EDUCATION PRACTICE. A 52-Year-Old Man With Heartburn: Should He Undergo Screening for Barrett s Esophagus? Clinical Scenario.
|
|
|
- Roderick Skinner
- 5 years ago
- Views:
Transcription
1 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2010;8: EDUCATION PRACTICE A 52-Year-Old Man With Heartburn: Should He Undergo Screening for Barrett s Esophagus? SETH D. CROCKETT, A. SIDNEY BARRITT IV, and NICHOLAS J. SHAHEEN Division of Gastroenterology and Hepatology, University of North Carolina at Chapel Hill, Chapel Hill, North Carolina A Clinical Scenario 52-year-old man is referred to your gastroenterology practice for a history of gastroesophageal reflux disease (GERD). The patient reports a long history of heartburn symptoms, dating back at least 5 years. His symptoms were responsive to over-the-counter remedies including antacid tablets and liquids, but eventually became such a regular occurrence that he sought medical care from his primary care physician. He was initially prescribed an H2 blocker, which was incompletely effective, so he was started on proton pump inhibitor therapy. He currently takes 20 mg of omeprazole daily which is effective, but notes that if he misses a dose, he sometimes experiences heartburn. He denies dysphagia, nausea or vomiting, blood in his stool, or unintentional weight loss. He has no other chronic medical conditions and takes no other medications. He is a nonsmoker who drinks alcohol in moderation, and has no family history of gastrointestinal cancer. Paperwork from the referring physician states that the reason for consultation is: screening for Barrett s esophagus. The Problem In the United States, GERD is a frequent disorder, affecting 10% to 20% of the population on a regular basis. 1 Barrett s esophagus (BE) is a metaplastic change of the normal esophageal mucosa, in which the normal squamous epithelium of the esophagus is transformed into columnar epithelium with goblet cells in response to chronic inflammation from reflux of acidic gastric contents. Barrett s esophagus is significantly less common than GERD in the general population, occurring in roughly 1 2 out of 100 persons in the US. 2,3 However, BE is quite common among GERD sufferers, occurring in 6% 18% of cases. 2,4,5 It is important to note that Barrett s epithelium is not necessarily associated with symptoms, and its effect on overall mortality is unclear, and may be negligible. 6 8 Therefore, BE is of interest because it is considered a premalignant condition. Pathologically, BE can progress to dysplasia of the esophageal mucosa and subsequently, to the development of invasive adenocarcinoma In epidemiologic studies, BE is associated with a substantially increased risk of esophageal adenocarcinoma (EAC), at least 40-fold higher than the general population. 12,13 Current estimates place the risk of EAC among patients with BE between 0.5% and 1% per patient per year. 14 Gastroesophageal reflux disease is also highly associated with esophageal adenocarcinoma, as has been shown by several case control studies Such studies also consistently show higher odds of esophageal cancer depending on duration and frequency of symptoms. Though the absolute risk of esophageal cancer in persons with GERD cannot be directly measured by such studies, it is undoubtedly quite low given the low incidence of esophageal cancer and the high prevalence of GERD. 18 Adenocarcinoma of the esophagus is a relatively rare condition, with 10,000 cases per year in the US. 19 However, EAC is on the rise, with several population-based cohort studies demonstrating a 300% 500% increase in incidence since the 1970s. 20,21 The reason for this increased frequency of EAC is uncertain, but may be due to increased rates of obesity. 22 Rates of esophageal cancer are highest among white men, while women and African Americans have lower rates. 21 African Americans have significantly higher esophageal cancer mortality than whites, however. 23 Esophageal adenocarcinoma is among the most lethal cancers, with an overall 5-year survival of 17%. 24 Most esophageal cancers are diagnosed at an advanced stage, when local resection is not possible. 19 The primary surgical treatment of advanced esophageal cancer is esophagectomy, which is associated with substantial morbidity and some decrement in quality of life. 25,26 Despite the fact that EAC is an uncommon cancer, a targeted screening approach is of interest because of the morbidity and mortality associated with this disease. Given the widespread use of upper endoscopy to manage GERD, large numbers of subjects with BE are likely to continue to be discovered serendipitously. The question, therefore, is whether a screening endoscopic examination in persons with GERD specifically to detect BE or EAC is a worthwhile pursuit, and whether this approach would lead to decreased burden of esophageal adenocarcinoma. Management Strategies and Supporting Evidence Controversy abounds over the issue of BE screening, particularly in regards to which patients should be screened, or if gastroenterologists should screen anyone at all. Screening for BE is typically performed via esophagogastroduodenoscopy (EGD) with biopsies of the esophagus if and when characteris- Abbreviations used in this paper: AGA, American Gastroenterological Association; ASGE, American Society for Gastrointestinal Endoscopy; BE, Barrett s esophagus; EAC, esophageal adenocarcinoma; EGD, esophagogastroduodenoscopy; GERD, gastroesophageal reflux disease by the AGA Institute /$36.00 doi: /j.cgh
2 566 CROCKETT ET AL CLINICAL GASTROENTEROLOGY AND HEPATOLOGY Vol. 8, No. 7 tic Barrett s-type mucosa is seen. Barrett s esophagus is diagnosed when these biopsies contain intestinal metaplasia. The rationale for such screening is that BE is a major risk factor for development of EAC, and that early detection may lead to improved survival. The initial enthusiasm of screening and surveillance programs for BE may have been in part fueled by early reports of cancer risk in BE. These reports might have overestimated the true cancer risk by 50% or more, due to publication bias. 27 Also, studies subject to length and lead time bias claimed early detection led to a survival benefit. 28,29 Over the past 2 decades, as understanding of the natural history of BE and EAC has evolved, several schools of thought have arisen with respect to screening, including: (1) screening all patients with GERD; (2) screening patients with specific clinical characteristics; and (3) no screening at all. Screening all patients with GERD symptoms is 1 option for detecting BE, but would represent an enormous challenge to medical resources and endoscopists time. Current estimates are that at least 20% of the US population suffers from heartburn on a weekly or monthly basis. 1,30 In some BE patients, esophageal acid exposure manifests with the classical symptoms of heartburn and acid reflux. However, many patients with longstanding acid exposure may have no symptoms at all. Such patients would presumably be missed by a strategy which focused endoscopic screening on those with GERD symptoms. Several prospective studies have demonstrated that a substantial proportion of incident BE occurs in persons without typical reflux symptoms (Table 1). 3,31 35 Thus, while patients with symptomatic heartburn may have a slightly increased incidence of BE, screening on the basis on GERD alone may miss more subjects with BE than it finds. Further evidence regarding the insensitivity of GERD symptoms as a criterion for entry into endoscopic screening programs comes from case-control studies demonstrating that up to half of subjects who develop adenocarcinoma of the esophagus do not have chronic GERD symptoms In light of the limitations of screening all patients with GERD for BE, other strategies have been proposed in support of screening GERD patients with certain symptoms or clinical characteristics. BE has been found to occur more often in Caucasian males over the age of 50 with longstanding GERD symptoms. 17 Inadomi et al (2003) have shown cost effectiveness for 1-time screening of such patients. 36 This screening strategy is only cost effective, however, if only those patients with BE and dysplasia undergo endoscopic surveillance. Furthermore, even using such patient characteristics to focus screening, the number of subjects necessary to screen to detect 1 cancer remains prohibitively high. 37 A primary question, then, is whether we should screen for BE at all. It should be noted that the case of screening for BE or EAC lacks many of the characteristics of a useful screening strategy by established criteria. 38,39 As discussed above, the burden of disease, while increasing, remains small, given the enormous pool of at risk subjects. The preclinical phase cannot be adequately identified or targeted as many patients with BE have no GERD symptoms. Finally, and most importantly, screening has not been sufficiently proven to improve outcomes such as mortality from esophageal cancer. 39 Areas of Uncertainty The benefits of screening and surveillance programs remain unclear. Several studies do show a potential benefit from endoscopic screening and surveillance in BE. Subjects who have their cancer diagnosed as part of a screening and surveillance program are less likely to have nodal involvement, and demonstrate a better 2-year survival than those presenting symptomatically. 28,40 However, such studies showing a benefit from screening and surveillance of patients with BE are largely retrospective and complicated by selection bias, lead time bias, and length bias. In fact, a recent nested casecontrol study performed in the US Veterans Affairs system demonstrated that subjects with adenocarcinoma who had had an upper endoscopy in the 5 years prior to diagnosis did not have significantly different survival than those presenting symptomatically. 41 The best evidence to establish the benefit of screening for BE would be a randomized controlled trial of endoscopic screening in GERD patients, measuring the outcome of esophageal cancer mortality. However, such a trial would be cumbersome and costly; given the rarity of esophageal adenocarcinoma and the long latency time between BE and development of cancer, a randomized trial of BE screening in all persons with GERD or in the general population would require large numbers of participants followed for a long period. Therefore, we must rely on indirect evidence that links screening GERD patients with reduced mortality from esophageal cancer. By applying US Preventative Services Task Force guidelines to the decision to perform endoscopy in this setting, one can see the number of unanswered questions to be addressed prior to understanding the utility of such screening and surveillance programs (Figure 1). 42 Table 1. Prospective Studies Comparing Prevalence of BE In GERD and Non GERD Patients Demonstrating Substantial Prevalence of BE In Subjects Who Do Not Have Typical GERD Symptoms Study Year Prevalence of BE in GERD patients (%) Prevalence of BE in non GERD patients (%) Prevalence of BE in the overall study cohort (%) Gerson et al 33,a 2002 n/a Rex et al Ronkainen et al Ward et al Zagari et al Gerson et al 32,b 2009 n/a 6 6 a Asymptomatic veterans only. b Asymptomatic women only.
