The incidence of esophageal adenocarcinoma has been rising rapidly over the past few
|
|
|
- Ralph Heath
- 5 years ago
- Views:
Transcription
1 Gastroesophageal Reflux Disease, Barrett Esophagus, and Esophageal Adenocarcinoma John T. Chang, MD; David A. Katzka, MD REVIEW ARTICLE The incidence of esophageal adenocarcinoma has been rising rapidly over the past few decades. The major risk factors predisposing to the development of adenocarcinoma are long-standing gastroesophageal reflux disease and Barrett esophagus, but other factors may be involved as cancer can occur in their absence. In patients with Barrett esophagus, the extent and degree of dysplasia influence the risk of esophageal adenocarcinoma. As neither medical nor surgical therapies have been proven to prevent adenocarcinoma, endoscopic screening of patients with chronic reflux and endoscopic surveillance of patients diagnosed with Barrett esophagus are usually performed in an effort to detect adenocarcinomas at earlier stages. The evidence supporting strategies in the management of patients with gastroesophageal reflux and Barrett esophagus is presented. Arch Intern Med. 2004;164: The incidence of esophageal adenocarcinoma (EAC) has risen faster than that of any malignancy in the United States, with an estimated rise of 300% to 350% since the 1970s. While the total incidence of all esophageal malignancies, which include squamous cell carcinoma and adenocarcinoma, has remained stable, the proportion of adenocarcinomas has risen dramatically. Specifically, the population incidence of esophageal squamous cell carcinoma declined from 3.4 per between 1974 and 1976 to 2.2 per between 1992 and 1994, whereas the incidence of EAC increased from 0.7 per to 3.2 per during the same period. 1 In 2002, there were an estimated cases of esophageal cancer, approximately 60% of which were adenocarcinomas. 2 Furthermore, the increasing rates of adenocarcinoma were more pronounced in older men, with a 2-fold increase in men younger than 65 years vs a 3- to 4-fold increase in men older than 65 years. Esophageal adenocarcinoma predominantly affects white men (whiteblack ratio, 5:1; male-female ratio, 8:1). 1 From the Department of Medicine (Dr Chang) and the Division of Gastroenterology (Dr Katzka), Hospital of the University of Pennsylvania, Philadelphia. Dr Katzka is a member of the speakers bureau of AstraZeneca Pharmaceuticals. There also appears to be regional variations in the increasing rates of EAC in the United States: the incidence rates recorded in the Seattle-Puget Sound registry for 1998, for example, are twice those recorded in the Utah registry for the same year. 3 The reasons for the rapidly rising incidence of EAC remain unclear. RISK FACTORS FOR ESOPHAGEAL ADENOCARCINOMA Gastroesophageal Reflux Disease Gastroesophageal reflux disease (GERD) is extremely common in Western countries. Its prevalence in the US population has not been studied; however, a population-based study in Minnesota found that 20% of patients reported having at least weekly symptoms of heartburn and/or regurgitation, 4 the most common manifestations of GERD, often occurring after meals. While the diagnosis can be made definitively by upper endoscopy and ambulatory 24-hour ph monitoring, patients presenting with symptoms typical of GERD are often empirically treated with either proton-pump inhibitors (PPI) or hydrogen receptor antagonists. 5 Further diagnostic evaluation is indicated when there 1482
2 is no response to empiric therapy or in the presence of warning symptoms of complicated GERD, ie, dysphagia, bleeding, weight loss, and/or chest pain. 5 However, evaluating only patients with warning symptoms may miss many, if not most, patients with Barrett esophagus (BE). Barrett Esophagus Barrett esophagus can be defined as the replacement of the squamous epithelium that normally lines the distal esophagus with columnarappearing epithelium on upper endoscopic examination, with histologic findings of specialized intestinal metaplasia. Traditionally, BE has been defined as columnar-appearing epithelium extending at least 3 cm above the gastroesophageal junction. However, it has become clear that shorter segments of columnarappearing epithelium may contain specialized intestinal metaplasia, and thus have malignant potential. No standardized definitions have been established. Generally, longsegment and short-segment BE are defined, respectively, as the presence of a specialized intestinal metaplasia 3 cm or greater, or less than 3 cm but the latter definition of short-segment BE may be problematic. As there is no gold standard of what defines an endoscopically normal-appearing squamocolumnar junction, distinguishing the intestinal metaplasia of BE from that of the proximal stomach, which is found in 18% of the healthy population, 6 can be difficult and lead to unnecessary surveillance. As a result, one must decide whether to sacrifice the sensitivity or the specificity of endoscopic criteria when determining whether longer ( 3 cm) or shorter ( 1 cm) segments of columnar-appearing mucosa are used to define BE morphologically. It is estimated that 5% to 15% of patients with GERD will have BE. Patients with long-standing GERD are at greatest risk for developing BE, which is considered the precursor lesion to adenocarcinoma. The presence of BE increases an individual s relative risk of cancer 30 to 120 times compared with persons without BE. 7-9 While the major risk factor for EAC is BE arising on the background of chronic GERD, several recent studies have shown that long-standing GERD is itself a risk factor for adenocarcinoma, even in the apparent absence of BE. 10,11 The largest of these studies, a population-based case-control study, found that the risk of EAC correlated with the frequency, severity, and duration of reflux symptoms. 10 In particular, among patients with frequent reflux symptoms, the adjusted odds ratio (OR) for EAC was 16.7 (95% confidence interval [CI], ) compared with asymptomatic controls. Similarly, among patients with a symptom duration of more than 20 years, the adjusted OR was 16.4 (95% CI, ). Among patients with both frequent symptoms and a symptom duration of more than 20 years, the adjusted OR was 43.5 (95% CI, ). The strength of these associations was independent of the presence of BE. It should be noted, however, that the apparent absence of BE in patients with EAC may have been due to tumor overgrowth. Genetic Factors The predilection of EAC to affect white men has triggered interest in the possible role of genetic factors in determining susceptibility to GERD, BE, and adenocarcinoma. In one study, relatives of patients with BE were 4.8 times as likely (95% CI, ) to have weekly reflux symptoms as relatives of asymptomatic control patients. 12 In another study, first-degree relatives of patients with BE completed a questionnaire to assess for reflux symptoms. Relatives with reflux symptoms who had not previously undergone endoscopy were invited to undergo endoscopy. The control group consisted of patients without a family history of either BE or EAC who were referred for endoscopy by their primary physician. Relatives of patients with BE were 1.5 times more likely to have BE than controls. 13 Although this finding did not reach statistical significance, probably because of the low number of patients ultimately found to have BE, these results are intriguing and underscore the need for additional investigation. Development of EAC Without Known Risk Factors Other risk factors that are less well substantiated than GERD and BE include obesity, smoking, alcohol use, use of acid-suppressing medications, and infection with Helicobacter pylori. Of these, obesity has been the best studied but has not been established as a definitive risk factor. For example, one study found that adenocarcinoma was 7 times more likely to develop in individuals with a body mass index (calculated as weight in kilograms divided by the square of height in meters) in the highest quartile (men 23.7, women 22.1) than in those with a body mass index in the lowest quartile (men 20.7, women 19.3). 14 However, it was unclear whether the observed effect of obesity in this study was direct, or indirect by exacerbating GERD. Thus, the major risk factors predisposing to the development of EAC are BE and longstanding symptomatic GERD. However, adenocarcinoma may develop in the absence of either. In the casecontrol study described above, which found a correlation between the risk of adenocarcinoma and the frequency, severity, and duration of reflux symptoms, 40% of patients diagnosed with adenocarcinoma did not have a history of reflux symptoms. Furthermore, 38% of patients with adenocarcinoma did not have BE. 10 These findings were supported by a population-based registry study which found that only 19% of patients who were diagnosed with EAC over a 5-year period had BE at subsequent endoscopic examination, surgery, or autopsy. 15 Similarly, a recent systematic review found that only 24% to 64% of patients undergoing surgery for EAC had BE. 16 It has been suggested that cancer may overgrow the Barrett segment from which it arises, thus causing to underestimate the prevalence of BE in patients with adenocarcinoma. 17 Nevertheless, taken together, these results suggest the possibility that 1483
3 EAC may develop in the absence of long-standing symptomatic GERD or BE. RISK OF EAC IN PATIENTS WITH BE The major risk factors that predispose patients with GERD to BE relate to the frequency and duration of reflux symptoms. One casecontrol study found that patients with reflux symptoms so severe as to wake them from sleep were more than 3 times more likely to develop BE than those without reflux. Such patients tended to have been younger at onset of symptoms, and they tended to have a longer symptom duration. 18 Another study found that patients with reflux episodes lasting more than 5 minutes or persistent reflux symptoms lasting longer than 5 years were at higher risk for BE. 19 However, it is important to recognize that BE can occur in patients without reflux symptoms. A population-based study published in 1990 showed that the prevalence of BE found on autopsy was 21 times greater than the expected prevalence based on endoscopically diagnosed cases. 20 This study was recently updated and showed that the prevalence of BE on autopsy was now only 5 times greater than the endoscopically diagnosed prevalence, which correlated with greater use of endoscopy in recent years. 21 Another study enrolled patients undergoing sigmoidoscopy screening for colon cancer for a concurrent upper endoscopy. In this population older than 50 years and without reflux symptoms, 25% were found to have BE. 22 Thus, while a longer duration and frequency of reflux symptoms increases one s risk of BE, the disease also commonly occurs in asymptomatic individuals. The prevalence of BE, and thus the number of individuals at risk for EAC, may be much higher than previously thought. Segment Length The risk of adenocarcinoma in individuals with BE is 30 to 120 times that of individuals without BE. Efforts have focused on identifying characteristics that can be used to further stratify the cancer risk of those with BE. One possible risk factor is the extent of BE. In the past, BE was defined as a segment of at least 3 cm. However, in recent years, the risk of adenocarcinoma of intestinal metaplasia involving shorter segments has been increasingly recognized. Although some studies found a lower risk of adenocarcinoma with shortsegment BE, 23,24 several other studies did not find a significant difference in the risk of adenocarcinoma between patients with shortsegment and long-segment BE This discrepancy may reflect the lack of standardization of the definition of short-segment BE, which in some studies is 2 cm or less above the esophagogastric junction and in other studies is 3 cm or less. Because there is no universally accepted definition of short-segment BE, and the natural history of shortsegment BE is unclear, shortsegment and long-segment BE should be considered to impart the same risk of adenocarcinoma. Low-Grade Dysplasia The most important predictor of cancer risk in patients with BE is the presence and degree of dysplasia. Biopsy specimens are graded as negative, indefinite for dysplasia, low-grade dysplasia (LGD), and high-grade dysplasia (HGD). 