical
The Role of Radiation in the Management of Gynecologic Cancers Scott Glaser, MD Nothing to disclose DISCLOSURE Outline The role of radiation in: Endometrial Cancer Adjuvant Medically inoperable Cervical
PENILE CANCER. Date Developed: January, Date Revised: February, 2012
 PENILE CANCER Date Developed: January, 2011 Date Revised: February, 2012 The recommendations contained in this guideline are a consensus of the Alberta Provincial Genitourinary Tumour Team synthesis of
PENILE CANCER Date Developed: January, 2011 Date Revised: February, 2012 The recommendations contained in this guideline are a consensus of the Alberta Provincial Genitourinary Tumour Team synthesis of
A phase II study of weekly paclitaxel and cisplatin followed by radical hysterectomy in stages IB2 and IIA2 cervical cancer AGOG14-001/TGOG1008
 A phase II study of weekly paclitaxel and cisplatin followed by radical hysterectomy in stages IB2 and IIA2 cervical cancer AGOG14-001/TGOG1008 NCT02432365 Chyong-Huey Lai, MD On behalf of Principal investigator
A phase II study of weekly paclitaxel and cisplatin followed by radical hysterectomy in stages IB2 and IIA2 cervical cancer AGOG14-001/TGOG1008 NCT02432365 Chyong-Huey Lai, MD On behalf of Principal investigator
Topics for Discussion. Malignant Melanoma. Surgical Treatment. Current Treatment of Cutaneous Melanoma 5/17/2013. Lymph Regional nodes:
 Topics for Discussion What is a sentinel lymph node (SLN)? Utility of sentinel lymph biopsies: therapeutic or staging? Current Treatment of Cutaneous Melanoma Carlos Corvera, M.D. Associate Professor of
Topics for Discussion What is a sentinel lymph node (SLN)? Utility of sentinel lymph biopsies: therapeutic or staging? Current Treatment of Cutaneous Melanoma Carlos Corvera, M.D. Associate Professor of
Da Costa was the first to coin the term. Marjolin s Ulcer: A Case Report and Literature Review. Case Report. Introduction
 E-Da Medical Journal 2016;3(2):24-28 Case Report Marjolin s Ulcer: A Case Report and Literature Review Yue-Chiu Su 1, Li-Ren Chang 2 Marjolin s ulcer is an aggressive cutaneous malignancy, which is common
E-Da Medical Journal 2016;3(2):24-28 Case Report Marjolin s Ulcer: A Case Report and Literature Review Yue-Chiu Su 1, Li-Ren Chang 2 Marjolin s ulcer is an aggressive cutaneous malignancy, which is common
Desmoplastic Melanoma: Surgical Management and Adjuvant Therapy
 Desmoplastic Melanoma: Surgical Management and Adjuvant Therapy Dale Han, MD Assistant Professor Department of Surgery Section of Surgical Oncology No disclosures Background Desmoplastic melanoma (DM)
Desmoplastic Melanoma: Surgical Management and Adjuvant Therapy Dale Han, MD Assistant Professor Department of Surgery Section of Surgical Oncology No disclosures Background Desmoplastic melanoma (DM)
No Benefit to Routine Completion Lymphadenectomy for Sentinel Lymph Node Positive Melanoma
 No Benefit to Routine Completion Lymphadenectomy for Sentinel Lymph Node Positive Melanoma Michael Lowe, MD Assistant Professor of Surgery Winship Cancer Institute Emory University School of Medicine July
No Benefit to Routine Completion Lymphadenectomy for Sentinel Lymph Node Positive Melanoma Michael Lowe, MD Assistant Professor of Surgery Winship Cancer Institute Emory University School of Medicine July
Invasive Cervical Cancer: Squamous Cell, Adenocarcinoma, Adenosquamous
 Note: If available, clinical trials should be considered as preferred treatment options for eligible patients (www.mdanderson.org/gynonctrials). Other co-morbidities are taken into consideration prior