3 July 2010 SHOULD GERD PATIENTS BE SCREENED FOR BE? 567 Figure 1. Important questions in considering whether GERD patients should be screened for BE to prevent esophageal adenocarcinoma. Questions labeled with asterisks are either poorly described or currently debated in the medical literature. Based on the US Preventive Health Service Task Force generic framework for screening topics Is there direct evidence that screening for Barrett s esophagus leads to reduced risk of morbidity or mortality from esophageal cancer?* 2. Is there direct evidence that screening for dysplasia in patients with BE leads to reduced risk of morbidity or mortality from esophageal cancer?* 3. Is there direct evidence that treatment of dysplasia leads to reduced risk of morbidity or mortality from esophageal cancer? 4. What is the prevalence of GERD? What is the prevalence of esophageal cancer in persons with GERD? Can a high risk group be identified? 5. What is the prevalence of BE? What is the prevalence of esophageal cancer in persons with BE? Can a high risk group be identified? 6. What is the prevalence of esophageal cancer? Does all esophageal cancer act the same way? Are there indolent forms of the disease?* 7. Can screening tests accurately identify BE? 8. Can screening tests accurately identify dysplasia?* 9. How effective are treatments for dysplasia? Does treatment of dysplasia reduce the risk of esophageal cancer? 10. How effective is treatment of esophageal cancer? Does treatment improve outcomes for people diagnosed by screening vs those diagnosed clinically?* 11. What are the adverse effects of screening for BE in people with GERD?* 12. What are the adverse effects of screening for dysplasia in people with BE?* 13. What are the adverse effects of treatment of dysplasia? 14. What are the adverse effects of treatment of esophageal cancer? Some recommendations for screening and surveillance may show efficacy in study settings but lack effectiveness in the real world. There are standardized techniques for taking biopsies of the esophagus, but clinical practice varies. In both Europe and the United States, professional associations recommend 4 quadrant biopsies every 2 centimeters within a segment of suspected BE. 43,44 However, a significant number of endoscopists fail to utilize proper biopsy technique or even identify standardized landmarks during endoscopy for BE. 45,46 In clinical practice, hiatal hernia, inflammation and tortuosity of the esophagus may make accurate technique difficult. Furthermore, biopsy of a normal gastroesophageal junction may lead to a false positive screen for BE (due to the high prevalence of goblet cells at the normal gastroesophageal junction in those with chronic GERD symptoms) and biopsies performed in the setting of inflammation may falsely identify dysplasia. 47,48 Once biopsies are obtained, expert pathologic assessment is required to accurately interpret BE specimens. Alikhan et al (1999) demonstrated considerable interoperator variability among community pathologists when interpreting standardized BE pathology. 49 High and low grade dysplasia were correctly identified by only 30% and 35% of pathologists, respectively, and many incorrectly identified gastric metaplasia as BE. Expert confirmation of BE pathology is only recommended for dysplastic BE and thus misclassified patients may receive inappropriate surveillance. Additionally, there are costs and risks to screening that are not often factored into the discussion of screening and surveillance programs for BE. These risks become important especially when the disease (esophageal cancer) is rare and the screening population (patients with GERD) is large. Therefore, the potential good done for the very few must outweigh the risks, costs, and inconvenience to the many. While uncommon, EGD has risks associated with sedation, perforation, infection, and bleeding. These small risks become significant when EGD is applied to millions of people to screen for a rare cancer. 18 There may be a risk in labeling patients with BE as well. 50 Quality of life is diminished for patients diagnosed with BE and those participating in surveillance programs compared with population norms. 51,52 Many patients overestimate their cancer risk and add psychological stress that is difficult to quantify. 53 Finally, patients with BE have increased insurance premiums compared with those without BE. 54 Screening for BE with or without subsequent surveillance remains a controversial topic. The current state of technology, available data in the published literature, and growing concern over costs in medical care all raise substantial concerns about the utility of such programs. Several potentially disruptive technologies hold the promise of changing this calculus. Ultrathin transnasal endoscopy may allow screening of unsedated patients, greatly lessening the cost of screening, and allowing higher throughput. 55 Capsule endoscopy or other novel imaging may also obviate the need for per oral endoscopy for screening. 56 Multiple imaging technologies hold the promise to improve our ability to detect dysplasia, perhaps allowing subsequent surveillance intervals to be lengthened or omitted altogether Ablative therapies may allow for intervention that would obviate the need for follow-up endoscopy and may change the natural history and downstream costs associated with the lesion. 60 All of these possibilities are intriguing, and may change our approach to cancer prevention, but the
4 568 CROCKETT ET AL CLINICAL GASTROENTEROLOGY AND HEPATOLOGY Vol. 8, No. 7 Table 2. Recommendations from Published Guidelines Regarding Screening for Barrett s Esophagus Society/organization American Gastroenterological Association American College of Gastroenterology American Society for Gastrointestinal Endoscopy British Society of Gastroenterology United States Preventive Services Taskforce Persons in whom endoscopic screening for BE is recommended Insufficient evidence Insufficient evidence Screening in high risk groups History of GERD 5 years White race Male sex Age 50 Family history of BE and/or esophageal cancer Screening not recommended No guideline potential of the interventions in the screening setting remains unproven. Published Guidelines There are a number of published guidelines that address the question of BE screening among persons with GERD (Table 2). The American Gastroenterological Association (AGA) published a medical position statement on the management of GERD in 2008, which utilized explicit evidentiary methodology. 61 The AGA guidelines determined that there was insufficient evidence to recommend for or against routine upper endoscopy in the setting of chronic GERD symptoms to diminish the risk of death from esophageal cancer. The AGA guidelines also determined that there was insufficient evidence to recommend for or against endoscopic screening for BE and dysplasia in adults 50 years or older with greater than 5 10 years of heartburn to reduce mortality from esophageal adenocarcinoma. The American College of Gastroenterology also published guidelines addressing the management of GERD and BE in 2005 and 2008, respectively. 43,62 These guidelines also recognize that screening for BE is controversial due to the lack of documented impact on esophageal cancer mortality. Similar to the AGA guidelines, the American College of Gastroenterology guidelines report inadequate evidence to recommend routine screening for BE in any specific high risk population (such as GERD patients or older individuals). The American Society for Gastrointestinal Endoscopy (ASGE) published guidelines on the role of endoscopy in BE and GERD in 2006 and 2007, respectively. 44,63 The ASGE recommends that screening for BE should be considered in selected patients with chronic, longstanding GERD. However, the ASGE does not recommend additional screening following a negative initial screening examination. Endoscopy at the time of presentation with GERD symptoms is also recommended for persons at risk of Barrett s esophagus, including patients with a prolonged history of GERD symptoms ( 5 years), white race, male sex, older age ( 50), and family history of BE and/or adenocarcinoma of the esophagus. However, the ASGE graded this recommendation 2C, indicating a very weak recommendation with unclear benefit. The British Society of Gastroenterology guidelines state that endoscopic screening of patients suffering from heartburn in order to detect BE is not recommended. 64 The United States Preventive Services Task Force (USPSTF) does not currently have any published guidelines addressing screening for esophageal cancer. There is perhaps no area in gastroenterology where the clinical practice is more at odds with the published data and guidelines than in endoscopic screening for BE. Although, as noted above, guidelines are either unsupportive or equivocal on such practices, data suggest that the overwhelming majority of gastroenterologists in the US enthusiastically support the practice of screening for BE. 65,66 Interestingly, fear of litigation from missed lesions appears to be a significant motivating factor of screening behavior. 66 Recommendations for this Patient The patient described in the scenario above has typical GERD symptoms, and received appropriate initial management including a trial of lifestyle modification. He is in a high risk category for BE in that he has a history of GERD for over 5 years, is over 50 years of age, and is a white male. However, he does not have any alarm symptoms that would prompt a diagnostic endoscopic exam. A simple algorithm summarizes an approach to BE screening in GERD patients (Figure 2). At Figure 2. Modified diagram for use of endoscopy in the setting of GERD, based on published AGA and ACG guidelines. ACG, American College of Gastroenterology.