28 The progression from BE to adenocarcinoma is thought to occur in a stepwise progression from metaplasia to dysplasia to adenocarcinoma. However, the time for progression of LGD to HGD and of HGD to adenocarcinoma has not been well characterized. A low degree of interobserver agreement makes the diagnosis of LGD difficult to reach, and thus studies of the natural history of LGD are highly variable and difficult to interpret. One study of 25 patients with LGD found that 20% of patients progressed to HGD in a median period of 11 months (range, 2-43 months). 29 Another study found that the mean time for progression from LGD to HGD was 29 months. 30 In addition, several studies have found that LGD may be a transient finding, because approximately 75% of patients with lowgrade dysplasia were found to have no dysplasia on a subsequent biopsy. 23,27 However, biopsy screening may reveal progression from intestinal metaplasia directly to HGD or carcinoma, without development of LGD. 31 Furthermore, one study showed that if 3 pathologists agreed on a diagnosis of LGD, there was an 80% rate of lesion progression to HGD or carcinoma. 29 High-Grade Dysplasia The degree of interobserver agreement in the diagnosis of HGD is excellent, approximately 85%. Previous studies having found that a high percentage of patients with HGD progressed to adenocarcinoma in a relatively short time, the use of prophylactic esophagectomy in the management of patients with HGD seemed reasonable. However, because these studies included adenocarcinomas that developed over the first 6 months of observation, subclinical cancers already present at the time of HGD diagnosis may have been recorded as new adenocarcinomas. When these prevalent cases were excluded, the percentage of patients whose HGD progressed to adenocarcinoma was lower. In one retrospective cohort study, 32% of patients with HGD developed adenocarcinoma in an average of 3 years; however, when prevalent adenocarcinomas were excluded, the rate of progression was 13%. 32 These results are supported by a recent large study of 1099 patients with BE. 33 Of the 75 patients who had HGD without carcinoma at entry into the study, only 12 (16%) developed carcinoma over the mean 7.3 years of follow-up. Of these 12 patients, 11 had early-stage cancer. These data have called into question the standard management for HGD, ie, prophylactic esophagectomy. Proponents of this approach cite the high rate of concurrent cancer found in patients undergoing surgery for HGD, which was reported to be 13 in a series of 32 patients. 34 Furthermore, there is inherent risk in allowing a premalignant lesion to progress beyond carcinoma in situ because metastasis may occur, even at very early stages. 35 However, the risks of esoph- 1484
4 agectomy are not inconsequential. These include an operative mortality rate of 3% to 12% and a perioperative morbidity rate of 30% to 50%. 34,36 Given these controversies, investigators have tried to identify subsets of HGD that may help to further stratify cancer risk. One study found that diffuse HGD, defined as dysplastic changes in more than 1 biopsy specimen or involving 5 crypts or more, was associated with a 3.7- fold increase in the risk of adenocarcinoma compared with focal HGD, defined as dysplasia limited to a single biopsy specimen or involving fewer than 5 crypts. 23,32 Furthermore, nodules found in areas of intestinal metaplasia were associated with a 2.5-fold increase in the risk of adenocarcinoma. 32 Other markers that may impart increased risk in patients with BE are under active investigation and include cell cycle regulators such as proliferating cell nuclear antigen and Ki-67, abnormalities in the DNA content of metaplastic cells, and tumor suppressor genes such as p53. 30,37 Thus, the management of HGD remains controversial and should be individualized. Esophagectomy continues to be recommended in patients with HGD, particularly those who are good surgical candidates and those with diffuse and nodular HGD. Frequent surveillance can be considered for patients who are not good surgical candidates and in those with focal HGD. PREVENTION OF EAC With the advent of PPI, reflux symptoms can be adequately controlled in most patients. However, it has become increasingly clear that a substantial proportion of patients with GERD or BE whose symptoms are controlled by medications still have abnormal acid reflux, as documented by 24-hour ambulatory ph monitoring. 38,39 While the addition of a bedtime hydrogen receptor antagonist to a maximal PPI regimen has been shown to control nocturnal gastric acid breakthrough, 40 the crucial issue is whether such aggressive control of acid reflux can prevent the development of BE in patients with GERD, cause regression of intestinal metaplasia in patients with BE, or prevent the development of EAC in patients with GERD and/or BE. Substantial and consistent regression of BE has not been observed, even in patients with documented normalization of ph by PPI therapy, 41 although aggressive acid control has been found to result in the replacement of columnar epithelium by macroscopic islands of squamous epithelium. This would suggest that partial regression of BE occurs; yet, in a recent study, histologic evidence of intestinal metaplasia in almost 40% of the patients with BE who had endoscopic evidence of macroscopic islands of squamous epithelium demonstrated that the development of squamous islands with aggressive acid control should not be interpreted as regression of BE or a reduction in the risk of cancer. 42 Both modern treatments of GERD medical (PPI) and surgical (fundoplication) are very effective at controlling reflux symptoms. However, no study has conclusively shown that either can effectively prevent the development of BE or EAC. Whereas several small surgical series of patients followed up for a mean of 5 years have reported a decreased incidence of dysplasia and/or EAC in those who underwent antireflux surgery, 43 other studies have found no significant differences in the development of EAC in patients treated medically or surgically after a mean of 7 years of follow-up. 44,45 Furthermore, long-term follow-up findings from a prospective randomized controlled trial originally reported in 1992 were recently published. 46,47 This trial randomized patients with complicated GERD to surgical (open Nissen fundoplication) or medical treatment consisting of hydrogen receptor antagonists, antacids, metoclopramide, or sucralfate. After a mean of 9 years of follow-up, the survival rate in the surgical group was worse because of an unexplained increase in cardiovascular complications. Furthermore, although the study was not designed to answer this question, no statistically significant differences were found between the medical and surgical groups in the development of EAC. These results are supported by a large retrospective cohort study, which showed similar rates of development of EAC in patients with GERD regardless of whether they were treated medically or surgically. 48 Thus, to date, neither medical nor surgical treatments for GERD and/or BE have been convincingly shown to prevent the development of EAC. Endoscopic ablative therapy is another strategy to prevent EAC in patients with BE, particularly those with HGD. This approach uses a laser or heat energy, with or without a cellular sensitizing agent, to ablate metaplastic or dysplastic mucosa for subsequent re-epithelialization with squamous epithelium. In one study, eradication of dysplastic mucosa was achieved in 80% of patients; of these, however, 34% developed strictures, and there was a high rate of recurrence, particularly in patients with HGD. 49 Thus, endoscopic ablative therapy may not completely eliminate dysplastic epithelium and it is associated with a relatively high rate of complications. It should not be used in patients with LGD but may be considered in patients with HGD, particularly those who are poor surgical candidates. SURVEILLANCE AND MORTALITY The major risk factors that predispose to the development of EAC are GERD and BE. Endoscopic screening of high-risk patients with GERD, with subsequent endoscopic surveillance of patients diagnosed with BE on screening, has been proposed as a strategy to identify patients at highest risk and detect adenocarcinoma at earlier stages, thus reducing mortality. To be effective, a screening and surveillance program must reduce mortality from the disease and be cost-effective. Small observational studies have found that EACs developing in patients with BE followed up in a surveillance program were detected at an earlier stage than EACs detected in symptomatic patients undergoing endoscopy for symptoms only. 31,50,51 One of these studies iden- 1485
5 tified 198 patients with EAC who had undergone resection. 31 From a review of medical records, it was determined that 54 of the patients had prior diagnoses of BE, and 16 had been enrolled in a surveillance program. More patients had advanced-stage EAC in the nonsurveillance group than in the surveillance group, which, presumably, resulted in a decreased mortality rate in the latter group. Similarly, a recent retrospective cohort study found that the patients with known BE and EAC detected by endoscopy in the context of a surveillance program tended to have earlier-stage disease and lower mortality rates than the patients whose EAC was diagnosed when they presented with symptoms. 52 However, these studies were subject to various methological flaws, including (1) selection bias, as younger, healthier patients more likely to survive esophagectomy may have been selected for surveillance programs, and (2) lead time bias, since EAC diagnosed earlier in the context of surveillance programs may have given the appearance of longer survival. Furthermore, several studies have found that cancer is not a common cause of death in patients with BE followed up in a surveillance program. In one, in which 409 patients with BE were followed up for 10 years, 137 patients died during follow-up but only 4 (2.9%) of the deaths occurred as a result of EAC. 53 Similarly, in a group of 155 patients with BE followed up for 9 years, 79 patients died during follow-up but only 2 (1.3%) of the deaths were due to esophageal cancer. 54 Thus, although it is clear that endoscopic surveillance programs detect adenocarcinoma at earlier stages, it is not clear whether they reduce mortality. The cost-effectiveness of screening and surveillance endoscopy for BE has been examined A recent study using a decision analytic model found that screening all white men with GERD who were older than 50 years, then surveillance only for patients with BE and dysplasia, would be a cost-effective approach. 58 This approach would be associated with an incremental costeffectiveness ratio of $10440 per quality-adjusted life-year (QALY) compared with no screening or surveillance. However, conducting surveillance in patients with BE but no dyplasia every 5 years was associated with an incremental costeffectiveness ratio of $ per QALY saved, making that approach prohibitively expensive. 