Note: If available, clinical trials should be considered as preferred treatment options for eligible patients (www.mdanderson.org/gynonctrials). Other co-morbidities are taken into consideration prior
Best Papers. F. Fusco
 Best Papers UROLOGY F. Fusco Best papers - 2015 RP/RT Oncological outcomes RP/RT IN ct3 Utilization trends RP/RT Complications Evolving role of elnd /Salvage LND This cohort reflects the current clinical
Best Papers UROLOGY F. Fusco Best papers - 2015 RP/RT Oncological outcomes RP/RT IN ct3 Utilization trends RP/RT Complications Evolving role of elnd /Salvage LND This cohort reflects the current clinical
Melanoma Patients and the Sentinel Lymph Node (SLN) Procedure: An Oncologic Surgeon s Perspective
 Melanoma Patients and the Sentinel Lymph Node (SLN) Procedure: An Oncologic Surgeon s Perspective Giorgos C. Karakousis, M.D. Associate Professor of Surgery Hospital of the University of Pennsylvania Disclosures
Melanoma Patients and the Sentinel Lymph Node (SLN) Procedure: An Oncologic Surgeon s Perspective Giorgos C. Karakousis, M.D. Associate Professor of Surgery Hospital of the University of Pennsylvania Disclosures
Radionuclide detection of sentinel lymph node
 Radionuclide detection of sentinel lymph node Sophia I. Koukouraki Assoc. Professor Department of Nuclear Medicine Medicine School, University of Crete 1 BACKGROUND The prognosis of malignant disease is
Radionuclide detection of sentinel lymph node Sophia I. Koukouraki Assoc. Professor Department of Nuclear Medicine Medicine School, University of Crete 1 BACKGROUND The prognosis of malignant disease is
category cm0. Category will ensure it T1 melanoma. 68 Retinoblastoma
 AJCC 8 th Edition Chapter 1 Principles of Cancer Staging: Node Status Not Required in Rare Circumstances Clinical Staging, cn Category For some cancer sites in which lymph node involvement is rare, patients
AJCC 8 th Edition Chapter 1 Principles of Cancer Staging: Node Status Not Required in Rare Circumstances Clinical Staging, cn Category For some cancer sites in which lymph node involvement is rare, patients
Talk to Your Doctor. Fact Sheet
 Talk to Your Doctor Hearing the words you have skin cancer is overwhelming and would leave anyone with a lot of questions. If you have been diagnosed with Stage I or II cutaneous melanoma with no apparent
Talk to Your Doctor Hearing the words you have skin cancer is overwhelming and would leave anyone with a lot of questions. If you have been diagnosed with Stage I or II cutaneous melanoma with no apparent
Primary Malignant Melanoma of the Vagina: Report of Two Cases and Review of the Literature
 Archives of Clinical and Medical Case Reports doi: 10.26502/acmcr.9655007 Volume 1, Issue 2 Case Report Primary Malignant Melanoma of the Vagina: Report of Two Cases and Review of the Literature Guler
Archives of Clinical and Medical Case Reports doi: 10.26502/acmcr.9655007 Volume 1, Issue 2 Case Report Primary Malignant Melanoma of the Vagina: Report of Two Cases and Review of the Literature Guler
CPC on Cervical Pathology
 CPC on Cervical Pathology Dr. W.K. Ng Senior Medical Officer Department of Clinical Pathology Pamela Youde Nethersole Eastern Hospital Cervical Smear: High Grade SIL (CIN III) Cervical Smear: High Grade
CPC on Cervical Pathology Dr. W.K. Ng Senior Medical Officer Department of Clinical Pathology Pamela Youde Nethersole Eastern Hospital Cervical Smear: High Grade SIL (CIN III) Cervical Smear: High Grade
is time consuming and expensive. An intra-operative assessment is not going to be helpful if there is no more tissue that can be taken to improve the
 My name is Barry Feig. I am a Professor of Surgical Oncology at The University of Texas MD Anderson Cancer Center in Houston, Texas. I am going to talk to you today about the role for surgery in the treatment