5 July 2010 SHOULD GERD PATIENTS BE SCREENED FOR BE? 569 Figure 3. Weighing the potential benefits and harms of screening for Barrett s esophagus among patients with GERD. this time, there is insufficient evidence to recommend routine screening for BE or esophageal cancer in persons with GERD, even those with risk factors for BE, and, based on the evidence and guidelines discussed above, this patient would not require endoscopic screening for BE. It is incumbent on physicians who elect to discuss endoscopic screening with patients to fully inform them of the potential pros and cons of this maneuver, as well as the weak nature of the data supporting endoscopic screening (Figure 3). Summary Whether persons with GERD should be screened for BE is a common question of both primary care physicians and gastroenterologists alike. Current guidelines recommend either no screening or screening only in individuals at high risk of esophageal cancer. Esophageal cancer is a relatively rare entity in patients with heartburn, and the vast majority of patients with GERD are unlikely to benefit from screening for BE. The evidence supporting screening efforts is weak and inconsistent. Therefore, wide scale endoscopic screening in its currently practiced form cannot be recommended on a routine basis. Further developments in technology may make screening more effective and cost effective. Finally, the changing epidemiology of this cancer demands that we revisit this issue frequently, as the value of effective screening would presumably increase as the incidence of esophageal cancer rises. While lack of evidence in favor of endoscopic screening does not indicate lack of efficacy, until more data are available to support this practice, screening efforts might be better directed at interventions with proven benefits. References 1. Locke GR 3rd, Talley NJ, Fett SL, et al. Prevalence and clinical spectrum of gastroesophageal reflux: a population-based study in Olmsted County, Minnesota. Gastroenterology 1997;112: Csendes A, Smok G, Burdiles P, et al. Prevalence of Barrett s esophagus by endoscopy and histologic studies: a prospective evaluation of 306 control subjects and 376 patients with symptoms of gastroesophageal reflux. Dis Esophagus 2000;13: Ronkainen J, Aro P, Storskrubb T, et al. Prevalence of Barrett s esophagus in the general population: an endoscopic study. Gastroenterology 2005;129: Lieberman DA, Oehlke M, Helfand M. Risk factors for Barrett s esophagus in community-based practice. GORGE consortium. Gastroenterology Outcomes Research Group in Endoscopy. Am J Gastroenterol 1997;92: Winters C Jr, Spurling TJ, Chobanian SJ, et al. Barrett s esophagus. A prevalent, occult complication of gastroesophageal reflux disease. Gastroenterology 1987;92: Anderson LA, Murray LJ, Murphy SJ, et al. Mortality in Barrett s oesophagus: results from a population based study. Gut 2003; 52: Eckardt VF, Kanzler G, Bernhard G. Life expectancy and cancer risk in patients with Barrett s esophagus: a prospective controlled investigation. Am J Med 2001;111: Moayyedi P, Burch N, Akhtar-Danesh N, et al. Mortality rates in patients with Barrett s oesophagus. Aliment Pharmacol Ther 2008;27: Hameeteman W, Tytgat GN, Houthoff HJ, et al. Barrett s esophagus: development of dysplasia and adenocarcinoma. Gastroenterology 1989;96: Hamilton SR, Smith RR. The relationship between columnar epithelial dysplasia and invasive adenocarcinoma arising in Barrett s esophagus. Am J Clin Pathol 1987;87: Miros M, Kerlin P, Walker N. Only patients with dysplasia progress to adenocarcinoma in Barrett s oesophagus. Gut 1991; 32: Drewitz DJ, Sampliner RE, Garewal HS. The incidence of adenocarcinoma in Barrett s esophagus: a prospective study of 170 patients followed 4.8 years. Am J Gastroenterol 1997;92: Spechler SJ, Robbins AH, Rubins HB, et al. Adenocarcinoma and Barrett s esophagus. An overrated risk? Gastroenterology 1984; 87: Falk GW. Barrett s esophagus. Gastroenterology 2002;122:
6 570 CROCKETT ET AL CLINICAL GASTROENTEROLOGY AND HEPATOLOGY Vol. 8, No Chow WH, Finkle WD, McLaughlin JK, et al. The relation of gastroesophageal reflux disease and its treatment to adenocarcinomas of the esophagus and gastric cardia. JAMA 1995;274: Farrow DC, Vaughan TL, Sweeney C, et al. Gastroesophageal reflux disease, use of H2 receptor antagonists, and risk of esophageal and gastric cancer. Cancer Causes Control 2000;11: Lagergren J, Bergstrom R, Lindgren A, et al. Symptomatic gastroesophageal reflux as a risk factor for esophageal adenocarcinoma. N Engl J Med 1999;340: Shaheen N, Ransohoff DF. Gastroesophageal reflux, barrett esophagus, and esophageal cancer: scientific review. JAMA 2002;287: SEER Cancer Statistics Review, Bethesda, MD: National Cancer Institute, Bytzer P, Christensen PB, Damkier P, et al. Adenocarcinoma of the esophagus and Barrett s esophagus: a population-based study. Am J Gastroenterol 1999;94: Devesa SS, Blot WJ, Fraumeni JF Jr. Changing patterns in the incidence of esophageal and gastric carcinoma in the United States. Cancer 1998;83: Wei JT, Shaheen N. The changing epidemiology of esophageal adenocarcinoma. Semin Gastrointest Dis 2003;14: Greenstein AJ, Litle VR, Swanson SJ, et al. Racial disparities in esophageal cancer treatment and outcomes. Ann Surg Oncol 2008;15: Cancer Facts & Figures Atlanta, GA: American Cancer Society, Djarv T, Lagergren J, Blazeby JM, et al. Long-term health-related quality of life following surgery for oesophageal cancer. Br J Surg 2008;95: Parekh K, Iannettoni MD. Complications of esophageal resection and reconstruction. Semin Thorac Cardiovasc Surg 2007;19: Shaheen NJ, Crosby MA, Bozymski EM, et al. Is there publication bias in the reporting of cancer risk in Barrett s esophagus? Gastroenterology 2000;119: van Sandick JW, van Lanschot JJ, Kuiken BW, et al. Impact of endoscopic biopsy surveillance of Barrett s oesophagus on pathological stage and clinical outcome of Barrett s carcinoma. Gut 1998;43: Corley DA, Levin TR, Habel LA, et al. Surveillance and survival in Barrett s adenocarcinomas: a population-based study. Gastroenterology 2002;122: Jaspersen D, Kulig M, Labenz J, et al. Prevalence of extraoesophageal manifestations in gastro-oesophageal reflux disease: an analysis based on the ProGERD Study. Aliment Pharmacol Ther 2003;17: Rex DK, Cummings OW, Shaw M, et al. Screening for Barrett s esophagus in colonoscopy patients with and without heartburn. Gastroenterology 2003;125: Gerson LB, Banerjee S. Screening for Barrett s esophagus in asymptomatic women. Gastrointest Endosc 2009;70: Gerson LB, Shetler K, Triadafilopoulos G. Prevalence of Barrett s esophagus in asymptomatic individuals. Gastroenterology 2002; 123: Ward EM, Wolfsen HC, Achem SR, et al. Barrett s esophagus is common in older men and women undergoing screening colonoscopy regardless of reflux symptoms. Am J Gastroenterol 2006; 101: Zagari RM, Fuccio L, Wallander MA, et al. Gastro-oesophageal reflux symptoms, oesophagitis and Barrett s oesophagus in the general population: the Loiano-Monghidoro study. Gut 2008;57: Inadomi JM, Sampliner R, Lagergren J, et al. Screening and surveillance for Barrett esophagus in high-risk groups: a cost-utility analysis. Ann Intern Med 2003;138: Lagergren J, Ye W, Bergstrom R, et al. Utility of endoscopic screening for upper gastrointestinal adenocarcinoma. JAMA 2000; 284: Sackett D, Haynes R, Guyatt G, et al. Early diagnosis in clinical epidemiology: a basic science for clinical medicine. Boston, MA: Little, Brown, Dellon ES, Shaheen NJ. Does screening for Barrett s esophagus and adenocarcinoma of the esophagus prolong survival? J Clin Oncol 2005;23: Peters JH, Clark GW, Ireland AP, et al. Outcome of adenocarcinoma arising in Barrett s esophagus in endoscopically surveyed and nonsurveyed patients. J Thorac Cardiovasc Surg 1994;108: ; discussion Rubenstein JH, Sonnenberg A, Davis J, et al. Effect of a prior endoscopy on outcomes of esophageal adenocarcinoma among United States veterans. Gastrointest Endosc 2008;68: Harris RP, Helfand M, Woolf SH, et al. Current methods of the US Preventive Services Task Force: a review of the process. Am J Prev Med 2001;20: Wang KK, Sampliner RE. Updated guidelines 2008 for the diagnosis, surveillance and therapy of Barrett s esophagus. Am J Gastroenterol 2008;103: Hirota WK, Zuckerman MJ, Adler DG, et al. ASGE guideline: the role of endoscopy in the surveillance of premalignant conditions of the upper GI tract. Gastrointest Endosc 2006;63: Amamra N, Touzet S, Colin C, et al. Current practice compared with the international guidelines: endoscopic surveillance of Barrett s esophagus. J Eval Clin Pract 2007;13: Ofman JJ, Shaheen NJ, Desai AA, et al. The quality of care in Barrett s esophagus: endoscopist and pathologist practices. Am J Gastroenterol 2001;96: Spechler SJ, Zeroogian JM, Antonioli DA, et al. Prevalence of metaplasia at the gastro-oesophageal junction. Lancet 1994; 344: Sharma P. Low-grade dysplasia in Barrett s esophagus. Gastroenterology 2004;127: Alikhan M, Rex D, Khan A, et al. Variable pathologic interpretation of columnar lined esophagus by general pathologists in community practice. Gastrointest Endosc 1999;50: Rubenstein JH, Inadomi JM. Defining a clinically significant adverse impact of diagnosing Barrett s esophagus. J Clin Gastroenterol 2006;40: Crockett SD, Lippmann QK, Dellon ES, et al. Health-related quality of life in patients with Barrett s esophagus: a systematic review. Clin Gastroenterol Hepatol 2009;7: Fisher D, Jeffreys A, Bosworth H, et al. Quality of life in patients with Barrett s esophagus undergoing surveillance. Am J Gastroenterol 2002;97: Shaheen NJ, Green B, Medapalli RK, et al. The perception of cancer risk in patients with prevalent Barrett s esophagus enrolled in an endoscopic surveillance program. Gastroenterology 2005;129: Shaheen NJ, Dulai GS, Ascher B, et al. Effect of a new diagnosis of Barrett s esophagus on insurance status. Am J Gastroenterol 2005;100: Preiss C, Charton JP, Schumacher B, et al. A randomized trial of unsedated transnasal small-caliber esophagogastroduodenoscopy (EGD) versus peroral small-caliber EGD versus conventional EGD. Endoscopy 2003;35: Bhardwaj A, Hollenbeak CS, Pooran N, et al. A meta-analysis of the diagnostic accuracy of esophageal capsule endoscopy for Barrett s esophagus in patients with gastroesophageal reflux disease. Am J Gastroenterol 2009;104:
7 July 2010 SHOULD GERD PATIENTS BE SCREENED FOR BE? Wolfsen HC. New technologies for imaging of Barrett s esophagus. Surg Oncol Clin N Am 2009;18: Haringsma J. Barrett s oesophagus: new diagnostic and therapeutic techniques. Scand J Gastroenterol Suppl 2002: Isenberg G, Sivak MV Jr, Chak A, et al. Accuracy of endoscopic optical coherence tomography in the detection of dysplasia in Barrett s esophagus: a prospective, double-blinded study. Gastrointest Endosc 2005;62: Inadomi JM, Somsouk M, Madanick RD, et al. A cost-utility analysis of ablative therapy for Barrett s esophagus. Gastroenterology 2009;136: , e1 e Kahrilas PJ, Shaheen NJ, Vaezi MF, et al. American Gastroenterological Association medical position statement on the management of gastroesophageal reflux disease. Gastroenterology 2008;135: , 1391, e1 e DeVault KR, Castell DO. Updated guidelines for the diagnosis and treatment of gastroesophageal reflux disease. Am J Gastroenterol 2005;100: Lichtenstein DR, Cash BD, Davila R, et al. Role of endoscopy in the management of GERD. Gastrointest Endosc 2007;66: Playford RJ. New British Society of Gastroenterology (BSG) guidelines for the diagnosis and management of Barrett s oesophagus. Gut 2006;55: Lin OS, Mannava S, Hwang KL, et al. Reasons for current practices in managing Barrett s esophagus. Dis Esophagus 2002;15: Rubenstein JH, Saini SD, Kuhn L, et al. Influence of malpractice history on the practice of screening and surveillance for Barrett s esophagus. Am J Gastroenterol 2008;103: Reprint requests Address requests for reprints to: Nicholas J. Shaheen, MD, MPH, Department of Medicine, Center for Esophageal Diseases and Swallowing, University of North Carolina School of Medicine, CB # 7080, Chapel Hill, North Carolina nshaheen@med.unc.edu; fax: (919) Conflicts of interest The authors disclose no conflicts.