58 Similarly, another study using a model evaluating screening 55-yearold men with BE every 1 to 5 years found that surveillance every 5 years would be associated with an incremental cost-effectiveness ratio of $27400 per QALY compared with no surveillance. 56 Decreasing the interval of surveillance to every 4 years would be more effective, but at a cost of $ per QALY. These analyses suggest that screening patients with chronic GERD, with subsequent surveillance for those diagnosed with BE every 5 years, might be cost-effective; however, these analyses are based on numerous assumptions, in particular the prevalence of BE and the incidence of cancer among patients with BE. Certain caveats must be kept in mind when considering screening and surveillance programs. First, the incidence of EAC in the US population is low, with an estimated 7860 new cases in 2002, compared with new cases of colon cancer and new cases of lung cancer for the same year. 59 Second, while longstanding GERD and BE greatly increase an individual s relative risk of cancer, the absolute risk is low, of the order of 0.5% per year. 27,54,60,61 Third, 40% of patients with EAC have no history or symptoms of reflux; these patients would be missed, as they would Patient With Long-standing Symptomatic Gastroesophageal Disease Consider Screening Endoscopy Barrett Esophagus With No Dysplasia Low-Grade Dysplasia High-Grade Dysplasia, Focal High-Grade Dysplasia, Multifocal not have been candidates for either screening or surveillance. RECOMMENDATIONS The American College of Gastroenterology has recently updated its guidelines for the management of patients with BE. 62 A screening endoscopy can be considered for patients with chronic GERD symptoms, although the duration of symptoms or the age of the patients are not specified. Proposed criteria for screening endoscopy are shown in the Table, although, as discussed above, there are no studies to support whether to screen or which patients to screen. Therefore, the decision to undergo screening endoscopy for chronic GERD symptoms should be individualized. Once BE has been identified, surveillance endoscopy is recommended with a frequency that is dependent on the presence and degree of dysplasia (Figure). A biopsy negative for dysplasia can be followed with surveillance every 3 years, and LGD can be followed up with annual endoscopy. Patients with HGD, particularly multifocal and nodular dysplasia, should be referred for esophagectomy. Patients with focal Proposed Criteria for Screening Endoscopy Age 50 y White race Male sex Duration of reflux 5 y Reflux symptoms at least twice per week Surveillance Endoscopy Every 3 Years Surveillance Endoscopy Every Year Surveillance Endoscopy Every 3 Months or Esophagectomy Consider Esophagectomy in Young, Fit Patients Consider Surveillance Endoscopy or Endoscopic Ablative Therapy in Older Patients American College of Gastroenterology management algorithm for the diagnosis and surveillance of Barrett esophagus
6 HGD, particularly those who are not surgical candidates, can be followed up with intensive surveillance every 3 months. CONCLUSIONS The major risk factors for the development of EAC are severe and longstanding symptomatic GERD and BE. Both are associated with an increased relative risk but low absolute risk of cancer compared with patients without these conditions. White race, older age, increased severity, and longer duration of symptoms appear to further increase the risk of cancer. Aggressive acid control with either medication or surgical fundoplication has not been shown to prevent EAC. Prospective randomized clinical trials are lacking, but our recommendations at this time are to consider a screening endoscopy in white men older than 50 years who have had symptomatic GERD longer than 5 years; in those diagnosed with BE, screening should be followed by endoscopic surveillance. Patients with HGD should be managed on an individual basis, either with surgery or intensive surveillance. Accepted for publication September 25, Correspondence: David A. Katzka, MD, Division of Gastroenterology, 3 Ravdin Bldg, 3400 Spruce St, Philadelphia, PA (katzka@mail.med.upenn.edu). REFERENCES 1. Devesa SS, Blot WJ, Fraumeni JF Jr. Changing patterns in the incidence of esophageal and gastric carcinoma in the United States. Cancer. 1998;83: Ries LAG, Eisner MP, Kosary CL, et al. SEER Cancer Statistics Review, Bethesda, Md: National Cancer Institute; Available at: http: //seer.cancer.gov/csr/1975_ Kubo A, Corley DA. Marked regional variation in adenocarcinomas of the esophagus and the gastric cardia in the United States. Cancer. 2002;95: Locke GR III, Talley NJ, Fett SL, Zinsmeister AR, Melton LJ III. Prevalence and clinical spectrum of gastroesophageal reflux: a population-based study in Olmsted County, Minnesota. Gastroenterology. 1997;112: DeVault KR, Castell DO. Updated guidelines for the diagnosis and treatment of gastroesophageal reflux disease: the Practice Parameters Committee of the American College of Gastroenterology. Am J Gastroenterol. 1999;94: Morales CP, Souza RF, Spechler SJ. Hallmarks of cancer progression in Barrett s oesophagus. Lancet. 2002;360: Miros M, Kerlin P, Walker N. Only patients with dysplasia progress to adenocarcinoma in Barrett s oesophagus. Gut. 1991;32: Cameron AJ, Ott BJ, Payne WS. The incidence of adenocarcinoma in columnar-lined (Barrett s) esophagus. N Engl J Med. 1985;313: Williamson WA, Ellis FH Jr, Gibb SP, et al. Barrett s esophagus: prevalence and incidence of adenocarcinoma. Arch Intern Med. 1991;151: Lagergren J, Bergstrom R, Lindgren A, Nyren O. Symptomatic gastroesophageal reflux as a risk factor for esophageal adenocarcinoma. N Engl J Med. 1999;340: Chow WH, Finkle WD, McLaughlin JK, Frankl H, Ziel HK, Fraumeni JF Jr. The relation of gastroesophageal reflux disease and its treatment to adenocarcinomas of the esophagus and gastric cardia. JAMA. 1995;274: Trudgill NJ, Kapur KC, Riley SA. Familial clustering of reflux symptoms. Am J Gastroenterol. 1999; 94: Romero Y, Cameron AJ, Schaid DJ, et al. Barrett s esophagus: prevalence in symptomatic relatives. Am J Gastroenterol. 2002;97: Lagergren J, Bergstrom R, Nyren O. Association between body mass and adenocarcinoma of the esophagus and gastric cardia. Ann Intern Med. 1999;130: Bytzer P, Christensen PB, Damkier P, Vinding K, Seersholm N. Adenocarcinoma of the esophagus and Barrett s esophagus: a populationbased study. Am J Gastroenterol. 1999;94: Dulai GS, Guha S, Kahn KL, Gornbein J, Weinstein WM. Preoperative prevalence of Barrett s esophagus in esophageal adenocarcinoma: a systematic review. Gastroenterology. 2002;122: Cameron AJ, Lomboy CT, Pera M, Carpenter HA. Adenocarcinoma of the esophagogastric junction and Barrett s esophagus. Gastroenterology. 1995;109: Eisen GM, Sandler RS, Murray S, Gottfried M. The relationship between gastroesophageal reflux disease and its complications with Barrett s esophagus. Am J Gastroenterol. 1997;92: Campos GM, DeMeester SR, Peters JH, et al. Predictive factors of Barrett esophagus: multivariate analysis of 502 patients with gastroesophageal reflux disease. Arch Surg. 2001;136: Cameron AJ, Zinsmeister AR, Ballard DJ, Carney JA. Prevalence of columnar-lined (Barrett s) esophagus: comparison of population-based clinical and autopsy findings. Gastroenterology. 1990; 99: Conio M, Cameron AJ, Romero Y, et al. Secular trends in the epidemiology and outcome of Barrett s oesophagus in Olmsted County, Minnesota. Gut. 2001;48: Gerson LB, Shetler K, Triadafilopoulos G. Prevalence of Barrett s esophagus in asymptomatic individuals. Gastroenterology. 2002;123: Weston AP, Badr AS, Hassanein RS. Prospective multivariate analysis of factors predictive of complete regression of Barrett s esophagus. Am J Gastroenterol. 1999;94: Hirota S, Nishida T, Isozaki K, et al. Familial gastrointestinal stromal tumors associated with dysphagia and novel type germline mutation of KIT gene. Gastroenterology. 2002;122: Sharma P, Morales TG, Bhattacharyya A, Garewal HS, Sampliner RE. Dysplasia in shortsegment Barrett s esophagus: a prospective 3-year follow-up. Am J Gastroenterol. 1997;92: Rudolph RE, Vaughan TL, Storer B. Segment length and risk for neoplastic progression in patients with Barrett esophagus [letter]. Ann Intern Med. 2000;133: O Connor JB, Falk GW, Richter JE. The incidence of adenocarcinoma and dysplasia in Barrett s esophagus: report on the Cleveland Clinic Barrett s Esophagus Registry. Am J Gastroenterol. 1999;94: Reid BJ, Haggitt RC, Rubin CE, et al. Observer variation in the diagnosis of dysplasia in Barrett s esophagus. Hum Pathol. 1988;19: Skacel M, Petras RE, Gramlich TL, Sigel JE, Richter JE, Goldblum JR. The diagnosis of low-grade dysplasia in Barrett s esophagus and its implications for disease progression. Am J Gastroenterol. 2000;95: Reid BJ, Blount PL, Rubin CE, Levine DS, Haggitt RC, Rabinovitch PS. Flow-cytometric and histological progression to malignancy in Barrett s esophagus: prospective endoscopic surveillance of a cohort. Gastroenterology. 1992;102: van Sandick JW, van Lanschot JJ, Kuiken BW, Tytgat GN, Offerhaus GJ, Obertop H. Impact of endoscopic biopsy surveillance of Barrett s oesophagus on pathological stage and clinical outcome of Barrett s carcinoma. Gut. 1998;43: Buttar NS, Wang KK, Sebo TJ, et al. Extent of highgrade dysplasia in Barrett s esophagus correlates with risk of adenocarcinoma. Gastroenterology. 2001;120: Schnell TG, Sontag SJ, Chejfec G, et al. Longterm nonsurgical management of Barrett s esophagus with high-grade dysplasia. Gastroenterology. 2001;120: Heitmiller RF, Redmond M, Hamilton SR. Barrett s esophagus with high-grade dysplasia: an indication for prophylactic esophagectomy. Ann Surg. 1996;224: O Sullivan GC, Sheehan D, Clarke A, et al. Micrometastases in esophagogastric cancer: high detection rate in resected rib segments. Gastroenterology. 1999;116: Swisher SG, Deford L, Merriman KW, et al. Effect of operative volume on morbidity, mortality, and hospital use after esophagectomy for cancer. J Thorac Cardiovasc Surg. 2000;119: Beilstein M, Silberg D. Cellular and molecular mechanisms responsible for progression of Barrett s metaplasia to esophageal carcinoma. Gastroenterol Clin North Am. 2002;31: , ix. 38. Katzka DA, Castell DO. Successful elimination of reflux symptoms does not insure adequate control of acid reflux in patients with Barrett s esophagus. Am J Gastroenterol. 1994;89: Ouatu-Lascar R, Triadafilopoulos G. Complete elimination of reflux symptoms does not guarantee normalization of intraesophageal acid reflux in patients with Barrett s esophagus. Am J Gastroenterol. 1998;93: Peghini PL, Katz PO, Castell DO. Ranitidine controls nocturnal gastric acid breakthrough on omeprazole: a controlled study in normal subjects. Gastroenterology. 1998;115: Sharma P, Sampliner RE, Camargo E. Normalization of esophageal ph with high-dose proton pump inhibitor therapy does not result in regression of 1487