My name is Barry Feig. I am a Professor of Surgical Oncology at The University of Texas MD Anderson Cancer Center in Houston, Texas. I am going to talk to you today about the role for surgery in the treatment
Sentinel Lymph Node Biopsy for Breast Cancer
 Sentinel Lymph Node Biopsy for Breast Cancer Registrar Tutorial Adam Cichowitz Surgical Registrar The Royal Melbourne Hospital Sentinel Lymph Node Biopsy Axillary LN status important prognostic factor
Sentinel Lymph Node Biopsy for Breast Cancer Registrar Tutorial Adam Cichowitz Surgical Registrar The Royal Melbourne Hospital Sentinel Lymph Node Biopsy Axillary LN status important prognostic factor
STAGE CATEGORY DEFINITIONS
 CLINICAL Extent of disease before any treatment y clinical staging completed after neoadjuvant therapy but before subsequent surgery TX Tis Tis (DCIS) Tis (LCIS) Tis (Paget s) T1 T1mi T1a T1b T1c a b c
CLINICAL Extent of disease before any treatment y clinical staging completed after neoadjuvant therapy but before subsequent surgery TX Tis Tis (DCIS) Tis (LCIS) Tis (Paget s) T1 T1mi T1a T1b T1c a b c
Cutaneous Melanoma: Epidemiology (USA) The Sentinel Node in Head and Neck Melanoma. Cutaneous Melanoma: Epidemiology (USA)
 The Sentinel Node in Head and Neck Melanoma Cutaneous Melanoma: Epidemiology (USA) 6 th leading cause of cancer among men and women 68,720 new cases of invasive melanoma in 2009 8,650 deaths from melanoma
The Sentinel Node in Head and Neck Melanoma Cutaneous Melanoma: Epidemiology (USA) 6 th leading cause of cancer among men and women 68,720 new cases of invasive melanoma in 2009 8,650 deaths from melanoma
Canadian Scientific Journal. Intraoperative color detection of lymph nodes metastases in thyroid cancer
 Canadian Scientific Journal 2 (2014) Contents lists available at Canadian Scientific Journal Canadian Scientific Journal journal homepage: Intraoperative color detection of lymph nodes metastases in thyroid
Canadian Scientific Journal 2 (2014) Contents lists available at Canadian Scientific Journal Canadian Scientific Journal journal homepage: Intraoperative color detection of lymph nodes metastases in thyroid
BLADDER CANCER: PATIENT INFORMATION
 BLADDER CANCER: PATIENT INFORMATION The bladder is the balloon like organ located in the pelvis that stores and empties urine. Urine is produced by the kidneys, is conducted to the bladder by the ureters,
BLADDER CANCER: PATIENT INFORMATION The bladder is the balloon like organ located in the pelvis that stores and empties urine. Urine is produced by the kidneys, is conducted to the bladder by the ureters,
Nodal Treatment in Melanoma: Snow to MSLT-II
 Nodal Treatment in Melanoma: Snow to MSLT-II Mark B. Faries, MD, FACS Director, Donald L. Morton Melanoma Research Program Program Director, JWCI Complex General Surgical Oncology Fellowship Director,
Nodal Treatment in Melanoma: Snow to MSLT-II Mark B. Faries, MD, FACS Director, Donald L. Morton Melanoma Research Program Program Director, JWCI Complex General Surgical Oncology Fellowship Director,
GUIDELINES ON NON-MUSCLE- INVASIVE BLADDER CANCER
 GUIDELINES ON NON-MUSCLE- INVASIVE BLADDER CANCER (Limited text update December 21) M. Babjuk, W. Oosterlinck, R. Sylvester, E. Kaasinen, A. Böhle, J. Palou, M. Rouprêt Eur Urol 211 Apr;59(4):584-94 Introduction
GUIDELINES ON NON-MUSCLE- INVASIVE BLADDER CANCER (Limited text update December 21) M. Babjuk, W. Oosterlinck, R. Sylvester, E. Kaasinen, A. Böhle, J. Palou, M. Rouprêt Eur Urol 211 Apr;59(4):584-94 Introduction
Prognostic factors associated with local recurrence in squamous cell carcinoma of the vulva