Accepted Manuscript. CGH Editorial: Sound the Alarm for Barrett s Screening! Tarek Sawas, M.D., M.P.H., David A. Katzka, M.D
 Accepted Manuscript CGH Editorial: Sound the Alarm for Barrett s Screening! Tarek Sawas, M.D., M.P.H., David A. Katzka, M.D PII: S1542-3565(18)31093-0 DOI: 10.1016/j.cgh.2018.10.010 Reference: YJCGH 56132
Accepted Manuscript CGH Editorial: Sound the Alarm for Barrett s Screening! Tarek Sawas, M.D., M.P.H., David A. Katzka, M.D PII: S1542-3565(18)31093-0 DOI: 10.1016/j.cgh.2018.10.010 Reference: YJCGH 56132
Barrett s Esophagus. Abdul Sami Khan, M.D. Gastroenterologist Aurora Healthcare Burlington, Elkhorn, Lake Geneva, WI
 Barrett s Esophagus Abdul Sami Khan, M.D. Gastroenterologist Aurora Healthcare Burlington, Elkhorn, Lake Geneva, WI A 58 year-old, obese white man has had heartburn for more than 20 years. He read a magazine
Barrett s Esophagus Abdul Sami Khan, M.D. Gastroenterologist Aurora Healthcare Burlington, Elkhorn, Lake Geneva, WI A 58 year-old, obese white man has had heartburn for more than 20 years. He read a magazine
Current Management: Role of Radiofrequency Ablation
 Esophageal Adenocarcinoma And Barrett s Esophagus: Current Management: Role of Radiofrequency Ablation Ketan Kulkarni, MD Regional Gastroenterology Associates of Lancaster INTRODUCTION The prognosis of
Esophageal Adenocarcinoma And Barrett s Esophagus: Current Management: Role of Radiofrequency Ablation Ketan Kulkarni, MD Regional Gastroenterology Associates of Lancaster INTRODUCTION The prognosis of
In 1998, the American College of Gastroenterology issued ALIMENTARY TRACT
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2012;10:1232 1236 ALIMENTARY TRACT Effects of Dropping the Requirement for Goblet Cells From the Diagnosis of Barrett s Esophagus MARIA WESTERHOFF,* LINDSEY HOVAN,
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2012;10:1232 1236 ALIMENTARY TRACT Effects of Dropping the Requirement for Goblet Cells From the Diagnosis of Barrett s Esophagus MARIA WESTERHOFF,* LINDSEY HOVAN,
Barrett s Esophagus: Old Dog, New Tricks
 Barrett s Esophagus: Old Dog, New Tricks Stuart Jon Spechler, M.D. Chief, Division of Gastroenterology, VA North Texas Healthcare System; Co-Director, Esophageal Diseases Center, Professor of Medicine,
Barrett s Esophagus: Old Dog, New Tricks Stuart Jon Spechler, M.D. Chief, Division of Gastroenterology, VA North Texas Healthcare System; Co-Director, Esophageal Diseases Center, Professor of Medicine,
ACG Clinical Guideline: Diagnosis and Management of Barrett s Esophagus
 ACG Clinical Guideline: Diagnosis and Management of Barrett s Esophagus Nicholas J. Shaheen, MD, MPH, FACG 1, Gary W. Falk, MD, MS, FACG 2, Prasad G. Iyer, MD, MSc, FACG 3 and Lauren Gerson, MD, MSc, FACG
ACG Clinical Guideline: Diagnosis and Management of Barrett s Esophagus Nicholas J. Shaheen, MD, MPH, FACG 1, Gary W. Falk, MD, MS, FACG 2, Prasad G. Iyer, MD, MSc, FACG 3 and Lauren Gerson, MD, MSc, FACG
Everything Esophagus: Barrett s Esophagus. Nicholas Shaheen, MD, MPH Center for Esophageal Diseases and Swallowing University of North Carolina
 Everything Esophagus: Barrett s Esophagus Nicholas Shaheen, MD, MPH Center for Esophageal Diseases and Swallowing University of North Carolina The Most Important Thing Stayed the Same Adenocarcinoma A
Everything Esophagus: Barrett s Esophagus Nicholas Shaheen, MD, MPH Center for Esophageal Diseases and Swallowing University of North Carolina The Most Important Thing Stayed the Same Adenocarcinoma A
The incidence rates of adenocarcinoma of the esophagus. The Risk of Esophageal Adenocarcinoma After Antireflux Surgery. Methods Study Design
 GASTROENTEROLOGY 2010;138:1297 1301 The Risk of Esophageal Adenocarcinoma After Antireflux Surgery JESPER LAGERGREN,* WEIMIN YE,*, PERNILLA LAGERGREN,* and YUNXIA LU*, *Upper Gastrointestinal Research,
GASTROENTEROLOGY 2010;138:1297 1301 The Risk of Esophageal Adenocarcinoma After Antireflux Surgery JESPER LAGERGREN,* WEIMIN YE,*, PERNILLA LAGERGREN,* and YUNXIA LU*, *Upper Gastrointestinal Research,
New Developments in the Endoscopic Diagnosis and Management of Barrett s Esophagus
 New Developments in the Endoscopic Diagnosis and Management of Barrett s Esophagus Prateek Sharma, MD Key Clinical Management Points: Endoscopic recognition of a columnar lined distal esophagus is crucial
New Developments in the Endoscopic Diagnosis and Management of Barrett s Esophagus Prateek Sharma, MD Key Clinical Management Points: Endoscopic recognition of a columnar lined distal esophagus is crucial
Definition of GERD American College of Gastroenterology
 Definition of GERD American College of Gastroenterology GERD is defined as chronic symptoms or mucosal damage produced by the abnormal reflux of gastric contents into the esophagus DeVault et al. Am J
Definition of GERD American College of Gastroenterology GERD is defined as chronic symptoms or mucosal damage produced by the abnormal reflux of gastric contents into the esophagus DeVault et al. Am J
Relative risk of dysplasia for patients with intestinal metaplasia in the distal oesophagus and in the gastric cardia
 Gut 2000;46:9 13 9 PAPERS Division of Gastroenterology, University of Kansas, VA Medical Center, Kansas City, Missouri, USA P Sharma A P Weston Department of Pathology, VA Medical Center, Kansas M Topalovski
Gut 2000;46:9 13 9 PAPERS Division of Gastroenterology, University of Kansas, VA Medical Center, Kansas City, Missouri, USA P Sharma A P Weston Department of Pathology, VA Medical Center, Kansas M Topalovski
Is intestinal metaplasia a necessary precursor lesion for adenocarcinomas of the distal esophagus, gastroesophageal junction and gastric cardia?
 Diseases of the Esophagus (2007) 20, 36 41 DOI: 10.1111/j.1442-2050.2007.00638.x Blackwell Publishing Asia Original article Is intestinal metaplasia a necessary precursor lesion for adenocarcinomas of
Diseases of the Esophagus (2007) 20, 36 41 DOI: 10.1111/j.1442-2050.2007.00638.x Blackwell Publishing Asia Original article Is intestinal metaplasia a necessary precursor lesion for adenocarcinomas of
Joel A. Ricci, MD SUNY Downstate Medical Center Department of Surgery
 Joel A. Ricci, MD SUNY Downstate Medical Center Department of Surgery Norman Barrett (1950) described the esophagus as: that part of the foregut, distal to the cricopharyngeal sphincter, which is lined
Joel A. Ricci, MD SUNY Downstate Medical Center Department of Surgery Norman Barrett (1950) described the esophagus as: that part of the foregut, distal to the cricopharyngeal sphincter, which is lined
Adherence to Surveillance Guidelines in Nondysplastic Barrett s Esophagus.
 Adherence to Surveillance Guidelines in Nondysplastic Barrett s Esophagus. Kunal S. Dalal, MD 1 ; Jessica Coffing, MPH 2 ; Thomas F. Imperiale, MD 1 Affiliations: 1 Indiana University School of Medicine,
Adherence to Surveillance Guidelines in Nondysplastic Barrett s Esophagus. Kunal S. Dalal, MD 1 ; Jessica Coffing, MPH 2 ; Thomas F. Imperiale, MD 1 Affiliations: 1 Indiana University School of Medicine,
Current Management of Low-Grade Dysplasia in Barrett Esophagus
 Current Management of Low-Grade Dysplasia in Barrett Esophagus Gary W. Falk, MD, MS Dr Falk is a professor of medicine in the Division of Gastroenterology at the University of Pennsylvania Perelman School
Current Management of Low-Grade Dysplasia in Barrett Esophagus Gary W. Falk, MD, MS Dr Falk is a professor of medicine in the Division of Gastroenterology at the University of Pennsylvania Perelman School
Symptoms suggestive of gastroesophageal reflux disease. Gastroesophageal Reflux Among Different Racial Groups in the United States
 GASTROENTEROLOGY 2004;126:1692 1699 Gastroesophageal Reflux Among Different Racial Groups in the United States HASHEM B. EL SERAG,*, NANCY J. PETERSEN, JUNAIA CARTER, DAVID Y. GRAHAM,* PETER RICHARDSON,
GASTROENTEROLOGY 2004;126:1692 1699 Gastroesophageal Reflux Among Different Racial Groups in the United States HASHEM B. EL SERAG,*, NANCY J. PETERSEN, JUNAIA CARTER, DAVID Y. GRAHAM,* PETER RICHARDSON,
The incidence of esophageal adenocarcinoma has been rising rapidly over the past few
 Gastroesophageal Reflux Disease, Barrett Esophagus, and Esophageal Adenocarcinoma John T. Chang, MD; David A. Katzka, MD REVIEW ARTICLE The incidence of esophageal adenocarcinoma has been rising rapidly
Gastroesophageal Reflux Disease, Barrett Esophagus, and Esophageal Adenocarcinoma John T. Chang, MD; David A. Katzka, MD REVIEW ARTICLE The incidence of esophageal adenocarcinoma has been rising rapidly
Barrett s Esophagus: What to Do for No Dysplasia, LGD, and HGD?