7 Barrett s esophagus. Am J Gastroenterol. 1997; 92: Sharma P, Morales TG, Bhattacharyya A, Garewal HS, Sampliner RE. Squamous islands in Barrett s esophagus: what lies underneath? Am J Gastroenterol. 1998;93: Katz D, Rothstein R, Schned A, Dunn J, Seaver K, Antonioli D. The development of dysplasia and adenocarcinoma during endoscopic surveillance of Barrett s esophagus. Am J Gastroenterol. 1998; 93: Parrilla P, Martinez de Haro LF, Ortiz A, et al. Longterm results of a randomized prospective study comparing medical and surgical treatment of Barrett s esophagus. Ann Surg. 2003;237: Csendes A, Braghetto I, Burdiles P, et al. Longterm results of classic antireflux surgery in 152 patients with Barrett s esophagus: clinical, radiologic, endoscopic, manometric, and acid reflux test analysis before and late after operation. Surgery. 1998;123: Spechler SJ, Lee E, Ahnen D, et al. Long-term outcome of medical and surgical therapies for gastroesophageal reflux disease: follow-up of a randomized controlled trial. JAMA. 2001;285: Spechler SJ. Comparison of medical and surgical therapy for complicated gastroesophageal reflux disease in veterans: the Department of Veterans Affairs Gastroesophageal Reflux Disease Study Group. N Engl J Med. 1992;326: Ye W, Chow WH, Lagergren J, Yin L, Nyren O. Risk of adenocarcinomas of the esophagus and gastric cardia in patients with gastroesophageal reflux diseases and after antireflux surgery. Gastroenterology. 2001;121: Overholt BF, Panjehpour M, Haydek JM. Photodynamic therapy for Barrett s esophagus: follow-up in 100 patients. Gastrointest Endosc. 1999; 49: Peters JH, Clark GW, Ireland AP, Chandrasoma P, Smyrk TC, DeMeester TR. Outcome of adenocarcinoma arising in Barrett s esophagus in endoscopically surveyed and nonsurveyed patients. J Thorac Cardiovasc Surg. 1994;108: Discussion Streitz JM Jr, Andrews CW Jr, Ellis FH Jr. Endoscopic surveillance of Barrett s esophagus; does it help? J Thorac Cardiovasc Surg. 1993;105: Discussion Corley DA, Levin TR, Habel LA, Weiss NS, Buffler PA. Surveillance and survival in Barrett s adenocarcinomas: a population-based study. Gastroenterology. 2002;122: Macdonald CE, Wicks AC, Playford RJ. Final results from 10 year cohort of patients undergoing surveillance for Barrett s oesophagus: observational study. BMJ. 2000;321: van der Burgh A, Dees J, Hop WC, van Blankenstein M. Oesophageal cancer is an uncommon cause of death in patients with Barrett s oesophagus. Gut. 1996;39: Wright TA, Gray MR, Morris AI, et al. Cost effectiveness of detecting Barrett s cancer. Gut. 1996; 39: Provenzale D, Kemp JA, Arora S, Wong JB. A guide for surveillance of patients with Barrett s esophagus. Am J Gastroenterol. 1994;89: Provenzale D, Schmitt C, Wong JB. Barrett s esophagus: a new look at surveillance based on emerging estimates of cancer risk. Am J Gastroenterol. 1999;94: Inadomi JM, Sampliner R, Lagergren J, Lieberman D, Fendrick AM, Vakil N. Screening and surveillance for Barrett esophagus in high-risk groups: a cost-utility analysis. Ann Intern Med. 2003;138: American Cancer Society. Cancer Facts & Figures Available at: /docroot/stt/stt_0.asp. 60. Drewitz DJ, Sampliner RE, Garewal HS. The incidence of adenocarcinoma in Barrett s esophagus: a prospective study of 170 patients followed 4.8 years. Am J Gastroenterol. 1997;92: Shaheen NJ, Crosby MA, Bozymski EM, Sandler RS. Is there publication bias in the reporting of cancer risk in Barrett s esophagus? Gastroenterology. 2000;119: Sampliner RE. Updated guidelines for the diagnosis, surveillance, and therapy of Barrett s esophagus. Am J Gastroenterol. 2002;97:
History. Prevalence at Endoscopy. Prevalence and Reflux Sx. Prevalence at Endoscopy. Barrett s Esophagus: Controversy and Management
 Barrett s Esophagus: Controversy and Management History Norman Barrett (1950) Chronic Peptic Ulcer of the Oesophagus and Oesophagitis Allison and Johnstone (1953) The Oesophagus Lined with Gastric Mucous
Barrett s Esophagus: Controversy and Management History Norman Barrett (1950) Chronic Peptic Ulcer of the Oesophagus and Oesophagitis Allison and Johnstone (1953) The Oesophagus Lined with Gastric Mucous
Barrett s Esophagus: Old Dog, New Tricks
 Barrett s Esophagus: Old Dog, New Tricks Stuart Jon Spechler, M.D. Chief, Division of Gastroenterology, VA North Texas Healthcare System; Co-Director, Esophageal Diseases Center, Professor of Medicine,
Barrett s Esophagus: Old Dog, New Tricks Stuart Jon Spechler, M.D. Chief, Division of Gastroenterology, VA North Texas Healthcare System; Co-Director, Esophageal Diseases Center, Professor of Medicine,
New Developments in the Endoscopic Diagnosis and Management of Barrett s Esophagus
 New Developments in the Endoscopic Diagnosis and Management of Barrett s Esophagus Prateek Sharma, MD Key Clinical Management Points: Endoscopic recognition of a columnar lined distal esophagus is crucial
New Developments in the Endoscopic Diagnosis and Management of Barrett s Esophagus Prateek Sharma, MD Key Clinical Management Points: Endoscopic recognition of a columnar lined distal esophagus is crucial
Barrett s Esophagus. Abdul Sami Khan, M.D. Gastroenterologist Aurora Healthcare Burlington, Elkhorn, Lake Geneva, WI
 Barrett s Esophagus Abdul Sami Khan, M.D. Gastroenterologist Aurora Healthcare Burlington, Elkhorn, Lake Geneva, WI A 58 year-old, obese white man has had heartburn for more than 20 years. He read a magazine
Barrett s Esophagus Abdul Sami Khan, M.D. Gastroenterologist Aurora Healthcare Burlington, Elkhorn, Lake Geneva, WI A 58 year-old, obese white man has had heartburn for more than 20 years. He read a magazine
Relative risk of dysplasia for patients with intestinal metaplasia in the distal oesophagus and in the gastric cardia
 Gut 2000;46:9 13 9 PAPERS Division of Gastroenterology, University of Kansas, VA Medical Center, Kansas City, Missouri, USA P Sharma A P Weston Department of Pathology, VA Medical Center, Kansas M Topalovski
Gut 2000;46:9 13 9 PAPERS Division of Gastroenterology, University of Kansas, VA Medical Center, Kansas City, Missouri, USA P Sharma A P Weston Department of Pathology, VA Medical Center, Kansas M Topalovski
Joel A. Ricci, MD SUNY Downstate Medical Center Department of Surgery
 Joel A. Ricci, MD SUNY Downstate Medical Center Department of Surgery Norman Barrett (1950) described the esophagus as: that part of the foregut, distal to the cricopharyngeal sphincter, which is lined
Joel A. Ricci, MD SUNY Downstate Medical Center Department of Surgery Norman Barrett (1950) described the esophagus as: that part of the foregut, distal to the cricopharyngeal sphincter, which is lined
Barrett s Esophagus in Women: Demographic Features and Progression to High-Grade Dysplasia and Cancer
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:1089 1094 Barrett s Esophagus in Women: Demographic Features and Progression to High-Grade Dysplasia and Cancer GARY W. FALK,* PRASHANTHI N. THOTA,* JOEL
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:1089 1094 Barrett s Esophagus in Women: Demographic Features and Progression to High-Grade Dysplasia and Cancer GARY W. FALK,* PRASHANTHI N. THOTA,* JOEL
Current Management: Role of Radiofrequency Ablation
 Esophageal Adenocarcinoma And Barrett s Esophagus: Current Management: Role of Radiofrequency Ablation Ketan Kulkarni, MD Regional Gastroenterology Associates of Lancaster INTRODUCTION The prognosis of
Esophageal Adenocarcinoma And Barrett s Esophagus: Current Management: Role of Radiofrequency Ablation Ketan Kulkarni, MD Regional Gastroenterology Associates of Lancaster INTRODUCTION The prognosis of
THE AMERICAN JOURNAL OF GASTROENTEROLOGY Vol. 97, No. 1, by Am. Coll. of Gastroenterology ISSN /02/$22.00
 THE AMERICAN JOURNAL OF GASTROENTEROLOGY Vol. 97, No. 1, 2002 2002 by Am. Coll. of Gastroenterology ISSN 0002-9270/02/$22.00 Published by Elsevier Science Inc. PII S0002-9270(01)03982-X ORIGINAL CONTRIBUTIONS
THE AMERICAN JOURNAL OF GASTROENTEROLOGY Vol. 97, No. 1, 2002 2002 by Am. Coll. of Gastroenterology ISSN 0002-9270/02/$22.00 Published by Elsevier Science Inc. PII S0002-9270(01)03982-X ORIGINAL CONTRIBUTIONS
Current challenges in Barrett s esophagus
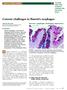 MEDICAL GRAND ROUNDS TAKE-HOME POINTS FROM LECTURES BY CLEVELAND CLINIC AND VISITING FACULTY Current challenges in Barrett s esophagus GARY W. FALK, MD * Director, Center for Swallowing and Esophageal
MEDICAL GRAND ROUNDS TAKE-HOME POINTS FROM LECTURES BY CLEVELAND CLINIC AND VISITING FACULTY Current challenges in Barrett s esophagus GARY W. FALK, MD * Director, Center for Swallowing and Esophageal
Is Radiofrequency Ablation Effective In Treating Barrett s Esophagus Patients with High-Grade Dysplasia?
 Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 12-2016 Is Radiofrequency Ablation Effective
Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 12-2016 Is Radiofrequency Ablation Effective
A bs tr ac t. n engl j med 365;15 nejm.org october 13,
 The new england journal of medicine established in 1812 october 13, 2011 vol. 365 no. 15 Incidence of Adenocarcinoma among Patients with Barrett s Esophagus Frederik Hvid-Jensen, M.D., Lars Pedersen, Ph.D.,
The new england journal of medicine established in 1812 october 13, 2011 vol. 365 no. 15 Incidence of Adenocarcinoma among Patients with Barrett s Esophagus Frederik Hvid-Jensen, M.D., Lars Pedersen, Ph.D.,
Is intestinal metaplasia a necessary precursor lesion for adenocarcinomas of the distal esophagus, gastroesophageal junction and gastric cardia?
 Diseases of the Esophagus (2007) 20, 36 41 DOI: 10.1111/j.1442-2050.2007.00638.x Blackwell Publishing Asia Original article Is intestinal metaplasia a necessary precursor lesion for adenocarcinomas of
Diseases of the Esophagus (2007) 20, 36 41 DOI: 10.1111/j.1442-2050.2007.00638.x Blackwell Publishing Asia Original article Is intestinal metaplasia a necessary precursor lesion for adenocarcinomas of
Adenocarcinoma of the Esophagogastric Junction and Barrett's Esophagus
 GASTROENTEROLOGY 1995;109:1541-1546 Adenocarcinoma of the Esophagogastric Junction and Barrett's Esophagus ALAN J. CAMERON,* CLIFFORD T. LOMBOY,* MANUEL PERA,* and HERSCHEL A. CARPENTER g *Division of
GASTROENTEROLOGY 1995;109:1541-1546 Adenocarcinoma of the Esophagogastric Junction and Barrett's Esophagus ALAN J. CAMERON,* CLIFFORD T. LOMBOY,* MANUEL PERA,* and HERSCHEL A. CARPENTER g *Division of
In 1998, the American College of Gastroenterology issued ALIMENTARY TRACT
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2012;10:1232 1236 ALIMENTARY TRACT Effects of Dropping the Requirement for Goblet Cells From the Diagnosis of Barrett s Esophagus MARIA WESTERHOFF,* LINDSEY HOVAN,
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2012;10:1232 1236 ALIMENTARY TRACT Effects of Dropping the Requirement for Goblet Cells From the Diagnosis of Barrett s Esophagus MARIA WESTERHOFF,* LINDSEY HOVAN,
Barrett s Esophagus: Review of Diagnostic Issues and Pre- Neoplastic Lesions
 Barrett s Esophagus: Review of Diagnostic Issues and Pre- Neoplastic Lesions Robert Odze, MD, FRCPC Chief, Gastrointestinal Pathology Associate Professor of Pathology Brigham and Women s Hospital Harvard
Barrett s Esophagus: Review of Diagnostic Issues and Pre- Neoplastic Lesions Robert Odze, MD, FRCPC Chief, Gastrointestinal Pathology Associate Professor of Pathology Brigham and Women s Hospital Harvard
Proton Pump Inhibitors Are Associated with Reduced Incidence of Dysplasia in Barrett s Esophagus
 American Journal of Gastroenterology ISSN 0002-9270 C 2004 by Am. Coll. of Gastroenterology doi: 10.1111/j.1572-0241.2004.30228.x Published by Blackwell Publishing ORIGINAL CONTRIBUTIONS Proton Pump Inhibitors
American Journal of Gastroenterology ISSN 0002-9270 C 2004 by Am. Coll. of Gastroenterology doi: 10.1111/j.1572-0241.2004.30228.x Published by Blackwell Publishing ORIGINAL CONTRIBUTIONS Proton Pump Inhibitors
The normal esophagus is lined with squamous epithelium.
 .. ALAN J. CAMERON, M.D. In Barrett's esophagus, the squamous lining of the lower esophagus is replaced by columnar epithelium. Barrett's esophagus is associated with gastroesophageal reflux and an increased
.. ALAN J. CAMERON, M.D. In Barrett's esophagus, the squamous lining of the lower esophagus is replaced by columnar epithelium. Barrett's esophagus is associated with gastroesophageal reflux and an increased
Barrett s Esophagus: What to Do for No Dysplasia, LGD, and HGD?