 Original Article J Gynecol Oncol Vol. 24, No. 3:242-248 pissn 2005-0380 eissn 2005-0399 Prognostic factors associated with local recurrence in squamous cell carcinoma of the vulva Sara Iacoponi, Ignacio
Original Article J Gynecol Oncol Vol. 24, No. 3:242-248 pissn 2005-0380 eissn 2005-0399 Prognostic factors associated with local recurrence in squamous cell carcinoma of the vulva Sara Iacoponi, Ignacio
Advances in Breast Surgery. Catherine Campo, D.O. Breast Surgeon Meridian Health System April 17, 2015
 Advances in Breast Surgery Catherine Campo, D.O. Breast Surgeon Meridian Health System April 17, 2015 Objectives Understand the surgical treatment of breast cancer Be able to determine when a lumpectomy
Advances in Breast Surgery Catherine Campo, D.O. Breast Surgeon Meridian Health System April 17, 2015 Objectives Understand the surgical treatment of breast cancer Be able to determine when a lumpectomy
Primary Cutaneous Melanoma Pathology Reporting Proforma DD MM YYYY. *Tumour site. *Specimen laterality. *Specimen type
 Primary Cutaneous Melanoma Pathology Reporting Proforma Includes the International Collaboration on Cancer reporting dataset denoted by * Family name Given name(s) Date of birth DD MM YYYY Sex Male Female
Primary Cutaneous Melanoma Pathology Reporting Proforma Includes the International Collaboration on Cancer reporting dataset denoted by * Family name Given name(s) Date of birth DD MM YYYY Sex Male Female
Disclosures. I have no conflicts of interest to disclose. Vulvar Disease. Precancer and Cancerous Vulvar Disease
 Precancer and Cancerous Vulvar Disease Stefanie M. Ueda, M.D. Disclosures I have no conflicts of interest to disclose. Assistant Clinical Professor Division of Gynecologic Oncology University of California,
Precancer and Cancerous Vulvar Disease Stefanie M. Ueda, M.D. Disclosures I have no conflicts of interest to disclose. Assistant Clinical Professor Division of Gynecologic Oncology University of California,
16/09/2015. ACOSOG Z011 changing practice. Presentation outline. Nodal mets #1 prognostic tool. Less surgery no change in oncologic outcomes
 ACOSOG Z011 changing practice The end of axillary US/FNA? Preoperative staging of the axilla in the era of Z011 Adena S Scheer MD MSc FRCSC Surgical Oncologist, St. Michael s Hospital Assistant Professor,
ACOSOG Z011 changing practice The end of axillary US/FNA? Preoperative staging of the axilla in the era of Z011 Adena S Scheer MD MSc FRCSC Surgical Oncologist, St. Michael s Hospital Assistant Professor,
Intra-operative frozen section analysis of common iliac lymph nodes in patients with stage IB1 and IIA1 cervical cancer
 Arch Gynecol Obstet (2012) 285:811 816 DOI 10.1007/s00404-011-2038-z GYNECOLOGIC ONCOLOGY Intra-operative frozen section analysis of common iliac lymph nodes in patients with stage IB1 and IIA1 cervical
Arch Gynecol Obstet (2012) 285:811 816 DOI 10.1007/s00404-011-2038-z GYNECOLOGIC ONCOLOGY Intra-operative frozen section analysis of common iliac lymph nodes in patients with stage IB1 and IIA1 cervical
Staging and Grading Last Updated Friday, 14 November 2008
 Staging and Grading Last Updated Friday, 14 November 2008 There is a staging graph below Blood in the urine is the most common indication that something is wrong. Often one will experience pain or difficulty
Staging and Grading Last Updated Friday, 14 November 2008 There is a staging graph below Blood in the urine is the most common indication that something is wrong. Often one will experience pain or difficulty
Risk assessment of lymph node metastasis before surgery in endometrial cancer: Do we need a clinical trial for low-risk patients?