 Barrett s Esophagus: What to Do for No Dysplasia, LGD, and HGD? Nicholas Shaheen, MD, MPH Center for Esophageal Diseases and Swallowing University of North Carolina 1 Outline What are the risks of progression
Barrett s Esophagus: What to Do for No Dysplasia, LGD, and HGD? Nicholas Shaheen, MD, MPH Center for Esophageal Diseases and Swallowing University of North Carolina 1 Outline What are the risks of progression
Present Day Management of Barrett s Esophagus
 Slide 1 Present Day Management of Barrett s Esophagus Kinnari R. Kher, M.D. Slide 2 Goals Risk factors for development of Barrett s esophagus Risks for progression to Esophageal Adenocarcinoma Current
Slide 1 Present Day Management of Barrett s Esophagus Kinnari R. Kher, M.D. Slide 2 Goals Risk factors for development of Barrett s esophagus Risks for progression to Esophageal Adenocarcinoma Current
Management of Barrett s Esophagus. Case Presentation
 Management of Barrett s Esophagus Lauren B. Gerson MD, MSc Associate Clinical Professor, UCSF Director of Clinical Research Gastroenterology Fellowship Program California Pacific Medical Center San Francisco,
Management of Barrett s Esophagus Lauren B. Gerson MD, MSc Associate Clinical Professor, UCSF Director of Clinical Research Gastroenterology Fellowship Program California Pacific Medical Center San Francisco,
Learning Objectives:
 Crescent City GI Update 2018 Ochsner Clinic, NOLA Optimizing Endoscopic Evaluation of Barrett s Esophagus What Should I Do in My Practice? Gregory G. Ginsberg, M.D. Professor of Medicine University of
Crescent City GI Update 2018 Ochsner Clinic, NOLA Optimizing Endoscopic Evaluation of Barrett s Esophagus What Should I Do in My Practice? Gregory G. Ginsberg, M.D. Professor of Medicine University of
History. Prevalence at Endoscopy. Prevalence and Reflux Sx. Prevalence at Endoscopy. Barrett s Esophagus: Controversy and Management
 Barrett s Esophagus: Controversy and Management History Norman Barrett (1950) Chronic Peptic Ulcer of the Oesophagus and Oesophagitis Allison and Johnstone (1953) The Oesophagus Lined with Gastric Mucous
Barrett s Esophagus: Controversy and Management History Norman Barrett (1950) Chronic Peptic Ulcer of the Oesophagus and Oesophagitis Allison and Johnstone (1953) The Oesophagus Lined with Gastric Mucous
Barrett s Esophagus: State of the Art. Food Getting Stuck
 Barrett s Esophagus: State of the Art Nicholas J. Shaheen, MD, MPH Center for Esophageal Diseases and Swallowing University of North Carolina SOM Food Getting Stuck 73-year-old retired Wilmington police
Barrett s Esophagus: State of the Art Nicholas J. Shaheen, MD, MPH Center for Esophageal Diseases and Swallowing University of North Carolina SOM Food Getting Stuck 73-year-old retired Wilmington police
Frequency of Barrett Esophagus in Patients with Symptoms of Gastroesophageal Reflux Disease
 Original Article Frequency of Barrett Esophagus in Patients with Symptoms of Gastroesophageal Reflux Disease From Military Hospital, Rawalpindi Obaid Ullah Khan, Abdul Rasheed Correspondence: Dr. Abdul
Original Article Frequency of Barrett Esophagus in Patients with Symptoms of Gastroesophageal Reflux Disease From Military Hospital, Rawalpindi Obaid Ullah Khan, Abdul Rasheed Correspondence: Dr. Abdul
Meta-analysis: the association of oesophageal adenocarcinoma with symptoms of gastro-oesophageal reflux
 Alimentary Pharmacology and Therapeutics Meta-analysis: the association of oesophageal adenocarcinoma with symptoms of gastro-oesophageal reflux J. H. Rubenstein*, & J. B. Taylor à *Veterans Affairs Center
Alimentary Pharmacology and Therapeutics Meta-analysis: the association of oesophageal adenocarcinoma with symptoms of gastro-oesophageal reflux J. H. Rubenstein*, & J. B. Taylor à *Veterans Affairs Center
Barrett's Esophagus: Sorting Out the Controversy
 Barrett's Esophagus: Sorting Out the Controversy Learning Objectives 1. Identify the challenges in screening for Barrett s esophagus 2. Demonstrate comprehension of the risk of progression of Barrett s
Barrett's Esophagus: Sorting Out the Controversy Learning Objectives 1. Identify the challenges in screening for Barrett s esophagus 2. Demonstrate comprehension of the risk of progression of Barrett s
This medical position statement considers a series of
 GASTROENTEROLOGY 2011;140:1084 1091 American Gastroenterological Association Medical Position Statement on the Management of Barrett s Esophagus The Institute Medical Position Panel consisted of the authors
GASTROENTEROLOGY 2011;140:1084 1091 American Gastroenterological Association Medical Position Statement on the Management of Barrett s Esophagus The Institute Medical Position Panel consisted of the authors
Current challenges in Barrett s esophagus
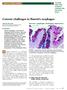 MEDICAL GRAND ROUNDS TAKE-HOME POINTS FROM LECTURES BY CLEVELAND CLINIC AND VISITING FACULTY Current challenges in Barrett s esophagus GARY W. FALK, MD * Director, Center for Swallowing and Esophageal
MEDICAL GRAND ROUNDS TAKE-HOME POINTS FROM LECTURES BY CLEVELAND CLINIC AND VISITING FACULTY Current challenges in Barrett s esophagus GARY W. FALK, MD * Director, Center for Swallowing and Esophageal
Barrett s esophagus. Barrett s neoplasia treatment trends
 Options for endoscopic treatment of Barrett s esophagus Patrick S. Yachimski, MD MPH Director of Pancreatobiliary Endoscopy Assistant Professor of Medicine Division of Gastroenterology, Hepatology & Nutrition
Options for endoscopic treatment of Barrett s esophagus Patrick S. Yachimski, MD MPH Director of Pancreatobiliary Endoscopy Assistant Professor of Medicine Division of Gastroenterology, Hepatology & Nutrition
Screening of Barrett: Is it cost-effective? Is there a high-risk population? T Ponchon Ed. Herriot Hospital Lyon, France
 Screening of Barrett: Is it cost-effective? Is there a high-risk population? T Ponchon Ed. Herriot Hospital Lyon, France Barrett s esophagus (BE) is an acquired condition in which the normal squamous epithelium
Screening of Barrett: Is it cost-effective? Is there a high-risk population? T Ponchon Ed. Herriot Hospital Lyon, France Barrett s esophagus (BE) is an acquired condition in which the normal squamous epithelium
Is Radiofrequency Ablation Effective In Treating Barrett s Esophagus Patients with High-Grade Dysplasia?
 Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 12-2016 Is Radiofrequency Ablation Effective
Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 12-2016 Is Radiofrequency Ablation Effective
T he incidence of adenocarcinoma of the oesophagus (AC)
 162 OESOPHAGUS Increasing incidence of Barrett s oesophagus in the general population E M van Soest, J P Dieleman, P D Siersema, M C J M Sturkenboom, E J Kuipers... See end of article for authors affiliations...
162 OESOPHAGUS Increasing incidence of Barrett s oesophagus in the general population E M van Soest, J P Dieleman, P D Siersema, M C J M Sturkenboom, E J Kuipers... See end of article for authors affiliations...
Achalasia is a rare disease with an annual incidence estimated REVIEWS. Erroneous Diagnosis of Gastroesophageal Reflux Disease in Achalasia
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2011;9:1020 1024 REVIEWS Erroneous Diagnosis of Gastroesophageal Reflux Disease in Achalasia BOUDEWIJN F. KESSING, ALBERT J. BREDENOORD, and ANDRÉ J. P. M. SMOUT
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2011;9:1020 1024 REVIEWS Erroneous Diagnosis of Gastroesophageal Reflux Disease in Achalasia BOUDEWIJN F. KESSING, ALBERT J. BREDENOORD, and ANDRÉ J. P. M. SMOUT
Hold the Wrap! There is so much more to be done!
 Hold the Wrap! There is so much more to be done! (Well, a few things that can be done.) (Well, not all that much, really ) (But Blair has never killed anyone with a PPI!) Nicholas Shaheen, MD, MPH Center
Hold the Wrap! There is so much more to be done! (Well, a few things that can be done.) (Well, not all that much, really ) (But Blair has never killed anyone with a PPI!) Nicholas Shaheen, MD, MPH Center
Barrett s Esophagus in Women: Demographic Features and Progression to High-Grade Dysplasia and Cancer
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:1089 1094 Barrett s Esophagus in Women: Demographic Features and Progression to High-Grade Dysplasia and Cancer GARY W. FALK,* PRASHANTHI N. THOTA,* JOEL
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:1089 1094 Barrett s Esophagus in Women: Demographic Features and Progression to High-Grade Dysplasia and Cancer GARY W. FALK,* PRASHANTHI N. THOTA,* JOEL
LIST OF ABBREVIATIONS
 Gastroenter oenterology 2005 Royal College of Physicians of Edinburgh Screening and surveillance for upper and lower gastrointestinal cancer JN Plevris Consultant Gastroenterologist and Honorary Senior
Gastroenter oenterology 2005 Royal College of Physicians of Edinburgh Screening and surveillance for upper and lower gastrointestinal cancer JN Plevris Consultant Gastroenterologist and Honorary Senior
P the esophagus may differ from those of squamous
 Incidence of Cancer of the Esophagus in the US by Histologic Type PAUL c. YANG, MD, MPH, AND SCOTT DAVIS, PHD' Data from nine US population-based cancer registries participating in the Surveillance, Epidemiology,
Incidence of Cancer of the Esophagus in the US by Histologic Type PAUL c. YANG, MD, MPH, AND SCOTT DAVIS, PHD' Data from nine US population-based cancer registries participating in the Surveillance, Epidemiology,
The Impact of Gender on the Symptom Presentation and Life Quality of Patients with Erosive Esophagitis and Non-Erosive Reflux Disease
 ARC Journal of Hepatology and Gastroenterology Volume 1, Issue 1, 2016, PP 3-8 www.arcjournals.org The Impact of Gender on the Symptom Presentation and Life Quality of Patients with Erosive Esophagitis
ARC Journal of Hepatology and Gastroenterology Volume 1, Issue 1, 2016, PP 3-8 www.arcjournals.org The Impact of Gender on the Symptom Presentation and Life Quality of Patients with Erosive Esophagitis
Photodynamic Therapy for High Grade Esophageal Dysplasia. California Technology Assessment Forum
 TITLE: AUTHOR: PUBLISHER NAME: Photodynamic Therapy for High Grade Esophageal Dysplasia Jeffrey A. Tice, M.D. Assistant Adjunct Professor of Medicine Division of General Internal Medicine Department of
TITLE: AUTHOR: PUBLISHER NAME: Photodynamic Therapy for High Grade Esophageal Dysplasia Jeffrey A. Tice, M.D. Assistant Adjunct Professor of Medicine Division of General Internal Medicine Department of
Identifying Intestinal Metaplasia at the Squamocolumnar Junction by Using Optical Coherence Tomography
 Identifying Intestinal Metaplasia at the Squamocolumnar Junction by Using Optical Coherence Tomography The Harvard community has made this article openly available. Please share how this access benefits
Identifying Intestinal Metaplasia at the Squamocolumnar Junction by Using Optical Coherence Tomography The Harvard community has made this article openly available. Please share how this access benefits
Barrett s Oesophagus Information Leaflet THE DIGESTIVE SYSTEM. gutscharity.org.