 Barrett s Esophagus: What to Do for No Dysplasia, LGD, and HGD? Nicholas Shaheen, MD, MPH Center for Esophageal Diseases and Swallowing University of North Carolina 1 Outline What are the risks of progression
Barrett s Esophagus: What to Do for No Dysplasia, LGD, and HGD? Nicholas Shaheen, MD, MPH Center for Esophageal Diseases and Swallowing University of North Carolina 1 Outline What are the risks of progression
Accepted Manuscript. CGH Editorial: Sound the Alarm for Barrett s Screening! Tarek Sawas, M.D., M.P.H., David A. Katzka, M.D
 Accepted Manuscript CGH Editorial: Sound the Alarm for Barrett s Screening! Tarek Sawas, M.D., M.P.H., David A. Katzka, M.D PII: S1542-3565(18)31093-0 DOI: 10.1016/j.cgh.2018.10.010 Reference: YJCGH 56132
Accepted Manuscript CGH Editorial: Sound the Alarm for Barrett s Screening! Tarek Sawas, M.D., M.P.H., David A. Katzka, M.D PII: S1542-3565(18)31093-0 DOI: 10.1016/j.cgh.2018.10.010 Reference: YJCGH 56132
Frequency of Barrett Esophagus in Patients with Symptoms of Gastroesophageal Reflux Disease
 Original Article Frequency of Barrett Esophagus in Patients with Symptoms of Gastroesophageal Reflux Disease From Military Hospital, Rawalpindi Obaid Ullah Khan, Abdul Rasheed Correspondence: Dr. Abdul
Original Article Frequency of Barrett Esophagus in Patients with Symptoms of Gastroesophageal Reflux Disease From Military Hospital, Rawalpindi Obaid Ullah Khan, Abdul Rasheed Correspondence: Dr. Abdul
Barrett s esophagus. Barrett s neoplasia treatment trends
 Options for endoscopic treatment of Barrett s esophagus Patrick S. Yachimski, MD MPH Director of Pancreatobiliary Endoscopy Assistant Professor of Medicine Division of Gastroenterology, Hepatology & Nutrition
Options for endoscopic treatment of Barrett s esophagus Patrick S. Yachimski, MD MPH Director of Pancreatobiliary Endoscopy Assistant Professor of Medicine Division of Gastroenterology, Hepatology & Nutrition
The incidence rates of adenocarcinoma of the esophagus. The Risk of Esophageal Adenocarcinoma After Antireflux Surgery. Methods Study Design
 GASTROENTEROLOGY 2010;138:1297 1301 The Risk of Esophageal Adenocarcinoma After Antireflux Surgery JESPER LAGERGREN,* WEIMIN YE,*, PERNILLA LAGERGREN,* and YUNXIA LU*, *Upper Gastrointestinal Research,
GASTROENTEROLOGY 2010;138:1297 1301 The Risk of Esophageal Adenocarcinoma After Antireflux Surgery JESPER LAGERGREN,* WEIMIN YE,*, PERNILLA LAGERGREN,* and YUNXIA LU*, *Upper Gastrointestinal Research,
Current Management of Low-Grade Dysplasia in Barrett Esophagus
 Current Management of Low-Grade Dysplasia in Barrett Esophagus Gary W. Falk, MD, MS Dr Falk is a professor of medicine in the Division of Gastroenterology at the University of Pennsylvania Perelman School
Current Management of Low-Grade Dysplasia in Barrett Esophagus Gary W. Falk, MD, MS Dr Falk is a professor of medicine in the Division of Gastroenterology at the University of Pennsylvania Perelman School
Present Day Management of Barrett s Esophagus
 Slide 1 Present Day Management of Barrett s Esophagus Kinnari R. Kher, M.D. Slide 2 Goals Risk factors for development of Barrett s esophagus Risks for progression to Esophageal Adenocarcinoma Current
Slide 1 Present Day Management of Barrett s Esophagus Kinnari R. Kher, M.D. Slide 2 Goals Risk factors for development of Barrett s esophagus Risks for progression to Esophageal Adenocarcinoma Current
AGA SECTION. Gastroenterology 2016;150:
 Gastroenterology 2016;150:1026 1030 April 2016 AGA Section 1027 Procedural intervention (3) Upper endoscopy indications 3 6 Non-response of symptoms to a 4 8 week empiric trial of twice-daily PPI Troublesome
Gastroenterology 2016;150:1026 1030 April 2016 AGA Section 1027 Procedural intervention (3) Upper endoscopy indications 3 6 Non-response of symptoms to a 4 8 week empiric trial of twice-daily PPI Troublesome
Proton-pump inhibitor therapy and the development of dysplasia in patients with Barrett s oesophagus
 Proton-pump inhibitor therapy and the development of dysplasia in patients with Barrett s oesophagus BARRETT S OESOPHAGUS is a premalignant condition, with dysplasia usually preceding the development of
Proton-pump inhibitor therapy and the development of dysplasia in patients with Barrett s oesophagus BARRETT S OESOPHAGUS is a premalignant condition, with dysplasia usually preceding the development of
Evaluating Treatments of Barrett s Esophagus That Shows High-Grade Dysplasia
 ...PRESENTATIONS... Evaluating Treatments of Barrett s Esophagus That Shows High-Grade Dysplasia Based on a presentation by Bergein F. Overholt, MD Presentation Summary Thermal ablation and surgery are
...PRESENTATIONS... Evaluating Treatments of Barrett s Esophagus That Shows High-Grade Dysplasia Based on a presentation by Bergein F. Overholt, MD Presentation Summary Thermal ablation and surgery are
ACG Clinical Guideline: Diagnosis and Management of Barrett s Esophagus
 ACG Clinical Guideline: Diagnosis and Management of Barrett s Esophagus Nicholas J. Shaheen, MD, MPH, FACG 1, Gary W. Falk, MD, MS, FACG 2, Prasad G. Iyer, MD, MSc, FACG 3 and Lauren Gerson, MD, MSc, FACG
ACG Clinical Guideline: Diagnosis and Management of Barrett s Esophagus Nicholas J. Shaheen, MD, MPH, FACG 1, Gary W. Falk, MD, MS, FACG 2, Prasad G. Iyer, MD, MSc, FACG 3 and Lauren Gerson, MD, MSc, FACG
Learning Objectives:
 Crescent City GI Update 2018 Ochsner Clinic, NOLA Optimizing Endoscopic Evaluation of Barrett s Esophagus What Should I Do in My Practice? Gregory G. Ginsberg, M.D. Professor of Medicine University of
Crescent City GI Update 2018 Ochsner Clinic, NOLA Optimizing Endoscopic Evaluation of Barrett s Esophagus What Should I Do in My Practice? Gregory G. Ginsberg, M.D. Professor of Medicine University of
Gregory G. Ginsberg, M.D.
 Radiofrequency Ablation for Barrett s Esophagus with HGD Gregory G. Ginsberg, M.D. Professor of Medicine University of Pennsylvania School of Medicine Abramson Cancer Center Gastroenterology Division Executive
Radiofrequency Ablation for Barrett s Esophagus with HGD Gregory G. Ginsberg, M.D. Professor of Medicine University of Pennsylvania School of Medicine Abramson Cancer Center Gastroenterology Division Executive
ORIGINAL ARTICLE. Adenocarcinoma of the Esophagus With and Without Barrett Mucosa
 ORIGINAL ARTICLE Adenocarcinoma of the Esophagus With and Without Barrett Mucosa Michael S. Sabel, MD; Kate Pastore, MD; Hannah Toon, MD; Judy L. Smith, MD Hypothesis: Previous studies have demonstrated
ORIGINAL ARTICLE Adenocarcinoma of the Esophagus With and Without Barrett Mucosa Michael S. Sabel, MD; Kate Pastore, MD; Hannah Toon, MD; Judy L. Smith, MD Hypothesis: Previous studies have demonstrated
Definition of GERD American College of Gastroenterology
 Definition of GERD American College of Gastroenterology GERD is defined as chronic symptoms or mucosal damage produced by the abnormal reflux of gastric contents into the esophagus DeVault et al. Am J
Definition of GERD American College of Gastroenterology GERD is defined as chronic symptoms or mucosal damage produced by the abnormal reflux of gastric contents into the esophagus DeVault et al. Am J
Hiatal Hernias and Barrett s esophagus. Dr Sajida Ahad Mercy General Surgery
 Hiatal Hernias and Barrett s esophagus Dr Sajida Ahad Mercy General Surgery Objectives Identify the use of different diagnostic modalities for hiatal hernias List the different types of hiatal hernias
Hiatal Hernias and Barrett s esophagus Dr Sajida Ahad Mercy General Surgery Objectives Identify the use of different diagnostic modalities for hiatal hernias List the different types of hiatal hernias
EDUCATION PRACTICE. A 52-Year-Old Man With Heartburn: Should He Undergo Screening for Barrett s Esophagus? Clinical Scenario.
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2010;8:565 571 EDUCATION PRACTICE A 52-Year-Old Man With Heartburn: Should He Undergo Screening for Barrett s Esophagus? SETH D. CROCKETT, A. SIDNEY BARRITT IV,
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2010;8:565 571 EDUCATION PRACTICE A 52-Year-Old Man With Heartburn: Should He Undergo Screening for Barrett s Esophagus? SETH D. CROCKETT, A. SIDNEY BARRITT IV,
The presence of intestinal-type goblet cells (ITGCs) in
 Goblet Cell Mimickers in Esophageal Biopsies Are Not Associated With an Increased Risk for Dysplasia Mamoun Younes, MD; Atilla Ertan, MD; Gulchin Ergun, MD; Ray Verm, MD; Margaret Bridges, MD; Karen Woods,
Goblet Cell Mimickers in Esophageal Biopsies Are Not Associated With an Increased Risk for Dysplasia Mamoun Younes, MD; Atilla Ertan, MD; Gulchin Ergun, MD; Ray Verm, MD; Margaret Bridges, MD; Karen Woods,
What s New in the Management of Esophageal Disease
 What s New in the Management of Esophageal Disease Philip O. Katz, MD Chairman, Division of Gastroenterology Einstein Medical Center Philadelphia Clinical Professor of Medicine Jefferson Medical College
What s New in the Management of Esophageal Disease Philip O. Katz, MD Chairman, Division of Gastroenterology Einstein Medical Center Philadelphia Clinical Professor of Medicine Jefferson Medical College
Ablation for Barrett s Esophagus: Burn or Freeze
 Ablation for Barrett s Esophagus: Burn or Freeze John R. Saltzman MD Director of Endoscopy Brigham and Women s Hospital Professor of Medicine Harvard Medical School Disclosures No relevant disclosures
Ablation for Barrett s Esophagus: Burn or Freeze John R. Saltzman MD Director of Endoscopy Brigham and Women s Hospital Professor of Medicine Harvard Medical School Disclosures No relevant disclosures
T he incidence of adenocarcinoma of the oesophagus (AC)
 162 OESOPHAGUS Increasing incidence of Barrett s oesophagus in the general population E M van Soest, J P Dieleman, P D Siersema, M C J M Sturkenboom, E J Kuipers... See end of article for authors affiliations...