 bs_bs_banner doi:10.1111/jog.12281 J. Obstet. Gynaecol. Res. Vol. 40, No. 2: 322 326, February 2014 Risk assessment of lymph node metastasis before surgery in endometrial cancer: Do we need a clinical
bs_bs_banner doi:10.1111/jog.12281 J. Obstet. Gynaecol. Res. Vol. 40, No. 2: 322 326, February 2014 Risk assessment of lymph node metastasis before surgery in endometrial cancer: Do we need a clinical
VULVAR CANCER GUIDELINES
 VULVAR ANER GUIDELINES www.esgo.org Broz_210x297_9_16_b.indd 1 13.09.16 21:48 The European Society of Gynaecological Oncology (ESGO) developed guidelines covering diagnosis and referral, preoperative investigations,
VULVAR ANER GUIDELINES www.esgo.org Broz_210x297_9_16_b.indd 1 13.09.16 21:48 The European Society of Gynaecological Oncology (ESGO) developed guidelines covering diagnosis and referral, preoperative investigations,
September 10, Dear Dr. Clark,
 September 10, 2015 Peter E. Clark, MD Chair, NCCN Bladder Cancer Guidelines (Version 2.2015) Associate Professor of Urologic Surgery Vanderbilt Ingram Cancer Center Nashville, TN 37232 Dear Dr. Clark,
September 10, 2015 Peter E. Clark, MD Chair, NCCN Bladder Cancer Guidelines (Version 2.2015) Associate Professor of Urologic Surgery Vanderbilt Ingram Cancer Center Nashville, TN 37232 Dear Dr. Clark,
New diagnostic and therapeutic options in early-stage vulvar cancer Oonk, Maaike Henrike Marije
 University of Groningen New diagnostic and therapeutic options in early-stage vulvar cancer Oonk, Maaike Henrike Marije IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF)
University of Groningen New diagnostic and therapeutic options in early-stage vulvar cancer Oonk, Maaike Henrike Marije IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF)
Omitting Preoperative Lymphoscintigraphy Does Not Decrease Sentinel Lymph Node Detection Rate in Vulvar Cancer
 International Journal of Clinical Oncology and Cancer Research 2018; 3(3): 30-34 http://www.sciencepublishinggroup.com/j/ijcocr doi: 10.11648/j.ijcocr.20180303.13 ISSN: 2578-9503 (Print); ISSN: 2578-9511
International Journal of Clinical Oncology and Cancer Research 2018; 3(3): 30-34 http://www.sciencepublishinggroup.com/j/ijcocr doi: 10.11648/j.ijcocr.20180303.13 ISSN: 2578-9503 (Print); ISSN: 2578-9511
Epithelial Cancer- NMSC & Melanoma
 Epithelial Cancer- NMSC & Melanoma David Chin MB, BCh, BAO, LRCP, LRCS (Ireland) MCh(MD), PhD (UQ), FRCS, FRACS (Plast) Plastic & Reconstructive Surgeon Visiting Scientist Melanoma Genomic Group & Drug
Epithelial Cancer- NMSC & Melanoma David Chin MB, BCh, BAO, LRCP, LRCS (Ireland) MCh(MD), PhD (UQ), FRCS, FRACS (Plast) Plastic & Reconstructive Surgeon Visiting Scientist Melanoma Genomic Group & Drug
Tumours of the Oesophagus & Gastro-Oesophageal Junction Histopathology Reporting Proforma
 Tumours of the Oesophagus & Gastro-Oesophageal Junction Histopathology Reporting Proforma Mandatory questions (i.e. protocol standards) are in bold (e.g. S1.01). S1.01 Identification Family name Given