 THE DIGESTIVE SYSTEM http://healthfavo.com/digestive-system-for-kids.html This factsheet is about Barrett s Oesophagus Barrett s Oesophagus is the term used for a pre-cancerous condition where the normal
THE DIGESTIVE SYSTEM http://healthfavo.com/digestive-system-for-kids.html This factsheet is about Barrett s Oesophagus Barrett s Oesophagus is the term used for a pre-cancerous condition where the normal
Barrett s esophagus (BE), originally described by Norman REVIEW
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:613 623 REVIEW Health-Related Quality of Life in Patients With Barrett s Esophagus: A Systematic Review SETH D. CROCKETT,*, QUINN K. LIPPMANN,* EVAN S. DELLON,*,
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:613 623 REVIEW Health-Related Quality of Life in Patients With Barrett s Esophagus: A Systematic Review SETH D. CROCKETT,*, QUINN K. LIPPMANN,* EVAN S. DELLON,*,
Barrett s Esophagus. Radiofrequency Ablation with the HALO Technology A Reference Book
 Radiofrequency Ablation with the HALO Technology A Reference Book 540 Oakmead Parkway, Sunnyvale, CA 94085 What is Barrett s esophagus? Barrett s esophagus is a change that occurs within the cellular lining
Radiofrequency Ablation with the HALO Technology A Reference Book 540 Oakmead Parkway, Sunnyvale, CA 94085 What is Barrett s esophagus? Barrett s esophagus is a change that occurs within the cellular lining
During the past 30 years, the incidence of esophageal ORIGINAL ARTICLES
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2006;4:38 43 ORIGINAL ARTICLES Optical Coherence Tomography to Identify Intramucosal Carcinoma and High-Grade Dysplasia in Barrett s Esophagus JOHN A. EVANS,* JOHN
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2006;4:38 43 ORIGINAL ARTICLES Optical Coherence Tomography to Identify Intramucosal Carcinoma and High-Grade Dysplasia in Barrett s Esophagus JOHN A. EVANS,* JOHN
Hiatal Hernias and Barrett s esophagus. Dr Sajida Ahad Mercy General Surgery
 Hiatal Hernias and Barrett s esophagus Dr Sajida Ahad Mercy General Surgery Objectives Identify the use of different diagnostic modalities for hiatal hernias List the different types of hiatal hernias
Hiatal Hernias and Barrett s esophagus Dr Sajida Ahad Mercy General Surgery Objectives Identify the use of different diagnostic modalities for hiatal hernias List the different types of hiatal hernias
Management of Barrett s: From Imaging to Resection
 Management of Barrett s: From Imaging to Resection Michael Wallace, MD, MPH, FACG Professor of Medicine Mayo Clinic Florida Goals of Endoscopic Evaluation in Barrett s Detect Barrett s and dysplasia Reduce/eliminate
Management of Barrett s: From Imaging to Resection Michael Wallace, MD, MPH, FACG Professor of Medicine Mayo Clinic Florida Goals of Endoscopic Evaluation in Barrett s Detect Barrett s and dysplasia Reduce/eliminate
What s New in the Management of Esophageal Disease
 What s New in the Management of Esophageal Disease Philip O. Katz, MD Chairman, Division of Gastroenterology Einstein Medical Center Philadelphia Clinical Professor of Medicine Jefferson Medical College
What s New in the Management of Esophageal Disease Philip O. Katz, MD Chairman, Division of Gastroenterology Einstein Medical Center Philadelphia Clinical Professor of Medicine Jefferson Medical College
ORIGINAL ARTICLE. Adenocarcinoma of the Esophagus With and Without Barrett Mucosa
 ORIGINAL ARTICLE Adenocarcinoma of the Esophagus With and Without Barrett Mucosa Michael S. Sabel, MD; Kate Pastore, MD; Hannah Toon, MD; Judy L. Smith, MD Hypothesis: Previous studies have demonstrated
ORIGINAL ARTICLE Adenocarcinoma of the Esophagus With and Without Barrett Mucosa Michael S. Sabel, MD; Kate Pastore, MD; Hannah Toon, MD; Judy L. Smith, MD Hypothesis: Previous studies have demonstrated
THE AMERICAN JOURNAL OF GASTROENTEROLOGY Vol. 97, No. 1, by Am. Coll. of Gastroenterology ISSN /02/$22.00
 THE AMERICAN JOURNAL OF GASTROENTEROLOGY Vol. 97, No. 1, 2002 2002 by Am. Coll. of Gastroenterology ISSN 0002-9270/02/$22.00 Published by Elsevier Science Inc. PII S0002-9270(01)03982-X ORIGINAL CONTRIBUTIONS
THE AMERICAN JOURNAL OF GASTROENTEROLOGY Vol. 97, No. 1, 2002 2002 by Am. Coll. of Gastroenterology ISSN 0002-9270/02/$22.00 Published by Elsevier Science Inc. PII S0002-9270(01)03982-X ORIGINAL CONTRIBUTIONS
Proton Pump Inhibitors Are Associated with Reduced Incidence of Dysplasia in Barrett s Esophagus
 American Journal of Gastroenterology ISSN 0002-9270 C 2004 by Am. Coll. of Gastroenterology doi: 10.1111/j.1572-0241.2004.30228.x Published by Blackwell Publishing ORIGINAL CONTRIBUTIONS Proton Pump Inhibitors
American Journal of Gastroenterology ISSN 0002-9270 C 2004 by Am. Coll. of Gastroenterology doi: 10.1111/j.1572-0241.2004.30228.x Published by Blackwell Publishing ORIGINAL CONTRIBUTIONS Proton Pump Inhibitors
AGA SECTION. Gastroenterology 2016;150:
 Gastroenterology 2016;150:1026 1030 April 2016 AGA Section 1027 Procedural intervention (3) Upper endoscopy indications 3 6 Non-response of symptoms to a 4 8 week empiric trial of twice-daily PPI Troublesome
Gastroenterology 2016;150:1026 1030 April 2016 AGA Section 1027 Procedural intervention (3) Upper endoscopy indications 3 6 Non-response of symptoms to a 4 8 week empiric trial of twice-daily PPI Troublesome
Histopathology of Endoscopic Resection Specimens from Barrett's Esophagus
 Histopathology of Endoscopic Resection Specimens from Barrett's Esophagus Br J Surg 38 oct. 1950 Definition of Barrett's esophagus A change in the esophageal epithelium of any length that can be recognized
Histopathology of Endoscopic Resection Specimens from Barrett's Esophagus Br J Surg 38 oct. 1950 Definition of Barrett's esophagus A change in the esophageal epithelium of any length that can be recognized
1. Introduction. Correspondence should be addressed to Wei-Chen Tai; Received 29 May 2013; Accepted 5 July 2013
 Gastroenterology Research and Practice Volume 2013, Article ID 480325, 6 pages http://dx.doi.org/10.1155/2013/480325 Clinical Study The Frequencies of Gastroesophageal and Extragastroesophageal Symptoms
Gastroenterology Research and Practice Volume 2013, Article ID 480325, 6 pages http://dx.doi.org/10.1155/2013/480325 Clinical Study The Frequencies of Gastroesophageal and Extragastroesophageal Symptoms
Barrett s esophagus (BE), a known complication of chronic
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2011;9:220 227 Patients With Nondysplastic Barrett s Esophagus Have Low Risks for Developing Dysplasia or Esophageal Adenocarcinoma SACHIN WANI,* GARY FALK, MATTHEW
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2011;9:220 227 Patients With Nondysplastic Barrett s Esophagus Have Low Risks for Developing Dysplasia or Esophageal Adenocarcinoma SACHIN WANI,* GARY FALK, MATTHEW
Barrett esophagus. Bible class Inselspital
 Barrett esophagus Bible class Inselspital 2015.08.10 Guidelines Definition? BSG: ACG: Definition? BSG: ACG: What are the arguments for and against IM as prerequisite for the Dg? What are the arguments
Barrett esophagus Bible class Inselspital 2015.08.10 Guidelines Definition? BSG: ACG: Definition? BSG: ACG: What are the arguments for and against IM as prerequisite for the Dg? What are the arguments
The increasing incidence of esophageal adenocarcinoma
 GASTROENTEROLOGY 2004;127:310 330 A Critical Review of the Diagnosis and Management of Barrett s Esophagus: The AGA Chicago Workshop PRATEEK SHARMA,* KENNETH MCQUAID, JOHN DENT, M. BRIAN FENNERTY, RICHARD
GASTROENTEROLOGY 2004;127:310 330 A Critical Review of the Diagnosis and Management of Barrett s Esophagus: The AGA Chicago Workshop PRATEEK SHARMA,* KENNETH MCQUAID, JOHN DENT, M. BRIAN FENNERTY, RICHARD
Barrett s Esophagus. lining of the lower esophagus that bears his name (i.e., Barrett's esophagus). We now
 Shamika Johnson Anatomy & Physiology 206 April 20, 2010 Barrett s Esophagus What is Barrett s Esophagus? Norman Barrett was a pathologist. In 1950, he described an abnormality in the lining of the lower
Shamika Johnson Anatomy & Physiology 206 April 20, 2010 Barrett s Esophagus What is Barrett s Esophagus? Norman Barrett was a pathologist. In 1950, he described an abnormality in the lining of the lower
July 19, Division of Dockets Management Food and Drug Administration 5630 Fishers Lane Room 1061, HFA-305 Rockville, Maryland 20852
 July 19, 2017 Division of Dockets Management Food and Drug Administration 5630 Fishers Lane Room 1061, HFA-305 Rockville, Maryland 20852 Re: Comments on Citizen s Petition #FDA-2017-P-2733 Herein, the
July 19, 2017 Division of Dockets Management Food and Drug Administration 5630 Fishers Lane Room 1061, HFA-305 Rockville, Maryland 20852 Re: Comments on Citizen s Petition #FDA-2017-P-2733 Herein, the
The relationship between length of Barrett s oesophagus mucosa and body mass index
 Alimentary Pharmacology and Therapeutics The relationship between length of Barrett s oesophagus mucosa and body mass index J. Abdallah*, C. Maradey-Romero*, S. Lewis, A. Perzynski & R. Fass* *Division
Alimentary Pharmacology and Therapeutics The relationship between length of Barrett s oesophagus mucosa and body mass index J. Abdallah*, C. Maradey-Romero*, S. Lewis, A. Perzynski & R. Fass* *Division
Quality ID #249 (NQF 1854): Barrett s Esophagus National Quality Strategy Domain: Effective Clinical Care
 Quality ID #249 (NQF 1854): Barrett s Esophagus National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE: Process DESCRIPTION: Percentage
Quality ID #249 (NQF 1854): Barrett s Esophagus National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE: Process DESCRIPTION: Percentage