162 OESOPHAGUS Increasing incidence of Barrett s oesophagus in the general population E M van Soest, J P Dieleman, P D Siersema, M C J M Sturkenboom, E J Kuipers... See end of article for authors affiliations...
Citation for published version (APA): Phoa, K. Y. N. (2014). Endoscopic management of Barrett s esophagus with dysplasia
 UvA-DARE (Digital Academic Repository) Endoscopic management of Barrett s esophagus with dysplasia Phoa, Nadine Link to publication Citation for published version (APA): Phoa, K. Y. N. (2014). Endoscopic
UvA-DARE (Digital Academic Repository) Endoscopic management of Barrett s esophagus with dysplasia Phoa, Nadine Link to publication Citation for published version (APA): Phoa, K. Y. N. (2014). Endoscopic
Symptoms suggestive of gastroesophageal reflux disease. Gastroesophageal Reflux Among Different Racial Groups in the United States
 GASTROENTEROLOGY 2004;126:1692 1699 Gastroesophageal Reflux Among Different Racial Groups in the United States HASHEM B. EL SERAG,*, NANCY J. PETERSEN, JUNAIA CARTER, DAVID Y. GRAHAM,* PETER RICHARDSON,
GASTROENTEROLOGY 2004;126:1692 1699 Gastroesophageal Reflux Among Different Racial Groups in the United States HASHEM B. EL SERAG,*, NANCY J. PETERSEN, JUNAIA CARTER, DAVID Y. GRAHAM,* PETER RICHARDSON,
Everything Esophagus: Barrett s Esophagus. Nicholas Shaheen, MD, MPH Center for Esophageal Diseases and Swallowing University of North Carolina
 Everything Esophagus: Barrett s Esophagus Nicholas Shaheen, MD, MPH Center for Esophageal Diseases and Swallowing University of North Carolina The Most Important Thing Stayed the Same Adenocarcinoma A
Everything Esophagus: Barrett s Esophagus Nicholas Shaheen, MD, MPH Center for Esophageal Diseases and Swallowing University of North Carolina The Most Important Thing Stayed the Same Adenocarcinoma A
Gland ducts and multilayered epithelium in mucosal biopsies from gastroesophageal-junction region are useful in characterizing esophageal location
 Diseases of the Esophagus (2005) 18, 87 92 2005 ISDE Blackwell Publishing, Ltd. Original article Gland ducts and multilayered epithelium in mucosal biopsies from gastroesophageal-junction region are useful
Diseases of the Esophagus (2005) 18, 87 92 2005 ISDE Blackwell Publishing, Ltd. Original article Gland ducts and multilayered epithelium in mucosal biopsies from gastroesophageal-junction region are useful
Speaker disclosure. Objectives. GERD: Who and When to Treat 7/21/2015
 GERD: Who and When to Treat Eugenio J Hernandez, MD Gastrohealth, PL Assistant Professor of Clinical Medicine, FIU Herbert Wertheim School of Medicine Speaker disclosure I do not have any relevant commercial
GERD: Who and When to Treat Eugenio J Hernandez, MD Gastrohealth, PL Assistant Professor of Clinical Medicine, FIU Herbert Wertheim School of Medicine Speaker disclosure I do not have any relevant commercial
Management of Barrett s Esophagus. Case Presentation
 Management of Barrett s Esophagus Lauren B. Gerson MD, MSc Associate Clinical Professor, UCSF Director of Clinical Research Gastroenterology Fellowship Program California Pacific Medical Center San Francisco,
Management of Barrett s Esophagus Lauren B. Gerson MD, MSc Associate Clinical Professor, UCSF Director of Clinical Research Gastroenterology Fellowship Program California Pacific Medical Center San Francisco,
Screening of Barrett: Is it cost-effective? Is there a high-risk population? T Ponchon Ed. Herriot Hospital Lyon, France
 Screening of Barrett: Is it cost-effective? Is there a high-risk population? T Ponchon Ed. Herriot Hospital Lyon, France Barrett s esophagus (BE) is an acquired condition in which the normal squamous epithelium
Screening of Barrett: Is it cost-effective? Is there a high-risk population? T Ponchon Ed. Herriot Hospital Lyon, France Barrett s esophagus (BE) is an acquired condition in which the normal squamous epithelium
Intestinal metaplasia at the gastro-oesophageal junction: Helicobacter pylori gastritis or gastro-oesophageal reflux disease?
 Gut 1998;43:17 21 17 Gastroenterology, Hepatology, and Infectious Diseases A Hackelsberger V Schultze G Manes J-E Dominguez-Muñoz P Malfertheiner Pathology, Otto-von-Guericke University, Magdeburg, Germany
Gut 1998;43:17 21 17 Gastroenterology, Hepatology, and Infectious Diseases A Hackelsberger V Schultze G Manes J-E Dominguez-Muñoz P Malfertheiner Pathology, Otto-von-Guericke University, Magdeburg, Germany
Is There Publication Bias in the Reporting of Cancer Risk in Barrett s Esophagus?
 GASTROENTEROLOGY 2000;119:333 338 Is There Publication Bias in the Reporting of Cancer Risk in Barrett s Esophagus? NICHOLAS J. SHAHEEN, MELISSA A. CROSBY, EUGENE M. BOZYMSKI, and ROBERT S. SANDLER Division
GASTROENTEROLOGY 2000;119:333 338 Is There Publication Bias in the Reporting of Cancer Risk in Barrett s Esophagus? NICHOLAS J. SHAHEEN, MELISSA A. CROSBY, EUGENE M. BOZYMSKI, and ROBERT S. SANDLER Division
Photodynamic Therapy for High Grade Esophageal Dysplasia. California Technology Assessment Forum
 TITLE: AUTHOR: PUBLISHER NAME: Photodynamic Therapy for High Grade Esophageal Dysplasia Jeffrey A. Tice, M.D. Assistant Adjunct Professor of Medicine Division of General Internal Medicine Department of
TITLE: AUTHOR: PUBLISHER NAME: Photodynamic Therapy for High Grade Esophageal Dysplasia Jeffrey A. Tice, M.D. Assistant Adjunct Professor of Medicine Division of General Internal Medicine Department of
Adenocarcinoma of the distal esophagus is a recognized
 ORIGINAL ARTICLE Adenocarcinomas of the Distal Esophagus and Gastric Cardia Are Predominantly Esophageal Carcinomas Parakrama Chandrasoma, MD, Kumari Wickramasinghe, MD, PhD, Yanling Ma, MD, and Tom DeMeester,
ORIGINAL ARTICLE Adenocarcinomas of the Distal Esophagus and Gastric Cardia Are Predominantly Esophageal Carcinomas Parakrama Chandrasoma, MD, Kumari Wickramasinghe, MD, PhD, Yanling Ma, MD, and Tom DeMeester,
Barrett s Esophagus: State of the Art. Food Getting Stuck
 Barrett s Esophagus: State of the Art Nicholas J. Shaheen, MD, MPH Center for Esophageal Diseases and Swallowing University of North Carolina SOM Food Getting Stuck 73-year-old retired Wilmington police
Barrett s Esophagus: State of the Art Nicholas J. Shaheen, MD, MPH Center for Esophageal Diseases and Swallowing University of North Carolina SOM Food Getting Stuck 73-year-old retired Wilmington police
Barrett s Esophagus: Ablate Everyone?
 Nicholas J. Shaheen, MD, MPH, FACG Barrett s Esophagus: Ablate Everyone? Nicholas J. Shaheen, MD, MPH, FACG Center for Esophageal Diseases and Swallowing University of North Carolina Greetings from UNC,
Nicholas J. Shaheen, MD, MPH, FACG Barrett s Esophagus: Ablate Everyone? Nicholas J. Shaheen, MD, MPH, FACG Center for Esophageal Diseases and Swallowing University of North Carolina Greetings from UNC,
Vital staining and Barrett s esophagus
 Marcia Irene Canto, MD, MHS Baltimore, Maryland Vital staining or chromoendoscopy refers to staining of endoscopic tissue or topical application of chemical stains or pigments to alter tissue appearances
Marcia Irene Canto, MD, MHS Baltimore, Maryland Vital staining or chromoendoscopy refers to staining of endoscopic tissue or topical application of chemical stains or pigments to alter tissue appearances
Patterns of recurrent and persistent intestinal metaplasia after successful radiofrequency ablation of Barrett s esophagus
 Patterns of recurrent and persistent intestinal metaplasia after successful radiofrequency ablation of Barrett s esophagus Robert J. Korst, MD, a,b Sobeida Santana-Joseph, MSN, a,b John R. Rutledge, MAS,
Patterns of recurrent and persistent intestinal metaplasia after successful radiofrequency ablation of Barrett s esophagus Robert J. Korst, MD, a,b Sobeida Santana-Joseph, MSN, a,b John R. Rutledge, MAS,
Original article INTRODUCTION
 Diseases of the Esophagus (2014), DOI: 10.1111/dote.12166 Original article A Barrett s esophagus registry of over 1000 patients from a specialist center highlights greater risk of progression than population-based
Diseases of the Esophagus (2014), DOI: 10.1111/dote.12166 Original article A Barrett s esophagus registry of over 1000 patients from a specialist center highlights greater risk of progression than population-based
Barrett s Esophagus. Radiofrequency Ablation with the HALO Technology A Reference Book
 Radiofrequency Ablation with the HALO Technology A Reference Book 540 Oakmead Parkway, Sunnyvale, CA 94085 What is Barrett s esophagus? Barrett s esophagus is a change that occurs within the cellular lining
Radiofrequency Ablation with the HALO Technology A Reference Book 540 Oakmead Parkway, Sunnyvale, CA 94085 What is Barrett s esophagus? Barrett s esophagus is a change that occurs within the cellular lining
Barrett esophagus. Bible class Inselspital
 Barrett esophagus Bible class Inselspital 2015.08.10 Guidelines Definition? BSG: ACG: Definition? BSG: ACG: What are the arguments for and against IM as prerequisite for the Dg? What are the arguments
Barrett esophagus Bible class Inselspital 2015.08.10 Guidelines Definition? BSG: ACG: Definition? BSG: ACG: What are the arguments for and against IM as prerequisite for the Dg? What are the arguments
Endoscopic therapy of Barrett s esophagus Oliver Pech and Christian Ell
 Endoscopic therapy of Barrett s esophagus Oliver Pech and Christian Ell Department of Internal Medicine 2, HSK Wiesbaden, Wiesbaden, Germany Correspondence to Oliver Pech, MD, PhD, Department of Gastroenterology,
Endoscopic therapy of Barrett s esophagus Oliver Pech and Christian Ell Department of Internal Medicine 2, HSK Wiesbaden, Wiesbaden, Germany Correspondence to Oliver Pech, MD, PhD, Department of Gastroenterology,
During the past 30 years, the incidence of esophageal ORIGINAL ARTICLES
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2006;4:38 43 ORIGINAL ARTICLES Optical Coherence Tomography to Identify Intramucosal Carcinoma and High-Grade Dysplasia in Barrett s Esophagus JOHN A. EVANS,* JOHN