Tumours of the Oesophagus & Gastro-Oesophageal Junction Histopathology Reporting Proforma Mandatory questions (i.e. protocol standards) are in bold (e.g. S1.01). S1.01 Identification Family name Given
Patient age and cutaneous malignant melanoma: Elderly patients are likely to have more aggressive histological features and poorer survival
 MOLECULAR AND CLINICAL ONCOLOGY 7: 1083-1088, 2017 Patient age and cutaneous malignant melanoma: Elderly patients are likely to have more aggressive histological features and poorer survival FARUK TAS
MOLECULAR AND CLINICAL ONCOLOGY 7: 1083-1088, 2017 Patient age and cutaneous malignant melanoma: Elderly patients are likely to have more aggressive histological features and poorer survival FARUK TAS
Prognostic factors in squamous cell anal cancers
 Prognostic factors in squamous cell anal cancers Zainul Abedin Kapacee Year 4-5 Intercalating Medical Student, University of Manchester Dr. Shabbir Susnerwala, Mr. Nigel Scott Dr. Falalu Danwata, Dr. Marcus
Prognostic factors in squamous cell anal cancers Zainul Abedin Kapacee Year 4-5 Intercalating Medical Student, University of Manchester Dr. Shabbir Susnerwala, Mr. Nigel Scott Dr. Falalu Danwata, Dr. Marcus
Evaluation of AJCC and an Alternative Tumor Classification System for Primary Vulvar Squamous Cell Carcinoma
 Original Research Evaluation of AJCC and an Alternative Tumor Classification System for Primary Vulvar Squamous Cell Carcinoma Sarah T. Le, MBBS (Hons), BMedSci (Hons) a,b ; Pritesh S. Karia, MPH a ; Beverley
Original Research Evaluation of AJCC and an Alternative Tumor Classification System for Primary Vulvar Squamous Cell Carcinoma Sarah T. Le, MBBS (Hons), BMedSci (Hons) a,b ; Pritesh S. Karia, MPH a ; Beverley
A study of incidence and management of carcinoma of penis
 Research Article A study of incidence and management of carcinoma of penis K C T Naik 1*, A Setu Madhavi 2 1 Associate Professor, 2 Assistant Professor, Department of Surgery, RIMS Medical College, Ongole
Research Article A study of incidence and management of carcinoma of penis K C T Naik 1*, A Setu Madhavi 2 1 Associate Professor, 2 Assistant Professor, Department of Surgery, RIMS Medical College, Ongole
UICC TNM 8 th Edition Errata
 UICC TNM 8 th Edition Errata ions are in italics Page 28 Oropharynx p16 positive Pathological Stage II,T2 N2 M0 T3 N0,N1 M0 Stage II,T2 N2 M0 T3,T4 N0,N1 M0 Page 61 Oesophagus Adenocarcinoma Pathological
UICC TNM 8 th Edition Errata ions are in italics Page 28 Oropharynx p16 positive Pathological Stage II,T2 N2 M0 T3 N0,N1 M0 Stage II,T2 N2 M0 T3,T4 N0,N1 M0 Page 61 Oesophagus Adenocarcinoma Pathological
Cervical Cancer Guidelines L and SC Network July Introduction:
 Cervical Cancer Guidelines L and SC Network July 2018 Introduction: There was a total number of 442 cases of cervix cancer diagnosed in Lancashire and South Cumbria Cancer Network in the period 2005 2009
Cervical Cancer Guidelines L and SC Network July 2018 Introduction: There was a total number of 442 cases of cervix cancer diagnosed in Lancashire and South Cumbria Cancer Network in the period 2005 2009