MANAGEMENT OF BARRETT S RELATED NEOPLASIA IN 2018
 MANAGEMENT OF BARRETT S RELATED NEOPLASIA IN 2018 Sachin Wani Medical Director Esophageal and Gastric Center Division of Gastroenterology and Hepatology University of Colorado Anschutz Medical Campus DISCLOSURES
MANAGEMENT OF BARRETT S RELATED NEOPLASIA IN 2018 Sachin Wani Medical Director Esophageal and Gastric Center Division of Gastroenterology and Hepatology University of Colorado Anschutz Medical Campus DISCLOSURES
Table 2.9. Case control studies of helicobacter pylori infection and oesophageal adenocarcinoma
 Characteristics of Characteristics of controls Detection Chow et al (1998) 1993-1995 129 of newly diagnosed oesophageal/gastric cardia (OGC) adenocarcinoma. 224 population controls selected by random digit
Characteristics of Characteristics of controls Detection Chow et al (1998) 1993-1995 129 of newly diagnosed oesophageal/gastric cardia (OGC) adenocarcinoma. 224 population controls selected by random digit
Quality ID #249 (NQF 1854): Barrett s Esophagus National Quality Strategy Domain: Effective Clinical Care
 Quality ID #249 (NQF 1854): Barrett s Esophagus National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL MEASURES: CLAIMS ONLY MEASURE TYPE: Process DESCRIPTION: Percentage
Quality ID #249 (NQF 1854): Barrett s Esophagus National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL MEASURES: CLAIMS ONLY MEASURE TYPE: Process DESCRIPTION: Percentage
RADIOFREQUENCY ABLATION OR CRYOABLATION FOR ESOPHAGEAL DISORDERS
 DISORDERS Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs are dependent
DISORDERS Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs are dependent
Disclosures. Gastroesophageal Reflux Disease. Gastroesophageal Reflux Disease
 Kunal Jajoo, MD Brigham and Women s Hospital July 2012 Disclosures Spouse is a physician employed by Boston Scientific Corporation The content of this lecture equitably discusses products of multiple companies
Kunal Jajoo, MD Brigham and Women s Hospital July 2012 Disclosures Spouse is a physician employed by Boston Scientific Corporation The content of this lecture equitably discusses products of multiple companies
Citation for published version (APA): Phoa, K. Y. N. (2014). Endoscopic management of Barrett s esophagus with dysplasia
 UvA-DARE (Digital Academic Repository) Endoscopic management of Barrett s esophagus with dysplasia Phoa, Nadine Link to publication Citation for published version (APA): Phoa, K. Y. N. (2014). Endoscopic
UvA-DARE (Digital Academic Repository) Endoscopic management of Barrett s esophagus with dysplasia Phoa, Nadine Link to publication Citation for published version (APA): Phoa, K. Y. N. (2014). Endoscopic
235 60th Street, West New York, NJ T: (201) F: (201) Main Street, Hackensack, NJ T: (201)
 235 60th Street, West New York, NJ 07093 T: (201) 854-4646 F: (201) 854-4647 810 Main Street, Hackensack, NJ 07601 T: (201) 488-0095 Barrett's Esophagus WHAT IS BARRETTT'S ESOPHAGUS? Barrett's esophagus
235 60th Street, West New York, NJ 07093 T: (201) 854-4646 F: (201) 854-4647 810 Main Street, Hackensack, NJ 07601 T: (201) 488-0095 Barrett's Esophagus WHAT IS BARRETTT'S ESOPHAGUS? Barrett's esophagus
Adenocarcinoma of the Esophagogastric Junction and Barrett's Esophagus
 GASTROENTEROLOGY 1995;109:1541-1546 Adenocarcinoma of the Esophagogastric Junction and Barrett's Esophagus ALAN J. CAMERON,* CLIFFORD T. LOMBOY,* MANUEL PERA,* and HERSCHEL A. CARPENTER g *Division of
GASTROENTEROLOGY 1995;109:1541-1546 Adenocarcinoma of the Esophagogastric Junction and Barrett's Esophagus ALAN J. CAMERON,* CLIFFORD T. LOMBOY,* MANUEL PERA,* and HERSCHEL A. CARPENTER g *Division of
GASTROESOPHAGEAL REFLUX
 SCIENTIFIC REVIEW AND CLINICAL APPLICATIONS CLINICIAN S CORNER Gastroesophageal Reflux, Barrett Esophagus, and Esophageal Cancer Clinical Applications Nicholas Shaheen, MD, MPH David F. Ransohoff, MD disease
SCIENTIFIC REVIEW AND CLINICAL APPLICATIONS CLINICIAN S CORNER Gastroesophageal Reflux, Barrett Esophagus, and Esophageal Cancer Clinical Applications Nicholas Shaheen, MD, MPH David F. Ransohoff, MD disease
The normal esophagus is lined with squamous epithelium.
 .. ALAN J. CAMERON, M.D. In Barrett's esophagus, the squamous lining of the lower esophagus is replaced by columnar epithelium. Barrett's esophagus is associated with gastroesophageal reflux and an increased
.. ALAN J. CAMERON, M.D. In Barrett's esophagus, the squamous lining of the lower esophagus is replaced by columnar epithelium. Barrett's esophagus is associated with gastroesophageal reflux and an increased
Barrett s Esophagus: Review of Diagnostic Issues and Pre- Neoplastic Lesions
 Barrett s Esophagus: Review of Diagnostic Issues and Pre- Neoplastic Lesions Robert Odze, MD, FRCPC Chief, Gastrointestinal Pathology Associate Professor of Pathology Brigham and Women s Hospital Harvard
Barrett s Esophagus: Review of Diagnostic Issues and Pre- Neoplastic Lesions Robert Odze, MD, FRCPC Chief, Gastrointestinal Pathology Associate Professor of Pathology Brigham and Women s Hospital Harvard
Faculty Disclosure. Objectives. State of the Art #3: Referrals for Gastroscopy (focus on common esophagus problems) 24/11/2014
 State of the Art #3: Referrals for Gastroscopy (focus on common esophagus problems) Dr. Amy Morse November 2014 Faculty: Amy Morse Faculty Disclosure Relationships with commercial interests: Grants/Research
State of the Art #3: Referrals for Gastroscopy (focus on common esophagus problems) Dr. Amy Morse November 2014 Faculty: Amy Morse Faculty Disclosure Relationships with commercial interests: Grants/Research
Vital staining and Barrett s esophagus
 Marcia Irene Canto, MD, MHS Baltimore, Maryland Vital staining or chromoendoscopy refers to staining of endoscopic tissue or topical application of chemical stains or pigments to alter tissue appearances
Marcia Irene Canto, MD, MHS Baltimore, Maryland Vital staining or chromoendoscopy refers to staining of endoscopic tissue or topical application of chemical stains or pigments to alter tissue appearances
Evolution of gastro-oesophageal reflux disease over 5 years under routine medical care the ProGERD study
 Alimentary Pharmacology and Therapeutics Evolution of gastro-oesophageal reflux disease over 5 years under routine medical care the ProGERD study P. Malfertheiner*, M. Nocon, M. Vieth à, M. Stolte, D.
Alimentary Pharmacology and Therapeutics Evolution of gastro-oesophageal reflux disease over 5 years under routine medical care the ProGERD study P. Malfertheiner*, M. Nocon, M. Vieth à, M. Stolte, D.
Adenocarcinoma of the distal esophagus is a recognized
 ORIGINAL ARTICLE Adenocarcinomas of the Distal Esophagus and Gastric Cardia Are Predominantly Esophageal Carcinomas Parakrama Chandrasoma, MD, Kumari Wickramasinghe, MD, PhD, Yanling Ma, MD, and Tom DeMeester,
ORIGINAL ARTICLE Adenocarcinomas of the Distal Esophagus and Gastric Cardia Are Predominantly Esophageal Carcinomas Parakrama Chandrasoma, MD, Kumari Wickramasinghe, MD, PhD, Yanling Ma, MD, and Tom DeMeester,
Gastrointestinal pathology 2018 lecture 2. Dr Heyam Awad FRCPath
 Gastrointestinal pathology 2018 lecture 2 Dr Heyam Awad FRCPath Eosinophilic esophagitis Incidence of eosinophilic gastritis is increasing. Symptoms: food impaction and dysphagia. Histology: infiltration
Gastrointestinal pathology 2018 lecture 2 Dr Heyam Awad FRCPath Eosinophilic esophagitis Incidence of eosinophilic gastritis is increasing. Symptoms: food impaction and dysphagia. Histology: infiltration
Management of dyspepsia and of Helicobacter pylori infection
 Management of dyspepsia and of Helicobacter pylori infection The University of Nottingham John Atherton Wolfson Digestive Diseases Centre University of Nottingham, UK Community management of dyspepsia
Management of dyspepsia and of Helicobacter pylori infection The University of Nottingham John Atherton Wolfson Digestive Diseases Centre University of Nottingham, UK Community management of dyspepsia
DISCLOSURES. This program meets the requirements for GI specific Category 1 contact hours. M
 DISCLOSURES Educational Dimensions is accredited as a provider of continuing nursing education by the American Nurses Credentialing Center s Commission on Accreditation. Successful completion: Participants
DISCLOSURES Educational Dimensions is accredited as a provider of continuing nursing education by the American Nurses Credentialing Center s Commission on Accreditation. Successful completion: Participants
Title Description Type / Priority
 Merit-based Incentive Payment system (MIPS) 2019 Qualified Clinical Data Registry (QCDR) Measure Specifications Summary Listing of QCDR measures supported by the NHCR Measure # NHCR4 NHCR5 GIQIC12 GIQIC15
Merit-based Incentive Payment system (MIPS) 2019 Qualified Clinical Data Registry (QCDR) Measure Specifications Summary Listing of QCDR measures supported by the NHCR Measure # NHCR4 NHCR5 GIQIC12 GIQIC15
Influence of Malpractice History on the Practice of Screening and Surveillance for Barrett s Esophagus
 American Journal of Gastroenterology ISSN 0002-9270 C 2008 by Am. Coll. of Gastroenterology doi: 10.1111/j.1572-0241.2007.01689.x Published by Blackwell Publishing Influence of Malpractice History on the
American Journal of Gastroenterology ISSN 0002-9270 C 2008 by Am. Coll. of Gastroenterology doi: 10.1111/j.1572-0241.2007.01689.x Published by Blackwell Publishing Influence of Malpractice History on the
The Role of Secondary Versus Tertiary Prevention in Decreasing the Incidence of. Esophageal Adenocarcinoma in Patients with Barrett s Esophagus.