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2006;4:38 43 ORIGINAL ARTICLES Optical Coherence Tomography to Identify Intramucosal Carcinoma and High-Grade Dysplasia in Barrett s Esophagus JOHN A. EVANS,* JOHN
Barrett's Esophagus: Sorting Out the Controversy
 Barrett's Esophagus: Sorting Out the Controversy Learning Objectives 1. Identify the challenges in screening for Barrett s esophagus 2. Demonstrate comprehension of the risk of progression of Barrett s
Barrett's Esophagus: Sorting Out the Controversy Learning Objectives 1. Identify the challenges in screening for Barrett s esophagus 2. Demonstrate comprehension of the risk of progression of Barrett s
Comparison of Endoscopic and Clinical Characteristics of Patients with Familial and Sporadic Barrett s Esophagus
 DOI 10.1007/s10620-011-1620-3 ORIGINAL ARTICLE Comparison of Endoscopic and Clinical Characteristics of Patients with Familial and Sporadic Barrett s Esophagus Samuel Ash Benjamin J. Vaccaro Mary Kay Dabney
DOI 10.1007/s10620-011-1620-3 ORIGINAL ARTICLE Comparison of Endoscopic and Clinical Characteristics of Patients with Familial and Sporadic Barrett s Esophagus Samuel Ash Benjamin J. Vaccaro Mary Kay Dabney
L was termed Barrett s esophagus (BE) after the
 ORIGINAL ARTICLES Barrett s Esophagus With High-Grade Dysplasia: An Indication for Esophagectomy? Manuel Pera, MD, Victor F. Trastek, MD, Herschel A. Carpenter, MD, Mark S. Allen, MD, Claude Deschamps,
ORIGINAL ARTICLES Barrett s Esophagus With High-Grade Dysplasia: An Indication for Esophagectomy? Manuel Pera, MD, Victor F. Trastek, MD, Herschel A. Carpenter, MD, Mark S. Allen, MD, Claude Deschamps,
GASTROESOPHAGEAL REFLUX
 SCIENTIFIC REVIEW AND CLINICAL APPLICATIONS CLINICIAN S CORNER Gastroesophageal Reflux, Barrett Esophagus, and Esophageal Cancer Clinical Applications Nicholas Shaheen, MD, MPH David F. Ransohoff, MD disease
SCIENTIFIC REVIEW AND CLINICAL APPLICATIONS CLINICIAN S CORNER Gastroesophageal Reflux, Barrett Esophagus, and Esophageal Cancer Clinical Applications Nicholas Shaheen, MD, MPH David F. Ransohoff, MD disease
Endoscopic Management of Barrett s Esophagus
 Endoscopic Management of Barrett s Esophagus Sammy Ho, MD Director of Pancreaticobiliary Services and Endoscopic Ultrasound Montefiore Medical Center Barrett s Esophagus Consequence of chronic GERD Mean
Endoscopic Management of Barrett s Esophagus Sammy Ho, MD Director of Pancreaticobiliary Services and Endoscopic Ultrasound Montefiore Medical Center Barrett s Esophagus Consequence of chronic GERD Mean
SAM PROVIDER TOOLKIT
 THE AMERICAN BOARD OF PATHOLOGY Maintenance of Certification (MOC) Program SAM PROVIDER TOOLKIT Developing Self-Assessment Modules (SAMs) www.abpath.org The American Board of Pathology (ABP) approves educational
THE AMERICAN BOARD OF PATHOLOGY Maintenance of Certification (MOC) Program SAM PROVIDER TOOLKIT Developing Self-Assessment Modules (SAMs) www.abpath.org The American Board of Pathology (ABP) approves educational
This medical position statement considers a series of
 GASTROENTEROLOGY 2011;140:1084 1091 American Gastroenterological Association Medical Position Statement on the Management of Barrett s Esophagus The Institute Medical Position Panel consisted of the authors
GASTROENTEROLOGY 2011;140:1084 1091 American Gastroenterological Association Medical Position Statement on the Management of Barrett s Esophagus The Institute Medical Position Panel consisted of the authors
Disclosures. Gastroesophageal Reflux Disease. Gastroesophageal Reflux Disease
 Kunal Jajoo, MD Brigham and Women s Hospital July 2012 Disclosures Spouse is a physician employed by Boston Scientific Corporation The content of this lecture equitably discusses products of multiple companies
Kunal Jajoo, MD Brigham and Women s Hospital July 2012 Disclosures Spouse is a physician employed by Boston Scientific Corporation The content of this lecture equitably discusses products of multiple companies
Meta-analysis: the association of oesophageal adenocarcinoma with symptoms of gastro-oesophageal reflux
 Alimentary Pharmacology and Therapeutics Meta-analysis: the association of oesophageal adenocarcinoma with symptoms of gastro-oesophageal reflux J. H. Rubenstein*, & J. B. Taylor à *Veterans Affairs Center
Alimentary Pharmacology and Therapeutics Meta-analysis: the association of oesophageal adenocarcinoma with symptoms of gastro-oesophageal reflux J. H. Rubenstein*, & J. B. Taylor à *Veterans Affairs Center
ORIGINAL ARTICLE. Laparoscopic Antireflux Surgery in the Treatment of Gastroesophageal Reflux in Patients With Barrett Esophagus
 ORIGINAL ARTICLE Laparoscopic Antireflux Surgery in the Treatment of Gastroesophageal Reflux in Patients With Barrett Esophagus Patrick Yau, MD, FRCSC; David I. Watson, MBBS, MD, FRACS; Peter G. Devitt,
ORIGINAL ARTICLE Laparoscopic Antireflux Surgery in the Treatment of Gastroesophageal Reflux in Patients With Barrett Esophagus Patrick Yau, MD, FRCSC; David I. Watson, MBBS, MD, FRACS; Peter G. Devitt,
Table 2.9. Case control studies of helicobacter pylori infection and oesophageal adenocarcinoma
 Characteristics of Characteristics of controls Detection Chow et al (1998) 1993-1995 129 of newly diagnosed oesophageal/gastric cardia (OGC) adenocarcinoma. 224 population controls selected by random digit
Characteristics of Characteristics of controls Detection Chow et al (1998) 1993-1995 129 of newly diagnosed oesophageal/gastric cardia (OGC) adenocarcinoma. 224 population controls selected by random digit
The Role of Secondary Versus Tertiary Prevention in Decreasing the Incidence of. Esophageal Adenocarcinoma in Patients with Barrett s Esophagus.
 The Role of Secondary Versus Tertiary Prevention in Decreasing the Incidence of Esophageal Adenocarcinoma in Patients with Barrett s Esophagus. Submitted by Lindsay West A project presented to the Department
The Role of Secondary Versus Tertiary Prevention in Decreasing the Incidence of Esophageal Adenocarcinoma in Patients with Barrett s Esophagus. Submitted by Lindsay West A project presented to the Department
MANAGEMENT OF BARRETT S RELATED NEOPLASIA IN 2018
 MANAGEMENT OF BARRETT S RELATED NEOPLASIA IN 2018 Sachin Wani Medical Director Esophageal and Gastric Center Division of Gastroenterology and Hepatology University of Colorado Anschutz Medical Campus DISCLOSURES
MANAGEMENT OF BARRETT S RELATED NEOPLASIA IN 2018 Sachin Wani Medical Director Esophageal and Gastric Center Division of Gastroenterology and Hepatology University of Colorado Anschutz Medical Campus DISCLOSURES
Quality ID #249 (NQF 1854): Barrett s Esophagus National Quality Strategy Domain: Effective Clinical Care
 Quality ID #249 (NQF 1854): Barrett s Esophagus National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE: Process DESCRIPTION: Percentage
Quality ID #249 (NQF 1854): Barrett s Esophagus National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE: Process DESCRIPTION: Percentage
The increasing incidence of esophageal adenocarcinoma
 GASTROENTEROLOGY 2004;127:310 330 A Critical Review of the Diagnosis and Management of Barrett s Esophagus: The AGA Chicago Workshop PRATEEK SHARMA,* KENNETH MCQUAID, JOHN DENT, M. BRIAN FENNERTY, RICHARD
GASTROENTEROLOGY 2004;127:310 330 A Critical Review of the Diagnosis and Management of Barrett s Esophagus: The AGA Chicago Workshop PRATEEK SHARMA,* KENNETH MCQUAID, JOHN DENT, M. BRIAN FENNERTY, RICHARD
P the esophagus may differ from those of squamous
 Incidence of Cancer of the Esophagus in the US by Histologic Type PAUL c. YANG, MD, MPH, AND SCOTT DAVIS, PHD' Data from nine US population-based cancer registries participating in the Surveillance, Epidemiology,
Incidence of Cancer of the Esophagus in the US by Histologic Type PAUL c. YANG, MD, MPH, AND SCOTT DAVIS, PHD' Data from nine US population-based cancer registries participating in the Surveillance, Epidemiology,
The relationship between length of Barrett s oesophagus mucosa and body mass index
 Alimentary Pharmacology and Therapeutics The relationship between length of Barrett s oesophagus mucosa and body mass index J. Abdallah*, C. Maradey-Romero*, S. Lewis, A. Perzynski & R. Fass* *Division
Alimentary Pharmacology and Therapeutics The relationship between length of Barrett s oesophagus mucosa and body mass index J. Abdallah*, C. Maradey-Romero*, S. Lewis, A. Perzynski & R. Fass* *Division
Tobacco Smoking Increases the Risk of High-Grade Dysplasia and Cancer Among Patients With Barrett s Esophagus
 GASTROENTEROLOGY 2012;142:233 240 CLINCAL ALIMENTARY TRACT Tobacco Smoking Increases the Risk of High-Grade Dysplasia and Cancer Among Patients With Barrett s Esophagus HELEN G. COLEMAN,* SHIVARAM BHAT,*
GASTROENTEROLOGY 2012;142:233 240 CLINCAL ALIMENTARY TRACT Tobacco Smoking Increases the Risk of High-Grade Dysplasia and Cancer Among Patients With Barrett s Esophagus HELEN G. COLEMAN,* SHIVARAM BHAT,*
Increased detection rates for Barrett s oesophagus without rise in incidence of oesophageal adenocarcinoma
 Original article Peer reviewed article SWISS MED WKLY 2003;133:507 514 www.smw.ch 507 Increased detection rates for Barrett s oesophagus without rise in incidence of oesophageal adenocarcinoma A ten-year
Original article Peer reviewed article SWISS MED WKLY 2003;133:507 514 www.smw.ch 507 Increased detection rates for Barrett s oesophagus without rise in incidence of oesophageal adenocarcinoma A ten-year
Histopathology of Endoscopic Resection Specimens from Barrett's Esophagus
 Histopathology of Endoscopic Resection Specimens from Barrett's Esophagus Br J Surg 38 oct. 1950 Definition of Barrett's esophagus A change in the esophageal epithelium of any length that can be recognized
Histopathology of Endoscopic Resection Specimens from Barrett's Esophagus Br J Surg 38 oct. 1950 Definition of Barrett's esophagus A change in the esophageal epithelium of any length that can be recognized
ACG Clinical Guideline: Diagnosis and Management of Gastroesophageal Reflux Disease
 ACG Clinical Guideline: Diagnosis and Management of Gastroesophageal Reflux Disease Philip O. Katz MD 1, Lauren B. Gerson MD, MSc 2 and Marcelo F. Vela MD, MSCR 3 1 Division of Gastroenterology, Einstein