 The Role of Secondary Versus Tertiary Prevention in Decreasing the Incidence of Esophageal Adenocarcinoma in Patients with Barrett s Esophagus. Submitted by Lindsay West A project presented to the Department
The Role of Secondary Versus Tertiary Prevention in Decreasing the Incidence of Esophageal Adenocarcinoma in Patients with Barrett s Esophagus. Submitted by Lindsay West A project presented to the Department
Esophageal Adenocarcinoma and Its Rare Association with Barrett s Esophagus in Henan, China
 Esophageal Adenocarcinoma and Its Rare Association with Barrett s Esophagus in Henan, China Shuzheng Liu 1., James Y. Dai 2., Lena Yao 2, Xiaohong Li 3, Brian Reid 3, Steve Self 2, Jie Ma 4, Yuxi Chang
Esophageal Adenocarcinoma and Its Rare Association with Barrett s Esophagus in Henan, China Shuzheng Liu 1., James Y. Dai 2., Lena Yao 2, Xiaohong Li 3, Brian Reid 3, Steve Self 2, Jie Ma 4, Yuxi Chang
Ablation for Barrett s Esophagus: Burn or Freeze
 Ablation for Barrett s Esophagus: Burn or Freeze John R. Saltzman MD Director of Endoscopy Brigham and Women s Hospital Professor of Medicine Harvard Medical School Disclosures No relevant disclosures
Ablation for Barrett s Esophagus: Burn or Freeze John R. Saltzman MD Director of Endoscopy Brigham and Women s Hospital Professor of Medicine Harvard Medical School Disclosures No relevant disclosures
National Digestive Diseases Information Clearinghouse
 Barrett s Esophagus National Digestive Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is Barrett s esophagus? Barrett s esophagus is
Barrett s Esophagus National Digestive Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is Barrett s esophagus? Barrett s esophagus is
SAMs Guidelines DEVELOPING SELF-ASSESSMENT MODULES TEST QUESTIONS. Ver. #
 SAMs Guidelines DEVELOPING SELF-ASSESSMENT MODULES TEST Ver. #5-02.12.17 GUIDELINES FOR DEVELOPING SELF-ASSESSMENT MODULES TEST The USCAP is accredited by the American Board of Pathology (ABP) to offer
SAMs Guidelines DEVELOPING SELF-ASSESSMENT MODULES TEST Ver. #5-02.12.17 GUIDELINES FOR DEVELOPING SELF-ASSESSMENT MODULES TEST The USCAP is accredited by the American Board of Pathology (ABP) to offer
Gregory G. Ginsberg, M.D.
 Radiofrequency Ablation for Barrett s Esophagus with HGD Gregory G. Ginsberg, M.D. Professor of Medicine University of Pennsylvania School of Medicine Abramson Cancer Center Gastroenterology Division Executive
Radiofrequency Ablation for Barrett s Esophagus with HGD Gregory G. Ginsberg, M.D. Professor of Medicine University of Pennsylvania School of Medicine Abramson Cancer Center Gastroenterology Division Executive
Chapter 2 Complications of Gastroesophageal Reflux Disease
 Chapter 2 Complications of Gastroesophageal Reflux Disease Patrick Yachimski Acute esophageal exposure to gastric and/or duodenal refluxate can result in pyrosis and symptomatic gastroesophageal reflux
Chapter 2 Complications of Gastroesophageal Reflux Disease Patrick Yachimski Acute esophageal exposure to gastric and/or duodenal refluxate can result in pyrosis and symptomatic gastroesophageal reflux
Health-related anxiety and the effect of open-access endoscopy in US patients with dyspepsia
 Aliment Pharmacol Ther 23; 17: 835 84. doi: 1.146/j.269-2813.23.1497.x Health-related anxiety and the effect of open-access endoscopy in US patients with dyspepsia A. QUADRI & N. VAKIL University of Wisconsin
Aliment Pharmacol Ther 23; 17: 835 84. doi: 1.146/j.269-2813.23.1497.x Health-related anxiety and the effect of open-access endoscopy in US patients with dyspepsia A. QUADRI & N. VAKIL University of Wisconsin
Disclosures. Heartburn and Barrett s Esophagus. Heartburn and Barrett s Esophagus. GERD is common in the U.S. None
 Heartburn and Barrett s Esophagus None Disclosures Christian Mathy, MD University of California, San Francisco 2015 Heartburn and Barrett s Esophagus Heartburn and GERD GERD therapy Extraesophageal GERD
Heartburn and Barrett s Esophagus None Disclosures Christian Mathy, MD University of California, San Francisco 2015 Heartburn and Barrett s Esophagus Heartburn and GERD GERD therapy Extraesophageal GERD
2019 COLLECTION TYPE: MIPS CLINICAL QUALITY MEASURES (CQMS) MEASURE TYPE: Process
 Quality ID #249 (NQF 1854): Barrett s Esophagus National Quality Strategy Domain: Effective Clinical Care Meaningful Measure Area: Transfer of Health Information and Interoperability 2019 COLLECTION TYPE:
Quality ID #249 (NQF 1854): Barrett s Esophagus National Quality Strategy Domain: Effective Clinical Care Meaningful Measure Area: Transfer of Health Information and Interoperability 2019 COLLECTION TYPE:
Performance measures for lower gastrointestinal endoscopy: a European Society of Gastrointestinal Endoscopy (ESGE) Quality Improvement Initiative
 Performance measures for lower gastrointestinal endoscopy: a European Society of Gastrointestinal Endoscopy (ESGE) Quality Improvement Initiative Name: Institution: Michal F. Kaminski, MD, PhD Dept. of
Performance measures for lower gastrointestinal endoscopy: a European Society of Gastrointestinal Endoscopy (ESGE) Quality Improvement Initiative Name: Institution: Michal F. Kaminski, MD, PhD Dept. of
Digestive Health Southwest Endoscopy 2016 Quality Report
 Digestive Health 2016 Quality Report Our 2016 our quality and value management program focused on one primary area of interest: Performing high quality colonoscopy High quality Colonoscopy We selected
Digestive Health 2016 Quality Report Our 2016 our quality and value management program focused on one primary area of interest: Performing high quality colonoscopy High quality Colonoscopy We selected
ACG Clinical Guideline: Diagnosis and Management of Barrett s Esophagus
 30 PRACTICE GUIDELINES nature publishing group CME ACG Clinical Guideline: Diagnosis and Management of Barrett s Esophagus Nicholas J. Shaheen, MD, MPH, FACG 1, Gary W. Falk, MD, MS, FACG 2, Prasad G.
30 PRACTICE GUIDELINES nature publishing group CME ACG Clinical Guideline: Diagnosis and Management of Barrett s Esophagus Nicholas J. Shaheen, MD, MPH, FACG 1, Gary W. Falk, MD, MS, FACG 2, Prasad G.
Gastroesophageal reflux disease (GERD) is among the
 Clinical Guideline Upper Endoscopy for Gastroesophageal Reflux Disease: Best Practice Advice From the Clinical Guidelines Committee of the American College of Physicians Nicholas J. Shaheen, MD, MPH; David
Clinical Guideline Upper Endoscopy for Gastroesophageal Reflux Disease: Best Practice Advice From the Clinical Guidelines Committee of the American College of Physicians Nicholas J. Shaheen, MD, MPH; David
Gland ducts and multilayered epithelium in mucosal biopsies from gastroesophageal-junction region are useful in characterizing esophageal location
 Diseases of the Esophagus (2005) 18, 87 92 2005 ISDE Blackwell Publishing, Ltd. Original article Gland ducts and multilayered epithelium in mucosal biopsies from gastroesophageal-junction region are useful
Diseases of the Esophagus (2005) 18, 87 92 2005 ISDE Blackwell Publishing, Ltd. Original article Gland ducts and multilayered epithelium in mucosal biopsies from gastroesophageal-junction region are useful
Proton-pump inhibitor therapy and the development of dysplasia in patients with Barrett s oesophagus
 Proton-pump inhibitor therapy and the development of dysplasia in patients with Barrett s oesophagus BARRETT S OESOPHAGUS is a premalignant condition, with dysplasia usually preceding the development of
Proton-pump inhibitor therapy and the development of dysplasia in patients with Barrett s oesophagus BARRETT S OESOPHAGUS is a premalignant condition, with dysplasia usually preceding the development of
Slide 1. Slide 2. Slide 3 DISCLOSURES EXPECTED OUTCOMES DIAGNOSIS AND TREATMENT
 Slide 1 DIAGNOSIS AND TREATMENT 1 Slide 2 DISCLOSURES Successful completion: Participants must attend the entire program, including any resulting Q & A, and submit required documentation. Conflict of interest:
Slide 1 DIAGNOSIS AND TREATMENT 1 Slide 2 DISCLOSURES Successful completion: Participants must attend the entire program, including any resulting Q & A, and submit required documentation. Conflict of interest:
Is There Publication Bias in the Reporting of Cancer Risk in Barrett s Esophagus?
 GASTROENTEROLOGY 2000;119:333 338 Is There Publication Bias in the Reporting of Cancer Risk in Barrett s Esophagus? NICHOLAS J. SHAHEEN, MELISSA A. CROSBY, EUGENE M. BOZYMSKI, and ROBERT S. SANDLER Division
GASTROENTEROLOGY 2000;119:333 338 Is There Publication Bias in the Reporting of Cancer Risk in Barrett s Esophagus? NICHOLAS J. SHAHEEN, MELISSA A. CROSBY, EUGENE M. BOZYMSKI, and ROBERT S. SANDLER Division
ESOPHAGEAL CANCER AND GERD. Prof Salman Guraya FRCS, Masters MedEd
 ESOPHAGEAL CANCER AND GERD Prof Salman Guraya FRCS, Masters MedEd Learning objectives Esophagus anatomy and physiology Esophageal cancer Causes, presentations of esophageal cancer Diagnosis and management
ESOPHAGEAL CANCER AND GERD Prof Salman Guraya FRCS, Masters MedEd Learning objectives Esophagus anatomy and physiology Esophageal cancer Causes, presentations of esophageal cancer Diagnosis and management
Patient-reported Outcomes
 3 Patient-reported Outcomes Ingela Wiklund Key points Many gastrointestinal diseases are symptomdriven, so the patient s perspective is particularly important in this area. Patient-reported outcomes (PROs)
3 Patient-reported Outcomes Ingela Wiklund Key points Many gastrointestinal diseases are symptomdriven, so the patient s perspective is particularly important in this area. Patient-reported outcomes (PROs)