ACG Clinical Guideline: Diagnosis and Management of Gastroesophageal Reflux Disease Philip O. Katz MD 1, Lauren B. Gerson MD, MSc 2 and Marcelo F. Vela MD, MSCR 3 1 Division of Gastroenterology, Einstein
Epidemiology of Esophageal Adenocarcinoma
 Journal of Surgical Oncology 2005;92:151 159 Epidemiology of Esophageal Adenocarcinoma MANUEL PERA, MD, PhD, 1 * CARLOS MANTEROLA, MD, PhD, 2 OSCAR VIDAL, MD, 1 AND LUIS GRANDE, MD, PhD 1 1 Section of
Journal of Surgical Oncology 2005;92:151 159 Epidemiology of Esophageal Adenocarcinoma MANUEL PERA, MD, PhD, 1 * CARLOS MANTEROLA, MD, PhD, 2 OSCAR VIDAL, MD, 1 AND LUIS GRANDE, MD, PhD 1 1 Section of
Endoscopic Radiofrequency Ablation or Cryoablation for Barrett s Esophagus
 Endoscopic Radiofrequency Ablation or Cryoablation for Barrett s Esophagus Policy Number: 2.01.80 Last Review: 6/2018 Origination: 6/2012 Next Review: 6/2019 Policy Blue Cross and Blue Shield of Kansas
Endoscopic Radiofrequency Ablation or Cryoablation for Barrett s Esophagus Policy Number: 2.01.80 Last Review: 6/2018 Origination: 6/2012 Next Review: 6/2019 Policy Blue Cross and Blue Shield of Kansas
Barrett s esophagus (BE), the premalignant condition
 GASTROENTEROLOGY 2009;136:2101 2114 A Cost-Utility Analysis of Ablative Therapy for Barrett s Esophagus JOHN M. INADOMI,*, MA SOMSOUK,*, RYAN D. MADANICK, JENNIFER P. THOMAS, and NICHOLAS J. SHAHEEN *Division
GASTROENTEROLOGY 2009;136:2101 2114 A Cost-Utility Analysis of Ablative Therapy for Barrett s Esophagus JOHN M. INADOMI,*, MA SOMSOUK,*, RYAN D. MADANICK, JENNIFER P. THOMAS, and NICHOLAS J. SHAHEEN *Division
Barrett s esophagus (BE), a known complication of chronic
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2011;9:220 227 Patients With Nondysplastic Barrett s Esophagus Have Low Risks for Developing Dysplasia or Esophageal Adenocarcinoma SACHIN WANI,* GARY FALK, MATTHEW
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2011;9:220 227 Patients With Nondysplastic Barrett s Esophagus Have Low Risks for Developing Dysplasia or Esophageal Adenocarcinoma SACHIN WANI,* GARY FALK, MATTHEW
Chapter 12: Training in Pathology. DDSEP Chapter 13: Question 19
 DDSEP Chapter 13: Question 19 A 70 year-old male with a history of celiac disease diagnosed in his forties reports abdominal pain, dark stools, and 20-pound weight loss. He reports complete compliance
DDSEP Chapter 13: Question 19 A 70 year-old male with a history of celiac disease diagnosed in his forties reports abdominal pain, dark stools, and 20-pound weight loss. He reports complete compliance
Long-term Outcome of Medical and Surgical Therapies for Gastroesophageal Reflux Disease. Follow-up of a Randomized Controlled Trial
 ORIGINAL CONTRIBUTION Long-term Outcome of Medical and Surgical Therapies for Gastroesophageal Reflux Disease Follow-up of a Randomized Controlled Trial Stuart Jon Spechler, MD Edward Lee, MD Dennis Ahnen,
ORIGINAL CONTRIBUTION Long-term Outcome of Medical and Surgical Therapies for Gastroesophageal Reflux Disease Follow-up of a Randomized Controlled Trial Stuart Jon Spechler, MD Edward Lee, MD Dennis Ahnen,
GERD DIAGNOSIS & TREATMENT DISCLOSURES 4/18/2018
 GERD DIAGNOSIS & TREATMENT Subhash Chandra MBBS Assistant Professor CHI Health Clinic Gastroenterology Creighton University, School of Medicine April 28, 2018 DISCLOSURES None 1 OBJECTIVES Review update
GERD DIAGNOSIS & TREATMENT Subhash Chandra MBBS Assistant Professor CHI Health Clinic Gastroenterology Creighton University, School of Medicine April 28, 2018 DISCLOSURES None 1 OBJECTIVES Review update
Quality ID #249 (NQF 1854): Barrett s Esophagus National Quality Strategy Domain: Effective Clinical Care
 Quality ID #249 (NQF 1854): Barrett s Esophagus National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL MEASURES: CLAIMS ONLY MEASURE TYPE: Process DESCRIPTION: Percentage
Quality ID #249 (NQF 1854): Barrett s Esophagus National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL MEASURES: CLAIMS ONLY MEASURE TYPE: Process DESCRIPTION: Percentage
Photodynamic Therapy of Barrett's Esophagus: Ablation of Barrett's Mucosa and Reduction in p53 Protein Expression after Treatment
 Photodynamic Therapy of Barrett's Esophagus: Ablation of Barrett's Mucosa and Reduction in p53 Protein Expression after Treatment MASOUD PANJEHPOUR 1, DOMENICO COPPOLA 2, BERGEIN F. OVERHOLT 1, TUAN VO-DINH
Photodynamic Therapy of Barrett's Esophagus: Ablation of Barrett's Mucosa and Reduction in p53 Protein Expression after Treatment MASOUD PANJEHPOUR 1, DOMENICO COPPOLA 2, BERGEIN F. OVERHOLT 1, TUAN VO-DINH
Esophageal cancer: Biology, natural history, staging and therapeutic options
 EGEUS 2nd Meeting Esophageal cancer: Biology, natural history, staging and therapeutic options Michael Bau Mortensen MD, Ph.D. Associate Professor of Surgery Centre for Surgical Ultrasound, Upper GI Section,
EGEUS 2nd Meeting Esophageal cancer: Biology, natural history, staging and therapeutic options Michael Bau Mortensen MD, Ph.D. Associate Professor of Surgery Centre for Surgical Ultrasound, Upper GI Section,
Greater Manchester & Cheshire Guidelines for Pathology Reporting for Oesophageal and Gastric Malignancy
 Greater Manchester & Cheshire Guidelines for Pathology Reporting for Oesophageal and Gastric Malignancy Authors: Dr Gordon Armstrong, Dr Sue Pritchard 1. General Comments 1.1 Cancer reporting: Biopsies
Greater Manchester & Cheshire Guidelines for Pathology Reporting for Oesophageal and Gastric Malignancy Authors: Dr Gordon Armstrong, Dr Sue Pritchard 1. General Comments 1.1 Cancer reporting: Biopsies
The New England Journal of Medicine
 The New England Journal of Medicine Copyright, 1999, by the Massachusetts Medical Society VOLUME 340 M ARCH 18, 1999 NUMBER 11 SYMPTOMATIC GASTRO REFLUX AS A RISK FACTOR FOR JESPER LAGERGREN, M.D., REINHOLD
The New England Journal of Medicine Copyright, 1999, by the Massachusetts Medical Society VOLUME 340 M ARCH 18, 1999 NUMBER 11 SYMPTOMATIC GASTRO REFLUX AS A RISK FACTOR FOR JESPER LAGERGREN, M.D., REINHOLD
Early detection and surgical treatment of adnocarcinoma of the oesophagus or oesophagogastric junction van Sandick, J.W.
 UvA-DARE (Digital Academic Repository) Early detection and surgical treatment of adnocarcinoma of the oesophagus or oesophagogastric junction van Sandick, J.W. Link to publication Citation for published
UvA-DARE (Digital Academic Repository) Early detection and surgical treatment of adnocarcinoma of the oesophagus or oesophagogastric junction van Sandick, J.W. Link to publication Citation for published
Intestinal Metaplasia of the Esophagus or Esophagogastric Junction Evidence of Distinct Clinical, Pathologic, and Histochemical Staining Features
 Anatomic Pathology / ESOPHAGEAL AND JUNCTIONAL INTESTINAL METAPLASIA Intestinal Metaplasia of the Esophagus or Esophagogastric Junction Evidence of Distinct Clinical, Pathologic, and Histochemical Staining
Anatomic Pathology / ESOPHAGEAL AND JUNCTIONAL INTESTINAL METAPLASIA Intestinal Metaplasia of the Esophagus or Esophagogastric Junction Evidence of Distinct Clinical, Pathologic, and Histochemical Staining
Barrett s Oesophagus Information Leaflet THE DIGESTIVE SYSTEM. gutscharity.org.
 THE DIGESTIVE SYSTEM http://healthfavo.com/digestive-system-for-kids.html This factsheet is about Barrett s Oesophagus Barrett s Oesophagus is the term used for a pre-cancerous condition where the normal
THE DIGESTIVE SYSTEM http://healthfavo.com/digestive-system-for-kids.html This factsheet is about Barrett s Oesophagus Barrett s Oesophagus is the term used for a pre-cancerous condition where the normal
LIST OF ABBREVIATIONS
 Gastroenter oenterology 2005 Royal College of Physicians of Edinburgh Screening and surveillance for upper and lower gastrointestinal cancer JN Plevris Consultant Gastroenterologist and Honorary Senior
Gastroenter oenterology 2005 Royal College of Physicians of Edinburgh Screening and surveillance for upper and lower gastrointestinal cancer JN Plevris Consultant Gastroenterologist and Honorary Senior
Endoscopic Radiofrequency Ablation or Cryoablation for Barrett`s Esophagus. Original Policy Date
 MP 2.01.52 Endoscopic Radiofrequency Ablation or Cryoablation for Barrett`s Esophagus Medical Policy Section Medicine Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature
MP 2.01.52 Endoscopic Radiofrequency Ablation or Cryoablation for Barrett`s Esophagus Medical Policy Section Medicine Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature
Changes to the diagnosis and management of Barrett s Oesophagus
 Changes to the diagnosis and management of Barrett s Oesophagus A review of the new BSG and NICE guidelines and best practice Anjan Dhar DM, MD, FRCPE, AGAF, MBBS (Hons.), Cert. Med. Ed Senior Lecturer
Changes to the diagnosis and management of Barrett s Oesophagus A review of the new BSG and NICE guidelines and best practice Anjan Dhar DM, MD, FRCPE, AGAF, MBBS (Hons.), Cert. Med. Ed Senior Lecturer
Sixteen-year follow-up of Barrett s esophagus, endoscopically treated with argon plasma coagulation
 Original Article Sixteen-year of Barrett s esophagus, endoscopically treated with argon plasma coagulation United European Gastroenterology Journal 2014, Vol. 2(5) 367 373! Author(s) 2014 Reprints and
Original Article Sixteen-year of Barrett s esophagus, endoscopically treated with argon plasma coagulation United European Gastroenterology Journal 2014, Vol. 2(5) 367 373! Author(s) 2014 Reprints and
Volumetric laser endomicroscopy can target neoplasia not detected by conventional endoscopic measures in long segment Barrett s esophagus
 E318 Volumetric laser endomicroscopy can target neoplasia not detected by conventional endoscopic measures in long segment esophagus Authors Institution Arvind J. Trindade, Benley J. George, Joshua Berkowitz,
E318 Volumetric laser endomicroscopy can target neoplasia not detected by conventional endoscopic measures in long segment esophagus Authors Institution Arvind J. Trindade, Benley J. George, Joshua Berkowitz,
